General practice evolution in New Zealand: hybridisation in action
Carol Atmore1 Department of General Practice and Rural Health, University of Otago, New Zealand
Correspondence to: Carol Atmore, Department of General Practice and Rural Health, University of Otago, Dunedin 9054, New Zealand. Email: carol.atmore@otago.ac.nz
Journal of Primary Health Care 9(3) 220-224 https://doi.org/10.1071/HC17043
Published: 25 September 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
This viewpoint outlines a brief history of primary care health reforms over the last 25 years, and how this history has influenced the business of caring. It also suggests where we should next look to improve the provision of equitable patient-centred care in the current climate of fiscal constraint, while meeting the challenges of an ageing population and increasing multimorbidity.
Introduction
General practice in New Zealand (NZ) has changed significantly over the last quarter of a century. In the early 1990s, general practice had no clear organisational structure beyond the stand-alone small business model, and general practitioners (GPs) were accountable for the clinical care of patients who chose to attend their practice. There was no collective clinical accountability for cost or quality of care, and little interface between general practice and hospital services.1 Now, general practice is locally organised through Primary Health Organisations (PHOs), and GP-led organisations and other networks provide regional and national structure. Clinical leaders from general practice and district health boards (DHBs) jointly commission and provide services for their areas in collaborative health alliances. Large groups of GPs through their PHOs are now accountable for the achievement of nationally set health targets for their enrolled populations.
So, what brought about these changes? How have they affected the business model of general practice and the clinical care that general practice teams provide to patients? And where do we need to go next? This viewpoint outlines a brief history of primary care health reforms over the last 25 years, and considers how this history has influenced the business of caring. It also suggests where we should next look to improve the provision of patient-centred care in the current climate of fiscal constraint, while meeting the challenges of an ageing population and increasing multimorbidity.2
The beginnings of organised general practice
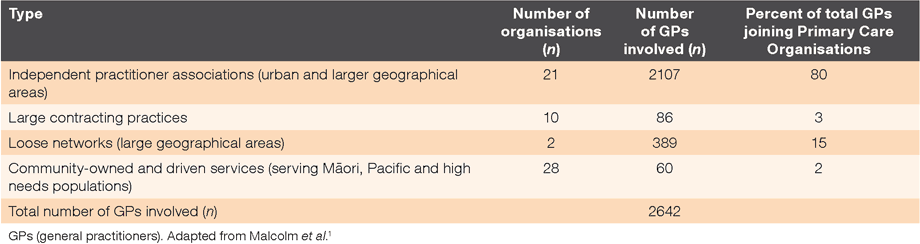
The health reforms of 1993 in NZ heralded budget holding for general practices. Some GPs saw this as a potential threat through competition if corporatized general practice developed, and others as an opportunity to strengthen the position of general practice and improve patient and community outcomes. In response, groups of GPs formed Primary Care Organisations, with most GPs belonging to large GP-controlled Independent Practitioner Associations.3 The early Primary Care Organisations generated savings from pharmaceutical and laboratory budget holding, which were used to fund new clinical programmes and local initiatives.4 This early success enticed other GPs and by 1999, 85% of all NZ GPs were members of one of four types of Primary Care Organisations, as shown in Table 1.1
|
This was the beginning of organised general practice. General practitioners began to receive information about how their practice compared with their colleagues and what was ‘best practice’ in prescribing and laboratory test ordering, which influenced doctor behaviour in patient consultations. One incentive behind changing prescribing and ordering behaviour was the ability to use discretionary funds, generated through savings, to provide locally relevant services. Groups of GPs worked collaboratively, often for the first time. New services emerged with a focus on population health or targeting unmet need, such as free palliative care services. Information systems started to develop. External relationships with community- and hospital-based providers grew. Integration projects developed, such as diabetes care, child health and health of older people.
Despite these developments, by the end of the 1990s inequalities in general practice access and lack of accountability around use of public funds (generated through savings) by private Primary Care Organisations were raising concern.1,3
The Primary Health Care Strategy and the establishment of the patient list
The NZ Primary Health Care Strategy of 2001 set out to improve access to general practice and primary care, reduce health inequalities, increase community participation in the governance of primary health care and develop a more multidisciplinary, team-based approach to primary healthcare delivery.5 It established PHOs, which became contract holders with DHBs for health funding for general practice.
For the first time, patients registered with their general practice, and through them, a PHO. Government funding for general practice was no longer fee-for-service, but by capitation. Extra funding was provided, aimed at reducing co-payment costs to patients, improving long-term conditions management, increasing the focus on population health, improving access and reducing inequalities.3,6
Regulations around PHO establishment were deliberatively permissive.7 In response, over 80 PHOs of diverse size, structure and differing priorities were established.6 These ranged from single practice PHOs immersed within their community, to large organisations closely linked with the pre-existing Independent Practitioner Associations. GPs lost the ability to contribute to locally available savings through altered prescribing and ordering behaviour. Community, Māori and primary care leaders now provided joint governance through PHO Boards to decide how to spend new government money to improve local health services.
These changes were not universally welcomed by GP leaders. They felt disengaged from PHO governance processes, and the Independent Practitioner Association Council was formed to negotiate with the Ministry of Health and represent the interests of GPs within the new PHO environment.3
These policy settings saw access to primary health care improve, with reduced patient co-payments.8 General practices had developed a stronger focus on proactive and preventative services, such as cervical and breast screening, and smoking cessation. Through the patient enrolment process, it was now clear to general practices whose care they were responsible for. Data were available about aspects of care and health promotion activities provided to their registered population. Financial incentives were targeted to specific areas such as the annual collection of data on diabetes care through free annual visits for people with diabetes.9
Financial constraints within the health system were increasing, and the need for more integration across different parts of the healthcare system was apparent. Both DHBs and PHOs were commissioning primary care services. Funding mechanisms were blocking service integration across DHB and PHO geographical boundaries. Strengthened clinical leadership within general practice and shared leadership with hospital clinicians was needed to advance integration.6,10
‘Better, Sooner, More Convenient’ and Alliancing
The ‘Better, Sooner, More Convenient’ health agenda of the late 2000s emphasised clinical leadership and engagement, improved health sector productivity and quality, and focused on community-based care to reduce pressure on hospital services. Nine pilot sites were established.11 ‘Alliance contracting’ was mandated as the vehicle to govern relationships between the DHBs and PHO alliance members undertaking the integration of services as specified in each pilot. Borrowed from the construction industry, alliancing aimed to more effectively deliver complex services by working collaboratively with common outcomes in a single overarching contract with shared accountability. It allowed collaboration rather than competition while maintaining separate organisations within the alliance.12,13
The underlying principles of working in an alliance are outlined in Box 1. A clinically led, patient-centred, whole-of-system approach was taken to maximise health gain with finite resources. A disputes resolution and exit process was established within each alliance’s charter.14
| Box 1. Key alliance principles | ||||||
| ||||||
The leadership and management structure and culture required for successful alliancing took time to be well understood and embedded.15 The author’s experience was that effective and timely implementation by management of decisions reached by the clinical leaders was essential to maintaining clinical engagement, while decisions reached by the clinical leaders needed to be implementable to succeed.
In 2011, the Ministry of Health rationalised the number of PHOs from over 80 to 36. Then, in 2013, all DHBs and PHOs were required to form health alliances to advance local integration.13
Alliance contracting has increased service integration in local health systems.12,13,16 It has provided the framework for clinical leaders and managers across local health systems to design, implement and monitor integrated systems together, in a high-trust, low-bureaucracy approach. There have been varying levels of success with DHB–PHO alliances to date. When working well,12,13 the ‘all succeed or all fail’ approach has allowed resources to be shifted to where they best meet people’s needs, as seen in the Canterbury Clinical Network Alliance.17
System Level Outcome Measures
From 2012 onwards, measures of integrated care began to be developed.18,19 At a local level, these allowed health care practitioners to see how their effort contributed to the whole system.18 Nationally, the Integrated Performance and Incentive Framework was the beginning of whole-of-system outcome measures across general practice, PHOs and DHBs. It had double aims of improving accountability of the system, and improving performance through a quality-improvement approach.19
This framework has evolved into the national System Level Measures programme, focused on outcomes across the whole health system. These are now part of regional, DHB and PHO annual planning processes. District Alliances, with their component DHB and PHO members, are responsible for driving the achievement of the System Level Measures programme in their local health system.20 GPs are responsible for their practice’s performance in measures that contribute to overall system performance, such as immunisation rates and smoking cessation.20 Financial rewards for general practices are attached to the achievement of these measures by their PHO.
Achievement of system-level outcome measures requires effective health alliances at the local level.19,21 A recent Ministry of Health System Level Measure Framework update noted that ‘Districts with mature alliances had strong clinical leadership and a system-wide approach to the development of their plans’.16
The policy and practice interface
The emergence of organised general practice and PHOs have been key in bringing a population health approach into general practice, and shifting some care from hospital into the community. National policy settings that promoted strong general practice clinical leadership and enabled wider system integration are outlined in Box 2. These have underpinned the culture change in general practice from stand-alone small businesses to organised networks where GPs and primary care nurses are key members of the team leading their local health system.
| Box 2. Key policy settings to develop strong, engaged clinical leadership in NZ general practice | |||||
| |||||
The ongoing challenge is how to balance the ‘big picture’ clinical leadership work that GP leaders in the sector are engaged in, with the realities of providing day-to-day patient care in general practices. As health practitioners, we are committed to providing best practice medicine and ensuring that our enrolled patients are accessing health and preventive services equally. But evidence of this is only collectable through data, and with ongoing time pressure, one does not always remember to tick the box in the patient management system that records that the question about smoking was asked. ‘Alert fatigue’ can creep in, so one forgets to record a patient’s weight, while addressing the several issues on the patient’s agenda in the 15 minute consultation. And that applies only to the patients who have actually been able to navigate the system to get an appointment. At a business ownership level, a broader range of services with a population health focus is required to meet the responsibilities that the general practice has to its PHO and local alliance. Providing these enhanced services can require more staff. This can challenge the financial sustainability of the business if funding does not follow the patient care pathway.
Where to next?
With increasing tensions between providing preventive, population health approaches and individualised person-centred care, and the need for appropriately staffed viable general practice businesses, new ways of organising care delivery are emerging. These include integrated family health services22 and patient-centred health care homes.23 Different ownership models are developing, such as corporate general practice and trust ownership, in addition to the traditional small business owner-operator model. Are these changes going to happen with enough scale and pace to manage the looming demographic changes of an ageing general practice workforce caring for an ageing population with increasing multimorbidity?24 Will changes increase equity, or will access to the system become disproportionately easier for people who are health literate and already well able to engage with the system?
Comparing our health system to our peers, New Zealand ranked fourth equal out of 11 high income countries in 2017, but was ranked seventh for access and eighth for equity. Our mortality rate amenable to health care was second worst, only better than the United States.25 Our health system is unusual among our peers, as general practice care still largely requires patient co-payments, while hospital care is free. Some efforts have been made by government in this regard, and general practice care for children aged ≤ 13 years is now largely free. While Very Low Cost Access (VLCA) practices provide more affordable general practice visits to people enrolled in those ‘high-needs’ practices, 44% of ‘high-needs’ New Zealanders – over 500,000 people – miss out on reduced fees as they are not enrolled in VLCA practices.26
We need to understand how new general practice service delivery, ownership and funding models can contribute to the achievement of New Zealand’s Triple Aim of improved patient experience, population health and equity, and value for money.27 We need to determine what makes well-functioning health alliances effective, and share these lessons. We need to explore what ‘funding following the patient’ really means. And we need to understand how the intimacy of the relationship between general practice teams and their patients and whanau can be preserved and strengthened in all this. Then we will be well placed to deliver a sustainable, high-quality health system that is fit for the 21st century.
COMPETING INTERESTS
The author declares no competing interests.
ACKNOWLEDGEMENTS
The author wishes to acknowledge and thank the West Coast District Health Board for funding her, and Professor Chris Ham and Hugh Alderwick for ideas while the initial work on this paper was undertaken during a sabbatical at the King’s Fund in the early phases of this paper’s genesis. This paper was completed while working within the Department of General Practice and Rural Health, University of Otago.
References
[1] Malcolm L, Wright L, Barnett P. The Development of Primary Care Organisations in New Zealand. Wellington: Ministry of Health; 1999.[2] Atmore C. The role of medical generalism in the New Zealand health system into the future. N Z Med J. 2015; 128 50–5.
[3] Thorlby R, Smith J, Barnett P, Mays N. Primary care for the 21st century. Learning from New Zealand’s independent practitioner associations. London: Nuffield Trust; 2012.
[4] Malcolm L. GP budget holding in New Zealand: lessons for Britain and elsewhere? BMJ. 1997; 314 1890–2.
| GP budget holding in New Zealand: lessons for Britain and elsewhere?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2szmslCgsQ%3D%3D&md5=b66c6c0ed27d0b74d936392e680093e5CAS |
[5] King A. The Primary Health Care Strategy. Wellington: Ministry of Health; 2001.
[6] Smith J, Cumming J. Where next for primary health organisations in New Zealand? Wellington: Victoria University of Wellington; 2009.
[7] King A. Minimum Requirements for Primary Health Organisations. Wellington: Ministry of Health; 2001.
[8] Hefford M, Crampton P, Foley J. Reducing health disparities through primary care reform: the New Zealand experiment. Health Policy. 2005; 72 9–23.
| Reducing health disparities through primary care reform: the New Zealand experiment.Crossref | GoogleScholarGoogle Scholar |
[9] Brady K. Ministry of Health and district health boards: effectiveness of the “Get Checked” diabetes programme. Wellington: Office of the Auditor-General; 2007.
[10] Smith J, McDonald J, Cumming J. Developing and implementing high impact changes for primary health care in New Zealand: a discussion document. Wellington: Victoria University of Wellington; 2008.
[11] Ministry of Health. Better, Sooner, More Convenient health care in the community. Wellington: Ministry of Health; 2011.
[12] Timmins N, Ham C. The quest for integrated health and social care: a case study in Canterbury, New Zealand. London: The King’s Fund; 2013.
[13] Gauld R. What should governance for integrated care look like? New Zealand’s alliances provide some pointers. Med J Aust. 2014; 201 S67–S68.
| What should governance for integrated care look like? New Zealand’s alliances provide some pointers.Crossref | GoogleScholarGoogle Scholar |
[14] DHB Shared Services. Alliance Agreement and Alliance Leadership Team Charter. Wellington: DHB Shared Services; 2013.
[15] Lovelock K, Martin G, Cumming J, Gauld R. The evaluation of the Better, Sooner, More Convenient Business Cases in MidCentral and the West Coast District Health Boards. Wellington: Victoria University of Wellington; 2014.
[16] Ministry of Health. System Level Measures Framework Update January 2017. Wellington: Ministry of Health; 2017.
[17] Canterbury Clinical Network. Alliancing in a health context. May 2015, Canterbury Clinical Network. [cited 2017 August 29]. Available from: http://ccn.health.nz/OurHealthSystem/OurWayofWorking.aspx
[18] Doolan-Noble F, Lyndon M, Hill A,, et al. Developing and implementing a framework for system level measures: lessons from New Zealand. Asia Pacific J Health Manag. 2016; 11 18–26.
[19] Ashton T. Measuring health system performance: a new approach to accountability and quality improvement in New Zealand. Health Policy. 2015; 119 999–1004.
| Measuring health system performance: a new approach to accountability and quality improvement in New Zealand.Crossref | GoogleScholarGoogle Scholar |
[20] Ministry of Health. Guide to Using the System Level Measures Framework for Quality Improvement. Wellington: Ministry of Health; 2016.
[21] Scott G, Horn M, Durie M, et al. Expert Advisory Group Report on the Integrated Performance and Incentive Framework. Wellington: Ministry of Health; 2014.
[22] West Coast PHO, West Coast DHB. Building a Better Buller Health System: Buller Integrated Family Health Centre Development Plan & Indicative/Strategic Business Case. Greymouth: West Coast DHB; 2011.
[23] Ernst & Young. Evaluation of the New Zealand Health Care Home, 2010–2016. Auckland: Ernst & Young; 2017.
[24] Ministry of Health. Health of the Health Workforce 2015. Wellington: Ministry of Health; 2016.
[25] Schneider EC, Sarnak DO, Squires D, et al. International Comparison Reflects Flaws and Opportunities for Better U.S. Health Care. The Commonwealth Fund, July 2017.
[26] Love T, Blick G. Primary care funding - a discussion paper. Wellington: Sapere Research Group; 2014.
[27] The Health Safety and Quality Commission. The Triple Aim. Wellington: The Health Safety and Quality Commission. [cited 2017 May 23]. Available from: http://www.hqsc.govt.nz/news-and-events/news/126/


