Outreach immunisation services in New Zealand: a review of service delivery models
Loretta Roberts 1 , Nikki Turner 1 , Barbara McArdle 1 , Mary Nowlan 1 , Lynn Taylor 1 , Rachel Webber 2 , Paul Rouse 31 Immunisation Advisory Centre, Department of General Practice and Primary Health Care, The University of Auckland, New Zealand
2 National Immunisation Programme, Ministry of Health, New Zealand
3 Department of Accounting and Finance, The University of Auckland, New Zealand
Correspondence to: Mary Nowlan, Immunisation Advisory Centre, Private Bag 92019, Auckland 1142, New Zealand. Email: m.nowlan@auckland.ac.nz
Journal of Primary Health Care 9(1) 62-68 https://doi.org/10.1071/HC16012
Published: 17 February 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Outreach Immunisation Services (OIS) enable children who have not been immunised on time at general practice to be immunised in the community, thereby improving immunisation coverage and reducing equity gaps.
AIM: To identify the most effective service delivery models and make recommendations for more effective and cost-efficient OIS delivery in New Zealand.
METHODS: Data collection and thematic analysis through a detailed review of OIS contracts and service specifications, an online survey and in-depth interviews with stakeholders and providers, and an analysis of cost data was conducted.
RESULTS: In total, 28 OIS providers completed survey questionnaires, 28 OIS staff were interviewed, and cost effectiveness data were obtained from 11 providers. The surveys and interviews identified key themes around identifying clients with the highest needs, effective engagement strategies, staffing requirements, and service challenges. On average, each OIS referral costs NZ$361 (median NZ$257), and each vaccination event costs NZ$636, ranging from NZ$145 to NZ$2403. Characteristics for two separate models of service delivery were identified based on provider size.
CONCLUSION: There is considerable range in costs and style of OIS delivery, and efficiencies can be gained. Models need to fit with locality needs and include adequate resourcing, staff with good local knowledge, close relationships with other key child health services and preferably co-location, sustainable funding, and regular service reviews. OIS are part of an effective integrated service that relies on accurate data, positive relationships and a rapid response when children fail to present for vaccination in a timely fashion.
KEYWORDS: Immunisation; vaccination; primary health care; family health care; equity
| WHAT GAP THIS FILLS |
| What is already known: Outreach Immunisation Services (OIS) are important to support the delivery of the early childhood national immunisation programme in New Zealand, particularly for children who do not access vaccination in a timely fashion from their primary healthcare provider, and to reduce equity gaps. The way these different models of service are provided varies widely across regions and providers. |
| What this study adds: This study identifies efficiencies in the types of service models and strategies that can be used to improve delivery of immunisation services to children who have not obtained their childhood vaccinations on time. The findings can be used to assist with the development of more efficient models of OIS delivery. |
Introduction
National immunisation targets have still not been met in New Zealand (NZ) despite excellent progress towards achieving high immunisation coverage over recent years.1 An important aspect of an effective service is the ability to find and offer services to children and their families who have not presented for vaccination in a timely fashion. Children from areas of higher deprivation and children of Māori and Pacific ethnicity are least likely to be immunised on time. This numerically small group is also most likely to be at risk of contracting vaccine-preventable diseases.1
Timely vaccination of children does not occur for several reasons, including challenges around transport and accessing services, other social and family priorities, lack of awareness of need, or perceived barriers at the practice level.2–4 Having effective outreach immunisation services (OIS) that are able to reach out to unvaccinated children is an important strategy to close equity gaps and maintain high immunisation coverage.5,6 As of September 2016, 93% of NZ children were fully immunised according to the National Immunisation Schedule (NIS) by the age of 8 months; the Ministry of Health target is 95%.7 OIS provide immunisations for children aged up to 6 years to support achieving the national immunisation coverage targets.8
Service specifications developed by the Ministry of Health describe the core requirements of OIS. OIS funding is provided by the District Health Boards (DHBs), and allowance is given to adapt and develop these requirements to fit the local context. The way OIS are provided varies between regions and providers.
The aim of this study was to identify different models of outreach services and to identify their most efficient and effective aspects. The research was funded by the Ministry of Health.
Methods
The study had three objectives: (1) to identify and analyse different OIS delivery models and approaches; (2) to analyse the cost-effectiveness of OIS services; and (3) to use the findings to make recommendations to improve OIS efficiencies and cost-effectiveness.
Ethics approval was granted by the University of Auckland Human Participants Ethics Committee on 31 March 2015.
Development of tools
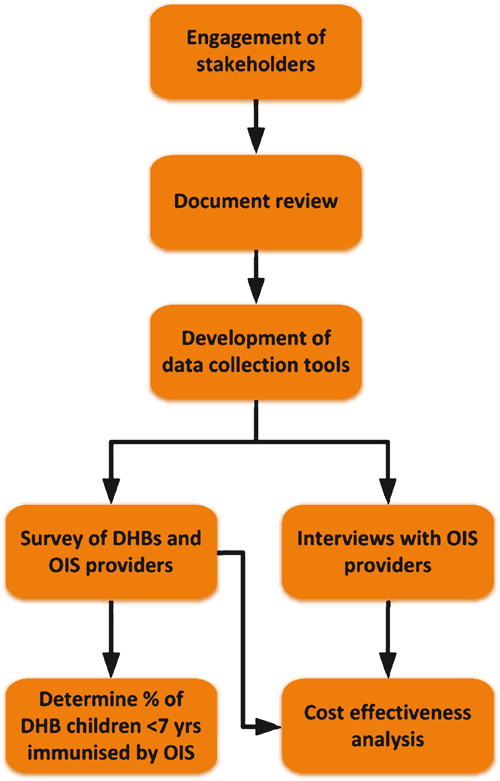
Development of the data collection tools was conducted, as shown in Fig. 1. Following an introductory letter from the Ministry of Health to key contacts in all 20 DHBs, consent for engagement of stakeholders was gained by a researcher.
|
Researchers reviewed all current DHB–OIS provider contracts and Ministry of Health Service Specifications to identify key performance expectations. This highlighted variations or additions in individual contracts, compared with standard OIS delivery requirements set out by the service specifications.
Topics based on key components identified by the document review were used to develop a 91-question survey to collect data from key stakeholders employed by DHBs and OIS providers. These topics included: contract details; characteristics of OIS area; staffing; service users; sources of referrals; vaccination processes and equipment; stakeholder engagement; service linkages; reporting; and evaluation of strengths and challenges.
A template was developed for face-to-face interviews with key informants based on the information from the service specifications reviews and pilot survey feedback. The interview questions varied depending on the role of the interviewee. Broadly, the topics were the same as in the survey, above.
Data collection
Surveys of DHBs and OIS providers: In total, 35 OIS providers across 20 DHBs were identified. DHBs were asked either to invite their OIS providers to take part in the survey or to provide a survey response(s) on behalf of their OIS providers. The survey format, in accordance to preference, was either online, an electronic document, or fully paper-based.
Face-to-face interviews with OIS providers: To sample across different delivery models, including small and larger providers and geographical range, 10 DHBs with 15 OIS providers were purposefully selected. Chosen OIS providers identified two key frontline and managerial staff to be interviewed.
Cost-effectiveness analysis: Analysis was based on data collected via the surveys and additional financial information requested during interviews. OIS managers were asked to complete a cost-effectiveness template.
Data analysis
Survey responses were entered into SurveyMonkey software (SurveyMonkey Inc.), either directly by survey respondents or by the researchers. Quantitative responses were analysed, depending on the question, to give averages (means or medians, as applicable). Qualitative responses were reviewed to identify key themes.
The interviews were recorded by a writer and analysed independently by two researchers to identify key themes.
For analysis of the percentage of children immunised by OIS services in each DHB, a proxy was calculated for the period 1 July 2013 to 30 June 2014 using the total number of children immunised by all OIS providers in each DHB as the numerator, and the number of children younger than 7 years old for the same period from the National Immunisation Register (NIR) DHB Registered Population reports for the denominator.
Within the scope of the study, data were not available to fully measure health outcomes, necessitating the use of proxy measures of effectiveness. Measures of effectiveness included ratios of referrals per general practice and percentage of vaccinations per referral. Referrals to OIS provide benefits that extend beyond immunisation, including engagement with other child services. Measures of cost-effectiveness included cost per referral using full cost, and cost per vaccination using both full cost and unit level costs, to focus on the variable cost of vaccinations.
Results
Surveys covering 28 OIS providers across 18 DHBs were received. Comprehensive responses were provided for 24 OIS providers, and four were incomplete. Interviews were conducted with 28 OIS staff from 15 OIS recruited providers, including 12 nurse vaccinators and 15 service managers. Cost-effectiveness data were obtained from 11 providers.
Common themes identified from survey responses
OIS clients and priority groups: Referred OIS clients were identified as vulnerable populations, mostly of Māori ethnicity and non-English speaking immigrants, generally with low socioeconomic status and many with low health literacy. Also identified were internal migrants relocating between DHBs due to changing employment or children moving between family members. In many cases, enrolling with a general practice and immunisation were seen as low priorities. Some areas had clusters of alternative lifestyle families who decline vaccination.
Generally, OIS providers felt that more intense effort was required to engage with some Māori families, with some expressing a higher level of suspicion of immunisation than other ethnicities. This appears to be related to engagement with services rather than anti-vaccination sentiment; many OIS staff reported that most Māori families accepted vaccination once they had visited the family home.
Many providers felt that 4-year-old children attending day-care at early childhood education centres were not well served by general practices. Children of working parents were often immunised late due to issues in accessing services during the working week. Some parents had to take annual leave to attend a general practice. Most services are offered in Monday to Friday working hours and very few practices immunise after 5 pm or at weekends.
Children under social service care with Child Youth and Family Services were often identified as under-immunised due to challenges in obtaining parental consent and delays in arranging relevant documentation.
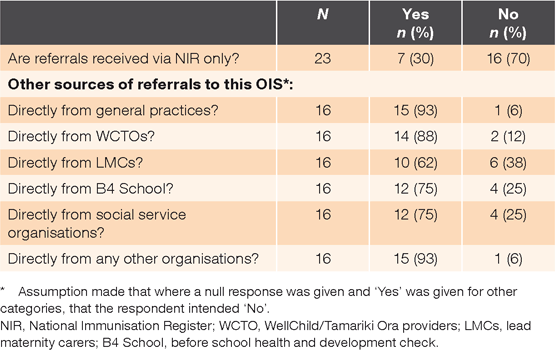
Source of OIS referrals: Referrals to OIS were received from a variety of sources, as shown in Table 1. Approximately one-third of all providers received referrals only from the NIR. The most common other referral sources were general practices, lead maternity carers and WellChild/Tamariki Ora providers.
|
Delays in referrals or referral of already vaccinated children and difficulty in finding families hinder OIS immunisations. Inability of OIS staff to directly access the NIR in the community, or access hospital and National Health Index databases were particularly linked to delays or unnecessary referrals.
More efficient and coordinated use of information technology was identified as needed to increase OIS productivity, by improving immunisation records and contact details across an OIS client database, the NIR and general practice electronic systems.
Wider system issues create unnecessary referrals. These include: receiving referrals for newborns not enrolled with a general practice, parental barriers to attend immunisation appointments such as outstanding medical bills at their general practice, missed opportunities to immunise in primary and secondary health care, and time-consuming consent issues; for example, for children in care.
Engaging clients: Smaller DHBs and communities rely on relationships with general practices to find and identify families, whereas larger DHBs have too many practices to maintain personal contact.
Difficulties in making appointments with transient families and long travel distances on rural roads pose challenges to access for OIS staff. Although time-consuming and requiring enormous persistence, it was frequently reported that cold calling, multiple visits and tracking down contact details were necessary to find referred children.
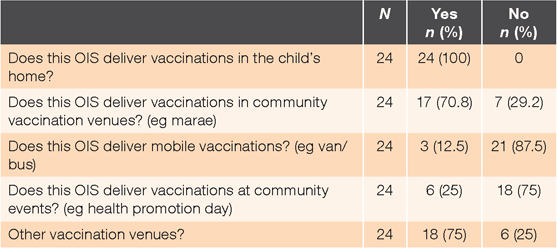
Due to privacy concerns about staff entering their home, some families decline home vaccination. Some providers arrange alternative venues, as shown in Table 2.
|
OIS funding and staffing: Small OIS providers experience funding challenges due to fewer economies of scale gains than larger providers and repeated uncertainties from short-term contract renewal. Resources can be wasted by small and isolated teams developing their own processes.
The success of the OIS is largely dependent on motivated staff with good communication skills, local knowledge and links to their community. Half of OIS providers reported having only one individual in the nurse vaccinator role. For more than one-third of the OIS providers, nurse vaccinators were employed at 0.6 full-time equivalents (FTE) or less. At the time of the survey, 49 individuals provided the equivalent work of 25 FTE staff across 24 OIS providers.
Managing and budgeting for many part-time staff was identified as an issue. Staff turnover and leave cover significantly impacted on provision of outreach immunisation by smaller providers. Within small teams, clinical staff with high skill levels are frequently required to undertake less skilful administrative tasks leading to reduced time for service delivery.
Other services: Most OIS provide services other than childhood vaccination, primarily conducted during the 20-min observational period post-vaccination. Many of these activities are defined components of the service, including support to re-engage with general practice and referrals to WellChild services and B4 School (health and development checks for 4-year-olds). However, services also commonly extend to screening and support for family violence and smoking cessation, and provision of more general health education.
Communications between funders and providers: Generally, effective interactions between the DHB and OIS providers occurred through immunisation steering groups, meetings with child health and social service providers, or interactions with the NIR team.
Cost-effectiveness
An estimated 4.0% of all children younger than 7 years old were immunised by OIS across DHBs (range: 0.7–14.8%). On average, a home vaccination event took 40 min (range: 25–60 min), including a post-vaccination observation period of 20 min.
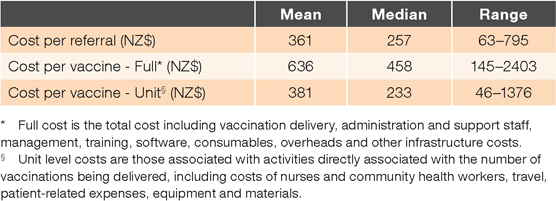
The cost-effectiveness analysis for 10 out of 11 OIS providers with sufficient data is summarised in Table 3. Taking all activities into account for the year ending June 2014, the mean full cost was NZ$361 (median NZ$257) per OIS referral and NZ$636 (median NZ$458) per vaccination event. Considering only activities associated with the number of vaccines delivered, the unit level cost of vaccination was NZ$381 (median NZ$233).
|
An alternative way to consider average costs is to sum across all 10 providers as if all results came from a single organisation, rather than to average across the outcome for each provider. In this way, the mean full cost per referral was NZ$214, and the mean unit and full cost per vaccination were NZ$218 and NZ$378, respectively. The differences between the two calculation methods emphasise the variability between providers, and likely reflects different cost structures.
OIS reporting
The time spent on quarterly performance reporting varied across providers. Most interviewees felt that the complexity of their OIS work was not adequately captured by the detailed reporting template provided by the Ministry of Health.
Models of service delivery
Two models of OIS service delivery were identified as the most effective approaches. For large urban areas with high volumes of referrals (DHB populations of >20,000 children aged 0–4 years), OIS operates most effectively as a stand-alone service based on referrals received directly from the NIR. Together with this is provision for broader access to services such as evening and regular weekend immunising, and clinics at after-hours medical centres or emergency departments. For effective action, appropriate staff need access to pertinent hospital patient records, National Health Index information and the NIR. Decisions around funding increases need to focus on extra staffing to support administration, processing of referrals by community healthcare workers, and effort in locating families before immunisation visits.
For smaller urban and rural areas, OIS is best co-located with NIR services and in close relationship to allied child-health services, immunisation coordinators and the local Medical Officer of Health. This allows small teams to share resources more effectively. In addition to the NIR, referrals may be received from other sources including general practice. Staff from co-located services are used to cover OIS staff absences. Strong relationships with local health and social service providers can facilitate finding children.
Discussion
In every system, there are children who do not access recommended immunisation in a timely fashion.9,10 There is a range of challenges for families in environments of poverty, including associations with sole parenting, certain ethnic groups, low health literacy, transport challenges, other costs to access services, and having other more pressing household priorities.9 Expanding access to healthcare services is well recognised as an effective mechanism for improving immunisation uptake.11 A systemic review on home visiting showed increases in immunisation coverage from 2 to 20% (median 13%).11 Home visiting interventions are resource-intensive, with adjusted cost-effectiveness ratios ranging from US$513 to US$13,020 per additional vaccination. Home visits are more likely to be most cost-effective when used as part of a multicomponent intervention.12
From this study, ~4% of children receive home vaccination (this varies per district from 0.7% to 14.8%), with an average time of 40 min spent per vaccination visit (25–60 min). The mean cost per referral was NZ$361 (ranging from NZ$63 to $795), and the full cost per immunisation event was a mean of NZ$636 (NZ$145 to $2,403). This demonstrates that outreach services are time-intensive and relatively expensive. Furthermore, the cost of delivery varies significantly with different delivery models. Two different models of delivery based on volumes of referral and efficiencies of scale were identified by this study.
To minimise the number of referrals to resource-intensive outreach services, primary care providers can increase access to vaccines. Effective multicomponent approaches include enrolment and engagement of newborn infants with a general practice, good recall and audit systems,13 good access to services with extended hours of access where possible, and minimising missed opportunities.14 These can all be built into practice quality-improvement processes.15 Making use of serendipitous or planned interactions between different child health providers can help increase opportunities to vaccinate.16,17
New Zealand is privileged to have excellent data systems making feasible efficient outreach services working alongside regular general practice delivery. This study identified some excellent models of OIS and primary care working well together to achieve high immunisation coverage. However, it has also demonstrated considerable variability in terms of costs and style of delivery processes, and that efficiencies can be gained.
Models of OIS service delivery need to fit with locality needs, and different mixes are required for smaller or larger areas. Close relationships between OIS, the NIR team and other immunisation, child health and social services were most effective. OIS staff with extensive local knowledge and well connected into communities is beneficial in gaining trust with families and health services. Effective service delivery can be hindered by fragmented and numerous small OIS providers with frequent short-term contracts. Regular reviews of service, performance and client satisfaction by OIS providers support effective quality-improvement models.
Conclusion
Outreach immunisation services are part of an integrated service that relies on effective use of good data, positive relationships and rapid response when children fail to present for their vaccination events in a timely fashion. However, the overarching principle of an outreach immunisation service should be for every child to be enrolled and fully immunised in general practice, both to minimise costs and to enable long-term engagement with the regular healthcare providers. Practices can support OIS by opportunistically immunising children to minimise missed vaccinations and ensuring that NIR records are kept up-to-date.
FUNDING
The review was commissioned by and funded by the Ministry of Health to inform a review of the Ministry of Health’s Services for Children and Young People – Outreach Immunisation Services Tier Level Two Service Specification. A detailed report is available on request from the Ministry of Health.
COMPETING INTERESTS
LT was previously the General Manager of MedTech New Zealand, one of the Practice Management Systems used by practices in this study. LT is currently the General Manager of DrINFO New Zealand, a practice audit tool used by ~50% of practices in NZ to assist them with the identification of patients requiring intervention, including children overdue for scheduled immunisations. None of the other authors have any potential conflicts of interest to declare.
ACKNOWLEDGEMENTS
The authors would like to acknowledge all the Immunisation Advisory Centre staff involved in this review, and would like to thank: staff from all DHB and OIS providers, Tina Noble from the Ministry of Health, and Dave Hebden from Mid Central DHB NIR for their assistance with accessing and acquiring data.
References
[1] Turner N. The challenge of improving immunization coverage: the New Zealand example. Expert Rev Vaccines. 2012; 11 9–11.| The challenge of improving immunization coverage: the New Zealand example.Crossref | GoogleScholarGoogle Scholar |
[2] Andrews B, Simmons P, Long I, et al. Identifying and overcoming the barriers to Aboriginal access to general practitioner services in Rural New South Wales. Aust J Rural Health. 2002; 10 196–201.
| Identifying and overcoming the barriers to Aboriginal access to general practitioner services in Rural New South Wales.Crossref | GoogleScholarGoogle Scholar |
[3] Bates AS, Fitzgerald JF, Dittus RS, et al. Risk factors for underimmunization in poor urban infants. JAMA. 1994; 272 1105–10.
| Risk factors for underimmunization in poor urban infants.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2M%2FhvVyqtA%3D%3D&md5=5b30677b33d18d26056fbb32c31b49c4CAS |
[4] Petousis-Harris H, Goodyear-Smith F, Godinet S, et al. Barriers to childhood immunisation among New Zealand mothers. N Z Fam Physician. 2002; 29 396–401.
[5] Grant CC, Turner N, Jones R. Eliminating ethnic disparities in health through immunisation: New Zealand’s chance to earn global respect. N Z Med J. 2009; 122 6–9.
[6] Drezner K, Newbern EC, Ossa A, et al. Evaluation of a community immunization outreach program–Philadelphia, Pennsylvania. J Public Health Manag Pract. 2015; 21 263–8.
| Evaluation of a community immunization outreach program–Philadelphia, Pennsylvania.Crossref | GoogleScholarGoogle Scholar |
[7] Ministry of Health. National and DHB immunisation data 2015 [updated 2016 Aug 1; accessed 2015 Sept 21]. Available from: www.health.govt.nz/our-work/preventative-health-wellness/immunisation/immunisation-coverage/national-and-dhb-immunisation-data
[8] Ministry of Health. Immunisation coverage 2015 [updated 08 Jul 2013; accessed 2015 Dec 1]. Available from: www.health.govt.nz/our-work/preventative-health-wellness/immunisation/immunisation-coverage
[9] Bosch-Capblanch X, Banerjee K, Burton A. Unvaccinated children in years of increasing coverage: how many and who are they? Evidence from 96 low-and middle-income countries. Trop Med Int Health. 2012; 17 697–710.
| Unvaccinated children in years of increasing coverage: how many and who are they? Evidence from 96 low-and middle-income countries.Crossref | GoogleScholarGoogle Scholar |
[10] Williams IT, Milton JD, Farrell JB, et al. Interaction of socioeconomic-status and provider practices as predictors of immunization coverage in Virginia children. Pediatrics. 1995; 96 439–46.
| 1:STN:280:DyaK2MzotVahsQ%3D%3D&md5=66cb6ff159aeca6426511d9f06a25980CAS |
[11] Briss PA, Rodewald LE, Hinman AR, et al. Reviews of evidence regarding interventions to improve vaccination coverage in children, adolescents, and adults. Am J Prev Med. 2000; 18 97–140.
| Reviews of evidence regarding interventions to improve vaccination coverage in children, adolescents, and adults.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c3msFalsA%3D%3D&md5=3b2a88061d9f819bede6bfa5fb26b80bCAS |
[12] Hambidge SJ, Phibbs SL, Chandramouli V, et al. A stepped intervention increases well-child care and immunization rates in a disadvantaged population. Pediatrics. 2009; 124 455–64.
| A stepped intervention increases well-child care and immunization rates in a disadvantaged population.Crossref | GoogleScholarGoogle Scholar |
[13] Ivers N, Jamtvedt G, Flottorp S, et al. Audit and feedback: effects on professional practice and healthcare outcomes. Cochrane Database Syst Rev. 2012; 6 1–227.
[14] Lewin S, Lavis JN, Oxman AD, et al. Supporting the delivery of cost-effective interventions in primary health-care systems in low-income and middle-income countries: an overview of systematic reviews. Lancet. 2008; 372 928–39.
| Supporting the delivery of cost-effective interventions in primary health-care systems in low-income and middle-income countries: an overview of systematic reviews.Crossref | GoogleScholarGoogle Scholar |
[15] Roberts JR, Freeland KD, Kolasa MS, et al. Do immunisation procedures match provider perception? A study from the South Carolina Pediatric Practice Research Network (SCPPRN). Qual Prim Care. 2011; 19 147–54.
[16] Fu LY, Zook K, Gingold J, et al. Frequent vaccination missed opportunities at primary care encounters contribute to underimmunization. J Pediatr. 2015; 166 412–7.
| Frequent vaccination missed opportunities at primary care encounters contribute to underimmunization.Crossref | GoogleScholarGoogle Scholar |
[17] Turner N, Grant C, Goodyear-Smith F, et al. Seize the moments: missed opportunities to immunize at the family practice level. Fam Pract. 2009; 26 275–8.
| Seize the moments: missed opportunities to immunize at the family practice level.Crossref | GoogleScholarGoogle Scholar |


