New screen on the block: non-invasive prenatal testing for fetal chromosomal abnormalities
Sara Filoche 1 , Beverley Lawton 1 , Angela Beard 2 , Anthony Dowell 3 , Peter Stone 41 Women’s Health Research Centre, Department of Obstetrics and Gynaecology, University of Otago Wellington, Wellington, New Zealand
2 Christchurch Obstetric Associates, Christchurch, New Zealand
3 Department of Obstetrics and Gynaecology, University of Otago Wellington, Wellington, New Zealand
4 School of Medicine, The University of Auckland, Auckland, New Zealand
Correspondence to: Sara Filoche, Women’s Health Research Centre, Department of Obstetrics and Gynaecology, University of Otago Wellington, Wellington 6023, New Zealand. Email: Sara.Filoche@otago.ac.nz
Journal of Primary Health Care 9(4) 248-253 https://doi.org/10.1071/HC16055
Published: 13 October 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
Non-invasive prenatal testing (NIPT) is a new screen for fetal chromosomal abnormalities. It is a screening test based on technology that involves the analysis of feto-placental DNA that is present in maternal blood. This DNA is then analysed for abnormalities of specific chromosomes (eg 13, 18, 21, X, Y). NIPT has a much higher screening capability for chromosomal abnormalities than current combined first trimester screening, with ~99% sensitivity for trisomy 21 (Down syndrome) and at least a 10-fold higher positive predictive value. The low false-positive rate (1–3%) is one of the most advertised advantages of NIPT. In practice, this could lead to a significant reduction in the number of false-positive tests and the need for invasive diagnostic procedures. NIPT is now suitable for singleton and twin pregnancies and can be performed from ~10 weeks in a pregnancy. NIPT is not currently publicly funded in most countries. However, the increasing availability of NIPT commercially will likely lead to an increase in demand for this as a screening option. Given the high numbers of women who visit a general practitioner (GP) in their first trimester, GPs are well-placed to also offer NIPT as a screening option. A GP’s role in facilitating access to this service will likely be crucial in ensuring equity in access to this technology, and it is important to ensure that they are well supported to do so.
Introduction
Prenatal testing for chromosomal abnormalities has been part of antenatal care in New Zealand for the last 40 years. Screening initially used maternal age as an indication for invasive procedures such as amniocentesis and, more recently, it combines the results from blood tests (B-HCG and Pregnancy Associated Plasma Protein A) and a Nuchal translucency ultrasound in the first trimester or maternal serum screening in the second trimester. In the last 4–5 years, a new technology has emerged for the screening of fetal chromosomal abnormalities – non-invasive prenatal testing (NIPT). The aim of this viewpoint article is to provide a summary of current understanding of NIPT, to discuss how NIPT may fit within general practice, and the role of general practitioners (GPs) in providing this new technology.
What is non-invasive prenatal testing (NIPT)?
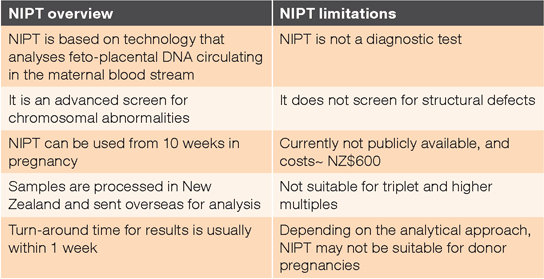
Non-invasive prenatal testing (NIPT) is a screening test based on technology that analyses the feto-placental DNA present in maternal blood (Table 1).1–3 This technology is based on the discovery in 1997 that cell-free DNA, including that from the fetus and placenta, can be isolated and analysed from the blood of pregnant women.1,2,4 NIPT was first released in Hong Kong in August 2011 and soon after was introduced commercially in the US in October 2011. Clinical translation of NIPT technologies has advanced rapidly. Commercially available NIPT identifies the most frequently observed chromosome aneuploidies, including Down syndrome (trisomy 21), Edward syndrome (trisomy 18), Patau syndrome (trisomy 13), and common sex chromosome aneuploidies such as Turner syndrome (X) and Klinefelter syndrome (XXY).1–3 NIPT is not a diagnostic test, but its high sensitivity (true positive rate) and specificity (true negative rate) make it an attractive alternative to the serum screens and ultrasound currently in use.
|
For determining both fetal sex and rhesus D status, NIPT is considered diagnostic.5 The National Institute for Clinical Excellence (NICE) has recommended it as a ‘cost-effective option to guide antenatal prophylaxis with anti-D immunoglobulin, provided that the overall cost of testing is £24 (approx. NZ$40) or less.’6 NIPT may prove beneficial in New Zealand, especially in light of the National Maternity Monitoring Group’s work around improving the management of rhesus disease.7 NIPT can also be used (where familial incidence indicates) to screen for single-gene disorders such as cystic fibrosis, Huntington’s disease and thanatophoric dysplasia.5 Furthermore, proof of concept has been demonstrated for sub-chromosomal abnormalities such as copy number variants or microdeletions, which may lead to a variety of conditions involving physical abnormality and cognitive delay.1 As of 2014, tests are commercially available for abnormalities on chromosomes 1p, 5p, 15q, 22q, 11q, 8q and 4p.40,41. The specificity and sensitivity of these tests, however, has not yet been validated. Proof of concept genome-wide screening has also been demonstrated, but again, not clinically validated.1,8
Clinical performance of NIPT
The clinical performance of NIPT is reported as 99% sensitive for trisomy 21, with positive predictive values ranging from 45% to 99%,4,9–12 which even at the lower range is 10-fold better than current antenatal screening.13 The low false-positive rate (1–3%) is one of the most advertised advantages of NIPT. In practice, this could potentially lead to a significant reduction in false-positive tests, and the need for invasive diagnostic procedures. In terms of other trisomic conditions, sensitivities (based on meta-analyses) for NIPT are reported to be between 91%10 to 93%12 for trisomy 18 and 90%10 to 95%12 for trisomy 13 (with positive predictive values at 84% and 87% respectively).9
Clinical and technical considerations
Non-invasive prenatal testing (NIPT) is not a diagnostic test, with confirmation required by invasive diagnostic procedures such as amniocentesis.2,4 NIPT cannot detect neural tube defects, but combining NIPT with a first trimester scan may overcome this potential disadvantage.14 False-positive results have been reported, although at much lower rates than current screening, and are thought to occur due to discrepancy between the chromosomal make-up of the cells in the placenta and the cells in the baby, the fetal death of a co-twin or maternal malignancy.2,4 Because feto-placental DNA is present early in pregnancy, NIPT can be performed from as early as 10 weeks in pregnancy or even earlier. The freely circulating fragments of DNA remain in the maternal circulation for only hours or, at most, a day or two after each pregnancy, making it suitable for pregnancy-specific testing.2,4
In terms of technical considerations, all tests have a limit of detection. For NIPT, this is linked directly to the amount of feto-placental DNA compared to all DNA, which includes maternal DNA.2,4 In turn, the amount of feto-placental DNA, the ‘fetal fraction’, is linked to gestational age (which increases over time) and influenced by maternal BMI (where feto-placental DNA is ‘diluted’ due to larger circulatory volume).2,4 The technical aspect of NIPT platforms and the way the risk result is generated (either comparing to a hypothetical or maternal genotype) also influences what type of pregnancy is amenable to NIPT screening.4 For example, NIPT screens based on SNP (single nucleotide polymorphism) technology, such as Panorama® (Natera Inc., USA) are not suitable for donor pregnancies. The issue of reporting fetal fraction is considered to be an important aspect of quality assurance to providers,15 and in counselling and reporting the results back to pregnant women.
As with all tests, NIPT does fail to produce a result, reportedly ~5% of the time.4 This is thought to be due to inadequate blood volume being drawn and hemolysis during transportation or storage.16 A failed result may be due to a failure in extracting DNA, amplification or sequencing, and may require another blood sample being taken, which could contribute to a negative experience for the expectant mother and delay in obtaining the result.16
Access to NIPT in New Zealand
Currently, NIPT is available to all women in New Zealand on a user-pays service (a for-profit-model) and it is not regulated. Anecdotal evidence suggests that NIPT is being accessed on an ad-hoc basis, with some District Health Boards (DHBs) offering an appointment at obstetric clinics for the blood draw, and others not. Women must also pay for a private obstetric consultation in addition to the NIPT screen. The cost of an NIPT screen is ~ $500–$600, rising to over $2000 with expanded screens, which for a large number of New Zealand women and whanau, would be prohibitive.
The National Screening Unit (NSU) and Ministry of Health are currently exploring the implementation of NIPT in New Zealand, and it is likely to be funded in some form. It may, for example, be offered only to women who have a risk result from serum and ultrasound screening, which is similar to the UK17 and Canada, but emerging evidence indicates that women want NIPT as a first-line option,18,19 as do maternity care providers.20
The American College of Medical Genetics and Genomics 2016 statement describes ‘New evidence strongly suggests that NIPS can replace conventional screening for Patau, Edwards, and Down syndromes across the maternal age spectrum, for a continuum of gestational age beginning at 9–10 weeks, and for patients who are not significantly obese.’21 In the Netherlands, NIPT has been offered since 2014 as an alternative option to invasive testing for pregnant women at increased risk of having a child with trisomy 21, 18 or 13 based on the first trimester combined test (cut-off 1:200) or because of a previous child with these trisomies.22 In 2016, the National Screening Committee in the UK announced that starting in 2018 (to allow time for training), NIPT will be publicly funded initially as a contingent screen dependent on selected risk cut-off scores. The introduction of NIPT in the UK has come about from a concerted and considerable amount of work and research over 10 years, covering areas such as detailed health economic evaluation, optimal ways to deliver education to women and healthcare professionals, and evaluation of sensitivity and specificity of NIPT for aneuploidy when performed in a NHS regional genetics laboratory.23 Although the UK could well-serve as a model for New Zealand, the increasing availability (influenced by increasing market pressure) of NIPT in New Zealand implies an urgent need for practice support around this technology.24
Requesting NIPT in New Zealand
There is no capability, as yet, for NIPT samples to be analysed in New Zealand, as all samples and resultant health information are analysed and stored overseas. Currently, at the time of publishing there are four options for NIPT analytical services available to New Zealand women: (1) Victorian Clinical Genetics Services (percept™, Australia); (2) BGI Diagnostics (Nifty™, China); (3) Southern Community Laboratories (SCL) (Harmony™, USA); and (4) sequenca (Sequenom tests: VisibiliT™, MaterniT®21, MaterniT21® PLUS and MaterniT™ GENOME). A referral by a GP, obstetric provider or midwife is required for SCL where an additional appointment needs to be made for the blood draw, and the test costs $675 (at the time of article submission). All of the testing companies require women to be at least 10 weeks gestation, as this usually means that there is sufficient fetal fraction for the test to be carried out. A typical turnaround time is ~7 days. Requesting clinicians usually provide pre- and post-test counselling.
What is the role of GPs and what do they need?
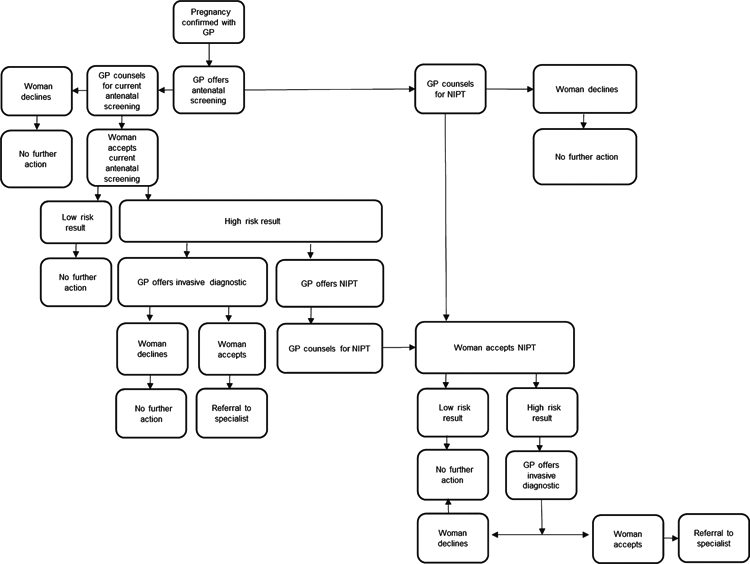
Although GPs are not usually lead maternity carers (LMCs) following changes to the maternity care system in 1996, they are still often the first point of contact and entry point to antenatal care with ~60% women seeing their GP in their first trimester of pregnancy.7 GPs may be asked to provide NIPT services by women and they are well-placed (as are midwives) to do so. It is plausible that GPs could provide NIPT before a woman books with her LMC, and make the referral to specialist care as appropriate (Fig. 1). This could be a component of a more integrated model of maternity care, with GPs supporting first trimester screening and navigation to a LMC, and fulfilling the recommendation of expedient access to antenatal screening.25
Currently, there are no clinical guidelines for the provision of NIPT and no framework for a publically funded service. A possible next step could be to develop a NIPT care pathway for general practices; for example, as outlined in Fig. 1. Determining what primary healthcare providers need in order to offer NIPT is paramount; for example, education around NIPT, ongoing support, information for women and their whanau. It is also important to establish whether GPs want to provide this service and how involved they want to be in the screening care pathway. In terms of fee structure for the practice, consideration of practice processes would also be needed for failed screens and communication of results.
Facilitating informed choice
Given that participation in antenatal screening is optional, informed choice about participation is crucial,26–33 and relationships that GPs have with women may benefit the counselling process. Informed choice is particularly important when an enhanced technology is being introduced alongside an existing service. A dichotomous service, as is currently in place (where a woman can choose current antenatal screening with some co-payment required for ultrasound, compared with NIPT where women pay all the costs), raises an important issue around equitable access. It may mean that providers will have to be flexible and mindful in their counselling and facilitation of informed choice so as not to promote one screen over another (because of the considerable differences in cost, balanced against the screening performance of NIPT). At the same time, women need to be aware that these options exist.
Summary
With such a high-performing screen, the clinical advantage of NIPT over current screening is clear. There is a high degree of urgency in ensuring equity in access to this technology, and given that GPs and other primary healthcare providers are well-placed to be at the forefront of offering NIPT, it is important to ensure that they are well supported to do so.
COMPETING INTERESTS
The authors declare no competing interests.
ACKNOWLEDGEMENT
Sara Filoche is supported by a Lotteries Health Research Board.
References
[1] Allyse M, Minear MA, Berson E, et al Non-invasive prenatal testing: a review of international implementation and challenges. Int J Womens Health 2015; 7 113–26.| Non-invasive prenatal testing: a review of international implementation and challenges.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC28Xns1Ggsbk%3D&md5=2650c0fdbdac5b46cd1669cd2c5d5362CAS |
[2] Benn P, Cuckle H, Pergament E. Non-invasive prenatal testing for aneuploidy: current status and future prospects. Ultrasound Obstet Gynecol 2013; 42 15–33.
| Non-invasive prenatal testing for aneuploidy: current status and future prospects.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3sjhvFKkug%3D%3D&md5=2329e06790be51badb739838ad8d5f8fCAS |
[3] Minear MA, Alessi S, Allyse M, et al Noninvasive prenatal genetic testing: current and emerging ethical, legal, and social issues. Annu Rev Genomics Hum Genet 2015; 16 369–98.
| Noninvasive prenatal genetic testing: current and emerging ethical, legal, and social issues.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC2MXhsFShs7vF&md5=882b447347d2a98ebc1731e393995161CAS |
[4] Bianchi DW, Wilkins-Haug L. Integration of noninvasive DNA testing for aneuploidy into prenatal care: what has happened since the rubber met the road? Clin Chem 2014; 60 78–87.
| Integration of noninvasive DNA testing for aneuploidy into prenatal care: what has happened since the rubber met the road?Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC2cXpslemsA%3D%3D&md5=7ddfe42da6d032bb736069535ed9d68dCAS |
[5] Mackie FL, Hemming K, Allen S, et al The accuracy of cell-free fetal DNA-based non-invasive prenatal testing in singleton pregnancies: a systematic review and bivariate meta-analysis. BJOG 2017; 124 32–46.
| The accuracy of cell-free fetal DNA-based non-invasive prenatal testing in singleton pregnancies: a systematic review and bivariate meta-analysis.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC28XitFGgt73E&md5=42400a8687629994e0fad8fd7490d475CAS |
[6] National Institute for Health and Care Excellence. High-throughput non-invasive prenatal testing for fetal RHD genotype. NICE; 2016. [cited 2017 July] Available from: https://www.nice.org.uk/guidance/dg25/chapter/1-Recommendations
[7] National Maternity Monitoring Group. National Maternity Monitoring Group Annual Report 2016. Wellington: Ministry of Health; 2016.
[8] Norton ME. Noninvasive prenatal testing to analyze the fetal genome. Proc Natl Acad Sci USA 2016; 113 14173–5.
| Noninvasive prenatal testing to analyze the fetal genome.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC28XitVyisrfN&md5=0128b945b9cf414b3860f705c19939faCAS |
[9] Dar P, Curnow KJ, Gross SJ, et al Clinical experience and follow-up with large scale single-nucleotide polymorphism-based noninvasive prenatal aneuploidy testing. Am J Obstet Gynecol 2014; 211 527.e1–527.e17.
| Clinical experience and follow-up with large scale single-nucleotide polymorphism-based noninvasive prenatal aneuploidy testing.Crossref | GoogleScholarGoogle Scholar |
[10] Gil MM, Quezada MS, Revello R, et al Analysis of cell-free DNA in maternal blood in screening for fetal aneuploidies: updated meta-analysis. Ultrasound Obstet Gynecol 2015; 45 249–66.
| Analysis of cell-free DNA in maternal blood in screening for fetal aneuploidies: updated meta-analysis.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2MrhsVSnsQ%3D%3D&md5=bc4505fd8d6f11bf2357bdff1d4f06b4CAS |
[11] Norton ME, Baer RJ, Wapner RJ, et al Cell-free DNA vs sequential screening for the detection of fetal chromosomal abnormalities. Am J Obstet Gynecol 2016; 214 727.e1–6.
| Cell-free DNA vs sequential screening for the detection of fetal chromosomal abnormalities.Crossref | GoogleScholarGoogle Scholar |
[12] Taylor-Phillips S, Freeman K, Geppert J, et al Accuracy of non-invasive prenatal testing using cell-free DNA for detection of Down, Edwards and Patau syndromes: a systematic review and meta-analysis. BMJ Open 2016; 6 e010002
| Accuracy of non-invasive prenatal testing using cell-free DNA for detection of Down, Edwards and Patau syndromes: a systematic review and meta-analysis.Crossref | GoogleScholarGoogle Scholar |
[13] Farrell RM, Agatisa PK, Mercer MB, et al The use of noninvasive prenatal testing in obstetric care: educational resources, practice patterns, and barriers reported by a national sample of clinicians. Prenat Diagn 2016; 36 499–506.
| The use of noninvasive prenatal testing in obstetric care: educational resources, practice patterns, and barriers reported by a national sample of clinicians.Crossref | GoogleScholarGoogle Scholar |
[14] McLennan A, Palma-Dias R, da Silva Costa F, et al Noninvasive prenatal testing in routine clinical practice - An audit of NIPT and combined first-trimester screening in an unselected Australian population. Aust N Z J Obstet Gynaecol 2016; 56 22–8.
| Noninvasive prenatal testing in routine clinical practice - An audit of NIPT and combined first-trimester screening in an unselected Australian population.Crossref | GoogleScholarGoogle Scholar |
[15] Takoudes T, Hamar B. Performance of non-invasive prenatal testing when fetal cell-free DNA is absent. Ultrasound Obstet Gynecol 2015; 45 112
| Performance of non-invasive prenatal testing when fetal cell-free DNA is absent.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2M3kslSltQ%3D%3D&md5=dd3354c5487f7a1f7917d12b92b547cbCAS |
[16] Yaron Y. The implications of non-invasive prenatal testing failures: a review of an under-discussed phenomenon. Prenat Diagn 2016; 36 391–6.
| The implications of non-invasive prenatal testing failures: a review of an under-discussed phenomenon.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC28XnslCqt78%3D&md5=2fc7f8721f8e0173af44c2493a14ca26CAS |
[17] Gil MM, Revello R, Poon LC, et al Clinical implementation of routine screening for fetal trisomies in the UK NHS: cell-free DNA test contingent on results from first-trimester combined test. Ultrasound Obstet Gynecol 2016; 47 45–52.
| Clinical implementation of routine screening for fetal trisomies in the UK NHS: cell-free DNA test contingent on results from first-trimester combined test.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC28zkvV2qsg%3D%3D&md5=f5046c32872bb1850a1129c6bc79ec6aCAS |
[18] Lewis C, Hill M, Chitty LS. Women’s experiences and preferences for service delivery of non-invasive prenatal testing for aneuploidy in a Public Health Setting: a mixed methods study. PLoS One 2016; 11 e0153147
| Women’s experiences and preferences for service delivery of non-invasive prenatal testing for aneuploidy in a Public Health Setting: a mixed methods study.Crossref | GoogleScholarGoogle Scholar |
[19] Vanstone M, Yacoub K, Giacomini M, et al Women’s experiences of publicly funded non-invasive prenatal testing in Ontario, Canada: considerations for health technology policy-making. Qual Health Res 2015; 25 1069–84.
| Women’s experiences of publicly funded non-invasive prenatal testing in Ontario, Canada: considerations for health technology policy-making.Crossref | GoogleScholarGoogle Scholar |
[20] Tamminga S, van Schendel RV, Rommers W, et al Changing to NIPT as a first-tier screening test and future perspectives: opinions of health professionals. Prenat Diagn 2015; 35 1316–23.
| Changing to NIPT as a first-tier screening test and future perspectives: opinions of health professionals.Crossref | GoogleScholarGoogle Scholar |
[21] Gregg AR, Skotko BG, Benkendorf JL, et al Noninvasive prenatal screening for fetal aneuploidy, 2016 update: a position statement of the American College of Medical Genetics and Genomics. Genet Med 2016; 18 1056–65.
| Noninvasive prenatal screening for fetal aneuploidy, 2016 update: a position statement of the American College of Medical Genetics and Genomics.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC28Xhs1aks77L&md5=00a634027df934727e16286052591549CAS |
[22] Tamminga S, van Dussen L, Verweij EJ, et al What do people want to know about NIPT? Content analysis of questions emailed to national NIPT information websites. Prenat Diagn 2017; 37 412–5.
| What do people want to know about NIPT? Content analysis of questions emailed to national NIPT information websites.Crossref | GoogleScholarGoogle Scholar |
[23] Hill M, Wright D, Daley R, et al Evaluation of non-invasive prenatal testing (NIPT) for aneuploidy in an NHS setting: a reliable accurate prenatal non-invasive diagnosis (RAPID) protocol. BMC Pregnancy Childbirth 2014; 14 229
| Evaluation of non-invasive prenatal testing (NIPT) for aneuploidy in an NHS setting: a reliable accurate prenatal non-invasive diagnosis (RAPID) protocol.Crossref | GoogleScholarGoogle Scholar |
[24] Filoche SK, Lawton BA, Beard A, et al Views of the obstetric profession on non-invasive prenatal testing in Aotearoa New Zealand: a national survey. Aust N Z J Obstet Gynaecol. 2017; In press
| Views of the obstetric profession on non-invasive prenatal testing in Aotearoa New Zealand: a national survey.Crossref | GoogleScholarGoogle Scholar |
[25] Health Quality and Safety Commission New Zealand. Improving quality and safety in maternity services: can we improve prevention, detection and management of congenital abnormalities in pregnancy? Auckland; 2012.
[26] Ahmed S, Bryant LD, Tizro Z, et al Interpretations of informed choice in antenatal screening: a cross-cultural, Q-methodology study. Soc Sci Med 2012; 74 997–1004.
| Interpretations of informed choice in antenatal screening: a cross-cultural, Q-methodology study.Crossref | GoogleScholarGoogle Scholar |
[27] Barr O, Skirton H. Informed decision making regarding antenatal screening for fetal abnormality in the United Kingdom: a qualitative study of parents and professionals. Nurs Health Sci 2013; 15 318–25.
| Informed decision making regarding antenatal screening for fetal abnormality in the United Kingdom: a qualitative study of parents and professionals.Crossref | GoogleScholarGoogle Scholar |
[28] de Jong A, de Wert GM. Prenatal screening: an ethical agenda for the near future. Bioethics 2015; 29 46–55.
| Prenatal screening: an ethical agenda for the near future.Crossref | GoogleScholarGoogle Scholar |
[29] de Jong A, Maya I, van Lith JM. Prenatal screening: current practice, new developments, ethical challenges. Bioethics 2015; 29 1–8.
| Prenatal screening: current practice, new developments, ethical challenges.Crossref | GoogleScholarGoogle Scholar |
[30] Dormandy E, Michie S, Hooper R, et al Low uptake of prenatal screening for Down syndrome in minority ethnic groups and socially deprived groups: a reflection of women’s attitudes or a failure to facilitate informed choices? Int J Epidemiol 2005; 34 346–52.
| Low uptake of prenatal screening for Down syndrome in minority ethnic groups and socially deprived groups: a reflection of women’s attitudes or a failure to facilitate informed choices?Crossref | GoogleScholarGoogle Scholar |
[31] Marteau TM, Dormandy E, Michie S. A measure of informed choice. Health Expect 2001; 4 99–108.
| A measure of informed choice.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3M3ns1WhsA%3D%3D&md5=2f81c027140ff4ff417237c2146d91b8CAS |
[32] Potter BK, O’Reilly N, Etchegary H, et al Exploring informed choice in the context of prenatal testing: findings from a qualitative study. Health Expect 2008; 11 355–65.
| Exploring informed choice in the context of prenatal testing: findings from a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[33] van den Berg M, Timmermans DR, ten Kate LP, et al Informed decision making in the context of prenatal screening. Patient Educ Couns 2006; 63 110–7.
| Informed decision making in the context of prenatal screening.Crossref | GoogleScholarGoogle Scholar |