Hunter and New England HealthPathways: a 4-year journey of integrated care
Jane S. Gray A , Judith R. Swan A E , Margaret A. Lynch A B , Tracey M. Tay A , Marika-Jane Mackenzie B , John H. Wiggers C , Karen A. Harrison A , Robert C. McDonald D , Ian P. O’Dea B , Louise M. Harrigan A , Sandra M. Fitzgerald B and on behalf of the Hunter and New England HealthPathways Steering CommitteeA Partnerships, Innovation & Research, Hunter New England Local Health District, 56 Stewart Avenue, Hamilton East, NSW 2303, Australia. Email: Jane.Gray@hnehealth.nsw.gov.au; Margaret.Lynch@hnehealth.nsw.gov.au; Tracey.Tay@hnehealth.nsw.gov.au; Karen.Harrison@hnehealth.nsw.gov.au; Louise.Harrigan.@hnehealth.nsw.gov.au
B Hunter New England Central Coast Primary Health Network, Suite 11, 125 Bull Street, Newcastle West, NSW 2302, Australia. Email: mmackenzie@hneccphn.com.au; IOdea@hneccphn.com.au; sfitzgerald@hneccphn.com.au
C Population Health Hunter New England Local Health District, School of Medicine and Public Health, University of Newcastle, Longworth Avenue, Wallsend, NSW 2287, Australia. Email: John.Wiggers@hnehealth.nsw.gov.au
D BMcD Consulting, Newcastle, NSW 2300, Australia. Email: bmcdonald@bmcdconsulting.com
E Corresponding author. Email: Judith.Swan@hnehealth.nsw.gov.au
Australian Health Review 42(1) 66-71 https://doi.org/10.1071/AH16197
Submitted: 31 August 2016 Accepted: 9 December 2016 Published: 20 February 2017
Journal compilation © AHHA 2018 Open Access CC BY-NC-ND
Abstract
Objective This paper describes the 4-year journey of Hunter and New England HealthPathways – a password-protected web-based portal designed to provide localised evidence-informed clinical and referral information to support general practice at the point of care.
Methods A process evaluation was conducted in 2013, with a case study comparison performed in 2014 to assess impact of HealthPathways on patient referral and access to specialist care, followed by a review in 2016 of utilisation of the online portal to assess whether healthcare providers continued to access HealthPathways.
Results Increased utilisation was correlated with an increase in the number of pathways published online. Clinical leadership and the process of developing pathways built relationships between primary care and specialist teams. Case studies indicated that a comprehensive approach to pathway implementation accompanied by service redesign resulted in higher pathway use and improved access to specialist care. Senior management support and a formal partnership between major health care providers led to strong governance of HealthPathways and the delivery of other integrated care initiatives. There was significant growth in utilisation over the 4 years, increasing to an average of 6679 sessions per month in 2016 and more general practices reported use of HealthPathways.
Conclusions HealthPathways is a vehicle for building strong foundations to support system change and integrated care. The critical elements for acceptability, growth and sustainability are the strong relationships between primary care and specialist clinicians, as well as formal partnerships that are built from the processes used to develop HealthPathways.
What is known about the topic? HealthPathways and similar web-based evidence-informed guidelines aimed at improving system integration are increasing in Australia. There are few published papers that describe approaches to inform the ongoing implementation of such programs.
What does this paper add? This paper describes iterative methodology for evaluating complex programs, such as HealthPathways, that identifies the critical factors required to build sustainable models of integrated care.
What are the implications for practitioners? The 4-year experience of Hunter and New England HealthPathways provides an approach to improve the implementation, sustainability and spread of similar programs and associated integrated care initiatives.
Introduction
Hunter and New England (H&NE) HealthPathways is a joint initiative between the Hunter New England Local Health District (HNELHD) and the Hunter New England Central Coast Primary Health Network (HNECCPHN). HealthPathways was designed to support general practice at the point of care through a single source of evidence-informed clinical and referral information that is developed, agreed and maintained locally. The different pathways are made available to clinicians in a standardised format via a password-protected web-based portal. HealthPathways originated in New Zealand as part of the Canterbury Initiative.1 The Hunter region in New South Wales (NSW) implemented the program in 2012, and was the first such partnership in Australia. Both HNELHD and the HNECCPHN considered HealthPathways to be a critical component in a range of strategies aimed at improving patient access to evidence-informed care at the right time in the right place. HealthPathways is now being implemented at 22 sites across Australia, nine regions in New Zealand and one in the UK.2
The need for local decision support tools was highlighted in the CareTrack Australia study,3 which found that adult Australians received appropriate care in 57% of healthcare encounters. However, accessing clinical guidelines was problematic for healthcare providers, with issues of volume, duplication, differing recommendations, inconsistent structure and currency.4 Internationally, it has been found that point-of-care online clinical decision support tools that are locally customised and combined with service redesign improve the appropriateness of referrals, decrease patient waiting times and reduce costs,5 and that referral guidelines improve appropriateness of care by improving prereferral investigation and treatment.6
In Canterbury (New Zealand), HealthPathways improved referral quality, triage and working relationships between clinicians.7 It also resulted in a wider range of conditions being investigated and treated in general practice.8 As well as the clinical benefits, the process of developing HealthPathways was a valuable change management tool for redesigning services and increasing healthcare integration.9
H&NE HealthPathways was developed in a clearly defined process. Individual pathways are written collaboratively by general practice and specialist teams, with the final product designed to be usable by general practice. Where there are disputes about the strength of evidence for a particular topic, the team agrees on a way of working locally. Pathways are then sent for wider consultation before publication online. The medical lead of relevant clinical areas endorses the final content. An important step in the process is to identify what is working well or not so well in both primary and tertiary care in order to identify opportunities for redesign.
To June 2016, over 230 pathways had been developed for the Hunter region HealthPathways initiative and were being localised for the New England region of NSW. The process has directly involved more than 350 clinicians, with more than another 1000 involved in wider consultation.
Evaluating HealthPathways is a challenge for those implementing such programs because the impact and outcomes cannot be measured independently of associated initiatives.10 The approach to evaluation of H&NE HealthPathways was formative and phased to ensure continuous learning and cycles of improvement.
Phases 1 and 2 of H&NE HealthPathways evaluations were conducted in 2013 and 2014 respectively, along with a review of utilisation in 2016. Phase 1 was a process evaluation to assess utilisation, stakeholder perceptions, the implementation approach, critical success factors and barriers.11 Phase 2 aimed to assess ongoing utilisation of HealthPathways and early indications of impact on patient referral and access to specialist care.12 The 2016 review of utilisation aimed to assess sustainability and spread of H&NE HealthPathways.
The aim of this paper is to describe the evaluation journey of H&NE HealthPathways, the key findings at each phase and how the results have informed ongoing integrated care initiatives.
Methods
Phase 1: 2013 process evaluation
Google analytics data
The number of sessions (individual visits) to H&NE HealthPathways was extracted for the period April 2012–August 2013 and correlated with the number of new live pathways in the period.
General practice surveys
A telephone survey was conducted of practice managers of all 129 medium (two to five GPs) -to-large practices (6 or more GPs) in the region, asking them ‘Do you use HealthPathways?’. In addition, a hardcopy survey was circulated to 105 general practitioners (GPs) at a local annual education event regarding the ease of HealthPathways navigation and its impact on practice. Respondents were asked whether they were likely to use HealthPathways while seeing patients and their level of agreement (rated using five-point Likert scale) with the statements that HealthPathways: (1) is easy to navigate; and (2) has ‘changed my clinical practice, the way I make referrals and the information I provide to my patients’.
Stakeholder perceptions
Thirty interviews were conducted with 11 GPs, nine specialist medical clinicians, five specialist nursing and allied health clinicians and five senior managers from both the Hunter Medicare Local (HML; previous organisation to the HNECCPHN) and the HNELHD, and two focus groups were conducted with key project staff (n = 6 in total for both groups). Informed consent was obtained and all interviews and focus groups were taped and transcribed. A thematic analysis was conducted using Dedoose software by SocioCultural Research Consultants, LLC (http://www.dedoose.com; accessed 19 December 2016).
Pathway development review by audit of existing documentation
The Phase 1 evaluation was conducted by an external consultant under the direction and support of the H&NE HealthPathways Evaluation Steering Committee.
Phase 2: 2014 impact evaluation
Google analytics data
Google analytics data for the total number of sessions on HealthPathways for the period January–March 2014 was extracted and collated and then compared with the same period in 2013.
General practice surveys
The Phase 1 telephone survey of practice managers was repeated for all 218 general practices (35 large (i.e. six or more GPs), 104 medium (i.e. two to five GPs) and 79 solo practices) in the region regarding their use of HealthPathways. Data from the large and medium-sized practices were compared with the results from the Phase 1 survey and the collated results were analysed using a Chi-square test.
Case studies
Case studies of three pathways were reviewed to assess the impact of HealthPathways on the quality of referrals and access to specialist care. Routine Antenatal Care, Persistent Non-Cancer Pain and Suicide Risk HealthPathways were selected based on the following criteria: (1) they had been complete and in operation for 12 months or more; (2) they had been developed to address a condition of high prevalence in the community; (3) they had higher utilisation compared with all H&NE HealthPathways; (4) there had been no major changes to the pathway in the previous 6 months; and (5) they had been developed according to the H&NE HealthPathways model.
The quality of referrals was assessed by audits of a random sample of referrals before and after implementation of each pathway: 50 referrals each before and after to maternity services for the antenatal pathway; 23 referrals before and 41 after to the local pain service for the pain pathway; 50 referrals each before and after for suicide or self-harm to the mental health service and another 50 referrals each before and after to the primary healthcare suicide and self-harm program for the Suicide Risk pathway. A standard audit tool was adapted from the Royal Australasian College of General Practitioner (RACGP) Standards for general practices (4th edition) Referral documents (Available at: https://www.racgp.org.au/your-practice/standards/standards4thedition/practice-services/1-6/referral-documents/; accessed 19 December 2016) with referral information items included from the relevant HealthPathway.
Access to specialist care was assessed via the referral audit process for referrals to the John Hunter Hospital Maternity Services and Pain Service using time between receipt of the referral and time of care provided. No indicator for access to specialist care was identified for the suicide risk pathway.
Document reviews, feedback from key stakeholders and checklists were developed to assess pathway development and implementation based on the critical success factors identified in Phase 1.
2016: review of website utilisation
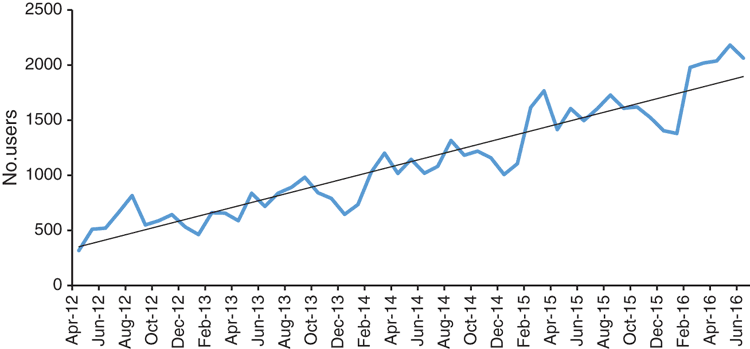
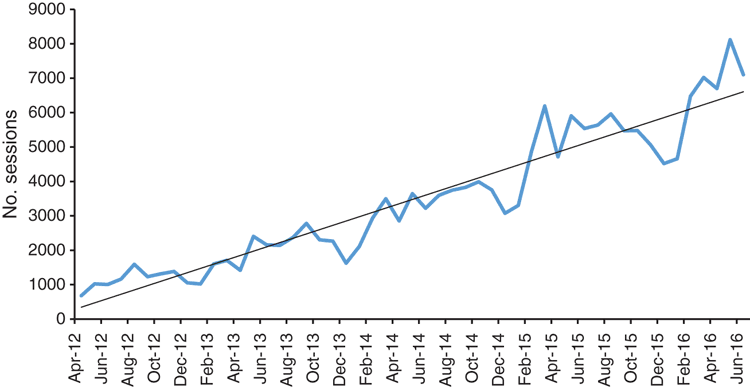
Google analytics data were trended from commencement of the program in April 2012 to June 2016 for the number of sessions and number of users per month. Regression analysis was conducted to assess whether the monthly growth in utilisation was statistically significant.
Phase 1 and 2 evaluations received ethics approval from the HNELHD Human Research Ethics Committee.
Results
Phase 1: process evaluation
Utilisation of HealthPathways doubled over the first 12 months and the increase in the number of sessions was correlated with the increase in the number of pathways going live (r = 0.749).
Of the 86 general practices that responded to the telephone survey (67% response rate), 37% used HealthPathways, 30% did not and 33% were unsure.
Of the 35 GPs who completed the survey (33% response rate), 71% said that they were likely to use HealthPathways while seeing patients, with 91% of these indicating the site was easy to navigate. Of those who used HealthPathways, 81% agreed it changed clinical practice, 61% agreed it changed the information provided to patients and 57% agreed it changed the way they made referrals.
Perceptions about HealthPathways from GPs, clinical leaders and senior managers involved in the process were positive. Themes from the interviews and focus groups were that HealthPathways strengthened relationships between organisations, as well as between the GPs and specialists working together as part of pathway development teams. Working together in this way increased awareness of each other’s views, processes and challenges, improved trust and respect, improved communication and increased GP empowerment. One GP stated:
Lots of people are good at describing what needs to change, not many groups have successfully set up a way of working together towards the change.
For GPs interviewed who did not use HealthPathways, the website had a non-existent or low profile, with communication efforts generally failing to reach them or convince them of its value.
Critical success factors for the development and implementation of pathways were identified as senior management support, senior clinical leadership, involvement of clinicians in development and implementation, the use of facilitated pathway development processes, the pathways adding value for clinicians, marketing and communication to end users and promotion and feedback by medical specialists.
Barriers to implementation were lack of integration with existing GP systems, the inability to make electronic referrals from within HealthPathways, gaining broad penetration across general practices, the busyness of GPs and specialists and limited capacity to write new pathways and to capitalise on redesign opportunities identified in the development process.
Phase 2: impact evaluation
Google analytics data showed that the number of sessions on HealthPathways doubled in January–March 2014 compared with the same period in 2013, from 4325 to 8544 sessions.
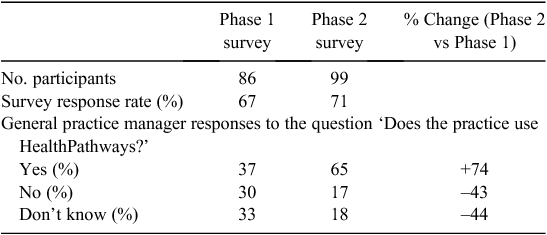
The general practice telephone survey indicated significant changes in the reported use of HealthPathways (χ2 = 13.9, p = 0.001). Use by medium-sized and large practices increased and the number of practices unsure whether they used HealthPathways or reported that they did not use HealthPathways decreased (Table 1).
|
Only 14 of the 79 solo practices (18%) responded to the telephone survey, with just six of these 14 reporting the use of HealthPathways.
Case studies
The review of three pathways suggested that the quality of referrals improved, that a comprehensive approach to implementation resulted in higher pathway use and that accompanying redesign initiatives led to improved access to care.
Quality of referrals
Following implementation of the HealthPathways, more of the recommended information was included on referrals to maternity, pain and mental health services.
For maternity services, 40% of the referrals audited used the referral form only available on HealthPathways. In addition, recording of past obstetric history, medications and naming of the specialist increased, with the latter increasing from 54% to 78%. For the 20 antenatal patients referred using the specific HealthPathways referral form, 95% included a named specialist.
For the pain service, recording of patient allergies and naming of a specialist on referrals to the pain service increased, with the latter increasing from 52% to 94%.
For the mental health service, recording of patient allergies and naming of a specialist increased, with the latter increasing from 18% to 62%. No marked changes were seen in the recording of information for referrals to the primary healthcare suicide and self-harm program.
Patient access to specialist care
For maternity services referrals, for the 20 women referred using the HealthPathways form, 80% were assessed within target time frames, compared with 57% referred using other forms. In addition, 92% of women were seen by the maternity services by 25 weeks gestation after implementation of the HealthPathway, compared with 74% before implementation.
An audit of pain service referrals indicated that the median patient waiting time to first contact was reduced from 56 to 41 days.
The two HealthPathways with indications of more timely access to care (i.e. Routine Antenatal Care and Persistent Non-Cancer Pain) had associated service redesign initiatives in the relevant Local Health District services. No clinical redesign initiatives associated with the development of the suicide risk pathway were identified.
For maternity services, the redesign initiatives involved the development of explicit triage, referral and risk criteria. These changes were accompanied by a strong communication and education strategy aimed at GPs using HealthPathways.
For pain services, there was redesign of discharge letters, pain management plans, associated programs, modification of triage criteria and waiting time estimates, patient questionnaire and initial assessment and approach to opioid management. Although these changes were communicated to GPs through HealthPathways, this vehicle was not the main focus of communication or education.
The Routine Antenatal Care pathway and associated referral pages to specialist maternity and gynaecology services are consistently the most accessed pages on H&NE HealthPathways.
Review of website utilisation: 2016
Since going live in April 2012 until 31 July 2016, over 32 782 individual users have accessed H&NE HealthPathways. These users have accessed the site 184 550 times (number of sessions) and there have been over one million (1 159 879) pages viewed.
From January to June 2016 there was an average of 6679 sessions per month on the website and an average of 1943 users per month.
As H&NE HealthPathways was embedded and spread, there was a significant increase in utilisation, with regression analysis showing that the monthly period was a highly significant predictor of both the number of sessions and the number of individual users accessing the site (Figs 1, 2), (R2 = 89.5% and 87.8% for sessions and users respectively; P < 0.001).
Discussion
With Australian GPs being one of the highest users of guidelines for certain common chronic conditions compared with international counterparts,13 providing reliable and localised information is an important strategy to better integrate and improve healthcare.
The continual increase in H&NE HealthPathways utilisation confirms that there is a demand for local information in the region. The large proportion of general practices reporting the use of HealthPathways provides support for the program and reinforces the suggested value of the approach in improving the quality of referral and patient access to care when comprehensively implemented.
The approach to pathway development that engages GPs and specialists using a team-based process is important to build relationships and gain acceptance and endorsement of the pathways. Implementation that is accompanied by service redesign is more likely to result in improvements, but is also a challenge due to the resourcing required.
Based on GP feedback and the learning that using HealthPathways information when making a referral can improve the timeliness of patient access to appropriate care, a smart eReferral solution that is integrated with H&NE HealthPathways is currently being implemented by the HNECCPHN and HNELHD partnership. A published HealthPathway, including referral information and criteria that have been agreed by local teams, is a prerequisite for inclusion in the roll-out of the eReferral system.
The next step in the H&NE HealthPathways journey is to evaluate the eReferral solution using the iterative cycles of improvement incorporated thus far. The first cycle of evaluation is to assess and monitor whether a high-quality eReferral improves access to specialist care.
The limitations of the approach are that it is not possible to make attributions about the impact of HealthPathways and that the study sizes have been small. However, the scale of access to the website indicates acceptability and the potential of HealthPathways for education and as a tool for system integration. The partnerships built from HealthPathways have led to associated integration initiatives, including the Hunter Alliance, which was established in 2014 (http://ouralliance.healthpathways.org.au; accessed 19 December 2016). Members of the Alliance agree to share their abilities, knowledge and specialist skills and establish processes by which collaboration and integration can occur with other partners to improve healthcare in the Hunter region.
Conclusion
HealthPathways is a vehicle that can build strong foundations to support system change and an integrated approach to care delivery. The critical elements for acceptability, growth and sustainability are the strong relationships and shared governance that are built from the processes used to develop HealthPathways.
H&NE HealthPathways is scaling up and spreading to the New England region of the HNECCPHN and HNELHD using the learnings from the phased evaluation that has accompanied the implementation of the program.
The lessons learnt from the 4-year experience of H&NE HealthPathways may be of value to others that are implementing HealthPathways, or for those considering implementation of this or similar web-based programs.
Competing interests
Robert McDonald was an independent consultant for Phase 1 of the work reported in this manuscript. Robert received financial payment for the work performed in phase 1 by NSW Health. There are no conflicts of interest in the preparation of this manuscript.
Acknowledgements
The guidance and support of the designers of HealthPathways, the Canterbury Initiative from New Zealand, is acknowledged, as well as Streamliners, the technical writers. The HealthPathways Steering Committee acknowledges all the clinicians and staff from the HNECCPHN, HNELHD and the Health Economics and Evaluation Team from the NSW Health Agency for Clinical Innovation who have provided advice and support to the evaluation of HealthPathways.
References
[1] HealthPathways Community Canterbury District Health Board and Streamliners NZ. HealthPathways Community Web Site. Available at: http://www.healthpathwayscommunity.org/About.aspx [verified 19 December 2016].[2] HealthPathways Community Canterbury District Health Board and Streamliners NZ. HealthPathways Community Newsletter: 2016 in numbers. Available at: http://www.healthpathwayscommunity.org/News/LatestNews/tabid/772/ArticleID/1581/Default.aspx [verified 17 January 2017].
[3] Runciman W, Hunt T, Hannaford N, Hibbert P, Westbrook J, Coiera E, Day R, Hindmarsh D, McGlynn E, Braithwaite J. CareTrack: assessing the appropriateness of health care delivery in Australia. Med J Aust 2012; 197 100–5.
| CareTrack: assessing the appropriateness of health care delivery in Australia.Crossref | GoogleScholarGoogle Scholar |
[4] Runciman W, Coiera E, Day R, Hannaford N, Hibbert P, Hunt T, Westbrook J, Braithwaite J. Towards the delivery of appropriate health care in Australia. Med J Aust 2012; 197 78–81.
| Towards the delivery of appropriate health care in Australia.Crossref | GoogleScholarGoogle Scholar |
[5] Brennan N, Mattick K, Ellis T. The map of medicine: a review of evidence for its impact on healthcare. Health Info Libr J 2011; 28 93–100.
| The map of medicine: a review of evidence for its impact on healthcare.Crossref | GoogleScholarGoogle Scholar |
[6] Clarke A, Blundell N, Forde I, Musila N, Spitzer D, Naqvi S, Browne J. Can guidelines improve referral to elective surgical specialties for adults? A systematic review. Qual Saf Health Care 2010; 19 187–94.
| Can guidelines improve referral to elective surgical specialties for adults? A systematic review.Crossref | GoogleScholarGoogle Scholar |
[7] McGeoch G, McGeoch P, Shand B. Is HealthPathways effective? An online survey of hospital clinicians, general practitioners and practice nurses. N Z Med J 2015; 128 36–46.
[8] Timmins N, Ham C. The quest for integrated health and social care: a case study in Canterbury New Zealand. London: The Kings Fund; 2013.
[9] McGeoch G, Anderson I, Gibson J, Gullery C, Kerr D, Shand B. Consensus pathways: evidence into practice. N Z Med J 2015; 128 86–96.
[10] Robinson S, Varhol R, Bell C, Quirk F, Durrington L. HealthPathways: creating a pathway for health systems reform. Aust Health Rev 2015; 39 9–11.
| HealthPathways: creating a pathway for health systems reform.Crossref | GoogleScholarGoogle Scholar |
[11] McDonald B. Process evaluation of the Hunter and New England HealthPathways. Newcastle: BMcD Consulting; 2013.
[12] Hunter and New England HealthPathways Evaluation Committee. Evaluation of Hunter and New England HealthPathways: Phase 2 Report. 2014.
[13] Harris M, Lloyd J, Krastev Y, Fanaian M, Davies G, Zwar N, Liaw S. Routine use of clinical management guidelines in Australian general practice. Aust J Primary Health 2014; 20 41–6.
| Routine use of clinical management guidelines in Australian general practice.Crossref | GoogleScholarGoogle Scholar |