Consumers’ and their supporters’ perspectives on barriers and strategies to reducing seclusion and restraint in mental health settings
Lisa M. Brophy A B , Catherine E. Roper C , Bridget E. Hamilton D E , Juan José Tellez F I and Bernadette M. McSherry F G HA Centre for Mental Health, Melbourne School of Population and Global Health, University of Melbourne, 4/207 Bouverie Street, Carlton, Vic. 3010, Australia. Email: lbrophy@unimelb.edu.au
B Mind Australia, 86–92 Mount Street, Heidelberg, Vic. 3084, Australia.
C Centre for Psychiatric Nursing, School of Health Sciences, The University of Melbourne, Level 6 Alan Gilbert Building, 161 Barry Street, Carlton, Vic. 3053, Australia. Email: croper@unimelb.edu.au
D Department of Nursing, School of Health Sciences, The University of Melbourne, Level 6 Alan Gilbert Building, 161 Barry Street, Carlton, Vic. 3053, Australia. Email: bh@unimelb.edu.au
E St. Vincent’s Mental Health, 41 Victoria Parade, Fitzroy, Vic. 3065, Australia.
F Melbourne Social Equity Institute, The University of Melbourne, 201 Grattan Street, Carlton, Vic. 3053, Australia.
G Melbourne Law School, University Square, 185 Pelham Street, Carlton, Vic. 3035, Australia. Email: bernadette.mcsherry@unimelb.edu.au
H Faculty of Law, Monash University, Wellington Road, Clayton, Vic. 3800, Australia.
I Corresponding author. Email: juan.tellez@unimelb.edu.au
Australian Health Review 40(6) 599-604 https://doi.org/10.1071/AH15128
Submitted: 5 July 2015 Accepted: 9 January 2016 Published: 3 March 2016
Journal Compilation © AHHA 2016
Abstract
Objective This paper examines the perspectives of consumers and their supporters regarding the use of seclusion and restraint in mental health settings.
Methods Five focus groups for consumers and five focus groups for supporters were conducted in four Australian cities and in one rural location. The 66 participants were asked about strategies to reduce or eliminate the use of seclusion and restraint in mental health settings.
Results All participants supported the reduction of the use of seclusion and restraint. Barriers to reducing these practices related to the environment, the effects of drug and alcohol issues, lack of a human rights focus and poor recognition of trauma, stigma and discrimination. Strategies for reducing or eliminating seclusion and restraint included workforce development, environmental and cultural changes.
Conclusions Participants clearly identified that the status quo needs to change and conveyed urgency for action. Participants suggested that the involvement of supporters and a range of consumer roles are integral to reducing the use of seclusion and restraint. The findings support the current policy emphasis of working towards the elimination of these practices.
What is known about the topic? Mental health policies across many jurisdictions support the reduction and elimination of restraint and seclusion. Evidence suggests those subjected to restraint and seclusion largely experience a range of harmful consequences. No studies focus on the views of supporters of consumers regarding the reduction and elimination of seclusion and restraint, whereas the views of consumers appear in a minority of international studies.
What does this paper add? The research enabled an opportunity to hear from people who have been personally affected by and/or have lived experience of these coercive practices. Participants identified local reforms that can uphold the human rights of consumers. They suggested practices to increase accountability, peer support and family involvement, areas that have not been analysed in depth in any of the seclusion and restraint literature.
What are the implications for practitioners? This paper will give healthcare services a deeper insight into how to reduce or eliminate restraint or seclusion from the perspective of those with lived experience.
Additional keywords: consumer voice, lived experience, qualitative research, service user perspective.
Introduction
Seclusion and restraint are interventions currently permitted for use in mental health services and other settings to control or manage a person’s behaviour. Seclusion generally refers to the deliberate confinement of a person alone in a room or area that cannot be freely exited. Restraint may encompass the use of bodily force (physical restraint) or a device (mechanical restraint) to control a person’s freedom of movement. Less commonly, the term ‘restraint’ is used to refer to the use of medication (chemical restraint) to control a person’s behaviour rather than to treat a mental disorder, and ‘emotional restraint’ whereby consumers feel constrained from expressing their views openly and honestly to staff for fear of the consequences.1
In Australia, serious concerns about the use of seclusion and restraint in mental health care have been raised at least since 1993,2 and in 2005 all Australian health ministers agreed to reduce the use of seclusion and restraint.3 Several studies have noted adverse consequences for those subjected to seclusion and mechanical restraint4–9 and raised concerns with human rights breaches.10 Many mental health practitioners, consumers and family members, friends and other supporters (supporters) have also embraced the aim to reduce and, where possible, eliminate seclusion and restraint.1
The United Nations Convention on the Rights of Persons with Disabilities11 details the human rights of those with disabilities and is a current driver for policy and legislative change to reduce all restrictive and coercive practices in countries such as Australia that have ratified this convention. In Australia, the federal government established the National Mental Health Commission in 2012 to provide independent advice regarding mental health issues and policies. In its first year the Commission made 10 recommendations for action, the third being: ‘Reduce the use of involuntary practices and work to eliminate seclusion and restraint’.12 It also called for all jurisdictions to provide regular data at a service agency level to enable national data collection. Following this report, in 2013 the Commission established the National Seclusion and Restraint Project.
There is minimal research evidence to inform the changes in practice required to support this policy direction and reduce the use of seclusion and restraint. Multiple factors influence how often and why these practices are used and their definition, use and oversight vary across and within jurisdictions. Consumer perspectives are reported in a minority of studies internationally. Most discussion indicates that consumers want to see a reduction in the use of seclusion and restraint in the context of the trauma and distress they generate.5,13 Many consumers do not think the use of seclusion and restraint is justifiable.14,15 There do not appear to be any studies focused on the views of the supporters of consumers regarding seclusion and restraint and its reduction or elimination. Some studies with partial relevance consider supporters’ views on restrictive practices from the Australian disability sector16 and in relation to the use and revocation of community treatment orders.17,18
As part of a larger study conducted by the Melbourne Social Equity Institute, The University of Melbourne, and funded by the National Mental Health Commission, five focus groups for consumers and five focus groups for supporters were conducted in four capital cities and one regional centre. This article analyses the perspectives of focus group participants related to barriers to reducing seclusion and restraint and the strategies for reducing these practices.
Methods
The project obtained ethics approval from The University of Melbourne (Ethics ID 1340647).
Five focus groups for family members, friends and other supporters (supporters) and five focus groups for people with lived experience of seclusion and restraint (consumers) were conducted. This was a convenience sample, although some purposive sampling was achieved by holding the focus groups in four Australian state capitals and a fifth group being held in a regional city to enable people living in that city, or the surrounding area, to attend. The focus groups did not attempt to have a representative sample; rather, the intent was to sample people who could contribute data from direct experience. This overall research design deliberately resourced focus groups with consumers and supporters placing those experiences at the centre of the investigation. Focus groups were included in the research design because they are a particularly good method for generating discussion and stimulating ideas.19 In-depth information and ideas related to the prevention of seclusion and restraint were elicited from the vantage point of people with direct experience of those interventions. Focus groups enabled the voices of consumers and supporters, which are relatively marginal in the research to date, to be highlighted in this research. It was expected that this would complement a concurrent nationwide online survey recruiting all stakeholders.
The supporter focus groups consisted of 36 participants (29 women, seven men) who had experienced a family member or person close to them being secluded or restrained. These included parents, siblings, marital partners and two people who had advocacy roles. The consumer focus group consisted of 30 adults (13 men, 17 women), all of whom had either experienced seclusion or restraint directly, witnessed these practices as in-patients or were consumer advocates who had directly supported people who had experienced seclusion and restraint.
The focus groups were all conducted in English, but participants indicated a variety of ethnic and cultural backgrounds. The participants ranged in age from 20 years old to one participant who was over 70 years of age. No Indigenous Australians attended, but people involved in supporting Indigenous people did attend. Participants self-selected and opted into the groups after receiving information through peak bodies and support services (including Indigenous health organisations) in each state where the focus groups were held. The facilitators had a brief discussion with each potential participant to confirm their eligibility to take part before the focus groups. Participants received an A$25 shopping voucher to express appreciation for their attendance.
The focus groups were conducted by an experienced qualitative researcher and mental health practitioner (LMB) and a consumer academic (CER). The involvement of a researcher with lived experience was a deliberate strategy to enable and support open and safe discussion of this sensitive topic. Although participants were reassured they were not being asked to speak of their personal experiences, many chose to share their direct experiences, and a facilitator who shared personal experience was considered to contribute to participants’ experiences being validated.
The overall aim of the focus groups was to give people an opportunity to share their perspectives as to how seclusion and restraint could be reduced or eliminated. Participants discussed their understanding of the use of seclusion and restraint and their effects on the people involved, their observations about poor practice and what contributes to it and ideas and recommendations regarding strategies to reduce or eliminate seclusion and restraint.
The focus group recordings were transcribed, then analysed using NVivo 10 qualitative data analysis software (QSR International, Melbourne, Vic., Australia). A general inductive approach was used to analyse the data.20 Each transcript was closely read and reread multiple times in order to identify categories, which were coded for words, phrases and meanings in the text by one member of the research team (JJT) who was independent of both focus group facilitators. Categories were continually refined through the analysis, with coding consistency checks performed by another team member to ensure trustworthiness of the data (LMB). Further confirmation of themes took place through team discussions that involved both facilitators. The emerging themes were also discussed with the full research team. The project’s two Lived Experience Advisory Groups for consumers and supporters also discussed and commented on the preliminary findings. The analysis enabled consideration of the responses to the key questions in the focus groups as well as identification of emerging themes.
Results
Barriers to reducing seclusion and restraint
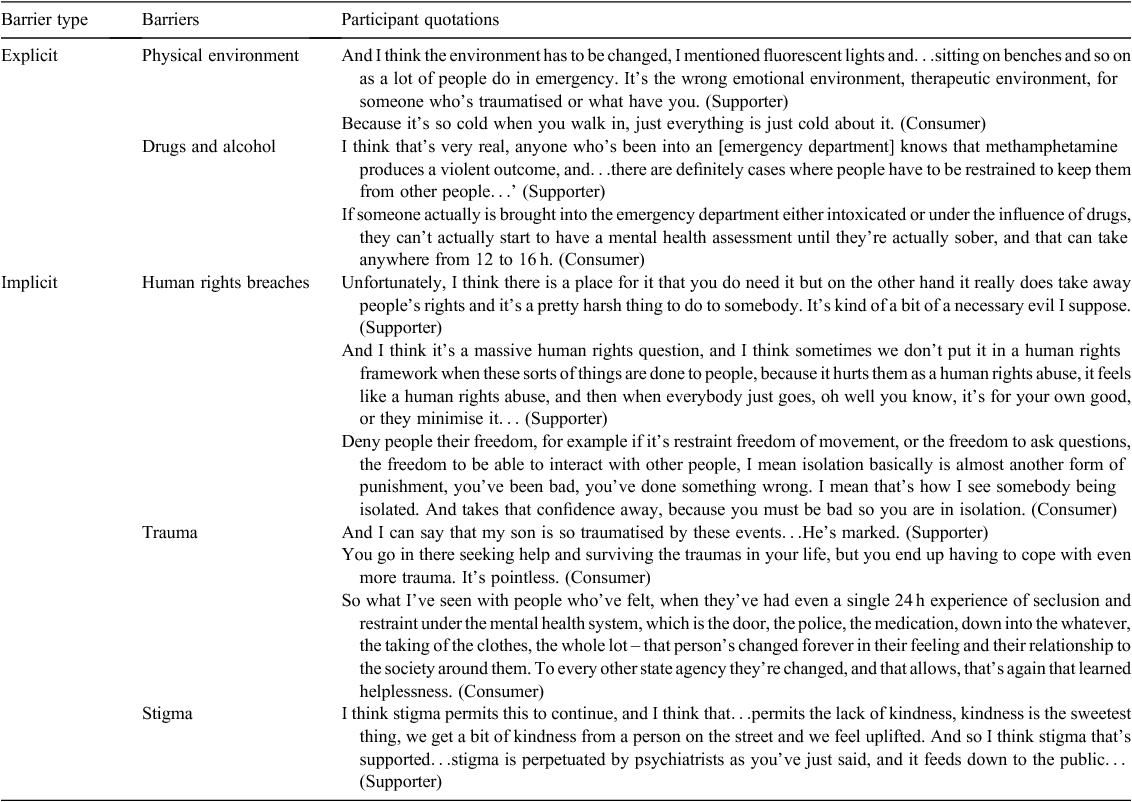
Participants discussed barriers either in a clear and explicit manner, or more implicitly through discussion about their observations and experience (Table 1).
|
Explicitly identified barriers
Participants identified the physical environment as a barrier to the reduction of seclusion and restraint in two main areas: the emergency department and the in-patient setting. Participants commented on features such as poor lighting, uncomfortable waiting areas and rooms being bare and cold. There were many criticisms of the environments people in mental distress or crisis were finding themselves in, and the difficulty of being able to respond therapeutically in these environments.
Participants in the supporter and, to a lesser extent, the consumer focus groups discussed how drugs and alcohol contribute to the use of seclusion and restraint. For example, the process of admission of an intoxicated person in the emergency department may also be a barrier to reducing seclusion and restraint in cases of acute mental health issues.
Implicitly identified barriers
Nine groups discussed the effect that seclusion and restraint have on consumers and carers. Through this discussion, several implicit barriers to the reduction of seclusion and restraint emerged. Even when deemed as necessary to manage risk, these practices were seen as breaching human rights, including basic freedoms. In addition, a lack of accountability and recognition from services for human rights breaches were concerns for participants, particularly because many of their supporters seemed powerless and may not be believed when they complain of abuse.
Participants discussed how trauma resulted from coercive practices, and how past traumas can be revisited during restraint or seclusion. Trauma experienced through restraint and seclusion was linked to the subsequent impact on a person’s recovery and ongoing relationship to services.
Paternalism was identified by participants as poor practice, encouraging the stigmatisation of consumers and contributing to a culture of fear and risk aversion, key factors in the overuse of coercive practices.
Strategies to prevent and eliminate seclusion and restraint
In both the consumer and supporter focus groups, strategies for the prevention of seclusion and restraint were discussed (Table 2). In the opinion of some participants, most often in the carer groups, seclusion and restraint may be necessary in some circumstances:

|
If a person is a severe and significant risk to either themselves or to another then I think that there is a duty on society to protect them, to protect them from committing offences against others or from doing those things to themselves. (Supporter)
However, others held strong views supporting elimination:
…it’s so appalling as somebody said…at the highest level of management, and the people with the power, what is going on. This should be absolutely banned. (Supporter)
There was considerable consensus that seclusion and restraint could be reduced and participants in both groups also discussed ways in which the elimination of seclusion and restraint could be realised.
Participants suggested that state and federal governments had an important role in leading change, as well as improving complaint systems, enabling public accountability and ensuring action is taken in relation to complaints. At the service level, participants proposed more opportunities to obtain advocacy, to complain and for services and staff to be accountable for their decisions and actions.
In seven of the 10 focus groups, peer support and advocacy were suggested as elimination or reduction strategies. There was strong consensus that peer support is vital to ensuring that understanding, empathy and recovery-oriented practice occur in the in-patient setting. Lived experience of seclusion and restraint gives peer support workers an important understanding of the traumatic effects of coercive interventions. Peer support workers can also assist in de-escalation, helping create a space of safety and understanding in a highly stressful environment.
Peer workers were also identified as having potential to influence practice and lead change more widely. In half the focus groups, it was suggested that more carer or family involvement could help reduce or eliminate seclusion and restraint. This was identified as particularly important for Indigenous people.
In over half the focus groups, strategies to improve the environment in the in-patient unit were encouraged. Changes such as non-fluorescent lighting, creating warmth by adding colour, pictures and quotes to walls and sensory modulation were suggestions that can be implemented within existing in-patient buildings. Unlocking the doors to the main ward and constructing a separate therapeutic environment connected to the emergency department were other suggestions by participants.
In nine of the 10 focus groups, respectful, recovery-oriented and sensitive care in crisis situations was recommended. Participants suggested that staff needed to be more prepared for responding to people who are distressed and there was confidence among participants that de-escalation strategies can work.
Improving staff culture was strongly linked to education and training, but also to steps such as ‘weeding out’ staff who appeared to lack skills and compassion and introducing more consumer feedback and involvement in services. Greater recognition of skills to calm and defuse situations was seen as a positive contribution to culture change.
Some participants suggested that improved support in the community would prevent involuntary admission and therefore result in less chance of seclusion and restraint being used.
Participants suggested that changing the language around seclusion and restraint may also change practice. Across consumer and supporter focus groups, participants commented that the violence of seclusion and restraint was disguised by the terminology used.
Discussion
The responses suggest that there is considerable consensus between both the consumer and supporter focus group participants about proposed strategies to reduce seclusion and restraint.
The findings indicate the importance of mental health services being recovery oriented such that every effort is made to offer respectful and non-coercive support to a person who is in crisis or involuntarily detained in hospital. As the recovery focus has grown in mental health care, the means of increasing recovery orientation in acute in-patient settings are emerging in the literature.21 However, these findings suggest that introducing more recovery-oriented service delivery is challenging when coercive practice is supported by workplace culture.
The need to improve the environment in which services are offered is a key finding. This included radical changes such as the total removal of seclusion rooms, through to improving relatively minor aspects of the environment. Research by Bowers et al.22 has also supported the importance of improving the physical environment of in-patient units and also noted that having some acute wards without a seclusion space in regions of the UK reduced seclusion rates overall.
Providing opportunities for support and connection, including having greater access to peer workers, family and other informal support for people in crisis situations and on in-patient units, is an important overarching theme in these findings, potentially supported by the inclusion of supporters in the study. Participants suggested this type of support was most likely to ensure that the person and their experience were respected. This is supported by the fifth of the six core strategies that were developed by Huckshorn encouraging peer roles in programs to reduce seclusion and restraint.23
Participants referred to the need for a change in the discourse surrounding seclusion and restraint, suggesting the current language appeared to support these practices as a legitimate use of power. Investigations of staff and consumer attitudes show language differs between these groups. Staff describe the impact of seclusion in more modest terms and use technical language that legitimises these practices.24 Implicit barriers to the reduction of coercive practices also need to be addressed to ensure trauma, stigma and discrimination are acknowledged and addressed.21
Strengths and limitations of the approach
These groups were deliberately small and based on participants opting in to participate, meaning the generalisability of the findings is limited. There were ethical and financial constraints on the project that limited the potential for more targeted purposive sampling of, for example, young people or people from different cultural and linguistic backgrounds. However, a broad range of participants did attend, the discussions were lengthy and fruitful and a safe environment for the discussion of such potentially sensitive issues was achieved. This was particularly supported by having a cofacilitator who had lived experience of the interventions under discussion.
Conclusion
Participants clearly identified that the current situation needs to change and a major contribution of the perspectives proffered is to inform a sense of urgency for action. It appears that many participant perspectives are in agreement with the United Nations Special Rapporteur on torture and other cruel, inhuman or degrading treatment or punishment, who has called for an absolute ban on all forced and non-consensual medical interventions.25 He has stated that ‘both prolonged seclusion and restraint may constitute torture and ill-treatment’ and that there can be no therapeutic justification for the use of them in psychiatric institutions.25 Consumers’ and their supporters’ perspectives regarding strategies for reducing or eliminating seclusion and restraint share similar concerns to those reported in previous research.21–24 These findings reinforce the emphasis on the need for accountability and the value of providing peer support and enabling the involvement of supporters. These strategies have the potential to assist with the policy direction in Australia of working towards the elimination of seclusion and restraint and are in need of further exploration. The strategies consumers and their supporters identified in the present study provide an important contribution to efforts to reduce coercive practices, improve recovery-oriented services and indicate the value of hearing the voices of those directly affected by the use of seclusion and restraint.
Competing interests
The authors report no competing interests.
Acknowledgements
This article presents independent research funded by the National Mental Health Commission. The views expressed in this article are those of the authors and not necessarily those of the National Mental Health Commission. The authors thank Andrew Butler for his research assistance with this paper. The authors also thank all the research participants and agencies that supported the research.
References
[1] National Mental Health Consumer and Carer Forum. Ending seclusion and restraint in Australian mental health services. Deakin West: National Mental Health Consumer and Carer Forum; 2009. Available at: http://www.nmhccf.org.au/documents/Seclusion%20&%20Restraint.pdf [verified 28 May 2014].[2] Australian Human Rights Commission. Report of the national inquiry into the human rights of people with mental illness. Canberra: Human Rights and Equal Opportunity Commission; 1993.
[3] National Mental Health Working Group. National safety priorities in mental health: a national plan for reducing harm. Canberra: Department of Health and Ageing, Commonwealth of Australia; 2005. Available at: http://www.health.gov.au/internet/main/publishing.nsf/Content/DB6FC7B04519D195CA257BF000217B28/$File/safety.pdf [verified 28 May 2014].
[4] Cano N, Boyer L, Garnier C, Michel A, Belzeaux R, Chabannes JM, Samuelian JC, Harle JR. Patients’ perception of seclusion in psychiatry: ethical perspectives. Encephale 2011; 37 S4–10.
| Patients’ perception of seclusion in psychiatry: ethical perspectives.Crossref | GoogleScholarGoogle Scholar | 21600332PubMed |
[5] Frueh BC, Knapp RG, Cusack KJ, Grubaugh AL, Sauvageot JA, Cousins VC, Yim E, Robins CS. Special section on seclusion and restraint: patients’ reports of traumatic or harmful experiences within the psychiatric setting. Psychiatr Serv 2005; 56 1123–33.
| Special section on seclusion and restraint: patients’ reports of traumatic or harmful experiences within the psychiatric setting.Crossref | GoogleScholarGoogle Scholar | 16148328PubMed |
[6] Gerace A, Pamungkas DR, Oster C, Thomson D, Muir-Cochrane E. The use of restraint in four general hospital emergency departments in Australia. Australas Psychiatry 2014; 22 366–9.
| The use of restraint in four general hospital emergency departments in Australia.Crossref | GoogleScholarGoogle Scholar | 24820291PubMed |
[7] Haw C, Stubbs J, Bickle A, Stewart I. Coercive treatments in forensic psychiatry: a study of patients’ experiences and preferences. J Forens Psychiatry Psychol 2011; 22 564–85.
| Coercive treatments in forensic psychiatry: a study of patients’ experiences and preferences.Crossref | GoogleScholarGoogle Scholar |
[8] Kontio R, Joffe G, Putkonen H, Kuosmanen L, Hane K, Holi M, Valimaki M. Seclusion and restraint in psychiatry: patients’ experiences and practical suggestions on how to improve practices and use alternatives. Perspect Psychiatr Care 2012; 48 16–24.
| Seclusion and restraint in psychiatry: patients’ experiences and practical suggestions on how to improve practices and use alternatives.Crossref | GoogleScholarGoogle Scholar | 22188043PubMed |
[9] Mayers P, Keet N, Winkler G, Flisher AJ. Mental health service users’ perceptions and experiences of sedation, seclusion and restraint. Int J Soc Psychiatry 2010; 56 60–73.
| Mental health service users’ perceptions and experiences of sedation, seclusion and restraint.Crossref | GoogleScholarGoogle Scholar | 20053723PubMed |
[10] Kumble S, McSherry B. Seclusion and restraint: rethinking regulation from a human rights perspective. Psychiatry Psychol Law 2010; 17 551–61.
| Seclusion and restraint: rethinking regulation from a human rights perspective.Crossref | GoogleScholarGoogle Scholar |
[11] United Nations. United Nations convention on the rights of persons with disabilities. Available at: http://www.un.org/disabilities/convention/conventionfull.shtml [verified 30 October 2014].
[12] National Mental Health Commission. A contributing life: the 2012 national report card on mental health and suicide prevention. Sydney: National Mental Health Commission; 2012.
[13] Grubaugh AL, Frueh BC, Zinzow HM, Cusack KJ, Wells C. Patients’ perceptions of care and safety within psychiatric settings. Psychol Serv 2007; 4 193–201.
[14] Duxbury J. An evaluation of staff and patient views of and strategies employed to manage inpatient aggression and violence on one mental health unit: a pluralistic design. J Psychiatr Ment Health Nurs 2002; 9 325–37.
| An evaluation of staff and patient views of and strategies employed to manage inpatient aggression and violence on one mental health unit: a pluralistic design.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD38zhslKlug%3D%3D&md5=3e6c688eb229b769a8b45f4f28662d7dCAS | 12060377PubMed |
[15] Meehan T, Vermeer C, Windsor C. Patients’ perceptions of seclusion: a qualitative investigation. J Adv Nurs 2000; 31 370–7.
| Patients’ perceptions of seclusion: a qualitative investigation.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c7jvVWhtQ%3D%3D&md5=f77c409f7b78767798d7135b54633978CAS | 10672095PubMed |
[16] Office of the Public Advocate. Restrictive interventions in Victoria’s disability sector. Issues for discussion and reform: discussion paper. Melbourne: Victorian Government; 2012. Available at: http://www.publicadvocate.vic.gov.au/our-services/publications-forms/55-restrictive-interventions-in-victorias-disability-sector-issues-for-discussion-and-reform?path= [verified 30 January 2016].
[17] Light EM, Robertson MD, Boyce P, Carney T, Rosen A, Cleary M, Hunt GE, O’Connor N, Ryan C, Kerridge IH. The lived experience of involuntary community treatment: a qualitative study of mental health consumers and carers. Australas Psychiatry 2014; 22 345–51.
| The lived experience of involuntary community treatment: a qualitative study of mental health consumers and carers.Crossref | GoogleScholarGoogle Scholar | 24963099PubMed |
[18] Owens N, Brophy L. Revocation of community treatment orders in a mental health service network. Australas Psychiatry 2013; 21 46–50.
| Revocation of community treatment orders in a mental health service network.Crossref | GoogleScholarGoogle Scholar | 23236095PubMed |
[19] Øvretveit J. Action evaluation of health programmes and changes: a handbook for a user-focused approach. Abingdon: Radcliffe Medical Press; 2002.
[20] Thomas DR. A general inductive approach for analyzing qualitative evaluation data. Am J Eval 2006; 27 237–46.
| A general inductive approach for analyzing qualitative evaluation data.Crossref | GoogleScholarGoogle Scholar |
[21] Jaeger M, Konrad A, Rueegg S, Rabenschlag F. Patients’ subjective perspective on recovery orientation on an acute psychiatric unit. Nord J Psychiatry 2015; 69 188–95.
| Patients’ subjective perspective on recovery orientation on an acute psychiatric unit.Crossref | GoogleScholarGoogle Scholar | 25241849PubMed |
[22] Bowers L, Van Der Merwe M, Nijman H, Hamilton B, Noorthorn E, Stewart D, Muir-Cochrane E. The practice of seclusion and time-out on English acute psychiatric wards: the City-128 study. Arch Psychiatr Nurs 2010; 24 275–86.
| The practice of seclusion and time-out on English acute psychiatric wards: the City-128 study.Crossref | GoogleScholarGoogle Scholar | 20650373PubMed |
[23] Huckshorn K. Reducing seclusion and restraint use in mental health settings: core strategies for prevention. J Psychosoc Nurs Ment Health Serv 2004; 42 22–33.
| 15493493PubMed |
[24] Van Der Merwe M, Muir-Cochrane E, Jones J, Tziggili M, Bowers L. Improving seclusion practice: implications of a review of staff and patient views. J Psychiatr Ment Health Nurs 2013; 20 203–15.
| Improving seclusion practice: implications of a review of staff and patient views.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC38fgslKnsw%3D%3D&md5=06aedf6c4273932e922c17e9a63dd798CAS | 22805615PubMed |
[25] United Nations Human Rights Council. Report of the Special Rapporteur on torture and other cruel, inhuman or degrading treatment or punishment, Juan E. Méndez. A/HRC/22/53. 2013. Available at: http://www.ohchr.org/Documents/HRBodies/HRCouncil/RegularSession/Session22/A.HRC.22.53_English.pdf [verified 1 January 2016].


