Self-care of Canterbury general practitioners, nurse practitioners, practice nurses and community pharmacists
Caroline Christie 1 , Susan Bidwell 1 , Andrea Copeland 1 , Ben Hudson 11 Pegasus Health (Charitable) Ltd, Christchurch, New Zealand
Correspondence to: Caroline Christie, Pegasus Health (Charitable) Ltd, PO Box 741, Christchurch 8140 (401 Madras Street, Christchurch 8013), New Zealand. Email: caroline.christie@pegasus.org.nz
Journal of Primary Health Care 9(4) 286-291 https://doi.org/10.1071/HC17034
Published: 13 October 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Pastoral care is recognised as an important aspect of a mature primary care network. Pegasus Health is now in its 25th year and has had a formal Pastoral Care Programme for doctors since 2009.
AIM: This study aimed to collect local data on the self-care of Canterbury (Christchurch, New Zealand) general practitioners (GPs), nurse practitioners (NPs), practice nurses (PNs) and community pharmacists (CPs).
METHODS: The survey was open to all participants in the Pegasus Small Group Education Programme in Canterbury. From a survey circulated to approximately 1100 primary care professionals, 504 responses were collected either electronically or as hard copies.
RESULTS: The themes that emerged were similar among all the health professional groups. A significant proportion of health professionals took minimal annual leave and even more worked while ill. CPs were the group with the highest rates in both these areas. Reasons given for this focused largely on a lack of locum cover.
DISCUSSION: Locum cover is a significant issue in Canterbury for all health professional groups in the study. The issue of locums is now being reviewed in Canterbury partly as a result of this study. Consideration is also being given to how the Pastoral Care Programme can be made more widely available.
| WHAT GAP THIS FILLS |
What is already known: International data suggest high rates of burnout and stress among doctors across both primary and secondary care. |
| What this study adds: This research expands knowledge about the self-care of general practitioners and adds previously unknown data about the self-care of nurse practitioners, practice nurses and pharmacists. This study explores reasons for stress in the workplace and provides possible solutions. This study adds local information on the self-care of Canterbury general practitioners, nurse practitioners, practice nurses and community pharmacists. |
Introduction
International research suggests high rates of burnout among doctors across both primary and secondary care.1–6 Community pharmacists (CPs) have also been shown to be increasingly stressed by high volumes of work, the perceived need to deliver services more quickly to patients and the expansion of CPs’ roles but without the level of control that an appointment system provides for general practitioners (GPs), nurse practitioners (NPs) and practice nurses (PNs).7–9 There is also considerable research on the level of burnout and stress in nurses, though this is largely limited to hospital settings rather than in primary care.10
Pegasus Health has had a formal Pastoral Care Programme since 2009. The programme offers rehabilitative and educational support to individual GPs and promotes a supportive culture and aims to reduce stressors in the workplace. The organisation had been looking for ways to systematise its approach and has been considering how the programme might be expanded to cater for NPs, PNs, and CPs. This paper reports on a Pegasus Health initiative to assess self-care among Canterbury primary healthcare professionals as a means of further informing and developing the Pastoral Care Programme.
Methods
A questionnaire (Appendix 1) was developed by the Pegasus Clinical Quality and Education (CQE) team on the topic of practitioner self-care to be distributed at their Small Group Education meetings.11 The questionnaire was distributed through the SurveyMonkey platform between August and October 2016, and was open to 1144 health professionals who were registered in the Small Group Education Programme. Responses were anonymous. Respondents were asked to indicate their professional group; GP, NP, PN, CP. To increase participation, paper copies were also made available at all Small Group Education meetings. To provide a higher level of anonymity, demographic data were not included.
To collate total responses, those from paper copies were manually entered into SurveyMonkey by a member of the CQE team. The analysis of quantitative results was conducted through the SurveyMonkey platform; responses to open questions were analysed separately for their content.
Results
There was a total of 504 responses, 495 of which were complete, giving a response rate of 43%. Fifty-one percent of respondents indicated they worked full time, 49% part time and 0.2% had not worked at all in the past 12 months.
Level of self-care among respondents
Enrolment with a GP was high at 95.8% (474/495), 4.2% were not enrolled with a GP, and nine respondents skipped this question. Almost half of the respondents (240, 48.2%), however, had consulted a colleague when unwell rather than attending their own GP, 258 (51.8%) had not done so, and six respondents did not answer this question.
Annual and sick leave
The amount of annual leave taken over the past 12 months varied widely among the 500 respondents who completed this question. The majority of respondents (215, 43%) had taken 2–4 weeks’ annual leave and 130 (26%) had taken more than 4 weeks. Of those who took less annual leave, 101 (20.2%) had taken 1–2 weeks, 24 (4.8%) had taken less than 1 week, and 30 (6%) had taken no leave at all. Four people did not answer this question.
From 498 responses, 210 (42.2%) people had taken no sick days in the past 12 months, 246 (49.4%) took 1–5 days, 27 (5.4%) took 6–10 days, and 15 (3%) took more than 10 days. Six respondents skipped this question. More than half the respondents (287/499, 57.5%) had worked while ill when they felt they should not have, 212 (42.5%) had not, and there were five missing responses. The reasons for working while ill were explored further. From 289 responses, 228 (78.9%) respondents did not want to let a colleague down, 112 (38.8%) were too busy to take time off, 79 (27.3%) did not want to let patients down, 48 (16.6%) could not afford to take time off, 28 (9.7%) wanted to avoid the stigma of being ill, 13 (4.5%) wanted to maintain personal privacy about illness, and 54 (18.7%) specified ‘other’ reasons. From a total of 250 comments, there were 95 comments (38%) about a lack of locum cover. When asked to specify the reason for working while ill, 35 out of 54 comments (64.8%) named the lack of locum cover as the reason to continue working while ill.
Compared with other health professional groups, community pharmacist respondents were less able to take leave, and worked when ill more frequently:
-
67% worked full time compared to 53% of GPs and 31% of PNs;
-
8% had taken no leave in the previous 12 months compared with 0.7% of GPs and 7% of PNs;
-
34% had taken less than 2 weeks’ leave in the previous 12 months compared with 10% of GPs;
-
64% had worked while ill compared with 53% of GPs and 37% of PNs.
Although many more PNs worked part time compared with the other professional groups, their rates of leave were also low; 7% did not take any leave and 40% took less than 2 weeks over the previous 12 months (Table 1). PNs were, however, less likely to report working when ill.

|
Workplace and professional support for self-care
Overall, 419/488 (85.9%) respondents to this question felt adequately supported in their own self-care, whereas 69 (14.1%) did not, and 16 respondents skipped this question. However, in answer to whether the workplace could be better at supporting health professionals to care for themselves, 129 of the 426 (30.3%) who responded felt there were ways it could. This question had the largest number of non-respondents (n = 78).
Two hundred and nine respondents (42.6%) had sought professional support for their self-care, including 185 (88.5%) who had sought help from a GP; 24 (11.5%) from a nurse; 12 (5.7%) from a psychologist; 16 (7.7%) from a counsellor; 8 (3.8%) from a professional body; 7 (3.3%) from a brief intervention counsellor; 3 (3.3%) from their Primary Health Organisation; and 25 (12.0%) from other services, mainly specialists.
Boundaries between professional and personal activities
From 493 responses, 322 (65.3%) respondents had used medications or supplies from their place of work for personal or family use. This included 75% of GPs and CPs, and 50% of PNs. More than one-third of all respondents (34.9%); however, indicated they had not done this, and 11 respondents skipped this question. Giving medical advice to friends and family was also explored in the survey. Results showed that 111 (22.5%) responders would give medical advice to family and friends, 84 (17%) would decline, and 300 (60.9%) would try not to, but sometimes find it hard to avoid. There were 495 responses and nine respondents skipped this question. The reasons for giving advice or treatment to friends or family included: triviality of the condition (324 responses, 65.5%), weekend or public holiday (212, 42.8%), non-availability of the person’s own GP (86, 17.3%), cost of medical care (75, 15.2%), the person not having time to see their GP (44, 8.9%), and other reasons (81, 16.4%).
In a question specifically for GPs, 116/143 (81.1%) of GP respondents were comfortable having other doctors as patients, 9 (6.3%) were not, and 18 (12.6%) were comfortable only in some situations. Further comments made in relation to this question suggested that health practitioners make good patients as they understand the information provided, while others felt that health professionals should be treated just like anybody else so no assumptions are made about their level of knowledge.
In relation to prescribing for friends and family, 142/496 (28.6%) of respondents had prescribed for themselves or their immediate family, 67 (13.5%) had not, and 287 (57.9%) did not have prescribing rights. Eight respondents skipped this question. The survey showed that 89% of GPs have prescribed for themselves or their immediate family. From 151 CPs responses, 74% indicated that receiving a script for a potential drug of abuse intended for the prescriber or a member of their family made them feel either uncomfortable or very uncomfortable.
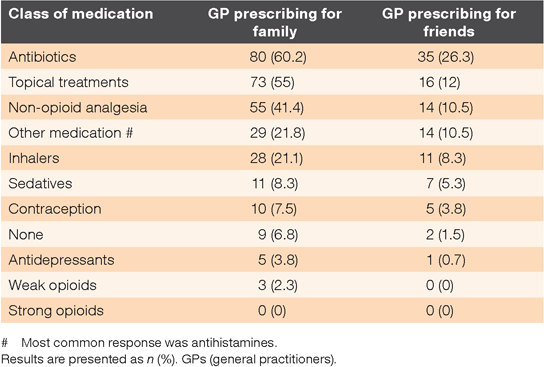
Table 2 shows prescribing patterns for GPs from 133 responses received.
|
Discussion
The survey showed that most respondents were enrolled with their own GP. Nevertheless, half had consulted a colleague rather than their own GP. The survey did not explore the reasons for this, but it may be that it was simply more convenient than making time outside of work commitments to see their own GP. The majority, especially the GPs, were also taking 2 weeks or more annual leave, but the 10.8% of health professionals who had taken no leave or less than 1 week (mostly CPs and PNs) was somewhat concerning. The most striking, though perhaps not surprising, finding was the high rate of working while ill among all professional groups, largely due to a lack of locum cover and not wanting to let colleagues or patients down. Pharmacists had the highest rates of working while ill (64.4%) as well as not taking adequate leave.
It has been shown previously that the negative impact of stress on health professionals’ personal and professional functioning, their patients, and the system as a whole, is considerable.12 Adverse effects reported include becoming detached and cynical towards patients, feeling emotionally exhausted, feeling devalued or unsupported by their organisation, decreased effectiveness and increased errors, and leaving the healthcare workforce altogether.2,3,5,10 The negative impact on personal and family life is also well documented.5,13 Sickness presenteeism (working while ill) has been shown to have similar negative effects; it has also been associated with a higher rate of future ill health, as well as far-reaching economic implications. One study referred to health professionals who worked while sick as ‘hazardous heroes’,14 who were endangering patient health and safety. However, there is clearly a very real tension between caring for oneself and having a profession that is focused on caring for others, including one’s colleagues.
While the findings from the GPs in this study are not entirely new, they underline and further support the concern that has been noted elsewhere; for example, in the recent booklet on GP self-care that was issued by the Royal New Zealand College of General Practitioners.15 In addition, this study shows that the same negative stressors also affect other primary health professionals. This appears to be the first multidisciplinary survey of this nature to be conducted, made possible through the wide reach of the Pegasus Small Group Education Programme. The overwhelming implication of the responses to the survey was the lack of available locums for all professional groups surveyed.
Limitations
This study represented the views of some groups of health practitioners in Canterbury and is not necessarily representative of other groups or areas in New Zealand. The response rate was relatively good for a survey of this nature.16,17 However, the decision not to include demographic data limited the amount of detailed analysis that could be carried out for subgroups of health professionals. An additional limitation was that the NP category was misinterpreted, with more respondents indicating they belonged to this category than there were NPs enrolled in the Small Group Programme.
Conclusion
The survey results showed that although the majority of health professionals are registered with a GP and take basic steps in self-care, there is an urgent and ongoing need for locum support in all disciplines, particularly among CPs. Findings from the study have been disseminated to relevant bodies in Canterbury responsible for the welfare of health professionals working in primary care, and these organisations are taking active steps to provide more satisfactory short- and long-term cover in all disciplines. More work is also being undertaken to expand the Pastoral Care Programme, currently only available to doctors, to all health professionals in the Canterbury community.
COMPETING INTERESTS
The authors declare no competing interests.
ACKNOWLEDGEMENTS
The authors thank the members of the CQE team who contributed to the development of the questionnaire that was used in the survey, and the health professionals of Canterbury for their responses.
References
[1] Arigoni F, Bovier PA, Sappino AP. Trend of burnout among Swiss doctors. Swiss Med Wkly. 2010; 140 w13070| 1:STN:280:DC%2BC3cjpt1CgsA%3D%3D&md5=cdf6b74dab7f031541af57b1d1155ed7CAS |
[2] Halbesleben JR, Rathert C. Linking physician burnout and patient outcomes: exploring the dyadic relationship between physicians and patients. Health Care Manage Rev. 2008; 33 29–39.
| Linking physician burnout and patient outcomes: exploring the dyadic relationship between physicians and patients.Crossref | GoogleScholarGoogle Scholar |
[3] Kay MP, Mitchell GK, Del Mar CB. Doctors do not adequately look after their own physical health. Med J Aust. 2004; 181 368–70.
[4] Pejuškovic B, Lecic-Tosevski D, Priebe S, et al. Burnout syndrome among physicians – the role of personality dimensions and coping strategies. Psychiatr Danub. 2011; 23 389–95.
[5] Riley GJ. Understanding the stresses and strains of being a doctor. Med J Aust. 2004; 181 350–3.
[6] Rø KE, Gude T, Tyssen R, et al. Counselling for burnout in Norwegian doctors: one year cohort study. BMJ. 2008; 337 a2004
| Counselling for burnout in Norwegian doctors: one year cohort study.Crossref | GoogleScholarGoogle Scholar |
[7] Gidman W. Increasing community pharmacy workloads in England: causes and consequences. Int J Clin Pharm. 2011; 33 512–20.
| Increasing community pharmacy workloads in England: causes and consequences.Crossref | GoogleScholarGoogle Scholar |
[8] Gidman WK, Hassell K, Day J, et al. The impact of increasing workloads and role expansion on female community pharmacists in the United Kingdom. Res Social Adm Pharm. 2007; 3 285–302.
| The impact of increasing workloads and role expansion on female community pharmacists in the United Kingdom.Crossref | GoogleScholarGoogle Scholar |
[9] Gaither CA, Kahaleh AA, Doucette WR, et al. A modified model of pharmacists’ job stress: the role of organizational, extra-role, and individual factors on work-related outcomes. Res Social Adm Pharm. 2008; 4 231–43.
| A modified model of pharmacists’ job stress: the role of organizational, extra-role, and individual factors on work-related outcomes.Crossref | GoogleScholarGoogle Scholar |
[10] Leiter MP, Maslach C. Nurse turnover: the mediating role of burnout. J Nurs Manag. 2009; 17 331–9.
| Nurse turnover: the mediating role of burnout.Crossref | GoogleScholarGoogle Scholar |
[11] Health P. Clinical quality and education. Christchurch: Pegasus Health 2016. [cited 2017 March 31]. Available from: http://www.pegasus.health.nz/clinical-quality-and-education.
[12] Institute of Medicine. Preventing Medication Errors. Washington, DC: Institute of Medicine; 2006.
[13] Shanafelt TD, Sloan JA, Habermann TM. The well-being of physicians. Am J Med. 2003; 114 513–9.
| The well-being of physicians.Crossref | GoogleScholarGoogle Scholar |
[14] Rosvold EO, Bjertness E. Physicians who do not take sick leave: hazardous heroes? Scand J Public Health. 2001; 29 71–5.
| Physicians who do not take sick leave: hazardous heroes?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD38%2FhtVWksg%3D%3D&md5=4aecb5ab1cce37d7332324ea023ca12cCAS |
[15] RNZCGP. Self care: caring for yourself and your colleagues. Wellington: Royal New Zealand College of General Practitioners; 2016.
[16] Cook JV, Dickinson HO, Eccles MP. Response raters in postal surveys of healthcare professionals between 1996 and 2005: an observational study. BMC Health Serv Res. 2009; 9 160
| Response raters in postal surveys of healthcare professionals between 1996 and 2005: an observational study.Crossref | GoogleScholarGoogle Scholar |
[17] VanGeest JB, Johnson TP, Welch VL. Methodologies for improving response rates in surveys of physicians: a systematic review. Eval Health Prof. 2007; 30 303–21.
| Methodologies for improving response rates in surveys of physicians: a systematic review.Crossref | GoogleScholarGoogle Scholar |
Appendix 1

|


