Not just tea and biscuits; the Gold Coast Primary Health Network process of designing, implementing and operating a Community Advisory Council
Jessica McClean A B and Kellie Trigger AA Primary Care Gold Coast (trading as Gold Coast Primary Health Network), Level 1, 14 Edgewater Court, Robina, Qld 4226, Australia.
B Corresponding author. Email: jess.mcclean@griffithuni.edu.au
Australian Journal of Primary Health 23(6) 504-508 https://doi.org/10.1071/PY16157
Submitted: 9 December 2016 Accepted: 14 March 2017 Published: 19 September 2017
Journal Compilation © La Trobe University 2017 Open Access CC BY-NC-ND
Abstract
Consumers are fast being acknowledged as a critical voice in the creation of sustainable health systems, and their ability and willingness to participate must be kept in mind by those eager to engage them. Federal health reform in Australia has mandated the formal involvement of communities in primary care through advisory committees in the newly established Primary Health Networks. Although there is clear progression towards increased consumer participation in Australia’s health services, scope exists to improve the evidence base around identifying and implementing the most appropriate approach in different settings. Gold Coast Primary Health Network has drawn on the principles of deliberative participation to design, implement and operate their Community Advisory Council. Although functioning well, further work is required to evaluate the efficiency of this approach.
| What is known about the topic? |
• Consumer involvement in health is increasing, requiring a new approach from health services. Australian health reform necessitates consumer involvement at the primary care level, limited evidence exists in this setting. |
| What does this paper add? |
• A practical real-world account of establishing and operating a formal mechanism for ongoing consumer input into primary care. |
Introduction
Consumers are commonly located at the centre of contemporary care models. Terms such as ‘consumer directed’ and ‘patient centred’ are driving the requirement for systems that enable the input of consumer experience and opinion (Janamian et al. 2016). In Australia, this movement towards consumer involvement coincides with the transformation of primary care delivery through the introduction of regional commissioning bodies known as Primary Health Networks (PHN). This Federal health reform has embedded consumer involvement through the requirement for Community Advisory Committees within all 31 Primary Health Networks.
The role of Community Advisory Committees (CAC) is to ‘…provide a community perspective to the PHN Board to ensure that decisions, investments and innovations are appropriately patient-centred, cost-effective, locally relevant and aligned to local care experiences and expectations’ (Australian Government Department of Health, Primary health networks standard funding agreement schedule, p. 46). CACs provide a structured mechanism for consumers to influence decision-making in primary care and support their right to participate in the planning of health services (ACSQHC 2008). Despite consensus in the literature regarding the merits of engaging consumers (Sankar 2005; Bossert and Mitchell 2011), conceptualisations remain inconsistent (Mittler et al. 2013) and evidence on effective tools and strategies for specific settings is limited (Sarrami-Foroushani et al. 2014). When coupled with the considerable flexibility around the construction and operation of CACs, this is likely to result in varied application of the concept across PHNs. More broadly, there is work to be done to reach a point where consumer involvement is a natural part of core-business, with a 2014 review of national safety and quality standards by the Australian Commission on Safety and Quality in Health Care (ACSQHC) finding the lowest scores across health services were in relation to partnering with consumers (Brandon and Popovich 2016). Although their review predominantly focussed on the tertiary setting, the interconnectedness of health supports the assumption that improvement is needed across other settings, including primary care. This article contributes a practical primary care account of designing, implementing and operating a CAC by outlining the process undertaken by Gold Coast Primary Health Network (GCPHN).
Background
The current CAC model has evolved from previous iterations. Prior to becoming a PHN, as the Gold Coast Medicare Local, the organisation sought to engage the local community and implemented an online forum. The intention behind the forum was to create a formal avenue for the community to provide input on local issues. Initially, following recruitment of 100 people and a face-to-face induction, there was great enthusiasm among both staff and participants. However, after operating for 1 year, the online forum was discontinued as it was resource intensive, had a significant decline in participation and was delivering limited outcomes.
Upon reflection, there were clear weaknesses in the approach taken with the online forum. Membership included representatives from the health and community industries, opinions were sought in relation to issues where there was little scope for action, feedback regarding the progression of issues was limited, there was misalignment between organisation and participant expectations in terms of the level of involvement and it was difficult to show contributors they were valued.
Late in 2014, a Community Advisory Committee replaced the online forum. In developing the model, key consideration was given to feedback from members of the online forum and related stakeholders and existing frameworks, namely the Health Consumers Queensland Consumer and Community Engagement Framework, Gold Coast Hospital and Health Service (GCHHS) Consumer Engagement Framework and the ACSQHC Standard 2 – Partnering with Consumers.
The 2014 committee functioned well and operated for ~6 months. Following the organisational transition to a PHN, the committee was reassessed and adjusted. To distinguish between these iterations, the group was also re-named as a Community Advisory Council.
Current approach
The public deliberation model has greatly influenced the GCPHN approach to designing, implementing and operating a CAC. There is considerable theoretical and case study literature to support deliberative processes as effective, feasible and useful for capturing informed public input into complex health issues and policies that are value-laden and lack simple solutions (Carman et al. 2014). Carcasson and Sprain (2016, p.5) describe deliberation as ‘…groups of individuals engaging in an inclusive, respectful, and reasoned consideration of information, views, experiences, and ideas’. The process involves a representative group of community members who are provided with balanced information on the topic at hand (Carcasson and Sprain 2016) and supported to consider diverse perspectives, learn from others and examine their own views before finalising their opinion (Carman et al. 2014). This culminates in the production of information from the community point of view that has progressed from top-of-mind opinion to considered judgement (Fishkin et al. 2004).
Given that true public deliberation can be time and resource intensive, often devoting days to a single issue, it is not practical for the GCPHN context where multiple topics are to be considered and regular and timely input needs to be fed to the Board. However, the underlying process of representation, neutral information and supported discussion have been adopted. Meetings are convened every 2 months, frequent enough to meet GCPHN needs without burdening participants, and run for a 4-h period. Discussion is usually limited to a maximum of two separate topics to allow time for understanding, questioning and reflecting.
Key to the successful use of deliberative techniques is a clear articulation of purpose and an appropriate selection of participants (Degeling et al. 2015). Determining membership of the CAC was acknowledged as a critical component for success. Advertising recruitment involved the dissemination of an expression of interest (EOI) form through all available channels. Reviewing the membership of the 2014 council identified insufficient representation of males, Aboriginal and Torres Strait Islander people and young people. During recruitment for the PHN council, specific actions were taken to access these groups, namely targeted distribution of the EOI through relevant stakeholders, with personalised follow up to engender support from key community figures.
Over 60 applications were received and a selection panel, comprising representation from GCPHN, Gold Coast Hospital and Health Service (GCHHS) and Griffith University was convened. To guide the selection process, a knowledge- and skills-based criterion was established along with specific demographic requirements to ensure membership was as representative of the local community as possible (Brownlea 1987; Irvin and Stansbury 2004; Carman et al. 2014). Further to this, applicants were viewed as experts in the consumer experience, and effort was made to ensure a diversity of interactions with the Gold Coast health system were included. Being aware that provider capture would dilute the community voice and be an inauthentic representation of true consumer interests, health professionals were actively excluded (Bossert and Mitchell 2011; ACSQHC 2012; Victorian Department of Health and Human Services 2013; Duckett 2015). Identifying non-clinicians was aided by the inclusion of a question on clinical experience in the EOI.
Payment is provided to CAC members as a means for GCPHN to demonstrate that their time and commitment are valued. A common argument against payment for consumers is that they will be motivated by self-interest (Callaghan and Wistow 2006); however, this assumes the perspective of someone who is incentivised by reimbursement is of less value, which GCPHN believe to be untrue. Providing payment for consumers’ time may, in fact, enable the participation of people who would otherwise be unable to contribute, and is therefore viewed as a critical component of the GCPHN approach. Providing adequate resourcing for consumer participation, including reimbursement, is widely accepted as important for successful engagement (Irvin and Stansbury 2004; Hinton 2010). Furthermore, the commitment of additional resources to pay for consumers’ time demonstrates recognition of their value, diminishing tokenism (Arnstein 1969; Brownlea 1987).
The successful involvement of consumers in health requires acknowledgement that there may be a gap between the expectations placed on consumers by services and their ability to participate (Gruman et al. 2010). Therefore, it is essential that the training and support needs of consumers are assessed and appropriate action taken to prepare them (Sarrami-Foroushani et al. 2014). GCPHN approached the participation needs of CAC members from two perspectives; orientation and training. Orientation involved the creation of hard copy induction materials and a corresponding online member portal where resources could be accessed by members at any time. The hard copy information folder contained contact details for appropriate staff, a welcome letter and overview details on the PHN, including policies and forms related to consumer participation, conflicts of interest, complaints and feedback and remuneration. It also provided information on primary care, the charter of consumer rights and two peak consumer health bodies (Health Consumers Queensland and Consumers Health Forum). The online member portal is kept up to date with relevant material uploaded following every meeting. Health Consumers Queensland provided formal training to CAC members. At the first meeting of the group, a session was focussed on introduction to being a health consumer, responsibilities, resources and support. Another training session was conducted 6 months later as a combined activity with consumers from GCHHS.
Oliver et al. (2008) identify that engagement methods should be selected based on purpose and type of information sought. GCPHN uses both facilitated discussion for eliciting ideas and opinions, and written questionnaires to produce quantitative material such as rankings (Oliver et al. 2008). The decision to include a written feedback component for every topic was also motivated by the engagement principles of accessibility and inclusiveness (Health Consumers Queensland 2012), and an understanding that not all participants are comfortable giving their true opinion in a group discussion. Feedback from members supported this and revealed appreciation of the opportunity to reflect on topic discussion and articulate their views on paper, which is consistent with the deliberative principle of informed decision-making.
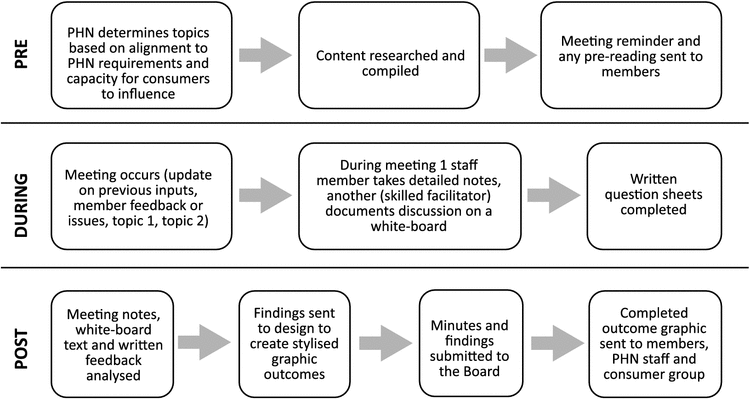
CAC meetings have a consistent structure and format (Fig. 1), creating a stable environment where members feel comfortable and know what to expect. Although this provides a level of formality required for the group to function effectively (McCabe et al. 2006), it is intentionally less rigid than a standard working group. This is to allow for adaptation to member needs and engender a convivial atmosphere. Critical to achieving this is the involvement of a skilled facilitator to read the room and encourage open and respectful discussion (Fishkin et al. 2004; Irvin and Stansbury 2004).
|
The importance of a closed feedback loop to successful consumer engagement cannot be overstated (McCabe et al. 2006; Oliver et al. 2008; Nimegeer et al. 2011) and was a key learning for GCPHN from the online forum experience. Care was taken to create realistic expectations among CAC members by clearly explaining the scope of influence they would have on different issues. To ensure the efforts of the CAC could have a meaningful effect and be easily demonstrated, the decision was made to actively determine the agenda, presenting only topics or issues directly related to GCPHN activity. This was a trade-off, as the decision resulted in a lower level of autonomy delegated to members and illustrates a power imbalance in favour of the GCPHN (Callaghan and Wistow 2006). Owing to the capacity-building nature of deliberative practice (Carcasson and Sprain 2016), it is hoped the ability of CAC members to identify appropriate topics will be strengthened, enabling more autonomy in the future. Evidence of this has already been observed, with many members actively relating their personal experiences and opinions to the broader context of community interests. Simple measures to track and share how member input is being used involve maintaining a basic spreadsheet and giving updates on previous topics at the beginning of every meeting. Information flow between the community and clinical councils is also encouraged, and supported through having a member of each council attend the meetings of the other and having standing updates on both agendas. Communication between the CAC and the GCPHN Board occurs through the submission of minutes and attendance of a Board member at CAC meetings. Although straightforward, these processes have ensured the effects of the CAC can be demonstrated to members, PHN staff and senior management.
Conclusion
Community engagement is often viewed as a continuum, moving from low to high in increments of participant involvement and effect. Myriad versions exist across disciplines and philosophies, resulting in a mix of broadly identified indicators of success (Sarrami-Foroushani et al. 2014), some of which are evident in the GCPHN approach. Elements associated with positive consumer engagement include a clear purpose, representative membership, adequate resourcing (inclusive of consumer reimbursement), training and support, face-to-face contact, a consistent structure with opportunity for consumers to share feedback, skilled facilitation and a closed feedback loop (Irvin and Stansbury 2004; McCabe et al. 2006; Oliver et al. 2008; Hinton 2010). These indicate that the GCPHN approach is achieving engagement around the collaborative middle area of the continuum, between passive one-way communication and full community-lead activity.
The GCPHN accept and acknowledge that, although the CAC appears to be functioning well, there are limitations to the chosen approach, and improvement can be made with attention now moving to evaluation of CAC member and GCPHN staff attitudes and overall council effectiveness. Effective engagement of consumers in health is not only achievable, it is essential to the creation of a sustainable system.
Conflicts of interest
Both authors are employees of the Gold Coast Primary Health Network and are directly involved with the Community Advisory Council.
Acknowledgements
The authors thank all current and past members of the GCPHN and GCML Community Advisory Councils and our colleagues at Gold Coast Health, Griffith University and Health Consumers Queensland; this could not have been achieved without your support and commitment.
References
ACSQHC (2008) Australian charter of healthcare rights. (Australian Commission on Safety and Quality in Health Care: Sydney, NSW, Australia). Available at https://www.safetyandquality.gov.au/national-priorities/charter-of-healthcare-rights/ [Verified 5 June 2017]ACSQHC (2012) Safety and quality improvement guide standard 2: partnering with consumers. Australian Commission on Safety and Quality in Health Care, Sydney, NSW, Australia.
Arnstein SR (1969) A ladder of citizen participation. Journal of the American Institute of Planners 35, 216–224.
| A ladder of citizen participation.Crossref | GoogleScholarGoogle Scholar |
Bossert TJ, Mitchell AD (2011) Health sector decentralization and local decision-making: decision space, institutional capacities and accountability in Pakistan. Social Science & Medicine 72, 39–48.
| Health sector decentralization and local decision-making: decision space, institutional capacities and accountability in Pakistan.Crossref | GoogleScholarGoogle Scholar |
Brandon L, Popovich S (2016) It’s not a one way street: Project Gauge alcohol and other drug client engagement and participation discussion paper. (Metro North Hospital and Health Service: Brisbane, Qld, Australia)
Brownlea A (1987) Participation: myths, realities and prognosis. Social Science & Medicine 25, 605–614.
| Participation: myths, realities and prognosis.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaL1c%2FntVOqtA%3D%3D&md5=570e300a0ff8e218290533760299f536CAS |
Callaghan G, Wistow G (2006) Publics, patients, citizens, consumers? Power and decision making in primary health care. Public Administration 84, 583–601.
| Publics, patients, citizens, consumers? Power and decision making in primary health care.Crossref | GoogleScholarGoogle Scholar |
Carcasson M, Sprain L (2016) Beyond problem solving: reconceptualizing the work of public deliberation as deliberative inquiry. Communication Theory 26, 41–63.
| Beyond problem solving: reconceptualizing the work of public deliberation as deliberative inquiry.Crossref | GoogleScholarGoogle Scholar |
Carman KL, Maurer M, Mallery C, Wang G, Garfinkel S, Richmond J, Gilmore D, Windham A, Yang M, Mangrum R, Ginsburg M, Sofaer S, Fernandez J, Gold M, Pathak-Sen E, Davies T, Siu A, Fishkin J, Rosenberg M, Fratto A (2014) ‘Community Forum Deliberative Methods Demonstration: Evaluating Effectiveness and Eliciting Public Views on Use of Evidence.’ (Agency for Healthcare Research and Quality: Rockville, MD, USA)
Degeling C, Carter SM, Rychetnik L (2015) Which public and why deliberate? A scoping review of public deliberation in public health and health policy research. Social Science & Medicine 131, 114–121.
| Which public and why deliberate? A scoping review of public deliberation in public health and health policy research.Crossref | GoogleScholarGoogle Scholar |
Duckett S (2015) Consumer and community engagement in primary health networks. Health Voices 16, 10–11.
Fishkin JS, Rosell SA, Shepherd D, Amsler T (2004) ChoiceDialogues and deliberative polls: two approaches to deliberative democracy. National Civic Review 93, 55–63.
| ChoiceDialogues and deliberative polls: two approaches to deliberative democracy.Crossref | GoogleScholarGoogle Scholar |
Gruman J, Rovner MH, French ME, Jeffress D, Sofaer S, Shaller D, Prager DJ (2010) From patient education to patient engagement: implications for the field of patient education. Patient Education and Counseling 78, 350–356.
| From patient education to patient engagement: implications for the field of patient education.Crossref | GoogleScholarGoogle Scholar |
Health Consumers Queensland (2012) Consumer and Community Engagement Framework. Health Consumers Queensland, Brisbane, Qld, Australia.
Hinton T (2010). Voices on choices: working towards consumer-led alcohol and drug treatment. (Anglicare: Hobart, Tas., Australia). Available at https://www.anglicare-tas.org.au/research-library/report/voices-choices [Verified 5 June 2017]
Irvin RA, Stansbury J (2004) Citizen participation in decision making: is it worth the effort? Public Administration Review 64, 55–65.
| Citizen participation in decision making: is it worth the effort?Crossref | GoogleScholarGoogle Scholar |
Janamian T, Crossland L, Wells L (2016) On the road to value co-creation in health care: the role of consumers in defining the destination, planning the journey and sharing the drive. The Medical Journal of Australia 204, 12–14.
| On the road to value co-creation in health care: the role of consumers in defining the destination, planning the journey and sharing the drive.Crossref | GoogleScholarGoogle Scholar |
McCabe AC, Keast RL, Brown KA (2006). Community engagement: towards community as governance. In ‘Governments and Communities in Partnership Conference’, 25–27 September 2006, Melbourne, Vic., Australia. Available at http://eprints.qut.edu.au/7497/ [Verified 5 June 2017]
Mittler JN, Martsolf GR, Telenko SJ, Scanlon DP (2013) Making sense of ‘consumer engagement’ initiatives to improve health and health care: a conceptual framework to guide policy and practice. The Milbank Quarterly 91, 37–77.
| Making sense of ‘consumer engagement’ initiatives to improve health and health care: a conceptual framework to guide policy and practice.Crossref | GoogleScholarGoogle Scholar |
Nimegeer A, Farmer J, West C, Currie M (2011) Addressing the problem of rural community engagement in healthcare service design. Health & Place 17, 1004–1006.
| Addressing the problem of rural community engagement in healthcare service design.Crossref | GoogleScholarGoogle Scholar |
Oliver SR, Rees RW, Clarke‐Jones L, Milne R, Oakley AR, Gabbay J, Stein K, Buchanan P, Gyte G (2008) A multidimensional conceptual framework for analysing public involvement in health services research. Health Expectations 11, 72–84.
| A multidimensional conceptual framework for analysing public involvement in health services research.Crossref | GoogleScholarGoogle Scholar |
Sankar M (2005) Bridging the gap between policy, research and practice: experiences from a Community Economic Development Action Research project in New Zealand. Social Policy Journal of New Zealand 26, 52–65.
Sarrami-Foroushani P, Travaglia J, Debono D, Braithwaite J (2014) Implementing strategies in consumer and community engagement in health care: results of a large-scale, scoping meta-review. BMC Health Services Research 14, 402
| Implementing strategies in consumer and community engagement in health care: results of a large-scale, scoping meta-review.Crossref | GoogleScholarGoogle Scholar |
Victorian Department of Health and Human Services (2013) Community advisory committee guidelines. (Rural and Regional Health and Aged Care Services, Division, Victorian Government Department of Human Services: Melbourne, Vic., Australia). Available at https://www2.health.vic.gov.au/getfile/?sc_itemid=%7b7D8E9161-5714-450A-ABE0-3DC6974280DE%7d&title=Community%20advisory%20committee%20guidelines [Verified 5 June 2017]


