Unmet need for referred services as measured by general practice
Graham McGeoch 1 , Kieran Holland 1 , Melissa Kerdemelidis 2 , Nikki Elliot 1 , Brett Shand 1 , Catherine Fink 1 , Anne Dixon 1 , Carolyn Gullery 21 Canterbury Initiative, Canterbury District Health Board, Christchurch, New Zealand
2 Planning and Funding and Decision Support, Canterbury District Health Board, Christchurch, New Zealand
Correspondence to: Graham McGeoch, Canterbury Initiative, Canterbury District Health Board, Christchurch, New Zealand. Email: graham.mcgeoch@cdhb.health.nz
Journal of Primary Health Care 9(4) 269-278 https://doi.org/10.1071/HC17044
Published: 12 December 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Unmet needs are a key indicator of the success of a health system. Clinicians and funders in Christchurch, Canterbury, New Zealand were concerned that unmet health need was hidden.
AIM: The aim of this survey was to estimate the proportion of patients attending general practice who were unable to access clinically indicated referred services.
METHODS: The survey used a novel method to estimate unserviced health needs. General practitioners (GPs, n = 54) asked their patients (n = 2135) during a consultation about any health needs requiring a referred service. If both agreed that a service was potentially beneficial and not available, this was documented on an e-referral system for review. The outcomes of actual referrals were also reviewed.
RESULTS: The patient group was broadly representative of the Canterbury population, but over-sampled female and middle-aged people and under-sampled Māori. Data adjusted to regional demographics showed that 3.6% of patients had a GP-confirmed unserviced health need. Elective orthopaedic surgery, general surgery and mental health were areas of greatest need. Unserviced health needs were significantly (P ≤ 0.05) associated with greater deprivation, middle-age, and receiving high health-use subsidies.
DISCUSSION: To our knowledge, this is the first survey of GP and patient agreement on unserviced referred health needs. Measuring unserviced health needs in this way is directly relevant to service planning because the gaps identified reflect clinically indicated services that patients want and need. The survey method is an improvement on declined referral rates as a measure of need. Key factors in the method were using a patient-initiated GP consultation and an e-referral system to collect data.
KEYWORDS: General practitioners; health research; health services; equity; doctor–patient relationships
| WHAT GAP THIS FILLS |
| What is already known: Numerous studies have attempted to measure unmet health needs in the community. There is no consensus on the best way to measure this need, with most studies using patient self-reported data, despite evidence that this may overestimate health needs. |
| What this study adds: We demonstrate a new method for estimating unserviced health needs, a component of total unmet health need relevant to service planning. The key factor in the process was agreement between a patient and their GP that a health condition would benefit from a referred service, but that this service was not available. Other important features were using a patient-initiated GP consultation and an e-referral system to collect data. |
Introduction
In most publicly funded health services, there is a gap between demand for care and supply of services. With increasing demand on public healthcare services, especially elective surgery, the issue of unmet healthcare needs in New Zealand has attracted considerable attention in health services research1–8 and the media.9,10 Identifying areas of unserviced health need is important for service planning and redesign, but has proved difficult for several reasons; (1) health needs incorporate the wider social and environmental determinants of health and there may be multiple reasons for one unserviced need;11–14 (2) patients’ and clinicians’ perceptions of unserviced need may differ;15,16 and (3) lack of consensus on how to measure these needs.
Numerous international studies have measured need using either population self-reported data obtained from questionnaires,17,18 face-to-face interviews,19–21 focus groups,22 telephone contact23 or from national databases,24 including audits of declined referrals and backlogs in treatment.25,26 Apart from the New Zealand Health Survey,27 the New Zealand Ministry of Health (MOH) National Patient Flow Programme28 and the Health and Independence Report,29 we are aware of only five population studies of unmet need in New Zealand. In 2009, the Survey of Family Income and Employment (SoFIE) carried out by Statistics New Zealand examined access to primary health care and showed financial barriers existed for many people.30 Another paper2 compared need for general practitioner (GP) services between Pacific peoples and other New Zealanders and showed associations of need with ethnicity, health condition and financial and time constraints. Two surveys were carried out in 20139 and 201610 by the private health sector, indicating that ~170,000 people in New Zealand met clinical thresholds for elective surgery, but were not on surgical waiting lists. Finally, 9.3% of people in a recent population questionnaire in Canterbury reported unmet need for secondary care.31
To manage patient flow through the health system, the MOH set a policy limiting maximum waiting times. This required the Canterbury District Health Board (DHB) to control demand by defining access criteria to hospital and community services, agreed between primary and secondary care clinicians and allied health.32,33 These criteria were made available on a website called Community HealthPathways (www.cdhb.health.nz/Hospitals-Services/Health-Professionals/Pages/Health-Pathways.aspx).34 The pathways are linked to an electronic request management system (ERMS; www.cdhb.health.nz/Patients-Visitors/Pages/Referrals.aspx) for public and private health services, including outpatient clinic requests and investigations such as radiology.35 Approximately 97% of referrals from general practice to any healthcare provider in Canterbury are now made through this system. The referrals are triaged before services are offered.
The tight management of the referral process in Canterbury has resulted in GPs tending not to refer patients with a high likelihood of the referral being declined. Counting declined hospital outpatient referrals does not give the full picture of unserviced health needs, so there is debate on the best way to measure the various components of ‘unmet health needs’. Most studies have used questionnaires or interviews to obtain self-reported information from patients.17–23 The aim of the research described in this paper was to measure unmet need for referred services in patients attending their general practice, where both patient and GP agreed that a health service was required but unavailable.
Methods
Definition of unserviced health need
Unmet need is the difference between services that are necessary to deal appropriately with health problems and services actually received,36 and is determined by the accessibility, availability or acceptability of services.37 Our research attempted to measure the component of ‘unmet need’ where patients’ medical condition would benefit from a referred service but this service was not available; that is, unserviced health need. A required service was defined as the situation where GPs thought a service was clinically indicated and included specialist advice, assessment, investigation, an allied health response or a clinical procedure. Clinical criteria were distinct from access criteria, which are informed by public system capacity.
Research design
A survey was carried out from August 2015 to May 2016, and data on the referrals reviewed until December 2016. The Health and Disabilities Ethics Committee provided ‘out-of-scope’ approval for the survey, as long as prospective signed consent was obtained from the patients. The ERMS38 was chosen to collect the survey data because GPs use this system routinely during daily practice and data required for the survey could be auto-populated in the referral form.
To identify an agreed unserviced health need, we used the question: ‘Today, do you and I agree you have a health need or needs that would benefit from referral and you want to be referred’. This question was based on the standard question on ‘unmet need’ of the European Union Statistics on Income and Living Condition survey.15,18–21,39 Our question differs in that it is phrased to record the patient’s perceived health needs on the day of the consultation. A second question confirmed whether a referral for the need, private or public, would be made at the consultation. The GPs discussed these two questions with their patients in an unscripted manner.
Two GPs carried out a pilot trial to determine the number of patients required to provide the survey with sufficient statistical power, and showed that 11 (9.6%) of the 114 patients surveyed had an unserviced health need. Using this prevalence and values reported for other countries,24 we assumed that at least 7% of patients may have an unserviced health need. To detect non-availability of individual services at this rate with a 95% confidence interval of ±0.5% requires 990 patients. To determine unserviced needs for common conditions and account for systematic recording errors and loss to follow up, we planned to enrol at least 2000 patients.
Recruitment of general practices
All Canterbury GPs were invited by post to participate in the survey. The first 54 GPs to accept were enrolled, planning that they would each survey at least 40 patients. Participating GPs could use the activity to complete a medical practice audit approved by the Royal New Zealand College of General Practitioners. There was partial reimbursement for the time spent completing the survey. A liaison person (AD) worked with general practice teams to ensure successful completion of the survey.
Patient recruitment
Patient inclusion criteria were: eligible for publicly funded health care, enrolled with a Primary Health Organisation (PHO) in Canterbury, and signed, informed consent in English. To avoid selection bias, each GP enrolled patients in a fixed sequence, commonly every fourth patient. The enrolment strategy varied between GPs, depending on their work schedule and patient load, but was always pre-agreed and systematic. Patients were provided with an information sheet and advised that taking part in the survey would not affect their access to services.
Data collection
The survey process is shown in Figure 1. If the patient and GP agreed a service would be beneficial and desired, but the patient did not meet local access criteria in the public system, this was recorded as ‘current need, not referred’. To ensure all unserviced needs were recorded, GPs were able to add any needs their patients had not identified. Referred patients were classified as ‘current need, referred’ (including public and private referrals) or ‘no current need’.
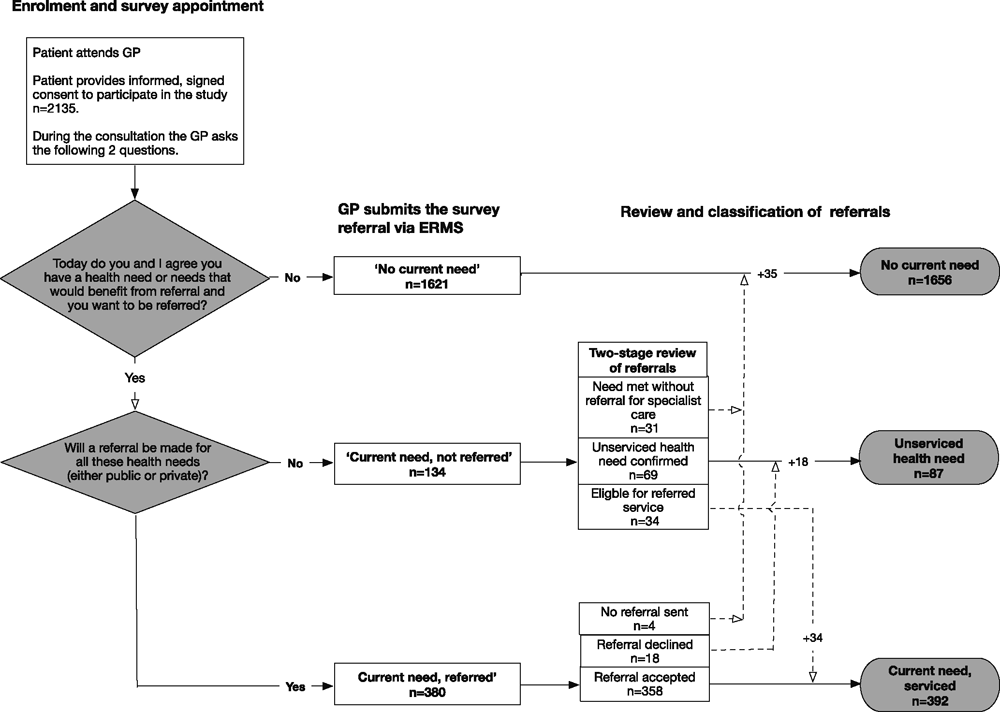
|
Data collected included age, gender, ethnicity, smoking history, enrolment in high health-use programmes (Community Services [CSC] and High Use Health [HUHC] cards, and Care Plus40) and deprivation index (NZDep2013) of the area of the patient’s address.41 Long-term medical conditions were recorded when available.
Review and classification of referrals
Referrals recorded as ‘current need, not referred’ were reviewed using a two-stage process: first by two medically qualified members of the research team (GM and KH) and then by two independent vocationally registered GPs. Patients with a confirmed healthcare need were classified as ‘unserviced health need’, and patients assessed as meeting the access criteria were reclassified as ‘current need, serviced’. Patients considered not to require a referred service were reclassified as ‘no current need’. The referring GPs were notified about reclassification of their referrals and given the opportunity to respond.
The outcome of referrals was examined by matching National Health Index (NHI) numbers to Canterbury DHB outpatient waitlist data and electronic records, and determining whether clinic appointments had been made, surgery undertaken or advice given. The records were reviewed for 4 months for first specialist assessments and 6 months for surgical procedures. Patients whose referrals were accepted were classified as ‘current need, serviced’ and patients declined service were added to the ‘unserviced health need’ group.
Statistical analysis
Chi-squared tests were used to examine if there were differences in the categorical variables between groups and Fisher’s exact test was used for comparison of categorical variables with low frequencies. We compared demographic characteristics of the study group and the Canterbury population using databases of PHO registration (Quarter 1, 2016, n = 498,108 and Canterbury DHB-funded, 2015–16, n = 529,905), and between patients with or without an unserviced health need. Relationships between unserviced health need and clinical and demographic variables were examined by univariate and multivariate logistic regression analyses.
The prevalence of unserviced need in Canterbury was estimated by extrapolation to the PHO-registered and Canterbury DHB-funded populations. Imbalances between the populations were corrected by assigning each patient with a post-stratification value constructed using gender and age that represented the weight for each subject in the statistical analyses.
Results
Demographics
Fifty-four GPs participated in the study (35 females, 19 males; 52 urban, 2 rural) representing ~10% of GPs in Canterbury. Forty-seven (87%) GPs enrolled at least 40 patients in the survey.
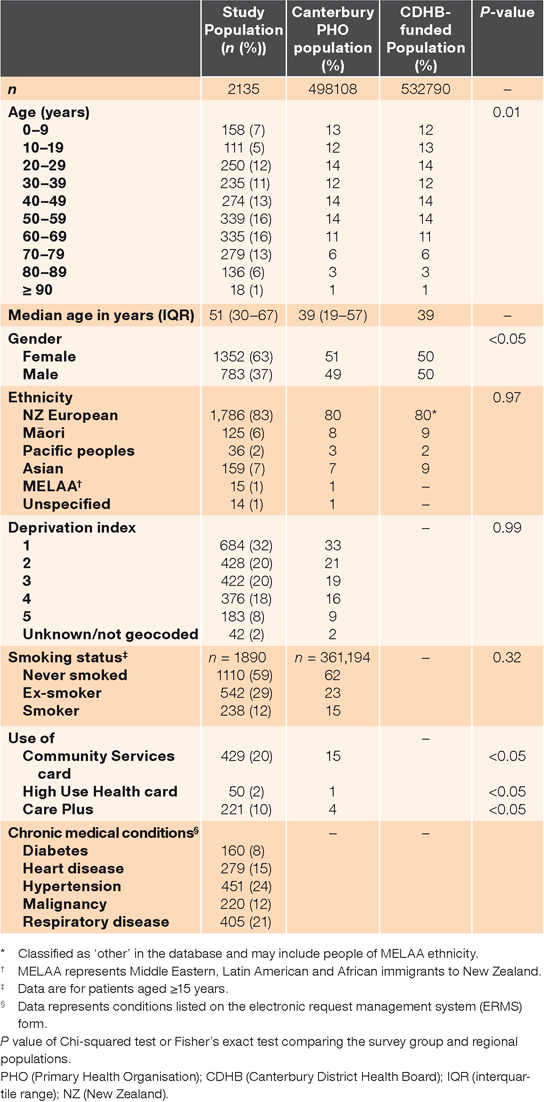
Table 1 shows that the characteristics of the 2135 patients in the study were broadly similar to the PHO-registered and Canterbury DHB-funded populations, but included more females (63%), elderly people, High Use Health Cared (HUHC) holders and patients on Care Plus, and fewer Māori, teenagers and children. This pattern reflects the 2014–15 New Zealand Health Survey.27 The distribution of NZDep2013 in the study group was similar to that in the PHO and Canterbury census populations,42 with ~10% of patients in the most deprived quintile. Approximately 15% of the survey group had at least one long-term medical condition.
|
Referral review and reclassification
The number of referrals reclassified is shown in Figure 1. Initially, 134 patients were classified in the ‘current need, not referred’ group. Review by the survey team reduced this to 87 patients, with reclassification most commonly due to referrals actually being made and accepted, patients being eligible for available services, or needs able to be met without referral for specialist care.
Patients in the ‘current need, referred’ group were followed up for an average of 244 days (interquartile range (IQR) 196–273). Initially, there were 380 patients in this group, although for four no referral could be found and were reclassified as ‘no current need’, while 18 had their referral declined and were reclassified into the ‘unserviced health need’ group.
Following these reclassifications, the final number of patients in the ‘unserviced health need group’ was 87 (4.1% of the survey population), 392 in the ‘current need, serviced’ group (18.3%) and 1656 (77.6%) in the ‘no current need’ group.
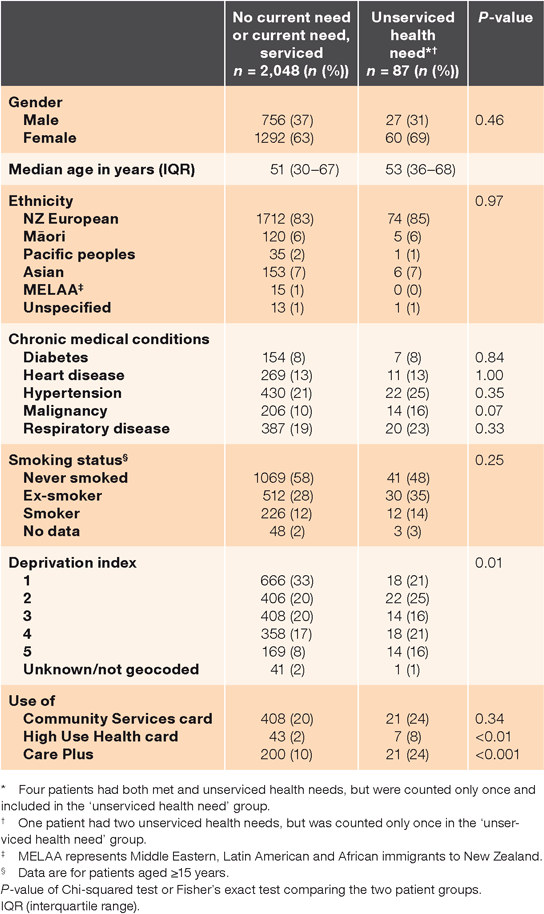
Characteristics of unmet need
Table 2 summarises study patients’ demographics, grouped according to unserviced health need as their final classification. Patients with an unserviced health need were more likely to be in the highest deprivation quintile or have received a subsidy for higher use of health services. Nearly two-thirds of unserviced health needs were for surgery, with referrals for hernia surgery being the most common, and orthopaedic surgery contributing one-half of surgery cases, mainly for problems of the knee, foot and back (Table 3).
|
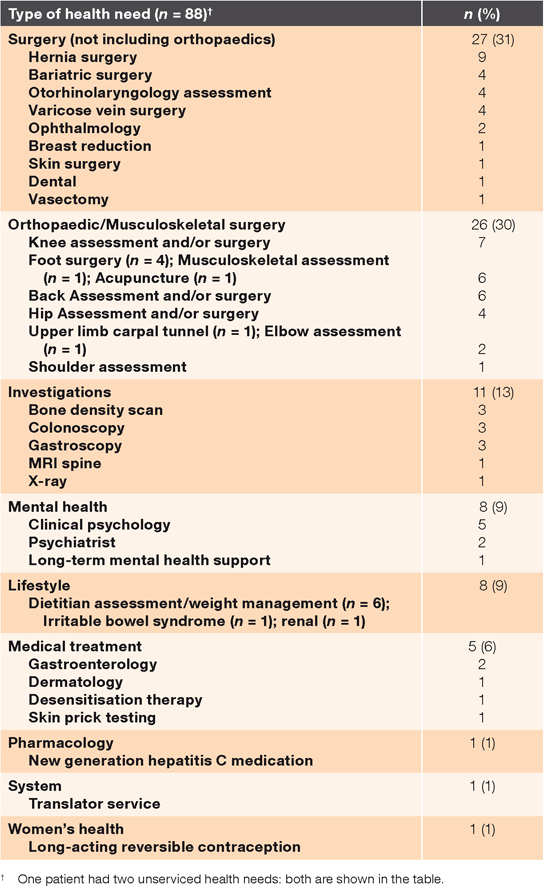
|
Univariate regression analysis showed significant associations (P ≤ 0.05) between unserviced need and middle age (40–69 years, odds ratio (OR) 8.37), highest NZDep2013 quintile (OR 3.1), use of a HUHC (OR 4.1) and enrolment in Care Plus (OR 2.9). With the exception of age and enrolment in Care Plus, these variables were independent determinants of unserviced health need in the multivariate regression model.
Estimation of unserviced health needs in Canterbury
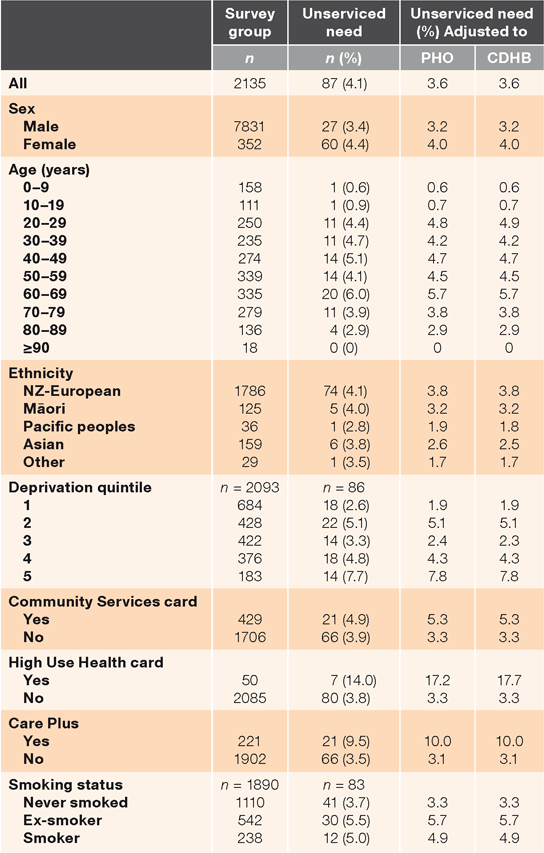
Adjustment to the PHO-registered and Canterbury DHB-funded populations showed a lower rate of unserviced health need (3.6%), which equates to 17,932 and 19,180 people respectively (Table 4). The adjusted data showed a close relationship between unserviced health need and the use of public healthcare funds targeted at low-income and high health-needs people, with rates of 10% for Care Plus and 17% for HUHC.
|
Discussion
Summary of findings
The study data, when adjusted to regional demographics, showed that 3.6% of patients who attended their GP were unable to access a clinically indicated referred service. This implies that health needs were not being met for ~19,000 people in Canterbury. The study confirmed local anecdotal information that elective surgery, particularly orthopaedics and general surgery, were the areas of greatest unserviced health need. Mental health care was also identified, but to a lesser extent than anticipated, in view of the marked increase in demand following the 2011 earthquakes.43
It is not possible to directly compare the rate of unserviced health need we observed to rates reported by population surveys collecting self-reported data. The term ‘unserviced health need’ covered services that were clinically indicated and actively sought by patients, and was distinct from the wider definition of unmet health need, which may include unrecognised health needs.
Strengths and weaknesses of the study
The survey used a novel way of estimating unserviced health needs, with the point of contact being general practices, patients identifying needs and their doctor verifying stated needs. Measuring unserviced health needs in this way is directly relevant to service planning because needs are linked to clinical criteria defined by local clinicians and assessed as being clinically indicated by the patient’s GP. We consider our method a more accurate estimation than the MOH method that uses the rate of declined referrals.
Other strengths of our method were: (1) many patients were well known to their GP and so true needs were likely to be well understood; (2) the GPs had clear local criteria for access to services to identify unmet need; (3) the data were collected during routine consultations using dedicated general practice software; autopopulation of clinical information ensured near complete data collection, probably to a greater extent than might have been achieved by other means; (4) referral review involved an independent two-stage process; and (5) the study team had existing goodwill with local general practices who were provided with support and acknowledgment of their work.
Weaknesses of our method were: addressing unmet need of patients not attending general practice requires a different strategy (19% of Māori and 6% of NZ Europeans are not enrolled with a PHO44) and the health needs of patients going to general practice may underestimate the wider health needs of the community. Patients may not disclose all of their needs, possibly for reasons such as cultural deference or stoicism, while GPs may have developed a higher threshold for referrals over time because of changes in access criteria. The GPs who participated were self-selected and may have introduced bias. The survey oversampled the unwell and elderly who were more likely to attend general practice and was in English, possibly reducing participation of non-English speaking people. The effect of private health care on unmet need was not investigated.
The process we used to review the referrals was a critical step in the study. To ensure this was transparent and objective, we used a two-stage, blinded process to review patients with unserviced health needs, first by the research team and then by two independent GPs. The GPs who participated in the survey had differing interpretations of unserviced health needs, with some not aware of recent changes in access to services. Care was taken not to exclude patients identified with a health need by their GP unless an error had been made and the service was available. In all cases, this was checked with the GP making the referral. The review team did not always agree with the GP, but erred on the side of inclusion in the unserviced health need group where doubt existed. Feedback was provided to GPs when a referral could have been made via another pathway and represented both quality control and education aspects. A limitation of the review process was that we did not examine the ‘no current need group’ to determine whether some patients had an unidentified health need requiring specialist care. Future research should include verification of this patient group.
Implications for healthcare policy
We are unaware of any other study that has used an agreement between a doctor and patient to identify unserviced health needs. This differs from surveys such as the MOH National Patient Flow Programme28 that reviews referral outcome for secondary care, or most of the published studies that used patient self-reported data. We chose our method because some studies have indicated self-reporting may overestimate health needs.15,16 Despite these differences in methodology, we observed associations between unserviced health need, greater deprivation and chronic illness similar to those reported by other studies.12,21,45
A recent pilot study of survey methods31 concluded that recording unmet secondary healthcare needs in primary care was not a reliable means of collecting these data, but could be made more effective by using dedicated resources to carry out data collection. Our results show that it is possible to collect data in primary care on verified unreferred health needs, and confirm that to obtain adequate and reliable data, it is necessary to have an easy method for collecting the data and establish a working relationship with study general practices.
In conclusion, our study achieved its aims of estimating the proportion of patients attending general practice who were unable to access clinically indicated referred services and identifying areas that would benefit from additional provision of services. In conjunction with population-based, self-reported surveys of health needs, the study provides more complete information to develop health services.11
COMPETING INTERESTS
The authors are all current or past employees or contractors of Canterbury DHB. Canterbury DHB funded the study and is responsible for the provision of publicly funded health care to the Canterbury population.
ACKNOWLEDGEMENTS
The Canterbury DHB funded the survey as part of the routine clinical review of the services it provides. We would like to thank the patients for providing their data and the general practice teams for their participation in the survey. We wish to thank Dr D. Holdgate and Dr B. Graham for their review of the referral classifications in the survey, and Dr K. Davey and Dr R. Yule for undertaking the pilot study for the survey. The assistance of Dr M. Yi, (Biostatistician, Canterbury DHB) with data analysis, G. Hamilton and S. Berry (Planning and Funding Department, Canterbury DHB) with data acquisition, and Dr M. Reid with manuscript preparation is gratefully acknowledged.
References
[1] Gauld R. Improving New Zealand’s health system performance: challenges for the way forward. Eurohealth 2009; 15 32–5.[2] Pledger MJ, Cumming J, Burnette M, Daubé J. Unmet need of GP services in Pacific people and other New Zealanders. N Z Med J 2011; 124 35–45.
[3] Ashton T, Tenbensel T. Health reform in New Zealand: short-term gain but long-term pain. Expert Rev Pharmacoecon Outcomes Res 2012; 12 579–88.
| Health reform in New Zealand: short-term gain but long-term pain.Crossref | GoogleScholarGoogle Scholar |
[4] Ministry of Health. Tupu Ola Moui Pacific Health Chart Book 2012. Wellington: Ministry of Health; 2012. [cited 2016 August]. Available from: http://www.health.govt.nz/publication/tupu-ola-moui-pacific-health-chart-book-2012
[5] Pfeifer M. The Canterbury Charity Hospital: facing the challenge of unmet need in healthcare. N Z Med J 2013; 126 9–11.
[6] Gauld R, Raymont A, Bagshaw PF,, et al. The importance of measuring unmet healthcare needs. N Z Med J 2014; 127 63–7.
[7] Horsfield E, Sheridan J, Kelly F,, et al. Filling the gaps: opportunities for community pharmacies to help increase healthcare access for young people in New Zealand. Int J Pharm Pract 2014; 22 169–77.
| Filling the gaps: opportunities for community pharmacies to help increase healthcare access for young people in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[8] Kahukura T. Māori Health Chart Book 2015, 3rd edn. Wellington: Ministry of Health; 2015. [cited 2016 August]. Available from: http://www.health.govt.nz/publication/tatau-kahukura-maori-health-chart-book-2015-3rd-edition
[9] Kantar TNS, New Zealand. Assessing the demand for elective surgery amongst New Zealanders. City: Health Funds Association of New Zealand and New Zealand Private Surgical Hospitals Association; 2013.
[10] Kantar TNS, New Zealand. Research into unmet need for elective surgery. Auckland: Health Funds Association of New Zealand and New Zealand Private Surgical Hospitals Association; 2016.
[11] Wright J, Williams R, Wilkinson JR. Development and importance of health needs assessment. BMJ 1998; 316 1310–3.
| Development and importance of health needs assessment.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1c3itlGkug%3D%3D&md5=0abf2bd11d292b35436caf377560d657CAS |
[12] Bickler S, Ozgediz D, Gosselin R,, et al. Key concepts for estimating the burden of surgical conditions and the unmet need for surgical care. World J Surg 2010; 34 374–80.
| Key concepts for estimating the burden of surgical conditions and the unmet need for surgical care.Crossref | GoogleScholarGoogle Scholar |
[13] Gosselin R, Ozgediz D, Poenaru D. A square peg in a round hole? Challenges with DALY-based “burden of disease” calculations in surgery and a call for alternative metrics. World J Surg 2013; 37 2507–11.
| A square peg in a round hole? Challenges with DALY-based “burden of disease” calculations in surgery and a call for alternative metrics.Crossref | GoogleScholarGoogle Scholar |
[14] Harrison JD, Young JM, Butow PN, Solomon MJ. Needs in health care: what beast is that? Int J Health Serv 2013; 43 567–85.
| Needs in health care: what beast is that?Crossref | GoogleScholarGoogle Scholar |
[15] Allin S, Masseria C. Unmet need as an indicator of health care access. Eurohealth 2009; 15 7–9.
[16] Marshall EG, Wong ST, Haggerty JL, Levesque J-F. Perceptions of unmet healthcare needs: what do Punjabi and Chinese-speaking immigrants think? A qualitative study. BMC Health Serv Res 2010; 10 46
| Perceptions of unmet healthcare needs: what do Punjabi and Chinese-speaking immigrants think? A qualitative study.Crossref | GoogleScholarGoogle Scholar |
[17] Nelson CH, Park J. The nature and correlates of unmet health needs in Ontario, Canada. Soc Sci Med 2006; 62 2291–300.
| The nature and correlates of unmet health needs in Ontario, Canada.Crossref | GoogleScholarGoogle Scholar |
[18] Sibley LM, Glazier RH. Reasons for self-reported unmet healthcare needs in Canada: a population-based provincial comparison. Healthc Policy 2009; 5 87–101.
[19] Thammatacharee N, Tisayaticom K, Suphanchaimat R,, et al. Prevalence and profiles of unmet healthcare need in Thailand. BMC Public Health 2012; 12 923
| Prevalence and profiles of unmet healthcare need in Thailand.Crossref | GoogleScholarGoogle Scholar |
[20] Cavalieri M. Geographical variation of unmet medical needs in Italy: a multivariate logistic regression analysis. Int J Health Geogr 2013; 12 27
| Geographical variation of unmet medical needs in Italy: a multivariate logistic regression analysis.Crossref | GoogleScholarGoogle Scholar |
[21] Pappa E, Kontodimopoulos N, Papadopoulos A,, et al. Investigating unmet health needs in primary health care services in a representative sample of the Greek population. Int J Environ Res Public Health 2013; 10 2017–27.
| Investigating unmet health needs in primary health care services in a representative sample of the Greek population.Crossref | GoogleScholarGoogle Scholar |
[22] Pieh-Holder KL, Callahan C, Young P. Qualitative needs assessment: healthcare experiences of underserved populations in Montgomery County, Virginia, USA. Rural Remote Health 2012; 12 1816
| 1:STN:280:DC%2BC38fhtl2ruw%3D%3D&md5=a607148deb891b5d45c4152b22769a67CAS |
[23] Bryant T, Leaver C, Dunn J. Unmet healthcare need, gender and health inequalities in Canada. Health Policy 2009; 91 24–32.
| Unmet healthcare need, gender and health inequalities in Canada.Crossref | GoogleScholarGoogle Scholar |
[24] World Health Organization. Health statistics and information systems. Disease and injury country estimates. Burden of disease. Geneva: World Health Organization; 2009. Available from: http://www.who.int/healthinfo/global_burden_disease/estimates_country/en/
[25] McBride D, Hardon S, Walters K,, et al. Explaining variation in referral from primary to secondary care: cohort study. BMJ 2010; 341 c6267
[26] Chevarley FM. Percentage of persons unable to get or delayed in getting needed medical care, dental care, or prescription medicines: United States 2007. Statistical Brief#282. April 2010. Rockville, MD, USA: Agency for Healthcare Research and Quality.
[27] Ministry of Health. New Zealand Health Survey. Wellington: Ministry of Health; 2011. Available from: http://www.health.govt.nz/nz-health-statistics/national-collections-and-surveys/surveys/current-recent-surveys/new-zealand-health-survey
[28] National Patient Flow. Prioritisation outcome of referrals for first specialist assessment tables (developmental). Wellington: Ministry of Health; 2016. Available from: http://www.health.govt.nz/publication/national-patient-flow-prioritisation-outcome-referrals-first-specialist-assessment-tables
[29] Ministry of Health. Health and Independence Report 2016. Wellington: Ministry of Health; 2017. Available from: http://www.health.govt.nz/publication/health-and-independence-report-2016
[30] Jatrana S, Crampton P. Primary health care in New Zealand: who has access? Health Policy 2009; 93 1–10.
| Primary health care in New Zealand: who has access?Crossref | GoogleScholarGoogle Scholar |
[31] Bagshaw P, Bagshaw S, Frampton C,, et al. Pilot study of methods for assessing unmet secondary health care need in New Zealand. N Z Med J 2017; 130 23–38.
[32] Timmins N, Ham C. The quest for integrated health and social care: a case study in Canterbury, New Zealand: The King’s Fund. London: The King’s Fund; 2013. Available at: http://www.kingsfund.org.uk/publications/quest-integrated-health-and-social-care
[33] Charles A. Developing accountable care systems. Lessons from Canterbury, New Zealand. London: The King’s Fund; 2017. [cited 2017 September]. Available at: www.kingsfund.org.uk/publications/developing-accountable-care-systems
[34] McGeoch G, Anderson I, Gibson J,, et al. Consensus pathways: evidence into practice. N Z Med J 2015; 128 86–96.
[35] Gu Y, Warren J, Orr M. The potentials and challenges of electronic referrals in transforming healthcare. N Z Med J 2014; 127 111–8.
[36] Carr W, Wolfe S. Unmet needs as sociomedical indicators. Int J Health Serv 1976; 6 417–30.
| Unmet needs as sociomedical indicators.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaE283lvFegtg%3D%3D&md5=d816e3beaddfe4952ff06c10b737d11fCAS |
[37] Chen J, Hou F. Unmet needs for healthcare. Health Rep 2002; 13 23–34.
[38] Gu Y, Warren J, Orr M. The potentials and challenges of electronic referrals in transforming healthcare. N Z Med J 2014; 127 111–8.
[39] Chaupain-Guillot S, Guillot O. Health system characteristics and unmet care needs in Europe: an analysis based on EU-SILC data. Eur J Health Econ 2015; 16 781–96.
| Health system characteristics and unmet care needs in Europe: an analysis based on EU-SILC data.Crossref | GoogleScholarGoogle Scholar |
[40] Ministry of Health. Care Plus. Wellington: Ministry of Health; 2017. [cited 2017 October 26]. Available at: http://www.health.govt.nz/our-work/primary-health-care/primary-health-care-subsidies-and-services/care-plus
[41] Ministry of Health. NZDep2013 Index of Deprivation. Wellington: Ministry of Health; 2017. [cited 2017 October 26]. Available at: http://www.health.govt.nz/publication/nzdep2013-index-deprivation
[42] Statistics New Zealand. 2013 Census. Wellington: Statistics New Zealand; 2017. [cited 2017 October 26]. Available at: http://www.stats.govt.nz
[43] Ardagh MW, Richardson SK, Robinson V,, et al. The initial health-system response to the earthquake in Christchurch, New Zealand, in February, 2011. Lancet 2012; 379 2109–15.
| The initial health-system response to the earthquake in Christchurch, New Zealand, in February, 2011.Crossref | GoogleScholarGoogle Scholar |
[44] Ministry of Health. Enrolment in a primary health organisation. Wellington, Ministry of Health; 2017. [cited 2017 October 26]. Available at: http://www.health.govt.nz/our-work/primary-health-care/about-primary-health-organisations/enrolment-primary-health-organisation
[45] Ahs AMH, Westerling R. Health care utilization among persons who are unemployed or outside the labour force. Health Policy 2006; 78 178–93.
| Health care utilization among persons who are unemployed or outside the labour force.Crossref | GoogleScholarGoogle Scholar |


