Hope headquarters: recovery college
Leighton Jay A E , Bruce Macadam B , Pamela Gardner C and Lyn Mahboub DA Sotica Pty Ltd, PO Box 8141, Hilton, WA 6163, Australia.
B Starfish Strategy Inc., PO Box 46, Duncraig East, WA 6023, Australia.
C PO Box 2137, Esperance, WA 6450, Australia.
D Curtin University, GPO Box U1987, Perth, WA 6845, Australia.
E Corresponding author. Email: leighton@sotica.com.au
Health Promotion Journal of Australia 28(2) 170-173 https://doi.org/10.1071/HE17034
Submitted: 30 March 2017 Accepted: 22 June 2017 Published: 25 July 2017
Journal Compilation © Australian Health Promotion Association 2017 Open Access CC BY-NC-ND
The mental health and well being of the Australian population remains an ongoing, unresolved issue. A 2007 survey of Australians aged 16–85 years estimated that almost half (45%, or 7.3 million people) had experienced mental ill health at some time in their lives and that approximately 20% of the population had experienced mental disorders in the 12 months before the survey.1 In addition, data from the 2013 National Mental Health Report indicated that 2–3% of all Australians, or around 600 000 people, had severe mental health disorders as determined by diagnosis, intensity, duration of symptoms and degree of functional impairment.2 This group included people with severe and disabling forms of depression and anxiety in addition to people experiencing psychoses. Another 4–6% of the population (or ~1 million) have moderate disorders, and a further 9–12% (~2 million) have mild disorders.2
Recovery and mental health
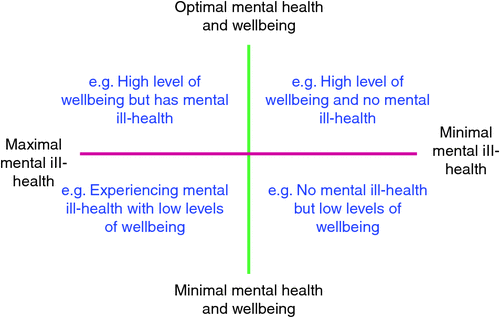
Numerous studies have demonstrated that ‘mental health’ and ‘mental illness’ are related but distinct dimensions that can be measured independently of each other. As Fig. 1 shows, one dimension measures the presence or absence of mental health, whereas the other axis measures the presence or absence of mental illness or distress.3
The model suggests that low mental health and well being can exist in the absence of a diagnosable mental condition and that people with defined mental illnesses can experience good mental health and well being. Therefore, clinical recovery from symptoms of mental ill health is possible and desirable for many people with a defined condition, especially when accompanied by a high level of mental well being. Westerhof and Keyes demonstrate that a substantial body of research evidence now supports this dual-continuum conceptualisation of mental health.4
In mental health, recovery is a personal journey that is understood to mean a process that enables people to create and ‘…live meaningful and contributing lives in a community of their choice with or without the presence of mental health symptoms and issues’.5 This is consistent with the UK’s Department of Health’s description of recovery as people having:
…a good quality of life [with] greater ability to manage their own lives, stronger social relationships, a greater sense of purpose, the skills they need for living and working, improved chances in education, better employment rates and a suitable and stable place to live.6
Clinical recovery and personal recovery are different in their approach. Clinical recovery reflects a medical model approach and focuses on the suppression of ‘symptoms’, whereas personal recovery has emerged as a more important dimension to people with lived experience of mental ill health due to its focus on living a life regardless of the presence or absence of ‘symptoms’.7 Beyond this, it is recognised that social recovery and functional recovery are key, with both being concerned with shifts towards hopefulness and taking up valued social roles in society.8 The challenge to health services is how to assist people on their journey of recovery.
It is clear that for consumers of mental health services, the dimensions of social and personal recovery represent an important balance to the medical model with its emphasis on diagnosis, deficits and pathology. Although the recovery journey is different for each person, consumers increasingly emphasise the need for it to revolve around what has meaning and value to the person and to incorporate elements of hope, self-determination, self-management, full community inclusion and empowerment.5
Recovery college
Recovery colleges (RCs) are a relatively new concept being increasingly recognised as an innovative approach to recovery-orientated mental health care.9 Around the world, RCs are formal learning institutions that strive to create environments in which people with a lived experience of mental distress feel safe, welcome and accepted. RCs aim to support their students to develop their own individual learning plans, with peer support if desired, that reflects their recovery journey and desired personal outcomes. McGregor et al.10 have identified seven key features of RCs, asserting that they need to be educational, collaborative, strength based, personalised, progressive, engaged with the community and inclusive.
Importantly, RCs offer complementary and alternative pathways for recovery that differ from the traditional clinical and therapeutic approaches to mental health (Table 1 distinguishes between therapeutic and educational recovery approaches). An RC has ‘pathways’ to learning, wellness, a new sense of identity and self-discovery.10 People at the college take on the socially valued role of ‘student’, something that many students in overseas colleges note has positive, empowering and layered effects on their recovery journeys.10

|
The courses and subjects offered by RCs reflect student demand and interest, and relate to many facets of a person’s recovery journey.11 Some courses may be only a few hours in length, whereas others may run for a full semester. A course’s duration is determined by its purpose and intended outcomes, with most students enrolling in and completing multiple courses in a year of study that reflects their own personal learning and recovery journey. A key feature of RCs is that people with a lived experience develop an identity as student and/or educator, which differs from the more usual identity of ‘patient’.
RCs can attract a wide range of students, including people on recovery journeys (at any stage of their journey), carers, family members, friends, professionals working in the mental health or associated fields and community members. Importantly, no one is ‘referred’ to a college by a service or health care professional. Exercising self-agency begins at the point of approaching the college, and college processes support this. Students may learn about the college through existing networks of support that could include community, public and private mental health services, educational institutions and local community networks and websites.
Several existing colleges have recognised the significant benefits associated with making some specific courses available to carers, significant others and professionals.12 In this way, the college is able to support and resource those who relate directly with people on a recovery journey in roles that include carer, family member, friend and professional who may also be on their own recovery journey. The fact that most people strive to increase their well being and have a meaningful, contributing life is a key connecting feature of the college.
Benefits of RCs
Although some formal evaluations of the effectiveness of RCs have been undertaken, there have not yet been opportunities to evaluate their benefits over extended time frames. This is an area requiring further research, including peer-reviewed studies. However, several shorter-term international studies13 have demonstrated that many students gain numerous benefits that include:
-
an improved sense of identity and empowerment
-
increased feelings of hopefulness
-
a greater sense of purpose and direction
-
increased knowledge about, and awareness of, their own determinants of mental well being
-
Reduced need for professional mental health services and reduced hospitalisations
-
skills and learning about their mental well being that contribute to increased self-mastery and coping strategies
-
specific knowledge about housing and personal welfare
-
specific skills and knowledge leading to employment and further mainstream education.14
Alignment with contemporary directions in mental health promotion
In Australia, there are currently RCs in Victoria, New South Wales (NSW) and South Australia. These colleges are working with people who want to learn and improve their mental health (see http://www.recoverycollege.org.au/enrol_now.html, accessed 20 September 2016, and http://www.seslhd.health.nsw.gov.au/Recovery_College/, accessed 20 September 2016).
There is a high level of convergence between the principles underpinning RCs and many of the key principles that underpin the directions embodied in government policy directions. At a national level, The Roadmap for National Mental Health Reform 2012–2022 references education and learning as an enabler of better outcomes across the sector.15 Evidence emerging in other countries increasingly demonstrates that RCs can play a central role in achieving this.10
The NSW Strategic Plan for Mental Health 2014–2024 is founded on values that include recovery, hope, citizenship and quality.16 It strives to promote and support self-agency and recovery, explicitly noting that RCs ‘…provide opportunities for consumers to live meaningful and contributing lives – and…promote the principles of recovery within mental health services and the community’.16
In Western Australia, progress towards establishing an RC is highly consistent with the policy directions elaborated in a range of documents guiding mental health services, including The Western Australian Mental Health, Alcohol and Other Drug Services Plan 2015–2025.17 This 10-year plan is based on ‘recovery’ practices and articulates the need to ‘…implement a range of system-wide improvements and initiatives to transform the mental health, alcohol and other drug service system’.17 Both the 10-year plan and Western Australia’s proposed RC: (1) endorse the centrality of cocreation,18 with consumers, families and supporters fully involved in coplanning, codesigning, codelivering and coreviewing policies and services; (2) focus on rebalancing services, moving them to the community as appropriate; and (3) advocate expanding services across regional Western Australia into locations where they are most required and closer to where people live17 (operating college campuses in regional communities fully aligns with this aspiration).
RCs that are community based, collaborative and intersectorial promote participation that is liberated from residency in particular geographic or service regions. Specifically, they aim to maximise students’ capacity to gain employment and create pathways that make this a more achievable goal.19 This particular benefit is closely aligned with Australian Government strategies and goals expressed in the National Disability Insurance Scheme Act 2013, the National Mental Health Strategy,20 the National Disability Strategy21 and the National Mental Health and Disability Employment Strategy.22
RCs apply a non-clinical pathway to support people to have a ‘good life’ using a specific life-affirming educational focus. They create opportunities for belonging by adopting a personal recovery philosophy and using coproduction principles. They support mental health promotion by building capacity and structural supports.12 RCs seek to recognise the limitations of a strictly individualised focus. They strive to create environments that support people to navigate normal problems in living while simultaneously addressing some of the social determinants of distress, such as poverty, discrimination, abuse and alienation.23
Acknowledgements
This article is based on the work and deliberations of a technical team established by the Western Australian (WA) Recovery College Steering Committee. The technical team did significant foundational work towards developing a WA Recovery College model and plan. Members of the team included Julie Jamieson, Kerry Hawkins, Carli Sheers, Andrew Markovs, Veronica Bruce and Coralie Flatters. Work undertaken by the group included input from the authors and was performed using coproduction principles. Helen Brown provided additional advice and expertise. The input and expertise of these people is gratefully acknowledged.
References
[1] Australian Bureau of Statistics (ABS). National survey of mental health and wellbeing: summary of results – Australia 2007. Canberra: ABS; 2008.[2] Department of Health and Ageing. National mental health report 2013: tracking progress of mental health reform in Australia 1993–2011. Canberra: Commonwealth of Australia; 2013.
[3] Tudor K. Mental Health Promotion: Paradigms and Practice. Routledge: London; 1996.
[4] Westerhof G, Keyes C (2010) Mental illness and mental health: the two continua model across the lifespan. J Adult Dev 17, 110–19.
| Mental illness and mental health: the two continua model across the lifespan.Crossref | GoogleScholarGoogle Scholar |
[5] Department of Health. National framework for recovery-oriented mental health services: policy and theory. Canberra: Australian Government; 2008.
[6] UK Department of Health. No health without mental health: a cross-government mental health outcomes strategy for people of all ages. UK Department of Health: London; 2011.
[7] Slade M. Personal recovery and mental illness: a guide for mental health professionals. Cambridge, UK: Cambridge University Press; 2009.
[8] Lloyd C, Waghorn G, Williams P (2008) Conceptualising recovery in mental health rehabilitation. Br J Occup Ther 71, 321–8.
| Conceptualising recovery in mental health rehabilitation.Crossref | GoogleScholarGoogle Scholar |
[9] Meddings S, Guglietti S, Lambe H, Byrne D (2014) Student perspectives: recovery college experience. Ment Health Soc Incl 18, 142–50.
| Student perspectives: recovery college experience.Crossref | GoogleScholarGoogle Scholar |
[10] McGregor J, Repper J, Brown H (2014) ‘The college is so different from anything I have done.’ A study of the characteristics of Nottingham Recovery College. J Ment Health Train Educ Pract 9, 3–15.
| ‘The college is so different from anything I have done.’ A study of the characteristics of Nottingham Recovery College.Crossref | GoogleScholarGoogle Scholar |
[11] Meddings S, Campbell E, Guglietti S, Lambe H, Locks L, Byrne D, Whittington A (2015) From service user to student – the benefits of recovery college. Clin Psych Forum 268, 32–7.
[12] Perkins R, Repper J, Rinaldi M, Brown H. Briefing: recovery colleges. Centre for Mental Health, NHS Confederation Mental Health Network; 2012. Available from: https://www.centreformentalhealth.org.uk/recovery-colleges-paper [Verified 30 Mar 2017].
[13] Dunn EC, Rogers ES, Hutchinson DS, Lyass A, MacDonald Wilson KL, Wallace LR, Furlong-Norman K (2008) Results of an innovative university-based recovery education program for adults with psychiatric disabilities. Adm Policy Ment Health 35, 357–69.
| Results of an innovative university-based recovery education program for adults with psychiatric disabilities.Crossref | GoogleScholarGoogle Scholar |
[14] Rinaldi M, Marland M, Wyburn S. Annual Report 2011–12, South West London Recovery College. 2012. Available from: http://rfact.org.au/wp-content/uploads/2015/05/SW-London-Recovery-College-evaluation-2011_12-v1-0.pdf [Verified 11 July 2017].
[15] Council of Australian Governments (COAG). The roadmap for national mental health reform 2012–2022. Canberra: Australian Government; 2012.
[16] NSW Mental Health Commission. Living well: a strategic plan for mental health in NSW 2014–2024. Sydney: Government of NSW; 2014.
[17] Western Australia Mental Health Commission. Better choices. Better lives. The Western Australian mental health, alcohol and other drug services plan 2015–2025. Perth: Western Australia Mental Health Commission; 2015.
[18] Gouillart F, Hallett T (2015) Co-creation in government. Stanf Soc Innov Rev 13, 40–7.
[19] Taggart H, Kempton J. The route to employment: the role of mental health recovery colleges. London: Centre Forum; 2015.
[20] Department of Health. National mental health strategy. 2014. Available from: http://www.health.gov.au/internet/main/publishing.nsf/Content/mental-strat [Verified 11 July 2017].
[21] Council of Australian Governments (COAG). National disability strategy 2010–2020. Canberra: Commonwealth of Australia; 2011.
[22] Government of Australia. National mental health and disability employment strategy. 2009. Available from: http://www.vicserv.org.au/images/PDF/Resources_and_links/National-Mental-Health---Disability-Ermployment-Strategy.pdf [Verified 25 October 2016].
[23] Jalleh G, Anwar-McHenry J, Donovan R, Laws A (2013) Impact on community organisations that partnered with the Act–Belong–Commit mental health promotion campaign. Health Promot J Austr 24, 44–8.