Standing order use in general practice: the views of medicine, nursing and pharmacy stakeholder organisations
Robyn Taylor 1 , Eileen McKinlay 2 , Caroline Morris 21 Karori Medical Centre, Karori, Wellington, New Zealand
2 Department of Primary Health Care & General Practice, University of Otago, Wellington, New Zealand
Correspondence to: Robyn Taylor, PO Box 17-264, Karori Wellington, New Zealand. Email: robyn.taylor@kmc.co.nz
Journal of Primary Health Care 9(1) 47-55 https://doi.org/10.1071/HC16023
Published: 10 February 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Standing orders are used by many general practices in New Zealand. They allow a practice nurse to assess patients and administer and/or supply medicines without needing intervention from a general practitioner.
AIM: To explore organisational strategic stakeholders’ views of standing order use in general practice nationally.
METHODS: Eight semi-structured, qualitative, face-to-face interviews were conducted with participants representing key primary care stakeholder organisations from nursing, medicine and pharmacy. Data were analysed using a qualitative inductive thematic approach.
RESULTS: Three key themes emerged: a lack of understanding around standing order use in general practice, legal and professional concerns, and the impact on workforce and clinical practice. Standing orders were perceived to extend nursing practice and seen as a useful tool in enabling patients to access medicines in a safe and timely manner.
DISCUSSION: The variability in understanding of the definition and use of standing orders appears to relate to a lack of leadership in this area. Leadership should facilitate the required development of standardised resources and quality assurance measures to aid implementation. If these aspects are addressed, then standing orders will continue to be a useful tool in general practice and enable patients to have access to health care and, if necessary, to medicines without seeing a general practitioner.
KEYWORDS: General practice; general practitioner, nurse, pharmacist, primary health care, standing orders
| WHAT GAP THIS FILLS |
| What is already known: There is little research within New Zealand or internationally on the use of standing orders in general practice. To date, it would appear that this is the first study to look at standing orders in general practice from an organisational strategic stakeholder perspective. |
| What this study adds: The use of standing orders in general practice is widespread, but stakeholder organisations believe there is little understanding by many general practitioners and practice nurses as to the legal and professional requirements around their use. This study draws attention to these discrepancies and suggests solutions to enable standing orders to be used in compliance with the legislation to protect those working with standing orders and to ensure patient safety. |
Introduction
Standing orders (SOs) for the administration of medicines are used in New Zealand (NZ) as a means of addressing general practice workforce shortages, which have an effect on patients’ abilities to access health care and medicines.1–3 This process is different to prescribing (Box 1). The former enables administration and/or supply of a medicine, while the latter results in a prescription.
| Box 1. Definition of a standing order1 |
| ‘a written instruction issued: by a medical practitioner… it authorises a specified person or class of people (eg registered nurses) who do not have prescribing rights to administer and/or supply specified medicines and some controlled drugs. The intention is for standing orders to be used to improve patients’ timely access to medicines.’ |
The original 2002 legislation4 was developed to facilitate access to medicines during an emergency in the hospital environment when a prescriber was not immediately available.5 Over time, SOs became regularly used in primary health-care settings and the legislation was amended accordingly.6
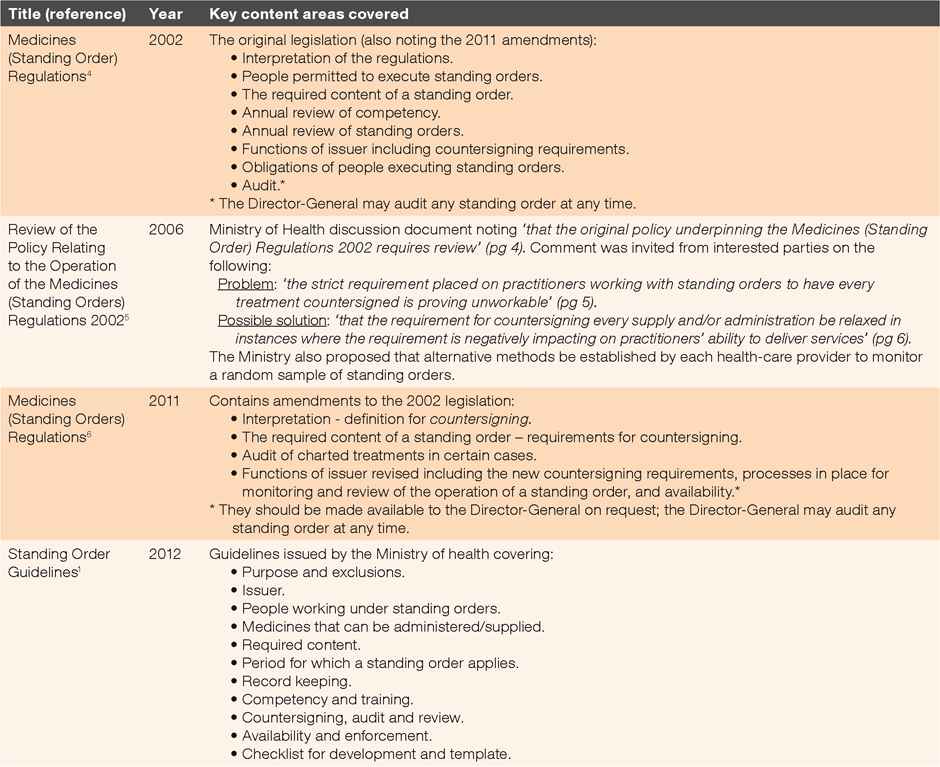
In the United Kingdom (UK), a similar function is fulfilled by patient group directions (PGDs).7 Although there are small differences between SOs and PGDs, they are generally agreed to be very similar,8 with PGDs defined as ‘written instructions for the supply and administration of named medicines in an identified clinical situation … [and] within the strict terms of a predetermined protocol’.9 In some countries, the legislation refers solely to medicines, while in others, it refers to ordering tests.10–12 National legislation covers the functions of the issuer, review of competency, mechanisms to review and audit, and obligations of the person supplying/administering the SO. The key legislation and documents are shown in Table 1.
|
Standing orders enable practice nurses (PNs) and other disciplines to make an assessment that the SO applies to a patient and to administer medicines; if necessary, without general practitioner (GP) involvement.1 Some query whether nurses are assessing or diagnosing when using SOs.13 Wilkinson’s survey reported that primary health care nurses were ‘making diagnostic decisions on a regular, if not daily basis in relation to implementing SOs. Even so, some expressed uncertainty about whether diagnosis was within the RN (registered nurse) scope of practice.’14
While used to administer and supply a range of medicines for common conditions (Table 2), the development process, by necessity, is complex and time-consuming to ensure patients are treated optimally and safely (Fig. 1).

|
Limited research has investigated SOs or PGDs in general practice settings. Interprofessional collaboration between GPs and PNs has been identified as an important factor in the successful use of SOs,2,3,14–19 with patients benefiting from the sharing of ideas and knowledge between health-care professionals.2 Although SOs are generally perceived as safe and effective, and enable nurses to develop clinical knowledge and skills in assessment,2,3,14–17 nurses sometimes misunderstand the term.14,15,19 Studies have found that nurses14,15 as well as nurses and GPs2 have identified a need for greater education and/or training around their use. Although it is a legal requirement that the SO issuer (usually a GP) annually checks the competence of the person carrying out the process,1 this does not always appear to happen.14
Historically and nationally, SOs have largely been developed in general practice settings for use by PNs. However, more recently, pharmacists have been responsible for monitoring and adjusting doses of warfarin in specific patients operating under SOs as part of the Community Pharmacy Anti-coagulation Management Service.20
Worldwide, research has focused solely on the views of individual practitioners, with no studies identified from the perspective of the key organisational stakeholders (eg professional organisations, colleges or regulators).
Over the last decade, there have been legislative changes nationally that have resulted in prescribing rights for several groups of nurses and allied health professionals.21–23 Some registered nurses practising in diabetes health,21 pharmacists22 and dietitians23 now hold designated prescriber status and are therefore legally allowed to prescribe within their area of practice from a specified list of medicines. In 2013, the designated prescriber status of nurse practitioners and optometrists was changed to put them on an equal footing with other authorised prescribers (doctors, dentists and midwives), allowing them to independently prescribe within their scope of practice.24 In 2013, the Nursing Council of New Zealand (NCNZ) also undertook a public consultation to gauge response to a proposal for two further levels of prescriber within the designated nurse prescriber class (‘specialist’ and ‘community’);25 regulatory changes are underway.
In addition to these changes,21–23 Health Workforce NZ has been involved in initiatives to increase the groups of those who prescribe; for example, diabetes nurse prescribers.26 Given that such changes and initiatives potentially have an impact on the use of SOs, it was timely to gain an understanding of the place of SOs from strategic stakeholder perspectives. This study aims to explore NZ organisational stakeholders’ views of SO use in general practice.
Methods
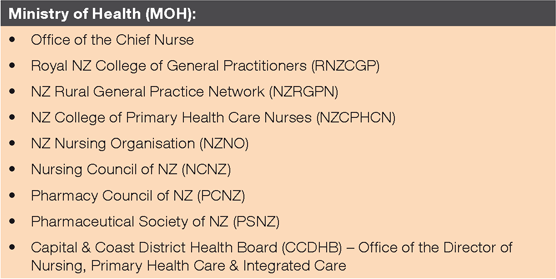
Face-to-face, semi-structured interviews were undertaken with representatives from relevant professional stakeholder organisations who have a national regulatory and/or advocacy role for their profession. As doctors are the issuer of SOs, nurses and pharmacists the most frequent users, and medicines an important feature, key strategic organisations representing medicine, nursing and pharmacy were purposively sampled. Nine stakeholder organisations were identified as potential participants (Table 3).
|
An invitation to participate, with a copy of the study information sheet, was sent by email to each organisation’s Chief Executive Officer. Those willing to participate were asked to nominate the most appropriate staff member for interview. Eight of the nine organisations approached agreed to participate. All interviews were undertaken by RT using a semi-structured interview schedule covering seven broad topic areas (Table 4).

|
Interviews of between 20 and 40 min were conducted between December 2013 and December 2014, audio-recorded and transcribed verbatim. All interviewees were provided with an opportunity to review the content of their transcribed interview.
Qualitative analysis was undertaken using an inductive thematic approach. This initially involved RT reading and re-reading the transcripts, coding categories and identifying emerging themes,27,28 followed by EM and CM independently doing the same. Transcripts were coded according to professional discipline (nursing, medical, pharmacy) rather than individual organisation to provide discipline-specific insights in relation to SOs. All three authors met to discuss and compare findings and agree on the final themes, with differences resolved by consensus. Some individuals representing an organisation were either former or current clinicians and we noted that they answered questions from a personal perspective rather than an organisational viewpoint. Furthermore, we accounted for the fact that participants’ views could not be assumed to reflect that of the organisation’s individual member practitioners during analysis.
Ethical approval was obtained from the University of Otago’s Human Ethics Committee (Reference: D13/357).
Results
Three key themes emerged from the data:
- •
-
A lack of understanding around SO use in general practice.
- •
-
Legal and professional concerns.
- •
-
The impact of SOs on workforce and clinical practice.
Each of these themes (with sub-themes where applicable) is described below with illustrative quotes.
Overall, there was general agreement from all participants that SOs are a useful and successful way of improving patient access to health care and to medicines if needed.
Lack of understanding around standing order use in general practice
Definition of standing orders: Despite being deemed the most appropriate person to speak on this subject, the majority of participants gave incorrect or confused versions of the official definition of SOs.
‘… it’s like an algorithm of medications, you can use for certain conditions that are defined…’ (Nursing Organisation 2)
Lack of resources or information: All organisations were supportive of the use of SOs; however, they believed SOs are not a priority in strategic planning or development. A lack of ownership by any one organisation resulted in a lack of strategies for developing, implementing, auditing and reviewing SOs in general practice. Similarly, there is no single place for GPs or PNs to obtain relevant information or education on how to implement SOs.
‘There is a lack of organisations to provide advice to people who are setting standing orders up about the clinical guidelines …’. (Nursing Organisation 4)
Variability of use: All participants believed there is significant variability in how SOs are used.
‘Sometimes [SOs] are used in compliance with the legislation and sometimes they’re not, so there’s variability ’. (General Practice Organisation 2)
Stakeholders described examples of both correct and incorrect use of SOs. Notably, some incorrectly described instances of nurses generating a prescription as a SO.
Legal and professional concerns
Most identified legal and professional risks as a major concern. Participants noted general risks as well as risks related to nurses’ competence to assess and diagnose, and also made a distinction between these and formal quality assurance measures.
General risk: Most participants acknowledged the variability as a risk. They felt this has the potential to put both health professionals and patients at risk.
‘I have questions around safety for the nurse, safety for the patient and safety for the issuer’. (Nursing Organisation 1)
Practice nurses’ lack of assessment and diagnosis skills: Concern was expressed about the level of PNs’ assessment and diagnosis skills. Some participants felt many PNs have not undertaken appropriate training, nor had the relevant experience to be able to diagnose and appropriately use a SO.
‘If you can’t make a diagnosis, you can’t use a standing order’. (General Practice Organisation 1)
However, one participant believed that PNs were competent to carry out SOs by virtue of their practice experience.
The perception existed that GPs in practice were unaware they are required to assess or be knowledgeable about nurses’ competence to carry out SOs. Furthermore, GPs may not know how to assess a nurse’s competence.
‘… even in some forward thinking practices …. a GP’s trust in a nurse’s competence is not founded on very scientific means’. (Nursing Organisation 1)
Lack of quality assurance measures: Although there is a high level of endorsement of SO use, some participants felt that few quality assurance measures are in place and that there is a lack of national standardisation for use:
‘I’ve done a little bit of work [to] actually develop a set of national standing orders … they are very supportive of the idea and keen to explore it … and would like to see the development of a national set’. (General Practice Organisation 3)
‘…some better information from the Ministry around examples …. or an audit template and where do they keep and store that information, and sign off the audit is done. Because if someone wants to audit where do they go. Most general practices don’t have a quality safety person’. (Nursing Organisation 4)
Despite high-level SO guidelines being available, these do not clearly set out the requirements for practical development and implementation.
Some participants considered insufficient funding and lack of ownership at an organisational level as reasons for this lack of quality assurance measures:
‘It’s not happening because no-one’s got the funds to do it, no-one’s got the ownership to do it…’. (Nursing Organisation 4)
Impact on workforce and clinical practice
The use of SOs was believed to have considerable impact on workforce capacity and utilisation. They were considered to support role extension, enhance interdisciplinary collaboration and lead to better use of health professional skill sets.
Workforce issues: Many participants noted the impact of an ageing professional population, a lack of younger replacement GPs and PNs, increasing patient co-morbidities and the relocation of some secondary care medical services into primary care as a driver for the use of SOs.
‘It [SO use] has potential workforce benefits … because it allows a practice to organise its workforce differently and nurses to work more independently’. (General Practice Organisation 1)
All participants recognised that SOs have extended PNs’ roles. They described PNs being able to work at a more advanced level of practice and offer a wider range of patient services.
‘It’s [use of SOs] a better utilisation of their [PNs] … skills … (and) it has improved nurses’ autonomy’. (Nursing Organisation 4)
Pharmacy participants could also see an increased role for pharmacists and allied health professionals in the future use of SOs.
‘… we know New Zealand is going to suffer an acute shortage of GPs and who better to step into those gaps than nurses and pharmacists, and be complementary to the GP’. (Pharmacy Organisation 1)
Enhanced relationships: Most stakeholder organisations felt SOs have encouraged more collegial working relationships between GPs and PNs.
‘[SOs] improve teamwork and improve access for patients to care … they do free up time within the team …’. (General Practice Organisation 3)
Discussion
This study explored organisational stakeholders’ views of SO use in general practice in NZ. Both benefits and challenges to the use of SOs were identified. While they were perceived to have a valuable role to play in the safe and timely access to medicines for patients, two key challenges emerged. First, stakeholders frequently misunderstand the use of SOs; second, no single organisation is taking responsibility for overseeing their use in this setting.
There is a general misunderstanding at a strategic organisational level about the definition and implementation of SOs. Although it is unclear why this confusion has occurred, there is a need for one organisation to promote and disseminate the correct definition.
Lack of clear understanding at an organisational level may have led to the variability of SO use in general practice and lack of understanding by both GPs and PNs of their legal responsibilities and professional accountabilities. This variability and lack of understanding was noted in 2013 by Scott-Jones, the then Chairman of the NZ Rural General Practice Network, stating that several general practices had stretched the bounds of SO legislation by developing ‘local solutions’ for use. He further stated ‘How they [SOs] are supposed to be used does not quite fit with how they are used in practice’.29
Both Jones15 in the UK and Wilkinson14 in NZ gave examples of nurses generating prescriptions for doctors to sign, mistakenly thinking these are SOs. Scott-Jones also acknowledged that PNs generating prescriptions for GPs to sign is common practice, with GPs and PNs both believing they are working under SOs.29
With a range of disciplines including pharmacists and podiatrists beginning to work with SOs, and proposed changes in who can issue SOs (nurse practitioners and optometrists),30 measures are needed to improve understanding of their use.31,32
Misunderstanding and misinterpretation of SO use may partially occur because no single organisation is taking the lead to support implementation and monitor use. Measures to improve the quality of usage would be worthwhile implementing, given their use is currently commonplace in general practice and likely to continue.
In line with recommendations made internationally,9,33 it makes sense these measures be coordinated and implemented by key stakeholder organisations. We suggest the Ministry of Health alongside the Royal New Zealand College of General Practitioners (RNZCGP) as organisations to potentially take a lead in developing standardised SOs, and for a nursing professional organisation to develop a standardised education framework.
Despite changes to health professional prescribing, stakeholders still endorsed the current use of SOs. They did, however, raise concerns about the lack of national quality assurance measures to ensure SOs are uniformly developed, implemented and quality assured. This aligns with previously published international findings.34,35
Despite a nationally available template for development and use of SOs,1 participants noted the practise of individual general practices developing, implementing and auditing their own versions, with a lack of strategic organisations able to provide the appropriate information or advice. This does not ensure that GPs and PNs are meeting the legal and professional standards for use. Similarly, participants perceived that some GPs did not understand their responsibilities regarding the issuing of SOs, or ensure regular quality checks in terms of use.
This study suggests that standardisation of education is important35 and the current practice of in-house training given by GPs to PNs regarding assessment and diagnosis3 is insufficient to ensure PNs have the necessary skills. While nurses are expected to be competent in terms of the NCNZ36 standards to administer medicines within the constraints of legislation (competency 2.1 and 2.9), previous studies have found2,14,15 a need for greater education and/or training around the development, implementation, use and audit of SOs.
Some ad hoc mechanisms were suggested by participants to address these issues; however, we propose a broad systems approach to change. This includes the promotion of the correct definition of SOs; formalisation of a standardised, clear set of up-to-date SO guidelines including detailed legal, professional and competence requirements for GPs and PNs; and establishment of a national standardised template of SOs for common conditions with agreed medicines and doses. As is common in the UK, a pharmacy professional body should be included in setting-up guidelines to ensure additional safety aspects are in place.7
As the RNZCGP already undertakes interdisciplinary quality assurance checks on general practices through the ‘Aiming for Excellence’ Cornerstone accreditation programme,37 they could take on a major role. They could advise on the training required to implement SOs in general practice, and Cornerstone accreditation could include measures to monitor that SOs are instigated, maintained and reviewed on a regular basis. Currently, only doctors issue SOs and it seems reasonable that a medical organisation provide information and advice on how to develop and implement legally and professionally sound SOs. It is unlikely that SO use will decline in the future; the importance of a national approach that ensures the safety of both patients and health-care practitioners should not be underestimated.
Strengths and limitations of the study
Although participants were nominated by their organisation’s Chief Executive Officer, not all appeared to have a clear perspective of the organisation’s view. It is therefore possible that some participants did not provide an accurate account of their parent organisations’ views. A second interview could have been sought with another person in their organisation to address this issue.
If time and resources had allowed, other potential stakeholder organisations could have been approached to ascertain their views on this issue; for example, the Medical Council or the College of Nurses Aotearoa. Similarly, views of other organisations could have been sought, such as Regional Public Health or Family Planning Association, both of which employ nurses using SOs.
Conclusion
This study has found a suboptimal understanding about SO use in general practice by some of the key strategic professional stakeholder organisations. It also identified a lack of standardised training or education on SO development, implementation or use, and no single organisation providing advice on these issues. It is therefore unsurprising that some GPs and PNs are less than clear about the legal requirements for development and implementation of SOs in general practice.
CONFLICTS OF INTEREST
The authors have no conflicts of interest to disclose.
COMPETING INTERESTS
Neither of Robyn Taylor’s funding sources (Wellington General Practice Research Trust and Karori Medical Centre) played any part in the design of the study, the interpretation of findings, the writing of this article or the decision to submit it for publication.
ACKNOWLEDGEMENTS
The authors gratefully acknowledge the stakeholder participants who willingly gave their time to participate in this research. This study formed the basis for Robyn Taylor’s Master Primary Health Care portfolio, undertaken through the University of Otago, Wellington. We also acknowledge the Wellington General Practice Research Trust and Karori Medical Centre who each part-funded her University tuition fees. We are also very grateful to Jill Wilkinson who reviewed a version of this paper.
References
[1] Ministry of Health. Standing Orders Guidelines. Wellington: Ministry of Health; 2012.[2] Scott-Jones J. Standing orders in New Zealand primary care. Master’s Research Portfolio, 2010. Auckland: University of Auckland; 2010. Portfolio link.
[3] Scott-Jones J, Young K, Keir D, Lawrenson R. Standing orders extend rural nursing practice and patient access. Nurs N Z. 2009; 15 14–15.
[4] New Zealand Parliamentary Counsel Office. Medicines (Standing Order). Wellington: New Zealand Government; 2002.
[5] Ministry of Health. Review of the Policy relating to the Operation of the Medicines (Standing Orders) Regulations 2002. Wellington: Ministry of Health; 2006.
[6] New Zealand Parliamentary Counsel Office. Medicines (Standing Orders) Amendment Regulations. Wellington: New Zealand Government; 2011.
[7] Medicines & Healthcare products Regulatory Agency. Patient group directions: who can use them. London: Medicines & Healthcare products Regulatory Agency; 2014.
[8] Wilkinson J. Extending the prescribing framework to nurses: lessons from the past. Collegian. 2011; 18 157–63.
| Extending the prescribing framework to nurses: lessons from the past.Crossref | GoogleScholarGoogle Scholar |
[9] Gielen SC, Dekker J, Francke AL, Mistiaen P, Kroezen M. The effects of nurse prescribing: a systematic review. Int J Nurs Stud. 2014; 51 1048–61.
| The effects of nurse prescribing: a systematic review.Crossref | GoogleScholarGoogle Scholar |
[10] Ornstein SM, Nemeth LS, Nietert PJ, Jenkins RG, Wessell AM, Litvin CB. Learning from primary care meaningful use exemplars. J Am Board Fam Med. 2015; 28 360–70.
| Learning from primary care meaningful use exemplars.Crossref | GoogleScholarGoogle Scholar |
[11] Nemeth LS, Ornstein SM, Jenkins RG, Wessell AM, Nietert PJ. Implementing and evaluating electronic standing orders in primary care practice: a PPRNet study. J Am Board Fam Med. 2012; 25 594–604.
| Implementing and evaluating electronic standing orders in primary care practice: a PPRNet study.Crossref | GoogleScholarGoogle Scholar |
[12] Ghorob A, Bodenheimer T. Building teams in primary care: a practical guide. Fam Syst Health. 2015; 33 182–92.
| Building teams in primary care: a practical guide.Crossref | GoogleScholarGoogle Scholar |
[13] Godlee F.. What skills do doctors and nurses need? BMJ. 2008; a1722
| What skills do doctors and nurses need?Crossref | GoogleScholarGoogle Scholar |
[14] Wilkinson J. Nurses’ reported use of standing orders in primary health care settings. J Prim Health Care. 2015; 7 34–41.
[15] Jones P. Patient group directions - the Salford primary care experience. J Clin Gov. 2002; 10 3–6.
[16] Scott-Jones J, Lawrenson R. Doctors and nurses: standing orders in primary care N Z Fam Physician. 2008; 35 107–11.
[17] Sinsky CA, Willard-Grace R, Schutzbank AM, Sinsky TA, Margolius D, Bodenheimer T. In search of joy in practice: a report of 23 high-functioning primary care practices. Ann Fam Med. 2013; 11 272–8.
| In search of joy in practice: a report of 23 high-functioning primary care practices.Crossref | GoogleScholarGoogle Scholar |
[18] Bodenheimer T, Ghorob A, Willard-Grace R, Grumbach K. The 10 building blocks of high-performing primary care. Ann Fam Med. 2014; 12 166–71.
| The 10 building blocks of high-performing primary care.Crossref | GoogleScholarGoogle Scholar |
[19] Lim A. Nurses as emergent prescribers in New Zealand: a descriptive comparative study using a multiple case approach. Auckland: University of Auckland; 2012.
[20] Pharmaceutical Society of New Zealand Incorporated. New Zealand National Pharmacist Services Framework. Wellington: Pharmaceutical Society of New Zealand Incorporated; 2014.
[21] New Zealand Parliamentary Counsel Office. Medicines (Designated Prescriber-Registered Nurses Practising in Diabetes Health) Regulations. Wellington: New Zealand Government; 2011.
[22] New Zealand Parliamentary Counsel Office. Medicines (Designated Pharmacist Prescribers) Regulations. Wellington: New Zealand Government; 2013.
[23] New Zealand Parliamentary Counsel Office. Medicines (Designated Prescriber-Dietitians) Regulations. Wellington: New Zealand Government; 2015.
[24] New Zealand Parliamentary Counsel Office. Medicines Amendment Act. Wellington: New Zealand Government; 2013.
[25] Nursing Council of New Zealand. Application for prescribing rights for registered nurses practising in primary care and speciality teams. Wellington: Nursing Council of New Zealand; 2014.
[26] Ministry of Health. Diabetes nurse prescriber. Wellington: Ministry of Health; 2016 [updated 24 February 2016].
[27] Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006; 3 77–101.
| Using thematic analysis in psychology.Crossref | GoogleScholarGoogle Scholar |
[28] Fereday J, Muir-Cochrane E. Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development. Int J Qual Methods. 2008; 5 80–92.
| Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development.Crossref | GoogleScholarGoogle Scholar |
[29] Scott-Jones J. Making standing orders work in practice and legislation. NZ Doctor. 2013; 2013 46
[30] Office of the Chief Nursing Officer. Sector Update. Wellington: Ministry of Health; 2016.
[31] Borthwick AM, Short AJ, Nancarrow SA, Boyce R. Non-medical prescribing in Australasia and the UK: the case of podiatry. J Foot Ankle Res. 2010; 3 1–10.
| Non-medical prescribing in Australasia and the UK: the case of podiatry.Crossref | GoogleScholarGoogle Scholar |
[32] Shaw J, Harrison J, Harrison J. A community pharmacist-led anticoagulation management service: attitudes towards a new collaborative model of care in New Zealand. Int J Pharm Pract. 2014; 22 397–406.
| A community pharmacist-led anticoagulation management service: attitudes towards a new collaborative model of care in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[33] Darvishpour A, Joolaee S, Cheraghi MA. A meta-synthesis study of literature review and systematic review published in nurse prescribing. Med J Islam Repub Iran. 2014; 28 77
[34] Price O, Baker J, Paton C, Barnes T. Patient group directives: a safe and effective practice Br J Nurs. 2012; 21 26–31.
| Patient group directives: a safe and effective practiceCrossref | GoogleScholarGoogle Scholar |
[35] Courtenay M, Carey N, Stenner K. Non medical prescribing leads views on their role and the implementation of non medical prescribing from a multi-organisational perspective. BMC Health Serv Res. 2011; 11 142
| Non medical prescribing leads views on their role and the implementation of non medical prescribing from a multi-organisational perspective.Crossref | GoogleScholarGoogle Scholar |
[36] Nursing Council of New Zealand. Competences for Registered Nurses. Wellington: Nursing Council of New Zealand; 2016 [updated March 2016; cited 27 May 2016].
[37] Royal New Zealand College of General Practitioners. Aiming for Excellence. Wellington: Royal New Zealand College of General Practitioners; 2002.



