Do Indigenous Australians age prematurely? The implications of life expectancy and health conditions of older Indigenous people for health and aged care policy
Philippa R. Cotter A E , John R. Condon B , Tony Barnes A , Ian P. S. Anderson C , Leonard R. Smith D and Teresa Cunningham AA The Northern Institute, Charles Darwin University, Casuarina Campus, Darwin, NT 0909, Australia. Email: tony.barnes@cdu.edu.au; teresa.cunningham@menzies.edu.au
B Menzies School of Health Research, Charles Darwin University, PO Box 41096, Casuarina, NT 0811, Australia. Email: john.condon@menzies.edu.au
C University of Melbourne, Melbourne School of Population Health, Level 4, 207 Bouverie Street, Carlton, Vic. 3010, Australia. Email: i.anderson@unimelb.edu.au
D Australian Demographic and Social Research Institute, Australian National University, Canberra, ACT 0200, Australia. Email: leonard.smith@anu.edu.au
E Corresponding author. Email: prcotter@bigpond.net.au
Australian Health Review 36(1) 68-74 https://doi.org/10.1071/AH11996
Submitted: 11 January 2011 Accepted: 27 April 2011 Published: 9 February 2012
Journal Compilation © AHHA 2012
Abstract
Objective. To assess whether Indigenous Australians age prematurely compared with other Australians, as implied by Australian Government aged care policy, which uses age 50 years and over for population-based planning for Indigenous people compared with 70 years for non-indigenous people.
Methods. Cross-sectional analysis of aged care assessment, hospital and health survey data comparing Indigenous and non-indigenous age-specific prevalence of health conditions. Analysis of life tables for Indigenous and non-indigenous populations comparing life expectancy at different ages.
Results. At age 63 for women and age 65 for men, Indigenous people had the same life expectancy as non-indigenous people at age 70. There is no consistent pattern of a 20-year lead in age-specific prevalence of age-associated conditions for Indigenous compared with other Australians. There is high prevalence from middle-age onwards of some conditions, particularly diabetes (type unspecified), but there is little or no lead for others.
Conclusion. The idea that Indigenous people age prematurely is not well supported by this study of a series of discrete conditions. The current focus and type of services provided by the aged care sector may not be the best way to respond to the excessive burden of chronic disease and disability of middle-aged Indigenous people.
What is known about the topic? The empirical basis for the Australian Government’s use of age 50 for Indigenous aged care planning, compared to age 70 for the non-indigenous population, is not well established. It is not clear whether Indigenous people’s poorer health outcomes and lower life expectancy are associated with premature ageing.
What does this paper add? This paper compares Indigenous and non-indigenous life expectancy and prevalence of health conditions. Only some conditions associated with ageing appear to affect Indigenous people earlier than other Australians. The proposition of premature ageing based on this explanatory framework is uncertain. The estimated gap between Indigenous and non-indigenous life expectancy in later life is ~6 years.
What are the implications for practitioners? The current rationale for using a lower Indigenous planning age is problematic; however, further research is required to assess the effectiveness of this policy measure. The much higher prevalence of preventable chronic conditions among Indigenous Australians in middle-age groups is clear. The ‘early ageing’ frame can imply irremediable disability and disease. The aged care sector may be filling gaps in other services. The community care services for this group require a more tailored approach than simply lowering the planning age for aged care services.
Introduction
The idea that Indigenous Australians age prematurely is embedded in policy: for over two decades the age 50 years and over has been used to plan and allocate aged care services for the Indigenous population in the same way as the age 70 years is used for the non-indigenous population. Government documents have offered various rationales for this policy measure: that ‘conditions associated with ageing generally affect Aboriginal and Torres Strait Islander people substantially earlier than other Australians’1 for example, or that the policy recognises Indigenous people’s ‘poor health status, reduced life expectancy and subsequent need for aged care services at a younger age’.2 Although some critiques do not accept the notion of early ageing3, the debate has lacked an empirical basis and the established rationale continues to be widely circulated in the aged care sector.4
In this paper, we examine the assumption that Australia’s Indigenous population ages earlier than the non-indigenous population. If this is not the case, questions arise about whether lowering the age for allocation of aged care services is a good way to respond to the health and care needs of Indigenous people in middle- and older-age groups. If the policy measure has some value – as a tool to increase resources for older Indigenous people, for example – it needs an evidence-based rationale. We probe the two components underpinning stated rationales: life expectancy and health conditions.
The gap between Indigenous and non-indigenous life expectancy of nearly 20 years has been an iconic statistic in our understanding of Indigenous health, but this understanding is being challenged. Methods for estimating Indigenous life expectancy are being refined5 and there are signs that Indigenous life expectancy may have improved.6 The latest estimates suggest Indigenous Australians may have ~11 years lower life expectancy at birth than other Australians.7 In this paper, we consider the use of the lower age benchmark in light of these shifts and also compare Indigenous and non-indigenous life expectancy in later life as this is more pertinent for aged care services.
The Indigenous population has worse health outcomes across all age groups relative to non-indigenous Australians. But it is not clear whether the lower life expectancy Indigenous people experience is associated with the pattern of disease that we commonly associate with ageing starting earlier or occurring at a faster rate. Although ‘ageing’ is a slippery concept, the ageing process can be defined by an increasing risk of irremediable disability and death. The age of onset and duration of this period of functional decline differs and is subject to social, behavioural and environmental factors that have cumulative and interacting effects over the lifespan.8 If the Indigenous population ages prematurely, we would expect to see the same set of conditions as the older non-indigenous population, but at a younger age. Ageing is a continuous process; no cut-off age can distinguish ‘old’ people from the non-elderly.9 We therefore compared the age-groups used in policy and examined whether Indigenous people showed a 20-year lead for conditions that are prevalent among the rest of the population aged over 70.
Investigating the health of older Indigenous people has been hindered by the lack of breakdown of older-age groups when reporting Indigenous health statistics. The few analyses that are available point to an age gap of ~20 years in self-reported health status between Indigenous and non-indigenous people. For instance, the proportion of Indigenous people reporting their health as fair or poor (compared to excellent or good) at ~50 years old is similar to that of non-indigenous people ~70 years of age.10 The prevalence of heart and circulatory diseases and of diabetes (type unspecified) reported by Indigenous people increases markedly from ~35 years of age onwards – ~10 years earlier than in the non-indigenous population.11 However, whereas a higher proportion of Indigenous Australians than non-indigenous Australians reported more than one long-term health condition in age groups between 25 and 54 years, older people (aged 55 years and over) in both populations had similar rates.12 A 2004 report examining Aged Care Assessment Program (ACAP) Indigenous client data from 2000 to 2001 provided information on client characteristics but did not examine health conditions.13 Our comparison of health conditions does not rely solely on self-reported data that may be affected by factors such as language spoken and employment status.14 We analysed multiple data sources to examine the age-specific prevalence of common health conditions of Indigenous Australians aged 50 years or over and compared these to the non-indigenous population aged 70 years or over.
Methods
We used national life tables for the Australian Indigenous and non-indigenous populations for 2005–07 published by the Australian Bureau of Statistics (ABS)7 to compare the life expectancy of Indigenous and non-indigenous people at different ages, particularly to assess at what age Indigenous people had the same life expectancy as non-indigenous people at age 70.
To examine prevalence of age-related conditions, we carried out the following analyses using summary tables from three data sources:
-
The Aged Care Assessment Program National Data Repository at La Trobe University provided data from the Aged Care Assessment Program Minimum Dataset Version 2 (ACAP MDSv2). Assessment by an Aged Care Assessment Team (ACAT) is mandatory for admission to residential care and also to access a range of community care packages. In 2006 there were 115 Australian Government funded ACATs regionally based throughout Australia.15 We analysed ACAP MDSv2 data from the last completed assessment during the 2005–06 financial year for individuals living in the community at the time of assessment with valid data on age and indigenous status (1668 Indigenous clients, 130 338 non-indigenous clients, 3727 (2.7%) indigenous status not recorded). Age-specific aged care assessment rates were calculated. The numerator was the number of people assessed by an ACAT, and people assessed more than once within the year were counted only once. We compared the prevalence of health conditions by age-group in Indigenous and non-indigenous people assessed by ACATs. The ACAT assessments record up to ten diagnosed conditions that have an effect on a person’s need for assistance with activities of daily living and social participation.16 We obtained summary data on the 12 conditions recorded most commonly in all ACAT assessments. Data on all conditions recorded were used, not just primary diagnosis.
-
The Australian Institute of Health and Welfare provided data from the National Hospital Morbidity Dataset.17 We compared age-specific hospital separation rates for Indigenous and non-indigenous people. Some of the 12 conditions compared in ACAT assessments could not be analysed because there were too few hospital admissions to provide reliable rates. We calculated age-specific hospital separation rates (excluding same day admissions) for arthritis, circulatory disease, dementia, diabetes and respiratory disease as the number of hospital separations with a relevant principal diagnosis in each age group, divided by the ERP in that age group. We used hospital separations data for the 2006–07 financial year for all jurisdictions except Tasmania and the Australian Capital Territory, as the quality of indigenous identification in these states and territories was not considered acceptable. Individuals who separated more than once in the year can have more than one record in the data.
-
The ABS provided data from the National Health Survey and the National Aboriginal and Torres Strait Islander Health Survey (NATSIHS) 2004–05.12,18 We compared age-specific prevalence of self-reported conditions for Indigenous and non-indigenous people for 7 of the 12 conditions examined in ACAT assessments. Data on the remaining conditions were not collected in these surveys.
Ten-year age groups were used because of the small number of Indigenous clients. The age groups 0–44, 45–54, 55–64, 65–74, 75–84 and 85 years and over were used for most analyses. All the datasets coded health conditions based on the 10th revision of the International Classification of Diseases (ICD-10).19 Age-specific assessment and prevalence rates were calculated as the number of people assessed or recorded with each condition in each age-group in the relevant time period divided by the Estimated Resident Population (ERP) in that age-group, separately for Indigenous and non-indigenous people. Rates are expressed per 1000 population. The ABS Experimental ERP for the Australian Indigenous and non-indigenous populations at 30 June 200620,21 were used to calculate age-specific rates.
Results
Life expectancy
The gap between Indigenous and non-indigenous life expectancy reduces with increasing age. In 2005–07, the further life expectancy of non-indigenous people aged 70 years was 17.4 years for women and 14.7 years for men. For Indigenous people, these further life expectancies were realised earlier: at age 63 for women and age 65 for men.
Prevalence of health conditions
ACAT assessments
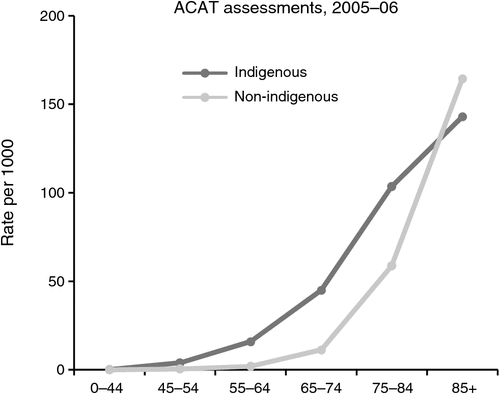
Compared to other Australians, Indigenous people have a higher rate of assessment by ACAT teams at every age-group except age 85+ (Fig. 1). Assessment rates for the Indigenous population were comparable to those for non-indigenous who were people 5 to 10 years older. These rates are important in the interpretation of the prevalence of health conditions in populations based on ACAT assessment, as the prevalence of health conditions in the Indigenous population may be overestimated to varying degrees.
|
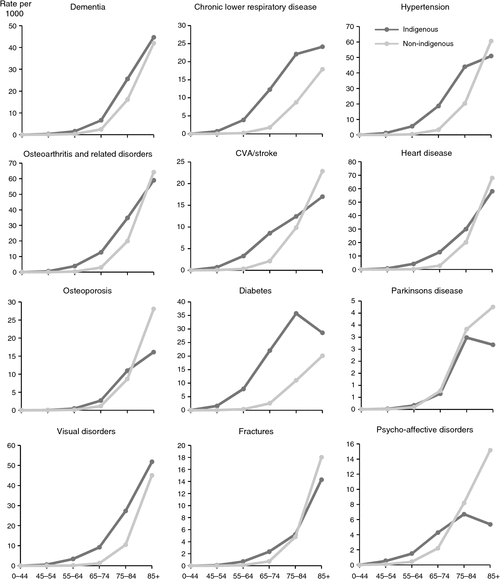
Indigenous people assessed by an ACAT did not consistently show a 20-year lead for the estimated population prevalence rates of these common conditions compared to non-indigenous people. The prevalence rates for dementia, Parkinson’s disease, osteoporosis and osteoarthritis, fractures, heart disease and psycho-affective disorders were similar or moderately higher than non-indigenous rates in most age groups, despite Indigenous people having much higher ACAT assessment rates (Fig. 2). There was little indication of earlier onset for these conditions or marked excess at any age among Indigenous Australians. Other conditions displayed a very different pattern. For example, the prevalence rates for hypertension, respiratory disease and diabetes were much higher than non-indigenous rates, particularly in younger-age groups (Fig. 2). These diseases affected Indigenous people 10–20 years earlier than non-indigenous people.
|
Hospital separations
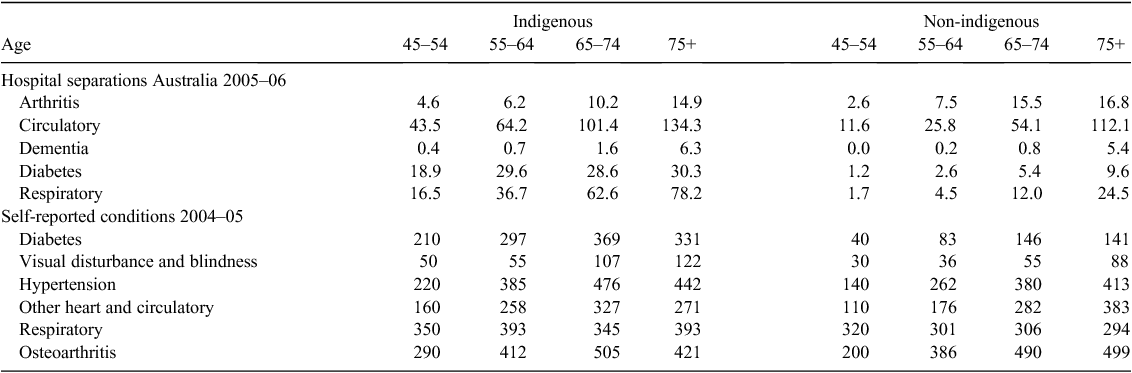
Indigenous hospital separation rates with a principal diagnosis of diabetes are much higher after age 45 than for non-indigenous people at any age (Table 1). The Indigenous population’s hospital separation rates for circulatory and respiratory diseases were also much higher than non-indigenous rates, particularly in younger-age groups. Rates among Indigenous people aged 45–54 years were close to rates for non-indigenous people ~20 years older. In contrast, the Indigenous population’s separation rate for arthritis was lower than for non-indigenous patients in all but the 45–54-year age group. Indigenous hospital separation rates for dementia were moderately higher than non-indigenous rates, but both groups had a similar pattern of increase with increasing age.
Self-reported conditions
Self-reported prevalence of health conditions from national surveys also showed a variable pattern (Table 1). Analysis of health survey data was restricted because data on some conditions (e.g. stroke and dementia) were not available and data on other conditions (e.g. osteoporosis) were unreliable for older-age groups. Nevertheless, among the conditions analysed, the patterns for diabetes, circulatory disease and arthritis matched that seen in hospital separation rates, whereas the prevalence rates among the Indigenous population of respiratory disease were higher than non-indigenous rates at all ages. Hypertension and visual disturbances affected Indigenous people ~10 years earlier than non-indigenous people.
Discussion
The gap in the Indigenous and non-indigenous age benchmarks used for planning does not reflect current estimates of the gap in life expectancy between these populations either at birth (~11 years) or our estimate of life expectancy in later life (~6 years). The Indigenous population aged over 50 does not have the same set of health conditions as the non-indigenous population aged over 70. Rather than a uniform pattern of earlier onset of age-associated conditions, we found earlier onset and high prevalence from middle-age onwards of only some conditions – particularly hypertension, respiratory disease and diabetes (type unspecified). Our findings are comparable with those of Vos et al.22 whose assessment of the Indigenous population’s burden of disease found that the largest proportion of the Indigenous health gap (the difference between levels of disease burden of the Indigenous and total Australian population) occurred in people aged 35–54 years and non-communicable diseases, particularly cardiovascular disease and diabetes (type unspecified), contributed most to the gap at these ages.
The current policy logic attributes the higher need for assistance of Indigenous people from age 50 to early ageing and therefore concludes that aged care services are needed. Our findings provoke a different conception about the type of services needed and who provides them. Rather than expecting community-based aged care services to provide rehabilitation and mental health services for example, primary care and community health services need to be strengthened. Like Jorm et al.,23 we would also suggest that the high rates of health conditions that are amenable to primary and secondary prevention among Indigenous ACAP clients present the potential for preventive healthcare programs to be implemented in the community-based aged care setting.
In our study, the prevalence of several health conditions among Indigenous people over 85 years was similar to, or lower than, their prevalence in non-indigenous people in this age-group. There are competing hypotheses about patterns of health disparities in later life. The ‘age as leveller’ hypothesis suggests a convergence in the health of those from different socioeconomic positions in late old age, but whether this can be explained by selective attrition (‘healthy survivor’ effect) is debated.24 The alternative hypothesis suggests inequalities persist or widen into older age due to cumulative disadvantage.25 Controlling for cohort and period effects to reach a consensus has proved problematic.8
Our analysis was limited to 12 conditions, few of which are ‘geriatric syndromes’. The term ‘geriatric syndrome’ is used to capture conditions in older people that do not fit into discrete disease categories. Geriatric syndromes such as delirium, falls, incontinence and frailty may occur as a consequence of certain conditions but also in the absence of identifiable specific disease.26,27 Despite lacking exact consensus about definitions and causes, the underlying concepts include complex interactions of an individual’s vulnerabilities, involvement of multiple risk factors (including those outside the biological framework) and multiple organ systems.27 However, whereas ‘older age’ is a risk factor shared by geriatric syndromes,27 in research on possible causative pathways, such as alterations to immunity, factors that are predictive of mortality for over 60 year olds have not been informative in younger-age groups.28 In their review of frailty, Fulop et al.26 suggest that there is insufficient evidence to dissect the role of ageing compared to the role of chronic disease. Nevertheless, it is worth investigating geriatric syndromes further in the Indigenous population given their increased prevalence of risk factors.
Our analysis is constrained by important limitations in the data. The conditions seen in older age could not be comprehensive. For example, there were insufficient hospital admissions with a principal diagnosis of Parkinson’s disease or osteoporosis to enable reliable comparisons by age-group and indigenous status. The presence of multiple health conditions was not able to be measured in these data. There is no indigenous indicator in the ABS Survey of Disability, Ageing and Carers – an important source of information on health conditions in the general older population – though even if this was available, the current sample size and coverage would not provide adequate information on Indigenous people. The NATSIHS does not include people living in residential care.
Indigenous identification is inaccurate or incomplete in some datasets and jurisdictions and indigenous rates are likely to be underestimated in these datasets. However, the degree of lack of completeness of indigenous status is likely to be similar across health conditions. The accuracy of diagnosis in the datasets may affect some health conditions more than others. For example osteoporosis may be under-reported unless diagnostic tests are specifically sought. Dementia is under-diagnosed at all levels of health presentations. A valid screening tool for assessing cognition in older Indigenous people has only recently been developed.29 A measure of Indigenous dementia prevalence (12.4% of those aged over 45 years) in the Kimberley region of Western Australia using this tool suggests that the condition may be under-diagnosed in our data.30 Differential access to services between Indigenous and non-indigenous people may confound some of our results; however, the range of datasets used helps to compensate for this limitation.
The cross-sectional data used in this study provide only a snapshot of prevalence. Longitudinal research or record linkage could provide useful evidence that tracks the factors associated with age-related changes in health and disability and demand for services among Indigenous people. Community level studies with validated tools to assess health conditions in older people may clarify some of the questions raised by this study.
Conclusions
It appears that current rationales for using a planning age for Indigenous people 20 years younger than the age used for non-indigenous people are not well substantiated. Only some conditions associated with ageing appear to affect Indigenous people earlier than other Australians and the construct of ‘early ageing’ based on this explanatory framework is uncertain. The estimated gap between Indigenous and non-indigenous life expectancy in later life is ~6 years. But does the policy also need to change or just the rhetoric used to justify it? A fuller understanding of the patterns of need for assistance and of aged care service use by Indigenous Australians aged 50–69 years and those aged 70 and over is required to determine whether age 50 is a good basis for defining the Indigenous target population for aged care services, and we are undertaking research to this end.
Our results raise questions about how the ‘early ageing’ concept shapes how needs are met and what is left out. The much higher prevalence of preventable chronic conditions among Indigenous Australians in middle-age groups needs to be addressed as such. The current focus and type of services provided by the aged care system may not be the best way to respond to the excessive burden of chronic disease and disability of middle-aged Indigenous people. The lower age criteria may contribute to the stereotyping of this group as passive and irreversibly reliant on care.9 Indigenous people in their fifties are not old. A decline into dependence at this age is not inevitable.
The greatest scope for future Indigenous life expectancy gains is through improving the health of middle- and older-age groups (ages 35 and over).6 The community supports that buttress this goal need a more tailored approach than simply lowering the aged care planning age. Efforts to improve life expectancy cannot sidestep the need to also improve quality of life for the increasing number of Indigenous Australians who live to old age.
Competing interests
The authors declare that they have no competing interests.
Acknowledgements
This project was funded by a National Health and Medical Research Council/Australian Research Council Ageing Well, Ageing Productively Strategic Award (#422501) with contributions from the CIPHER (Capacity Building in Indigenous Policy-relevant HEalth Research) NHMRC Population Health Capacity Building Grant (#236235). Funding for the Onemda VicHealth Koori Health Unit is provided by the Victorian Health Promotion Foundation, Department of Health and Ageing and Cooperative Research Centre for Aboriginal Health. The authors thank Anna Howe for her insightful comments on an early draft of the manuscript. We are also grateful to the many people who assisted us in obtaining data.
References
[1] Report on the Operation of the Aged Care Act 1997, 1 July 2008 to 30 June 2009. Canberra: Commonwealth of Australia; 2009.[2] Government response to the Commonwealth Grants Commission Report on Indigenous funding 2001. Canberra: Department of Immigration and Multicultural and Indigenous Affairs; 2002.
[3] Gibson D, Griew R. New models and approaches to care. Research paper, The Myer Foundation 2020 Vision Project. Melbourne: The Myer Foundation; 2002.
[4] National Indigenous Aged Care, Issues paper. Aged and Community Services Australia; 2006. Available at http://www.agedcare.org.au/POLICIES-&-POSITION/Position-and-discussion-papers/Indigenous_Issues_Paper.pdf [verified 10 March 2010].
[5] Discussion paper: Assessment of methods for developing life tables for Aboriginal and Torres Strait Islander Australians. Canberra: Australian Bureau of Statistics; 2006. Cat. No. 3302.0.55.002.
[6] Wilson T, Condon J, Barnes T. Northern Territory Indigenous life expectancy improvements, 1967–2004. Aust N Z J Public Health 2007; 31 184–8.
| Northern Territory Indigenous life expectancy improvements, 1967–2004.Crossref | GoogleScholarGoogle Scholar | 17461012PubMed |
[7] Experimental life tables for Aboriginal and Torres Strait Islander Australians, 2005–2007. Canberra: Australian Bureau of Statistics; 2009. Cat. No. 3302.0.55.003.
[8] Higgs P, Jones IR. Medical sociology and old age. Towards a sociology of health in later life. Oxford, UK: Routledge; 2009.
[9] Breda J, Schoenmaekers D. Age: a dubious criterion in legislation. Ageing Soc 2006; 26 529–47.
| Age: a dubious criterion in legislation.Crossref | GoogleScholarGoogle Scholar |
[10] Cotter P, Anderson I, Smith L. Indigenous Australians: ageing without longevity? In: Borowski A, Encel S, Ozanne E, editors. Longevity and social change in Australia. Sydney: UNSW Press; 2007. pp. 65–98.
[11] The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples. Canberra: Australian Bureau of Statistics and Australian Institute of Health and Welfare; 2008. Cat. No. 4704.0.
[12] National Aboriginal and Torres Strait Islander Health Survey, Australia 2004–05. Canberra: Australian Bureau of Statistics; 2006. Cat. No. 4715.0.
[13] Lincoln Centre for Ageing and Community Care Research. Aged Care Assessment Program National Report on Indigenous client data, July 2000–June 2001. Melbourne: La Trobe University; 2004.
[14] Cunningham J, Sibthorpe B, Anderson I. Occasional paper: Self-assessed health status, Indigenous Australians, 1994. Canberra: Australian Bureau of Statistics; 1997. Cat. No. 4707.0.
[15] Steering Committee for the Review of Government Service Provision. Report on Government Services 2007. 2007. Available at http://www.pc.gov.au/gsp/reports/rogs/2007 [verified 24 February 2010].
[16] Aged care assessment program data dictionary version 1. Canberra: Australian Institute of Health and Welfare; 2002. Cat. No. AGE 27.
[17] Australian Hospital Statistics 2006–07. Canberra: Australian Institute of Health and Welfare; 2008. Cat. No. HSE 55.
[18] National Health Survey summary of results, Australia 2004–05. Canberra: Australian Bureau of Statistics; 2006. Cat. No. 4364,0.
[19] International statistical classification of diseases and related health problems, 10th revision, Australian Modification, Australian Classification of Health Interventions and Australian Coding Standards, 5th edn. Sydney: National Centre for Classification in Health, University of Sydney; 2006.
[20] Australian Demographic Statistics, June quarter 2006. Canberra: Australian Bureau of Statistics; 2006. Cat. No. 3101.0.
[21] Experimental estimates of Aboriginal and Torres Strait Islander Australians June 2006. Canberra: Australian Bureau of Statistics; 2008. Cat. No. 3238.0.55.001.
[22] Vos T, Barker B, Stanley L, Lopez A. The burden of disease and injury in Aboriginal and Torres Strait Islander peoples 2003. Brisbane: School of Population Health, The University of Queensland; 2007. Available at http://lowitja.org.au/files/crcah_docs/Indigenous-BoD-Report.pdf [verified 14 December 2011].
[23] Jorm LR, Walter SR, Lujic S, Byles JE, Kendig HL. Home and community care services: a major opportunity for preventive health care. BMC Geriatr 2010; 10 26
| Home and community care services: a major opportunity for preventive health care.Crossref | GoogleScholarGoogle Scholar | 20492704PubMed |
[24] Beckett M. Converging health inequalities in later life – an artefact of mortality selection? J Health Soc Behav 2000; 41 106–9.
| Converging health inequalities in later life – an artefact of mortality selection?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c3htl2juw%3D%3D&md5=4a8c373832b9413d00dc4033f6f36e7bCAS | 10750325PubMed |
[25] Willson A, Shuey K, Elder G. Cumulative advantage processes as mechanisms of inequality in life course health. AJS 2007; 112 1886–924.
[26] Fulop T, Larbi A, Witkowski J, McElhaney J, Loeb M, Mitnitski A, Pawelec G. Aging, frailty and age-related diseases. Biogerontology 2010; 11 547–63.
| Aging, frailty and age-related diseases.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3cjns1aqtw%3D%3D&md5=c36737ecd8a5c7dfa1ec28303fe0fbd6CAS | 20559726PubMed |
[27] Inouye SK, Studenski S, Tinetti ME, Kuchel GA. Geriatric syndromes: clinical, research and policy implications of a core geriatric concept. J Am Geriatr Soc 2007; 55 780–91.
| Geriatric syndromes: clinical, research and policy implications of a core geriatric concept.Crossref | GoogleScholarGoogle Scholar | 17493201PubMed |
[28] Wikby A, Mansson I, Johansson B. The immune risk profile is associated with age and gender: findings from three Swedish population studies of individuals 20–100 years of age. Biogerontology 2008; 9 299–308.
| The immune risk profile is associated with age and gender: findings from three Swedish population studies of individuals 20–100 years of age.Crossref | GoogleScholarGoogle Scholar | 18369735PubMed |
[29] LoGiudice D, Smith K, Thomas J, Lautenschlager N, Almeida O, Atkinson D, Flicker L. Kimberley Indigenous Cognitive Assessment tool (KICA): development of a cognitive assessment tool for older indigenous Australians. Int Psychogeriatr 2006; 18 269–80.
| Kimberley Indigenous Cognitive Assessment tool (KICA): development of a cognitive assessment tool for older indigenous Australians.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD28zgslOluw%3D%3D&md5=1ac1487621584797f6283b0195e54480CAS | 16403247PubMed |
[30] Smith K. Assessment and prevalence of dementia in Indigenous Australians. 2009. PhD thesis, University of Western Australia, Perth. Available at http://repository.uwa.edu.au/R/-?func=dbin-jump-full&local_base=GEN01-INS01&object_id=6052 [verified 24 February 2010].