Building and expanding interprofessional teaching teams
Ben Darlow 1 , Eileen McKinlay 1 , Peter Gallagher 2 , Louise Beckingsale 3 , Karen Coleman 4 , Meredith Perry 5 , Sue Pullon 11 Department of Primary Health Care & General Practice, University of Otago, Wellington, New Zealand
2 Education Unit, University of Otago, Wellington, New Zealand
3 Department of Human Nutrition, University of Otago, Christchurch, New Zealand
4 Department of Radiation Therapy, University of Otago, Wellington, New Zealand
5 School of Physiotherapy, University of Otago, New Zealand
Correspondence to: Ben Darlow, Department of Primary Health Care & General Practice, University of Otago, Wellington, New Zealand. Email: ben.darlow@otago.ac.nz
Journal of Primary Health Care 9(1) 29-33 https://doi.org/10.1071/HC16053
Published: 29 March 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Interprofessional education (IPE) aims to prepare learners to work in collaborative health-care teams. The University of Otago, Wellington has piloted, developed and expanded an IPE programme since 2011. An interprofessional teaching team has developed alongside this programme.
AIMS: This study aimed to understand the development of a university-based interprofessional teaching team over a 4-year period and generate insights to aid the development of such teams elsewhere.
METHODS: Two semi-structured audio-recorded educator focus groups were conducted at key times in the development of the IPE programme in 2011 and 2014. The programme focused on long-term condition management and involved students from dietetics, medicine, physiotherapy and radiation therapy. Focus group transcripts were independently analysed by two researchers using Thematic Analysis to identify broad themes. Initial themes were compared, discussed and combined to form a thematic framework. The thematic framework was verified by the education team and subsequently updated and reorganised.
RESULTS: Three key themes emerged: (i) development as an interprofessional educator; (ii) developing a team; and (iii) risk and reward. Teaching in an interprofessional environment was initially daunting but confidence increased with experience. Team teaching highlighted educators’ disciplinary roles and skill sets and exposed educators to different teaching approaches. Educators perceived they modelled team development processes to students through their own development as a team. Interprofessional teaching was challenging to organise but participation was rewarding. Programme expansion increased the risks and complexity, but also acted as a stimulus for development and energised the teaching team.
DISCUSSION: Interprofessional teaching is initially challenging but ultimately enriching. Interprofessional teaching skills take time to develop and perspectives of role change over time. Educator team development is aided by commitment, understanding, enthusiasm, leadership and trust.
KEYWORDS: Interprofessional education; health professional education; faculty development; focus group; qualitative research
| WHAT GAP THIS FILLS |
| What is already known: Interprofessional teaching can be challenging and associated with initial anxiety. Confidence and ability grow with experience, and education teams role-model interprofessional behaviours and team development to students. |
| What this study adds: Exposure to different teaching approaches through participating in interprofessional education can help educators to develop their teaching skill set. Expanding interprofessional programmes can increase risk and complexity but also stimulate development and enthusiasm. |
Introduction
Interprofessional education (IPE) aims to prepare learners to work in collaborative health-care teams that use multiple skill sets to provide well-coordinated, high-quality, patient-centred care.1 Interprofessional practice is particularly important in the context of people living longer with long-term, complex and co-morbid conditions. Their multifaceted needs cannot be met by a single disciplinary skill set.2
The University of Otago, Wellington piloted an IPE programme involving dietetics, medicine and physiotherapy in 2011.3 This programme continued, developed and expanded over subsequent years to include the discipline of radiation therapy in 2014. The expansion increased class size from ~30 to 80 students. The education team also grew from an initial core group of five (professional backgrounds of dietetics, medicine, nursing and physiotherapy) to eight (additional backgrounds of education psychology, midwifery and radiation therapy). All education team members were experienced tertiary teachers with variable levels of IPE experience. The programme includes an initial workshop, visits in interdisciplinary groups of three students to a person living in the community with one or more long-term conditions, and an interdisciplinary group presentation to student peers about the person visited, clinicians involved in these people’s care and interprofessional educators. The experiences and outcomes of learners in this programme have been described previously.3–5
This programme has developed a community of interprofessional educators, which includes patients-as-teachers and their health-care providers. This study explored the perspective of the university-based education team that developed alongside the programme. The aim of this study was to understand the development of an interprofessional teaching team and generate insights that may aid the development of such teams elsewhere.
Methods
Two focus groups of educators were conducted at key time points in the IPE programme’s evolution. The first (n = 5) was conducted after the programme’s inception and delivery to the first cohort of students in 2011. The second (n = 6) was conducted in 2014 after the expansion of the programme to include students and educators from the discipline of radiation therapy.
Semi-structured audio-recorded focus groups were facilitated by an experienced educationalist. Focus group recordings (2011) or transcripts (2014) were analysed using Thematic Analysis.6 The facilitator and another researcher independently identified broad themes emerging from each group. These two researchers then compared, discussed and subsequently combined themes to form a thematic framework. Data were then coded by theme with nVivo10 software (QSR International Pty Ltd, Melbourne, VIC, Australia). Themes and representative data were summarised and presented anonymously to the education team for verification and comment. Following education team feedback, themes were reorganised and a summary written for further team review and discussion that informed final themes and interpretation. This study was approved by the University of Otago Ethics Committee (D13/186).
Results
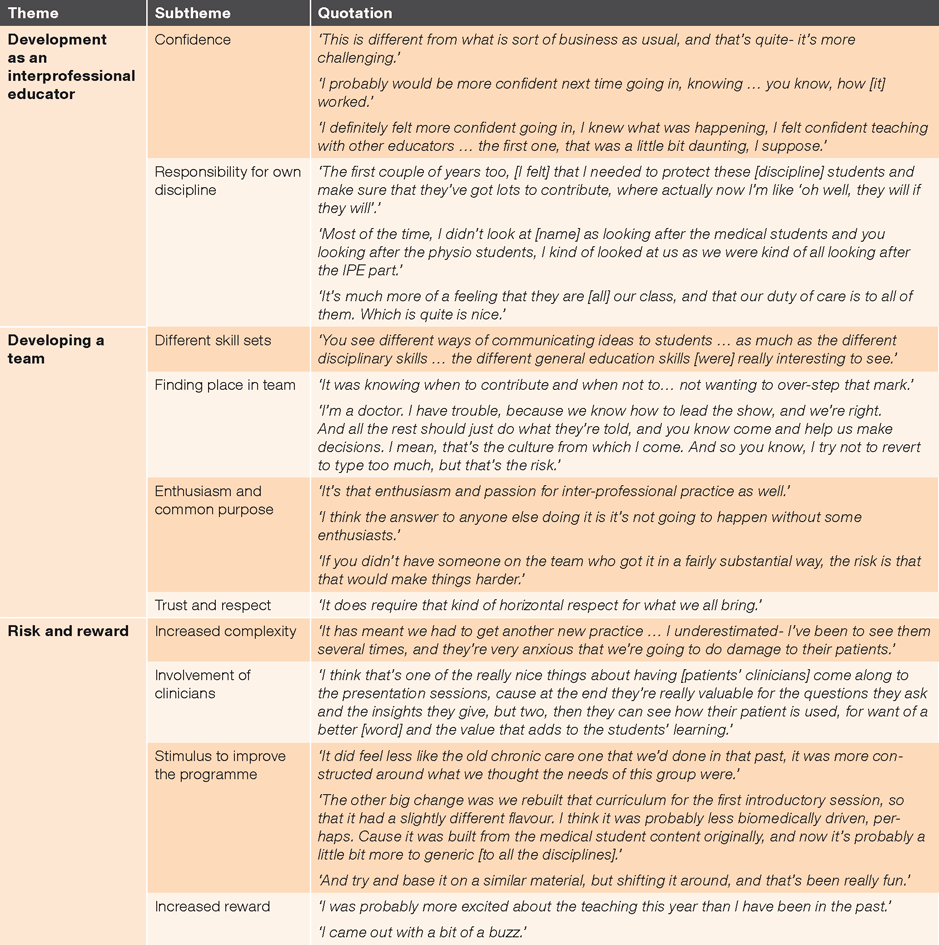
Three themes emerged. Data supporting the findings are presented in Table 1.
|
Development as an interprofessional educator
Teaching in an interprofessional environment for the first time was daunting. Confidence increased through experience teaching on the programme over several years. Educators new to the programme discussed feeling responsible for the students from their discipline. In contrast, educators with more interprofessional experience felt confident students from their discipline did not require specific facilitation and considered they were contributing experience and generic interprofessional teaching skills rather than discipline-specific skills.
Developing a team
Forming an interprofessional teaching team highlighted educators’ different disciplinary roles and skill sets. Exposure to different approaches was beneficial for educators’ teaching practice, even if at times it was challenging to change from ingrained habits.
Educators discussed the process of finding their own place within the teaching team. Educators new to the programme reported sitting back to watch how the team worked, whereas experienced educators reflected on the need to mitigate natural tendencies to take over the team and the influence of traditional hierarchies. Prior interprofessional practice experience and relationships were integral to developing working rapport. Educators understood they were modelling team development processes to students through their own development as a team.
It was considered vital that all IPE team members understood the concept, principles and ethos of IPE and the reason for the IPE programme, as well as being enthusiastic about it. This meant they all worked in the same direction and were willing to undertake the extra work required to enable the programme. It was clear from both focus groups that educators understood the importance of the IPE programme. The need for leadership (provided by one team member over the 4 years of the programme) was recognised, but also recognised was the requirement for this leader to be supported by team members and the institution.
Trust and respect were identified as required both in the immediate teaching team and also in the broader community of educators (encompassing the health-care providers who recruited patients and the patients themselves as teachers).
Risk and reward
Interprofessional teaching was challenging to organise within crowded curricula that provided limited opportunities for students from different disciplines to learn together. Challenges were compounded by the IPE programme running over several weeks and requiring multiple time points when students could interact or attend teaching contact sessions. Although many key constructs associated with providing care to people with long-term conditions were consistent across disciplines, this programme highlighted differences in explicit models and terminology that had to be reconciled. Despite these challenges, the 2011 focus group commented on educators’ enjoyment of the experience and their motivation to continue the programme.
Expansion added to the programme’s risks and complexity. More students and more disciplines increased difficulties associated with organising the teaching sessions and students finding opportunities to undertake independent learning activities. To enable the ‘patient-as-teacher’ model, the number of involved patients increased from seven in 2011 to 28 in 2014 and primary health-care practices from one to four. It was considered very important to involve the same primary health-care practice partners over a period of time and having these clinicians contribute to the presentation sessions, so that they could share additional knowledge and witness the value of these learning opportunities.
The increased size and complexity of the programme in 2014 also provided a stimulus to adapt the curriculum and find efficiencies to make the programme more sustainable. The development of a revised curriculum and refined delivery model made the 2014 programme more enjoyable and energised the education team. Educators commented that the revised curriculum seemed to better meet the needs of learners by integrating student suggestions from previous programme iterations and being purpose developed for an interprofessional class rather than an adapted medical module.
The 2014 focus group reflected that the programme provided a learning environment that enriched participants. The team felt that real progress had been made in the development of IPE and this gave confidence to try to integrate more disciplines and create new IPE activities.
Discussion
This study found that interprofessional teaching skills take time to develop and perspectives of role change over time. Educator team development is aided by commitment, understanding, enthusiasm, leadership and trust. There are risks and challenges associated with conducting and expanding interprofessional programmes, but these are balanced by considerable rewards.
Educators involved in teaching the IPE programme self-selected to take part and developed the programme from a shared interest in preparing learners to practice in an interprofessional collaborative manner. Previous studies have found that prior interprofessional clinical experience helps educators understand the importance of IPE.7,8 In the current study, the tenor of comments in the focus groups reflected educators’ enthusiasm. Educators with different experiences and motivations may have responded to challenges associated with the programme in different ways. Notwithstanding this, most educators had no prior experience of teaching as part of an interprofessional team.
Anxiety associated with initial interprofessional teaching and subsequent increased confidence as a result of experience is consistent with previous findings.8,9 IPE facilitation has been found to be more demanding than other forms of teaching, but also enriching from educational and clinical perspectives.7,10 Educators understand they are interprofessional role models for their students and can set a positive example for these learners’ future careers by role-modelling interprofessional behaviours and team development.8,11
This study highlights interprofessional teaching as initially challenging, but ultimately enriching. Educators are often not trained in interprofessional teaching but confidence and ability grow with experience; new teachers should be supported through this process. With time, educator focus shifts from representing a discipline to meeting the needs of the whole class.
Exploration of education team development was made possible by the stability of the teaching team. Despite this, findings emerged from only two focus groups and should be tested through future in-depth investigation. This programme integrates a community of interprofessional educators where people living in the community with long-term conditions and health professionals involved in their care are integral members of the education team. The focus groups described in this paper present the views of only the university-based educators. Future research will explore the views of community-based members of the education team.
COMPETING INTERESTS
All authors state that no potential conflicts of interest exist.
FUNDING
Aspects of this research were funded by a Committee for the Advancement of Learning and Teaching (CALT) Grant from the University of Otago.
ACKNOWLEDGEMENTS
The authors wish to acknowledge the members of the Wellington Interprofessional Teaching Initiative who have been integral to the development of this programme – Sarah Donovan, Ben Gray and Hazel Neser.
References
[1] Canadian Interprofessional Health Collaborative. A national interprofessional competency framework. Vancouver: College of Health Disciplines, University of British Columbia; 2010.[2] Thistlethwaite J. Interprofessional education: a review of context, learning and the research agenda. Med Educ. 2012; 46 58–70.
| Interprofessional education: a review of context, learning and the research agenda.Crossref | GoogleScholarGoogle Scholar |
[3] Pullon S, McKinlay E, Beckingsale L, et al. Interprofessional education for physiotherapy, medical and dietetics students: a pilot programme. J Prim Health Care. 2013; 5 52–8.
[4] Darlow B, Coleman K, McKinlay E, et al. The positive impact of interprofessional education: a controlled trial to evaluate a programme for health professional students. BMC Med Educ. 2015; 15 98
| The positive impact of interprofessional education: a controlled trial to evaluate a programme for health professional students.Crossref | GoogleScholarGoogle Scholar |
[5] Darlow B, Donovan S, Coleman K, et al. What makes an interprofessional education programme meaningful to students? Findings from focus group interviews with students based in New Zealand. J Interprof Care. 2016; 30 355–61.
| What makes an interprofessional education programme meaningful to students? Findings from focus group interviews with students based in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[6] Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006; 3 77–101.
| Using thematic analysis in psychology.Crossref | GoogleScholarGoogle Scholar |
[7] Lindqvist SM, Reeves S. Facilitators’ perceptions of delivering interprofessional education: a qualitative study. Med Teach. 2007; 29 403–5.
| Facilitators’ perceptions of delivering interprofessional education: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[8] Derbyshire JA, Machin AI, Crozier S. Facilitating classroom based interprofessional learning: a grounded theory study of university educators’ perceptions of their role adequacy as facilitators. Nurse Educ Today. 2015; 35 50–6.
| Facilitating classroom based interprofessional learning: a grounded theory study of university educators’ perceptions of their role adequacy as facilitators.Crossref | GoogleScholarGoogle Scholar |
[9] Egan-Lee E, Baker L, Tobin S, et al. Neophyte facilitator experiences of interprofessional education: implications for faculty development. J Interprof Care. 2011; 25 333–8.
| Neophyte facilitator experiences of interprofessional education: implications for faculty development.Crossref | GoogleScholarGoogle Scholar |
[10] Forte A, Fowler P. Participation in interprofessional education: an evaluation of student and staff experiences. J Interprof Care. 2009; 23 58–66.
| Participation in interprofessional education: an evaluation of student and staff experiences.Crossref | GoogleScholarGoogle Scholar |
[11] Selle KM, Salamon K, Boarman R, Sauer J. Providing interprofessional learning through interdisciplinary collaboration: the role of “modelling”. J Interprof Care. 2008; 22 85–92.
| Providing interprofessional learning through interdisciplinary collaboration: the role of “modelling”.Crossref | GoogleScholarGoogle Scholar |


