Coproducing Aboriginal patient journey mapping tools for improved quality and coordination of care
Janet Kelly A B C , Judith Dwyer A , Tamara Mackean A , Kim O’Donnell A and Eileen Willis AA Faculty of Medicine, Nursing and Health Sciences, Flinders University, GPO Box 2100, Adelaide 5001, Australia.
B Adelaide Nursing School, University of Adelaide, Adelaide, SA 5006, Australia.
C Corresponding author. Email: janet.kelly@adelaide.edu.au
Australian Journal of Primary Health 23(6) 536-542 https://doi.org/10.1071/PY16069
Submitted: 31 May 2016 Accepted: 7 October 2016 Published: 8 December 2016
Journal Compilation © La Trobe University 2017 Open Access CC BY-NC-ND
Abstract
This paper describes the rationale and process for developing a set of Aboriginal patient journey mapping tools with Aboriginal patients, health professionals, support workers, educators and researchers in the Managing Two Worlds Together project between 2008 and 2015. Aboriginal patients and their families from rural and remote areas, and healthcare providers in urban, rural and remote settings, shared their perceptions of the barriers and enablers to quality care in interviews and focus groups, and individual patient journey case studies were documented. Data were thematically analysed. In the absence of suitable existing tools, a new analytical framework and mapping approach was developed. The utility of the tools in other settings was then tested with health professionals, and the tools were further modified for use in quality improvement in health and education settings in South Australia and the Northern Territory. A central set of patient journey mapping tools with flexible adaptations, a workbook, and five sets of case studies describing how staff adapted and used the tools at different sites are available for wider use.
Additional keywords: Aboriginal health services, action research, continuity of patient care, hospitals, patient-centred care, rural health.
| What is known about the topic? |
• Aboriginal patient journeys from home to hospital are often complex involving multiple care providers and settings. Patient journeys are one of seven priority areas in the Closing the Gap program. |
| What does this paper add? |
• Bringing together the perspectives of patients, families and staff into a mapping framework can enable more timely and responsive care and support strategies to be developed. |
Introduction
Many Aboriginal people living in rural and remote locations of Australia experience lengthy and complex patient journeys for both emergency and planned care. Their care pathways are often clinically complex due to a higher incidence of comorbidities, and logistically complex because of the vast geographic distances, the number of healthcare locations and extensive travel required. One Aboriginal person may interact with 50 or more health professionals as they travel from home, to hospital to home, with most of these conversations occurring in English, which may be their second or third language. Access to interpreters may not be available at some sites, and they may or may not be accompanied by family members. Aboriginal people in these situations are sometimes required to make significant and life-changing decisions while alone and a long way from home (Lawrence et al. 2009). In addition, patients’ own priorities and commitments may or may not be recognised and respected by the healthcare professionals and services they encounter (Willis et al. 2010; Dwyer et al. 2011; Australian Government 2013).
Australia has a world-class healthcare system with publicly funded primary, secondary and tertiary care, accessible to all citizens. However, this system operates in silos, with poor interservice communication and significant coordination gaps. Generally, there are no designated health professionals or support persons to coordinate the entire patient journey from home to hospital to home (Lawrence et al. 2009). Staff in rural and remote healthcare settings prepare patients for journeys as best they can, but often the exact diagnosis and treatment options depend on the results of tests undertaken while in the city. Staff in urban hospitals provide required specialist care, but may experience difficulty effectively explaining the details and options to patients. Urban staff may be unaware of exactly what health care is and isn’t available in the patient’s home community, making discharge planning and referral challenging (Lawrence et al. 2009).
In response to these challenges, the Managing Two Worlds Together (MTWT) Project was undertaken at Flinders University to identify the barriers and enablers, gaps and strategies to care, funded through SA Health and Lowitja Institute grants. This project brought together the experiences of Aboriginal patients and their families, the perspectives of healthcare professionals in a range of urban, rural and remote healthcare settings, and a multidisciplinary, cross-cultural research team. The research team initially sought to use existing patient journey models and tools to analyse four Aboriginal patient journeys to better understand the entire experience for individual patients. They considered mapping real patient’s journeys from diagnosis to completion, focusing on specific conditions (Lawrence et al. 2009; Rolley et al. 2009) or adapting within-hospital care processes originally used to analyse patient flow (Richardson et al. 2007; Ben-Tovim et al. 2008a, 2008b). The team also considered Wagner’s chronic care model (Wagner 1998) and quality and safety frameworks (Australian Commission on Safety and Quality in Health Care 2010). However, none of these models or frameworks were able to adequately record and convey the complexities and gaps in cultural care described in interviews and focus groups, or the challenges and strategies within and across healthcare and geographic sites. It was clear that the team needed to bring together the experiences and priorities of Aboriginal patients and their families, and the perspectives of primary, secondary and tertiary care providers, Aboriginal and mainstream, in urban, rural and remote locations. Over the three stages of the project, a new framework and set of mapping tools were developed, initially to assist the team to better understand patient journey stories, and then, with the encouragement and participation of health and education professionals and managers, the tools were further developed for use in clinical practice, quality improvement and education contexts. This paper outlines the processes the team engaged in, the outcomes, and further research needs.
Methods
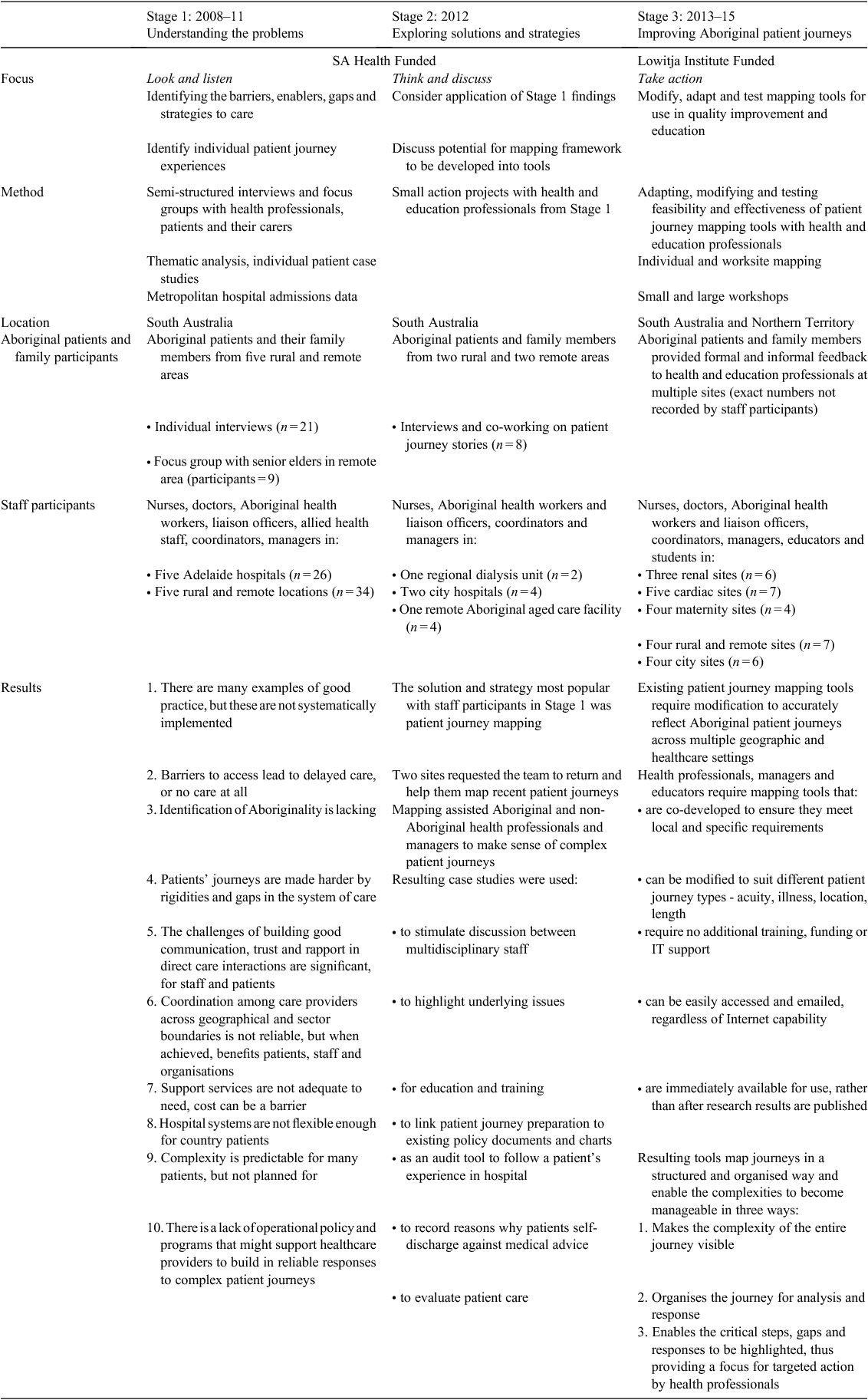
A collaborative participatory action research (PAR) approach with repeated cycles of Look and Listen, Think and Discuss and Take Action guided the project. This method was co-created with Aboriginal community women in an earlier study (Kelly 2009), informed by community-based action research (Stringer 2007). It emphasises the importance of Dadirri deep listening (Atkinson 2002), Ganma-knowledge sharing (O’Donnell and Kelly 2011), and culturally safe approaches to research (Browne and Smye 2002). The project was undertaken in three stages from 2008 to 2015 in South Australia and the Northern Territory (Table 1), with the aim of better understanding and improving communication, coordination, collaboration, and cultural safety in Aboriginal patient journeys.
|
Recruitment and conduct of interviews and focus groups
Health professional participants in urban, rural and remote locations were recruited in all three stages via flyers pinned to notice boards, email invitations passed on by ward, unit and service managers, and word of mouth. Patients and their family members were told about the research and invited to be involved by health staff in rural and remote Aboriginal health services and hospitals in Stages 1 and 2. If interested, the patients contacted the research team, or the health staff did so on their behalf. In Stage 3, interested patients were invited to work directly with their healthcare professionals to adapt and test the tools. This recruitment occurred locally within a health service as part of internal quality improvement activities. No financial payment was given to any participant; however, transport assistance was provided to patient and family participants if required. Interpreters were offered, but not required by patient and family participants. Patients and family members and carers were also offered a choice of an Aboriginal or non-Aboriginal researcher for interviews in Stage 1; all participation was voluntary. Patients and carers were adults aged 18 years to 80 years, with approximately two-thirds being female and approximately half being from remote and very remote areas. Interviews and focus groups in Stage 1 and 2 were semi-structured, using prompts related to individual journeys and practice experiences.
Aboriginal health professionals shared both work-related and personal accounts, and these accounts were analysed separately (as staff, as patients, and as family members).
Ethics and confidentiality
Ethical approvals were received from the Aboriginal Health Research Ethics Committee (SA), Flinders University Social and Behavioural Research Ethics Committee, and The Human Research Ethics Committee – The Queen Elizabeth Hospital. In Stage 3, additional approval was received from the Central Australian Human Research Ethics Committee and Human Research Ethics Committee of the Northern Territory Department of Health and Menzies School of Health Research as the research included Northern Territory sites. Governance agreements were negotiated with health service organisations for all three stages.
Healthcare staff provided de-identified versions of mapped journeys to the research team, to preserve confidentiality. An intellectual property agreement enabled each staff participant to keep the version of the tools that they personally developed with the assistance of the research team, and to continue using it within and beyond the MTWT project. Evaluation of the process of developing, adapting and testing the tools, and of the tools themselves occurred both within workshops and as an integral part of the PAR process in Stage 3.
Results
Coproduction of responsive mapping tools
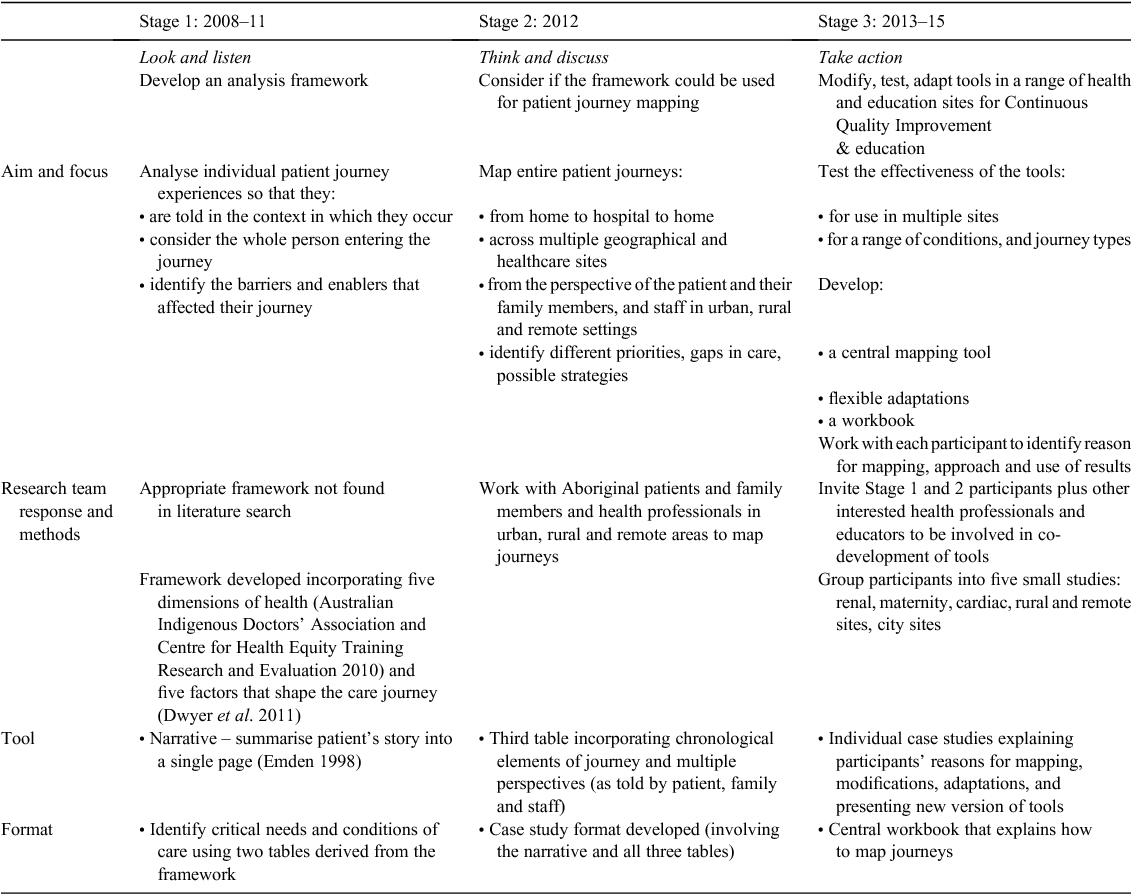
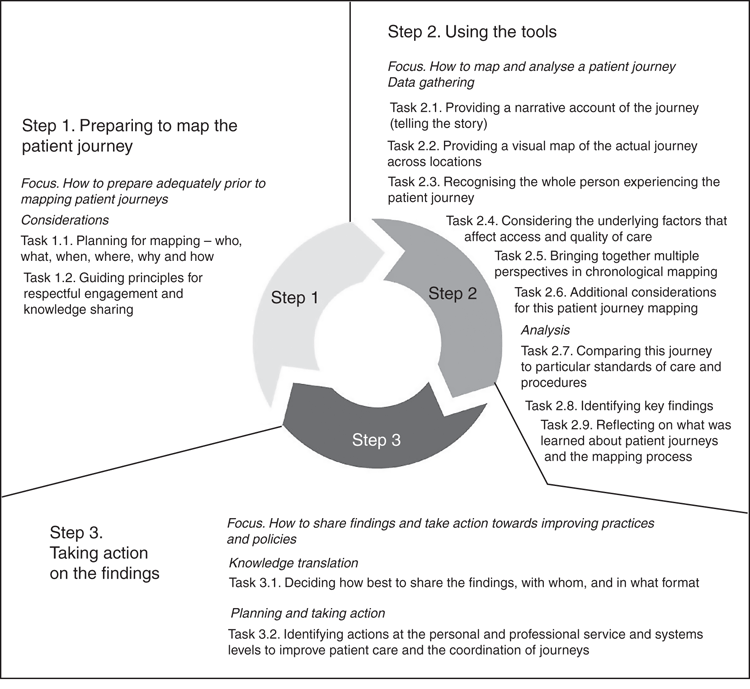
The patient journey mapping results and tools in the MTWT project were informed by extensive discussion and problem solving between Aboriginal patients and their families, healthcare professionals, managers and support workers, educators, and a multidisciplinary, cross-cultural research team (Table 1). The tools were then tested within multiple sites, ensuring their wide applicability across urban, rural and remote locations. Table 2 presents the results of the coproduction process for each of the three stages. The research coordinator shared de-identified versions of tools and emerging mapping ideas between staff participants across the different study groups (with permission), enabling shared learning and a central set of mapping tools to be developed (Fig. 1).
|
|
Ease of use
Participants stressed that any tools needed to be simply formatted, accessible to a diverse range of people with different skill levels and information technology support, be easily transferable via email, and adaptable to include different journey types, levels of complexity and priorities. The tools were therefore developed in Microsoft Word and Microsoft Excel (Microsoft Corporation, Redmond, WA, USA).
Knowledge translation
Writing the journeys into case studies enabled the issues, strategies and mapping processes to be more effectively shared with colleagues, managers, key stakeholders and a wider audience. A central workbook was developed, drawing from all case studies and mapping activities across the project. It was designed with a writable PDF section, a set of guiding principles, trigger questions, tables and diagrams. The reports and workbook remain available on Flinders University and Lowitja Institute websites at http://www.flinders.edu.au/medicine/sites/health-care-management/research/mtwt/ and https://www.lowitja.org.au/lowitja-publishing (accessed 24 November 2016).
During workshops and discussions, the need to diagrammatically present the entire patient journey across primary and tertiary care, and compare individual patient journey results to standards of care was identified. A range of approaches were trialled, with the most successful included in the workbook (Fig. 2). This version is representative, and can be further refined to reflect specific illnesses and actual journeys. In this figure, the vertical axis combines two concepts: Risk and Standard (referring to variations from standard care).
Participant reflection on the process of co-developing tools and mapping journeys
A benefit of co-producing patient journey mapping tools ‘from the ground up’ is that the tools inherently make sense, not only to those who developed them, but also to their colleagues. Staff participants, particularly nurses and Aboriginal staff, identified that previously when they noticed a gap in service delivery, they filled it themselves as best they could, or tried to raise an issue with management, but were often unsuccessful (Dwyer et al. 2014. The patient journey mapping tools have assisted them, and their colleagues, to identify practice issues, communicate them effectively, and seek strategies at personal, professional, organisation, and system levels. The structured framework of the tools assisted them to make sense of what was happening, and to articulate this clearly to others. For example, renal nurses have used the tools to highlight issues of Friday night discharges for rural patients, and used the case study as evidence to change policy and practice. They have also mapped end-of-life journeys and strategies for assisting patients to get home in time, in a supported manner (Kelly et al. 2016). Midwives and Aboriginal family birthing practitioners have mapped journeys and written case studies that highlight support and coordination issues, and presented these to unit managers (Kelly et al. 2015a). A remote Aboriginal aged care facility used the mapping tool to highlight funding and communication issues for their board and government funders, and mental health practitioners have used the tools to plan a community-wide response to suicide (Kelly et al. 2015b).
The barriers to using the tools were generally two-fold: (1) finding the time within busy clinical and education schedules; and (2) initially grasping the concepts involved in patient journey mapping.
The mapping tools continue to be adapted and used in even more diverse healthcare, research and education settings. They have been adapted to map the journeys of Aboriginal patients experiencing cancer, cardiovascular events, and burns. The outcomes of each stage are detailed in Table 2.
Discussion
Previous patient journey mapping tools and processes have focused on healthcare redesign within an organisation (Ben-Tovim et al. 2008a) or on individual disease processes such as cardiac care (Lawrence et al. 2009). Few tools have the capacity to map a diverse range of Aboriginal patient journeys from the perspective of Aboriginal patients and their family members, and the healthcare professionals caring for them within and across several healthcare sites. It is necessary to bring all of these perspectives together to highlight the complexity of journeys and the need for quality cultural care, which includes quality clinical care. The National Aboriginal and Torres Strait Islander Health Plan 2013–2023 highlights the need for ‘coordinated, culturally appropriate services across the health system, including primary health care, hospital care and aged care’ in order to improve both patient journeys and health outcomes for Aboriginal and Torres Strait Islander people and their families (Australian Government 2013, p. 14).
The MTWT mapping tools focus centrally on Aboriginal patients, following their journey across the health system, enabling a primary focus on the person rather than the system. This enables healthcare professionals and support staff to identify where they and their services fit in relation to the person’s journey, and what they need to do to ensure continuity of care. This approach could also be applied to other patient care journeys more broadly.
The processes of development and testing in this project affirmed the applicability of the framework and tools as assessed by participants in health services; and highlighted the importance of ease of use and adaptation. Stage 3 reinforced our findings from Stages 1 and 2 regarding the need both to consider the full complexity of care journeys for this group of patients and to separate out elements and processes in a way that renders them amenable to action for quality improvement (Emden 1998; Australian Indigenous Doctors’ Association and Centre for Health Equity Training Research and Evaluation 2010).
Conflicts of interest
The authors declare that they have no conflicts of interest.
Acknowledgements
We acknowledge the contribution of Brita Pekarsky, Natalie McCabe, Jacene Wiseman and Charlotte de Crespigny in the development of the patient journey mapping tools. We also acknowledge the many Aboriginal people (patients and their families) who shared their experiences of health care, and the many health professionals and support staff who are committed to improving access, quality and coordination of care. We also thank the Lowitja Institute and SA Health who funded this research.
References
Atkinson J (2002) ‘Trauma Trails, Recreating Song Lines: the Transgenerational Effects of Trauma in Indigenous Australia.’ (Spinifex Press: North Melbourne)Australian Commission on Safety and Quality in Health Care (2010) Patient-centred care: improving quality and safety by focusing care on patients and consumers. ACSQHC, Canberra, ACT, Australia.
Australian Government (2013) National Aboriginal and Torres Strait Islander Health Plan 2013–2023. (Department of Health and Aging: Canberra, ACT, Australia) Available at http://www.health.gov.au/internet/main/publishing.nsf/content/B92E980680486C3BCA257BF0001BAF01/$File/health-plan.pdf [Verified 18 October 2016]
Australian Indigenous Doctors’ Association and Centre for Health Equity Training Research and Evaluation (2010) Health impact assessment of the Northern Territory emergency response. (Australian Indigenous Doctors’ Association Ltd, Canberra, ACT, Australia) Available at https://www.aida.org.au/wp-content/uploads/2015/03/AIDA_HIA.pdf [Verified 18 October 2016]
Ben-Tovim DI, Dougherty M, O’Connell T, McGrath K (2008a) Patient journeys: the process of clinical redesign. The Medical Journal of Australia 188, S14–S17.
Ben-Tovim DI, Bassham JE, Bennett DM, Dougherty ML, Martin MA, O’Neill SJ, Sincock JL, Szwarcbord MG (2008b) Redesigning care at the Flinders Medical Centre: clinical process redesign using ‘lean thinking’. The Medical Journal of Australia 188, S27–S31.
Browne AJ, Smye V (2002) A post-colonial analysis of healthcare discourses addressing Aboriginal women. Nurse Researcher 9, 28–41.
| A post-colonial analysis of healthcare discourses addressing Aboriginal women.Crossref | GoogleScholarGoogle Scholar |
Dwyer J, Kelly J, Willis E, Glover J, Mackean T, Pekarsky B, Battersby M (2011) Managing Two Worlds Together: city hospital care for country Aboriginal people – Project Report. (The Lowitja Institute: Melbourne, Vic., Australia) Available at https://www.flinders.edu.au/medicine/fms/sites/health_care_management/mtwt/documents/Project%20Report_WEB.pdf [Verified 24 November 2016]
Dwyer J, Willis E, Kelly J (2014) Hospitals caring for rural Aboriginal patients: holding response and denial. Australian Health Review 38, 546–551.
Emden C (1998) Conducting a narrative analysis. Collegian (Royal College of Nursing, Australia) 5, 34–39.
| Conducting a narrative analysis.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1M7gsVKlsA%3D%3D&md5=957e915262f9d82b501c22d245245a49CAS |
Kelly J (2009) Moving Forward Together in Aboriginal Women’s Health. PhD thesis. Flinders University, Adelaide, SA, Australia.
Kelly J, Medway P, Miller D, Catt L, Lawrence M (2015a) Managing Two Worlds Together: stage 3: improving Aboriginal patient journeys – maternity case studies. The Lowitja Institute, Melbourne, Vic., Australia. Available at http://www.flinders.edu.au/medicine/fms/sites/health_care_management/mtwt/documents/M2WT-CaseStudy-Maternity-WEB_b.pdf [Verified 24 November 2016]
Kelly J, Wiseman J, Mazzone S, Miller D, Newham J, Ryan B, Thomas K, Martinez M (2015b) Managing Two Worlds Together: stage 3: improving Aboriginal patient journeys: rural and remote sites case studies. (Lowitja Institute: Melbourne, Vic., Australia) Available at http://www.flinders.edu.au/medicine/fms/sites/health_care_management/mtwt/documents/M2WT-CaseStudy-Rural-WEB_b.pdf [Verified 24 November 2016]
Kelly J, Wilden C, Herman K, Martin G, Russell C, Brown S (2016) Bottling knowledge and sharing it –using patient journey mapping to build evidence and improve Aboriginal renal patient care. The Renal Society of Australasia Journal 12, 48–55.
Lawrence M, Dodd Z, Mohor S, Dunn S, de Crespigny C, Power C, Mackean L (2009) Improving the patient journey. Cooperative Research Centre for Aboriginal Health, Darwin, NT, Australia.
O’Donnell K, Kelly J (2011) Using Gamma knowledge sharing as a decolonising approach to conference planning and facilitation. Action Learning and Action Research Journal 17, 137–156.
Richardson S, Casey M, Hider P (2007) Following the patient journey: older person’s experiences of emergency departments and discharge. Accident and Emergency Nursing 15, 134–140.
| Following the patient journey: older person’s experiences of emergency departments and discharge.Crossref | GoogleScholarGoogle Scholar |
Rolley JX, Davidson P, Salamonson Y, Fernandez R, Dennison C (2009) Review of nursing care for patients undergoing percutaneous coronary intervention: a patient journey approach. Journal of Clinical Nursing 18, 2394–2405.
| Review of nursing care for patients undergoing percutaneous coronary intervention: a patient journey approach.Crossref | GoogleScholarGoogle Scholar |
Stringer E (2007) ‘Action Research.’ (Sage: Thousand Oaks, CA, USA)
Wagner EH (1998) Chronic disease management: what will it take to improve care for chronic illness? Effective Clinical Practice 1, 2–4.
Willis J, Wilson G, Renhard R, Chong A, Clarke A (2010) Improving the culture of hospitals. (Australian Institute for Primary Care, Latrobe University) Available at http://www.lowitja.org.au/sites/default/files/docs/ICHP_Final_Report_August_2010.pdf [Verified 24 November 2016]



