Self-management of health care: multimethod study of using integrated health care and supportive housing to address systematic barriers for people experiencing homelessness
Cameron Parsell A C , Charlotte ten Have A , Michelle Denton B and Zoe Walter AA Institute for Social Science Research, The University of Queensland, St Lucia, Qld 4072, Australia. Email: c.tenhave@uq.edu.au; z.walter@uq.edu.au
B School of Nursing, Midwifery and Social Work, The University of Queensland, St Lucia, Qld 4072, Australia. Email: m.denton@uq.edu.au
C Corresponding author. Email: c.parsell@uq.edu.au
Australian Health Review 42(3) 303-308 https://doi.org/10.1071/AH16277
Submitted: 8 December 2016 Accepted: 1 March 2017 Published: 7 April 2017
Journal compilation © AHHA 2018 Open Access CC BY-NC-ND
Abstract
Objectives The aims of the present study were to examine tenants’ experiences of a model of integrated health care and supportive housing and to identify whether integrated health care and supportive housing improved self-reported health and healthcare access.
Methods The present study used a mixed-method survey design (n = 75) and qualitative interviews (n = 20) performed between September 2015 and August 2016. Participants were tenants of permanent supportive housing in Brisbane (Qld, Australia). Qualitative data were analysed thematically.
Results Integrated health care and supportive housing were resources for tenants to overcome systematic barriers to accessing mainstream health care experienced when homeless. When homeless, people did not have access to resources required to maintain their health. Homelessness meant not having a voice to influence the health care people received; healthcare practitioners treated symptoms of poverty rather than considering how homelessness makes people sick. Integrated healthcare and supportive housing enabled tenants to receive treatment for health problems that were compounded by the barriers to accessing mainstream healthcare that homelessness represented.
Conclusions Extending the evidence about housing as a social determinant of health, the present study shows that integrated health care and supportive housing enabled tenants to take control to self-manage their health care. In addition to homelessness directly contributing to ill health, the present study provides evidence of how the experience of homelessness contributes to exclusions from mainstream healthcare.
What is known about the topic? People who are homeless experience poor physical and mental health, have unmet health care needs and use disproportionate rates of emergency health services.
What does the paper add? The experience of homelessness creates barriers to accessing adequate health care. The provision of onsite multidisciplinary integrated health care in permanent supportive housing enabled illness self-management and greater control over lifestyle, and was associated with self-reported improved health and life satisfaction in formerly homeless tenants.
What are the implications for practitioners? Integrated health care and supportive housing for the formerly homeless can improve self-reported health outcomes, enable healthier lifestyle choices and facilitate pathways into more appropriate and effective health care.
Introduction
People who are homeless experience poorer physical and mental health than the broader population.1–3 They are also at greater risk of premature mortality.4 As homelessness endures, health deteriorates.5 Moreover, poverty driving homelessness means that health care is unaffordable6,7 and homeless people experience unmet health care needs.8 Kertesz et al.9 describe a paradox: homeless people have poor health and unmet health care needs, yet they use disproportionate emergency health services. Drawing on administrative data, Australian research shows that people who move from chronic homelessness into supportive housing use less emergency health care, and reduced health care offsets the costs of supportive housing.10
Reflected in the observation that it is pointless to treat a homeless patient and send them back to the social conditions that make them sick, housing is a social determinant of health.11 Housing is the most powerful prescription a physician could write for a homeless person.12
However, when people exit chronic homelessness and enter housing, they report only modest improvements in health.9,13 The complexity of ill health and previous experience of homelessness means that people’s health needs are not sufficiently met by mainstream health care.14
Integrated health care provided by an onsite multidisciplinary team combined with permanent supportive housing (PSH) for people who exit chronic homelessness aims to overcome long-term barriers to accessing mainstream health care.15 In Australia and internationally, PSH with integrated health care is adopted as a solution to chronic homelessness.16 However, the existing evidence does not demonstrate if and how people who exit chronic homelessness into PSH will use integrated health care.2
From the perspectives of tenants, the present study contributes to knowledge in two ways: first, by demonstrating how homelessness is experienced as a barrier to adequate healthcare; and, second, by examining how people exiting homelessness use and benefit from integrated health care and supportive housing.
Methods
Between September 2015 and August 2016, a mixed-methods study was conducted with a sample of tenants from one single-site PSH building in Brisbane (Qld, Australia). A survey (n = 75) was conducted first, followed by in-depth qualitative interviews (n = 20).
In the present study we draw on normative and theoretical literature on patients as co-designers of health care17,18 to locate the importance of taking seriously people’s first-hand experiences accessing health care. People’s positions as homeless or PSH tenants provides a fundamental perspective on what it means to access, or be excluded from, appropriate health care.
All 146 PSH tenants were invited to complete the survey. Seventy-five tenants voluntarily consented and completed the survey, administered face-to-face using an iPad (Apple) by two authors (CP, CtH). After surveys were completed, a maximum variation method was adopted to sample qualitative interview participants.19 The researchers sourced a list of tenants who had positive and negative experiences with integrated health care and who used the service for different reasons (chronic pain management, health literacy etc.). Tenants were recruited to ensure people with diverse experiences with healthcare were included. Ethics approval for the study was obtained from The University of Queensland’s Behavioural & Social Sciences Ethics Review Committee (Reference 2015001083 and 2016000409).
The survey measured perceptions of healthcare access and self-reported health, life satisfaction and autonomy. Survey items (Table 1) were selected to generate evidence to respond to the literature showing that people who are homeless report poor health and limited access to healthcare, and these problems are not immediately addressed with the provision of housing. Informed by survey data, qualitative interviews sought to understand how people used integrated health care, what it meant to them and how integrated health care differed from accessing healthcare as a homeless person. One author (CtH) conducted interviews face-to-face with tenants in a private office in the PSH building; interviews lasted 20–60 min. After 20 in-depth interviews, saturation was reached, whereby no new themes emerged.20

|
Interviews were professionally transcribed verbatim. Two authors (CP, CtH) read and reread the transcripts to identify initial codes and tentative themes. These two authors (CP, CtH) iteratively discussed themes and checked for the analytical link to transcripts.21 Then, all four authors scrutinised and discussed the data, explicitly searching for negative case analysis before refining themes.19 Rigour was further promoted through prolonged engagement by one of the authors (CP) with the tenants over 3 years.20 In-depth interviews and the survey achieved method triangulation;19 in-depth interviews add meaning to help explain survey results.
Survey data were analysed using mean (± s.d.), zero-order correlations and regressions. All analyses were performed in SPSS version 23 (IBM).
Results
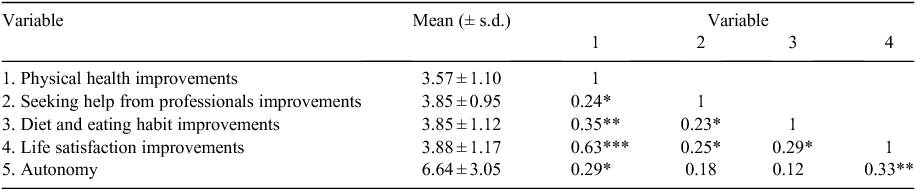
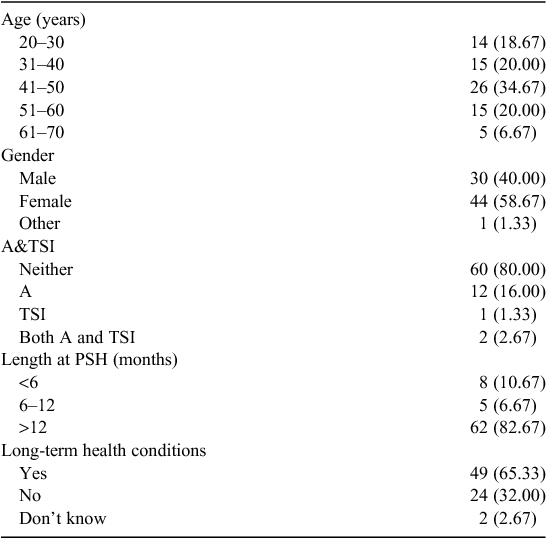
The characteristics of the tenants taking part in the survey are summarised in Table 2. Of the participants taking part in the in-depth interviews, 18 were female, 16 were non-Indigenous and the mean sample age was age 49 years (range 22–69 years). The survey results revealed that most tenants reported that living in PSH, compared with being homeless, was associated with improvements in seeking help from medical professionals, diet and eating, physical health and life satisfaction (Table 3). Several significant correlations were found (Table 4). Improvement in seeking help from medical professionals was associated with greater reported improved diet, physical health and life satisfaction. Improved diet was also positively associated with improved physical health and life satisfaction. Similarly, perceived autonomy was positively associated with improvements in health and life satisfaction, such that higher levels of perceived autonomy were associated with a greater perceived improvement in physical health and life satisfaction. Perceived autonomy accounted for 9% of the variance in improved physical health. Regression analysis found that improved diet was a stronger unique predictor of improved physical health (β = 0.31, t72 = 2.81, p = 0.006) compared with changes in help seeking from medical professionals (β = 0.16, t72 = 1.45, p = 0.152).
|

|
Improved physical health was a strong predictor of improved life satisfaction, accounting for 39% of the variance in life satisfaction improvements (β = 0.63, R2 = 0.39, F1,73 = 47.27, p < 0.001).
Gender, age, the presence of chronic health conditions and the length of PSH tenancy did not have an effect on the variables or the associations between variables.
Qualitative themes
Three themes were identified from the qualitative analysis: (1) homelessness as a barrier to adequate health care; (2) integrated health care solved barriers to access; and (3) integrated health care enabled illness self-management and control.
Homelessness as a barrier to adequate health care
To understand the meaning and function of integrated health care, it is necessary to grasp the living conditions that people experienced when homeless and how these created barriers to accessing adequate health care. Homelessness was experienced as a physical and symbolic assault to people’s sense of self:
I think when you’ve been on the streets a long time you sort of almost become a bit like an animal.
I noticed when it was really stormy and that I felt really good about myself being inside, because I’ve been underneath the church just before I came here. There were other squatters and I got really freaked out. I ended up on a toilet floor for about 3 days before I was here.
The descriptions of deprived living conditions when homeless foregrounds people’s experiences with integrated health care. The deprivations associated with homelessness undermined people’s sense of self-worth. This, in turn, limited people’s confidence to access health care and, importantly, to feel they had a say in the health care they received:
Well they just put you on medication and knock you out all day. You didn’t get to say a thing.
Homelessness meant not having a voice to influence how medical professionals saw and treated the homeless person’s presenting problems. As homeless, people perceived medical professionals would medicate without considering the consequences of housing exclusion. A tenant recalls:
…always just gave more medication. All right, it did work, but it’s no use just giving more medication when you don’t know what’s causing it.
The health care accessed, even when it did treat the presenting problem, did not consider ill health as symptomatic to homelessness. With the limited social power that comes with homelessness, people were not in a position to advocate for adequate health care, much less to advocate to have ‘the causes of the causes of ill health’ treated.11
Integrated health care solved barriers to health care access
Tenants experienced integrated health care and supportive housing as solving accessibility barriers to appropriate health care.
Well I can get everything I need here [at the PSH]. On the street you couldn’t. You had to wait in lines in hospital.
Yeah, because [support provider] will drop you off at your doctor’s and they pick you up if you can’t [walk]. With my emphysema I can’t walk that far, and my asthma, so they’ll drop me off and pick me up, which is good.
Solving accessibility barriers was critical because the consequences of homelessness compounded ill health. Ill health, in turn, further excluded people from adequate health care:
Tenant: I did have a [general practitioner], but he no longer wanted me to go to him.
Researcher: Why is that?
Tenant: Because I kept cancelling on him all the time; I wasn’t well. I was very sick and I was due for an operation and that’s why I couldn’t go anywhere. I couldn’t walk a certain distance.
Another tenant had a similar experience:
I was homeless a lot I used to have to make my way all the way to the [community organisations]. I used to see [general practitioner], she’s a really good doctor, but often you wouldn’t get around to it because you’d have to walk up these big stairs.
Healthcare resources located in PSH and the means by which transport to mainstream healthcare was facilitated made a demonstrable difference to people. Solving what are simple barriers meant that tenants no longer went without the health care they required. Illuminating the link between prolonged homelessness and deteriorating health,5 ill health when homeless was experienced as a barrier to health care access.
Illness self-management and control
People experienced homelessness as an inability to manage their day-to-day lifestyle to keep themselves healthy. The experience of homelessness prevented illness self-management. Homelessness resulted in exclusion from resources that are necessary to achieve a reasonable standard of positive health, well being and life satisfaction:
Because I was homeless before that…I was getting a lot of chafing and not keeping clean and dirty and unhygienic and even the bus driver basically threw me off the bus once recently, before I came in here, because I stunk. Well, he told me I stunk as I got off the bus.
Integrated health care and supportive housing was a practical resource for tenants to control the conditions of their lives that directly affected the self-management of their health care needs.
Researcher: How has taking your medication changed since moving to [PSH]?
Tenant: I take it a lot more now. Before I just used to take a bit here and there.
Researcher: So why is that different now to what it was before?
Tenant: Because in the boarding house you’ve got to share a toilet and bathroom and you can’t put your medication anywhere and some boarding houses don’t even have fridges in the room. With my diabetes and stuff, my insulin, I’ve got to put that in the fridge.
The tenant explained how having a refrigerator affected health not only by providing a safe place to store insulin, but also by providing a place to safely store food, and thus the capacity to eat a healthy diet, compared with living in a boarding house, where food was stolen.
Another tenant highlighted the importance of physical resources to promote security to self-manage their illness:
Researcher: So could you just explain a bit more about the biggest differences between living on the street and living here?
Tenant: Well the difference is it’s more safe. I don’t get stuff stolen anymore, you don’t get your [medications] taken.
Integrated health care enabled tenants access to knowledge so they could use the physical resources to control their health:
I had to change my diet because when I went to the hospital they just said, ‘You have very high potassium, extremely high.’ I went, ‘Okay.’ They said, ‘You just eat low potassium,’ I thought, ‘Well what’s potassium?’ I got all the help from here with my diet. We printed out potassium [information], the high levels of potassium, what’s in it. I now eat lower level potassium. That simple. I changed my diet around.
Integrated health care worked to translate information so tenants could act on specialist medical advice.
Tenant: I don’t understand all doctors [but the integrated health care provider] comes to my appointments.
Researcher: Why does he come to the appointments?
Tenant: Just so he can listen in, because sometimes I don’t understand it fully. He explains it on the way home because I don’t always understand everything my specialist says. It’s a bit hard for me. When we come back here he explains everything to me and then I understand it better.
When homeless, it is easy to conceptualise how exposure to the elements damages health and, in turn, how shelter is protective,15 but tenants added nuance to explain how homelessness meant exclusion from resources necessary to live a healthy lifestyle. Integrated health care was a resource actively used to access and benefit from healthcare professionals.
Discussion
In addition to the material deprivation of homelessness directly contributing to ill health, the present study provides evidence of how homelessness contributes to exclusions from mainstream healthcare. Developing the evidence about affordability barriers to accessing health care,6,7 homelessness was experienced as a devalued identity with limited power to be heard22 and thus to access and benefit from appropriate health care.9 From a devalued social position, being homeless meant that medical professionals treated the symptoms of their poverty, for example, treatment did not take account of how the social conditions of homelessness caused the ill-health. Perversely, the ill health exacerbated by homelessness5 constituted physical, often mobility, barriers to accessing mainstream healthcare. Ill health and homelessness worked in unison to prevent people from using mainstream healthcare.
Although we sought to have diverse tenants represented in the present study, our analysis is biased by including people engaged with integrated health care and who chose to participate. Thus, the data are not able to draw conclusions about people who are not engaged with integrated health care and for whom integrated health care may not address access barriers. Further, despite being advised that the research was interested in participants’ experiences, both positive and negative, in responding to the survey and interview questions participants may have felt compelled to offer positive and socially desirable reports of integrated health care and supportive housing.
Empowerment to control one’s life requires people to be enabled to access appropriate health care. The present data show how tenants actively used the resources available in integrated health care and supportive housing to access mainstream healthcare. The pattern of results in the quantitative analyses correspond to and reflect the themes of the qualitative analysis. Matching the in-depth interviews, most survey participants reported improved access to medical professionals, which predicted improved physical health and life satisfaction. Further, the finding that improved diet was a key predictor of physical health outcomes is reflected in the theme that integrated health care allows greater control over aspects of an individual’s life and self-management. In addition, having a sense of autonomy and control, a key theme in the qualitative analysis, was quantitatively related to increases in physical health and life satisfaction.23
The resources provided through integrated health care meant that people were no longer reliant on emergency or inadequate health care; rather, they were enabled to take control to manage their health needs. Integrated health care worked by acting as a conduit between tenants and mainstream healthcare systems. Coupled with the resources that housing enables, by providing transport, access to medical practitioners, advice and understanding of health care directions, integrated health care created the conditions for tenants to control their day-to-day lives and health care needs.
Autonomous decision making is an individual action enabled or constrained by the social context. Promoting autonomous health care decision making requires healthcare professionals to actively support patients rather than to leave them to make choices independently.24 In addition to the need to structure a personalised healthcare system to meet the needs of people with chronic and complex conditions,25 designing healthcare informed by the social position of marginalised groups is fundamental to enable them to take responsibility for their health care. Tenants were not passive recipients of health care services and their agency and experience need to inform how healthcare can be designed to meet their needs.17
Given that the conditions of homelessness are so detrimental to health, integrating health care with homelessness practice responses that do not end homelessness will be inadequate. Contemporary approaches that provide people living on the streets with basic hygiene resources, such as laundries and showers, are manifestly inadequate and perpetuate their devalued social position. As a social determinant of health, housing is a critical factor, but in the absence of mechanisms to address long-term exclusions, people who exit chronic homelessness will likely experience ongoing barriers to accessing mainstream healthcare. Integrating health care with supportive housing is a practical resource to address systematic barriers; the resources provided through integrated health care create the conditions for people to self-manage their health care.
Competing interests
None declared.
Acknowledgements
The research was funded by a grant from Micah Projects. Micah Projects funds and employs some of the healthcare professionals examined in the article. Micah Projects facilitated access to the tenants. Other than funding and enabling access, Micah Projects played no role in study design, data collection, analysis or writing. The researchers were independent of the funding body. Cameron Parsell receives funding from the Australian Research Council through a Discovery Early Career Researcher Award.
References
[1] Chin CN, Sullivan K, Wilson SFA. ‘Snap shot’ of the health of homeless people in inner Sydney: St Vincent’s Hospital. Aust Health Rev 2011; 35 52–6.| ‘Snap shot’ of the health of homeless people in inner Sydney: St Vincent’s Hospital.Crossref | GoogleScholarGoogle Scholar |
[2] Henwood BF, Cabassa LJ, Craig CM, et al Permanent supportive housing: addressing homelessness and health disparities? Am J Public Health 2013; 103 S188–92.
| Permanent supportive housing: addressing homelessness and health disparities?Crossref | GoogleScholarGoogle Scholar |
[3] O’Connell JJ, Swain S, Daniels C, et al. The health care of homeless persons: a manual of communicable diseases and common problems in shelters and on the streets. Boston: Boston Health Care for the Homeless Program; 2004.
[4] O’Connell JJ. Raging against the night: dying homeless and alone. J Clin Ethics 2005; 16 262–6.
[5] Johnson G, Tseng Y-P. Health and homelessness. In: Chigavazira A, Johnson G, Moschion J, et al., editors. Findings from Waves 1 to 5: special topics. Journeys Home Research Report No. 5. Melbourne: Melbourne Institute of Applied Economic and Social Research; 2014. Available at: http://melbourneinstitute.com/journeys_home/assets/pubs/2014/Scutella%20et%20al%20Journeys%20Home%20Research%20Report%20W5.pdf [verified November 2016].
[6] Bevitt A, Chigavazira A, Herault N, et al. Journeys Home Research Report No. 6: complete findings from Waves 1 to 6. Melbourne: Melbourne Institute of Applied Economic and Social Research; 2015. Available at: http://melbourneinstitute.com/journeys_home/assets/pubs/2015/Scutella%20et%20al%20Journeys%20Home%20Research%20Report%20W6.pdf [verified November 2016].
[7] Saunders P, Davidson P. Rising poverty is bad for our health. Med J Aust 2007; 187 530–1.
[8] Kertesz SG, McNeil W, Cash JJ, et al Unmet need for medical care and safety net accessibility among Birmingham’s homeless. J Urban Health 2014; 91 33–45.
| Unmet need for medical care and safety net accessibility among Birmingham’s homeless.Crossref | GoogleScholarGoogle Scholar |
[9] Kertesz S. Homelessness and health care. In Cockerham W, Dingwall R, Quah S, editors. The Wiley Blackwell Encyclopaedia of Health, Illness, Behavior, and Society. Chichester, West Sussex: John Wiley & Sons; 2014: pp. 1–11.
[10] Parsell CS, Petersen M, Culhane D. Cost offsets of supportive housing: evidence for social work. Br J Soc Work 2017;
| Cost offsets of supportive housing: evidence for social work.Crossref | GoogleScholarGoogle Scholar |
[11] Marmot M. Social determinants of health inequalities. Lancet 2005; 365 1099–104.
| Social determinants of health inequalities.Crossref | GoogleScholarGoogle Scholar |
[12] Doran K, Misa E, Shah N. Housing as health care – New York’s boundary-crossing experiment. N Engl J Med 2013; 369 2374–7.
| Housing as health care – New York’s boundary-crossing experiment.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC2cXhslGjs7Y%3D&md5=b91f50a27cb16f0cbe2570341ce5d300CAS |
[13] Hwang S, Gogosis E, Chambers C, et al Health status, quality of life, residential stability, substance use, and health care utilization among adults applying to a supportive housing program. J Urban Health 2011; 88 1076–90.
| Health status, quality of life, residential stability, substance use, and health care utilization among adults applying to a supportive housing program.Crossref | GoogleScholarGoogle Scholar |
[14] Hauff A, Secor-Turner M. Homeless health needs: shelter and health service provider perspective. J Community Health Nurs 2014; 31 103–17.
| Homeless health needs: shelter and health service provider perspective.Crossref | GoogleScholarGoogle Scholar |
[15] Henwood B, Stanhope V, Brawer R, et al Addressing chronic disease with supportive housing programs. Prog Community Health Partnersh 2013; 7 67–75.
| Addressing chronic disease with supportive housing programs.Crossref | GoogleScholarGoogle Scholar |
[16] Parsell CS, Petersen M, Moutou O. Single-site supportive housing: tenant perspectives. Housing Stud 2015; 30 1189–209.
| Single-site supportive housing: tenant perspectives.Crossref | GoogleScholarGoogle Scholar |
[17] Robert G, Cornwell J, Locock L, et al Patients and staff as codesigners of healthcare services. BMJ 2015; 350
| Patients and staff as codesigners of healthcare services.Crossref | GoogleScholarGoogle Scholar |
[18] Rose D. The contemporary state of service-user-led research. Lancet Psychiatry 2015; 2 959–60.
| The contemporary state of service-user-led research.Crossref | GoogleScholarGoogle Scholar |
[19] Kitto S, Chesters J, Grbich C. Quality in qualitative research. Med J Aust 2008; 188 243–6.
[20] Padgett DK. Qualitative methods in social work research. 3rd edn. New York: Sage; 2016.
[21] White B, Willmott L, Close E, et al What does ‘futility’ mean? An empirical study of doctors’ perceptions. Med J Aust 2016; 204 318
| What does ‘futility’ mean? An empirical study of doctors’ perceptions.Crossref | GoogleScholarGoogle Scholar |
[22] Lister R. Poverty. Cambridge: Polity; 2004.
[23] Marmot M. Social determinants and the health of Indigenous Australians. Med J Aust 2011; 194 512–13.
[24] Entwistle VA, Carter SM, Cribb A, et al Supporting patient autonomy: the importance of clinician–patient relationships. J Gen Intern Med 2010; 25 741–5.
| Supporting patient autonomy: the importance of clinician–patient relationships.Crossref | GoogleScholarGoogle Scholar |
[25] Dwyer JM, Duckett SJ. Restructuring primary health care in Australia. Med J Aust 2016; 205 435–6.
| Restructuring primary health care in Australia.Crossref | GoogleScholarGoogle Scholar |