Collaborative arrangements and privately practising nurse practitioners in Australia: results from a national survey
Jane Currie A B , Mary Chiarella A and Thomas Buckley AA Sydney Nursing School, University of Sydney, 88 Mallett Street, Camperdown, NSW 2050, Australia. Email: mary.chiarella@sydney.edu.au; tom.buckley@sydney.edu.au
B Corresponding author. Email: jane.currie@sydney.edu.au
Australian Health Review 41(5) 533-540 https://doi.org/10.1071/AH16051
Submitted: 24 February 2016 Accepted: 26 July 2016 Published: 9 September 2016
Journal Compilation © AHHA 2017 Open Access CC BY-NC-ND
Abstract
Objective Since the introduction of legislative changes in 2010, services provided by privately practising nurse practitioners (PPNPs) in Australia have been eligible for subsidisation through the Medicare Benefits Schedule (MBS) and Pharmaceutical Benefits Scheme (PBS). To provide eligible services, PPNPs must collaborate formally with a medical practitioner or an entity that employs medical practitioners. This paper provides data from a national survey on these collaborative arrangements in Australia. The aim of the study was to evaluate the impact of PPNP services on patient access to care in Australia.
Methods PPNPs in Australia were invited to complete an electronic survey. Quantitative data were analysed using descriptive statistics, whereas qualitative data were analysed using thematic analysis. Seventy-three surveys were completed.
Results Ninety-three per cent of participants reported having a collaborative arrangement in place. Frequency of communication ranged from daily (27%) to never (1%). Participants reported that collaborative arrangements facilitate learning, patient care and offer support to PPNPs. However, for some PPNPs, organising a formal collaborative arrangement is demanding because it is dependent on the availability and willingness of medical practitioners and the open interpretation of the arrangement. Only 19% of participants believed that collaborative arrangements should be a prerequisite for PPNPs to access the MBS and PBS.
Conclusion Although there are benefits to collaborative arrangements, there is also concern from PPNPs that mandating such arrangements through legislation presents a barrier to establishing PPNP services and potentially reduces patient access to care. Collaboration with medical practitioners is intrinsic to nursing practice. Thus, legislating for collaborative arrangements is unnecessary, because it makes the normal abnormal.
What is known about the topic? To access the MBS and PBS, PPNPs are required by law to have a collaborative arrangement with a medical practitioner or entity that employs medical practitioners. To date, the effects of these collaborative arrangements on PPNP services in Australia have not been known.
What does the paper add? This paper provides unique data from a national survey on collaborative arrangements between PPNPs and medical practitioners in Australia.
What are the implications for practitioners? Although there are benefits to collaborative arrangements, there is also concern that mandating such arrangements presents a barrier to establishing PPNP services and potentially reduces patient access to care.
Additional keywords: primary health care, nurse-led clinics.
Introduction
Since the introduction of legislative changes in 2010, services provided by privately practising nurse practitioners (PPNPs) in Australia have been eligible for subsidisation through the Medicare Benefits Schedule (MBS) and the Pharmaceutical Benefits Scheme (PBS). As a condition of their access to the MBS and PBS, each PPNP must establish a collaborative arrangement with a medical practitioner or an entity that employs medical practitioners. This paper examines these mandated collaborative arrangements between PPNPs and medical practitioners in Australia.
Collaboration between health professionals is fundamental to health care delivery both in Australia and internationally. Yet, for Australian PPNPs to provide services subsidised through the MBS or prescribe medications subsidised by the PBS, they must fulfil legislative requirements to collaborate with a medical practitioner. To date, the effects of these collaborative arrangements on PPNP services have not been known. This paper forms part of an evaluation of PPNP services in Australia.1,2 The data presented here address the collaborative arrangements of PPNP services in Australia.
Collaborative arrangements
The development of PPNP services in Australia has been relatively slow compared with the US or UK. Lack of access to the MBS and PBS for nurse practitioners (NPs) has been a significant barrier to the development of NPs in primary care settings in Australia.3 The National Health and Hospitals Reform Commission4 reported that the Australian healthcare system was under increasing pressure and acknowledged issues of equity of access to health care, particularly primary care. Australian nursing leaders continued to lobby for access for NPs to the MBS and PBS.5 The collaborative arrangement requirement was accepted to reduce Australian Medical Association (AMA) opposition to PPNP access.5 The primary concern of the AMA was reported to be that PPNP access may cause medical practitioners to be ‘…left out of the loop’.6
The Health Legislation Amendment (Midwives and Nurse Practitioners) Act 2010 (Cth) allowed NP services to be subsidised through the MBS, including certain diagnostic imaging and pathology, and NPs to prescribe certain medicines under the PBS. For PPNPs to be eligible providers within the MBS and PBS, they must have a Medicare provider number and/or a PBS prescriber number, be working in private practice, have professional indemnity insurance and have a collaborative arrangement in place.7,8 Subsidised medicine prescription is restricted to an approved list and guided by a NP’s scope of practice, and sometimes further controlled and limited by state or territory prescribing legislation.
A collaborative arrangement is an arrangement between an eligible NP and a specified medical practitioner that must provide for consultation, referral and transfer of care as clinically relevant.7,8 Collaborative arrangements can be demonstrated by being employed or engaged by a medical practitioner or an entity that employs medical practitioners, receiving patients on written referral from medical practitioners, a signed written agreement with a specified medical practitioner or an arrangement in the NP’s written records.7,8
The obligation for PPNPs to have collaborative arrangements has created significant discussion.3,5,9,10 Opponents argue that collaboration is innate to nursing practice, thus NPs naturally collaborate with a range of health professionals, including medical practitioners.9 Furthermore, mandating collaboration as a prerequisite to access presents impediments to NPs establishing themselves in private practice. PPNPs are marginalised because power and control over PPNP services reside in the hands of a medical practitioner (who may not welcome additional services).3,10
In Australia, none of the other health professionals that have access to MBS and PBS provider numbers, including physiotherapists and psychologists, are required by law to establish collaborative arrangements.3 The only exceptions are some specified PBS items (Section 100 Highly Specialised Drugs Program),11 whereby medical practitioners are mandated to collaborate with certain medical specialists in order to prescribe these medications.
Methods
Design
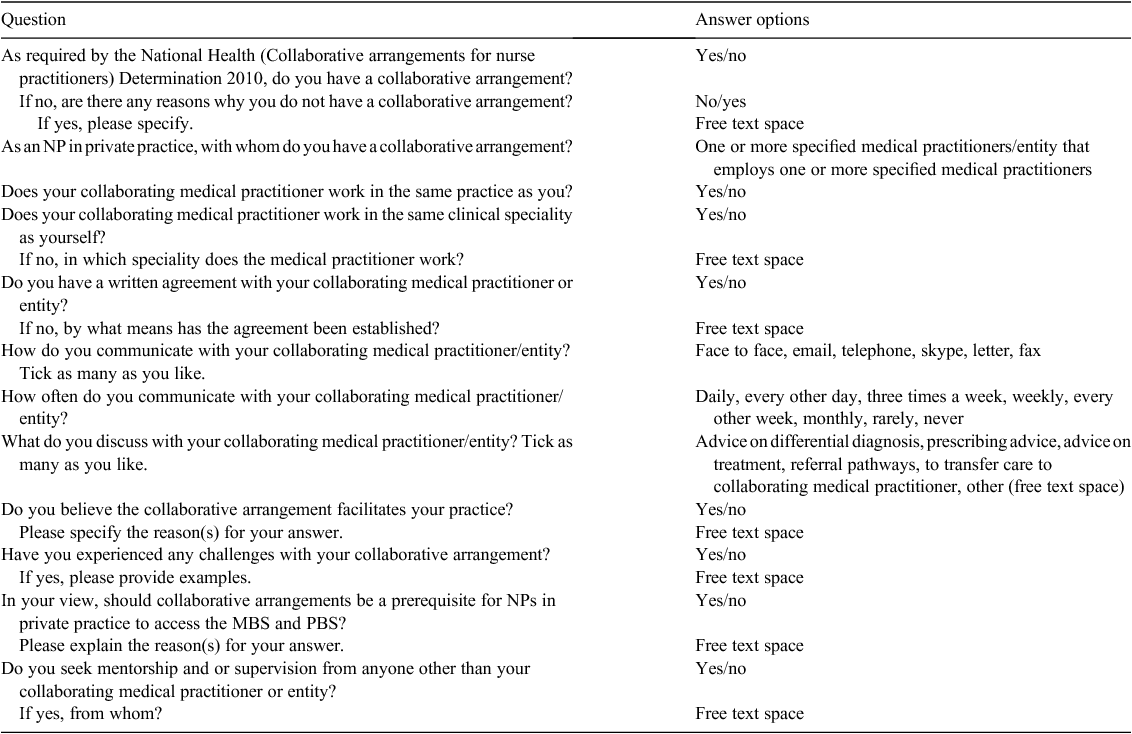
An electronic survey was designed to evaluate the impact of PPNP services in Australia on patient access to care. The survey questions were informed by current literature and focused on the following aspects of PPNP practice: workforce characteristics,2 collaborative arrangements, access to MBS and PBS and practice activities.12 Participants responded to 13 questions related to collaborative arrangements, nine focused on eliciting quantitative responses and four focused on eliciting qualitative responses (Table 1). To confirm the clarity of the survey, a pilot study was conducted (n = 6) and several minor amendments were made to the survey questions before administration of the national survey.
|
Realist evaluation (RE) provides the overarching theoretical framework of the present evaluation of PPNPs.1 RE is a theory-driven form of evaluation that places emphasis on the context in which the subject of the study operates and on the mechanisms (decision and reasoning processes) through which outcomes are produced. REs are iterative in the collection of data and in the development and refinement of theories that articulate why something works, how it works, for whom it works and under which circumstances it works.13 The stages of the present RE of PPNPs in Australia are: (1) literature review (conducted in 2014); (2) national survey (disseminated in 2015); and (3) interviews with PPNPs and their collaborating medical practitioners ( being conducted in 2016). After each stage of data collection, theories are refined and further developed. The findings of the present RE cannot be fully reported until completion of each stage of the RE data collection cycle. Therefore, this paper reports only the findings of the national survey, with a focus on collaborative arrangements.
Study participants
Eligible participants included NPs currently working in private practice in Australia and those who had previously worked in private practice. To recruit participants, the authors requested key organisations, including the Australian College of Nurse Practitioners, Australian College of Nursing and the Australian Practice Nurse Association, and the Chief Nursing and Midwifery Officers of each state and territory to disseminate an email invitation to endorsed NPs or to advertise a flyer on their website.
Data collection and analysis
Data were collected using an electronic questionnaire on the SurveyMonkey platform over 6 weeks between February and March 2015. In all, 76 PPNPs responded to and commenced the survey, and 73 provided complete data for analysis; three surveys answered no questions other than demographics. Quantitative data were imported into SPSS version 22.0 (SPSS Inc.) for analysis using descriptive statistics and the Chi-squared test. A thematic analysis was undertaken of the qualitative data by one of the authors (JC). The process of extracting themes was reviewed by all authors and unanimous agreement reached on the interpretation of these themes. The themes were developed inductively to provide as accurate a reflection of the data as possible.14
Ethics
The study was approved by the University of Sydney Ethics Committee (2014/696). All participants were provided with written information about the study upon invitation to participate, and all provided informed consent before partaking in the study.
Results
Ninety-three per cent of participants (n = 68) stated that they had a collaborative arrangement in place (four did not provide an answer to this question and one reported that private practice did not involve access to the MBS or PBS). Sixty-two per cent (n = 45) reported that they collaborated with one or more specified medical practitioners and 30% (n = 22) collaborated with an entity that employed or engaged one or more specified medical practitioners (six did not provide an answer to this question).
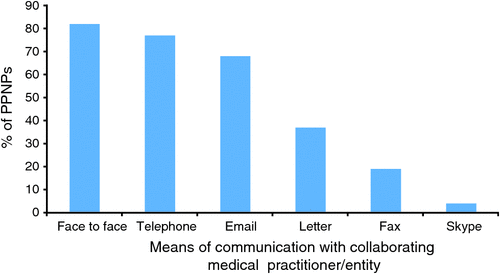
Sixty per cent of participants (n = 44) had a written collaborative agreement. Frequency of communication ranged from daily (27%) to never (1%), and 9% communicated up to three times each week, 25% communicated weekly and 18% communicated monthly. Means of communication are shown in Fig. 1.
|
Forty-five participants responded to the question whether their collaborator worked in the same speciality and practice as themselves. Of these 45, just under half (n = 22) stated they worked in the same practice setting. In addition, 66.7% of these 45 participants (n = 30) stated they worked in the same clinical speciality as their collaborating medical practitioner. Further analysis of these 45 participants suggested a relationship between working in the same practice and speciality and the frequency of communication. Twenty-one of these 45 participants who worked in the same speciality were more likely to communicate at least weekly, whereas only six of those not working in the same speciality communicated at least weekly (χ2 P = 0.053). Similarly, 18 participants who worked in the same practice as their collaborating medical practitioner communicated at least weekly, compared with nine participants who had not worked in the same practice and communicated at least weekly (χ2 P = 0.003).
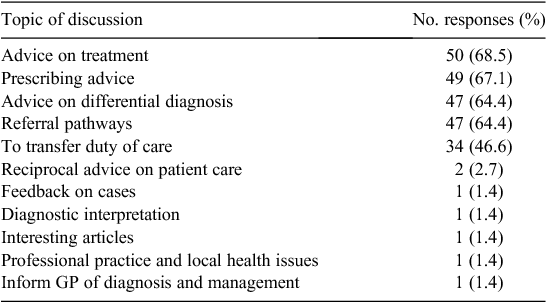
Participants were asked to identify the topics they discussed with their collaborating medical practitioners, and these are presented in Table 2.
|
One respondent identified the reciprocal nature of their collaborative arrangement:
I advised them on management plans…[General practitioners] and medical specialists send patients to me, it is a two way relationship. (Participant 27)
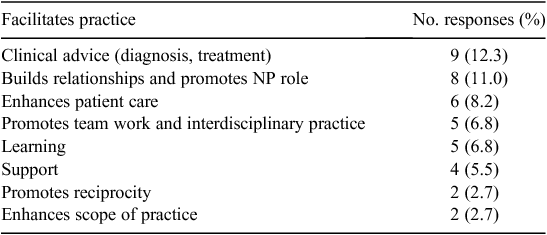
Two-thirds of participants (n = 48) believed that the collaborative arrangement facilitated their practice. Their reasons were varied (Table 3). One participant identified that their collaborative arrangement enhanced patient care as a:
|
…method to circumvent the restrictions placed on my prescribing of medications and ordering of investigations etc. or to prevent patients from being unreasonably out of pocket. (Participant 61)
Twenty-five per cent (n = 18) of participants reported challenges with their collaborative arrangement; analysis of these data revealed six themes: understanding of collaborative arrangements; understanding of PPNP role; resistance; accessibility; reciprocation; and difference in clinical opinion. Examples of these themes are presented in Table 4. A comparative analysis was undertaken of participants who believed collaborative arrangements facilitated their practice and the time these participants had been endorsed as a NP. Further analysis revealed no significant relationship between time endorsed as a NP and participants’ perceptions about whether collaborative arrangements facilitated practice.

|
Critical to the success of collaborative arrangements appeared to be the medical practitioner’s level of understanding of the NP’s role and of the pertinent legislation. One participant stated that her collaborating medical practitioner understood the NP’s role:
I am lucky and have an agreement with a medical practitioner who was a nurse and paramedic. He allows me to practise at [the] highest level of practice I can. (Participant 71)
In circumstances where medical practitioners did not fully understand the legislation, the collaborative arrangements were open to interpretation, especially that they may be supervisory:
It gives the medical practitioners and the others the impression we need supervision and that they might be responsible for our decisions. We would collaborate without it. (Participant 27)
One GP said I will not collaborate with you because the AMA told me nurse practitioners are a danger to clients. (Participant 29)
As an independent clinician in the hospital setting I can work as an independent practitioner. In the private setting, I have constraints and restrictions that reduce my capacity to practise. (Participant 1)
There was also a sense that collaborative arrangements were perceived as a way for medicine to control nursing:
There is a need to separate the financial and clinical connection in collaborative arrangements or NPs will continue [to] be subject to unfair power imbalances brought on by medical associations/medical practitioners. (Participant 81)
There is absolutely no reason to have enforced collaborative arrangements, it is a misconception that they somehow keep [a] NP under medical supervision. (Participant 61)
Participants also perceived collaborative arrangements as insulting:
It is in my nature to collaborate. I wouldn’t operate otherwise and it’s insulting to be ‘mandated’ to do so when pharmacists are in Queensland providing health assessments and vaccinations without any collaborative arrangements. (Participant 7)
I maintain it purely because the law says I must. However, my supervising psychiatrist and I both agree that it is quite a ridiculous legislative requirement. (Participant 3)
Working in the same speciality as the collaborating medical practitioner was identified as being important:
In many cases if you work with supporting doctors in the same field as you it could be excellent but that is not always the case. In some cases there is more benefit in peer support in your specialty area. (Participant 19)
…nurse practitioners in some areas do not have access to well-informed doctors that understand their specialty… (Participant 49)
Nineteen per cent (n = 14) of participants believed that collaborative arrangements should be a prerequisite for PPNPs to access the MBS and PBS. Among the participants who supported the collaborative arrangement legislation, four believed collaboration to be necessary when working in a healthcare team. Of the 74% (n = 54) participants who identified that collaborative arrangements should not be a prerequisite to access to MBS and PBS, 19 stated that it is unnecessary because collaboration is already an accepted norm of PPNPs practice. Comments from one participant identify that it can be extremely difficult to establish a collaborative arrangement:
If [a] NP is working in a one-doctor town and there is a fall out, then the NP may not be able to continue working in that role. No other allied health provider, i.e. dietitians, mental health workers, psychologist, physios, are subject to a collaborative arrangement. (Participant 81)
Two-thirds (n = 48) of participants reported receiving mentorship and/or supervision from a person other than their collaborating medical practitioner (Table 5).

|
Discussion
This paper presents the results of a national survey of PPNPs, with a specific focus on collaborative arrangements with medical practitioners. The data in this study are unique and the first from Australia to report the benefits of and barriers to collaborative arrangements. They also go some way to suggest circumstances that facilitate and/or impede collaboration between PPNPs and medical practitioners. Below we discuss the themes arising from the data in relation to the benefits, barriers and facilitation of collaboration and the impact of collaborative arrangements on patient access to care.
Benefits of collaboration
Although almost two-thirds of the 73 participants believed collaboration facilitates practice, only 19.2% (n = 14) believed the arrangements should be mandated for PPNP access to the MBS and PBS. The benefits of collaboration are not new: participants in the present study reported support, learning, enhancing patient care, building relationships and promoting the NP’s role. International research reports that collaboration reduces patient waiting times, improves prescribing processes, reduces treatment periods and reduces the cost of care delivery.15–17 Australian research also reports on the benefits of collaboration for NPs working in public practice as enablers to the implementation of NP roles.18,19 It has been reported that NPs working in public practice seek out collaborative professional relationships, despite not being mandated through legislation to do so.19 The reason collaborative arrangements have received attention in relation to PPNP services in Australia is because here collaboration is mandated for PPNPs through legislation, but it is a one-way street. A PPNP cannot get access to the MBS without a collaborative agreement, but there is no mandate for a medical practitioner to collaborate with a PPNP who may identify the need for a service in order to facilitate the establishment of improved patient access.
Barriers to collaboration
Participants in the present study similarly identified medical practitioners’ level of understanding of the NP role and of the collaborative arrangement itself as a challenge. Some medical practitioners perceive collaboration as a form of supervision with concomitant legal responsibility for care delivery rather than a reciprocal working relationship. Such an interpretation has the potential to limit PPNPs’ scope of practice. The barriers medical practitioners historically erected to the establishment of NPs, in both private and public practice, are well documented in the international literature.20–22 Notwithstanding this opposition, the need for NPs was recognised by many enlightened medical practitioners, and NP roles are now widely established in the public sector. The clarity of NP roles and scope of practice were the most frequently identified barriers and facilitators to collaborative practice reported in a recent integrative review of NP collaborative practice in primary care in the US, Canada, UK, the Netherlands, Sweden, Ireland and New Zealand.23
Difficulty in receiving patient data, such as results or current medication prescribing and notification of discharge, are practical challenges of collaborative arrangements identified by the present study. In hospital services, general practitioners are still documented as patients’ primary practitioners, even when this may not be correct.
The availability and accessibility of medical practitioners with whom to collaborate remains a challenge for some PPNPs, for example in rural and remote locations. Under such circumstances, a NP may forge a collaborative arrangement with a medical practitioner in another geographical area but, if this is not possible, the mandate for the collaborative arrangement may preclude the establishment of a PPNP service, thereby reducing patient access to care. Part of the impetus for establishing NP roles in Australia was to increase patient access to care specifically in rural and remote settings, and the collaborative arrangement legislation presents a potential barrier to this. In the present study, 28 (38.4%) of the PPNPs worked in rural and remote settings, compared with 35 (47.9%) and 31 (42.5%) who work in suburban and metropolitan settings respectively.2 Although the number of PPNPs working in rural and remote settings shows potential for further development, the collaborative arrangement legislation poses a potential barrier.
Difficulty recruiting a medical practitioner to collaborate with and resistance to referrals is problematic for some PPNPs. Even though NP services have been in existence for more than 50 years in the US and 15 years in Australia, medical practitioner acceptance of NP services continues to be a matter of personality, not policy.24,25 Medical practitioners’ available time for collaboration may also be an impediment for some PPNPs. There is evidence that collaborating with a NP may increase a medical practitioner’s workload as a consequence of consultation with, and ‘supervision of’, a NP.21,26 This concern may be a deterrent to medical practitioners who would otherwise be prepared to collaborate.
The findings of the present study also suggest that there may be circumstances under which PPNPs and medical practitioners may not concur with regard to optimal treatment for patients. PPNPs are usually highly specialised in a specific area of practice;2 the medical practitioner may override the PPNP’s treatment plan, even though the medical practitioner may be the generalist and the NP the specialist.
Facilitation of collaboration
Working closely and belonging to the same clinical speciality appear to facilitate collaboration. The participants in the present study communicated far more frequently with their medical counterparts if they worked at the same location and/or were in the same speciality. A period of 3–6 months has been identified as a sufficient period to build trust and understanding between a NP and collaborating medical practitioner working in the same practice and speciality.20 The geography of some Australian-based PPNP services means that the NPs work alone and may not have the opportunity to work at the same practice, which may affect the relationship.
Impact of collaborative arrangements on patient access to care
The main intent of enabling PPNPs to have access to the MBS and PBS was to increase patient access to care by fostering greater flexibility of the healthcare workforce. The data in the present study go some way to suggesting that mandating collaborative arrangements affects patients’ access to PPNP services, primarily as a result of the practical challenges of establishing and maintaining the arrangement. There is abundant evidence that NPs provide care that is of an equal quality to that of medical practitioners.27–29 Collaboration is already an intrinsic component of registered nurse standards for practice.30 Therefore, mandating collaborative arrangements seems both superfluous and potentially counter-productive to the establishment of much needed community and primary care services.
There is opposition to the collaborative arrangement legislation from key Australian nursing groups.10 Opponents identify that there is no evidence base to support the introduction of collaborative arrangements.11 There is also no evidence that collaborative arrangements are being evaluated through government in terms of their impact or quality. When completing the application form for a provider or prescriber number, practitioners are not even asked whether they have a collaborative arrangement. The main concerns regarding collaborative arrangements are that they may be restrictive and may affect patient access to care.3,10
Conclusion
Although there are clear benefits to interprofessional collaboration, there is concern that mandating collaborative arrangements through legislation creates a barrier to establishing PPNP services and thereby potentially reduces patient access to care. The aim of NP eligibility for the MBS and PBS was to facilitate equity of access to health care for patients, particularly in primary care. The condition of collaborative arrangements appears to run counter to this aim because, for some, they restrict the ability of PPNPs to establish themselves in private practice. The success of a collaborative arrangement is not guaranteed and is underpinned by many variables, such as the medical practitioner’s understanding of the NP role and collaborative relationship, and their availability and willingness to collaborate. These variables present multiple impediments to PPNPs’ clinical practice and therefore patient access to care. Based on these findings, and the fact that there is no evidence that mandating collaboration is required for patient safety, the collaborative arrangement requirement needs to be reviewed to enable PPNPs to reach their full potential to affect patient access to care.
Competing interests
None declared.
Acknowledgement
The authors thank the Australian College of Nursing, Australian College of Nurse Practitioners, Australian Practice Nurse Association and the Offices of the Chief Nurse and Midwife for their assistance in the dissemination and advertisement of this survey.
References
[1] Currie J, Chiarella M, Buckley T. Preparing a realist evaluation to investigate the impact of privately practising nurse practitioner services on patient access to care in Australia. Int J Nurs 2015; 2 1–10.[2] Currie J, Chiarella M, Buckley T. Workforce characteristics of privately practising nurse practitioners in Australia. Results of a national survey. J Am Acad Nurs Pract 2016,;
| Workforce characteristics of privately practising nurse practitioners in Australia. Results of a national survey.Crossref | GoogleScholarGoogle Scholar |
[3] Harvey C. Legislative hegemony and nurse practitioner practice in rural and remote Australia. Health Sociol Rev 2011; 20 269–80.
| Legislative hegemony and nurse practitioner practice in rural and remote Australia.Crossref | GoogleScholarGoogle Scholar |
[4] National Health and Hospitals Reform Commission. A healthier future for all Australians, final report June 2009. 2009. Available at: http://www.health.gov.au/internet/nhhrc/publishing.nsf/content/nhhrc-report [verified 12 January 2016].
[5] Cashin A. Collaborative arrangements for Australian nurse practitioners: a policy analysis. J Am Acad Nurs Pract 2014; 26 550–4.
[6] Australian Medical Association. Collaborative arrangements: what you need to know. 2010. Available at: https://ama.com.au/sites/default/files/documents/Collaborative_Arrangements_What_you_need_to_know.pdf [verified 22 December 2015].
[7] Department of Health Australia. Collaborative arrangements for participating midwives and nurse practitioners. 2012. Available at: http://www.health.gov.au/internet/main/publishing.nsf/Content/midwives-nurse-pract-collaborative-arrangements [verified 1 December 2015].
[8] Australian Government. National health (collaborative arrangements for nurse practitioners). Determination (Cth). 2010. Available at: http://www.comlaw.gov.au [verified 1 December 2015].
[9] Carrigan C. Collaborative arrangements: are expanded roles for nurses and midwives being stifled? Aust Nurs J 2010; 18 24–7.
[10] Carter M, Owen-Williams E, Della P. Meeting Australia’s emerging primary care needs by nurse practitioners. J Nurse Pract 2015; 11 647–52.
| Meeting Australia’s emerging primary care needs by nurse practitioners.Crossref | GoogleScholarGoogle Scholar |
[11] Australian Government Department of Health. Pharmaceutical Benefits Scheme. Section 100 highly specialised drugs program. Available from: http://www.pbs.gov.au/info/browse/section-100/s100-highly-specialised-drugs [verified 15 January 2016].
[12] Currie J, Chiarella M, Buckley T. An investigation of the international literature on nurse practitioner private practice models. Int Nurs Rev 2013; 60 435–47.
| An investigation of the international literature on nurse practitioner private practice models.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2c%2FltFGjsg%3D%3D&md5=bf9c0dd67db24bc7a5bb99290258c7d7CAS | 24131230PubMed |
[13] Pawson R, Tilley N. Realistic evaluation. London: Sage; 1997.
[14] Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol 2006; 3 77–101.
| Using thematic analysis in psychology.Crossref | GoogleScholarGoogle Scholar |
[15] McCaffrey R, Hayes R, Stuart W, Cassell A, Farell C, Miller-Reyes C. Program to improve communication and collaboration between nurses and medical residents. J Contin Educ Nurs 2010; 41 172–8.
| Program to improve communication and collaboration between nurses and medical residents.Crossref | GoogleScholarGoogle Scholar | 20411889PubMed |
[16] Zwarenstein M, Goldman J, Reeves S, Interprofessional collaboration Effects of practice-based interventions on professional practice and healthcare outcomes. Cochrane Database Syst Rev 2009; 3 CD000072
| Effects of practice-based interventions on professional practice and healthcare outcomes.Crossref | GoogleScholarGoogle Scholar | 19588316PubMed |
[17] Cowan M, Shapiro M, Hays R, Abdelmonem A, Vazirani S, Ward C, Ettner S. The effect of a multidisciplinary hospitalist/physician and advanced practice nurse collaboration on hospital costs. J Nurs Admin 2006; 36 79–85.
| The effect of a multidisciplinary hospitalist/physician and advanced practice nurse collaboration on hospital costs.Crossref | GoogleScholarGoogle Scholar |
[18] Desborough J, Parker R, Forrest L. Nurse satisfaction with working in a nurse led primary care walk-in centre: an Australian experience. Aust J Adv Nurs 2013; 31 11–19.
[19] Desborough J. How nurse practitioners implement their roles. Aust Health Rev 2012; 36 22–6.
| How nurse practitioners implement their roles.Crossref | GoogleScholarGoogle Scholar | 22513015PubMed |
[20] Legault F, Humbert J, Amos S, Hogg W, Ward N, Dabrouge S, Ziebell L. Difficulties encountered in collaborative care: logistics trumps desire. J Am Board Fam Med 2012; 25 168–76.
| Difficulties encountered in collaborative care: logistics trumps desire.Crossref | GoogleScholarGoogle Scholar | 22403197PubMed |
[21] Main R, Dunn N, Kendall K. Crossing professional boundaries: barriers to the integration of nurse practitioners in primary care. Educ Prim Care 2007; 18 480–7.
| Crossing professional boundaries: barriers to the integration of nurse practitioners in primary care.Crossref | GoogleScholarGoogle Scholar |
[22] Bailey P, Jones L, Way D. Family physician/nurse practitioner: stories of collaboration. J Adv Nurs 2006; 53 381–91.
| Family physician/nurse practitioner: stories of collaboration.Crossref | GoogleScholarGoogle Scholar | 16448481PubMed |
[23] Schadewaldt V, McInnes E, Hiller J, Gardner A. Investigating characteristics of collaboration between nurse practitioners and medical practitioners in primary healthcare: a mixed methods multiple case study protocol. J Adv Nurs 2014; 70 1184–93.
| Investigating characteristics of collaboration between nurse practitioners and medical practitioners in primary healthcare: a mixed methods multiple case study protocol.Crossref | GoogleScholarGoogle Scholar | 24138114PubMed |
[24] MacLellan L, Higgins I, Kevtt-Jones T. Medical acceptance of the nurse practitioner role in Australia: a decade on. J Am Acad Nurs Pract 2015; 27 152–9.
[25] DeGuzman A, Ciliska D, DiCenso A. Nurse practitioner role implementation in Ontario public health units. Canad J Pub Hlth 2010; 101 309–13.
[26] Fletcher C, Baker S, Copeland L, Reeves P, Lowery J. Nurse practitioners’ and physicians’ views of NPs as providers of primary care to veterans. J Nurs Schol 2007; 39 358–62.
| Nurse practitioners’ and physicians’ views of NPs as providers of primary care to veterans.Crossref | GoogleScholarGoogle Scholar |
[27] Stantik-Hutt J, Newhouse R, White M, Johantgen M, Bass E, Zangaro G, Wilson R, Fountain L, Steinwachs DM, Heindel L, Weiner JP. The quality and effectiveness of care provided by nurse practitioners. J Nurse Pract 2013; 9 492–500.
| The quality and effectiveness of care provided by nurse practitioners.Crossref | GoogleScholarGoogle Scholar |
[28] Dinh M, Walker A, Parameswaran A, Enright N. Evaluating the quality of care delivered by an emergency department fast track unit with both nurse practitioners and doctors. Australas Emerg Nurs J 2012; 15 188–94.
| Evaluating the quality of care delivered by an emergency department fast track unit with both nurse practitioners and doctors.Crossref | GoogleScholarGoogle Scholar | 23217651PubMed |
[29] Jennings N, O’Reilly G, Lee G, Cameron P, Free B, Bailey M. Evaluating outcomes of the emergency nurse practitioner role in a major urban emergency department, Melbourne Australia. J Clin Nurs 2008; 17 1044–50.
| Evaluating outcomes of the emergency nurse practitioner role in a major urban emergency department, Melbourne Australia.Crossref | GoogleScholarGoogle Scholar | 18321270PubMed |
[30] Nursing and Midwifery Board of Australia. Registered Nurse Standards for Practice. 2016, June 1. Available at: http://www.nursingmidwiferyboard.gov.au/Codes-Guidelines-Statements/Professional-standards.aspx [verified 8 August 2016].


