The burdensome logistics of data linkage in Australia – the example of a national registry for congenital heart disease
Larissa K. Lloyd A B C , Calum Nicholson A B C , Geoff Strange A B C and David S. Celermajer A B C *
A B C , Calum Nicholson A B C , Geoff Strange A B C and David S. Celermajer A B C *
A
B
C
Abstract
Data linkage is a very powerful research tool in epidemiology, however, establishing this can be a lengthy and intensive process. This paper reports on the complex landscape of conducting data linkage projects in Australia.
We reviewed the processes, required documentation, and applications required to conduct multi-jurisdictional data linkage across Australia, in 2023.
Obtaining the necessary approvals to conduct linkage will likely take nearly 2 years (estimated 730 days, including 605 days from initial submission to obtaining all ethical approvals and an estimated further 125 days for the issuance of unexpected additionally required approvals). Ethical review for linkage projects ranged from 51 to 128 days from submission to ethical approval, and applications consisted of 9–25 documents.
Major obstacles to conducting multi-jurisdictional data linkage included the complexity of the process, and substantial time and financial costs. The process was characterised by inefficiencies at several levels, reduplication, and a lack of any key accountabilities for timely performance of processes. Data linkage is an invaluable resource for epidemiological research. Further streamlining, establishing accountability, and greater collaboration between jurisdictions is needed to ensure data linkage is both accessible and feasible to researchers.
Keywords: congenital heart disease, data linkage, epidemiology, ethics, population health, registry.
Introduction
Data linkage is a valuable research tool, which involves the bringing together of information from various sources, creating a new, more comprehensive dataset.1 Linked data is thus a very powerful resource in epidemiological research, and its benefits have been widely reported.2–6 Data linkage allows for the study of disease groups across a population.7–9 Matching records from the same individual across different data sources allows researchers to capture a ‘whole of life’ picture of a patient’s journey through a healthcare system.
The Australian Government reported on the substantial advantages of utilising linked administrative data in health research as part of the National Research Infrastructure Roadmap in 2006.10 This Roadmap also proposed the development of a coordinated national data linkage framework, resulting in the establishment of the Population Health Research Network (PHRN) in 2009.11 The PHRN facilitates a network of the seven data linkage units (DLUs) representing the Australian states and territories, and a national DLU, the Australian Institute of Health and Welfare (AIHW), supporting researchers who wish to access linked population data. Multi-jurisdictional research projects are advised to apply via the PHRN.
Most administrative health service datasets involve hospital-based health care, such as admitted patient data. Much data on outpatient care can be obtained via linkage with the Medicare Benefits Schedule (MBS) and the Pharmaceutical Benefits Scheme (PBS) data. Linking of registry data to administrative datasets allows for analysis of the economic burden of disease, access to and patterns of care, and assessment of outcomes in a contextualised manner – taking into consideration the impact of health determinants such as ethnicity, remoteness, and socioeconomic status.12
In 2020, we were awarded an Australian Government Medical Research Future Fund grant, to analyse the burden of congenital heart disease (CHD) in Australia. The project involves the establishment of a National CHD Registry and includes funding for data linkage.13 The aim of our linkage project is to understand the burden of CHD from a healthcare provision perspective, and to provide more accurate monitoring of healthcare utilisation for CHD.
The study population consists of patients with a diagnosis of CHD derived from the 10 major CHD referral centres across Australia. The total cohort was defined as either Cohort 1, consisting of patients known to the clinics contributing to the Registry, or Cohort 2, patients not already known to the centres, but identified as having CHD by the DLUs through patient encounters associated with CHD diagnosis codes.
We have previously described the major bureaucratic inefficiencies in the establishment of a national disease registry in Australia.14 In this companion paper, we now examine the process of attempting to obtain data linkage for such projects.
The process of data linkage is currently complex and lengthy. For a national study, it can take >3 years to gain all required approvals, involving up to 8 DLUs, over 10 ethics committees, and numerous data custodians.15 This linkage project commenced at the end of 2021, with linkage unlikely to commence until early 2024. Although linked health data is an invaluable asset for researchers, the process of obtaining the necessary approvals is a major burden to applicant resources. This paper provides insight into the process of undertaking multi-jurisdictional data linkage in Australia.
Methods
Data collection
We reviewed the processes, required documentation, and applications required to conduct multi-jurisdictional data linkage across Australia.
Applying for multi-jurisdictional data linkage was a stepwise process (Table 1, Fig. 1). The first stage of the multi-jurisdictional linkage application process commenced with submission of an expression of interest (EOI) to the PHRN, via their online system. Once the DLUs are satisfied that the project is feasible, the project can proceed to jurisdiction-specific applications. Approval must be granted from each DLU linking the dataset, the data custodian governing the database, and the relevant ethics committee, and any other required bodies before linkage can commence.
| Consultation |
| |
| Review |
| |
| Application | ||
| Approvals | ||
| Data linkage |
CHAANZ, Congenital Heart Alliance of Australia and New Zealand; DLU, Data Linkage Unit; PHRN, Population Health Research Network.
Flowchart of the application phase for all linkage units involved in the CHAANZ CHD Registry Data Linkage project. AIHW, Australian Institute of Health and Welfare; CVDL, Centre for Victorian Data Linkage; HREC, Human Research Ethics Committee; NT, Northern Territory; PHRN, Population Health Research Network; MBS, Medicare Benefits Schedule; PBS, Pharmaceutical Benefits Schedule; SA, South Australia; WA, Western Australia.
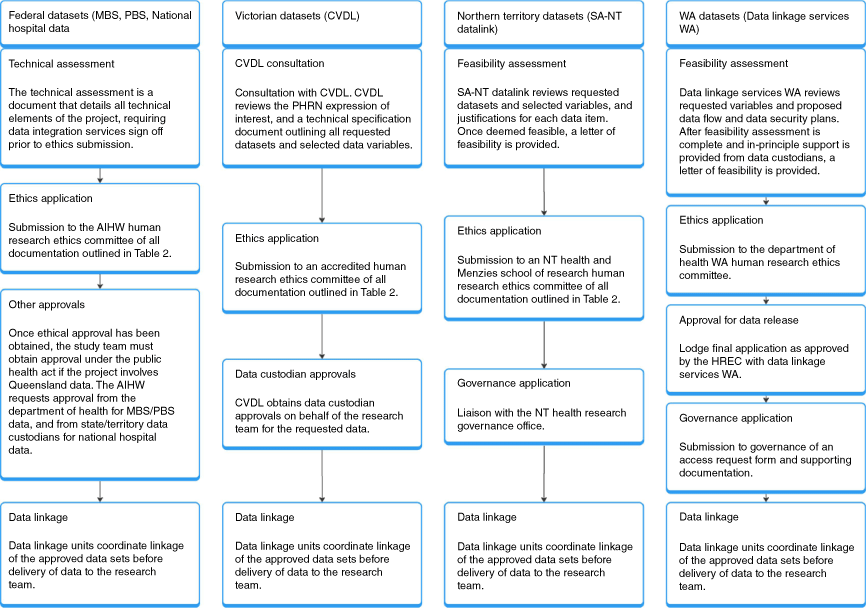
The AIHW National Hospital datasets are compiled from data previously supplied to the AIHW by state and territory health authorities. The Northern Territory (NT) does not participate in National Mutual Acceptance (NMA) for data linkage, and therefore NT data required a direct application to SA-NT Datalink and submission to a NT Human Research Ethics Committee (HREC). Also of importance to our study aims was the Victorian Cost Data Collection maintained by the Centre for Victorian Data Linkage. This dataset is not covered under the AIHW HREC, requiring submission to an additional NMA-participating accredited HREC.
The Western Australia (WA) DLU underwent major reform over 2022–2023, resulting in major delays and an extended closure of services. Due to these lengthy delays, Western Australian linkage was put ‘on hold’ until WA Research Data Service recommenced. The team re-engaged the WA linkage team in June 2023, although the WA DLU had a substantial backlog of requests, and our application has not yet been addressed at the time of writing and hence data pertaining to this process is not included in the results.
Results
Our EOI was first submitted to the PHRN on 1 December 2021. This commenced the consultation phase (Table 1). The project was authorised to commence jurisdictional ethics and governance applications on the 26 July 2022 (238 days from submission of the EOI), and the consultation and review phases were deemed complete on 13 March 2023 (468 days from submission of EOI).
Each DLU has its own processes within the application phase, as outlined in Fig. 1. The entire process took a total of 605 days from initial submission to final approval from all ethics committees.
Data linkage framework
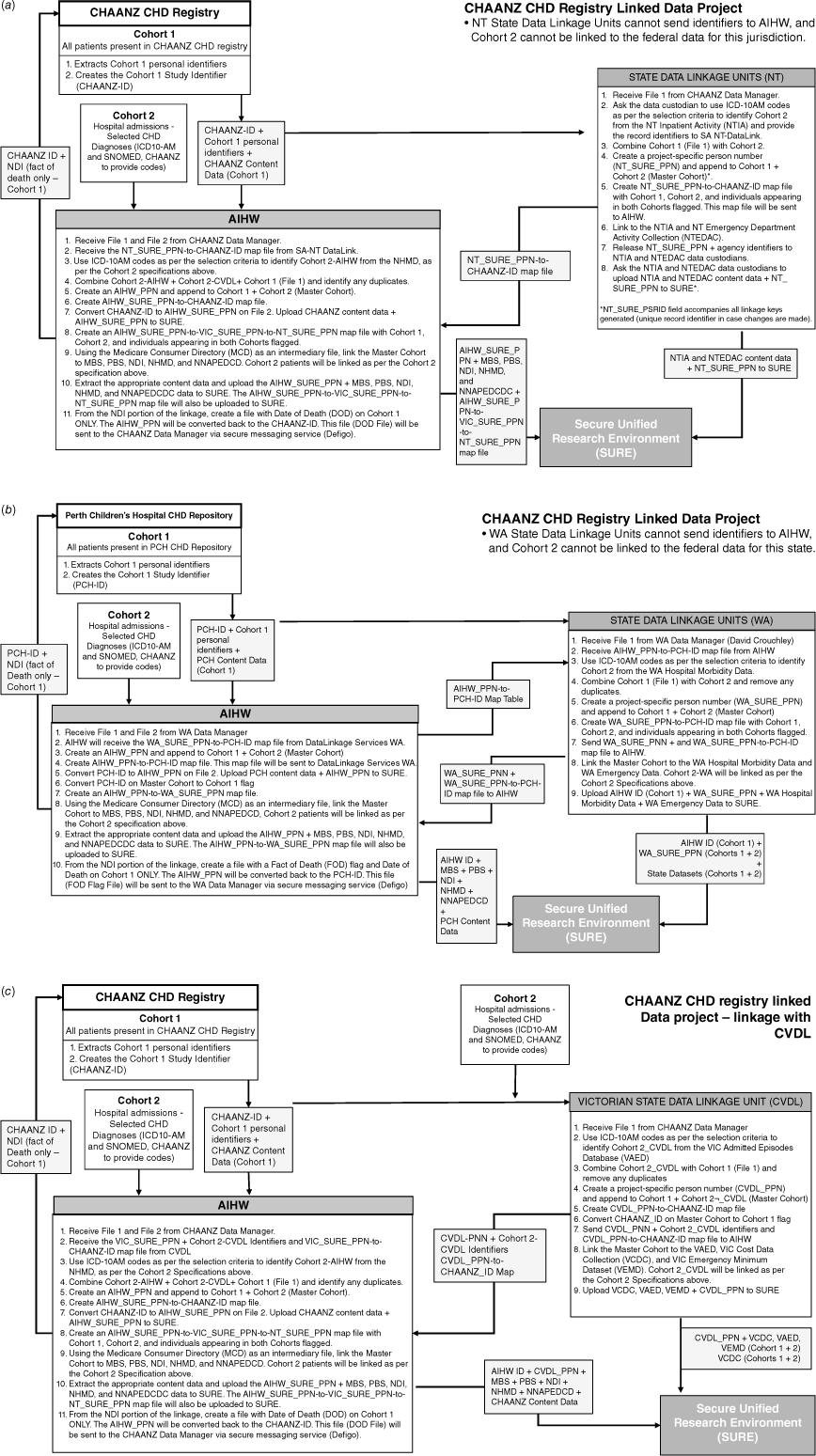
Much of the consultation and review phases was spent developing and editing the data linkage framework, or data flow, of the linkage project (Fig. 2). This dataflow was complex, given that the project involved not only linkage of individuals in Cohort 1 whose identifiers were to be provided to DLUs, but also of the unknown Cohort 2. The data flow also had to be tailored to each state/territory DLU that was involved. The data flow went through several rounds of feedback with the DLUs. This feedback was seldom through the central PHRN feedback, with numerous requested changes being made via direct email or phone calls. Each time the data flow methodology changed, all documents involving the data flow had to be updated in the PHRN online system, as well as the direct communications being had with each DLU and ethics committees.
The data linkage framework required for data linkage for the CHAANZ CHD Registry linkage project. (a) Outline of the data flow for linkage with the AIHW and the Northern Territory DLU, (b) outline of the data flow for linkage with the AIHW and the Western Australian DLU, and (c) outline of the data flow for linkage with the AIHW and the Victorian DLU. AIHW, Australian Institute of Health and Welfare; CHAANZ, Congenital Heart Society of Australia and New Zealand; CHD, Congenital Heart Disease; CVDL, Centre for Victorian Data Linkage; FOD, Fact of Death; ID, identification; MBS, Medicare Benefit Scheme; MCD, Medicare Consumer Directory; NDI, National Death Index; NHMD, National Hospital Minimal Dataset; NNAPEDDC, National Non-Admitted Patient Emergency Department Data Collection; NT, Northern Territory; NTDL, Northern Territory Data Linkage; PBS, Pharmaceutical Benefit Scheme; PPN, Person Project Number; SURE, Secure Unified Research Environment; VAED, Victorian Admitted Episode Database; VCDC, Victorian Cost Data Collection; VEMD, Victorian Emergency Minimum Dataset.
Ethics approvals
Grant reporting timelines were greatly challenged by the coronavirus disease 2019 (COVID-19) pandemic. In the interest of meeting already delayed reporting milestones, the team opted to collect hospital inpatient and emergency department data via the AIHW National Hospital datasets, as compared to the alternative option of applying to each state and territory DLU and their associated ethics committees and data custodians. This decision streamlined the application process significantly, reducing the DLU applications required from 7 to 3, and ethics applications from 5 to 3. There were other considerations involved in this decision, summarised in Table 2.
| Pros | Cons | |
|---|---|---|
| Streamlined application process, reducing number of data linkage unit applications required from 7 to 3, and ethics applications from 5 to 3. | As most of the data linkage is funnelled through the AIHW DLU and their ethics team, progression of linkage is limited by their response/approval time. | |
| Uniform variable list for datasets across states and territories. | Loss of some variables of interest from some datasets. | |
| Presumably lesser cost, however, as accurate quotes were not obtained from DLUs once decision to take National Hospital data route was made, this cannot be verified. | Significantly increased cost of AIHW linkage from initially budgeted amount. |
The application for NT data linkage ethical approval was submitted to the NT Health and Menzies School of Research HREC on 16 January 2023, with approval received on 7 March 2023 (51 days). This application consisted of nine documents (Table 3), and went through one additional round of review, wherein the ethics committee asked for additional information regarding data collection, recruitment, and stakeholder involvement.
CHAANZ, Congenital Heart Alliance of Australia and New Zealand; CHD, congenital heart disease; CVDL, The Centre for Victorian Data Linkage; CV, curriculum vitae; HREA, Human Research Ethics Application; HREC, Human Research Ethics Committee; NSW, New South Wales; NT, Northern Territory; SA, South Australia.
Application to the AIHW HREC was submitted on 23 March 2023, with approval received on 28 July 2023 (128 days). This application consisted of 25 documents (Table 3) and went through five additional rounds of feedback prior to the HREC meeting. This feedback involved revisions to the Technical Assessment, queries about study personnel, and updates to the proposed data flow.
Application to the NSW Population and Health Services Research Ethics Committee (PHSREC) was submitted on 29 May 2023, with approval received on 18 July 2023 (52 days). This application consisted of 22 documents (Table 3) and went through one additional round of feedback prior to the HREC meeting, and one round of review post-meeting. This feedback involved recommendations for consultation with experienced data linkage researchers, and queries about requested variables.
Delays in submission to the relevant HRECs were experienced during the approval stage outlined in Table 1, due to lengthy response times from DLUs. For example, with all other documentation prepared, a requirement for one signature from a data custodian for the Victorian Cost Data delayed application to the PHSREC by 60 days.
Other approvals
After the relevant ethical approvals had been obtained, additional approvals were required prior to linkage. For Queensland hospitals' data, it is required that an application for data release under the Public Health Act 2005 (Qld) (PHA) be approved by each data custodian relevant to the project and the Director General of Queensland Health. This was fortunately swift for our project, as we had obtained data custodian signatures whilst awaiting ethics approval. The PHA application was submitted on 29 August 2023, with approval received on 6 September 2023 (9 days).
Lastly, when we thought that all the appropriate approvals for the project had been obtained, after 646 days, we received an email from the AIHW informing us of a further and unforeseen delay. The AIHW National Hospitals’ team obtains the remaining jurisdiction’s data custodian approvals on the research team’s behalf once AIHW ethics is approved. In the meantime, the AIHW was to submit the approved project to the Department of Health and Aged Care for them to issue a Public Interest Certificate (PIC) for the use of MBS/PBS data. The AIHW estimated that it would be a few weeks until they submitted that request, owing to the Department being ‘understaffed recently and unable to progress new requests’. At that point, the time estimate was a further 3–4 months for the PIC to be issued. Only then could linkage begin.
Discussion
There are obvious important advantages of data linkage for national or state-based Registry projects, as this enables a complete picture of patient interactions with the healthcare system. This information is invaluable for patients, families, healthcare providers, systems planners, and governments. In this paper, we describe the continuing and substantial bureaucratic hurdles to data linkage in Australia, 15 years after the establishment of a centralised body which aims to streamline this process. These delays frustrate researchers but also, importantly, reduce Australia’s ability to generate meaningful data and reduce our international competitiveness in epidemiological research.
Without national data linkage capabilities, research cannot make use of cross-jurisdictional data linkage. Data linkage infrastructure has progressed since its inception,16 however, much duplication and complexity in the application process remains. Conducting research involving national data linkage in a timely manner is thus virtually impossible.
The difficulty in establishing cross-jurisdictional linkage problems lies, in part, within the complex multi-jurisdictional nature of Australia’s health system. Australia’s federal, state and territory, and local governments share responsibility for the health system, and consequently health data is not held centrally. Navigating the legal framework governing these systems, while achieving standardisation of data and linkage methodology across jurisdictions, is complicated.
Although all efforts were made to expedite our linkage applications, expected timelines were pushed back repeatedly. The PHRN online cross-jurisdictional application form was designed to enable a more centralised application process, but it is unclear if this system streamlines applications as intended. The central EOI process meant DLUs had some familiarity with the project once we progressed to the application phase, but nevertheless we had to undertake the same processes outlined by each individual DLU for single jurisdictional linkage (Fig. 1), not circumventing any steps after the lengthy consultation and review period.
The application phase involved substantial duplication of effort. Each time the data flow or application documentation was amended during consultation with individual DLUs, these changes had to be uploaded to the PHRN online form. This also occurred in the other direction, with changes in the PHRN form needing to be relayed back to DLUs. Multiple places to update versions led to confusion amongst the team and DLUs about document versions and changes to data flow.
Another limitation of this centralised process is that the progression of the consultation and review process is limited by the availability of all parties to meet and discuss the project. Feedback was not released to the research team until all DLUs had provided their feedback; this was thus limited by the slowest party. Significant delays were experienced due to the WA DLU undergoing reform, with the WA portion of the linkage eventually being placed on indefinite hold. This extended closure highlights the need for lasting resources to ensure the longevity of Australia’s linkage infrastructure. Unpredictable responsiveness added further delays to the project, with no expected response time outlined by most DLUs.
The research team was responsible for developing the data flow (Fig. 2), at times feeling like guesswork via many iterations of data flow documentation. It seemed counterintuitive that the data flow was not initially proposed to us by the DLUs conducting the linkage, who were the experts in data linkage, and were charging considerable dollar amounts for the linkage.
Other groups have also found that, although data linkage in Australia has overcome some challenges in developing the infrastructure for cross-jurisdictional data linkage, national data linkage projects are hindered by the complexity of the process.15,17 A recent publication by Dutch researchers reported on obstacles similar to those faced in the Australian data linkage landscape.18 There is an urgent need for a truly streamlined application process with reduced duplication and greater consistency of procedures.7,15,17,19
Improving Australia’s data linkage infrastructure requires greater homogeneity and simplification of the legislative framework governing health data. The Australian Government 2017 Productivity Commission inquiry report noted a risk-averse culture has led to ‘overly cautious interpretation of relevant legislation … and complex and lengthy approval processes’ (p. 55).20 The 2017 report also noted a lack of national leadership and longwinded bureaucratic processes for data release.20 While protecting patient privacy and ensuring ethical conduct is undoubtedly a critical element of research, the current approval process is a source of major inefficiency and limits the accessibility of data linkage.
Greater oversight from the PHRN could be considered. The PHRN provided excellent resources on navigating the complicated application phase, however, the requirements themselves were oftentimes unclear. One common application, such as the existing online PHRN EOI form, could be utilised by all DLUs, centralising the process.
The AIHW has been developing new data asset initiatives that should address some of the issues faced in accessing cross-jurisdictional health data, by integration of existing linked AIHW datasets to enable access in a more timely manner.21 This initiative is underway, with assets such as the National Integrated Health Services Information available for application, and the National Disability Data Asset being finalised.22
Ultimately, the establishment of the data linkage project was a lengthy and intensive process. Access to linked data is invaluable to a National Registry, allowing for longitudinal analysis of population groups, however, the costly and time-consuming process of achieving the necessary approvals remains a challenge to both grant funding and timelines. Further streamlining, key accountabilities, and greater collaboration between jurisdictions is needed to ensure data linkage is feasible to researchers.
Acknowledgements
We thank the numerous contacts we had at the various data linkage units and the PHRN for their countless emails and the time they spent aiding us through this challenging process and answering our many queries. Without their experience and guidance this project would not have been possible.
References
1 Hobbs MS, McCall MG. Health statistics and record linkage in Australia. J Chronic Dis 1970; 23(5): 375-81.
| Crossref | Google Scholar | PubMed |
2 Brook EL, Rosman DL, Holman CD. Public good through data linkage: measuring research outputs from the Western Australian Data Linkage System. Aust N Z J Public Health 2008; 32(1): 19-23.
| Crossref | Google Scholar | PubMed |
3 Hall SE, Holman CD, Finn J, Semmens JB. Improving the evidence base for promoting quality and equity of surgical care using population-based linkage of administrative health records. Int J Qual Health Care 2005; 17(5): 415-20.
| Crossref | Google Scholar | PubMed |
4 Sibthorpe B, Kliewer E, Smith L. Record linkage in Australian epidemiological research: health benefits, privacy safeguards and future potential. Aust J Public Health 1995; 19(3): 250-6.
| Crossref | Google Scholar | PubMed |
5 Bohensky MA, Jolley D, Sundararajan V, Evans S, Pilcher DV, Scott I, et al. Data linkage: a powerful research tool with potential problems. BMC Health Serv Res 2010; 10: 346.
| Crossref | Google Scholar | PubMed |
6 Holman CD, Bass AJ, Rouse IL, Hobbs MS. Population-based linkage of health records in Western Australia: development of a health services research linked database. Aust N Z J Public Health 1999; 23(5): 453-9.
| Crossref | Google Scholar | PubMed |
7 Young A, Flack F. Recent trends in the use of linked data in Australia. Aust Health Rev 2018; 42(5): 584-90.
| Crossref | Google Scholar | PubMed |
8 Tew M, Dalziel KM, Petrie DJ, Clarke PM. Growth of linked hospital data use in Australia: a systematic review. Aust Health Rev 2017; 41(4): 394-400.
| Crossref | Google Scholar | PubMed |
9 Dinh NTT, Cox IA, de Graaff B, Campbell JA, Stokes B, Palmer AJ. A Comprehensive Systematic Review of Data Linkage Publications on Diabetes in Australia. Front Public Health 2022; 10: 757987.
| Crossref | Google Scholar | PubMed |
10 Australian Government, Department of Education. National Collaborative Research Infrastructure Strategy Strategic Roadmap 2006. Australian Government; 2006. Available at https://www.education.gov.au/national-research-infrastructure/resources/national-collaborative-research-infrastructure-strategy-strategic-roadmap-2006
11 Boyd JH, Ferrante AM, O’Keefe CM, Bass AJ, Randall SM, Semmens JB. Data linkage infrastructure for cross-jurisdictional health-related research in Australia. BMC Health Serv Res 2012; 12: 480.
| Crossref | Google Scholar | PubMed |
12 Tervonen HE, Purdie S, Creighton N. Using data linkage to enhance the reporting of cancer outcomes of Aboriginal and Torres Strait Islander people in NSW, Australia. BMC Med Res Methodol 2019; 19(1): 245.
| Crossref | Google Scholar | PubMed |
13 Celermajer D, Strange G, Cordina R, Selbie L, Sholler G, Winlaw D, et al. Congenital Heart Disease Requires a Lifetime Continuum of Care: A Call for a Regional Registry. Heart Lung Circ 2016; 25(8): 750-4.
| Crossref | Google Scholar | PubMed |
14 Lloyd LK, Nasir R, Nicholson C, Strange G, Celermajer DS. Obstacles in establishing a national disease registry in Australia: lessons from the development of the CHAANZ Congenital Heart Disease Registry. Aust Health Rev 2023; 47: 410-7.
| Crossref | Google Scholar | PubMed |
15 Andrew NE, Sundararajan V, Thrift AG, Kilkenny MF, Katzenellenbogen J, Flack F, et al. Addressing the challenges of cross-jurisdictional data linkage between a national clinical quality registry and government-held health data. Aust N Z J Public Health 2016; 40(5): 436-42.
| Crossref | Google Scholar | PubMed |
16 Smith M, Flack F. Data Linkage in Australia: The First 50 Years. Int J Environ Res Public Health 2021; 18(21):.
| Crossref | Google Scholar | PubMed |
17 Palamuthusingam D, Johnson DW, Hawley C, Pascoe E, Fahim M. Health data linkage research in Australia remains challenging. Intern Med J 2019; 49(4): 539-44.
| Crossref | Google Scholar | PubMed |
18 Smit J-A, van der Graaf R, Mostert M, Vaartjes I, Zuidgeest M, Grobbee D, et al. Overcoming ethical and legal obstacles to data linkage in health research: stakeholder perspectives. Int J Popul Data Sci 2023; 8(1):.
| Crossref | Google Scholar |
19 Mitchell RJ, Cameron CM, McClure RJ, Williamson AM. Data linkage capabilities in Australia: practical issues identified by a Population Health Research Network ‘Proof of Concept project’. Aust N Z J Public Health 2015; 39(4): 319-25.
| Crossref | Google Scholar | PubMed |
20 Productivity Commission. Data Availability and Use. Report No. 82. Canberra: Productivity Commission; 2017. Available at https://www.pc.gov.au/inquiries/completed/data-access/report/data-access-overview.pdf
21 Australian Research Data Commons. Linked Data Asset for Australian Health Research. NCRIS; 2022. Available at ardc.edu.au/project/linked-data-asset-australian-health-research/
22 Australian Institute of Health and Welfare. AIHW linked data assets. 2023. Available at https://www.aihw.gov.au/about-our-data/linked-data-assets


