General practitioner referrals to paediatric specialist outpatient clinics: referral goals and parental influence
Marina Kunin 1 , Erin Turbitt 1 , Sarah A. Gafforini 1 , Lena A. Sanci 2 , Neil A. Spike 2 , Gary L. Freed 11 Centre for Health Policy, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia
2 General Practice and Primary Health Care Academic Centre, Melbourne Medical School, The University of Melbourne, Melbourne, Australia
Correspondence to: Gary L. Freed, Centre for Health Policy, Melbourne School of Population and Global Health, The University of Melbourne, Level 4, 207 Bouverie Street, Carlton, Vic. 3053, Australia. Email: gary.freed@unimelb.edu.au
Journal of Primary Health Care 10(1) 76-80 https://doi.org/10.1071/HC17030
Published: 29 March 2018
Journal Compilation © Royal New Zealand College of General Practitioners 2018.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Previous research on general practitioner (GP) referrals in adult populations demonstrated that patient pressure influenced referral practice. No research has been conducted to investigate how involvement of a parent influences paediatric referrals.
AIM: To investigate whether GPs who report parental influence on their decision to refer paediatric patients differ in their referral patterns from GPs who do not report parental influence.
METHOD: A mail survey of 400 GPs who had referred at least two children to paediatric specialist outpatient clinics during 2014 was distributed.
RESULTS: The response rate was 67% (n = 254). For initial referrals, 27% of GPs stated that parental request frequently or almost always influenced their referral decision. For returning referrals, 63% of GPs experienced parental influence to renew a referral because a paediatrician wanted a child to return; 49% of GPs experienced influence to renew a referral because a parent wanted to continue care with a paediatrician. Experiencing parental influence was associated with increased likelihood for frequent referrals in order for a paediatrician to take over management of a child’s condition.
DISCUSSION: GPs who frequently refer with a goal for a paediatrician to take over management of a child’s condition also report that parental request almost always influences their decision to refer.
KEYWORDS: Primary care; secondary care; outpatients; child care; continuity of patient care; delivery of health care
| WHAT GAP THIS FILLS |
| What is already known: Previous research on GP referrals in adult populations demonstrated that patient pressure influenced referral practice. No research has been conducted to investigate how involvement of a parent influences paediatric referrals. |
| What this study adds: GPs who frequently refer with a goal for a paediatrician to take over management of a child’s condition also report that parental request almost always influences their decision to refer. |
Introduction
In Australia, ~20% of children (birth –14 years) consult specialists during any one year. Approximately one-quarter of these visits are to paediatric specialist outpatient clinics.1
Similar to countries where general practitioners (GPs) are an individual’s first point of contact with the health system (e.g. New Zealand,2 UK,3 Canada4), paediatric patients in Australia are referred to specialist care at private or public specialist clinics by GPs, other specialists, emergency departments (EDs) or at hospital discharge. While previous Australian research found the proportion of referrals from general paediatricians and hospital discharge is considerable, GPs are still the most common referral source for paediatric specialist care.5 Whereas in some health systems (eg New Zealand), patients referred to the publicly funded clinics first undergo triage where a specialist decides whether specialist assessment is required, in Australia, all eligible-for-Medicare-benefits referrals are accepted.2,6
There are multiple factors that may influence the decision of a GP to refer a patient to a specialist. The decision to refer is not always based solely on clinical considerations.7 One non-clinical factor is a patient request for a referral for an initial or returning consultation. Research on GP referrals in adult populations in the UK and Canada demonstrated that patient pressure influenced referral practice,8 and that GPs with a high referral rate reported significantly greater perceived pressure from patients for referral than their counterparts with lower referral rate.9 No similar research has been conducted in paediatric care to investigate how involvement of a parent influences the referral process.
The GP’s reason for referral is ideally specified by a GP through communication with a specialist. The main referral purpose usually relates to diagnosis and treatment of a condition, and may result in arranging shared care with a specialist for a specific problem or fully delegating the management of a condition to a specialist. The stated purpose of the referral may play a decisive role in defining the future relationship and communication between a GP, the referred patient and a specialist. It may signal to a specialist the degree of continued involvement desired by the referring GP and may provide an indication of who will have ongoing responsibility for management of a condition in the future. Thus, it is important to understand factors associated with GPs stating a particular referral purpose.
The aim of this study was to investigate whether GPs who report parental influence in their decision to refer paediatric patients differ in their referral patterns from GPs who do not report parental influence. Understanding any potential link between parental request for referral and referral purpose, stated or not, may improve the efficiency in primary and specialist care utilisation by preventing unnecessary referrals.
Methods
This report is part of a wider study to investigate multiple aspects of referrals from GPs to public outpatient paediatricians in Melbourne, Australia.
Sample and recruitment
The sampling frame for this study consisted of GPs who had referred at least two children to the paediatric specialist outpatient clinics at either The Royal Children’s Hospital (RCH) or Monash Children’s Hospital within the 2014 calendar year. Lists of eligible GPs were provided by the respective hospitals. From each list, a random sample of 200 GPs was generated using computer-generated random number sequence. The sample size was calculated for chi-square analysis to detect a difference of 25%, with 80% power at the 5% significance level.
A questionnaire was administered to the sample via registered mail. The dates of the first, second and third mailings were 18 May, 4 June and 18 June of 2015 respectively. At the first mailing, GPs were provided with a co-branded (University of Melbourne and the two hospitals) information sheet about the study, a survey, a Reply Paid envelope and AU$5 cash incentive to participate. GPs were informed that returning the anonymous survey would constitute consent to participate. The information sheet advised GPs that non-respondents would receive up to three further mailings, but that they could contact the research team should they not wish to receive further correspondence. At the two subsequent mailings, GPs received a modified information sheet and another copy of the survey.
Questionnaire
The questionnaire was developed by the research team in consultation with GPs currently engaged in practice. Responses were provided on Likert scales, or as single/multiple choices. With regard to factors associated with referral goals or parental influence, respondents were asked to rate the frequency of these as a proportion of their referrals to public specialist paediatricians over the past 5 years. The rationale for choosing a 5-year period was based on the notion that the number of referrals to paediatric specialist outpatient clinics would have been too few if asked about experiences over a shorter time period. Participants were given response options that included a four-point Likert scale (rarely [< 10%], sometimes [10–50%], frequently [51–90%] and almost always [> 90%]). Other responses were provided as multiple choice options.
Data analysis
Initially, frequency distributions were performed, followed by bivariate analyses using chi-square statistics to determine the differences, if any, among respondents based on referral goals and experiencing parental request to refer. All analyses were completed using STATA 13.0 (StataCorp. 2013; Stata Statistical Software: Release 13. StataCorp LP, College Station, TX).
The project was approved by the Ethics Committees at the University of Melbourne and at the two participating hospitals.
Results
Invitations to participate in this study were sent to 377 GPs (postal addresses could not be sourced for 23 of the GPs from the random generated list). The response rate was 67% (n = 254). We received roughly equal numbers of responses from GPs who had referred to Monash Children’s Hospital or The RCH (n = 128, n = 126 respectively).
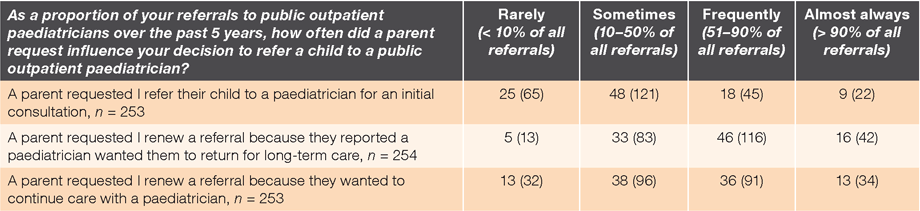
We asked GPs how often parental request influenced their decision to refer a child to a public outpatient paediatrician over the past 5 years. For initial referrals, 27% (n = 67) of GPs stated that parental request frequently or almost always influenced their decision to issue referrals. For returning referrals, 63% (n = 158) of GPs reported frequently or almost always experiencing parental influence to renew a referral because parents reported a paediatrician wanted a child to return for long-term care; 49% (n = 125) of GPs experienced parental influence to renew a referral because a parent wanted to continue care with a paediatrician for an existing condition (Table 1).
|
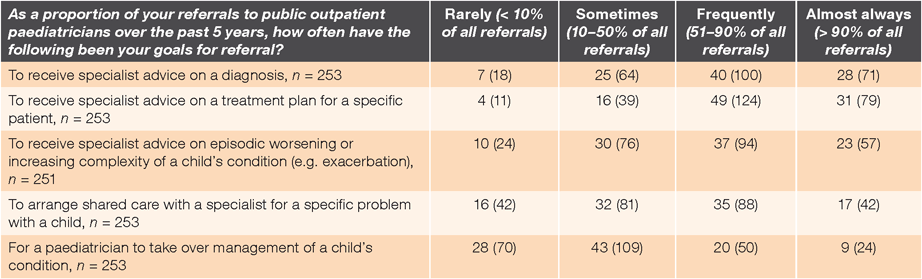
We also asked about referral goals. Respondents rated the importance of each goal individually. The most frequent (combining the responses ‘frequently and ‘almost always’) goal stated by GPs was to receive specialist advice on a treatment plan for a specific patient (80%, n = 203), followed by advice on a diagnosis (68%, n = 171), advice on episodic worsening or increasing complexity of a child’s condition (60%, n = 151), arranging shared care with a specialist for a specific problem with a child (51%, n = 130) and for a paediatrician to take over management of a child’s condition (29%, n = 74) (Table 2).
|
The only statistically significant comparisons from bivariate analysis related to: GPs who almost always experienced parental influence on their decision to refer; GPs influenced to refer because parents reported paediatricians wish to take over a child’s care management (n = 42); and GPs influenced by parents’ request to renew a referral because they wanted to continue care with a paediatrician (n = 34). All comparisons were made with all other GPs. GPs who experienced parental influence on their decision to refer were more likely than other GPs to arrange shared care with a specialist (P = 0.003), and to refer patients for a paediatrician to take over management of a child’s condition (P < 0.001). GPs who were influenced by parents’ request to renew a referral because a paediatrician wanted the patient to return for long-term care (n = 42) were more likely than other GPs to arrange shared care with a specialist (P < 0.001), and to refer for a paediatrician to take over management of a child’s condition (P < 0.001). GPs influenced by parents’ request to renew a referral because they wanted to continue care with a paediatrician (n = 34) were more likely than other GPs to arrange shared care with a specialist (P = 0.002), and refer for a paediatrician to take over management of a child’s condition (P < 0.001). Associations with other referral goals were not statistically significant.
Discussion
The most important finding from this study is that GPs who frequently refer with the goal for a paediatrician to take over management of a child’s condition almost always experience requests from parents to refer. Taking into consideration a parents’ request to refer their child is an appropriate and ethical response by a GP, and demonstrates respect for the parent’s wishes. Similarly, referring patients with a goal to delegate management of their condition to a paediatrician may be an appropriate professional decision depending on the severity of the medical condition. However, the link between these two situations may reflect a more nuanced tendency of some GPs not feeling comfortable in treating certain paediatric conditions and parents not being confident in their GP in providing care in specific instances. This is plausible given recent trends in Australia for a decreasing proportion of a GP’s patient load to consist of children and the potential effect this could have on competency and confidence of GPs to provide primary care for acute and chronic illness in children.10
Previous research into GP referral behaviour suggested that psychological factors are of central importance to understand the referral decision-making process.11 For example, experiencing pressure to refer is a subjective feeling that relates to GPs’ perception of parental wishes. It reflects the interaction between patients’ behaviour and its interpretation by a doctor.9 Research in the adult population in the UK found that perceived pressure from patients was a strong independent predictor of GPs’ decisions to refer.12 A Norwegian study involving adults examining GP referrals to secondary care showed that less medically necessary referrals were more frequently associated with patient pressures influencing GPs’ decisions.13 Our findings imply that in paediatric care, perceived pressure to refer plays an important role also in determining goals of referrals; in particular, the goal of delegating management of the condition to a paediatrician.
The GP decision of handing over permanent care to paediatricians or arranging shared care is also influenced by paediatrician perceptions of the process. A recent study on parental preference for paediatric speciality follow-up care found that the advice of the consulting paediatrician in support of follow-up care with a GP contributes significantly to the willingness of parents to return to primary care and to seek treatment from their GP for a slight worsening of their child’s condition. Thus, paediatricians have a significant influence on care arrangements for paediatric patients with GPs.14
We found that 52% of GPs frequently or almost always refer to arrange shared care with a specialist for a specific problem with a child. These GPs were also more likely to report that parental request to renew a referral almost always influences their decision to refer. Future research should investigate whether parental pressure, actual or perceived by GPs, to issue a referral for a return visit to a paediatric specialist leads to increases in shared care arrangements between GPs and paediatricians.
Limitations
In this study, GPs were asked to recall referrals made within the previous 5 years; thus, recall bias is possible. The study sample were GPs who had referred at least two patients in the past year for paediatric speciality care; thus, the findings may not be generalisable to all GPs, but rather reflect the perceptions of those who have actual recent paediatric referral experience. The study sample consisted of GPs who had referred their patients for paediatric speciality care at public hospitals; thus, the results may not capture referral patterns to private paediatricians. The study was conducted in only one state and thus may not be reflective of patterns of care in other states. However, the main strength of our study is a 67% response rate among GPs, which decreases the potential for response bias.
Conclusion
GPs who frequently refer with a goal for a paediatrician to take over management of a child’s condition also report that parental request almost always influences their decision to refer. Future research should investigate whether this association is linked to potential issues of GP confidence in treating paediatric patients and a diminution of parental confidence in GPs. Also, it is important to understand the contribution of parental preferences to the arrangement of shared care between GPs and paediatric specialists, especially in light of the recent emphasis on coordination of care for chronic patients in Australia.
FUNDING
This study was funded by the Victorian Government’s Department of Health and The Royal Children’s Hospital Foundation.
COMPETING INTERESTS
None.
ACKNOWLEDGEMENTS
We thank the participants of this study for their time answering the survey.
References
[1] Australian Bureau of Statistics. Australian Health Survey: Health Service Usage and Health Related Actions 2011–12. Canberra: ABS; 2013.[2] Cumming J, McDonald J, Barr C, et al. New Zealand: health system review. Health Syst Transit. 2014; 4 1–244.
[3] Cylus J, Richardson E, Findley L, et al. United Kingdom: health system review. Health Syst Transit. 2015; 17 1–126.
[4] Marchildon G. Canada: health system review. Health Syst Transit. 2013; 15 1–179.
[5] Kunin M, Turbitt E, Gafforini S, et al. What proportion of paediatric specialist referrals originates from general practitioners? J Paediatr Child Health. 2017; Sept 6
| What proportion of paediatric specialist referrals originates from general practitioners?Crossref | GoogleScholarGoogle Scholar |
[6] Healy J, Sharman E, Lokuge B. Australia: health system review. Health Syst Transit. 2006; 8 1–158.
[7] Newton J, Hayes V, Hutchinson A. Factors influencing general-practitioners referral decisions. Fam Pract. 1991; 8 308–13.
| Factors influencing general-practitioners referral decisions.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK387pt1ektA%3D%3D&md5=02fb9ce72c33752bbf82b5943da6e814CAS |
[8] Langley GR, Maclellan AM, Sutherland HJ, Till JE. Effect of nonmedical factors on family physicians decisions about referral for consultation. CMAJ. 1992; 147 659–66.
| 1:STN:280:DyaK38zptlKltA%3D%3D&md5=19459a948a04d1786c7c1a99a7b87451CAS |
[9] Armstrong D, Fry J, Armstrong P. Doctors’ perceptions of pressure from patients for referral. BMJ. 1991; 302 1186–8.
| Doctors’ perceptions of pressure from patients for referral.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK3M3lsFOltQ%3D%3D&md5=7db6b6bae56c410d1e6a1fd32b89de6fCAS |
[10] Freed GL, Sewell J, Spike N, et al. Changes in the demography of Australia and therefore general practice patient populations. Aust Fam Physician. 2012; 41 715–9.
[11] Dowie R. General practitioners and consultants: a study of outpatient referrals. London: King Edward’s Hospital Fund for London; 1983.
[12] Little P, Dorward M, Warner G, et al. Importance of patient pressure and perceived pressure and perceived medical need for investigations, referral, and prescribing in primary care: nested observational study. BMJ. 2004; 328 444–6.
| Importance of patient pressure and perceived pressure and perceived medical need for investigations, referral, and prescribing in primary care: nested observational study.Crossref | GoogleScholarGoogle Scholar |
[13] Ringberg U, Fleten N, Forde OH. Examining the variation in GPs’ referral practice: a cross-sectional study of GPs’ reasons for referral. Br J Gen Pract. 2014; 64 e426–33.
| Examining the variation in GPs’ referral practice: a cross-sectional study of GPs’ reasons for referral.Crossref | GoogleScholarGoogle Scholar |
[14] Kunin M, Turbitt E, Gafforini S, et al. Parental preferences for paediatric specialty follow-up care. Aust Health Rev. 2017; 41 401–6.
| Parental preferences for paediatric specialty follow-up care.Crossref | GoogleScholarGoogle Scholar |


