Cheques and challenges: business performance in New Zealand general practice
Richard Greatbanks 1 , Fiona Doolan-Noble 2 , Alex McKenna 11 Department of Management, Otago Business School, University of Otago, Dunedin 9054, New Zealand
2 Rural Aotearoa Research Network, Department of General Practice and Rural Health, University of Otago, New Zealand
Correspondence to: Fiona Doolan-Noble, Rural Aotearoa Research Network, Department of General Practice and Rural Health, University of Otago, New Zealand. Email: fiona.doolan-noble@otago.ac.nz
Journal of Primary Health Care 9(3) 185-190 https://doi.org/10.1071/HC17047
Published: 25 September 2017
Journal Compilation © Royal New Zealand College of General Practitioners 2017.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: New Zealand general practice mainly functions as small businesses, usually owned by a single or small group of doctors. Consequently, owners often have to balance the provision of patient care with varying funding priorities, changing patient needs and the pressures of running a sustainable business. Such balancing inevitably leads to tensions developing between these factors.
AIM: To explore and understand these tensions and responses to them, by examining the business performance measurements used by general practice.
METHODS: For this study, the unit of analysis and focus were individual practices, but qualitative semi-structured interviews with general practitioners (GPs) and practice managers were used to gather the data.
RESULTS: All participating practices had some form of governance or board review, where high-level aggregated business performance data were presented. More sophisticated business performance measures were evident in the larger, more developed practices and in practices functioning as community trusts. Examples of such measures included doctor utilisation and efficiency, appraisal of risk, patient satisfaction with services and responses to changes in patient demand.
DISCUSSION: As the number of general practices based on the traditional model decrease, a corresponding increase is likely in the establishment and development of ‘super practices’ based on a corporatized, multi-service, single-location model. Consequently, service delivery will become increasingly complex and will drive a need for increased sophistication in how general practice measures its business performance, thus ensuring a balance between high-quality, safe patient care and the maintenance of a sustainable business.
KEYWORDS: New Zealand; general practice; business performance; hybridization tension
| WHAT GAP THIS FILLS |
There is a dearth of academic research examining how general practices respond to increasing levels of change within the sector. Responding to such changes can exacerbate the tension of balancing patient care with operating a small business. |
| What is already known: New Zealand general practice is facing increasing changes in patient needs and expectations, in government policy and funding, and in general practitioner employment preferences. These changes are already resulting in new business models of general practice. |
| What this study adds: This research presents a unique analysis of how a small sample of New Zealand general practices have implemented different business performance measures in response to changes in patient need, funding policy and employee expectations. |
Introduction
In New Zealand (NZ), general practices mainly operate as small businesses, usually owned by a single or small group of doctors. This traditional model means owners are frequently challenged with having to balance the provision of care to patients with the pressures of running a sustainable business. Most general practitioners (GPs) have little formal business training. This lack of business understanding can potentially create tension between delivering care and performing as a business. We describe this as a hybridity tension.1 Hybridity tensions typically arise when organisations attempt to retain traditional models of service delivery in the face of increasing sector-wide change, causing tensions to develop between the delivery mission of the organisation and the externally imposed pressures for change. In NZ, external pressures include changes in population demographics, government funding and policy, and a growing preference for GPs to be employees rather than practice owners. Increases in hybridity tensions have been associated with lower performing general practices in other countries.2
There is a dearth of academic literature regarding business performance focused on general practice, with a few notable exceptions.3–5 Most literature in this area is from industry-, professional- or practitioner-based sources. Of the few academic research papers found,3–5 these considered general practice from a health network or system view, with none examining hybridity tensions at the practice level.
When faced with changing circumstances, most businesses tend to respond to hybridity tensions by developing new performance measures6 that reflect the nature of the external changes, allowing business owners to gauge the effectiveness of their response.7,8 The overall aim of this research, therefore, was to investigate emerging hybridization tensions in NZ general practice by focusing on business performance measures used in general practice, and to determine if, and how, practices are responding to hybridization tensions.
Methods
This qualitative study had four research questions:
-
How do general practices measure business performance?
-
What types of measures do practice owners find useful from a business perspective?
-
How are these measures collected and analysed?
-
What are the motivations for measuring business performance within the sector?
Secondary to these, the level of sophistication of business performance measurement adopted at the practice level was also examined.
Following a review of the literature, an interview schedule was developed,9 refined and finalised through discussion within the research team. The sampling frame10 engaged a variety of general practice stakeholders, such as owner-doctors, practice managers, community trust chief executives and general practice network owners. In addition, the study aimed to sample the 78 practices in the Southern region to ensure variation in practice type, including small and large practices, urban and rural, Very Low Cost Access (VLCA) and private and commercially owned entities. The unit of analysis and focus of this work were individual practices, and a purposive sample of 35 practices meeting the criteria was selected.
Semi-structured interviews with GPs and practice managers were used to gather the data.9 All respondents answered the questions from their practice’s perspective. Each interview lasted 30–60 min and was digitally recorded. Interviews were professionally transcribed verbatim. Each transcript was analysed by at least two members of the research team, with differences of opinion resolved through discussion. The results section describe the deductive analysis of the text data.11
Results
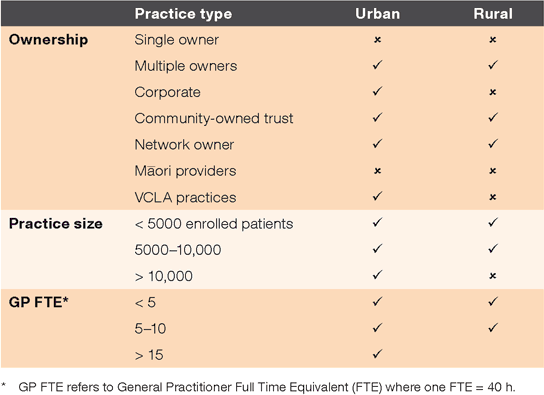
Of 35 practices contacted, 17 responded and six were not interviewed for reasons including timing of the research project and illness of the potential interviewee. Eleven practices participated, with a total of 12 participants. Table 1 provides an overview of participating stakeholders and practices. Data collection was completed between 1 December 2016 and the end of February 2017. Category B ethical approval for this research was granted in December 2016 by the University of Otago Ethics Committee, reference number: D16/404.
|
The first research question sought to determine how general practices measure business performance. Most respondents discussed the use of financial management accounting methods, such as profit-and-loss reports, cash flow, income statements and practice annual budgets. Each of these measures was usually discussed in relation to capitation funding and patient co-payments. Both funding streams formed the primary income to practices. All practices, regardless of size, had these basic measures in place and usually reviewed them in monthly Board meetings. Other business-level performance measures discussed in Board meetings included staff turnover, patient enrolment and demographic trends.
At a more detailed level most, but not all, respondents discussed their use of strategic and business planning. Strategic planning processes were normally based on a 2- or 3-year horizon, with business plans developed annually. In this way, practices translated their longer-term plans into short-term specific activities, which could then be actioned in the current year.
The second and third research questions focused on the types of measures practice owners found useful, and how these were collected and analysed. The measure most often mentioned for its usefulness was capitation, with one practice manager commenting:
‘Capitation income - you know how much [money] you have to run your business. Capitation covers all fixed expenses.’ [Practice Manager 4]
While capitation and patient co-payments were identified as the two most useful measures of income, respondents identified other income streams, including Accident Compensation Corporation (ACC) and immunisation claims. The more progressive practices identified further forms of income, such as District Health Board (DHB)-specific funding initiatives. Conversely, these practices also identified the precarious nature of such funding.
‘A lack of long-term planning from the Ministry of Health and uncertainty with contracting with the DHB makes it really difficult to invest in programmes. We’re forever setting up particularly nurse-led programmes, in response to health targets or encouragement from the DHB and PHO, to have them run for a couple of years and then the funding is pulled completely, but we’re still expected to do the work’. [General Practitioner 3]
Two practices provided evidence of more sophisticated performance measurement; for example, one practice discussed measuring efficiency of individual GPs and correlating this with patient satisfaction data.
‘We do key performance indicators (KPIs), which might be doctors’ utilisation. All the sessions are based on 12 appointments per doctor, and then we’ll watch the trends of a particular person, or we’ll separate it out between locations, and so monitor it with income per doctor, and wait times.’ [Practice Manager 6]
Some practices distinguished between practice-owner and non-owner GPs, particularly from a patient allocation and utilisation perspective.
‘We have talked about having some sort of bonus system. We don’t do that currently and the majority of the owners are pretty much 100 per cent utilised, and now most of our assistants are as well.’ [General Practitioner 1]
Another practice undertook measurement of consultations, after-hours consultations and phone calls to nurses to indicate population and consumer demand. The practice manager commented:
‘I pretty much daily look at the numbers … we know how many clinics we run, how many appointments are in each clinic, and whether they are fully booked. That’s a review that happens every day, whether we’re fully booked and where the gaps are. We now have clinics that start at eight o’clock in the morning, whereas everybody was starting at nine, but the demand was for earlier than that.’ [Practice Manager 7]
Accessing data to undertake this detailed level of measurement was noted as challenging.
‘It’s quite time consuming to do even those [KPIs] because Medtech, our PMS (practice management software) is not administration-friendly. It’s good from a clinical aspect, but as far as trying to extract data, it’s not totally reliable.’ [Practice Manager 6]
In terms of the frequency for reviewing performance, practice managers in particular discussed the monthly reporting of operational budgets to ensure day-to-day spend was controlled. One practice manager, however, indicated reviewing performance against budget was a daily and ongoing activity within their practice.
The final research question explored motivations for measuring business performance. The ability to keep providing a quality health service in their community was the leading motivator, as illustrated below:
‘We are not aiming to be an innovative company, we’re not aiming to grow, we think of ourselves as a service. We’re not trying to make more money, we’re just trying to keep going and offer the best service we can.’ [Practice Manager 1]
Another practice explicitly discussed patient satisfaction as a motivator and how they noticed its correlation with practice profitability.
‘We’ve been measuring it [patient satisfaction] more intensively for the past four of five years. It’s got a direct relationship to profitability. Of all the measures that we have been using, we found that’s the closest to identify profitability in the organisation.’ [General Practitioner 2]
Another practice mentioned the desire to reduce their exposure to risk and the process of using risk analysis to determine risk from new projects or planned services.
‘The business plan that the CEO produces is normally a good 20 pages; everything’s just broken down. Then we have aims and goals and risks - low, medium, high risks. If this is happening, what we’re going to do to prevent that or minimise it if it does happen.’ [General Practitioner 1]
Discussion
This research makes the subtle, but important distinction between two different aspects of business performance – performance measurement of the practice itself, and performance measurement of processes that operate within the practice.7 In the first instance, this research found many examples where practices measured the performance of their business; that is, the value of its patient roll as an income stream. Focusing on capitation and patient co-payments is not surprising, and provides evidence of a basic level of business performance measurement, particularly where this is the only perspective used to understand key business processes at the individual practice level.
Typically, management accounting approaches such as profit and loss (or earnings before interest and tax) were used to assess business value. These were normally reviewed in Board meetings.12 Such accounting-based measures tend to use aggregated measures over longer time periods, so they are not considered useful to measure key business processes, hence the need for short-term, process-based measurement.7,12 As most general practices are still relatively small businesses, exposure to financial risk could be damaging to their sustainability. The apparent lack of a risk management process is therefore of concern, and highlights an area where further training, education and support might be valuable to smaller practices.
Most practices distinguished between strategic and business planning, with the former being a governance or Board responsibility and the latter more of a managerial responsibility undertaken by practice managers. Two practices, however, did not discuss these processes despite interviewer prompting. This is of some concern, as strategic planning is a key primary mechanism for setting the long-term direction of a practice. The absence of business planning routines in general practice is reflected in the literature5,13 and can partly be explained by the day-to-day nature of general practice distracting from planning for the longer term.13
There was less compelling evidence to indicate that practices measured key business processes, but some practices did. For instance, the measurement of efficiency and utilisation of GPs is a reasonably sophisticated interpretation of performance, and implies there are emerging pressures acting on the practice to ensure efficiency in utilisation of key staff. Monitoring practice demand to this degree implicitly speaks to the need to ensure customers are satisfied; a fundamental premise of good business. Patient satisfaction, and the means to measure and track it, is an important component of a successful practice, particularly in urban areas where patients have a wide choice of general practices.
The undertaking of a risk analysis by a practice indicates a maturity of business practice. Risk analysis is an essential tool for any business as it assists the business in managing risk and consequently minimising the impact of these on the business.
Study limitations, conclusion and further research
The sample size in this study was small (12 respondents from 11 general practices) and localised, with most participants drawn from the Otago and Southland regions. This research, however, was designed to explore a theory, so notwithstanding these limitations, it has highlighted some useful and interesting perspectives.
First, all participating practices had some form of governance or Board review, who normally met monthly, to which high-level aggregated business performance data were presented. As general practices are often small businesses, this is a positive finding. However, in two practices in our sample, business performance measurement did not go beyond this basic legal requirement for any form of business entity, suggesting that in these practices, performance measurement could be developed further.
When looking for evidence of more sophisticated performance measurement of key business processes, it was only the larger more developed practices and the community trust-owned practices that appeared to consider other aspects of performance, such as doctor utilisation and efficiency, risk management or responses to patient demand. This evidence of more sophisticated forms of measurement being adopted implies that some practices are responding by necessity to measure these functions because of external sector, patient or funding pressures. We see this as emerging evidence that hybridity tensions exist in general practice in this region of NZ. Further, we postulate that such tensions are likely to become more prevalent as practices feel the impact of demographic changes, changing Ministry requirements and consequent changes to DHB funding policies.
Finally, there is a potential point of debate about whether these identified hybridity tensions can be considered ‘emerging’ or if they have been ‘present’ within general practice for some time. Our interpretation, arising from experience in the non-profit or Third sector,1 is that rapidly changing business environments produce organisational performance discomfort (hybridity tension), which in turn drives an emerging change in performance measurement. This research has focused on these performance measurement changes. Perhaps the issue is not one of either ‘emerging’ or ‘pre-existing’ tensions, but rather the degree of change in such tensions that the general practice sector and profession is currently witnessing.
Several areas for further research have emerged from this study. As an example, if doctor utilisation and efficiency are being measured, then linking such performance to a bonus payment could be possible. However, this could potentially introduce ethical or gaming dysfunctionalities – often an unintended outcome of more detailed performance measurement – so the potential for such bonus payments needs further research. There also appears to be little academic research considering business performance measurement specifically at the practice level, and so this research appears to be unique in its focus.
As the number of general practices based on the traditional small business model begin to decrease, a corresponding increase is likely in the establishment and development of ‘super practices’ based on a corporatized, multi-service, single-location model, which provide employment, rather than ownership, opportunities for GPs. The increasing complexity of service delivery will likely drive the need for increased sophistication in how general practice measures its business performance to ensure the balance between patient care and a sustainable business.
We anticipate that however hybridity tensions shape general practice over the next decade, the degree of change will be at levels not previously experienced within this sector. The cumulative effects of these managerial and organisational changes are not fully understood, and will require the continued engagement of researchers and general practice across a broad range of academic fields.
COMPETING INTERESTS
Dr Richard Greatbanks is a faculty member of the Otago Business School, University of Otago, and a member of the Alliance South Leadership Team. Dr Fiona Doolan-Noble is a faculty member of the Department of General Practice and Rural Health, Dunedin School of Medicine and is the Director of the Rural Research Network.
ACKNOWLEDGEMENTS
This research was initially funded as a summer student project through the Otago Business School, University of Otago. The research team wish to acknowledge the time given by all participants.
References
[1] Billis D. Hybrid organisations and the third sector. Challenges for practice, theory and policy. Basingstoke, UK: Palgrave; 2010.[2] van den Hombergh P, Kunzi B, Elwyn G, et al. High workload and job stress are associated with lower practice performance in general practice: an observational study in 239 general practices in the Netherlands. BMC Health Serv Res 2009; 9 118
| High workload and job stress are associated with lower practice performance in general practice: an observational study in 239 general practices in the Netherlands.Crossref | GoogleScholarGoogle Scholar |
[3] Rogan L, Boaden R. Understanding performance management in primary care. Int J Health Care Qual Assur. 2017; 30 4–15.
| Understanding performance management in primary care.Crossref | GoogleScholarGoogle Scholar |
[4] Grice N, Wilson J, Foster G, Padgett G. The nature of business planning undertaken by general practitioner fundholding practices in the North West Region. Public Money Manag. 1998; 18 31–40.
| The nature of business planning undertaken by general practitioner fundholding practices in the North West Region.Crossref | GoogleScholarGoogle Scholar |
[5] Majeed FA, Voss S. Performance indicators for general practice. BMJ 1995; 311 209–10.
| Performance indicators for general practice.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2MzltlWjtA%3D%3D&md5=f2a81472c65d8518d14a8f6324911cd1CAS |
[6] Neely A. Business Performance Measurement. Theory and Practice. Cambridge, UK: Cambridge University Press; 2002.
[7] Bourne M, Neely A, Platts K, Mills J. The success and failure of performance measurement initiatives. Int J Oper Prod Manage. 2002; 22 1288–310.
| The success and failure of performance measurement initiatives.Crossref | GoogleScholarGoogle Scholar |
[8] Bryman A. Chapter 18: Sampling in qualitative research. In: Social Research Methods, 4th edn. Oxford, UK: Oxford University Press; 2012. p. 415–429.
[9] Bryman A. Chapter 20. Interviewing in qualitative research. In: Social Research Methods, 4th edn. Oxford, UK: Oxford University Press; 2012. p. 468–498.
[10] Bryman A. Chapter 2. Social research strategies. Social Research Methods. 4th edn. Oxford, UK: Oxford University Press; 2012. p. 18–4.
[11] Brignall S, Modell S. An institutional perspective on performance measurement and management in the ‘new public sector’. Manage Account Res. 2000; 11 281–306.
| An institutional perspective on performance measurement and management in the ‘new public sector’.Crossref | GoogleScholarGoogle Scholar |
[12] Currie G. The influence of middle managers in the business planning process: a case study in the UK NHS. Br J Manage. 1999; 10 141–55.
| The influence of middle managers in the business planning process: a case study in the UK NHS.Crossref | GoogleScholarGoogle Scholar |
[13] Kath . A worthwhile plan - Business plans help practices focus on their long-term goals. Med J Aust. 2012; 196 2 Available from: https://www.mja.com.au/journal/2012/196/2/worthwhile-plan-business-plans-help-practices-focus-their-long-term-goals cited 15/06/2017.


