Identifying factors behind the general practice use of the term ‘decline’ for the childhood immunisation programme in New Zealand
Nikki Turner 1 , Lynn Taylor 1 , Angela Chong 1 , Barbara Horrell 11 Department of General Practice and Primary Care, University of Auckland, Private Bag 92019, Victoria Street West, Auckland 1142, New Zealand
Correspondence to: Nikki Turner, Department of General Practice and Primary Health Care, University of Auckland, Private Bag 92019, Victoria Street West, Auckland 1142, New Zealand. Email: n.turner@auckland.ac.nz
Journal of Primary Health Care 9(1) 69-77 https://doi.org/10.1071/HC16031
Published: 17 February 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: The role of healthcare providers and their use of systems is one of the most important factors in vaccination uptake.
AIM: To identify reasons and find patterns behind why immunisation providers code the word ‘decline’ in their system for childhood immunisation events.
METHODS: A qualitative study involving face-to-face semi-structured interviews with staff members involved in immunisation delivery. General practices were purposively selected for having either high or low rates of registered children coded on the electronic practice management system as having declined immunisation events. Thematic analysis was undertaken using an inductive approach to link themes to the data.
RESULTS: A total of 35 interviews were conducted with practice nurses; 21 were from practices with high rates of registered children recorded as having declining immunisation events, and 14 practices with low rates of declining. Common themes were: effective use of systems, early and ongoing engagement, adequate health care practitioner time and practitioner experience. Practices with low rates of coded decliners had stronger approaches for early and ongoing engagement, and were less likely to use formalised decline forms. As practice immunisation coverage rates improved over time, there was perceived to be less expressed vaccine hesitancy from families.
CONCLUSIONS: The reasons for coding individuals as ‘decliners’ are a complex mixture of individual, community, practitioner and practice systems. Front-line providers need adequate tools, time and resourcing to support effective and ongoing engagement with families. Community factors have influence but can change over time.
KEYWORDS: Immunisation, Immunisation coverage, Primary care, Systems
| WHAT GAPS THIS FILLS |
| What is already known: Provider behaviour and use of provider systems is known to be an important part of vaccination uptake. |
| What this study adds: This study adds further understanding about why some providers code individuals as declining vaccination. Early engagement with families of infants, keeping dialogue open, less use of official declination forms and practitioner experience and time all are likely to lead to a reduction in patients coded as declining vaccination. |
Introduction
Despite compelling evidence of the benefits of childhood immunisation programmes, immunisation attempts internationally have failed to achieve high immunisation coverage targets.1 Much of the published literature has been around the contribution of communities and individuals, but a systematic review across all domains also noted the importance of health systems as part of the mix.2 Significant variability in immunisation coverage is associated with service delivery and with practitioners.3,4 The role of healthcare systems is an important factor in vaccination uptake, alongside the knowledge and attitude of front-line healthcare providers.5–7 Even within one system, there is significant variability between immunisation provider services in their ability to achieve and maintain high immunisation coverage.8 This variability may be due to characteristics of practices and practitioners, as well as parents, caregivers and the community they live in.9
The childhood immunisation programme in New Zealand (NZ) is delivered primarily through general practice by practice nurses, and occasionally by general practitioners. Children who have not responded to recall are referred to outreach immunisation services that are available through a range of local providers and offer flexible arrangements for vaccination; for example, by providing services in home or community settings. Reasons for failure to immunise are coded in an electronic system called a Practice Management Systems (PMS). The word ‘decline’ is used when healthcare providers entering the data assume that caregivers have actively chosen not to vaccinate, and ‘non-responder’ is used when families have not responded to messages to bring children in for vaccination.
This study was designed to identify reasons and find patterns behind why immunisation providers use the word ‘decline’. The study was deliberately designed not to focus on practices centred in communities where there are geographically high rates of decliners, but to consider approaches at the provider level, and to compare practices with high and low rates of childhood vaccination decline status.
Methods
Ethical approval was obtained from the Northern A Health and Disability Ethics Committee, reference 12/NTA/90/AM02.
In this qualitative study, structured interviews were undertaken with the key staff member(s) involved in immunisation systems and delivery in general practices. This is almost always a practice nurse. Practices were purposively selected for having high rates of registered children aged six weeks to two years of age coded as ‘decline’ (high decline) on their PMS. Comparator practices were from a similar geographical location and selected for having low rates of ‘decline’ (low decline).
Identifying participating general practices
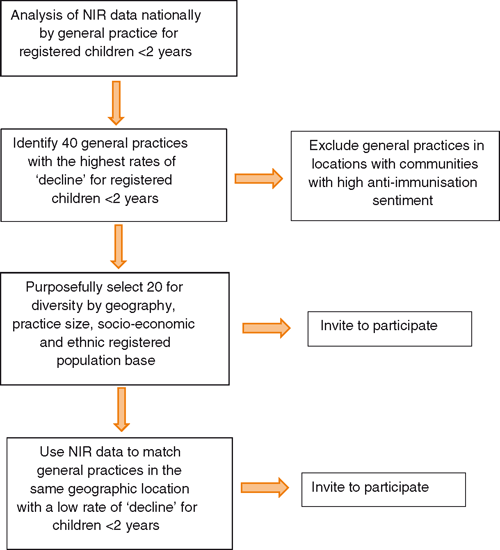
An ideal sample size of 20 high decline practices and 20 comparator low decline practices was based on previous research where theme saturation was reached well before interviews had been completed with 20 practitioners (Immunisation Advisory Centre, University of Auckland, unpubl. data). Figure 1 shows the recruitment process.
|
Immunisation decline rates were defined using National Immunisation Register data. Decline rates at the milestone ages of 6, 8, 12 and 24 months were listed by practice. Practices with high decline rates were defined as greater than, or equal to, twice the national average rate. The final list of practices was reviewed and study practices were selected to ensure a diverse range of registered patients based on practice size, geographical spread and socioeconomic and ethnic diversity.
Identified practices were matched one-to-one with practices that had low decline rates. These were defined as having less than, or equal to, half the national average for any of the milestones above, geographically located in the same district health board region and the same Primary Health Organisation as the matched practice selected with a high decline rate. The national average decline rates for the milestone ages for 6, 8, 12 and 24 months were 3.2%, 3.1%, 3.4% and 4.1%, respectively.
Practices in geographical areas where there were communities with high rates of immunisation hesitancy and refusal were excluded. These areas were defined by the regional immunisation advisors’ local knowledge of their communities. Also excluded were practices with less than 10 children born in the previous 12 months.
Recruitment of participants
Selected general practices were approached initially by the Ministry of Health. Written consent to participate was supplied by practice managers or their delegate. Each practice selected the study interviewees, who were Practice Nurses actively involved in the vaccination process. Excluded were non-vaccinating nurses, nurses working less than one day a week and temporary employees.
Data collection tools
A pre-visit questionnaire was used to gain general demographic background information on study practices including the patient population size, staff numbers and roles, locality and type of PMS. An interview questionnaire was developed based on earlier research that identified important components of immunisation service delivery in New Zealand general practice (Immunisation Advisory Centre, University of Auckland, unpubl. data). The areas covered in the interview included practice policy around enrolment processes, entering data and using codes in the PMS, beliefs around contraindications, and views on the reasons why families chose not to vaccinate or to selectively vaccinate. Table 1 shows the interview guide.

|
Semi-structured interviews with prompted questions were conducted onsite at the general practice by three researchers (LT, AC and BH). The interview times ranged from 35 min to 1 h.
Data entry and analysis
The researchers took written notes during each interview that were reviewed immediately following the interview to ensure data clarity and completeness. Notes were entered into Microsoft Excel spreadsheets (Microsoft Corporation, Redmond, WA, USA) alongside the questions from the interview schedule. Tabulating the data in this way highlighted commonalities and differences within high and low decline practices, thereby enabling comparisons between the two groups. Using thematic analysis,10 patterns (themes) within the entire dataset were identified. BH began the analysis by repeatedly reading the interviews to become familiar with the data, which were then organised according to the most interesting features. An inductive approach was used to link themes to the data11 rather than trying to fit the data into a pre-existing coding frame. In this sense, the analysis was data-driven. The themes were validated by a second reviewer, and refined by the other researchers during the writing process.
Results
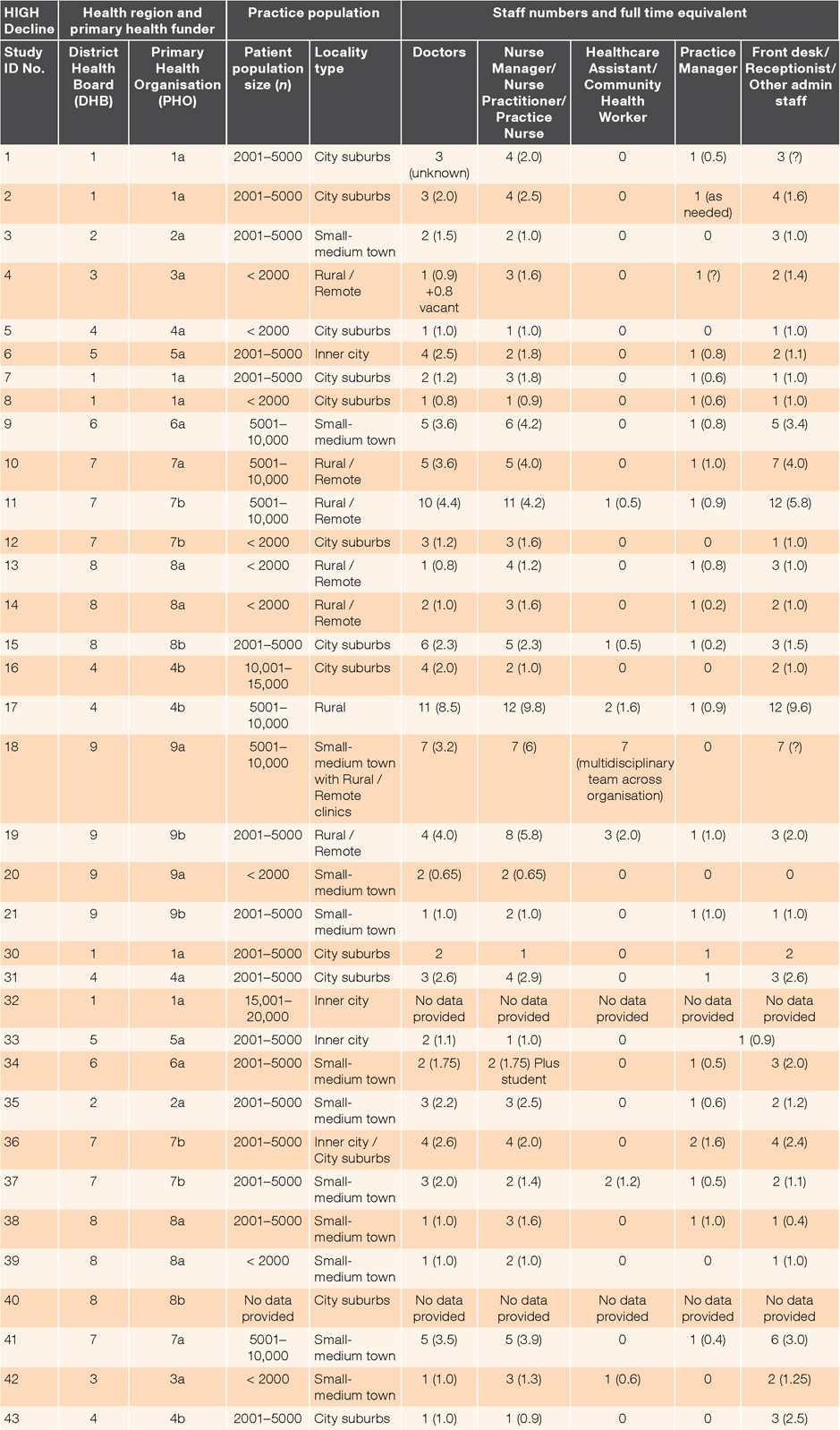
Thirty-five interviews were conducted in nine District Health Board regions; 21 were from practices identified as having high decline rates and 14 from practices with low decline rates. Table 2 shows characteristics of study practices. There were seven practices for which a low decline comparator practice was not able to be included. For two practices in one District Health Board area, no comparator practices could be identified (decline rates were all high), four comparator practices declined to participate (‘too busy’ or felt the approach to participate should have come via their Primary Health Organisation) and two comparator practices did not respond to the invitation or follow up.
|
Perceived reasons for family/caregivers declining immunisations
Similar challenges were identified by practice nurses in both high and low decline practices. These included particular communities with similar interests within the practice population whose natural lifestyles or religious beliefs did not match with the immunisation programme.
The influence of local anti-immunisation lobbyists and peer pressure via social media, coffee groups and the internet were all noted. One of the interviewers noted that natural remedies were being offered for sale at a high decline practice and, unlike other practices, this practice had no immunisation promotional posters in the waiting room.
Changes over time
Many participants noted changes over time. Participants from low decline practices in particular reported they were having less conversations around vaccine hesitancy than in past years, and they felt that not immunising was becoming less socially acceptable in many instances.
‘[we] aren’t having the same discussions that we had seven years ago’
‘[it is seen as] more socially acceptable now’
‘It is [now] irresponsible to not vaccinate’
A local measles outbreak was considered a turning point at one practice, where a shift in attitudes had been observed.
Practice procedures
Overall, high and low decline practices follow similar procedures with regard to recording declines in their PMS. However, there was a difference between practices in the use of formal decline forms, with just over half (52%) of high decline practices saying that they used a decline form, compared to just over one-quarter (28%) of low decline practices. Face-to-face conversations are the preferred form of communication between practice staff and parents, although phone conversations are also routinely used. Very few practices send text reminders to parents. Most participants said they make several attempts (usually at least three documented contacts) to talk about immunisations with parents and that conversations must be with nurses or doctors, rather than with receptionists or practice managers. Needing to take a gentle approach and not wanting to ‘get parents’ backs up’ was commonly stressed. While participants appeared willing to expend a great deal of effort in talking to parents about immunisation, and chasing overdue patients, one made the following observation:
‘The time/cost burden on the practice of managing decliners and catch up schedules for patients who have previously declined immunisations is significant. I find that parents who are wary of immunisation require extensive time – sometimes over several presentations to build the trust relationship where they feel comfortable deciding to go ahead with vaccinations. As a nurse who is passionate about education and advocacy for young children, I happily give this time but am aware it is at a cost to my employer’ [low decline practice]
Participants consistently reported that there needed to be prior evidence of discussion attempts and the offer of information to parents before recording a decline outcome. Using opportunistic moments (eg when parents come into the practice for other reasons) to discuss the benefits of immunisation or overdue vaccinations and having an ‘open door’ policy whereby parents are given the opportunity to change their minds, were commonly mentioned. Only one practice (a high decline practice) accepts a decline form with no prior face-to-face contact.
Both high and low decline practices use the outreach immunisation service to assist with immunisations. Most practices wait to see if receiving vaccination via the outreach service is successful in reaching reluctant and overdue patients before coding them as a decline.
There were some differences in the approach to registering newborn infants on their PMS. While notifications for newborns come electronically to the practice via the National Immunisation Register, all the high decline practices register infants only after they have received a signed enrolment form by the family. Practices with a low rate of decline were more likely to accept a nomination without the family needing to attend to sign up, particularly if the family was known to the practice.
Healthcare Practitioner
Experience
Staff experiences and longevity was perceived as a positive contributor to relationship building. Many practitioners in the low decline practices had been in their role for a substantial amount of time, with one mentioning she had held her role for 20 years.
‘…time to build up the knowledge’
‘…share life experience of seeing the disease in NZ’
One participant reported a child dying of meningococcal disease at 8 weeks of age, and another shared that her sister had been affected by their mother contracting rubella during pregnancy. In this way, personal lived experiences add to nurses’ views on immunisation and what they share with their patients. Additionally, many participants were mothers themselves. One stated that parents query her stance on immunisation, asking if she vaccinated her own children.
Discussion
The model of determinants of vaccine hesitancy endorsed by the World Health Organization endorsed identified the challenges around three key domains: contextual influences, individual and group influences, and vaccine and vaccination-specific influences.2 While healthcare providers frequently assume vaccine hesitancy is mostly related to community and family influences, the NZ experience has shown that provider and provider systems are likely to have the greater influence.9,12
Although this study was designed to identify differences between practices with high and low rates of decliners, it was notable that all practices took a similar systematic approach with most practice procedures. This included active and regular pre-call and recall, electronic recording and a stated commitment to the importance of face-to-face communication and documenting all contacts. Almost all have an ‘open door’ policy for parents to re-discuss, at any time, alongside using opportunistic moments to discuss overdue vaccinations. All practices actively used outreach immunisation services and see important benefit in this service.
Overall, there was little systematic difference in practices’ systems between practices with high or low rates of decliners. However, one exception was the enrolment process, which is the first step in patients’ engagement with general practice. Practices with lower rates of decline were more likely to accept nominated babies without further efforts required from the family. This is likely to enable early engagement, an important feature of an effective system.13
While there were no differences in terms of practice policy for decliners, many more of the practices with high rates of decline used an actual decline form, often requiring signatures of parents or guardians. This raises the possibility that use of ‘declination’ forms may not be the most useful approach at the practice level. Many practices noted the importance of keeping the dialogue open and using opportunistic moments to continue the discussion, whereas the use of official forms may shut down ongoing dialogue. Declination forms have been used effectively in adult influenza vaccination strategies,14 but these approaches may not translate to childhood programmes where repeated engagement with families is likely.
Most practices identified the Practice Nurse as the key person who recorded decliners, with this rarely being a task for general practitioners. This is consistent with all our earlier research on the importance of giving support and recognition to the role of the primary vaccinator in managing the systems for immunisation.15 Of note was the recurrent theme identifying the significant and often unrecognised time commitment to follow-up children who are overdue for vaccination and engage in conversations with caregivers who have vaccine hesitancy.
While all practices recognised members of their practice population who have divergent views on immunisation, there were differences in practitioner language around responses to this and the practice environment. At one practice with a higher decline rate, the interviewer noted there was less official promotional material and more interest in natural remedies apparent. The attitude of practices towards complementary or natural therapies could be worthy of further investigation in future research. Health practitioners are influenced by their own belief models and by the communities they live in.2 Both the confidence and knowledge of healthcare providers and their interactional skills in decision-making processes is known to be important.5 In many practices with lower decline rates, the Practice Nurses had been in the role for a very long period of time, up to 20 years in one instance, and were experienced parents themselves. This possible difference is worth consideration for future research, and these insights highlight the importance of ongoing support to front-line vaccinators to support both their knowledge base and their commitment to the importance of their work.16
In line with extensive international research, the practitioner-perceived range of challenges for families was similar across all practices. These included family and local community belief systems, effects of local anti-immunisation lobbyists, misinformation and the use of private research on the internet, anxiety of vaccines, lack of awareness of diseases and barriers to accessing the practice.2,17,18
An interesting finding was the reported reduction in community vaccine hesitancy over time and the issues apparently becoming more confined to identifiable populations and communities. New Zealand historically has had mediocre childhood immunisation coverage and has seen impressive gains in coverage with fully immunised 2-year-old rates improving by more than 15% in just over 10 years and almost complete closure of traditional socioeconomic status and ethnicity equity gaps.12 This improvement was driven almost entirely by a focus on targets, systems and provider education, but the result has also shown a significant shift in community attitudes and confidence in vaccination.12
We note several limitations in this study. First, as a qualitative study of healthcare professionals’ views, we cannot claim the views are fully representative or generalisable. We based our analysis on their perceived views. Practices usually have more than one Practice Nurse and we did not ascertain the views across the whole practice. Neither did we interview other members of the general practice team. While we can identify themes, we cannot quantify the relative merits of each theme. Furthermore, while this study attempted to exclude practices in communities that had high rates of vaccine refusal to avoid the effect of local communities on practices and practice systems, we could not fully control for this.
Conclusions
The reasons for coding ‘decliners’ are a complex mixture of individual, community, practitioner and practice systems. Reducing vaccine hesitancy requires focus on all aspects of the system. This study highlights the importance of providers in their active use of early and ongoing family engagement. Supporting front-line providers are the electronic systems, the tools, the time and resourcing decisions. We identified the importance of a systematic approach that does not close down the decision-making process with a single declination form, but allows re-engagement of conversations with vaccine-hesitant families. And finally, this study suggests that community factors do have influence but this can change over time, with support from confident providers making effective use of good general practice systems.
CONFLICTS OF INTEREST
LT was previously the General Manager of MedTech New Zealand, one of the PMS used by practices in this study. LT is currently the General Manager of DrINFO New Zealand, a practice audit tool used by ~50% practices in NZ to assist them to identify patients requiring intervention, including children overdue for scheduled immunisations.
ACKNOWLEDGEMENTS
Funding for this research was provided by the New Zealand Health Research Council in partnership with the New Zealand Ministry of Health.
We wish to acknowledge the support from the New Zealand Ministry of Health, the Primary Health Organisations and all the participating General Practices and their staff.
References
[1] World Health Organization Meeting of the Strategic Advisory Group of Experts on Immunization, October 2014 - conclusions and recommendations. Wkly Epidemiol Rec. 2014; 89 561–76.[2] Larson HJ, Jarrett C, Eckersberger E, et al. Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: a systematic review of published literature, 2007–2012. Vaccine. 2014; 32 2150–9.
| Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: a systematic review of published literature, 2007–2012.Crossref | GoogleScholarGoogle Scholar |
[3] Goodyear-Smith F, Grant C, Petousis-Harris H, Turner N. Immunization champions. Characteristics of general practitioners associated with better immunization delivery. Hum Vaccin. 2009; 5 403–11.
| Immunization champions. Characteristics of general practitioners associated with better immunization delivery.Crossref | GoogleScholarGoogle Scholar |
[4] Desmond N, Grant CC, Goodyear-Smith F, et al. Nurses make a difference in immunisation delivery. Aust J Adv Nurs. 2011; 29 28–35.
[5] Wang E, Baras Y, Buttenheim AM. “Everybody just wants to do what’s best for their child”: understanding how pro-vaccine parents can support a culture of vaccine hesitancy. Vaccine. 2015; 33 6703–9.
| “Everybody just wants to do what’s best for their child”: understanding how pro-vaccine parents can support a culture of vaccine hesitancy.Crossref | GoogleScholarGoogle Scholar |
[6] O’Leary ST, Allison MA, Fisher A, et al. Characteristics of physicians who dismiss families for refusing vaccines. Pediatrics. 2015; 136 1103–11.
| Characteristics of physicians who dismiss families for refusing vaccines.Crossref | GoogleScholarGoogle Scholar |
[7] Grant CC, Petousis-Harris H, Turner N, et al. Primary care practice and health professional determinants of immunisation coverage. J Paediatr Child Health. 2011; 47 541–9.
| Primary care practice and health professional determinants of immunisation coverage.Crossref | GoogleScholarGoogle Scholar |
[8] Pert H. An immunisation success story N Z Med J. 1999; 112 327 [letter].
| 1:STN:280:DyaK1MvitFWqsA%3D%3D&md5=4b7c8c98f111e1ad5d628da12ff0b376CAS |
[9] Grant CC, Turner NM, York DG, et al. Factors associated with immunisation coverage and timeliness in New Zealand. Br J Gen Pract. 2010; 60 e113–20.
| Factors associated with immunisation coverage and timeliness in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[10] Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006; 3 77–101.
| Using thematic analysis in psychology.Crossref | GoogleScholarGoogle Scholar |
[11] Patton M. Qualitative evaluation and research methods. SAGE Publications, Inc.; 1990.
[12] Turner N. The challenge of improving immunization coverage: the New Zealand example. Expert Rev Vaccines. 2012; 11 9–11.
| The challenge of improving immunization coverage: the New Zealand example.Crossref | GoogleScholarGoogle Scholar |
[13] Goodyear-Smith F, Grant C, Poole T, et al. Early connections: effectiveness of a pre-call intervention to improve immunisation coverage and timeliness. J Prim Health Care. 2012; 4 189–98.
[14] Jaiyeoba O, Villers M, Soper DE, et al. Association between health care workers’ knowledge of influenza vaccine and vaccine uptake. Am J Infect Control. 2014; 42 69–70.
| Association between health care workers’ knowledge of influenza vaccine and vaccine uptake.Crossref | GoogleScholarGoogle Scholar |
[15] Desmond N, Grant CC, Goodyear-Smith F, et al. Nurses make a difference in immunisation service delivery. Aust J Adv Nurs. 2011; 28 27–35.
[16] Turner N, Grant C, Goodyear-Smith F, Petousis-Harris H. Seize the moments: missed opportunities to immunize at the family practice level. Fam Pract. 2009; 26 275–8.
| Seize the moments: missed opportunities to immunize at the family practice level.Crossref | GoogleScholarGoogle Scholar |
[17] Pearce A, Marshall H, Bedford H, Lynch J. Barriers to childhood immunisation: findings from the longitudinal study of Australian children. Vaccine. 2015; 33 3377–83.
[18] Omer SB, Salmon DA, Orenstein WA, et al. Vaccine refusal, mandatory immunization, and the risks of vaccine-preventable diseases. N Engl J Med. 2009; 360 1981–8.
| Vaccine refusal, mandatory immunization, and the risks of vaccine-preventable diseases.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BD1MXlsFCqtL0%3D&md5=6d16d7ab6f48406ce4b27f99c6ebacb8CAS |


