‘I think I’d get a lot out of something where my views count and I could help other people’ – co-designing a family project-based intervention with people with lived experience of traumatic brain injury
Lynn Grayson A B , Marian C. Brady
A B , Marian C. Brady  A , Leanne Togher C * and Myzoon Ali A D
A , Leanne Togher C * and Myzoon Ali A D
A
B
C
D
Abstract
Meaningful engagement with families who have lived experience of traumatic brain injury (TBI) is essential if interventions are to more closely align with their needs. The aim of this study was to co-design a family project-based intervention including people with lived experience of TBI and explore participant experience.
People with cognitive-communication disorders following severe TBI, and their family members, were recruited from three Scottish brain injury services. The co-design teams participated in Microsoft Teams focus groups (October 2022 to January 2023). A range of adapted communication tools were developed to facilitate the co-design process, and e-surveys about the co-design experience were completed. Qualitative data arising from the focus groups were analysed thematically, and survey data were analysed descriptively.
Thirteen participants (6 people following TBI and 7 family members) attended the co-design groups. The concept of a family project-based intervention was positively received and adaptions to content identified: inclusion of real-life examples, family support resources and a toolkit of strategies. A range of perceived personal benefits of being involved in the co-design groups was also reported; peer support, feeling heard and helping others.
People with cognitive–communication disorders following severe TBI, and their families, can make a valuable contribution to co-design research and benefit from the process. Following development of the adapted content, progression to the next design stage will involve feasibility testing of the co-designed family project-based intervention.
Keywords: acquired communication disorders, co-design, cognitive-communication disorders, family intervention, lived experience expertise, project-based intervention, rehabilitation of speech and language disorders, traumatic brain injury.
Introduction
Worldwide, more than 50 million people sustain a traumatic brain injury (TBI) each year (Maas et al. 2017), resulting in a wide range of devastating and enduring effects for both the person following TBI, and their family (Downing et al. 2022; Dams-O’Connor et al. 2023). Altered communication is common following TBI, with reported incidence rates of >75% following moderate to severe injuries (MacDonald 2017). Cognitive-communication disorders (CCD) resulting from disrupted cognitive processes rather than a specific language disorder are the most prevalent communication difficulties following TBI (Togher et al. 2023a). The clinical presentation of a person with CCD following TBI is highly heterogeneous, and can include changes to information processing, social communication and conversational discourse (MacDonald 2017). The effects of CCD are chronic and pervasive (Kelly et al. 2023; Togher et al. 2023b), negatively impacting upon the person’s ability to reintegrate into previous life roles (Struchen et al. 2011; Douglas et al. 2016; Tran et al. 2018), family functioning and relationships (Anderson et al. 2002; Knox et al. 2015; Grayson et al. 2021).
Access to family support following TBI reduces levels of family stress and improves outcomes for the TBI survivor (Winstanley et al. 2006; Vangel et al. 2011). Communication partner training (CPT) enables family members to facilitate conversations with the person following TBI more effectively (Behn et al. 2020; Wiseman-Hakes et al. 2020), and is therefore recommended as best practice for speech and language pathologists (SLP; Togher et al. 2023a). CPT delivers positive communication outcomes in a variety of formats, such as dyad, group and via telehealth (Togher et al. 2013; Rietdijk et al. 2020), although the majority of CPT evidence has been generated by one group of Australian researchers testing adapted versions of the TBI Express program (Togher et al. 2013, 2016): TBIconneCT (Rietdijk et al. 2019, 2020). Studies exploring family perception of CCD rehabilitation have highlighted that a single CPT approach may not suit the learning style of all families affected by TBI, with some participants indicating a preference for family-led, solution-focused learning (Grayson et al. 2020, 2021). Interventions that support the family unit’s varying communication needs across the recovery trajectory rather than focusing on supporting a single (primary) caregiver at a single recovery stage are also required (Grayson et al. 2020, 2021).
One intervention that uses a participant-led, solution-focused approach to communication therapy is project-based intervention (PBI; Feeney et al. 2001; Ylvisaker et al. 2007). PBI encourages collaborative teamwork, raised awareness of communication changes and generation of supports for the person with CCD to successfully complete a project with others (Behn et al. 2022). Use of PBI with groups of people with CCD in the chronic phase of recovery following TBI is evidence informed (Behn et al. 2019a, 2022; Hoepner et al. 2022), although there are no published reports to date of a PBI delivered to the family unit.
To increase the likelihood of a family-PBI meeting the needs of people with CCD and their family members, meaningful input from key stakeholders is essential (Moore et al. 2021). Co-design is a research approach in which researchers collaborate with the target population to study, and plan and develop an intervention (Masterson et al. 2022). Meaningful engagement can result in a better product-user fit, materials with higher applicability and end-user acceptability (Slattery et al. 2020). Co-design is time and resource intensive, however, and a balance between end-user preference and methodological rigour can be difficult to achieve (Grindell et al. 2022). Tokenistic involvement can also result in service users feeling unheard and marginalised (D’Cruz et al. 2022). Recent reviews have identified a lack of definitions, methodological descriptions and empirical evaluation of the outcomes (Slattery et al. 2020; Grindell et al. 2022; Masterson et al. 2022). Transparent reporting of the co-design methods used and evaluation of the impact of these methods on outcomes is required (D’Cruz et al. 2022).
Detailed descriptions of co-design processes (Benz et al. 2024), a theoretical model of co-design mechanisms of change (Palmer et al. 2015, 2023), and reporting the feasibility and acceptability of different approaches are emerging (Lamontagne et al. 2021). The need for co-design reporting guidelines to supplement existing public and patient involvement guidance (Staniszewska et al. 2017) has been identified (D’Cruz et al. 2022; Munce et al. 2023), and a tool to support participation research discussions with service users has been developed (Smits et al. 2020).
The value of engaging stakeholders in intervention development and adaption for people following TBI is increasingly acknowledged (Volkmer 2022) with the inclusion of healthcare professionals (How et al. 2017; Hwang et al. 2024), service users and family members (Bould and Callaway 2021; Nunnerley et al. 2023). To date, reporting the co-design methods and impacts has been limited. Exceptionally, a cyber scam resource development qualitatively explored the co-design experience for people following brain injury, providing valuable insights into the perceived benefits and challenges of the codesign process, and the support required to enable meaningful participation (Carminati et al. 2023).
Co-design approaches are becoming more prevalent in the development of communication partner interventions for people following TBI. Consultation with service users has informed development of a new digital health intervention for conversation skills after brain injury (Avramović et al. 2023), and digital health implementation strategies for online communication support tools (Miao et al. 2023). Involving people with CCD in co-design research requires careful planning to ensure processes are inclusive, safe and enjoyable for those taking part (Volkmer 2022). Although few TBI co-design studies have reported on the inclusive practices used to facilitate meaningful involvement of people with CCD, communication accessible co-design has been described in the context of aphasia interventions (Volkmer et al. 2021; Cruice et al. 2022), and alternative and augmentative communication (Broomfield et al. 2021). The communication support tools that were identified to positively impact and support meaningful participation of people with CCD include: visual agendas, illustrated minutes, visual prompt cards, talking mats and the use of metaphor, although it is unclear whether these tools would work for groups of people following TBI with their family members.
Families managing communication changes following TBI report unmet communication needs, and to date, their inclusion in the design of CPT interventions has been limited (Grayson et al. 2020; Avramović et al. 2023). This is despite recognition that meaningful engagement with people who have lived experience as active, equal partners in the design process is essential to ensure new interventions are closely aligned with the needs of potential users (Grayson et al. 2021; Volkmer 2022). The recent use of co-design approaches offers a new and, as yet, untested way to engage families living with TBI in the process of developing customised cognitive communication interventions. Investigating this approach, combined with transparent reporting of the co-design methods used, is the focus of this preliminary study.
Methods
Study design
An iterative, focus group methodology enabled people with lived experience to collectively make decisions regarding the content and design of a family-PBI. Mixed methods (a survey and focus group) explored the participants co-design experience. This study was approved by the West of Scotland NHS ethics review (IRAS number 305543], and Glasgow Caledonian University School of Health and Life sciences Ethics Committee (HLS/NCH/21/021).
Recruitment
Eligible participants were identified from two National Health Service health boards – Lanarkshire, and Greater Glasgow and Clyde – and one independent brain injury service – Graham Anderson House in Scotland, UK. At each site, SLPs screened for eligible participants, and informed them about the study by phone, email or during a usual appointment. An accessible participant information sheet that contained contact details for the research team was provided to interested parties. Potential participants who initiated contact with the research team were provided with more information about the study and at least 48 h to consider whether they wished to participate, prior to being contacted by the research team again to confirm participation. The lead author (LG) completed the University of California, San Diego Brief Assessment of Capacity to Consent (Jeste et al. 2007) with all people interested in study participation to confirm their cognitive capacity to understand the study and what participation would entail; for example, to advise on the content of a new intervention, not take part in the intervention itself. All participants completed the written consent form prior to the study.
Participants
Eligible participants with CCD were aged >18 years, medically stable, at least 12 months following severe TBI and had an SLP-documented CCD diagnosis defined as ‘difficulty with any aspect of communication that is affected by disruption of cognition’ (College of Audiologists and Speech-Language Pathologists of Ontario 2015). Severe TBI was defined as a brain injury caused by a road traffic accident, assault or fall with a score on the Glasgow Coma Scale of ≤8 and/or a period of post-traumatic amnesia ≥24 h (Greenbaum 1982). Eligible family members were aged >18 years and in daily contact with the person following TBI. Exclusion criteria were severe aphasia, dysarthria or other communication problems that prevented conversational participation; a co-occurring degenerative neurological condition; or lacking capacity to provide informed consent.
Advisory group
An advisory group was formed to support the co-design process. This included international expert SLPs and researchers with experience of working with people following TBI and PBI.
Survey development
Short, pre- and post-co-design experience surveys, informed by National Institute for Health Research guidance on evaluating the impact of co-design research (NIHR 2024), were created using Microsoft Forms (Microsoft Corporation). Suitable survey questions were identified from the Western Australian Involving Consumers in Health and Medical Research handbook; resource 8 ‘why get involved in research’ and resource 27 ‘evaluating the involvement’ (Tuffrey et al. 2021). Survey questions from the handbook were adapted, to reflect the study context: no financial remuneration and need for accessible content. This involved reducing the number of questions from 13 to 9, using shorter, simplified questions and response options. Both surveys contained nine closed questions, and one open question distributed across one page in the paper copy (one screen in the online version). Respondents were asked to rate each item along one dimension: not important, quite important, very important in the pre-survey and not really, somewhat, yes in the post-survey. Both surveys were piloted with two people with CCD and two family members who were unconnected with the study. Minor changes to question wording were made to enhance the clarity of the survey.
Intervention adaption
Program content from a manualised PBI for people following acquired brain injury informed the co-design group sessions (Behn et al. 2019b). Core components of PBI – communication goals, expert roles, completion of a meaningful project – were introduced to the co-design team to promote discussion about how these components might work with family groups. The co-design team also considered family adaptions for PBI in relation to the four elements of the rehabilitation treatment specification system : aims, targets, ingredients and mechanisms of action (Hart et al. 2019).
Pre-group orientation
One week prior to the co-design groups, the team members (one to one sessions) and the advisory group (group meeting) participated in a Microsoft Teams-based induction session (led by LG). Participants were provided with support to access Microsoft Teams using practice links and telephone assistance. Guidance on what to expect, time to ask questions and examples of group activities were provided to help co-design team members feel more prepared for their role. All then received a link to the pre-group survey via email. Where requested, a hardcopy of the survey and stamped addressed return envelope was posted to their home address. The same process was used for the post-group survey 1 week following the final focus group.
Co-design focus groups
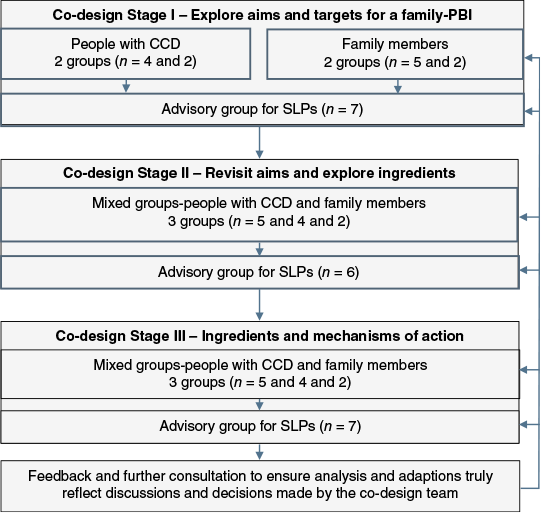
Online focus groups followed by an advisory group meeting were conducted across three family-PBI design stages (Fig. 1). More than one co-design focus group was facilitated at each stage to accommodate participants’ availability and communication support needs. People with CCD and family members attended separate groups at stage I followed by mixed groups at all subsequent stages (Fig. 1).
Co-design focus groups lasted approximately 1–1.5 h, and were facilitated by two female SLPs (LG and HMacL) with >15 years of experience working with people following TBI and their families. The role of the facilitator was to remain neutral during conversations, introduce discussion topics and encourage all group members to express their opinion. Reflective field notes were completed by LG following each group, and the reflections were shared with co-design and advisory group members to optimise the participant-led process in subsequent groups. Focus group topic guides containing information on group set up and open-ended questions relating to the core components of PBI were drafted, reviewed by the wider research team and finalised for each design stage to ensure parity across all groups (Supplementary Material S1). The final focus group topic guide also explored participants’ co-design experience, perceived barriers and facilitators.
Following piloting (with 2 people with CCD and 2 family members unconnected to the study), adapted communication tools facilitated group discussion, enabled the relevance of different intervention ingredients to be rated and supported collaborative decision making. Examples of communication tools included simple visual choice making systems, image rather than text-heavy minutes and visual conversation aids (Supplementary Material S2).
Advisory group involvement
The role of the advisory group was to support interpretation of co-design group data and advise on communication supports for subsequent sessions. Each group consisted of a short PowerPoint presentation that summarised focus group findings followed by group discussion. An agenda was sent via email to advisory group members 1 week prior to each group, and minutes were sent following each group meeting.
Data collection and analysis
All focus groups were digitally recorded, and transcribed verbatim. Concurrent qualitative data analysis following each focus group was completed to enable iterative planning and development for the following group in consultation with advisory group and co-design team members. Qualitative data and the survey responses were analysed using a thorough, six-stage thematic analysis (Braun and Clarke 2006). Transcripts were read and re-read to get an overall sense of the data prior to grouping the responses to each question and ‘coding’ the main ideas (research team). Comments were selected and put into ‘nodes’, resulting in a list of open codes (research team). The different codes were sorted into potential themes, and LG worked with the wider research team, and advisory and co-design groups to identify and refine the themes. Suitable extracts were then identified for each theme (research team). Member checking was completed during and after each group to support trustworthiness of the data. Facilitators summarised the information provided by participants during groups to confirm whether their message had been understood correctly. Co-design team members provided feedback on transcripts, themes and quotes, and results were then summarised into pictorial minutes that were disseminated to all team members prior to the next group. A reflective log was completed by LG throughout the study to document any consequences arising and responsive adaptions. Quantitative data arising from surveys were analysed descriptively post-study (sum, frequency, percentages), and feedback was provided to the co-design and advisory groups. The study was reported in accordance with Guidance for Reporting Involvement of Patients and the Public; GRIPP2 (Staniszewska et al. 2017; Supplementary Material S3).
Results
Aim 1: seek perspectives of people with lived experience of severe TBI in the co-design of a family-PBI in relation to intervention content and design
Thirteen people with lived experience of CCD following severe TBI (6 people following TBI and 7 family members) participated in the co-design process. Most participants were men (62%, n = 8/13), a median of age of 48 years (range 18–67 years) and 5 years living with TBI (range 2–12 years). Family members were a parent (14%, n = 1), child (29%, n = 2), spouse (29% n = 2) or sibling (29% n = 2) of the person with TBI. All participants were British and resided within Scotland. The advisory group consisted of seven SLPs and researchers with >15 years of experience of working in the field of brain injury and a special interest in delivering PBI with people following TBI. Ten co-design groups (and four advisory groups) were held to enable all voices to be heard (Fig. 1).
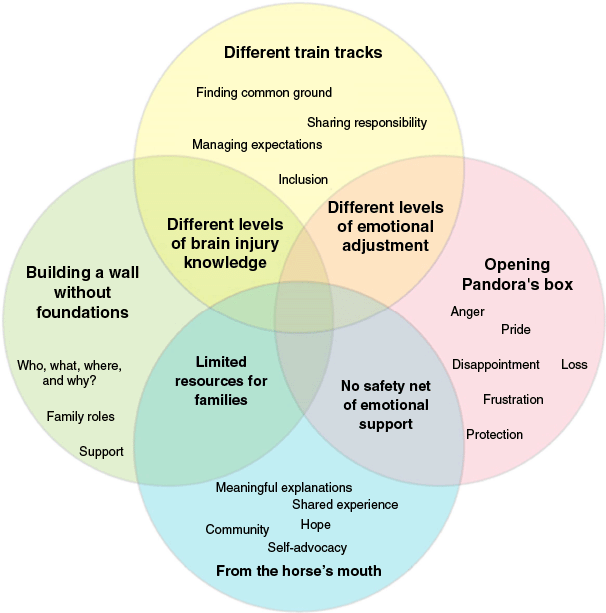
Analysis of transcripts generated from design stage 1 (n = 4 groups) generated four themes that encapsulated the co-design team’s hopes and concerns for an adapted family-PBI: ‘different train tracks’, ‘from the horse’s mouth’, ‘opening Pandora’s box’ and ‘building a wall without foundations’. Fig. 2 represents the interconnected nature of these themes as a Venn diagram.
Different train tracks
Working together on a family-PBI was perceived by people with CCD (P) as a positive way of sharing the responsibility of therapy and managing expectations. Family members (FM) also welcomed the inclusivity of family-PBI, particularly participants who were not the primary caregiver and had experienced limited contact with TBI services
It wouldn’t just be down to me, because other people would be there to help you remember and encourage you to do it (P1)
If my family could see first-hand where I’m struggling, we could figure it out together rather than someone telling them this is what he struggles with (P2)
I think my dad got to be more involved, but my dad’s not a big talker, so I wasn’t really in the loop (FM1, son)
Me and my sister didn’t know what was going on. I still don’t really know (FM3, son)
Concerns about encouraging an open dialogue about brain injury were highlighted, as these discussions were not happening frequently within the family group. Potential pressure points included mismatched expectations and differing levels of insight:
If I’m honest, we don’t have many conversations where we talk about the brain injury at all. I just try to hold my tongue (FM4, wife)
So, I think everybody is almost separate and on their own. I’m trying to protect my wife and son, and my wife is protecting me (P2)
We’re not all on the same page, even within the family, my husband sees it differently to me (FM5, mother)
I think my views and my relatives’ views are a bit different to be honest (P6)
From the horse’s mouth
Hearing directly from people with lived experience of TBI was identified as a very valuable, but under utilised, therapeutic tool by the co-design team. The mechanism of action worked both ways; as a means of supporting family adjustment following brain injury and as a way to empower people with lived experience expertise:
To hear it from people who have walked the walk makes more sense. A lot of people can talk the talk, but it’s more important to put those shoes on and have walked the walk (FM2, wife)
I was bobbing about in this world with nobody. Just to hear from someone else and think they know, they are living my life (FM5, mother)
Brain injury is not well spoken about, so it would feel good to help somebody else in that situation (P4)
Opening Pandora’s box
Co-design team members were concerned about the emotions that working on a project together would raise; each member of the family might be at a different stage of emotional adjustment/acceptance of the long-term effects of brain injury.
For us to get good common ground and move forward, you would have to accept Pandora’s box might open, because I know it would bring up a lot of emotions for me (FM2, wife)
Before my family could take part in anything like that, everybody would have to accept that the brain injury is here, it’s real and it’s forever (P1)
I’m grateful still to have him, but I’m also distraught and angry, which spills over into everything (FM5, mother)
Building a wall without foundations
Co-design members identified areas that could impact on the effectiveness of a family-PBI if they were not addressed. This included difficulty understanding the abstract nature of PBI, conflicting opinions about therapy goals and which family members to include:
It’s about the terminology, how we explain a project to people, so I think that’s maybe one of the building blocks as well (P5)
I’d say not parents, as mine are drama all over, but then they would be upset if they were not involved (P4)
He had very fixed goals about return to work and driving, whereas my goal was just to get through the day so I’m not sure how we could meet in the middle (FM4, wife)
The advisory group discussion following design stage I reframed the concerns raised by the co-design team as potential intervention targets rather than barriers to participation. This shift helped the co-design team transform stage I themes into concrete aims and targets during design stage II.
Analysis of co-design group transcripts from design stage II (n = 3) generated three aims for a family-PBI: supporting families to develop a shared brain injury narrative, identifying helpful communication solutions and advocating for other families affected by TBI. (Table 1).
P = person with CCD; FM = family member.
Tangible targets included the creation of brain injury resources to help other families and a personalised toolkit of CCD supports that each family could refer to following completion of the intervention (Table 1).
The advisory group discussion following design stage II facilitated the development of communication tools to support collaborative decision making during design stage III. Co-design team members reviewed PBI manual ingredients to identify components that could be retained and any new ingredients required to support families participating in the intervention.
Many of the original features of PBI were identified as a good fit for families: creating an expert role for people with CCD, practising real life conversations and the need for SLP guidance to keep things on track.
Additional materials included the development of interactive explanatory videos from people with lived experience to help families understand the concept of family-PBI, normalise the process of family communication changes following TBI and support insight. The need for emotional supports was also identified. Table 2.
P = person with CCD; FM = family member.
Aim 2: evaluate the co-design experience in relation to the people involved
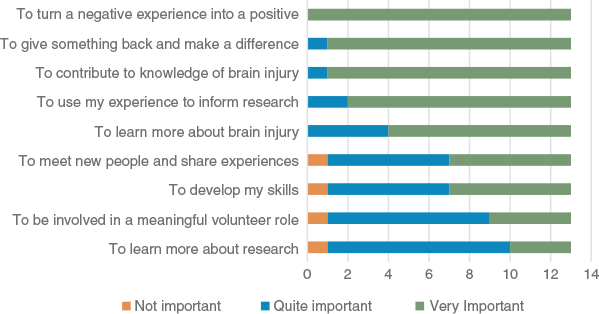
People with CCD and their family members identified ‘turning a negative experience into a positive’ (n = 13, 100%), ‘giving something back’ (n = 12, 90%) and ‘contributing to knowledge of brain injury’ (n = 12, 90%) as their most important reasons for participation (Fig. 3).
Analysis of co-design group transcripts from design stage III (n = 3) and open survey questions (n = 6 responses) revealed three themes about co-design participation: personal benefits of involvement, perceived positive impacts on future families and positive effects for SLPs (Table 3).
| Illustrative quotes | ||
|---|---|---|
| Personal benefit | ||
| Peer support | ||
| Being heard | ||
| Making a difference | ||
| Benefit for future families | ||
| Relatable content | ||
| Person- centred resources | ||
| Benefit for SLPs | ||
| Greater consideration of end-user perspective | ||
P = person with CCD; FM = family member.
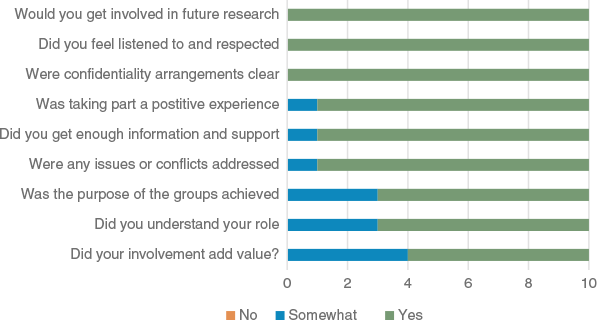
Co-design team members also identified barriers and facilitators to participation during the groups (n = 10). Facilitators included small group size, structured communication activities and memory support tools. Barriers involved time constraints, the online format of the group and challenges in understanding the co-design team role (Table 4). The reflective log offered valuable insights into both the intended and unintended consequences of the co-design process, as well as adaptive responses developed by the research team in collaboration with co-design and advisory team members (Table 5). Among post-survey responses, 100% (n = 10) of participants expressed willingness to engage in future research. However, a minority (n = 3/10, 2 people with CCD) reported that their understanding of the co-design role and the value of their contributions was only ‘somewhat’ achieved (Fig. 4).
| Illustrative quotes | ||
|---|---|---|
| Barriers | ||
| Time constraints | ||
| Online nature of group | ||
| Difficulty understanding role | ||
| Facilitators | ||
| Communication support tools and experienced facilitators | ||
| Small groups | ||
| Group mix | ||
| Option to be in a different group from relative | ||
P = person with CCD; FM = family member.
| Anticipated consequences | Pre-study mitigation strategies (identified by research team and university PPI group) | |
|---|---|---|
| Power inequalities | ||
| Group accessibility | ||
| Wide range of CCD | ||
| Understanding of role | ||
| Diverse expectations and differences in opinion |
| Unintended consequences | During study responsive adaptions (identified by authors, co-design and advisory teams) | |
|---|---|---|
| Difficulty ensuring the involvement is participant- and not researcher-led | ||
| Time and labour required | ||
| The positive impact of mixed peer support |
PPI = public and patient involvement.
Discussion
Our co-design study sheds light on factors that may support people with lived experience of CCD following TBI to become involved in participatory research. To our knowledge, it is the first study that has adapted a PBI for use with families, and the findings provide a road map for how an intervention can be adapted for family groups.
Core components of PBI were well suited to family group work, and the concept of a communication intervention that could support several family members at once was positively received (Grayson et al. 2020, 2021). Empowering people with CCD by creating expert roles and developing a resource that could support other families affected by TBI was rated highly. This resonates with previous studies exploring the impact of advocacy projects on sense of self (Hoepner et al. 2022), insight (Behn et al. 2022) and quality of life (Behn et al. 2019a).
Adaptions to PBI included the addition of explanatory materials by people with lived experience of TBI. This reinforces the findings from peer support studies that highlight the benefits of vicarious learning through the stories of others with lived experience of TBI (Bellon et al. 2017; Lau et al. 2021), and other co-creation studies that report improved user friendly materials as an outcome (Carminati et al. 2023; Miao et al. 2023; Benz et al. 2024).
Co-design participants also emphasised that family-PBI should acknowledge and normalise the emotional experiences of participants, as cognitive-communication rehabilitation cannot be considered in isolation from emotional adjustment and recovery following TBI. The impact of emotions on identity, narrative surrounding the brain injury, and recovery for people following TBI (Douglas 2013; Ownsworth and Haslam 2016; Hoepner et al. 2022) and their families (Whiffin et al. 2017, 2021) has been well documented. Each family member may be in a different place emotionally with a different brain injury recovery narrative. Therefore, development of a shared brain injury narrative that is inclusive of the person with CCD and all members of the family was considered an important outcome for family-PBI, as it would support a common vocabulary through which to discuss the way forward (Whiffin and Ellis-Hill 2022). Written support materials, signposting to specialist support services and optional one-to-one check-ins for family members during the intervention would further support family members’ emotional needs during family-PBI (Townshend and Norman 2018; Holloway et al. 2019).
Involvement in the co-design process was considered as positive and personally beneficial by all involved, reinforcing other co-design studies’ findings (Palmer et al. 2015, 2023; Carminati et al. 2023). Co-design team members enjoyed the peer support within the groups, while the group discussion format allowed ideas to grow and develop over the study. Peer discussion has been identified as an effective mechanism of change in other co-design studies, as it enables dynamic development of viewpoints in response to others (Palmer et al. 2015; Lamontagne et al. 2021; Carminati et al. 2023).
Novel to this study were the steps taken to address potential power imbalances between stakeholders (Greenhalgh et al. 2019). Involving professional stakeholders in an advisory capacity rather than as part of the co-design focus groups enabled people with lived experience to express their views unmodified by professional constraints (Palmer et al. 2015). A separate focus group for people with CCD and family members, and the option to be in a different mixed group from their loved ones enabled co-design team members to express opinions more openly. Building flexibility into the focus group design with concurrent data analysis and advisory group support enabled responsive adaptions to the direction and content of the focus groups to be made. This allowed the perspectives of professional stakeholders to be incorporated into the intervention design, and enabled the co-design team to take the lead on decisions. Meaningful involvement at the level of partner and decision maker could, therefore, be achieved (Smits et al. 2020).
Additional focus groups to accommodate for the CCD needs and availability of team members were required, resulting in increased time taken for data collection and analysis (Miller et al. 2017; Slattery et al. 2020). People with CCD and family members responded well to the visual choice-making frameworks, and these activities provided structure and focused attention during the groups. Co-design team members also appreciated the visual agendas and minutes, as this enabled planning of ideas prior to the group and supported memory of group decisions post-group. The clinical experience of the group facilitators was beneficial when it came to managing diverse expectations and communication needs within a group setting, and context specific tools (rather than a one size fits all approach) optimised authenticity of the data gathered (Greenhalgh et al. 2019).
Understanding the co-design role was challenging for some team members. This was particularly noticeable during activities exploring the personal impact of TBI, where participants found it difficult to stay focused on the broader goal of developing an intervention for others. Additionally, the lack of tangible outcomes at this early design stage may have hindered participants’ ability to appreciate the significance of their contributions. Although general feedback on study outcomes was shared with all team members, offering personalised feedback may have been more meaningful for participants. Study updates will continue to be shared following each design stage, along with further consultation opportunities for those wishing to remain involved. Further development of inclusive engagement strategies and guidelines are required to ensure people with lived experience of TBI understand their role and feel valued during participatory research (Slattery et al. 2020; D’Cruz et al. 2022).
Study strengths and limitations
This study enhances our understanding of inclusive co-design research practices for people with CCD following severe TBI and their families. Combining quantitative survey data with qualitative focus group insights enabled detailed information about participant experience to be gathered. A sample size of 13 co-design participants, along with measures to ensure that the voices of those with lived experience were not overshadowed by other stakeholders, enabled the collection of a diverse range of perspectives on family-PBI. The use of a flexible, iterative focus group methodology enabled responsive adaptions to group size and communication materials to be made during the study.
As this project was part of a larger PhD study, time constraints and lack of remuneration for co-design team members impacted on the number of groups, the number of participants recruited and the amount of pre-group training that could be provided. Further support to help co-design team members to understand their role and how their input added value would have been beneficial. Although the adaptations to PBI identified during co-design were clearly documented, their effect on outcomes remains untested. Future design stages are needed to assess the feasibility, acceptability, and clinical and economic effectiveness of family-PBI. The outcomes from this study are context-specific and may not reflect the experiences of people from different sociocultural or geographical backgrounds.
Clinical implications
People with CCD can contribute meaningfully to co-design projects and value that opportunity (Elwyn et al. 2020; Bould and Callaway 2021; Volkmer 2022). Learning from the lived experience of others, acknowledging the emotional impact of TBI on families and supporting the communication needs of the wider family were identified as beneficial for families by the participants in this study. Training one communication partner does not guarantee that the information will filter to other members of the family, and SLPs should consider how information about CCD can be shared more widely (Grayson et al. 2020). Having permanent access to information about CCD, either online or in paper format, is also important for families, as it allows strategies to be reviewed and discussed when more unsettled periods arise in the future (Grayson et al. 2021). SLPs can support the person with CCD and their family to develop a more strengths-based identity following the brain injury (Lyon et al. 2021; Hoepner et al. 2022), and promote exploration of positive, as well as negative, post-injury narratives (D’Cruz et al. 2020; Whiffin and Ellis-Hill 2022). The inclusion of real-life examples from people with lived experience should be included in brain injury resources, and SLPs should provide families with information about peer support/other support services.
Research implications
Descriptions of inclusive co-design practices that enable people with CCD to participate successfully in collaborative research should be transparently reported, including the communication tools used, participation barriers and facilitators, and the degree of participation (Smits et al. 2020). Consensus terminology, descriptions of participatory research and co-design-specific reporting guidelines would support direct comparison between studies and a stronger evidence base for co-design methodologies to be developed (D’Cruz et al. 2022; Masterson et al. 2022; Munce et al. 2023). Empirical evaluation of co-designed intervention adherence and outcomes compared with other intervention development approaches is required (O’Cathain et al. 2019; Grindell et al. 2022). Further evaluation of what co-design approaches work best with different participants and at different stages in the intervention development process would also be beneficial (Slattery et al. 2020; Lamontagne et al. 2021).
Conclusion
This study involved the co-design of a family-PBI with people with CCD following TBI, and their families. Co-design team members identified several helpful adaptions to the aims, content and outcomes of PBI to make it more suitable for use with families. Co-design team members valued the opportunity to make a positive difference and enjoyed the peer support aspect of the groups, although the need for more support to understand the co-design role was highlighted. This study adds to the theoretical development of using participatory co-design with people with lived experience of TBI, and demonstrates that people with CCD can make a valuable contribution to co-design research and enjoy the process.
Data availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to their containing information that could compromise the privacy of research participants.
Conflicts of interest
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
Ethics
This study was approved by the West of Scotland NHS ethics review (IRAS number 305543], and Glasgow Caledonian University School of Health and Life sciences Ethics Committee (HLS/NCH/21/021).
Acknowledgements
The authors acknowledge and thank the people with lived experience of traumatic brain injury who participated in the co-design groups and informed this research. The authors also thank the professional advisory group members and SLP facilitator Helen MacLean for their time and expertise.
References
Anderson MI, Parmenter TR, Mok M (2002) The relationship between neurobehavioural problems of severe traumatic brain injury (TBI), family functioning and the psychological well-being of the spouse/caregiver: path model analysis. Brain Injury 16(9), 743-757.
| Crossref | Google Scholar | PubMed |
Avramović P, Rietdijk R, Kenny B, Power E, Togher L (2023) Developing a Digital Health Intervention for Conversation Skills After Brain Injury (convers-ABI-lity) Using a Collaborative Approach: Mixed Methods Study. Journal of Medical Internet Research 25, e45240.
| Crossref | Google Scholar | PubMed |
Behn N, Marshall J, Togher L, Cruice M (2019a) Feasibility and initial efficacy of project-based treatment for people with ABI. International journal of language & communication disorders 54(3), 465-478 https://doi-org.gcu.idm.oclc.org/10.1111/1460-6984.12452.
| Google Scholar | PubMed |
Behn N, Francis J, Togher L, Hatch E, Moss B, Hilari K (2020) Description and Effectiveness of Communication Partner Training in TBI: A Systematic Review. The Journal of Head Trauma Rehabilitation 36, 56-71.
| Crossref | Google Scholar | PubMed |
Behn N, Hoepner J, Meulenbroek P, Capo M, Hart J (2022) Core components of project-based intervention after acquired brain injury: Delivering meaningful groups online. International Journal of Language & Communication Disorders 59, 572-590.
| Crossref | Google Scholar | PubMed |
Bellon M, Sando S, Crocker R, Farnden J, Duras M (2017) Information, connection and giving back: peer support outcomes for families following acquired brain injury in South Australia. Health & Social Care in the Community 25, 204-214.
| Crossref | Google Scholar | PubMed |
Benz C, Scott-Jeffs W, Mckercher KA, Welsh M, Norman R, Hendrie D, Locantro M, Robinson S (2024) Community-based participatory-research through co-design: supporting collaboration from all sides of disability. Research Involvement and Engagement 10, 47.
| Crossref | Google Scholar | PubMed |
Bould E, Callaway L (2021) A co-design approach to examine and develop pathways to open employment for people with acquired brain injury. Brain Impairment 22, 50-66.
| Crossref | Google Scholar |
Braun V, Clarke V (2006) Using thematic analysis in psychology. Qualitative Research in Psychology 3, 77-101.
| Crossref | Google Scholar |
Broomfield K, Craig C, Smith S, Jones G, Judge S, Sage K (2021) Creativity in public involvement: supporting authentic collaboration and inclusive research with seldom heard voices. Research Involvement and Engagement 7, 17.
| Crossref | Google Scholar | PubMed |
Carminati J-YJ, Ponsford JL, Gould KR (2023) “This group… I felt like I was medicating myself from this cyberscam illness that was living with me.” A qualitative evaluation of co-designing cybersafety training resources with and for people with acquired brain injury. Disability and Rehabilitation 45, 3719-3729.
| Crossref | Google Scholar | PubMed |
College of Audiologists and Speech-Language Pathologists of Ontario (2015) Practice standards and guidelines for acquired cognitive communication disorders. Available at https://www.caslpo.com/sites/default/uploads/files/PSG_EN_Acquired_Cognitive_Co mmunication_Disorders.pdf
Cruice M, Aujla S, Bannister J, Botting N, Boyle M, Charles N, Dhaliwal V, Grobler S, Hersh D, Marshall J, Morris S, Pritchard M, Scarth L, Talbot R, Dipper L (2022) Creating a novel approach to discourse treatment through coproduction with people with aphasia and speech and language therapists. Aphasiology 36, 1159-1181.
| Crossref | Google Scholar |
Dams-O’Connor K, Juengst SB, Bogner J, Chiaravalloti ND, Corrigan JD, Giacino JT, Harrison-Felix CL, Hoffman JM, Ketchum JM, Lequerica AH, Marwitz JH, Miller AC, Nakase-Richardson R, Rabinowitz AR, Sander AM, Zafonte R, Hammond FM (2023) Traumatic brain injury as a chronic disease: insights from the United States Traumatic Brain Injury Model Systems Research Program. Lancet Neurology 22, 517-528.
| Crossref | Google Scholar | PubMed |
D’Cruz K, Douglas J, Serry T (2020) Narrative storytelling as both an advocacy tool and a therapeutic process: Perspectives of adult storytellers with acquired brain injury. Neuropsychological Rehabilitation 30, 1409-1429.
| Crossref | Google Scholar | PubMed |
D’Cruz K, Antonopoulos S, Rothman R, Douglas J, Winkler D, Oliver S (2022) Co-designing with adults with acquired neurological disability in the community: a scoping review protocol. BMJ Open 12, e064921.
| Crossref | Google Scholar | PubMed |
Douglas JM (2013) Conceptualizing self and maintaining social connection following severe traumatic brain injury. Brain Injury 27, 60-74.
| Crossref | Google Scholar | PubMed |
Douglas JM, Bracy CA, Snow PC (2016) Return to Work and Social Communication Ability Following Severe Traumatic Brain Injury. Journal of Speech, Language, and Hearing Research 59, 511-520.
| Crossref | Google Scholar | PubMed |
Downing MG, Hicks AJ, Braaf S, Myles DB, Gabbe BJ, Ponsford J (2022) “It’s been a long hard road”: challenges faced in the first three years following traumatic brain injury. Disability and Rehabilitation 44, 7439-7448.
| Crossref | Google Scholar | PubMed |
Elwyn G, Nelson E, Hager A, Price A (2020) Coproduction: when users define quality. BMJ Quality & Safety 29, 711-716.
| Crossref | Google Scholar | PubMed |
Feeney TJ, Ylvisaker M, Rosen BH, Greene P (2001) Community supports for individuals with challenging behavior after brain injury: an analysis of the New York state behavioral resource project. The Journal of Head Trauma Rehabilitation 16, 61-75.
| Crossref | Google Scholar | PubMed |
Grayson L, Brady MC, Togher L, Ali M (2020) A survey of cognitive–communication difficulties following TBI: are families receiving the training and support they need? International Journal of Language & Communication Disorders 55, 712-723.
| Crossref | Google Scholar | PubMed |
Grayson L, Brady MC, Togher L, Ali M (2021) The impact of cognitive-communication difficulties following traumatic brain injury on the family; a qualitative, focus group study. Brain Injury 35, 15-25.
| Crossref | Google Scholar | PubMed |
Greenbaum R (1982) Management of Head Injuries. By Jennett B and Teasdale G. Contemporary Neurology Series. Published by F. A. Davis Company, Philadelphia Pp. 361, illustrated, indexed. Price £22 50. British Journal of Anaesthesia 54, 371-372.
| Crossref | Google Scholar |
Greenhalgh T, Hinton L, Finlay T, Macfarlane A, Fahy N, Clyde B, Chant A (2019) Frameworks for supporting patient and public involvement in research: Systematic review and co-design pilot. Health Expectations 22, 785-801.
| Crossref | Google Scholar | PubMed |
Grindell C, Coates E, Croot L, O’Cathain A (2022) The use of co-production, co-design and co-creation to mobilise knowledge in the management of health conditions: a systematic review. BMC Health Services Research 22, 877.
| Crossref | Google Scholar | PubMed |
Hart T, Dijkers MP, Whyte J, Turkstra LS, Zanca JM, Packel A, Van Stan JH, Ferraro M, Chen C (2019) A Theory-Driven System for the Specification of Rehabilitation Treatments. Archives of Physical Medicine and Rehabilitation 100, 172-180.
| Crossref | Google Scholar | PubMed |
Hoepner JK, Yingst H, Harder B, Zehm C (2022) “I never thought I would be an international speaker but I am”: an interpretive qualitative analysis of experiences of a project-based advocacy intervention. Neuropsychological Rehabilitation 32, 2077-2101.
| Crossref | Google Scholar | PubMed |
Holloway M, Orr D, Clark-Wilson J (2019) Experiences of challenges and support among family members of people with acquired brain injury: a qualitative study in the UK. Brain Injury 33, 401-411.
| Crossref | Google Scholar | PubMed |
How T-V, Hwang AS, Green REA, Mihailidis A (2017) Envisioning future cognitive telerehabilitation technologies: a co-design process with clinicians. Disability and rehabilitation: Assistive Technology 12, 244-261.
| Crossref | Google Scholar | PubMed |
Hwang JHA, Downing MG, Specht RAG, Ponsford JL (2024) Co-designing for behavioural change: understanding barriers and enablers to addressing sexuality after traumatic brain injury and mapping intervention strategies in a multi-disciplinary rehabilitation unit. Brain Impairment 25, IB23068.
| Crossref | Google Scholar | PubMed |
Jeste DV, Palmer BW, Appelbaum PS, Golshan S, Glorioso D, Dunn LB, Kim K, Meeks T, Kraemer HC (2007) A New Brief Instrument for Assessing Decisional Capacity for Clinical Research. Archives of General Psychiatry 64, 966-974.
| Crossref | Google Scholar | PubMed |
Kelly C, Cornwell P, Hewetson R, Copley A (2023) The Pervasive and Unyielding Impacts of Cognitive-Communication Changes Following Traumatic Brain Injury. International Journal of Language & Communication Disorders 58, 2131-2143.
| Crossref | Google Scholar | PubMed |
Knox L, Douglas JM, Bigby C (2015) ‘The biggest thing is trying to live for two people’: Spousal experiences of supporting decision-making participation for partners with TBI. Brain Injury 29, 745-757.
| Crossref | Google Scholar | PubMed |
Lamontagne M-E, Gagnon M-P, Perreault K, Gauthier V (2021) Evaluating the Acceptability, Feasibility, and Outcomes of Two Methods Involving Patients With Disability in Developing Clinical Guidelines: Crossover Pilot Study. Journal of Participatory Medicine 13, e24319.
| Crossref | Google Scholar | PubMed |
Lau SKC, Luong D, Sweet SN, Bayley M, Levy BB, Kastner M, Nelson MLA, Salbach NM, Jaglal SB, Shepherd J, Wilcock R, Thoms C, Munce SEP (2021) Using an integrated knowledge translation approach to inform a pilot feasibility randomized controlled trial on peer support for individuals with traumatic brain injury: A qualitative descriptive study. PLoS One 16, e0256650.
| Crossref | Google Scholar | PubMed |
Lyon I, Fisher P, Gracey F (2021) “Putting a new perspective on life”: a qualitative grounded theory of posttraumatic growth following acquired brain injury. Disability and Rehabilitation 43, 3225-3233.
| Crossref | Google Scholar | PubMed |
Maas AIR, Menon DK, Adelson PD, Andelic N, Bell MJ, Belli A, et al. (2017) Traumatic brain injury: integrated approaches to improve prevention, clinical care, and research. The Lancet Neurology 16(12), 987-1048.
| Crossref | Google Scholar |
MacDonald S (2017) Introducing the model of cognitive-communication competence: A model to guide evidence-based communication interventions after brain injury. Brain Injury 31, 1760-1780.
| Crossref | Google Scholar | PubMed |
Masterson D, Areskoug Josefsson K, Robert G, Nylander E, Kjellström S (2022) Mapping definitions of co‐production and co‐design in health and social care: A systematic scoping review providing lessons for the future. Health Expectations 25, 902-913.
| Crossref | Google Scholar | PubMed |
Miao M, Morrow R, Salomon A, Mcculloch B, Evain J-C, Wright MR, Murphy MT, Welsh M, Williams L, Power E, Rietdijk R, Debono D, Brunner M, Togher L (2023) Digital Health Implementation Strategies Coproduced With Adults With Acquired Brain Injury, Their Close Others, and Clinicians: Mixed Methods Study With Collaborative Autoethnography and Network Analysis. Journal of Medical Internet Research 25, e46396.
| Crossref | Google Scholar | PubMed |
Miller CL, Mott K, Cousins M, Miller S, Johnson A, Lawson T, Wesselingh S (2017) Integrating consumer engagement in health and medical research - an Australian framework. Health Research Policy and Systems 15, 9.
| Crossref | Google Scholar | PubMed |
Moore G, Campbell M, Copeland L, Craig P, Movsisyan A, Hoddinott P, Littlecott H, O’Cathain A, Pfadenhauer L, Rehfuess E, Segrott J, Hawe P, Kee F, Couturiaux D, Hallingberg B, Evans R (2021) Adapting interventions to new contexts—the ADAPT guidance. BMJ 374, n1679.
| Crossref | Google Scholar | PubMed |
Munce SEP, Steele Gray C, Pomeroy BC, Bayley M, Kokorelias KM, Luong D, Biddiss E, Cave T, Bragge P, Chew-Graham CA, Colquhoun H, Dadich A, Dainty KN, Elliott M, Feng P, Goldhar J, Hamilton CB, Harvey G, Kastner M, Kothari A, Langley J, Jeffs L, Masterson D, Nelson MLA, Perrier L, Riley J, Sellen K, Seto E, Simpson R, Staniszewska S, Srinivasan V, Straus SE, Tricco AC, Kuluski K (2023) Development of the Preferred Components for Co-Design in Research Guideline and Checklist: Protocol for a Scoping Review and a Modified Delphi Process. JMIR Research Protocols 12, e50463.
| Crossref | Google Scholar | PubMed |
NIHR (2024) Guidance on co-producing a research project. Available at NIHR Guidance on co-producing a research project [last accessed 1 April 2025]
Nunnerley J, King M, Hodge K, Hopkins P, Stockwell R, Thorne N, Snell D, Gozdzikowska K (2023) Co-design of a therapeutic virtual reality tool to increase awareness and self-management of cognitive fatigue after traumatic brain injury. Disability and Rehabilitation: Assistive Technology 18, 1404-1410.
| Crossref | Google Scholar | PubMed |
O’Cathain A, Croot L, Sworn K, Duncan E, Rousseau N, Turner K, Yardley L, Hoddinott P (2019) Taxonomy of approaches to developing interventions to improve health: a systematic methods overview. Pilot and Feasibility Studies 5, 41.
| Crossref | Google Scholar | PubMed |
Ownsworth T, Haslam C (2016) Impact of rehabilitation on self-concept following traumatic brain injury: An exploratory systematic review of intervention methodology and efficacy. Neuropsychological Rehabilitation 26, 1-35.
| Crossref | Google Scholar | PubMed |
Palmer VJ, Chondros P, Piper D, Callander R, Weavell W, Godbee K, Potiriadis M, Richard L, Densely K, Herrman H, Furler J, Pierce D, Schuster T, Iedema R, Gunn J (2015) The CORE study protocol: a stepped wedge cluster randomised controlled trial to test a co-design technique to optimise psychosocial recovery outcomes for people affected by mental illness in the community mental health setting. BMJ Open 5, e006688.
| Crossref | Google Scholar | PubMed |
Palmer VJ, Bibb J, Lewis M, Densley K, Kritharidis R, Dettmann E, Sheehan P, Daniell A, Harding B, Schipp T, Dost N, Mcdonald G (2023) A co-design living labs philosophy of practice for end-to-end research design to translation with people with lived-experience of mental ill-health and carer/family and kinship groups. Frontiers in Public Health 11, 1206620.
| Crossref | Google Scholar | PubMed |
Rietdijk R, Power E, Brunner M, Togher L (2019) A single case experimental design study on improving social communication skills after traumatic brain injury using communication partner telehealth training. Brain Injury 33, 94-104.
| Crossref | Google Scholar | PubMed |
Rietdijk R, Power E, Attard M, Heard R, Togher L (2020) Improved Conversation Outcomes After Social Communication Skills Training for People With Traumatic Brain Injury and Their Communication Partners: A Clinical Trial Investigating In-Person and Telehealth Delivery. Journal of Speech, Language, and Hearing Research 63, 615-632.
| Crossref | Google Scholar | PubMed |
Slattery P, Saeri AK, Bragge P (2020) Research co-design in health: a rapid overview of reviews. Health Research Policy and Systems 18, 17.
| Crossref | Google Scholar | PubMed |
Smits D-W, Van Meeteren K, Klem M, Alsem M, Ketelaar M (2020) Designing a tool to support patient and public involvement in research projects: the Involvement Matrix. Research Involvement and Engagement 6, 30-37.
| Crossref | Google Scholar | PubMed |
Staniszewska S, Brett J, Simera I, Seers K, Mockford C, Goodlad S, Altman DG, Moher D, Barber R, Denegri S, Entwistle A, Littlejohns P, Morris C, Suleman R, Thomas V, Tysall C (2017) GRIPP2 reporting checklists: tools to improve reporting of patient and public involvement in research. BMJ 358, j3453.
| Crossref | Google Scholar | PubMed |
Struchen MA, Pappadis MR, Sander AM, Burrows CS, Myszka KA (2011) Examining the Contribution of Social Communication Abilities and Affective/Behavioral Functioning to Social Integration Outcomes for Adults With Traumatic Brain Injury. Journal of Head Trauma Rehabilitation 26, 30-42.
| Crossref | Google Scholar | PubMed |
Togher L, Mcdonald S, Tate R, Power E, Rietdijk R (2013) Training communication partners of people with severe traumatic brain injury improves everyday conversations: a multicenter single blind clinical trial. Journal of Rehabilitation Medicine 45, 637-645.
| Crossref | Google Scholar | PubMed |
Togher L, Mcdonald S, Tate R, Rietdijk R, Power E (2016) The effectiveness of social communication partner training for adults with severe chronic TBI and their families using a measure of perceived communication ability. NeuroRehabilitation 38, 243-255.
| Crossref | Google Scholar | PubMed |
Togher L, Douglas J, Turkstra LS, Welch-West P, Janzen S, Harnett A, Kennedy M, Kua A, Patsakos E, Ponsford J, Teasell R, Bayley MT, Wiseman-Hakes C (2023a) INCOG 2.0 Guidelines for Cognitive Rehabilitation Following Traumatic Brain Injury, Part IV: Cognitive-Communication and Social Cognition Disorders. The Journal of Head Trauma Rehabilitation 38, 65-82.
| Crossref | Google Scholar | PubMed |
Togher L, Elbourn E, Kenny B, Honan C, Power E, Tate R, Mcdonald S, Macwhinney B (2023b) Communication and Psychosocial Outcomes 2-Years After Severe Traumatic Brain Injury: Development of a Prognostic Model. Archives of Physical Medicine and Rehabilitation 104, 1840-1849.
| Crossref | Google Scholar |
Townshend J, Norman A (2018) The Secondary Impact of Traumatic Brain Injury: An Interpretative Phenomenological Analysis of the Experiences of Family and Friends. The Family Journal 26, 77-85.
| Crossref | Google Scholar |
Tran S, Kenny B, Power E, Tate R, Mcdonald S, Heard R, Togher L (2018) Cognitive-communication and psychosocial functioning 12 months after severe traumatic brain injury. Brain Injury 32, 1700-1711.
| Crossref | Google Scholar | PubMed |
Tuffrey T, Wilkie J, Parker R (2021) Involving Consumers in Health and Medical Research: A practical handbook for organisations, researchers, consumers and funders. The University of Western Australia, Perth, WA.
| Crossref | Google Scholar |
Vangel SJ, Rapport LJ, Hanks RA (2011) Effects of family and caregiver psychosocial functioning on outcomes in persons with traumatic brain injury. The Journal of Head Trauma Rehabilitation 26, 20-29.
| Crossref | Google Scholar | PubMed |
Volkmer A, Spector A, Swinburn K, Warren JD, Beeke S (2021) Using the Medical Research Council framework and public involvement in the development of a communication partner training intervention for people with primary progressive aphasia (PPA): Better Conversations with PPA. BMC Geriatrics 21, 642.
| Crossref | Google Scholar | PubMed |
Whiffin CJ, Ellis-Hill C (2022) How does a narrative understanding of change in families post brain injury help us to humanise our professional practice? Brain Impairment 23, 125-133.
| Crossref | Google Scholar |
Whiffin CJ, Ellis-Hill C, Bailey C, Jarrett N, Hutchinson PJ (2017) We are not the same people we used to be: An exploration of family biographical narratives and identity change following traumatic brain injury. Neuropsychological Rehabilitation 29, 1256-1272.
| Crossref | Google Scholar | PubMed |
Whiffin CJ, Gracey F, Ellis-Hill C (2021) The experience of families following traumatic brain injury in adult populations: A meta-synthesis of narrative structures. International Journal of Nursing Studies 123, 104043.
| Crossref | Google Scholar | PubMed |
Winstanley J, Simpson G, Tate R, Myles B (2006) Early Indicators and Contributors to Psychological Distress in Relatives During Rehabilitation Following Severe Traumatic Brain Injury: Findings From the Brain Injury Outcomes Study. Journal of Head Trauma Rehabilitation 21, 453-466.
| Crossref | Google Scholar | PubMed |
Wiseman-Hakes C, Ryu H, Lightfoot D, Kukreja G, Colantonio A, Matheson FI (2020) Examining the Efficacy of Communication Partner Training for Improving Communication Interactions and Outcomes for Individuals With Traumatic Brain Injury: A Systematic Review. Archives of Rehabilitation Research and Clinical Translation 2, 100036.
| Crossref | Google Scholar | PubMed |
Ylvisaker M, Feeney T, Capo M (2007) Long-Term Community Supports for Individuals With Co-Occurring Disabilities After Traumatic Brain Injury: Cost Effectiveness and Project-Based Intervention. Brain Impairment 8, 276-292.
| Crossref | Google Scholar |