Beyond the four walls: an exploratory survey of location, employment and roles of pharmacists in primary health care
Chloë Campbell 1 2 , Rhiannon Braund 1 , Caroline Morris 21 School of Pharmacy, University of Otago, Dunedin, New Zealand
2 Department of Primary Health Care and General Practice, University of Otago, Wellington, New Zealand
Correspondence to: Chloë Campbell, School of Pharmacy, University of Otago, Dunedin, New Zealand. Email: chloe.campbell@postgrad.otago.ac.nz
Journal of Primary Health Care 9(4) 297-310 https://doi.org/10.1071/HC17022
Published: 28 August 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Recognition of the need to reduce harm and optimise patient outcomes from the use of medicines is contributing to an evolution of pharmacy practice in primary health care internationally. This evolution is changing community pharmacy and leading to new models of care that enable pharmacist contribution beyond traditional realms. There is little information about the extent of these changes in New Zealand.
AIM: The aim of this study was to investigate emerging roles of pharmacists in primary health care.
METHODS: A 10-question electronic survey was used to collect quantitative data about location, employment and roles of pharmacists practising in primary health care.
RESULTS: There were 467 survey responses. Although most pharmacists are employed by (78%, n = 357/458) and located in (84%, n = 393/467) community pharmacies, small numbers are dispersed widely across the primary health care sector. Of the 7% (n = 31/467) working in general practices, most are employed by Primary Health Organisations or District Health Boards. Limited cognitive pharmacy service provision is evident in the sector overall, but is much greater for pharmacists spending time located within general practices.
DISCUSSION: The large proportion of pharmacists practising in community pharmacies emphasises the importance of the Community Pharmacy Services Agreement in facilitating increased cognitive pharmacy service provision to optimise patient outcomes. The small numbers of pharmacists located elsewhere in the primary health care sector suggest there is scope to improve collaboration and integration in these areas. Flexible funding models that promote innovation and support sustainable practice change are key.
KEYWORDS: Primary health care; pharmacy services; integration; general practice; clinical services
| WHAT GAP THIS FILLS |
| What is already known: Optimising patient health outcomes by ensuring that medicine use achieves maximal benefit with minimal harm is a goal of health systems internationally. Recognition of the need to make better use of the pharmacist workforce to help achieve this is driving change in pharmacy practice, yet there is little information on the evolution and delivery of pharmacy services in New Zealand primary health care. |
| What this study adds: While most pharmacists are practising in and employed by community pharmacies, small numbers are dispersed widely across primary health care, including a small number spending time in general practices. Overall, the extent of cognitive pharmacy service provision in primary health care is low, emphasising a need to develop models of care that support sustainable practice change and enhance patient outcomes from medicines use. |
Introduction
Widespread recognition of the need to optimise patient outcomes from the use of medicines is contributing to changes in pharmacy practice within primary health care (PHC) internationally.1 A key aspect of this evolution is movement beyond traditional roles in medicines supply towards increasing provision of ‘cognitive pharmacy services’ (ie services that specifically draw on pharmacists’ specialised knowledge to promote safe, effective use of medicines).2 In practical terms, this means new roles for pharmacists within community pharmacies,3–6 as well as new models of care that facilitate pharmacist contributions in other parts of PHC.7–10
Foundation cognitive services implemented in community pharmacy internationally have centred around two areas: medication adherence support and medication review. As cognitive pharmacy services mature, comprehensive medication management roles with or without prescribing rights are also developing.11,12 Medication adherence support services aim to improve patients’ understanding of and adherence to prescribed medicines, while medication reviews involve a clinical review and the provision of recommendations on therapy adjustments, as necessary, with the goal of optimising patient outcomes.
Community pharmacy-based cognitive services were introduced in the United Kingdom (UK) in 2005 with government funding of ‘Medicine Utilisation Review’, a medicines adherence support service.13,14 The ‘New Medicines Service’ was introduced in 2011 to improve medicines adherence in patients with newly prescribed treatments for long-term conditions.15 Cognitive services delivered within this setting in the UK are likely to develop further following a recent National Health Service-commissioned report that recommended redesign of adherence support services to incorporate on-going monitoring.4 The addition of a medication review service using independent pharmacist prescribers was also mooted.4 In Canada, government-funded, community pharmacy-led adherence support services began in Ontario in 2007.16 Other provinces have since developed adherence support services and several also run funded medication review services.1 In contrast to other countries that began with adherence support services, Australia commenced with ‘Home Medication Reviews’ in 2001.17 These medication reviews are funded on a fee-for-service basis as part of the national community pharmacy agreement.18 The ‘Residential Medication Management Review’ was introduced in 2005 and adherence support services in 2012.1,19
Pharmacist contribution outside the traditional realm of community pharmacy has also evolved with changing models of care in PHC internationally.7 Pharmacists have been employed in population-level primary care management organisations8 similar to New Zealand (NZ) Primary Health Organisations (PHOs) and, more recently, the concept is emerging of pharmacists being fully integrated within general practice teams.10–12,20–23 In the UK, a successful £30 million pilot project has facilitated nearly 500 clinical pharmacists to be employed directly by general practices.12 A further £100 million funding was announced in December 2016 for another 1500 clinical pharmacists to be working in general practice by 2020/21.9 The UK National Health Service vision is for pharmacists in general practice to support patients to self-manage their wellbeing and long-term conditions through optimising medicines, and to facilitate improved medicine-related communication at interfaces of care.12 Similar integrated care models have been described in Canada10,22,24 and Australia,11,20,23 where the concept is supported by the Australian Medical Association.25
In NZ, available cognitive pharmacy services include the adherence support service, ‘Medicines Use Review’ and the medication review service, ‘Medicines Therapy Assessment’.26 Both may be provided by accredited pharmacists but have not gained consistent funding by individual District Health Boards (DHBs). Likewise, the Community Pharmacy Anti-Coagulation Management Service is funded in only some DHB areas.5 A new Community Pharmacy Services Agreement in 2012 introduced, at a national level, a form of adherence service known as the ‘Long-Term Conditions’ service. Eligible patients are identified, registered and managed by community pharmacies to encourage better medicines adherence; funding is via a monthly fee per registered service user.27
The recently released Pharmacy Action Plan outlines actions to be taken to enable better use of the pharmacy workforce.28 Grounded in the principles of the NZ Health Strategy and closely aligned with the NZ Medicines Strategy, its vision is for pharmacists to work collaboratively in integrated teams across health and social care sectors, helping to improve health outcomes through a comprehensive range of medicines management services.28–30
To date, there is little national information about the provision of cognitive pharmacy services in NZ. The aim of this study was therefore to investigate the physical location and employment situation of pharmacists and to identify the range and extent of cognitive pharmacy services being provided.
Methods
A 10-question electronic survey was used to collect quantitative data about location, employment and roles of pharmacists working in primary care (see Appendix 1). To assess content validity, the survey was piloted by two practising pharmacists, resulting in minor adjustments to improve flow and readability. Following ethical approval (University of Otago, D16/230), an email invitation was sent by the Chief Pharmacist Advisor at the Pharmaceutical Society of New Zealand to all 3482 pharmacists on the members’ mailing list. As it is mandatory for all practising pharmacists to be active in a continuing professional development programme, and the Pharmaceutical Society is the sole provider, our sampling strategy included all pharmacists practising nationally. The email invitation specified the inclusion criteria of working in PHC and contained a link to the e-survey, which was open for 4 weeks. Two email reminders were sent; one after 2 weeks and one 5 days before the survey closing date.
Results
There were 467 survey responses. It was not possible to identify a definitive response rate because the number of pharmacists working within the wider PHC sector is unknown. However, an approximate response rate of 16% (n = 467/2951) was calculated using publicly available data.31 The denominator (2951) was derived by subtracting pharmacists known to be working in hospital pharmacy (491) or the pharmaceutical industry (40) from the total number invitations sent (3482). Female pharmacists accounted for 70% of the respondents. The average number of years in practice was 20 years and the range was from less than 1 year to 55 years.
Physical location of work
Most respondents (74%) practised solely within a community pharmacy. Of the remaining 26%, 12% worked in a single location other than a community pharmacy, 10% worked in more than one location including community pharmacy, and 4% worked in a combination of locations that did not include community pharmacy. Figure 1 presents the physical locations across the PHC sector where respondents reported working. The ‘other’ category included locations such as academia, private hospitals, and organisations such as the Best Practice Advocacy Centre. For pharmacists spending time located in general practice, the average was 21 h/week (range 1–50 h/week). For pharmacists working in patients’ homes, the average was 5 h/week (range 1–20 h/week).
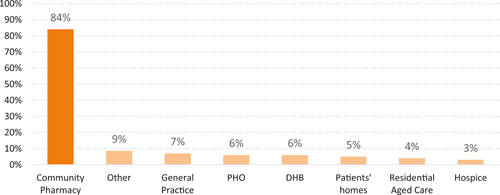
|
Employment
Most respondents were employed by community pharmacies (Figure 2). Independent contractors or self-employed pharmacists were the next largest group at 9%. Apart from community pharmacies, few participants were employed directly by individual providers.
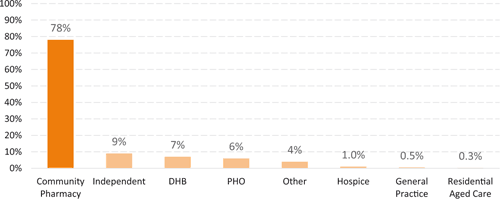
|
Roles and services
Most (88%) responding pharmacists who spend time working in community pharmacy answer medicines information questions from other health professionals (Figure 3). All other cognitive roles and services investigated in this study were undertaken by less than one-third of respondents. The Community Pharmacy Anti- Coagulation Management Service, accredited supply of emergency contraception, trimethoprim and sildenafil, administration of vaccinations, and advice to patients were the roles or services most commonly mentioned in the ‘other’ category.
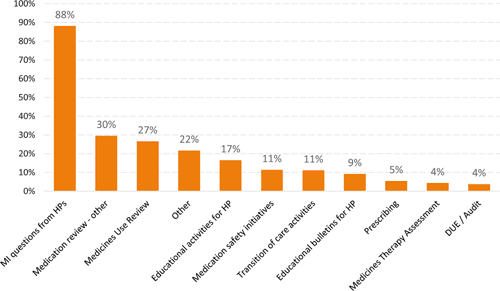
|
Pharmacists spending time in general practice
As integration and collaboration within PHC are key foci of NZ health policy, we specifically examined the roles and employment situation of the pharmacists spending time physically located in general practices (n = 31). One-third worked solely in general practices, one-third worked in general practice and one other setting such as a PHO, a community pharmacy or patient homes; and one-third worked in a combination of three or more locations.
In contrast to the overall findings, all cognitive services are provided by at least one-third of pharmacists spending time in general practice, and most by over half (Figure 4). Nearly one-third reported providing ‘other’ services, which included working with practice nurses on diabetic medication management, medicines reconciliation and involvement in the maintenance of electronic medication records.
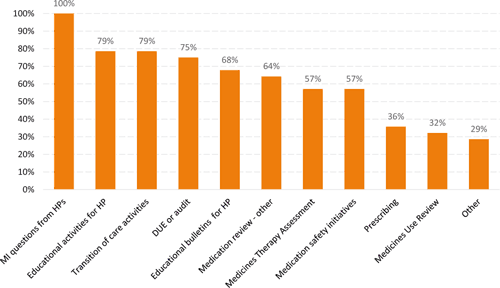
|
Both PHOs and DHBs employed the greatest number of pharmacists who spend time physically located within general practice (Figure 5). A small number were employed by a general practice in combination with either a DHB or PHO, but none were employed solely by a general practice.
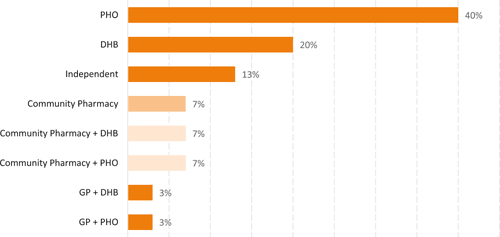
|
Discussion
While most pharmacists working in primary care are based in community pharmacies, these results show there is movement beyond the four walls, with one-quarter of respondents involved in work outside traditional pharmacy premises. The 2016 Pharmacy Action Plan expresses a vision for pharmacists to be located across health and social care sectors.28 The ideal arrangement will harness the benefits of accessibility when pharmacists are located within community pharmacies32 to strengthen contribution in areas such as self-care33 and minor ailment management,34 medicines adherence,35 health literacy,36 and public health.6 Yet, it will also position pharmacists in other areas of the sector to capitalise on different skills. Some will be ideally located within general practices for close involvement in practice-level medicines management activities, some may work with patients in their homes,37 some within residential aged care facilities,38 and some will contribute at the system level, within PHOs.8 While our data indicate that small numbers of pharmacists are already working in these different areas of primary care, the ideal composition for optimal pharmacist contribution requires ongoing consideration.
Although expected, the finding that most pharmacists in PHC are employed by community pharmacies underlines the potential of the national Community Pharmacy Services Agreement in supporting use of pharmacist expertise to optimise patient outcomes from the use of medicines. Cognitive pharmacy services such as Medicines Use Review and Medicines Therapy Assessment are not included in the current national Community Pharmacy Services Agreement.39
To reduce fragmentation of care and promote efficient use of limited health resources, there is a strong drive for effective multidisciplinary integration and collaboration in national health policy and from professional organisations.28–30,40 Internationally, momentum is building for pharmacists to be integrated within individual general practices.11,12,20,24 In this study, a small number of respondents reported spending time physically located in a general practice. Co-location of pharmacists and general practitioners enabling regular face-to-face communication is an important factor in successful interprofessional working for medicines optimisation.7,20,22,41
In this study, most pharmacists who spent time located in general practices were employed by PHOs or DHBs. This employment model has the advantage of supporting a range of cognitive services, as illustrated by our results where most of these pharmacists are involved in a range of otherwise unfunded activities – transition of care liaison, education for other health professionals and drug utilisation evaluations. Employment and funding are important and interrelated considerations in optimising pharmacist contribution in a sustainable way. Although a medication review service is funded nationally in Australia, a 2014 study indicated that most pharmacists working in general practices were providing additional services for no remuneration, an undeniably unsustainable model.20 Isolated single-service funding could thwart achievement of the full potential of pharmacist involvement in PHC teams. A flexible approach to funding that supports different models of practice is needed, similar to the needs of other allied health professionals working towards enhanced integration.42 The UK National Health Service has provided a seeding subsidy of pharmacist salary in order to facilitate direct employment of pharmacists by general practices.12 The Australian Medical Association has suggested government provision of incentive funding for general practices to develop a practice pharmacist workforce.25 Health Workforce New Zealand has already had a role in funding demonstration projects for new pharmacy services such as the Community Pharmacy Anti-Coagulation Management Service, pharmacist prescribing and checking technicians.
A strong focus of the NZ Pharmacy Action Plan is to remedy chronic underuse of pharmacists’ expertise, moving beyond the supply of medicines towards greater provision of cognitive services.28 Apart from responding to medicines information questions from other health professionals, our findings suggest that overall involvement in cognitive service provision by pharmacists in NZ PHC is low. Although some participants highlighted their provision of the Community Pharmacy Anti-Coagulation Management Service by including it in the ‘other’ category, we did not include it as a separate cognitive role in our survey due to the availability of uptake data from previous research.5 The provision of a range of cognitive services is much increased for pharmacists spending time physically located in a general practice. This is consistent with the international literature and is expected given that cognitive service provision is the primary reason for pharmacists choosing to work in general practices.7,20,22
The low overall provision of cognitive services generally does not signify impossibility. Instead, it draws attention to the challenges of practice change and suggests that successful expansion of such services will need to be preceded by infrastructure changes that support new ways of working. Changes that release pharmacists from traditional technical roles are already being pursued in NZ, with the development of accredited checking technicians.43 Further practical innovations and enhanced collaboration between general practitioners and community pharmacists will be needed to support practice to keep up with evidence.3,44,45
The high proportion of pharmacists responding to medicines information questions from other health professionals is notable considering there is no remuneration for this role. This suggests it is a role driven by demand and is an established role for pharmacists that is recognised by other health professionals. There is little documented literature regarding community pharmacists’ provision of medicines information to health professionals, but access to resources and variable information literacy among pharmacists are areas that may need attention.46,47 For pharmacists integrated within general practices, the high proportion responding to medicines information questions from other health professionals is consistent with reports that 89% of practice pharmacists respond to clinical queries from general practitioners and 77% from other health professionals.20
The low response rate is a limitation of this study. However, the emphasis of this research was to explore emerging roles of pharmacists in PHC as opposed to obtaining a ‘generalisable’ sample. An overestimation of the proportion of pharmacists working in roles outside community pharmacy is possible because we relied on invitees to self-identify as working in PHC. Pharmacists in roles outside traditional community pharmacies may have a stronger identification with working in PHC and thus would be more likely to participate. A key strength of this study is the valuable overview it provides of cognitive pharmacy service provision in NZ PHC. The study provides information for policymakers that has not previously been available, and a useful baseline to track practice change.
Further research is needed to better understand the emerging collaborative practice models in operation locally, their effect on patient and population level outcomes, and the features that lead to success.
Conclusion
This study provides an overview of the current NZ PHC pharmacist workforce in terms of location, employment and roles. It will help to inform workforce planning and policy development in pharmacy and the wider health system, and provides a platform for further research. Pharmacists provide services in a variety of PHC locations, though most are based in and employed by community pharmacies where cognitive pharmacy service provision remains low. Both DHBs and PHOs are key employers for the small numbers of pharmacists who provide a wide range of cognitive pharmacy services. The impact of pharmacist location and employment on optimising contribution to patient health outcomes is an important consideration in the development of future funding models.
FUNDING
This study forms a part of Chloë Campbell’s PhD undertaken through the University of Otago, Dunedin, New Zealand.
COMPETING INTERESTS
The authors have no conflicts of interest to declare.
ACKNOWLEDGEMENTS
We gratefully acknowledge the pharmacists who participated in this study.
References
[1] Houle SK, Grindrod KA, Chatterley T, et al. Paying pharmacists for patient care: a systematic review of remunerated pharmacy clinical care services. Can Pharm J. 2014; 147 209–32.| Paying pharmacists for patient care: a systematic review of remunerated pharmacy clinical care services.Crossref | GoogleScholarGoogle Scholar |
[2] Moullin JC, Sabater-Hernández D, Fernandez-Llimos F, et al. Defining professional pharmacy services in community pharmacy. Res Social Adm Pharm. 2013; 9 989–95.
| Defining professional pharmacy services in community pharmacy.Crossref | GoogleScholarGoogle Scholar |
[3] Jokanovic N, Tan ECK, Sudhakaran S, et al. Pharmacist-led medication review in community settings: an overview of systematic reviews. Res Social Adm Pharm. 2017; 13 661–85.
| Pharmacist-led medication review in community settings: an overview of systematic reviews.Crossref | GoogleScholarGoogle Scholar |
[4] Murray R. Community pharmacy clinical services review. London: NHS England; 2016.
[5] Harper P, McMichael I, Griffiths D, et al. The community pharmacy-based anticoagulation management service achieves a consistently high standard of anticoagulant care. N Z Med J. 2015; 128 31–41.
[6] Brown TJ, Todd A, O’Malley C, et al. Community pharmacy-delivered interventions for public health priorities: a systematic review of interventions for alcohol reduction, smoking cessation and weight management, including meta-analysis for smoking cessation. BMJ Open. 2016; 6 e009828
| Community pharmacy-delivered interventions for public health priorities: a systematic review of interventions for alcohol reduction, smoking cessation and weight management, including meta-analysis for smoking cessation.Crossref | GoogleScholarGoogle Scholar |
[7] Tan ECK, Stewart K, Elliott RA, et al. Pharmacist services provided in general practice clinics: a systematic review and meta-analysis. Res Social Adm Pharm. 2014; 10 608–22.
| Pharmacist services provided in general practice clinics: a systematic review and meta-analysis.Crossref | GoogleScholarGoogle Scholar |
[8] Silcock J, Raynor DKT, Petty D. The organisation and development of primary care pharmacy in the United Kingdom. Health Policy. 2004; 67 207–14.
| The organisation and development of primary care pharmacy in the United Kingdom.Crossref | GoogleScholarGoogle Scholar |
[9] Anon. Clinical pharmacy scheme set to benefit patients across England. NHS England; 2016. [cited 2017 March 1]. Available from: www.england.nhs.uk/2016/12/clinical-pharmacy/
[10] Dolovich L, Pottie K, Kaczorowski J, et al. Integrating family medicine and pharmacy to advance primary care therapeutics. Clin Pharmacol Ther. 2008; 83 913–7.
| Integrating family medicine and pharmacy to advance primary care therapeutics.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1czit1Wguw%3D%3D&md5=aaea10225e52ac85c02d5e9e19dd5d08CAS |
[11] Freeman C, Rigby D, Williams I. The practice pharmacist: a natural fit in the general practice team. Aust Prescr. 2016; 39 211–4.
| The practice pharmacist: a natural fit in the general practice team.Crossref | GoogleScholarGoogle Scholar |
[12] Snow-Miller R. Clinical pharmacists in general practice pilot. London: NHS England; 2015.
[13] Department of Health. The Pharmaceutical Services Directions (Advanced and Enhanced Services). United Kingdom: Department of Health; 2005.
[14] Medicines Use Review. Pharmaceutical Services Negotiating Committee. [cited 2017 March 1]. Available from: http://psnc.org.uk/services-commissioning/advanced-services/murs/
[15] New Medicines Service. Pharmaceutical Services Negotiating Committee. [cited 2017 March 1]. Available from: www.psnc.org.uk/services-commissioning/advanced-services/nms/
[16] Pechlivanoglou P, Abrahamyan L, MacKeigan L, et al. Factors affecting the delivery of community pharmacist-led medication reviews: evidence from the MedsCheck annual service in Ontario. BMC Health Serv Res. 2016; 16 666
| Factors affecting the delivery of community pharmacist-led medication reviews: evidence from the MedsCheck annual service in Ontario.Crossref | GoogleScholarGoogle Scholar |
[17] Chen TF. Pharmacist-led Home Medicines Review and Residential Medication Management Review: the Australian model. Drugs Aging. 2016; 33 199–204.
| Pharmacist-led Home Medicines Review and Residential Medication Management Review: the Australian model.Crossref | GoogleScholarGoogle Scholar |
[18] Anon. Management Reviews. Australian Department of Health. [cited 2017 March 1]. Available from: www.health.gov.au/internet/main/publishing.nsf/Content/medication_management_reviews.htm
[19] Australian Department of Health. MedsCheck/Diabetes MedsCheck Pilot. [cited 2017 March 1]. Available from: www.health.gov.au/internet/main/publishing.nsf/Content/fifth-community-pharmacy-agreement-medscheck)
[20] Freeman C, Cottrell N, Rigby D, et al. The Australian practice pharmacist. J Pharm Pract Res. 2014; 44 240–8.
| The Australian practice pharmacist.Crossref | GoogleScholarGoogle Scholar |
[21] Ackermann E, Williams ID, Freeman C. Pharmacists in general practice: a proposed role in the multidisciplinary team. Aust Fam Physician. 2010; 39 163–4.
[22] Farrell B, Ward N, Dore N, et al. Working in interprofessional primary health care teams: what do pharmacists do? Res Social Adm Pharm. 2013; 9 288–301.
| Working in interprofessional primary health care teams: what do pharmacists do?Crossref | GoogleScholarGoogle Scholar |
[23] Tan ECK, Stewart K, Elliott RA, et al. Pharmacist consultations in general practice clinics: The Pharmacists in Practice Study (PIPS). Res Social Adm Pharm. 2014; 10 623–32.
| Pharmacist consultations in general practice clinics: The Pharmacists in Practice Study (PIPS).Crossref | GoogleScholarGoogle Scholar |
[24] Farrell B, Pottie K, Haydt S, et al. Integrating into family practice: the experiences of pharmacists in Ontario, Canada. Int J Pharm Pract. 2008; 16 309–15.
| Integrating into family practice: the experiences of pharmacists in Ontario, Canada.Crossref | GoogleScholarGoogle Scholar |
[25] Australian Medical Association. General Practice Pharmacists – Improving patient care. Canberra: Australian Medical Association; 2015.
[26] Pharmaceutical Society of New Zealand. New Zealand National Pharmacist Services Framework. Wellington: Pharmaceutical Society of New Zealand; 2014.
[27] Moore D, Love T, Boyle R, et al. Community pharmacy services agreement 2012 evaluation. Wellington: Sapere Research Group; 2015.
[28] Ministry of Health. Pharmacy Action Plan 2016 to 2020. Wellington: Ministry of Health; 2016.
[29] Minister of Health. New Zealand Health Strategy: Future Direction. Wellington: Ministry of Health; 2016.
[30] Ministry of Health. Implementing Medicines New Zealand 2015 to 2020. Wellington: Ministry of Health; 2015.
[31] Pharmacy Council of New Zealand. 2016 Workforce Demographic. Wellington: Pharmacy Council of New Zealand; 2016.
[32] Lindsey L, Husband A, Steed L, et al. Helpful advice and hidden expertize: pharmacy users’ experiences of community pharmacy accessibility. J Public Health. 2016; 1–7.
| Helpful advice and hidden expertize: pharmacy users’ experiences of community pharmacy accessibility.Crossref | GoogleScholarGoogle Scholar |
[33] Rutter P. Role of community pharmacists in patients’ self-care and self-medication. Integr Pharm Res Pract 2015; 4 57–65.
| Role of community pharmacists in patients’ self-care and self-medication.Crossref | GoogleScholarGoogle Scholar |
[34] Porteous T, Ryan M, Bond C, et al. Managing minor ailments: the public’s preferences for attributes of community pharmacies. A discrete choice experiment. PLoS One. 2016; 11 e0152257
| Managing minor ailments: the public’s preferences for attributes of community pharmacies. A discrete choice experiment.Crossref | GoogleScholarGoogle Scholar |
[35] Barnett N. Medication adherence: where are we now? A UK perspective. Eur J Hosp Pharm Sci Pract. 2014; 21 181–4.
| Medication adherence: where are we now? A UK perspective.Crossref | GoogleScholarGoogle Scholar |
[36] Malatest International. Health literacy medication project - measurement and evaluation. Wellington: Health Quality and Safety Commission; 2013.
[37] Castelino RL, Hilmer SN, Bajorek BV, et al. Drug burden index and potentially inappropriate medications in community-dwelling older people: the impact of Home Medicines Review. Drugs Aging. 2010; 27 135–48.
| Drug burden index and potentially inappropriate medications in community-dwelling older people: the impact of Home Medicines Review.Crossref | GoogleScholarGoogle Scholar |
[38] Nishtala PS, Hilmer SN, McLachlan AJ, et al. Impact of residential medication management reviews on Drug Burden Index in aged-care homes. Drugs Aging. 2009; 26 677–86.
| Impact of residential medication management reviews on Drug Burden Index in aged-care homes.Crossref | GoogleScholarGoogle Scholar |
[39] Anon. Consolidated New Zealand Community Pharmacy Services Agreement. 2016. [cited 2017 Mar 1]. Available from: www.centraltas.co.nz/community-pharmacy/community-pharmacy-services-agreement/
[40] Pharmaceutical Society of New Zealand and New Zealand Medical Association. Vision 2020 - Partnership for care - doctors and pharmacists working together. Wellington: Pharmaceutical Society of New Zealand and New Zealand Medical Association; 2015.
[41] Bradley F, Elvey R, Ashcroft DM, et al. The challenge of integrating community pharmacists into the primary health care team: a case study of local pharmaceutical services (LPS) pilots and interprofessional collaboration. J Interprof Care. 2008; 22 387–98.
| The challenge of integrating community pharmacists into the primary health care team: a case study of local pharmaceutical services (LPS) pilots and interprofessional collaboration.Crossref | GoogleScholarGoogle Scholar |
[42] Beckingsale L, Fairbairn K, Morris C. Integrating dietitians into primary health care: benefits for patients, dietitians and the general practice team. J Prim Health Care. 2016; 8 372–80.
[43] Quigley and Watts. Evaluation of the pharmacy checking technician demonstration site project. Wellington: Ministry of Health; 2015.
[44] Spinks J, Jackson J, Kirkpatrick CM, et al. Disruptive innovation in community pharmacy - impact of automation on the pharmacist workforce. Res Social Adm Pharm. 2017; 13 394–7.
| Disruptive innovation in community pharmacy - impact of automation on the pharmacist workforce.Crossref | GoogleScholarGoogle Scholar |
[45] Bardet J-D, Vo T-H, Bedouch P, et al. Physicians and community pharmacists collaboration in primary care: a review of specific models. Res Social Adm Pharm. 2015; 11 602–22.
| Physicians and community pharmacists collaboration in primary care: a review of specific models.Crossref | GoogleScholarGoogle Scholar |
[46] Rutter PM, Warren S, Rutter J. Medicine-related questions handled by community pharmacists: an exploratory study. Int J Pharm Pract. 2009; 17 313–5.
| Medicine-related questions handled by community pharmacists: an exploratory study.Crossref | GoogleScholarGoogle Scholar |
[47] Peterson-Clark G, Aslani P, Williams KA. Pharmacists’ online information literacy: an assessment of their use of Internet-based medicines information. Health Info Libr J. 2010; 27 208–16.
| Pharmacists’ online information literacy: an assessment of their use of Internet-based medicines information.Crossref | GoogleScholarGoogle Scholar |
Appendix 1 – Survey Questions
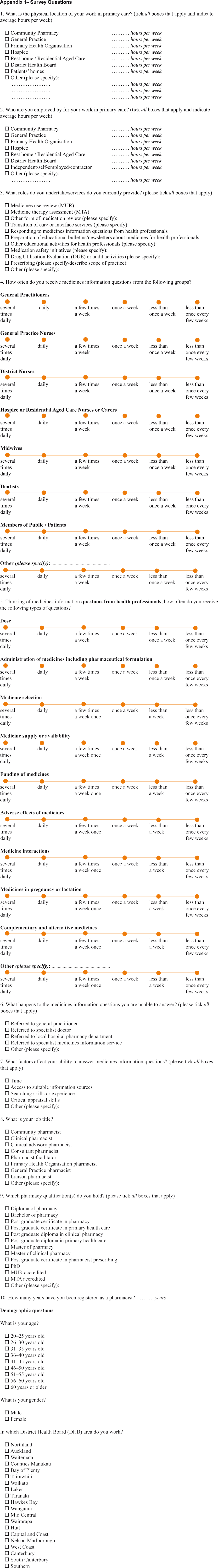
|


