Growth of linked hospital data use in Australia: a systematic review
Michelle Tew A , Kim M. Dalziel A , Dennis J. Petrie A B and Philip M. Clarke AA The University of Melbourne, Centre for Health Policy, Melbourne School of Population and Global Health, Level 4, 207 Bouverie Street, Carlton, Vic. 3053, Australia. Email: michelle.tew@unimelb.edu.au; kim.dalziel@unimelb.edu.au; philip.clarke@unimelb.edu.au
B Corresponding author. Email: dennis.petrie@unimelb.edu.au
Australian Health Review 41(4) 394-400 https://doi.org/10.1071/AH16034
Submitted: 5 February 2016 Accepted: 5 June 2016 Published: 22 July 2016
Journal Compilation © AHHA 2017 Open Access CC BY-NC-ND
Abstract
Objective The aim of the present study was to quantify and understand the utilisation of linked hospital data for research purposes across Australia over the past two decades.
Methods A systematic review was undertaken guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2009 checklist. Medline OVID, PsycINFO, Embase, EconLit and Scopus were searched to identify articles published from 1946 to December 2014. Information on publication year, state(s) involved, type of data linkage, disease area and purpose was extracted.
Results The search identified 3314 articles, of which 606 were included; these generated 629 records of hospital data linkage use across all Australian states and territories. The major contributions were from Western Australia (WA; 51%) and New South Wales (NSW; 32%) with the remaining states and territories having significantly fewer publications (total contribution only 17%). WA’s contribution resulted from a steady increase from the late 1990s, whereas NSW’s contribution is mostly from a rapid increase from 2010. Current data linkage is primarily used in epidemiological research (73%).
Conclusion More than 80% of publications were from WA and NSW, whereas other states significantly lag behind. The observable growth in these two states clearly demonstrates the underutilised opportunities for data linkage to add value in health services research in the other states.
What is known about the topic? Linking administrative hospital data to other data has the potential to be a cost-effective method to significantly improve health policy. Over the past two decades, Australia has made significant investments in improving its data linkage capabilities. However, several articles have highlighted the many barriers involved in using linked hospital data.
What does this paper add? This paper quantitatively evaluates the performance across all Australian states in terms of the use of their administrative hospital data for research purposes. The performance of states varies considerably, with WA and NSW the clear stand-out performers and limited outputs currently seen for the other Australian states and territories.
What are the implications for practitioners? Given the significant investments made into data linkage, it is important to continue to evaluate and monitor the performance of the states in terms of translating this investment into outputs. Where the outputs do not match the investment, it is important to identify and overcome those barriers limiting the gains from this investment. More generally, there is a need to think about how we improve the effective and efficient use of data linkage investments in Australia.
Introduction
Linked administrative health data in Australia have been recognised as an important resource for health services research and informing health policies.1 Data linkage represents a platform enabling longitudinal health studies, epidemiological surveillance on rare diseases,2 the examination of variations in healthcare3 and the capture and comparison of healthcare costs across populations and over time.4 It also allows researchers to assess health outcomes on specific cohorts, such as Indigenous populations5,6 and children, who are generally difficult to recruit.7 Data linkage circumvents loss to follow-up problems common in longitudinal studies because patients are tracked retrospectively8 and long-term outcomes, such as survival, can be assessed via linkage to mortality databases.9,10 It can be an efficient and cost-effective11 approach to research and health service improvement because data are acquired from routinely collected hospital data.
Western Australia (WA) was the first state to initiate data linkage in the 1970s,12 but its use was limited in scope and purpose. Over the years, specific health databases, such as mortality and births, were developed, giving rise to small clusters of linked data for specific populations.13 In 1995, using an infrastructure grant, WA established a full-population-based data linkage system. A decade later, New South Wales (NSW) followed suit with the establishment of the Centre for Health Record Linkage (CHeReL) in 2006, providing linkage services for NSW and the Australian Capital Territory (ACT). The linkage of NSW hospital data to a large-scale cohort study of individuals aged 45 years and over14 has been particularly valuable.15
In 2009, the Population Health Research Network (PHRN) was initiated to further improve Australia’s data linkage capabilities. Since its establishment, approximately A$93 million from various sources, including government, state and academic partners, has been allocated to the PHRN to fulfil its purpose.16 As a result, all Australian states have established data linkage units with the capacity to provide population-wide linked data.
Although considerable progress has been made, significant barriers remain that are impeding the effective and efficient use of data linkage.17,18 In Australia and within each state, health data are collected by different organisations and at various levels of government,19 prolonging approvals from numerous data custodians to link and access databases.20–22 In addition, the use of cross-jurisdictional linked datasets is particularly difficult. The lack of a streamlined process and excessive duplication were identified as key issues for researchers.23 Further, differences in legislative protocols surrounding confidentiality between ethics committees and operating procedures between linkage units can create discord in research progress.20,24,25
Given the public investments in data linkage, it is important to monitor and evaluate the outputs from this investment. In the present study, we sought to quantify and understand the adoption of linked hospital data for health research purposes over time and by Australian state. We conducted a systematic review of the published literature that uses linked Australian hospital data. The findings provide an overview of the use of linked hospital data in Australia and inform on the uniformity of its use between states. To our knowledge, no study has collated and quantified research publication outputs arising from the use of hospital data linkage in Australia.
Methods
Information source and search strategy
Following Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2009 guidelines,26 five electronic databases, namely Medline OVID, PsycINFO, Embase, EconLit and Scopus, were systematically searched between June and July 2015 to identify all relevant articles published between 1946 and December 2014. Hospital data linkage was defined as linkage of individual patient data that are routinely collected from a patient’s hospital admission to an external or secondary source, such as state or national registers, administrative databases or state records. The search terms were hospital*, data*, link*, record* and Australia*. The full search strategy can be found in Appendix S1, available as Supplementary Material to this paper.
Study selection and eligibility criteria
The results were compiled using reference management software (Mendeley Desktop 1.13; Mendeley Ltd) and duplicates removed. The remaining articles were imported into an online database (Covidence; Veritas Health Innovation Ltd), where two investigators (MT and DP) independently screened titles and abstracts against the inclusion and exclusion criteria as defined below. Full-text screening was performed where it was unclear whether hospital data linkage was used based on the abstract. Although unconventional, both abstract and full-text screening were conducted concurrently because of the atypical research question and the broad search specificity required to capture relevant articles. A third reviewer (KD) resolved any discrepancies.
To be eligible for inclusion, articles had to be journal articles written in English that used individual patient-level data linked with Australian hospital records. The type of data linkage used could be manual, through an established linkage service or a probabilistic technique.
Articles that did not use or involve any data linkage to hospital records or did not specify the state(s) were excluded, as were those that did not have full text available or did not involve original data on which analysis was performed, such as conference abstracts, reviews, comments, discussions or letters.
Data extraction
The template used to record the data extracted included the Australian state(s) in which the data linkage was conducted, publication year, the type of linkage used, research area (classified according to International Statistical Classifications of Diseases and Related Health Problems 10th Revision Australian Modification) (ICD-10-AM) (http://www.aihw.gov.au/hospitals-data/national-hospital-morbidity-data/coded-clinical-data/, accessed 17 July 2015) and type of study. Studies with multiple states data counted as one publication for each state. To illustrate the diversity of groups contributing to the publications from each state, the names of the last author on the publications were collated and assessed.
Data validation and analysis
The PHRN website (http://www.phrn.org.au/, accessed 22 January 2016) provides a publication repository where data linkage units may list peer-reviewed publications arising from their data between 2010 and 2014. This list was subjected to the same screening process based on the above eligibility criteria and was compared with the systematic search list from the same period. This allowed the comparison and validation of our search strategy, and these results are reported in Appendix S2.
Data collected were counted and collated descriptively. To test the significance of differences in proportions between states over time and across research areas, Chi-squared tests were used. All data analyses were managed using STATA IC version 13 (StataCorp).
Quantifying data linkage funding by state
Finally, because available resources are a key factor in determining capacity to undertake linkage and support research, we quantified the data linkage funding in each state where available. The funding included grants from the National Collaborative Research Infrastructure Strategy (NCRIS) and from the Department of Industry, Innovation, Science, Research and Tertiary Education (DIISRTE), as well as state cash contributions. These were based on PHRN Annual Reviews 2011–14,16,27,28 years where funding was broken down by institution.
Results
The systematic search results are provided in Fig. 1. Of the 3314 articles identified, 1704 were duplicated articles identified from different databases and 343 were not journal publications. The remaining 1267 articles were screened against the eligibility criteria; 661 articles were excluded and, of these, 371 (56%) did not involve hospital data and data linkage or used hospital data but did not involve any linkage or vice versa. Seventy articles (11%) did not have full-text or involve original data and 123 (19%) were not Australian or did not specify the state. The remaining articles excluded were not related to population health (15%). The final analysis included 606 studies, and this generated 629 records of hospital data linkage usage across all Australian states.
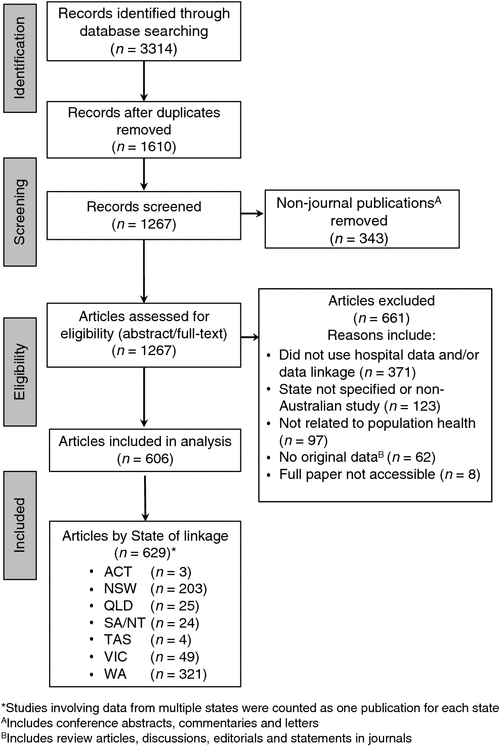
|
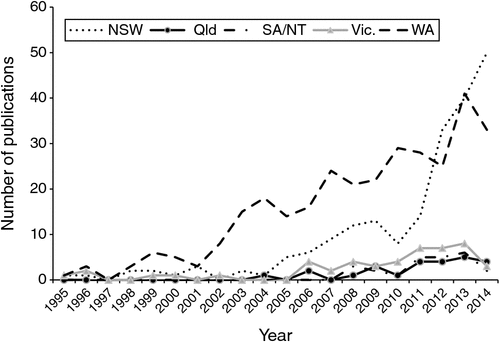
Since 1996, the number of publications using hospital data linkage across Australia has increased (Fig. 2), with more than 80% contributed from two states alone, namely WA (51%) and NSW (32%). The surge of publications from WA coincides with the establishment of the data linkage system in WA in 1995. Prior to this, there were fewer than 10 publications using data linkage (data not shown).
|
The number of publications from NSW has increased steadily in the past decade, but more considerably in the past 5 years, with only one publication in 2004 increasing to 13 in 2009 and to 50 by 2014. Small increases in publications in the past 5 years have also been observed from Victoria, South Australia (SA) and the Northern Territory (NT) and Queensland (Qld).
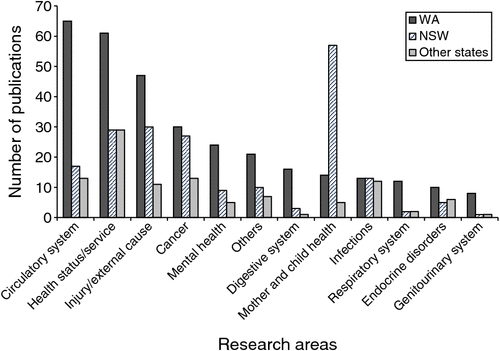
Figure 3 shows the publication numbers by state across different research areas. The most common research area using hospital data linkage was on factors affecting health status or the use of health services (n = 119). Circulatory diseases (n = 95) and injury and external causes (n = 88) were also frequently researched disease areas. WA publications focused primarily on the circulatory system, whereas NSW publications focused primarily on maternal and child health (n = 57). The research areas across all states differed significantly (P < 0.001), thus highlighting the disparity in data linkage usage across Australia. Further analysis to demonstrate the diversity of authors and the extent of data access showed 31% and 38% of publications from WA and NSW respectively were contributed by the top 10 last authors.
|
Linkage between hospital databases or from hospital to external health databases (56%) were the most common data linkage employed. This includes all mentions of state-wide linked data, administrative data or any hospital database. Hospital data linkage to other governmental database (non-hospital) such as Police Road Traffic Accident reports, PBS, MBS, ABS, Child Protection Service records make up 8% of reported data linkage while the remaining 36.2% were from non-specified birth or death records, registries, existing studies or survey populations.
Most publications (73%) were descriptive and analytical epidemiological studies, such as those that assessed mortality from rheumatic heart disease on the Aboriginal Australian population,29 time trends in risk of stroke among elderly Victorians30 and studies exploring respiratory infection hospitalisations for children.31 The smallest contributions came from costing studies, economic evaluations, healthcare evaluations and those informing health services planning (12.9%); the rest were validation studies (13.7%). Some examples of data linkage use in health services planning include assessing the suitability of using emergency department discharge diagnosis in evaluating performance32 and evaluating access to general practitioner services by mental health service users in WA.33 Validation studies are those examining the consistency or variations of patient information between two or more data sources,34–36 which is helpful in assessing the appropriateness of the source.
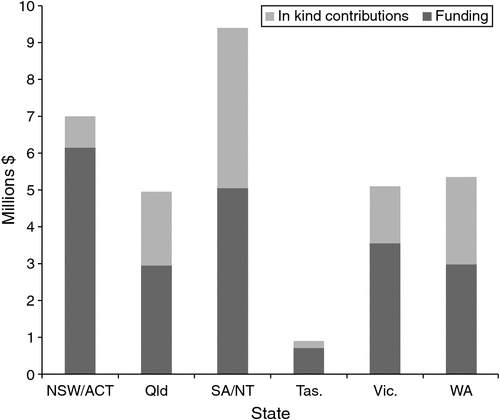
The total funding identified for data linkage by state for the period 2011–13 is shown in Fig. 4. Direct funding ranged from A$0.7 million for Tasmania to around A$6.15 million for NSW (an average of A$3.5 million per state). With the exception of WA and SA, ‘in-kind’ funding was significantly lower than direct funding and was, on average, A$1.8 million per state.
|
Discussion
The present study has documented, for the first time, the research outputs that have flowed from the significant investment in hospital data linkage by Australian Governments over the past two decades. The results indicate a great unevenness in the use of linked administrative hospital data in Australia. Clearly there is enormous variation across states and disease areas in publication quantity with outputs being dominated by two states (WA and NSW). The results show only 10 publications used data from multiple states, thus implying barriers in conducting multistate research with data linkage. The results also demonstrate uneven growth, with a marked rise in publications from NSW not matched by any other Australian state.
Which factors explain the increase in publications from NSW in recent years? Much of the increased research appears to have been driven by the additional datasets that enhance the use of linked hospital data, including the development of a large cohort through the 45 and Up study14 and NSW Perinatal Data Collection.37 It would be important to coordinate the development of supplementary data collection and additional linkage across states in order for Australia to maximise the potential research arising from these efforts. This could include facilitating cross-state comparisons outputs,23 particularly when there is practice variation or when the timing of legislative changes creates a natural experiment, in a similar manner to recent work on the timing of gun buybacks and the effect on firearm-related suicide.38
Despite a decade of significant infrastructure support for data linkage and the development of the PHRN, several Australian states appear to have very few research publications involving use of their linked hospital data. The funding breakdown by state indicates that, with the exception of Tasmania, all Australian states received a total of A$5–9.5 million in direct and ‘in-kind’ funding to support data linkage between the 2011 and 2013 financial years. For most of these states, the published research outputs using these data remain modest. For example, in 2014 (the most recent year in the present study), there were only an average of three publications per year across SA and the NT, Qld and Victoria, and there were no identified publications using Tasmanian linked hospital data. It is hard to determine whether the barriers are due primarily to failures of the linkage units to supply data or to there not being a sufficient demand from researchers for linked datasets. It may also be a ‘chicken and egg’ story, because states where units have no established record of supplying data may not have a critical mass of skilled analysts to make the best use of linked data for research. Beyond developing the infrastructure for comprehensive administrative datasets, there is clearly a need to provide training and funding for analysis if data linkage is to translate into research and further impact. In this regard, it would be worth revisiting the recommendations of the McKeon review regarding ways to promote health economics, biostatistics and health services research alongside investments in data linkage infrastructure.39
It is also important to note that these problems are not confined to health data. A recent Victorian Auditor General’s report indicates that many government departments do not provide the ‘public with the full and open access to the information to which they are entitled’.40 Although there have been several big data strategies developed by various Australian Government departments,41 these have generally not been undertaken in consultation with the research community or involved integration with bodies such as the National Health and Medical Research Council of Australia (NHMRC), which could facilitate aligned research funding.
It is recognised that researchers face numerous barriers to gain data access through the current data linkage processes. In some cases the direct financial barriers are minimal, but a significant time investment from the researcher is needed and even then timely data access is not guaranteed. This was highlighted in a recent proof-of-concept project assessing the practical issues faced by researchers conducting national data linkage.23 Thus, it is helpful to describe how administrative processes between Australian states differ to better understand opportunities to improve data linkage. Therefore, we directly contacted each state data linkage unit for information. Appendix S3 shows significant variation across the states in the provision of linked data in terms of whether they link all hospitals, and the provision of private and emergency data. Few data linkage units provide hospital out-patient data. Although there does not appear to be a clear relationship between the length of establishment of data linkage units and their quantum of research outputs, the results do show that for productive units (NSW and WA) there was only a small lag between the year of establishment and the start of their upward trend in publications. This indicates the potential for newer units to grow rapidly and provide supportive data linkage for research like NSW.
The most productive data linkage units (e.g. NSW and WA) tend to charge for their services, which may indicate the reality that resourcing is required to support research. Likewise, to support quality research, data linkage units will need to be adequately resourced with skilled personnel. More productive data linkage units were more likely to list publication outputs on their websites and had more comprehensive websites in general. This may be in recognition of research and their ability to contribute, and may also indicate resourcing. Along with the comprehensiveness of websites comes the clarity of procedural guidelines. The more productive units all have clear and established guides and processes for researchers available online.
Although the present study is a one-off study, it collected information that should be routinely reported both by data linkage units and the PHRN. Statistics showing increasing trends of activity (e.g. linked datasets being made available for researchers) and a database of outputs (e.g. publications) would build a compelling case for additional funding. Furthermore, the comparable reporting of outcomes by all data linkage units will facilitate comparison across different jurisdictions. Ultimately, we should report a measure that captures both resources and outcomes, such as cost per publication, which would facilitate the evaluation of data linkage units in producing research outputs.
The present study has limitations. First, a pragmatic search approach that balances specificity and sensitivity was adopted to optimise as well as limit the search. As such, some studies using hospital linked data may have been missed. However, the validation result shows that the search strategy were likely to have captured most of the articles. Second, the search was limited to peer-reviewed articles only; hence, grey literature was excluded. Reports from state- or federal-funded data linkage projects would have been missed, but some states may be more likely to make reports public. Third, the PHRN publication list was only available from 2010 onwards; therefore, prior validation could not be conducted. In addition, the funding reported based on PHRN annual reviews does not capture all funding for data linkage in Australia, but provides a useful lower bound on the resources available by state. Finally, it is recognised that there is a lag time between accessing data and publication; hence, this systematic review is not able to fully capture the current linkage capacity and research output from each data linkage unit.
Conclusion
There is uneven use of linked administrative hospital data in Australia, with published outputs being dominated by two states (WA and NSW). Given certain states have demonstrated their effectiveness in using data linkage, it may be possible for others to draw on their expertise. Record linkage to support cross-jurisdictional research can help generalise findings and better inform health outcomes at an Australian level. Policies need to be developed that promote greater use of these data in providing research evidence to make better decisions and improve the healthcare system across Australia.
Competing interests
PMC has previously published using WA, Qld and Department of Veterans’ Affairs (DVA) linked data and all authors are likely to want to use linked data in the future. The authors have no other conflicts of interest to report.
Acknowledgements
The study received no explicit funding, but the authors acknowledge an NHMRC Research Fellowship for PMC (APP 1079621), the 2013 Melbourne University McKenzie Fellowship for KMD and the Australian Research Council’s Discovery Early Career Awards funding scheme (Project DE150100309) for DJP. The authors also thank the following the personnel at the data linkage units for their assistance in completing and verifying the information relevant to their units: Nicky O’Brien, Jasna Tepsic and Chris Radbone (SA/NT DataLink), Jessica Hehir (Centre for Health Record Linkage), Trisha Johnston (Queensland Health – Health Statistics Unit), Katy Greenland and Peter Carver (Victorian Data Linkages) and Janine Alan (Data Linkage Western Australia). The authors thank Merran Smith and Felicity Flack from the Population Health Research Network for their kind help in providing information to supplement this research. The views expressed herein are those of the authors and the authors take responsibility for all remaining errors in the paper.
References
[1] Moore HC, Guiver T, Woollacott A, de Klerk N, Gidding HF. Establishing a process for conducting cross-jurisdictional record linkage in Australia. Aust N Z J Public Health 2015; 40 159–64.| Establishing a process for conducting cross-jurisdictional record linkage in Australia.Crossref | GoogleScholarGoogle Scholar | 26559155PubMed |
[2] Gibson A, Jorm L, McIntyre P. Using linked birth, notification, hospital and mortality data to examine false-positive meningococcal disease reporting and adjust disease incidence estimates for children in New South Wales, Australia. Epidemiol Infect 2015; 143 2570–9.
| Using linked birth, notification, hospital and mortality data to examine false-positive meningococcal disease reporting and adjust disease incidence estimates for children in New South Wales, Australia.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2MvltFClsw%3D%3D&md5=a6cf57ca57f63cad02adeb4349e54d4eCAS | 25573266PubMed |
[3] Hall SE, Holman CDJ, Hendrie DV, Spilsbury K. Unequal access to breast-conserving surgery in Western Australia 1982–2000. ANZ J Surg 2004; 74 413–19.
| Unequal access to breast-conserving surgery in Western Australia 1982–2000.Crossref | GoogleScholarGoogle Scholar | 15191470PubMed |
[4] Clarke P, Leal J, Kelman C, Smith M, Colagiuri S.. Estimating the cost of complications of diabetes in Australia using administrative health-care data. Value Health 2008; 11 199–206.
| Estimating the cost of complications of diabetes in Australia using administrative health-care data.Crossref | GoogleScholarGoogle Scholar | 18380631PubMed |
[5] Katzenellenbogen JM, Vos T, Somerford P, Begg S, Semmens JB, Codde JP. Burden of stroke in Indigenous Western Australians: a study using data linkage. Stroke 2011; 42 1515–21.
| Burden of stroke in Indigenous Western Australians: a study using data linkage.Crossref | GoogleScholarGoogle Scholar | 21493909PubMed |
[6] Katzenellenbogen JM, Sanfilippo FM, Hobbs MS, Knuiman MW, Bessarab D, Durey A, Thompson SC. Voting with their feet – predictors of discharge against medical advice in Aboriginal and non-Aboriginal ischaemic heart disease inpatients in Western Australia: an analytic study using data linkage. BMC Health Serv Res 2013; 13 330
| Voting with their feet – predictors of discharge against medical advice in Aboriginal and non-Aboriginal ischaemic heart disease inpatients in Western Australia: an analytic study using data linkage.Crossref | GoogleScholarGoogle Scholar | 23962275PubMed |
[7] McCallum LK, Liu B, McIntyre P, Jorm LR. Estimating the burden of pertussis in young children on hospitals and emergency departments: a study using linked routinely collected data. Epidemiol Infect 2014; 142 695–705.
| Estimating the burden of pertussis in young children on hospitals and emergency departments: a study using linked routinely collected data.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3snjs1enug%3D%3D&md5=ce232a5f9a341cc134c9eabf74afb959CAS | 23672837PubMed |
[8] Wilson CL, Cohn RJ, Johnston KA, Ashton LJ. Late mortality and second cancers in an Australian cohort of childhood cancer survivors. Med J Aust 2010; 193 258–61.
| 20819041PubMed |
[9] Williams TA, Dobb GJ, Finn JC, Knuiman M, Lee KY, Geelhoed E, Webb SA. Data linkage enables evaluation of long-term survival after intensive care. Anaesth Intensive Care 2006; 34 307–15.
| 1:STN:280:DC%2BD28zos1antw%3D%3D&md5=36916978b13c296d24366a370764d5ecCAS | 16802482PubMed |
[10] Kinner SA, Degenhardt L, Coffey C, Hearps S, Spittal M, Sawyer SM, Patton GC. Substance use and risk of death in young offenders: a prospective data linkage study. Drug Alcohol Rev 2015; 34 46–50.
| Substance use and risk of death in young offenders: a prospective data linkage study.Crossref | GoogleScholarGoogle Scholar | 25066461PubMed |
[11] Rotermann M, Sanmartin C, Trudeau R, St-Jean H. Linking 2006 census and hospital data in Canada. Health Rep 2015; 26 10–20.
| 26488823PubMed |
[12] Hobbs MS, McCall MG. Health statistics and record linkage in Australia. J Chronic Dis 1970; 23 375–81.
| Health statistics and record linkage in Australia.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaE3M%2FnvFOlsQ%3D%3D&md5=4670459fd46277525eeea20f0aea63f3CAS | 5492967PubMed |
[13] Holman CD, Bass AJ, Rosman DL, Smith MB, Semmens JB, Glasson EJ, Brook EL, Trutwein B, Rouse IL, Watson CR, de Klerk NH, Stanley FJ. A decade of data linkage in Western Australia: strategic design, applications and benefits of the WA data linkage system. Aust Health Rev 2008; 32 766–77.
| A decade of data linkage in Western Australia: strategic design, applications and benefits of the WA data linkage system.Crossref | GoogleScholarGoogle Scholar | 18980573PubMed |
[14] Banks E, Redman S, Jorm L, Armstrong B, Bauman A, Beard J, Beral V, Byles J, Corbett S, Cumming R, Harris M, Sitas F, Smith W, Taylor L, Wutzke S, Lujic S. Cohort profile: the 45 and Up Study. Int J Epidemiol 2008; 37 941–7.
| Cohort profile: the 45 and Up Study.Crossref | GoogleScholarGoogle Scholar | 17881411PubMed |
[15] Jorm L, Walter S, Lujic S, Mealing N, Byles J, Kendig H. The 45 and Up Study: exploring the health of home and community care clients in New South Wales. Sydney: Operational Performance Directorate Ageing, Disability and Home Care Department of Family and Community Services NSW; 2012.
[16] Population Health Research Network. Annual report 2013–14. Perth: Population Health Research Network Program Office; 2015. Available at: http://www.phrn.org.au/media/80709/annual-report-2013-2014_final.pdf [verified 1 February 2016].
[17] Roder DM, Fong KM, Brown MP, Zalcberg J, Wainwright CE. Realising opportunities for evidence-based cancer service delivery and research: linking cancer registry and administrative data in Australia. Eur J Cancer Care (Engl) 2014; 23 721–7.
| Realising opportunities for evidence-based cancer service delivery and research: linking cancer registry and administrative data in Australia.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2M7jsVGgtg%3D%3D&md5=425d3ecb1b3ac18b37e6a2e82bc3ef2eCAS |
[18] Olver IN. Linking data to improve health outcomes. Med J Aust 2014; 200 368–9.
| Linking data to improve health outcomes.Crossref | GoogleScholarGoogle Scholar | 24794653PubMed |
[19] Kelman CW, Bass AJ, Holman CDJ. Research use of linked health data: a best practice protocol. Aust N Z J Public Health 2002; 26 251–5.
| Research use of linked health data: a best practice protocol.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD38zpt1Oitg%3D%3D&md5=0902bd682de4e7fcae9eadb484f0f30aCAS | 12141621PubMed |
[20] Glasson EJ, Hussain R. Linked data: opportunities and challenges in disability research. J Intellect Dev Disabil 2008; 33 285–91.
| Linked data: opportunities and challenges in disability research.Crossref | GoogleScholarGoogle Scholar | 19039688PubMed |
[21] Mitchell RJ, Cameron CM, Bambach MR. Data linkage for injury surveillance and research in Australia: perils, pitfalls and potential. Aust N Z J Public Health 2014; 38 275–80.
| Data linkage for injury surveillance and research in Australia: perils, pitfalls and potential.Crossref | GoogleScholarGoogle Scholar | 24890486PubMed |
[22] Whop LJ, Cunningham J, Condon JR. How well is the National Cervical Screening Program performing for Indigenous Australian women? Why we don’t really know, and what we can and should do about it. Eur J Cancer Care (Engl) 2014; 23 716–20.
| How well is the National Cervical Screening Program performing for Indigenous Australian women? Why we don’t really know, and what we can and should do about it.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2M7jtVCltQ%3D%3D&md5=b04590a0d06fa87221cff86019f63cceCAS |
[23] Mitchell RJ, Cameron CM, McClure RJ, Williamson AM. Data linkage capabilities in Australia: practical issues identified by a Population Health Research Network ‘proof of concept project’. Aust N Z J Public Health 2015; 39 319–25.
| Data linkage capabilities in Australia: practical issues identified by a Population Health Research Network ‘proof of concept project’.Crossref | GoogleScholarGoogle Scholar | 25716143PubMed |
[24] Xafis V, Thomson C, Braunack-Mayer AJ, Duszynski KM, Gold MS. Legal impediments to data linkage. J Law Med 2011; 19 300–15.
| 1:STN:280:DC%2BC383hvF2gtA%3D%3D&md5=06e897c35c77c6b02997146dc58e5aafCAS | 22320005PubMed |
[25] Nadathur SG. Maximising the value of hospital administrative datasets. Aust Health Rev 2010; 34 216–23.
| Maximising the value of hospital administrative datasets.Crossref | GoogleScholarGoogle Scholar | 20497736PubMed |
[26] Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 2009; 151 264–9.
| Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement.Crossref | GoogleScholarGoogle Scholar | 19622511PubMed |
[27] Population Health Research Network. Annual review 2011/2012. Perth: Population Health Research Network Program Office; 2013. Available at: http://www.phrn.org.au/media/80633/annual-report-2011v10.pdf [verified 1 February 2016].
[28] Population Health Research Network. Annual review 2012/2013. 2014. Available at: http://www.phrn.org.au/media/80631/annual-report-201213v2.pdf [verified 1 February 2016].
[29] Davies SB, Hofer A, Reeve C. Mortality attributable to rheumatic heart disease in the Kimberley: a data linkage approach. Intern Med J 2014; 44 1074–80.
| Mortality attributable to rheumatic heart disease in the Kimberley: a data linkage approach.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2cbmsleqtA%3D%3D&md5=fc8c5adc47dcde11c2517085001d3461CAS | 25070793PubMed |
[30] Sundararajan V, Thrift AG, Phan TG, Choi PM, Clissold B, Srikanth VK. Trends over time in the risk of stroke after an incident transient ischemic attack. Stroke 2014; 45 3214–18.
| Trends over time in the risk of stroke after an incident transient ischemic attack.Crossref | GoogleScholarGoogle Scholar | 25256181PubMed |
[31] Moore HC, de Klerk N, Keil AD, Smith DW, Blyth CC, Richmond P, Lehmann D. Use of data linkage to investigate the aetiology of acute lower respiratory infection hospitalisations in children. J Paediatr Child Health 2012; 48 520–8.
| Use of data linkage to investigate the aetiology of acute lower respiratory infection hospitalisations in children.Crossref | GoogleScholarGoogle Scholar | 22077532PubMed |
[32] Howell SC, Wills RA, Johnston TC. Should diagnosis codes from emergency department data be used for case selection for emergency department key performance indicators? Aust Health Rev 2014; 38 38–43.
| Should diagnosis codes from emergency department data be used for case selection for emergency department key performance indicators?Crossref | GoogleScholarGoogle Scholar | 24308873PubMed |
[33] Mai Q, Holman CDAJ, Sanfilippo FM, Emery JD, Stewart LM. Do users of mental health services lack access to general practitioner services? Med J Aust 2010; 192 501–6.
| 20438420PubMed |
[34] Havard A, Jorm LR, Lujic S. Risk adjustment for smoking identified through tobacco use diagnoses in hospital data: a validation study. PLoS One 2014; 9 e95029
| Risk adjustment for smoking identified through tobacco use diagnoses in hospital data: a validation study.Crossref | GoogleScholarGoogle Scholar | 24736621PubMed |
[35] Lee YYC, Roberts CL, Jane Y, Dobbins T. Using hospital discharge data to identify incident pregnancy-associated cancers: a validation study. BMC Pregnancy Childbirth 2013; 13 37
| Using hospital discharge data to identify incident pregnancy-associated cancers: a validation study.Crossref | GoogleScholarGoogle Scholar |
[36] Chamberlain C, Fredericks B, McLean A, Davis B, Eades S, Stewart K, Reid CM. Gestational diabetes mellitus in far north Queensland, Australia, 2004 to 2010: midwives’ perinatal data most accurate source. Aust N Z J Public Health 2013; 37 556–61.
| Gestational diabetes mellitus in far north Queensland, Australia, 2004 to 2010: midwives’ perinatal data most accurate source.Crossref | GoogleScholarGoogle Scholar | 24892154PubMed |
[37] Australian Bureau of Statistics (ABS). NSW perinatal data collection (PDC). Canberra: ABS; 2011. Available at: http://www.abs.gov.au/ausstats/abs@.nsf/7d12b0f6763c78caca257061001cc588/43487e1fe03beaaeca25732c00192874!OpenDocument [verified 1 February 2016].
[38] Leigh A, Neill C. Do gun buybacks save lives? Evidence from panel data. Am Law Econ Rev 2010; 12 509–57.
| Do gun buybacks save lives? Evidence from panel data.Crossref | GoogleScholarGoogle Scholar |
[39] McKeon R, Alexander E, Brodaty H, Ferris B, Frazer I, Little M. Strategic review of health and medical research in Australia: better health through research. 2013. Available at: http://www.mckeonreview.org.au/downloads/Strategic_Review_of_Health_and_Medical_Research_Feb_2013-Final_Report.pdf [verified 1 February 2016].
[40] Victorian Auditor-General. Access to public sector information. 2015. Available at: http://www.audit.vic.gov.au/publications/20151210-Public-Sector-Info/20151210-Public-Sector-Info.pdf [verified 28 January 2016].
[41] Australian Government. Australian public service big data strategy. 2013. Available at: https://www.finance.gov.au/sites/default/files/Big-Data-Strategy.pdf [verified 1 February 2016].


