Pacific island health inequities forecast to grow unless profound changes are made to health systems in the region
Don Matheson A D , Kunhee Park B and Taniela Sunia Soakai CA Griffith University School of Medicine, 170 Kessels Road, Nathan, Qld 4111, Australia.
B World Health Organization, Level 4, Provident Plaza One, Downtown Boulevard, 33 Ellery Street, Suva, Fiji. Email: parkku@who.int
C Pacific Community BP D5, 98848, Noumea, New Caledonia. Email: sunia@spc
D Corresponding author. Email: donmathes@gmail.com
Australian Health Review 41(5) 590-598 https://doi.org/10.1071/AH16065
Submitted: 9 May 2016 Accepted: 23 August 2016 Published: 20 February 2017
Journal Compilation © AHHA/World Health Organization 2017 Open Access CC BY-NC-ND
Abstract
Objective Twenty years ago the Pacific’s health ministers developed a ‘Healthy Islands’ vision to lead health development in the subregion. This paper reports on a review of health development over this period and discusses the implications for the attainment of the health related Sustainable Development Goals.
Methods The review used qualitative and quantitative methods. The qualitative review included conducting semi-structured interviews with Pacific Island Government Ministers and officials, regional agencies, health workers and community members. A document review was also conducted. The quantitative review consisted of examining secondary data from regional and global data collections.
Results The review found improvement in health indicators, but increasing health inequality between the Pacific and the rest of the world. Many of the larger island populations were unable to reach the health Millennium Development Goals. The ‘Healthy Islands’ vision remained an inspiration to health ministers and senior officials in the region. However, implementation of the ‘Healthy Islands’ approach was patchy, under-resourced and un-sustained. Communicable and Maternal and Child Health challenges persist alongside unprecedented levels of non-communicable diseases, inadequate levels of health finance and few skilled health workers as the major impediments to health development for many of the Pacific’s countries.
Conclusions The current trajectory for health in the Pacific will lead to increasing health inequity with the rest of the world. The challenges to health in the region include persisting communicable disease and maternal and child health threats, unprecedented levels of NCDs, climate change and instability, as well as low economic growth. In order to change the fortunes of this region in the age of the SDGs, a substantial investment in health is required, including in the health workforce, by countries and donors alike. That investment requires a nuanced response that takes into account the contextual differences between and within Pacific islands, adherence to aid effectiveness principles and interventions designed to strengthen local health systems.
What is known about the topic? It is well established that the Pacific island countries are experiencing the double disease burden, and that the non-communicable disease epidemic is more advanced.
What does this paper add? This paper discusses the review of 20 years of health development in the Pacific. It reveals that although progress is being made, health development in the region is falling behind that of the rest of the world. It also describes the progress made by the Pacific countries in pursuit of the ‘Healthy Islands’ concept.
What are the implications for practitioners? This paper has significant implications for Pacific countries, donor partners and development partners operating across and within Pacific countries. It calls for a substantial increase in health resourcing and the way development assistance is organised to arrest the increasing inequities in health outcomes between Pacific people and those of the rest of the world.
Additional keywords: health promotion, health system evaluation, health system strengthening, Healthy Islands, Pacific island health development, settings approach, sustainable development goals.
Introduction
The Pacific island countries have a population of 10 million people living in 22 nations and territories spread over more than 25 000 islands and islets occupying an ocean covering one-third of the Earth’s surface. These countries vary considerably in population size, growth and density, the non-communicable disease (NCD) burden, the wider burden of disease, resource availability for health and local capacity. Rates of obesity and diabetes in many Pacific countries are higher than anywhere else in the world and continue to increase.1 Although NCDs dominate the disease burden in many Polynesian and Micronesian countries, the disease burden in most of Melanesia is shared with communicable diseases and maternal and child health issues, as evidenced by outbreaks of cholera, high maternal death rates and low levels of child nutrition; this is the only region in the world where the number of underweight children increased over the past 25 years.2 The maternal and child health-related Millennium Development Goals (MDGs) 4 and 5 (http://www.unmillenniumproject.org/goals/gti.htm, verified 13 October 16) have not been reached in the Pacific’s most populous countries; basic necessities of life, such as clean water supplies, are accessible to only half the population and only one-third of people use any type of improved sanitation facility.3 The recent El Niño weather pattern exposed the fragility of food security for many Pacific communities, where stunting rates were already high. Added to this is the effect of climate change, starkly demonstrated by high-intensity cyclones hitting the region, costing lives, devastating dwellings and crops and further damaging weak economies. As sea levels rise, the very existence of some Pacific states and cultures is threatened because, in many countries, the entire population lives at <5 m above sea level.
Twenty years ago, Pacific health ministers declared their vision for ‘Healthy Islands’ in the Yanuca Island Declaration.4 They envisioned Healthy Islands as places where children are nurtured in body and mind, environments invite learning and leisure, people work and age with dignity, ecological balance is a source of pride and the ocean which sustains us is protected.5
The health ministers returned to Yanuca Island, Fiji, in April 2015 and reviewed the progress made over the past 20 years. They reaffirmed their commitment to Healthy Islands as their vision for health development for the 21st century.6 In September 2015, the world’s political leaders confirmed their commitment to 17 Sustainable Development Goals (SDGs),7 with health featuring directly in Goal 3: ‘Ensure healthy lives and promote well-being for all at all ages’.
The purpose of this paper is to report on the findings of a review of the past 20 years of health development in the Pacific across 22 countries and territories,8 and to discuss the implications of these findings for future health development in the subregion if the health-related SDGs are to be achieved.
Methods
The review used qualitative and quantitative methods. The qualitative review included conducting semi-structured interviews and a document review. The interview questions were derived from the five elements describing a ‘Healthy Island’ and explored its strength as a vision, a catalyst for change and its effects. The recruitment process for interviewees was purposeful, initially involved identifying key informants through contacts in the respective Pacific island governments and regional health agencies (World Health Organization (WHO), the Secretariat of the Pacific Community, Pacific Island Health Officers Association). Snowballing was then used to identify further key informants to be interviewed. Participants were interviewed in person at a regional meeting of health ministers held in Manila from 13–17 Oct 2014 during country visits to Fiji, Samoa and Vanuatu or by telephone. In all, 79 people were interviewed, including six ministers of health, 20 senior health officials, development partners at national and regional levels and other national and sub-national health workers in the three countries visited. Interviews were recorded manually and then entered into NVivo software (QSR International), where data were coded according to the initial questionnaire, then further coded to capture emerging themes and concepts. Participants included people from all three Pacific groupings: Melanesia, Polynesia and Micronesia.
The quantitative review consisted of examining secondary data from regional and global data collections. Indicators were sought according to the following criteria: data available to assess trends over a 20-year time frame; data covering both the subregion and individual countries; and data reflecting progress on one of the original Healthy Island descriptors. National reports from specific countries were used to fill the gaps in global data collections.
Results
Child survival
Measurable outcome indicators, such as life expectancy and child survival, show health improvement in the Pacific over the 20-year period. However, the progress is slower than the world average.
Figure 1 shows the death rate in children under 5 years of age. Overall, this death rate is decreasing for the Pacific. However, comparisons show that the mortality rate for children under 5 years of age was lower in the Pacific than the rest of the world in 1995, but is now higher. Differences between the Pacific countries and the rest of the world are increasing and, if the current trends continue, the inequality in child mortality will intensify. MDG4 was not met for Pacific Children.
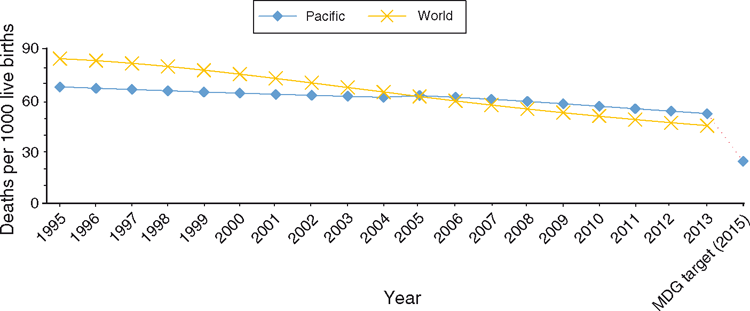
|
The child mortality rate in Melanesia is much higher than that in Polynesia or Micronesia (Fig. 2). (Melanesia includes Fiji, Papua New Guinea (PNG), Solomon Islands and Vanuatu. Micronesia includes Kiribati, Marshall Islands, Federated States of Micronesia, Nauru and Palau. Polynesia includes Cook Islands, Niue, Samoa, Tonga and Tuvalu.) When the three major groupings in the Pacific are examined, there are very marked differences between them. The mortality rate for children under 5 years of age is highest in Melanesia, largely influenced by PNG, with its under-5 population of 1 million children.
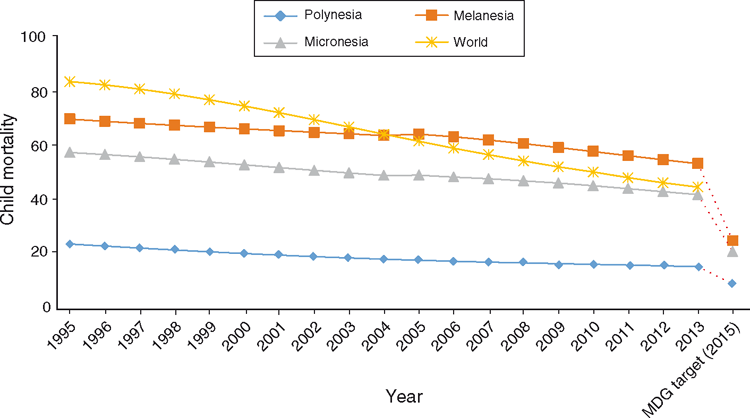
|
Water and sanitation
Figure 3 shows the proportion of the population using improved water sources. This is lower for the Pacific than the rest of the world, and the gap is not closing. A similar pattern is seen for the proportion of the population with improved sanitation facilities, with the world at 64% and the Pacific at 36% at 2012 and the gap increasing. There is a strong correlation between the state of water and sanitation and the mortality rate for children under 5 years of age. Melanesia again has the lowest level of coverage (data not shown).
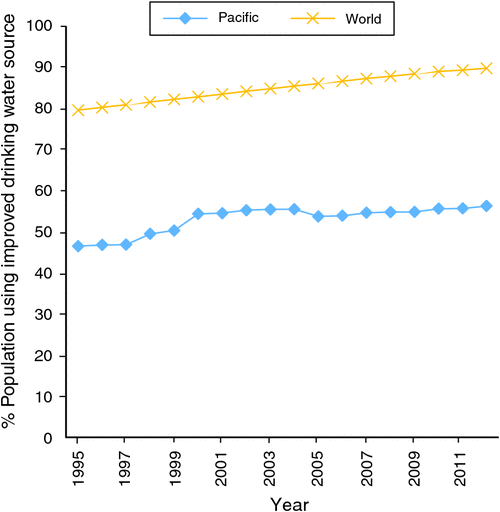
|
Non-communicable diseases
The differences between the Pacific and the rest of the world are most marked when it comes to NCDs. Figure 4 shows that the rates of obesity for adults over 18 years of age for many Pacific Countries far exceeds the world average. Obesity reduces life expectancy, as it is a major risk factor for NCDs such as diabetes, heart disease and some cancers. The negative effects on families of losing parents at a young age are considerable. The negative economic effect is also large, not only through the cost of health care, but also through loss of labour productivity. Almost half of all deaths (48%) in Tonga occur below the age of 64 years as a result of cardiovascular disease, resulting in large losses of labour productivity among the country’s most skilled workers.9
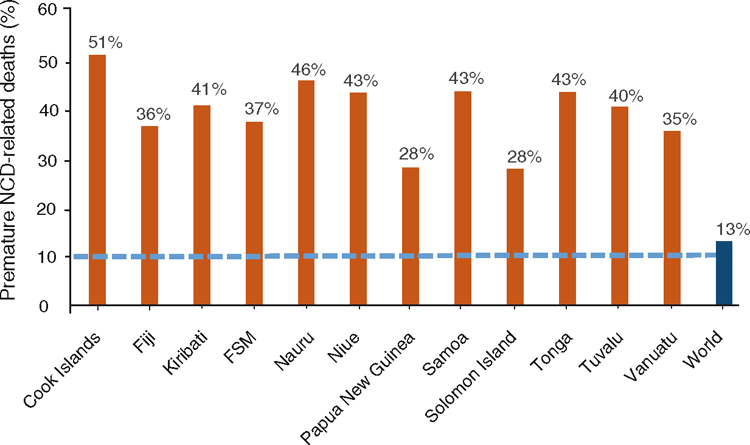
|
The WHO STEPwise approach to Surveillance (STEPS) surveys (WHO Office, Suva, pers. comm) and other studies show that the NCD epidemic in the Pacific has not yet reached its peak. Living with diabetes is now becoming the norm for adults in some Pacific communities.
Health resourcing
Health in the Pacific, as elsewhere, is strongly affected by the wider determinants of health, as well as the health system response. Gross domestic product (GDP) growth per capita from 1992 to 201210 has been slow in the Pacific, and negative in some periods. Only PNG is showing significant growth, due to the effect of the extraction industry, but recent predictions of high growth in this economy have not materialised because of the current low price for oil and gas. Pacific economies have a narrow economic base, are geographically isolated from global markets, rely on few commodities for export (agriculture, forestry, fishing, minerals and gas) and are prone to interruption because of the frequency of natural disasters.
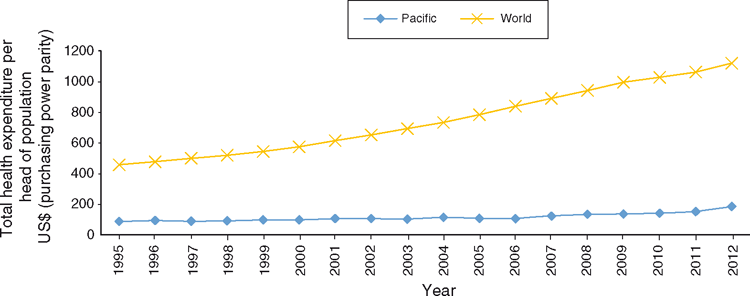
Investment in health per head of population in the Pacific began at one-fifth of the global spend in 1995, but by 2012 this proportion had decreased, with Pacific health spending now one-sixth of the world average, reflecting increased inequality in health resourcing (Fig. 5).
|
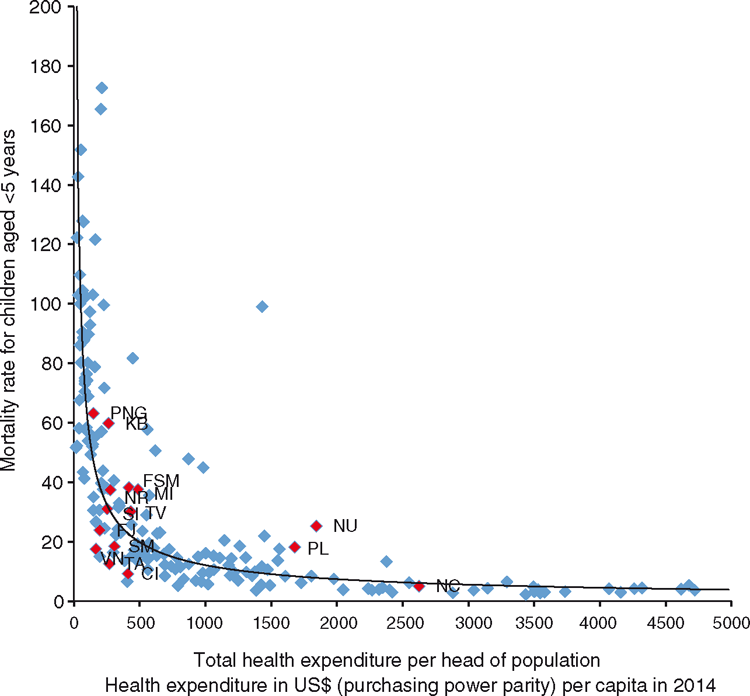
There is wide variation in the expenditure on health service provision per capita and the efficiency of the health spend between different Pacific countries. PNG (with 75% of the region’s population) spends USD100 per person per year, whereas New Caledonia spends US$2600 (data not shown). Figure 6 shows the relationship between health expenditure and the mortality rate of children under 5 years of age, with improved mortality associated with increased expenditure. Many Pacific states (Cook Islands, Tonga, Vanuatu, Fiji, Solomon Islands) have achieved lower levels of child mortality than the world trend line (Fig. 6), despite their geographic and demographic challenges. Other countries (Federated States of Micronesia, Marshal Islands, Kiribati, Palau) have expenditures above the trend line (Fig. 6). A full examination of the drivers of these differences has not been conducted.
|
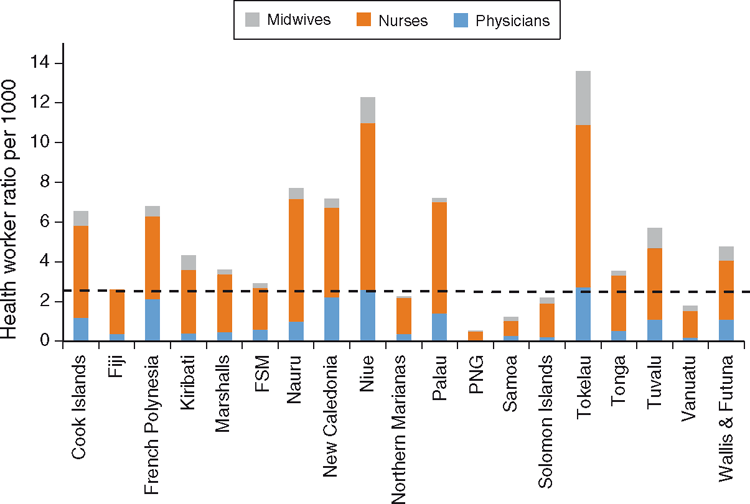
The health workforce profile in Pacific countries (Fig. 7) shows that although many of the countries have at least the critical threshold11 required to meet the MDGs, the exceptions (PNG, Vanuatu, Solomon Islands and Samoa) involve some of the biggest populations. In PNG, it is estimated that 3.5 million people do not have access to a doctor within their district.12 The country requires 17 600 additional skilled health workers.13 The global critical threshold of 2.3 skilled health workers per 1000 population12 does not take into account the workforce required to meet the overwhelming NCD challenge or the workforce required for isolated island populations. The critical thresholds for a health workforce in the Pacific to meet global goals has yet to be determined.
|
Qualitative findings
The interviewees strongly supported ‘Healthy Islands’ as the overarching vision for Pacific health development. The meaning associated with Healthy Islands was the articulation of a high-level vision steeped in Pacific understanding of health and the environment. This view was consistently articulated by ministers and senior health officials. Interviewees reported a heartfelt message arising from Healthy Islands, using words such as ‘utopia’, ‘unifying’, ‘spiritual’, ‘freedom’, ‘wisdom’ and ‘heart’ to describe its meaning. Healthy Islands was used in practice to refer to a settings approach, primary health care, health promotion and working across sectors. Recent evidence suggests that Pacific youth also share this holistic view of health.14
Healthy Islands played a significant role in the advocacy by Pacific ministers to address NCDs globally, and the adoption of inter-sectoral approaches at the national level. The vision framed the approach Pacific health leaders have taken to engage with other sectors, and continues to inspire health ministers and senior health officials across the Pacific. As one official noted, ‘Healthy Islands was ahead of its time, and its time has now come’. A joint agreement has been forged15 between Pacific health and economic ministers on the approach to NCDs, including an agreement to increase excise duties on tobacco products and to consider an increase in taxation of alcohol products, as well as introducing policies that reduce the consumption of local and imported food and drink products high in sugar, salt and fat. Several Pacific countries have already developed this approach for tobacco control16 and it could be extended further across the region to include alcohol, gambling and some foods.
There was a broad consensus that although the vision was strong, more could have been achieved had greater attention been paid to the implementation barriers over the 20-year period. These barriers included the fragmented approach taken by development partners. Interviewees commented that even existing funds, such as Global Alliance for Vaccines and Immunization (GAVI), the Global Fund to Fight AIDS, Tuberculosis and Malaria, and the Gates Foundation are too frequently off plan, off budget and have separate reporting arrangements, severely limiting their future sustainability and the opportunity to strengthen local systems. In addition, barriers identified by participants included political upheaval, vertical programs driving system inefficiencies, lack of sustained momentum in programs, lack of sub-national health system development and local management failures, including the lack of adequate information systems and reporting.
Discussion
The review of the past 20 years of health development in Pacific island countries has found that despite improvements, gaps are increasing between health outcomes in the Pacific and those in the rest of the world. The region has a well-supported vision, Healthy Islands, but implementation has fallen short. Inadequate finances, workforce and fragmented implementation are the main implementation barriers identified.
From the perspective of Pacific ministers and senior officials, the problem has not been the lack of a clear vision, or the cross-sectoral approaches required, but the challenges of implementation. Resourcing for health has been low for most countries, reflecting weak economic growth. Efficiency of health service provision does not differ markedly from global trends, although there is considerable variation within the region. The strategic frameworks developed by the Pacific and global leaders are unlikely to reverse the current trajectory for health in the Pacific unless the implementation mechanism, including resourcing the health systems in the region, is strengthened considerably.
The prospects of economic growth closing the gap in health development between the Pacific and the rest of the world are slim. Economic growth is attracted to scale and concentration, and deterred by isolation and dispersal.17 The Pacific reality is small populations, isolated from markets and reliant on finite and diminishing commodities, such as forests, fish, minerals and gas. The island nations have experienced considerable downsides to globalisation to date. Pacific food supplies have seen nutritious local food consumption replaced by low-quality imported food, high in fat, salt and sugar. The number of underweight children is increasing18 and water and sanitation coverage lags behind the rest of the world. Deteriorating food security remains a major health challenge.19 The by-product of the rest of the world’s global economic growth, climate change, now threatens the existence of some Pacific island nations, and associated climate instability further curbs economic growth.
What needs to change over the next 15 years?
The global SDGs have now been set for 2030. These goals have made strong links between different dimensions of development. Health benefits are likely to accrue from attainment of most of the goals. Of special significance to the Pacific is Goal 13: ‘Take urgent action to combat climate change and its impacts’.7 The Pacific ministers, 20 years earlier, had envisaged health as being intrinsically connected to work, the learning environment, ecological balance and the protection of oceans. The SDGs also affirm a strong focus on equity. ‘No one left behind’ and ‘Universal Health Coverage’ (http://www.who.int/dg/speeches/2015/universal-health-coverage/en/, verified 13 October 2016) imply that there needs to be a system response that delivers on equity.
Both Healthy Islands and the SDGs call for an integrated view of health development. The past has seen a disconnection between economic, environmental and social progress in the Pacific (as they have elsewhere). For example, trade agreements have been largely negotiated without assessing their health and environmental effects on the Pacific peoples.20 An integrated view of health development needs to be put into practice by both the countries themselves and the development partners.
For much of the past 20 years, the bulk of the Pacific population’s health services had insufficient levels of financing and human resources to achieve global health goals. Island governments’ contributions to health have increased over the period and, for most countries, health is now predominantly government funded. Given the economic headwinds being faced, it is unlikely there will be sufficient growth in these economies to fund health services in the Pacific to the level that is required to meet the health SDGs, as happened with the MDGs.
On their own, many Pacific countries cannot afford universal health coverage. Given the global origins of many of the challenges faced (NCDs, global warming), developed countries should take more responsibility in addressing health challenges in the Pacific.
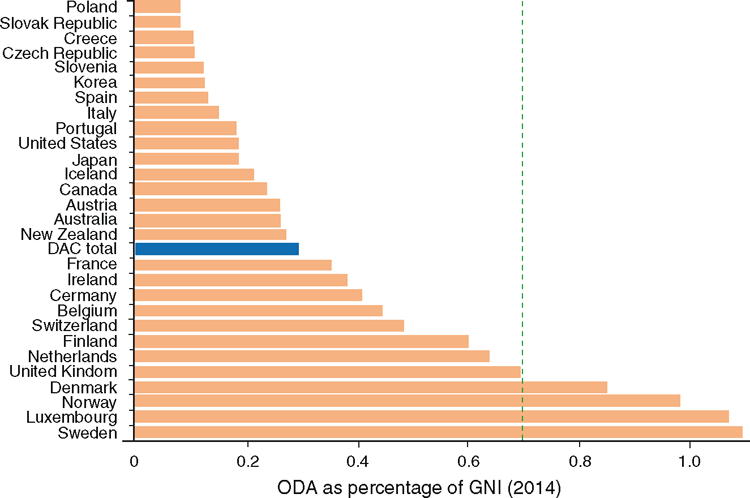
As indicated in Fig. 8, the level of overseas development assistance for most of the region’s largest donors21 (Australia, USA, New Zealand, Japan, Korea) is currently below the Organization for Economic Cooperation and Development (OECD) average of 0.29% of gross national income,21 and well less than half of the 1970 United Nations commitment to 0.7%. France is the only major Pacific island donor country that contributes above the OECD average. The commitment to 0.7% has recently been refreshed at a meeting of small island developing states22 and as a central tool for meeting global development goals.23 Any move that major donors in the Pacific make towards 0.7% could substantially address the financing deficit for health in the region.
|
The number of actors providing support for Pacific countries is increasing rapidly. There is a strong likelihood of further fragmentation, and resulting frustration,24 with the potential addition to the development architecture of the Green Climate Fund (www.greenclimate.fund, verified 15 February 2016), Asian Infrastructure Investment Bank (www.aiib.org, verified 15 February 2016), the Global Infrastructure Hub (www.globalinfrastructurehub.org, verified 15 February 2016) , the New Development Bank (www.ndbbrics.org, verified 15 February 2016), the Asia Pacific Project Preparation Facility (www.adb.org/documents/asia-pacific-project-preparation-facility, verified 15 February 2016), the World Bank Group’s Global Infrastructure Facility (www.worldbank.org/en/programs/global-Infrastructure-facility, verified 15 February 2016), Global Financing Facility in support of Every Woman, Every Child (www.globalfinancingfacility.org, verified 15 February 2016), a Technology Facilitation Mechanism (www.sustainabledevelopment.un.org/topics/technology/facilitationmechanism, verified 15 February 2016) and the Technology Bank for Least Developed Countries (www.unohrlls.org/technologybank, verified 15 February 2016). This list is not exhaustive, because it omits the global growth of private philanthropic efforts. Pacific health leaders have identified fragmentation of development efforts as a major impediment to implementation over the past 20 years, so this latest wave of development modalities risks further exacerbating this problem, overwhelming local capacity and consequently failing to achieve health development goals. What is required is better coordination, and a focus on how development assistance in the Pacific can best meet the development needs of these unique populations in this unique setting. This renewed interest in financing modalities is welcomed, but its effect will be limited unless aid effectiveness principles25 and cognizance of the Pacific context are applied from the start.
The response to the health care worker deficit also requires a nuanced response to the different island contexts. PNG’s deficit requires a substantial boost to its local health training capacity. Currently, 45 doctors are trained in the country per year (G. Mola, pers. comm.), and this needs to increase to 300 per year if there is to be any chance of meeting universal health coverage requirements. Effective deployment of these doctors will also require resources for salaries, infrastructure and supplies. Other countries, such as the Solomon Islands, will double their doctor numbers in the next 5 years by increasing the number trained outside the country, such as in Cuba.26 Their challenge is to build the necessary district infrastructure so that they can deploy these new graduates to areas where their skills are most needed.
The NCD epidemic also calls for a response commensurate with the size of the disease threat, and the state of knowledge of effective interventions. The Pacific is already pioneering public health responses to NCDs27 that will have important lessons for the rest of the world. The current package of essential NCD interventions for primary health care approach is an important start, but much more is required in adapting chronic disease management approaches for Pacific island contexts.
Conclusion
The current trajectory for health in the Pacific will lead to increasing inequity with the rest of the world. The challenges to health in the region include persisting communicable disease and maternal and child health threats, unprecedented levels of NCDs, climate change and instability, as well as low economic growth.
In order to change the fortunes of this region in the age of the SDGs, a substantial investment in health is required, including in the health workforce, by countries and donors alike. That investment requires a nuanced response that takes into account the contextual differences between and within Pacific islands, adherence to aid effectiveness principles and interventions designed to strengthen local health systems.
Competing interests
The lead author is a health systems consultant and the co-authors work for the World Health Organisation and the Pacific Community respectively.
Acknowledgements
This article uses some of the findings of The First 20 Years of the Journey towards the Vision of Healthy Islands in the Pacific, which was supported financially by the World Health Organization (WHO) and is available at http://iris.wpro.who.int/bitstream/10665.1/10928/3/9789290617150_eng.pdf, verified 14 October 2016], and The State of Human Development in the Pacific; A Report on Vulnerability and Exclusion in a Time of Rapid Change’, available at: http://www.unescap.org/resources/state-human-development-pacific-report-vulnerability-and-exclusion-time-rapid-change [verified 2 May 2015]. The authors thank Vivian Lin, who provided valuable commentary at the drafting stage, and Junsoo Ro, who assisted with the compilation of indicators. The views expressed in this paper are those of the authors and do not necessarily reflect the official policy or position of the World Health Organization or Pacific Community.
References
[1] Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 2015; 384 766–81.[2] United Nations. The millennium development goals report 2015. 2015 Available at: http://www.un.org/millenniumgoals/2015_MDG_Report/pdf/MDG%202015%20rev%20%28July%201%29.pdf [verified June 2016].
[3] World Health Organization, Regional Office for the Western Pacific. Sanitation, drinking-water and health in Pacific island countries: 2015 update and future outlook. Manila: WHO Regional Office for the Western Pacific; 2016.
[4] World Health Organization (WHO), Regional Office for the Western Pacific. Yanuca Island declaration: March 1995. WHO; 1995. Available at: http://www.pihoa.org/fullsite/newsroom/wp-content/uploads/downloads/2012/09/WPR_RC46_INF_DOC1.pdf [verified 14 October 2016].
[5] World Health Organization, Regional Office for the Western Pacific. Recommendations of the meeting of the Ministers of Health of the Pacific islands Koror, Republic of Palau, 18–19 March 1999. Available at: http://iris.wpro.who.int/bitstream/handle/10665.1/5565/WPR_HRH_DHI_99.1_eng.pdf [verified 14 October 2016]
[6] Pacific Health Ministers. 2015 Yanuca Island Declaration on health in Pacific island countries and territories 15–17 April 2015. In Eleventh Pacific Health Ministers Meeting, 2015. Available at: http://www.wpro.who.int/southpacific/pic_meeting/2015/phmmdeclaration2015_english_final_nov3.pdf. [verified 13 October 2016].
[7] United Nations. Transforming our world by 2030: a new agenda for global action. 2015. Available at: https://sustainabledevelopment.un.org/post2015/transformingourworld [verified 14 October 2016].
[8] World Health Organization (WHO), Western Pacific Region. The first 20 years of the journey towards the vision of Healthy Islands in the Pacific. Manila: WHO; 2015. Available at: http://iris.wpro.who.int/bitstream/10665.1/10928/3/9789290617150_eng.pdf [verified 14 October 2016]
[9] Anderson I. The economic costs of non-communicable diseases in the Pacific Islands. A rapid stocktake of the situation in Samoa, Tonga and Vanuatu. Final report, November 2012. 2012. Available at: http://www.worldbank.org/content/dam/Worldbank/document/the-economic-costs-of-noncommunicable-diseases-in-the-pacific-islands.pdf [verified 14 October 2016].
[10] Asian Development Bank (ADB). Estimates based on data from World Bank’s world development indicators online. Extracted from ADB, Key Indicators for Asia and the Pacific. 2014. Available at: www.adb.org/statistics [verified 15 February 2016].
[11] World Health Organization. Achieving the health-related MDGs. It takes a workforce! 2010 Available at: http://www.who.int/hrh/workforce_mdgs/en/ [15 Oct 2016].
[12] Mills D. Mending the road behind and building the road ahead. In: National Rural Health Alliance. Proceedings of the 13th National Rural Health Conference, Port Moresby, 2–3 Sept 2015. Available at: http://www.ruralhealth.org.au/13nrhc/images/paper_Mills%2C David.pdf [verified 15 February 2016].
[13] Morris IP, Somanathan A. Papua New Guinea (PNG) health workforce crisis: a call to action. Washington, DC: The Worldbank; 2012. Available at: http://documents.worldbank.org/curated/en/216511468332461651/Papua-New-Guinea-PNG-health-workforce-crisis-a-call-to-action World Bank [verified 31 October 2016].
[14] Sheridan S, Brolan CE, Fitzgerald L, Tasserei J, Maleb M-F, Rory J-J, Hill PS. Facilitating health and wellbeing is ‘everybody’s role’: youth perspectives from Vanuatu on health and the post-2015 sustainable development goal agenda. Int J Equity Health 2014; 13 80
| Facilitating health and wellbeing is ‘everybody’s role’: youth perspectives from Vanuatu on health and the post-2015 sustainable development goal agenda.Crossref | GoogleScholarGoogle Scholar |
[15] Joint forum economic and Pacific health ministers meeting outcomes statement, Honiara, Solomon Islands, 11 July 2014. 2014. Available at: http://www.forumsec.org/resources/uploads/attachments/documents/2014_Joint_FEMM_PHMM_%20Meeting_Outcomes_Statement_July14_approvedbyMinisters.pdf [verified 31 October 2016].
[16] World Health Organization. Pacific tobacco taxation project. 2015. Available at: http://www.wpro.who.int/tobacco/pacifictobaccotaxationproject/en/ [verified 15 February 2016].
[17] Haque T. Economic transitions in Solomon Islands. 2013 Available at: http://bellschool.anu.edu.au/sites/default/files/publications/attachments/2016-04/ssgm_ib_2013_16.pdf [15 February 2016].
[18] United Nations. The millennium development goals report. 2015. Available at: http://www.un.org/millenniumgoals/2015_MDG_Report/pdf/MDG%202015%20rev%20%28July%201%29.pdf [verified Oct 2016].
[19] World Health Organization. Towards a food secure Pacific. 2010. Available at: https://pacenet.eu/system/files/documents/Food Secure Pacific Framework for Action.pdf [verified 15 Feb 2016].
[20] Friel S, Hattersley L, Townsend R. Trade policy and public health. Annu Rev Public Health 2015; 36 325–44.
| Trade policy and public health.Crossref | GoogleScholarGoogle Scholar |
[21] Organization for Economic Cooperation and Development (OECD). Official development assistance 2014. 2015. Available at: http://www.compareyourcountry.org/oda?cr=oecd&lg=en [verified 28 January 2016].
[22] United Nations General Assembly. Resolution adopted by the General Assembly on 14 November 2014. 69/15. SIDS Accelerated Modalities of Action (SAMOA) Pathway 2014. Available at: http://www.un.org/ga/search/view_doc.asp?symbol=A/RES/69/15&Lang=E [verified 31 December 2016].
[23] United Nations. (2015). Third international conference on financing for development outcome document of the Third International Conference on Financing for Development: Addis Ababa Action Agenda Annex Addis Ababa Action Agenda of the Third International Conference on Financing (Vol. 1, pp. 1–39). Available at: http://www.un.org/esa/ffd/ffd3/documents.html [verified 15 February 2016].
[24] SciDevNet. Island states slam climate fund red tape. 2015. Available at: http://www.scidev.net/global/funding/news/pacific-island-states-climate-fund-red-tape.html [verified 15 February 2016].
[25] Organization for Economic Cooperation and Development. The Busan partnership for effective development co-operation. 2011. Available at: http://www.oecd.org/dac/effectiveness/49650173.pdf [verified 12 December 2015].
[26] National Health Strategic Plan 2016–2020. (2016). Honiara. Available at: http://daisi.com.au/wp-content/uploads/2016/09/Strategic-Plan-for-Solomon-Islands-2016-2010.pdf. [verified 13 October 2016].
[27] Snowdon W, Thow AM. Trade policy and obesity prevention: challenges and innovation in the Pacific Islands. Obes Rev 2013; 14 150–8.
| Trade policy and obesity prevention: challenges and innovation in the Pacific Islands.Crossref | GoogleScholarGoogle Scholar |


