A project to improve the quality of care for overweight and obese patients in a Nelson general practice
Jennifer Naper 1 , Luis Manetto 2 , Diane Wiren 21 Nelson Marlborough District Health Board, Nelson, New Zealand
2 Nelson Medical and Injury Centre, Nelson, New Zealand
Correspondence to: Jennifer Naper, Nelson Marlborough District Health Board, Nelson, New Zealand. Email: jennaper86@gmail.com
Journal of Primary Health Care 9(4) 321-327 https://doi.org/10.1071/HC17009
Published: 12 December 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Local guidelines exist in Nelson to assist general practitioners (GPs) in supporting overweight and obese patients with weight loss and improvements in their overall health. This audit measures whether this role is fulfilled in a Very Low Cost Access practice in Nelson, in which 76% of enrolled patients reside in New Zealand social deprivation index quintiles 4 and 5.
AIM: This study measured whether Nelson Marlborough District Health Board Health Pathways and the Ministry of Health Clinical Guidelines are followed in identifying risk and initiating management, including treatment of additional risk factors, lifestyle modification and dietitian referral.
RESULTS: Although limited by sample size and consecutive patient screening methodology, the results of this study indicate that overweight and obesity rates in this practice are comparable with the national average, with Māori and Pacific Island populations more likely to be affected compared to their New Zealand European counterparts. Of the patients who had their body mass index recorded, 65% were overweight or obese. Risk factors were assessed and treated in all, green prescriptions were issued in 4%, and 23% were referred to a dietitian.
DISCUSSION: Audit findings were presented at an intervention session where strategies for improvement were considered including routine waist circumference measurement, dietitian referral, exercise on prescription and providing individualised tailored approaches that integrate patients’ cultural and social context. While risk factors are being managed appropriately, improvements can be made in identifying high-risk patients, promoting lifestyle modifications and early dietitian referral.
KEYWORDS: Obesity; general practitioner; cardiovascular risk factors; exercise; weight management
| WHAT THIS GAP FILLS |
| What is already known: It is well recognised that high obesity rates place a significant health, social, economic, emotional and financial burden on patients and healthcare systems, and obesity rates are highest among the most deprived populations. |
| What this study adds: This audit provides an insight into rates of obesity in a Very Low Cost Access practice in Nelson, New Zealand, with particular emphasis on specific patient demographics, assessment of individual risk factors and individualised management according to the resources available locally. |
Introduction
New Zealand (NZ) is now the third most obese country in the Organisation for Economic Cooperation and Development (OECD), with nearly two-thirds of adults either overweight (35%) or obese (32%). Obesity rates are particularly high among Māori (47%) and Pacific Islands people (PI) (67%),1 and in people at greatest deprivation levels.2 Rates of overweight and obesity are projected to increase and may potentially be the greatest public health threat we face over the next decade as they are risk factors for many non-communicable diseases including type 2 diabetes, cardiovascular disease, musculoskeletal problems and many cancers. Overweight and obesity also has an effect on individuals’ self-esteem and is associated with anxiety, social isolation and mood problems. As well as the health, emotional and social consequences, obesity places a significant financial burden on our healthcare system. This has been shown in a 2006 study, which found that as a percentage of total healthcare expenditure, the healthcare costs of overweight and obesity in NZ are among the highest in the world.3 Reasons for the increased obesity prevalence in our society are complex, but include the increased availability of cheap, energy-rich, nutrient-poor food combined with reduced levels of physical activity.
Body mass index (BMI) is an index of weight adjusted for height and is calculated by dividing the weight in kilograms by height in metres squared. The NZ Ministry of Health uses the World Health Organization (WHO) BMI cut-off points to classify adults into underweight (BMI < 18.5), healthy range (BMI 18.5–24.9), overweight (BMI 25–29.9), obese class I (BMI 30–34.9), obese class II (BMI 35–39.9) and obese class III or ‘extreme obesity’ (BMI ≥ 40),4 and these figures have been used to identify overweight and obese patients for this audit. The risk of adverse health conditions increases with rising BMI.
General practitioners (GPs) are vital in identifying at-risk patients and instigating management to help address the obesity epidemic. It is well recognised that individuals living in the most deprived areas are more likely to suffer adverse health outcomes5 and have much higher levels of unmet need for health care,6 indicating that people at greatest risk may be less likely to receive appropriate support. This audit was carried out to measure the burden of obesity in a Very Low Cost Access (VLCA) practice in Nelson and identify whether local guidelines are being followed in terms of assessment, management and referral. The aim of this audit was to quantify obesity rates, evaluate current management strategies and identify further measures that could be put in place to assist obese and overweight patients with weight loss and improvements in their overall health.
Nelson Medical and Injury Centre is a VLCA practice for enrolled patients within the catchment area. It differs from other practices in the region in terms of ethnicity, social deprivation index (SDI) and age distributions of the enrolled population. Māori and PI ethnic groups make up 43% of the practice population, but only 12% of the total District Health Board (DHB) population. High-needs patients comprise 70% of this practice’s total enrolled patient population, with Māori and PI patients making up 61% of the high-needs population despite Nelson having a lower proportion of Māori and PI people living in the region compared to the national average. While the Nelson–Marlborough region has a very low proportion of people living in the most deprived quintiles of the population (9% overall living in SDI quintile 5) compared to the national average, 46% of this practice’s population live in SDI quintile 5 areas. The practice population is much younger than the DHB average (86% of the DHB population is aged <70 years),7 with 98% of patients attending this practice aged <65 years. This practice is also different in that it operates as the only after-hours accident and medical centre for the Nelson region. This audit included only enrolled patients aged 18–65 years who presented between 9am to 5pm on standard working days.
In terms of resources available to the practice, free dietitian appointments can be provided monthly. Green prescriptions are available through the Nelson Primary Health Organisation (PHO) and are utilised as a motivation tool to assist with weight loss.8 Te Piki Oranga, a regional Māori Health Provider, is also a useful resource for weight loss services and health promotion for Māori and Pacific Island patients in particular.
Assessment of problems
Nelson Marlborough Health Pathways contains a comprehensive guide for assessing, managing and supporting adults who are overweight or obese in primary care. It states that all patients who are identified as overweight or obese should have risk factors assessed, including weight history, waist circumference, BMI-to-waist circumference ratio, blood pressure (BP), lipids, haemoglobin A1c (HbA1c), smoking status and cardiovascular risk factors including Total Cardiovascular Risk (TCVR) score. It states that management should be guided by patients’ levels of motivation, but should include practice nurse review, dietitian review, green prescription, smoking cessation support and risk factor management. Weight-reducing drug treatment and bariatric surgery are also mentioned in the guideline for patients who are compliant with lifestyle modifications, engaged with all appropriate support services and meet access criteria.9
The standards set were guided by the primary care guidelines set out in Nelson Marlborough DHB Health Pathways and shown in Box 1. These guidelines as standards were considered to be achievable and realistic by the practice, but some potential barriers were identified. A practice nurse review was not considered achievable for all overweight or obese patients due to the high numbers of such patients attending the practice, often for issues perceived to be unrelated to their weight. While free monthly dietitian appointments are available, this is not realistically achievable for all patients, and compliance with dietitian follow up can be affected by accessibility, motivation and cultural acceptability. The Green Prescription pathway is specifically available to patients who are ready to make changes to self-manage and benefit their health,10 making this an unrealistic option for patients who lack motivation, are unable to actively engage in physical activity or have an unstable health condition.11 Furthermore, the National Institute for Health and Care Excellence (NICE) guidelines recommend that GPs should not refer sedentary or inactive patients who are otherwise healthy to exercise referral schemes, and specific criteria exist for referring sedentary or inactive patients with existing health conditions to exercise on prescription programmes.12
| Box 1. Weight management in adults, Health Pathways Consensus23 | ||||
| ||||
Methods
All enrolled patients aged 18–65 years who presented to the practice over a 5-day period were identified by MedTech software (MedTech Global, Auckland, New Zealand), and their age, sex and ethnicity was recorded on a Microsoft Excel spreadsheet. BMI was also recorded, and relevant patients were classified as either overweight or obese accordingly. The documentation of risk factors and all management strategies that had been instigated were also recorded, and the results were collated and analysed using Microsoft Excel.
Results
A group of 53 enrolled patients with an average age of 36.6 years were studied. Of these, 64.2% (34/53) were female and 35.8% (19/53) were male. In terms of ethnicity, 54.7% (29/53) were NZ European, 20.8% (11/53) were Māori, 7.5% (4/53) were of PI ethnicity, 15.1% (8/53) were Asian (Chinese, Burmese, Thai and Indian) and 1.9% (1/53) were of other European ethnicity.
Of the 53 presenting patients, 75.5% (40/53) had their BMI recorded and 84.9% (45/53) had their weight documented. The 24.5% (13/53) who did not have their BMI recorded were excluded from the audit. Of these excluded patients, 38.5% (5/13) had been weighed but BMI was not documented, 46.2% (6/13) were of Māori or PI ethnicity, 38.5% (5/13) were NZ European and 15.4% (2/13) were Asian.
Of the 40 patients who did have their BMI checked, 35% (14/40) had a BMI of <25. Overweight patients (BMI 25–30) made up 25% (10/40) of the group, and obese patients (BMI > 30) made up 40% (16/40). Over one-third of audited patients therefore had a BMI of >30 and nearly two-thirds had a BMI of >25.
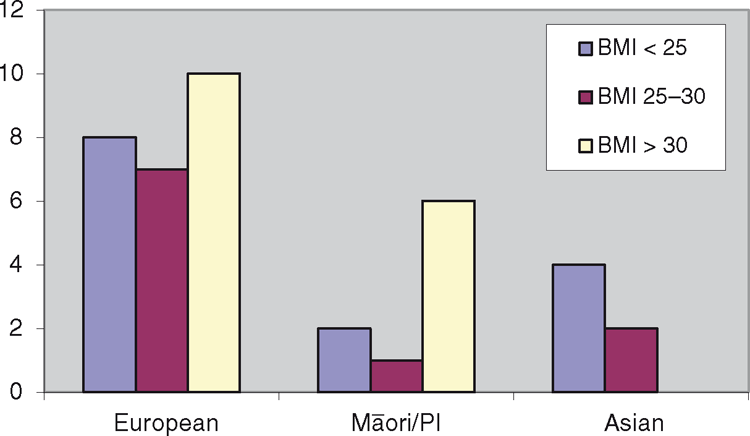
Audited patients were further classified by their ethnicity, as shown in Fig. 1. Of the patients of European ethnicity who had their BMI checked, 40% (10/25) had a BMI of >30, 28% (7/25) had a BMI of 25–30 and 32% (8/25) had a BMI of <25. Of the NZ Māori and PI patients who had their BMI checked, 66.7% (6/9) had a BMI of > 30, 11.1% (1/9) had a BMI of 25–30 and 22.2% (2/9) had a BMI of <25. One-third (2/6) of the audited patients of Asian ethnicity had a BMI of 25–30 and two-thirds (4/6) had a BMI of <25.
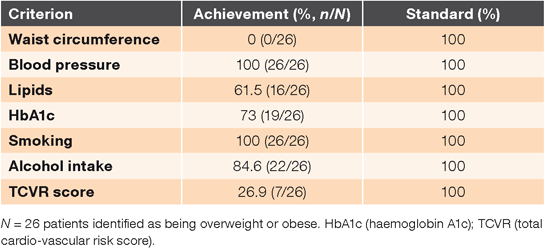
Table 1 shows the numbers and proportions of overweight and obese patients who had risk factors assessed. Additional risk factors were identified in 69.2% (18/26), while no additional risk factors were identified in 30.8% (8/26) of the audited overweight or obese individuals.
|
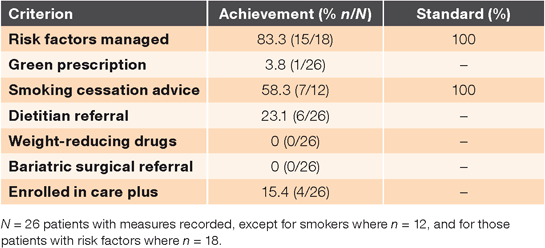
Table 2 includes the numbers and proportions of obese or overweight patients who received management according to the guideline-based standards. Of the 18 patients who had additional risk factors identified, 83.3% (15/18) had them addressed through smoking cessation advice or treatment, anti-hypertensives, statin therapy, antiplatelet agents and diabetes management. Just 1 of the 26 overweight or obese patients received a green prescription; this was a 24-year-old female of NZ European ethnicity with a BMI of 30.1 and no identified additional risk factors. Referral to the dietitian occurred for 23.1% (6/26).
|
Strategies for quality improvement or change
Audit findings were presented to staff at the practice at an educational session that was attended by the practice manager, clinical director, clinical nurse leader and practices nurses. Introducing waist circumference measurement into routine practice was considered due to the evidence that waist circumference coupled with BMI is better at predicting health risk than BMI alone13 and therefore may help with risk stratification and the direction of resources towards those patients most at-risk. The benefits and limitations of potential effective intervention strategies were discussed and included increased practice nurse input, dietitian referral and rates of green prescription. Resource limitation, the normalisation of obesity in our society and low rates of compliance with long-term follow up were identified as barriers to change. It was particularly recognised that participation rates with such interventions are often affected by the broader cultural and community context, and that ongoing dialogue with patients, their families, the wider community and society as a whole is required to bring about sustainable improvements in rates of overweight and obesity in this Nelson practice.
Lessons and messages
This audit identified that improvements can be made in identifying at-risk obese patients. Almost one-quarter of patients audited did not have their BMI checked, and waist circumference, a measure of central (abdominal) obesity, is not being routinely checked for overweight and obese patients. The gap in frequency of coding of BMI in obese patients is recognised, and obese patients tend not to have BMI values recorded regularly.14 The gap observed in measuring waist circumference is also common, despite good evidence that excess abdominal obesity and fat correlates most strongly with risk of disease, in particular diabetes and cardiovascular disease, but also cancer.15 Waist circumference measurement also provides a simple method of identifying people at increased risk of obesity-associated illness due to abdominal distribution of fat.16
Improvements can also be made in measuring risk factors. Commendably, BP and smoking status has been addressed in all patients, but there has been variable assessment of other cardiovascular risks. While risk factors have been appropriately managed, dietitian referral is not routine and green prescription is an underutilised tool, although this may be affected by motivational factors, readiness to change, ability to participate, pre-existing health conditions and restrictions in the international literature. An educational session with staff at the practice has increased awareness and motivated staff to address the problem in a sensitive manner while considering the additional multidisciplinary resources that may be underutilised at present.
Discussion
Nelson Medical and Injury Centre is a VLCA practice with a large proportion of high-needs patients, high numbers of patients living in socially deprived areas of Nelson, and higher numbers of Māori and PI patients than the local or national average. As obesity is a condition that is more prevalent among the most deprived in our society and Māori and PI populations, it was unsurprising the patients audited have similar rates of overweight and obesity to the national average, with Māori and PI people attending this practice more likely to be overweight or obese than their European or Asian counterparts.
The NZ primary care sector has been identified as being an important contributor to the prevention and management of overweight and obesity rates,17 as most NZ adults visit their GP at least once per year.18 Weight loss advice in primary care has been shown to have a statistically significant positive effect on patient weight loss behaviour.19 Despite this, GPs and primary care providers often feel disempowered regarding their ability to manage obesity, with barriers including the rooting of weight management in personal issues, social stigma, the normalisation of overweight and obesity in society, a lack of efficacious interventions and a lack of available resources identified in a 2014 qualitative study carried out in the Wellington region.20
At a primary care level, local guidelines are useful for supporting GPs to help individuals living with obesity, but a tailored approach may be most appropriate, taking into consideration patients’ levels of motivation to change their lifestyle, their physical wellbeing, the significance of risk determined by additional risk factors, the availability of local resources and the wider social and cultural context. An integrated government response to the obesity epidemic is also necessary to facilitate and complement primary care and community-based approaches to obesity, combining legislation, regulations and policies to counter our obesogenic environment and improve health literacy.21
Limitations
This audit screened consecutive enrolled patients who attended one general practice over a 5-day period. It is therefore unlikely to be a representative sample of the practice population, as patients were not randomly sampled. This audit is also limited by its small sample size, so the results cannot necessarily be generalised to make conclusions about the practice population or the wider community.
BMI is widely used as an indirect measure of body adipose tissue, as it is simple to measure and is correlated with total body fat. It is a reasonable indicator of body fatness in most individuals and within populations; however, for an audit like this, we needed to take into account that BMI varies according to age, gender, ethnicity and other factors, such as body build. This variation is accounted for by the fact that BMI cannot differentiate between lean and fat mass and does not give any information on the distribution of body fat. BMI is a continuous variable with a continuous relationship between BMI and health outcomes. There is no threshold at which the risk of disease suddenly increases and so the specific cut-off points used by the Ministry of Health and WHO to define BMI category is somewhat arbitrary.22
Conclusion
The patients audited in this VLCA practice in Nelson have similar rates of overweight and obesity to the national average, with highest rates among Māori and PI populations. Small individual practice audits such as this can help to increase awareness and implement improvements in measuring BMI, weight circumference, assessing risk factors and utilising multidisciplinary management approaches.
COMPETING INTERESTS
The authors declare no conflicts of interest.
ACKNOWLEDGEMENT
The authors wish to thank Graham Mc Geoch, Chief Clinical Editor, Health Pathways, Canterbury District Health Board.
References
[1] Ministry of Health NZ. Obesity statistics. [cited 2017 August 7]. Available from: http://www.health.govt.nz/nz-health-statistics/health-statistics-and-data-sets/obesity-statistics[2] Ministry of Health. Understanding excess body weight: New Zealand health survey. Wellington: Ministry of Health; 2015. [cited 2017 June 29]. Available from: http://www.health.govt.nz/system/files/documents/publications/understanding-excess-body-weight-nzhs-apr15-v2.pdf
[3] Lal A, Moodie M, Ashton T, Siahpush M, Swinburn B. Health care and lost productivity costs of overweight and obesity in New Zealand. Aust N Z J Public Health. 2012; 36 550–6.
| Health care and lost productivity costs of overweight and obesity in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[4] Ministry of Health. Clinical Guidelines for Weight Management in New Zealand Adults. Wellington: Ministry of Health; 2009. p. 13.
[5] Ministry of Health. Atlas of Socioeconomic Deprivation in New Zealand NZDep2006. Wellington: Ministry of Health; 2008. p. 7.
[6] Ministry of Health. Annual update of key results 2015/16: New Zealand Health Survey. [cited 2017 August 10]. Available from: http://www.health.govt.nz/publication/annual-update-key-results-2015-16-new-zealand-health-survey
[7] Ministry of Health NZ. Population of Nelson Marlborough DHB 2016. [cited 2017 August 10]. Available from: http://www.health.govt.nz/new-zealand-health-system/my-dhb/nelson-marlborough-dhb/population-nelson-marlborough-dhb
[8] Nelson Marlborough HealthPathways. Green Prescription (GRx). 2015. [cited 2017 June 29]. Available from: https://nm.healthpathways.org.nz/index.htm
[9] Nelson Marlborough HealthPathways. Weight Management in Adults. 2015. [cited 2017 June 29]. Available from: https://nm.healthpathways.org.nz/index.htm
[10] Nelson Bays Primary Health. Green Prescription. 2016. [cited 2017 June 29]. Available from: http://nbph.org.nz/new-page
[11] Ministry of Health. The Green Prescription (GRx) Process for Primary Health Care. 2016. [cited 2017 June 29]. Available from: http://www.health.govt.nz/system/files/documents/pages/greenprescriptionprocess-forprimaryhealthcare.pdf
[12] National Institute for Health and Care Excellence. Physical activity: exercise referral schemes. Guidance and guidelines. NICE. 2014. [cited 2017 June 29]. Available from: https://www.nice.org.uk/guidance/ph54
[13] Janssen I, Katzmarzyk P, Ross R. Waist circumference and not body mass index explains obesity-related health risk. Am J Clin Nutr. 2004; 79 379–84.
| 1:CAS:528:DC%2BD2cXhslOht7w%3D&md5=5ab82022467995f8cc35b183c6e8a233CAS |
[14] Booth HP, Prevost AT, Gulliford MC. Epidemiology of clinical body mass index recording in an obese population in primary care: a cohort study. J Public Health. 2013; 35 67–74.
| Epidemiology of clinical body mass index recording in an obese population in primary care: a cohort study.Crossref | GoogleScholarGoogle Scholar |
[15] Turley M, Tobias M, Paul S. Non-fatal disease burden associated with excess body mass index and waist circumference in New Zealand adults. Aust N Z J Public Health. 2006; 30 231–7.
| Non-fatal disease burden associated with excess body mass index and waist circumference in New Zealand adults.Crossref | GoogleScholarGoogle Scholar |
[16] World Health Organization. Obesity: preventing and managing the global epidemic. Geneva: WHO; 2000. p. 7. [cited 2017 June 29]. Available from: http://www.who.int/nutrition/publications/obesity/WHO_TRS_894/en/
[17] The Royal New Zealand College of General Practitioners. Tackling the growing obesity epidemic: a general practice perspective. Wellington: The Royal New Zealand College of General Practitioners; 2014; p. 1. [cited 2017 June 29]. Available from: https://www.rnzcgp.org.nz/RNZCGP/Publications/Policy_briefs/RNZCGP/Publications/Policy_briefs.aspx?hkey=20017639-9b5a-4ff1-b6e6-bebfc01b47bd
[18] Ministry of Health. New Zealand Health Survey: Annual update of key findings 2012/13. Wellington: Ministry of Health; 2013. p. 6.
[19] Rose SA, Poynter PS, Anderson JW, et al. Physician weight loss advice and patient weight loss behaviour change: a literature review and meta-analysis of the survey data. Int J Obes. 2013; 37 118–28.
| Physician weight loss advice and patient weight loss behaviour change: a literature review and meta-analysis of the survey data.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC38vpvVWnsQ%3D%3D&md5=943d1dd2850c088afaeaae49c1f200c5CAS |
[20] Claridge R, Gray L, Stubbe M, Tester R, Dowell A. General practitioner opinion of weight management interventions in New Zealand. J Prim Health Care. 2014; 6 212–20.
[21] New Zealand Medical Association. Tackling obesity. Wellington: New Zealand Medical Association; 2014. pp. 12–28. [cited 2017 June 29]. Available from: https://www.nzma.org.nz/__data/assets/pdf_file/0015/32082/NZMA-Policy-Briefing-2014_Tackling-Obesity.pdf
[22] Ministry of Health. Understanding excess body weight: New Zealand Health Survey. Wellington: Ministry of Health; 2015. p. 4.
[23] Nelson Marlborough HealthPathways. Weight management in adults. 2015. [cited 2017 August 11]. Available from: https://nm.healthpathways.org.nz/index.htm