Understanding the structure and processes of primary health care for young indigenous children
Natalie A. Strobel 1 2 , Kimberley McAuley 1 , Veronica Matthews 3 , Alice Richardson 2 , Jason Agostino 4 , Ross Bailie 3 , Karen M. Edmond 1 , Daniel McAullay 1 51 Medical School, The University of Western Australia, Crawley, Western Australia, Australia
2 National Centre for Epidemiology & Population Health, Research School of Population Health, Australian National University, Canberra, ACT, Australia
3 University Centre for Rural Health, The University of Sydney, Lismore, NSW, Australia
4 Academic Unit of General Practice, College of Health and Medicine, Australian National University, Canberra, ACT, Australia
5 Kurongkurl Katitjin, Centre for Indigenous Australian Education and Research, Edith Cowan University, Mt Lawley, Western Australia, Australia
Correspondence to: Natalie A. Strobel, School of Biomedical Sciences, The University of Western Australia, 35 Stirling Highway, Crawley, WA 6009, Australia. Email: natalie.strobel@uwa.edu.au
Journal of Primary Health Care 10(3) 267-278 https://doi.org/10.1071/HC18006
Published: 28 August 2018
Journal Compilation © Royal New Zealand College of General Practitioners 2018.
This is an open access article licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Abstract
INTRODUCTION: Primary health care organisations need to continuously reform to more effectively address current health challenges, particularly for vulnerable populations. There is growing evidence that optimal health service structures are essential for producing positive outcomes.
AIM: To determine if there is an association between process of care indicators (PoCIs) for important young indigenous child health and social issues and: (i) primary health-care service and child characteristics; and (ii) organisational health service structures.
METHODS: This was a cross-sectional study of 1554 clinical child health audits and associated system assessments from 74 primary care services from 2012 to 2014. Composite PoCIs were developed for social and emotional wellbeing, child neurodevelopment and anaemia. Crude and adjusted logistic regression models were fitted, clustering for health services. Odds ratios and 95% confidence intervals were derived.
RESULTS: Overall, 32.0% (449) of records had a social and emotional wellbeing PoCI, 56.6% (791) had an anaemia PoCI and 49.3% (430) had a child neurodevelopment PoCI. Children aged 12–23 months were significantly more likely to receive all PoCIs compared to children aged 24–59 months. For every one point increase in assessment scores for team structure and function (aOR 1.14, 95% CI 1.01–1.27) and care planning (aOR 1.14, 95% CI 1.01–1.29) items, there was a 14% greater odds of a child having an anaemia PoCI. Social and emotional wellbeing and child neurodevelopment PoCIs were not associated with system assessment scores.
DISCUSSION: Ensuring young indigenous children aged 24–59 months are receiving quality care for important social and health indicators is a priority. Processes of care and organisational systems in primary care services are important for the optimal management of anaemia in indigenous children.
KEYWORDS: Indigenous health; health services; health systems; paediatrics; epidemiology
| WHAT GAP THIS FILLS |
| What is already known: Organisational health service structures have enabled primary health-care services to improve their quality of care for indigenous adult chronic disease management and maternal care; however, there is little information on how the organisation of health systems structures influences the processes of care for important health and wellbeing indicators for young indigenous children. |
| What this study adds: This research highlights that organisational health service structures are important for the delivery and management of anaemia for indigenous children. Primary health-care services should be supported in delivering social and emotional wellbeing, child neurodevelopment and anaemia care for children aged 25–59 months. |
Introduction
Internationally, the health and social wellbeing of young indigenous children are of major concern.1 In Australia, young Aboriginal and Torres Strait Islander children (hereafter ‘indigenous’) remain a high-risk group for experiencing adverse health and social outcomes such as otitis media,2 child neurodevelopment delay3 and birth outcomes such as prematurity and low birthweight4 compared to non-indigenous Australian children. Despite this, improvements in primary health care, coupled with major policy and funding changes, has resulted in an increase of important child health indicators including child health assessments and vaccination coverage.4–7
Primary health care plays an important role in the delivery of community and preventive health services. However, providing high-quality care remains an ongoing challenge.8 Detailed measurement and evaluation of the quality of care delivered to indigenous children is needed to track and improve service delivery. This can be determined through understanding the relationship and interplay between the three categories of quality of care: structure (attributes and organisational structures that define a health system); processes (delivering and receiving care); and outcomes (the consequences or effect of care on health status).9 Good structural systems are expected to lead to good processes of care and ultimately improved outcomes.9 It is therefore important to objectively assess the relationship between these three categories and service delivery to children in real world situations.
The Assessment of Chronic Illness Care (ACIC) tool was developed to help health services understand the organisation of care within their systems, identify areas for improvement and evaluate the level and nature of these changes for people living with a chronic disease.10 The ACIC team identified six areas of system change: delivery system design, self-management, clinical information systems, linkages to community resources, decision support, and organisation of the health system.10 In 2005, the Audit and Best Practice for Chronic Disease (ABCD) programme (a continuous quality improvement (CQI) programme in Australia) modified the ACIC tool, added three items (cultural competence, laboratory management and pharmacy management) and developed the Systems Assessment Tool (SAT).11 The SAT has enabled indigenous health services to assess their health-care systems and improve the quality of care they provide.11,12
To date, the SAT has been used to assess the quality of care for diabetes and pregnancy.11,13,14 The SAT has yet to be used to assess on a broad scale the quality of care delivered through organisations of care (structures) for indigenous children and key process of care indicators (PoCIs) for important childhood health and social issues, in particular, social and emotional wellbeing, anaemia and child neurodevelopment. Therefore, the objectives of this study were to determine whether there was an association between social and emotional wellbeing, anaemia and child neurodevelopment PoCIs and: (i) primary health-care service and child characteristics; and (ii) organisational health service structures. It was hypothesised that fully supported organisations and structures within health services would result in increased improvement in processes of care for indigenous children.
Methods
Study setting
This was a retrospective cross-sectional study of 1554 child health audits that included SAT data from remote, rural and urban primary health-care services that participated in the ABCD programme in Queensland, Northern Territory, South Australia and Western Australia from 2012 to 2014. The most recent record for each child was included.
Data collection
ABCD audits
Annual child health audits from participating primary health-care services were completed by primary care staff who had received training by ABCD educators.15,16 Files had to meet the following criteria to be eligible for auditing: (1) child is aged 3 months to 14 years at the audit date; (2) child is a resident in the community for at least 6 months (or half of the time since birth if aged <6 months); and (3) child has no major health anomalies such as heart defects or inherited disorders.
A random sample of at least 30 files was selected for audit from each participating primary health-care service. The sampling process included stratification of sex to ensure similar numbers. The auditors read each client file (electronic and paper) and recorded information in a standardised pre-coded data collection tool. Child characteristics included: date of birth, age, sex, indigenous status, attendance at the primary care centre in the previous 12 months, reason for the last attendance (acute care, health check, vaccination, other) and receipt of any child health checks in the last 12 months (Australian Commonwealth funded [Medicare 715] or other child health check). Health centre characteristics included governance (Aboriginal community-controlled health service or government operated), location (urban, rural or remote) and number of CQI audits the primary care centre had completed. The auditors scored ‘yes’ in the audit tool if there had been any documentation in the client file in the last 12 months, ‘no’ if there was no documentation and ‘not applicable’ if a service was not recommended or scheduled within that jurisdiction.
The ABCD audit tool included 11 pre-coded items about social and emotional wellbeing services, seven on anaemia and six on child neurodevelopment. Descriptions of these items are provided in Supplementary material table 1 (available at journal’s website).
|
SAT audit
The SAT (Supplementary material table 2) included five components (delivery system design; information systems and decision support; self-management support; links with community, other health service and other services; and organisational influence and integration), with multiple items for each component. The SAT was self-completed in each primary health-care service by staff and a trained CQI facilitator. Each item within a component was scored as 0–2 (limited), 3–5 (basic), 6–8 (good) and 9–11 (fully developed) by the health service. The tool included a brief description of each component and item to help health service staff decide on their existing support. The CQI facilitator helps health service staff reach agreement about what best represents their health system. Each component score was calculated as the mean of the individual items. The overall organisation of the health system score was the mean of the four component scores. We did not include the self-management component of the SAT due to perceptions that this was of limited relevance to the study outcomes.

|
Definitions
We defined PoCIs as:
-
Social and emotional wellbeing : using four items comprising advice provided to parents or carers at least once in the last 12 months about: domestic environment, social support, housing condition and child stimulation for all children aged 3–59 months.
-
Anaemia : using two items comprising advice provided at least once in the last 12 months about nutrition and haemoglobin, documented in the last 12 months for all children aged 6–59 months.
-
Child neurodevelopment : using five items comprising assessment provided in the last 12 months for parent–child interaction (<2 years), developmental milestones, vision and hearing testing for all children aged 3–59 months. Advice about physical and mental stimulation of the child was also included for all children aged 3–59 months.
The PoCIs were developed using the Primary Clinical Care Manual for Queensland,17,18 the Central Australian Rural Practitioners Association (CARPA) standard treatment manuals for Northern Territory and South Australia19 and the Kimberley Aboriginal Medical Service guidelines.20,21 The Medicare Benefits Schedule (MBS) child health check22 and the National guide to a preventive health assessment for Aboriginal and Torres Strait Islander people23 were also consulted in the development of the PoCIs. To develop the PoCIs, there had to be commonality in individual items between jurisdictions. The PoCIs were dichotomised into a score of ‘yes’ if an audit record showed evidence that all items had been completed or ‘no’ if records were partially or not completed (Supplementary material table 3).

|
Statistical analysis
Descriptive statistics were calculated as counts and percentages for all categorical data, and median and interquartile ranges (IQR, 75% percentile – 25% percentile) for continuous data. Data analyses were conducted using STATA 13.1 (StataCorp, College Station, TX, USA).
PoCIs and child and primary health service characteristics
To examine the effect of primary health-care service and child characteristics on the probability of having a PoCI, multilevel binomial models with an exchangeable correlation structure and robust standard errors were used. Adjusted logistic regression models were fitted using generalised estimating equations and the primary health-care service as the clustering variable. Odds ratios and 95% confidence intervals (95% CI) were derived. Important explanatory variables were constructed a priori and included: sex, year of data collection, geographic location, governance and CQI participation.
PoCIs and SAT components
To assess associations between SAT components and the three PoCIs, crude and adjusted logistic regression models were fitted using generalised estimating equations and the primary health-care service as the clustering variable. Multilevel binomial models with an exchangeable correlation structure and robust standard errors were also constructed, and odds ratios and 95% CIs were derived. Important explanatory variables were constructed a priori and included: year of data collection, geographical location, governance, CQI participation and the number of health areas SAT was related to.
Ethics approval
Ethics approval was obtained from all Human Research Ethics Committees in the states and territories involved: the Human Research Ethics Committee of the Northern Territory Department of Health and Menzies School of Health Research (HREC-205 EC00153); Central Australian Human Research Ethics Committee (HREC-12–53); Queensland Human Research Ethics Committee of the Darling Downs Health Services District (HREC/11/QTDD/47); South Australian Indigenous Health Research Ethics Committee (04–10–319); Curtin University Human Research Ethics Committee (HR140/2008); Western Australian Country Health Services Research Ethics Committee (2011/27); Western Australian Aboriginal Health Ethics Committee (111–8/05); University of Western Australia Human Research Ethics Committee (RA/4/1/5051); and the Australian National University (2017/560).
Results
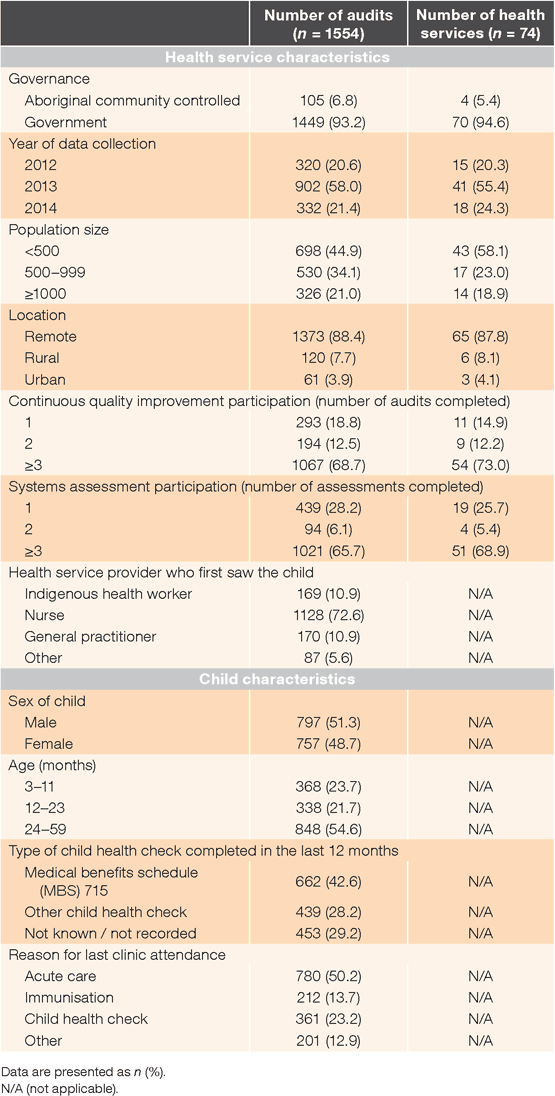
During 2012–14, there were 1554 records audited from 74 primary health-care services that completed the SAT (Table 1). Most health services (94.6%, 70/74) were government run, serviced a population of <500 people (58.1%, 43/74), were in remote locations (87.8%, 65/74) and had participated in three or more CQI cycles (73.0%, 54/74) (Table 1). Approximately half (54.6%, 848/1554) of records audited were for children aged between 24 and 59 months.
PoCIs and child and primary health service characteristics
Less than one-third of records (32.0%, 449) had a social and emotional wellbeing PoCI, 56.6% (791) had an anaemia PoCI and just under half (49.3%, 430) had a child neurodevelopment PoCI (Table 2). Children aged 12–23 months had increased odds of receiving a PoCI for social and emotional wellbeing (aOR 1.35, 95% CI 1.01–1.49), anaemia (aOR 1.68, 95% CI 1.30–2.18) and child neurodevelopment (aOR 1.80, 95% CI 1.12–2.90) compared to children aged 24–59 months (Table 2). Children who received acute care were less likely to have a PoCI for social and emotional wellbeing (aOR 0.74, 95% CI 0.57–0.96), anaemia (aOR 0.62, 95% CI 0.49–0.77) and child neurodevelopment (aOR 0.61, 95% CI 0.44–0.85) than children who received a child health check (Table 2).
PoCIs and SAT components
Two items within the delivery system design SAT component were significantly associated with the anaemia PoCI. For every one point increase in the team structure and function item, there was a 14% greater odds of having an anaemia PoCI (aOR 1.14, 95% CI 1.01–1.27) (Table 3). A similar trend was shown for care planning where for every one point increase in the care planning item, there was also a 14% greater odds of having the anaemia PoCI (aOR1.14, 95% CI 1.01–1.29) (Table 3). Social and emotional wellbeing and child neurodevelopment PoCIs were not influenced by delivery systems design (Table 3). There was no association between information systems and decision support, links with community and other health and non-health services or organisational influence and integration on any of the three PoCIs (Table 4–6). For all three PoCIs, there was little difference in the median and interquartile ranges for each system assessment item and component between children receiving the PoCI and children who did not (Supplementary material table 4).

|

|

|
Discussion
There was wide variation on the delivery of PoCIs, with 32.0% of children receiving PoCIs for social and emotional wellbeing, 56.6% for anaemia and 49.3% for child neurodevelopment. Children who were aged 12–23 months were more likely to receive the PoCIs than children aged 24–59 months. Contrary to our expectations, there was little association between an organisation’s health structures and processes of care for social and emotional wellbeing and child neurodevelopment. However, we found that the delivery system design component, which included items for team structure and function and care planning, were associated with the process of care provided for anaemia.
Based on the reporting of child health indicators, CQI has improved the delivery of many child health milestones and brief interventions over time.4 As a result, we anticipated that 50% of records would achieve our PoCIs. However, social and emotional wellbeing (32%) fell well short of this. In contrast, anaemia (60%) and child neurodevelopment (49%) reached the expected target. Our data also indicate that the provision of care varies greatly, depending on the routine service provided.
There has been much concern in primary health-care centres about the high levels of iron-deficiency anaemia in young indigenous children.24 Substantial emphasis in recent years on improving these rates in remote regions has included improving primary and secondary prevention through implementing CQI initiatives, health sector forums and community engagement. In our study, elements of team structure and functioning including team leadership, defining roles and responsibilities and building capacity, as well as care planning that includes planning as part of routine practice, and consistency with best practice guidelines, were shown to be positive in improving anaemia care. Capacity building with health service providers for anaemia care has fostered important changes in health services and provided quality care to children.25 Alternatively, non-adherence to guidelines has resulted in poor management of children with anaemia.26
In contrast, there has been little focus on the more complex processes of care needed for social and emotional wellbeing and child neurodevelopment, and this is reflected in the lower PoCIs that we reported for these two conditions.27 The delivery of child neurodevelopment assessments has been shown to vary across primary health-care services, and researchers have recently called for a more system-wide approach to improve delivery, recording and monitoring.28 There has been a recent emphasis on the importance of child neurodevelopment and the delivery of social and emotional services in family-centred care practice. Thus, it is expected that we will see improvements in the provision of care for these important areas in the coming years.29,30
It is our understanding that this is the first study to investigate associations between a standardised SAT assessment of quality of care and the processes of care delivered to indigenous children in primary health care. It has previously been shown that a health-care system’s organisational influence and integration is positively associated with the quality of care provided to adults for diabetes control (HbA1C), blood pressure and total cholesterol levels.31 However, we found no association between the organisation of health systems and the provision of care for children as measured by our neurodevelopment and social and emotional wellbeing PoCIs. Almost 70% of the health services had completed at least three or more SAT cycles, thus this may have improved the organisation of all the health-care systems in terms of these PoCIs over time. It is also possible that other factors have resulted in this lack of association, including lack of assessment of communication and patient-centred care, which were not included in our analysis and the potential for under-reporting in health records. Despite this, processes of care and organisational systems in primary care services were shown to be important for the optimal management of anaemia in indigenous children and should be enhanced.
There are several limitations to this study. Although guidance and facilitation was provided to local health centre staff and managers to complete the SAT, in practice, they were largely completed by front-line primary health-care teams without direct standardised support. This is likely to influence how the tool was completed. It was decided that the process of care delivered should be maximal and therefore included all elements documented. Although the PoCIs have not been validated, we believe this study has demonstrated an important use of them. In addition, we constructed them through ensuring that they were specific, measurable, attainable, relevant and trackable. It is also possible that for some levels of care, there was no or little documentation of this in the health-care records.
This was a cross-sectional study so we could only report associations and could not assess causality. The positive results seen in our analyses may be the result of type 1 error; however, given that our P values were not borderline and we have narrow confidence intervals, we are confident in our results. Due to the voluntary nature of participation by primary health-care services in this study, the findings are not necessarily generalisable to all primary health-care services. Most of the health services were government-run (94.6%), located in remote areas (87.8%) and serviced populations of <500 (58.1%) people. This also limits the potential generalisability of findings to other health services, in particular Aboriginal Community-Controlled Health Organisations.
Conclusion
Our study found that organisational health service structures, which included items for team structure and function and care planning, were associated with quality of anaemia care. This study provides evidence that organisation of health services is associated with the prevention and management of anaemia for young indigenous children. In addition, our young indigenous children aged 24–59 months are not receiving care for important social and health indicators. Child health checks are an important avenue to ensuring quality care is provided.
FUNDING
This research was supported by an Australian Government Research Training Program (RTP) Scholarship. This study was also funded by the National Health and Medical Research Council of Australia. The funders had no role in the design of the study and collection, analysis and interpretation of data, and in writing the manuscript.
COMPETING INTERESTS
The authors declare that they have no competing interests.
ACKNOWLEDGEMENTS
We would like to thank the ABCD team, participating health services and CQI facilitators for the data collection for this project.
References
[1] Anderson I, Robson B, Connolly M, et al. Indigenous and tribal peoples’ health (The Lancet-Lowitja Institute Global Collaboration): a population study. Lancet. 2016; 388 131–57.| Indigenous and tribal peoples’ health (The Lancet-Lowitja Institute Global Collaboration): a population study.Crossref | GoogleScholarGoogle Scholar |
[2] Leach AJ, Wigger C, Andrews R, et al. Otitis media in children vaccinated during consecutive 7-valent or 10-valent pneumococcal conjugate vaccination schedules. BMC Pediatr. 2014; 14 200–10.
| Otitis media in children vaccinated during consecutive 7-valent or 10-valent pneumococcal conjugate vaccination schedules.Crossref | GoogleScholarGoogle Scholar |
[3] Brinkman SA, Gialamas A, Rahman A, et al. Jurisdictional, socioeconomic and gender inequalities in child health and development: analysis of a national census of 5-year-olds in Australia. BMJ Open. 2012; 2 e001075
| Jurisdictional, socioeconomic and gender inequalities in child health and development: analysis of a national census of 5-year-olds in Australia.Crossref | GoogleScholarGoogle Scholar |
[4] McAullay D, McAuley K, Bailie R, et al. Sustained participation in annual continuous quality improvement activities improves quality of care for Aboriginal and Torres Strait Islander children. J Paediatr Child Health. 2018; 54 132–40.
[5] Cashman PM, Allan NA, Clark KK, et al. Closing the gap in Australian Aboriginal infant immunisation rates – the development and review of a pre-call strategy. BMC Public Health. 2016; 16 514–20.
| Closing the gap in Australian Aboriginal infant immunisation rates – the development and review of a pre-call strategy.Crossref | GoogleScholarGoogle Scholar |
[6] Australian Institute of Health and Welfare. Aboriginal and Torres Strait Islander Health Performance Framework 2012: detailed analyses. Cat. no. IHW 94. Canberra: AIHW; 2013.
[7] Commonwealth of Australia, Department of the Prime Minister and Cabinet. Closing the Gap - Prime Minister’s Report 2017. Canberra: Commonwealth of Australia; 2017.
[8] Donabedian A. The seven pillars of quality. Arch Pathol Lab Med. 1990; 114 1115–8.
[9] Donabedian A. The quality of care. How can it be assessed? JAMA 1988; 260 1743–8.
| The quality of care. How can it be assessed?Crossref | GoogleScholarGoogle Scholar |
[10] Bonomi AE, Wagner EH, Glasgow RE, VonKorff M. Assessment of chronic illness care (ACIC): a practical tool to measure quality improvement. Health Serv Res. 2002; 37 791–820.
| Assessment of chronic illness care (ACIC): a practical tool to measure quality improvement.Crossref | GoogleScholarGoogle Scholar |
[11] Si D, Bailie R, Connors C, et al. Assessing health centre systems for guiding improvement in diabetes care. BMC Health Serv Res. 2005; 5 56–64.
| Assessing health centre systems for guiding improvement in diabetes care.Crossref | GoogleScholarGoogle Scholar |
[12] Cunningham FC, Ferguson-Hill S, Matthews V, Bailie R. Leveraging quality improvement through use of the Systems Assessment Tool in Indigenous primary health care services: a mixed methods study. BMC Health Serv Res. 2016; 16 583–593.
| Leveraging quality improvement through use of the Systems Assessment Tool in Indigenous primary health care services: a mixed methods study.Crossref | GoogleScholarGoogle Scholar |
[13] Gibson-Helm ME, Rumbold AR, Teede HJ, et al. Improving the provision of pregnancy care for Aboriginal and Torres Strait Islander women: a continuous quality improvement initiative. BMC Pregnancy Childbirth 2016; 16 118–28.
| Improving the provision of pregnancy care for Aboriginal and Torres Strait Islander women: a continuous quality improvement initiative.Crossref | GoogleScholarGoogle Scholar |
[14] Gibson-Helm ME, Teede HJ, Rumbold AR, et al. Continuous quality improvement and metabolic screening during pregnancy at primary health centres attended by Aboriginal and Torres Strait Islander women. Med J Aust. 2015; 203 369–70.
| Continuous quality improvement and metabolic screening during pregnancy at primary health centres attended by Aboriginal and Torres Strait Islander women.Crossref | GoogleScholarGoogle Scholar |
[15] Bailie R, Sibthorpe B, Gardner K, Si D. . Quality improvement in Indigenous Primary Health Care: history, current initiatives and future directions. Aust J Primary Health. 2008; 14 53–7.
| Quality improvement in Indigenous Primary Health Care: history, current initiatives and future directions.Crossref | GoogleScholarGoogle Scholar |
[16] Bailie R, Si D, Shannon C, et al. Study protocol: national research partnership to improve primary health care performance and outcomes for Indigenous peoples. BMC Health Serv Res. 2010; 10 129–39.
| Study protocol: national research partnership to improve primary health care performance and outcomes for Indigenous peoples.Crossref | GoogleScholarGoogle Scholar |
[17] Queensland Health. Statewide Health Check Forms 2016. Cairns: Queensland Government. [cited 2016 April 20]. Available from: https://www.health.qld.gov.au/rrcsu/html/health-check-forms
[18] Queensland Health, Royal Flying Doctor Service. (Queensland Section). Primary Clinical Care Manual, 9th edn. Cairns: The Rural and Remote Clinical Support Unit, Torres and Cape Hospital and Health Service; 2016.
[19] Remote Primary Health Care Manuals. CARPA Standard Treatment Manual, 7th edn. Alice Springs, NT: Centre for Remote Health; 2017.
[20] Kimberley Aboriginal Medical Services Council (KAMSC). WA Country Health Service (WACHS) Kimberley. Anaemia in Children. Kimberley: Kimberley Aboriginal Medical Services Council; 2015.
[21] Kimberley Aboriginal Medical Services Council (KAMSC). WA Country Health Service (WACHS) Kimberley. Healthy Kids. Kimberley: Kimberley Aboriginal Medical Services Council; 2011.
[22] Department of Health. Health assessment for Aboriginal and Torres Strait Islander people (MBS Item 715). Medicare Benefits Schedule - Note AN.0.44. Canberra: Commonwealth of Australia; 2016. [cited 2016 April 9] Available from: http://www9.health.gov.au/mbs/fullDisplay.cfm?type=note8qt=NoteID8q=AN.0.44
[23] NACCHO/RACGP. National guide to a preventive health assessment for Aboriginal and Torres Strait Islander people, 2nd edn. South Melbourne: The RACGP; 2012. [cited 2016 April 8]. Available from: http://www.naccho.org.au/download/aboriginal-health/1.National%20guide%20to%20a%20preventive%20health%20assessment%20for%2 0Aboriginal%20and%20Torres%20Strait%20Islander%20people%20%282%29.pdf
[24] Khambalia AZ, Aimone AM, Zlotkin SH. Burden of anemia among indigenous populations. Nutr Rev. 2011; 69 693–719.
| Burden of anemia among indigenous populations.Crossref | GoogleScholarGoogle Scholar |
[25] Shet AS, Rao A, Jebaraj P, et al. Lay health workers perceptions of an anemia control intervention in Karnataka, India: a qualitative study. BMC Public Health. 2017; 17 720–28.
| Lay health workers perceptions of an anemia control intervention in Karnataka, India: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[26] Bar-Zeev SJ, Kruske SG, Barclay LM, et al. Adherence to management guidelines for growth faltering and anaemia in remote dwelling Australian Aboriginal infants and barriers to health service delivery. BMC Health Serv Res. 2013; 13 250–61.
| Adherence to management guidelines for growth faltering and anaemia in remote dwelling Australian Aboriginal infants and barriers to health service delivery.Crossref | GoogleScholarGoogle Scholar |
[27] Langham E, McCalman J, Matthews V, et al. Social and emotional wellbeing screening for Aboriginal and Torres Strait Islanders within primary health care: a series of missed opportunities? Front Public Health. 2017; 5 159–67.
| Social and emotional wellbeing screening for Aboriginal and Torres Strait Islanders within primary health care: a series of missed opportunities?Crossref | GoogleScholarGoogle Scholar |
[28] D’Aprano A, Silburn S, Johnston V, et al. Challenges in monitoring the development of young children in remote Aboriginal health services: clinical audit findings and recommendations for improving practice. Rural Remote Health. 2016; 16 3852.
[29] McCalman J, Heyeres M, Campbell S, et al. Family-centred interventions by primary healthcare services for Indigenous early childhood wellbeing in Australia, Canada, New Zealand and the United States: a systematic scoping review. BMC Pregnancy Childbirth. 2017; 17 71–91.
| Family-centred interventions by primary healthcare services for Indigenous early childhood wellbeing in Australia, Canada, New Zealand and the United States: a systematic scoping review.Crossref | GoogleScholarGoogle Scholar |
[30] Department of Health. National Framework for Health Services for Aboriginal and Torres Strait Islander Children and Families. Canberra: Australian Government; 2016.
[31] Si D, Bailie R, Dowden M, et al. Assessing quality of diabetes care and its variation in Aboriginal community health centres in Australia. Diabetes Metab Res Rev. 2010; 26 464–73.
| Assessing quality of diabetes care and its variation in Aboriginal community health centres in Australia.Crossref | GoogleScholarGoogle Scholar |


