A review of the economic impact of mental illness
Christopher M. Doran A B and Irina Kinchin AA Centre for Indigenous Health Equity Research, School of Health, Medical and Applied Sciences, Central Queensland University, Level 4, 160 Ann Street Brisbane Qld 4000, Australia. Email: i.kinchin@cqu.edu.au
B Corresponding author. Email: c.doran@cqu.edu.au
Australian Health Review 43(1) 43-48 https://doi.org/10.1071/AH16115
Submitted: 25 May 2016 Accepted: 1 September 2017 Published: 13 November 2017
Journal Compilation © AHHA 2019 Open Access CC BY-NC-ND
Abstract
Objective To examine the impact and cost associated with mental illness.
Methods A rapid review of the literature from Australia, New Zealand, UK and Canada was undertaken. The review included literature pertaining to the cost-of-illness and impact of mental illness as well as any modelling studies. Included studies were categorised according to impact on education, labour force engagement, earlier retirement or welfare dependency. The well-accepted Drummond 10-point economic appraisal checklist was used to assess the quality of the studies.
Results A total of 45 methodologically diverse studies were included. The studies highlight the significant burden mental illness places on all facets of society, including individuals, families, workplaces and the wider economy. Mental illness results in a greater chance of leaving school early, a lower probability of gaining full-time employment and a reduced quality of life. Research from Canada suggests that the total economic costs associated with mental illness will increase six-fold over the next 30 years with costs likely to exceed A$2.8 trillion (based on 2015 Australian dollars).
Conclusions Mental illness is associated with a high economic burden. Further research is required to develop a better understanding of the trajectory and burden of mental illness so that resources can be directed towards cost-effective interventions.
What is known about the topic? Although mental illness continues to be one of the leading contributors to the burden of disease, there is limited information on the economic impact that mental illness imposes on individuals, families, workplaces and the wider economy.
What does this paper add? This review provides a summary of the economic impact and cost of mental illness. The included literature highlights the significant burden mental illness places on individuals, families, workplaces, society and the economy in general. The review identified several areas for improvement. For example, only limited information is available on the impact of attention deficit hyperactivity disorder, anxiety, cognitive function, conduct disorder, eating disorder and psychological distress. There was also a dearth of evidence on the intangible elements of pain and suffering of people and their families with depressive disorders. More research is required to better understand the full extent of the impact of mental illness and strategies that may be implemented to minimise this harm.
What are the implications for practitioners? Knowing the current and future impact of mental illness highlights the imperative to develop an effective policy response.
Additional keywords: mental health, health economics, health policy.
Introduction
The term mental illness describes a diverse range of behavioural, psychological and low-prevalence conditions including eating disorders and severe personality disorder.1,2 Mental and substance use disorders are responsible for 24% of the non-fatal disease burden in Australia and 12% of the total disease burden, reflecting the disabling nature of these conditions.3 Other data suggest that one in five Australians aged 16–85 years experienced mental illnesses in the last 12 months.4 People with severe mental disorders represent a vulnerable and socially excluded population and are more likely to be affected by lower educational and social opportunities, social alienation, and increased morbidity and mortality rates.5
The economic cost of mental illness in the community is high, with the National Mental Health Report 2013 suggesting that outlays by governments and health insurers on mental health services in 2010–11 totalled A$6.9 billion, representing 7.7% of all government health spending.6 Over the period 1992–93 to 2010–11, total government expenditure on mental health has increased by 178% in real terms. These figures reflect the cost of operating the mental health service system, with an additional A$4.63 billion spent by the Australian Government on providing other support services for people with mental illness, including income support, housing assistance, community and domiciliary care, and employment and training opportunities.
Australian and international cost-of-illness (COI) studies suggest that in addition to government expenditures, mental illness imposes a significant burden on families, businesses and other non-government organisations through out-of-pocket personal expenses, carer or family costs and lost productivity costs. The evidence suggests that these costs are at least equal to, if not more, than total government expenditures.7–9
The Mental Health Commission of NSW is an independent body that engages with the mental health community to bring about sustained change regarding all aspects of mental illness. To inform the development of the Commission’s strategic plan a rapid review of the costs and impacts on the economy and productivity due to mental illness was undertaken. This article provides a synthesis of the methods and main findings of that rapid literature review.10
Methods
A rapid literature review is a streamlined approach to accessing and synthesising literature on a focussed topic in a timely way.11 The Mental Health Commission of NSW predetermined the scope of the review to include studies related to the impact that mental illness imposes on individuals, families, workplaces and the wider economy. A search strategy for both the peer-reviewed and grey literature was developed in consultation with an accredited librarian.
The search was limited to papers on people with mental illness of working age in employment. Consequently, conditions involving dementia, intellectual disability, substance use and abuse or behavioural problems in youth (except attention deficit hyperactivity disorder; ADHD) were excluded. The search was also limited to countries that shared relatively comparable healthcare systems, namely, Australia, the United Kingdom (UK), Canada and New Zealand. The checklist for international comparisons of health-related data was used to make this judgement.12
A comprehensive search of a range of databases was conducted for studies published over the period 2000–2013 (inclusive). Databases searched were: Medline; Embase; PsycINFO; Cochrane Database of Systematic Reviews; The Campbell Library; APAIS-Health; CINAHL; Global Health; EconLit; PAIS International; and ABI/INFORM Global. Each database was searched using the following keywords, or combinations thereof:
-
Mental health OR mental disorders OR anxiety disorders OR mood disorders OR affective disorders OR depressive disorders OR schizophrenia disorders OR bipolar disorder OR depression OR post-traumatic stress disorder OR obsessive compulsive disorder OR phobia OR panic disorders OR eating disorders OR personality disorders OR mental illness OR ADHD OR conduct disorders OR oppositional defiant disorder.
-
Costs OR impact OR productivity OR workforce OR economy.
-
Australia OR United Kingdom OR Canada OR New Zealand.
-
AND combination of 1–3.
Articles were classified using the accepted Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement.13 Data extraction and quality assessment were conducted by the lead author (CD) and checked by the second author (IK). Data extraction included: characteristics (such as type of mental disorder and study population), first author, year published, country, aim, key findings and recommendations; and methodological features such as costing approach, perspective, data collection, measurement and valuation.
Although several guidelines exist to aid the appraisal of economic evaluations,14–16 the Drummond 10-point checklist is perhaps the most widely used and had been previously used by the lead author.17 This checklist considers 10 items: the research question; description of study; how effectiveness was established; study design; identification, measurement and valuation of costs and consequences; discounting; presentation of results; and, discussion of results in the context of policy relevance and existing literature. Each item included in the paper is given a score of 1, and studies then categorised based on their total score as poor quality (scores ranging from 1–3), average quality (scores ranging from 4–7) or good quality (scores ranging from 8–10).
The main characteristics of each included study was also summarised using a narrative synthesis approach. Studies were classified as either COI studies, impact analysis or modelling studies. Impact analysis studies were further classified as education, labour force engagement, earlier retirement or welfare dependency. Short-term studies were defined as ranging between 6 months and 2 years, with medium- to long-term referring to 2 years or more.
Results
Two hundred and seventy-eight studies were identified in the initial search (Fig. 1). Both authors independently reviewed the abstracts of all studies and excluded 229 for a range of reasons including: country outside study parameters; not a cost or impact study; papers were thesis, commentary or editorial; alcohol study; and duplicate of another study. The lead author reviewed full copies of the remaining 49 studies and excluded a further 21 due to: duplicates; country; commentary; not a cost or impact study; and study conducted outside of study timeframe. The grey literature search resulted in an additional 17 studies that were subsequently added to the included peer-reviewed literature resulting in a total of 45 studies (see Table S1 available as supplementary material to this paper).
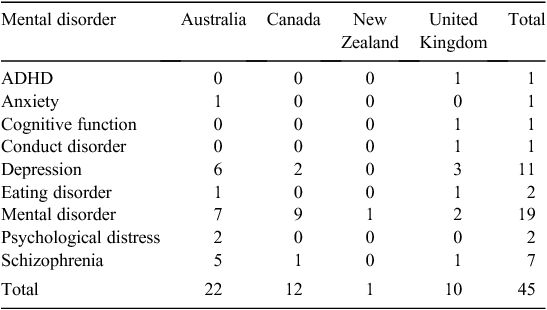
Table 1 provides an overview of studies by country and mental health disorder. The majority of studies were from Australia (n = 22), followed by Canada (n = 12), the UK (n = 10) and New Zealand (n = 1). Nineteen studies were classified under the general heading of mental disorder, 11 studies focussed on depression, seven on schizophrenia, and two each on eating disorders and psychological distress. ADHD, anxiety, cognitive function and conduct disorder had one study each.
|
Of the 45 studies, 26 were COI studies followed by impact and/or review studies (n = 12) and modelling studies (n = 7). The majority of the COI studies adopted a social perspective (n = 14) or health sector viewpoint (n = 6). All 26 COI studies were rated as good quality. This rating reflected that all of the COI studies had identified a research question, implemented an appropriate methodology for the question at hand, interpreted and discussed the results.
Cost
The COI studies defined costs as direct and indirect (or productivity) costs.14 The measurement of direct costs was standard in all studies. Of those studies that valued indirect costs (n = 16), the majority (n = 10) followed the human capital approach that measures lost productivity as discounted earnings, with earnings reflecting productivity at the margin.
COI studies were based on either prevalence or incidence figures. Prevalence-based estimates can be used as an indication of the costs of providing healthcare, as they consider the cost of providing care for both existing and new cases in a given population over a defined period, usually a year. Incidence-based estimates are more useful for estimating the potential benefits of prevention programs as they consider the lifetime economic burden of new cases of a disease occurring in a given population in a defined period, again usually a year. The prevalence-based approach was the more common method used.
COI studies generally used a combination of top-down and bottom-up approaches to costing. The top-down approach apportions national or regional expenditures by number of cases, whereas the bottom-up approach applies unit-cost estimates (i.e. for each element of service use) to each individual, which are then aggregated. Those studies that relied on survey data facilitated a more precise bottom-up approach, whereas those studies that relied on national estimates, particularly using administrative data, used the top-down approach.
Impact
The majority of studies that assessed impact considered short-term time- frames. These studies commonly relied on administrative or survey data to explore annual impacts of mental disorders. A limited number of studies (n = 9) were able to take advantage of linked data to examine a more medium to longer-term impact of mental disorders (see Table S1).
Educational outcomes
Three studies examined the impact of poor mental health on school completion. Leach et al. found that age of onset of mental disorders is an important factor in predicting the course of illness and psychosocial factors such as educational attainment.18 Evidence further suggests that those who complete high school are more likely to be employed in higher skilled occupations and to obtain other (non-school) educational qualifications.19
In New Zealand, Gibb et al. used longitudinal data to examine whether common psychiatric disorder between ages 18 and 25 was associated with negative economic and educational outcomes at age 30.20 The authors found that, after adjusting for confounding factors, increasing episodes of psychiatric disorder have negative effects on life outcomes. The authors suggest there is a need to develop targeted interventions for those with multiple psychiatric disorders to reduce the risks of negative life outcomes.20
An Australian study by Laplagne et al. used data from Household, Income and Labour Dynamics in Australia (http://melbourneinstitute.unimelb.edu.au/hilda, accessed 12 October 2017) to examine labour force participation effects associated with health and education variables.21 Using an integrated modelling framework, the authors found that a mental health condition was associated with the lowest likelihood of being in the labour force, especially for men. The authors do contend however, that causality between mental health and labour force participation is bi-directional: poor mental health may lead to a reduced likelihood of labour force participation and labour force participation can, in turn, influence a person’s mental health (i.e. working may have a positive or negative impact on mental health).
Labour force engagement
An Australian study conducted by Schofield et al. found that individuals with a mental health condition have unemployment rates up to four times higher than healthy Australians and were in general reluctant or unable to join the labour force.19 Schofield et al. also found that employees in the workforce that have a mental disorder tend to work less productively (presenteeism) and take more sick leave (absenteeism).19
Work presenteeism
Hilton et al. used the health and performance at work questionnaire to examine the relationship between psychological distress and workplace productivity.8,22 In the first study, Hilton et al. found that high psychological distress increased absenteeism by 1.7%, decreased employee performance at work by 6.1%, with the net result being a productivity loss of 6.7%.8 In the 2010 study, Hilton et al. estimated that psychological distress produces a reduction of A$5.9 billion (equivalent to A$7.8 billion in 2015) in Australian employee productivity per annum.
Work absenteeism
Two UK studies examined the association between mental disorders and long-term sick leave in adult life. Stansfeld et al. used data from the Longitudinal Whitehall II Study of British Civil Servants to examine the association of common mental disorders with psychiatric and non-psychiatric sickness absence.23 The authors reported that clinical mental disorders were associated with an increased risk of psychiatric sickness absence for men, but not for women, after adjusting for covariates. Henderson et al. used data from various UK cohort studies to examine the association between childhood cognitive function and long-term sick leave in adult life and whether this association was mediated by educational attainment, adult social class or adult mental ill-health.24 The authors found a clear dose–response relationship between lower cognitive function in childhood and increased odds of being on long-term sick leave in adulthood. The authors contend that this relationship is mediated, in part, by education attainment suggesting that improved education, especially for those with lower cognitive abilities, might help lower the risk of long-term sickness absence.
Earlier retirement
Two Australian studies, Paradise et al. and Schofield et al. examined the association and impact of mental disorders on earlier and ill retirement. Paradise et al. used data from the 45 and Up Study to examine the association of heart disease, depression and ill-health retirement in a large community sample.25 The authors found that a prior diagnosis of depression was associated with a three-fold increase in the risk of ill-health retirement.25 Schofield et al. developed a microsimulation model of health and disability and found that individuals who retired early due to a diagnosis of depression had an income that was 73% lower than their full-time employed counterparts.19 Schofield et al. estimated the national cost of this early retirement at A$278 million (A$367 million in 2015) in lost income taxation revenue, A$407 million (A$537 million in 2015) in additional transfer payments and around A$1.7 billion (A$2.2 billion in 2015) in gross domestic product.26
Welfare dependency
An Australian study by Morgan et al. relied on data from the 2010 national survey of psychotic illness and found that government pensions were the main source of income for 85% of the sample.27
Modelling mental health expenditure
Four studies adopted a longer-term timeframe to estimate the impact of mental illness. McCrone et al. estimated the cost of mental health expenditure in England for the next 20 years to 2026.28 The authors used a prevalence-based approach and derived estimates for depression, anxiety disorders, schizophrenic disorders, bipolar disorder and related conditions, eating disorders, personality disorder, child and adolescent disorders and dementia. The authors estimate the number of people in England who experience a mental health problem will increase by 14.2%, with health service costs estimated to increase by 45% to £32.6 billion in 2026 (at 2007 prices). A Canadian study by Smetanin et al. used modelling to generate an estimate of the current and future cost associated with major mental illness.29 The authors estimate that the total cumulative costs of mental illness over the next 30 years could exceed C$2.5 trillion dollars (equivalent to A$2.8 trillion in 2015). A separate study conducted by Schlander, examined future trends (2002–2012) of ADHD-related drug expenditures in Germany and the UK.30 The authors suggested a more than six-fold increase of pharmaceutical spending for children and adolescents is predicted over the decade from 2002 to 2012. Scott et al. assessed the costs to the public sector in dealing with children with different levels of antisocial behaviour.31 By the age of 28, costs for individuals with conduct disorder are 10.0 times higher than for those with no problems and 3.5 times higher than for those with conduct problems.
Discussion
This article provides a synthesis of a larger rapid review of the evidence for what is known about the potential short-, mid- and longer-term economic impact and cost of mental illness. The studies included in this review highlight the significant impact mental illness has on individuals, families, workplaces, society and the economy. A mental illness reduces the likelihood of: completing school, getting a full-time job, having a highly paid professional career and good quality of life. The findings suggest that people with psychotic illness have substantially poorer physical health than the general population and remain at considerably greater risk of higher levels of obesity, smoking, alcohol and drug use.27
Several gaps and unanswered questions are evident from this review. First, given the high prevalence of mental illness in our society, the review found limited research relating to the costs and impact of mental illness. In particular, more research is urgently required on disorders including ADHD, anxiety, cognitive function, conduct disorder, eating disorder and psychological distress, to better understand the economic impact of these illnesses. Second, although several studies assessed the relationship between mental illness and lost productivity, only one study had examined the economic impacts of supported employment.32 Given the potential importance of employment programs to mediate the negative impacts of mental disorders, further investigation into this area is warranted. Third, no evidence was found of the impact mental illness may have on intangible elements such as pain and suffering. Although it is important to understand direct and indirect costs, it is also important to develop a better understanding of the intangible suffering associated with mental illness. Fourth, although Canada and the UK have attempted to develop assessments of current and projected economic impacts of mental illness, no such estimates exist for Australia.
Understanding the burden of disease and economic cost of a disease provides the platform by which policy makers can make effective and informed decisions about priority areas and allocate resources to strategies (preferably cost-effective options) to reduce this burden.
Limitations
This research adopted a rapid-review approach; therefore, all key literature may not have been captured. Further, given that the majority of studies were identified from the peer-reviewed literature, there may be some possibility of publication bias in favour of research that publishes positive outcomes. Publication bias, or more specifically the inability to identify studies that report negative results, such as low- or no-cost implications, may distort any conclusions or recommendations. Further, as with any review process, there are potential problems with comparing studies conducted over different time and geographical region due to various methods and measures used. For example, in the review of published COI studies of depression, Luppa et al. found that across all studies, perspectives and methods differed substantially with only a few studies reporting indirect costs.33 The authors acknowledge that methodological differences restricted comparison across studies and recommend that results of COI should be linked to outcome data to increase effectiveness and efficiency in depression management.
Conclusion
The evidence generated from this rapid review highlight the significant impact mental illness has on the economy. With research suggesting that the economic costs associated with mental illness will increase six-fold over the next 30 years, it is imperative that we develop a better understanding of the impact of mental illness and cost-effective strategies to reduce this burden.
Competing interests
The authors declare no competing interests exist.
Acknowledgements
The New South Wales Mental Health Commission provided funding for this review.
References
[1] Department of Health and Ageing. National mental health report 2010: summary of 15 years of reform in Australia’s mental health services under the national mental health strategy 1993–2008. Canberra: Commonwealth of Australia; 2010.[2] Murray CJ, Vos T, Lozano R, Naghavi M, Flaxman AD, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, et al Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380 2197–223.
| Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010.Crossref | GoogleScholarGoogle Scholar |
[3] Australian Institute of Health and Welfare (AIHW). Australian burden of disease study: impact and causes of illness and death in Australia 2011. Canberra: AIHW; 2016.
[4] Australian Bureau of Statistics (ABS). National survey of mental health and wellbeing: summary of results. ABS Catalogue No. 4326.0. Canberra: ABS; 2008.
[5] Becker AE, Kleinman A. Mental health and the global agenda. N Engl J Med 2013; 369 66–73.
| Mental health and the global agenda.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC3sXhtFygu7zI&md5=082e83cc73fc40baa478f1aabb2126d7CAS |
[6] Department of Health and Ageing. National mental health report 2013: tracking progress of mental health reform in Australia 1993–2011. Canberra: Commonwealth of Australia; 2013.
[7] Degney J, Hopkins B, Hosie A, Lim S, Rajendren AV, Vogl G. Counting the cost: the impact of young men’s mental health on the Australian economy. Canberra: Inspire Foundation and Ernst & Young; 2012.
[8] Hilton M, Scuffham P, Sheridan J, Cleary C, Whiteford HA. Mental ill-health and the differential effect of employee type on absenteeism and presenteeism. J Occup Environ Med 2008; 50 1228–43.
| Mental ill-health and the differential effect of employee type on absenteeism and presenteeism.Crossref | GoogleScholarGoogle Scholar |
[9] Jacobs P, Dewa C, Lesage A, Vasiliadis HM, Escober C, Mulvale G, Yim, R. The cost of mental health and substance abuse services in Canada: a report of the Mental Health Commission of Canada. Alberta: Institute of Health Economics; 2010.
[10] Doran CM. The evidence on the costs and impacts on the economy and productivity due to mental ill health: an evidence check rapid review brokered by the Sax Institute for the Mental Health Commission of NSW. 2013. Available at: https://www.saxinstitute.org.au/wp-content/uploads/The-evidence-on-the-costs-and-impacts-on-the-economy-and-productivity-due-to-mental-ill-health-a-rapid-review.pdf. [verified 12 October 2017]
[11] Khangura S, Konnyu K, Cushman R, Grimshaw J, Moher D. Evidence summaries: the evolution of a rapid review approach. Syst Rev 2012; 1 10
| Evidence summaries: the evolution of a rapid review approach.Crossref | GoogleScholarGoogle Scholar |
[12] Australian Institute of Health and Welfare (AIHW). A working guide to international comparisons of health. Canberra: AIHW; 2012.
[13] Moher D, Liberati A, Tetzlaff J, Altman D, The PRISMA Group Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 2009; 6 e1000097
| Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement.Crossref | GoogleScholarGoogle Scholar |
[14] Drummond M, Torrance G, O’Brien B, Stoddart GL. Methods for the economic evaluation of health care programmes. New York: Oxford University Press; 2005.
[15] Mason J, Eccles M, Freemantle N, Drummond M. Incorporating economic analysis in evidence-based guidelines for mental health: the profile approach. J Ment Health Policy Econ 1999; 2 13–9.
| Incorporating economic analysis in evidence-based guidelines for mental health: the profile approach.Crossref | GoogleScholarGoogle Scholar |
[16] Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 2009; 6 e1000097
| Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement.Crossref | GoogleScholarGoogle Scholar |
[17] Doran CM. Economic evaluation of interventions to treat opiate dependence: a review of the evidence. Pharmacoeconomics 2008; 26 371–93.
| Economic evaluation of interventions to treat opiate dependence: a review of the evidence.Crossref | GoogleScholarGoogle Scholar |
[18] Leach L, Butterworth P. The effect of early onset common mental disorders on educational attainment in Australia. Psychiatry Res 2012; 199 51–7.
| The effect of early onset common mental disorders on educational attainment in Australia.Crossref | GoogleScholarGoogle Scholar |
[19] Schofield D, Kelly S, Shrestha R, Callander E, Percival R, Passey ME. How depression and other mental health problems can affect future living standards of those out of the labour force. Aging Ment Health 2011; 15 654–62.
| How depression and other mental health problems can affect future living standards of those out of the labour force.Crossref | GoogleScholarGoogle Scholar |
[20] Gibb S, Fergusson D, Horwood L. Burden of psychiatric disorder in young adulthood and life outcomes at age 30. Br J Psychiatry 2010; 197 122–7.
| Burden of psychiatric disorder in young adulthood and life outcomes at age 30.Crossref | GoogleScholarGoogle Scholar |
[21] Laplagne P, Glover M, Shomos A. Effects of health and education on labour force participation. Melbourne: Productivity Commission; 2007.
[22] Hilton M, Scuffham P, Vecchio N, Whiteford H. Using the interaction of mental health symptoms and treatment status to estimate lost employee productivity. Aust N Z J Psychiatry 2010; 44 151–61.
| Using the interaction of mental health symptoms and treatment status to estimate lost employee productivity.Crossref | GoogleScholarGoogle Scholar |
[23] Stansfeld S, Fuhrer R, Head J. Impact of common mental disorders on sickness absence in an occupational cohort study. Occup Environ Med 2011; 68 408–13.
| Impact of common mental disorders on sickness absence in an occupational cohort study.Crossref | GoogleScholarGoogle Scholar |
[24] Henderson M, Richards M, Stansfeld S, Hotopf M. The association between childhood cognitive ability and adult long-term sickness absence in three British birth cohorts: a cohort study. BMJ Open 2012; 2 e000777
| The association between childhood cognitive ability and adult long-term sickness absence in three British birth cohorts: a cohort study.Crossref | GoogleScholarGoogle Scholar |
[25] Paradise M, Naismith S, Davenport T, Hickie IB, Glozier NS. The impact of gender on early ill-health retirement in people with heart disease and depression. Aust N Z J Psychiatry 2012; 46 249–56.
| The impact of gender on early ill-health retirement in people with heart disease and depression.Crossref | GoogleScholarGoogle Scholar |
[26] Schofield D, Shrestha R, Percival R, Passey M, Callander E, Kelly S. The personal and national costs of mental health conditions: impacts on income, taxes, government support payments due to lost labour force participation. BMC Psychiatry 2011; 11 72
| The personal and national costs of mental health conditions: impacts on income, taxes, government support payments due to lost labour force participation.Crossref | GoogleScholarGoogle Scholar |
[27] Morgan VA, Waterreus A, Jablensky A, Mackinnon A, McGrath JJ, Carr V, Bush R, Castle D, Cohen M, Harvey C, Galletly C, Stain HJ, Neil A, McGorry P, Hocking B, Shah S, Saw S. People living with psychotic illness 2010: report on the second Australian national survey. Canberra: Commonwealth of Australia; 2011. Available at: http://www.health.gov.au/internet/main/publishing.nsf/content/717137a2f9b9fcc2ca257bf0001c118f/$file/psych10.pdf [verified 17 October 2017]
[28] McCrone P, Dhanasiri S, Patel A, Knapp M, Lawton-Smith S. Paying the price: the cost of mental health care in England to 2026. London: King’s Fund; 2008.
[29] Smetanin P, Stiff D, Briante C, Adair CE, Ahmad S, Khan M. The life and economic impact of major mental illnesses in Canada: 2011 to 2041. Toronto: RiskAnalytica, on behalf of the Mental Health Commission of Canada; 2011. Available at: https://www.mentalhealthcommission.ca/sites/default/files/MHCC_Report_Base_Case_FINAL_ENG_0_0.pdf [verified 12 October 2017]
[30] Schlander M. Impact of attention-deficit/hyperactivity disorder (ADHD) on prescription dug spending for children and adolescents: Increasing relevance of health economic evidence. Child Adol Psychiatry Mental Health. 2007; 1 13
| Impact of attention-deficit/hyperactivity disorder (ADHD) on prescription dug spending for children and adolescents: Increasing relevance of health economic evidence.Crossref | GoogleScholarGoogle Scholar |
[31] Scott S, Knapp M, Henderson J, Maughan B. Financial cost of social exclusion: follow up study of antisocial children into adulthood. BMJ 2001; 323 191
| Financial cost of social exclusion: follow up study of antisocial children into adulthood.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3MvislWgsQ%3D%3D&md5=b64cc389739b2d17cc9330c040673cbdCAS |
[32] Latimer E. Economic impacts of supported employment for persons with severe mental illness. Can J Psychiatry 2001; 46 496–505.
| Economic impacts of supported employment for persons with severe mental illness.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3MvosV2gtA%3D%3D&md5=5d540b8e125370f59e889d4402bdbc4cCAS |
[33] Luppa M, Heinrich S, Angermeyer M, König H, Riedel-Heller S. Cost of illness studies of depression: a systematic review. J Affect Disord 2007; 98 29–43.
| Cost of illness studies of depression: a systematic review.Crossref | GoogleScholarGoogle Scholar |



