Primary healthcare utilisation among adults with mood and anxiety disorders: an analysis of the New Zealand Health Survey
Helen Lockett 1 2 , Jennifer Lai 3 , Charito Tuason 3 , Angela Jury 3 , David Fergusson 41 The Wise Group, Hamilton, New Zealand
2 Department of Psychological Medicine, The University of Auckland, Auckland, New Zealand
3 Te Pou o te Whakaaro Nui, Auckland, New Zealand
4 Department of Psychological Medicine, University of Otago, Christchurch, New Zealand
Correspondence to: Helen Lockett, The Wise Group, 293 Grey Street, PO Box 307, Hamilton 3240, New Zealand. Email: Helen.Lockett@wisegroup.co.nz
Journal of Primary Health Care 10(1) 68-75 https://doi.org/10.1071/HC17077
Published: 29 March 2018
Journal Compilation © Royal New Zealand College of General Practitioners 2018.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: In New Zealand, as in other OECD countries, there is a high and growing prevalence of mental health problems, particularly anxiety and depression. These conditions are associated with a range of physical illnesses, and as a result this population have high and often complex needs for healthcare services, particularly through primary care.
AIM: To use data from the New Zealand Health Survey (NZHS) to examine the associations between internalising disorders (including anxiety, depression and bipolar disorder) and measures related to the utilisation of primary healthcare services.
METHODS: The study was based on responses from 13,719 adults who took part in the 2015–16 NZHS. Logistic regression analyses adjusted for sociodemographic variables were undertaken to examine the effect of having an internalising disorder on each measure related to primary healthcare utilisation. The strength of associations was indicated by odds ratios (ORs).
RESULTS: Adults with an internalising disorder were more likely to utilise primary health services (OR = 1.43–2.56, P < 0.001) compared to adults without an internalising disorder. However, they were more likely to have unmet needs due to cost or transport (OR = 2.45–3.38, P < 0.001), unfilled prescriptions due to cost (OR = 3.03, P < 0.001) and less likely to report positive experiences with general practitioners (OR = 0.67–0.79, P < 0.01).
DISCUSSION: Adults with internalising disorders require a higher level of support from primary healthcare, yet experience more barriers to accessing these services, and report less positive experiences with general practitioners. The NZHS may be a useful source of routinely collected data for understanding, monitoring and improving primary health service utilisation among people with internalising disorders.
KEYWORDS: Primary healthcare; depression; anxiety disorders; bipolar disorder; health service utilisation; health service access
| WHAT GAP THIS FILLS |
| What is already known: The New Zealand Health Survey is conducted annually to assist with the development of health services, policy and strategy. It has not been used specifically to investigate the utilisation of primary healthcare services for people with mental health problems. |
| What this study adds: Adults with internalising disorders are more likely to access primary healthcare services, to experience greater levels of unmet need for these services and higher levels of dissatisfaction with the primary care services they receive. The New Zealand Health Survey may be a useful source of routinely collected data for informing and monitoring the development of primary mental healthcare policy and practice over time. |
Introduction
In New Zealand, as in other OECD (Organisation for Economic and Co-operation and Development) countries, there is a high prevalence of mental health problems,1 and this population have multiple and often complex needs for both mental and physical healthcare. To better meet the needs of people with mental health problems within primary healthcare services, New Zealand’s Ministry of Health funded the first wave of Primary Mental Health Initiatives (PMHIs) in 2005.1 This involved the development of different service delivery models across the country, with elements specific to local needs.1 The Ministry of Health now funds primary mental healthcare across all district health boards (DHBs), with the total funding in 2015–16 being NZ$29.3 million.2 This funding targets priority groups who have a higher prevalence of mild-to-moderate mental health and addiction problems, such as people who are Māori, Pacific or have low incomes.3 Components of primary mental healthcare include extended consultations, assessments, brief interventions (including counselling), other psychosocial interventions and medication reviews.4
The physical health of people with mental health problems is a sizeable issue. The lifetime prevalence rates of anxiety and mood disorders are estimated at 25% and 20% of the population respectively, and this is coupled with high levels of co-morbidity with physical health problems.5 It is important, therefore, to understand and monitor the effect of the government’s primary mental healthcare initiatives and any unmet needs for primary care services. To address this need for information, the New Zealand Health Survey (NZHS) may be a useful source of data on primary healthcare utilisation among people with mental health problems. The NZHS has been conducted each year since 2011, and is used to examine the primary healthcare utilisation of the general population to inform the development of health services, policy and strategy.6 The survey also collects information on mental health problems, including depression, anxiety and bipolar disorders.6 However, to date, it has not been used to specifically investigate the utilisation of primary care services among people with mental health problems.
Against this background, the objective of the study was to use data from the 2015–16 NZHS to examine the following issues: (i) the associations between internalising disorders (depression, anxiety and bipolar disorders) and measures related to the utilisation of primary healthcare services; and (ii) to adjust these associations for sociodemographic factors including age, gender, ethnicity and socioeconomic status. More generally, the study aimed to provide contemporary data on the associations between internalising disorders and primary healthcare utilisation in New Zealand.
Methods
Study design
This investigation was carried out using 2015–16 NZHS data. The NZHS survey had a multi-stage, stratified, probability-proportional-to-size sampling design and was administered face-to-face with computer assistance to a sample of 13,719 adults (aged 15 years and over) living in the community.7 Ethical approval for the 2015–16 NZHS was granted by the New Zealand Health and Disability Multi-Region Ethics Committee. The questions used to enquire about mental health diagnosis and primary healthcare utilisation were validated through cognitive testing undertaken by an external agency, and then tested. For most questions, a 12-month recall period was used to capture contacts with services. However, questions about patient experience (like satisfaction, confidence and trust with a general practitioner) relate to visits that occurred in the last 3 months to reduce recall bias.7
Measures
The following measures from the 2015–16 NZHS were included in the analysis.
Internalising disorders: Self-report diagnosis, based on the participants response to being asked if they had ever been told by a doctor that they have depression, bipolar disorder (sometimes called manic depression) or an anxiety disorder (including panic attacks, phobia, post-traumatic stress disorder and obsessive-compulsive disorder).
Self-perceived health status: Current health status was rated on a five-point scale ranging from 1 (Excellent) to 5 (Poor). Low self-perceived health was based on responses of 4 or 5.
Primary health service utilisation: Participants were asked about their general practitioner (GP) visits, practice nurse (PN) visits and after-hours medical centre visits (excluding public hospital emergency departments) in the past 12 months (Yes/No; three items) and also whether they had a usual healthcare provider (such as a GP clinic or medical centre) they go to when feeling unwell or injured (Yes/No).
Barriers to access: Participants were asked whether they had experienced unmet needs for GP services (having a medical problem but not visiting a GP) due to cost or lack of transport; and unmet needs for after-hours services due to cost or lack of transport in the past 12 months (Yes/No; four items). Participants were also asked whether they had been unable to collect prescription items from the pharmacy or chemist due to cost in the past 12 months (Yes/No).
Experience using primary healthcare services: Participants who had visited their GP in the past 3 months were asked whether they had definite confidence and trust in their GP, if their GP was good at explaining health conditions and treatments, and good at involving them in decisions about care and treatment options (Yes/No; three items).
Psychiatrist visits: Participants were asked to indicate whether they had seen a psychiatrist in the past 12 months (Yes/No).
Sociodemographic characteristics: Sociodemographic characteristics examined included gender (female/male), age (years), ethnicity (Māori; Pacific; Asian; European; and Other) and socioeconomic status, as indicated by the New Zealand Index of Deprivation 2013 (NZDep2013).
Statistical methods
Descriptive analysis: In the first stage of the analysis, the number of people with and without internalising disorders was examined. The sociodemographic characteristics among respondents with and without internalising disorders, were investigated using chi-square tests of association. In the group with internalising disorders, visits to psychiatrists in the last 12 months were also examined using chi-square tests of association.
Bivariate analysis: In the second stage of the analysis, chi-square tests were conducted to determine whether there were any significant associations between having an internalising disorder and each dependent variable examined. Odds ratios (OR) were calculated through logistic regression analysis to examine the strength of the association. An OR >1 indicates people with an internalising disorder had increased odds associated with the dependent variable, and an OR <1 indicates reduced odds.
Multivariate analysis: Multiple logistic regression analyses were conducted to examine the odds of each dependent variable being associated with having an internalising disorder, while controlling for age, gender, ethnicity and socioeconomic status. The analysis did not control for comorbidities of long-term conditions.
All analyses were performed using Stata version 12 (StataCorp LP, College Station, TX, USA), using listwise deletion.
Results
Internalising disorders
Of the 13,719 respondents, 2,957 (18.8%) people reported having been diagnosed by a doctor, sometime in their life, as having one or more of the following diagnosis: anxiety, depression or bi-polar. Of these people 6.3% had seen a psychiatrist in the past 12 months.
Adults with an internalising disorder were significantly more likely to be female (64%, P < 0.001) compared to adults without a disorder (48% female), and were on average older (mean age: 47 vs. 45 years respectively, P < 0.001). Adults with an internalising disorder were significantly more likely to identify as European (89 vs. 74%, P < 0.001) and less likely to identify as Pacific (3 vs. 7%, P < 0.001) or Asian (4 vs. 14%, P < 0.001), compared to adults without a disorder. There was no significant difference in the proportion of people who identified as Māori, and no significant difference between groups in relation to socioeconomic status.
Self-perceived health status
Compared with adults without an internalising disorder, adults with a disorder were at least three-fold more likely to perceive their health status as fair or poor (unadjusted OR = 2.93, 95% CI [2.55–3.36], P < 0.001; adjusted OR = 3.17, 95% CI [2.75–3.67], P < 0.001).
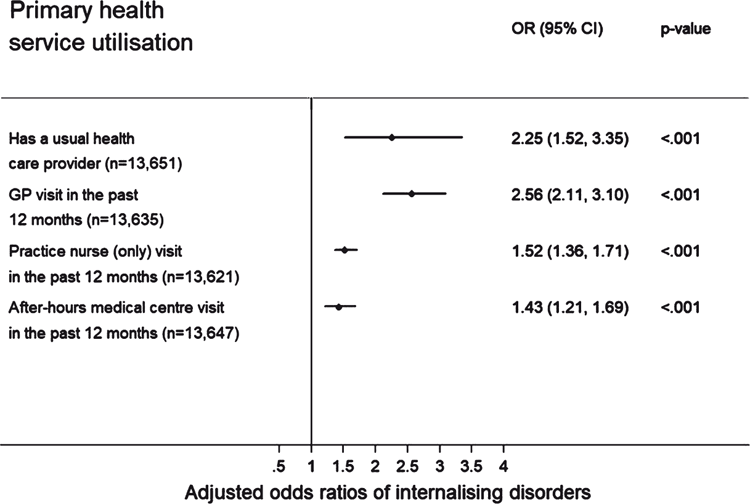
Primary health service utilisation
Figure 1 shows stem leaf plots for the adjusted associations between internalising disorders and primary health service utilisation. Adults with an internalising disorder were more likely to have a usual primary care provider than people without an internalising disorder (unadjusted OR = 3.27, 95% [2.22–4.81], P < 0.001; adjusted OR = 2.25, 95% CI [1.52–3.35], P < 0.001).
The odds of visiting a GP in the past 12 months was higher among adults with an internalising disorder compared to people without a disorder (unadjusted OR = 3.02, 95% [2.51–3.62], P < 0.001; adjusted OR = 2.56, 95% CI [2.11–3.10], P < 0.001). Adults with an internalising disorder were also more likely to have visited a practice nurse (unadjusted OR = 1.81, 95% CI [1.63–2.00], P < 0.001; adjusted OR = 1.52, 95% CI [1.36–1.71], P < 0.001) and an after-hours medical centre (unadjusted OR = 1.46, 95% CI [1.24–1.72], P < 0.001; adjusted OR = 1.43, 95% CI [1.21–1.69], P < 0.001).
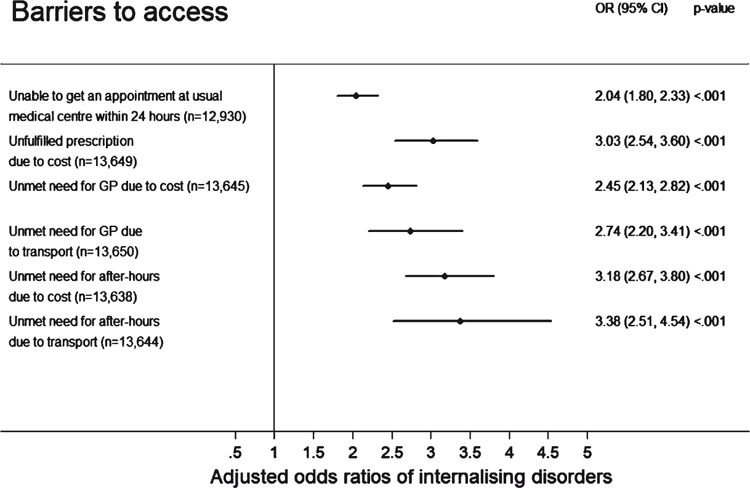
Barriers to accessing primary healthcare services
As shown in Figure 2, adults with an internalising disorder were two times more likely to be unable to get an appointment at their usual medical centre within 24 hours (unadjusted OR = 2.21, 95% CI [1.95–2.51], P < 0.001; adjusted OR = 2.04, 95% CI [1.80–2.33], P < 0.001) and three times more likely to be unable to collect prescription items from their pharmacy or chemist due to cost (unadjusted OR = 2.76, 95% CI [2.34–3.24], P < 0.001; adjusted OR = 3.03, 95% CI [2.54–3.60], P < 0.001).
Compared with adults without an internalising disorder, adults with a disorder were more likely to have an unmet need for GP services due to cost (unadjusted OR = 2.54, 95% CI [2.22–2.89], P < 0.001; adjusted OR = 2.45, 95% CI [2.13–2.82], P < 0.001). Unmet needs for GP services due to transport were also higher (unadjusted OR = 2.53, 95% CI [2.05–3.13], P < 0.001; adjusted OR = 2.74, 95% CI [2.20–3.41], P < 0.001).
The odds of having an unmet need for after-hours medical services due to cost was three times higher in adults with an internalising disorder (unadjusted OR = 3.07, 95% CI [2.60–3.63], P < 0.001; adjusted OR = 3.18, 95% CI [2.67–3.80], P < 0.001). They were also three times more likely to have an unmet need for after-hours medical services due to transport (unadjusted OR = 2.92, 95% CI [2.14–4.00], P < 0.001; adjusted OR = 3.38, 95% CI [2.51–4.54], P < 0.001).
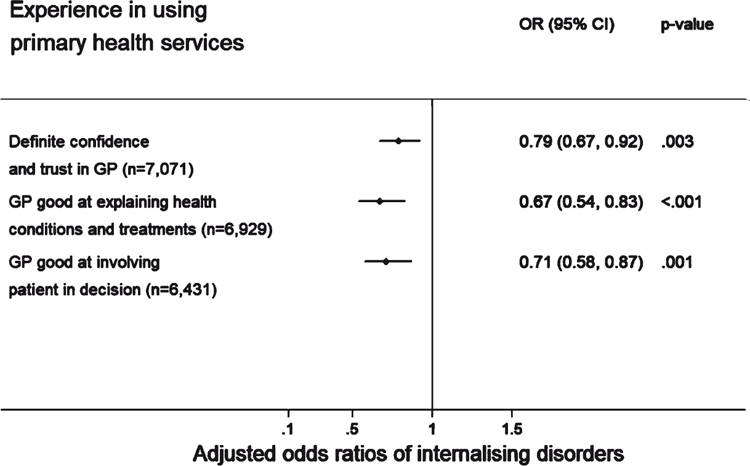
Experience in using primary health services
Figure 3 shows people with an internalising disorder who visited their primary health service in the past 3 months (n = 1,964) were less likely to report definite confidence and trust in their GP (unadjusted OR = 0.78, 95% CI [0.67–0.91], P = 0.002; adjusted OR = 0.79, 95% CI [0.67–0.92], P = 0.003). Adults with an internalising disorder were less likely to report their GPs were good at explaining health conditions and treatments (unadjusted OR = 0.67, 95% CI [0.54–0.82], P < 0.001; adjusted OR = 0.67, 95% CI [0.54–0.83], P < 0.001) and less likely to involve them in making decisions about their care and treatment options (unadjusted OR = 0.72, 95% CI [0.59–0.88], P = 0.001; adjusted OR = 0.71, 95% CI [0.58–0.87], P = 0.001).
Discussion
This analysis of the NZHS indicates adults with internalising disorders are more likely to access primary care services, to experience greater levels of unmet need for these services, and have higher levels of dissatisfaction with the primary care services they receive.
Use of primary healthcare services
In line with Te Rau Hinengaro,5 only a small proportion of adults diagnosed with internalising disorders had seen a psychiatrist in the past 12 months. Post-hoc analysis, removing this group from the multivariate analysis, resulted in no material change in the results. This further highlights the importance of primary care services in addressing both the person’s mental and physical health needs. Findings also corroborate previous research showing that people with internalising disorders tend to have poorer self-perceived health8,9 and higher levels of primary health service utilisation,5 compared to people without an internalising disorder. This is likely to reflect the higher prevalence of somatic symptoms and comorbid physical health conditions among adults with an internalising disorder, and the higher level of support needed.5
Barriers to accessing primary health services
Adults with internalising disorders were less likely to experience timely access to services. This unmet need for care may have been due to no appointments being available, unsuitable appointment times or preferred doctors being unavailable.10 Having an internalising disorder was also associated with higher levels of unmet need for primary healthcare services due to cost and transport, including the collection of prescription items from a chemist or pharmacy.
New Zealand has various centrally led funding initiatives aimed at reducing cost barriers to primary care access, particularly for people with higher health needs and low income. Initiatives are currently in place to help reduce the costs of primary healthcare services and prescriptions, provide extended hours, walk-in services without the need to reserve appointments, easily accessible clinics and additional care (such as emergency dental care and lifestyle changes).11–14 However, issues have been raised about the ability of some of these initiatives to support people with multimorbidities.15,16 There is growing evidence that models of collaborative care, which include delivery system re-design, use of clinical information systems, decision support tools and good links with community resources and services, are effective in improving access to primary care, satisfaction with care, and health outcomes.17
Experience in using primary healthcare services
The likelihood of reporting positive experiences with primary care services was lower among adults with internalising disorders. These people had lower confidence and trust in their GP compared to people without a disorder, and were also less likely to feel their GP was good at explaining health conditions and treatments or involving them in making decisions about their care and treatment options. Given that GP services are the first point of contact with the health system, this finding has important implications.
While use of primary care is comparatively higher among people with mental health problems, they tend to receive fewer physical health checks and screening,18 which can lead to the delayed diagnosis of physical health problems. In a recent New Zealand cohort study, later diagnosis was identified as one major factor contributing to the lower levels of breast and colorectal cancer survival among people accessing specialist mental health services.19 Issues of delayed diagnosis can be improved by increasing service providers’ awareness of comorbid health problems and the reasons behind them, actively avoiding diagnostic overshadowing, empowering people’s efforts to seek treatment, collaborating with other providers, encouraging regular check-ups and providing extended consultation times.20
Recent qualitative data indicate ‘feeling listened to’ and having a trusted healthcare practitioner that provides clear information is highly valued by people with multimorbidities, and is likely to influence how they manage their conditions.16
Implications
The findings from this analysis of the NZHS make two important contributions to understanding the linkages between mental health problems and primary healthcare. First, they provide contemporary data on a range of outcomes relating to primary health service utilisation, barriers to service access and experiences with these services, which may be used to motivate and inform policy and practice development in this area. Second, the findings provide benchmarks against which to evaluate the success of policy changes and initiatives.
In New Zealand, there is increasing focus on primary mental healthcare in policies and from healthcare practitioners,2,21 in part because this is an issue that affects a substantial proportion of the population and is recognised as a growing health need.1 In any year, one in five New Zealanders will experience a mental health problem, and the absolute number of people affected is increasing amid a growing population.22 This growing demand for mental healthcare within primary care services is an issue also being faced by other countries. The World Health Organization’s Mental Health Action Plan 2013–202023 proposed that service re-organisation and expanded coverage is needed, shifting the focus of care into non-specialised settings and increasing coverage of evidence-based interventions, which incorporate stepped-care approaches. The action plan also identifies the need for funding, workforce development and the integration of primary and community healthcare services.23
Similarly, New Zealand’s recently published Mental Health and Addiction Workforce Action Plan 2017–202124 indicated a competent and capable workforce will require training and development programmes to strengthen awareness and understanding of comorbidities, and a stepped-care model for the integration of primary, community and specialist services. Moreover, a recent collaboration between New Zealand’s four largest primary health organisations (PHOs) and Platform Trust described a future vision of primary mental healthcare in Closing the Loop.2 This vision involves a system of care that is person-centred, integrated and considers people’s first point of contact through to the outcome.
Limitations
The data from the NZHS is self-reported, which has likely underestimated the prevalence of internalising disorders. Furthermore, while internalising disorders may affect use of primary health services, the NZHS data does not indicate whether consultations were sought mainly to address physical health or mental health problems. As a result, ORs may be underestimated in this analysis; first, because people in the sample who were identified as having no internalising disorder may have undiagnosed mental health problems; and second, in contrast to previous findings from Te Rau Hinengaro,5 the 2015/2016 NZHS did not find that Māori, Pacific and Asian people were more likely to have an internalising disorder. In addition, binary responses to many of the questions relating to service utilisation provide a limited measure to explore complex issues such as satisfaction with GP explanations.
Conclusion
Data from the 2015–16 NZHS show the higher need for primary healthcare among adults with internalising disorders. Findings indicate that even though adults with internalising disorders have greater need for primary healthcare services, they experience more barriers to accessing these services, and report less positive experiences with GPs, than people without an internalising disorder. As the utilisation of primary mental healthcare continues to grow, and clinicians continue to develop new models of care, this study indicates the NZHS may be a useful source of routinely collected data for understanding and monitoring primary health service utilisation and experiences among people with internalising disorders.
COMPETING INTERESTS
The authors report no competing interests. The authors alone are responsible for the content and writing of the paper.
References
[1] Dowell AC, Garrett S, Collings S, et al. Evaluation of the Primary Mental Health Initiatives: Summary Report 2008. Wellington, New Zealand: University of Otago and Ministry of Health; 2009.[2] O’Connell J, Swanson Dobbs A, Bolden F, et al. (2016) Closing the loop: a person-centred approach to primary mental health and addictions support. Auckland: New Zealand Network Four.
[3] Ministry of Health. Primary Mental Health. Wellington, New Zealand: Ministry of Health; 2017 [cited 2017 September 12]. Available from: http://www.health.govt.nz/our-work/primary-health-care/primary-health-care-subsidies-and-services/primary-mental-health
[4] Bagnall C (2016) Developing a service model for primary mental health support for moderate need: an evidence review developed by network 4 in partnership with platform trust. Auckland: New Zealand Network Four.
[5] Oakley Browne MA, Wells JE, Scott KM. Te Rau Hinengaro: The New Zealand Mental Health Survey. Wellington, New Zealand: Ministry of Health; 2006.
[6] Ministry of Health. Annual Update of Key Results 2015/16: New Zealand Health Survey. Wellington, New Zealand: Ministry of Health; 2016.
[7] Ministry of Health. Sample Design from 2015/16: New Zealand Health Survey. Wellington, New Zealand: Ministry of Health; 2016.
[8] Kroenke K. Patients presenting with somatic complaints: epidemiology, psychiatric comorbidity and management. Int J Methods Psychiatr Res. 2003; 12 34–43.
| Patients presenting with somatic complaints: epidemiology, psychiatric comorbidity and management.Crossref | GoogleScholarGoogle Scholar |
[9] Watson D, Pennebaker JW. Health complaints, stress, and distress: exploring the central role of negative affectivity. Psychol Rev. 1989; 96 234–54.
| Health complaints, stress, and distress: exploring the central role of negative affectivity.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaL1M3itFChuw%3D%3D&md5=001c4d66ef28b0afc131794aa13c1f73CAS |
[10] Ministry of Health. The Health of New Zealand Adults 2011/12: Key Findings of the New Zealand Health Survey. Wellington, New Zealand: Ministry of Health; 2012.
[11] Ministry of Health. Care Plus: An Overview. Wellington, New Zealand: Ministry of Health; 2004.
[12] Ministry of Health. Care Plus. Wellington, New Zealand: Ministry of Health; 2014 [cited 2017 September 12]. Available from: http://www.health.govt.nz/your-health/services-and-support/health-care-services/care-plus
[13] Ministry of Health. Better, Sooner, More Convenient Health Care in the Community. Wellington, New Zealand: Ministry of Health; 2011.
[14] Ministry of Health. Community Services Card and High Use Health Card. Wellington, New Zealand: Ministry of Health; 2016 [cited 2017 September 12]. Available from: http://www.health.govt.nz/our-work/primary-health-care/primary-health-care-subsidies-and-services/community-services-card-and-high-use-health-card
[15] Stokes T, Tumilty E, Doolan-Noble F, Gauld R. Multimorbidity, clinical decision making and health care delivery in New Zealand Primary care: a qualitative study. BMC Fam Pract. 2017; 18 51
| Multimorbidity, clinical decision making and health care delivery in New Zealand Primary care: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[16] Signal L, Semper K, Stairmand J, et al. A walking stick in one hand and a chainsaw in the other: patients’ perspectives of living with multimorbidity. NZ Med J. 2017; 130 65–76.
[17] Woltmann E, Grogan-Kaylor A, Perron B, et al. Comparative effectiveness of collaborative chronic care models for mental health conditions across primary, specialty, and behavioral health care settings: systematic review and meta-analysis. Am J Psychiatr. 2012; 169 790–804.
| Comparative effectiveness of collaborative chronic care models for mental health conditions across primary, specialty, and behavioral health care settings: systematic review and meta-analysis.Crossref | GoogleScholarGoogle Scholar |
[18] De Hert M, Correll CU, Bobes J, et al. Physical illness in patients with severe mental disorders. I. Prevalence, impact of medications and disparities in health care. World Psychiatr. 2011; 10 52–77.
| Physical illness in patients with severe mental disorders. I. Prevalence, impact of medications and disparities in health care.Crossref | GoogleScholarGoogle Scholar |
[19] Cunningham R, Sarfati D, Stanley J, et al. Cancer survival in the context of mental illness: a national cohort study. Gen Hosp Psychiatr. 2015; 37 501–506.
| Cancer survival in the context of mental illness: a national cohort study.Crossref | GoogleScholarGoogle Scholar |
[20] Royal New Zealand College of General Practitioners. Policy Brief: Equally Well. Wellington, New Zealand: Royal New Zealand College of General Practitioners; 2017.
[21] Ministry of Health. Rising to the Challenge: The Mental Health and Addiction Service Development Plan 2012–2017. Wellington, New Zealand: Ministry of Health; 2012.
[22] Moffitt TE, Caspi A, Taylor A, et al. How common are common mental disorders? Evidence that lifetime prevalence rates are doubled by prospective versus retrospective ascertainment. Psychol Med. 2010; 40 899–909.
| How common are common mental disorders? Evidence that lifetime prevalence rates are doubled by prospective versus retrospective ascertainment.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3czgvFCrsQ%3D%3D&md5=546515cff189ad42a9a2b92894713559CAS |
[23] World Health Organization. Mental Health Action Plan 2013–2020. Geneva, Switzerland: World Health Organization; 2013.
[24] Ministry of Health. Mental Health and Addiction Workforce Action Plan 2017–2021. Wellington, New Zealand: Ministry of Health; 2017.