Social networks of patients with multimorbidity: a qualitative study of patients’ and supporters’ views
Eileen McKinlay 1 , Janet McDonald 1 , Ben Darlow 1 , Meredith Perry 11 University of Otago, Wellington, New Zealand
Correspondence to: Eileen McKinlay, Associate Professor, Department of Primary Health Care and General Practice, University of Otago, Wellington, New Zealand. Email: eileen.mckinlay@otago.ac.nz
Journal of Primary Health Care 9(2) 153-161 https://doi.org/10.1071/HC16062
Published: 17 May 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Multimorbidity impacts on patients’ health and wellbeing, but relationships experienced within social networks can support people to live well.
AIM: This study sought to elicit the views of New Zealanders with multimorbidity about their social networks and the views of their nominated supporters.
METHODS: Ten patients with multimorbidity and their nominated supporters each independently recorded their views of the patient’s social network on a five-concentric-circle template, indicating supporting role and importance to each patient. Sets of patients’ and nominated supporters’ templates were compared followed by comparing matched pairs of patient–supporter templates. Nominated supporters’ views about the patients’ networks and why they were nominated were collated.
RESULTS: Three patients nominated family members as supporters and seven nominated health professionals. Nominated family members identified a greater range of supporters than nominated health professionals. Nominated family members perceived that they played an integral role, whereas health professionals were less comfortable viewing relationships with patients in this way. Family members were not surprised to be nominated as supporters, and some described a considerable burden of care. Health professionals described themselves as coordinators of support and having positive relationships with patients.
DISCUSSION: Patients with multimorbidity have rich and diverse social networks. They view partners, family and health professionals as providing significant support. Family members are more aware of their role and have a deeper understanding of other network members than health professionals. Further research is needed on the use of social networks in clinical practice to support the health and wellbeing of those with multimorbidity.
KEYWORDS: Health professionals; long-term conditions; multimorbidity; patients; social networks
| WHAT GAP THIS FILLS |
| What is already known: Patients with multimorbidity benefit from the support of social networks. Internationally, social networks have been examined using a structured social network template, but no such research has been completed in New Zealand. |
| What this research adds: Patients with multimorbidity recorded varied social networks and they nominated partners, family members and health professionals from the network as providers of significant support. If health professionals have a deeper understanding of patients’ social networks, they could use this information to support the efforts of patients and their families. |
Introduction
Multimorbidity (multiple long-term conditions) is a rising challenge around the world and is associated with reduced quality of life, increased mortality, polypharmacy and greater health service use.1 Past and current relationships, often experienced within a social network, influence health and wellbeing. The concept of health and wellbeing is now more broadly defined as the ‘ability to adapt and to self-manage, in the face of social, physical and emotional challenges’.2 Positive relationships improve health literacy, self-efficacy, self-management and patient activation for people with multimorbidity.2–8
Social networks are ubiquitous across all countries and settings, and typically include partners, family, friends, community-based organisations9–13 and, to a lesser extent, professionals.13,14 Informally and yet in a connected fashion, network members can act to support an individual with health and social needs.15 Irrespective of socioeconomic status12 or country,16 social networks can or have the potential to collectively enable patients to self-manage17,18 and enhance feelings of social integration and individual identity.18 Social networks yield benefits to people, health systems, health professionals and the economy.19
To date, multimorbidity research has focused on exploring individual interactions between patients and health professionals, usually within healthcare consultations, rather than exploring relationships between patients and people in their social networks.9,10,20,21 Studies exploring social networks typically use a visual template of concentric circles, indicating relative degree and importance of interaction from a patient’s perspective.12,13,17,22 In New Zealand (NZ), research with medical students has examined the use of similar templates to facilitate understanding of patients’ Communities of Clinical Practice, an approach somewhat akin to social networks,23–25 and patients’ and clinicians’ views of Communities of Clinical Practice.26 No research involving the social networks of patients with multimorbidity and that of their supporters appears to have been undertaken, although the need to do so has been recognised.27
This exploratory study sought to elicit the views of NZ patients with multimorbidity about their social networks, and the views of their nominated significant supporters.
Health system context
New Zealand has comparable multimorbidity prevalence to other Western countries,28 although people of Maori and Pacific descent have higher rates of multimorbidity and overall lower life expectancy.28–31 The care of patients with multimorbidity generally involves both primary and secondary healthcare providers, with primary care assumed to take the lead role in coordination.32,33
Context of data collection
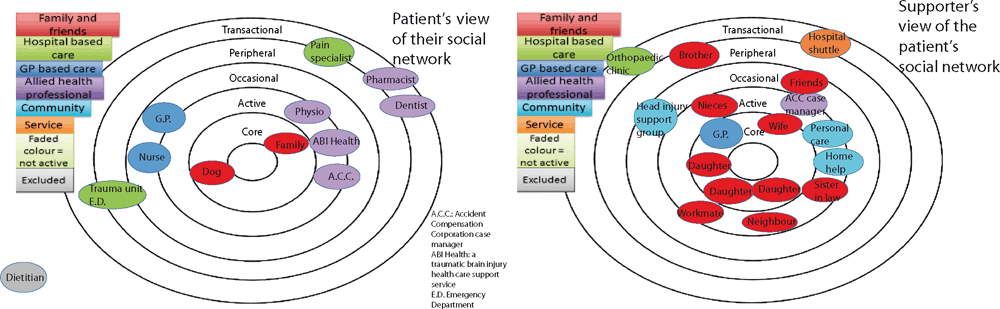
This study was built around an existing pre-vocational registration teaching programme. A long-term conditions management module is included in an interprofessional programme for dietetic, medicine, physiotherapy and radiation therapy students.34 As part of this module, interprofessional groups of three students visited a patient with multimorbidity in their home to explore the patient’s experience of multimorbidity. A social network template comprising five concentric circles (adapted from E & B Wenger-Trayner35) was used to record each patient’s network.25 Colour-coded categories identified possible groups of network supporters. Proximity to the centre (Core, Active, Occasional, Peripheral, Transactional) indicated the relative degree of interaction or importance of individuals within patients’ social networks.
This study was approved by the University of Otago ethics committee (No. H16/007).
Methods
Researchers phoned the patients and sent written information, consent and demographic forms to patients who expressed an interest in participating in the study. Consenting patients were asked to nominate an individual who provided significant support to them. Throughout the rest of this paper, this nominated individual will be referred to as ‘the supporter’.
Student groups interviewed each patient about their experience of multimorbidity and, using a broad list of question prompts, asked patients to complete a social network template (with or without the assistance of the students). They then prepared a PowerPoint presentation (which included the social network template) to represent this information. The presentation was retained for analysis (with the students’ consent).
The research team then approached and interviewed the nominated supporters about the patient’s social network and asked them to also complete the social network template, with or without assistance. Nominated supporters were not shown the patients completed templates so that the supporters could record their own perspective on each patient’s social network and their role in supporting the health and wellbeing of the patient, without being influenced by the patient’s view. All interviews were audio recorded, transcribed verbatim and field notes were retained.
Data analysis
The theoretical framework for this study drew on social network analysis focusing on relational data, including contacts, ties, connections and attachments within patients’ social networks.36
The data analysis included collating information on who was in the patient’s social network. Sets of patients’ and then supporters’ templates were analysed for similarity and difference. Then, pairs of social network templates relating to each patient were independently analysed by JM and EM, who compiled and compared summary frameworks of patients and supporters.
We compared patients’ and supporters’ views about proximity and the relative importance of people named in the social network, and the sufficiency of patients’ social networks. This was undertaken through analysis of the social network templates, summary frameworks and transcribed interview data. We collated information on why supporters thought they had been nominated.
As the above steps progressed, the research team met regularly to discuss the analysis of the social network templates, to review the qualitative interview data and to contribute to the synthesis of the datasets.
Results
Of the 21 patients with multimorbidity involved in the teaching programme, 11 agreed to take part in the study, and nominated a supporter who provided significant support. One nominated supporter (a nurse) subsequently left her place of employment and could not be contacted for interview. Thus, 10 patients and 10 nominated others were included in the analysis (Table 1), with nine pairs of social network templates for comparison (one student group did not supply a PowerPoint presentation or a social network template).

|
Five females and five males aged between 35 and 86 years (five were aged 65 years or over) participated in the study, along with their nominated supporters. Supporters included family members (sister, daughter, wife) and health professionals (exercise physiologist, practice nurse, three general practitioners (GPs), a renal physician and an endocrinologist). Three patients lived alone and the remainder lived with one or more family members. Eight patients were NZ European, one Maori and one Cook Islands Maori. All patients had at least three long-term conditions.
Who is in the patient’s social network? The views of patients and nominated supporters
Patients’ social networks varied in number and range of supporters. Family supporters nominated more supporters and placed these supporters nearer to the Core circle, indicating greater perceived support. Health professional supporters tended to focus on other health professionals, who they placed in the Active and Occasional circle, although one had a broad understanding of the patient’s family and community-based supporters. The colour-coded categories provided a starting point, but participants could include whatever was meaningful to them. For example, a patient recorded a pet and a health professional recorded a patient’s interests.
Two paired examples were chosen as examples for this paper: the first where the supporter was a family member and the second, a health professional. In Figure 1, the social network templates were recorded by Patient 7 and the nominated supporter, his wife. His wife recorded more people with a wider range of support roles. Compared with her husband’s view, she indicated that additional people were more closely involved nearer to the Core circle.
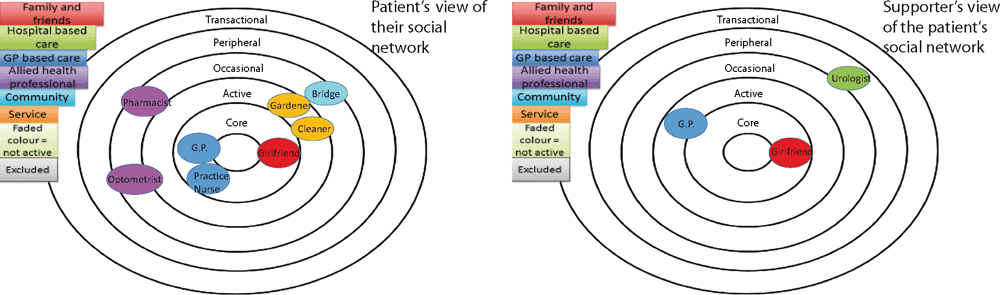
In Figure 2, the social networks were recorded by Patient 3 and the nominated supporter, his GP. His GP knew about this patient’s girlfriend, but very little else about him and recorded only two others involved (he and another health professional). In contrast, the patient noted more and wider supports, including his girlfriend, community supporters (gardener, cleaner), interests (bridge) and health professionals (e.g. pharmacist).
Comparison of views about proximity of participants in the social network to patients, why supporters believe they were nominated and the sufficiency of patients’ social networks
In relation to the template centre (i.e. the patient), all except one patient placed the nominated supporter in the Core circle (one placed in the Active circle), indicating a high degree of perceived importance and interaction (Table 1). The three family member supporters also placed themselves in the Core circle. Five of the seven health professional supporters placed themselves in the Active circle, while the other two positioned themselves in the Occasional circle. Supporters’ views on why they were nominated ranged from surprise (supporter 10); role as coordinator (supporters 2, 4); relationship (supporters 3, 5, 8, 9); family affiliation (supporters 1, 7); to community affiliation (supporter 6).
Most health professional supporters thought that patients’ social networks were sufficient (patients 2, 4, 6, 8, and 10) or had some minor shortcomings (patients 3 and 9), such as; ‘No. I don’t think he needs anything at the moment…. the big thing is his cognition’ (supporter, patient 3); ‘because it’s a fairly small family network and he lives alone, the challenge will be if he gets more (unwell)’ (supporter, patient 9).
The three family member supporters (patients 1, 5 and 7) directly or indirectly expressed major or significant concerns about social network sufficiency. The sister of patient 1 was under substantial pressure and described her own life as being ‘on hold’. The daughter of patient 5 described a limited network: ‘It’s just about (her) going to appointments and me, which is a bit sad’. The wife of patient 7 noted her role as: ‘I just have had to do everything, so I am definitely in that caring mode compared with (our previous) relationship’, but noted previously, ‘I think people genuinely want to help. But I suppose I always think … you’ve got to be self-sufficient’.
Discussion
This study reports the views of patients with multimorbidity regarding their social networks and the views of their nominated supporters regarding the patients’ social networks. As well as describing who is in the patients’ social networks, it highlights the range of people supporting patients with multimorbidity. Internationally, social networks are receiving increasing attention,12,14,37 and this exploratory study signals a similar importance in NZ. The study builds on international research (typically asking only patients to identify their social networks12,14) by also asking patients to nominate a significant supporter, and exploring the supporter’s view of the patient’s social network. This approach provides insight into a patient’s social network from both perspectives.
Most patients recorded diverse and rich social networks. When each pair (patient and supporter) of templates was compared, it was evident that the role and level of involvement of the supporter appeared to influence who was recorded on their template. Nominated family member supporters tended to record family, friends and community supporters, although they were also aware of the key health professionals involved. Nominated health professional supporters mainly included other health professionals, except for one who had a broader understanding of the patient’s network.
Two-thirds of the patients in this study nominated health professionals as significant supporters. All patients, except one, categorised the health professional supporters in the Core circle. In comparison, the health professionals categorised themselves as Active or Occasional supporters, possibly signalling that they perceived themselves as being central or essential in providing support. Health professional supporters typically recorded a more limited range of people in patients’ social networks, and this may be due to a lack of knowledge about patients’ family and social circumstances. Because of this, health professionals may have misjudged the degree of sufficiency of the social network. In two instances where they described the social networks as being sufficient but with minor shortcomings, this was probably not so. These patients, both elderly men, lived alone with one having no close-living family members and the other with only one close friend; one of these men was reported to have cognitive decline.
When patients nominated family members as providing significant support and placed them in the Core circle, they signalled a high level of importance and reliance on that relationship. However, it is possible that patients may have underestimated the degree of physical or emotional involvement given; the qualitative comments supported the effect on the family supporter’s quality of life. Patients may also not appreciate the reliance that family supporters have on others within their network.
The three family members expected to be involved in the patient’s care and either lived with the patient or had daily contact. However, two expressed stress, loneliness and isolation in their supporting role, accompanied by the belief that they needed to remain self-sufficient.38,39 It is possible that the expectation of family involvement in NZ is influenced by the collectivist culture of both the indigenous Maori peoples and people of Pasifika ethnicity.40,41 Despite being keen to be involved, there are likely to be limitations to the amount of work family members are able to undertake. A study by Mays notes it is unwise to regard informal care provided by social networks ‘as a straightforward source of care that can be switched on or off to meet gaps in paid care’ and cautions that people can be reluctant to accept help from family or neighbours unless they can reciprocate.42
Health professionals are generally considered to be weak ties in social networks, akin to acquaintances, with relationships characterised as transient, briefer, transactional and with less connection (contrasting to the strong ties of family or close friends where trust and bonds exist).22,43 Weak ties are important in social networks, as they allow patients to seek specific, yet socially distanced support without the constraints of close relationships.43 This study shows it is possible for patients to categorise health professionals as being in the Core circle, yet still meet the definition of being a weak tie. It also shows that health professionals either underestimate their importance in a patient’s social network or do not want to be too important to the patient. Despite being seen as Core by patients, there was no suggestion that these patients unduly called on the health professionals’ time and care.
Health professionals are not always aware of their patients’ social networks and do not actively use them as a resource, particularly to encourage self-management.44 Understanding the nature of the support given by social networks is important, as not all health professionals appreciate the ‘hard work’ and effect of multimorbidity45,46 or the time, effort and self-efficacy required to self-care.47,48 Some health professionals are unrealistic about how much patients can self-manage.49 This study suggests that social network information is not easily recalled by health professionals, perhaps because they do not ask about it, or if elicited, it is then not specifically recorded in the patient’s clinical record. It is also not clear if and how information about social networks should be used by health professionals to support or influence care, particularly when working within a family-centred model of care.50 There seems considerable potential to do so. For example, when working with family, friends and others to encourage patient self-management, defining social networks would acknowledge or explore work being undertaken on behalf of the patient or help assess the burden of care on family members. Further work is needed to explore patients’ views of confidentiality and information-sharing, as well as how and when the health professionals may or might contact the social network members.
There are limitations and strengths to this study. Although students were supplied a list of question prompts to help patients complete the social network template, they may not have uniformly used these. They may have also misinterpreted the patients’ view of their social network or not recorded the information accurately. One group of students did not return the patient’s social network template. The multiple categories included in the network diagrams were useful for prompting students, but a simpler design may be easier for patients to complete. It is possible that having 10 patients and nominated supporters may limit who the study represents, but a gender balance and age range of patients was achieved, as was a balance of nominated supporters between family members and health professionals. A further methodological strength was the use of multiple sources of data, enabling data triangulation, although there may have been advantages in interviewing both health professional and family supporters about each patient.
Conclusion
Social networks are important to patients with multimorbidity and can include a diverse range of family, friends, community organisations, health professionals, interests and pets. Relationships formed are often very helpful to patients in managing their health and wellbeing. Unknown to health professionals, patients include them in their social networks and regard them as significant supporters in their care. Although health professionals know about other health professionals in patients’ social network, they have more limited knowledge about family, friends or community organisations and do not appear to actively use this information to enhance care. Patients and health professionals are not always aware of the pressure family supporters are under, how much support these family supporters also need, or the extent to which they rely on others within the patient’s social network. More research is required on how best to use information about social networks when supporting the care of people with multimorbidity.
FUNDING
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
COMPETING INTERESTS
The authors have no competing interests to declare.
ACKNOWLEDGEMENTS
The authors sincerely thank the patients and staff who took part from Johnsonville Medical Centre, Karori Medical Centre & Newtown Union Health Service, and staff from Capital and Coast District Health Board and Massey University. We also thank the 2016 February/March interprofessional student class and the Wellington Interprofessional Teaching Initiative: Louise Beckingsale, Karen Coleman, Sarah Donovan, Ben Gray, Hazel Neser, Sue Pullon and Christine Wilson. The authors acknowledge the work of the Community of Clinical Practice researchers: Jess Young, Chrys Jaye and Tony Egan.
References
[1] National Institute for Health and Care Excellence (NICE). Multimorbidity: clinical assessment and management. London: NICE; 2016.[2] Huber M, van Vliet M, Giezenberg M, et al. Towards a ‘patient-centred’ operationalisation of the new dynamic concept of health: a mixed methods study. BMJ Open. 2016; 6 e010091
| Towards a ‘patient-centred’ operationalisation of the new dynamic concept of health: a mixed methods study.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC28rpvVSltA%3D%3D&md5=e5dbd02aa08f4064df327f4d1c156d61CAS |
[3] Afshar S, Roderick PJ, Kowal P, et al. Multimorbidity and the inequalities of global ageing: a cross-sectional study of 28 countries using the World Health Surveys. BMC Public Health. 2015; 15 776
| Multimorbidity and the inequalities of global ageing: a cross-sectional study of 28 countries using the World Health Surveys.Crossref | GoogleScholarGoogle Scholar |
[4] Van Hecke A, Heinen M, Fernández-Ortega P, et al. Systematic literature review on effectiveness of self-management support interventions in patients with chronic conditions and low socio-economic status. J Adv Nurs. 2017; 73 775–93.
[5] Greene J, Hibbard J. Why does patient activation matter? An examination of the relationships between patient activation and health-related outcome. J Gen Intern Med. 2012; 27 520–6.
| Why does patient activation matter? An examination of the relationships between patient activation and health-related outcome.Crossref | GoogleScholarGoogle Scholar |
[6] Flickinger TE, Saha S, Moore RD, Beach MC. Higher quality communication and relationships are associated with improved patient engagement in HIV care. J Acquir Immune Defic Syndr. 2013; 63 362–6.
| Higher quality communication and relationships are associated with improved patient engagement in HIV care.Crossref | GoogleScholarGoogle Scholar |
[7] Ward MC, Miller BF, Marconi VC, et al. The role of behavioral health in optimizing care for complex patients in the primary care setting. J Gen Intern Med. 2016; 31 265–7.
| The role of behavioral health in optimizing care for complex patients in the primary care setting.Crossref | GoogleScholarGoogle Scholar |
[8] Gonzalez JS, Tanenbaum ML, Commissariat PV. Psychosocial factors in medication adherence and diabetes self-management: implications for research and practice. Am Psychol. 2016; 71 539–51.
| Psychosocial factors in medication adherence and diabetes self-management: implications for research and practice.Crossref | GoogleScholarGoogle Scholar |
[9] Muth C, van den Akker M, Blom JW, et al. The Ariadne principles: how to handle multimorbidity in primary care consultations. BMC Med. 2014; 12 223
| The Ariadne principles: how to handle multimorbidity in primary care consultations.Crossref | GoogleScholarGoogle Scholar |
[10] Wallace E, Salisbury C, Guthrie B, et al. Managing patients with multimorbidity in primary care. BMJ. 2015; 350 h176
| Managing patients with multimorbidity in primary care.Crossref | GoogleScholarGoogle Scholar |
[11] Smith SM, Soubhi H, Fortin M, O’Dowd T. Interventions for improving outcomes in patients with multimorbidity in primary care and community settings: systematic review. Cochrane Database Syst Rev 2012; 4 CD006560
[12] Vassilev I, Rogers A, Blickem C, et al. Social networks, the ‘work’ and work force of chronic illness self-management: a survey analysis of personal communities. PLoS One. 2013; 8 e59723
| Social networks, the ‘work’ and work force of chronic illness self-management: a survey analysis of personal communities.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC3sXmtVeit7c%3D&md5=520d859c800ef764559e9592fd386bb1CAS |
[13] Morris RL, Kennedy A, Sanders C. Evolving ‘self’-management: exploring the role of social network typologies on individual long-term condition management. Health Expect. 2016; 19 1044–61.
| Evolving ‘self’-management: exploring the role of social network typologies on individual long-term condition management.Crossref | GoogleScholarGoogle Scholar |
[14] Rogers A, Vassilev I, Sanders C, et al. Social networks, work and network-based resources for the management of long-term conditions: a framework and study protocol for developing self-care support. Implement Sci. 2011; 6 56
| Social networks, work and network-based resources for the management of long-term conditions: a framework and study protocol for developing self-care support.Crossref | GoogleScholarGoogle Scholar |
[15] Crossley N. Small-world networks, complex systems and sociology. Sociology. 2008; 42 261–77.
| Small-world networks, complex systems and sociology.Crossref | GoogleScholarGoogle Scholar |
[16] Kennedy A, Rogers A, Vassilev I, et al. Dynamics and nature of support in the personal networks of people with type 2 diabetes living in Europe: qualitative analysis of network properties. Health Expect. 2015; 18 3172–85.
| Dynamics and nature of support in the personal networks of people with type 2 diabetes living in Europe: qualitative analysis of network properties.Crossref | GoogleScholarGoogle Scholar |
[17] Reeves D, Blickem C, Vassilev I, et al. The contribution of social networks to the health and self-management of patients with long-term conditions: a longitudinal study. PLoS One. 2014; 9 e98340
| The contribution of social networks to the health and self-management of patients with long-term conditions: a longitudinal study.Crossref | GoogleScholarGoogle Scholar |
[18] Vassilev I, Rogers A, Kennedy A, Koetsenruijter J. The influence of social networks on self-management support: a metasynthesis. BMC Public Health. 2014; 14 719
[19] Forbes H, Sutton M, Richardson G, Rogers A. The determinants of time spent on self-care. Chronic Illn. 2016; 12 98–115.
| The determinants of time spent on self-care.Crossref | GoogleScholarGoogle Scholar |
[20] Smith SM, Wallace E, O’Dowd T, Fortin M. Interventions for improving outcomes in patients with multimorbidity in primary care and community settings. Cochrane Database Syst Rev. 2016; CD006560
[21] Cottrell E, Yardley S. Lived experiences of multimorbidity: an interpretative meta-synthesis of patients’, general practitioners’ and trainees’ perceptions. Chronic Illn. 2015; 11 279–303.
| Lived experiences of multimorbidity: an interpretative meta-synthesis of patients’, general practitioners’ and trainees’ perceptions.Crossref | GoogleScholarGoogle Scholar |
[22] Rogers A, Vassilev I, Brooks H, et al. Brief encounters: what do primary care professionals contribute to peoples’ self-care support network for long-term conditions? A mixed methods study. BMC Fam Pract. 2016; 17 21
| Brief encounters: what do primary care professionals contribute to peoples’ self-care support network for long-term conditions? A mixed methods study.Crossref | GoogleScholarGoogle Scholar |
[23] Jaye C, Egan T. Communities of clinical practice: implications for health professional education. Focus Health Prof Educ. 2006; 8 1–10.
[24] Egan T, Jaye C. Communities of clinical practice: the social organization of clinical learning. Health. 2009; 13 107–25.
| Communities of clinical practice: the social organization of clinical learning.Crossref | GoogleScholarGoogle Scholar |
[25] Young J, Egan T, Williamson M, et al. An exercise to map patient-centred care networks. Clin Teach. 2016; 13 448–50.
| An exercise to map patient-centred care networks.Crossref | GoogleScholarGoogle Scholar |
[26] Young J, Jaye C, Egan T, et al. Communities of clinical practice in action: doing whatever it takes. Health. 2017; 1–19.
| Communities of clinical practice in action: doing whatever it takes.Crossref | GoogleScholarGoogle Scholar |
[27] Carryer J, Doolan-Noble F, Gauld R, Budge C. New Zealand patients’ perceptions of chronic care delivery. J Integr Care. 2014; 22 71–80.
| New Zealand patients’ perceptions of chronic care delivery.Crossref | GoogleScholarGoogle Scholar |
[28] Schoen C, Osborn R, Squires D, et al. New 2011 survey of patients with complex care needs in eleven countries finds that care is often poorly coordinated. Health Aff. 2011; 30 2437–48.
| New 2011 survey of patients with complex care needs in eleven countries finds that care is often poorly coordinated.Crossref | GoogleScholarGoogle Scholar |
[29] Kerse N, Teh R, Moyes SA, et al. Cohort profile: Te puawaitanga o Nga tapuwae Kia Ora tonu, life and living in advanced Age: a cohort study in New Zealand (LiLACS NZ). Int J Epidemiol. 2015; 44 1823–32.
| Cohort profile: Te puawaitanga o Nga tapuwae Kia Ora tonu, life and living in advanced Age: a cohort study in New Zealand (LiLACS NZ).Crossref | GoogleScholarGoogle Scholar |
[30] Ministry of Health. Tagata Pasifika in New Zealand 2016. [cited 2016 November 18]. Available from http://www.health.govt.nz/our-work/populations/pacific-health/tagata-pasifika-new-zealand
[31] Yon Y, Crimmins EM. Cohort morbidity hypothesis: health inequalities of older Maori and non-Maori in New Zealand. N Z Popul Rev. 2014; 40 63–83.
[32] Bower P, Macdonald W, Harkness E, et al. Multimorbidity, service organization and clinical decision making in primary care: a qualitative study. Fam Pract. 2011; 28 579–87.
| Multimorbidity, service organization and clinical decision making in primary care: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[33] Mangin D, Heath I, Jamoulle M. Beyond diagnosis: rising to the multimorbidity challenge. BMJ 2012; 344 e3526
[34] Darlow B, Donovan S, Coleman K, et al. What makes an interprofessional education programme meaningful to students? Findings from focus group interviews with students based in New Zealand. J Interprof Care. 2016; 30 355–61.
| What makes an interprofessional education programme meaningful to students? Findings from focus group interviews with students based in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[35] Wenger-Trayner E, Wenger-Traynor B. Social learning: levels of participation. 2015. [cited 2016 October 14]. Available from http://wenger-trayner.com/project/levels-of-participation/
[36] Scott J. Social Network Analysis, 3rd edn. Singapore: Sage Publications Ltd; 2013.
[37] Dwarswaard J, Bakker E, van Staa A, Boeije HR. Self-management support from the perspective of patients with a chronic condition: a thematic synthesis of qualitative studies. Health Expect. 2016; 19 194–208.
| Self-management support from the perspective of patients with a chronic condition: a thematic synthesis of qualitative studies.Crossref | GoogleScholarGoogle Scholar |
[38] Deeken JF, Taylor KL, Mangan P, et al. Care for the caregivers: a review of self-report instruments developed to measure the burden, needs, and quality of life of informal caregivers. J Pain Symptom Manage. 2003; 26 922–53.
| Care for the caregivers: a review of self-report instruments developed to measure the burden, needs, and quality of life of informal caregivers.Crossref | GoogleScholarGoogle Scholar |
[39] Kendall M, Carduff E, Lloyd A, et al. Different experiences and goals in different advanced diseases: comparing serial interviews with patients with cancer, organ failure, or frailty and their family and professional carers. J Pain Symptom Manage. 2015; 50 216–24.
| Different experiences and goals in different advanced diseases: comparing serial interviews with patients with cancer, organ failure, or frailty and their family and professional carers.Crossref | GoogleScholarGoogle Scholar |
[40] Duke NN, Azzahir A. Creating culturally relevant and responsive health care models. J Comm Engage Higher Educ. 2016; 8 53–65.
[41] Oetzel J, Simpson M, Berryman K, et al. Managing communication tensions and challenges during the end-of-life journey: perspectives of Maori kaumatua and their whanau. Health Commun. 2015; 30 350–60.
| Managing communication tensions and challenges during the end-of-life journey: perspectives of Maori kaumatua and their whanau.Crossref | GoogleScholarGoogle Scholar |
[42] Mays N. Reorienting the New Zealand health care system to meet the challenge of long-term conditions in a fiscally constrained environment. Paper prepared for New Zealand Treasury Long-term Fiscal External Panel, November 2012. London: Victoria University & London School of Hygiene and Tropical Medicine, University of London; 2013. Available from www.victoria.ac.nz/sacl/about/cpf/publications/pdfs/Nick-Mays-Revised-Conference-Paper-Jan-2013-website-version.pdf
[43] Rogers A, Brooks H, Vassilev I, et al. Why less may be more: a mixed methods study of the work and relatedness of ‘weak ties’ in supporting long-term condition self-management. Implement Sci. 2014; 9 19
| Why less may be more: a mixed methods study of the work and relatedness of ‘weak ties’ in supporting long-term condition self-management.Crossref | GoogleScholarGoogle Scholar |
[44] Soubhi H, Bayliss EA, Fortin M, et al. Learning and caring in communities of practice: using relationships and collective learning to improve primary care for patients with multimorbidity. Ann Fam Med. 2010; 8 170–7.
| Learning and caring in communities of practice: using relationships and collective learning to improve primary care for patients with multimorbidity.Crossref | GoogleScholarGoogle Scholar |
[45] May C. The hard work of being ill. Chronic Illn. 2006; 2 161–2.
| The hard work of being ill.Crossref | GoogleScholarGoogle Scholar |
[46] Sav A, Kendall E, McMillan SS, et al. ‘You say treatment, I say hard work’: treatment burden among people with chronic illness and their carers in Australia. Health Soc Care Community. 2013; 21 665–74.
[47] Jowsey T, McRae IS, Valderas JM, et al. Time’s up. Descriptive epidemiology of multi-morbidity and time spent on health related activity by older Australians: a time use survey. PLoS One. 2013; 8 e59379
| Time’s up. Descriptive epidemiology of multi-morbidity and time spent on health related activity by older Australians: a time use survey.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC3sXmtVemu7s%3D&md5=103f3840af0ed5e277e1d27aa4e65581CAS |
[48] Jowsey T. Time and chronic illness: a narrative review. Qual Life Res. 2016; 25 1093–102.
| Time and chronic illness: a narrative review.Crossref | GoogleScholarGoogle Scholar |
[49] Coventry PA, Fisher L, Kenning C, et al. Capacity, responsibility, and motivation: a critical qualitative evaluation of patient and practitioner views about barriers to self-management in people with multimorbidity. BMC Health Serv Res. 2014; 14 536
| Capacity, responsibility, and motivation: a critical qualitative evaluation of patient and practitioner views about barriers to self-management in people with multimorbidity.Crossref | GoogleScholarGoogle Scholar |
[50] Neuwelt P, Matheson D. New Zealand’s journey towards people-centred care. Int J Pers Cent Med. 2012; 2 73–9.