Changing perspectives of the role of community pharmacists: 1998 – 2012
Linda Bryant 1 , Joanne Maney 2 , Nataly Martini 21 Department of General Practice and Primary Health Care, Faculty of Medical and Health Sciences, The University of Auckland, Private bag 92019, Auckland, New Zealand
2 School of Pharmacy, Faculty of Medical and Health Sciences, The University of Auckland, Private bag 92019, Auckland, New Zealand
Correspondence to: Nataly Martini, School of Pharmacy, Faculty of Medical and Health Sciences, The University of Auckland, Private bag 92019, Auckland 1010, New Zealand. Email: n.martini@auckland.ac.nz
Journal of Primary Health Care 9(1) 34-46 https://doi.org/10.1071/HC16032
Published: 10 February 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: In New Zealand, extended medicines management roles proposed for pharmacists include the optimisation and monitoring of medicines in patients with long-term conditions through greater collaboration with general practitioners (GPs). Although some collaborative roles have been successfully implemented in hospitals, barriers for both pharmacists and GPs hinder interprofessional working relationships in the community.
AIM: To compare data from a 2012 study with two previous studies (1998, 2002) examining perceptions of community pharmacists and GPs of the expanding medicines management roles of community pharmacists.
METHODS: In 2012, a survey, modelled on the 1998 and 2002 studies, was sent to 600 community pharmacists and 600 GPs. Analyses considered the five-point Likert scale to be a continuous variable. A change of ≥ 10% between any two surveys indicated a relevant change for comparison.
RESULTS: Increasing agreement, which differed considerably between professions, was apparent for most expanding medicine management roles over the 14 study years. In all three studies, pharmacists were open to expanding their roles to include monitoring, screening, advisory and prescribing roles. GPs were most accepting of the traditional dispensing role with a positive shift towards pharmacists’ involvement in medicines management over time.
DISCUSSION: Over 14 years, GPs became more accepting of community pharmacists’ involvement in extended medicines management roles, although still had low acceptance of the more clinical roles. Pharmacists considered increased involvement in medicines management as their role, but appeared to lack confidence in their ability to do this role.
KEYWORDS: Pharmacy services; general practitioners; primary health care; workforce
| WHAT GAP THIS FILLS |
| What is already known: Successful, collaborative, interprofessional relationships between general practitioners and community pharmacists require positive endeavour and communication from both parties. Implementation of practical systems to standardise practice are required for pharmacists to have credibility in extended roles. |
| What this study adds: There is a gradual shift by both general practitioners and pharmacists in accepting the expanding roles of community pharmacists. Although levels of acceptance differ considerably between the two professions, certain barriers still exist. Pharmacists remain concerned about how medicines management will be implemented, and whether their clinical knowledge and training is adequate to undertake this role. |
Introduction
Proposed extended roles for community pharmacists in New Zealand include prevention of drug-related adverse events,1 optimising and monitoring medicines in patients with long-term health conditions through greater collaboration with general practitioners (GPs),2 promotion of patients’ health, wellbeing and self-care,2 and a collaborative prescribing role.3 Some of these extended roles have been successful in hospitals, where doctors are familiar with clinical pharmacists participating in drug management,3 but relationships between community pharmacists and GPs are less formalised. Perceived professional barriers prevent comprehensive interprofessional working relationships.3
Pharmacist-perceived barriers to expansion of their roles include a lack of orientation to take on new roles,4–7 and perceptions that some roles are not legitimate for pharmacists.6 Other pharmacists perceive they lack knowledge and clinical problem-solving skills, so feel uncomfortable with the accountability that is integral to these services.6,8,9 External factors include beliefs that pharmacists do not have the mandate from the government, GPs, or patients to undertake new roles.5,6
GPs’ perceptions of pharmacists may determine their willingness to collaborate.10 Historically, the ‘shop keeping’ role of community pharmacists has resulted in their being perceived as tainted health professionals1,11 who might act for commercial gain and not in the patients’ best interests.3,12,13 GPs report more distrust of pharmacists practicing in pharmacy chains,11 and many GPs preferred an interprofessional model that involves pharmacists located within their practices and working directly with GPs.3 Furthermore, GPs’ lack of knowledge regarding pharmacists’ professional training, responsibilities and continuing professional development obligations,3,11,14 and their professional skills and strengths, has resulted in contributions made by pharmacists to patient-focused services being undervalued.6,15 GPs have also expressed concerns about pharmacists taking on GP roles such as screening, monitoring and prescribing.2,3,11,16,17
In part, the issue is that pharmacists’ roles appear ill-defined and on the periphery of primary healthcare teams,3 so pharmacists have been viewed as subordinates to GPs who consider themselves the decision-makers and ultimately responsible for patient outcomes.11,18 Pharmacists’ attempts to re-professionalise have been reported as threatening to GPs’ status, autonomy and control.2,11 When working collaboratively, role clarification for both professions is paramount.8,18–21
GPs have also been reluctant to use services led by pharmacists they did not trust, respect or have confidence in, with regard to competence and quality of cognitive services.1,11,12,14,18 Good communication19,21–23 and effort from both parties is required to build successful collaborative, interprofessional relationships.12,18 For pharmacists to have credibility in extended roles, practical systems need to be implemented to standardise practice.11
In 1998 and 2002, surveys of GPs’ and community pharmacists’ perceptions of the role of community pharmacists and barriers to increasing their roles were undertaken across New Zealand.5,24 The aim of this 2012 study was to repeat the survey to determine whether perceptions had changed over time and in what domains this might have occurred. A focus of all three surveys was on the role of pharmacists in medicines management, which ‘… identif[ies] potential and actual medicines therapy problems including non-compliance, adverse effects and monitoring for effectiveness. The aim is to optimise the use and benefit of medicines … by pharmacists and GPs working together using a structured, documented process and regular meetings.’5 This definition aligns with the concept of pharmaceutical care, as originally defined by Hepler and Strand.25
Methods
The study approved by the University of Auckland Human Participants Ethics Committee (Reference: 8231).
Participant selection
Questionnaires were sent to 600 community pharmacists and 600 GPs, based on power calculations from the 1998 and 2002 surveys. Pharmacists were randomly selected from a list of 1300 community pharmacists who held a current Annual Practicing Certificate and agreed to release their address for research. GPs were selected via random selection from the Medimedia® database of all New Zealand GPs. Exclusion criteria included ‘specialist’ practice; for example, Poisons Centre and travel medicine.
Questionnaire design
The original questionnaire was developed through key informant interviews and refined through piloting.5 Using statements and level of agreement, Part A explored perceived roles that community pharmacists should be involved in. Part B explored potential barriers to involvement of community pharmacists in medicines management services, using five-point Likert scales. Comments were encouraged in free-text boxes (not reported in this paper).
Data collection and entry
In 2012, two mailings of the survey were sent 3 weeks apart with a prepaid return envelope addressed to a Justice of Peace (JP) who marked off the returns against a master sheet of names and unique identifiers. The JP forwarded to the researcher the list of non-responders to allow for resending and, for analysis, completed questionnaires identified only by a uniquely assigned number.
For each of the three studies, survey data were double entered into two separate databases by JM and an independent party. The two entry sets were compared for accuracy. Discrepancies were corrected by referral to original survey documents, and data were converted to SPSS® Version 20 (IBM SPSS Inc., IL, USA) for analysis.
Data analysis and statistical applications
Quantitative analysis assumed five-point Likert scales to represent continuous variables.
Attempting to update original files from the 1998 and 2002 surveys, analysed with IBM SPSS® Version 15, corrupted those files, and so prohibited statistical tests comparing the three surveys. Consequently, positive responses (strongly agree and agree) were grouped as ‘yes’ and negative responses (strongly disagree and disagree) were grouped as ‘no’ and presented as a percentage using published data from the 1998 and 2002 surveys.5,24
Changes of ≥ 10% in the ‘yes’ percentage of respondents between any two surveys was deemed an important change in perception. The rationale for this came after analysis of variance was applied to the 1998 and 2002 data and significant outcomes were further explored using the method of Tukey to preserve an overall significance of 5%; this was then fixed at 10% due to the multiple survey questions. Multiple linear regression was used to build models explaining the association between responses after adjustment. The same criteria were used to enable comparisons between the three studies.
A role was considered ‘acceptable’ if more than 75% of respondents definitely or probably agreed (1 and 2 on the Likert scale); ‘ambivalent’ when 50–75% of respondents definitely or probably agreed; and when fewer than 50% definitely or probably agreed, the respondents were deemed to ‘oppose’ the role.
From the previous surveys, themes for the barriers emerged, and were confirmed by factor analysis.24 The main themes were mandate, legitimacy, adequacy, effectiveness and change.5,24
Results
Survey response rates and demographics
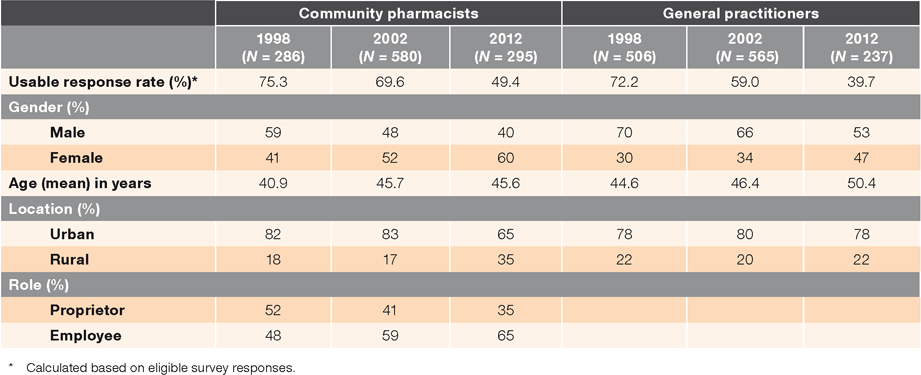
For both professions, there was a steady and substantial decline in response rates, and the number of male responses declined by 20% between 1998 and 2012 (Table 1). A significant (P < 0.0001) decrease in the percentage of proprietor pharmacists was seen between 1998 and 2002, which continued to decline in 2012. For both professions, there was a significant increase in the age of respondents between 1998 and 2002 (pharmacists: P < 0.0001; GPs: P = 0.002), with a further increase in the 2012 survey for GPs.
|
Comparison of pharmacists’ and GPs’ responses to the role of community pharmacists
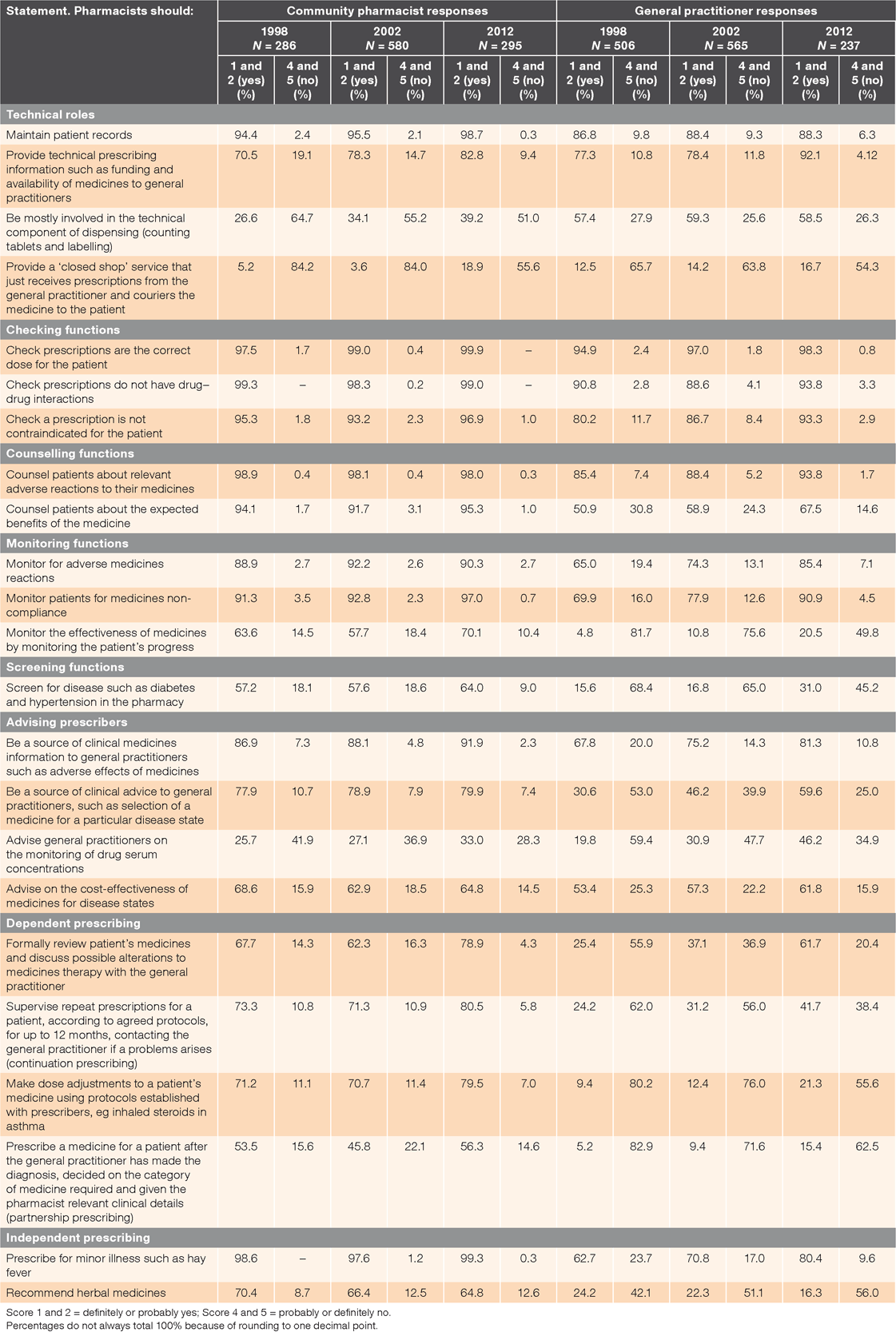
Pharmacists’ agreement increased for four of the 23 roles discussed: three technical roles and the dependent prescribing role. GPs’ agreement increased for 14 roles and moved from opposition to ambivalence regarding pharmacists’ involvement with medicines management (Table 2).
|
Technical and checking roles
Both professions increasingly found it acceptable for pharmacists to provide technical prescribing information to GPs and remained opposed to pharmacists receiving prescriptions from GPs and couriering medication to patients; however, pharmacists showed increasing agreement for this role in 2012. Although opposed to being mostly involved in the technical aspects of dispensing, pharmacists showed increasing agreement with this role; GPs remained ambivalent.
Counselling, monitoring and screening
Both groups accepted that patient counselling on adverse effects was a pharmacist role. However, whether pharmacists should counsel on expected benefits of medicines was still ‘ambivalent’ in 2012 by GPs, despite a 16.6% increase between 1998 and 2012.
Important changes were seen for monitoring for adverse medicine reactions and medicines non-compliance, which saw GPs move from ambivalence to acceptance. This 10% increase was also seen for monitoring of patients’ progress – a pharmacist role still opposed by GPs in 2012.
GPs were consistently opposed to pharmacists screening for conditions such as diabetes and hypertension, but a 15.4% increase in agreement was seen from the first survey.
Advising prescribers
There was little change in pharmacists’ responses regarding their medicines advisory role. GPs moved from ambivalence to acceptance (+13.5%) between 1998 and 2012, and from opposition to ambivalence (+29.0%) for pharmacists being a source of clinical medicines information and advice on medicines selection, during the same timeframe. Both professions opposed pharmacists advising on therapeutic drug monitoring, although GPs increased agreement over time. Pharmacists moved from ambivalence to acceptance (+11.2%) and GPs from opposition to ambivalence (+36.3%) in accepting pharmacists formally reviewing patients’ medicines and discussing alterations with GPs.
Dependent prescribing
In 2012, continuation prescribing of medicines was considered an acceptable role by pharmacists, while GPs remained in opposition, despite a 17.5% increase since 1998. Similarly, making dosage adjustments to patients’ medicines was considered acceptable by most pharmacists, but although an 11.9% acceptance increase was seen since 1998, GPs remained opposed.
Pharmacists remained ambivalent regarding partnership prescribing. In 2012, only 15.4% of GPs considered this an acceptable role (+10.2%).
Independent prescribing
Pharmacists agreed that prescribing for minor illness was a recognised and regular component of their daily work, with agreement from GPs in 2012 (+17.7%). Pharmacists remained ambivalent about herbal products, with GPs becoming more strongly opposed to this.
Barriers to increased community pharmacist involvement in medicines management
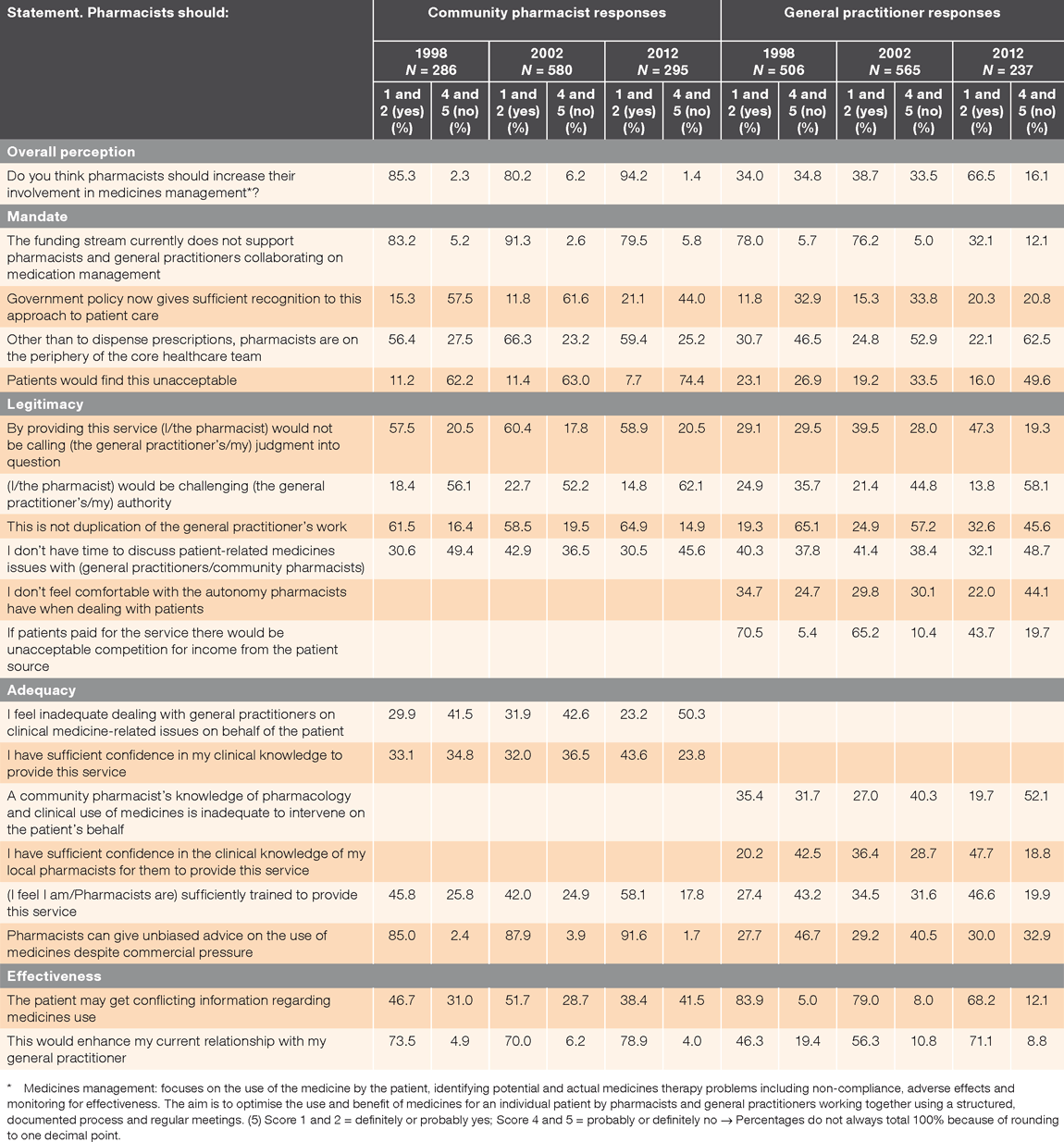
Pharmacists changed their level of agreement for eight of the 23 statements, and GPs increased their level of agreement for 17 barriers (Table 3). Neither profession perceived that pharmacists had a mandated role in the medicines management service or that it was a legitimate role for community pharmacists, or that pharmacists have adequate knowledge and skills to be effective in providing this service. Potential resistance to change for both professions was high, although GPs appeared to be more accepting of change. Pharmacists accepted increased involvement in medicines management, while GPs moved from initial opposition in 1998 (34.0%) to ambivalence (66.5%) in 2012.
|
Mandate
Pharmacists agreed that government funding did not support medicines management services. Conversely, only 32.1% of GPs agreed with this statement, a 45.9% decline from 1998.
Almost 60% of pharmacists still felt that they were on the periphery of the healthcare team in 2012, while only 22.1% of GPs thought so.
Legitimacy
GPs moved towards ambivalence that medicines management would not question their judgment, and although 13.8% still agreed that pharmacists would challenge their authority, this declined from 24.9% (–11.1%). Pharmacists were ambivalent about the service duplicating GPs’ work, but GPs remained hesitant. Over time, GPs became less uncomfortable with pharmacists’ autonomy with patients, even though responses consistently demonstrated disquiet. In 2012, less than half of GPs believed that there would be competition for income from patients, a marked change from 70.5% in 1998.
Adequacy
Less than half of both professions were confident that pharmacists’ clinical knowledge was sufficient to provide a medicines management service. Pharmacists agreed they were able to provide unbiased advice; GPs remained doubtful.
Effectiveness
GPs demonstrated substantially higher concern that medicines management services may result in patients receiving conflicting medicines information, although they became less concerned over time. Pharmacists accepted that medicines management would enhance intercollegial relationships and improve patient medicine-related health outcomes. GPs moved from opposition to ambivalence for both these statements, with a 24.8% and 23.6% change in agreement over time, respectively.
Change
Pharmacists were consistently ambivalent as to whether the current health environment provided a good opportunity to refine roles, while GPs remained opposed to this statement. GPs indicated less resistance to adapting to new roles over the time period, with 60.7% agreeing in 1998 that there were enough changes in the health system without having to cope with new changes, compared to 29.2% in 2012.
Discussion
Over the past decade, an increase in demand for healthcare services constrained by limited resources has resulted in major changes in primary health care.26,27 Recognition of under-utilisation of community pharmacists’ training and skills has presented opportunities for developing the profession through provision of services beyond the traditional supply function.28 This study aimed to examine the effects of time and a dynamic healthcare environment on the perceived role of community pharmacists.
Technical, checking, counselling and monitoring roles
Both GPs and pharmacists generally accept the traditional community pharmacist roles of dispensing, checking and counselling, and also for increased involvement in more clinical aspects of medicines management. Exceptions to the agreement between pharmacists and GPs were: counselling on expected benefits of medicines and monitoring for the effectiveness of medicines.
Advisory role
More divergence was seen around perceived clinical roles, which may be expected, as this has traditionally been considered GP territory. Community pharmacists in all three studies agreed with the role of advising GPs on the adverse effects of medicines, with GPs increasing their agreement over time. This may be due to escalation in the complexity of medication regimens, a result of an ageing population, an increase in the number of patients with multiple chronic conditions, and the advent of new medicines. GPs remained opposed to this role, but the level of disagreement diminished over time, consistent with the advent of practice and Primary Health Organisation pharmacist facilitators, an evolving role for pharmacists.
Medication review and continuation prescribing
Performing in-depth clinical medication reviews is a departure from traditional community pharmacist roles. Results demonstrated an increase in the percentage of respondents agreeing that pharmacists should increase their involvement in medicines management services. However, during this time, an adherence support service (Medicines Use Review) was introduced, and some respondents may have interpreted this statement to refer to the adherence support service rather than full clinical medication reviews. Success of medication review services depends on adequate training for pharmacists,7 appropriate patient selection,29,30 quality assurance of the service through peer review,31 communication and collaboration with GPs, allocation of sufficient time to undertake the service,29 and adequate remuneration. Pharmacists’ heavy involvement in the dispensing process, commercial intent, and patients’ lack of awareness of pharmacists’ ability to offer this service constrain the effectiveness of the service.32
Both professions showed increased agreement with the extended roles of continuation and protocol prescribing, although GPs remained opposed to this role. Pharmacist-led repeat and continuation prescribing implemented in the United Kingdom since 2004 has been well received by GPs,33 is logistically feasible, identifies and addresses clinical problems, and has resulted in cost savings.34 Pharmacist involvement in repeat or continuation prescribing has overcome many of the documented problems associated with traditional systems for repeat prescribing (including medicine stockpiling and inappropriate treatment), resulting in improved patient outcomes.33
In this study, an apparent conflict was noted in the perceptions of community pharmacists and their perceived clinical roles, and their view of adequacy to undertake this role. Part B of the survey found feelings of inadequacy, lack of confidence in clinical knowledge, and less than 60% of pharmacists felt sufficiently trained. Although perceptions of inadequacy have been identified previously, this discrepancy in perceived roles versus perceived ability needs to be explored further, but may explain why, when opportunities are presented, extensive implementation fails.5 Concerns were also noted regarding the need for adequate training, appropriateness of the role for community, as opposed to specialist, pharmacists and the need for unambiguous delegation of overall responsibility.
Investigation of the culture of the pharmacy profession35,36 has revealed characteristics including lack of confidence, aversion to change, and apparent unwillingness to leave the comfort of the dispensary. This may be impeding the profession’s advancement; attitudes held by pharmacists may be sabotaging the development of the profession.
In June 2013, New Zealand legislation permitted the role of prescribing pharmacists. This is a specialist and not a community pharmacist role, and possibly a reason for an increase in agreement over time by pharmacists for all dependent prescribing roles apart from formal review services. Conversely, although GPs remained opposed to all dependent prescribing roles, except for the formal review service, the decrease in the level of opposition over time was noteworthy. The pharmacist prescriber role is uncharted territory for New Zealand’s pharmacy profession and has been viewed as a major advance in the recognition of pharmacists’ skills and a positive step towards their inclusion into core healthcare teams. Nevertheless, many issues discussed previously need to be resolved so that prescribing pharmacists can be effective in their new role.
Prescribing for minor illness and recommending herbal medicines
Pharmacists prescribing through the Pharmacist Only Medicine classification allows pharmacists to select appropriate medication for specific conditions in accordance with guidelines and after consultation with patients, providing some recognition of skills to undertake this cognitive service.37 Convenience,38 accessibility39 and trustworthiness39,40 have resulted in local pharmacies often being the triage centre for healthcare advice, a valid (mandated) role acknowledged in this study by GPs. Over time, GPs’ opinions went from ambivalence (1998) to agreement (2012) for this role.
GPs remained opposed to pharmacists recommending herbal medicines, suggesting pharmacists would rather make a sale than adhere to evidence-based practice for particular remedies. The tainted ‘shopkeeper’ role has been well documented.1,11 Although pharmacists remained ambivalent over time, results concurred with the requirement for scientific evidence and better training when recommending herbal medicines.
Study limitations
The poorer response rate from pharmacists in the 2012 survey may have been due to the timing of the survey coinciding with the implementation of the new community pharmacist national contract, which caused distress among community pharmacists. The difference in the pharmacist demographics across the studies may also have influenced response rate and responses.
The low GP response rate may be attributed to a lack of time and the policies of some general practices, which avoid survey participation. A potential bias may be introduced if more ‘pharmacy-friendly’ GPs responded to the survey.
Responses may have been skewed by the tendency of survey respondents to provide socially desirable responses; however, participant anonymity is likely to have minimised this effect.
The inability to undertake comparative statistical analysis of the 2012 results with previous surveys limited analysis to the identification of trends, but still provides useful information on changes in perceptions over time, and barriers that remain if community pharmacists are to extend their role in health care.
Conclusion
Over a 14-year period, this study has shown increased agreement by both GPs and pharmacists for expanding roles for community pharmacists, but levels of agreement differed considerably between the two professions. Pharmacists were open to expanding their role to include services such as medicines management, monitoring, screening, advisory and prescribing roles, but expressed concern on how this would be implemented and identified a lack of confidence in their clinical knowledge and training. Only about half considered they have adequate skills to undertake clinical roles. GPs demonstrated less agreement for all roles. While accepting of the traditional dispensing role, they were less supportive of other roles, although there was a gradual shift towards agreement concerning pharmacists’ involvement in medicines management.
With the evolution of pharmacists’ roles, the future focus of research is likely to change to the general practice environment. For the pharmacy profession and universities, there is a need to explore the contrasting perception of the community pharmacists and the roles that they think they should be undertaking, and the lack of confidence in their adequacy to do these roles.
Conflicts of interest
None.
Acknowledgements
The authors would like to thank Professor Janie Sheridan for editing the manuscript.
References
[1] Rigby D. Collaboration between doctors and pharmacists in the community. Aust Prescr 2010; 33 191–3.| Collaboration between doctors and pharmacists in the community.Crossref | GoogleScholarGoogle Scholar |
[2] Edmunds J, Calnan MW. The reprofessionalisation of community pharmacy? An exploration of attitudes to extended roles for community pharmacists amongst pharmacists and General Practitioners in the United Kingdom. Soc Sci Med 2001; 53 943–55.
| The reprofessionalisation of community pharmacy? An exploration of attitudes to extended roles for community pharmacists amongst pharmacists and General Practitioners in the United Kingdom.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3MvnvVKntQ%3D%3D&md5=76859536d68ad95a4a687237fd2d572eCAS |
[3] Hughes CM, McCann S. Perceived interprofessional barriers between community pharmacists and GPs: a qualitative assessment. Br J Gen Pract 2003; 53 600–6.
[4] Zellmer WA. Pharmacy’s future: transformation, diffusion, and imagination. Am J Health Syst Pharm 2010; 67 1199–204.
| Pharmacy’s future: transformation, diffusion, and imagination.Crossref | GoogleScholarGoogle Scholar |
[5] Bryant LJ, Coster G, Gamble GD, McCormick RN. GPs’ and pharmacists’ perceptions of the role of community pharmacists in delivering clinical services. Res Social Adm Pharm 2009; 5 347–62.
| GPs’ and pharmacists’ perceptions of the role of community pharmacists in delivering clinical services.Crossref | GoogleScholarGoogle Scholar |
[6] Bryant L, Coster G, McCormick R. Community pharmacist perceptions of clinical medication reviews. J Prim Health Care 2010; 2 234–42.
[7] Scahill S, Harrison J, Sheridan J. Pharmacy under the spotlight: New Zealand pharmacists’ perceptions of current and future roles and the need for accreditation. Int J Pharm Pract 2010; 18 59–62.
| Pharmacy under the spotlight: New Zealand pharmacists’ perceptions of current and future roles and the need for accreditation.Crossref | GoogleScholarGoogle Scholar |
[8] Howard M, Trim K, Woodward C, et al Collaboration between community pharmacists and family physicians: lessons learned from the Seniors Medication Assessment Research Trial. J Am Pharm Assoc (Wash DC) 2003; 43 566–72.
| Collaboration between community pharmacists and family physicians: lessons learned from the Seniors Medication Assessment Research Trial.Crossref | GoogleScholarGoogle Scholar |
[9] Dunlop JA, Shaw JP. Community pharmacists’ perspectives on pharmaceutical care implementation in New Zealand. Pharm World Sci 2002; 24 224–30.
| Community pharmacists’ perspectives on pharmaceutical care implementation in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[10] Kucukarslan S, Lai S, Dong Y, et al Physician beliefs and attitudes toward collaboration with community pharmacists. Res Social Adm Pharm 2011; 7 224–32.
| Physician beliefs and attitudes toward collaboration with community pharmacists.Crossref | GoogleScholarGoogle Scholar |
[11] Bryant L, Coster G, McCormick R. General practitioner perceptions of clinical medication reviews undertaken by community pharmacists. J Prim Health Care 2010; 2 225–33.
[12] Rubio-Valera M, Jové A, Hughes C, et al Factors affecting collaboration between GPs and community pharmacists: a qualitative study. BMC Health Serv Res 2012; 12 188
| Factors affecting collaboration between GPs and community pharmacists: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[13] Ambler S. GPs and community pharmacists: times they are a-changing. Br J Gen Pract 2003; 53 594–5.
[14] Bradley F, Elvey R, Ashcroft DM, et al The challenge of integrating community pharmacists into the primary health care team: a case study of local pharmaceutical services (LPS) pilots and interprofessional collaboration. J Interprof Care 2008; 22 387–98.
| The challenge of integrating community pharmacists into the primary health care team: a case study of local pharmaceutical services (LPS) pilots and interprofessional collaboration.Crossref | GoogleScholarGoogle Scholar |
[15] Scahill S, Harrison J, Carswell P, Shaw J. Health care policy and community pharmacy: implications for the New Zealand primary health care sector. N Z Med J 2010; 123 41–51.
[16] Muijrers P, Knottnerus JA, Sijbrandij J, et al Changing relationships: attitudes and opinions of GPs and pharmacists regarding the role of the community pharmacist. Pharm World Sci 2003; 25 235–41.
| Changing relationships: attitudes and opinions of GPs and pharmacists regarding the role of the community pharmacist.Crossref | GoogleScholarGoogle Scholar |
[17] Hatah E, Braund R, Duffull S, Tordoff J. GPs’ perceptions of pharmacists’ new services in New Zealand. Int J Clin Pharm 2012; 34 364–73.
| GPs’ perceptions of pharmacists’ new services in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[18] Snyder ME, Zillich AJ, Primack BA, et al Exploring successful community pharmacist-physician collaborative working relationships using mixed methods. Res Social Adm Pharm 2010; 6 307–23.
| Exploring successful community pharmacist-physician collaborative working relationships using mixed methods.Crossref | GoogleScholarGoogle Scholar |
[19] Bradley F, Ashcroft DM, Noyce PR. Integration and differentiation: a conceptual model of general practitioner and community pharmacist collaboration. Res Social Adm Pharm 2012; 8 36–46.
| Integration and differentiation: a conceptual model of general practitioner and community pharmacist collaboration.Crossref | GoogleScholarGoogle Scholar |
[20] Pojskic N, MacKeigan L, Boon H, et al Ontario family physician readiness to collaborate with community pharmacists on drug therapy management. Res Social Adm Pharm 2011; 7 39–50.
| Ontario family physician readiness to collaborate with community pharmacists on drug therapy management.Crossref | GoogleScholarGoogle Scholar |
[21] Zillich AJ, Doucette WR, Carter BL, Kreiter CD. Development and initial validation of an instrument to measure physician-pharmacist collaboration from the physician perspective. Value Health 2005; 8 59–66.
| Development and initial validation of an instrument to measure physician-pharmacist collaboration from the physician perspective.Crossref | GoogleScholarGoogle Scholar |
[22] Norton D, Measday J, Grenfell R, et al GP-pharmacist liaison: a rural case study. Aust Fam Physician 2003; 32 191–2.
[23] Blenkinsopp A, Tann J, Evans A, Grime J. Opportunity or threat? General practitioner perceptions of pharmacist prescribing. Int J Pharm Pract 2008; 16 29–34.
| Opportunity or threat? General practitioner perceptions of pharmacist prescribing.Crossref | GoogleScholarGoogle Scholar |
[24] Bryant L. Evaluation of the barrier to, and implementation of, comprehensive pharmaceutical care in New Zealand [Thesis]. Auckland: University of Auckland; 2006.
[25] Hepler CD, Strand LM. Opportunities and responsibilities in pharmaceutical care. Am J Hosp Pharm 1990; 47 533–43.
| 1:STN:280:DyaK3c7ps1Sgsw%3D%3D&md5=bed47e0e73e3e5f19c8c9d77401ddaa1CAS |
[26] Ministry of Health. New Zealand Health Strategy: future direction [Internet]. Wellington: Ministry of Health; 2016. [cited 2016 September 2]. Available from: www.health.govt.nz/new-zealand-health-system/new-zealand-health-strategy-future-direction
[27] Mays N. Reorienting the New Zealand health care system to meet the challenge of long term conditions in a fiscally constrained environment. Paper prepared for New Zealand Treasury Long-term Fiscal External Panel, Nov 2012, and Chair of Public Finance, Victoria University of Wellington and New Zealand Treasury conference, Affording our Future, Wellington, 10–11 December 2013. Available from: www.hiirc.org.nz/page/37816
[28] Hook S, Windle J. Community pharmacy influenza immunisation increases vaccine uptake and gains public approval. Aust N Z J Public Health 2013; 37 489–90.
| Community pharmacy influenza immunisation increases vaccine uptake and gains public approval.Crossref | GoogleScholarGoogle Scholar |
[29] Rigby D. Medication review: learnings from Old Blighty. Aust J Pharmacy 2010; 91 34–5.
[30] Krska J, Cromarty J, Arris F, et al Pharmacist-led medication review in patients over 65: a randomized, controlled trial in primary care (statistical data included). Age Ageing 2001; 30 205–11.
| Pharmacist-led medication review in patients over 65: a randomized, controlled trial in primary care (statistical data included).Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3MzovVKnsA%3D%3D&md5=ae1f200a86e95b74dcac0c29d72db060CAS |
[31] Harding G, Wilcock M. Community pharmacists’ perceptions of medicines use reviews and quality assurance by peer review. Pharm World Sci 2010; 32 381–5.
| Community pharmacists’ perceptions of medicines use reviews and quality assurance by peer review.Crossref | GoogleScholarGoogle Scholar |
[32] Latif A, Pollock K, Boardman HF. The contribution of the Medicines Use Review (MUR) consultation to counseling practice in community pharmacies. Patient Educ Couns 2011; 83 336–44.
| The contribution of the Medicines Use Review (MUR) consultation to counseling practice in community pharmacies.Crossref | GoogleScholarGoogle Scholar |
[33] Porteous T, Bond C. Evaluation of a pharmacist-managed repeat dispensing system: the GP perspective. Int J Pharm Pract 2005; 13 41–6.
| Evaluation of a pharmacist-managed repeat dispensing system: the GP perspective.Crossref | GoogleScholarGoogle Scholar |
[34] Bond C, Matheson C, Williams S, et al Repeat prescribing: a role for community pharmacists in controlling and monitoring repeat prescriptions. Br J Gen Pract 2000; 50 271–5.
| 1:STN:280:DC%2BD3cvgtVyitQ%3D%3D&md5=bed4ccb92cfe3712f0c7e1846413e842CAS |
[35] Scahill S, Harrison J, Sheridan J. The ABC of New Zealand’s ten year vision for pharmacists: awareness, barriers and consultation. Int J Pharm Pract 2009; 17 135–42.
| The ABC of New Zealand’s ten year vision for pharmacists: awareness, barriers and consultation.Crossref | GoogleScholarGoogle Scholar |
[36] Rosenthal M, Austin Z, Tsuyuki RT. Are pharmacists the ultimate barrier to pharmacy practice change? Can Pharm J 2010; 143 37–42.
| Are pharmacists the ultimate barrier to pharmacy practice change?Crossref | GoogleScholarGoogle Scholar |
[37] Kay OC, Bajorek BV, Brien JA. Pharmacist prescribing activities – an electronic survey on the opinions of Australian pharmacists. J Pharmacy Pract Res 2006; 36 199–203.
| Pharmacist prescribing activities – an electronic survey on the opinions of Australian pharmacists.Crossref | GoogleScholarGoogle Scholar |
[38] Gidman W, Ward P, McGregor L. Understanding public trust in services provided by community pharmacists relative to those provided by GPs: a qualitative study. BMJ Open 2012; 2 e000939
| Understanding public trust in services provided by community pharmacists relative to those provided by GPs: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[39] Anscombe J, Thomas M, Plimley J. The future of community pharmacy in England. London: A.T. Kearney’s Health Practice; 2012. Available from: www.atkearney.com/documents/10192/649132/The+Future+of+Community+Pharmacy.pdf/1838dede-b95a-4989-8600-6b435bd00171
[40] Silcock J, Raynor DK, Petty D. The organisation and development of primary care pharmacy in the United Kingdom. Health Policy 2004; 67 207–14.
| The organisation and development of primary care pharmacy in the United Kingdom.Crossref | GoogleScholarGoogle Scholar |


