STI & HIV 2025 World Congress Conference Abstracts
Abstract
26–30 July 2025, Montreal, Canada
The theme of the 2025 Congress is “Sexual Health for All”, and we hope to gather together an inclusive group of researchers, clinicians, laboratorians, public health practitioners, community members, and advocates from around the world to share ground-breaking clinical and basic science, innovative public health interventions, and evidence-based best practices in STI/HIV.
To cite the full set of abstracts: (2025) Abstracts from STI & HIV 2025 World Congress Conference. Sexual Health 22, SHv22n4abs. doi:10.1071/SHv22n4abs
To cite individual abstracts use the following format: McClarty L et al. (2025) OA10.05 - Expanded Polling Booth Surveys (ePBS) as a Rapid, Innovative, and Community-Engaged Tool for Routine Monitoring and Refinement of HIV/STI Programs for Criminalized and Other Marginalized Populations in Lower-Resourced Contexts: Findings from a Program Science-Guided Outcome Assessment in Nairobi County, Kenya [Conference abstract]. Sexual Health 22, SHv22n4abs.
OA10.05 – Expanded Polling Booth Surveys (ePBS) as a Rapid, Innovative, and Community-Engaged Tool for Routine Monitoring and Refinement of HIV/STI Programs for Criminalized and Other Marginalized Populations in Lower-Resourced Contexts: Findings from a Program Science-Guided Outcome Assessment in Nairobi County, Kenya
Dr. Leigh McClarty1, Stella Leung1, Dr. Joshua Kimani2, Antony Kinyua2, Rhoda Kabuti2, Jaffred Okoyana3, Virjinia Ndukuyu3, Dr. Helgar Musyoki4, Anthony Kiplagat5, Dr. Peter Arimi2, Dr. Shajy Isac6, Dr. Souradet Shaw1, Dr. Marissa Becker1, Parinita Bhattacharjee1,2
1Institute for Global Public Health, University of Manitoba, Winnipeg, Canada.
2Partners for Health and Development in Africa, Nairobi, Kenya.
3Sex Workers Outreach Programme (SWOP), Nairobi, Kenya.
4The Global Fund to Fight AIDS, Tuberculosis, and Malaria, Nairobi, Kenya.
5Nairobi County Health Department, Nairobi, Kenya.
6India Health Action Trust, Delhi, India.
Background: In many lower-resourced settings, comprehensive surveillance systems for HIV/STI are sub-optimal. Countries often depend upon resource-intensive population-based surveys that are implemented sporadically, leaving them reliant on outdated data to support epidemic responses. To better inform (sub-)national policy/programming, lower-cost, rapid, and flexible methods that retain methodological rigour are needed to maintain up-to-date HIV/STI estimates. Our team pioneered the expanded polling booth survey (ePBS) method with female sex workers (FSW) and men who have sex with men (MSM) in Nairobi County, Kenya to rapidly generate relevant data for programmatic refinement.
Description: The ePBS is a nimble, community-engaged method comprising three modules – polling booth surveys (anonymous, ballot-based group surveys); individual questionnaires linked to biological samples; and focus group discussions – that uses population- and location-based random sampling to generate representative samples. Descriptive equity analyses of ePBS data presented examine programmatically relevant outcomes – e.g., HIV prevalence, service coverage – by sub-county.
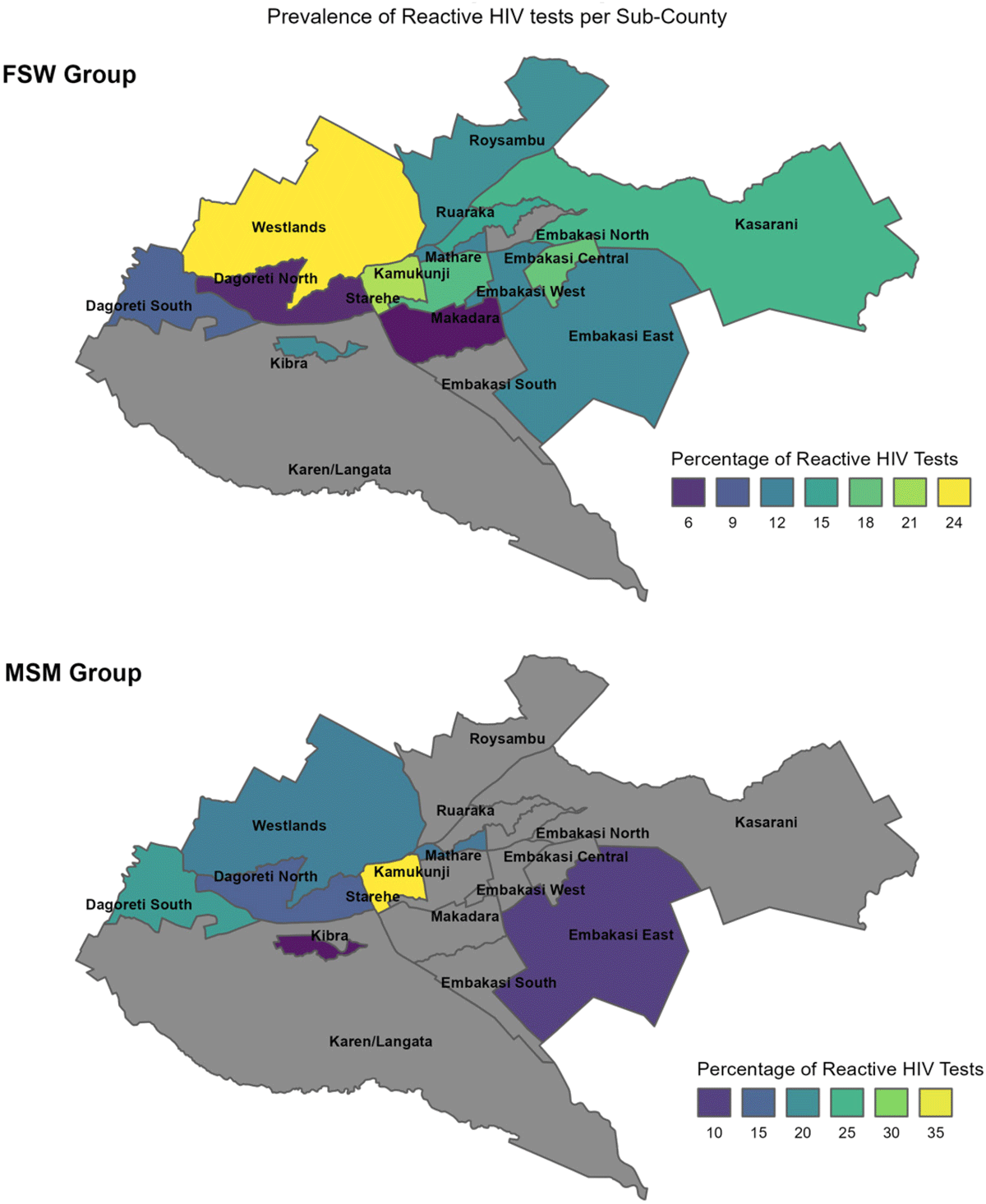
Results: Over 30 days in 2023, ePBS data were collected from 759 FSW and 398 MSM across 15 and 9 sub-counties of Nairobi, respectively. Inequalities in outcomes by sub-county were stark. HIV prevalence range: 0–24.2% (FSW) and 0–36.3% (MSM); contact with outreach (last quarter) range: 47.2–100% (FSW) and 52.1–91.7% (MSM); taken PrEP (last quarter) range: 4.6–19.1% (seronegative FSW) and 1.7–44.9% (seronegative MSM). Additional, ongoing analyses will be presented to examine inequalities by key variables (age, typology, years identifying as FSW/MSM); equiplots and choropleth maps (Fig. 1) will illustrate heterogeneity in inequalities.
Conclusion: ePBS is a rapid, rigorous, and lower-cost tool that can be regularly implemented to supplement routine program data. Through meaningful community engagement, ePBS enhances program monitoring and response to changes in local HIV/STI epidemiology, and service users’ needs over time and space. The flexibility, adaptability, and modular nature of ePBS is conducive to incorporating new surveillance and biomedical technologies and tracking emerging epidemiological trends rapidly, at relatively low cost.
Sub-county heterogeneity in HIV prevalence among female sex worker and men who have sex with men participating in the Expanded Polling Booth Survey study in Nairobi County, Kenya.
LBA01.01 – Can STI Testing Help Prioritise Use of Long-Acting PrEP in Rural South Africa? Process Data from the LAPIS Cluster Randomised Controlled Trial
Prof. Maryam Shahmanesh1,2, Mr Jacob Busang, Dr Thembelihle Zuma, Ms Carina Herbst, Ms Nonhlanhla Okesola, Dr Natsayi Chimbindi, Mr Jaco Dreyer, Ms Nqobile Ngoma, Dr Theresa Smit, Mr Lucky Mtolo, Dr Limakatso Lebina, Prof Janet Seeley, Dr Jana Jarolimova, Dr Andrew Copas, Dr Kathy Baisley
1University College London, London, United Kingdom.
2Africa Health Research Institute, Durban, South Africa.
Background: There are limited supplies of efficacious long-acting HIV pre-exposure prophylaxis (PrEP). We use a trial of long-acting PrEP delivery through mobile sexual health services to investigate if Sexually Transmitted Infections (STIs) diagnosis offers a way to prioritise long-acting PrEP amongst adolescents and young adults (AYA) in rural South Africa.
Methods: LAPIS (NCT066250504) is a cluster randomized controlled trial comparing offering a choice of oral PrEP, two monthly injectable cabotegravir (CABLA), or post-exposure prophylaxis (PEP), compared to offering oral PrEP alone, through mobile sexual health services. AYA aged 15–30 are offered testing for STIs (GeneXpert for gonorrhoea, chlamydia and trichomonas and point of care syphilis testing). We describe the pattern of STIs amongst AYA offered PrEP and the association with uptake and retention of different PrEP modalities in both arms. Uptake is defined as proportion of participants who initiate PrEP/PEP and retention as returning for the 1 month follow-up visit.
Results: June 2024 to April 2025, 2105 AYA were screened for PrEP suitability. 139 (7%) were living with HIV and 1404 (67%) were at risk of HIV acquistion and offered PrEP. 1307 (86%) initiated PrEP/PEP (n = 710; 83% in women). 588 (45%) chose CABLA (n = 365; 51% in women). 350/1422 (25%) tested positive for at least one STI (gonorrhoea, chlamydia, trichomonas, or syphilis). STI prevalence was 31% (181/588) amongst those who chose CABLA compared to 21% (135/650) and 15% (10/69) amongst those who took oral PrEP and PEP, respectively and 27% (172/636) among those retained on PrEP. Any STI diagnosis was associated with increased odds of CABLA uptake; OR = 1.69 (95% CI: 1.04–2.73) and age and gender adjusted OR = 1.79 (95% CI: 1.10–2.92).
Conclusions: Curable STIs are common and associated with increased uptake of long-acting PrEP. STI services offer an opportunity to prioritise those at highest risk of sexually acquired HIV with newer PrEP agents.
LBA01.02 – Trends in Bacterial STI Diagnoses Among Gay and Bisexual Men Before and After Emergent DoxyPEP Guidance
Research Fellow Michael Traeger1,2, Jason Asselin1,2,3, Hetin Linn Aung3, Vincent Cornelisse4, Dash Heath-Paynter5, Eric Chow6,7,9, Jason Ong6,7, Tom Rees8, Brendan Quinn1, Bridget Haire3, Basil Donovan3, Rebecca Guy3, Margaret Hellard1,2, Mark Stoove1,2
1Burnet Institute, Melbourne, Australia.
2School of Public Health and Preventive Medicine, Monash University, Australia.
3The Kirby Institute, UNSW Sydney, Australia.
4Mid North Coast & Northern NSW Local Health Districts, NSW Health, Australia.
5Health Equity Matters, Australia.
6Melbourne Sexual Health Centre, Alfred Health, Australia.
7School of Translational Medicine, Monash University, Australia.
8SA Health, Australia.
9Melbourne School of Population and Global Health, The University of Melbourne, Australia.
Background: Doxycycline post-exposure prophylaxis (doxyPEP) reduced bacterial STI incidence among gay and bisexual men (GBM) in clinical trials. The Australian DoxyPEP Consensus Statement released in September 2023 recommended prescribing doxyPEP to GBM with recent STIs. We evaluated changes in STIs among GBM following the release of doxyPEP trial findings and national prescribing recommendations.
Methods: We analysed testing data from GBM attending primary care/sexual health services in the ACCESS surveillance network (n = 27) between January 2022 and December 2024. Interrupted time-series analyses of monthly infectious syphilis, chlamydia and gonorrhoea diagnoses estimated trends in three periods (period 1 = January 2022–April 2023, period 2 = May 2023–September 2023, and period 3 = October 2023–December 2024) delineated by two interruptions: April 2023 [prominent RCT findings highlighting doxyPEP efficacy] and October 2023 [Australian doxyPEP recommendations released]. We estimated the relative change in diagnoses in December 2024 due to doxyPEP guidance by comparing the fitted value of observed data (period 3 trend) with the expected value under the counterfactual of no doxyPEP guidance (period 1 trend).
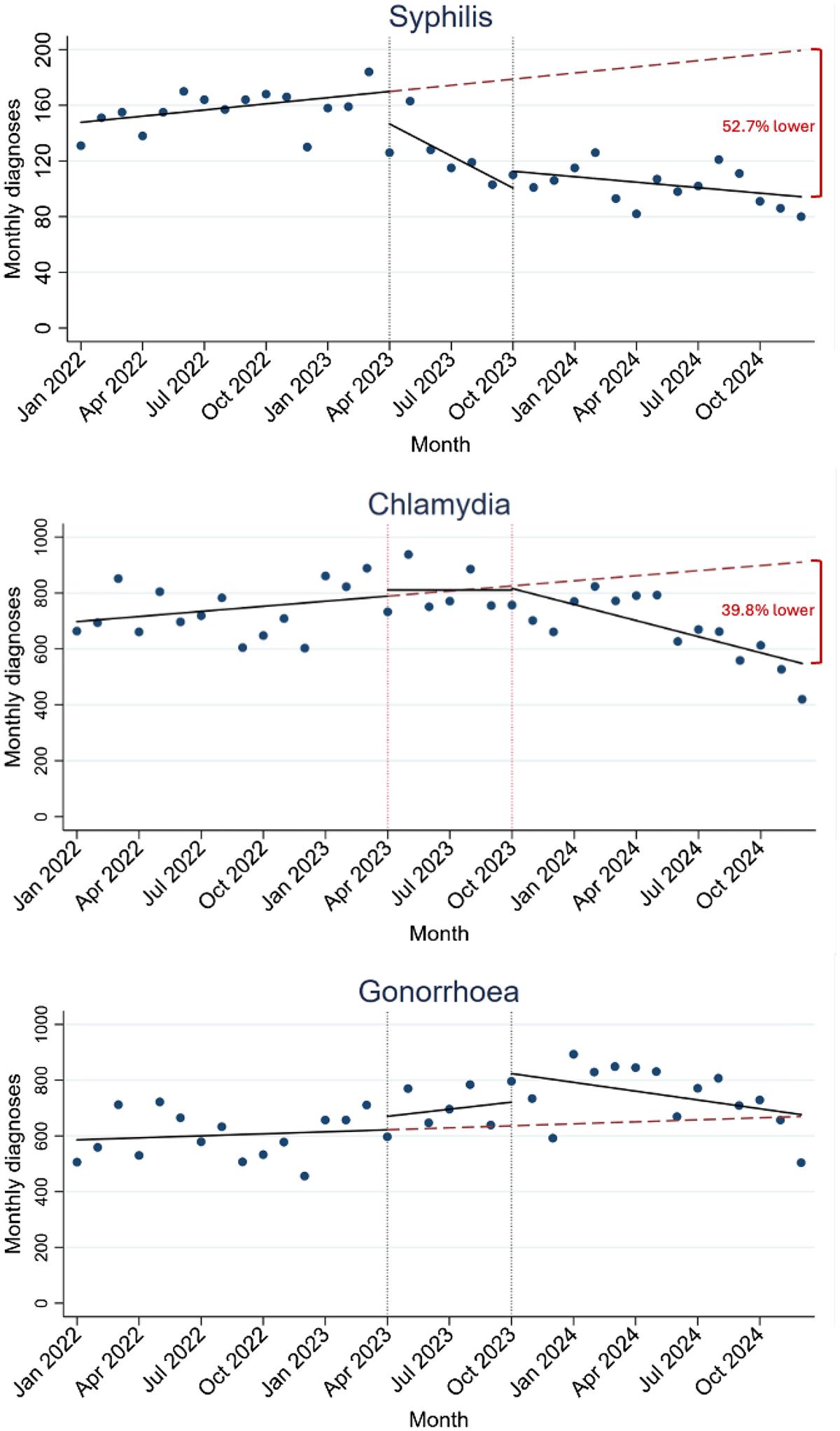
Results: 8,075 syphilis, 40,773 chlamydia and 36,074 gonorrhoea cases were diagnosed among 36,027 GBM. Monthly syphilis diagnoses increased in period 1 by 1.6/month (P = 0.049), declined by 7.7/month in period 2 (P = 0.022), and were stable in period 3 (β = 1.3/month, P = 0.106). Chlamydia diagnoses were stable in periods 1 (β = 6.1, P = 0.26) and 2 (β = 0.0, P = 0.99), and declined by 19.2/month in period 3 (P = 0.001). No significant trends in gonorrhoea were detected. The estimated change in diagnoses in December 2024 from expected to observed data was 199 to 94 for syphilis (52.7% lower, P < 0.001), 910 to 548 for chlamydia (39.8% lower, P < 0.001), and 669 to 676 for gonorrhoea (non-significant).
Conclusion: Diagnoses of syphilis and chlamydia declined following the release of doxyPEP prescribing guidance. These ecological data suggest doxyPEP may be having an impact on population-level STI incidence among GBM attending sexual health clinics.
Monthly number of STI diagnoses among gay and bisexual men attending ACCESS clinics from 2022 to 2024, with trend interruptions at April 2023 (US DOXYPEP trial findings published) and October 2023 (ASHM doxyPEP guidelines released).
LBA01.03 – Contribution of Increased STI Screening to Increased Rate of Gonorrhea and Chlamydia Diagnoses After PrEP Initiation
Ms. Anna Marie Parker1, Dr. Benjamin John Singer1, Mr. Chungman Chae1, Mrs. Tara Wood2, Dr. Joseph A. Lewnard1, Dr. Katia J. Bruxvoort2
1University of California, Berkeley, Berkeley, United States.
2University of Alabama at Birmingham, Birmingham, United States.
Background: HIV preexposure prophylaxis (PrEP) users experience higher rates of chlamydia and gonorrhea diagnoses compared to non-users. However, the contribution of increased STI screening after PrEP initiation to this increase in STI diagnoses remains unclear.
Methods: We conducted a case-crossover study using data from the Merative MarketScan® Research Databases (2016–2019) to estimate the risk of chlamydia and gonorrhea diagnoses associated with PrEP initiation. To quantify the contribution of increased case ascertainment, we assessed the proportion of infections attributable to extragenital screening integrated into routine PrEP care.
Results: PrEP initiation was associated with nearly threefold increases in gonorrhea (adjusted risk ratio [aRR] = 3.21 [95% CI: 2.42–4.15]) and chlamydia diagnoses (aRR = 4.00 [2.74–5.63]). However, enhanced case detection was the primary driver of these associations: we estimated that increased screening alone accounted for 3.18-fold (1.23–7.91) and 3.78-fold (1.19–13.60) increases in rates of ascertaining asymptomatic gonorrhea and chlamydia infections, respectively. Overall, increased screening accounted for 68.6% (27.7%–100%) and 64.7% (18.5%–100%) of the increase in gonorrhea and chlamydia diagnoses observed after PrEP initiation.
Conclusions: Our findings suggest that increased case ascertainment is the primary driver of elevated rates of chlamydia and gonorrhea diagnoses observed after PrEP initiation.
LBA01.04 – Human Papillomavirus (HPV) Screening Utilising HPV Self-Testing in New Zealand): a Cluster-randomised Non-inferiority Trial
Prof. Bev Lawton1, Dr Melanie Gibson1, Dr Tania Slater1, Ms Varsha Parag2, Dr Kendall Stevenson1, Dr Anna Adcock1, Dr Jo-Anne Stanton1, Ms Maxine Schmidt1, Ms Mary-Ann Stevenson3, Ms Koha Aperahama4, Ms Carissa Thompson5, Ms Alison Carlin6, Dr Kristy Wolff6, Professor Stacie Geller7, Mr Charles Lambert1, Mr Matthew Bennett1, Professor Merilyn Hibma8, Associate Professor Peter Sykes9, Professor Marion Saville10, Professor David Hawkes10, Dr Jane MacDonald1
1Te Tatai Hauora O Hine (ncwhra) - Victoria University of Wellington, Wellington, New Zealand.
2National Institute for Health Innovation, University of Auckland, Auckland, New Zealand.
3Mahitahi Hauora Primary Health Entity, Whangarei, New Zealand.
4Te Whatu Ora, New Zealand.
5Ngā Tohianga, Kaitaia, New Zealand.
6Colposcopy Team, Te Whatu Ora, Whangarei, New Zealand.
7Department of Obstetrics and Gynaecology, Centre for Research on Women and Gender, College of Medicine, University of Illinois, USA.
8Department of Pathology, University of Otago, New Zealand.
9Christchurch Hospital and University of Otago, Christchurch, New Zealand.
10Australian Centre for the Prevention of Cervical Cancer, Melbourne, Australia.
Background: The opportunistic offer of HPV self-testing (self-collection) in under-screened women has been shown to increase uptake of screening. What is not known is whether “Universal offer of HPV self-testing “increases program coverage. The objective of this study is to assess whether implementing a universal offer of HPV self-testing for cervical screening achieves non-inferior screening coverage compared to standard care (cervical cytology by vaginal speculum examination).
Methods: Cluster-randomised, non-inferiority trial. Fourteen primary health care practices (seven per arm).
Participants: Women and people with a cervix aged 24.5–69.9 years due or overdue for cervical screening attending participating practices.
Intervention –“universal offer of HPV self-testing” included community engagement, clinic education, and an offer of HPV self-testing (self-collection).
Main outcome measures: The primary outcome was screening coverage.
Results: 22,511 people were in the main analysis: 10,727 in the intervention arm, 11,784 in the comparison arm. The mean absolute difference in screening coverage between intervention compared to comparison was 10.8% (95% CI: 4.7 to 16.9, P = 0.0006), higher for the intervention. This demonstrated both non-inferiority and superiority of the intervention. Non-inferiority and superiority were demonstrated in subgroup analyses for equity. Full details will be described in presentation.
Conclusions: These findings of superior and equitable screening coverage, suggest cervical screening programmes can have confidence that implementing a universal offer of HPV self-testing will not decrease coverage and is likely to increase coverage leading to reduced preventable morbidity and mortality from cervical cancer.
LBA01.05 – Unpacking Chemsex in Amsterdam: What Distinguishes Non-Users, Non-Problematic, and Problematic Users?
Ms. Doortje van den Dungen1, Assistant Professor Mark Assink2, Professor Henny Bos2, Doctor Elske Hoornenborg1, Doctor Udi Davidovich1,3, Prof. Henry de Vries1,5, Doctor Vita Jongen1,4
1Department of Infectious Diseases, Public Health Service Amsterdam (GGD Amsterdam), Amsterdam, the Netherlands.
2Research Institute of Child Development and Education (RICDE), University of Amsterdam, Amsterdam, the Netherlands.
3Department of Social Psychology, University of Amsterdam, Amsterdam, the Netherlands.
4Stichting HIV Monitoring, Amsterdam, the Netherlands.
5Department of Dermatology, Amsterdam UMC, University of Amsterdam, Amsterdam, the Netherlands.
Background: Chemsex – the use of specific substances to enhance sex – is predominantly described among gay, bisexual, and other men who have sex with men (GBMSM). While chemsex is linked to increased STIs and mental health concerns, not all chemsex is problematic. Problematic chemsex is characterized by negative impacts on relationships, work, and mental health. This study aimed to identify psychological factors associated with problematic chemsex and examine differences between non-users, non-problematic, and problematic chemsex users.
Methods: A cross-sectional survey was conducted in Amsterdam (April–July 2024) among GBMSM recruited via health clinics, social media, dating apps, and community outreach. Chemsex was defined as the use of methamphetamine, mephedrone, GHB/GBL, ketamine, cocaine, speed, 3-MMC, and designer drugs, in sexual settings. The survey assessed gay community stress, psychological distress, loneliness, interpersonal awareness, and internalized homophobia, and compared these across non-chemsex users (NCS), non-problematic users (NPCS), and problematic users (PCS) using Kruskal–Wallis and pairwise Wilcoxon tests.
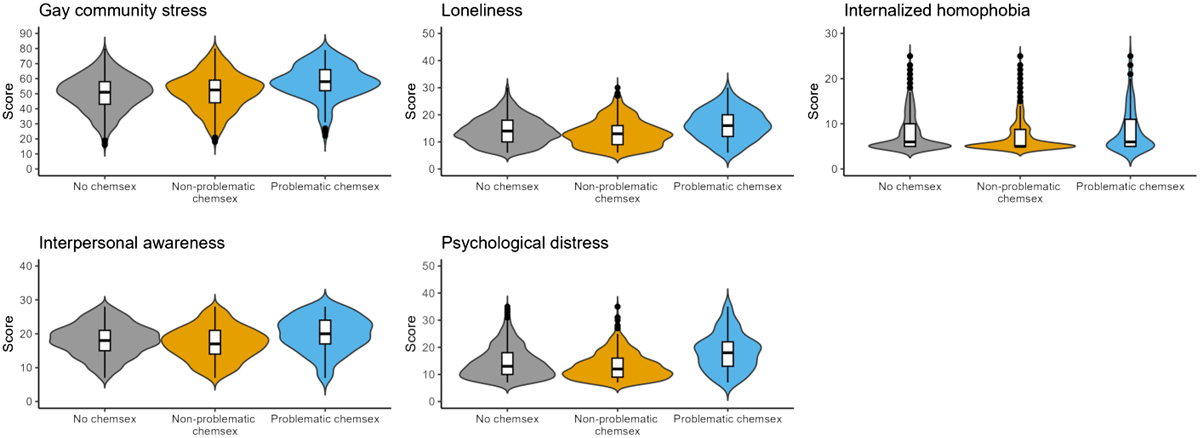
Results: Of the 2,984 participants who initiated the survey, 1,888 (63%) completed it (NCS = 1,077; NPCS = 650; PCS = 161). Median age was 39 years (IQR = 31–52). Of these 1,888 participants, 203 (10.8%) reported living with HIV. Gay community stress was high overall (median = 52, IQR = 44-59), differed significantly across groups (P < 0.001) (Fig. 1), and was highest in PCS. Similarly, loneliness (median = 13, IQR = 10–17), internalized homophobia (median = 5, IQR = 5–9), interpersonal awareness (median = 18, IQR = 15–21), and psychological distress (median = 13, IQR = 10–18) differed between groups (all P <0.001), and were highest in PCS.
Conclusion: Problematic chemsex is associated with greater psychological burden. Further research into psychosocial factors may help identify predictors for PCS, supporting early detection and tailored interventions. These findings highlight the need for targeted mental health support and integrated care addressing both substance use and underlying psychological challenges.
Psychological stressors among non-chemsex, non-problematic chemsex, and problematic chemsex users.
LBA01.06 – Exploring Challenges Faced by Female Sex Workers Using the Dapivirine Vaginal Ring: Insights from BHESP’s (Bar Hostess Empowerement and Support Program) Implementation in Mowlem, Kenya
Miss Maureen Waithira1, Miss Janeffer Gacheru1
1Bhesp, NAIROBI, Kenya.
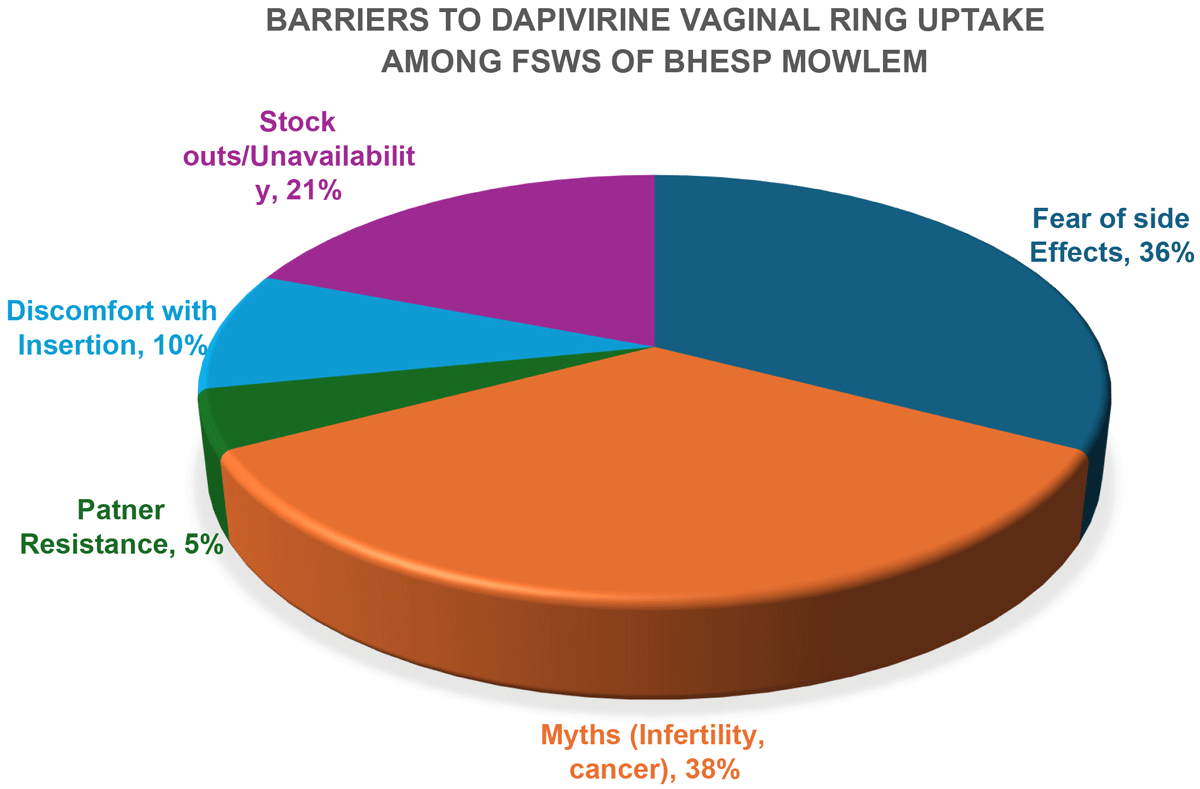
Background: Female sex workers (FSWs) in Kenya are at a heightened risk of acquiring HIV due to various biological, structural, and social vulnerabilities. In response to these challenges and as part of a national effort to introduce biomedical HIV prevention methods, the BHESP implemented the dapivirine vaginal ring intervention in Mowlem, Nairobi. This intervention aimed to expand HIV prevention options for women in a community with a persistent HIV prevalence and significant stigma, where traditional oral PrEP has limitations regarding adherence and discretion.
Description: The intervention was rolled out through a drop-in center offering integrated HIV prevention and SRHR services. Peer educators conducted community sensitizations and supported ring uptake through tailored counseling and follow-up visits. BHESP collaborated with LVCT, who trained clinicians in ring insertion and removal. Data on uptake and user experiences was collected the clinic, focus group discussions were also conducted.
Results: While there was moderate initial interest in the intervention, uptake remained low, with only 21% of eligible FSWs accepting the ring (Fig. 1). Major challenges affecting uptake included fear of side effects (reported by 63% of non-users), myths regarding infertility and cancer, and discomfort with self-insertion. Users who continued using the ring cited discretion and the convenience of monthly dosing as significant benefits. Peer support was identified as critical for acceptance and sustained use. Additionally, structural issues such as limited clinic hours, and stockouts were also reported. Qualitative insights emphasized the necessity for more robust demand creation efforts and interventions aimed at dispelling myths.
Conclusion: The introduction of the dapivirine ring among FSWs revealed important acceptability and access challenges that require targeted responses. Community-led education, provider sensitization, and stronger follow-up mechanisms are essential for successful rollout. Lessons from BHESP’s implementation can inform scale-up efforts and guide integration of new PrEP options in national HIV prevention programs targeting FSWs.
OA01.01 – PrEP-Surfing: HIV Pre-Exposure Prophylaxis (PrEP) Use of Sexual Partners as HIV Prevention Strategy Among Men Who Have Sex with Men
Ms. Carien Blomaard1,2,3,4, Jeffrey Koole1,2,3,4, Elske Hoornenborg1,2,3,4, Maria Prins1,2,3,4, Janneke Heijne1,2,3,4, Udi Davidovich1,5, Maarten Schim van der Loeff1,2,3,4
1Public Health Service Amsterdam, Amsterdam, Netherlands.
2Amsterdam UMC location University of Amsterdam, Department of Internal Medicine, Amsterdam, Netherlands.
3Amsterdam Institute for Immunology and Infectious Diseases, Amsterdam, Netherlands.
4Amsterdam Public Health Research Institute, Amsterdam, Netherlands.
5University of Amsterdam, Department of Social Psychology, Amsterdam, Netherlands.
Background: Having condomless anal sex (CAS) while relying on the HIV pre-exposure prophylaxis (PrEP) use of one’s sex partner is referred to as PrEP-surfing. Frequency of PrEP-surfing and characteristics of men-who-have-sex-with-men (MSM) practicing it are unknown. We aimed to estimate the frequency of PrEP-surfing, intention to practice it, and determinants of both.
Methods: We included MSM of the Amsterdam Cohort Studies participating in 2021–2023. Participants completed six-monthly questionnaires about recent (=preceding 6 months) sexual behaviour, including PrEP use and PrEP-surfing, and intention for PrEP use and PrEP-surfing in coming 6 months (assessed on a 7-point Likert scale; high intention was defined as ≥6). Eligible were HIV-negative MSM not using exclusively daily PrEP. We assessed determinants of PrEP-surfing with logistic regression and determinants of intention to PrEP-surfing with linear regression.
Results: We included 562 participants, who contributed 1,779 visits. Median age was 45 (IQR = 33–52) years, number of recent sex partners 4 (IQR = 1–9) and 190 (34%) participants reported recent PrEP use. In 449/1,779 visits (25%) recent PrEP-surfing was reported. In multivariable analysis, CAS with a partner with unknown HIV status and ≥3 recent sex partners were associated with recent PrEP-surfing, while older age and having a steady partner were inversely associated (Table 1). In 1,061 visits by 385 participants without high PrEP use intention, the median intention to PrEP-surfing was 3 (IQR = 1–5); in 194/1,061 visits (18%) intention to PrEP-surfing was high. CAS with a casual partner (β = 1.4, 95% CI = 1.0–1.8) and high perceived probability of contracting HIV (β = 0.8, 95% CI = 0.4–1.1) were associated with surfing intention; age ≥45 was inversely associated with surfing intention (45-54: β = –0.9, 95% CI = –1.3,–0.4; ≥55: β = –0.6, 95% CI = –1.1,–0.1).
Conclusion: PrEP-surfing is a common HIV prevention strategy among MSM in Amsterdam, particularly among younger MSM. Further research is needed to assess motives, settings, and possible risks, in order to optimize HIV prevention care for MSM.
| n/N (%) | Univariable model | Multivariable model | |||||
|---|---|---|---|---|---|---|---|
| OR | 95% CI | aOR | 95% CI | P | |||
| Age group | |||||||
| 18–34 years | 135/405 (33.3%) | REF | – | REF | – | – | |
| 35–44 years | 117/363 (32.2%) | 0.95 | 0.63–1.42 | 1.02 | 0.67–1.55 | 0.932 | |
| 45–54 years | 115/612 (18.8%) | 0.46 | 0.3–0.68 | 0.44 | 0.29-0.65 | <0.001 | |
| ≥55 years | 82/399 (20.6%) | 0.52 | 0.33–0.81 | 0.42 | 0.27-0.68 | <0.001 | |
| Steady partnera | |||||||
| Yes | 261/1215 (21.5%) | REF | – | REF | – | – | |
| No | 188/564 (33.3%) | 1.83 | 1.37-2.44 | 1.51 | 1.11–2.06 | 0.009 | |
| Number of sex partnersa | |||||||
| 0–2 | 64/745 (8.6%) | REF | – | REF | – | – | |
| 3–8 | 204/577 (35.4%) | 5.82 | 4.06–8.34 | 4.86 | 3.33–7.11 | <0.001 | |
| ≥9 | 181/457 (39.6%) | 6.98 | 4.67–10.42 | 4.70 | 2.97–7.44 | <0.001 | |
| CAS with partner with unknown HIV statusA | |||||||
| No | 243/1292 (18.8%) | REF | – | REF | – | - | |
| Yes | 206/487 (42.3%) | 3.16 | 2.39–4.23 | 1.80 | 1.27–2.54 | 0.001 | |
| Rectal STI or syphilisA | |||||||
| No | 367/1610 (22.8%) | REF | – | REF | – | – | |
| Yes | 82/169 (48.5%) | 3.19 | 2.24–4.55 | 1.81 | 1.23–2.66 | 0.003 | |
OA01.02 – HIV Stigma Beliefs Associated with PrEP Willingness and Status Disclosure Among Adolescents in Kenya
Prof. Hong-Ha M. Truong1, Ms. Sayo Amboka2, Ms. Elsa Heylen1, Ms. Beatrice Otieno3, Mr. Kevin Kadede2, Mr. Hanningtone Odhiambo2, Ms. Damaris Odeny2, Ms. Marion Hewa2, Mr. Maurice Opiyo2, Mr. Fidel Opondo2, Mr. David Ogolla2, Ms. Lara Miller1, Prof. Elizabeth Bukusi2, Prof. Craig Cohen1
1University of California, San Francisco, United States.
2Kenya Medical Research Institute, Kisumu, Kenya.
3University of California Global Programs, Kisumu, Kenya.
Background: Fear of HIV stigmatization may hinder pre-exposure prophylaxis (PrEP) use and status disclosure by adolescents. We assessed HIV stigma beliefs and willingness to use PrEP and disclose HIV status among adolescents in Kenya.
Methods: The Maneno Yetu study enrolled adolescents aged 15–19 (N = 3,061) residing in Kisumu for a cross-sectional survey. HIV stigma beliefs were assessed via three statements. Participants self-reporting as HIV-negative (n = 3,011) were asked their willingness to use PrEP and disclose their HIV status if they tested positive.
Results: Overall, 55% of adolescents agreed “most people are uncomfortable around persons living with HIV (PLWH)”, 37% agreed “most people think PLWH is disgusting”, and 31% agreed “most people think PLWH brought it on themselves”. Endorsement of “most people think PLWH are disgusting” was higher among girls than boys (P = 0.02). HIV-negative participants were willing to use PrEP (53%) and disclose their HIV status if they tested positive (66%). Higher endorsement of “most people are uncomfortable around PLWH” was associated with higher willingness to consider PrEP use (P = 0.03). Lower endorsement across stigma belief statements was associated with higher willingness to disclose HIV status (P < 0.01).
Conclusion: HIV stigma remains pervasive among adolescents despite decades of educational efforts. Many adolescents believe people in their communities have negative perceptions about PLWH. Interestingly, adolescents who believe people are uncomfortable around PLWH were more willing to consider using PrEP, suggesting fear of stigmatization may be a motivating factor for PrEP use. Adolescents who disagreed with stigmatizing statements about PLWH were more willing to disclose their HIV status if they tested positive, suggesting they believe HIV stigma is not widespread in their communities. Our findings highlight the need for continued HIV stigma reduction efforts. Peer influence is important during adolescence, therefore education delivered by peers may be persuasive in changing HIV stigma beliefs and expanding PrEP use.
OA01.03 – Reinvigorating Condom Programming Is the Way to Ensure Sexual Health for All in the Increasing Trend of Consumption of Pre-Exposure Prophylaxis (PrEP) by MSM in Delhi and Mumbai
Dr. V Sam Prasad1, Ms. Elizabeth Michael1, Mr. Mohnish Kumar1, Mr. Shivam Dwivedi1, Mr. Lyle Honig Mojica2
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
2AIDS Healthcare Foundation (AHF), Los Angeles, United States of America.
Background: The increasing availability of Pre-Exposure Prophylaxis (PrEP) has led to a decline in condom use among Men who have Sex with Men (MSM), resulting in a rising trend of Sexually Transmitted Infections (STIs) in Delhi and Mumbai.
Description: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across ten states. The study recruited participants (n = 300) who identified as MSM and were taking PrEP. Qualitative in-depth interviews were also conducted (n = 20) with MSM in Delhi and Mumbai.
Results: Quantitative findings revealed:
-
60% of participants reported inconsistent condom use.
-
40% reported never using condoms during oral sex.
-
75% of participants had limited knowledge about STI risks and its association with HIV.
-
50% reported experiencing stigma associated with condom use.
-
30% of participants reported using PrEP irregularly, only 10% reported consistent condom use while on PrEP.
-
25% of participants reported having multiple sexual partners in the past 6 months.
Qualitative findings highlighted:
-
Perceived reduced risk of STI/ HIV transmission with PrEP.
-
Lack of awareness about STI /HIV risks.
-
Stigma associated with condom use and its availability are major barriers to consistent condom use.
-
Difficulty accessing condoms, especially in rural and sub-urban locations.
-
Limited availability of STI testing and treatment services.
Conclusion: This study underscores the urgent need for robust condom programming among MSM populations in Delhi and Mumbai. Policymakers, healthcare providers, and community organizations must work together to promote comprehensive STI education and awareness, increase condom availability and accessibility, address stigma associated with condom use, and integrate STI testing and treatment services into existing healthcare infrastructure. Additionally, targeted interventions for MSM populations using PrEP, are necessary which may be spear headed by community-based organizations and peer support groups.
OA01.04 – High Interest in the PrEP (Dapivirine) Ring Among US, Low-Income Latina Women: Results from a Community Clinic
Dr. Erica Gollub1, Ms. Elena Finver1, Ms. Lauren Pizzella1, Ms. Cinthya Raposo1, Mr Jesus Hernandez1
1Pace University, Pleasantville, United States.
Background: The long-acting PrEP/Dapivirine ring is not yet US-approved. PrEP coverage among US Latinas (<10%) indicates an urgent need for additional PrEP choices. We report results from a hypothetical acceptability study among a low-income, predominantly Latina population.
Methods: This study was approved by Pace University IRB. Women (> = 18 years of age, heterosexually active) were recruited from a community clinic waiting room by a bilingual research assistant. Following a brief informational session, participants handled a placebo ring, then completed a one-time survey via audio computer-assisted self interview (Spanish or English). Multivariate analysis explored predictors of interest in future ring use.
Results: Of 152 participants. 90% were Hispanic/Latino; a majority (77%) elected Spanish survey language (SLS). Most women had children (73%), and a main sexual partner (91%); 13% reported casual partner/s. Only 47% had health insurance. Two-thirds had at least a high school diploma; 23% had a college degree or higher. Anal sex was common (43% main partner, 57% casual partner). One-quarter reported a “main partner would get angry if asked to use a condom”; 44% of those with casual partners felt at risk for STDs. Substantial numbers cited ring concerns, including ease of use (42%); fear of side effects (51%) or discomfort for self (49%) or partner (42%) during sex; ring “falling out” (51%); ring “getting stuck” (58%). Nevertheless, the majority (76%) reported wanting to try the PrEP ring when available. Upwards of 90% of women liked ring aspects: discreet protection; relief from daily PrEP pill burden; women’s control of the ring. In multivariate modeling, ring interest was associated with SLS (P < 0.002), high perceived HIV risk (P < 0.035), and health insurance (P < 0.057).
Conclusion: Interest in the PrEP ring was high, especially among SLS participants and despite ring concerns or fears. The PrEP ring provides an urgently-needed additional choice for US women.
OA01.05 – Support for Over-The-Counter HIV PrEP Among Cisgender Women in the United States
Dr. Lauren R. Violette1,2, Dr. Rebecca Schnall3,4, Dr. Mirjam-Colette Kempf5,6,7, Dr. Amy K. Johnson8, Ms. Maeve Brin3, Ms. Fengdi Xiao3, Dr. Douglas S. Krakower1,2, Dr. Julia L. Marcus1,2
1Harvard Medical School, Boston, United States.
2Harvard Pilgrim Health Care Institute, Boston, United States.
3School of Nursing, Columbia University, New York, United States.
4Columbia University Mailman School of Public Health, New York, United States.
5School of Public Health, University of Alabama at Birmingham, Birmingham, United States.
6School of Nursing, University of Alabama at Birmingham, Birmingham, United States.
7Heersink School of Medicine, University of Alabama at Birmingham, Birmingham, United States.
8Ann & Robert H Lurie Children’s Hospital of Chicago, Chicago, United States.
Background: Over-the-counter (OTC) availability of HIV PrEP could improve access, use, and impact, but it is unknown if populations likely to benefit from PrEP would support this policy change.
Methods: We analyzed data from the American Women: Assessing Risk Epidemiologically prospective cohort study from June-December 2024. Participants were US cisgender women aged 14–64, were HIV-negative, and reported condomless sex with a male in the past 6 months and ≥1 other factor associated with HIV seroconversion. In the 12-month survey, participants were asked whether they would support making daily oral PrEP available OTC in pharmacies or online, without the need for a prescription, if research showed it was safe and effective. We used modified Poisson regression to compute unadjusted prevalence ratios (PR) to identify correlates of support for OTC PrEP.
Results: Among 251 respondents, median age was 36 years, 71% were White, 15% were Hispanic or Latina, and 94% were PrEP-naïve. Overall, 83% supported OTC PrEP; 4% did not support it and 13% were unsure (Table 1). Support for OTC PrEP did not differ by age but was higher among Asian (PR = 1.05, 95% confidence interval [CI] = 1.02–1.09) and Black (PR = 1.05, 95% CI = 1.02–1.09) respondents compared with White respondents, and among uninsured respondents compared with those with private insurance (PR = 1.05, 95% CI = 1.01–1.10). Among those with no intention to start PrEP soon, support for OTC PrEP was higher among those who did not want PrEP because they believed it would not be covered by their health insurance (PR = 1.05, 95% CI = 1.02–1.08). Participants who would be motivated to initiate PrEP if there were fewer monitoring appointments had greater support for OTC access (PR = 1.05, 95% CI = 1.02–1.08).
Conclusion: Support for OTC PrEP was high among cisgender women, especially those facing barriers related to insurance coverage. Future research should explore interest in OTC PrEP use in populations that could benefit most from expanded access.
| Supports OTC PrEP N = 209 | Does not support OTC PrEP N = 9 | Unsure about support for OTC PrEP N = 33 | ||
|---|---|---|---|---|
| Age (years) – median [IQR] | 35 [29–41] | 38 [24–43] | 39 [33–45] | |
| Ethnicity | ||||
| Hispanic or Latina | 30 (14%) | 2 (22%) | 5 (15%) | |
| Non-Hispanic | 177 (85%) | 7 (78%) | 28 (85%) | |
| Refuse to answer | 2 (1%) | 0 (0%) | 0 (0%) | |
| Race | ||||
| American Indian/Alaskan Native | 2 (1%) | 0 (0%) | 1 (3%) | |
| Asian | 8 (4%) | 0 (0%) | 1 (3%) | |
| Black or African American | 28 (13%) | 0 (0%) | 8 (24%) | |
| Multiracial | 17 (8%) | 1 (11%) | 3 (9%) | |
| White | 151 (72%) | 8 (89%) | 20 (61%) | |
| Another group not listed | 3 (1%) | 0 (0%) | 0 (0%) | |
| Housing status | ||||
| Has housing | 204 (98%) | 7 (78%) | 32 (97%) | |
| Does not have housing | 4 (2%) | 2 (22%) | 0 (0%) | |
| Refuse to answer | 1 (0%) | 0 (0%) | 1 (3%) | |
| Highest level of education | ||||
| Less than high school | 3 (1.4%) | 0 (0%) | 0 (0%) | |
| High school diploma or GED | 28 (13%) | 0 (0%) | 1 (3%) | |
| More than high school | 177 (85%) | 9 (100%) | 32 (97%) | |
| Refuse to answer | 1 (0%) | 0 (0%) | 0 (0%) | |
| Current employment status | ||||
| Not employed | 21 (10%) | 1 (11%) | 3 (9%) | |
| Part-time or temporary work | 46 (22%) | 2 (22%) | 5 (15%) | |
| Full-time work | 116 (56%) | 4 (44%) | 22 (67%) | |
| Not seeking work | 24 (11%) | 2 (22%) | 2 (6%) | |
| Refuse to answer | 2 (1%) | 0 (0%) | 1 (3%) | |
| Type of health insurance | ||||
| No insurance | 26 (12%) | 0 (0%) | 3 (%) | |
| Public insurance | 71 (34%) | 3 (33%) | 8 (%) | |
| Private insurance | 111 (53%) | 6 (67%) | 20 (%) | |
| Refuse to answer | 1 (0%) | 0 (0%) | 2 (%) | |
| PrEP use | ||||
| PrEP-naïve | 196 (94%) | 8 (89%) | 33 (100%) | |
| PrEP-experienced (current or past) | 10 (5%) | 0 (0%) | 0 (0%) | |
| Refuse to answer | 3 (1%) | 1 (11%) | 0 (0%) |
OA01.06 – Addressing Barriers to HIV Prevention Among Men Who Have Sex with Men (MSM) in Kenya: A Focus on PrEP Uptake
Mr. Harrison Wanjohi1,2
1Hoymas Kenya.
2Fahari Ya Jamii Project, Nairobi, Kenya.
Background: Men who have sex with men (MSM) in Kenya face a heightened risk of HIV acquisition due to high-risk sexual behaviors and stigma that limits access to healthcare services. Pre-exposure prophylaxis (PrEP) has proven effective in preventing HIV transmission, yet uptake among MSM remains suboptimal. This study explores the unique barriers and facilitators influencing PrEP use among MSM, aiming to provide insights for improving HIV prevention strategies in this key population.
Methods: A cross-sectional study was conducted among 300 MSM participants recruited from Nairobi, Kisumu, and Mombasa. Quantitative data were collected through structured surveys covering topics such as sexual risk behavior, HIV knowledge, and PrEP awareness. Additionally, in-depth qualitative interviews were conducted with 30 MSM participants to gain insights into their personal experiences with HIV prevention services. Quantitative data were analyzed using logistic regression, while thematic analysis was used for qualitative data to explore key themes related to PrEP use.
Results: Among the MSM surveyed, 74% were aware of PrEP, but only 27% reported current use. Barriers to PrEP uptake included fear of stigma (55%), misconceptions about PrEP (43%), and lack of access to LGBTQ-friendly health services (39%). Facilitators of PrEP uptake included peer support groups (66%), integration of PrEP into general health services (58%), and the availability of PrEP information via social media. Participants expressed a preference for accessing PrEP through community-based clinics, which they perceived as more confidential and inclusive.
Conclusions: While awareness of PrEP is high among MSM in Kenya, uptake remains limited due to stigma, misconceptions, and lack of LGBT-competent health services. Interventions that address these barriers, such as expanding community-based clinics, increasing peer support networks, and providing culturally sensitive health education, are crucial for improving PrEP uptake and reducing HIV transmission among MSM in Kenya.
OA02.03 – Community Pharmacy Users in Kampala Continue Sexual Activity Despite STI Symptoms
Miss Vivian Nakate1, Dr Annet Onzia Aketoko1, Miss Irene Bagaya1, Prof Yukari C Manabe2, Dr Johan H Melendez2, Dr Rosalind Parkes Ratanshi1, Dr Matthew M Hamill2, Dr Agnes Kiragga1
1Infectious Diseases Institute, Kampala, Uganda.
2Division of Infectious Diseases, Department of Medicine; Johns Hopkins University School of Medicine, Baltimore, MD, USA.
Background: Community pharmacies (CP) are accessible with shorter waiting times than clinics, provide trusted healthcare services in Ugandan communities and could be a point of access to healthcare for STI/HIV care. The relationship between sexual activity and the presence of STI-related symptoms in CP users remains underexplored. We examined associations with ongoing sexual activity in CP users with STI symptoms.
Methods: Clients purchasing treatment for STI-syndromes and non-STI-related conditions in 18 CPs in urban Uganda were enrolled and tested for STIs. Trained researchers administered a structured questionnaire which collected clinical, sociodemographic, STI knowledge, and sexual behavior information. Bivariate and multivariable Poisson model was used to determine factors associated with sexual behavior since symptom onset.
Results: Between May 2021 and June 2022, 450 participants were recruited (female, 62.2%), median (IQR) age 28 (24–35). 238/450 (52.9%) had STI symptoms; of those, 126/238 (52.9%) had ≥2 symptoms, 87/238 (36.9%) had symptoms for >2 weeks. 117/238 (49.2%) reported sexual activity since symptom onset; 66/117 (56.4%) were female, 94/117 (80.3%) aged ≥25 years, 69/117 (59.0%) were engaging in transactional sex, 67/117 (57.3%) had low STI knowledge, and 35/117 (30.0%) tested positive for syphilis, gonorrhea, chlamydia, or trichomoniasis (Table 1).
Factors significantly associated with having sex despite symptoms adjusted for age, partner status, transactional sex, STI knowledge, STI status, partner notification, recent antibiotic use, and symptom duration, were age 25–34 years, engagement in transaction sex, STI knowledge, duration of symptoms >2 weeks.
Conclusion: Individuals who engaged in transactional sex, had prolonged symptoms, and low STI knowledge were more likely to have sex despite STI symptoms. This emphasizes the need for targeted education and interventions in community pharmacy settings to reduce behaviours associated with STIs. CPs can serve as key access points for those at risk of STIs/HIV and reduce time to initiate treatment.
| Had sex since developed symptoms 117/238 (49.2%) | Unadjusted PR (95% CI) | P-value | Adjusted PR (95% CI) | P-value | ||
|---|---|---|---|---|---|---|
| Overall | N/A | N/A | N/A | N/A | ||
| Gender | ||||||
| Female | 51/103 (49.5) | Ref | Ref | |||
| Male | 66/135 (48.9) | 1.01 (0.70–1.46) | 0.946 | – | – | |
| Age (years) | ||||||
| 17–24 | 23/67 (34.3) | Ref | Ref | – | ||
| 25–34 | 57/102 (55.9) | 1.63 (1.00–2.64) | 0.049 | 1.63 (1.01–2.66) | 0.050 | |
| ≥35 | 37/69 (53.6) | 1.56 (0.93–2.63) | 0.093 | 1.45 (0.86–2.47) | 0.159 | |
| Partner status | ||||||
| Have no sex partner | 9/36 (25.0) | Ref | Ref | |||
| Have a sex partner | 108/202 (53.5) | 2.13 (1.08–4.22) | 0.028 | 1.95 (0.95–4.00) | 0.069 | |
| Highest level of education | ||||||
| Primary or below | 40/70 (57.1) | Ref | – | – | ||
| Post primary | 77/159 (48.4) | 0.96 (0.65–1.40) | 0.819 | – | – | |
| Employment | ||||||
| Employed | 99/196 (50.5) | Ref | – | – | ||
| Non-employed | 18/42 (42.9) | 0.85 (0.51–1.40) | 0.521 | – | – | |
| Condom use | ||||||
| Never | 5/10 (50.0) | Ref | – | – | ||
| Sometimes | 32/69 (46.4) | 0.99 (0.40–2.45) | 0.989 | – | – | |
| Always | 80/159 (50.3) | 0.92 (0.61–1.39) | 0.697 | – | – | |
| Engagement in transactional sex | ||||||
| No/unknown | 48/117 (41.0) | Ref | Ref | |||
| Yes | 69/121 (57.0) | 1.39 (0.96–2.01) | 0.080 | 1.64 (1.07–2.51) | 0.021 | |
| STI knowledge | ||||||
| None/Low | 67/122 (54.9) | Ref | Ref | |||
| High | 50/116 (43.1) | 0.78 (0.54–1.13) | 0.195 | 0.64 (0.43–0.95) | 0.026 | |
| Alcohol use in the past 12 months | ||||||
| No | 77/163 (47.2) | Ref | – | – | ||
| Yes | 40/75 (53.3) | 1.13 (0.77–1.65) | 0.534 | – | – | |
| Antibiotic use in the past 30 days | ||||||
| No/unsure | 71/159 (44.7) | Ref | Ref | |||
| Yes | 46/79 (58.2) | 1.30 (0.89–1.89) | 0.161 | 1.16 (0.77–1.76) | 0.479 | |
| STI statusA | ||||||
| Negative | 82/152 (43.9) | Ref | Ref | – | ||
| Positive | 35/86 (40.7) | 0.75 (0.51–1.12) | 0.163 | 0.82 (0.55-1.23) | 0.337 | |
| Symptom duration (weeks) | ||||||
| ≤2 | 61/149 (40.9) | Ref | Ref | |||
| >2 | 55/87 (63.2) | 1.54 (1.07–2.22) | 0.019 | 1.75 (1.20-2.56) | 0.004 | |
| Presence of symptomsB | ||||||
| 1 symptom | 60/112 (53.6) | Ref | – | – | ||
| ≥2 symptoms | 57/126 (45.2) | 0.84 (0.59–1.21) | 0.361 | – | – | |
| Partner notified about STI symptoms | ||||||
| Yes | 77/132 (58.3) | 1.54 (1.04–2.25) | 0.028 | 1.49 (0.99–2.26) | 0.057 | |
| No | 40/106 (37.7) | Ref | Ref |
OA02.01 – Prevalence and Correlates of Chlamydia Trachomatis and Neisseria Gonorrhoeae Among Adolescent Girls and Young Women Seeking Contraception at Pharmacies in Kenya
Miss Omolara Akingba1, Dr. Elizabeth Bukusi1,2, Dr. Connie Celum1, Dr. David Katz1, Dr. Zachary Kwena2, Mr. Harison Lagat1,2, Miss Meena Lenn1, Mr. Felix Mogaka2, Dr. Melissa Mugambi1, Dr. Kenneth Mugwanya1, Mr. Bernard Nyerere2, Mr. Victor Omollo2, Miss Josephine Odoyo2, Dr. Katrina Ortblad1,3, Dr. Barbra Richardson1,3, Mr. Bernard Rono2, Dr. Greshon Rota2, Dr. Monisha Sharma1, Dr. Jillian Pintye1
1University of Washington, Seattle, United States.
2Kenya Medical Research Institute, Nairobi, Kenya.
3Fred Hutch Cancer Research Centre, Seattle, United States.
Background: Adolescent girls and young women (AGYW) often access contraception at pharmacies in Kenya, a setting where HIV PrEP is scaling up. Evaluating sexually transmitted infections (STIs) among AGYW accessing sexual and reproductive health services in pharmacies could guide pharmacy-based STI testing models.
Methods: We evaluated the prevalence of Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) among AGYW in an ongoing cluster-randomized trial (NCT05467306) on HIV PrEP delivery at 20 retail pharmacies in Kisumu, Kenya. Participants were HIV-negative AGYW (ages 15–24) purchasing contraception (emergency contraception [EC], oral contraceptives, injectables, implants, or condoms). A subset was offered CT/NG testing using Xpert® nucleic acid amplification. Poisson regression was used to identify correlates of CT and NG, adjusting for pharmacy-level clustering.
Results: As of December 2024, 563 AGYW were offered CT/NG testing. The median age was 20 years (IQR: 18–22), 38% of AGYW were in school, and 58% had prior pregnancies. EC was the most commonly purchased contraceptive (46%) and 80% accepted HIV PrEP. Overall, 88% accepted CT/NG testing, with results returned in a median of 3 days (IQR: 2–6). CT prevalence was 21%, NG 6%, and co-infection 3%; 78% of infections were asymptomatic. Among 133 AGYW with CT or NG, 86% received treatment and 89% accepted expedited partner therapy (EPT); untreated AGYW were unreachable. CT prevalence was higher in AGYW who experienced intimate partner violence vs those who did not (43% vs 20%; PR = 2.17, CI: 1.29–3.64, P = 0.003) and those with recent condomless sex vs without (23% vs 10%; PR = 2.26, CI: 1.14–4.48, P = 0.02). NG prevalence was higher in rural vs urban residents (10% vs 2%; PR = 5.26, CI: 1.31–21.0, P = 0.019).
Conclusion: AGYW accessing contraception at pharmacies frequently accepted STI testing and STIs were common, with high treatment and EPT uptake. Pharmacies in Kenya are a promising platform for reaching AGYW likely to benefit from STI testing and HIV PrEP.
OA02.02 – Advancing Sexual Health Through Pharmacy-Health Department Partnerships in the United States: Findings from Demonstration Projects
Miss Melissa Habel1, Ms. Rebekah Horowitz2
1U.S. Centers for Disease Control and Prevention, Atlanta, United States.
2National Association of County and City Health Officials, Washington, United States.
Background: Patients visit pharmacies nearly twice as often as other healthcare providers. When local health departments (LHDs) face overwhelming demand or public health emergencies, pharmacies may be critical for delivering STI/HIV care. Effective practice models must be evaluated for their feasibility of expanding access in these settings.
Description: From January 2022–July 2024, 5 LHDs were funded to design and implement a partnership model with community pharmacies to expand STI/HIV services and care. Each model was evaluated to understand the specific STI needs addressed through these collaborations; feasibility of the partnership itself, including barriers and facilitators to implementation and lessons learned; and community response and uptake of services. The evaluation utilized qualitative methods to identify key themes and analyze findings from reports, recipient calls, and in-depth interviews conducted with LHD and pharmacy staff.
Results: Models were designed to complement existing STI care, alleviating pressure on LHDs by leveraging the strengths of pharmacies while engaging individuals who might otherwise avoid care. The partnership models generally fell into 2 categories: 1) self-collection STI testing kits and 2) more accessible or faster medication dispensing to the patient and/or their partner(s). Assessments of feasibility indicated that integrating STI services into pharmacists’ daily workflows could occur without significant burden. Changes to medication dispensing (e.g., adding injectables) was easier to implement than expanding patient-pharmacist interactions e.g. adding testing onsite). Challenges included staff turnover at both entities, navigating legal barriers, and adapting to new processes and data systems. Across the models, patient demand was low, but return and positivity rates showed that when reached, there was need in communities served. LHDs and pharmacies alike appreciated the partnership and would do it again stating that they were “stronger together.”
Conclusion: Further efforts are needed to ensure successful models are replicable and there is adequate reimbursement for pharmacists to sustain these collaborations.
OA02.05 – Impact of Result Displays in an Anogenital Symptom Checker App on Health-Seeking Behaviours: A Cross-Sectional, Vignette-Based Study
Dr. Nyi Nyi Soe1,2, Dr. Phyu Mon Latt1,2, Dr. David Lee1, Dr. Janet M Towns1,2, Dr. Alicia King1,2, Dr. Eric P.F. Chow1,2,3, Dr. Jason J Ong1,2, Dr. Lei Zhang1,2,4, Dr. Christopher K. Fairley1,2
1Melbourne Sexual Health Centre, Melbourne, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
4Clinical Medical Research Center, Children’s Hospital of Nanjing Medical University, Nanjing, China.
Background: The Melbourne Sexual Health Centre (MSHC) developed an AI-powered app called AiSTI to help the public identify potential STI-related anogenital lesions. This research sought to explore how individuals respond to the application’s result displays and recommendations and how this might affect their health-seeking behaviour.
Methods: From April to July 2024, participants completed an anonymous online survey, responding to hypothetical scenarios related to STI and non-STI conditions before and after viewing the randomised AiSTI application’s result displays. They were asked how soon they would seek health care and how concerned they would be about each scenario. We reported descriptive statistics and used logistic regression analyses to explore associations between result displays and health-seeking behaviours.
Results: Our study included 512 participants (median age of 32 years, IQR: 25–40.5). Approximately 65% (n = 330) were assigned male at birth. For the STI scenario, intention to seek care within 24 h increased from 75% to over 90% after viewing probable STI diagnosis displays (P < 0.001). For the non-STI scenario, 46% initially intended to seek urgent care, but this was significantly reduced to below 25% after viewing non-STI result displays (P < 0.001). All result displays (concise text, full text, and meter) significantly increased the likelihood of seeking care within 24 h for the STI scenario (Adjusted ORs: 3.6–4.0, P < 0.001) and within a week for the non-STI scenario (Adjusted ORs: 2.4–2.5, P < 0.001).
Conclusion: Our study found that digital health interventions with effective result displays could encourage urgent care-seeking for STI cases.
OA02.06 – Characteristics of Users of GetCheckedOnline, British Columbia’s Digital Sexually Transmitted and Blood-Borne Infection Testing Service Who Are Testing for the First Time Ever
Dr. Mark Gilbert1,2, Aidan Ablona, Heather Pedersen, Devon Haag, Pierce Gorun1,2, Dr. Ihoghosa Iyamu1,2, Hsiu-Ju Chang1,2, Dr. Kirsty Bobrow, Karmen Olson, Dr. Troy Grennan1,2
1University of British Columbia, Vancouver, Canada.
2University of British Columbia Centre for Disease Control, Vancouver, Canada.
Background: British Columbia’s digital sexually transmitted and blood-borne infection (STBBI) testing service GetCheckedOnline aims to improve uptake of STBBI testing among people at greater risk of infection facing barriers accessing local services. We examined use by people reporting no prior lifetime experience of STBBI testing (first-time testers, FTT) to evaluate these aims.
Methods: We reviewed GetCheckedOnline data for initial testing visits (June 2021–May 2023). We measured the proportion of FTT and using univariable bivariate logistic regression identified associated characteristics.
Results: Of 19,517 records analyzed, 4,353 (22.3%) were FTT, with significant differences between seven communities where GetCheckedOnline is available (range 12–30% FTT). Higher odds of FTT were found in younger age groups (vs ≥ 40 years) and people of colour (Odds Ratio = 1.77 [95% CI 1.63–1.91]; vs White), with lower odds among women (OR = 0.64 [0.59–0.68]) and gender-diverse users (OR = 0.61 [0.49–0.77]; vs men). Compared to heterosexual women, the odds of FTT were higher among heterosexual men (OR = 1.69 [1.57, 1.83]) and lower among homosexual men (OR 0.74 [0.64–0.68]), bisexual women (OR = 0.55 [0.44–0.68]), and women with other partner types (OR = 0.56 [0.41, 0.75]). Odds of FTT were higher among users reporting a partner with an STI (OR = 1.14 [1.02–1.28]), and lower among users with more partners (vs 1 partner) and condomless sex with > 1 partner (OR = 0.64 [0.59–0.68]; vs not) in the past 3 months.
Conclusion: One in five users at their initial use of GetCheckedOnline report testing for STBBI for the first time, confirming service aims to increase testing uptake are being met. We found higher odds among some groups that face systemic barriers accessing testing (people of colour, heterosexual men) and lower odds among some groups who may have different motivations to test or access testing in other ways (e.g., older ages, females, homosexual men). Differences between communities may relate to local testing access.
OA03.01 – The Multi-Country Aetiology Study of Genital Ulcer Disease in Sub-Saharan Africa
Professor Yaw Adu-Sarkodie, Dr Edith Nakku-Joloba, Professor Chelsea Morroni, Dr Michael Owusu, Ms Ethel Dauya, Ms. Aamirah Mussa, Ms Rebecca Handley, Dr Sarah Burl, Dr Matthew Beale, Professor Nicholas Thomson, Professor Rashida Ferrand, Professor Michael Marks1
1London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: In most African countries, patients with Genital Ulcer Disease (GUD) are managed syndromically without diagnostic testing. This approach relies on accurate data on the major causes of GUD which may vary by country and other factors such as HIV status. There have been very few studies of the causes of GUD in Africa in the last 20 years.
Methods: Participants presenting with genital ulcer(s) were recruited from primary care and specialist clinics in Botswana, Ghana, Uganda and Zimbabwe. From each individual, we collected detailed socio-demographic and clinical data including HIV status and previous history of GUD. Genital ulcer swabs were collected from all participants. A multiplex PCR for HSV, syphilis and chancroid was used to determine the aetiology of the ulcers.
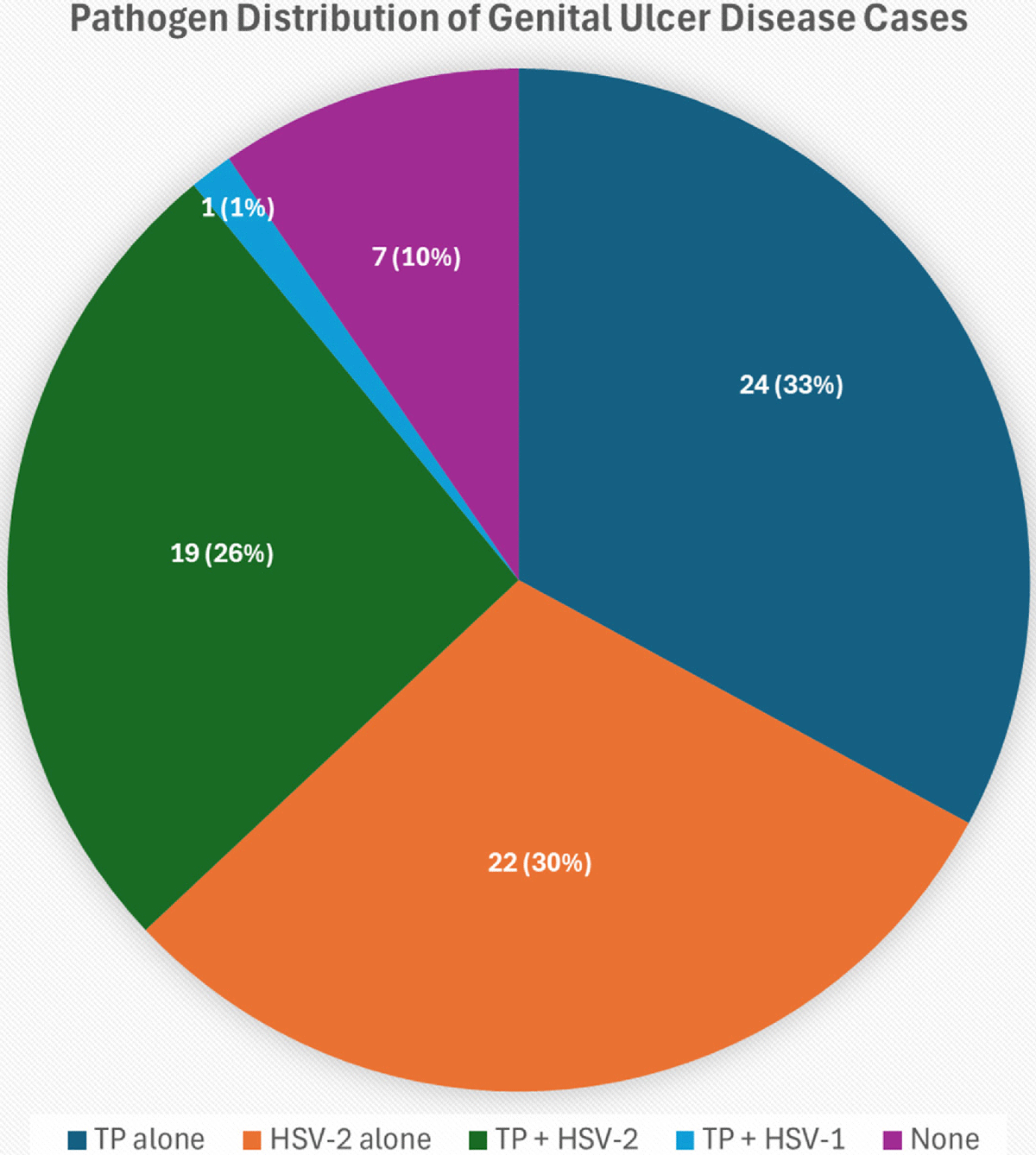
Results: Between June 2022 and December 2023, 1,198 participants enrolled in the study; 597 (53.6%) were female and the median age was 28 (IQR 23–37). Overall, 305 (29.0%) reported they were living with HIV. One hundred and thirty-six individuals (11.4%) reported a previous diagnosis of syphilis and 404 (33.7%) reported recent treatment with antibiotics before being seen at the clinic. The majority of individuals reported only heterosexual intercourse (>95%) except for in Ghana where 9.8% of individuals identified as men who have sex with men. HSV was the most common cause of genital ulcer disease in 46% of individuals. Syphilis was diagnosed in 7% of cases. No cases of chancroid were detected. A substantial proportion of patients did not have a cause identified, and this proportion varied by country.
Conclusion: HSV and syphilis remain major causes of GUD across Africa. Many patients received treatment before they were seen for at a health centre and despite using molecular testing many patients remain undiagnosed. Near patient diagnostics are required to enable aetiologically guided therapy in place of current syndromic approaches to management.
OA03.02 – How Spaces Impact Cases: A Spatial Analysis of Declining Gonorrhea Case Rates in the United States, 2021–2022
Ms. Brittany Liebhard1, Dr. David M. Kline2, Dr. Abigail Norris Turner1, Dr. William C. Miller3
1The Ohio State University, Columbus, United States.
2Wake Forest University School of Medicine, Winston-Salem, United States.
3University of North Carolina at Chapel Hill, Chapel Hill, United States.
Background: Gonorrhea case rates decreased in the United States in 2022 for the first time in over 10 years. While this decrease occurred in 41 states, it is unknown how trends changed at more granular spatial scales. We aimed to describe county-level trends in gonorrhea case rates in the continental US between 2021 and 2022 by urbanicity and region.
Methods: Using publicly available data from the U.S. Centers for Disease Control and Prevention (CDC), we computed county-level, global empirical Bayesian-smoothed gonorrhea case rates for 2021 and 2022. We calculated standardized morbidity ratios (SMRs) and exceedance probabilities for 2021 and the relative percent changes in county-level case rates between 2021 and 2022. We describe the frequency and proportion of counties with increasing (>10% increase), decreasing (>10% decrease), and stable (within-10% change) case rates. Finally, we performed a hot spot analysis using the Getis-Ord Gi* statistic to identify clusters of counties with changing case rates above and below the national average.
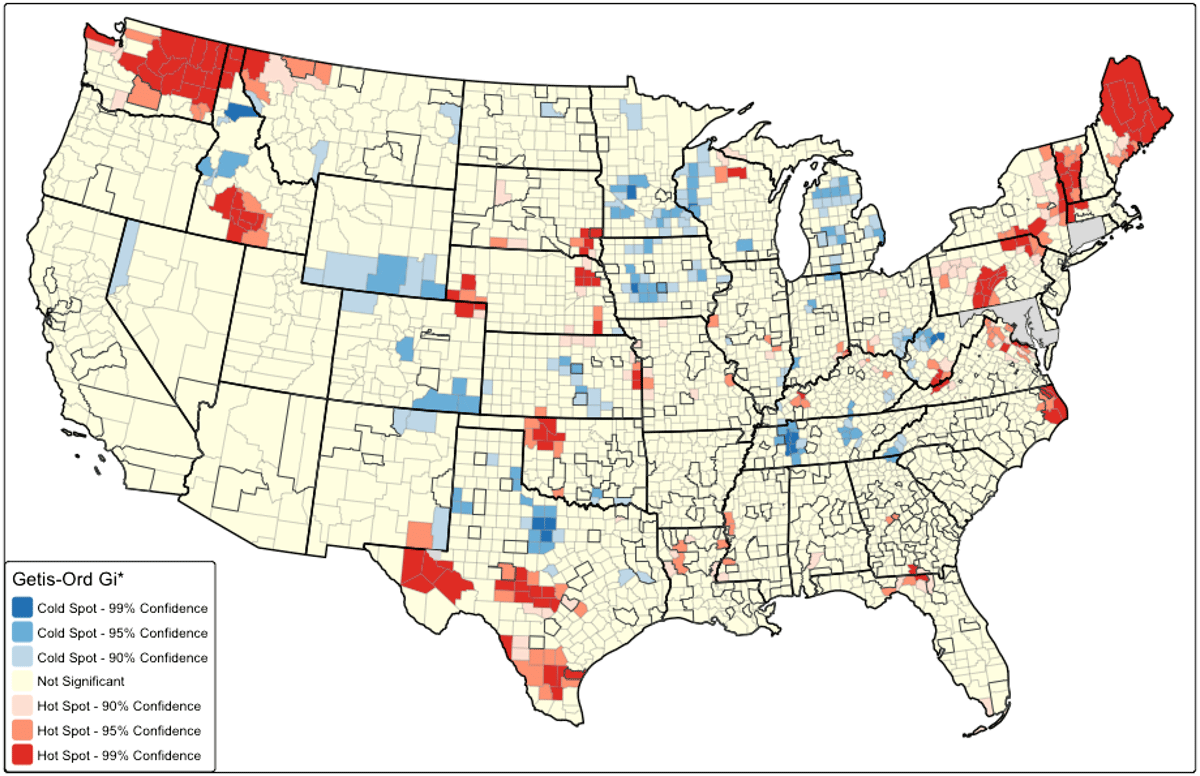
Results: Around half (55%) of all counties experienced a decrease in gonorrhea case rates between 2021 and 2022; the remainder had stable (24%) or increased rates (21%). Over half of counties in the rural Northeast (65%), urban Northeast (65%), and urban South (52%) had stable or increasing case rates. Cold spots – clusters of counties experiencing significant declines in case rates – were primarily found in areas throughout the U.S. that had expected or lower-than-expected baseline morbidity in 2021 (Fig. 1).
Conclusion: Despite an overall national decrease in gonorrhea case rates in 2022, nearly half of all counties (representing 57% of the population) had stable or even increasing case rates; this varied by urbanicity and region. Counties with increasing case rates, particularly those with higher-than-expected morbidity in 2021, may be targets for future intervention. Surveillance data for 2023 indicates that the national decrease in gonorrhea is continuing.
Getis-Ord Gi* hot spot analysis of the county-level percent change in gonorrhea case rate between 2021 and 2022. Hot spots represent clusters of counties with percent change in case rate above the mean (e.g. small decrease, no change, or increase). Cold spots represent clusters of counties with percent change in case rate below the mean (e.g. large decrease). Counties with higher-than-expected baseline morbidity in 2021 are outlined. States represented in gray (Connecticut and Maryland) had suppressed gonorrhea case data and are excluded from analyses.
OA03.03 – Global Spread of a Novel Ceftriaxone and Multidrug Non-Susceptible Neisseria Gonorrhoeae with PenA 60.001 Allele: A Wake-Up Call for Surveillance and Treatment
Assoc. Prof. Meiping Ye1,2, Miss Linyin Yao2, Miss Tingli Tian2, Miss Danyang Zou2, Miss Xinying Lu1,2, Prof. Yi Lin3, Prof. Zhen Ning3, Prof. Liang Chen4, Dr. Jianping Jiang5, Prof. Pingyu Zhou1,2
1Department Of Dermatology, Xinhua Hospital, Shanghai Jiaotong University School Of Medicine, Shanghai, China.
2STD Institute, Shanghai Skin Disease Hospital, Tongji University School of Medicine, Shanghai, China.
3Division of Tuberculosis and HIV/AIDS Prevention, Shanghai Municipal Center for Disease Control and Prevention, Shanghai, China.
4School of Pharmacy and Pharmaceutical Sciences, University at Buffalo, Buffalo, USA.
5Institute of Antibiotics, Huashan Hospital, Fudan University, Shanghai, China.
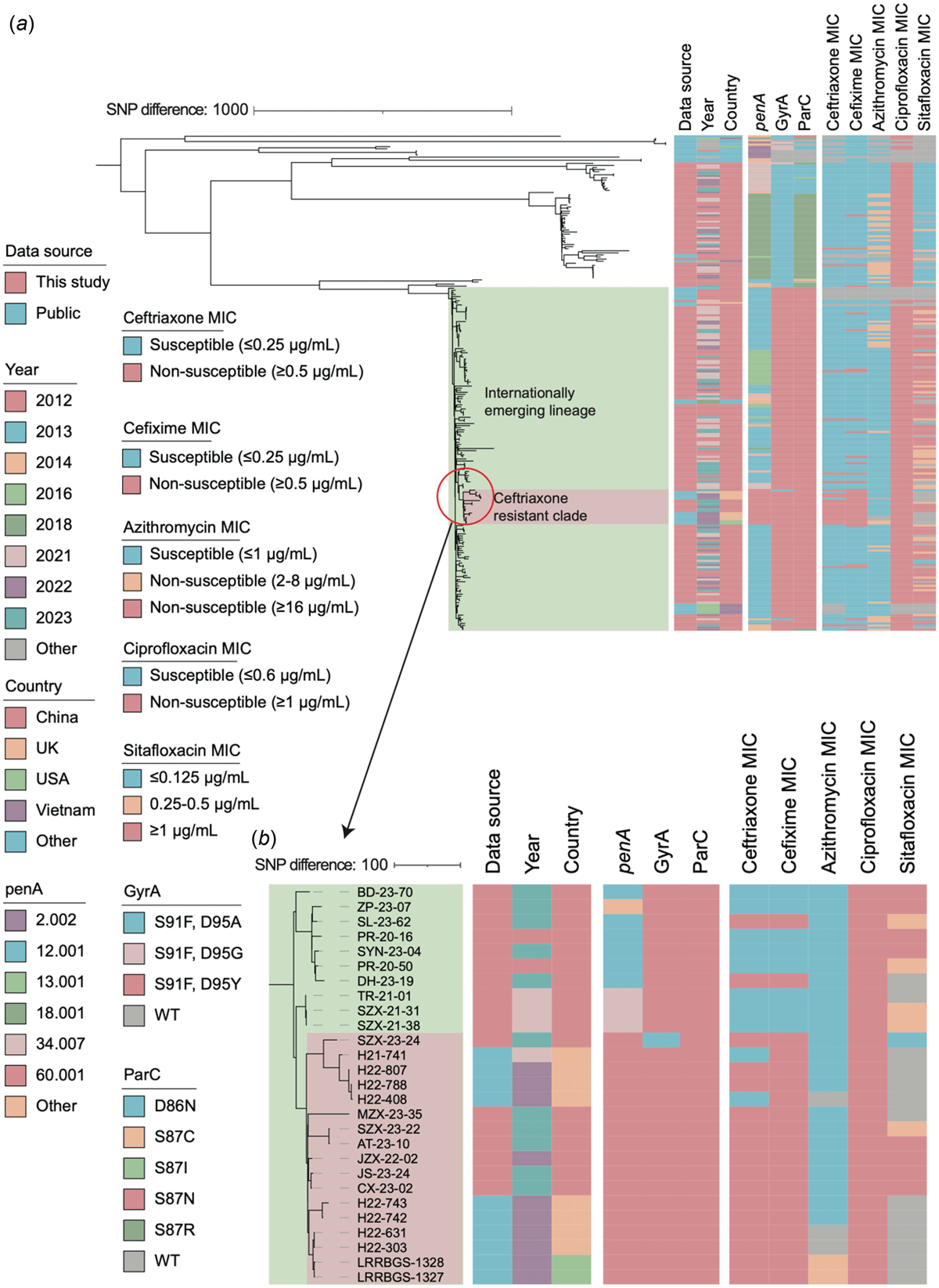
The emergence of a novel multidrug-resistant Neisseria gonorrhoeae strain harboring the penA 60.001 allele has raised global concern due to its association with high-level resistance to ceftriaxone. This study highlights the alarming detection of these strains in Shanghai, China, where 1,774 N. gonorrhoeae isolates collected between 2020 and 2023 were analyzed as part of the Shanghai Gonococcal Resistance Surveillance Programme (SH-GRSP). Among these, seven isolates belonging to MLST 8123 were identified as multidrug-resistant, with six isolated in 2023, a year marked by the aftermath of the COVID-19 pandemic. The strains demonstrated significant non-susceptibility to ceftriaxone (MICs 0.5–>2 μg/mL), cefixime (MICs 2–>2 μg/mL), and ciprofloxacin (MICs 8–>8 μg/mL). Genomic analysis uncovered a newly emerging international lineage (IEL) within MLST 8123, positioning these strains as part of a broader global threat. Phylogenomic analysis of 197 MLST 8123 strains identified three major lineages, with IEL being the most prevalent, characterized by a distinctive combination of mutations in penA, gyrA, and parC. Notably, IEL isolates, including those harboring the GyrA D95Y mutation, exhibited decreased susceptibility to novel fluoroquinolones such as sitafloxacin, as well as to experimental antibiotics like gepotidacin and zoliflodacin. The emergence of these multidrug-resistant strains coincides with shifts in sexual behavior following the pandemic, further elevating the risk of gonococcal transmission. This study underscores the urgent need for enhanced global surveillance, improved diagnostic tools, and concerted international efforts to combat the spread of these novel multidrug-resistant N. gonorrhoeae strains.
Recombination-adjusted phylogenetic tree of 238 MLST 8123 N. gonorrhoeae strains (a) and the penA 60.001 novel strain clade (b). A core genome phylogeny was created with the genomic sequences of 197 MLST 8123 strains in this study and 41 MLST 8123 strains from PubMLST. Colored bars represent data source, year, country, penA alleles, GyrA genotypes, ParC genotypes, ceftriaxone MIC, cefixime MIC, azithromycin MIC, ciprofloxacin MIC, and sitafloxacin MIC. The internationally emerging lineage was highlighted in green and ceftriaxone resistant clade was highlighted in red. Antimicrobial susceptibility data were not available for some isolates (grey boxes). MIC = minimum inhibitory concentration. MLST = multilocus sequence type.
OA03.04 – European Gonococcal Antimicrobial Surveillance Programme Findings 2023
Dr. Melissa Jansen van Rensburg1, Dr Susanne Jacobsson2, Mr Daniel Schröder2, Dr Sarah Alexander1, Dr Csaba Ködmön3, Prof Magnus Unemo2, Dr Michelle Cole1, The Euro-GASP Network
1UK Health Security Agency, London, United Kingdom.
2WHO Collaborating Centre for Gonorrhoea and other STIs, Örebro University, Örebro, Sweden.
3European Centre for Disease Prevention and Control, Stockholm, Sweden.
Background: Treatment options for gonorrhoea are now limited; therefore, surveillance of antimicrobial resistance (AMR) is critical. The European Gonococcal Antimicrobial Surveillance Programme (Euro-GASP) monitors AMR trends across the European Economic Area (EEA). Here we present key Euro-GASP findings from 2023.
Methods: Participating countries collected Neisseria gonorrhoeae isolates from consecutive patients, predominantly between September and November 2023. Susceptibility to ceftriaxone, cefixime, azithromycin, ciprofloxacin, and tetracycline was determined with minimum inhibitory concentration (MIC) gradient strip tests or agar dilution using EUCAST clinical breakpoints. Linked epidemiological data were also provided. The statistical significance of differences in resistance relative to 2022 Euro-GASP results was determined using the Z-test.
Results: In 2023, 3184 N. gonorrhoeae isolates were collected from 24 EEA countries. One isolate was resistant to ceftriaxone (compared to two in 2022), which also displayed high-level azithromycin resistance (HL-AziR, MIC >256 mg/L). Cefixime resistance was observed in 0.2% of isolates, which was comparable to 2022 (0.3%, P = 0.212). Azithromycin resistance decreased to 23.1% (25.6% in 2022, P = 0.013); however, 39 isolates from 15 countries exhibited HL-AziR compared to 13 isolates from five countries in 2022. HL-AziR isolates were not restricted to a particular demographic group, although they were more common among men who have sex with men (61.9%). Ciprofloxacin resistance also decreased to 62.7% (65.9%, P = 0.003). Tetracycline susceptibility testing was added to Euro-GASP in 2023, and resistance was at 58.4%.
Conclusions: Resistance to ceftriaxone and cefixime remained rare in the EEA in 2023. Azithromycin and ciprofloxacin resistance decreased slightly; however, azithromycin resistance continues to threaten the effectiveness of dual therapy, and the increased number and geographic distribution of HL-AziR isolates is also worrying. The inclusion of tetracycline susceptibility testing in 2023 confirmed that resistance is high in the EEA, providing an important baseline for monitoring the impact of doxycycline post-exposure prophylaxis.
OA03.05 – Trends in Gonorrhoea Testing and Incidence Among Gay and Bisexual Men in Australia Over a Decade Spanning HIV PrEP Implementation
Hein Htet Aung1,2, Rebecca Guy3, Eric Chow2,4,5, Christopher Fairley4,5, Rick Varma3,6, Caroline Thng7, Marcus Shaw8, David Templeton3,9, Vincent Cornelisse10, Dash Heath-Paynter11, Htein Linn Aung3, Jason Asselin1,3, Basil Donovan3, Margaret Hellard1,12, Mark Stoove1,12, Research Fellow Michael Traeger1,12
1Burnet Institute, Melbourne, Australia.
2School of Population and Global Health, University of Melbourne, Melbourne, Australia.
3The Kirby Institute, UNSW Sydney, Sydney, Australia.
4Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
5School of Translational Medicine, Monash University, Melbourne, Australia.
6Sydney Sexual Health Centre, Sydney, Australia.
7Gold Coast Sexual Health Service, Gold Coast Health, Gold Coast, Australia.
8M Clinic, Perth, Australia.
9Department of Sexual Health Medicine, Sydney Local Health District, Sydney, Australia.
10HIV and Sexual Health Services, Mid North Coast & Northern NSW Local Health Districts, NSW Health, Australia.
11Health Equity Matters, Sydney, Australia.
12School of Public Health and Preventive Medicine, Monash University, Sydney, Australia.
Background: Changes in sexual networks associated with HIV PrEP and treatment-as-prevention may be influencing gonorrhoea transmission among gay and bisexual men (GBM). We describe trends in gonorrhoea testing and incidence among GBM in Australia over a decade spanning PrEP implementation.
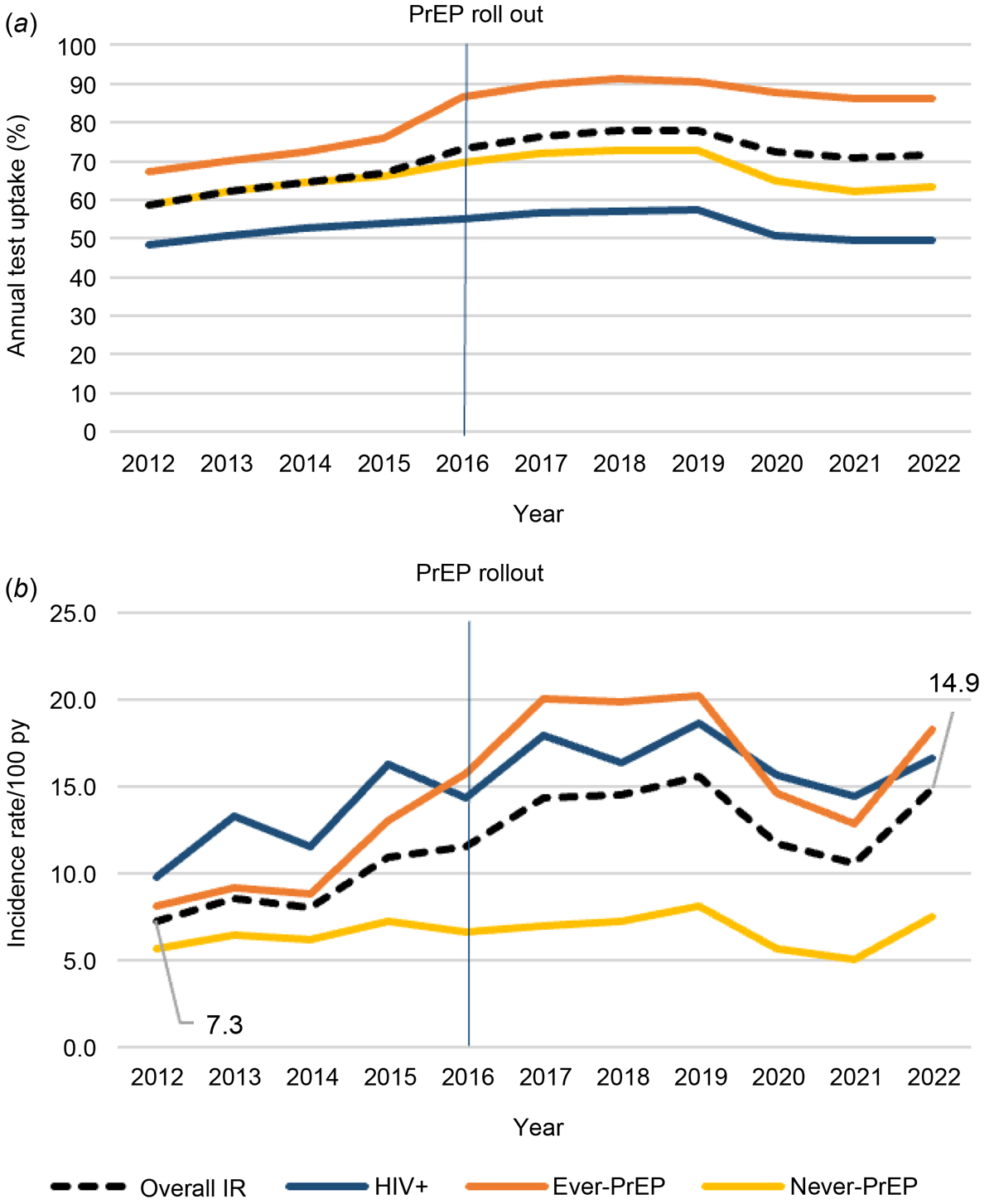
Methods: Linked clinical data were extracted from 64 services in the ACCESS surveillance network. GBM attending a clinic between 01 January 2013 and 31 December 2022 were included. We calculated annual test uptake (proportion of attendees with ≥1 test event in a year) and, among those with ≥2 tests during the study period, gonorrhoea incidence per 100 person-years. Annual testing and incidence rates were stratified by HIV status and evidence of PrEP prescription (categorised into ever/never-PrEP users). Multivariable Poisson regression explored associations between HIV status, PrEP use and incident gonorrhoea, adjusted for calendar year and age.
Results: In total, 175,655 GBM attended a clinic during the study period, of which 90.5% were tested for gonorrhoea at least once. The annual testing rate increased from 58.7% to 71.7% from 2012 to 2022, largely driven by testing increases among ever-PrEP users (Fig. 1). Among 111,846 GBM with ≥2 test events, 59,672 gonorrhoea infections were diagnosed over 480,815 person-years (overall incidence = 12.4/100py). Incidence among HIV-negative ever-PrEP users increased from 8.2/100 to 18.3/100py, and among GBM with HIV increased from 9.8 to 16.6/100py. 13,196 (11.8%) GBM had ≥2 infections, accounting for 71.8% of all diagnoses; 2,248 (2.0%) GBM with ≥5 infections accounted for 24.8% of diagnoses. In multivariable Poisson regression, ever being prescribed PrEP (aIRR = 2.41, 95% CI = 2.37–2.46) and living with HIV (aIRR = 2.94, 95% CI = 2.87–3.02) were associated with gonorrhoea diagnosis.
Conclusion: In this large cohort of GBM, gonorrhoea incidence increased during PrEP implementation, however incidence was increasing before large-scale PrEP roll-out in 2016. GBM living with HIV, using PrEP, or with a prior gonorrhoea infection should be prioritised biomedical risk-reduction strategies (i.e., vaccination).
Annual (a) test uptake and (b) incidence per 100 person-year of gonorrhoea among gay and bisexual men attending an ACCESS clinic. Footnote: Large-scale PrEP roll out began in early 2016 through demonstration studies.
OA03.06 – High Neisseria Meningitidis Oropharyngeal Carriage Trends in Men Who Have Sex With Men: A Public Health Warning
Miss Aminah Memon1, Dr Manik Kohli2, Dr Emmi Suonpera2, Miss Yomna Gharib2, Mr Christos Karathanasis2, Miss Fowsiya Nur2, Professor Richard Gilson2, Dr. Odile B. Harrison1
1University of Oxford, Oxford, United Kingdom.
2University College London & Central and NorthWest London NHS Foundation Trust, London, United Kingdom.
Background: Invasive meningococcal disease can occur in men who have sex with men (MSM), particularly caused by ST-11 serogroup C N. meningitidis (Nme). An increased incidence of meningococcal urethritis has also been reported in the UK consistent with oral-urogenital transmission.
Methods: Oropharyngeal charcoal-amies swabs were obtained from MSM attending the Mortimer Market Centre, a sexual health clinic located in London. Following microbiology culture, Gram-negative, oxidase-positive diplococci (GND) were isolated and whole-genome sequenced. Genome assemblies were uploaded to PubMLST for species identification. Both chromosomally-encoded and plasmid-encoded AMR genes were characterised. Patient data were collected including smoking and sexual behaviour. Univariate, unadjusted odds ratios (OR) were calculated.
Results: 173 oropharyngeal swabs were obtained from which 37 GND were found, all of which Nme, a carriage rate of 21.4%. 58.3% were in men aged 25 to 44, 41.7% aged 45 to 74; the majority (80.6%) non-smokers. Condomless, anal sex with 3 or more partners 3 months prior to the study was associated with oropharyngeal Nme (OR 6.7, CI 3.67–12.27). Individuals reporting taking HIV-pre-exposure prophylaxis (HIV-PrEP) had higher odds of Nme carriage compared to those not taking HIV-PrEP (OR 2.61 CI 1.41–4.06). 18 Nme were serogroups B, C, W, X, and Y; 5 were ST-11 (4 group W, 1 group C), and 3 were ST-4821 (all B). One Nme carried the tetM conjugative plasmid, conferring tetracycline resistance.
Conclusion: A high Nme carriage rate was found that included Nme from hyperinvasive clonal complexes increasing the risk of IMD. With planned implementation of doxycycline post-exposure prophylaxis (‘doxyPEP’) for prevention of bacterial STIs in MSM, our observation of a tetM+ Nme raises concerns about Nme acquiring tetracycline resistance as already seen at a high rate in N. gonorrhoeae. The preliminary data collected here suggest that HIV-PrEP use and associated patterns of sexual behaviour may be risk factors for oropharyngeal Nme carriage.
OA04.01 – Cristi: A Suite of CRISPR-Based Point-Of-Care Tests for Sexually Transmitted Infections
Dr Soo Jen Low1, Mr Matthew O’Neill1,2, Mr Janath Fernando1, Mr William Kerry2, Ms Natasha Wild2, Ms Jacqueline Prestedge1,3, Ms Georgina Papadakis3, Ms Marcelina Krysiak1, Ms Simran Chahal1, Dr Eloise Williams1,3, Ms Francesca Azzato1,3, Mr Thomas Tran3, Prof Christopher Fairley4, Dr Chuan Kok Lim3, Prof Catriona Bradshaw4,5, Prof Marcus Chen4,5, Prof Deborah Williamson1, Dr. Shivani Pasricha1,2
1The University of Melbourne at the Peter Doherty Institute for Infection and Immunity, Melbourne, Australia.
2Walter and Eliza Hall Institute of Medical Research, Parkville, Australia.
3Victorian Infectious Diseases Reference Laboratory, The Royal Melbourne Hospital at The Peter Doherty Institute for Infection and Immunity, Melbourne, Australia.
4Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
5Central Clinical School, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
Background: Early diagnosis and prompt treatment are essential for effectively mitigating STIs. However, approved diagnostic tests for both STIs and antimicrobial resistance (AMR) require specialized laboratory equipment and trained personnel. This severely limits access to testing in low-resourced settings where the burden of infection is greatest. The objective of this study was to develop a portfolio of multiplexed CRISPR-based tests for STI detection (CRISTI) and perform clinical validation on a deployment-ready portable, point-of-care (PoC) device.
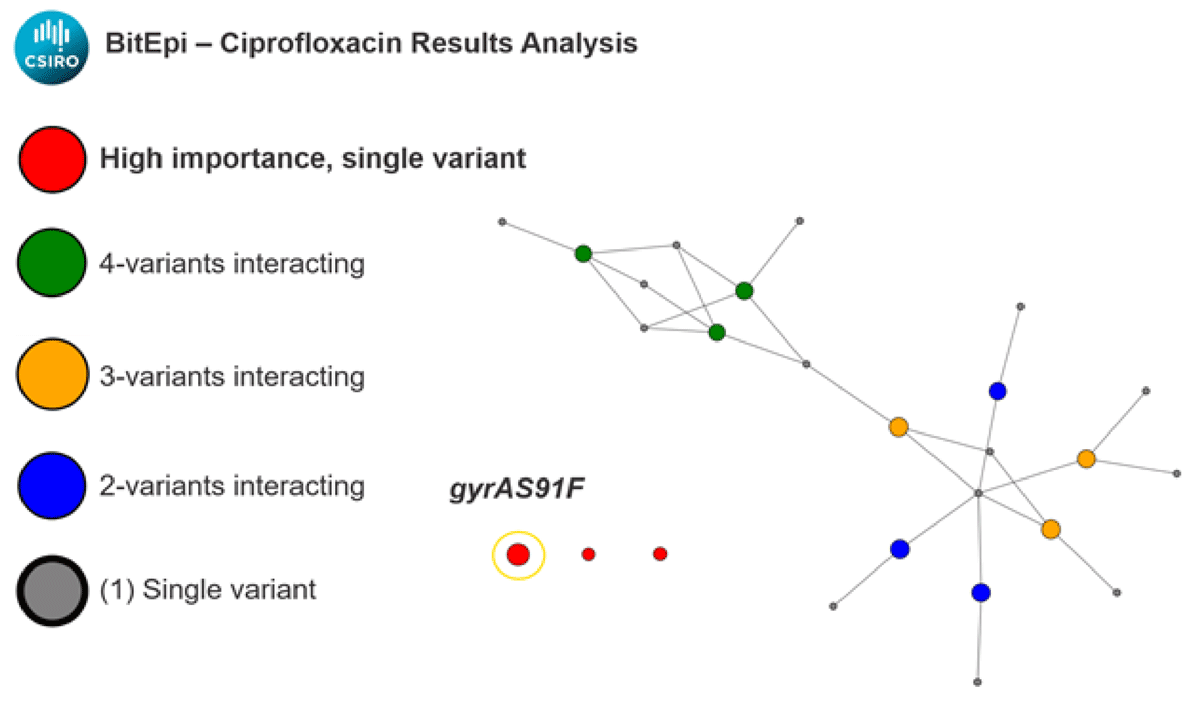
Methods: Multiplexed CRISPR-Cas tests with isothermal pre-amplification were developed for the detection of (1) Treponema pallidum and Herpes simplex virus (TP/panHSV), with reflexed distinction between HSV-1 and HSV-2 infection (HSV-1/HSV-2) and (2) Neisseria gonorrheoa and Chlamydia trachomatis (NG/CT), with reflexed AMR test for detecting gyrA mutation S91F (NG/gyrA), indicative of ciprofloxacin resistance. Candidate primer and guide RNA sets were designed using an in-house bioinformatic pipeline, and multiplexed sets producing the strongest signal using a fluorescence-based readout were selected. Tests were evaluated for analytical sensitivity and specificity using serial dilutions of target and non-target gDNA. Blinded clinical validation was conducted on gDNA from multiple body sites, with over 200 specimens tested per pathogen.
Results: Integrated onto a PoC device, the test takes 45 min, detects single copies per µL of pathogen gDNA and displays 100% analytical specificity against a panel of relevant bacterial and viral pathogens. Results from the clinical validation align with the World Health Organisation’s (WHO) target product profile for STI PoCTs.
Conclusion: We demonstrated the use of CRISPR technology on a portable diagnostic device for both pathogen and AMR detection, with clinical validation on what is, to the best of our knowledge, the largest clinical STI sample cohort to date used for rapid diagnostics. CRISTI represents a comprehensive diagnostic suite for WHO priority bacterial STIs, paving the way for rapid deployment.
OA04.02 – Clinical Evaluation of a Novel, Rapid Point of Care Test for the Detection of Treponema Pallidum in Genital Ulcers – A Case Study In, South Africa
Mrs. Mildred Mandisa Mdingi1,2, Dr Ranjana Gigi1,3, Dr Hyunsul Jung2, Dr Matthew Burton4, Ms. Marleen Kalk4, Dr. Joost Gazendam4
1Foundation For Professional Development, East London, South Africa.
2Department of Medical Microbiology, University of Pretoria, Pretoria, South Africa.
3Institute of Social and Preventive Medicine, University of Bern, Bern, Switzerland.
4Detact Diagnostics BV, Groningen, The Nertherlands.
Background: Syphilis, caused by Treponema pallidum subspecies pallidum (TP), remains a growing public health concern. Standard serological diagnostics for syphilis may be false-negative in early infection and cannot distinguish past from active infections. SpiroTact® (Detact Diagnostics BV) a novel, rapid point of care test targeting treponemal protease, was evaluated in a pilot study of patients with genital ulcer disease.
Methods: This evaluation was conducted from June to September 2024 at one primary healthcare facility in East London, South Africa. Adults (≥18 years) with genital ulcers were enrolled followed by on-site SpiroTact test. Genital ulcer swabs were collected for TP detection by SpiroTact® and by real-time PCR. Whole blood was collected for TP testing (Abbott GmbH Alinity i syphilis TP assay) and Treponemal serology was performed with (Chromotest RPR-Carbon, Linear Chemicals S.L.U, Montgat-Barcelona).
Results: We enrolled 10 patients with genital ulcer. TP PCR and Spirotact were positive in the same 4/10 cases (40%) resulting in 100% positive and negative test agreement. Serological testing was also positive in these four cases with RPR titres of 1:32, 1:4, 1:4 and 1:2. There was one additional case with positive serology (titre 1:2) but negative TP PCR and Spirotact. No cross-reaction between SpiroTact and HSV in three patients with positive HSV PCR. SpiroTact® median result time was 38 min (range 32–59) vs >7 days for PCR.
Conclusion: SpiroTact® showed 100% concordance with TP PCR, highlighting its potential for diagnosing primary syphilis. Its high technical specificity was confirmed in patients with HSV-associated ulcers. While further clinical performance evaluation is needed, these results demonstrate the test’s initial feasibility.
OA04.03 – A Novel Highly Sensitive Target for Treponema Pallidum DNA Detection: Advancing Syphilis Diagnosis with TMF7-Based PCR
Dr. Meiping Ye1,2, Miss Mengya Shang2, Miss Chunjie Liao2, Miss Xinying Lu1,2, Miss Danyang Zou2, Miss Xin Feng2, Dr. Jianping Jiang3, Prof. Pingyu Zhou1,2
1Department Of Dermatology, Xinhua Hospital, Shanghai Jiaotong University School of Medicine, Shanghai, China.
2STD Institute, Shanghai Skin Disease Hospital, Tongji University School of Medicine, Shanghai, China.
3Institute of Antibiotics, Huashan Hospital, Fudan University, Shanghai, China.
Background: PCR has been increasingly used for Treponema pallidum DNA (TP-DNA) detection in syphilis patients. However, the sensitivity is far from satisfactory and the method remains to be improved.
Description: Multiple-copy fragments (TMFs) on T. pallidum genome were identified by K-mer based genomic analysis. The analytical sensitivities and specificities were estimated by PCR. 178 patients with different stages of syphilis were enrolled, and samples including saliva, plasma, cerebrospinal fluid (CSF) and extrudate were collected. All the samples were detected by nested PCR.
Results: A 7-copy TMF (TMF7) on the genome were identified and it achieved a substantially increased analytical sensitivity (≥6 copies/ml) compared to Tpp47/polA (≥1000 copies/mL). By using TMF7, TP-DNA was detected in at least 1 study sample in 100% (7/7) patients with primary syphilis (7/7 plasma, 4/7 saliva, and 2/6 CSF); in 100% (40/40) patients with secondary syphilis (31/40 plasma, 40/40 saliva, and 9/39 CSF); in 67.9% (36/53) patients with latent syphilis (17/53 plasma, 22/53 saliva, and 14/53 CSF), and in 80.8% (63/78) patients with neurosyphilis (19/78 plasma, 29/78 saliva, and 57/78 CSF), which were significantly higher than those of Tpp47/polA. Furthermore, 67.4% (31/46) of late latent syphilis were positive for TP-DNA. In CSF, TP-DNA detection rates were positively correlated with neurosyphilis progress. TP-DNA turned negative in all the 68 follow-up patients with neurosyphilis after therapy.
Conclusions: TMF7 is a highly sensitive target for TP-DNA detection, and it achieved better performances in both analytical and practical tests compared to the commonly used targets. TMF7-based PCR is a promising tool for routine syphilis diagnosis and management.
OA04.04 – Performance of a Novel Molecular-Phenotypic Assay for Viability and Antibiotic Susceptibility Assessment of Neisseria Gonorrhoeae (NG)
Dr. Nicole Lima1,2, Dr Athur Wong3,4, Dr Rick Varma3,4, Ms Kasia Strojny1, Ms Ingrid Aneman1, Dr Tamika Blair1, Dr Tina Lonergan1, Dr Hannah Lowes1, Professor Rebecca Guy4, Dr Tanya Applegate4, Professor Catriona Bradshaw5,6, Professor Alison Todd1,7
1SpeeDx Pty Ltd, EVELEIGH, Australia.
2School of Life Sciences, University of Technology Sydney, Sydney, Australia.
3Sydney Sexual Health Centre, Sexual Health & Bloodborne Viruses Service, South Eastern Sydney Local Health District, Sydney, Australia.
4The Kirby Institute, University of New South Wales, Sydney, Australia.
5School of Translational Medicine, Monash University, Melbourne, Australia.
6Melbourne Sexual Health Centre, Alfred Hospital, Melbourne, Australia.
7School of Biotechnology & Biomolecular Sciences, University of New South Wales, Sydney, Australia.
Background: Simple and fast methods for determining viability and antibiotic susceptibility are needed for NG infections. InSignia®, an innovative all-in-one NAAT, compares the ratio of RNA to DNA in an organism, enabling pathogen detection, viability assessment and antibiotic susceptibility testing (AST). Viability status is measured as an Index, reflective of the level of active transcription. Antibiotic susceptibility is determined by the change in Index, following a brief exposure to antibiotic, resulting from shifts in RNA transcription that are different between susceptible and resistant organisms. Feasibility of the SpeeDx InSignia® CT/NG workflow was tested on characterised isolates and within a cross-sectional cohort study.
Methods: In vitro, genetically and geographically diverse isolates were analysed. This was followed by in vivo prospective clinical samples from a cohort of cisgender men (rectal swabs in Amies charcoal gel (Copan) and neat urine). The InSignia® CT/NG workflow was performed by transferring samples into relevant buffer, followed by a 5 min incubation with ciprofloxacin and extraction on an automated platform. Results from InSignia® CT/NG RT-qPCR assay were compared to gold standard methods (culture and genotypic NAAT).
Results: Characterised NG isolates (n = 110) tested with InSignia® demonstrated 99.1% concordance for ciprofloxacin susceptibility profiling. In clinical samples, all urine (n = 23) and rectal (n = 34) samples tested with InSignia® demonstrated high concordance with NAAT for NG detection (96.5%) and culture for viability assessment (92.9%). For ciprofloxacin AST, a 93% agreement was obtained in comparison to commercially available genotypic NAAT for gyrA testing.
Conclusion: The ability to perform pathogen detection, viability assessment and AST with a single NAAT makes InSignia® CT/NG a useful rapid tool for screening and test of cure to support antibiotic stewardship efforts, as well as inform treatment in situations where changes to antibiotic prescription is possible. Future studies will focus on asymptomatic infections and demonstrating the pan-antibiotic abilities of the technology.
OA04.05 – Treponema Pallidum PCR (TPPCR) Re-Staging for Latent Syphilis of Unknown Duration in Vancouver, Canada: A Pilot Project
Dr. Rohit Vijh1,2,3, Ms. Kristina Mendoza-Martin1, Ms. Elly Blake1, Dr. Hasan Hamze2, Dr. Adrianna Gunton2, Mr. Brendan Bakos1, Ms. Doris Chang1, Min-Kuan Lee4, Dr. Barbra Arnold3, Dr. Sarah Malleson3, Dr. Vincent Valdrez3, Dr. Rochelle Stimpson3, Dr. Muhammad Morshed2,4, Dr. Troy Grennan3, Dr. Althea Hayden1,2
1Vancouver Coastal Health, Vancouver, Canada.
2University of British Columbia, Vancouver, Canada.
3BC Centre for Disease Control, Vancouver, Canada.
4BC Public Health Laboratory, Vancouver, Canada.
Background: In Vancouver Coastal Health (VCH) region, over 37% of patients diagnosed with syphilis are staged as Latent Syphilis of Unknown Duration (LSUD). In these patients, Treponema pallidum DNA testing (TPPCR), can provide evidence of early syphilis infection. Universal TPPCR testing may improve diagnostic accuracy and conserve public health resources.
Description: For all LSUD cases from 11/2023 to 10/2024 we prospectively recommended collecting oral, rectal, vaginal or lesion swabs for TPPCR testing. Patients with a positive test were restaged to early syphilis infection. A chart review was conducted for relevant lab, clinical and demographic information.
Results: There were 232 patients initially staged as LSUD; 112 (48%) had a TPPCR test of which 34 (30%) were positive. These clients were restaged to early latent syphilis (n = 23), secondary syphilis (n = 9) and primary syphilis (n = 2). Swab positivity varied by site with majority being oral (28/101) then lesions (10/22), rectal (3/14) and vaginal (3/16). Individuals with positive TPPCR swabs were more likely to have a lower EIA assay index (consistent with a newer, less-established infection) on initial syphilis serology (median: 17.2 vs 44.4, P < 0.001) and were more likely to be identified with signs/symptoms of syphilis during follow up (44% vs 13%, P < 0.001). All individuals (12/12) who were restaged based on a positive TPPCR and had follow-up serology ≥ 3 months from treatment demonstrated adequate treatment response (four-fold RPR titer decrease). The overall cohort identified predominantly as male (55%) and heterosexual (57%) (Table 1).
Conclusion: Recommending TPPCR testing allowed 15% of patients initially staged as LSUD to be restaged to early syphilis (30% of swabbed patients). This simplified treatment regimens and improved patient care. Unexpectedly, this intervention also improved the diagnosis of early syphilis by prompting more comprehensive physical examinations. Jurisdictions responding to a syphilis outbreak should consider TPPCR testing of all clients initially staged as LSUD
| TPPCR result | |||||
|---|---|---|---|---|---|
| Negative | Positive | Overall | P-valueA | ||
| N | 78 | 34 | 112 | ||
| Age (year, median [IQR]) | 37.00 [30.00, 42.00] | 34.50 [30.25, 38.00] | 35.50 [30.00–41.00] | 0.121 | |
| Sex (n, %) | |||||
| Male | 41 (52.6) | 21 (61.8) | 62 (55.4) | 0.413 | |
| Sexual Orientation (n, %) | 0.596 | ||||
| Heterosexual | 44 (56.4) | 20 (58.8) | 64 (57.1) | ||
| MSM | 17 (21.8) | 10 (29.4) | 27 (24.1) | ||
| Bisexual | 3 (3.8) | 1 (2.9) | 4 (3.6) | ||
| Unknown | 14 (17.9) | 3 (8.8) | 17 (15.2) | ||
| HIV Infection (n, %) | 0.324 | ||||
| No | 73 (93.6) | 32 (94.1) | 105 (93.8) | ||
| Yes | 5 (6.4) | 1 (2.9) | 6 (5.4) | ||
| Unknown | 0 (0.0) | 1 (2.9) | 1 (0.9) | ||
| Symptoms compatible with syphilis (n, %) | <0.001 | ||||
| Yes (%) | 10 (12.8) | 15 (44.1) | 25 (22.3) | ||
| Contact to syphilis case (n, %) | 0.168 | ||||
| Yes | 5 (6.4) | 5 (14.7) | 10 (8.9) | ||
| Syphilis EIA IndexB(median [IQR]) | 44.36 [28.71, 46.00] | 17.17 [14.01, 22.23] | 35.21 [19.65, 46.00] | <0.001 | |
| Syphilis EIA IndexB(n, %) | <0.001 | ||||
| >45.00 | 38 (48.7) | 2 (5.9) | 40 (35.7) | ||
| Syphilis RPR titer (median [IQR]) | 64.00 [16.00, 128.00] | 64.00 [32.00, 256.00] | 64.00 [32.00, 128.00] | 0.093 | |
| Syphilis RPR titer (n, %) | 0.055 | ||||
| >1:32 | 55 (70.5) | 30 (88.2) | 85 (75.9) | ||
| Treatment received (n, %) | |||||
| Benzathine Penicillin G (BPG) | 69 (88.5) | 33 (97.1) | 102 (91.1) | 0.725 | |
| BPG & Doxycycline | 1 (1.3) | 0 (0.0) | 1 (0.9) | ||
| BPG & IV Pen G | 3 (3.8) | 0 (0.0) | 3 (2.7) | ||
| Doxycycline | 5 (6.4) | 1 (2.9) | 6 (5.4) | ||
| Treatment completed (n, %) | |||||
| Yes | 67 (85.9) | 33 (97.1) | 100 (89.3) | 0.102 | |
| Partial | 11 (14.1) | 1 (2.9) | 12 (10.7) | ||
| No | 0 (0) | 0 (0) | 0 (0) | ||
| Serological treatment response | 0.436 | ||||
| YesC | 26 (33.3) | 12 (35.3) | 38 (33.9) | ||
| No | 1 (1.3) | 0 (0.0) | 1 (0.9) | ||
| Too earlyD | 20 (25.6) | 10 (29.4) | 30 (26.8) | ||
| UnknownE | 20 (25.6) | 11 (32.4) | 31 (27.7) | ||
| Unable to assess due to partial treatment | 11 (14.1) | 1 (2.9) | 12 (10.7) | ||
OA04.06 – Novel Use of a Treponema Pallidum Nucleic Acid Amplification Test to Restage Cases of Unknown Duration to Early Latent Syphilis: The Syphilis Staging Quality Improvement Using Novel Diagnostics with Polymerase Chain Reaction (SQuID-PCR) Study
Ms. Katrina Yuen1,2, Maya Tharp1,2, Barbra Arnold1, Hasan Hamze2, Sarah Malleson1, Min-Kuang Lee3, Rochelle Stimpson1, Vincent Valdrez1, Rohit Vijh1,4, Muhammad Morshed2,3, Troy Grennan1,2
1British Columbia Centre for Disease Control, Vancouver, Canada.
2University of British Columbia, Vancouver, Canada.
3British Columbia Centre for Disease Control Public Health Laboratory, Vancouver, Canada.
4Vancouver Coastal Health, Vancouver, Canada.
Background: Roughly a third of syphilis cases in British Columbia (BC), Canada, are staged as latent syphilis of unknown duration (LSUD), which are treated as late-stage cases with longer treatment duration. Treponema pallidum (TP) polymerase chain reaction (PCR) is a direct syphilis test typically used on lesions, though if reactive from mucocutaneous sites (e.g. oral, anogenital) in asymptomatic individuals, it can confirm early infection. This study examines the role of TP-PCR in restaging LSUD to early latent (i.e. infectious) syphilis. We conducted a retrospective cohort study of all LSUD cases with TP-PCR results in BC from 06/2022 to 05/2024, focusing on LSUD cases restaged to early latent. Demographic, clinical and laboratory data were analyzed using descriptive statistics, and logistic regression was used to identify predictors associated with restaging. One such predictor is the enzyme immunoassay (EIA) index, an indirect measure of infection status (i.e. index >45, established infection; index ≤45, recent infection).
Results: There were a total of 1282 LSUD cases during the study period, of which 179 (14.0%) had a TP-PCR performed. Of these, 48 (26.8%) were TP-PCR positive and were therefore restaged to early latent. Restaged individuals were statistically significantly more likely to have an RPR >1:32, and an EIA index ≤45 when compared to non-restaged individuals (Table 1), both of which are more consistent with early infection. All 29 (100%) restaged cases with 12-month follow-up serology demonstrated an appropriate treatment response (i.e. at least 4-fold decrease in RPR titre). In this study population, a positive TP-PCR resulted in the restaging of over a quarter of LSUD cases to early latent syphilis. These findings support the use of TP-PCR in cases of LSUD, with the goal of more accurately staging syphilis infection. This approach could help shorten treatment duration, prevent antibiotic overuse, and enable more targeted public health management.
| Characteristics | Not Restaged (n = 131) | Restaged (n = 48) | P-value | |
|---|---|---|---|---|
| Gender, n (%) | ||||
| Female | 52 (39.69) | 23 (47.92) | ||
| Male | 77 (58.78) | 24 (50.00) | 0.574 | |
| MSM | 43 | 14 | ||
| Transgender | 2 (1.53) | 1 (2.08) | ||
| Age group, n (%)A | ||||
| 15–19 years | 3 (2.29) | 0 (0.00) | ||
| 20–24 years | 6 (4.58) | 5 (10.42) | ||
| 25–29 years | 34 (25.95) | 7 (14.58) | 0.0171 | |
| 30–39 years | 50 (38.17) | 30 (62.50) | ||
| 40–59 years | 36 (27.48) | 6 (12.50) | ||
| 60+ years | 2 (1.53) | 0 (0.00) | ||
| EIA Index, n (%)A,B | ||||
| ≤45.00 | 90 (68.70) | 43 (91.49) | 0.00205 | |
| >45.00 | 41 (31.30) | 4 (8.51) | ||
| RPR titre, n (%)A,B | ||||
| ≤1:32 | 57 (43.51) | 9 (17.02) | ||
| >1:32 | 68 (51.91) | 38 (80.85) | 0.00188 | |
| Nonreactive | 6 (4.58) | 0 (0.00) | ||
| HIV status, n (%) | ||||
| Positive | 11 (8.40) | 2 (4.17) | ||
| Negative | 105 (80.15) | 42 (87.50) | 0.462 | |
| Unknown | 15 (11.45) | 4 (8.33) |
OA05.01 – HIV and STD Testing Among Adolescents Experiencing Sexual Violence in 2021
Mr. Darsh Patel1
1University of Georgia, Athens, United States.
Background: Adolescents who experience sexual abuse in relationships are at increased risk of sexually transmitted diseases (STDs) and HIV. This study examines the relationship between physical abuse in dating relationships and HIV/STD testing behaviors, focusing on age, gender, and racial disparities.
Methods: Using data from the ABES (7705 participants), we analyzed demographic variables (age, gender, race, and sexual identity), experiences of sexual dating violence and condom use, and self-reported HIV and STD testing. Statistical associations were analyzed and evaluated using Chi-square tests through SPSS statistics software.
Results: Among the 7705 adolescents surveyed, the most prevalent age group reported testing was 17 (34.9%). Overall, females displayed a higher HIV and STD testing rate (56.4% and 61.4%) than males (43.6% and 38.6%), respectively. The overall demographic showed American Indian/Alaska Native (1.5%), Native Hawaiian (0.3%), and Hispanic (3.1%) adolescents having lower rates of STD testing compared to White (45.1%) and African American (24.7%). Of the respondents who reported having sexual intercourse, 73.4% and 84.9% reported HIV and STD testing, respectively. Among the 756 reported experiencing sexual violence, the testing percentage for HIV was 22.3% and STDs were 25.9%. Among adolescents reporting sexual violence and no condom use, only 35.3% and 32.6% reported HIV and STD testing, respectively.
Conclusion: Adolescents experiencing sexual violence report low HIV and STD testing rates, especially when not using condoms, despite their increased risk. Racial disparities further highlight inequities, with American Indian/Alaska Native, Native Hawaiian, and Hispanic adolescents having significantly lower testing rates compared to White and African American peers. These findings emphasize the critical need for targeted, culturally sensitive interventions to improve access to testing and address barriers for vulnerable populations.
OA05.02 – Youth-Friendly Mobile Sexual Health Services Reach Adolescents with High STI Risk in Rural South Africa: Baseline Data from the Thetha Nami Cluster-Randomized Trial
Dr. Jana Jarolimova1, Jacob Busang2,3, Nqobile Ngoma2, Thembelihle Zuma2,3,4, Carina Herbst2, Nonhlanhla Okesola2, Natsayi Chimbindi2,3,4, Jaco Dreyer2, Theresa Smit2, Lucky Mtolo2, Osee Behuhuma2, Willem Hanekom2,3,4, Ingrid Bassett1, Kobus Herbst2,5, Limakatso Lebina2,3,6, Janet Seeley2,3,7, Andrew Copas3, Kathy Baisley2,7, Maryam Shahmanesh2,3,4, Thetha Nami ngithethe nawe research group
1Massachusetts General Hospital, Boston, USA.
2Africa Health Research Institute, Mtubatuba, South Africa.
3University College London, London, United Kingdom.
4University of KwaZulu-Natal, Durban, South Africa.
5DSI-SAMRC South African Population Research Infrastructure Network (SAPRIN), Durban, South Africa.
6University of the Witwatersrand, Johannesburg, South Africa.
7London School of Hygiene & Tropical Medicine, London, United Kingdom.
Background: Adolescents and young adults (AYA) in South Africa (SA) have a high burden of curable sexually transmitted infections (STIs). Identifying AYA with asymptomatic STIs who would benefit from treatment, HIV prevention, and other sexual and reproductive health (SRH) services is a challenge in rural settings. We use a cluster-randomized trial in rural SA to compare STI prevalence among AYA accessing mobile sexual health services with population-representative estimates.
Methods: Between May 2022–February 2023, we conducted a baseline survey among a randomly selected sample of 15–30-year-olds. Between June 2022–November 2024, peer navigators mobilized community-dwelling AYA to attend youth-friendly mobile clinics for SRH services. At both time points, AYA were offered testing for chlamydia, gonorrhea, and trichomoniasis using GeneXpert on self-collected vaginal swabs or urine. We compared STI prevalence by sex and age group within each sample (survey participants and SRH clinic attendees) and between samples using chi-square tests.
Results: A total of 2090 AYA participated in the baseline survey; among the 1350 (64.6%) who consented to STI testing and had results available, STI prevalence was 22.7%; lower among 15–19-year-olds (14.9%) than 20–24-year-olds (31.1%) or 25–30-year-olds (22.8%, P < 0.001), and lower among males than females (15.0% vs 28.8%, P < 0.001) (Table 1). Among 3877 AYA seen in mobile clinics, 2486 provided STI specimens and had results available. STI prevalence was 29.8%, lower among males than females (18.4% vs 37.4%, P < 0.001). Prevalence in mobile clinics was significantly higher than in the population-representative survey among adolescents aged 15–19 years (28.3% vs 14.9%, P < 0.001), driven primarily by significantly higher prevalence among female adolescents (40.1% vs 22.1%, P < 0.001).
Conclusions: Mobile SRH services in rural SA reached adolescents aged 15–19 years, particularly girls, with higher STI prevalence than the general population. Mobile sexual health services are a potential way to deliver comprehensive SRH and HIV prevention to adolescents at highest risk.
| Sex | Age | Baseline survey: prevalence of any STI | SRH clinics: prevalence of any STI | |||||
|---|---|---|---|---|---|---|---|---|
| n | % (95% CI) | P-value* | n | % (95% CI) | P-value* | |||
| Overall | 15–19 | 484 | 14.9% (11.8%–18.4%) | <0.001 | 829 | 28.3% (25.3%–31.5%) | <0.001 | |
| 20–24 | 437 | 31.1% (26.8%–35.7%) | 909 | 34.5% (31.5%–37.7%) | ||||
| 25–30 | 429 | 22.8% (19.0%–27.1%) | 748 | 25.7% (22.6%–29.0%) | ||||
| All ages | 1350 | 22.7% (20.5%–25.0%) | 2486 | 29.8% (28.0%–31.6%) | ||||
| Male | 15–19 | 244 | 7.8% (4.8%–11.9%) | <0.001 | 368 | 13.6% (10.3%–17.5%) | 0.001 | |
| 20–24 | 187 | 21.4% (15.7%–28.0%) | 355 | 24.2% (19.9%–29.0%) | ||||
| 25–30 | 169 | 18.3% (12.8%–25.0%) | 270 | 17.4% (13.1%–22.5%) | ||||
| All ages | 600 | 15.0% (12.2%–18.1%) | 993 | 18.4% (16.1%–21.0%) | ||||
| Female | 15–19 | 240 | 22.1% (17.0%–27.9%) | <0.001 | 461 | 40.1% (35.6%–44.8%) | 0.001 | |
| 20–24 | 250 | 38.4% (32.3%–44.7%) | 554 | 41.2% (37.0%–45.4%) | ||||
| 25–30 | 260 | 25.8% (20.6%–31.5%) | 478 | 30.3% (26.2%–34.7%) | ||||
| All ages | 750 | 28.8% (25.6%–32.2%) | 1493 | 37.4% (34.9%–39.9%) | ||||
*P-values for chi-squared tests testing for variability by age within each sample.
OA05.03 – HIV Self-Testing Awareness and Use Among Adolescents in Kenya
Prof. Hong-Ha M. Truong1, Ms. Sayo Amboka2, Mr. Kevin Kadede2, Mr. Hanningtone Odhiambo2, Ms. Beatrice Otieno3, Ms. Elsa Heylen1, Ms. Marion Hewa2, Mr. Maurice Opiyo2, Mr. Fidel Opondo2, Ms. Damaris Odeny2, Mr. David Ogolla2, Ms. Lara Miller1, Prof. Elizabeth Bukusi2, Prof. Craig Cohen1
1University of California, San Francisco, United States.
2Kenya Medical Research Institute, Kisumu, Kenya.
3University of California Global Programs, Kisumu, Kenya.
Background: HIV self-testing (HIVST) provides a convenient alternative to facility-based testing. HIVST has been a component of national testing guidelines in Kenya since 2015, yet gaps remain in awareness and use. We assessed awareness, prior use and willingness to consider using HIVST among adolescents.
Methods: The Maneno Yetu study enrolled adolescents aged 15–19 (N = 3,061) residing in Kisumu for a cross-sectional survey using respondent-driven sampling. Associations were assessed by logistic regression.
Results: Overall, 60% of participants heard of HIVST and 9% had used HIVST. Boys were more likely than girls (P = 0.001) and adolescents aged 18–19 were more likely than those aged 15–17 (P < 0.001) to have heard of HIVST. Among 275 adolescents with HIVST experience, girls compared to boys (P = 0.048) and adolescents aged 18–19 compared to 15–17 (P < 0.001) were more likely to have used HIVST. Among 1528 adolescents who heard of HIVST but had no prior use, 58% were willing to consider using HIVST. Willingness to use HIVST did not differ by sex or age group. Perceived benefits associated with willingness to consider using HIVST included greater convenience (P < 0.001), not needing to go to health facilities (P = 0.018) and greater privacy (P = 0.026).
Conclusion: HIVST use by adolescents in Kenya remains low despite awareness of its availability. More boys than girls had heard of HIVST, a surprising finding given HIV testing and prevention efforts in sub-Saharan Africa have focused primarily on adolescent girls and young women. Maneno Yetu participants expressed willingness to consider using HIVST, noting greater convenience and privacy as key benefits. Our findings of limited uptake despite awareness and willingness to use HIVST suggest the need to provide clearer instructions for use, make tests available at schools and community venues such as youth clubs where adolescents gather, and leverage peer support so more adolescents can conveniently access and feel confident using HIVST.
OA05.04 – Prevalence of Four Sexually Transmitted Infections Among Adolescents and Young People Aged 15 to 24 in Lusaka, Zambia
Dr. Mwelwa Muleba Phiri1, Ms Sophie Inambwae1, Ms Lucheka Malisawa Sigande1, Mr Bxyn Kangololo1, Mr Ab Schaap1,2, Ms Maina Cheeba1, Ms Kwitaka Maluzi1, Ms Ngosa Mwanza1, Mr Felix Chilambe1, Mr Steve Belemu1, Dr Jennifer Fitzpatrick1, Ms Vicky Cuylaerts3, Dr Irith De Baetselier3, Professor Helen Ayles1,4, Dr Bernadette Hensen3
1Zambart, Lusaka, Zambia.
2Department of Infectious Disease Epidemiology, London School of Hygiene and Tropical Medicine, London, United Kingdom.
3Institute of Tropical Medicine, Sexual Health Unit., Antwerp, Belgium.
4Clinical Research Department, London School of Hygiene and Tropical Medicine., London, United Kingdom.
Background: There is limited data on the burden of STIs among adolescents and young people (AYP) in southern African countries, including Zambia. This study estimates the prevalence of chlamydia, gonorrhoea, trichomoniasis, and syphilis among AYP aged 15 to 24 in Lusaka, Zambia.
Methods: A cross-sectional survey among AYP was conducted in an urban community (population ~200,000) from May–September 2024. For a geographically representative sample, two-stage sampling was applied to randomly select 10 blocks of 20–40 households each. All households in a block were visited and all AYP aged 15–24 invited to participate. Consenting AYP completed a questionnaire, provided a self-collected sample (vaginal swab or urine) for diagnosis of chlamydia, gonorrhoea or trichomoniasis, among adolescent girls and young women (AGYW) an additional vaginal swab for bacterial vaginosis (BV) diagnosis, and were offered dual HIV/syphilis rapid testing in the household. When reactive for syphilis, a blood sample was collected for RPR testing. AYP were provided their test results and referred for treatment. We present the prevalences of STIs (chlamydia, gonorrhoea, trichomoniasis, or syphilis), by sex, and of BV among AGYW.
Results: Among 606 AYP, 18.5% (n = 111) were diagnosed with any STI. By sex, prevalence was 25.1% (73/305) among AGYW and 12.0% (38/301) among adolescent boys and young men; prevalence increased with age (Fig 1). Among all AYP, chlamydia was most common (10.4%) followed by trichomoniasis (6.4%). Over two-thirds of the infections (70.3%) were asymptomatic and 92.8% had never been treated for an STI. Among AGYW, 65.8% diagnosed with an STI were also diagnosed with BV compared to 46.8% undiagnosed with an STI (P = 0.01).
Conclusion: One-fifth of AYP, and one-quarter of AGYW, were diagnosed with an STI, with AGYW also experiencing a high burden of BV. Effective strategies for STI diagnosis and treatment are crucial to improving the sexual health of AYP.
Prevalence of four sexually transmitted infections among adolescents and young people by age and sex.
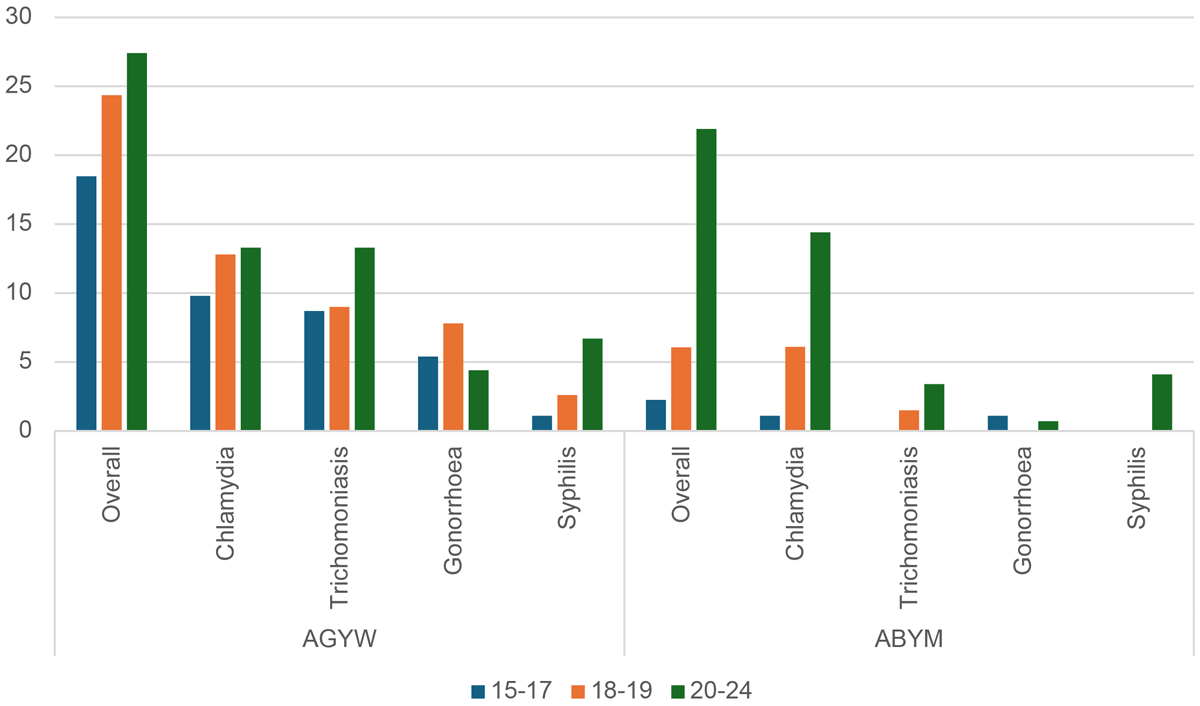
OA05.05 – Sexual Behaviours and Condom Use Among Adolescent Girls and Young Women in Nigeria: Urban-Rural Disparities and Implications for Sexual and Reproductive Health
Dr. Rose Aguolu1, ThankGod Zachariah Kums1
1National Agency for the Control of AIDS, Abuja, Nigeria.
Background: Understanding sexual behaviours and condom use patterns among adolescent girls and young women (AGYW) is crucial for developing effective sexual and reproductive health interventions in Nigeria. This study examined urban-rural disparities in sexual behaviours and condom usage among AGYW aged 15–24 years, utilizing data from the 2021 Multiple Indicator Cluster Survey (MICS).
Methods: Nationally representative data from 14,821 AGYW with 57.3% aged 15–19 years and 42.7% aged 20–24 years were analyzed, focusing on sexual debut, multiple sexual partnerships, and condom use patterns. The sample represented both rural (55.3%) and urban (44.7%) populations, with most participants having never married (71.0%) and nearly half (47.5%) attaining secondary education.
Results: The findings revealed distinct behavioural patterns between urban and rural populations. Urban AGYW reported lower rates of sexual experience (37.0%) compared to their rural counterparts (56.8%). Early sexual debut before age 15 was three times more prevalent in rural areas (12.0%) than in urban settings (4.0%). While multiple sexual partnerships were relatively low in both settings, 37.7% of all respondents engaged in sexual activity with non-marital, non-cohabiting partners within the past year. Condom use showed marked urban-rural disparities. Among AGYW engaging in sexual activity with non-marital, non-cohabiting partners, urban residents demonstrated higher rates of condom use during their last sexual encounter (59.8%) compared to rural residents (45.9%). Similar patterns were recorded in general condom use during most recent sexual activity, with urban AGYW (58.9%) showing higher usage rates than rural AGYW (43.6%).
Conclusion: These findings highlight significant vulnerabilities to sexually transmitted infections and unintended pregnancies, particularly among rural AGYW. The study underscores the critical need for targeted interventions that address these disparities through expanded access to reproductive health services and enhanced comprehensive sexuality education with particular attention to the more vulnerable rural populations.
OA05.06 – Knowledge of Sexually Transmitted Infections Among Rural Adolescents in Bangladesh: A Community-Based Survey
Dr. Farah Naz Rahman1, Mr Shafayatul Islam Shiblee1, Dr Anadil Alam1, Iffat Sharmin1, Dr Quamrun Nahar1
1Maternal and Child Health Division, International Centre For Diarrhoeal Disease Research Bangladesh (icddr,b), Dhaka, Bangladesh.
Background: Adolescents in rural Bangladesh remain a vulnerable and under-researched group in sexually transmitted infection (STI) studies. Limited access to sexual health education in these settings heightens their risk of STIs. This study investigates STI knowledge among unmarried adolescents in Baliakandi upazila, Rajbari district, to inform tailored intervention strategies.
Methods: This community-based cross-sectional survey was conducted in January 2024, using a random sample from an existing adolescent cohort in Baliakandi Upazila. A total of 2,156 unmarried adolescents (1,109 girls and 1,047 boys), aged 14 to 17 years, were interviewed at home. The questionnaire assessed familiarity with the term “Sexually Transmitted Infections” in English and Bangla, awareness of common infections (HIV, syphilis, gonorrhea, chlamydia, herpes), and knowledge of transmission methods. Descriptive statistics were used to analyze the data.
Results: Among the 2,156 adolescents, only 19.4% (n = 420) had heard of STIs. Awareness was slightly higher among 16-year-olds (24.3%) compared to 14-year-olds (14.8%), but no substantial differences were observed between boys and girls or across education levels, as most lacked basic knowledge. HIV was the most recognized infection (33.1% unprompted, 51.9% prompted), while awareness of other STIs was very low. Only 7.6% identified syphilis, 14.2% gonorrhea, 10.9% chlamydia, and 4.7% herpes when prompted. Among those aware of STIs, 75.2% (n = 316) did not know how they are transmitted. Knowledge of sexual transmission (15.9%) and blood transfusion (32.3%) was limited, with recognition of other routes below 5%.
Conclusion: This large community-based survey highlights a critical gap in STI knowledge among rural adolescents in Bangladesh, indicating an urgent need for comprehensive, community-based sexual health education programs to equip adolescents with accurate information and reduce their risk of STIs.
OA06.01 – Impact of Penile-Vaginal Sex on the Microbiome and Immunology of the Penile Urethra
Mr. Marcio Gabriel Amancio De Carvalho1, Dr. Avid Mohammadi1, Sareh Bagherichimeh1, Dr. Yoojin Choi1, Azadeh Fazel1, Elizabeth Tevlin2, Sanja Huibner1, Dr. Eric Armstrong1, Dr. Daniel Park3, Dr. Cindy Liu3, Wangari Tharao2, Dr. Bryan Coburn1
1University of Toronto, Toronto, Canada.
2Women’s Health in Women’s Hands Community Health Center, Toronto, Canada.
3George Washington University, Washington, USA.
Background: Penile HIV acquisition occurs primarily through the inner foreskin and the distal urethra. Genital inflammation, epithelial disruption and microbiome composition affect HIV acquisition risk in both the vagina and penile coronal sulcus, and penile-vaginal sex has a major impact on these parameters. However, while the penile urethra is a key HIV acquisition site in circumcised men, the impact of sex at this tissue site has been less explored.
Methods: The Sex, Couples and Science (SECS) study examined the short-term impact of penile-vaginal sex on the genital immunology and microbiome of established couples. First-void urine was collected at baseline and immediately, +1, +7 and +72 h after penile-vaginal sex to characterise the penile urethra microbiome (16S sequencing and quantitative gene Polymerase Chain Reaction (qPCR)) and immune milieu (multiplex chemiluminescent immunoassay) (Fig. 1).
Results: Male participants were an average of 25 years old, and predominantly of Asian (40.5%) or White (40.5%) ethnicities. Sex immediately induced urethral inflammation and enrichment of the common vaginal species Lactobacillus crispatus and L. jensenii, with resolution within 7 h. Interestingly, non-optimal bacterial species that increase inflammation and HIV risk in the vagina – namely L. iners and Gardnerella vaginalis – were present in the urethra prior to sex, and their levels were not altered by sex.
Conclusion: Penile-vaginal sex caused transient urethral inflammation and transfer of vaginal bacteria from the vagina into the urethra, with potential implications for penile HIV susceptibility. However, key “non-optimal” vaginal bacteria associated with higher HIV risk in women were already present in the urethra, suggesting stable colonization and that the urethra may play an important role as a reservoir for these non-optimal vaginal bacteria.
Relative Abundance of Key Vaginal Bacteria in the Penile Urethra Before and After Sex. Modified relative abundances plot showing each individual participant’s total microbiome with species of interest highlighted in color. Blank columns represent excluded or unavailable samples. Background shading indicates participant grouping based on condom use. Samples ordered based on L. crispatus relative abundance at 1 h timepoint.
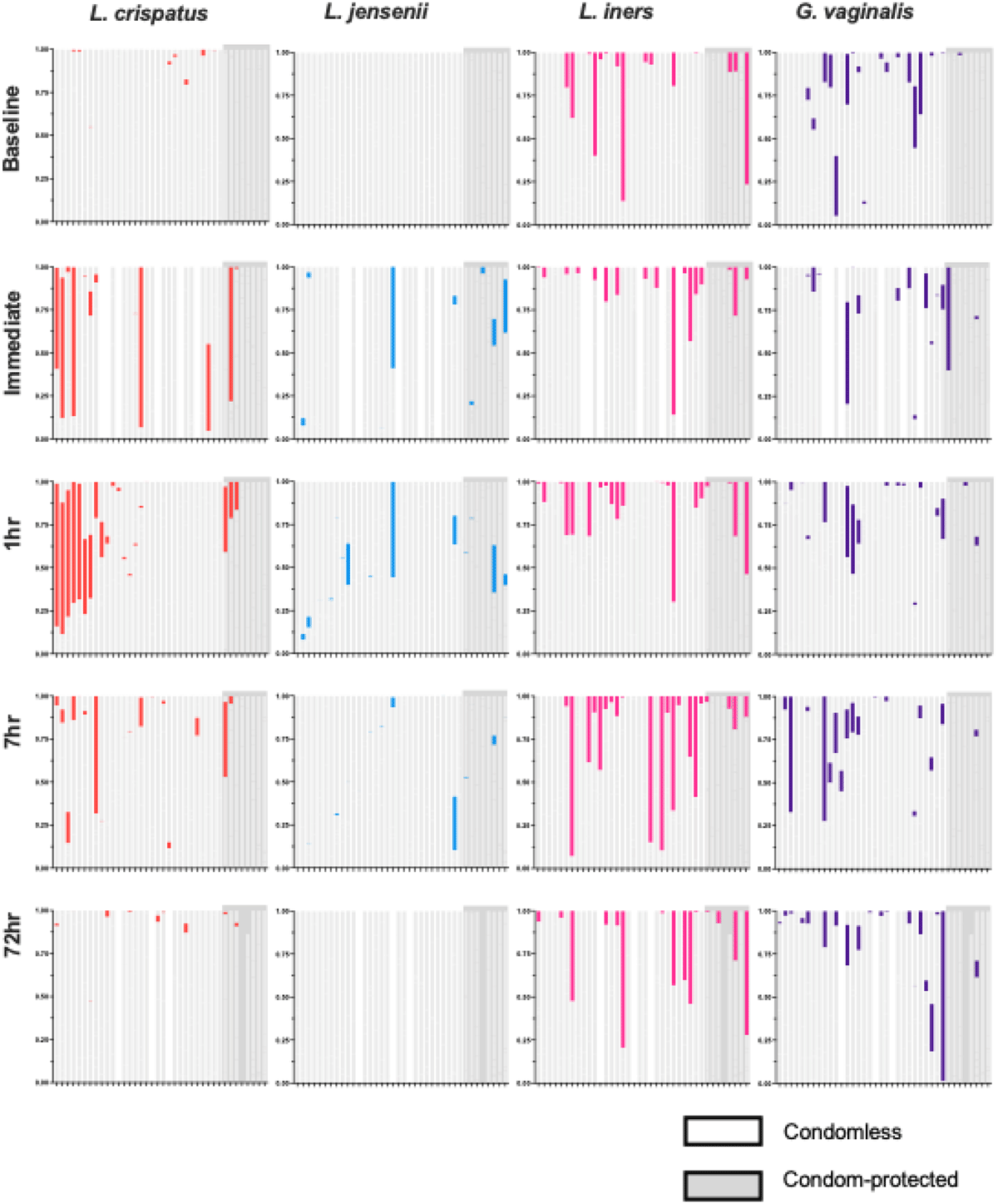
OA06.02 – Role of Microrna Regulation in Vaginal Epithelial Cells: Effect of Sex Hormones and Microbiota on HIV Susceptibility
Miss Shreya Joshi1, Dr. Aisha Nazli1, Dr. Charu Kaushic1
1McMaster Immunology Research Centre, McMaster University, Hamilton, Canada.
Background: HIV disproportionately affects women, with about 40% of infections occurring in the female reproductive tract. Factors such as sex hormones and vaginal microbiota (VMB), regulate HIV susceptibility. Our lab has demonstrated that estrogen (E2) confers protection, whereas progesterone (P4) increases susceptibility to HIV. Similarly, eubiotic Lactobacillus crispatus (LC)-dominated VMB is protective, while dysbiotic Gardnerella vaginalis (GV), increases HIV risk. The mechanisms leading to differential protection remain unclear. MicroRNAs, small non-coding RNAs that regulate gene expression, are modulated by hormones and microbiota and can influence disease outcomes. We investigated the role of sex hormones and VMB in modulating the effects on HIV susceptibility through differential microRNA expression in vaginal epithelial cells (VK2).
Methods: In separate experiments, VK2 cells were exposed to eubiotic (LC) and dysbiotic (GV) bacteria, for varying durations (0.5–22 h) and HIV-1 (1–24 h), to evaluate their impact on microRNA expression. The effects of physiological range of E2 (10^-9-10^-10M) and P4 (10^-7–10^-8M) were assessed to determine the optimal hormone concentration capable of modulating microRNA expression. The expression of seven microRNAs-hsa-miR-146a, hsa-miR-155, hsa-miR-125b, hsa-miR-23a, hsa-miR-27b, hsa-miR-193b and hsa-miR-130a was quantified by qRT-PCR.
Results: LC and GV significantly altered the expression of hsa-miR-23a-3p, hsa-miR-193b-3p, hsa-miR-146a-5p, hsa-miR-155-5p, hsa-miR-27b-3p, and hsa-miR-130a-3p in VK2 cells at various time points. Pathway analysis of all microRNAs revealed enrichment of TNF-α, NF-κB and MAPK signaling pathways indicating their potential involvement in regulating inflammatory responses. LC and GV significantly upregulated IL-6 and IL-8 within 30 min, followed by increased TNF-α and IL-1β expression over 11 h. E2(10^-9M) significantly upregulated hsa-miR-146a-5p, a known anti-inflammatory microRNA, while P4 showed no effect. HIV significantly downregulated hsa-miR-155-5p, a known pro-inflammatory microRNA and upregulated hsa-miR-146a-5p, potentially suppressing inflammation.
Conclusion: These findings indicate potential role of microRNAs in modulating differential effect of hormones and VMB on HIV susceptibility, offering potential therapeutic targets.
OA06.03 – Prediction of Discharge-Causing Sexually Transmitted Infections and Bacterial Vaginosis Using Vaginal Inflammation Biomarkers: Evidence from the Genital InFlammation Test (GIFT) Clinical Study in Madagascar, Zimbabwe and South Africa
Miss Micaela Lurie1, M Sinkala1, R Tanko1, K Gill1,2, K Kranzer3,4, LG Bekker1,2, T Mayouya-Gamana5, T Mwaturura4,6, A Madikida2, K Mahlangu2, N Thomas2, C Dziva Chikwari3,4,6, J van de Wijgert7, C Fortas8,9, BT Huynh8,9, A Harimanana5, S Randrianjatovo5, S Rasoanandrianina10, MT Manhanzva1, F Khumalo1, T Pidwell1, D Anderson1, T Crucitti5, JS Passmore1,12,13, L Masson1,11,13,14,15
1Institute of Infectious Disease and Molecular Medicine (IDM), University of Cape Town, South Africa.
2Desmond Tutu HIV Centre, University of Cape Town, South Africa.
3London School of Hygiene & Tropical Medicine, England, United Kingdom.
4The Biomedical Research and Training Institute, Zimbabwe.
5Institut Pasteur de Madagascar, Madagascar.
6Organization for Public Health Interventions and Development, Zimbabwe.
7University Medical Center Utrecht, Netherlands.
8Institut Pasteur, France.
9UVSQ, Inserm, France.
10Centre Hospitalier Universitaire de Gynécologie et Obstétrique de Befelatanana, Antananarivo, Madagascar.
11Maternal Child and Adolescent Health Program, Public Health Discipline, Burnet Institute, Australia.
12National Health Laboratory Service, South Africa.
13Centre for the AIDS Programme of Research in South Africa, South Africa.
14Disease Elimination Program, Life Sciences Discipline, Burnet Institute, Australia.
15Central Clinical School, Monash University, Australia.
Background: Bacterial vaginosis (BV) and sexually transmitted infections (STIs) increase HIV and reproductive health risks. IL-1α, IL-1β, and IP-10 were identified as biomarkers for detecting BV and STIs in sub-Saharan Africa, with elevated IL-1α/IL-1β indicating STI/BV and decreased IP-10 differentiating BV. We conducted a study comprising 675 women from Madagascar, Zimbabwe and South Africa to test this biomarker panel to improve STI/BV management in regions with varying HIV burdens.
Methods: IL-1α, IL-1β, and IP-10 were measured in vaginal swabs from women aged 18–40 using ELISA. STIs, including Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), Trichomonas vaginalis (TV) and Mycoplasma genitalium (MG), were detected via NAATs, BV by Nugent scoring, and vaginal pH with strips. Thirty-four machine learning models used cytokines and pH to predict STI/BV status.
Results: Among 675 women, 96 had CT, 37 NG, 78 TV, 30 MG, and 458 BV, with most STIs co-occurring with BV. IL-1α and IL-1β levels were significantly higher in women with CT, TV, and BV but not NG, compared to those without STIs/BV. BV was the most inflammatory condition in all three countries, especially when combined with an STI. IP-10 concentrations were significantly higher in women with CT (but not NG or TV) and lower in those with BV, compared to women without STIs/BV. IP-10 decreased with higher Nugent scores. Using machine learning, the three cytokines predicted STI/BV with 79.4% accuracy (sensitivity 85.54%, specificity 60.84%). Models incorporating vaginal pH and excluding IP-10, achieved 81.5% accuracy (sensitivity 92.57%, specificity 48.19%) with IL-1β and pH, and 80.9% accuracy (sensitivity 93.57%, specificity 42.77%) with IL-1α and pH.
Conclusion: Vaginal inflammation was observed in women with STIs and BV in Madagascar, Zimbabwe and South Africa. The most accurate model combined IL-1b with vaginal pH. Work is ongoing to develop a lateral flow test using these biomarkers to detect undiagnosed STIs/BV.
OA06.04 – Longitudinal Dynamics of the Vaginal Microbiota Before and After Hyperosmolal Lubricant Use in Patients Referred for TVUS
Dr. Sarah E. Brown1,2, Dr. Xin He3, Dr. Laurence Magder1, Dr. Christina A. Stennett1,2, Dr. Sarah J. Robbins1,2, Elizabeth D. Johnston4, Dr. Daniel Morgan1, Dr. Khalil G. Ghanem5, Dr. Jacques Ravel2,6, Dr. Katrina Mark7, Dr. Rebecca M. Brotman1,2
1Institute For Genome Sciences, University of Maryland School of Medicine, Baltimore, United States.
2Department of Epidemiology and Public Health, University of Maryland School of Medicine, Baltimore, United States.
3Department of Epidemiology and Biostatistics, University of Maryland College Park, College Park, United States.
4University of Maryland, Faculty Physicians Inc, Baltimore, United States.
5Division of Infectious Diseases, Johns Hopkins School of Medicine, Baltimore, United States.
6Department of Microbiology and Immunology, University of Maryland School of Medicine, Baltimore, United States.
7Department of Obstetrics and Gynecology, University of Maryland School of Medicine, Baltimore, United States.
Background: Hyperosmolal vaginal lubricants are commonly used during sex and clinical procedures like transvaginal ultrasound (TVUS); however, they may disrupt beneficial vaginal Lactobacillus spp. This study evaluated changes in vaginal microbiota composition following a single lubricant exposure during TVUS.
Methods: N = 104 participants referred for TVUS self-collected mid-vaginal swabs daily for ~1 week before TVUS. During TVUS, 2.7 g of hyperosmolal lubricant (GLIDE lubricating jelly, Athena Medical Products, ~2400 mOsm/kg) was used. Vaginal swabs were collected immediately before TVUS, 6–12 h afterward, and then twice-weekly for 9 weeks. Microbiota composition was characterized by 16S rRNA gene amplicon sequencing (V3–V4) and assigned to community state types (low-Lactobacillus, CST IV vs Lactobacillus-dominated, CSTs I/II/III/V). Yue-Clayton theta indices defined compositional similarity of daily successive samples and microbiota stability. Generalized linear mixed models evaluated the within-participant odds of having a CST IV microbiota in their post-TVUS samples versus their pre-TVUS samples.
Results: There was no immediate change in the vaginal microbiota composition and structure in daily successive samples immediately following TVUS. Longer-term analyses over 10 weeks indicated the vaginal microbiota was less stable within 3-week intervals post-TVUS versus before TVUS. While overall odds of CST IV did not change after TVUS in all participants, stratified analyses found peri-/post-menopausal participants (N = 19, aOR 3.22, 95% CI: 1.16–8.98) and those with prior BV (N = 58, aOR 1.73, 95% CI: 1.10–2.72) were more likely to exhibit CST IV microbiota post-TVUS. These changes to CST IV persisted throughout follow-up (9 weeks).
Conclusions: Peri-/post-menopausal women and those with prior BV were more likely to exhibit a low-Lactobacillus vaginal microbiota up to 9 weeks after a single exposure to hyperosmolal lubricant during TVUS, while the vaginal microbiota of premenopausal women and those without prior BV appeared more resilient against perturbations. Reformulating lubricant products to reduce osmolality and mitigate antimicrobial effects may help preserve vaginal microbiota health.
Odds of CST IV versus Lactobacillus-dominated (CSTs I/II/III/V) vaginal microbiota after exposure to exposure to lubricant during TVUS versus before.
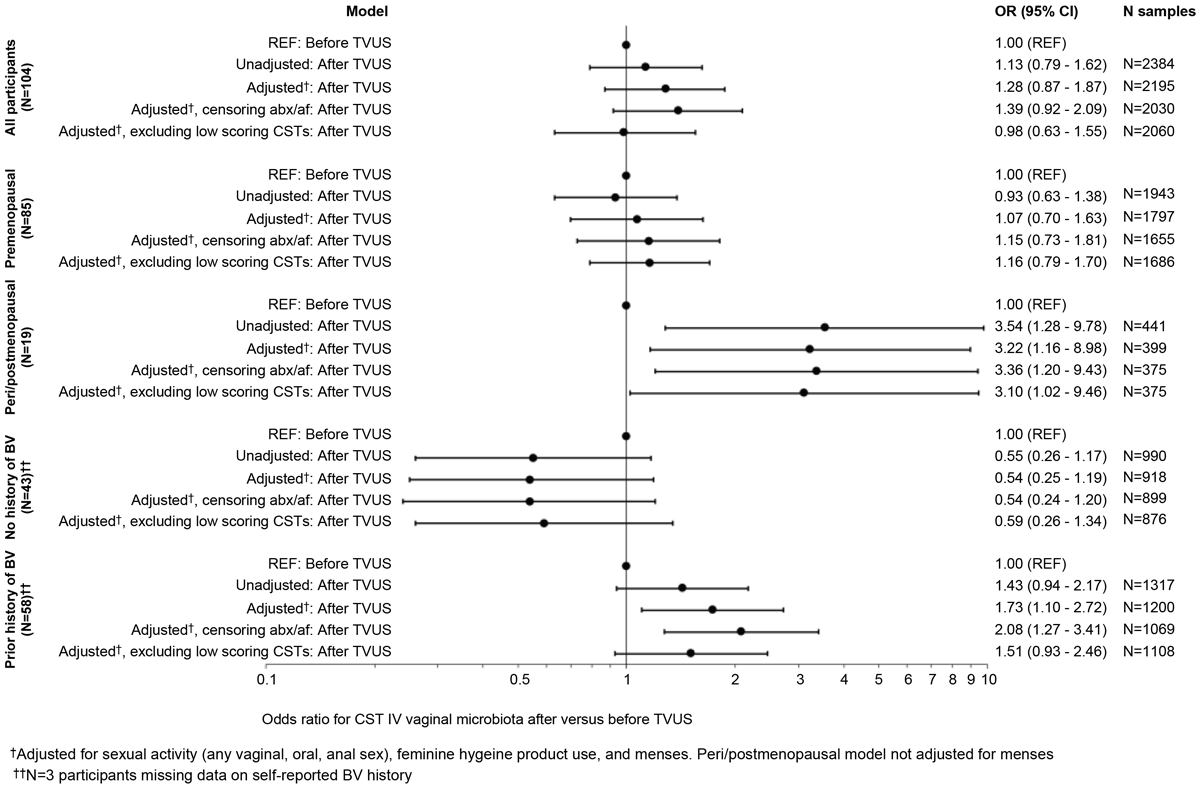
OA06.05 – Contribution of the Cervicovaginal Microbiome to Chlamydia Trachomatis Spontaneous Clearance: Evidence from a Longitudinal Study
Dr. Kayla Carter1, Dr. Sarah Brown1, Lindsay Rutt1, Christina Barrett1, Rishi Jindal1, Prof. Michelle Shardell1, Prof. Andrew Macintyre2, Dr. Yukari Manabe3, Dr. Susan Tuddenham3, Dr. Khalil Ghanem3, Prof. Jacques Ravel1, Prof. Rebecca Brotman1
1Institute for Genome Sciences, University of Maryland School of Medicine, Baltimore, United States.
2Duke Human Vaccine Institute, Duke University Medical Center, Durham, United States.
3Johns Hopkins University School of Medicine, Baltimore, United States.
Background: Urogenital Chlamydia trachomatis (CT) spontaneously clears without antibiotics in up to 26% of women between screening and treatment initiation. While the vaginal microbiome is linked to increased CT risk, its role in spontaneous clearance remains unclear. Identifying factors that influence clearance may inform interventions to reduce CT burden.
Methods: The Longitudinal Study of Vaginal Flora (1999–2002) followed reproductive-age women quarterly for one year. Endocervical swabs were collected at all visits. Baseline chlamydia screening began in 2001 with commercial introduction of ligase chain reaction assays; untested swabs were screened after study completion. Empiric treatment and symptomatic CT testing were implemented throughout the study. Excluding visits with chlamydia-active antibiotics, we constructed a nested case-control study, defining persistence as two consecutive chlamydia-positive visits (n = 310) and spontaneous clearance as a chlamydia-positive followed by a chlamydia-negative visit (n = 301). We used archived cervicovaginal lavages for whole metagenome sequencing, lactic acid (LA) isomer quantification, and NAAT for Candida, Mycoplasma genitalium, Neisseria gonorrhoeae, and Trichomonas vaginalis. We used logistic regression with generalized estimating equations to estimate associations of behaviors, microbiota and co-infection exposures with chlamydia persistence versus spontaneous clearance.
Results: Microbiota dominated by Candidatus Lachnocurva vaginae (adjusted odds ratio [aOR] = 3.46, 95% confidence interval [CI]: 1.61–7.45) or Gardnerella (aOR = 2.29, 95% CI: 1.20–4.36) were significantly associated with chlamydia persistence 3 months later compared to those dominated by D-LA-producing lactobacilli (Lactobacillus crispatus, Lactobacillus gasseri, Lactobacillus jensenii). Low D-LA (aOR = 2.83, 95% CI: 1.54–5.21) and low L-LA (aOR = 1.68, 95% CI: 1.14–2.47) concentrations were significantly associated with chlamydia persistence; D-LA:L-LA ratio was not. M. genitalium co-infection was significantly associated with chlamydia persistence among non-Lactobacillus-dominated microbiota in unadjusted models (OR = 1.76, 95% CI: 1.10–2.84), but not in the study overall. Self-reported behaviors were non-significant.
Conclusion: Bacterial vaginosis-associated microbial factors were associated with chlamydia persistence. Potential interactions between M. genitalium and C. trachomatis warrants further study.
Candidatus Lachnocurva vaginae-dominated microbiota, Gardnerella-dominated microbiota, low D-LA concentration, low L-LA concentration, and Nugent-BV are associated with subsequent CT persistence versus spontaneous clearance. (a) Whole metagenome sequencing relative abundances for all index visits were determined by mapping to VIRGO2. mgCSTs were assigned using the published classifier. Mycoplasma genitalium (MG) data are from Hologic Aptima testing. Spontaneous clearance index visits are presented on the left side of the plot, and persistence index visits on the right. (b) pH, D-LA and L-LA concentrations, and D-LA:L-LA concentration ratios at spontaneous clearance and persistence index visits. pH was measured via test strip and is a discreet measure (i.e., not continuous), and points are jittered around the discreet values for ease of viewing. LA isomer concentrations are in g/L. Values below the LLOQ (0.01 g/L) were imputed as half the LLOQ, and points are jittered for ease of viewing.
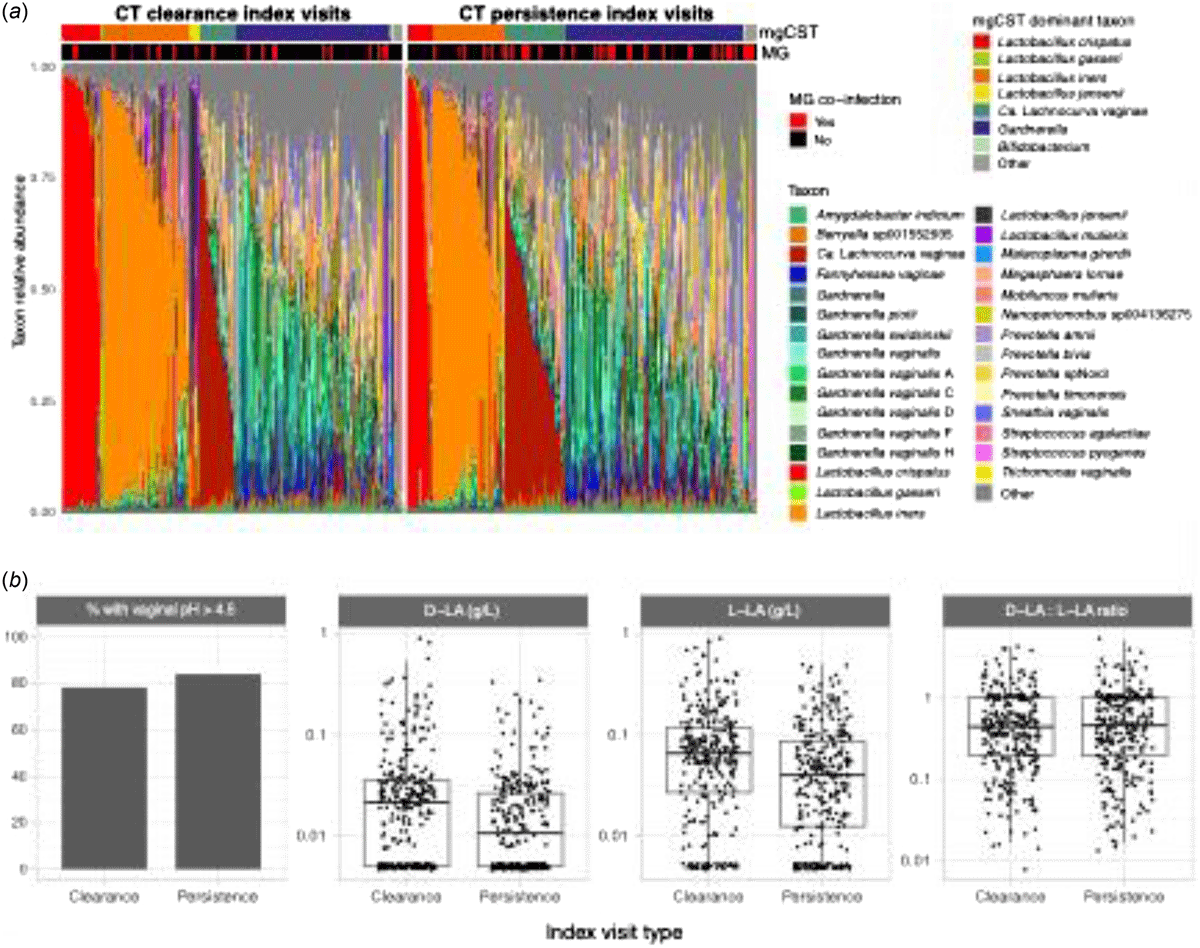
OA06.06 – Chlamydia Trachomatis Infection Is Preceded by Depletion of Genital Lactobacillus Crispatus and Higher Abundances of Specific Bacterial Vaginosis-Associated Bacteria
Dr. Smritee Dabee1,2, Omola Akingba3, Juma Shafi4, Dr. Daniel Raftery3, Dr. Jennifer Balkus3, Dr. Scott McClelland3,4, Dr. Heather Jaspan3,5,6
1University of British Columbia, Vancouver, Canada.
2McMaster University, Hamilton, Canada.
3University of Washington, Seattle, USA.
4University of Nairobi Institute for Tropical and Infectious Diseases, Nairobi City, Kenya.
5Seattle Children’s Research Institute, Seattle, USA.
6University of Cape Town, Cape Town, South Africa.
Background: With 130 million infections each year, Chlamydia trachomatis (CT) is the most prevalent bacterial sexually transmitted infection (STI) globally. Prevalence is highest among reproductive-age women and is linked to serious adverse health outcomes, including pelvic inflammatory disease, infertility, ectopic pregnancy, and HIV infection. Epidemiological studies have shown an association between genital microbial dysbiosis and a higher prevalence of CT infections. However, the directional relationship between CT and specific genital bacteria remains unclear. Using a nested case-control study design, we characterized the microbial changes preceding acquisition of new CT infections.
Methods: N = 231 Kenyan women (from the Mombasa Cohort) were compared using a matched case-control design using a 1:2 ratio. Longitudinal 3-monthly samples for these women were available. The presence of CT and the total 16S bacterial load were determined using qPCRs. 16S rRNA sequencing was used to characterize the genital microbiome at the visit immediately preceding CT acquisition among cases and their matched controls. Bacterial vaginosis (BV) status was determined using Nugent scoring.
Results: Women with BV had 2.18 higher odds of acquiring CT at the next visit. Women who subsequently acquired CT had a statistically significantly more diverse genital microbiota at the previous visit, but interestingly, the CT infection itself did not lead to an increase in genital microbial diversity. More specifically, CT acquisition was preceded by a lower fold-change in the optimal Lactobacillus crispatus and increased fold-changes in the BV-associated bacteria Dialister micraerophilus, Prevotella amnii, Prevotella timonensis, and Sneathia sanguinegens. The absolute concentrations of the different taxa identified with 16S rRNA sequencing were derived using the total bacterial load concentration. The same differences found using 16S rRNA sequencing were present when comparing the total bacterial concentrations rather than relative abundances.
Conclusion: These findings suggest a potential directional relationship where microbial dysbiosis precedes/increases susceptibility to C. trachomatis.
OA07.01 – Potential Impact of Catch-Up HPV Vaccination for Women Living with HIV in South Africa
Dr. Carla Doyle1, Dr. Minttu Rönn2, Dr. Cari van Schalkwyk3, Dr. Marc Brisson4,5, Dr. Leigh Johnson6, Dr. Marie-Claude Boily7, Dr. Mathieu Maheu-Giroux1
1Mcgill University, Montreal, Canada.
2Harvard University, Boston, United States.
3Stellenbosch University, Stellenbosch, South Africa.
4Centre de recherche du CHU de Quebec, Quebec, Canada.
5Universite Laval, Quebec, Canada.
6University of Cape Town, Cape Town, South Africa.
7Imperial College London, London, United Kingdom.
Background: Women living with HIV (WLHIV) are at higher risk of cervical cancer (CC). In high HIV prevalence settings, synergies between HIV and HPV challenge CC control.
Methods: We evaluated the potential impact of including catch-up HPV vaccination for WLHIV in South Africa using two dynamic transmission models of HPV/CC and HIV parameterized and calibrated to South African data. Two scenarios adding 90% catch-up vaccination for WLHIV aged 15–24 (two models; Sc1) or 15+ years (one model; Sc2) were compared to 90% routine vaccination of girls aged 9–14. All vaccination was initiated in 2020 using a nonavalent vaccine (100% effective, lifelong protection). Sensitivity analyses considered lower coverage, bivalent vaccines, and 20–30 years protection. We predicted the age-standardized relative reduction in annual vaccine-type high-risk (VT-HR) HPV prevalence and cumulative fraction of CC averted among WLHIV.
Results: Sc1 increased vaccination coverage among WLHIV compared to routine vaccination alone (7–9-fold in 2020) but remained substantially below that among all women unless the catch-up age expanded to 15+ (Sc2) (Fig. 1a, b). From 26% in 2020, routine vaccination alone reduced VT-HR HPV prevalence among WLHIV by 50% and 90% by 2040 and 2085, respectively. Sc1 further reduced VT-HR HPV prevalence by 10% by 2025 and a maximum of 10%–25% by 2060 compared to 25% in 2025 and a maximum of 36% by 2050 with Sc2 (Fig. 1c). Sc1 and Sc2 averted a maximum of 3%–9% and 14% CCs among WLHIV by 2080 and 2050–2065, respectively (Fig. 1d). Sensitivity analysis (Sc1) indicated that 50% catch-up vaccination, bivalent vaccines, or shorter protection duration would reduce the maximum cumulative fraction averted by 44%–47%, 15%–36%, and 45%–62%, respectively.
Conclusions: Catch-up HPV vaccination of WLHIV can help reduce the CC burden among WLHIV, especially if offered to WLHIV of all ages. Prioritizing nonavalent vaccines and achieving high coverage are important for maximizing benefits.
Estimated impact of adding HPV vaccination for women living with HIV (WLHIV) compared to routine vaccination in South Africa. The panels present the median estimates under each scenario (Basecase [two models]: 90% routine vaccination of girls aged 9–14; Sc1 [two models]: adding 90% catch-up vaccination for WLHIV aged 15–24; and Sc2 [one model]: adding 90% catch-up vaccination for WLHIV aged 15+ years) and model (Model 1: Det_HPV-HIV, Model 2: MicroCOSM-HPV). Line colours indicate the model and linetype indicate the scenario. The predicted relative reduction in annual vaccine-type high-risk (VT-HR) HPV (HPV6/11/16/18/31/33/45/52/58) prevalence (panel c) and cumulative fraction of cervical cancers (CC) averted among WLHIV (panel d) are age-standardized to the South African UN Population Projections.
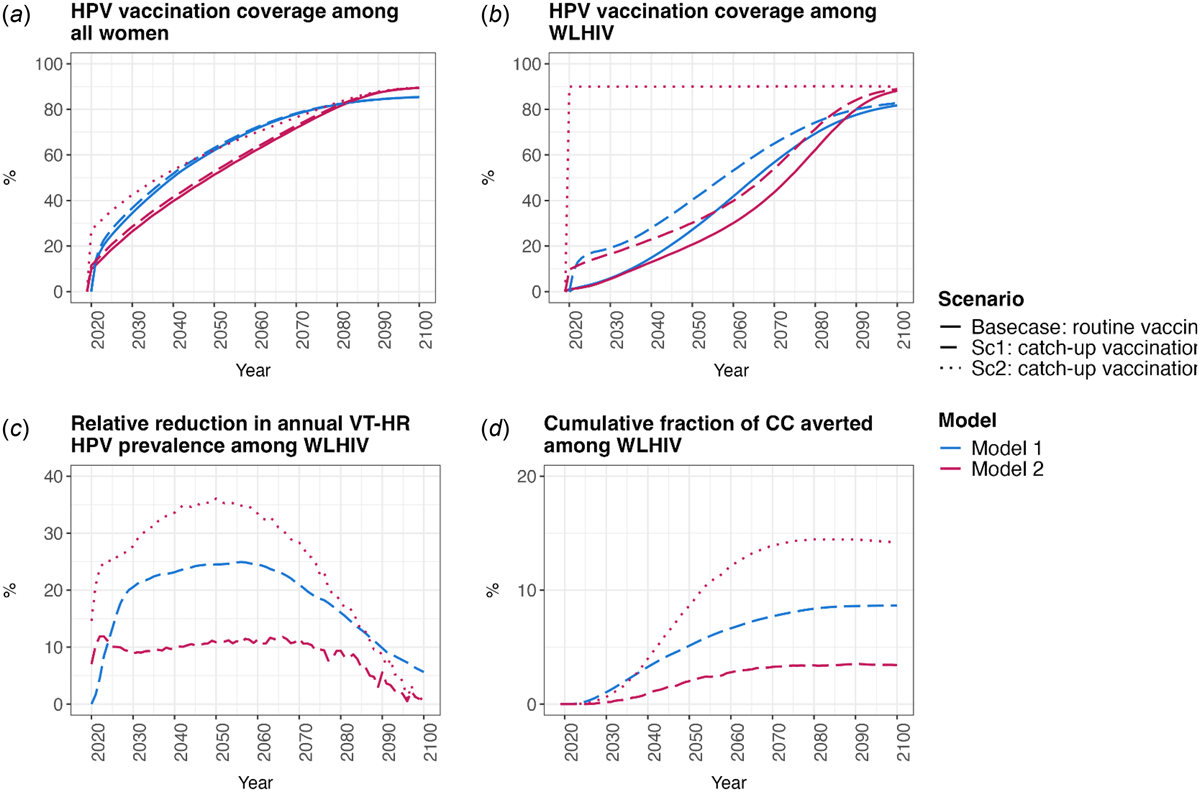
OA07.02 – Comparing Strategies to Introduce Two New Antibiotics That Minimize Drug Resistance in Gonorrhea: A Modeling Study
Miss Madeleine Kline1, Dr. Kirstin Oliveira Roster1, Dr. David Helekal1, Dr. Yonatan Grad1
1Harvard T.H. Chan School of Public Health, Boston, United States.
Background: Drug resistance is a major threat to the management of gonorrhea. Reduced susceptibility to ceftriaxone, the last remaining first-line therapy, has already been detected worldwide, emphasizing the need for more treatment options. Two first-in-class oral antibiotics successfully completed phase III trials and will likely be approved to treat gonorrhea. Prior modeling showed that holding a new treatment in reserve until resistance to the current antibiotic reaches 5% population prevalence results in a shorter clinically useful drug lifespan than rapid introduction of the new antibiotic and combination strategies. However, there are many more ways to introduce two new antibiotics, and there is a lack of research to indicate which is optimal.
Methods: We use a deterministic, compartmental model to simulate two implementation strategies: a) sequential and b) equal allocation. In the sequential strategy, the first new drug is introduced when the current therapy reaches a 5% resistance prevalence threshold, at which point it is phased out. When the second drug reaches 5% resistance prevalence, it is phased out and the third drug is phased in. In the equal allocation strategy, all drugs are used in equal allocation and phased out when they reach the resistance threshold. We measure the time until a 5% resistance prevalence threshold is met for all three drugs (TOL) and compare implementation strategies.
Results: The equal allocation strategy prolongs the TOL by 19 years (TOL = 36.2 in equal allocation, 13.6 in sequential) compared to the sequential strategy (Fig. 1a). This TOL extension stays between 17 and 19 years over a range of relative fitness and resistance evolution parameters for strain C (Fig. 1b).
Conclusions: Preliminary results suggest that balancing selective pressures at a population level rather than reserving new drugs reduces overall gonorrhea drug resistance, which aligns with prior modeling but contradicts classical antibiotic stewardship dogma.
(a) Equal allocation strategy compared to the sequential strategy. (b) The TOL extension stays between 17 and 19 years over a range of relative fitness and resistance evolution parameters for strain C.
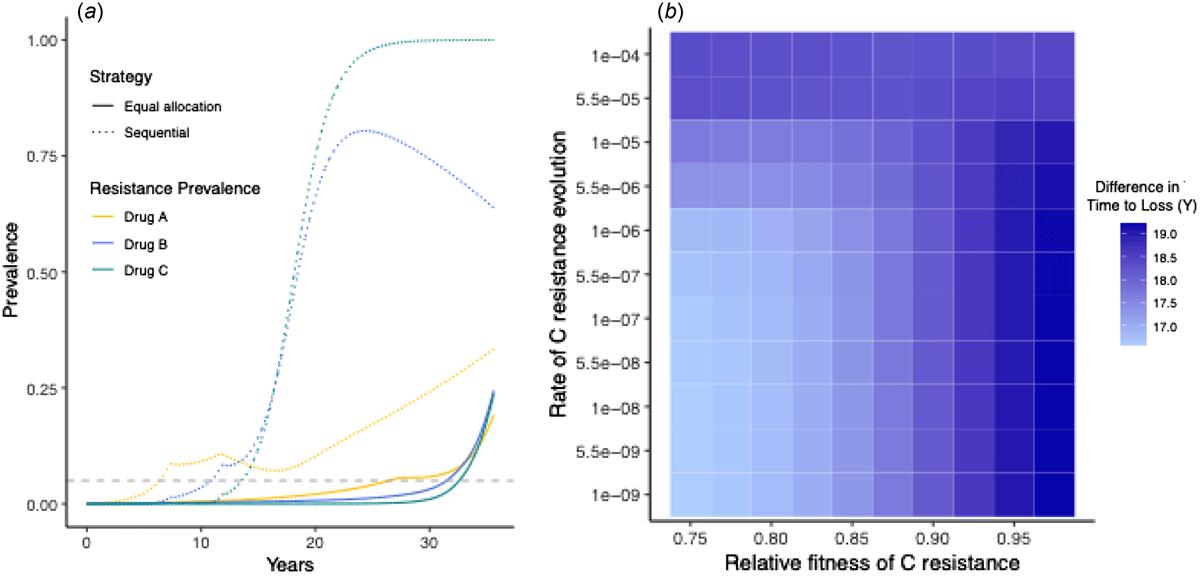
OA07.03 – Modelling the HIV Epidemic in South Africa’s Sex Workers: Impact of Key Assumptions
Dr. Nanina Anderegg1, Prof. Matthias Egger1, Prof. Leigh Johnson2
1University of Bern, Bern, Switzerland.
2University of Cape Town, Cape Town, South Africa.
Background: Thembisa is a widely used mathematical model predicting HIV dynamics in South Africa. It considers key populations, including female sex workers (FSW), but like many models for generalized HIV epidemics, relies on simplifying assumptions about key populations. As UNAIDS and national HIV strategies increasingly focus on key populations, assessing these assumptions is crucial. We examined the impact of key assumptions for FSW.
Methods: We assumed FSW age and sex work (SW) duration were either a) constant or b) increasing over time. For per-act HIV transmission risk, we considered: 1) constant, 2) declining exponentially, or 3) dynamically changing dependent on exposure to HIV-positive clients. This yielded six scenarios (1a, 1b, 2a, 2b, 3a, 3b) implemented in Thembisa. Each was calibrated separately using HIV prevalence surveys in FSW, antenatal clinics, and the general population. Finally, we validated modelled estimates of HIV prevalence, incidence and viral load suppression (VLS) in FSW against a 2019 national survey.
Results: Assuming constant transmission risk (1a,1b) produced highest modelled HIV incidence and lowest VLS (denominator: all FSW living with HIV), with prevalence peaking around 2002 before declining (Fig. 1). In other scenarios, prevalence plateaued in 2002 and declined only slightly in recent years. Allowing for increases in FSW age and SW duration (1b,2b,3b) resulted in lower HIV incidence and slightly higher VLS. The 2019 national survey estimates of HIV incidence (4.6 per 100 pyrs) and prevalence (62.1%) matched scenario 2b most closely (5.0 per 100 pyrs; 62.0%), with similar results in 3b (5.0 per 100 pyrs; 61.0%). VLS for both scenarios (60.3%) were lower than the survey estimate (64.4%) but still provided best fit across scenarios.
Conclusion: Allowing for increases in FSW age, SW duration, and declining transmission risk improves model accuracy compared to static assumptions commonly used in models. This highlights the importance of critically evaluating assumptions to enhance model reliability.
Estimates of HIV incidence, HIV prevalence, and viral load (VL) suppression in South African female sex workers (FSW) under different assumptions about FSW age, sex work duration, and per-act HIV transmission risk. Scenarios 1a, 1b assume constant transmission risk, while 2a, 2b, 3a, 3b allow for changes over time. ‘a’ scenarios assume constant FSW age and sex work duration, while ‘b’ scenarios allow for increases over time.
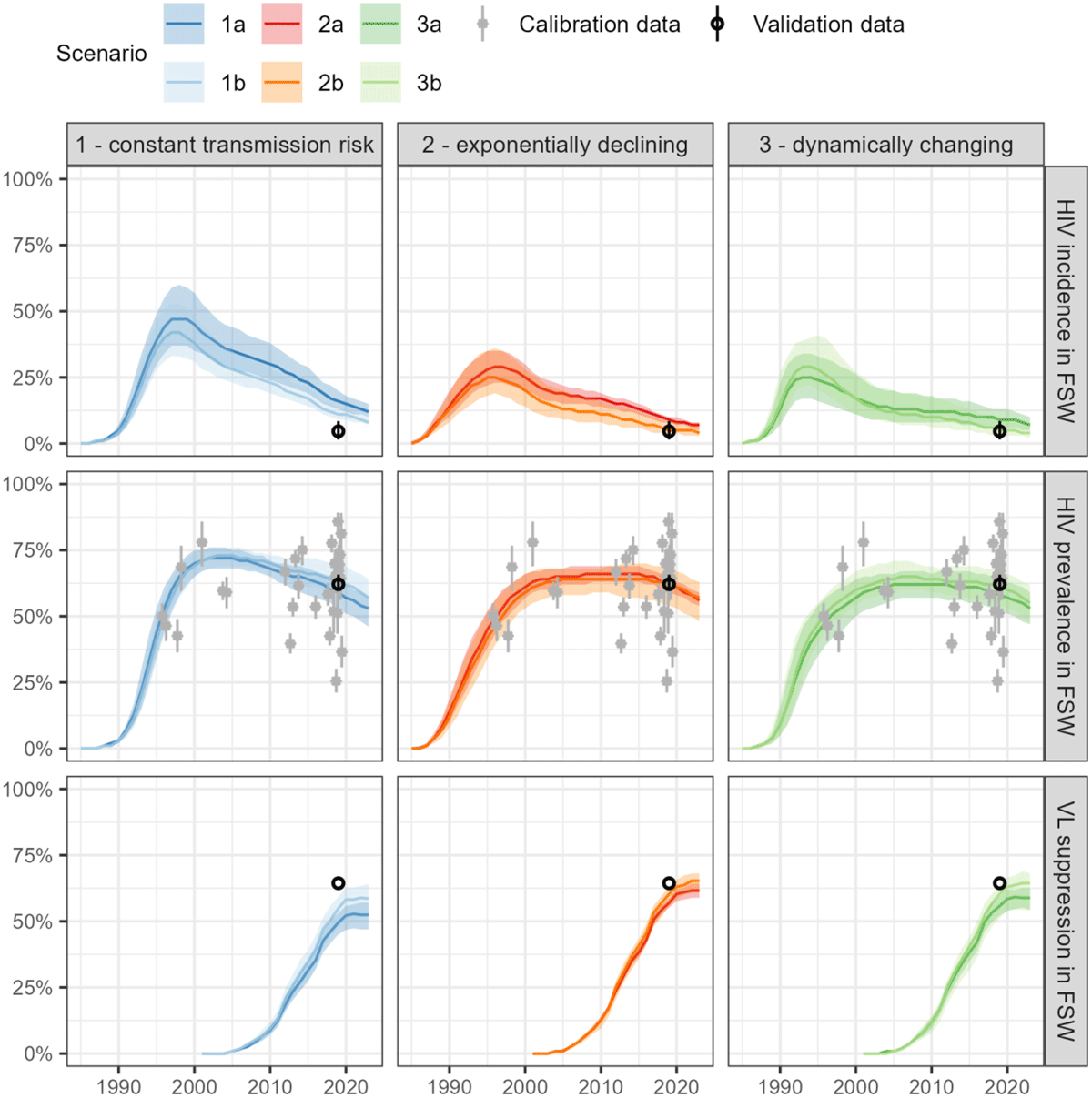
OA07.04 – Modelling the Impact and Cost-Effectiveness of Long-Acting Injectable PrEP Among Men Who Have Sex with Men in Cotonou, Benin
Dr. Mike Pickles1, Dr. Trystan Leng, Dr. Leon Kessou, Dr. Jesse Heitner, Dr. Luc Behanzin, Dr. Souleymane Diabaté, Dr. Carin Ahouada, Dr. Fernand Guedou, Dr. René Keke, Dr. Kate Mitchell, Mr. Marius Olodo, Dr. Romain Silhol, Dr. Dobromir Dimitrov, Prof. Marie-Claude Boily
1Imperial College London, London, United Kingdom.
Background: Estimating impact and cost-effectiveness of long-acting injectable pre-exposure prophylaxis (LA-PrEP) for men who have sex with men (MSM) is important to inform policy-making.
Methods: We used a deterministic MSM HIV transmission model, including daily/on-demand oral PrEP and LA-PrEP (Cabotegravir (CAB-LA) or Lenacapavir (LEN-LA)), parameterised to Cotonou, Benin using bio-behavioural and cost data from an MSM oral PrEP demonstration study. Daily/on-demand oral PrEP was introduced in 2022, with 19%/29% effectiveness based on low observed study adherence. CAB-LA/LEN-LA effectiveness was 91%/96%. Assumed annual LA-PrEP drug costs were 3× oral PrEP drug costs. Using a Bayesian framework, the model was fitted to HIV prevalence and treatment outcomes. We considered four scenarios, with LA-PrEP introduced in 2025 and overall PrEP coverage (oral + LA-PrEP) among MSM increasing to ~30% (50% for Scenario-4) by 2045 (Fig. 1a). We report median (and 95% uncertainty interval, 95%UI) percentages of infections averted and cost (in US$2021) per disability-adjusted life year (DALY) averted (both discounted at 3%) from 2025 to 2045, compared to base-case (no PrEP from 2025).
Results: Predicted HIV incidence in 2024 was 1.8 (95%UI 0.5–4.0)/100 person-years. Median (95%UI) % infections averted and cost/DALY averted were: 13% (7–18%), $2,024 ($378–26,060); 29% (20–38%), $1,312 ($185–16,400); 31% (21–39%), $1,037 ($119–13,344); and 40% (28–51%), $1,501 ($235–15,737), for Scenarios 1–4 respectively. Fig. 1b presents cost-effectiveness by whether estimated HIV incidence was above/below median in 2024, as cost/DALY averted was negatively correlated with incidence.
Conclusions: Neither LA-PrEP nor oral PrEP are expected to be cost-effective for MSM in Benin compared to 1xGDP threshold if HIV incidence is low, but both should be cost-effective if current incidence is above 1.8/100person-years. Introducing CAB-LA/LEN-LA with oral PrEP is likely more cost-effective than oral PrEP alone due to low oral PrEP adherence. For similar drug costs, LEN-LA is more cost-effective than CAB-LA due to higher effectiveness and fewer clinic visits.
(a) Coverage of PrEP among all sexually active MSM in 2025 and 2045, by PrEP regimen. (b) Cost per DALY averted over 2025–2045 for each scenario, stratified by whether modelled baseline HIV incidence in 2024 was above or below median modelled HIV incidence of 1.8 per 100 person-years (y-axis truncated at $8000). Solid bar shows median, boxes show interquartile range, and whiskers show 95% uncertainty interval of model estimates. Dotted line shows nominal cost-effectiveness threshold of 1xGDP per capita for Benin ($1,225).
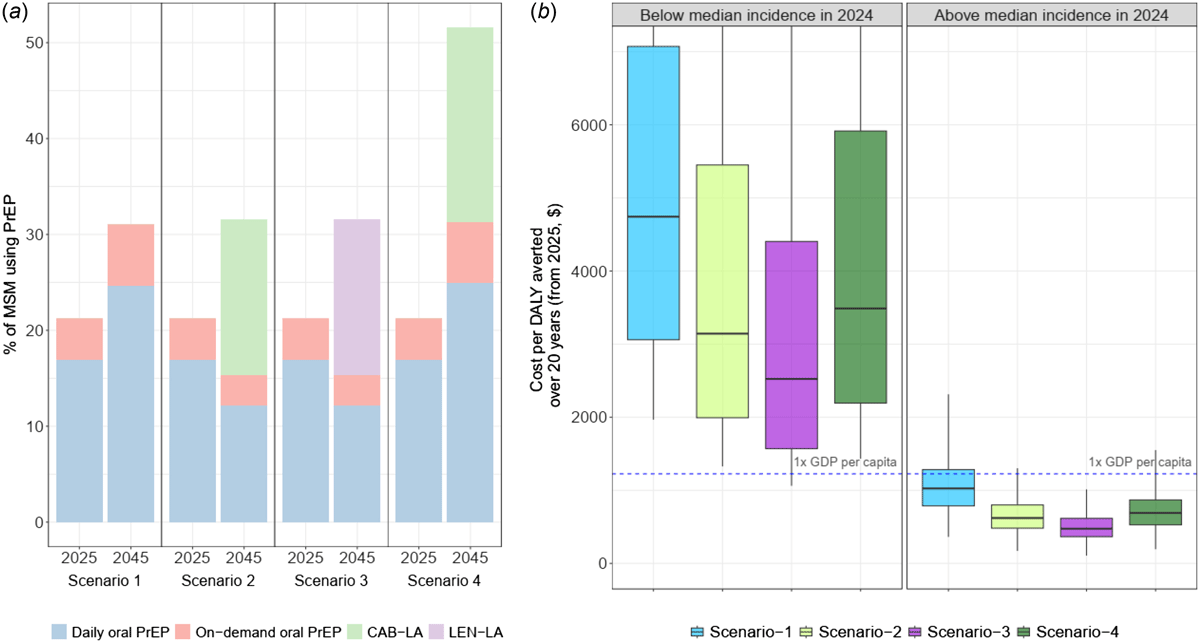
OA07.05 – Prevalent Asymptomatic Mpox Infection and Extensive Under-Reporting of Cases Among Men Who Have Sex with Men Following JYNNEOS Vaccine Implementation: A Prospective Surveillance and Modeling Study
Assoc. Prof. Joseph Lewnard1, Miguel Paredes, Matan Yechezkel, Gregg Davis, Jessica Skela, Vennis Hong, Nicola Mueller, Magdalena Pomichowski, Iris Reyes, Lauren Granskog, Noah Parker, Isabel Rodriguez Barraquer, Sara Tartof
1University of California Berkeley, Berkeley, United States.
Background: Sporadic clade II mpox cases, often without known transmission links, continue to occur among MSM and other high-risk populations since implementation of JYNNEOS vaccination in response to the 2022 mpox outbreak. Factors driving this persistent transmission pattern remain poorly understood.
Description: We undertook prospective surveillance testing for mpox infection in rectal swabs obtained from males undergoing routine gonorrhea/chlamydia testing in Kaiser Permanente Southern California clinics in Los Angeles between May and October, 2024. We used inverse propensity weighting to adjust for demographic, clinical, and epidemiologic characteristics of the sample captured by testing. We used estimates of the expected duration of PCR-positive shedding to project incidence rates from prevalent infections and estimate reporting fractions. We confirmed our findings through two ancillary analyses: first, estimating the ratio of reported cases to the effective population size of all mpox infections in Los Angeles based on phylogenetic sequence data, and second, estimating the same quantity via a meta-analysis of previously-published prospective serological or molecular surveillance studies undertaken during the 2022 outbreak.
Results: We estimate that mpox infections outnumber clinically ascertained and reported cases by a factor of 24.0 (95% CI: 15.0–39.2). This reporting fraction varies according to characteristics expected to influence disease severity: we estimate one out of every 9.4 (5.0–18.2) infections among unvaccinated persons and one out of every 34.6 (18.6–63.7) infections among previously-vaccinated persons is detected, while one out every 8.5 (3.8–20.3) infections among HIV-positive individuals and one out of every 28.9 (17.1–48.5) infections among HIV-negative individuals is detected. Ancillary phylogenetic analyses and our meta-analysis of 2022 surveillance studies in other settings provide comparable estimates of reporting fractions.
Conclusion: Most clade II mpox infections do not result in clinical care-seeking or detection even among MSM connected to sexual health services. Our findings suggest reported cases vastly underestimate true infections.
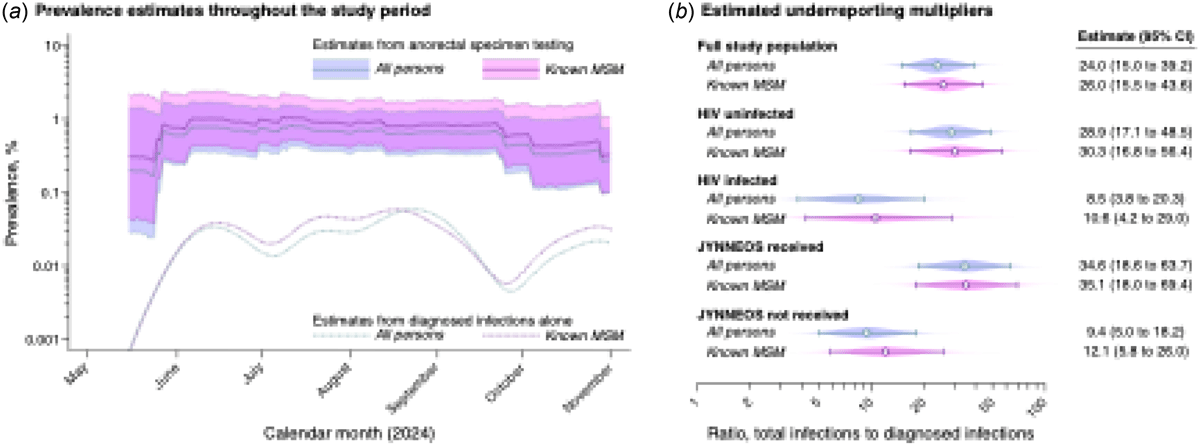
OA07.06 – HPV Genotype Distribution and STI Co-Infections Among MSM in Agadir, Morocco: Insights from a Respondent-Driven Sampling Study
Miss Rokaya Aitlhaj-mhand1,2, Dr Bahija Bellaji3, Miss Chaimae Remz1, Dr Reda Charof4, Professor Hanaa Abdelmoumen2, Dr Amina Hançali3, Professor Hicham Oumzil5
1Virology Department, National Institute of Hygiene, Rabat, Morocco.
2Microbiology and Molecular Biology Team, Research Center for Plant and Microbial Biotechnology, Biodiversity and Environment, Faculty of Sciences, Mohammed V University in Rabat, Rabat, Morocco.
3STIs Reference Laboratory, Medical Bacteriology Department, National Institute of Hygiene, Rabat, Morocco.
4Epidemic Diseases Laboratory, Medical Bacteriology Department, National Institute of Hygiene, Rabat, Morocco.
5Medical Biotechnology Laboratory, School of Medicine and Pharmacy, University Mohammed V in Rabat, Rabat, Morocco.
Background: Sexually transmitted infections (STIs), including human papillomavirus (HPV), represent a major global health challenge, particularly in developing countries, and are closely linked to an increased risk of HIV acquisition and transmission. Within the population of men who have sex with men (MSM), these infections are notably widespread, attributable to a complex interaction of biological, behavioral, and structural determinants. While data on HPV prevalence among women, particularly in relation to cervical cancer, is available in Morocco, findings on HPV and other STIs in MSM is under-researched, despite the significant health risks associated with these infections.
In response to this challenge, the objective of this study is to assess the prevalence of HPV genotype distribution and co-infections with NG, CT and TV among MSM in Morocco.
Methods: In 2021, a cross-sectional study was conducted involving 245 participants, using respondent-driven sampling (RDS) to recruit MSM, aged 18 years and older, who had lived in Agadir for at least 6 months, regardless of nationality. Participants were required to have engaged in sexual activity in the past 6 months. Anal swab samples were collected and analyzed using the GeneXpert molecular testing system (Cepheid, USA).
Results: Among the 245 MSM included in the survey, 5.71% were identified as HPV16, 6.53% as HPV18/45, and 22.44% as other HPV types. Regarding co-infections with other STIs, 7.75% had co-infection with Neisseria gonorrhoeae (NG), 5.71% with Chlamydia trachomatis (CT), and 2.44% had dual co-infection with both NG and CT. However, no cases of co-infection with Trichomonas vaginalis (TV) were recorded.
Conclusion: The results reveal a significant prevalence of HPV and co-infections with NG and CT among MSM, highlighting the need for targeted screening and prevention efforts. The absence of TV co-infection suggests its limited relevance in this population.
Keywords: HPV, NG, CT, MSM, prevalence.
OA08.01 – Examining Social-Structural Conditions Impacting STI Testing Access Among Migrant Sex Workers in Metro Vancouver, Canada: A Mixed Methods Study
Dr. Ran Hu1, Assistant Professor Andrea Krüsi2, Professor Kate Shannon3, Statistician Charlie Zhou2, Doctoral candidate Sarah Moreheart2, Research Coordinator Melody Wise3, Associate Professor Shira Goldenberg4
1The Ohio State University, Columbus, United States.
2Simon Fraser University, Vancouver, Canada.
3University of British Columbia, Vancouver, Canada.
4San Diego State University, San Diego, United States.
Objectives: Prior research has shown that in Canada, migrant women sex workers face substantial health inequities stemming from stigma, criminalization, precarious immigration status, and gaps in health insurance, including low utilization of primary health care, limited access to justice, and unmet HIV/STI prevention needs. This mixed-methods study aimed to identify how social-structural factors influence migrant sex workers’ utilization and lived experiences of STI testing.
Methods: Our mixed-methods analyses began with descriptive, bivariate, and multivariable generalized estimating equation (GEE) analyses to examine social-structural factors associated with STI testing access; Data were from 167 migrant sex workers enrolled in a community-based cohort study, An Evaluation of Sex Workers Health Access (AESHA) between 2015 and 2024. The quantitative analysis was followed by a reflexive thematic analysis of semi-structured interviews with 22 indoor migrant sex workers collected from 2022–2023.
Results: Lack of access to sex work outreach services, gaps in healthcare coverage, being a racialized person, condom refusal, and limited English fluency were associated with reduced odds of receiving STI testing at community sites, compared to not getting tested; additionally, limited English fluency, and being a racialized person were associated with reduced odds of receiving testing by the AESHA team, compared to not getting tested. Qualitative interviews further unpacked how intersecting language and cultural barriers, stigma and privacy concerns, and lack of awareness of testing resources reinforced inequitable access to STI testing and treatment among Chinese migrant sex workers.
Conclusion: To promote equitable access to STI-testing for migrant sex workers, our study shows an urgent need for culturally responsive, linguistically-tailored, sex worker-friendly, confidential, and voluntary STI testing and health system navigation resources for migrants, including via scale-up of outreach services. Structural changes including decriminalization of sex work and shifting away from policies that conflate migrant sex work with trafficking, are also recommended.
OA08.02 – Access to Sexual Health Services Among Ethnic Minorities Under the Age of 25 Years in the Netherlands
Dr. Ymke Evers1,2, Amanja Verhaegh1,2, Dr. Aiman Ibrahim3, Dr. Nicole Dukers-Muijrers1,3, Dr. Rianne Reijs1,2, Prof.Dr. Christian Hoebe1,2,5
1Department of Sexual Health, Infectious Diseases and Environmental Health, Living Lab Public Health Mosa, Public Health Service South Limburg, Heerlen, The Netherlands.
2Department of Social Medicine, Care and Public Health Research Institute (CAPHRI), Maastricht University/Maastricht UMC+, Maastricht, The Netherlands.
3Department of Sexual Health, Municipal Public Health Service Rotterdam-Rijnmond, Rotterdam, The Netherlands.
4Department of Health Promotion, Care and Public Health Research Institute (CAPHRI), Maastricht University/Maastricht UMC+, Maastricht, The Netherlands.
5Department of Medical Microbiology, Infectious Diseases and Infection Prevention, Care and Public Health Research Institute (CAPHRI), Maastricht University Medical Centre (MUMC+), Maastricht, The Netherlands.
Introduction: Migration is a growing phenomenon and has impact on sexual and reproductive health outcomes, such as an increased risk for STIs, sexual violence and unintended pregnancies. Equitable access to sexual health care is of great importance for young people from ethnic minorities (EMs). In this study, we aimed to determine the proportional representation of first- and second-generation EMs under 25 years at Dutch Sexual Health Centers (SHCs) and compare this to ethnic Dutch citizens.
Methods: In this retrospective cohort study, coded surveillance data of 270.927 persons under the age of 25 visiting SHCs between 2016 and 2021 were included. This data was combined with population numbers from the Statistics Netherlands to calculate consultation rates. Consultation rates were calculated as dividing the number of first consultations of a patient in the study period belonging to a specific EM by the total number of citizens in the age group of 15 till 24 years belonging to that EM in the Netherlands in 2021, multiplied by 1000.
Results: The consultation rate for ethnic Dutch patients was 22.0 per 1000 person-years (95% CI: 21.8–22.2, 18.9, 19.8 (95% CI: 19.8–20.4) for first-generation EMs and 18.4 (95% CI: 18.0–18.8) for second-generation EMs. In both first- and second-generation EMs, consultation rates for patients from Turkey, Morocco, Eastern Europe and Asia were lower than for ethnic Dutch patients. Consultation rates among patients from Africa were lower for first-generation EMs than ethnic Dutch patients. Consultation rates among patients from Indonesia, Suriname/Dutch Antilles, Latin America and other western countries were equal or higher than among ethnic Dutch patients.
Conclusion: Our study showed that several EMs were underrepresented in Dutch sexual health care, indicating the need for culturally sensitive approaches to increase access. Using consultation rates is informative to indicate inequalities in access to sexual health care among EMs.
OA08.03 – Associations Between Extreme Weather Events and HIV and STI Vulnerabilities Among Refugee Youth Living in a Ugandan Refugee Settlement: Cross-Sectional Survey Findings
Dr. Carmen Logie1, Dr. Miranda Loutet1, Dr. Moses Okumu2, Mr. Simon Odong Lukone3, Mr. Nelson Kisubi3, Dr. Peter Kyambadde4, Dr. Lawrence Mbuagbaw5, Ms. Frannie MacKenzie1, Dr. Zerihun Admassu1
1University of Toronto, Toronto, Canada.
2University of Illinois at Urbana-Champaign, Urbana, USA.
3Uganda Refugee and Disaster Management Council, Yumbe, Uganda.
4Uganda Ministry of Health, Kampala, Uganda.
5McMaster University, Hamilton, Canada.
Background: There is growing evidence of associations between extreme weather events (EWE) and HIV and STI vulnerabilities, yet this is understudied in humanitarian settings. We examined associations between EWE and HIV/STI vulnerabilities among refugee youth in Bidi Bidi Refugee Settlement, Uganda.
Methods: We collected baseline (February–March 2024) cohort data with refugee youth aged 16–24 years in Bidi Bidi. We conducted linear and logistic regression to assess associations between a) number of past-year EWE types, and b) frequency of past-year EWE, with HIV/STI vulnerabilities (sexual relationship power [SRP], reproductive autonomy, condom use self-efficacy [CUSES], transactional sex, intimate partner violence [IPV], multiple sex partners [MSP]), adjusted for age, gender, education, and employment.
Results: Among 400 participants (50% women; mean age: 19, standard deviation: 2.3), a higher number of past-year EWE types (vs 1 EWE type) was significantly associated with reduced: SRP (2–4 EWE: adjusted beta [aβ]: –2.96, 95% confidence interval [CI]: –5.17, –0.74; >5 EWE: aβ: –4.92, 95% CI: –7.29, –2.56), reproductive autonomy (2–4 EWE: aβ: –0.32, 95% CI: –0.56, –0.09; >5 EWE: aβ: –0.42, 95% CI: –0.67, –0.17), CUSES (2–4 EWE: aβ: –3.02, 95% CI: –4.47, –1.58; aβ: >5 EWE: –3.04, 95% CI: -4.58, –1.50), and increased: transactional sex (>5 EWE: adjusted odds ratio [aOR]: 8.70, 95% CI: 1.10, 68.61), IPV (>5 EWE: aOR: 3.13, 95% CI: 1.36, 7.20), and MSP (>5 EWE: aOR: 4.7, 95% CI: 1.8, 12.0). Increased past-year EWE frequency (reference: 1 EWE, ≥once) was associated with reduced: SRP (>1 EWE [once]: aβ = –5.79, 95% CI: –8.50, –2.08; >1 EWE [>once]: aβ = –3.33, 95% CI: –5.56, –1.10); reproductive autonomy (>1 EWE [>once]: aβ = –0.40, 95% CI: –0.63, –0.17), and CUSES (>1 EWE [once]: aβ = –4.29, 95% CI: –4.49, –1.61; >1 EWE [>once]: aβ = –3.05, 95% CI: –4.49, –1.61).
Conclusion: EWE experiences were associated with multiple HIV/STI vulnerabilities among refugee youth in Uganda. Climate-informed HIV and STI prevention strategies are urgently needed.
| Crude regression coefficient (95% CI) | P-value | AdjustedA regression coefficient (95% CI) | P-value | ||
|---|---|---|---|---|---|
| Sexual relationship powerB | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | –3.46 (–5.70, –1.22) | 0.003 | –2.96 (–5.17, –0.74) | 0.009* | |
| 5+ | –5.19 (–7.57, –2.81) | <0.001 | –4.92 (–7.29, –2.56) | <0.001** | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | –6.54 (–9.20, –3.87) | <0.001 | –5.79 (–8.50, –3.08) | <0.001** | |
| more than 1 type of weather event, at least one occurred >1 | –3.74 (–5.97, –1.50) | 0.001 | –3.33 (–5.56, –1.10) | 0.003* | |
| Reproductive autonomyC | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | –0.34 (–0.57, –0.11) | 0.004 | –0.32 (–0.56, –0.09) | 0.006* | |
| 5+ | –0.40 (–0.64, –0.16) | 0.001 | –0.42 (–0.67, –0.17) | 0.001** | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | –0.05 (–0.32, 0.23) | 0.739 | –0.04 (–0.32, 0.24) | 0.789 | |
| more than 1 type of weather event, at least one occurred >1 | –0.41 (–0.64, –0.18) | <0.001 | –0.40 (–0.63, –0.17) | 0.001** | |
| Condom use self-efficacyD | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | –3.52 (–4.98, –2.07) | <0.001 | –3.02 (–4.47, –1.58) | <0.001** | |
| 5+ | –3.34 (–4.88, –1.79) | <0.001 | –3.04 (–4.58, –1.50) | <0.001** | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | –4.73 (–6.46, –3.00) | <0.001 | –4.29 (–6.05, –2.54) | <0.001** | |
| more than 1 type of weather event, at least one occurred >1 | –3.38 (–4.83, –1.94) | <0.001 | –3.05 (–4.49, –1.61) | <0.001** | |
| Transactional sex in past yearE | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | 2.83 (0.37, 21.83) | 0.318 | 2.61 (0.33, 20.51) | 0.360 | |
| 5+ | 7.59 (0.99, 58.45) | 0.052 | 8.70 (1.10, 68.61) | 0.040* | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | 2.30 (0.25, 21.47) | 0.466 | 2.34 (0.24, 22.61) | 0.463 | |
| more than 1 type of weather event, at least one occurred >1 | 4.49 (0.60, 33.86) | 0.145 | 4.24 (0.55, 32.50) | 0.165 | |
| Intimate partner violence in past yearF | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | 1.14 (0.55, 2.37) | 0.721 | 1.21 (0.57, 2.55) | 0.623 | |
| 5+ | 2.76 (1.23, 6.17) | 0.014 | 3.13 (1.36, 7.20) | 0.007* | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | 0.56 (0.23, 1.39) | 0.211 | 0.58 (0.22, 1.48) | 0.255 | |
| more than 1 type of weather event, at least one occurred >1 | 1.91 (0.92, 3.98) | 0.084 | 1.95 (0.92, 4.14) | 0.083 | |
| Mutiple sexual partners in past yearG | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | 0.98 (0.44, 2.2) | 0.953 | 1.3 (0.57, 3.2) | 0.497 | |
| 5+ | 3.0 (1.3, 7.2) | 0.012 | 4.7 (1.8, 12.0) | 0.002* | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | 1.4 (0.52, 3.7) | 0.509 | 1.6 (0.51, 4.7) | 0.437 | |
| more than 1 type of weather event, at least one occurred >1 | 1.3 (0.58, 2.9) | 0.525 | 1.8 (0.77, 4.4) | 0.174 | |
| HIV test in the past yearH | |||||
| Number of extreme weather events in past year | |||||
| 1 | Ref. | Ref. | |||
| 2 to 4 | 0.99 (0.48, 2.0) | 0.975 | 1.0 (0.46, 2.2) | 0.970 | |
| 5+ | 1.3 (0.60, 2.8) | 0.509 | 1.3 (0.55, 3.0) | 0.561 | |
| Frequency of extreme weather events in past year | |||||
| 1 type of weather event, occurring at least once | Ref. | Ref. | |||
| more than 1 type of weather event, each only occurred once | 0.60 (0.25, 1.4) | 0.244 | 0.53 (0.21, 1.4) | 0.194 | |
| more than 1 type of weather event, at least one occurred >1 | 1.3 (0.62, 2.7) | 0.494 | 1.2 (0.57, 1.4) | 0.599 |
*P < 0.05, **P ≤ 0.001.
OA08.04 – Prevalence, Drivers, and Recurrence of Genital Infections Among Symptomatic Syrian Refugee Women: A Longitudinal Cohort Study
Dr. Sasha Fahme1,2, Dr. Ghina Mumtaz2, Ms. Maria Lteif2, Dr. Myung Hee Lee1, Dr. Ali Ghassani3, Professor Laith Abu-Raddad1,4, Dr. Jennifer Downs1, Professor Jocelyn DeJong2, Professor Daniel Fitzgerald1
1Weill Cornell Medicine, New York, United States.
2American University of Beirut, Beirut, Lebanon.
3Amel Association, Beirut, Lebanon.
4Weill Cornell Medicine-Qatar, Qatar Foundation-Education City, Doha, Qatar.
Background: Genital infection symptoms are prevalent, poorly characterized, and inadequately treated among Syrian refugee women. Current guidelines insufficiently address genital infection recurrence. This study identified etiologies of genital infection symptoms and determined rates and drivers of infection recurrence, defined as a positive test for a pathogen diagnosed at a prior visit.
Methods: This longitudinal cohort study was conducted among sexually-active Syrian refugee women with gynecologic symptoms in refugee camps along the Lebanese-Syrian border. Community health workers administered a baseline survey of demographic, clinical, and psychosocial factors, and followed women over 3 months. At baseline, 1-, and 3-months, a midwife conducted a comprehensive pelvic examination and evaluated participants for Chlamydia trachomatis, Neisseria gonorrhoeae, Trichomonas vaginalis, bacterial vaginosis (BV), and vaginal candidiasis using WHO guidelines, Xpert CT/NG assays, and point-of-care tests for trichomonas and BV.
Results: Of 204 women enrolled, 171 (83.8%) were retained at 3-months. The mean age was 34.3 (SD + 8.6) years; 99.5% were married. Gender-based violence (65.7%) and self-prescribed antimicrobial use (67.2%) were common. At baseline, 65.0% (n = 133) were diagnosed with an infection/disease, including candidiasis (40.2%), BV (38.2%), pelvic inflammatory disease (3.9%), trichomoniasis (2.5%), and chlamydia (0.5%) (Fig. 1). Frequencies of diagnoses improved over time. On average, women had 1.7 ([1.5–2.0]; P < 0.001) fewer symptoms at 3-months as compared with baseline. Overall, 104 women (56.8%) had recurrent reproductive tract infections (RTIs); two (10.0%) had recurrent STIs. Women with a sexual violence history had 4.3× greater odds of an STI ([1.3–14.1]; P = 0.01). Contraceptive use was associated with 4.0× greater odds of any RTI ([1.5–10.7]; P < 0.01). Intrauterine device (IUD) use conferred 2.3× greater odds of BV ([1.0–5.2]; P < 0.05).
Conclusion: Genital infection prevalence and recurrence are common among Syrian refugee women and may be associated with sexual violence and IUD use. Community-based interventions addressing genital infections and sexual violence are urgently needed.
Trends in genital infection diagnoses over 3 months. BV, bacterial vaginosis; PID, pelvic inflammatory disease; RTI, reproductive tract infection; STI, sexually transmitted infection; TV, Trichomonas vaginalis.
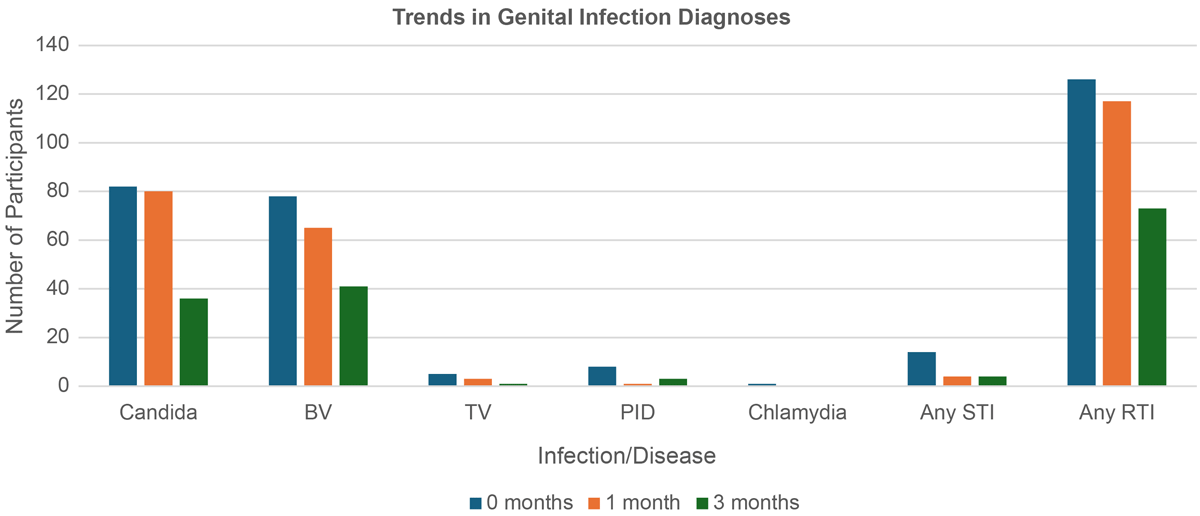
OA08.05 – Factors Associated with Early Attendance (<6 Months) to an Urban Sexual Health Service Among Migrant Gay & Bisexual Men (GBM) and Trans & Gender Diverse (TGD) Patients in Sydney, Australia
Mr. Anik Ray1, Mrs. Alison Mahoney1, Ms. Lisa McCann1, Ms. Rebecca Houghton1, Mr. Brent Mackie3, Mr. Joubert Van Der Merwe3, Dr. Rick Varma1,2, Dr. Arthur Wong1,2
1Sydney Sexual Health Centre, Sydney, Australia.
2Kirby Institute, Sydney, Australia.
3AIDS Council of NSW (ACON), Sydney, Australia.
Background: Improving migrant access to HIV testing and prevention services is a key strategy in the virtual elimination of HIV. Asian, Latin/South American born GBM/TGD people have the highest proportion of HIV notifications in Sydney. They are priority populations to promote early engagement with sexual health services (SHS).
Methods: This cross-sectional study used data from the largest government funded SHS in Sydney. GBM/TGD patients arriving in Australia between 01/01/2022 and 01/01/2024 were included. The time between arrival in Australia and first contact with our SHS was classified as early (<6 months) or late (>6 months). Chi-squared test was used to find factors associated with early attendance. A multivariable logistic regression model was used to examine associations between early attendance with clinical and demographic factors.
Results: Of 1,290 patients, 1,238 (96.0%) were cisgender GBM. Median days between arrival and service attendance was 148 days (IQR 64–306). 56% attended <6 months after arrival. Factors associated with early attendance include previous sexually transmitted infections (aOR 3.81, P < 0.001), previous PrEP use (aOR 2.97, P < 0.001), previous HIV testing before arrival (aOR 2.39, P < 0.001) and requirement for an interpreter (aOR 1.43, P = 0.03). Compared to patients fro North America, Europe and New Zealand – patients from Asia (OR 0.46, P < 0.001) and Latin/South America (OR 0.67, P = 0.009) were less likely to attend early in univariable analysis – however this was not significant in the multivariable model. Patients reporting sexualised drug use were more likely to attend early in the univariable (OR 1.76, P = 0.013) but not multivariable (P = 0.196) analysis.
Conclusion: Prior experience with SHS before arriving in Australia was the strongest predictor of early engagement with Australian SHS, irrespective of the patient’s country of origin. Public health interventions should focus on identifying and supporting GBM/TGD individuals who have never accessed SHS to enhance early engagement with Australian testing and prevention services.
OA08.06 – Barriers and Facilitators to Availing Targeted Interventions, Testing and Treatment Services by People Who Inject Drugs Under National AIDS Control Program India in Districts Along the Indo-Nepal Border
Dr. Manish Kumar Singh1, Dr Ayush Lohiya2, Dr SD Kandpal1, Dr Aditi Mohta3, Dr Pradeep Kharya4, Dr Ramashankar Rath4
1Dr. RMLIMS, Lucknow, UP, Lucknow, India.
2KSSSCI, Lucknow, India.
3IIMS&R, Lucknow, India.
4AIIMS, Gorakhpur, India.
Background: India and Nepal share a porous border, with border districts of Indian state of Uttar Pradesh (UP) having an estimated HIV prevalence of 1.5 to 3 times more than state average. The objective of our study was to assess perceived barriers and facilitators to availing Targeted Interventions (TI), testing and treatment services under National AIDS Control Program, India by People Who Inject Drugs (PWID) and service providers in districts of UP along Indo Nepal border.
Methods: 16 In Depth Interview with service providers at TI sites and 6 Focused Group Discussion with PWID were done across 6 districts of India along Indo Nepal border. Thematic analysis was done using grounded theory approach and inductive reasoning.
Results: Easy accessibility of TI site, supportive staff, liaison and networking of TI sites, facilitation by peer/Outreach Worker (ORW), Free availability of needles/syringes with Peer, transport were major facilitators perceived by PWID. Perceived barriers were Irregular supply of condoms, non-accessibility to OST (Opioid Substitution Therapy) drugs, lack of flexible timings and approach amounting to loss of livelihood, stigma and prejudice. Service providers perceived barriers were inability and lack of motivation of PWID to seek services, roping in family and neighbors for support, additional expenditure on travel and facilitating services at ART centre, lack of training of peers and ORW. Facilitators were free of cost services, availability of ICTC services and supportive staff/doctor, Trained Project Managers, availability of Effective Information Education Communication material.
Conclusion: Ensuring easy access of testing and treatment, prioritization, flexible timings, wider outreach via trained peer workers, quality services, working on stigma and prejudice faced by PWID are essential steps to mitigate the epidemic. The study paves way for further operational and implementational research to address perceived gaps in service delivery.
OA09.01 – Treponema Pallidum PEPtidoglycan Provides Insights Into Bacterial Growth and Pathogenesis
Ms. Kathryn Hayes1,2, Dr. Richard Helm3, Dr. Brandon Jutras2
1Driskill Graduate Program in Life Sciences, Northwestern University, Chicago, United States.
2Department of Microbiology and Immunology, Feinberg School of Medicine at Northwestern University, Chicago, United States.
3Department of Biochemistry, Virginia Tech, Blacksburg, United States.
Background: The synthesis of peptidoglycan, a major component of the bacterial cell wall, must be tightly regulated for proper bacterial growth and division, making it a powerful antibiotic target. Additionally, some bacteria shed peptidoglycan during infection where it may act as an immunomodulatory factor and in some instances even as toxins. As such, understanding the previously uncharacterized peptidoglycan of Treponema pallidum could provide not only insight into syphilis treatment, but it could also fill critical knowledge gaps in bacterial pathogenesis.
Methods: In this study we conducted LCMS analysis on purified T. pallidum peptidoglycan to determine its chemical features and architecture. Peptidoglycan modifying enzymes responsible for the unusual features were discovered and validated through biochemical approaches, further confirming the accuracy of our LCMS results. In depth in silico analysis of the T. pallidum genome failed to identify any of the highly conserved components required for peptidoglycan recycling. Pulse-chase experiments using fluorescent peptidoglycan synthesis probes, along with classical radio-labeling methods, show that T. pallidum is unable to recycle liberated muropeptides during growth and instead sheds them into the environment.
Results: We found that T. pallidum peptidoglycan has unique chemical features that differentiate it from the spirochete phylum; alteration that may impact immune recognition and/or host response(s). Recombinant expression of putative peptidoglycan modification enzymes confirms not only their function in T. pallidum but also complements our LCMS analysis using an alternative approach. Additionally, we found that T. pallidum releases muropeptides fragments as a normal function of growth.
Conclusion: This study provides novel insight into the complexity of T. pallidum peptidoglycan 1) synthesis, 2) turnover, and 3) possible role in pathogenesis. Our findings have broad translational implications for pathogenesis, treatment, and possibly diagnosis of a re-emerging threat to public health.
OA09.02 – The Impact of Treponema Pallidum on Endothelial Cells; Time-Course Transcriptomics Reveals Insight into Syphilis Symptoms
Mr. Sean Waugh1, Dr Mara C. Goodyear1, Mr. Alloysius Gomez1, Mr. Akash Ranasinghe1, Dr. Karen V. Lithgow1, Mr. Reza Falsafi2, Dr. Robert E.W. Hancock2, Dr. Amy H. Lee3, Dr. Caroline E. Cameron1,4
1Department of Biochemistry and Microbiology, University of Victoria, Victoria, Canada.
2Department of Microbiology and Immunology, University of British Columbia, Vancouver, Canada.
3Department of Molecular Biology and Biochemistry, Simon Fraser University, Burnaby, Canada.
4Department of Medicine, University of Washington, Seattle, USA.
Background: Treponema pallidum (Tp) spreads through the bloodstream and traverses the endothelium to establish a systemic and multi-stage infection that is lifelong in the absence of treatment. To increase our understanding of both the pathogenic mechanisms employed by Tp to infect the host and the corresponding host cellular response to Tp infection, we performed systems-level analyses of the molecular responses of endothelial cells to Tp exposure. These analyses provide novel insight into Tp infection and enhance our understanding of Tp dissemination through the body, immune system evasion, and disease symptom causation.
Methods: We performed time-course transcriptome sequencing of hCMEC/d3 human brain microvascular endothelial cells exposed to viable Tp or a background control lacking the pathogen at time points spanning 45 min to 24 h. This systems biology-focused approach to investigating Tp-host interactions allows us to characterize the cellular pathways that are engaged in the host response to Tp infection.
Results: Our analyses showed correlation of increasing dysregulation of genes and cellular pathways with increasing Tp exposure times. Altered host cellular pathways included extracellular matrix and cytoskeletal organization, immunity, growth factor signaling, and cell stress. These processes overlap with transcriptional alterations observed in endothelial to mesenchymal transition, a cellular phenomenon where endothelial cells reduce contact with neighbouring cells and develop a fibroblast-like phenotype. Importantly, these altered cellular pathways support clinical observations of syphilis disease manifestations, including chancre formation, ocular syphilis, and gumma development.
Conclusion: An increased understanding of the host response to Tp infection is needed to develop effective syphilis biomedical interventions. Our systems biology approach provides insight into cellular pathways engaged in response to Tp, and how they contribute to the development of systemic infection and syphilis disease symptoms. Additionally, our work may inform syphilis vaccine design by describing key cellular processes and pathways engaged during Tp infection.
OA09.03 – High-Throughput Profiling of the IgG and IgA Response to the Treponema Pallidum Subsp. Pallidum Proteome in Syphilis Patients
Prof. Lorenzo Giacani1, Linda Xu1, Amit Oberai2, Jozelyn V. Pablo2, Christopher Hung2, Andy A. Teng2, Adam D. Shandling2, Emily Romeis1, Kelika A. Konda3, Silver K. Vargas3, Michael Reyes Diaz3, Carlos F. Caceres3, Jeffrey D. Klausner4, Joseph J Campo2
1University of Washington, Seattle, USA.
2Antigen Discovery, Inc., Irvine, USA.
3Universidad Peruana Cayetano Heredia, Lima, Peru.
4University of Southern California, Los Angeles, USA.
Background: Syphilis is a chronic sexually transmitted infection that can result in severe clinical outcomes without adequate treatment. Furthermore, vertical transmission of its etiological agent, the spirochete Treponema pallidum subsp. pallidum (T. pallidum), is significantly associated with stillbirth and neonatal death. Syphilis serodiagnosis requires the combined use of lipoidal tests for screening and treponemal tests to confirm the screening result. Unlike lipoidal assays, treponemal tests cannot monitor response to treatment. Neither type of test can stage syphilis.
Description: To identify antigens and reactivity patterns that could facilitate early syphilis diagnosis, and possibly serve as markers for disease staging and monitoring response to treatment, we developed an array carrying 98.8% of the annotated proteomes of two T. pallidum strains (Nichols and SS14). We probed the array with 217 sera collected pre- and post-treatment from 120 syphilis patients for detection of IgG and IgA antibodies.
Results: Although a very limited IgA response was detected in these sera, significantly higher IgG reactivity allowed us to define the most recognized antigens during natural infection and identify a subset of targets differentially recognized by baseline (pre-treatment) sera when factoring in covariates such as syphilis stage, syphilis history, and HIV status. Differential reactivity to a subset of antigens was also detected in sera collected pre-and post-treatment.
Conclusion: These antigens could be further evaluated to improve the performance of treponemal serological tests. Additionally, antigens inducing a detectable IgA response during infection in adults, albeit few, could be evaluated as diagnostic markers for congenital syphilis in future studies using serum samples from newborns.
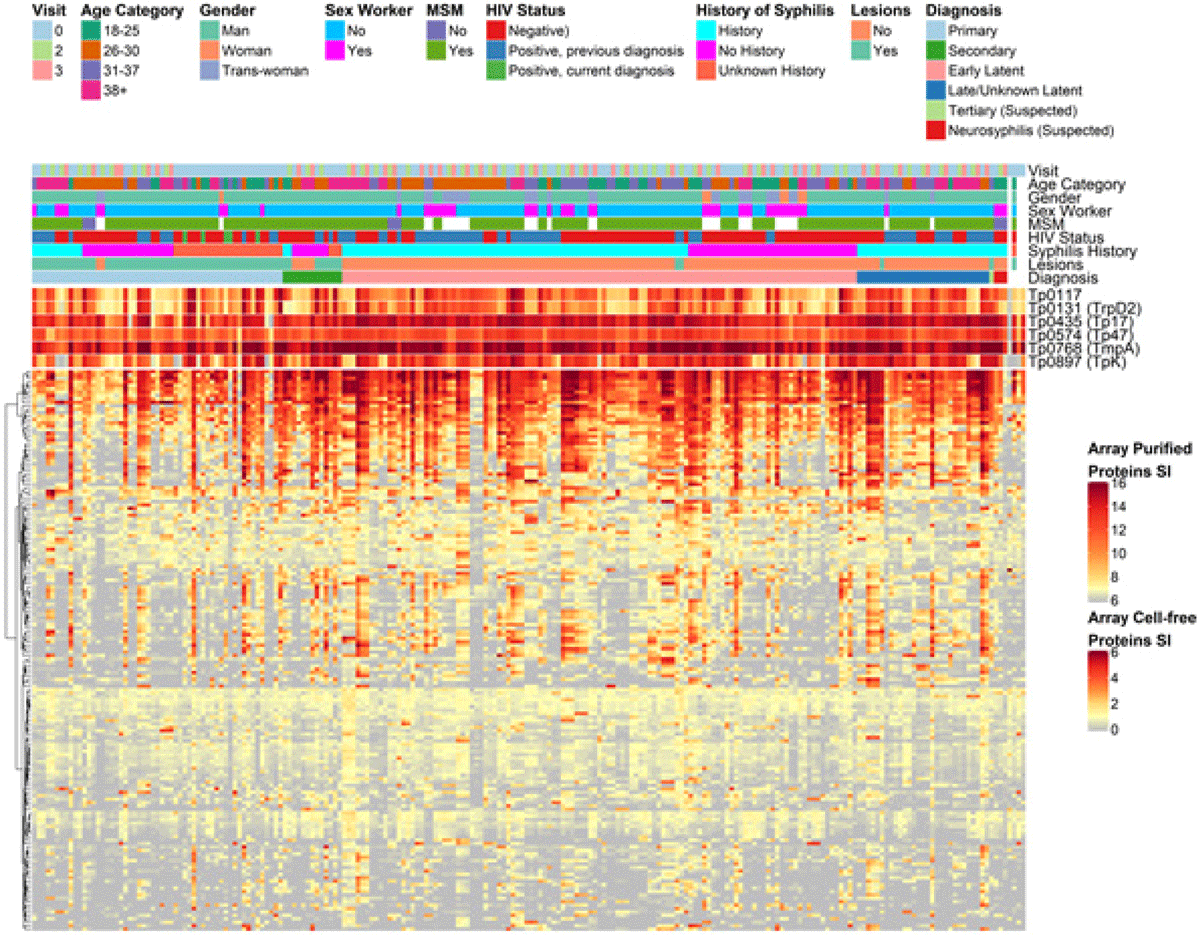
OA09.04 – Single-Cell RNA-seq and TCR/BCR Repertoire Analysis Unveil Immune Responses to Tp Infection During Progression of Syphilis in Lesions and Peripheral Blood
Dr. Xuan Yi1, Yan Zhang1, Xiaoyuan Xie1, Jun Xian1, Jianwei Liao2,3, Haobin Chen1, ZhiJia Li1, Litian Zhang1, Zhenglai Zhu1, Tao Huang1, Yinbo Jiang1, Wentao Chen1, Liuyuan Wang1, Xiaohui Zhang1, Ligang Yang1, Arlene C Seña6, Kelly L. Hawley7, Michael Anthony Moody8, Yingping Xu1, Zhili Rong1,4,5, Justin D. Radolf9, Bin Yang1,2,3
1Dermatology Hospital, Southern Medical University, Guangzhou, China.
2Department of Dermatology, Guangdong College of Clinical Dermatology, Anhui Medical University, Guangzhou, China.
3The Fifth School of Clinical Medicine, Anhui Medical University, Heifei, China.
4Cancer Research Institute, School of Basic Medical Sciences, Southern Medical University, Guangzhou, China.
5State Key Laboratory of Organ Failure Research, National Clinical Research Center of Kidney Disease, Key Laboratory of Organ Failure Research (Ministry of Education), Guangzhou, China.
6Division of Infectious Diseases, Institute for Global Health and Infectious Diseases, University of North Carolina at Chapel Hill, Chapel Hill, USA.
7Departments of Pediatrics, Medicine, and Immunology, UConn Health, Farmington, Connecticut USA and Division of Pediatric Infectious Diseases, Connecticut Children’s, Hartford, USA.
8Departments of Pediatrics and Integrative Immunobiology, Duke University, Durham, USA.
9Departments of Medicine, Pediatrics, Genetics and Genomic Science, Molecular Biology and Biophysics, and Immunology, UConn Health, Farmington, USA.
Background: Syphilis, caused by Treponema pallidum (Tp), remains a significant public health challenge. Although the histopathology of syphilitic lesions has been studied extensively, the immunological mechanisms underlying the infection remain understood.
Methods: We utilized single-cell RNA, T-cell and B-cell receptor sequencing to profile the immune landscape in both lesions and peripheral blood from 6 early syphilis patients enrolled in China, and validated core findings by flow cytometry and immumohistochemical staining.
Results: Elevated endogenous antigen presentation was observed in primary syphilis (PS) lesions and secondary syphilis (SS) peripheral blood mononuclear cells (PBMCs), with strong activation of cytotoxic CD4+ and CD8+ T cells. In SS lesions, we observed impaired antigen presentation through MHC II by myeloid cells, which was compensated for by non-myeloid cells. Notably, a potential Tp-specific cytotoxic T-cell response was identified, characterized by GZMB_Cytotoxic_CD4_T and GZMK_Cytotoxic_CD8_T cells. CellChat analysis indicated that this response may facilitate the cDC1 response, which is critical for antigen cross-presentation. Additionally, we found elevated expression of CX3CR1 on cytotoxic CD4+ T cells, suggesting a potential role in enhancing HIV susceptibility in syphilis patients. B-cell function was found to be impaired in both PS PBMCs and SS skin lesions, potentially contributing to early dissemination of Tp and the progression from PS to SS. We also observed defective antibody affinity maturation in B cells, alongside the presence of inducible skin-associated lymphoid tissue-like structures in both PS and SS lesions, validated by CXCR5/CXCL13 staining.
Conclusion: This comprehensive single-cell analysis revealed dynamic shifts in immune responses across different stages of syphilis. Our findings suggest that impaired antigen presentation, altered T-cell responses, and compromised B-cell function play key roles in disease progression and spirochete persistence. These insights not only improve our understanding of syphilis pathogenesis but also have potential implications for the development of novel targeted therapies and vaccine strategies.
OA09.05 – Persons with Early Syphilis Make Antibodies That Differentially Recognize Extracellular Loops of Treponema Pallidum Outer Membrane Proteins
Dr. Michael Anthony Moody1, Arlene C. Seña2, Mitch M. Matoga3, Eduardo Lopez4, Kristina N. Delgado5, Everton Bettin5, Farhang Aghakhanian2, Isabel C. Orbe5, Melissa J Caimano5, Jonny Alejandro Garcia-Luna4,6, Lady Ramirez4,6, Irving F. Hoffman2, Jonathan B. Parr2, Juan C. Salazar5,7, Justin D. Radolf5,7, Kelly L. Hawley5,7
1Duke University School of Medicine, Durham, United States.
2University of North Carolina at Chapel Hill, Chapel Hill, United States.
3UNC Project Malawi, Lilongwe, Malawi.
4CIDEIM, Cali, Colombia.
5UConn Health, Farmington, United States.
6Universidad Icesi, Cali, Colombia.
7Connecticut Children’s, Hartford, United States.
Background: Persons with syphilis produce treponemal antibodies during infection with Treponema pallidum (TPA), which are often insufficient for spirochete clearance, hence TPA’s designation as ‘the stealth pathogen’. Deconvoluting surface-directed antibody responses will provide insights into spirochete persistence and guide TPA antigen selection for vaccine development.
Methods: We enrolled patients with early syphilis from clinics in Colombia and Malawi between November 2019–May 2022. Sera from 90 participants were tested for ELISA reactivity to two TPA lipoproteins and 62 predicted extracellular loops (ECLs) of Nichols strain outer membrane proteins (OMPs) displayed on a Pyrococcus furiosus thioredoxin (PfTrx) scaffold. Reactivity to an empty PfTrx scaffold was subtracted from reactivity of the scaffolded ECL. For 47 participants, the genome of the infecting TPA strain was sequenced and ECLs in the infecting strain compared to the Nichols strain.
Results: All participant sera reacted to at least one lipoprotein. In contrast, most predicted ECLs were not recognized, although strong reactivity to some ECLs (e.g., TP0856 ECL4, TP0858 ECL2, BamA ECL4) was observed for many participants. Minimal reactivity differences were observed based on participant’s sex and clade (Nichols vs SS14) of the infecting strain. Surprisingly, we observed higher reactivity for ECLs in participants with primary than secondary syphilis. Among sequenced strains, 16/62 (26%) ECLs were variable. Shorter and more variable ECLs were weakly associated with lower responses. Sequenced isolates formed six genomic clusters (subclades); for some invariant ECLs, patients had higher antibody responses when infected by specific subclades.
Conclusion: This is the first large-scale screening of human reactivity to predicted TPA OMP ECLs. Contrary to current concepts of antibody production in syphilis, we found that ECL responses develop during primary syphilis in parallel with lipoprotein responses. Further studies will be needed to evaluate the mechanism for these observed differences and their importance for spirochete clearance vs persistence.
OA09.06 – Single Cell Analysis Allows Phenotypic and Clonotypic Analysis of Treponema Pallidum-Specific CD4+ T Cells
Dr. Tara Reid1, Charmie Godornes1, Victoria Campbell1, Dr. Lichen Jing1, Dr. Emily Ford1,2, Dr. Anna Wald1,2, Dr. David Koelle1,2,3
1University of Washington, Seattle, United States.
2Fred Hutchinson Cancer Research Center, Seattle, United States.
3Benaroya Research Institute, Seattle, United States.
Background: Syphilis is a major public health threat, but we have limited understanding of what constitutes a protective immune response in humans. Treponema pallidum (Tp)-specific CD4 T cell responses are likely important to heal syphilis lesions and are persistent in blood and in the rash skin rash of secondary syphilis. We sought to define the Tp-specific CD4 T cell phenotypes that may contribute to Tp clearance.
Methods: After stimulating peripheral blood mononuclear cells (PBMC) with Tp sonicate, individual Activation Induced Marker positive CD4 T cells were isolated and expanded as candidate Tp-specific T cell clones (TCC). From these TCC, we confirmed Tp-specificity by proliferation and IFNγ secretion. From Tp-specific clones, we obtained paired TCRα/β sequences and multiplexed cytokine analysis (IFNγ, IL10, IL13, IL17A, IL21, and IL5).
Results: We detected CD4 T cell responses to Tp from PBMC of participants with recently treated secondary syphilis, active early latent syphilis and remotely treated early latent syphilis. Functionally, the Tp-reactive CD4 TCC were mostly Th1-like (106/136, 77.9%), with examples of Th2 (8/136, 5.9%), Treg (9/136, 6.6%), Tfh (7/136, 5.1%) and Th17 phenotypes (6/136, 4.4%). Initial TCR analysis from 53 of the 136 TCC revealed clusters of sequence-related TCRs, suggesting an immunodominance hierarchy of clonotypes within individuals. We were further able to identify peptide epitopes for three of these TCC with unique TCR sequences.
Conclusions: We have defined Tp-specific CD4 phenotypes, refining our current understanding of CD4 T cell function during Tp infection and after treatment, to inform vaccine design.
OA10.01 – A National Snapshot of HIV Stigma: Key Findings from the Canadian People Living with HIV Stigma Index
Mr. Alex Tran1, James R. Watson1, Jason M. Lo Hog Tian1, Kristin McBain1, Arthur D. Miller2, Anthony R. Boni1, Lynne Cioppa1, Michael Murphy1, Deborah Norris1, Danita Wahpoosewyan1,3,4, Jennifer Demchuk5, Catherine M. L. Pearl6, Adrian Betts7, Jacqueline Gahagan8, Maureen Owino9, Darren Lauscher5, Sean B. Rourke1,10
1MAP Centre For Urban Health Solutions, St. Michael’s Hospital, Unity Health Toronto, Toronto, Canada.
2Sexual Health and Gender Research (SHaG) Lab, Faculty of Health, Dalhousie University, Halifax, Canada.
3Wellness Wheel Medical Clinic, Regina, Canada.
4AIDS Programs South Saskatchewan (APSS), Regina, Canada.
5PAN, Canada.
6Mount Royal University, Calgary, Canada.
7AIDS Committee of Durham Region, Oshawa, Canada.
8Mount Saint Vincent University, Halifax, Canada.
9York University, Toronto, Canada.
10Department of Psychiatry, University of Toronto, Toronto, Canada.
Background: HIV stigma significantly affects the health and well-being of people living with HIV. This study explores the experiences of people living with HIV in Canada, highlighting key findings related to participant characteristics, HIV stigma, and status disclosure.
Methods: From 2018 to 2024, 1,438 people living with HIV across Canada participated in the People Living with HIV Stigma Index 2.0, an international, standardized tool developed by and for people living with HIV to document the impact of stigma and discrimination. Descriptive analyses examined participant demographics, disclosure behaviors, experiences of stigma (internalized, enacted, and anticipated), and actions taken to challenge stigma.
Results: Participants averaged 48 years old and had lived with HIV for 16 years. Most were cisgender male (60%), heterosexual (44%), and gay/lesbian (41%). The majority identified as white (51%), African, Caribbean, or Black (21%), or Indigenous (21%). Most disclosed their HIV status to partners (87%) and family (75%). However, many found status disclosure to be challenging (61%), and 40% regret past disclosures. Notably, 59% hid their status, and 46% delayed HIV care or treatment, as they were not ready to accept their status. Reflecting on the 12 months prior to survey completion, 41% experienced stigmatizing conversations and 45% avoided sexual relationships due to their status. Encouragingly, during this same period, 36% challenged stigma and 33% supported others in coping with stigma.
Conclusion: This study highlights the urgent need to address HIV stigma in Canada, revealing its persistent impact on the lives of people living with HIV. These findings offer insights to support evidence-based interventions and community-led initiatives to challenge stigma. Addressing stigma supports greater engagement in STI/HIV prevention, testing, and treatment, ultimately improving health outcomes. Continued collaboration among researchers, healthcare providers, policymakers, and community members are essential to creating a supportive environment for all people seeking sexual healthcare.
OA10.02 – Impact of Anti-LGBTQ+ Campaigns on STI Incidence Among MSM and Transgender Persons in Mombasa, Kenya: A Case Study of ICRHK
Mr. Simon Mwangi1, Mr. David Muchiri1, Mr. Abel Mokua1, Ms Aurelia Vose1, Ms Pamphillas Samia1, Mr. Mathew Ogutu1, Dr. Susan Ontiri1, Dr. Dismas Ouma1
1International Centre for Reproductive Health, Kenya.
Introduction: The Supreme Court ruling in March 2023, which granted the LGBTQIA+ community the right to associate, sparked a wave of homophobic protests and anti-LGBTQIA+ agitation in Mombasa, Kenya. These protests led to the profiling of MSM and TG individuals, forcing many into hiding and creating barriers to accessing HIV/STI services. This case study is to examine the association between anti-LGBTQ campaigns and the incidence of STIs among MSM and TG individuals in Kenya.
Methods: ICRHK conducted a retrospective review and analysis of clinical data collected between January 2023 and April 2024 from key population Drop-in Centers in Mombasa to identify the effects of anti-LGBTQ campaigns on STI incidence among MSMs. We compared trends before and during the anti-LGBTQ campaigns.
Results: The findings revealed a significant increase in STI incidence among men who have sex with men (MSM), rising from 1.1% (9/799) to a peak of 4.4% (39/880) in September 2023, with the highest recorded incidence at 5.5% (24/435) in December 2023, coinciding with the peak of anti-LGBT protests and campaigns in Mombasa. For transgender individuals, STI incidence increased from 0.7% (2/277) in January to 3.2% (11/34) in September, peaking at 3.7% (7/189) in April 2024. Following ICRHK’s intervention to establish a gender-based violence (GBV) response mechanism, the prevalence decreased to 2.1% (18/866) by September 2024.
Conclusion: The significant increase in STI incidence among MSM and transgender individuals during periods of heightened anti-LGBT sentiment indicates a strong correlation between social and political factors and health outcomes. The peak incidences during anti-LGBT protests suggest that stigma, discrimination, and violence can lead to increased vulnerability to STIs due to limited access to reproductive health services including STI/HIV prevention services.
Keywords: LGBTQ, Men Who Have Sex with Men, Gender-Based Violence, Sexually Transmitted Infections.
OA10.03 – Hidden Lives, Unseen Risks: STI Transmission Among Closeted Young Gay Men in Forced Marriages in India
Dr. V Sam Prasad1, Ms. Elizabeth Michael1, Mr. Mohnish Kumar1, Mr. Shivam Dwivedi1, Mr. Lyle Honig Mojica2
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
2AIDS Health Care Foundation (AHF), Los Angeles, United States of America.
Background: In India, societal pressure and stigma often force young gay men into heterosexual marriages, putting themselves and their spouses at risk of STI/ HIV transmission. This hidden epidemic requires urgent attention to prevent further transmission and protect the health and well-being of all.
Description: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across 10 states. This study combined quantitative (n = 1050) and qualitative in-depth interviews (n = 30) with closeted young gay men in forced marriages in India. Participants who identified themselves as closeted Gay man during counselling were recruited. 1050 were recruited from 6500 STI /HIV tests conducted among MSMs for 2 years. It assessed STI/HIV prevalence, sexual behavior, and marriage dynamics. Interviews explored the experiences of living with the secret, the impact of forced marriage on mental and physical health, and the challenges of disclosing one’s sexual orientation.
Results: Quantitative findings revealed that:
-
35% of participants reported having an STI, with 20% transmitting it to their spouse.
-
60% of participants reported engaging in high-risk sexual behaviors, such as unprotected anal sex.
-
40% of participants reported experiencing mental health issues, such as depression and anxiety.
Qualitative findings highlighted:
-
The psychological distress, feelings of guilt and shame, and fear of discovery associated with living a closeted life.
-
Difficulty accessing STI testing and treatment due to fear of stigma and being judged
-
The need for safe spaces for disclosure, accessible STI testing and treatment, and inclusive, non-judgmental healthcare services.
Conclusion: This study underscores the urgent need for targeted interventions by
-
Creating safe spaces for disclosure and providing accessible STI testing and treatment.
-
Promoting inclusive, non-judgmental healthcare services and training healthcare providers on LGBTQ+ issues.
-
Implementing comprehensive sexuality education and awareness campaigns to address stigma and promote acceptance.
OA10.04 – A Qualitative Examination of Community Health Workers’ Experience in Sexual Health Care in the US
Dr. Germysha Little1, Joan Ferguson1, Dr. Hilary Reno1
1Washington University, St. Louis, United States.
Background: A community health worker (CHW) is a frontline public health worker who lives in or is trusted by the community. CHWs are essential to providing non-clinical support to contribute to the continuum of sexual health care services. While the network of community health workers is continuing to expand, their experience and training is not well understood. This article describes the role of CHWs in the community, their experience, and their contribution to sexual health care. The purpose of this study was to understand CHW training, their work in sexual health care, and preferred learning styles.
Methods: We conducted structured interviews with a convenience sample of 15 CHWs from the Midwestern US. Participants were interviewed on their passion for becoming a CHW, training, role in health care, and experience in sexual health work including trauma-informed care, gender affirming care, prevention counseling, and syndemic-based care. A thematic analysis was conducted using Nvivo.
Results: Findings suggest that CHWs have a strong passion for their work in the community and occupy many roles beyond their in-classroom training programs. They serve not only as an advocate but also as educators, providers of emotional support, resource access navigators, and champions of civil and human rights. While there is a desire for additional training in sexual health, only 47% of participants reported job-associated shadowing opportunities. In addition, 60% of participants reported a desire for additional hands-on experience regarding trauma-informed care, gender-affirming care, and HIV prevention.
Conclusion: This study offers a comprehensive overview of community health workers’ diverse role, training, and experience in sexual health care. It provides evidence that CHWs fulfill many responsibilities in healthcare but there are many opportunities for improvement in training in sexual health. The data will be used to inform the design of a learning collaborative designed for CHWs by CHWs.
OA10.04 – Optimizing HIV Self-Testing Service Delivery for Key Populations in Nigeria: A Discrete Choice Experiment
Assoc. Prof. Alex Dubov1, Dr Olumide Abiodun
1Loma Linda University, Los Angeles, United States.
Background: This study addresses the critical issue of increasing HIV testing among key populations in Nigeria—men who have sex with men (MSM), female sex workers (FSW), and people who inject drugs (PWID). These groups, though only 3.4% of the population, account for nearly 40% of new HIV infections. With only 65% of Nigerian MSM ever tested, there is a clear need for strategies to promote HIV testing that are client-centered and culturally tailored. This research examines the preferences of MSM, FSW, and PWID for HIVST programs to improve uptake and linkage to care.
Methods: Between May and July 2024, a cross-sectional online discrete choice experiment (DCE) was conducted in Ogun State, Nigeria, among 683 MSM, PWID, and FSW. Participants completed 14 choice tasks involving six HIVST program attributes: test type, pickup location, price, testing support, included items, and results disclosure incentive. Latent class analysis then estimated the relative importance of each attribute.
Results: Of 683 respondents equally split among MSM, FSW, and PWID, only 10.8% had never tested for HIV. The top-ranked HIVST attribute was pickup location (26.7%) – pharmacies or hospitals – followed by included items (21.1%) like condoms, and test type (19.9%) favoring oral tests. Preferences clustered into five groups. Group 1 (3.7%) preferred hospital testing and faced the highest HIV risk. Group 2 (15.1%) was price-sensitive (up to 2000 Naira). Group 3 (8%), predominantly low-risk men, showed minimal interest in HIVST. Group 4 (59.1%) was interested in HIVST across all scenarios, especially with condoms included. Finally, Group 5 (13.8%) strongly preferred oral tests and was highly interested in HIVST.
Conclusion: HIVST acceptability among Nigeria’s key populations was high but varied by scenario and subgroup. Uptake can be maximized by offering HIVST in pharmacies, prioritizing affordable oral tests, and including HIV prevention items. These findings can inform tailored interventions to enhance testing.
OA10.06 – Characterizing Sub-Group Heterogeneity Among Informal Sex Workers to Tailor Differentiated HIV Interventions in a Low-Level HIV Epidemic: Results from a Latent Class Analysis
Dr. Isabel Tavitian-Exley1, Ms Vanessa Ho, Ms Sally Low, Ms Shannon Low, Dr Chen Seong Wong
1National Centre For Infectious Diseases, Singapore, Singapore.
Background: With declining HIV incidence in the Asia-pacific region, informal sex workers (SWs) and their clients remain key populations at risk of HIV transmission. Informal SWs not covered by the Medical Surveillance Scheme (MSS) represent a heterogeneous and insufficiently defined population. This study examines client-seeking methods among SWs and associations with socio-demographics, risk behaviours, and prevention service coverage.
Methods: Data from a 2023 behavioural survey of SWs were analysed using latent class analysis (LCA) to identify sub-groups based on client-seeking methods, including physical venues (massage parlours, streets, brothels, clubs, karaoke lounges) and digital platforms (websites, apps, social media). Associations between sub-groups, socio-demographics, risk behaviours, and programmatic coverage were assessed using multinomial logistic regression.
Results: Five sub-groups were identified: (1) massage-centric (34%), (2) street-centric (16%), (3) brothel-based (10%), (4) club-centric (10%), and (5) online and social media (30%) (Table 1, Fig. 1). Sub-group characteristics varied significantly. The club-centric class, predominantly young, female, and non-Singaporean, reported low condom use and minimal prevention service access. The online and social media class, similarly young, showed greater awareness of pre-exposure prophylaxis (PrEP) but similar service gaps. SWs in the massage-centric and brothel-based classes were older, reported higher client volumes and less PrEP knowledge. Across all classes, access to testing and consistent condom use with non-client partners remained suboptimal.
Conclusion: Heterogeneity among SWs highlights the need for tailored, differentiated HIV prevention strategies. Vulnerable sub-groups, such as younger SWs on digital platforms and transient non-Singaporeans in entertainment venues, require targeted interventions. Enhanced HIV/STI prevention strategies integrating peer-led outreach and education, anonymous testing and expanded access to PrEP need to address individual and structural barriers to sustain recent declines in HIV incidence and reduce STI prevalence among SW. These findings emphasize the importance of granular data to inform targeted, inclusive, and sustainable HIV/STI prevention strategies in low-level epidemics.
| Massage centric (C1, n = 126) | Street-centric (C2, n = 61) | Brothel-based (C3, n = 36) | Clubs and street (C4, n = 38) | Online (C5, n = 110) | ||
|---|---|---|---|---|---|---|
| Class probabilities | 34% | 16.4% | 10% | 10% | 29.6% | |
| Item response probabilities by meeting place | ||||||
| Massage parlour | 100.0% | 0.0% | 0.0% | 0.0% | 7.1% | |
| Clubs and KTV lounges | 2.4% | 0.0% | 0.0% | 100.0% | 4.6% | |
| Brothels | 0.8% | 0.0% | 100.0% | 0.0% | 5.5% | |
| On the streets | 4.0% | 100.0% | 27.9% | 10.6% | 2.2% | |
| Web and online | 0.1% | 12.8% | 0.2% | 0.0% | 77.1% | |
| Mobile dating apps | 0.7% | 0.0% | 0.0% | 0.0% | 33.3% | |
| Social media | 0.6% | 1.5% | 0.0% | 0.0% | 48.7% | |
| Instant messaging | 0.5% | 0.0% | 0.0% | 0.0% | 53.1% |
Note: (1) Conditional probabilities are the probability that a respondent falls in a given class, conditional on their answer “yes” to a specific question item (i.e. observed variable).
Respondent profiles based on places where they find clients (five-class solution of Latent Class model). Notes: The estimated probabilities for places used to find clients are plotted based on latent class (C1-C5) membership shown in Table 1.
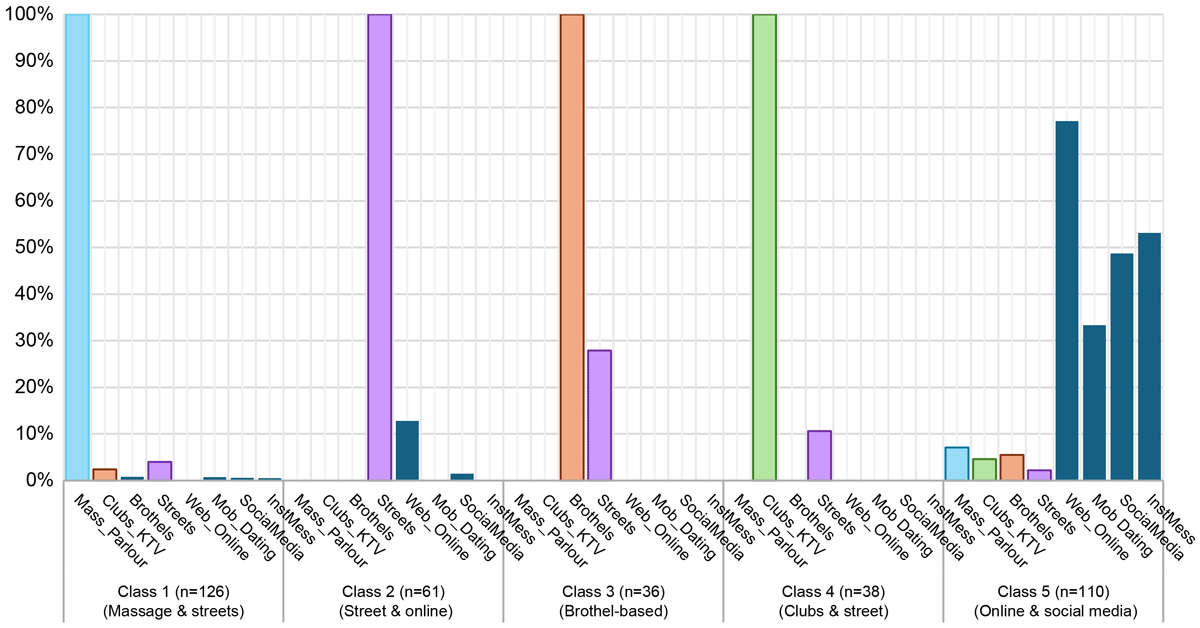
OA11.01 – Emergent Informal Use of Doxycycline Post- and Pre-Exposure Prophylaxis (DoxyPEP/PrEP) Among Men Who Have Sex with Men and Transgender and Gender Diverse People in the Netherlands
Mr. Buhari Teker1,2, Dr. Elske Hoornenborg1,4, Prof. Dr. Maarten Schim van der Loeff1,3,4,5, Dr. Anders Boyd1,5,6, Dr. Janneke Heijne1,3,4,5, Prof. Maria Prins1,3,4,5, Dr. Udi Davidovich1,6, Prof. dr. Henry de Vries1,2,4,5, Dr. Vita Jongen1,4,6
1Department of Infectious Diseases, Public Health Service of Amsterdam, Amsterdam, the Netherlands.
2Department of Dermatology, Amsterdam UMC location University of Amsterdam, Amsterdam, the Netherlands.
3Department of Internal Medicine, Amsterdam UMC location University of Amsterdam, Amsterdam, the Netherlands.
4Amsterdam Institute for Immunology & Infectious Diseases (AI&I), Amsterdam, the Netherlands.
5Amsterdam Public Health research institute (APH), Amsterdam, the Netherlands.
6Department of Social Psychology, Amsterdam, the Netherlands.
Background: Doxycycline post- and pre-exposure prophylaxis (doxyPEP/PrEP) are novel prevention strategies for bacterial sexually transmitted infections (STIs). In the Netherlands, doxyPEP/PrEP is not part of standard practice, but might be used informally (i.e., without a prescription for doxycycline use as prophylaxis). This could lead to incorrect use and related adverse events. We assessed awareness, intention-to-use, and informal use of doxyPEP/PrEP among men who have sex with men (MSM) and transgender and gender diverse people in the Netherlands.
Methods: Between 26 February 2024 and 6 May 2024, we conducted an online survey in the Netherlands on awareness, informal use in the preceding 6 months, and intention-to-use of doxyPEP/PrEP. High intention-to-use was defined as score 6–7 on a 7-point Likert-scale. We assessed the determinants of informal doxyPEP/PrEP use and high intention-to-use using relative risk regression.
Results: A total of 1,633 individuals (96.7% MSM) were included. Of these, 246 (15%) participants reported recent informal use, 1,037 (63.5%) were aware, and 1,063 (65.1%) had a high intention-to-use doxyPEP/PrEP. Informal use was more common among participants who used HIV PrEP or were living with HIV, had ≥15 anonymous sexual partners, engaged in chemsex, wanted to protect oneself, got advice from others to use doxyPEP/PrEP, and believed doxyPEP/PrEP is safe. A total of 1,063 (65%) had high intention-to-use. High intention-to-use was more common among participants using HIV PrEP or living with HIV, who wanted to have condomless sex, who wanted to protect others from STIs, and who perceived doxyPEP/PrEP as effective and safe.
Conclusion: Although doxyPEP/PrEP is not formally accessible in the Netherlands, survey participants reported significant informal use of doxyPEP/PrEP and a high intention-to-use. These findings, combined with the global increase of antimicrobial resistance, stress the need for (inter)national guidelines on the use and monitoring of individual and population-effects of doxyPEP/PrEP.
OA11.02 – Evaluation of Rpr Titer Differences at Early Syphilis Diagnosis in Doxy-PEP Users vs Non-Users
Dr. Chase Cannon1,2, Dr. Timothy Menza1,2, Christina Thibault2, Dr. Matthew Golden1,2, Dr. Julie Dombrowski1,2
1University of Washington, Seattle, United States.
2Public Health - Seattle & King County, Seattle, United States.
Background: Doxy-PEP prevents syphilis in men who have sex with men and transgender women. Intermittent doxycycline exposure may impact syphilis titer dynamics and thus the ability to diagnose new syphilis, but to what extent this occurs is currently unknown.
Methods: Using routinely collected clinic data from PrEP patients at the Seattle-King County sexual health clinic from 2023/04/01 (when providers began prescribing doxy-PEP) to 2024/12/01, we characterized demographics, self-reported doxy-PEP, syphilis history, clinical details of early syphilis (ES) diagnoses (including primary and secondary [P&S] and early latent stages). The Wilcoxon rank sum test was used to compare median RPR titers at ES diagnosis, stratified by doxy-PEP use.
Results: 1777 PrEP patients attended 6843 clinic visits, most of which (5120, 75%) were routine PrEP appointments. Patients were median age 32 [IQR: 27–38], majority cisgender men (91%), of White (52%) or Asian (13%) race, and non-Hispanic ethnicity (72%). History of syphilis was common (437, 25%) – 34% among doxy-PEP users vs 24% among non-users. Over one-third (643, 36%) of patients reported recent doxy-PEP use at ≥1 visits. There were 59 new syphilis cases in 56 patients, including 42 (71%) cases in non-users and 14 (24%) in doxy-PEP users. Early latent was the commonest stage (56%) at diagnosis; a much higher proportion of P&S cases were in non-users vs users (88% vs 12%). The distribution of RPR titers at ES diagnosis (Fig. 1) differed for non-users vs users in both mode (1:128 vs 1:2) and median values (1:32 vs 1:8, P = 0.0285).
Conclusion: Median RPR titers were 2 dilutions lower in doxy-PEP users compared to non-users, but the extent to which this is attributable to doxy-PEP use vs syphilis history is unclear. Longitudinal data are necessary to better characterize titer trends in doxy-PEP users and any potential impact on the clinical diagnosis of new syphilis.
OA11.03 – A Few Antimicrobial-Resistant Mycoplasma Genitalium Clones Circulate Among MSM on PrEP in the ANRS DOXYVAC Trial
Prof. Cecile Bebear1, Pr Beatrice Berçot2, Dr Lambert Assoumou3, Mr Moussa Ouattara3, Mrs Carla Balcon1, Dr Jennifer Guiraud1, Dr Olivia Peuchant1, Mr Aymeric Braille2, Mrs Marie Maynardis2, Mrs Aissata Kaba3, Dr Emma Rubinstein2, Pr Gilles Pialoux4, Pr Christine Katlama5, Dr Laure Surgers6, Dr Laurence Slama7, Dr Juliette Pavie7, Dr Claudine Duvivier9, Dr Beatrice Loze2, Pr Jade Ghosn8, Pr Dominique Costagliola3, Pr Jean-Michel Molina2
1Bordeaux University hospital and University of Bordeaux, Bordeaux, France.
2Assistance-Publique Hôpitaux de Paris, Saint-Louis and La Riboisière hospital, Paris, France.
3Sorbonne Université, INSERM, Paris, France.
4Assistance-Publique Hôpitaux de Paris, Tenon hospital, Paris, France.
5Assistance-Publique Hôpitaux de Paris, Pitié Salpétrière hospital, Paris, France.
6Assistance-Publique Hôpitaux de Paris, Saint-Antoine hospital, Paris, France.
7Assistance-Publique Hôpitaux de Paris, Hotel-Dieu Hospital, Paris, France.
8Assistance-Publique Hôpitaux de Paris, Bichat Hospital, Paris, France.
9Necker Pasteur Infectiology Center, Paris, France.
Background: To address the circulation of different antimicrobial-resistant (AMR) Mycoplasma genitalium (MG) strains among MSM on PrEP, using or not doxycycline post-exposure prophylaxis (PEP) in the French ANRS DOXYVAC trial. From January 2021 to February 2023, 356 MG infections were diagnosed by PCR in urine, pharyngeal or anal samples (138 at baseline, and 88 in the no-PEP group, 130 in the PEP group during follow-up). Rates for macrolide resistance ranged between 93.6 and 82.3% in both arms while fluoroquinolone-resistance rates were similar in both groups (46.7% to 51.6%). Tetracycline-resistance associated mutations were found in the 16S rRNA for around 15% of MG-positive patients at baseline and in both arms.
Methods: Molecular typing was performed using SNP analysis of the mgpB adhesin gene. P-values were calculated using Fisher’s exact test.
Results: Twenty-eight different mgpB types were identified for 133 samples (54 no-PEP, 79 PEP) obtained from 122 patients MG-positive at baseline or with an incident infection during follow-up. No difference in sequence type (ST) distribution was identified between both arms (PEP vs no-PEP, Fisher exact P = 0.91). The mpgB phylogenetic construction revealed several clusters according to AMR profile. ST 159 harboring both the A2058T 23S rRNA and the S80I ParC mutations was the most frequent one representing 32.3% of samples. ST4 (21.1%) was associated with only macrolide resistance (A2059G mutation) while ST153 (6.8%) was associated with 23S rRNA (A2058G) and 16S rRNA (G966T, G967T) mutations. Four strains (3.0%), from which three belonged to ST3, harbored resistance-associated mutations in the three antibiotic targets.
Conclusion: We report a low diversity of mgpB MG types among French MSM on PrEP in the Paris area, which reflects the easier spread of a few MG multi-drug resistant clones in this population. No impact of PEP was observed on the ST distribution of MG strains.
OA11.04 – Population-Level Impact of Doxy-PEP on Syphilis Diagnoses, King County, WA, USA, 2021–2024
Dr. Tim Menza1,2, Anna Berzkalns2, Dr. Chase Cannon1,2, Dr. Jen Balkus1,2, Dr. Roxanne Kerani1,2, Dr. Julie Dombrowski1,2, Dr. Matthew Golden1,2
1University of Washington, Seattle, United States.
2Public Health--Seattle & King County, Seattle, United States.
Background: Data suggest that use of doxy-PEP among men who have sex with men and transgender women has a population-level effect on incident syphilis diagnoses. Whether doxy-PEP’s impact will be generalizable across the US and ultimately affect cisgender women and congenital syphilis (CS) diagnoses is unknown.
Description: Using interrupted time series analyses, we evaluated county-wide trends in syphilis (all stages) overall and by gender between January 2021 and December 2024, before and after the implementation of doxy-PEP in a large sexual health clinic in King County, WA began in March 2023.
Results: The total quarterly number of syphilis cases increased 65% from 308 in Q1 2021 to 508 in Q1 2023 (+20 cases per quarter [cpq]; 95% CI: +10, +30; P = 0.001) and then declined 54% to 233 in Q4 2024 (–32 cpq; 95% CI: –43, –20; P = 0.001) (Fig. 1). Between Q1 2021 and Q1 2023, cases among cisgender men rose 47% from 253 to 372 (+11 cpq; 95% CI: +4, +18; P = 0.006), while cases in cisgender women increased 137% from 51 to 121 (+8 cpq; 95% CI: +5, +11; P < 0.001). After doxy-PEP implementation in Q1 2023, syphilis cases in cisgender men and cisgender women declined to 195 (48% decline vs Q1 2023; –25 cpq; 95% CI: –35, –14; P < 0.001) and 81 (33% decline vs Q1 2023; –6 cpq; 95% CI: –9, –4; P < 0.001) in Q4 2024, respectively. The number of syphilis cases among transgender and nonbinary patients remained stable. In contrast, syphilis cases is pregnant persons rose from 21 in 2021 to 33 and 34 in 2022 and 2023, respectively, while the number of CS cases increased from 11 in 2021 to 20 in 2023.
Conclusions: Doxy-PEP implementation in King County was associated with a dramatic decline in syphilis diagnoses, including among cisgender women, a group we do not believe is receiving significant amounts of doxy-PEP, yet this has not affected the number of cases of syphilis in pregnant persons or CS.
OA11.05 – Population Impact and Cost-Effectiveness of Doxycycline Post-Exposure Prophylaxis in Preventing the Sexually Transmitted Infections Among Gay, Bisexual, and Other Men Who Have Sex with Men in Australia: A Mathematical Modelling Study
Mr Hao Lai2, Prof Jason Ong1, Prof Mingwang Shen2, Prof. Lei Zhang1
1Monash University, Carlton, Australia.
2Xi’an Jiaotong University, Xi’an, China.
Background: WHO aims to reduce gonorrhoea and syphilis incidence by 90% and chlamydia by 50% by 2030 (compared to 2020). Doxycycline post-exposure prophylaxis (doxy-PEP) can reduce the incidence of sexually transmitted infections (STIs), but potential antimicrobial resistance (AMR) raises concerns.
Methods: We developed an individual-based stochastic network model simulating the transmission, progression, and treatment of gonorrhoea, chlamydia, and syphilis among 10,000 gay, bisexual, and other men who have sex with men (GBMSM) in Australia. The model incorporated demographic, behavioural, and AMR factors and was calibrated with annual STI positivity rates (2012–2023) from the Australian Collaboration for Coordinated Enhanced Sentinel Surveillance network and AMR trends (2013–2022) from the Melbourne Sexual Health Centre. We compared a base case (no doxy-PEP) to seven doxy-PEP strategies with eligibility criteria informed by HIV status, PrEP use, and STI history. Outcomes included incidence of STI and doxycycline-resistant gonorrhoea, quality-adjusted life-years (QALYs) gained, incremental cost-effectiveness ratios (ICERs), and benefit-cost ratios (BCRs).
Results: All doxy-PEP strategies reduced cumulative incident STIs over 10 years by 9.7–46.3% compared to the base case. Only the most inclusive strategy – providing doxy-PEP to all HIV+ or PrEP-using GBMSM attendees regardless of STI history – achieved the WHO’s targets for chlamydia and syphilis but not for gonorrhoea. This approach increased doxycycline-resistant gonorrhoea by 31.3%, causing a rebound in incidence of gonorrhoea from 2028. Except for this most inclusive strategy, all other strategies were cost-saving, with positive QALYs gained and high BCRs from 1.8–3.8. The strategy targeting HIV+ or PrEP-using individuals diagnosed with syphilis decreased overall STI incidence by 8.0%, reduced doxycycline-resistant gonorrhoea by 5.9%, and had the highest BCR.
Conclusion: Doxy-PEP can substantially reduce chlamydia and syphilis incidence and be cost-saving among GBMSM in Australia, but its limited impact on gonorrhoea and potential to increase AMR highlight targeted implementation.
OA11.06 – Weekly Doxycycline Prophylaxis for Prevention of Sexually Transmitted Infections Among Cisgender Women in Kenya
Dr. Jenell Stewart1,2, Dr. Felix O. Mogaka3, Dr. Lauren R. Violette4,5,7, Dr. Deborah Donnell6, Dr. Victor Omollo3, Daisy Eugine Anyango3, John Bosco Tsetso3, Purity Kwamboka3, Beatrice Obonyo3, Violet Kwach3, Bernard Rono3, Josephine Odoyo3, Marya Abdel Hadi1, Dr. Jared M. Baeten7, Dr. Elizabeth A. Bukusi3,7
1Hennepin Healthcare, Minneapolis, United States.
2University of Minnesota, Minneapolis, United States.
3Kenya Medical Research Institute, Centre for Microbiology Research, Kisumu, Kenya.
4Harvard Pilgrim Health Care Institute, Cambridge, United States.
5Harvard Medical School, Cambridge, United States.
6Fred Hutchinson Cancer Center, Seattle, United States.
7University of Washington, Seattle, United States.
Background: Bacterial sexually transmitted infections (STIs) are responsible for severe clinical outcomes among cisgender women with rising incidence globally. Doxycycline postexposure prophylaxis (DoxyPEP) prevents STIs among cisgender men and transgender women; however, the recently-completed dPEP Kenya Study of doxyPEP among cisgender women did not demonstrate efficacy in the setting of low use of doxycycline. Pharmacokinetic modeling of doxycycline in the vagina suggests time above minimum inhibitory concentration for Chlamydia trachomatis is greater than 96 h suggesting that weekly dosing may be sufficient for combination pre- and post- exposure prophylaxis.
Methods: In June 2025, we will conclude an open-label trial of 200 mg doxycycline hyclate given weekly by directly observed therapy in Kenya. Participants were tested for bacterial STIs (chlamydia, gonorrhea, and syphilis) at enrollment and every 3 months for 6 months. We aimed to compare incident STIs with the standard of care group of the PEP Kenya Study. In both studies we enrolled Kenyan women, 18–30 years old, who were taking HIV pre-exposure prophylaxis. At the time of this preliminary abstract, 32 (53.3%) participants had exited the study.
Results: Among 60 participants at 86 follow-up study visits over 6 months, two incident chlamydia and two incident gonorrhea cases were detected among four participants with a chlamydia incidence of 9.2 per 100 person-years and combined incidence of 18.4 per 100 person-years. Among 225 assigned to standard of care in the dPEP Kenya Study at 439 follow-up study visits over 6 months, 30 incident chlamydia and 7 incident gonorrhea cases were detected among 33 participants with a chlamydia incidence of 28.9 per 100 person-years and combined incidence of 31.8 per 100 person-years.
Conclusion: In preliminary results, chlamydia incidence and combined STI incidence were lower with weekly doxycycline prophylaxis when retrospectively compared with participants assigned to standard of care in the dPEP Kenya Study.
| Characteristics | Weekly Doxycycline DoxyDOT Study N = 60 | Standard of Care dPEP Kenya Study N = 225 | |
|---|---|---|---|
| Age | |||
| 18–24 | 38 (63.3%) | 127 (56.4%) | |
| 25–30 | 22 (36.7%) | 98 (43.6%) | |
| Education level | |||
| Primary School | 5 (8.3%) | 55 (24.4%) | |
| Secondary School | 36 (60.0%) | 128 (56.9%) | |
| Post-Secondary School | 19 (31.7%) | 42 (18.7%) | |
| Participant earns own income | 32 (53.3%) | 143 (63.6%) | |
| Marital status | |||
| Never Married | 43 (71.7%) | 139 (61.8%) | |
| Married | 14 (23.3%) | 53 (23.6%) | |
| Previously Married | 3 (5.0%) | 33 (14.7%) | |
| Has a primary sex partner | 58 (96.7%) | 184 (81.8%) | |
| New sex partners* | 12 (20.0%) | 72 (32.0%) | |
| Number of partners, median (IQR)* | 1 (1-1) | 2 (1-4) | |
| Transactional sex* | 14 (23.3%) | 76 (33.8%) | |
| Condom use at last vaginal sex act+ | 23 (38.3%) | 67 (29.8%) | |
| Months on HIV PrEP, median (IQR) | 9 (4-15) | 7 (4-14) | |
| Contraception use^ | 38 (63.3%) | 135 (60.0%) | |
| Parity | |||
| None | 17 (28.3%) | 65 (28.9%) | |
| 1 live birth | 29 (48.3%) | 83 (36.9%) | |
| 2 or more live births | 14 (23.3%) | 77 (34.2%) | |
| Sexually transmitted infection | |||
| C. trachomatis | 8 (13.3%) | 33 (14.7%) | |
| N. gonorrhoeae | 4 (6.7%) | 7 (3.1%) | |
| T. pallidum | 0 (0%) | 2 (0.9%) | |
| Any STI | 11 (18.3%) | 40 (17.8%) |
OA12.01 – The Association Between HIV and Antimicrobial Resistance in Curable Sexually Transmitted Infections: Systematic Review and Meta-Analysis
Dr. Amajida F Ratnasari1, Dr. Sophie Kelly2, Dr. Ioana D Olaru1,2, Professor Rashida A Ferrand1,2, Professor Katharina Kranzer1,2,3, Professor Michael Marks1, Dr. Kevin Martin1,2
1London School of Hygiene & Tropical Medicine, London, United Kingdom.
2The Health Research Unit Zimbabwe, Biomedical Research and Training Institute, Harare, Zimbabwe.
3LMU University Hospital, LMU Munich, Munich, Germany.
Background: People living with HIV (PLWH) may have an increased risk of antimicrobial resistance (AMR) in curable sexually transmitted infections (STIs) due to differing risk of acquiring infections and more frequent antimicrobial use for STIs and/or other infections. This review investigates the association between HIV and AMR in curable STIs: infections with Neisseria gonorrhoeae, Treponema pallidum, Mycoplasma genitalium, Chlamydia trachomatis, and Trichomonas vaginalis.
Methods: Searches were conducted in databases (including MEDLINE and EMBASE) and surveillance websites up to May 10 2024. Abstracts and full-text articles were screened independently by two reviewers. Studies were eligible if they reported AMR prevalence in curable STIs, stratified by HIV status. Meta-analysis to estimate pooled odds ratios was performed using random-effects models. When data were available, subgroup meta-analyses by sexual orientation were conducted.
Results: Of 5162 articles identified by the search, there were 44 eligible studies (Fig. 1), pertaining to N. gonorrhoeae (n = 34), M. genitalium (n = 7) and T. pallidum (n = 3). No eligible studies covered C. trachomatis or T. vaginalis. Most studies were conducted in high-income countries (n = 39; 88.6%). PLWH had 1.19 (95% CI: 1.01, 1.40) higher odds of penicillin resistance and 1.88 (95% CI: 1.35, 2.60) higher odds of resistance to tetracyclines in N. gonorrhoeae than people without HIV. No differences in AMR prevalence were observed in T. pallidum and M. genitalium. Subgroup meta-analyses showed differences in resistance to penicillin (P = 0.04) and tetracyclines (P = 0.02) by sexual orientation with higher odds among heterosexual populations than in men who have sex with men.
Conclusion: There is increased risk of penicillin and tetracyclines resistance in N. gonorrhoeae among PLWH than people without HIV. The increased risk of tetracyclines resistance has potential implications regarding differential effectiveness of doxycycline prophylaxis for STIs. This review also highlights geographical evidence gaps and the need for more data from low- and middle-income countries.
OA12.02 – New HIV, HCV and HBV Infections Due to Unsafe Medical Injections in Low and Middle-Income Countries: An Analysis Based on Demographic and Health Surveys
Asst. Prof. Adelina Artenie1,2, Dr Anna L. McNaughton2, Mr. Joshua Dawe2, Dr Daniel Low-Beer3, Dr Niklas Luhmann3, Dr Catherine de Martel3, Dr Homie Razavi4, Ivane Gamkrelidze4, Prof. Matthew Hickman2, Prof. Peter Vickerman2
1Universite De Montreal, Montreal, Canada.
2University of Bristol, Bristol, UK.
3World Health Organization, Switzerland.
4Polaris Observatory, Colorado, United States.
Background: Recent data on the extent to which unsafe medical injections contribute to new HIV, hepatitis C virus (HCV) and hepatitis B virus (HBV) infections are lacking. We estimated the annual number and rate (for HIV/HCV/HBV) and fraction (HIV/HCV only) of new infections attributed to unsafe medical injections. This analysis was restricted to adults aged 15–49 based in 60 low- and middle-income countries (LMICs) with Demographic and Health Survey (DHS) data on medical injection safety.
Methods: For each viral infection and country, we fitted a mass action model to data on: medical injection safety (i.e., average number of medical injections/year; probability that last injection was safe), HIV/HCV/HBV prevalence, HIV/HCV/HBV transmission probability using accidental needlestick injury data among healthcare workers, and susceptible population size (i.e., adults uninfected with HIV/HCV/HBV and – additionally for HBV – previously unexposed and unvaccinated). Data were retrieved through multiple sources, including DHS, UNAIDS, Centre for Disease Analysis and Global Burden of Disease. Uncertainty was assessed using Monte Carlo simulations. For HCV/HBV, we estimated new acute (total) and new chronic infections; only the former are shown.
Results: The countries included account for 55% of adults aged 15–49 in LMICs. Overall (across all 60 countries), 2,016 (95%UI: 299–4,065), 50,523 (95% UI: 27,472–86,081) and 448,886 (95% UI: 280,636–688,025) new HIV, HCV and HBV infections were estimated to occur annually because of unsafe medical injections, respectively. The 10 countries with the largest absolute rates (per 100,000 people) are shown (Fig. 1). Overall, the estimated fraction of HIV and HCV infections attributed to unsafe medical injections was 0.4% (95%UI: 0.3–0.5) and 5.1% (95% UI: 3.8–6.8), respectively; these fractions were highest in Pakistan (HIV: 1.5%; HCV: 44.9%).
Conclusions: New HIV, HCV, and HBV infections persist due to unsafe medical injections, with substantial variation in the number, rate, and fraction of cases across countries and viral infection type.
OA12.03 – Intimate Partner Violence (IPV) and Subsequent Bacterial Sexually Transmitted Infection (STI) Diagnoses Among Gay, Bisexual, and Other Men Who Have Sex with Men (GBM) in Canada
Dr. James Stannah1, Mr. Jorge Luis Flores Anato1, Mr Stephen Juwono1, Milada Dvorakova2, Tin D Vo3, Paolo A Parma4, David Moore5, Alain Fourmigue2, Nathan J Lachowsky6, Trevor A Hart3, Shayna Skakoon-Sparling4,7, Darrell H S Tan8, Daniel Grace3, Terri Zhang4, Aki Gormezano6, Joseph Cox1,2,9, Mathieu Maheu-Giroux1
1McGill University, Montreal, Canada.
2Research Institute of the McGill University Health Centre, Montreal, Canada.
3University of Toronto, Toronto, Canada.
4Toronto Metropolitan University, Toronto, Canada.
5BC Centre for Excellence in HIV/AIDS, Vancouver, Canada.
6University of Victoria, Victoria, Canada.
7University of Guelph, Guelph, Canada.
8Unity Health Toronto, Toronto, Canada.
9Direction Regionale de Sante Publique de Montreal, Montreal, Canada.
Background: GBM experience high rates of IPV. However, most of the evidence linking IPV to STI comes from studies of women. We aimed to estimate the effect of physical and/or sexual IPV on bacterial STI diagnosis among GBM in Canada’s three largest cities.
Methods: We used longitudinal data on GBM recruited through respondent-driven sampling in Montréal, Toronto, and Vancouver (Engage Cohort Study, 2017–2024). Among partnered GBM, we fit logistic generalised estimating equations to estimate the crude (OR) and adjusted odds ratios (aOR) of recent IPV (past 6 months) on laboratory-confirmed bacterial STI (gonorrhoea, chlamydia, syphilis) at the same and the subsequent (i.e., lagged effect) study visit as IPV measurement. We adjusted for city, age, education, income, HIV status, baseline number of sexual partners and mental health, lifetime IPV experience and perpetration, history of STI, and childhood sexual abuse. We accounted for missing data using multiple imputation and loss-to-follow-up with inverse probability of censoring weights.
Results: Of 2,518 GBM recruited at baseline, 1,324 partnered GBM attended at least one follow-up (4,313 visits). During follow-up, 95 GBM (7%) reported incident IPV at least once and 221 received incident bacterial STI diagnoses (275 visits). The crude STI incidence rate was over two-fold higher for GBM with recent IPV experience during follow-up (30 vs 12/100 person-years, Table 1). GBM who experienced IPV were more likely to be diagnosed with STI at the same follow-up visit (OR = 2.26, 95% confidence interval [CI] 1.34–3.84; aOR = 1.82, 1.09–3.04), but not the subsequent visit (OR = 1.64, 0.80–3.38; aOR = 1.32, 0.63–2.74).
Conclusion: GBM who recently experienced IPV are at increased risk of bacterial STIs. STI prevention efforts for GBM should include services to address IPV alongside the syndemic factors driving this association to reduce infection risk and improve health outcomes for GBM.
| Experienced IPV in the P6M? | N | Incidence rate (/100PY) | ||||||
|---|---|---|---|---|---|---|---|---|
| (participants) | (visits) | Number of STI diagnoses (n) | PY at risk | Crude | RDS-II adjusted | RDS-II-IPCW adjusted | ||
| No | 1,311 | 4,188 | 257 | 2099 | 12.2 | 9.1 | 9.0 | |
| Yes | 95 | 125 | 18 | 59 | 30.3 | 18.3 | 17.4 | |
IPCW, inverse probability of censoring weights; IPV = intimate partner violence; PY, person-years; RDS, respondent-driven sampling; STI, sexually transmitted infections.
OA12.04 – An Initial Epidemiological Analysis of HIV Incidence, Adolescent Pregnancy, and Sex and Gender-Based Violence to Inform Kenya’s “End the Triple Threat” Campaign
Dr. Murugi Micheni2, Dr. Souradet Shaw1, Dr. Ruth Laibon-Masha2, Dr. Celestine Mugambi2, Dr. Joshua Gitonga2, Dr. Peter Arimi3, Mr. Japheth Kioko3, Dr. Banadakoppa Ramesh1, Dr. Parinita Bhattacharjee1, Dr. James Blanchard1
1Institute For Global Public Health, University of Manitoba, Winnipeg, Canada.
2National Syndemics Disease Control Council, Nairobi, Kenya.
3Partners for Health and Development in Africa, Nairobi, Kenya.
Background: In 2022, Kenya’s National Syndemics Disease Control Council embarked on the “End the Triple Threat” campaign, which sought to decrease the rates of new HIV infections, adolescent pregnancies, and sexual and gender-based violence (SGBV) by the year 2030. This study presents initial epidemiological analyses of all three indicators of interest.
Methods: Indicators were captured across Kenya’s 47 counties: HIV incidence for 15–19 year-old females was estimated from mathematical models for 2018 and 2022; SGBV (10–17 year-old males and females; 2020–2022) and pregnancy (15–19 year old females; 2018–2022) rates were from program data. Rates were calculated using the appropriate mid-point populations and visualized using choropleth mapping. Geographic inequality at the county level was assessed using the Gini coefficient, with 95% confidence intervals (95% CI) calculated.
Results: Between 2018 and 2022, HIV incidence decreased from 16.6 (95% CI: 16.1–17.1) to 10.2 (95% CI: 9.9–10.6) per 10,000 female population. In this same time period, pregnancy rates decreased from 140.2 to 60.4 per 1,000 female population, while from 2020 to 2022, SGBV decreased from 24.8 to 17.4 per 1,000 population (Fig. 1). However, decreases in the three indicators were not uniform across counties; for example, HIV incidence increased in Nairobi and flatlined in several counties. Some counties, such as West Pokot and Tana River consistently had the highest SGBV and pregnancy rates. Inequality analyses revealed that in 2022, HIV had the highest geographic inequality (Gini: 0.422, 95% CI: 0.318–0.525), followed by pregnancy (Gini: 0.178, 95% CI: 0.134–0.221), and SGBV (Gini: 0.160, 95% CI: 0.117–0.203), suggesting greater geographic dispersion among the latter two indicators.
Conclusion: As Kenya begins to address pregnancy, SGBV, and HIV in tandem, these preliminary results suggest an expanded geographic focus will be required, with several rural counties consistently having the highest rates of SGBV and pregnancy.
OA12.05 – The Impact of Chlamydia Trachomatis on Male Infertility: A Systematic Review and Meta-Analysis
Dr. Nicola Luigi Bragazzi1,2,3, Dr. Valerie Bosch Castells4, Dr. Qi Deng2, Dr. Grégoire Ranson2,5, Dr. Edward Thommes6,7, Prof. Dr. Jianhong Wu2, Dr. Sandra S. Chaves4
1University of Parma, Parma, Italy.
2Laboratory for Industrial and Applied Mathematics (LIAM), Department of Mathematics and Statistics, York University, Toronto, Canada.
3Saarland University, Saarbrücken, Germany.
4Sanofi, Lyon, France.
5Institut Camille Jordan (Inria), Université Claude Bernard Lyon 1, Villeurbanne, France.
6Sanofi, Toronto, Canada.
7University of Guelph, Guelph, Canada.
Background: Male infertility accounts for up to 50% of infertility cases globally, with approximately 15% linked to genitourinary infections. Despite the high prevalence of Chlamydia trachomatis (CT), its impact on male infertility remains underexplored. This study aimed to synthesize existing evidence on the association between CT infection and male infertility.
Methods: A systematic literature review and meta-analysis were conducted according to PRISMA guidelines. A comprehensive search was conducted in PubMed/MEDLINE, Scopus, Cochrane, and Embase. A time filter was applied, focusing on articles from 2000. Meta-analytic computations were performed using random-effects models, with subgroup analyses by geography, case definition, diagnostic methods, and matching criteria. All computations were carried out in the open-source R environment.
Results: Out of 2,941 items initially retrieved, 26 case-control studies published between 2003–2024 and involving 11,706 participants (7,934 cases and 3,772 controls) were retained. Seven studies originated from Iran, four from China, three from Egypt, two from Iraq, two from Mexico, and two from Turkey. Single studies were conducted in Argentina, Bulgaria, India, Jordan, Nigeria, and Kuwait. Sample size from the various studies included in the meta-analysis varied from 76 to 3,950. Most studies used molecular diagnostics (n = 23), with only three employing immunoassays to ascertain CT exposure. A significant association between CT infection and male infertility was observed (pooled odds ratio (OR) 3.68 [95% CI 2.24–6.04]), with substantial heterogeneity (I2 = 64.75%) (Fig. 1). Studies with age-based matching reported higher effect sizes (OR 6.77 [95% CI 3.65–12.55]). Funnel plot asymmetry suggested publication bias, with a trimmed effect size of 2.75 [95% CI 1.74–4.35].
Conclusion: CT significantly impairs male fertility by affecting key semen parameters. These findings underscore the need for targeted public health interventions and clinical practices to address CT-associated infertility. Moreover, further high-quality research is warranted to enhance evidence reliability and representativeness.
Forest Plot of the impact of Chlamydia trachomatis on male infertility. Abbreviations: ES (effect size); CI (confidence interval); W (weight); N (total sample size); N1 (cases); N2 (controls).
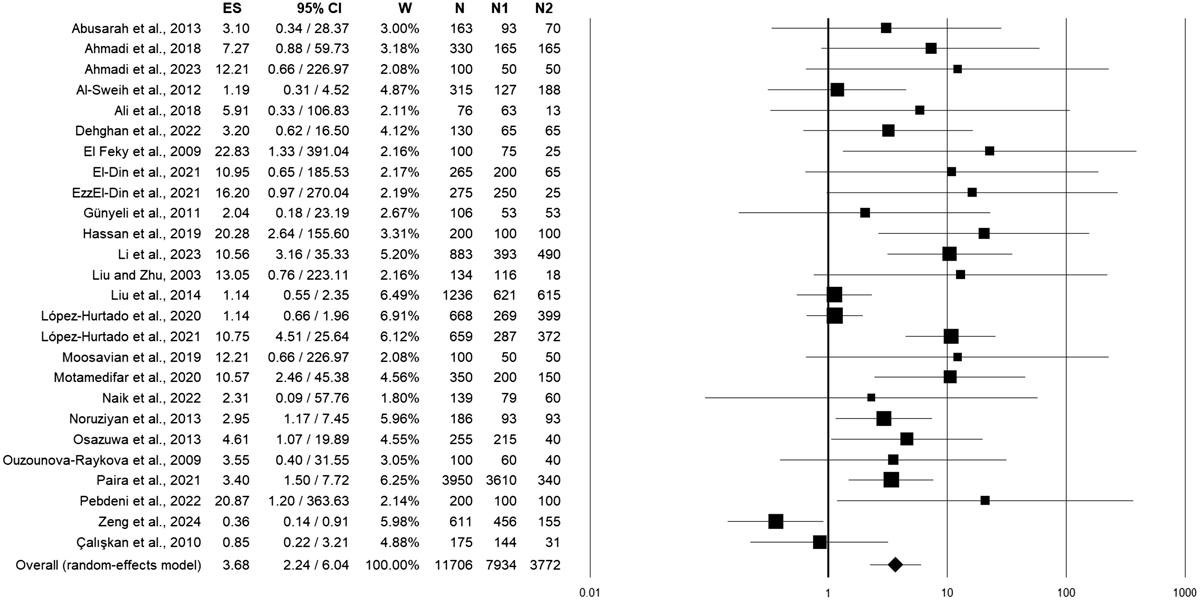
OA12.06 – The HIV and Sexually Transmitted Infection Syndemic Following Mass Scale-Up of Combination HIV Interventions in Two Communities in Southern Uganda: A Population-Based Cross-Sectional Study
Miss Jacqueleen Kyolaba1, Dr Isaac Ddumba1
1African Research Center 4 Ageing & Dementia, Kampala, Uganda.
Background: Combination HIV prevention and treatment interventions (CHIs) have led to substantial declines in HIV incidence in sub-Saharan Africa; however, population-level data on non-HIV sexually transmitted infections (STIs) in the context of CHIs are rare. We aimed to assess STI burden following scale-up of CHIs in Uganda.
Methods: The Sexually Transmitted Infection Prevalence Study (STIPS) was a cross-sectional study nested within a population-based cohort among inland agrarian and Lake Victoria fishing populations in southern Uganda. STIPS enrolled consenting residents aged 18–49 years in two communities (one inland and one fishing) between May and October, 2019, and measured the prevalence of chlamydia, gonorrhoea, trichomonas, syphilis, and herpes simplex virus 2 (HSV-2).
Results: Between May 27, 2019 and Oct 25, 2019, STIPS enrolled 1825 participants. HIV prevalence was 14.0% among the inland population and 39.8% among the fishing population, with about 90% HIV viral load suppression in both communities. Among inland and fishing populations, chlamydia prevalence was 9.6% (95% CI 7.9–11.7) and 9.9% (8.1–12.0), gonorrhoea prevalence 5.0% (3.8–6.7) and 8.4% (6.8–10.5), trichomonas prevalence 9.4% (7.7–11.5) and 12.2% (10.2–14.5), and HSV-2 prevalence 43.0% (39.9–46.3) and 64.4% (61.3–67.6), respectively. In the fishing population, syphilis seropositivity was 24.2% (21.5–27.2) with 9.4% (7.7–11.5) having high-titre (rapid plasma reagin ≥1:8) infection, including 16.9% (11.9–24.0%) of men living with HIV. Prevalence of at least one curable STI (chlamydia, gonorrhoea, trichomonas, or high-titre syphilis) was 51% higher among people living with HIV (vs HIV negative; adjusted prevalence risk ratio [PRR] 1.51; 95% CI 1.27–1.78), including among pregnant women (adjusted PRR 1.87, 1.11–3.17), with no differences by HIV suppression status.
Conclusion: Despite near universal HIV treatment, STI burden remains extremely high in southern Uganda, particularly among people living with HIV. There is an urgent need to integrate STI care with HIV services in African settings.
OA13.01 – Features of Mpox in Fully Vaccinated People: An Outbreak Investigation, New South Wales, Australia, June – November 2024
Dr. Ned Latham1, Ms Jennifer Pett1, Dr Anthea L. Katelaris2, Prof David J. Templeton3,4,5, Ms Ellen J. Donnan1,5, Prof Janaki Amin1,4,6, Dr Jen Kok7,8, Dr Jessica Wells1, Dr Kingsley King-Gee Tam5,7, Dr Leena Gupta3, A/Prof Matthew O'Sullivan5,7,8, Dr Phillip Read2,4, Dr Rebecca J. Rockett58, Dr Vendula Blaya-Novakova3, Dr Vicky Sheppeard2,5, A/Prof Vincent J. Cornelisse4,9, Prof Vitali Sintchenko5,8, Prof William Rawlinson8,10, Dr Christine E. Selvey1
1NSW Ministry of Health, Sydney, Australia.
2South Eastern Sydney Local Health District, Sydney, Australia.
3Sydney Local Health District, Sydney, Australia.
4The Kirby Institute UNSW, Sydney, Australia.
5The University of Sydney, Sydney, Australia.
6Macquarie University, Sydney, Australia.
7Western Sydney Local Health District, Sydney, Australia.
8NSW Health Pathology, Sydney, Australia.
9Mid North Coast Local Health District, Port Macquarie, Australia.
10The University of New South Wales, Sydney, Australia.
Background: Since 2022, clade IIb mpox outbreaks have occurred in previously non-endemic countries, primarily amongst men who have sex with men. Two doses of modified vaccinia Ankara vaccine (MVA) are recommended for people at risk. Infections in fully vaccinated people have been infrequently described. Consequently, evidence that MVA-induced antibodies wane within a year remains of unclear clinical significance. We aimed to describe mpox cases arising during an outbreak in New South Wales (NSW), and to determine whether vaccination was associated with less severe disease.
Methods: We included all mpox cases notified in NSW between 20 June and 20 November 2024 in this outbreak investigation. Cases and their clinicians were interviewed to obtain epidemiologic and clinical information. We used logistic regression to explore the relationship between factors indicative of exposure risk and/or likelihood of testing and being fully vaccinated. Risk ratios were calculated for clinical outcomes. Some specimens underwent whole genome sequencing.
Results: There were 674 confirmed cases notified. All sequenced specimens (n = 102, 15.1%) were clade IIb. Vaccination status was ascertained for most (n = 663, 98.4%) with 37.9% fully vaccinated, 10.9% partially vaccinated, and 51.3% unvaccinated. Median time between vaccination and symptom onset was 21.8 months (IQR 19.5–23.0 months). Factors independently associated with being fully vaccinated (Table 1) included sex on premises venue attendance (aOR 1.69 [95% CI 1.15–2.48]) and having a sexually transmissible infection notified in the past year (aOR 1.63 [1.14–2.33]). Compared to unvaccinated cases, those who received two MVA doses were less likely to be hospitalised (RR 0.11 [95% CI 0.03–0.43]), have extragenital lesions (RR 0.45 [0.36–0.56]) or prodromal symptoms (RR 0.72 [0.64–0.80]).
Conclusion: Being fully vaccinated was associated with factors suggestive of greater exposure risk and/or likelihood of testing. Two MVA doses reduced the risk of disseminated disease and hospitalisation, including amongst cases vaccinated more than 1.5 years prior.
| Fully vaccinatedA | Univariable analysis | Multivariable analysis | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Yes n = 251B | No n = 412B | OR | 95% CI | P-value | aORC | 95% CI | P-value | ||
| Age group | <0.001 | 0.002 | |||||||
| 19–29 yrs | 21 (8.4%) | 96 (23.3%) | — | — | — | — | |||
| 30–39 yrs | 119 (47.4%) | 179 (43.4%) | 3.04 | 1.83, 5.25 | <0.001 | 2.44 | 1.42, 4.33 | 0.002 | |
| 40–49 yrs | 68 (27.1%) | 82 (19.9%) | 3.79 | 2.17, 6.83 | <0.001 | 2.90 | 1.59, 5.44 | <0.001 | |
| 50 yrs + | 43 (17.1%) | 55 (13.3%) | 3.57 | 1.95, 6.73 | <0.001 | 2.95 | 1.51, 5.87 | 0.002 | |
| Born overseas | 111 (45.5%) | 212 (53.1%) | 0.74 | 0.53, 1.01 | 0.060 | 0.74 | 0.52, 1.05 | 0.10 | |
| Postcode IRSAD quintile | <0.001 | 0.5 | |||||||
| 5 (most advantaged) | 193 (77.8%) | 245 (60.9%) | — | — | — | — | |||
| 4 | 37 (14.9%) | 89 (22.1%) | 0.53 | 0.34, 0.80 | 0.003 | 0.73 | 0.43, 1.22 | 0.2 | |
| 3 | 8 (3.2%) | 28 (7.0%) | 0.36 | 0.15, 0.78 | 0.014 | 0.53 | 0.19, 1.36 | 0.2 | |
| 2 | 5 (2.0%) | 23 (5.7%) | 0.28 | 0.09, 0.68 | 0.010 | 0.52 | 0.14, 1.55 | 0.3 | |
| 1 (least advantaged) | 5 (2.0%) | 17 (4.2%) | 0.37 | 0.12, 0.96 | 0.057 | 0.65 | 0.19, 1.93 | 0.5 | |
| Resident of postcode with >5% gay male population | 179 (72.2%) | 215 (53.3%) | 2.27 | 1.62, 3.20 | <0.001 | 1.70 | 1.07, 2.71 | 0.024 | |
| Recent sex on premises venue attendance | 88 (35.2%) | 89 (22.2%) | 1.90 | 1.34, 2.71 | <0.001 | 1.69 | 1.15, 2.48 | 0.008 | |
| STI notified within the past year | 155 (61.8%) | 184 (44.7%) | 2.00 | 1.45, 2.76 | <0.001 | 1.63 | 1.14, 2.33 | 0.007 | |
| Diagnosed at a public sexual health or s100 clinic | 209 (83.3%) | 286 (69.4%) | 2.19 | 1.49, 3.27 | <0.001 | 2.34 | 1.54, 3.61 | <0.001 | |
OR, odds ratio; CI, confidence interval; aOR, adjusted odds ratio; IRSAD, Index of Relative Socio-economic Advantage and Disadvantage; STI, sexually transmissible infection (N. gonorrhoea, C. trachomatis, or syphilis of less than 2 years duration); s100, section 100 provider (a clinician accredited to prescribe specialised drugs including antiviral medications for HIV and viral hepatitis.
OA13.02 – Evaluating Presumptive Antibiotic Treatment for Gonorrhea: Towards a Tailored Approach
Dr. Dieuwertje L. Horsten1,3,4,5, Dr. Ymke J. Evers1,3, Dr. Petra F. G. Wolffs3, Dr. Nicole H. T. M. Dukers-Muijrers1,3, Prof. Dr. Christian J. P. A. Hoebe1,3,5
1South Limburg Public Health Service, Heerlen, The Netherlands.
2Consortium of Academic WorkplacesCollaborative Academic practice for Public health Infectious diseases (CAPI), Heerlen, The Netherlands.
3Maastricht University, Maastricht, The Netherlands.
4Brabant-Zuidoost Public Health Service, Eindhoven, The Netherlands.
5Collaborative Academic practice for Public health Infectious diseases (CAPI).
Introduction: Gonorrhea, caused by Neisseria gonorrhoeae (NG), poses a significant global health challenge due to increasing incidence and growing antimicrobial resistance. While international guidelines recommend presumptive antibiotic treatment before laboratory-confirmed diagnosis, this practice is increasingly debated in well-resourced settings like the Netherlands. Concerns center around overtreatment and its contribution to antibiotic resistance. This study aims to optimize presumptive treatment for NG by examining its prevalence, accuracy, and behavioral and clinical factors influencing its accuracy.
Methods: This retrospective cohort study analyzed systematically registered consultation data (2014–2023) from a public health STI clinic in the Netherlands. Variables included demographics, sexual history, symptoms, antibiotic treatments, and laboratory test results. Presumptive treatment was defined as NG testing and treatment with intramuscular ceftriaxone performed simultaneously, or treatment occurring before laboratory confirmation. Accurate presumptive treatment was defined as presumptive treatment corresponding to a positive NG test result. Descriptive statistics assessed treatment accuracy, and logistic regression will identify factors associated with accurate presumptive treatment.
Results: Among 82,695 consultations, 4.2% (n = 3693) involved treatment with intramuscular ceftriaxone. In 3377 cases, testing and treatment dates were available: 44.8% (n = 1514) was presumptively treated, and 55.2% (n = 1863) was treated based on laboratory results. Of those presumptively treated, 67.4% (n = 1021) tested NG positive, indicating accurate presumptive treatment, while 32.6% (n = 493) was NG negative, representing inaccurate presumptive treatment. Statistical analyses to identify predictors of accurate presumptive treatment are ongoing.
Conclusion: These results indicate that presumptive treatment accurately targets NG in most cases but also leads to significant overtreatment. Optimizing presumptive treatment strategies is critical to balancing timely care with antimicrobial stewardship. Further analyses will provide insights into factors influencing treatment accuracy to guide evidence-based practices.
OA13.03 – Real-World Outpatient Diagnostic Testing and Treatment Patterns Among People with Vaginitis Symptoms in the United States
Dr. Rebecca Lillis1, Mr. Justin Chen2, Ms. Jenny Tse2, Dr. Mindy Cheng3, Dr. Diane Kawa3, Mr. Liucheng Shi2, Ms. Aimee Near2
1LSU Health Sciences Center, New Orleans, United States.
2IQVIA, Durham, United States.
3Cepheid, Sunnyvale, United States.
Background: Despite available vaginitis diagnostic tests, including traditional methods, direct probe, and nucleic acid amplification tests (NAATs), longer turnaround times for laboratory tests may result in empiric treatment. This study retrospectively assessed real-world treatment patterns for bacterial vaginosis (BV), vulvovaginal candidiasis (VVC) and trichomoniasis (TV) relative to test result timing.
Methods: Analysis was conducted using IQVIA’s Ambulatory EMR (AEMR) linked to longitudinal prescription (LRx) and outpatient medical (Dx) claims databases. Patients were identified from 1/1/2018 to 12/2/2023. The date of first vaginitis diagnosis or related symptom presentation was the index visit. Patients with or without evidence of pregnancy were stratified into mutually exclusive subgroups by test type (NAAT panel [BV, VVC and TV], direct probe, or traditional methods) performed at index visit. Treatments filled before (empiric) and up to 7 days after (informed) the test result date were assessed.
Results: The study identified 1,465 pregnant and 13,447 non-pregnant patients with vaginitis test results. Of these, 31.7%, 26.3% and 2.0% of the pregnant and 26.6%, 16.1% and 2.0% of the non-pregnant cohorts tested positive for BV, VVC and TV, respectively; fewer positive results were documented for traditional methods (Table 1). Empiric treatment was common across pregnant (35.5–66.7%) and non-pregnant (52.2–74.2%) cohorts. Among patients who later had positive BV/VVC/TV results, empiric treatments for other etiologies were observed. For example, 6.5–8.2% of pregnant and 11.7–13.0% of non-pregnant patients who tested BV-positive by NAAT panel or direct probe had empiric treatment indicated for VVC or TV only. Among pregnant and non-pregnant subgroups with BV+VVC mixed infection, empiric treatment typically did not address both etiologies.
Conclusion: The high rates of empiric treatment and evidence of inappropriate treatment highlight an unmet need for rapid and accurate tests to diagnose the most common vaginal infections, including mixed infections, and inform clinical decision-making and results-guided prescribing at point-of-care.
| Pregnant cohort (N = 1,465) | Non-pregnant cohort (N = 13,447) | ||||||
|---|---|---|---|---|---|---|---|
| Subgroup 1 NAAT panel N = 509 | Subgroup 2 Direct probe A N = 807 | Subgroup 3 Traditional methods B N = 149 | Subgroup 1 NAAT panel N = 3,800 | Subgroup 2 Direct probe N = 7,790 | Subgroup 3 Traditional methods N = 1,857 | ||
| With evidence of treatment from index date to test result date + 7 days (n, %)A | 231 (45.4%) | 389 (48.2%) | 72 (48.3%) | 1,846 (48.6%) | 4,066 (52.2%) | 717 (38.6%) | |
| With evidence of empiric treatmentD | 127 (55.0%) | 138 (35.5%) | 48 (66.7%) | 1,028 (55.7%) | 2,122 (52.2%) | 533 (74.2%) | |
| With evidence of informed treatmentE | 126 (54.5%) | 280 (72.0%) | 33 (45.8%) | 1,036 (56.1%) | 2,468 (60.7%) | 261 (36.4%) | |
| Among patients with specific positive test result, evidence of empiric treatment4(i.e., before test result date) | |||||||
| Patients who tested positive for BV (n, %) | 124 (24.4%) | 340 (42.1%) | 1 (0.7%) | 617 (16.2%) | 2,939 (37.7%) | 15 (0.8%) | |
| With no empiric treatment | 83 (66.9%) | 269 (79.1%) | 0 (0%) | 424 (68.7%) | 2,004 (68.2%) | 6 (40.0%) | |
| With BV treatmentF | 33 (26.6%) | 43 (12.6%) | 1 (100.0%) | 121 (19.6%) | 553 (18.8%) | 9 (60.0%) | |
| With other treatment (i.e., for TV or VVC) | 8 (6.5%) | 28 (8.2%) | 0 (0%) | 72 (11.7%) | 382 (13.0%) | 0 (0%) | |
| Patients who tested positive for VVC (n, %) | 128 (25.1%) | 228 (28.3%) | 29 (19.5%) | 817 (21.5%) | 1,204 (15.5%) | 139 (7.5%) | |
| With no empiric treatment | 85 (66.4%) | 167 (73.2%) | 19 (65.5%) | 500 (61.2%) | 672 (55.8%) | 60 (43.2%) | |
| With VVC treatmentG | 38 (29.7%) | 50 (21.9%) | 9 (31.0%) | 285 (34.9%) | 481 (40.0%) | 71 (51.1%) | |
| With other treatment (i.e., for BV or TV) | 5 (3.9%) | 11 (4.8%) | 1 (3.4%) | 32 (3.9%) | 51 (4.2%) | 8 (5.8%) | |
| Patients who tested positive for TV (n, %) | 18 (3.5%) | 11 (1.4%) | 0 (0%) | 121 (3.2%) | 143 (1.8%) | 5 (0.3%) | |
| With no empiric treatment | 10 (55.6%) | 9 (81.8%) | – | 85 (70.2%) | 85 (59.4%) | 3 (60.0%) | |
| With TV treatmentH | 5 (27.8%) | 1 (9.1%) | – | 21 (17.4%) | 37 (25.9%) | 1 (20.0%) | |
| With other treatment (i.e., for BV or VVC) | 3 (16.7%) | 1 (9.1%) | – | 15 (12.4%) | 21 (14.7%) | 1 (20.0%) | |
| Patients who tested positive for BV + VVC (n, %) | 16 (3.1%) | 101 (12.5%) | 0 (0%) | 88 (2.3%) | 499 (6.4%) | 0 (0%) | |
| With no empiric treatment | 11 (68.8%) | 71 (70.3%) | – | 57 (64.8%) | 277 (55.5%) | – | |
| With BV + VVC treatmentI | 1 (6.3%) | 7 (6.9%) | – | 8 (9.1%) | 37 (7.4%) | – | |
| With other treatment (i.e., for TV or only one of BV or VVC) | 4 (25.0%) | 23 (22.8%) | – | 23 (26.1%) | 185 (37.1%) | – | |
OA13.04 – Are Clinicians Open to Less Asymptomatic STI Testing for Chlamydia and Gonorrhoea in Men Who Have Sex with Men (MSM) and the Possibility of Not Treating Positive Diagnoses? A Qualitative Study from Australia
Dr. Teralynn Ludwick1, Ethan T. Cardwell1, Dr. Tin Vo2, Dr. Eric P.F. Chow3,4, Benjamin Riley5, Dr. Jane S. Hocking1, Dr. Daniel Grace2, Dr. Fabian YS Kong1
1University of Melbourne, Melbourne, Australia.
2University of Toronto, Toronto, Canada.
3Melbourne Sexual Health Centre, Melbourne, Australia.
4Monash University, Melbourne, Australia.
5AHSM Health, Syndey, Australia.
Background: New evidence from real-world studies suggests that 3 × 3 screening for asymptomatic chlamydia/gonorrhoea is not reducing incidence. Further, frequent testing may drive unnecessary treatment of asymptomatic infections, antibiotic over-consumption and antimicrobial resistance (AMR). Consequently, some countries are considering less frequent testing recommendations. This study explored clinicians’ openness to changing practices around asymptomatic testing for chlamydia/gonorrhoea in MSM and attitudes around not automatically treating positive diagnoses.
Methods: We conducted content analysis of 17 semi-structured interviews with Australian sexual health clinicians working in public/private practice. Interview domains covered: evidence on ‘test and treat’, perspectives on reducing testing and treatment for chlamydia/gonorrhoea in MSM, AMR, and managing patient conversations.
Results: Clinicians acknowledged that ‘test and treat’ has been a mainstay of their practice, but had variable knowledge of the evidence. Many were open to reduced testing, noting lack of clinical harm to MSM and that 3-monthly screening is largely a ‘comfort thing’. Given challenges in reducing medical interventions, clinician time required for patient education, and the ‘emotional response’ to testing, they recommended public education to drive changes in testing frequency.
While some clinicians questioned their ‘knee jerk’ reaction to treating patients and support patient dialogue in electing treatment/‘waiting and seeing’, most clinicians felt uncomfortable not treating. Concerns included: ideas about their role as doctors; onward transmission (particularly to women); and, complications/uncomfortable symptoms/patient psychological well-being. Concerns did not focus on AMR.
Conclusion: While the ‘test and treat’ paradigm is engrained, clinicians were open to reduced testing, if provided with clear evidence, but were generally reluctant to not treat. A flexible approach that supports patient empowerment in decision-making about testing frequency and choices around treatment may represent a productive way forward. Changing practice requires education to shift patient/clinician mindsets around what it means to have a positive chlamydia/gonorrhoea diagnosis and if medical interventions are needed.
OA13.05 – Absence of Viable Chlamydia Trachomatis (CT) Among Men with Rectal Exposures Who Test NAAT-Positive for Rectal CT
Assoc. Prof. Christine Khosropour1, Mr. Robert J. Suchland1, Assoc. Prof. Lucia Vojtech1, Assoc. Prof. Olusegun O. Soge1, Dr. Lindley A. Barbee1
1University of Washington, Seattle, United States.
Background: Behaviors other than receptive anal sex (e.g.,rimming) can lead to positive nucleic acid amplification tests (NAAT) for rectal CT. However, it is unknown how often positive rectal CT NAATs represent true infections (with viable CT) versus detection of nonviable bacteria or cell-free nucleic acid.
Methods: In Seattle, Washington, 2019–2022, we enrolled individuals assigned male sex at birth who reported sex with men and denied receptive anal sex (RAS) in the past 2 years or reported RAS 1–2 years ago but were tested and treated since then. Participants completed a survey that asked about 13 non-RAS rectal exposures and self-collected rectal swabs for CT NAAT, CT culture, and viability-PCR (vPCR). We classified NAAT-positive infections as “viable” if either culture or vPCR were positive. We identified factors associated with viable versus non-viable rectal CT.
Results: Of 277 enrolled men, 28 (10%) tested positive for rectal CT by NAAT but only 36% (n = 10/28) of NAAT-positive specimens were viable. The distribution of most reported behaviors (i.e.,oral-anal contact, use of sex toys, fingering) was similar among those with viable rectal CT vs non-viable rectal CT, though individuals with viable rectal CT more often reported engaging in perianal exposure (partner’s penis touching respondent’s perianal region) compared to those with non-viable rectal CT (60% vs 27%; P = 0.09). Individuals with viable rectal CT also more often had CT at another anatomic site (30% vs 6%; P = 0.08), reported more sex partners in the past 12 months (median 10 vs 2 partners; P = 0.57), and reported more recent rectal exposure (median 21 days before testing vs 42 days; P = 0.39) compared to those without viable CT.
Conclusion: Most rectal CT NAAT-positive results from men with rectal exposures other than RAS are not viable infections. Screening for rectal CT among individuals who report rectal exposures other than RAS is likely not warranted.
OA13.06 – Assessing the Accuracy of Symptomatic Syndrome Screening for Sexually Transmitted Infections: A Comparative Study with Laboratory-Based Diagnostic Testing
Ms. Kyokushaba Judith Ainemukama1, Ms Namusoosa Rita1, Ms Kasone Viola1, Dr. Achii Pamela3, Ms Namakula Aidarayaan1, Dr. Nabadda Susan1, Dr. Mudiope Peter2
1National Health Laboratory and Diagnostic Services, Ministry of Health, Kampala, Uganda.
2AIDS Control Program, Ministry of Health Uganda, Kampala, Uganda.
3Department of Pharmaceuticals and Nature Medicine, Ministry of Health, Kampala, Uganda.
Background: Sexually transmitted infections (STIs) are a significant public health concern in Uganda, often leading to adverse reproductive health outcomes. Symptomatic syndrome screening is widely used in low-resource settings due to its simplicity and cost-effectiveness, but its accuracy compared to laboratory diagnostics remains uncertain. This study assessed the sensitivity, specificity, and reliability of syndromic STI screening among adults in Uganda.
Methods: A cross-sectional study was conducted at six regional referral hospitals in Uganda, enrolling 120 participants presenting with symptoms suggestive of STIs. Syndromic STI screening followed Uganda’s Ministry of Health guidelines, while Gene Xpert® CT/NG and TV assays were used for laboratory confirmation. Gene Xpert®, introduced in Uganda over a decade ago, can be integrated to provide an alternative rapid, cheaper, and accurate test for STI diagnosis. Data analysis was performed to determine the sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) of the syndromic diagnostic testing.
Results: The median age of participants was 28 years (IQR: 24–37); 52% were females, and 26% were people with a positive HIV status, The common symptoms were itching and vaginal discharge (38% each), burning sensation (34%), dysuria (32%), lower abdominal pain (20%), and urethral discharge (8%). 42% of participants had a confirmed positive laboratory STI test result: Neisseria gonorrhoeae (11%), Chlamydia trachomatis (8%), and Trichomonas vaginalis (2%). The syndromic screening had a sensitivity of 87.5%, specificity of 25.8%, PPV of 23.73%, and NPV of 88.68%.
Conclusions: The syndromic test’s low sensitivity, specificity, and positive predictive value, with resultant underdiagnosis or misdiagnosis. This underscores the need for integrating rapid, affordable diagnostic technologies into primary healthcare settings to improve STI management, reduce further transmission and complications.
OA14.01 – Surveillance of Antimicrobial Resistance in Mycoplasma Genitalium, Treatment Outcomes and Factors Associated with Resistance
Miss Kirsty Bennet1, Dr James E C Johnson1, Dr Rachel Pitt-Kendall1, Sandra David1, Dr Michaela J Day1, Fahima Rashid1, Emma Callan1, Dr Laura Viviani1, Dr Katy Sinka1, Dr Sarah Alexander1, Dr Hamish Mohammed1, Dr Helen Fifer1, Dr Michelle J Cole1
1UK Health Security Agency, London, United Kingdom.
Background: Mycoplasma genitalium is a bacterial sexually transmitted infection which can cause serious complications if untreated. There is global public health concern about antimicrobial resistance (AMR) to the recommended first- and second-line treatments of azithromycin (a macrolide) and moxifloxacin (a fluoroquinolone) but data on the prevalence and risk factors of AMR are limited.
Methods: From 1 March to 30 June 2023, M. genitalium-positive specimens were collected at 28 sexual health services in England. Specimens were tested for molecular markers predictive of macrolide and fluoroquinolone resistance in the 23S rRNA and parC genes, respectively. AMR data were linked to patient demographic and treatment outcome data. Risk factors for AMR were assessed through multivariable logistic regression.
Results: Of the specimens included, 62.2% (523/841) showed macrolide resistance, 12.1% (98/807) exhibited fluoroquinolone resistance, and 10.1% (78/772) demonstrated dual resistance.
Resistance frequency differed between demographic groups (Table 1). Specimens from GBMSM had increased odds of macrolide resistance compared to those from heterosexual men (adjusted odds ratio (aOR) 3.07; P < 0.001). When compared to those of white ethnicity, macrolide resistance was more likely among those of Asian (aOR 2.44; P = 0.034) or mixed (aOR 2.04; P = 0.017) ethnic groups. Fluoroquinolone resistance was more likely in specimens from those of Asian ethnicity (aOR 2.34; P = 0.037).
Most individuals (89.6%) were prescribed the recommended first or second-line treatments. Despite high levels of macrolide resistance, 69.8% of those with macrolide-resistant infections were known or assumed to be clinically cured with azithromycin. Among fluoroquinolone-resistant infections, 79.4% had or were assumed to have successful treatment with moxifloxacin.
Conclusion: This is the largest dataset examining AMR in M. genitalium in England, confirming widespread macrolide resistance and concerning levels of fluoroquinolone and dual resistance. As well as providing data to inform treatment guidelines, this analysis has identified factors associated with AMR.
| Antimicrobial | Factors | Resistant (n) | Susceptible | Total (N) | Resistant (n of N), % | Adjusted odds ratio | 95% confidence intervals | P-value | |
|---|---|---|---|---|---|---|---|---|---|
| Macrolide resistance | Gender and sexual orientation | ||||||||
| Het. men | 204 | 156 | 360 | 56.67 | reference | ||||
| GBMSM | 103 | 28 | 131 | 78.63 | 3.07 | 1.86–5.04 | <0.001 | ||
| Women | 127 | 88 | 215 | 59.07 | 1.08 | 0.75–1.57 | 0.671 | ||
| Ethnic group | |||||||||
| White | 196 | 131 | 327 | 59.94 | reference | ||||
| Asian | 30 | 8 | 38 | 78.95 | 2.44 | 1.07–5.55 | 0.034 | ||
| Black | 105 | 88 | 193 | 54.40 | 0.92 | 0.63–1.35 | 0.667 | ||
| Mixed | 52 | 19 | 71 | 73.24 | 2.04 | 1.14–3.65 | 0.017 | ||
| Other | 20 | 13 | 33 | 60.61 | 0.96 | 0.45–2.03 | 0.912 | ||
| Fluoroquinolone resistance | Ethnic group | ||||||||
| White | 39 | 255 | 294 | 13.27 | reference | ||||
| Asian | 10 | 28 | 38 | 26.32 | 2.34 | 1.05–5.18 | 0.037 | ||
| Black | 14 | 171 | 185 | 7.57 | 0.54 | 0.28–1.02 | 0.056 | ||
| Mixed | 5 | 62 | 67 | 7.46 | 0.53 | 0.20–1.39 | 0.197 | ||
| Other | 2 | 25 | 27 | 7.41 | 0.52 | 0.12–2.30 | 0.391 | ||
OA14.02 – Revealing the Importance of gyrA, gyrB, parC and parE Genes Against Fluoroquinolone Resistance in Mycoplasma Genitalium by in Vitro Selection
Ms. Tessa Doelman1,2, Ms. Nikki Adriaens2,3, Ms. Anisha Bhaggan1, Dr. Sylvia Bruisten2,3, Dr. Brenda Westerhuis2,3, Ms. Fenna Bouwman3, Dr Clarissa Vergunst3,4, Dr. Alje van Dam1,2,3
1Amsterdam University Medical Center, Amsterdam, Netherlands.
2Amsterdam Institute for Immunology and Infectious Diseases, Amsterdam, Netherlands.
3Public Health Service of Amsterdam, Amsterdam, Netherlands.
4NWZ, Den Helder, Netherlands.
Background: Mycoplasma genitalium (MG) is sexually transmitted and associated with urethritis in men. A global increase of fluoroquinolone resistant MG has been found in recent years. Fluoroquinolone resistant-associated mutations (FRAM) in parC and gyrA genes have been primarily found through molecular techniques, but are phenotypically not well defined. We aimed to discover the relation between in vitro fluoroquinolone resistance and mutations found in the gyrA, gyrB, parC and parE genes of MG using in vitro selection.
Methods: Reference strain G37 and isolate MG182 containing a parC mutation (S83I) isolated from a patient were tested on their MIC against fluoroquinolones. These isolates were then subjected to subinhibitory concentrations of levofloxacin, moxifloxacin and sitafloxacin. Isolates were subcultured in the presence of stepwise twofold increasing concentrations of antibiotics until the isolate was able to grow beyond the previously measured MIC. Isolates were then sequenced for mutations in gyrA, gyrB, parC and parE regions. Mutated isolates were retested for MIC against fluoroquinolones.
Results: In total 16 mutated isolates were created. Four isolates of the mutated reference strain contained a single codon insertion in the parE gene (+M469/+L471). This extra codon increased the MIC for levofloxacin (4 to 16–32), moxifloxacin (0.25 to 1–4) and sitafloxacin (0.25 to 1) (Table 1). Eleven subsequently obtained isolates contained secondary mutations in the gyrA (D99Y/G93C/M95I/M95V/D94G) or gyrB (D443N/D443G/P462S/E483D) genes. Combinations of the additional parE codon and gyrA or gyrB mutations further increased the MIC for levofloxacin (≥64), moxifloxacin (4–>16) and sitafloxacin (>2). One secondary mutation in gyrA (G93C) was obtained into isolate MG182, increasing MIC for levofloxacin (8 to 64), moxifloxacin (0.5 to 16) and sitafloxacin (0.25 to >2).
Conclusion: Using in vitro selection culture we provided evidence for the importance of secondary mutations as well as the involvement of parE and gyrB mutations in fluoroquinolone resistance.
| Strain/isolate | Primary mutation (parC/parE) | Secondary mutation (gyrA/gyrB) | Antibiotic selection | MIC LVX (mg/L) | MIC MXF (mg/L) | MIC STFX (mg/L) | |
|---|---|---|---|---|---|---|---|
| G37 | Wildtype | Wildtype | – | 2 | 0.25 | 0.25 | |
| +M469 (parE) (n = 4) | Wildtype (n = 3) | LVX | 16–32 | 1–4 | >0.25–1 | ||
| M95V (gyrA) (n = 1) | LVX | 64 | 4 | >1 | |||
| +L471 (parE) (n = 7) | G93C (gyrA) (n = 1) | LVX | >64 | 16 | >2 | ||
| M95I (gyrA) (n = 1) | LVX | >64 | >16 | 2 | |||
| P462S (gyrB) (n = 1) | MXF | 64 | 16 | 2 | |||
| D443G (gyrB) (n = 1) | LVX | >64 | 16 | >0.25 | |||
| D443N (gyrB) (n = 1) | MXF | >64 | >16 | >0.5 | |||
| E483D (gyrB) (n = 2) | MXF | 64 | 16 | 1->2 | |||
| G81C (parC) (n = 1) | D99Y (gyrA) (n = 1) | MXF | >64 | 16 | >2 | ||
| MG182 | S83I (parC) (n = 2) | Wildtype (n = 1) | – | 8 | 0.5 | 0.25 | |
| G93C (gyrA) (n = 1) | MXF | 64 | 16 | >2 |
OA14.03 – Impact of Antibiotic Treatment on Pena Diversity in Oropharyngeal Neisseria Species
Mr. Sem Vellema1,2, Prof. Dr. Christian Hoebe1,3, Mr. Mayk Lucchesi1,2, Prof. Dr. Paul Savelkoul1,2, Dr. Petra Wolffs1,2
1Care and Public Health Research Institute, Maastricht University, Maastricht, Netherlands.
2Maastricht University Medical Center, Maastricht, Netherlands.
3Living Lab Public Health Mosa, South Limburg Public Health Service, Heerlen, Netherlands.
Background: Ceftriaxone-resistant Neisseria gonorrhoeae (NG) poses a significant challenge to effective first-line empirical treatment of gonorrhoea. Resistance is partially conferred through mosaic penA alleles, primarily acquired via transformation of DNA from commensal Neisseria species (CNS) colonizing the oropharynx. CNS may act as reservoirs for resistance; however, not much is known about the impact of ceftriaxone exposure on the penA resistome of CNS. This study aims to assess the genetic diversity of the penA gene among commensal Neisseria species in the oropharynx before and after antibiotic treatment.
Methods: 96 oropharyngeal swabs were collected from 10 patients attending the STI clinic of the Public Health Service South-Limburg between 2019 and 2021, selected based on frequency of positive PCR tests for NG. Samples taken before and after antibiotic treatment resulted in 34 sample pairs. Targeted sequencing of the penA gene was performed using Nanopore sequencing, including flanking regions for Neisseria species identification. Sequence alignment was conducted using Clustal Omega, and genetic distances were calculated using TN93 metrics to quantify variations in penA sequences. Analysis of Molecular Variance (AMOVA) was utilized to evaluate genetic variance attributable to antibiotic treatment.
Results: AMOVA analysis across 34 sample pairs (before and after treatment) revealed a mean R2 value of 0.603 [95% Confidence Interval 0.488–0.718], indicating that 60.3% of the variation in genetic distances was explained by treatment status.
Conclusion: Our research suggests that treatment with ceftriaxone may lead to significant genetic differentiation of penA alleles in commensal Neisseria species. This highlights the potential role of CNS as reservoirs for antimicrobial resistance (AMR) and emphasizes the importance of genetic monitoring of CNS. Future research should focus on linking specific commensal species to genetic differentation and assessing whether post-treatment genetic variation correlates with AMR.
OA14.04 – In Vitro Activity and Resistance Mechanism of Gepotidacin Against Neisseria Gonorrhoeae with Decreased Susceptibility or Resistance to Extended-Spectrum Cephalosporins in Nanjing, China (2013 to 2021)
MD.PhD Jiaojiao Zhong1, MS Wenjing Le1, PhD Caroline Genco2, MD. Peter Rice3, MD.PhD Xiaohong Su1
1Hospital for Skin Diseases and Institute of Dermatology, Chinese Academy of Medical Sciences, Nanjing, China.
2Department of Immunology, Tufts University School of Medicine, Boston, USA.
3Division of Infectious Diseases and Immunology, Department of Medicine, University of Massachusetts Chan Medical School, Worcester, USA.
Background: Gepotidacin, a novel triazaacenaphthylene bacterial type II topoisomerase inhibitor, exhibits potent bactericidal activity against Neisseria gonorrhoeae (Ng).
Methods: 283/1526 (19%) Ng isolates collected in Nanjing (2013 to 2021), exhibited decreased susceptibility or resistance to extended cephalosporins (ESCs) and were tested for susceptibility to gepotidacin. N. gonorrhoeae with gepotidacin MICs ≥ 1 mg/L were evaluated for synergy of gepotidacin combined with ceftriaxone, cefixime, spectinomycin or gentamicin and fractional inhibitory concentration indices (FICIs) determined to classify synergy. Sub-inhibitory concentrations of gepotidacin were used to induce resistance of strain ATCC 49226 by successive passages: antimicrobial resistance (AMR) genes were sequenced and amino acid counterparts determined.
Results: The MIC range, MIC50, and MIC90 of gepotidacin for the 283 ESC-resistant isolates were 0.03-4 mg/L, 0.25 mg/L, and 1 mg/L, respectively. 35 isolates with gepotidacin MICs ≥1 mg/L tested in combination with ceftriaxone, cefixime, spectinomycin or gentamicin showed synergistic effects in 54.3%, 68.6%, 22.9% and 25.7% of isolates, respectively. The mean FICI values of the antibiotic combinations were 0.580, 0.494, 0.714 and 0.608 respectively, indicating synergy for the gepotidacin/cefixime combination and indifference in the others. Twenty successive subpassages of Ng ATCC 49226 resulted in an increase of gepotidacin MIC from 0.5 mg/L to 20 mg/L. By the 3rd subpassage, mutations had developed in GyrA (S91F and D95A), ParC (G85C) and Protein-Binding Protein 2 (PBP 2) (the penA gene product) (N513Y), which remained at the 20th subpassage. A loss of a mutation in PBP 2 (A517G) also occurred.
Conclusions: Gepotidacin demonstrated potent in vitro antimicrobial activity (MICs 1 mg/L) against 248/283 (87.6%) Ng isolates that exhibited decreased susceptibility or resistance to ESCs. The remaining 35 gepotidacin-resistant (MICs ≥1 mg/L) isolates showed synergy when tested in combination with cefixime. Successive passage of Ng ATCC 49226 in subinhibitory concentrations of gepotidacin produced incremental MICs.
OA14.05 – Comparing Cefixime and Penicillin G for Early Syphilis: Rapid Plasma Reagin Titer Decline and Preliminary Treatment Outcomes
Ms. Gjermayne Wilson1, Ms. Kori Keith1, Chrysovalantis Stafylis, Kelika Konda, Jeffrey Klausner
1University of Southern California, Los Angeles, United States.
Background: Syphilis is a global health problem. Benzathine penicillin G (penicillin) is the standard treatment for early syphilis; however, a prior pilot study found oral cefixime likely efficacious, leading us to conduct a larger clinical trial to evaluate cefixime as a potential treatment alternative.
Methods: We are conducting a randomized, open-label, non-inferiority multisite clinical trial comparing the efficacy of cefixime (400 mg orally, twice daily for 10 days) to penicillin (2.4 million units intramuscularly) in participants with and without human immunodeficiency virus (HIV). During penicillin shortages, doxycycline hyclate (100 mg orally, twice daily for 14 days) was used instead of penicillin. Participants were evaluated at 3-, 6-, and 9-months. Primary outcome is defined as ≥4-fold decline in rapid plasma reagin (RPR) titers by 6 months. Treatment failure is defined as insufficient RPR decline, a ≥4-fold increase, or symptom recurrence.
Results: As of December 17, 2024, 156 participants were enrolled (78 received cefixime, 70 received penicillin, and 8 received doxycycline), with 67.3% living with HIV and 93.5% identifying as men who have sex with men or transgender women. Reported 10-day cefixime adherence was 92.3% (62/67).
Treatment success across treatment arms by 6 months is: 89.5% for cefixime, 96.0% for penicillin, and 100% for doxycycline (Fig. 1).
Eight participants (7.0%) experienced treatment failure: 6 cefixime participants – 2 without HIV (≥4-fold increase) and 4 with HIV (insufficient RPR decline by 6 months), and 2 penicillin participants, both with HIV (insufficient RPR decline by 6 months). There were no observed doxycycline failures (N = 7).
Conclusion: Cefixime and penicillin demonstrated similar efficacy at 6 months. These preliminary findings support study continuation.
Treatment response by 3- and 6- months after treatment initiation among cefixime, penicillin, and doxycycline participants.
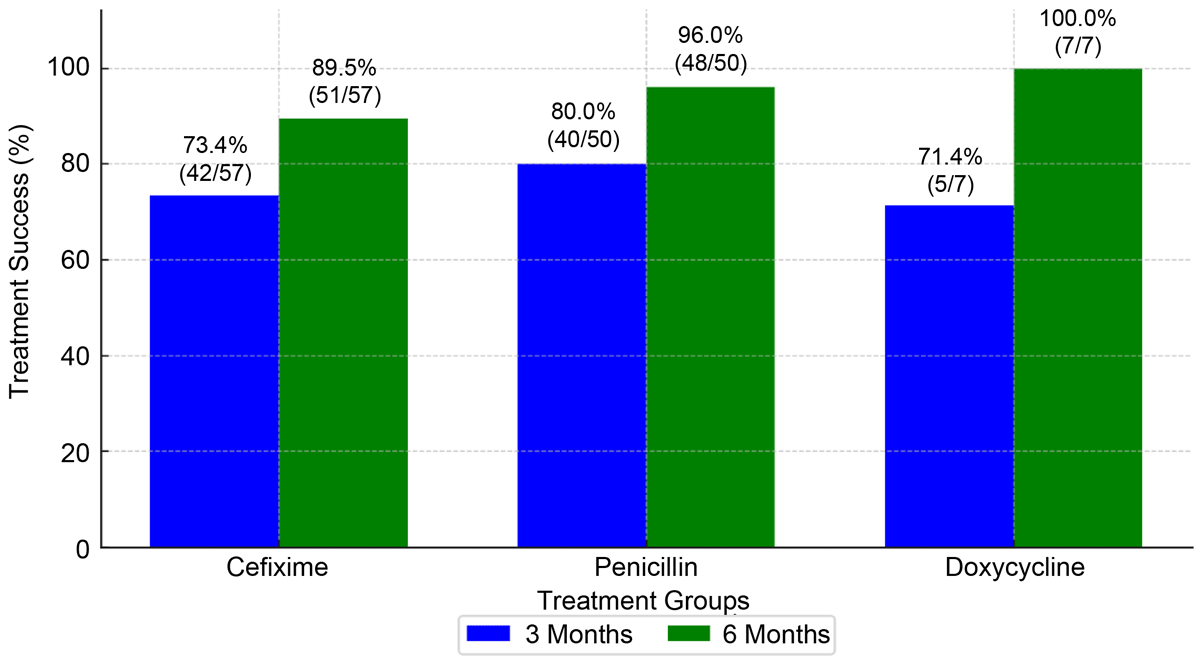
OA14.06 – Screening Antimicrobial Fatty Acids for Treating Oral Gonorrhoea Using a Validated 2D Human Oral Cell Model
Dr. Syed Ameer Hamza1, Ms Rita Paolini1, Ms Caroline Moore1, Prof. Micheal McCullough1, Ms Alyce Mayfosh2, Dr. Thomas Rau2, Prof. Magnus Unemo3,4, Prof. Jane Hocking5, Dr. Antonio Celentano1, Assoc. Prof. Fabian YS Kong5
1Melbourne Dental School, The University of Melbourne, Melbourne, Australia.
2Wintermute Biomedical, Melbourne, Australia.
3WHO Collaborating Centre for Gonorrhoea and other STIs, Örebro University Hospital, Örebro, Sweden.
4Institute for Global Health, University College London, London, UK.
5Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Oropharyngeal Neisseria gonorrhoeae (NG) is associated with higher rates of treatment failure, though the underlying reasons remain unclear. Resistance to the last remaining treatment option, ceftriaxone, is rising, and emerging treatments like zoliflodacin and gepotidacin demonstrate <95% efficacy against oral NG. There is an urgent need for novel therapeutic strategies. To address this, we developed and validated a 2D human oral cell model to study NG infection dynamics and assess the efficacy of five novel fatty acids compounds against a susceptible NG strain (FA1090).
Methods: We infected five human oropharyngeal cell lines (floor of mouth, gingiva, cheek, tonsil, and posterior oropharynx) with susceptible (FA1090) and resistant (WHO-R) NG strains. Model validation included clearing intracellular infections with azithromycin, ceftriaxone, cefixime (but not tetracycline or gentamicin) and demonstrating low invasion rates for the oral commensal N. oralis. The minimum inhibitory concentrations (MIC90), minimum bactericidal concentration (MBC), and cellular cytotoxicity for five fatty acid compounds were determined. The most promising compounds (low MIC and toxicity) were tested for their ability to clear NG infections after 30, 60 and 120 min of exposure.
Results: Undecanoic and lauric acid emerged as the most effective fatty acid compounds, demonstrating bactericidal activity against FA1090 and WHO-R strains, with MIC90 values of ~22 µg/mL and 42 µg/mL, respectively. Both compounds exhibited no cytotoxicity to oral cells. At 150 µg/mL, lauric acid achieved dose-dependent killing, clearing NG within 60 min, while undecanoic acid displayed time-dependent killing, eradicating NG at 120 min. Importantly, both fatty acids are classified as safe for human consumption by the FDA.
Conclusion: Our findings highlight the potential of lauric and undecanoic acids as effective, non-cytotoxic prevention or treatments for oropharyngeal NG. These compounds could be formulated into chewing gum for pre- or post-exposure use to prevent oral NG transmission, representing a practical approach to reducing NG incidence.
OA15.01 – Evaluating a New in Bacterial STI Partner Management Strategy in Amsterdam, The Netherlands
Mr. Buhari Teker1,2, Prof. dr. Maarten Schim van der Loeff1,3,4,5, Ms. Lois Deden1, Mr. Jason Schouten1, Dr. Elske Hoornenborg1,4, Dr. Vita Jongen1,4,6, Prof. dr. Henry de Vries1,2,4,5
1Public Health Service Of Amsterdam, Amsterdam, The Netherlands.
2Department of Dermatology, Amsterdam UMC location University of Amsterdam, Amsterdam, The Netherlands.
3Department of Internal Medicine, Amsterdam UMC location University of Amsterdam, Amsterdam, The Netherlands.
4Amsterdam Institute for Immunology & Infectious Diseases (AI&I), Amsterdam, The Netherlands.
5Amsterdam Public Health Research Institute (APH), Amsterdam, The Netherlands.
6Stichting HIV Monitoring, Amsterdam, The Netherlands.
Background: Previously at the Centre for Sexual Health Amsterdam, we offered presumptive antibiotic treatment to clients notified for chlamydia or gonorrhoea infection by both steady and non-steady partners. To reduce antibiotic consumption, from 1 March 2020 onwards, presumptive treatment was limited to clients notified by steady partners only. From that moment on, treatment for non-steady partners followed later and was based on positive test results. We evaluated the effects of this new approach on antibiotic consumption and the number of lost-to-follow-up consultations.
Methods: We included consultations with a partner notification between 2017 and 2023. We compared the proportion of consultations where presumptive antibiotic treatment was prescribed before and after 1 March 2020. Additionally, we assessed the time to return to the clinic for treatment of confirmed but not presumptively treated chlamydia and/or gonorrhoea infections.
Results: The proportion of consultations in which individuals received presumptive antibiotic treatment for (later) confirmed chlamydia infections increased from 553/1,368 (40.4%) before 1 March 2020 to 290/614 (47.2%) afterwards (P = 0.005), and for confirmed gonorrhoea infections from 406/1,173 (34.6%) to 250/591 (42.3%) (P = 0.002). After 1 March 2020, chlamydia and gonorrhoea infections were ruled out in 327/441 (74.2%) and 396/496 (79.8%) partner notification consultations, respectively, where presumptive treatment would have previously been provided. In 114/441 (25.9%) and 100/496 (20.2%) of these consultations, chlamydia and gonorrhoea were confirmed, respectively, but no presumptive treatment was provided. After 1 March 2020, individuals who did not receive presumptive treatment but were later diagnosed with chlamydia or gonorrhoea returned for treatment after a median of 6 days (interquartile range, 4–8) following the initial consultation. Three participants with chlamydia (2.6%) and two with gonorrhoea (2.0%) did not return for treatment.
Conclusion: The implementation of the new partner management protocol led to a substantial reduction in unnecessary antibiotic use for clients notified for chlamydia and/or gonorrhoea. The vast majority of confirmed infections were successfully treated.
OA15.02 – A Qualitative Exploration of STI Partner Notification Services Delivery Models Among Key Stakeholders in Rural Southwestern Uganda
Dr. Pooja Chitneni1, Moran Owembabazi2, Eunice Kanini2, Rosemary Kansiime2, Winnie Muyindike2, Lynn Matthews3, Jessica Haberer4
1Brigham And Women’s Hospital, Boston, United States.
2Mbarara University of Science and Technology, Mbarara, Uganda.
3University of Alabama at Birmingham, Birmingham, Alabama, United States.
4Massachusetts General Hospital, Boston, United States.
Background: Comprehensive STI care requires not only patient treatment but STI partner notification (PN) and evaluation to prevent ongoing STI transmission and reinfection. In rural, southwestern Uganda, we explored healthcare practitioners’ views on three STI PN models that focused on task-shifting to non-physician practitioners to inform the development of a novel STI PN services delivery system.
Methods: From September to November 2023, we conducted individual in-depth interviews with 32 participants from 4 categories (8 participants from each category): patients with a self-reported history of having an STI in Uganda, healthcare workers (physicians, nurses, and community health workers), pharmacists, and healthcare administrators (Ministry of Health officials and regional referral hospital administrators). Interviews explored participants’ views on a nursing-based, pharmacy-based, and community-based STI PN models as well as healthcare system tools and needs to facilitate PN (Fig. 1). We used inductive and deductive approaches to generate a codebook guided by the Consolidated Framework for Implementation Research in a thematic analysis.
Results: Ten female and twenty-two male participants participated in individual in-depth interviews. The median age of the patient and healthcare practitioner participants was 32 and 34 years, respectively. We found that 1) the nursing model was widely supported as nurses are trusted to perform a variety of tasks, 2) pharmacies are well-positioned to engage in STI PN as they are early points of contact for patients, incentivized monetarily by PN and patient-delivered partner medication, and have the potential to physically restructure to create private spaces and increase counseling training, 3) the community-based model should center on village health teams and focus on advocacy and education.
Conclusion: Given the high STI incidence globally and in sub-Saharan Africa, exploring innovative STI care models that resonate with patients and healthcare practitioners will be important. Future work includes a Delphi method to refine these models for testing.
OA15.03 – The Impact of Patient Delivered Digital Partner Services Following a Diagnosis of Syphilis
Dr. Anatole Menon-johansson1
1SXT Health CIC, London, United Kingdom.
Background: Syphilis is increasing whilst the number of Disease Intervention Specialists (DIS) delivering partner services is falling. An anonymous digital Partner Notification tool (dPNt) was updated in mid-2024 to provide more detailed partner outcome information. We therefore assessed the contribution of index patients to partner service delivery.
Description: Data from July 14–November 30, 2024, for patients diagnosed with syphilis from United Kingdom clinics was obtained on January 5, 2025. Partner notification outcomes were analysed using spreadsheet pivot tables.
Results: Partners services were delivered using dPNt with 590 patients diagnosed with syphilis across 39 clinics. Seventy nine percent [469/590] of index patients received a dPNt link from the DIS so that they could inform partners using their mobile phone. In both Table 1 columns, 0.59 partners were informed per index patient (PpIP).
Conclusion: When the DIS used dPNt alone, 3× more partners were verified as tested at the time that partner services were initiated when compared to index patients send the dPNt link. When the index patient was enabled to inform partners too, nearly one partner was informed per index patient. Further work is required with DIS, index patients and clinics to improve engagement and verification of partners.
| Partner testing verification | DIS using dPNt [121 index patients] Number (%) | DIS and index patient using dPNt [469 index patients] Number (%) | |
|---|---|---|---|
| Partners reported as tested prior to initiation of partner notification by DIS | 37 (51) | 43 (16) | |
| Partners who self-verify via dPNt | 13 (18) | 177 (64) | |
| Partners verified in clinic via dPNt | 3 (4) | 20 (7) | |
| Partners verified in dPNt follow-up questionnaire by index patient | 0 (0) | 24 (9) | |
| Partners verified during DIS follow-up call | 19 (26) | 13 (5) | |
| Total partners verified as seen and tested | 72 | 277 | |
| Partners notified via dPNt | 48 (0.40 PpIP) | 445 (0.95 PpIP) |
OA15.04 – Factors Associated with Treatment Failure Following Male Partner-Treatment for Bacterial Vaginosis
Dr. Lenka Vodstrcil1,2,3, Dr Erica Plummer1,2, Professor Jane Hocking3, Professor Christopher Fairley1,2, Sid Atkinson2, Natasha Wild1,2, Laura Matthews1,2, Dr Kay Htaik1,2, Professor Matthew Law4, Professor Kathy Petoumenos4, Professor Eric Chow1,2,3, Professor Catriona Bradshaw1,2,3
1School of Translational Medicine, Monash University, Carlton, Australia.
2Melbourne Sexual Health Centre, Carlton, Australia.
3Melbourne School of Population and Global Health, The University of Melbourne, Parkville, Australia.
4Kirby Institute, UNSW Sydney, Kensington, Australia.
5University of Sydney, Camperdown, Australia.
Background: Bacterial vaginosis (BV) recurrence after recommended antimicrobials in women with an ongoing regular sex partner approaches 80%. We have shown by randomised controlled trial (RCT) that male partner-treatment with combination antibiotics reduces recurrence over 3-months (hazard ratio = 0.37, 95% CI: 0.22–0.61, P < 0.001), demonstrating that reinfection is a significant driver and amenable to an intervention. We hypothesised that some women may experience BV persistence following antibiotics and not derive the same benefit from partner-treatment. We combined data from participants in our RCT and pilot studies of male partner-treatment to examine factors associated with detection of BV at Week 4.
Description: Women received recommended therapy and men received combination therapy with oral metronidazole 400 mg and topical 2% clindamycin (for penile application) twice daily for 7 days. Participants completed questionnaires at enrolment, Day 8 and Week 4. Women provided vaginal smears for Nugent scoring. We used Cox regression to assess factors associated with week 4 BV (defined as Nugent score [NS] = 7–10).
Results: Across 165 treated couples, 35 (21%, 95% CI: 15–28%) women had BV at Week 4. At Day 8, 10 women (6%, 95% CI: 3–11%) had a NS of 7–10 and 58 (35%, 95% CI: 28–43%) had NS of 4-10. Having a Day 8 NS of 4–10 was associated with a 4.5-fold increased risk of BV at Week 4, relative to NS of 0–3 (adjusted [A] HR = 4.53, 95% CI: 2.05–10.04, Fig. 1). Women with an intrauterine device (IUD) had an elevated risk of BV at Week 4 (AHR = 2.15, 95% CI: 0.98–4.73) that was of borderline significance.
Conclusion: Male partner-treatment had a substantial impact on reinfection and recurrence, however, the association between non-optimal Day 8 Nugent scores and Week 4 BV, suggests persistence is occurring in a sub-group of women, which may be in part mediated by IUD-use. Partner-treatment in combination with prolonged/alternative regimens for women to target persistent BV-organisms may further improve cure rates.
Factors associated with Bacterial vaginosis (BV) at Week 4, following concurrent female and male partner-treatment. Legend: The rates of BV at Week 4 within each stratum were compared using Cox regression. Adjusted hazard ratios and 95% confidence intervals are displayed for each variable. Couple adherence was defined as <100% if one or both people in the relationship were not 100% adherent to all of the prescribed therapy. Sex during treatment represents self-report of condomless penile-vaginal sex. Hazard ratios were adjusted for all other variables displayed and study group (RCT or pilot study). Due to a correlation with Day 8 NS = 4–10, the adjusted HR for Day 8 NS = 7–10 is derived from a second model that contained all other variables except Day 8 NS = 4–10. **Indicates significantly increased risk of BV at Week 4 (P < 0.001, Day 8 NS of 4–10 vs NS of 0–3); *Indicates increased risk of BV at Week 4 that is of borderline-significance (P = 0.056; IUD-use vs no IUD-use). Key: BV, bacterial vaginosis; CI, confidence interval; IUD, intrauterine device; NS, Nugent score; Rx, treatment; UPVS, unprotected (condomless) vaginal sex.
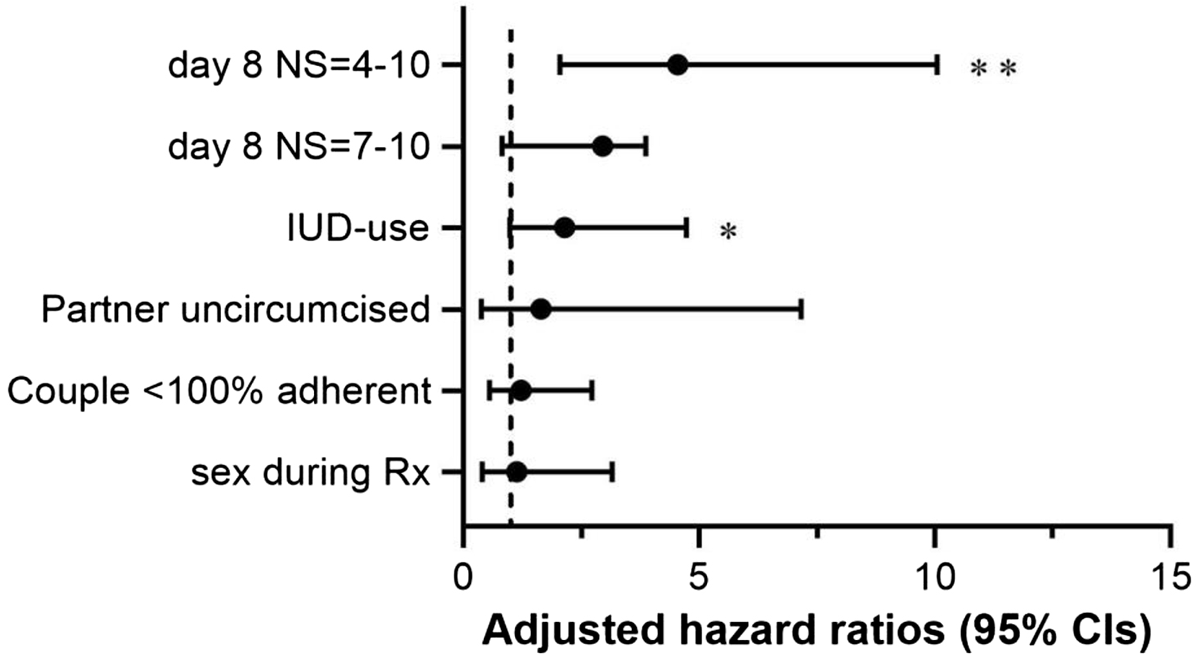
OA15.05 – Acceptance of and Experiences with Delivery of Expedited Partner Therapy for STIs Among Adolescent Girls and Young Women Using Oral PrEP in Johannesburg, South Africa
Dr. Jennifer Balkus1,2, Krishnaveni Reddy3, Nkosiphile Ndlovu3, Rebecca Howett2, Brian Pfau2, Nompumelelo Sigcu3, Reolebogile Kgoa3, Lindsay Kew3, Jennifer Ross2, Jennifer Velloza4, Thesla Palanee-Phillips2,3
1Public Health - Seattle & King County, Seattle, United States.
2University of Washington School of Public Health, Seattle, United States.
3Wits RHI, University of Witwatersrand, Johannesburg, South Africa.
4University of California, San Francisco, San Francisco, United States.
Background: Adolescent girls and young women (AGYW) utilizing oral PrEP for HIV prevention frequently experience high rates of sexually transmitted infections (STIs). We conducted a prospective cohort study to assess implementation of same-day lab-based STI testing, treatment and expedited partner therapy (EPT) among AGYW in Johannesburg, South Africa. We previously reported high EPT acceptance at enrollment. We now present data on participant experiences through 12-months of follow-up.
Methods: Between February 2022 and December 2023, HIV-negative, non-pregnant, sexually active, cisgender AGYW aged 18–25 years, interested in or already using PrEP underwent same-day testing for C. trachomatis (CT) and N. gonorrhoeae (GC) by GeneXpert and T. vaginalis (TV) by OSOM. AGYW positive for these STIs received treatment, were eligible to enroll and completed quarterly visits for 12 months. At enrollment and each subsequent STI+ visit, participants were offered EPT. Those who accepted engaged in counseling to support delivery; those who declined were offered partner referral cards (standard of care). Descriptive statistics were used to summarize STI positivity, EPT acceptance, and delivery experiences over the course of follow-up.
Results: Among 257 AGYW who enrolled and returned for follow-up, 79% had CT at enrollment, 19% had GC and 19% had TV. Across quarterly visits, STI positivity was 12–14%. EPT acceptance and delivery were high at all quarterly visits (Table 1). Participant-reported partner reactions to EPT delivery were mostly neutral or positive, with one report of a violent partner reaction.
Conclusions: Among AGYW using PrEP, EPT acceptance was high at quarterly visits, with a substantial proportion reporting successful partner delivery. Despite treatment and EPT, STI positivity was also high, demonstrating the need for wider access to STI diagnostics for AGYW and their partners. As access to STI testing improves, EPT should be considered for inclusion in a comprehensive STI treatment and prevention package for AGYW using PrEP.
| Enrollment A | 3-month visit | 6-month visit | 9-month visit | 12-month visit A | ||
|---|---|---|---|---|---|---|
| STI+ | 257/257 (100%) | 34/250 (14%) | 30/247 (12%) | 32/250 (13%) | 32/246 (13%) | |
| Accepted EPT | 239/257 (93%) | 31/34 (91%) | 29/30 (97%) | 30/32 (94%) | 29/31 (93%) | |
| Delivered EPTB | 227/239 (95%) | 30/31 (97%) | 28/29 (97%) | 28/30 (93%) | 29/29 (100%) |
OA15.06 – Preliminary Implementation of the New York City Expedited Partner Therapy Medication Program, 2023–2024
Ms. Jennifer Slutsker1, Dr. Diana Sanchez1, Justin Toro2, Dr. Julian Torres2,3, Dr. Virginia Robertson4, Dr. Chris Ka Wing Pak4, Dr. Marie Abdallah5, Dr. Michael Augenbraun5, Maris Mosley6, Dr. Michele Elliott6, Dr. Preeti Pathela1
1New York City Department of Health and Mental Hygiene, Long Island City, United States.
2Montefiore Medical Center, Bronx, United States.
3Albert Einstein College of Medicine, Bronx, United States.
4New York University Student Health Center, New York, United States.
5New York City Health + Hospitals/Kings County, Brooklyn, United States.
6The Door – A Center of Alternatives, New York, United States.
Background: Expedited partner therapy (EPT) is an efficacious, yet underutilized, approach to prevent chlamydia and gonorrhea reinfection. The Centers for Disease Control and Prevention (CDC) recommend providing index patients with packaged oral medication for their sex partners (medication-EPT); however, myriad barriers prevent widespread adoption of this recommendation. There remains an urgent need to implement and evaluate programs that increase access to medication-EPT.
Description: The NYC Health Department launched a program in June 2023 to expand access to free medication-EPT. We recruited health facilities that diagnosed over 100 chlamydia and gonorrhea infections among people 15–24 years in 2021 to participate. Facilities ordered free medications for chlamydia, gonorrhea, and trichomoniasis through a web-based portal, and then dispensed these for index patient and sex partner treatment according to customized protocols. The Health Department and facilities monitored the number of medications ordered, stocked, and distributed. We analyzed preliminary data using descriptive statistics to quantify the initial reach of the program.
Results: Five health facilities participated in the Medication-EPT Program; each was unique in setting, location, and patient population. In the first 6 months, facilities ordered 1,722 courses of CDC-recommended medications (655 doxycycline, 330 azithromycin, 310 cefixime, and 427 metronidazole) (see Table 1). Facilities reported distributing 434 courses of medication (241 doxycycline, 67 azithromycin, 49 cefixime, and 77 metronidazole), including 254 to index patients (58.5%) and 180 (41.5%) to sex partners. Facilities varied widely in the proportion of medication distributed, dispensing between 5.3% to 69.1% of stock ordered through the program.
Conclusion: Diverse healthcare settings participated in the Medication-EPT Program, highlighting broad interest and need for free EPT. Facilities distributed more medication to index patients than sex partners. Despite all diagnosing high volumes of chlamydia and gonorrhea, facilities showed substantial variation in medication distribution. Implementation research is needed to better understand optimal implementation of medication-EPT.
| Health facility | Description | Courses ordered by health facility | Dispensed for index patient treatment | Dispensed for sex partner treatment | |||
|---|---|---|---|---|---|---|---|
| Number | Number | Percent | Number | Percent | |||
| A | Adolescent health center | 435 | 116 | 26.7% | 74 | 17.0% | |
| B | University student health center | 692 | 40 | 5.8% | 43 | 6.2% | |
| C | Community health center | 110 | 33 | 30.0% | 43 | 39.1% | |
| D | Public hospital-affiliated STI clinic | 260 | 55 | 21.2% | 18 | 6.9% | |
| E | Community-based sexual health clinic | 225 | 10 | 4.4% | 2 | 0.9% | |
| Total | 1,722 | 254 | 14.8% | 180 | 10.5% | ||
OA16.01 – Gender Disparities in Opioid Agonist Therapy’s Effect on Hepatitis C Virus Risk: A Prospective Cohort Study of People Who Inject Drugs in Montréal, Canada
Ms. Milca Meconnen1, Dr. Sarah Larney1, Dr. Julie Bruneau1, Ms. Geng Zang1, Ms. Bluma B. Kleiner1, Dr. Valérie Martel-Laferrière1, Dr. Nanor Minoyan1, Dr. Adelina A. Artenie2, Dr. Jack Stone2, Dr. Peter Vickerman2
1University of Montreal, Montréal, Canada.
2University of Bristol, Bristol, England, United Kingdom.
Background: Some evidence suggests that the benefits of opioid agonist therapy (OAT) in preventing hepatitis C virus (HCV) acquisition are stronger in men than women. However, existing analyses have used crude OAT exposure measures. We aimed to estimate the effect of OAT on HCV acquisition among women and men who inject drugs using detailed OAT exposure data.
Methods: Data were from the Hepatitis Cohort (HEPCO) study, March 2011–March 2024. Eligible participants were over 18 years old, reported past 6-month injection drug use, and resided in the greater Montréal region. Approximately every 3 months, participants completed a questionnaire and provided blood samples for HCV antibody testing. Using data from participants who were HCV-antibody negative at baseline, we performed Cox regression analyses with gender as an interaction term to estimate the associations between recent OAT participation (time-updated) and primary HCV infection. In multivariable analyses, we adjusted for baseline injecting drug use duration, past-month stimulant injecting and prescription opioid injecting, and past 3-month sharing of injecting paraphernalia.
Results: There were 66 HCV seroconversions among 315 participants (258 men, 57 women) over 1082.5 person-years (p-y). HCV incidence was 6.09 (4.62–7.56) per 100 p-y overall, 11.63 (6.26–17.00) per 100 p-y in women, and 5.17 (3.71–6.63) per 100 p-y in men. In the model including only the OAT variable and its interaction with gender, the hazard ratio (HR) for women was 0.81 (95% CI: 0.31–2.09), while the HR for men was 1.25 (95% CI: 0.50–4.76). Adjusted HRs were 0.49 (95% CI: 0.18–1.31) for women and 0.95 (95% CI: 0.61–6.23) for men.
Conclusion: OAT participation reduces primary HCV acquisition risk among people who inject drugs in Montréal. Although confidence intervals were wide, results suggest a stronger reduction among women compared to men, indicating possible gender-specific protective effects of OAT that require further study.
OA16.02 – Increased Days of Housing Insecurity Elevates Risk of Bacterial STIs Among Transgender Women: Results from the Lite Study
Ms. Dorothy Apedaile1, Sari L Reisner2, Erin Cooney3, Tonia Poteat4, Susan Bondy1, Amaya Perez-Brumer1, Andrea L Wirtz3
1University of Toronto Dalla Lana School of Public Health, Toronto, Canada.
2University of Michigan School of Public Health, Ann Arbor, USA.
3Johns Hopkins Bloomberg School of Public Health, Baltimore, USA.
4Duke University School of Nursing, Durham, USA.
Background: Transgender women experience high rates of lifetime homelessness and housing insecurity, which can lead to vulnerability to sexually transmitted infections (STIs). This analysis investigates the effect of past year housing insecurity on bacterial STI positivity among a cohort of transgender women in the United States.
Methods: A total of 725 transgender women without HIV were recruited from March 2018 to May 2020 in a multisite, prospective cohort study in 6 cities in the eastern and southern United States. Participants completed surveys every 3 months and bacterial STI testing (rectal, vaginal, and urogenital chlamydia and gonorrhea; syphilis) annually. Past year housing insecurity was defined as a continuous variable representing the total number of days with difficulty finding a safe place to sleep in the past 3 months, summed across four visits. We used Poisson regression with robust standard errors to estimate the effect of 7 additional days of housing insecurity over the past year on testing positive for ≥1 bacterial STI, adjusting for baseline sociodemographic, behavioural, and psychosocial characteristics.
Results: Among the 425 participants who completed an STI test at month 12, the median age was 30 (IQR: 24–40) and 48.5% reported lifetime homelessness at baseline. At 12 months, 11.2% of participants tested positive for a bacterial STI and 19.2% reported ≥1 day of housing insecurity in the past year. After adjusting for confounding, an increase in 7 days of housing insecurity in the past year was associated with testing positive for ≥1 bacterial STI (aRR = 1.09, 95% CI = 1.02–1.16).
Conclusion: In a population with high levels of lifetime homelessness, increased days of housing insecurity in the past year increased levels of bacterial STIs. Transgender women experiencing housing insecurity need improved access to safe, stable, and secure housing as well as access to STI testing and prevention options (e.g., DoxyPEP).
OA16.03 – Experiences Accessing HIV and STI Prevention Services Among South Asian Gay, Bisexual, and Other Queer Men in Toronto, Canada
Mr. Joshun Dulai1, Laila Vahed1, Vaibhav Sawhney2, Praney Anand2, Dr. Ananya Banerjee1,3, Dr. Darrell Tan1,4, Dr. Amaya Perez-Brumer1, Dr. Daniel Grace1
1University of Toronto, Toronto, Canada.
2Alliance for South Asian AIDS Prevention, Toronto, Canada.
3McGill University, Montreal, Canada.
4Unity Health Toronto, Toronto, Canada.
Background: Canadian gay, bisexual, and other queer men (GBQM) are disproportionately affected by sexually transmitted and blood-borne infections (STBBI). However, access to testing, treatment, vaccinations for HPV, and pre- and post-exposure prophylaxis for HIV can reduce STBBI in this understudied population. We conducted a qualitative study guided by intersectionality to explore experiences with STBBI prevention services in the Greater Toronto Area (GTA).
Methods: From July to November 2024, SA GBQM participants ≥18 years old and residing in the GTA were recruited using posters distributed by community organizations serving SA and/or GBQM communities. We used a semi-structured interview guide to probe on social identities (ethnicity, class, gender, sexuality, etc.), knowledge of STBBI prevention services, and experiences with access (barriers and facilitators). Interviews lasted 60 to 90 min and were recorded and transcribed verbatim. Transcripts were analyzed using reflexive thematic analysis following Cuadraz and Uttal’s approach to intersectional qualitative analysis.
Results: The sample consisted of 30 SA GBQM (see table). Most participants identified as gay (67%), Indian (67%), and Muslim (37%) (Table 1). Participants reported interpersonal, institutional, and structural barriers in accessing STBBI prevention services. Migration histories intersected with class to produce barriers related to cost, geography, and awareness, with intersecting experiences of racism, cisheterosexism, and xenophobia from providers also noted as barriers. Solutions included increasing awareness, reducing costs, providing cultural competency training to healthcare professionals, hiring and training more SA and/or queer healthcare providers, and expanding access outside of downtown Toronto.
Conclusion: Systems of oppression are embedded within institutions that produce barriers to accessing STBBI prevention services for SA GBQM with diverse intersecting identities. Structural changes are required to increase affordability of services, provide consistent funding to provide services at no cost, build additional sites outside of downtown Toronto, and dismantle oppression within institutions to meet the sexual health needs of SA GBQM.
| Sociodemographic characteristic | Number (%) | |
|---|---|---|
| Sexual orientationa | ||
| Gay | 20 (67%) | |
| Queer | 10 (33%) | |
| Bisexual | 5 (17%) | |
| Racial/ethnic/cultural identity | ||
| South Asian | 25 (83%) | |
| South Asian & Indo-African | 2 (7%) | |
| South Asian & West Asian | 2 (7%) | |
| Indo-Caribbean | 1 (3%) | |
| Ancestral countries of originA | ||
| India | 20 (67%) | |
| Pakistan | 7 (23%) | |
| Sri Lanka | 5 (17%) | |
| Bangladesh | 2 (7%) | |
| Other | 2 (7%) | |
| Born in Canada? | ||
| No | 24 (80%) | |
| Yes | 6 (20%) | |
| Religious identityA | ||
| Muslim | 11 (37%) | |
| Agnostic/Atheist | 6 (20%) | |
| Hindu | 5 (17%) | |
| Christian | 3 (10%) | |
| Other | 3 (10%) | |
| Spiritual | 2 (7%) | |
| Buddhist | 1 (3%) | |
| Sikh | 1 (3%) | |
| Sex/gender assigned at birth | ||
| Male | 26 (87%) | |
| Female | 4 (13%) | |
| Current gender identityA | ||
| Man | 21 (70%) | |
| Non-binary | 7 (23%) | |
| Genderqueer | 4 (13%) | |
| Genderfluid | 2 (7%) | |
| Agender | 1 (3%) | |
| Hijra or similar term | 1 (3%) | |
| Other | 1 (3%) | |
| Has a disability? | ||
| No | 20 (67%) | |
| Yes | 9 (30%) | |
| Prefer not to answer | 1 (3%) | |
| Highest level of education | ||
| Above a bachelor’s degree | 17 (57%) | |
| Bachelor’s degree | 9 (30%) | |
| High school or equivalent | 3 (10%) | |
| Post-secondary certificate | 1 (3%) | |
| Relationship status | ||
| Single | 16 (53%) | |
| Married/partnered to one person and monogamous | 9 (30%) | |
| Married/partnered to one person and in an open relationship | 3 (10%) | |
| Partnered to more than one person and in an open relationship | 2 (7%) | |
| GTA region | ||
| Toronto | 22 (73%) | |
| Peel | 4 (13%) | |
| Durham | 2 (7%) | |
| Halton | 1 (3%) | |
| Toronto and York | 1 (3%) | |
| Living with HIV | ||
| No | 26 (87%) | |
| Yes | 4 (13%) | |
| Age | ||
| 20–29 | 13 (43%) | |
| 30–39 | 12 (40%) | |
| 40+ | 5 (17%) |
OA16.04 – Food Insecurity: Impacts on HIV/STI Risk and Variations by Working Conditions and Police Harassment in a Cohort of Sex Workers in Vancouver, Canada (2010–2024)
Mrs Kayla Saadeh1, Dr. Kate Shannon2, Dr. Andrea Krusi3, Ms. Wiebke Bartels4, Dr. Shira Goldenberg1
1San Diego State University, San Diego, United States.
2The University of British Columbia School of Social Medicine, Vancouver, Canada.
3Simon Fraser University School of Criminology, Burnaby, Canada.
4The University of British Columbia Centre for Gender and Sexual Health Equity, Vancouver, Canada.
Background: Food insecurity is a known driver of HIV/STI risk; limited research has evaluated the potentially heterogeneous relationship between food insecurity and client condom refusal by exposure to police harassment and across diverse work environments. Building on prior research demonstrating food insecurity as a predictor of HIV/STI risk in young sex workers, we evaluated the association between food insecurity and client condom refusal in a large, prospective cohort of sex workers, including stratified effects by work environment and police harassment.
Description: Data were from an open community-based longitudinal (2010–2024) cohort of women sex workers (AESHA) in Vancouver, Canada. Bivariate and multivariable modified Poisson regression estimated risk ratios (RRs) and 95% confidence intervals (CIs) for food insecurity and client condom refusal in the past 6 months; analyses were stratified by work environment and exposure to police harassment (without arrest).
Results: Of 1,013 participants, 173 (17.1%) experienced client condom refusal and 727 (71.8%) reported food insecurity at least once during the study. After adjusting for age, sexual orientation, racialization, education, and immigration, those facing food insecurity faced higher risk of client condom refusal (RR = 1.75, 95% CI = 1.32, 2.32). This effect was strongest amongst those experiencing recent police harassment (without arrest) (RR = 4.15, 95% CI = 2.88, 5.99) and those working in outdoor/public workspaces (RR = 2.02, 95% CI = 1.41, 2.90), compared to indoor spaces.
Conclusion: In this large, prospective cohort of sex workers, food insecurity was associated with risk of client condom refusal, and this effect was strongest amongst sex workers experiencing police harassment and working in outdoor/public spaces. To meet the HIV/STI prevention needs of sex workers, structural interventions that address food insecurity, access to safer indoor occupational environments, and sex work decriminalization are recommended.
OA16.05 – “Should We Continue to Hide?” Examining the Potential Effects of the Introduction of the Anti-LGBTQ+ Bill on HIV & AIDS Programs for Men Who Have Sex with Men (MSM) in Ghana
Mr. Samuel Elliot Owusu1, Mrs. Hellen Mawuli Quarshie1
1Maritime Life Precious Foundation, Takoradi, Ghana.
Background: Men who have sex with men (MSM) are disproportionately affected by HIV due to stigma, discrimination, and violence. Anti-LGBTQ+ laws further exacerbate these challenges, hindering access to essential HIV&AIDS services for MSM, a key population at high-risk. The introduction of an anti-LGBTQ+ bill in Ghana raises concerns about its potential impact on HIV response efforts, as it criminalizes same-sex relationships and penalizes advocacy for LGBTQ+ rights, including the provision of HIV services to LGBTQ+ individuals. This study examines the potential effects of the bill on HIV&AIDS programs targeting MSM in Ghana.
Methods: A qualitative cross-sectional survey was conducted to assess the potential influence of the anti-LGBTQ+ bill on HIV programs for MSM. Directors of three organizations working with MSM and 30 MSM individuals were purposively selected and interviewed between March and April 2023. In-depth individual and focus group interviews were conducted using semi-structured interview guides. Data were transcribed verbatim and analyzed using inductive thematic analysis.
Results: Findings revealed a significant decline in MSM’s uptake of HIV&AIDS services. Participants expressed concerns about accessing healthcare due to fears of discrimination and exposure of their sexual orientation. Many MSM reported avoiding health services and community programs that promote HIV prevention, testing, and treatment due to fear of being outed. HIV organizations also reported low turnout for group programs and shifted to one-on-one sessions to reduce the risk of public harassment. Increased stigma and retaliatory attacks against organizations were noted, leading some to scale down activities for staff and MSM safety.
Conclusion: The introduction of the anti-LGBTQ+ bill poses a grave threat to the fight against HIV in Ghana. It violates human rights, heightens stigma, and undermines public health efforts. Advocacy for LGBTQ+ rights, legal protections, and continued access to HIV services are essential to safeguard the health of MSM and ensure ongoing progress in HIV prevention and treatment.
OA16.06 – Racial Disparities in Doxy-PEP-To-Need Ratios Among a Sexually Transmitted Infection (STI) Clinic Population in San Francisco, USA
Mr. Jason Melo1, Dr. Trang Q Nguyen1, Dr. Oliver Bacon1, Mr. Christopher Ruiz1, Dr. Stephanie E Cohen1
1San Francisco Department of Public Health, San Francisco, United States.
Background: PrEP-to-need ratios have identified disparities in HIV PrEP use relative to HIV rates. We applied the framework to assess doxy-PEP use relative to doxy-PEP need at a municipal STI clinic, San Francisco City Clinic (SFCC).
Methods: The study population included cis men, trans women, and non-binary people assigned male at birth who reported sex with men in the past year and who sought care at SFCC from October 2022, when citywide doxy-PEP guidelines were released, through September 2024. Within this group, we assessed doxy-PEP uptake, defined as prescription receipt or self-reported current use at the current or previous SFCC visit, and doxy-PEP need, defined as the number of incident chlamydia, gonorrhea, or early syphilis cases. We divided doxy-PEP uptakes by total combined cases to calculate the doxy-PEP-to-need ratio (DPnR). Doxy-PEP uptake and DPnR were calculated by race/ethnicity for the overall and quarter-stratified analysis period.
Results: We analyzed 4709 Asian, Black, Latine, and White patients, excluding races with low visit counts. Overall, doxy-PEP uptake was 43% among patients (2015/4709; range: 30%, Blacks to 47%, Asians). There were 951 chlamydia, 1992 gonorrhea, and 343 early syphilis cases. The combined case rate was 63/100 patients (range: 57/100, Asians to 71/100, Latines). Compared to Whites, doxy-PEP uptake was 1.15 times higher among Latines, but DPnR was 0.95 times lower. Doxy-PEP uptake and DPnR among Blacks were respectively 0.73 and 0.72 times those among Whites. Doxy-PEP uptake increased quarterly across all races/ethnicities but remained lowest among Blacks. The DPnR disparity increased between Blacks and all others in recent quarters (Fig. 1).
Conclusion: This ecologic analysis of SFCC patients reveals a widening disparity in doxy-PEP uptake relative to the burden of STIs among Black patients compared to other races/ethnicities. DPnRs can identify actionable disparities in doxy-PEP uptake that are not evident through measuring uptake alone.
Among cis men, trans women, and non-binary people assigned male at birth that reported sex with men in the past year: quarterly doxy-PEP uptake1 rate and doxy-PEP-to-need Ratio (DPnR)2 by race/ethnicity3, San Francisco City Clinic, 2022-Q4 to 2024-Q3. 1Uptake is defined based on a doxy-PEP prescription or self-reported history of use at the current or previous San Francisco City Clinic visit. 2DPnR is calculated as the total number of doxy-PEP uptakes divided by the combined number of incident chlamydia, gonorrhea, and early syphilis cases, reported among patients of each race/ethnicity within a given quarter. A patient diagnosed with multiple infections at the same visit counts as one case. 3Races/ethnicities with visit counts too low to calculate stable quarter-stratified DPnRs were excluded from analysis, which were patients who identified as multi-racial, Native American, or Pacific Islander.
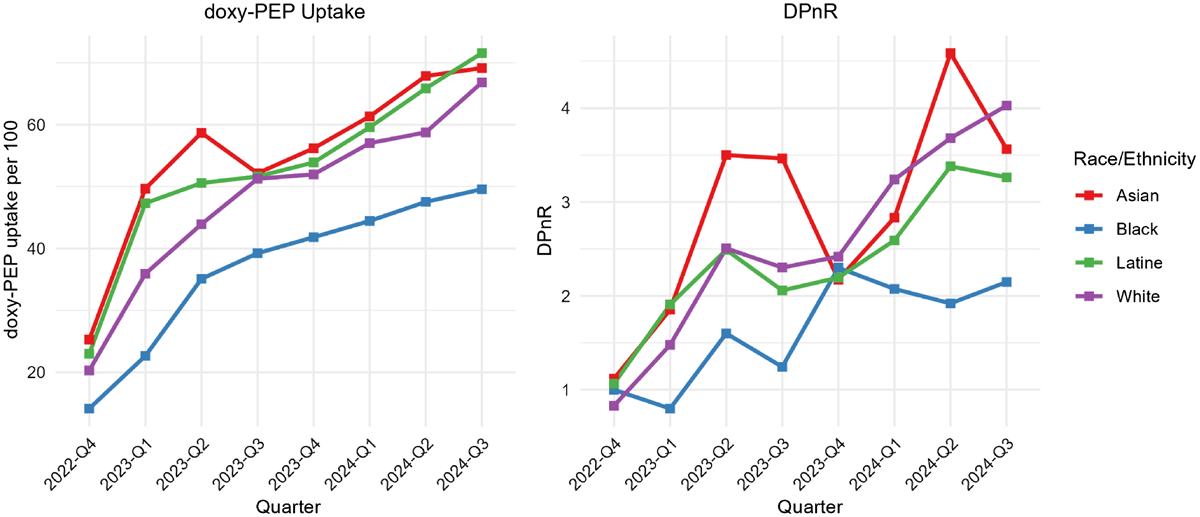
OA17.01 – Computational Modeling to Inform Syphilis Vaccine Development
Dr. Caroline E. Cameron1,2, Steven Marshall1, Austin Miller1, Dr. Javier Alfaro1,3, Dr. Simon Houston1
1University of Victoria, Victoria, Canada.
2University of Washington, Seattle, USA.
3University of Edinburgh, Edinburgh, UK.
Background: Thirty percent of Treponema pallidum (Tp) proteins lack amino acid sequence similarity with proteins from other pathogens, resulting in their function remaining unknown. Of particular interest, Tp outer membrane proteins (OMPs) located at the pathogen-host interface are targets of protective antibodies and comprise leading vaccine candidates. This study used artificial intelligence-assisted computational modeling to reveal structure-conferred functions of Tp proteins of unknown function, identify new Tp OMPs, and enhance understanding of known Tp OMPs, with the goal of providing new insight into Tp pathogenesis and informing syphilis vaccine development.
Methods: Amino acid sequences of 342 Tp proteins of unknown function, including 30 previously identified known or potential OMPs, were modelled using RoseTTAFold (RF) and AlphaFold 3 (AF3). DALI analysis identified high confidence structural orthologs, allowing inference of protein function. Novel Tp OMPs were identified by RF/AF3 structure modeling, DALI structure comparative analyses, and structure- and sequence-based bioinformatics analyses. Tp OMP inter-strain amino acid differences from Nichols & SS14 strains were identified via EMBOSS Needle sequence alignments and mapped onto structure models.
Results: Models with DALI high-confidence structural orthologs were generated for 93% (28/30) of previously identified Tp OMPs, and eight novel Tp OMPs were predicted. Most Tp OMPs adopted structural folds similar to OMPs from Gram-negative bacteria, with functions including protein export/secretion, host adhesion, and immune evasion. Of significance, 61% (23/38) of the known or predicted OMPs contained inter-strain amino acid sequence differences, primarily localizing to protein loops at the pathogen-host interface.
Conclusion: This study provides insight into Tp pathogenesis via structure modeling of proteins of unknown function, allowing prediction of eight novel OMPs and identification of sequence variance in surface-exposed, host-facing loop regions. Overall this study informs syphilis vaccine development by identifying new Tp vaccine candidates and defining OMP loop regions that vary between globally circulating Tp strains.
OA17.02 – Patterns of Genetic, Antigenic and Structural Diversity in the Neisseria Gonorrhoeae Outer Membrane Protein Porb: Implications for Vaccine Design
Dr. Odile B. Harrison1, Professor Margaret Bash2, Dr Fidel Ramirez-Bencomo3, Dr Rebekah Jones4, Dr Lenka Stejskal3, Professor Eduard Sanders5, Professor Ian M Feavers6, Professor Ann Jerse7, Professor Jeremy P Derrick3, Professor Christoph M Tang4, Professor Martin CJ Maiden6
1Nuffield Department of Population Health, University of Oxford, Oxford, United Kingdom.
2Laboratory of Bacterial Polysaccharides, Division of Bacterial, Parasitic, and Allergenic Products, Center for Biologics Evaluation and Research, US Food and Drug Administration, Silver Spring, Maryland, USA.
3School of Biological Sciences, Faculty of Biology, Medicine, and Health, University of Manchester, Manchester, United Kingdom.
4William Dunn School of Pathology, University of Oxford, Oxford, United Kingdom.
5The Aurum Institute, Johannesburg, South Africa.
6Department of Biology, University of Oxford, Oxford, United Kingdom.
7Department of Microbiology and Immunology, Uniformed Services University, Bethesda, USA.
Background: Vaccines targeting Neisseria gonorrhoeae (Ng) are needed to reduce disease burden and help address the problem of AMR. An understanding of the relationship between Ng genetics and the molecules influencing diversity, infection and immune responses is essential for developing effective vaccine formulations.
Description: The genetic diversity of PorB, a major Ng antigen, essential for viability and abundantly expressed in the outer membrane, was analysed in 5,760 porB alleles found in 22,227 N. gonorrhoeae isolates. The diversity of all 8 surface-exposed outer membrane loops, or variable regions (VR), was catalogued, leading to the development of a PorB subtyping scheme. Machine learning employing association rule mining was used to identify interactions between VRs. Protein microarray data containing diverse PorB subtypes, was used to assess PorB IgG responses elicited in sera obtained from participants vaccinated with 4CMenB and sera obtained during and after infection.
Results: Subtyping identified 328 unique PorB VR subtypes, many of which associated with genome lineages (Fig. 1). Association rule mining identified interactions between VRs, with results showing epistasis and positive selection for VR combinations that persist over time. Ng microarray analyses on sera following vaccination demonstrated skewed anti-PorB IgG VR responses directed towards distinct VR subtypes, indicative of structured, strain-specific antibody responses. Cross-reactive immune responses were found using convalescent sera.
Conclusions: The deconstruction of PorB into each surface exposed loop provides a powerful approach for detecting non-random VR associations and linkage disequilibrium in an otherwise highly diverse antigen. Shared PorB subtypes may contribute to the cross-reactive immunity observed such that infection with one gonococcus will provide partial protection against infection by another genetically diverse gonococcus, should they share PorB VR subtypes. These approaches will be invaluable in identifying and characterising further gonococcal vaccine candidates and in unmasking the complexity of the gonococcal population structure.
OA17.03 – Treponema Pallidum Subsp. Pallidum Hijacks Human Factor H to Avoid Killing by the Complement Alternative Pathway: Implications for Syphilis Pathogenesis and Vaccine Development
Aldo Trejos1,2, Keith Wycoff3, Lauren Tantalo2, Linda Xu2, Yi-Pin Lin4,5, Lorenzo Giacani1,2
1Department of Global Health, University of Washington, Seattle, United States.
2Department of Medicine, Division of Allergy and Infectious Diseases, University of Washington, Seattle, United States.
3Planet Biotechnology Inc., Hayward, United States.
4Division of Infectious Disease, Wadsworth Center, New York State Department of Health, Albany, United States.
5Department of Biomedical Sciences, State University of New York at Albany, Albany, United States.
Background: A key aspect of syphilis pathogenesis is the rapid hematogenous dissemination of its causative agent, Treponema pallidum subsp. pallidum (T. pallidum), to virtually all bodily organs during early infection. Dissemination via the bloodstream suggests that T. pallidum can evade killing by the complement alternative pathway (CAP). However, the molecular basis for this phenomenon is not clear. We hypothesize that T. pallidum might employ a surface-exposed virulence factor to recruit factor H (FH), a potent inhibitor of the CAP, thus enabling evasion of complement-mediated killing.
Methods: A functional assay using intact T. pallidum cells assessed FH binding to the pathogen’s surface. Since there are two common microbial binding sites on FH, namely the short consensus repeat (SCR) modules 6-7 and SCR19-20, we used chimeric constructs carrying SCR6-7 and SCR19-20 fused to the human IgG Fc portion to perform complement-activated binding/killing and opsonophagocytic assay in presence of complement to determine whether T. pallidum recognizes one SCR or both. Lastly, we used affinity ligand binding immunoblotting (ALBI) to identify possible FH-binding proteins from T. pallidum lysates.
Results: The binding/killing assay showed that FH binding by T. pallidum occurs through the SCR19-20 modules. Opsonophagocytic assay with the SCR19-20 chimeric construct further confirmed the above result and supported that the T. pallidum FH binding factor is on the pathogen’s outer membrane. Lastly, the ALBI assay identified a 43 kDa putative FH-binding protein in T. pallidum lysates.
Conclusion: Our findings suggest that T. pallidum evades complement-mediated killing by recruiting human FH to its surface via a 43 kDa virulence factor yet to be fully characterized. Future directions will focus on identifying the gene encoding the 43 kDa putative outer membrane protein and assessing its potential as a vaccine candidate.
OA17.04 – Developing Engineered Protein-Based Vaccines Targeting Nutritional Uptake Systems Against Neisseria Gonorrhoeae
Dr. Jamie Fegan1, Dr. Epshita Islam1, Ms. Natalie Au1, Dr. David Curran1, Dr. Dixon Ng1, Ms. Laura-lee Caruso1, Dr. Anthony Schryvers2, Dr. Trevor Moraes1, Dr. Scott Gray-Owen1
1University of Toronto, Toronto, Canada.
2University of Calgary, Calgary, Canada.
Background: Neisseria gonorrhoeae is the causative agent of the sexually transmitted infection gonorrhea. This highly host adapted pathogen utilizes various human specific nutrient uptake systems to acquire essential micronutrients, including the bacterial transferrin receptor composed of transferrin binding protein A and B (TbpA and TbpB) which allows for uptake of iron from human transferrin during infection. TbpB has been previously identified as a promising candidate vaccine antigen, however challenges remain to identify the optimal variants to include, engineering the antigens to be ideal immunogens, and to identify efficacious adjuvant formulations to elicit broad protection at relevant mucosal sites.
Methods: A novel software program, Navargator, was developed to utilize sequence diversity data to select the most representative protein variants to include in a vaccine formulation. The selected variants have been expressed, purified, and immunized into small animal models to evaluate immunogenicity, cross-reactivity, and protection from experimental infection by N. gonorrhoeae. Protein variants have been engineered to abolish binding to their host ligand, transferrin, and evaluated in transgenic mice to determine changes in efficacy between native and mutant immunogens. Protein variants have been formulated with different vaccine adjuvants and evaluated for immunogenicity and protection from bacterial colonization on relevant mucosal surfaces.
Results: Sera from animals immunized with different identified TbpB variants have been evaluated for immunogenicity, cross-reactivity, and functional activity across a broad panel of Neisserial TbpBs. Engineered proteins lacking transferrin binding have been shown to be superior immunogens when tested in transgenic mice during challenge studies. Formulations containing different types of adjuvants have been evaluated to determine the type of immune response, the resulting immunogenicity, and the protective capability.
Conclusions: Taken together, these data support the potential of a TbpB-based vaccine against N. gonorrhoeae and aid in identifying optimal vaccine formulations for robust protection.
OA17.05 – Syphilis Vaccine Development: Insight into Vaccine-Induced Antigen-Specific B Cell Responses and Cytokine Profiles
Mr. Alloysius Gomez1, Francesca Urselli2, Ayman Haimour1, Ethan Schovanek1, Bridget Mateyko1, Ellis Evans1, Charmie Godornes3, Dr. Lorenzo Giacani3, Dr. Sheila Lukehart3, Dr. Tara Reid3, Dr. Anna Wald3, Dr. David Koelle3, Dr. Justin Taylor4, Dr. Caroline E. Cameron1
1University of Victoria, Victoria, Canada.
2Fred Hutchinson Cancer Center, Seattle, USA.
3University of Washington, Seattle, USA.
4University of Virginia, Charlottesville, USA.
Background: Prior studies have demonstrated the importance of humoral and Th1/Th17 cellular immune responses in T. pallidum (Tp) clearance. Further, previous pre-clinical studies by our group achieved reproducible levels of protection from chancre development and Tp dissemination in rabbits immunized with cocktail- and chimera-based vaccine constructs and challenged with infectious Tp. In the current study we report a novel pipeline for isolation and characterization of vaccine-specific monoclonal antibodies (mAbs) from protected rabbits and characterized the cytokine profiles induced by immunization with the cocktail- and chimera-based vaccine constructs.
Methods: Vaccine antigen-specific B cells were enriched from peripheral blood mononuclear cells of immunized rabbits that exhibited reduced chancre development and dissemination to distant organ sites. Vaccine-specific mAbs were mapped to the molecular structure of the vaccine construct and tested for their ability to inhibit Tp attachment to endothelial cells via epitope mapping and attachment inhibition assays, respectively. Splenocytes harvested from immunized and control challenged rabbits were stimulated with vaccine constructs, and expression levels of Th1 (IFN-γ and TNF-α), Th17 (IL-22), and regulatory (IL-10) cytokines were quantified using RT-qPCR and antigen-capture assays.
Results: We isolated ten vaccine antigen-specific mAbs from rabbits that were fully or partially protected from Tp dissemination. All mAbs inhibited Tp endothelial attachment, with a range of inhibition of 20-50%. A trend between extent of vaccine construct binding and level of endothelial attachment inhibition was observed for the mAbs. Cytokine profiles from immunized and challenged animals showed upregulation of IFN-γ, TNF-α, and IL-22 and downregulation of IL-10 expression compared to unimmunized, challenged animals.
Conclusion: We developed first-in-field methodology to isolate and characterize vaccine-specific mAbs from protected animals. This study also defined a streamlined methodology for assessing cytokine profiles induced in the pre-clinical vaccine model. These tools will assist with identifying correlates of protection for effective syphilis vaccine development.
OA17.06 – Revolutionizing STI Vaccines: Artificial Intelligence-Driven Discovery of Vaccine Candidates in Mycoplasma Genitalium
Dr. Jyoti Taneja1, Dr. Ravi Kant2, Prof. Daman Saluja2
1Department of Zoology, Daulat Ram College, University of Delhi, New Delhi, India.
2Dr. B.R.Ambedkar Centre for Biomedical Research, University of Delhi, Delhi, India.
Background: Mycoplasma genitalium is a significant sexually transmitted pathogen associated with non-gonococcal urethritis, pelvic inflammatory disease, and infertility. The increasing prevalence of antibiotic-resistant strains demands urgent alternative intervention strategies. Despite its clinical relevance, many hypothetical proteins (HPs) in the M. genitalium genome remain uncharacterized. These HPs may serve as promising vaccine candidates, yet their potential has yet to be fully explored. The goal of this study was to apply artificial intelligence (AI)-driven reverse vaccinology to identify and prioritize novel vaccine candidates to combat M. genitalium.
Methods: An AI-enhanced reverse vaccinology approach was employed, utilizing various computational tools, including ProtParam, CELLO, PSORTb, TMHMM, SignalP, and VirulentPred. These tools assessed the physicochemical properties, subcellular localization, transmembrane domains, and virulence potential of HPs. Additionally, BepiPred was used to predict B-cell epitopes to evaluate the immunogenicity of the proteins. HPs that met critical criteria – surface exposure, stability, immunogenicity, and potential involvement in virulence – were shortlisted for experimental validation.
Results: Out of 74 HPs analysed, 23 were identified as high-priority vaccine candidates. These candidates were predominantly membrane-associated and exhibited favorable stability indices. Functional annotation highlighted their potential roles in host-pathogen interactions, emphasizing their involvement in virulence mechanisms. Immunogenic epitopes were predicted within these proteins, further supporting their vaccine potential.
Conclusion: This study demonstrates the application of AI-driven reverse vaccinology as a transformative method for identifying novel vaccine candidates for M. genitalium. The prioritized HPs provide a strong foundation for future experimental validation and vaccine development, addressing the critical need for new therapeutic strategies against antibiotic-resistant sexually transmitted infections. Congress attendees will gain insights into how AI can revolutionize STI vaccine discovery and how these findings can be leveraged for global STI prevention strategies, with potential applications in communities facing high STI burdens.
Keywords: Artificial Intelligence, Reverse Vaccinology, Mycoplasma genitalium, Vaccine Development, Hypothetical Proteins, Antibiotic Resistance.
OA18.01 – Preferences for In-Person Sexual Health Services Among Middle-Aged and Older Adults: Findings from Discrete Choice Experiments Conducted in the UK and China
Ms Yoshiko Sakuma1, Ms Chuquing Cao2, Mr Dongya Wang3, Dr Stephen W Pan2, Ms Warrittha Tieosapjaroen4, Professor Jason J Ong1,4, Professor Fern Terris-Prestholt5, Professor Joseph D Tucker1,6, Professor Dan Wu1,7, Dr. Eneyi Kpokiri1
1London School of Hyigiene and Tropical Medicine, London, United Kingdom.
2Xi’an Jiaotong-Liverpool University, Suzhou, China.
3University of Miami, Miami, United States.
4Monash University, Clayton, Australia.
5University of Warwick Medical School, Coventry, United Kingdom.
6University of North Carolina at Chapel Hill, Chapel Hill, United States.
7Nanjing Medical University, Nanjing, China.
Background: Sexual health impacts physical and mental well-being, and must be considered alongside general health regardless of age. Sexual health needs of middle-aged and older adults remain largely overlooked in many settings. This study explores the preferences for sexual health services among middle-aged and older adults (aged 45 and above) in the UK and China, addressing a significant gap in research. Despite structural differences in their healthcare systems, both countries face similar challenges in providing sexual health services to this demographic group.
Methods: We employed a discrete choice experiment (DCE) survey to explore the preferences among middle-aged and older adults for accessing sexual health services in the UK and China. To develop the full-scale DCEs and elicit potential attributes and levels, we conducted semi-structured and in-depth interviews. Common attributes across both UK and China surveys were mode of delivery (in-person, telephone, and video consultation), location (general practitioner, sexual health hospital), cost (middle-range, high range) and communication and consultation style (patient-centred, not-patient-centred).
Results: We received 339 eligible responses to the Chinese DCE and 200 responses to the UK DCE survey. The results revealed similarities in preferences across the two countries (Fig. 1). Key findings were a preference for in-person consultations over tele-conference consultations, and respondents in both countries showed a willingness to pay a moderate out-of-pocket expense for sexual health services (UK: $60–130, China: $30), even with publicly funded healthcare systems available.
Conclusion: Our findings question prevailing assumptions about middle-aged and older adults’ engagement with online sexual health services, particularly in the wake of the global shift towards online services prompted by the COVID-19 pandemic. Further research is needed to understand older adults’ preferences at a more granular level and how the voices of middle-aged and older adults can inform more tailored and locally appropriate services.
Preferences for sexual health services from the UK and Chinese participants (China n = 339, UK n = 200). ****P < 0.001, ***P < 0.01, **P < 0.05, *P < 0.10.
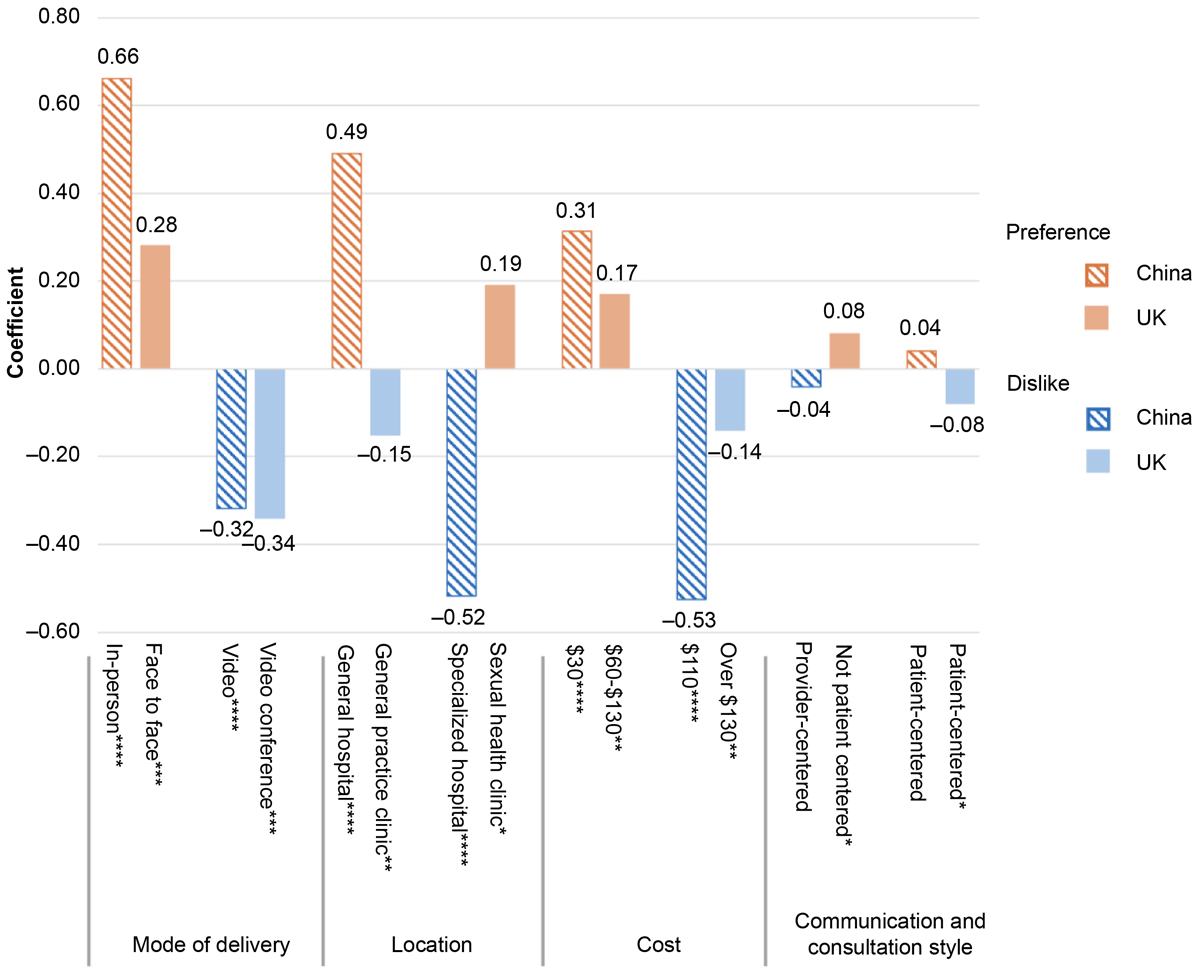
OA18.02 – Evaluation of Artificial Intelligence (AI) Chatbots for Providing Sexual Health Information: A Consensus Study Using Real-World Clinical Queries
Dr. Phyu Mon Latt1,2, Dr. Ei Thu Aung1,2, Dr. Kay Htaik1,2, Dr. Nyi Nyi Soe1,2, Dr. David Lee2, Dr. Alicia King1,2, Dr. Ria Fortune2, Prof Jason Ong1,2,3, Prof Eric Chow1,2,4, Prof Catriona Bradshaw1,2, Mr Rashidur Rahman2, Mr Matthew Deneen5, Ms Sheranne Dobinson2, Ms Claire Randall2, Prof Lei Zhang1,2,6, Prof Christopher Fairley1,2
1Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Melbourne, Australia.
3Department of Clinical Research, London School of Hygiene and Tropical Medicine, London, United Kingdom.
4Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
5Alfred Health, Melbourne, Australia.
6Clinical Medical Research Centre, Children’s Hospital of Nanjing Medical University, Nanjing, China.
Introduction: Artificial Intelligence (AI) chatbots could provide information on sexual health to the public. However, their performance in sexual health compared to human clinicians and across different AI chatbots remains understudied. This study evaluated the performance of three AI chatbots – two prompt-tuned (Alice and Azure) and one standard chatbot (ChatGPT by OpenAI) – in providing sexual health information, compared to clinicians.
Methods: We analysed 195 anonymised sexual health questions received by the Melbourne Sexual Health Centre phone line. Using a consensus-based approach, a panel of experts evaluated responses to these questions generated by the three AI chatbots in a blinded order. Performance was assessed based on overall correctness and five specific measures: guidance, accuracy, safety, ease of access, and provision of necessary information. We conducted subgroup analyses for clinic-specific and general sexual health questions and a sensitivity analysis excluding questions that Azure could not answer.
Results: Alice demonstrated the highest overall correctness (85.2%; 95% confidence interval (CI), 82.1%–88.0%), followed by Azure (69.3%; 95% CI, 65.3%–73.0%) and ChatGPT (64.8%; 95% CI, 60.7%–68.7%). Prompt-tuned chatbots outperformed the base ChatGPT across all measures. Azure achieved the highest safety score (97.9%; 95% CI, 96.4%–98.9%), indicating the lowest risk of providing potentially harmful advice. In subgroup analysis, all chatbots performed better on general sexual health questions compared to clinic-specific queries. Sensitivity analysis showed a narrower performance gap between Alice and Azure when excluding questions Azure could not answer.
Conclusions: Prompt-tuned AI chatbots demonstrated superior performance in providing sexual health information compared to base ChatGPT, with high safety scores particularly noteworthy. However, all AI chatbots showed susceptibility to generating incorrect information. These findings suggest the potential for AI chatbots as adjuncts to human healthcare providers while highlighting the need for continued refinement and human oversight. Future research should focus on larger-scale evaluations and real-world implementation.
OA18.03 – What Do People Want from an Artificially-Intelligence-Assisted Screening App for Sexually Transmitted Infection-Related Anogenital Lesions: A Discrete Choice Experiment
Dr. Nyi Nyi Soe1,2, Dr. Phyu Mon Latt1,2, Dr. Alicia King1,2, Dr. David Lee1, Dr. Tiffany R. Phillips1,2, Dr. Christopher K. Fairley1,2, Dr. Lei Zhang1,2,3, Dr. Jason J. Ong1,2,4
1Melbourne Sexual Health Centre, Melbourne, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Clinical Medical Research Centre, Children’s Hospital of Nanjing Medical University, Nanjing, China.
4Faculty of Infectious Diseases, London School of Hygiene and Tropical Medicine, London, UK.
Background: Melbourne Sexual Health Centre (MSHC) developed an artificially intelligence (AI) assisted screening app (AiSTI) for the detection of common STI-related anogenital skin conditions. This study aims to understand the community’s preference for using the app.
Methods: A discrete choice experiment (DCE) was used to understand community preferences regarding the attributes of the app for checking anogenital skin lesions. The DCE design included the attributes: data type; AI accuracy; verification of result by a clinician; details of result; speed; professional support; and cost. The anonymous DCE survey was conducted between January and March 2024. Participant preferences on various app attributes were examined using random parameters logit (RPL) and latent class analysis (LCA) models.
Results: The median age of 411 participants was 32 years (IQR: 26–40 years), with 64.0% assigned male at birth. Of the participants, 177 (43.1%) identified as same-sex attracted and 137 (33.3%) as heterosexual. In the RPL model, the most influential attribute was the cost of using the app (relative importance: 24.1%), followed by the clinician’s verification of results (20.4%), the AI accuracy (19.5%) and the speed of receiving the result (19.1%). The LCA identified two distinct groups: ‘all-rounders’ (class size 88%), who considered every attribute as important, and a ‘cost-focused’ group (12%), who mainly focussed on the price. The predicted uptake, based on the current app attributes, was 72%. In the short term, improving AI accuracy to 80–89% with clinician verification at $5 could increase uptake to 90%. An optimistic long-term scenario with AI accuracy over 95%, without clinician verification and cost, could increase it to 95% (Figs 1–4).
Conclusions: Participants would prefer an AI-assisted screening app targeting STI-related anogenital skin lesions that is low-cost, clinician-verified, highly accurate and provides results rapidly. An app with these key qualities would substantially improve user uptake.
A total of 24 discrete choice sets were generated. An example of a discrete choice set is as follows. Imagine that you suspect a genital skin lesion you have might be a sexually transmitted infection. You decide to use an online tool to evaluate your skin lesion image. Of the options presented below, which would you choose?

Simulation scenarios and predicted uptake. Scenario D assumes the app with 80-89% AI accuracy, clinician verification, and a $5 cost. Scenario E assumes the app with over 95% AI accuracy, no clinician verification, and no cost.
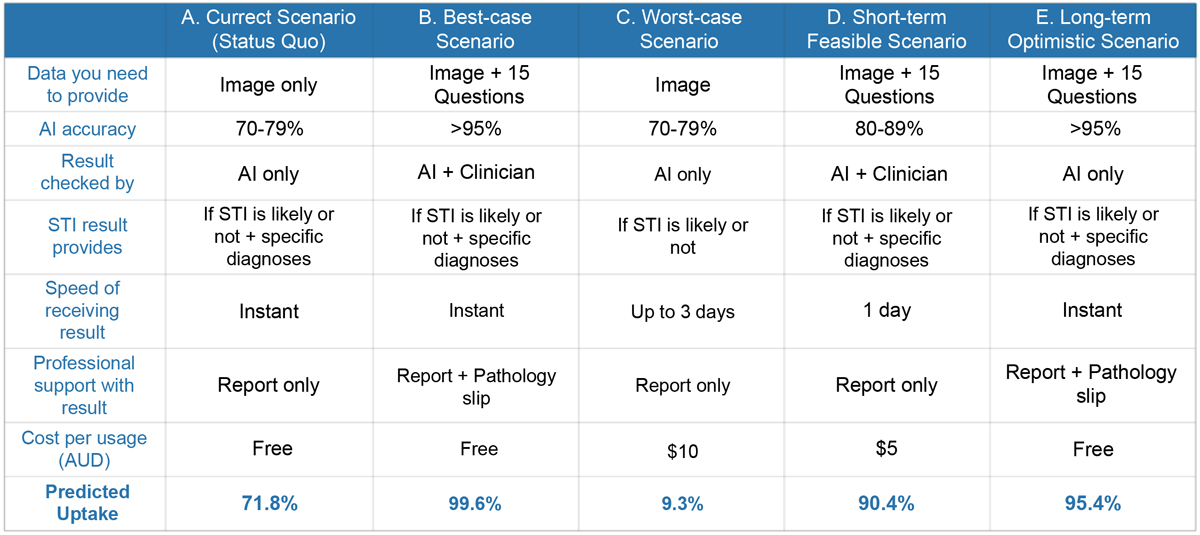
OA18.04 – Using Online Media to Increase the Awareness and Uptake of Pre-Exposure Prophylaxis Among Asian-Born Men Having Sex with Men: A Randomised Controlled Trial
Mrs Warittha Tieosapjaroen1,2, Dr Tiffany R. Phillips1,2, Prof Eric P.F. Chow1,2,3, Prof Chritopher K. Fairley1,2, Dr Satrio Nindyo Istiko4,5,6, Dr Jason Wu1,7, Mr James Tapa2, Prof Limin Mao8, Prof Lei Zhang1,2, Mr David Wang9, Mr Budiadi Sudarto2, Prof Jason J. Ong1,2,10
1Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia, Melbourne, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Melbourne, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
4Bradford Institute for Health Research, Bradford Teaching Hospitals NHS Foundation Trust, Bradford, UK.
5Bristol Medical School, University of Bristol, Bristol, UK.
6School of Public Health, Faculty of Medicine, The University of Queensland, Brisbane, Australia.
7Kings Park Medical Centre – Hillside, General Practice, Melbourne, Australia.
8Centre for Social Research in Health, University of New South Wales, Sydney, Australia.
9Burnet Institute, Melbourne, Australia.
10Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, UK.
Background: Asian-born men having sex with men (ABMSM) are a key population for ending HIV transmission in Australia. However, most existing campaigns were not designed for them. We assessed the acceptability of a community-based audio drama, developed through a designathon, compared to written information on a PAN website (PAN.org.au) to increase PrEP awareness and uptake among ABMSM in Australia.
Methods: This open-label-two-arm pilot stratified randomised controlled trial was conducted between April and July 2024. ABMSM were randomised 1:1 to receive either the Hot Peach Tea 30-min audio drama (intervention), depicting a PrEP journey of an ABMSM who newly arrived in Australia, or the PAN website (control), commonly suggested by clinicians in Victoria to gain PrEP-related information. An intention-to-treat analysis was used to evaluate the data. Outcomes are shown in Table 1.
Results: Among the 200 participants, 96 received the control, and 104 received the intervention. Extreme satisfaction was expressed by 74% (71/96) and 77% (80/104) in the control and intervention arms, respectively. Full engagement was 22% (21/96) and 85% (88/104) in the control and intervention arms, respectively (P < 0.001). The median score increase in attitude towards PrEP was 4 (interquartile (IQR) 0,7) and 7 (3,12.5) in the control and intervention arms, respectively (P = 0.023). Both online media increased the uptake of PrEP, with no significant differences observed between the two arms. At the 2-month follow-up, 18% (17/96) and 22% (23/104) initiated PrEP in the control and intervention arm, respectively (P = 0.0133). The most reported reasons for not initiating PrEP were PrEP side effects (20%, 19/96) in the control arm and perceived inconvenience of PrEP use (16%, 17/104) in the intervention arm.
Conclusions: The Hot Peach Tea audio drama effectively engaged and positively influenced ABMSM’s attitudes towards PrEP. Strategies to link individuals to care post-audio drama are needed to increase the uptake of PrEP.
| Outcomes | Measures | Post-intervention (Time point 0) | 1-month follow-up (Time point 1) | 2-month follow-up (Time point 2) | ||
|---|---|---|---|---|---|---|
| Primary outcomes | ||||||
| Acceptability | Satisfaction | Participants’ satisfaction with the intervention and control. | X | |||
| Engagement | The percentage of participants who complete the intervention and control. | X | ||||
| Uptake of PrEP | Intention to use PrEP | Changes in participants’ intention to use PrEP using a 3-item PrEP intention questionnaire by Walsh. | X | |||
| Awareness | Attitudes toward PrEP | Changes in participants’ attitudes toward PrEP using a survey adapted from the 5-item PrEP attitudes questionnaire by Walsh. | X | |||
| Secondary outcomes | ||||||
| Change in knowledge of PrEP | Change in knowledge of PrEP using a survey adapted from Walsh’s questionnaire. | X | ||||
| PrEP initiation after 1 month | The percentage of individuals who take further actions to obtain PrEP or initiate PrEP at 1 and 2 months after receiving the intervention or control. | X | ||||
| PrEP initiation after 2 months | X | |||||
| Adherence to PrEP after 1 month | If participants initiate PrEP after receiving the intervention or control, we will ask how participants take PrEP (i.e., daily or on-demand), how many pills they have taken after they receive PrEP and their reasons for discontinuing PrEP if they stop using PrEP. | X | ||||
| Adherence to PrEP after 2 months | X | |||||
OA18.05 – Partnerships Between Public Health and Dating Apps Lead to Increased Access for HIV and STI Self-Testing
Ms. Jen Hecht1, Steph Niaupari
1BHOC, Richmond, United States.
2Springboard HealthLab, Richmond, United States.
Background: In 2023, WHO called for the expanded use of HIV self-testing. Building Healthy Online Communities (BHOC) is a consortium of public health organizations partnering with dating apps to improve sexual health. With Emory University, BHOC determined that 85% of MSM in the US reported using dating apps to meet a recent partner, and within this group, 22% had never tested for HIV.
Description: BHOC developed TakeMeHome.org to enable dating app users to order a free HIV self-test. BHOC partnered with many dating apps, most notably Grindr, to promote the program.
Results: Over 4 years of messaging, Grindr directed users to TakeMeHome, and 33% of participants reported their first-ever HIV test and 70,000 self-tests were distributed. BHOC worked with Emory and CDC to scale nationally in the US. With this expansion, Grindr added prominent in-app buttons to direct users to the program. These buttons were incredibly successful in driving traffic, yielding 50% of orders, and leading to 650,000 kits distributed in 18 months.
Grindr has users in 197 countries, and Grindr4Equality has built relationships with many organizations. This self-testing recruitment model has been expanded to Ireland, Georgia, New Zealand, Australia and Namibia, and in development in Cambodia, Mexico, Spain and other locations.
Conclusions: There is significant demand and acceptability among dating app users for self-testing. By building local relationships with health ministries and NGOs, BHOC and Grindr have successfully recruited non-testers through prominent in-app buttons. Success has hinged upon funding for kits, adapting delivery mechanisms and ordering platforms to local environments, approval of testing technologies, and competitive pricing for kits.
Building on a strong public-private partnership and leveraging digital technology, this program has reached people vulnerable to HIV/STIs, engaging thousands of new testers. BHOC and Grindr aim to add 10–20 countries in 2025 and 2026.
OA18.06 – Exploring the Role of Digital Health Literacy in Awareness and Use of Digital Sexually Transmitted Infections Testing Interventions: Insights from a Structural Equation Modelling of the 2022 Getcheckedonline Community Survey
Dr. Ihoghosa Iyamu1,2, Pierce Gorun1,2, Hsiu-Ju Chang2, Dr. Rodrigo Sierra-Rosales1,2, Devon Haag2, Heather Pedersen2, Dr. Sofia Bartlett1,2, Dr. Nathan Lachowsky3, Dr. Geoffrey McKee1,2, Dr. Catherine Worthington3, Dr. Troy Grennan4, Dr. Daniel Grace5, Dr. Mark Gilbert1,2
1School of Population and Public Health, University of British Columbia, Langley, Canada.
2BC Centre for Disease Control, Vancouver, Canada.
3School of Public Health and Social Policy, Victoria, Canada.
4Division of Infectious Diseases, University of British Columbia, Vancouver, Canada.
5Dalla Lana School of Public Health, University of Toronto, Toronto, Canada.
Background: Digital health literacy (DHL) influences access to digital STI testing services. Popular DHL tools, including the eHealth Literacy Scale (eHEALS), are often unidimensional and insufficient for guiding programs. This study examined how refined DHL measures based on eHEALS influence disparities in awareness and use of GetCheckedOnline, British Columbia’s publicly funded digital STI testing service.
Methods: We analyzed data from GetCheckedOnline’s 2022 community survey of English-speaking BC residents aged ≥16 years and sexually active in the past year. Outcomes were awareness and use of GetCheckedOnline (both yes/no). Latent DHL factors were identified using exploratory factor analyses from the eHEALS questionnaire, followed by confirmatory factor analysis using weighted least squares mean variance-adjusted models. Factor models were evaluated using standard indices. Structural equation modeling assessed associations between latent DHL factors, sociodemographic characteristics and main outcomes.
Results: Among 1,657 respondents (mean age: 33.0 years, SD: 11.77), 52.5% (784) were women. Three latent DHL factors were identified: Factors 1 (information navigation), two (resource appraisal) and three (confidence in use). Information navigation (β = 0.162, P < 0.001 and β = 0.063, P = 0.020) and confidence in use (β = 0.206, P = 0.014 and β = 0.115, P = 0.020) were positively associated with awareness and use of GetCheckedOnline. Resource appraisal was negatively associated with awareness and use of GetCheckedOnline (β = −0.263, P = 0.006 and β = −0.150, P = 0.010). DHL factors mediated the effect of age, income, education and digital access on awareness and use of GetCheckedOnline.
Conclusions: Findings suggest that users’ information vavigation and confidence in use DHLS are positively associated with awareness and use of GetCheckedOnline. In contrast, resource appraisal DHL may constrain awareness and use, potentially due to heightened criticality, skepticism, or concern about online stigma. Findings highlight the role of DHLs in existing inequities in uptake of digital STI testing. Future research should explore how DHLs interact with trust, stigma, and service design to influence use, particularly among populations marginalized populations.
OA19.01 – Syphilis and HIV Among Parturient Women in Brazil: Could Duo Testing Prevent Missed Diagnoses During Pregnancy?
Dr. Angelica Espinosa Miranda1, Dr Pamela Cristina Gaspar, Dr Marcos André Schörner, Dr Fernando Hartmann Barazzetti, Dr Alisson Bigolin, Dr Italo Vinicius Albuquerque Diniz, Dr Draurio Barreira, Dr Maria Luiza Bazzo
1Universidade Federal do Espírito Santo, Vitoria, Brazil.
Background: Syphilis and HIV pose significant public health challenges during pregnancy, increasing risks of adverse maternal and neonatal outcomes. Dual tests enable simultaneous testing for HIV and syphilis in pregnant women and could improve diagnosis access. This study estimated the prevalence of syphilis and HIV among parturient women in Brazil, using secondary data from a national implementation study on molecular STI diagnostics.
Methods: This cross-sectional analysis used data from 2022, encompassing parturient women from diverse Brazilian regions. Prevalence rates of syphilis and HIV were determined through point-of-care (POC) and serological tests. Sociodemographic and clinical characteristics were analyzed, highlighting gaps in antenatal testing. Health surveillance data were provided by Brazilian Ministry of Health.
Results: Among 2,728 women aged 15–49 years from public antenatal clinics, and different geographical regions: North 284 (10.4%), Northeast 572 (21%), Center-West 149 (5.5%), Southeast 1167 (42.8%) and South 556 (20.4%). Key characteristics included: 39.6% aged 15–24 years, 57.0% identifying as Black or mixed race, and 72.7% with family incomes ≤US$800. Early sexual initiation (<15 years) was reported by 21.6%, while 3.3% experienced first pregnancies under 15 years. Despite low STI reporting (1.1%), 29.7% reported STI-related symptoms, and 21.0% (573) was positive for at least Chlamydia trachomatis, Neisseria gonorrhoeae, Trichomonas vaginalis, and/or Mycoplasma genitalium. Stillbirths were reported by 2.1%. Syphilis prevalence was 2.2% and HIV prevalence was 0.5%. However, 143 women (5.2%) lacked HIV test results, and 311 (11.4%) lacked syphilis results despite single POC test availability in the public clinics.
Conclusion: The study reveals a significant burden of syphilis among parturient women in Brazil, compounded by notable gaps in antenatal testing. These findings emphasize the need to strengthen maternal health programs by integrating dual HIV-syphilis testing to ensure comprehensive screening, reduce vertical transmission, and improve maternal and neonatal outcomes.
OA19.02 – Missed Treatment Opportunities Following Antenatal Syphilis Screening in Kenya
Dr. Jerusha N Mogaka1, Ms Salphine Watoyi1, Ms Mary Marwa2, Mr. Felix Abuna2, Dr. Melissa Mugambi1, Dr Irene Njuguna1, Dr. Barbra Richardson1, Ms Laurén Gomez1, Ms. Eunita Akim2, Dr. Nancy Ngumbau2, Ms Tessa Concepcion1, Mr. Ben Odhiambo2, Dr. John Kinuthia1,2, Dr. Grace C. John-Stewart1, Dr. Jillian Pintye1, Miss Omolara Akingba
1University of Washington, Seattle, United States.
2Kenyatta National Hospital, Nairobi, Kenya.
Background: Implementation of rapid point-of-care (POC) HIV/syphilis dual test kits improved coverage of universal screening for HIV and syphilis at first antenatal care (ANC) visits in Kenya. However, few recent data exist on syphilis screening and treatment outcomes from the era of rapid POC testing in this setting.
Methods: We abstracted syphilis data from maternal health records from pregnant women enrolled in ongoing studies of HIV treatment and prevention who were seeking ANC services at 5 public clinics in Western Kenya – a region with 20% HIV prevalence among women. Per national guidelines, laboratory-based non-treponemal tests (Rapid Plasma Reagin[RPR]/Venereal Disease Research Laboratory [VDRL]) or rapid POC HIV/syphilis dual tests are used for syphilis screening at first ANC visits, based on availability. If screened positive, an initial dose of intramuscular benzathine penicillin G (IM pen G) is indicated while confirmatory testing is performed.
Results: A total of 1330 pregnant women enrolled in the parent studies between October 2020 and December 2024 at a median gestational age of 26 weeks (IQR: 23–29). Median age was 26 (IQR:22–30), and 43% were living with HIV. Overall, 1273 (95.7%) women had syphilis screening documented at first ANC visits (80.2% RPR/VDRL alone and 15.5% rapid POC dual tests with or without RPR/VDRL); 4.3% were missing any syphilis screening results. In total, 76 (6%) women tested positive on either rapid POC dual test or RPR/VDRL. Syphilis positivity was higher among women living with HIV (WLHIV) compared to those without HIV (16.6% vs 1.1%, prevalence ratio 14.5, CI 95% 7.9–29.8, P < 0.001). Only 55% of those who screened positive had documentation of any IM pen G treatment.
Conclusions: Despite high syphilis screening rates, nearly half of women who screened positive were inadequately treated per national guidelines. Antenatal syphilis programs urgently need strengthening in Kenya.
OA19.03 – Contextual Facilitators to Public Health Units’ Adoption of the Rapid Syphilis “Test and Treat” Outreach Model of Care
Mr. Sina Sayyad1, Ms. Jillian Antoun1, Ms. Lucy Mackrell1, Dr. Megan Carter2, Dr. Sahar Saeed1
1Queen’s University, Kingston, Canada.
2Kingston, Frontenac and Lennox & Addington (KFL&A) Public Health, Kingston, Canada.
Background: Canada has experienced a heterogenous surge of syphilis cases in the last 5 years. Eight public health units (PHUs) across Ontario implemented a “rapid test and immediate treatment” outreach model of care to combat the outbreak. Using the implementation science framework, The Practical, Robust Implementation and Sustainability Model (PRISM), we identified contextual barriers and facilitators to adopting this new model of care.
Methods: An instrumental case study using Yin’s constructivist paradigm was selected to explore decision-making processes at one of the PHUs. A comprehensive literature review and expert testimony informed the creation of a semi-structured interview guide. Six interviews with front-line and decision-making staff at the PHU were transcribed and, alongside 20 internal reports, abductively coded to generate the results.
Results: Preliminary results identified five key facilitators. (1) Innovation drivers and (2) a flatter organizational structure. All participants noted “an overall organizational culture… more action-oriented.” These drivers enabled frontline staff to bring solutions to decision-makers keen on adopting new initiatives and “physician leadership being OK with the medical, legal risk of these initiatives”. The significance of (3) relying on existing infrastructure, such as task-shifting and leveraging “outreach models… for COVID-19 made the team more familiar… and comfortable with the outreach model”. (4) Existing relationships with community-based organizations (CBOs) were also highlighted as a catalyst for adoption. (5) The perceived urgency further propelled adoption due to high incidence rates. Participants noted the “biggest benefit is the reduction of the loss to follow up problem at our PHU.” No barriers to adoption emerged. Insights from regional CBOs, collected through focus groups with staff, will be incorporated by the conference.
Conclusion: Distinct facilitators emerged for adopting a new model of care at a PHU, offering solutions that can aid other PHUs adopting this new model of care to address the rising syphilis epidemic.
OA19.04 – Decentralizing Integrated Hepatitis B, HIV, and Syphilis Services to Accelerate Uptake Among Pregnant Women in Vietnam
Dr. Bao Vu Ngoc1, Dr. Kimberly Green2, Dr. Kim Do Tuan1, Dr. Kieu Hoang Quoc3, Dr. Hang Le Thi3, Dr. Trang Chu Trong3, Dr. Lien Tran Thi Huong1, Mr. An Tran Khanh1
1PATH, Hanoi, Vietnam.
2PATH, Geneva, Switzerland.
3Provincial Center for Disease Control, Vinh City, Vietnam.
Background: Although universal hepatitis B (HBV), HIV, and syphilis screening is recommended for all pregnant women (PW) at first antenatal care (ANC) visit, testing coverage in Vietnam remains low (50.6%, 48.4%, 30.2%, respectively [2023]) due to centralized laboratory-based services. We introduced an integrated and decentralized model to increase uptake of HBV, HIV, and syphilis screening and care among PW in two districts of Nghe An.
Description: Our model leveraged rapid, multiplex, point-of-care testing to decentralize HBV/HIV/syphilis screening to the primary health care level. We trained providers at 46 commune health stations (CHS), two private facilities, and two district hospitals to systematically screen PW during ANC appointments using rapid HBV surface antigen and dual HIV/syphilis tests. Providers used referral slips and telephone follow-up to proactively refer/link those with positive/reactive results for confirmatory diagnosis and treatment. CHS staff and village health workers promoted early uptake of testing and treatment among PW through counseling sessions, community meetings, and social media group chats.
Results: From July 2022 through September 2024, we reached 8,275 PW with integrated screening and linkage services (see Table 1), with slightly higher acceptance of HBV screening (99.3%) than HIV and syphilis (98.9%) due to stigma. We observed higher uptake of screening across all three diseases, particularly for syphilis (98.9% [our model] versus 28.8% [standard-of-care]), due to increased convenience of accessing services at PHC sites than a centralized laboratory. Our decentralized model, coupled with community promotion through pregnant women, facilitated earlier screening, with 6,027 (73.4%) women screened in their first two trimesters.
Conclusion: Our integrated, decentralized approach enabled higher and earlier uptake of HBV/HIV/syphilis screening and treatment among pregnant women. Evidence from our project informed advocacy efforts to approve Nghe An’s provincial triple elimination action plan and include HBV, HIV, and syphilis testing within the standard ANC package at CHSs in Vietnam.
| Accepted/provided screening services | Screened positive/reactive | Received confirmatory testing | Confirmed positive | Initiated on treatment | ||
|---|---|---|---|---|---|---|
| Hepatitis B | 8,215 (99.3%) | 474 (5.8%) | 411 (86.7%) | 103 (25.1%) | 61 (59.2%) | |
| HIV | 8,188 (98.9%) | 1 (0.01%) | 1 (100%) | 1 (100%) | 1 (100%) | |
| Syphilis | 4 (0.05%) | 4 (100%) | 4 (100%) | 4 (100%) |
OA19.05 – Evaluating the Feasibility and Effectiveness of Routine Opt-Out Syphilis Testing Among Women of Childbearing Age in Jails
Ms. Fanta Nani Drame1, Mr Dayne Collins1, Ms Daisha Washington2, Mr Robert McDonald1, Ms. Rebekah Horowitz
1Centers For Disease Control & Prevention, Atlanta, United States.
2National Association of County and City Health Officials, Washington D.C, United States.
Background: Primary and secondary syphilis (P&S) rates among women aged 15–44 in the U.S. surged 580% from 2014 to 2023, contributing to 3,882 congenital syphilis (CS) cases in 2023. Expanding testing and treatment beyond clinics, including jails, is crucial for early detection and increased access to STI and prenatal care. From 2021 to 2022, incarceration among women rose 9%, and 17% of women with P&S syphilis in 2022 reported incarceration within the prior year. Rising syphilis and incarceration rates among women highlight the potential impact of syphilis testing and treatment in jails to help reduce transmission and prevent CS.
Description: To enhance our capacity to detect and treat new cases of syphilis and evaluate the viability of routine syphilis testing in different settings, we conducted a demonstration project in women’s jails across three states in the U.S. Three local health departments (LHD) received funding to implement a protocol assessing the practicality and efficacy of routine opt-out syphilis testing within jails. Using the RE-AIM Framework, we assessed this approach’s feasibility, effectiveness, and sustainability in real-world settings.
Results: During the project, testing uptake was low; only 9.1% (1,564/17,161) of women who have been incarcerated were tested. Among those tested, 2.1% were newly diagnosed with syphilis, and 78.8% received treatment. Qualitative feedback from LHD reports identified challenges in policy adherence, data access, protocol alignment, staffing, and testing acceptance, impacting adoption, implementation, and sustainability. Strong partnerships with LHDs, integrated health services within jails, and rapid point-of-care tests helped improve safety and efficiency.
Conclusion: Addressing implementation challenges and building strong partner support are essential for implementing routine opt out syphilis testing in jails and other high-priority settings. Despite the challenges, new cases of syphilis were identified underscoring the potential of routine opt-out syphilis testing in jails to limit syphilis transmission and build accessible health solutions for disproportionately impacted populations.
OA19.06 – 20 Years Since the Introduction of Rapid Testing for HIV and Syphilis in Brazil: A Key Tool in Expanding Access to Diagnosis
Ms. Ana Philippus1, Mr. Alisson Bigolin1, Ms. Pamela Gaspar1
1Brazilian Ministry of Health, Brasília, Brazil.
Background: HIV and syphilis remain major public health concerns in Brazil, particularly vulnerable populations. Rapid tests (RT) are crucial to increase testing access and early diagnosis.
Description: Since 2005, the Brazilian Ministry of Health (MoH) has distributed over 251 million RT, recommending them as the primary tool for diagnosing HIV and syphilis. In 2011, RT expanded to include testing for pregnant women, decentralizing testing to primary health care – previously restricted to specialized clinics. Testing is permitted for non-laboratory professionals (e.g., nurses and technicians). By 2024, new strategies were introduced, including dual tests for simultaneous detection of anti-HIV and treponemal antibodies, and the implementation of RT in private pharmacies (representing >40 thousand health services in Brazil).
Results: RT has led to significant advances, including improved access, reduced costs, faster diagnoses, and the ability to conduct tests in areas with limited infrastructure, like Amazon region. The decentralization of testing and expanded diagnostic access contributed to a marked increase in the proportion of people living with HIV/AIDS (PLWHA) diagnosed, rising from 69% in 2012 to 96% in 2024. Considering the high prevalence of syphilis in the country, a reactive result in a rapid test already allows treatment to be started in pregnant women and in people who are more vulnerable. Thus, early diagnosis through RT has helped reduce the incidence of congenital syphilis, with a 4.7% (1,511 cases) decrease between 2022 and 2023, despite a rising trend in syphilis rates among pregnant women since 2013.
Conclusions: The implementation of RT for HIV and syphilis in Brazil has significantly improved diagnostic and treatment outcomes. However, the continued rise in syphilis and HIV cases highlight the need for ongoing efforts in prevention, education, and care access. To further reduce the burden of these infections, it is essential to address stigma, regional healthcare disparities, and social inequalities.
PP01.03 – Performance of a Research-Use-Only Prototype of a Highly Multiplexed Sample-to-Answer Diagnostic System for Identification of Sexually Transmitted Infections from Vaginal Swabs and Penile Urine
Mr. Jeremiah Antosch1, Kerrin Koch1, Sarah Gross1, Ray Kirby Jennings1, Jenifer Einstein1, Marta Mangifesta1, Tanner Robinson1, Matt Jones1, Tyler Healy1, Alex Taylor1, Cody Firmage1, Toma Todorov1, Matt Poulson1, Russell Green1, Caitlin Castaneda1, Lorin Brookes1, Cameron Hill1, Justin Keener1, Jeffrey Bastar1, Ashley Ky1, Dr. John Kriesel2, Dr. Aaron Ermel3, Dr. Barbara Van Der Pol4, Dr. LaShonda Crane5
1Biomerieux, Salt Lake City, United States.
2University of Utah, Salt Lake City, United States.
3Indiana University School of Medicine, Indianapolis, United States.
4University of Alabama at Birmingham, Birmingham, United States.
5Planned Parenthood Gulfcoast, Houston, United States.
Background: Sexually transmitted infections are highly prevalent, symptomatically similar conditions spread through sexual activity causing sexual health complications and, if untreated, adverse reproductive outcomes.
bioMérieux is developing the BIOFIRE® SPOTFIRE® Sexually Transmitted Infection (STI) Panel, a <20-min molecular test designed for a point-of-care setting to provide detection of Chlamydia trachomatis, Mycoplasma genitalium, Neisseria gonorrhoeae, and Trichomonas vaginalis from vaginal swabs (Vswabs) or first-catch penile urine collected in eNAT® media. The Research-Use-Only (RUO) BIOFIRE SPOTFIRE® STI Panel was evaluated against a composite agreement between three nucleic acid amplification tests (NAATs) in a pilot study.
Methods: The study was performed at four Institutional Review Board approved sites in the US. Symptomatic subjects with relevant clinician-ordered test(s) were included after providing informed consent/assent/parental permission. Between April 2024 and January 2025, 787 subjects provided penile urine, and 783 subjects provided Vswabs in test-specific media. Three FDA-cleared NAATs and a bioMérieux-developed NAAT served as comparators. Sequencing was used to resolve discrepancies.
Results: The sensitivity/specificity of the RUO BIOFIRE SPOTFIRE® STI Panel for every analyte was 97.69%/98.63% or greater in Vswabs, and 98.86%/99.58% or greater in urine (see Table 1). Testing resulted in 4 false negatives, likely due to near-LoD organism load, 16 positives which either had ambiguity among comparators or were confirmed as true positives by sequencing, and 12 false positives which are still being investigated.
Conclusions: This study showed that the RUO- BIOFIRE SPOTFIRE® STI Panel combines ease-of-use with accurate and rapid detection of key STI agents.
This abstract contains data regarding a device that has not been reviewed or approved by regulatory agencies for in vitro diagnostic use.
| Analyte | Vswab | Penile Urine | |||
|---|---|---|---|---|---|
| Detections | Sensitivity(%)/Specificity(%) | Detections | Sensitivity(%)/Specificity(%) | ||
| C. trachomatis | 48 | 97.69/99.32 | 72 | 98.63/99.58 | |
| M. genitalium | 112 | 99.12/98.63 | 102 | 100.0/99.7 | |
| N. gonorrhoeae | 13 | 100.0/99.87 | 45 | 100.0/99.86 | |
| T. vaginalis | 70 | 98.59/99.3 | 13 | 100.0/99.74 | |
PP01.04 – Comparative Genomics of the Sexually Transmitted Parasite Trichomonas Vaginalis Reveals Virulence and Pathogenesis Genes Involved in its Jump from Birds to the Human Reproductive Tract
Prof. Jane Carlton1
1Johns Hopkins University, Baltimore, United States.
Background: Trichomonas vaginalis is a parasite that infects people globally causing the disease trichomoniasis. T. vaginalis infections are associated with serious outcomes during pregnancy, increased risk of HIV-1 infection, and cancers of the human reproductive tract. Other species of Trichomonas infect a range of hosts in addition to humans including birds, livestock, and pets. Phylogenetic studies of Trichomonas samples from birds have provided evidence that a spillover event from pigeons and doves likely gave rise to T. vaginalis in humans. There are few genome sequences of Trichomonas species, and the first T. vaginalis genome sequence in 2007 was highly fragmented and with low quality gene finding and functional analyses. This study aimed to produce high-quality chromosome-scale reference genomes for T. vaginalis and its closest relative in birds Trichomonas stableri, plus genome sequences of five other species that infect birds and mammals.
Methods: The latest techniques in long-read sequencing, chromosomal conformation sequencing, and genome assembly algorithms, were employed to generate high-quality chromosome-scale reference genomes for human T. vaginalis and bird T. stableri, and short read assemblies of several other species that infect cats, dogs, birds, monkeys, and humans.
Results: Trichomonas species that infect humans have undergone an expansion in the size of their genomes compared to their sister species found in birds, a result of expansions of gene families and transposable elements. Trichomonas species are thought to have independently host-switched twice from birds to mammals/humans. We identified gene functions implicated in the transition, including those involved in adherence to host tissue, parasite phagocytosis, extracellular vesicle formation, and CAZyme virulence factors.
Conclusion: This study provides insights into the evolution of T. vaginalis, including evidence for natural selection accompanying the host switch from birds into humans. Virulence and pathogenesis genes involved in its jump from birds to the human reproductive tract are now candidates for further investigation.
PP01.05 – Genital Microbial and Inflammation Changes Among Women Using 30-Day L. Rhamnosus/L. Reuteri Probiotic, in Combination with Intravaginal Estradiol
Dr. Smritee Dabee1,2, Dr. Maysa Niazy1, Dr. Biban Gill1, Dr. Jocelyn M. Wessels1,3, Dr. Christina L. Hayes1, Dr. Jenna Ratcliffe1, Junic Wokuri4, Dr. Gregor Reid5, Dr. Rupert Kaul6,7, Dr. Jesleen Rana4, Dr. Muna Al-Khaifi4, Wangari Tharao4, Dr. Fiona Smaill8, Dr. Charu Kaushic1
1McMaster Immunology Research Centre and Department of Medicine, McMaster University, Hamilton, Canada.
2University of British Columbia, Vancouver, Canada.
3Afynia Laboratories, Hamilton, Canada.
4Women’s Health in Women’s Hands Community Health Centre, Toronto, Canada.
5Departments of Microbiology & Immunology and Surgery, Western University, and Canadian Research and Development Centre for Human Microbiome and Probiotics, The Lawson Health Research Institute, London, Canada.
6Departments of Immunology and Medicine, University of Toronto, Toronto, Canada.
7Department of Medicine, University Health Network, Toronto, Canada.
8Department of Pathology and Molecular Medicine and Michael G. DeGroote Institute for Infectious Disease Research, McMaster University, Hamilton, Canada.
Background: Probiotic Lactobacillus species have been shown to improve the genital microbial milieu, particularly among women with bacterial vaginosis (BV). Further, the hormone estradiol is associated with mucosal health and better Lactobacillus adhesion. In a prospective, randomized, phase I trial, we assessed the impact of treatment with intravaginal estradiol, with/without concurrent use of probiotic Lacticaseibacillus rhamnosus and Limosilactobacillus reuteri administered vaginally or orally, on the genital microbiome.
Methods: African, Caribbean, and Black women (N = 41) aged 18–49, living in Greater Toronto Area, were randomized to four study arms: intravaginal estradiol (Estring©; 7.5 mg/day); vaginal probiotic (RepHresh™ Pro-B™) administered twice daily; combination of Estring© and vaginal RepHresh™ Pro-B™ (twice daily); or the Estring© and oral RepHresh™ Pro-B™ (twice daily), for 30 days. Cervicovaginal lavages were collected at baseline, mid-intervention, end-of-intervention, and follow-up (after 7 days) for 16S rRNA microbiome sequencing and measuring 43 cytokines. BV was determined using vaginal swabs (Nugent scoring). A composite inflammation score was generated using eight inflammatory markers (IL-1α, IL-1β, IL-8, IL-18, MIG, IL-6, IP-10, TNF-α).
Results: By mid-intervention, there were statistically-significantly higher abundances of probiotic lactobacillus species in both vaginal probiotic arms (P < 0.05), which persisted till end-of-treatment, although abundances returned to baseline levels a week later at follow-up. 51.2% (N = 21) of women experienced an overall positive shift in microbial composition from baseline to end of treatment. At follow-up, despite the decrease in probiotic species abundances, the overall relative abundance of other lactobacilli, mostly L. iners, remained higher compared to baseline. Further, there was a consistent decrease in inflammation score from baseline to end-of-intervention, and 7-days post-treatment among those with an overall positive microbial shift (P < 0.05 at all visits).
Conclusion: Overall, treatment with probiotic lactobacilli with/without intravaginal estradiol led to a significant increase in genital Lactobacillus abundance, with half the participants experiencing an improved microbial composition, and significantly lower inflammatory cytokine levels.
PP01.06 – Proteolytic Bacterial Vaginosis-Associated Bacteria Target Complement Factor C3
Miss Ana D’aubeterre1,2,3, Lauren Over1,2,3, Karen V. Lithgow1,2,3, Kenzie Birse1,2,3, Shaelen Konschuh1, Dr. Antoine Dufour2,5, Dr. Laura K. Sycuro1,2,3,4,6
1Department of Microbiology, Immunology and Infectious Diseases, Cumming School of Medicine, University of Calgary, Calgary, Canada.
2Calvin, Phoebe & Joan Snyder Institute for Chronic Diseases, University of Calgary, Calgary, Canada.
3Alberta Children’s Hospital Research Institute, Cumming School of Medicine, University of Calgary, Calgary, Canada.
4Department of Obstetrics and Gynaecology, Cumming School of Medicine, University of Calgary, Calgary, Canada.
5Department of Physiology and Pharmacology, Cumming School of Medicine, University of Calgary, Calgary, Canada.
6International Microbiome Centre, University of Calgary, Calgary, Canada.
Background: Bacterial vaginosis (BV) is linked to adverse sexual and reproductive health outcomes including an increased risk of sexually transmitted infections (STIs). The mechanisms by which BV-associated bacteria (BVABs) impair host immunity to facilitate STI acquisition are poorly understood. STI pathogens have evolved to evade the complement system, indicating this key branch of the innate immune system is important for their control. However, interactions between BVABs and complement remain uncharacterized. Proteolytic BVABS including Prevotella bivia and Porphyromonas asaccharolytica are related to complement disruptors in the oral niche. We hypothesize that these bacteria secrete complement-targeting proteases that alter the function of complement factor C3 in the vaginal niche, affecting C3 cleavage and release of inflammatory anaphylatoxin C3a, which may impact STI risk.
Methods: To investigate the effects of secreted bacterial proteases on C3, we exposed human C3 to cell-free bacterial supernatants +/- protease inhibitor, observed cleavages via Western blot, and measured subsequent production of C3a using ELISA. Cell-shaving proteomics was used to isolate surface-associated and secreted proteins from P. bivia enabling identification of protease candidates.
Results: We demonstrate that both P. bivia and P. asaccharolytica exhibit secreted protease activity towards C3. Similar cleavage products and visible degradation of the C3 α-chain were observed across both species including the production of a 109 kDa band suggesting liberation of C3a. Preliminary C3a ELISAs indicate the production and subsequent degradation of C3a over time. The serine protease inhibitor PMSF partially blocked protease activity in P. asaccharolytica. In contrast, complement-targeting activity in P. bivia was inhibited by the cysteine protease inhibitor E64; P. bivia encodes only one secreted cysteine protease identified by cell-shaving proteomics.
Conclusions: The discovery and identification of complement-targeting proteases in P. bivia and P. asaccharolytica highlight a novel immunomodulatory role for BVABs in the cervicovaginal niche that could contribute to STI risk.
PP01.07 – Development of a Point-of-Care, Field-Deployable CRISPR-Based Assay for Predicting Neisseria gonorrhoeae Phenotypic Susceptibility to Cefixime
Miss Sakshi Garg1,2, Elizabeth Caso2, Gordon Adams2,3, Sreekar Mantena3, Dr. Nisha Gopal3, Dr. Jeffrey D. Klausner4, Dr. Pardis C. Sabeti3,5,6,7,8, Dr. Jacob E. Lemieux2,3, Dr. Lao-Tzu Allan-Blitz1,2,3
1Brigham & Women’s Hospital, Boston, United States.
2Massachusetts General Hospital, Boston, United States.
3Broad Institute of Massachusetts Institute of Technology and Harvard, Boston, United States.
4Keck School of Medicine, University of Southern California, Los Angeles, United States.
5Massachusetts Institute of Technology, Cambridge, United States.
6Harvard University, Cambridge, United States.
7Harvard T.H. Chan School of Public Health, Boston, United States.
8Howard Hughes Medical Institute, Chevy Chase, United States.
Background: Antibiotic resistance in Neisseria gonorrhoeae is an urgent global health threat. Treatment diversification using rapid molecular assays to guide management may reduce selective pressure towards the emergence of N. gonorrhoeae resistance. The absence of six mutations in the penA gene (mosaic codons 375–377 and non-mosaic codons 501, 542 and 555) reliably predict susceptibility to cefixime – an oral antibiotic that can facilitate non-clinic-based care and expedited partner therapy.
Methods: We aimed to develop a point-of-care assay to detect the absence of mutations at penA codons 375–377 using CRISPR-Cas13a detection paired with isothermal recombinase polymerase amplification (RPA). We leveraged a machine-learning algorithm to design CRISPR-Cas13a guide RNA (gRNA) sequences with maximal on-target and minimal off-target activity. We also designed RPA primers with >90% homology among a database of 2,274 N. gonorrhoeae genomes. We evaluated and optimized performance of the gRNAs and primers using synthetic DNA and assessed the best performing assay design on 29 isolates (n = 17 with cefixime minimum inhibitory concentration (MIC) > 0.125). We ran the CRISPR-Cas13a assay on a field-deployable fluorometric device (DxHub; DxLabs, United States), comparing results with phenotypic resistance and penA genotyping determined by in-house PCR.
Results: We evaluated four wildtype and four mutant gRNA sequences, as well as eight RPA primer sets. The selected CRISPR-based assay demonstrated 100% concordance with PCR penA genotyping and 96.6% (95% CI 82.2–99.9%) concordance (28/29) with phenotypic susceptibility testing (Table 1); one isolate had an MIC of 0.125 and a mutated penA genotype. The median time-to-result was 12.5 min (IQR 5.0).
Conclusion: A field-deployable CRISPR-based assay correctly and rapidly identified the absence of mutation at penA codons 375–377 among N. gonorrhoeae isolates. Further work can evaluate assay performance among diverse clinical specimens and incorporate gRNAs for detecting additional penA mutations to improve concordance with phenotypic testing.
| Isolate | Cefixime MIC µg/mL | PenA codons 375-377 (PCR) | PenA codons 375-377 (CRISPR) | Concordant with PCR? | Concordant with MIC? | Time to detection (min) | |
|---|---|---|---|---|---|---|---|
| FQ009 | 0.125 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 24.8 | |
| FQ023 | ≤0.015 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 9.0 | |
| FQ027 | 0.060 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 10.8 | |
| FQ030 | ≤0.015 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 12.0 | |
| FQ038 | ≤0.015 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 12.5 | |
| FQ043 | 0.060 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 15.5 | |
| FQ047 | ≤0.015 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 15.8 | |
| FQ049 | 0.060 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 11.4 | |
| FQ056 | 0.060 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 15.3 | |
| FQ059 | ≤0.015 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 9.2 | |
| FQ093 | 0.060 (S) | Non-Mutated | Non-Mutated | Yes | Yes | 32.7 | |
| FQ091 | 0.125 (S) | Mutated | Mutated | Yes | No | ||
| FQ041 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ045 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ048 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ050 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ053 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ069 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ071 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ057 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ060 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ062 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ074 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ076 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ078 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ081 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ083 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ085 | 0.250 (R) | Mutated | Mutated | Yes | Yes | ||
| FQ088 | 0.250 (R) | Mutated | Mutated | Yes | Yes |
† Phenotypic resistance defined in accordance with the European Committee on Antimicrobial Susceptibility Testing MIC breakpoint of > 0.125 µg/mL.
PP01.08 – Glycome Degradation by the Vaginal Microbiome: A Risk Factor for Chlamydia Infection?
Ms. Katherine Heger1, Dr. Karen Lithgow1,2, Ms. Shaelen Konschuh1, Ms. Sahar Bagheri3, Mr. Nicholas Twells4,5, Dr. Nelly Mugo6,7, Dr. Alison Roxby7,8,9,10, Dr. Lara Mahal4,5, Dr. Laura Sycuro1,2,3
1Department of Microbiology, Immunology and Infectious Diseases, Cumming School of Medicine, University of Calgary, Calgary, Canada.
2Alberta Children’s Hospital Research Institute, Cumming School of Medicine, University of Calgary, Calgary, Canada.
3International Microbiome Centre, University of Calgary, Calgary, Canada.
4Department of Chemistry, University of Alberta, Edmonton, Canada.
5Glycomics Institute of Alberta, University of Alberta, Edmonton, Canada.
6Kenya Medical Research Institute, Nairobi, Kenya.
7Department of Global Health, University of Washington, Seattle, United States of America.
8Department of Medicine, University of Washington, Seattle, United States of America.
9Department of Epidemiology, University of Washington, Seattle, United States of America.
10Vaccine and Infectious Disease Division, Fred Hutchinson Cancer Research Center, Seattle, United States of America.
Background: Chlamydia, the most common bacterial sexually transmitted infection, disproportionately affects adolescents and young adults (AYA) assigned female at birth. A diverse vaginal microbiome, clinically known as bacterial vaginosis (BV), increases risk of chlamydia through uncertain mechanisms. Yet, AYA display low rates of BV. Sialidase-producing Gardnerella and Prevotella spp. commonly precede BV and, we hypothesize, may act as “Gateway Bacteria” – cleaving terminal sialic acids to expose chlamydial docking sites for efficient binding and invasion.
Study Design: To investigate vaginal niche shifts that precede infection, we profiled the microbiome and cell-associated/soluble host glycomes in longitudinal vaginal samples collected from 40 low-risk Kenyan participants at baseline, preceding infection, and at incident chlamydia. Vaginal microbiome composition was determined using 16S rRNA gene amplicon sequencing while the glycome was quantified using a lectin microarray.
Results: Preceding infection, protective L. crispatus decreased (Wilcoxon signed-rank test, P = 0.0054) while sialidase-producing Prevotella spp. increased (Wilcoxon signed-rank test, P = 0.0024). Concurrently, sialic decreased 50% in both cell-associated and soluble glycomes (Wilcoxon signed-rank test, P = 0.0056 and 0.0072). Microbiomes with Lactobacillus depletion displayed a decrease in sialic acid, protective high mannose, and an increase in Type II LacNAc residues. Overall, the niche became less protective, with a significant decrease in vaginal IgG1 (Mann-Whitney U Test, IgG1 P = 0.0172) and total lactic acid (Mann-Whitney U Test, P = 0.0384). Finally, Galectin-1, an endogenous lectin chlamydia hijacks to facilitate binding, increased significantly at incident chlamydia (Mann-Whitney U Test, P = 0.0198) and was negatively correlated with total lactic acid (Spearman ρ = –0. 2555; P = 0.0129).
Conclusion: We observed a decrease in protective characteristics within the vaginal microbiome, glycomes, and biomolecular composition preceding infection. These findings suggest lactic acid and microbiome screening may provide new avenues for public health and therapeutic strategies to alleviate the burden of chlamydia infection.
PP01.09 – Understanding the Interaction Between the Vaginal Microbiome and Host Immune Response in the Progression of Papillomavirus-Mediated Cervical Cancer
Mr. Akash Hirgond1, Ms Deesha Nayar1, Mr Debjyoti Thakur1, Ms Sarah Brendle3, Dr Alicia Berard1,2, Dr Deanna Santer1, Dr Adam Burgener2,1, Dr Jiafen Hu3, Dr Thomas Murooka1
1University of Manitoba, Winnipeg, Canada.
2Case Western Reserve University, Cleveland, United States of America.
3Pennsylvania State Cancer Institute, Hershey, United States of America.
Background: The female genital tract (FGT) is comprised of a specialized immune system that maintains homeostasis, protects against infections and supports reproductive health. A healthy vaginal microbiome is dominated by Lactobacillus species but a shift to specific anaerobic bacterial species is associated with inflammation and increased acquisition risk for STBBIs. High-risk human papillomavirus (HPV) infection is the leading cause of cervical cancer in women in Canada and across the globe. Current HPV vaccines are strictly prophylactic, indicating that people already infected are at risk of spreading the disease and developing cancer. Studies show strong associations between the presence of inflammation-causing vaginal bacteria and cervical cancer progression, but the mechanistic understanding of HPV+ cervical cancer development is incomplete. Here, we will test the hypothesis that vaginal anaerobic bacteria will increase viral HPV persistence and enhanced cancer progression through the modulation of T cell function.
Methods: Using a mouse model of vaginal murine papillomavirus (MmuPV1) infection, we aim to understand how specific anerobic bacteria may induce immune cell recruitment, immune activation and cancer development in vivo. We will evaluate mucosal T cell responses in the lower FGT after bacteria/viral co-infection. We will perform immunohistochemistry to look for cancer progression with markers associated with cervical cancer as p16INKA4a+, suprabasal p63+ localization, Ki67+ in the lower FGT.
Results: Our studies show that the presence of anaerobic bacteria causes inflammation, epithelial barrier dysfunction in vivo. However, we show that the presence of inflammation-associated anaerobes does not enhance susceptibility to vaginal MmuPV1 infection. We are currently evaluating whether these bacteria accelerate MmuPV1-induced cervical cancer development in vivo.
Conclusions: Our study will demonstrate the role of vaginal microbiome in HPV mediated cervical cancer progression. It will address the critical role of mucosal T cells in clearing the viral infection in vivo contributing to papillomavirus-associated cancer development.
PP01.10 – The Role of Mutations in the Mycoplasma genitalium 16S rRNA Gene for the In-vitro Activity of New and Old Tetracyclines
Miss Simone Høstgaard1,2, Doctor Suhella Tulsiani Drud1, Mr Thomas Roland Pedersen1, Doctor Kirsten Salado-Rasmussen1,2, Doctor Lars Haukali Omland1,3, Mrs Christina Nørgaard1, Doctor Jørgen Skov Jensen1
1Research Unit for Reproductive Microbiology, Department of Bacteria Parasites and Fungi, Statens Serum Institut, Copenhagen, Denmark.
2Department of Dermato-venereology, Bispebjerg University Hospital, Copenhagen, Denmark.
3Department of Infectious Diseases, Copenhagen University Hospital, Rigshospitalet, Copenhagen, Denmark.
Background: Mycoplasma genitalium (MG) infections are difficult to treat due to antimicrobial resistance. Doxycycline (DOX), commonly used prior to resistance-guided therapy, has low cure-rates. We evaluated in-vitro minimal inhibitory concentrations (MICs) of tetracyclines against MG and associations with 16S rRNA gene mutations.
Methods: Fifty-five clinical MG isolates were analyzed. MICs for tetracycline (TET), DOX, minocycline (MIN), omadacycline (OMA), and eravacycline (ERA) were determined. Partial 16S rRNA gene sequences were examined for TET resistance (TETR) associated mutations (MIC>4 µg/mL).
Results: Fifteen of 55 isolates (27%) were TETR. DOX MICs among TETR isolates were 1-2 mg/mL as compared to a median of 0.5 µg/ml (range 0.125 µg/mL to 2) for Tetracycline sensitive (TETS) isolates. Median MIC’s were as follows: TET (n = 55) 1 (range 0.25 to 16 µg/mL) DOX (n = 56) 0.5 (range 0.125 to 2 µg/mL), MIN (n = 54) 0.5 (range 0.125 to 1 µg/mL), OMA (n = 54) 0.5 (range 0.25 to 1 µg/mL), and ERA (n = 33) 0.125 (range ≤0.03 to 1 µg/mL) (Fig. 1). High TET MICs predicted high DOX and MIN MIC, whereas OMA and ERA MICs were unaffected. 16S rRNA gene sequencing revealed two isolates with a G1054T mutation with corresponding TET MICs of 8 µg/mL and 16 µg/mL. The remaining 13 TETR isolates did not have mutations near the TET binding site.
Conclusion: Isolates with G1054T mutations – associated with DOX resistance in Mycoplasma hominis – were TETR. However, most TETR lacked 16S mutations, suggesting other resistance mechanisms. MIN was more active than DOX, and ERA and OMA appeared to be active even in TETR isolates with median MICs as follows: OMA 0.5 (range 0.25 to 1) in TETS isolates, compared to OMA 0.5 (range 0.25 to 1) in TETR isolates, and ERA 0.125 (range <0.03 to 0.5) in TETS compared to ERA 0.25 (range 0.125 to 1) in TETR isolates.
In vitro minimal inhibitory concentration (MIC) values in μg/mL (x-axis) for doxycycline, eravacycline, minocycline, omadacycline, and tertacycline in MG isolates.
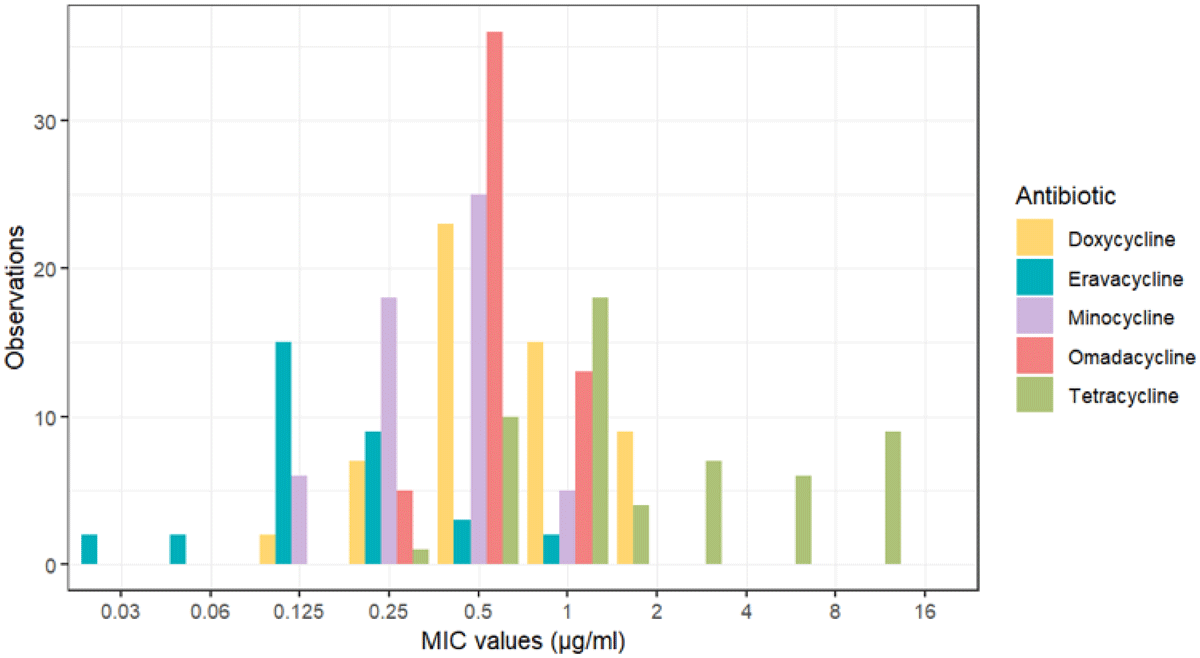
PP01.11 – Evaluation of the Performance of the Sysmex UF-5000 Urinary Flow Cytometer to Detect Urethral Inflammation in Men: A Pilot Study
Dr. Evelyn Toh1, Xiaoli Zhang1, Tina Nitsos1, Dr Caleb Ardizzone1, Waleed Alrebdi1, Dr David Nelson1, Dr. Stephen Jordan1
1Indiana University, Indianapolis, United States.
Background: Urethritis diagnosis requires urethral inflammation confirmation, indicated by the presence of urethral discharge, elevated polymorphonuclear leukocytes on either centrifuged urine or urethral swab Gram stain microscopy, or elevated leukocyte esterase (LE) on urinalysis. We evaluated the performance of the Sysmex UF-5000 urinary flow cytometer, compared to LE and urethral swab Gram stain, in symptomatic and asymptomatic men.
Description: Remnant urine was obtained from men attending the Indianapolis Bell Flower sexually transmitted infection (STI) clinic for STI evaluation or treatment. After an aliquot of urine was taken for chlamydia and gonorrhea NAAT, the remaining urine was used to measure White blood cell (WBC) count per µL using the UF-5000 and LE by urinalysis. Demographic and clinical data, including urethral swab Gram stain results, were abstracted from the electronic medical record. T-tests were used for statistical analysis, with P-values less than 0.05 considered significant.
Results: Two hundred sixty-five remnant urine specimens were included in this study. The median participant age was 33 years (range: 18–71); 50% were Black, 30% White, and 20% other race; 80% not Hispanic. No urethral symptoms were reported in 74% (195/265) of men. A urethral swab was obtained for Gram stain microscopy in 66% (46/70) of symptomatic men. Gonorrhea and chlamydia prevalence were 3% and 5%, respectively. The mean UF-5000 WBC count was significantly higher in men with a positive LE (1544 vs 34 WBC/µL, P < 0.0001), presence of urethral symptoms (213 vs 37 WBC/µL, P = 0.0016), and a urethritis diagnosis (509 vs 34 WBC/µl, P < 0.0001) (Fig. 1).
Conclusion: The Sysmex UF-5000 urine flow cytometer detected increased WBCs in urine from men with positive LE, urethral symptoms, and urethritis. Future studies are needed to evaluate the assay sensitivity and specificity, relative to LE and Gram stain microscopy, and evaluate the potential of the UF-5000 to detect urethritis at the point-of-care setting.
PP01.12 – Investigating the Antimicrobial Resistance Profile of Biofilms Formed by Neisseria Gonorrhoeae
Miss Joyce Kuipers1, Dr. Cezar Khursigara1
1University of Guelph, Guelph, Canada.
Background: Neisseria gonorrhoeae is the causative bacterial agent of the sexually transmitted infection gonorrhea. Over half of infections present asymptomatically, contributing to the transmission of this pathogen. As the total number of infections steadily increases, so does the incidence of complicated gonorrheal infections-which can impact fertility or be life-threatening. Further, rates of antimicrobial resistance (AMR) are becoming increasingly concerning as treatment options are limited. It is largely unknown why these asymptomatic infections persist, but research suggests they are mediated by biofilms. As an acquired mechanism of AMR, biofilms may play a key role in the development and persistence of AMR determinants.
Methods: The objective of this study is to characterize the degree of AMR of biofilms formed by N. gonorrhoeae. We evaluated this using an extended panel of antimicrobials including azithromycin, ceftriaxone, ciprofloxacin, tetracycline, penicillin, spectinomycin and gentamicin tested against 4 strains of N. gonorrhoeae including ATCC 49226, FA1090, CH811 and F62. (Fig. 1).
Results: We applied a high-throughput minimum inhibitory concentration (MIC) assay to measure AMR profiles and crystal violet assays to determine the minimum biofilm inhibition concentration (MBIC). Further, we investigated using DNase I the degree of resistance the extrapolymeric substance (EPS) contributes for biofilms. It was determined that biofilms conveyed varying degrees of resistance between strains and antimicrobials, with fold-change differences between MICs and MBICs of a minimum 1000-fold. Accordingly, the application of DNase I to these biofilms significantly reduced the MBIC values for three of our strains, though still demonstrating a significant fold-change to the MIC values.
Conclusion: These results demonstrate that biofilms formed by N. gonorrhoeae convey high levels of resistance to antimicrobials and that this resistance is largely due to the presence of the EPS. This knowledge will inform the continued research into the contribution that biofilm formation has to the development of AMR determinants in N. gonorrhoeae.
Comparison of minimum inhibitory concentration to minimum biofilm inhibition concentration of 4 strains of Neisseria gonorrhoeae to the antimicrobial ceftriaxone. N. gonorrhoeae strains ATCC 49226, FA1090, F62 and CH811 were tested against the antimicrobial ceftriaxone between 0.001-0.25 µg/mL for minimum inhibitory concentrations (MICs) using agar dilution (a) and 4-2048 µg/mL for minimum biofilm inhibition concentrations (MBICs) with and without the application of 0.5 µg/mL of DNAse I using crystal violet biomass assays (b).
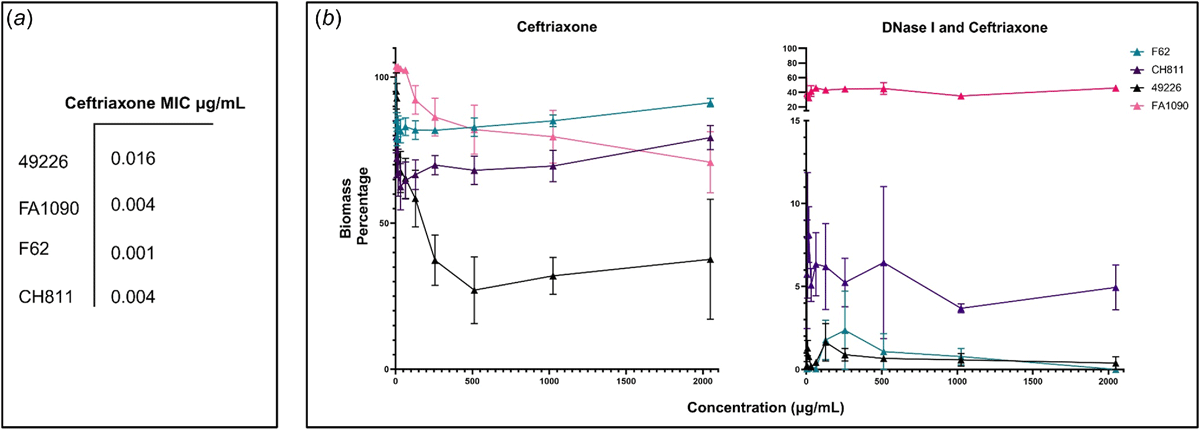
PP01.13 – MiR-330-3p Downregulates NAT10 Expression to Promote T Cell Ferroptosis and Inhibit IFN-γ Production in Neurosyphilis
Dr. Fu-quan Long1
1Shanghai Skin Disease Hospital, Shanghai, China.
Background: Neurosyphilis (NS) is a severe neurological infection caused by Treponema pallidum that can lead to irreversible central nervous system damage. CD4+ T cells play a crucial role in the immune response to NS, but the mechanisms underlying T cell dysfunction and IFN-γ dysregulation remain unclear. MicroRNAs (miRNAs) are known to regulate immune responses, and miR-330-3p has been shown to be upregulated in neurosyphilis patients. However, its specific role and mechanisms in NS pathogenesis are not well understood.
Methods: We collected peripheral blood and CSF samples from 30 neurosyphilis patients and 30 healthy controls. CD4+ T cells were isolated, and miR-330-3p expression was analyzed by RT-qPCR. The effects of miR-330-3p on T cell ferroptosis and IFN-γ production were investigated using in vitro experiments with Jurkat-E6-1 cells and primary CD4+ T cells. Mechanistic studies included dual-luciferase assays, RNA immunoprecipitation (RIP), and ac4C dot blot assays to elucidate the role of miR-330-3p and NAT10 in ferroptosis regulation.
Results: We found that miR-330-3p was significantly upregulated in CD4+ T cells from neurosyphilis patients, correlating with increased T cell ferroptosis. miR-330-3p directly targeted NAT10 mRNA, leading to decreased NAT10 expression and reduced acetylation of GPX4 mRNA, which destabilized GPX4 and promoted ferroptosis. Overexpression of NAT10 or activation of GPX4 reversed the pro-ferroptotic effects of miR-330-3p. Additionally, miR-330-3p enhanced IFN-γ production independently of NAT10.
Conclusion: Our study reveals that miR-330-3p promotes T cell ferroptosis in neurosyphilis through the miR-330-3p/NAT10/GPX4 axis and regulates IFN-γ production via a NAT10-independent pathway. These findings provide novel insights into the pathogenesis of neurosyphilis and highlight potential therapeutic targets for mitigating T cell dysfunction and immune dysregulation in this disease.
PP01.14 – Emergence and Sustained Transmission of Neisseria Gonorrhoeae with High-Level Resistance to Azithromycin in Kampala, Uganda
Dr. Johan Melendez1, Dr. Herve Tetellin2, Ms Adamaris Muniz Tirado1, Dr. Annet Onzia3, Ms Brenda Dawa3, Dr. Peter Kyambadde4, Dr. Francis Kakooza3, Dr. Matthew Hamill1, Dr. Rosalind Parkes-Ratanshi3, Dr. Yukari Manabe1
1Johns Hopkins University School of Medicine, Baltimore, United States.
2Institute for Genome Science, University of Maryland, Baltimore, United States.
3Infectious Diseases Institute, Kampala, Uganda.
4Ugandan Ministry of Health, Kampala, Uganda.
Background: EGASP (Enhanced Gonococcal Antimicrobial Surveillance Programme) has reported very high rates of antimicrobial resistance (AMR) in Uganda,but never reported Neisseria gonorrhoeae (NG) with high-level resistance to azithromycin (HLR-AZM). We report on the emergence, sustained transmission, and characteristics of HLR-AZM NG in Kampala, Uganda.
Methods: Within a cross-sectional study of men seeking treatment for urethritis from July 2020 to August 2023 at five government health clinics in Kampala, urogenital and pharyngeal samples were collected and cultured for NG. NG isolates underwent antimicrobial susceptibility testing by E-test (all isolates) and agar dilution (HLR-AZM NG), whole genome sequencing, and multilocus sequence typing (MLST).
Results: Of 182 isolates, 25 were AZM-resistant; of those, 24/182 (13.2%) from 22 participants, collected over 3 years, median [IQR] 24 years [20, 29], displayed HLR-AZM (MIC ≥ 256 µg/mL). All HLR-AZM NG had resistance/intermediate resistance to ciprofloxacin, tetracycline, and penicillin, but were susceptible to ceftriaxone and cefixime. Of participants with HLR-AZM NG, 22.7% (n = 5) had ≥ 2 isolates with different AZM susceptibility (one HLR-AZM and the other(s) AZM-susceptible). Of the sequenced HLR-AZM NG isolates (n = 14), 85.7% (n = 12) belonged to MLST ST11994, demonstrated close relatedness to each other, and relatedness to other AZM-susceptible strains. The other two HLR-AZM NG belonged to MLST ST1588, and to a novel ST. The 23S rRNA A2047G mutation was present in 92.9% (13/14) of HLR-AZM NG; one isolate harbored the novel 23S rRNA C2404T mutation. None of the 22 participants with HLR-AZM NG reported AZM use in the 14 days prior to clinic visit.
Conclusions: The close genetic relatedness of NG with HLR-AZM, collected over a three-year period during the COVID pandemic, suggests local, undetected sustained transmission. The emergence of resistance and HLR to AZM in Kampala highlights the rapid evolution of AMR in NG and warrants enhanced surveillance practices and antimicrobial stewardship.
| ID # | Site of isolation (Isolate #) | Age | HIV | Date of visit | AZM | CEF CRO | CIP | PEN | TET | 23S rRNA A2047G (# of alleles) | MLST ST | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| MN220 | Penile (1) | 32 | Neg | 7/27/20 | HLR | S | R | I | R | Yes (4/4) | 11994 | |
| Penile (2) | S | S | R | R | R | N/A | TBD | |||||
| Pharynx | S | S | I | I | S | N/A | TBD | |||||
| MN221 | Penile | 24 | Neg | 7/28/20 | HLR | S | R | I | R | Yes (4/4) | 11994 | |
| Pharynx | S | S | R | R | I | N/A | 1597 | |||||
| MN228 | Penile | 23 | Neg | 8/6/20 | HLR | S | R | I | R | Yes (4/4) | 11994 | |
| Pharynx | S | S | R | I | R | N/A | 11368 | |||||
| SA093 | Penile | 39 | Pos | 2/18/22 | HLR | S | R | I | R | Yes (4/4) | 11994 | |
| SA098 | Penile | 26 | Neg | 2/23/22 | HLR | S | R | I | R | TBD | TBD | |
| SA100 | Penile | 43 | Neg | 2/24/22 | R | S | R | R | R | C2599T (4/4) | 16145 | |
| SA105 | Penile | 20 | Neg | 3/3/22 | HLR | S | R | I | R | Yes (4/4) | 11994 | |
| SA120 | Penile | 25 | Neg | 3/17/22 | HLR | S | R | I | R | Yes (4/4) | 11994 | |
| Pharynx | HLR | S | R | I | R | Yes (4/4) | 11994 | |||||
| SA204 | Penile | 24 | Pos | 4/6/23 | HLR | S | R | R | R | TBD | TBD | |
| SA257 | Penile | 43 | Pos | 5/23/23 | HLR | S | R | R | R | TBD | TBD | |
| SA275 | Penile | 29 | Neg | 6/6/23 | HLR | S | R | R | R | TBD | TBD | |
| SA276 | Penile | 24 | Neg | 6/7/23 | HLR | S | R | R | R | TBD | TBD | |
| SA277 | Penile | 30 | Neg | 6/7/23 | HLR | S | R | R | R | TBD | TBD | |
| SA279 | Penile | 52 | NA | 6/7/23 | HLR | S | R | R | R | TBD | TBD | |
| SA212 | PenileA | 23 | Neg | 6/8/23 | HLR | S | R | R | R | Yes (4/4) | 11994 | |
| SA240 | Penile | 20 | Neg | 6/19/23 | HLR | S | R | R | R | Yes (2/4) | New | |
| Pharynx | HLR | S | R | R | R | C2404T (4/4) | 1588 | |||||
| SA283 | Penile | 25 | Neg | 6/21/23 | HLR | S | R | R | R | TBD | TBD | |
| SA284 | Penile | 18 | Neg | 6/22/23 | HLR | S | R | R | R | Yes (4/4) | 11994 | |
| SA285 | Penile | 17 | Neg | 6/22/23 | S | S | R | I | R | N/A | 1588 | |
| Pharynx (1) | HLR | S | R | R | R | TBD | TBD | |||||
| Pharynx (2) | S | S | R | I | R | N/A | TBD | |||||
| SA324 | Penile | 23 | Neg | 7/31/23 | HLR | S | R | R | R | TBD | TBD | |
| SA314 | Penile | 19 | Neg | 8/3/23 | HLR | S | R | R | R | Yes (4/4) | 11994 | |
| SA328 | Penile | 24 | Pos | 8/8/23 | HLR | S | R | R | R | Yes (4/4) | 11994 | |
| SA331 | Penile (1) | 20 | Neg | 8/21/23 | S | S | R | R | R | N/A | TBD | |
| Penile (2) | HLR | S | R | R | R | Yes (3/4) | 11994 |
PP01.15 – Investigating the Interplay Between the Vaginal Microbiota and Papillomavirus Infection in Vivo
Ms. Deesha Nayar1, Mr. Paul Lopez1, Dr. Jiafen Hu1, Dr. Thomas Murooka1
1University of Manitoba, Winnipeg, Canada.
2Pennsylvania State University, Hershey, United States.
Background: Human papillomavirus (HPV) infection is one of the most common sexually transmitted diseases worldwide and the causative factor for most cervical cancers. We and others have reported strong associations between the vaginal microbiome and HPV acquisition, persistence, and cervical neoplasm in women. Notably, a polymicrobial vaginal microbiota dominated by Gardnerella, Prevotella and Mobiluncus spp, among others, is common in bacterial vaginosis (BV) and is associated with high-risk HPV (HR-HPV) persistence and high-grade lesions. In contrast, a Lactobacillus spp. dominant vaginal microbiota is associated with protection against HR-HPV infection. Thus, we hypothesize that BV-associated bacteria directly enhance HPV infection and accelerate cervical cancer development by inducing a prolonged inflammatory state within the female reproductive tract (FRT).
Methods: We have previously described a BV-like mouse model that recapitulates key biological features of vaginal inflammation, epithelial barrier function and immune activation. We have overlayed the vaginal murine papillomavirus (MmuPV-1) infection challenge model to address how BV-associated bacteria impacts papillomavirus infection in the FRT. Our primary readouts include: (1) viral DNA/RNA measurements in vaginal lavage by qPCR and: (2) immunohistochemistry to localize infected cells with markers of heightened cell proliferation, abnormal epithelial differentiation, biomarkers of cervical cancer development.
Results and Conclusion: MmuPV-1 viral load and persistence dynamics was not altered in the presence of BV-associated bacteria species, and mice proceeded to cervical cancer development within 4–6 months. While M. mulieris inoculated challenge did not significantly increase viral replication in the lower FRT, the presence of L. crispatus showed a remarkable reduction in MmuPV1 replication. Current studies are focused on determining whether reduction in viral replication kinetics reduces cervical cancer progression. These studies represent efforts to better understand the mechanistic underpinnings of bacteria/viral co-infections during cervical cancer development.
PP01.16 – Comparative Transcriptomic Profiling of Mycoplasma genitalium Reveals Growth Phase Dynamics and Strain Specific Responses to Antibioticsveals Growth Phase Dynamics and Strain Specific Responses to Antibiotics
Miss Hannah Nugent1, Dr Laurence Luu1,2, Dr Gerald L Murray3,4,5, Professor Catriona S Bradshaw6,7,8, Professor Wilhelmina M Huston1,9
1University of Technology Sydney, Sydney, Australia.
2School of Biotechnology and Biomolecular Sciences, University of New South Wales, Sydney, Australia.
3Department of Obstetrics, Gynaecology and Newborn Health, University of Melbourne, Parkville, Australia.
4Molecular Biology Research Group, Murdoch Children’s Research Institute, Parkville, Australia.
5Centre for Women’s Infectious Diseases, The Royal Women’s Hospital, Parkville, Australia.
6Melbourne Sexual Health Centre, Alfred Health, Cartlon, Australia.
7Central Clinical School, Monash University, Melbourne, Australia.
8Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, Parkville, Australia.
9Faculty of Science, University of Melbourne, Parkville, Australia.
Background: Little is known regarding the transcriptional activity of Mycoplasma genitalium, a fastidious organism with increasing antibiotic resistance. We investigated this using RNA sequencing to elucidate transcriptional dynamics throughout the growth cycle and in response to antibiotic treatment.
Methods: To characterise growth dynamics, M. genitalium G37 was cultured in Vero cells and sampled at Days 3, 7, 10, 12, & 19; timepoints corresponding to the lag, exponential, and stationary growth phases. Antibiotic response was characterised using G37, and G512, a clinical isolate with 23s rRNA gene and gyrA resistance mutations, which were cultured in Vero cells for 7 days and then treated with 4 mg/L of azithromycin, doxycycline, or moxifloxacin, for 24 and 72 h.
Results: Exponential growth phase associated timepoints (Days 7–10) showed significant changes in gene expression, with 46% of genes showing significant upregulation and 47% showing significant downregulation (P > 0.05). Upregulated genes were associated with cell division, protein synthesis and DNA replication, e.g., scpA (log2FC = 2.52, adj P < 0.001) and rpsM (log2FC = 2.80, adj P < 0.001), whereas downregulated genes were associated with the metabolism, translation, and adhesin, e.g,. mgpA (log2FC = −1.57, adj P < 0.001) and msrA (log2FC = 2.43, adj P < 0.001).
Hierarchical clustering of the transcriptomic profile in response to azithromycin treatment showed that for G37, the treated and untreated samples formed distinct clusters; in contrast, the treated and untreated G512 samples co-clustered tightly. Interestingly, G37 samples treated with azithromycin, doxycycline, and moxifloxacin each clustered separately from doxycycline and moxifloxacin-treated G512 samples.
Conclusions: M. genitalium significantly upregulates replication and protein synthesis genes while downregulating metabolic and adhesion genes during exponential growth (Day 7-10), reflecting a shift from host attachment toward rapid biomass accumulation.
Azithromycin treatment elicited minimal transcriptional changes in G512, suggesting no bacterial impact from treatment. Conversely, doxycycline and moxifloxacin elicited unique gene expression profiles for G37 and G512, indicating a strain-specific antibiotic response.
PP01.17 – Reduced TPPA Confirmation of New Syphilis Cases in High Prevalence Settings: Manitoba, Canada
Miss Alice Van Wyk1,2, Mr Wyman Mar2, Doctor Paul Van Caeseele1,2, Doctor Derek Stein1,2
1The University of Manitoba, Winnipeg, Canada.
2Cadham Provincial Laboratory, Winnipeg, Canada.
Background: Manitoba employs the reverse algorithm method for syphilis testing, which includes a chemiluminescent microparticle immunoassay (CMIA) to detect treponemal antibodies, followed by a rapid plasma reagin (RPR) and a Treponema pallidum particle agglutination (TPPA) to confirm. Other jurisdictions in Canada, due to higher test volumes (Saskatchewan and Ontario), have implemented a policy in which TPPA testing is only performed on CMIA-positive, RPR negative, specimens with no previous syphilis history which could indicate a false positive, an early infection or a very latent infection. Therefore, we underwent a review of current diagnostic practices concerning TPPA testing.
Methods: This study used all TPPA results from January 1, 2020, to September 31, 2024, along with the CMIA and RPR results from the Cadham laboratory information management system. The results were tabulated by positive/negative RPR and TPPA, respectively. CMIA and RPR titers were also plotted to determine if a threshold could accurately predict the need for further TPPA testing.
Results: Of all the TPPA tests performed, 8780 were positive, and 2285 were negative through RPR testing. An additional 186 specimens were cancelled due to insufficient specimen volume or incorrect specimen type. Of the negative RPR specimens, 1506 were positive or borderline, while 779 were negative by TPPA testing. Of the positive RPR specimens, 8764 were positive or borderline, while 16 were negative by TPPA testing. These 16 negative TPPA specimens would represent 16 false positives.
Conclusion: Data collected from the past 5 years indicated that 99.8% of CMIA-positive and RPR-positive specimens with no previous history were confirmed positive by TPPA (8764/8780). Performing TPPA only on new syphilis positives with a negative RPR or CMIA S/Co < 5 will reduce turn around time, testing costs, and labour without affecting patient care. It should be considered for implementation in high-prevalence settings like the prairies.
PP01.18 – First Evaluation of Performance of the Liat CT/NG Assay for Point-of-Care Detection of Chlamydia Trachomatis (CT) and Neisseria Gonorrhoeae (NG) on Extragenital Samples
Dr. Petra Wolffs1, Julia Hintzen1, Selma Herngreen1, Prof. Dr. Christian Hoebe2
1Maastricht University Medical Center, Maastricht, Netherlands.
2Maastricht University, Department of Social Medicine, Maastricht, Nethelands.
Background: Point-of-care testing (POCT) of sexually transmited infections is increasingly of interest. Testing can be performed at clinics while the patient waits for results, after which treatment can be directly administered. Recently a new POCT test for detection of CT and NG in genital samples has been released. The test is however not validated for extragenital samples which are part of the routine work-up for patients such as MSM. The goal of this study was to provide a first evaluation of the use of the Liat CT/NG test for extragenital samples. Here we report the results for the first 75 anal samples.
Methods: A validation set of 75 samples was selected to contain 15 samples that were CT+/NG−, 15 samples NG+/CT−, 5 samples that were CT+/NG+ and 40 samples CT−/NG−. Self-collected samples were obtained from patients attending local Public Health Services. Samples were obtained in Roche PCR media and routinely analysed by Cobas 4800 CT/NG (Roche Diagnostics). The novel Liat CT/NG was evaluated in this study and compared to routine results.
Results: Overall, the results for CT showed 100% agreement with routine diagnostics while for NG results showed 93% agreement. All NG positive results were detected but 5 negative samples were found to be positive with Liat testing. When observing the Ct values for both tests, the Liat tests showed Ct values of 8–12 Ct earlier than those detected in COBAS 4800, potentially indicating a higher analytical sensitivity of the Liat.
Conclusion: This first evaluation shows promising results for the POCT Liat CT/NG test to be used on extragenital samples. Possible false-positive Liat results for NG will have to be investigated, but could be due to a higher analytical sensitivity. Future work will focus on the evaluation of the Liat test in oral samples.
PP01.19 – Genomic Sequencing of Treponema Pallidum Strains to Improve Understanding of Syphilis Epidemiology in Low- and Middle-Income Countries
Dr. Farhang Aghakhanian1, Dr. Nicole Lieberman2, Mr. Christopher Hennelly1, Dr. Jane Chen1, Dr. Everton Bettin3, Dr. Wentao Chen4, Dr. Ligang Yang4, Dr. Mitch Matoga5, Dr. Irving Hoffman1, Dr. Jonathan Juliano1, Dr. M. Anthony Moody6, Dr. Juan Salazar3,7, Dr. Justin Radolf3,7, Dr. Lorenzo Giacani2, Dr. Kelly Hawley3,7, Dr. Alexander Greninger2, Dr. Arlene Seña1, Dr. Jonathan Parr1
1University of North Carolina at Chapel Hill, Chapel Hill, United States.
2University of Washington, Seattle, United States.
3UConn Health, Farmington, United States.
4Southern Medical University, Guangzhou, China.
5UNC Project Malawi, Lilongwe, Malawi.
6Duke University, Durham, United States.
7Connecticut Children’s, Hartford, United States.
Background: Syphilis, caused by Treponema pallidum subsp. pallidum (TPA), has seen a global resurgence. Understanding TPA genomic epidemiology, particularly in low- and middle-income countries (LMICs), is crucial for addressing the syphilis epidemic.
Methods: We conducted a genomic analysis of TPA, incorporating 298 newly sequenced genomes from early syphilis patients across 14 countries on five continents, including LMICs such as Argentina, Colombia, Malawi, Madagascar, Sri Lanka, and Vietnam. By integrating these genomes with 1,409 publicly available sequences, we assembled a collection of 1,707 TPA genomes. Our analyses focused on characterizing the genetic structure of TPA populations, identifying unique single nucleotide variants (SNVs) within subpopulations, and exploring the genotype-phenotype correlation between outer membrane protein variability and antigenicity using paired syphilitic serum samples.
Results: We identified eight distinct subpopulations within the Nichols lineage and five within the SS14 lineage, exhibiting geographical clustering as shown by principal component analysis. Notably, we discovered novel TPA subpopulations from Malawi and Tanzania, highlighting Africa’s overlooked genetic diversity. Significant genetic variation was found in the Nichols lineage, particularly within genes TP0462 (an antigenic putative lipoprotein) and TP0865 (a fatty acid transporter homolog, FadL). In the SS14 lineage, notable variation was observed in TP0705 (mrcA), a penicillin-binding protein, especially in genomes from South America, Oceania, and Asia. Genotype-phenotype analyses are ongoing.
Conclusions: This study enhances our understanding of TPA by significantly increasing the available genomic data and shedding light on its global genetic diversity and population structure. Further investigation is needed to determine the biological impact of these genetic differences and their implications for developing effective vaccines and therapeutic strategies.
PP01.20 – Prevalence of Trichomonas Vaginalis Among MSM Attending an STI Clinic in Kumasi, Ghana
Dr Thomas Agyarko-Poku1,2, Dr Albert Adusei Dua2, Prof Yaw Adu-Sarkodie1,2
1Kwame Nkrumah University of Science and Technology, Kumasi, Ghana.
2APT Foundation for Sexual Health, Kumasi, Ghana.
Introduction: Trichomonas vaginalis is a common sexually transmitted infection globally, but its prevalence among men who have sex with men (MSM) is not well-documented in sub-Saharan Africa. This study aims to determine the prevalence of T. vaginalis among MSM at the STI Clinic in Suntreso Government Hospital, Kumasi, Ghana, and explore its association with having female sexual partners.
Methods: A cross-sectional study was conducted from January to June 2024 with 157 self-identified MSM, aged 18 to 70, who attended the STI Clinic. Participants were recruited through convenience sampling and completed surveys about their sexual behaviour over the past 24 months, particularly their interactions with female partners. Urine samples were tested for T. vaginalis using nucleic acid amplification testing (NAAT). Chi-square tests and logistic regression were used to analyze the relationship between sexual behaviours and T. vaginalis infection.
Results: Of the participants, 81.3% (128/157) reported sexual intercourse with at least one woman in the last 2 years, and 68.6% (108/157) had current female partners, with some married (25.7%) or cohabiting (30.2%). T. vaginalis prevalence was 4.3% (7/157). Notably, 71.4% (5/7) of those infected were married or cohabiting with a woman. There was a statistically significant link between T. vaginalis infection and having a female sexual partner, especially among those who were married or cohabiting (P < 0.05).
Conclusions: The study reveals a low prevalence (4.3%) of T. vaginalis among MSM in Kumasi. Still, it indicates a significant correlation with sexual relationships with female partners, particularly in marital or cohabiting contexts. These findings suggest the need for targeted STI prevention strategies that include both MSM and their female partners, emphasizing education and regular screening to curb transmission.
PP01.21 – Advancing Molecular Diagnostic Access: In-House Real-Time PCR for Detecting Neisseria Gonorrhoeae in Anal Specimens from Outpatient Recruits in Morocco
Miss Rokaya Aitlhaj-mhand1,2, Dr Bahija Bellaji3, Miss Chiamae Remz1, Dr Reda Charof4, Professor Hanaa Abdelmoumen2, Dr Amina Hançali3, Professor Hicham Oumzil5
1Virology Department, National Institute Of Hygiene, Rabat, Morocco.
2Microbiology and Molecular Biology Team, Research Center for Plant and Microbial Biotechnology, Biodiversity and Environment, Faculty of Sciences, Mohammed V University in Rabat, Rabat, Morocco.
3STIs Reference Laboratory, Medical Bacteriology Department, National Institute of Hygiene, Rabat, Morocco.
4Epidemic Diseases Laboratory, Medical Bacteriology Department, National Institute of Hygiene, Rabat, Morocco.
5Medical Biotechnology Laboratory, School of Medicine and Pharmacy, University Mohammed V in Rabat, Rabat, Morocco.
Background: Gonorrhea is one of the most prevalent sexually transmitted infections (STIs) worldwide. In Morocco, the laboratory diagnosis of Neisseria gonorrhoeae (NG) primarily depends on microscopy and, in some facilities, culture methods. However, nucleic acid amplification tests (NAATs) have not yet been implemented for routine gonorrhea diagnosis. Objective: This study aims to assess the performance of an in-house real-time PCR assay for detecting NG DNA, with the goal of establishing it as a routine diagnostic tool in healthcare laboratories. This approach seeks to enable broad-spectrum testing while addressing supply challenges associated with the high cost of the GeneXpert test.
Methods: NG infection was evaluated using anal swabs subjected to molecular testing. The Xpert® CT/NG assay (Cepheid, USA) was utilized as the primary test and reference standard. Subsequently, an in-house qRT-PCR, optimized for its applicability, was conducted as an alternative diagnostic method. The performance characteristic, including sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV), were compared with those of the GeneXpert CT/NG assay (Cepheid, USA).
Results: The evaluation of the PCR test revealed high sensitivity, capable of detecting N. gonorrhoeae DNA at concentrations as low as 1 pg/µL. The in-house real-time PCR assay demonstrated a sensitivity of 80% and a specificity of 100%. The positive predictive value (PPV) was 100%, confirming that all positive results were true positives, while the negative predictive value (NPV) was 97.3%, indicating a high likelihood that negative results were true negatives.
Conclusion: The findings show that the in-house real-time PCR test has high sensitivity and specificity for detecting Neisseria gonorrhoeae in extragenital samples. This makes it a reliable diagnostic tool for healthcare labs. Using this test could improve diagnostic accuracy and accessibility, especially in resource-limited areas.
Keywords: Neisseria gonorrhoeae, real time PCR, porA pseudogene, Morocco.
PP01.22 – Fifteen Years of Molecular Diagnostic Services for Syphilis: What Does the Laboratory Data Show?
Dr. Sarah Alexander1, Dr Michelle Cole1, Mr Jack Minshull1, Dr Helen Fifer1, Dr Rachel Pitt1
1United Kingdom Health Security Agency, London, United Kingdom.
Background: The United Kingdom has limited commercially available molecular tests for the detection of Treponema pallidum (TP) DNA. Consequently, these diagnostic services are often restricted to larger specialist laboratories, that have the resources and specimen flow to validate and quality control in-house assays. This study examines the breadth of TP Real-Time PCR (RT-PCR) data obtained over a 15-year testing period from a wide-range of different clinical specimens.
Methods: Clinical specimens, sourced from patients who were clinically suspected to have syphilis, were referred for TP RT-PCR between 2010 and 2024. DNA was extracted from the specimens and tested using an in-house TP RT-PCR with a 47kDa lipoprotein gene target and internal control. The extraction methods and TP RT-PCR chemistry were modified over the 15-year period (adapting to changing technologies) however the primer and probe sequences were consistent throughout.
Results: In total 16,343 clinical specimens were tested, from 194 referring centres, representing 90 different clinical specimen types. 13,080 (80.0%) specimens were from genital sites; TP was more commonly detected in specimens from males [2300/9714, 23.7%] than females [144/2788, 5.2%]; (Fishers Exact Test: P = <0.001) and genital specimens from patients of unknown sex [42/578, 7.3%] were excluded from this analysis. An additional 3,263 specimens were received from non-genital sites and variation in TP rates were observed between different sample types (Table 1). Importantly, 47 specimens were received for investigations for congenital syphilis and 19 (40.4%) were TP RT-PCR positive.
Conclusion: Syphilis can cause many complex clinical presentations. To allow investigation of more unusual presentations it is important that diagnostic laboratories (where quality and regulatory systems allow) are flexible as to which specimens are accepted for TP RT-PCR assays. Finally, this data highlights that testing of more common specimen types can result in high rates of detection of TP DNA.
| Specimen Group [Sample Types] | % TP Positive (Total no.) | % Inhibition (Total no.) | |
|---|---|---|---|
| Oral specimens[Mouth/Lip; Oral ulcer swabs; pharyngeal swabs; Throat/Tongue Swabs] | 19.7%(73/369) | 1.9%(7/369) | |
| Rectal[Anal Swabs; Rectal Swabs; Perianal swab; Rectal biopsy’s] | 21%(198/941) | 2%(19/941) | |
| Ocular Samples[Vitreous Fluid; Eye Swabs; Conjunctival swab] | 14.3%(2/14) | 0%(0/14) | |
| Cerebrospinal fluid | 0%(0/8) | 0%(0/8) | |
| Tissue Biopsies[Lymph node; Liver; Pancreas; Lung; testicular; Abscess fluid] | 25.8%(16/62) | 1.6%(1/62) | |
| Blood[Whole Blood; Plasma; Serum] | 17.4%(16/92) | 0%(0/92) | |
| Unknown[Other; Information Not Provided] | 21.4%(125/583) | 1.5%(9/583) | |
| Nasal[Nose swab; Nasopharyngeal secretions] | 0(0/8) | 12.5(1/8) | |
| Skin[Skin Swabs; Rash Swabs] | 19.6%(223/1139) | 2%(23/1139) | |
| Paediatric samples[Amniotic Fluid; Placenta; Nose swab; mouth swab; Nasopharyngeal secretions; Endotracheal secretions; Spleen; Liver; Skin Lesion Biopsies; Other Swab] | 40.4%(19/47) | 0.0%(0/47) |
PP01.23 – Ureaplasma Parvum Infection Could Alter the Oxidative Stress State and Contribute to Spontaneous Abortion
Sra. Fernanda Karoline1, Doutora Caline Novais Teixeira Oliveira, Sra Lara Fabiana Luz Malheiro, Teacher Thiago Macedo Lopes Correia, Sra Beatriz A. Sampaio, Teacher Lucas Miranda Marques, Teacher Liliany S. de Brito Amaral, Teacher Guilherme Barreto Campos
1Federal University of Bahia, Vitória da Conquista, Brasil.
Background: Spontaneous abortion (SA) is a public health issue with various causes, including infections. Vaginal infections can reach the uterine-placental cavity, disrupting redox status and gestational homeostasis. This study investigated whether Mollicutes infections contribute to SA development.
Methods: Placental tissue from 89 women with SA and 20 women with full-term delivery (FD) were studied. The samples were submitted to qPCR to identify Mollicutes. We also selected positive samples for the pathogen most related to SA (Ureaplasma parvum – UP) to investigate whether the infection was related to SA in the context of redox status (lipid peroxidation – TBARS, protein carbonylation, nitrite levels, and defense antioxidants: superoxide dismutase – SOD, catalase – CAT, and glutathione peroxidase – GPX). Four subgroups were considered: SA without UP infection (SA), SA with UP infection (SA+UP), FD without infection (FD), and FD with UP infection (FD+UP).
Results: UP was the most prevalent pathogen in the SA group (66.3%), followed by Mycoplasma genitalium (41.6%). A positive association was found between UP detection in placental tissue and SA (PR = 5.90, CI 1.9–17.8; P < 0.05), with significantly higher UP microbial loads in SA compared to FD groups (P < 0.01). UP-infected subgroups showed altered redox status compared to non-infected groups. TBARS levels were reduced in SA+UP versus SA (0.2309 ± 0.3170; 0.1083 ± 0.0050; P < 0.0001), while protein carbonylation (2.704 ± 0.5783; 3.873 ± 1.535; P < 0.01) and nitrite levels (1.566 ± 0.4899; 2.577 ± 0.5547; P < 0.05) were elevated. SOD levels increased (2.341 ± 0.2216; 2.563 ± 0.2470; P < 0.05), and CAT levels decreased (0.4644 ± 0.1060; 0.3584 ± 0.0963; P < 0.01) in SA+UP.
Conclusion: These findings highlight that UP infection, an underexplored sexually transmitted infection during pregnancy, disrupts redox status, increasing the risk of spontaneous abortion.
PP01.24 – Advancing Diagnostics for Neisseria Gonorrhoeae Through Explainable Machine Learning
Mr. Andrey Verich1,2, Dr Priya Ramarao-Milne2, Dr Letitia Sng2, Dr Ella Trembizki4, Dr Elisa Mokany3, Assoc. Prof. Tanya Applegate1, Dr Denis Bauer2
1The Kirby Institute, University of New South Wales, Kensington, Australia.
2Transformational Bioinformatics Group, Commonwealth Scientific and Industrial Research Organisation, Sydney, Australia.
3SpeeDx Pty. Ltd., Sydney, Australia.
4Centre for Clinical Research, University of Queensland, Brisbane, Australia.
Background: Neisseria gonorrhoeae (NG) is a global health priority due to increasing prevalence and antimicrobial resistance (AMR) limiting treatment options. Improving treatment outcomes is critical as NG disproportionately affects vulnerable populations. Molecular diagnostics utilising NG resistance-gene targets can improve treatment; however, this requires optimal and adaptable target selection. This study utilises an easily interpretable machine learning pipeline to identify resistance-associated gene variants and their interaction networks, aiming to enhance diagnostic target selection to improve treatment outcomes.
Methods: Whole-genome sequencing data and resistance profiles were systematically collected from publications. A curated dataset of ~7,500 NG sequences underwent reference-based assembly and analysis through the following pipeline: 1) VariantSpark, a random forest machine learning platform, identified resistance-associated gene variants for ciprofloxacin, azithromycin, tetracycline, and penicillin. 2) RFlocalfdr controlled for false positives, and 3) BitEpi assessed variant interactions (up to groups of four) contributing to resistance outcomes.
Results: VariantSpark identified key resistance-associated gene variants, including known markers within: gyrAS91F for ciprofloxacin and rspJ for tetracycline. Additionally, some novel genes were highlighted including, truA for tetracycline. And iles, miab, and tgt for ciprofloxacin, previously unlinked to NG resistance but associated with resistance in other bacteria. BitEpi analysis revealed that the gyrAS91F mutation is a singular, critical mutation for ciprofloxacin resistance (see Fig. 1), while tRNA synthesis pathway genes and chaperone gene variants (hscA and hemW) interact within networks to potentially contribute to resistance outcomes.
Conclusion: This machine learning pipeline allows for easy and rapid identification of potential diagnostic targets and their networks. These targets can now be validated for future study. With its ease of use and adaptability, this approach can drive the development of general and population-specific diagnostics to address resistance, thus improving sexual health and treatment outcomes for all.
PP01.25 – Gardnerella Vaginalis and Prevotella Bivia Embedded in Dual Species in Vitro Bacterial Vaginosis Biofilm Model Exhibit Survival at High Antibiotic Concentrations
Miss Mansi Apreja1, Dr. Rachna Singh2, Dr. Rashmi Bagga1, Dr Archana Angrup1, Dr. Rakesh Yadav1, Ms. Kiran Bala1, Ms. Karamjeet Kaur1, Ms. Nandita Sharma1, Dr. Sunil Sethi1
1Post Graduate Institute of Medical Education and Research, Chandigarh, India.
2Panjab University, Chandigarh, India.
Background: Bacterial vaginosis (BV) is associated with the presence of a polymicrobial biofilm on the vaginal epithelium. It is hypothesized that this polymicrobial biofilm might increase the survival of BV associated bacteria exposed to antibiotics. However, most studies on in vitro bacterial biofilms base their work around main causative agent, since cultivating multispecies biofilms for prolonged time periods, especially with anaerobic bacteria involved, poses significant challenges.
Objective: We aimed to develop and optimize a defined multispecies biofilm model using representative bacterial species associated with BV to depict the efficacy of conventional therapeutics in vitro.
Methods: The dual-species biofilm model was optimized in terms of incubation conditions and duration to ensure successful incorporation of both bacterial species. Bacterial incorporation within the biofilm was assessed using culture (colony counting) and molecular (qPCR) methods. Scanning electron microscopy (SEM) and confocal laser scanning microscopy (CLSM) were performed to visualize ultrastructure of the biofilm. MTT viability assay was performed to evaluate the effect of antibiotic on single and dual-species biofilms.
Results: A compact biofilm structure was confirmed by both SEM and CLSM analysis. In dual-species biofim, both G. vaginalis and P. bivia were found to co-exist with 8.2 log10 cfu/mL and 7.4 log10 cfu/mL respectively. The planktonic MIC (pMIC) of metronidazole (MET) against G. vaginalis was 256 µg/mL. 65% ± 8.6% viable cells and 80% ± 20% viable cells were detected respectively in G. vaginalis monospecies biofilm and in dual-species biofilms treated with 1x pMIC. 20% ± 11% and 29% ± 17% viable cells were detected in mono and dual-species biofilms respectively when treated with 8× pMIC MET.
Conclusion: Our results showing viable bacterial cells in BV associated monospecies and dual-species biofilms treated with antibiotic concentration upto 8× pMIC support the idea of involvement of polymicrobial biofilms in the clinically observed high BV recurrence rates.
PP01.26 – Differential Urinary IgG and IgA Responses in Men with Chlamydia Trachomatis Urethral Infection Before and After Treatment
Dr. Caleb Ardizzone1, Dr. John Ryan1, Dr. Aaron Ermel1, James Williams1, Waleed Alrebdi1, Evelyn Toh1, Dr. David Nelson1, Dr. Stephen Jordan1
1Indiana University School of Medicine, Indianapolis, United States.
Background: The role of antibodies in the urethral immune response to Chlamydia trachomatis (CT) infection in men is unclear. We recently developed a method to accurately quantify IgG and IgA antibodies that recognize CT elementary bodies (EB) in first-catch urine (FCU). Here, we measured and compared the concentrations of anti-EB antibodies in men with and without CT-associated nongonococcal urethritis (NGU) and pre- and post-treatment.
Methods: FCU was collected from men with acute NGU due to CT or other causes at enrollment and at 1-month post-treatment; asymptomatic men without STI or urethritis served as controls. At enrollment, all men with NGU were symptomatic with documented urethritis, as assessed by counting white blood cells on urethral smears. At 1-month post-treatment, all men tested negative for CT and 32% had persistent urethritis. Anti-EB IgG and IgA was quantified by ELISA.
Results: More anti-EB IgG and IgA was detected in enrollment specimens from the men with CT-NGU compared to controls. Comparing enrollment and post-treatment specimens from the men with CT-NGU, the concentration of anti-EB IgG remained elevated in the men with persistent urethritis but declined in the men who resolved urethritis. In contrast, anti-EB IgA remained elevated at follow-up in men who did and did not have persistent urethritis.
Conclusion: After cure of CT infection and urethritis, urinary anti-EB IgA levels, but not IgG, remained elevated for a least one month, suggesting stable mucosal IgA production. Anti-EB IgG declined in men who resolved inflammation, suggesting that IgG does not provide long-term protection against urethral CT infection. Our findings suggest that vaccine development should focus on activating mucosal antibody responses. Prospective studies are needed to determine if these antibodies protect against CT reinfection and transmission.
PP01.28 – Validation of Point of Care Bacterial STI Diagnostic Rapid Tests as Self-Testing Options for Adolescent Girls and Young Women in South Africa
Miss Krishnaveni (Surina) Reddy1, Dr Jiaying Hao2, Ms Nompumelelo Sigcu1, Ms Merusha Govindasami1, Ms Nomasonto Matswake1, Ms Busisiwe Jiane1, Dr Reolebogile Kgoa1, Dr Lindsay Kew1, Dr Nkosiphile Ndlovu1, Ms Reginah Stuurman1, Ms Hlengiwe Mposula1, Dr Jennifer Balkus3, Prof Renee Heffron2, Prof Thesla Palanee-Phillips1,3
1Wits RHI, University of the Witwatersrand, Johannesburg, South Africa.
2University of Alabama at Birmingham, Heersink School of Medicine, Birmingham, USA.
3University of Washington, School of Public Health, Seattle, USA.
Adolescent girls and young women (AGYW) experience high rates of asymptomatic and symptomatic sexually transmitted bacterial infections (STIs). Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG) and Trichomonas vaginalis (TV) increase HIV transmission risk. Young women prefer discrete self-testing for HIV and pregnancy, however STI self-testing options are limited.
We validated seven CT, NG and/or TV single use diagnostic test kits (six antigen-based and one polymerase chain reaction (PCR)-based) for use with self-collected vaginal samples in PROVE, a cross-sectional validation study enrolling AGYW aged 16-25. CEPHEID GeneXpert® NG/CT and OSOM® TV testing using nurse-collected endocervical and vaginal samples served as gold standards to calculate sensitivity, specificity and predictive values. We further validated the most sensitive and specific test (Visby Medical™ Sexual Health Test) for non-clinic self-testing using self-collected vaginal samples in PALESA, a longitudinal follow-up study enrolling AGYW aged 16–18. Here, CEPHEID GeneXpert® NG/CT and TV testing with nurse-collected vaginal samples served as gold standards.
In PROVE, 314 AGYW (median age = 21, IQR 19–23) contributed 558 paired samples (matched self-collected vaginal samples and nurse-collected endocervical/vaginal samples) and the Visby Medical™ Sexual Health Test exhibited highest sensitivity (CT = 78.78%, NG = 100%, TV = 66.67%). In PALESA, 28 AGYW (median age = 18, IQR 17–18) contributed 84 paired samples (matched self-collected and nurse-collected vaginal samples) and the Visby Medical™ Sexual Health Test was 100% sensitive for all three STIs. This kit also demonstrated high specificity and negative predictive value (NPV) in both validation studies. The positive predictive values were low (33–84%) in the longitudinal study.
The discrete Visby Medical™ Sexual Health test was shown to be a viable potential self-test option where AGYW can self-collect vaginal samples, test for three STIs concurrently and receive their own results. Further work is required to confirm these findings and test acceptability, utility and feasibility of STI self-testing in a larger sample of AGYW.
| Validation metrics | PROVE cross-sectional validation (558 paired samples) | PALESA longitudinal validation (84 paired samples) | |||||
|---|---|---|---|---|---|---|---|
| CT | NG | TV | CT | NG | TV | ||
| Sensitivity | 78.78% | 100% | 66·67% | 100% | 100% | 100% | |
| Specificity | 80% | 100% | 90.91% | 88.24% | 87.50% | 92.59% | |
| NPV | 66.67% | 100% | 90.91% | 100% | 100% | 100% | |
| PPV | 87.50% | 100% | 66.67% | 84.62% | 57.14% | 33.33% | |
PP01.29 – Performance Characteristics of Chembio DPP Dual Rapid Test for HIV and Syphilis Using Whole Blood, Oral Swab, and Oral Fluid
Mr. M. Harris Bayan1, Dr. Matthew M. Hamill1, Alec Boudreau1, Tanique Bennett1, Nisha Ramdeep1, Elizabeth Nielsen1, Nyah Johnson2, Caroline Tran1, Jen Jiang1, Robin J. MacGowan3, Nathalie Gonzalez Jimenez3, Debra Daugherty3,4, Dr. Kevin P. Delaney3, Dr. Richard Rothman2, Dr. Yu-Hsiang Hsieh2, Dr. Yukari C. Manabe1
1Division of Infectious Diseases, Johns Hopkins University, Baltimore, United States.
2Department of Emergency Medicine, Johns Hopkins University, Baltimore, United States.
3Centers for Disease Control and Prevention, Atlanta, United States.
4DLH Corporation, Atlanta, United States.
Background: Assays with excellent performance characteristics, easy availability and usability in diverse contexts are critical for the accurate assessment of patients for prevention and treatment of syphilis and HIV. We evaluated the performance of Chembio DPP HIV-syphilis, a rapid, point-of-care HIV and syphilis dual test using whole blood, oral swab, and oral fluid specimens.
Methods: From 08/2021 to 06/2024, participants were enrolled in a randomized controlled trial in Baltimore, Maryland. Eligibility criteria for enrollment was aged 18 or older, having risk factors for HIV infection and not taking pre-exposure prophylaxis, or living with HIV and not in care. Participants answered a sociodemographic questionnaire and provided blood, oral fluid or oral swab specimens collected using manufacturer-provided swabs. Testing was performed according to the manufacturer’s instructions and results were interpreted using the Chembio automated reader. Oral fluid and swab specimens results were read at 15 and 30 min. We used Stata to determine sensitivity and specificity, along with their 95% confidence intervals from participants who had a valid Chembio test result.
Results: Performance characteristics of the assay using whole blood, oral swab, and oral fluid samples collected from 368 participants are presented in Table 1. The one blood-based false-negative HIV result was due to a person with acute HIV infection. The two blood-based false-negative syphilis results were from individuals previously treated for syphilis with negative plasma reagin (non-treponemal antibody) results.
Conclusion: In this population, using whole blood with the Chembio DPP HIV/Syphilis test yielded the highest overall sensitivity and specificity for both infections, followed by samples collected using oral swabs. Waiting an additional 15 min to read the oral swab and oral fluid tests did not significantly alter interpretation of results. Pending further studies, these results highlight the potential utility of using this test and the impact of specimen type on test performance.
| Test | N | False Positive/False Negative | Sensitivity % (95% CI) | Specificity % (95% CI) | |
|---|---|---|---|---|---|
| HIV | |||||
| Blood-based | 368 | 7/1 | 98.8 (93.4–100) | 97.6 (95.0–99.0) | |
| Oral swab 15-min | 284 | 6/5 | 91.5 (81.3–97.2) | 97.3 (94.3–99.0) | |
| Oral swab 30-min | 284 | 5/5 | 91.5 (81.3–97.2) | 97.8 (94.9–99.3) | |
| Oral fluid 15-min | 92 | 10/5 | 82.1 (63.1–93.9) | 84.4 (73.1–92.2) | |
| Oral fluid 30-min | 92 | 7/7 | 75 (55.1–89.3) | 89.1 (78.8–95.5) | |
| Syphilis | |||||
| Blood-based | 368 | 22/2 | 96.1 (86.5–99.5) | 93.1 (89.7–95.6) | |
| Oral swab 15-min | 284 | 8/2 | 94.7 (82.3–99.4) | 96.7 (93.7–98.6) | |
| Oral swab 30-min | 284 | 9/2 | 94.7 (82.3–99.4) | 96.3 (93.2–98.3) | |
| Oral fluid 15-min | 92 | 4/5 | 70.6 (44.0–89.7) | 94.7 (86.9–98.5) | |
| Oral fluid 30-min | 92 | 3/4 | 76.5 (50.1–93.2) | 96.0 (88.8–99.2) | |
CI, confidence interval.
PP01.30 – Genomic Epidemiology of African Syphilis as a Window Into Global Transmission Dynamics of Treponema Pallidum
Dr. Mathew Beale1, Professor Michael Marks, Rebecca Handley, Dr Sarah Burl, Kirsty Ambridge, Ethel Dauya, Aamirah Mussah, Dr Michael Owusu, David Kateete, Rogers Kamulegeya, Edgar Kigozi, Dennis Kimbugwe, Mahlape Mahlangu, Johanna Venter, Bianca Da Costa Dias, Professor Yaw Adu-Sarkodie, Dr Chelsea Morroni, Dr Edith Nakku-Joloba, Dr Etienne Muller, Professor Rashida Ferrand, Professor Nicholas Thomson
1Wellcome Sanger Institute, Hinxton, United Kingdom.
Background: Over the last two decades, syphilis rates have risen dramatically globally, yet genomics is only beginning to catch up. With more Treponema pallidum genomes to enhance epidemiological surveillance, comes novel insights into transmission and data to guide public health interventions. Genomes can also be used to inform rational vaccine design by considering allele frequencies in genes coding for antigenic proteins, ensuring vaccines have broad global utility. However, although >1000 T. pallidum genomes are now available from high-income countries, there are relatively few genomes from Africa.
Methods: We combined samples from 1198 patients recruited into a genital ulcer aetiology study (2022–2023) in Botswana, Ghana, Uganda and Zimbabwe with samples from national syphilis surveillance in South Africa (2006–2023) to generate 147 novel African T. pallidum genomes. Combining these with 167 publicly available African genomes and 1062 genomes from 24 non-African countries, we performed contextual population genomic analyses to understand the T. pallidum genomic diversity and transmission within and between African countries and the rest of the world.
Results: Contrasting with previous studies showing global circulation of highly similar T. pallidum, we found remarkable diversity amongst African T. pallidum. We identified 25 sublineages from 6 African countries, compared to 36 sublineages from 24 non-African countries. Sharing of sublineages between African countries and the rest of the world was rare, and 83.8% of African syphilis was caused by locally circulating sublineages exclusive to Africa. Moreover, just 20.1% of African syphilis was resistant to macrolides; where resistance occurred, this was strongly associated with introduction of global sublineages into Africa.
Conclusion: African T. pallidum is characterised by locally circulating strains not found globally. Since sublineage sharing between countries is low, cataloguing African T. pallidum diversity will require intense local sampling in many countries. These findings will inform ongoing strategies for genomic surveillance and vaccine design.
PP01.31 – In Vitro Evaluation of the Activity of Gepotidacin Against Chlamydia Trachomatis
Dr Olivia Peuchant1,2, Dr Arabella Touati1, Dr Chase A. Weikel3, Prof. Cecile Bebear1,2
1Bordeaux University hospital, Bordeaux, France.
2University of Bordeaux, Bordeaux, France.
3GSK, Collegeville, USA.
Background: Gepotidacin is a novel, first-in-class triazaacenaphthylene antibiotic that selectively inhibits type IIA topoisomerases through a distinct binding site and unique mechanism not utilized by any currently approved human therapeutic agent. It has been shown to be active in vitro against Neisseria gonorrhoeae and Mycoplasma genitalium, including antibiotic-resistant isolates. However, its activity against Chlamydia trachomatis remained unknown.
The aim of this study was to evaluate gepotidacin activity in vitro against C. trachomatis, in comparison to levofloxacin, azithromycin and doxycycline.
Methods: Eight C. trachomatis strains were tested: 2 reference strains (D/UW-3/Cx (ATCC VR-885) and L2/434-Bu (ATCC VR-902B), 1 ofloxacin-resistant mutant of the reference strain L2/434-Bu (OFX-R) selected in vitro, and 5 clinical isolates (genovar D (n = 2), E (n = 2), L2b (n = 1).
To assess drug activity, minimum inhibitory concentration (MIC) determinations were performed on infected monolayers of McCoy cells in 12 mm glass shell vials. Chlamydial inclusions were detected using IMAGEN Chlamydia (OXOID) utilizing a fluorescein-conjugated monoclonal antibody. The following dilution scheme was used: 1–256 µg/mL for gepotidacin, 0.0075-1 µg/mL for doxycycline, 0.0075–1 µg/mL for azithromycin, and 0.03–4 µg/mL for levofloxacin (1–128 µg/mL for OFX-R strain).
Results: All 8 strains of C. trachomatis tested displayed gepotidacin MICs >256 µg/mL. In comparison, azithromycin MICs ranged from 0.125 to 0.5 µg/mL and doxycycline MICs ranged from 0.015 to 0.03 µg/mL. For levofloxacin, the MICs ranged from 0.25 to 0.5 µg/mL for all isolates, with the exception of the L2/434-Bu OFX-R strain, which had a levofloxacin MIC of 64 µg/mL.
Conclusion: In this study, no antibacterial activity was observed for gepotidacin against C. trachomatis at concentrations up to 256 µg/mL. All gepotidacin MICs observed were off scale at >256 µg/mL for all strains tested. These results demonstrate that gepotidacin is not active in vitro against C. trachomatis.
PP01.32 – Sequence Variability of BamA and FadL Orthologs Suggests Divergent Evolutionary Paths of Treponema Pallidum Outer Membrane Proteins
Dr. Everton Bettin1, Farhang Aghakhanian2, Chris Hennelly2, Wentao Chen3, Timothy Davenport4, Simon Hackl5, Andre Grassmann1, Jonny García6,7, Lady Ramirez6,7, Sebastián Silva6,7, Yinbo Jiang3, Joseph Tucker2, Ligang Yang3, Heping Zheng3, Bin Yang3, Petra Pospíšilová8, David Šmajs8, Mitch Matoga9, Irving Hoffman2, Eduardo López-Medina6,7, Kay Nieselt5, M. Anthony Moody10, Arlene Sena2, Juan Salazar1,11, Jonathan Parr2, Dr. Melissa Caimano1,11, Kelly Hawley1,11, Justin Radolf1,11
1Uconn Health, Farmington, United States.
2University of North Carolina at Chapel Hill, Chapel Hill, USA.
3Southern Medical University, Guangdong Provincial Center for Skin Diseases and STD Control, Guangzhou, China.
4Duke University, School of Medicine, Department of Molecular Genetics and Microbiology, Durham, USA.
5Institute for Bioinformatics and Medical Informatics, University of Tübingen, Tübingen, Germany.
6CIDEIM, Cali, Colombia.
7Universidad Icesi, Cali, Colombia.
8Masaryk University, Brno, Czech Republic.
9UNC Project Malawi, Lilongwe, Malawi.
10Duke University Meical Center, Durham, USA.
11Connecticut Children’s, Hartford, USA.
Background: Knowledge of Treponema pallidum subspecies pallidum (TPA) outer membrane protein (OMP) sequence variability is essential for understanding spirochete persistence and designing a global syphilis vaccine. Our group identified extracellular loops (ECLs) of TPA BamA and members of the FadL family as potential components of a multivalent vaccine cocktail.
Methods: We performed whole-genome sequencing of 186 TPA strains collected from early syphilis patients enrolled in Malawi (n = 117), China (n = 37), and Colombia (n = 32) between November 2019 and May 2022. Sequences for BamA and FadLs (TP0548, TP0856, TP0858, TP0859, and TP0865) were compared to the Nichols and SS14 reference strains, and sequence variants were mapped onto Alphafold models. Proteoforms for all six OMPs within the same strain were concatenated and a minimum spanning tree was generated using GrapeTree.
Results: The 186 genomes grouped into eight subclades (five Nichols lineage and three SS14 lineage) with substantial geographic clustering. Single nucleotide variants accounted for the vast majority of identified proteoforms, with variability notably higher among Nichols-like strains. Most mutations occurred in regions predicted to be extracellular, suggesting that host immune pressure drives OMP diversity. The number of unique proteoforms identified for the six OMPs ranged from four to 17: TP0856 (n = 4), TP0859 (n = 5), TP0858 (n = 10), BamA (n = 15), TP0865 and TP0548 (n = 17), highlighting the uneven distribution of evolutionary pressures across the OMPeome. Concatenated OMP profiles largely clustered by subclades within geographic areas. Candidate vaccinogen ECLs (BamA ECL4, TP0856 and TP0858 ECLs 2 and 4) were well conserved, indicating that these regions are under structural and/or functional constraints.
Conclusion: Our study suggests that host immune pressures and host-pathogen interactions at the population level drive TPA OMP diversity. It also provides a structural framework for analyzing the forces shaping the host-pathogen interface in syphilis on a global scale while informing the selection of targets for vaccine development.
PP01.33 – Comparison of Single- and Multi-Valent Scaffolds Displaying Treponema Pallidum Outer Membrane Protein ECL Candidate Syphilis Vaccinogens
Dr. Everton Bettin1, Ms. Kristina Delgado1, Ms. Renee Pontbriant1, Dr. Justin Radolf1,2, Dr. Kelly Hawley1,2, Dr. Melissa Caimano1
1UConn Health, Farmington, United States.
2Connecticut Children’s, Hartford, United States.
Background: Increases in the incidence of syphilis highlight the urgent need for a vaccine to prevent transmission of Treponema pallidum (Tp). An efficacious syphilis vaccine should elicit ‘functional’ (i.e., opsonic and/or neutralizing) antibodies (Abs) against extracellular loops (ECLs) from the spirochete’s limited repertoire of outer membrane proteins (OMPs). Long-lasting protection likely will require a vaccine cocktail comprised of multiple ECLs displayed in a native conformation. Accordingly, we engineered single- and multi-ECL scaffolds and compared the antibody responses they elicit following immunization.
Methods: Individual ECLs from the FadL-like transporters TP0856 and TP0858 and the 8-stranded beta-barrel TP0698 were displayed on a Pyrococcus furiosus thioredoxin (PfTrx) scaffold (Fig. 1). These same ECLs also were grafted onto Escherichia coli OmpA (Ec OmpA) in place of the protein’s native ECLs (Fig. 1). The corresponding recombinant PfTrx and OmpA scaffolds then were used to immunize rabbits and mice. The resulting immune sera were characterized for ECL-specific Ab titers using an unrelated TbpB scaffold based on transferrin binding protein C-lobe. The functionality of antisera also was tested in vitro using our recently developed Tp Nichols strain expressing green fluorescent protein (GFP+).
Results: Both single- and multi-ECL scaffolds produced comparable titers against linear and/or discontinuous epitopes. Importantly, the presence of multiple ECLs from the same OMP did not diminish the production of Abs against the individual ECL components. In vitro assays using Abs generated using PfTrx single-ECL scaffolds showed strong opsonic and/or neutralizing activity. A head-to-head comparison of Abs generated using single- and multi-ECL scaffolds against GFP+ Tp strain are underway.
Ribbon diagrams showing computational models for Pyrococcus furiosus thioredoxin (PfTrx) scaffold (left) containing individual Treponema pallidum OMP extracellular loops (ECLs) for TP0698 versus a multi-loop scaffold based on Escherichia coli OmpA containing all four ECLs (right).
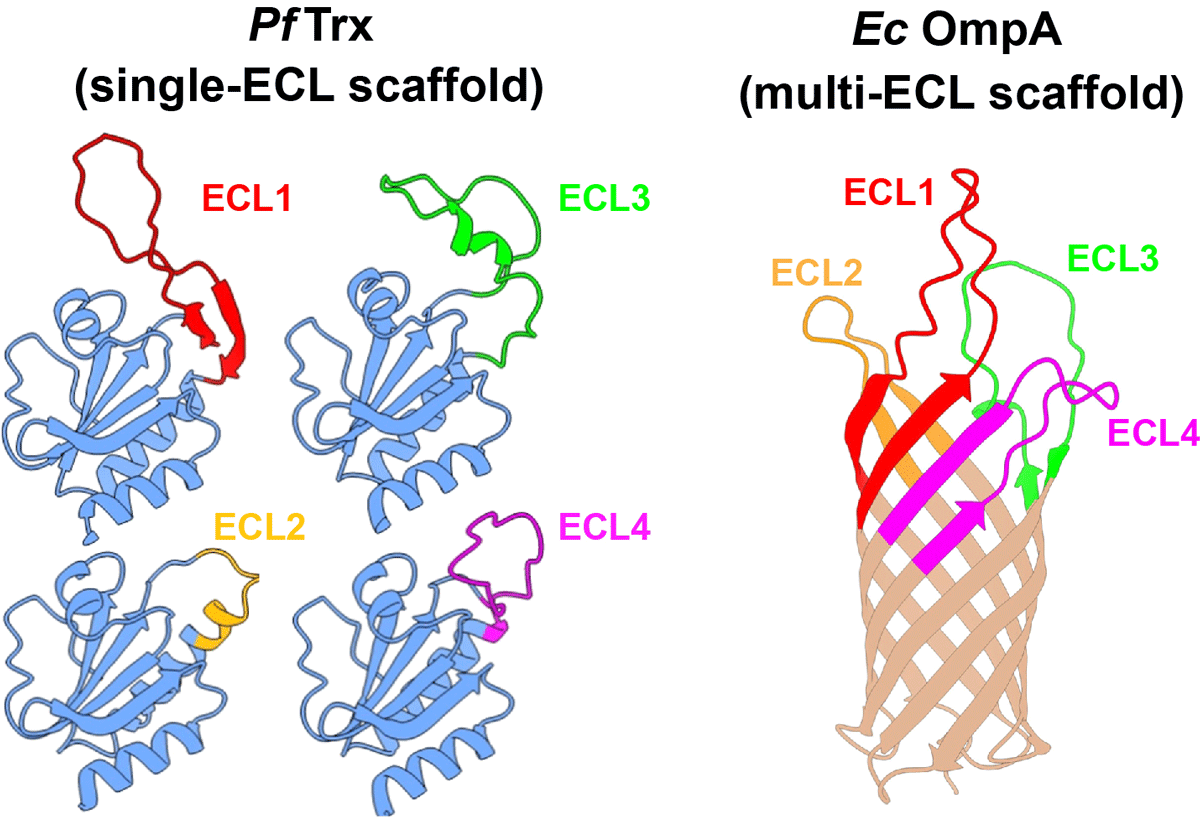
PP01.34 – Performance and Workflow of Allplex™ Assays for the Detection of Mycoplasma Genitalium and Macrolide Resistance Associated Mutations in Self-Collected Vaginal Swabs and First Void Urinef-Collected Vaginal Swabs and First Void Urine
Dr. Max Chernesky1, Dr David J Speicher1, Mr Dan Jang1, Dr Sam Ratnam1
1McMaster University/St Josephs Healthcare, Hamilton, Canada.
Background: Self collected vaginal swabs(VS) and first-void urine(FVU) are convenient samples for identifying women with Mycoplasma genitalium (MG) infection and macrolide resistance-associated mutations (MRAM).
Methods: We compared the ability of Seegene Allplex™CT/NG/MG/TV (STI-4) and Allplex™MG&AziR to detect MG on archived specimens from 300 women. Extraction was on a Microlab STARlet (Hamilton) and amplification on a CFX96 thermocycler (Bio-Rad).The accuracy of Allplex™ MG&AziR was determined for MRAM. Workflow was measured for manual and automated components of each procedure. The reference comparator test was SpeeDx Resistance Plus MG (RPMG) with extraction on an m2000 (Abbott) and PCR on ABI 7500 (ThermoFisher).
Results: Prevalence of MG infection by testing VS was 15% by STI-4, 14.7% by MG&AziR and 15.3% by RPMG; results for FVU were 9,7%,9.7% and10.3% respectively. Agreement between the 2 Seegene assays for MG detection was very good for VS (Kappa 0.960) and FVU (Kappa 0.885). Both of the Seegene assays showed very good agreements with RPMG for both specimen types. Allplex™MG&AziR detected MRAM in 63.6% (28/44) VS and 65.5% (19/29) FVU. RPMG values were 58% (27/46) VS and 48.4% (15/31) FVU. Overall agreements of the 2 assays for MRAM were 97% (Kappa 0.82) for VS and 96.7% (Kappa 0.688) for FVU. For small batches of 10 samples the time to results for MG and MRAM identification was 4.5 h for RPMG compared to 3.5 h for the Allplex™ assays.Larger batches of 90 specimens required more than 9 h to results. Daily maintenance was 3 min for Allplex compared to 25 min for RPMG.
Conclusions: VS testing detected more positive patients than FVU. Both Allplex™ assays demonstrated good agreement with RPMG for detecting MG and MRAM.All of the assays showed desirable turn around times to results. Larger prospective comparisons are required to demonstrate the clinical value of identifying MG infections with or without MRAM using laboratory-efficient commercial assays.
PP01.35 – Neutrophil Extracellular Traps Impair Vaginal Barrier Function and Increase HIV Acquisition in Response to Non-Optimal Bacteria Species
Miss Marina Costa Fujishima1, Ms Deesha Nayar1, Mr Morgan Taverner1, Ms Oluwaseun Ajibola1, Ms Riley Greenslade1, Mr Thomas Murooka1
1University of Manitoba, Winnipeg, Canada.
Background: Analysis from >700 women from the CAPRISA004 cohort show that women with a non-Lactobacillus dominant vaginal microbiome (non-optimal microbiome) were at significantly higher risk of sexual HIV acquisition, and that this strongly correlated with loss of barrier integrity, inflammation and neutrophil accumulation. Despite these strong associations, the cellular and molecular mechanisms that mediate this risk remain largely unknown. Here, we will test that hypothesis that neutrophil recruitment and neutrophil extracellular traps (NETs) in response to non-optimal bacterial species initiate an inflammatory cascade that results in vaginal barrier dysfunction and enhances HIV acquisition.
Methods: Balb/c mice were intravaginally inoculated with either PBS, Lactobacillus crispatus, Mobiluncus mulieris or Gardnerella vaginalis. Vaginal barrier integrity was assessed in the presence or absence of NETs (DNAse I treatment) by inoculating mice with lucifer yellow (0.45 Da) and measuring dye penetration into the submucosa by immunohistochemistry. Finally, to evaluate the impact of different bacteria species on HIV transmission, humanized BLT (bone marrow/liver/thymus) mice were weekly challenged with a low dose of HIV transmitted/founder (T/F) REJO.c virus and plasma viremia was monitored by RT-qPCR.
Results: We found that the presence of non-optimal bacteria species in the vaginal mucosa causes substantial damage to the vaginal epithelium and results in high neutrophil recruitment along with an increase in the release of NETs. Excitingly, we also show that NET formation directly impacts the FGT biology and drives barrier breakdown in the vaginal mucosa. Finally, we demonstrate that these changes in barrier dysfunction directly impact HIV acquisition rates by ~10–14 days compared to PBS controls, suggesting that increased HIV translocation across the FGT barrier contribute to systemic viremia.
Conclusions: Together, our work provides a mechanistic understanding of how non-optimal bacteria species can alter innate immune responses and increase barrier breakdown in the vaginal mucosa to modulate HIV acquisition risk in vivo.
PP01.36 – Spatial Organization of Gardnerella Species and Fannyhessea Vaginae in the Bacterial Vaginosis Biofilm
Mrs Sheridan George1, Dr. Megan Amerson-Brown1, Dr. Kristal Aaron1, Dr. Olivia Van Gerwen1, Dr. Ashutosh Tamhane1, Dr. Paweł Łaniewski2, Dr. Melissa Herbst-Kralovetz2, Dr. Christopher Taylor3, Dr. Nuno Cerca4, Dr. Christina Muzny1
1University of Alabama at Birmingham, Birmingham, United States.
2University of Arizona, Phoenix, United States.
3Louisiana State University, New Orleans, United States.
4University of Minho, Braga, Portugal.
Background: Key BV-associated bacteria hypothesized to be important in incident BV (iBV) pathogenesis are Gardnerella species and Fannyhessea vaginae. We investigated the spatial organization of these bacteria within clue cells and surrounding extracellular matrix in longitudinal vaginal specimens from women who developed iBV using peptide nucleic acid-fluorescence in situ hybridization (PNA-FISH).
Methods: Women with optimal vaginal microbiota (no Amsel criteria, Nugent score 0–3) self-collected twice daily vaginal specimens for 60 days. iBV was defined as a Nugent score of 7–10 on ≥4 consecutive specimens. Fluorescent PNA probes were used to quantify Gardnerella spp. (Alexa fluor 594) and F. vaginae (Alexa fluor 633) within the layers of the BV biofilm from iBV case specimens 2 days before iBV, on the day of iBV, and 2 days after iBV using the NanoZoomer S60 Slide Scanner. For each day, z-stack images were taken at –4 μm, –2 μm, 0 μm, 2 μm, and 4 μm and analyzed using Fiji ImageJ 1.8.0. Statistical analysis was performed using GraphPad Prism 10.0.2.
Results: Thirty vaginal specimens have been imaged from 10 iBV case participants. On 2 days before, day of, and 2 days after iBV, mean Gardnerella spp. counts were significantly higher than mean F. vaginae counts on the bottom layer of the biofilm (–4 μm) (P ≤ 0.031, 0.039, 0.031, respectively). Additionally, on the day of iBV and 2 days after iBV, mean Gardnerella spp. counts were significantly higher than mean F. vaginae counts on layers –2 μm (P ≤ 0.011, 0.015) and 0 μm (P ≤ 0.011, 0.046) (Fig. 1). F. vaginae counts became comparable to Gardnerella spp. counts at layers 2 μm and 4 μm on the day of iBV and 2 days after iBV.
Conclusion: These data suggest that Gardnerella spp. may be an initial colonizer of the BV biofilm while F. vaginae may be a secondary colonizer.
Mean Gardnerella spp. and F. vaginae counts at different layers of the BV biofilm on 2 days before iBV (a), on the day of iBV (b), and 2 days after iBV (c). Layers of the biofilm are listed in order from bottom layer to top layer: –4 μm, –2 μm, 0 μm, 2 μm, and 4 μm. *P ≤ 0.05. Error bars represent the minimum value to the maximum value recorded. Abbreviations: iBV, incident bacterial vaginosis.
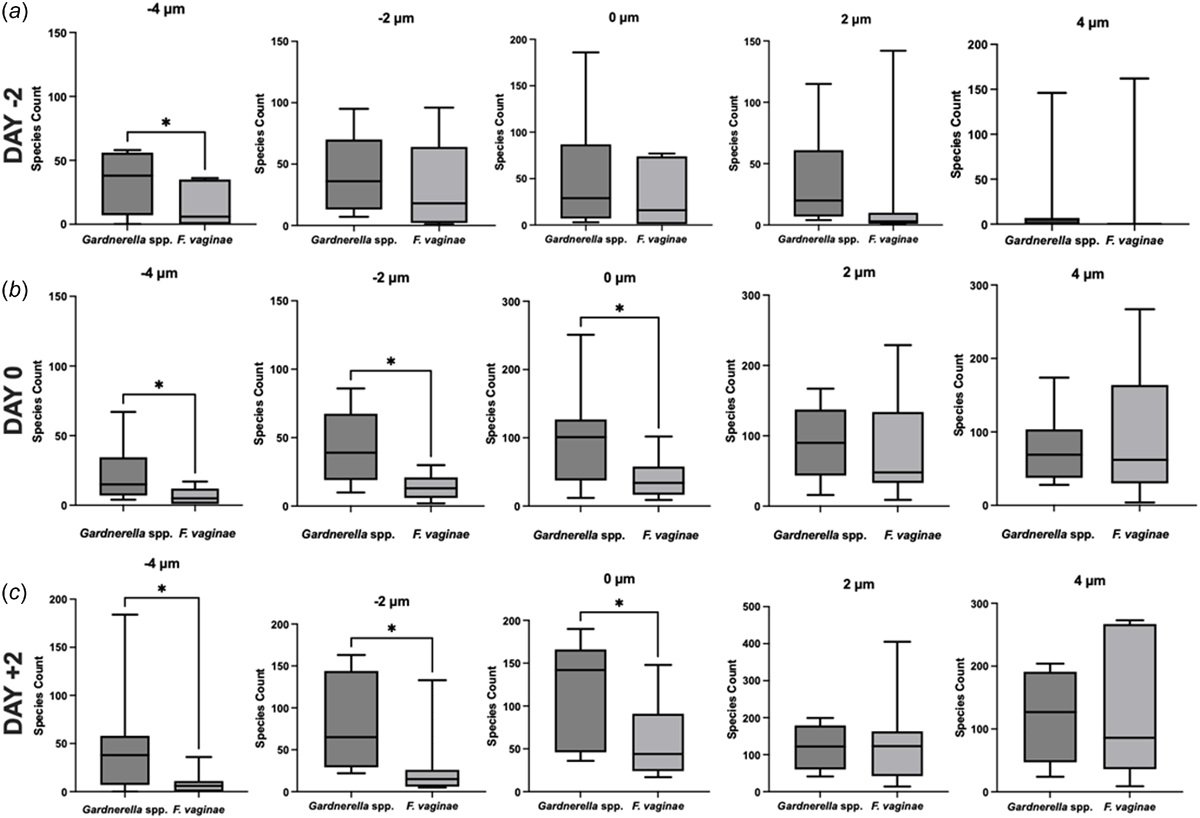
PP01.37 – Multi-Omics Analysis of Clinical Samples from Individuals Diagnosed with First-Time or Repeat Syphilis Infections
Dr. Mara C. Goodyear1, Ramin Azmin2, Jennifer Dechka3, Derek Smith3, Dr. David R. Goodlett1,3, Dr. Troy Grennan2,4, Dr. Amy H. Lee5, Dr. Caroline E. Cameron1,6
1University of Victoria, Victoria, Canada.
2British Columbia Centre for Disease Control, Vancouver, Canada.
3University of Victoria Genome BC Proteomics Centre, Victoria, Canada.
4University of British Columbia, Vancouver, Canada.
5Simon Fraser University, Burnaby, Canada.
6University of Washington, Seattle, United States of America.
Background: Syphilis is a multistage infection caused by the bacterium Treponema pallidum ssp. pallidum (Tp). The correlates of protection for syphilis are incompletely understood and must be identified to help guide development of an effective syphilis vaccine. Infection with Tp does not provide protection from future exposures and, in the absence of antibiotic treatment, Tp is able to persist in the body for a person’s lifetime. Individuals with a repeat syphilis infection have been observed to have reduced symptoms, which may indicate partial protection to Tp infection. Our aim is to apply a multi-omics approach to profile the host response during first-time and repeat syphilis infections to identify host responses that may provide insight into correlates of protection for syphilis.
Methods: Participants were enrolled through an informed consent process in three cohorts: 1) first-time infection, latent stage; 2) repeat infection, latent stage; and 3) diagnosis-free, no history of syphilis. Eligibility criteria included age 19–60, no coinfections, and assigned male sex at birth. Whole blood and plasma were collected for transcriptomics (RNA-sequencing) and proteomics analysis, respectively. In this pilot study, samples from five participants per cohort were analyzed.
Results: Differentially expressed genes and proteins were identified by comparing the latent syphilis cohorts (1 and 2) with the diagnosis-free cohort. Bioinformatic analyses, including pathway enrichment and integration of transcriptomic and proteomic data, were used to identify host pathways that are exploited by Tp to facilitate first-time, but not repeat, infections, and to identify host processes that may provide protection and reduce symptoms during repeat infections.
Conclusions: This study is the first multi-omic analysis of clinical samples from individuals with syphilis and provides an unbiased, systems-level understanding of host responses during infection. The identification of host components and pathways that may provide partial protection to infection will inform syphilis vaccine design.
PP01.38 – Antigen Stimulation Drives Clonal Expansion of Latent CD4+ T Cells Under Art Suppression
Miss Riley Greenslade1, Nnamdi Ikeogu1, Oluwaseun Ajibola1, Wan Koh2, Xinyun Liu1, Dr. Mario Ostrowski2, Dr. Thomas Murooka1
1University of Manitoba, Winnipeg, Canada.
2University of Toronto, Toronto, Canada.
Background: Successful antiretroviral therapy (ART) reduces mortality rates by suppressing Human Immunodeficiency Virus-1 (HIV) to undetectable levels in people living with HIV (PLWH). However, ART is not curative due to the establishment of the HIV reservoir that continues to persist despite prolonged ART suppression. Long-lived memory T cells represent the most important HIV reservoir population which is predominantly composed of CD4+ T cell clones that are established early after infection and increase during ART treatment. Our data points to cognate dendritic cell:T cell interactions as the main driver of clonal expansion of latent T cell subsets through TCR-dependent signaling and cytokines that support a pro-survival state in these cells. Depending on the nature of the stimulus, latent T cell proliferation can occur in the absence of virus reactivation. However, a remaining gap in knowledge is how antigen stimulation regulates opposing biological processes of (i) proliferation leading or clonal expansion or (ii) viral production leading to cell death.
Methods: We utilized a dual-fluorescent HIV latency reporter and human CD4+ T cell clones to modulate TCR signaling strengths using a panel of altered peptide ligands (APLs), and directly examined the relationship between TCR signals and proliferative responses by latent T cells.
Results: Adding anti-PD-1 increased virus reactivation and reduced the latently infected population, suggesting that blocking negative regulatory signals to enhance TCR signaling may promote latency reversal and reduce latent CD4+ T cell proliferation. Modulation of peptide binding affinity supports that high affinity TCR stimulation triggers virus reactivation and cell death, while low-affinity APL stimulation may promote latent T cell expansion and survival.
Conclusion: Our data argue that a critical balance between stimulatory and inhibitory pathways dictate which T cell subsets clonally expand under ART suppression. These studies have implications on stimulatory signals that can be therapeutically targeted to reduce the HIV reservoir size in PLWH.
PP01.39 – Integrative Genomic, Transcriptomic, and Ai-Driven Analysis Expands the Repertoire of Outer Membrane Protein Candidates for Syphilis Vaccine Development
Dr. Linda Grillova1
1Wellcome Sanger Institute, Cambridge, United Kingdom.
Background: The increasing incidence of syphilis, caused by Treponema pallidum (TPA), underscores the urgent need for a vaccine. Unlike Escherichia coli, TPA present unique challenges, as many TPA proteins resist heterologous expression. Numerous TPA genes are hypothetical with unknown functions, presenting opportunities for novel vaccine targets discovery. Understanding the diversity and function of OMP-encoding genes is crucial for advancing syphilis vaccine development.
Methods: We integrated deep transcriptome sequencing of cultured TPA with AI-driven protein predictions using an ESM2-based model, AlphaFold3, and Foldseek to identify genes active at the host-pathogen interface. We assessed sequence variability of potential OMP targets using approximately 1,700 global Treponema genomes, encompassing diverse syphilis strains and those causing yaws and bejel. Vaccine candidates were further analyzed through amino acid profiling.
Results: In our recent RNA-seq study, we reconstructed TPA’s complete transcriptional profile, confirming transcripts for hypothetical genes and identifying discrepancies with current annotations. Using machine learning, we trained an ESM2-based model to predict protein coding sequences in the TPA genome by analyzing all possible amino acid sequences in its genome. We validated the model with high-quality annotations from Mycoplasma genomes, which include 737 genes verified experimentally. ESM-Annotator successfully predicted over 98% of proteins with high confidence. Applying this model to the TPA genome, combined with our transcriptional data and presence of open reading frames, we identified 49 regions as potential new mRNA coding for proteins. Furthermore, we modeled the effects of amino-acid replacements found in these regions and previously identified OMPs, resulting in 50 candidate genes ranked by conservation and antigenicity.
Conclusion: By integrating genomic, transcriptomic, and structural approaches, we expanded the list of syphilis vaccine candidates and identified OMPs potentially capable of eliciting protective immune responses across diverse TPA strains and related subspecies. This research advances syphilis vaccine development with promising targets for experimental validation.
PP01.40 – HIV-1 Proviral Sequences with Large Internal Deletions Arise Through Distinct Strand Transfer Mechanisms
Mr. Jarryt Hardy1, Mrs. Delfien Staelens1, Mrs. Els Demecheleer1, Mrs. Marlies Schauvliege1, Mrs. Virginie Mortier1, Ms. Ciel Vermeersch1, Prof. Dr. Elizaveta Padalko1,2, Prof. Dr. Chris Verhofstede1
1Ghent University, Aids Reference Laboratory, Ghent, Belgium.
2Ghent University Hospital, Laboratory of Medical Microbiology, Ghent, Belgium.
Background: Curative interventions for HIV-1 seek to reduce the size of the replication-competent viral reservoir. Characterizing defective proviral sequences, however, could provide relevant insights that help refine the methods used to assess replication competence. In this study, a substantial set of proviral sequences with large internal deletions was characterized to understand the mechanisms behind their origin.
Methods: DNA sequences were obtained using an in-house full-length individual proviral sequencing technique and were supplemented with sequences from two published studies. Sequences that were no more than 200 nucleotides shorter than the primer coverage length were discarded. Also, incomplete sequences, sequences with more than one deletion, regions in reverse complement, or those harboring non-HIV-related sequences were omitted from the dataset. Ultimately, 395 selected sequences, each with a single deletion of over 200 nucleotides, were studied in detail.
Results: In-depth analysis demonstrated that aberrant strand transfers occur most frequently in the untranslated region (UTR) of the HIV genome. Proportional to the size of the different genomic regions, 56.6% of the deletion start sites were observed in the 5′UTR, and 62.6% of the deletion stop sites were found in the 3′UTR. A second hotspot, observed in 41 sequences (10.4%), was identified in a region close to the central polypurine tract. All observerd deletion junctions were matched to six hypothetical mechanisms of aberrant strand transfer during reverse transcription: premature first-strand transfer (Fig. 1a), aberrant first-strand transfer (Fig. 1b), minus-strand transfer (Fig. 1c), premature second-strand transfer (Fig. 1d), tRNA insertion due to aberrant second-strand transfer (Fig. 1e), and plus-strand transfer (Fig. 1f).
Conclusions: Our findings demonstrate that deletions predominantly extend across the UTRs, suggesting that PCR primer selection may lead to a skewed representation of the reservoir. In addition, we propose six distinct mechanisms that contribute to the heterogeneous pool of proviruses with internal deletions.
PP01.41 – A Murine Model to Identify Potentially Protective Treponema Pallidum Outer Membrane Proteins for Syphilis Vaccine Development
Kristina N. Delgado1, Crystal F. Vicente1, Carson J. La Vake1, Dr. Justin D. Radolf1, Dr. Melissa J. Caimano1, Dr. Kelly L. Hawley1,2
1Uconn Health, Farmington, United States.
2Connecticut Children’s, Hartford, United States.
Background: Treponema pallidum’s (TPA’s) repertoire of outer membrane proteins (OMPs) contains the principal candidates for syphilis vaccine design. To circumvent problems associated with full-length OMPs, we recently described the use of Pyrococcus furiosus thioredoxin (PfTrx) as a scaffold for assessing the reactivity of TPA OMP ECLs with immune rabbit sera and generating loop-specific antibodies. Herein we describe development of an inbred murine model to expedite vaccine development.
Methods: A/J, Balb/c, C3H/HeJ, and C57BL/6 mice were infected with TPA Nichols. Tissues and sera were collected, spirochete burdens were quantified by qPCR, and seroconversion was assessed using TPA lysates. Reactivity of mouse syphilis sera (MSS) to scaffolded extracellular loops (ECLs) was evaluated by ELISA. Day 84 sera were tested for opsonization, in vitro growth inhibition, and inhibition of attachment to Sf1EP cells.
Results: All strains seroconverted following infection, although at different timepoints. C57BL/6 and Balb/c mice initially supported TPA infection but exhibited declining bacterial burdens. In contrast, A/J mice showed the highest burdens and C3H/HeJ the lowest during the course of infection. All MSS demonstrated opsonic activity. C57BL/6 and C3H/HeJ MSS were more effective at inhibiting TPA growth and cellular attachment. TP0858 ECL4 antibodies emerged early (Day 21) in C57BL/6 and Balb/c mice but later in C3H/HeJ mice (Day 42). C57BL/6 MSS exhibited the strongest reactivity to BamA ECL4 (Days 42 and 84), whereas other strains showed minimal responses. Antibodies against TP0865 ECL3 increased over time in C3H/HeJ and Balb/c mice. A/J mice generated antibodies only to TP0856 ECLs 2 and 4, which appeared late (Day 84). TP0858 ECL2 showed minimal reactivity in all strains.
Conclusion: C3H/HeJ mice may aid in identifying surface-reactive antibodies post-infection, while A/J mice could assess the protective efficacy of ECL-based immunization. Further optimization and evaluation of protective responses are needed to support future protective ECL-epitope mapping studies.
PP01.42 – Sequencing Cultured Isolates of Mycoplasma Genitalium Using Oxford Nanopore
Dr. Jose Luis Alfredo Huaman Torres1,2,3, Dr. Jennifer A Danielewski1,2,3, Dr Erica L Plummer2,4,5, Dr Lenka A Vodstrcil4,5,6, Dr. Catriona S Bradshaw4,5,6, Dr. Suzanne M Garland1,2,3, Gerald L Murray1,2,3
1The University of Melbourne, Parkville, Australia.
2Centre for Women’s Infectious Diseases, The Royal Women’s Hospital, Parkville, Australia.
3Molecular Microbiology Research Group, Murdoch Children’s Research Institute, Parkville, Australia.
4Melbourne Sexual Health Centre, Alfred Health, Carlton, Australia.
5Central Clinical School, Monash University, Melbourne, Australia.
6Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, University of Melbourne, Parkville, Australia.
Background: Mycoplasma genitalium has gained notoriety due to rapidly increasing rates of antibiotic resistance. Comprehensive genomic characterization is crucial for elucidating resistance mechanisms and improving therapeutic strategies. Our laboratory has successfully isolated M. genitalium from clinical samples through co-culture with Vero cells. In this study, we used Nanopore long-read sequencing to investigate the genomic landscape of these M. genitalium isolates.
Methods: Genomic DNA (gDNA) was extracted using Zymo Quick-DNA HMW MagBead Kit. Sequencing libraries were generated from 400 ng of gDNA with the Ligation Sequencing Kit SQK-NBD114.96, with up to 5 samples were multiplexed on one flow cell. The prepared libraries were sequenced on a R10.4.1 flow cell and MinION device for 72 h. Pod5 output files were basecalled using Dorado with the super accuracy model. Coverage and depth were obtained using Minimap2 and SAMtools. Filtered reads were subjected to de novo assembly using Flye and polished with Medaka.
Results: Across 13 analysed samples, we observed 98.5% of the reads aligned to the Vero cell genome. Although the average proportion of reads mapping to M. genitalium was relatively low (0.82%), we obtained complete genomes with length ranging from 579 to 582 kbp and an alignment depth from 32 to 62-fold. Interestingly, a translocation comprising 16S, 23S and 5S ribosomal RNA was identified in 7 samples. This rearrangement translated into a longer genome length 581–582 kbp compared to 579–581 kbp in samples with genomic structure like the reference genome. Further analysis is ongoing to elucidate the significance of this event.
Conclusion: This study demonstrates the utility of Nanopore long-read sequencing for comprehensive genomic characterization of M. genitalium isolates. Moreover, our data will contribute to expand genomic resources for future research in combating this emerging pathogen.
PP01.43 – High Levels of Anti-HHV-8 IgG Binding Capacity Are Linked with Low HHV-8 Viremia in People with and Without HI
Dr. Stephane Isnard1,2, Dr Léna Royston1,2,3, Mrs Tsoarello Mabanga1,2, Ms Milada Dvorakova9, Dr Carolina A Berini1,2, Dr Bluma Brenner4, Dr Cecilia T Costiniuk1,2, Dr Sean Yaphe2,5, Dr Bertrand Lebouché1,2, Dr Réjean Thomas5, Dr Jean-Guy Baril6, Dr Marc Steben7, Dr Daniel Grace8, Dr Daniel Grace9, Dr Joseph Cox1,2,9,10, Dr Jean-Pierre Routy1,2,11
1Research Institute of the Mcgill University Health Centre, Montreal, Canada.
2Chronics Viral Illness Service, McGill University Health Centre, Montreal, Canada.
3Geneva University Hospitals, Geneva, Switzerland.
4Lady Davis Institute, McGill University, Montreal, Canada.
5Clinique L’Actuel, Montreal, Canada.
6Clinique Médicale du Quartier Latin, Montreal, Canada.
7Canadian Network for HPV prevention, Montreal, Canada.
8Dalla Lana School of Public Health, Social and Behavioural Health Sciences, Toronto, Canada.
9Engage Cohort Study, Montreal, Canada.
10Epidemiology Department, McGill University, Montreal, Canada.
11Division of Hematology, McGill University Health Centre, Montreal, Canada.
Introduction: The human herpes virus 8 (HHV-8) causes Kaposi Sarcoma (KS) and is linked with some type of B-cell proliferation disorders that develop upon aging and immunosuppression, including in people living with HIV (PLWH).
HHV-8 establishes latency in cellular and anatomical reservoirs in epithelial cells as well as B-cells. Factors controlling latency and replication remain seldomly described. We developed HHV-8 specific serological and virological assays to assess ex-vivo whether antibodies targeting HHV-8 could control replication.
Methods: Serum and cell lysate were obtained from cis and transgender men of the Engage cohort in Montreal. Participants with active KS (11 PWH on ART [HIV KS] and 11 HIV-negative classic KS [cKS]) were included from the McGill biobank. Circulating levels of IgG binding to BCBL1 HHV-8-infected cells were quantified by flow cytometry. Digital-droplet-PCR was used to assess HHV-8 DNA levels in blood extracts and biopsies.
Results: In absence of KS, HHV-8 seropositivity was higher in PWH than HIV-negative participants (67.5% vs 41.8%, P < 0.001). Moreover, in 106 HHV-8 seropositive participants, levels of anti-HHV-8 IgG were higher in PLWH than in 260 HIV-negative controls (median 1.5 vs 1.2AU, P = 0.03). Levels of anti-HHV-8 IgG were negatively correlated with HHV-8 viremia in whole blood extracts (r = –0.48, P = 0.004, n = 39).
Patients with KS were all seropositive for HHV-8. HIV KS had higher levels of anti-HHV-8 IgG levels than cKS (3.7 vs 1.8AU, P = 0.02). Interestingly, HIV KS had lower circulating HHV-8 viremia than cKS (695 vs 8405 copies/106 cells, P = 0.04). However, HHV-8 DNA levels were similar in KS lesion biopsies for the 2 groups (HIV KS: 68.103 vs cKS: 323.103 copies/106 cells, P = 0.89).
Conclusion: In both symptom-free carrier and KS patients, high levels of anti-HHV-8 IgG were associated with low circulating viremia. Whether higher anti-HHV-8 IgG levels contribute to prevent KS development should be further studied.
PP01.44 – Impact of Penile-Vaginal Sexual Debut on the Immune Milieu and Bacterial Load of the Penile Urethra in Adolescent Males from Rakai, Uganda
Miss Rameen Jamil1, Ms. Sanja Huibner1, Mr. James Pollock1, Mr. James Nnamutete2, Mr. Ping Yang3, Ms. Jodie L. White3, Lori Sokoll3, Dr. Ronald Galiwango2, Dr. Bryan Coburn1, Dr. Cindy Liu4, Dr. Jessica Prodger5, Dr. Aaron A.R. Tobian3, Dr. Rupert Kaul1
1University of Toronto, Toronto, Canada.
2Rakai Health Sciences Program, Kalisizo, Uganda.
3John Hopkins University, Baltimore, USA.
4George Washington Milken Institute School of Public Health, Washington DC, USA.
5Western University, London, Canada.
Background: Genital inflammation increases HIV susceptibility in the foreskin, and a key driver of inflammation at this site is the local microbiome. The latter is also true in the penile urethra, although the immune correlates of HIV acquisition at this tissue site are unknown. Epidemiologic studies suggest that components of the urethral microbiome are acquired during penile-vaginal sex. The current study characterized the impact of sexual debut on the immune milieu and microbiome of the urethra.
Methods: A cohort of 200 sexually naive adolescent males were enrolled into a longitudinal study in Rakai, Uganda. Follow-up visits occurred every 3 months for 3 years. Urethral swabs were collected annually; participant-reported circumcision status and serum testosterone was ascertained at each visit. Urethral levels of 9 soluble immune factors (IL-1α, IL-1β, IL-8, MIP-1β, sEcad, resistin, TIMP-1, VEGF, and MMP-9) were quantified by chemiluminescent multiplex immunoassay, and total bacterial load was measured using 16S rRNA gene quantitative PCR. Impact of sexual debut independent of serum testosterone and circumcision was assessed by mixed-effects models.
Results: Median participant age at enrollment was 16 years, and during the follow-up period 81/189 participants (43%) reported sexual debut. Sexual debut was independently associated with increased levels of all urethral soluble immune factors and total bacterial load (Table 1). Furthermore, serum testosterone was independently associated with elevated urethral levels of IL-1α, IL-1β, TIMP-1, and VEGF. Circumcision was not associated with immune changes, but with a decrease in urethral bacterial load.
Conclusion: Sexual debut has important independent effects on urethral inflammation that may impact HIV susceptibility; future studies from this cohort may link these changes to the urethral microbiome.
| Fixed effect estimates | ||||
|---|---|---|---|---|
| Urethral parameters | Sexual debut | Serum testosterone | Circumcision status | |
| Soluble immune factors (Log10 pg/ml) | ||||
| Soluble E-cadherin | 1.31E−01* | 6.57E-05 | –6.42E-02 | |
| IL-1α | 1.61E-01** | 1.65E−04** | –6.12E-01 | |
| IL-1β | 2.07E-01 *** | 1.40E−04* | –9.41E-02 | |
| IL-8 | 2.60E-01** | 1.45E-04 | 6.80E−02 | |
| MMP-9 | 3.91E-01*** | 1.77E-04 | 1.66E-01 | |
| Resistin | 3.68E-01*** | 1.86E-04 | 7.84E-02 | |
| TIMP-1 | 3.24E-01*** | 2.99E−04** | 9.55E-03 | |
| VEGF | 2.77E-01*** | 2.88E−04** | 3.79E-02 | |
| Total bacterial load (Log10 16S/swab) | ||||
| Total 16S rRNA | 3.05E-01** | −1.89E−05 | –4.17E-01*** | |
*P ≤ 0.05, **P ≤ 0.01, ***P ≤ 0.001.
PP01.45 – Exploring the Antiviral Effects of DDX21 Overexpression in Vaginal Epithelial Cells During HSV-2 Infection
Miss Lauren Jirik1,2, Dr. Aisha Nazli1,2, Dr. Charu Kaushic1,2
1McMaster Immunology Research Centre, Hamilton, Canada.
2Department of Medicine, McMaster University, Hamilton, Canada.
Background: Herpes simplex virus type 2 (HSV-2) is the leading cause of genital herpes and one of the most prevalent sexually transmitted infections worldwide. Women, particularly in Sub-Saharan Africa, experience disproportionately high rates of HSV-2, with prevalence reaching 70–80% in some areas. HSV-2 primarily spreads through direct contact, infecting genital epithelial cells at mucosal surfaces. Transcriptomic analysis using DNA microarrays on a vaginal epithelial cell line (VK2) revealed significant downregulation of DDX21 expression following HSV- 2 infection. DDX21, a DEAD-box RNA helicase is involved in immune response modulation, has been shown to play a dual role in viral infections. Given its involvement in type I interferon (IFN) signaling, this study aimed to explore the functional role of DDX21 in HSV-2 infection.
Methods: To investigate the role of DDX21, we established stable overexpression (OE) of DDX21 in VK2 cells. We assessed viral replication through fluorescent imaging of GFP tagged HSV-2 and evaluated immune responses by measuring the mRNA expression of type I IFNs and interferon-stimulated genes (ISGs) using q-PCR.
Results: DDX21 OE in VK2 cells significantly reduced HSV-2 replication. Additionally, DDX21 OE cells showed elevated levels of IFN-alpha expression both prior to and after HSV-2 infection compared to wild-type VK2 cells. Several ISGs, including IFIT3, ISG15, MX1, and RSAD2, were significantly upregulated in DDX21 OE cells, particularly post-infection. These responses were markedly stronger than in wild-type cells, indicating that DDX21 plays a critical role in enhancing antiviral immune responses against HSV-2.
Conclusion: From our findings we can conclude that DDX21 acts as an antiviral factor during HSV-2 infection of vaginal epithelial cells by suppressing HSV-2 replication through activating type I interferon signaling and upregulating key ISGs. This highlights DDX21 as a potential therapeutic target to enhance innate immunity and control HSV-2, with implications for clinical management and prevention in high-prevalence areas.
PP01.46 – Improving Trichomonas Vaginalis Detection: Evaluating Wet PrEP and Point-Of-Care Testing in an Urban Emergency Department
Ms. Nyah Johnson Nyah Johnson1, Gaby Dashler1, Dr. Kendall Maliszewski1, Dr. Yukari C. Manabe1, Dr. Charlotte Gaydos1, Dr. Edana Mann1, Dr. Mustapha Saheed1, Dr. Eili Klein1, Spencer Mann1, Katelyn Mann1, Dr. Richard Rothman1, Dr. Yu-Hsiang Hsieh1
1Johns Hopkins University, Baltimore, United States.
Background: Trichomonas vaginalis (TV), an infection that increases the risk of HIV co-infection and PID, often goes undiagnosed in urban emergency departments (EDs) which serve as critical access points for underserved populations. Wet mount preparation (wet prep), the most widely-used diagnostic method has surprisingly low sensitivity estimated from 44% to 66%. The recently FDA-cleared Visby Medical Sexual Health Test, a 30-min point-of-care (POC) Real-Time PCR (RT-PCR) assay with a sensitivity of 99.3% and a specificity of 96.7% for TV detection (compared to reference molecular gold standard NAAT), enhances diagnostic efficiency. This study aims to evaluate diagnostic performance of the wet prep compared to Visby in detecting TV in EDs.
Methods: Secondary data analysis of female patients testing for TV in an urban ED in Baltimore, Maryland from January to April 2023 was performed. Positive percent agreement (PPA) and negative percent agreement (NPA) between wet prep and POC RT-PCR testing were calculated.
Results: Overall, 204 patients were tested for TV using both tests. Of them, 189 tested negative on both, 6 tested positive on both, and 9 tested positive by POC RT-PCR but were negative by wet prep. PPA and NPA of the wet prep was 40% (95% CI: 16.3%, 67.7%) and 100% (95% CI: 98.1%, 100%), respectively, compared to the POC RT-PCR test. All 15 TV-positive patients reported relevant symptoms (Table 1). A significantly higher proportion of wet prep-negative but POC RT-PCR-positive patients reported vaginal itching as compared to those positive for both (56% vs 0%, P = 0.042, mid-P exact test).
Conclusion: While wet prep is highly specific, this study underscores the diagnostic limitations of wet prep in missing 60% of TV cases in ED settings where it remains widely-used. The POC RT-PCR test, with a higher sensitivity and a 30-minute turnaround, can improve detection rates and patient outcomes in EDs.
| Symptoms | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Subject | Wet prep | POC-PCR | Age group | Race/ethnicity | Lower abd. pain | Vag. bleeding | Vag. discharge | Vag. odor | Vag. itching | Painful urination | Pain during sex | Bumps, blisters, sores | Nausea/vomiting | Other | |
| 1 | Negative | Positive | 30–34 | NH-Black | No | No | Yes | Yes | Yes | Yes | No | No | No | No | |
| 2 | Negative | Positive | 25–29 | NH-Black | Yes | No | Yes | No | Yes | No | No | No | No | No | |
| 3 | Negative | Positive | 35–39 | NH-Black | No | No | No | No | No | No | No | No | No | YesA,D | |
| 4 | Negative | Positive | 18–24 | NH-Black | No | No | Yes | No | Yes | No | No | No | No | No | |
| 5 | Negative | Positive | 18–24 | NH-Black | Yes | Yes | No | No | No | No | No | No | No | No | |
| 6 | Negative | Positive | 25–29 | NH-NB-POC | Yes | Yes | No | No | No | No | No | No | No | No | |
| 7 | Negative | Positive | ≥ 40 | NH-Black | No | No | Yes | No | Yes | No | No | No | Yes | YesA,B | |
| 8 | Negative | Positive | 18–24 | NH-Black | No | No | Yes | Yes | Yes | No | No | No | No | No | |
| 9 | Negative | Positive | 30–34 | NH-Black | Yes | No | No | No | No | No | No | No | Yes | No | |
| 10 | Positive | Positive | 18–24 | NH-Black | Yes | No | Yes | No | No | No | No | No | Yes | No | |
| 11 | Positive | Positive | 35–39 | NH-Black | Yes | No | No | No | No | No | No | No | No | No | |
| 12 | Positive | Positive | 18–24 | NH-Black | Yes | Yes | No | No | No | Yes | No | No | No | No | |
| 13 | Positive | Positive | 18–24 | NH-Black | Yes | No | Yes | No | No | No | No | No | No | YesC | |
| 14 | Positive | Positive | 18–24 | NH-Black | Yes | No | Yes | No | No | Yes | No | No | No | YesD | |
| 15 | Positive | Positive | ≥ 40 | NH-Black | No | No | No | No | No | No | No | No | No | YesB | |
| Total number of symptomatic patients | 9/15 | 3/15 | 8/15 | 2/15 | 5/15 | 3/15 | 0/15 | 0/15 | 3/15 | 5/15 | |||||
PP01.47 – Impact of Prior Chlamydia Trachomatis Infection on Urethral Antibody Responses and Organism Load in Men with Acute Chlamydial Nongonococcal Urethritis
Caleb Ardizzone1, Waleed Alrebdi1, John Ryan1, Evelyn Toh1, Teresa Batteiger1, David Nelson1, Dr. Stephen Jordan1
1Indiana University, Indianapolis, United States.
Background: Chlamydia trachomatis (CT) infection rates in the United States are near an all-time high, and existing knowledge gaps in anti-chlamydial immunity limit vaccine development. As CT immunity has been poorly described in men, we investigated the relationship between prior CT infection, anti-chlamydial antibody responses, and CT organism loads using first-catch urine (FCU) specimens from men with CT-associated nongonococcal urethritis (CT-NGU).
Methods: A total of 108 men with CT-NGU were included in this analysis. FCU was collected at enrollment, along with clinical and demographic information. STI testing was performed on FCU by nucleic acid amplification testing (NAAT). Men with a positive Neisseria gonorrhoeae NAAT result were excluded. Urinary IgG and IgA against CT elementary bodies (EB) were quantified by EB-ELISA, and CT load was measured by quantitative PCR.
Results: Men reporting prior CT infection had significantly lower CT loads and higher anti-EB IgA concentrations compared to those without prior infection. However, CT loads did not inversely correlate with anti-EB IgA concentrations in men reporting prior CT infection. CT loads positively correlated with anti-EB IgG concentrations in all men with CT-NGU and with anti-EB IgA concentrations only in men without prior CT.
Conclusions: These findings suggest that prior CT infections confer some degree of immune protection in the urethra, although the functional role of anti-chlamydial antibody remains unclear. The unexpected positive correlation between anti-EB antibodies and CT loads may reflect differences in immune dynamics during acute urethral versus prevalent cervical infections, given that this study did not include men with asymptomatic CT infection. Importantly, this study demonstrates that urethral antibody responses can be non-invasively monitored using FCU, supporting its use in prospective studies investigating whether and how anti-chlamydial antibodies contribute to protection against CT reinfection.
PP01.48 – Comparison of Dried Blood Spots Versus Microvolume Blood Tubes in Serological Testing for Sexually Transmitted Bloodborne Pathogens
Dr. Stephen Jordan1, Samantha Hawkins2, Lauren Maier2, Ryan Kinsella2, Matthew McVeigh2, Patrycja Szybowska2, Carly Lattimore2, Barbara Van Der Pol3
1Indiana University, Indianapolis, United States.
2Preventx, Sheffield, United Kingdom.
3University of Alabama at Birmingham, Birmingham, United States.
Background: Remote testing for sexually transmitted infections may increase access to underserved and high-risk individuals who are unlikely to present to a health clinic for screening. Remote testing for sexually transmitted bloodborne pathogens (BBP) typically involves transfer of finger-pricked blood onto either dried blood spot (DBS) cards or into microvolume blood tubes (MVBT), but the performance of these devices in serological testing for BBPs remains unclear. We evaluated the performance of DBS vs MVBT using spiked samples in order to identify the optimal collection device for remote serological testing.
Methods: Whole blood from four BBP-negative individuals was obtained by venipuncture, pooled, and separated into 420 aliquots. Mock samples were generated by spiking thirty aliquots in quintuplicate with increasing concentrations of BBP in human serum (very low – very high) per device; unspiked samples served as controls. 600 uL of mock blood were dispensed to MVBT. Two DBS/analyte were loaded with 50 uL of mock blood/spot, allowed to air dry, and then 3 punches were eluted using 300 uL of PBS. Serological testing for HIV-1 and HIV-2 antibodies, HIV p24 antigen, syphilis, hepatitis C (HCV) antibody and hepatitis B core antibody (HBVcAb) and HBV surface antigen (HBVsAg) was performed on the Roche cobas e801 platform.
Results: Compared to MVBT, all serological tests of DBS samples resulted in a significant loss of sensitivity. By analyte, the percent positive agreements were: HIV antibodies 100%, HIV antigen 25%, syphilis treponemal antibody 40%, HCV antibody 28%, HBVcAb 0% and HBVsAg 100%. All analytes had 100% negative agreement (Table 1).
Conclusion: Compared to MVBT, using DBS for serological testing resulted in a significant loss in assay performance; these results confirm recent findings from Europe. The unacceptable false negative rate from DBS puts clients at increased risk for missed diagnoses, complications of untreated infections, and BBP transmission to partners.
| Spiked assay target concentration | ||||||||
|---|---|---|---|---|---|---|---|---|
| Antigen | Negative | Very Low | Low | Medium | High | Very high | Positive mean | |
| HIV-1 Ab | 100% | 100% | 100% | 80% | 100% | 100% | 96% | |
| HIV-2 Ab | 100% | 60% | 60% | 100% | 60% | 100% | 76% | |
| HIV Ag | 100% | 0% | 0% | 0% | 40% | 80% | 24% | |
| HB Core Ab | 100% | 0% | 0% | 0% | 0% | 0% | 0% | |
| HB sAg | 100% | 100% | 100% | 60% | 60% | 100% | 84% | |
| HCV Ab | 100% | 0% | 0% | 0% | 40% | 100% | 28% | |
| Syphilis Ab | 100% | 0% | 0% | 0% | 100% | 100% | 40% | |
PP01.49 – Investigation of the Genetic Basis Reduced Gentamicin Susceptibility in Neisseria Gonorrhoeae Isolates from Mice Given Sub-Inhibitory Levels of Gentamicin
Dr. Adriana Le Van1,2, Mr. Vincent J. Oliver1,2, Ms. Brittany Bivens1, Dr. William M. Shafer3, Dr. Kristie L. Connolly1, Mr. III Lenise G. Solieau1, Dr. Ann E. Jerse1
1Department of Microbiology and Immunology, Uniformed Services University, Bethesda, United States.
2Henry M. Jackson Foundation for the Advancement of Military Medicine, Inc., Bethesda, USA.
3School of Medicine, Emory University, Decatur, USA.
Background: The rapid development of antimicrobial resistance in Neisseria gonorrhoeae (Ng) is an urgent threat to public health. Ceftriaxone is the only remaining first-line treatment for gonorrhea in the US; however, CDC and WHO guidelines recommend gentamicin (GEN) as an alternative antibiotic for patients with ceftriaxone-resistant infection or allergy. We recently reported decreasing GEN susceptibility among Ng isolates from Kenya and Georgia, and little is known about the evolution of GEN resistance in Ng.
Methods: To select for mutations associated with decreased GEN susceptibility, we infected female Balb/C mice with Ng strain WHO X and treated them with sub-inhibitory concentrations of GEN. Vaginal swabs were cultured on media containing increasing concentrations of GEN over the course of 8 days. Whole genome sequence (WGS) analysis was conducted on isolates with a >2-fold increase in the minimal inhibitory concentration (MIC) of GEN.
Results: Passage of the multi-drug resistant, GENIR strain WHO X (GEN MIC, 8 µg/mL) through GEN-treated mice allowed isolation of a GENR mutant (13R; MIC, 64 µg/mL), which carries a mutation in the gene encoding the refolding chaperone protein (SpyC/CpxP). Subsequent passage of strain 13R in GEN-treated mice selected for two additional independent mutants (13R-8 and 13R-17) with GEN MICs of 256 µg/mL and mutations in the genes encoding FusA, LgtG, ModA13 and the SMI1/KNR4 family protein.
Conclusions: Serial passage of WHO X lineage Ng strains through mice treated with sub-inhibitory doses of GEN selected for increased GEN resistance. Several novel mutations have been identified that may contribute to in vivo-selected increased in GEN resistance. We conclude that widespread use of non-prescription GEN may promote the emergence of GENR Ng strains and possibly facilitate the spread of resistant Ng observed in surveillance clinical isolates.
PP01.50 – Critical Residues in the N-Terminus of FtsI of Neisseria Gonorrhoeae Modulate Penicillin Binding
Oluwatobi E Oladele1,2, Dr Michal T Boniecki1,3, Mr. Griffin Lehnert1,2, Dr Jenny Wachter1,2, Professor Jo-Anne R Dillon1,2
1Department of Microbiology, Immunology and Microbiology, University of Saskatchewan, Saskatoon, Canada.
2Vaccine and Infectious Disease Organization, University of Saskatchewan, Saskatoon, Canada.
3Protein Characterization and Crystallization Facility, University of Saskatchewan, Saskatoon, Canada.
Background: Penicillin-binding protein 2 (PBP2/FtsINg) of Neisseria gonorrhoeae (Ng) is an essential cell division protein and the primary target for β-lactam antibiotics. FtsI is a transpeptidase involved in cell wall synthesis present across bacterial species. While mutations around the active site of the C-terminal transpeptidase domain of FtsINg are well-characterized for their effects on chromosomally-mediated β-lactam resistance, the function of the N-terminal domain is poorly understood. In the present analysis we report on the conservation of N-terminal FtsI amino acid residues across proteobacterial species and their role in penicillin binding for FtsINg.
Methods: Protein sequences of FtsINg and homologs from proteobacterial species were retrieved from the NCBI protein database and aligned to identify conserved residues. Site-directed mutagenesis was performed on FtsINg to introduce single amino acid substitutions at the identified conserved residues. Recombinant histidine-tagged wild-type and mutant FtsINg were analyzed for structural integrity using size exclusion chromatography multi-angle light scattering (SEC-MALS), dynamic light scattering (DLS), and circular dichroism (CD). The effects of mutations on penicillin binding were ascertained by isothermal titration calorimetry (ITC).
Results: Amino acid residues R75, R167, G180, and E193 were 100% conserved in the N-terminus of FtsI from 2132 Proteobacteria species and 19 Neisseria species. DLS and SEC-MALS methods demonstrated that both wild-type and mutant FtsINg were monomeric, monodisperse, and free from aggregation. CD analysis confirmed the structural integrity of these proteins. ITC experiments indicated that recombinant FtsINg mutated at R75A, R75G, R167A, R167G, and G180R increased penicillin binding by 2.6-fold, 4-fold, 2.9-fold, 2.1-fold, and 2-fold, respectively, as compared to wild-type FtsINg (P < 0.05).
Conclusions: The discovery of four conserved residues in the N-terminus of FtsINg as critical sites modulating penicillin binding reveals unexpected nuances to penicillin resistance mediated by this protein. Their conservation across Proteobacteria raises exciting questions regarding horizontal gene transfer in Gram-negative bacteria.
PP01.51 – Disseminated Syphilis Caused by Two Recombining Treponema Pallidum Strains in a Patient with Untreated HIV
Dr. Nicole Lieberman1, Shah Bakhash1, Ethan Nunley1, Dr. Muyi Li2, Dr. Brian Mau3, Dr. John Pauk4, Dr. Paul Swanson1, Dr. Anand Baxi2, Dr. Joshua Lieberman1, Dr. Alexander Greninger1,5
1Department of Laboratory Medicine and Pathology, University of Washington School of Medicine, Seattle, United States.
2Department of Gastroenterology and Hepatology, University of Washington School of Medicine, Seattle, United States.
3Department of Pathology and Laboratory Medicine, Oregon Health & Science University School of Medicine, Portland, United States.
4Infectious Disease, Swedish Medical Center, Seattle, United States.
5Vaccine and Infectious Disease Division, Fred Hutchinson Cancer Center, Seattle, United States.
Background: Recent efforts to catalog the global genomic diversity of Treponema pallidum subspecies pallidum (Tp), the causative agent of syphilis, have revealed variation in genes encoding antigens and putative virulence factors consistent with inter-subspecies and inter-clade recombination. However, direct evidence of inter-strain recombination in Tp has not previously been seen, and its role in enhancing Tp fitness is unknown.
Methods: Tp in patient-derived specimens was characterized by hybrid-capture whole genome sequencing (WGS) and quantified by digital droplet PCR. Consensus genomes were assembled and contextualized within a maximum likelihood phylogeny of Tp samples. WGS results were confirmed with an amplicon sequencing approach.
Results: We carry out ongoing molecular surveillance of Tp clinical specimens. We recently found the first known case of co-infection with strains from both Nichols-like and SS14-like clades, a necessary pre-condition for inter-strain recombination, in gastric and colon biopsies from a patient in Seattle, WA, with untreated HIV and widely disseminated syphilis. Using strain-specific droplet PCR, we found a ratio of 43:57 Nichols-clade:SS14-clade in the gastric biopsy and 97:3 in the colon. Both strains were closely related to others circulating contemporaneously in Seattle. The SS14-clade strain had recombined with the Nichols-clade strain within TP0705/mrcA, a penicillin-binding protein. The Nichols-clade strain in the colon, but not the stomach, underwent extensive recombination with the SS14-clade strain to generate multiple variants of the outer membrane protein TP0865, a fadL homolog (Fig. 1).
Conclusions: Our finding of inter-strain recombination in the first known case of Tp co-infection highlights the evolutionary plasticity by which new strains can emerge, providing a possible mechanism for development and spread of antimicrobial resistance and other factors that confer enhanced fitness. Furthermore, this study demonstrates the central role of molecular epidemiology to track the emergence and spread of Tp sequence variants.
Genomic and molecular studies reveal T. pallidumco-infection with two strains and recombination between strains. (a) Coverage of lineage-defining single nucleotide variants in stomach and colon. The number of reads supporting Nichols-clade (blue) and SS14-clade (red) are shown. (b) Digital droplet PCR of the lineage-specific locus TP0136 reveals 56.6% SS14-clade strain and 43.4% Nichols-clade strain in the stomach, and 2.7% SS14-clade and 97.3% Nichols-clade in the colon. (c) SS14-clade and Nichols-clade strains recovered from the patient are closely related to strains circulating contemporaneously in the same city, Seattle, WA, during 2021-2022. Reference strains are denoted by triangles. Nodes with >95% bootstrap support are labeled with grey circles. A node with 94% bootstrap support defines a heterosexual cluster to which the patient’s SS14-clade strain is closely related. (d) Frequencies of Nichols-clade and SS14-clade alleles at and adjacent to the penicillin binding protein mrcA/TP0705. Genome position is relative to the SS14 reference strain, NC_021508.1. (e) TP0865 haplotypes present in stomach and colon. Sequences that originated in the Nichols parental strain are shown in blue, and SS14 parental in red. Extracellular loop (ECL)1 and ECL5 are invariant between Nichols- and SS14-clade strains and are shown in white. All variants were supported by amplicon and WGS approaches. The relative proportions of variants 1a, 1b, 2a and 2b, could not be determined precisely due to methodological limitations, therefore combined results are presented and ECL4 made opaque to convey uncertainty.
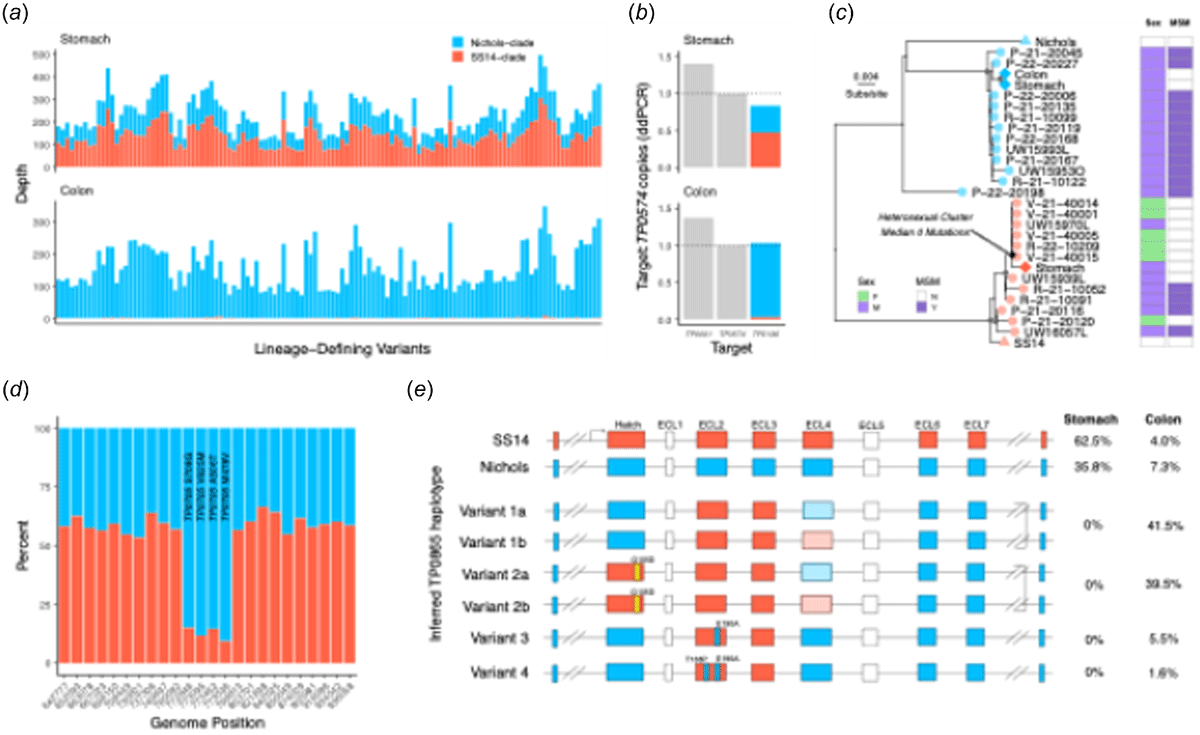
PP01.52 – Predicting Response to Syphilis Treatment Using Cytokines and Clinical Characteristics
Miss Jillian Max1, Janet Siebert2, Dr. Silver Vargas3, Michael Reyes-Diaz3, Dr. Carlos Caceres3, Dr. Lorenzo Giacani4, Dr. Kelika Konda1, Dr. Jeffrey D Klausner1
1Department of Population and Public Health Sciences, University of Southern California, Los Angeles, United States.
2Cyto Analytics, San Diego, United States.
3Center for Interdisciplinary Studies in Sexuality, AIDS, and Society, Universidad Peruana Cayetano Heredia, Lima, Peru.
4Department of Medicine, University of Washington, Seattle, United States.
Background: Recently, cytokine expression analysis has become of interest as an approach to facilitate syphilis diagnosis. Infection with Treponema pallidum is treatable but can be difficult to diagnose due to the limitations of lipoidal tests, especially in cases of repeated infections. We sought to compare cytokine levels in patients at baseline and post-treatment taking covariates such as syphilis history, HIV status, and stage into account.
Methods: We characterized the longitudinal patterns of 45 cytokines in samples from a cohort of individuals from Peru diagnosed with syphilis based on serologic and clinical criteria. The analysis included 192 individuals tested quarterly up to 12 months post-treatment. Cytokines were measured in duplicate using a Luminex Flex3D-H2 instrument (Thermo Fisher, Waltham, MA) at the Immunology Laboratory at Stanford University, and the average median fluorescence intensity (MFI) values from each sample were used for analysis. We estimated the changes in cytokine levels 1) at baseline by syphilis history (ANOVA), 2) at baseline by HIV stage (t-test), 3) at baseline by syphilis stage (ANOVA), and 4) between baseline and 1-month post-treatment (linear mixed models with Bonferroni corrected P-values).
Results: We were able to identify statistically significant differences in cytokines by history (5 cytokines including IL10, IL18, Leptin, RANTES.CCL5, and TNFA), HIV (6 cytokines including RANTES.CCL5, TGFA, TRAIL.TNFSF10, Leptin, IL22, IL10, and GROA.KC.CXCL1), and stage (3 cytokines including IL18, RANTES.CCL5, and EOTAXIN.CCL11). We were also able to identify differences from pre to 1-month post treatment in cytokines: EGF, GROA.KC.CXCL1, IL3, IL7, IL10, IL18, IP.10.CXCL10, MIP1B.CCL4, TNF-α, and VEGF (Fig. 1).
Conclusion: Cytokines have significantly different values comparing pre-post treatment, syphilis stage, syphilis history, and HIV status. These characteristics may be able to lead to improvements in syphilis diagnosis, including exploration of machine learning models.
Selected cytokine MFI values comparing (a) Syphilis history for IL-10, (b) HIV status for GROA.KC.CXCL1, (c) Syphilis stage for EOTAXIN.CCL11, and (d) Stage by study visit for EGF. (a) Average MFI values for cytokine IL10 with syphilis history (H) and no history (NH). Cytokine GROA.KC.CXCL1 mean MFI values in samples without HIV (“no” x-axis) and with HIV (“yes” x-axis). (b) Cytokine EOTAXIN.CCL11 mean MFI values in samples with primary (I), secondary (II), early latent (EL), and late latent (LL) syphilis. (c) Cytokine EGF mean MFI values at baseline, visit 1 (1-month), and visit 3 (3-month) post treatment as time passed (tp), differentiating between primary, secondary, early latent, and late latent syphilis samples. Estimated mean MFI value recorded as decreasing by 183 over 1 month.
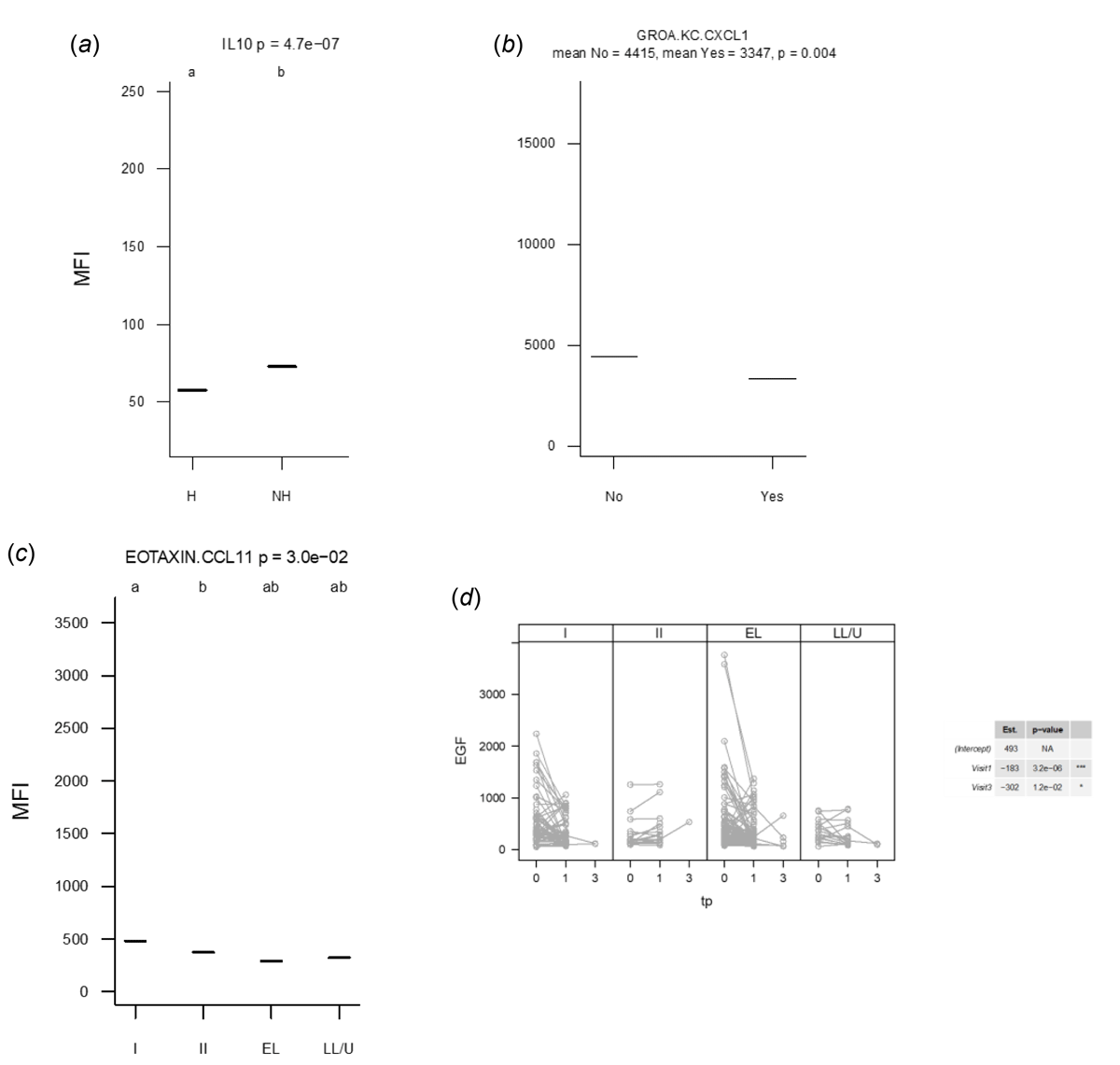
PP01.53 – Rates and Characterization of Urogenital and Pharyngeal Neisseria Gonorrhoeae Strain Differences in Ugandan Men
Dr. Johan Melendez1, Dr. Annet Onzia2, Adamaris Muniz Tirado1, Brenda Dawa2, Emmanuel Mande2, Dr. Peter Kyambadde3, Dr. Matthew Hamill1, Dr. YH Hsieh1, Dr. Rosalind Parkes-Ratanshi2, Dr. Herve Tettelin4, Dr. Yukari Manabe1
1Johns Hopkins University School Of Medicine, Baltimore, United States.
2Infectious Diseases Institute, Kampala, Uganda.
3Ministry of Health, Uganda.
4University of Maryland Baltimore, Baltimore, Maryland, United States.
Background: Africa has the highest prevalence of gonorrhea globally, but studies on pharyngeal Neisseria gonorrhoeae (pNG) are extremely scarce. We report on the characteristics of pNG and urogenital NG (uNG) in Ugandan men with urethral discharge syndrome.
Methods: Participants were recruited at six government clinics in Kampala, Uganda between October 2019 and July 2023. Penile-meatal and pharyngeal samples were cultured for NG and tested by nucleic acid amplification test (NAAT). NG isolates were subjected to antimicrobial susceptibility testing, whole genome sequencing (WGS), and multilocus sequence typing (MLST).
Results: Of 338 participants, median [IQR] age 25.0 [22, 32] years, 16.6% (n = 56) were living with HIV. By NAAT and/or culture, 67.5% (228/338) and 8% (27/338) were positive for uNG and pNG, respectively. Of those with uNG, 11.8% (27/228) were NAAT-positive for pNG; 74.1% (20/27) were culture-positive for both uNG and pNG. All isolates were susceptible to cefixime and ceftriaxone and >96% were resistant to ciprofloxacin, penicillin, and tetracycline. Eight isolates were azithromycin-resistant, seven from participants positive for both pNG and uNG, and 62.5% (5/8) belonged to MLST sequence type (ST) 11994. WGS revealed that 50% (n = 10) of participants had different STs between the urethra and pharynx; 35% (7/20) of paired uNG and pNG (same participant) had different susceptibility profiles (Table 1). The 119 uNG and 20 pNG isolates belonged to 31 and 10 different STs, respectively; the most common STs were ST1587 for uNG and ST1588 for pNG. A WGS-based global phylogeny of NG revealed that 96.4% (134/139) of isolates clustered into 5 clusters.
Conclusions: Pharyngeal NG is common in men with uNG, both displaying high rates of antimicrobial resistance. The finding of increasing rates of azithromycin-resistant NG in this setting and of NG with different susceptibility profiles at separate anatomical sites might be of great importance for treatment and surveillance purposes.
| ID | MLST ST | Azithromycin | Cefixime & Ceftriaxone | Ciprofloxacin | Penicillin | Tetracycline | |
|---|---|---|---|---|---|---|---|
| Same MLST ST | Minimum inhibitory concentration (MIC) (µg/mL) | ||||||
| SA_005-P | Unknown | S | S | R | R | R | |
| SA_005-Ph | Unknown | S | S | R | R | R | |
| SA_014-P | 11368 | S | S | R | I | R | |
| SA_014-Ph | 11368 | S | S | R | I | R | |
| SA_030-P | 1587 | S | S | R | R | R | |
| SA_030-Ph | 1587 | S | S | R | R | R | |
| SA_041-P | 11365 | S | S | R | R | I | |
| SA_041-Ph | 11365 | S | S | R | R | I | |
| SA_102-P | Unknown | S | S | R | R | R | |
| SA_102-Ph | Unknown | S | S | R | R | R | |
| SA_120-P | 11994 | R (>4) | S | R | I | R | |
| SA_120-Ph | 11994 | R (>4) | S | R | I | R | |
| SA_121-P | 11365 | S | S | R | R | I | |
| SA_121-Ph | 11365 | S | S | R | R | I | |
| SA_171-P | 1587 | S | S | R | R | R | |
| SA_171-Ph | 1587 | S | S | R | R | R | |
| SA_241-P | 1588 | S | S | R | R (2) | R | |
| SA_241-Ph | 1588 | S | S | R | R (8) | R | |
| SA_281-P | 1588 | S | S | R | I (<0.25) | R | |
| SA_281-Ph | 1588 | S | S | R | R (8) | R | |
| Different MLST ST | |||||||
| SA_057-P | 13778 | S | S | R | R (>32) | R | |
| SA_057-Ph | 13781 | S | S | R | I (<0.25) | R | |
| SA_110-P | 11365 | S | S | R | I | R | |
| SA_110-Ph | 13781 | S | S | R | I | R | |
| SA_166-P | 13778 | S | S | R (2) | I (<0.25) | R | |
| SA_166-Ph | 13765 | S | S | R (8) | R (>32) | R | |
| SA_240-P | Unknown | R (>4) | S | R | R | R | |
| SA_240-Ph | 1588 | R (>4) | S | R | R | R | |
| SA_285-P | 1588 | S | S | R | I | R | |
| SA_285-Ph | Unknown | S | S | R | I | R | |
| SA_290-P | 1901 | S | S | R | R (8) | R | |
| SA_290-Ph | 1588 | S | S | R | R (32) | R | |
| MN-102-P | Unknown | S | S | R | R | R (32) | |
| MN-102-Ph | 11367 | S | S | R | R | I (0.5) | |
| MN_220-P-1 | 11994 | R (>4) | S | R (16) | I (<0.25) | R (>32) | |
| MN_220-P-2 | Unknown | S (0.125) | S | R (4) | R (>32) | R (32) | |
| MN_220-Ph | Unknown | S (0.03) | S | I (0.125) | I (<0.25) | I (0.125) | |
| MN_221-P | 11994 | R (>4) | S | R (16) | I (<0.25) | R (>32) | |
| MN_221-Ph | 1597 | S (0.25) | S | R (4) | R (>32) | I (0.5) | |
| MN_228-P | 11994 | R (>4) | S | R (16) | I | R | |
| MN_228Phh | 11368 | S (0.25) | S | R (4) | I | R | |
MLST ST, Multilocus Sequence Type, Sequence Type; P, penile; Ph, pharyngeal; S, susceptible; I, intermediate resistance; R, Resistant. Antimicrobial susceptibility testing was performed by agar dilution and CLSI (Clinical and Laboratory Standards Institute) guidelines were used. Isolates with MIC ≥ 2.0 µg/mL were classified as azithromycin resistant. The penile culture of participant MN_220 had two distinct NG strains. For simplicity, the MIC has been excluded if the MIC was identical for both the urogenital and pharyngeal isolate.
PP01.54 – Antimicrobial Resistance Profiles of Neisseria Gonorrhoeae in Kampala, Uganda: A Retrospective Analysis of the National Antimicrobial Resistance Surveillance Data (2022–2023)
Miss Ritah Namusoosa1, Mr Benedict Kanamwanji3, Mr Micheal Ssekyanzi4, Mr Jonathan Kabazzi3, Dr Grace Najjuka3
1Uganda National Institute of Public Health, Kampala, Uganda.
2National Health Laboratory and Diagnostic Services - Ministry of Health, Kampala, Uganda.
3National Microbiology Reference Laboratory, Kampala, Uganda.
4Makerere University, College of Natural Sciences, Kampala, Uganda.
Background: Gonorrhea, caused by Neisseria gonorrhoeae, remains a major global health concern, with an estimated 86.9 million new cases annually, primarily in the Pacific and African regions. Effective management relies on antimicrobial treatment, but increasing antimicrobial resistance (AMR) complicates control efforts. This study aimed to characterize AMR profiles of N. gonorrhoeae in Kampala, Uganda, using retrospective data from the National Microbiology Reference Laboratory (October 2022–December 2023).
Methods: We conducted a retrospective analysis of routine AMR testing data at the National Microbiology Reference Laboratory from 2022 to 31 December 2023 for samples collected from 10 healthcare facilities in Kampala, Uganda. Susceptibility profiles for the priority antibiotics; ceftriaxone, ciprofloxacin, tetracycline, cefixime, spectinomycin, and penicillin G, were analyzed. Patient demographics; age, sex, signs, and symptoms were included to contextualize the findings.
Results: All 148 isolates analyzed were from male patients with a mean age of 23 years (SD 6.8). 92 (62.2%) were culture-positive, 96 (64.9%) showed microscopic evidence of gonorrhea and 7.4% (11/148) reported having HIV. Resistance rates were highest for ciprofloxacin (100%), tetracycline (91.6%), and Penicillin G (88.1%). Ceftriaxone showed significantly lower resistance (8.7%) while resistance to spectinomycin was minimal (5.5%), and no resistance was observed for cefixime, maintaining its efficacy as a treatment option based on disk diffusion. Among the isolates that underwent detailed characterization using Etest, 57/92(61.5%) of the culture-positive, 56/60(93.3%) were ciprofloxacin-resistant, 57/60 (95.0%) were azithromycin-sensitive, and 58/60 (96.7%) gentamicin-sensitive. Resistance profiles were comparable between methods except for ceftriaxone (disk diffusion: 58/60, 96.7%; Etest: 57/60, 95%) and gentamicin (disk diffusion: 4/15, 26.7%; Etest: 58/60, 96.7%) sensitivity.
Conclusion: The findings highlight the importance of continued surveillance to monitor evolving AMR patterns, particularly for Neisseria gonorrhoeae. Cefixime and ceftriaxone remain reliable treatment options, but emerging resistance to other antibiotics demands revised treatment protocols and enhanced stewardship efforts.
PP01.55 – Generalizable Segment Anything Model Via Selection Strategy for Skin Lesion Segmentation in Sexual Transmitted Infection Cases
Mr. Jiajun Sun1,2, Dr. Zhen Yu5,6, Mr. Siyuan Yan5,6, Mr. Cheng Luo5,6, Dr. Janet Towns1,2, Dr. Lin Zhang3,4, Prof. Dr. Jason Ong1,2, Dr. Zongyuan Ge5,6, Dr. Lei Zhang1,2,7
1Melbourne Sexual Health Centre, Carlton, Australia.
2The School of Translational Medicine (STM), Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Suzhou Industrial Park Monash Research Institute of Science and Technology, Suzhou, China.
4School of Public Health and Preventative Medicine, School of Medicine, Nursing and Health Sciences, Monash University, Clayton, Australia.
5AIM for Health Lab, Monash University, Clayton, Australia.
6Faculty of IT, Monash University, Clayton, Australia.
7China-Australia Joint Research Center for Infectious Diseases, School of Public Health, Xi’an Jiaotong University Health Science Center, Xi’an, China.
Background: Accurate segmentation of skin lesions is essential for the diagnosis, monitoring, and treatment of dermatological conditions, particularly those associated with sexually transmitted infections (STIs). STI-related skin lesions often exhibit special visual patterns, irregular borders, and varying sizes, adding to the complexity of manual segmentation. These challenges are further compounded by complex contrasts between lesions and surrounding skin, as well as diverse backgrounds in clinical settings.
Methods: To address these challenges, we introduce an innovative point-selection strategy for the Segment Anything Model (SAM) to improve its generalization in skin lesion segmentation. Specifically, we first identify the uncertain areas by SAM, which may contain lesion parts, and learn the distribution of these uncertain areas. With this learned prior, complementary points are selected as prompts to refine the segmentation results. Furthermore, to avoid segmentation regions overlapping benign areas, we constrain the segmentation results through pseudo-boxes crafted by the selected points.
Results: Our proposed techniques collectively result in skin lesion segmentation with more precise, completed, and compact lesion areas compared to standard SAM and previous methods. Extensive experiments on the ISIC2016, ISIC2017, PH2, Dermofit, and STI Atlas public datasets demonstrate that our method can achieve superior performance. For example, compared to nnU-Net, our model achieves an average improvement of +0.82% on dermoscopic images and a +5.85% increase in zero-shot capability when segmenting rare skin infection regions captured in clinical settings (Figs 1–6; Tables 1–5).
Conclusion: Our PSAM introduces a well-designed framework based on SAM to optimize the model’s mask output for point prompts. We further improve the model’s ability to recognize skin lesions by adding adapters to the transformer module in the mask decoder. We successfully used the SAM in the skin lesion segmentation task, especially in the STI-caused skin lesion. We hope our work can promote further research on community segmentation models for skin images.
Comparison of results produced by (b) nnU-Net, (c) ScribbleSaliency (with scribble prompts), (d) SAM (with point prompts), (e) One-Prompt (with point prompts), (f) Medical SAM (with box prompts), and (g) our proposed prompt-enhanced SAM (PASM). (I) represents dermatologic cases, while (II) represents skin infection cases captured in clinical settings. The red curve represents the model’s segmentation results, while the green curve indicates the ground truth. Red boxes highlight prediction failures. The right section presents the quantitative comparisons, with validation results displayed at the top and test results at the bottom.
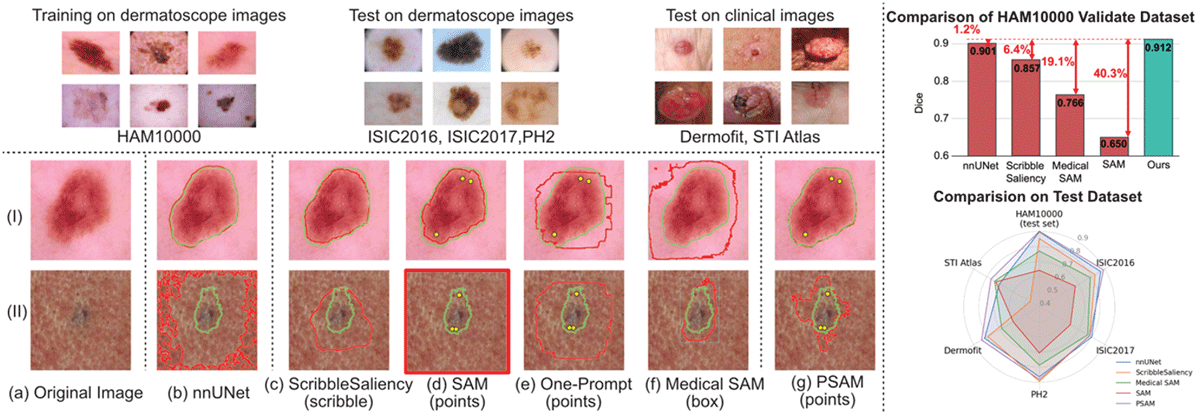
Overview of our proposed PSAM framework. We introduce an edge feature augmentation module to generate uncertain regions for identifying ambiguous boundary areas, and a point supplementation and refinement module to select additional complementary prompts within the uncertain regions. The initial prompts, together with the supplementary prompts, jointly constrain the final refined lesion boundaries.
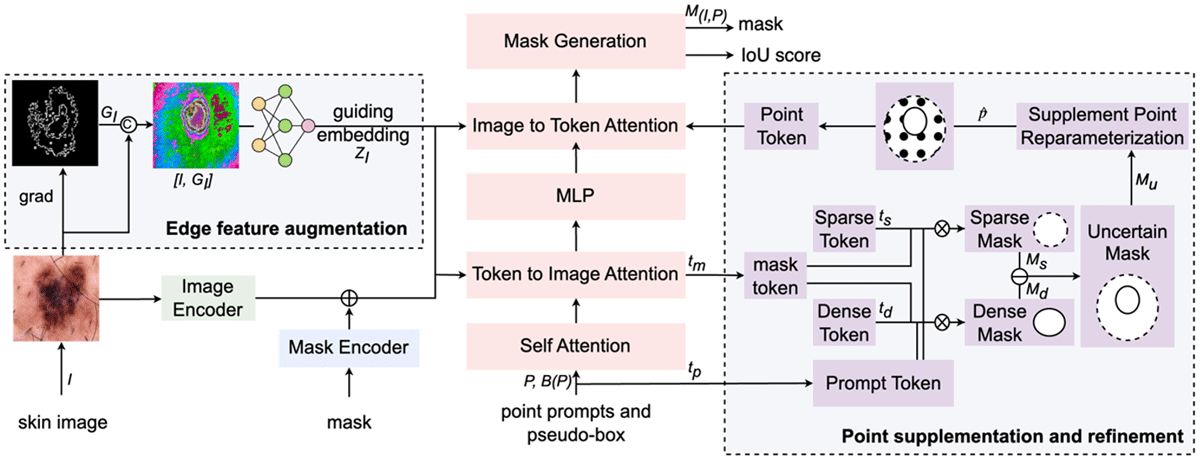
Visualization of the uncertain mask and supplemental points. The initial points are marked with green stars. The uncertain mask, shown on the right, is generated based on the uncertain mask. Four positive and four negative supplemental points, indicated by pink and blue stars respectively, are calculated from uncertain masks. The final output, displayed on the left, is represented by the red curve.
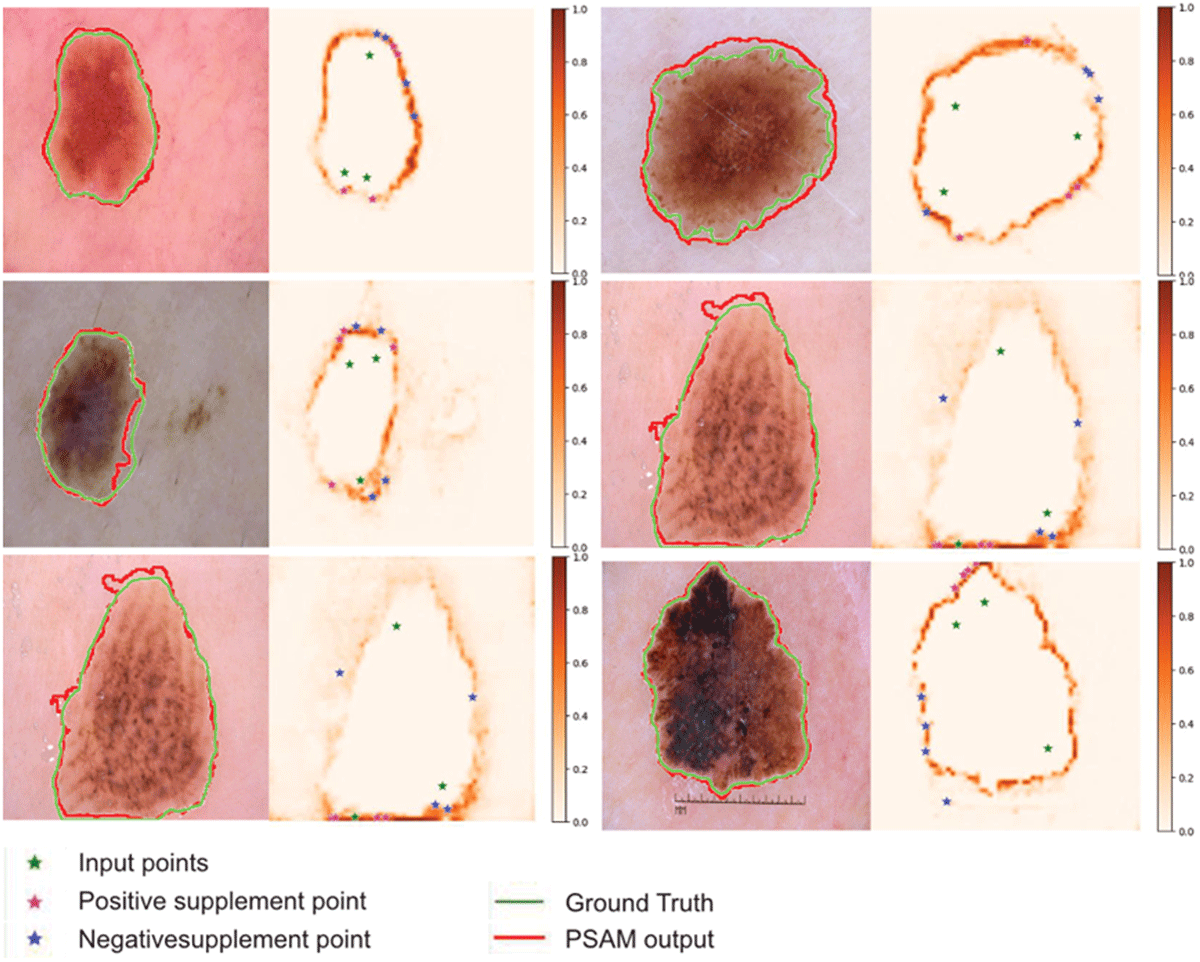
Visual comparison of several segmentation methods results (in red) and corresponding ground truth (in green) on the six skin lesion image datasets. Point prompt marked as the yellow star. Red boxes mark prediction failure.
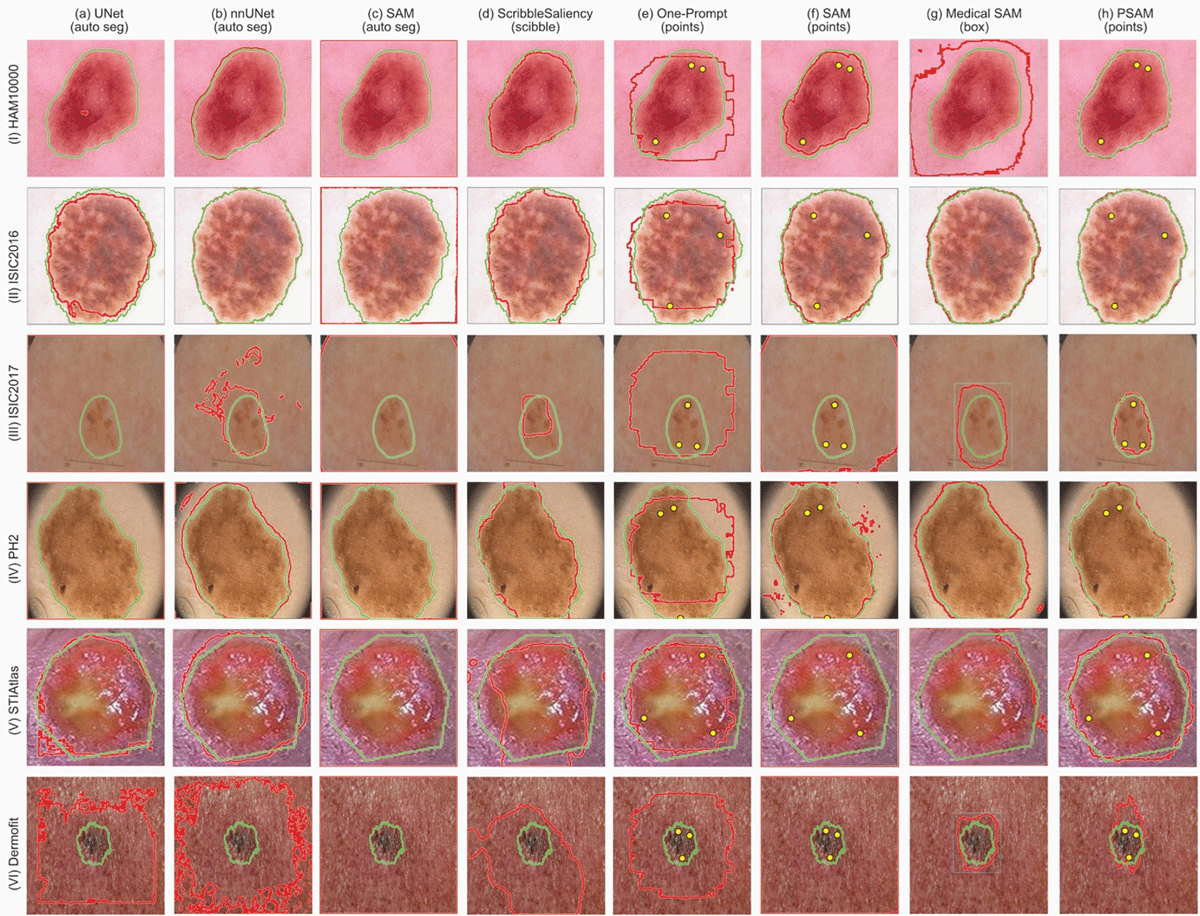
Model Performance on the validation dataset. The best results were marked in bold and the second best results were marked in underline.
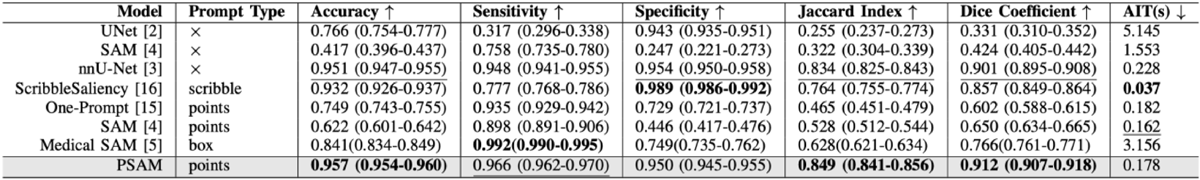
PP01.56 – HIV Resistance to ARVs in Patients with Therapeutic Failure in Cuba, 2022–2024
Prof. Lissette Perez1, MSc Yanet Pintos1, Bachellor Gabriela Diaz1, MSc Rosario Gravier1, Bachellor Eslin Dominguez1, MD, MSc Jorge Perez1, MD, MSc Carlos Fonseca1, MD, MSc Darien Fonseca1, PhD Yudira Soto1, Karla Fernandez Bachellor1, PhDs Vivian Kouri1
1Pedro Kouri of Tropical Medicine Institute, La Habana, Cuba.
Background: In 2009, Cuba introduced resistance testing in clinical practice, in 2016 it changed its first-line therapy (Atripla), in 2018 it started using DTG in patients with therapeutic failure, and in 2019 it changed its first-line therapy again and introduced DTG. The Cuban epidemic has been characterized by the circulation of numerous subtypes and CRFs. This work aims to investigate the level and profile of ARV resistance and subtype distribution among HIV-1 patients failing therapy from 2022 to 2024.
Methods: Protease, reverse transcriptase and integrase were amplified and sequenced using the Sanger methodology and resistance interpretation was performed using the Stanford database. HIV-1 subtyping was performed with Los Alamos db.
Results: The laboratory received 35, 40 and 23 plasmas from patients with therapeutic failure from the years 2022, 2023 and 2024, respectively. A significant increase in resistance to NRTIs was observed between 2022 and 2024 (P < 0.01). The highest resistance values in the 3 years were quantified to 3TC/FTC, followed by ABC, among NRTIs, to EFV and NPV among NNRTIs and to CAB, followed by DTG, BIC and EVG among NNRTIs. The most frequent mutations were M184V (NRTI), Y181C and K103N (NNRTI), Q58E (IPR) and E138K and R263K (IINT). Resistance to IPRs has remained very low during the years of study (<4%). The most frequently detected subtypes were B, CRF_BG, CRF19_cpx, CRF18_cpx and URF.
Conclusions: The high levels of resistance to NNRTIs show the risk of using other members of this family in future treatments. The highest levels of resistance were detected to the ARVs used in the country, with an increase observed for TDF. Resistance to IPRs has decreased due to their limited use. Close monitoring of resistance to IINTs is necessary because its increase may put first-line therapy at risk.
PP01.57 – Implementation of Next-Generation Sequencing for the Detection of HIV-1 Resistance Mutations to Antiretroviral in Cuba
MD Yolanda Polanco1, Prof. Lissette Perez1, MSc Rosario Gravier1, Gabriela Diaz Bachellor1, Bachellor Eslin Dominguez1, MD, MSc Jorge Perez1, MD, MSc Milena Duque1, MD, MSc Darien Fonseca1, PhD Yudira Soto1, Bachellor Karla Fernandez1, PhDs Vivian Kouri1
1Pedro Kouri of Tropical Medicine Institute, La Habana, Cuba.
Introduction: Antiretroviral drug resistance testing is essential for therapeutic efficacy in HIV-infected patients. Sanger sequencing is the gold standard and detects viral populations greater than 20%, while next-generation sequencing (NGS) technologies can detect minority populations (1%).
Objective: To implement the NGS assay for HIV-1 genotypic studies in untreated Cuban patients infected with different viral variants.
Materials and Methods: Plasma from 28 patients was sequenced using the Sanger method and NGS Sentosa® SQ. Sequences were analyzed in the Stanford HIVdb database for the detection of total mutations, mutations associated with drug resistance (MDR), antiretroviral resistance levels, and other parameters. Performance indicators of the implemented NGS assay were calculated.
Results: NGS detected more unique mutations (P = 0.0006) and MDR (P = 0.0104) in the protease/reverse transcriptase region. There was no difference between the mean levels of resistance to the drugs used in therapy for the sequence methods analyzed. Good agreement was observed between NGS and the Sanger method (88.0%). Complete protein sequences were obtained by NGS, however, with the Sanger method, 78.6% (22/28) for protease, 85.7% (24/28) for reverse transcriptase and 89.3% (25/28) for integrase. Only stop codons were found in the sequences obtained by NGS. The most frequent protease/reverse transcriptase and integrase subtypes were URF, CRF_BGs, CRF19_cpx, B, CRF18_cpx, and C.
Conclusions: The Sentosa NGS method demonstrated good performance and a more optimized workflow for HIV-1 genotyping compared to the reference method. These findings support its usefulness in improving antiretroviral therapy outcomes in the care of patients living with HIV.
PP01.58 – Performance of Softcup® Menstrual Cup and Vulvovaginal Swab Samples for Detection and Quantification of Genital Cytokines
Mr. Nashlin Pillay1,2, Dr. Gugulethu Favourate Mzobe1,2, Mr. Marothi Letsoalo1, Miss Asavela Olona Kama1, Dr. Andile Mtshali1,2, Mr. Stanley Nzuzo Magini1, Mrs. Nikkishia Singh1, Mrs. Vani Govender1,2, Dr. Natash Samsunder1, Dr. Megeshinee Naidoo1, Prof. Dhayendre Moodley1,2, Dr. Cheryl Baxter1,3, Prof. Derseree Archary1,2, Dr. Sinaye Ngcapu1,2
1Centre for the AIDS Programme of Research in South Africa (CAPRISA), Durban, South Africa.
2University of KwaZulu-Natal (UKZN), Durban, South Africa.
3Centre for Epidemic Response and Innovation (CERI) - Stellenbosch University, Stellenbosch, South Africa.
Background: Cytokines are important mediators of immunity in the female genital tract, and their levels may be associated with various reproductive health outcomes. However, the measurement of cytokines and chemokines in vaginal fluid samples may be influenced by a variety of factors, each with the potential to affect the sensitivity and accuracy of the assay, including the interpretation and comparison of data.
Description: We measured and compared cytokine milieu in samples collected via Softcup® menstrual cup versus vulvovaginal swabs. One hundred and eighty vulvovaginal swabs from CAPRISA 088 and 42 Softcup supernatants from CAPRISA 016 cohorts of pregnant women were used to measure the concentrations of 28 cytokines through multiplexing.
Results: Cytokines measured in this study were detectable in each of the methods however, SoftCup supernatants showed consistently, higher detectability, expression ratios, and mean concentration of cytokines than vulvovaginal swabs. While mean concentrations differed, the majority of cytokines correlated between SoftCup supernatants and vulvovaginal swabs. Additionally, there were no significant differences in a number of participants between the two sampling methods for the classification of genital inflammation.
Conclusion: Our findings suggest that SoftCup supernatants and vulvovaginal swab samples are suitable for the collection of genital specimens to study biological markers of genital inflammatory response. However, the Softcup menstrual cup performs better for the detection and quantification of soluble biomarkers that are found in low concentrations in cervicovaginal fluid.
Cytokine concentrations by biological sample type in pregnant women. A t-test was used to compare cytokine concentrations (pg/mL) in SoftCup super-natants versus vulvovaginal swabs of women with the cytokines detected above threshold of detection (blue color) while B was from those with cytokines below threshold of detection (green color). (For interpretation of the references to color in this figure legend, the reader is referred to the web version of this article.).
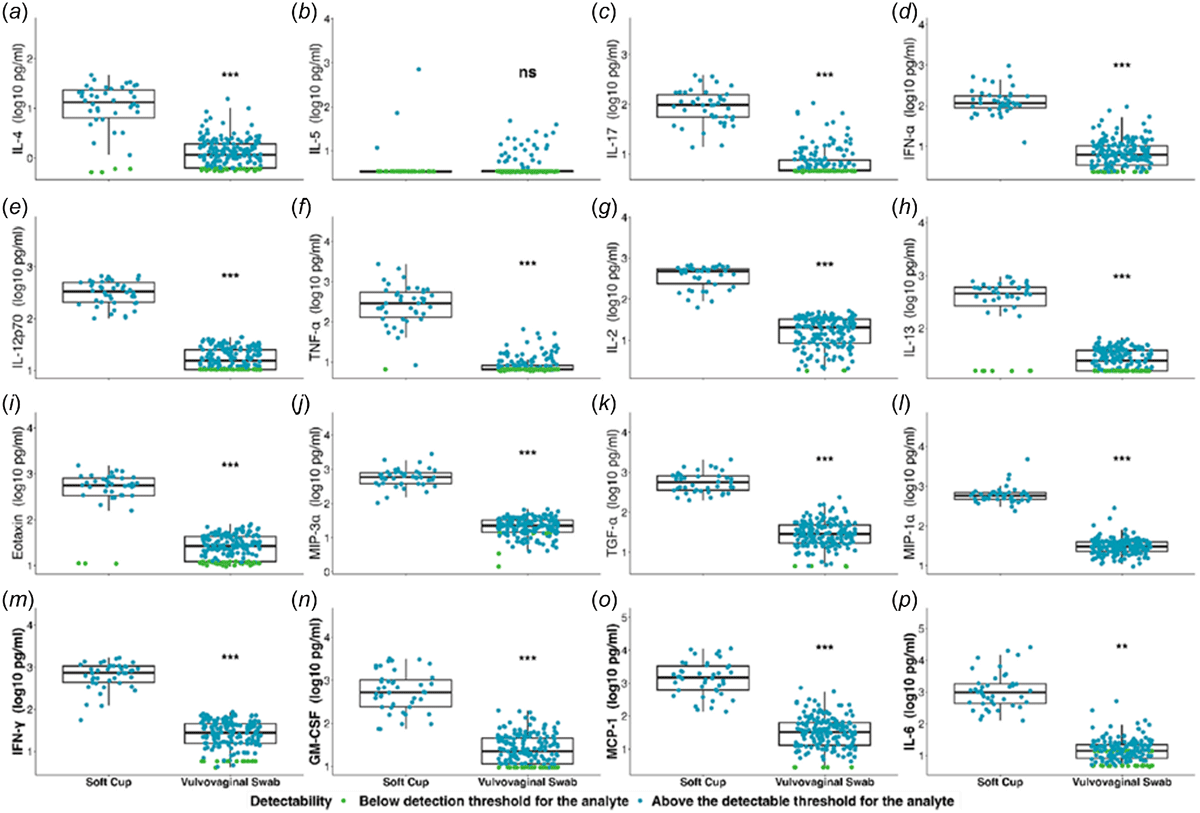
PP01.59 – Comparability of Gradient Strip and Agar Dilution Methods for Antimicrobial Susceptibility Testing of Neisseria Gonorrhoeae
Dr. Rachel Pitt-Kendall1, Dr Anna Vickers1, Suzy Sun1, Sandra David1, Sandhya Vivekanand1, Prarthana Narayanan1, Emma Callan1, Dr Hamish Mohammed1, Dr Katy Sinka1, Dr Michelle Cole1, Dr Helen Fifer1, Dr Sarah Alexander1
1UK Health Security Agency, London, United Kingdom.
Background: Antimicrobial susceptibility testing (AST) of Neisseria gonorrhoeae (Ng) is imperative for surveillance of resistance and to inform management of complex cases. AST of Ng for case management commonly uses gradient strip testing, whilst surveillance programmes, such as the Gonococcal Resistance to Antimicrobials Surveillance Programme, use agar dilution.
We undertook a comparison of minimum inhibitory concentration (MIC) results from gradient strip and agar dilution methods to establish validation data for the use of gradient strips (Etest® specifically) off-licence for AST of Ng.
Methods: Gradient strip (Etest®) AST was performed in triplicate for azithromycin, cefixime, ceftriaxone, ciprofloxacin, gentamicin, penicillin and tetracycline, using six well-characterised Ng control strains (WHO G, K, M, O, P and Q), on GCVIT agar (GC agar, 1% Vitox). Modal MICs were compared to published data and those obtained via agar dilution on DST agar (DST agar, 5% lysed horse blood, 1% Vitox). MICs were interpreted using EUCAST breakpoints and Cohen’s Kappa statistic.
Results: Etest® MICs for all combinations were within one doubling-dilution of the agar dilution MIC, and within essential agreement. Where variance was observed, there was a systematic shift to higher MICs for azithromycin and lower MICs for cefixime, gentamicin and tetracycline with Etest®. Most (40/42, 95.2%) Etest® MICs were within one doubling-dilution of the published MICs. For 2/42 combinations (WHO K, azithromycin; WHO Q, tetracycline) the Etest® MIC was two doubling-dilutions lower than the published MIC. The susceptibility categorisation was concordant for 27/30 (90.0%) combinations where EUCAST breakpoints were available (κ = 0.8).
Conclusion: High concordance was seen between two AST methodologies for Ng. However, method variation did result in some systematic shifts in MICs. These differences should be considered when comparing and interpreting susceptibility data from different laboratories.
PP01.60 – Detection of Treponema Pallidum Subspecies Pallidum in Plasma Samples from Blood Donors Using Real-Time PCR
Dr. Rachel Pitt-Kendall1, Zilan Ersoy1, Victoria Maddox2, Dr. Michelle Cole1, Dr. Helen Fifer1, Dr. Heli Harvala2, Dr. Sarah Alexander1
1UK Health Security Agency, London, United Kingdom.
2NHS Blood and Transplant, London, United Kingdom.
Background: Blood donations in England are screened for Treponema pallidum subspecies pallidum (Tp) using a treponemal test and positives are excluded from donation. If a donor screens positive, a lookback is performed of previous donations to confirm prior negative status.
We performed a feasibility study to understand the utility of molecular detection of Tp in plasma samples from blood donors.
Methods: DNA was extracted from 55 screen-negative plasma samples from donors who had later seroconverted on subsequent donation, using the DSP Virus/Pathogen mini-kit (Qiagen) on the Qiasymphony platform (Qiagen). Extracts were tested in triplicate on a T. pallidum 47 kDa lipoprotein gene RT-PCR on the Quantstudio platform (Applied Biosystems). Where Tp DNA was detected in at least 2/3 replicates, specimens were categorised as positive. Where Tp DNA was detected in 1/3 or no replicates, specimens were categorised as inconclusive or negative respectively. RT-PCR results were analysed in context of the linked serology results.
Results: Three (3/55, 5.5%) plasma extracts were positive for Tp DNA and 1/55 (1.8%) plasma extract was inconclusive (Table 1). The RT-PCR was negative for all remaining (51/55, 92.7%) extracts. Further serological results, using a panel of tests (Table 1), for the PCR positive and inconclusive samples were consistent with Tp infection. However, the PCR was more reliably detected when the IgM and RPR assays were also positive, likely indicating more recent infection.
Conclusions: We have demonstrated proof-of-concept of detection of Tp DNA in plasma specimens from blood donors with positive Tp serology results. The Ct values for all reactions indicated very low DNA load. Transfusion transmission risk of Tp, through refrigerated blood-products, is very low and there was no evidence of transmission in these cases. Further work is required with clinically staged Tp infections to explore the full benefit of this assay in blood donor screening.
| Tp 47 kDa RT-PCR result (Ct value) | RT-PCR overall resultA | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Plasma sample | Replicate 1 | Replicate 2 | Replicate 3 | IgG/IgM Ab EIAsκ | IgMκ | TPHAκ (≥1:32 = positive) | RPRκ | INNO-LIAκ | ||
| 1 | − | − | + (38.79) | Inconclusive | Positive | Negative | 1:64 | Negative | Positive | |
| 2 | + (33.72) | + (33.44) | − | Positive | Positive | Positive | 1:64 | Positive - neat | Positive | |
| 3 | + (31.90) | − | + (35.55) | Positive | Positive | Positive | 1:512 | Positive - 1:2 | Positive | |
| 4 | + (33.62) | − | + (34.67) | Positive | Positive | Positive | 1:128 | Positive - 1:2 | Positive | |
APositive - Tp detected on at least 2 occasions, inconclusive - Tp detected on 1 occasion, negative - Tp not detected
κ Total Ab EIA - CapitaTM Syphilis Total Aantibody EIA (Trinity Biotech) and ICE Syphilis (Diasorin);
IgM - CapitaTM Syphilis NMT IgM (Trinity Biotech); TPHA (Fortress Diagnostics); RPR (NewBio); INNO-LIA (Fujirebio).
PP01.62 – Transforming HIV Care: Real-Time SMS Alerts for Critical Viral Load Results in Rural Mozambique
Mrs Deonilde Sarmento1, Dr. Irenio Gaspar1, Dr. Isidoro Nobre1, Dr. Aleny Couto1
1Ministry of Health of Mozambique, Maputo, Mozambique.
Background: To monitor the response to antiretroviral therapy (ART) through HIV viral load (VL) analysis, molecular biology devices are utilized. However, due to limited resources for distributing VL testing equipment across all health facilities (HFs), Mozambique has implemented a sample referral system where samples are collected at peripheral health facilities, sent to provincial hubs, and then forwarded to reference laboratories. Results are subsequently returned to the requesting facilities.
Description: Interoperability was established between the laboratory information system, the mobile phone service provider, and the mobile phone allocated to health facility in a rural area of Maputo Province. Tools were provided to record information on the sending of SMS notifications. Patients’ mobile numbers were collected at the time of sample collection for HIV viral load testing.
Results: Overall, from August to October, 771 samples were tested for HIV viral load. Of these, 53 samples (6.9%) showed critical results, indicating the need for rapid intervention. Many SMS notifications were successfully sent to patients, with 49 out of 53 cases (92.5%) receiving messages. However, 4 SMS (7.5%) were not sent, suggesting a small gap in the communication process. These results highlight that, while most patients with critical viral load levels were promptly informed, there remains a small but noticeable percentage of cases where SMS notifications were not delivered.
Conclusion: The data collected from August to October demonstrate that the system for notifying patients with critical HIV viral load results via SMS is generally effective. With 92.5% of critical cases receiving messages, the communication process functions well. However, the 7.5% of cases where SMS were not sent indicates room for improvement. Future efforts should focus on optimizing these areas to enhance the system’s reliability and effectiveness, ultimately leading to better health outcomes for people living with HIV in Mozambique.
PP01.63 – Comparison of Nugent Score Versus Molecular Quantification of Gardnerella Vaginalis and Fannyhessea Vaginae Loads to Predict Bacterial Vaginosis
Dr. Sunil Sethi1, Dr. Mansi Apreja1, Dr. Rashmi Bagga2, Dr. Archana Angrup1, Dr. Rakesh Yadav1
1PGIMER, Chandigarh, India.
2Department of Obstetrics and Gynecology PGIMER, Chandigarh, India.
Background: Bacterial vaginosis is a highly prevalent infection among the women of reproductive age. In BV, reduction of beneficial lactobacilli and overgrowth of Gardnerella vaginalis, Fannyhessea vaginae, etc. occurs. Current gold standard for BV diagnosis is Gram stain based Nugent criteria. However, it has some disadvantages like inter-observer variability, misidentification of F. vaginae, presenting a variable morphology. We have compared qPCR assay targeting G. vaginalis and F. vaginae with the Nugent score for diagnosis of BV.
Description: Vaginal swabs were collected from women of reproductive age presenting with complaint of abnormal vaginal discharge. Two swabs were collected from each woman, one of the swabs was rolled onto a glass slide and used for nugent scoring and the second swab was used for DNA extraction. The quantitative real time PCR targeted Gardnerella vaginalis and Fannyhessea vaginae. For each microorganism, a standard curve depicting copies per mL versus cycle threshold (Ct) value was prepared.
Results: A total of 60 vaginal samples were included in the study. The Nugent score and molecular quantification of G. vaginalis, F. vaginae were successfully obtained for each sample. 9/60 (15%) women had BV according to nugent score. 16/60 (26%) women had both an F. vaginae DNA level > 108 copies/mL and a G. vaginalis DNA level > 109 copies/mL. Out of 16 samples positive by qPCR, 8 were intermediate BV and 3 were BV negative based on nugent score.
Conclusion: qPCR assay targeting G. vaginalis and F. vaginae is a reliable tool for diagnosis of BV. Our findings reveal, 50% of samples demonstrating intermediate flora satisfied quantitative criteria used to define BV. F. vaginae was detected by qPCR in 56% of patients with BV and in only 8.5% of those with normal nugent socre, suggesting that quantification of F. vaginae is a good predictor of BV.
PP01.64 – ATP-Conjugated Gold Nanoparticles with Enhanced Antibacterial Efficacy Against Multidrug-Resistant Neisseria Gonorrhoeae
Prof. Aleksandra Sikora1, Dr. Mansab Saleemi1
1Oregon State University College of Pharmacy, Corvallis, United States.
Background: Gonorrhea, caused by Neisseria gonorrhoeae (Ng), poses a significant public health threat due to its high prevalence, severe health complications, increased susceptibility to HIV, and the alarming rise of multidrug-resistant (MDR) strains. The absence of a gonorrhea vaccine and the diminishing efficacy of current antibiotics necessitate innovative therapeutic strategies. Gold nanoparticles (AuNPs) have demonstrated antimicrobial activity against various pathogens, yet their potential against pathogenic Neisseria remains under explored. This study evaluates the synergistic antibacterial effects of AuNPs conjugated with adenosine triphosphate (ATP) against Ng.
Methods: AuNPs were synthesized at pH 6 and pH 9.5, functionalized with ATP (AuNPs-ATP), and characterized using UV-vis spectroscopy, dynamic light scattering, zeta potential analysis, Fourier transform infrared spectroscopy, and transmission electron microscopy. Antibacterial efficacy against Ng FA1090 and MDR WHO X strains was assessed using minimum inhibitory concentration (MIC), minimum bactericidal concentration (MBC), and time-kill kinetic assays.
Results: AuNPs-ATP exhibited significantly enhanced antigonococcal activity compared to AuNPs or free ATP. Against Ng FA1090, the MIC and MBC values of AuNPs-ATP (pH 9.5) were 0.0058 ± 0.00 mg/mL and 0.047 ± 0.00 mg/mL, respectively, while those for AuNPs-ATP (pH 6) were 0.0058 ± 0.00 mg/mL and 0.012 ± 0.00 mg/mL. For MDR WHO X, the MIC and MBC values of AuNPs-ATP (pH 9.5) were 0.37 ± 0.00 mg/mL and 0.75 ± 0.00 mg/mL, respectively, and for AuNPs-ATP (pH 6), 0.18 ± 0.00 mg/mL and 0.37 ± 0.00 mg/mL. Compared to standard antibiotics polymyxin B sulfate and ceftriaxone, AuNPs-ATP demonstrated superior efficacy, particularly in time-kill assays where AuNPs-ATP (pH 6 and pH 9.5) achieved rapid bacterial inhibition within 2 h.
Conclusion: The conjugation of AuNPs with ATP offers a novel and promising strategy to combat gonorrhea infections. Future studies will evaluate the in vivo efficacy of AuNPs-ATP in a murine model of gonococcal infection.
PP01.65 – Extragenital Screening Reveals Asymptomatic STI Burden in MSM in Indian Setting
Prof. Seema Sood1, Prof. Somesh Gupta2, Mr. Diwakar Sharma1, Dr. Rachna Verma1, Mr. Rajendra Singh1
1Department of Microbiology, All India Institute of Medical Sciences, New Delhi, India.
2Department of Dermatology & Venereology, All India Institute of Medical Sciences, New Delhi, India.
Background: Men who have sex with men (MSM) are disproportionately affected by anorectal and pharyngeal infections caused by Neisseria gonorrhoeae (NG) and Chlamydia trachomatis (CT). These are usually asymptomatic and found in absence of simultaneous infection at genital sites. However, they contribute significantly to the overall burden of sexually transmitted infections (STIs), heighten the risk of HIV transmission, and exacerbate development of antimicrobial resistance (AMR). The current study was undertaken to investigate the anatomic distribution of NG & CT infections in MSM as limited data is available from India.
Methods: This study recruited 257 MSM patients attending the STI clinic at AIIMS between May, 2023 and November, 2024. Oropharyngeal, urethral, and rectal swab samples were collected in triplicate and processed using standard diagnostic techniques. In-house polymerase chain reaction (PCR) assays were employed for NG and CT, with NG additionally tested by conventional methods.
Results: A total of 80% MSM were asymptomatic. The prevalence of NG infections by PCR was 24.9%, with site-specific rates of 14.4% (urethral), 9.7% (rectal), and 0.8% (pharyngeal). CT infections were identified in 6.2% of participants, with site-specific rates of 3.5% (urethral), 2% (rectal), and 0.8% (pharyngeal). Extragenital infections accounted for 42% of NG and 44% of CT cases. No individual tested positive for NG or CT at all three anatomical sites. Co-infections with NG and CT were observed in 1.5% of participants. Further, culture positive for NG was seen only in 4.2% of cases, at urethral site. Additionally, 9.7% were HIV-positive.
Conclusion: More than 40% of NG and CT infections would have been missed if screening had been limited to genital sites only. An expanded screening, incorporating extragenital sites, is essential for management and control of STIs in MSM. Implementation of NAAT based testing significantly increases the yield and should continue to be endorsed.
PP01.66 – Estimating the Sensitivity of Non-Treponemal Testing Among Patients with Primary Syphilis
Dr. Stephanie Sweitzer1, Dr. Jane Chen1, Mitch Matoga2, Ligang Yang3, Eduardo Lopez-Medina4,5, Jonny Garcia-Luna4,7,8, Christopher Hennelly1, Irving Hoffman1, Bin Yang3, Juan Salazar4,6,9, Justin Radolf6,9, Dr. Jonathan Parr1, Dr. Arlene Sena1
1Division of Infectious Diseases, Department of Internal Medicine, University of North Carolina, Chapel Hill, United States.
2UNC Project Malawi, Lilongwe, Malawi.
3Dermatology Hospital, Southern Medical University, Guangzhou, China.
4Centro Internacional de Entrenamiento e Investigaciones Medicas - CIDEIM, Cali, Columbia.
5Department of Pediatrics, Universidad del Valle, Cali, Columbia.
6University of Connecticut School of Medicine, Farmington, United States.
7Universidad ICESI, Cali, Columbia.
8Division of Dermatology, School of Medicine, Universidad del Valle, Cali, Columbia.
9Connecticut Children’s, Hartford, United States.
Background: Diagnosis of primary syphilis (PS) is challenging. Darkfield microscopy (DFM) was traditionally used but newer polymerase chain reaction (PCR) assays are not widely available. Serologic testing is the mainstay of diagnosis; however, further investigation is needed to refine sensitivity estimates of nontreponemal antibody tests for PS.
Methods: This observational, cross-sectional study enrolled participants >18 years with PS in China, Colombia, and Malawi from November 28, 2019 to May 27, 2022 as part of a parent study. Clinical data were collected through self-report and medical record review. Point-of-care testing was performed for HIV and syphilis. Laboratory testing included DFM, rapid plasma reagin (RPR) or toluidine red unheated serum tests (TRUST), treponemal tests, and quantitative polA PCR for Treponema pallidum.
Results: Across the four sites, 2820 participants were screened and 233 enrolled. Of those, 79 (34%) had PS. Most were cisgender men (61, 77%), and the remainder cisgender women (18, 23%). Age ranged from 18 to 58 years. Race/ethnicity was reported as Black by most (44, 56%), followed by Asian (18, 23%), and Hispanic/Latino (17, 22%). A minority (13, 17%) were living with HIV, and 9 (11%) had a prior history of syphilis or genital ulcer disease. Median number of days since appearance of an ulcer was 9. Among those with positive DFM, RPR demonstrated a sensitivity of 78% (38/49) and TRUST had a sensitivity of 55% (6/11) (Table 1). Among those with a positive PCR assay, RPR demonstrated a sensitivity of 94% (43/46) and TRUST had a sensitivity of 60% (9/15).
Conclusion: RPR showed moderate sensitivity compared to DFM and high sensitivity compared to PCR, while TRUST demonstrated low sensitivity compared to both DFM and PCR. These findings underscore the importance of using nucleic acid amplification tests for diagnosing PS given the limitations of nontreponemal tests for this syphilis stage.
| Number of positive tests | Total number tested | Sensitivity | ||
|---|---|---|---|---|
| Sensitivity as compared to DFM | ||||
| RPR | 38 | 49 | 77.6% | |
| TRUST | 6 | 11 | 54.5% | |
| Sensitivity as compared to PCR | ||||
| RPR | 43 | 46 | 93.5% | |
| TRUST | 9 | 15 | 60.0% | |
PCR, polymerase chain reaction; DFM, darkfield microscopy; RPR, rapid plasma reagin test; TRUST, toluidine red unheated serum test.
PP01.67 – Prompt Point-Of-Care HIV Viral Load Testing
Dr. Alexander Trick1, Preston Zimprich1, Mei Jin1, Dilawer Singh1, Alana Germroth1, Dr. Jeffrey Burke1
1Prompt Diagnostics, Baltimore, United States.
Background: Viral load monitoring is essential to tracking treatment adherence and efficacy for patients with HIV. Existing clinical workflows require phlebotomists for blood draws, shipment to centralized laboratory facilities, and testing on expensive equipment which can result in significant delays to results and treatment decisions. These delays can further aggravate development of drug resistance in patients with poor adherence and lead to increased complications and spread of infections.
Methods: We developed a streamlined method for handling fingerstick volumes of blood (100 μL) for plasma filtration coupled with nucleic acid extraction and PCR (Fig. 1). Contrived samples were created with spiked HIV viral standards into whole blood and processed with a manual filtration tool such that plasma was dispensed directly into our magnetofluidic assay cartridges. Magnetic bead manipulation and HIV RNA quantification in the cartridges was performed on portable Prompt Dx instrumentation with automated capture and transfer of HIV RNA on magnetic beads into PCR amplification reagents.
Results: Real-time PCR results with our portable platform enabled detection down to 1000 copies/mL of plasma. Overall time-to-result was completed in under 40 min including 90 s for blood separation. Successful filtration and sample processing was confirmed with the inclusion of a bacteriophage lysis control. Quantitative linearity of cartridges results was demonstrated with R2 > 0.95.
Conclusion: Our HIV assay demonstrates promising results towards accessible point-of-care viral load testing to guide immediate treatment decisions in the clinic and enable patients to monitor their viral load status at-home. Continuing efforts include further integration of blood sample processing for more streamlined and automated user experience, improved limit of detection, and even faster results to fit within existing clinical workflows.
HIV viral load testing workflow. Fingerstick blood added to a filtration module (left) is separated into red blood cells (RBCs) and plasma using a combination of magnetic separation and filtration. The filtered plasma is dispensed into a cartridge followed by loading the cartridge into a portable instrument that automates sample preparation and PCR quantification of HIV RNA.

PP01.68 – The Immune Correlates of HIV and STI Induced by Penile-Vaginal Sex Is Enhanced in the Context of Relative Genital Immunoquiescence
Miss Jinny Tsang1, Dr. Avid Mohammadi2, Sareh Bagherichmeh2,3, Dr. Yoojin Choi1, Dr. Azadeh Fazel2, Elizabeth Tevlin4,5, Sanja Huibner2, Dr. Sara V. Good6, Wangari Tharao4, Dr. Bryan Coburn2,7, Dr. Rupert Kaul2
1Department of Immunology, University of Toronto, Toronto, Canada.
2Department of Medicine, University of Toronto, Toronto, Canada.
3Department of Pathology and Laboratory Medicine at Schulich Medicine and Dentistry, University of Western Ontario, London, Canada.
4Women’s Health in Women’s Hands Community Health Center, Toronto, Canada.
5Street Health Community Nursing, Toronto, Canada.
6Department of Biology, University of Winnipeg, Canada.
7Toronto General Hospital Research Institute, University Health Network, Toronto, Canada.
Background: Penile-vaginal sex causes vaginal epithelial disruption and an immediate increase in vaginal pro-inflammatory cytokines and chemokines, all of which are associated with increased HIV and STI acquisition risk. However, there is considerable heterogeneity in the degree of vaginal inflammation experienced following sex. We hypothesize that the degree of sex-induced inflammation would depend on the preexisting immune milieu, with enhanced impact in women with an immunoquiescent vaginal immune environment at baseline.
Description: We employed multiplex and single-plex immunoassays to quantify HIV-associated soluble immune factors within cervicovaginal secretions of HIV-uninfected, STI-free women before and 1hr after condomless (n = 29) or condom-protected (n = 8) penile-vaginal sex. Cytokine concentrations in the upper tertile of baseline levels are defined as elevated, and inflammation is defined as elevations of ≥5/10 cytokines. Co-primary endpoints are (a) genital inflammation and (b) vaginal epithelial damage (i.e., elevated sEcad levels), 1hr after penile-vaginal sex.
Results: Penile-vaginal sex induces vaginal inflammation (P = 0.0126) and epithelial damage (p < 0.0001), regardless of condom use, but they are restricted to participants with low/no vaginal inflammation and sEcad levels (P < 0.0001; elevated sEcad, P = 0.4697) at baseline. Specifically, sex significantly induced vaginal HIV-associated immune markers IP-10, MIG, MIP-1β, IL-6, IL-1α, IFNα-2a and MMP-9 only within participants with low concentrations at baseline. Baseline vaginal IgG concentrations are greater than IgA levels (P < 0.0001), and both increase after sex (P < 0.0001 and P = 0.002, respectively). Elevated baseline concentrations of IgA are associated with baseline vaginal inflammation (P = 0.0093), but not with epithelial disruption (P = 0.1123).
Conclusion: Women with low vaginal inflammation at baseline experience increased vaginal inflammation after penile-vaginal sex, suggesting a heightened risk of HIV and STI acquisition during this period. In contrast, women with vaginal inflammation at baseline may have similar HIV and STI risks both before and after sex. Vaginal antibodies do not seem to play an anti-inflammatory role and warrant further investigation.
PP01.69 – Identifying Viable Neisseria Gonorrhoeae Through Validation and Application of Viability PCR
Mr. Sem Vellema1,2, Prof. Dr. Christian Hoebe1,3, Mr. Mayk Lucchesi1,2, Prof. Dr. Paul Savelkoul1,2, Dr. Petra Wolffs1,2
1Care and Public Health Research Institute, Maastricht University, Maastricht, Netherlands.
2Maastricht University Medical Center, Maastricht, Netherlands.
3Living Lab Public Health Mosa, South Limburg Public Health Services, Heerlen, Netherlands.
Background: The incidence of gonorrhoea, caused by the bacterial pathogen Neisseria gonorrhoeae (NG), is increasing globally, accompanied by rising antimicrobial resistance, including resistance to first-line treatment. Current molecular diagnostic methods, such as nucleic acid amplification tests, cannot differentiate between viable and non-viable bacteria. Bacterial culture – an inherent viability assessment – is challenged by the organism’s fastidious nature and sensitivity to environmental factors. Molecular viability assays have been developed, but to our knowledge not yet applied to NG. This study aims to validate and apply a viability PCR (V-PCR) method for NG, while correlating the results to successful culture recovery in clinical samples.
Methods: Viability was assessed using PMAxx, a membrane-impermeable dye that selectively binds to nucleic acids in non-viable cells, allowing for discrimination between viable and non-viable cells. Technical validation employed dilution series of viable NG mixed with heat-killed NG, treated or untreated with PMAxx, followed by PCR targeting the porA gene to determine delta Ct-values based on PMAxx status. Clinical samples (anorectal, oropharyngeal, and urogenital) were subsequently analysed using V-PCR, and results were compared with standard diagnostic culture results.
Results: Validation demonstrated that V-PCR eliminated 99.97% of DNA from non-viable NG, with strong correlation in viability detection (R2 = 0.973) across dilution series. Clinical samples showed a significantly higher median log viable load of 3.69 log10 copies/mL (IQR: 0.872–7.39) in culture-positive samples than culture-negative samples (10.7 log10 copies/mL; IQR: 6.05–13.1, P = 0.0003). Median viability percentage was significantly higher in culture-positive samples (16.4%; IQR: 0.887–37.7%) compared to culture-negative samples (0.31%; IQR: 0.01–11.9%, P = 0.0003).
Conclusion: V-PCR effectively discriminates viable NG from non-viable cells and performs well across varying bacterial concentrations. V-PCR reliably assesses viability in clinical specimens, with higher absolute and relative viability shown in culture-positive samples. V-PCR holds potential for improving diagnostic stewardship and provides insights into factors affecting culture recovery and infection dynamics.
PP01.70 – Commensal Oropharyngeal Rothia Mucilaginosa Inhibits the Growth of Neisseria Gonorrhoeae
Ms. Rebecca Villa1, Dr. Olusegun Soge1
1University of Washington, Seattle, United States.
Background: The growing threat of multidrug resistant Neisseria gonorrhoeae has prompted a need to develop alternative strategies to prevent and treat gonorrhea. Rothia mucilaginosa is a common commensal bacterium in the oropharynx and has been shown to inhibit the growth of other bacteria. We explored the potential of R. mucilaginosa to serve as an antagonist against N. gonorrhoeae.
Method: We investigated the ability of 72 commensal oropharyngeal R. mucilaginosa isolates to antagonize N. gonorrhoeae by standard co-culture methods using the N. gonorrhoeae strains WHO L, WHO U, or ATCC 49226. Each bacterium was suspended in Mueller-Hinton broth (MHB), mixed at a 1:1, 1:2, or 1:5 R. mucilaginosa to N. gonorrhoeae ratio, pooled onto chocolate II agar, and incubated overnight at 36°C with 5% CO2. Co-culture growth was suspended in MHB, serially diluted, plated onto chocolate II agar, and incubated for 48 h. Colonies were observed for their ability to form engulfing-like shapes surrounding N. gonorrhoeae colonies. Furthermore, 5 of the R. mucilaginosa isolates were assessed for their ability to inhibit N. gonorrhoeae growth. Colony counts were analyzed with one-way ANOVA.
Results: Of the 72 R. mucilaginosa isolates co-cultured with N. gonorrhoeae, 52 (72.22%) isolates formed engulfing-like shapes around N. gonorrhoeae colonies, indicating an antagonistic relationship. Of the 5 isolates tested for N. gonorrhoeae growth inhibition, 3 isolates significantly decreased N. gonorrhoeae colony counts (Fig. 1), and 2 of these isolates formed engulfing-like shapes surrounding N. gonorrhoeae colonies.
Conclusion: R. mucilaginosa reduces N. gonorrhoeae colony counts when co-cultured and forms engulfing-like shapes around N. gonorrhoeae colonies, indicating an antagonizing relationship. These results highlight the potential of novel bacterial-derived inhibitory agents from R. mucilaginosa to combat multidrug-resistant gonorrhea.
Average colony counts of Rothia mucilaginosa (RM) isolate 3MTM1 and Neisseria gonorrhoeae (NG) strain WHO L co-culture at 1:5 ratio. Dark red line is RM colony counts on co-cultured plates; dark blue is NG counts on co-cultured plates; light red is RM counts on control plate; light blue is NG counts on control plate. (n = 4; F = 24.35, P < 0.001; Tukey HSD P = 0.002, 95% CI = [44.29, 147.15]).
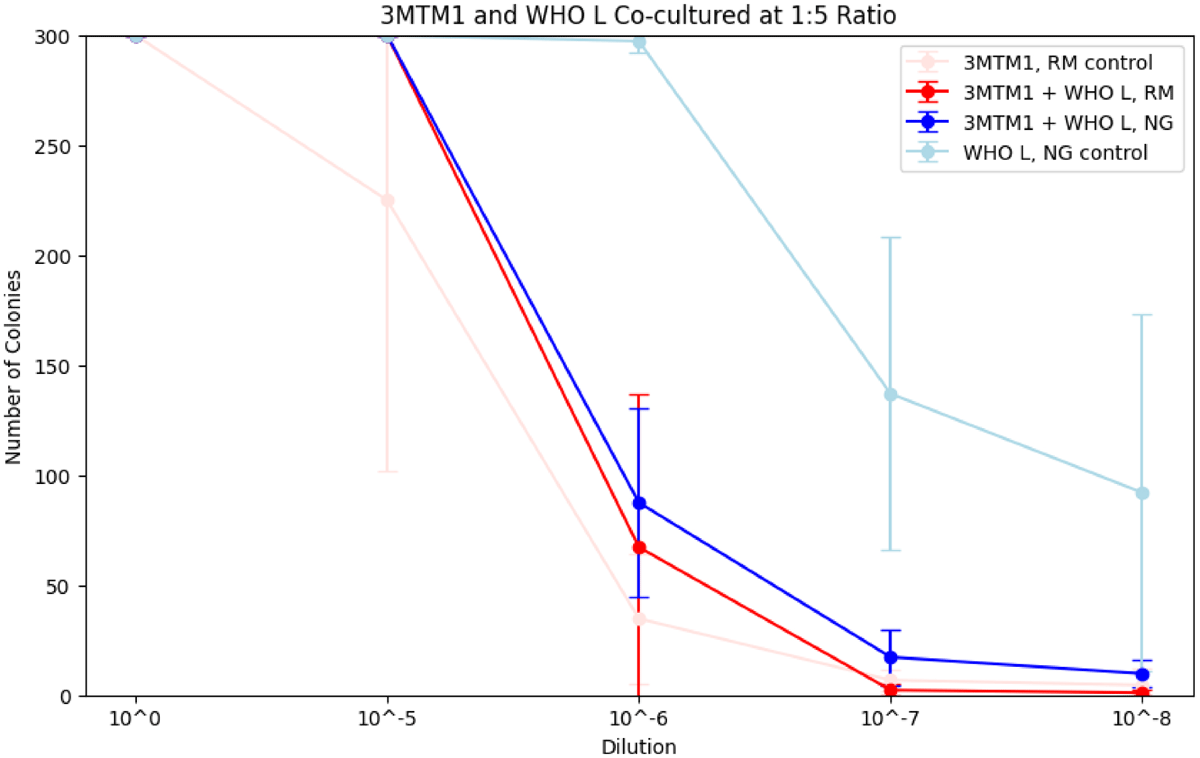
PP01.71 – Exploring the Diversity of Sexual Acts in Chinese Men Who Have Sex with Men and Its Impacts on the Risk of HIV and Sexually Transmitted Infections
Ms. Yu Liu1, Mr. Bingyang She1, Dr. Rui Zhao1, Ms. Gaixia Li1, Mr. Yawu Hu1, Ms. Fang Lu1, Dr. Shu Su2, Prof. Lei Zhang1,3
1Xi’an Jiaotong University, Xi’an, China.
2The Second Affiliated Hospital of Chongqing Medical University, Chongqing, China.
3Monash University, Carlton, Australia.
Background: High-risk sexual behaviour contributes to sexually transmitted infections (STIs), but the diversity of sexual acts in men who have sex with men (MSM) was understudied. We aimed to identify the diversity of sexual acts in Chinese MSM and its impacts on HIV/STI risk.
Methods: Between January and September 2022, the study was conducted in Xi’an, China, to identify sexual acts performed during the last sexual episode, which was measured by the Shannon diversity index.
Results: Of the 931 MSM, 2.9 % tested positive for HIV, 5.7 % for syphilis, 13.6 % for gonorrhoea and 12.9 % for chlamydia. The Shannon diversity index for individual sexual acts was 1.609 (IQR 0.693–1.946), whereas the index for sexual act pairs was 1.386 (IQR 0–1.792). MSM infected with gonorrhoea exhibited significantly greater diversity in individual sexual acts (1.792 vs 1.609) and sexual act pairs (1.609 vs 1.386) than otherwise. Compared with MSM having one partner over the past 3 months, MSM with 2–5 partners was 69.7 % more diverse in individual sexual acts (aOR = 1.697, 1.489–1.935) and 59.4 % more diverse in sexual act pairs (aOR = 1.594, 1.401–1.811). For MSM with >5 partners, the corresponding percentages were 84.8 % (aOR = 1.848, 1.624–2.104) and 56.2 % (aOR = 1.562, 1.368–1.782). Compared with those who did not use saliva as a lubricant, MSM who did were less diverse in individual sexual acts (aOR = 0.763, 0.662–0.878) and sexual act pairs (aOR = 0.752, 0.654–0.866).
Conclusion: MSM infected with gonorrhoea and those with multiple sexual partners are more diverse in sexual acts during sexual episodes.
PP01.72 – Associations Between Antibacterial Mouthwash Use with Sexual Behaviours and Sexually Transmitted Infections Among Chinese Men Who Have Sex with Men
Mr. Yawu Hu1, Dr. Rui Zhao1, Ms. Gaixia Li1, Ms. Yu Liu1, Ms. Fang Lu1, Mr. Bingyang She1, Dr. Min Zhao1, Prof. Lei Zhang1,2
1Xi’an Jiaotong University, Xi’an, China.
2Monash University, Carlton, Australia.
Background: Mouthwash is a commonly used product with the potential to prevent the transmission of STIs. This study aims to determine the association between mouthwash use frequency with sexual behaviours and STIs among Chinese MSM.
Methods: A cross-sectional study was conducted among MSM in Xi’an, China, from January to September 2022. Data on sexual behavioural information, including the number of sexual partners in the past 3 months, the use of protective measures, and the diversity of sexual acts in the most recent sexual episode, were collected and analyzed. Participants were categorized into non-mouthwash users, occasional, and frequent mouthwash users based on their usage frequency in the past 3 months. Multinomial logistics regression was performed to identify the association between mouthwash use frequency with STIs and sexual behaviours.
Results: Of the 838 MSM included in the analysis, 621 (74.11%) reported never used mouthwash, while 47 (5.60%) used it occasionally and 170 (20.29%) used it frequently. Frequent mouthwash users had a lower prevalence of Chlamydia compared to occasional users (8.33% vs 23.93%, P < 0.05). In comparison to participants who consistently used condoms, those who used condoms occasionally and never used condoms were 1.8 (aOR = 1.838, 1.011–3.375) and 4.5 (aOR = 4.538, 1.259–16.362) times more likely to be frequent mouthwash users. Participants with more sexual partners engaged in kissing (aOR = 1.060, 1.019–1.103), receptive masturbation (aOR = 1.061, 1.029–1.093), insertive masturbation (aOR = 1.040, 1.012–1.068), receptive oral sex (aOR = 1.065, 1.024–1.108), insertive oral sex (aOR = 1.043, 1.014–1.072), and receptive anal sex (aOR = 1.076, 1.027–1.127) were more likely to be frequent mouthwash users.
Conclusion: MSM with more sexual partners engaged in six types of sexual acts or lower condom use frequency were more likely to be frequent mouthwash users. However, frequent mouthwash users had a lower Chlamydia prevalence, suggesting potential STIs prevention among MSM. Further research is needed to confirm these findings and clarify the underlying mechanisms.
PP01.73 – Coupling Rabbit Infectivity Test with the in Vitro Cultivation of Treponema Pallidum from Patients with Early Syphilis in Cali, Colombia
Mrs Lady Giovanna Ramírez1,2, Mr Sebastian Alejandro Silva1,2, Mrs Ana Milena Folleco2, Mrs Kristina Delgado3, Mrs Carson La Vake4, Mrs Crystal Vicente4, Mr Jose David Ramirez1,2, Mr Jonny Alejandro Garcia-Luna1,2, Dr. Juan Carlos Salazar1,4,5,6,7, Dr. Justin D Radolf3,4,5,6,7, Dr. Kelly L. Hawley3,4,5,6,7
1CIDEIM, Cali, Colombia.
2Universidad ICESI, Cali, Colombia.
3Department of Medicine, University of Connecticut School of Medicine, Farmington, USA.
4Department of Pediatrics, University of Connecticut School of Medicine, Farmington, USA.
5Division of Infectious Diseases, Connecticut Children’s, Hartford, USA.
6Department of Immunology, University of Connecticut School of Medicine, Farmington, USA.
7Connecticut Children’s Research Institute, CT Children’s, Hartford, USA.
Introduction: The recent development of an in vitro cultivation system for Treponema pallidum subsp. pallidum (TPA), the causative agent of syphilis, creates new opportunities to explore TPA biology, syphilis pathogenesis, and syphilis epidemiology on a population-wide basis. Obtaining circulating clinical isolates for experimentation is essential for these efforts. Herein, we report the isolation of TPA in an endemic area using rabbit infectivity testing (RIT) followed by successful in vitro propagation of the isolated strains.
Methods: Whole blood from patients with early syphilis was injected into New Zealand White rabbits housed in a customized temperature-controlled cage. Animals were monitored weekly for seroconversion, assessed via rapid diagnostic testing and RPR titers. Isolated spirochetes were cultured in vitro using Sf1Ep cells in TPA Culture Medium 2 (TpCM2) and maintained under a low-oxygen environment (1.5% O2, 3.5% CO2, and 95% N2). Spirochetes were enumerated via darkfield microscopy and passaged weekly to maintain growth.
Results: Three TPA strains were isolated from polA qPCR-negative blood samples. Seroconversion (Rapid Treponemal test positivity and RPR ≥1:4) occurred after an average of 52.2 ± 26.34 days. The three isolates were successfully propagated in vitro for 100, 105, and 77 days, respectively. Cultures were terminated for cost-related reasons. Rabbits inoculated with samples from two other early syphilis patients are being monitored for seroconversion with plans to initiate in vitro cultivation once strains have been isolated and passaged to high density (Fig. 1).
Conclusion: This study demonstrates the feasibility of combining RIT with in vitro cultivation to achieve long-term propagation of TPA clinical isolates. It also underscores the extraordinary sensitivity of RIT. This advancement provides a transformative platform for studying patient immune responses to their own infecting strains (‘dyads’) in order to obtain new insights into how TPA flourishes within endemic populations.
PP02.01 – A Simulated Patient Study Investigating the Accessibility of HIV Self-Tests from Australian Community Pharmacies
Dr. Jack Collins1, Dr. Jessica Pace1, A/Prof Carl Schneider1
1The University of Sydney School of Pharmacy, Sydney, Australia.
Background: Access to regular testing is a critical component of strategies to promote early detection and reduced transmission of HIV. Self-testing kits offer an alternative to traditional HIV testing options and were made available via community pharmacies in Australia in 2021. Limited evidence regarding the experience of accessing these kits from community pharmacies exists. This study aims to explore the availability and accessibility of HIV self-testing kits from Australian community pharmacies using the simulated patient method.
Methods: A random, representative sample of 365 community pharmacies from Australian states and territories with accessible registers of pharmacy premises was generated and stratified according to location (Metropolitan/Region, Rural, Remote). A standardised telephone script was developed and the researchers telephoned pharmacies to enquire about the availability of HIV self-testing kits, acting as a member of the public. Primary data collection commenced in April 2024 and is ongoing. Telephone calls were documented and analysed descriptively.
Results: To date, 183 of 365 planned calls have been conducted. Nine pharmacies (4.9%) stocked HIV self-testing kits. Ten pharmacies (5.5%) were able to order in the kits for the next delivery. Many pharmacy staff (n = 79, 43.2%) were unfamiliar with the testing kits and 24 (13.1%) gave erroneous information regarding the availability of the kits. When self-testing kits were not stocked, pharmacy staff most frequently referred callers to another pharmacy (n = 58, 31.7%), a doctor (n = 32, 17.5%), or provided no advice (n = 20, 10.9%).
Conclusion: Interim results indicate that consumers may not be able to readily access self-testing kits from community pharmacies. Pharmacy staff lack familiarity with such kits and may not be equipped to provide adequate advice to consumers seeking HIV testing.
PP02.02 – Factors Influencing Willingness to Accept STI Prophylaxis Among Patients with Genital Ulcer Diseases in Uganda
Dr. Yuka Iijima1, Dr. Annet Onzia2, Brenda Dawa2, Beatrice Magoro2, Dr. Johan H. Melendez3, Dr. Rosalind Parkes-Ratanshi2,4, Dr. Yukari C. Manabe2,3, Dr. Matthew Hamill1,3
1Johns Hopkins Bloomberg School of Public Health, Baltimore, United States.
2Infectious Diseases Institute, Makerere University, Kampala, Uganda.
3Johns Hopkins School of Medicine, Baltimore, United States.
4Queen’s University Belfast, Belfast, United Kingdom.
Background: Sexually transmitted infections (STI) prophylaxis remains underutilized in high burden settings in sub-Saharan Africa. This study assessed sociodemographic and perceptual factors influencing willingness to accept STI prophylaxis among adults with genital ulcer disease (GUD) in Uganda where syndromic STI management is the norm.
Methods: Cross-sectional study among 104 participants with clinician-confirmed GUD attending public health facilities and via community outreach in Kampala, Wakiso, and Kalangala Uganda. Structured interviews captured demographic and sociobehavioral factors, and STI prevention preferences prior to STI results. Point-of-care tests for HIV/syphilis antibodies (Bioline duo, Abbott, Chicago, IL) and nucleic acid tests for Neisseria gonorrhoeae (NG) and Chlamydia trachomatis (CT) (GeneXpert, Cepheid, Sunnyvale, CA) were performed. Logistic regression was used to examine factors associated with willingness to use STI prophylaxis; Firth-penalized models were fitted separately within the High and Low perceived risk strata.
Results: Syphilis prevalence was 11.5%, NG 8.7%, CT 8.7%, and HIV 38.5%. 80.8% expressed willingness to use STI prophylaxis if available. The most common reason (70.2%) to consider prophylaxis was to protect against STIs, followed by feeling of being at high risk for STIs (36.9%). The most common barriers were lack of perceived risk and fear of side effects (both 35.0%). Willingness to use STI prophylaxis was lower among those with laboratory-confirmed bacterial STI in adjusted models (aOR 0.31; 95% CI: 0.10–0.97; P = 0.041). Among participants with bacterial STI, 53.8 % (14/26) self-classified as Low-risk versus 46.2 % (12/26) as High-risk. Differences in acceptability of STI prophylaxis by risk stratum are described in Table footnote.
Conclusion: STI prophylaxis acceptability was high in Ugandan adults with GUD; however, poor risk awareness possibly reflects limited access to routine diagnostic testing. Integrating STI prophylaxis with etiological diagnosis and educational counseling within existing HIV/STI programs may improve uptake by addressing low perceived risk and safety concerns.
| Characteristic | Level | Overall n (%) | Willingness to accept STI prophylaxis Yes No | P-value | Crude OR (95% CI) | Adjusted OR (95% CI) | ||
|---|---|---|---|---|---|---|---|---|
| N | 104 | 84/104 (80.8%) | 20/104 (19.2%) | |||||
| Age (median [IQR]) | 29.0 [23.8, 37.0] | 28.5 [23.8, 36.0] | 30 [22.5, 39.8] | 0.418 | ||||
| Age group (%) | 18–24 | 32 (30.8%) | 26/32 (81.3%) | 6/32 (18.8%) | 0.030 | 1.23 (0.44–3.78) | 0.66 (0.18–2.37) | |
| 25-34 | 39 (37.5%) | 33/39 (84.6%) | 6/39 (15.4%) | |||||
| 35-44 | 25 (24.0%) | 22/25 (88.0%) | 3/25 (12.0%) | |||||
| 45+ | 8 (7.7%) | 3/8 (37.5%) | 5/8 (62.5%) | |||||
| Gender (%) | Male | 28 (26.9%) | 25/28 (89.3%) | 3/28 (10.7%) | 0.264 | |||
| Female | 76 (73.1%) | 59/76 (77.6%) | 17/76 (22.4%) | |||||
| HIV status by POCT | Positive | 40 (38.5%) | 28/40 (70.0%) | 12/40 (30.0%) | 0.051 | 0.33 (0.12–0.90) | 0.53 (0.15–1.82) | |
| Negative | 64 (61.5%) | 56/64 (87.5%) | 8/64 (12.5%) | |||||
| Education (%)A | <P7 | 50 (48.1%) | 37/50 (80.5%) | 13/50 (19.5%) | 0.151 | |||
| ≥P7 | 54 (51.9%) | 47/54 (81.8%) | 7/54 (18.2%) | |||||
| Employment (%) | Employed | 59 (56.7%) | 50/59 (84.7%) | 9/59 (15.3%) | 0.354 | |||
| Unemployed | 45 (43.3%) | 34/45 (75.6%) | 11/45 (24.4%) | |||||
| Heard of HIV PrEP (%) | Yes | 41 (39.4%) | 34/41 (82.9%) | 7/41 (17.1%) | 0.845 | |||
| No | 63 (60.6%) | 50/63 (79.4%) | 13/63 (20.6%) | |||||
| Heard of HIV PEP (%) | Yes | 28 (26.9%) | 23/28 (82.1%) | 5/28 (17.9%) | 1 | |||
| No | 76 (73.1%) | 61/76 (80.3%) | 15/76 (19.7%) | |||||
| STI risk perception (%)B | HighC | 42 (40.4%) | 35/42 (83.3%) | 7/42 (16.7%) | 0.296 | |||
| LowD | 62 (69.6%) | 49/62 (79.0%) | 13/62 (21.0%) | |||||
| Condom use | Yes | 19 (18.3%) | 13/19 (68.4%) | 6/19 (31.6%) | 0.235 | |||
| No | 85 (81.7%) | 71/85 (83.5%) | 14/85 (16.5%) | |||||
| Engaged in transactional sex | Yes | 30 (28.8%) | 20/30 (66.7%) | 10/30 (33.3%) | 0.040 | 0.31 (0.11–0.86) | 0.57 (0.17–1.97) | |
| No | 74 (71.2%) | 64/74 (86.5%) | 10/74 (13.5%) | |||||
| Neisseria gonorrhoeae | Positive | 9 (8.7%) | 4/9 (44.4%) | 5/9 (55.6%) | 0.012 | 0.24 (0.08–0.66) | 0.31 (0.10–0.97) | |
| Negative | 95 (91.3%) | 80/95 (84.2%) | 15/95 (15.8%) | |||||
| Syphilis POCT | Positive | 12 (11.5%) | 6/12 (50.0%) | 6/12 (50.0%) | 0.013 | |||
| Negative | 92 (88.5%) | 78/92 (84.8%) | 14/92 (15.2%) | |||||
| Chlamydia trachomatis | Positive | 9 (8.7%) | 1/9 (11.1%) | 8/9 (88.9%) | 1 | |||
| Negative | 95 (91.3%) | 76/95 (80.0%) | 19/95 (20.0%) | |||||
| Alcohol use in last 3 months | Yes | 43 (41.3%) | 30/43 (69.8%) | 13/43 (30.2%) | 0.033 | 0.30 (0.10–0.81) | 0.46 (0.11–1.69) | |
| No | 61 (58.7%) | 54/61 (88.5%) | 7/61 (11.5%) | |||||
PP02.03 – Barriers and Facilitators to Gonorrhea and Chlamydia Screening in Women Veterans: A Qualitative Study
Asst. Prof. Shimrit Keddem1, Omaris Caceres, Tammara Dixon
1University of Pennsylvania, Philadelphia, United States.
Background: Rates of sexually transmitted infection (STI), especially gonorrhea and chlamydia, have increased dramatically over the past decade, and women are more vulnerable to their negative effects. Several studies examining STI rates in active duty and Veteran women suggest that both rates of STI and risk factors are high, especially due to elevated prevalence of sexual trauma. Moreover, screening rates are low among women Veterans served by the US Veterans Health Administration (VHA).
Methods: We used qualitative interviews with women Veterans and clinicians across a national sample of six facilities to explore contextual factors impacting gonorrhea and chlamydia screening at the VHA. Interviews were conducted virtually, transcribed, and coded using qualitative data analysis software. Data collection and analysis was guided by the P3 Model, using key constructs of health behavior theory.
Results: We conducted 38 interviews with 8 clinicians and 30 women Veterans. We identified four overarching themes: screening is underutilized due to communication challenges, patients have positive attitudes but varying levels of comfort with testing, patient satisfaction with testing is high despite barriers, and provider burden is a barrier to screening reminders. Providers are uncomfortable discussing sexual health, which can lead to missed discussion opportunities. Patient comfort levels vary and are based on familiarity with their provider. Women Veterans report overall satisfaction with testing and highlight the importance of Veteran-specific services that address the unique needs of women Veterans.
Conclusions: These findings highlight the complex barriers and facilitators surrounding sexual health screenings for women Veterans. By addressing communication challenges, patient comfort, and provider burden, healthcare systems can improve the utilization of screenings and overall patient satisfaction. These findings can help inform strategies for enhancing provider-patient interactions, ensuring that services are more accessible, comfortable, and tailored to meet the unique needs of this population.
PP02.04 – Preliminary Insights Into Developing a Nursing Intervention Program for Successful Aging Among Older Adults Living with HIV: A Theoretical Framework and Systematic Review of Healthy Aging Models
Mr. Hatem Laroussi1, Dr Marie-Soleil Hardy1,2, Dr Clémence Dallaire1
1Laval University- School Of Nursing, Quebec, Canada.
2VITAM- Centre de recherche en santé Durable, Canada.
Background: Older adults living with HIV (PLWH) are considered “elderly” at age 50 due to premature physical aging caused by antiretroviral treatments. While these individuals may live longer, aging introduces various challenges, including complex healthcare needs, comorbidities, and social isolation. Addressing physiological and psychosocial issues is critical for successful aging among this population. Concurrently, healthy aging (HA) is a multidimensional concept defined by various theoretical models emphasizing person-environment interactions, adaptive processes, and health promotion.
Methods: This project aims to develop a nursing intervention program to promote successful aging among older PLWH. Roy’s Adaptation Model and Flood’s theory serve as the theoretical framework. The exploratory study follows Sidani and Braden’s methodological process in three phases: (1) literature review and semi-structured interviews; (2) defining intervention characteristics; and (3) theorizing the nursing intervention program. This abstract presents preliminary results from the first theoretical phase, including a systematic review of HA models analyzing 65 definitions published since 1960 across multiple dimensions and disciplines.
Preliminary Findings: The initial theoretical phase highlights the complexity of aging with HIV and HA as multidimensional phenomena requiring tailored interventions. For PLWH, understanding successful aging adapted to their realities will enhance nursing practices. The systematic review of HA models revealed various types, including health-state outcomes, life-course adaptations, and combined approaches. These findings provide insights into harmonizing terms and dimensions to guide subsequent research phases.
Potential Implications: The completed nursing intervention program is expected to empower PLWH to achieve better mental health outcomes and avoid aging-related complications. The comprehensive model classification from the theoretical phase supports the development of targeted interventions and will inform future empirical comparisons and policy development for diverse populations, including older PLWH.
PP02.05 – Navigating Digital Health Systems for Sexual Health: A Caes Study of Consensual Non-Monogamy
Ms. Caitlin Learmonth1
1Swinburne University of Technology, Melbourne, Australia.
Background: The diverse and increasingly privatised nature of digital clinical support systems in Australian healthcare settings has resulted in data siloes, inconsistencies in data capabilities, and lack of interoperability across health services (Bjørnstad & Ellingsen, 2019; Bossen etal., 2019).
For sexual health (and other primary health services) digital systems often rely on binary sexuality and gender categorisations (Carrotte etal., 2016). This impacts STI and HIV clinical targeting and continuity of care for patients falling outside of normative risk categorisations. In response, marginalised consumers may change or withhold information to mitigate potential stigma.
This paper draws on qualitative research presenting a case study of data frictions across digital health systems for consensually non-monogamous (CNM) sexual health consumers in Australia. It highlights strategies used by health consumers and healthcare providers to navigate digital system limitations.
Methods: Interviews were conducted with CNM adults about their experiences of accessing sexual healthcare (n = 17). Sense-checking interviews (n = 4) and workshops with healthcare professionals (n = 11) developed a multifaceted understanding of digital health systems and the impacts of everyday data practices on sexual health-seeking and service provision.
Results: CNM participants (including heterosexual women) often found it difficult to make their identities and practices legible to data collection systems. They detailed a range of strategic practices used to work around digital health system limitations. Healthcare stakeholders similarly identified strategies to overcome system limitations to provide patient-appropriate sexual health testing but expressed concern regarding lack of interoperability between health data systems.
Conclusion: The data frictions imposed by digital health systems have significant implications for sexual health continuity of care. Lack of interoperability between healthcare settings limit the extent to which healthcare professionals can provide patient-centred ongoing sexual healthcare. However, it is also acknowledged that intentional fragmentation of data by consumers and providers may be a protective strategy.
PP02.06 – Long-time Survivorship, and Regimen Perspectives, Adaptations, and Uptake of Long-acting Medications among Black Women Living with HIV Infection in New York State
Dr. Natalie Leblanc1, Dr. Keosha T. Bond2, Dr. Osman W. Shamrock1, Dr. Kandis Backus3
1University of Rochester School of Nursing, Rochester, United States.
2City University of New York, New York, United States.
3Gilead Health Sciences, New York, United States.
Background: U.S. Black women experience the greatest years of life lost due to HIV infection and inability to attain viral load suppression. Recent advancements in long-acting injectable (LAI) HIV therapies, such as Lenacapavir (LEN), present promising opportunities to shift treatment paradigms.
Methods: As part of a larger ethno-phenomenological study of Black women living with HIV (BWLWH) in New York State, this analysis explores perspectives and preferences for novel LAI HIV treatments, focusing on LEN. Beginning May 2024 to April 2025, serial qualitative interviews (up to three/participant) were conducted among 13 BWLWH.
Results: All women were living with HIV for 20+ years, currently in HIV care, over the age of 40, and reported being undetectable. Many reported childhood sexual assault esperiences; few had a substance use history, prior treatment resistance and had relocated from the Southern U.S. Analysis led to the emergence of three main themes: treatment initiation decisions; regimen changes and adaptations; and perspectives on and experiences with LAI. Treatment initiation did not always begin at diagnosis, partly due to regimen recommendations. Once engaged in care, substance use and difficulty accessing empathetic providers posed as barriers. Despite early challenges, all participants sought affirming HIV care. Many described “drug holidays”, due to travel, substance use, or to just “take a break.” Most participants used oral ART, while a few had transitioned to LAIs. No intertest in LAI was due to current treatment satisfaction, dislike for injections and potential side effects. Hesitant willingness involved wanting to observe others’ experiences before deciding on uptake.
Conclusion: Findings inform LAI implementation and expansion of LEN uptake among BWLWH. These results support the development of long-acting modalities and reinforce the importance of equitable access for sustained viral suppression. Attendees will gain actionable knowledge to address treatment needs and preferences of BWLWH in clinical and community practice.
PP02.07 – Prevalence of HIV/AIDS in Disaster-Ravaged Communities in Nigeria
Mr. Promise Ebubechukwu Nnaoma1, Mr Promise Ebubechukwu Nnaoma1
1University of Port Harcourt, Port Harcourt, Nigeria.
Background: There have been growing concerns that conflicts and disasters exacerbate the HIV epidemic yet there is little or no empirical evidence to ascertain the prevalence of HIV among people living in conflict-affected areas. Since persons living in conflict-affected areas may not have access to adequate medical supplies and facilities, then it is safe to believe that conflict can cause a rise in the number of HIV patients.
Method: This study was carried out between the 1 September and the 27 November, 2024 in 12 flood-ravaged States. A community cross-sectional study design was adopted. The population consisted of 230 men and women aged 20–49 years residing in internally displaced persons (IDP) camps in Rivers State. The instrument for data collection was a pretested questionnaire with a reliability coefficient of 0.87. A sample size of 230 was selected using a census since the population was manageable. Participants were provided informed consent, and the instrument covering demographics, sexual risk, reproductive health behaviour, and history of gender-based violence was administered. Participants also provided a blood specimen for HIV and other STD testing and were referred to HIV counselling and testing services established for this study to learn their HIV status.
Results: Results showed that HIV prevalence was significantly higher among men in the IDP population compared to women in the environment. Also, the result further revealed that STIs such as syphilis and gonorrhoea were prevalent in the flood-ravaged IDP camps, though they were more prevalent among women aged 20–28 years.
Conclusion: The study concluded that disaster, conflicts and other related vices have a significant influence on the prevalence of HIV and other STDs.
PP02.08 – The Art of Human Immunodeficiency Virus Wellness: Assessing the Impact of Therapeutic Art on Self-Management in Persons Living with Human Immunodeficiency Virus
Miss Rica Abbott1, Mr Michael DeWitt1, Mr Chad Downard2, Dr. Robert Rominger1, Miss Juhi Saxena1, Dr. Candice McNeil1
1Wake Forest University, School of Medicine, Winston Salem, United States.
2University of North Carolina, School of the Arts, Winston Salem, United States.
Background: Human Immunodeficiency Virus (HIV) is a chronic condition that affects millions of people worldwide. Previous research has suggested that creative therapies such as art can improve well-being in various patient populations. However, the impact of art therapy on the quality of life (QoL) of people living with HIV (PLWH) remains underexplored. The objective of this study is to study the impact of a therapeutic art program on the QoL of PLWH.
Methods: A single-arm observational study was conducted among PLWH. The art therapy program was implemented over a 6-week period consisting of painting and talk therapy. The QoL assessment was completed by participants at baseline, Week 3, and Week 6. Descriptive data analysis was performed to assess QoL scores at these specific time points. Correlation analysis was performed using the initial survey responses to assess relationships between psychometric measures. Qualitative analysis was performed to assess common themes during talk therapy.
Results: 17 participants completed the baseline survey with 4 completing all of the follow-up surveys. Participants who completed all follow-up surveys were majority non-Hispanic (n = 3), had at least some college education (n = 3), and evenly divided between Black and White. Ultimately, 75% improved in their baseline Spirituality/Religion/Personal belief theme following the WHO Quality of Life instrument. No change or declines were observed among the majority of the other themes for the Quality of Life, Rosenberg Self-esteem scale, Spielberger state-trait anxiety inventory, and the Healthy Days Inventory (Fig. 1).
Conclusion: This study indicates that the effects of Art therapy could result in multidimensional effects across health and wellbeing inventories. Further research with a larger sample size and longer follow-up is needed to assess the sustainability of these improvements. Ultimately, these findings can inform healthcare practice, supporting the use of complementary therapies to improve patient outcomes among PLWH.
Abbreviations: STAI, State-Trait Anxiety Inventory.
(a) Correlation plot of the different psychometric measures at baseline (N = 17). Positively associated values are shown in blue while negatively associated values are shown in red. (b) Art paintings performed by participants enrolled in the art therapy program. Participant artwork includes sumi ink on paper.
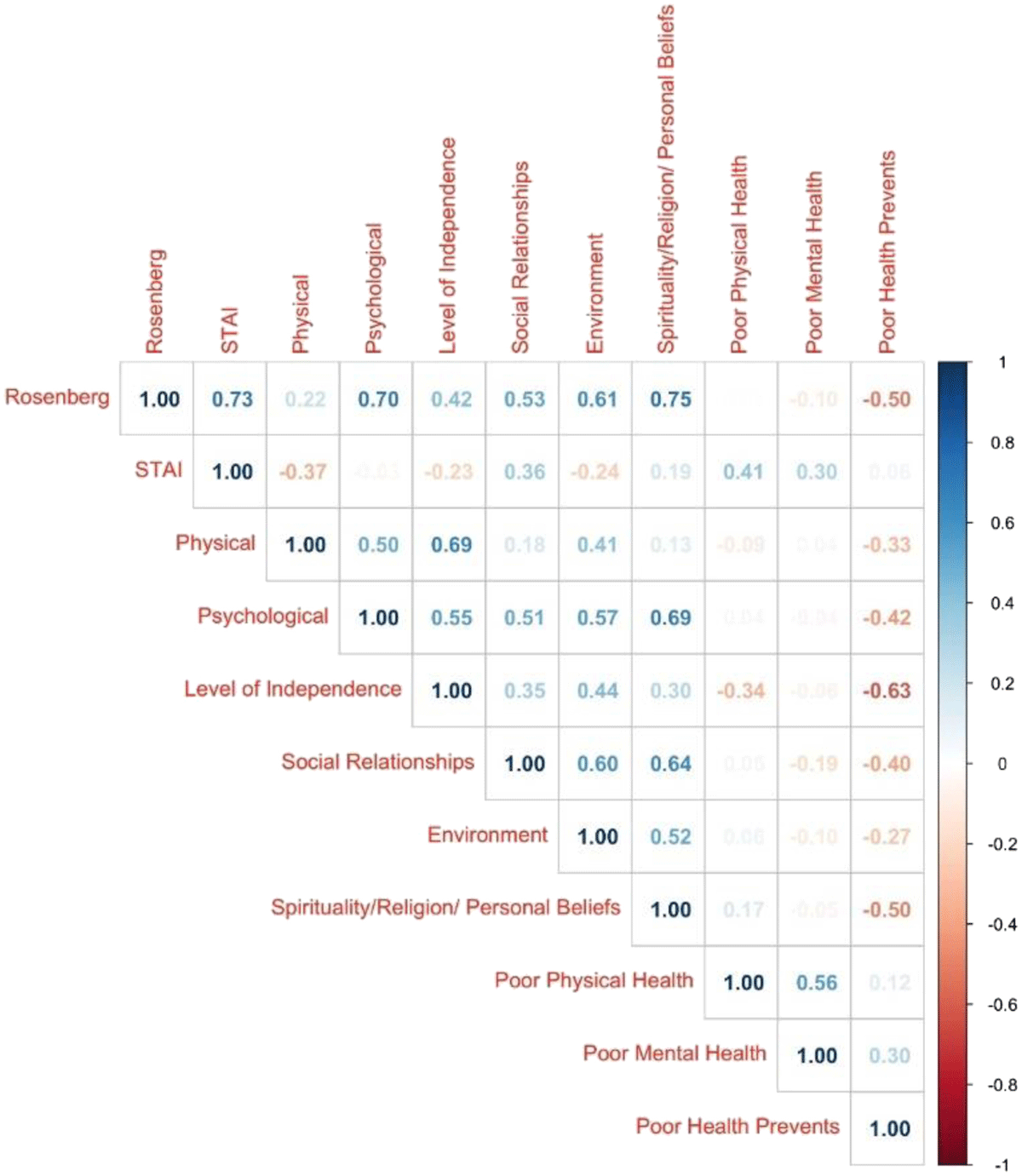

PP02.09 – Intersectional Stigma Among Migrant Women from Sub-Saharan African Communities Living with HIV in Australia
Mr. Collins Adu1, Scientia Professor Carla Treloar1, Professor Loren Brener1, Dr. Timothy Broady1
1Centre For Social Research in Health, The University of New South Wales Sydney, Sydney, Australia.
Background: Stigma poses significant challenges for people from culturally and linguistically diverse (CALD) communities, particularly migrant women living with HIV. These migrant women experience intersecting stigmas shaped by race, gender, HIV status, and immigration status which hinder access to essential healthcare services. Despite the profound impact of these intersecting stigmas, limited research has been conducted on the lived experiences of migrant women from high prevalence countries living with HIV. This study explored the intersectional nature of HIV-related stigma among migrant women from sub-Saharan Africa (SSA) living with HIV in Australia.
Methods: The study utilised semi-structured interviews conducted in-person or via Zoom with ten migrant women from SSA living with HIV with at least 6 months of stay in Australia. The audio recordings were transcribed, coded into NVivo 12, and analysed thematically.
Results: Findings indicated that stigma was experienced at the intersections of race, gender, HIV status, and immigration status. Three themes emerged:
The first theme, ‘race and migrant identity’ reflected participants’ feelings of “otherness” and racial prejudice associated with being SSA migrants and living in Australia. The second theme, ‘gendered experiences’ explored how participants felt judged for their HIV status, which was perceived as a failure to adhere to traditional social roles. The third theme, ‘immigration and policy impacts’ captured how visa-related uncertainties exacerbate mental health struggles and feelings of instability.
Conclusion: The study underscores how intersecting identities such as race, migrant status, gender, and HIV status shape the unique challenges experienced by migrant women from SSA living with HIV in Australia. The study’s insights into intersectional stigma among migrant women from SSA living with HIV in Australia offer valuable implications for other high-income countries. These findings emphasize the need for tailored policies and culturally appropriate interventions that address stigma faced by this vulnerable population within diverse socio-political contexts.
PP02.10 – Types and Experiences of Stigma and Discrimination Among People Living with HIV in Nigeria: A Cross-Sectional Study
Dr. Rose Aguolu1, ThankGod Zachariah Kums1
1National Agency for the Control of AIDS, Abuja, Nigeria.
Background: HIV-related stigma and discrimination remain significant barriers to effective HIV prevention, treatment, and care in Nigeria, despite advances in antiretroviral therapy and public health interventions. This study examined the types and experiences of stigma and discrimination faced by PLHIV in Nigeria.
Methods: We conducted a cross-sectional study that assessed the extent, types, and experiences of stigma and discrimination among PLHIV in Nigeria. Using the standardized Stigma Index Survey 2.0 tool, data were collected from 1,240 PLHIV across sixteen states and the Federal Capital Territory between May and June 2021. The study population comprised both general and key population groups. Both descriptive and inferential statistics were conducted on the data.
Results: Of the participants surveyed, 75.9% were from the general population; 13.0% female sex workers (FSW); 6.5% men who have sex with men (MSM); and 4.6% people who use drugs (PWUD). The majority of participants were female, with 33.2% aged 35–44 years. 24.5% of adults aged 35–44 years and 21.7% of those aged 18–24 years reported experiencing stigma and discrimination within the last 12 months. KPs, particularly PWUD and MSM (26% and 31% respectively), reported higher rates of stigma and discrimination compared to other groups. The most common types of discrimination were verbal abuse, discriminatory remarks, and gossip. Physical harassment was reported by 5.4% of respondents, while less than 5% experienced employment refusal or exclusion from social and religious gatherings within the last year.
Conclusion: These findings underscore the persistent stigma and discrimination faced by PLHIV in Nigeria, particularly among key populations. Despite the existence of the anti-stigma law, there remains a critical need to evaluate its implementation across all states and enhance public awareness to combat HIV-related stigma and discrimination. This suggests a gap between policy and practice that requires attention to protect the well-being of PLHIV in Nigeria.
PP02.11 – Examining the Discrepancy: MSM In Ghana and Their Heterosexual Identities – a Cross-Sectional Study at an STI Clinic in Kumasi, Ghana
Dr. Thomas Agyarko Poku1, Prof Yaw Adu-Sarkodie2,3, Dr Albert Adusei Duah2,3
1Ghana Health Service, Kumasi, Ghana.
2Kwame Nkrumah University of Science & Technology, Kumasi, Ghana.
3APT Foundation for Sexual Health, Kumasi, Ghana.
Background: The sexual identities and behaviours of men who have sex with men (MSM) in Ghana remain complex. They are not widely understood, partly due to the prevailing social stigma around same-sex relationships. Understanding the interaction between heterosexual and homosexual behaviours is essential for addressing sexual health risks in MSM. This study aimed to explore the sexual behaviours and partner relationships of MSM attending an STI clinic in Kumasi, Ghana.
Methods: This cross-sectional study involved 157 self-identified MSM who attended the STI clinic at Suntreso Government Hospital in Kumasi, Ghana, between January and June 2024. Participants provided data on their sexual behaviours over the past 24 months. Data were statistically analysed to examine relationships between sexual identity and partner choice.
Results: Of the participants, 81.4% (128/157) reported having had sexual relations with a woman, and 72.2% (113/157) had engaged in sexual activity with both male and female partners within the past 24 months. A smaller proportion, 27.7% (44/157), reported engaging exclusively in sexual relations with men. The study found statistically significant associations between sexual identity and partner selection (P < 0.05).
Conclusions: The findings illustrate the fluidity of sexual behaviours among MSM in Kumasi, emphasising the need for comprehensive sexual health interventions that cater to this diverse population. Sexual health programs must target both MSM and their heterosexual partners to reduce the risk of STI transmission, addressing the unique dynamics within this population.
PP02.12 – Knowledge and Attitudes Regarding HIV Pre- and Post-Exposure Prophylaxis (PrEP and PEP) of Healthcare Workers: A Cross-Sectional Study
Dr. Lissa Alexandra Balinas1, Dr. Juanita Carmela Co Buenviaje1, Dr. Lian C Jamisola1, Dr. Gilbert C. Yang1, Dr. Camille B Angeles1
1UERM Medical Center, Quezon city, Philippines.
Background: Human immunodeficiency virus (HIV) infection remains a significant global public health issue. Among the strategies recommended to combat this disease are pre-exposure prophylaxis (PrEP) and post-exposure prophylaxis (PEP). However, limited data exists on healthcare providers’ perspectives on PrEP and PEP prescribing, particularly in the local setting. Hence, the objective of this study is to determine the knowledge and attitudes regarding HIV pre- and post-exposure prophylaxis among healthcare workers of a tertiary hospital in Metro Manila, Philippines.
Methods: This study is a descriptive cross-sectional study involving healthcare workers, chosen through proportionate stratified random sampling. A self-administered questionnaire with 5 main segments (demographics, knowledge on PrEP and PEP, attitudes towards PrEP and PEP) was adapted from validated survey forms used in previous similar studies.
Results: A total of 132 respondents completed the questionnaire, with 68.9% being female. Among respondents, 77.3% were aware of HIV PrEP, while only 65.9% had heard of PEP. Healthcare professionals were the primary source of information for both PrEP (68.9%) and PEP (48.5%). Overall, only 26.5% of participants exhibited good knowledge about PrEP, and 22.7% for PEP. Just over half of the respondents displayed a positive attitude toward PrEP (53.2%) and PEP (59.2%).
Conclusion: The results of the study highlight the need for comprehensive educational programs aimed at enhancing healthcare workers’ knowledge and attitudes toward HIV prevention. Understanding the perspectives of healthcare providers is pivotal in developing targeted interventions and ensuring the success of PrEP and PEP implementation.
Keywords: HIV, pre-exposure prophylaxis, post-exposure prophylaxis.
PP02.13 – Factors Contributing to Missed Art Appointments and Re-Engagement of HIV Clients at Hetauda Hospital, Makwanpur, Nepal
Mr. Amrit Lamichhane1, Mr. Amrit Bikram Rai1, Dr. Adele Benzaken
1Aids Healthcare Foundation, Bharatpur, Nepal.
Background: Adherence to antiretroviral therapy (ART) is crucial for managing HIV, reducing viral load, and preventing disease progression. However, many people living with HIV (PLHIV) miss ART appointments, jeopardizing their health and increasing the risk of HIV transmission. Understanding the reasons behind missed visits is essential for developing targeted interventions.
Methods: This study involved in-depth counseling sessions with HIV-positive clients who missed their ART appointments at Hetauda Hospital from June to September 2024. Direct counseling was offered to clients who visited the hospital, while home visits were arranged for those unable to attend, with their consent. For clients who declined home visits, attempts were made to reach them via phone to discuss their reasons for missed appointments. This multifaceted approach aimed to identify the factors contributing to missed visits and assess the effectiveness of counseling in re-engaging clients in care.
Results: After counseling, 4 of the 10 clients were successfully re-engaged and have been attending their ART appointments regularly. The remaining six clients cited various reasons for missing appointments: one believed exercise and meditation could suppress HIV without ART; another experienced emotional distress from a divorce; a third struggled with drug addiction; a female client engaged in high-risk sexual behavior could not be located; one avoided treatment due to fear of stigma; and one client was unreachable despite multiple attempts.
Conclusion: Missed ART appointments stem from a complex mix of social, emotional, and personal factors. Tailored interventions, including mental health support, substance abuse treatment, and stigma reduction strategies, are vital for improving ART adherence. While effective counseling can help re-engage clients, addressing underlying barriers is critical for long-term success.
PP02.14 – The Impact of Sources of Stigma and Stigma Sensitivity on Healthcare Avoidance Among Gay and Bisexual Men in Australia
Prof. Loren Brener1, Dr Tim Broady1, Dr Elena Cama1, Prof Carla Treloar1
1University of New South Wales, Kensington, Australia.
Background: Research suggests that gay and bisexual men (GBM) may experience stigma by association, because they are perceived to be at risk of HIV, and are thus less likely to engage in HIV testing. Interventions to reduce l negative attitudes towards GBM, including those with HIV and STIs, may be effective in improving healthcare access. This study aimed to assess the association between sources of stigma and healthcare avoidance amongst a sample of GBM, and to establish whether healthcare avoidance is more likely to occur among those who report heightened sensitivity to stigma around their sexuality.
Methods: The sample consisted of 1116 GBM in Australia recruited via targeted social media advertising, who completed the online survey.
Results: 20% of participants reported health service avoidance due to sexuality-related stigma. Those reporting any experience of stigma were likely to avoid healthcare services and avoiding different types of healthcare was related to the source of the stigma. For example, participants who had avoided sexual health services were more likely to report any stigma from sexual health services. Younger participants were also found to be more likely to avoid GPs and sexual health services due to anticipated stigma. Greater sensitivity to perceived stigma was associated with avoidance of all healthcare services.
Conclusion: The findings suggest that stigma sensitivity is linked to avoidance of healthcare services. GBM may come to health services with complex and recurrent experiences of stigma. Understanding this context for GBM will increase the ability of services to work sensitively with GBM clients and increase healthcare access. It is important to target services to ensure access for young GBM. Addressing stigma within healthcare services is critical to promote access to all healthcare services and increase HIV testing and healthcare for GBM so as to achieve the UNAIDS targets towards HIV elimination.
PP02.15 – High Interest in Long-Acting Injectable Antiretroviral Therapy Among Gay and Bisexual Venezuelan Migrant Men Living with HIV in Colombia: Qualitative Insights
Dr. Julien Brisson1, Dr. Mariangela Castro-Arteaga1, Dr. Amaya Perez-Brumer1
1Dalla Lana School of Public Health, University of Toronto, Toronto, Canada.
Background: Colombia hosts the largest population of Venezuelan migrants globally. For these migrants living with HIV, access to antiretroviral treatment (ART) is severely constrained. Despite the urgency of this issue, limited research has explored the interest in and potential advantages of long-acting injectable antiretroviral therapy (LAI-ART) among gay and bisexual Venezuelan migrant men in Latin America.
Methods: Between October and December 2024, we conducted 28 virtual individual semi-structured interviews with gay and bisexual Venezuelan migrant men living with HIV across Colombia. Purposive recruitment was facilitated through Mas Que Tres Letras, a community-based organization supporting gay and bisexual men living with HIV. Interview guide probed on: ART access and interest in LAI-ART based on participant healthcare needs. A thematic analysis was conducted.
Results: Participants ranged in age from 23 to 60 years (mean: 35). Eleven were diagnosed with HIV in Venezuela, while 17 were diagnosed in Colombia. Most participants experienced substantial delays and interruptions in ART access and care. Barriers included gaps in health insurance coverage associated with migration status, financial constraints, and occasional adherence challenges like forgetfulness. Most participants were unfamiliar with LAI-ART but expressed strong interest in it if it were available and cost-accessible. Participants perceived LAI-ART as a potential solution to improve treatment access and adherence by reducing the need for daily medication. However, the inconsistent availability of physician oversight for LAI-ART, driven by healthcare access instability and interruptions in insurance coverage associated with migrant status, raises concerns about drug resistance stemming from treatment disruptions or inconsistent supervision.
Conclusions: While LAI-ART is unavailable in Colombia, integrating LAI-ART could enhance migrant treatment access and ensure sustained and equitable HIV care, provided it is economically accessible. Migrants whose healthcare access is interrupted and insurance coverage is limited face significant barriers to sustained ART care, making LAI-ART a critical option.
PP02.16 – Mobilizing Indigenous Community-Led STBBI Research to Increase Impact and Advance New Knowledge
Miss Angie Carriere1, Connor Reid1
1CAAN Communities Alliances And Networks, Fort Qu’appelle, Canada.
Background: CAAN Communities, Alliances, and Networks (CAAN) has successfully led 53 community-based research projects focused on sexually transmitted and blood-borne infections (STBBIs), significantly enhancing the landscape of Indigenous health research. This initiative aims to mobilize STBBI research findings to develop and implement effective Indigenous knowledge translation (KT) strategies that not only disseminate research findings but also resonate with Indigenous communities. By incorporating the lived experiences and narratives of these communities into broader discussions, the initiative seeks to promote healing and advance reconciliation efforts.
Methods: CAAN is currently undertaking a comprehensive review of its prior projects to identify successful knowledge translation strategies and the challenges encountered in their execution. By analyzing various Indigenous KT methodologies across diverse cultural contexts, the initiative aims to deepen its understanding and enhance the practical application of these critical approaches. Valuable insights have been extracted and synthesized from previous research endeavours to illuminate health experiences related to HIV and STBBIs. Emphasizing the interconnectedness of mental, physical, and spiritual health, CAAN advocates for a holistic approach to well-being that empowers Indigenous Peoples in their pursuit of health and healing. An Indigenous-grounded data analysis process has been adopted that respects the contextual integrity of the narratives, ideas, and dialogues captured in CAAN’s past research. The resulting findings will be disseminated in community-centric formats and peer-reviewed academic journals, reflecting CAAN’s commitment to integrating both Indigenous and Western epistemologies.
Preliminary Results: Recent investigations have highlighted the critical role of social determinants of health and underscored the necessity for improved dissemination of research findings. CAAN’s mobilizing STBBI project emphasizes the integration of Indigenous methodologies by engaging community members, Elders, and individuals with lived experiences throughout the research process. This participatory approach ensures that the research remains culturally relevant and authentically reflects the perspectives and needs of Indigenous populations.
PP02.17 – Awareness and Perspectives of Sexually Transmitted Infections and Vaccine Willingness Among Young Adults in Australia
Dr. Sandra Chaves1, Ms Valerie Bosch Castell1, Ms Sophie Wagué1, Ziqi Tian2, Alison Eglentals2, Andrew Ward2, Shane Compton2
1Sanofi Vaccines, Lyon, France.
2Social Research Centre, Melbourne, Australia.
Background: Sexually transmitted infections (STIs) are the most frequently reported conditions to Australia’s National Notifiable Diseases Surveillance System, with chlamydia being particularly prevalent among young people aged 15–25 years. This study assesses the knowledge, attitudes, and practices related to sexual behaviour and STI prevention, including vaccine willingness, to enhance public health education and guide future STI vaccine trials.
Methods: In August 2024, an online survey was conducted with Australian youth aged 18–29 years using the Social Research Centre’s probability-based panel, Life in Australia™, complemented by the i-Link non-probability panel. Data from both samples were statistically blended and weighted to ensure they represent sexually active Australians aged 18–29 years.
Results: A total of 1,002 surveys were completed and included in this weighted analysis. Awareness of STIs was high (93.3%), particularly for chlamydia (88.4%), though with misconceptions about transmission. Overall, 46.1% had undergone STI testing and 27.9% considered themselves at risk of STIs. Among those tested, chlamydia was the most frequently reported infection at 14.7%. HIV was the greatest concern for those perceiving themselves at risk of STIs (43.0%), followed by concerns about genital herpes (15.8%). Notably, 84.1% expressed willingness to receive a multi-STI vaccine, and 79.7% were willing to take a chlamydia-only vaccine. One quarter (26.9%) of respondents mentioned prevention of new infections and reduction in transmission (25.8%) as the main reasons to be vaccinated against chlamydia.
Conclusion: While young Australians generally demonstrate high awareness of STIs, specific knowledge gaps about infections like chlamydia exist. Despite moderate testing rates, the relatively low risk perception suggests the need for better public health communication and knowledge-raising campaigns. The strong willingness to vaccinate against multiple STIs and specifically for chlamydia, shows promising potential for future vaccine development and research.
PP02.18 – Awareness, Usage, Beliefs and Concerns of Doxycycline Prophylaxis for STI Prevention Among Gay and Bisexual Men, Transgender and Non-Binary People in Australia
Prof. Eric Chow1,2,3, Ei Aung1,2, Ms Kate Maddaford1,2, Professor Kai Jonas4, Professor Christopher Fairley1,2, Dr Sarah Martin5,6, Dr Carole Khaw7,8, Dr Rick Varma9,10, Dr Caroline Thng11,12, Dr Manoji Gunathilake10,13, Associate Professor Vincent Cornelisse2,10,14, Dr Teralynn Ludwick3, Mr Ethan Cardwell3, Dr Michael Traeger15,16, Professor Catriona Bradshaw1,2,3, Mr Dash Heath-Paynter17, Associate Professor Daniel Grace18, Associate Professor Fabian Kong3, on behalf of the DoxyAWARE Study Group
1Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
4Department of Work and Social Psychology, Maastricht University, Maastricht, The Netherlands.
5Canberra Sexual Health Centre, Canberra Health Services, Canberra, Australia.
6School of Medicine and Psychology, Australian National University, Canberra, Australia.
7Adelaide Sexual Health Centre, Infectious Diseases Unit, Royal Adelaide Hospital, Adelaide, Australia.
8School of Medicine, Faculty of Health Sciences, The University of Adelaide, Adelaide, Australia.
9Sydney Sexual Health Centre, South Eastern Sydney Local Health District, Sydney, Australia.
10The Kirby Institute, UNSW Sydney, Sydney, Australia.
11Gold Coast Sexual Health, Gold Coast Hospital and Health Service, Southport, Australia.
12Institute for Biomedicine and Glycomics, Griffith University, Gold Coast, Australia.
13Sexual Health and Blood Borne Virus Unit, Centre for Disease Control, Northern Territory Department of Health, Darwin, Australia.
14HIV and Sexual Health Services, Mid North Coast & Northern NSW Local Health Districts, Australia.
15Burnet Institute, Melbourne, Australia.
16School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia.
17Health Equity Matters, Sydney, Australia.
18Dalla Lana School of Public Health, The University of Toronto, Toronto, Canada.
Background: The Australian Consensus Statement on doxycycline prophylaxis (doxyPEP) for STI prevention was published in September 2023. This study aimed to examine the awareness, usage, and concerns of doxyPEP in Australia.
Methods: A cross-sectional national survey was conducted between July and November 2024. Participants were recruited from sexual health clinics, general practice, social media and dating apps. Eligible participants were ≥18 years, living in Australia and self-identified as a man, transgender or non-binary person who had sex with men.
Results: We included 2095 participants who completed the survey. Half (51.6%, 1080/2095) had heard of doxyPEP. Of those, 29.9% (323/1080) had ever used doxyPEP, and 28.5% (306/1080) used it in the past 12 months (recent users). DoxyPEP awareness and usage varied by HIV status and PrEP use (Fig. 1, P < 0.0001). Most users took the recommended 200 mg within 72 h after sex (63.6%, 206/322); however, 14.4% (46/322) took 100 mg daily, and 21.7%(70/322) followed other regimens. Among recent doxyPEP users, 33.6% (94/280) reported recent syphilis or ≥2 chlamydia/gonorrhoea diagnosis. Of the 323 ever doxyPEP users, 41.8% obtained prescriptions from doctors in Australia, 5.3% obtained it online without prescriptions, and 8.7% obtained it overseas (in-person) without prescriptions. Of the 1080 participants who had heard of doxyPEP, 45.6% (490/1080) planned to use DoxyPEP in the next 12 months, primarily to prevent chlamydia (93.9%, 460/490), gonorrhoea (86.1%, 422/490) or syphilis (78.8%, 386/490). Some intended to prevent Mycoplasma genitalium (18.8%, 92/490) or mpox (7.4%, 36/490). Of those who had never used doxyPEP, 40.5% (306/756) worried about antibiotic resistance.
Conclusion: Only half the participants in this survey were aware of doxyPEP and one-fifth of those used a regimen not currently recommended. Some used it to prevent certain infections with no evidence supporting its effectiveness. More educational resources are needed to ensure individuals use doxyPEP accurately and effectively.
Doxycycline prophylaxis (a) awareness among all 2095 participants; and (b) current and future use among 1080 participants who were aware of doxycycline prophylaxis, by HIV status and PrEP use.
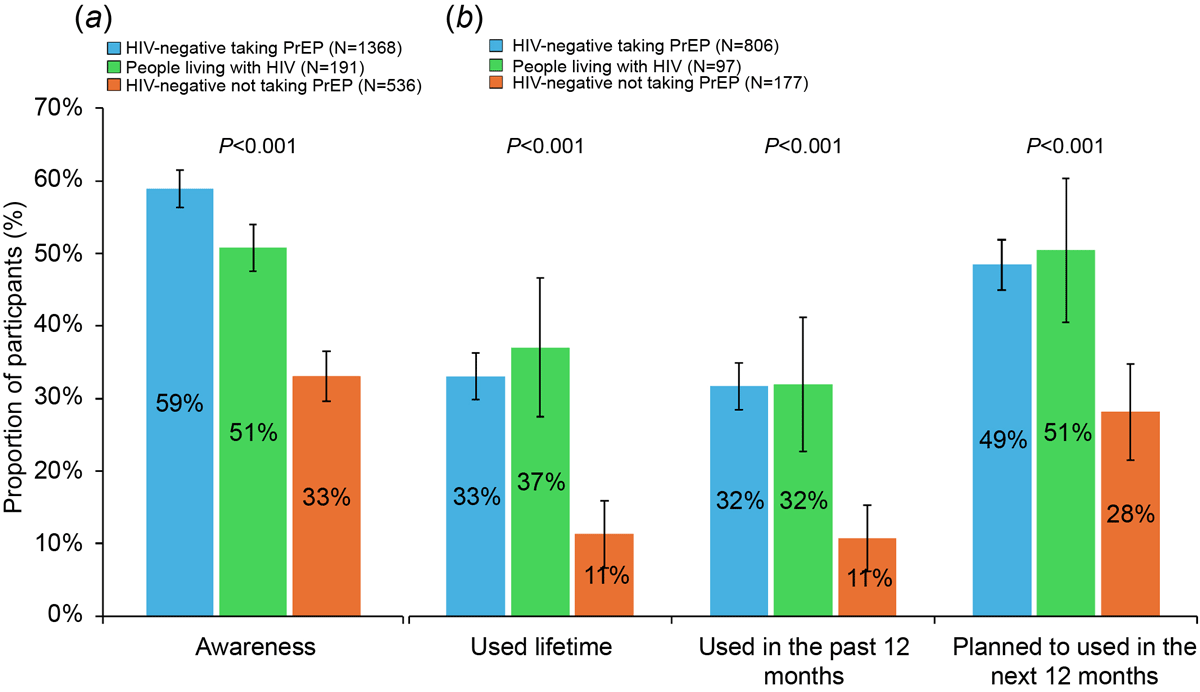
PP02.19 – Facilitators and Barriers to Syphilis Vaccine Trial Participation: A Qualitative Analysis of Perceptions from Malawi to Inform Trial Design
Dr. Suzanne Day1, Annie Thom2, Twambilile Phanga2, Arlene Seña1, Justin Radolf3, Joseph Tucker1,4, Irving Hoffman1,2, Mitch Matoga2, Agatha Bula2
1Department of Medicine, Division of Infectious Diseases, University of North Carolina at Chapel Hill, Chapel Hill, United States.
2UNC Project Malawi, Lilongwe, Malawi.
3Department of Medicine, UConn Health, Farmington, United States.
4Clinical Research Department, Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: Understanding perspectives of priority groups likely to be recruited in early-phase syphilis vaccine trials can help address socio-cultural, organizational, and ethical issues in trial design. We explored facilitators and barriers to future syphilis vaccine trial participation among individuals diagnosed with a sexually transmitted infection (STI) in Malawi.
Methods: In-depth interviews were conducted with individuals >18 years old recruited from an STI clinic in Malawi from Dec 2022 to July 2023. Eligibility criteria included any syndromic STI diagnosis at recruitment. The semi-structured interview guide examined views on syphilis vaccines, trial participation, and community involvement in vaccine research. A post-interview survey collected demographic data. Interviews were audio recorded, translated from Chichewa to English and transcribed verbatim, then coded using NVivo by three independent coders and thematically analyzed using a social-ecological framework.
Results: Thirty individuals were interviewed; 15 (50%) were women, 24 (80%) were aged 18–34, and 3 (10%) were living with HIV. Most (27, 90%) indicated immediate interest in syphilis vaccine trial participation; two were unsure, and one declined. Key facilitators included contributing to scientific advancement to help Malawians, and personal benefits (medical care, knowledge, compensation). Important trial design considerations also emerged as facilitators, including community outreach to foster buy-in, counseling participants, and building trust through transparency in trial processes. A common barrier was concern about vaccine side effects; however, additional barriers involved precarity in participants’ lives, with scheduling, insufficient compensation, and transportation potentially hindering daily subsistence. Syphilis-related stigma and mistrust in researchers were also concerns. Community involvement in research was highlighted as essential to fostering trust and vaccine acceptance.
Conclusions: While persons with STIs are interested in syphilis vaccine trial participation, several important barriers exist. Meaningful community engagement is needed to design trials that leverage facilitators while addressing community concerns, as are administrative structures to support participation in resource-constrained settings.
PP02.20 – U.S. Adolescents’ Views on Participating in HIV Clinical Research During Pregnancy
Ms. Hadas Baron1, Dr. Rita Masese1, Dr. Anne Lyerly1, Dr. Suzanne Day2
1University of North Carolina At Chapel Hill, Department of Social Medicine, Center For Bioethics, Chapel Hill, United States.
2University of North Carolina at Chapel Hill, Department of Medicine, Division of Infectious Diseases, Chapel Hill, United States.
Background: Pregnant adolescents are often excluded from participating in clinical HIV research, resulting in less evidence to inform safe and effective treatment/prevention strategies for this population. To inform inclusion strategies that center adolescents’ concerns and priorities regarding research participation, we explored adolescents’ perspectives on enrollment in HIV prevention/treatment studies during pregnancy.
Methods: We conducted in-depth interviews with ever-pregnant adolescents living with HIV (age 15–24 years) and at-risk of HIV (age 15–20 years) recruited from clinical settings across the U.S. The interview guide explored decision-making around enrollment during pregnancy using two vignettes depicting hypothetical HIV studies: (1) testing the pregnancy specific dosage of a medication to prevent/treat HIV, and (2) a randomized control trial comparing an existing daily pill vs a new injectable. Interviews were transcribed verbatim, coded using NVivo qualitative analysis software, and analyzed for emergent themes in adolescents’ reasons for being willing or unwilling to join the vignette studies.
Results: Forty adolescent interviews were conducted (20 living with HIV, 20 at-risk). Participants’ mean age was 20 years old. The majority reported willingness to join vignette 1 (32, 80%) while interest in vignette 2 was mixed, with a majority declining participation (23, 57.5%). Adolescents’ motivations for wanting to participate included a desire to promote their health and the health of their baby, to benefit others in the future, and to gain health-related knowledge. Among those who shared concerns about study participation, reasons were centered on the uncertainty of randomization processes and concerns about unknown side effects.
Conclusion: Adolescents’ willingness to participate in at least one study vignette and their ability to assess studies’ risks and benefits suggests a disjunct between current practices of routine exclusion of pregnant adolescents from research and their interests/capacities. These findings can inform guidance to promote ethical inclusion of this population in HIV research.
PP02.21 – Call the Shots: A Vignette Study Investigating the Influence of Partner Characteristics on Condom Use Decision-Making in Casual Partners
Ms. Alcira de Vries1, Dr Janneke Heijne2,3, Prof. Dr. John de Wit4, Dr. Chantal den Daas5
1National Institute For Public Health And The Environment (RIVM), Bilthoven, The Netherlands.
2Public Health Service of Amsterdam, Amsterdam, The Netherlands.
3Amsterdam institute for Immunology & Infectious Diseases (AII) and Amsterdam Public Health research institute (APH), Amsterdam UMC, Amsterdam, The Netherlands.
4Utrecht University, Utrecht, The Netherlands.
5University of Aberdeen, Aberdeen, United Kingdom.
Background: Increasing condom use among youth is crucial to improve sexual health. Since condom use involves interactions between two partners, condom use decision-making may be influenced by either or both individuals. As studies on partner influences on condom use in casual relationships are lacking, we aimed to gain more insights into condom use decision-making during vaginal sex in casual relationships.
Methods: Dutch youth aged 16–24 were recruited online in 2023. Using vignettes, we examined the partner’s influence in condom use decision-making during casual vaginal sex. Participants indicated the likeliness of using a condom for one of six randomly assigned partner vignettes: attitudes (positive/negative), norms (condom use norm/condom nonuse norm) or risk behavior (higher risk: multiple short-term partners/lower risk: one long-term partner). We performed three ANOVA analyses; the dependent variable was the participant’s condom use decision, the three manipulated constructs were categorical between-participant independent variables. We also explored interactions between the conditions and individual factors, i.e. demographic, psychosocial and sexual behavior.
Results: We included 1070 participants. Youth indicated being more likely to use a condom if the partner had positive attitudes towards condom use F(1, 347) = 69.01, P < 0.01, indicated condom use as the norm F(1, 367) = 4.04, P < 0.05, or engaged in more risk behavior F(1, 350) = 7.34, P = 0.01 (Fig. 1). Different sexual behavior- and psychosocial factors moderated these effects, e.g. all condition effects were stronger in persons with more lifetime sexual partners or negative attitudes towards condom use.
Conclusion: Our findings suggest that individuals likely go along with their partner’s attitudes or norms, and may be more inclined to use a condom based on higher risk behavior of the partner. When improving sexual health, considering the influence of a partner and promoting positive attitudes towards condom use, specifically, but also promoting condom use as the norm may positively impact condom use.
PP02.22 – How Many Adolescents Received Sexually Transmitted Infection Testing or Diagnosis in School Based Health Centers? A Descriptive Analysis in King County, Washington
Dr. Claudia Douglas1,2, Dr. Matthew P. Kronman3, Sara Rigel4, Dr. Julia C. Dombrowski1
1University of Washington, Seattle, United States.
2Seattle Children’s Research Institute, Seattle, United States.
3Division of Infectious Diseases, Seattle Children’s Hospital, Seattle, United States.
4Public Health Seattle & King County, Seattle, United States.
Background: School based health centers (SBHC) represent a potential opportunity for adolescents to receive confidential and convenient STI related care. Our objective for this study was to evaluate STI testing among high school students who utilize school-based health center services in King County, Washington.
Methods: We analyzed SBHC health records from 31 high schools in King County, WA from 2017 to 2021 to identify encounters where a chlamydia (CT), gonorrhea (GC), syphilis, or HIV test or diagnosis was documented by a medical provider, defined by use of the relevant ICD-10 codes for the visit.
Results: Of 63,135 SBHC medical encounters, 6,425 (10.2%) were associated with one or more STI-specific ICD codes over the 5-year study period (Table 1). Of these encounters, 88.8% were associated with STI or HIV “screening”; the remaining 11.2% of STI encounters were associated with a STI diagnosis. Among students who had STI or HIV screening, 73.1% and 65.8% respectively were 15–17-years-old, 4.8% and 8.9% respectively were 11–14-years-old, and 21.5% and 25.3% respectively were 18–21-years-old. For students with a STI “diagnosis”, most were for CT (92.5%), followed by GC (6.0%), and syphilis (1.5%). Female students accounted for 78.9% of STI screenings, and 79.8% and 60.6% of CT and GC diagnosis, respectively. Students who had STI screening were most commonly White (33.6%), multi-racial (30.5%), and Black (21.2%). Students who had a CT or GC diagnosis were most commonly Black (35.2% and 42.4% respectively) or multi-racial (29.7% and 27.3% respectively). Among students with more than one STI encounter, 15.1% had more than 10 encounters and 6.2% had more than 20 STI encounters over the study period.
Conclusion: Our study highlights Black, multi-racial, 15–17-year-olds, and female students are over-represented among STI care in SBHC encounters. SBHCs have potential to reach disproportionately impacted adolescents and should be explored as an avenue to improve STI care.
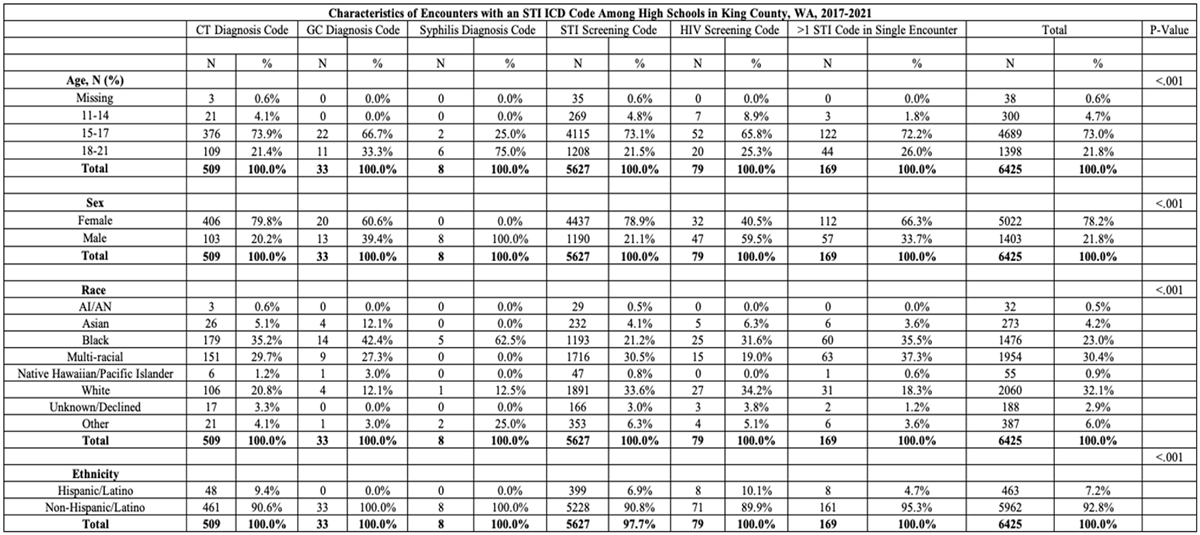
PP02.23 – Relationships Between Problematic Pornography Consumption and Anxiety, Depression and Aggression Among Adolescents in the United States: A Systematic Review
Mr. Ahmed Elaghoury1, Professor Jan Dimmitt Champion1
1University of Texas at Austin, School of Nursing, Austin, United States.
Background: The aim of this review was to synthesize the current knowledge about the relationships between problematic pornography consumption and mental health outcomes (anxiety, depression, and aggression) among adolescents in the US.
Methods: We conducted this systematic review following the PRISMA (Preferred Reporting Items for Systematic Reviews) guidelines and initially registered it with the PROSPERO database (registration number: CRD42024602759) in November 2024.We included studies that meet the following criteria: assessed the relationship between Problematic Pornography Consumption (PPC) and any of the mental health outcomes (anxiety, depression, and aggression); quantitative, qualitative, or mixed studies focused on adolescents (13–18 years) in the United States, published in English in peer-reviewed journals within the past 10 years. Three databases (PubMed, PsycINFO & CINAHL) were searched to extract the eligible publications (Fig. 1). One reviewer independently screened and extracted the required data using Rayyan software and then evaluated the study’s quality and risk of bias using Joanna Briggs Institute critical appraisal tools.
Results: We included 16 studies with a total of 20,209 participants. Our results showcased a significant positive correlation between PPC and various aggression forms: sexual aggression, acceptance of rape myths, intimate partner violence, online aggressive behaviours, and cyberbullying perpetration. PPC was also correlated with increased levels of depression, low self-esteem, eating disturbances and suicidal behaviours. Finally, our results indicated a weak positive correlation between anxiety and pornography among Asian American/Pacific Islander, Latin, and White male adolescents.
Conclusion: Our review concluded that adolescents with higher frequency of pornography consumption are more likely to manifest aggressive behaviours, have higher depressive symptoms, low self-esteem, eating disturbances, and suicidal ideations. We found a weaker correlation between PPU and anxiety, underscoring the importance of culturally sensitive approaches in addressing the pornography utilization issue. Future research must address the effect of PPC among adolescents considering gender differences, sexual orientations and minorities.
PP02.24 – HIV/STIs Risks and Health Disparities Among Black LGBTQ+ University Students
Dr. Zahra Fazli Khalaf1, Ms. Camryn Goins1
1North Carolina A&T State University, Greensboro, United States.
Background: The risk of HIV and sexually transmitted infections (STIs) is significantly higher among the LGBTQ+ population, with Black/African American communities facing disproportionately high rates. Alarmingly, Black men who have sex with men (MSM) demonstrate the highest lifetime risk of HIV diagnosis, according to the Centers for Disease Control and Prevention (CDC).
Methods: This research, conducted between 2024 and 2025, utilized a phenomenological qualitative approach to investigate the factors contributing to HIV/STIs risk behaviors among Black LGBTQ+ university students. Participants were selected using purposive sampling through online advertisements and social media recruitment strategies.
Results: The findings highlight the intersectional factors that contribute to increased risk behaviors, healthcare utilization, and barriers to accessing healthcare services. These challenges include the underutilization of essential preventive measures, such as HIV testing, pre-exposure prophylaxis (PrEP), and post-exposure prophylaxis (PEP).
Conclusions: This research advocates for enhanced university health services to address these disparities and promote equitable access to STIs/HIV prevention and care. Addressing these inequities requires intersectional approaches that integrate education, community support, and systemic change. Such interventions are critical to reducing the disproportionate burden of STIs and HIV on marginalized populations within higher education institutions.
PP02.26 – “Some Fear Injection, Others Don’T Want to Swallow Tablets, While Others Forget”: Ugandan Health Providers’ Perspectives on PrEP Ring Introduction Among Young Mothers in Rural Settings
Dr. Erica Gollub1, Dr Marie Charles, Ms. Esther Nakyaze, Dr. Marc Sklar, Dr. Daniel Murokora
1Pace University, Pleasantville, United States.
Background: Choice in PrEP methods is essential for young mothers in rural sub-Saharan Africa (SSA) where pill uptake is low. The Dapivirine ring or PrEP ring is now approved in eleven SSA countries including Uganda. Implementation studies are underway ahead of market introduction. Numerous studies focus on potential users; few have focused on healthcare providers. Providers of diverse cadres play an important role and their attitudes towards the PrEP ring will impact uptake.
Methods: We conducted a qualitative study of nurses, midwives and community health workers (CHWs) serving young mothers in rural Uganda to assess their perspectives on the ring, including challenges and opportunities. IRB approval was granted by Pace University (USA) and Mildmay Uganda Research & Ethics Committee with further approval by the Uganda National Council for Science and Technology. Participants consisted of 60 government health workers from the Rakai and Kyotera districts recruited from the directory of a locally-led, non-governmental organization focused on Maternal and Newborn Health systems strengthening. Following informed consent, they attended an onsite focus group discussion (~1.5 h, total of 6 sessions), jointly moderated in a hybrid format.
Results: Study participants comprised of 26 nurses, 18 midwives, and 16 CHWs (45 females, 15 males). Themes included: advantages of the PrEP ring as a discreet, non-hormonal method without pill-related burden or side effects; concern regarding size and texture of the ring; the vital role of men as method champions; the value of CHWs and peer counselors to reduce stigma and tailor counseling; the need to distinguish the PrEP ring from contraceptives, especially the IUD; concern about PrEP ring stockouts; and the importance of collaboration across healthcare workers.
Conclusion: Participants highlighted important topics for educating healthcare professionals from all cadres. The emerging cultural and attitudinal perspectives can help tailor outreach to young mothers in rural SSA settings.
PP02.27 – Is It Partner Number or Group Sex? STI Risk Among Urban Gay, Bisexual, and Other Men Who Have Sex with Men in Montreal, Toronto, and Vancouver: A Matched Comparison Analysis
Dr. Aki Gormezano1,2, Dr. David M Moore2,3, Lu Wang2, Justin Barath2, Santiago Aguilera-Mijares2,3, Jason Trigg2, Paul Sereda2, Allan Lal2, Dr. Paolo Palma4, Dr. Tin D. Vo5, Dr. Shayna Skakoon-Sparling6, Dr. Daniel Grace5, Dr. Trevor Hart4,5, Dr. Joseph Cox7, Dr. Darrell H. S. Tan5,8, Jody Jollimore9, Milada Dvorakova7, Terri Zhang4, Nathan J Lachowsky1,2
1University of Victoria, Victoria, Canada.
2British Columbia Centre for Excellence in HIV/AIDS, Vancouver, Canada.
3University of British Columbia, Vancouver, Canada.
4Toronto Metropolitan University, Toronto, Canada.
5University of Toronto, Toronto, Canada.
6University of Guelph, Guelph, Canada.
7Research Institute of McGill University Health Centre, Montréal, Canada.
8St. Michael’s Hospital, Toronto, Canada.
9CATIE, Toronto, Canada.
Background: Group sex is associated with acquisition of bacterial sexually transmitted infections (B-STI) among gay, bisexual, and other men who have sex with men (GBM). However, whether this is driven by increased numbers of sexual partners alone or other factors is unclear. We compared B-STI diagnoses among GBM with group sex participation to non-group sex controls matched on partner number.
Methods: We recruited sexually-active GBM aged 16+ in Vancouver, Toronto, and Montreal through respondent-driven sampling from 02/2017 to 08/2019. Participants completed computer-assisted self-interviews and B-STI tests (chlamydia, gonorrhea, syphilis) at enrolment and every 6–12 months through 08/2023. B-STI period prevalence included any diagnoses at study visits or self-reported in the previous 6 months (P6M). We created a matched control group with no group sex but similar P6M sexual partner number and other key characteristics (e.g., HIV status; substance use) using “nearest neighbour” propensity score matching (Rosenbaum & Rubin, 1985). We used generalized linear-mixed effects models to compare B-STIs among three groups of GBM: 1) any self-reported bareback/Party-and-Play (PnP) group sex, 2) other group sex, and 3) the matched controls.
Results: We matched 767 group sex participants (median = 10 P6M sex partners; 15.6% HIV+) to 767 controls (median = 7 P6M sex partners; 12.7% HIV+). The proportion of GBM who had a B-STI in groups 1, 2, and 3 across all visits were: 76.4% (95% CI: 72.0-80.9), 45.1% (40.3–49.9), and 41.6% (38.1–45.1), respectively. P6M odds of B-STIs were higher among bareback/PnP group sex participants than controls, aOR = 1.89 (95% CI: 1.51–2.37). Odds were similar among other group sex participants and controls, aOR = 0.97 (0.78–1.21).
Conclusions: Only bareback/PnP group sex participants had higher B-STIs independent of partner number, and should be supported with emerging/novel STI prevention. Future research should examine how norms facilitating condom use and limiting substance use may ameliorate the impacts of group sex on B-STI transmission.
PP02.28 – Provider Perceptions of the Updated Texas Prenatal Syphilis Screening Policies
Dr. Stacey Griner1, Ms. Idara Akpan1, Ms. Sophia Garza1, Ms. Kaeli Johnson1, Ms. Amanda Brosnan1, Dr. Malinee Neelamegam1, Dr. Meaghan Nelsen1
1University of North Texas Health Science Center, Fort Worth, United States.
Background: Congenital syphilis (CS) rates are increasing in Texas. In 2019, Texas revised its prenatal syphilis screening policy to include additional screening at delivery. However, there is limited evidence on the translation of this policy to clinical settings, and rates of CS remain high. The purpose of this study was to explore prenatal providers’ perceptions of the CS policy using an implementation science framework.
Methods: In-depth interviews were conducted with 18 prenatal care providers. The interview guide was framed in the Consolidated Framework for Implementation Research, particularly focusing on the innovation domain. We explored provider perceptions of the policy characteristics, including the evidence strength and quality, the perceived need for the change, the relative advantage of the policy change compared to the previous recommendations, costs associated with implementation, and the provider’s individual perception of the CS policy as a whole.
Results: Overall, participants desired more information about the evidence base that was used to guide the CS policy change, both to understand the context as to why the policy was changed and to inform their patients about this evidence. Participants had a variety of perceptions of the need for the CS policy change – some identified the prevention of the negative outcomes as a reason to change the policy, but others questioned the cost-effectiveness of the additional point of screening based on their practice experience of seeing very few diagnoses.
Conclusion: Without evidence supporting this change, providers were hesitant to implement the policy into practice. Public health and policymakers should incorporate policy dissemination strategies when releasing new information to health care providers. Furthermore, identifying barriers to policy implementation can inform strategies to increase adoption of policies in health care settings.
PP02.29 – Future Gonorrhea Vaccines: Acceptability, Behaviors, and Barriers Among Young Adults
Dr. Stacey Griner1, Idara N. Akpan, Sarah A. Alkhabtib, Amanda Brosnan, Kaeli C. Johnson, Sophia Garza, Alexandra N. Farris, Dr. Malinee Neelamegam
1University of North Texas Health Science Center, Fort Worth, United States.
Background: As Neisseria gonorrhoeae continues to develop multidrug resistance, innovative strategies are needed for primary prevention. While potential vaccines are currently in development, their acceptability is unknown and developing strategies that may increase vaccination rates could facilitate future uptake. As a first step, we assessed acceptability, behaviors, and barriers related to gonorrhea vaccines among young adults.
Methods: Using an online survey panel, we recruited sexually active young adults (18–24 years) in the United States (n = 379). We assessed the hypothetical likelihood of being vaccinated with or without a provider recommendation and engaging in additional discussion or research about the gonorrhea vaccine. The five response options were collapsed into two categories, not likely and likely. Barriers included costs, vaccine effectiveness, and social concerns. Descriptive analyses were conducted in SPSS.
Results: The average respondent age was 21.1 years (SD = 1.9). Roughly 49% were men, and 13% of all respondents had previously contracted a sexually transmitted infection. Almost 41% were likely to get vaccinated, which increased to 48% if the vaccine was recommended by their healthcare provider. Over 31% of participants were likely to ask their provider about the gonorrhea vaccine in the future, 29% were likely to discuss the vaccine with their provider, and 35% were likely to do additional research about the vaccine. Potential barriers included concerns regarding vaccine effectiveness (69%), vaccine costs (68%), and the possibility of contracting gonorrhea through the vaccine (66%) (Table 1).
Conclusion: There was moderate acceptability of gonorrhea vaccines among young adults, which increased when recommended by their healthcare provider. Additional research to qualitatively understand the salient barriers to vaccine uptake can guide communication strategies that address young adults’ concerns and inform successful vaccine roll-out. Incorporating the perspectives of the ultimate end users into future gonorrhea vaccine campaigns could bolster vaccine adoption and uptake among this priority population.
| N(%) | ||
|---|---|---|
| Acceptability | ||
| If a safe and effective vaccine for gonorrhea was available, how likely are you to be vaccinated? | ||
| Not likely | 221 (58.3) | |
| Likely | 154 (40.6) | |
| If a safe and effective vaccine for gonorrhea was available and your doctor recommended it, how likely are you to be vaccinated? | ||
| Not likely | 191 (50.4) | |
| Likely | 183 (48.3) | |
| Future behaviors | ||
| In the future, how likely are you to ask a doctor about the gonorrhea vaccine? | ||
| Not likely | 257 (67.8) | |
| Likely | 118 (31.1) | |
| In the future, how likely are you to discuss the gonorrhea vaccine with your doctor? | ||
| Not likely | 264 (69.7) | |
| Likely | 111 (29.3) | |
| In the future, how likely are you to do additional research on the gonorrhea vaccine? | ||
| Not likely | 241 (63.6) | |
| Likely | 134 (35.4) | |
| Barriers: Would the following things discourage you from getting you vaccinated for gonorrhea? | ||
| Having to pay for the gonorrhea vaccine. | ||
| Not at all | 122 (32.5) | |
| A little/A lot | 253 (67.5) | |
| Concern you might get gonorrhea as a result of the vaccine. | ||
| Not at all | 126 (33.6) | |
| A little/A lot | 249 (66.4) | |
| Concern that a gonorrhea vaccine would not work. | ||
| Not at all | 115 (30.7) | |
| A little/A lot | 260 (69.3) | |
| Concern that someone would think poorly of you for getting a gonorrhea vaccine. | ||
| Not at all | 174 (46.8) | |
| A little/A lot | 199 (53.2) | |
Not likely: not at all likely, not very likely, somewhat likely; Likely: very likely, extremely likely.
PP02.30 – HIV Prevention Knowledge and Behaviour Among Corporate Commercial Sex Workers; a Case Study of Kampala Metropolitan Area – Uganda
Mr. Isaac Gulemye1
1Anchoring Communities Uganda, Kampala, Uganda.
Background: Numbers of corporate sex workers in Uganda have grown exponentially. Despite this, no interventions have been documented targeting corporate sex workers which threatens gains made in the fight against new HIV infections, especially among most at risk populations. For this study, corporate sex workers are defined as women/men who engage in transactional sex by sourcing clients through digital platforms as opposed to traditional parading in brothels and along streets.
Description: This cross-sectional study examined the knowledge and behaviors of corporate sex workers towards HIV prevention. The study was conducted from June 2023 to May 2024, reaching 219 respondents (173 female, 46 male). Respondents were randomly selected from six websites listing services of corporate sex workers (Escorts) in Kampala, Mukono & Wakiso districts. Researchers who disguised themselves as potential clients contacted the respondents through phone calls and instant messaging Apps. Data was recorded using an observation checklist. Data were analyzed using Microsoft Office Excel.
Conclusion: There is a glaring knowledge gap and low uptake of HIV prevention interventions among corporate commercial sex workers, resulting in high-risk sexual behavior. The sex workers are not stationed in brothels, therefore conventional interventions can not reach them hence a need for novel strategies targeting them.
Findings
| Knowledge of | Female (n = 173) | Male (n = 46) | |||
|---|---|---|---|---|---|
| Yes | No | Yes | No | ||
| Pre-Exposure Prophylaxis (PrEP) | 57 (32.9%) | 116 (67.1%) | 11 (23.9%) | 35 (76.1%) | |
| HIV self-testing | 79 (45.7%) | 94 (54.3%) | 27 (58.7%) | 19 (41.3%) | |
| Post Exposure Prophylaxis (PEP) | 118 (68.2%) | 55 (31.8%) | 46 (100) | 0 (0%) | |
| Own HIV status | 84 (48.6%) | 89 (51.4%) | 5 (10.9%) | 41 (89.1%) | |
| Behaviour | |||||
| Currently using PrEP | 5 (2.9%) | 168 (97.1%) | 0 (0%) | 46 (100%) | |
| Agree to sex without a condom for extra money | 136 (78.6%) | 37 (21.4%) | 21 (45.7%) | 25 (54.3%) | |
| Requires HIV test before sex | 64 (37%) | 109 (63%) | 13 (28.3%) | 33 (71.7%) | |
| Anal sex for extra money | 77 (44.5%) | 96 (55.5%) | 14 (30.4%) | 32 (69.6%) | |
| Ever used PEP | 38 (22.0%) | 135 (78.0%) | 8 (17.4%) | 38 (82.6%) | |
Virtual peer to peer support to enhance Antiretroviral adherence among young people living with HIV.
Background: Although the region has a relatively low prevalence of HIV, East central Uganda has continued to register an increase in the number of people living with HIV (PLHIV) with Unsuppressed viral load. This pilot intervention was in response to an increase in the number of adolescents and young people with unsuppressed HIV viral load majorly as a result of the effects of COVID-19.
Methodology: The target group was adolescents and young people age 13 to 24 years. Client files and ministry of health registers were reviewed at 24 health facilities in Kamuli, Buyende and Luuka districts to identify clients in the target group who had an unsuppressed viral load during the previous year. A total of 257 young people living with HIV (YPLHIV) were recruited into the study. These were paired with trained expert peer counsellors from another district other than their own. The pilot intervention was from November 2021 to October 2022. The last viral load for each enrolled young person was captured as baseline.
During the intervention year, using virtual platforms such as instant messaging application and phone calls, expert peer counsellors provided intensive adherence counselling, psychosocial support to the participants. Each expert peer counsellor had 4–6 young people to support. Qualitative data was analysed thematically while quantitative data was analysed using SPSS 27.
Results: Female 154. Male 103.
Conclusion: https://bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-021-12366-4.
Keywords: Right to choice, UHC, Diversity, Meaningful involvement, Agency.
PP02.31 – Addressing Inequities in HIV Prevention in British Columbia, Canada: Findings from a Community-Based Qualitative Study with People Newly Diagnosed With HIV
Mr. Evan Hall1,2, Mr. Ben Klassen2, Mr. Jean Carlos Reyes2, Mr. Robert Dean3, Mr. Andy Lessard2, Mr. Chris Draenos2, Mr. Mark Hull4, Mr. Nathan Lachowsky2,5
1University of British Columbia, Vancouver, Canada.
2Community Based Research Centre, Vancouver, Canada.
3Ribbon Community, Vancouver, Canada.
4BC Centre for Excellence in HIV/AIDS, Vancouver, Canada.
5University of Victoria, Victoria, Canada.
Background: Systemic gaps in HIV prevention result in sub-optimal intervention uptake and ongoing HIV transmission, particularly among communities experiencing intersectional social inequities. This study explored how HIV prevention can be improved from the perspectives of people newly diagnosed with HIV (PLHIV) in British Columbia (BC), Canada, where a publicly funded PrEP (pre-exposure prophylaxis) program has been available since 2018.
Methods: Guided by Greater Involvement/Meaningful Engagement of PLHIV and community-based research principles ensured all project aspects were led by PLHIV. Recruitment was conducted through HIV service organizations and care providers. Semi-structured peer-led interviews were conducted in English (n = 20) and Spanish (n = 11) with PLHIV diagnosed between 2018 and 2023, residing in BC, and aged 18+.
Results: Most participants (n = 27/31) were Two-Spirit/Gay, Bisexual, Trans, Queer Men and non-binary individuals, while four were straight women; one-third were Latinx (n = 12/31), and ages ranged from 24–62. Social determinants of health such as housing, financial security, and immigration status influenced participants’ access to HIV prevention and testing services. HIV knowledge varied across social locations and was shaped by persistent stigma and misconceptions about HIV risk. Testing access was often limited by geographic proximity to urban, affirming health services. Barriers to PrEP uptake included low awareness, difficulty perceiving oneself as a PrEP candidate, complexity in navigating health systems, and adherence challenges linked to mental health and substance use.
Conclusion: Effective HIV prevention in BC must address structural drivers and inequities. Prevention efforts can improve through tailored education for key populations, adaptations to PrEP services to reduce barriers, the promotion of accurate risk assessment tools, and upstream interventions targeting health inequities affecting priority populations, including newcomers. These outcomes in BC can provide greater understanding to service delivery in high resource settings internationally. Systemic barriers must be tackled through structural interventions to enhance accessibility and equity in HIV prevention.
PP02.32 – Sex Worker’s Safety-Making in Ukraine: A Secondary Qualitative Analysis Using a Feminist Political Economy Approach
Ms. Nicole Herpai1, Dr. Lisa Lazarus1, Dr. Dasha Pavlova1, Dr. Leigh M. McClarty1, Dr Evelyn L. Forget1, Dr Rob Lorway1, Dr Marissa L. Becker1
1University of Manitoba, Winnipeg, Canada.
Background: Ukraine has the highest prevalence of HIV in Europe, and women who do sex work have a prevalence three times the national average. Women who do sex work also have higher sexually transmitted and blood-borne infections (STBBI) associated vulnerabilities, connected to their gender and the criminalization of sex work. Periods of political conflict can trigger significant social and economic shifts, intensifying existing health and safety challenges. This project seeks to answer the question: How have women engaged in sex work in Dnipro, Ukraine navigated health and occupational risks during a period of protracted political conflict?
Methods: We conducted a secondary qualitative analysis of interview and diary data collected from 43 sex workers in Ukraine in 2018. Translated texts were open coded for key themes and emergent categories, followed by further in-depth thematic analyses. Thematic analysis was guided by a feminist political economy theoretical lens, a critical materialist approach that acknowledges the socially constructed nature of gender and critiques the sexual division of labour. This approach is used to understand the downstream health effects of complex settings and illuminate the processes that produce gendered health inequities.
Results: Participants discussed utilizing a range of safety-making strategies to navigate health and occupational risks in an environment shaped by criminalization, stigma, political conflict, and economic instability. Three key themes emerged from participant narratives: 1) adaptive risk management and fluid safety-making strategies (identifying and responding to threats); 2) emotional labor of client management (assessing client moods and dynamics); and 3) structural security measures (e.g., security-guards).
Conclusion: These findings bring insights into the additional labour required to keep safe and well in a dynamic industry that exists outside the formal economy. The themes highlighted by our participants raise important considerations for how to structurally support safety-making for sex workers in Ukraine and other contexts globally.
PP02.33 – Pre-Exposure Prophylaxis and Sexual Quality of Life in MSM: Pre-Pandemic Insights from the Brazilian Amazon
Dr. Eduardo Honorato1, Dr Djane Baia-da-Silva2, sr Mario Felipe Bosco Santos1, Dr Daniel Cerdeira de Souza4, Dr Erica da Silva Carvalho1, Dr Marcus Vinicius Guimarães Lacerda3
1Universidade do Estado do Amazonas, Manaus, Brazil.
2Fundação de Medicina Tropical Dr. Heitor Vieira Dourado, Manaus, Brazil.
3Instituto Leônidas e Maria Deane FIOCRUZ-AM, Manaus, Brazil.
4Universidade Federal do Amazonas, Benjamim Constant, Brazil.
Background: HIV Pre-Exposure Prophylaxis (PrEP) has demonstrated significant efficacy in preventing HIV infections. However, little is known about its social and behavioral impact, particularly on the quality of sexual life. This study evaluates the sexual quality of life of men who have sex with men (MSM) during early PrEP adherence in the Brazilian Amazon. Notably, these data were collected months before the COVID-19 pandemic, which devastated the region, and are being presented only now, as the city recovers partially post-pandemic.
Methods: This prospective longitudinal study included MSM aged 18 years or older initiating daily PrEP. Participants completed the Sexual Quality of Life Questionnaire-Male (SQoL-M) at baseline (D0) and after 120 days (D120) of adherence. Qualitative data were collected through open-ended questions, and responses were analyzed using Bardin’s Content Analysis.
Results: Of 98 participants, 72 completed follow-ups. A 22.97% improvement in sexual quality of life was observed, with the greatest increases in future expectations (93.86%) and reduced anxiety. Safety and trust emerged as the most mentioned themes, with 41 references. Adherence (fewer missed doses) was significantly associated with better outcomes (P < 0.05).
Conclusion: PrEP significantly enhances the quality of sexual life among MSM, impacting psychological and social aspects such as anxiety, fear, and self-esteem. These findings underscore the importance of PrEP in improving overall well-being, extending beyond its biological role in HIV prevention. The study offers critical insights into the intersection of behavioral health and HIV prevention, emphasizing the need for integrating psychosocial support into PrEP programs, particularly in vulnerable regions recovering from large-scale crises.
PP02.34 – What Do Pregnant Women Know About Syphilis During Pregnancy? Findings from a Mixed Methods Survey
Ms. Rachel Kachur1, Dr. Rebecca Schlaff2, Ms. Megan Higdon2, Krissy Leahy2, Ms. Rebekah Horowitz3
1CDC, Atlanta, United States.
2Altarum, Washington, United States.
3NACCHO, Washington, United States.
Background: Syphilis during pregnancy can cause significant infant morbidity and death. CDC recently reported a 755% increase of congenital syphilis (CS) cases during 2012–2021, mostly because a lack of prenatal care or timely testing and treatment during pregnancy. To inform future, empowerment-framed messages, we conducted a mixed-methods survey with women who recently received prenatal care to explore syphilis/CS knowledge and awareness, and prenatal care experiences.
Methods: In November 2024, women from 5 states were recruited into an online, asynchronous survey. Women answered questions about syphilis/CS knowledge and awareness, barriers, and facilitators to prenatal care, and recent prenatal experiences. Data analysis included descriptive statistics for close-ended questions and inductive thematic analysis of open-ended questions.
Results: A convenience sample of 87 pregnant (28%) or recently pregnant (72%, past 12 months) women participated. Most (63%) were aged 21–29 years and identified as Black/African American (57%). One third identified as Hispanic/Latino. A majority knew syphilis is a STI (81.8%) and they should be tested while pregnant (84.4%); fewer knew it was curable (49.4%). About 25% didn’t know syphilis can pass from mother to fetus, 16.9% had not heard of syphilis. Many (55.8%) stated a clinician talked to them about syphilis, however 30% reported never hearing or not knowing if they ever heard the word “congenital” before. Barriers to receiving wanted care included appointment availability (12.3%), lack of transportation (7.4%), and competing priorities (6.2%). Most women reported positive prenatal care experiences such as feeling respected by providers (71.8%) and comfortable asking questions (79.5%). Negative experiences included not being listened to (6.4%), feeling judged (2.6%) or distrusting the provider (2.6%).
Conclusion: Most women knew of syphilis and the recommended testing during pregnancy; they also reported positive prenatal care experiences. However, there is room to improve knowledge and conversations about syphilis among pregnant women and their providers.
PP02.35 – Amplifying Voices, Destigmatizing HIV: The Journey of Call Me Shamsz and Its Media Tour
Mr. Samsudeen Kareem1, Mr Geoff Brown1
1Association of Positive Youths Living with HIV in Nigeria (APYIN), Abuja, Nigeria.
Background: HIV-related stigma remains one of the most significant barriers to achieving optimal health outcomes for people living with HIV (PLHIV), particularly among adolescents and young adults. Call Me Shamsz is a groundbreaking documentary that provides a deeply personal and unfiltered account of living with HIV, chronicling the challenges of disclosure, the societal stigma faced, and the resilience needed to overcome these barriers. This documentary aims to humanize the experiences of PLHIV, foster empathy, and catalyze global conversations around stigma reduction and support for vulnerable populations.
Methods: Funded by Dr. Mike Dybul, former PEPFAR Coordinator, the documentary’s launch is strategically accompanied by a media tour designed to amplify its impact. The media tour employs a multipronged approach, leveraging television, radio, social media platforms, and live Q&A events to engage diverse audiences. It serves as a platform to disseminate actionable insights from recent HIV conferences and mobilize stakeholders – including policymakers, healthcare providers, and community leaders – to intensify efforts in addressing HIV stigma.
Results: Preliminary evaluations of the documentary’s screenings and media tour indicate increased awareness about HIV-related stigma, improved community attitudes, and the empowerment of PLHIV to embrace disclosure and seek support. This presentation will highlight the documentary’s creation, its strategic dissemination, and measurable outcomes from the media tour. It will conclude with actionable recommendations for using media as a tool for public health advocacy and stigma reduction.
Conclusion: This abstract seeks to inspire further collaborations in utilizing creative media to achieve the UNAIDS 2030 goals of ending the HIV epidemic by normalizing conversations around HIV and reinforcing the rights and dignity of PLHIV.
PP02.36 – Exploratory Thematic Analysis of Knowledge and Barriers to Sexual Health Among Street-Based Sex Workers in Bangladesh
Mr. Farhan Khandakar1, Mr Khandaker Imrul2
1Department of Public Health Sciences, Queen’s University, Kingston, Canada.
2Shishuder Jonno Aamra, Dhaka, Bangladesh.
Background: Sex workers (SW) in Bangladesh face significant barriers to sexual and reproductive health (SRH) services, yet limited research exists on street-based (floating) SW. This study examines the experiences of floating cisgender female sex workers (FSW) and Hijra (transgender or intersex) SW, focusing on their knowledge of sexual health and access to SRH services.
Methods: Participants were recruited using snowball sampling facilitated by a trusted community partner. October 2024, three focus group discussions were conducted in Bengali with 13 participants (aged 18–65) from various backgrounds, including 2 retired FSW, 1 Hijra community member, 8 current FSW, and 2 current Hijra SW. Interviews were audio-recorded, translated, transcribed, and analyzed using thematic analysis to identify key themes.
Results: SW affiliated with Non-Governmental Organizations (NGOs) demonstrated basic knowledge of sexually transmitted blood-borne infections (STBBIs), particularly HIV. All participants lacked awareness of long-term health implications. FSW and Hijra SW were more likely to engage in unprotected sex, often driven by economic needs. Misconceptions about condom use and protective measures were common. None of the participants had knowledge of pre- or post-exposure prophylaxis; however, almost all current SW reported receiving regular HIV point-of-care testing through NGOs. Most FSW reported treatment for symptoms of gonorrhea and chlamydia, although they could not clearly identify the STBBI. FSW reported better healthcare experiences when accompanied by NGO representatives, whereas Hijra SW were prioritized in healthcare settings due to stigma and fear among providers and society. Most participants also reported recent exasperated verbal and physical harassment in public due to Bangladesh’s current political climate.
Conclusion: This study highlights critical gaps in sexual health knowledge and inequities in healthcare access for floating SW in Dhaka, Bangladesh. Addressing misinformation, enhancing education on STBBIs, and reducing stigma in healthcare are essential to improve SRH outcomes.
PP02.37 – Innovative Financing to Support STI Testing: A Mixed Methods Analysis of Donations to a Pay-It-Forward Program in China
Miss Ye Liu1, Miss Ke Zhou1, Miss Gayed Salma2, Miss Gifty Marley1, Dr Tom Fitzpatrick2, Professor Weiming Tang2, Dr. Lan Li, Professor Joseph Tucke2,3
1Sesh Global Llc, Guangzhou, China.
2University of North Carolina at Chapel Hill, North Carolina, America.
3London School of Hyigene and Tropical Medicine, London, UK.
Background: Many STI testing services are underfunded. Pay-it-forward is an innovative approach to support STI testing which has participants donate money or write postcards to spur others to receive STI testing. We performed a secondary analysis of data from a mixed-methods study evaluating a pay-it-forward intervention in China to explore correlates of monetary and non-monetary (postcards) donation.
Methods: We used a convergent parallel mixed-methods approach to analyze quantitative data from a randomized controlled trial and qualitative data from semi-structured interviews. Correlates of making a monetary or non-monetary donation were identified using logistic regression. For the qualitative component, we conducted semi-structured interviews with participants and using thematic analysis the interview data to contextualize determinants of monetary and non-monetary donations.
Results: From 4 cities, there are 800 men who satisfied recruitment criteria has been recruited. Among the 800 participants offered the pay-it-forward intervention, 154 (19.3%) made a monetary donation. The mean donation amount was $4.04 USD. The total amount of all donations was $622.61 USD, covering XX% of STI testing costs. Men with higher incomes (>$8280 USD/year) were more likely to donate money (aOR = 1.65, 95% CI = 1.01–2.74) compared to men with lower incomes. 86/388 (22.16%) donated a postcard, and there was no correlation between those who made monetary and non-monetary donations. Men from CBO-led clinic were less likely to donate postcards compared to men from public STD clinic (aOR = 0.37, 95% CI = 0.21–0.65). Many men noted that clear messaging and transparency increased the understanding of pay-it-forward and facilitated monetary donations
Conclusion: Our data have implications for structuring innovative financing to support STD testing. Only by adopting targeted donation strategies for different groups of people can the sustainability of pay it forward be ensured.
PP02.38 – The Emotional Context of STI Testing: A Secondary Analysis Focused on Gratitude for a Pay-It-Forward Intervention from an RCT in China
Dr. Lan Li1, Dr Gifty Marley1, Miss Ye Liu1, Dr Weiming Tang3, Prof Joseph Tucker2,3
1University of North Carolina Project-China, Guangzhou, China.
2London School of Hygiene and Tropical Medicine, London, United Kingdom.
3University of North Carolina at Chapel-Hill, Chapel Hill, USA.
Background: The emotional context of STI testing is important. Pay-it-forward is an implementation strategy in which a person receives a free gonorrhea/chlamydia test, postcards, and can then support others to donate money or postcards. This secondary analysis aims to understand the emotional context of gratitude for pay-it-forward using mixed methods.
Methods: Data was collated from a randomised controlled trial conducted in China involving 783 recipients of a pay-it-forward intervention. Qualitative data explored participants’ feelings about the intervention through open-ended questions capturing words describing immediate feelings among donors and non-donors. Gratitude for pay-it-forward was measured using a 10-item validated scale across three domains: feeling cared for, warm glow, and a desire to share with others. Logistic regression assessed the association between gratitude domains and testing and monetary/non-monetary gift-giving behaviours.
Results: The average participant age was 35.4 years and 54.0% (n = 423) had ever had sex with men (MSM). Content analysis showed that “gratitude“(87/783, 11.1%) and “satisfaction” (65/783, 8.3%) were the most cited terms used to describe participant feelings after receiving pay-it-forward. 10.3% (16/155) of donors expressed gratitude, often linked to themes like “sharing” and “passing-it-on”. 11.3% (71/630) of non-donors expressed gratitude, in association with “free testing” and “government support”. Regression analysis showed that feeling grateful was not significantly associated with testing. Feeling cared for, a warm glow, and a desire to share services with others were each positively associated with giving monetary gifts and feeling cared for was associated with giving non-monetary gifts (Table 1).
Conclusion: Specific emotional and motivational aspects of gratitude significantly enhanced monetary and non-monetary donations. Emotional cues matter in service delivery, and future research should explore innovative ways to leverage this in intervention design.
| Testing behavior | Monetary donation | Non-monetary donation | |||||
|---|---|---|---|---|---|---|---|
| Odds ratio [95% CI] | P-value | Odds ratio [95% CI] | P-value | Odds ratio [95% CI] | P-value | ||
| Feeling cared for | 0.84 [0.34, 1.71] | 0.674 | 2.35 [1.38, 4.46] | 0.004 | 0.50 [0.28, 0.84] | 0.013 | |
| Feelings of warm glowA | 0.54 [0.14,1.41] | 0.288 | 2.00 [1.13, 3.94] | 0.028 | 0.77 [0.44, 1.25] | 0.317 | |
| Desire to share service with others | 1.32 [0.64, 2.41] | 0.408 | 2.05 [1.22,3.79] | 0.012 | 0.74 [0.45, 1.16] | 0.212 | |
PP02.39 – Generosity in the STI Clinic: A Mixed-Methods Analysis of Health Professionals in China
Miss Ke Zhou1, Dr. Ruby Congjiang Wang2,6, Mr. Dorian Ho3, Dr. Thomas Fitzpatrick1,4, Dr. Gifty Marley1, Dr. Weiming Tang5, Dr. Joseph D. Tucker5,6, Dr. Lan Li
1University of North Carolina Project - China, Guangzhou, China.
2Digital Health Council at the UK Royal Society of Medicine, London, UK.
3Department of Health Policy & Management, University of North Carolina at Chapel Hill, Chapel Hill, USA.
4Division of Allergy and Infectious Diseases, University of Washington, Washington, USA.
5University of North Carolina at Chapel Hill, Chapel Hill, USA.
6London School of Hygiene and Tropical Medicine, London, UK.
Background: Generosity among health professionals has been shown to improve patient relationships and improve outcomes. However, STI professionals are overworked and underpaid. This paper examined how providers define and enact generosity, as well as facilitators and barriers to acting generously in STI clinics, aiming to support health professionals and to improve care quality for patients.
Methods: This study used a mixed-methods approach. In-depth interviews and focus group discussions were conducted with doctors, nurses, laboratory technicians, and medical students. Factors influencing generosity were identified using a six-phase inductive thematic analysis. A crisp-set qualitative comparative analysis (csQCA), a mixed-methods approach that views each case as a combination of conditions and outcomes, was applied to identify potential drivers of generosity.
Results: We interviewed 27 health professionals from five hospitals in Guangdong Province, China. The average clinical experience was 16 years, and specialties included dermatology, gynecology, and STD. Generosity was defined as the social behaviour of giving emotional or material resources to others without expecting anything in return. In STI clinics, generous acts were rooted in a sense of moral obligation and manifested as allocating extra time, providing emotional care, and offering lower-cost treatment. Patient rapport and colleague support enabled clinicians to enact greater generosity in their work. csQCA found that non-discriminatory attitudes and teamwork drove generosity. The complexity associated with STI and related stigmas further encouraged societal expectations for generosity. However, some health professionals were expected to do too much, leading to burnout, overstepped boundaries, and job dissatisfaction, which limited generosity.
Conclusion: Health professionals regarded generosity in the STI clinical setting as a moral duty that can enhance patient care. However, unrealistic clinic expectations and social roles may contribute to burnout. Healthcare systems should promote non-stigmatizing attitudes and team support to encourage more generosity in the clinical setting.
PP02.40 – Seizing the Moment: Using Ecological Momentary Assessment to Capture Variability in Sexual Behaviors Among Sexual Minority Men
Ms. Brittany Liebhard1, Dr. JaNelle M. Ricks1, Mr. Morgan Spahnie1, Dr. William C. Miller2, Dr. Abigail Norris Turner1
1The Ohio State University, Columbus, United States.
2University of North Carolina at Chapel Hill, Chapel Hill, United States.
Background: Ecological momentary assessment (EMA) can measure sexual behaviors in near-real time. We included between-visit ecological momentary assessments in a prospective cohort study of factors associated with syphilis transmission among sexual minority men (SMM) in Columbus, Ohio. In preparation, we piloted the EMA component among a sample of SMM.
Methods: Participants downloaded an EMA app to their personal smartphones and were asked to complete daily surveys (regardless of their sexual activity for that day) for 4 weeks. The survey included questions about anal and oral sex, use of apps to meet partners, and other behaviors in the past 24 h, and plans for these behaviors in the next 24 h.
Results: Thirty-nine of 40 enrolled men submitted 706 surveys (5–31 each). Twenty-two percent of all surveys included reports of anal or oral sex in the past 24 h (Table 1). Most men reporting anal sex had only one partner (87%) and knew their last partner for more than one month (83%). Fifteen men reported anal sex only once and with one male partner, and four never reported sex during the 4-week study. Four men had sex with a female partner (1 anal and oral, 3 oral only); the participant reporting anal sex never reported sex with a male. From the 548 surveys where men reported no sex, less than 10% had plans to have sex or use an app to look for sex in the next 24 h.
Conclusion: Most men in this sample reported low sexual frequency in EMA surveys, and they typically had only one partner whom they knew. The findings may be limited by varying participant responsiveness to the surveys. Nevertheless, these pilot data give important insights on how to use EMA in combination with more conventional longitudinal data to better understand sexual behaviors and syphilis risk.
| Individual surveys with reported behavior | Participants ever reporting each behaviorA | ||||
|---|---|---|---|---|---|
| n | % | n | % | ||
| In the last 24 h: | n = 706 | n = 39 | |||
| Had anal and oral sex | 62 | 9 | 23 | 59 | |
| Had anal sex only | 16 | 2 | 7 | 18 | |
| Had oral sex only | 79 | 1 | 29 | 74 | |
| Did not have anal or oral sex | 548 | 7 | 38 | 97 | |
| Had anal sex only or anal and oral sex | n = 78 | n = 23 | |||
| Num. male partners last 24 h | |||||
| 0 | 4 | 5 | 1 | 4 | |
| 1 | 61 | 78 | 20 | 87 | |
| 2 | 10 | 13 | 5 | 22 | |
| 3 | 2 | 3 | 1 | 4 | |
| 6+ | 1 | 1 | 1 | 4 | |
| Num. female partners last 24 h | |||||
| 0 | 4 | 5 | 22 | 96 | |
| 1 | 74 | 95 | 1 | 4 | |
| Last partner: where first met | |||||
| Website or mobile app | 25 | 31 | 14 | 61 | |
| Public or private setting | 21 | 27 | 8 | 35 | |
| At work or through friends | 22 | 28 | 9 | 39 | |
| Other or don’t know | 10 | 13 | 4 | 17 | |
| Last partner: how long known | |||||
| Just met when had sex | 9 | 12 | 6 | 26 | |
| Less than 1 month | 5 | 6 | 4 | 17 | |
| More than 1 month | 64 | 82 | 19 | 83 | |
| Had oral sex only | n = 79 | n = 29 | |||
| Num. male partners last 24 h | |||||
| 0 | 20 | 25 | 4 | 14 | |
| 1 | 56 | 71 | 25 | 86 | |
| 2 | 3 | 4 | 3 | 10 | |
| Num. female partners last 24 h | |||||
| 0 | 58 | 73 | 25 | 86 | |
| 1 | 20 | 25 | 3 | 10 | |
| 2 | 1 | 1 | 1 | 3 | |
| Last partner: where first met | |||||
| Website or mobile app | 47 | 59 | 15 | 52 | |
| Public or private setting | 12 | 15 | 8 | 28 | |
| At work or through friends | 16 | 20 | 11 | 38 | |
| Other or don’t know | 4 | 5 | 3 | 10 | |
| In the next 24: | n = 548 | n = 38 | |||
| Plan to have anal or oral sex | 36 | 7 | 22 | 58 | |
| Plan to use an app to look for sex | 40 | 7 | 17 | 45 | |
PP02.41 – Examining the Relationship Between Sociodemographic Variables and Sexually Transmitted Infections: A Cross-Sectional Study in the All of Us Research Program
Dr. Germysha Little1, Ben Cooper1, Dr Hilary Reno1
1Washington University, St. Louis, United States.
Introduction: The NIH All of Us Research Program has enrolled over 849,000 participants across the U.S. with 80% of participants from underrepresented groups in biomedical research providing unique opportunities. Sexually transmitted infections (STIs) remain high and disparities in infection rates persist. The purpose of this study was to examine the relationship between sociodemographic characteristics and STIs in a diverse health dataset.
Methods: This study utilized data from 791,573 participants in the All of Us Research Program with electronic health record data to determine the relationship between sociodemographic variables and STIs (HIV, syphilis, gonorrhea, and chlamydia). Chi-square tests were completed using R.
Results: Among the participants, 2% had been diagnosed with HIV at some point in their lifetime, while 2% had experienced a syphilis infection, 1% a gonorrhea infection, and 1% a chlamydia infection. Participants diagnosed with chlamydia or gonorrhea were more likely to be between the ages of 30 and 34, non-Hispanic, Black, and female while CDC data indicates that 48% of STIs are in 15- to 24-year-olds. Participants diagnosed with syphilis were more likely to be over 65, non-Hispanic, Black, and male. Participants diagnosed with HIV were more likely to be between the ages of 55–64, non-Hispanic, Black, and male. Over 50% of all cases of chlamydia, gonorrhea, HIV, and syphilis were among non-Hispanic Black persons, a departure from CDC data reports less than 33%.
Conclusion: Disparities in STIs remain significant, but previously available public datasets may not capture the scope of the issue. The All of Us Research Program addresses this gap by recruiting from populations often underrepresented in biomedical research. This dataset should be used in STI research to advance efforts to enable equitable approaches to care. Through the collection of diverse data the program aims to provide a more comprehensive understanding of individuals affected by STIs.
PP02.42 – Associations Between Extreme Weather Events and Resource Insecurities with HIV and STI Vulnerabilities Among Adolescent Girls and Young Women in Nairobi and Kisumu, Kenya
Dr. Carmen Logie1, Dr. Zerihun Admassu1, Ms. Aryssa Hasham1, Mr. Humphres Evelia2, Dr. Julia Kagunda3, Ms. Beldine Omondi2, Ms. Clara Gachoki3, Ms. Mercy Chege3, Dr. Lesley Gittings4, Dr. Caetano Dorea5, Dr. Lawrence Mbuagbaw6
1University of Toronto, Toronto, Canada.
2Centre for the Study of Adolescence, Nairobi, Kenya.
3Elim Trust, Nairobi, Kenya.
4University of Western Ontario, London, Canada.
5University of Victoria, Victoria, Canada.
6McMaster University, Hamilton, Canada.
Background: There is increased focus on relationships between extreme weather events (EWE) and HIV vulnerabilities, yet this is understudied with climate-affected adolescent girls and young women (AGWY). We examined associations between EWE, resource insecurities, and HIV vulnerabilities among AGWY in Nairobi and Kisumu, Kenya.
Methods: We collected cross-sectional data (April–June 2024) with a purposive sample of AGYW aged 16–24 in Nairobi and Kisumu. We conducted linear and logistic regression with backward stepwise methods to examine associations between socio-demographics, resource insecurities (food, water, sanitation), and EWE (past-year EWE types and frequency, ecoanxiety) with HIV vulnerabilities (past 12-month transactional sex; past 12-month intimate partner violence [IPV]; sexual relationship power [SRP]; pre-exposure prophylaxis [PrEP] awareness, use, and acceptability).
Results: Among participants (n = 597; mean age: 20.13 years; standard deviation: [SD] = 2.5), half (51.9%) reported 2–4 past 12-month EWE, one-third (31.8%) >5, and 16.2% one. In adjusted analyses, results include: sanitation insecurity (adjusted odds ratio [AOR] = 1.02, 95% confidence interval [CI]: 1.01–1.04) and water insecurity (AOR: 2.26, 95% CI: 1.51–3.39) were associated with increased transactional sex odds. Increased past-year EWE types (>5 vs 1) (AOR = 1.76, 95% CI: 1.08–2.88) and eco-anxiety (aβ = 1.05, 95% CI: 1.02–1.08) were associated with higher IPV odds. Sanitation insecurity (AOR = 0.97, 95% CI: 0.95–0.99) and EWE frequency (>1 vs 1) (AOR = 0.32, 95% CI: 0.11–0.91) were associated with reduced, and water insecurity with increased (AOR: 1.84, 95% CI: 1.11–3.06), PrEP awareness. Sanitation insecurity (AOR: 10.2, 95% CI: 1.00–1.03) and EWE frequency (>1 vs 1) (AOR: 3.64, 95% CI: 1.16–11.43) were associated with PrEP acceptability. Food insecurity (aβ = −0.14, 95% CI: –0.27, –0.01), sanitation insecurity (aβ = –0.08, 95% CI: –0.16, –0.02), and EWE frequency (>5 vs 1) (aβ = –3.52, 95% CI: –5.32, –1.72), were associated with reduced SRP.
Conclusion: Resource scarcities and EWE were associated with HIV vulnerabilities as well as PrEP acceptability among AGYW. Future climate-informed HIV prevention research can integrate EWE and resource insecurity-related priorities.
| Variables | Transactional sex | PrEP awareness | Lifetime PrEP use | PrEP acceptability | SRP | Recent IPV | |
|---|---|---|---|---|---|---|---|
| Adjusted OR (95% CI) | Adjusted OR (95% CI) | Adjusted OR (95% CI) | Adjusted OR (95% CI) | Adjusted β (95% CI) | Adjusted OR (95% CI) | ||
| Socioeconomic factors | |||||||
| Age 20–25 (ref = 16–19) | 0.88 (0.56, 1.39) | 2.28 (1.26, 4.12)** | 2.61 (1.43, 4.76)** | 1.94 (1.23,3.06)** | –0.56 (–2.50, 1.39) | 1.04 (0.64, 1.69) | |
| Educational level (ref < secondary) | |||||||
| Secondary school or higher | 2.19 (1.21, 3.98)* | 1.23 (0.74, 2.05) | 1.22 (0.76, 1.95) | ||||
| Employment (ref = Employed full or part-time) | |||||||
| Unemployed/student | 0.66 (0.37, 1.15) | 0.59 (0.27, 1.31) | 0.48 (0.26, 0.90)* | 0.90 (0.47, 1.74) | –0.68 (–3.08, 1.71) | 0.64 (0.32, 1.28) | |
| Relationship status (ref = No current partner) | |||||||
| Married | 0.80 (0.42, 1.52) | 0.33 (0.16, 0.65)** | 1.12 (0.49, 2.59) | 2.42 (0.18, 4.65)* | |||
| Dating | 2.09 (1.43, 3.05)** | 1.39 (0.79, 2.44) | 1.50 (0.90, 2.48) | 0.21 (–1.67, 2.10) | |||
| Casual dating/multiple | 6.58 (1.34, 32.36)* | 3.12 (0.92, 10.53) | –2.75 (–8.07, 2.56) | ||||
| Young parenthood (yes vs no) | 1.55 (1.05, 2.28)* | 3.17 (1.80, 5.57)** | 1.77 (1.10, 2.83)* | –4.92 (–6.71, –3.12)** | 1.69 (1.10, 2.60)* | ||
| Weather-related events | |||||||
| Number of extreme weather types experienced last year (ref = 1) | |||||||
| 2 to 4 | 0.60 (0.34, 1.09) | 1.52 (0.57, 4.08) | 0.85 (0.51, 1.41) | 0.67 (–3.15, 4.50) | 0.80 (0.44, 1.45) | ||
| 5+ | 0.67 (0.33, 1.33) | 1.12 (037, 3.34) | –3.52 (–5.32, –1.72)** | 1.76 (1.08, 2.88)* | |||
| Frequency of extreme weather events last year (ref = 1 type of weather event, once in last year) | |||||||
| 1 type of weather, >once in last year | 2.77 (0.78, 9.81) | 3.42 (0.96, 12.16) | –0.51 (–5.05, 4.02) | ||||
| >1-type, all only once in the last year | 0.32 (0.11, 0.91)* | 3.13 (0.71, 13.71) | –1.65 (–5.64, 2.34) | ||||
| >1-type, at least 1 occurred more than once in last year | 3.64 (1.16, 11.43)* | ||||||
| Eco-anxiety | 1.02 (0.99, 1.04) | 1.02 (0.99,1.06) | 1.02 (0.99, 1.05) | 1.01 (0.98, 1.04) | 0.03 (–0.08, 0.15) | 1.05 (1.02, 1.08)** | |
| Resource insecurities | |||||||
| Food insecurity | 1.03 (0.99, 1.07) | 1.02 (0.98, 1.07) | 1.03 (0.99, 1.07) | 1.00 (0.97, 1.04) | –0.14 (–0.27, –0.01)* | 1.02 (0.98,1.06) | |
| Water insecurity | 2.26 (1.51, 3.39)** | 1.84 (1.11, 3.06)* | 1.05 (0.64,1.74) | –1.09 (–2.99, 0.80) | 1.04 (0.64, 1.67) | ||
| Sanitation insecurity | 1.02 (1.01,1.04)** | 0.97 (0.95, 0.99)** | 1.02 (1.00, 1.03)* | –0.08 (–0.16, –0.02)* | 1.01 (0.99, 1.02) | ||
Note: OR, odds ratio; CI, confidence interval; PrEP, pre-exposure prophylaxis; SRP, sexual relationship power; recent IPV, intimate partner violence in the past 12 months. Variables with P < 0.2 in bivariate analysis and participants location were included in the initial multivariate model. Final model selection used backward stepwise regression with P < 0.05. (*P < 0.05, **P < 0.01 in multivariate).
PP02.43 – Changes in Traditional Risk Factors for Cardiovascular Diseases in People Living with HIV in Tanzania Using LS7
Dr. Gloria James Manyangu1,2, Safah Khan Khan3, Dr. Robert Peck2,4,5
1Bugando Medical Centre, Mwanza, Tanzania.
2Catholic University of Health and Allied Sciences, Mwanza, Tanzania.
3Weill Cornell Medical College, Qatar, Qatar.
4Weill Cornell Medicine, New York, United States.
5Center of Global Health, New York, United States.
Background: Since the wide coverage of antiretroviral therapy (ART) globally, people living with HIV (PLWH) are living longer and are faced with non-AIDS related comorbidities such as cardiovascular diseases (CVD). We sought to understand the changes in cardiovascular health (CVH) profiles among PLWH after 5 years of ART compared to HIV-negative adults using the American Heart Association’s Life’s Simple 7 (LS7) to guide primary prevention efforts.
Methods: A cross-sectional analysis was conducted using the HTN& HIV datasets with PLWH and HIV-negative adults recruited from 2015 to 2021 in HIV clinics in Mwanza, Tanzania. Participants were screened every 3 months at the study sites. Modified Life’s Simple 7 (LS7) definitions were applied to the cohorts. Difference in Difference model were employed to investigate associations between HIV status and each individual LS7 metric.
Results: A total of 402 adult PLWH and 430 HIV-negative adults were included in the analysis with a median age of 39 (IQR 32, 46) years. Women accounted for 70% and 44% of participants had overall ideal CVH (>4 total ideal). At baseline, the prevalence of ideal body mass index (75.6%, P = 0.002), blood pressure (56.3%, P < 0.001), and total cholesterol (76%, P < 0.001) were higher among PLWH than HIV-negative. However, after 5 years of ART, the prevalence of ideal blood pressure (56.47%, P = 0.005) and physical inactivity (37.31%, P < 0.001) was higher among PLWH than HIV-negative. The positive and statistically significant coefficient for time (Coefficient: 0.349, P = 0.001) suggests that total LS7 scores increased over time across all participants, with an average increase of about 0.35 points from baseline to the later period (Fig. 1).
Conclusion: PLWH’s CVH profiles significantly changed following the use of ART. Our results suggest the need for primary prevention strategies such as weight management. Future research should investigate how to integrate cardiovascular primary prevention in HIV clinics.
Ilustrates the average LS7 scores at baseline and endling for both the HIV-positive and HIV-negative groups.
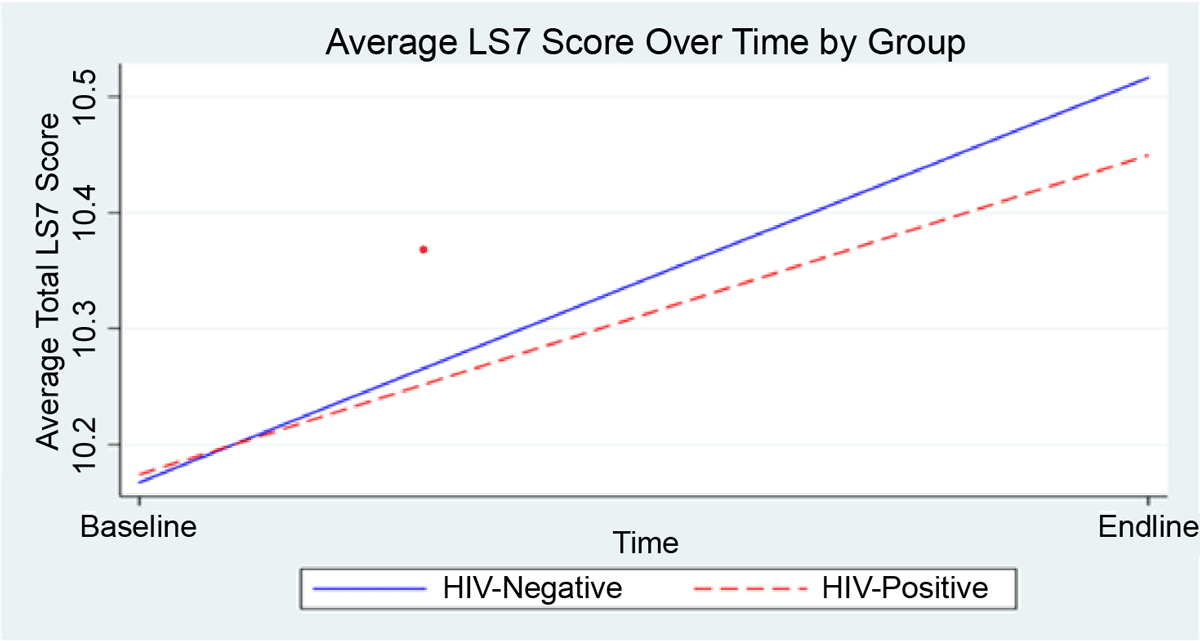
PP02.44 – Pay-It-Forward Gonorrhea and Chlamydia Testing: A Sequential Mixed Method Rct Among Men in China
Dr. Gifty Marley1, Dr Rayner Tan1,2, Ms Ye Liu1, Ms Zixuan Zhu1, Ms Ke Zhou1, Dr Lan Li1, Prof Kurt Gray3, Dr Dan Wu5, Prof David Van Duin3, Prof Roman Xu4, Dr Rohit Ramaswamy6, Dr Laura Forastiere7, Ms Camille Liu3, Mr Thomas Fitzpatrick8, Dr Weiming Tang1,3, Prof Joseph Tucker1,3,9
1UNC - Project China, Guangzhou, China.
2National University of Singapore, University Town, Singapore.
3University of North Carolina at Chapel Hill, Chapel Hill, USA.
4Southern Medical Uinversity, Guangzhou, China.
5Nanjing Medical University, Nanjing, China.
6Cincinnati Children’s Hospital Medical Center, Cincinnati, USA.
7Yale University, New Haven, USA.
8University of Washington, Seattle, UK.
9London School of Hygiene and Tropical Medicine, UK.
Background: Gonorrhea and chlamydia testing is underfunded and has poor community engagement among men. Pay-it-forward offers STD testing as a gift and peer messages to encourage testing and an opportunity to donate. This study evaluates the effectiveness of a pay-it-forward strategy to improve chlamydia/gonorrhoea test uptake among men compared to standard-of-care.
Methods: PIONEER is a cluster randomized controlled trial (NCT05723263) evaluating a pay-it-forward strategy (a donated free test accompanied by personalized messages) to promote chlamydia/gonorrhoea testing among men in China. This sequential mixed methods approach analysed quantitative data from the RCT and qualitative data from semi-structured interviews with participants and healthcare providers. We recruited men ≥18 years old who had not tested for gonorrhoea in the last 12 months and were seeking STD services at community-led or public STD clinics. Chi-square test and GEE analyses compared test uptake between the two arms, followed by a thematic analysis of the qualitative data.
Results: From October 2023 to June 2024, we recruited 1200 men into the standard-of-care (n = 400) and pay-it-forward (n = 800) arms. Mean age was 35 years (±12.16 S.D) and 51.8% (n = 621) ever had sex with other men. Chlamydia/gonorrhea testing uptake was 94%(751/800) in the pay-it-forward arm and 3% (12/400) in the standard-of-care arm [adjusted probability difference = 9%1, 95% CI = 90–92]. Among pay-it-forward recipients,19% (156/800) donated money, and 10% (87/800) wrote personalized messages encouraging testing and/or donations. Qualitative findings showed that “feeling cared for and loved” and “gratitude toward donors” were motivators for testing while “warm glow” and “needing to pragmatically help other men in the same community” motivated donation among interviewed participants. Comparatively, “not feeling at risk of infection” and “test cost being too high” were the main reasons for not testing.
Conclusion: A pay-it-forward strategy increased STD test uptake. These data suggest that prosocial health services and emotional cues from community engagement may increase testing uptake.
PP02.45 – Sliding into Socials to Stop the Spread of STIs: Using Social Media Channels in South Africa to Reach Young People with Information and Linkage to Care for STI Management
Ms. Elmari Briedenhann1, Ms. Nakita Sheobalak1, Dr. Catherine Martin1, Prof Saiqa Mullick1
1Wits RHI, Johannesburg, South Africa.
Background: Sexually transmitted infections among young people remain unacceptably high. Condom use is inconsistent, barriers to healthcare access remain, and low awareness about STIs is still prevalent. Using social media platforms focused on comprehensive HIV prevention information sharing in South Africa, we aimed to provide accurate, youth-friendly information about STIs to young people.
Description: The MyPrEP South Africa social media channels on Facebook (since 2018) and Instagram (since 2019) are designed in collaboration with technical experts, the National Department of Health and youth from three provinces in South Africa, and share an average of four posts per week covering a range of HIV prevention topics. The focus is on generating reach and facilitating engagement to support information sharing and linkage to services; selected posts are boosted through paid advertising to optimise reach and engagement with the target audience. We conducted a descriptive analysis of posts relating to STIs between May and October 2024. STI-specific posts were defined as such if they mentioned STIs, STI screening, or condom use. We describe the unique user reach (users who see a post) and engagement (users interacting with content through comments, reactions, WhatsApp chats, shares, clicks).
Results: Between May and October 2024, 163 (total) posts were shared on Instagram and Facebook, 36/163 (22%) related to STIs. Overall, STI-related posts reached 524,973 (14,583 average per post) and engaged (total) 5,481, of which 964/5,481 (17.6%) resulted in WhatsApp chats with a trained, project staff member. These WhatsApp chats either resulted in private information sharing or linkage of a young person to their closest STI screening service.
Conclusion: Social media provides a platform to inform and engage young people on STI management. Ensuring users can ask further questions through an individual online chat, such as WhatsApp, is important in providing additional information, support and linkage to care.
PP02.46 – Examining the Effects of Art Duration on the Choice of Multi-Month Drug Dispensing Model Amongst HIV Positive Children and Adolescents in Eswatini
Mr. Themba Matsebula1
1Young Heroes Organisation, Hhohho, Eswatini.
Background: The Sub-Saharan Africa region is the world has the greatest number of people eligible to receive antiretroviral treatment (ART). Multi-month dispensing (MMD) of antiretroviral treatment (ART) aims to reduce patient-related barriers to access long-term treatment and improve health system efficiency. In Eswatini however, few children and adolescents are on MMD. Young Heroes is implementing an HIV program that aims to avert new HIV infections in children and youth and improve treatment outcomes for children and adolescents living with HIV (C/ALHIV: 0–19 Years).
Objectives: To ascertain factors that are associated with the assignment of MMD model on C/ALHIVs.
Description: The project provides treatment adherence support through well trained community cadres (HVs) at both community and health facility levels. During door-to-door, HVs track all C/ALHIV enrolled in the project monthly and refer any who might have interrupted treatment. C/ALHIV with unsuppressed viral load are supported through case conferencing and teen clubs. A quantitative cross-sectional analysis was conducted using STATA for children and adolescents living with HIV enrolled in the project from January 2024 to December 2024.
Results: Data for 4011 C/ALHIV (0–19 Years) was analyzed in STATA. Results show a strong association between (duration on ART, Age, being in teen club) and enrolment in an MMD model. Duration on ART is a major predictor for the choice of MMD model at (95% CI: 0.0012905–0.0039812; P = <0.0001). C/ALHIV who have been on ART for less than a year are less likely to be on MMD. C/ALHIVs who are 1 or years on ART are more likely to be in 3 months dispensation while those who are 5 years are most likely to be in 6 months model.
Conclusion: The more number of years on ART, the mostly likely to be put on a upper MMD model.
PP02.47 – Predictors of Treatment Interruption Among Patients on Antiretroviral Therapy from an HIV Prevention Program in Eswatini
Mr. Themba Matsebula1
1Young Heroes Organisation, Hhohho, Eswatini.
Background: The Sub-Saharan Africa region is the world has the greatest number of people eligible to receive antiretroviral treatment (ART). Consistency on antiretroviral therapy (ART) remains the most effective intervention in the global HIV response. Understanding the factors associated with interrupting antiretroviral therapy (ART) is therefore critical for designing client-centered services to ensure optimal outcomes. Young Heroes is implementing an HIV program that aims to avert new HIV infections in children and youth and improve treatment outcomes for children and adolescents living with HIV (C/ALHIV: 0–19 Years) with HIV prevention and impact mitigation interventions that prevents new HIV infections and reduce vulnerability.
Aim: To assess predictors of treatment interruption amongst Sabelo Sensha enrolled CALHIVs in Eswatini.
Description: The project provides treatment adherence support through well trained community cadres (HVs) at both community and health facility levels. HVs track all C/ALHIV enrolled in the project monthly and refer any who might have stopped or interrupted treatment. We reviewed records of HIV-positive patients aged ≥19 years who are on ART since January to 31 December 2024. We determined treatment status over 12 months as either active, or interrupted treatment. Potential predictors of interruption were assessed using regression models.
Results: Overall, 1597 patients were on ART and 329 (20%) patients had ART interruptions. Retention at 1, 3, 6, 9, and 12 months was 87%, 83%, 79%, 76%, and 69%, respectively. From regression analysis, refiling in rural areas (P = 0.003), being an older CALHIV (15–17 years) (P < 0.005), and residing outside the clinic catchment area (P = 0.02) were major contributors of treatment interruption.
Conclusion: Treatment interruption was common amongst the CALHIVs but can be improved by focusing on supporting elder CALHIVs (15+ years), CALHIV refiling in rural areas and providing client-centred HIV services for those who live further from clinics
PP02.48 – An Evaluation of Factors Associated with Completing an HIV Testing Linkage Amongst Adolescent Girls at Risk of HIV Acquisition in Eswatini
Mr. Themba Matsebula1
1Young Heroes Organisation, Hhohho, Eswatini.
Background: Eswatini has a high HIV rate compared to any other Southern Africa country. Even though the country have achieved much, it still records new HIV infections more especially amongst young women aged 25–29 years. This calls for more efficient and effective ways to reach, diagnose and link them to HIV care. Sabelo Sensha project implemented by Young Heroes Organization supports the government of Eswatini to prevent new HIV infections and reducing the HIV vulnerabilities among adolescent girls (AGYW).
Objectives: 1) To ascertain the factors associated with completing an HIV testing service referral amongst adolescent girls at HIV risk.
Description: A quantitative cross-sectional data analysis was conducted for December 2023–December 2024 implementation period. Trained Mentors identify AGYWs in their communities and provide enrolment consents where an HIV risk assessment is administered. AGYW found to be at HIV risk (sexual intercourse under the influence of alcohol, sexual abuse exposure, STI experience, having multiple sexual partners and transactional sex) acquisition are referred for HIV testing and linkage services.
Results: About 5,001 AGYW took part in a HIV risk assessment, 26% (1,301/5,001) had never tested for HIV whilst 74% (3,700/5,001) have had an HIV test before. Of the 5,001 AGYW, 28% (1,411/5,001) were at risk of contracting HIV. Out of the AGYW at risk, 51% (738/1,411) were referred for HIV testing and 31% (231/738) completed HTS referral. From regression analysis, AGYW with STIs experience were most likely complete HIV testing and linkage services (AOR = 0.62; 95% CI = 0.52, 0.74) compared to the other HIV risk factors (sexual intercourse under the influence of alcohol, having multiple sexual partners, transactional sex).
Conclusion: Having an STI experience improves chances of HIV services linkages. There is a need for targeted HIV programs to ensure that all AGYW having any other HIV risk factors completes referrals for HTS.
PP02.49 – Assessing the Cost-Effectiveness of Households Visitation on HIV Affected Children’s Health Outcomes in Eswatini
Mr. Themba Matsebula1, Mr Dumisa Thwala
1Young Heroes Organisation, Hhohho, Eswatini.
Background: HIV infection and undernutrition remain significant public health concerns for young children. Proper management of nutrition and related nutrition complications in these groups with increased nutrition needs are prominent challenges in Eswatini. Efforts to improve child health and nutrition status culminated in different strategies being employed, which amongst them is household nutrition support and care. Sabelo Sensha project implemented by Young Heroes Organization supports the government of Eswatini to prevent new HIV infections and reducing the HIV vulnerability for orphans and vulnerable children.
Objective: To measure the effects of Home visitation on Eswatini HIV affected children’s health outcome.
Description: Secondary data analysis of routine data collected from June 2024 to December 2024 within ongoing implementation of Sabelo Sensha project was explored. Trained Home Visitors (HVs) identify vulnerable children, provide consent to identified households for enrollment into the project and provide health education, nutritional screening and support, linkages to clinical and social services. Through phone calls and constant households visitations, caregivers are linked to services as per need and provided health education.
Findings: June 2024 about 7396 children less than 5 years were assessed by HVs where 1970 (27%) were malnourished, in which 70 of 294 (24%) were malnourished HIV positive children. The cohort received monthly HIV and nutrition education and support and linkages to care from HVs. Over a 6 month period the number of malnourished children decreased by 15%, and after a year about 53% (1052/1970) of the young children in the intervention showed an acceptable weight-for-age and faster catch-up growth.
Conclusion: Home visitation by HVs is an effective strategy that improves development and health outcomes for malnourished children. There is a need for future studies to determine the intensity of the intervention required to generate long-lasting benefits.
PP02.50 – Assessing the Concurrent Use of Herbal Concoctions and Antiretroviral Therapy Among Persons Living with HIV/AIDS in Tamale, Ghana
Mr. Haris Sualah Musah1, Dr (PhD) Osman Adamu Dufailu2, Mrs. Alimatu-Sadia Mohammed3
1University For Development Studies, Tamale, Ghana.
2University of Greenwich, Medway, United Kingdom.
3Tamale Teaching Hospital, Tamale, Ghana.
Background: In 2023, Ghana had over 330,000 HIV/AIDS patients, while deaths due to the disease were approximately 11,000. Herbal treatment of diseases, though primordial, remains a significant source of medication for many Ghanaians. The increasing burden of HIV/AIDS in lower-income countries may have driven the use or simultaneous use of herbal concoctions and antiretroviral (ART) drugs. The interactions of herbal concoctions with ART medications can affect the effectiveness of the latter, thus, the overall health of HIV/AIDS patients. The concurrent use of herbal concoctions may lead to non-adherence to ART drugs, which can occasion treatment failures and drug-resistant HIV strains. This research aimed to assess the simultaneous use of herbal and ART medications among HIV/AIDS persons in Tamale, Ghana.
Methods: The study employed a cross-sectional design to collect and analyse data from 120 HIV/AIDS patients attending sexually transmitted infections (STI) clinics in Tamale. The questionnaire was self-administered or assisted, ensuring strict confidentiality. The questions focused on the prevalence of combined use of herbal concoctions and ART drugs as well as influencing factors, including sociocultural reasoning.
Results: Preliminary findings from 53 respondents indicate that 47% still combine herbal treatment with ART therapy, 21% had prior usage, and 32% never used. Of the patients using herbal treatment, the primary reasons included perceived synergistic effects (34%), improving overall health 32%), mitigating adverse effects associated with ART drugs (30%) and others (4%). All respondents using herbal treatment with ART have not disclosed their practice to their physicians. Approximately 64 % of herbal treatment respondents are unsure of its effectiveness.
Conclusion: Although the study is expected to be concluded by February 5, tentative data highlights the challenges of managing HIV/AIDS in Ghana. It also prompts further studies to evaluate the clinical outcomes of patients on ART therapy in Ghana to avert probable complications.
SURVEY QUESTIONNAIRE TO ASSESS THE CONCURRENT USE OF HERBAL AND ANTIRETROVIRAL THERAPY AMONG PERSONS LIVING WITH HIV/AIDS IN TAMALE, GHANA.
This form has been designed to collect data from persons living with HIV/AIDS to assess their use or otherwise of herbal concoctions with antiretroviral (ART) drugs. This questionnaire is particularly interested in your honest responses to these questions; thus, no traceable information about you or your family will be required. Your honest responses will contribute to the knowledge of herbal and ART combined usage in Tamale.
The survey is also interested in any experiences and observations you might provide.
I would greatly appreciate it if you could spend about 3 minutes responding to these questions. Thank you.
Kindly tick against the appropriate option applicable.
Section 1: Demographics
1. Age:
- 18–24
- 25–34
- 35–44
- 45–54
- 55 and above
2. Gender:
- Male
- Female
3. Educational Level:
- No formal education
- Primary school
- Secondary school
- Tertiary education
- Other (please specify)
4. Duration of HIV Diagnosis:
- Less than 1 year
- 1–5 years
- 6–10 years
- More than 10 years
Section 2: ART Usage
5. Are you currently on antiretroviral therapy (ART)?
- Yes
- No
6. If yes, which ART medications are you taking? (Select all that apply)
- Tenofovir Disoproxil Fumarate (TDF)
- Abacavir Disoproxil Fumarate (ADF)
- Emtricitabine (FTC)
- Other (please specify)
Section 3: Herbal Treatment Usage
7. Do you use herbal treatments in addition to your ART medications?
- Yes
- No
8. If yes, how often do you use herbal treatments?
- Daily
- Weekly
- Monthly
- Occasionally
9. Which herbal treatments do you use? (Select all that apply)
- Traditional herbal concoctions
- Herbal capsules or tablets
- Herbal teas
- Other (please specify)
10. Why do you use herbal treatments? (Select all that apply)
- To enhance the effectiveness of ART
- To manage the side effects of ART
- Cultural or traditional beliefs
- Personal preference
- Recommendations from others
- Other (please specify)
Section 4: Perception of Herbal Treatments
11. How effective do you believe herbal treatments are in managing HIV/AIDS?
- Very effective
- Somewhat effective
- Not effective
- Not sure
12. Do you believe there are any risks associated with using herbal treatments alongside ART?
- Yes
- No
- Not sure
13. If yes, what risks do you believe are associated with using herbal treatments alongside ART? (Select all that apply)
- Reduced effectiveness of ART
- Adverse side effects
- Interactions with ART medications
- Other (please specify)
14. How comfortable do you feel discussing your use of herbal treatments with your healthcare provider?
- Very comfortable
- Somewhat comfortable
- Not comfortable
- Not sure
Section 5: Symptoms of Complications
15. Have you experienced any symptoms or complications since combining herbal treatments with ART? (Select all that apply)
- Nausea or vomiting
- Diarrhea
- Fatigue
- Jaundice (yellowing of the skin or eyes)
- Abdominal pain
- Skin rashes
- Other (please specify):
16. If yes, which treatment do you believe is the cause?
- ART drug
- Herbal treatment
- Not sure
Section 6: Cultural Influences
17. How important are cultural or traditional beliefs in your decision to use herbal treatments?
- Very important
- Somewhat important
- Not important
- Not sure
18. Do you consult with traditional healers while using herbal treatments?
- Yes
- No
- Sometimes
19. How do you perceive the advice of traditional healers compared to modern healthcare providers?
- More trustworthy
- Equally trustworthy
- Less trustworthy
- Not sure
20. Have you experienced any cultural or family pressures to use or not use herbal treatments?
- Yes, to use
- Yes, not to use
- No
- Not sure
21. How do you balance the use of traditional and modern treatments for HIV/AIDS?
- Primarily traditional treatments
- Primarily modern treatments
- Both equally
- Not sure
Section 7: Sources of Information
22. Where do you get information about herbal treatments? (Select all that apply)
- Healthcare providers
- Friends or family
- Traditional healers
- Internet or social media
- Books or pamphlets
- Other (please specify)
Section 8: Suggestions and Comments
23. What suggestions do you have for improving information and guidance on using herbal treatments with ART?
- ___________________________________________________________
24. Do you have any additional comments or experiences you would like to share about using herbal treatments with ART?
- ___________________________________________________________
PP02.51 – Female Sex Workers’ Leadership in Addressing PrEP Continuation Barriers in Kilifi County – A Case Study of ICRH-Kenya
Mr. Simon Mwangi1, Ms Marion Asike1, Mr. David M Muchiri1, Dr. Dismas Congo1
1Icrhk, Nairobi, Kenya.
Background: Despite the proven efficacy of oral pre-exposure prophylaxis (PrEP) in reducing HIV transmission among high-risk individuals, low continuation rates remain a significant challenge among female sex workers. While PrEP holds immense potential for ending the HIV epidemic, its effectiveness relies on successful integration with community-centered approaches. We developed innovative, community-driven interventions to address the barriers to PrEP continuation and ensure equitable access to PrEP for all sex workers attending our Mtwapa drop in centre.
Methods: Female sex workers receiving services at Mtwapa drop in centre took charge by forming voluntary, hotspot-based community PrEP groups to improve oral PrEP uptake. Capped at 20 members, these groups met on shared refill dates, offering peer support, health education (focused on PrEP), comprehensive clinical services (STI treatment, TB screening, etc.), and tailored counseling. This proactive approach aimed to scale up and retain FSWs on PrEP, empowering them to lead the fight against HIV.
Results: Between January and April 2024, 12 community oral PrEP groups for female sex workers were established at hotspot locations to address barriers and improve PrEP continuation rates. Prior to the intervention, PrEP refill rates at the Mtwapa Drop-In Centre were alarmingly low. From January to April 2023, month one refills were 39%, 45%, 40%, and 61%, while month three refills were even lower at 33%, 8%, 26%, and 29%. Following the intervention, month one refill rates improved significantly, rising to 90%, 51%, 69%, and 89%, while month three refill rates increased to 94%, 52%, 73%, and 32% for the same months in 2024.
Conclusion: The power of peer support, as sex workers have become champions in raising awareness, reminding each other about refills, and demystifying myths surrounding PrEP and HIV. This community-driven initiative proves that empowering sex workers can lead to a sustainable fight against HIV.
PP02.52 – The Impact of Integrated Mental Health Services on ART Uptake and Viral Suppression Among Transgender Persons in Mombasa, Kenya, During Anti-LGBTQ Campaigns: A Case Study of ICRH
Mr. Simon Mwangi1, Mr David Muchiri1, Ms Millicent Okello1, Mr Mathew Ogutu1, Ms. Aurelia Vose1, Ms. Pamphillas Samia1, Dr. Susan Ontiri1, Dr. Dismas Ouma1
1International Centre for Reproductive Health, Kenya.
Background: In Kenya, transgender persons encounter significant mental health challenges that impede their access to HIV prevention and treatment services. The objective of this study is to determine the impact of mental health services on the uptake of ART and the achievement of HIV viral suppression among Transgenders.
Methods: The Kenya Supreme Court ruling in March 2023 granting the LGBTQIA+ community the right of association sparked a wave of homophobic protests and anti-LGBTQIA+ agitation in Mombasa. At the height of anti- rights anti- gender demonstration, ICRH implemented Peer Mental Health Support and conducted interpersonal group therapy (IPT) for transgender persons living with HIV. 10 sessions were done for 55 TG who exhibited high levels of distress based on the Patient Health Questionnaire (PHQ4 and 9) screening. TG scoring 3 or higher on the PHQ-4, or those scoring 10 or higher on the PHQ-9, were grouped into the IIPT sessions. IPT is a therapeutic approach that aims to alleviate symptoms of depression by enhancing interpersonal relationships and social functioning.
Results: A retrospective analysis of the program data revealed that, despite the mental health challenges faced by marginalized sexual minorities during the anti-LGBTQ campaigns in Kenya, ICRHK successfully sustained high ART uptake and viral suppression. 96% of transgender individuals (n = 53/55) who received mental health support adhered to ART and achieved 100% viral suppression. (VL < 200 copies/mL). There was 0% missed appointment. This was an improvement comparing the same period in 2022 where Viral load uptake was at 42% and a suppression rate of 89%.
Conclusion: This case study provides evidence that integrating mental health services into HIV care and treatment is essential for success. Providing mental health interventions for transgender individuals has led to enhanced coping strategies for the challenges affecting their HIV care, resulting in improved treatment outcomes.
PP02.53 – Factors Associated with Late Presentation to Care Among People Living with HIV: A Qualitative Comparative Analysis of Men Who Have Sex with Men and Heterosexuals in Singapore
Ritu Jain1,2, Wen Zhi Ng3, Pin Zhong Chan3, Rayner Kay Jin Tan3
1School of Humanities, Nanyang Technological University, Singapore.
2Lee Kong Chian School of Medicine, Nanyang Technological University, Singapore.
3Saw Swee Hock School of Public Health, National University of Singapore, Singapore.
Background: Early detection of HIV, initiation of antiretroviral therapy, and achieving viral suppression are key to ending onward transmission of HIV. This study evaluates the narratives of late-presenting People Living with HIV(PLHIV) to identify factors associated with late presentation to care for HIV.
Methods: Semi-structured interviews were conducted with 32 late-presenting PLHIV (15 men who have sex with men [MSM], 14 heterosexual men, and 3 heterosexual women; CD4 <200 at diagnosis) and 17 stakeholders including healthcare professionals between July 2021 and January 2022. Participants were recruited through community group networks and a specialist outpatient HIV clinic. Thematic analysis was conducted to identify themes across MSM and heterosexual PLHIV.
Results: Denial emerged as a common theme but was rooted in distinct experiences and manifested in different ways among MSM and heterosexual participants. Heterosexual participants exhibited a denial of HIV-related risk when discussing their own sexual histories. This denial is rooted in a general lack of knowledge on HIV, its transmission mechanisms, and misconceptions around which one’s susceptibility to HIV is based on one’s heterosexual identity. In contrast, while HIV knowledge was more prevalent among MSM, denial manifested in avoidance of testing to maintain one’s ignorance of being at risk of, or the possibility of having acquired HIV. The absence of knowledge of their HIV status or their risk was construed as a different form of denial that facilitated avoidance of an HIV identity and associated discrimination. One common theme across both groups was the idea of fatalism - that one had no future living with HIV, therefore refusing to get tested in hopes of delaying the perceived inevitable fallout.
Conclusion: While there are similar barriers to testing between late-presenting heterosexual individuals and MSM, there were clear differences in the type of denial associated with testing behaviours, which will allow for meaningful and targeted intervention.
PP02.54 – HIV Prevalence Among High School Teenagers in Anambra State, Nigeria: A Cross-Sectional Design
Ms. Josephine Ita Okon1
1University of Port Harcourt, Port Harcourt, Nigeria.
Background: The human immunodeficiency virus (HIV) remains a major public health concern worldwide, and Nigeria is one of the countries with the highest burden of HIV infections. Adolescent populations are particularly vulnerable to HIV due to a combination of factors, including limited access to sexual education and healthcare services. This abstract focuses on the prevalence of HIV among high school teenagers in Anambra State, Nigeria.
Methods: The study utilized a cross-sectional design, and a total of 500 high school students from various schools in Anambra State were randomly selected to participate in the study. Data were collected using a pretested structured questionnaire and analyzed using descriptive and inferential statistics.
Results: The findings revealed that the prevalence of HIV among high school teenagers in Anambra State was 2.4%. Furthermore, the study found that the level of knowledge about HIV transmission and prevention was generally low among the participants, with only 41.2% of the respondents reporting that they had ever received HIV education.
Conclusion: These findings underscore the urgent need for targeted interventions aimed at improving HIV education and prevention among high school teenagers in Anambra State. Such interventions could include the incorporation of comprehensive sexual education into the school curriculum and the provision of youth-friendly healthcare services that prioritize HIV prevention and treatment. By implementing these measures, it may be possible to reduce the burden of HIV among high school teenagers in Anambra State and ultimately contribute to the overall control of the HIV epidemic in Nigeria.
PP02.55 – Preferences and Willingness to Use Pre-Exposure Prophylaxis for HIV Among Men Who Have Sex with Men in Mainland China and Hong Kong
Mr. Jiajun Sun1,2, Prof. Dr. Jason Ong1,2,3, Dr. Heather-Marie Schmidt4,5, Mr. Curtis Chan6, Dr. Benjamin Bavinton6, Dr. Kimberly Green7, Dr. Nittaya Phanuphak8,9, Dr. Midnight Poonkasetwattana10, Dr. Nicky Suwandi11, Dr. Doug Fraser6, Dr. Weiming Tang12, Dr. Michael Cassell13, Dr. Hua Boonyapisomparn11, Dr. Edmond Choi14, Dr. Lei Zhang1,2, Miss Warittha Tieosapjaroen1,2
1School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Melbourne, Australia.
2Melbourne Sexual Health Centre, Melbourne, Australia.
3Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, United Kingdom.
4Joint United Nations Programme on HIV/AIDS (UNAIDS), Geneva, Switzerland.
5World Health Organization, Geneva, Switzerland.
6Kirby Institute, University of New South Wales, Sydney, Australia.
7PATH, Hanoi, Vietnam.
8Institute of HIV Research and Innovation (IHRI), Bangkok, Thailand.
9Centre of Excellence in Transgender Health (CETH), Chulalongkorn University, Bangkok, Thailand.
10Asia Pacific Coalition on Male Sexual Health (APCOM), Bangkok, Switzerland.
11Asia Pacific Transgender Network, Thailand.
12The University of North Carolina at Chapel Hill Project-China, Guangzhou, China.
13Family Health International (FHI) 360, North Carolina, United States.
14School of Nursing, LKS Faculty of Medicine, The University of Hong Kong, Hong Kong, China.
Background: Pre-exposure prophylaxis (PrEP) uptake remains low in mainland China and Hong Kong. We examined preferences for different PrEP modalities among men who have sex with men (MSM) in mainland China and Hong Kong.
Methods: We conducted a cross-sectional online survey from May to November 2022 in mainland China and Hong Kong. Eligible participants were aged ≥18 years, identified as MSM and self-reported HIV-negative or unknown. Random forest models and SHAP (SHapley Additive exPlanations) analysis were used to identify key factors influencing preferences for six PrEP options: daily oral, on-demand oral, monthly oral, 2-monthly injectable, 6-monthly injectable, and implant PrEP (Fig. 1).
Results: Among 2,142 participants, the mean age was 28.4 (±7.0) years in mainland China and 34.7 (±9.5) years in Hong Kong. Current PrEP use was similar between mainland China and Hong Kong (18.0% vs 17.8%, P = 0.93), with an additional 10.5% and 8.0% reporting past PrEP use (P = 0.11), respectively. Oral PrEP options were most preferred. A greater proportion of participants from mainland China preferred on-demand PrEP compared to those from Hong Kong (55.7% vs 48.1%, P < 0.01), while more participants from Hong Kong preferred monthly oral PrEP (53.2% vs 47.3%, P = 0.02) (Figs 2–8). Willingness to use non-oral options was lower, with 2-monthly injectable PrEP preferred by 21.1% (19.1%–23.1%) in mainland China and 15.4% (12.3%–18.5%) in Hong Kong (P < 0.01). Among Hong Kong participants, condom use frequency and migration status were important predictors of willingness to use both oral and injectable PrEP options. Peer influence played a more significant role for Chinese participants. Current PrEP use status and initial PrEP attitudes were consistently important predictors. Individuals who preferred 6-monthly injectable PrEP tended to dislike the two-monthly option (Tables 1–4).
Conclusion: While oral PrEP remains the preferred choice among MSM in both mainland China and Hong Kong, factors influencing PrEP preferences differ between mainland China and Hong Kong.
Radar and bar charts comparing preferences for different PrEP options in Mainland China and Hong Kong. *PrEP: Pre-Exposure Prophylaxis.
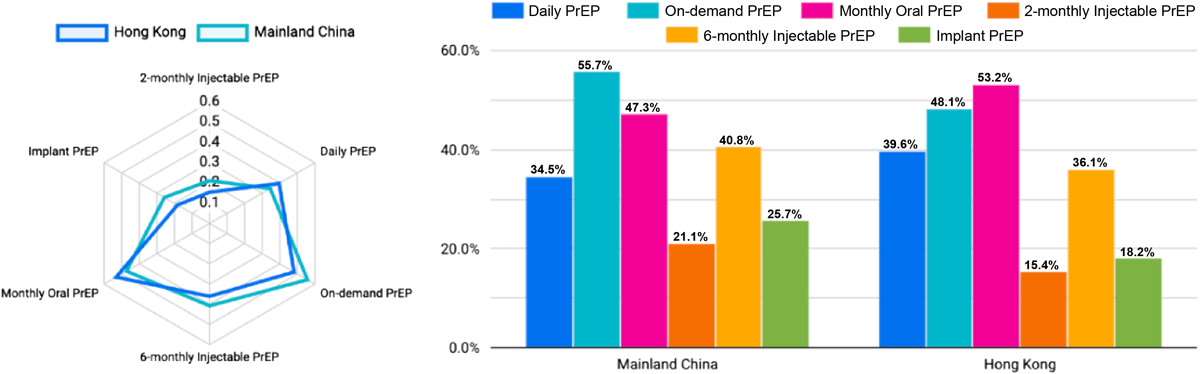
| Mainland China | Hong Kong | ||||
|---|---|---|---|---|---|
| n | % | n | % | ||
| Age | Mean 28.4 | SD 7.0 | Mean 34.7 | SD 9.5 | |
| Sex at birth | |||||
| Male | 1604 | 100.0 | 537 | 99.8 | |
| Female | 0 | 0.0 | 1 | 0.2 | |
| Sexual identity | |||||
| Gay or homosexual | 1302 | 81.2 | 451 | 83.8 | |
| Bisexual or pansexual | 230 | 14.3 | 76 | 14.1 | |
| Heterosexual or straight | 17 | 1.1 | 1 | 0.2 | |
| I don’t usually use a term | 45 | 2.8 | 8 | 1.5 | |
| I use a different term | 10 | 0.6 | 2 | 0.4 | |
| Education level | |||||
| No schooling | 2 | 0.1 | 0 | 0.0 | |
| Primary/Elementary school | 3 | 0.2 | 0 | 0.0 | |
| Junior high school | 20 | 1.2 | 9 | 1.7 | |
| Senior high school | 125 | 7.8 | 79 | 14.7 | |
| Diploma/trade/vocational certificate | 141 | 8.8 | 97 | 18.0 | |
| Undergraduate degree | 982 | 61.2 | 206 | 38.3 | |
| Postgraduate degree | 316 | 19.7 | 145 | 27.0 | |
| Missing | 15 | 0.9 | 2 | 0.4 | |
| Employment | |||||
| Full time | 1076 | 67.1 | 407 | 75.7 | |
| Part time | 92 | 5.7 | 42 | 7.8 | |
| Unemployed | 107 | 6.7 | 26 | 4.8 | |
| Student | 309 | 19.3 | 51 | 9.5 | |
| Retired | 3 | 0.2 | 6 | 1.1 | |
| Other | 13 | 0.8 | 5 | 0.9 | |
| Missing | 4 | 0.2 | 1 | 0.2 | |
| PrEP awareness and use | |||||
| Never heard of PrEP | 64 | 4.0 | 20 | 3.7 | |
| Heard of PrEP but never used PrEP | 1009 | 62.9 | 358 | 66.5 | |
| Used in the past but not currently | 168 | 10.5 | 43 | 8.0 | |
| Currently using PrEP | 289 | 18.0 | 96 | 17.8 | |
| Missing | 74 | 4.6 | 21 | 3.9 | |
| Chemsex in the last 6 months | |||||
| No sexual partner | 1162 | 72.4 | 430 | 79.9 | |
| No chemsex | 359 | 22.4 | 85 | 15.8 | |
| Had chemsex | 78 | 4.9 | 22 | 4.1 | |
| Missing | 5 | 0.3 | 1 | 0.2 | |
| STI diagnosis in the last 6 months | |||||
| No | 1525 | 95.1 | 504 | 93.7 | |
| Yes | 77 | 4.8 | 34 | 6.3 | |
| Missing | 2 | 0.1 | 0 | 0.0 | |
| Involvement in commercial sex in the last 6 months | |||||
| No | 1521 | 94.8 | 523 | 97.2 | |
| Yes | 82 | 5.1 | 15 | 2.8 | |
| Missing | 1 | 0.1 | 0 | 0.0 | |
| Sexual partner in the last 6 months | |||||
| Single | 149 | 9.3 | 44 | 8.2 | |
| One partner | 510 | 31.8 | 92 | 17.1 | |
| Multiple partners | 945 | 58.9 | 402 | 74.7 | |
| Condomless anal sex in the last 6 months | |||||
| No sex | 275 | 17.1 | 99 | 18.4 | |
| Always used condoms | 644 | 40.1 | 140 | 26.0 | |
| Not always used condoms | 684 | 42.6 | 298 | 55.4 | |
| Missing | 1 | 0.1 | 1 | 0.2 | |
| Sharing injecting equipment in the last 6 months | |||||
| Not injecting drugs | 1531 | 95.4 | 497 | 92.4 | |
| Injecting drug without sharing equipment | 69 | 4.3 | 40 | 7.4 | |
| Injecting drug and sharing equipment | 2 | 0.1 | 1 | 0.2 | |
| Missing | 2 | 0.1 | 0 | 0.0 | |
SD, standard deviation; PrEP, pre-exposure prophylaxis; STI, sexually transmitted infection.
| Definition | Type | Description | |
|---|---|---|---|
| Age | Continuous | ||
| Comfortable discussing PrEP with healthcare worker | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Discrimination by healthcare providers | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Prefer discussing with MSM healthcare worker | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Concern about PrEP-hormone interaction | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Disclosure to healthcare providers | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Worried about the side effects of PrEP | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Taken PrEP to prevent getting HIV. | Continuous | The values range from 1 to 5, indicating a scale from “Strongly disagree” to “Strongly Agree.” | |
| Anal sex condom use frequency (6 months) | Continuous | The values range from 1 to 5, indicating a scale from “I did not have anal sex with any casual partners” to “Always used condoms.” | |
| Vaginal sex condom use frequency (6 months) | Continuous | The values range from 1 to 5, indicating a scale from “I did not have vaginal sex with any casual partners” to “Always used condoms.” | |
| Chemsex drug use frequency (6 months) | Continuous | The values range from 1 to 3, indicating a scale from “Never” to “Often” | |
| Number of sexual partners (6 months) | Continuous | The values range from 1 to 7, representing a scale from “None” to “More than 50.” | |
| Education | Continuous | The values range from 1 to 7, representing a scale from “No schooling” to “Postgraduate degree.” | |
| Number of LGBTQ+ friends | Continuous | The values range from 1 to 5, indicating a scale from “None” to “All.” | |
| Time spent with LGBTQ+ friends | Continuous | The values range from 1 to 5, indicating a scale from “None” to “All.” | |
| Last time of HIV test | Continuous | The values range from 1 to 7, indicating a scale from “I have never had an HIV test” to “More than 5 years ago.” | |
| Proportion of friends currently taking PrEP | Continuous | Replace “don’t know” as N/A. The values range from 1 to 7, indicating a scale from “None” to “All.” | |
| Residence | Continuous | The values range from smallest to largest, representing a gradient from the capital city to the countryside. | |
| Place of birth | Categorical | 13 categories | |
| Employment | Categorical | 6 categories | |
| Gender identity | Categorical | 5 categories | |
| Heard 2 months PrEP | Categorical | Yes/No/Don’t know | |
| Heard daily PrEP | Categorical | Yes/No/Don’t know | |
| Heard on-demand PrEP | Categorical | Yes/No/Don’t know | |
| Heard of PrEP | Categorical | Yes/No/Don’t know | |
| Type of currently take PrEP | Categorical | Daily/On-demand/Others PrEP | |
| Friends have positive attitude toward PrEP | Categorical | Yes/No/Don’t know | |
| Currently taking PrEP | Categorical | Yes/Temporarily stop/Permanently stop | |
| Sexual orientation | Categorical | 5 categories | |
| HIV status | Categorical | negative/don’t know/not to say | |
| Source for PrEP pills/prescription | Categorical | Combine from where prep tgw (for TGW) and where prep msm (for MSM), 10 categories | |
| Born in the current country | Binary | Yes/No | |
| STI diagnosis (excluding HIV) (6 months) | Binary | Yes/No | |
| Injected drug use frequency (6 months) | Binary | Yes/No | |
| Like to take PrEP but have not | Binary | Yes/No | |
| Exchanged sex for money/gifts (6 months) | Binary | Yes/No | |
| In a romantic relationship | Binary | Yes/No | |
| Sex with men (last 6 months) | Binary | Yes/No | |
| Sex with non-binary/gender queer (last 6 months) | Binary | Yes/No | |
| Sex with transgender men (last 6 months) | Binary | Yes/No | |
| Sex with transgender women (last 6 months) | Binary | Yes/No | |
| Sex with women (last 6 months) | Binary | Yes/No | |
| Gender at birth | Binary | Male/Female | |
| Sex worker | Binary | Yes/No | |
| Shared injecting equipment | Binary | Yes/No | |
| Ever taken PrEP | Binary | Yes/No | |
| Spoken to a doctor about starting PrEP | Binary | Yes/No | |
| Know where and how to get oral PrEP | Binary | Yes/No | |
| Willing to use 2 months PrEP | Binary | Yes/No | |
| Willing to use daily PrEP | Binary | Yes/No | |
| Willing to use on-demand PrEP | Binary | Yes/No | |
| Willing to use 1 year PrEP | Binary | Yes/No | |
| Willing to use monthly PrEP | Binary | Yes/No | |
| No willing to use PrEP | Binary | Yes/No | |
| Willing to use other types of PrEP | Binary | Yes/No | |
| Willing to use 6 months PrEP | Binary | Yes/No | |
| Willing to use monthly vaginal ring | Binary | Yes/No |
TGW, transgender women; MSM, men who have sex with men; PrEP, pre-exposure prophylaxis.
| Coef. | Std.Err. | z | P>|z| | [0.025] | [0.975] | ||
|---|---|---|---|---|---|---|---|
| On-demand PrEP in Mainland China | |||||||
| Currently take on-demand PrEP | 0.355 | 0.109 | 3.245 | 0.001 | 0.141 | 0.569 | |
| Like to take PrEP but have not | 0.362 | 0.079 | 4.605 | 0 | 0.208 | 0.516 | |
| Education | 0.098 | 0.036 | 2.714 | 0.007 | 0.027 | 0.168 | |
| Age | −0.019 | 0.007 | –2.835 | 0.005 | –0.032 | –0.006 | |
| Willing to use monthly oral PrEP | 0.367 | 0.115 | 3.179 | 0.001 | 0.141 | 0.593 | |
| Heard on-demand PrEP | 0.365 | 0.119 | 3.06 | 0.002 | 0.131 | 0.598 | |
| Daily PrEP in Mainland China | |||||||
| const | 0.957 | 0.428 | 2.236 | 0.025 | 0.118 | 1.796 | |
| Heard daily PrEP | 1.064 | 0.166 | 6.423 | 0 | 0.739 | 1.388 | |
| Willing to use 6-monthly injectable PrEP | −0.469 | 0.139 | –3.369 | 0.001 | –0.743 | –0.196 | |
| Worried about the side effects of PrEP | −0.246 | 0.054 | –4.583 | 0 | –0.352 | –0.141 | |
| PrEP from online | −0.414 | 0.195 | –2.122 | 0.034 | –0.796 | –0.032 | |
| Age | −0.046 | 0.01 | –4.796 | 0 | –0.064 | –0.027 | |
| Willing to use implant PrEP | –0.42 | 0.152 | –2.752 | 0.006 | –0.719 | –0.121 | |
| Number of LGBTQ+ friends | −0.173 | 0.074 | –2.352 | 0.019 | –0.318 | −0.029 | |
| Willing to use monthly oral PrEP | 0.293 | 0.127 | 2.301 | 0.021 | 0.043 | 0.543 | |
| Number of sexual partners (6 months) | 0.184 | 0.061 | 3.025 | 0.002 | 0.065 | 0.303 | |
| PrEP from a friend or sex partner | 0.606 | 0.248 | 2.448 | 0.014 | 0.121 | 1.092 | |
| Monthly Oral PrEP in Mainland China | |||||||
| const | −1.301 | 0.366 | –3.551 | 0 | –2.019 | –0.583 | |
| Willing to use 6-monthly injectable PrEP | 0.355 | 0.128 | 2.771 | 0.006 | 0.104 | 0.605 | |
| Vaginal sex condom use frequency (6 months) | −0.104 | 0.036 | –2.915 | 0.004 | –0.175 | –0.034 | |
| Willing to use 2-monthly injectable PrEP | 0.551 | 0.155 | 3.544 | 0 | 0.246 | 0.856 | |
| Taken PrEP to prevent getting HIV | 0.114 | 0.058 | 1.982 | 0.047 | 0.001 | 0.227 | |
| Prefer discussing with MSM healthcare worker | 0.095 | 0.048 | 2.005 | 0.045 | 0.002 | 0.189 | |
| Willing to use on-demand PrEP | 0.3 | 0.119 | 2.519 | 0.012 | 0.067 | 0.533 | |
| Number of LGBTQ+ friends | 0.148 | 0.068 | 2.178 | 0.029 | 0.015 | 0.282 | |
| PrEP from Hospital | 0.359 | 0.124 | 2.895 | 0.004 | 0.116 | 0.602 | |
| Like to take PrEP but have not | 0.324 | 0.095 | 3.407 | 0.001 | 0.138 | 0.511 | |
| 2-monthly Injectable PrEP in Mainland China | |||||||
| const | −4.784 | 0.59 | –8.104 | 0 | –5.941 | –3.627 | |
| Willing to use 6-monthly injectable PrEP | 1.429 | 0.169 | 8.444 | 0 | 1.098 | 1.761 | |
| Willing to use implant PrEP | 0.796 | 0.166 | 4.802 | 0 | 0.471 | 1.121 | |
| Willing to use monthly oral PrEP | 0.554 | 0.159 | 3.494 | 0 | 0.243 | 0.865 | |
| PrEP from a friend or sex partner | 0.586 | 0.145 | 4.045 | 0 | 0.302 | 0.87 | |
| Taken PrEP to prevent getting HIV. | 0.18 | 0.085 | 2.126 | 0.034 | 0.014 | 0.345 | |
| Comfortable discussing PrEP with healthcare worker | 0.172 | 0.074 | 2.32 | 0.02 | 0.027 | 0.317 | |
| Place of birth (Taiwan) | −0.902 | 0.382 | –2.361 | 0.018 | –1.651 | –0.153 | |
| Willing to use daily PrEP | 0.686 | 0.163 | 4.212 | 0 | 0.367 | 1.005 | |
| 6-monthly Injectable PrEP in Mainland China | |||||||
| const | −1.372 | 0.468 | –2.932 | 0.003 | –2.29 | –0.455 | |
| Willing to use implant PrEP | 1.054 | 0.148 | 7.139 | 0 | 0.765 | 1.343 | |
| Willing to use 2-monthly injectable PrEP | 1.432 | 0.169 | 8.468 | 0 | 1.101 | 1.763 | |
| Taken PrEP to prevent getting HIV. | 0.171 | 0.067 | 2.547 | 0.011 | 0.039 | 0.302 | |
| Place of birth (Mainland China) | 0.802 | 0.27 | 2.968 | 0.003 | 0.272 | 1.332 | |
| Willing to use monthly oral PrEP | 0.403 | 0.133 | 3.037 | 0.002 | 0.143 | 0.664 | |
| Willing to use daily PrEP | −0.652 | 0.145 | –4.491 | 0 | –0.937 | –0.368 | |
| Comfortable discussing PrEP with healthcare worker | 0.155 | 0.058 | 2.695 | 0.007 | 0.042 | 0.268 | |
| Vaginal sex condom use frequency (6 months) | −0.115 | 0.04 | –2.85 | 0.004 | –0.194 | –0.036 | |
| PrEP from Hospital | 0.339 | 0.104 | 3.267 | 0.001 | 0.136 | 0.543 | |
| Number of sexual partners (6 months) | 0.127 | 0.063 | 2.032 | 0.042 | 0.005 | 0.25 | |
| Implant PrEP in Mainland China | |||||||
| const | −2.325 | 0.245 | –9.506 | 0 | –2.805 | –1.846 | |
| Willing to use 6-monthly injectable PrEP | 1.056 | 0.144 | 7.339 | 0 | 0.774 | 1.338 | |
| Willing to use 2-monthly injectable PrEP | 0.775 | 0.161 | 4.819 | 0 | 0.46 | 1.09 | |
| Willing to use daily PrEP | –0.506 | 0.151 | –3.341 | 0.001 | –0.802 | –0.209 | |
| Comfortable discussing PrEP with healthcare worker | 0.157 | 0.06 | 2.625 | 0.009 | 0.04 | 0.274 | |
| Friends have positive attitude toward PrEP | 0.301 | 0.134 | 2.248 | 0.025 | 0.039 | 0.563 |
| Coef. | Std.Err. | z | P>|z| | [0.025] | [0.975] | ||
|---|---|---|---|---|---|---|---|
| On-demand PrEP in Hong Kong | |||||||
| Currently take on-demand PrEP | 2.363 | 0.541 | 4.37 | 0 | 1.303 | 3.423 | |
| Like to take PrEP but have not | 0.435 | 0.156 | 2.779 | 0.005 | 0.128 | 0.741 | |
| Age | –0.029 | 0.008 | –3.799 | 0 | –0.043 | –0.014 | |
| PrEP from online | 0.588 | 0.29 | 2.028 | 0.043 | 0.02 | 1.157 | |
| Currently take other PrEP types | –3.682 | 0.77 | –4.785 | 0 | –5.19 | –2.174 | |
| Daily PrEP in Hong Kong | |||||||
| PrEP from online | 0.565 | 0.174 | 3.256 | 0.001 | 0.225 | 0.905 | |
| Worried about the side effects of PrEP | –0.242 | 0.082 | –2.956 | 0.003 | –0.403 | –0.082 | |
| Place of birth (Mainland China) | –0.397 | 0.149 | –2.669 | 0.008 | –0.689 | –0.106 | |
| Taken PrEP to prevent getting HIV | 0.135 | 0.068 | 1.991 | 0.046 | 0.002 | 0.269 | |
| Monthly oral PrEP in Hong Kong | |||||||
| const | –1.875 | 0.673 | –2.788 | 0.005 | –3.194 | –0.557 | |
| Vaginal sex condom use frequency (6 months) | –0.219 | 0.068 | –3.21 | 0.001 | –0.353 | –0.085 | |
| Like to take PrEP but have not | 0.381 | 0.123 | 3.09 | 0.002 | 0.139 | 0.622 | |
| Taken PrEP to prevent getting HIV | 0.212 | 0.096 | 2.198 | 0.028 | 0.023 | 0.401 | |
| Education | 0.216 | 0.09 | 2.391 | 0.017 | 0.039 | 0.392 | |
| Proportion of friends currently taking PrEP | 0.156 | 0.065 | 2.398 | 0.016 | 0.029 | 0.284 | |
| Willing to use 2-monthly injectable PrEP | 0.921 | 0.314 | 2.931 | 0.003 | 0.305 | 1.538 | |
| 2-monthly injectable PrEP in Hong Kong | |||||||
| const | –4.157 | 0.928 | –4.48 | 0 | –5.976 | –2.339 | |
| Willing to use 6-monthly injectable PrEP | 2.232 | 0.362 | 6.159 | 0 | 1.521 | 2.942 | |
| Willing to use implant PrEP | 1.205 | 0.344 | 3.498 | 0 | 0.53 | 1.88 | |
| Willing to use monthly oral PrEP | 0.903 | 0.349 | 2.584 | 0.01 | 0.218 | 1.587 | |
| Age | –0.055 | 0.018 | –3.033 | 0.002 | –0.09 | –0.019 | |
| Disclosure to healthcare providers | 0.387 | 0.129 | 2.989 | 0.003 | 0.133 | 0.64 | |
| Discrimination by healthcare providers | 0.374 | 0.15 | 2.485 | 0.013 | 0.079 | 0.668 | |
| 6-monthly injectable PrEP in Hong Kong | |||||||
| const | –3.424 | 0.613 | –5.581 | 0 | –4.626 | –2.221 | |
| Willing to use 2-monthly injectable PrEP | 2.593 | 0.36 | 7.212 | 0 | 1.888 | 3.297 | |
| Age | 0.046 | 0.012 | 3.762 | 0 | 0.022 | 0.07 | |
| Vaginal sex condom use frequency (6 months) | –0.228 | 0.08 | –2.861 | 0.004 | –0.383 | –0.072 | |
| Number of LGBTQ+ friends | 0.345 | 0.127 | 2.716 | 0.007 | 0.096 | 0.593 | |
| Proportion of friends currently taking PrEP | 0.183 | 0.073 | 2.508 | 0.012 | 0.04 | 0.327 | |
| Implant PrEP in Hong Kong | |||||||
| const | –1.387 | 0.228 | –6.091 | 0 | –1.833 | –0.941 | |
| Willing to use 2-monthly injectable PrEP | 1.624 | 0.3 | 5.417 | 0 | 1.037 | 2.212 | |
| Vaginal sex condom use frequency (6 months) | –0.292 | 0.104 | –2.797 | 0.005 | –0.497 | –0.087 |
PP02.56 – Overseas-Born Trans and Gender Diverse People’s Experiences with the Australian Sexual Health Services: A Qualitative Study
Mx. Budi Sudarto1, Dr Eric PF Chow1,2,3, Dr Tiffany R Phillips1,2, Prof. Dr. Jason Ong1,2,4
1School of Translational Medicine, Faculty of Medicine, Nursing, and Health Sciences, Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Melbourne, Australia.
3Melbourne School of Population and Global Health, University of Melbourne, Melbourne, Australia.
4London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: Overseas-born trans and gender diverse people is an often-overlooked population in Australia’s HIV and other sexually transmitted infection (STI) prevention strategy, treatment, and care. They faced an intersecting unique challenges, including limited gender-affirming resources, fear of multiple forms of discrimination by health professionals, limited income and concern of costs. These could result in delaying access to HIV and other STI test, treatment, and care. This study aimed to investigate their experiences with sexual health services in Australia.
Methods: An in-depth, semi-structured qualitative interview was conducted between July 2024 and November 2024. We were guided by the social-ecological model and conducted a reflexive thematic analysis to interpret the data.
Results: 11 participants were involved in the study, with the majority (n = 8) were in the 30s age group. Participants were born in Southeast Asia, South Asia, South America, and Western Europe. All participants reported mixed experiences with sexual health services. Some participants shared positive experiences, such as being addressed by their pronouns, and practitioners referring to their body using words that they were comfortable with (e.g., ‘front hole’, ‘bonus hole’). Others, however, had negative experiences, such as practitioners making assumptions about their sexual identity and the gender/s of their sexual partners, referring to their body using medical terms, and not providing adequate sexual health information specific to their gender identity. Nearly all participants recommended a standardised gender-affirming care training for all sexual health professionals to ensure safety and accessibility.
Conclusion: Education about the specific circumstances and health needs of overseas-born trans and gender diverse people is needed to ensure gender-affirming and anti-discriminatory sexual health services in Australia. We recommend a strong commitment from the relevant regulatory bodies, such as the Australian Health Practitioner Regulation Agency, to make such a training compulsory based on the human rights principle of health for all.
PP02.57 – Virtual Avatars for Enhancing Human Immunodeficiency Virus Prevention Access and Education Among MSM of Color: Service Provider Perceptions
Mr. Gilbert Orta Portillo1, Dr. Joseph Daniels2, Dr. Kelika Konda1, Dr. Jeffrey Klausner1,3, Dr. Jesse Fletcher4
1Keck School of Medicine of the University of Southern California, Department of Population and Public Health Sciences, Los Angeles, United States.
2Arizona State University, Edson College of Nursing and Health Innovation, Tempe, United States.
3Keck School of Medicine of the University of Southern California, Department of Medicine, Los Angeles, United States.
4Friends Research Inc., Baltimore, United States.
Background: HIV pre-exposure prophylaxis (PrEP) uptake is lower among men who have sex with men (MSM) of color compared to their white counterparts in the United States. Common barriers to PrEP access include stigma, limited awareness, and lack of trust or familiarity with healthcare contexts. User-controlled avatars may help overcome these barriers by increasing feelings of privacy and safety, potentially facilitating engagement with HIV prevention services.
Methods: We developed a web-based interactive PrEP experience (e.g., museum-style exhibit featuring PrEP infotainment, sex-positive messaging, and HIV stigma art), to educate MSM of color about PrEP, explored via avatars. This was demonstrated over three iterations to staff from three HIV service providers in Los Angeles County (Feb–Mar 2024). After the demonstrations, we conducted three focus groups (N = 32 participants) and a Stakeholder Advisory Board meeting (N = 13 participants). After obtaining verbal consent, all communications were audio-recorded, transcribed via Sonix transcription services, and analyzed using inductive coding to assess feasibility and identify software preferences.
Results: The 45 participants (58% male, 49% Hispanic/Latinx, 62% gay, 56% aged 25–34) reported they felt the Avatar platform was feasible for helping users learn about HIV prevention and offering personalized services, such as role-playing to practice skills (e.g., sharing and discussing personal information) (Table 1). Providers suggested improvements, including enhanced security features (e.g., clearing history and enabling ‘trigger’ words for emergency situations) and emphasized the need for human interaction in certain contexts, such as receiving diagnoses or finding peer support. Logistical barriers to PrEP adoption (e.g., finances, travel) remained a persistent challenge.
Conclusions: Service providers working with MSM of color find avatars a promising tool to engage patients remotely seeking information about HIV prevention services. This approach could improve engagement and access to PrEP, though further improvements are needed in areas such as security and human interaction.
| N (%) or median | ||
|---|---|---|
| Age (years) | ||
| 18–24 | 6 (13%) | |
| 25–34 | 25 (56%) | |
| 35–44 | 12 (27%) | |
| 45 or older | 2 (4%) | |
| Gender identity | ||
| Man | 21 (47%) | |
| Non-binary | 11 (24%) | |
| Trans woman | 7 (16%) | |
| Woman | 6 (13%) | |
| Racial identity | ||
| Black | 15 (33%) | |
| White | 13 (29%) | |
| Prefer not to say | 8 (18%) | |
| Multiracial/other | 6 (13%) | |
| American Indian/Alaskan Native | 3 (7%) | |
| Ethnic identity | ||
| Hispanic/Latinx-Identified | 22 (49%) | |
| Sexual orientation | ||
| Gay | 28 (62%) | |
| Heterosexual | 9 (20%) | |
| Bisexual | 6 (13%) | |
| Queer | 2 (4%) | |
| Avatar models of care | ||
| Appropriate | 4 out of 5 | |
| YMC would be comfortable | 4 out of 5 | |
| Engage new YMC | 4 out of 5 | |
| Intuitive | 4 out of 5 | |
| Improve HIV knowledge | 4 out of 5 | |
| Recommend to YMC clients | 5 out of 5 | |
| Exciting potential for HIV services | 5 out of 5 |
PP02.58 – Social Vulnerabilities of Women Living with HIV in Mozambique: An Insight into the Study “Why Art Was Stopped”
Mrs Edna Paunde Xavier1, Dr Aleny Couto1, Dr Irenio Gaspar1
1Moh Mozambique, Maputo, Mozambique.
Background: In Mozambique, although more and more people living with HIV (PLHIV) are successfully undergoing antiretroviral treatment, keeping them on treatment for a long period of time remains a challenge. Women in particular present many challenges due to their social, economic and financial dependence.
Description: in-depth interviews were carried out with 159 patients in six districts with low retention rates in the provinces of Nampula, Zambézia and Maputo City). 105 of these patients had never abandoned treatment, while the remaining 104 had abandoned once or more for more than 3 months and then restarted or never restarted up to the date of the interview. These groups were further divided into four subgroups: men under and over 30 and women under 30 who were pregnant at the time of diagnosis or not.
Results: social situation of women influences adherence to HIV services. Women with abusive partners were very reluctant to disclose their status to their husbands, fearing abandonment and loss of their home and economic status, which resulted in delays in appointments and picking up medication.
Single mothers without secure employment were identified as another group likely to abandon treatment, due to the fact that they have to carry out different tasks, often without any support, they chose to deal with what they consider to be the most urgent, the need to earn money.
All the women whose partners died of an HIV-related illness said they had abandoned treatment at least once, and most of them several times.
Conclusion: Women’s special vulnerabilities are mainly linked to their more precarious economic situation, which is a result of the unbalanced gender roles in the country.
In conclusion, it can be said that women have to face various barriers to treatment, mainly economic or strongly influenced by their lower access to financial resources.
PP02.59 – Psychosocial Support: The Path to Understanding the Needs of Women Living with HIV in Mozambique Context
Mrs Edna Paunde Xavier1, Dr Aleny Couto, Dr Irenio Gaspar1, Mr Fernando Boene1
1Moh Mozambique, Maputo, Mozambique.
2MoH Mozambique, Maputo City, Mozambique.
Background: The impact of HIV in Mozambique is visible in women, with the epidemic in the country being more feminised. According to spectrum data (version 6.36) by December 2023 in Mozambique 60 per cent of people living with HIV are women. In Mozambique 1,470,000 women are living with HIV and of these 125,000, 8.5% are pregnant women. Psychosocial support is an established standard of care for people living with HIV in different age groups, where all people diagnosed positive must be prepared for the start of treatment and during follow-up to achieve viral suppression.
Description: a follow-up flow has been drawn up and standardised which recommends that all pregnant and breastfeeding women living with HIV who are diagnosed in the antenatal clinic or at-risk child clinic, or who arrive at these clinics with the diagnosis, receive psychosocial support according to their needs. At every monthly consultation, pregnant and breastfeeding women should be assessed for risk factors for adherence, asked to consent to calls and visits, offered positive prevention messages and identify forms of support. The maternal and child health nurses at the health centres have been trained tas part of the one-stop shop.
Results: By the end of 2024, 72 per cent of women living with HIV on antiretroviral treatment had received integrated psychosocial support in prenatal consultations for pregnant women and in specific psychosocial support services for non-pregnant women. This follow-up is carried out by different categories of professionals, including counsellors, maternal health nurses, psychologists and general practitioners.
Conclusion: Psychosocial support is therefore an essential tool for women living with HIV, helping them to deal with the emotional, social and psychological challenges. This support not only improves mental and emotional health, but also contributes to adherence to treatment, strengthening autonomy, reducing stigma and improving quality of life.
PP02.60 – Sexual Health for All – a Distant Dream for Women in Rural India
Miss Elizabeth Michael1, Dr. V Sam Prasad1, Mr. Mohnish Kumar1, Mr. Shivam Dwivedi1, Mr. Lyle Honig Mojica2
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
2AIDS Healthcare Foundation (AHF), Los Angeles, United States of America.
Background: Sexually transmitted infections (STIs) disproportionately affect women, particularly in rural India, where social and economic determinants exacerbate vulnerability. Limited access to STI services, stigma, low levels of knowledge, and gender-based violence hinder women’s ability to seek STI prevention, diagnosis, and treatment.
Description: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across ten states. The retrospective study analysed the tests conducted among women 342,217 women between the age of 18–49 years. This was supplemented by in-depth interviews with 36 women and 9 healthcare providers. The study explored the barriers to accessing STI services. During the testing and in-depth interviews, comprehensive awareness of STIs was provided to these women.
Results: The study revealed that the HIV prevalence among these women was 1.3% and over 47.4% of women reported at least one symptom of STI. Out of these 16% have at least one symptom for the last 2 years, while 14.5% have symptoms for less than a year. Almost 76% of women were reluctant and felt ashamed to consult a medical doctor for treatment. 15% of the women consulted a doctor as they were pregnant. Qualitative findings highlighted women’s limited knowledge about STIs, fear of stigma, and experiences of gender-based violence and forced sex.
Conclusion: This study emphasizes the critical need for comprehensive STI prevention and care services tailored to the needs of rural Indian women. The findings indicate the importance of addressing social and economic determinants, stigma, and gender-based violence to reduce women’s vulnerability to STIs. Women’s sexual health is critical in determining the quality of health of the next generation of a nation.
PP02.61 – The Hidden Epidemic: Anal STIs Among Men Who Have Sex with Men (MSM) in India – a Call to Action – Sexual Health for All!
Mr. Shivam Dwivedi1, Dr. V Sam Prasad1, Ms. Elizabeth Michael1, Mr Mohnish Kumar1, Mr Lyle Honig Mojica2
1AIDS Healthcare Foundation (AHF) - India Cares, New Delhi, India.
2AIDS Healthcare Foundation (AHF), California, United States of America.
Background: Men who have sex with men (MSM) in India are disproportionately affected by anal sexually transmitted infections (STIs), which significantly increase the risk of HIV transmission. Despite this, anal STIs remain largely neglected by the community due to reluctance of consulting and get a physical examination by a medical practitioner.
Description: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across ten states. The quantitative study was conducted during the pre and post-test counselling for STI/HIV testing among the men who identified as MSM. The study assessed symptoms of anal STIs, HIV risk behaviors, and healthcare access. Interviews explored the lived experiences of MSM with anal STIs and their perceptions of healthcare services.
Results: The study revealed that 42% of participants reported anal STI symptoms, with 6.1% testing positive for HIV. The Counselling sessions highlighted the stigma, shame, and social isolation associated with anal STIs, leading to delayed healthcare-seeking practices. Over 92% of the participants have managed anal STI symptoms through over-the-counter medicine of which 37% have managed the symptoms through over-the-counter medicines and by visiting quacks multiple times. The major reasons are difficulty in accessing anal STI testing and treatment due to fear of discrimination and ashamed of physical examination by a physician, and fear of others in the community knowing by which they may lose their friends. 56% of the respondents felt that there is a lack of awareness among healthcare providers.
Conclusion: This study underscores the urgent need for targeted interventions addressing anal STIs among MSM in India. Immediate actions are required to scale up community-friendly anal STI testing and treatment, HIV prevention services, and healthcare provider training. Policymakers, healthcare providers, and community organizations must work together to address the social determinants of health and promote inclusive, equitable care for MSM in India.
PP02.62 – Leveraging Social Media to Connect High-Risk Female Sex Workers (FSWs) in Ghana’s Western Region with HIV&AIDS Services
Mrs. Hellen Mawuli Quarshie1, Mr Samuel Elliot Owusu1
1Maritime Life Precious Foundation, Kumasi, Ghana.
Background: Social media has become a prominent platform for communication among female sex workers (FSWs) in Ghana, with many increasingly using it to solicit clients instead of traditional physical hotspots. While Ghana’s national HIV prevention program for key populations typically relies on physical outreach, certain high-risk FSWs especially those engaging in risky sexual behaviors remain underserved. This gap in service delivery highlights the need for a more integrated approach that incorporates social media to enhance outreach, education, and support.
Description: MLPF conducted a rapid assessment to identify the most popular social media platforms used by FSWs for finding sexual clients, including Facebook, Snapchat, Tiktok, and Tinder. Tailored content on HIV prevention, testing, and treatment options was shared across these platforms to raise awareness, reduce stigma, and encourage service uptake. FSWs who engaged with this content were directed to a dedicated landing page on MLPF website, where they could book confidential appointments with healthcare professionals. Participants were also encouraged to visit Drop-In-Centers for in-person services. Data were collected and analyzed, comparing the effectiveness of social media outreach versus physical outreach.
Results: Social-media outreach was more successful in reaching high-risk FSWs than physical outreach. Among FSWs recruited via social media, 57% had never been tested for HIV, compared to 35% reached through physical outreach. 61% of social media recruits reported engaging in unprotected sex with non-paying partners, compared to 46% recruited through physical outreach (Figs 1, 2). Additionally, 2100 FSWs tested for HIV through social media; 370 were diagnosed HIV+ (17.6%). Comparatively, 4960 FSWs tested for HIV through physical outreach; 298 were diagnosed HIV+ (6%).
Conclusions: Social-media has proven effective in reaching high-risk, underserved FSWs and should be integrated into future HIV prevention strategies. Investing in innovative, technology-based approaches is crucial to enhancing HIV prevention and care programs in the changing social and community dynamics.
The data below shows the comparison between Female Sex Workers (FSWs) reached through social media outreach and physical outreach in Ghana.
HIV positivity rate was higher among those tested through social media outreach compared to hotspot outreach.
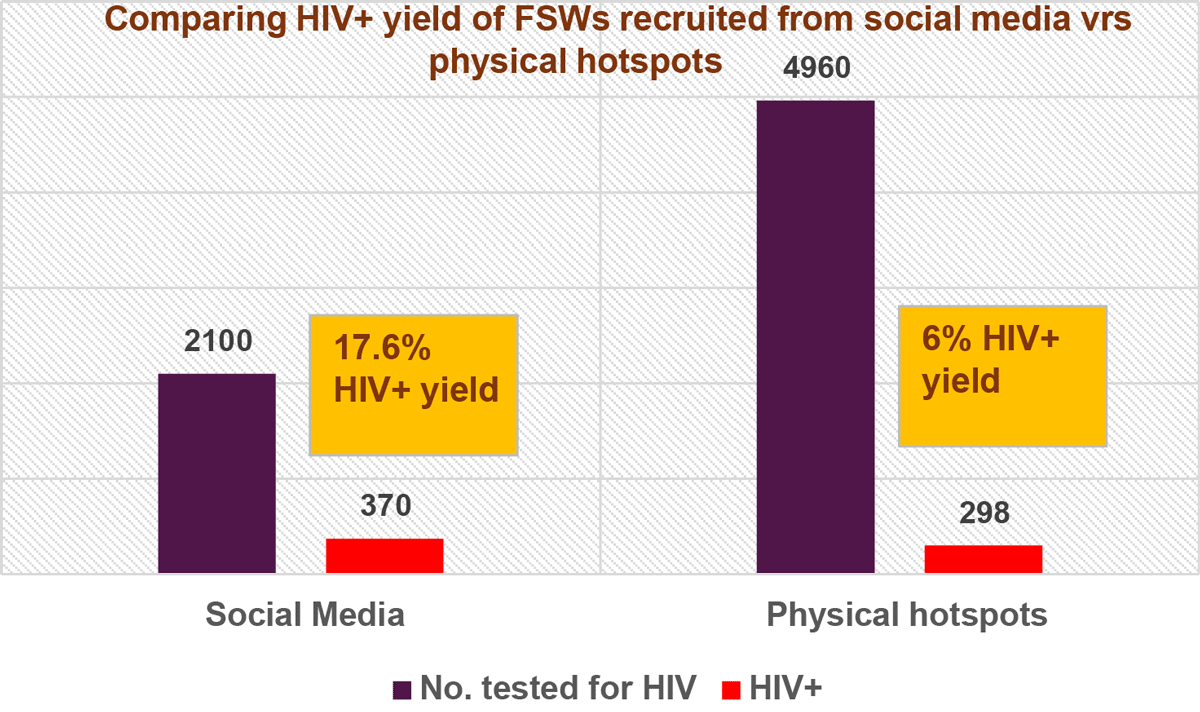
PP02.63 – Perception on HIV and Sexual Behavior: A Cross-Sectional Study Among Future Judges and Lawyers of School of Law of Bhaktapur
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
Background: In 1981, US Center for Disease Control reported a sudden rise in HIV infections among young gay men, which spread globally. Today, HIV is more public health threat in developing countries like Nepal, where it was first reported in 1988 and continues to increase annually.
Methods: This study “Perception on HIV and Sexual Behavior: A cross-sectional study among future Judges and lawyers of School of Law of Bhaktapur, 2024”, has been carried out the cross-sectional study based on the primary data collected through census sampling in school of law. The main objective of the study is to assess the Perception on HIV and Sexual Behavior among Students of School of Law. The sample size was 104 including 45 male and 59 female respondents.
Results: All respondents were found the students among them the 19 to 24 age group of respondents were as more (89.4%). All respondents had heard about HIV and AIDS and Radio/TV and Books/Newspapers were the major source for information. Nearly all respondents considered HIV transmitted through unprotected sexual intercourse with an infected person and 95.2 per cent were known that HIV is preventable. About 96 per cent answered that awareness is the best way to reduce the infection of HIV. And 90.4 per cent of respondents had answered that pre-marital sex is not good.
The respondents were aware of HIV and AIDS but lacked knowledge about transmission and preventive measures. Some had misconceptions about HIV and infected individuals. They were aware of high-risk groups for HIV transmission but needed more knowledge. They also believed pre-marital sex was unsuitable.
Conclusion: The awareness program should be strengthened to address misconceptions about HIV among future judges and lawyers, and teachers should be trained for effective education, and curriculum should include HIV content at college level.
PP02.64 – HIV Prevention and Care: A Comparative Study of Medical Students in the South and Midwest
Mr. Kyle Roe1, Mr. Colton Boney1, Mr. Zachary Montgomery2, Dr. Rahul Garg1, Dr. III R. Wayne Parker1
1Alabama College of Osteopathic Medicine, Dothan, United States.
2Tom and Julie Wood College of Osteopathic Medicine, Indianapolis, United States.
Background: The U.S. Department of Health and Human Services aims to reduce new HIV infections by 90% by 2030. Achieving this goal requires future physicians to be equipped to provide HIV prevention and care, including pre-exposure prophylaxis (PrEP). This study investigates changes in medical student perceptions, attitudes, and preparedness for PrEP and HIV care during their education.
Methods: Medical students in years 1–4 from two U.S. osteopathic medical schools – one in the South and one in the Midwest – completed an anonymous online survey during the Fall 2024 semester. The survey assessed perceptions, comfort levels, and preparedness to care for patients with HIV and those at high risk. Chi-square and Fisher’s Exact Test compared scores across groups; P-values <0.05 were considered significant.
Results: A total of 122 students participated (South: 77 [63%]; Midwest: 45 [37%]). Significant differences were noted across region and training level:
-
Regional Differences: Students in the South reported greater preparedness for PrEP care (P = 0.0019) and overall HIV prevention (P < 0.0001).
-
Training Level: Clinical students were significantly more prepared to integrate PrEP into routine visits (P = 0.0051) and take sexual histories (P = 0.018).
-
Impact of Education: Students with prior HIV/PrEP education showed significantly higher preparedness for HIV prevention (P < 0.0001).
-
Education Adequacy: Students who perceived their education was adequate correlated with increased preparedness (P = 0.0016).
Conclusions: Regional disparities and clinical training influence preparedness for PrEP and HIV prevention. Prior education enhances readiness, but gaps remain in comfort with HIV care. Targeted educational interventions are needed to meet national HIV prevention goals.
PP02.65 – Exploring the Impact of Remote Consultations in Sexual and Reproductive Health Services in England and Wales
Dr. Charlotte Spurway1, Dr Tom Witney2, Professor Fiona Burns2, Professor Louise Jackson1, Prof. Jonathan Ross
1University of Birmingham, Birmingham, United Kingdom.
2University College London, London, United Kingdom.
Background: Recent years have seen substantial reductions in Sexual and Reproductive Health Services (SRHS) funding in England and Wales and an increase in remote (via telephone or video) service delivery. Remote services were critical in maintaining access during COVID-19 pandemic restrictions, however, there remains limited evidence on their impact and how they may address or exacerbate health inequalities. This study aimed to explore the equity, acceptability, and appropriateness of remote sexual health consultations.
Methods: We conducted semi-structured interviews across three case study areas with 51 service users and potential service users and 35 healthcare professionals and other stakeholders. Participants were purposively sampled to ensure diversity in demographics and service experiences. Data were thematically analysed, with findings interpreted collaboratively with public and patient involvement groups.
Results: Provision of remote consultations were sometimes driven by non-clinical considerations, including large local catchment areas, lack of clinical space, and commissioning models that prioritised in-person consultation. Some service users expressed a preference for the trust and reassurance provided by in-person interaction, others preferred the speed and flexibility of online interaction. Remote consultations could improve access for people who face challenges attending a clinic in person, e.g., those with reduced mobility and caregiving responsibilities. However, concerns were raised about accessibility for those with limited internet connectivity, people with English as an additional language, and vulnerable populations. Healthcare professionals noted challenges assessing safeguarding remotely, emphasising the risk of missing information and being unable to assure the privacy and confidentiality of a remote service user’s environment.
Conclusion: This study suggests remote consultations can be acceptable and appropriate, but that their equity is potentially impacted by barriers that disproportionately affect certain groups. Services should balance the convenience of remote consultations with the need for accurate clinical assessment and patient comfort. Diverse service delivery models are crucial to address inequalities.
PP02.66 – Perceptions of HIV Risk and Prevention Among Pregnant and Non-Pregnant Heterosexual Couples in Baltimore, Maryland
Ms. Sydney R. Santos1, Ms. Crystal Christie1, Ms. Jayelin N. Parker2, Dr. Jamie Perrin1, Dr. Okeoma Mmeje2, Dr. Jenell S. Coleman1
1Johns Hopkins School of Medicine, Department of Gynecology and Obstetrics, Baltimore, United States.
2University of Michigan School of Medicine, Department of Obstetrics and Gynecology, Ann Arbor, United States.
Background: In 2022, nearly one in four new HIV diagnoses in the United States were attributed to heterosexual contact. This study assessed individual and dyadic correlates of perceived HIV risk among pregnant and non-pregnant heterosexual couples.
Methods: Female cisgender patients (FPs) and their male partners (MPs) were recruited from four OB/GYN clinics in Baltimore, Maryland, an Ending the HIV Epidemic jurisdiction. Eligibility included FPs aged 15–65 years and at risk of HIV acquisition. Participants completed a 23-item perceived HIV risk survey. Wilcoxon rank sum and two sample Student’s t-test were performed by gender and pregnancy status. Cohen’s Kappa evaluated agreement within couples.
Results: As of December 2024, 58 couples (71% (n = 41) pregnant) were enrolled, with FP mean age of 27.8 years, and 29.3 for MPs. Most FPs (76%) and MPs (71%) identified as Black/African-American. 76% of FPs and 62% of MPs reported having one sexual partner. Compared to FPs, MPs felt more likely to become infected with HIV (P = 0.031). MPs were less confident communicating with their FP about regular HIV testing (P = 0.004), making decisions about using condoms (P = 0.01) or participating in regular testing (P = 0.013), and acting with their FP to get regular testing (P = 0.006) or prevent transmission to their children (P = 0.019). Non-pregnant FPs and their MPs were more likely to agree on completing regular testing (P = 0.029) compared to those in pregnant couples. Notable non-significant trends included non-pregnant FPs and their MPs also agreeing more on their concern about (P = 0.071) or picturing themselves (P = 0.06) acquiring HIV.
Conclusion: Among heterosexual couples, MPs felt an increased risk for acquiring HIV and were less confident about implementing prevention methods in their relationship compared to FPs. Non-pregnant FPs and their MP agreed more on risk reduction than pregnant couples. Tailoring interventions to address these gender and pregnancy-based differences may encourage the prevention of heterosexual transmission.
PP02.67 – Monitoring the HIV “PrEP Gap” to Inform Implementation and Policy Using Behavioural Surveillance in New Zealand
Assoc. Prof. Peter Saxton1, Cameron Leakey2, Dr Adrian Ludlam1, Dr Janine Paynter1, Dr Susan McAllister3, Kevin Haunui2, Koson Tony Sriamporn1, Brooke Hollingshead2, Mark Fisher4, Assoc Prof Stephen Ritchie1, Prof Patricia Priest3
1University of Auckland, Auckland, New Zealand.
2Burnett Foundation Aotearoa, Auckland, New Zealand.
3University of Otago, Dunedin, New Zealand.
4Body Positive Inc, Auckland, New Zealand.
Background: Governments have an obligation to ensure HIV pre-exposure prophylaxis (PrEP) is delivered sufficiently and equitably to eliminate HIV transmission. A challenge for public health planners is that similar PrEP dispensing between population subgroups can mask unmet prevention needs. PrEP coverage may be inadequate depending on behavioural risk factors, and clinically-indicated PrEP suitability may vary between subgroups. Identifying the gap between those already using PrEP, and those not on PrEP but suitable and willing to take it (the “PrEP gap”), is essential to improve uptake and reduce inequities. We estimated the PrEP gap among gay, bisexual and other men who have sex with men (GBM) in New Zealand (NZ).
Methods: We used data from NZ’s HIV behavioural surveillance programme among GBM (SPOTS 2022). Current NZ guidelines were used to define participants deemed suitable for PrEP. Willingness to use oral PrEP was a survey question. PrEP uptake was determined by reported use <6 months. We estimated the size of the PrEP gap, and whether this was associated with participant characteristics using chi-squared tests.
Results: Of 2,857 participants, 22.8% were suitable and on PrEP, 18.9% were suitable and willing but not on PrEP (the PrEP gap), 6.5% were suitable but unwilling to take PrEP. The PrEP gap was significantly higher among GBM who were Māori or Pacific, living outside NZ’s largest city, identified as bisexual, had lower disposable incomes, had 2–10 sexual partners, reported inconsistent condom use, reported any casual sex partners, engaged in sex work, were not out to their GP, engaged in chemsex or injected drugs.
Conclusion: Behavioural surveillance can identify unmet PrEP needs and can improve implementation. Of participants in the PrEP gap, almost half reported only moderate sexual partner change, who clinicians may not view as priority PrEP candidates. Focusing on this subpopulation could help reduce other inequities.
PP02.68 – Barriers to Antiretroviral Treatment Success: Exploring Predictors of Virologic Failure Among Adolescents Living with HIV in Northern Tanzania
Mr. Anthony Sebastian Charles1, Ms Irene Nkonoki2
1Management And Development For Health- Temeke specialized laboratory, Dar Es Salaam, Tanzania.
2Kilimanjaro Christian Medical University College, Kilimanjaro, Tanzania.
Background: Despite the availability and use of ART in most parts of the world, virologic failure is still a problem especially among adolescents who are on ART. Several interventions have been put into actions to improve viral suppression but it has only been achieved to a greater percent among adults while adolescents fall behind. The study aimed to determine the prevalence and determinants of virologic failure among HIV positive adolescents under ART and came up with appropriate measures that will address treatment failure and prevent unnecessary switch to second line regimens.
Methods: A cross-sectional design conducted at KCMC and Mawenzi Hospitals in Kilimanjaro Region. The study population was HIV adolescents attending CTC clinics, Questionnaires were administered, data was prepared, cleaned and entered into SPSS Software Version 25 to obtain prevalence and predictors of virologic failures.
Results: A total of 216 participants enrolled. Their median age was 17 (IQR 14–18); 60.2% were males and 39.8% were females. Of total, 13.9% had VF. After adjustment of other covariates, the likelihood of having VF was higher among adolescents who were consuming alcohol (RR = 3.49, 95% CI 1.58–7.72), smoking cigarette (RR = 7.0, 95% CI 4.19–11.69), poor ART adherence (RR = 14.46, 95% CI 7.63–27.3) and having HIV/TB co-infection (RR = 1.43, 95% CI 0.55–3.70).
Conclusions: The proportion of adolescents living with HIV in this study who were virally suppressed was relatively high at 86.1%. However, this proportion falls short of the UNAIDS’ 95% target for on treatment viral suppression. Findings from this study indicate that programs targeting younger adolescents and adolescents in transition from pediatric to adult clinics with a range of interventions including psycho socio support and treatment counselling could further improve viral suppression outcomes among this young population.
PP02.69 – Inadequate HIV Prevention Services in Substance Use Disorder Treatment Facilities That Do Not Have HIV-Specific Care for People with HIV
Dr. Khairul Siddiqi1, Samiha Nahar Tuli, Rima Nath, Sharmin Akter, Gazi Sakir Mohammad Pritom, A M Khairul Islam, Mary A Hatch, Michael G McDonell
1Washington State University Elson S. Floyd College of Medicine, Spokane, United States.
Background: People with substance use disorder (SUD) are at increased risk of HIV acquisition, yet many SUD treatment programs lack HIV-specific preventive and care services, including facilities not having specialized programs for people with HIV (PWH). This study aims to assess the availability of HIV-related services in SUD treatment facilities in the United States (US) with no HIV-specific programs.
Methods: The 2023 National Substance Use and Mental Health Services Survey (N-SUMHSS) was used to examine the availability of HIV-related services in US SUD treatment facilities that do not have specific programs/groups for clients with HIV or AIDS (PWH-specialized) compared to other facilities. Descriptive statistics and bivariate comparisons using chi-square tests assessed the differences in services across facility types, with statistical significance set at P < 0.01: SUD treatment only (n = 5,873) and a mix of mental health and SUD treatment services (n = 7,655).
Results: PWH-specialized SUD treatment facilities offer more HIV-related services than non-PWH-specialized facilities, both in SUD-only and mixed settings. Compared to PWH-specialized facilities, HIV testing was less prevalent in non-PWH-specialized SUD-only (31.3% vs 47.3%) and mixed facilities (29.2% vs 48.8%). HIV counseling and education were less common in non-specialized settings, with 62.4% (vs 81.50%) in SUD-only settings and 52.1% (vs 72.53%) in mixed settings than in PWH-specialized settings. Ancillary HIV interventions and Hepatitis C and HIV PrEP medication were also less prevalent in non-specialized facilities. Additionally, non-PWH-specialized facilities test less for Hepatitis B, C, and STDs and have fewer programs for the LGBTQ+ population.
Conclusion: Non-PWH-specialized SUD treatment offers fewer HIV-related services than specialized settings, representing missed opportunities to identify at-risk clients and engage them in HIV care. Given that people with SUD are equally at risk of HIV, prevention efforts should be directed to both types of SUD facilities to prevent the HIV epidemic in the US.
PP02.70 – Exploratory Cost and Cost-Effectiveness of a Point-Of-Care Genital Inflammation Test for Asymptomatic STIs and BV in Women
Mrs Elise Smith1, Ms Aina Harimanana2, Ms Tinashe Mwaturura3,4, Ms Vaomalala Raharimanga2, Ms Theodora Mayouya Gamana2, Dr Katherine Gill5, Dr Emma Harding-Esch6, Dr Tania Crucitti2, Dr Lindi Masson7,8,9,10,11, Professor Jo-Ann Passmore7,10,12, Professor Edina Sinanovic1
1University of Cape Town, Cape Town, South Africa.
2Institut Pasteur de Madagascar, Antananarivo, Madagascar.
3Organization for Public Health Interventions and Development, Harare, Zimbabwe.
4The Biomedical Research and Training Institute, Harare, Zimbabwe.
5Desmond Tutu HIV Centre, University of Cape Town, Cape Town, South Africa.
6London School of Hygiene & Tropical Medicine, London, England, United Kingdom.
7Institute of Infectious Disease and Molecular Medicine (IDM), University of Cape Town, Cape Town, South Africa.
8Maternal Child and Adolescent Health Program, Public Health Discipline, Burnet Institute, Melbourne, Australia.
9Disease Elimination Program, Life Sciences Discipline, Burnet Institute, Melbourne, Australia.
10Centre for the AIDS Programme of Research in South Africa, South Africa.
11Central Clinical School, Monash University, Melbourne, Australia.
12National Health Laboratory Service, South Africa.
Background: Genital inflammation from bacterial vaginosis (BV) and sexually transmitted infections (STIs) increases women’s HIV risk. However, asymptomatic STIs are largely missed due to syndromic management (SM), the standard-of-care in low-and middle-income countries (LMICs). To address this, an observational study is evaluating the effectiveness of a point-of-care Genital InFlammation Test (GIFT) for identifying inflammation linked to Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), Trichomonas vaginalis (TV), Mycoplasma genitalium, and BV in Madagascar, South Africa, and Zimbabwe. We assessed GIFT’s cost and cost-effectiveness for STI screening in asymptomatic women.
Methods: The ingredients-based cost per asymptomatic woman screened using GIFT was estimated from the health service perspective in each country. Static decision tree modeling calculated the cost/STI and BV case correctly diagnosed and treated across seven diagnostic strategies for asymptomatic women, including: no screening (1), universal diagnostic testing (2–4), and GIFT screening followed by confirmatory testing (5-7) (see table 1). STI/BV prevalence was obtained from the observational study. GIFT’s sensitivity (77%) and specificity (71%) were adopted from previous validation studies. Sensitivity and threshold analyses explored variations in test performance, prevalence rates and cost inputs.
Results: The study enrolled 676 women across the three countries. BV prevalence was 44% in Madagascar, 57% in South Africa, and 50% in Zimbabwe, with STI prevalence between 20% and 36%. With a GIFT device priced at $5.00, the average cost per asymptomatic woman screened was $6.37, $9.10, and $8.34, respectively. Sensitivity analysis revealed that cost-effectiveness was highly contingent on GIFT’s specificity. At higher specificities (80%–86%), the most cost-effective strategy was GIFT screening followed with confirmatory GeneXpert (CT/NG), OSOM TV and microscopy testing. Cost-effectiveness increased at higher STI/BV prevalence (Table 1).
Conclusion: Achieving high specificity is key to GIFT’s cost-effectiveness as an STI/BV screening tool in LMICs. Exploring alternative genital inflammation screening use cases may reveal more cost-effective applications of GIFT.
| Madagascar | South Africa | Zimbabwe | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| GIFT sensitivity: 77%, specificity 80% | GIFT sensitivity: 77%, specificity 86% | GIFT sensitivity: 77%, specificity 81% | ||||||||
| Diagnostic strategy (model comparator) | Cost per STI/BV case correctly diagnosed and treated* | STI/BV cases missed | STI/BV cases overtreated | Cost per STI/BV case correctly diagnosed and treated* | STI/BV cases missed | STI/BV cases overtreated | Cost per STI/BV case correctly diagnosed and treated* | STI/BV cases missed | STI/BV cases overtreated | |
| 1. Standard of care (no screening for STIs/BV) | – | 74 | – | – | 127 | – | – | 136 | – | |
| 2. Laboratory-based PCR (CT/NG/TV) & microscopy (BV) | $ 90.69 | 25 | – | $ 72.33 | 43 | – | $ 118.32 | 47 | – | |
| 3. GeneXpert (CT/NG and TV) & microscopy (BV) | $ 69.65 | 1 | 2 | $ 56.61 | 0.4 | 4 | $ 72.44 | 0.4 | 5 | |
| 4. GeneXpert (CT/NG), OSOM TV & microscopy (BV) | $ 63.93 | 4 | 2 | $ 49.93 | 3 | 3 | $ 61.12 | 3 | 4 | |
| 5. GIFT-positive followed by PCR (CT/NG/TV) & microscopy (BV) | $ 90.61 | 35 | – | $ 73.32 | 61 | – | $ 114.38 | 66 | – | |
| 6. GIFT-positive followed by GeneXpert CT/NG & TV + microscopy | $ 67.21 | 16 | 0.4 | $ 53.99 | 28 | 0.5 | $ 70.59 | 30 | 0.9 | |
| 7. GIFT-positive followed by GeneXpert CT/NG, OSOM TV & microscopy | $ 63.64 | 11 | 0.4 | $ 49.67 | 30 | 0.4 | $ 60.99 | 30 | 0.8 | |
Note: PCR, polymerase chain reaction; CT, Chlamydia trachomatis; NG, Neisseria gonorrhoeae; TV, Trichomonas vaginalis. Mycoplasma genitalium has not been included in the analysis as this stage. GIFT specificity represents the minimum (threshold) value where any GIFT screening strategy (5-7) was the most cost-effective. The cost for the standard of care (do-nothing strategy) is zero, with the cost per STI/BV case correctly diagnosed and treated for model comparators 2–7 being incremental to this baseline.
PP02.71 – “It’s Like a Party” – HPV Self-Sampling Perspectives Among End-Users: A Qualitative Systematic Review
Ms. Kaja Swenson1
1Independent Researcher (LSHTM MSc Student), Tokyo, Japan.
Background: Human papillomavirus (HPV) is a common sexually transmitted infection, with high-risk types linked to cancers, especially cervical cancer. Despite its prevalence, screening rates remain low, particularly in low- and middle-income countries. Self-sampling offers a private, accessible alternative to clinician-performed screening, potentially increasing uptake. This review synthesises qualitative data on HPV self-sampling experiences since 2018, focusing on values, barriers, and facilitators to its use.
Methods: A systematic literature search identified studies using qualitative data from people with cervixes who have direct experience with HPV self-sampling. Studies were included if published post-October 2018 and involved participants with lived experiences of HPV self-sampling. The data were analysed using the framework method with thematic analysis to uncover key themes regarding user values, barriers, and facilitators.
Results: Of 935 articles screened, eight met the criteria, with seven conducted in high-income countries and one in a low-income country. Findings indicated that HPV self-sampling was valued for its privacy, bodily autonomy, and empowerment. Concerns included unclear results delivery and lack of support. Barriers involved doubts about proper sample collection, limited knowledge, and cultural sensitivities. Facilitators included the method’s simplicity, convenience, and non-invasive nature. These findings underscore the need for improved health education, clear communication, and culturally sensitive approaches to boost confidence and acceptance of HPV self-sampling. Enhanced post-test support is essential for a positive experience.
Conclusion: HPV self-sampling is valued for its convenience, privacy, and empowerment potential, making it a promising approach to increasing cervical cancer screening. However, barriers like concerns about sample collection accuracy, limited HPV knowledge, and cultural issues must be addressed through targeted education, clear communication, and supportive measures during result delivery.
PP02.72 – Complementing HIV-Related Services: A Qualitative Study on the Adoption of Generative AI Chatbots for HIV Self-Testing Among Men Who Have Sex with Men in China
Mr. Zhuoheng Yin1, Zihan Wang2, Dr. Weiming Tang3, Dr. Bolin Cao2, Ms. Yusha Tao
1UNC Project-china, Guangzhou, China.
2Shenzhen University, Shenzhen, China.
3University of North Carolina at Chapel Hill, Chapel Hill, USA.
Background: Generative AI chatbots are increasingly used for HIV prevention services. This qualitative study, grounded in the Unified Theory of Acceptance and Use of Technology, explores the acceptance and utilization of generative AI chatbots in facilitating HIV self-testing (HIVST) among men who have sex with men (MSM) in China.
Methods: Between May and October 2024, we conducted online interviews with 15 MSMs in China, recruited through community organizations and snowball sampling. Participants engaged with AI platforms on HIVST topics before interviews. Data were coded deductively, with two participants validating the interpretation. Those who completed the study received 7 USD compensation. Ethical approval was obtained from corresponding author’s University.
Results: We interviewed 13 gay and two bisexual men. The average age was 25.7 years; 12 had prior HIVST experience, and eight had used AI chatbots for over a year. We identified three key domains (Table 1). The performance expectancy domain highlighted the chatbot’s effective provision of HIVST knowledge and personalized responses, reducing stigma, promoting safe sex, and boosting user confidence. However, its non-medical nature limited credibility and testing assistance. It failed to provide emotional support and restricted sensitive topics. The effort expectancy domain indicated the chatbot’s destigmatizing discourse and anonymity eased privacy concerns and encouraged self-disclosure. Its ease of use mirrored familiar tools like search engines, though the quality of responses depended on users’ ability to provide precise prompts. The social influence and facilitating conditions domain revealed that while AI integration in healthcare has increased acceptance of chatbots for HIVST, particularly among first-time testers, the limited adoption within the broader community hinders wider diffusion.
Conclusion: AI chatbots can address gaps in HIVST education, provide personalized HIVST support, and reduce stigma in China. Future efforts should optimize models, improve users’ media literacy, and integrate AI chatbots into community practices to enhance their medical and emotional support roles.
| Category | Sub-theme | Description | Quotation | |
|---|---|---|---|---|
| Positive Performance Expectancy | Provides integrated knowledge and personalized advice | AI integrates HIV knowledge effectively and delivers personalized solutions by analyzing user-provided details. | “My view of AI chat content…better at organizing information and integrating resources.” (010) | |
| “AI helps visualize problems before solving them.” (003) | ||||
| Positive Performance Expectancy | Reduces stigmatization and privacy concerns | AI's friendly, anonymous nature avoids stigmatization in HIV testing and alleviates privacy worries, creating a safe environment for users. | “This way…he does not have to be afraid of other people.” (012) | |
| “AI doesn’t know who you are…doesn’t know your last name.” (006) | ||||
| Negative Performance Expectancy | Identified as non-medical entity with limited support | AI clarifies that it is not a medical substitute and provides only limited informational support, leaving gaps in practical assistance. | “He always adds…better consult regular healthcare providers for specifics.” (005) | |
| “He provided methods…but not specifics like saliva or blood tests.” (015) | ||||
| Negative Performance Expectancy | Closure conversation and regulation on prompts | AI provides closed-ended answers, and its responses are restricted due to regulatory oversight, limiting the scope of discussions. | “He just answered my question and then it was gone.” (012) | |
| “I asked if gay men are more infected..AI offered reasonable advice after rephrasing the question.” (004) | ||||
| Neutral Effort Expectancy | Similar to search engines | AI chatbots resemble search engines in logic and usability, offering a familiar and easy-to-use interface. | “There doesn’t seem to be much difference between using AI and a search engine.” (010) | |
| Negative Effort Expectancy | Requires communication skills | Users’ media literacy impacts the quality of AI responses, with challenges arising from misinterpretations or input errors. | “AI only gave me accurate answers when I typed ‘PreEP’ correctly with the right capitalization.” (004) | |
| Positive Effort Expectancy | Non-judgmental environment | AI promotes value-free disclosure, reducing user self-judgment and encouraging open communication. | “AI doesn’t associate your self-test with inappropriate behavior…it's just a test.” (016) | |
| Mixed Social Influence and Facilitating Conditions | Commonly used healthcare technology but not widely accepted | AI chatbot adoption reflects the rise of healthcare technologies, but its acceptance remains limited due to skepticism or perceived lack of utility. | “BJ University introduced AI glasses for surgery…AI self-tests are becoming the norm.” (009) | |
| “People think chatting with AI is pointless…but it has value for specific uses.” (015) |
PP02.73 – Partner Notification Practices Among Transgender Women Diagnosed with Sexually Transmitted Infection in Lima, Peru: A Mixed Methods Study
Dr. Tijana Temelkovska1, Jessica Gutierrez2, Edson Linares2, Yahaira Pimentel2, Dr. Narendar Kumar2, Jose Ipanaque2, Dr. Jordan E Lake3, Dr. Cherie Blair4, Dr. Robinson Cabello2, Dr. Jesse L Clark4
1Department of Obstetrics & Gynecology, University of Colorado, Denver, United States.
2Asociacion Civil de Via Libre, Lima, Peru.
3Department of Internal Medicine, McGovern Medical School at UTHealth, Houston, United States.
4Department of Medicine, Division of Infectious Diseases, David Geffen School of Medicine at UCLA, Los Angeles, United States.
Background: Partner management can link at-risk individuals to HIV and STI care, but its utility among transgender women (TW) is unknown. We investigated sexual partnership contexts, HIV/STI communication, and partner notification (PN) practices among TW in Lima, Peru.
Methods: TW in Lima completed a cross-sectional survey and STI screening between September 2022 and January 2024. Forty-one participants diagnosed with STI completed additional surveys regarding sexual networks and PN practices. A random selection was invited to participate in qualitative interviews addressing similar themes.
Results: Among 181 TW screened, the prevalence of HIV-1 was 62%, syphilis 54%, chlamydia 19%, and gonorrhea 13%. Among TW with STI, 25% of participants notified their last primary partner, 12.5% their last casual partner, and 5% their last commercial sex client. 80% of participants who notified their primary partner did so in person. Of all sexual partners identified by this group, 43% of primary partners were notified, 6% of casual partners, and 0.7% of clients. Anticipated versus actual PN outcomes were similar. Qualitative interviews revealed that TW are integral to partner access for HIV/STI education, screening, and treatment. Most TW interviewed had notified a prior partner of STI diagnosis, though rarely informed partners about HIV. TW who did not explicitly notify their partners reported indirectly encouraging HIV/STI testing or insisting on condom use. Fears of rejection or violence, social stigma, and low partner knowledge of HIV/STIs were principal barriers to notification. Preferred tools to support notification included in-person visits, partner counseling, and psychological support instead of third-party notification, expedited partner therapy, or at-home test kits.
Conclusions: TW have complex partnership contexts and often engage in discussions about HIV/STIs and even PN, particularly with primary partners. Leveraging TW’s roles in their community and facilitating access to in-person counseling may empower TW and better reach their sexual partners.
PP02.74 – Meanings of Sexual Health Among Gay Men in Singapore: A Baseline Qualitative Study Pre-Dating the Repeal of Penal Code 377A
Mr. Daniel Teo1
1Nanyang Technological University, Singapore.
Gay men in Singapore are faced with socio-structural barriers which reduce their access to sexual health resources and increase incidence of STIs, especially HIV. However, in 2022, Penal Code 377A, a British colonial legacy ruling which criminalises sex between men, was finally repealed. This study was conducted as part of a Masters Thesis in 2013, and now forms an important baseline before the repeal of 377A. The study explores the meanings of sexual health among self-identified gay men. In their everyday lives, gay men actively negotiate with these constraints in making choices about their sexual health; within this context, their interpretations of sexual behaviour, sexual identity and sexual rights are constituted, negotiated, and communicated through stories of their life experiences. This study adopts a narrative approach to yield gay men’s meanings of sexual health situated in the context of their everyday lives. The central research questions of the study are: What are the meanings of sexual health among gay men in Singapore? And how do gay men negotiate their sexual health in the context of Singapore? Semi-structured interviews were conducted with 19 gay men in 2013. The participants, in dialogue with the researcher, co-constructed narratives of sexual behaviour, sexual identity, and sexual rights. The narratives revealed the complex, conflicting and co-existing meanings within the participants’ stories, as well as a culture of secrecy within which the participants operated, challenged and resisted structural barriers in maintaining their sexual health. These findings now create a window into the recent past, and with the subsequent repeal of 377A, creates a point of reference with which an evolution of the meanings of sexual health with the passage of time and the removal of a significant structural barrier can be illuminated.
PP02.75 – Crowdsourcing Strategies to Improve Access to HIV Pre-Exposure Prophylaxis (PrEP) in Australia, the Philippines, Thailand and China: A Multi-Country Crowdsourcing Study
Mrs Warittha Tieosapjaroen1,2, Mr Jr Arturo M. Ongkeko3,4, Mr Zhuoheng Yin5, Ms Krittaporn Termvanich6, Mr Artit Wongsa6, Prof Joseph D. Tucker7,8, Prof Weiming Tang5, Dr Chunyan Li9, Miss Ying Zhang1,2, Dr Nina T. Castillo-Carandang4,10, Prof Jason J. Ong1,2,8
1Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
2The School of Translational Medicine, Monash University, Melbourne, Australia.
3National Institutes of Health, University of the Philippines, Manila, The Philippines.
4Foundation for the Advancement of Clinical Epidemiology, Inc., Manila, The Philippines.
5University of North Carolina Project China, Guangzhou, China.
6Institute of HIV Research and Innovation, Bangkok, Thailand.
7Institute for Global Health and Infectious Diseases, University of North Carolina at Chapel Hill, Chapel Hill, US.
8Clinical Research Department, Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, UK.
9Tokyo College, The University of Tokyo, Tokyo, Japan.
10Department of Clinical Epidemiology, College of Medicine, University of the Philippines, Manila, The Philippines.
Background: Many Asian countries have yet to scale up HIV pre-exposure prophylaxis (PrEP). Crowdsourcing has a group of individuals solving all or part of a problem before sharing solutions with the public. We used crowdsourcing to seek innovative strategies to optimise PrEP access by increasing the uptake and effective use of PrEP. This study compares crowdsourcing to develop PrEP campaigns in four Asian countries.
Methods: Four crowdsourcing open calls were conducted between 2021 and 2023 in Australia, the Philippines, Thailand and China according to a WHO/TDR guide. All open calls included the following: 1) problem identification; 2) committee formation with local groups; 3) community engagement for idea submission (e.g., texts, posters, pitches); 4) evaluation of submissions; 5) recognition of finalists; and 6) online dissemination of solutions. We examined the number of total and high-quality submissions. We also identified themes across countries.
Results: The Australian, Philippines, Thai and Chinese teams received 9, 22, 9 and 19 eligible submissions, respectively. A total of 3, 10, 7 and 8 submissions had a mean score of 6/10 or greater. Three common solutions emerged across all the finalist ideas: enhanced service access, optimising promotional campaigns, and person-centred promotional materials. The winning ideas from the Australian, Filipino, Thai and Chinese teams were an anonymous online PrEP service, a printed ready-to-wear garment to create awareness about PrEP, PrEP and HIVST dispensing kiosks and a poster on PrEP effectiveness, respectively (Fig. 1).
Conclusions: Crowdsourcing can be a promising and versatile tool for developing PrEP strategies in Asia. We conducted clinical trials to bridge the gap between idea generation and implementation, and to create the empirical evidence pivotal for the policy adoption of these innovations.
PP02.76 – A Narrative Inquiry into the Experiences Related to Pre-Exposure Prophylaxis (PrEP) Access Among Young Men Who Have Sex with Men (YMSM) in Canada
Dr. Jose Benito Tovillo1
1University of Victoria, Edmonton, Canada.
Background: Young men who have sex with men (YMSM) in Canada and globally are disproportionately impacted by human immunodeficiency virus (HIV). Pre-exposure prophylaxis (PrEP) is an effective strategy for reducing transmission and acquisition of HIV infection among high-risk populations, including YMSM. However, there is a limited number of studies exploring YMSM’s PrEP access experiences and the different social, structural, behavioural, and clinical factors that influence their PrEP access and use. The purpose of this narrative inquiry study was to explore and understand the experiences of Canadian YMSM in relation to their PrEP access.
Methods: Using a narrative inquiry approach, the researcher worked collaboratively with three Canadian YMSM between the ages of 21 and 24 over 24 months. With relational ethics at the center, the participants and the researcher engaged in multiple conversations in person and virtually and collected field texts that provided insights into their experiences across time, places, and social contexts.
Results: The intensive and long-term researcher-participant relationships allowed them to co-compose narrative accounts that reflected the participants’ unique experiences, especially those that shaped their overall PrEP access. Through the continuous telling and retelling of the participants’ stories and by reflecting on and laying their narrative accounts side by side, the researcher identified resonant threads that highlighted their experiences of accessing PrEP in relation to and in the contexts of identity-making and social responsibility.
Conclusion: This narrative inquiry research provided new understandings and knowledge of Canadian YMSM’s PrEP access experiences, specifically in the contexts of identity-making and social responsibility. The new knowledge from this research can be utilized to inform PrEP programs, research, education, policies, and practice guidelines that will improve PrEP access and help decrease the rate of new HIV infections among Canadian YMSM.
PP02.77 – Barriers and Facilitators to STI/HIV Prevention Among MSM in Ibadan: A Qualitative Study on Access and Awareness
Dr. Aishat Bukola Usman1, Dr Olubunmi Akinboye, Prof Olufunmilayo Fawole
1West African Health Organization, FCT, Nigeria.
Background: Men who have sex with men (MSM) face higher risks of STIs and HIV due to individual behaviors and community factors, including underreporting and low testing rates. In Nigeria, STI rates are elevated among MSM compared to the general population, particularly for syphilis, chlamydia, and gonorrhea. However, healthcare services often fail to address these needs adequately, especially for asymptomatic extra-genital infections. This study explores the risk factors, barriers, and facilitators for STI and HIV prevention among MSM in Ibadan, Nigeria.
Methods: The study conducted eight focus group discussions with 77 MSM, ages 18–43, who are HIV-positive on ART and have prior experience with STI services. Participants were quota-sampled by age, gender, and sexual orientation. Discussions in community settings were analyzed using thematic analysis to identify patterns of risk, barriers to care, and potential facilitators for prevention.
Results: Participants identified multiple risk factors, including recent new partnerships, multiple sexual partners, and the use of online platforms to find partners. Limited health education was noted, leaving many MSM unaware of available STI services. Barriers to care included stigma, discrimination, and confidentiality issues at health facilities, all of which deterred MSM from seeking appropriate care and increased the likelihood of STI and HIV transmission. Many participants incorrectly believed that taking antibiotics post-exposure would prevent infections, a practice that risks developing antibiotic-resistant strains of STIs. Key facilitators for care included flexible clinic hours, confidential services, non-judgmental healthcare providers, and free access to STI medications, condoms, and lubricants.
Conclusions: To mitigate STI and HIV risks in this vulnerable population, public health strategies must combine integrated prevention approaches, regular extra-genital screenings, and inclusive healthcare practices. Interventions should emphasize early STI diagnosis and treatment, along with improved healthcare access through non-stigmatizing environments, to enhance health outcomes among MSM in Ibadan.
PP02.78 – Exploring the Impact of New Chlamydia Testing Guidelines on STI Testing Preferences in the Netherlands
Miss Ilja van Bergen1, Dr. Janneke Heijne2,3,4, Prof. Dr. Marijn de Bruin5, Dr. Daphne van Wees1
1National Institute For Public Health And The Environment, Bilthoven, The Netherlands.
2Public Health Service of Amsterdam, Amsterdam, The Netherlands.
3Amsterdam Institute for Immunology and Infectious Diseases and Amsterdam Public Health Research Institute, Amsterdam, The Netherlands.
4Amsterdam University Medical Center, Amsterdam, The Netherlands.
5Radboud University Medical Centre, Nijmegen, The Netherlands.
Background: From January 2025, restrictive chlamydia testing guidelines for asymptomatic individuals will apply at Dutch Sexual Health Centers (SHCs). Testing guidelines for other sexually transmitted infections (STI) remain unchanged. We aimed to assess the potential impact of this guideline change on STI testing preferences and explore associations between demographic and psychosocial characteristics and (changes in) preferences.
Methods: An online survey among heterosexuals aged 16–34 years was conducted between April-June 2024, including a hypothetical scenario involving condomless sex with a partner with unknown STI-status. STI testing preferences in this scenario before and after the anticipated guideline change were assessed. For statistical analyses, preferences before and after the change were categorized into four groups: 1) SHC before and after (“SHC”), 2) SHC before and other location after (“SHC-other”), 3) other locations than the SHC (“Other”) before and after, and 4) no test (anymore) after (“No test”). Univariable multinomial logistic regression models were used to explore associations between demographic and psychosocial characteristics and preferences.
Results: Of the 1159 participants, 15% was categorized into SHC, 47% in SHC-other, 9% in No test, and 28% in the Other group. Participants in the SHC-other group were more likely to be female (OR = 1.45, 95% CI 1.02–2.06), and participants in the No test group were less likely to be aged >22 years (vs <21 years, OR = 0.46, 0.23–0.91), with migration background (vs Dutch origin, OR = 0.38, 0.21–0.71), and more likely to report low perceived importance of health (OR = 2.05, 1.26–3.34) compared to participants in the SHC group.
Conclusion: STI testing preferences may shift towards other test locations or not testing at all after chlamydia guidelines have changed at SHCs, even though testing guidelines for other STI remain unchanged. Tailored communication to sustain STI testing uptake is of important, especially for young, Dutch natives with low perceived importance of health.
PP02.79 – The Relationship Between Trauma and Sexual Health Outcomes Among Transgender Women in the US Deep South
Ms. Katelyn S. Day1, Dr. Kristal Aaron2, Dr. Bulent Turan5, Dr. D. Scott Batey4, Dr. Gabe H. Miller3, Hannah M. Lindl3, Dr. Christina Muzny2, Dr. Olivia Van Gerwen2
1UAB Heersink School of Medicine, Birmingham, United States.
2UAB Heersink School of Medicine, Division of Infectious Diseases, Birmingham, United States.
3UAB College of Arts and Sciences, Department of Sociology, Birmingham, United States.
4Tulane University, School of Social Work, New Orleans, United States.
5Koc University, Istanbul, Turkey.
Background: Transgender women are disproportionately affected by STIs and experience unique life traumas that may further negatively impact their sexual health outcomes. We aimed to identify associations between trauma and sexual health outcomes in this population, hypothesizing that trauma is associated with worse sexual health outcomes.
Methods: We developed a multi-item trauma measure for transgender women (Table 1), including subscales for healthcare, sexual/relationship, general trauma, gender dysphoria, and discrimination-related trauma. We administered this measure along with questions about sexual health outcomes and socio-demographics to adult transgender women in clinical and community settings in Birmingham, Alabama. We estimated univariate logistic regressions to examine relationships between trauma and sexual health outcomes including HIV PrEP awareness/use, condom use, and self-reported lifetime STI history/testing. Age and race were adjusted for in all models and backward selection with a significance of P = 0.2 was employed for other variables to stay in the model, with a P-value <0.05 considered statistically significant. Analysis was performed using SAS v9.4.
Results: Between April-September 2024, 105 participants enrolled. Median age was 30 years (range 19–73), with 52.4% being White (n = 55). There were no significant associations between any trauma subscales and PrEP awareness, history of PrEP use, or condom use during receptive anal sex. High trauma scores for healthcare, gender dysphoria, and discrimination-related experiences were not associated with negative sexual health outcomes. Significant associations were found between self-reported lifetime STI history and high general trauma experiences score (OR 1.74 [1.29–2.35], P < 0.001) as well as self-reported STI testing in the last year and high general trauma experiences score (OR 1.33 [1.14–1.56], P < 0.001).
Conclusion: Traumatic experiences appear to be a contributing factor to the STI epidemic facing transgender women. Patient-centered, trauma-informed care is essential to promote the uptake of sexual health care services among this population.
PP02.80 – Vital Priority Improving Anal Health for Gay Men in Kenya
Mr. Harrison Wanjohi1
1 Hoymas Kenya, Kenya.
2FAHARI YA JAMII, Kenya.
Introduction: Anal health issues among gay men in Kenya are becoming more common but often overlooked. This abstract highlights the urgent need to focus on improving anal health services for this group.
Objectives: To raise awareness about the importance of anal health for gay men in Kenya. To identify the key challenges and risks associated with poor anal health. To propose recommendations for addressing these issues effectively.
Methods: This abstract presents findings from an ongoing research initiative focusing on anal health among gay men in Kenya. The research employs a mixed-methods approach, including one-on-one interviews and focus group discussions (FGDs). These methods are chosen to ensure privacy and encourage open dialogue on sensitive topics related to anal health.
Results: Preliminary results from interviews and FGDs highlight a concerning lack of awareness among gay men in Kenya regarding anal health. Many participants express limited knowledge about the importance of anal health and preventive measures. This shows the need for education and support to help them learn more and take care of their anal health.
Recommendations: Integrate routine anal health screenings into primary care services for gay men. Provide comprehensive education and prevention programs to promote healthy anal practices.
Train healthcare providers to deliver culturally sensitive care that respects the dignity of gay men.
Support community-based initiatives to raise awareness and de stigmatize discussions about anal health.
Advocate for policy reforms and resource allocation to establish dedicated anal health clinics and expand access to affordable treatments.
Conclusion: In conclusion, addressing anal health disparities among gay men in Kenya requires a multifaceted approach that prioritizes awareness, education, and policy reforms. By taking proactive steps to improve anal health services, we can enhance the well-being and quality of life for this marginalized population.
PP02.81 – Enhancing HIV Prevention Among People Who Use Drugs (PWUD) in Kenya: Integrating Harm Reduction and PrEP Services
Mr. Harrison Wanjohi1
1Hoymas Kenya, Kenya.
2FAHARI YA JAMII, Kenya.
Background: People who use drugs (PWUD) are disproportionately affected by HIV in Kenya, with needle sharing and risky sexual behavior driving high rates of transmission. While harm reduction services such as needle exchange programs (NEP) have been introduced, uptake of HIV prevention tools like pre-exposure prophylaxis (PrEP) remains low. This study assesses the impact of integrating PrEP with harm reduction services to improve HIV prevention outcomes among PWUD.
Methods: A cohort of 200 PWUD from Nairobi and Mombasa was followed over a 12-month period. Participants were enrolled in a program that provided NEP alongside HIV testing, counseling, and PrEP. Data on PrEP initiation, adherence, and HIV incidence were collected at baseline, 6 months, and 12 months. Qualitative interviews were also conducted with 40 participants to explore their perceptions of integrated services. Statistical analysis was performed using Cox proportional hazards models, and thematic analysis was used for qualitative data.
Results: At baseline, 60% of participants were aware of PrEP, but only 20% had initiated it. After integrating PrEP with NEP services, PrEP uptake increased to 55% at the 6-month follow-up, with 70% adherence among those who initiated it. The HIV incidence rate declined by 30% over 12 months. Qualitative findings revealed that participants appreciated the convenience of receiving both clean needles and PrEP in one location, which minimized stigma and reduced logistical barriers to accessing HIV prevention services.
Conclusions: Integrating PrEP with harm reduction services significantly increases PrEP uptake and adherence among PWUD in Kenya, while also reducing HIV incidence. Expanding such integrated programs, particularly in urban areas with high PWUD populations, offers a promising approach to controlling HIV transmission in this vulnerable group. Scaling up these interventions, coupled with peer support and community outreach, will be key to achieving long-term HIV prevention success.
PP02.82 – Knowledge, Behaviour, and Perceptions of STI Screening Programs in Hamilton Shelter Clients
Miss Kelly Waters1, Ms Jodi Gilchrist1,2, Ms Zayn Brar1, Ms Alex Martindale1, Ms Keltie Baldwin1, Dr. Kerry Beal3, Dr. Marek Smieja1,2,4
1Research St. Joseph’s - Hamilton, Hamilton, Canada.
2Department of Health Research Methods, Evidence and Impact, McMaster University, Hamilton, Canada.
3Shelter Health Network, Hamilton, Canada.
4Department of Pathology and Molecular Medicine, McMaster University, Hamilton, Canada.
Background: Those experiencing unstable housing face an increased risk for acquiring infectious diseases including sexually transmitted and blood borne infections (STBBIs), and encounter barriers to testing and treatment. This study assessed the knowledge, behaviour, and perceptions of STBBIs and screening programs in unhoused individuals in Hamilton, Ontario.
Methods: Clients accessing one of 9 shelter locations in Hamilton, ON were invited to participate in an anonymous survey of their attitudes, beliefs, and knowledge regarding STBBIs, including their transmission, diagnosis, and treatment.
Results: A total of 285 individuals participated (58.9% male, 37.5% female, 1.1% non-binary, 0.7% transgender female, 0.7% transgender male, 1.1% unspecified). Of these, 8.4% reported having one or more partners in the past 6 months and 5.3% reported 10 or more partners. Roughly 30% of participants reported that STBBI testing was: accessible but required some assistance (22.8%); difficult to access (4.9%); or very difficult to access (2.8%). Of the 62% who reported that STBBI testing was easy to access (25.6%) or very easy to access (36.5%), only 33% were tested for STBBIs in the previous 12 months. Participants selected that they “weren’t sure where to get tested” (31.9%) and stigma associated with STBBIs (16.8%) as their biggest barriers when seeking testing. A total of 46.1% of participants reported that they are worried about contracting an STI. Of the 56.2% who reported that they felt they are well-educated on STBBIs, 27.0% incorrectly answered that “you only need to get tested if you have symptoms” and 35.2% incorrectly answered that “you can determine if you have an STBBI based just on how you feel”.
Conclusion: Overall individuals accessing shelter services in Hamilton reported that they are well-educated on STBBIs and STBBI testing was easy to access. However, STBBI screening remains low despite the number of individuals with at least one sexual partner.
PP02.83 – Stigma, Perceptions, and Social Conditioning in HIV PEP Uptake Among Sexual Assault Survivors: Implications for Trauma-Informed Care
Miss Tequila Porter3, Miss Patricia Fernandez2, Mrs Lakyn Webb1, Miss Jocelyn C. Anderson1, Mrs. Jessica Draughon Moret2
1The University of Arkansas for Medical Sciences, Little Rock, United States.
2Betty Irene Moore School of Nursing, University of California, Davis, Sacramento, United States.
3UC San Diego Health System: San Diego, United States.
Background: Survivors of sexual assault face a higher risk of sexually transmitted infections (STIs), including human immunodeficiency virus (HIV). Post-exposure prophylaxis (PEP) can prevent HIV if taken within 72 h of exposure, but many survivors hesitate to start or finish treatment due to stigma, fear, and unfavorable healthcare experiences. Beliefs about HIV – such as the misconception that it primarily affects homosexual men – create additional barriers to care. This study looks at how survivors’ beliefs and experiences shape their decisions about PEP and highlights ways to make STI prevention more compassionate and trauma-informed.
Methods: We interviewed 42 sexual assault survivors who sought care within the 72-h window when PEP could still be effective. The semi-structured interviews focused on their experiences with PEP, thoughts on HIV-related stigma, and interactions with healthcare providers. The thematic analysis helped us identify patterns in survivors’ decisions about PEP, especially why some accepted it and others declined.
Results: Three key themes emerged from the interviews (Table 1):
Stigma and Fear: Many survivors felt shame and fear about taking HIV PEP, driven by societal stigma around HIV.
Provider Influence: Trust in healthcare providers made survivors more likely to accept PEP, but coercive communication – such as warnings that they would “get HIV” if they did not take it – created more fear and stigma.
Perceptions of Risk: Survivors often underestimated their own HIV risk, influenced by societal messages that HIV was a problem for other groups, not them.
Conclusion: The decision to take HIV prevention medication after sexual assault is not easy. Survivors face stigma, fear, and outdated ideas about HIV risk that create barriers to care. They need providers who listen, offer clear information, and treat them empathetically. Breaking down stigma through trauma-informed care can build trust, improve PEP use, and help survivors take steps to protect their health.
| Theme | Quote | Demographics | |
|---|---|---|---|
| Stigma and Fear | “It felt like taking the medication meant admitting to something shameful, even though I didn’t do anything wrong.” | Black female, insured | |
| Stigma and Fear | “It was pretty scary ‘cause there was a lot of folks around.. I didn’t want everyone knowing my business.” | White female, employed, insured | |
| Stigma and Fear | “In the beginning, I wanted to keep it private.. I didn’t want anybody to know because I was embarrassed.” | White female, employed, insured | |
| Provider Influence | “The doctor said, ‘If you don’t take this, you’ll get HIV,’ and it made me feel like I was dirty or already infected.” | White female, insured | |
| Provider Influence | “They just said just follow what the specialist says, because if you don’t, you could catch something that you might not know how to handle.” | White male, employed, insured | |
| Provider Influence | “I guess I mean more extensive details and information.. I don’t even know what it really was treating.” | White male, employed, insured | |
| Perception of Risk | “I’ve never been with someone who uses drugs or prostitutes, so I didn’t think it was something I had to worry about.” | Hispanic female, employed | |
| Perception of Risk | “He told me he had a family and kids, so I thought he wasn’t the type to give me anything.” | White female, insured |
PP02.85 – Community Mobilization for Prevention of Mother-to-Child Transmission of HIV Services: Empowering Pregnant Women in South-South Nigeria Through Information, Education and Communication Materials and Media Campaigns
Mrs Hidayat Bukola Yahaya1, Dr Babayemi Olakunde2, Dr Mojisola Mobolaji Bello3, Mrs Ibironke Adeoye1, Mrs Tolulope Adebisi1, Mr Yomi Olatunji1, Dr James Anenih1
1National Agency for the Control of AIDS, Abuja, Nigeria.
2College of Public Health, University of North Texas Science Centre, Fort Worth, United State of America.
3National AIDS, Viral Hepatitis and STI Control Programme, Abuja, Nigeria.
Background: To achieve the UNAIDS 95-95-95 targets in Nigeria, the wide gap in the prevention of mother-to-child HIV transmission (PMTCT) which drives the increasing burden of HIV amongst children is being addressed through the National PMTCT Scale-up approach. This approach includes demand creation services to target women who do not receive any form of care or receive care from non-health sector service providers during pregnancy. This report highlights the implementation in the South-South geopolitical zone of Nigeria.
Description: A critical mass team of People Living with HIV network, Ward Development Committees, and Community Health Influencers and Promoters within the Primary Health Care Agency was identified, trained, and engaged as Community Mobilizers (CMs). Their role was to facilitate pregnant women’s access to PMTCT services, ensuring those identified as HIV-positive are enrolled and retained in care. A total of 1,710 CMs across states utilized information, education, and communication (IEC) materials to create demand for PMTCT. A media campaign featuring posters and radio jingles complemented the CMs’ efforts. These initiatives targeted women of childbearing age, traditional and religious leaders in each local government areas. A data reporting tool, powered by Kobo Toolbox, was utilized to monitor activities over a three-month period.
Results: The CMs utilized social behavior change communication strategies, including IEC materials, advocacy, and dialogue to raise awareness about PMTCT services. A total of 35,997 pregnant women were reached, and 20,636 linked to healthcare facilities for PMTCT services. Notably, 1,681 pregnant women were referred from birth homes to healthcare facilities for PMTCT services. Myths and misconceptions about HIV persist in these areas.
Conclusion: Social behavior change communication serves as an effective strategy for bridging gaps in PMTCT services. CMs engagement in demand creation demonstrated that community involvement is crucial in addressing service delivery and structural barriers that hinder uptake of PMTCT services.
PP02.86 – Infection by HIV and Other Sexually Transmitted Infections Among Men Who Have Sex with Men in Kazakhstan: Associations with Community Connectedness, HIV Stigma, and Internalized Homophobia
Ms. Xiaotong Yang1, Dr. Emily Allen Paine2,3, Dr. Yong Gun Lee4, Mr. Vitaliy Vinogradov5, Dr. Gaukhar Mergenova5, Ms. Sholpan Primbetova5, Dr. Assel Terlikbayeva5, Dr. Elwin Wu1
1Columbia School of Social Work, New York, United States.
2New York State Psychiatric Institute, New York, United States.
3Columbia University, New York, United States.
4The University of Hong Kong, China.
5Columbia University Global Health Research Center of Central Asia, Kazakhstan.
Background: Men who have sex with men (MSM) in Kazakhstan experienced an 88% increase in HIV incidence from 2010–2021 and a concomitant increase in sexually transmitted infections (STIs). An earlier study found that HIV testing among MSM from three cities in Kazakhstan – Almaty, Nur-Sultan, and Shymkent – was associated with greater connectedness to the MSM community (“MSM community connectedness”), lower HIV stigma, and lower internalized homophobia. We follow up these results with an examination of whether HIV infection or other STIs are associated with MSM community connectedness, HIV stigma, and internalized homophobia.
Methods: From the same three-city clinical trial with MSM in Kazakhstan, we conducted secondary analyses using data from structured interviews that assessed MSM community connectedness, HIV stigma, and internalized homophobia (higher scale scores indicate greater levels for each construct) and those who completed biological assays to confirm infection by HIV or other STIs (specifically, chlamydia, gonorrhea, and syphilis). Hypothesis testing utilized binary logistic regression
Results: Among the 625 participants, 117 (19%) were confirmed to be living with HIV and 227 (36%) with an STI. The association between HIV infection and MSM community connectedness was significant (OR = 1.06; 95% CI = 1.00–1.13; P = 0.046) in bivariate models and suggestive after controlling for sociodemographics (aOR = 1.06; 95% CI = 1.00–1.13; P = 0.063). No significant associations were observed between HIV infection and HIV stigma nor internalized homophobia. The association between STIs and HIV stigma was significant (OR = 1.04; 95% CI = 1.00–1.09; P = 0.030) in bivariate models and suggestive after controlling for sociodemographics (aOR = 1.04; 95% CI = 1.00–1.09; P = 0.083). The association between STIs and internalized homophobia was significant after controlling for sociodemographics (aOR = 1.03; 95% CI = 1.00–1.06; P = 0.038). No significant associations were observed between STIs and MSM community connectedness.
Conclusion: Results support the potential impact and value of addressing community context and a stigmatizing culture with respect to the disproportionate psychosocial and sexual health burden experienced by MSM in Kazakstan.
PP02.87 – Clustering Analysis of Sexual Behavioral Patterns and Risk of Sexually Transmitted Infections in Chinese Men Who Have Sex with Men
Mr Bingyang She2, Mr Yiming Liu2, A/Prof Shu Su3, Prof. Lei Zhang1
1Monash University, Carlton, Australia.
2Xi’an Jiaotong University, Xi’an, China.
3The Second Affiliated Hospital of Chongqing Medical University, Chongqing, China.
Background: This study identifies clusters in Chinese men who have sex with men (MSM) by sexual behavioral patterns and investigates its association with gonorrhea and chlamydia infections.
Methods: We conducted a longitudinal study of Chinese MSM from November 2020 to January 2022. Data on sequential sexual act patterns from the most recent sexual encounter, gonorrhea and chlamydia infections, were collected weekly over 12 consecutive weeks. Hierarchical clustering was used to identify clusters based on sexual behavioral patterns, while survival analysis was employed to calculate infection incidence within each cluster.
Results: We identified three main clusters (n = 91, 100, 62), one small cluster (n = 8) and 41 unclustered participants. Participants in cluster 1 assumed both insertive and receptive roles in oral, anal sex and rimming during sexual episodes, whereas participants in cluster 2 predominately conducted insertive sexual acts and participants in cluster 3 conducted receptive sexual acts. During follow-up, cluster 1 exhibited a significantly higher incidence of overall gonorrhea infection (581.51/100,000 person-days), pharyngeal (355.45/100,000 person-days) and anorectum gonorrhea (487.63/100,000 person-days) while comparing with cluster 2 and 3. Consistently, cluster 1 was significantly more likely to engage in kissing (40.08%) and rimming (6.77%) and being rimmed (7.18%), in sexual act pairs such as ‘receptive oral sex-insertive oral sex’ (8.71%), ‘being rimmed-insertive anal sex’ (4.59%), ‘kissing-receptive oral sex’ (13.62%), ‘insertive anal sex-receptive anal sex’ (5.38%) and ‘rimming-being rimmed’ (6.83%).
Conclusion: The sexual role preferred by participants is a key to the clustering of Chinese MSM. MSM who assume both insertive and receptive roles demonstrate a substantial higher risk of gonorrhea infection.
PP02.88 – Identifying Subgroups of Chinese Men Who Have Sex with Men Based on Sexual Behavior and Drug Use Patterns Using a Clustering Analysis Approach
Mr Bingyang She2, Mr Jiajun Sun1, Prof Weiming Tang3, A/Prof Shu Su4, Prof. Lei Zhang1
1Monash University, Carlton, Australia.
2Xi’an Jiaotong University, Xi’an, China.
3University of North Carolina at Chapel Hill, Chapel Hill, USA.
4The Second Affiliated Hospital of Chongqing Medical University, Chongqing, China.
Introduction: Sexualized drug use (SDU) refers to using drugs before and during sex to enhance experiences, increasing high-risk behaviors among men who have sex with men (MSM). This study explores how SDU affects sexual behavior in Chinese MSM.
Methods: We collected information on demographics, sexual acts, drug use, and condom attitudes among 890 MSM in six Chinese cities via WeChat ads through community-based organizations from March 23 to April 22, 2022. Cluster analysis using Gower’s distance and hierarchical clustering explored differences in sexual acts among MSM who reported SDU in their last encounter and otherwise.
Results: Cluster analysis categorized 890 participants into three clusters. Cluster 3 (n = 155) reported 100% SDU in their last sexual encounter (poppers use at 83.87%,), whereas Clusters 1 (n = 581) and 2 (n = 154) reported none. Compared with other clusters, Cluster 3 demonstrated significantly higher PrEP use (34.90% vs 17.02% vs 8.00%, P < 0.0001), more sexual acts over the past 12 months (35.80–61.30 vs 31.30–56.10 and 4.37–21.22, P < 0.001), more regular (3.16 ± 4.37 vs 2.27 ± 3.52 vs 2.51 ± 2.53, P = 0.028) and casual sexual partners (4.55 ± 6.55 vs 2.48 ± 3.21 vs 2.74 ± 3.66, P < 0.0001), more partners with STIs (8.39% vs 3.79% vs 3.90%, P = 0.029), and lower consistent condom use over the past 6 months (48.53% vs 59.41% vs 72.28%, P < 0.0001). Comparing Clusters 1 and 2, Cluster 1 had a higher frequency in all sexual acts except self-masturbation. Self-masturbation was the most common act across all clusters, especially in Cluster 2, which was primarily characterized by this act.
Conclusion: SDU is a stratum for identifying MSM subgroups, and MSM who reported SDU demonstrated higher sexual risk behaviors and PrEP usage. Among those not practicing SDU, self-masturbation is a key behavioral indicator for subgrouping.
PP02.89 – Examining the Effects of PrEP Use on Sexual Behaviors and Sexually Transmitted Infections Among Chinese Men Who Have Sex with Men: A Cross-Sectional Study
Mr Bingyang She2, Ms Fang Lu2, A/Prof Shu Su3, Prof. Lei Zhang1
1Monash University, Carlton, Australia.
2Xi’an Jiaotong University, Xi’an, China.
3The Second Affiliated Hospital of Chongqing Medical University, Chongqing, China.
Background: Men who have sex with men (MSM) is a high-risk population for HIV and sexually transmitted infections (STIs). Pre-exposure prophylaxis (PrEP) is effective in HIV prevention. This study aims to examine the differences in sexual behaviors, STI prevalence and HIV/STI testing across subgroups of MSM with various PrEP use.
Methods: Data were collected via a cross-sectional survey in an MSM community in Xi’an, Shaanxi, from 2022.01 to 2022.09. Participants were categorized as ‘PrEP-naïve and unwilling to use’, ‘PrEP-naïve but willing to use’, and ‘current or former PrEP users’. Shannon index was used to assess sexual act diversity and multivariate logistic regression analyzed factors associated with PrEP use.
Results: Of the 1,131 MSM participants, 23.52% were PrEP-naïve and unwilling, 64.98% were PrEP-naïve but willing, and 11.49% were current or former PrEP users. The PrEP-naïve but willing group had the highest recent STI testing rates at 73.06% and showed greater sexual act diversity (Shannon index 1.61). This group also had the highest syphilis rates (7.49% vs 6.47% and 2.54%, P < 0.01). Younger age (18–30: OR = 0.39 (0.18–0.85); 31–40: OR = 0.43 (0.20–0.96)) and lower education (high school/vocational: OR = 0.15 (0.04–0.58); associate degree: OR = 0.21 (0.06–0.71)) were factors that negatively influenced PrEP use. Current or former PrEP users had the highest oropharyngeal gonorrhea (14.39% vs 9.68% and 5.80%, P < 0.01) and overall gonorrhea rates (20.86% vs 17.17% and 8.37%, P < 0.001).
Conclusion: ‘PrEP-naïve but willing’ participants consistently demonstrated high-risk sexual behavior, increased STI testing, and more diverse sexual acts, whereas PrEP users had the highest STI prevalence.
PP03.01 – Distinct Metabolic Profiles Characterized Paired Maternal-Cord Blood and Placental Tissues Among Individuals with Treated vs Untreated Syphilis and Congenital Syphilis
Dr. Emily Adhikari1,2, Andrea Woods1, Kyra Solis-Beach1, Ana Espinosa1, Claudia Brock1, Dr. Jessica Pruszynski1, Dr. Ashley Solmonson1
1UT Southwestern Medical Center, Dallas, United States.
2Parkland Health, Dallas, United States.
Background: Metabolic reprogramming is involved in the innate immune response to infection, triggering changes in metabolic pathways to allow rapid response upon encountering a pathogen. Mechanisms involved in early response to infection with Treponema pallidum, the organism that causes congenital syphilis, are poorly understood. We explored whether metabolites are detected in paired maternal-cord blood samples and placental tissues, and whether altered serum and placental metabolites differentiate treated vs untreated syphilis and congenital syphilis.
Methods: Pregnant individuals were prospectively consented at a high-volume Maternal-Fetal Medicine clinic for infectious diseases in pregnancy. Additional individuals were recruited after presenting at delivery with untreated syphilis. Maternal serum and paired umbilical cord blood were collected; placental samples were flash frozen within 4 h of delivery. Metabolomic analysis was performed using a Vanquish UHPLC coupled to a Thermo Scientific QExactive HF-X hybrid quadrupole orbitrap high-resolution mass spectrometer. Relative metabolite abundance was compared between paired maternal-cord blood specimens and placental tissues for adequately treated versus confirmed or highly probable congenital syphilis, compared to uninfected negative controls delivering at term. Available longitudinal pre- and post-treatment samples were compared.
Results: Of 37 individuals consented with syphilis in pregnancy, median gestational age at enrollment was 17 weeks (IQR 14–22) among those recruited before delivery. Nine had early syphilis (1 primary, 3 secondary, 5 early latent) and 22 late latent infection. Of 34 delivered patients, 4 delivered preterm, including one set of twins. Immunohistochemical presence of Treponema pallidum was confirmed in 3 of 10 placentas including dichorionic twins. Distinct metabolic profiles characterized maternal, cord blood and placental tissues among individuals with early vs latent and treated vs untreated syphilis with congenital syphilis.
Conclusion: Elucidating metabolic drivers of syphilis pathogenesis in pregnancy may shed light on potential therapeutic targets for this devastating disease.
PP03.02 – Rapid Detection of Four STI Bacteria and Associated Antibiotic Resistance Markers Enabling Specific Treatment at the Point-of-Care
Mr. Sonny Michael Assennato1, Dr. Odeta Villaruel Villaruel2, Dr. John White White3, Mr. Nikolai Kirkby4, Dr. Lourdes Nadala1, Dr. Helen Lee1
1Diagnostics For the Real World, Cambridge, United Kingdom.
2Social Hygiene Clinic, Iloilo City, Philippines.
3Northern & Western Health and Social Care Trusts, Londonderry, United Kingdom.
4Dept of Clinical Pathology, Rigshospitalet, Copenhagen, Denmark.
Background: Antibiotic resistance to Neisseria gonorrhoeae and Mycoplasma genitalium is a growing global health threat with significant implications for both individual and public health. Delayed and Ineffective treatment can lead to adverse outcomes and onward transmission. Rapid implementation of resistance-guided therapy using molecular point-of-care is recommended.
Methods: The SAMBA III STI Discharge panel identifies 4 main targets – Neisseria gonorrhoeae (NG), Chlamydia trachomatis (CT), Mycoplasma genitalium (MG), Trichomonas vaginalis (TV) and two important antibiotic resistance markers (to quinolones for NG and macrolides for MG) with time to result of 50 min. We evaluated its performance in comparison with CE-marked multiplex molecular assays (cobas® CT/NG and MG/TV, Roche). Resistance-associated mutations (RAMs) for MG and NG were confirmed with the R/MG Elite MGB assay (ELItech InGenius) and sequencing, respectively. Vaginal or urethral swabs were collected from consenting participants attending a social hygiene clinic in Iloilo city, Philippines.
Results: We tested specimens from 243 participants (216 female sex workers, 13 female and 14 male walk-in patients). Results are shown in Table 1 below:
Overall, 112 participants (46.1%) tested positive for one or more STI targets: 64 CT (26.3%), 38 NG (15.6%), 36 TV (14.8%) and 28 MG (11.5%). 71 participants had monoinfections and 41 had multiple STIs: CT/NG (12), CT/TV (8), CT/MG (6), MG/TV (3), NG/MG (1), CT/NG/MG (6), CT/NG/TV (3) and CT/MG/TV (2). NG quinolone RAMs were present in 94.7% of the NG positive samples whereas macrolide RAMs were detected in only 10.7% of the 28 MG-positive samples. All samples identified as antibiotic resistant were confirmed by alternative assay or sequencing.
Conclusion: The SAMBA III Discharge panel provides high diagnostic accuracy and rapid turn-around time allowing clinicians to promptly and accurately diagnose STIs at the point-of-care and provide with resistance-guided therapy while patients still on site.
| SAMBA III/COMPARATOR | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Site | Target | No. of specimens | +/+ | +/− | −/+ | −/− | PPA (95% CI) | NPA (95% CI) | |
| Philippines | CT | 243 | 63 | 0 | 1 | 179 | 98.46% (91.72–99.96) | 100% (97.96–100) | |
| NG | 243 | 37 | 0 | 1 | 205 | 97.44% (86.52–99.94) | 100% (98.22–100) | ||
| MG | 243 | 27 | 0 | 1 | 215 | 96.55% (82.24–99.91) | 100% (98.3–100) | ||
| TV | 243 | 35 | 0 | 1 | 207 | 97.03% (85.84–99.93) | 100% (98.23–100) | ||
PP03.03 – Factors Associated with PrEP Referral Acceptance and PrEP Linkage-to-Care
Mr. Alec Boudreau1, Ms. Pallavi Menon1, Mr. M. Harris Bayan1, Nisha Ramdeep1, Tanique Bennett1, Nyah Johnson1, Jennifer Jiang1, Caroline Tran3, Zoe Demko1, Debra Daughtery2, Dr. Yu-Hsiang Hsieh1, Dr. Richard Rothman1, Robin MacGowan2, Dr. Kevin Delaney2, Nathalie Gonzalez-Jimenez2, Dr. Yukari Manabe1, Dr. Matthew Hamill1
1Johns Hopkins School of Medicine, Baltimore, United States.
2Centers for Disease Control and Prevention, Atlanta, United States.
3Johns Hopkins University, Baltimore, United States.
Background: Pre-exposure prophylaxis (PrEP) is a key strategy for preventing HIV transmission and mitigating the HIV epidemic. We used data from a clinical trial which evaluated the impact of rapid HIV diagnostic tests on linkage-to-care conducted in Baltimore, Maryland. Using the PrEP care cascade, we analyzed factors associated with PrEP navigation among participants from a clinical trial who were at risk of HIV infection.
Methods: From 08/2021 through 12/2024, 245 participants were recruited from an Emergency Department, through online platforms, and through other sources. Participants were included in the analysis if they tested HIV-negative, reported no PrEP use in the past 3 months, and completed at least one follow-up interview at 4 and/or 12 weeks. Logistic regression was used to calculate odds ratios for PrEP referral acceptance and linkage to PrEP based on demographic and behavioral factors. Adjusted regression models included variables selected based on statistical significance in bivariate analyses and relevance to HIV risk factors.
Results: Participant drop-offs were observed at both the referral and linkage stages. Of the 245 enrolled participants, 34 (13.9%) participants declined referral, and 102 of 211 referred (48.3%) were not linked to PrEP care. Participants were more likely to accept PrEP referrals if they identified as not being heterosexual (See Table 1), had experienced homelessness in the previous 12 months, or were recruited from online platforms. Participants with education beyond high school or without a regular healthcare provider were less likely to accept referrals. Participants recruited from online platforms were more likely to be linked to PrEP (Adjusted Odds Ratio 5.17).
Conclusion: Increased efforts may be needed to encourage people who may not perceive themselves to be at risk of infection to accept PrEP referrals. People recruited through emergency departments may require additional support to accept PrEP referrals and be linked to services.
| Demograhpic and behavioral factors | Step 1: Enrolled | Step 2: Referred to PrEP | Step 3: Linked to PrEP | |||||
|---|---|---|---|---|---|---|---|---|
| Total N = 245 (100%) | Total N = 211 (100%) | Unadjusted OR (95% CI) P-value | Adjusted† OR (95% CI) P-value | Total N = 109 (100%) | Unadjusted OR (95% CI) P-value | Adjusted‡ OR (95% CI) P-value | ||
| Age range (Ref:<25) | 44 (18%) | 39 (18%) | 18 (17%) | |||||
| 25–40 | 105 (43%) | 88 (42%) | 0.66 (0.21–1.82) 0.451 | 47 (43%) | 1.34 (0.63–2.87) 0.451 | |||
| >40 | 96 (39%) | 84 (40%) | 0.90 (0.27–2.60) 0.848 | 44 (40%) | 1.28 (0.60–2.77) 0.521 | |||
| Sex (Ref: male) | 128 (52%) | 109 (52%) | 58 (53%) | |||||
| Female | 117 (48%) | 102 (48%) | 1.19 (0.57–2.49) 0.648 | 51 (47%) | 0.88 (0.51–1.51) 0.641 | |||
| Racial identity (Ref: White) | 78 (32%) | 67 (32%) | 31 (28%) | |||||
| Black | 123 (50%) | 107 (51%) | 1.10 (0.47–2.49) 0.825 | 53 (49%) | 1.14 (0.62–2.11) 0.675 | |||
| Other | 44 (18%) | 37 (18%) | 0.77 (0.28–2.27) 0.628 | 25 (23%) | 2.03 (0.87–4.89) 0.105 | |||
| Sexual orientation (Ref: heterosexual) | 134 (55%) | 111 (53%) | 48 (44%) | |||||
| Not heterosexual | 111 (45%) | 100 (47%) | 2.55 (1.17–6.02) 0.023 | 3.36 (1.18–10.77) 0.03 | 61 (56%) | 2.06 (1.19–3.61) 0.011 | 1.42 (0.72–2.84) 0.312 | |
| Education (Ref: high school or less) | 120 (49%) | 103 (49%) | 48 (44%) | |||||
| Some college or more | 125 (51%) | 108 (51%) | 0.66 (0.26–1.56) 0.36 | 0.33 (0.11–0.95) 0.046 | 61 (56%) | 1.73 (0.96–3.14) 0.069 | 0.87 (0.41–1.82) 0.715 | |
| Drug use (Ref: no) | 221 (90%) | 190 (90%) | 101 (93%) | |||||
| Yes | 24 (10%) | 21 (10%) | 1.15 (0.37–5.09) 0.825 | 0.36 (0.07–2.09) 0.219 | 8 (7%) | 0.53 (0.20–1.32) 0.179 | ||
| Has health insurance (Ref: yes) | 213 (87%) | 190 (90%) | 96 (88%) | |||||
| No | 32 (13%) | 21 (10%) | 13 (12%) | 1.61 (0.65–4.23) 0.315 | 2.24 (0.70–8.04) 0.191 | |||
| Has a regular healthcare provider (Ref: yes) | 202 (82%) | 177 (84%) | 97 (89%) | |||||
| No | 43 (18%) | 34 (16%) | 0.60 (0.26–1.52) 0.254 | 0.33 (0.12–1.00) 0.045 | 12 (11%) | 0.45 (0.20–0.95) 0.04 | 0.42 (0.14–1.16) 0.102 | |
| Tested for HIV before enrolment (Ref: yes) | 210 (86%) | 182 (86%) | 97 (89%) | |||||
| No | 35 (14%) | 29 (14%) | 0.71 (0.27–2.24) 0.517 | 0.40 (0.13–1.19) 0.106 | 12 (11%) | 0.67 (0.27–1.61) 0.377 | ||
| HIV test frequency (Ref: every 1–6 months) | 81 (33%) | 73 (35%) | 43 (39%) | |||||
| Every 1–2 years | 63 (26%) | 56 (27%) | 0.88 (0.30–2.64) 0.81 | 30 (28%) | 0.81 (0.40–1.63) 0.545 | |||
| No pattern | 66 (27%) | 53 (25%) | 0.45 (0.17–1.14) 0.096 | 24 (22%) | 0.58 (0.28–1.18) 0.132 | |||
| Missing | 35 (14%) | 29 (14%) | 0.53 (0.17–1.73) 0.276 | 12 (11%) | 0.49 (0.20–1.17) 0.112 | |||
| Reason for HIV testing (Ref: proactive*) | 77 (31%) | 66 (31%) | 33 (31%) | |||||
| Retroactive due to worry** | 56 (23%) | 48 (23%) | 1.00 (0.38–2.76) 1.00 | 26 (24%) | 1.18 (0.56–2.50) 0.66 | |||
| Free and convenient | 81 (33%) | 69 (33%) | 0.96 (0.39–2.33) 0.925 | 35 (32%) | 1.03 (0.52–2.03) 0.933 | |||
| Refuse/other/missing | 31 (13%) | 28 (13%) | 1.56 (0.44–7.26) 0.521 | 15 (14%) | 1.15 (0.48–2.83) 0.751 | |||
| Homelessness in past 12 months (Ref: no) | 208 (85%) | 176 (84%) | 94 (86%) | |||||
| Yes | 37 (15%) | 35 (16%) | 3.18 (0.91–20.20) 0.124 | 11.3 (1.54–250.6) 0.045 | 15 (14%) | 0.65 (0.31–1.35) 0.256 | 0.66 (0.28–1.54) 0.34 | |
| Hispanic/Latin identity (Ref: yes) | 29 (12%) | 23 (11%) | 17 (16%) | |||||
| No | 216 (88%) | 188 (89%) | 1.73 (0.60–4.41) 0.273 | 2.47 (0.65–8.50) 0.161 | 92 (84%) | 0.34 (0.12–0.85) 0.029 | 0.56 (0.16–1.72) 0.326 | |
| Participant source (Ref: emergency department) | 71 (29%) | 57 (27%) | 13 (12%) | |||||
| Online recruitment | 158 (64%) | 141 (66%) | 2.04 (0.93–4.41) 0.071 | 3.55 (1.26–10.46) 0.018 | 88 (81%) | 5.62 (2.84–11.76) <0.001 | 5.17 (2.30–12.43) <0.001 | |
| Other^ | 16 (7%) | 13 (6%) | 0.98 (0.27–4.73) 0.98 | 2.31 (0.42–19.38) 0.376 | 7 (6%) | 4.74 (1.30–18.53) 0.019 | 3.57 (0.87–15.34) 0.077 | |
*Proactive Reasons, such as: ‘Before having sex with someone new’ or ‘I get tested on a regular schedule and it was time for me to get tested again’.
**Retroactive Reasons, such as: ‘I had sex with someone new’ or ‘I was worried I might have been exposed to HIV’.
^Other: Participant recruitment sources include an outpatient STI clinic, local health department, posted fliers, and referrals from previously enrolled participants.
†Regression model adjusted for: Sexual Orientation, Education, Drug Use, Has Health Insurance, Has a Regular Healthcare Provider, Tested for HIV Before Enrollment, Homelessness in the Last 12 Months, Hispanic/Latin Identity, & Participant Source.
‡Regression model adjusted for: Sexual Orientation, Education, Has Health Insurance, Has a Regular Healthcare Provider, Homelessness in the Last 12 Months, Hispanic/Latin Identity, & Participant Source.
PP03.04 – LIMIT Trial - Lidocaine with Intramuscular Injection of Benzathine Penicillin G for Treponema pallidum Treatment
Dr. Joseph Cherabie1, Dr. Germysha Little1, Dr. Patrick Kojima1, Dr. Donald Hong1, Dr. Aditi Ramakrishnan1, Dr. Andy Brand1, Mr Caleb Bender1, Dr. Lauren Karpman1, Dr. Rachel Presti1, Dr. Hilary Reno1
1Washington University St. Louis, St. Louis, United States.
Background: There is evidence to suggest that lidocaine can help reduce the pain associated with intramuscular injections of benzathine penicillin G (BPG) or bicillin, used to treat syphilis infections. The objective of this study was to examine if there is any benefit of adding 0.5 mL 1% lidocaine to prepackaged Benzathine Penicillin G, with respect to pain, compared to standard of care, in the treatment of Treponema pallidum infections, both 10 min and 24 h after injection.
Methods: This study is a double blinded randomized placebo control trial of addition of the effect on pain of the addition of 0.5 mL 1% lidocaine solution to prepackaged benzathine Penicillin G injection, compared to addition of 0.5 mL normal saline solution, in adults being treated for syphilis (Treponema pallidum) infections, within the Infectious Diseases Clinic at Washington University in St. Louis.
Results: Preliminary analysis included 13 participants. A Wilcoxon Signed-Rank Test indicated a statistically significant reduction in pain 10 min after lidocaine injection compared to the saline injection (z = −2.46, P = 0.014) (Table 1). The median pain score following administration of the lidocaine solution was 2.77, compared to 6.62 for the saline solution. Overall, 92% of participants reported a reduction in pain scores with lidocaine relative to saline. However, while there was a trend to less pain in the lidocaine BPG solution injection compared to the saline BPG solution at 24 h follow up, this difference was not statistically significant.
Conclusion: Additional data is being collected in this study, but this trial demonstrates that lidocaine can help reduce the pain associated with intramuscular injections of BPG. This may provide evidence that could change standard clinical practice with respect to how we perform BPG injections in the US that may improve patient comfort during minor procedures or interventions.
| Mean | Median | ||
|---|---|---|---|
| Saline-10 min | 6.62 | 7 | |
| Lidocaine-10 min | 2.77 | 3 | |
| Saline-24 h | 4.13 | 4 | |
| Lidocain-24 h | 3.25 | 4 |
| Wilcoxon Signed-Rank Test comparing pain scores after Lidocaine and Saline injections after 10 min | ||||
|---|---|---|---|---|
| N | P-value | Z-Score | ||
| Negative ranks | 12 | 0.014 | –2.46 | |
| Positive ranks | 1 | |||
| Ties | 0 | |||
| Total | 13 | |||
| AIndicates that Lidocaine pain score was lower than Saline pain score | ||||
| BIndicates that Lidocaine pain score was higher than Saline pain score | ||||
| CIndicates that Lidocaine pain score was equal to Saline pain score | ||||
| Wilcoxon Signed-Rank Test comparing pain scores after Lidocaine and Saline injections after 24 h | ||||
|---|---|---|---|---|
| N | P-value | Z-Score | ||
| Negative ranksa | 4 | 0.317 | –1.00 | |
| Positive ranks | 2 | |||
| Ties | 2 | |||
| Total | 8 | |||
| AIndicates that Lidocaine pain score was lower than Saline pain score | ||||
| BIndicates that Lidocaine pain score was higher than Saline pain score | ||||
| CIndicates that Lidocaine pain score was equal to Saline pain score | ||||
PP03.05 – Pregnancy of an HIV-Positive Patient Using Implanon®: Case Report
Dr Gabriel Antonio Cabriott Dumbra1, Ms Marina Passoni1, Ms Mariana Mayumi Ishizava1, Dr Paula Ferreira Pinheiro2, Dr Marília Colturato Cleto2, Dr Samelline Ramos Albuquerque2, Dr Amanda de Oliveira Rodrigues2, Mrs Carolina De Marqui1
1Faceres, São José do Rio Preto, Brasil.
2Santa Casa de Misericórdia, Araçatuba, Brasil.
Background: Etonogestrel implant is a highly effective contraceptive method, with an estimated failure rate of 0.05%. Pregnancy in women using this method, although rare, may occur due to factors such as inadequate insertion and drug interactions, which it’s mechanism have not yet been elucidated.
Methods: Descriptive Observational Study.
Results: A.C.F.S., 24 years old, HIV-positive, undetectable since 2017, on antiretroviral treatment using a combination of Tenofovir (TDF) 300 mg, Lamivudine (3TC) 300 mg and Dolutegravir (DTG) 50 mg, with a dosage of 1 2-in-1 tablet of DTG+3TC and 1 tablet of TDF, in a single daily dose, chose to have a long-acting implant placed as a contraceptive method. On October 18, 2022, after a negative beta HCG test, a subdermal etonogestrel contraceptive implant (Implanon®) was inserted, with due guidance to the patient. On February 21, 2024, the patient was admitted for consultation, when a beta HCG test was performed due to a delayed menstrual period, with a positive result with a value of 14,041.00 mIU/mL, indicating an ongoing pregnancy, despite the use of the contraceptive implant. The patient underwent a transvaginal ultrasound on February 22, revealing a topical pregnancy compatible with 6 weeks and 2 days and an embryo identified with BCF present. The implant was removed on March 5, 2024, without complications, shortly after the pregnancy diagnosis and was found to be correctly inserted, allowing to rule out a possible error during insertion.
Conclusion: This case report presents a rare but possible pregnancy in a woman with HIV who was using Implanon®. Contraceptive failure may be influenced by drug interactions, especially if patient is using certain antiretrovirals that may affect the metabolism of hormones released by the implant.
PP03.06 – The Future of PrEP: Long-Acting Injectable Lenacapavir in HIV Type 1 Prevention
Mrs Carolina De Marqui1, Dr Gabriel Antonio Cabriott Dumbra1
1Faceres, São José do Rio Preto, Brasil.
Introduction: Pre-exposure prophylaxis (PrEP) has proven to be an extremely important tactic in preventing the human immunodeficiency virus (HIV) infection. New long-term therapeutic strategies revealed the potential to enhance treatment adherence, as well as its effectiveness. Lenacapavir, an HIV-1 capsid inhibitor, is notable for its revolutionary method of action, binding to the NTD-CTD interface of the capsid and inhibiting several steps of viral replication, including capsid disassembly and assembly, nuclear transportation and virus production, in addition to biannual administration, which simplifies its application. This research aims to evaluate the efficacy of long-acting injectable lenacapavir in HIV type 1 prevention.
Materials and Methods: Integrative review using two databases: Pubmed/Medline (n = 32) and Virtual Health Library (VHL) (n = 11). With a controlled vocabulary in the search strategy, the following terms were used: “Lenacapavir” and “HIV-1 Prevention”, as well as their synonyms and combinations.
Results: Clinical research has shown efficacy rates greater than 90% in preventing type 1 HIV among high-risk people, with consistent adherence to biannual treatment. In research conducted in African countries, a 94% decrease in the rate of new infections was observed among individuals who received treatment with lenacapavir compared to the control group. Furthermore, the drug has shown high tolerability, with most adverse events ranging from mild to moderate. The dosage analyzed in the studies involved subcutaneous application of 927 mg, followed by maintenance doses of 463 mg every 6 months.
Conclusion: Lenacapavir stands out as an efficient and practical alternative to HIV-1 PrEP, exhibiting high prevention success rates and a favorable safety profile. Biannual administration simplifies treatment, especially in high-risk populations, increasing its effectiveness, as adherence is the basis for successful pre-exposure prophylaxis.
PP03.07 – Relationship Between Vaginal Microbiota Composition, STI Susceptibility and Potential Therapeutic Approaches Based on Microbial Modulation
Mrs Carolina De Marqui1, Dr Gabriel Antonio Cabriott Dumbra1
1Faceres, São José do Rio Preto, Brasil.
Background: Vaginal microbiota plays an essential role in gynecological health maintenance and sexually transmitted infections (STIs) protection. Predominance of Lactobacillus spp. contributes to an acidic and protective environment. Otherwise, an imbalanced microbiome can increase pathogens vulnerability. This study aims to explore the relationship between vaginal microbiota composition, STI susceptibility, and potential therapeutic approaches based on microbial modulation.
Methods: Integrative review using two databases: Pubmed/Medline (n = 11) and Virtual Health Library (BVS) (n = 5). With a controlled vocabulary in the search strategy, the following terms were used: “Sexually Transmitted Infections” and “Vaginal Microbiota” and “Probiotics” as well as their synonyms and combinations.
Results: Vaginal flora composition has a considerable impact on STIs occurrence and evolution. Women with a microbiota formed mainly by Lactobacillus crispatus have reduced rates of HIV and HPV infection, in addition to a more effective local immune response, marked by increased production of lactic acid and maintenance of an acidic vaginal pH, which prevents pathogens multiplication. In contrast, predominance of vaginal dysbiosis is associated with higher risk of HPV infection and persistence, and greater susceptibility to HIV. In a prospective study, women with persistent HPV who were given oral supplements with Lactobacillus crispatus had significantly higher rates of virus clearance than controls. In HIV prevention, instability of the vaginal flora can impair the effectiveness of preventive measures, such as pre-exposure prophylaxis (PrEP) use. Women with vaginal dysbiosis tend to retain and activate less antiretrovirals administered vaginally, which can reduce the effectiveness of these measures.
Conclusion: Vaginal microbiota plays a crucial role in STI vulnerability, affecting infection incidence, treatments effectiveness and prevention strategies. Microbiome regulation appears to be a promising strategy to reduce HPV persistence and possibly improve the effectiveness of PrEP in HIV combat.
PP03.08 – Enrollment Experience and Prevalence of Sexually Transmitted Infections Upon Enrollment Into a Clinical Trial of a Gonorrhea Vaccine Candidate at Two Sites in Thailand
Dr Eric Garges5, Dr Pathariya Promsena1, Dr Trevor A. Crowell2,6, Dr Carlo Sacdalan1, Praporn Savaraj3, Dr Somchai Sriplienchan1, Dr Sorachai Nitayapan3, Dr Eugene Kroon1, Dr Sangsulee Thamakaison2, Haoyu Qian2,6, Dr Thanyawee Puthanakit4, Sandra Waggoner2,7
1SEARCH Research Foundation, Bangkok, Thailand.
2Henry M. Jackson Foundation for the Advancement of Military Medicine, Bethesda, USA.
3Royal Thai Army, Armed Forces Research Institute of Medical Sciences, Bangkok, Thailand.
4Division of Infectious Diseases, Department of Pediatrics, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand.
5Department of Retrovirology, Armed Forces Research Institute of Medical Sciences, Bangkok, Thailand.
6U.S. Military HIV Research Program, CIDR, Walter Reed Army Institute of Research, Silver Spring, USA.
7Infectious Disease Clinical Research Program, Department of Preventive Medicine and Biostatistics, Uniformed Services University of the Health Sciences, Bethesda, USA.
Background: The NIAID-sponsored Meningococcal Vaccine Against Gonococcal Infection (MAGI) clinical trial is a phase IIb randomized, placebo-controlled trial evaluating the efficacy of GSK’s Bexsero® vaccine in preventing Neisseria gonorrhoeae infection. Originally developed for Neisseria meningitidis, Bexsero® may provide cross-protection against genital and rectal gonorrhea in populations vulnerable to infection. This analysis summarizes recruitment and sexually transmitted infection (STI) prevalence among 1,100 participants enrolled from the Thai Red Cross/Search Research Foundation (TRC) and Royal Thai Army (RTA) sites in Thailand.
Methods: We enrolled sexually active men and women aged 18–50 years who were disproportionately vulnerable to gonococcal infection. At screening for study eligibility, voided urine, anorectal swabs, and oropharyngeal swabs were tested for gonorrhea and/or chlamydia using NAAT assays.
Results: From 2020–2024, participants were recruited from distinct populations between the two study sites including government clinic sites, existing research studies, and community engagement activities. HIV positivity was noted in 7% and 28% of enrollment populations. Primary screen failure occurred in 24% and 33% of participants from the TRC and RTA sites, respectively. The primary reason for screen failure was concurrent STI, with pharyngeal gonorrhea and rectal chlamydia being most common. Rescreening and enrollment were common in primary screen failures. Overall population demographics are presented in the accompanying Table 1.
Conclusions: Successful recruitment of a largely male volunteer population vulnerable to gonococcal infection was achieved in Thailand. Gonorrhea and chlamydia were highly prevalent at screening for study eligibility, and rescreening and enrollment was common after treatment. The age, sex, HIV and STI infection status at baseline were variable between the two study sites, achieving the goal of increasing representation in the study population to improve external validity of study results.
| Characteristics | Total (N = 1,100) | RTA site (N = 500) | TRC site (N = 600) | |
|---|---|---|---|---|
| Age (years) | ||||
| Median (IQR) | 31.0 (26.0–38.0) | 35.0 (29.0–42.0) | 29.0 (24.0–34.0) | |
| Age categories | ||||
| 18–24 | 194 (17.6%) | 32 (6.4%) | 165 (27.5%) | |
| 25–34 | 503 (45.7%) | 209 (41.8%) | 297 (49.5%) | |
| 35+ | 403 (36.6%) | 259 (51.8%) | 138 (23.0%) | |
| Sex | ||||
| Female | 146 (13.3%) | 100 (20.0%) | 46 (7.7%) | |
| Male | 954 (86.7%) | 400 (80.0%) | 554 (92.3%) | |
| HIV status | ||||
| Not living with HIV | 897 (81.5%) | 464 (92.8%) | 433 (72.2%) | |
| Living with HIV | 203 (18.5%) | 36 (7.2%) | 167 (27.8%) | |
| Prevalent Ng | ||||
| Pharyngeal Ng | 52 (4.7%) | 16 (3.2%) | 36 (6.0%) | |
| Rectal Ng | 37 (3.4%) | 15 (3.0%) | 22 (3.7%) | |
| Urogenital/vaginal Ng | 6 (0.5%) | 2 (0.4%) | 4 (0.7%) | |
| Prevalent CT | ||||
| Rectal CT | 99 (9.0%) | 38 (7.6%) | 61 (10.2%) | |
| Urogenital/vaginal CT | 48 (4.4%) | 26 (5.4%) | 21 (3.5%) |
PP03.09 – A case-control study to investigate the aetiology of pelvic inflammatory disease (PID)
Dr. Kay Htaik1, Dr Lenka Vodstrcil1,2,3, Dr Erica Plummer1,2, Ms Natasha Wild1, Ms Laura Matthews1, Ms Nisha Malhotra1, Professor Eric Chow1,2,3, Professor Catriona Bradshaw1,2,3
1Melbourne Sexual Health Centre, Melbourne, Australia.
2School of Translational Medicine, Monash University, Melbourne, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) are established causes of acute pelvic inflammatory disease (PID). However, less is known about the association of M. genitalium and bacterial vaginosis (BV) with PID. We aimed to determine the contribution of known STIs (CT and NG) and potential emerging causes (M. genitalium and BV) to PID.
Methods: Case control study conducted at Melbourne Sexual Health Centre (MSHC) between 2023 and 2025. Cases (n = 208) were women presenting to MSHC with symptoms of PID who fulfilled CDC clinical criteria for PID on examination. Two control groups comprised: 1) asymptomatic women attending MSHC for STI screening (n = 208,“clinic-controls”) and 2) asymptomatic women recruited from the community through expressions of interest (n = 100, “community-controls”). All participants were tested for CT, NG, and M. genitalium using a NAAT and assessed for BV using the Nugent method.
Results: Cases were significantly more likely than both control groups to have chlamydia [13% (95% CI: 8%–18%) versus 1% (95% CI: 5%–13%, P < 0.001) and 0% (95% CI: 0%–3%, P < 0.001)] and gonorrhoea [6% (95% CI: 3%–11%) versus 1% (95% CI: 0%–3%, P < 0.001) and 0%(95% CI: 0%–4%, P < 0.001)] detected, respectively. M. genitalium was more commonly detected in cases than both control groups [12% (95% CI: 8%–18%) versus 8% (95% CI: 5%–13%, P = 0.234) and 2% (95% CI: 0.2%–7%, P = 0.003)], but this was only significant compared to community-controls. BV was commonly detected in cases [29% (95% CI: 22%–36%)] and clinic-controls [25% (95% CI: 19%–31%, P = 0.354)] but was significantly less common in community controls [10% (95% CI: 4%–16%, P < 0.001)]. 57% of cases had none of the four infections detected compared to 70%–90% of the controls.
Conclusions: This study, using CDC criteria to diagnose PID, confirms an association with both chlamydia and gonorrhoea and PID. Neither M. genitalium nor BV was significantly more commonly detected in PID than clinic-controls. More than 50% of cases had no infection detected, highlighting the need for sequencing studies to identify novel infectious causes of PID to improve testing and care.
PP03.10 – Syphilis prevalence among people living with HIV in Nepal and its association with sociodemographic and sexual behaviors
Mr Yuba Raj Sapkota1, Mr Upendra Shrestha1, Ms. Shristi Rijal1, Ms Neeti Sedhain1, Mr Bhagawan Shrestha1, Mr Pradeep Kumar Thakur2, Mr Micheal Cassell2, Ms Mary Kariuki2
1FHI360 Nepal, Kathmandu, Nepal.
2FHI360, Durham, United state America.
Background: Syphilis is a sexually transmitted infection (STI) and a common co-infection among people living with HIV (PLHIV). The status of syphilis co-infection among PLHIV is not known in Nepal. The abstract aims to examine the status syphilis among PLHIV and correlated behaviors among PLHIV who are receiving community care through outreach workers of FHI360 Nepal working in 37 districts of Nepal.
Methods: We conducted a descriptive study followed by statistical data analysis of PLHIV receiving community care services from FHI360 Nepal project. Secondary program data collected between October 2023 and September 2024 was used for the analysis. Syndromic STI screening data followed by Rapid Plasma Reagin (RPR) test results were extracted from DHIS2 system.
Results: During the reporting period, 17,261 PLHIV were reached through community care services. Of these, 1,496 (9%) were screened for STIs using syndromic chart followed by etiological testing at EpiC Nepal supported clinic and ART sites. Of those screened, 262 (18%) were diagnosed with at least one STI.
Out of total screened, 206(14%) ever had presence of syphilis (95% CI, 12.1–15.6). The prevalence of active syphilis was 8.4% (95% CI, 7.1–9.8) among screened. The active syphilis prevalence was 10.3 % (95% CI, 8.5–12.4) among male and 5.2% (95% CI, 3.6–7.4) among females. Male were 53% more likely to have active syphilis. The active syphilis prevalence was higher among young population (19–25 years) than older groups (13.7% vs 6.9%). The younger population were 54% more likely to acquired active syphilis than old population. Similarly, illiterate populations were 1.3 times more suspectable to acquire syphilis than its odds (AOR 1.3, P < 0.05).
Conclusion/Next steps: Syphilis prevalence among PLHIV remains high among younger male PLHIV. PLHIV, specially from younger group required regular counselling on comprehensive HIV checkup that includes syphilis screening and treatment. Controlling STIs, especially syphilis, is crucial for preventing new HIV transmission.
PP03.108 – Successful Implementation of PCR Directed Neisseria Gonorrhoeae Culture: Results from a Large 5-Year Prospective Study
Dr. Merel J.M. Boderie1, Dr. Helke A. Van Dessel1,2, Dr. Nicole H.T.M. Dukers-Muijrers2,3, Dr. Christian J.P.A. Hoebe2,3, Dr. Luuk T.J. Levels4, Dr. Inge H.M. van Loo1,2, Dr. Petra Wolffs1,2
1Maastricht Umc, Maastricht, The Netherlands.
2Maastricht University, Maastricht, The Netherlands.
3Public Health Service South Limburg, Heerlen, The Netherlands.
4Limburg North Public Health Service, Venlo, The Netherlands.
Background: Due to the growing emergence of multidrug resistant Neisseria gonorrhoeae (NG) worldwide, it is important to monitor antimicrobial resistance (AMR) data of this difficult to culture microorganism. NG culture recovery rates depend on the bacterial load, by proxy of the cycle threshold (Ct) value obtained by quantitative polymerase chain reaction (qPCR), irrespective of the anatomic site of infection. In this 5 year prospective study we have implemented the use of qPCR data from routine NG diagnostics with the aim to optimize the NG culture recovery rate.
Methods: Data were obtained from routine qPCRs on COBAS 4800 (Roche diagnostics) for detection of NG and from corresponding NG cultures performed between January 2017 and December 2021 for two sexually transmitted infections (STI) clinics in Limburg, The Netherlands. STI clinic 1 was advised to only culture an anatomic site of infection when the qPCR Ct value was ≤32. STI clinic 2 continued culture practice as usual.
Results: 2498 NG qPCR positive samples were analyzed. NG culture was performed in 686 (27%) of these samples, of which 227 were positive (mean culture recovery rate 33%). The median Ct value of samples sent by STI clinic 1 and 2 were 28.9 (IQR 2.8) and 32.5 (IQR 8.1) respectively. STI clinic 1 sent in 344 of their 1814 (19%) NG qPCR positive samples for NG culture of which 180 were positive (culture recovery rate 52%). STI clinic 2 sent in 342 of their 684 (50%) NG qPCR positive samples for NG culture of which 47 were positive (culture recovery rate 14%). We were unable to retrieve information on transport times.
Conclusion: This 5-year study demonstrated that routinely obtained qPCR data can be used to maximize culture effectivity by guiding which samples to submit for NG culture and subsequent AMR testing.
PP03.109 – Multimodal Approach for Optimal Treatment Outcomes in Condyloma Acuminata
Dr. Rey Tristan Joshua Unay1,2, Dr. Marion Odette Alonzo1,2, Dr Jolene Kristine Dumlao1,2
1Southern Isabela Medical Center, Philippines.
2Philippine Dermatological Society, Philippines.
Background: Condyloma acuminata, or genital warts, is a common sexually transmitted infection caused by human papillomavirus (HPV). While various treatment modalities exist, a multimodal approach may be necessary for optimal outcomes, especially in cases of extensive or refractory lesions. This case report presents a patient with condyloma acuminata who was successfully treated with a combination of surgical excision, cautery, chemical cauterization, and topical imiquimod therapy.
Methods: A 64-year-old male presented with multiple erythematous to grayish verrucous hyperkeratotic plaques on the perianal and right inguinal area associated with pruritus on a background of pertinent sexual history of multiple female sexual partners with occasional condom use. He denied any MSM encounters nor anal plays. Serology testing yielded negative to Syphilis and HIV. He is a known diabetic and hypertensive and is maintained on medications. Histopathological examination showed exophytic structure with hyperkeratosis and parakeratosis, papillomatosis, acanthosis with bulbous rete ridges, presence of koilocytes, dilated blood vessels in the dermal papillae, consistent with condyloma acuminata. He was treated initially with serial debulking excision surgery with cautery and trichloroacetic acid (TCA) 30% as hemostatic agents. Patient was given topical imiquimod post-op as continued topical medications and was advised safe sexual practices.
Results: At 2- and 4-week follow up visits, the patient reported marked improvement in the previous lesions and consequently with satisfactory results.
Conclusion: This case highlights the efficacy of a multimodal approach in the management of condyloma acuminata. By combining surgical excision, cautery, chemical cauterization, and topical imiquimod therapy, complete resolution of the lesions was achieved. This case report underscores the importance of tailoring treatment plans to individual patient needs and considering a combination of therapeutic modalities for optimal outcomes.
PP03.11 – A Multisite Pilot Study Evaluating Linezolid for Early Syphilis Treatment
Dr. Chrysovalantis Stafylis1, Ryan Mikaela Nguyen1, Jacob Gizamba1, Kelika Konda1, Michael Reyes2, Kori Keith1, Keith Stokes4, Catherine Creticos3, Byron Johnson4, Ebony Philips3, Jeffrey D Klausner1
1University of Southern California, Los Angeles, United States.
2Universidad Peruana Cayetano Heredia, Lima, Peru.
3Howard Brown Health, Chicago, United States.
4Open Arms HealthCare, Jackson, United States.
Background: Linezolid is an FDA-approved, safe, low-cost, oral antibiotic that is efficacious against Treponema pallidum in in vitro and animal studies. Pharmacological simulations show that linezolid 600 mg, twice a day for 10 days, may be efficacious for syphilis treatment. We are assessing the clinical efficacy of linezolid 600 mg for cases of early syphilis.
Methods: We are conducting a randomized, non-comparative pilot study enrolling adults with primary, secondary, or early latent syphilis. We will enroll 24 patients (18 linezolid, 6 penicillin) from clinical sites in the United States. The linezolid arm receives oral linezolid 600 mg twice daily for 10 days, while the penicillin arm receives benzathine penicillin G 2.4 million units intramuscularly once. The primary outcome is a ≥4-fold RPR titer decline by 6 months after treatment. Linezolid participants are monitored for adherence and adverse events during treatment. Clinical and serological response is evaluated through 3-month, and 6-month follow-up visits. A 1-month visit for linezolid participants ensures safety.
Results: Fifteen out of 24 participants are enrolled in the study (11 linezolid arm, 4 penicillin arm). Fourteen participants had early latent syphilis, while 1 participant had secondary syphilis. To date, 9/10 eligible linezolid participants participated in the 1-month visit; one participant was retreated due to increasing RPR titer, 5 showed lower RPR titer and 3 the same RPR titer compared to enrollment. Eight participants reached and completed their 3-month and 6-month visit. Of the eleven linezolid participants, four achieved treatment success, one treatment failure (4-fold RPR titer increase), and six are awaiting three or 6-month follow-ups. Among the penicillin participants, all 3 had successful treatment outcomes. No serious adverse reactions have been reported.
Conclusion: With 1 case of linezolid failure among 10 participants at 1-month, and the majority of participants showing serological response, linezolid shows promise. Study enrollment continues.
PP03.12 – Evaluating the Non-Reportable Rate of Clinician Collected Samples When Tested with BD Vaginal Panel on the BD COR System
Ms. Elizabeth Stonebraker1, Mr. Brendan Dunphy1, Ms. Brandy Garzel1, Ms. Courtney Passow
1Becton Dickinson and Company, Sparks, United States.
Background: Vaginitis is a common complaint, traditionally diagnosed either empirically or using Amsel’s criteria and wet mount microscopy. Compared to traditional methods, molecular-based assays have a high analytical sensitivity and have shown good clinical sensitivity for vaginitis detection. However, improper specimen collection and specimen contamination can lead to high non-reportable (NR) rates (defined as any result that is not positive or negative) when performing molecular assays. High NR rates can contribute to a specimen backlog, reduced revenue, and low user satisfaction. Here, we determine the sample NR rate while performing BD Vaginal Panel (VP) when run on the high-throughput BD COR™ system (COR).
Materials and Methods: NR results on COR occur as either unresolved (UNR) or indeterminate (IND). Three hundred (300) clinician-collected specimens (according to manufacturer’s package insert) were obtained from women, symptomatic of vaginitis. Specimens were stored per the package insert (2–30°C for ≤21 days) prior to testing with VP on COR.
Results: An initial UNR rate of 0.33% [95% CI: 0.00, 1.86] was obtained for the 300 samples on COR during performance of VP. After retesting all XX UNR specimens returned a valid result, leaving a final UNR rate of 0.00% [95% CI: 0.00, 1.26]. An initial IND rate of 0.0% [95% CI: 0.00, 1.26] was observed; thus no specimen retesting was required due to IND results. After all testing was complete, the initial NR rate was 0.33% [95% CI: 0.00, 1.86] and the final NR rate was 0.00% [95% CI: 0.00, 1.26].
Conclusions: When specimens are collected according to the manufacturer’s package insert, VP produced a NR rate of less than 1%. This highlights the importance of proper specimen collection – especially prior to a speculum exam; avoiding specimen exposure to lubricants, which might be applied to the speculum, is an important precaution.
PP03.13 – ABI-1179, a Novel, Orally Administered, Long-Acting HSV Helicase-Primase Inhibitor: Interim Analysis of Safety and Pharmacokinetic Data from a Phase 1a Study in Healthy Participants
Prof. Edward Gane1, Dr Christian Schwabe2, Dr. Grace Wang3, Mr Jieming Liu3, Mr Steven Knox3, Ms Kathryn Kitrinos3, Dr Anuj Gaggar3, Ms Katie Zomorodi3
1University of Auckland, Auckland, New Zealand.
2New Zealand Clinical Research, Auckland, New Zealand.
3Assembly Biosciences, South San Francisco, United States.
Background: Herpes simplex virus type 2 (HSV-2), the primary cause of genital herpes, is estimated to infect 491.5 million people aged 15–49 years worldwide. Recurrences associated with pain and psychological stress are frequent and suppressive therapy with nucleoside analogues is suboptimal. ABI-1179 is a potent, orally administered, investigational agent that interferes with the HSV helicase-primase enzyme complex and is under development for suppression of recurrent genital herpes (RGH). Here we report single-dose safety and PK data in healthy participants.
Methods: ABI-1179-101 (NCT06698575) is a randomized, blinded, placebo-controlled Phase 1 study. Part A is ongoing and is evaluating the safety and PK of single, oral ABI-1179 doses in healthy participants. Within each dose group participants were randomized in a 6:2 ratio to ABI-1179 or placebo with 10-day post-dose follow-up. Safety was assessed by physical examination, adverse events (AEs), and laboratory parameters. ABI-1179 plasma concentrations were quantified by LC-MS.
Results: 24 participants received treatment in three ABI-1179 dose groups (50, 100, 300 mg). Most were male (20/24), white (17/24), aged 18–52 years with BMI 19.1–31.0 kg/m2. Treatment was well tolerated. AEs, generally Grade 1, were reported in 11/18 and 2/6 ABI-1179 and placebo recipients respectively. No Grade 3/4 AEs, treatment-related lab abnormalities, serious AEs or deaths were reported. ABI-1179 plasma exposure increased nearly dose proportionally from 50 to 300 mg (Fig. 1). The PK profile indicates a t1/2 of approximately 4 days with projected Ctrough values in excess of protein-adjusted EC50 for HSV replication achievable at all dose levels with once weekly dosing.
Conclusion: ABI-1179 was well tolerated when administered orally as single doses up to 300 mg. Plasma exposures exceeded protein-adjusted EC50’s for inhibition of HSV replication and the observed t1/2 of approximately 4 days supports once weekly dosing. Phase 1b will explore safety, PK and antiviral activity following multiple doses in participants with RGH.
PP03.14 – Impact of Comorbidity of HIV infection and Chronic Cocaine Use on Brain Aging and Cognitive Impairment
Dr. Hong Gu1, Dr. Betty Jo Salmeron1, Dr. Danni Wang1, Dr. Nanyu Kuang1, Dr. Hui Zheng1, Dr. Shenghan Lai2, Dr. Yihong Yang1
1National Institute on Drug Abuse, Baltimore, United States.
2University of Maryland School of Medicine, Baltimore, United States.
Background: While substance use disorders (SUDs) are known to be highly prevalent in people living with HIV (PLWH), the impact of comorbidity of HIV infection and SUD on brain aging and related cognitive impairment is unknown. In this study, we investigated the combined impact of comorbid chronic cocaine exposure in PLWH on brain aging and neurocognitive impairment (NCI).
Methods: A brain aging model was built based on network-wise cortical metrics in the brain MRI of Human Connectome Project in Aging (HCP-A) (N = 725, age range = 36–100 years) using a machine learning approach. The model was applied to a community cohort of HIV-infected and uninfected participants with or without cocaine use (N = 186, age range = 35–76.6 years) to predict their brain ages. Brain age gap (BAG) was defined as the difference between the predicted brain age and chronological age, with a positive BAG indicating accelerated brain aging. Cognitive performance was evaluated by NIH Toolbox cognition battery and NCI was defined present if the fully adjusted T scores in at least two cognitive domains was 1.0 SD below the mean.
Results: Cognitively, BAG was significant higher in participants with NCI than without NCI (P = 0.013). Compared with controls, PLWH showed larger BAG (P = 0.00061) and higher risk of NCI (OR = 3.36, P = 0.019). Similarly, participants who reported cocaine use showed larger BAG (P = 0.0031) and marginally higher risk of NCI (OR = 2.80, P = 0.052). Furthermore, PLWH using cocaine showed marginally significantly larger BAG (P = 0.088) compared to PLWH without cocaine use. When compared to HIV-uninfected participants with cocaine use, PLWH using cocaine showed larger BAG (P = 0.032).
Conclusion: This study demonstrated that both HIV infection and chronic cocaine use contribute individually to accelerated brain aging and increased risk of neurocognitive impairment, and chronic cocaine use further exacerbates neurobiological aging in PLWH.
PP03.15 – Antibiotic Resistance Mutations and Treatment Outcomes in Men with (Persistent) Mycoplasma Genitalium Urethritis
Miss Nikki Adriaens1,2, Dr Sylvia Bruisten1,2, Dr Alje van Dam1,2,3, Dr Brenda Westerhuis1,2, Ms Fenna Bouwman1, Ms Tessa Doelman2,3, Prof Henry de Vries1,2,3, Dr Clarissa Vergunst1,4
1Public Health Service of Amsterdam, Amsterdam, Netherlands.
2Amsterdam Institute for Immunology and Infectious Diseases, Amsterdam, Netherlands.
3Amsterdam UMC Location University of Amsterdam, Amsterdam, Netherlands.
4NWZ, Den Helder, Netherlands.
Background: Mycoplasma genitalium (MG) is a leading cause of non-gonococcal urethritis (NGU) in men. Over 70% of MG infections harbor macrolide-resistance associated mutations (MRAMs), reducing azithromycin efficacy, while fluoroquinolone-resistance associated mutations (FRAMs) may limit moxifloxacin effectiveness. Dutch guidelines recommend presumptive azithromycin treatment and awaiting symptom clearance for at least 4 weeks before considering MG testing and moxifloxacin treatment, despite limited evidence. This study evaluates the clinical and microbiological effectiveness of this treatment regimen and its association with antibiotic resistance-associated mutations.
Methods: Urine samples from men with NGU at the Amsterdam Centre for Sexual Health were tested for MG, Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) (Fig. 1). MG-positive participants were invited for follow-up at Weeks 2, 4 and 6 for clinical assessment and repeated urine testing. MRAMs and FRAMs were identified in MG-positive samples. Participants recorded symptoms and antibiotic-related side-effects in a diary. Moxifloxacin was prescribed if MG-NGU persisted at Week 4.
Results: Preliminary results revealed a high prevalence of MG, identified in 15/46 participants (32.6%) compared to CT in 12/46 (26.1%). MRAMs were detected in 66.7% (33.3% non-typable), while FRAMs were identified in 13.3% (40.0% non-typable) of MG-cases. Following presumptive azithromycin treatment, MG persisted in 7/11 (63.3%) at Week 2 of follow-up and 6/9 (66.7%) at Week 4. After moxifloxacin treatment, 4/9 participants (44.4%) remained MG-positive at Week 6 of follow-up, with three cases testing negative for FRAM. In 2/4 participants with persistent MG-NGU, symptoms, particularly dysuria, did not improve over the course of 6 weeks.
Conclusion: The high prevalence of MG and the presence of MRAMs and FRAMs highlight the challenges in managing MG-NGU. The three cases of persistent MG positivity following moxifloxacin treatment, despite testing negative for FRAM, underscore the need for further investigation into additional mutations that may lead to fluoroquinolone treatment failure.
Urine samples from men with NGU at the Amsterdam Centre for Sexual Health were tested for MG, Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG).
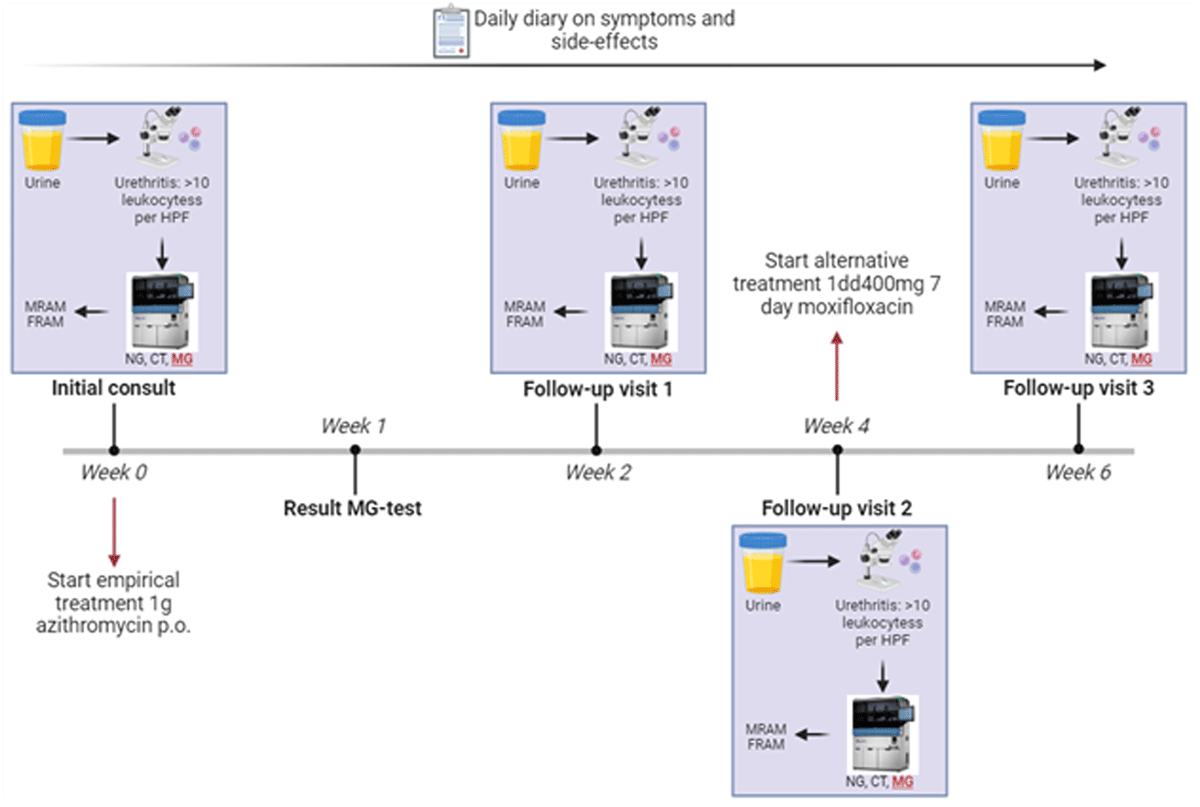
PP03.16 – Survey on the Difficulties and Questions of Healthcare Professionals in Addressing Syphilis in Brazil, 2024
Dr. Luiz Fernando Aires Junior1, Ana Paula Betaressi da Silva1, Pâmela Cristina Gaspar1, Marcia Rejane Colombo1, Mayra Gonçalves Aragón1, Romina Oliveira1
1Health Ministery, Brasilia, Brazil.
Background: Syphilis is a bacterial infection that can be transmitted sexually and vertically, and it can progress to severe forms, complications during pregnancy, and congenital alterations. In Brazil, syphilis is an important public health issue, with a growing increase in the detection rates of acquired syphilis and syphilis in pregnant women, reflecting in a high incidence of congenital syphilis. The aim of this study was to identify the main questions that healthcare professionals have regarding the management of this disease.
Materials/Methods: Between 04/25 and 05/20/24, an anonymous public electronic survey was conducted through the federal management platform. The form contained eight fields: state, municipality of residence, and professional category of the participant; and two fields for questions about syphilis, categorized into the following themes: “Diagnosis,” “Monitoring,” “Prevention,” “Surveillance,” “Treatment,” or “Other.” The responses were exported and analyzed using Microsoft Excel®.
Results: A total of 392 questions were received across 316 forms. Of these, 62.3% (197/316) were from nurses, 11.4% (36/316) from doctors, and 37.3% (118/316) from 13 other healthcare professional categories. The highest percentage of questions was about acquired syphilis (38.4%), followed by syphilis in pregnant women (32.8%) and congenital syphilis (28.8%). The most frequently addressed theme was treatment. About the federative units (UF), 81.4% (22/27) participated in the survey, with lower participation from the northern region of the country. Two of the three federative units with the highest participation also have some of the highest incidence rates of syphilis.
Conclusions: The results revealed gaps in knowledge among various healthcare professionals across the country. This survey may serve as a foundation for future training and the development of strategies to reduce the burden of infection in the territory, improve health indicators, empower professionals through knowledge, and provide comprehensive care for patients.
PP03.17 – Secondary Syphilis in Primigravidas: A Case Series
Dr. Sittie Junainah Ali1, Dr Christine Remar Concepcion1
1Las Pinas General Hospital- Satellite Trauma Center, Las Pinas, Philippines.
Background: In the Philippines, health often takes a backseat as a societal priority, reflected in the lack of official data on syphilis in pregnancy. Syphilis, caused by the spirochetal bacterium Treponema pallidum, is a sexually transmitted disease with severe implications for maternal and fetal health. Despite the World Health Organization (WHO) reporting 8 million new syphilis cases among adults aged 15–49 and 700,000 congenital syphilis cases globally in 2022, the condition remains undiagnosed and underreported in the Philippines.
Methods: We present three rare cases of secondary syphilis in teenage pregnancies during the third trimester. Two patients initially presented with labor pains and physical examination revealed condyloma lata and maculopapular rash on the hands and soles. Both delivered preterm stillborn infants. The third patient, not in labor, consulted for vulvar lesions (condyloma lata) and was discharged clinically improved after treatment.
Results: Serological tests, including the Venereal Disease Research Laboratory (VDRL) test and Treponema pallidum hemagglutination assay (TPHA), confirmed the diagnosis.
All patients tested reactive for VDRL and TPHA, confirming secondary syphilis. Clinical presentations included vulvar lesions, maculopapular rash, and adverse pregnancy outcomes such as preterm stillbirth, underscoring the severe impact of untreated syphilis in pregnancy.
Conclusions: These cases highlight the critical need for routine syphilis screening during pregnancy to prevent adverse outcomes, including stillbirth and congenital syphilis. Efforts must also focus on educating communities about sexually transmitted diseases and promoting safe sexual practices. Hospitals must establish comprehensive tracking systems for syphilis cases to improve surveillance, guide public health interventions, and allocate resources effectively. Such initiatives would enable the adoption of evidence-based practices from the international community, improving maternal and fetal health outcomes. Addressing this preventable yet overlooked condition is vital for safeguarding maternal and neonatal health.
PP03.18 – A Scoping Review of Strategies to Diversify Treatment of N. Gonorrhoeae Infection to Mitigate the Emergence of Antimicrobial Resistance
Dr. Lao-Tzu Allan-Blitz1, Dr. Paul Adamson2, Prof Jeffrey D. Klausner3
1Harvard Medical School, Boston, United States.
2Division of Infectious Diseases, School of Medicine, University of California, Los Angeles, United States.
3Department of Population and Public Health Sciences, Keck School of Medicine, University of Southern California, United States.
Background: Antimicrobial-resistant N. gonorrhoeae is an urgent global public health threat. Novel antibiotics have been developed, while rapid molecular resistance assays to guide therapy are increasingly available. Both can facilitate treatment diversification – a key strategy for mitigating resistance emergence.
Methods: We conducted a scoping review of emerging strategies that may support diversifying treatment of N. gonorrhoeae infection. We searched PubMed for reports published in the last 10 years of a) clinical treatment trials, or b) antimicrobial resistance testing for N. gonorrhoeae infection. We included non-peer reviewed reports of recent phase III trials for two new antimicrobials.
Results: A 3 g dose of oral zoliflodacin and two 3 g doses of oral gepotadicin 12 h apart both demonstrated non-inferiority to a combination of ceftriaxone 500 mg plus azithromycin 1 g for urogenital N. gonorrhoeae infection. Notably, 79% of pharyngeal infections were cured with zoliflodacin, and 78% with gepotadicin. Cefixime 800 mg plus doxycycline 100 mg twice daily for 7 days had a 14.5% increased risk of treatment failure compared with ceftriaxone 1 g plus azithromycin 2 g; all failures were attributed to pharyngeal infection. Modeling work estimated that time to resistance after introduction of novel antimicrobials was longest if new treatments are introduced in parallel or combination with current therapy.
Incorporation of gyrase A genotyping (predicting ciprofloxacin resistance) into routine care significantly decreased ceftriaxone use in settings across the US and UK. Modeling studies demonstrated prolonged ceftriaxone effectiveness after incorporation of genotypic resistance testing.
Conclusion: With the development of novel therapeutics and the increasing availability of molecular resistance testing, treatment diversification for N. gonorrhoeae is becoming possible. Given that most ceftriaxone treatment failures to date involve the pharynx, and that the efficacy of novel antimicrobials at the pharynx remains to be determined, outcomes data are necessary for pharyngeal infections.
PP03.19 – Comparison of Self-Sampling and Physician-Sampling of Anal Swabs for Anal Cancer Screening
Dr. Naokatsu Ando1, Dr. Daisuke Mizushima1, Dr Misao Takano1, Seitaro Abe1, Akira Kawashima1, Ryo Kuwata1, Dr Takato Nakamoto1, Dr Daisuke Shiojiri1, Dr Takahiro Aoki1, Dr. Shinichi Oka1, Dr Hiroyuki Gatanaga1
1National Center for Global Health and Medicine, Shinjuku-ku, Japan.
Background: Self-sampling is increasingly promoted for its potential to improve screening accessibility and acceptability. This study evaluates the concordance, sensitivity, and specificity of self-sampling (SS) compared to physician-sampling (PS) for detecting high-risk HPV and cytology in men who have sex with men (MSM).
Methods: This cross-sectional study involved MSM at the National Center for Global Health and Medicine in Japan. Participants collected self-sampled (SS) and physician-sampled (PS) specimens in sequence – first SS, then PS – and underwent tissue biopsy under high-resolution anoscopy on the same day. Kappa statistics and McNemar’s tests were used to assess agreement and systematic differences between the two methods; sensitivity and specificity were also calculated (Table 1).
Results: A total of 136 participants (median age: 48 years, IQR: 40–53) were analyzed, of whom 125 (91.2%) were living with HIV. High-risk HPV was detected in 82.4% (95% CI: 74.9–87.9) using SS and 88.2% (95% CI: 81.6–92.7) with PS. High-risk HPV detection showed substantial agreement between self-sampling and physician-sampling (κ = 0.651, P < 0.001). Sensitivity for high-risk HPV was 98.2% (95% CI: 93.7–99.8), while specificity was 58.3% (95% CI: 36.6–77.9). For HPV16, agreement was even stronger (κ = 0.861, P < 0.001), with a sensitivity of 92.3% (95% CI: 74.9–99.1) and a specificity of 96.4% (95% CI: 91.0–99.0). Cytology showed moderate agreement (κ = 0.512, P < 0.001). Sensitivity for cytology was 73.2% (95% CI: 59.7–84.2), and specificity was 77.9% (95% CI: 66.2–87.1).
Conclusions: Self-sampling demonstrates high concordance with physician-sampling for detecting high-risk HPV, particularly for specific genotypes such as HPV16. The moderate agreement observed for cytology highlights the potential utility of self-sampling in detecting cytological abnormalities, although further refinements in this approach may improve its accuracy. Implementing self-sampling could facilitate broader participation in anal cancer screening programs, especially among high-risk populations.
| Agreement (%) | kappa coeefecient | P-value | McNemar test (P-value) | Sensitivity (%) | 95% CI | Specificity (%) | 95% CI | Positive predictive value (%) | 95% CI | Negative predictie value (%) | 95% CI | ROC area | 95% CI | ||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| High-risk HPV | 91.18 | 0.6507 | <0.001 | 0.0209 | 98.2 | 93.7-99.8 | 58.3 | 36.6-77.9 | 91.7 | 85.2-95.9 | 87.5 | 61.7-98.4 | 0.78 | 0.68-0.88 | |
| HPV16 | 95.59 | 0.8614 | <0.001 | 0.4142 | 92.3 | 74.9-99.1 | 96.4 | 91.0-99.0 | 85.7 | 67.3-96.0 | 98.1 | 93.5-99.8 | 0.94 | 0.89-1.00 | |
| HPV18 | 96.32 | 0.8073 | <0.001 | 0.1797 | 92.3 | 64.0-99.8 | 96.7 | 91.9-99.1 | 75 | 47.6-92.7 | 99.2 | 95.4-100.0 | 0.95 | 0.87-1.00 | |
| HPV31 | 97.79 | 0.9228 | <0.001 | 0.5637 | 95.7 | 78.1-99.9 | 98.2 | 93.8-99.8 | 91.7 | 73.0-99.0 | 99.1 | 95.1-100.0 | 0.97 | 0.93-1.00 | |
| HPV33 | 97.06 | 0.8023 | <0.001 | 0.3173 | 90 | 55.5-99.7 | 97.6 | 93.2-99.5 | 75 | 42.8-94.5 | 99.2 | 95.6-100.0 | 0.94 | 0.84-1.00 | |
| HPV45 | 97.06 | 0.7843 | <0.001 | 0.3173 | 88.9 | 51.8-99.7 | 97.6 | 93.3-99.5 | 72.7 | 39.0-94.0 | 99.2 | 95.6-100.0 | 0.93 | 0.82-1.00 | |
| HPV52 | 92.65 | 0.8258 | <0.001 | 0.0578 | 94.7 | 82.3-99.4 | 91.8 | 84.5-96.4 | 81.8 | 67.3-91.8 | 97.8 | 92.4-99.7 | 0.93 | 0.89-0.98 | |
| HPV58 | 90.44 | 0.7681 | <0.001 | 0.7815 | 84.6 | 69.5-94.1 | 92.8 | 85.7-97.0 | 82.5 | 67.2-92.7 | 93.8 | 86.9-97.7 | 0.89 | 0.82-0.95 | |
| HPV06 | 97.06 | 0.92 | <0.001 | 0.3173 | 91.2 | 76.3-98.1 | 99 | 94.7-100.0 | 96.9 | 83.8-99.9 | 97.1 | 91.8-99.4 | 0.95 | 0.90-1.00 | |
| HPV11 | 99.26 | 0.9614 | <0.001 | 0.3173 | 100 | 76.8-100.0 | 99.2 | 95.5-100.0 | 93.3 | 68.1-99.8 | 100 | 97.0-100.0 | 1 | 0.99-1.00 |
PP03.20 – High Test-Of-Cure Positivity After Cefixime Treatment for Gonorrhea in Hanoi, Vietnam
Dr. Paul Adamson1, Hollie David1, Hao TM Bui2, Loc Q Pham2, Assoc Prof Giang Minh Le2, Prof Jeffrey D Klausner3, Assoc. Prof. Tanya Applegate
1Division of Infectious Diseases, University of California, Los Angeles School of Medicine, Los Angeles, United States.
2Hanoi Medical University, Hanoi, Vietnam.
3Department of Population and Public Health Sciences, Keck School of Medicine, University of Southern California, Los Angeles, USA.
Introduction: Antimicrobial resistance in Neisseria gonorrhoeae (NG) is a global health challenge. Ceftriaxone is the first-line treatment, while cefixime, given as a single oral dose, is recommended as an alternative. Data on cefixime treatment outcomes are limited, especially in areas with emerging cefixime resistance.
Methods: We conducted a secondary analysis from a study on Chlamydia trachomatis and NG testing within an HIV PrEP program in Hanoi, Vietnam. Eligible participants were males, aged ≥16 years, with ≥1 male sex partner in the past 12 months. Between May 2022 and February 2023, participants with NG infections, detected via culture or nucleic acid amplification test (NAAT), at pharyngeal, rectal, or urogenital sites were treated with a single 800 mg oral dose of cefixime. A test-of-cure (TOC) visit was done 10–21 days post-treatment, with specimens obtained for culture and NAAT. Multivariate logistic regression was used to evaluate factors associated with TOC positivity.
Results: There were 24 participants treated with cefixime, including 12 rectal, 17 pharyngeal, and 7 urethral infections. Twenty participants (83.3%) returned for TOC, with a median of 12 days [IQR: 11.5–14]. Overall TOC positivity by NAAT was 45% (9/20); TOC positivity was 60% (9/15) in pharyngeal, 10% (1/10) at rectal, and 0% at urogenital sites. All TOC cultures were negative. Initial NAAT cycle thresholds were associated with TOC positivity (aOR = 0.82; 95% CI 0.70–0.92). Time from treatment to TOC and symptoms at treatment were not associated with TOC positivity.
Conclusions: Our findings indicate a high TOC positivity by NAAT, particularly at pharyngeal sites, among NG infections treated with oral cefixime in Vietnam. Higher NAAT cycle thresholds at treatment were less likely to have a positive TOC. No infections were culture-positive at TOC, suggesting that NAAT results might reflect non-viable bacterial DNA. These results raise concerns about the utility of NAATs for TOC.
PP03.21 – Leveraging Digital Health Innovations to Improve Adolescent Sexual Health in Underserved Remote Areas of West Africa Countries
Dr. Oluwatomiyin Bassey Ekong1
1Nigeria LNG Limited (NLNG) Residential Hospital, Bonny Island, Nigeria.
The adolescents in the remote communities of West African countries are disadvantaged in terms of receiving appropriate sexual health education and services. Cultural barriers, inadequate health facilities and a shortage of competent healthcare personnel in the rural areas compound all these. As a result, adolescents are at higher risk of STI infections, early pregnancies, and poor knowledge of sexual health. Solving these issues calls for innovative approaches to ensure that the gap in health care is closed and adolescents are reached where other methods are ineffective. This research proposal assesses how new technologies, including mobile applications, telemedicine and Short Message Service (SMS) based programmes, can enhance adolescent sexual health knowledge and services in the less developed remote regions of West Africa. This study will adopt a systematic review approach, extracting data from published articles, reports, and case studies between 2010 and 2024. The review will be mainly on awareness of useful tools in digital health and its influence on youth sexual health and limitations in implementing digital health in West Africa. The expected outcomes include defining the major digital health interventions that have been effective in enhancing sexual health, and emerging issues such as digital literacy, access to the internet, and cultural barriers. The study’s results will be useful for policymakers, healthcare organizations, and NGOs to show how digital health solutions can revolutionize adolescent sexual health and close gaps in care in rural areas of West Africa.
PP03.22 – Ocular Chlamydia Trachomatis (CT) and Neisseria Gonorrhoeae (NG): No Need to Confirm Positive Nucleic Acid Amplification Tests (NAAT) Results
Dr. Olivier Bédard1, Dr. Julie Vadboncoeur1,2, Dr. Émilie Vallières1,4, Dr. Patrick Hamel1,4, Dr. Christian Lavallée1,2,3, Dr. Brigitte Lefebvre5, Dr. Judith Fafard1,5, Dr. Annie-Claude Labbé1,2,3
1Université de Montréal, Montréal, Canada.
2Hôpital Maisonneuve-Rosemont, Montréal, Canada.
3Centre hospitalier de l’Université de Montréal, Montréal, Canada.
4Centre hospitalier universitaire Ste-Justine, Montréal, Canada.
5Laboratoire de Santé Publique du Québec, Sainte-Anne-de-Bellevue, Canada.
Background: Laboratory diagnosis of CT/NG conjunctivitis is made by NAAT. Diagnosis of ocular NG infections can also be made by culture, which is less sensitive than NAAT. Since regulatory agencies have not approved CT/NG NAAT for ocular specimens, a local validation is required. Among challenges are the lack of a gold standard with equivalent performance and the rarity of positive ocular samples. The objective of this retrospective case-series is to combine clinical with microbiological data to strengthen our validation process.
Methods: All positive local CT/NG NAAT results from ocular samples collected between October 2012 and September 2024 were extracted from the Laboratory Information System. Testing was performed using the Roche cobas®4800 (until March 2022), and subsequently with the cobas®8800 analyzer. Clinical files were reviewed by an ophthalmologist, and confirmatory CT/NG NAAT results were obtained from the Laboratoire de Santé Publique du Québec (LSPQ) (PCR targeting the porA and opa genes for NG and cryptic plasmid for CT).
Results: A total of 70 ocular samples (58 CT+ and 12 NG+) were identified among 53 distinct individuals (45 CT infections and 8 NG infections). Twenty CT+ samples (13 individuals) were sent to the LSPQ, all confirmed as positive. Additionally, 6 samples (6 individuals) were considered confirmed by a concomitant CT+ NAAT from a genital sample. Among the remaining samples, clinical information was available for 21 (17 individuals). All had a compatible clinical presentation (follicular or purulent conjunctivitis). For 11 samples (nine individuals), there was no laboratory confirmation test, and clinical information was not available. All NG+ samples were sent to LSPQ and confirmed as positive.
Conclusion: In this case-series, 47 CT+ and 12 NG+ ocular samples were either laboratory or clinically confirmed. We conclude that positive results obtained with the Roche cobas CT/NG assay on ocular samples do not need confirmatory testing.
PP03.23 – Factors Associated with Loss to Follow-Up Among People Living with HIV at Public Health Facilities in Manaus, Brazil: A Multicentric Study
Dr. Zeca Manuel Salimo1,2, Dr. Elizangela Farias da Silva3, Dr. Michael Nosano Yakubu1,4, Miss Yamile Alves Silva Vilela5, Dr. Raquel Maria Navarro6, Dr. Paulo Afonso Nogueira7,8, Dr. Adele Benzaken1,9
1Programa de Pós-Graduação em Medicina Tropical, Universidade do Estado do Amazonas, Manaus, Brazil.
2Faculdade de Ciências de Saúde, Universidade Lúrio, Nampula, Mozambique.
3Centro de Estudos Superiores de Tabatinga, Universidade do Estado do Amazonas, Tabatinga, Brazil.
4Department of Microbiology, Federal University Wukari, Wukari, Nigeria.
5AIDS Healthcare Foundation (AHF), São Paulo, Brazil.
6Departamento de Infecções Sexualmente Transmissíveis, Fundação Hospitalar Alfredo da Matta, Manaus, Brazil.
7Instituto Leônidas e Maria Deane, Fundação Oswaldo Cruz, Manaus, Brazil.
8Programa de Pós-Graduação em Imunologia Básica e Aplicada, Universidade Federal do Amazonas, Manaus, Brazil.
9AIDS Healthcare Foundation (AHF), Los Angeles, USA.
Background: Loss to follow-up (LTFU) among people living with HIV (PLHIV) impact on the quality of life of PLHIV, and consequently on the ineffectiveness of strategies to control the HIV/AIDS epidemic. The aim of the study was to investigate the factors associated with LTFU among PLHIV treated at referral health facilities in Manaus.
Methods: This was a multicenter cohort study that involved the review of 2085 medical records. Sociodemographic, epidemiological, behavioral, diagnostic and clinical follow-up variables of all study participants were analyzed. Cox proportional hazards regression was used to determine factors associated with LTFU. Semi-structured interviews were conducted with PLHIV in LTFU status to explore reasons for LTFU.
Results: Of the 2085 PLHIV enrolled, 1534 (73.58%) were male, the median age was 36.75 years, and 1226 (58.80%) were single. A total of 465 (22.30%) PLHIV who did not collect ARVs in a period of more than 90 days or did not attend a scheduled appointment in 6 months were considered LTFU. The main factors associated with LTFU included being single (hazard ratio (HR) = 3.51, 95% confidence interval (CI): 1.69–7.36, P = 0.01), low education level (HR = 2.1, 95% CI: 0.62–1.36, P = 0.00), and having an undetectable last viral load result (HR = 2.04; 95% CI, 1.05–3.95; P = 0.04). Discrimination, stigma, lack of family or social support, illicit drug use, low economic conditions, adverse effects of antiretroviral therapy, and poor patient-provider relationship were the main reasons for LTFU reported from semi-structured interviews.
Conclusions: LTFU among PLHIV in health facilities in Manaus can occur at any stage of clinical follow-up. To mitigate the LTFU rate among PLHIV in Manaus, it is recommended to reinforce appropriate measures for risk groups and improve the quality-of-service provision to PLHIV.
Keywords: Public health facilities, PLHIV, HIV care, Loss to follow-up, Predictors, Manaus.
PP03.24 – Pritelivir for Resistant HSV Infections: Phase 3 Progress and Expanding Therapeutic Horizons
Dr. Alexander Birkmann1, Dr. Alessandra Marini1, Melanie Sumner1, Dr. Cynthia Wat1
1Aicuris Anti-infective Cures AG, Wuppertal, Deutschland.
Background: Pritelivir, an anti-herpes simplex virus (HSV) helicase primase inhibitor, addresses an unmet medical need for the treatment of acyclovir-resistant HSV infections in immunocompromised patients. We will provide an update on the ongoing Phase 3 PRIOH-1 trial, the early access program (EAP), and explore potential broader applications of pritelivir in HSV management.
Methods: The PRIOH-1 trial is a randomized, open-label study comparing pritelivir (100 mg orally) with investigator’s choice (foscarnet, cidofovir IV or topically, and imiquimod) in patients with acyclovir-resistant HSV infection. The treatment duration is up to 42 days. Safety, efficacy and tolerability data are being collected and analyzed to inform future research directions. In addition, an EAP is active globally with 209 treatments in 124 subjects to date.
Results: Data from the Phase 2 portion of the trial demonstrated promising efficacy and safety for pritelivir with 83% of pritelivir treated subjects showing full resolution of their HSV lesions within the treatment period. The PRIOH-1 trial has been expanded to include 55 sites in 14 countries reflecting the widespread nature of this clinical challenge. Interim analysis from the EAP indicates lesion resolution rates and safety profile consistent with the Phase 2 results. The data may support potential applications beyond the current study population and warrant further investigation in various HSV management scenarios.
Conclusion: The ongoing Phase 3 trial aims to evaluate pritelivir as a treatment for resistant HSV infections in immunocompromised patients. Future studies will evaluate long-term safety and efficacy in various clinical settings, potentially expanding the therapeutic scope of pritelivir and informing new strategies for HSV management across different patient populations and treatment paradigms.
PP03.25 – Treatment Variability Among People Assigned Male at Birth with Complicated Mycoplasma Genitalium Infections, Public Health – Seattle and King County Sexual Health Clinic, 2023–2024
Dr. Chase Cannon1,2, Dr. Timothy Menza1,2, Christina Thibault2, Dr. Lisa Manhart1
1University of Washington, Seattle, United States.
2Public Health - Seattle & King County, Seattle, United States.
Background: Mycoplasma genitalium (Mgen) antimicrobial resistance (AMR) frequently leads to complicated infections and treatment failure. Sparse guidance exists for treating complicated infections and antibiotic options in the US are limited. We assessed treatment regimens used for complicated Mgen in a public sexual health clinic (SHC).
Methods: We conducted a case series of SHC patients assigned male at birth in Seattle, Washington, with ≥2 positive Mgen nucleic acid amplification tests (NAAT) within any 6-month period between 2023/1/1 to 2024/11/30. We classified patients as either recurrent (symptom recurrence within 2 months of appropriate treatment and positive Mgen NAAT at the same anatomic site after negative test of cure) or persistent (positive Mgen NAAT within 6 months of appropriate treatment without interval sexual exposure) infection.
Results: Overall, 293/2361 (12%) patients had Mgen. Sixteen patients met inclusion criteria (Table 1). Fourteen (88%) had NGU and 2 (12%) had proctitis. 10/14 (71%) patients with NGU had persistent (1) or recurrent (9) infection; both patients with proctitis experienced persistent Mgen. Mean time between visits/testing was 93 days. For complicated NGU and proctitis, patients completed a median of 2 (range = 1–7) and 4 (range = 3–4) antibiotic courses over a median of 34 (range = 7–134) and 65.5 (range = 64–67) days, respectively. 10/14 NGU cases received sequential doxycycline+moxifloxacin (DOX+MOX) more than once. Subsequent regimens included minocycline (NGU 4/14, proctitis 2/2), tinidazole (NGU 2/14, proctitis 2/2), azithromycin (NGU 5/14, proctitis 2/2), or pristinamycin (NGU 1/10, proctitis 0/2). Three NGU patients were probably re-infected; one was lost-to-follow-up. Confirmed cure occurred in 4/10 (40%) after their second DOX-MOX course, and 3/3 (100%) with NGU and 1/1 with proctitis who received minocycline+tinidazole. Minocycline alone was effective in 1 each with NGU and proctitis.
Conclusion: Treatment of recurrent/persistent Mgen varies considerably. Mgen treatment trials and clinically useful AMR testing are needed to inform clinical guidance on treating complicated Mgen infections.
| Case | Persistent or recurrent M gen | Gender of sex partners | Reinfection likely? | Infection Number and Antimicrobials Received | Total antibiotic days | Outcome after Final Regimen | |
|---|---|---|---|---|---|---|---|
| 1 | Neither | Men | Probable | Doxy (7d) + moxifloxacin (10d) | 34 | Clinical and microbiological cure | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 2 | Recurrent | Men | Possible | Doxy (7d) + moxifloxacin (10d) | 34 | Presumed clinical cure; gap between doxy and moxi, imperfect adherence | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 3 | Persistent at 3 months | Men | Possible | Doxy (7d) + azithromycin (3d) | 35 | Clinical and microbiological cure after final regimen. Tested partner had macrolide resistance mutation. Anaphylaxis to moxifloxacin | |
| Doxy (7d) + azithromycin (4d) | |||||||
| Minocycline (14d) | |||||||
| 4 | Neither | Women | Probable | Doxy (7d) + moxifloxacin (10d) | 34 | Presumed clinical cure | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 5 | Neither | Men | Probable | Doxy (7d) + moxifloxacin (10d) | 34 | Presumed clinical cure | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 6 | Persistent at 3 months | Women | Unlikely | Doxy (7d) + moxifloxacin (2d) | 38 | Presumed clinical cure; did not take moxi during first 2 courses due to nausea and concerns about side effects | |
| Doxy (7d) + moxifloxacin (0d) | |||||||
| Azithro 3g (5d) + doxy (7d) + moxifloxacin (10d) | |||||||
| 7 | Persistent at 3 and 6 months | Women | Unlikely | Doxy (7d) + moxifloxacin (10d) | 65 | Clinical and microbiologic cure | |
| Minocycline (14d) | |||||||
| Doxy (7d) + azithro (10d) | |||||||
| Doxy (7d) + pristinamycin (10d) | |||||||
| 8 | Persistent at 3 and 6 months | Men | Probable (second infection) and unlikely (subsequent infections) | Doxy (7d) + moxifloxacin (10d) | 134 | Clinical cure | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| Doxy (7d) + azithro 2.5g (4d) | |||||||
| Doxy (7d) + moxifloxacin (10d) | |||||||
| Doxy (7d) + azithro 2.5g (4d) | |||||||
| Doxy (7d) + minocycline (14d) | |||||||
| Minocycline (30d) + tinidazole 11g (10d) | |||||||
| 9 | Neither | Women | Probable | Doxy (7d) + moxifloxacin (10d) | 34 | Presumed clinical cure; lost to follow-up after 2nd antibiotic course | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 10 | Persistent at 6 months | Men, Nonbinary | Possible | Doxy (7d) + moxifloxacin (10d) | 34 | Presumed clinical cure | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 11 | Persistent at 6 months | Men | Unlikely | Doxy (7d) + moxifloxacin (10d) | 34 | Presumed clinical cure | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 12 | Persistent at 3 and 6 months | Men | Possible | Doxy (7d) + moxifloxacin (10d) | 34 | Microbiological cure (NGU 4.5 months after completing last antibiotic course) | |
| Doxy (7d) + moxifloxacin (10d) | |||||||
| 13 | Persistent at 3 and 6 months | Men, Women | Possible | Doxy (7d) + moxifloxacin (0d) | 7 | Took only doxycycline. Symptom resolution but positive test of cure | |
| 14 | Persistent at 3 and 6 months | Women | Unlikely | Doxy (7d) + moxifloxacin (10d) | 87 | Microbiologic and clinical cure after 4th antibiotic course; S83I mutation in ParC gene on research-based molecular sequencing | |
| Doxy (7d) + azithro 2.5g (4d) | |||||||
| Mino (14d) + tinidazole 11g (10d) | |||||||
| Mino (21d) + tinidazole 15g (14d) | |||||||
| 15 | Persistent at 3 months | Men | Probable (#2), unlikely (#3 and #4) | Doxy (7d) + moxifloxacin (7d) | 64 | Microbiologic cure (recurrent symptoms with negative test of cure 4 weeks after 4th antibiotic course) | |
| Doxy (14d) + azithro 3g (5d) | |||||||
| Doxy (7d) + tinidazole 11g (10d) | |||||||
| Minocycline (14d) | |||||||
| 16 | Persistent at 3 months | Men | Probable (#2); Unlikely (#3) | Moxifloxacin (10d) | 67 | Cure after first antibiotic course; presumed clinical cure but lost-to-follow-up with subsequent antibiotic courses | |
| Doxy (14d) + azithro 3g (5d) | |||||||
| Minocycline (28d) + tinidazole 11 g (10d) |
PP03.26 – A Case of Mpox in a 32-Year-Old Immunocompromised Male: A Case Report
Dr. Naphi Yaen Caymo1, Dr. Louella Fatima Ramos-Bascos1, Dr. Jolene Kristine Dumlao1
1Southern Isabela Medical Center, Santiago City, Philippines.
Background: Mpox virus is a zoonotic virus which belongs to the Orthopoxvirus genus of the Poxviridae family. The incubation period is 5 to 21 days. The illness begins with fever, headache, myalgia, and lymphadenopathy. In immunocompetent patients, lesions presents initially as monomorphic macules and papules which progress to become vesicles and pustules that umbilicate, crust, and desquamate. In immunocompromised patients however, lesions may present as multiple, large, rounded ulcers with necrotic centers and raised border. Hospitalization is reserved for patients with moderate to severe illness due to the risk for complications that may require more intensive pain management.
Description: We report a case of a 32-year-old immuncompromised male who initially presented with 2 skin-colored papules with central umbilication on the perioral area preceded by undocumented fever, headache, and body malaise (Fig. 1). Lesion progressed to become multiple skin-colored papules and plaques with central umbilication, ulceration, erosions and brown crusts on the face, trunk, back, upper and lower extremities, gluteal, anal and scrotal area. Past medical history revealed non-compliance to ARV medications with latest CD4+ count at <5 cells/uL and a viral load of 555,000. Sexual history revealed a history of casual sexual encounter. Family and social history were non-contributory. Mpox RT-PCR and 4mm skin punch biopsy on 2 sites was done. Management through an interdisciplinary approach consisting of dermatologists, infectious disease physicians, gastroenterologists, ophthalmologists, surgeons and psychiatrists was employed.
Results: Mpox RT-PCR revealed positive for Mpox clade II. The histopathological examination showed epidermal hyperplasia with viral cytopathic changes.
Conclusion: This case report discusses the interplay between skin manifestations, histopathologic findings, and management in patients diagnosed with mpox in an immunocompromised patients. Through a comprehensive analysis, we highlight the clinical presentation, the histopathologic features, and the interdisciplinary approach aimed at managing the disease.
PP03.28 – Feasibility, Acceptability & Fidelity of a Rapid Switch to B/F/TAF in Art-Experienced Migrants with HIV (Asap-Switch Study)
Dr. MHD Amir Chalati1, Arnaud Godin2, David Lessard1, Kim Engler1, Dominic Chu1, Moustafa Laymouna Laymouna1,2,3, Joel Ishak1, Dr Sean Yaphe4, Dr Jean-Pierre Routy4, Dr Alexandra DePokomandy3,4, Sebastien Landry4, Serge Vicente2,3, René-Pierre Lorgeoux5, Bertrand Lebouché1,3,4
1Centre for Outcomes Research and Evaluation, Research Institute of the McGill University Health Centre (MUHC), Montreal, Canada.
2Faculty of Medicine and Health Science, McGill University, Montreal, Canada.
3Department of Family Medicine, Faculty of Medicine and Health Sciences, McGill University, Montreal, Canada.
4Chronic Viral Illness Service, Division of Infectious Disease, Department of Medicine, McGill University Health Centre, Montreal, Canada.
5Gilead Sciences Canada; Inc, Mississauga, Canada.
Background: Migrant populations represent an increasing proportion of new referrals for HIV care in Canada. Many migrants living with HIV (MLWH) are referred with limited known clinical history and with antiretroviral treatments (ART) that cannot be renewed locally. We assessed the feasibility, acceptability, and fidelity of a free-of-charge rapid ART switch among MLWH.
Methods: In May 2024, we initiated a 52-week prospective cohort at a hospital-based clinic in Montreal. ART-experienced MLWH recently arrived in Quebec (<2 years) were switched to Bictegravir/Emtricitabine/Tenofovir-Alafenamide (B/F/TAF) free-of-charge. Feasibility was defined as ≥75% of participants starting B/F/TAF within 7 days of first study visit. Acceptability of the switch was defined as a mean sample score (MSS) ≥4/5 on the 4-item Acceptability of Intervention Measure (AIM) and of 8/10 on a scale of readiness to start B/F/TAF. Fidelity was defined as self-reported adherence ≥90% and 100% in the past 30 and 7 days, respectively. All above variables, sociodemographic information and viral load were collected at baseline and/or Week 4.
Results: As of December 2024, 20 participants (40% of target of 50) were recruited and prescribed B/F/TAF. 17/20 (85%) are active participants who completed at least 4/72 weeks of follow-up (3 withdrawals). Among these, 9/17 (53%) are female; 13/17 (76%) aged <50 years; and 10/17 (59%) are heterosexual. Concerning the switch, 17/17 (100%) participants started B/F/TAF within 7 days of their first visit. The MSS for acceptability of the rapid and free-of-charge components of the switch were respectively 4.8/5 and 4.6/5, and the MSS for readiness was 9.5/10. As for fidelity, mean adherence was 100% and 95% in the past 30 and 7 days, respectively. Most participants 12/17(71%) had undetectable viral loads at baseline, which increased to 14 (82%) at Week 4.
Conclusion: Our preliminary results indicate that a rapid free-of-charge switch to B/F/TAF among MLWH is highly feasible and acceptable, and shows fidelity.
PP03.29 – Unmet Needs for Diagnostic Testing and Treatment of Chlamydia Trachomatis, Neisseria Gonorrhoeae, and Mycoplasma Genitalium
Dr. Jayne Smith-Palmer1, Mr. Richard F Pollock1, Dr. Avneet Hansra2, Dr. Susan N Chang2
1Covalence Research Ltd, Harpenden, United Kingdom.
2Roche Molecular Systems, Inc., Pleasanton, United States.
Background: Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), and Mycoplasma genitalium (MG) are clinically important pathogens that present with similar symptoms and contribute to the substantial global burden of sexually transmitted infections (STIs). When left untreated, STIs can lead to complications such as pelvic inflammatory disease (PID) and infertility, and have been associated with increased risk of HIV transmission. A greater understanding of unmet needs in the care pathway for CT, NG, and MG is needed to improve diagnosis, treatment, and outcomes.
Methods: A narrative literature review was performed to identify relevant publications. Searches were conducted in PubMed using Medical Subject Headings and free-text terms, supplemented with grey literature searches. Reference sections of included articles were also searched.
Results: 45 relevant publications were identified, covering multiple unmet needs. Barriers to testing need to be addressed, as they disproportionately affect underserved, high-risk and hard-to-reach groups; initiatives are needed to reduce access barriers, as already acknowledged in national strategic plans. There is an unmet need for rapid, accurate point-of-care diagnostic tests that can distinguish CT, NG, and MG infection and provide results within a timeframe that can inform immediate decision-making. The turnaround times of current laboratory-based approaches can delay treatment initiation, or lead to use of empiric therapy. In turn, this can lead to inappropriate treatment, increasing antibiotic resistance risk. It may also lead to additional contacts/visits, potentially increasing loss to follow-up (LTFU), leading to some infections going untreated, and increasing long-term risk of complications like PID and infertility.
Conclusion: Action is urgently needed to address the unmet needs and burden of STIs. Innovative solutions like point-of-care multiplex diagnostic tests, outreach programs to reduce LTFU, greater focus through national action plans, and systemic efforts to invest in expanded STI care capabilities can bring efficiencies and improve care delivery for people with STIs.
PP03.30 - Usability Evaluation of Simpli-COLLECT Urine Collection Kit for STI Testing
Dr. Richard Cullum1, Dr. Danijela Lucic1
1Abbott, Des Plaines, United States.
Background: The increasing prevalence of STIs poses a significant public health challenge, with millions of new cases of chlamydia, gonorrhea, and trichomoniasis reported annually. An innovative approach to address this issue is the use of STI home collection kits. By offering a discreet and convenient testing option, these kits can encourage more individuals to get tested, leading to earlier detection and treatment. This study evaluates the usability of the simpli-COLLECT Urine Collection IUO Kit (sC kit) in a simulated home environment for STI testing using urine samples.
Methods: The sC kit was assessed through simulated use, knowledge-based questions, and subjective feedback during individual, in-person sessions. Usability data were collected from 162 participants (81 male and 81 female), divided into three age groups: adolescents (14–17 years), adults (18–64 years), and older adults (65+ years). Participants were evaluated on their ability to complete critical tasks (e.g., collecting urine sample, transferring urine to sample tube) and essential tasks (e.g., opening kit, inspecting contents, applying mailing label).
Results: Across all participants, the mean score for the ease of use of the sC kit was 4.6 out of 5 (SD = 0.52), and the instructional materials scored an average of 4.5 out of 5 (SD = 0.61). The pass rate for critical tasks ranged from 94.4% to 100.0%, while the pass rate for essential tasks ranged from 86.2% to 100.0% across all age groups.
Conclusion: This study provides insights into the usability of the sC kit, with high scores for ease of use and instructional materials. The high pass rates for both critical and essential tasks (≥ 86.2%) indicate that STI home collection kits, particularly those using urine samples, can play a role in STI prevention efforts.
PP03.31 – Assessing the Usability of Simpli-COLLECT STI Home Collection Kit for Vaginal STI Testing
Dr. Richard Cullum1, Dr. Danijela Lucic1
1Abbott, Des Plaines, United States.
Background: The rise of STIs is a significant public health concern, with millions of new cases of chlamydia, gonorrhea and trichomoniasis reported each year. One innovative strategy which may aid in addressing this issue is the implementation of STI home collection kits. By providing a discreet and convenient option, more individuals are likely to get tested, leading to earlier detection and treatment of infections. Here, we evaluated the usability of simpli-COLLECT Swab Collection IUO Kit (sC kit) in a simulated home environment for vaginal STI testing.
Methods: The sC kit was evaluated through simulated use, knowledge-based questions, and subjective feedback in individual, in-person sessions. Usability data was evaluated from 61 female participants that were divided into 3 age groups: adolescents (age 14–17), adults (age 18–64), and older adults (65+). Each participant was evaluated on the ability to complete critical tasks (e.g., uncapping sample tube, opening swab packet, collecting swab sample) and essential tasks (e.g., opening kit, inspecting kit, placing mailing label on box).
Results: Across all participants, the mean score for the ease of use of the sC kit was 4.8 (out of 5) with an SD of 0.46 and the mean score for the ease of use of the instructional material was 4.7 (out of 5) with an SD of 0.49. Across all age groups, the pass rate for critical tasks ranged from 92.6% to 100.0% and the pass rate for essential tasks ranged from 88.5% to 100.0%.
Conclusion: This study demonstrated that the participants found the sC kit easy to use with a score of 4.8. Similar feedback was obtained for instructional materials. Critical and essential tasks pass rate was ≥88.5%. STI home collection kits are a vital tool in the fight against the rising tide of STIs and contributing to the global goal of STI prevention.
PP03.32 – A Novel Point-Of-Care Rapid IgM Test for the Diagnosis of Congenital Syphilis
Assoc. Prof. Irene Stafford1, Dr. Sabrina DaCosta1, Dr Diana Villarreal2, Dr Jeffrey Klausner2, Dr Leandro Mena3, Dr Gary Lehnus4
1The University of Texas Health Science Center, Houston, TX, United States.
2The University of Southern California, Los Angeles, CA, United States.
3All-In Health Solutions LLC, Atlanta, GA, United States.
4Lehnus and Associates Consulting LLC, East Stroudsburg, PA, United States.
Background: Neonatal syphilis-specific IgM immunoglobulins are fetal in origin and may reflect congenital syphilis. This pilot study aims to determine the test performance of a point-of-care anti-treponemal IgM test for the diagnosis of congenital syphilis.
Methods: Sera from 2 uninfected and 37 pregnant patients with syphilis and their newborns with sonographic evidence of congenital syphilis were collected between May 2022 and June 2024. Serum aliquots (20 µL) were tested using a research-use-only rapid 15-min point-of-care lateral flow test developed by Diagnostics Direct, LLC (Stone Harbor, NJ) for the detection of anti-treponemal IgM. Serum aliquots (50 µL) from the samples were also tested for treponemal IgM using two Commune-Europe-marked immunoblot tests as comparators (ViraMed, Germany and Euroimmun, Germany) and a commercial IgM ELISA (Euroimmun, Germany). The composite IgM reference comparator was based on these three tests. If at least two of three were positive, this was considered a positive reference comparator, and two negative tests constituted a negative comparator. The point-of-care anti-treponemal IgM test was also compared to Mother-newborn dyads at delivery for additional test performance. Dyads were staged for syphilis according to national guidelines.
Results: The positive percent agreement was 93.0% (CI: 68.0–99.8%) and the negative percent agreement was 88.0% (CI: 87.5–97.3%) versus the composite IgM reference comparator (Table 1). Based on maternal and neonatal clinical diagnosis, the positive percent agreement was 100% (73.5–100%) and the negative percent agreement was 82.0% (61.9–93.7%).
Conclusion: The syphilis point-of-care IgM test demonstrated excellent test performance when compared to a composite reference standard and with clinical cases and non-cases. Further studies evaluating this point-of-care anti-treponemal IgM test as a neonatal diagnostic test for congenital syphilis are warranted.
| Composite IgM Reference StandardA | |||||||
|---|---|---|---|---|---|---|---|
| + | − | Total | PPA (%) | NPA (%) | |||
| IgM POC test | + | 14 | 3 | 17 | 93.0 | 88.0 | |
| − | 1 | 21 | 22 | ||||
| Total | 15 | 24 | 39 | (68.0-99.8) | (87.5-97.3) | ||
| Test Results of Novel IgM Rapid Assay Test Compared to Mother and Neonatal Syphilis Infection StatusB | |||||||
|---|---|---|---|---|---|---|---|
| + | − | Total | PPA (%) | NPA (%) | |||
| IgM POC test | + | 14 | 3 | 17 | 100.0 | 88.0 | |
| − | 0 | 22 | 22 | ||||
| Total | 14 | 25 | 39 | (76.8-100) | (68.8-97.5) | ||
PP03.33 – A Novel Single-Visit Point-Of-Care Multiplex Diagnostic Test for Chlamydia Trachomatis and Neisseria Gonorrhoeae
Miss Violette Defourt1, Dr Peter Rahfeld1, Dr Sara Foreman1, Mr Aman Urazov1, Mrs Haarika Bhamidipati1
1Rapidemic, Leiden, Netherlands.
Background: In 2020, the WHO reported 211 million Chlamydia trachomatis (CT) and Neisseria gonorrhea (NG) infections worldwide. The golden standard for diagnosis of CT/NG in most countries are nucleic acid amplification tests (NAAT), where samples are analyzed in central diagnosis laboratory facilities. In many settings (like rural settings), this is suboptimal as it is logistically demanding, requires trained personnel, and is slow (2 to >7 days). Recent developments in the point-of-care diagnostic field have shown promising potential to tackle the rise in STI infections, but current technologies are either inaccurate, too slow, or costly. Rapidemic has developed a novel assay that enables decentralized lysis, amplification and detection of CT/NG. The device is a stand-alone and single-use, which works independently of additional equipment. Here, we present proof-of-concept and analytical data of this groundbreaking assay, which provides opportunities for ultra-rapid and accurate molecular multiplex diagnosis of CT/NG in (a)symptomatic patients.
Methods: We tested Rapidemic’s assay system for its effective lysis of NG and CT (N = 3) in relevant patient matrix in comparison to a 95°C heat treatment. Additionally, analytical sensitivity for the detection of NG bacteria or CT gDNA in negative urine was measured. The readout was performed on a lateral flow strip.
Results: We have shown effective lysis of NG and CT bacteria in urine and vaginal swab matrix using our lysis buffer. The analytical LOD for the detection of NG in urine samples using the assay is <10 CFU/ml and for CT is <10 pg/mL.
Conclusion: Rapidemic’s test successfully lysed and detected very low amounts of CT/NG bacteria in <15 min in relevant sample matrix. The Rapidemic test fits the WHO’s ASSURED criteria and could be a promising tool for improving STI management in primary healthcare settings around the world.
PP03.34 – The Role of Nod Gene Polymorphism in the Pathogenesis of Tube Infertility in Patients with Past Chlamydial Infection
Prof. Svetlana Dubrovina1, Oksana Ardintseva1, Elena Mashkina2
1Rostov State Medical University, Rostov, Russian Federation.
2Southern Federal University, Rostov-on-Don, Russian Federation.
Improving the management of patients with peritoneal infertility after chlamydial infection based on the study of polymorphic variants rs6958571 of NOD1 gene (A>C) and s2066847 of NOD2 (CCC>CC).
93 patients with infertility were divided into groups depending on the infertility factor. Subgroup 1A consisted of 32 women with tube pathology, subgroup 1B 25 women with a history of chlamydial infection and no pathology of the fallopian tubes during diagnostic laparoscopy. The control group included 35 patients with unspecified infertility and without history of previous chlamydial infection. DNA was isolated from peripheral blood using the commercial Genomic DNA Mini Kit PureLink. Gene polymorphism analysis was performed using TaqMan MGB probes by real-time polymerase chain reaction (TaqMan SNP Genotyping Assays, Thermo Fisher Scientific). Statistical processing of the results was carried out using Statistica 12.5.
There were no statistically significant differences in the frequency of rs6958571 polymorphism of the NOD1 gene (A>C) between subgroups of group 1 (P > 0.05) and in comparison the control group with subgroups (group 2 versus subgroup 1A (P > 0.05) and group 2 versus subgroup 1B (P > 0.05). When analyzing the rs2066847 gene NOD2 (CCC>CC), there were also no statisoftically significant differences between subgroups of group 1 (P > 0.05) and in comparison of the control group with subgroups (group 2 versus subgroup 1A (P > 0.05) and group 2 versus subgroup 1B (P > 0.05). The absence of statistically significant differences in the frequency of registration of NOD1, NOD2 gene polymorphisms between patients with past chlamydial infection and fallopian tube pathology and without it, as well as when compared with patients with unspecified infertility and without indicating a history of STIs do not confirm the previous assumption that variations in these genes may be responsible for ascending chlamydial infection and, as a consequence, tubal-peritoneal infertility.
PP03.35 – Progression Factors and Survival of Cuban Patients with Advanced HIV Disease
Dr. Milena Duque1, Dr. Armando La Rosa, Dr C Lissette Perez
1Pedro Kouri Tropical Medicine Institute, La Habana, Cuba.
2Santiago de Cuba Provintial Hospital, Santiago de Cuba, Cuba.
3Pedro Kouri Tropical Medicine Institute, La Habana, Cuba.
Introduction: The proportion of people presenting for care with advanced HIV disease has remained constant over the past 5 years. Individuals presenting with advanced HIV disease are at very high risk of AIDS-related morbidity and mortality. Identifying progression factors reducing survival of HIV is imperative. The present study aims to determine an assessment of survival of advanced HIV disease patients and its’ related progression factors.
Methods: Observational retrospective cohort study was conducted based on patients with advanced HIV disease admitted in Pedro Kourí Tropical Medicine Institute, La Havana, Cuba, between 2023 and 2024. Kaplan Meyer and Cox regression model were applied for bivariate and multivariate analyses. Data were analyzed using SPSS-21.0.
Results: Factors identified as high risk for progression to Advanced HIV disease were CD4 count <349 cells/mm3 (OR: 21,200), late diagnosis (OR: 9,505), non-stability during antiretroviral treatment (OR: 6,236) and anemia (OR: 5,882), these factors were part of a stable risk model for the development of opportunistic infections in an average of 120 months and 42,2% of survival.
Conclusion: Cuban patients with severe immunosuppression, late HIV diagnosis, non-stability on antiretroviral treatment and anemia have at increased risk for progression to advanced HIV disease and limited survival.
The present investigations contribute to identify risk factor for diagnosis, managment and prevention of several conditions that can prevent progression to advanced HIV disease and reduces morbidity and mortality.
PP03.36 – Ocular Syphilis: Case Series (2016–2023) from Two Tertiary Care Centers in Montreal, Canada
Dr. Evangelina Esposito1, Dr. Mélanie Hébert2, Adam Hocini3, Yacine Zaffour3, Nicole Moussa3, Anne-Sophie Boucher3, Dr. Laurence Jaworski4, Dr. Julie Vadboncoeur5, Dr. Annie-Claude Labbé6, Dr. Claude Fortin6, Dr. Marie-Josée Aubin7
1Department of Ophthalmology, Faculty of Medicine, Université de Montréal, Montreal, Canada.
2Department of Ophthalmology, Faculty of Medicine, Université Laval, Quebec City, Qc, Canada.
3Université de Montréal, Faculty of Medicine, Montreal, Qc, Canada.
4Department of Ophthalmology, Faculty of Medicine, Montreal, Qc; University Ophthalmology Center, Centre Hospitalier de l’Université de Montréal (CHUM), Montréal, Qc, Canada.
5Department of Ophthalmology, Faculty of Medicine, Montreal, Qc; University Ophthalmology Center, Maisonneuve-Rosemont Hospital, Montreal, Qc, Canada.
6Department of Microbiology, Infectious Diseases and Immunology, Faculty of Medicine, Montreal, Qc; Division of Infectious Diseases and Medical Microbiology, Hôpital Maisonneuve-Rosemont (HMR), CIUSSS de l’Est-de-l'Île-de-Montréal, Montreal, Qc, Canada.
7Department of Ophthalmology, Faculty of Medicine, Montreal, Qc; University Ophthalmology Center, Maisonneuve-Rosemont Hospital, CIUSSS de l’Est-de-l'Île-de-Montréal, Montreal, Qc; Department of Social and Preventive Medicine, School of Public Health, Université de Montreal, Montreal, Qc, Canada.
Background: To describe the clinical characteristics and management of patients with ocular syphilis at two tertiary care centers in Montreal, Canada.
Methods: Patients with ocular syphilis were identified by extracting positive syphilis serology results from laboratory databases from 2016 to 2023, and chart review of those who had a visit at the ophthalmology clinic of two Montreal university hospitals.
Results: Of 102 patients with a true positive syphilis serology and a visit in ophthalmology, 33 were excluded because of missing information (n = 5), syphilis treated in the past (n = 23) or absence of active ocular signs (n = 5). Among the 69 included patients, 57 (83%) were males. Thirty-one were reported as being heterosexual (45%) and 20 (29%) as having sex with other men (MSM). Syphilis stage was determined as secondary (n = 34; 49%), early latent (n = 5; 7%), late latent (n = 11; 16%) or tertiary (n = 15; 22%). HIV serology was negative for 47 (68%) patients and positive for 16 (23%); 6 (9%) patients were not tested. The preferred treatment was penicillin (n = 65, 94%); one patient was treated with doxycycline and another with ceftriaxone. Ocular involvement was unilateral in 37 (54%) patients and bilateral in 32 (46%). Among HIV-infected patients, panuveitis was the most common presentation (n = 8; 53%). Improvement in visual acuity was significant for patients with secondary syphilis (P = 0.01) and tertiary syphilis (P = 0.04).
Conclusion: Syphilis diagnosis should be considered when facing ocular inflammation. In the presence of syphilis, eye symptoms and signs should be addressed. In ocular syphilis, the recommended treatment is the neurosyphilis regimen (intravenous penicillin G for 2 weeks). This treatment has proven successful, significantly improving visual acuity in both the secondary and tertiary stages. This outcome highlights the importance of prompt diagnosis and treatment of syphilis along with identification of potential HIV co-infection.
PP03.37 – Jarisch-Herxheimer Reaction in Neurosyphilis: Incidence, Clinical Features, and Management in Penicillin and Ceftriaxone Treatments
Dr. Xin Feng1, Miss Junjun Yu1, Prof Pingyu Zhou1
1Institute of Sexually Transmitted Disease, Shanghai Skin Disease Hospital, School of Medicine, Tongji University, Jingan, China.
Background: Neurosyphilis, an infection of the central nervous system (CNS) caused by Treponema pallidum, often leads to the Jarisch-Herxheimer reaction (JHR) after antibiotic treatment. This study investigates the incidence, clinical manifestations, and management of JHR in patients treated with penicillin or ceftriaxone.
Methods: A retrospective study was conducted at the Shanghai Skin Disease Hospital, China, involving 1010 inpatients diagnosed with neurosyphilis, among whom 103 developed JHR. Statistical analyses included Student’s t-test or Mann-Whitney test for continuous variables and Fisher’s exact test for categorical data.
Results: The overall incidence rate of JHR among neurosyphilis patients was 10.20% (103/1010), with similar rates observed in penicillin-treated 10.20% (92/902) and ceftriaxone- treated (10.19%, 11/108) cohorts. Amon the 103 JHR patients, febrile reactions were reported in 102 patients (98.9%), and neuropsychiatric symptoms occurred in 23 patients (22.3%) (Tables 1–3). Fever onset was earlier in penicillin-treated patients (8.92 h vs 14.00 h, P < 0.05) and resolved faster (16.35 h vs 20.80 h, P < 0.05) compared to ceftriaxone-treated patients (Figs 1, 2). Notably, all neuropsychiatric JHR cases occurred in penicillin group [25%, (23/92)] and none in ceftriaxone [0%, (0/11)] group, although this difference did not reach statistical significance. Effective management strategies included physical cooling, indomethacin suppositories, and supportive treatment for neuropsychiatric symptoms. Neuropsychiatric manifestations of JHR resolved within 2–7 days of initiating antibiotic therapy.
Conclusions: JHR is a notable complication of antibiotic treatment for neurosyphilis, characterized by febrile reactions and various neuropsychiatric symptoms. While the incidence of JHR is comparable between penicillin and ceftriaxone treatments, penicillin appears to trigger earlier onset and potentially more severe reactions. JHR is typically temporary and manageable with appropriate interventions. This study advances the understanding of JHR and and provides insights into the therapeutic effects of penicillin and ceftriaxone in neurosyphilis management.
| Variable | Antibiotic treatment | P value | ||
|---|---|---|---|---|
| Penicillin (N = 92) | Ceftriaxone (N = 11) | |||
| Male, n (%) | 71 (77.2%) | 8 (72.7%) | 0.715 | |
| Age, median [IQR] | 57 [52–62.75] | 57 [46–69] | 0.767 | |
| Types of neurosyphilis, n (%) | ||||
| General paresis | 80 (87.0%) | 8 (72.7%) | 0.199 | |
| Asymptomatic neurosyphilis | 9 (9.8%) | 1 (9.1%) | >0.999 | |
| Meningovascular syphilis | 1 | 1 | ||
| Tabes dorsalis | 1 | 0 | ||
| General paresis plus Tabes dorsalis | 0 | 1 | ||
| Gummatous syphilis | 1 | 0 | ||
| Peripheral blood plasma | ||||
| TRUST titre, median [IQR] | 1:48 [1:16-1:112] | 1:32 [1:32-1:64] | 0.851 | |
| Cerebrospinal fluid | ||||
| TRUST titre, median [IQR] | 1:4 [1:2–1:8] | 1:4 [1:2–1:4] | 0.145 | |
| VDRL titer, median [IQR] | 1:8 [1:4–1:16] | 1:8 [1:2–1:8] | 0.131 | |
| WBC count (cells/µl), median [IQR] | 44.0 [20.5–70.0] | 48.0 [22.0–100.0] | 0.645 | |
| Protein concentration (mg/L), median [IQR] | 1187 [916.5–1518] | 794 [738–1154] | 0.013 | |
Normality test was conducted for all continuous variables. The titres of plasma TRUST, CSF TRUST and VDRL were normalized by log2 transformation. Student’s t or Mann-Whitney test was performed for continuous data appropriately. Fisher’s exact test in categorical data. Abbreviations: SD, standard deviation; IQR, interquartile range; TRUST, toluidine red unheated serum test; VDRL, venereal disease research laboratory test; WBC, white blood cell; JHR, Jarisch-Herxheimer reaction.
| Variable | Antibiotic treatment | P value | |||
|---|---|---|---|---|---|
| Overall (N = 102) | Penicillin (N = 91) | Ceftriaxone (N = 11) | |||
| Maximum temperature, mean (SD) ℃ | 38.81 (0.62) | 38.81 (0.61) | 38.75 (0.75) | 0.755 | |
| Fever onset timing, mean (SD), h | 9.47 (5.29) | 8.92 (4.98) | 14.00 (5.90) | 0.004 | |
| Peak temperature timing, mean (SD), h | 10.41 (4.80) | 9.91 (4.45) | 14.55 (5.79) | 0.006 | |
| Fever recover timing, mean (SD), h | 16.83 (5.49) | 16.35 (5.48) | 20.80 (3.79) | 0.002 | |
| Duration timing of fever, mean (SD), h | 7.36 (4.18) | 7.43 (4.13) | 6.82 (4.73) | 0.635 | |
P-value were determined by Mann-Whitney test, two-tailed.
Clinical characteristics ad management strategies of the 23 patients manifested as neuropsychiatric symptoms.

Temp.: The peak body temperature.
PP03.38 – Assessing Doxycycline Postexposure Prophylaxis Comfort and Familiarity Among Pediatric Providers in the United States
Dr. John Flores1,2, Trenton Lam3, Dr. Jose Paredes Sosa4, Sebastian Otero2, Dr Aniruddha Hazra1,5
1University of Chicago Medicine, Chicago, United States.
2University of Chicago Comer Children’s Hospital, Chicago, United States.
3Pritzker School of Medicine of University of Chicago, Chicago, United States.
4Advocate Illinois Masonic Medical Center, Chicago, United States.
5Howard Brown Health, Chicago, United States.
Background: Doxycycline post-exposure prophylaxis (doxyPEP) has been shown to reduce the risk of acquisition of syphilis, gonorrhea, and chlamydia in high-risk sexual encounters among high-priority groups. Young adults 18–24 years old, a particularly vulnerable demographic, often seek routine health care from pediatric infectious diseases (ID), adolescent, or general pediatric providers. Our study sought to investigate the perspectives and prescribing practices of doxyPEP through a nationwide survey of pediatric providers in the United States.
Methods: Providers were recruited July–August 2024 from a medical organization database, within the sections of adolescent medicine and pediatric infectious diseases. Questions were rated on a 5-point Likert scale related to comfort and familiarity with clinical care related to sexual health, STI diagnosis and management, and doxyPEP use. Analyses compared Pediatric ID and non-ID providers’ responses.
Results: 164 providers completed the survey, including 75 (45.7%) Pediatric ID and 89 (54.3%) non-ID providers (Table 1). There were no statistically significant differences in Likert scale scores between the two provider groups with age, gender identity, years in practice, geographic region of practice, comfort or familiarity with discussing sexual health, or STI diagnosis and management. 95 of 164 (57.9%) were very comfortable or somewhat comfortable prescribing doxyPEP: 54 (60%) of PID and 51 (55%) of non-PID, with no statistical difference between the groups (P = 0.961)
Conclusion: Our nationwide survey-based study among pediatric ID and pediatric non-ID providers found no differences between groups regarding DoxyPEP familiarity or prescribing practices. While most respondents, on average, reported some comfort or familiarity with DoxyPEP, Likert scale scores did not reveal generalized confident responses. Given there is a strong cohort of high-risk individuals who primarily visit pediatric providers and may benefit from DoxyPEP, and ongoing clinical trials looking at DoxyPEP use in adolescents, future outreach interventions are pivotal in continuing to reduce the burden of STIs.
| Variable | Not familiar with doxyPEP, N(%) | Familiar with doxyPEP, N(%) | Odds ratio (95% CI) | P-value | |
|---|---|---|---|---|---|
| Provider type | 0.96 | ||||
| PID | 29 (39.2) | 45 (60.8) | 1.02 (0.54–1.90) | ||
| Non-PID | 36 (39.6) | 55 (60.4) | 1 | ||
| Age | 0.39 | ||||
| <40 | 21 (44.7) | 26 (55.3) | 0.94 (0.41–2.15) | ||
| 41–50 | 19 (43.2) | 25 (56.8) | 1 | ||
| 51–60 | 7 (25.9) | 20 (74.1) | 2.17 (0.76–6.19) | ||
| 61+ | 18 (38.3) | 29 (61.7) | 1.22 (0.53–2.83) | ||
| Gender | 0.03 | ||||
| Male | 16 (28.1) | 41 (71.9) | 1 | ||
| Female | 44 (43.6) | 57 (56.4) | 0.51 (0.2–-1.02) | ||
| Non-Binary | 5 (71.4) | 2 (28.6) | omitted | ||
| Region | 0.43 | ||||
| West | 7 (33.3) | 14 (66.7) | 1.80 (0.63–5.12) | ||
| Midwest | 14 (34.2) | 27 (65.9) | 1.74 (0.76–3.98) | ||
| Northeast | 15 (34.1) | 29 (65.9) | 1.74 (0.78–3.91) | ||
| South | 27 (47.4) | 30 (52.6) | 1 | ||
| Non USA | 2 (100.0) | 0 (0.0) | Omitted | ||
| Directly or indirectly assist in the management of patients who are 18 years old or older | 0.03 | ||||
| Yes | 45 (34.9) | 84 (65.1) | 2.33 (1.10–4.94) | ||
| No | 20 (55.6) | 16 (44.4) | 1 | ||
| Comfort with discussing sexual orientation | |||||
| Not comfortable | 40 (76.9) | 12 (23.1) | 1 | <0.001 | |
| Comfortable | 25 (22.3) | 87 (77.7) | 11.6 (5.30–25.40) | ||
| Comfort with discussing gender identity | <0.001 | ||||
| Not comfortable | 41 (71.9) | 16 (28.1) | 1 | ||
| Comfortable | 23 (21.5) | 84 (78.5) | 9.36 (4.47–19.60) | ||
| Comfort with discussing sexual activities | <0.001 | ||||
| Not comfortable | 41 (80.4) | 10 (19.6) | 1 | ||
| Comfortable | 10 (21.0) | 90 (79.0) | 15.4 (6.74–35.08) | ||
| Comfort with discussing sexual activities with the knowledge and/or involvement of parents | <0.001 | ||||
| Not comfortable | 43 (72.9) | 16 (27.1) | 1 | ||
| Comfortable | 21 (20.0) | 84 (80.0) | 10.8 (5.09–22.69) | ||
| Comfort with discussing sexual activities without the knowledge and/or involvement of parents | <0.001 | ||||
| Not comfortable | 45 (75.0) | 15 (25.0) | 1 | ||
| Comfortable | 20 (19.1) | 85 (80.9) | 12.75 (5.95–27.28) | ||
| Comfort with screening STIs | <0.001 | ||||
| Not comfortable | 39 (78.0) | 11 (22.0) | 1 | ||
| Comfortable | 26 (22.6) | 89 (77.4) | 12.14 (5.46–26.99) | ||
| Comfort with treating STIs | <0.001 | ||||
| Not comfortable | 41 (80.4) | 10 (19.6) | 1 | ||
| Comfortable | 24 (21.2) | 89 (78.8) | 15.20 (6.67–34.70) |
Familiar with doxyPEP was defined as being very familiar or somewhat familiar with doxyPEP; Not familiar with doxyPEP was defined as being Neutral, Somewhat Unfamiliar or Very Unfamiliar with doxyPEP; Comfortable was defined as very comfortable or somewhat comfortable and not comfortable as neutral, Somewhat Uncomfortable, Very Uncomfortable; 95% CI = 95% Confidence Interval. Non-binary omitted due to low N of participants. Data collected from pediatric providers across all regions of the United States May 1, 2024 – June 12 2024.
PP03.39 – Acceptability of a Chlamydia Vaccine Among Young Women and Men
Ms. Bria Gamble1, Dr. Kanupriya Gupta1, Ms. Madison D’Amico1, Ms. Rebecca Shiry1, Dr. Muhan Hu1, Ms. Aamuktha Pentala1, Dr. Kristal Aaron1, Dr. Janeen Arbuckle1, Dr. Samantha Hill1, Dr. Barbara Van Der Pol1, Dr. William M. Geisler1
1The University of Alabama at Birmingham, School of Medicine, Birmingham, United States.
Background: Chlamydia remains a global health concern, justifying need for a chlamydia vaccine. Chlamydia rates are highest amongst young women and men; thus, they would be a target population for vaccination. Chlamydia vaccine availability does not ensure its acceptability. We conducted a survey in young women and men to identify factors that may influence chlamydia vaccine acceptability.
Methods: Women and men aged 16–29 seen for care in adolescent, gynecology, student health and STD clinics completed a computer survey that collected information on sexual health, healthcare utilization, and vaccine history, as well as other factors related to chlamydia and vaccine acceptability.
Results: 334 women and 119 men completed the survey to date. Most (94%) heard of chlamydia, 20% reported prior chlamydia, and 45% believed they could acquire chlamydia. Interest in receiving a chlamydia vaccine was reported by 44% of females and associated with ethnicity, clinic site, receiving HPV, flu or COVID-19 vaccines, and chlamydia awareness. Among males, 49% reported chlamydia vaccine interest, associated with clinic site, previous chlamydia, and possibility of acquiring chlamydia. Most participants (83%) reported the main motivation for receiving a chlamydia vaccine was to protect themselves. Main reason for females not wanting it was safety concerns (33%) and for males it was cost (30%). Majority of participants (68%) reported conversations with healthcare providers as the main resource for vaccine information.
Conclusion: Preliminary findings suggest only about half of young women and men were interested in receiving a chlamydia vaccine. Findings will help guide strategies for chlamydia vaccine implementation.
PP03.40 – Results from a Single-Arm Phase 1 Trial Evaluating Low Iron MTbLF Formulated with Zn and Mn for Preventing Recurrence of Symptomatic Bacterial Vaginosis Following Treatment with Metronidazole
Dr. Gary A. Gelbfish1,2, Dr. Catherine Insley3, Sue Garnett1, Zafeiria Athanasiou1, Claudia Bustos1, Maura-Ann Matthews1
1Metrodora Therapeutics, Brooklyn, United States.
2Department of Surgery, Mount Sinai School of Medicine, New York, United States.
3East Sydney Doctors, Darlinghurst, Australia.
Background: Bacterial vaginosis (BV) is a dysbiotic condition with high rates of recurrence after antibiotic treatment. It is a stubborn problem for which new therapeutic approaches are warranted.
Methods: Metrodora Therapeutics’ bovine Lactoferrin (Low Iron MTbLF) formulated with Zn and Mn was evaluated in a single arm, Phase 1b, study (MT300V-103, Reg: ACTRN12622000548730) that enrolled premenopausal females aged 18–45 with symptomatic BV (Amsel ≥3 and Nugent ≥4). Within 48 h after treatment with metronidazole, (0.75% intravaginal QD 5 days), participants began a 12-week course of Low Iron MTbLF self-administered daily and were followed for an additional 12 weeks after study drug. Participants attended clinic visits at Weeks 0, 2, 4, 8, 12, and 24 after completion of antibiotics, phone visits at Weeks 16 and 20, collected home swabs weekly for the duration of the study, and completed e-diaries.
Results: Of the 19 women enrolled, 14 completed study drug administration, 2 withdrew, and 3 were lost to follow up. No deaths or serious adverse events were reported, and no subjects withdrew from the study due to an adverse event. One of 14 participants (7%) had a recurrence of BV during the 12-week Low Iron MTbLF dosing period. Five of 14 participants (35.7%) had BV recurrence during the 12-week follow-up period, including the participant that had BV recurrence during the dosing phase.
Conclusions: Although the results of this study are limited by the small sample size and open label design, the 7% rate of BV recurrence by week 12 compares favorably other trials with recurrence rates of 30–50%. The 35.7% recurrence rate during the follow-up phase suggests Low Iron MTbLF with Zn and Mn may have stabilized the vaginal microbiome during the dosing phase but that the effect did not persist in the follow-up period. A randomized, placebo-controlled trial is planned.
PP03.41 – Dequalinium Chloride Vaginal Tablets in the Treatment of Inflammatory Vaginitis
Dr. Deborah Goode1, Dr. Emma Street1
1Calderdale & Huddersfield NHS Foundation Trust, Halifax, United Kingdom.
Background: Inflammatory vaginitis (IV), including desquamative inflammatory vaginitis, can cause chronic symptoms of pain and discharge and has an unclear aetiology. Treatment options are limited to antibiotics or intravaginal steroids. Antibiotics can have significant unwanted side effects, such as promoting candidiasis or gastro-intestinal side effects. In the UK intra-vaginal prednisolone foam is not readily available and also has a significant cost implication.
Dequalinium chloride vaginal tablets have been awarded a license for use in bacterial vaginosis. It is known to have anti-inflammatory and anti-microbial properties. The side effect profile is favourable and the cost is less than one tenth of that of prednisolone foam.
Methods: We have seen six patients with inflammatory vaginitis. Of these patients, three were trans-men, the other three were post menopausal cis-women. Symptoms had been present for between 1 week to 12 months.
A clinical decision was made with the first patient to use dequalinium for symptomatic relief whilst awaiting the results of the sexual health screen. In this first case a 6-day course of dequalinium was sufficient to resolve the symptoms, and so this was used with subsequent patients.
Microscopy was performed before and after treatment to assess response to the treatment as well as a sexual health screen.
Results: Five out of six patients had a symptomatic response tablets used for between 6 and 12 days. One of the patients did not benefit. No STIs were identified in any of the cases. Microscopic improvement was also documented in three of the cases.
No adverse side effects were reported.
Conclusion: In this case series, dequalinium has been successful at managing inflammatory vaginitis. We believe dequalinium should be a treatment option for these cases.
PP03.42 – A Novel Syphilis Point-Of-Care Test Is Accurate and Feasible for Syphilis Screening in a Population of Individuals Receiving Sexually Transmitted Infection Care at an Urban Canadian Sexual Health Clinic
Ms. Kathleen Whyte3, Ms. Katrina Yuen1,2, Ms. Maya Tharp1,2, Mr. Ramin Azmin1,2, Mr. Ian Hunter1, Mr. Brody Lyons1,4, Ms. Eri Flores1,2, Dr. Raymond Tsang3, Dr. Muhammad Morshed2,5, Dr. Troy Grennan1,2
1BC Centre for Disease Control, Vancouver, Canada.
2University of British Columbia, Vancouver, Canada.
3Public Health Agency of Canada - National Microbiology Laboratory Branch, Winnipeg, Canada.
4University of Calgary, Calgary, Canada.
5BC Centre for Disease Control Public Health Laboratory, Vancouver, Canada.
Background: Globally, syphilis rates are increasing substantially, and impacting new, previously-unaffected populations, highlighting the need for rapid diagnostics to maximize engagement in care and treatment completion. We performed a validation study of a Treponema pallidum (syphilis) antibody point-of-care test (POCT) in a population seeking sexually transmitted infection (STI) care at a high-volume clinic in Vancouver, Canada, compared to standard syphilis serology.
Methods: The Reveal Rapid TP Antibody POCT was offered to adult patients attending a high-volume STI clinic and requiring conventional syphilis serology (enzyme immunoassay; EIA) as part of routine STI screening. Participants provided a fingerstick blood specimen for POCT, and completed a brief feasibility survey. POCT performance characteristics were calculated by comparing POCT results with syphilis EIA.
Results: There were 525 POCTs completed between 05/2023 and 12/2024. Median age was 32 years, and 66.9% were male. The performance characteristics of the POCT in detecting antibodies to treponemal antigens were: sensitivity 71.3% (95% confidence interval [CI]: 63.0% to 78.7%); specificity 97.9% (95% CI: 96.0% to 99.1%); positive predictive value 92.4% (95% CI: 85.8% to 96.0%); and negative predictive value 90.7% (95% CI: 88.2% to 92.7). The POCT was reactive for 8/13 (61.5%) cases of newly-diagnosed infectious syphilis cases, but was nonreactive in 5/6 (83.3%) new primary syphilis cases. Most participants (81.6%) were satisfied with the overall POCT experience.
Conclusion: When used along with clinical assessment and patient history, the Reveal Rapid TP Antibody POCT performed very well for identifying both new and prior syphilis in an urban STI clinic. It may not be reliable for very early (i.e. primary) infections, though this would need replication with larger sample size. Given EIA’s lifelong positivity, it is also of limited use for reinfection. Participants considered the POCT to be acceptable, suggesting that this assay is a feasible option in select populations seeking STI screening.
PP03.43 – Sensitivity and Specificity of the BD Affirm™ VPIII Compared to Xpert® Xpress MVP and BD MAXTM Vaginal Panel for Diagnosis of Vaginitis/Vaginosis
Prof. Sharon Hillier1,2, Lisa Cosentino2, May A Beamer2, Melinda Petrina2, Tracy Zamborsky2, Leslie Meyn1,2, Katherine Bunge1
1University of Pittsburgh, Pittsburgh, United States.
2Magee-Womens Research Institute, Pittsburgh, United States.
Background: BD Affirm™ VPIII, a non-amplified molecular test for the detection of Candida, Trichomonas vaginalis (TV) and Gardnerella vaginalis, was compared to nucleic acid amplification tests (NAATs), Xpert® Xpress MVP and BD MAX™ Vaginal Panel to estimate the sensitivity and specificity of this platform for vaginitis/vaginosis diagnosis.
Methods: 200 people ≥18 years age, assigned female sex at birth, seeking care with symptoms of vaginitis (vaginal discharge, odor, vulvar or vaginal itch, irritation, burning) provided self-collected vaginal samples for the Xpert® Swab Specimen Collection (Xpert® Xpress MVP), BD Molecular Swab Collection (BD MAXTM Vaginal Panel), and BD Affirm™ Ambient Temperature Transport System (ATTS) (BD Affirm™ VPIII). True positive and negative results were defined as concordant results on both NAATs.
Results: Participants (n = 200) with median age of 33 years (range 17–76); 45% self-reporting black race, 39% white and 16% other. Twelve (6%) participants were pregnant. Agreement between the NAATs was 97% for bacterial vaginosis (BV), 91% for Candida and 100% for TV. Based on both NAATs, the prevalence of BV in the population was estimated to be 46.8% (88/188), 5.2% (10/192) for TV, and 33.5% (59/176) for Candida. After excluding 5 invalid Affirm results, the sensitivity and specificity of the BD Affirm™ VPIII system was 78/88 (88.6%, 95% confidence interval (CI): 80.1–94.4%) and 76/100 (76.0%, 95% CI: 66.4–84.0%) for BV, 4/10 (40%, 95% CI: 12.2–73.8%) and 182/182 (100%, 95% CI: 98–100%) for TV, and 33/59 (55.9%, 95% CI: 42.4–68.8%) and 116/117 (99.1%, 95% CI: 95.3–99.9%) for Candida.
Conclusion: The BD Affirm™ VPIII detected only 40% of TV and 56% of Candida, suggesting unacceptably low sensitivity for use in clinical settings for women seeking care for vaginitis. The specificity of G. vaginalis for diagnosis of BV could result in false positives and women without BV receiving unwarranted treatment.
PP03.44 – The Role of Symptoms in Gonorrhea Detection Among Men: Asymptomatic Screening Remains Important
Dr. Dieuwertje L. Horsten1,2,3,4, Dr. Ymke J. Evers1,3, Dr. Petra F. G. Wolffs3, Dr. Nicole H. T. M. Dukers-Muijrers1,3, Prof. Dr. Christian J. P. A. Hoebe1,2,3
1South Limburg Public Health Service, Heerlen, The Netherlands.
2Collaborative Academic practice for Public Health Infectious diseases (CAPI), Heerlen, The Netherlands.
3Maastricht University, Maastricht, The Netherlands.
4Brabant-Zuidoost Public Health Service, Eindhoven, The Netherlands.
Background: The rising incidence of gonorrhea highlights the critical need for timely detection and treatment to curb transmission and prevent complications. Public health testing policies increasingly target symptomatic individuals. Therefore, understanding symptom presentation is crucial: how many men with gonorrhea experience symptoms, which symptoms are associated with gonorrhea, and can these inform targeted testing?
Methods: This retrospective cohort study used consultation data from a public health STI clinic in the Netherlands (2011–2023), including demographics, symptoms, and laboratory test results. High quality data collection involved systematically inquiring about STI symptoms, with each symptom explicitly presented to each patient for confirmation. Associations between symptoms and gonorrhea were analyzed using logistic regression, stratified by target group (men who have sex with men [MSM], men who have sex with women [MSW]) and infection site (genital, anorectal, oropharyngeal).
Results: Of 44,283 men, 10.6% of MSM and 2.0% of MSW tested positive for gonorrhea, with 44.4% and 64.0%, respectively, reporting symptoms. For urethral gonorrhea, the strongest associations were with urethral discharge (MSM: 27.4%; OR9.0, 95% CI 8.0–10.2; MSW: 52.3%; OR11.3, 95% CI 9.3–13.8), pain during urination (MSM: 29.3% OR4.2, 95% CI 3.7–4.7; MSW: 57.3%, OR4.8, 95% CI 3.9–5.8), and frequent urination (MSM: 13.3%; OR2.2, 95% CI 1.9–2.6; MSW: 22.4%; OR2.5, 95% CI 2.0–3.1). Anal discharge (11.0%; OR7.4, 95% CI 6.1–9.0), pain during sex (4.8%; OR2.7, 95% CI 2.0–3.3), and anal itching (13.9%; OR2.5, 95% CI 2.0–3.3) were strongly associated with anal gonorrhea in MSM. Associations between throat symptoms and oropharyngeal gonorrhea were weak (MSM: 10.5%; OR1.5, 95% CI 1.2–1.8) or insignificant (MSW). Symptom-directed testing would detect 42.0% of genital and 26.1% of anal gonorrhea infections.
Conclusion: Specific genital and anorectal symptoms were strongly associated with gonorrhea, providing indicators for testing. However, as a substantial proportion of gonorrhea-positive men are asymptomatic, symptom-based testing may miss many infections. Asymptomatic testing remains important for timely detection and treatment.
PP03.45 – Weak Symptom Correlations Undermine Symptom-Based Testing for Gonorrhea in Women: A Retrospective Cohort Study
Dr. Dieuwertje L. Horsten1,2,3,4, Dr. Ymke J. Evers1,3, Dr. Petra F.G. Wolffs3, Dr. Nicole H.T.M. Dukers-Muijrers1,3, Prof. Dr. Christian J.P.A. Hoebe1,2,3
1South Limburg Public Health Service, Heerlen, The Netherlands.
2Collaborative Academic practice for Public health Infectious Diseases (CAPI), Heerlen, The Netherlands.
3Maastricht University, Maastricht, The Netherlands.
4Brabant-Zuidoost Public Health Service, Eindhoven, The Netherlands.
Introduction: Gonorrhea rates are rising among women, underscoring the importance of timely detection and treatment to halt transmission and prevent complications. Simultaneously, shifting testing policies emphasize testing individuals with physical symptoms. Understanding gonorrhea symptom presentation is crucial: how many women experience symptoms, which symptoms are associated with gonorrhea, and can these symptoms reliably guide testing?
Methods: This retrospective cohort study analyzed consultation data (2011–2023) from a public health STI clinic in the Netherlands, including demographics, symptoms, and laboratory test results. High quality data collection involved systematically inquiring about STI symptoms, with each symptom explicitly presented to each patient for confirmation. Logistic regression analyzed associations between symptoms and gonorrhea, stratified by infection site (genital, anorectal, oropharyngeal).
Results: Of 40,343 women 1.8% (n = 717) tested positive for gonorrhea; 51.0% of gonorrhea-positive women reported symptoms. Genital gonorrhea was associated with hematuria (6.9%; OR 1.80, 95% CI 1.33–2.45; P < 0.01), frequent urination (19.8%; OR 1.48, 95% CI 1.22–1.79; P < 0.01), pain during urination (26.2%; OR 1.32, 95% CI 1.11–1.58; P < 0.01), and abdominal pain (18.3%; OR 1.30, 95% CI 1.06–1.58; P < 0.01). Genital discharge showed a weaker association (16.7%; OR 1.25, 95% CI 1.01–1.53; P = 0.04). No significant associations were found between symptoms and anorectal or oropharyngeal gonorrhea. Testing based on the previously mentioned symptoms would detect 47.5% of genital gonorrhea diagnoses.
Conclusion: Nearly half of women with gonorrhea are asymptomatic. Contrary to common ideas, no strong associations were found between specific genital symptoms and genital gonorrhea. Anorectal and oropharyngeal symptoms showed no associations. Symptom-based testing would miss many gonorrhea infections.
PP03.46 – Does Pre-Treatment with Doxycycline Improve the Efficacy of Combination Minocycline and Metronidazole for Macrolide Resistant Mycoplasma Genitalium Infections?
Dr. Kay Htaik1, Dr. Lenka Vodstrcil1,2,3, Dr. Erica Plummer1,2, Ms Laura Matthews1,2, Ms Ivette Aguirre1, Prof Eric Chow1,2,3, Prof Christopher Fairley1,2, Prof Catriona Bradshaw1,2,3
1Melbourne Sexual Health Centre, Melbourne, Victoria, Australia.
2School of Translational Medicine, Monash University, Melbourne, Victoria, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Victoria, Australia.
Background: Curing Mycoplasma genitalium is challenging due to rising antimicrobial resistance and limited therapeutic options. There is an urgent need for more therapeutic options. A recent series of patients attending Melbourne Sexual Health Centre (MSHC) found 14 days of minocycline and metronidazole (minocycline+metronidazole) achieved microbial cure in 76.7% (95% CI, 65.4–85.8%) of macrolide-resistant infections, indicating it may be more effective than 14 days of minocycline (67.5%; 95% CI, 58.4–75.6%). Doxycycline has been shown to reduce M. genitalium load and is used for STI syndromes and in resistance-guided therapy. We hypothesized that the addition of 7 days of oral doxycycline prior to minocycline+metronidazole may further enhance cure and provide an effective and affordable therapeutic option.
Methods: We evaluated microbial cure and tolerability of 7 days of oral doxycycline 100 mg twice daily followed by oral minocycline 100 mg BD and metronidazole 400 mg BD for 14 days for macrolide-resistant M. genitalium infections at MSHC. Microbial cure was defined as a negative test-of-cure (TOC) using transcription mediated amplification 14–90 days after completing the regimen. Data on side effects and adherence were collected at TOC visits.
Results: Between September 2021 and November 2024, 69 patients were treated with doxycycline followed by minocycline+metronidazole; 61/69 (88.4%, 95% CI, 78.4–94.9%) achieved microbial cure. Cure was significantly higher than that achieved with minocycline monotherapy (88.4% vs 67.5%, P = 0.002) (Tables 1, 2). Preliminary data suggests it may be more effective than minocycline+metronidazole without doxycycline (88.4 vs 76.7%, P = 0.080). Central nervous system and gastrointestinal side effects were commonly reported for all regimens.
Conclusion: The efficacy of the minocycline+metronidazole regimen appears to be enhanced by pre-treatment with 7 days of oral doxycycline with cure rates of 88%. This regimen may offer an effective and affordable option for patients with contraindications to quinolones or limited options. Clinicians should be aware of side effects.
PP03.47 – Cognitive Concerns and Uncertainty Among People Aging with HIV
Ms. Jenny Hui1,2, Ms. Teresa Kern2,3,5, Ms. Carley Moore4, Mr. Nelson Pang2,5, Ms. Marvelous Muchenje2,5, Ms. Kate Murzin3, Dr. Soo Chan Carusone6, Dr. Francisco Ibáñez-Carrasco4, Dr. Kristina Kokorelias7, Dr. Andrew D. Eaton2,5
1Ontario Institute For Studies In Education (OISE), University of Toronto, Toronto, Canada.
2Faculty of Social Work – Saskatoon Campus, University of Regina, Saskatoon, Canada.
3Realize Canada, Toronto, Canada.
4Dalla Lana School of Public Health, University of Toronto, Toronto, Canada.
5Factor-Inwentash Faculty of Social Work, University of Toronto, Toronto, Canada.
6Collaborative for Health and Aging, McMaster University, Hamilton, Canada.
7Division of Geriatric Medicine, Department of Medicine, Sinai Health System and University Health Network, Toronto, Canada.
Background: Cognitive challenges and uncertainty about cognitive aging are frequently reported by people aging with HIV. Uncertainty is further exacerbated by experiences of HIV-related stigma, ageism, social isolation, and concerns about potential discrimination in healthcare settings. This study explored individuals’ experiences and needs at the intersection of HIV, aging, and cognitive health concerns.
Methods: We purposively recruited 45 PAHIV (aged 40+) with self-identified cognitive concerns in two Canadian provinces. Participants completed an online demographic survey and a two-hour, peer-led focus group (3–7 participants each) conducted via Zoom. Three coders used thematic content analysis to identify emergent themes across the 10 focus group transcripts, incorporating input from both people aging with HIV and service providers.
Results: All participants reported experiencing at least five cognitive challenges, with memory and attention issues being the most common (n = 41), yet only 4 reported a dementia diagnosis. Across focus groups, participants highlighted concerns related to memory, concentration, and mental health. Feelings of uncertainty were prominent as participants navigated overlapping challenges of cognitive symptoms and aging with HIV. They also described factors that negatively and positively influenced healthcare experiences and identified gaps in existing supports/services. Critically, participants provided practical recommendations to address unmet needs at the intersection of cognition, aging, and HIV.
Conclusion: Aging is often fraught with uncertainty; for people aging with HIV, this uncertainty can present early due to cognitive difficulties in middle-age. In this study, many participants reported relying on informal support networks due to insufficient formal resources for HIV, aging, and cognition. Congress attendees will learn about the importance of implementing tailored psychosocial supports, ensuring earlier and routine cognitive screening, and providing education on cognitive health to people aging with HIV. Addressing these gaps is critical to enhancing affirming care for people aging with HIV.
PP03.48 – Expedited Partner Therapy Uptake and STI Clearance Rates Among Cisgender Women in Doxycycline Post-Exposure Prophylaxis (dPEP) Study
Mr. Lawrence Juma1, Sangeitha Thayalan2, Benard Rono1, Victor Omollo1, Kevin Oware1, Lauren Violette3,4, Deborah Donnel5, Josephine Odoyo1, Felix Mogaka1, Lianne Siegel6, Sarah Hoffman6, Elizabeth Bukusi1,4, Jared Baeten4, Jenell Stewart2,6
1Kenya Medical Research Institute, Kisumu, Kenya.
2Hennepin Healthcare, Minneapolis, USA.
3Harvard University, Boston, USA.
4University of Washington, Seattle, USA.
5Fred Hutchinson Cancer Center, Seattle, USA.
6University of Minnesota, Minneapolis, USA.
Background: We examined factors associated with the uptake of expedited partner therapy (EPT) and sexually transmitted infection clearance among participants diagnosed with Chlamydia trachomatis (CT) and/or Neisseria gonorrhoeae (NG) participating in a doxycycline post-exposure prophylaxis (dPEP) study in Kenya.
Methods: Cisgender women in the dPEP study (N = 449) were tested for CT/NG every 3 months for one year; following any positive test, participants were treated, offered EPT, and returned for a test-of-cure 2 to 4 weeks after treatment. Using chi-squared tests, baseline characteristics were compared between participants with any versus no EPT uptake. We used generalized estimating equation (GEE) models to compare visit-level EPT uptake by participant characteristics and test of cure results by EPT uptake to account for participants who were treated at more than one visit.
Results: Our analysis included 140 participants who tested positive for CT and/or NG at 209 study visits. Among women who tested positive, 75% (n = 105) accepted EPT during the study. Women who accepted EPT were more likely (61.9%) to have an income compared to 37.1% who did not (P = 0.018) and more likely (54.3%) to report recent transactional sex (P = 0.032). Using visit-level covariates across baseline and follow-up visits, having a primary sex partner within the past 3 months (91/105, 86.7%) was positively correlated with EPT uptake (OR = 2.17, 95% CI 1.01–4.65, P = 0.047). Reporting intimate partner violence (3/103, 2.9%) was associated with less EPT uptake (OR = 0.25, 95% CI 0.06–1.01, P = 0.051). In a multivariable analysis with both factors, intimate partner violence was associated with less EPT uptake (OR = 0.23, 95% CI 0.06–0.95 P = 0.042). EPT uptake was not significantly associated with a negative test of cure result (N = 174, OR = 2.42, 95% CI 0.89–6.56, P = 0.082).
Conclusion: Findings suggested that despite high overall uptake, EPT did not significantly associate with test of cure results. Results demonstrated important implications for partner engagement.
PP03.49 – Overview of the Current Penicillin Use for the Treatment of Syphilis in Geneva, Switzerland and the Hospital Management to Prevent Future Shortages
Dr. Myriam Lamrayah1, Dr Soufiene Krifa3, Dr Antoine David2, Pr Laurence Toutous Trellu2
1University of Geneva, Geneva, Switzerland.
2University Hospital of Geneva, Dermatology Unit, Geneva, Switzerland.
3University Hospital of Geneva, Pharmacy Unit, Geneva, Switzerland.
Since the discovery and commercialization of penicillin in 1940’s, syphilis is efficiently treatable at all stages. Despite access to testing centers, large safety campaigns and prevention tools against STIs, the WHO estimates 8 million adults acquired syphilis in 2022. One probable cause is the successive global shortages of penicillin, a consequence of supply and demand imbalances, explaining by the upsurge opposed to fewer active pharmaceutical ingredient manufacturers. Two different forms of penicillin are used for treating syphilis depending on the status of the patient and the stage of the disease: benzyl penicillin (BP) or penicillin G, an aqueous solution for intravenous injection; and the long-acting salt option benzathine BP for intramuscular route uniquely. The latter, which is the first line recommended treatment, is the most affected by the stock-outs: during 2014–2016, over 40 countries worldwide globally reported shortages in benzathine BP. The case of congenital syphilis is then crucial in a such situation. Here, we evaluate the management of the syphilis treatment in the University Hospitals of Geneva to elaborate a standard operating procedure (SOP) of penicillin uses. It will be useful to 1) mitigate strategies for potential future storages and to 2) avoid the use of inappropriate treatments leading to serious therapeutic failures. In this way, we monitor regional stock levels, the quantity of active authorized suppliers, the number and type of centers authorized to deliver. Even if Treponema pallidum resistance to penicillin has never been reported, we can notice increasing levels of general genotypic resistance thanks to recent large genomic sequencing, and clinical treatment failure to macrolides such as azithromycin (99.2 % of resistance in the USA). Nevertheless, latest in vitro studies highlighted various antibiotic classes would be potential candidates for expanding the current therapeutic repertoire for syphilis. A such SOP will be transposable to next anti-syphilis antibiotics.
PP03.50 – The Association Between Material Deprivation, Sociodemographic Factors and HIV Outcomes Among Migrants with HIV in the ASAP Study
Dr. Moustafa Laymouna1,2,3, Dr Kim Engler2,3, Dr Melchior Belin2,3,5, Dr David Lessard2,3,4, Dr Tibor Schuster1, Dr Joel Ishak2,3,4, Dr Joseph Cox2,3,4,6, Dr Sean Yaphe4, Dr Amir Chalati2,3,4, Dr Bertrand Lebouché1,2,3,4
1Department of Family Medicine, Faculty of Medicine and Health Sciences, McGill University, Montreal, Canada.
2Centre for Outcomes Research and Evaluation, Research Institute of the McGill University Health Centre, Montreal, Canada.
3Infectious Diseases and Immunity in Global Health Program, Research Institute of McGill University Health Centre, Montreal, Canada.
4Chronic and Viral Illness Service, Division of Infectious Disease, McGill University Health Centre, Montreal, Canada.
5Department of General Medicine, Faculty of Medicine, University of Lille, Sciences of Health and Sport, Lille, France.
6Department of Epidemiology, Biostatistics and Occupational Health, Faculty of Medicine and Health Sciences, McGill University, Montreal, Canada.
Background: Migrant people are disproportionately affected by the HIV epidemic in Montreal, Canada. Material deprivation (MD), the inability to access basic necessities, may hinder timely care and optimal outcomes among migrants with HIV (MWH). This study examines MD prevalence in this population and its association with sociodemographic factors and HIV clinical outcomes.
Description: This secondary analysis used data from 63 antiretroviral therapy (ART)-naïve MWH enrolled in the Antiretroviral Speed Access Program (ASAP) Study, which investigated free-of-charge, rapid ART initiation in a multidisciplinary HIV care setting. MD was assessed using the Canadian Material Deprivation Index (CMDI), scored 0–17, treated as continuous for descriptive analyses and dichotomized (high: ≥7, low: <7) for regression analyses. T-tests compared mean MD scores across sociodemographic groups, with median and interquartile ranges (IQR) reported for highly variable scores. Logistic regression assessed associations between MD and clinical outcomes: CD4 count (<200 vs ≥200 cells/μL), time to ART initiation (>7 vs ≤7 days), and time to viral suppression (>84 vs ≤84 days).
Results: Participants were on average 39.3 ± 11.0 years old, 68% male, 61% from Africa/Caribbean, and 76% with annual income <40,000 CAD. The mean MD score was 7.0 ± 4.8 (median: 7; IQR: 4–12). Participants with high MD included unemployed individuals (9.8 ± 3.7), those living alone (8.9 ± 4.1), and participants with a secondary education or less (8.7 ± 4.2). Female participants had significantly higher MD scores than males (9.1 ± 4.9 vs 6.3 ± 4.5, P = 0.02). Clinical outcomes revealed associations with high MD: delays >7 days (OR: 2.4; 95% CI: 1.2–4.8; P = 0.01); suppression >84 days (OR: 2.6; 95% CI:1.5–4.3; P < 0.01); and baseline CD4 T-cell count <200 cells/μL (OR:2.2; 95% CI: 1.1–4.0; P = 0.02).
Conclusion: Among ART-naïve MWH, MD was more prevalent among unemployed, less-educated, female participants, and those living alone. MD significantly contributed to delayed ART initiation, slower viral suppression, and lower CD4 counts. Tailoring interventions to address social determinants is critical to achieve equitable outcomes.
PP03.51 – A 5-Year Retrospective Study of Prevalence and Antimicrobial Susceptibility Patterns of Genital Mycoplasmas in Hanoi, Vietnam
Dr. Hai Ha Long Le1,2, Dr Paul C. Adamson3, Dr Hung Van Le1,2, Dr Hoang Huy Le4, Dr An Van Nguyen5, Dr Luong Huy Vu1,2, Dr Vinh Thi Ha Nguyen1,2, Dr Hoa Quynh Pham2, Dr Viet Hoang Nguyen1
1Hanoi Medical University, Hanoi, Vietnam.
2National Hospital of Dermatology and Venereology, Hanoi, Vietnam.
3David Geffen School of Medicine, Los Angeles, US.
4National Institute of Hygiene and Epidemiology, Hanoi, Vietnam.
5Military Hospital 103, Hanoi, Vietnam.
Background: Mycoplasmas, including Mycoplasma hominis and Ureaplasma urealyticum, are associated with genital infections in both men and women. These bacteria naturally resist several antibiotics, leaving limited treatment options available. Furthermore, studies have shown that antibiotic resistance in these bacteria increases and varies geographically. This study aims to investigate the prevalence and antimicrobial resistance patterns of mycoplasmas in Hanoi, Vietnam.
Methods: From January 2018 to December 2022, a survey was conducted on outpatients with STI-related symptoms in the clinical microbiology laboratory at the National Hospital of Dermatology and Venereology, Hanoi, Vietnam. Urethral or cervical samples were collected, followed by cultivation, identification, and antibiotic susceptibility testing using the Mycoplasma IST2 assay (bioMérieux, France). Intermediate susceptible isolates were grouped with resistant isolates. The Cochran-Armitage test was used to assess the significance of annual trends.
Results: A total of 1,510 patients were recruited, including 1,085 males and 425 females. Of these, 430 (28.5%) samples tested positive for genital mycoplasmas (Table 1). The prevalence of single U. urealyticum infection, single M. hominis infection, and co-infection was 20.6% (311), 0.7% (11), and 7.2% (108), respectively. During the study period, the highest susceptibility rates for genital mycoplasmas were observed for pristinamycin (90.2%), followed by doxycycline (87.9%), josamycin (84.9%), and tetracycline (73.7%). In contrast, ciprofloxacin and ofloxacin exhibited the lowest activity against these bacteria, with resistant rates of 92.6% and 88.6%, respectively. Interestingly, genital mycoplasmas showed a significantly increasing trend of resistance to erythromycin and tetracycline, while trends in resistance to clarithromycin approached significance.
Conclusions: This study revealed a high prevalence of genital mycoplasmas and a high antibiotic resistance rate compared to other studies. The high prevalence of resistance to ciprofloxacin and ofloxacin highlights the need for improved management of these infections. While pristinamycin demonstrated high efficacy against mycoplasmas, overall susceptibility to other antibiotics was low.
| 2018 (n = 116; %) | 2019 (n = 95; %) | 2020 (n = 71; %) | 2021 (n = 87; %) | 2022 (n = 61; %) | Total (n = 430) | ZA | P-trendA | ||
|---|---|---|---|---|---|---|---|---|---|
| Doxycycline | 12 (10.3) | 8 (8.4) | 11 (15.5) | 13 (14.9) | 8 (13.1) | 52 (12.1) | 1.18 | 0.24 | |
| Josamycine | 15 (12.9) | 8 (8.4) | 14 (19.7) | 16 (18.4) | 12 (19.7) | 65 (15.1) | 1.89 | 0.59 | |
| Ofloxacine | 100 (86.2) | 87 (91.6) | 64 (90.1) | 79 (90.8) | 51 (83.6) | 381 (88.6) | -0.15 | 0.88 | |
| Erythromycine | 50 (43.1) | 39 (41.1) | 43 (60.6) | 53 (60.9) | 38 (62.3) | 223 (51.9) | 3.50 | <0.001 | |
| Tetracycline | 26 (22.4) | 20 (21.1) | 19 (26.8) | 29 (33.3) | 19 (31.1) | 113 (26.3) | 2.02 | 0.04 | |
| Ciprofloxacine | 104 (89.7) | 93 (97.9) | 65 (91.5) | 79 (90.8) | 57 (93.4) | 398 (92.6) | 0.16 | 0.87 | |
| Azithromycine | 54 (46.6) | 48 (50.5) | 40 (56.3) | 42 (48.3) | 35 (57.4) | 219 (50.9) | 1.10 | 0.27 | |
| Clarythromycin | 35 (30.2) | 18 (18.9) | 25 (35.2) | 28 (32.2) | 25 (41.0) | 131 (30.5) | 1.93 | 0.054 | |
| Pristinamycine | 7 (6.0) | 7 (7.4) | 10 (14.1) | 12 (13.8) | 6 (9.8) | 42 (9.8) | 1.67 | 0.09 |
PP03.52 – Real-World Observations on the Diagnosis of Syphilis After Initation of Doxycycline Post-Exposure Prophylaxis
Dr. Alice Lehman1, Pamela Layton2, Susan Mishkulin2, Dr. Jenell Stewart1,3
1University of Minnesota, Minneapolis, United States.
2Hennepin County Public Health Clinic, Minneapolis, United States.
3Division of Infectious Diseases, Hennepin Healthcare, Minneapolis, United States.
Background: Doxycycline post-exposure prophylaxis (doxyPEP) is proven to prevent bacterial sexually transmitted infections among persons who were assigned male sex at birth (AMAB). Syphilis diagnoses require interpretation of RPR titers and clinical assessments; recent exposure to noncurative antibiotics can decrease quantitative RPR. The impact of intermittent or partner-selective doxyPEP use on the diagnosis of syphilis remains undescribed.
Methods: Syphilis diagnoses among all AMAB persons were compared in 12-month pre-period (N = 4880) and post-period following doxyPEP initiation in December 2023 (N = 3570), at the Red Door Clinic, a public health clinic in Minneapolis, Minnesota. New syphilis diagnoses were defined via ICD10 code (Table 1 footnote). The first new diagnosis per unique person within each time-period were analyzed by stage, treponemal antibody, quantitative RPR, and doxyPEP prescription. Descriptive statistics were calculated with Chi-squared test.
Results: Among persons who received doxyPEP (n = 596), new syphilis diagnoses decreased to 9/596 (1.5%) in the post-period compared with all AMAB in pre-period, 165/4880 (3.4%), P = 0.013. There was no decline among all AMAB in post-period 108/3570 (3.0%) (P = 0.361). Of the nine breakthrough syphilis diagnoses with doxyPEP prescription, 6/9 (66%) had a clinical diagnosis with no reactive RPR and median RPR titer was 1:4 among the 3/9 (33%) with an RPR titer ≥1:1. Diagnosis of syphilis is often made on clinical presentation without RPR >1:1 (pre-period 111/165 67% vs post-period 62/108, 57%, P = 0.098). There was no change in the median RPR titer (pre 1:16 vs post 1:16) or when stratified by stage of syphilis (Table 1).
Conclusion: New syphilis diagnoses decreased among people who were prescribed doxyPEP in the 12 months following doxyPEP initiation. Clinical, non-laboratory confirmed diagnoses were frequent in pre-period and post-period. Potential impact of intermittent use of doxyPEP on decreases in RPR titers cannot be directly concluded in setting of low incidence of syphilis.
| Pre-doxyPEP 12/11/2022 – 12/10/2023 | Post-doxyPEP 12/11/2023 – 12/10/2024 | Persons prescribed doxyPEP 12/11/2023 – 12/10/2024 | ||
|---|---|---|---|---|
| Number of syphilis screening tests | 8010 | 7610 | 4146 | |
| Number of syphilis screening tests among unique persons | 4880 | 3570 | 596 | |
| New syphilis diagnosis (% screening tests) | 165 (3.4) | 108 (3.0) | 9 (1.5)* | |
| New syphilis diagnosis with reactive RPR (% new dx) | 126 (76.3) | 78 (72.2) | 3 (33.3)** | |
| New syphilis diagnosis with reactive RPR and treponemal antibody | 123 (74.5) | 78 (72.2) | 3 (33.3)** | |
| New syphilis diagnosis with RPR > 1:1 (% new dx) | 111 (67.2) | 62 (57.4) | 2 (22.2)** | |
| Stage of Syphilis Diagnosis | ||||
| Primary syphilis (% new dx) | 20 (12.1) | 7 (6.4) | 1 (11.1)** | |
| Secondary syphilis (% new dx) | 20 (12.1) | 9 (8.2) | 0 | |
| Early latent or early not specified (% new dx) | 36 (21.8) | 15 (13.9) | 2 (22.2)** | |
| Late latent (% new dx) | 18 (10.9) | 17 (15.7) | 0 | |
| Unspecified (% new dx) | 71 (43.0) | 60 (55.6) | 6 (66.7)** | |
| Median RPR | ||||
| Median RPR, all | 1:8 | 1:2 | Negative | |
| Median RPR, if reactive | 1:16 | 1:16 | 1:4 | |
| Primary median RPR | 1:2 | Negative | Negative | |
| Secondary median RPR | 1:32 | 1:16 | - | |
| Early latent or early not specified median RPR | 1:1 | 1:4 | 1:4 | |
| Late latent median RPR | 1:8 | 1:2 | - | |
| Unspecified median RPR | 1:4 | 1:2 | Negative | |
*percentage from unique screening tests among persons prescribed doxyPEP.
**percentages from new diagnoses among persons prescribed doxyPEP.
Foot Note
ICD 10 Dx codes for new syphilis diagnosis:
PP03.53 – Efficacy Among Antiretroviral Treatment-Naïve Individuals Initiating Albuvirtide-Based Antiretroviral Therapy: A Real-Word Study
Ms. Huanxia Liu1, Dr. Shenghua HE1, Dr. Yuanhong He1, Dr. Tongtong Yang1, Dr. xia Zhao1
1Public Health Clinical Center of Chengdu, Sichuan, China.
Background: Albuvirtide (ABT) is the first long-acting HIV-1 fusion inhibitor. As a peptide, ABT is not metabolized by CYP450 enzymes and is expected to undergo catabolism to amino acid residues, resulting in fewer drug-drug interactions. A prospective cohort study demonstrated that ABT-based regimens exhibited excellent tolerability and good clinical effectiveness in ART-naïve patients with HIV-1 in China. We evaluated its effectiveness in a real-life setting.
Methods: We collected the relevant data of ART-naïve people living with HIV (PLWH) in Chengdu public health clinical medical center initiating ABT-based regimens for 24 weeks between July 2021 and July 2023. The primary outcome was viral suppression (HIV RNA <50 copies/mL) at 24 weeks, and we utilized logistic regression analysis to explore the factors affecting virological suppression. Analysis-of-variance for repeated measures was used to examine changes in CD4 and CD4/CD8 ratio from baseline to Week 24.
Results: All 112 patients included in this study were complicated with severe opportunistic infections. 112 ART-naïve PLWH initiated ABT+DTG/3TC (80.36%), ABT+DTG (19.64%). The median HIV-1 RNA levels significantly decreased from 5.39 log10copies/mL to 2.27 log10copies/mL, 1.73 log10copies/mL and 1.40 log10copies/mL after 4, 12 and 24 weeks of treatment, respectively (P < 0.001). 83 (74.11%) patients achieved viral suppression of <50 copies/mL after 24 weeks of treatment. Compared with the baseline, the CD4/CD8 ratio increased by 0.1 (0.04, 0.25) and CD4 increased by 115.50 (63.00, 194.50) after 24 weeks of treatment, and both showed statistically significant differences (P < 0.0001). The multivariate regression analysis revealed that baseline HIV-1 RNA and CD4 + T-cell counts were associated with successful virological suppression (P < 0.05).
Conclusions: ABT-based regimens is effective for ART-naïve patients with HIV-1. Baseline HIV-1 RNA and CD4 independently predicted successful virological suppression.
PP03.54 – Safety and Efficacy of Albuvirtide and Dolutegravir for HIV Post-Exposure Prophylaxis in MSM Population: A Prospective Controlled Study
Ms. Huanxia Liu1, Dr. Shenghua He1, Dr. Tongtong Yang1
1Public Health Clinical Center of Chengdu, Sichuan, China.
Background: There are no prospective clinical studies of adherence and tolerance to HIV post-exposure prophylaxis (PEP) in Men who have sex with men (MSM) in China. The simplified two-drug regimen can reduce adverse drug reactions and drug interactions. Thus, We aimed to explore the efficacy, safety, and adherence of the simplified regimen of Albuvirtide (ABT) + Dolutegravir (DTG) for HIV PEP in the MSM population.
Methods: A prospective, open-label, single-center, cohort study was conducted, enrolling participants who received PEP for HIV at the Chengdu Public Health Clinical Medical Center from June 2021 to December 2023 and met the inclusion criteria. Participants were divided into two groups based on their preference: the study group received ABT + DTG for PEP, while the control group received TDF/3TC or TDF/FTC + DTG. All enrolled participants received PEP within 72 h after exposure and continued for 28 days, and were followed up for 12 weeks.
Results: A total of 120 MSM participants were enrolled and stratified into two groups: the study group and the control group, with 60 and 60 participants in each group, respectively (Tables 1–3). Baseline characteristics were similar between groups (P > 0.05). The overall completion rate for 28 days of treatment among all 120 participants was 91.67%, with the study group showing a higher completion rate than the control group (96.67% vs 86.67%, P = 0.048). No serious adverse events occurred in either of the two groups of subjects. The total incidence of clinical adverse events in the digestive system was lower in the study group than that in the control group (13.33% vs 36.67%, P = 0.003). All participants in both groups had negative HIV screening antibody results during the study period.
Conclusion: The ABT+DTG simplified regimen for PEPin MSM populations showed no cases of treatment failure and demonstrated good adherence and safety.
| Total (N, %) | Study group (N, %) | Study group (N, %) | P | |||
|---|---|---|---|---|---|---|
| Age (years) | ≤20 | 12 (10.00) | 8 (13.33) | 4 (6.70) | 0.684 | |
| 21–40 | 96 (80.00) | 43 (71.67) | 53 (83.33) | |||
| ≥40 | 12 (10.00) | 9 (15.00) | 3 (5.00) | |||
| Ethnicity | Han Chinese | 115 (95.83) | 58 (96.67) | 57 (95.00) | 0.648 | |
| Minority Ethnic | 5 (4.17) | 2 (3.33) | 3 (5.00) | |||
| Comorbidities | Hypertension | 1 (0.83) | 1 (1.67) | 0 (0.00) | 0.315 | |
| Hypertension | 1 (0.83) | 0 (0.00) | 1 (1.67) | 0.315 | ||
| Hepatitis B | 6 (5.00) | 5 (8.33) | 1 (1.67) | 0.094 | ||
| Syphilis | 6 (5.00) | 4 (6.67) | 2 (3.33) | 0.402 | ||
| Syphilis | Married | 14 (11.67) | 6 (10.00) | 8 (13.33) | 0.351 | |
| Divorced | 5 (4.17) | 4 (6.67) | 1 (1.67) | |||
| Single | 101 (84.16) | 50 (83.33) | 51 (85.00) | |||
| Education Level | College and above | 107(89.17) | 51 (85.00) | 56 (93.33) | 0.142 | |
| College and above | 13 (10.83) | 9 (15.00) | 4 (6.67) | |||
| HIV Exposure Time (h) | Exposure Time [M(P25, P75)] | 19.00 (12.00, 30.00) | 22.00 (12.00, 32.00) | 17.00 (12.00, 28.0) | ||
| ≤24 | 77 (64.17) | 37 (61.67) | 40 (66.67) | 0.489 | ||
| 24–48 | 41 (34.17) | 21 (35.00) | 20 (33.33) | |||
| 48–72 | 2 (1.67) | 2 (3.33) | 0 (0.00) | |||
Among the study group, 6 participants had coexisting HBV infection, with 1 participant showing mild baseline liver function abnormalities. However, there was no worsening of liver function abnormalities during the treatment process. In the control group, 1 participant had coexisting HBV infection and received regular antiviral treatment for hepatitis B. No liver function abnormalities were observed at baseline or during the treatment period. None of the study participants with HBV infection in either the study or control group experienced any worsening of liver function during or after the study. Additionally, no participants in either the study or control group had hyperlipidemia or tested positive for anti-hepatitis C virus (HCV) antibodies.
2.2 Adherence of Study Participants (Completion of 28-Day Medication Regimen)
Among the 120 study participants, the completion rate of the 28-day medication regimen was 91.67% (110/120). The study group had a 28-day medication completion rate of 96.67% (58/60), which was significantly higher than the control group’s rate of 86.67% (52/60), with a statistically significant difference (P = 0.048).
| Study Group | Study Group | P | |||
|---|---|---|---|---|---|
| ABT | 100%(60/60) | TDF/FTC或TDF/3TC | 86.67 (52/60) | – | |
| DTG | 96.67 (58/60) | DTG | 86.67 (52/60) | – | |
| Total | 96.67 (58/60) | Total | 86.67 (52/60) | 0.048 |
2.3 Efficacy of Study Participants (HIV Antibody Seroconversion Rate)
During the study, no participants in either the study group or the control group experienced seroconversion to HIV initial screening antibody positivity. A total of 120 study participants were tested for HIV initial screening antibodies at 2 weeks, 4 weeks, and 12 weeks after receiving their first preventive medication dose.
2.4 Safety
The study group had a significantly lower overall incidence of gastrointestinal clinical adverse events compared to the control group (13.33% vs 36.67%, P = 0.003). There were no significant differences in the occurrence of other clinical adverse events or laboratory adverse events. No participants in either group experienced severe adverse events, and no participants withdrew from the study due to serious drug-related adverse reactions. Additionally, no participants in the study group experienced injection site reactions.
| Adverse events | Total (N, %) | Study group (N, %) | Study group (N, %) | P | |
|---|---|---|---|---|---|
| Laboratory Adverse Events | |||||
| ALT Elevation | |||||
| Grade 1 | 12 (10.00) | 6 (10.00) | 7 (11.67) | 0.215 | |
| Grade 2 | 2 (1.67) | 0 (0.00) | 2 (3.33) | ||
| AST Elevation | |||||
| Grade 1 | 7 (5.83) | 4 (6.67) | 3 (5.00) | 0.593 | |
| Grade 2 | 7 (5.83) | 3 (5.00) | 4 (6.67) | ||
| Elevated Uric Acid | |||||
| Grade 1 | 18 (15.00) | 9 (15.00) | 9 (15.00) | 0.364 | |
| Grade 2 | 4 (3.33) | 1 (1.67) | 3 (5.00) | ||
| Elevated Urea | |||||
| Grade 1 | 11 (9.17) | 5 (8.33) | 6 (10.00) | 0.752 | |
| Thrombocytopenia | |||||
| Grade 1 | 3 (2.50) | 1 (1.67) | 2 (3.33) | 0.559 | |
| Decreased Hemoglobin | |||||
| Grade 1 | 2 (1.67) | 1 (1.67) | 1 (1.67) | 1.000 | |
| Proteinuria | |||||
| Grade 1 | 6 (5.00) | 2 (3.33) | 4 (6.67) | 0.402 | |
| Clinical Adverse Events | |||||
| Gastrointestinal System | 30 (25.00) | 8 (13.33) | 22 (36.67) | 0.003* | |
| -Nausea | 6 (5.00) | 2 (3.33) | 4 (6.67) | 0.402 | |
| -Abdominal Pain, Diarrhea | 13 (10.83) | 4 (6.67) | 9 (15.00) | 0.142 | |
| -Changes in Stool Consistency | 11 (9.17) | 2 (3.33) | 9 (15.00) | 0.027* | |
| Nervous System | |||||
| Dizziness, Headache | 9 (7.55) | 4 (6.67) | 5 (8.33) | 0.729 | |
| Others | |||||
| -Joint and Muscle Pain | 10 (8.33) | 4 (6.67) | 6 (10.00) | 0.509 |
Note: The hepatitis B status of participants in the study group and the control group was 8.33% vs 1.67%, respectively (P = 0.094), with no worsening of liver function observed after discontinuation of the medication. Gastrointestinal clinical adverse events were defined as the total number of participants who experienced nausea, abdominal pain, diarrhea, or changes in stool consistency. During the study, no participants in either group developed fever.”
PP03.55 – Is Antimicrobial Resistance a Big Enough Part of the Conversation About Prescribing Doxy-PEP? A Qualitative Study of Australian Sexual Health Clinicians
Dr. Teralynn Ludwick1, Ethan T. Cardwell1, Dr. Tin Vo2, Dr. Eric P. F. Chow3,5, Benjamin Riley4, Dr. Jane S. Hocking1, Dr. Daniel Grace2, Dr. Fabian YS Kong1
1University of Melbourne, Melbourne, Australia.
2University of Toronto, Toronto, Canada.
3Melbourne Sexual Health Centre, Melbourne, Australia.
4ASHM Health, Sydney, Australia.
5Monash University, Melbourne, Australia.
Background: While there is growing interest in doxycycline post-exposure prophylaxis (doxy-PEP), many countries lack clear guidance on patient eligibility for prescribing and messaging around antimicrobial resistance (AMR). This study aimed to understand Australian sexual health clinicians’ decision-making around prescribing doxy-PEP, including assessment of individual and population-level benefits/harms.
Methods: Using content analysis, we analyzed 17 semi-structured interviews with Australian sexual health clinicians working in public/private practice. Interview domains covered: knowledge of doxy-PEP’s effectiveness, considerations for prescribing, navigating patient conversations, and information/resource needs.
Results: Clinicians generally deemed doxy-PEP effective in preventing bacterial STIs, discounting lower effectiveness against gonorrhoea relative to its utility in preventing syphilis. Doxy-PEP was seen as most appropriate for high-risk patients (e.g. repeated STI diagnoses/many sex partners), though clearer guidelines on eligibility were of interest. Clinicians believed that ‘nuanced’ discussion with patients (particularly low-risk individuals) about benefits/harms was important, with some patients ultimately declining use. However, most clinicians were better able to articulate concrete side effects (e.g. photosensitivity) to patients than the vague concept of AMR which was described as ‘airy, nebulous’, lacking long-term data on real effects, and of less concern to patients. While clinicians supported antimicrobial stewardship generally, the level of concern with AMR related to doxy-PEP varied considerably across participants, and for many did not have a large bearing on prescribing. Clinicians expressed the need for community-based awareness/education campaigns on AMR and doxy-PEP as an important building block to support clinician-led conversations.
Conclusion: Clear, immediate benefits of doxy-PEP for individual patients in contrast with the ‘abstract’ nature of AMR renders AMR less prominent in clinician mental models/logics for prescribing. For AMR to factor more prominently in clinical decision-making, we need to think of ways to make it more compatible with clinical prescribing logics (such as providing quantifiable estimates of AMR risk/outcomes), while simultaneously raising community awareness.
PP03.56 – Factors Correlated with High Rates of STI Syndromic Diagnosis and Trends Among Clients Attending Wellness Centre at Lamvelase Clinic: Retrospective Cohort Study
Miss Phumlile Ndlovu1, Mrs Khetsiwe L. Maseko1, Dr. Yves Mafulu1, Miss Bongiwe Matsebula1, Mr Ncedo Mhlanga1, Dr. Adele Benzaken1, Mr Nkululeko Dube1
1Aids Healthcare Foundation- Eswatini, Nhlangano, Eswatini.
Background: In Eswatini, Ministry of Health recommends syndromic management approach for clients with Sexually Transmitted Infections (STIs). There is a high burden of STIs in Eswatini and key populations are at higher risk due to behavioral factors. A rise of PrEP uptake with high STI prevalence have been observed. The study hypothesized there are factors correlated with STI diagnosis, therefore aims to explore factors and identify trends.
Methods: A retrospective facility-based study, with client data purposively collected from Wellness Centre Registers (September 2024 to December 2024).
Results: A total of 1369 clients were included. Out of 1369 clients, over half (62.4%, n = 871) were females, and 40.1% (n = 560) were aged from 25–34 years, median age 28. Among key populations seen, 9%, (n = 126) were female sex workers and public transport operators (1.2%, n = 17). Almost half (43.1%, n = 602) verbalized STI symptoms, while 36.5% (n = 510) came for PrEP. Nearly half (47.1%, n = 645) had STI syndromic diagnosis, vaginal discharges mostly reported (18.4%, n = 257), 11.5% with urethral discharges (n = 161). 37.8% (n = 528) clients did Syphilis test and 4.4% (n = 62) reported with a reactive syphilis (RPR) result. In Chia-square, gender, reason for visiting wellness center, key population, client category, HIV test result, syphilis test and PrEP follow-up were significantly associated with STI syndromic diagnosis.
Conclusion: This study highlights that STI remains a burden among females of reproductive age, key populations and clients who come for PrEP follow-up. There is need to strengthen etiological and syndromic STI management. Future research is needed STI burden in other regions.
PP03.57 – Prevalence of Asymptomatic, Sporadic Symptomatic, Recurrent, and Refractory Bacterial Vaginosis at a Vaginitis Clinic
Mrs Erica Mann1, Dr. Olivia T Van Gerwen2, Dr. Kristal J Aaron2, Dr. Lorenzo Corsini3, Dr. Christina A Muzny2
1University of Alabama at Birmingham Heersink School of Medicine, Birmingham, United States.
2Division of Infectious Diseases, University of Alabama at Birmingham, Birmingham, United States.
3BioNTech Research & Development, Austria.
Background: Bacterial vaginosis (BV), the leading cause of vaginal discharge, is divided into subtypes which inform treatment recommendations: asymptomatic BV, uncomplicated/sporadic (symptomatic) BV, recurrent BV, and refractory BV. We aimed to evaluate the prevalence of these subtypes at a tertiary care Vaginitis Clinic to better understand the burden of BV among women.
Methods: Data were collected through chart review of all patients ≥18 years old who attended a Vaginitis Clinic at least once since its inception (June 2021). Data abstracted included demographics, number of clinic visits, symptoms, and vaginal infection diagnoses, including subtype(s) of BV, trichomoniasis (TV), and vulvovaginal candidiasis (VVC). Analysis was performed using SAS v9.4.
Results: Between June 2021 and December 2024, 149 patients were seen, of which 102 had their records reviewed. Median age was 35 years (IQR: 17–44); 96% were non-Hispanic. There was a total of 262 clinic visits with a median of 2 visits per patient. Of 221 vaginal infections diagnosed, 79/221 (35.7%) were due to BV alone, 50/221 (22.6%) due to BV/VVC co-infection, 13/221 (5.9%) due to BV/TV co-infection, and 12/221 (5.4%) due to BV/VVC/TV co-infection. In total, 154/221 (69.7%) visits with a vaginal infection diagnosis included BV, with some patients fitting the criteria for more than one BV subtype at a visit. Among visits where BV was diagnosed, 37 (24%) included asymptomatic BV, 88 (57.1%) included sporadic/uncomplicated symptomatic BV, 95 (61.7%) included recurrent BV, and 20 (13.0%) included refractory BV. Black race was associated with increased likelihood of recurrent BV (OR 6.54; 95% CI: 2.09–20.54, P = 0.001).
Conclusion: BV was highly prevalent in this population, frequently occurring in the setting of mixed vaginal infections. Most BV visits were due to recurrent BV followed by sporadic, symptomatic BV. These findings can inform future studies on which sub-populations of women will benefit most from novel therapeutic interventions.
PP03.58 – Impact of Simplification of Hepatitis C Treatment on the Evolution of Themes Discussed in Telementoring Sessions
Dr. Valérie Martel-Laferrière1,2,3, Jocelyne Parent3, Dominic Martel1,2,3, Dr. Geneviève Huard2,3, Barbara Kotsoros2, Dr. Ziad Hassoun2,3, Dr. Suzanne Brissette1,2,3
1Centre de recherche du Centre hospitalier de l’Université de Montréal, Montréal, Canada.
2Centre hospitalier de l’Université de Montréal, Montréal, Canada.
3Université de Montréal, Montréal, Canada.
Background: The Extension for Community Healthcare Outcomes (ECHO) model™ was initially developed to improve access to complex treatments such as hepatitis C (HCV) treatment. Real-life cases which pose challenges (investigation, diagnostic, treatment) are presented by participants, and a hub of specialists leads the discussion, focusing on the presenter’s questions. An ECHO program was set up at the Centre hospitalier de l’Université de Montréal in 2017. Since then, the arrival of pangenotypic direct-acting antiviral agents (Fall 2017) and the lifting of restrictions on treatment reimbursement in Québec (March 2018) have considerably simplified the management of this disease. To determine whether the program remains relevant in 2025, we conducted a comparative analysis of the themes addressed in the sessions between the pre- and post-universal hepatitis C treatment eras.
Methods: All the cases presented since the beginning of the program were revised to identify the theme of the questions addressed. Proportions of cases addressing specific themes were compared between the pre- (2017–2018) and post-universal treatment (2018–2024) periods.
Results: A total of 151 cases have been presented since the start of the program (pre: 41 vs post: 110). For most themes, there was no difference between the two periods (Table 1). In 2017–2018, however, there were less questions about the natural history of the disease, such as spontaneous clearance, (2.4% vs 29.1%; P < 0.001), and issues related to substance use disorders (0% vs 11.8%; P = 0.02). Issues of resistance and concomitant medical conditions trended to be addressed more often in 2017–2018, while specific treatment choice, patient and medication management, and liver fibrosis evaluation trended to be addressed more often in 2018–2024.
Conclusion: Our results suggest that, with the simplification of treatments, participants are more concerned with concrete management issues than with specific medical issues. Nevertheless, the themes addressed remain diverse and justify the continuation of the program.
| 2017–2018 (n = 41) | 2018–2024 (n = 110) | P | ||
|---|---|---|---|---|
| Hepatitis C natural history | 1 (2.4%) | 32 (29.1%) | <0.001 | |
| Fibrosis staging | 7 (17.1%) | 35 (31.8%) | 0.07 | |
| Concomitant medical concerns | 11 (26.8%) | 25 (22.7%) | 0.60 | |
| Substance use disorders | 0 (0%) | 13 (11.8%) | 0.02 | |
| Hepatitis B co-infection | 4 (9.8%) | 13 (11.8%) | 1.00 | |
| Cirrhosis | 6 (14.6%) | 10 (9.1%) | 0.24 | |
| Treatment eligibility | 10 (24.4%) | 13 (14.5%) | 0.15 | |
| Treatment choice | 21 (51.2%) | 74 (67.2%) | 0.07 | |
| Treatment timing | 3 (7.3%) | 19 (17.3%) | 0.19 | |
| Drug-drug interactions | 5 (12.2%) | 22 (20%) | 0.27 | |
| Resistance | 4 (9.8%) | 6 (5.5%) | 0.46 | |
| Pre-treatment evaluation, side effects and monitoring | 8 (19.5%) | 35 (31.8%) | 0.14 | |
| Medication and patient management | 2 (4.9%) | 19 (17.3%) | 0.06 | |
| Post-treatment follow up | 6 (14.6%) | 22 (20%) | 0.45 | |
| Re-treatment | 2 (4.9%) | 11 (10%) | 0.52 |
PP03.59 – How Do Asymptomatic Patients Feel About Deferring Empiric Treatment After Gonorrhea Exposure? Analysis of Participant Survey After Empiric Ceftriaxone Deferral
Dr. Stephanie E. McLaughlin1,2, Kate Holzhauer1,2, Lindley A. Barbee1,2, Olusegun O. Soge1,2, Matthew Golden1,2
1University of Washington, Seattle, United States.
2Public Health Seattle King County, Seattle, United States.
Background: Prompted by increasing concerns related to antimicrobial stewardship, a growing number of sexual health providers are discontinuing or questioning the empiric treatment of persons presenting after sexual exposure to a person with gonorrhea or chlamydia. We evaluated willingness to defer empiric treatment among persons seeking care after sexual contact to a person with gonorrhea in a sexual health clinic (SHC) in Seattle, WA.
Methods: Study participants included persons offered enrollment in a study to evaluate the performance of SpeeDx ResistancePlus® GC testing to guide antibiotic therapy enrolled 3/2022–7/2024. We collected data on patients’ willingness to defer treatment until they received test results as part of initial study enrollment screening. Participants who consented to defer treatment as part of the study completed a self-administered survey on their experience.
Results: A total of 120 asymptomatic NG-contacts were offered enrollment in the study. Seventy-eight (65%) refused participation, including 53 who did not want to defer treatment (68% of those who declined and 44% of those offered enrollment). Forty-two (35%) people consented to participate and defer treatment, 27 (64%) of whom completed the study survey; 8 (19%) of 27 tested positive for NG. Most survey respondents stated they would defer treatment again in the future, and a majority also reported a desire to limit antibiotic exposure (see Table 1).
Conclusions: At least within the context of a study, over one third of SHC patients are willing to defer therapy while they await test results, and 81% of NG-contacts who deferred treatment were spared unnecessary antibiotic therapy. Our findings support SHCs offering patients who present as contacts to gonorrhea the option of deferring empiric therapy. Routinely deferring empiric treatment among contacts to gonorrhea will require additional efforts to understand and address patient concerns and make receipt of delayed treatment easy for patients who test NG-positive.
| NG Positive (n = 5) | NG Negative (n = 22) | Total (n = 27) | ||
|---|---|---|---|---|
| The time it took to get my gonorrhea test results was __________. | ||||
| Just right | 4 (80%) | 20 (91%) | 24 (89%) | |
| Too long | 1 (20%) | 1 (5%) | 2 (7%) | |
| I would wait for my gonorrhea test results again instead of receiving same-day gonorrhea treatment. | ||||
| Strongly Agree | 3 (60%) | 7 (32%) | 10 (37%) | |
| Agree | 1 (20%) | 12 (55%) | 13 (48%) | |
| Neutral | 0 | 1 (5%) | 1 (4%) | |
| Disagree | 0 | 1 (5%) | 1 (4%) | |
| Strongly Disagree | 1 (20%) | 0 | 1 (4%) | |
| What are your thoughts on antimicrobial (aka antibiotic) resistance and the role of antibiotic overuse in antimicrobial resistance? | ||||
| I don’t know anything about antimicrobial resistance | 2 (40%) | 3 (14%) | 5 (19%) | |
| I care about antibiotic resistance, and try to limit my antibiotic usage | 3 (60%) | 19 (86%) | 22 (81%) | |
| Why did you participate in this study? (can choose multiple reasons) | ||||
| The money | 1 (20%) | 5 (17%) | 5 (19%) | |
| To possibly avoid a shot | 0 | 7 (33%) | 7 (26%) | |
| To possibly avoid antibiotics | 0 | 10 (50%) | 10 (37%) | |
| To help advance science | 5 (100%) | 16 (58%) | 21 (78%) | |
PP03.60 – Trends in Mycoplasma Genitalium Consultations Received Through the STD Clinical Consultation Network
Dr. Jacob McLean1,6, Dr. Nick Van Wagoner2, Dr. Wyatt Hanft3, Dr. Kelly Johnson3,7, Dr. Jacqueline Sherbuk4, Barbara Wilgus5, Dr. William Geisler2
1Columbia University Vagelos College of Physicians and Surgeons, New York, United States.
2University of Alabama at Birmingham Heersink School of Medicine, Birmingham, United States.
3University of California San Francisco, San Francisco, United States.
4University of South Florida, Tampa, United States.
5Johns Hopkins University, Baltimore, United States.
6NYC STI/HIV Prevention Training Center, New York, United States.
7California Prevention Training Center, San Francisco, United States.
Background: Mycoplasma genitalium (Mgen) is an emerging sexually transmitted pathogen. Mgen is often asymptomatic but can cause urethritis and is associated with cervicitis, PID, infertility, and possibly premature labor. Although multiplex STI testing platforms including Mgen are available, screening for asymptomatic infection is not recommended as the potential impacts of undiagnosed/untreated asymptomatic infection are unknown. Leveraging the STD Clinical Consultation Network (STDCCN) – an STI consultation service for healthcare and public health professionals in the United States – this study aimed to characterize provider training needs by analyzing general, geographic, and temporal trends in Mgen consultations.
Methods: Consults referencing “mycoplasma,” “genitalium,” and “mgen” between 2015 and 2024 were accessed through STDCCN. Date, location, and verbatim consult were extracted. Consults were reviewed by two subject matter experts (with a third reviewer to adjudicate disagreements) and categorized by theme(s) and patient symptom status. Multiple themes may be present in a single consult. Findings were recorded in REDCap® and analyzed using R software.
Results: 331 Mgen consults were identified, of which 90% occurred after January 2021. Consults were from all US regions. Common themes were Mgen management in pregnancy (N = 138, 41.7%), management of initial episode of Mgen (N = 117, 35.3%), and management of Mgen treatment failure (N = 117, 35.3%). 41.1% of Mgen consults involved people who were asymptomatic (or without specified symptoms) (Table 1).
Conclusion: The STDCCN observed a substantial increase in consultations related to Mgen since 2021. Screening for Mgen in asymptomatic people and in pregnancy is not recommended in the US yet 41.1% of consults were related to Mgen management in people without specified symptoms, often in the context of pregnancy. 35.3% of consults inquired about Mgen management after treatment failure. This study highlights the need for provider education about appropriate use of Mgen diagnostics, indications for Mgen screening/testing, and management of Mgen treatment failures.
| 2015 (from June 15) | 2016 | 2017 | 2018 | 2019 | 2020 | 2021 | 2022 | 2023 | 2024 (through June 30) | Full study period | ||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mgen consults as a proportion of total STDCCN consults n/N (%) | 1/267 (0.4) | 8/565 (1.4) | 5/648 (0.8) | 7/909 (0.8) | 6/909 (0.7) | 7/707 (1.0) | 16/953 (1.7) | 31/1087 (2.9) | 177/1400 (12.6) | 74/754 (9.7) | 332/8204 (4.0) | |
| Mgen consults with theme “Management of Mgen in pregnant person” (n/N, %) | 0/1 (0.0) | 0/8 0.0 | 1/5 (20.0) | 0/7 (0.0) | 0/6 (0.0) | 1/7 (14.3) | 1/16 (6.3) | 13/31 (41.9) | 96/176 (54.5) | 26/74 (35.1) | 138/331 (41.7) | |
| Mgen consults with the theme “Management of Mgen initial episode (not recurrence/treatment failure)” n/N (%) | 0/1 (0.0) | 0/8 (0.0) | 1/5 (20.0) | 0/7 (0.0) | 0/6 (0.0) | 4/7 (57.1) | 6/16 (37.5) | 2/31 (6.5) | 73/176 (41.5) | 32/74 (43.2) | 117/331 (35.3) | |
| Mgen consults with theme “Management of Mgen treatment failure” n/N (%) | 0/1 (0.0) | 0/8 (0.0) | 0/5 (0.0) | 4/7 (57.1) | 1/6 (16.7) | 3/7 (42.9) | 6/16 (37.5) | 8/31 (25.8) | 58/176 (33.0) | 37/74 (50.0) | 117/331 (35.3) | |
| Mgen clinical case consults in which patient is asymptomatic or symptoms are not specified n/N (%) | 0/1 (0.0) | 1/3 (33.0) | 0/3 (0.0) | 2/5 (40.0) | 0/2 (0.0) | 1/5 (20.0) | 2/10 (20.0) | 10/26 (38.5) | 71/165 (43.0) | 33/72 (45.8) | 120/292 (41.1)* |
*Only questions directly referencing a patient (N = 292) were included.
PP03.61 – Missed Syphilis Diagnosis by Rapid Treponemal Antibody Testing of Individuals with Treponema Pallidum PCR-Positive Genital Ulcers and Condylomata Lata, East London, South Africa
Mrs. Mildred Mandisa Mdingi1,2, Dr Ranjana M. S. Gigi1,3, Dr Andy Liu4, Dr Hyunsul Jung2, Professor Remco P. H. Peters1,2,5, Professor Jeffery D Klausner4
1Foundation For Professional Development, East London, South Africa.
2University of Pretoria, Pretoria, South Africa.
3University of Bern, Bern, Switzerland.
4University of Southern California, Los Angeles, California, United States of America.
5University of Cape Town, Cape Town, South Africa.
Background: Rapid point-of-care treponemal antibody tests are increasingly used to screen patients for syphilis. Laboratory-based treponemal antibody tests may also be used for screening or confirmation of syphilis. Performance of these tests in diagnosing patients with syphilitic lesions is unknown.
Methods: We recruited adults with syphilitic skin lesions in an ongoing study at five primary healthcare facilities in East London, South Africa. The Abbott DetemineTM Syphilis Treponema pallidum (TP) rapid test was performed on finger prick capillary blood specimens. We compared the performance of the rapid versus in-house laboratory-based test among patients with TP PCR positive lesions. We report the sensitivity and specificity of the rapid TP test with 95% confidence intervals (CI).
Results: From October 2023 to November 2024, we recruited 100 participants. Of these, 73 presented with genital ulcers and 27 with condylomata lata. The median age was 26 years; 38% were living with HIV. For those with TP PCR+ genital ulcers, the rapid test versus the laboratory test was 61% (23/38; 95% CI 43.4–76.0%) vs 97% (37/38; 95% CI 86.19%–99.93%) sensitive and 94% (33/35; 95% CI 80.8–99.3%) vs 77% (27/35; 95% CI 59.86%–89.58%) specific. While in those with TP PCR+ condylomata lata, the rapid test was 79% (15/19; 95% CI 54.4–94.0%) vs 95% (18/19; 95% CI 73.97%–99.87%) sensitive and 100% (8/8; 95% CI 63.1–100%) vs 63% (5/8; 95% CI 24.49%–91.48%) specific.
Conclusion: The rapid treponemal test showed lower sensitivity, particularly for genital ulcers, compared to lab-based testing. The Abbott Determine rapid test may be falsely negative in those with syphilitic lesions while laboratory-based testing may be positive in patients with negative TP PCR. Clinical interpretation of syphilis test results is needed.
PP03.62 – Sexually Transmitted Infections Burden and Pre-Exposure Prophylaxis Uptake Among Young Women During Pregnancy in a High HIV Burden Setting
Miss Nqobile Ngoma1,2,3, Mr Jacob Busang1,3, Dr Jana Jarolimova4, Dr Natsayi Chimbindi1,6, Ms Theresa Smit1, Ms Thandeka Danisa1, Mr Nkosinathi Ngcobo1, Ms Carina Herbs1, Ms Nonhlanhla Okeseola1, Prof Janet Seeley1,3,7, Mr Kobus Herbs1,5, Prof Andrew Copas3, Prof Willem Henekom1,3,6, Dr Lemakatso Lebina1,3, Prof Maryam Shahmanesh1,3,6
1Africa Health Research Institute, Sandton, South Africa.
2University of Pretoria, Pretoria, South Africa.
3University College London, London, United Kingdom.
4Massachusetts General Hospital, Boston, United States of America.
5DSI-SAMRC South African Population Research Infrastructure Network, Durban, South Africa.
6University of KwaZulu-Natal, Durban, South Africa.
7London School of Hygiene & Tropical Medicine, London, UK.
Background: Sexually transmitted infections (STIs) among women of reproductive age can lead to pregnancy complications, and pregnancy is a time of heightened HIV risk. We conducted a cluster-randomized trial in rural South Africa to explore the relationship between pregnancy and STI acquisition among adolescent girls and young women (AGYW) aged 15–30 years attending mobile sexual and reproductive health (SRH) services.
Methods: Between June 2022 and November 2024, AGYW were mobilized by peer navigators to attend youth-friendly mobile clinics offering STI testing (Xpert CT/NG), HIV testing (dry blood spot ELISA), and pregnancy testing. We compared characteristics of pregnant and non-pregnant women using chi-squared tests and assessed the association between pregnancy and STI acquisition using logistic regression.
Results: Of 2006 AGYW, 10% (n = 191) were pregnant. Among 1506 with STI results, 37% (n = 560) tested positive, with a significantly higher burden among pregnant women (46% vs 36%, P = 0.015) and those aged 15–24 years (52.4%–56.9%) compared to 25–30 years (28%). Most were treated (84%). HIV prevalence was slightly higher among pregnant women (19% vs 16%), but not statistically significant (P = 0.311). PrEP eligibility was higher among pregnant women (58% vs 48%, P = 0.013), though uptake was low across both groups (26.6% vs 25.7%). Pregnancy was associated with 1.52 times higher odds of STI (95% CI: 1.08–2.13); after adjusting for age, PrEP eligibility and previous history of pregnancy the association was attenuated 1.39 (95% CI: 0.91–2.12, P = 0.24).
Conclusions: There is a substantial burden of curable STIs among pregnant AGYW in this rural setting, highlighting the need for routine STI testing during pregnancy. Despite high STI prevalence and PrEP availability, uptake remains low, underscoring the need for targeted interventions, including long-acting PrEP, to improve prevention among this key population.
Keywords: Sexually transmitted infections, PrEP uptake, pregnancy, HIV prevention, rural South Africa, maternal health.
PP03.63 – Mycoplasma Genitalium Treatment Failures: Insights from a National Registry on Clinical Outcomes
Dr. Jessica Penney1, Dr. Priyanka Anand1, Dr. Laura A. S. Quilter1, Dr. Laura H. Bachmann1, Dr. Lindley A. Barbee1, Professor Ina Park1,2
1Centers For Disease Control and Prevention, Atlanta, United States.
2University of California San Francisco School of Medicine, San Francisco, United States.
Background: Increasing Mycoplasma genitalium (Mgen) resistance to azithromycin and fluoroquinolones has been paralleled by increasing clinical treatment failures. To better understand treatment failure management, the US Centers for Disease Control and Prevention (CDC) created a registry for reporting of suspected cases; we describe treatment regimens and clinical outcomes of these cases.
Methods: Cases were reported from December 1, 2022, to September 30, 2024; data included demographics, clinical presentations, treatment courses and clinical outcomes. We limited our analysis to symptomatic cases reported by a provider with complete data. We adjudicated final status of each case as either clinical treatment failure which we defined as continued symptoms despite CDC-recommended treatment (doxycycline followed by moxifloxacin) or clinical cure. Clinical cure was classified as: 1) clinical cure only [symptoms resolved, nucleic acid amplification test (NAAT) not performed]; 2) clinical cure without microbiologic cure (symptoms resolved, positive NAAT); 3) clinical cure with microbiologic cure (symptoms resolved, negative NAAT).
Results: Eighty-eight cases were reported, of which 40 met inclusion criteria. Over half were classified as clinical treatment failure (n = 24/40; 60%); the remainder were clinically cured with or without microbiologic cure (n = 16; 40%). Median age was 30 years (IQR 26–33), and the majority were male (n = 35; 87.5%). Approximately half of cases received 2–3 antibiotic courses (n = 21; 52.5%; range 1–8) (Table 1). Among 16 cases achieving clinical cure, the most common final treatment regimens were minocycline monotherapy (n = 5; 31.3%) or doxycycline followed by moxifloxacin (n = 4; 25%).
Conclusion: Mgen is increasingly challenging to treat; in this cohort, most cases experienced ongoing symptoms despite multiple courses of antibiotics. Minocycline monotherapy or doxycycline followed by moxifloxacin were the most common final treatment in cases with clinical cure. Research for novel or repurposed drugs to treat Mgen is needed.
| N = 40 | ||
|---|---|---|
| Clinical Presentation, n(%) | ||
| Urethritis | 34 (85) | |
| Cervicitis/vaginal discharge | 5 (12.5) | |
| Proctitis | 1 (2.5) | |
| Clinical Outcome, n(%) | ||
| Clinical treatment failure (symptoms did not resolve despite additional treatments) | 24 (60.0) | |
| Clinical cure | 16 (40) | |
| Clinical cure only (symptoms resolved, repeat NAAT not documented) | 4 (10.0) | |
| Clinical cure without microbiologic cure (symptoms resolved, repeat NAAT persistent positive) | 3 (7.5) | |
| Clinical cure with microbiologic cure (symptoms resolved, repeat NAAT negative) | 9 (22.5) | |
| Number of Treatment Courses Received, median (IQR) | 3 (2-4.3) | |
| Number of Treatment Courses Received, n(%) | ||
| 1 | 2 (5) | |
| 2 | 13 (32.5) | |
| 3 | 8 (20) | |
| 4 | 7 (17.5) | |
| 5 | 5 (12.5) | |
| 6 | 1 (2.5) | |
| ≥ 7 | 4 (10) | |
| Final Treatment Prescribed in Cases with Clinical Cure, n(%) | N = 16 | |
| Monotherapy Regimens | ||
| Azithromycin 1gm PO once | 1 (6.3) | |
| Minocycline 100mg PO BID for 14 days | 5 (31.3) | |
| Moxifloxacin 400 mg PO daily for 7–14 days | 2 (12.5) | |
| Omadacycline 300 mg daily for 10 days | 1 (6.3) | |
| Combination therapy | ||
| Doxycycline 100 mg PO BID for 7 days followed by moxifloxacin 400 mg PO daily for 7 days | 4 (25) | |
| Doxycycline 100 mg PO BID for 7 days followed by azithromycin 1 gm PO initial dose followed by 500 mg daily for 3 additional days | 1 (6.3) | |
| Minocycline 100 mg PO BID for 21 days followed by moxifloxacin 400 mg PO daily for 14 days | 1 (6.3) | |
| Minocycline 100 mg PO BID for 7 days followed by pristinamycin 1 g QID for 10 days | 1 (6.3) |
PP03.64 – Utilizing the Behavioral Risk Factor Surveillance System to Characterize the Adequacy of HIV Screening in a Rural New England State
Dr. Finlay Pilcher1,2, Bradley Tompkins2, Dr. Andrew Hale1,2, Dr. Devika Singh1,2
1University of Vermont Medical Center, Burlington, United States.
2University of Vermont Larner College of Medicine, Burlington, United States.
Background: Human immunodeficiency virus (HIV) screening is lower in rural areas of the US compared with urban settings. Correspondingly, people in rural areas are more likely to present with advanced HIV. It is not well-described which groups are most impacted by reduced rural HIV screening. This study examined data from the Centers for Disease Control and Prevention (CDC) Behavioral Risk Factor Surveillance System (BRFSS) to characterize HIV screening in a rural New England state and describe its variation with demographic factors.
Methods: Our study included participants who responded to the three HIV/AIDS questions in Vermont’s BRFSS from 2010 to 2019. Chi-square analysis was applied to determine if adequate HIV screening varied by sex, sexual orientation, gender identity, and race/ethnicity.
Results: The adequacy of HIV screening varied significantly with sex (adequate screening in 30.2% of female compared to 31.6% of male participants, P = 0.003), sexual orientation, and race/ethnicity (adequate screening in 30.3% of White participants compared to 41.4% of participants that were Black, Indigenous, and People of Color, P < 0.001) (Table 1). Adequacy of HIV screening did not vary significantly with gender identity.
Conclusion: Our results indicate that Vermonters are less likely to be adequately screened for HIV if they are female, heterosexual, and White. Though these groups are less represented in new HIV infections nationally, demographics of HIV transmission may differ substantially in rural areas.
It is also possible that the BRFSS is not an appropriate tool for evaluating HIV screening in rural areas due to its requirement of 20-30 min of spare time and, prior to 2014, a stable landline telephone. This methodology may introduce selection bias by underrepresenting respondents with unstable housing or inconsistent access to a telephone. Many rural areas also have challenges related to cellular reception that may further restrict telephone survey participation.
| Adequate HIV screening | Inadequate HIV screening | Chi-square analysis | ||
|---|---|---|---|---|
| n(%) | n(%) | χ2 (P-value) | ||
| Sex Assigned at Birth | ||||
| Male | 11,560 (68.4) | 5,338 (31.6) | 8.5 (0.003) | |
| Female | 15,679 (69.8) | 6,789 (30.2) | ||
| Sexual Orientation | ||||
| Heterosexual | 14,078 (67.9) | 6,643 (32.1) | 141.4 (<0.001) | |
| Homosexual | 207 (49.4) | 212 (50.6) | ||
| Bisexual | 291 (50.2) | 289 (49.8) | ||
| Other | 132 (66.7) | 66 (33.3) | ||
| Gender Identity | ||||
| Transgender Assigned Male at Birth | 21 (61.8) | 13 (38.2) | 1.8 (0.611) | |
| Transgender Assigned Female at Birth | 15 (68.2) | 7 (31.8) | ||
| Gender Nonconforming | 11 (55.0) | 9 (45.0) | ||
| Cisgender | 14,840 (67.2) | 7,268 (32.8) | ||
| Race/Ethnicity | ||||
| White, Non-Hispanic | 25,638 (69.7) | 11,128 (30.3) | 112.3 (<0.001) | |
| Black, Indigenous, or Person of Color | 1,191 (58.6) | 842 (41.4) |
PP03.65 – Defining the Impact of Non-Ulcerative Sexually-Transmitted Infections on the Genital Immune Milieu of Female Sex Workers in Nairobi, Kenya: A Prospective Study
Sanja Huibner1, Mr. James Pollock1, Suji Udayakumar1, Rhoda Kabuti2, Mary Kung’u2, Hellen Babu2, Erastus Irungu2, Polly Ngurukiri2, Peter Muthoga2, Wendy Adhiambo2, Helen A Weiss3, Janet Seeley3, Tanya Abramsky3, Joshua Kimani2, Tara S Beattie3, Rupert Kaul1
1University of Toronto, Toronto, Canada.
2Partners for Health and Development in Africa, Nairobi, Kenya.
3London School of Hygiene & Tropical Medicine, London, United Kingdom.
Background: Female sex workers (FSWs) in sub-Saharan Africa are a key population at risk of HIV acquisition. This risk is increased by inflammation and epithelial barrier disruption in the female genital tract, both of which may be caused by STIs. Here we investigate the effect of three STIs on genital biomarkers of inflammation and epithelial barrier disruption among HIV-uninfected Kenyan FSWs.
Methods: This study was nested within the Maisha Fiti study, a longitudinal mixed-method study that investigated the impact of violence and mental health problems on genital immunology among FSWs in Nairobi, Kenya. Behavioural and socio-demographic data were collected from 746 HIV-uninfected participants at up to three study visits. Participants were tested for the non-ulcerative STIs Chlamydia trichomonas, CT; Neisseria gonorrhoeae, NG; and Trichomonas vaginalis, TV; genital secretions were collected by menstrual cup to quantify inflammatory protein markers. We prospectively evaluated the effect of these STIs on (1) genital inflammation, defined by a clinically validated inflammation score of inflammatory protein markers, and (2) epithelial barrier disruption (soluble E-cadherin; sE-cad), in a mixed effects model.
Results: The baseline prevalence of CT, GC and TV infection was 64/726 (8.6%), 20/746 (2.7%) and 20/746 (2.7%) participants, respectively. After controlling for potential confounders, CT infection (P = 0.034) was associated with genital inflammation, while GC infection (P = 0.072) and TV infection (P = 0.647) were not. None of the tested STIs were associated with differences in epithelial damage (sE-cad levels).
Conclusion: In this unique cohort of Kenyan female sex workers, CT infection was the most common STI detected and most strongly associated with inflammation among the STIs investigated in this study; no non-ulcerative STI was associated with epithelial damage. These findings highlight the need to reduce the prevalence of STI co-infections as a strategy for tackling the HIV pandemic.
PP03.66 – Accessing the Impact of Same-Day Antiretroviral Therapy (ART) Initiation on Early Retention Among Men Who Have Sex with Men in Sekondi-Takoradi, Ghana
Mrs. Hellen Mawuli Quarshie1, Mr Samuel Elliot Owusu1, Dr Edward Azalemah2, Mr George Laryeh2
1MLPF, Kumasi, Ghana.
2GHS, Sekondi-Takoradi, Ghana.
Introduction: Retention in HIV care is essential for optimal outcomes, particularly for men who have sex with men (MSM) living with HIV. In Ghana, stigma, discrimination, and healthcare barriers often hinder ART uptake, making retention critical for effective treatment. Although national guidelines recommend same-day ART initiation for newly diagnosed individuals, its impact on early retention in public sector settings is underexplored. This study examines how same-day ART initiation, compared to delayed initiation, affects early retention (within 3-months) among MSM in Sekondi-Takoradi, Ghana.
Methods: A retrospective cohort study was conducted among HIV-positive MSM aged 18+ who initiated ART under the Treat-all policy at five clinics in Sekondi-Takoradi between January and December 2023. Participants were grouped by ART initiation timing: same-day (0 days post-diagnosis) and delayed (≥1–10 days post-diagnosis). The primary outcome was retention, defined as failure to return for care within 3-months of ART initiation. We used log-binomial regression and targeted maximum likelihood estimation (TMLE) to assess the impact of same-day ART on early retention, calculating adjusted relative risks (aRR) and 95% confidence intervals (CIs).
Results: Among 690 MSM, 448 (64.9%) initiated ART on the same day, and 242 (35.1%) had delayed initiation. Of the same-day initiators, 45% failed to return for the first follow-up visit, compared to 62% of delayed initiators. After adjusting for age, testing year, and healthcare facility, same-day initiators had a higher risk of non-return (aRR = 1.48, 95% CI: 1.16–1.89). TMLE analysis showed that after one year, 29.7% of same-day initiators would experience higher likelihood of poor retention compared to 22.4% for delayed initiators (difference: 7.3%, 95% CI: 1.5%–13.2%).
Conclusion: Same-day ART initiation was associated with lower early retention rates compared to delayed initiation among MSM in Sekondi-Takoradi. These findings underscore the need for tailored interventions to improve long-term retention, particularly for high-risk groups like MSM.
PP03.67 – Herpes Simplex Virus 1 and Late Latent Syphilis as Underlying Causes of Recurrent Erythema Multiforme in a 34-Year-Old Male: A Case Report
Dr. Jessica Grace Ran˜ola1, Dr. Camille Angeles1, Dr. Katrina Canlas-Estrella1, Dr. Juanita Carmela Buenviaje1, Dr. Lian Jamisola1, Dr. Gilbert Yang1
1UERM Medical Center, Quezon City, Philippines.
Background: Erythema multiforme (EM) is a rare benign mucocutaneous condition characterized by targetoid lesions usually triggered by infections, commonly herpes simplex virus (HSV). In some case reports, syphilis can also lead to EM. This case reports an atypical manifestation of recurrent EM triggered by two concomitant infections (HSV-1 and syphilis).
Description/Case Report: A 34-year-old male presented with 15-year history of recurrent blisters and erosions on the extremities and mucosae of 1-week duration, occurring once to twice yearly (Fig. 1). First episode was allegedly diagnosed as Stevens-Johnson Syndrome secondary to HSV, post-biopsy. His recent flare involves a 4-day history of erythematous patches and papules progressing to generalized violaceous plaques, and flaccid bullae with erosions associated with mucosal erosions, periorbital edema and purulent eye discharge. Nikolsky and Asboe-Hansen signs were positive. Biopsy revealed intraepidermal blister with re-epithelialization, and negative direct immunofluorescence. Given the recurrent lesions, negative drug history, supported by histopathology, EM was the impression. A multidisciplinary approach, and supportive treatment with systemic and topical corticosteroids, and topical antibiotics provided complete resolution. Further work-up revealed positive FTA-Abs, VDRL and HSV1 IgG. He completed 3 weekly doses of penicillin 2.4Mü IM for late-latent syphilis, and 1 month acyclovir 400 mg BID as HSV prophylaxis. No recurrences in the next 18 months concludes this interesting case of recurrent EM potentially secondary to HSV1 and late-latent syphilis.
Conclusion: EM is a rare dermatologic recurrent condition warranting an extensive investigation of the underlying causes. Addressing the precipitating causes is crucial for resolution and prevention of recurrences.
PP03.68 – Usability Evaluation of the Simpli-Collect Urine Collection Kit Across Different Demographic Characteristics
Dr. Mark Sasaki1, Dr. Danijela Lucic1, Dr. Charles Sailey1
1Abbott, Des Plaines, United States.
Background: Sexually transmitted infection (STI) prevalence is increasing with millions of new cases of chlamydia, gonorrhea, and trichomoniasis reported annually. This presents a significant public health challenge for which STI home collection kits offer a discreet and convenient testing option to encourage more individuals to get tested, leading to earlier detection and treatment. This study evaluates the usability of the simpli-COLLECT Swab Collection IUO Kit (sC kit) in a simulated home environment for STI testing using vaginal swab samples.
Methods: The sC kit was assessed through simulated use and subjective feedback during individual, in-person sessions from 74 participants (30 females, 44 males). Usability data was analyzed across age, race, and education.
Results: Across all participants, the mean score for ease of use of the sC kit was 4.81 out of 5 (SD = 0.46); the mean score was 4.84 for 18-64 year olds and 4.50 in those over 65 years old. Mean score ranged from 4.00 to 5.00 across race and 4.67 to 5.00 across education. For ease of use of instructional material the mean score was 4.66 out of 5 (SD = 0.64) for all participants. The mean score was 4.68 for 18-64 year olds and 4.33 for those over 65 years old. Mean score ranged from 4.00 to 5.00 across race and 4.25 to 5.00 across education.
Conclusion: This study provides insights into the usability of the sC kit, with high scores for ease of use of the sC kit and instructional materials indicating that STI home collection kits, such as those for urine samples investigated for this study, can play a role in STI prevention efforts.
PP03.69 – Usability Evaluation of the Simpli-Collect Vaginal Swab Collection Kit Across Different Demographic Characteristics
Dr. Mark Sasaki1, Dr. Danijela Lucic1, Dr. Charles Sailey1
1Abbott, Des Plaines, United States.
Background: Sexually transmitted infection (STI) prevalence is increasing with millions of new cases of chlamydia, gonorrhea, and trichomoniasis reported annually. This presents a significant public health challenge for which STI home collection kits offer a discreet and convenient testing option to encourage more individuals to get tested, leading to earlier detection and treatment. This study evaluates the usability of the simpli-COLLECT Swab Collection IUO Kit (sC kit) in a simulated home environment for STI testing using vaginal swab samples.
Methods: The sC kit was assessed through simulated use and subjective feedback during individual, in-person sessions from 48 female participants. Usability data was analyzed across age, race, and education.
Results: Across all participants, the mean score for ease of use of the sC kit was 4.82 out of 5 (SD = 0.39); the mean score was 4.83 for 18-64 year olds and 4.50 in those over 65 years old. Mean score ranged from 4.50 to 5.00 across race and 4.60 to 5.00 across education. For ease of use of instructional material the mean score was 4.61 out of 5 (SD = 0.67) for all participants. The mean score was 4.63 for 18-64 year olds and 5.00 for those over 65 years old. Mean score ranged from 4.50 to 5.00 across race and 4.33 to 5.00 across education.
Conclusion: This study provides insights into the usability of the sC kit, with high scores for ease of use of the sC kit and instructional materials indicating that STI home collection kits, such as those for vaginal samples investigated for this study, can play a role in STI prevention efforts.
PP03.70 – Contact Tracing Prevalence Among Men Who Have Sex with Men Diagnosed with an STI: Behavioural Surveillance in New Zealand
Assoc. Prof. Peter Saxton1, Dr Adrian Ludlam1, Dr Janine Paynter1, Brooke Hollingshead2, Dr Susan McAllister3, Koson Tony Sriamporn1, Kevin Haunui2, Mark Fisher4, Associate Professor Stephen Ritchie1, Professor Patricia Priest3
1University of Auckland, Auckland, New Zealand.
2Burnett Foundation Aotearoa, Auckland, New Zealand.
3University of Otago, Dunedin, New Zealand.
4Body Positive Inc, Auckland, New Zealand.
Background: Contact tracing is crucial to sexually transmitted infection (STI) control. Contact tracing is routinely recorded by publicly-funded sexual health clinics (SHCs). However, an increasing proportion of STIs are diagnosed by general practitioners (GP), point-of-care testing or self-screening, and it is unknown how much contact tracing is initiated following positive disease tests in these settings. We estimate the prevalence of contact tracing among a community sample of gay, bisexual and other men who have sex with men (GBM) in New Zealand (NZ).
Methods: We examined data from a cross-sectional HIV behavioural surveillance programme among GBM (SPOTS 2022). Participants self-reporting an STI <12 months were asked if contact tracing had occurred and by whom. We report the prevalence of contact tracing overall and by test setting, then examined whether the prevalence of any contact tracing was associated with select characteristics using odds ratios with 95% confidence intervals (OR, 95% CI).
Results: Among n = 3347 participants, 61.6% reported a sexual health check and 16.9% one or more STI diagnoses <12 months. Of these, 44.6% had their last check at a GP, 46.4% at a SHC, 9.1% somewhere else. Among the n = 548 providing information, 89.2% reported any contact tracing <12 months, including 12.6% by a SHC, 6.8% by a GP, 75% by themselves, 3.1% didn’t know and 8.6% stated none. Any contact tracing prevalence was significantly lower among Asian participants (OR 0.4, 0.2-0.7), participants diagnosed with warts (OR 0.1, 0.1–0.3) or non-specific urethritis (OR 0.4, 0.2–0.97), and greater among participants taking PrEP (OR 2.3, 1.3–4.1) or diagnosed with chlamydia (OR 1.7, 1.0-2.9). Contact tracing was not associated with age, region, sexual partnering, setting last tested, or symptoms.
Conclusion: STI contact tracing was common in this NZ community sample and was mostly initiated by GBM themselves. Reassuringly, contact tracing did not vary by test setting.
PP03.71 – Schistosomiasis and HIV Co-Infection: An Intersectional Public Health Concern for Women in Rural Tanzania
Mr. Anthony Sebastian Charles1, Mr Ally Baghayo2, Ms Aziza Ndwata2
1Management And Development for Health-Temeke specialized laboratory, Dar Es Salaam, Tanzania.
2Kilimanjaro Christian Medical University College, Kilimanjaro, Tanzania.
Background: Schistosomiasis infection has been associated with increased risk of HIV infection in African women. The co-infection between schistosomiasis and HIV/AIDS infection can be mediated through some social behavioral factors. Cases show that over 200 million people are infected worldwide with a disproportionate burden in Africa, about 90% cases are found alongside co-infection with HIV/AIDS. The aim of the study was to assess the prevalence and associated risk factors of schistosomiasis among HIV/AIDS women in lower Moshi.
Methodology: This study was a cross-sectional hospital based analytical study, which was conducted in lower Moshi (Pasua, TPC, Arusha chini, Mabogini) from April to June 2021.The study population was HIV/AIDS infected women aged (15–49) years. A minimum of 260 women was enrolled in this study with a simple random sampling technique. A questionnaire was a tool for data collection. Data was entered and analyzed using SPSS version 20. Microscopic examination was performed to test for schistosome infection where urine sample was used for detection of Schistosoma haematobium by membrane filtration method.
Results: A total of 260 participants were enrolled. The prevalence of schistosomiasis among HIV/AIDS positive women is 5% (13/260). There was an association between the outcome (schistosomiasis) and the previous infection with a P-value <0.01.
Conclusion: There is low prevalence of Schistosomiasis among HIV/AIDS women is 5%Only previous infection were associated with schistosomiasis. So strategic plans such as provision of Praziquantel drugs in the CTC and health seminars should be provided to residents in lower Moshi Kilimanjaro, also an immediate interventional programs should be established in rural Tanzania to cut the Neglected tropical diseases emergences.
PP03.72 – Evolving Epidemic of Sexually Transmitted Infections Among Men Who Have Sex with Men in Lagos, Nigeria: Identifying Risk Factors for Prevention
Mrs. Elizabeth Shoyemi, Dr Oluwatayo Oluwadamilola, Mr Kanayochukwu Okeke, Dooshima Uganden
1Centre For Population Health Initiatives, Lagos, Nigeria.
Background: This study aimed to enhance understanding of the evolving epidemic of sexually transmitted infections (STIs) among men who have sex with men (MSM) in Lagos, Nigeria. It focused on identifying risk factors contributing to this epidemic to inform future prevention strategies.
Methods: A cross-sectional design was employed, utilizing snowball sampling to select 202 MSM participants in Lagos. Respondents completed a pre-tested semi-structured questionnaire to gather data on socio-demographic characteristics, sexual behaviors, and experiences with STIs. Descriptive statistics and the Chi-square test were used for data analysis.
Results: The mean age of respondents was 25.4 ± 6.2 years, with 87.4% single and 89.7% having tertiary education. The average age at sexual initiation was 19.6 ± 5.6 years, with initial partners being boyfriends (10.2%), girlfriends (56.4%), or sex workers (3.3%). Most (86.4%) reported having at least two male sexual partners, while 12.9% also had female partners.
Concerning condom use, 47.8% of respondents expressed dislike for condoms, and only 23.7% used them during their last sexual encounter with male partners. 34.8% reported doing nothing to protect themselves from STIs. Most of the respondents (87.6%) did not perceive themselves at risk for STIs, including HIV, and 45.9% believed they were currently STI-free. Some (23.7%) had been counseled by a health worker to get tested for STIs.
In the last 12 months, 12.6% of the respondents had experienced pus-like discharge, and 15.4% reported itching in the penile area.
Conclusion: Many respondents did not perceive themselves as being susceptible to sexually transmitted infections, including HIV, despite engaging in risky sexual behavior. It is crucial to implement behavioral change intervention programs to help respondents accurately assess their vulnerability and self-appraisal of HIV-related risk.
PP03.73 – Using Deep Learning Systems for Diagnosing Common Skin Lesions in Sexual Health
Dr. Nyi Nyi Soe1,2, Dr. Phyu Mon Latt1,2, Dr. David Lee1, Dr. Zhen Yu2,3, Dr. Martina Schmidt1, Dr. Melanie Bissessor1, Dr. Ei T Aung1,2, Dr. Zongyuan Ge3,4, Dr. Jason J Ong1,2, Dr. Christopher K. Fairley1,2, Dr. Lei Zhang1,2,5
1Melbourne Sexual Health Centre, Melbourne, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Augmented Intelligence and Multimodal analytics (AIM) for Health lab, Faculty of Information Technology, Monash University, Melbourne, Australia.
4Data Science And AI (DASI), Faculty of Information Technology, Monash University, Melbourne, Australia.
5Clinical Medical Research Centre, Children’s Hospital of Nanjing Medical University, Nanjing, China.
Background: Early identification and treatment of sexually transmitted infections (STIs) prevent complications and improve STI control. A deep learning system (DLS) that automates the diagnosis of skin lesions may facilitate access to health care but has not been evaluated across a comprehensive range of sexual health-related skin conditions.
Methods: We developed a DLS using 15,891 clinical images from public repositories and the Melbourne Sexual Health Centre (MSHC) to classify 33 anogenital dermatoses. We prospectively collected 336 images to evaluate the DLS’s accuracy and compared it to the clinician’s diagnosis. We also evaluated whether DLS recommendations aligned with clinical urgency for seeking care based on the diagnosis.
Results: On the hold-out test dataset, the DLS achieved an accuracy of 59.2% (SD 0.7%) (top-1) and the correct diagnosis was included in the top five diagnoses (top-5) with an accuracy of 82.1% (SD 13.3%). On the 8-month prospective dataset at MSHC, the DLS achieved a top-1 accuracy of 52.1%, top-3 of 73.8%, and top-5 of 89.9%. The highest accuracy was achieved for tinea curitis, discharge-associated gonorrhoea or chlamydia, molluscum contagiosum, and mpox. The DLS recommendation based on top-5 diagnoses for seeking care maintained 100% sensitivity for urgent cases (e.g. syphilis) but had a lower positive predictive value (59.5%). The recommendation based on top-1 diagnosis provided more balanced sensitivity (85.0%) and PPV (80.5%).
Conclusions: The DLS demonstrated satisfactory statistical accuracy and could enhance the sexual health intervention for early diagnosis and treatment. When the actual diagnosis was included in the top 5 diagnoses predicted by DLS, the recommendation for the urgency of seeking health care was highly sensitive but not specific. Future work should evaluate the DLS’s performance across expanded populations and skin conditions from multiple clinics in different countries and determine how such tools could be used for the public good.
PP03.74 – Impact of Treatment on High-Risk HPV Detection and HPV16 Viral Quantity in Anal and Vulvar High-Grade Squamous Intraepithelial Lesions
Dr. Helen Stankiewicz Karita1, Amalia Magaret2, Jessica Moreno2, Matthew Seymour2, Dana Varon2, Stacy Selke2, Meei-Li Huang2,3, Margaret Madeleine2,3, Anna Wald2,3
1University of California San Francisco, San Francisco, United States.
2University of Washington, Seattle, United States.
3Fred Hutchinson Cancer Center, Seattle, United States.
Background: Anal and vulvar high-grade squamous intraepithelial lesions (HSIL) are premalignant epithelial changes driven by persistent high-risk human papillomavirus (hr-HPV), with recurrence rates of up to 50% after treatment. The dynamics of HPV persistence after treatment for anal and vulvar HSIL are not well understood. We aimed to evaluate hr-HPV detection rates and HPV16 quantity following treatment for anal and vulvar HSIL.
Methods: We enrolled persons with histologically-confirmed anal or vulvar HSIL who were scheduled for treatment. Following collection of anal or vulvar swabs by both clinicians and participants at enrollment, participants self-collected up to 4 weekly swabs pre-treatment and 8 weekly swabs post-treatment. Swabs were tested for quantitative HPV16 DNA, with additional qualitative hr-HPV PCR performed if HPV16 was undetected. HPV detection rates were calculated as the proportion of HPV-positive swabs pre-versus post-treatment, and changes in HPV16 load were assessed using the Wilcoxon signed-rank test.
Results: Overall, 164 swabs (141 anal, 23 vulvar) were collected from 16 participants. Perfect concordance was observed between clinician-collected (n = 21) and participant-collected (n = 21) swabs (Kappa = 1) (Fig. 1). Among the 10 participants who completed the study, hr-HPV was detected in 119 of 132 samples (90.2%). On average, the hr-HPV detection rate decreased after HSIL treatment, from 100% (45 of 45 samples) to 88% (74 of 87 samples) (P = 0.03). Among the 6 participants with quantifiable HPV16, the average pre-treatment viral load was 235909.8 copies, compared to the average post-treatment viral load of 90334.1 copies (P = 0.46).
Conclusions: Although hr-HPV detection rates were lower after HSIL treatment, treatment did not eliminate hr-HPV or significantly reduce HPV16 viral load in swabs. This hr-HPV persistence likely contributes to the high recurrence rates of anal and vulvar HSIL after treatment. Our findings highlight the potential of using HPV persistence for evaluation of novel antivirals and therapeutic vaccines in anal and vulvar HPV disease.
PP03.75 – Asymptomatic and Symptomatic Bacterial Vaginosis: Associations with STI Risk
Dr. Susan Tuddenham1, Associate Professor Xin He2, Professor Jacques Ravel2, Professor Rebecca Brotman3
1Johns Hopkins, Baltimore, United States.
2University of Maryland, College Park, College Park, United States.
3University of Maryland, Baltimore, Baltimore, United States.
Background: Bacterial vaginosis (BV), characterized by low vaginal Lactobacillus spp. relative abundance, an overgrowth of strict and facultative bacterial anaerobes, and elevated vaginal pH, has been associated with increased susceptibility to sexually transmitted infections (STIs), including HIV. Most BV cases are asymptomatic (aBV); however, screening and treatment for aBV are not currently recommended. To evaluate the risks associated with aBV, we compared incident STI data among individuals with aBV, sBV, and no BV in a large, longitudinal cohort.
Methods: We utilized data from the Longitudinal Study of Vaginal Flora, conducted between 1999–2002 in Birmingham, Alabama. Participants were followed quarterly for one year. Clinicians identified BV using Amsel’s criteria and diagnosed sBV if participants reported vaginal symptoms or aBV if no symptoms were reported. sBV was treated with metronidazole (500 mg or 2 g regimens). STI testing at each visit included ligase chain reaction for chlamydia, culture for gonorrhea, and InPouch culture or microscopy for trichomonas. Logistic mixed-effects models estimated the associations between antecedent aBV, sBV, and no Amsel-BV exposures and STI incidence over a 3-month period to the next visit.
Results: Data included 2,864 participants with 524 sBV observations, 2,771 aBV, and 5,819 without Amsel-BV; resulting 98 gonorrhea, 355 chlamydia and 300 trichomonas incident cases. In adjusted analyses, aBV was associated with increased incidence of STIs (gonorrhea, chlamydia or trichomonas composite; aOR:1.42, 95% CI: 1.15–1.74) compared to no Amsel-BV. Evaluating individual STIs, aBV was specifically associated with trichomonas (aOR:1.69, 95% CI: 1.27–2.24). In contrast, sBV was associated only with chlamydia (aOR:1.71, 95% CI: 1.08–2.71). See Table 1.
Conclusion: aBV was significantly associated with an increased risk of incident STIs, particularly trichomonas. sBV estimates might have been diminished due to BV treatment. As new, more efficacious treatments for BV are developed, additional research on preventing aBV to reduce STI risk is warranted.
| Incident STI | BV at the prior visit | Unadjusted | AdjustedA | |||
|---|---|---|---|---|---|---|
| OR | 95% CI | aOR | 95% CI | |||
| CT, TV or GC (Any)B | Symptomatic BV | 1.37 | (0.93, 2.00) | 1.35 | (0.92, 2.00) | |
| Asymptomatic BV | 1.72 | (1.41, 2.09) | 1.42 | (1.15, 1.74) | ||
| No BV (Ref.) | – | – | – | – | ||
| CT onlyB | Symptomatic BV | 1.63 | (1.08, 2.47) | 1.71 | (1.08, 2.71) | |
| Asymptomatic BV | 1.27 | (1.01, 1.61) | 1.15 | (0.87, 1.50) | ||
| No BV (Ref.) | – | – | – | – | ||
| TV onlyC | Symptomatic BV | 0.96 | (0.52, 1.79) | 0.92 | (0.50, 1.70) | |
| Asymptomatic BV | 2.28 | (1.73, 3.00) | 1.69 | (1.27, 2.24) | ||
| No BV (Ref.) | – | – | – | – | ||
| GC onlyB,D | Symptomatic BV | 0.73 | (0.29, 1.87) | 0.45 | (0.14, 1.46) | |
| Asymptomatic BV | 1.36 | (0.93, 1.98) | 1.22 | (0.82, 1.83) | ||
| No BV (Ref.) | – | – | – | – | ||
Statistically significant associations are bolded.
PP03.76 – Asymptomatic Versus Symptomatic Bacterial Vaginosis: Comparing the Vaginal Microbiota and Lactic Acid Concentrations
Associate Professor Xin He2, Assistant Professor Golsa Yazdy1, Professor Carl Yeoman4, Professor Khalil Ghanem1, Associate Professor Daniel Erchick5, Research Assistant Alexis Taylor1, Research Assistant Karen Griffin1, Assistant Professor Johanna Holm3, Professor Jacques Ravel3, Professor Rebecca Brotman3, Dr. Susan Tuddenham1
1Johns Hopkins, Baltimore, United States.
2University of Maryland, College Park, College Park, United States.
3University of Maryland, Baltimore, Baltimore, United States.
4Montana State University, Bozeman, United States.
5Johns Hopkins School of Public Health, Baltimore, United States.
Background: Bacterial vaginosis (BV), characterized by scarce vaginal lactobacilli, an overgrowth of strict and facultative bacterial anaerobes, and elevated pH, results in vaginal symptoms in half of individuals. Irrespective of symptoms, BV has been associated with increased risk of sexually transmitted infections (STIs) and HIV. However, treatment for asymptomatic BV (aBV) is not currently recommended; whether aBV and symptomatic BV (sBV) confer the same STI/HIV risk is not well studied. We compared vaginal microbiota and lactic acid isomer concentrations in aBV and sBV to understand whether biological factors distinguish these conditions and ultimately their potential contributions to STI/HIV acquisition.
Methods: This secondary analysis utilized data from the Longitudinal Study of Vaginal Flora. Clinicians classified participants with Amsel-BV as sBV if they reported vaginal symptoms and aBV if no symptoms were reported. Cervicovaginal lavage fluid underwent 16S rRNA gene amplicon sequencing, broad-range qPCR, and lactic acid isomer quantitative assays. Wilcoxan rank sum and Chi-squared tests compared Amsel’s criteria, Nugent scores, bacterial absolute abundance, community state types (CSTs) and D- and L-lactic acid concentrations, and elastic net modeling assessed differences between aBV and sBV.
Results: Data were available from N = 70 with sBV and N = 270 with aBV. Clinician-assessed homogeneous discharge was more frequent in sBV (85.7%) than aBV (70.6%), P = 0.01. All samples were classified as Lactobacillus iners-dominated (CST III) or low-Lactobacillus CST IV (subtypes IV-A, IV-B, IV-C), with no significant difference between aBV and sBV (Table 1). No significant differences were found for other Amsel’s criteria, Nugent scores, or relative abundance of taxa. Similarly low D- and L-lactic acid concentrations were observed in sBV and aBV.
Conclusion: No significant differences were observed in vaginal microbiota or lactic acid between sBV and aBV. Additional research is needed to understand whether other biological factors differentiate these conditions and assess their respective associations with STI/HIV acquisition.
| sBV (n = 70) | aBV (n = 270) | P-value | |||
|---|---|---|---|---|---|
| CST* | III | 11 (15.7%) | 48 (17.8%) | 0.47 | |
| IV-A | 32 (45.7%) | 102 (37.8%) | |||
| IV-B | 26 (37.1%) | 118 (43.7%) | |||
| IV-C | 1 (1.4%) | 2 (0.7%) | |||
*Fisher's exact test.
PP03.77 – Factors Associated with Ocular, Otic and Neurosyphilis Cases Diagnosed in Vancouver Coastal Health, British Columbia (2018–2024)
Dr. Rohit Vijh1, Mr. Nick Pang3, Ms. Harmeet Gill3, Dr. Rowan Laird3, Ms. Doris Chang1, Mr Brendan Bakos1, Ms. Laura Zerr1, Dr. Althea Hayden1,3
1Vancouver Coastal Health, Vancouver, Canada.
2BC Centre for Disease Control, Vancouver, Canada.
3University of British Columbia, Vancouver, Canada.
Background: Neurosyphilis is clinically complex to diagnose and resource intensive to treat. As syphilis outbreaks continue to affect marginalized communities with a high burden of neurological and psychiatric comorbidities, there is an urgent need for low barrier clinical tools to aid in diagnostic decision making.
Methods: A cohort was constructed of all syphilis cases who underwent a lumbar puncture (LP) with VDRL testing from January 1, 2018, to July 31, 2024. A chart review was undertaken to describe their medical history, presenting symptoms, and laboratory findings. Individuals were categorized as cases if they were clinically assessed to have either have confirmed or probable ocular, otic or neurosyphilis, and controls if not. Univariable logistic regressions were used to calculate odds ratios (OR).
Results: Our cohort comprised of 198 individuals (3.6% of total syphilis cases), with 48% (n = 96) cases and 52% (n = 102) controls; the cohort identified largely as male (72%), gay, bisexual, or other men who have sex with men (gbMSM) (42%) and were housing secure (88%). Cases were significantly more likely to experience blurry/reduced vision (OR: 3.25, 95% CI: 1.54–6.83), photophobia (OR: 6.47, 95% CI: 1.40–30.00), eye pain (OR: 13.07, 95% CI: 1.66–103.22), red eye (OR: 5.17, 95% CI: 1.09–24.58), and neck stiffness (OR: 13.07, 95% CI: 1.66–103.22). Controls were more likely to experience cognitive impairment (OR: 0.34, 95% CI: 0.15–0.77) and have an anxiety (OR: 0.37, 95% CI: 0.15–0.92), primary psychotic (OR: 0.21, 95% CI: 0.08–0.59) or opioid use (OR: 0.42, 95% CI: 0.19–0.91) disorder. Controls were more likely to have a previously treated syphilis infection (OR: 0.20, 95 %CI: 0.11–0.37). Cases were more likely to have an RPR titer greater than 1:16 at time of diagnosis (OR: 3.07, 95% CI: 1.70–5.54).
Conclusions: Our findings highlight factors that can be used by clinicians in their decision making about which patients require additional investigations or empiric treatment for neurosyphilis. Additional research is needed to develop and validate non-invasive clinical risk predication tools for neurosyphilis based on clinical and lab findings.
PP03.78 – Prevalence of Mycoplasma Genitalium and Antibiotic Resistance-Associated Mutations in Sti-Clinic Patients at Three Healthcare Regions in Sweden
Ms. Mimmi Wänn1,2, Karin Sanner1,2, Sofia Fall3, Elisabet Eriksson4, Alfred Åhman1,2, Daniel Schröder3, Daniel Golparian3, Karolina Gullsby4, Magnus Unemo3, Björn Herrmann1,2
1Uppsala University, Uppsala, Sweden.
2Uppsala University Hospital, Uppsala, Sweden.
3Örebro University Hospital, Örebro, Sweden.
4Region Gävleborg, Gävle, Sweden.
Background: This study aimed to demonstrate the current prevalence of Mycoplasma genitalium (MG) and commonly used antibiotics (macrolides and quinolones) in three healthcare regions in Sweden. MG191-MG309 genotyping data also to be included. At deadline for abstract submission only preliminary data for the Uppsala region is presented (data from Region Gävle and Örebro to be included).
Methods: Patients visiting the STI clinic at Uppsala University Hospital (inclusion 09-2022 and ongoing) were tested if symptomatic or showing signs of infection and were subsequently included in the study if MG-positive. Samples included vaginal swabs, first-void urine and/or rectal swabs, screened for MG in Abbott Alinity STI-m. Positive samples were analyzed for macrolide resistance-associated mutations (MRMs) using ResistancePlus MG (SpeedX). Additionally, droplet digital PCR (MgPa-gene) was applied for bacterial quantification. Patients were treated according to Swedish guidelines.
Results: Among the MG-positive cases (n = 197), 45% were women and 55% were men. Of these, 44% (n = 86) tested positive for MRMs while 42% (n = 83) were macrolide sensitive and 14% (n = 28) were excluded from MRM testing due to low bacterial load. MG concentrations were lower in urine samples compared to vaginal and rectal specimens (index mean: 36, 213 and 532 copies/µL, respectively). The index median concentration in urine was significantly lower than for vaginal and rectal samples (0.6, 60 and 796 copies/µL, respectively), although vaginal swabs exhibited a broader range. Extended data on quinolone resistance and genotyping will be shown at the STI & HIV 2025 World Congress.
Conclusion: Prevalence data indicate an increase in MRMs compared to previous studies in Sweden, although this study focuses on a more targeted population suspected of MG infection. The findings are valuable for enhancing the knowledge base and improving the treatment of MG infections.
PP03.79 – Limited Impact of a Direct-To-Consumer Offer for Chlamydia and Gonorrhea Screening to Patients in a Healthcare System
Dr. Harold Wiesenfeld1, Dr. Glenn Updike, Jennifer Chaney, Loren Sutton
1University of Pittsburgh, Pittsburgh, United States.
Background: Chlamydia and gonorrhea screening is recommended for all sexually active women 24 years of age and younger in the U.S., yet many women are not screened. Innovative approaches to facilitate screening are needed. We created a novel program offering chlamydia and gonorrhea screening to women under care by providers in Western Pennsylvania. Screening was no cost to patients and did not require an office visit with a provider.
Methods: We identified women 18–24 years old who had received care from a provider in our OBGYN department 6–24 months prior to January 2024. We then selected those who did not have an order for a chlamydia test in the electronic medical record in the prior 365 days. A secured message was sent electronically to each of these patients via their health portal. The message described the importance of chlamydia and gonorrhea screening and offered urine-based screening without a medical evaluation. Patients interested in screening replied affirmatively to the message and were contacted by a staff member. Patients desiring screening were then ordered a chlamydia and gonorrhea test on a urine sample at the patient’s preferred laboratory.
Results: An offer for free chlamydia and gonorrhea screening was sent to 11,050 patients. In the 6 weeks following the offer, 109 (1%) responded with an interest in screening, and 40 (0.4%) ultimately requested an order for screening. Only 14 patients pursued screening, all testing negative for infection.
Conclusion: Acceptance and uptake of a direct-to-consumer offer for chlamydia and gonorrhea screening was surprisingly low. Eliminating an office visit and the cost of screening had little impact on screening in this cohort of women. Other novel approaches to improve the rate of chlamydia and gonorrhea screening in women are needed.
PP03.80 – Closing the Window Between Collection and Culture: Does Direct Plating of Swabs in the Clinic Improve Yield of Neisseria Gonorrhoeae?
Dr. Arthur Wong1,2, A/Prof Tanya Applegate2, Mrs. Alison Mahony1, Mr. George Xu1, Ms. Rebecca Houghton1, Dr. Tiffany Hogan3,4, Prof Monica Lahra3,4
1Sydney Sexual Health Centre, Sexual Health & Bloodborne Viruses Service, South Eastern Sydney Local Health District, Sydney, Australia.
2The Kirby Institute, University of New South Wales, Sydney, Australia.
3WHO Collaborating Centre for STI and AMR, Sydney, Australia.
4Department of Microbiology, NSW Health Pathology Randwick, Sydney, Australia.
Background: Culture remains optimal for antimicrobial resistance (AMR) surveillance in Neisseria gonorrhoeae. Data from our centre showed that up to 39% of anorectal culture from nucleic acid amplification testing (NAAT)-confirmed infections did not yield gonorrhoea growth. We investigated if reducing the time to plating swabs on culture media improved yield.
Methods: We conducted a cross-sectional study in men with urethral and/or anorectal gonorrhoea (suspected on microscopy and/or confirmed by NAAT) in an inner-urban sexual health clinic in Sydney, Australia. Our centre is located 8 km from our reference laboratory with samples couriered 3 times daily. Cultures were sent from gonorrhoea-infected sites concurrently via two transport.
Methods: (i) swab placed in Amie’s medium (Copan) then sub-cultured onto agar at the laboratory and (ii) direct inoculation onto agar then placed into a sealed CO2-enriched transport system (Bio-BagTM Type C, Becton Dickinson). Associations between culture yield and participant and transport characteristics were examined.
Results: 57 pairs of gonorrhoea cultures were included (24 urethral and 33 anorectal). Overall culture positivity was 82% (urethral 100% vs anorectal 70%, P = 0.003) (Table 1). There was 100% concordance between the two transport systems in urethral samples. One anorectal sample was negative in Amie’s gel but positive in CO2-enriched system (concordance 97.0%). The time between culture collection in Amie’s gel and sub-culture was short (median 6.7 h, range 2.7–10.7 h). Positive anorectal culture was associated with time to sub-culture of <5 h (100% vs 61.54%, P = 0.049) and last intercourse >10 days prior to sampling (87.0% vs 22.2%, P < 0.001).
Conclusion: No significant difference was observed in our setting between gonorrhoea cultures transported in simple Amie’s medium compared to a CO2-encirhced system. However, shorter time between collection and sub-culture was a significant predictor of growth – suggesting that expediency between sampling and delivery may be a crucial aspect in the optimisation of culture.
| Total | Culture positive (Amie’s gel) | % | P-value (χ2) | ||
|---|---|---|---|---|---|
| All samples | |||||
| Total | 57 | 47 | 82% | ||
| Anatomical site | |||||
| Urethral | 24 | 24 | 100% | ||
| Anorectal | 33 | 23 | 69.70% | 0.003 | |
| Symptoms | |||||
| No | 29 | 19 | 66% | ||
| Yes | 28 | 28 | 100% | 0.001 | |
| Anorectal samples only | |||||
| Total | 33 | 23 | 70% | ||
| Symptoms | |||||
| No | 29 | 19 | 83% | ||
| Yes | 4 | 4 | 100% | 0.159 | |
| Time from collection to sub-culture | |||||
| Within 5 h | 7 | 7 | 100% | ||
| More than 5 h | 26 | 16 | 61.54% | 0.049 | |
| Number of days since last sexual intercourse | |||||
| Within 10 days | 9 | 2 | 22.22% | ||
| More than 10 days | 23 | 20 | 86.96% | <0.001 |
PP03.81 – What Proportion of Asymptomatic Rectal Neisseria Gonorrhoeae (NG) Infections Are Non-Viable? A Study Combining Culture and a Novel Molecular Viability Test
Dr. Arthur Wong1,2, Dr. Nicole Lima3,4, Dr Rick Varma1,2, Dr Kasia Strojny3, Dr Ingrid Aneman3, Dr Tamika Blair3, Dr Tina Lonergan3, Dr Hannah Lowes3, Prof Catriona S Bradshaw5,6, Prof Rebecca Guy2, A/Prof Alison V Todd3,7, A/Prof Tanya L Applegate2
1Sydney Sexual Health Centre, Sexual Health & Bloodborne Viruses Service, South Eastern Sydney Local Health District, New South Wales Health, Sydney, Australia.
2The Kirby Institute, UNSW, Sydney, Australia.
3SpeeDx Pty Ltd, Sydney, Australia.
4School of Life Sciences, University of Technology Sydney, Sydney, Australia.
5School of Translational Medicine, Monash University, Melbourne, Australia.
6Melbourne Sexual Health Centre, Alfred Hospital, Melbourne, Australia.
7School of Biotechnology & Biomolecular Sciences, University of New South Wales, Sydney, Australia.
Background: Nucleic acid amplification tests (NAAT), which are used to screen and diagnose NG, detect both viable and non-viable organisms. New assays to rapidly determine NG viability from clinical samples may reduce unnecessary treatment by distinguishing between remnant nucleic acids and true infections.
Methods: We conducted a prospective study on men with NAAT-confirmed rectal NG. Participants were recruited during their treatment visit. Pre-antibiotic, clinician-collected anal swab was transferred onto agar for culture followed by a swab in Amie’s gel with charcoal for testing via a novel molecular viability test (InSignia®) that analyses the RNA-to-DNA ratio and a repeat NAAT. We defined non-viable NG as infections with negative culture and negative via InSignia® (NG undetectable or non-viable). Association between time since last intercourse and non-viability was examined.
Results: Among 33 NAAT-confirmed rectal NG infections, 29 were asymptomatic. Among asymptomatic infections the median time between initial screening NAAT and viability testing was 6 days (IQR 4–7 days). Within these, 20 (69.0%) were culture positive and 17 (58.6%) were InSignia® viable. Among culture negative samples (n = 9), InSignia® test determined 6 had no detectable NG, 2 had detectable but non-viable NG and 1 had indeterminate viability. In total, 8 samples (27.6%) were negative/non-viable on both culture and InSignia®, while 4 of these remained NG positive by repeat NAAT. Non-viability was associated with timing between last intercourse and viability test of <=14 vs >14 days (42.1% vs. 0%, P = 0.016).
Conclusions: By combining culture and a novel viability test, we found that approximately a quarter of asymptomatic rectal NG were non-viable and potentially treated unnecessarily. Agreement between culture and InSignia® was high but further studies are needed to understand discordant results. The potential of this assay to offer an alternative determination of viability, including in settings where timely culture is not possible, warrants further investigation to improve NG screening programs.
PP03.82 – Multiplex Testing for HIV, Viral Hepatitis, and STIs at the Point-Of-Care: A Scoping Review
Miss Sandra Olisakwe1, Sahar Bajis2, Aliza Monroe-Wise2, Emma C O’Hagan1, Bhekumusa Lukhele1, Renee Heffron1, Cheryl C Johnson2, Katia Bruxvoort1, Ms. Tara Wood
1University of Alabama At Birmingham, Birmingham, United States.
2World Health Organization, Geneva, Switzerland.
Background: Multiplex testing, whereby a device detects different analytes in a single specimen, is becoming more important for sexually transmitted infections (STIs), as programs aim to be client-centered and deliver services as part of primary care. Most recently, dual HIV/syphilis rapid diagnostic tests (RDT) and self-tests (ST) have been shown to increase access to and uptake of HIV and syphilis testing services especially in pregnant women. This scoping review examines recent data on these multiplex testing platforms’ feasibility, usability, and diagnostic accuracy.
Methods: A systematic search of published and grey literature was conducted across PubMed, Embase, Scopus, Web of Science, and MEDLINE for studies published between January 2019 and July 2024. Inclusion criteria focused on rapid (<90 min) multiplex testing for HIV, STIs, and hepatitis B and C, prioritizing studies comparing outcomes between individuals using point-of-care multiplex testing services and those using single testing services. We reviewed and synthesized findings from the included studies for recurring themes.
Results: A total of 3,948 records were screened by two independent reviewers, and 114 studies were included. Multiplex testing methods included molecular diagnostics, serology-based rapid diagnostic tests (RDTs), and ST platforms. Molecular tests were commonly used for multiplex testing of STIs like chlamydia and gonorrhea, reducing time to treatment and improving care delivery, while serology RDTs for HIV/syphilis demonstrated high diagnostic accuracy, with HIV sensitivity reaching 100%. Uptake among priority populations, such as pregnant women exceeded 85%. ST platforms demonstrated feasibility and the potential to improve accessibility and autonomy. Geographical gaps were evident, with limited studies from the Eastern Mediterranean and Southeast Asia WHO regions.
Conclusion: Multiplex testing has great potential for integrating the diagnosis of HIV, viral hepatitis, and STIs, offering high accuracy and user acceptance. However, more work is needed to optimize test combinations for specific populations and settings.
PP03.83 – National Consultation Service to Inform Management of Trichomoniasis Clinical Treatment Failure
Dr. Laura A. S. Quilter1, Dr. Priyanka Anand1, Peter Augostini2, Dr. W. Evan Secor2, Jane E. Yang1, Yan Yuan1, Matthew Pooser1, Dr. Laura H. Bachmann1, Dr. Lindley A. Barbee1, Prof. Kimberly Workowski1,3
1Division of STD Prevention, National Center for HIV, Viral Hepatitis, STD, and TB Prevention, US Centers for Disease Control and Prevention, Atlanta, United States.
2Division of Parasitic Diseases and Malaria, National Center for Emerging and Zoonotic Infectious Diseases, US Centers for Disease Control and Prevention, Atlanta, United States.
3Department of Medicine, Emory University, Atlanta, United States.
Background: Nitroimidazoles are the only class of antimicrobials that have demonstrated clinical efficacy against Trichomonas vaginalis infections; however, nitroimidazole treatment failure has been reported in up to 10% of infections. Data are limited regarding alternative therapies for nitroimidazole-resistant trichomoniasis. US Centers for Disease Control and Prevention (CDC) provides clinical consultation on T. vaginalis treatment failure cases concerning for nitroimidazole-resistant trichomoniasis.
Methods: During April 1, 2023–September 12, 2024, clinicians reported cases of persistent T. vaginalis to CDC to request in vitro nitroimidazole susceptibility testing through CDC’s Parasites Lab and clinical consultation. Reporting clinicians sought consultation by submitting clinical history information including patient demographics, prior treatment courses, and nitroimidazole susceptibility results. Alternative treatment recommendations were provided based on these data; follow up information was collected on clinical outcomes. Resistance categories were set according to minimal lethal concentration (MLC; Table 1).
Results: During the study period, clinical consultation was requested for 52 cases of T. vaginalis treatment failure among cisgender women. The median age was 36 years [IQR 28–44.3] and eight (15.4%) were pregnant at the time of consultation. Clinicians reported a median of 4 treatments [IQR 3–5.3] prior to pursuing consultation. Among cases with susceptibility results (n = 50), 34 (68.0%) had moderate or high-level in vitro nitroimidazole resistance (metronidazole, 68%; tinidazole, 38.0%). Follow-up information was available for 16 (30.8%) cases. Of the cases with follow-up information, 13 (81.3%) achieved clinical or microbiological cure; among those with high-level nitroimidazole resistance (n = 6), 83.3% achieved cure after treatment with consultation-recommended regimen (Table 1).
Conclusion: Most T. vaginalis treatment failure cases reported to CDC for clinical consultation had moderate to high-level nitroimidazole resistance. However, cure was high following receipt of recommended alternative treatment, highlighting importance of susceptibility testing to inform treatment recommendations. Further studies are needed to inform alternative treatment recommendations for nitroimidazole-resistant T. vaginalis infections.
| n (%) | ||||
|---|---|---|---|---|
| Sex Assigned at Birth | ||||
| Female | 52 (100) | |||
| Gender Identity | ||||
| Female | 52 (100) | |||
| Age (Median, IQR) | 36 (28-44.3) | |||
| Weight, in pounds (Mean, SD) | 195.9 (61.7) | |||
| Pregnant | 8 (15.4) | |||
| Race and Hispanic Ethnicity | ||||
| Hispanic or Latino | 7 (13.5) | |||
| Non-Hispanic Black | 22 (42.3) | |||
| Non-Hispanic White | 18 (34.6) | |||
| Non-Hispanic Other Race | 3 (5.8) | |||
| Non-Hispanic Multi-race | 1 (1.9) | |||
| Number of Antimicrobial Treatment Courses Completed Prior to CDC Consultation (Median, IQR) | 4 (3-5.3) | |||
| Susceptibility Results* (n = 50) | ||||
| Metronidazole | ||||
| Susceptible (MLC <50) | 4 (8.0) | |||
| Minimal Level Resistance (MLC 50–100) | 12 (24.0) | |||
| Moderate Level Resistance (MLC 200) | 10 (20.0) | |||
| High Level Resistance (MLC ≥400) | 24 (48.0) | |||
| Tinidazole | ||||
| Susceptible (MLC ≤6.3) | 6 (12.0) | |||
| Minimal Level Resistance (MLC 12.5–50) | 25 (50.0) | |||
| Moderate Level Resistance (MLC 100-200) | 10 (20.0) | |||
| High Level Resistance (MLC ≥400) | 9 (18.0) | |||
| Clinical Outcome Following Recommended Treatment Among Consultations with Follow Up Information (n = 16) | Minimal Nitroimidazole Resistance* (n = 5) | Moderate Nitroimidazole Resistance* (n = 5) | High-Level Nitroimidazole Resistance* (n = 6) | |
|---|---|---|---|---|
| Cure ƚ, n (%) | Cure ƚ, n (%) | Cure ƚ, n (%) | ||
| Tinidazole 1g PO three times a day for 14 days PLUS intravaginal boric acid capsules 600mg twice a day for 28 days¶ | 1/1 (100) | 0 | 4/5 (80) | |
| Tinidazole 1g PO two times a day for 14 days PLUS intravaginal boric acid capsules 600mg twice a day for 60 daysƚƚ | 0 | 1/1 (100) | 0 | |
| Tinidazole 1g PO two times a day for 14 days | 1/2 (50) | 2/3 (66.7) | 1/1 (100) | |
| Tinidazole 1g PO twice a day for 7 days | 1/1 (100) | 0 | 0 | |
| Tinidazole 2g PO daily for 7 days | 0 | 1/1 (100) | 0 | |
| Tinidazole 1 g PO three times a day for 14 days | 1/1 (100) | 0 | 0 |
IQR, interquartile range; SD, standard deviation; MLC, minimal lethal concentration.
*Nitroimidazole susceptible was defined as an in vitro aerobic metronidazole MLC of <50 µg/mL or tinidazole MLC ≤6.3 µg/mL; minimal resistance as an metronidazole MLC of 50 to 100 µg/mL or tinidazole MLC of 12.5 to 50 µg/mL; moderate resistance as an metronidazole MLC of 200 µg/mL or tinidazole MLC of 100–200 µg/mL; and high-level resistance as an metronidazole MLC of ≥400 µg/mL or tinidazole MLC of ≥400 µg/mL.
ƚCure was defined as either a negative T. vaginalis nucleic acid amplification test (NAAT) at least 4 weeks after treatment or negative trichomonas culture 1 to 4 weeks after treatment and/or complete resolution of trichomoniasis signs and symptoms if test-of-cure NAAT or culture was not performed.
ƚƚThe patient experienced treatment failure after initial recommended treatment with tinidazole 1 g PO twice a day for 14 days and was recommended to complete high dose tinidazole regimen combination therapy with intravaginal boric acid.
¶One patient was pregnant at time of consultation; completed intravaginal boric acid capsules 600 mg two times a day until delivery followed by high dose tinidazole combination regimen with intravaginal boric acid.
PP04.01 – Epidemiology of Neisseria Gonorrhoeae in South-East Asia: Systematic Review, Meta-Analyses, and Meta-Regressions
Miss Rwedah Ali Ageeb1, Ms. Sawsan Al-mukdad1,2, Ms. Huda Alalami1, Ms. Manale Harfouche1, Prof. Laith Abu-Raddad1,3,4,5
1Infectious Disease Epidemiology Group, Weill Cornell Medicine-Qatar, Cornell University, Qatar Foundation - Education City, Doha, Qatar, Doha, Qatar.
2Interprofessional Education Office, QU Health Sector, Qatar University, Doha, Qatar, Doha, Qatar.
3Department of Population Health Sciences, Weill Cornell Medicine, Cornell University, New York, New York, USA, New York, USA.
4Department of Public Health, College of Health Sciences, QU Health, Qatar University, Doha, Qatar, Doha, Qatar.
5College of Health and Life Sciences, Hamad bin Khalifa University, Doha, Qatar, Doha, Qatar.
Background: The epidemiology of Neisseria gonorrhoeae (NG) infection in South-East Asia remains inadequately understood, despite the disease burden and the global threat posed by gonococcal antimicrobial resistance. This study aimed to provide an analytical description of the epidemiology of NG infection in South-East Asia.
Methods: The study conducted a systematic review, synthesizing and analyzing NG prevalence data up to September 3, 2024, with findings reported in accordance with PRISMA guidelines. Random-effects meta-analyses were employed to estimate the pooled mean NG prevalence across different population types and anatomical sites. Meta-regressions were used to investigate associations, time trends, and sources of heterogeneity across studies.
Results: A total of 475 publications were included, encompassing 885 overall and 1,136 stratified measures. The pooled mean prevalence of urogenital NG infection was 0.5% (95% CI: 0.3–0.8%) in general populations, 13.9% (95% CI: 11.9–16.1%) in female sex workers (FSWs), 16.8% (95% CI: 12.6–21.5%) in sexually transmitted infection (STI) clinic attendees, and 38.5% (95% CI: 31.8–45.3%) in symptomatic men. Among male sex workers, men who have sex with men, and transgender people, the pooled mean prevalence was 0.9% (95% CI: 0.4–1.9%) for urogenital infection, 12.0% (95% CI: 8.8–15.7%) for anorectal infection, and 7.1% (95% CI: 4.0–10.9%) for oropharyngeal infection. Meta-regression analyses explained more than 50% of the variation in prevalence, indicating a higher prevalence among symptomatic men, FSWs, and STI clinic attendees compared to the general population. The analyses also revealed a higher prevalence in men than in women and a slow annual decline in prevalence at a relative rate of 1%.
Conclusion: NG prevalence in South-East Asia is comparable to that in other regions, highlighting an underrecognized disease burden. The region is unlikely to meet the World Health Organization’s target of a 90% reduction in NG incidence by 2030.
PP04.02 – Prevalence and Incidence of External Genital Warts in State of Qatar 2019–2023
Dr. Samya Abushaikha1, Dr Hissa Almarri1, Dr Afraa Almohannadi1, Dr Hend Alobaidli1, Dr Sara Al-Khawaga1, Dr Mohamed Sherbash1
1Hamad Medical Corporation, Doha, Qatar.
Background: Genital warts, predominantly induced by low-risk human papillomavirus (HPV) genotypes 6 and 11, constitute a significant burden in dermatology and venereology, with implications for public health and patients quality of life. This study aims to provide a detailed analysis of genital wart incidence, prevalence, and associated comorbidities in Qatar, utilizing national data to inform targeted prevention and management efforts.
Methods: Aims and Objectives: The primary aim of this study is to establish the first national epidemiological database on genital warts in Qatar, spanning the period from 2016 to 2023. Specific objectives include evaluating the incidence and prevalence of genital warts among Qataris and non-Qataris, identifying associated demographic and clinical characteristics.
Patients: Inclusion Criteria: All patients diagnosed with genital warts during the study period were included. Data were extracted retrospectively from electronic health records in the Cerner database.
Data Analysis: Statistical analyses, including chi-square tests, were performed using SPSS Statistics Software (IBM) to identify associations between demographic factors and disease metrics.
Results: The incidence and prevalence of genital warts in Qatar reveal significant disparities by nationality and gender, with Qataris consistently experiencing higher incidence rates than non-Qataris throughout the study period. Among Qataris, the incidence rate peaked at 23 per 100,000 in 2019, declined to 13 in 2020 due to potential pandemic-related healthcare disruptions, and partially recovered to 19 by 2023 (Figs 1–6, Tables 1–6). Non-Qataris maintained stable incidence rates between 4 and 7 per 100,000, with a slight increase in 2023.
Conclusions: The study highlights significant disparities in the incidence and prevalence of genital warts in Qatar, with Qataris and females bearing a disproportionately higher burden.
The incidence rate of genital warts was consistently higher among Qataris compared to non-Qataris throughout the study period. Among Qataris, the incidence rate peaked in 2019 at 23 per 100,000 population, followed by a decline to 13 in 2020 and a gradual recovery to 19 in 2023. In contrast, non-Qataris maintained relatively stable rates, ranging between 4 and 7 per 100,000, with a slight increase in 2023. These trends underscore notable disparities in incidence rates by nationality.
Gender-specific differences in incidence rates were observed, with females generally exhibiting higher rates than males. In 2019, females experienced their highest incidence rate of 0.6 per 100,000, which decreased to 0.3 in 2020 before recovering to 0.7 by 2023. For males, the highest incidence rate was also in 2019 at 0.8 per 100,000, dropping to 0.6 in 2023. These findings highlight potential variations in exposure or healthcare-seeking behaviors between genders.
The incidence rate for the total population increased slightly from 7 per 100,000 in 2016 to a peak of 8 in 2019. A noticeable decline occurred in 2020, with the rate falling to 5 per 100,000, followed by a gradual rebound to 8 per 100,000 in 2023. These fluctuations could reflect broader public health factors, including pandemic-related disruptions in healthcare services.
The prevalence rate of genital warts showed a sharp increase over time among both Qataris and non-Qataris. Qataris exhibited a significant rise from 21 per 100,000 in 2016 to 139 in 2023, indicating a substantial cumulative disease burden. Non-Qataris also experienced an increase, though at a slower rate, from 6 per 100,000 in 2016 to 41 in 2023. These patterns suggest a growing prevalence gap between the two nationality groups.
Prevalence rates among females were consistently higher than among males. Female prevalence rose from 12 per 100,000 in 2016 to 74 in 2023, while male prevalence increased from 6 to 42 per 100,000 during the same period. The widening gender disparity indicates a potential difference in disease progression or diagnosis rates.
The total population prevalence rate of genital warts demonstrated a steady upward trend, increasing from 7 per 100,000 in 2016 to 53 in 2023. This growth reflects an accumulating number of cases over time, emphasizing the need for targeted public health interventions.
| Year | Cases (Qatari) | Population (Qatari) | Incidence/100,000 | Cases (Non-Qatari) | Population (Non-Qatari) | Incidence/100,0002 | |
|---|---|---|---|---|---|---|---|
| 2016 | 65 | 314116 | 21 | 128 | 2303518 | 6 | |
| 2017 | 72 | 326953 | 22 | 137 | 2397653 | 6 | |
| 2018 | 60 | 331220 | 18 | 158 | 2428950 | 7 | |
| 2019 | 76 | 335904 | 23 | 147 | 2463298 | 6 | |
| 2020 | 45 | 341534 | 13 | 112 | 2504584 | 4 | |
| 2021 | 57 | 340041 | 17 | 94 | 2493638 | 4 | |
| 2022 | 51 | 329779 | 15 | 125 | 2418383 | 5 | |
| 2023 | 68 | 355914 | 19 | 169 | 2610038 | 6 |
| Year | Cases (Males) | Population (Males) | Incidence/100,000 | Cases (Females) | Population (Females) | Incidence/100,0002 | |
|---|---|---|---|---|---|---|---|
| 2016 | 115 | 1975536 | 6 | 78 | 642098 | 12 | |
| 2017 | 119 | 2046047 | 6 | 168 | 678559 | 25 | |
| 2018 | 135 | 2048206 | 7 | 251 | 711964 | 35 | |
| 2019 | 128 | 2064276 | 6 | 346 | 734926 | 47 | |
| 2020 | 97 | 2025902 | 5 | 406 | 807777 | 50 | |
| 2021 | 87 | 1970649 | 4 | 470 | 777513 | 60 | |
| 2022 | 105 | 2121336 | 5 | 541 | 810905 | 67 | |
| 2023 | 144 | 2206546 | 7 | 634 | 856459 | 74 |
| Year | Cases (Total) | Population (Total) | Incidence/100,000 | |
|---|---|---|---|---|
| 2016 | 193 | 2617634.0 | 7 | |
| 2017 | 209 | 2724606.0 | 8 | |
| 2018 | 218 | 2760170.0 | 8 | |
| 2019 | 223 | 2799202.0 | 8 | |
| 2020 | 157 | 2846118.0 | 6 | |
| 2021 | 151 | 2833679.0 | 5 | |
| 2022 | 176 | 2748162.0 | 6 | |
| 2023 | 237 | 2965952.0 | 8 |
| Year | Cases (Qatari) | Population (Qatari) | Prevalence/100,000 | Cases (Non-Qatari) | Population (Non-Qatari) | Prevalence/100,0002 | |
|---|---|---|---|---|---|---|---|
| 2016 | 65 | 314116 | 21 | 128 | 2303518 | 6 | |
| 2017 | 137 | 326953 | 42 | 265 | 2397653 | 11 | |
| 2018 | 197 | 331220 | 59 | 423 | 2428950 | 17 | |
| 2019 | 273 | 335904 | 81 | 570 | 2463298 | 23 | |
| 2020 | 318 | 341534 | 93 | 682 | 2504584 | 27 | |
| 2021 | 375 | 340041 | 110 | 776 | 2493638 | 31 | |
| 2022 | 426 | 329779 | 129 | 901 | 2418383 | 37 | |
| 2023 | 494 | 355914 | 139 | 1070 | 2610038 | 41 |
| Year | Cases (Males) | Population (Males) | Prevalence/100,000 | Cases (Females) | Population (Females) | Prevalence/100,0002 | |
|---|---|---|---|---|---|---|---|
| 2016 | 115 | 1975536 | 6 | 78 | 642098 | 12 | |
| 2017 | 234 | 2046047 | 11 | 168 | 678559 | 25 | |
| 2018 | 369 | 2048206 | 18 | 251 | 711964 | 35 | |
| 2019 | 497 | 2064276 | 24 | 346 | 734926 | 47 | |
| 2020 | 594 | 2025902 | 29 | 406 | 807777 | 50 | |
| 2021 | 681 | 1970649 | 35 | 470 | 777513 | 60 | |
| 2022 | 786 | 2121336 | 37 | 541 | 810905 | 67 | |
| 2023 | 930 | 2206546 | 42 | 634 | 856459 | 74 |
| Year | Cases (Total) | Population (Total) | Prevalence/100,000 | |
|---|---|---|---|---|
| 2016 | 193 | 2617634.0 | 7 | |
| 2017 | 402 | 2724606.0 | 15 | |
| 2018 | 620 | 2760170.0 | 22 | |
| 2019 | 843 | 2799202.0 | 30 | |
| 2020 | 1000 | 2846118.0 | 35 | |
| 2021 | 1151 | 2833679.0 | 41 | |
| 2022 | 1327 | 2748162.0 | 48 | |
| 2023 | 1564 | 2965952.0 | 53 |
PP04.03 – An Assessment of the HIV Epidemic in Nigeria: A Gender Perspective
Dr. Rose Aguolu1, Joy Egwuonwu1
1National Agency for the Control of AIDS, Abuja, Nigeria.
Background: Nigeria’s HIV epidemic is significantly influenced by gender inequalities, prompting various national interventions. This study aimed to evaluate the gender-specific dimensions of Nigeria’s HIV epidemic and identify strategic investment opportunities to enhance gender equality.
Description: We conducted a cross-sectional study from August 2021 to March 2022 in partnership with the Federal Ministry of Women Affairs, UN Women, and UNAIDS. Quantitative data was collected using the UNAIDS Gender Assessment Tool (GAT) through a comprehensive desk review of national documents, relevant literature, and HIV and gender databases. Data analysis was performed using Excel.
Results: Our findings revealed marked gender disparities in HIV prevalence and transmission patterns. Women represented 60% of adults (15–49 years) living with HIV, with a prevalence rate of 1.6% compared to 1.0% among men. Notably, women initiated sexual activity approximately 4.5 years earlier than men. Between 2010 and 2020, new HIV infections among adult females (15+ years) decreased from 50,000 to 39,000, representing a 22% reduction. In contrast, new infections among adult males showed a more substantial decline from 41,000 to 25,000, marking a 39% reduction. Antiretroviral therapy (ART) coverage demonstrated significant improvements across both genders from 2015 to 2020, with men’s coverage increasing from 36% to 73% and women’s coverage rising from 62% to nearly complete coverage at 98%.
Conclusion: Despite approaching universal ART coverage among women and comparable increases in coverage rates between genders, women continue to experience disproportionately higher rates of new HIV infections. These findings underscore the urgent need to re-evaluate and strengthen HIV prevention strategies targeting women, with particular emphasis on interventions for adolescent girls and young women. Such targeted approaches are essential for addressing the persistent gender disparities in HIV transmission and advancing toward more equitable health outcomes.
PP04.04 – High-Risk Sexual Behaviours and HIV Vulnerability Among Key Populations in Nigeria: Implications for Prevention Strategies
Dr. Rose Aguolu1, ThankGod Zachariah Kums1, Adediran Adesina2
1National Agency for the Control of AIDS, Abuja, Nigeria.
2University of Manitoba, Abuja, Nigeria.
Background: Key populations (KPs) in Nigeria, including men who have sex with men (MSM), female sex workers (FSW), people who inject drugs (PWID), and transgender individuals (TG), account for a very significant proportion of new HIV infections in Nigeria. Identifying the sexual behaviours that increase HIV risk in these groups is crucial to improving prevention efforts.
Method: This study was carried out in twelve Nigerian states from October to November 2020, using a multi-stage probability sampling method. Participants were recruited from both in-person and online platforms. Behavioural data were collected using a structured questionnaire from MSM, FSW, PWID, and TG individuals and analyzed using STATA 16.0.
Results: A total of 17,975 KPs participated, with 4,974 FSW, 4,397 MSM, 4,414 PWID, and 4,190 TG. Over 75% of respondents had at least a secondary education, and most were unmarried. The average age ranged from 24 to 30 years. The HIV prevalence among these populations was highest among TG (28.8%), followed by MSM (25.0%), FSW (15.5%), and PWID (10.9%). Condom use in the past 6 months was low, particularly with regular and casual partners. Only 53.4% of FSW and 51.1% of PWID used condoms during their last sexual encounter with a regular partner. About 71.2% of MSM and 85% of TG reported unprotected receptive anal intercourse, while 60% of PWID shared syringes. STI prevalence in the past year was 55.6% among FSW, 30.2% among MSM, 34.0% among PWID, and 30.9% among TG; meanwhile, access to HIV testing and STI services was limited across all groups.
Conclusions: This study highlights significant high-risk sexual behaviours among KPs, increasing their vulnerability to HIV. There is an urgent need to reassess HIV prevention strategies and improve accessibility for these populations. Further research into the drivers of risky behaviours is essential for refining prevention programs.
PP04.05 – Individual and Community-Level Determinants of HIV/AIDS Knowledge and Discriminatory Attitudes Among Women of Reproductive Age in Pakistan: A Multilevel Approach
Miss Iqra Akram1,2, Dr. Misbah Kanwal1, Dr. Umaima Khan1, Dr. Aalima Fatima1, Dr. Safura Awais1, Dr. Owais Raza1
1BMY Health, Lahore, Pakistan.
2Simon Fraser University, Burnaby, Canada.
Background: HIV/AIDS remains a significant public health challenge in Pakistan, with an estimated 240,000 people living with HIV in 2023. Women of reproductive age are a critical demographic, as their knowledge and attitudes shape health outcomes within families and communities. Understanding individual and community-level determinants of HIV/AIDS knowledge and discriminatory attitudes is crucial for targeted interventions that enhance awareness, reduce stigma, and promote health equity.
Methods: This study analyzed data from the 4th cohort (2017–18) of the Pakistan Demographics and Health Survey (PDHS), which employed a stratified two-stage sample design. A total of 12,811 ever-married women aged 15–49 were interviewed across 561 clusters, excluding 19 due to security concerns. Outcome variables included comprehensive knowledge of HIV and discriminatory attitudes toward people living with HIV (PLHIV). Independent variables encompassed individual factors (e.g., age, education, media exposure) and community factors (e.g., regional wealth, urban/rural residence). Multilevel logistic regression was performed using STATA v17, with sampling weights applied to reduce bias.
Results: Among 12,364 women, 95.81% lacked comprehensive HIV knowledge, and 60.1% held discriminatory attitudes. Greater HIV knowledge was observed among women aged 25+, with secondary education, media exposure, and a higher wealth index. Non-discriminatory attitudes were more common in urban areas, among educated women, and those with decision-making authority. Education and wealth index strongly influenced both knowledge and attitudes.
Conclusion: Both individual and community-level factors significantly impacted HIV knowledge and attitudes. Enhanced HIV knowledge was associated with reduced stigma, emphasizing the need for targeted interventions addressing educational and socio-economic disparities.
PP04.06 – Mpox Cases in Toronto, 2024: Shifts in Epidemiology?
Mrs. Dana Al-Bargash Dana Al-Bargash1
1Toronto Public Health, Toronto, Canada.
Background: After 2 years combating the mpox outbreak in Toronto, mpox activity increased again in 2024. While the outbreak continues to primarily affect gay, bisexual, and other men who have sex with men (GBMSM), there is some evidence this increase is partly attributed to changes in transmission or screening patterns among females and males with only opposite-sex partners.
Methods: Data on probable and confirmed Toronto mpox cases from January 1 2023 to November 30 2024 were extracted from Ontario’s integrated Public Health Information System on December 18, 2024. Analyses were conducted in SAS 9.4.
Results: From January 1 to November 30, 2024, Toronto reported 230 mpox cases, 784% increase from 26 cases in 2023 for the same period.
Cases in 2024 peaked in July, shortly after Toronto’s Pride Festival. Most were male (n = 216, 94%):165 (76%) reporting only same-sex partners, seven (3%) both opposite- and same-sex partners, five (3%) only opposite-sex partners, and 39 (18%) did not report either. Six female cases were reported, all after June 23 and reporting opposite-sex partners. Seven transgender cases (3%) were reported, five reported same-sex partners and two did not specify. One case had an unknown sex. Twenty-eight cases (all male, most reported same-sex partners) reported travel during their incubation period. Thirty-three cases (14%), all male, received two Imvamune® doses; only one reported opposite-sex partners, along with same-sex partners.
All 26 cases in 2023 were male, 23 (88%) reporting only same-sex partners, one (4%) opposite-sex partners, and two (8%) did not report either.
Conclusion: While GBMSM continue to be most affected by mpox in Toronto, 2024 data show an increase in cases among other groups, including women and men with opposite-sex partners. This shift may reflect changes in transmission patterns or increased screening. Therefore, continued vaccination, strengthened surveillance, and targeted public health measures are needed.
PP04.07 – Diagnosis of Early Syphilis: Support for Reverse Sequence Testing
Ms. Alexandra Aubee1, Dr. Heather Elder1, Lauren Molotnikov1, Erin Wade1, Colleen Beatriz1, Nikki Gilani1, Jennifer Delmonte1, Kaitlin Nichols1, Dr. Peter Collin1,2, Betsey John1, Dr. Katherine Hsu1, Dr. Lao-Tzu Allan-Blitz1,3
1Massachusetts Department of Public Health, Jamaica Plain, United States.
2Beth Israel Deaconess Medical Center, Boston, United States.
3Brigham and Women’s Hospital, Boston, United States.
Background: The incidence of infectious syphilis in Massachusetts rose by 106% since 2013. Serologic testing is used to support diagnosis, either via the traditional algorithm using a non-treponemal test confirmed by a treponemal test, or the reverse-sequence algorithm using a treponemal test confirmed by a non-treponemal test. The reverse-sequence algorithm, more commonly used in Massachusetts, may have a higher sensitivity for early syphilis, but limited data are available on testing algorithm performance.
Methods: To describe testing algorithm performance in early-stage syphilis, we retrospectively reviewed all primary infectious syphilis diagnoses from January 2022 to December 2023 in Massachusetts. We assessed treponemal and non-treponemal test positivity frequencies. Among those identified with discordant results, we report relevant test results and sociodemographic data.
Results: Five hundred thirty-six primary infectious syphilis cases had serologic testing results available. Of those, 507 (94.6%) had dual treponemal and non-treponemal test positivity; 12 (2.2%) did not have a second test available for analysis. Seventeen cases (3.2%) had discordant test results, 14 had positive treponemal and negative non-treponemal tests, 1 of which subsequently became dual test positive; 3 cases had negative treponemal and positive non-treponemal tests, 2 of which had RPR titers of <1:8. All 17 individuals with discordant testing had a documented lesion at time of testing and were treated for primary syphilis, predominantly in emergency department or urgent care settings (7/17, 41.2%).
Conclusion: In a statewide surveillance system, the majority of reported primary syphilis cases had dual test positivity around time of diagnosis. Reverse-sequence algorithm testing supported the diagnosis of 14 cases of primary syphilis that would have been negative using traditional algorithm; however, the traditional algorithm supported the diagnosis of 3 cases of primary syphilis infections that would have been negative using reverse sequence. Discordant serologic testing did not appear to impede presumptive treatment of primary syphilis.
PP04.08 – Identifying Without Stigmatizing: Individuals of Transgender Experience Differ from Men Who Have Sex with Men
Ms. Colleen Beatriz1, Erin Wade1, Alexandra Aubee1, Lauren Molotnikov1, Laura Kersanske1, Nikki Gilani1, Betsey John1, Dr. Katherine Hsu1,2, Dr. Lao-Tzu Allan-Blitz1,3, Dr. Heather Elder1
1Massachusetts Department of Public Health, Jamaica Plain, United States.
2Section of Pediatric Infectious Diseases, Boston Medical Center, Boston, United States.
3Division of Global Health Equity, Brigham and Women’s Hospital, Boston, United States.
Background: Syphilis disproportionately affects sexual minority populations. Since 2014, the World Health Organization has called for recognition of individuals of transgender experience (ITE) as a distinct population; however, many analyses continue to conflate ITE, particularly transgender women, with men who have sex with men (MSM), limiting our understanding of unique syphilis risk factors and experiences within each group.
Methods: We explored differences between ITE (both transgender men and women) and cisgender MSM (inclusive of MSM who also reported sex with women or ITE) diagnosed with infectious syphilis and interviewed by field epidemiologists in Massachusetts from 2021 to 2023. We compared age, HIV status (through HIV surveillance cross-match), social vulnerability index, and self-reported behaviors. For individuals who completed multiple interviews, we distilled whether a behavior was ever reported and used the most complete information available for remaining variables.
Results: Between 2021–2023, 99 ITE and 1,693 cisgender MSM were diagnosed with infectious syphilis and completed at least one interview with a field epidemiologist.
For ITE compared to cisgender MSM, respectively, mean age at first diagnosis was 30.8 vs 37.7 years (P < 0.0001); HIV co-infection rate 33.3% vs 32.4% (P > 0.05); residence in an area of high social vulnerability 56.8% vs 42.2% (P < 0.05); and report of transactional sex 14.1% vs 2.7% (P < 0.0001), sex while intoxicated 34.3% vs 19.3% (P < 0.001), and substance use 34.3% vs 22.5% (P < 0.05). Similarities were observed with other behaviors including majority of individuals in both groups reporting inconsistent condom use and anonymous sex.
Conclusions: ITE with infectious syphilis in Massachusetts may be younger, more socially vulnerable, and more likely to be involved in transactional sex or use substances than cisgender MSM. In spite of younger age, HIV co-infection rates were similar in syphilis-infected ITE and cisgender MSM. Understanding unique drivers of exposures among ITE can inform future tailored HIV/ STI prevention strategies.
PP04.09 – Trends in HIV Self-Testing Uptake and Behaviors in Africa: A Mathematical Modeling Study Combining Population-Based Surveys and Program Data
Miss Aishi Aratrika1, Dr. Carla M Doyle1, Dr. Cheryl C Johnson2, Mr. Olanrewaju Edun2,3, Dr. Jeffrey W Imai-Eaton3,4, Dr. Mathieu Maheu-Giroux1
1McGill University, Montreal, Canada.
2World Health Organization, Geneva, Switzerland.
3Imperial College London, London, United Kingdom.
4Harvard T.H. Chan School of Public Health, Boston, United States.
Background: HIV self-testing (HIVST) can increase testing coverage by reaching underserved populations and help achieve the UNAIDS goal of 95% of people living with HIV knowing their status. Several African countries, the region with the highest HIV burden, have scaled-up this modality since the 2016 HIVST recommendation from the World Health Organization. We aim to estimate country-level and regional trends in HIVST uptake and behaviors in Africa.
Method: We collated information from all population-based surveys on the proportion of individuals who used HIVST and country-level programmatic data on annual HIVST kit distribution (up to 2024). We developed a hierarchical Bayesian framework to triangulate surveys with program data using a compartmental model of HIVST behaviors. We used country-level random effects to pool information across countries for the sex-specific rate ratios, the re-testing rates, and the proportion of distributed kits being used. The model estimates sex-specific trends in HIVST uptake and the number of HIVST kits used.
Results: Forty-seven surveys from 35 countries, encompassing 915,697 participants and country-level information on 20 million distributed HIVST kits, were triangulated to inform the model (Fig. 1). We estimate that, in 2024, 7% (95%CrI: 6%–9%) of the population in these countries ever used an HIVST, increasing from <0.1% in 2011. The proportion varied substantially across countries, reaching a maximum of 44% (95%CrI: 43%–46%) in Lesotho. The HIVST male-to-female rate ratio was 1.1 (95%CrI: 0.9–1.2). Individuals who have previously used an HIVST were 40% (95%CrI: –2%, 87%) more likely to re-use an HIVST; although this specific estimate was imprecise due to limited overlap between survey and program data. Finally, we estimate that 79% (95%CrI: 67–90%) of all HIVST distributed were used.
Conclusion: Our study provides insights into HIVST uptake patterns. These can be integrated into epidemiological models to understand the impact of HIVST scale-up in high HIV prevalence settings.
Sex-specific temporal trends of HIVST uptake in Africa (Panel A; shaded areas correspond to 95% credible intervals), and country-specific and overall estimates of HIVST male-to-female rate ratios (Panel B), HIVST re-testing rate ratios (Panel C), and proportion of distributed HIVST kits being used (Panel D); horizontal lines represent 95% credible intervals in Panel B, C and D.
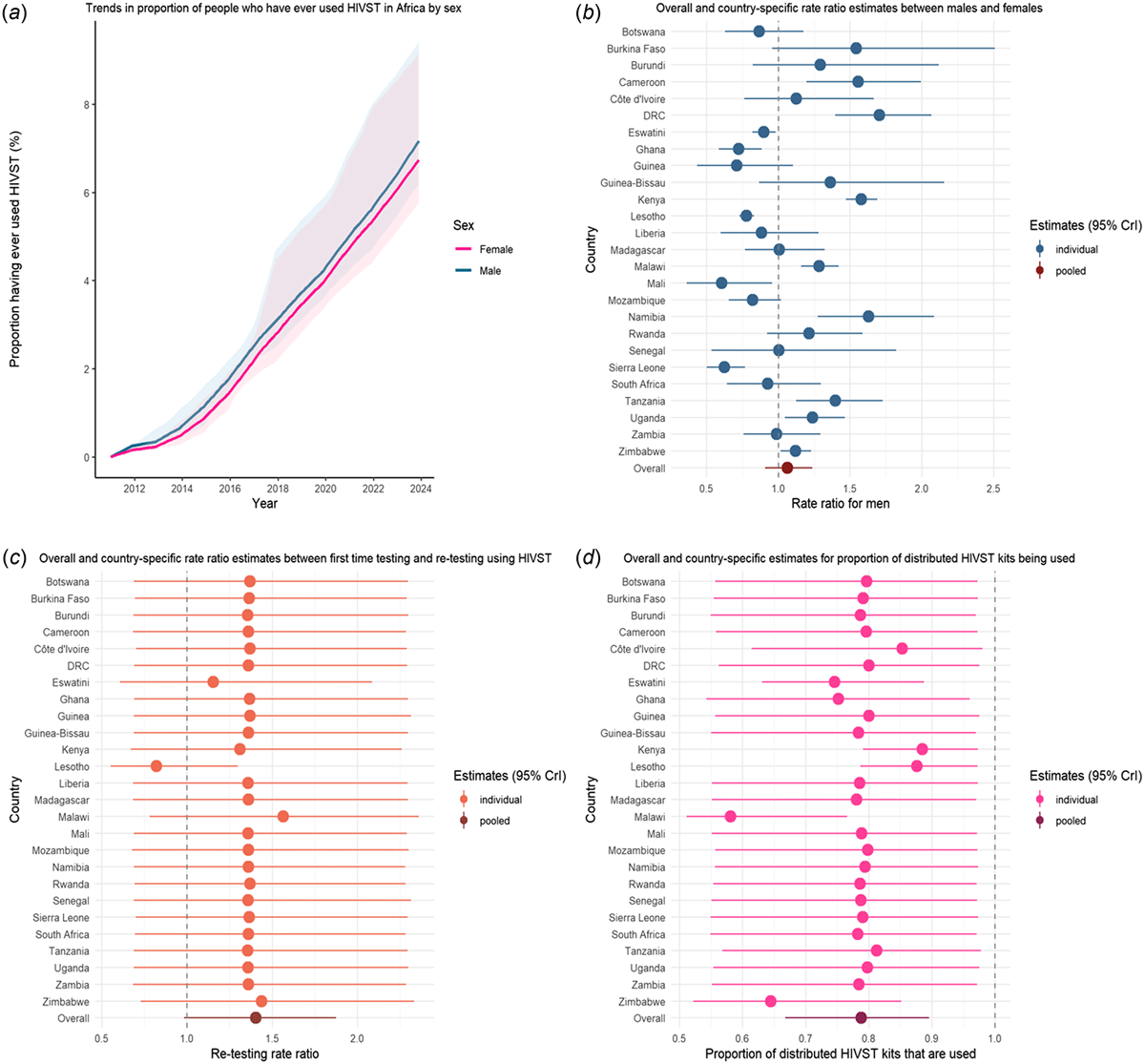
PP04.10 – Adverse Birth Outcomes in Pregnant Women Receiving Fewer vs Standard 3-Dose Benzathine Penicillin G for Late Latent or Syphilis of Unknown Duration
Dr. Chibuzor M. Babalola1, Mandisa Mdingi2, Freedom Mukomana2, Msindisi Gqirana2, Dr Christina A. Muzny3, Dr Christopher M. Taylor4, Dr Andrew Medina-Marino5, Dr Jeffrey D. Klausner1
1University of Southern California, Los Angeles, United States.
2Foundation for Professional Development, East London, South Africa.
3University of Alabama at Birmingham, United States.
4Louisiana State University, United States.
5Desmond Tutu Health Foundation, Cape Town, South Africa
Background: In South Africa, syphilis screening in pregnancy is routine, with a 3-dose regimen of intramuscular benzathine penicillin G (BPG) administered weekly after a positive rapid treponemal diagnostic test. Pregnant women with syphilis are treated as having late latent or unknown-duration disease due to limited clinical history and delayed confirmatory results. However, patient- and healthcare-related factors, including missed visits and supply shortages, can result in incomplete regimens by delivery. We explored whether fewer BPG doses increase the risk of adverse birth outcomes.
Methods: Nested within the Philani study (NCT04446611) in East London, South Africa, which investigates screening strategies for sexually transmitted infections and impact on adverse birth outcomes, we conducted a chart review of women with singleton pregnancies treated for syphilis per routine care. We identified preterm birth, low birth weight, or stillbirth outcomes, comparing women who received fewer doses (2 or 1) of BPG before delivery to those who received the full 3-dose regimen.
Results: Among 1,888 pregnancies, 92 (4.9%) were treated for syphilis. Of these, 24 (26.1%) experienced an adverse birth outcome. Dosing data have been retrieved for 38 women to date. Among the 38, 10 received fewer doses (2 doses: n = 2; 1 dose: n = 8), while 28 received 3 doses. Adverse outcomes (all being preterm birth or low birth weight) occurred in 26.3% of this subset (10/38); 20% in the fewer-dose group (2/10) vs 28.6% in the 3-dose group (8/28) (Risk Difference: –8.6%; 95% CI: −38.5%, 21.3%; Relative Risk: 0.70; 95% CI: 0.18, 2.73).
Conclusion: In this small cohort, receiving fewer BPG doses was not associated with worse adverse-birth-outcomes. Although limited by a small sample and statistical uncertainty, our findings preliminarily support the potential non-inferiority of reduced-dose regimens in late maternal syphilis or syphilis of unknown duration. Larger studies are needed to clarify these findings and optimize syphilis care in this population.
PP04.100 – Sexual Behavior, Microbiome Composition, and HPV16 Prevalence in Newly Formed Couples from Montréal Canada
Dr. Ruth Mwatelah1
1McGill University, Montreal, Canada.
Background: Vaginal dysbiosis has been associated with human papillomavirus (HPV) infection. We assessed among newly formed couples the association of 1) sexual behavior and douching with the microbiome and 2) microbiome with HPV16 prevalence.
Methods: The HITCH Cohort Study followed 18–24-year-old female university students and their male partners in Montréal, Canada (2005–2011). Current analyses are based on a pilot study of 256 samples obtained at the 2nd study visit (192 self-collected vaginal, 64 nurse-collected penile/scrotal). The microbiome was characterized using 16s rRNA, sequencing the V5-V6 region. Bioinformatics analysis was done using the ANCHOR pipeline. We used logistic regression models to estimate odds ratio (OR) and 95% confidence intervals (CI). We used the Jaccard index to measure beta diversity and the Shannon index to measure alpha diversity of the microbiome.
Results: The median age (interquartile range) was 21 (20,22) for women and 22 (20,24) for men. Among men, 34% had Corynebacterium tuberculostearicum, 20% had Lactobacillus crispatus and Lactobacillus iners, 13% had Finegolda magna, and 7% had Gardnerella spp. Most women (70%) had Lactobacillus dominant microbiome; 29% had Gardnerella and Prevotella species combined. The prevalence of HR-HPV and HPV16 among men and women was 36% (93/256) and 15% (37/256), respectively. The mean Jaccard dissimilarity was similar between the couples (0.83) and among random dyads (0.78). Alpha and beta diversity were not associated with HPV16 positivity in males (Alpha: OR:1.47, CI: 0.17–12.97; Beta: OR:1.23, CI: 0.53–2.82) and females (Alpha: OR:1.09, CI: 0.44–2.68; Beta: OR: 1.09, CI: 0.84–1.42). Douching among females was associated with increased alpha diversity (OR: 2.4, CI: 0.39–4.45).
Conclusion: This pilot study lays the groundwork for further exploration for microbiome transmission and HPV dynamics; additional data (2180 vaginal, 946 penile, from 5 study visits) and longitudinal analyses of the cohort are forthcoming.
PP04.101 – Determinants Sexual Behavior and STIs Among Youths in Molyko-Buea in Cameroon: A Cross-Sectional Study
Mr. Cyril Abane Ndumbe1, Dr Betrand Tambe Ayuk1, Dr Julie Nchung Ashu1
1University of Buea, Buea, Cameroon.
Background: Reproductive health is a very important aspect of public health. Young people go into sexual activities without knowing various aspects of their reproductive health. This therefore leads most of them to unwanted pregnancies, abortion, and sexually transmitted infections. The objective of this study is to assess the determinants of sexual and reproductive health among youths in Molyko-Buea.
Description: This study is a community-based cross-sectional study that was conducted among youths in Molyko-Buea selected using a multistage sampling method. Data was collected using a questionnaire made up of 4 sections that is socio-demographic characteristics, knowledge, attitude, and practice. Statistical package for social sciences (SPSS) version 26 was used to analyze descriptive statistics, chi-square test, and logistic regression, with a P-value < 0.05 considered significant.
Results: Among the 700 youths who participated in this study, 62% of the participants had good knowledge of reproductive health, 58% had a positive attitude towards reproductive health, and 84% had poor practices towards reproductive health. Some of the factors that were significantly associated with sexually transmitted infections were the low level of education, use of injectable contraceptives and involvement in sexual intercourse (P < 0.05).
Conclusion: The findings of this study show that more than half of the participants had good knowledge and positive attitudes towards reproductive health, but there are still some gaps in such knowledge, and attitude which still needs interventions. Also, most of the participants had poor practices towards reproductive health. Finally, the findings also show that low level of education, use of injectable contraceptives and involvement in sexual intercourse were some associated risk factors for sexually transmitted infection.
PP04.102 – Assessing Parameter Importance in Models Guiding the Rollout of a New Gonorrhea Treatment in Varying Country Contexts
Dr. Kirstin Oliveira Roster1, Ms Eva Gorenburg2, Mr Dennis Partl3,4,5, Dr Nanina Anderegg5, Prof. Pia Abel zur Wiesch6, Prof. Roger Kouyos3,4, Prof Nicola Low5, Prof Yonatan Grad1
1Harvard T. H. Chan School of Public Health, Boston, United States.
2Program in Human Biology, Stanford, United States.
3University of Zurich, Zurich, Switzerland.
4University Hospital Zurich, Zurich, Switzerland.
5University of Bern, Bern, Switzerland.
6University of Tromsø, Tromsø, Norway.
Background: Gonorrhea is a major public health concern, due to its high global incidence of infections and increasing challenges in treatment. Zoliflodacin, a new gonorrhea treatment in development for global use promises to reduce reliance on ceftriaxone, the only remaining antibiotic for gonorrhea treatment. However, the optimal strategy for introduction of a new antibiotic to minimize infections and resistance is unknown. Decision-making is complicated by limited surveillance of resistance, uncertainty in the natural history of gonorrhea, and wide variation in epidemiology and sexual behavior among countries.
Methods: We used a compartmental model of gonorrhea transmission among men who have sex with men to evaluate the sensitivity of antibiotic rollout strategies to changes in epidemiological and behavioral variables. We considered several zoliflodacin rollout strategies against a baseline scenario of ceftriaxone monotherapy and ranked strategies by gonorrhea incidence and useful lifespan of antibiotics. The strategies included combination therapy of ceftriaxone and zoliflodacin; random allocation of zoliflodacin to 50% or 20% of cases; reserve strategies with either slow or quick introduction of 50% or 100% zoliflodacin treatment after the prevalence of ceftriaxone resistance reaches 5%; and gradual introduction to 50% or 100% use without holding zoliflodacin in reserve.
Results: Combination therapy and 50% allocation of zoliflodacin were the highest-performing strategies in most parameter regimes (Fig. 1). Both the policy objective and the parameter regime influenced strategy rankings. Asymptomatic screening frequency and the starting prevalence of ceftriaxone resistance had the highest impact of the parameters we considered, while population heterogeneity and sexual behavior did not alter rankings.
Conclusion: Epidemiological settings, including the prevalence of ceftriaxone resistance, influenced the optimal antibiotic rollout strategy, suggesting that introduction of zoliflodacin should be targeted to country-specific contexts. Focused data collection, including surveillance of resistance, will reduce uncertainty in decision-making.
Ranking of zoliflodacin rollout strategies for varying parameter values. Strategies are ranked best (top) to worst (bottom) by their average performance along two outcome measures, the total gonorrhea incidence and the useful lifespan of zoliflodacin, for varying levels of (a) starting prevalence of ceftriaxone resistance, (b) the assortativity of mixing among sexual activity groups, (c) multiples of partner change rates, (d) the symptomatic proportion of gonococcal infections, (e) the asymptomatic screening frequency, and (f) the number of sexual activity population subgroups stratified by partner change rates. Colors represent rankings for different strategies: combination therapy of ceftriaxone and zoliflodacin (yellow); random allocation strategies, where a share of patients – either 50% (dark red) or 20% (light red) – is treated with zoliflodacin and the remaining cases are treated with ceftriaxone; gradual introduction strategies, where zoliflodacin becomes available gradually to either 50% (light purple) or 100% (dark purple) of the population over the course of 8 years; and finally, reserve strategies, where zoliflodacin is held in reserve until the prevalence of ceftriaxone resistance reaches 5%, and then is introduced either quickly (light green) or gradually to either 50% (is introduced to replace all or some ceftriaxone use.
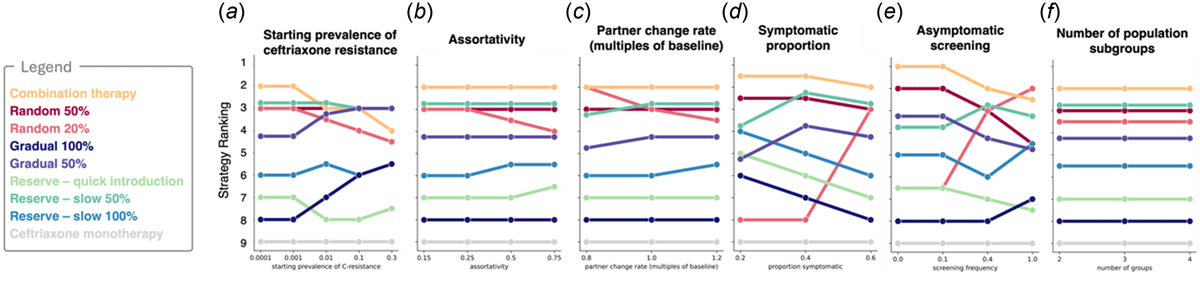
PP04.103 – The Prevalence of Adverse Drug Reactions and Associated Factors Among Pediatric Patients Living with HIV on Antiretroviral Therapy in Sub-Saharan African Countries – A Systematic Review and Meta-Analysis
Dr. Bukola Omotoso1
1University of The Free State Bloemfontein 9300, South Africa, Bloemfontein, South Africa.
Background: Despite the remarkable progress towards achieving the UNAIDS 95-95-95 (Joint United Nations Program on HIV/AIDS) targets in people living with HIV, the pediatric population seems to be lagging, especially in developing countries such as sub-Saharan Africa (SSA). Notably, the greatest burden of HIV infection is in the SSA countries. This systematic review aims to map out the prevalence of adverse drug reactions (ADRs) and associated factors among HIV-positive pediatric patients on ART in SSA countries.
Methods: This review is based on a systematic and extensive search of PubMed, Scopus, CINAHL, Web of Science, EBSCOHost, and Google Scholar. The protocol for this review was registered in PROSPERO (Registration ID CRD42024535907).
Results: A total of 9 articles were included. The pooled estimate of ADRs among children on ART was statistically significant (0.26 (95% CI 0.15, 0.36); P-value <0.001) with high heterogeneity. The types of ADRs reported in the included studies are gastrointestinal, dermatology, central nervous system, hematology, liver pathology, metabolic disorder, heart disease, and hormonal imbalance symptoms. Some of the factors associated with the occurrence of ADRs include treatment duration, the combination of ART used, sex, age, malnutrition, and compliance. The pooled prevalence of mortality among children on ART was statistically significant, with high heterogeneity.
Conclusion: The study highlighted the prevalence and factors associated with ADRs in HIV-positive children on ART in the SSA countries. The prevalence of adverse drug reactions to antiretroviral therapy in children is highly significant in the meta-analyzed studies. As the SSA countries battle to achieve the UNAIDS 95-95-95 targets in this vulnerable population, findings from this review can help inform policies on integrating spontaneous reporting of ADRs and pharmacovigilance into the service delivery component of pediatric ART. This intervention will support patient retention in care, as ADRs are a significant cause of medication non-adherence.
PP04.104 – Preferences of Men Who Have Sex with Men Towards the Distribution of HIV Self-Test Kits Through Social Networks: A Discrete Choice Experiment
Ms. Ying Zhang1,2, Prof Eric PF Chow1,2,3, Dr Tiffany R. Phillips1,2, Prof Christopher K. Fairley1,2, Prof. Dr. Jason Ong1,2,4
1Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
4London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: Social network distribution of HIV self-test (HIVST) kits utilizes personal connections within social networks to increase HIV testing among marginalized populations, such as men who have sex with men (MSM), especially those hard to reach through traditional methods. Using a discrete choice experiment (DCE), we identified factors influencing MSM preferences for distributing HIVST kits.
Description: An online DCE survey was conducted among MSM in Australia (December 2023–May 2024), recruited via online/offline advertisements. Participants completed seven choice sets, each containing two hypothetical scenarios related to distributing HIVST kits described by attributes such as cost, location, training, support system, and self-reporting methods. Mixed logit models with interactions and latent class analysis explore preference heterogeneity.
Results: There were 251 participants, including 140 overseas-born MSM, with a mean age of 36.5 (SD = 11.9). Participants who did not speak English as their first language (29/251, 12%) showed a lower preference for paid HIVST kits ($30 or $60 out-of-pocket cost for three kits) and online video chats with sexual health professionals as pre-test support. Overseas-born participants also preferred not to attend 30-min or 1-h training sessions on distributing HIVST kits to social contacts. Instead of accessing HIVST kits from hospitals, they favoured obtaining them from pharmacies. Class 1 participants (61.7%) were willing to pay up to AUD 30 for three kits, while Class 2 (38.3%) strongly resisted costs and self-reporting results by phone.
Conclusion: To increase participation in social network HIVST kit distribution, kits should be free or subsidized. Tailored support systems should prioritize overseas-born MSM with limited English proficiency.
PP04.105 – HIV, Viral Hepatitis, and Syphilis Self-Testing Among Adolescents and Young Adults: A Systematic Review and Meta-Analysis
Ms. Ying Zhang1,2, Mr James Tapa1,2, Dr Cheryl C. Johnson3, Dr Tiffany R. Phillips1,2, Prof Christopher K. Fairley1,2, Dr Wole Ameyan3, Dr Maeve B. Mello3, Prof Eric PF. Chow1,2, Dr Thato Chidarikire4, Prof. Dr. Jason Ong1,2,5
1School of Translational Medicine, Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
3Global HIV, Hepatitis and STI Programmes, World Health Organization, Geneva, Switzerland.
4South Africa Country Office, World Health Organization, Pretoria, South Africa.
5Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: Adolescents and young adults (age 10–24 years) bear a substantial burden of HIV and sexually transmitted infections (STI) globally. Self-testing has been shown to increase access to and uptake of testing and enhance engagement in onward prevention and/or treatment services. We systematically reviewed literature regarding self-testing for HIV, viral hepatitis (HBV/HCV), and syphilis among adolescents and young adults, focusing on its usability, feasibility, and acceptability.
Description: We searched six databases between January 2010 and October 2023 and included all studies investigating self-testing for HIV, viral hepatitis and syphilis among adolescents and young adults. A random-effects meta-analysis was conducted to pool data across the infections, as the evidence was deemed sufficiently similar. Outcomes assessed included testing uptake, the proportion of first-time testers and linkage to prevention/care. Qualitative data were narratively synthesized.
Results: We identified 89 relevant studies, of which most were in Africa (57/89, 64%) and lower-middle-income countries (34/89, 38%). Meta-analysis of 27 studies (n = 28,787 individuals) demonstrated that 79% (95% CI: 69–87%, I2 = 99%) of adolescents and young adults who were offered HIV or syphilis self-test completed the test. Meta-analysis of five studies (n = 4117) indicated 62% (95% CI: 53–71%, I2 = 83%) were first-time testers. No studies reported completion rates for viral hepatitis self-testing. Adolescents and young adults were highly accepting of self-testing and found it easy to use.
Conclusion: Self-testing is a safe, acceptable and effective way to increase access to HIV, viral hepatitis and syphilis testing among adolescents and young adults. Countries should review and revise their national policies to support self-testing access and uptake among young people to maximize public health impact.
PP04.106 – Sexually Transmitted Infections Among Young Women Employed in Domestic Work in Central Uganda
Dr. Annet Onzia Aketoko1, Dr Matthew M. Hamill2, Miss Vivian Nakate1, Mr Joseph Musaazi1, Dr. Justine Bukenya3, Dr. Eric Ssegujja3, Dr. Rosalind Parkes-Ratanshi1, Dr. Ajeru Patricia4, Dr. Agnes Kiragga5, Dr. Andrew Kambugu1, Dr. Yukari C. Manabe2, Dr. Barbara Castelnuovo1
1Infectious Diseases Institute, Makerere University, Kampala, Uganda.
2Division of Infectious Diseases, Johns Hopkins University, Baltimore, Unites States of America.
3Makerere University School of Public Health, Kampala, Uganda.
4Kampala International University, Kampala, Uganda.
5African Population and Health Research Center, Nairobi, Kenya.
Introduction: Adolescent girls and young women (AGYW) employed in household domestic work in low-income settings remain an understudied, vulnerable population due to inequitable power dynamics and social isolation which may increase their risk of acquiring sexually transmitted infections (STIs). We determined STI prevalence and associated demographic and socio-behavioural factors in this population.
Methods: A community-based cross-sectional study enrolled female domestic workers aged 14–24 years in Kampala metropolitan area. Structured questionnaires were used to collect demographic and behavioural characteristics and self-collected vaginal swabs to test for Neisseria gonorrhoeae (NG) and Chlamydia trachomatis (CT) using a molecular test, GeneXpert (Cepheid, HBDC, Maurens-Scopont, France). HIV and syphilis antibody testing were conducted using the SD Bioline HIV/Syphilis Duo-testing kit (Abbott, Illinois, US), with confirmatory rapid algorithmic testing done for any reactive HIV screening assay. Sexual abuse was defined as non-consensual conduct involving forcing or coercion into vaginal, anal and oral sex. Summary statistics were calculated and modified Poisson regression assessed factors associated with having an STI by calculating prevalence ratios (PR).
Results: Of 262 participants enrolled the median (IQR) age was 20 years (18–23), 33.2% had at least 1 STI: 2% NG, 28% CT, 6% had a reactive treponemal antibody for syphilis, and 5% HIV; 14.9% had > one STI. Lower education level (aPR: 1.73, 95% CI: (1.16–2.57); P = 0.007), non-cash remuneration (aPR: 2.26, 95% CI: 1.04–4.92; P = 0.04), transactional sex in past 12 months (aPR: 1.43, 95% CI: 1.01–2.04; P = 0.045) and alcohol consumption in past 6 months (aPR: 1.72, 95% CI: 1.12–2.64; P = 0.013) were associated with STIs. Reported sexual abuse was negatively associated with STIs (aPR: 0.48, 95% CI: 0.28–0.83; P = 0.008) as shown in Table 1.
Conclusion: The high prevalence of undiagnosed STIs and behaviours associated with STI acquisition in AGYW employed in domestic work warrants advocacy for expanded testing and treatment opportunities and targeted STI/HIV prevention interventions to reduce incident HIV in this population.
PP04.107 – Genital Herpes Trends in Commercially Insured Patients, Merative Marketscan, United States (2012–2022)
Dr. Sancta St. Cyr1, Brian Emerson1, Dr. William Pearson1, Dr. Lindley Barbee1, Professor Ina Park1
1U.S. Centers for Disease Control and Prevention (Division of STD Prevention), Atlanta, United States.
Background: Genital herpes (GH), caused by herpes simplex virus types 1 and 2 (HSV-1 and HSV-2), is a life-long sexually transmitted infection frequently presenting with painful anogenital lesions. In the United States (US), 572,000 estimated incident GH cases occur annually among 18–49-year-olds. Since GH is not a reportable condition in the US, large datasets are often used to monitor trends.
Methods: The 2022 Merative MarketScan healthcare administrative claims dataset, covers ~20% of employer-insured patients in the US. We used 2012–2022 data to characterize trends in diagnosed GH-related episodes in this population. GH-related episodes were identified using five International Classification of Diseases (ICD)-9 (2012–2022) and 10 ICD-10 (2015–2022) codes that represent diagnoses of herpes lesions at any anogenital site. Changes across years were analyzed with Joinpoint by sex, age group, and US region.
Results: The total number of GH-related episodes decreased 45% (2012: 82,121; 2022: 45,411), but the overall proportion of the population with at least one GH-related episode annually increased (2012: 0.20%; 2022: 0.26%, P-value: <0.001). The proportion of men (2012: 0.12%; 2022: 0.14%, P-value: <0.001), women (2012: 0.27%; 2022: 0.35%, P-value: <0.001) and age groups 35–44 (2012: 0.30%; 2022: 0.35%, P-value: <0.001), 45–54 (2012: 0.22%; 2022: 0.33%, P-value: <0.001), and 55–64 (2012: 0.15%; 2022: 0.27%, P-value: <0.001) with GH-related episodes all increased. The regions with statistically significant increases in the proportion of the population with GH-related episodes were the South (2012: 0.22%; 2022: 0.28%, P-value: <0.001) and Midwest (2012: 0.14%; 2022: 0.21%, P-value: <0.001).
Conclusion: The proportion of the population with GH-related episodes among these commercially-insured patients increased between 2012-2022, except among those <35 years and in the Northeast and West. Additional data are needed to understand the fluctuations in MarketScan participation and possible causes of these GH patterns, including testing changes, sexual practice shifts, and incidence/prevalence of HSV-1 and HSV-2 caused infections.
PP04.108 – Neisseria Gonorrhoeae Antimicrobial Resistance in South Africa, 2007–2023: Implications for National Sentinel Surveillance
Mr. Dennis K. Partl1,2,3, Dr. Nanina Anderegg3, Dr. Etienne E. Müller4, Ms. Venessa Maseko4, Dr. Tendesayi Kufa4,5, Dr. Kirstin Oliveira Roster6, Prof. Yonatan H. Grad6, Prof. Pia Abel zur Wiesch7, Prof. Roger D. Kouyos1,2, Prof. Nicola Low3
1University of Zurich, Zurich, Switzerland.
2University Hospital Zurich, Zurich, Switzerland.
3University of Bern, Bern, Switzerland.
4National Institute for Communicable Diseases, Johannesburg, South Africa.
5University of the Witwatersrand, Johannesburg, South Africa.
6Harvard University, Boston, United States of America.
7University of Tromsø, Tromsø, Norway.
Background: South Africa has among the highest levels of gonorrhea worldwide. Neisseria gonorrhoeae resistance develops readily and recommended first line gonorrhea treatments in South Africa have changed accordingly: in 2008, from ciprofloxacin to cefixime, and in 2014 to ceftriaxone. Azithromycin has been in the regimen for genital discharge syndrome since 2014.
Methods: We analyzed sentinel surveillance data collected by the South African National Institute for Communicable Diseases from 2007 to 2023. Samples from patients with male urethritis syndrome were cultured. Confirmed N. gonorrhoeae isolates had minimum inhibitory concentrations (MIC, mg/L) of antimicrobials determined by Etest or agar dilution, interpreted using European Committee on Antimicrobial Susceptibility Testing (EUCAST) breakpoints. We described MICs using medians (interquartile range, IQR) and percentages resistant (95% confidence intervals, CI). For antimicrobials with sufficient data, we estimated resistance trends using logistic regression models, incorporating splines to allow flexibility in the shape of the distribution.
Results: MIC data were available for: ceftriaxone (n = 4844, 2007–2023), cefixime (n = 4496, 2008–2023), ciprofloxacin (n = 2121, 2007–2016) and azithromycin (n = 2824, 2011 and 2014–2023). MIC distributions were stable for ceftriaxone (2023 median 0.004 mg/L, IQR 0.002–0.004) and cefixime (0.016, 0.016–0.016), with the last resistant isolate in 2019 (cefixime, 0.25) (Fig. 1). Ciprofloxacin resistance increased from 27% (95% CI 21–35%) in 2007 to 75% (69–80%) in 2016 and was predicted at 91% (69–98%) in 2023. Azithromycin resistance increased from 0.2% (0–0.6%) in 2020 to 3.3% (1.5–5.2%) in 2023.
Conclusion: N. gonorrhoeae MICs to ceftriaxone are not increasing in South Africa. Azithromycin resistance is increasing, reducing potential effectiveness of a combination regimen. Nearly all N. gonorrhoeae isolates were predicted to be resistant to ciprofloxacin by 2023. This finding is consistent with reports of ongoing prescribing, despite its longstanding absence from guidelines. Routine enhancement of sentinel surveillance with prescription data, and interventions for South African physicians could improve antimicrobial stewardship.
MICs for N. gonorrhoeae isolates from patients with male urethritis syndrome in South Africa, for ceftriaxone (a), cefixime (b), ciprofloxacin (c) and azithromycin (d). Colored areas from blue through red show proportions of isolates with MIC at each doubling dilution for years with available data. Panels C and D: black lines show the predicted proportion of resistance (EUCAST breakpoints) from logistic regression models, incorporating splines; confidence intervals shown as grey shaded area bordered by black dashed lines for ciprofloxacin, extrapolated to 2023 (panel C) and azithromycin, with inset enlarged for 2020–2023 (d). The white dashed line in panel C in 2008 is when ciprofloxacin was removed from treatment guidelines.
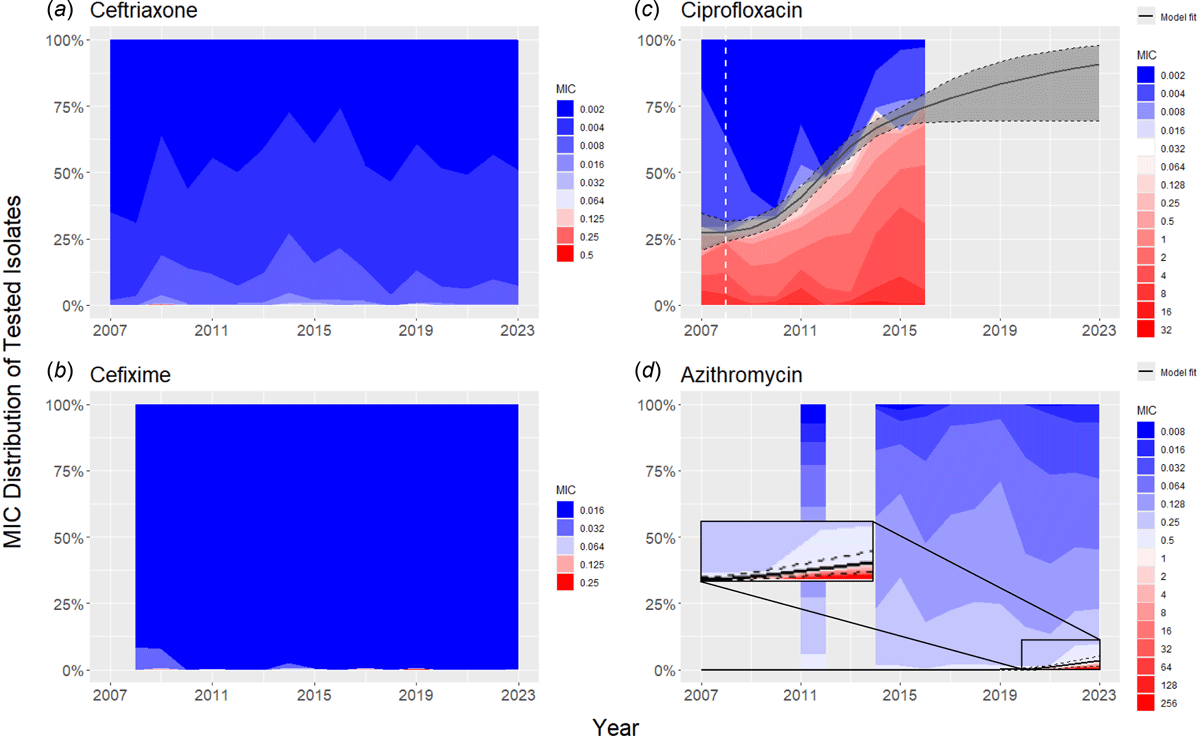
PP04.109 – Factors Associated with Chlamydia Trachomatis and Neisseria Gonorrhoeae Infection in Brazil, 2022–2024
Dr. Amanda Krummenauer1, Dr. Ana Pascom1, Dr Álisson Bigolin1, Dr Amanda Alencar Cabral Morais1, Dr Leonor Henriette de Lannoy1, Dr Mayra Gonçalves Aragón1, Dr Luiz Fernando Aires Junior1, Dr Pâmela Cristina Gaspar1
1Brazilian Ministry Of Health, Brazilia, Brazil.
Background: Early detection and treatment of Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) are essential to prevent complications and reduce transmission. Since 2022, the Brazilian Ministry of Health has been monitoring molecular tests for CT/NG detection in national laboratories. This study describes the profile of people with CT/ NG infections and associated factors.
Methods: Data from the national laboratory management platform were analyzed from September/2022 to November/2024. Specimens for molecular tests were collected from public health services, including people living with HIV/Aids, PrEP users, and symptomatic individuals. Logistic regression identified factors associated with CT/NG infection, calculating Odds Ratios (OR) and Adjusted Odds Ratios (aOR) for age, race/ethnicity, geographic region, Municipal Human Development Index (IDHM), and Social Vulnerability Index (IVS).
Results: Among 79,229 tested individuals, 5,652 (7.1%) were detected for CT, 5,413 (6.8%) for NG; of these, 1,301 (1.6%) were co-infections (Table 1). Most infected individuals (64.2%) were male and 48.8% identified as white. Detection rates for CT and NG were 7.0% and 2.9% in women, and 7.2% and 9.0% in men, respectively. Factors associated with higher likelihood of infection (CT and/or NG) included age ≤24 years (aOR: 2.00, 95% CI: 1.91–2.09), male sex (aOR: 1.43, 95% CI: 1.36–1.50), and non-white race/ethnicity. The Midwest region (aOR: 1.92, 95% CI: 1.74–2.12), along with higher IVS and IDHM strata were also associated with increased infection risk.
Conclusion: Young people, men, and those of non-white race/ethnicity were more likely to be infected with CT and/or NG. Associations with higher IDHM strata, which reflect longevity, education, and income, as well as with higher IVS, indicating the degree of social inequality, showed that although these cases are linked to more developed municipalities, they are also unequal. These findings highlight the importance of addressing both sociodemographic and geographic inequalities when designing prevention strategies and improving public health policies for STI control.
| Characteristic | CT Only (N = 4,351) | NG Only (N = 4,112) | CT/NG coinfected (N = 1,301) | CT/NG uninfected (N = 69,465) | Crude OR (95% CI) | Adjusted OR (95% CI) | |
|---|---|---|---|---|---|---|---|
| Age, years | |||||||
| ≤24 | 1,690 | 1,251 | 613 | 15,968 | 1.94 (1.87–2.01) | 2.00 (1.91–2.09) | |
| >24 | 2,559 | 2,758 | 651 | 51,985 | Reference | ||
| NA | 102 | 103 | 37 | 1,512 | |||
| Sex | |||||||
| Female | 1,697 | 538 | 288 | 25,777 | Reference | ||
| Male | 2,651 | 3,573 | 1,013 | 43,646 | 1.69 (1.66–1.72) | 1.43 (1.36–1.50) | |
| NA | 3 | 1 | 0 | 42 | |||
| Race/ethnicity | |||||||
| White | 1,853 | 1,591 | 434 | 34,817 | Reference | ||
| Black | 495 | 441 | 173 | 5,407 | 1.84 (1.78–1.91) | 1.42 (1.32–1.54) | |
| Mixed | 1,476 | 1,485 | 512 | 21,211 | 1.47 (1.44–1.50) | 1.25 (1.18–1.31) | |
| Asian | 468 | 538 | 170 | 7,231 | 1.46 (1.42–1.51) | 1.25 (1.16–1.35) | |
| Indigenous | 9 | 4 | 1 | 193 | |||
| NA | 50 | 53 | 11 | 606 | |||
| Region of residence | |||||||
| South | 1,408 | 704 | 211 | 26,205 | Reference | ||
| Midwest | 241 | 355 | 116 | 3,227 | 2.49 (2.41–2.58) | 1.92 (1.74–2.12) | |
| Southeast | 1,840 | 2,298 | 736 | 25,690 | 2.14 (2.07–2.21) | 1.79 (1.68–1.89) | |
| Northeast | 643 | 532 | 184 | 7,734 | 1.98 (1.92–2.05) | 1.55 (1.41–1.69) | |
| North | 219 | 223 | 54 | 6,609 | 0.84 (0.82–0.88) | 0.68 (0.61–0.76) | |
| Municipal Human Development Index | |||||||
| Very high (0.800–1.000) | 1,418 | 1,579 | 480 | 22,711 | Reference | ||
| High (0.700–0.799) | 2,493 | 2,136 | 697 | 38,153 | 0.91 (0.88–0.94) | 0.75 (0.71–0.79) | |
| Medium (0.600–0.699) | 358 | 317 | 94 | 6,791 | 0.74 (0.71–0.77) | 0.64 (0.58–0.70) | |
| Low (0.500–0.599) | 79 | 78 | 28 | 1,715 | 0.70 (0.69–0.73) | ||
| Very low (0.000–0.499) | 2 | 2 | 0 | 72 | |||
| NA | 1 | 0 | 2 | 23 | |||
| Social Vulnerability Index | |||||||
| Very low (0–0.199) | 394 | 182 | 56 | 8,128 | Reference | ||
| Low (0.200–0.299) | 2,628 | 2,559 | 815 | 42,129 | 1.83 (1.77–1.90) | 1.37 (1.26–1.48) | |
| Medium (0.300–0.399) | 1,162 | 1,197 | 380 | 15,086 | 2.33 (2.26–2.42) | 1.95 (1.77–2.14) | |
| High (0.400–0.499) | 114 | 122 | 33 | 2,669 | 1.30 (1.25–1.34) | 1.27 (1.07–1.51) | |
| Very high (0.500–1.000) | 52 | 52 | 15 | 1,430 | |||
| NA | 1 | 0 | 2 | 23 | |||
NA: Data Not Available; CT: Chlamydia trachomatis; NG: Neisseria gonorrhoeae; 95% CI: 95% confidence interval; OR: odds ratio; P-value ≤0.05.
Source: National Laboratory Management Platform.
PP04.11 – Adverse Birth Outcomes Among Syphilis-Treated Versus Syphilis-Seronegative Pregnant Women in East London, South Africa
Dr. Chibuzor M. Babalola1, Mandisa Mdingi2, Freedom Mukomana2, Msindisi Gqirana2, Dr Christina A. Muzny3, Dr Christopher M. Taylor4, Dr Andrew Medina-Marino5, Dr Jeffrey D. Klausner1
1University of Southern California, Los Angeles, United States.
2Foundation for Professional Development, East London, South Africa.
3University of Alabama at Birmingham, United States.
4Louisiana State University, United States.
5Desmond Tutu Health Foundation, Cape Town, South Africa.
Background: Syphilis in pregnancy remains a leading cause of adverse birth outcomes globally. Screening and treatment with benzathine penicillin G is highly effective. However, residual risks may exist in treated mothers due to factors such as delayed treatment initiation, reinfection, or inadequate maternal immune response.
Methods: We compared adverse birth outcomes in syphilis-treated versus syphilis-seronegative mothers, using data from singleton pregnancies (2021–2024) across four primary healthcare facilities in East London, South Africa. Women were identified by syphilis serostatus at their first antenatal visit (<27 weeks) and/or a third trimester visit (30–34 weeks). We calculated frequencies and risk differences (RDs) in both groups with 95% confidence intervals (CIs) for preterm birth (<37 weeks) or low birth weight (<2,500 g) among live births, and for stillbirths.
Results: Among 1,888 singleton pregnancies, 92 (4.9%) were treated for syphilis based on a positive rapid treponemal antibody test, with 78% (n = 72) diagnosed and treated at the first antenatal visit. Overall, adverse birth outcomes were observed in 22.5% (n = 425). Comparing syphilis-treated to syphilis-seronegative pregnancies (Table 1), adverse birth outcomes occurred in 26.1% vs 22.3% (RD: +3.8%; 95% CI: –5.4%, 12.9%). Preterm birth was observed in 15.4% vs 16.5% (RD: –1.1%; 95% CI: –8.8%, 6.5%), low birth weight in 14.7% vs 11.6% (RD: +3.1%; 95% CI: –4.4%, 10.7%), composite preterm birth or low birth weight in 25.3% vs 20.3% (RD: +5.0%; 95% CI: –4.1%, 14.1%), and stillbirth in 1.1% vs 2.6% (RD: –1.5%; 95% CI: –3.7%, 0.8%).
Conclusion: In this South African cohort with a relatively high syphilis prevalence, adverse birth outcomes were frequent. However, no excess risks were observed among syphilis-treated pregnancies; the majority treated before the third trimester. Our findings reinforce the effectiveness of antenatal syphilis screening and treatment in mitigating risks to the fetus. Prioritizing syphilis screening and treatment programs remains essential in high-prevalence settings.
| Birth Outcomea | Total | Treated for Syphilisb | Seronegative | Risk Difference (95% CI) | |
|---|---|---|---|---|---|
| Preterm Birth (N = 1841) | 303 (16.5%) | 14 (15.4%) | 289 (16.5%) | –1.1% (–8.8, +6.5) | |
| Low Birth Weight (N = 1756) | 207 (11.8%) | 13 (14.7%) | 194 (11.6%) | +3.1% (–4.4, +10.7) | |
| Preterm Birth or Low Birth Weight (N = 1841) | 378 (20.5%) | 23 (25.3%) | 355 (20.3%) | +5.0% (–4.1, 14.1) | |
| Stillbirth (N = 1888) | 47 (2.5%) | 1 (1.1%) | 46 (2.6%) | –1.5% (–3.7, +0.8) | |
| Any Adverse Birth Outcome (N = 1888) | 425 (22.5%) | 24 (26.1%) | 401 (22.3%) | +3.8% (–5.4, +12.9) |
Footnotes
a) Denominators:
- Stillbirth and any adverse birth outcome: N = 1888 (All pregnancies).
- Preterm Birth and composite preterm birth or low birth weight: N = 1841 (Live births only).
- Low birth weight: 85 Live births missing birthweight data are excluded.
b) Syphilis Cases:
- 92 treated for syphilis among all 1888 pregnancies (4.9%).
- 91 treated for syphilis among all 1841 live births (4.9%).
- 88 treated for syphilis among the 1756 live births contributing birthweight data (5.0%).
PP04.110 – Epidemiological Profile of Coinfections by Chlamydia Trachomatis and Neisseria Gonorrhoeae in Brazil, 2022–2024
Dr. Amanda Krummenauer1, Dr. Ana Pascom1, Dr Álisson Bigolin1, Dr Amanda Alencar Cabral Morais1, Dr Leonor Henriette de Lannoy1, Dr Mayra Gonçalves Aragón1, Dr Luiz Fernando Aires Junior1, Dr Pâmela Cristina Gaspar1
1Ministry of Health of Brazil, Brazilia, Brazil.
Background: The World Health Organization estimates 82 million gonorrhea and 129 million new chlamydia cases annually worldwide among adults. In Brazil, these infections are among the most prevalent STIs, highlighting the need for epidemiological studies. This study describes the profile of coinfected individuals in the country.
Methods: Cross-sectional study using data from the public national laboratory management platform for molecular biology tests detecting Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) from September/2022 to November/2024. Variables included age, sex, race/ethnicity, region, and sample type.
Results: A total of 79,229 individuals were tested for CT/NG, with 5,652 (7.1%) detected for CT infection and 5,413 (6.8%) for NG (Table 1). Among them, 1,301 (1.6%) were coinfected and included in this analysis. The median age of coinfected individuals was 25 years (IQR: 21–30), younger than the median of 29 years (IQR: 24–37) for all tested. Most coinfected cases were male (n = 1,013; 98.25%). The highest number of cases occurred among individuals who identified as mixed-race (n = 512; 2.07%), followed by white individuals (n = 434; 1.12%). Black individuals had the highest proportion of coinfections, with 173 cases (2.66%) among 6,516 tested. Nationwide, 341 municipalities across 26 federative units conducted sample collection. The Midwest and Southeast regions had the highest proportions of coinfections, with rates of 2.94% and 2.41%, respectively. Urine was the most collected sample (n = 738), but the highest proportion of coinfections was found in anorectal samples (2.88%).
Conclusion: Higher coinfection proportions were observed among men, youth, and Black or Mixed-race individuals. Additionally, the regions with the highest sample collections (South and Southeast) also had the highest white population proportions. These findings underscore the disproportionate burden of STIs on marginalized populations and emphasize the need to expand access to testing, particularly in underdiagnosed regions and groups, with the goal of reducing inequalities and strengthening STI surveillance in Brazil.
| Characteristic | CT/NG coinfected (N = 1,301) | Tested individuals (N = 79,229) | Proportion (%) | |
|---|---|---|---|---|
| Sex | ||||
| Female | 288 | 28,300 | 1.02 | |
| Male | 1,013 | 50,883 | 2.00 | |
| NA | 0 | 46 | 0 | |
| Race/ethnicity | ||||
| White | 434 | 38,695 | 1.12 | |
| Black | 173 | 6,516 | 2.66 | |
| Mixed | 512 | 24,684 | 2.07 | |
| Asian | 170 | 8,407 | 2.02 | |
| Indigenous | 1 | 207 | 0.48 | |
| NA | 11 | 720 | 1.53 | |
| Region of residence | ||||
| South | 211 | 28,528 | 0.74 | |
| Midwest | 116 | 3,939 | 2.94 | |
| Southeast | 736 | 30,564 | 2.41 | |
| Northeast | 8 | 9,093 | 0.09 | |
| North | 54 | 7,105 | 0.76 | |
| Type of biological sample | ||||
| Urine | 738 | 45,124 | 1.64 | |
| Anorectal swab | 306 | 10,620 | 2.88 | |
| Oropharyngeal swab | 44 | 8,798 | 0.50 | |
| Vaginal swab | 45 | 5,666 | 0.79 | |
| Endocervical swab | 41 | 5,368 | 0.76 | |
| Other | 127 | 3,653 | 3.48 | |
NA: Data Not Available; CT: Chlamydia trachomatis; NG: Neisseria gonorrhoeae.
Source: National Laboratory Management Platform.
PP04.111 – Routine Reporting of Negative Syphilis Test Results to Improve Estimation of Screening Coverage Among People Exposed to Syphilis – New York City (NYC)
Dr. Preeti Pathela1, Kimberly Johnson1
1NYC Department of Health and Mental Hygiene, New York, United States.
Background: NYC Health Code required reporting of all positive and indeterminate syphilis test results, and only some negative test results, for NYC residents until December 2023. A health code amendment requires laboratories to now report all negative syphilis test results also, which we used to examine screening coverage among sex partners of syphilis case-patients.
Methods: We extracted surveillance, case investigation, and partner services data on reported syphilis case-patients in NYC from March to July 2024. We examined syphilis screening among their named partners, by self-reported testing status collected through partner interview versus recorded tests. We then examined variability in screening coverage among partners by race/ethnicity, age, and neighborhood poverty level (NPL), classified by the proportion of residents in a ZIP code with household incomes below federal poverty level: very high (>30%), high (20–<30%), medium (10–<20%), low (<10%).
Results: A total of 872 syphilis case-patients (292 cismen who have sex with men, 254 cismen who have sex with women only, 293 ciswomen, 3 transgender, 30 with unknown gender) had 204 named partners, of whom 149 (73%) were screened for syphilis, yielding 17 new diagnoses. Forty-one percent (61/149) of partners were identified as having been screened solely via negative test reporting, for an additional 69% ascertainment over what was available through interviews alone. Screening rates among non-Hispanic white partners (61%) were lower than among Hispanic (78%) and non-Hispanic Black (71%) partners. Screening coverage increased with increasing age (73% for ages <25 to 84% for ages >45 years). By NPL, screening coverage was lowest for partners living in very high poverty neighborhoods (72%).
Conclusions: Integration of negative syphilis test results into routine surveillance resulted in substantially improved documentation of syphilis screening among people exposed to syphilis. Such data can be used to identify areas and populations with lower screening levels for outreach and education.
PP04.112 – Syphilis Among Women of Reproductive Age and Pregnant Women – New York City (NYC), 2014–2023
Dr. Sarah Wondmeneh1, Kimberly Johnson2, Dr. Preeti Pathela2
1Centers For Disease Control and Prevention, Atlanta, United States.
2New York City Health Department, New York City, United States.
Background: Syphilis has increased among women of reproductive age (WRA) and pregnant women (PW) in the United States, corresponding with increases in congenital syphilis (CS) to levels not observed since the 1990s. We characterize WRA and PW with syphilis and describe CS cases potentially averted among PW with syphilis to better understand NYC’s syphilis epidemic.
Methods: We analyzed case reports among non-pregnant WRA (including persons with a reported sex or sex at birth of female) and PW aged 15–44 during 2014–2023. We described demographic and clinical characteristics of WRA and PW with syphilis (all stages); behaviors of those with primary and secondary (P&S) syphilis; and proportion of CS cases potentially averted among PW with syphilis, by neighborhood poverty level (Low/Medium: 0–20% below federal poverty level (FPL), High/Very High: >20% below FPL) and race/ethnicity.
Results: During 2014–2023, annual syphilis case reports increased 132% (473 to 1,095) among WRA and 78% (114 to 203) among PW. About 70% of WRA and PW identified as non-Hispanic Black or Hispanic/Latino. Most were staged with unknown duration/late (WRA: 55%, PW: 65%) or early non-primary non-secondary (WRA: 30%, PW: 27%) syphilis. Almost all WRA and PW with P&S syphilis and available sex partner data reported sex with male partner(s); only 2% reported sex with male partner(s) who have male sex partner(s). The proportion of CS cases potentially averted was similar across poverty levels; differences were noted by race/ethnicity with the lowest proportion among non-Hispanic Black PW in both groups (Table 1).
Conclusion: Syphilis among WRA and PW is increasing, predominantly affecting racial/ethnic minority groups. Most are staged with latent syphilis, emphasizing the importance of screening and thorough clinical evaluation for accurate staging. Assessing for intersectional effects of race and social determinants of health is needed to address context-specific barriers to syphilis prevention and care among PW.
| Pregnant Women with Syphilis | Reported CS Cases among Pregnant Women with Syphilis | Proportion of CS Cases Potentially Avertedb | ||
|---|---|---|---|---|
| n | n | % | ||
| All Syphilis Casesc | 1,223 | 129 | 89% | |
| Low/Medium Poverty Neighborhoods (0–20% below Federal Poverty Level) | ||||
| All Cases | 590 | 71 | 88% | |
| Asian, non-Hispanic | 32 | 3 | 91% | |
| Black, non-Hispanic | 196 | 33 | 83% | |
| Hispanic/Latino | 223 | 20 | 91% | |
| Multiracial, non-Hispanic | 75 | 5 | 93% | |
| White, non-Hispanic | 32 | 5 | 84% | |
| High/Very High Poverty Neighborhoods (>20% below Federal Poverty Level) | ||||
| All Cases | 629 | 57 | 91% | |
| Asian, non-Hispanic | 31 | 0 | 100% | |
| Black, non-Hispanic | 189 | 27 | 86% | |
| Hispanic/Latino | 253 | 20 | 92% | |
| Multiracial, non-Hispanic | 103 | 7 | 93% | |
| White, non-Hispanic | 18 | 1 | 94% |
PP04.113 – Analysis and Forecasting of Gonorrhea Trends Among the Elderly Population in the Chinese Mainland
Dr. Rui-Rui Peng1, Dr. Fu-Quan Long1, Dr. Xiang-Dong Gong2
1Clinical Center for Sexually Transmitted Disease, Shanghai Skin Disease Hospital, School of Medicine, Tongji University, China.
2Department of STD Epidemiology, Institute of Dermatology, Chinese Academy of Medical Sciences and Peking Union Medical College, Naijing, China.
Background: The challenge of population aging is emerging as a global concern due to the increasing human life expectancy. Older adults continue to experience sexual desires, and sexual health remains a critical component of their overall well-being. We aimed to analyze the incidence of gonorrhea trends and forecast the incidence in the next 5 years among the elderly population in the Chinese mainland.
Methods: The annual cases of national gonorrhea among the elderly population from 2004 to 2023 were obtained from National Center for STD Control, China CDC. Annual population data were sourced from the China Statistical Yearbooks. Temporal trends in gonorrhea incidence were analyzed using Joinpoint regression, estimating the average annual percent change (AAPC) along with the corresponding 95% confidence interval (95% CI). Subsequently, an optimized LSTM model was employed to forecast the incidence trends for the subsequent five-year period.
Results: The incidence of gonorrhea among the elderly population in the Chinese mainland has shown a consistent downward trend from 2004 to 2022, with a more significant decrease noted since 2018. The Average Annual Percent Change (AAPC) figures was –5.9805 (95% CI: –7.7098 to –4.2187) for elderly males and –4.5296 (95% CI: –6.4869 to –2.5314) for elderly females. Following the global declaration of the end of the COVID-19 pandemic, there has been an increase in the incidence of gonorrhea in 2023, particularly among elderly males. It is anticipated that the incidence of gonorrhea among elderly males will stabilize over the next 5 years, while it is expected to continue its gradual decline among elderly females.
Conclusion: Given the growing elderly population, characterized by compromised immune systems and reduced awareness of sexual health, the prevention and control of gonorrhea among older adults, particularly elderly males, cannot be overlooked.
PP04.114 – Spread of a Dual Resistant Mycoplasma Genitalium Clone Harboring an A2058T Substitution in 23S rRNA in Men in France
Prof. Sabine Pereyre1,2, Mrs Cécile Laurier-Nadalié2, Mrs Carla Balcon2, Mrs Nadège Hénin1, Mrs Amandine Dolzy2, Mrs Marie Gardette2, Dr Jennifer Guiraud2, Prof. Cécile Bébéar1,2, Investigator group
1University of Bordeaux - CNRS, Bordeaux, France.
2CHU Bordeaux - National Reference Centre for Bacterial Sexually Transmitted Infections, Bordeaux, France.
Background: Macrolide resistance has been rapidly increasing worldwide in Mycoplasma genitalium. The spread of macrolide resistance has been reported to be polyclonal. However, a few resistant clones may be circulating, particularly in men. To search for the potential spread of M. genitalium macrolide-resistant clones in men in France, we performed a nationwide survey to investigate the mgpB type of macrolide-resistant strains.
Methods: A 1-month systematic prospective collection of M. genitalium-positive specimens in men was performed between 15 Sept. and 15 Oct. 2021 and 2022 in French diagnostic laboratories.
Resistance-associated mutations were detected using 23S rRNA, parC, and gyrA gene sequencing. Typing was performed using SNP analysis of the mgpB adhesin gene on all macrolide-resistant strains.
Results: M. genitalium-positive specimens were collected from 229 and 191 male patients from 38 and 37 French laboratories in 2021 and 2022, respectively. The overall prevalence of macrolide-resistance associated mutations was 53.2% (95% CI 47.9–58.3%) and the percentage of fluoroquinolone resistance-associated mutations was 25.2% (95% CI 20.8%–30.1%). The most frequent macrolide-resistance associated mutation was A2059G (Escherichia coli numbering) (46.6%) followed by the A2058T substitution (33.5%) and the A2058G mutation (19.5%). The proportion of A2058T transversion increased significantly compared to a similar previous study in 2018 (18.8% in 2018 vs 34.2% in 2022, P = 0.02).
MgpB typing of macrolide-resistant strains revealed 47 distinct sequence types (STs), including 16 new STs. ST159 was the most frequent ST representing 20.2%. All ST159 strains harbored both the A2058T transversion in 23S rRNA and the S83I fluoroquinolone-resistance associated mutation in ParC. Moreover, 94.1% of ST159 were from bisexual or men who have sex with men, and 63.6% were from the Paris region.
Conclusion: We report the emergence of the A2058T transversion among macrolide-resistant strains in France and the spread of a dual resistant A2058T-S83I ST159 clone more likely circulating in MSM from Paris.
PP04.115 – Unveiling the Overlooked: A Retrospective Cohort of Asymptomatic STI Detection in Women Via Multiplex PCR
Ms. Thunyapon Pipattaweepon1, Ms. Kannapat Phanjaroen1, Ms. Irin Srila-or1, Ms. Warapron Eiamyoung1, Mr. Thanawin Leabchan1, Mr. Supphadith Barisri1, Ms. Pintip Jomja1, Ms. Pasathorn Sirithiranont1, Ms. Walaiporn Canda1, Ms. Daranit Triyawong1, Doctor Nuntana Chumpa2
1Thai Red Cross Aids Research Centre (anonymous Clinic), Bangkok, Thailand.
2Thai Red Cross Emerging Infectious Diseases Clinical Center, King Chulalongkorn Memorial Hospital, Bangkok, Thailand.
Background: Over one million new cases of Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), Trichomonas vaginalis (TV), and Treponema pallidum (TP) were reported globally in 2020. Asymptomatic infections in women may remain undetected, leading to delayed treatment, severe complications, and increased transmission. Women without symptoms are often overlooked by themselves and healthcare providers, whereas men typically present clearer signs. Yet multiplex PCR usually requires self-payment, limiting access.
Methods: A retrospective cohort study was conducted from March 1 to November 30, 2024, at an STI clinic in Bangkok. A total of 701 asymptomatic individuals (369 men, 332 women) aged 16–76 years were included. Samples from sexual intercourse sites were pooled and tested via multiplex PCR, allowing simultaneous detection of multiple pathogens in one assay, thus reducing costs compared to separate tests or delayed treatments. Descriptive statistics and logistic regression were applied, with P < 0.05 indicating significance.
Results: Of 701 participants, 77 (10.98%) tested positive for STIs. Chlamydia trachomatis was significantly more prevalent in women (34/332, 10.24%) than men (22/369, 5.96%) (P = 0.04) (Table 1). No significant sex-based differences were observed for NG, TV, or TP. Key risk factors included age <45 years (OR = 4.15), PrEP use (OR = 4.31), female sex (OR = 4.29), and having a partner with STI symptoms or diagnosis (OR = 7.02). Most (76.75%) had no prior STIs, and only 3.71% reported a high-risk partner.
Conclusion: CT was notably more prevalent among asymptomatic women. Implementing multiplex PCR with pooled sampling minimized diagnostic expenses by detecting multiple pathogens simultaneously, reducing costs tied to delayed diagnoses. Younger age, PrEP use, female sex, and a high-risk partner were significant predictors. Integrating multiplex PCR could enhance early detection and reduce the global STI burden. These findings underscore the need for routine multiplex PCR screening among asymptomatic women to prevent complications.
| 1. Risk Factors and Corresponding Odds Ratios among Asymptomatic Participants | ||||
|---|---|---|---|---|
| Risk Factors | Comparison (Ref.) | Odd ratio (95% CI) | P-value < 0.05 | |
| Age <45 years | Age ≥ 45 years | 4.15 (0.99–33.7) | 0.0416 | |
| Previous of Sextually transmitted infections (STIs) | No history of STIs | 0.69 (0.40–1.43) | 0.4063 | |
| Partner with STIs symptoms/diagnosis | No Partner with STIs symptoms/diagnosis | 7.02 (1.09–8.24) | 0.0081 | |
| Pre-exposure prophylaxis drug (PrEP) use | No PrEP use | 4.31 (0.90–4.98) | 0.0380 | |
| Patient living with HIV (PLWH) | None PLWH | 0.02 (0.23–2.69) | 0.8811 | |
| Female | Male | 4.26 (1.00–2.76) | 0.0390 | |
| 2. Distribution of Pathogen Infections in 701 Asymptomatic Participants by gender | ||||
|---|---|---|---|---|
| Pathogen | Gender | P-value | ||
| Male (N 369) | Female (N 332) | |||
| Chlamydia trachomatis | 22 (3.14%) | 34 (4.85%) | 0.037* | |
| Neisseria gonorrhea | 12 (1.71%) | 14 (2.00%) | 0.636 * | |
| Trichomonas vaginalis | 2 (0.29%) | 4 (0.57%) | 0.430 ** | |
| Treponema pallidum | 1 (0.14%) | 1 (0.14%) | 1.000 ** | |
| Mycoplasma genitalium | 16 (2.28%) | 28 (3.99%) | 0.026 * | |
| Ureaplasma urealyticum | 50 (7.12%) | 105 (14.96%) | 0.000 * | |
| Candida albicans | 9 (1.28%) | 47 (6.7%) | 0.000 * | |
| Gardnerella vaginalis | 58 (8.26%) | 211 (30.06%) | 0.000 * | |
| Herpes simplex type 1 | 2 (0.28%) | 4 (0.57%) | 0.430 ** | |
| Herpes simplex type 2 | 7 (0.99%) | 9 (1.28%) | 0.475 * | |
Note: *Pearson’s Chi-squared test; **Fisher’s exact test; P < 0.05 = significant.
PP04.116 – Prevalence of HIV Among Sexual Partners of High-Risk Key Populations and HIV Positive People: Overview of 2-Years Rapid Testing Program in Russia
Mrs Elena Sklyarskaya1, Mrs Polina Supronenko1, Mr Alexander Chuykov1, Dr. V Sam Prasad1
1AIDS Healthcare Foundation, Saint-Petersburg, Russian Federation.
Background: AIDS Healthcare Foundation (AHF) pioneered rapid HIV testing program in Russia in 2012. Program is implemented in cooperation with NGOs at health facilities and community settings in 11 regions. Following WHO recommendations, testing of sexual partners of high-risk key populations (KP) and of PLHIV is one of the AHF’s core priorities.
Description: Anonymous free rapid HIV testing and consulting is performed by medical staff. Client receives pre- and post-test consultations and provides information about age, risk behavior, belonging to risk groups, etc. The procedure takes 15-30 min. In the end client gets prevention materials, condoms and in case of positive result is referred to care. During post-test consultation staff motivate clients, especially HIV-positive, to bring in their partners.
Results: From January 1, 2023 to December 31, 2024 overall 180 777 people were screened for HIV with 9 264 (5.1%) positive results. Among these 66 614 sexual partners of identified KP at higher risk and of PLHIV with 3 254 (4.9%) positive results. The highest positivity rate (8.5%) was found among sexual partners of PLHIV. The most HIV affected age group was 40–49 y/o clients (37.4% of positive cases) followed by 30–39 y/o clients (35.2%). Linkage to care was 92.0% on average, women from these groups and of all ages are linked to care more eagerly than men (93.3%). The most frequent reasons of unsuccessful linkage were loss (45.5%), refuse (20.1%), move (17.3%).
Conclusions: Results of this work prove the need to continue testing sexual partners and explore motivations that make clients bring in their partners. Awareness of motivations allows to improve methods of engaging new clients at risk into testing. Post-test consultations should be an integral part of effective linkage. Social orientation and understanding clients’ needs by NGO staff are crucial to achieve high rates of linkage.
| Number of tests | Number of positive cases | Positivity | Linkage | ||
|---|---|---|---|---|---|
| All populations | 180,777 | 9264 | 5.1% | 92.8% | |
| Male | 107,008 | 5928 | 5.5% | 91.8% | |
| Female | 73,769 | 3336 | 4.5% | 94.7% | |
| Partners of high risk KP | 53,948 | 2174 | 4.0% | 91.4% | |
| Male | 31,755 | 1196 | 3.8% | 90.6% | |
| Female | 22,193 | 978 | 4.4% | 92.3% | |
| Partners of PLHIV | 12,666 | 1080 | 8.5% | 93.4% | |
| Male | 5801 | 510 | 8.8% | 91.6% | |
| Female | 6865 | 570 | 8.3% | 95.1% |
PP04.117 – Incidence of Bacterial Sexually Transmitted Infections Among People with Opioid Use Disorder and the Impact of Opioid Agonist Treatment
Ms. Olivia Price1, Dr Chrianna Bharat1, Mrs Nikky Jones1, Mrs Nimnaz Ghouse1, A/Prof Amy Peacock1,2, Dr Phillip Read3,4, Prof Matthew Hickman5,1, Prof Louisa Degenhardt1
1National Drug and Alcohol Research Centre, Sydney, Australia.
2School of Psychological Sciences, Hobart, Australia.
3Kirketon Road Centre, Sydney, Australia.
4Kirby Institute, Sydney, Australia.
5Bristol Medical School, Bristol, United Kingdom.
Background: Substance use has been identified as a risk factor for bacterial sexually transmitted infections (STIs). In this study, we examined the incidence of STIs among people who had been prescribed opioid agonist treatment (OAT; treatment for opioid use disorder).
Methods: We conducted a retrospective population-based cohort study of all OAT recipients (N = 53,987) in New South Wales, Australia between 2001 and 2022, using linked administrative data. Incidence rates for STI notifications (chlamydia, gonorrhea, and infectious syphilis) were estimated per 1000 person years (PY), and compared over the study period and by sex. We also compared incidence to priority populations (female sex workers and HIV-positive and HIV-negative gay and bisexual men who have sex with men). Poisson regression models with generalized estimating equations estimated the impact of OAT exposure on notification rates.
Results: In total, there were 2,775 STI notifications (2,066 individuals), equivalent to 3.80 (95% confidence interval [CI]: 3.66–3.95) per 1000 PY. There were more notifications for chlamydia (2.46 per 1000 PY, 95% CI: 2.35–2.58), than gonorrhoea (1.18 per 1000 PY, 95% CI: 1.11–1.27) and syphilis (0.16 per 1000 PY, 95% CI: 0.13–0.19). Overall notifications were higher for females than males (rate ratio: 1.54, 95% CI: 1.43–1.66). Notification of any STI increased over the study period (2.2 per 1000 PY in 2001 to 5.8 per 1000 PY in 2022). STI incidence among this cohort was higher than female sex workers, but lower than gay and bisexual men who have sex with men (both HIV positive and negative). Analysis of the impact of OAT exposure on notifications is ongoing and will be presented at the conference.
Conclusion: Increasing STI incidence warrants targeted screening for people with opioid use disorder.
PP04.118 – Growth of HIV Molecular Clusters of Rapid Transmission by Level of Viral Suppression at Detection, United States
Dr. Karen Schlanger1, Dr. Anne Marie France1, Dr. Kathryn G. Curran1, Fathima N. Farhan Ahmed2, Dr. Alexandra M. Oster1, Dr. Hilary Reno1
1Centers for Disease Control and Prevention, Atlanta, United States.
2DLH Corporation, Atlanta, United States.
Background: HIV molecular clusters of rapid transmission detected using surveillance data are known to be a subset of full clusters, which also include undiagnosed infections and diagnosed infections without sequences available. Because >90 clusters are detected in the United States each year and health departments have limited response resources, identifying prioritization criteria is important. To determine whether deprioritizing responding to clusters with high viral suppression (VS) is a reasonable strategy, we compared growth in molecular clusters with and without high VS at detection.
Methods: We used December 2023 National HIV Surveillance System data to assess growth of clusters (at a 0.5% genetic distance threshold) first detected in national quarterly analyses during 2018–2021 with ≥5 diagnoses (≥3 for low morbidity jurisdictions) in the most recent 12 months. We compared growth in the 24 months after detection in clusters with high VS (i.e., ≥80% of cluster members with <200 copies/mL) at detection to growth in clusters without high VS.
Results: During 2018–2021, 303 molecular clusters were detected; 98 (32%) had high VS at detection. Median size (range) at detection was 6.5 cases (3–18) for clusters with high VS and 8 (3–16) for other clusters; median growth at 24 months was 5 cases (0–31) for clusters with high VS and 6 (0–72) for other clusters. Similar proportions of clusters with and without high VS did not grow (9.2% and 8.3%, respectively), and levels of cluster growth were similar.
Conclusion: Nearly all molecular clusters of rapid transmission grow in the 24 months after detection. We did not identify differences in growth between clusters with and without high VS at detection, suggesting growth may be driven primarily by undiagnosed or non-sequenced infections and health departments should mount similar levels of response for clusters regardless of baseline VS.
PP04.119 – Applying an Intersectional Lens to Examine Associations Between Drug Use and Sexually Transmitted Infections
Dr. Joy Scheidell1, Bedis Elkamel, Dr Typhanye Dyer
1University of Central Florida, Orlando, United States.
Background: Drug use and STI risk vary among people with intersecting gender, racial, ethnic, and sexual identities, but limited research has examined these associations specifically within these marginalized populations.
Methods: We conducted a secondary data analysis of baseline data from Project Aware, a randomized controlled trial in nine U.S. STI clinics (n = 5012). Participants were categorized as cisgender women, men who have sex with men (MSM), and men who do not (non-MSM). Race and ethnicity were classified as non-Hispanic White, non-Hispanic Black, and Hispanic. Participants reported illicit drug use, injection drug use (IDU), and drug use severity based on the DAST-10 (no/low/moderate <6 vs severe ≥6). Bacterial STIs (chlamydia, gonorrhea, syphilis) were measured via self-report, clinical records, and laboratory diagnosis. Prevalence of drug use and STIs and the association between drug use and STIs were calculated among the intersecting populations.
Results: Half of participants reported illicit drug use, with the highest prevalence among White women and MSM (60%) and lowest among Black and Hispanic women (42%). IDU prevalence was 2%, and 9% reported severe drug use. STI prevalence varied by group: self-reported STIs were highest among Black women (23%) and lowest among White non-MSM (3%); clinical STIs were most prevalent among Black MSM (15%); and laboratory-confirmed STIs were highest among Black women (34%). Illicit drug use was associated with higher STI prevalence across all groups, notably Black men, White women and White MSM. IDU was associated with twice the STI prevalence, particularly among White and Hispanic MSM. Severe drug use was linked to higher STI prevalence among White participants.
Conclusion: Drug use is disproportionately associated with STI prevalence in marginalized groups, with notable variations by intersecting gender, race and ethnicity, and sexual identity. Interventions addressing drug use and STI prevention in these populations are critical to reducing inequities and improving health.
PP04.12 – Evaluating a New Approach to Capturing Housing Status Information as Part of Public Health STI Reporting in King County, Washington: A Focus on Cisgender Girls and Women Diagnosed with Gonorrhea
Dr. Jennifer Balkus1,2, Anna Berzkalns1, Christina Thibault1, Chase Cannon1,2, Tim Menza1,2, Matthew Golden1,2
1Public Health - Seattle & King County, Seattle, United States.
2University of Washington, Seattle, United States.
Background: Homelessness is a key social determinant of health; however, the burden of homelessness among people diagnosed with bacterial STIs uncertain. To improve data collection related to housing status, in December 2022 a check box was added to the STI case report form in King County, Washington to capture “unhoused or unstably housed in the past 3 months.” Here we describe Neisseria gonorrhoeae (GC) reports by housing status.
Methods: The analysis population included cisgender girls and women (≥14 years) diagnosed with GC between December 2022–June 2024 based on public health surveillance data. Housing status at diagnosis was defined as “housed” (residential address provided), unhoused (unhoused box checked or address matches a local shelter or supportive housing) and missing (no address and box not checked). Descriptive statistics were used to summarize select characteristics by housing status.
Results: During the evaluation period, there were 1,064 GC diagnoses of which 135 (13%) were classified as unhoused at diagnosis (Table 1) compared to 1% of King County residents being unhoused. Of 135 GC reports among unhoused persons, 64 (47%) were identified by the new check box rather than address data alone. Unhoused at diagnosis was most prevalent among 35–44 year-olds (Table 1). Within racial/ethnic strata, the proportion unhoused was highest among White (18%), American Indian/Alaska Native (14%) and Latina (13%) identified persons. The proportion diagnosed at an Emergency Room or Urgent Care was 27% for both unhoused and unhoused persons.
Conclusions: Including a check box on STI case reports to capture housing status improved county data collection for GC. These data showed a disproportionate burden of being unhoused among cis-girls and women diagnosed with GC and important trends in housing status by age, race and ethnicity, which can be used to inform public health action. Other jurisdictions should consider collecting housing data as part of STI case reporting.
| Age (years) | Unhoused N = 135 | Housed N = 913 | Missing N = 16 | Race and ethnicityB | Unhoused N = 135 | Housed N = 913 | Missing N = 16 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 14–19 | 10 | 8% | 112 | 89% | 4 | 3% | AIAN | 6 | 14% | 36 | 82% | 2 | 5% | |
| 20–24 | 15 | 6% | 226 | 93% | 3 | 1% | Asian | 4 | 6% | 61 | 94% | 0 | 0% | |
| 24–29 | 20 | 9% | 199 | 90% | 2 | 1% | Black | 24 | 8% | 273 | 91% | 3 | 1% | |
| 30–34 | 25 | 15% | 143 | 83% | 4 | 2% | Latinx | 16 | 13% | 108 | 86% | 2 | 2% | |
| 35–44 | 51 | 24% | 155 | 74% | 3 | 2% | NHPI | 2 | 6% | 34 | 94% | 0 | 0% | |
| 45–54 | 12 | 17% | 58 | 83% | 0 | 0% | White | 84 | 18% | 365 | 80% | 9 | 2% | |
| >55 | 2 | 9% | 20 | 91% | 0 | 0% | Another race | 11 | 10% | 102 | 89% | 1 | 1% | |
| Unknown/refused | 7 | 8% | 77 | 91% | 1 | 1% | ||||||||
PP04.120 – High Prevalence of Asymptomatic Sexually Transmitted Infections and Moderate Same-Day Treatment Rates in Pregnant Women in South Africa
Ms. Natalie Shaetonhodi1, Dr Jeffrey D. Klausner2, Dr Andrew Medina-Marino3,4, Prof. Dr Remco P. H. Peters5, Dr Alex de Voux1, Dr Dvora Joseph-Davey6,1, Ms. Mandisa M. Mdingi5,7, Dr Ranjana M. S. Gigi8,5, Dr Chibuzor Babalola2, Mr Freedom Mukomana5
1School of Public Health and Family Medicine, University of Cape Town, Cape Town, South Africa.
2Keck School of Medicine, University of Southern California, Los Angeles, United States.
3Perelman School of Medicine, University of Pennsylvania, Philadelphia, United States.
4Desmond Tutu HIV Centre, University of Cape Town, Cape Town, South Africa.
5Research Unit, Foundation for Professional Development, East London, South Africa.
6Geffen School of Medicine, University of California Los Angeles, Los Angeles, United States.
7University of Pretoria, Pretoria, South Africa.
8Institute of Social and Preventive Medicine, University of Bern, Bern, Switzerland.
Background: Curable sexually transmitted infections (STIs) contribute to adverse maternal and neonatal outcomes. Syndromic management is the standard of care for STIs in South Africa. We evaluated STI prevalence, symptomology, and the role of point-of-care testing in optimizing STI treatment among pregnant women.
Methods: We analysed baseline data from a randomized trial on pregnant women attending their first antenatal care visit in East London (2021–2024), South Africa. Women were tested for Chlamydia trachomatis (CT), Neisseria gonorrhea (NG), Trichomonas vaginalis (TV) using GeneXpert (Cepheid, Sunnyvale, CA; turnaround time 60–90 min) and for syphilis using a rapid treponemal diagnostic test (<20 min). We assessed symptoms through self-report and clinical examination. Adjusted prevalence ratios were estimated using Poisson regression with robust standard errors.
Results: Among 1,494 pregnant women (median age: 23 years, IQR: 24–34; gestational age: 13 weeks, IQR: 8–18; HIV prevalence: 30%), the prevalence of any STI was 27.6% (95% CI: 25.3–29.9): CT 14.7%, NG 5%, TV 10.2%, syphilis 3.4%. Women living with HIV had higher prevalence of any STI (32.8% vs 25.3%, P = 0.003), TV (17% vs 7.3%, P < 0.001), and coinfection with multiple STIs (7.1% vs 4.2%, P = 0.025). Most STIs (74.3%) were asymptomatic, and 63% of women who reported vaginal discharge did not have an STI. Clinically-identified vaginal discharge was associated with an STI (aPR 1.46, 95% CI: 1.1–1.86) while self-reported vaginal discharge was not (aPR 1.21, 95% CI: 0.86–1.69). Most (95%) women with CT, NG, or TV received treatment; 51% same-day; 100% of those with syphilis were treated the same-day.
Conclusion: Prevalence of STIs in pregnancy was high. The high proportion of asymptomatic STIs and symptoms among women without STIs highlight gaps in current STI care. Same-day treatment was higher with syphilis rapid tests versus CT/NG/TV tests. How to best use point-of-care STI testing in low-resource settings remains to be determined.
PP04.121 – Heterogeneity in Covid-19 Vaccine Uptake Among People with STBBI Diagnoses: A Population-Based Analysis
Dr. Souradet Shaw1, Dr. Alyson Mahar2, Dr. Derek Stein3,4, Dr. Jason Kindrachuk4, Dr. Christine Kelly4, Mr. Kevin John Friesen5, Mr. Mohammad Nazmus Sakib5, Mr. Isuru Dharmasena5, Dr. Charles N. Bernstein4, Dr. Joss Reimer6, Dr. Nathan C. Nickel5
1Institute For Global Public Health, University of Manitoba, Winnipeg, Canada.
2Queen’s University, Kingston, Canada.
3Cadham Provincial Laboratory, Winnipeg, Canada.
4University of Manitoba, Winnipeg, Canada.
5Manitoba Centre for Health Policy, University of Manitoba, Winnipeg, Canada.
6Winnipeg Regional Health Authority, Winnipeg, Canada.
Background: Prior to the COVID-19 pandemic, Manitoba, Canada, was experiencing a crisis associated with sexually transmitted and bloodborne infections (STBBI). As STBBI and COVID-19 share similar healthcare access barriers, this study investigated the association between previous STBBI exposure and COVID-19 vaccination.
Methods: This was a retrospective cohort analysis using linkable population-based healthcare databases in Manitoba. Cohorts of individuals alive and registered with Manitoba’s single-payer insurance provider on March 1, 2020, and with a positive laboratory test for syphilis, chlamydia/gonorrhea (CT/GC), or HIV in the 4 years prior to the pandemic (i.e., 2016–2020) were assembled. Cohorts were not mutually exclusive, and individuals with positive tests for different pathogens could be included in multiple cohorts. COVID-19 vaccination (up to March 31, 2022) was captured using Manitoba’s vaccine registry. Poisson regression estimated relative rates (RRs) and 95% confidence intervals (95% CIs) for vaccination by age group, income quintile (IQ), and geography (Fig. 1).
Results: 4,527 individuals testing positive for syphilis, 24,414 for CT/GC, and 1,372 for HIV were included. Vaccination with 1+ doses was 77%, 81%, and 86% in the syphilis, CT/GC, and HIV cohorts, respectively, while uptake of 2+ doses was 70%, 76%, and 82% in the same cohorts. Within cohorts, uptake of 2+ vaccines ranged from 63%–79% from the lowest to the highest urban income quintile (RR highest vs lowest income quintile: 1.24, 95% CI: 1.01–1.54), 69%–84% (RRhi_vs_loIQ: 1.23, 95% CI: 1.15–1.32), and 81%–95% (RRhi_vs_loIQ: 1.17, 95% CI: 0.88–1.55) for syphilis, CT/GC, and HIV cohorts, respectively. Uptake was higher in Manitoba’s northern and remote health regions, compared to the Winnipeg health region for syphilis and CT/GC cohorts, but not HIV.
Conclusion: COVID-19 vaccination was lower in syphilis and CT/GC cohorts, while higher in the HIV cohort. Within STBBI cohorts, considerable heterogeneity in vaccination exists, structured around age group, residence, and area-level economic measures.
Poisson regression estimated relative rates (RRs) and 95% confidence intervals (95% CIs) for vaccination by age group, income quintile (IQ), and geography.
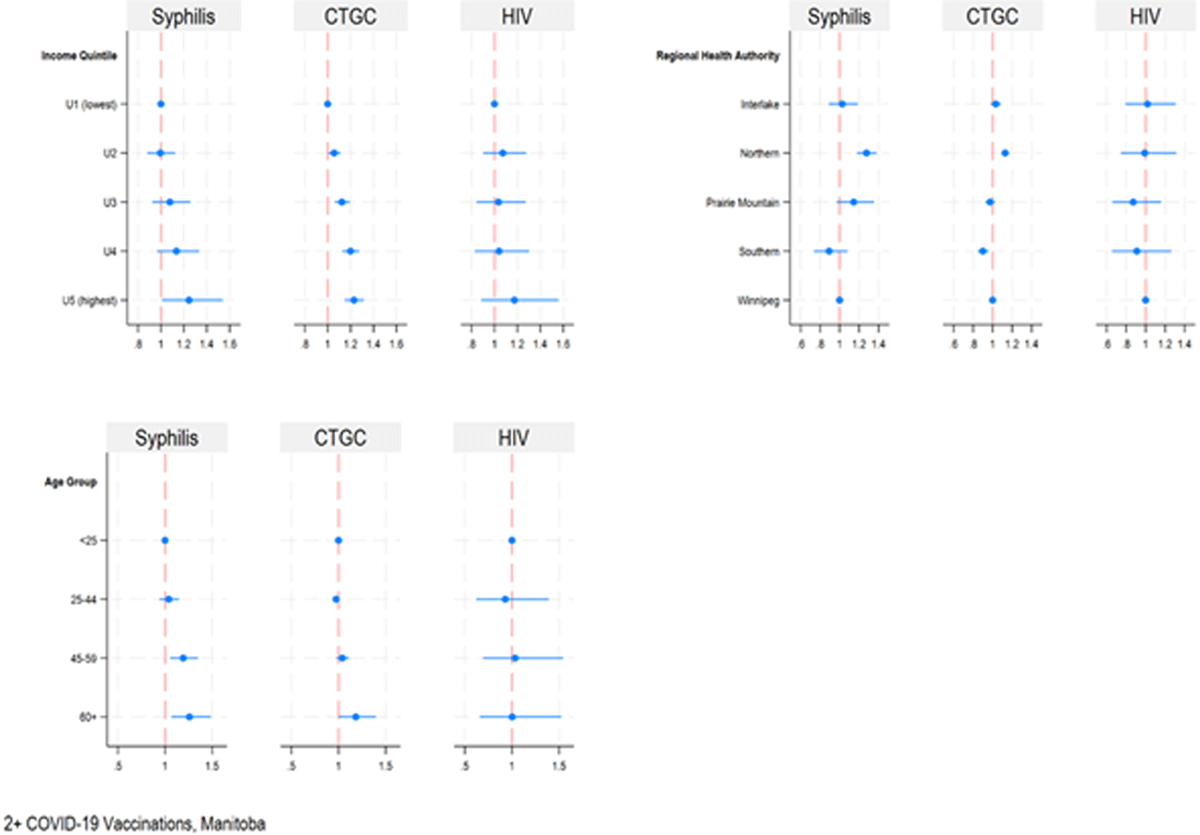
PP04.122 – The Epidemiology of HIV and Injection Practices Among People Who Inject Drugs in Nigeria: Results from the 2020 Integrated Biological and Behavioural Surveillance Survey
Dr. Souradet Shaw1, Dr. Kalada Green2, Mr. Chukwuebuka Ejeckam2, Mr. Adediran Adesina2, Dr. Gambo Aliyu3, Dr. Gregory Ashefor3, Dr. Rose Aguolu3, Dr. Shajy Isac1, Dr. Faran Emmanuel1, Dr. Lisa Lazarus1, Dr. Leigh McClarty1, Dr. Marissa Becker1, Dr. James Blanchard1
1Institute For Global Public Health, University of Manitoba, Winnipeg, Canada.
2West Africa Centre for Public Health and Development, Abuja, Nigeria.
3National Agency for the Control of AIDS, Abuja, Nigeria.
Background: Nigeria has one of the largest HIV epidemics globally. Relative to other key populations, epidemiological understanding of people who inject drugs (PWID) in Nigeria is limited. Using data from the largest key population survey ever conducted in Nigeria, we sought to describe and examine the correlates of HIV and injection/sharing practices of PWID.
Methods: Data were from a cross-sectional bio-behavioural survey conducted across 12 states in 2020 (Fig. 1). HIV seroprevalence was based on testing, with self-reported data on socio-demographic and injection/sharing practices. Modified Poisson regression models were used to estimate adjusted prevalence ratios (aPRs) and 95% confidence intervals (95% CIs) of factors associated with HIV prevalence, and injection and sharing practices.
Results: Among 4,358 participants, weighted HIV prevalence was 10.9%. Median age was 30 years (interquartile range: 25–35) with two-thirds reporting <75 months of injection drug use. 80% reported injecting in the last month, and of those, 21% reported injecting at least once a day; 15% reported “every time/almost every time” to sharing/lending syringes/needles; while 9% reported back/front-loading, sharing paraphernalia, or drawing up from common containers “every time/almost every time”. In multivariable models, female sex (aPR: 1.6, 95% CI: 1.2–2.1) and less than secondary education (aPR: 1.4, 95% CI: 1.1–2.0) was associated with HIV. Less than secondary education (aPR: 3.0, 95% CI: 2.0–4.6), pentazocine (aPR: 1.7, 95% CI: 1.2–2.4), and crack cocaine (aPR: 2.0, 95% CI: 1.4–2.8) injection were associated with riskier injection practices. Risky sharing practices were associated with less than secondary education (aPR: 2.7, 95% CI: 1.6–4.7), pentazocine (aPR: 2.5, 95% CI: 1.6–4.0), pethidine (aPR: 2.7, 95% CI: 1.4–5.3) and cocaine (aPR: 2.1, 95% CI: 1.4–3.3) injection.
Conclusion: HIV prevalence was highly heterogeneous across states, as were riskier injection and sharing practices, with social determinants like education being associated with both, challenging prevention and intervention programs for PWID.
Data taken from a cross-sectional bio-behavioural survey conducted across 12 states in 2020.
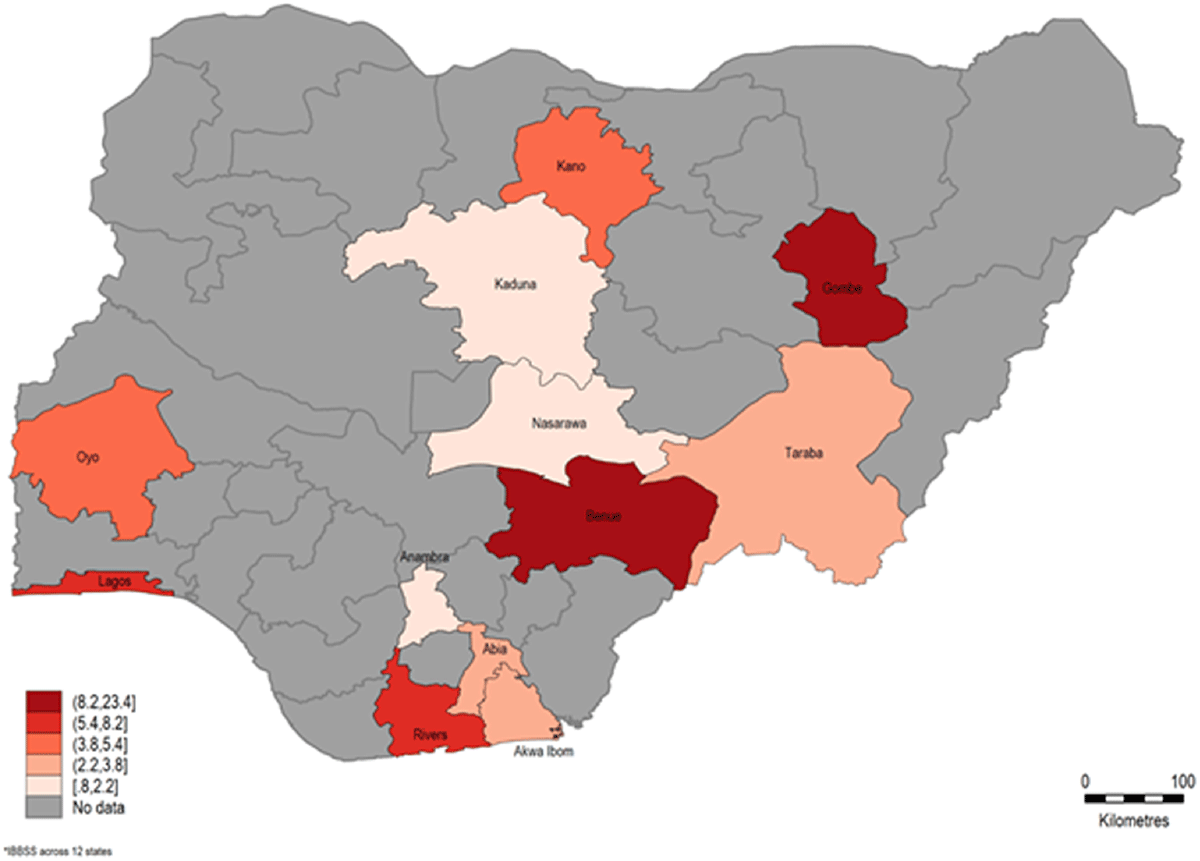
PP04.123 – Mpox and Mpox Prevalence in People Living with HIV/AIDS: A Cross-Sectional Study in Brazil’s Interior
Senhor. João Victor Soares Coriolano Coutinho1,2,3
1Instituto de Patologia Tropical e Saúde Pública (IPTSP) da Universidade Federal de Goiás (UFG), Goiânia, Brasil.
2Hospital Estadual de Doenças Tropicais Dr. Anuar Auad (HDT), Goiânia, Brasil.
3Centro de Testagem e Aconselhamento (CTA) e Serviço de Atendimento Especializado (SAE) de Goiânia, Goiânia, Brasil.
Context: Identified in 1958 in non-human primates, the Mpox virus was later identified in a 9-year-old child in the Democratic Republic of Congo. By 2022, the virus had spread internationally, posing a unique clinical and epidemiological profile. It predominantly affected men who have sex with men, featuring genital and anal lesions, and disproportionately impacted people living with human immunodeficiency virus (HIV)/acquired immunodeficiency syndrome (AIDS) (PLWHA). This study aimed to compare the epidemiological and clinical characteristics of Mpox/HIV/AIDS co-infected patients with those infected by Mpox alone.
Methods: This was a cross-sectional study that analysed all confirmed patients with Mpox from Goiânia, Goiás, Brazil, between June 2022 and June 2023 (Fig. 1). The patients were divided into three groups: Mpox only, Mpox and HIV, and Mpox and AIDS; the epidemiological and clinical characteristics were compared between the different groups.
Findings: Out of 398 patients with confirmed infection, 223 (52%) occurred in PLWHA, including 14 (6%) in the AIDS stage. Among 175 patients with Mpox-only, 37 (21.14%) used HIV pre-exposure prophylaxis (PrEP). Clinical differences included more frequent localized lymphadenopathy in patients with Mpox-only and genital lesions in the Mpox/AIDS group, both statistically significant (Figs 2, 3, Tables 1–4, Supplementary material). Co-infection with another STI was more common in the Mpox/HIV group. All infections were resolved.
Interpretation: The Mpox outbreak predominantly impacted PLWHA in Goiânia, who often had another STI, more genital involvement, and less frequent localized lymph node enlargement. Few patients with only Mpox were on PrEP for HIV.
Anatomical sites of the lesions in the three groups analysed according to the percentage of incidence in each area. Patients living in Goiânia, Goiás, Brazil, diagnosed with Mpox between June 2022 and June 2023.
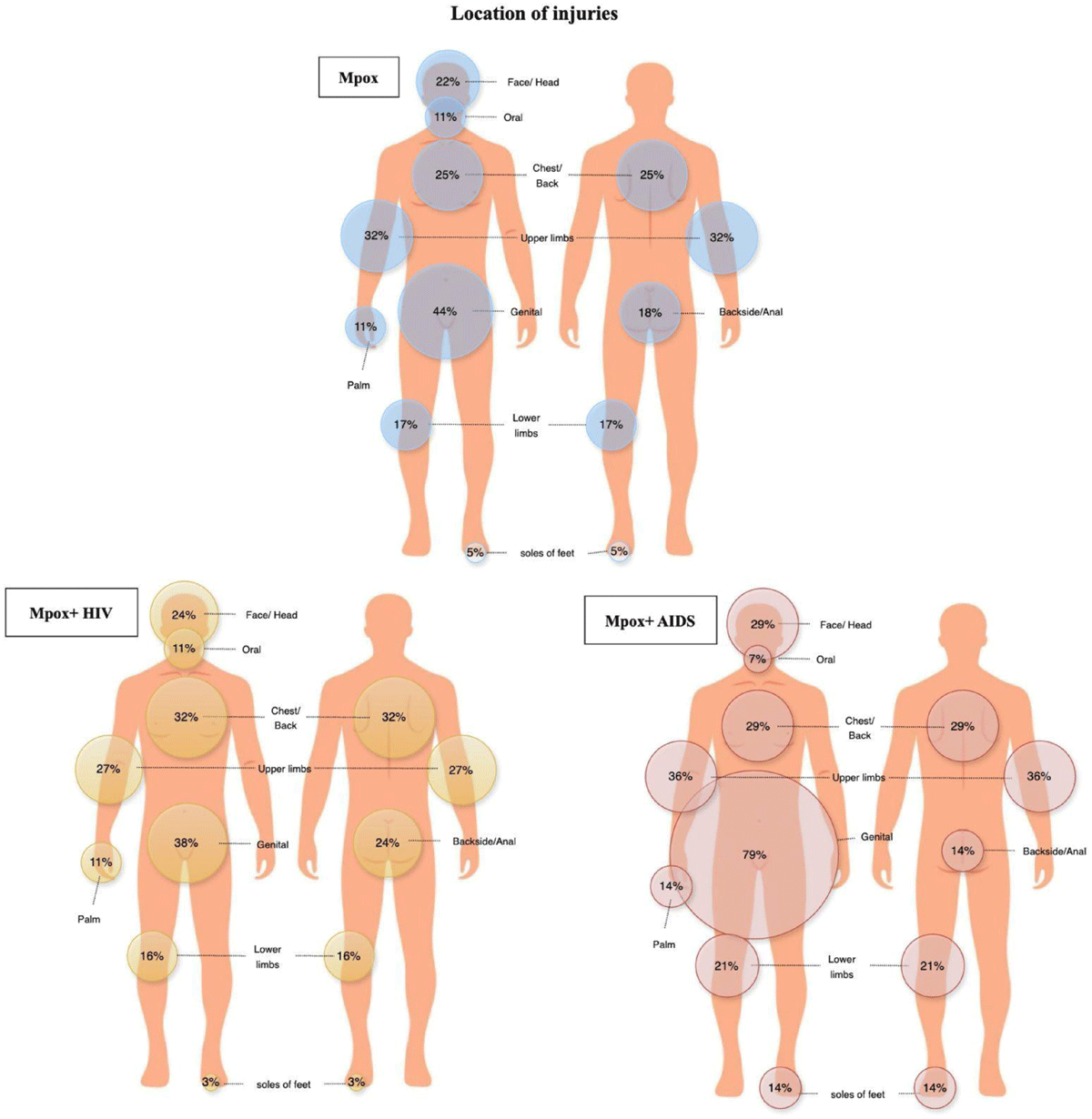
Ct values of the Mpox PCR in the groups with Mpox, Mpox + HIV, and Mpox + AIDS. Patients living in Goiânia between June 2022 and June 2023.
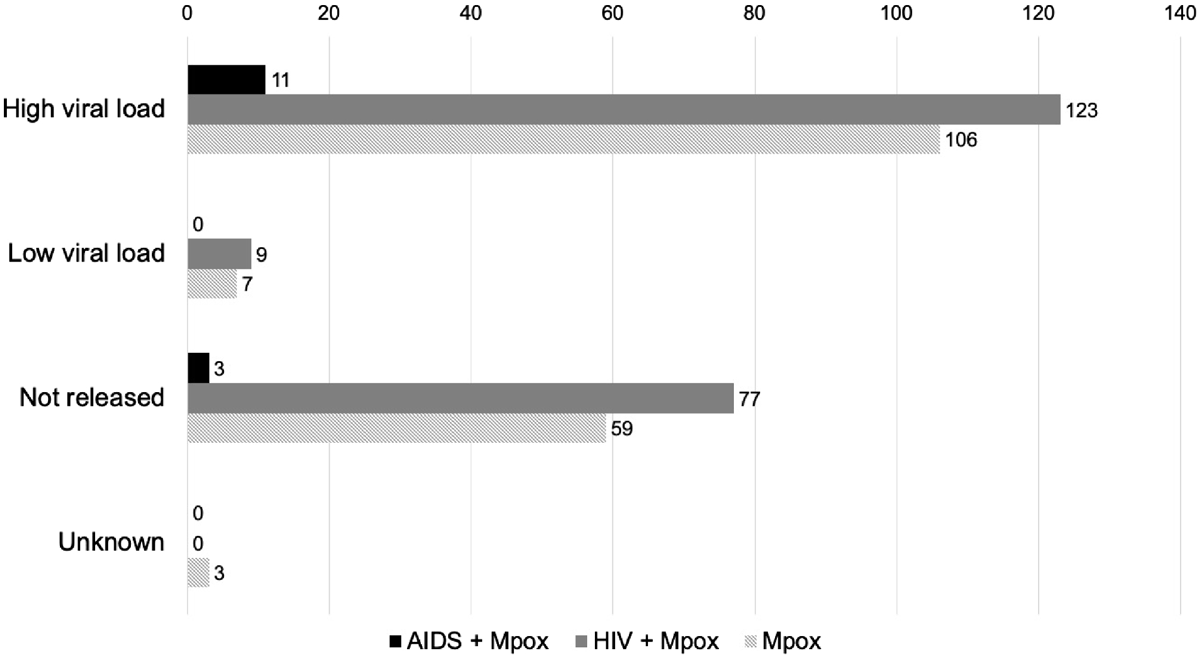
Supplementary Appendix 1
Supplementary Fig. 1. Flowchart of reported patients with Mpox living in Goiânia, Goiás, from June 2022 to June 2023.
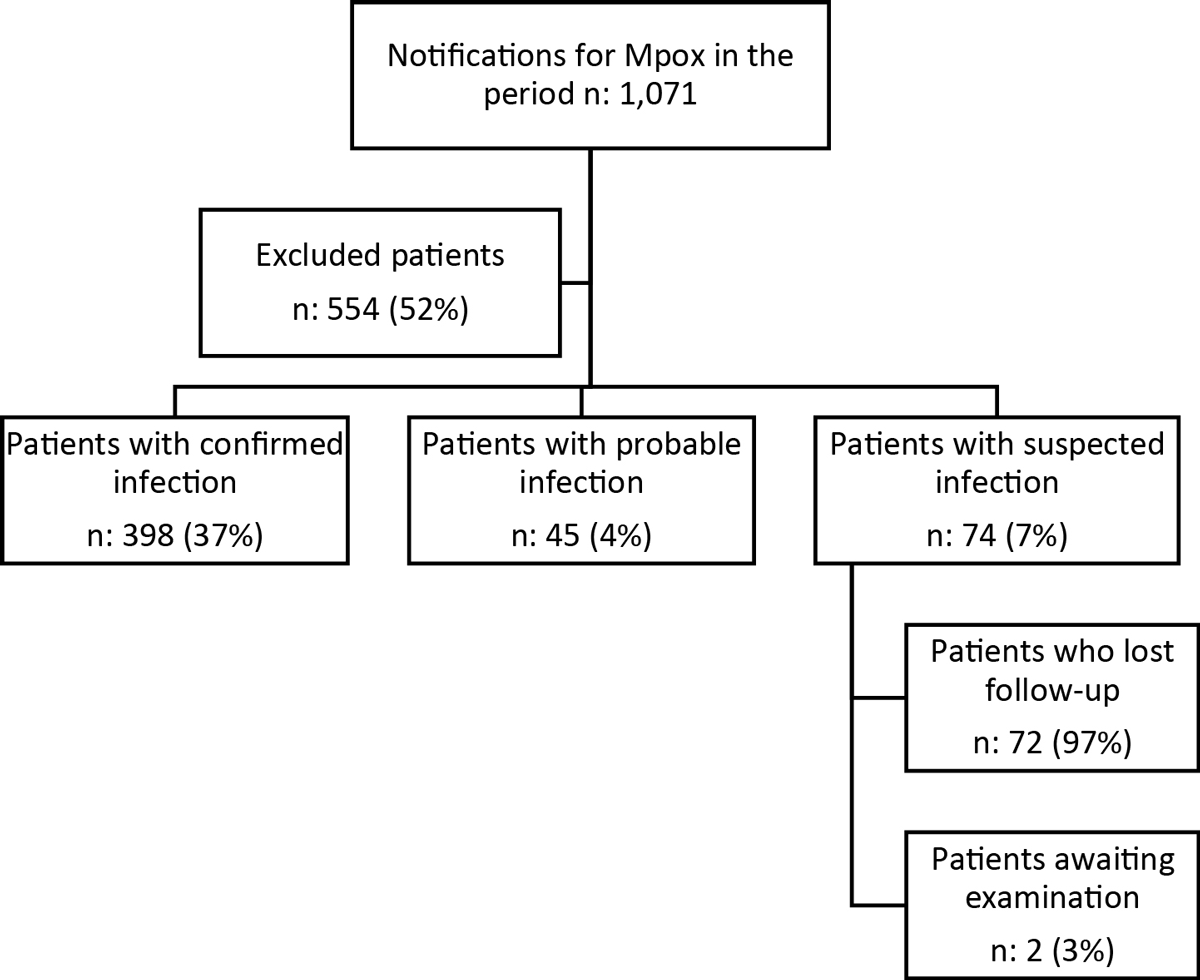
Supplementary Fig. 2. Flowchart of confirmed patients with Mpox living in Goiânia, Goiás, between June 2022 and June 2023, with stratification for HIV co-infection.
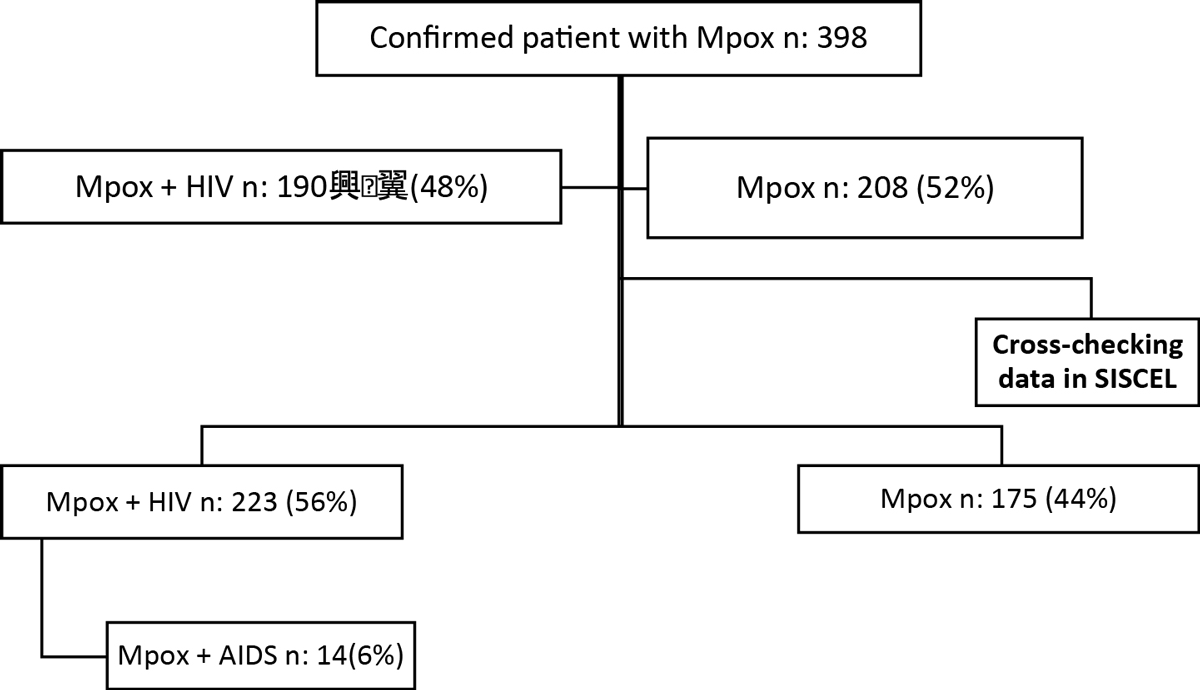
Acronyms: AIDS-Acquired Immunological Deficiency Syndrome. HIV- Human Immunodeficiency Virus.
Supplementary Table 1. Degree of immunosuppression measured by the number of TCD4 lymphocytes/mm3 of the 14 patients with AIDS co-infected with Mpox, living in Goiânia from June 2022 to June 2023.
| Patient | Number of cells/mm3 | |
|---|---|---|
| Patient 1 | 33 | |
| Patient 2 | 151 | |
| Patient 3 | 173 | |
| Patient 4 | 204 | |
| Patient 5 | 231 | |
| Patient 6 | 242 | |
| Patient 7 | 245 | |
| Patient 8 | 260 | |
| Patient 9 | 271 | |
| Patient 10 | 277 | |
| Patient 11 | 294 | |
| Patient 12 | 294 | |
| Patient 13 | 325 | |
| Patient 14 | 336 |
Supplementary Fig. 3. Plot of patients with Mpox taking PrEP for HIV and living in Goiânia between June 2022 and June 2023.
Acronyms: PrEP - Pre-Exposure Prophylaxis.
Supplementary Table 2. Hospitalization data for the 13 patients with Mpox who required hospital admission, living in Goiânia, between June 2022 and June 2023.
| patients | HIV | CD4 | VL | Reason for admission | Complications | Surgical approach | Antimicrobials | ICU | |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Yes | 732 | 159,376 | Clinical | No access | No access | No access | No | |
| 2 | No | - | - | Clinical | No access | No access | No access | No | |
| 3 | Yes | 388 | 360,152 | Clinical | Secondary skin infection | No | Amoxicillin + Clavulanate | No | |
| 4 | No | - | - | Clinical | Submandibular abscess | Abscess draining | Ceftriaxone + Clindamycin Meropenem + Vancomycin | No | |
| 5 | Yes | 877 | 284 | Clinical | Proctitis | No | Amoxicillin + Clavulanate | No | |
| 6 | Yes | 852 | 201 | Clinical | Anal abscess | No | Ceftriaxone + Metronidazole | No | |
| 7 | Yes | 2685 | Undetected. | Clinical | Anal abscess + Scrotal cellulitis | No | Ceftriaxone + Metronidazole Amoxicillin + Clavulanate | No | |
| 8 | Yes | 204 | Undetected. | Clinical | No access | No access | No access | Yes | |
| 9 | Yes | 474 | Undetected. | Clinical | Paraphimosis and cellulitis on the penis | Postectomy | Ceftriaxone + Clindamycin | No | |
| 10 | Yes | 805 | 66 | Isolation | No | No | No | No | |
| 11 | No | - | - | Clinical | Proctitis | No | Azithromycin | No | |
| 12 | Yes | 532 | 80 | Clinical | No | No | No | No | |
| 13 | No | - | - | Clinical | Perianal abscess + Anal fissure | Fissurectomy | Ceftriaxone + MetronidazoleAmoxicillin +Clavulanate | No |
Acronyms: AIDS-Acquired Immunological Deficiency Syndrome. HIV- Human Immunodeficiency Virus. VL - Viral load. ICU - Intensive Care Unit.
Supplementary Fig. 4. Hospital admission time (in days) of patients with Mpox + HIV co-infection and Mpox only, patients living in Goiânia, between June 2022 and June 2023.
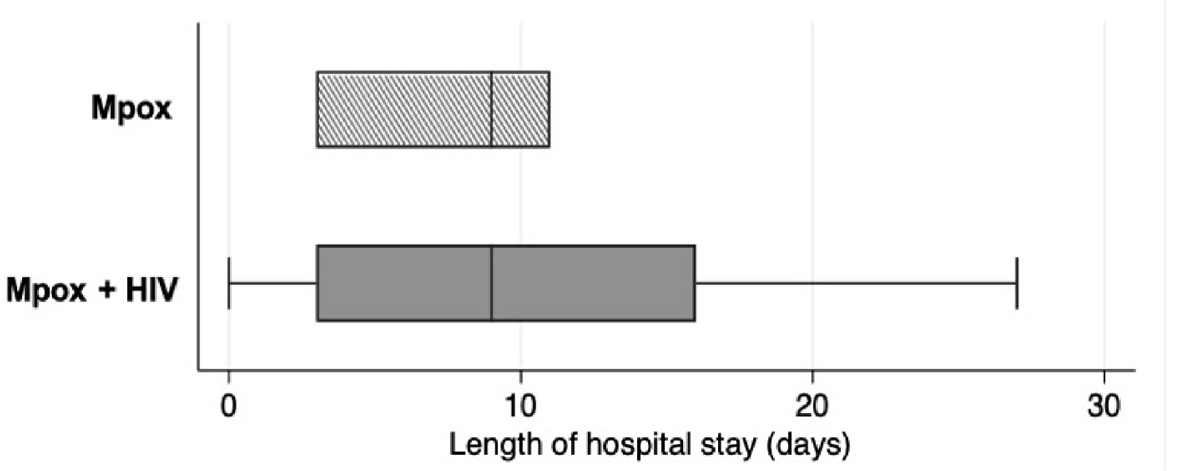
*Patients admitted to the hospital, except for patients with Mpox + AIDS. Acronyms: PLWHA - People Living with HIV/AIDS.
Supplementary Fig. 5. Time between onset of symptoms and cure in the Mpox, Mpox + HIV, and Mpox + AIDS groups. Patients living in Goiânia between June 2022 and June 2023.
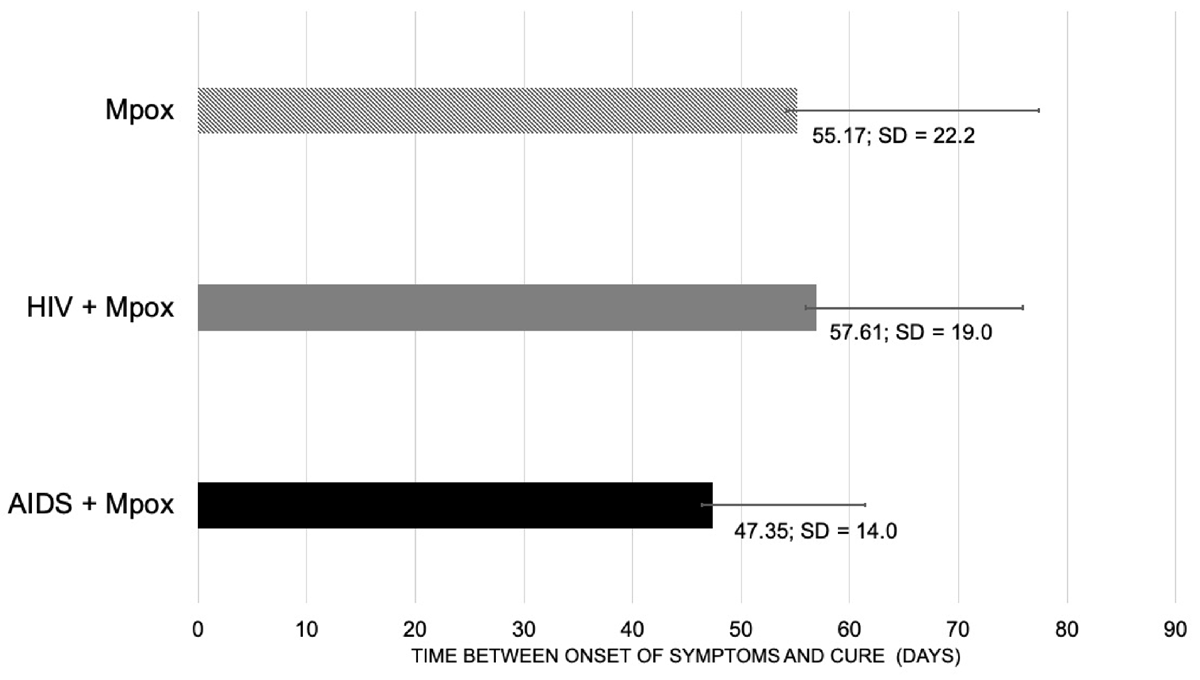
Acronyms: AIDS-Acquired Immunological Deficiency Syndrome. HIV- Human Immunodeficiency Virus.
Table 2. Signs and symptoms, and characteristics and anatomical location of lesions of the Mpox, Mpox + AIDS, and Mpox + HIV groups living in Goiânia between June 2022 and June 2023.
| Mpox (n = 175) | Mpox + AIDS (n = 14) | Mpox + HIV (n = 209) | P-value | |||||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | N | % | |||
| Sudden onset of fever | 115 | 65.7 | 11 | 78.6 | 140 | 67 | 0.664 | |
| Adenomegaly | 61 | 34.9 | 6 | 42.9 | 87 | 41.6 | 0.377 | |
| Acute skin rash | 139 | 79.4 | 10 | 71.4 | 156 | 74.6 | 0.468 | |
| Headache | 101 | 57.7 | 7 | 50.0 | 102 | 48.8 | 0.217 | |
| Dorsalgia | 42 | 24.0 | 2 | 14.3 | 51 | 24.4 | 0.788 | |
| Asthenia | 83 | 47.4 | 7 | 50.0 | 89 | 42.6 | 0.568 | |
| Myalgia | 62 | 35.4 | 3 | 21,4 | 76 | 36.4 | 0.597 | |
| Conjunctivitis | 3 | 1.7 | 0 | 0.0 | 6 | 2.9 | 0.652 | |
| Nausea and vomiting | 28 | 16.0 | 2 | 14.3 | 24 | 11.5 | 0.421 | |
| Photosensitivity | 13 | 7.4 | 0 | 0.00 | 12 | 5.7 | 0.634 | |
| Sweating/chills | 57 | 32.6 | 6 | 42.9 | 68 | 32.5 | 0.731 | |
| Odynophagia | 47 | 26.9 | 4 | 28.6 | 49 | 23.4 | 0.691 | |
| Bleeding | 5 | 2.9 | 0 | 0.0 | 11 | 5.3 | 0.480 | |
| Arthralgia | 19 | 10.9 | 2 | 14.3 | 20 | 9.6 | 0.718 | |
| Cough | 19 | 10.9 | 3 | 21,4 | 23 | 11.0 | 0.401 | |
| Generalized lymphadenopathy | 2 | 1.1 | 0 | 0.0 | 4 | 2 | 0.752 | |
| Localized Lymphadenopathy | 57 | 32.6 | 1 | 7.1 | 49 | 23.4 | 0.031 | |
| Genital/perianal lesion | 86 | 49.1 | 10 | 71.4 | 107 | 51.2 | 0.287 | |
| Oral lesion | 25 | 14.3 | 0 | 0.0 | 27 | 13 | 0.365 | |
| Penile edema | 26 | 14.9 | 3 | 21,4 | 21 | 10 | 0.160 | |
| Proctitis | 18 | 10.3 | 1 | 7.1 | 35 | 16.7 | 0.148 | |
| Itching | 8 | 4.6 | 0 | 0.00 | 3 | 1.4 | 0.188 | |
| Diarrhoea | 1 | 0.6 | 0 | 0.0 | 1 | 0.5 | 1.000 | |
| Exanthema | 0 | 0.0 | 0 | 0.0 | 3 | 1.4 | 0.330 | |
| Coryza | 0 | 0.0 | 0 | 0.0 | 1 | 0.5 | 1.000 | |
| Abdominal/pelvic pain | 1 | 0.6 | 0 | 0.00 | 4 | 2 | 0.483 | |
| Characteristics of lesions | ||||||||
| Single | 17 | 9.7 | 1 | 7.1 | 17 | 8.1 | 0.905 | |
| Multiple | 110 | 62.9 | 12 | 85.7 | 128 | 61.2 | 0.642 | |
| Unknown | 43 | 24.6 | 1 | 7.1 | 59 | 28.2 | ||
| Location of lesions | ||||||||
| Face/ Head | 39 | 22.3 | 4 | 28.6 | 51 | 24.4 | 0.806 | |
| Torso | 44 | 25.1 | 4 | 28.6 | 66 | 31.6 | 0.382 | |
| Lower limbs | 30 | 17.1 | 3 | 21,4 | 33 | 15.8 | 0.804 | |
| Upper limbs | 56 | 32 | 5 | 35.7 | 57 | 27.3 | 0.501 | |
| Genital | 77 | 44.0 | 11 | 78.6 | 79 | 37.8 | 0.010 | |
| Buttocks/ Anal | 32 | 18.3 | 2 | 14.3 | 51 | 24.4 | 0.291 | |
| Oral | 20 | 11.4 | 1 | 7.1 | 24 | 11.5 | 1.000 | |
| Palms of hands | 20 | 11.4 | 2 | 14.3 | 23 | 11 | 0.878 | |
| Soles of feet | 9 | 5.1 | 2 | 14.3 | 6 | 2.9 | 0.075 | |
Acronyms: AIDS-Acquired Immunological Deficiency Syndrome. HIV- Human Immunodeficiency Virus.
Table 3. Evaluation of CD4 and VL counts in patients with Mpox + HIV/AIDS co-infection in patients living in Goiânia between June 2022 and June 2023.
| Mpox + HIV/AIDS (n = 223) | |||
|---|---|---|---|
| n | % | ||
| TCD4 lymphocytes (cells/mm3) | |||
| ≤200 | 3 | 1·3 | |
| 201–350 | 11 | 4·9 | |
| 351–500 | 36 | 16·1 | |
| ≥501 | 153 | 68·6 | |
| Not available | 20 | 9 | |
| Viral load (copies/mL) | |||
| Undetectable | 124 | 55·6 | |
| Below the minimum detection limit | 32 | 14·3 | |
| ≤50 | 11 | 4·9 | |
| 51–1000 | 14 | 6·3 | |
| ≥1001 | 20 | 9 | |
| Not available | 22 | 10 | |
Acronyms: AIDS-Acquired Immunological Deficiency Syndrome. HIV- Human Immunodeficiency Virus.
Table 4. Co-infection with other STIs at the time of Mpox diagnosis in the groups with Mpox, Mpox + AIDS, and Mpox + HIV. Patients living in Goiânia between June 2022 and June 2023.
| Mpox (n = 175) | Mpox + AIDS (n = 14) | Mpox + HIV (n = 209) | P-value | |||||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | |||
| STI co-infection | 15 | 8·6 | 2 | 14·3 | 22 | 10·5 | 0·584 | |
| Syphilis | 11 | 6·3 | 1 | 7·1 | 16 | 7·7 | 0·825 | |
| HTLV | 0 | 0·0 | 0 | 0·0 | 1 | 0·5 | 1·000 | |
| Genital herpes simplex | 0 | 0·0 | 0 | 0·0 | 1 | 0·5 | 1·000 | |
| Urethral discharge | 3 | 1·7 | 1 | 7·1 | 6 | 2·9 | 0·261 | |
| Hepatitis C | 0 | 0·0 | 0 | 0·0 | 1 | 0·5 | 1·000 | |
| HPV | 1 | 0·6 | 0 | 0·0 | 0 | 0·0 | 0·475 | |
Acronyms: AIDS-Acquired Immunological Deficiency Syndrome. HIV- Human Immunodeficiency Virus. HTLV- Human T-cell Lymphotropic Virus. HPV- Human Papilloma Virus.
PP04.124 – Overcoming Health Disparities Associated with the HIV PrEP Initiation Cascade Though Provider Feedback, Baltimore City Health Department Sexual Health Clinics, 2016–2023
Mr. Norberth Stracker IV1, Sarah Rives2, Christina Schumacher1, Dr. Matthew Hamill2,3, Dr. Adena Greenbaum3, Dr. Amanda Rosecrants2,3
1Center for Child and Community Health Research, Division of Pediatrics, School of Medicine, Johns Hopkins University, Baltimore, United States.
2Division of Infectious Diseases, School of Medicine, Johns Hopkins University, Baltimore, United States.
3Division of Clinical Services and HIV/STI Prevention, Baltimore City Health Department, Baltimore, United States.
Background: Increasing PrEP uptake while ensuring health equity is critical to reach Ending the HIV Epidemic goals. We investigated disparities in PrEP discussions and prescriptions among demographic groups and risk categories at high-volume sexual health clinics at the Baltimore City Health Department over three periods of programmatic change: 2016–2019, program establishment and scale-up; 2020–2021, COVID-19-impacted; 2022–2023, expansion of rapid PrEP and targeted feedback to clinicians about missed opportunities for PrEP discussions.
Methods: We utilized routinely collected patient demographic, sexual history, substance use, clinical, and treatment data from electronic health records at Baltimore City Health Department Sexual Health Clinics from 2016 to 2023. We defined a “priority for PrEP initiation” group based on clinical and epidemiologic indications for PrEP. We analyzed disparities in i) patient-clinician discussions about PrEP and ii) PrEP prescriptions using multivariable regression across three time periods: 2016–2019, 2020–2021, and 2022–2023.
Results: From 2016 to 2023 PrEP discussions among priority patients increased by 163% (Fig. 1). Overall, among 8672 priority patients, 4045 (47%) had documented discussions with a provider and 1369 (16%) were prescribed PrEP. During 2016–2019, we observed significant racial/ethnic disparities among MSM in both discussions and prescriptions. Among MSM, racial/ethnic disparities in prescriptions decreased by 28% by 2022–2023. By 2022–2023, disparities in discussions between Black MSM under 30 and other population groups decreased substantially or remained non-significant, but cis women and straight cis men remained significantly less likely to initiate PrEP.
Conclusion: Expansion of access to PrEP and usage of PrEP initiation ‘priority patient’ criteria, with direct feedback to clinicians, can reduce racial disparities: in PrEP discussions among all population groups, and in prescriptions among MSM. Disparities between MSM and cis women/straight cis men remain substantial and highlight areas for continued public health intervention.
Trends from 2016 to 2023 among six key demographic groups at Baltimore City Health Department Sexual Health Clinics: the number of patients already on PrEP (a); the number of patients not already on PrEP but priority for PrEP initiation (b); the percent of priority patients with documented discussions with sexual health providers about PrEP (c); and percent of priority patients prescribed PrEP (d).
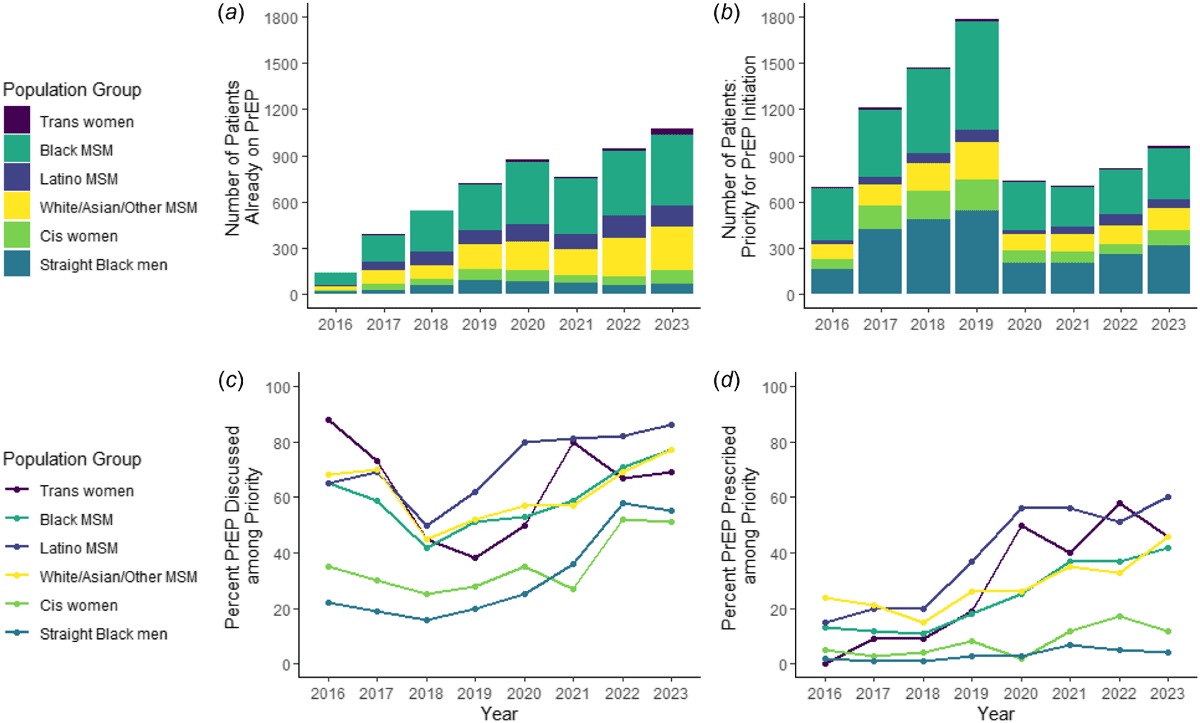
PP04.125 – Modeling the Implementation of Syndromic Management and the Value of Point-Of-Care Testing for Gonorrhea and Chlamydia in Zimbabwe
Dr. Robyn Stuart1, Lori Newman1, Griffins Manguro1, Chido Dziva Chikwari2,3, Remco P. H. Peters4, Daniel Klein1, Lauren Snyder1, Cliff Kerr1, Darcy Rao1
1Bill & Melinda Gates Foundation, Seattle, USA.
2Department of Infectious Disease Epidemiology, London School of Hygiene & Tropical Medicine, London, UK.
3Biomedical Research and Training Institute, Harare, Zimbabwe.
4Department of Global HIV, Hepatitis and STI Programmes, World Health Organization, Geneva, Switzerland.
Background: Zimbabwe’s national guidelines for STI management recommend that high-risk women presenting with vaginal discharge syndrome (VDS) are prescribed antibiotics for gonorrhea (NG), chlamydia (CT), trichomoniasis (TV), and bacterial vaginosis (BV). The performance of this approach depends on prevalence of symptoms, patterns of care-seeking, and implementation of treatment guidelines. Here, we investigate the role of these factors, and elucidate how they influence the potential impact of a point-of-care (POC) testing for NG/CT.
Methods: We created an agent-based model with an age-risk-stratified sexual network and modeled co-circulation of NG, CT, and TV as well as occurrence of BV. Our baseline model uses symptomatic proportions of 10%/20%/40% for women with NG/CT/TV, assumes that 75% of women with symptoms seek care, and that 100% of those seeking care are treated for all 3 STIs. We then created alternative scenarios with lower/higher symptomaticity, care-seeking, and treatment receipt. For each scenario we estimate over/undertreatment rates assuming continuation of the standard of care with/without a POC NG/CT test available over 2025–2040.
Results: We estimate high coinfection rates in Zimbabwe, with ~45% of women presenting with VDS having >1 infection (inclusive of BV). Per-guidelines prescription of STI treatment to all cases implies 70–80% of antibiotics for NG/CT are given to women without these infections; a sensitive POC test for these infections would reduce overtreatment to <5%, but would not impact transmission. However, if we assume lower treatment coverage in current syndromic practice, a POC test would reduce both over/undertreatment and could imply a 10–15% reduction in incident NG/CT cases over 2025–2040.
Conclusion: POC testing holds potential to improve antimicrobial management and reduce NG/CT transmission. Evaluating the impact of new diagnostics depends crucially on understanding the performance of the standard of care.
PP04.126 – Trends, Associated Factors and Reasons for Late and Advanced HIV Diagnoses in 2011–2022 in Melbourne, Australia
Mrs Warittha Tieosapjaroen1,2, Mr Arron Tran1,3, Mr Marcus Maisano1, Ms Cham Kim2,3, Dr Christopher K. Fairley1,2, Dr Eric P. F. Chow1,2,4, Dr Lei Zhang1,2, Dr Tiffany R. Phillips1,2, Ms Melanie Bissessor1, Dr Jason J Ong1,2,5
1Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia, Melbourne, Australia.
2The School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Melbourne Medical School, The University of Melbourne, Faculty of Medicine Dentistry and Health Sciences, Melbourne, Australia.
4Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
5Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, UK.
Background: Late (LHD) and advanced HIV diagnoses (AHD) remain high in many countries despite a global reduction in new notifications. This retrospective study examined trends, associated factors and reasons for LHD (CD4 < 350 cells/µL) and AHD (CD4 < 200 cells/µL) between 2011–2022 at Melbourne Sexual Health Centre (MSHC), Australia, to inform strategies for earlier detection of HIV.
Methods: Two independent researchers reviewed e-medical records of new HIV diagnoses at MSHC. We used chi-square trend tests for trends in proportions of LHD or AHD, univariable and multivariable multinomial regression analyses for associated factors for LHD and AHD. We report risks of HIV infection, initial testing reasons and barriers to earlier testing.
Results: Among 606 new diagnoses, 25% (n = 152) were LHD, 11% (n = 65) were AHD, and 94% (n = 568) were among men who have sex with men (Fig. 1). Among 352 overseas-born individuals, LHD and AHD increased from 22% (4/18) in 2011 to 56% (5/9) in 2022 (Ptrend = 0.017). No significant change was observed among Australian-born individuals. LHD was associated with being born in Latin America (adjusted relative risk ratio (aRRR) 2.66, 95% Confidence interval 1.10–6.43) or in East Asia and Pacific (aRRR 1.98, 1.14–3.43), having no prior sexually transmitted infection (STI) diagnosis in lifetime (aRRR 2.32, 1.36–3.96), and no drug use in lifetime (aRRR 2.12, 1.30–3.44). AHD was associated with being born in East Asia and Pacific (aRRR 2.38, 1.02–5.56), no prior STI (aRRR 4.60, 2.14–9.92), older age (aRRR 1.05, 1.02–1.09), Medicare-ineligibility (aRRR 3.19, 1.33–7.65), and unknown condom use history in the last year (aRRR 2.45, 1.09–5.54). Key barriers to earlier testing included LGBT-related stigma (19%; 41/217) and recent arrival (<5 years) in Australia (19%; 41/217). The primary risk for contracting HIV was condomless anal sex (27%; 80/217).
Conclusions: One in three new HIV diagnoses was late or advanced, with increased risk among overseas-born, Medicare-ineligible or those with perceived low risk.
Adjusted relative importance of factors associated with late and advanced HIV diagnoses. RRR, relative risk ratio; STI, sexually transmitted infection.
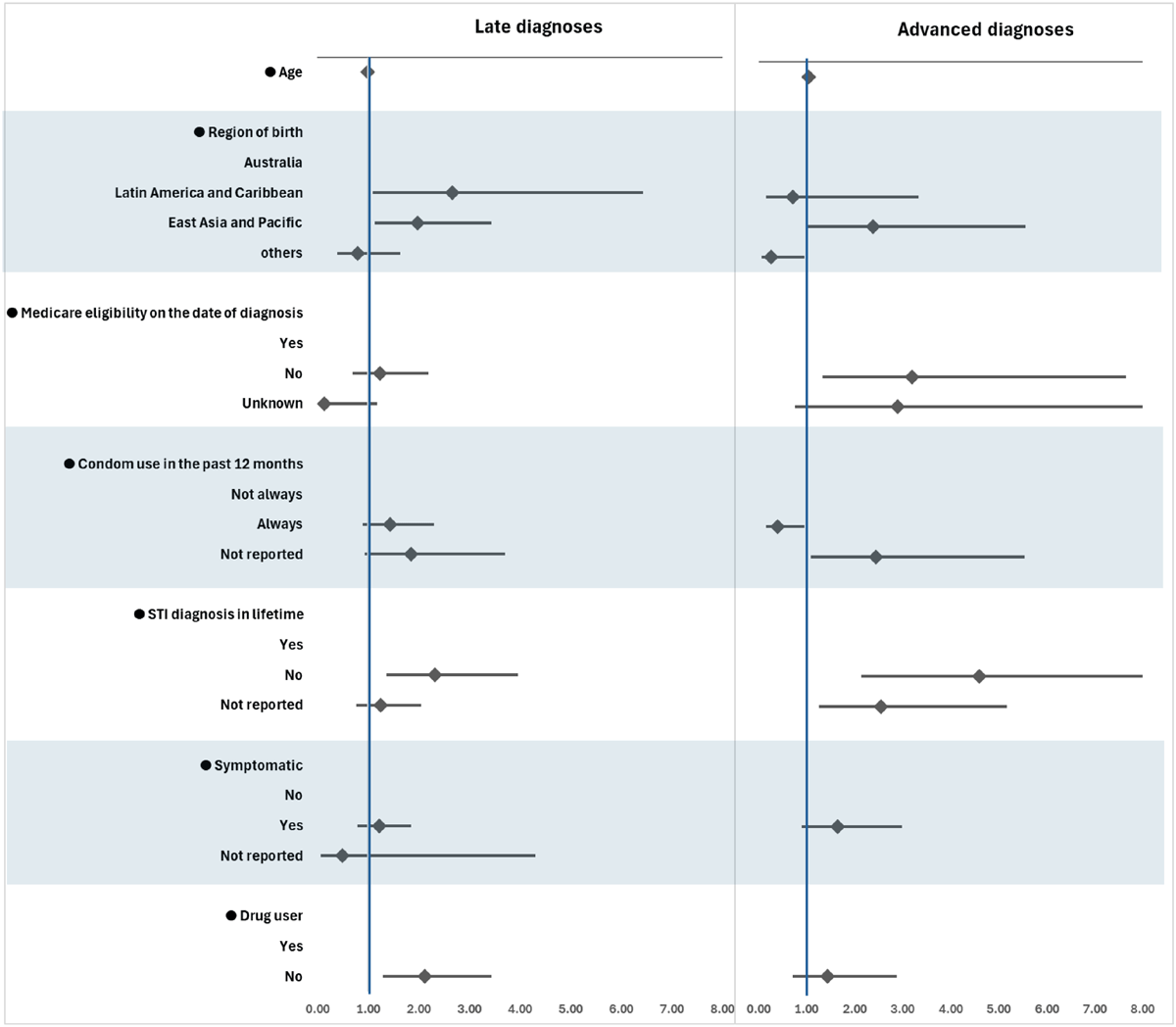
PP04.127 – “If Someone Has Information That Could Help Someone’s Health, Don’t They Have a Responsibility to Share It?” Survey Findings on Young People’s Preferences for Partner Notification of Sexually Transmissible Infections in Australia
Dr. Steph Munari1,2, Research Fellow Michael Traeger1, Dr Jane Goller2, Dr Jacqueline Coombe2, Ana Orozco1, Sarah Eddy1, Prof Jane Hocking2, Prof Margaret Hellard1,3,4,5, A/Prof Megan Lim1,2,4
1Burnet Institute, Melbourne, Australia.
2Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
3Department of Infectious Diseases, Alfred Hospital, Melbourne, Australia.
4Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, Australia.
5Doherty Institute and School of Population and Global Health, University of Melbourne, Melbourne, Australia.
Background: Partner notification for Sexually Transmissible Infections (STI) is an important step in the overall management of STIs, helping to reduce transmission and the risk of complications. As STIs continue to be present at high rates among young people in Australia, this study aimed to determine the preferences and motivations for partner notification among this priority population.
Methods: Data were collected through the 2024 Sex Drugs and Rock ‘n’ Roll survey, an annual online cross-sectional survey conducted among people aged 15–29 years old in Victoria, Australia. Closed-ended responses in the form of counts and percentages determined preferences by regular and casual sexual partners, and method of communication. Inductive content analysis was used to analyse motivations within open-ended free-text responses.
Results: Survey questions within the partner notification module were completed by 1,163 people (60.3% identified as women, 40.2% as heterosexual), including a total of 1,720 free-text responses. The large majority stated they would notify a sexual partner of an STI risk (1,056; 90.8%), and even more stated they would want to be notified (1,142; 98.2%). Most preferred to notify regular partners face-to-face (941; 80.9%) and casual partners via text message (785; 67.5%). Social media was more preferred for notifying (280; 24.1%) and being notified by (327; 28.1%) casual partners compared to notifying (176; 15.1%) and being notified by (181; 15.6%) regular partners.
Conclusion: Almost all young people in our survey want to notify and be notified by partners of an STI risk, regardless of age, gender or sexual identity. Tailoring resources by communication method and partner type is one way in which public health practitioners can support young people in undertaking this important step in STI control.
PP04.128 – Prevalence and Associated Risk Factors of Curable Bacterial STIs in Key Populations (MSM and FSW) Visiting STD Clinics in North India
Ms. Tenzin Tsephel1, Dr Tarun Narang1, Dr Rakesh Yadav1, Dr P. V. M. Lakshmi1, Miss Nandita Sharma1, Dr Sunil Sethi1
1Postgraduate Institute of Medical Education and Research (PGIMER), Chandigarh, Chandigarh, India.
Background: Studies on the key populations encompassing both men who have sex with men (MSM) and Female Sex workers (FSW), have been extensively documented in countries such as the US, UK, and Australia, yet they remain relatively scarce in the Indian context. This study aims to evaluate the prevalence of curable bacterial STIs and identify associated risk factors among key population groups in North-India. Prevalence of antimicrobial resistance is increasing tremendously both in Neisseria gonorrhoeae (NG) and Mycoplasma genitalium (MG) worldwide.
Methods: A prospective study was conducted between February 2022 and January 2024 at the regional STI reference center, at Postgraduate Institute of Medical Education and Research (PGIMER), Chandigarh. A total of 375 participants comprising of 213 MSMs and 162 FSWs were enrolled. Genital or extra-genital samples were collected from each patient along with demographic details. The samples were screened for Neisseria gonorrhoeae (NG), Mycoplasma hominis (MH) and Ureaplasma urealyticum (UU) by culture as well as by NAAT method and Mycoplasma genitalium (MG) by in house PCR. Macrolide and fluoroquinolone resistance-associated mutations were studied using Sanger sequencing in MG and NG.
Results: The prevalence of MG was 8.2% (31/375), NG 2.9% (11/375), MH 18.6% (70/375), UU 20.2% (76/375), HIV 1.06% (4/375), Treponema pallidum 4.53% (17/375). The prevalence of all STIs in total population was higher in the below 30 years of age group. A co-infection of MG and GC was found in 0.8% (3/375) participant. 5/31 (16.12%) showed macrolide associated mutation in Mycoplasma genitalium. All NG positive isolates showed fluoroquinolone resistance in gyrA gene.
Conclusion: In this study, STIs were found to be more prevalent in MSM who had bisexual behaviors compared to those who engaged only in homosexual behaviors. Among all sample types, urine was found to be the most commonly infected source in both MSMs and FSWs.
PP04.129 – Prevalence, Knowledge, and Treatment-Seeking Behavior for Sexually Transmitted Infections Among Men Who Have Sex with Men in Ibadan, Oyo State Nigeria, 2023
Dr Olubunmi Akinboye1, Dr. Aishat Bukola Usman2, Prof Olufunmilayo Fawole1
1Department of Epidemiology and Medical Statistics, University of Ibadan, Nigeria.
2West African Health Organization, Bobo Dioulasso, Burkina Faso.
Background: This study examines the knowledge, prevalence, and treatment-seeking behaviors regarding sexually transmitted infections (STIs) among men who have sex with men (MSM) in Ibadan, Nigeria. Due to the stigma and hidden nature of MSM in Nigeria, limited research exists on their STI knowledge and behaviors.
Methods: To address this gap, a cross-sectional study recruited 551 MSM aged 18 and above through Respondent-Driven Sampling. Participants provided data on demographics, sexual practices, STI knowledge, and treatment sources via a semi-structured questionnaire, analyzed using descriptive statistics and multivariate regression.
Results: The participants’ ages ranged from 18 to 47, with a mean age of 26.4 years. Most respondents identified as bisexual (71.6%), were students (48.6%), and had tertiary education (66.9%). Despite 68.4% reporting condom use in the last month, risky behaviors were noted, including multiple sexual partnerships (62.9%) and transactional sex (50.5%). The self-reported lifetime prevalence of STIs was 18.9%, though 27% were unsure of past infections. STI knowledge was generally low (64.9%), with a significant association between knowledge levels and factors such as occupation, healthcare contact, and condom use. Most MSM (76.5%) preferred seeking STI treatment from Patent Medicine Vendors (PMVs), while only 3.4% used clinics, mainly due to stigma concerns (42.8%).
Conclusion: The study concludes that low STI knowledge, high STI prevalence, and reliance on informal treatment sources like PMVs underscore a critical need to reduce stigma and improve healthcare access for MSM. Targeted education and outreach are recommended to support STI prevention and appropriate treatment-seeking among this vulnerable population.
Keywords: Men who have sex with men (MSM), sexually transmitted infections (STIs), knowledge, prevalence, treatment-seeking behavior, Nigeria.
PP04.13 – Assessing the Association Between Bacterial Vaginosis and Cervicitis Among Female Sex Workers in Kenya
Dr. Fredericka Albertina Sesay1, Dr. Jennifer Balkus1,2, Dr Walter Jaoko3, Dr Marianne Mureithi3, Dr Kishorchandra Mandaliya1, Khamis Mwinyikai6, Dr Michelle C. Sabo1, Dr Elizabeth A. Bukusi1,3, Dr Jenell Stewart4,5, Dr Olusegun O. Soge1, Dr R. Scott McClelland1
1University of Washington, Seattle, United States.
2Seattle & King County, HIV/STI/HCV Program, Seattle, United States.
3University of Nairobi, Nairobi, Kenya.
4Hennepin Healthcare Research Institute, Minneapolis, United States.
5University of Minnesota, Minneapolis, United States.
6Pwani Research Centre, Mombasa, Kenya.
Background: Cervicitis, an inflammatory condition of the cervix, is often caused by Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (GC), but its etiology remains unexplained in approximately 50% of cases. Studies examining the relationship between the vaginal microbiota, including bacterial vaginosis (BV), and cervicitis, have yielded conflicting results.
Methods: We analyzed data from an open cohort study of cisgender women who engage in sex work in Mombasa, Kenya (2004–2023). BV was assessed via Gram stain using Nugent and Hillier criteria (normal = 0–3; intermediate = 4–6; BV = 7–10), and cervicitis as ≥30 polymorphonuclear cells per high-power field on cervical Gram stain. BV and cervicitis were assessed monthly; CT/GC testing occurred quarterly. Modified Poisson regression with generalized estimating equations was used to assess the association between BV and cervicitis while adjusting for known or suspected confounders, including CT/NG infections, assuming negative results between quarterly tests (Table 1).
Results: There were 1,615 participants, contributing 25,322 visits. At enrollment, the median age was 28 years, and the median duration of sex work was 2 years. Across all visits, BV prevalence was 30.2%, and intermediate microbiota was 15.6%. Cervicitis was identified at 5.8% of visits with normal microbiota compared to 9.1% (adjusted RR = 1.32; 95% CI: 1.18–1.48) at visits with intermediate microbiota and 6.8% (adjusted RR = 1.12; 95% CI: 1.01–1.25) at visits with BV. These findings remained consistent across multiple sensitivity analyses (Table 1).
Conclusion: Our findings show that intermediate microbiota was associated with the highest risk of cervicitis. Prior studies have shown that a Lactobacillus-dominated vaginal microbiota is associated with higher concentrations of CXCL10, while BV is associated with higher concentrations of a group of pro-inflammatory cytokines (but not CXCL10). Intermediate microbiota may be a state in which the combination of higher CXCL10 and other pro-inflammatory cytokines leads to more cervical inflammation. This hypothesis should be explored in future studies.
| Analysis/BV Status | Number of Events/Visits (%) | Unadjusted RR (95% CI) | Adjusted RR (95% CI)1 | |
|---|---|---|---|---|
| Primary Analysis (N = 25,322)2 | ||||
| Normal (Reference) | 796/13739 (5.8%) | 1.00 | 1.00 | |
| Intermediate | 359/3946 (9.1%) | 1.39 (1.24–1.56) | 1.32 (1.18–1.48) | |
| BV | 522/7637 (6.8%) | 1.14 (1.02–1.26) | 1.12 (1.01–1.25) | |
| Sensitivity AnalysisA (N = 19,218) | ||||
| Normal (Reference) | 648/10393 (6.2%) | 1.00 | 1.00 | |
| Intermediate | 316/3108 (10.2%) | 1.42 (1.25–1.60) | 1.35 (1.19–1.53) | |
| BV | 427/5717 (7.5%) | 1.13 (1.01–1.27) | 1.12 (1.00–1.26) | |
| Sensitivity AnalysisB (N = 11,329) | ||||
| Normal (Reference) | 304/6005 (5.1%) | 1.00 | 1.00 | |
| Intermediate | 164/1820 (9.0%) | 1.64 (1.38–1.95) | 1.53 (1.28–1.83) | |
| BV | 230/3504 (6.6%) | 1.26 (1.08–1.47) | 1.23 (1.05–1.45) | |
| Sensitivity AnalysisC (N = 10,776) | ||||
| Normal (Reference) | 282/5758 (4.9%) | 1.00 | 1.00 | |
| Intermediate | 147/1726 (8.5%) | 1.62 (1.35–1.93) | 1.53 (1.27–1.83) | |
| BV | 201/3292 (6.1%) | 1.22 (1.04–1.44) | 1.21 (1.02–1.43) |
PP04.130 – Digital Innovations for Youth Sexual and Reproductive Health Knowledge and Behaviour: Evidence from a Systematic Review
Miss Olivia Vaikla1,2, Dr. Angela Karellis2, Miss Elizabeth Woolhouse2, Dr. Roni Deli-Houssein2, Miss Melisa Eraslan2, Miss Hani Rukh-E-Qamar1,2, Dr. Suma Nair3, Dr. Qihuang Zhang1, Dr. Nitika Pant Pai1,2
1McGill University, Montreal, Canada.
2Research Institute of the McGill University Health Centre, Montreal, Canada.
3D.Y. Patil University, Navi Mumbai, India.
Background: Adolescents and young adults often lack access to quality, evidence-based sexual and reproductive health and rights (SRHR) education. Innovative digital interventions provide SRH tools, services, and resources, offering promise and potential to catalyze change. However, evidence on the effectiveness of innovations to guide World Health Organization policy remains limited. We conducted a systematic review to address this gap.
Methods: For the period June 2017–April 2023, reviewers independently searched PubMed and Embase for publications and abstracts, retrieving 11,556 citations. Data abstraction and quality critique were performed on a final set of 112 studies.
Results: We abstracted data from 50,658 participants across 24 countries, with most studies conducted in the United States (US; 66.1%, 74/112) (Fig. 1). Studies reported on knowledge uptake (62.5%, 70/112) and behaviour change (69.6%, 78/112), across 47 randomized controlled trials (RCTs; 42.0%), 26 pilot RCTs (23.2%), 18 quasi-experimental trials (16.1%), and 21 observational studies (18.8%).
Multi-modal innovations (n = 14), combining at least two digital components to deliver SRH content, proved most effective. A trial demonstrated increased pre-exposure prophylaxis adherence (Mean 0.02 to 0.05, possible range: 0–1, P < 0.001) and reduced condom use errors (Mean 4.04 to 3.70, possible range: 0–9, P < 0.05).
General SRH knowledge improved in all studies where assessed (38.6%, 27/70), with increases ranging from 8.1%–76.0% reported in Nicaragua, Thailand, and the US.
Behavioural changes varied, with notable US-based trials reporting increased STI testing (P = 0.016), improved contraception and condom use (IRR = 1.39 [95% CI 1.09–2.11]), higher clinic attendance and follow-up (aOR = 1.6 [1.1–2.3], P = 0.01), and reduced sexual risk-taking (PR = 0.83 [0.70–0.99], P = 0.04).
Conclusion: Digital innovations effectively enhanced SRH knowledge and promoted safer behaviours in young, underserved populations. While these tools demonstrated significant promise, wide variability in outcomes underscores the need for a standardized evaluation framework that will ensure reliable reporting and comparisons across studies to steer normative guidance.
Registration: PROSPERO CRD42021258889
PP04.131 – STI Positivity Among Home-Based Female Sex Workers Compared to Female Sex Workers in Indoor Sex Venues and Escorts in the Netherlands
Mrs Amanja Verhaegh-Haasnoot1, Ms. Charlotte Peters1,2, Dr. Ymke Evers1,2, Ms. Marita Werner1, Dr. Nicole Dukers-Muijrers1,3, Prof. Christian Hoebe1,4
1Department of Sexual Health, Infectious Diseases and Environmental Health, Living Lab Public Health Mosa, South Limburg, Heerlen, Netherlands.
2Department of Social Medicine, Care and Public Health Research Institute (CAPHRI), Maastricht University/Maastricht UMC+, Maastricht, Netherlands.
3Department of Health Promotion, Care and Public Health Research Institute (CAPHRI), Maastricht University/Maastricht UMC+, Maastricht, Netherlands.
4Department of Medical Microbiology, Infectious Diseases and Infection Prevention, Care and Public Health Research Institute (CAPHRI), Maastricht University Medical Centre (MUMC+), Maastricht, Netherlands.
Background: Home-based female sex workers (FSW) have been an increasing population over the last decade. Professionals at a Dutch STI clinic noticed relatively more STI among home-based female sex workers (FSW) than among other FSW. Limited scientific research is available on STI among home-based FSW. This study aims to assess STI positivity among FSW working in different sex work locations, specifically home-based sex work.
Methods: A retrospective cohort study included 1180 routinely collected STI consultations from 406 FSW visiting our Dutch STI Clinic between 2014–2019. Positivity for STI (chlamydia/gonorrhea/infectious syphilis/infectious hepatitis B/HIV) was compared among home-based FSW, FSW working in indoor sex venues and escort FSW, using chi-squared tests and multivariate logistic regression analyses adjusting for age and ethnicity.
Results: STI positivity was 10% overall, 6% for chlamydia and 5% for gonorrhea. Syphilis, infectious hepatitis B and HIV were diagnosed in <0.4% of the consultations. Overall STI positivity differed significantly by sex work location, with infections being more prevalent among home-based FSW (16% versus 9%, P < 0.05). Sociodemographic factors, including age, ethnicity, and education, as well as sexual behaviors, such as condom use, varied significantly among FSW by work location. Working as a home-based FSW was associated with diagnosis of a new STI (aOR 1.9, 95% CI 1.2–3.2) compared to FSW in indoor sex venues.
Conclusion: STI positivity is substantial among home-based FSW versus escort FSW, highlighting the importance of targeted (online) outreach strategies that engage home-based FSW.
PP04.132 – A Bayesian Clinical Risk Prediction Model to Pre-Screen Key Populations Prior to Multiplexed Testing: Results from a Canadian Study
Mx. Fio Vialard1,2, Qihuang Zhang1, Duncan Webster3, Stefanie Materniak3, Alexandre Dumont Blais4, Suma Nair5, Susan Bartlett1,2, Nitika Pant Pai1,2
1McGill University, Montreal, Canada.
2Research Institute of the McGill University Health Centre, Montreal, Canada.
3Saint John Regional Hospital, Saint John, Canada.
4RÉZO, Montreal, Canada.
5DY Patil University, Navi Mumbai, India.
Background: Multiplexed rapid screening programs that detect sexually transmitted infections (STI) are becoming popular worldwide. Pre-screening key populations for STI risk could improve case finding with multiplexed testing. For this, we developed and validated a diagnostic clinical risk prediction model (CRPM) to estimate an overall STI risk from Hepatitis C virus (HCV), HIV and syphilis infections. We used secondary data from a multiplexed study (n = 400) conducted in key populations (i.e. people who use injection drugs, trans- and gender-diverse people, gay and bisexual men who have sex with men) recruited from two Canadian provinces (New Brunswick and Québec).
Methods: In R, using clinic-stratified sampling, we randomly split data into development (n = 300) and validation (n = 100) datasets. Using development data, we performed a Bayesian predictive projection to select predictors for STI risk. Using validation data, we measured the performance of candidate CRPMs with area under the receiver operating curve (AUC), sensitivity, specificity with 89% Credible Intervals (89%CrI) and calculated the Odds Ratios (OR) and risk by predictor of the highest performing candidate.
Results: Of 400 participants, 73 were infected with HCV (n = 60), HIV (n = 16), and/or syphilis (n = 5). The final internally validated CRPM with the highest AUC (0.79; 89%CrI: 0.66–0.79), sensitivity (0.85; 89%CrI: 0.79–0.91), and specificity (0.30; 89%CrI: 0.15–0.50) contained two predictors: 1) Past drug injections (OR = 7.62; 89%CrI: 4.41–13.07), and 2) Past STI test (Unspecified OR = 3.84; 89%CrI: 1.06–10.97 & Specified OR = 1.65; 89%CrI: 0.97–3.15). In Table 1, we present a hypothetical screening decision based on STI risk by predictors of the final CRPM.
Conclusion: This Bayesian CRPM demonstrates that history of drug injections and STI tests were sufficient to estimate STI risk (HCV, HIV, and syphilis) in these key populations. It is a promising pre-screening tool to optimize case finding in combination with rapid multiplexed screening programs. However, its validation in diverse key populations is recommended before its widespread use.
| Pre-screening questions | Results | Hypothetical screening decision | ||
|---|---|---|---|---|
| Does the individual have a history of past drug injection? | Has the individual previously been tested for STIs? | Predicted STI risk (89%CrI) A | Should a multiplex test be offered? | |
| No | No | 0.06 (0.04–0.10) | No | |
| Yes | No | 0.31 (0.15–0.59) | Yes | |
| No | Yes, with type of test unspecified | 0.19 (0.04–0.55) | Yes | |
| No | Yes, with type of test specified | 0.09 (0.04–0.26) | No | |
| Yes | Yes, with type of test unspecified | 0.64 (0.16–0.94) | Yes | |
| Yes | Yes, with type of test specified | 0.43 (0.15–0.82) | Yes | |
PP04.133 – Sequential Sex Practices and the Likelihood of Bacterial Sexually Transmitted Infections and Urethritis in Men Who Have Sex with Women
Ms. Mary Bridget Waters1, Dr. Laura C. Chambers2, Dr. Lisa E. Manhart1, Dr. Christine M. Khosropour1
1University of Washington, Seattle, United States.
2Brown University, Providence, United States.
Background: Mathematical modeling studies suggest that sequential sex practices (SSP) among men who have sex with men are necessary to produce observed rates of bacterial sexually transmitted infections (STIs). The frequency of SSP and their associations with bacterial STIs among men who have sex with women (MSW) is not well-characterized.
Methods: We utilized data from a cohort study examining the role of the urethral microbiota and sexual behaviors in male urethritis in Seattle, WA (2014–2018). Participants provided monthly urine samples, which were tested for Chlamydia trachomatis (CT), Mycoplasma genitalium (MG), and Neisseria gonorrhoeae (NG) via nucleic acid amplification testing, and completed questionnaires ascertaining SSP at six monthly follow-up visits. This analysis included males age ≥16 years who reported exclusively female partners in the past year and had at least one follow-up visit. We identified the most frequent SSP reported at participants’ last sexual encounter before testing and used generalized estimating equations to estimate probability of positive urethral STI test (CT, MG, or NG) and urethritis.
Results: Overall, 205 participants reported 715 sexual encounters; 76% of sexual encounters included >1 sex act. The most frequently reported SSP were insertive oral sex followed by vaginal sex (57.8%), vaginal sex only (19.6%), and vaginal sex followed by insertive oral sex (9.2%) (Table 1). In total, participants had 17 positive urethral STI tests and 15 urethritis cases. The probability of a positive STI test (6.4%) and urethritis (3.1%) was highest among those who reported vaginal sex followed by insertive oral sex.
Conclusion: Among MSW, there are clear patterns in SSP and potentially elevated transmission probabilities associated with particular sequences. Future work could apply this data in STI modeling studies or explore similar outcomes in a larger sample.
| Percent of sexual encounters (95% CI) | Probability, percent (95% CI) | |||
|---|---|---|---|---|
| Positive CT, MG, or NG NAAT A (n = 17) B | Urethritis (n = 15) | |||
| Overall (N = 715 sexual encounters among 205 participants) | -- | 2.64 (1.37, 5.03) | 2.09 (1.29, 3.38) | |
| Insertive oral sex → vaginal sex (n = 413) | 57.8 (54.0, 61.4) | 2.12 (0.83, 5.26) | 2.17 (1.15, 4.06) | |
| Vaginal sex (n = 140) | 19.6 (16.8, 22.7) | 2.14 (0.69, 6.39) | 2.91 (1.14, 7.23) | |
| Vaginal sex → insertive oral sex (n = 66) | 9.2 (7.3, 11.6) | 6.39 (2.37, 16.09) | 3.11 (0.77, 11.77) | |
PP04.134 – Factors Associated with Acquired Syphilis in Southern Brazil: Results from the SIM Study
Dr Thayane Martins Dornelles1, Dr Rafael Steffens Martins1, Dr Gustavo Eidt1, Dr Augusto Bacelo Bidinotto1, Dr. Eliana Wendland1
1Hospital Moinhos de Vento, Porto Alegre, Brasil.
2Federal University of Health Sciences of Porto Alegre, Porto Alegre, Brazil, Brasil.
Background: Syphilis rates are increasing globally, particularly in high-income countries and Latin America. In Brazil, both acquired and congenital syphilis rates exceed WHO targets and have risen since 1990, with the southern region reporting the highest prevalence. This study aimed to identify factors associated with syphilis diagnosis in Porto Alegre, southern Brazil.
Methods: The Health, Information, and Monitoring of Sexually Transmitted Infections (SIM) study was a cross-sectional survey conducted via a mobile testing unit between 2021 and 2023. Adults (≥18 years) were recruited on a walk-in basis and completed a semi-structured questionnaire on sociodemographic and behavioral characteristics, followed by rapid and confirmatory syphilis testing. Active syphilis was defined as a reactive treponemal test (TR) and a positive VDRL, combined with specific diagnostic or treatment criteria. Descriptive and chi-square statistical analyses were performed.
Results: Of 10,878 rapid syphilis tests, 1,559 (14.3%) were reactive. Confirmatory testing revealed an active syphilis prevalence of 6.4% (701 cases). Active syphilis was associated with male sex (67.3%, P = 0.004), lower educational attainment (70.9%, P < 0.001), self-identification as pardo (71.09%, P = 0.002), and lower socioeconomic status (71.43%, P = 0.005). Behavioral factors such as alcohol consumption or drug use were not significantly associated with syphilis. However, unprotected vaginal sex (62.47%, P = 0.04) and commercial sex (78.7%, P = 0.01) were associated with higher prevalence.
Conclusion: High syphilis rates in Porto Alegre are significantly linked to sociodemographic vulnerabilities. Public health interventions are essential to address disparities by reducing barriers to education and healthcare and improving access to preventive measures for at-risk populations.
PP04.135 – Prevalence of Unsuppressed HIV Viraemia in Rio Grande Do Sul, Brazil: Results from the Atitude Serological Household Survey
Dr Gustavo Eidt1, Dr Bruna Angelo Vieira1, Msc Giovana Petracco de Miranda1, Dr Aniúsca Vieira dos Santos1, Dr Augusto Bacelo Bidinotto1, Dr. Eliana Wendland1,2
1Hospital Moinhos De Vento, Porto Alegre, Brasil.
2Federal University of Health Sciences of Porto Alegre, Porto Alegre, Brazil, Brasil.
Background: In the southernmost Brazilian state, the HIV epidemic has historically been more severe, with the metropolitan health macroregion presenting a generalized epidemic in the adult population. Undiagnosed HIV is associated with increased rates of disease transmission and increased mortality. This likely contributes to the prevalence of unsuppressed viraemia (PUV) and aggravates the HIV epidemic. Therefore, we aimed to evaluate the PUV among adults.
Methods: A population-based household survey was conducted (2020–2022) among general adult residents of Rio Grande do Sul who answered questionnaires and provided capillary blood samples for HIV testing, using dried blood spots and microtainers with gel separators. Xpert® HIV-1 (Cepheid®) was used for HIV viral load analysis. Unsuppressed viraemia was defined as having a viral load ≥1000 copies/mL. Prevalence estimates used survey-weighted methods with regional stratification based on health macroregions.
Results: From 7,978 analyzed individuals, over one-third (37%) of the diagnosed people living with HIV remain unaware of their serological status. The overall rate of unsuppressed viremia was 271.3 (95% CI 143.4–512.6) per 100,000 population reaching the 400.6 (95% CI 365.9–438.4) per 100,000 at metropolitan health macroregion. One fifth of all diagnosed HIV cases presented unsuppressed viraemia, with most of them (15 out of 17) being unaware of their HIV status before the survey.
Conclusion: We found high prevalence of unsuppressed viraemia in the adult population, which indicates high transmission risk, pointing to the need for enhanced community-based HIV detection strategies in southern Brazil. A national serological household survey to explore these findings across other Brazilian states is highly advisable.
PP04.136 – Prevalence of Unsuppressed HIV Viraemia in Rio Grande Do Sul, Brazil: Results from the Atitude Serological Household Survey
Dr. Gustavo Eidt1, Dr. Bruna Angelo Vieira1, MSc Giovana Petracco de Miranda1, Dr. Aniúsca Vieira dos Santos1, Dr. Augusto Bacelo Bidinotto1, Dr. Eliana Wendland1,2
1Hospital Moinhos De Vento, Porto Alegre, Brazil.
2Federal University of Health Sciences of Porto Alegre, Porto Alegre, Brazil.
Background: In the southernmost Brazilian state, the HIV epidemic has historically been more severe, with the metropolitan health macroregion presenting a generalized epidemic in the adult population. Undiagnosed HIV is associated with increased rates of disease transmission and increased mortality. This likely contributes to the prevalence of unsuppressed viraemia (PUV) and aggravates the HIV epidemic. Therefore, we aimed to evaluate the PUV among adults.
Methods: A population-based household survey was conducted (2020–2022) among general adult residents of Rio Grande do Sul who answered questionnaires and provided capillary blood samples for HIV testing, using dried blood spots and microtainers with gel separators. Xpert® HIV-1 (Cepheid®) was used for HIV viral load analysis. Unsuppressed viraemia was defined as having a viral load ≥1000 copies/mL. Prevalence estimates used survey-weighted methods with regional stratification based on health macroregions.
Results: From almost eight thousand analyzed individuals, over one-third (37%) of the diagnosed people living with HIV remain unaware of their serological status. The overall rate of unsuppressed viremia was 271.3 (95% CI 143.4–512.6) per 100,000 population reaching the 400.6 (95% CI 365.9–438.4) per 100,000 at metropolitan health macroregion. One fifth of all diagnosed HIV cases presented unsuppressed viraemia, with most of them (15 out of 17) being unaware of their HIV status before the survey.
Conclusion: We found high prevalence of unsuppressed viraemia in the adult population, which indicates high transmission risk, pointing to the need for enhanced community-based HIV detection strategies in southern Brazil. A national serological household survey to explore these findings across other Brazilian states is highly advisable.
PP04.137 – Help-Seeking Behaviors in Adults Reporting Genital Lesions: Results from the Atitude Household Survey
Msc Giovana Petracco De Miranda1, Msc Igor Terra1, Dr Bruna Angelo Vieira1, Dr Gustavo Eidt1, Ana Carolina Monteiro da Rocha1, Dr Augusto Bacelo Bidinotto1, Dr. Eliana Wendland1,2
1Hospital Moinhos de Vento, Porto Alegre, Brasil.
2Federal University of Health Sciences of Porto Alegre, Porto Alegre, Brazil, Brasil.
Background: Genital lesions, such as sores, blisters, or warts, are a common manifestation of sexually transmitted infections (STI) and a recognized risk factor for their transmission. Therefore, this study aimed to estimate the prevalence of self-reported genital lesions and help-seeking behaviors among adults in Brazil’s southernmost state, stratified by gender.
Methods: A population-based household survey (2020–2022) was conducted, targeting adults aged 18 years or older in Rio Grande do Sul, Brazil. Participants completed a structured questionnaire to assess knowledge, attitudes, and practices related to STI, including whether and where they sought assistance and treatment for genital lesions. The prevalence of genital lesions was estimated using survey-weighted methods, based on participants’ self-reported lifetime occurrence of sores, blisters, or warts.
Results: Among 7,976 participants, the overall prevalence of self-reported genital lesions was 6.8% (95% CI 5.3–8.5%), being 7.3% (5.5–9.6%) in females and 5.7% (4.5–7.1%) in males. Among individuals with genital lesions, the proportion of males who underwent treatment was 65.4% (56.9–73.9%), significantly lower than females (80.2% [77.2–83.2%]). This might be partly explained by the higher proportion of males who didn’t seek assistance 21.7% (12.6–30.8%), compared to 9.0% (5.6–12.4%) for females. Doctor visits represented 92.9% (88.7–97.0%) of help-seeking behaviors.
Conclusion: No significant difference was observed in the prevalence of self-reported genital lesions between genders. However, a significant gender gap in help-seeking behaviors and treatment access highlights men’s lower engagement with their own sexual health. This issue may be exacerbated by societal perceptions of masculinity, which discourage men from prioritizing and addressing their health needs.
PP04.138 – Chlamydia, Gonorrhea, Mycoplasma, and Trichomonas Infections Among Young Adults in Brazil: Results from Pop-Brazil Study
Dr Michele Bertoni Mann1, Dr Ana Paula Muterle Varela1, Dr Rafael Steffens Martins1, Fernanda Rodrigues Girard Abdallah Abdallah1, Dr Gustavo Eidt1, Dr Thayane Martins Dornelles1, Msc Camila Bonalume Dall’ Aqua1, Amanda de Carvalho Robaina1, Dr Natália Luiza Kops1, Dr Luana Giongo Pedrotti1, Dr Augusto Bacelo Bidinotto1, Dr. Eliana Wendland1
1Hospital Moinhos de Vento, Porto Alegre, Brasil.
2Federal University of Health Sciences of Porto Alegre, Porto Alegre, Brazil, Brasil.
Background: The 2022–2030 Global Health Strategies for sexually transmitted infections (STIs) aim to reduce the incidence of Chlamydia trachomatis, Neisseria gonorrhoeae, Trichomonas vaginalis, and Mycoplasma genitalium. However, these infections remain neglected and under-monitored in Brazil, with national prevalence data unavailable. This study estimated the prevalence of these STIs among young individuals in Brazil over recent years.
Methods: Data from two cross-sectional surveys (POP-Brazil I: 2016–2017; POP-Brazil II: 2020–2023) were analyzed. Participants were sexually active individuals aged 16–25 years from 26 state capitals and the Federal District. Genital samples were collected using Digene kits, DNA was extracted with MagNA Pure, and samples were analyzed using the Allplex™ CT/NG/MG/TV Assay. Survey-weighted methods were used to estimate prevalence.
Results: We analyzed 4,735 cervical and 1,734 penile samples in the first survey and 4,164 cervical and 2,300 penile samples in the second. Among women, prevalence rates remained stable for C. trachomatis (14.86% vs 14.59%), N. gonorrhoeae (2.49% vs 2.77%), and T. vaginalis (3.83% vs 4.74%), while M. genitalium increased significantly (4.85% vs 8.03%). Among men, no significant changes were observed for C. trachomatis (11.76% vs 8.07%), N. gonorrhoeae (2.66% vs 4.36%), M. genitalium (2.08% vs 1.99%), or T. vaginalis (3.60% vs 2.97%).
Conclusion: The high prevalence of all evaluated STIs, particularly the doubling of N. gonorrhoeae rates compared to previous Latin American studies and the rising M. genitalium rates among women, underscores the urgency of targeted public health interventions. Enhanced STI awareness, condom promotion, regular screening, and timely treatment are essential to address this persistent burden among young Brazilians.
PP04.139 – Finding Optimal Strategies for Targeting Gonorrhea Vaccination, Balancing Impact with Cost-Effectiveness: A Modeling Analysis
Dr Trystan Leng1, Dr Lilith Whittles1, Ms Dariya Nikitin1, Prof. Peter White1
1Imperial College London, London, United Kingdom.
Background: Vaccination for UK men who have sex with men (MSM) at increased gonorrhea risk has been advised, but not yet implemented. The key question is how to effectively target vaccination to maximize coverage of at-risk MSM without compromising cost-effectiveness by vaccinating low-risk people. Previously-examined targeting approaches have disadvantages: only vaccinating people with current gonorrhea infection (“Vaccination-on-Diagnosis”, VoD) achieves low coverage (limiting the impact of vaccination), and expanding eligibility to include people with self-reported high numbers of partners (“Vaccination-according-to-Risk”, VaR) requires asking sensitive questions about sexual behavior, which is not always feasible.
Methods: We developed a new transmission-dynamic model to assess novel targeting strategies based on a recent but not necessarily current gonorrhea infection (“Vaccination-according-to-History”, VaH) and/or being a notified partner of a gonorrhea case (“Vaccination-according-to-partner-Notification”, VaN). We evaluated cost-effectiveness, comparing the net monetary benefit (NMB) of each strategy over 10 years.
Results: Combining VaH+VaN, offering vaccination to MSM who are either notified partners of gonorrhea cases or were diagnosed themselves in the past 2 years, averts 1.6× more cases [48,700 (95%CrI: 21,900–85,000) vs 29,400 (15,600–47,200) with 20% vaccine protection; or 92,000 (46,800–149,200) vs 57,200 (33,100–86,200) with 40% protection] and is more cost-effective than VoD [NMB £3.3M (–0.7–9.0) vs £1.7M (–0.6–4.7) with 20% protection; £10.2M (3.0–19.4) vs £6M (2.0–11.2) with 40% protection] (Fig. 1). Even if vaccine protection is only 20%, lasting only 1.5 years after primary vaccination and 3 years after revaccination, the VaH, VaN, and VaH+VaN strategies are cost-effective at the estimated UK cost of £18/dose administered. Higher levels and longer durations of protection make vaccination cost-effective at higher prices.
Conclusion: Effective targeting towards at-risk MSM is essential to gonorrhea vaccination program success, and can be achieved using information readily-available to clinicians, without asking sensitive questions about sexual behavior. The novel strategies considered are cost-effective and have important advantages over previously-examined approaches, achieving greater impact than VoD, and without the feasibility issues of VaR.
Cost-effectiveness over the first 10 years of a vaccination program under different targeting strategies, for a vaccine costing £18/dose administered, and providing 20% or 40% protection lasting 1.5 years after 2-dose primary vaccination and 3 years after single-dose booster vaccination. Vaccination strategies considered are Vaccination-on-Diagnosis (VoD); Vaccination-according-to-partner-Notification (VaN); Vaccination-according-to-History (VaH) offering vaccination to those with a diagnosis in the last year [VaH(1yr)] or in the last 2 years [VaH(2yrs)]; VaN combined with VaH(1yr) or VaH(2yr); and Vaccination-according-to-Risk (VaR). (a,b) Cost-effectiveness planes, showing Quality-Adjusted Life Years (QALYs) gained and net costs (which are negative because vaccination is cost-saving) for vaccines offering (a) 20% protection and (b) 40% protection. Point markers show mean values, while outlined regions show high density regions which include 80% of model predictions. (c,d) Box plots of the net monetary benefit (net cost savings + value of health gains with a QALY valued at £20,000) of each strategy for vaccines offering (c) 20% protection and (d) 40% protection. Whiskers indicate the 2.5th and 97.5th centiles, boxes the 25th and 75th centiles, and the central line the median (50th centile). Note that the uncertainty in the estimates is due to primarily due to uncertainty in epidemiological parameters, and there is little uncertainty in the relative effectiveness of the different targeting strategies: each strategy is more effective than the previous one in the series presented.
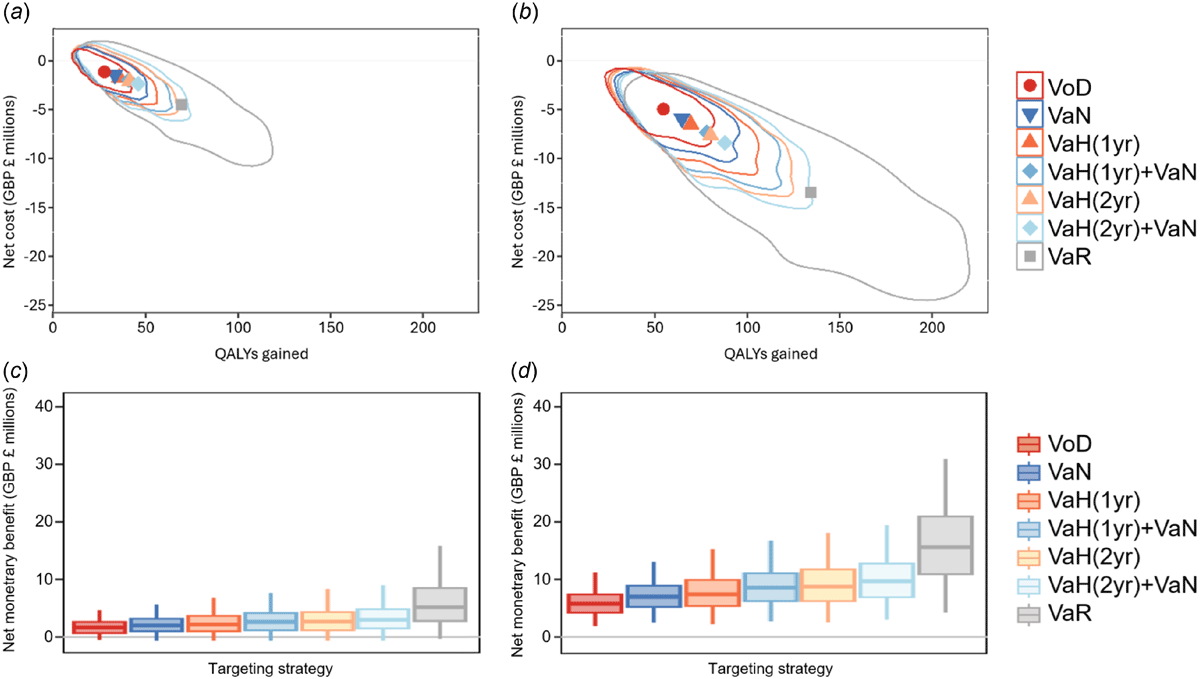
PP04.14 – Willingness to Use Bacterial STI Specimen Self-Collection Kits Among Transgender Women – Transgender Women’s Internet Survey and Testing Study
Iaah L Lucas2, Mariah Valentine-Graves2, Savannah Winter2, Joanna A. Caldwell2, Prof. Stefan Baral3, Dr. Travis Sanchez2
1U.S. Centers for Disease Control and Prevention, Atlanta, United States.
2Emory University, Atlanta, United States.
3Johns Hopkins University, Baltimore, United States.
Background: Transgender women (TGW) are disproportionately burdened by bacterial sexually transmitted infection (STIs) like gonorrhea, chlamydia, and syphilis, yet testing remains low. Bacterial STI specimen self-collection kits can increase testing because they are convenient, increase privacy, and mitigate barriers like stigma, discrimination, and cisgenderism that TGW. We sought to evaluate willingness to use bacterial STI specimen self-collection kits among TGW.
Methods: We obtained data from the Transgender Women’s Internet Survey and Testing, an online survey of U.S. TGW. The analytical sample included TGW, ≥15 years who reported sex in the past 12 months. We calculated descriptive statistics and estimated unadjusted odds ratio (OR) and 95% confidence intervals (CI) using ordinal regression to assess willingness to use bacterial STI testing (willing/neither willing nor unwilling/unwilling).
Results: Of 1,667 TGW, majority were White, non-Hispanic (74.6%) and aged 15–24 years (51.1%); 61.3% were willing to use bacterial STI specimen self-collection kits; and 7.9% used a bacterial STI specimen self-collection kit in the past 12 months. Willingness to use bacterial STI specimen self-collection kits was negatively associated with ≤high school education (OR = 0.58, 95% CI = 0.45–0.74) and younger age, 15–24 years, (OR = 0.62, 95% CI = 0.14–0.41), but positively associated with a bacterial STI test in the past 12 months (OR = 1.56, 95% CI = 1.27–1.93), condomless anal sex (OR = 1.24, 95% CI = 1.01–1.52), gender identity disclosure to a healthcare provider (OR = 1.68, 95% CI = 1.24–2.27), hormone therapy for medical gender affirmation/transition (OR = 1.39, 95% CI = 1.08–1.77), and HIV pre-exposure prophylaxis use in the past 12 months (OR = 1.57, 95% CI = 1.04–2.37).
Conclusion: Majority of TGW in this sample were willing to use bacterial STI specimen self-collection kits with variations in willingness by socio-demographic, behavioral, and healthcare engagement factors. Expanding access to bacterial STI specimen self-collection kits among TGW may increase testing and ultimately linkage to treatment and mitigate the disproportionate bacterial STI burden among TGW.
PP04.140 – Associations Between Frequency of Chlamydia and Gonorrhoea Screening and Ceftriaxone Consumption in Australian Gay and Bisexual Men (GBM) Attending Sexual Health Clinics (SHCs)
Dr. Arthur Wong1,2, Dr Michael Trager3, Dr Htein Aung2, Dr Rick Varma1,2, Prof David Templeton4, Dr Alison Nikitas5, Dr Sarah Martin6, Prof Louise Owen7, Prof Christopher Fairley9, Prof Catriona S. Bradshaw9, Prof Eric Chow9,10,11, Prof Rebecca Guy2, Dr Nicholas Medland2
1Sydney Sexual Health Centre, Sexual Health & Bloodborne Viruses Services, South Eastern Sydney Local Health District, Sydney, Australia.
2The Kirby Institute, University of New South Wales, Sydney, Australia.
3Burnet Institute, Melbourne, Australia.
4RPA Sexual Health, Sydney, Australia.
5Murrumbidgee Local Health District, Wagga Wagga, Australia.
6Canberra Health Service, Canberra, Australia.
7Statewide Sexual Health Service Tasmania, Hobart, Australia.
8Townsville Sexual Health Service, Townsville, Australia.
9Melbourne Sexual Health Centre, Melbourne, Australia.
10School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
11Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Population-level benefits and harms of asymptomatic chlamydia/gonorrhoea screening in GBM remain unclear. We sought to examine the association between asymptomatic screening frequency and ceftriaxone consumption in Australian GBM.
Methods: We conducted a retrospective cohort study using data from 16 sexual health centers (SHCs). Chlamydia/gonorrhoea testing events and ceftriaxone doses prescribed to GBM between 2016–2023 were extracted and categorized as screening-related (no symptoms and no contact with STI at time of test/prescription) versus non-screening-related. GBM with >1 screening-related test in a year contributed one person-year of follow-up. We calculated the annual number of ceftriaxone doses per person-year. Multivariable Poisson regression adjusting for PrEP use, HIV status, injecting drug use (IDU), history of STI (chlamydia/gonorrhoea) in the same year was used to examine associations between screening frequency (categorized as 1, 2, 3 or >4 screening-related tests per year) with number ceftriaxone doses per year. We also adjusted for clustering of observations within individuals.
Results: Of 99,022 GBM attending SHCs, 65,261 (65.9%) had >1 screening visit and contributed 133,848 person-years (PY) (Table 1). There were 216,092 screening-related test events. Of 23,449 ceftriaxone doses administered, 11,330 (48.3%) were screening-related.
Most people received one (62.9%) or two (21.5%) screening-related tests in a year. The mean number of ceftriaxone doses increased from 0.117/PY in 2016 to 0.210/PY in 2023 (P-trend < 0.001). Compared to having one screening-related test in a year, having 2 (aRR 1.39, CI = 1.34–1.43), 3 (aRR 1.60, CI = 1.53–1.66) and >=4 (aRR 1.71, CI = 1.63–1.79) screening-related tests in a year were associated with increase in ceftriaxone doses. PrEP use (aRR = 1.82), HIV (aRR = 1.73) and IDU (aIRR = 1.48) were also associated with increased ceftriaxone doses.
>=2 chlamydia/gonorrhoea screening per year was associated with an increase in ceftriaxone consumption. PrEP users and people with HIV, cohorts undergoing regular screening, also experienced a similar increase – suggesting this as the driver for ceftriaxone consumption in these groups.
Doses of screening-related and non-screening related ceftriaxone between 2016 and 2023 using Poisson regression.
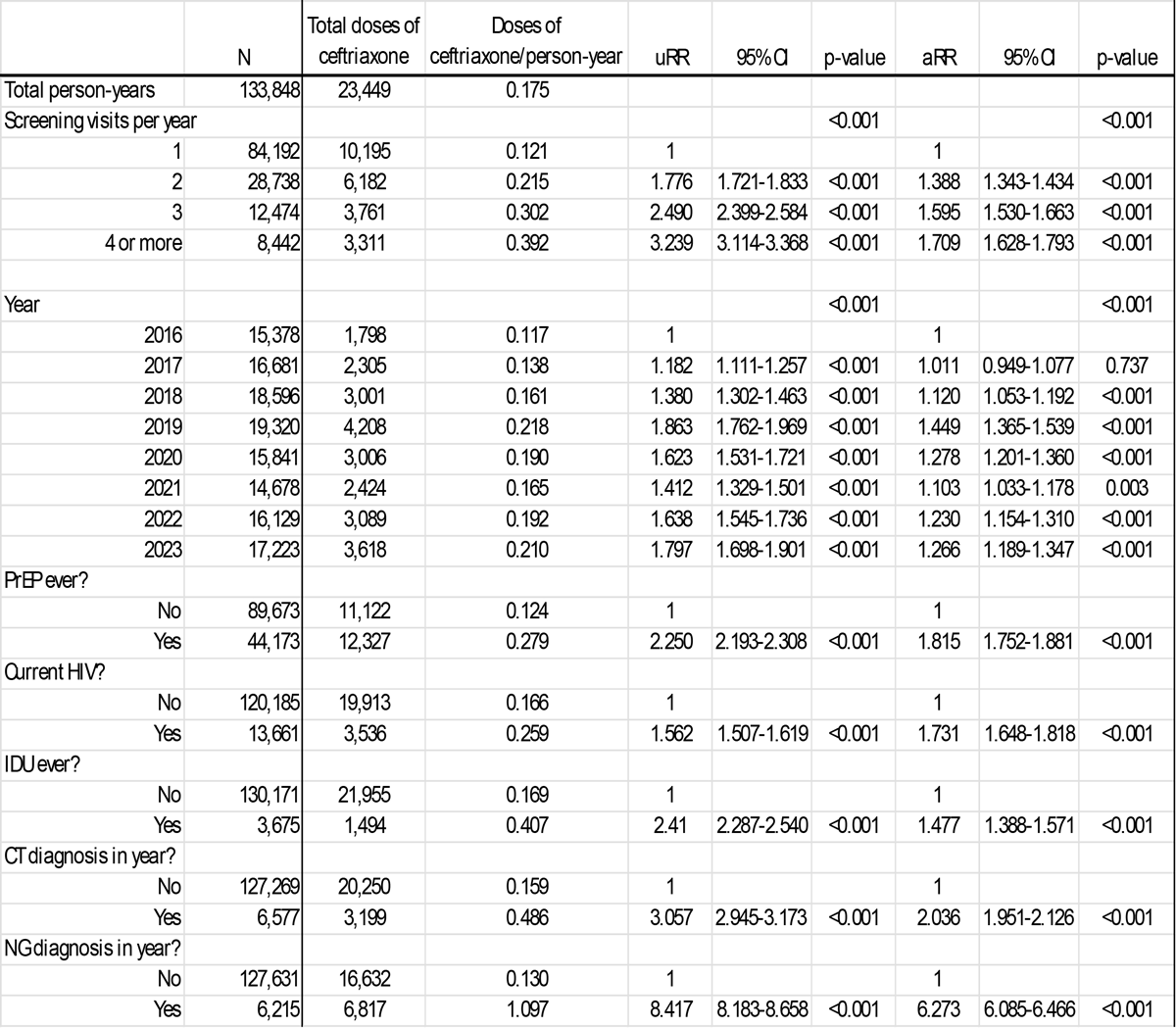
uRR, unadjusted risk ratio | aRR, adjusted risk ratio.
PP04.141 – Prenatal Syphilis Screening Among Commercially-Insured Women in the United States
Ms. Tara Wood1, Dr. Jodie Dionne1, Mr. Ligong Chen1, Dr. Joe Lewnard2, Dr. Katia Bruxvoort1
1University of Alabama at Birmingham, Birmingham, United States.
2University of California, Berkeley, Berkeley, United States.
Background: Congenital syphilis cases increased by 183% in the United States (US) between 2017–2022. The US Centers for Disease Control and Prevention recommend syphilis screening for pregnant women at the first prenatal visit and at delivery, but inconsistent state guidelines and poor compliance may lead to inadequate screening rates in this population.
Methods: Using the Merative MarketScan Research Database, a US-wide collection of longitudinal, patient-level healthcare claims data, we examined syphilis screening rates among a cohort of commercially-insured pregnant women aged 15–44 years. Women were included if they had a documented pregnancy resulting in a live birth, stillbirth, or spontaneous abortion during 2017–2021 and were continuously enrolled in commercial medical plans during the year prior to pregnancy end. We described demographic characteristics (age and US region) and used ICD-10 codes to identify substance use disorder, mental health disorder, and prior year STI (syphilis, gonorrhea, and chlamydia) diagnoses. The primary outcome was prenatal syphilis screening based on healthcare procedure codes.
Results: Among 770,877 pregnant women, median (IQR) age was 31 (27–34 y) and 15.3%, 20.9%, 48.2%, and 15.5% were in the Northeast, North Central, South, and West regions, respectively. Few women had ≥1 STI (0.25%) or substance use (1.3%) diagnosis in the year prior to pregnancy start, and 10.8% had a mental health disorder diagnosis. Overall, 80.4% of women received ≥1 syphilis test during pregnancy; 45.1% received multiple tests. Syphilis screening increased approximately 4.7% between 2017–2021. In the first, second, and third trimester, 41.4%, 17.6%, and 34.6% were screened, respectively.
Conclusion: These data demonstrate a systematic gap in syphilis screening among pregnant women, especially in the first trimester, when timely screening may allow for early intervention. Additionally, a majority of pregnant women are only screened once, reducing providers’ ability to identify cases. Closing this gap is essential to addressing the congenital syphilis epidemic.
| Variable | Overall | 2017 | 2018 | 2019 | 2020 | 2021 | |
|---|---|---|---|---|---|---|---|
| (N = 770877) | (N = 160255) | (N = 158957) | (N = 159277) | (N = 145524) | (N = 146864) | ||
| Any prenatal syphilis screening | 619,368 (80.4%) | 125,332 (78.2%) | 124,926 (78.6%) | 128,790 (80.9%) | 120,008 (82.5%) | 120,312 (81.9%) | |
| Number of prenatal syphilis tests | |||||||
| . 0 | 151,509 (19.7%) | 34,923 (21.8%) | 34,031 (21.4%) | 30,487 (19.1%) | 25,516 (17.5%) | 26,552 (18.1%) | |
| . 1 | 271,915 (35.3%) | 73,788 (46%) | 71,393 (44.9%) | 38,390 (24.1%) | 38,077 (26.2%) | 50,267 (34.2%) | |
| . >1 | 347,453 (45.1%) | 51,544 (32.2%) | 53,533 (33.7%) | 90,400 (56.8%) | 81,931 (56.3%) | 70,045 (47.7%) | |
| Screening by pregnancy trimester | |||||||
| . 1st trimester | 318,893 (41.4%) | 68,858 (43%) | 64,682 (40.7%) | 65,107 (40.9%) | 60,112 (41.3%) | 60,134 (41%) | |
| . 2nd trimester | 135,256 (17.6%) | 26,155 (16.3%) | 25,277 (15.9%) | 27,020 (17%) | 27,219 (18.7%) | 29,585 (20.1%) | |
| . 3rd trimester | 266,752 (34.6%) | 47,402 (29.6%) | 46,433 (29.2%) | 54,280 (34.1%) | 56,766 (39%) | 61,871 (42.1%) |
PP04.142 – Gender-Specific Syphilis Screening Strategies in a Canadian High Transmission Setting: A Mathematical Modeling Study
Miss Yiqing Xia1, Dr. Cedric Yansouni2,3,4, Dr. Jean-Sébastien Touchette5, Dr. Yassen Tcholakov1,5, Mrs Chelsea Caya2,3, Miss Mariana Pico2, Dr. Mathieu Maheu-Giroux1
1McGill University, Montreal, Canada.
2Research Institute of the McGill University Health Centre, Montreal, Canada.
3McGill Interdisciplinary Initiative in Infection and Immunity, Montreal, Canada.
4McGill University Health Centre, Montreal, Canada.
5Nunavik Regional Board of Health and Social Services, Nunavik, Canada.
Background: Some Canadian communities experience high rates of syphilis transmission. In such settings, a proportion of the population could have developed temporary infection-derived immunity resulting from diagnosis/treatment delays. Options to control syphilis outbreaks include mass screening using rapid diagnostic tests. However, misaligned screening strategies could lead to paradoxical increases in incidence through immunity reductions. We evaluated the population-level impact of mass syphilis screening strategies in a small high-transmission community.
Methods: An individual-based model was developed, parameterized, and calibrated using real-world survey, laboratory, and surveillance data from an anonymized community, simulating syphilis transmission with 1,050 sexually active individuals (2017–2022). Based on previous literature, individuals treated later than the secondary stage are assumed to gain temporary immunity, which duration was calibrated and model outputs cross-validated with the proportion of reinfections. Gender-specific and universal mass screening strategies with different frequencies were examined using the annual median fractions of cumulative new infections averted (2023–2032) (Fig. 1).
Results: In this setting, men test at ~50% the rate of women and are more likely to be treated late. The model projected an incidence of 0.044 (0.015–0.066) among sexually active population in 2023. Screening men once per year could cause an increase in syphilis transmission due to decreased population immunity against reinfection. Nevertheless, screening women once per year instead could avert a cumulative 10% (0–22%) infections as this strategy has less impact on their temporary immunity (~2 years), given their already high testing rates. By screening the whole community once a year, a cumulative 29% (12–40%) could be averted, with the effect increased to 57% (46–67%) if being screened twice a year.
Conclusion: Despite uncertainties in the extent and duration of post-infection immunity to syphilis, the existence of this phenomenon could lead to paradoxical effects. Prioritizing groups with unmet testing needs should be accompanied by concomitant overall testing efforts.
Fractions of cumulative new syphilis infections averted over 2023 to 2032 by population prioritized (men, women, or both) and screening frequency (once or twice a year). Negative fractions indicate higher transmission in the intervention scenario with screening.
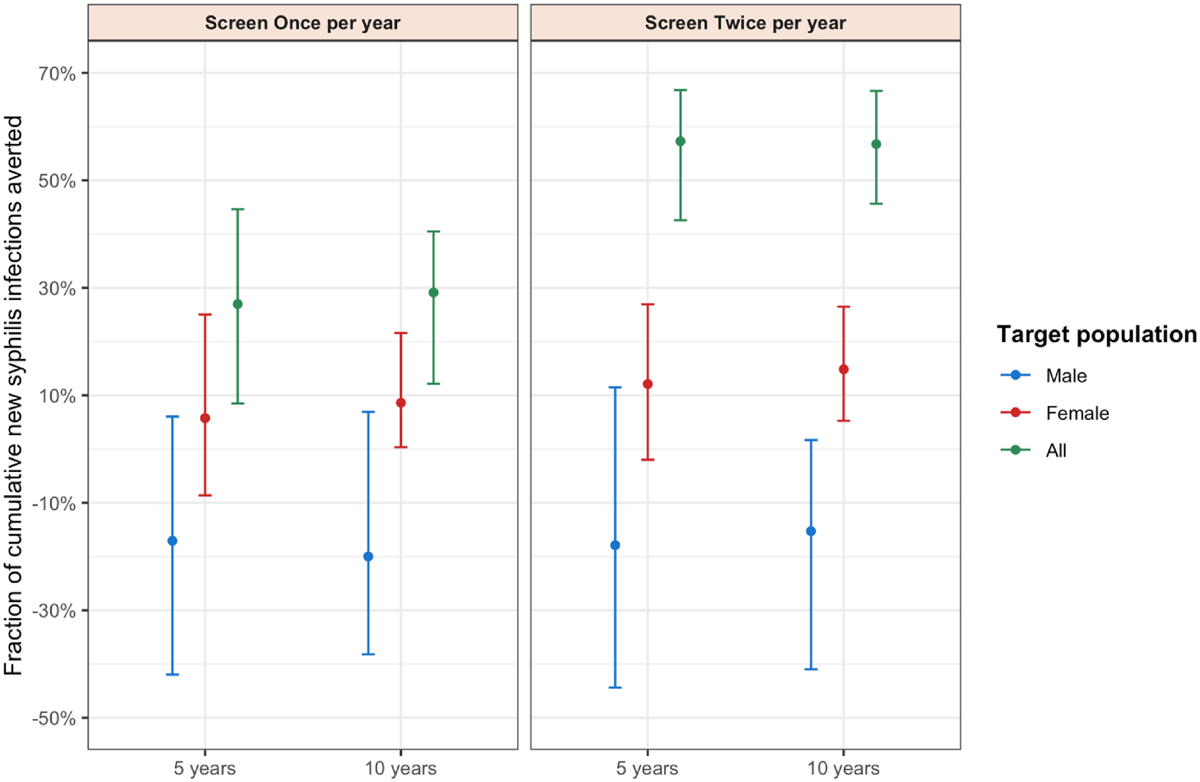
PP04.143 – Urine-Based Human Papillomavirus Screening: Performance, Challenges, and Opportunities to Expand Access in the United States
Miss Lily Yang1, Dr. Chibuzor Babalola1, Dr. Jeffrey D. Klausner1
1Keck School of Medicine, University of Southern California, Los Angeles, United States.
Background: In the United States, about 12,000 new cases of cervical cancer are diagnosed each year, largely due to 30% of eligible women remaining unscreened. Underscreening is most common in rural populations and in populations where healthcare access is difficult. Urine-based testing for Human Papillomavirus (HPV) offers a non-invasive, self-sampling method that could improve access to screening. FDA-approved tests detect HPV in cervical and vaginal samples, but none are currently approved for urine detection. We conducted a narrative review of urine-based HPV testing, focusing on diagnostic performance and feasibility.
Methods: Studies were identified through PubMed using combinations of search terms including ‘urine,’ ‘screening,’ ‘diagnostic tests,’ and ‘HPV’ from January 1, 2006, to December 31, 2024. Studies reporting test performance for detecting HPV and acceptability of urine-based HPV testing compared to current cervical/vaginal detection were included. Studies comparing detection to precancerous lesions were excluded. Weighted averages for sensitivity and specificity were calculated based on study performance values and sample sizes.
Results: We identified 14 studies (N = 67 to N = 561) evaluating test performance for detecting any HPV in urine specimens. Weighted sensitivity was 57% (range 56.6 to 98.6%), and specificity was 82% (range 61 to 100%), compared to vaginal/cervical sampling. In studies that reported higher sensitivities, the samples were processed more promptly after collection and preservatives were added. Regarding acceptability (n = 5 studies), one quantitative study reported that 95% of participants felt comfortable with urine sampling compared to 82% for cervical sampling, and qualitative assessments ranked urine as the easiest collection method.
Conclusion: Urine-based HPV testing has variable performance and high acceptability among patients eligible for cervical HPV detection. The lack of FDA-approved urine-based HPV tests represents a gap in improving accessibility to under-screened populations.
PP04.144 – Prevalence and Risk Factors of Six Common Sexually Transmitted Infections Among People Receiving HIV Pre-Exposure Prophylaxis at Public Health Facilities and Pharmacies in Western Kenya
Ms. Zoïe Alexiou1, Mr Aarman Sohaili2, Dr. Victor Ocholla Omollo3, Mr. Benn Kwach3, Mr. Bernard Rono3, Dr. Sander Ouburg2, Mr. Roel Heijmans2, Prof. Dr. Servaas A. Morré1,2, Prof. Dr. Elizabeth Bukusi3, Dr. Pierre P. M. Thomas1, Dr. Felix Mogaka3
1GROW Research Institute for Oncology and Reproduction, Maastricht University, Maastricht, The Netherlands.
2Microbe&Lab B.V., Amsterdam, The Netherlands.
3Centre for Microbiology Research, Kenya Medical Research Institute, Kisumu, Kenya.
Background: In resource-limited settings, sexually transmitted infections (STIs) are underreported, and accessible diagnostics are lacking. This study assesses the prevalence of six STIs in people receiving pre-exposure prophylaxis (PrEP) using a unique point-of-care (POC) testing device.
Methods: HIV-negative people ≥15 years, receiving PrEP at public health facilities or pharmacies in western Kenya were included. Self-collected urine samples were tested for Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), Trichomonas vaginalis (TV), Mycoplasma genitalium (MG), Mycoplasma hominis (MH), and Ureaplasma species (US). All STIs were detected in triplicate in one reaction using the research-use-only FlashDx semi-solid PCR chip-based POC device. FlashDx results were validated with Mikrogen PCR; CT/NG detection and treatment followed Cepheid results. Limit of detection (LOD) for FlashDx was assessed. Prevalence estimates were compared across at-risk groups.
Results: Between March 24 and April 30, 2025, 324 participants enrolled, who identified as men who have sex with men (MSM) (n = 100), men (n = 100), or women (n = 124). The median age was 24 years (IQR 21–29). Most participants were never married (65.4%) and were informally employed (77.1%). Condom use was 48.2% for vaginal sex and 44.2% for anal sex. Prevalence was 25.5% (CI: 21.5–29.5%) for multiple STIs, 13.9% (CI 11.2–16.5%) for CT, 2.6% (CI: 1.3–4.0%) for NG, 5.2% (CI: 3.1–7.3%) for TV, 4.6% (CI: 2.5–6.7%) for MG, 18.3% (CI: 15.3–21.3%) for MH, and 56.3% (CI: 51.7–60.9%) for US. TV, MH, US and NG were more common in women (P < 0.02, P < 0.001, P < 0.001, P = 0.11). MSM had higher MG prevalence (P = 0.13). No differences were observed for CT (P = 0.77). FlashDx detected 10 targets per PCR in LOD analyses. Concordance was high between FlashDx and Cepheid.
Conclusion: Using a POC test, CT/NG and other STIs were commonly detected in people receiving PrEP, with the highest prevalence in women. Field studies are needed to assess the (cost-) effectiveness of this diagnostic tool.
PP04.145 – The Lasting Impact of COVID-19 on Mail-In STI Testing: A Long-Term View from Baltimore City, MD (2017–2025)
Miss Tanique Bennett1, Mr. Alec Boudreau1, Dr. Johan Melendez1, Dr. Mathew Hamill1, Mrs. Gretchen Armington1, Dr. Yukari Manabe1
1Johns Hopkins School of Medicine, Baltimore, United States.
Background: Examining changes in the characteristics of users of a mail-in STI testing service across the COVID-19 pandemic reveal the pandemic’s temporal impact which may guide future on-line STI programs’ response to future STI clinic service disruptions.
Methods: User data from Baltimore City, MD was analyzed from the mail-in testing program I Want The Kit (IWTK), using WHO’s pandemic declaration (03/11/2020) and end (05/05/2023) as cutoffs. Genital and extragenital swabs were tested for N. gonorrhoeae, C. trachomatis, and Trichomonas vaginalis (vaginal swabs only) using nucleic acid amplification. Weighted multinomial regression assessed differences in user characteristics by period; t-tests evaluated daily order volume changes (Table 1).
Results: Variety of user characteristics and order volume increased during the pandemic and, despite a post-pandemic decline, remain above pre-pandemic levels. During the pandemic, mean daily order volume rose from 1.63 to 8.33, then dropped to 5.69 post-pandemic.
Compared to pre-pandemic, users aged 14–25 were more likely to engage with IWTK during (OR = 3.52, P < 0.001) and post-pandemic (OR = 4.71, P < 0.001). Male users (OR = 1.71, P = 0.007) also showed increased post-pandemic engagement compared to pre-pandemic. Black users engaged more during (OR = 1.78, P < 0.001) and post-pandemic (OR = 1.22, P = 0.027), as did American Indian/Alaska Native users (during: OR = 4.12, P = 0.006; post: OR = 3.61, P = 0.015). Post-pandemic users were less likely to report multiple partners (OR = 0.77, P < 0.001). Despite these shifts, STI positivity did not differ significantly by period (P = 0.926).
Conclusion: In Baltimore City, post-pandemic mail-in STI users are younger, more likely to identify as Black, report fewer partners, and more likely to be male. Despite these shifts in demographics, there is not a statistically significant difference in STI positivity.
| Variable (n = 14077) | Pre-Pandemic (Reference, n = 987) vs Pandemic (n = 9,359) [OR] | Pandemic (Reference, n = 9,359) vs Post-Pandemic (n = 3,731) [OR] | Pre-Pandemic (Reference, n = 987) vs Post-Pandemic (n = 3,731) [OR] | |
|---|---|---|---|---|
| Unique User (N = 8931) | 1.81(n = 529 vs 6355)CI: 1.57–2.09 P < 0.001 | 0.62(n = 6355 vs 2047)CI: 0.57–0.68 P < 0.001 | 0.92(n = 529 vs 2047)CI: 0.78–1.07 P = 0.287 | |
| Age | ||||
| 14-25(N = 3043) | 3.52(n = 56 vs 2023)CI: 2.62–4.73 P < 0.001 | 1.25(n = 2023 vs 964)CI: 1.13–1.38 P < 0.001 | 4.71(n = 56 vs 964)CI: 3.48–6.38 P < 0.001 | |
| 26-35(N = 7565) | reference(n = 517 vs 5151) | reference(n = 5151 vs 1897) | reference(n = 517 vs 1897) | |
| 36-45(N = 2550) | 0.55(n = 311 vs 1577)CI: 0.47–0.64 P < 0.001 | 1.167(n = 1577 vs 662)CI: 1.04–1.31 P = 0.007 | 0.63(n = 311 vs 662)CI: 0.53–0.76 P < 0.001 | |
| 46-55(N = 601) | 0.708(n = 65 vs 397)CI: 0.53–0.94 P = 0.019 | 1.12(n = 397 vs 139)CI: 0.90–1.40 P = 0.291 | 0.79(n = 65 vs 139)CI: 0.57–1.09 P = 0.153 | |
| 56+(N = 318) | 0.68(n = 38 vs 211)CI: 0.48–0.96 P = 0.028 | 1.12(n = 211 vs 69)CI: 0.83–1.52 P = 0.451 | 0.7(n = 38 vs 69)CI: 0.48–1.01 P = 0.059 | |
| Race | ||||
| American Indian or Alaskan Native(N = 108) | 4.12(n = 3 vs 72)CI:1.50–11.29 P = 0.006 | 0.86(n = 72 vs 33)CI: 0.57–1.32 P = 0.501 | 3.61(n = 3 vs 33)CI: 1.29–10.12P = 0.015 | |
| Asian(N = 753) | 0.85(n = 53 vs 514)CI: 0.59–1.21 P = 0.365 | 0.75(n = 514 vs 186)CI: 0.62–0.90 P = 0.003 | 0.61(n = 53 vs 186)CI: 0.42–0.90 P = 0.012 | |
| Black or African American(N = 7488) | 1.78(n = 498 vs 5166)CI: 1.51–2.09 P < 0.001 | 0.86(n = 5166 vs 1824)CI: 0.78–0.95 P = 0.002 | 1.22(n = 498 vs 1824)CI: 1.02–1.45 P = 0.027 | |
| Native Hawaiian or Other Pacific Islander(N = 44) | N/A* | 2.35(n = 19 vs 25)CI: 1.25–4.42 P = 0.008 | N/A* | |
| Two or More Races(N = 950) | 1.05(n = 79 vs 653)CI: 0.78–1.42 P = 0.730 | 0.71(n = 653 vs 218)CI: 0.59 - 0.85 P < 0.001 | 0.65(n = 79 vs 218)CI: 0.47–0.90 P = 0.009 | |
| Unknown(N = 523) | 2.2(n = 20 vs 361)CI: 1.31–3.73 P = 0.003 | 0.86(n = 361 vs 142)CI: 0.69–1.07 P = 0.175 | 1.72(n = 20 vs 142)CI: 0.99–2.97 P = 0.052 | |
| White(N = 4211) | reference(n = 987 vs 9359) | reference(n = 2574 vs 1303) | reference(n = 334 vs 1303) | |
| Gender | ||||
| Male(N = 6101) | 1.94(n = 457 vs 4149)1.35–2.81 P < 0.001 | 0.97(n = 4149 vs 1495)CI: 0.75–1.26 P = 0.834 | 1.71(n = 457 vs 1495)CI:1.16–2.53 P = 0.007 | |
| Unknown(N = 556) | 4.26(n = 11 vs 350)CI: 2.22–8.19 P < 0.001 | 1.22(n = 350 vs n = 195)CI: 0.99–1.52 P = 0.067 | 5.39(n = 6 vs 162)CI: 2.80–10.23 P < 0.001 | |
| Female(N = 7420) | reference(n = 519 vs 4860) | reference(n = 4860 vs 2041) | reference(n = 519 vs 2041) | |
| User with at Least 1 Positive Swab for either Gonorrhea, Chlamydia, or Trichomoniasis (N = 827) | 1.07(n = 47 vs 600)CI: 0.78–1.48 P = 0.42 | 0.96(n = 600 vs 180)CI: 0.80–1.16 P = 0.693 | 0.98(n = 47 vs 180)CI: 0.69–1.40 P = 0.926 | |
| Currently Has More Than One Sex Partner (N = 4333) | N/A* | 0.77(n = 2724 vs 1609)CI: 0.70–0.86 P < 0.001 | N/A* | |
| How Many Partners in the last 90 days | ||||
| 0–1 Partners (N = 4057) | reference | reference(n = 2637 vs 1420) | N/A* | |
| 2–4 Partners (N = 5684) | N/A* | 0.82(n = 3742 vs 1942)CI: 0.74–0.91 P < 0.001 | N/A* | |
| 5–9 Partners (N = 735) | N/A* | 0.75(n = 478 vs 257)CI: 0.62–0.91 P = 0.004 | N/A* | |
| 10 or More Partners (N = 278) | N/A* | 0.89(n = 167 vs 111)CI: 0.68–1.18 P = 0.420 | N/A* | |
| Mean Daily Order Volume (# of orders per day) | T-Test (Mean) | |||
| Pre-Pandemic | 1.64 orders per day | |||
| Pandemic | 8.33 orders per day | |||
| Post-Pandemic | 5.70 orders per day |
*Variable/Category did not exist in the registration process prior to the pandemic.
PP04.146 – Implementing DOXY-PEP in a Community-Based HIV Care Setting: A Retrospective Study
Miss Elizabeth Bolton1
1WSUSOM, Detroit, United States.
2The Horizon’s Project, Detroit, United States.
Background: Rates of bacterial sexually transmitted infections (STIs), including chlamydia, gonorrhea, syphilis, are rising in the U.S., disproportionately affecting transgender women (TGW) and men who have sex with men (MSM). In 2025, Detroit reported the highest STI rates nationally, with nearly half of cases in individuals aged 15–24. Doxycycline post-exposure prophylaxis (DOXY-PEP) clinical trials have demonstrated >70% reduction in syphilis and chlamydia, and ~50% in gonorrhea. The CDC now recommends DOXY-PEP for MSM and TGW with recent STIs or multiple partners, but uptake among urban adolescents remains understudied.
Methods: A retrospective chart review (2022–2024) analyzing STI history, DOXY-PEP adherence, and post-initiation STI incidence was conducted on 72 eligible MSM and TGW Horizon’s Project HIV Clinic patients aged 14–27. Adherence was based on prescription pickup, follow-up attendance, and repeat labs.
Results: Among 150 patients, 72 met inclusion criteria (6 TGW, 66 MSM; 3 non-binary, 63 cisgender). Most were Black (n = 69), and all were HIV-positive, with 71 on ART. Of those eligible, 76.4% (n = 55) were prescribed DOXY-PEP, with 36.3% (n = 20) demonstrating adherence; 10 were lost to follow-up. Overall STI incidence dropped from 0.467 to 0.217 cases/person-year after DOXY-PEP (IRR: 0.466; 95% CI: 0.284–0.763; P < 0.05), a 53.3% reduction. Among those prescribed, chlamydia and syphilis incidence fell by 56.1% and 65.7%, respectively. Among adherent patients, reductions were 36.6% (chlamydia) and 53.6% (syphilis). Gonorrhea incidence declined by 44.6% (prescribed) and 28.7% (adherent), possibly due to emerging tetracycline resistance. Common barriers to adherence included forgetfulness and prescription delivery errors.
Conclusions: DOXY-PEP significantly reduced STI incidence among high-risk MSM and TGW patients in Detroit. However, challenges related to adherence and antimicrobial resistance warrant further investigation. As STI rates continue to rise, integrating DOXY-PEP into comprehensive sexual health strategies could play a crucial role in improving public health outcomes.
STI incidence for patients prescribed (n = 45) and adherent (n = 20) to DOXY-PEP. Incidence data is calculated as cases per person-years. * Denotes statistical significance (p < 0.05).
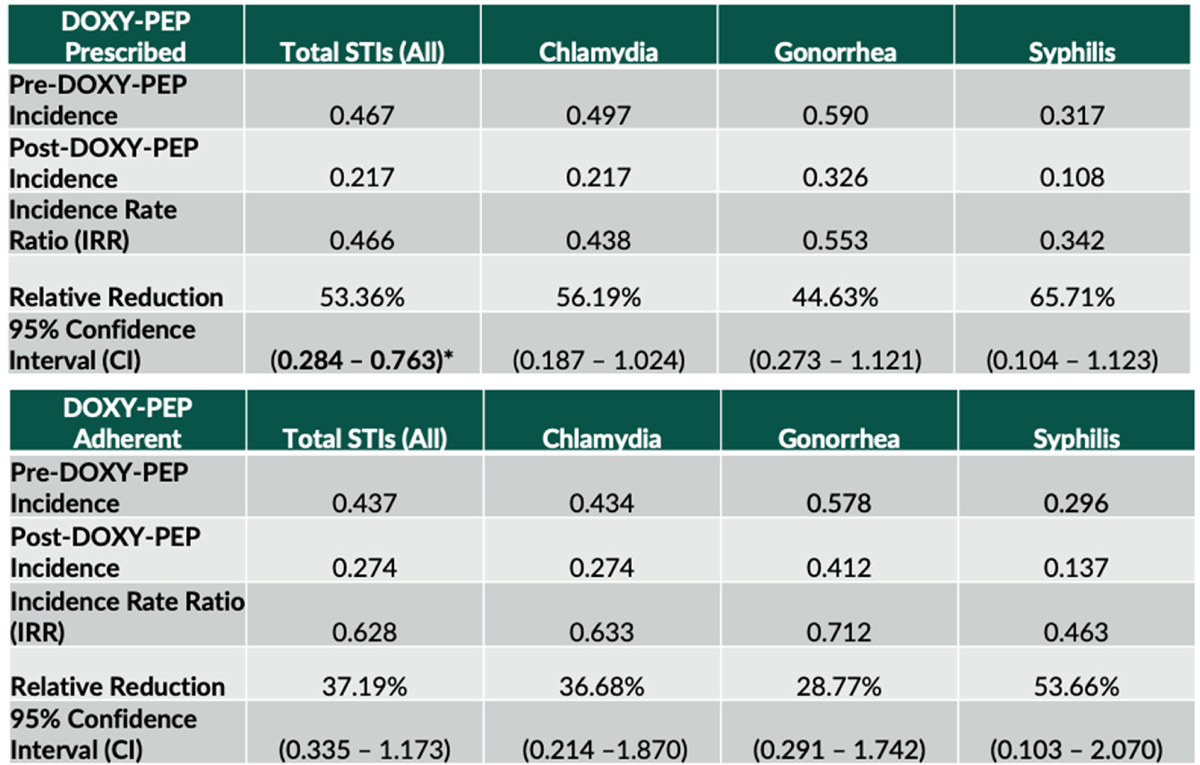
PP04.147 – Are Populations most at Risk of Bacterial Sexually Transmitted Infections willing to take Presumptive Medical Treatments: Results from a Systematic Literature Review and Findings from an Australian Sexual Health Survey
Dr. Julie-Anne Carroll1, Professor Philip Baker1, Professor Amy Mullens2, Dr Daniel Demant3
1Queensland University of Technology, Toowong, Australia.
2University of Southern Queensland, Toowoomba, Australia.
3University of Technology Sydney, Sydney, Australia.
Background: This paper will present the findings from the first and second phases of research funded by the Sexual Health Research Fund in Queensland, Australia. Researchers from three different Australian universities collaborated to undertake a systematic review of the literature (SLR), and quantitative, population data collections to assess the acceptability and feasibility of Doxy-PrEP as an ongoing preventative approach for STIs in high-risk sexually active groups.
Methods: The SLR was undertaken by adhering to PRISMA-P guidelines, a comprehensive search strategy was developed and executed in August 2023 across six databases with additional citation screening. The survey had 250 participants from GBSM, Indigenous, CALD, youth, and sex worker groups. A univariate analyses examined the relationships between several independent variables and three dependent variables in this population sample: the appropriateness of Doxy PrEP, its consistency with perceived risk, and the availability of better treatment options.
Results: In the SLR, only 8 of the 912 retrieved studies met the inclusion criteria. These studies were all conducted in high-income countries, used various methods, and all focused on sexual minority men. Findings consistently identified moderate to high levels of acceptability of Doxy PrEP among GBMSM (54.3%–67.5%) In the cross-sectional population survey, age was a consistent predictor across all three dependent variables. Older participants were more likely to perceive Doxy-PrEP as appropriate (rs = 0.201, P = 0.002). A history of PrEP use also showed significant associations. Additionally, the frequency of antibiotic prescriptions was positively correlated with perceptions of Doxy-PrEP’s appropriateness (rs = 0.185, P = 0.006).
Conclusion: The SLR findings showed that due to the limited and homogenous research in this area, vast gaps in preventative approaches knowledge remain. The survey results underscore the importance of age, PrEP use history, and antibiotic familiarity in shaping perceptions of Doxy-PrEP.
PP04.148 – Biological Influences in Vaginal Microbiome Composition and STI Outcomes
Ms. Kirsti Gilmore1, Dr. Mufaro Kanyangarara1, Dr. Madeline Meyer, Kia Zellars1,2, Dr. Melissa Nolan1,2
1Arnold School of Public Health, University of South Carolina, Columbia, United States.
2Institute for Infectious Disease Translational Research, University of South Carolina, Columbia, United States.
Background: Research gaps persist regarding how sexual activity and sexual partnerships contribute to bacterial vaginosis (BV), a known risk factor for sexually transmitted infections (STIs). Conflicting findings, particularly across racial backgrounds, highlight the need for further research among racially and ethnically diverse patient populations.
Methods: By examining the vaginal microbiome composition, sexual health practices, and STI diagnosis, we will be able to identify associative causes of STI diagnosis.
The Sexually Transmitted Infection Concomitance and Kinetics (STICK) study enrolled 48 women aged 18–24 years seeking clinical management for STIs or nonmarital pregnancy. Serial vaginal samples were prospectively collected over one year for STI testing and vaginal microbiome analysis, resulting in 65 samples across 36 women. Microbial DNA was extracted using a Zymo protocol and sequenced with Illumina® NextSeq™ technology. At the genus level, patient alpha diversity of the vaginal microbiome were quantified via multinomial logistic regression to assess associations between bacterial community composition and patient characteristics, Shannon Index, and alpha-beta diversity statistics are to be employed.
Results: None of the predictors are statistically significant at α = 0.05 level (Fig. 1). However, the variable “Dr_noted_unprotected” representing notation of unprotected sexual activity is the closest to statistical significance (P = 0.1773) to a history of sexual transmitted infection contraction.
Conclusion: Preliminary findings demonstrate significant bacterial composition differences between women with and without current or historical STIs. Understanding these microbiome patterns is essential to developing targeted BV and STI prevention strategies, particularly for women of African descent, who are often disproportionately impacted. Addressing racial differences in BV pathogenesis may ultimately support more equitable STI prevention efforts through microbiome-informed interventions. At the genus level no epidemiological risk factors associated with lactobacillus. Further research is being conducted at the family and species level to identify microbial predictors of STI diagnosis.
None of the predictors (race, Medicaid insurance status, and Dr. noting unprotected sex) are statistically significant at α = 0.05 level. However, the variable “Dr_noted_unprotected” representing notation of unprotected sexual activity is the closest to statistical significance (P = 0.1773) to a history of sexual transmitted infection contraction. There is no evidence of Lactobacillus having an epidemiological significance when associated with a history of sexually transmitted infection amongst women between the ages of 18–26.
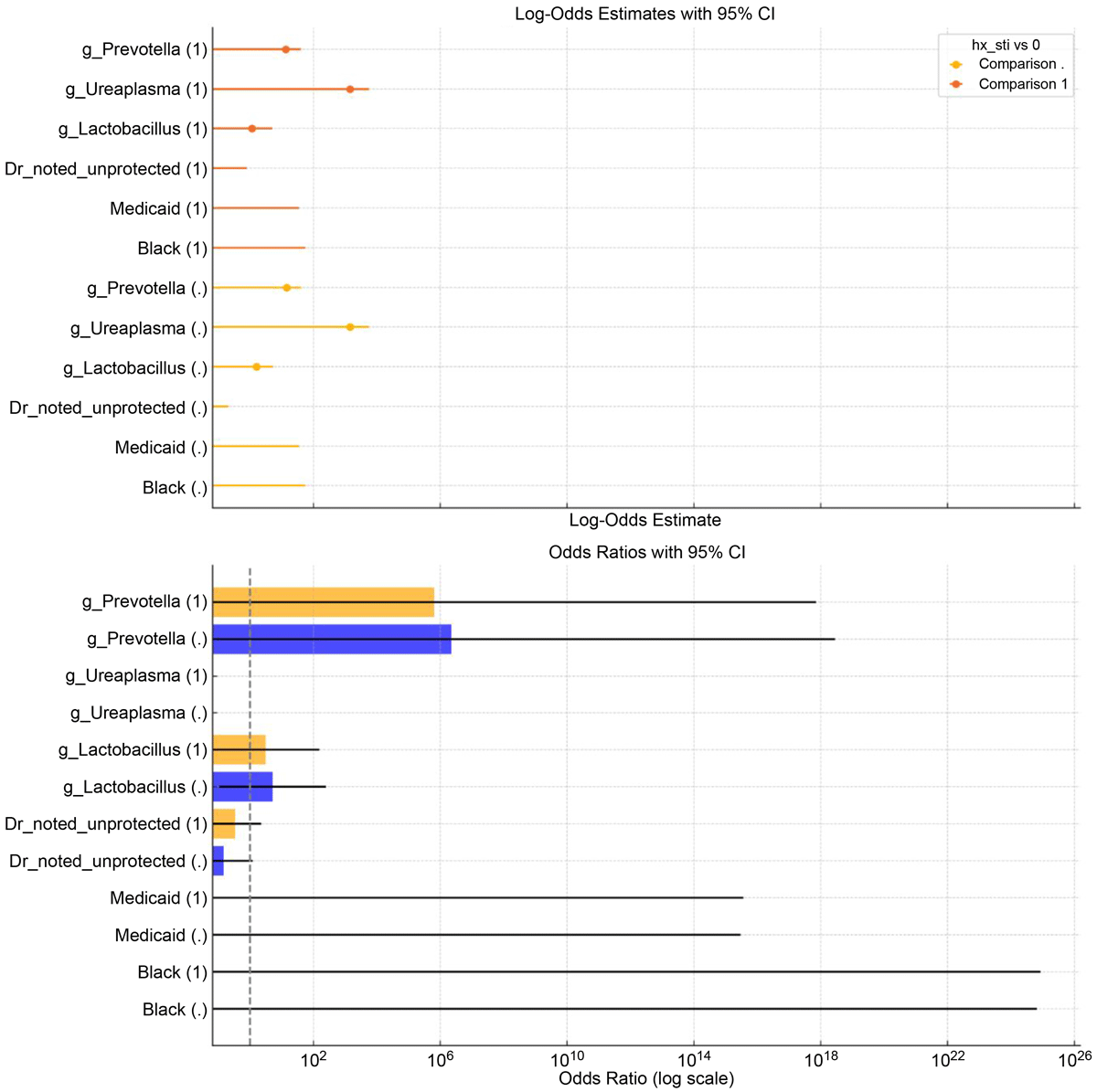
PP04.149 – High-Risk Human Papillomavirus (HPV) Prevalence in Women from the Caribbean Island of Montserrat
Miss Caroline Harris1, Dr Tiffannie Skerritt-Flemming2, Dr Dorothea Hazel-Blake2, Ms Penny Maloney2, Ms Kimona Daniel-Bourne2, Mr John Lee3, Dr Sharra Greenaway-Duberry2, Dr Petra Manley3
1UK Field Epidemiology Training Programme, UK Health Security Agency, London, United Kingdom.
2Montserrat Ministry of Health and Social Services, Montserrat.
3UK Overseas Territories Team, UK Health Security Agency, London, United Kingdom.
Background: Montserrat is a UK Overseas Territory in the Caribbean with a population of 4,386. There is no universal HPV vaccination programme in place and colposcopy and cervical cancer screening services are limited. HPV is sexually transmitted, and some high-risk (hrHPV) subtypes are associated with cervical cancer; with HPV16 and HPV18 being most prevalent globally. We aimed to determine the prevalence of hrHPV and associated demographic risk factors in women in Montserrat to inform preventive strategies.
Methods: Using 2023 census, we applied random spatial sampling to select 520 buildings to recruit the 207 women required to estimate a hrHPV prevalence of 20%, with 5% precision at 5% significance level, accounting for a 40% response. Resident women aged 25–64 years were invited to participate and samples were tested with the GeneXpert assay for 14 hrHPV subtypes. Sampling weights were applied to reflect the age distribution in the population. Demographic characteristics were collected via questionnaire and differences assessed using logistic regression.
Results: Of 225 eligible women, 213 (95%) consented to participate though only 185 women submitted a sample despite reminders (82% of those eligible). All age groups were represented in the study population. Three women were vaccinated against HPV. Overall hrHPV prevalence was 14.7% (95% CI: 10.3–20.6); prevalence of HPV16 was 2.0% (95% CI: 0.7–5.2) and HPV18/45 was 1.6% (95% CI: 0.5–4.8) respectively (Table 1). Preliminary analysis shows that the 55–64 years age group was associated with lower hrHPV prevalence (OR = 0.26, 95% CI: 0.05–0.93, P = 0.05).
Conclusions: Overall hrHPV prevalence in Montserrat women was consistent with findings from previous Caribbean Island studies. Although HPV16 and 18 are not predominate in our sample unlike other countries, our findings suggest that hrHPV virus is present in the Montserrat population thus universal screening and vaccination programmes should be considered to reduce HPV prevalence in the overall population.
| Genotype | Prevalence (%) | 95% CI | |
|---|---|---|---|
| HPV 16 | 2.0 | 0.7–5.2 | |
| HPV 18 or 45 | 1.6 | 0.5–4.8 | |
| HPV Other High Risk | 11.2 | 7.3–16.6 | |
| Overall High Risk | 14.7 | 10.3–20.6 |
PP04.15 – Awareness of and Willingness to Use Doxycycline Post-Exposure Prophylaxis Among Transgender Women – Transgender Women’s Internet Survey and Testing Study
Iaah L. Lucas2, Mariah Valentine-Graves2, Savannah Winter2, Joanna A Caldwell2, Prof. Stefan Baral3, Dr. Travis Sanchez2
1U.S. Centers for Disease Control and Prevention, Atlanta, United States.
2Emory University, Atlanta, United States.
3Johns Hopkins University, Baltimore, United States.
Background: Doxycycline post-exposure prophylaxis (doxy-PEP) is recommended for bacterial sexually transmitted infection (STI) prevention among transgender women (TGW) if taken within 72 h after sex. TGW are disproportionately burdened by bacterial STIs, yet there is little research about doxy-PEP awareness or willingness in this population. The objective of this study was to evaluate awareness of and willingness to use doxy-PEP to reduce bacterial STI risk among sexually active TGW.
Methods: We obtained data from the Transgender Women’s Internet Survey and Testing. The analytical sample included TGW, ≥15 years who reported sex in the past 12 months. We calculated unadjusted prevalence ratios (PR) and 95% confidence intervals (CI) using log-binomial regression for doxy-PEP awareness (yes/no); and unadjusted odds ratios (OR) and 95% CI using ordinal regression for doxy-PEP willingness (willing/neither willing nor unwilling/unwilling).
Results: Of 1,667 TGW, majority were White, non-Hispanic (74.6%) and aged 15–24 years (51.1%); 15.3% were aware of doxy-PEP and 72.2% were willing to use doxy-PEP. Doxy-PEP awareness was negatively associated with ≤high school education (PR = 0.61, 95% CI = 0.45–0.83) but positively associated with disclosing gender identity to a healthcare provider (PR = 2.27, 95% CI = 1.35–3.82), hormone therapy for medical gender affirmation/transition (PR = 1.54, 95% CI = 1.10–2.16), bacterial STI test (PR = 1.61, 95% CI = 1.29–2.03), HIV PrEP use (PR = 2.04, 95% CI = 1.53–2.72), or bacterial STI (PR = 2.02, 95% CI = 1.35–3.02). Willingness to use doxy-PEP was associated with bacterial STI test history (PR = 1.41, 95% CI = 1.12–1.77) and HIV PrEP use (PR = 1.98, 95% CI = 1.21–3.23).
Conclusion: Doxy-PEP awareness was low, although willingness to use doxy-PEP was high in this sample. Differences in doxy-PEP awareness and willingness were associated with socio-demographic, behavioral, and healthcare factors. Increasing awareness, willingness, and eventually coverage of doxy-PEP as an STI prevention strategy necessitates individual and system-level STI interventions tailored to TGW.
PP04.150 – Resurgence of Sexually Transmitted and Blood-Borne Infections (STBBIs): Epidemiological Trends and Rising Cases in Alberta, Manitoba, Saskatchewan, and Canada, 1980–2024
Dr. Mariana Herrera Diaz1, Mrs Maria Arango1, Ms Zipporah Gitau1, Mr Camilo Suarez1, Mrs Angela Copete1, Ms Camila Oda1, Ms Rotem Keynan1, Dr. Ameeta E Singh1, Dr. Stuart Skinner1, Dr. Cara Spence1, Dr. Lauren J MacKenzie1, Dr. Ken Kasper1, Dr. Laurie Ireland1, Dr. Jared Bullard1, Dr. Irene Martin1, Dr. David Alexander1, Dr. Diana Marin1, Dr. Lucelly Lopez1, Mrs Margaret Haworth-Brockman1, Dr. Yoav Keynan1, Dr. Zulma Rueda1
1University of Manitoba, Winnipeg, Canada.
Background: STBBIs have increased in Canada.
Objective: To describe the epidemiology of Chlamydia trachomatis, Neisseria gonorrhoeae, hepatitis B (HBV) and C (HCV) viruses, and syphilis in Prairie Provinces compared to Canada, 1980–2024.
Methods: This ecological study used publicly available data from Canadian and provincial governments. We analyzed the incidence rates/100,000 people/year in general and by sex, age, ethnicity, and mode of STBBIs acquisition.
Results: STBBIs rates have steadily increased over the past 15–30 years, reaching the highest rates in the last 5–7 years. The three provinces have highest STBBI rates compared to Canada. STBBIs are most prevalent in those 20–30 y. Highest coinfection detection: Chlamydia–Gonorrhea (20.85%, 2006); HIV–HCV (24.4%, 1999).
Chlamydia is the most frequently reported STBBI. In 2019, Saskatchewan had the highest rates (534.6/100,000), followed by Manitoba (402.7/100,000), and Alberta (399.9/100,000). Females accounted for 60% of diagnoses.
Gonorrhea reached the highest rates between 2019 and 2022, with Manitoba (272.7/100,000) and Saskatchewan (271.9/100,000) reporting the highest rates, compared to Canada (94.31/100,000) and Alberta (122.0/100,000). Males accounted for 60% of infections in Canada, but 40% in Saskatchewan and Manitoba.
In Canada, the lowest rate recorded for syphilis was 0.4/100,000 (1995–1996), and in 2022, the rate was 36.1/100,000. The highest rates were reported in Saskatchewan (164.2/100,000, 2021) and Manitoba (143.2/100,000, 2019), followed by Alberta (73.2/100,000, 2022). Diagnoses among females surpassed 55%. Congenital syphilis is rising nationally.
HCV incidence in 1991 in Canada was 3.3/100,000 and 19.7/100,000 in 2021. Manitoba (42.3/100,000) and Saskatchewan (38.3/100,000) had higher rates than Alberta (14.7/100,000). Males accounted >60% of infections (2022).
Following vaccination (1990s), HBV rates declined nationally from 10.8/100,000 to 0.3/100,000 (2021). However, Alberta recorded the highest HBV rates (2008–2019). Males, 40–59y, represented most diagnoses.
Conclusion: Canada and its provinces are facing unacceptable STBBIs rates. There is an urgent need for intensified national and provincial public health responses to halt rising STBBIs.
PP04.151 – Uptake and Impact of Revised Screening Recommendations for Syphilis During Pregnancy in Massachusetts, 2016–2024
Mr. Christian Hague1, Dr. Michael Klompas, Catherine Rocchio, Liisa Randall, Kathleen Roosevelt, Dr. Katherine Hsu, Noelle Cocoros
1Harvard Pilgrim Health Care Institute, Boston, United States.
Background: The Massachusetts Department of Public Health (MDPH) issued a clinical alert on June 30, 2020, recommending a second syphilis screening test during the third trimester for all pregnancies. Previous guidelines recommended one syphilis screening during pregnancy at the first prenatal visit. We evaluated syphilis screening and positive tests during pregnancy in the 4 years before versus after the alert.
Methods: We assessed syphilis screening of pregnant patients from three large clinical practice groups, from January 2016 through December 2024, using the Electronic medical record Support for Public health (ESP; esphealth.org) platform.
Results: Among 50,964 pregnancies, 84.2% (42,922/50,964) had ≥1 syphilis screening recorded. The proportion of pregnancies with ≥2 screenings increased from 12.4% (3,225/25,915) to 67.8% (16,990/25,049). Approximately 95% of pregnancies had a third trimester medical encounter in both periods but the proportion who had a syphilis screening during the third trimester increased from 15.5% (3,830/24,654) to 77.8% (18,449/23,725). The proportion of pregnancies with positive syphilis screenings in the third trimester increased from 0.2% (46/25,915 pregnancies) to 0.9% (231/25,049 pregnancies). Of 62 pregnancies with a positive confirmatory assay in the third trimester, 80.6% (50/62) had not been tested previously. This corresponds to 369 pregnancies-needed-to-screen during the third trimester to detect one new syphilis case.
Conclusion: We observed a large increase in the proportion of pregnancies with multiple syphilis screenings following state recommendations to rescreen for syphilis in the third trimester. Our findings suggest high rates of provider compliance with MPDH’s revised syphilis screening recommendations. Multiple syphilis cases were detected only during the third trimester. Our analysis demonstrates the value of public health surveillance platforms that leverage electronic health record data drawn from multiple practices to monitor screening tests in addition to positive tests along with pregnancy dates to generate a richer picture of the impact of public health recommendations.
PP04.152 – Trends in Infections Detected in Women with Pelvic Inflammatory Disease over a Decade
Dr. Kay Htaik1,2, Prof. Catriona Bradshaw1,2,3, Dr. Erica Plummer1,2, Ms Laura Matthews1,2, Ms Nishtha Malhotra1, Ms Natasha Wild1, Professor Eric PF Chow1,2,3, Dr Lenka Vodstrcil1,2,3
1Melbourne Sexual Health Centre, Melbourne, Australia.
2School of Translational Medicine, Monash University, Clayton, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) are established causes of pelvic inflammatory disease (PID), but in up to 70% of cases there is no pathogen detected. We aimed to describe infections detected among PID cases over a decade and establish the prevalence of Mycoplasma genitalium (MG) and bacterial vaginosis (BV) among non-chlamydial/non-gonococcal cases to inform testing and treatment practices.
Methods: We conducted a retrospective case-series to determine the number of PID cases diagnosed with genital infections (CT, NG, MG, BV) among individuals attending MSHC from 2014–2024. We determined the proportion of PID cases with >=1 genital infection detected, and a chi- square trend test was used to explore trends in detection of infections over time.
Results: Among 2907 PID cases, 1302 (45%, 95% CI: 43%–47%) had no infection detected; 294/2722 (11%, 95% CI: 10%–12%) had MG, 796/2533 (31%, 95% CI: 28%–35%) had BV, 422/2792 (15%, 95% CI:14%–17%) had CT, and 93/2784 (3%, 95% CI: 1%–3%) had NG. Of the 2374 (82%) cases tested for all four infections, 852 (36%) had one and 467 (20%) had >1 infection detected. Of the 2018/2374 (85%) non-chlamydial/non-gonococcal cases, 547/2018 (27%) had BV and 107/2018 (7%) had MG as the only infection detected while 68 cases (3%) were co-infected with BV and MG. Over the decade, the proportion of cases assessed for BV was high (80%–90%) and stable (P < 0.001) but detection increased from 23% to 40% (Ptrend < 0.001). MG testing was high (91%–98%) and stable (P < 0.001) but detection increased from 5% to 14% (Ptrend < 0.001).
Conclusion: Within this STI clinic population, CT and NG were not detected in ∼85% of PID cases. Among non-chlamydial/non-gonococcal cases, BV and MG were common, and both increased in prevalence over time. These data highlight the importance of testing for BV and MG in people diagnosed with PID in the STI clinic setting.
PP04.153 – Human Immunodeficiency Virus-1 Subtypes and Drug Resistance Among Children Under DTG Antiretroviral Regimen in Morocco
Mme Ghita Jouf1, Mme Alae Bekkouri Alami1, Mme Najwa Maazaz2, Mr Hassan Ihazmade3, Dr Imane Belbacha3, Dr Samira Benkerroum3, Mme Siham Amghar3, Mme Soumiya Ouedrhiri3, Mme Nezha El omari3, Mme Boushra NOURI3, Mme Hajar Elmrabet3, Pr Soumia Benchekroun4, Dr Elmir Elharti3, Pr Rachid El jaoudi1, Pr Zineb Rchiad2, Pr Hicham Oumzil1,5
1Medical Biotechnology Laboratory, Faculty of Medicine and Pharmacy. Mohammed V University, Rabat, Morocco.
2Corelab. University Mohammed VI Polytechnic, Benguérir, Morocco.
3Department of Virology, National Institute of Hygiene, Rabat, Morocco.
4Faculty of Medicine and Pharmacy. Mohammed V University, Rabat, Morocco.
5Centre for Biological Sciences. University Mohammed VI Polytechnic, Benguérir, Morocco.
Background: HIV drug resistance in children is often due to poor adherence or transmitted drug resistance during mother-to-child transmission. In Morocco, Dolutegravir (DTG)-based antiretroviral therapy (ART) was introduced in 2022 without prior evaluation of resistance mutation profiles. This study aims to determine the HIV-1 subtypes circulating among children and to establish the drug resistance mutation profile for protease (PR), reverse transcriptase (RT), and integrase (IN) genes.
Methods: Genetic analysis was conducted on 28 children and adolescents receiving DTG-based ART with detectable viral loads. HIV-1 pol genes (RT, PR, IN) were sequenced using Ion Torrent next-generation sequencing (S5, ThermoFisher, USA). Drug resistance was assessed using the Stanford HIV Drug Resistance Database algorithm.
Results: The majority of participants were infected with HIV-1 CRF_02 AG (64%), followed by subtype B (21%) and subtype A1 (15%). Overall resistance prevalence was 25% (95% CI: 11–45%), with the highest resistance found in nucleoside reverse transcriptase inhibitors (NRTIs) at 60% (95% CI: 39–79%), followed by non-nucleoside reverse transcriptase inhibitors (NNRTIs) at 40% (95% CI: 21–61%). No resistance mutations were observed for protease or integrase inhibitors. Among NRTIs, resistance was highest for Emtricitabine, Lamivudine, and Zidovudine, while Nevirapine and Efavirenz had the highest resistance among NNRTIs. The most common RT mutations were M184V (26%), K103N (16%), M41L (8%), K70R (8%), and T215Y (4%).
Conclusion: These findings highlight the importance of genotypic resistance monitoring to guide ART decisions and ensure optimal therapeutic outcomes in children. This research provides valuable insights into resistance patterns and supports the need for resistance testing to improve pediatric HIV care in Morocco.
PP04.154 – Low Rates of Vaccine Uptake Undermine Opportunities for Human Papillomavirus (HPV) Associated Cancers for Prevention
Ms. Rotem Keynan1, Mrs. Maria Arango1, Ms. Zipporah Gitau1, Mr. Camilo Suarez1, Mrs. Angela Copete1, Ms. Camila Oda1, Dr. Ameeta E Singh2, Dr. Stuart Skinner3,5, Dr. Cara Spence4,5, Dr. Lauren J MacKenzie6,7, Dr. Ken Kasper6,7,10, Dr. Laurie Ireland7,11,12, Dr. Jared Bullard1,8,9, Dr. Lucelly Lopez13, Dr. Diana Marin13, Dr. Margaret Haworth-Brockman14,15, Dr. Yoav Keynan1,6,14,15, Dr. Zulma Rueda1,13, Dr. Mariana Herrera1
1Department of Medical Microbiology and Infectious Diseases, University of Manitoba, Winnipeg, Canada.
2Department of Medicine, University of Alberta, Edmonton, Canada.
3Department of Medicine, University of Saskatchewan, Regina, Canada.
4Department of Medicine, University of Saskatchewan, Saskatoon, Canada.
5Wellness Wheel Clinic, Regina, Canada.
6Department of Internal Medicine, University of Manitoba, Winnipeg, Canada.
7Manitoba HIV Program, Winnipeg, Canada.
8Cadham Provincial Laboratory, Shared Health, Winnipeg, Canada.
9Department of Pediatrics and Child Health, University of Manitoba, Winnipeg, Canada.
10Health Sciences Centre, Winnipeg, Canada.
11Department of Family Medicine, University of Manitoba, Winnipeg, Canada.
12Nine Circles Community Health Centre, Winnipeg, Canada.
13School of Medicine, Universidad Pontificia Bolivariana (UPB), Medellin, Colombia.
14Department of Community Health Sciences, University of Manitoba, Winnipeg, Canada.
15National Collaborating Centre for Infectious Diseases (NCCID), University of Manitoba, Winnipeg, Canada.
Background: HPV-associated malignancies include anogenital and oropharyngeal cancers. Vaccination can decrease prevalence and associated malignancies in females and males. We determined the rates of HPV vaccine uptake, HPV infection, and HPV-associated malignancies in Alberta, Saskatchewan, and Manitoba, Canada, between 1980 and 2024.
Methods: We searched publicly available HPV reports published by Governments of Manitoba, Saskatchewan, Alberta, and Canada, Canadian Cancer Statistics and the International Cancer Agency. Variables: Number of HPV diagnoses per year (new), proportion of diagnoses by sex, age, HPV-associated malignancies (cervical, oral, ano-rectal, oropharynx), and vaccine intake (number of doses, by sex, age, and region).
Results: HPV-associated malignancies increased over time in Alberta: cervical cancer: 541 cases in 1980 to 4557 in 2009; oral cancer: <105 in 1980 to 1454 in 2009; and rectal cancer: <79 in 1980 to 721 in 2009. Saskatchewan reported increasing anorectal cancer among females (1.27/100,000 in 2021) and stable rates among males (0.42/100,000 in 2021) since 2009. Rates of oropharyngeal cancer in both sexes and cervical cancer were unchanged. Manitoba reports did not include HPV-related cancer rates; however, from 1990 to 2011 HPV infection rates decreased among females (163/100,000 population to 120/100,000) but increased in males (136/100,000 population to 167.1/100,000). Data was not disaggregated by age, race/ethnicity, or geographic location. Alberta reported lower rates of vaccination among males, compared to females (40.9% vs 42.6%). Saskatchewan reported that females aged 15 had highest rates of full vaccination in 2014 with 78.5% coverage. Manitoba vaccination rates declined from 64.3% in 2020 to 58.5% in 2021.
Conclusion: We documented a marked increase in HPV infection rates and HPV-related malignancies across Manitoba, Saskatchewan, and Alberta. Concerning low rates of vaccination among females and males with decreased rates in recent years suggest that education to address post-COVID-19 vaccine reluctance is required. Limited reporting and data disaggregation prohibit population-specific interventions.
PP04.155 – Tetracycline-resistant Neisseria gonorrhoeae Global Estimates – Impacts on doxyPEP Implementation and Monitoring
Kim Do1, M Unemo2,3, C Kenyon4,5, JS Hocking6, Assoc. Prof. Fabian YS Kong6
1Notre Dame University, Australia.
2WHO Collaborating Centre for Gonorrhoea and other STIs, Örebro University Hospital, Örebro, Sweden.
3Institute for Global Health, University College London, London, United Kingdom.
4Institute of Tropical Medicine, Antwerp, Belgium.
5Division of Infectious Diseases and HIV Medicine, University of Cape Town, Cape Town, South Africa.
6Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Doxycycline is recommended as post-exposure prophylaxis (doxyPEP) for sexually transmitted infections including gonorrhoea in multiple countries for men who have sex with men (MSM) and transgender women. However, its effectiveness depends on existing tetracycline resistance (TcR) in Neisseria gonorrhoeae (NG) within each country. Importantly, in countries implementing doxyPEP, existing surveillance systems should be able to monitor antimicrobial resistance (AMR), using standardized and quality-assured methods. In this systematic review, we estimate the proportion of NG isolates with tetracycline resistance by country/region and describe the contribution of sex and infection site to these estimates.
Methods: Bibliographic databases were searched between 1 January 2000 to 26 August 2024. Eligible studies were in English language, sample size >10 isolates and reported tetracycline MIC among NG isolates. Country, year of isolate collection, number of isolates, sex, infection site was collected. Country level data was aggregated into 7 World Bank Regions. TcR (MIC >1 mg/L) was reported by country, region and over time (2011–2023 vs 1996–2010).
Results: 66 included studies from 26 countries studying 75,858 isolates (91% from 2011 to 2023) were analysed (Table 1). Overall median tetracycline resistance was 54.5% (4.0–100.0%). The highest TcR was reported in East Asia/Pacific (82.1%, 18–100%) and Sub-Saharan Africa (81.6%,44–100%), while the lowest was in North America (26.5%, 4–78%). Only 17% (11/66) of studies provided data from MSM, 18% (12/66) included oropharyngeal isolates and 9% (6/66) provided data from women. Median TcR increased by 3-4-fold in South Asia (RR 3.8) and North America (RR 3.5) in 2011–2023 (vs 1996–2010).
Conclusion: With existing high levels of NG TcR, and substantial increases in South Asia and North America, doxyPEP is unlikely to be effective in preventing incident gonococcal infections globally. Prospectively, more data is needed from isolates from MSM, women and from the oropharynx to ensure we understand AMR development in NG and the impacts of transmission between MSM and women.
| World Bank Region Total isolates: 75,858 | 1996–2010 (% Resistance) | 2011–2023 (% Resistance) | Overall (1996–2023) (% Resistance) | Relative resistance increases between 2011–2023 versus 1996–2010 | ||||
|---|---|---|---|---|---|---|---|---|
| Median | Range | Median | Range | Median | Range | |||
| East Asia and Pacific(n = 16, 6304 isolates) | 82.1(n = 4, 659 isolates) | 17.6–100 | 82.1(n = 12, 5645 isolates) | 24.3–98.7 | 82.1 | 17.6–100 | 1.0 | |
| Sub-Saharan Africa(n = 10, 1733 isolates) | 75.0(n = 2, 241 isolates) | 54.0–77.0 | 81.6(n = 8, 1492 isolates) | 44.0–100 | 81.6 | 44.0–100 | 1.1 | |
| Latin America and Caribbean (n = 7, 2344 isolates) | 63.6(n = 2, 211 isolates) | 54.2–83.5 | 61.6(n = 5, 2123 isolates) | 22.6–100 | 61.6 | 22.6–100 | 0.97 | |
| Europe and Central Asia(n = 19, 6027 isolates) | 33.8(n = 5, 1062 isolates) | 17.4–54.0 | 50.5(n = 14, 4965 isolates) | 16.9–100 | 50.5 | 16.9–100 | 1.5 | |
| Middle East and North Africa (n = 1, 46 isolates) | 41.3(n = 1, 46 isolates) | 41.3 | – | – | ||||
| South Asia(n = 3, 168 isolates) | 12.0(n = 1, 50 isolates) | – | 45.0(n = 2, 118 isolates) | 38.9–51.0 | 38.9 | 12.0–51.0 | 3.8 | |
| North America(n = 10, 59246 isolates) | 7.5(n = 2, 4275 isolates) | 4.0–10.9 | 31.1(n = 8, 54,971 isolates) | 18.9–77.7 | 26.5 | 4.0–77.7 | 3.5 | |
PP04.156 – STI Burden and Co-Infection Patterns in Schistosomiasis-Endemic Settings: Findings from the MAP-FGS Study in Tanzania
Ms. Sarah Sullivan1, Dr. Diana Wilfred2, Ms. Elizabeth Long1, Ms. Elizabeth Long1, Dr Crecencia Chiombola2, Dr Amina Yussuph5, Dr Edgar Ndamboine5, Dr Godfrey Kaizilege5, Dr Crispin Mukerebe3, Dr John Changalucha3, Dr Jane Maganga3, Mr Titus Leeyio2, Dr Jennifer Downs4, Prof Humphrey Mazigo2
1Task Force for Global Health, Atlanta, United States.
2Catholic University of Health and Allied Sciences, Mwanza, Tanzania.
3National Institute of Medical Research, Mwanza, Tanzania.
4Cornell University, Ithaca, USA.
5Bugando Medical Centre, Mwanza, Tanzania.
Background: The Multi-Country Assessment of Prevalence for Female Genital Schistosomiasis (MAP-FGS) is the first large-scale study to estimate the burden of female genital schistosomiasis (FGS) across sub-Saharan Africa, which fills crucial data gaps to guide regional interventions for at-risk women and girls. Key objectives include: estimating prevalence of confirmed FGS cases in women aged 15-60 and identifying feasible, accurate, and locally-tailored diagnostic algorithms and screening procedures for diagnosing FGS and sexually transmitted infections (STI).
Methods: Nearly 10,000 women and girls aged 10–60 were enrolled across six countries (Tanzania, Mali, Madagascar, Senegal, Ghana, and Nigeria). In Tanzania, 1,288 women aged 18–60 from two districts (Itilima and Meatu) were included in the study. In addition to FGS prevalence, study data includes spatial modeling, reported HIV, HPV and STI results, and health-seeking behavior. This abstract highlights STIs results by PCR analysis for 1,271 women aged 18–60.
Results: Small though clinically important numbers of women tested positive for chlamydia (n = 132, 10.3%) and gonorrhoea (n = 51, 4.0%), whereas almost half tested positive for Trichomoniasis (n = 569, 45%). Women diagnosed with chlamydia were an average of 3.3 years younger than their peers without chlamydia (P = 0.002). While the number of reported pregnancies did not differ between women who tested positive or negative for STIs, reported infertility was significantly higher among women positive for trichomoniasis than those without trichomoniasis (47.6% vs 41.6% respectively, P = 0.016). Prevalence of trichomoniasis also varied significantly between the two districts in the study (Itilima = 62.8%, Meatu = 26.2%, P < 0.001) despite a shared border and similar populations.
Conclusion: STI data, especially in the context of schistosomiasis-endemic settings, is exceptionally limited. This presentation will allow Congress attendees to gain unique insights into STI prevalence, co-infection with schistosomiasis, and HPV through the results of Tanzania.
PP04.157 – Prevalence of Gonorrhea and Chlamydia Among Symptomatic and Asymptomatic Vulnerable Women Screened for the Bexsero Vaccine Efficacy Trial in Lilongwe, Malawi
Dr. Mitch Matoga1, Dr Jane S. Chen2, Dr. Gomezgani Lukhanda1, Mr. Claightone Chirombo1, Mrs Beatrice Ndalama1, Miss Jacqueline Mbendera1, Mrs Naomi Nyirenda1, Mrs Naomi Bonongwe1, Mrs. Yvonne Makala1, Mrs. Esther Mathiya1, Mr Edward Jere1, Mr Chalimba Lusewa1, Mr Gabriel Banda1, Mr Lloyd Singogo1, Dr Eric Garges3, Prof. Irving Hoffman4
1University of North Carolina Project Malawi, Lilongwe, Malawi.
2UNC Gillings School of Global Public Health, Chapel Hill, United States of America.
3Division of Global Public Health, Uniformed Services University of Health Sciences, Bethesda, United States of America.
4Department of Medicine, Institute of Global Health and Infectious Diseases, Chapel Hill, United States of America.
Background: Neisseria gonorrhoeae (Ng) and Chlamydia trachomatis (Ct) infections are common in Malawi, particularly among women with abnormal vaginal discharge (AVD) and/or lower abdominal pain (LAP) seeking STI services. However, there is limited data on the prevalence of Ng/Ct, including in extragenital sites, among asymptomatic women in Malawi.
Methods: This cross-sectional analysis compares the prevalence of Ng/Ct among symptomatic and asymptomatic women vulnerable to STIs in Lilongwe, Malawi. During the screening process for DMID 19-0004, a phase II study for Ng prevention (ClinicalTrials.gov ID NCT 04350138), we conducted urogenital Ng/Ct NAAT testing (GeneXpert) on symptomatic women presenting to Bwaila STI clinic with AVD or LAP or rectal discharge; and asymptomatic women considered vulnerable to gonococcal infection due to one or more of the following: age ≤25 years, multiple sexual partners or STI treatment within the past year or current HIV PrEP use.
Results: Between February and November 2024, 449 total women were screened for Ng/Ct. The median age was 26 (interquartile range: 23, 32). Of these, 181 (40%) were symptomatic with AVD or LAP but no rectal symptoms and 268 (60%) were asymptomatic. The overall prevalence of Ng and/or Ct was 123 (27%): 75 (17%) with Ng, 72 (16%) with Ct and 24 (5%) co-infected. The prevalence was higher among symptomatic compared to asymptomatic women Ng: (22% vs 13%), Ct: (21% vs 13%) and co-infection: (8% vs 4%), respectively. Both Ng and Ct prevalence was higher in rectal compared to pharyngeal sites (11% vs 1%).
Conclusion: Ng and Ct are highly prevalent among symptomatic and asymptomatic women at risk in Malawi. The high prevalence of asymptomatic infection, including extragenital sites, highlights the limitations of syndromic management and emphasizes the need for affordable rapid point-of-care diagnostics, scalable programs of comprehensive treatment and prevention strategies such as targeted Ng/Ct screening, Doxy PrEP/PEP and potential vaccination.
PP04.158 – Unmasking Versus Paradoxical IRIS in Pregnancy: Demographic Predictors and Outcomes, a Kaplan Meier and Cox-regression Analysis
Asst. Prof. John Muthuka1
1Kenya Medical Training College, Nairobi, Kenya.
2Meharry Medical College, Nashville, USA.
Background: This study aimed to address the gap in understanding the incidence, predictors, and types of immune reconstitution inflammatory syndrome (IRIS) among ART-naïve pregnant women, its survival time, and correlation with adverse pregnancy outcomes (APOs). The findings provide critical insights into health risks faced by this population, potentially guiding strategies to improve maternal and fetal health.
Methods: Conducted between June 2019 and March 2020, the study assessed IRIS following the International Network for Studies Against HIV-Associated IRIS criteria. Data analysis included Kaplan-Meier survival analysis to estimate time to APOs, multivariate Cox regression analysis for pre-ART demographic predictors of IRIS incidence, and decision tree modeling to predict APOs based on demographics.
Results: IRIS occurred in 25% (n = 133) of participants, with unmasking IRIS accounting for 72.9% and significantly associated with APOs [χ2 (1) = 4.911, P = 0.027]. Over 80% survived IRIS events for 6 weeks, with 50% diagnosed at approximately 2 months. Kaplan-Meier analysis showed longer survival before APOs among unmasking IRIS cases (χ2 = 5.292, Log Rank test = 0.021) (Fig. 1). Hazard ratios for cumulative risk were 0.18 for unmasking IRIS and 0.4 for paradoxical IRIS. Decision tree analysis identified women aged 30–39 as having the highest incidence of APOs (P = 0.688).
Conclusion: Unmasking IRIS was the most common type and strongly linked to APOs, with older age as a significant predictor. Women with unmasking IRIS survived longer before experiencing APOs compared to paradoxical IRIS cases. Further research on paradoxical IRIS is crucial. Healthcare providers should monitor ART-naïve pregnant women, particularly older women, and develop targeted interventions to mitigate IRIS-related risks.
| Group | Survival Rate | Statistical Test | Result | |
|---|---|---|---|---|
| Unmasking IRIS | Higher | χ2 (Chi-Squared) | 5.292 | |
| Log Rank Test | 0.021 | |||
| Paradoxical IRIS | Lower |
Hazard plot based on hazard function Kaplan Meir curve on APO between unmasking and paradoxical IRIS.
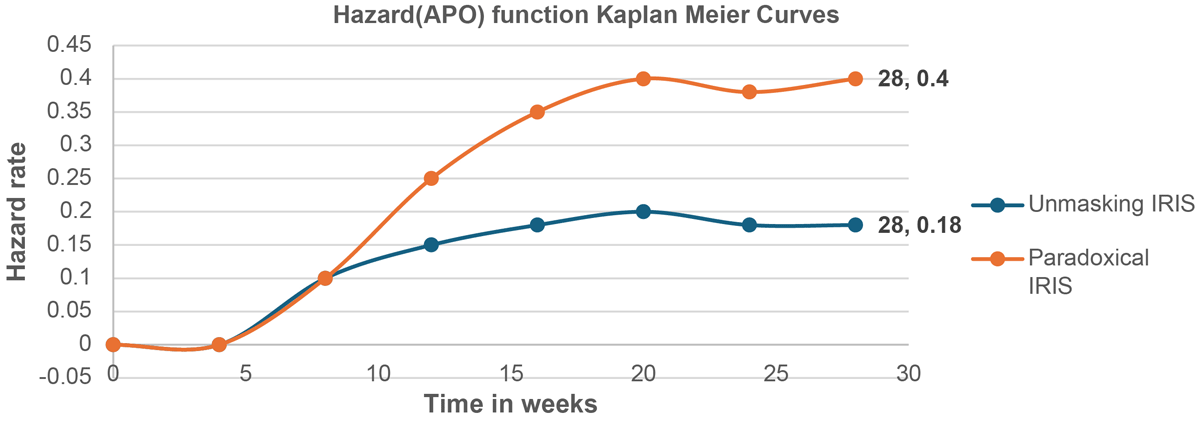
PP04.159 – Molecular Evolution and Phylodynamic of Human Immunodeficiency Virus-1 in Morocco: Insights from Two Decades of Sequence Data
Miss Maazaz Najwa1, Miss Jouf Ghita2, Miss Bekkouri Alami Alae1,2, Dr Laamarti Mariem1, Mr Ihazmade Hassan3, Mr Bouragba Elmaslouhi Ayman1, Dr Belbacha Imane3, Dr Benkerroum Samira3, Amghar Siham3, Ouedrhiri Soumiya3, El Omari Nezha3, Nouri Bouchra3, Elmrabet Hajar3, Benyaich Latifa4, Mountassir Meryem5, Dr Hassaini Nadia6, Elmeliani Fatima6, Dr Elharti Elmir3, Pr. El Fatimy Rachid7, Pr El Jaoudi Rachid2, Pr Rchiad Zineb1, Pr Oumzil Hicham1,2
1University Mohammed VI Polytechnic, Benguerir, Morocco.
2Medical Biotechnology Laboratory, Faculty of Medicine and Pharmacy. Mohammed V University, Rabat, Morocco.
3Department of Virology, National Institute of Hygiene, Rabat, Morocco.
4Medical Laboratory, Mohammed V Regional Hospital, Tangier, Morocco.
5Medical Laboratory, Ibn Zohr Regional Hospital, Marrakech, Morocco.
6Medical Laboratory, Hassan II Regional Hospital, Agadir, Morocco.
7Faculty of Medical Sciences, UM6P Hospital, Mohammed VI Polytechnic University, Morocco.
Background: The molecular evolution of HIV-1 is essential for informing public health interventions and optimizing treatment strategies. However, such molecular epidemiological analyses remain scarce in Morocco. This study aims to investigate the molecular evolution and diversity of HIV-1 in the Moroccan population using publicly available sequencing data.
Description: A total of 723 HIV-1 pol gene sequences (protease, reverse transcriptase, and integrase regions) were retrieved from both our research and public databases, representing Moroccan patients between 2005 and 2024. Computational analyses were conducted to assess temporal subtype evolution, phylodynamics, and date estimations using a Markov Chain Monte Carlo (MCMC)-based molecular clock approach.
Results: Over the past two decades, a notable shift in circulating HIV-1 subtypes in Morocco was observed — from a predominance of subtype B to an increasing presence of the recombinant form CRF_02 AG. This evolution was accompanied by the emergence of additional subtypes, including C, G, and A1.
Phylodynamic analysis revealed that Moroccan subtype B strains were closely linked to Western European and North American lineages, whereas CRF_02 AG strains clustered with viruses from West and Central Africa. Molecular clock estimates dated the most recent common ancestor of CRF_02 AG to 1953 (95% highest posterior density [HPD]: 1915–1984), and that of subtype B to 1969 (95% HPD: 1936–1988).
Conclusion: These findings underscore Morocco’s position as a genetic and epidemiological bridge between North Africa and sub-Saharan HIV-1 networks, contributing to regional viral diversity. They highlight the urgent need to strengthen molecular surveillance systems and to tailor HIV prevention and treatment strategies to the evolving local epidemiological landscape.
PP04.16 – Increase in Syphilis Antibody Detection Among People Who Tested Positive for Hepatitis C Antibodies in British Columbia, Canada from 2018 to 2023
Asst. Prof. Sofia Bartlett1,2, Dr. Theodora B. Consolacion1, Amanda Yu1, Dr. Julia MacIsaac3,4, Victor Lei1, Katherine Twohig1,5, Chloe Xavier1, Samie Lawal1, Hannah Baer1, Heather Burgess1,6, Robert Higgins1, Justin Sorge1,7, Venessa Ryan1, Dr. Jennifer Vines1, Dr. Mark Gilbert1,2, Dr. Muhammad Morshed8,9, Dr. Agatha Jassem8,9, Dr. Adriana Airo8,9, Dr. Eric Eckbo8,9, Dr. Troy Grennan1,3, Dr. Kirsty Bobrow1
1Clinical Prevention Services, British Columbia Centre for Disease Control, Vancouver, Canada.
2School of Population and Public Health, University of British Columbia, Vancouver, Canada.
3Department of Medicine, University of British Columbia, Vancouver, Canada.
4St. Paul’s Hospital, Providence Health Care, Vancouver, Canada.
5Canadian Field Epidemiology Program, Public Health Agency of Canada, Ottawa, Canada.
6Canadian Public Health Service, Public Health Agency of Canada, Ottawa, Canada.
7Centre for Communicable Diseases and Infection Control, Infectious Diseases and Vaccination Programs Branch, Public Health Agency of Canada, Ottawa, Canada.
8Public Health Laboratory, British Columbia Centre for Disease Control, Vancouver, Canada.
9Department of Pathology and Laboratory Medicine, University of British Columbia, Vancouver, Canada.
Background: Increasingly, syphilis cases have been reported among people experiencing substance use or mental health (SU/MH) challenges in British Columbia (BC), Canada. Hepatitis C virus (HCV) rates have been consistently elevated in this population, resulting in high routine HCV screening rates among people accessing (SU/MH) care in BC. To assess trends in syphilis screening, we evaluated syphilis antibody (anti-syphilis) testing and test positivity after a positive HCV antibody (anti-HCV) test in BC from 2018–2023.
Methods: All syphilis and >95% of anti-HCV tests in BC are conducted by BC Centre for Disease Control (CDC) Public Health Laboratory (PHL). We therefore used BC CDC PHL data on anti-HCV tests to identify positive anti-HCV episodes (all anti-HCV tests conducted per person within 24-h) from 2018 to 2023 (Fig. 1). Next, we determined if persons testing anti-HCV positive also received syphilis screening (anti-syphilis enzyme linked immunoassay [EIA]) that calendar year, and how many screened positive.
Results: There were 74,644 positive anti-HCV test episodes identified from 2018 to 2023. During this period, 27% (20,352/74,644) of people with a positive anti-HCV test were then screened for syphilis that calendar year, and 9% (1,853/20,352) of those screened anti-syphilis positive. Syphilis EIA test positivity increased by 170% from 2018 (6%) to 2023 (16%), with an absolute increase of 10.24 percentage points. While the proportion of people with an anti-HCV positive test episode who were then screened for syphilis increased by 63%, the absolute number of anti-syphilis tests performed decreased by 25% during this period.
Conclusions: The declining number of anti-HCV positive episodes suggests encouraging progress towards HCV elimination in BC. However, further efforts to increase awareness of the need for syphilis screening among providers that frequently screen for and diagnose HCV, such as SU/MH care providers, is warranted. Reflexively screening anti-HCV positive specimens for syphilis by BC CDC PHL may increase syphilis diagnosis.
Number of positive hepatitis C virus (HCV) antibody (anti-HCV) enzyme-linked immunoassay (EIA) test episodes among all anti-HCV tests conducted by British Columbia Centre for Disease Control Public Health Laboratory in British Columbia, Canada from 2018 to 2023 are represented by the dark blue bars (left y-axis). The number of syphilis antibody (anti-syphilis) EIA tests performed among people after an anti-HCV positive test each year are represented by the lighter blue bars (left y-axis). The proportion of positive anti-syphilis EIA tests (percent positivity) among those conducted each year (number represented by the light blue bars) are represented by the lighter blue line (right y-axis).
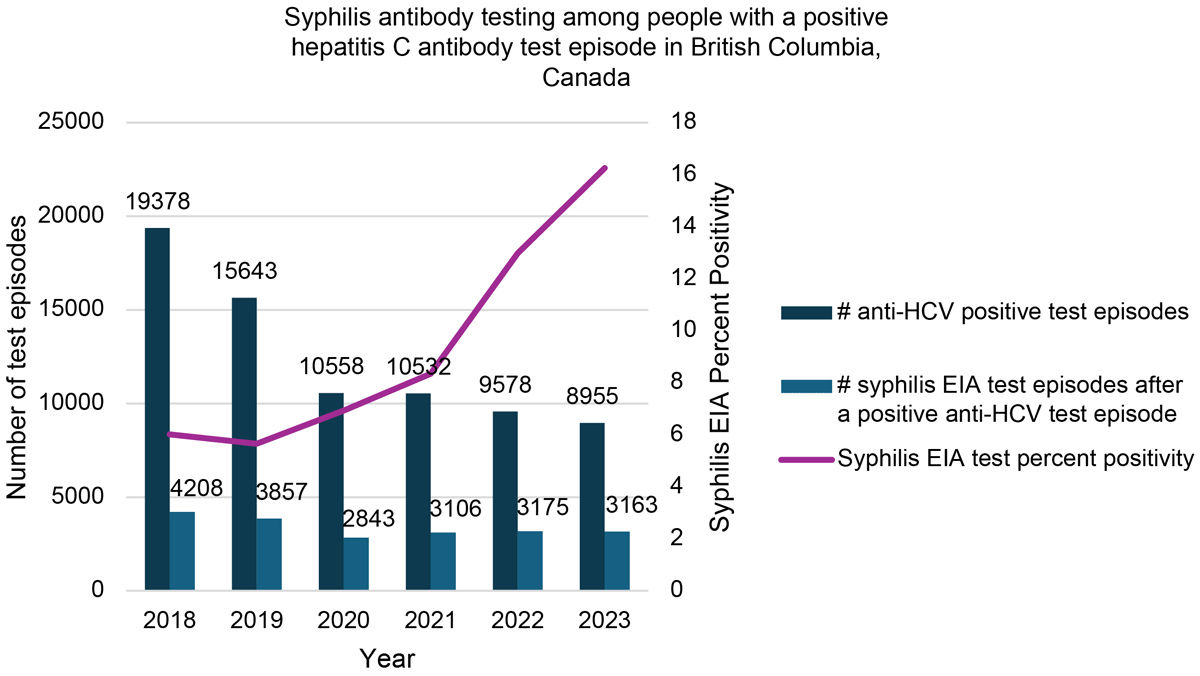
PP04.160 – Bacterial Sexually Transmitted Infections and Related Antibiotic Use Among Individuals Eligible for Doxycycline Post-exposure Prophylaxis in the United States
Ms. Anna Marie Parker1, Dr. Jennifer Chang2, Mrs. Laura M. King1, Dr. Sandra I. McCoy1,3, Dr. Joseph A. Lewnard1, Dr. Katia J. Bruxvoort4
1University of California, Berkeley, Berkeley, United States.
2Los Angeles Medical Center, Southern California Permanente Medical Group, Los Angeles, United States.
3Gilead Sciences, Inc., Foster City, United States.
4University of Alabama at Birmingham, Birmingham, United States.
Background: Doxycycline postexposure prophylaxis (doxyPEP) can prevent bacterial sexually transmitted infections (STIs) among men who have sex with men (MSM) and transgender women. However, concern surrounds the volume of tetracycline use needed to realize these benefits, and whether potential risks of increased tetracycline exposure outweigh benefits of doxyPEP for specific populations.
Methods: We estimated incidence rates of gonorrhea, chlamydia, and syphilis and related antibiotic prescribing among commercially-insured US males and transgender individuals using the Merative MarketScan® Research Databases during 2016–2019. We evaluated potential impacts of doxyPEP implementation under risk-based prioritization schemes focusing on HIV pre-exposure prophylaxis (PrEP) recipients, people living with HIV (PLWH), and people with prior STI diagnoses.
Results: Incidence rates of gonorrhea, chlamydia, and syphilis among PLWH and PrEP recipients with ≥1 STI diagnosis in the prior year totaled 33.3–35.5 episodes per 100 person-years. Direct effects of doxyPEP could prevent 7.4–9.6 gonorrhea diagnoses, 7.3-8.1 chlamydia diagnoses, and 3.1–5.9 syphilis diagnoses per 100 person-years within these populations. Expected increases in tetracycline consumption resulting from doxyPEP implementation were equivalent to 271.9–312.9 additional 7-day doxycycline treatment courses (resembling current standards for chlamydia treatment) per 100 person-years of use. This increase corresponded to the equivalent of 36.5–37.0, 37.0–38.7, and 46.1–100.2 additional 7-day doxycycline treatment courses for each prevented chlamydia, gonorrhea, and syphilis episode, respectively. These increases in doxycycline use exceeded anticipated reductions in STI-related prescribing of cephalosporins, macrolides, and penicillins by 16–69 fold margins.
Conclusions: Estimates of changes in antibiotic use and STI incidence resulting from doxyPEP implementation in differing populations may inform priority-setting for this intervention.
PP04.161 – Chlamydia and Gonorrhoea Testing and Positivity Among Women on Opioid Agonist Therapy Attending Primary Care Clinics in Australia
Ms. Samara Griffin1,2,3, Mr Jason Asselin1,2,4, Dr Anna Wilkinson1,2,5, Dr Michael Traeger1,2, Dr Rebecca Winter1,2,3, Ms Nyssa Watson1, Dr. Brendan Quinn1, Mr Vincent Cornelisse6, Dr Nathan Ryder6, Dr Eugene Athan7, Prof Jenny McCloskey8, Dr David A Baker9, Dr Louise Owen10, Prof Eric Chow5,11,12, Prof Rebecca Guy4, Prof Mark Stoove1,2,13, Prof Margaret Hellard1,2,4,14
1Burnet Institute, Melbourne, Australia.
2School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia.
3Department of Gastroenterology, St Vincent’s Hospital Melbourne, Melbourne, Australia.
4Kirby Institute, Sydney, Australia.
5University of Melbourne School of Population and Global Health, Melbourne, Australia.
6NSW Department of Health, Sydney, Australia.
7Barwon Health, Geelong, Australia.
8WA Department of Health, Perth, Australia.
9East Sydney Doctors, Sydney, Australia.
10Tasmanian Department of Health, Hobart, Australia.
11Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
12School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
13Australian Research Centre in Sex, Health and Society, La Trobe University, Melbourne, Australia.
14Department of Infectious Diseases, The Alfred and Monash University, Melbourne, Australia.
Background: People who use drugs experience higher rates of sexually transmitted infections (STIs), however there is limited understanding of the patterns of testing and STI positivity among women who use drugs. We aim to describe chlamydia and gonorrhoea testing and positivity among women prescribed opioid agonist therapy (OAT) in Australia.
Methods: Data were from women aged 15–55 years attending any of 69 primary care clinics from 01 January 2012 to 31 December 2024, with evidence of OAT prescription during the study period across a network of primary care services. We report total test uptake (proportion of women tested during the study period) and annual test positivity. We determined post-diagnosis re-testing and reinfection. Outcomes were stratified by a binary age grouping of <30 or ≥30.
Results: Among 6,581 women prescribed OAT, 2,159 (33%) were tested for chlamydia or gonorrhoea at least once during the study period. Test uptake was 29% (2008/6581) for gonorrhoea and 32% (2134/6581) for chlamydia. Gonorrhoea test positivity was 6.5% for women <30 years and 4.6% for women ≥30 years (P < 0.001) (Fig. 1). Chlamydia test positivity was 12% for women <30 years and 4.7% for women ≥30 years (P = 0.09). Annual test positivity increased from 2.6 to 4.3% between 2012 and 2024 for chlamydia (P-value [test of trend] = 0.02) and 0.3–2.7% between 2012 and 2024 for gonorrhoea (P-value [test of trend] < 0.01). Among 94 gonorrhoea positives, 59 (63%) had subsequent gonorrhoea testing and nine had ≥1 additional positive gonorrhoea test. Among 148 chlamydia positives, 110 (74%) had subsequent chlamydia testing and 24 had ≥1 additional positive chlamydia test.
Conclusion: Despite high test positivity, particularly among young women, two-thirds of women on OAT were not tested for gonorrhoea or chlamydia at a participating service during the study period. Among those tested after a positive test, positivity was high, indicating either high rates of reinfection or sub-optimal rates of effective treatment.
Test positivity for chlamydia and gonorrhoea, by year, for women aged 15–55 with at least one electronic prescription for OAT, ACCESS, Australia, 2012–2024 (n = 2,159).
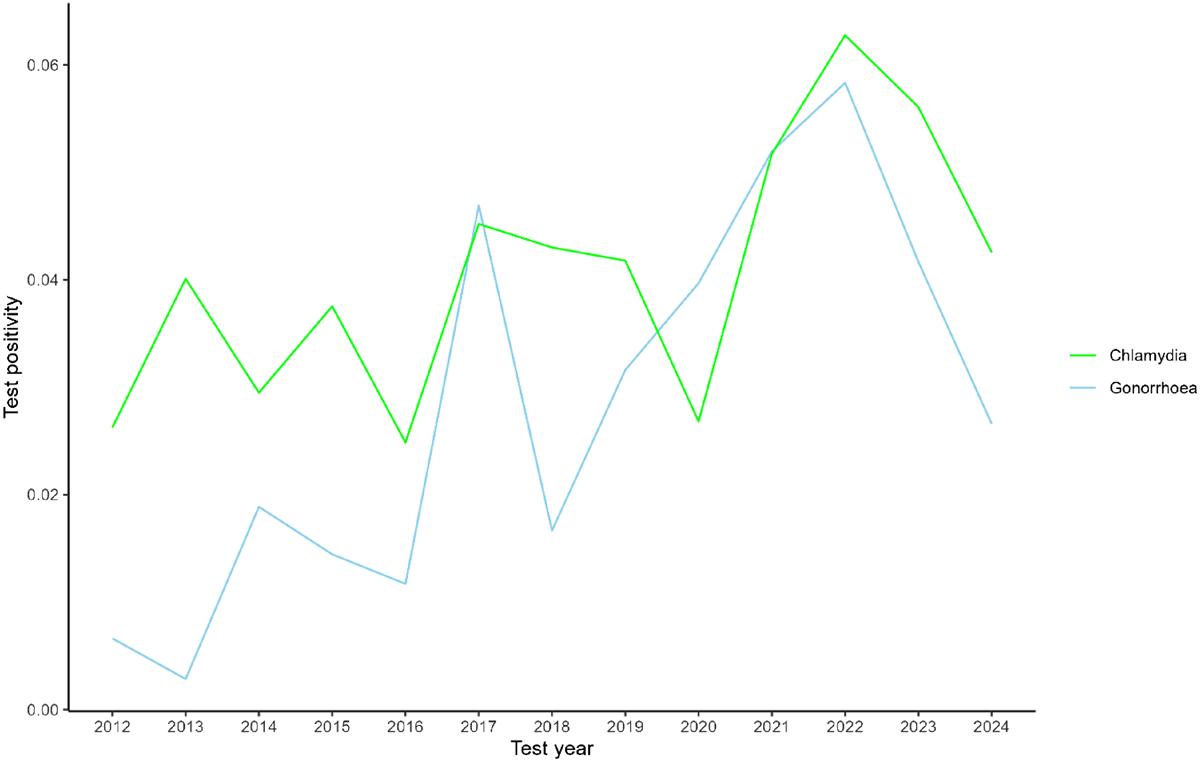
PP04.162 – Infectious Syphilis Test Uptake and Positivity Among Australian Women Ever Prescribed Opioid Agonist Therapy
Dr. Brendan Quinn1, Mr Jason Asselin1,2,3, Dr Anna Wilkinson1,2,4, Dr Brendan Harney1,2,5, Nyssa Watson1, Samara Griffin1,2,6, Louise Owen7, Eric Chow8, Jason Ong8, David Baker9, Sharon Chen10, Sherelle Iuretigh11, Christopher Carmody12, Charlotte Bell13, Phillip Read14, Caroline Lade15, David Templeton3,16, Donna Mak17, Jenny McCloskey17, Eugene Athan18, Nathan Ryder19, Vincent Cornelisse3,20,21, Htein Linn Aung3, Basil Donovan3, Belinda Hengel3, Rebecca Guy3, Margaret Hellard1,2,3,22, Mark Stoové1,2,11, Michael Traeger1
1Burnet Institute, Melbourne, Australia.
2School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia.
3Kirby Institute, University of New South Wales, Sydney, Australia.
4University of Melbourne School of Population & Global Health, Melbourne, Australia.
5Centre de recherche du Centre hospitalier de l’Université de Montréal, Montreal, Canada.
6Department of Gastroenterology, St Vincent’s Hospital, Melbourne, Australia.
7Tasmanian Sexual Health Service, Hobart, Australia.
8Melbourne Sexual Health Centre, Carlton, Australia.
9East Sydney Doctors, Sydney, Australia.
10Centre for Infectious Diseases & Microbiology Laboratory Services, NSW Health Pathology, Sydney, Australia.
11Alice Springs Sexual Health Centre, Alice Springs, Australia.
12Liverpool Sexual Health Centre, Liverpool, Australia.
13Adelaide Sexual Health Centre, Adelaide, Australia.
14Kirketon Road Centre, Kings Cross, Australia.
15Gold Coast Sexual Health Centre, Gold Coast, Australia.
16Department of Sexual Health Medicine, Sydney Local Health District, Sydney, Australia.
17Department of Health, East Perth, Australia.
18Barwon Health, Geelong, Australia.
19NSW Department of Health, Sydney, Australia.
20North Coast Health Services, NSW Health, Australia.
21School of Translational Medicine, Monash University, Melbourne, Australia.
22Department of Infectious Diseases, The Alfred & Monash University, Melbourne, Australia.
Background: Increased syphilis transmission among women is a growing concern. Injecting drug use has been associated with syphilis incidence, yet Australia’s STI Strategy does not consider people who use drugs a priority population. To inform integrated care and targeted testing and prevention, we estimated testing uptake and positivity for infectious syphilis among women attending primary care services ever prescribed opioid agonist therapy (OAT), compared to those never prescribed OAT.
Methods: Consultation, OAT and syphilis test data were extracted from a sentinel surveillance network of general practice, community health and alcohol and other drug services (n = 25) for women aged 15–55 years between 2014 and 2024. We report test uptake (number individuals tested/number attending) and test positivity (number diagnoses/tests) for infectious syphilis, stratified by evidence of ever having OAT prescribed (a proxy for ever injecting drugs). Associations between test positivity and OAT prescription were explored using logistic regression, adjusted for age and Indigenous status.
Results: Among 257,370 women, 5,667 (2.2%) were ever prescribed OAT. Of these, 1,100 (19.4%) were tested for syphilis at least once (vs 12.6% of women never prescribed OAT). Of 32,933 women tested for syphilis (median = 1 test/person; IQR = 1–20), 116 (0.24%) tested positive (no reinfections). Women ever prescribed OAT were more likely to test positive for syphilis (3.6% vs 0.2%; aOR = 11.4, 95% CI: 7.3, 17.8). The percentage of women ever prescribed OAT and tested for syphilis at least once per calendar year declined from 7.6% to 5.7% between 2014 and 2024.
Conclusion: Women ever prescribed OAT and tested for syphilis were over 11 times likely to test positive than women never prescribed OAT. Despite substantial increased syphilis notifications among women over the observation period Australia-wide, annual syphilis testing rates declined for women receiving OAT. Our findings strongly support greater integration of sexual health in models of care for people who use drugs.
PP04.163 – Multi-Level Determinants of STI Incidence in a Community-Based Cohort of Women Sex Workers in Vancouver, Canada: Findings of a Recurrent Event Analysis (2010–2024)
Mrs. Kayla Saadeh1,5, Dr. Kate Shannon2, Dr. Andrea Krusi3, Jennie Pearson4, Wiebke Bartels4, Dr. Shira Goldenberg1
1San Diego State University School of Public Health, San Diego, United States.
2The University of British Columbia School of Social Medicine, Vancouver, Canada.
3Simon Fraser University School of Criminology, Burnaby, Canada.
4The University of British Columbia, Vancouver, Canada.
5UC San Diego School of Public Health, San Diego, United States.
Background: Sex workers face disproportionate burdens of stigma, criminalization, violence, and HIV/STIs. A growing body of research elucidates individual-level determinants of STIs, but few prospective studies comprehensively assess contributions of macro-structural, community, and occupational-level factors on recurrent STIs among sex workers in high-income contexts. We aimed to 1) describe recurrent STI events over 14 years, and 2) evaluate the relationship between macro-structural, community, and occupational risk exposures and recurrent STI infections in a prospective cohort of sex workers.
Description: Data were from an open community-based longitudinal (2010–2024) cohort of women sex workers (AESHA) in Vancouver, Canada. Bivariate and multivariate models using a marginal means/rates approach were used to generate rate ratios (RRs) and 95% confidence intervals (CIs) for macro-structural, community, and occupational exposures and STI events.
Results: Among 770 participants reporting exchanging sex for money in the last 6 months, 192 (24.9%) experienced at least one STI (chlamydia, gonorrhea, or syphilis), with an event rate of 17.74 per 100 person-years. In adjusted models, working, volunteering, or participating in community organizations, ranging from sex-worker-specific organizations to other community initiatives, was associated with lower STI infection rates (RR = 0.62, 95% CI = 0.45, 0.85); use of sex work outreach programs (RR = 2.56, 95% CI = 1.90, 3.44) and client condom refusal (RR = 1.49, 95% CI = 1.01, 2.21) were associated with higher rates.
Conclusion: In this cohort, participating in community-based initiatives was associated with reduced STI rates, potentially due to increased social support and better access to prevention resources through such initiatives. Utilizing sex work outreach was positively associated, potentially due to effectiveness of such programs in reaching highly marginalized and street-based workers. Scale-up of sex worker-led initiatives and policy changes to remove structural barriers to community mobilization and safer occupational conditions via decriminalization are recommended.
| Unadjusted RR (95% CI) | Adjusted RRA (95% CI) | ||
|---|---|---|---|
| Macro-structural factorsB | |||
| Housing insecurity | 1.48 (1.16, 1.89) | 1.20 (0.95, 1.52) | |
| Detention/prison/jail overnight or longer | 1.26 (0.75, 2.13) | 1.02 (0.62, 1.67) | |
| Community factors | |||
| Working, volunteering, or participating in community organizations/peer-based initiativesB | 0.56 (0.39, 0.79) | 0.62 (0.45, 0.85) | |
| Use of sex work outreach programsC | 2.88 (2.16, 3.83) | 2.56 (1.90, 3.44) | |
| Occupational factors and exposuresC | |||
| Informal indoor primary place of service (vs outdoor) | 0.83 (0.61, 1.12) | 0.91 (0.67, 1.23) | |
| Formal indoor primary place of service (vs outdoor) | 0.48 (0.30, 0.79) | 0.78 (0.37, 1.65) | |
| Police encounters while working | 1.28 (1.01, 1.63) | 1.11 (0.88, 1.39) | |
| Rushed negotiations with client due to police presence | 1.40 (1.10, 1.80) | 1.14 (0.89, 1.45) | |
| Any physical/sexual violence with clients | 1.18 (0.84, 1.66) | 1.03 (0.74, 1.43) | |
| Client condom refusal | 1.57 (1.05, 2.35) | 1.49 (1.01, 2.21) | |
AAdjusted for controlled for age, race, minoritized gender, injection drug use, and whether interviews were conducted during COVID-19.
BSample 1 (n = 797 participants, 7,040 observations) – Entire sample with complete outcome data.
CSample 2 (n = 770 participants, 5,039 observations) – Restricted to participants reporting exchanging sex for money in the last 6 months.
PP04.164 – Prevalence of Quinolone Resistance-Associated Mutations in the United States Varies Geographically, but Overall Was Stable from 2020–2023
Dr. Olusegun Soge1, Avery Tuggle1, Professor William Geisler2, Dr. Stephen Jordan3, Associate Professor Candice McNeil4, Dr. Preeti Pathela5, Professor Hilary Reno6, Professor Karen Wendel7, Gina Leipertz8, Anika Parker1, Dr. Damon Getman9, Professor Matthew Golden1, Professor Lisa Manhart1
1University of Washington, Seattle, United States.
2University of Alabama at Birmingham, Birmingham, United States.
3Indiana University, Indianapolis, United States.
4Wake Forest University School of Medicine, Winston-Salem, United States.
5New York City Department of Health and Mental Hygiene, Queens, NY, United States.
6Washington University, St. Louis, United States.
7Public Health Institute at Denver Health, Denver, United States.
8Washington State University, Spokane, United States.
9Hologic Inc., San Diego, United States.
Background: Mycoplasma genitalium (MG) azithromycin resistance has been widely reported in the US but quinolone resistance-associated mutation (QRAM) data are limited. We describe QRAM prevalence in sexual health clinics (SHCs) in 7 US cities from 2020–2023.
Methods: We tested remnant Aptima urogenital specimens from symptomatic/asymptomatic males/females attending SHCs in Birmingham, Denver, Greensboro, Indianapolis, New York, Seattle, and St. Louis for MG and macrolide resistance using Aptima assays. We detected parC mutations by PCR and Sanger sequencing and calculated adjusted prevalence ratios (aPR) controlling for site, sex and symptom status using Poisson regression with robust standard errors.
Results: Overall, 1128 (95.1%) of 1186 MG-positive remnant specimens had sufficient volume for QRAM testing (Table 1). Of those, 420 (35.4%) did not amplify; 38 (3.2%) yielded an amplicon inadequate for sequencing; 43 (3.6%) had inconclusive sequences. Failure to amplify was associated with site, urine versus swab samples, and asymptomatic versus symptomatic status (P < 0.05 for all). Among 627 specimens with conclusive parC sequences, 422 (67.3%) had no parC mutations; 169 (27%) had mutations not associated with treatment failure; 36 (5.7%; 95% CI = 4.1–7.9) had QRAMs (S83I [n = 20], S83N [n = 4], S83R [n = 3], D87Y [n = 3], D87N [n = 6]). Most with QRAMs also had macrolide resistance (29/36 [80.6%]). QRAM prevalence was higher in men who have sex with men (MSM) than men who have sex with women (23.5% vs 2.7%, aPR = 8.96; 95% CI = 3.12–25.71), but did not differ significantly by sex, symptom status, race/ethnicity, or age. Prevalence ranged from 1.8% in Indianapolis to 22.2% in Seattle, but there was no significant difference after adjusting for prevalence in MSM. QRAM prevalence did not vary over time (P = 0.31).
Conclusion: QRAM prevalence was 5.7% in 7 US cities and substantially higher in MSM. Higher prevalence in selected geographic areas likely reflects the distribution of MSM in each location. Ongoing surveillance is needed to monitor trends.
| Site | TOTAL NUMBER SPECIMENS TESTEDN = 627N (%)D | QRAMN = 36N (%) | WT or otherN = 591N (%) | P-valueC | |
|---|---|---|---|---|---|
| Overall | 627 | 36 (5.7) | 591 (94.3) | - | |
| Birmingham, AL | 115 (18.3) | 3 (2.6) | 112 (97.4) | 0.002 | |
| Denver, CO | 113 (18.0) | 4 (3.5) | 109 (96.5) | ||
| Greensboro, NC | 120 (19.1) | 9 (7.5) | 111 (92.5) | ||
| Indianapolis, IN | 57 (9.1) | 1 (1.8) | 56 (98.3) | ||
| New York City, NY | 76 (12.1) | 7 (9.2) | 69 (90.8) | ||
| Seattle, WA | 36 (5.7) | 8 (22.2) | 28 (77.8) | ||
| St. Louis, MO | 110 (17.5) | 4 (3.6) | 106 (96.4) |
PP04.165 – Neisseria Gonorrhoeae Antimicrobial Resistance Among Kenyan Women Enrolled in the Doxycycline Post-Exposure Prophylaxis Study
Dr. Fredericka Albertina Sesay1, Avery Tuggle1, Dr Jenell Stewart2,3, Dr Jennifer E Balkus1,4, Tia Nguyen1, Dr Felix O Mogaka5, Dr Elizabeth A Bukusi1,5, Dr Olusegun O Soge1
1University of Washington, Seattle, United States.
2Hennepin Healthcare Research Institute, Minneapolis, United States.
3University of Minnesota, Minneapolis, United States.
4Public Health – Seattle & King County, HIV/STI/HCV Program, Seattle, United States.
5Centre for Microbiology Research, Kenya Medical Research Institute (KEMRI), Kisumu, Kenya.
Background: Antimicrobial resistance (AMR) in Neisseria gonorrhoeae poses a significant challenge globally. Data on AMR patterns in the context of doxycycline post-exposure prophylaxis (doxyPEP) in African settings are limited. We determine the prevalence of genetic markers associated with AMR in N. gonorrhoeae and identify associated demographic, behavioral, and clinical factors among cisgender women in the doxyPEP Kenya Study.
Methods: We conducted a cross-sectional analysis of 42 N. gonorrhoeae-positive endocervical swabs from 37 women in a randomized trial comparing doxyPEP to standard-of-care (SOC). Samples underwent genomic DNA extraction and PCR assays to detect genetic markers associated with resistance to tetracyclines (tet(M)), fluoroquinolones (gyrA S91F), macrolides (23S rRNA mutations, C2611T and A2059G), and decreased susceptibility to cephalosporins (penA N513Y). Modified Poisson regression with generalized estimating equations was used to assess factors associated with fluoroquinolone resistance, given its sufficient variability for meaningful analysis.
Results: The tet(M) gene conferring high-level tetracycline-resistance was detected in 100% of samples (95% CI: 92–100%), while fluoroquinolone resistance was present in 91% (95% CI: 77–97%). One sample demonstrated decreased susceptibility to cephalosporin, and no low-level and high-level macrolide resistance was detected (Table 1). Resistance to ≥2 antimicrobial classes occurred in 91% of samples, predominantly as fluoroquinolone-tetracycline co-resistance. No significant differences in resistance patterns were observed between doxyPEP and SOC groups (P = 1.00, Fisher’s Exact Test). We found no significant associations between fluoroquinolone resistance and age, recent antibiotic use, number of sexual partners, or condomless sex.
Conclusion: The high prevalence of tetracycline and fluoroquinolone resistance in this population is consistent with other Kenyan studies. Despite universal tetracycline resistance, decreased cephalosporin susceptibility was minimal, and macrolide resistance was absent. No differences in resistance patterns were observed between study groups, although doxycycline use was low among those randomized to doxyPEP. Ongoing surveillance remains essential to monitor AMR trends in N. gonorrhoeae.
| Marker | Marker Description | Positive Samples | Negative Samples | Total Tested | Prevalence | 95% CI (Lower) | 95% CI (Upper) | |
|---|---|---|---|---|---|---|---|---|
| gyrA_S91F | (Ciprofloxacin Resistance) | 38 | 4 | 42 | 90.48% | 77.4% | 97.3% | |
| rRNA_C2611T | (Low-level Azithromycin Resistance) | 0 | 42 | 42 | 0.00% | 0.0% | 8.4% | |
| rRNA_A2059G | (High-level Azithromycin Resistance) | 0 | 41 | 41 | 0.00% | 0.0% | 8.6% | |
| penA_513Y | (decreased cephalosporin susceptibility) | 1 | 37 | 38 | 2.63% | 0.1% | 13.8% | |
| tet(M) | high-level tetracycline-resistance | 42 | 0 | 42 | 100% | 92% | 100% |
AConfidence intervals were calculated using the exact (Clopper-Pearson) method, which is particularly suitable for small sample sizes and provides conservative bounds for binomial proportions.
BIndeterminate results were excluded from prevalence calculations. The number of indeterminate results for each marker were: rRNA_A2059G (n = 1) and penA_513Y (n = 4).
PP04.166 – Treatment of Chlamydia with Azithromycin Leads to Macrolide Resistance in Mycoplasma Genitalium
Dr. Suhella Tulsiani Drud1, Mr. Thomas Roland Pedersen1, Dr. Simone Hostgaard1,2, Dr. Kirsten Salado-Rasmussen1,2, Mr. Mikkel Lindegaard3, Ms. Majda Attauabi3, Dr. Jorgen Skov Jensen1
1Research Unit for Reproductive Microbiology, Department of Bacteria, Parasites and Fungi, Statens Serum Institut, Copenhagen, Denmark.
2Sexual Health Clinic, Department of Dermato-venereology, Bispebjerg Hospital, Copenhagen, Denmark.
3National Reference Lab for AMR and Staphylococci, Department of Bacteria, Parasites and Fungi, Statens Serum Institut, Copenhagen, Denmark.
Background: Mycoplasma genitalium (MG) infection is indistinguishable from Chlamydia trachomatis (CT) and treatment for both has traditionally included azithromycin. We aimed to determine the effect of a previous infection with CT on macrolide-resistance mutations (MRM) in MG in the Danish population over 14 years (2011–2024).
Methods: Data was extracted from the Danish microbiological database (MiBa) which collects all microbiological test results at a person-identifiable level from the total Danish population (6 million inhabitants). The first episode of MG was identified from 2014 to 2024. Each episode was then matched with previous CT infections stratified according to the time interval between infections: i) CT infection between 15–365 days prior to MG; ii) CT infection between 366 and 1095 days prior to MG and iii) control – individuals with longer interval than 1095 days or no prior CT infection. Population data on antibiotic use was extracted from the Register of Pharmaceutical Sales based on prescriptions issued for STIs. All data were analyzed and statistical analysis was performed using R.
Results: Since 2011, MRM rates in MG increased from 48% to 64% in 2024. For individuals that had a CT infection within 365 days (one year group) prior to the MG episode, an MRM rate of 76% (95% CI:71%–85%) was observed compared to individuals that had a prior CT infection from within 1–3 years 66% (53%–73%) and the control group 56% (45%–60%) (P = 2.933e-10 for 1 year vs control; P = 0.046 for 1–3 years vs control; P = 0.001 for 1 year vs 1–3 years)). This effect was seen in each year separately (Fig. 1). Until 2020, nearly 100% of CT prescriptions were azithromycin 1g single dose whereas nearly 50% of the CT prescriptions have been doxycycline since 2021.
Conclusion: Treatment of CT with azithromycin strongly influences MRM in MG.
Macrolide-resistance (MRM) rates in Mycoplasma genitalium (MG)-infected individuals (2011–2024) in the context of a previous episode of Chlamydia trachomatis (CT). Columns indicate MRM rates across the years for the three study groups: an episode of CT between 15–365 days preceding MG, between 366 and 1095 days, and no CT or more than 1096 days since CT. 95% Confidence Interval bars indicated for each group.
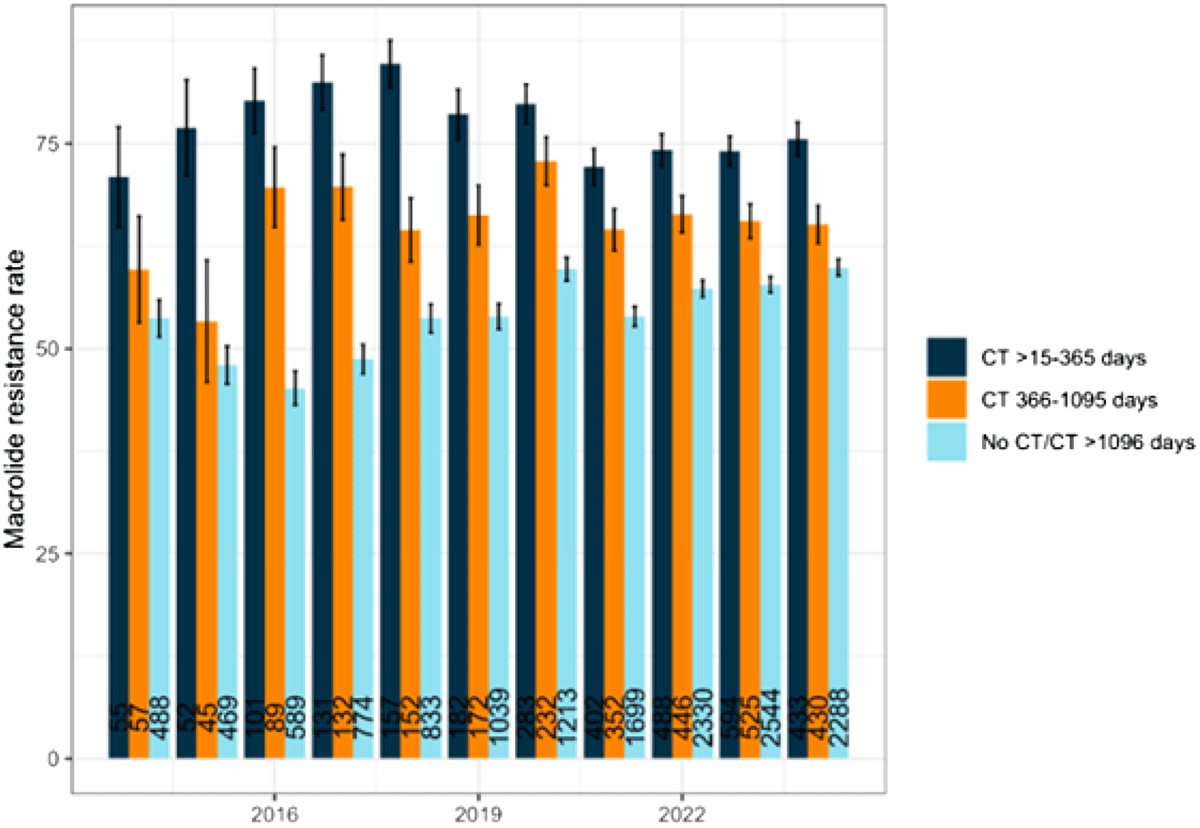
PP04.167 – Prevalence of Neisseria gonorrhoeae and Chlamydia trachomatis Among Ugandan Adults and Adolescents Vulnerable to HIV
Madelaine Ouellette1, Natalie Burns2,3, Roger Ying2,3, Immaculate Nakabuye4, Grace Mirembe4, Ronald Ephraim Wasswa4, Justine Nalunga4, Emmanuel Wasswa4, Prossy Naluyima4, Michelle Imbach2,3, Hannah Kibuuka4, James Tielsch1, Margaret Yacovone5, Betty Mwesigwa4, Trevor A. Crowell2,3
1George Washington University, Washington, USA.
2U.S. Military HIV Research Program, Walter Reed Army Institute of Research, Silver Spring, USA.
3Henry M. Jackson Foundation for the Advancement of Military Medicine, Bethesda, USA.
4Makerere University Walter Reed Program, Kampala, Uganda.
5National Institute of Allergy and Infectious Diseases, National Institutes of Health, Rockville, USA.
Background: Chlamydia and gonorrhea are common bacterial sexually transmitted infections (STIs) in populations with behavioral vulnerability to HIV. In Uganda, syndromic STI management is routine but underdiagnoses infections. We evaluated STI prevalence and associated factors to inform targeted screening and prevention strategies.
Methods: Between October 2022 and October 2024, we enrolled participants in Kampala, Uganda, aged 14–55 years without HIV, who reported a recent STI, injection drug use, transactional sex, condomless sex, or anal sex with male partners. Behavioral data were collected via audio computer-assisted self-interviews. Voided urine, anorectal swabs, and oropharyngeal swabs were tested for chlamydia and gonorrhea using the GeneXpert platform (Cepheid). Multivariable robust Poisson regression with purposeful variable selection was used to estimate adjusted prevalence ratios (aPRs) and 95% confidence intervals (CIs) for factors potentially associated with each STI.
Results: Among 420 participants, the median age was 21 (interquartile range 19–24) and 241 (57.4%) were female. Chlamydia was more prevalent than gonorrhea (21.9% vs 13.1%, P < 0.001). Each STI was most common at the anorectal site (Fig. 1). Hypothetical urogenital-only screening would have missed 51.1% and 58.2% of chlamydia and gonorrhea cases, respectively, while combined urogenital and anorectal screening would have missed 1.1% and 0%, respectively. In adjusted models, male sex was associated with increased prevalence of chlamydia (aPR 1.99 [95% CI 1.31–3.01], P = 0.001) and gonorrhea (aPR 3.16 [95% CI 1.70–5.86]. Chlamydia was also more common among participants aged 14–24 years (as compared to 25–55, aPR 2.52 [95% CI 1.17–5.46], P = 0.019). Gonorrhea was less common among participants who had ever used HIV pre-exposure prophylaxis (aPR 0.50 [95% CI 0.27–0.91], P = 0.023).
Conclusions: Chlamydia and gonorrhea were common, with many cases occurring at extra-genital sites. Healthcare providers and policy-makers should consider prioritizing multi-site STI screening, including anorectal testing, and targeted interventions for young people and males to improve STI detection and reduce transmission.
PP04.169 – Investigating Mediators in the Relationship Between Interpersonal Gendered Violence and Antiretroviral Therapy Use: Implications for Strength-Focused Interventions
Dr. Kathleen Deering1, Mr. Haoxuan Zhou2
1University of British Columbia, Vancouver, Canada.
2Simon Fraser University, Burnaby, Canada.
Background: Globally, women living with HIV experience disproportionately high levels of gendered social and structural violence. This study investigated mediators in the relationship between interpersonal gendered violence and optimal antiretroviral therapy (ART) use consistency.
Methods: We drew on data from the SHAWNA Project, a longitudinal cohort study among women living with HIV in Metro Vancouver, Canada. We used path analysis to investigate complex pathways from interpersonal gendered violence (“violence”, physical, sexual violence by any perpetrator) to multiple outcomes of ART use consistency (adherence); only results for the outcome, >=95% ART use consistency in the last 3–4 weeks are reported. Mediators were grouped as HIV stigma (internalized, perceived, anticipated) [Model 1] and psychosocial (HIV medication self-efficacy, depression, social support) [Model 2], in separate path models. All variables were time-updated and measured in the last 6 months. In each path model, we adjusted for hypothesized confounders. Standardized coefficients and p-values are presented for each direct relationship. Path analysis model fit was assessed using chi-square, root mean square error of approximation (RMSEA), and comparative fit index (CFI).
Results: The sample of 360 women had 2898 observations over 11.5 years (September/2014–February/2025). Final model fit indices suggest models fit well to the data. Violence had a significant negative direct effect on >=95%ART use (β = –0.160; P < 0.001), and a significant positive effect on internalized (β = 0.094; P = 0.001), perceived (β = 0.088; P = 0.004) and anticipated (β = 0.133; P < 0.001) HIV stigma. Internalized HIV stigma had a significant negative effect on >=95%ART use consistency (β = –0.151; P < 0.001). Violence had a significant negative direct effect on >=95%ART use consistency (β = –0.093; P = 0.002), social support (β = –0.144; P < 0.001) and medication self-efficacy (β = –0.112; P = 0.002). Medication self-efficacy had a significant positive direct effect on >=95%ART use (β = 0.690; P < 0.001). Internalized HIV stigma and medication self-efficacy partially mediated the relationship between violence and >=95%ART.
Conclusion: This study identified multiple intervention points to mitigate relationships between violence and sub-optimal antiretroviral therapy use, including strength-focused, multi-level anti-stigma interventions and improved access to social/peer support.
PP04.17 – National Surveillance of Neisseria Gonorrhoeae Antimicrobial Susceptibility Across Brazil, 2023–24: Partial Results
Prof. Maria Luiza Bazzo1, PhD Marcos André Schörner1, PhD Jéssica Motta Martins1, M.Sc. Fernando Hartmann Barazzetti1, Miss Julia Kinetz Wachter1, Miss Bianca Padilha Cassiano1, Miss Natália Groders da Costa1, Mrs Manoela Valmorbida1, M.Sc. Felipe de Rocco1, Miss Thábata da Rosa Sant’Ana1, Dr. Mayra Gonçalves Aragón2, Mr. Adson Belem Ferreira da Paixão2, PhD Alisson Bigolin2, PhD Pâmela Cristina Gaspar2, Dr. Draurio Barreira2
1Federal University of Santa Catarina, Florianópolis, Brazil.
2Department of HIV/Aids, Tuberculosis, Viral Hepatitis, and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
Background: In 2020, sentinel surveillance of male urethral discharge syndrome was institutionalized in Brazil. Sentinel sites are registered in the Brazilian Gonococcal Antimicrobial Surveillance Programme (Brazilian-GASP) and notify all cases of male urethral discharge attended at designated centers spread across the country.
Methods: Brazilian-GASP is structured with twelve sentinel sites present in all major Brazilian regions. Brazil begins a third round of surveillance of Neisseria gonorrhoeae (NG) susceptibility to antimicrobials in late 2023. Samples are collected at sentinel sites and the NG isolates are sent to the national reference laboratory (NRL). At the NRL, the isolates are identified using Maldi-Tof or PCR and the minimum inhibitory concentrations (MIC) are determined using agar dilution method for azithromycin, ceftriaxone, cefixime, gentamicin, and tetracycline. If the azithromycin MICs are greater than 4 mg/L and ceftriaxone MICs are above 0.125 mg/L in agar dilution, MICs are confirmed with Etest.
Results: Since the last round of surveillance in Brazil in 2018–20, two new sentinel sites have been included in the Center-west and Southeast regions. Up to now, 764 samples were collected and from those 384 NG were isolated. No isolates resistant to ceftriaxone have been identified, but resistance to azithromycin has remained consistently high, keeping the levels observed between 2018 and 2020 (approximately 11%). Furthermore, four isolates with a high-level resistance to azithromycin (>256 μg/mL) were identified in isolates from the Southeastern, three from São Paulo and one from Belo Horizonte. Those are the first isolates with high-level resistance to azithromycin identified since the beginning of Brazilian-GASP in 2015.
Conclusion: The partial results demonstrate a high resistance rate to azithromycin, which should be continuously monitored to support treatment protocols for STIs in Brazil. To date, among the isolates collected by this surveillance programme, no ceftriaxone-resistant isolates have been found.
PP04.18 – Evaluation of Fluoroquinolone and Macrolide Resistance in Mycoplasma Genitalium in South of Brazil
Dr. Marcos André Schörner1, MSc. Fernando Hartmann Barazzetti1, PharmB Julia Kinetz Wachter1, Dr. Jéssica Motta Martins1, Rafael Emmanuel Godoy Martinez1, PharmB Manoela Valmorbida1, MSc. Felipe de Rocco1, Mr. Osmar Guesser2, Mr. Felipe Barbosa Busnello2, MSc. Pattrícia da Rosa Damiani2, Tatiana Vieira Fraga2, Dr. Ronaldo Zonta2, Dra. Patrícia de Almeida Vanny1, Dr. Alisson Bigolin3, Dr. Pâmela Cristina Gaspar3, Prof. Maria Luiza Bazzo1
1Molecular Biology, Microbiology, and Serology Laboratory, Federal University of Santa Catarina, Florianópolis, Brazil.
2Polyclinic center - Rapid Response and Testing Center, Florianópolis, Brazil.
3Department of HIV/Aids, Tuberculosis, Viral Hepatitis, and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
Background: Resistance to macrolides and fluoroquinolones in Mycoplasma genitalium (MG) has been underexplored and the etiological approach does not encompass the detection of this bacterium in Brazil. The aim of this study was to evaluate macrolide and fluoroquinolone resistance in MG in one Brazilian sentinel site for Gonococcal Antimicrobial Surveillance Programme.
Methods: The samples analysed were collected from urethral, vaginal, rectal, and oropharynx between October 2021 and September 2024 in seven primary health care units in Florianópolis, Santa Catarina, Southern Brazil. DNA purification was performed with ReliaPrep™ Blood gDNA Miniprep System kit (Promega®, USA) and Allplex CT/NG/MG/TV Assay kit (Seegene®) was used to detect Chlamydia trachomatis, Neisseria gonorrhoeae, MG, and Trichomonas vaginalis. Allplex MG & AziR Assay (Seegene®) and Allplex MG & MoxiR Assay kit (Seegene®) were used to detect macrolide and fluoroquinolone mutations, respectively. Genotyping was performed with the MG191/MG309 scheme.
Results: During the study period, 29 samples were positive for MG: 58,6% (n = 17) from urethra 31.0% (n = 9) from vagina; 6.9% (n = 2) from rectum; e 3.5% (n = 1) from oropharynx. Coinfection was observed with C. trachomatis or N. gonorrhoeae in 24.1% (n = 7) samples. Out of 29 samples, two had invalid results for mutation detection. Macrolide resistance was observed in 85.2% (23/27) of samples. A2059G was the most common mutation (14/23). For fluoroquinolones, the percentage of samples with mutation was 29.6% (8/27), six of which had the G248T mutation and two had the G259T mutation in parC. Furthermore, six samples have mutations in both the 23S rRNA and parC. Genotyping reveals new MG191/MG309 types and new combinations that must be assigned as new sequence types.
Conclusion: These findings reinforce the importance of STI testing, especially in cases where symptoms persist. A second-line treatment option should be discussed to update the Brazilian Clinical Protocol and Therapeutic Guidelines for STI Treatment, regarding MG.
PP04.19 – Prevalence of Bacterial Sexually Transmissible Infections in Incarcerated Populations: A Systematic Review and Meta-Analysis
Dr. Gabrielle Beaudry1, Dr. Brendan Harney2,3,4,5, Dr. Sarah Larney5,6, Dr. Emma Plugge7,8, Dr. Anne C Spaulding9, Dr. Nadine Kronfli10,11
1Faculty of Medicine and Health Sciences, McGill University, Montréal, Canada.
2Burnet Institute, Melbourne, Australia.
3School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia.
4Department of Infectious Diseases, Monash University, Melbourne, Australia.
5Centre de recherche du CHUM, Montréal, Canada.
6Department of Family Medicine and Emergency Medicine, Université de Montréal, Montréal, Canada.
7UK Health Security Agency, London, UK.
8Primary Care, Population Sciences and Medical Education, Faculty of Medicine, University of Southampton, Southampton, UK.
9Rollins School of Public Health, Emory University, Atlanta, USA.
10Department of Medicine, Division of Infectious Diseases and Chronic Viral Illness Service, McGill University Health Centre, Montréal, Canada.
11Centre for Outcomes Research and Evaluation, Research Institute of the McGill University Health Centre, McGill University Health Centre, Montréal, Canada.
Background: Sexually transmitted and blood-borne infections (STBBIs) are common among people in prison, a population recognized by the World Health Organization as critical to the global STBBI response. As recent estimates are lacking, we aimed to determine the global prevalence of bacterial sexually transmitted infections (bSTIs; chlamydia, gonorrhea, and syphilis) among people in prison.
Methods: A global systematic review and random-effects meta-analysis were conducted by searching online databases and grey literature to identify unique articles published from January 2000 to June 2023 without language restrictions. Studies evaluating the prevalence of bSTIs in incarcerated populations were included. Two independent reviewers screened eligible full texts. Disagreements were resolved by a third reviewer. Analyses were aggregated separately for each bSTI, by age (i.e. adults and adolescents [≤19 years]), and sex (i.e. male and female). Potential sources of heterogeneity were examined by meta-regression and subgroup analyses.
Results: A total of 2,627 unique articles were identified, 274 were eligible for full-text review, and 195 studies were included (1,318,590 individuals; 441,545 [34%] females, 766,753 [58%] males, and 110,292 [8.4%] unknown). Among eligible studies, 91% were conducted in high- or upper-middle income countries. The mean age was 33.5 years (SD = 9.7) among adults and 15.6 years (SD = 1.1) among adolescents. The prevalence of chlamydia, gonorrhea, and syphilis was 6.5% (95% CI 5.0%–8.5%), 1.7% (1.0%–3.0%), and 6.2% (4.3%–8.9%), respectively, among female adults, versus 4.5% (3.5%-5.8%), 0.6% (0.2%–1.4%), and 3.3% (1.7%–6.2%) among male adults. Among adolescents, the prevalence of chlamydia, gonorrhea, and syphilis was 16.9% (14.0%–20.2%), 6.0% (4.5%–7.9%), and 1.9% (0.1%–26.4%), respectively, among females vs 7.4% (6.3%–8.8%), 2.0% (1.4%–2.7%), and 1.8% (0.5%–6.5%), among males.
Conclusion: High bSTI prevalence among incarcerated individuals, particularly adolescents, underscores significant public health concerns and unmet needs. Enhanced testing and treatment for bSTIs both within and beyond carceral settings is imperative to address these disparities globally.
PP04.20 – Previous Syphilis Diagnosis as a Predictor of Subsequent Early Non-Primary Non-Secondary Syphilis
Dr. Roxanne Kerani1,2, Ms. Anna Berzkalns2, Dr. Timothy Menza1,2, Dr. Rachel Amiya3, Dr. Chase Cannon1,2, Dr. Matthew Golden1,2, Dr. Adele Benzaken
1University of Washington, Seattle, United States.
2Public Health - Seattle and King County, Seattle, United States.
3Washington State Department of Health, Olympia, United States.
Background: Observational data suggest that previous syphilis may decrease primary/secondary (PS) syphilis symptoms, leading to more early non-primary non-secondary (ENPNS) syphilis diagnoses. Regular STI testing among PrEP patients may also result in increased ascertainment of ENPNS syphilis. We evaluated the association of previous syphilis with subsequent ENPNS syphilis, adjusting for PrEP use.
Methods: The study population included early syphilis cases (primary, secondary, ENPNS) diagnosed in King County January 1, 2011–Oct 31, 2022, and recorded in Washington State surveillance data. Prior syphilis diagnoses were ascertained from the same database 2007–2022. PrEP use was consistently collected beginning March 1, 2020. We used multivariate binomial log regression to examine the association between previous infection and ENPNS syphilis and conducted a subgroup analysis of infections diagnosed March 1, 2020-Oct 31, 2022 to adjust for the impact of PrEP use on ENPNS diagnosis.
Results: From 1/1/2011 to 10/31/2022, 5663 individuals had 7570 cases of early syphilis; 44% (N = 3301) were ENPNS. Thirty-one percent of cases were in people with >1 previous infection. Among ENPNS cases, 43% (1404/3301) occurred in persons with >1 previous infections, compared to 21% (914/4269) among PS syphilis cases (P < 0.0001). Among diagnoses 3/1/2020–10/31/2022, 43% (1092/2558) were ENPNS. In a model adjusted for age, race, ethnicity, sex at birth, gender of sex partners, current diagnosis year, HIV status, and PrEP use, prevalence of ENPNS syphilis was 47% higher in patients with prior syphilis (prevalence ratio PR = 1.47, 95% CI = 1.31–1.65) compared to those without prior syphilis (Table 1). In this model, compared to people with HIV, PrEP users had a similar prevalence of ENPNS syphilis (PR = 1.03, 95% CI = 0.91–1.16) while ENPNS syphilis prevalence was lower in patients not using PrEP (PR = 0.71, 95% CI = 0.64–0.79).
Conclusions: Previous T. pallidum infections may change the natural history of syphilis leading to more infections diagnosed as ENPNS. This association is independent of more frequent HIV or PrEP-related screening.
| Total Analytic Study Period:2011–2022 AN = 7570 | Subgroup Analysis Period:2020–2022 B, CN = 2155D | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N | % | AdjustedPrevalence Ratio | 95% Confidence Interval | N D | % | AdjustedPrevalence Ratio | 95% Confidence Interval | |||
| Prior syphilisinfection | Yes | 2318 | 31 | 1.53 | 1.43–1.63 | 716 | 33 | 1.47 | 1.32–1.65 | |
| No | 5252 | 69 | 1.0 | 1439 | 67 | 1.0 | ||||
| PrEP use and HIV status | Living with HIV | 773 | 36 | 1.0 | ||||||
| Using PrEP | 614 | 28 | 1.03 | 0.91–1.16 | ||||||
| Not using PrEP | 768 | 35 | 0.71 | 0.64–0.79 | ||||||
PP04.21 – Gender-Based Differences in Clinical Presentation, Testing, and Test Positivity Yield in STI Wellness Centers
Dr. Vivian Avelino-Silva1, Betty Biwot1, Fernanda Fonseca1, Wilfred Odoke1, Jan van den Hombergh1, Dr. Adele Benzaken1
1AIDS Healthcare Foundation, Los Angeles, United States.
Background: Sexually transmitted infections (STIs) are pervasive across different demographic groups. However, the clinical presentation, access to STI diagnostic tests, and likelihood of coinfections may vary according to gender identity.
Methods: AIDS Healthcare Foundation supports 36 STI wellness centers (WCs) providing walk-in, free-of-charge STI care in 22 low- and middle-income countries. We extracted de-identified data from WC visits to investigate clinical presentation, access to syphilis and HIV tests, and test positivity yield according to gender identity (cisgender-men; cisgender-women; transgender).
Results: We identified 71,181 visits from January-October/2024, including 35,154 first-time and 36,027 return visits. Cisgender-men, cisgender-women, and transgender persons comprised 69.3%, 29.7%, and 0.9%, respectively. Frequent clinical presentations included genital warts (10.6%) and urethral discharge (8.4%) among cisgender-men; vaginal discharge (20.6%) and genital warts (3.4%) among cisgender-women; and genital warts (19.3%) and genital ulcers (2.7%) among transgender persons. The proportion of visits that included a syphilis test and its positivity yield were 41.2% and 20.1% among cisgender-men; 49.7% and 13.0% among cisgender-women; and 29.3% and 36.1% among transgender persons. The proportion of visits that included HIV tests among those with syndromic STIs and HIV test positivity yield was 27.4% and 6.6% for cisgender-men; 32.5% and 3.6% for cisgender-women; and 28.4% and 16.4% for transgender persons. Visits provided to transgender persons included syphilis tests less frequently compared to cisgender-men (P < 0.001) and women (P < 0.001). HIV test positivity was higher in the transgender group compared to cisgender-men (P < 0.004) and cisgender-women (P < 0.001).
Conclusion: Our results highlight gender-based differences in the clinical presentation at STI WCs. Transgender persons were less often tested for syphilis despite high positivity rate. HIV tests were done in <1/3 of syndromic STI visits for all groups, with significantly higher positivity among transgender persons. Expanding STI testing and care programs could help reduce gender-based gaps in access to STI diagnosis and care.
PP04.22 – The Epidemiological Characteristics of Mpox Cases in 2023–2024: Insights from Public Health – Seattle and King County
Ms. Anna Berzkalns1, John Chang Lang1, Chase Cannon1,2, Tim Menza1,2, Jennifer Balkus1,2, Roxanne Kerani1,2, Matthew Golden1,2
1Public Health Seattle & King County, Seattle, United States.
2University of Washington, Seattle, United States.
Background: While the United States saw declining mpox infections in Q4 2024, community transmission persists. In contrast to national trends, mpox diagnoses in Seattle-King County, Washington have increased from January to December 2024. Understanding the sociodemographics, vaccination status, and behavioral patterns of reported cases is necessary to refine local public health prevention strategies.
Methods: We analyzed routinely collected mpox surveillance data from King County, WA for 2023–2024 broken down by four-month periods (January–April, May–August, September–December).
Results: Overall, 129 King County residents were diagnosed with mpox in 2023 (63 diagnoses) and 2024 (66 diagnoses), of which 126 (98%) were assigned male sex at birth (Fig. 1). The median age was 34, and 17 (13%) infections were diagnosed among people living with HIV. In both years, few diagnoses occurred from May to August (3 in 2023 and 13 in 2024), and over half of diagnoses occurred from September to December (2023, 52% and 2024, 74%). Overall, 48 (37%) individuals were unvaccinated, 18 (14%) had received one dose of the JYNNEOS vaccine, and 63 (48%) had received two doses prior to mpox diagnosis. No hospitalizations or deaths were reported. Public health staff interviewed 86 (67%) of persons diagnosed with mpox, of which 73 (85%) identified as cisgender men who have sex with men (MSM) and 8 (9%) identified as transgender (TG)/non-binary (NB) persons who have sex with men. Among the persons diagnosed with mpox in September–December 2024, five reported attending the same sex party, and four cases reported exposure at the same sauna.
Conclusion: The continued diagnosis of mpox suggests that the infection is now an endemic sexually transmitted infection concentrated among MSM and TG/NB persons who have sex with men. The month-to-month variation in cases with a predominance of cases in late summer to early winter suggests that infections occur in episodic clusters, sometimes linked to specific events, or possibly seasonal occurrences.
PP04.23 – Impact of PrEP on Microbiome and STI Dynamics in Adolescent MSM and TGW in Brazil: Evidence from the PrEP15-19 Study
Dra. Rafaela Bittencourt1, M.Sc Caio Oliveira1, Ph.D Anne Brito1, Ph.D Fabiane Soares1, Ph.D Laio Magno1,2, Ph.D Inês Dourado1, PhD Danielle Medeiros1, Ph.D Guilherme Campos1, Ph.D Lucas Marques1
1Federal University of Bahia, Salvador, Brazil.
2State University of Bahia, Salvador, Brazil.
Background: Pre-exposure prophylaxis (PrEP) is effective against HIV, but its effects on dysbiosis remain underexplored. Dysbiosis facilitates bacterial sexually transmitted infections (bSTIs), influencing occurrence, persistence, and recurrence. This study aims to assess the effects of HIV pre-exposure prophylaxis (PrEP) on the microbiome and the dynamics of bSTIs in adolescent men who have sex with men (AMSM) and transgender women (ATGW).
Methods: PrEP1519 was a single-arm cohort study of daily oral PrEP among AMSM/ATGW aged 15–19 in three Brazilian cities (2019–2022). Ten participants from Salvador were followed quarterly for 28 months. PrEP adherence was confirmed via Tenofovir-diphosphate (TFV-DP) levels in dried blood spots. Swab samples (oral, anal, urethral) underwent metagenomic sequencing to assess microbiome impacts, focusing on α-diversity (Shannon index, ANOVA, Tukey). Additionally, qPCR was conducted for Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), Mycoplasma genitalium (MG), M. hominis (MH), Ureaplasma parvum (UP), and U. urealyticum (UU) to assess the frequency of persistence/recurrence of bSTIs.
Results: The participants analyzed showed good adherence (Median TFV-DP 1395 fmol/punch). No significant differences in α-diversity were observed in oral, anal, or urethral microbiomes when comparing initial visits to follow-up visits (Shannon Index: overall P = 0.878, Comparison visits 1 to 2: P = 0.923, Comparison visits 1 to 4: P = 0.937, Comparison visits 1 to 8: P = 0.403). There were significant differences between intermediate visits (P = 0.682). Regarding persistence/recurrence of bISTs, UU was the pathogen with the highest frequency, with recurrence in 80% of participants, followed by MH (20%), MG (10%), and MH (10%). No persistence/recurrence was observed for NG or UP.
Conclusion: These findings highlight that PrEP does not directly affect microbiota and reinforces its safety. However, the high frequency of persistence/recurrence of bSTIs emphasizes the need for integrated surveillance and enhanced management of infections in sexual and gender minority adolescents.
PP04.24 – HIV and STI Incidence and Condomless Anal Sex, Before and After Oral HIV PrEP Implementation: Results from the Amsterdam Cohort Studies
Ms. Carien Blomaard1,2,3,4, Anders Boyd1,2,3,4,5, Maria Prins1,2,3,4, Janneke Heijne1,2,3,4, Udi Davidovich1,6, Sonia Boender1,2,3,4,7, Maarten Schim van der Loeff1,2,3,4, Vita Jongen1,3,5
1Department of Infectious Diseases, Public Health Service Amsterdam, Amsterdam, The Netherlands.
2Amsterdam UMC location University of Amsterdam, Department of Internal Medicine, Amsterdam, The Netherlands.
3Amsterdam Institute for Immunology and Infectious Diseases, Amsterdam, The Netherlands.
4Amsterdam Public Health Research Institute, Amsterdam, The Netherlands.
5Stichting HIV monitoring, Amsterdam, The Netherlands.
6University of Amsterdam, Department of Social Psychology, Amsterdam, The Netherlands.
7Department of Health Sciences, Faculty of Science, Vrije Universiteit, Amsterdam, The Netherlands.
Background: HIV incidence among men who have sex with men (MSM) greatly reduced after the introduction of biomedical-preventive strategies, including oral pre-exposure prophylaxis (PrEP) and Treatment as Prevention (TasP). We assessed trends in HIV and STIs incidence and condomless anal sex (CAS), before and after PrEP implementation in the Netherlands.
Methods: The Amsterdam Cohort Studies is an open observational cohort study initiated in 1984. We included HIV-negative MSM participating between 2009 and 2023. Biannually, men completed online questionnaires about sexual behavior, and were tested for HIV and STIs. Date of HIV infection was defined as the midpoint between date of last negative and first positive test. Any STI was defined as diagnosed syphilis, gonorrhea or chlamydia. Trends over time were assessed using exponential survival models. We highlight 2018 in our analysis as the year prior to the launch of the National PrEP program in the Netherlands.
Results: We included 1,040 men (median age 41 years); total follow-up time was 8697.7 person-years. During follow-up, 48 incident HIV infections occurred, HIV incidence rate per 100 person-years decreased from 1.9 (95% CI = 1.0–3.7) in 2009 to 0.4 (95% CI = 0.1–1.4) in 2018 and 0 (95% CI = 0.0–0.6) in 2023 (ptrend = 0.049) (Fig. 1). The incidence rate for any STI per 100 person-years increased from 15.9 (95% CI = 12.6–19.9) in 2009 to 27.6 (95% CI = 24.0–31.9) in 2018 and 40.7 (95% CI = 35.9–46.1) in 2023 (ptrend <0.001) (Fig. 1). In 2009, 16.3% of participants reported CAS with an unknown casual partner which increased to 27.2% in 2018 and 47.5% in 2023 (ptrend <0.001).
Conclusion: CAS with casual partners and STIs strongly increased, while HIV incidence strongly decreased over a 15-year period; these trends were coinciding with gradually increasing availability of HIV PrEP and gradually increasing knowledge on TasP in the Netherlands. Contrary, the increase in STI incidence highlights the need for attention to STI prevention.
HIV and any STI incidence per 100 person-years between 2009 and 2023 among 1,040 men who have sex with men participating in the Amsterdam Cohort Studies, the Netherlands.
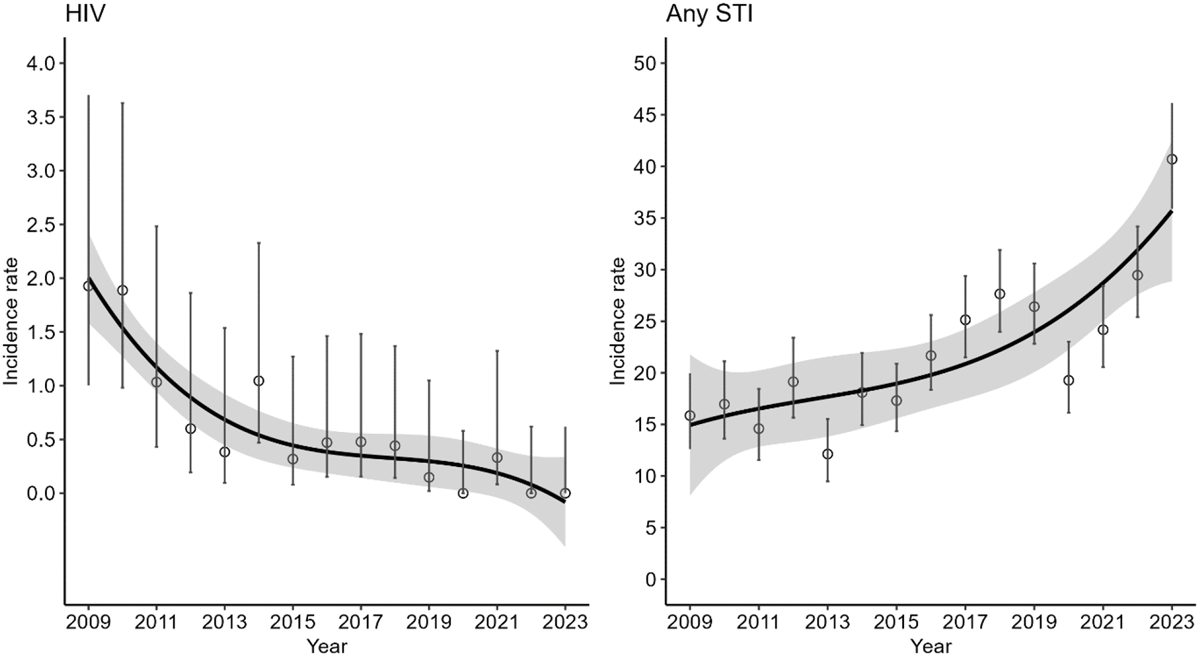
PP04.25 – Doxy-PEP Awareness and Use Among Trans Women Lags Behind Men Who Have Sex with Men in San Francisco
Rachel Brandão Raskin1, Gabriel Tariq Xavier Salomão de Pina1, Erikka Palafox2, Iris R. O’Neal2, Bow Suprasert2, Raul Ruiz2, Moranda Tate2, Glenda Baguso2, Stephanie Cohen2, Maria Amélia de Sousa Mascena Veras1, Willi McFarland2,3, Erin C. Wilson2,3
1Santa Casa of São Paulo School of Medical Sciences, São Paulo, Brazil.
2San Francisco Department of Public Health, San Francisco, USA.
3University of California San Francisco, San Francisco, USA.
Background: In October 2022, The San Francisco Health Department pioneered the release of guidelines on the use of doxycycline post-exposure prophylaxis (doxy-PEP) for sexually transmitted infection (STI) prevention. Guidelines recommended doxy-PEP to transgender women (TGW) and men who have sex with men (MSM) with a history of bacterial STI and condomless anal or oral sex in the last year. Our study aims to assess doxy-PEP awareness and uptake among TGW in San Francisco.
Methods: Data originate from the CDC-led National HIV Behavioral Surveillance (NHBS) survey, conducted among TGW recruited through respondent-driven sampling in San Francisco, from July 2023 to March 2024 — spanning eight to 17 months after the doxy-PEP guidelines were released. An in-person interview recorded demographics, behaviors, HIV serostatus, and history of STI, as well as doxy-PEP awareness, discussion with a health care provider, and use in the last year. Comparison is made to MSM participating in a contemporaneous NHBS survey.
Results: Among 339 TGW, 37% were aware of doxy-PEP, 20% discussed it with a provider, and 11% used doxy-PEP in the previous year (Table 1). Higher proportions of use were observed among younger TGW (14% among 18–29-year-olds), those tested for an STI (17%), testing positive for an STI (33%), using HIV PrEP (22%), and living with HIV (16%). Doxy-PEP awareness was associated with younger age (43% aged 18–29), engaging in sex work (49%), testing for STI (48%), testing positive for STI (61%), and using HIV PrEP (59%). Among MSM, 70% were aware of doxy-PEP, 32% discussed doxy-PEP with a provider, and 21% used doxy-PEP in the last year.
Conclusion: Doxy-PEP awareness and use among TGW lags substantially behind MSM despite guidelines prioritizing both populations, mirroring historic delays in promoting HIV PrEP for TGW. Future campaigns should use differentiated delivery models to better reach and meet the needs of TGW.
| Characteristics | Used doxy-PEP N = 38 (11.2%) | Has not used doxy-PEP N = 301 (88.8%) | X2 value | P-value A | Aware of doxy-PEP N = 125 (36.9%) | Not aware of doxy-PEP N = 214 (63.1%) | X2 value | P-valueA | |
|---|---|---|---|---|---|---|---|---|---|
| Demographics | |||||||||
| Age group18–2930–3940–4950+ | 7 (13.7)10 (12.3)13 (18.3)8 (5.9) | 44 (86.3)71 (87.7)58 (81.7)128 (94.1) | 7.91 | 0.048 | 22 (43.1)37 (45.7)33 (46.5)33 (24.3) | 29 (56.9)44 (54.3)38 (53.5)103 (75.7) | 15.66 | 0.001 | |
| Race/EthnicityHispanicBlack/African AmericanWhiteOther | 18 (12.2)6 (9.0)7 (11.5)7 (12.3) | 130 (87.8)61 (91.0)54 (88.5)50 (87.7) | 0.52 | 0.913 | 62 (41.9)17 (25.4)22 (36.1)22 (38.6) | 86 (58.1)50 (74.6)39 (63.9)35 (61.4) | 5.49 | 0.139 | |
| Had health care visit in the past 12 monthsNoYes | 038 (12.0) | 22 (100.0)278 (88.0) | 2.09 | 0.084 | 6 (27.3)119 (37.7) | 16 (72.7)197 (62.3) | 0.95 | 0.329 | |
| EducationHigh school or lessSome collegeBachelor’s degree or more | 17 (9.7)14 (12.8)7 (13.5) | 159 (90.3)95 (87.2)45 (86.5) | 0.97 | 0.614 | 56 (31.8)45 (41.3)24 (46.1) | 120 (68.2)64 (58.7)28 (53.9) | 4.74 | 0.093 | |
| Sexual Behaviors and STI | |||||||||
| Had sex in the past 12 monthsNoYes | 038 (14.4) | 76 (100.0)225 (85.6) | 12.36 | 0.000 | 12 (15.8)113 (43.0) | 64 (84.2)150 (57.0) | 18.70 | 0.000 | |
| Engaged in sex work in the past 12 monthsNoYes | 20 (9.0)18 (15.4) | 201 (90.0)99 (84.6) | 3.07 | 0.079 | 67 (30.3)57 (48.7) | 154 (69.7)60 (51.3) | 11.15 | 0.001 | |
| Had an STI test in the past 12 monthsNoYes | 1 (0.86)37 (17.2) | 115 (99.1)178 (82.8) | 19.81 | 0.000 | 21 (18.1)103 (47.9) | 95 (81.9)112 (52.1) | 28.56 | 0.000 | |
| Tested positive for bacterial STIs in the past 12 monthsNoYes | 17 (6.2)21 (32.8) | 258 (93.8)43 (67.2) | 36.99 | 0.000 | 86 (31.3)39 (60.9) | 189 (68.7)25 (39.1) | 19.62 | 0.000 | |
| Has tested positive for HIVNoYes | 20 (8.8)18 (16.4) | 208 (91.2)92 (83.6) | 4.28 | 0.038 | 86 (37.7)39 (35.4) | 142 (62.3)71 (64.6) | 0.16 | 0.686 | |
| Used HIV PrEP in the past 12 monthsNoYes | 020 (22.0) | 137 (100.0)71 (78.0) | 33.00 | 0.000 | 32 (23.4)54 (59.3) | 105 (76.6)37 (40.7) | 30.13 | 0.000 | |
| Used PEP in the past 12 monthsNoYes | 18 (8.2)2 (22.2) | 201 (91.8)7 (77.8) | 2.11 | 0.146 | 79 (36.1)7 (77.8) | 140 (63.9)2 (22.2) | 6.40 | 0.011 |
PP04.26 – Characterizing Sexual Partnership Dynamics in a Longitudinal Cohort of STI Clinic Patients in Lilongwe, Malawi
Ms. Cara Broshkevitch1, Kimberly A Powers1, Jane S Chen1, Edward Jere2, Esther Mathiya2, Naomi Nyirenda2, Gabriel Banda2, Mina C Hosseinipour1,2, Irving F Hoffman1, Mitch Matoga2, Beatrice Ndalama2, Naomi Bonongwe2, Sarah E Rutstein1
1University of North Carolina at Chapel Hill, Chapel Hill, USA.
2UNC Project Malawi, Lilongwe, Malawi.
Background: Population-level incidence of sexually transmitted infections (STIs) and the impact of transmission prevention interventions depend on sexual partnership dynamics, including patterns of partner acquisition and overlap. We characterized these aspects of partnership dynamics among patients initiating HIV pre-exposure prophylaxis (PrEP) at an urban STI clinic in Lilongwe, Malawi.
Methods: We conducted a secondary analysis of sexual behavior data collected at 0 (baseline), 1, 3, and 6 months in a longitudinal cohort of 174 STI clinic patients initiating PrEP between March and December 2022. Primary outcomes were the number of partners in the prior month reported at each visit and the rate of new partner acquisition during follow-up. Participants could designate up to one primary (i.e., main regular) partner at each visit. We characterized outcomes overall and stratified by whether a primary partner was reported at baseline.
Results: Approximately half (53%; n = 92) of participants reported a primary partner at baseline. The median number of reported prior-month partners was 1 (interquartile range: 1, 2) at baseline, and remained consistent across study visits and when stratified by baseline report of a primary partner. The percentage of participants reporting only one prior-month partner ranged from 51% to 62% across visits (Fig. 1), but most participants (63%) had at least one change in the reported number of prior-month partners during follow-up. Participants acquired new partners at an overall rate of 0.9 new partners per person-month, with a slightly lower rate among those with versus without a primary partner at baseline (0.8/person-month versus 1.0/person-month).
Conclusion: STI clinic patients in Lilongwe reported frequent new partners in the 6 months after STI services and PrEP initiation, indicating the potential for ongoing STI acquisition and transmission. Transmission modeling analyses parameterized with partnership dynamics data can quantify these risks and the potential impacts of transmission prevention strategies in this population.
Distribution of participants reporting 0, 1, or ≥2 partners in the prior month across study visits at 0 (baseline), 1, 3, and 6 months.
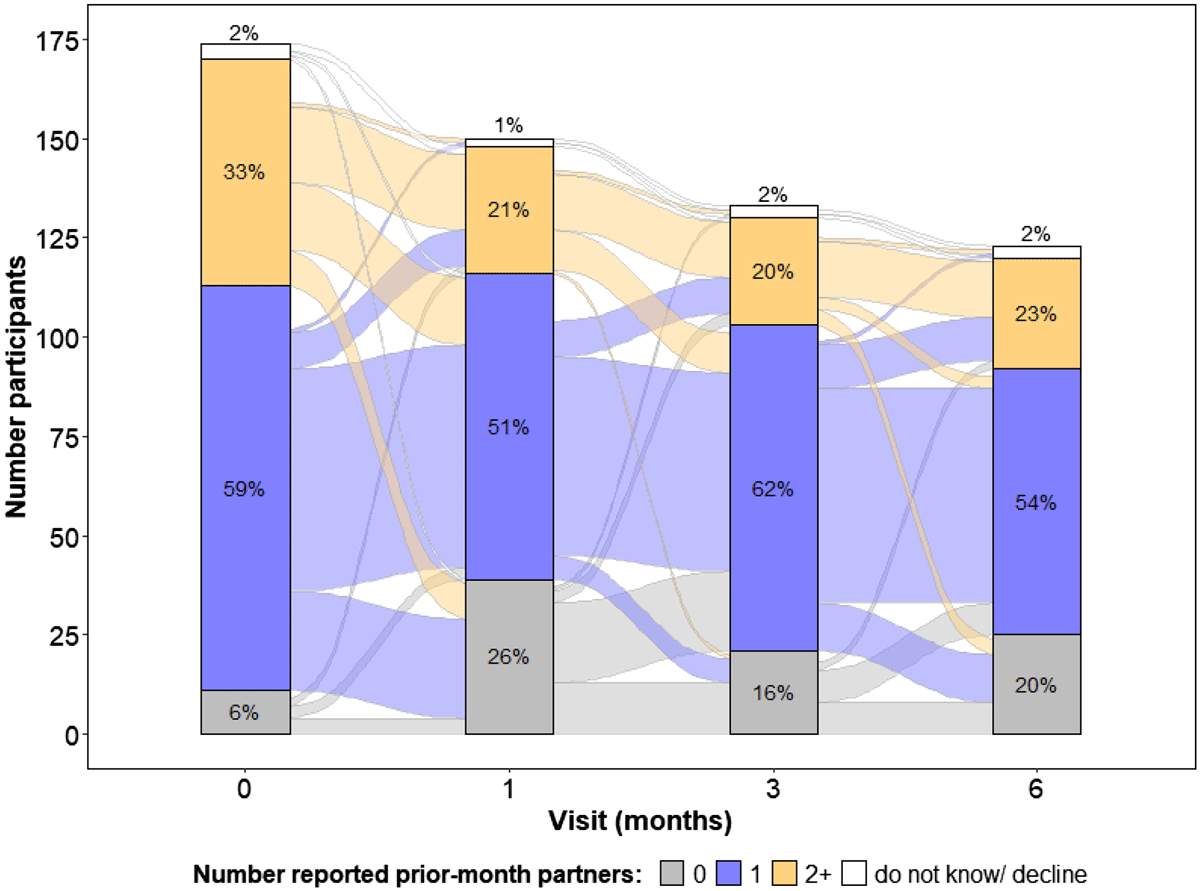
PP04.27 – Epidemiological Profile of Neurosyphilis in Congenital Syphilis Cases: São Paulo State, Brazil (2007–2024)
Dra. Carmen Silvia Bruniera Domingues1,2, Dra. Mariza Vono Tancredi1, Ângela Tayra1, Rosa Alencar1, Carla Gianna Luppi1, Alexandre Gonçalves1
1Health Secretariat of the State of São Paulo, STD/AIDS Reference and Training Center, São Paulo, Brasil.
2Ministry of Health, Department of HIV/AIDS, Tuberculosis, Viral Hepatitis, and Sexually Transmitted Infections, Brasília, Brasil.
Background: In Brazil, 309,824 cases of congenital syphilis (CS) were reported (2007–2024). Among these, neurosyphilis was diagnosed in 23,875 newborns (7.7%). São Paulo State (SPS) accounted for 16.1% (50,035/309,824) of the country’s CS cases. This study aims to analyze the epidemiological profile of CS cases with neurosyphilis in SPS during 2007–2024.
Methods: A descriptive study was conducted using data on CS cases with neurosyphilis (Brazilian case definition) from SPS’s epidemiological surveillance system. Trend analysis employed a polynomial regression model with moving average (MA) of neurosyphilis cases (2007–2024). The dependent variable (Y) was the MA, and the independent variable(X) was time (diagnosis year), centralized at the midpoint of the series. The goodness-of-fit was assessed using r2, residual analysis, and P-values (<0.05).
Results: Among 50,035 CS cases reported in SPS, 89.8% (44,916) were live births. Cerebrospinal fluid (CSF) testing was performed in 76.7% (34,449/44,916) of cases, diagnosing neurosyphilis in 18.3% (6,312/34,449). An increasing trend in the MA of neurosyphilis cases was observed with first-order modeling [Y = 339.58 + 55.58X; r2 = 0.94; P < 0.001], reflecting diagnostic improvements. Most newborns with neurosyphilis (3,623; 57.4%) were asymptomatic. Main clinical findings included jaundice (572; 9.1%), long bone abnormalities (355; 5.6%), and hepatomegaly (215; 3.4%). A reactive CSF VDRL was observed in 28.3% of cases, while 71.5% showed cellular/protein abnormalities. Crystalline penicillin was administered in 81.2% of cases. A total of 88 newborns died. Maternal characteristics: 50.4% were Black/mixed race; 56.8% were aged 20–29 years; 86.6% attended prenatal care; 72.4% were diagnosed during pregnancy; and 64.6% of mothers received inadequate/no treatment.
Conclusions: The increase in neurosyphilis cases reflects more frequent CSF testing. CSF analysis is critical for appropriate evaluation and management. Although neurosyphilis requires crystalline penicillin treatment, some cases remain inadequately treated. High prenatal care coverage and maternal syphilis diagnosis have not translated into effective maternal treatment, which remains a key challenge to reducing the burden of CS.
PP04.28 – Syphilis Reported Cases in Sao Paulo State, Brazil, 2011–2023
Asst. Prof. Carla Gianna Luppi1, Angela Tayra1, Roberto José Carvalho Silva1, Rosa de Alencar Souza1, Amanda Cristina Santos Jesuino1, João Luiz Grandi1, Laura Marques Azevedo1, Lourdes Helena Braga Andrade1, Mariza Vono Tancredi, Dra. Carmen Silvia Bruniera Domingues3
1Centro de Referência e Treinamento de Doenças Sexualmente Transmissíveis e Aids/SES/SP, Sao Paulo, Brazil.
2Universidade Federal de São Paulo, Sao Paulo, Brazil.
3Health Secretariat of the State of São Paulo, STD/AIDS Reference and Training Center, São Paulo, Brazil.
Introduction: In Brazil, there has been an increase in reported cases of syphilis, and São Paulo was the state with the highest number of cases. The aim of this study is to analyze the trends of syphilis reported cases rate in the state of São Paulo from 2011 to 2023.
Methods: Time series of all reported cases of syphilis per 100,000 inhabitants were conducted. Syphilis cases at all stages and pregnant women with syphilis were included. The trends were calculated using multiple jointpoint regression to estimate the annual percentage change (APC) and the average annual percentage change (AAPC).
Results: In 2023, 80,617 cases of syphilis were reported: 43,129 female cases (22,101 non-pregnant and 21,028 pregnant) and 37,488 male cases. By sex, the reported rates of syphilis per 100,000 were: 186.7 (female) and 174.9 (male). In the period from 2011 to 2023, the percentage increase in the reported rate was 440.9: 433.1 (female); 449.5 (male). The AAPC from 2011 to 2023 were: (female) 14.66 (95% CI 12.50–16.56); (male) 14.88 (95% CI 13.01–16.78). In the last period analyzed, it was observed that by sex/age group, the APC at 20/24 and 25/29 years among women was 15.48 and 26.86; and among men at same age groups 11.16 and 21.92 (Fig. 1).
Conclusion: Differences were found in the trend of syphilis notification rates by sex among younger people. The periods of inflection in the trend suggest that prevention policies may have impacted the data temporarily, but not in a sustainable way.
Syphilis* - Rates of Reported Cases by sex/age group and year - Multiple Jointpoint Models. Sao Paulo-Brazil. 2011–2023.
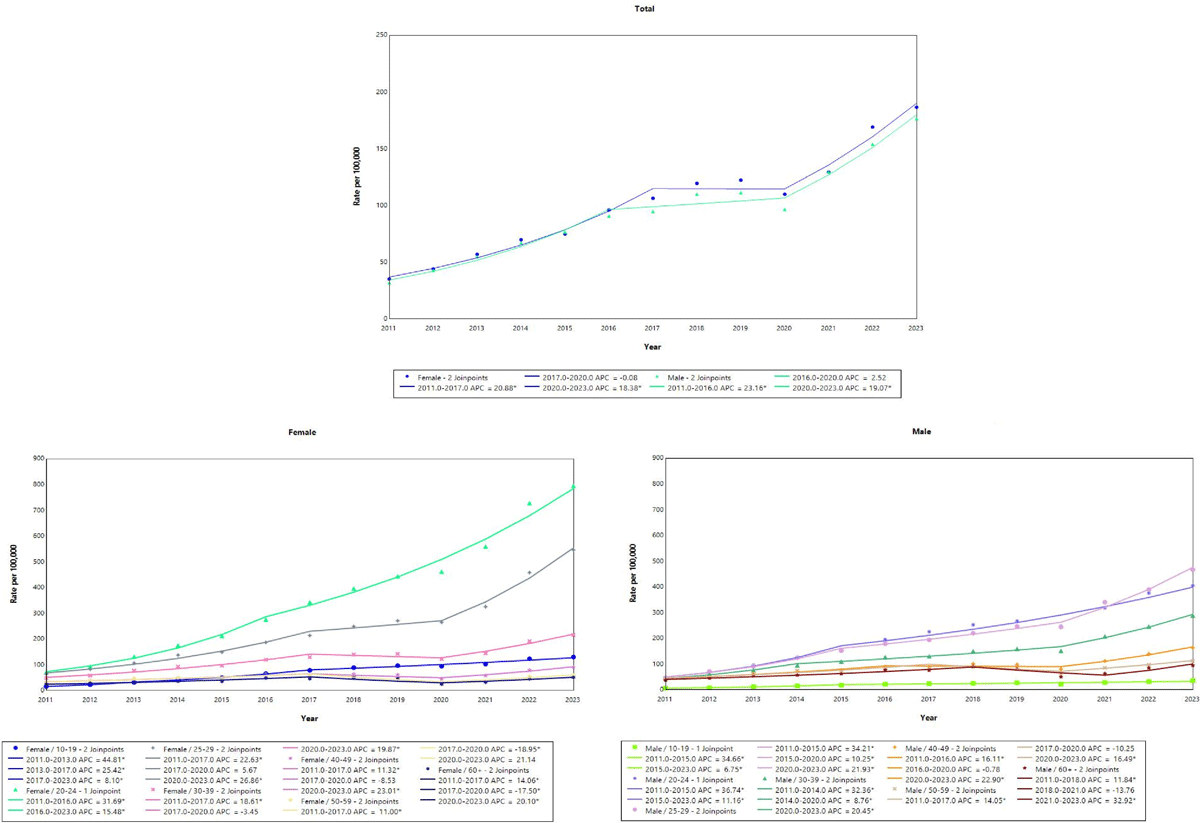
PP04.29 – Factors Associated with Mortality Among People with Advanced HIV Disease in Rural Uganda, 2018–2021
Mr. Kabali Bwogi1, Dr. Catherine Nassozi Lwanira2, Dr. Ivan Kasamba3, Dr. Joseph Baruch Baluku3, Ms Justine K. Nakiwala3, Ms Regina Ndagire2, Ms Catherine Nassolo3, Mr. Gerald Wabomba3, Mr. Christopher Bwanika3, Dr. Jane Nakawesi3, Dr. Grace Namayanja4, Dr. Joseph Kabanda4, Dr. Julius N Kalamya4, Dr. Julius Ssempiira4, Dr. Catherine Ssenyimba3, Dr. Ronald Mulebeke3, Dr. Arthur G. Fitzmaurice4, Dr. Barbara Mukasa3
1C-care Uganda (IHK), Wakiso, Uganda.
2Department of Research, School of Graduate Studies, Research and Innovations, Clarke International University, Kampala, Uganda.
3Mildmay Uganda, Kampala, Uganda.
4Division of Global HIV and TB, Global Health Center, U.S. Centers for Disease Control and Prevention (CDC), Kampala, Uganda.
Background: Despite global efforts to improve HIV care, late identification and delayed antiretroviral therapy (ART) initiation continue to pose mortality risks among people living with HIV (PLHIV) with advanced HIV disease (AHD). This study investigated factors associated with mortality among PLHIV with AHD in rural North-Central Uganda from January 2018 to December 2021.
Methods: We conducted a retrospective review of records from 18 health facilities, obtaining data from patients seen between January 2018 and December 2021 on patient demographics and clinical characteristics including baseline CD4 count, baseline ART regimen, current ART regimen, ART adherence, body mass index (BMI), tuberculosis (TB) status, TB preventive therapy (TPT) use, WHO clinical stage, and viral load status. AHD was defined as CD4 cell count ≤200 cells/mm3. A Cox proportional hazard model was fitted to identify factors associated with mortality among individuals with AHD. Factors were summarized by adjusted hazard ratios (aHRs) with their 95% confidence intervals (CIs) and considered statistically significant at 5%.
Results: Records of 1,161 PLHIV with AHD were analyzed, contributing 1,565.56 person-years of observation (pya). Of these, 84 (7.2%) deaths were reported, equivalent to a mortality rate of 5.37 deaths per 100 pya (95% CI: 4.33–6.64). Factors significantly associated with mortality included PLHIV aged ≥50 years (aHR = 4.36, 95% CI: 1.86–10.23), never having a viral load test (aHR = 16.06, 95% CI: 7.36–35.05), viral load non-suppression (≥1,000 copies/mL; aHR = 9.54, 95% CI: 3.55–25.62), baseline CD4 count ≤50 (aHR = 1.84, 95% CI: 1.03–3.27), and never having taken TPT (aHR = 3.57, 95% CI: 1.85–6.86).
Conclusion: Despite advancements in HIV programs, the mortality rate among patients with AHD indicates ongoing challenges. Concentrating on identifying AHD patients early, promoting TPT, and ensuring regular viral load testing, ART optimization, and adherence may improve lives of PLHIV, including reducing mortality, improving patient outcomes, and ending HIV as a public health threat by 2030.
PP04.30 – Prevalence of Bacterial Sexually Transmitted Infections Among Young Men Who Have Sex with Men (MSM) Aged 15 to 24 in a City in Northeast Brazil
Dr. Guilherme Campos1, M.Sc. Thaise Rocha1, M.Sc. Monica Carnaúba2, M.Sc. Stefanie Cairo1, B.Sc. Agatha Silva1, Dr Laio Magno3, Dr Fabiane Soares2, Dr Inês Dourado2, Dr Lucas Marques1, Dr Danielle Medeiros1
1Universidade Federal da Bahia, Vitoria da Conquista, Brazil.
2Universidade Federal da Bahia, Salvador, Brazil.
3Universidade do Estado da Bahia, Salvador, Brazil.
Background: Bacterial sexually transmitted infections (bSTIs) among young men who have sex with men (MSM) are a critical public health issue in Brazil. This study assessed the prevalence of Neisseria gonorrhoeae (NG), Chlamydia trachomatis (CT), and Mollicutes among MSM aged 15–24 in Vitória da Conquista, Brazil.
Methods: A cross-sectional study using respondent-driven sampling recruited 106 MSM at an STI reference center between 2021 and 2022. Samples from anal, urethral, and oral sites were analyzed by qPCR for pathogen detection. Associations were evaluated using chi-square, Fisher’s exact test, and Poisson regression with 95% confidence intervals.
Results: NG prevalence was 8.1%, predominantly in the anal site (6.7%), while CT prevalence was 8.5%, varying across anatomical sites. Ureaplasma spp. were more prevalent (39.8%–36.8% for U. urealyticum and 4.8% for U. parvum) than Mycoplasma spp (28.1%–21.8% for M. hominis and 9.5% for M. genitalium) in the urethral site. Homosexual orientation (PR = 9.15; 95% CI 1.05–79.8) and group sex (PR = 3.56; 95% CI 1.07–11.84) were associated with NG. Younger age (PR = 6.93; 95% CI 2.14–22.46) and multiple sexual partners (PR = 11.37; 95% CI 1.45–88.98) correlated with CT. For Mycoplasma spp., it was associated with inconsistent condom use (PR = 3.2, 95% CI 1.24–8.71), transactional sex (PR = 4.08, 95% CI 1.23–13.52), and signs or symptoms in the urethral and anal region (PR = 2.55, 95% CI 1.01–6.45). For Ureaplasma spp., associations were observed with transactional sex (PR = 2.46, 95% CI 1.20–5.04), discrimination in healthcare settings due to sexual orientation or gender identity (PR = 4.00, 95% CI 1.89–8.46), and coinfection with HIV (PR = 2.72, 95% CI 1.42–5.21).
Conclusion: These findings highlight the interplay between bSTIs, risk behaviors, and sociostructural factors. Professional training focused on comprehensive testing and counseling tailored to LGBTQIA+ individuals is key to fostering inclusive, humanized care. Including extragenital screening is essential to address asymptomatic infections and reduce transmission.
PP04.31 – Prevalence and Risk Factors for Human Papillomavirus Infection Among Female Sex Workers in Two Large Cities in Zimbabwe
Dr. Sungai T Chabata1,2, Mr Pardon Masuka1, Ms Tsitsi Hove1, Ms Tatenda Kujeke1, Ms Memory Makamba1, Ms Primrose Matambanadzo1, Dr Owen Mugurungi3, Dr Elizabeth Fearon4, Prof James R Hargreaves5, Prof Frances M Cowan1,2
1Centre For Sexual Health and HIV/AIDS Research (ceshhar), Harare, Zimbabwe.
2Liverpool School of Tropical Medicine, Liverpool, United Kingdom.
3Ministry of Health and Child Care Zimbabwe, Harare, Zimbabwe.
4University College London, London, United Kingdom.
5London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: Female sex workers (FSWs) are at high risk of human papillomavirus (HPV) infections and cervical cancer due to their high number of sexual partners. We determine the prevalence of HPV and identify risk factors for high-risk HPV infection among FSWs.
Methods: Between June and August 2023, we recruited 3006 FSWs aged ≥18 in 2 large cities in Zimbabwe using respondent-driven sampling. A random sample of 1346 FSWs was screened for 14 high-risk HPV types (16/18/31/33/35/39/45/51/52/56/58/59/66/68) using Allplex™ HPV HR Detection. We estimated the prevalence of any high-risk HPV, HPV-16/18, and HPV-35/58 by age and HIV status. We assessed whether these prevalences differ by risk of HIV acquisition/transmission using a 6-question programmatic microplanning risk assessment tool (Fig. 1A). Factors associated with high-risk HPV infection were identified using multivariable modified Poisson regression models, adjusted for socio-demographic, sexual behaviours, and HIV status. All analyses were RDS-weighted.
Results: The overall prevalence of any high-risk HPV, HPV-35/58, and HPV-16/18 infection was 59.8%, 21.7%, and 34.8%, respectively, similar among FSWs aged 18–24 and ≥25, and by risk of HIV acquisition/transmission (Fig. 1B). Multiple HPV infections were identified in 576/1346 participants (42.7%). HPV-16 was the most prevalent (12.5%), followed by HPV-58 (12.2%). Any high-risk HPV was higher among HIV-positive FSW compared to HIV-negative FSW (68.9% vs 53.3%, P < 0.001). FSW who were ever married (adjusted prevalence-ratio [aPR]: 1.15, 95% confidence interval [CI]: 1.02–1.35) had a higher prevalence of high-risk HPV infection compared to those who were never married. Also, a single increase in the number of clients per week was associated with a 5% increase in the prevalence of any high-risk HPV.
Conclusion: Nearly two-thirds of FSWs in the 2 cities were infected with high-risk HPV. This highlights the importance of HPV vaccination and screening, particularly in HIV programming, to prevent cervical cancer in this high-risk group.
(a) Microplanning risk assessment tool (b) Prevalence of any high-risk HPV by risk of HIV acquisition/transmission.
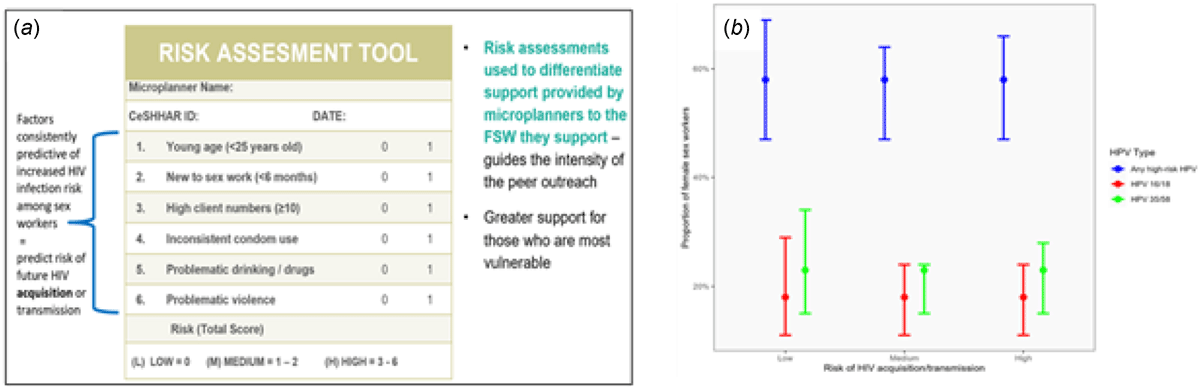
PP04.32 – Syphilis in Migrant Workers: A Nationwide Assessment in Qatar
Dr. Hiam Chemaitelly1,2, Prof Laith J. Abu-Raddad1,2
1Infectious Disease Epidemiology Group, Weill Cornell Medicine-Qatar, Doha, Qatar.
2Department of Population Health Sciences, Weill Cornell Medicine, Cornell University, New York, USA.
Background: Scant data are available on syphilis infection within migrant populations worldwide and in the population of the Middle East and North Africa region. This study investigated the prevalence of both lifetime and recent syphilis infections among migrant craft and manual workers (MCMWs) in Qatar, a diverse demographic representing 60% of the country’s population.
Methods: Sera specimens collected during a nationwide cross-sectional survey of SARS-CoV-2 seroprevalence among the MCMW population, conducted between July 26 and September 9, 2020, were analyzed. Treponema pallidum antibodies were detected using the Mindray CL-900i Chemiluminescence Immunoassay Analyzer. To differentiate recent infections, rapid plasma reagin (RPR) testing was performed, with an RPR titer of ≥1:8 considered indicative of recent infection. Logistic regression analyses were employed to identify factors associated with lifetime syphilis infection. Sampling weights were incorporated into all statistical analyses to obtain population-level estimates.
Results: T. pallidum antibodies were identified in 38 of the 2,528 tested sera specimens. Prevalence of lifetime infection was estimated at 1.3% (95% CI: 0.9%–1.8%). Among the 38 treponemal-positive specimens, 15 were reactive by RPR, with 3 having titers ≥1:8, indicating recent infection. Prevalence of recent infection was estimated at 0.09% (95% CI: 0.01–0.3%). Among treponemal-positive MCMWs, the estimated proportion with recent infection was 8.1% (95% CI: 1.7–21.4%). The adjusted odds ratio for lifetime infection increased with age, reaching 8.68 (95% CI: 2.58–29.23) among those aged ≥60 years compared to those ≤29 years of age. Differences in prevalence were observed by nationality and occupation, but no differences were found by educational attainment or geographic location.
Conclusions: Syphilis prevalence among MCMWs in Qatar is consistent with global levels, highlighting a disease burden with implications for health and social well-being. These findings underscore the need for programs addressing both sexually transmitted infections and the broader sexual health needs of this population.
PP04.33 – Neisseria Gonorrhoeae Prevalence Among Women with Abnormal Vaginal Discharge or Lower Abdominal Pain at a Malawian STI Clinic
Dr. Jane Chen1, Gomezgani Lukhanda2, Edward Jere2, Beatrice Ndalama2, Naomi Nyirenda2, Esther Mathiya2, Naomi Bonongwe2, Gabriel Banda2, Robert Krysiak1,2, Mitch Matoga2, Irving Hoffman1,2
1University of North Carolina, Chapel Hill, United States.
2UNC Project Malawi, Lilongwe, Malawi.
Background: Understanding the etiologies of sexually transmitted infection (STI) syndromes is crucial for countries utilizing syndromic management. In Malawi, most studies on STI etiologies have been conducted in men, with few and sporadic assessments in women. This study aimed to estimate the prevalence of Neisseria gonorrhoeae at vaginal and pharyngeal sites, among women presenting with high-risk abnormal vaginal discharge (AVD+) and/or lower abdominal pain (LAP), the syndromes that prompt treatment for N. gonorrhea.
Methods: In 2022, this cross-sectional pilot study enrolled women presenting to the Bwaila STI clinic in Lilongwe, Malawi with AVD+ and/or LAP. Vaginal and pharyngeal swabs were collected and tested for N. gonorrhoeae using the Cepheid GeneXpert® platform. All participants were treated according to the Malawi Standard Treatment Guidelines.
Results: Sixty women enrolled in the study: 27 with AVD+, 13 with LAP, and 20 with AVD+ and LAP. The median age was 29 years (IQR: 23, 36) and most (67%) women were married. Most women (68%) reported having only 1 primary sexual partner in the past 3 months, and 73% reported never or rarely using condoms. Half (55%) reported no prior STI history. Overall, the prevalence of vaginal N. gonorrhoeae was 33% (AVD+/LAP: 40%; AVD+ only: 33%; LAP only: 23%) (Fig. 1). Only 1 of 60 participants (5%) had a concurrent pharyngeal infection; no woman had only pharyngeal infection.
Conclusion: N. gonorrhoeae continues to be a significant cause of high-risk abnormal vaginal discharge and lower abdominal pain syndromes, but still only accounts for about one-third of the cases that are treated for it. The need for point-of-care test options is critical for the adequate treatment of women with AVD+ and/or LAP. The presence of pharyngeal gonorrhea in this pilot study underscores the need for a larger trial to estimate the burden of extragenital gonorrhea and surveillance for antimicrobial resistance.
PP04.34 – Impact of Increased PrEP Prescriptions on STI Notifications from the DSC Clinic, Singapore
Dr. Terrence Chiew, Dr Benson Yeo
1The Department of STI Control (DSC) Clinic, National Skin Centre, Singapore, Singapore.
Background: Sexually transmitted infections (STIs) continue to be a significant public health concern with a considerable economic burden on healthcare systems. Pre-exposure Prophylaxis (PrEP) has emerged as a promising biomedical intervention to reduce the risk of acquiring HIV. It involves the use of antiretroviral medications by those at high risk of contracting HIV but are not infected.
Description: We compared the total number of PrEP prescriptions to the total number of notifiable STIs from the DSC clinic. The STIs included in the review are syphilis, gonorrhoea and chlamydia infections.
Results: There was an increase in the number of PrEP prescription. In 2017, there were only 38 prescriptions followed by 70 in 2018. From 2019, there was stark increase in total number of annual PrEP prescriptions – 418 in 2019, 442 in 2020, 659 in 2021 followed by a drop to 584 in 2022 before increasing to 729 in 2023. However, the trend of STI notification from DSC remained stable, if not, reducing. In 2017, there were a total number of 8585 STI cases, followed by a decrease to 7684 in 2018 and 7533 in 2019. There were only 5591 cases documented in 2020, followed by an increase to 6038 in 2021, 6456 in 2022 and 6570 in 2023.
Conclusion: The DSC clinic is the only public STI clinic and accounts for at least half of all notified STIs in Singapore. This preliminary review suggests that even with a 10-fold increase in PrEP prescription, the number of notifiable STIs seen in the clinic remains stable. This highlights the importance of a comprehensive STI prevention program that integrates PrEP into existing healthcare services. A holistic approach that combines PrEP with other preventive measures, such as condom use, regular STI screening, and health education, can yield better outcomes in controlling STI rates.
PP04.35 – Understanding the Epidemiology, Clinical Characteristics and Infection Severity of Mpox Cases in 2024 Outbreaks in Victoria, Australia
Dr. Ei Aung1,2, Dr Soo Jen Low3,4, Dr Janet Towns1,2, Prof Christopher Fairley1,2, Dr Chuan Kok Lim3,4, Prof. Eric Chow1,2,3
1Melbourne Sexual Health Centre, Alfred Health, Carlton, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Victorian Infectious Diseases Reference Laboratory, Royal Melbourne Hospital, Doherty Institute for Infection and Immunity, Melbourne, Australia.
4Department of Infectious Diseases, Doherty Institute of Infection and Immunity, The University of Melbourne, Melbourne, Australia.
5Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Following the global mpox outbreak in 2022, clusters of clade II mpox cases have continued to emerge in 2024 in many countries, including Australia. This study describes the epidemiology, characteristics, and severity of mpox cases presented to a public sexual health clinic in Victoria during the 2024 outbreaks.
Methods: We conducted a retrospective cross-sectional study of mpox-confirmed cases using mpox polymerase chain reaction test at the Melbourne Sexual Health Centre, Australia between January and September 2024. We collected data on demographic characteristics, sexual behavioural data, and vaccination history, clinical characteristics, and infection severity. We examined the factors associated with mpox clinical severity (mild, moderate, severe) using ordered logistic regression.
Results: We included 156 mpox confirmed cases (155 men and 1 woman) with the median age of 35 (IQR: 31–40), and most were MSM (98%, n = 153). More than half (59%, n = 91) had at least one mpox vaccine. Mpox vaccination was highest in PrEP users (74%, n = 67), followed by persons living with HIV (PLHIV) (19%, n = 17), and HIV-negative non-PrEP users (8%, n = 7). One person had a previous mpox infection in 2022.
Most (94%, n = 147) had mild or moderate symptoms, and 5% (n = 8) had severe symptoms requiring hospitalisations. One was lost to follow-up. The median of lesions per case was 3 (IQR: 1–9). Vaccinated group (n = 91) had lower odds of severe disease than unvaccinated group (n = 64) (odds ratio[OR]: 0.32, 95%confidence interval [CI]: 0.15–0.67, P = 0.002). An increase in the number of lesions was associated with more severe disease (OR: 1.07, 95% CI: 1.01–1.13, P = 0.02). PrEP use, HIV status, and age were not associated with clinical severity.
Conclusion: Our findings suggest mpox vaccination reduces disease severity. However, the notable number of unvaccinated PLHIV and non-PrEP users highlighted the need for increased awareness and public health campaigns to boost vaccine uptake among MSM.
PP04.36 – Comparing HIV Testing and PrEP Uptake Between a Fixed-Site Clinic and Mobile Outreach Locations in Memphis, TN
Mr. David Closs1
1Friends For All, Memphis, United States.
Background: In 2023, Memphis ranked second in the U.S. for the highest rates of new HIV infections. Friends for All (FFA) is a Memphis-based community organization focused on preventing the spread of HIV and improving health outcomes for individuals living with HIV. To reduce new HIV infections in Memphis, FFA launched a HIV testing and linkage to PrEP protocol at its fixed-site clinic (FSC) and mobile/outreach locations (MOL).
Methods: From December 1, 2023, to September 30, 2024, we implemented an HIV testing and linkage to PrEP protocol at both the FSC and MOL. At the FSC, clients were required to schedule appointments but were offered immediate access to PrEP during testing. MOL testing occurred in community settings where clients were already gathered. At these locations, clients could walk in for testing; however, if they wanted PrEP, they were scheduled for an appointment at the FSC within 7 days.
Results: A total of 2,999 individuals (569 from MOL, 2,430 from FSC) were screened for HIV. Of the 2,874 who tested negative, 312 started PrEP. Of these, 98% were from the FSC, while less than 2% were from MOL.
MOL outperformed the FSC in screening women and people of color. At the FSC, 47% of clients identified as African American, compared to 60% at MOL (Table 1). Similarly, 13% of FSC clients were Hispanic non-white, while 24% were at MOL. Additionally, 25% of women were screened at the FSC, versus 62% at MOL locations.
Conclusion: These results suggest that collocating PrEP and screening services, as well as offering same-day access, can enhance effectiveness. Additionally, they indicate that walk-in screenings in community settings effectively reach women and people of color. To further increase PrEP access within these populations, we are exploring the use of a nurse practitioner at our MOL to provide immediate PrEP access.
| Populations Screened by Site Type | FSC | MOL | |
|---|---|---|---|
| Black/African American | 47% | 60% | |
| Hispanic non-White | 13% | 24% | |
| White non-Hispanic | 26% | 10% | |
| Women | 25% | 62% |
PP04.37 – The Ability of European Economic Area Countries to Respond to the Threat of Multi-Drug Resistant Neisseria Gonorrhoeae Has Weakened
Dr. Michelle Cole1, Dr Melissa Jansen van Rensburg1, Dr Susanne Jacobsson2, Dr Sarah Alexander1, Dr Csaba Ködmön3, Prof Magnus Unemo2
1UK Health Security Agency, London, United Kingdom.
2Örebro University Hospital, Örebro, Sweden.
3European Centre for Disease Prevention and Control, Stockholm, Sweden.
Background: The European Centre for Disease Prevention and Control response plan to control and manage the threat of multi- and extensively drug-resistant Neisseria gonorrhoeae (MDR/XDR-NG) was updated and published in 2019. The effectiveness and value of the response plan is assessed periodically to identify and address areas for improvement.
Methods: During 2024, EU/EEA countries were invited to provide information on the response plan indicators for 2023, using 2019 as a baseline. The indicators assessed a country’s ability to perform gonococcal antimicrobial surveillance and to clinically manage gonorrhoea, including treatment failure monitoring. Additionally, indicators assessing the European Gonococcal Antimicrobial Surveillance Programme (Euro-GASP) were completed.
Results: All 30 countries responded, however only 24 countries participated in the Euro-GASP surveillance in 2023, two less than 2019. Similarly, 24 laboratories participated in the 2023 EQA, 13 fewer than in 2019. In contrast, increasing numbers of gonococcal isolates were submitted to Euro-GASP; 5,269 vs 4,166 isolates in 2019, representing a 27% increase.
There was a lower proportion of STI clinics with access to antimicrobial susceptibility testing (AST) and culture; 97% in 2019 vs 83% in 2023. Also, the proportion of gonorrhoea cases with AST decreased by 9%, as well a 15% decrease in patients receiving appropriate treatment.
There was little change in the reporting and completeness of Euro-GASP epidemiological variables, as well as treatment failure monitoring.
Conclusion: Euro-GASP, like many other programmes and services, faced unprecedented circumstances in 2019–2021 due to COVID-19. We may still experience the impact of this pandemic, as the ability to respond to MDR/XDR-NG seems to have weakened in the EU/EEA. This is concerning as we are currently observing increases in gonorrhoea cases, as well as cases of MDR/XDR NG in Europe. Renewed efforts to go back to basics, to improve obtaining cultures and linked patient metadata, are now underway.
PP04.38 – Chlamydia And/Or Gonorrhea Case Demographics Correlations with Later Syphilis Diagnosis in British Columbia (BC), 2014–2023
Dr. Theodora B. Consolacion1, Amanda Yu1, Dr. Hannah M. Baer1, Heather Burgess1,2, Robert Higgins1, Justin Sorge1,2, Venessa Ryan1, Ina Chen1, Sven Dong1, Dr. Jennifer Vines1, Dr. Sofia R. Bartlett1,3
1British Columbia Centre for Disease Control, Vancouver, Canada.
2Public Health Agency of Canada, Vancouver, Canada.
3University of British Columbia, Vancouver, Canada.
Background: Infectious syphilis (IS) diagnoses (Dx) rates in BC have risen from 11.7 per 100,000 population in 2014 to 37.4 in 2023. Left untreated, about 33% of people will develop complications related to IS. Rates are much higher in Chlamydia (CT) and gonorrhea (GC). The study’s purpose is to examine relationships between more prevalent CT and/or GC (CT/GC) Dx to subsequent IS Dx.
Methods: All genital CT, GC and IS Dx in 2014–2023 from the provincial Electronic Medical Record system were selected. A dataset with sex, age, CT/GC counts, first CT Dx date, first GC Dx date, first IS Dx date, and a flag denoting subsequent IS Dx after first CT/GC Dx. Logistic regressions with IS after a CT/GC Dx as the outcome and sex, age, and CT/GC Dx counts as predictors were calculated.
Results: Final dataset was N = 141,994 with sex (males = 64,168; females = 77,390), and age (median = 26, IQR: 21, 33.) Sex, age and CT/GC Dx count were significantly associated with subsequent IS Dx. Adjusted odds ratios (aOR) for males was 2.4 (95% CI: 2.2, 2.6) higher than females. Using the median age (26 years) to create age categories, people ≥26 years were 2.4 (95% CI: 2.1, 2.6) higher than those <26 years. Multiple CT/GC Dx were 2.1 (95% CI: 2.0, 2.1) higher to be diagnosed with IS Dx later.
Interactions between sex and age-group and sex and CT/GC count were significant. With the number of CT/GC Dx at 1.1, males ≥26 years were 3.2 (95% CI: 32.6, 4.0) higher than females of the same age-group, while males < 26 years were 1.8 (95% CI: 1.3, 2.4) higher than females in the same age-group.
Conclusion: Data suggest CT/GC diagnosis among males ≥26 years with a previous CT/GC diagnosis are at elevated risk for syphilis. Universal syphilis screening should be considered after CT/GC diagnosis in this group.
PP04.39 – Perceived STI Seriousness and Subsequent Acquisition of Chlamydia, Gonorrhea or Syphilis Among Urban Gay, Bisexual and Other Men Who Have Sex with Men in Canada, 2019–2024
Dr. Joseph Cox1,2,3, Mrs. Milada Dvorakova3, Dr. Alain Fourmigue3, Miss Sophie Brunelle-Newman3, Dr. Mathieu Maheu-Giroux2, Dr. Erica EM Moodie2, Dr. Daniel Grace4, Dr. Trevor A. Hart4,5, Dr. David Moore6,7, Dr. Nathan Lachowsky6,8, Dr. Darrell H. S. Tan9,10, Dr. Paolo A. Palma5, Dr. Shayna Skakoon-Sparling5,11, Mr. Jody Jollimore12, Terri Zhang5, Mr. Allan Lal6, Dr. Aki Gormezano8, Dr. Tin D. Vo10, Dr. Gilles Lambert
1Direction régionale de santé publique, CIUSSS Centre-Sud-de-l'île-de-Montréal, Montréal, Canada.
2School of Population and Global Health, McGill University, Montréal, Canada.
3Research Institute of the McGill University Health Centre, Montréal, Canada.
4Dalla Lana School of Public Health, University of Toronto, Toronto, Canada.
5Toronto Metropolitan University, Toronto, Canada.
6BC Centre for Excellence in HIV/AIDS, Vancouver, Canada.
7University of British Columbia, Vancouver, Canada.
8School of Public Health and Social Policy, University of Victoria, Victoria, Canada.
9Saint Michael’s Hospital, Toronto, Canada.
10University of Toronto, Toronto, Canada.
11University of Guelph, Guelph, Canada.
12Canadian AIDS Treatment Information Exchange (CATIE), Toronto, Canada.
Background: Perceptions of the seriousness of chlamydia (CT), gonorrhea (GN), and syphilis among gay, bisexual, and other men who have sex with men (GBM) may shape health behaviors and related outcomes. We examined STI seriousness perceptions and the impact on STI acquisition.
Methods: Sexually active GBM aged 16+ years were recruited through respondent-driven sampling (2017–2019) in Montreal, Toronto and Vancouver. Participants completed a computer-assisted self-interview and tests for CT, NG, and syphilis at enrollment and every 6–12 months. Perceived seriousness of each STI was assessed and responses were dichotomized (serious/somewhat serious versus neutral/somewhat not serious/not serious). Crude proportions of perceived seriousness of each STI were calculated. Poisson regressions with robust standard errors were used to estimate the effect (rate ratios and 95% confidence intervals) of perceived CT, NG and syphilis seriousness on one-year STI-specific acquisition risk. Models were weighted to account for the recruitment method (RDS-II weights) and loss-to-follow-up. We adjusted for potential confounders (inverse probability weighting) Fig. 1; common mediators (e.g. condomless sex, number of partners) were excluded from the analysis.
Results: Of 2,449 participants, 1,142 answered the perceived STI seriousness question and attended a follow-up visit within the subsequent year. CT, NG and syphilis were perceived as “serious/somewhat serious” by 44.0%, 45.2%, and 56.3% of participants, respectively. The effects of perceiving CT, NG and syphilis as “serious/somewhat serious” on acquiring each STI were: aRR = 0.7 (95% CI: 0.4–1.1), 0.8 (0.5–1.3), and 0.3 (0.1–0.7), respectively.
Conclusions: More participants perceived syphilis as serious, compared to CT and NG. Perceiving syphilis as serious lowered risk of its acquisition among GBM. Syphilis prevention efforts may benefit from health education that informs perceptions of seriousness based on accurate STI information.
Causal diagram of the effect of perceived STI seriousness on acquisition of bacterial STIs (chlamydia, gonorrhea, and syphilis) within 1 year.
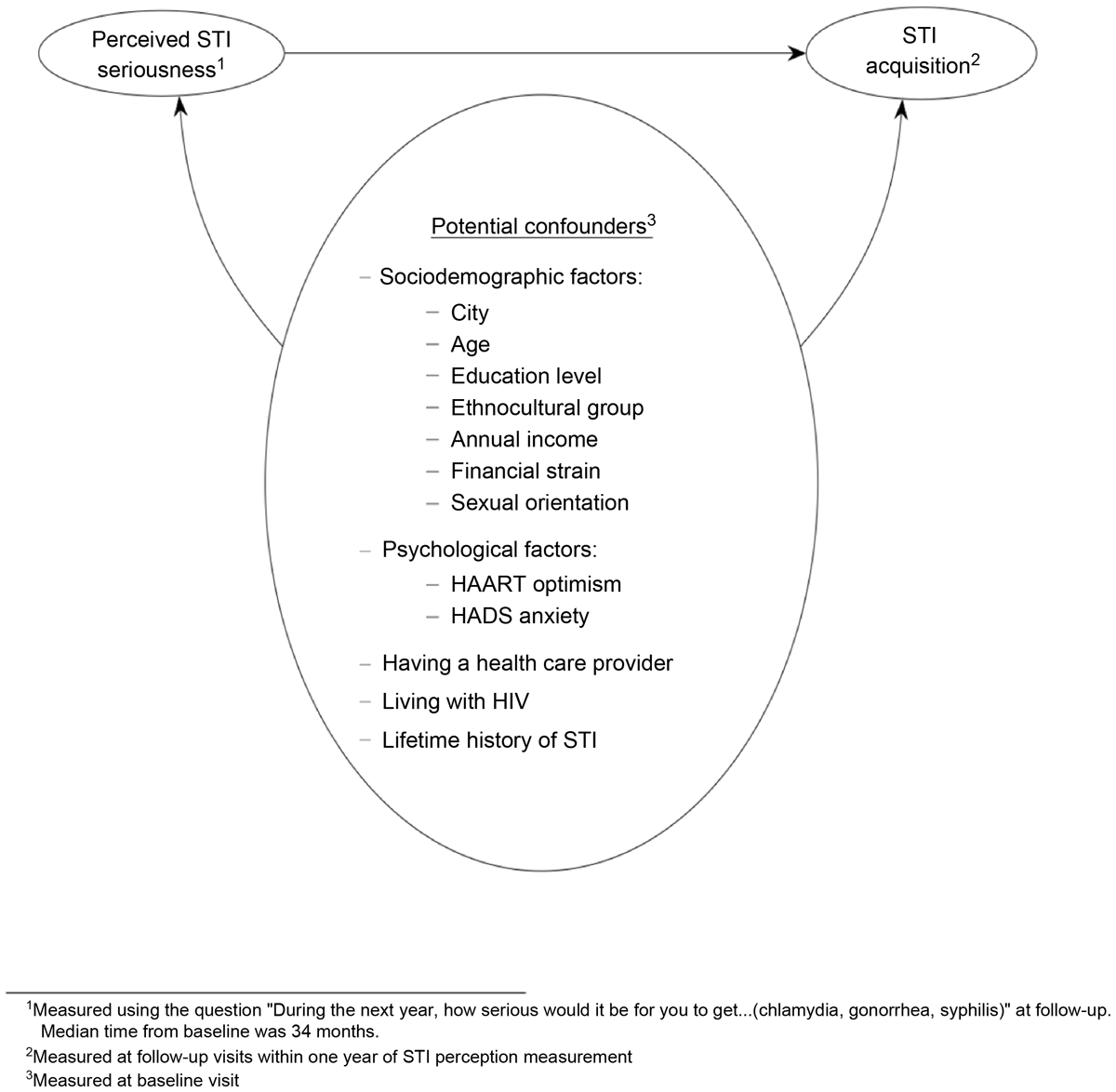
PP04.40 – Trends in All-Cause and Cause-Specific Mortality, Including HIV, Among People Who Inject Drugs in Montreal, 1989–2018
Dr. Harika Dasari1,2, Dr. Adelina Artenie2, Dr. Sarah Larney2,3
1Centre de recherche du Centre hospitalier de l’Université de Montréal (CRCHUM), Montréal, Canada.
2Département de Biomedical Sciences, Université de Montréal, Montreal, Canada.
3Département de Médicine Familiale et Médecine d’Urgence, Université de Montréal, Montreal, Canada.
Background: HIV has historically been a major contributor to mortality among people who inject drugs (PWID), alongside overdose, liver disease, cancer, and other comorbidities. Examining all-cause and cause-specific mortality trends in the HEPCO cohort, a long-standing prospective study of PWID in Montreal provides insights into the changing burden of disease and the effectiveness of public health interventions.
Methods: HEPCO cohort data (1989–2018) were linked to Québec mortality records. Age–sex–standardized mortality rates (ASSRs), standardized to the cohort’s average age and sex profile, were calculated for all-cause and cause-specific mortality, including HIV, drug overdose, cancer, cardiovascular disease (CVS), and liver disease. Annual Percent Change (APC) was used to evaluate trends. Proportions of deaths by cause were analyzed to assess shifts in mortality patterns over time.
Results: Among 3,747 participants contributing 67,071 person-years, 1,273 deaths were recorded. ASSRs declined from 8,000 per 1,000 person-years in 1989 to below 500 in 2018, reflecting reductions in HIV-related mortality and other causes. HIV, the second leading cause until 2001, became less prominent following widespread access to antiretroviral therapy (APC: –8.2%). Drug overdoses, the leading cause of death (19.4%), peaked in the mid-2000s, with fluctuations reflecting harm reduction interventions. Liver-related deaths (9.19%), closely linked to chronic Hepatitis C Virus (HCV) infection, emerged as a significant contributor after 2001, alongside cancer (10.37%) and CVS (10.05%). Mortality among PWID remained significantly higher than in the general population, particularly among males.
Conclusion: This study highlights trends in all-cause and cause-specific mortality among PWID. While HIV-related deaths declined dramatically due to treatment advances, drug overdoses persisted as the leading cause. The growing burden of liver-related deaths linked to HCV, as well as cancer and CVS, underscores the need for integrated care and harm reduction strategies. Findings support targeted public health interventions to improve outcomes for PWID.
PP04.41 – Patterns and Gaps in Co-Infection Testing: Retrospective Study of Female Patients Tested for Chlamydia and Gonorrhea in the Emergency Department
Gaby Dashler1, Nyah Johnson1, Kendall Maliszewski1, Edana Mann1, Mustapha Saheed1, Spencer Mann1, Brooke Peterman1, Katelyn Mann1, Eili Klein1, Richard E. Rothman1, Yu-Hsiang Hsieh1
1Johns Hopkins University School of Medicine, Baltimore, United States.
Background: The emergency department (ED) serves as a critical access point for individuals seeking care for STIs, including chlamydia (CT) and gonorrhea (NG). The co-occurrence of other STIs, such as HIV and syphilis, underscores the need for comprehensive testing in this setting. We sought to understand co-infection testing rates for ED patients receiving CT/NG testing, and what clinical factors may influence additional testing.
Methods: This is a retrospective analysis of co-infection testing for female patients receiving CT/NG testing in the ED (August 1 to November 30, 2022 and January 9 to April 28, 2023). The analysis included co-infection testing during the visit by demographic and clinical characteristics using chi-square test.
Results: Overall, 792 female patients underwent CT/NG testing. Of these, 245 (30.9%) received additional co-infection testing, including HIV only (73.9%), syphilis only (6.5%), or both (19.6%) (Table 1). No new HIV cases were identified, but 6 of 64 patients (9.4%) tested for syphilis had positive antibody screens, and 5 had positive RPR results. 4 out of the 5 were confirmed new infections, in which 3 were in patients of childbearing age. Factors significantly associated with co-infection testing included self-reported pregnancy status (P < 0.001), known HIV status (P < 0.001), lower abdominal pain (P = 0.004), vaginal discharge (P = 0.002), and vaginal itching (P < 0.01). Among 52 (6.6%) patients with CT/NG positive results, 36.5% underwent HIV testing, and 7.7% underwent syphilis testing, compared to 28.8% and 8.1% respectively for 740 patients with negative CT/NG results (both P > 0.05, respectively).
Conclusion: Many patients did not receive co-infection testing, but those tested were more likely to have STI symptoms, self-reported pregnancy status, or positive CT/NG results. Four new syphilis cases were identified, highlighting the importance of comprehensive testing. Consistent, targeted co-infection testing in EDs is crucial for timely STI diagnosis and treatment.
| STI Co-Testing [HIV, Syphilis] | |||||
|---|---|---|---|---|---|
| Characteristics | Category | Total | Yes | No | |
| Overall | 792 | 245 | 547 | ||
| A. Socio-demographics | |||||
| Age (years) | Mean | 32.4 ± 11.5 | 32.0 ± 11.7 | 32.5 ± 11.5 | |
| Median | 30 [24, 37] | 29 [23, 37] | 31 [24, 37] | ||
| 18–24 | 231 | 76 (32.9) | 155 (67.1) | ||
| 25–29 | 145 | 51 (35.2) | 94 (64.8) | ||
| 30–34 | 156 | 42 (26.9) | 114 (73.1) | ||
| 35–39 | 98 | 23 (23.5) | 75 (76.5) | ||
| ≥40 | 161 | 53 (32.9) | 108 (67.1) | ||
| Missing | 1 | 0 (0.0) | 1 (100) | ||
| Gender | Female | 787 | 241 (30.6) | 546 (69.4) | |
| Transgender | 3 | 2 (66.7) | 1 (33.3) | ||
| Non-Binary | 2 | 2 (100) | 0 (0.0) | ||
| Race/Ethnicity | White, Non-Hispanic | 94 | 28 (29.8) | 66 (70.2) | |
| Black, Non-Hispanic | 503 | 163 (32.4) | 340 (67.6) | ||
| Other Race, Non-Hispanic | 69 | 22 (25.4) | 47 (74.6) | ||
| Hispanic | 126 | 32 (31.9) | 94 (68.1) | ||
| Insurance Payor | Medicaid | 402 | 127 (31.6) | 275 (68.4) | |
| Medicare | 53 | 17 (32.1) | 36 (67.9) | ||
| Private | 138 | 37 (26.8) | 101 (73.2) | ||
| Self-Pay | 88 | 25 (28.4) | 63 (71.6) | ||
| Unknown | 111 | 39 (35.1) | 72 (64.9) | ||
| Having PCP | Yes | 370 | 101 (27.3) | 269 (72.7) | |
| No | 328 | 110 (33.5) | 218 (66.5) | ||
| Unknown | 94 | 34 (36.2) | 60 (63.8) | ||
| Housing | Permanent | 536 | 159 (29.7) | 377 (70.3) | |
| Staying with Friends | 23 | 11 (47.8) | 12 (52.2) | ||
| Unstable or Homeless | 61 | 20 (32.8) | 41 (67.2) | ||
| Unknown | 172 | 55 (32.0) | 117 (68.0) | ||
| B. Clinical Characteristics | |||||
| Self-Reported | Yes | 175 | 31 (17.7) | 144 (82.3) | |
| Pregnancy | No | 129 | 40 (31.0) | 89 (69.0) | |
| Unknown | 488 | 174 (35.7) | 314 (64.3) | ||
| HIV Status | Previously Diagnosis | 11 | 2 (18.2) | 9 (81.8) | |
| Negative | 556 | 233 (41.9) | 323 (58.1) | ||
| Unknown | 225 | 10 (4.4) | 215 (95.6) | ||
| HCV Status | Positive | 14 | 7 (50.0) | 7 (50.0) | |
| Negative | 400 | 132 (33.0) | 268 (67.0) | ||
| Unknown | 378 | 106 (28.0) | 272 (72.0) | ||
| Past STIs | Chlamydia | 140 | 43 (30.7) | 97 (69.3) | |
| Gonorrhea | 85 | 27 (31.8) | 58 (68.2) | ||
| Trichomonas | 104 | 36 (34.2) | 68 (65.4) | ||
| Syphilis | 23 | 7 (30.4) | 16 (69.6) | ||
| Herpes | 33 | 9 (27.3) | 24 (72.7) | ||
| HPV | 35 | 11 (31.4) | 24 (68.6) | ||
| Any STI Above | 274 | 86 (31.4) | 188 (68.6) | ||
| Symptoms | Lower Abdominal Pain | 494 | 135 (27.3) | 359 (72.7) | |
| Vaginal Bleeding | 216 | 53 (24.5) | 163 (75.5) | ||
| Vaginal Discharge | 204 | 81 (39.7) | 123 (60.3) | ||
| Nausea or Vomiting | 197 | 57 (28.9) | 140 (71.1) | ||
| Painful Urination | 141 | 47 (33.3) | 94 (66.7) | ||
| Vaginal Itching | 69 | 34 (49.3) | 35 (50.7) | ||
| Vaginal Odor | 37 | 14 (37.8) | 23 (62.2) | ||
| Bumps, Blisters or Sores | 7 | 5 (71.4) | 2 (28.6) | ||
| Pain During Sex | 7 | 4 (57.1) | 3 (42.9) | ||
| Any Symptom Above | 726 | 217 (29.9) | 509 (70.1) | ||
| STI Testing | Central Lab NAAT | 501 | 161 (32.1) | 340 (67.9) | |
| POC PCR | 291 | 84 (28.9) | 207 (71.1) | ||
| STI Results | CT Positive | 38 | 16 (42.1) | 22 (57.9) | |
| NG Positive | 21 | 8 (38.1) | 13 (61.9) | ||
| Any Positive | 52 | 20 (38.5) | 32 (61.5) | ||
| No CT, NG | 740 | 225 (30.4) | 515 (69.6) | ||
* ‘Central Lab Testing’ whereby a central laboratory tested for chlamydia (CT) and gonorrhea (NG) with nucleic acid amplification test (NAAT). ‘ED POC PCR Testing’ whereby an ED POC laboratory tested for CT and NG with Visby Medical Sexual Health Test.
P < 0.05: Self-reported pregnancy (17.7% (yes) vs 31.0% (no) vs 35.7% (unknown), P < 0.001), HIV status [18.2% (known) vs 41.9% (negative) vs 4.4% (unknown), P < 0.001], Symptom – Lower Abdominal Pain (27.3% vs 36.9%, P = 0.005), Symptom – Vaginal Bleeding (24.5% vs 33.3%, P = 0.017), Symptom –Vaginal Discharge (39.7% vs 27.9%, P = 0.002), Symptom – Vaginal Itching (49.3% vs 29.2%, P < 0.001), Symptom – Bumps, Blisters or Sores (71.4% vs 31.1%, P = 0.032), Symptom – Any Symptom (29.9% vs 42.4%, p = 0.035).
0.1 < P ≤ 0.05: Having PCP (27.6% (yes) vs 34.5% (no) vs 36.2% (known), P = 0.085); HCV status [50.0% (known) vs 33.0% (negative) vs 28.0% (unknown), P = 0.097].
PP04.42 – The Association Between Experiences of Physical and Sexual Violence and HIV Seroprevalence Among Female Sex Workers: A Global Systematic Review and Meta-Analysis
Mr. Joshua Dawe1, Dr Khadimul Mazhar1, Ms Saher A Khan1, Ms Lucy Barrass1, Ms Julie Ambria1, Dr Adam Trickey1, Ms Victoria Bendaud2, Dr Keith Sabin2, Dr Adelina Artenie1, Associate Professor Jack Stone1, Professor Matthew Hickman1,3, Professor Peter Vickerman1,3
1Bristol Medical School, Bristol, United Kingdom.
2Data for Impact, The Joint United Nations Program on HIV/AIDS (UNAIDS), Geneva, Switzerland.
3Health Protection Research Unit, Bristol, United Kingdom.
Background: Female sex workers (FSW) are a key population with a high HIV burden, who commonly experience multiple forms of violence. Studies suggest that experiences of violence are associated with increased HIV risk behaviours and transmission, but no study has yet systematically reviewed this association. We assessed whether FSW with recent (previous year) or lifetime experiences of physical and/or sexual violence had higher odds of HIV infection.
Methods: We searched multiple databases for studies reporting an association between experiences of violence and HIV infection among FSW published between January 2010 and March 2024. We extracted estimates of the association between experiences of recent and lifetime physical and/or sexual violence and HIV seroprevalence. We used adjusted estimates when available, and otherwise used unadjusted estimates. We pooled data using random-effects meta-analysis.
Results: A total of 56 cross-sectional studies reported an association between violence and HIV seroprevalence. The majority of studies were from the African region (32/56, 57%). Pooled effects of sexual violence showed strong evidence of an association with HIV seroprevalence for both recent exposure (n = 17 studies; OR: 1.79; 95% CI: 1.38–2.33; I2: 71%) and lifetime exposure (n = 20; OR: 1.39; 95% CI: 1.19–1.49; I2: 52%) (Fig. 1). We also found strong evidence of an association between recent (n = 14; OR: 1.36; 95% CI: 1.14–1.63; I2: 60%) and lifetime (n = 16; OR: 1.44; 95% CI:1.27–1.63; I2:42%) exposure to physical violence and HIV seroprevalence. Similarly, among studies reporting combined estimates for physical and sexual violence, we found evidence that both recent (n = 9; OR: 1.26; 95% CI: 1.02–1.57; I2: 61%) and lifetime (n = 11; OR: 1.26; 95% CI: 1.08–1.47; I2: 53%) exposure are associated with HIV seroprevalence.
Conclusion: Our findings indicate that recent and lifetime experiences of physical and sexual violence are associated with HIV infection among FSW. Our systematic review underscores the need for HIV interventions and policy and legal environments to acknowledge and address violence as a structural determinant of HIV infection among FSW.
PP04.43 – Results of a Pooled Screening Method to Monitor Mpox Circulation Among Men Who Have Sex with Men Attending a Sexual Health Service to Test for Chlamydia/Gonorrhea in Belgium, 2023–2024
Dr. Irith De Baetselier1, Dr. Jasmine Coppens1, Dr. Christophe Van Dijck1, Prof. Dr. Chris Kenyon1, Prof. Dr. Laurens Liesenborghs1, Dorien Van den Bossche1, Koen Vercauteren1, Dr Marjan Van Esbroeck1
1Institute Of Tropical Medicine, Antwerp, Belgium.
Background: Mpox continues to circulate globally. Most cases outside of Africa belong to clade IIb and are associated with sexual contact among gay and bisexual men who have sex with men. Cases may remain undiagnosed due to unrecognized, mild or subtle clinical presentations and decreased awareness. Monitoring these cases is important as they may lead to onward transmission. Wastewater monitoring is one example of a surveillance method. Here, we describe another, low-cost and potentially highly sensitive surveillance method to detect silent circulation of mpox. The method involved directly detecting monkeypox virus (MPXV) DNA in clinical samples from individuals at risk for mpox attending a sexual health clinic for chlamydia/gonorrhea screening in Antwerp, Belgium.
Methods: From January 2023 to November 2024, we tested leftover DNA extracts from male samples initially used for chlamydia/gonorrhea molecular testing or screening (anorectal swabs, or pooled urine + anorectal + oropharyngeal swabs). The DNA extracts were combined in pools (further called ‘COMBO pools’) of maximum five, and were tested by PCR for MPXV. PCR-positive COMBO pools underwent additional clade differentiation. The results were compared with the overall number of mpox cases reported in Belgium during the same period.
Results: Of 826 COMBO pools, 12 (1.5%) tested positive for MPXV clade II (Fig. 1). The majority (10/12; 83.3%) of infections were detected in August–November 2024, highlighting increased circulation which coincided with the monthly reported number of mpox cases in Belgium.
Conclusion: Pooled MPXV PCR testing of leftover DNA-extracts from samples collected for chlamydia/gonorrhea testing in a sexual health clinic accurately reflects trends in national mpox case reporting in Belgium, and helps to alert physicians and public health agencies of continued mpox circulation. Importantly, using our strategy to combine DNA extracts used for chlamydia/gonorrhea testing, we mitigated the financial and logistical burdens of additional surveillance methods.
Number of negative (grey) and positive (orange) COMBO pools from January 2023 until November 2024. The total number of mpox cases reported in Belgium is shown in blue.
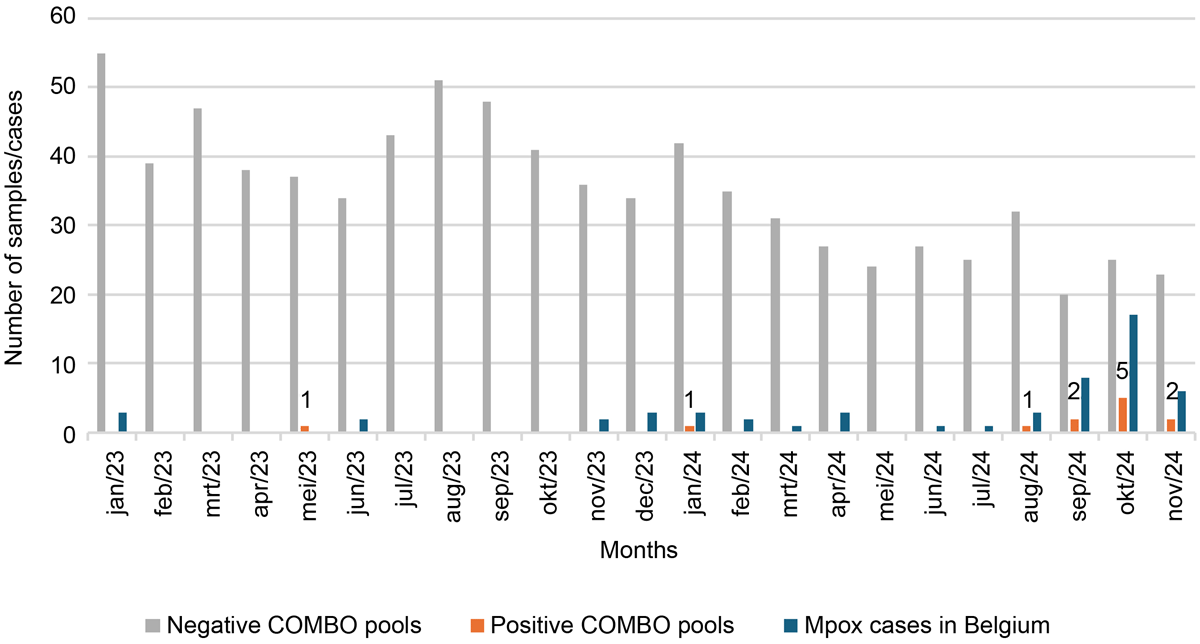
PP04.44 – Impact of Prenatal Care Gaps on the Congenital Syphilis Cases in Brazil: An Analysis Based on Syphilis in Pregnant Women
Dr. Leonor Henriette De Lannoy1, Mr Ítalo Vinicius Albuquerque Diniz1, Mr Ana Paula Betaressi1, Dr Angélica Espinosa Miranda2, Dr Pâmela Gaspar1, Dr Drauri Barreira1
1Department of HIV/Aids, Tuberculosis, Viral Hepatitis, and Sexually Transmitted Infections, Ministry of Health of Brazil., Brasília, Brazil.
2Federal University of Espírito Santo, Vitória, Brazil.
Background: The elimination of congenital syphilis (CS) as a public health problem is a national priority, aligned with the 2030 national health goals. Despite the availability of well-established prevention measures for the entire population, challenges such as the high prevalence of syphilis in pregnant women (PW), complexities in diagnosing and monitoring PW with syphilis, and limitations in defining a PW case contribute to the persistence of CS as a public health problem. Our objective was to analyze the incidence rate of CS considering the detection rate of PW.
Methods: The prevalence of syphilis in PW was estimated based on the detection rate, alongside the number of PW potentially generating a case of CS under the prenatal care cascade, assuming a 95% success rate at each stage: prenatal coverage; testing; and adequate treatment. Based on the number of pregnant women with care failure, the projected incidence of CS, considering care failures, was then compared with the current incidence.
Results: In 2023, the incidence of CS was 9.9/1,000 live births and the syphilis detection rate in PW was 3.4% (prevalence), equivalent to 3,400 PW in 100,000 women. Assuming 95% (3,230) of PW accessing prenatal care, of which 95% (3,068) are tested for syphilis, and 95% (2,915) receive adequate treatment, 485 women would still lack access to adequate care, potentially resulting in CS cases. This translates to an incidence of 4.8/1000 live births, half the national rate reported in 2023.
Conclusion: Even with 95% coverage of prevention measures for CS, Brazil would still face a CS incidence rate 10 times higher than the 2030 elimination target of 0.5 per 1000 live births. These findings reinforce the urgent need to strengthen syphilis prevention efforts across the general population, leading to a reduction of syphilis rates during pregnancy and improving maternal and child health outcomes.
PP04.45 – Surveillance of Children with HIV Infection Aiming at the Elimination of Mother-To-Child Transmission of HIV in Brazil
Dr. Leonor Henriette De Lannoy1, Mr Ítalo Vinicius Albuquerque Diniz1, Dr Angélica Espinosa Miranda2, Dr Pâmela Gaspar1, Dr Draurio Barreira1
1Department of HIV/Aids, Tuberculosis, Viral Hepatitis, and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
2Federal University of Espírito Santo, Vitória, Brazil.
Background: Brazil, with a population of approximately 216 million, has an estimated HIV prevalence in pregnant women of 0.4/1000 live births. The country’s universal health system offers free access to HIV diagnostic tests, antiretroviral treatment, pre-exposure prophylaxis, and pos-exposure prophylaxis. Since 1989, Brazil’s HIV/AIDS response has integrated all available technologies to reduce Mother-to-child transmission (MTCT). Epidemiological monitoring is conducted via the Notifiable Diseases Information System (SINAN). However, underreporting in SINAN, particularly of children exposed to or infected with HIV, poses a significant challenge to achieving MTCT elimination. To address this issue, a national routine was established to reduce underreporting and enhance data accuracy to ensure the achievement of the goal of eliminating MTCT in the country.
Description: The strategy involved (1) linking multiple information systems, including SINAN, the Mortality Information System, the Laboratory Test Control System, and the Medication Logistics Control System; (2) Creating a centralized Excel database identifying the source system Federative Unit (UF) of each child; (3) Tasking coordinators from all 27 UFs to investigate, verify, and report cases not previously included in SINAN; and (4) Providing feedback to the Ministry of Health regarding the investigation process and outcomes.
Results: A total of 458 children born in 2021–2022, were identified as infected or potentially infected with HIV. By June 2023, 121(26.4%) were registered in SINAN. Following investigation across all UFs, 326(71.1%) cases were confirmed, comprising 180 born in 2021 and 146 in 2022. Excluded cases included non-children, HIV-exposed but uninfected children, or duplicates records.
Conclusion: This investigative routine facilitates early detection of HIV infection in children, improving their retention in health services and supporting enhanced prevention and control strategies. It also identifies regions with significant gaps in reporting and demonstrates Brazil’s efficient program for preventing MTCT of HIV.
PP04.46 – Cervical Cancer in Women Living with HIV in Brazil: Epidemiological Analysis
Mrs Carolina De Marqui1, Dr Gabriel Antonio Cabriott Dumbra1
1Faceres, São José do Rio Preto, Brasil.
Background: Cervical cancer is closely associated with human papillomavirus (HPV) infection. It is the most common cancer among women living with HIV. The increase in risk is related to the reactivation of the previous infection, and could vary according to the oncogenic subtype. The HPV vaccine was introduced into the Brazilian vaccination calendar in 2014 and expanded to people living with HIV with the intention of reducing the incidence and mortality of the disease.
Methods: This is an epidemiological, descriptive, cross-sectional study. The data were obtained via the Notifiable Diseases Information System (SINAN) and the Cancer Information System (SISCAN), analyzing cases reported from 2019 to 2023, covering race, age group and clinical evolution.
Results: The data showed an overlap between HIV and human papillomavirus infection. In Brazil, 215,793 cases of cervical cancer were registered between 2019 and 2023, based on data from SISCAN. During the period, the prevalence of cervical HPV infection in HIV-positive women was approximately 57.8% (26,503). Furthermore, 17.3% (7,932) presented cervical intraepithelial neoplasia (CIN) on cytology, with a higher incidence in the Northeast and Southeast regions. The most affected group were women aged 35 to 45 (55.43%). Additionally, 53.89% of cases occurred in individuals who declared themselves mixed race.
Conclusion: Data showed a relevant association, highlighting the high rate of HPV infection in HIV-positive women and the occurrence of cervical intraepithelial tumors, particularly in women between 35 and 45 years and in more susceptible subgroups. The inclusion of the HPV vaccine for women living with HIV in the vaccination schedule in Brazil represents significant progress in prevention, however, other epidemiological factors can interfere with the development of cervical cancer.
PP04.47 – Syphilis Screening and Birth Outcomes Among Pregnant Oral HIV Pre-Exposure Prophlyaxis Users, Cape Town, South Africa, 2024
Dr. Alex de Voux1, Ms Kalisha Bheemraj1, Ms Rufaro Mvududu1, Dr Sumaya Dadan1, Professor Landon Myer1, Dr Dvora Joseph Davey1,2,3
1Division of Epidemiology & Biology, School of Public Health, University of Cape Town, Cape Town, South Africa.
2Division of Infectious Diseases, David Geffen School of Medicine, University of California Los Angeles, Los Angeles, United States of America.
3Department of Epidemiology, Fielding School of Public Health, University of California Los Angeles, Los Angeles, United States of America.
Background: Syphilis is a sexually transmitted infection caused by Treponema pallidum, which during pregnancy is associated with adverse birth outcomes, including stillbirth. We determined syphilis seropositivity and its association with adverse birth outcomes among pregnant oral HIV PrEP users in Cape Town, South Africa.
Methods: We enrolled HIV-negative pregnant women on oral PrEP (TDF/FTC) ≥16 years between September 2023 and May 2024 into a randomized controlled trial evaluating biofeedback on oral PrEP adherence. We obtained antenatal syphilis screening and birth outcomes from pregnancy and birth records. We determined the prevalence and correlates of syphilis seropositivity (past-treated: TPHA+/RPR- or active: TPHA+/RPR+) and used multivariable logistic regression to evaluate adverse birth outcomes – stillbirth, neonatal or infant death, preterm birth, and low birthweight (<2500 g)—by syphilis seropositivity (TPHA+ versus TPHA-).
Results: We ascertained birth outcomes for 737 of 750 participants (98%) – median age 26 years (IQR 21–32) and median gestational age 29 weeks (IQR 23–35). Syphilis seropositivity (TPHA+) was 11% (n = 83) overall, with 47% (n = 39) also RPR+. Stillbirth prevalence was 2% among TPHA+ and 0.8% among TPHA- participants (odds ratio [OR] = 3.2; 95% CI: 0.6–16.8). Active syphilis in pregnancy was associated with younger age (<25 versus ≥25 years, OR = 2.6; 95% CI: 1.3–5.3), primigravidity (OR = 1.9; 95% CI: 1.0–3.8), and any alcohol use in the last year (OR = 2.2; 95% CI: 1.1–4.2). Overall, 14% of participants had an adverse birth outcome (n = 97) with no difference by syphilis seropositivity (TPHA+ versus TPHA–) (aOR = 1.0; 95% CI:0.5–1.9), adjusting for maternal age and relationship status.
Conclusion: We report a high prevalence of syphilis and adverse birth outcomes in a cohort of pregnant oral PrEP users. Syphilis seropositivity was not associated with an increased prevalence of adverse birth outcomes, though stillbirths were more prevalent among seropositive compared to seronegative participants. High gestational syphilis seroprevalence emphasizes the importance of antenatal syphilis screening and treatment for pregnant women and partners.
Table 1_Syphilis Screening and Birth Outcomes.pdf (could not be inserted).
PP04.48 – Estimating Genital Herpes Prevalence and Treatment Patterns Among US Healthcare-Engaged Individuals: Insights from Claims DataEstimating Genital Herpes Prevalence and Treatment Patterns Among U.S. Healthcare-Engaged Individuals: Insights from Claims Data
Dr. Lian Liu2, Dr Christine Johnston3, Dr Min Seo4, Dr. Katie Kitrinos1, Dr. Anuj Gaggar1, Mr. Jason Deer1
1Assembly Biosciences, South San Francisco, United States.
2Clearview Healthcare Partners, New York, United States.
3University of Washington, Seattle, United States.
4Adsum Consulting, San Carlos, United States.
Background: Genital herpes (GH), caused by Herpes simplex virus types 1 and 2 (HSV-1 and HSV-2), is a prevalent sexually transmitted infection in the US, associated with significant morbidity, psychosocial burden, and increased HIV acquisition risk. Traditional epidemiological methods can underestimate real-world healthcare patterns. This study analyzed claims-based data to evaluate GH prevalence, recurrence, and treatment trends.
Methods: Using Forian’s hybrid claims and electronic health record (EHR) database (01/01/2021–12/31/2023), 40,428,823 individuals with consistent medical and pharmacy claims were analyzed. GH cases in 2023 were identified via ICD-10-CM codes: A60% for GH (including 2021-2022 confirmed cases receiving antiviral therapy) and B00% for HSV with GH symptoms or EHR-confirmed diagnoses. Recurrent GH (RGH) was defined as ≥90 days of annual antiviral use or ≥2 care episodes ≥28 days apart. Treatment patterns were categorized as chronic suppressive (≥180 days), intermittent suppressive (90–179 days), or episodic therapy (<90 days).
Results: In 2023, 262,457 GH cases and 148,067 RGH cases were identified, with the highest prevalence in females and individuals aged 18–39. Among all GH patients, 32% received chronic or intermittent suppressive therapy, 40% used episodic therapy, and 28% received no treatment. Among RGH cases, 97% received pharmacologic treatment (57% chronic or intermittent suppressive; 40% episodic). Standardized prevalence rates were 714 (95% CI: 703–725) per 100,000 person-years for GH and 408 (95% CI: 402–415) for RGH. Extrapolated to the U.S. population, approximately 2.39 million seek care for GH, including 1.35 million for recurrent GH, with 763,017 on a suppressive regimen.
Conclusions: This analysis highlights a substantial burden of GH in the U.S., with variable antiviral usage patterns. The true burden is likely greatly underestimated due to undiagnosed cases and those outside the healthcare system. Findings emphasize the need for improved diagnostics, treatment options, and targeted interventions for sexually active individuals.
PP04.49 – Exploring the Potential Impact of a Chlamydia Vaccine in the US Population Using an Agent-Based Model
Dr. Qi Deng1, Grégoire Ranson1,2, Nicola Luigi Bragazzi1,3,4, Valerie Bosch Castells5, Sandra Chaves5, Edward Thommes6,7, Jianhong Wu1
1York University, Toronto, Canada.
2Université Claude Bernard Lyon 1, Lyon, France.
3University of Parma, Parma, Italy.
4Saarland University, Saarbrücken, Germany.
5Sanofi, Lyon, France.
6Sanofi, Toronto, Canada.
7University of Guelph, Guelph, Canada.
Background: Chlamydia trachomatis (CT) infection is the most reported bacterial sexually transmitted infection in the United States (US). Despite many cases being asymptomatic, infection can lead to complications such as pelvic inflammatory disease (PID) in females, and infertility in both females and males. Using a transmission dynamics model, we evaluated the impact of a potential CT vaccine on the prevalence of CT infections and associated PID in the US population.
Methods: An agent-based model with an evolving sexual contact network that considers heterogeneous partnership preferences was developed to simulate the individual-level dynamics of CT infection in the US. The calibration was performed in two steps: first, to US national-level, age- and sex-specific CT prevalence rates estimated from the 2015_2018 cycles of the National Health and Nutrition Examination Survey (NHANES); and then, to age-specific prevalence of female PID estimated from 2013_2016 cycles of the NHANES. With the calibrated model, we evaluated the impact of different scenarios of vaccination coverage and targeting, assuming a vaccine with 80% efficacy against infection and a 5-year duration of protection.
Results: The impact of different scenarios can be seen in Fig. 1. A vaccination coverage rate of 60% across the US population in ages 15–44 could result in 62.9 (60.9, 64.9)% reduction in CT prevalence, and for females, a 19.9 (17.1, 22.7)% reduction in all-cause PID. Prioritizing only females would require very high vaccination coverage (90%) to achieve similar reduction in CT prevalence in the general population (58.9 (53.9, 63.9)%) and PID prevalence in females (12.8 (10.5, 15.1)%).
Conclusion: A gender-neutral vaccine recommendation is projected to achieve the highest impact, even with moderate vaccination coverage. These findings highlight the critical role vaccination could play in controlling CT and its complications, offering actionable guidance for policymakers and vaccine developers.
PP04.50 – Vagisim: Modeling the Interplay Between Vaginal and Penile Microbiomes in Sexual Activity to Predict BV Prevalence and HIV Risk
Miss Lillian Dillard1, Robyn Stuart2, Daniel Klein1, Francesca Mazzola4, Sharon Achilles3, Jamie Cohen1
1Institute for Disease Modeling, Global Health Division, Bill & Melinda Gates Foundation, Seattle, United States.
2Gender Equality Division, Bill Melinda Gates Foundation, Seattle, United States.
3Discovery and Translational Sciences, Global Health Division, Bill & Melinda Gates Foundation, Seattle, United States.
4Foundation Strategy Office, Bill & Melinda Gates Foundation, Seattle, United States.
Background: Bacterial Vaginosis (BV) increases risk of HIV and other sexually transmitted infections (STIs) and is linked to new and concordant sexual partners. Historically, BV has not been classified as an STI, but emerging evidence implicates the penile microbiome (PMB) in BV incidence and recurrence in female partners. Bidirectional transmission of vaginal microbiota (VMB) to partner’s PMB is also supported, with shared taxa associated with both BV and HIV seroconversion risk. This study uses VagiSim, an agent-based model of VMB compositional changes, to explore the impact of sexual transmission of BV and its secondary impact on HIV risk.
Methods: Using VagiSim, we simulated within-agent VMB dynamics using two model structures: one assuming bidirectional BV-associated microbe sexual transmission, and another assuming BV occurrence is driven by new and recent sexual partners but not explicitly sexually transmitted. The transmission-based model evaluates how connectivity and sexual history affect BV prevalence and recurrence. Agents are assigned durable community state types (CST), based on CST distributions from the South African FRESH cohort, which moderate the risk of CST transitions. Comparing these models clarifies BV recurrence drivers and evaluates interventions with or without sexual network transmission.
Results: The sexual-network transmission model explains high BV recurrence rates by capturing the role of sexual partner history. It also highlights how shared VMB and PMB taxa amplify HIV risk for both sexes showing the potential for BV-associated PMB microbes to facilitate HIV seroconversion. Interventions, like male circumcision and vaginal probiotics reduce BV prevalence more effectively in the transmission model, emphasizing the impact of VMB interventions to mitigate HIV risk.
Conclusion: Investigating BV transmission within sexual networks is critical for understanding recurrence and HIV burden. VagiSim provides a framework for evaluating targeted interventions for reducing BV prevalence and improving HIV prevention. Further research into PMB and VMB interactions is essential.
PP04.51 – Prevalence of Condyloma Acuminatum and Genital Herpes Ulcers in the Population Attended at an STI Referral Service in Amazonas, Brazil
Dr Carolina Talhari, Dr. Angelica Espinosa Miranda1, Dr Maria das Graças Barbosa Guerra, Celilia Lima Borges, Dr Jose Carlos Sardinha, Dr Valderiza Lourenço Pedrosa, Ana Claudia Chaves Camilo, Silvana Paiva da Costa, Jamile Izan Lopes Palheta Júnior, Camila Gurgel Santos Silva, Cynthia Oliveira Ferreira, Dr Sinesio Talhari
1Universidade Federal Do Espírito Santo, Vitoria, Brazil.
Background: Understanding the epidemiology of genital warts and ulcers is essential to prevent associated complications and develop effective control strategies, such as vaccination and health education. This study aimed to estimate the prevalence of condyloma acuminatum and genital ulcers caused by herpes simplex virus over a historical series at a referral service for sexually transmitted infections (STIs) in the state of Amazonas, Brazil.
Methods: This was a descriptive and retrospective study based on the analysis of medical records of patients attended at the Alfredo da Matta Foundation, a referral center for STIs in Amazonas, Brazil, from January 2014 to December 2023. Sociodemographic, behavioral, and clinical data were analyzed to identify the presence of genital warts and vesicular-associated genital ulcers suggestive of herpes. Descriptive analyses were performed to determine absolute and relative frequencies and trends in patient profiles and diagnostic patterns over time.
Results: During the analyzed period, 22,160 individuals sought care, with a reduction observed during the COVID-19 pandemic years. The diagnostic pattern for condyloma acuminatum and genital ulcers remained constant throughout the historical series. Among those attended, 72.1% were male, 25.9% were married or reported living together, 13.4% reported homosexual relations, 41.6% had casual partners, and 46.0% reported they did not use condoms. Genital warts were identified in 6,184 cases (27.9%), while genital ulcers suggestive of herpes were observed in 1,239 cases (5.6%).
Conclusion: The prevalence of condyloma acuminatum and genital ulcers underscores the substantial burden of these conditions within the attended population. Since most HPV and genital herpes infections are asymptomatic, the actual frequency of these conditions could be significantly higher. These findings reinforce the role of specialized services in managing STIs to control and mitigate the impact of symptomatic STIs on public health.
PP04.52 – Substantial Increase in the Proportion of Heterosexual Females Who Ever Had Anal Sex Over Generations in Canada
Mr. Sullivan Evain1,2, Dr Melanie Drolet1, Prof Marc Brisson1,2
1Centre de recherche du CHU de Québec - Université Laval, Québec, Québec, Canada, Québec, Canada.
2Université Laval, Québec, Canada.
Background: Although anal sex has mostly been associated with homosexuality, this practice seems to be increasing among heterosexuals, which would have important public health implications. However, little quantitative data exist to document age-cohort changes in the proportion of heterosexuals that have anal sex. We aimed to examine the evolution of anal sex across generations, among Canadian heterosexual females.
Description: CONNECT is a pan Canadian population-based study of social/sexual contacts conducted in 2018–2019. Participants were recruited by random digit dialing and data was collected using self-administered online questionnaires. Questionnaires documented sociodemographic, behavioral and sexual characteristics (including insertive/receptive anal sex). Our main analysis focussed on receptive anal sex among heterosexual females. Anal sex among heterosexual/non-heterosexuel males was examined in additional anayses. The main outcome was the proportion of females who ever had receptive anal sex by age (e.g., age 20, 30,…, 60 yrs) by generation (silent generation, baby boomers, and generations X, Y and Z). Sociodemographic and behavioral characteristics associated with ever having anal sex were examined by generation.
Results: The study included 1,288 heterosexual females. The lifetime proportion of females who ever had anal sex increased substantially over generations (Fig. 1). For example, the propropotion of heterosexual females who ever had anal sex by age 20yrs was 1% for the silent generation, 3% for baby boomers, 8% for generation X, and >20% for generations Y and Z. Factors associated with ever having anal sex were smoking, alcohol/drug use, and having had an STI. Patterns were similar for heterosexual males, but there were little differences for non-heterosexual males (incertive/receptive) over generations.
Conclusion: Ever having anal sex increased dramatically over generations among Canadian females, with earlier age of initiation. Better understanding the evolution of anal sex behaviours is essential to predict the evolution of STIs linked to this practice, and optimise prevention strategies.
PP04.53 – Factors Associated with Universal Prenatal Syphilis Screening: A Population-Based Retrospective Cohort Study in Ontario, Canada
Ms. Amanda Featherstone1, Hannah Willms2, Dr. Megan Carter1,3, Dr. Maria B. Ospina1, Dr. Maria P. Velez4, Dr. T Hugh Guan3, Dr. Melissa Richard-Greenblatt5, Dr. Vanessa Tran6,7, Dr. Jennifer Flemming1,8, Dr. Sahar Saeed1
1Department of Public Health Sciences, Queen’s University, Kingston, Canada.
2ICES, Queen’s University, Kingston, Canada.
3Kingston, Frontenac and Lennox & Addington Public Health (KFL&A), Kingston, Canada.
4Department of Obstetrics and Gynecology, McGill University Health Centre, Montreal, Canada.
5Hospital for Sick Children (SickKids), Toronto, Canada.
6Public Health Ontario, Toronto, Canada.
7Department of Laboratory Medicine and Pathobiology, University of Toronto, Toronto, Canada.
8Department of Medicine, Queen’s University, Kingston, Canada.
Background: Since 2018, rates of congenital syphilis in Canada have increased by 599%. Canadian prenatal syphilis screening guidelines recommend universal screening for all pregnant people during the first trimester or initial prenatal visit. This study evaluated adherence to first-trimester syphilis screening and investigated individual-, provider-, and system-level factors influencing screening practices.
Methods: We conducted a retrospective cohort study using administrative health data from Ontario, Canada, including residents with universal provincial health insurance (approximately 97% of 16 million residents). Inpatient birth admission records were used to identify eligible pregnant people between January 2018 and March 2023. Provincial laboratory records of syphilis serology screening (chemiluminescent microparticle immunoassay) were used to determine receipt of prenatal syphilis screening. Using a modified Poisson regression with robust standard error estimates, we examined the association between non-adherence to screening guidelines and the following risk factors: maternal age, socioeconomic status by neighbourhood-level income, health region, receipt of prenatal care, and trimester of prenatal care initiation. Adjusted relative risks (aRR) and 95% confidence intervals (CI) were reported.
Results: In this study, we included 476,342 pregnancies, the median maternal age at conception was 31 years (interquartile range, 28–34), of which 374,053 (78.5%) received first-trimester prenatal syphilis screening. No first-trimester syphilis screening was associated with the absence of prenatal care (aRR, 2.76; 95% CI, 2.71–2.81), initiation of prenatal care after the first trimester (2.71; 2.68–2.74), younger age at conception (15–19 years: 1.50; 1.46–1.54; 20–24 years: 1.24; 1.22–1.26, compared to ages 30–34), living in neighbourhoods with the lowest income quintile (1.13; 1.11–1.15), and living in Northern Ontario (1.05; 1.03–1.07).
Conclusion: More than 1 in 5 pregnant people in Ontario were not screened for syphilis during their first trimester and there were significant socio-demographic and geographic inequities. Public health response efforts should focus on evaluating and strengthening syphilis-targeted programs and interventions to increase fidelity to universal guidelines.
PP04.54 – Congenital Syphilis in England: from Awareness to Action
Dr. Helen Fifer1, Professor Margaret Kingston2, Professor Hermione Lyall3, Professor Claire Thorne4, Dr Katy Sinka1
1UKHSA, London, United Kingdom.
2Manchester University NHS Foundation Trust, Manchester, UK.
3Imperial College Healthcare NHS Trust, London, UK.
4UCL Institute of Child Health, London, UK.
Background: In 2023 there were 9,513 diagnoses of infectious syphilis in England, the highest number since 1948. Most infections are diagnosed in men who have sex with men (MSM), but since 2019, infections in women have risen 36% (from 272 to 825 cases). Systematic surveillance of congenital syphilis (CS) in England started in 2020, with a look-back to 2015. Here we review lessons learned.
Description: Detailed information is collected for all cases by the Integrated Screening Outcomes Surveillance Service within the NHS Infectious Diseases in Pregnancy Screening Programme, including: maternal treatment, relevant social and safeguarding issues, laboratory results, infant presentation and treatment. Cases are reviewed by a clinical panel and contributing factors identified.
Results: Between January 2015 and September 2023, 55 confirmed cases of CS were reported. Most mothers were English of white ethnicity, >50% with adverse social circumstances. 35% were diagnosed antenatally; CS occurred due to: booking late and delivering before treatment could be completed, declining treatment, incorrect management (including use of macrolides in penicillin allergy) and re-infections. Of those diagnosed postnatally, most had a negative screen in early pregnancy and acquired syphilis in later pregnancy, most had no identifiable risk factors. Some women presented with symptoms/signs of syphilis but were not offered repeat testing.
Conclusion: Actions have included: new national guidelines on the management of syphilis in pregnancy and children; removal of macrolides as a treatment option; updated guidance on the investigation of rashes in pregnancy, to include syphilis testing; new laboratory guidelines to include syphilis PCR for investigation of possible CS; education of healthcare professionals to increase awareness of syphilis; and a review of the screening programme to consider repeat screening for syphilis in later pregnancy. Ultimately measures are needed to tackle the wider syphilis epidemic in England, which will include doxycycline post-exposure prophylaxis in MSM.
PP04.55 – Frequency of and Factors Associated with Frequent Sexually Transmitted Infection Testing in Gay, Bisexual, and Other Men Who Have Sex with Men, United Kingdom, 2023
Miss Lucy Findlater1,2, Mr George Baldry2, Ms Ana Karina Harb2, Ms Dolores Mullon2, Ms Dawn Phillips2, Ms Erna Buitendam2, Ms Catherine M. Lowndes2, Mr David Reid3, Professor Catherine H. Mercer3, Dr John Saunders2, Ms Dana Ogaz2, Dr Hamish Mohammed2,3,4
1UK Field Epidemiology Training Programme, UK Health Security Agency, London, United Kingdom.
2Division of Blood Safety, Hepatitis, STIs and HIV, UK Health Security Agency, London, United Kingdom.
3Institute for Global Health, University College London, London, United Kingdom.
4National Institute for Health and Care Research Health Protection Research Unit in Blood Borne and Sexually Transmitted Infections at University College London in partnership with the UK Health Security Agency, London, United Kingdom.
Background: In the UK, gay, bisexual, and other men who have sex with men (GBMSM) with high-risk sexual behaviours are recommended to test quarterly for sexually transmitted infections (STIs), but it is not known how many are following this recommendation. We describe the prevalence and correlates of frequent STI testing amongst GBMSM in the UK.
Methods: We analysed data on participants of the community-based Reducing Inequalities in Sexual Health (RiiSH) online survey of GBMSM, all of whom were recruited from November to December 2023 via social media and dating apps. Participants were UK residents aged over 16 years. We described the frequency of STI testing amongst individuals who would be recommended quarterly testing following national guidelines. This was assessed using proxies for quarterly testing eligibility (any of the following over the past 3 months: any new male sexual partner, condomless anal sex (CAS), 10+ male partners, or chemsex). We explored factors associated with frequent testing (defined as having at least four tests in a year) using univariate and multivariable logistic regression.
Results: Among 1106 participants (median age 44 years, 89% white), we estimated 918 individuals (83%) would be recommended quarterly STI testing. In this group, over the past year, 196 individuals (21%) tested at least 4 times, 461 (50%) tested 1–3 times, and 261 (28%) did not test (Fig. 1). Factors associated with frequent testing were use of HIV pre-exposure prophylaxis (HIV-PrEP) in the past year (adjusted odds ratio 9.51 (95% confidence intervals 5.89–16.10)), STI diagnosis in the past 3 months (2.46 (1.49–4.08), and younger age (2.07 (1.17–3.62), aged 16–29 years vs ≥45 years).
Conclusion: Our findings suggest that only 1 in 5 eligible GBMSM test frequently for STIs, and those that do are more likely to engage in preventive interventions such as HIV-PrEP.
Frequency of STI testing in the last year amongst GBMSM in the UK who would be recommended to test quarterly, 2023 (n = 917).
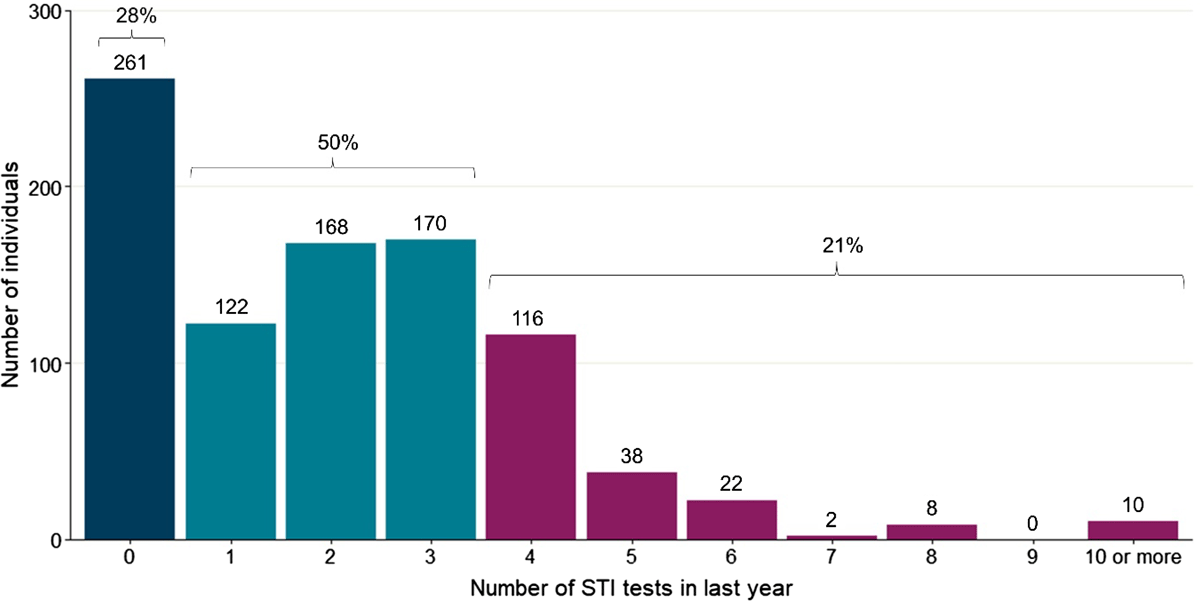
Figure legend: Graph showing the number of STI tests taken in the last year by individuals in the RiiSH 2023 survey. The graph is annotated with the percentage of the sample who had 0, 1-3, or at least 4 tests in the past year. The graph includes 917/918 individuals who would be recommended quarterly testing. One individual who had tested in the last year but did not remember the number of times was excluded.
PP04.56 – Disparities in Hawaiʻi STI Counseling: Assessing Disparities in Self-Reported STI Counseling Pre-Pregnancy Using Hawaiʻi Pregnancy Risk Assessment Monitoring System (PRAMS), 2019–2022
Miss Breena Gaskov1, Jane Awakuni2, Dr. Jonathan Huang1, Dr. Alan R. Katz1
1University of Hawaiʻi at Mānoa, Honolulu, United States.
2Hawaiʻi Department of Health, Honolulu, United States.
Background: Sexually transmitted infections (STI), especially congenital syphilis (CS), are a growing public health concern in the United States. In Hawaiʻi, there has been an 188% rise in syphilis and 575% increase in CS from 2018 to 2022, ranking Hawaiʻi 10th in the nation for CS prevalence. Native Hawaiian and Pacific Islander populations experience disproportionately higher CS prevalence. The aim of this study was to examine disparities in self-reported receipt of pre-pregnancy STI counseling to assess missed opportunities for CS interventions.
Methods: Data from the 2016–2022 Hawaiʻi Pregnancy Risk Assessment Monitoring System (PRAMS) were used to examine the frequency of receipt of healthcare providers’ counseling regarding STIs amongst PRAMS respondents who reported any healthcare visits. Survey-weighted counts, proportions, and logistic regression models were used to describe and assess associations between counseling receipt and maternal race/ethnicity, county of residence, and age group.
Results: Overall, 27.5% of participants who reported any pre-pregnancy healthcare visits reported receiving STI counseling at those visits. Although less likely to report any pre-pregnancy healthcare visits, Other Pacific Islanders were significantly more likely to receive STI counseling (OR = 2.72, 95% CI: 1.49–4.97), and Japanese participants (OR = 0.76, 95% CI: 0.47–1.24) were less likely to receive STI counseling compared to White participants.
Conclusion: This study highlights differences in STI counseling prevalence among reproductive-age women in Hawaiʻi by race, county, and age. While Other Pacific Islanders reported relatively higher proportions of STI counseling, a minority reported having any pre-pregnancy healthcare visits, which may mask larger disparities. Congress attendees will gain insights into identifying and addressing hidden disparities through disaggregated data and can apply this knowledge to promote provider education, reduce biases, and improve sexual healthcare delivery within their communities.
PP04.58 – Assessing the Impact of Population Testing Patterns on Observed Infectious Syphilis Surveillance Case Rates, 2010–2022, British Columbia, Canada
Dr. Mark Gilbert1,2,3, Shabnam Fahni1, Hsiu-Ju Chang1,3, Venessa Ryan1, Elaine Chan1, Amanda Yu1, Dr. Jason Wong1,2, Dr. Kirsty Bobrow1, Dr. Troy Grennan1,2,3, Dr. Sofia Bartlett1,2,3
1British Columbia Centre for Disease Control, Vancouver, Canada.
2University of British Columbia, Vancouver, Canada.
3University of British Columbia Centre for Disease Control, Vancouver, Canada.
Background: Population syphilis rates based on surveillance case reports are a commonly used proxy for incidence yet dependent on population testing patterns. While adjusting for testing may be more valid, comprehensive data is often unavailable. We aimed to assess the impact of testing patterns on infectious syphilis case rates using comprehensive provincial data in British Columbia (BC).
Methods: We used infectious syphilis case and syphilis laboratory testing data from the BC Centre for Disease Control and Laboratory (which conducts >99% of all syphilis testing in BC) from 2010 to 2022. We examined two time periods of rising cases: 1) 2010–2017, outbreak concentrated among men who have sex with men (MSM); 2) 2018–2022, outbreak among MSM and heterosexual populations. We compared case rates (cases/100,000 population) and percent positivity (cases/individuals tested) by overall trends and the magnitude of change (ratio between values at start and end years of each period), stratified by gender.
Results: The trends for both measures were similar for both time periods (Fig. 1). During period 1, percent positivity ratios were 22–37% lower (2017:2010 case rate and percent positivity ratios respectively: BC 4.06, 2.92; males 4.19, 2.63; females 2.50, 1.93.) During period 2, ratios were more similar (2022:2018 case rate and percent positivity ratios respectively: BC 2.00, 1.92; males 1.53, 1.56; females 9.78, 9.11).
Conclusion: Trends being similar for both measures during both periods affirms the validity of infectious syphilis case rates as a proxy measure for incidence. However, adjusting for population testing patterns using percent positivity reduced the observed magnitude of the increasing trend during period 1 only (GBMSM outbreak), which may be related to population differences in testing frequency during these two time periods. Development of further measures accounting for population testing patterns may be helpful (e.g., linking case and laboratory data to account for testing frequency on case rates).
Comparison of infectious syphilis case rates and percent positivity*, British Columbia, 2010–2022.
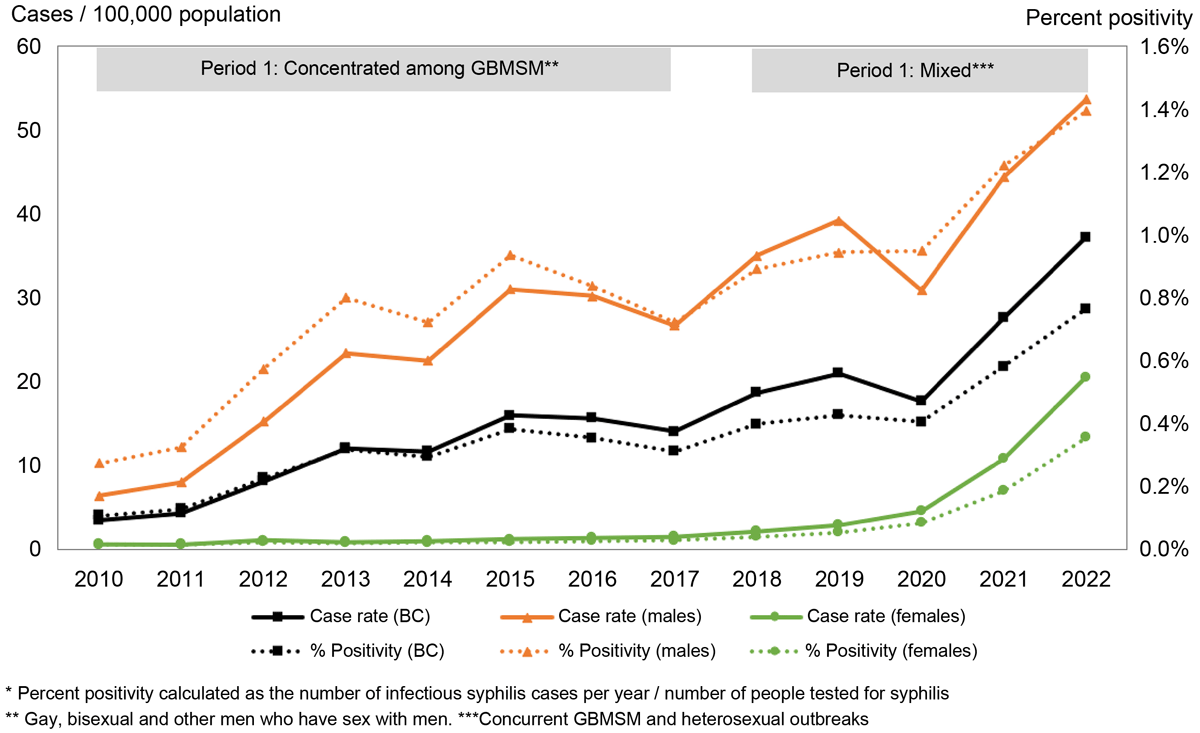
PP04.59 – Evaluating Sexually Transmitted and Blood-Borne Infection Prevalence and Screening Needs in Hamilton Shelter Clients
Ms. Jodi Gilchrist1,2, Kelly Waters2, Sarah Marttala2, Doris Williams2, Zayn Brar1,2, Alex Martindale2, Julio Diaz L’Hoeste1,2, Ian Restall2, Amjad Arrabi2, Kerry Beal3, Marek Smieja1,2
1McMaster University, Hamilton, Canada.
2Research St. Joseph’s - Hamilton, Hamilton, Canada.
3Shelter Health Network, Hamilton, Canada.
Background: Individuals experiencing homelessness face a disproportionate risk for acquiring infectious diseases including sexually transmitted and blood-borne infections (STBBIs) like Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), and Mycoplasma genitalium (MG). A recent systematic review found that people experiencing homelessness in Canada and the United States are at an increased risk of CT, NG, Treponema pallidum, and Trichomonas vaginalis (TV), highlighting the need for improved STBBI screening services. This study was undertaken to assess the prevalence of STBBIs in those accessing shelter services in Hamilton, ON and evaluate the need for integrated screening and treatment strategies.
Methods: Clients from nine shelter locations in Hamilton, ON participated in this two-part study. Part one involved an anonymous survey on attitudes, beliefs, and knowledge regarding STBBIs. Part two involved self-collected urine (male) or self-collected urine and vaginal swab (female), tested for CT, NG, MG, TV, and human papillomavirus (HPV) using the Panther Fusion® and BD MaxTM.
Results: To date 265 participants (59.6% male, 40.4% female) have been recruited. Roughly 67% of participants reported not having been tested for an STBBI in the last 12 months; of those who have been tested (33%), 14% were tested 3 or more times. About 50.5% of participants have had at least one sexual partner in the last year and 4.5% have had 10 or more partners. Roughly 25% of participants had at least one infection and the prevalence of CT, NG, MG, TV, and HPV was 1.6%, 1.2%, 5.5%, 3.6%, and 4.4%, respectively. In women, the prevalences were 4.3%, 4.3%, 10.9%, 9.1%, and 18.7%, respectively.
Conclusion: Overall, the prevalence of these five STBBIs was relatively low in the population screened. However, women accessing shelter services appear to be at an increased risk of acquiring one or more STBBI, underscoring the need for advanced screening strategies at these sites.
PP04.60 – Risk of Stroke in People with Syphilis: A Nationwide Population-Based Matched Cohort Study
MD, MSc TMIH Laura Glismann1,2, BMSc Emilie With Hall Petersen3, MD Simone Høstgaard1,2, MD, DMSc Steen Hoffmann2, MD, DMSc Jørgen Skov Jensen2, MD PhD Jan Gorm Lisby4, MD DMSc Terese Katzenstein3, MD, PhD Maria Wessman2, MD PhD Kirsten Salado-Rasmussen1,2,5, MD, DMSc Lars Haukali Omland2,3,5
1Bispebjerg University Hospital, Copenhagen, Denmark.
2Statens Serum Institut, Copenhagen, Denmark.
3Rigshospitalet University Hospital, Copenhagen, Denmark.
4Copenhagen University Hospital, Amager and Hvidovre, Copenhagen, Denmark.
5Copenhagen University, Copenhagen, Denmark.
Background: Syphilis disseminates to the central nervous system shortly after inoculation and an association with stroke has been proposed. As syphilis has re-emerged in recent decades, and previous studies have been biased by the use of healthy comparators, updated data on the risk of stroke after syphilis diagnosis is highly needed.
Methods: We conducted a nationwide population-based matched cohort study of all people with syphilis (defined as a positive test for non-treponemal and treponemal antibodies) in Denmark from 2000 to 2023 compared with a cohort of people with negative syphilis serology, matched 1:1 on sex and age. As a measure of relative risk, Cox regression was used to calculate hazard ratios (HRs) and corresponding 95% confidence intervals (CIs) for diagnosis of stroke in a time-updated analysis. Individuals with stroke before study inclusion were excluded from the analyses.
Results: We identified 5,085 persons for each of the two cohorts, of whom 50 and 63 were diagnosed with stroke before study inclusion, which left 5,035 people in the syphilis cohort and 5,022 people in the negative cohort for analyses. The median age was 35 years and 78% were male. We observed no difference in risk of stroke between the two cohorts, neither in the entire study period (HR: 1.2 (95% CI: 0.8–1.9) or in the time-updated analyses (HR<5 years: 1.0 (95% CI: 0.6–3.4) and HR>=5 years: 1.7 (95% CI: 0.8–3.4)) (Fig. 1).
Conclusion: Contrary to previous reports, we did not demonstrate any increased risk of stroke among people with syphilis, which could be explained by the more appropriate use of comparator in our study. Our study should serve as a reassurance for people with syphilis.
PP04.61 – Detection of Treponema Pallidum Nucleic Acid by Anatomic Site and Syphilis Stage and Association of Detection with Prior Syphilis
Dr. Matthew Golden1,2, Anna Berzkalns2, Kate Holzhauer1, Dr. Sheila Lukehart1, Dr. Damon Getman3, Dr. Paul Swenson2, Dr. Olusegun Soge1
1University of Washington, Seattle, United States.
2Public Health - Seattle & King County, Seattle, United States.
3Hologic, San Diego, USA.
Background: Nucleic acid amplification test positivity is a surrogate for bacterial shedding during T. pallidum (Tp) infection. Prior studies have documented Tp shedding patterns among men who have sex with men (MSM) and suggest that Tp infection confers partial immunity from symptomatic re-infection. Tp shedding patterns among women are ill-defined, and the impact of prior infection on shedding is unknown.
Methods: We used a Tp transcription-mediated assay to test remnant specimens from persons diagnosed with syphilis in a sexual health clinic in Seattle, WA, July 2021–November 2024. Specimens included serum, rectal, pharyngeal swabs, and urine from MSM and transgender(TG)/nonbinary(NB) persons assigned male at birth (AMAB) who have sex with men (MSM/TGNB); serum and urine from men and other AMAB with female sex partners (MSW/AMAB); and serum, pharyngeal and vaginal specimens from persons assigned female at birth (AFAB).
Results: The study population included 500 MSM/TGNB, 99 MSW/AMAB, and 114 AFAB with new syphilis diagnoses. Among MSM/TGNB, detection in pharyngeal and rectal samples was highest in secondary syphilis (Fig. 1). Tp detection in vaginal specimens was 50%, 75%, and 43% in primary, secondary, and early latent infection, respectively. Tp detection in urine was higher in P&S syphilis in MSW/AMAB than in MSM (P = 0.0012). Compared to MSM/TGNB with no history of syphilis, MSM/TGNB with a history of syphilis were less likely to have detectable Tp in serum (4% vs 15%, P = 0.004), urine (4% vs 11%, P = 0.20), pharyngeal swabs (20% vs 30%, P = 0.02), and rectal swabs (16% vs 30%, P = 0.01).
Conclusions: Nucleic acid detection of Tp varies by anatomic site, syphilis stage, and between populations. The high frequency of Tp detection in the vagina among persons with latent infection suggests that the period of genital tract transmissibility may be relatively long in this population. Repeated episodes of syphilis may be associated with decreased Tp transmissibility.
PP04.62 – Substantial Rise in Anal Cancer Projected Among Heterosexual Females Due to Increasing Anal Sex Practice Over Generations in Canada: A Modeling Study
Ms. Marianne Gratton1, M. Sullivan Evain1,2, Dr. Jean-François Laprise1, Dr. Mélanie Drolet1, Prof. Marc Brisson1,2
1Centre de recherche du CHU de Québec - Université Laval, Québec, Canada.
2Université Laval, Québec, Canada.
Background: The CONNECT study estimated that the percentage of heterosexual females who ever had anal sex (ASex) is increasing in Canada; from 8%/17% by age 30yrs among the silent/baby boomer generations, to 34% among generation X, to >50% for generation Y. Currently, anal cancer (AC) is rising among females in high income countries. Given the long lag time between HPV infection and AC, current trends are driven by females from the silent/baby boomer generations. The substantial increase in receptive ASex over generations could lead to an accelerated rise in female AC in the next decades. Our aim was to project AC incidence among Canadian females.
Methods: A mathematical model of trends in AC incidence among females was developed, based on 1) trends among heterosexual females who ever had ASex by birth-cohort (CONNECT), and 2) Canadian age-specific trends in AC (Statistics Canada). To reproduce past and project future trends in age-specific AC incidence, key model parameters include: 1) distribution of ASex debut by birth-cohort, 2) time between ASex debut and HPV infection, 3) proportion of infections that progress to AC, and 4) distribution of time from infection to AC. Least squares were used to fit the model to yearly age-specific AC incidence (1992–2017). For projections, sexual behavior of future birth-cohorts was assumed stable. HPV vaccination impact was examined using a best-case scenario, where individuals born after 1995, eligible for vaccination, would be 100% protected against HPV/AC.
Results: The model projects a 3-fold increase in AC incidence among females between 2020 and 2050, which would not be mitigated by HPV vaccination (Fig. 1). In 2050, AC incidence would be comparable to 2017 cervical cancer incidence.
Conclusion: Increased practice of ASex over generations is projected to raise AC incidence substantially amongst females over the next decades. Screening and additional preventive measures should be explored.
Projected increase in anal cancer among heterosexual females. Solid lines and shaded area represent, respectively, the median and the range of model projections for the 10 best model fits. The blue curve represents the model projections without vaccination, assuming 100% protection against HPV infections and AC for individuals born after 1995 (best-case scenario). The red dashed line represents the projections from linear extrapolation of the observed data. Red and gray dots represent, respectively, the observed incidence of anal and cervical cancer among females (Statistics Canada DOI: https://doi.org/10.25318/1310011101-eng).
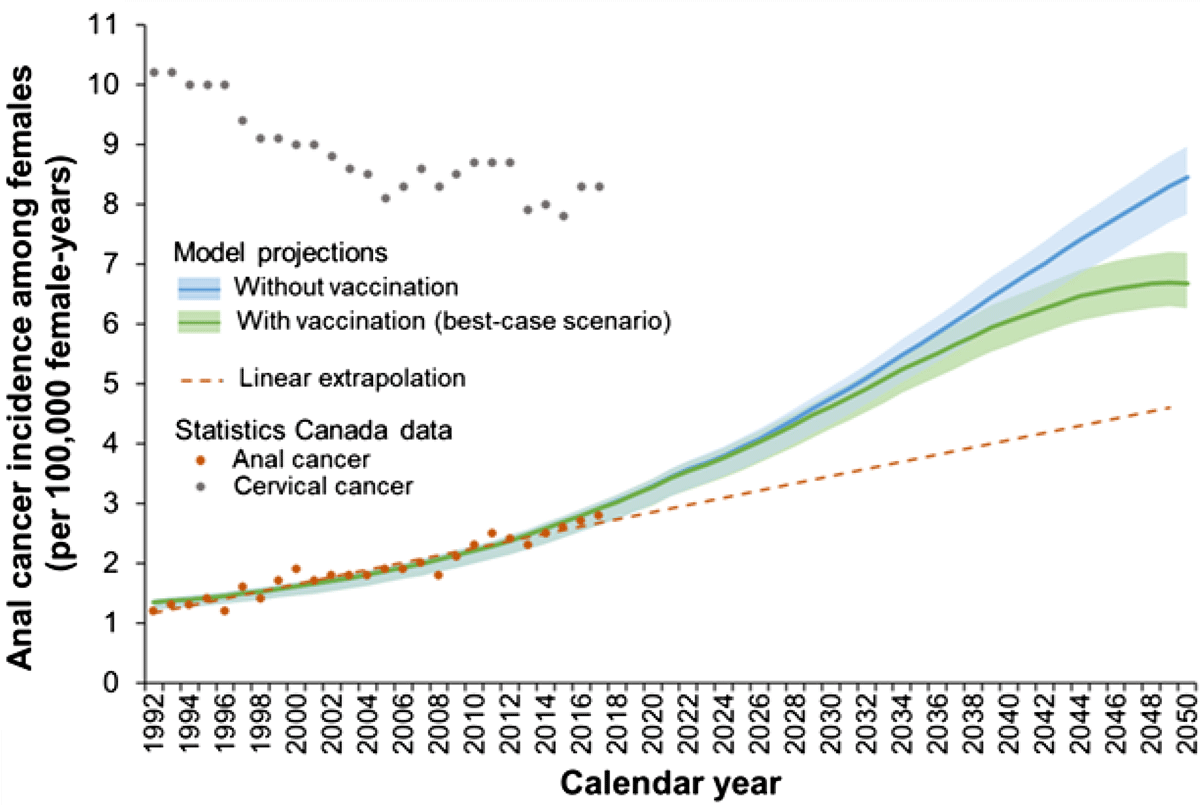
PP04.63 – Tampons or Swabs? An Acceptability Study for Sexually Transmitted Infection (STI) Testing Sample Collection Methods
Ms. Sophie Nash1,2, Ms Valerie Adjei-Darko3, Dr Adele Wolujewicz4,5, Dr Suneeta Soni3,6, Dr. Emma Harding-Esch1
1London School of Hygiene and Tropical Medicine, London, United Kingdom.
2Royal Free NHS Foundation Trust, London, United Kingdom.
3Brighton & Sussex Medical School, Brighton, United Kingdom.
4University Hospitals Bristol and Weston NHS Foundation Trust, Bristol, United Kingdom.
5North Bristol NHS Trust, Bristol, United Kingdom.
6Royal Sussex County Hospital, Brighton, United Kingdom.
Background: In recent years in the UK, online service provision and sexually transmitted infection (STI) testing have increased. Self-collected vaginal swab is the optimum sample for individuals assigned-female-at-birth; however, tampons have been suggested as an alternative sample type. We aimed to explore the acceptability of these two different sample types for STI testing.
Methods: An online questionnaire captured information about STI test sample collection preferences, use of period products, and previous online STI testing use. Survey participants were recruited via university events and professional networks. Upon survey completion, they were invited to participate in a follow-up in-depth interview (IDI).
Results: Overall, 234 people completed the questionnaire; 162 were recruited from professional networks and 72 from student events. When asked about acceptability of swabs and tampons as sample types, the acceptability of swabs was higher than for tampons (82% vs 62%). When asked to choose their preference between the sample types for STI testing, there was an overall preference for swabs (68%, 95% CI: 62%–74%). Strong evidence of a positive association was found between: tampon use and tampon sample preference, tampon use and tampon sample acceptability, and ever-use of online STI swab testing and swab acceptability. One in five respondents had used an online STI swab test before (22%, 52/234). The top cited reasons for their use were: trusted provider (n = 17), recommended to them (n = 15); had used them before (n = 12).
During the 15 IDIs, emerging themes were: familiarity with swabs since the pandemic (n = 4), swabs feeling medical (n = 5) or being painful (n = 4), and either being very familiar with tampons (n = 6) or never using tampons (n = 9) (Fig. 1).
Conclusion: While most participants in this study would prefer swabs to tampons for STI sampling, tampons were found to be an acceptable sample type. New STI sampling methods should be co-designed with service users.
PP04.64 – Private Sexually Transmitted Infection Testing Providers in the United Kingdom: Healthcare Worker Perspectives and Impact on Sexual Health Services
Ms. Sophie Nash1,2, Dr. Emma Harding-Esch1, Dr David Phillips3, Dr Matt Phillips4, Ms Kat Smithson5, Mr Simon Whalley6, Dr Suneeta Soni7,8
1London School of Hygiene and Tropical Medicine, London, United Kingdom.
2Royal Free NHS Foundation Trust, London, United Kingdom.
3Croydon Health Services NHS Trust, London, United Kingdom.
4North Cumbria Integrated Care NHS Foundation Trust, Cumbria, United Kingdom.
5British Association for Sexual Health and HIV, London, United Kingdom.
6M&F Health, United Kingdom.
7Royal Sussex County Hospital, Brighton, United Kingdom.
8Brighton and Sussex Medical School, Brighton, United Kingdom.
Background: Since COVID-19, both the number of private sexually transmitted infection (STI) testing providers (PSTIP) in the UK and users accessing these services have increased. This clinical audit sought to understand National Health Service (NHS) healthcare worker (HCW) views and the impact of private STI testing on sexual health services (SHS) in the UK.
Methods: British Association for Sexual Health and HIV (BASHH) members were invited to complete an online survey, which captured information on their experiences of patients who had tested through PSTIP and their views on PSTIP. Upon survey completion, participants were invited to take part in in-depth interviews (IDI).
Results: Eighty-five HCWs from 60 SHSs across all four UK nations completed the survey (Table 1) and 18 agreed to participate in IDI. Most respondents (95%) reported that they had seen ≥1 patient who had attended their SHS following PSTIP testing, and the most common (96%) reason for attendance was to seek treatment. Based on reported number of patients seen, where reported, most patients were asymptomatic when tested privately (94%, 214/227) and most tests were not recommended according to BASHH guidelines (79%, 258/327). When sample type was known, 75% (43/57) were inappropriate. Respondents had mixed views on the gap PSTIP fill and whether patients should be signposted to the NHS. Consistent views included that PSTIP should not test for Ureaplasmas or Mycoplasmas, should report diagnoses for national surveillance purposes, and should be subject to regulation.
Conclusion: PSTIP practices reported by survey respondents demonstrate widespread inappropriate use, resulting in unnecessary antimicrobial treatment and additional burden on the NHS. PSTIP have an important role to play, and public providers should work collaboratively with them to encourage better practice including compliance with national guidelines and contributing data to national surveillance systems. Future work will include the IDI to gain deeper insights.
| Variable | Number of respondents | % of respondents | |
|---|---|---|---|
| Country | |||
| England | 63 | 74 | |
| Northern Ireland | 5 | 6 | |
| Scotland | 9 | 11 | |
| Wales | 8 | 9 | |
| Number of patients seen in the past year who attended SHS because of a private STI test | |||
| 0 | 4 | 5 | |
| 1 | 1 | 1 | |
| 2 | 10 | 12 | |
| 3 | 11 | 13 | |
| 4 or more | 59 | 69 | |
| Reason for attending sexual health services following private STI test (respondents could select multiple answers) | |||
| To get treatment for an infection they have tested positive for | 78 | 96 | |
| Seeking medical explanation/implication of the test and/or result | 53 | 65 | |
| They were a partner of someone who tested positive from private STI provider | 43 | 53 | |
| Repeat STI testing – confirming/verifying a positive test result | 24 | 30 | |
| Test of cure | 17 | 21 | |
| To support them with partner notification | 12 | 15 | |
| Repeat STI testing – confirming/verifying a negative test result | 2 | 2 | |
| Other reason | 5 | 6 | |
| Do not remember | 1 | 1 | |
| Views of private providers of STI testing (respondents could select multiple answers) | |||
| Offer patients welcome choice in addition to what is available in NHS services | |||
| Agree | 21 | 25 | |
| Neutral | 22 | 26 | |
| Disagree | 42 | 49 | |
| Do more harm than good | |||
| Agree | 61 | 72 | |
| Neutral | 20 | 24 | |
| Disagree | 4 | 5 | |
| Fill gaps in STI testing that exist in the NHS | |||
| Agree | 22 | 26 | |
| Neutral | 18 | 21 | |
| Disagree | 45 | 53 | |
| Should include Ureaplasma and Mycoplasma testing in a routine sexual health screen | |||
| Agree | 3 | 4 | |
| Neutral | 3 | 4 | |
| Disagree | 79 | 93 | |
| Should be exempt from following national guidelines, as they are independent providers | |||
| Agree | 1 | 1 | |
| Neutral | 4 | 5 | |
| Disagree | 80 | 94 | |
| Are not needed because the NHS provides an adequate online postal sampling service and face to face clinic service | |||
| Agree | 26 | 31 | |
| Neutral | 20 | 24 | |
| Disagree | 39 | 46 | |
| Offer service users value for money because they test for more infections | |||
| Agree | 1 | 1 | |
| Neutral | 5 | 6 | |
| Disagree | 79 | 93 | |
| Offer service users value for money because they provide results quickly | |||
| Agree | 23 | 27 | |
| Neutral | 17 | 20 | |
| Disagree | 45 | 53 | |
| Should report STI diagnoses for national surveillance purposes | |||
| Agree | 81 | 95 | |
| Neutral | 3 | 4 | |
| Disagree | 1 | 1 | |
| Should signpost to NHS sexual health services for treatment and partner notification | |||
| Agree | 44 | 52 | |
| Neutral | 18 | 21 | |
| Disagree | 23 | 27 | |
| Should be subject to regulation of their testing practices from an external body | |||
| Agree | 84 | 99 | |
| Neutral | 0 | 0 | |
| Disagree | 1 | 1 | |
| Total | 85 | ||
STI, sexually transmitted infection; NHS, National Health Service.
PP04.65 – High Sexually Transmitted Infection and Bacterial Vaginosis Prevalences Among Women Attending Family Planning in South Africa, Madagascar and Zimbabwe
Dr. Aina Harimanana1, Katharina Kranzer2,3, Tinashe Mwaturura2,4,5, Linda-Gail Bekker6, Katherine Gill6, Theodora Mayouya Gamana1, Dr Rindra Vatosoa Randremanana1, Reziky Mangahasimbola1, Nicola Thomas6, David Anderson7, Micaela Lurie8, Anda Madikida6, Karabo Mahlangu6, Fezile Khumalo8, Tanya Pidwell8, Monalisa T Manhanzva8, Chido Dziva Chikwari2,4,5, Soamiangaly Randrianjatovo1, Solange Bienvenue Randianarivo9, Camille Fortas10,11, Bich-Tram Huynh10,11, Emma Harding-Esch2, Janneke HHM van de Wijgert12, Lindi Masson7,13, Jo-Ann S Passmore8,1,4, Tania Crucitti1
1Institut Pasteur De Madagascar, Antananarivo, Madagascar.
2London School of Hygiene & Tropical Medicine, London, England.
3Medical Center of the University of Munich, Munich, Germany.
4Organization for Public Health Interventions and Development, Harare, Zimbabwe.
5The Biomedical Research and Training Institute, Zimbabwe.
6Desmond Tutu HIV Centre, University of Cape Town, Cape Town, South Africa.
7Disease Elimination Program, Life Sciences Discipline, Burnet Institute, Melbourne, Australia.
8Institute of Infectious Disease and Molecular Medicine, University of Cape Town, Cape Town, South Africa.
9Centre Hospitalier Universitaire de Gynécologie Obstétrique de Befelatanana, Antananarivo, Madagascar.
10Institut Pasteur, Université Paris Cité, Biodiversity and Epidemiology of Bacterial Pathogens, Paris, France.
11Université Paris-Saclay, Université Versailles Saint-Quentin, Villejuif, France.
12Julius Center University Medical Center Utrecht, University of Utrecht, Utrecht, The Netherlands.
13Central Clinical School, Monash University, Victoria, Australia.
14National Health Laboratory Service, Cape Town, South Africa.
Background: As part of a multi-country diagnostic evaluation of a novel point-of-care test for genital inflammation (GIFT), we sought to determine the prevalence of, and factors associated with, sexually transmitted infections (STIs) and bacterial vaginosis (BV) in South Africa (SA), Madagascar (MG), and Zimbabwe (ZW).
Methods: We recruited from family planning services women who were: sexually active, non-pregnant, aged 18–35 years, and untreated for STIs or BV in the past month (Table 1). Participants completed questionnaires covering demographics, sexual behaviour, hygiene practices, and reproductive history. Medical staff performed clinical examinations, conducted HIV testing, and collected vaginal swabs for Nugent scoring and STI testing (Chlamydia trachomatis, Neisseria gonorrhoeae, Trichomonas vaginalis, Mycoplasma genitalium).
Results: Among 676 participants (median age: SA 25y, MG 27y, ZW 29y, P < 0.001), participants in MG had significantly lower education levels and income than the participants in SA and ZW (P < 0.001). Contraceptive use was 100% in MG, 84% in SA, and 51% in ZW (P < 0.001). Abnormal vaginal discharge was reported by 52% in MG, 37% in ZW, and 9% in SA (P < 0.001). HIV positivity was 20% in SA, 7.5% in ZW, and 0.4% in MG. PrEP was used by 12% in SA, 5% in ZW, and absent in MG.
Overall, STIs were found in 29% of participants (SA: 36%, MG: 32%, ZW: 20%, P < 0.001). C. trachomatis and N. gonorrhoeae prevalence was highest in SA (23%, 8%), followed by MG (13%, 5%) and ZW (10%, 4%). T. vaginalis was most prevalent in MG (18%), compared to SA (10%) and ZW (7%). BV affected half of all participants (SA: 57%, MG: 44%, ZW: 48%) while M. genitalium prevalence was 4.5% overall.
Conclusions: STI prevalence, sociodemographic, and behavioural characteristics varied significantly across the three countries. The high prevalences of BV and STIs underscore the urgent need for improved management strategies in these settings.
| South AfricaN = 225 | MadagascarN = 225 | ZimbabweN = 226 | TotalN = 676 | ||
|---|---|---|---|---|---|
| Socio-demographics | |||||
| Age (year) Median (IQR) | 24.9 (21.5–29.7) | 26.5 (22.4–29.8) | 28.6 (24.9–32.4) | 27.1 (22.8–30.6) | |
| Marital status | |||||
| Married or as if married | 26 (11.5) | 199 (88.4) | 182 (80.5) | 407 (60.2) | |
| Never married | 197 (87.6) | 14 (6.2) | 23 (10.2) | 234 (34.6) | |
| Divorced, widow, separated, prefer not to say | 2 (0.9) | 12 (5.3) | 21 (9.3) | 35 (5.2) | |
| Average income of household ($) Median(IQR) | 250 (84-350) | 46.2 (33–77) | 200 (120–300) | 105 (120–264) | |
| Highest level of education | |||||
| Higher education | 60 (26.7) | 15 (6.7) | 44 (19.5) | 119 (17.6) | |
| High school or vocational | 147 (65.3) | 49 (21.8) | 176 (77.9) | 372 (55.0) | |
| Middle school or below | 18 (8.0) | 161 (71.6) | 6 (2.7) | 185 (27.4) | |
| Occupation | |||||
| Student | 27 (12.0) | 6 (2.7) | 4 (1.8) | 37 (5.5) | |
| Formal occupation | 23 (10.2) | 18 (8.0) | 47 (20.8) | 88 (13.0) | |
| Informal occupation | 37 (16.4) | 108 (48.0) | 119 (52.7) | 264 (39.1) | |
| Housemaker/No occupation | 138 (61.3) | 93 (41.3) | 56 (24.8) | 287 (42.5) | |
| Sexual history | |||||
| Age of sexual debut (year) Range | 11–22 | 12–24 | 5–27 | 5–27 | |
| Number of sexual partners to date Range | 1–88 | 1-51 | 1–150 | 1–150 | |
| Number of times the participant used condom with a casual sexual partner in the last 3 months | |||||
| Always | 18 (8.0) | 0 | 14 (6.2) | 32 (4.7) | |
| Sometimes | 156 (69.3) | 5 (2.2) | 54 (23.9) | 215 (31.8) | |
| Never | 35 (15.6) | 44 (19.6) | 139 (61.5) | 218 (32.3) | |
| No casual partners/no data | 16 (7.1) | 176 (78.2) | 19 (8.4) | 221 (31.2) | |
| Sexual hygiene | |||||
| Ever inserts liquids inside vagina for vaginal cleansing | 99 (44.0) | 14 (6.2) | 129 (57.1) | 242 (35.8) | |
| Plain water | 72 (72.7) | 10 (71.4) | 129 (100) | 211 (87.2) | |
| Water and soap | 69 (69.7) | 0 | 6 (4.7) | 75 (31.0) | |
| Lemon/lime juice, vinegar, commercial products for genital cleansing, other | 4 (4.0) | 4 (28.6) | 9 (7.0) | 17 (7.0) | |
| Lifestyle | |||||
| Cigarette consumption | 52 (23.1) | 21 (9.3) | 1 (0.4) | 74 (11.0) | |
| Alcohol consumption | 174 (77.3) | 91 (40.4) | 63 (27.9) | 328 (48.5) | |
| Pregnancy | |||||
| Ever been pregnant | 86 (38.2) | 5 (2.2) | 19 (8.4) | 110 (16.3) | |
| Use a method to prevent pregnancy (Yes) | 189 (84.0) | 225 (100) | 115 (50.9) | 529 (78.3) | |
| Symptoms and Clinical signs | |||||
| Self-reported abnormal vaginal discharge | 20 (8.9) | 118 (52.4) | 83 (36.7) | 221 (32.7) | |
| Observed unusual vaginal discharge | 74 (32.9) | 137 (60.9) | 47 (20.8) | 258 (38.2) | |
| Vaginal pH | |||||
| <3.8 | 44 (19.6) | 60 (26.8) | 34 (15.0) | 138 (20.4) | |
| 3.8-4.5 | 46 (20.4) | 72 (32.1) | 39 (17.3) | 157 (23.3) | |
| >4.5 | 135 (60.0) | 92 (41.1) | 153 (67.7) | 380 (56.3) | |
| Bacterial vaginosis | 128 (56.9) | 98 (43.6) | 111 (49.1) | 337 (49.9) | |
| Chlamydia trachomatis* | 51 (22.7) | 28 (12.5) | 22 (9.9) | 98/672 (14.6) | |
| Neisseria gonorrhoeae* | 17 (7.6) | 11 (4.9) | 10 (4.5) | 38/672 (5.7) | |
| Trichomonas vaginalis* | 23 (10.2) | 40 (17.9) | 16 (7.2) | 79/672 (11.8) | |
| Mycoplasma genitalium* | 10 (4.4) | 11 (4.9) | 9 (4.0) | 30/672 (4.5) | |
| HIV positive | 45 (20.0) | 1 (0.4) | 17 (7.5) | 63 (9.3) | |
| Of which newly confirmed during study | 7 (3.1) | 1 (0.4) | 5 (2.2) | 13 (1.9) | |
| Taking PreP | 28 (12.4) | 0 | 8 (3.5) | 36 (5.3) |
Legend: * 1 vaginal specimen from Madagascar, 3 vaginal specimens from Zimbabwe were not suitable for PCR testing, Prep: pre-exposure prophylaxis.
PP04.66 – An Intersectional Exploratory Analysis of Syphilis Prevalence Among People Who Inject Drugs in Montreal, Canada
Dr. Brendan Harney1, Dr Julie Bruneau1, Dr Valerie Martel-Laferrière1, Dr Sarah Larney1
1University of Montreal/CRCHUM, Montreal, Canada.
Background: Syphilis notifications have increased among women and heterosexual men in Canada and people who inject drugs (PWID) are an emerging group at risk. However, there is a limited understanding of syphilis specifically among PWID. We examined syphilis prevalence and how this varied by intersecting population groups and environmental factors.
Methods: Data were from HEPCO, a cohort study of PWID in Montreal. Syphilis testing via venipuncture was added in November 2022 with treponemal testing reflexed to non-treponemal testing if positive. We included the result at each person’s first test and Fisher’s exact test was used to examine differences in the prevalence of any syphilis exposure, inclusive of current or past infection.
Results: As of March 2024, 386 people (16.1% women, 2.6% non-binary/transgender/two-spirit) had a syphilis test. Two people (0.52% [95% CI 0.1–2.1]), one man and one woman had current syphilis and 33 (8.6% [95% CI 6.1–11.8] had any syphilis exposure. Men and women both had a prevalence of 8.1% (Table 1). Among men, prevalence was higher among those identifying as gay, bisexual and other MSM (gbMSM), those with HIV, and those who reported recent sex work (all P < 0.001). All women with syphilis identified as heterosexual and none were living with HIV. Prevalence was higher among women reporting recent sex work and recent unstable housing; however, this was not statistically significant.
Conclusion: Current syphilis infection was uncommon among this cohort of PWID; however, any syphilis exposure was higher than anticipated. Among men, there is an intersection and overlap among those who identify as gbMSM and are living with HIV. Among women, there was a possible link to sex work and unstable housing however caution is needed due to the small sample size. Periodic syphilis testing among PWID may be justified alongside testing for other STBBIs.
| Total | n, % (95% CI) | P-value | ||
|---|---|---|---|---|
| Men overall | 310 | 25, 8.1% (5.5–11.7) | ||
| Sexual identity | ||||
| Heterosexual | 271 | 15, 5.5%, 95% CI 3.4–9.0 | ||
| Gay/bisexual/MSM | 31 | 10, 32.3% (18.3–50.4) | <0.001 | |
| HIV status | ||||
| Without HIV | 271 | 14, 5.2% (3.1–8.6) | ||
| With HIV | 37 | 10, 27.0% (15.2–43.4) | <0.001 | |
| Sex work in past 3 months | ||||
| No | 290 | 18, 6.2% (3.9–9.7) | ||
| Yes | 19 | 7, 36.8% (18.6–59.8) | <0.001 | |
| Unstable housing past 3 months | ||||
| No | 178 | 13, 7.3% (4.3–12.2) | ||
| Yes | 131 | 12, 9.2% (5.3–15.5) | 0.67 | |
| History of incarceration | ||||
| No | 71 | 10, 14.1% (7.7–24.3) | ||
| Yes | 238 | 15, 6.3% (3.8–10.2) | 0.05 | |
| Women overall | 62 | 5, 8.1% (3.3–18.2) | ||
| Sex work in past 3 months | ||||
| No | 47 | 3, 6.4%, (2.0–18.4) | ||
| Yes | 14 | 2, 14.3%, (3.5–43.4) | 0.32 | |
| Unstable housing past 3 months | ||||
| No | 33 | 2, 5.6%, (1.4–20.1) | ||
| Yes | 29 | 3, 11.5%, (3.7–30.8) | 0.66 | |
| History of incarceration | ||||
| No | 26 | 2, 11.5%, (3.7–30.8) | ||
| Yes | 35 | 3, 5.7%, (1.4–20.6) | 0.64 | |
| Non-binary, transgender, Two-spirit | 14 | 4, 29%, (8.3-67.1) |
PP04.67 – Increased Internet-Based Chlamydia Trachomatis Testing in Sweden Leads to a Change in Testing Practises?
Siri Westborg1,2, Karin Elfving3, Ylva Lindroth4, Lisa Stark5, Karolina Gullsby6, Åsa Gylfe7, Prof. Björn Herrmann1,2
1Uppsala University, Uppsala, Sweden.
2Uppsala University Hospital, Uppsala, Sweden.
3Falu Hospital, Falun, Sweden.
4Lund University, Lund, Sweden.
5County Hospital Ryhov, Jönköping, Sweden.
6Region Gävleborg, Gävle, Sweden.
7Umeå University, Umeå, Sweden.
Objectives: To assess chlamydia testing and diagnostic outcomes in different types of clinics, including internet-based self-sampling (IBSS), as part of a nationally available public health service in Sweden.
Methods: Data on Chlamydia trachomatis (CT) testing activities were retrieved from six healthcare regions representing 29% of the population. Data included the number of tests and the number of tested persons in different clinic types between 2016–2023.
Results: The number of CT cases detected through IBSS increased by 85% from 2016 (n = 1967) to 2023 (n = 3644) when it accounted for 43% of all cases. The proportion of positive tests for IBSS was 5.3% for the study years (range 4.7%–5.6% per year); this rate was 4.3% (3.6%–5.0%) for clinic-based testing (P < 0.0001). The proportion of CT-positive individuals of all tested persons per category was equally high for IBSS (7.0%–8.5% per year); STI clinics (8.5%–9.9%) and youth clinics (9.7%–10.9%). In contrast, genecology clinics had a low proportion of CT-positive individuals (1.8%–2.3%), and primary healthcare clinics have a decreasing proportion of CT-positive persons (4.8% in 2016 and 3.0% in 2023). The number of tests per person and year was similar for all clinic types except STI clinics, where extragenital testing increased in later years.
The proportion of internet-based samples of all samples increased from 19% (n = 36,148) in 2016 to 33% (n = 64,782) in 2023. Primary healthcare clinics decreased their proportion from 30% (n = 57,395) in 2016 to 21% (n = 44,573) in 2023. Youth clinics decreased from 20% (n = 37,510) to 11% (n = 22,448). For STI clinics, a constant proportion was noted between 2016 (14%, n = 26,852) and 2023 (16%, n = 31,891).
Conclusions: IBSS has become the most important CT case detector. Testing in primary care and gynaecology clinics have lower positivity rates. Therefore, reduced testing may be justified.
PP04.68 - Increasing Risk of Human Immunodeficiency Virus Among Those Diagnosed with Multiple Sexually Transmitted Infections in Chicago, 2013–2023
Dr. Casey Luc1, Ms. Taylor Holly2, Jeff Lauritsen2, Colleen Leonard2, David Kern2, Dr. Irina Tabidze2
1CDC Foundation assigned to Chicago Department of Public Health, Syndemic Infectious Disease Bureau, Atlanta, USA.
2Chicago Department of Public Health, Syndemic Infectious Disease Bureau, Chicago, USA.
Background: Previous population-level research has shown human immunodeficiency virus (HIV) incidence to be high among those diagnosed with a sexually transmitted infection (STI) in urban settings. Despite advances in the prevention of HIV transmission, men who have sex with men (MSM) are disproportionally affect by the HIV epidemic. We described demographic and behavioral characteristics of individuals at risk for HIV acquisition following STI diagnosis, and identified factors associated with HIV acquisition to inform targeted interventions in Chicago.
Methods: STI (e.g., gonorrhea, chlamydia, primary & secondary syphilis) surveillance data reported between 2013 and 2023 were matched with HIV surveillance data using a 12 step SAS matching algorithm. The risk of more than one STI infection and related risk factors for HIV infection was assessed using cox proportional hazards models.
Results: From 2013 to 2023, annual HIV incidence was higher after syphilis infection (0.70%), followed by gonorrhea (0.26%), and chlamydia (0.09%) (Table 1). HIV risk increased by 14% per additional chlamydia infection (aHR: 1.14, 95% CI: 1.05, 1.24), 76% per gonorrhea infection (aHR: 1.76, 95% CI: 1.64, 1.90), and 77% per syphilis infection (aHR: 1.77, 95% CI: 1.14, 2.73). Compared to Non-Hispanic (NH) White individuals with any STI infection, HIV risk was higher among Hispanic and NH Black individuals. For syphilis, MSM had a 2.6-fold increased risk of HIV compared to heterosexual individuals (aHR: 2.63, 95% CI: 1.51, 4.59).
Conclusions: HIV incidence was disproportionately higher among all cases with multiple STI infections. Multipronged approaches (e.g., screening for STIs, counseling on prevention, vaccination, barrier protection) are urgently needed for STI/HIV prevention. Other prevention strategies such as antiretroviral treatment as prevention, HIV pre- and post-exposure prophylaxis and doxycycline post-exposure prophylaxis at the point of care for those diagnosed with any STI, particularly among MSM and racially and ethnically diverse populations, may help reduce risk of future STI and HIV acquisition.
| Chlamydia, N = 197,234 | Gonorrhea, N = 79,474 | Syphilis, N = 6537 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Study Variable | STI Cases, N (%) | HIV, N | Person-Years at Risk | HIV Incidence (%) | STI Cases, N (%) | HIV, N | Person-years at Risk | HIV Incidence (%) | STI Cases, N (%) | HIV, N | Person-years at Risk | HIV Incidence (%) | |
| Age | |||||||||||||
| <35 | 171768 (87.1) | 782 | 867461.0 | 0.09 | 64897 (81.7) | 826 | 308674.2 | 0.27 | 1912 (29.3) | 91 | 7625.7 | 1.19 | |
| ≥35 | 25466 (12.9) | 104 | 117588.5 | 0.09 | 14577 (18.3) | 126 | 61510.2 | 0.20 | 4625 (70.8) | 140 | 25291.5 | 0.55 | |
| Race/Ethnicity | |||||||||||||
| Hispanic | 33486 (17.0) | 143 | 146649.7 | 0.10 | 8013 (10.1) | 147 | 31094.4 | 0.47 | 1192 (18.3) | 44 | 5946.3 | 0.74 | |
| NH Black | 87222 (44.2) | 434 | 432563.0 | 0.10 | 44436 (55.9) | 484 | 209838.5 | 0.23 | 2634 (40.3) | 95 | 11945.0 | 0.80 | |
| NH White | 21708 (11.0) | 112 | 102586.8 | 0.11 | 9751 (12.7) | 148 | 39246.6 | 0.38 | 1514 (23.2) | 40 | 8116.0 | 0.49 | |
| NH Other/Unknown | 54818 (27.8) | 197 | 303250.1 | 0.06 | 17274 (21.7) | 173 | 90002.1 | 0.19 | 1197 (18.3) | 52 | 6910.0 | 0.75 | |
| Sex at Birth | |||||||||||||
| Male | 80782 (41.0) | 718 | 385106.8 | 0.19 | 47607 (59.9) | 864 | 209343.2 | 0.41 | 5552 (84.9) | 224 | 28964.8 | 0.77 | |
| Female | 116452 (59.0) | 168 | 599942.7 | 0.03 | 31867 (40.1) | 88 | 160841.2 | 0.05 | 985 (15.1) | 7 | 3952.4 | 0.18 | |
| Site of Infection | |||||||||||||
| Genito-urinary | 182861 (92.7) | 591 | 924505.8 | 0.06 | 65024 (81.8) | 598 | 318334.5 | 0.19 | -- | -- | -- | -- | |
| Rectal | 8361 (4.2) | 228 | 26370.6 | 0.86 | 4245 (5.3) | 138 | 13601.4 | 1.01 | -- | -- | -- | -- | |
| Pharyngeal | 1614 (0.8) | 19 | 4760.4 | 0.40 | 5259 (6.6) | 75 | 16379.8 | 0.46 | -- | -- | -- | -- | |
| Multi | 2203 (1.1) | 30 | 7292.6 | 0.41 | 4085 (5.1) | 128 | 13307.6 | 0.96 | -- | -- | -- | -- | |
| Other/Unknown | 2195 (1.1) | 18 | 22120.1 | 0.08 | 861 (1.1) | 13 | 8561.1 | 0.15 | -- | -- | -- | -- | |
| Anonymous Sexual Partners | -- | -- | -- | -- | -- | -- | -- | -- | 2096 (32.1) | 98 | 12745.7 | 0.77 | |
| Transmission Category | |||||||||||||
| Heterosexual | -- | -- | -- | -- | -- | -- | -- | -- | 1609 (24.6) | 21 | 7348.1 | 0.29 | |
| IDU | -- | -- | -- | -- | -- | -- | -- | -- | 7 (0.1) | 0 | 35.5 | 0 | |
| MSM | -- | -- | -- | -- | -- | -- | -- | -- | 3404 (52.1) | 159 | 19592.5 | 0.81 | |
| MSM+IDU | -- | -- | -- | -- | -- | -- | -- | -- | 67 (1.2) | 3 | 400.6 | 0.75 | |
| Unknown/Other | -- | -- | -- | -- | -- | -- | -- | -- | 1450 (22.2) | 46 | 5976.6 | 0.77 | |
| Previous STI Infection | |||||||||||||
| None | 142551 (72.3) | 599 | 773178.0 | 0.08 | 59334 (74.6) | 590 | 302347.3 | 0.20 | 6015 (92.0) | 218 | 30905.0 | 0.71 | |
| 1 | 33462 (17.0) | 172 | 144343.0 | 0.12 | 12544 (15.8) | 202 | 47455.3 | 0.43 | 439 (6.7) | 9 | 1816.4 | 0.50 | |
| 2 | 11785 (6.0) | 59 | 41617.1 | 0.14 | 4121 (5.2) | 82 | 12475.2 | 0.66 | 64 (1.0) | 3 | 162.3 | 1.85 | |
| 3+ | 9436 (4.8) | 56 | 25911.3 | 0.22 | 3475 (4.4) | 78 | 7906.6 | 0.99 | 19 (0.3) | 1 | 33.6 | 2.98 | |
| Other STI Infection | |||||||||||||
| None | 150242 (76.2) | 368 | 782036.2 | 0.05 | 32634 (41.1) | 419 | 159573.4 | 0.26 | 3121 (47.7) | 92 | 16429.1 | 0.56 | |
| Chlamydia | -- | -- | -- | -- | 44318 (55.8) | 420 | 201122.0 | 0.21 | 894 (13.7) | 26 | 4410.1 | 0.59 | |
| Gonorrhea | 44318 (22.5) | 420 | 192704.1 | 0.22 | -- | -- | -- | -- | 742 (11.4) | 41 | 3677.8 | 1.11 | |
| Syphilis | 894 (0.5) | 26 | 4075.0 | 0.64 | 742 (0.9) | 41 | 3157.8 | 1.30 | -- | -- | -- | -- | |
| Both | 1780 (0.9) | 72 | 6234.1 | 1.15 | 1780 (2.2) | 72 | 6331.2 | 1.14 | 1780 (27.2) | 72 | 8400.2 | 0.86 | |
PP04.69 – Uptake of Sex Work Outreach Programmes Among a Longitudinal, Community-Based Cohort of Sex Workers Over a 15-Year Period
Assoc. Prof. Shira Goldenberg1,2,4, Assistant Prof. Andrea Krüsi2,3, Ms. Jennie Pearson2, Ms. Melody Wise2, Mr. Charlie Zhou2, Dr. Ran Hu2,5, Prof. Kate Shannon2
1Division of Epidemiology and Biostatistics, School of Public Health, San Diego State University, San Diego, United States.
2Division of Social Medicine, Department of Medicine, University of British Columbia, Vancouver, Canada.
3School of Criminology, Simon Fraser University, Burnaby, Canada.
4University of California, San Diego, La Jolla, United States.
5College of Social Work, Ohio State University, Columbus, United States.
Background: Sex workers face a disproportionate burden of HIV/STIs as a result of criminalization and other forms of structural violence. Community mobilization interventions, including community outreach, are global best practices for HIV/STI prevention with sex workers. Although Canada has been a site of strong sex worker advocacy and community mobilization, few quantitative studies have evaluated utilization of sex work-led programmes. The aim of this study was to evaluate uptake and structural factors linked to utilization of sex work outreach programmes in a prospective cohort of sex workers over 15 years.
Methods: Baseline and semi-annual questionnaire data were drawn from a community-based cohort of women sex workers in Vancouver (2010–2024). We used bivariate and multivariable GLMM to model relationships between structural factors (violence, criminal legal system contact, migration) and the utilization of sex worker outreach programmes.
Results: Analyses included 1035 participants interviewed between 2010 and 2024. At baseline, 10.2% (n = 106) were STI-seropositive. 57.0% recently used sex work outreach services at baseline, and 69.5% did so at least once during the 15-year study. In adjusted models, uptake of outreach services was highest amongst those experiencing workplace (AOR: 1.82, 95% CI: 1.37, 2.40), neighborhood (AOR: 1.63, 95% CI: 1.22, 2.19), or interpersonal violence (AOR: 1.52, 95% CI: 1.26, 1.85), as well as police encounters (AOR: 2.37, 95% CI: 1.91, 2.95) or harassment (AOR: 1.84, 95% CI: 1.31, 2.56); whereas im/migrants faced reduced access (AOR: 0.33, 95% CI: 0.18-0.59).
Conclusion: Sex work outreach programmes represent a critical health promotion intervention for sex workers impacted by structural violence policing, all of which shape HIV/STIs. With reduced HIV program funding in recent years and increasing STIs among key populations in North America, there is an urgent need to resource sex worker-led community outreach and mobilization programmes. Scale-up of outreach programmes serving sex workers facing criminalization, violence, and language barriers is especially recommended.
PP04.70 – HHV-8 Seropositivity Among Gay, Bisexual, and Other Men Who Have Sex with Men in Montreal
Dr. Stephane Isnard1,2, Dr Léna Royston1,2,3, Mrs Tsoarello Mabanga1,2, Ms Milada Dvorakova9, Dr Carolina A Berini1,2, Dr Bluma Brenner4, Dr Cecilia T Costiniuk1,2, Dr Sean Yaphe2,5, Dr Bertrand Lebouché1,2, Dr Réjean Thomas5, Dr Jean-Guy Baril6, Dr Marc Steben7, Dr Daniel Grace8, Dr Gilles Lambert9, Dr Joseph Cox9,10, Dr Jean-Pierre Routy1,2,11, Study group the Montreal ENGAGE study team9
1Research Institute of the McGill University Health Centre, Montreal, Canada.
2Chronic Viral Illness Service, McGill University Health Centre, Montreal, Canada.
3Geneva University Hospitals, Switzerland.
4Lady Davis Institute, McGill University, Montreal, Canada.
5Cinique médicale l’Actuel, Montreal, Canada.
6Clinique médicale du Quartier Latin, Montreal, Canada.
7Canadian Network for HPV Prevention, Montreal, Canada.
8University of Toronto, Dalla Lana School of Public Health, Social and Behavioural Health Sciences, Toronto, Canada.
9Engage Cohort Study, Montreal, Canada.
10Department of Epidemiology, Biostatistics and Occupational Health, McGill University, Montreal, Canada.
11Division of Hematology, McGill University Health Centre, Montreal, Canada.
Background: HHV-8 is a gammaherpesvirus associated with Kaposi sarcoma, some B lymphoproliferative disorders and inflammatory cytokine syndrome, mostly in older and immunosuppressed men. Lack of validated serological tests has hampered the assessment of its seroprevalence. Using our in-house serology assay, we assessed demographic and sexual behaviour factors linked with HHV-8 seropositivity in men.
Methods: 802 Cis and transgender gay, bisexual and other men who have sex with men (GBM) from the Engage study in Montreal were included. 33 HIV-negative heterosexual men from the McGill HIV cohort were included. HHV-8 serology was assessed by flow cytometry quantifying IgG binding to HHV-8 infected BCBL1 cells. Comparisons of demographics and sexual behaviours in GBM were performed using Kruskal Wallis’, t- and binomial tests.
Results: From a total of 802 participants, 157 (19.6%) were living with HIV. HHV-8 seropositivity was elevated in GBM with HIV as compared to GBM without HIV (67.5% vs 41.8%, P < 0.001), independently of ethnicity. Conversely, HHV-8 seropositivity was low at 9.1% in heterosexual men compared to GBM, regardless of HIV (P < 0.001) (Table 1).
HHV-8 seropositive HIV-negative GBM were older (median age 35 vs 32, P < 0.001), and had more lifetime (8 vs 5, P < 0.001) and recent (<6 months) sexual partners (6 vs 3, P < 0.01) than their HHV-8 seronegative counterparts. HHV-8 seropositive GBM living with HIV had similar age (52 vs 50, P > 0.99), but tended to have more sexual partners in their lifetime (10 vs 4, P = 0.054) than their HHV-8 seronegative counterparts. Irrespective of HIV, HHV-8 seropositive GBM had more often been diagnosed with an STI in their lifetime (HIV-: 70 vs 56%, HIV+: 94 vs 82%, P < 0.001).
Conclusion: HHV-8 seropositivity appears elevated among this large sample of Montreal GBM compared to heterosexuals. Older HIV-negative GBM and those living with HIV may be more at risk for the development of HHV-8-induced diseases.
| Engage Study | McGill HIV Cohort | |||
|---|---|---|---|---|
| HIV– GBM | HIV+ GBM | HIV– Heterosexuals | ||
| Number of participants | 645 | 157 | 33 | |
| Age average (range) | 36 (18–80) | 48 (23–72) | 55 (24–89) | |
| Non white, n (%) | 153 (23.8%) | 23 (14.6%) | 1 (3.0%) | |
| HHV-8 seropositive, n (%) | 270 (41.8%) | 106 (67.5%) | 3 (9.1%) | |
| HHV-8 serology indeterminate, n | 23 | 7 | 0 | |
| Lifetime partners, n (range) | 13 (0–300) | 9.4 (0–150) | Not done | |
| New partners last 6 months, n (range) | 10.1 (0–200) | 14 (0–100) | Not done | |
GBM, Gay, bisexual and other men who have sex with men.
PP04.71 – High Prescriber Adherence to National and Jurisdictional Gonorrhea Treatment Guidelines Among Provinces and Territories Participating in the Enhanced Surveillance of Antimicrobial-Resistant Gonorrhea (ESAG) System in Canada, 2018–2022
Ms. Carmen Issa1, Geneviève Gravel1, Irene Martin2, Dr. Andrea Chittle1, Ms. Maria Guirguis1, Shelley Peterson2, Robyn Thorington2, Norman Barairo2, Charity Maritim1, Debbie Nowicki3, Ms. Sara Perlman-Arrow1, Dr. Molly Trecker4, Ms. Colleen Ryan4, Ms. Jennifer Gratrix5, Ms. Sarah Jeffrey6, Ms. Lillian Lourenço1
1Centre for Communicable Diseases and Infection Control, Public Health Agency of Canada, Ottawa, Canada.
2National Microbiology Laboratory, Public Health Agency of Canada, Winnipeg, Canada.
3Manitoba Health, Seniors and Long-Term Care, Winnipeg, Canada.
4Nova Scotia Health, Halifax, Canada.
5Alberta Health Services, Edmonton, Canada.
6Department of Health and Social Services, Yellowknife, Canada.
Background: Neisseria gonorrhoeae has demonstrated resistance to all current gonorrhea (GC) therapies, limiting treatment options. To help curb antimicrobial-resistant (AMR)-GC emergence, the Public Health Agency of Canada’s (PHAC’s) Enhanced Surveillance of Antimicrobial-resistant Gonorrhea (ESAG) system monitors the appropriateness of antimicrobial use.
Methods: Prescription data reported between 2018 and 2022 were analyzed for anogenital or pharyngeal gay, bisexual, or other men who reported having sex with men (GBMSM) (n = 1,781) or ‘Other Adult (OA)’ (i.e., female or heterosexual male) (n = 1,676) ESAG cases. We calculated the proportion of prescriptions that met contemporaneous PHAC and provincial/territorial (PT) treatment guidelines, stratified by infection site and GBMSM/OA status (as guidelines varied by infection site and client sex/sexual behaviour). Data were provided by Alberta, Manitoba, Nova Scotia and the Northwest Territories.
Results: From 2018 to 2022, annual prescriber adherence to PHAC/PT guidelines was consistently high among GBMSM anogenital (5-year average (avg.): 92.8% PHAC, 93.7% PT), GBMSM pharyngeal (avg.: 88.3% PHAC, 88.9% PT), and OA anogenital (avg.: 93.8% PHAC, 94.1% PT) cases. Annual adherence among OA pharyngeal cases varied slightly but remained high overall (avg.: 90.8% PHAC, 91.5% PT). Most GBMSM cases were prescribed the PHAC/PT preferred regimen of ceftriaxone 250 mg and azithromycin 1 g (avg.: 83.4% anogenital, 86.9% pharyngeal). Similarly, OAs with anogenital infections were mostly prescribed the preferred regimen of PHAC and 3 PTs, cefixime 800mg and azithromycin 1g (avg.: 88.2%). However, among OA pharyngeal cases, the PHAC/PT alternative regimen (cefixime 800 mg and azithromycin 1 g) was prescribed more (avg.: 50.2%) than the preferred regimen (ceftriaxone 250 mg and azithromycin 1 g) (avg.: 41.3%).
Conclusion: Annual prescriber adherence to PHAC and PT gonorrhea treatment guidelines was consistently high among ESAG cases from 2018 to 2022, supporting efforts to curb AMR. Although no specific adherence target exists, maintaining high guideline adherence is crucial to minimizing AMR development.
PP04.72 – Efficacy of Oral Cefixime Versus Benzathine Penicillin G for Early Syphilis by HIV Status
Gjermayne Wilson3, Ms. Kori Keith1, Chrysovalantis Stafylis1, Kelika Konda2, Michael Reyes-Diaz2, Jeffrey Klausner1
1University of Southern California, Los Angeles, United States.
2Universidad Peruana Cayetano Heredia, Lima, Peru.
3AIDS Healthcare Foundation, Los Angeles, United States.
Background: Rising syphilis rates pose significant public health challenges. Decline in rapid plasma reagin (RPR) titer is a key indicator of syphilis treatment effectiveness. Evidence suggests that people living with human immunodeficiency virus (HIV) experience slower RPR decline compared to those without HIV. We investigated RPR decline timelines by comparing treatment outcomes for cefixime and penicillin in early syphilis by HIV status.
Methods: In our clinical trial, patients with early syphilis were randomized to receive cefixime (400 mg orally, twice daily for 10 days) or penicillin (2.4 million units intramuscularly). Participants living with HIV must have undetectable HIV viral load <200 copies/mL or CD4 T cell count >350 cells/mm3 and be on antiretroviral treatment. Participants are followed at 3, 6, and 9 months for clinical evaluation and RPR testing. The primary outcome is a ≥4-fold decline in RPR titer by 6 months.
Results: As of December 17, 2024, 114 participants (32 without HIV; 75 living with HIV) completed 6 months of observation. Of those without HIV, 20 received cefixime, and 12 received penicillin. Among participants with HIV, 37 received cefixime, and 38 received penicillin. Fig. 1 shows treatment outcomes by HIV status and treatment arm.
Conclusion: Participants without HIV appear to achieve faster RPR declines across treatment arms. By 3 months, most participants without HIV achieved treatment success with both cefixime and penicillin, while success rates over time for those with HIV appear lower for cefixime than those with penicillin. Our preliminary analysis highlights the importance or considering HIV status in syphilis treatment evaluations. Future analysis will look at history of prior syphilis and its relationship to titer decline and HIV status.
Rapid Plasma Reagin (RPR) titer treatment rates by HIV status and treatment arm at 3 and 6 months.
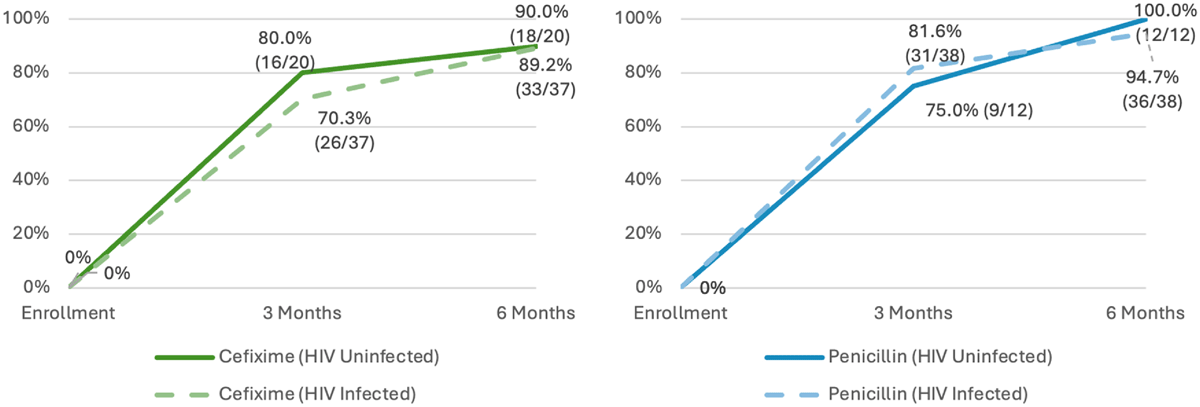
PP04.73 – Impact of Additional Antibiotic Use on Rapid Plasma Reagin Titer Declines in Early Syphilis Treatment
Gjermayne Wilson3, Ms. Kori Keith1, Chrysovalantis Stafylis1, Kelika Konda2, Michael Reyes-Diaz2, Jeffrey Klausner1
1University of Southern California, Los Angeles, United States.
2Universidad Peruana Cayetano Heredia, Lima, Peru.
3AIDS Healthcare Foundation, Los Angeles, United States.
Background: Syphilis has reemerged as a global health problem. Benzathine penicillin G (penicillin) is the standard treatment for early syphilis. We evaluated oral cefixime as a potential alternative and assessed the impact of additional antibiotic use on rapid plasma reagin (RPR) decline.
Methods: Participants with early syphilis were randomized to cefixime (400 mg twice daily for 10 days) or benzathine penicillin G (2.4 million units intramuscularly). Doxycycline hyclate (100 mg twice daily for 14 days) was used during penicillin shortages. Those on recent antibiotics or at baseline were excluded. Treatment success was defined as a ≥4-fold RPR decline by 6 months (Fig. 1). We evaluated whether additional antibiotic use after treatment influenced treatment success, with antibiotic use self-reported at 3-, 6-, and 9-month follow-ups by treatment arm and time to response.
Results: Of 114 participants, 14 (12.3%) reported additional antibiotic use. Of cefixime participants with additional antibiotics (n = 8), 4 succeeded by 3 months (3 doxycycline, 1 penicillin), and 4 by 6 months (3 doxycycline, 1 unknown) versus among those allocated to cefixime (n = 49) 39 succeeded by 3 months and 43 by 6 months. For penicillin (n = 5 who received azithromycin, levofloxacin, amoxicillin, doxycycline, or unknown) all succeeded by 3 months versus 35 of 45 succeeded by 3 months, and 43 by 6 months of in those not receiving additional antibiotics (n = 45).
For doxycycline (n = 1) all succeeded by 6 months. Among those without additional antibiotics (n = 6), 5 succeeded by 3 months, and all by 6 months.
Conclusions: All participants reporting additional antibiotic use achieved treatment success, while some without additional antibiotics did not achieve treatment success by 6 months. These findings suggest that additional antibiotics may accelerate RPR decline.
Treatment Success (With and Without Additional Antibiotics) by Treatment Group at 3 or 6 Months.
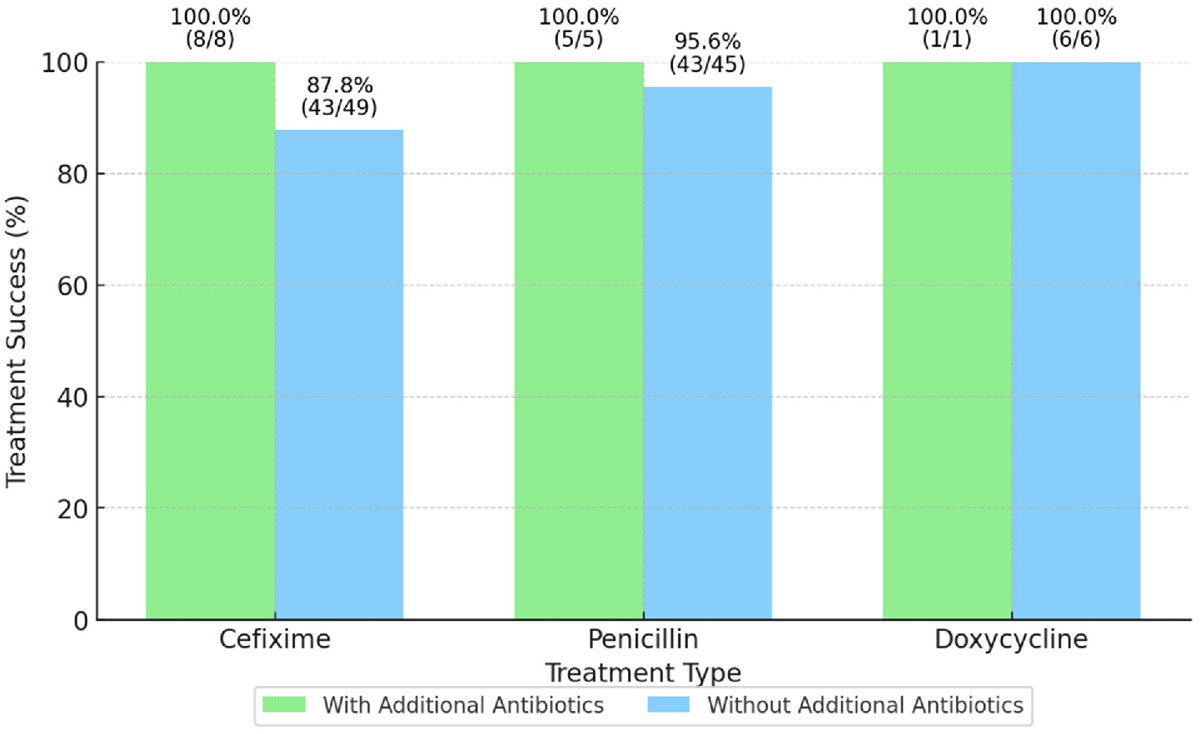
PP04.74 – Membership in Multiple Priority Groups for Hepatitis C Elimination in Canada: Common Intersections in a National Database Cohort
Medical Student Andréa Khabazeh1, Stine Hoj2, Haris Imsirovic4, Hongqun Q Liu5, Dr. Jordan J Feld6,7, Dr. Sam S Lee5, Dr. Curtis L Cooper4, Dr. Valérie Martel-Laferrière1,2,3, on behalf of the Canadian Network Undertaking against Hepatitis C (CANUHC) investigators
1Université de Montréal, Montréal, Canada.
2Centre de recherche du Centre hospitalier de l’Université de Montréal, Montréal, Canada.
3Centre hospitalier de l’Université de Montréal, Montréal, Canada.
4University of Ottawa, Ottawa, Canada.
5University of Calgary, Calgary, Canada.
6University of Toronto, Toronto, Canada.
7Toronto General Hospital Research Institute, Ottawa, Canada.
Background: The Blueprint to inform hepatitis C elimination efforts in Canada recognizes that intervention to achieve hepatitis C (HCV) elimination should focus on six priority populations disproportionately affected by HCV and/or facing challenges in accessing care: people who use/used drugs (PWUD); Indigenous peoples; those with experience in federal or provincial prisons; immigrants and newcomers from countries where HCV is common; gay, bisexual, and other men who have sex with men (gbMSM); and the 1945–1975 birth cohort (baby boomers). While data on overlapping categories are limited, recognizing common combinations could enable more targeted approaches.
Methods: Data were extracted from the Canadian Network Undertaking against Hepatitis C (CANUHC), a prospective cohort of HCV infected patients from 17 Canadian publicly funded clinics. We described the distribution of participants across priority groups, identified most common intersections (>10% of the cohort), and discussed frequent overlaps.
Results: Data on membership to at least one category was available for 3258 participants (Table 1). On average, individuals belong to 2.07 (95% CI: 2.05–2.09) priority populations, with 199 (6.1%) participants belonging to 4 or more. Most common categories were baby boomers+PWUD (14.4%), baby boomers+PWUD+incarceration (12.9%), baby boomers alone (12.0%) and PWUD+incarceration (11.0%). Over 50% of individuals in the 6 priority groups were baby boomers. Among them, 73% use/used drugs, and 40% have been incarcerated. Furthermore, about 90% of Indigenous people, incarcerated individuals, and gbMSM use/used drugs, while 57% of PWUD have a history of incarceration.
Conclusion: Data indicate that many individuals belong to multiple priority groups, amplifying their vulnerability to hepatitis C. This highlights the importance of personalized and focused interventions that effectively address these overlapping risks and enhance access to HCV care and services.
| Identified as member of this group | PWUD | Indigenous people | Incarceration | gbMSM | Newcomers | Baby boomers | ||
|---|---|---|---|---|---|---|---|---|
| PWUD | 2198/2799 (78.5%) | 498/2131(23.3%) | 1154/2043(56.5%) | 78/1876(4.2%) | 125/2008(6.2%) | 1235/2166(57%) | ||
| Indigenous people | 571/3163 (18.1%) | 498/547(91%) | 345/532(65%) | 21/499(4.2%) | 5/542(0.9%) | 292/569(51.3%) | ||
| Incarceration | 1310/2944 (44.5%) | 1154/1244(92.7%) | 345/1278(27%) | 35/1180(3%) | 56/1210(4.63%) | 733/1290(56.8%) | ||
| gbMSM | 98/2826 (3.5%) | 78/88(88.6%) | 21/97(21.6%) | 35/93(37.6%) | 16/96(16.7%) | 54/95(56.8%) | ||
| Newcomers | 519/2957 (17.6%) | 125/376(33.2%) | 5/511(0.98%) | 56/445(12.6%) | 16/431(3.71%) | 332/514(64.6%) | ||
| Baby boomers | 2025/3214 (63.0%) | 1235/1682(73%) | 292/1963(14.9%) | 733/1812(40.5%) | 54/1611(3.35%) | 332/1799(18.5%) |
PP04.75 – Chlamydia and Gonorrhea Trends Before and After the Pandemic: Assessing Service Disruptions in British Columbia and Ontario
Mr. Farhan Khandakar1, Dr. Nichole Austin2, Dr. Sahar Saeed1
1Department of Public Health Sciences, Queens University, Kingston, Canada.
2School of Health Administration, Dalhousie University, Halifax, Canada.
Background: Chlamydia and gonorrhea infections increased in Canada between 2011 and 2019, with young adults disproportionately affected. We examined the impact of the COVID-19 pandemic on reported chlamydia and gonorrhea cases among young adults in Ontario, Canada.
Methods: Data on laboratory confirmed chlamydia and gonorrhea cases among young adults under 25 years of age were obtained from the integrated Public Health Information System database by Public Health Ontario between 2016 and 2021. Immediate impact of the pandemic was estimated using an Interrupted Time Series analysis. Linear regression models assessed trends in infections before and after the onset of the pandemic (March 2020) and were sex stratified.
Results: A total of 138,812 chlamydia cases (92,064 females and 46,748 males) and 16,338 gonorrhea cases (7,575 females and 8,763 males) were reported over the observation period. Pre-pandemic chlamydia and gonorrhea cases were increasing between 2016 and 2020 (Fig. 1). Onset of the pandemic resulted in immediate and statistically significant reductions in reported chlamydia and gonorrhea cases. Chlamydia cases declined by 1,064 cases (95% CI: –1,278, –851) between February to March 2020. Among males there was a decrease of 394 cases (–468, –320), while the reduction among females was by 670.2 cases (–816, –525). Similarly, gonorrhea cases declined, by 109 cases overall (–141, –77); and decreased by 73 cases among males (–93, –53) and 36 case among females (−52, –20). Post-pandemic trends for both infections did not significantly differ from pre-pandemic slopes.
Conclusion: The pandemic significantly disrupted access to sexual health services. Disproportionately larger reduction in reported cases among males underscores pre-existing gaps in screening strategies for this group, which were further exacerbated by the pandemic. Further studies will investigate if cases have since returned to pre-pandemic levels and if the gap can be leveraged to apply a correction factor to post-pandemic infection rates.
PP04.76 – Revisiting the Disulfiram-Like Reaction Between Alcohol and Oral Metronidazole
Dr Patricia Kissinger1, Dr Ifeoluwa Orire1, Ms Momi Sagoe1, Dr Christina Muzny2
1Tulane University, New Orleans, United States.
2University of Alabama, Birmingham, United States.
Background: Metronidazole (MTZ) is a widely used antimicrobial agent effective against anaerobic bacteria and protozoa. Since its introduction in the 1950s, a longstanding debate exists regarding its potential to induce a disulfiram-like reaction (DLR) when combined with alcohol. Early observations suggested that MTZ inhibits aldehyde dehydrogenase (ALDH), mimicking disulfiram-like effects, suggesting that alcohol should not be ingested concurrently with metronidazole. Alcohol restrictions may serve as a barrier to MTZ use. We aimed to conduct a systematic review to evaluate the evidence for a MTZ-induced DLR.
Methods: Databases searched included PubMed, Embase, and the Cochrane Library. Inclusion criteria encompassed clinical trials, retrospective studies, mechanistic studies, animal studies, and case reports that evaluated concurrent use of oral MTZ and alcohol from 1970 to 2024. Keywords searched were: “Disulfiram-Like Reaction”.
Results: The search resulted in 137 papers, of which 11 met study eligibility criteria. Four case reports and a clinical trial suggested positive DLR during concurrent oral MTZ and alcohol use with symptoms including headache, nausea, vomiting, flushing, and tachycardia. In contrast, multiple experimental studies (n = 5) and a retrospective chart review (case control study) have largely failed to replicate these findings. These studies measured ethanol and acetaldehyde levels in human and animal models which revealed no significant inhibition of hepatic ALDH by MTZ. Instead, alternative mechanisms of action were suggested, including altered intestinal alcohol metabolism, with increased intracolonic acetaldehyde concentrations potentially contributing to symptoms. Additionally, Most of the studies largely provided no evidence of DLR in patients who consumed alcohol concurrently with oral MTZ.
Conclusions: Available data don’t robustly support the existence of a clinically significant DLR between oral MTZ and alcohol. Observed reactions may be due to alternative mechanisms or a side effect of alcohol use itself. These findings challenge longstanding clinical recommendations to avoid alcohol use during treatment with oral MTZ.
| Article | Study setting | Age | Gender | Subject | Timeline | Sample Size | DLR +/− | Location | |
|---|---|---|---|---|---|---|---|---|---|
| Taylor (1964) | Case Report | 59 | M | Human | N/A | 1 | + | Los Angeles U.S.A | |
| Lehmann (1966) | Clinical Trial | 22-50 | M,F | Human | N/A | 23 | + | California U.S.A | |
| Gelder (1968) | Controlled Trial | N/A | M,F | Human | 10 days | 10 | − | London U.K | |
| Strassman (1970) | Clinical Trial | N/A | M,F | Human | 45 | − | S. California U.S.A | ||
| Tillonen (2000) | Experimental study | N/A | Animal (Rats) | 6 weeks | 32 | − | Helsinki Finland | ||
| Visapaa (2002) | Clinical Trial | N/A | M,F | Human | 5 days | 12 | − | Helsinki Finland | |
| Karamanakos (2007) | Experimental Study | 4 months | Animal (Rats) | N/A | 60 | − | Kuopio Finland | ||
| Sharma (2009) | Case Report | 48 | M | Human | N/A | 1 | + | Delhi India | |
| Guler (2015) | Case report | 30 | M | Human | N/A | 1 | + | Antalya Turkey | |
| Alonzo (2019) | Case Report | 14 | F | Human | N/A | 1 | + | Texas U.S.A | |
| Feldman (2023) | Retrospective chart review | ~46 | M,F | Human | 10 years | 36 | − | San Francisco U.S.A |
DLR +/− attests to a disulfiram-like reaction due to an interaction between oral MTZ and alcohol being positive or negative in the findings of the study.
PP04.77 – Neonatal Herpes Simplex Virus in the US: Regional Trends and Comparison 2017–2021
Dr. Che’ Harris, PhD Candidate Katherine Lewis, Dr. Jeffrey Klausner
1Herpes Cure Advocacy, Baltimore, United States.
Background: Neonatal Herpes Simplex Virus (HSV) infection is one of the most serious complications of genital HSV infection. However, recent disease burden estimates using nationally representative data are lacking. We address this gap by comparing US trends in neonatal HSV infection by region from 2017–2021.
Methods: We identified neonatal HSV infection cases from the National Inpatient Sample (NIS) database using ICD-10 codes. Disease incidence was calculated by comparing the number of cases yearly to the total number of live births using NIS sample weights. We used linear regression with an interaction term to compare 5-year incidence trends by region.
Results: We identified 1,895 neonatal HSV infection cases, for an average of 379 cases per year and an average annual incidence of 10.28 cases per 100,000 live births. Of these, 47% were in the South, 19% in the Midwest, 19% in the West, and 15% in the Northeast. Total number of cases in the South was persistently higher than in other regions, and half of all cases in the South were in zip codes of the lowest household income quartile. There was no significant change in national neonatal HSV incidence over the 5-year period (coefficient = 0.06, P = 0.801), but there was significant moderation in incidence by region. In the Northeast, incidence decreased by an average of 1.52 cases per 100,000 live births (P = 0.018). Relative to the Northeast, the slope for incidence was increased significantly higher in the Midwest and West (interaction coefficients: 2.84 [P = 0.003], 2.17 [P = 0.017]).
Conclusion: Neonatal HSV infection incidence was stable and varied by region. Neonatal HSV has been widely neglected in pediatric infectious disease and sexual health research and policy but remains an important cause of infant morbidity. Improved national data and attention to this condition are needed to inform targeted risk reduction programs and provider education efforts.
PP04.78 – Increased Hepatitis C and HIV Incidence Among People Who Inject Drugs in Montreal, Canada, 2011–2024
Ms. Bluma Blake Kleiner1, Dr. Adelina Artenie2, Dr. Valérie Martel-Laferrière1,3, Dr. Nanor Minoyan1, Dr. Marleine Azar1, Geng Zang1, Milca Meconnen1, Dr. Didier Jutras-Aswad1,4, Dr. Julie Bruneau1,5, Dr. Sarah Larney1,5
1Centre de recherche du Centre hospitalier de l’Université de Montréal (CRCHUM), Montréal, Canada.
2Population Health Sciences, Bristol Medical School, Bristol, United Kingdom.
3Département de microbiologie, infectiologie et immunologie, Faculté de médecine, Université de Montréal, Montréal, Canada.
4Département de psychiatrie et d’addictologie, Faculté de médecine, Université de Montréal, Montréal, Canada.
5Département de médecine familiale et médecine d’urgence, Université de Montréal, Montréal, Canada.
Background: In Montreal, as in many other high-income settings, HIV and hepatitis C virus (HCV) incidence rates were decreasing before the COVID-19 pandemic due to improvements in comprehensive harm reduction services and effective treatments Disruptions to these services during the COVID-19 pandemic may have affected HCV and HIV acquisition among people who inject drugs. We aimed to estimate and describe patterns in HCV and HIV incidence in people who inject drugs in Montreal, 2011–2024, accounting for the impacts of the pandemic on recruitment and retention in our incidence estimations.
Methods: The Hepatitis Cohort (HEPCO) is an open prospective cohort study that engages people who inject drugs aged ≥ 18 living in Montreal. Every 3 months, participants complete a comprehensive interview and provide blood samples. We calculated annual and overall HCV (primary infection) and HIV incidence from 2011 to 2024. We used two different approaches to calculate person-time at risk, using both a midpoint and a random point method.
Results: Over 2011–2024, 313 participants at risk of primary HCV acquisition were followed, of whom 68 acquired HCV (21.7%); 773 participants at risk of HIV acquisition were followed, of whom 10 acquired HIV (1.3%). Incidence rates estimated using the random point method are reported in Table 1. Similar results were obtained using the midpoint method.
Conclusion: Primary HCV incidence increased among people who inject drugs in Montreal following the COVID-19 pandemic. The HIV incidence trend is consistently very low despite signals that require ongoing monitoring. Confidence intervals around estimates after 2022 are wide due to limited observation time. Enhanced efforts are needed to ensure people who inject drugs are prioritized in HCV and HIV elimination.
| Year | HCV | HIV | |
|---|---|---|---|
| 2011B | 6.40 (1.07–21.15) | 0.00 (0.00–2.43) | |
| 2012 | 12.39A (5.76–23.54) | 1.06A (0.27–2.87) | |
| 2013 | 9.59 (5.04–16.67) | 0.26 (0.013–1.26) | |
| 2014 | 9.11 (4.79–15.84) | 0.24 (0.012–1.17) | |
| 2015 | 4.00 (1.47–8.87) | 0.00 (0.00–0.69) | |
| 2016 | 6.11 (2.84–11.60) | 0.00 (0.00–0.69) | |
| 2017 | 6.06 (2.65–11.98) | 0.00 (0.00–0.79) | |
| 2018 | 4.82 (1.77–10.67) | 0.31 (0.015–1.53) | |
| 2019 | 1.10 (0.055–5.41) | 0.00 (0.00–1.09) | |
| 2020 | 1.40 (0.07–6.91) | 0.48 (0.024–2.36) | |
| 2021 | 0.00 (0.00–4.74) | 0.52 (0.026-2.58) | |
| 2022B | 0.00 (0.00–5.60) | 0.00 (0.00-1.91) | |
| 2023–2024B | 11.55A (5.63–21.19) | 1.00A (0.17–3.30) | |
| Overall | 5.84 (4.57–7.36) | 0.26 (0.13–0.47) |
PP04.79 – Impact of Mpox on Sexual Health Behaviors in Key Populations
Ms Ellen J. Klingler1, Dr. Zoe R. Edelstein1, Dr Devon M. Price1, Dr Preeti Pathela1
1NYC Department Of Health, New York City, United States.
Background: New York City (NYC) primary and secondary syphilis rates in men rose from 1.6/100,000 in 1999 to 49.8/100,000 in 2022 but dropped to 39.0/100,000 in 2023. NYC was an epicenter of the 2022 mpox outbreak; most cases occurred among men who have sex with men (MSM). We investigated behavior changes related to mpox that could impact syphilis trends.
Methods: In March 2023, the NYC Health Department conducted a probability-based survey of sexually active NYC residents (ages 18+) that included demographics, healthcare experiences, and sexual behaviors during the mpox outbreak. Proportions were weighted to NYC’s sexually active population. Logistic regression models examined factors associated with reported decreases in sex partners and increased STI testing (June–September 2022) among respondents reporting mpox-related concerns or impacts on sexual health.
Results: Among 2,192 respondents (representing ~4.5 million NYC residents), 48% were cis-men, 50% cis-women, and 2% reported another gender identity (TGNCNB) (Table 1). Most (91%) were aware of the mpox outbreak, with higher awareness among cis-men and TGNCNB people than cis-women. Twenty percent reported concern about mpox, 5% reported impact on sexual healthcare, and 9% reported impact on sexual activity, with cis-men and TGNCNB people more likely than cis-women to report these issues.
Among those reporting impacts from mpox (n = 491), 34% reported reduced number of sex partners, more common among cis-men (OR: 5.6; 95% CI: 5.6–5.7) than cis-women, and among MSM (OR: 7.5; 95% CI: 7.4–7.6) than other cis-men. Seven percent reported increased STI testing, higher among cis-men (OR: 3.9; 95% CI: 3.8–4.0) and TGNCNB-people (OR: 2.2; 95% CI: 2.1–2.2) than cis-women, and MSM (OR: 15.1; 95% CI: 14.5–15.7) than other cis-men.
Conclusions: During the mpox outbreak, cis-men and TGNCNB individuals reported mpox-related impact and adoption of prevention strategies similar to those recommended for syphilis prevention. Research is needed on how to sustain prevention strategies for effective public health action.
| Unweighted N | overall | awareness of mpox | impact on sexual activity | Unweighted N - affected by mpox | Decreased Sexual Partners; Freq 34%3 | Increased STI Checks; Freq 7%3 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| count | Freq %3 | 95% CI | Freq %3 | 95% CI | Freq %3 | 95% CI | Odds Ratio3 | 95% CI | Odds Ratio3 | 95% CI | |||
| NYC overall | 2,192 | 100 | 91.29 | 89.56-92.75 | 8.90 | 7.06–11.16 | 491 | ||||||
| Gender Identity1 | |||||||||||||
| cisWomen | 1,298 | 48.49 | 45.73–51.27 | 90.49 | 88.27–92.32 | 2.90 | 1.91–4.37 | 256 | reference | reference | |||
| cisMen | 855 | 49.63 | 46.84–52.42 | 91.86 | 88.95–94.06 | 13.55 | 10.37–17.51 | 212 | 5.64 | 5.58–5.70 | 3.89 | 3.82–3.98 | |
| TGNCNB | 39.0 | 1.88 | 1.18–2.97 | 97.05 | 86.43–99.42‡ | 36.91 | 15.88–64.46*†‡ | 23.0 | 6.96 | 6.82–7.09 | 2.15 | 2.06–2.23 | |
| Race Ethnicity | |||||||||||||
| Asian/Native Hawaiian/Pacific Islander, non–Latina/o | 279 | 14.16 | 12.40–16.12 | 91.44 | 86.64–94.63 | 5.67 | 3.13–10.06 | 66 | 0.26 | 0.26–0.26 | 0.22 | 0.21–0.23 | |
| Black, non–Latina/o | 381 | 18.80 | 16.65–21.17 | 92.26 | 88.05–95.06 | 7.22 | 4.18–12.19 | 95 | 0.47 | 0.46–0.47 | 2.44 | 2.38–2.51 | |
| Latina/o | 625 | 28.23 | 25.68–30.94 | 87.80 | 83.34–91.19 | 12.52 | 7.81–19.48 | 186 | 0.71 | 0.70–0.71 | 3.67 | 3.58–3.75 | |
| Native American/Alaskan Native/Multi/Another, non-Latina/o | 109 | 5.93 | 4.69–7.47 | 90.52 | 82.44–95.10 | 6.30 | 2.79–13.63* | 17 | 1.16 | 1.14–1.19 | 1.10 | 1.04–1.17 | |
| White, non-Latina/o | 788 | 32.88 | 30.58–35.25 | 94.03 | 91.60–95.79 | 8.85 | 6.57–11.83 | 125 | reference | reference | |||
| MSM | |||||||||||||
| cisMSM2 | 191 | 21.91 | 18.36–25.94 | 95.37 | 86.36–98.53 | 51.04 | 41.12–60.87 | 133 | 7.53 | 7.44–7.62 | 15.10 | 14.55–15.68 | |
| Other cisMen | 664 | 78.09 | 74.06–81.64 | 90.87 | 87.54–93.38 | 2.51 | 1.30–4.79* | 79 | reference | reference | |||
1. Gender Identity: derived from sex at birth and gender identity; TGNCNB indicates discordant sex at birth and gender identity; reporting transgender, genderqueer, gender non-conforming, or gender non-binary; or reporting another gender identity.
2. CisMSM: cisgender men who have sex with men; determined by sex at birth, gender identity, and self-reported gender of sex partner from the last 12 months.
3. Estimate is weighted.
*Estimate should be interpreted with caution. RSE is greater than 30%.
†Estimate should be interpreted with caution. The 95% Confidence Interval half-width is greater than 10.
‡Estimate should be interpreted with caution. The sample size is too small.
^Data to be suppressed due to imprecise and unreliable estimates.
For Impact of Mpox on Sexual Health Behaviors in Key Populations.
PP04.80 – A Retrospective Multi-Centre Analysis of Neisseria Meningitidis Urethritis in Men Attending Sexual Health Clinics in London, United Kingdom – an Outbreak?
Dr. Manik Kohli1,2, Eliza Gil3, Sandra Coombes1,2, Vitasta Raina4, Maithili Varadarajan4, Risata Kufour4, Su Mei Goh4, Jack Kerwin4, Michael Rayment4, Daniel Trotman5, Shara Palanivel3, Harry Coleman2, Joseph Heskin4, John Saunders6, Helen Fifer6, Odile Harrison7, Gilson Richard1,2
1Institute for Global Health, University College London, London, United Kingdom.
2Central and North West London NHS Foundation Trust, London, United Kingdom.
3University College London Hospitals NHS Foundation Trust, London, United Kingdom.
4Chelsea and Westminster Hospital NHS Foundation Trust, London, United Kingdom.
5Kingston and Richmond NHS Foundation Trust, London, United Kingdom.
6Blood Safety, Hepatitis, STI & HIV Division, UK Health Security Agency, United Kingdom.
7Nuffield Department of Population Health, University of Oxford, Oxford, United Kingdom.
Background: Sexual transmission of Neisseria meningitidis (N.men) can cause urethritis in men. Outbreaks of meningococcal urethritis and invasive meningococcal disease have been reported in men who have sex with men (MSM). This study aimed to characterise cases of N.men urethritis seen in sexual health clinics in London.
Methods: Electronic health records of men diagnosed with N.men urethritis at 7 London sexual health clinics from January 2014 to July 2024 were reviewed. Clinics covered North (Archway), Central (Mortimer Market Centre/56 Dean Street), West (John Hunter Clinic/10 Hammersmith Broadway), South-West (Wolverton) London, and Surrey (Buryfields). Demographic, sexual history, clinical, and microbiological data were extracted. N.men urethritis was defined as urethral symptoms with/without positive in-clinic microscopy (>5 polymorphonuclear leukocytes with/without gram-negative intracellular diplococci), plus positive N.men culture, and negative tests for other urethral sexually transmitted infections.
Results: 101 cases of N.men urethritis were identified from 2014–2024. Median age was 28 (IQR 23.5–34), 56.6% (n = 56/99) were MSM, and 51.1% (n = 46/90) White. Urethral discharge, dysuria, and positive microscopy were present in 92.0% (n = 93/101), 79.2% (n = 80/101), and 71.3% (n = 72/101) respectively. Most (n = 73/101) were treated with ceftriaxone. The highest number of cases (n = 28) was seen in 2023 (Fig. 1), representing 27.7% of all cases. Of these, 60.1% (n = 17/28) were in heterosexual men, and 12/17 were diagnosed at a single clinic (Archway). The overall rate of positive N.men per 100 Neisseria gonorrhoeae also increased at Archway from 0.2 in 2022 to 2.3 in 2023. The number of cases diagnosed in 2023 at other clinics ranged from 2–4.
Discussion: We identified an increase in N.men urethritis in 2023, primarily among heterosexual men attending a single sexual health clinic in North London. No increase was noted elsewhere. Surveillance and characterisation of urogenital N.men is needed, with the UK Health Security Agency now recommending the transfer of urogenital/anorectal N.men isolates to the Meningococcal Reference Unit.
Confirmed Neisseria meningitis urethritis cases in men at 7 sexual health clinics in London January 2014 to July 2024, by sexual orientation. MSM, men who have sex with men.
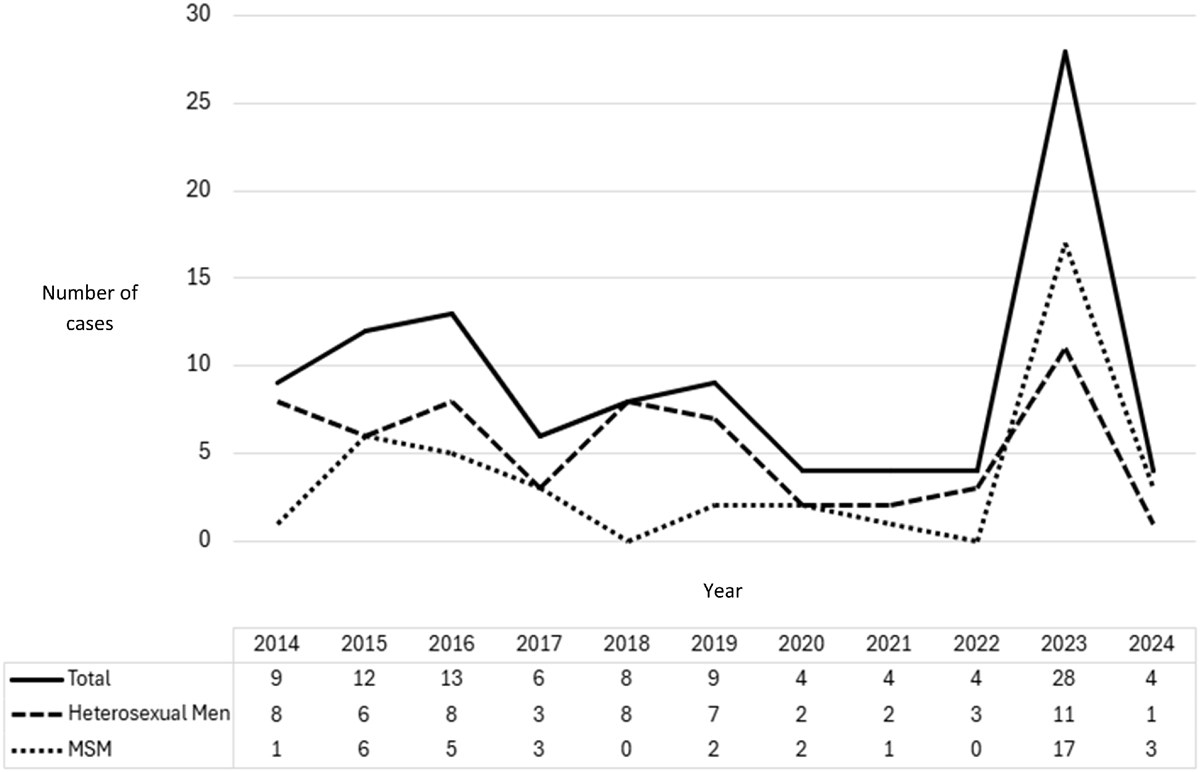
PP04.81 – Machine Learning for Personalised Risk Assessment of HIV, Syphilis, Gonorrhoea, and Chlamydia: A Systematic Review and Meta-Analysis
Dr. Phyu Mon Latt1,2, Dr Nyi Nyi Soe1,2, Prof. Christopher Fairley1,2, Prof. Eric Chow1,2,3, Dr. Cheryl Johnson1,2,4, Dr. Purvi Shah1,2,4, Dr. Ismail Maatouk1,2,4, Prof Lei Zhang1,2,5, Prof. Jason Ong1,2,6
1Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Melbourne, Australia.
3Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
4Global HIV, Hepatitis and STIs Programmes, World Health Organization, Geneva, Switzerland.
5Clinical Medical Research Centre, Children’s Hospital of Nanjing Medical University, Nanjing, China.
6Department of Clinical Research, London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: Optimising sexually transmitted infection (STI) risk estimation remains challenging. Machine learning (ML) approaches promise to enhance STI risk estimation. This study systematically evaluated the performance of ML models in estimating individual risk for HIV, syphilis, gonorrhoea, and chlamydia.
Methods: Following PRISMA guidelines, we systematically searched six electronic databases, three preprint archives, and conference proceedings from January 2010 to April 2024. Studies were eligible if they reported performance metrics for supervised ML-based STI risk prediction models. Two independent reviewers assessed the risk of bias using PROBAST (Prediction Model Risk Of Bias Assessment Tool). We employed bivariate random-effects meta-analysis to estimate pooled sensitivity, specificity, and area under the curve (AUC) with 95% confidence intervals. We conducted sequential analyses of studies with complete and reconstructed confusion matrices. Subgroup analyses and meta-regression explored potential sources of heterogeneity.
Results: Among 3,877 records screened, 25 studies comprising 45 unique models met inclusion criteria, with sample sizes ranging from 547 to 4,384,178 participants across 14 countries. For HIV risk estimation, the SROC curve analysis of studies reporting complete confusion matrices (7 studies with 9 contingency tables) demonstrated a summary AUC of 0.91 (95% CI: 0.88–0.93), with a pooled sensitivity of 0.84 (0.76–0.90) and specificity of 0.84 (0.70–0.93). The analyses demonstrated substantial heterogeneity (I2 > 98%). Limited evidence was available for meta-analysis of other STIs, with AUCs ranging from 0.75 to 0.87 for syphilis (N = 5), 0.73–1.00 for gonorrhoea (N = 6), and 0.67–1.00 for chlamydia (N = 6). Despite comprehensive subgroup analyses, substantial statistical heterogeneity persisted across all analyses.
Discussion: While ML models show promising performance, particularly for HIV risk estimation, significant heterogeneity complicates interpretation. Only four studies transformed their research into an accessible clinical tool, highlighting the gap between model development and real-world application. Future research should prioritise external validation, standardised reporting following TRIPOD-AI guidelines, and robust implementation studies.
PP04.82 – Multiplex PCR for Genital Ulcer Disease Etiology in East London, South Africa
Mr. Andy Liu1, Ms Mandisa Mdingi2, Dr. Hyunsul Jung3, Dr. Ranjana Gigi2, Dr. Remco Peters2,3, Dr. Jeffrey Klausner1
1Keck School of Medicine of USC, Los Angeles, United States.
2Foundation for Professional Development, East London, South Africa.
3University of Pretoria, Pretoria, South Africa.
Background: Genital ulcer disease (GUD) remains a significant public health challenge in sub-Saharan Africa, contributing to an increased risk of HIV acquisition. Understanding the microbial etiology of GUD may help facilitate treatment, control, and prevention of sexually transmitted infections.
Methods: As part of an ongoing genomic study of syphilis in sub-Saharan Africa, we enrolled patients with syphilitic skin lesions at primary healthcare facilities in East London, South Africa. Lesion swabs were collected and analyzed using an in-house multiplex PCR assay to detect Haemophilus ducreyi (HD), Treponema pallidum (TP), and herpes simplex virus types 1 (HSV-1) and 2 (HSV-2). Positive detection was defined as a cycle threshold value below 40. Chi-squared analysis was performed to assess differences in pathogen distribution by sex and HIV status.
Results: Between October 2023 and November 2024, 73 participants presenting with genital ulcers were recruited. Of these, 39 (53.4%) were female, and 25 (34.2%) were living with HIV. Pathogens were detected in 35/39 (89.7%) ulcers in females (Fig. 1). Of these, 13 (37.1%) tested positive for TP alone, 13 (37.1%) tested positive for HSV-2 alone, and 9 (25.7%) were co-infected with TP and HSV-2. Pathogens were detected in 31/34 (91.2%) ulcers in males. Of these, 11 (35.5%) tested positive for TP alone, 9 (29.0%) tested positive for HSV-2 alone, 10 (32.3%) were co-infected with TP and HSV-2, and 1 (3.2%) was co-infected with TP and HSV-1. All ulcers were negative for HD. Chi-squared analysis revealed no significant differences in the pathogen distribution (TP alone, HSV-2 alone, and TP/HSV-2 coinfection) by sex (P = 0.75) or HIV status (P = 0.21).
Conclusion: Our findings highlight the substantial burden of TP and HSV-2 in GUD cases in this population, with frequent co-infections, regardless of sex or HIV status. These results underscore the importance of molecular diagnostics to guide effective STI management and prevention strategies.
PP04.83 – Impact of Mycoplasma Hominis on Trichomonas Vaginalis in Pregnancy and Gestational Age at Birth: Cohort Study, South Africa
Prof. Nicola Low1, Dr. Ranjana MS Gigi1,2, Ms. Mandisa M Mdingi2, Dr. Hyunsul Jung3, Dr. Jean-Benoît Rossel1, Dr. Lydia Braunack-Mayer1, Dr. Eric Mensah3, Ms. Annika Henry3, Dr. Chibuzor M Babalola4, Prof. Christina A Muzny5, Ass. Prof. Christopher M Taylor6, Dr. Andrew Medina-Marino7, Prof. Jeffrey D Klausner4, Prof. Janneke HHM van de Wijgert8, Prof. Remco PH Peters2,3
1University of Bern, Bern, Switzerland.
2Foundation for Professional Development, East London, South Africa.
3University of Pretoria, Pretoria, South Africa.
4University of Southern California, Los Angeles, United States of America.
5University of Alabama at Birmingham, Birmingham, United States of America.
6Louisiana State University Health Sciences Center, New Orleans, United States of America.
7University of Pennsylvania, Philadelphia, United States of America.
8University Medical Center Utrecht, Utrecht, The Netherlands.
Background: Trichomonas vaginalis (TV) during pregnancy is associated with preterm birth. Mycoplasma hominis (MH) is associated with preterm birth and increases the pathogenicity of TV in vitro. We aimed to investigate TV and MH co-infection among pregnant women and associations with preterm birth.
Methods: We conducted a cohort study in East London, South Africa. Pregnant women were enrolled at <27 weeks gestation, confirmed by ultrasound. Chlamydia trachomatis, Neisseria gonorrhoeae (GeneXpert, Cepheid) and HIV testing occurred on-site, with treatment as appropriate. Baseline vaginal swabs were PCR-tested for TV, MH, M. genitalium and Ureaplasma urealyticum at the end of the study, so specific treatment during pregnancy was not given. The prespecified outcome was gestational age at birth, in days (preterm birth, <37 weeks = <259 days). Among women with known delivery date, we conducted regression analyses, adjusting for baseline sociodemographic, clinical and microbiological covariates, incorporating an interaction term between TV and MH (Table).
Results: From March 2021 to October 2023, 603 pregnant women were enrolled (median gestation 13 weeks, interquartile range, IQR 10–19), 581/603 (96.4%) were followed post-delivery. Median age was 28 years (IQR 24–33) and 156/581 (26.9%) were living with HIV. MH (427/581, 73.5%) was more common among women with TV (62/581, 10.7%, MH+TV+ 53/62, 85.5%) than without (MH+TV- 374/519, 72.1%). Median gestational ages at birth and percentages preterm were: women with TV+/MH+ (n = 53, 39 weeks + 0 days, 17.6%); TV+/MH− (n = 9, 37+4, 22.2%); TV-MH+ (n = 374, 39+0.5, 19.5%); TV-MH– (n = 145, 38+6, 22.3%). In multivariable analysis for women both with and without TV, gestational age at birth did not differ by MH status (Table 1, P-value for interaction = 0.41).
Conclusion: MH was highly prevalent in pregnancy and was associated with TV. TV was, however, not associated with shorter gestation and MH did not modify the effect. These findings, among prospectively followed South African pregnant women, challenge existing published research.
| TV-positive | TV-negative | |||||
|---|---|---|---|---|---|---|
| MH-positive | MH-negative | MH-positive | MH-negative | |||
| Number of women | 53 | 9 | 374 | 145 | ||
| Baseline characteristics | ||||||
| Age in years | ||||||
| Median | 29 | 26 | 28 | 29 | ||
| (IQR) | (23, 32) | (22, 32) | (23, 33) | (25, 33) | ||
| Living with HIV, n (%) | ||||||
| No | 32 (60.4%) | 5 (55.6%) | 268 (71.7%) | 120 (82.8%) | ||
| Yes | 21 (39.6%) | 4 (44.4%) | 106 (28.3%) | 25 (17.2%) | ||
| Birth outcome, univariable analysis | ||||||
| Gestational age, in weeks+days | ||||||
| Median | 39+0 | 37+4 | 39+.5 | 38+6 | ||
| (IQR) | (37+3, 40+0) | (37+2, 39+4) | (37+5, 40+2) | (37+1, 40+1) | ||
| Missing | 2 | 0 | 20 | 6 | ||
| Preterm birth, n (%) | ||||||
| Yes | 9 (17.6%) | 2 (22.2%) | 69 (19.5%) | 31 (22.3%) | ||
| No | 42 (82.4%) | 7 (77.8%) | 285 (80.5%) | 108 (77.7%) | ||
| Missing | 2 | 0 | 20 | 6 | ||
| Birth outcome, multivariable analysisa | P-valueb | |||||
| Mean differencec in gestational age, in weeks+days | ||||||
| All births (95% CI) | –0+3 (−2+6, 2+0) | 0+5 (–0+4, 2+0) | 0.41 | |||
| Live births (95% CI) | 0+6 (−0+5, 2+3) | –0+0 (–0+4, 0+3) | 0.27 | |||
| Risk differencec in preterm birth, % | ||||||
| All births (95% CI) | –8.1% (–38.8%, 22.6%) | –2.1% (–10.2%, 6.0%) | 0.43 | |||
| Live births (95% CI) | –12.1% (–43.1%, 18.9%) | 1.7% (–5.2%, 8.7%) | 0.33 | |||
a. Linear regression model, adjusted for baseline covariates, including an interaction between TV and MH exposure. Baseline covariates: age, level of education, alcohol consumption, at least one prior pre-term birth, living with HIV, C. trachomatis, N. gonorrhoeae, M. genitalium, U. urealyticum;
b. P-value from Wald test for interaction;
c. Differences are calculated as MH-positive minus MH-negative;
CI, confidence interval; IQR, interquartile range; MH, M. hominis; TV, T. vaginalis.
PP04.84 – HPV and Syphilis Infection Among Men Who Have Sex with Men Living with or Without HIV in Tianjin, China: A Biological Behavioral Study
Dr. Ping Ma1,2, Dr. Ziyu Wang1, Dr. Yiyao Zhang1, Dr. Jianyun Bai3, Dr. Mengdi Wan1, Manager Zhengwei Ding4, Dr. Maohe Yu3, Dr. Hao Wu5
1Tianjin Second People’s Hospital, Tianjin, China.
2Association for STDs & AIDS Prevention and Control, Tianjin, China.
3Tianjin Center for Disease Control and Prevention, Tianjin, China.
4AIDS Health Foundation(AHF), Beijing, China, Beijing, China.
5Beijing You’an Hospital of Capital Medical University, Beijing, China.
Background: Men who have sex with men are at higher risk of sexually transmitted diseases, such as syphilis and HPV. In China, the prevalence of STIs in MSM populations has risen sharply. We aimed to investigate the prevalence of HPV and syphilis in MSM populations living with or without HIV in Tianjin, providing reference data for policy makers.
Methods: The study was conducted from June to November 2024, using a cross-sectional study design. It was conducted simultaneously at three project sites in Tianjin, including an infectious diseases hospital, where AHF wellness center located, a municipal center for disease control and treatment, and a MSM community organization. Genital exfoliated cells and plasma were collected for HPV testing and syphilis antibody testing in two groups. Data were analyzed using SPSS 24.0.
Results: A total of 2,300 MSM people were recruited, of whom 1,229 were HIV-negative from a local MSM community, and 1,071 HIV-positive who received long-term follow-up of antiviral therapy in the designated hospital. The prevalence of syphilis (including either positive or double positive of syphilis antibodies and non-treponemal antibodies) and HPV in HIV-positive MSM were 40.1% and 42.6% respectively. And these two indicators were 11.2% and 37.8% respectively in HIV negative MSM. There was a significant difference with statistical significance in the syphilis infection rate between the two groups (40.1% vs 11.2% P < 0.001)
Conclusion: The prevalence of syphilis and HPV in the MSM population in Tianjin, China is relatively high, and the prevalence of syphilis in the HIV-positive population is significantly higher than that in the HIV-negative population. It is necessary to pay attention to the publicity and education of HIV and STD prevention and treatment in the MSM population to improve the screening and treatment rate.
The Ethics approval is TJCDC-R-2023-013.
PP04.85 – Intersecting Risks: Heightened Syphilis Seropositivity Among Equity-Deserving Populations in Ontario, Canada
Ms. Lucy Mackrell1, Dr. Megan Carter1,2, Ms. Natasha Larkin1,3, Dr. Patrick O’Byrne4, Dr. Vanessa Tran5,6, Ms. Nicole Szumlanski2, Ms. Maggie Hoover1, Ms. Kira Mandryk7, Mr. Farhan Khandakar1, Ms. Jessica Burnside1, Dr. Sahar Saeed1
1Queen’s University, KINGSTON, Canada.
2Kingston, Frontenac and Lennox & Addington Public Health, Kingston, Canada.
3Kingston Community Health Centres, Kingston, Canada.
4University of Ottawa, Ottawa, Canada.
5Public Health Ontario, Toronto, Canada.
6University of Toronto, Toronto, Canada.
7Ottawa Public Health, Ottawa, Canada.
Background: Infectious syphilis has reemerged as a global public health threat. Since 2013, the incidence of infectious syphilis in Ontario, Canada has surged by 345%, alongside significant demographic shifts. We evaluated intersecting risk factors associated with seropositivity in an equity-deserving population in Ontario.
Methods: We used data from the Syphilis Point of Care Rapid Test and Immediate Treatment Evaluation (SPRITE) study- a community-based study across eight Ontario public health units (PHUs). Sociodemographic and risk factor data such as being un(der)housed, using drugs (PWUD), or engaging in survival sex work, was collected from public health intake forms along with lab-based syphilis serology (treponemal antibodies (IgG and IgM)). Syphilis seroprevalence was stratified by risk factors, and a mixed-effects regression with a log-binomial distribution was used to estimate the adjusted prevalence ratio (aPR) controlling for age and sex and clustering by PHUs.
Results: From April to November 2024, 407 participants with serological results were included: median age 38 (IQR 31–48); 42% female; 62% un(der)housed; 34% reported a sexual risk factor; 63% PWUD, 47% of whom used crystal meth. Syphilis seroprevalence was 7.6% (95% CI 5.5, 9.7); higher among women (aPR 1.7 (1.0, 2.9)) and PWUD (aPR 2.3 (0.9,5.50)). Crystal meth use (aPR 2.9 (1.3, 6.3) was independently association with seropositivity compared to other illicit drugs. Fig. 1a illustrates a significant overlap of risk factors; 57% of the participants reported at least two risk factors. Seropositivity was highest at 19.2% (11.2, 29.7) among participants who reported having sexual risk factors, PWUD, and being un(der)housed (Fig. 1b).
Conclusion: Syphilis burden is heightened at the intersection of sexual risk factors, illicit drug use, and housing instability among equity-deserving populations. This signals a significant shift in Ontario’s syphilis epidemiology, highlighting the urgency of developing targeted prevention, screening, and intervention strategies to address the unique needs of this population.
The number (n) of SPRITE participants by self-reported risk factors, reflected by circle size. Fig. 1b: Syphilis seroprevalence (%) by risk factor(s).
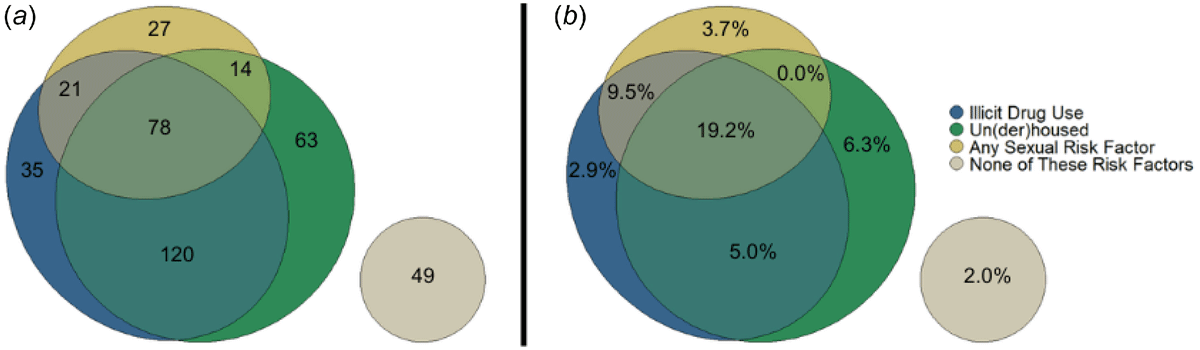
PP04.86 – Antimicrobial Resistance of Neisseria Gonorrhoeae in France From 2018 to 2023
Dr François Caméléna1,2, Miss Manel Mérimèche1,2, Miss Mary Mainardis1,2, M Aymeric Braille1,2, Miss Fabienne Meunier1,2, Dr Emilie Chazelle3, Pr Cécile Bébéar4, Prof. Beatrice Bercot1,2, on the behalf of th EnGON Study Group
1Associated Lab of French National Center for Bacterial Sexually Transmitted Infections, Bacteriology Department, St Louis and Lariboisière Hospital, AP-HP, Paris, France.
2IAME, UMR 1137, INSERM, Paris Cité University, Sorbonne Paris Cité, Paris, France.
3Santé publique France, Saint-Maurice, France.
4Bacteriology Department, French National Center for Bacterial Sexually Transmitted Infections, CHU de Bordeaux, Bordeaux, France.
Background: In France, annual national surveys (ENGON) have been established to monitor gonococcal resistance, combining clinical, phenotypic and genotypic strain data. Neisseria gonorrhoeae (NG) strains were collected in public and private laboratories over a period running from September to December 2018 to 2023. Ceftriaxone(CRO)-resistant strains isolated outside the survey periods have been added to this surveillance.
Description: Between 2018 and 2023, laboratories participating in 104-ENGON sent 2,972 NG isolates to the National Reference Center for bacterial STIs. MICs were measured using the MICstrip test (bioMérieux). Results were interpreted according to the EUCAST breakpoint table version 13.0. Whole genome sequencing of NG isolates was performed by the Illumina technology.
Results: In total, 2,972 isolates were tested from 2018 to 2023. Of these, 80.2% were from men; median age was 28 years. Most isolates were obtained urethral (49.8%), followed by vaginal (17.3%), anal (17.1%) and oral samples (10.8%). NG antimicrobial resistance prevalence is high for tetracycline (85.4%–90.5%) and ciprofloxacin (62%–70.9%). Azithromycin resistance was steadily increasing up to 10% in 2022, but only 1.9% of isolates had mutations in the 23S rRNA gene, associated with higher azithromycin MICs (2 to 256 mg/L).
Cefixime (CFX)- and Ceftriaxone(CRO)-resistance was stably low. Six isolates from patients returning from Asia were resistant to CRO and CFX and carried the penA-60 allele.
However, we also observed a recent increase in reduced susceptibility and/or resistance to CFX (MIC > 0.032 mg/L), rising from 4.5% in 2022 to 12.1% in 2023. This increase was significantly associated with the acquisition of the penA-34 mosaic allele and the ST16676 sequence type clone (P < 0.00001).
Conclusion: A worrying increase in NG strains with reduced CFX susceptibility was observed in France in 2023. These data are linked to the presence of clones carrying the penA34 mosaic gene and this trend has to be monitored over time and in other European countries.
PP04.87 – Survey of Neisseria Gonorrhoeae Susceptibility in French Polynesia (2021–2023)
Miss Mary Mainardis1,2, Dr Stephane Lastere3, Dr François Camelena1,2, Miss Jeanne Petiot1, Miss Manel Mérimèche1,2, M Aymeric Braille1,2, Mrs Fabienne Meunier1,2, Dr Marc Levy3, Pr Béatrice Berçot1,2
1Associated Lab of French National Center for Bacterial Sexually Transmitted Infections, Bacteriology Unit, St Louis and Lariboisière Hospital, Paris, France.
2IAME, UMR 1137, INSERM, Paris Cité University, Sorbonne Paris Cité, Paris, France.
3Microbiology Unit, Clinical Lab, French Polynesia Referral Hospital, Papeete, French Polynesia.
Background: In 2020, the WHO estimated 82.4 million new infections by Neisseria gonorrhoeae (NG) and recognized gonorrhea as a major public health problem. The genomic surveillance of NG in the French overseas departments and regions is particularly complicated by geographical constraints. This study presents the epidemiological and microbiological data of NG infection from the French Polynesia Referral Hospital (FPRH) located in Tahiti, French Polynesia.
Methods: Between May 2021 and November 2023, 48 strains from 48 patients isolated in FPRH were sent to the STI French National Reference Center for gonococcal expertise located in Saint-Louis hospital (Paris, France).
Isolates were cultured on chocolate agar and MIC were determined with E-tests (Biomérieux). Whole-Genome-Sequencing (WGS) of the isolates was performed using Illumina technology.
Results: Patients with NG infection were mostly men (73%); median age was 25 years old. Most patients (50%) were diagnosed following a visit to the emergency department. The localization of the infection was mostly genital (92%) and 52% of patients had symptoms.
NG isolates were resistant to tetracycline, ciprofloxacin and azithromycin in 96%, 92% and 17%, respectively. All isolates were susceptible to spectinomycin, gentamicin, cefixime and ceftriaxone.
The WGS revealed that all ciprofloxacin-resistant isolates had S91F and D95A GyrA mutations. All tetracycline-resistant isolates showed V57M RpsJ mutation. The tetM plasmid gene was present in 4.2% (all highly resistant to tetracycline). All penA genes were non-mosaic. The most frequent ST were ST9362 (43.8%) followed by ST11200 (43.8%). These ST are part of the clones circulating in France between 2021 and 2023.
Conclusion: NG infections were mostly genitals and found in male. Almost all NG isolates were resistant to ciprofloxacin and tetracycline. The NG clones circulating in Tahiti were similar to those circulating in metropolitan France. Repeating survey would allow for improved surveillance and an update of gonococcal infection data in French Polynesia.
PP04.88 – Rectal Mycoplasma Genitalium (MG) Infection, Proctitis and Antimicrobial Resistance in the United States (US) from 2023 to 2024
Dr. Lisa Manhart1, Dr. Olusegun Soge1, Dr. Stephen Jordan2, Dr. Candice McNeil3, Dr. Preeti Pathela4, Dr. Hilary Reno5, Dr. Karen Wendel6, Dr. William Geisler7, Ms. Anika Parker1, Ms. Gina Leipertz8, Dr. Damon Getman9
1University of Washington, Seattle, United States.
2Indiana University, Indianapolis, United States.
3Wake Forest University, Winston-Salem, United States.
4New York City Department of Health and Mental Hygiene, New York City, United States.
5Washington University at St. Louis, St. Louis, United States.
6Public Health Institute at Denver Health, Denver, United States.
7University of Alabama at Birmingham, Birmingham, United States.
8Washington State University, Spokane, United States.
9Hologic, Inc., San Diego, United States.
Background: MG surveillance in the US has demonstrated ~16% and ~58% prevalence of urogenital infection and macrolide resistance, respectively. Data on rectal infections are limited.
Methods: We collected remnant rectal specimens during 2023–2024 from males and females tested for chlamydia (CT) and gonorrhea (GC) in sexual health clinics in Denver CO, Greensboro NC, Indianapolis IN, New York NY, Seattle WA, and St. Louis MO. Specimens were tested for MG (Aptima Mycoplasma genitalium Assay) and macrolide resistance mutations (MRMs) (analyte-specific reagents; Hologic, Inc). We estimated rectal and macrolide resistance prevalence and calculated adjusted prevalence ratios (aPR) using Poisson regression with robust standard errors.
Results: Of 1,586 persons with rectal specimens, 160 (10.2%) reported rectal symptoms. MG was detected in 253 (148/877 males [16.9%]; 105/709 females [14.8%]: combined prevalence = 16.0%; 95% CI = 14.18%–17.85%). Adjusting for city, rectal MG prevalence declined as age increased (adjusted prevalence ratio [aPR] = 0.98per year; 95% CI = 0.969–0.996, P = 0.01). Rectal MG was not associated with year, sex, same-sex partners, race-ethnicity, or rectal CT/GC but was three times more common in those with than without a proctitis diagnosis (14/38 [36.8%] vs 236/1540 [15.3%]: aPR = 3.1; 95% CI = 1.62–5.89, adjusted for rectal CT/GC and city). MRMs were detected in 129/236 MG-positive rectal specimens (combined prevalence = 54.7%; 95% CI = 48.07%–61.13%). From 2023–2024, rectal MRM prevalence declined by 22% (64.5% [2023] vs 48.3% [2024]; aPR = 0.78; 95% CI = 0.61–0.98, P = 0.03, adjusting for city) whereas urogenital MRM prevalence over the same time period did not (58.8% [2023] vs 54.1% [2024]; aPR = 0.98; 95% CI = 0.88–1.10, P = 0.76). Prevalence of rectal MRMs was not associated with age, sex, same-sex partners or rectal CT/GC, but varied significantly by race/ethnicity (P < 0.01) (Table 1).
Conclusion: Rectal MG was common in both MSM and cis-women. Despite stable rectal MG prevalence from 2023–2024, macrolide resistance declined. MG may cause proctitis but prospective studies should confirm this. Ongoing surveillance is needed.
| Characteristic | M. genitalium PrevalenceN = 1,586 | Macrolide Resistance PrevalenceN = 236 | |||
|---|---|---|---|---|---|
| N (%) | P-value | N (%) | P-value | ||
| Year | |||||
| 2023 | 109 (15.9) | 0.99 | 60 (64.5) | 0.01 | |
| 2024 | 144 (16.0) | 60 (64.5) | |||
| Age | |||||
| <25 | 58 (20.6) | 0.02 | 35 (63.6) | 0.13 | |
| ≥25 | 195 (15.0) | 94 (51.9) | |||
| Sex | |||||
| Male | 148 (16.9) | 0.26 | 80 (59.7) | 0.08 | |
| Female | 105 (14.8) | 49 (48.0) | |||
| MSM vs. MSW | |||||
| MSM | 141 (17.4) | 0.67 | 78 (60.5) | 0.08 | |
| MSW | 5 (20.8) | 0 (0) | |||
| WSW vs. WSM | |||||
| WSW | 17 (15.5) | 0.94 | 11 (64.7) | 0.13 | |
| WSM | 80 (15.2) | 34 (44.2) | |||
| Race/ethnicity | |||||
| NH Black | 74 (19.0) | 0.36 | 31 (49.2) | <0.01 | |
| NH White | 24 (15.4) | 52 (61.9) | |||
| NH Another | 90 (15.4) | 16 (80.0) | |||
| Hispanic | 52 (13.7) | 21 (37.5) | |||
| Unknown | 13 (17.1) | 9 (69.2) | |||
| Rectal CT/NG | |||||
| No | 212 (15.5) | 0.37 | 113 (57.1) | 0.16 | |
| Yes | 38 (17.9) | 16 (44.4) | |||
| Proctitis | |||||
| No | 236 (15.3) | <0.001 | 121 (55.3) | 0.89 | |
| Yes | 14 (36.8) | 8 (57.1) | |||
Abbreviations: MSM, men who have sex with men; MSW, men who have sex with women; WSW, women who have sex with women; WSM, women who have sex with men; NH, non-Hispanic; CT, Chlamydia trachomatis; NG, Neisseria gonorrhoeae.
PP04.89 – Prevalence of Mollicutes in Pregnant Women Undergoing High-Risk Prenatal Care at a Maternal and Child Reference Unit in Bahia, Brazil
Dr. Lucas Marques1, Dr. Fabricia Santana2, Dr. Jéssica Almeida1, Miss Mariana Ferraz1, Miss Victória Cardoso1, Miss Jassy Borges1, Dr Danielle Medeiros1, Dr Mauricio Grijó Junior1, Dr Guilherme Campos1
1Universidade Federal Da Bahia, Vitoria Da Conquista, Brazil.
2Universidade Estadual de Santa Cruz, Ilhéus, Brazil.
Background: This study investigated the prevalence of Mycoplasma hominis, M. genitalium, Ureaplasma parvum, and U. urealyticum in pregnant women receiving high-risk prenatal care and associated factors.
Methods: The study included 164 pregnant women aged 18 years or older, with exclusions for antibiotic use within 14 days before sample collection. Data were collected to determine epidemiological profiles (EP) and cervical samples taken by gynecologists/obstetricians. Mollicutes species were identified using qPCR. Associations between EP and Mollicutes prevalence were analyzed using chi-square or Fisher’s exact tests and Poisson regression with robust variance to estimate prevalence ratios, considering statistical significance at P < 0.05 with a 95% confidence interval.
Results: The prevalence of Mollicutes was 60.97%, with specific rates of 48.78% for U. parvum, 11.59% for U. urealyticum, 18.9% for M. hominis, and 1.22% for M. genitalium. Factors associated with Mollicutes colonization included having 12 or more years of schooling (PR = 1.36, CI 1.04–1.78), age at first sexual intercourse up to 14 years (PR = 1.41, CI 1.07–1.84), and infertility treatment (PR = 0.32, CI 0.14–0.75). Specific findings showed associations for Ureaplasma spp. with early sexual debut (PR = 1.37, CI 1.03–1.81) and infertility treatment (PR = 0.27, CI 0.09–0.76). Mycoplasma spp. was linked to ages between 20 and 34 years (PR = 2.61, CI 1.10–6.20). U. urealyticum was associated with the third trimester of pregnancy (PR = 0.24, CI 0.08–0.77), history of STIs (PR = 2.58, CI 1.09–6.12), and groin lymph nodes (PR = 3.07, CI 1.04–9.04). For U. parvum, significant factors included schooling of 12 years or more (PR = 1.60, CI 1.11–2.30), early sexual debut (PR = 1.60, CI 1.13–2.26), and infertility treatment (PR = 0.30, CI 0.11–0.82). M. hominis was linked to ages 20–34 years (PR = 2.57, CI 1.08–6.11).
Conclusion: These results highlight the need for screening and interventions to reduce adverse pregnancy outcomes associated with these infections.
PP04.90 – Prevalence of Extragenital Neisseria Gonorrhoeae and Chlamydia Trachomatis Among Persons Assigned Female Sex at Birth in Seattle, WA
Dr. Stephanie E. McLaughlin1, Krstine Lan, Dr. Margaret Green, Dr. Eve Lake, Dr. Raaka Kumbhaka, Shireesha Dhanireddy, Dr. Maria A. Corcorran
1University of Washington, Seattle, United States.
Background: The CDC recommends screening for extragenital (rectal and oropharyngeal) bacterial STIs in sexually active men who have sex with men (MSM) and allows for shared decision-making regarding screening at these sites in women and other persons assigned female sex at birth (AFSB).
Methods: We quantified the prevalence of Neisseria gonorrhea (NG) and Chlamydia trachomatis (CT) infections in patients AFSB seen at the Safe. Healthy. Empowered. (SHE) low-barrier care clinic in Seattle, WA. In addition to cervicovaginal screening by urine or vaginal swab (Aptima NAATs), patients AFSB were offered extragenital (rectal and oropharyngeal) screening for NG and CT in an opt-out system as part of routine clinical care. Positive tests were recalled to clinic and treated with ceftriaxone and/or doxycycline as per clinical guidelines, although antibiotic treatment completion data were not incorporated into this analysis. We used descriptive statistics to describe the proportion of oropharyngeal and rectal NG and CT test that were positive at each anatomic site.
Results: From December 2021 to December 2023, there were 739 NG/CT NAAT tests performed among 114 patients AFSB. Nearly all had cervicovaginal testing (95%), 61% had oropharyngeal testing, and 37% had rectal testing. The overall prevalence of NG was 5.7% (42 infections) and CT was 6.9% (51 infections). Among those tested, 4.4% of oropharyngeal samples were positive for NG and 2.2% were positive for CT. Among rectal samples, 5.6% were positive for NG and 7.8% for CT (Table 1). Half (51%) of CT, and one third (33%) of NG infections would have been missed by cervicovaginal testing alone.
Conclusions: In a population of patients AFSB at high risk for STIs, screening only for cervical NG/CT may miss a significant number of isolated extragenital infections.
| NG Prevalence (n) | CT Prevalence (n) | ||
|---|---|---|---|
| Cervical | 3.7% (26) | 5.3% (37) | |
| Oropharyngeal | 4.4% (20) | 2.2% (10) | |
| Isolated Oropharyngeal (neg cervical) | 2.7% (11) | 1.0% (4) | |
| Rectal | 5.6% (15) | 7.8% (21) | |
| Rectal Isolated (neg cervical) | 1.7% (4) | 4.7% (11) | |
| Isolated Rectal and/or Oropharyngeal (neg cervical) | 3.4% (14) | 5.6% (26) |
PP04.91 – How Anti-Indigenous Racism and Global Exploitation Impact the Rate of HIV Cases Among Indigenous Women in Canada
Mr. Albert Mcleod1
12spirit Consultants Of Manitoba, Winnipeg, Canada.
Indigenous women in Canada are consistently and progressively over-represented in HIV epidemiology reports due to the impacts of anti-Indigenous racism, ongoing resource extraction, and colonial exploitation of traditional land-based territories. This presentation will review recent federal and provincial HIV epidemiological reports that show a steep increase among Indigenous women, specifically in the Prairie provinces (Manitoba HIV Program, 2024). Historically, HIV/AIDS stigma has prevented the inclusion of sexual health information and HIV-STBBI prevention, treatment, and support information to reach Indigenous women in a timely manner. Canada’s National Inquiry into Murdered and Missing Indigenous Women and Girls (2016–2019) has established the bias against First Nations, Inuit, and Metis women due to patriarchal structures and the inherent misogyny and racism in the state’s history and institutions.
In Manitoba, Indigenous ethnic identifiers were included in Manitoba’s annual HIV epi update beginning in 2001. The rate of HIV transmission reported Indigenous people increased from 27% in 2021 to 73% in 2024 (Manitoba Health). HIV prevention and awareness promotion campaigns have declined drastically since the 1990s, leaving many Indigenous women oblivious to interventions like the female condom, PrEP, PEP, harm reduction information and supplies, and the HIV self-test. Further, Indigenous communities are now targeted by international drug cartels and organized crime syndicates for the distribution and habitual use of drugs like prescription opiates, meth, fentanyl, heroin, and cocaine. In rural communities, this situation has led to a public health crisis where Indigenous communities are ill-prepared to deal with HIV outbreaks.
To respond effectively to the lack of political will to effectively address this growing HIV pandemic faced by Indigenous women, a national inquiry into the over-representation of Indigenous people (particularly women) in HIV epidemiologic reports is needed.
| 2018 (%) | 2019 (%) | 2020 (%) | 2021 (%) | ||
|---|---|---|---|---|---|
| Indigenous | 51.4 | 57.7 | 71.9 | 73.4 | |
| White/European | 18.0 | 15.4 | 12.3 | 11.2 | |
| African/Black | 21.6 | 18.7 | 7.9 | 5.9 | |
| East/Southeast Asian | 6.3 | 3.3 | 5.3 | 2.4 | |
| Latin American | 0.9 | 1.6 | 0.0 | 2.4 | |
| South Asian | 1.8 | 0.8 | 0.0 | 1.8 | |
| Middle Eastern | 0.0 | 1.6 | 0.0 | 0.6 | |
| Not reported/no data | 0.0 | 0.8 | 2.6 | 2.4 | |
| Total | 111 | 123 | 114 | 169 |
PP04.92 – BV or Not BV: The Association Between Mycoplasma Genitalium and Vaginitis and Other Female Genital Syndromes
Dr. Candice McNeil1, Mr. Michael DeWitt1, Dr. Olusegun Soge2, Dr. William Geisler3, Dr. Stephen Jordan4, Dr. Preeti Pathela5, Dr. Hilary Reno6, Dr. Karen Wendel7, Ms. Anika Parker2, Ms. Gina Leipertz8, Dr. Damon Getman9, Dr. Matthew Golden2, Dr. Lisa Manhart2
1Wake Forest University School of Medicine, Winston-salem, United States.
2University of Washington, Seattle, United States.
3University of Alabama at Birmingham, Birmingham, United States.
4Indiana University, Indianapolis, United States.
5New York City Department of Health and Mental Hygiene, Queens, United States.
6Washington University, St. Louis, United States.
7Public Health Institute at Denver Health, Denver, United States.
8University of Washington, Seattle, United States.
9Washington State University, Spokane, United States.
10Hologic, Inc, San Diego, United States.
11University of Washington, Seattle, United States.
Background: Data on M. genitalium (MG) in females are inconsistent, and CDC guidelines only recommend MG testing in women with persistent/recurrent cervicitis and pelvic inflammatory disease (PID). We evaluated MG, vaginitis, and other female genital syndromes in a large surveillance program.
Methods: From 2020 to 2024, urogenital specimens from symptomatic and asymptomatic females attending US sexual health clinics (Birmingham, Denver, Greensboro, Indianapolis, New York City, Seattle, and St. Louis) were tested for MG using the Aptima Mycoplasma genitalium Assay and macrolide resistance mutations (MRM) using analyte-specific reagents (Hologic, Inc.). We utilized Poisson regression with robust standard errors to estimate prevalence ratios for associations of urogenital MG with clinical diagnoses of vaginitis, bacterial vaginosis (BV; 2022–2024 only), cervicitis, and PID, adjusting for study site, and gonorrhea and chlamydia.
Results: Overall, 9,487 females had MG results, of whom 4,792 (50.5%) were symptomatic. MG was detected in 1,607 (16.9%; 95% CI = 16.19%–17.71%). Ninety-five (1.0%) had PID, 99 had cervicitis (1.0%), and 3,073 had vaginitis (32.4%). BV was diagnosed in 1,231/6,244 (19.7%). Demographics are shown in Table 1. MG prevalence did not differ in females with or without cervicitis (adjusted prevalence ratio [aPR = 1.1; 95% CI = 0.66–1.70, P = 0.82); it was higher in women with than without PID (aPR] = 1.4; 95% CI = 0.95–2.15, P = 0.09) but not significantly. Conversely, MG prevalence was significantly higher in females with than without BV (22.0% vs 15.1%; aPR = 1.3; 95% CI = 1.13–1.55, P = 0.001) and with than without vaginitis (19.7% vs 15.5%; aPR = 1.2; 95% CI = 1.04–1.31, P = 0.01), but not associated with vaginitis in absence of BV (aPR = 1.1; 95% CI = 0.92–1.24, P = 0.37). MRMs were detected in 789/1,422 (55.5%) but not associated with vaginitis, BV, cervicitis, or PID (P > 0.10 for all).
Conclusion: Women with BV had a higher MG prevalence. Macrolide resistance was uniformly high, irrespective of symptoms. Larger prospective studies of PID using rigorous definitions are needed to assess associations with MG.
| Characteristic | Overall,N = 9,4871 | MG Negative,N = 7,880A | MG Positive,N = 1,607A | P-valueB | |
|---|---|---|---|---|---|
| Age (years) | 28 (23–34) | 29 (24–35) | 25 (21–30) | <0.001 | |
| Age group (years) | <0.001 | ||||
| <18 | 187 (2.0) | 138 (1.8) | 49 (3.0) | ||
| 18–24 | 2,805 (30) | 2,142 (27) | 663 (41) | ||
| 25–29 | 2,498 (26) | 2,039 (26) | 459 (29) | ||
| 30–39 | 2,582 (27) | 2,253 (29) | 329 (20) | ||
| >=40 | 1,408 (15) | 1,301 (17) | 107 (6.7) | ||
| Race/Ethnicity | <0.001 | ||||
| Asian, non-Hispanic | 310 (3.3) | 271 (3.4) | 39 (2.4) | ||
| Black, non-Hispanic | 5,054 (53) | 4,018 (51) | 1,036 (64) | ||
| Hispanic/Latinx | 1,709 (18) | 1,490 (19) | 219 (14) | ||
| Other, non-Hispanic | 271 (2.9) | 227 (2.9) | 44 (2.7) | ||
| White, non-Hispanic | 1,896 (20) | 1,666 (21) | 230 (14) | ||
| Unknown | 247 (2.6) | 208 (2.6) | 39 (2.4) | ||
| Symptoms at visit | 4,792 (51) | 3,958 (50) | 834 (52) | 0.22 | |
| Bacterial Vaginosis | <0.001 | ||||
| no BV | 5,013 (80) | 4,257 (82) | 756 (74) | ||
| BV | 1,231 (20) | 960 (18) | 271 (26) | ||
| Vaginitis | 3,073 (33) | 2,467 (31) | 606 (38) | <0.001 | |
| Non-BV Vaginitis | 1,872 (23) | 1,531 (22) | 341 (26) | 0.006 | |
| Urogenital gonorrhea NAAT | <0.001 | ||||
| Neg | 7,112 (96) | 6,077 (96) | 1,035 (92) | ||
| Pos | 315 (4.2) | 226 (3.6) | 89 (7.9) | ||
| Urogenital chlamydia NAAT | <0.001 | ||||
| Neg | 6,798 (91) | 5,853 (92) | 945 (83) | ||
| Pos | 670 (9.0) | 483 (7.6) | 187 (17) | ||
| Urogenital gonorrhea or chlamydia NAAT | 894 (12) | 655 (10) | 239 (21) | <0.001 | |
| Cervicitis | 99 (1.2) | 79 (1.1) | 20 (1.5) | 0.22 | |
| Pelvic Inflammatory Disease | 95 (1.2) | 76 (1.1) | 19 (1.5) | 0.25 |
Abbreviations: BV, bacterial vaginosis; NAAT, Nucleic Acid Amplification Test; Neg, negative; MG, Mycoplasma genitalium; Pos, positive.
AMedian (IQR); n (%); BWilcoxon rank sum test; Pearson's Chi-squared test; Fisher’s exact test.
PP04.93 – 20 Years of Gonorrhea Evolution: A Whole Genome Sequencing Study in Western Kenya, 2002 to 2022
Dr. Supriya Mehta1,2, Robyn Thorington3, Walter Agingu4, Dr. Fredrick Otieno4, Dr. Anastasia Unitt5, Laura Rusie2, Dr. Adriana Le Van6,7, Irene Martin3, Dr. Ann Jerse7, Dr. Odile Harrison5
1University of Illinois Chicago, Chicago, United States.
2Rush University, Chicago, United States.
3Public Health Agency of Canada, Winnipeg, Canada.
4Nyanza Reproductive Health Society, Kisumu, Kenya.
5University of Oxford, Oxford, United Kingdom.
6Henry M Jackson Foundation, Bethesda, United States.
7Uniformed Services University, Bethesda, United States.
Background: Using isolates collected 2002–2009 and 2020–2022 from Kisumu, Kenya, we conducted whole genome sequencing (WGS) to understand the evolution and epidemiology of Neisseria gonorrhoeae (NG). Our objectives were to: (1) characterize AMR genes and alleles over time; (2) compare NG over time using novel and conventional typing; (3) explore individual-level data in relation to AMR and phylogeny to gain insight on transmission.
Methods: Isolates were collected in 2002–2009 (n = 108) and 2020–2022 (n = 110) from men with urethral discharge and/or dysuria. Phenotypic AMR was determined by agar dilution (2002–2009) or E-test and agar dilution (2020-2022). Predicted minimum inhibitory concentrations (MICs), multi-locus sequence typing (MLST), multi-antigen ST (NG-MAST), NG-STAR, and AMR genetic determinants were determined using WGS and Detection of Molecular Markers (WADE) in R. Meta-data (e.g., age, circumcision status, HIV status) were compared by genes associated with AMR, housekeeping, and iron acquisition or metabolism (using PubMLST), stratified by time period. Novel typing used LIN codes (cgMLST scheme categorizing isolates at hierarchical levels of allele combinations).
Results: Resistance to penicillin, ciprofloxacin, and tetracycline were common 2002–2022. In 2020–2022, azithromycin resistance (n = 2; both with four A2059 mutations) and cephalosporin alert values (n = 5) were observed; no genetic markers typically associated with increased cephalosporin MIC were observed. Phylogenetic clusters were identified that were congruent with LINcode lineage, though other typing schemes (MLST, NG-STAR, NG-MAST) did not align as well (Fig. 1). There were major shifts over time in lineages and genetic determinants. Circumcision status and HIV status were associated with several AMR, housekeeping, metabolism, and iron acquisition genetic determinants.
Discussion: WGS provided insight on the evolution of NG over a 20-year period in Kenya, and confirmed determinants of recently emerged macrolide resistance but not cephalosporin alerts. Epidemiologic analyses suggest novel behavioral and biological factors to examine in association with circulating NG and AMR emergence.
Phylogenetic tree of NG Isolates aligned with study time period, LIN lineage and sub-lineage and standard typing, and results of comparison of epidemiologic analyses by genetic determinants, stratified by time period.
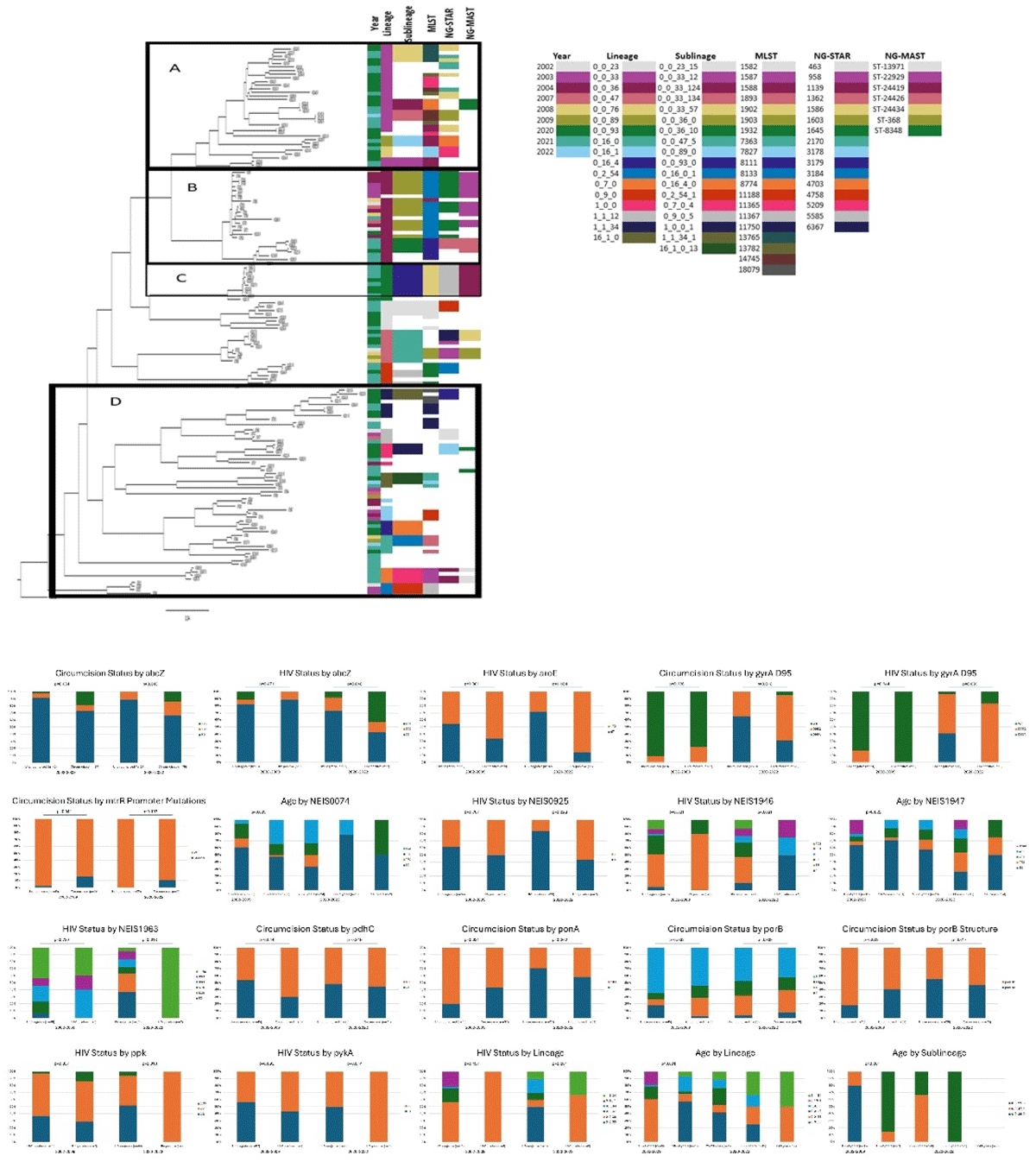
PP04.94 – Poor Mental Health, Salivary Cortisol, Serum Estradiol, and the Vaginal Microbiome
Dr. Supriya Mehta1,2, Debarghyah Nandi1, Dr. Garazi Zulaika4, Walter Agingu3, Elizabeth Nyothach5, Dr Runa Bhaumik1, Dr Stefan Green2, Dr Anna Maria van Eijk4, Dr Fredrick Otieno3, Prof Penelope Phillips-Howard4
1University of Illinois Chicago, Chicago, United States.
2Rush University, Chicago, United States.
3Nyanza Reproductive Health Society, Kisumu, Kenya.
4Liverpool School of Tropical Medicine, Liverpool, United Kingdom.
5Kenya Medical Research Institute, Kisumu, Kenya.
Background: The increasing frequency of population-level crises, like the COVID-19 pandemic, have led to epidemic impacts on mental health. Cortisol is released in response to stress, subsequently inhibiting estrogen, which in turn can lead to reduced vaginal lactobacilli. We measured the association of poor mental health on cortisol, estradiol, and vaginal microbiome (VMB) among adolescent girls and young women (AGYW) during the COVID-19 pandemic.
Methods: 50 AGYW were randomly selected from a prospective cohort of 436 AGYW in western Kenya. We assessed mental health measures, cortisol, estradiol, and VMB every 6 months over a 2-year period. Validated tools assessed mental health: depressive symptoms, anxiety, stress, and thoughts of self-harm. Cortisol was measured via ultrasensitive ELISA in saliva using a single-day, 6-time point protocol. Estradiol was measured via ELISA in serum. VMB was assessed from self-collected vaginal swabs via DNA-based 16S rRNA gene amplicon sequencing. Associations were estimated via mixed effects models adjusted for age, economic status, menstrual hygiene, hormonal contraception, hours awake, and study time.
Results: Participants were median age 19.1 at initial assessment. Estradiol (mean 61.4 ng/mL, SD 59.9) correlated strongly with Lactobacillus crispatus (mean relative abundance [RA] 17.6%; SD 32.0%): as estradiol increased, so did L. crispatus RA (β = 0.16; P < 0.001). Analyses demonstrated a strong negative association between cortisol (mean total AUC 33.4; SD 25.8) and estradiol (β = –0.30, P = 0.035). Participants expressing thoughts of self-harm (expressed at 15% of observations across time points) had on average 10.9% (P = 0.006) lower RA of L. crispatus. Longitudinal sequential mediation analyses are ongoing.
Conclusions: Poor mental health and elevated cortisol were associated with lower estradiol and reduced L. crispatus. This has implications for treatment of non-optimal VMB related infections (e.g., BV, STIs): the extent to which non-optimal VMB is hormonally mediated could negatively impact antibiotic and biotherapeutic treatment effectiveness.
Results of mixed effects longitudinal multivariable modeling: associations between poor mental health: salivary cortisol, serum estradiol, and relative abundance of L. crispatus, N = 121.
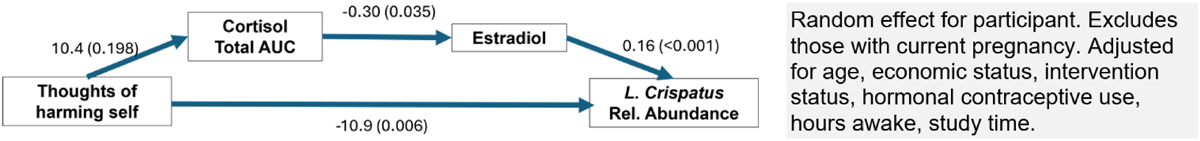
PP04.95 – HIV-1 Drug Resistance Among Key Populations in Nigeria: Results from the 2020 Integrated Biological and Behavioural Surveillance Survey
Miss Stephanie Melnychuk1,2, Alexandria Reimer1, Chantal Munyuza1, Rayeil Chua1, Xuefen Yang1, Kalada Green2, Gambo Aliyu3, Gregory Ashefor3, Rose Aguolu3, Adediran Adesina4, Chukwuebuka Ejeckam4, Leigh McClarty2, Shajy Isac5, Faran Emmanuel2, James F. Blanchard2, Paul Sandstrom1,4, Hezhao Ji1,4, Marissa L. Becker2, Souradet Y. Shaw2,4, Francois Cholette1,4
1National Sexually Transmitted and Blood-Borne Infections Laboratory, J.C. Wilt Infectious Diseases Research Centre, Public Health Agency of Canada, Winnipeg, Canada.
2Institute for Global Public Health, Community Health Sciences, University of Manitoba, Winnipeg, Canada.
3National Agency for the Control of AIDS, Abuja, Nigeria.
4West African Centre for Public Health and Development, Abuja, Nigeria.
5India Health Action Trust, Delhi, India.
6Department of Medical Microbiology and Infectious Diseases, University of Manitoba, Winnipeg, Canada.
Background: HIV-1 drug resistance mutations (DRMs) compromise the effectiveness of antiretroviral therapy (ART) and lead to treatment failure. While DRMs have been extensively studied in many parts of the world, data from African countries, including Nigeria, remains limited.
Methods: A cross-sectional integrated biological and behavioural surveillance survey was conducted across 12 states, representing two states from each of Nigeria’s geo-political zones, among female sex workers, men who have sex with men, people who inject drugs (PWID), and transgender individuals. Dried blood spot specimens were collected from 2,309 participants, of whom 719 (31.1%) were HIV-1 viremic (>1,000 copies/mL). Partial HIV-1 pol genes were sequenced from viremic specimens using an in-house DRM genotyping assay. DRMs were identified from MiSeq reads with HyDRA Web and resistance levels were interpreted using the Stanford HIVdb program. Pearson Chi-square tests assessed associations between sociodemographic factors and DRMs.
Results: Of the 414 HIV-1 genotyped specimens, 16.7% contained at least one DRM. The most common DRMs were K103N, M41L, and M184V, with 9.2% showing high-level resistance to both efavirenz and nevirapine. DRMs were most prevalent among PWID (21.6%) and in the North Central zone (25.8%). Older age was significantly associated with the presence of DRMs (P < 0.001). Notably, over half (58.7%) of participants reported being unaware of their HIV-positive status and having never received ART.
Conclusion: Our findings suggest the presence of transmitted drug resistance, given most participants reported never receiving ART. The association between older age and DRMs may be indicative of HIV-1 chronicity and/or sub-optimal ART adherence. While the high-level resistance to efavirenz supports the transition to dolutegravir-based regimens in Nigeria, parallel efforts should be made to improve adherence and ensure sustained ART access to prevent the emergence and spread of drug-resistant strains. Ongoing surveillance remains essential to address these challenges and guide effective interventions.
PP04.96 – HPV Prevalence Among Transgender Women and Travestis with Neovagina in Five Brazilian Capital Cities
Perder Camila Moraes1,2, Katia Cristina Bassichetto1,2, Aline Borges Moreira Rocha1,2, Luana Vasconcelos Freitas1,2, Maria Amelia Veras1,2
1Faculdade de Ciências Médicas da Santa Casa de São Paulo, São Paulo, Brazil.
2Núcleo de Pesquisa em Direitos Humanos e Saúde da População LGBT+, São Paulo, Brazil.
Introduction: Data regarding the prevalence of sexually transmitted infections (STIs) among transgender women and travestis (TWTr) with neovagina are limited in the existing literature. Studies conducted across various countries have reported the incidence of high-risk HPV in TWTr with neovagina ranging from 8.3% to 20%, highlighting a significant prevalence. In Brazil, there is a lack of information concerning HPV among TWTr following gender reassignment surgery.
Methods: We used data from “TransOdara” a cross-sectional study, conducted in five Brazilian capital cities between 2019 and 2021. Respondent-driven sampling was used to assemble 1317 TWTr. For this analysis, we are using the socioeconomic and demographic data of 21 participants who had undergone gender reassignment surgery and provided vaginal and anal swab samples for HPV. Descriptive and bivariate analysis was performed using Fisher’s exact test, considering a 95% confidence interval.
Results: Of the 21 TWTr in the study, 52.4% were aged 18–34 years, 57.1% Black/Mixed-race, 42.9% had completed 12 or more years of education, and 52.4% earned less than one minimum wage. Sex work was reported by 52.4%, with 14.3% in the last 6 months. Of the 16 who provided valid vaginal swab samples (76.2%), 12 (75.0%) had detectable HPV, seven high-risk (58.3%). Of the 15 provided valid anal swabs (71.4%), 14 (93.3%) had detectable anal HPV, 13 high-risk (92.9%) (Table 1). Factors associated with higher vaginal HPV frequency were age over 35 years (P = 0.019) and not having a history of sex work (P = 0.015). For anal HPV, we found no associated factors, as almost all samples were detectable for high-risk HPV.
Conclusion: A high HPV positivity rate among TWTr with neovagina was observed in this study, mostly high-risk carcinogenic types. Further studies are needed, such as HPV rates before and post neovagina, to generate information to improve prevention, diagnosis, and monitoring strategies for this infection.
| City | n | % | HIV Status | n | % | |
| São Paulo | 13 | 61.9 | Reactive | 7 | 33.3 | |
| Porto Alegre | 5 | 23.8 | Non-reactive | 14 | 66.7 | |
| Campo Grande | 0 | 0.0 | ||||
| Salvador | 1 | 4.8 | Anal collection | |||
| Manaus | 2 | 9.5 | Self-collection | 10 | 47.6 | |
| Professional | 11 | 52.4 | ||||
| Age group (median = 34) | ||||||
| Up to 34 years | 11 | 52.4 | Anal HPV (n = 15) | |||
| 35 years or over | 10 | 47.6 | Positive | 14 | 93.3 | |
| Negative | 1 | 6.7 | ||||
| Race/Skin color | ||||||
| White | 9 | 42.9 | Anal HPV high risk (n = 14) | |||
| Black/Mixed-race | 12 | 57.1 | Alto risco | 13 | 92.9 | |
| Baixo risco | 1 | 7.1 | ||||
| Level of education | ||||||
| Up to 8 years | 5 | 23.8 | Vaginal collection | |||
| 8 to 12 years | 7 | 33.3 | Self-collection | 11 | 52.4 | |
| More than 12 years | 9 | 42.9 | Professional | 10 | 47.6 | |
| Income (in minimum wages) | Vaginal HPV (n = 16) | |||||
| < 1 | 11 | 52.4 | Positive | 12 | 75.0 | |
| 1 to 2 | 6 | 28.6 | Negative | 4 | 25.0 | |
| > 2 | 4 | 19.0 | ||||
| Vaginal HPV high risk (n = 12) | ||||||
| Sex work | Positive | 7 | 58.3 | |||
| Only in the past | 8 | 38.1 | Negative | 5 | 41.7 | |
| Current | 3 | 14.3 | ||||
| No | 10 | 47.6 |
PP04.97 – What Do the Patterns and Services Offered to a STI Clinic Attendees Tell About the Responses to End HIV Epidemic as an Important Public Health Problem in a Country? Observations from a Retrospective Audit at a Referral Hospital’s STI Clinic in Malawi
Dr. Kelvin Mponda1,2,3, Dr Patrick Nachipo3,4, Chifuniro Nindi3, Peter Mthimbwa3, Felix Mwalule3, Fortune Chipatala3
1Johns Hopkins Project, Blantyre, Malawi.
2Department of Dermatology, Queen Elizabeth Central Hospital, Blantyre, Malawi.
3Kamuzu University of Health Sciences, Blantyre, Malawi.
4Department of Medicine, Queen Elizabeth Central Hospital, Blantyre, Malawi.
Background: To end HIV as a public health problem, intervention that promote detection and reduction of new HIV infections, including sexually transmitted disease (STI) services are crucial. This study aimed to assess current patterns of STIs and services offered in a referral STI clinic.
Methods: We conducted a retrospective audit utilizing data covering 1 January 2018 to 31 December, 2022 at Malawi’s Queen Elizabeth Central Hospital’s STI clinic to estimate frequencies. Variables collected were age category, sex, pregnancy status, HIV status, client type (index/partner) and syndromic diagnosis.
Results: A total of 23,776 clients, 14,867 (62.5%) female, were attended. Young clients aged 0–19 years representing 4.2 %, and 20–24 years (15.5%) were fewer than individuals aged ≤25 years (80.3 %). HIV negative clients were 14,121 (59.3%), HIV positive 9115 (38.3%) while 540 (2.3%) had unknown HIV status. Index clients (20,194, 85%), were in majority, then asymptomatic partners 2932 (12.3%), and symptomatic partners 650 (2.7%). Over the 5 years, 12,301 (51.7%), were issued partner notification slips. Diagnosed disease syndromes were abnormal vaginal discharge – high risk (6056, 25.4%), urethral discharge (3636, 15.2%), abnormal vaginal discharge – low risk (2739, 11%), syphilis (2707, 10.8%), low abdominal pain (1683, 7%), genital ulcer disease (2057, 8%), and others (4007, 16%).
Conclusion: Increased number of clients were diagnosed with both STIs and HIV but the high ascertainment of HIV status is encouraging. The yield from partner notification was however low and fewer young people were accessing STI care services, raising concerns as to if and what quality of care these individuals are otherwise getting. Future studies should focus on the access by young people, an important population in HIV control, to STI services and on use of cost effective interventions to motivate partners come for care.
PP04.98 – Everyday Racial Discrimination and Sexual Pleasure: Examining the Experiences of Women Living with and Without HIV in Canada
Ms. Charity V. Mudhikwa1,2,3, Dr João Bastos1, Dr Allison Carter1,4, Dr Notisha Massaquoi5, Ms Patience Magagula6, Ms Zoe Osborne1, Dr Kalysha Closson1,7, Dr Elizabeth King1,2,3, Dr Hélène Côté2,8,9,10, Dr Melanie Murray2,3,9,10,11, Dr Angela Kaida1,2
1Faculty of Health Sciences, Simon Fraser University, Burnaby, Canada.
2Women’s Health Research Institute, Vancouver, Canada.
3Oak Tree Clinic, Vancouver, Canada.
4Kirby Institute, The University of New South Wales, Sydney, Australia.
5Department of Health and Society, University of Toronto, Scarborough, Canada.
6Afro-Canadian Positive Network of British Columbia, Burnaby, Canada.
7Centre on Gender Equity and Health, University of California, San Diego, USA.
8Department of Pathology and Laboratory Medicine, University of British Columbia, Vancouver, Canada.
9Centre for Blood Research, University of British Columbia, Vancouver, Canada.
10Edwin S.H. Leong Healthy Aging Program, University of British Columbia, Vancouver, Canada.
11Faculty of Medicine, University of British Columbia, Vancouver, Canada.
Background: Research suggests women living with HIV (WLWH) experience poor sexual health outcomes, including reduced levels of pleasure. Everyday racial discrimination affects a range of health outcomes and potentially underlies sexual health-related inequities. We assessed the association between racial discrimination and sexual pleasure among women in British Columbia (BC), Canada, including the extent to which HIV status modifies this association.
Methods: We used survey data from the BC CARMA-CHIWOS Collaboration study of WLWH and women without HIV. Participants who had any sexual experience in the past month reported frequency of experiencing sexual pleasure (never, seldom, sometimes, usually, and always). They also reported frequency of race-based mistreatment, using the 9-item Everyday Discrimination Scale. Using ordinal logistic regression, we examined the association between racial discrimination and sexual pleasure by estimating odds ratios (OR), adjusting for confounders, and testing for interaction by HIV status.
Results: Among the 355 sexually active women (median age = 45.6 y [IQR: 35.2–55.2]), 58% were racialized, and 37.5% were WLWH. Overall, 67.6% “always/usually”, 13.2% “sometimes”, and 19.2% “seldom/never” experienced sexual pleasure, with similar figures for both WLWH and women without HIV. Experiencing everyday racial discrimination was negatively associated with sexual pleasure, whereby for every unit increase in the discrimination score, the odds of being in a higher category of sexual pleasure (e.g. moving from ‘sometimes’ to ‘usually’) decreased by 5% (adjusted OR = 0.95; 95% CI = 0.93–0.98). HIV status did not modify this association (interaction term adjusted OR = 0.96; 95% CI = 0.97–1.01).
Conclusion: Over two-thirds of sexually active WLWH reported always/usually experiencing pleasure, challenging deficit-based narratives about the sexual lives of women with HIV. Contrary to past studies, frequency of pleasure did not differ by HIV status. Our findings also suggest that racism drives sexual pleasure inequities, highlighting the urgent need to address it as a system of oppression that undermines women’s sexual health and rights in Canada.
PP04.99 – Prevalence of Three Curable Sexually Transmitted Infections Among Syrian Refugee Women in Lebanon with Gynecological Symptoms
Dr. Ghina R. Mumtaz1,2, Ms. Iman Fakih1, Dr. Nada Fares1, Dr. Ali Ghassani3, Prof. Laith Abu-Raddad4,5,6,7,8, Dr. Sasha Fahme1
1Department of Epidemiology and Population Health, American University of Beirut, Beirut, Lebanon.
2Center for Infectious Diseases Research, American University of Beirut, Beirut, Lebanon.
3Community Research Department, Amel Association, Beirut, Lebanon.
4Infectious Disease Epidemiology Group, Weill Cornell Medicine-Qatar, Cornell University, Doha, Qatar.
5World Health Organization Collaborating Centre for Disease Epidemiology Analytics on HIV/AIDS, Sexually Transmitted Infections, and Viral Hepatitis, Weill Cornell Medicine–Qatar, Cornell University, Doha, Qatar.
6Department of Population Health Sciences, Weill Cornell Medicine, Cornell University, New York, USA.
7Department of Public Health, College of Health Sciences, QU Health, Qatar University, Doha, Qatar.
8College of Health and Life Sciences, Hamad bin Khalifa University, Doha, Qatar.
Background: Syrian refugee women in Lebanon are a vulnerable population disproportionately affected by overlapping humanitarian crises. Data on the burden of sexually transmitted infections (STIs) among this population remain scarce. We previously determined a low prevalence of STIs among pregnant Syrian refuges, despite a high prevalence of self-reported symptoms. This study focuses on symptomatic Syrian refugee women, investigating the prevalence of Chlamydia trachomatis, Neisseria gonorrhoeae, and Trichomonas vaginalis.
Methods: This cross-sectional study was conducted at three public clinics in Beirut (urban) and two in the Bekaa valley (semi-rural). Participants were adult, married, non-pregnant Syrian refugee women seeking care for STI symptoms. Sociodemographic and sexual behavior data were collected through an interviewer-administered survey. STI testing was done using Xpert NG/CT and TV assays on urine specimens.
Results: A total of 276 participants were enrolled, with a mean age of 32 years (range: 18–56 years). Approximately 86% of participants had less than a secondary-level education. The mean age at marriage was 18 years (range: 12–41 years), and 93% reported having one lifetime sexual partner. Additionally, 77% reported never using condoms. The most commonly reported symptoms were pelvic pain (86.2%), abnormal vaginal discharge (76.4%), and dysuria (74.6%). Three women (1.4%) were diagnosed with Trichomoniasis. No cases of chlamydia or gonorrhea were identified.
Conclusions: Our results suggest that curable STIs are uncommon among Syrian refugees in Lebanon, even among symptomatic women engaged in care. This may reflect a low-risk sexual environment and, possibly, the widespread, unregulated use of antimicrobials within the community. Further research is needed to examine the etiology of reported symptoms. Such studies will guide tailored interventions to address the specific health needs of this vulnerable, displaced population and improve health outcomes.
PP05.01 – Community Consultations to Meaningfully Address Sexually Transmitted and Blood-Borne Infections (STBBIs): Inclusive Research
Dr. Zulma Vanessa Rueda1, MSc Monica Cyr2, Ms. Tessa Whitecloud3, Mr. Paul Loewen3, Dr. Katharina Maier4, MSc Margaret Haworth-Brockman5,10, MD Lauren MacKenzie6, Dr. Ken Kasper6,7,11, Ms. Kimberly Templeton7, MD Laurie Ireland8, Mr. Mike Payne8, Mrs. Marjorie Schenckels9, Mrs. Heather Pashe1,9, Ms. Sykes Maya1, Dr. Mariana Herrera-Diaz1, Mrs. Maria Arango1, Mrs. Angela Copete-Rengifo1, Mr. Camilo Suarez1, Ms. Zipporah Gitau1, Dr. Catherine Card1, Dr. Yoav Keynan1,5,6,10
1Department of Medical Microbiology and Infectious Diseases, University of Manitoba Rady Faculty of Health Sciences, Winnipeg, Canada.
2Aboriginal Health & Wellness Centre of Winnipeg, Winnipeg, Canada.
3Siloam Mission, Winnipeg, Canada.
4Criminal Justice, The University of Winnipeg, Winnipeg, Canada.
5Department of Community Health Sciences, University of Manitoba, Rady Faculty of Health Sciences, Winnipeg, Canada.
6Department of Internal Medicine, University of Manitoba Rady Faculty of Health Sciences, Winnipeg, Canada.
7The Manitoba HIV Program, Winnipeg, Canada.
8Nine Circles Community Health Centre, Winnipeg, Canada.
9AllTogether4IDEAS Peer Research Team, University of Manitoba Rady Faculty of Health Sciences, Winnipeg, Canada.
10National Collaborating Centre for Infectious Diseases, Rady Faculty of Health Sciences, University of Manitoba, Winnipeg, Canada.
11Health Science Centre Winnipeg, Shared Health, Winnipeg, Canada.
Background: Manitoba is facing the highest increase in new HIV infections, and the highest HIV rates in Canada. We envisioned ‘community-driven research’ rather than exclusively researcher-driven priorities. Therefore, we invited the community to share their ideas for new research on HIV, STBBI, and other non-STBBI co-infections.
Description: The AllTogether4Ideas research team and four Manitoban community-based organizations co-developed community consultations using 10 different strategies to meaningfully engage and listen to people experiencing houselessness, people who use drugs, Indigenous and other minority groups, service providers and staff, and policy- and decision-makers between June and October 2024. We followed Indigenous research methodologies and collected information using 16 questions (12 open-ended and 4 closed-ended questions, varied by target group); these included, “What is the biggest risk to your health and wellbeing?”, “What do you know about sexual health”? and best ways of creating safe, inclusive, culturally appropriate spaces to provide healthcare.
Results: 229 clients/community relatives, 58 staff and providers, 15 directors, program managers and public health workers participated in these consultations. The main needs identified in order of frequency mentioned were: 1) Housing programs, including transitional housing, shelters, temporary housing, and prevention of houselessness. 2) Drug abuse, STBBI, infectious and non-infectious risks of drug use, and safety of street drugs, and harm reduction programs. 3) Mental health support programs. 4) Healthcare services and clinics ‘where people are at’. Participants also wanted to learn more about health issues, sexual health, and STBBI differences between females and males. Clients and providers preferred to learn by watching and listening to recorded materials.
Conclusion: Results from the community consultations informed our research objectives to address the full range of individual, social-structural, and contextual factors driving HIV/STBBI in Manitoba. Participants suggested sex- and gender-responsive strategies, and intersectional and equitable approaches to care and their preferences to learn.
PP05.02 – Implementation and Informal Use of Doxycycline Prophylaxis for Bacterial Sexually Transmitted Infections in the European Union and European Economic Area – Results of a 2024 Survey
Dr. Lina Nerlander1, Ms Sarah North1, Dr Otilia Mardh1
1European Centre for Disease Prevention and Control, Stockholm, Sweden.
Background: Although use of 200 mg doxycycline taken 24–72 h after sex (doxy-PEP) has proven effective to prevent sexually transmitted infections (STIs) among MSM and transgender women at high-risk for bacterial STIs, concerns remain related to the development of antimicrobial resistance. Some countries, including the United States, Canada and Australia have published guidelines on its use. While few such guidelines have been published in Europe, doxy-PEP, obtained through different channels, may still be used. This study aimed to describe the current state of guidance and use of doxy-PEP in the European Union (EU) and the European Economic Area (EEA).
Methods: To monitor progress towards STI prevention and control the European Centre for Disease Prevention and Control (ECDC) requested that national Public Health Authorities in EU/EEA complete a questionnaire October–December 2024 on STI prevention, testing and treatment, including doxy-PEP.
Results: A national guidance, policy or recommendation on doxy-PEP exists in 4 (Austria, Czechia, Germany and Ireland) of the 29 countries (14%) that responded to this question. In Belgium, a statement of the Research on AIDS and HIV consortium (BREACH) advises against widespread doxy-PEP use. Of the 25 countries without national guidance, 10 (36%) reported anecdotal or other evidence of doxy-PEP being prescribed by clinicians, including Belgium. Use of doxy-PEP without prescription or obtained by prescription for another purpose was reported from 13/29 countries (45%) based on information from community organisations and STI clinicians.
Conclusion: There is evidence of doxy-PEP use beyond the four EU/EEA countries that have issued a guidance, policy or recommendation either through clinical prescriptions or other channels. This presents a challenge, as doxy-PEP, if used, should ideally be provided as part of a comprehensive sexual health package. Monitoring at national and EU/EEA levels is warranted to assess doxy-PEP use, its impact on STI incidence and antimicrobial resistance.
PP05.03 – Multi-Stakeholder Engagement for Scaling Up Prevention of Mother-To-Child Transmission of HIV in Nigeria: Insights from the Global Fund TB/HIV Program
Dr. Opeyemi Adebayo1, Dr Joseph Daniel1, Ms Rifkatu Aimu1, Dr Kenneth Atoi1, Ms Kelechi Nzaedibe1, Mr Benjamin Pillatar1, Dr Uchenna Ugwoke1, Ms Hasiya Bello Raji1, Dr Vincent Emmanuel1, Dr Adekola Adekunle1, Dr Temitope Adetiba1, Dr Evaezi Okokoro2, Pharm Chiagozie Mgbemena1, Dr Olayemi Olupitan1,3,4, Ms Fati Murtala-Ibrahim1,3, Dr Aderonke Agbaje1,3, Dr Charles Mensah4, Dr Patrick Dakum3, Dr Nibretie Workneh5, Pharm Janet Kimeu5, Dr Kazuaki Tsujii5, Margaret Zamzu5, Dr Jean-Thomas Nouboussi5
1GF N-THRIP, Insitute of Human Virology Nigeria, Abuja, Nigeria.
2International Research Centre of Excellence, Abuja, Nigeria.
3Institute of Human Virology Nigeria, Office of the COO, Abuja, Nigeria.
4Institute of Human Virology Nigeria, Office of the CEO, Abuja, Nigeria.
5The Global Fund to Fight AIDS, Tuberculosis and Malaria, Global Health Campus, Geneva, Switzerland.
Background: Nigeria’s Global Fund TB/HIV program initiated a scale-up of Prevention of Mother-to-Child Transmission of HIV (PMTCT) services across 36 states + the Federal Capital Territory (FCT) at informal care settings in January 2024 to enhance HIV testing services (HTS) and treatment for PWH in healthcare facilities and informal care settings, like home-based care and birth centres. A structured roadmap centred on strategic planning, stakeholder engagement, and community interventions was essential for streamlined implementation.
Methods: A multi-stakeholder approach facilitated the rollout of HTS for PWH in informal care settings, involving key stakeholders like community-based organizations and government agencies. Key milestones included a pre-implementation meeting, mapping of service delivery points (SDPs), and community volunteers’ engagement for integrated TB/HIV testing. Mentor mothers were recruited for community mobilization, linking PWH to treatment and support services. From February to May 2024, the focus was on clarifying reporting pathways and logistics. A boot camp in May brought all stakeholders together to confirm HTS pathways, commodity flow and reporting processes. The Training-of-Trainers model ensured knowledge transfer to SDPs, and bi-weekly meetings in August 2024 fostered feedback and near-realtime problem-solving.
Results: By August 2024, PMTCT activities were implemented in both formal and informal healthcare settings across the states. Out of 88,454 PWH screened for HIV, 71% were tested in informal care settings. Co-infections were detected in 0.2% (39/17,625) for Syphilis and 2.9% (20/695) for Hepatitis B. Although 30% of facilities experienced logistical delays that affected TB test results, the TB-HIV Integrated screening allowed for early co-infection identification and achieved 100% linkage to care.
Conclusions: The multi-stakeholder engagement and the structured roadmap for the PMTCT scale-up were crucial in integrating TB/HIV testing in informal care settings. These initiatives are essential for the global efforts to eradicate the HIV epidemic by 2030.
PP05.04 – Sexual and Reproductive Health (SRH) Needs for Forcibly Displaced Girl Child and Young Women in Humanitarian Settings in Northern Nigeria
Mrs Rashidat Jogbojogbo1, Mrs Tolulope Adebisi, Mr Emmanuel Clement, Mrs Ronke Adeoye
1NATIONAL AGENCY FOR THE CONTROL OF AIDS, Abuja, Nigeria
Background: In Northern Nigeria particularly in the northeast region, approximately 2.2 million individuals are currently displaced due to the ongoing Boko Haram insurgency with women and girls constituting nearly half of this population. The unique vulnerabilities faced by forcibly displaced adolescent girls and young women in humanitarian settings are exacerbated by limited access to sexual and reproductive health services, increased risks of gender-based violence (GBV), and adverse health outcomes such as unsafe abortions and high maternal mortality rates. The unsecured living conditions in internally displaced persons (IDP) camps significantly hinder these young women’s ability to meet their SRH needs, leading to a cycle of health risks and unmet needs.
Method: This study employs a mixed-methods approach, combining qualitative interviews and quantitative surveys conducted in various IDP camps across Northern Nigeria. Data were collected from a purposive sample of 2,341 adolescent girls and young women, focusing on their experiences with SRH services, barriers to access, and coping strategies. The interviews were designed to elicit detailed accounts of their SRH needs, including contraception, maternal health services, and experiences of GBV. Data analysis utilized thematic coding to identify key issues and trends.
Results: Findings shows the primary SRH needs among displaced girls and young women to include access to contraceptives, safe abortion services, and comprehensive maternal health care. Many respondents reported using traditional remedies or seeking help from untrained providers due to the lack of available medical services. Financial constraints, cultural stigmas around contraceptive use, and fear of GBV were significant barriers to accessing formal healthcare services.
Conclusion: The study emphasizes the urgent need for targeted interventions to address the SRH needs of forcibly displaced girls and young women in Northern Nigeria. Current humanitarian responses are insufficient in providing comprehensive SRH care, leaving this vulnerable population at heightened risk for adverse health outcomes.
PP05.05 – Gender and Human Rights Response Team: Experience from Upholding Rights and Dignity of Nigerians Towards Ending HIV Epidemic in South West Zone Nigeria
Mrs Ibironke ADEOYE1, Hidayat Bukonla Yahaya, Dr Omolola Sule, Mrs Tolulope Adebisi
1National Agency for the Control of AIDS, FCT, Nigeria.
2Lagos State Agency for the Control of AIDS, Lagos, Nigeria.
3Oyo State Agency for the Control of, Ibadan, Oyo State, Nigeria.
Background: In Nigeria, integrating gender and human rights into HIV programming is essential to address systemic inequalities and improve access to HIV prevention, care, and treatment services. Evidence have shown that there is a strong intersect between HIV and GBV, gender based violence is a risk factor for the transmission of HIV because of inability to negotiate condom use, child sexual abuse and other forms of sexual violence. It also undermines the victims of sexual abuse to assert themselves in building healthy relationship and refusing unwanted advances.
Description: In the South West Zone of the country, comprising of six states, the establishment of a gender and human rights response team aims to ensure that HIV interventions are inclusive, equitable, and uphold the dignity of all individuals, particularly vulnerable and marginalized populations.
NACA in response to increased risk of gender-based violence and work place discrimination amongst Persons living with HIV (PLHIV) has coordinated domestication of HIV anti-discrimination law in Nigeria. In addition, a multi-sectoral approach was adopted to establish a well-coordinated structure in the South-Western region, aiming to break the cycle of violence, reduce HIV transmission, and combat HIV-related stigma in these states.
Results: Amidst rising cases of gender-based violence, rape, discrimination by healthcare workers, and workplace stigma against persons living with HIV (PLHIV), the response team has achieved remarkable success, with over 90% of cases being addressed promptly. These efforts include swift emergency responses, prosecuting offenders, linking survivors to care, integrating mental health into healthcare counselling services, and providing comprehensive psychosocial support for affected individuals.
Conclusion: The efforts of states in the South-West region to address the intersection of HIV and GBV have demonstrated significant effective result. However, response mechanisms across the states must be further strengthened through enhanced policy support to eliminate stigma, discrimination, and gender-based violence.
PP05.06 – Policy Gaps and Rising HIV Incidence in Canada: Insights for Effective Community Engagement
Ms Mariam Ally Ngoya2, Mr. Frederick Okello1
1Balsillie School Of International Affairs (university Of Waterloo), Halifax, Canada.
2Africa Initiative for Rural Development (AiRD), Tanzania.
Background: While global HIV infection rates are declining, Canada has seen a significant rise in new cases, posing a unique public health challenge. This study examines potential policy gaps and explores how community engagement can mitigate the upward trend in HIV incidence.
Methods: We conducted a mixed-methods analysis, combining epidemiological data from national health surveys with policy reviews and focus group discussions involving public health officials and community leaders. Key areas of focus included prevention programs, access to healthcare, and public awareness initiatives.
Results: Our analysis revealed critical shortcomings in policy implementation, particularly in underserved populations such as Indigenous communities and recent immigrants. Prevention efforts, including needle exchange programs and PrEP (pre-exposure prophylaxis) accessibility, remain insufficiently funded and poorly distributed. Community focus groups highlighted a disconnect between governmental policies and local needs, with stigma and misinformation acting as significant barriers to effective engagement.
Conclusion: Addressing the rise in HIV incidence in Canada requires targeted policy reforms and robust community collaboration. This study underscores the need for culturally tailored public health strategies and improved resource allocation. Congress attendees will gain actionable insights into fostering effective policy-community synergies, potentially applicable to similar challenges in other high-income nations.
PP05.07 – Progress and Remaining Challenges in Eliminating HIV Mother-To-Child Transmission in Brazil: A Narrative Review
Mrs Andrea M B Beber1, Dr Ximena Pamela D Bermúdez1, Mrs Francisca Lidiane S Freitas2, Dr Elisangela Silva3, Dr Leila P Garcia4, Dr Lino N Da Silveira5, Dr. Adele Benzaken6
1Public Health Postgraduate Program, University of Brasilia, Brasília, Brazil.
2Health Surveillance Secretariat, Brazilian Ministry of Health, Brasília, Brazil.
3Tropical Medicine Postgraduate Program, Amazonas State University, Manaus, Brazil.
4Jorge Duprat Figueiredo Foundation for Occupational Safety and Health, Advanced Office in Santa Catarina, Florianópolis, Brazil.
5Health Department of the Federal District, Brasília, Brazil.
6Aids Healthcare Foundation, Los Angeles, United States.
Background: Since the 1990s, Brazil has made significant progress in preventing MTCT-HIV through public policies aimed at reducing pediatric HIV/AIDS. Despite these advancements, challenges persist in achieving global elimination targets. This study analyzes progress in Brazilian MTCT prevention programs and identifies barriers to eliminating MTCT-HIV as a public health problem.
Description: Literature review and documentary research were conducted on PubMed, Virtual Health Library, and the Brazilian Ministry of Health (MoH) website, following the STARLITE framework. Titles and publication years were used to search for official documents and pediatric AIDS data. We used MeSH terms for scientific articles: ‘Infectious Disease Transmission’, ‘Mother-to-Child Transmission’, ‘Vertical Transmission’, ‘HIV’, and ‘Brazil’. Historical documents on Brazilian MTCT-HIV prevention policies and epidemiological data (1995-2024), and scientific articles (2019–2024) were included. Articles unrelated to the topic or lacking relevant information on MTCT-HIV prevention gaps in Brazil were excluded. Analysis was organized into four historical periods (1985–1995, 1995–2002, 2002–2011, 2011–2022).
Results: MTCT-HIV increased from 0.0/100,000 live births (LB) (1985) to 3.7/100,000LB (1995), then rose by 72.9% to 6.4/100,000LB (2002). It subsequently declined by 46.8% to 3.4/100,000LB (2011) and 55.8% to 1.5/100,000LB (2022). Evidence-based policies, such as ensuring free universal treatment, comprehensive PMTCT-HIV care, and strategic programs (e.g., Projeto Nascer, Rede Cegonha), improve life quality for women and children. Fig. 1 illustrates the effects of national policy over the analyzed periods. However, regional disparities in antenatal care, gaps in surveillance systems, and persistent social inequities – poverty, low education, and discrimination – continue to challenge equitable HIV elimination.
Conclusion: Brazil has achieved the global target of <2% of MTCT-HIV rate. This result reflects the effectiveness of evidence-based policies. Nevertheless, addressing regional barriers remains crucial to ensuring equity and sustaining progress. The Subnational Certification process and the National Pact for Eliminating MTCT provide scalable strategies and represent promising initiatives for achieving the complete elimination of MTCT-HIV.
PP05.08 – Increasing Diagnosis of Syphilis in Argentine Key Populations: Effectiveness of the Etiological Approach
Dr. Miguel Pedrola1, Engineer Florencia Bagilet1, Ms. Natalia Haag1, Dr. Adele Benzaken2
1Aids Healthcare Foundation, Buenos Aires, Argentina.
2Aids Healthcare Foundation, Los Angeles, United States.
Background: Argentina is transitioning from a syndromic to an etiological approach to STIs. This study aimed to evaluate the number of new syphilis diagnoses using two different approaches in a community-run Sexual Health Center focused on key populations.
Methods: Data on syphilis diagnoses were collected from clients of the Community Sexual Health Center (CCSS) of AHF Argentina in Buenos Aires. We are comparing the syndromic approach (SA) implemented in the clinic from January 1, 2023, to December 31, 2023, involving rapid syphilis testing (Determine® Syphilis TP) for clients presenting with genital ulcers, signs of secondary syphilis, or who were sexual partners of individuals diagnosed with syphilis. The etiological approach (EA) was applied from January 1, 2024, to December 31, 2024, to all individuals attending the CCSS for a rapid HIV test and/or STI symptoms were tested for syphilis (Bioline® HIV/Syphilis DUO). Positive results were confirmed with a VDRL test.
Results: In 2023, using the SA, 120 new syphilis diagnoses were made. In 2024, using the EA, 297 new syphilis diagnoses were identified, with 45% being asymptomatic. This represents a 148% year-on-year increase in syphilis diagnoses. No significant differences were observed in terms of gender or age among the new diagnoses (see Table 1).
Conclusions: The etiological approach significantly increases the detection of syphilis in key populations, reducing missed opportunities for diagnosis. Continued monitoring of results in the coming years is essential to evaluate and refine strategies to address this epidemic.
| 2023 | 2024 | General total | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Male | Female | Trans Fem. | Total | % | Male | Female | Trans Fem. | Trans Masc. | Total | % | |||
| Age range | |||||||||||||
| 15–20 | 2 | 2 | 2 | 9 | 2 | 11 | 4 | 13 | |||||
| 20–24 | 20 | 1 | 1 | 22 | 18 | 26 | 6 | 2 | 54 | 18 | 76 | ||
| 25–29 | 36 | 8 | 44 | 37 | 75 | 15 | 1 | 91 | 31 | 135 | |||
| 30–39 | 27 | 2 | 1 | 30 | 25 | 69 | 7 | 3 | 2 | 81 | 27 | 111 | |
| 40–49 | 13 | 1 | 14 | 12 | 37 | 4 | 1 | 42 | 14 | 56 | |||
| Mas 50 | 7 | 1 | 8 | 7 | 13 | 5 | 18 | 6 | 26 | ||||
| Total | 105 | 13 | 2 | 120 | 249 | 39 | 7 | 2 | 297 | 417 | |||
| 88% | 11% | 2% | 84% | 13% | 2% | 1% | |||||||
PP05.09 – Relationship Between Vaccination Protocols and Their Effectiveness Against Cervical Cancer: Integrative Literature Review
Mrs Carolina De Marqui, Dr Gabriel Antonio Cabriott Dumbra1
1Faceres, São José do Rio Preto, Brasil.
Background: Cervical cancer occurs in up to 90% of cases due to previous exposure to the human papilloma virus (HPV). Some oncogenic subtypes act on cell proliferation and decrease control mechanisms. According to UNAIDS, HIV and cervical cancer are inextricably linked, as women living with HIV are more likely to develop this type of tumor. Vaccine prophylaxis measures have been implemented and demonstrate a protective effect. In this review, we seek to evaluate the relationship between different HPV vaccination protocols and their effectiveness against cervical cancer.
Methods: This is an integrative review using two databases: Pubmed/Medline (n = 101) and Virtual Health Library (VHL) (n = 105). With a controlled vocabulary in the search strategy, the following terms were used: “Cervical Cancer” and “Vaccine Efficiency” as well as their synonyms and combinations.
Results: In our review, 206 references were found during the electronic search. At the end of the process, 16 articles were selected for inclusion. The articles demonstrate that different HPV vaccination protocols are targets of studies to evaluate their effectiveness. Regarding the quadrivalent vaccine, the results demonstrated that there was no difference in the protective effect between the 1, 2 or 3 dose regimens. Regarding the age at which the vaccine is administered, studies indicate that there is an inversely proportional relationship with the effectiveness of the vaccine. One of the possible justifications for the reduced effectiveness of the vaccine in the older group of women is the greater probability of previous exposure to HPV. In general, a substantial reduction in the occurrence of cervical tumors can be observed among vaccinated women.
Conclusion: Vaccination against the human papillomavirus has proven to be an effective tool for reducing the incidence of neoplastic lesions of the cervix, regardless of the protocol used.
Figura 1.docx.pdf (could not be inserted).
PP05.10 – Connection, Care, Community: Strengthening Harm Reduction for Gay, Bisexual, Trans, Two-Spirited People and Queer People Who Use Drugs in Canada
Mr. Richard Elliott1
1HIV Legal Network, Halifax, Canada.
Background: Gay, bisexual, trans, two-spirited and queer (“GBT2Q”) people have higher rates of substance use. One aspect of this public health concern is greater risk of acquiring and transmitting HIV and other STIs, particularly in the context of sexualized drug use (chemsex) among GBT2Q people who have sex with men. As a population, men who both have sex with men and use drugs face heightened risk of HIV, HCV, and other STBBIs, and other harms sometimes associated with substance use. Meanwhile, both GBT2Q people and people who use drugs face barriers to health care, including harm reduction services; GBT2Q people who use drugs have particular needs and face additional barriers. Until recently, this public health and human rights issue has received little attention in drug policy discussions or from 2SLGBTQ+ advocacy organizations.
Description: The HIV Legal Network undertook a literature review, key informant interviews, and a scan of services and (federal) strategies and funding in Canada. In 2024, it released *Connection, Care, Community: Strengthening Harm Reduction for GBT2Q People who Use Drugs in Canada*, two companion resources aimed at challenging stigma and protecting the health of GBT2Q people who use drugs.
Findings: The first is a Summary Report reviewing the evidence about substance use — including problematic use — among GBT2Q people and includes insights from GBT2Q people working in harm reduction.
Conclusions: The second is an Agenda for Action with nearly 30 recommendations for action in multiple areas, including:
-
improving data collection;
-
challenging stigma through public education;
-
making services more accessible, including through enhancing cultural competence of service providers;
-
ensuring 2SLGBTQ+ communities are more inclusive and strengthen their advocacy for sensible drug policy;
-
enhancing funding for the health of GBT2Q people who use drugs; and
-
enacting key legal and policy reforms.
PP05.11 – Syndromic Management of Sexually Transmitted Infections in a Reference Care Unit in Amazonas, Brazil (2014–2023)
Dr José Carlos Sardinha, Dr Angelica Espinosa Miranda1, Dr Carolina Talhari, Ana Claudia Chaves Camilo, Dr Valderiza Lourenço Pedrosa, Celilia Lima Borges, Silvana Paiva da Costa, Jamile Izan Lopes Palheta Júnior, Camila Gurgel Santos Silva, Cynthia Oliveira Ferreira, Dr Maria das Graças Barbosa Guerra, Dr Sinesio Talhari
1Universidade Federal Do Espírito Santo, Vitoria, Brazil
Background: The syndromic approach is widely used in the management of sexually transmitted infections (STIs), particularly in resource-limited settings. It is based on the identification of clinical signs and symptoms, such as discharge, genital ulcers, or pelvic pain, to initiate immediate treatment, often without etiological confirmation. This study aimed to evaluate the frequency of syndromic diagnoses over a historical series in a reference service for STIs in the state of Amazonas, Brazil.
Methods: This descriptive, retrospective study analyzed medical records of patients treated at the Alfredo da Matta Foundation, a reference center for STIs in Amazonas, Brazil, between January 2014 and December 2023. Sociodemographic, clinical, and diagnostic data based on the syndromic approach were assessed. The criteria included vaginal discharge, cervical discharge, genital ulcers, urethral discharge, and genital warts. Descriptive analyses were performed to identify absolute and relative frequencies and trends in patient profiles and diagnostic patterns over time.
Results: A total of 22,160 individuals sought care during the study period, with a reduction observed during the COVID-19 pandemic years. Among the patients, 72.1% were men, 25.9% were married or in cohabiting relationships, 13.4% reported homosexual relationships, 41.6% had casual partners, 46.0% reported never using condoms, and 15,220 (68,7%) presented STIs signs and symptoms. Syndromic diagnoses included 345 cases (2.3%) of vaginal discharge, 590 cases (3.9%) of cervical discharge, 3,215 cases (21.1%) of genital ulcers, 4,886 cases (32.1%) of urethral discharge, and 6,184 cases (40.6%) of genital warts.
Conclusion: Despite its limitations, the syndromic approach remains a vital strategy in resource-constrained settings, enabling rapid treatment initiation and improved access to healthcare. Its integration with etiological diagnosis is essential to ensure more accurate and effective STI management, particularly in contexts where laboratory testing is unavailable or delayed.
PP05.12 – Global R&D Funding for HIV and STIs: The Need for Centering LMIC Accessibility in Funding Efforts
Dr. Alison Footman1, Dr. Cécile Ventola2, Dr. Amelia Hynen2
1AVAC, New York, United States.
2Impact Global Health, Sydney, Australia.
Background: Funding for HIV and STIs is crucial in ending these epidemics, globally. Robust HIV funding along with advocacy efforts has led to the development of new products to better prevent and treat infections. At the same time, STI prevention and treatment options and funding have remained limited. In exploring HIV and STI funding, there is a lot to learn in how funding can advance the development and implementation of new tools, especially for low- and middle-income countries (LMICs), disproportionately impacted by these infections.
Methods: The G-FINDER survey collects global R&D funding data every year for several global health areas, including HIV and STIs, through datamining and surveying funders and industry stakeholders. Funding data for drugs, biologics, diagnostics, vaccines, and microbicides was collected. Funding trends were compared and connected to pipeline developments.
Results: In 2023, a total of $1,269m and $218m was dedicated to HIV and STI R&D, respectively. This represented a 10% ($143m) decrease in HIV and 36% ($58m) increase in STI funding, since 2022. While HIV R&D funding decreased, there were several pipeline developments showing the success of coordinated efforts and sustained funding for products, including lenacapavir. The majority of STI funding was dedicated to biologics ($58m) and vaccines ($84m) for gonorrhea and HSV-2. However, investments in STI diagnostics, particularly needed in low resource settings, have decreased by 31% ($6.8m) since 2018.
Conclusion: This data highlights the importance of funding for the development of vaccines, biologics, and other prevention and treatment options for HIV and STIs. While HIV investment has led to several new products, including lenacapavir, limited STI funding hinders the development of new tools. Advocacy efforts are needed to push for investments and products to end these epidemics, especially in LMICs where infections continue to be prevalent with few resources available for prevention and treatment.
PP05.13 – HTLV in Brazil: Bringing It Out of Invisibility Through Community Engagement
Miss Mayra Gonçalves Aragón1, Mr Jair Brandão de Moura Filho1,2, Mr Luiz Fernando Aires Júnior1, Dr Pâmela Cristina Gaspar1, Miss Romina do Socorro Marques de Oliveira1, Miss Adijeane Oliveira de Jesus3, Miss Márcia Carneiro Brandão3
1Ministry Of Health Of Brazil, Brasilia, Brazil.
2Federal University of Espírito Santo, Vitória, Brazil.
3Association HTLVida, Salvador, Brazil.
Background: It is estimated that 800,000 people are living with HTLV (PLHTLV) in Brazil. Despite this, HTLV remains largely underrecognized, and HTLVida is currently the only CSO (civil society organization) representing PLHTLV in the country.
Description: This report outlines the experience of workshops conducted across Brazilian states in 2023 and 2024. These events were organized by the Ministry of Health (MoH), local HIV/STI health managers, scientific community, and HTLVida.
Findings: The “HTLV: Coming out of Invisibility” workshops aimed to raise awareness about HTLV through a single-day program. The morning session included presentations on national and local HTLV public policies, as well as a lecture by a local HTLV expert on diagnosis, prevention, and clinical management. In the afternoon, a discussion circle was held, starting with a presentation from HTLVida, followed by dialogue among participants. Seven workshops were held across seven states, with a total of 340 participants, averaging 50 individuals per event. Attendees included health managers, healthcare professionals from HIV care services and HIV/STI testing and counseling centers, and HIV, tuberculosis, viral hepatitis, LGBTQIA+, sex workers, youth, women, and Black community CSOs. CSOs highlighted the need for improved health communication regarding HTLV and the need to build an HTLV care line in their territories. Challenges included organizing a compact one-day event that ensured the attendance of health managers and care providers, while maintaining accessibility for CSOs members.
Conclusion: The workshops were deemed successful, providing a valuable opportunity to bring together health managers, care providers, researchers, and CSOs in bringing HTLV out of invisibility. It is expected that the information will reach more people after the workshops, as each participant has the potential to be a multiplier among their peers. In 2025, the MoH plans to expand the workshops to other states across Brazil and hold a national HTLV meeting.
PP05.14 – Enhancing Anal Health Care, HPV Care, and Anal STI Care Through Community-Led Research and Policy Advocacy for GBMSM in Kenya
Mr. Samuel Gorigo1, Mr. John Mathenge1, Professor Robert Lorway2, Dr. Lisa Lazarus2, Mr. Pascal Macharia3, Miss Jedidah Wanjiku3
1HOYMAS KENYA, Nairobi, Kenya.
2Institute for Global Public Health, University of Manitoba, Winnipeg, Canada; Department of Anthropology, University of Manitoba, Winnipeg, Canada.
3HOYMAS, Nairobi, Kenya; Partners for Health and Development in Africa (PHDA), Nairobi, Kenya.
Background: Gay, bisexual, and other men who have sex with men (GBMSM) in Kenya face disproportionate challenges in accessing human papillomavirus (HPV)-related, anal sexually transmitted infections (STIs) and other anal healthcare services due to stigma, discrimination, and a lack of inclusive health policies. Despite the high prevalence of anal warts, anal STIs, and HPV among GBMSM, existing guidelines inadequately address their unique needs. This research aimed to explore the knowledge and perceptions of GBMSM regarding anal health and advocate for policy reforms to integrate comprehensive HPV and anal STI care.
Description: Using a community-engaged research approach, data were gathered through creative space workshops, in-depth interviews, and body mapping exercises involving GBMSM across several counties in Kenya. These methods facilitated candid discussions, allowing participants to share lived experiences and barriers in seeking anal health services. Stakeholder consultations contextualized findings within structural and systemic frameworks. Collaborative workshops with healthcare providers, policy experts, and community representatives co-developed standard operating procedures (SOPs) and advocacy materials targeting anal health.
Findings: Key insights revealed significant knowledge gaps about HPV and anal health among GBMSM, compounded by stigma and discrimination. Structural barriers, including a lack of anal health guidelines and insufficient provider training, delayed care-seeking behaviors, leading to advanced anal diseases. Collaborative efforts led to SOP development for anal examinations and surgical excisions, endorsed by Nairobi County Health Management Teams. These SOPs and a comprehensive screening tool were incorporated into advocacy campaigns for policy reforms, highlighting the need for HPV vaccine accessibility and integrated anal health care within Kenya’s HIV/STI guidelines.
Conclusion: Engaging GBMSM communities in shaping health policies is critical. Integrating comprehensive anal health care services, including HPV vaccination, can significantly improve health outcomes and serve as a replicable model for resource-constrained settings globally.
Keywords: HPV, GBMSM, anal health, health policy, community engagement, Kenya.
PP05.15 – Prioritizing Black/African American Transitional Age Youth: Testing an Educational Video to Increase PrEP Use at an HBCU
Dr. Tyesha Karume1
1Coppin State University - Helene Fuld School of Nursing, Baltimore, United States.
Background: Young Black/African Americans (YBA) continue to contract human immunodeficiency virus (HIV) at alarmingly higher rates than other racial/ethnic groups. Pre-exposure prophylaxis (PrEP) is often not prescribed to Black/African Americans despite indication. Students at Historically Black Colleges/Universities (HBCU) exhibit less PrEP awareness do not believe sexual activity could result in HIV, and are unwilling to take PrEP. The study aimed to develop and test an educational video intervention to promote PrEP awareness, awareness of sexual risk behaviors, and willingness to take PrEP among YBA Transitional Age Youth (TAY: age 18–24) attending an HBCU.
Description: A pre/post-test design using the Health Belief model including an educational video created with CDC and AltaMed content. Demographics, PrEP awareness, sexual risk awareness, and willingness to take PrEP were also collected. A survey link was sent to students at one Maryland HBCU. Data from Black/African American students aged 18–24 was analyzed.
Findings: Thirty-three students participated (30 females & 3 males) (Table 1). Paired t-tests were used to analyze the data. Participants indicated statistically significant increases in PrEP awareness from pretest to posttest (pretest mean = 1.2963; posttest mean = 1.1481; Sig = 0.043). No statistically significant increases were determined in awareness of sexual risk behaviors (pretest mean = 2.5556; posttest mean = 2.6667; Sig = 0.502) or willingness to take PrEP (pretest mean = 5.5926; posttest mean = 5.5185; Sig = 0.779) within the sample. On pretest, 75.8% indicated awareness of PrEP and 87.9% did not think they were at risk of HIV based on sexual behaviors. Regarding willingness to take PrEP, 54.5% were willing to take a daily pill, 45.5% were willing to take a monthly injection and the same for an injection every 2 months.
Conclusion: Concerns remain about sexual risk and willingness to take PrEP among TAYs. Future research should explore potentially overlooked factors that may be improved to address HIV awareness and decrease acquisition in this population.
| Demographics | Total, N = 33 | ||
|---|---|---|---|
| Gender | Male | 3 (9.1) | |
| Female | 30 (90.9) | ||
| Age (in years) | 18 | 5 (15.2) | |
| Mean: 20.4 years | 19 | 10 (33.3) | |
| 20 | 2 (6.1) | ||
| 21 | 3 (9.1) | ||
| 22 | 7 (21.2) | ||
| 23 | 2 (6.1) | ||
| 24 | 3 (9.1) | ||
| Sexual Orientation | Gay | ||
| Lesbian | 2 (6.1) | ||
| Bisexual | 6 (18.2) | ||
| Transgender | |||
| Queer | |||
| Heterosexual | 21 (63.6) | ||
| Not sure | 1 (3) | ||
| Decline to answer | 3 (9.1) | ||
| Class | Freshman | 15 (45.5) | |
| Sophomore | 3 (9.1) | ||
| Junior | 7 (21.2) | ||
| Senior | 7 (21.2) | ||
| No Response | 1 (3) | ||
| N (%) | ||||
|---|---|---|---|---|
| Pre-Test | Post-Test | 2 -Tailed Paired-T | ||
| PrEP Awareness | .043 | |||
| “Have you heard of the once-daily pill to prevent HIV (a.k.a PrEP, Truvada)?” | ||||
| Yes | 25 (75.8) | 23 (69.7) | ||
| No | 8 (24.2) | 4 (12.1) | ||
| Did not respond | 6 (18.2) | |||
| If Yes, where did you hear about PrEP from? | Not asked on post test | |||
| A friend or a sex partner | 2 (6.1) | |||
| An advertisement/commercial (TV, magazine, online, billboard) | 15 (45.5)% | |||
| Student Health | 2 (6.1) | |||
| A health promotion event on campus | 2 (6.1) | |||
| A student organization on campus | ||||
| Social media | ||||
| Other (write in) | 5 (15.2) | |||
| Decline to answer | 2 (6.1) | |||
| Did not respond | 3 (9.1) | |||
| If Yes, how long ago did you hear about PrEP? | Not asked on post test | |||
| Within the last 3 months | 12 (36.4) | |||
| 3–6 months ago | 5 (15.2) | |||
| 6–12 months ago | 2 (6.1) | |||
| Over 1 year ago | 5 (15.2) | |||
| Over 2 years ago | 5 (15.2) | |||
| Did not respond | 4 (12.1) | |||
| Awareness Sexual Risk | .502 | |||
| Based on your behavior over the past 3 months, how much do you think you are at risk for getting HIV? | ||||
| Not at risk | 29 (87.9) | 24 (72.7) | ||
| A little bit at risk | 4 (12.1) | 2 (6.1) | ||
| Somewhat at risk | Not Selected | 1(3) | ||
| Very much at risk | Not Selected | Not Selected | ||
| Did not respond | 6 (18.2) | |||
| How likely do you think you are to get HIV in your lifetime? | ||||
| Not at risk | 17 (51.5) | 17 (51.5) | ||
| A little bit at risk | 13 (39.4) | 6 (18.2) | ||
| Somewhat at risk | 3 (9.1) | 4 (12.1) | ||
| Very much at risk | Not Selected | Not Selected | ||
| Did not respond | 6 (18.2) | |||
| Willingness to take PrEP | .779 | |||
| Would you take a pill once a day, every day to protect yourself from getting HIV? | ||||
| Yes | 18 (54.5) | 12 (36.4) | ||
| No | 6 (18.2) | 7 (21.1) | ||
| Not Sure | 9 (27.3) | 8 (24.2) | ||
| Did not respond | 6 (18.2) | |||
| Would you take an injection once a month to protect yourself from getting HIV? | ||||
| Yes | 15 (45.5) | 12 (36.4) | ||
| No | 10 (30.3) | 8 (24.2) | ||
| Not Sure | 8 (24.2) | 7 (21.1) | ||
| Did not respond | 6 (18.2) | |||
| Would you take an injection once every 2 months to protect yourself from getting HIV? | ||||
| Yes | 15 (45.5) | 12 (36.4) | ||
| No | 10 (30.3) | 7 (21.1) | ||
| Not Sure | 8 (24.2) | 8 (24.2) | ||
| Did not respond | 6 (18.2) | |||
| If you were to take a medication to prevent yourself from getting HIV, which method would you prefer to use? | ||||
| A pill once a day, every day | 11 (33.3) | 12 (36.4) | ||
| An injection once a month | 8 (24.2) | 7 (21.1) | ||
| An injection once every 2 months | 14 (42.4) | 8 (24.2) | ||
| Did not respond | 6 (18.2) | |||
PP05.16 – What Do People Who Care About Herpes Want?
Dr. Jeffrey Klausner1
1Johns Hopkins Bayview Medical Center, Baltimore, United States
Background: Herpes Cure Advocacy (HCA) is a community-based volunteer organization committed to helping to find a cure, new treatment, and vaccines for herpes simplex viruses (HSV) 1 and 2. The organization launched in 2021 and today has over 5,000 members from various backgrounds, including patients, researchers, healthcare providers, and policymakers.
Methods: Given the growth of HCA’s membership and the organization’s impact on governmental funding and research for HSV, we surveyed HCA members. The survey sought to understand members’ current demographics and preferences for intra-membership interactions and their hopes for the direction of future HSV policies and research. A 14-item survey was distributed via email and online to HCA members over 3 weeks in October 2024. Following the initial distribution, one weekly reminder was sent over the remaining 2 weeks.
Results: Four hundred members responded to the survey (~8% response rate). Over 70% (>280) were 35 years and older. Sixty-four percent (257) identified as female, and 62.5% (252) lived in the U.S. Most members, 43% (171), preferred Zoom events to connect with other members on National Herpes Day.
On a ranking scale, members ranked ‘Increasing HSV research’ at 93.3% (373), ‘Increasing HSV awareness and education’ at 85.6% (342), and ‘Enhancing HSV prevention strategies’ at 68.5% (274) as their highest policy priorities. Goals for ‘Finding a cure’ 99.1% (396), ‘developing HSV vaccines’ 95.3% (381), and increasing research funding’ 60.5% (242) were chosen as their highest research priorities.
Conclusion: HCA members selected funding research, finding a cure, increasing education and awareness, and prevention as their top HSV policy and research priorities. Ongoing and future HSV advocacy efforts that target membership needs and preferences are essential for engagement and promoting the future direction of the HSV field.
PP05.17 – What Do People Who Care About Herpes Want?
Ms. Kim Neff, Ms. Karly Kern, Nicole Hanley, Dr. Simon Delgrave, Dr. Luis Schang, Dr. Che Harris, Dr. Gary Richwald, Dr. Jeffrey Klausner
1Herpes Cure Advocacy, Baltimore, United States
Background: Herpes Cure Advocacy (HCA) is a community-based volunteer organization committed to helping to find a cure, new treatment, and vaccines for herpes simplex viruses (HSV) 1 and 2. The organization launched in 2021 and today has over 5,000 members from various backgrounds, including patients, researchers, healthcare providers, and policymakers.
Methods: Given the growth of HCA’s membership and the organization’s impact on governmental funding and research for HSV, we surveyed HCA members. The survey sought to understand members’ current demographics and preferences for intra-membership interactions and their hopes for the direction of future HSV policies and research. A 14-item survey was distributed via email and online to HCA members over 3 weeks in October 2024. Following the initial distribution, one weekly reminder was sent over the remaining 2 weeks.
Results: Four hundred members responded to the survey (~8% response rate). Over 70% (>280) were 35 years and older. Sixty-four percent (257) identified as female, and 62.5% (252) lived in the U.S. Most members, 43% (171), preferred Zoom events to connect with other members on National Herpes Day.
On a ranking scale, members ranked ‘Increasing HSV research’ at 93.3% (373), ‘Increasing HSV awareness and education’ at 85.6% (342), and ‘Enhancing HSV prevention strategies’ at 68.5% (274) as their highest policy priorities. Goals for ‘Finding a cure’ 99.1% (396), ‘developing HSV vaccines’ 95.3% (381), and increasing research funding’ 60.5% (242) were chosen as their highest research priorities.
Conclusion: HCA members selected funding research, finding a cure, increasing education and awareness, and prevention as their top HSV policy and research priorities. Ongoing and future HSV advocacy efforts that target membership needs and preferences are essential for engagement and promoting the future direction of the HSV field.
PP05.19 – Chlamydia Testing and Care Experiences Among Two-Spirit, Queer, Trans, Disabled Indigenous, Black and People of Colour in Ontario, Canada
Ms. Marie Geoffroy2, Mx. Malek Yalaoui2, Dr. Maryam Khan1, Ms. Anu Radha Verma2, Mr. Jessy Dame2, Prof. Nathan Lachowsky3, Dr. Ciann L. Wilson1
1Wilfrid Laurier University, Waterloo, Canada.
2Community-Based Research Centre, Vancouver, Canada.
3University of Victoria, Victoria, Canada.
Background: The history of 2S/LGBTQ+ STBBI research in Canada has often overlooked the unique experiences of Indigenous, Black, people of color (IBPOC) who are disabled and are trans and cis queer women, femme-presenting Two-Spirit, and non-binary individuals. This research gap is particularly concerning for marginalized populations who face intersecting forms of discrimination (including ableism, racism, sexism, and cisheteronormativity) especially considering that chlamydia is the most commonly reported bacterial STI in Canada.
Methods: In partnership with Community-Based Research Centre, a community-based mixed methods (qualitative and Critical Discourse Analysis) research project informed by, disability justice, and critical feminist perspectives was undertaken to explore the experiences of IBPOC disabled trans and cis queer women and femme-presenting Two-Spirit and non-binary individuals in accessing Ontario chlamydia screening and care. The presentation will focus on themes generated by the qualitative data with approximately 23 participant interviews using a semi-structured format.
Results: Presenters will share data on the participants’ lived experiences, including barriers to care, experiences of discrimination, and recommendations for improving access for IBPOC disabled trans and cis queer women and femme-presenting Two-Spirit and non-binary individuals. Findings on accessibility and the need for culturally relevant and inclusive approaches to chlamydia prevention and care guidelines and practices will be discussed.
Conclusion: From this presentation, attendees will gain an understanding of the unique challenges faced by marginalized 2S/LGBTQ+ disabled IBPOC individuals; identify barriers to chlamydia screening and care; and will learn about strategies to improve access to chlamydia screening and care, including culturally relevant and inclusive approaches.
PP05.20 – Analysis of Asymptomatic and Symptomatic Sexually Transmitted Infections and the Impact on Clinical Outcomes in a Student-Run Free Clinic
Mr. Gabriel Lee1, Ms. Hayley Dunlop1, Mr. Gunnar Meyer3, Ms. Yuehe Wang1, Ms. Frances Trezza3, Ms. Nisha Makkar3, Ms. Isabella Donelley3, Dr. Robert Cooper1, Dr. Courtney Shihabuddin2
1The Ohio State University College of Medicine, Columbus, United States.
2The Ohio State University College of Nursing, Columbus, United States.
3The Ohio State University, Columbus, United States.
Background: Over one million curable STIs are acquired daily among individuals aged 15–49, most of whom are asymptomatic. Patients with lower socioeconomic status (SES) are disproportionately affected and less likely to access STI care, emphasizing the critical role of free clinics in STI screening and treatment. While literature highlights the importance of asymptomatic testing, little focuses on uninsured patients. This study aimed to evaluate symptomatic and asymptomatic STI testing outcomes at a student-run free clinic in a large Midwestern medical school. We hypothesized that symptomatic tests would yield higher positive rates than asymptomatic tests.
Methods: This was an IRB-approved retrospective review of 296 patient records from October 2019 to November 2023. Demographics, symptoms, collection sites, and results were assessed. Incomplete records were excluded from final analysis. Symptomatic versus asymptomatic status was determined retrospectively. Pearson’s Chi-Square, Fisher Exact, and Kruskal-Wallis tests were used for intergroup analyses, with a 2-sample test for equality of proportions examining positivity and negativity differences. Statistical significance was set at P < 0.05.
Results: Gonorrhea and Chlamydia were the most common tests (197), followed by Human-Immunodeficiency Virus (HIV) (185), Syphilis (173), Trichomonas (86), Candida (80), Gardnerella (80), and HPV (46). The most common demographics tested were patients identifying as female and Black/African American. There was no statistical difference between asymptomatic and symptomatic testing on both positive and negative testing rates for any STI (Table 1).
Conclusion: In this study, we observed no difference in positivity or negativity rates of STI tests between asymptomatic and symptomatic patients. Given the sequelae of untreated STIs and the limited contact that uninsured or underinsured patients may have with the healthcare system, availability of free STI testing for patients with and without STI symptoms is essential to reduce the rates of STIs, especially amongst underinsured and uninsured patient populations.
| Symptomatic (positive) | Asymptomatic (positive) | P-value | Symptomatic(negative) | Asymptomatic (negative) | P-value | ||
|---|---|---|---|---|---|---|---|
| Gonorrhea | 4 (3.4%) | 4 (3.7%) | 1 | 101 (85.6%) | 88 (81.5%) | 0.5128 | |
| Chlamydia | 8 (6.7%) | 6 (5.6%) | 0.9292 | 97 (81.5%) | 86 (79.6%) | 0.8491 | |
| HIV | NA | ||||||
| Syphilis | 6 (6.8%) | 4 (4.2%) | 0.6527 | 78 (88.6%) | 85 (89.5%) | 1 | |
| Garnerella | 31 (47.7%) | 12 (46.2%) | 1 | 27 (41.5%) | 10 (38.5%) | 0.9731 | |
| Candida | 11 (17.7%) | 2 (6.9%) | 0.2909 | 44 (71.0%) | 23 (79.3%) | 0.5577 | |
| Trichomonas | 5 (7.7%) | 1 (3.1%) | 0.6674 | 53 (81.5%) | 27 (84.4%) | 0.951 | |
| HPV | 3 (6.1%) | 6 (12.5%) | 0.4369 | 17 (34.7%) | 20 (41.7%) | 0.6186 |
PP05.21 – Six-Month Sexually Transmitted Infections Trends at a Novel Wellness Clinic Implemented in a High-Burdened Sexually Transmitted Infections Setting in Eswatini
Dr. Yves Mafulu1, Mrs. Nonkululeko Dlamini1, Sr. Khetsiwe Maseko1, Dr. Adele Benzaken, Dr. Nkululeko Dube1
1AIDS Healthcare Foundation, Manzini, Eswatini.
Background: Eswatini faces a significant challenge with STI diagnosis and treatment due to service access and stigma. Studies report a 25% STI prevalence rate among HIV-positive females and an overall prevalence of 22%. Nearly 29% of these cases are asymptomatic. In response, the AHF Eswatini implemented a novel STI wellness clinic to increase access to diagnosis and treatment for STIs in a time-flexible, stigma-free and non-judgemental environment. We analyze trends in STI diagnoses over 6 months, from June to December 2024, to assess the effectiveness of this new initiative.
Methods: We conducted a retrospective analysis using routinely collected data collected, focusing on various syndromic diagnoses and service utilization. The evaluation examined trends in STI consultations before and after implementation of a comprehensive marketing plan in September 2024.
Results: From June to September 2024, client numbers increased gradually. Following the implementation of a comprehensive marketing plan in September, attendance surged. The total number of clients increased from 20 in June to 445 in December, indicating a growth of 2,125%. New attendance for STI consultations increased from 14 in June to 119 by December, marking an increase of over 750%. Clients consulting for urethral discharge rose from 11 to 45 (an increase of 309%), while vaginal discharge cases peaked at 100 in October before declining to 52 in December. While all clients seen in June consulted for STIs (100%), this figure decreased to 134 out of 445 (30%) by December, due to utilization of other offered services such as HIV prevention and SRH.
Conclusion: The rise of clinical attendance after the implementation of new marketing strategies highlights effective outreach and marketing efforts while demonstrating that the message reached the target populations. These results give insights into the importance of targeted interventions and community engagement in addressing STI burdens effectively.
PP05.22 – A Case Scenario of How Amalgamated Transport Workers Union (ATGWU) at the Busia Boarder District Sustained Access to HIV Prevention and Reproductive Health Services Amongst Key and Priority Populations Following Enactment of the Anti-Homosexuality Act in Uganda
Dr. Peter Mikago1, Dr Nelson Mahulo1, Dr Hillary Alima1, Mr. Michael Mugweri1, Mr. Henry Kasadha1, Mr. Aramanzan Mulira2
1Uganda Protestant Medical Bureau, Jinja, Uganda.
2Amalgamated Transport and Workers Union, Busia, Uganda.
Background: Community-led solutions are necessary to mitigate public health threats including HIV. According to the Uganda Aids Commission Annual Joint AIDS review report, Nov 2023 Key Populations (KP) and Priority Populations (PP) remained an important target group for prevention interventions since HIV prevalence is high among them (between 11 and 34%). This is partly due to the discriminatory access to services in some of the areas following passing of the Anti-Homosexuality Act in Uganda.
Description: We embraced the Ministry of Health adaptation plan and modified service delivery approaches by leveraging on the partnerships of the Civil Society Organizations. Amalgamated Transport Workers Union (ATGWU) one of the 18 Civil society organizations serving at the Uganda Kenya Busia Border, Busia Municipality profiled was supported to profile Key and Priority population peers who were to report incidents of gender-based violence and ensure timely reporting of barriers to access of services at the various facilities. The peers were supported with transport to deliver integrated services testing services lubricants, Anti-retroviral therapy medicines, Pre-exposure Medicines, Post exposure Medicines, Family planning amongst others at various hotspots with in the communities and multi-coordinated household targeted visits.
Findings: In a period of 12 months, 5452 key populations and priority populations were reached with different integrated services including testing, Pre-Exposure Prophylaxis, PEP and Family planning (Table 1). A total of female 118 clients were diagnosed newly positive and initiated on treatment.
Conclusion: Civil society Organizations offer an opportunity to reach out to the Key and priority populations amongst the Private Not for Profit Faith based Health facilities.
Leveraging on Civil Society organizations is essential for offsetting barriers to access and utilization of prevention and sexual reproductive health services amongst the Key and Priority and populations in restrictive challenging environments.
| Oct-23 | Nov-23 | Dec-23 | Jan-24 | Feb-24 | Mar-24 | Apr-24 | May-24 | Jun-24 | Jul-24 | Aug-24 | Sept-24 | TOTAL | ||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Key and Priority Populations served | 299 | 174 | 679 | 645 | 466 | 536 | 467 | 555 | 356 | 485 | 480 | 396 | 5538 | |
| Key and Priority Populations Identified Positive and started on Anti-Retroviral treatment | 4 | 1 | 14 | 12 | 14 | 15 | 9 | 8 | 10 | 11 | 9 | 6 | 113 |
PP05.23 – Leveraging Community Health Workers to Improve Case Identification Through Maternal Retesting During Pregnancy, Labour and Breastfeeding at Private Not for Profit Health Facilities in Uganda; a Lesson from Uganda Protestant Medical Bureau
Dr. Peter Mikago1, Dr Nelson Mahulo1, Dr. Hillary Alima1, Mr. Michael Mugweri1, Mr. Edgar Tusubira1, Dr Racheal Kikansa1, Mr. Henry Kasadha1, Mrs. Dorcas Musubaho2, Miss Joweriah Namakula3
1Uganda Protestant Medical Bureau, Jinja, Uganda.
2Uganda Catholic Medical Bureau, Jinja, Uganda.
3Uganda Moslem Medical Bureau, Jinja, Uganda.
Introduction: The Mother To Child Ttransmission (MTCT) is the primary source of HIV infections for children in Uganda accounting for 18% of new infections (Uganda Ministry of Health National Elimination Plan II (2018–2023). Maternal resting for early identification of incident infections can potentially reduce Mother to Child transmission rate. By December 2022, Uganda Protestant Medical Bureau LSDA supported 197 Private Not for Profit Health Facilities had only 47% of the eligible women who were retested for HIV during pregnancy, Labour and breastfeeding period. This was due to heavy work load midwives and frontline staffs were experiencing, low demand creating at the supported facilities, reporting gaps and stock challenges of testing kits and knowledge gaps amongst service providers.
Methodology/Description: A total of 380 community Health workers (Peer mothers, para-social workers, mentor mothers, Young Adolescent and Peer supporters, Group Antenatal peers, Linkage facilators) were identified at the supported 197 health facilities. These were empowered through structured mentorships, coaching and facility Continuous Medical Education sessions about Maternal retesting. They were oriented on utilization of Maternal retesting trackers to follow through eligible women and also conducted routine health education sessions about maternal retesting. HIV testing kits were redistributed across health facilities that lacked to minimize missed opportunities during stock outs. During mentorships, project technical staffs emphasized proper data capture and coding while using the primary tools (registers).
Results: Gradually, Maternal retesting gradually improved from 47% as of October 2022 to 94 % as of September 2024 as detailed in the table of results.
Recommendations/Conclusions: Community Health workers should be empowered through trainings and mentorships to improve their knowledge on sustainable service provision of services.
In order to minimize Mother to Child Transmission of HIV, Health facilities should track maternal resting routinely among the Pregnant, those in labor and breastfeeding women.
Results of the Intervention
PP05.24 – Understanding the Landscape: Barriers to Effective Sexually Transmitted Infections Prevention and Treatment in Zimbabwe
Mrs Cleopatra Mpaso1, Mr Joseph Murungu1, Miss Imelda Mahaka1, Mr Joseph Njowa1, Miss Alison Footman2
1Pangaea Zimbabwe, Harare, Zimbabwe.
2AVAC, United States of America.
Background: Sexually transmitted infections (STIs) remain a significant public health challenge in Zimbabwe, despite progress in HIV management. While the country has met the 95-95-95 HIV targets, STI responses lag behind. The incidence of STIs among females increased from 33 per 1,000 in 2015 to 41 per 1,000 in 2018. Although reported STI cases declined by 28% from 2018 to 2022 due to increased awareness, gaps in testing and prevention persist. This assessment aimed to evaluate the STI prevention and treatment landscape and recommend improvements.
Methods: Qualitative methods were employed, including focus group discussions and semi-structured interviews with 93 participants and 27 key informants. Participants included adolescent girls and boys, sex workers, pregnant and lactating women, persons with disabilities, men who have sex with men, and transgender individuals across nine out of provinces (Fig. 1). Topics included access to services, barriers to care, and prevention strategies. Data were transcribed and analyzed using thematic coding.
Results: Access to STI treatment was hindered by stigma, medication stockouts, long waiting periods, and the cost of services. A significant proportion of the population lacked comprehensive knowledge about STIs and did not seek medical advice or treatment. Gaps in policy implementation and community outreach resulted in limited access to high-quality information, testing, and treatment services. The COVID-19 pandemic further disrupted healthcare services and funding, exacerbating these issues.
Conclusion: At the individual level, increasing education and addressing low-risk perceptions are crucial. At the community level, enhancing outreach and reducing stigma is essential. Strengthening health systems, improving supply chains, and integrating STI services with other health programs are needed. At the policy level, addressing socio-economic factors and targeting high-risk populations, including adolescent girls and young women, and men who have sex with men, is vital for reducing STI prevalence and improving sexual health outcomes.
PP05.25 – Impact Evaluation of Laboratory Health Products Evaluation and Validation on Policy Formulation, Review and Program Implementation
Ms. Namakula Aidah Rayaan Aidah Rayaan Namakula1, Ms Judith Kyokushaba1, Ms Susan Nambozo1, Mr Sulaiman Ikoba1, Ms Viola Kasone1
1Ministry of Health-nhlds, Kampala, Uganda.
Background: Laboratory health products validation and evaluation in Uganda are considered a systematic process that assesses the effectiveness, efficiency, and impact of laboratory health products introduced into the country serving as an essential tool for informing policy and programmatic decisions. This multifaceted approach not only evaluates the performance of laboratory testing kits and reagents but also examines their usability within the country settings. This study assessed the impact evaluation of laboratory testing kits within the country for policy formation and program design.
Methods: A mixed methods study was conducted for the last 11 new testing kits introduced into the country by 2024 and their impact on policy review and program implementation using convergent parallel design. Uganda has received several testing kits for the last 4 years for Mpox, Ebola and Hemorrhagic fevers. Testing Kits in the table below have been very critical in Laboratory testing policy review.
Data reviewed was from the 11 sampled testing kits with performance of 80% ≥ for specificity and sensitivity on both lab and field validation. Of the 11 randomly selected kits, 4 were Lab validated and field evaluated in 2022–2023, and 8 in 2023–2024.
Findings: Table 1: Refer to the attached table. 100% of all the 11selected testing kits were validated in the lab and field evaluations conducted in last 4 years provided vital information for policy review and program strategic directions.
Conclusion: Laboratory test kits field and lab validation within the specific country settings are indispensable in policy formulation and review for improved patient care.
| HIV testing kits | Validation status | Policy status | Testing Protocal | |
|---|---|---|---|---|
| Wondfo | Yes | Reviewed-HIV testing Algorithm | Screening | |
| One step | Yes | Reviewed-HIV testing Algorithm | Tie braker | |
| Meriscreen | Yes | Reviewed-HIV testing Algorithm | Confirmatory | |
| Syphillis Duo | Yes | Reviewed-EMTCT policy | Testing for all pregnant mothers | |
| Visitect RDT-Advanced CD4 | Yes | Reviewed-AHD strategy | All HIV patients | |
| Mpox Outbreak | Laboratory testing | |||
| RADI kit | Yes | Reviewed-Reference Testing strategy | Confirmatory | |
| NOVAPLEX | Yes | Reviewed-Reference Testing strategy | Confirmatory | |
| CDC Atlanta Inhouse kit | Yes | Reviewed-Reference Testing strategy | Screening Test | |
| Bioperfectus | Yes | Reviewed-Reference Testing strategy | Confirmatory | |
| Ebola Outbreak | ||||
| Altona Ebola | Yes | Reviewed-Reference Testing strategy | Confirmatory for Ebola | |
| Filovirus tests | Yes | Reviewed-Reference Testing strategy | Screening and confirmatory for Ebola and Marburg |
PP05.26 – Prevalence of HIV/AIDS in Disaster-Ravaged Communities in Nigeria
Mr. Promise Ebubechukwu Nnaoma1
1University of Port Harcourt, Port Harcourt, Nigeria.
There have been growing concerns that conflicts and disasters exacerbate the HIV epidemic, yet there is little or no empirical evidence to ascertain the prevalence of HIV among people living in conflict-affected areas. Since persons living in conflict-affected areas may not have access to adequate medical supplies and facilities, then it is safe to believe that conflict can cause a rise in the number of HIV patients.This study was carried out between the 1 of September and the 27 of November, 2024 in twelve flood-ravaged States. A community cross-sectional study design was adopted. The population consisted of 230 men and women aged 20–49 years residing in internally displaced persons (IDP) camps in Rivers State. The instrument for data collection was a pretested questionnaire with a reliability coefficient of 0.87. A sample size of 230 was selected using a census since the population was manageable. Participants were provided informed consent, and the instrument covering demographics, sexual risk, reproductive health behaviour, and history of gender-based violence was administered. Participants also provided a blood specimen for HIV and other STD testing and were referred to HIV counselling and testing services established for this study to learn their HIV status. Results showed that HIV prevalence was significantly higher among men in the IDP population compared to women in the environment. Also, the result further revealed that STIs such as syphilis and gonorrhoea were prevalent in the flood-ravaged IDP camps, though they were more prevalent among women aged 20–28 years. The study concluded that disasters, conflicts, and other related vices have a significant influence on the prevalence of HIV and other STDs.
PP05.27 – Closing the Gaps — Integrating HIV Testing Into TB Programs: A Scalable Model for Maternal and Pediatric Health in Nigeria
Dr. Opeyemi Adebayo1, Ms Aimu Rifkatu1, Dr Opeyemi Adebayo1, Ms Miriam Bathna2, Dr Uchenna Ugwoke1, Dr Emmanuel Vincent1, Dr Joseph Daniel1, Dr Temitope Adetiba1, Dr Adekola Adekunle1, Mrs Comfort Ochigbo1, Mr Benjamin Pillatar1, Pharmacist Adeyinka Aderounmu1, Pharmacists Arinze Nwadukwe1, Pharmacists Ritmwa Gurumnan1, Pharmacist Sunday Attah1, Pharmacist Chiagozie Mgbemena1, Dr Fati Murtala-Ibrahim1, Dr Evaezi Okpokoro2, Dr. Olayemi Kinmilola Olupitan1, Dr Aderonke Agbaje3, Dr Charles Mensah4, Dr Patrick Dakum3, Mr Nibretie Workneh5, Ms Janet Kimeu5, Mr Kazuaki Tsujii5, Ms Margaret Zamzu5, Mr Jean-Thomas Nouboussi5
1Global Fund NTHRIP Institute of Human Virology Nigeria (IHVN), Abuja, Nigeria.
2International Research Centre of Excellence, Institute of Human Virology, Nigeria (IHVN), Abuja, Nigeria.
3Institute of Human Virology Nigeria (IHVN), Office of the CEO, Abuja, Nigeria.
4Institute of Human Virology Nigeria (IHVN), Office of the COO, Abuja, Nigeria.
5The Global Fund to Fight AIDS, Tuberculosis and Malaria, Global Health Campus, Geneva, Switzerland.
Background: Nigeria accounts for 14% of global pediatric HIV infections, with a 23.4% vertical-transmission rate in 2023, driven by low antenatal care coverage and poor PMTCT uptake. Additionally, 62% of deliveries occur outside formal-health facilities, often without skilled-care. To address these gaps, the IHVN Global Fund Grant cycle-7 implements community-based testing and referral systems as part of TB/HIV integration efforts. This study evaluates the effectiveness of these interventions in reducing pediatric HIV infections through community engagement.
Description: The project, spanning from January 2024 to December 2026, is implemented across Nigeria’s 36 states and the Federal-Capital-Territory. It employs two approaches: Approach 1 operates in community-settings- Homes, Internally-Displaced-Persons camps, and Slums—integrating HIV/Syphilis/Hepatitis-B screening into TB case-finding for pregnant women (PW) through community teams and mentor mothers. Approach 2 targets unconventional care settings, training caregivers at traditional-birth facilities, healing homes, and religious centres incorporating HIV-testing into routine services, with structured tools for documentation and reporting.
Findings: Between January and November 2024, the program identified 278,592 PW, testing 219,093 (79%) for HIV. Of these, 1,098 (0.5%) tested positive and were linked to care and ANC. Additional cases included 553 syphilis, 53 hepatitis B, and 13 HIV-HBV co-infections. Compared to 2023, the project accounted for 14% of newly identified HIV-positive PW and an 8% increase in PW aware of their HIV status.
Key successes include strengthened TB-HIV collaboration, improved ANC attendance, and local ownership. Best practices include integrated disease testing and expanded logistics delivery points. While Challenges include TB-worker resistance, dual test kit shortages, and limited commodity access.
Conclusions: The findings highlight the effectiveness of integrating HIV-testing into TB programs and leveraging community-based interventions to enhance HIV prevention, treatment, and ANC attendance, while identifying co-infections and addressing gaps in service delivery, offering a scalable model for improving maternal health outcomes and reducing pediatric HIV infections.
PP05.28 – Strengthening Screening Services: Barriers and Facilitators to Cervical Cancer Prevention Among Women Living with HIV in Kilimanjaro, Tanzania
Mr. Anthony Sebastian Charles1, Prof Michael Mahande2
1Management And Development For Health- Temeke specialized laboratory, Dar Es Salaam, Tanzania.
2Kilimanjaro Christian Medical University College, Kilimajaro, Tanzania.
Background: Cervical cancer is the fourth most common cancer globally among women in incidence and mortality and one of the most common cancers affecting women in Tanzania. HIV-Positive women are disproportionately at higher risk of developing the disease, The aim of this study was to assess the knowledge, practices and barriers to cervical cancer screening among HIV- Positive women in Moshi Municipality, Kilimanjaro in northern Tanzania.
Method: A cross-sectional study was conducted in the Kilimanjaro region among 215 HIV-Positive women attending care and treatment centers (CTC) at Mawenzi regional hospital and KCMC hospital between 8 July and 21 July 2021. A questionnaire was used for data collection using face-to-face interviews. The study population were women living with HIV aged 18 to 49. Data were analyzed using SPSS version 20.0. Frequencies and percentages summarized categorical variables and numerical variables summarized using median and interquartile range (IQR).
Results: Over half 60.9% of the participants had knowledge on cervical cancer risk factors, 69.3% had good level of knowledge on cervical cancer preventive methods. Over half 64% of HIV-Positive women in this study had ever screened for cervical cancer. And among these 29.9% had their cervical cancer screening in the past 12 months. HIV status, advice from health care providers and screening campaigns were the reasons for undergoing cervical cancer screening. 85.0% received information on cervical cancer from health professionals and 47.7% from medias and 20.1% of them from family/relatives. Barriers to cervical cancer screening, afraid for the badresults (71.5%), afraid for the test procedure (59.8%), lack of disease symptoms were commonly mentioned by the participants.
Conclusions: For successful implementation of cervical screening program, the health care workers should intervening at the community level and compliance of HIV-Positive women.
PP05.29 – Community Support and HIV Testing Through the Role of Peer-Client Bonds in Self-Test Kit Uptake and Return Among Key and Vulnerable Groups in Tanzania
Mr. Anthony Sebastian Charles1
1Management And Development For Health – Temeke specialized laboratory, Dar Es Salaam, Tanzania.
Background: HIV self-test is an approach to get current testing services, both assisted and unassisted are recommended by WHO to Key populations. In Tanzania, by 2022 the rate of return of unassisted kits among KVPs was 66% compared with the established which is 100%. Low return rate can lead to stigma, and barriers to HIV care and treatment services, the program aimed to investigate the effectiveness of peer client bond in returning of unassisted self test kits among FSW participated in community HIV testing and services.
Description: Peer client bond introduced among targeted female sex worker groups, groups of ages, locality and friendships were established. Peers were capacitated and demanded for kits distributions, pre counselling, dealing with client perceptions on tests and following up for the return of results using unassisted kits distributions modalities.
Lessons learned: Improved rates of unassisted kits from 66% to 95% from January to October 2023, and hence contributed in identifications of new cases for HIV. Peer beneficiary attachment is a key model worked effectively in improving the return of rates of unassisted HIV kits as it removes barriers and experience sharing in removing fear, stigma and improve HIV care and treatment services.
Conclusions/Next steps: Adapting peer client bond work effectively in improving community HIV interventions for KVPs, adapting HIVST is the best interventions for KVP services and case identifications for linkage, it is recommended for partners and other stakeholders who are implementing HIV testing services to adopt peer client bond model to improve HIV care and treatment services.
PP05.30 – Demand Creation Through Local Government Sensitization to Unwavering Commitment: Lessons from Climate Challenges to Enhance Community HIV Interventions for Key and Vulnerable Populations in Tanzania
Mr. Anthony Sebastian Charles1
1Management And Development For Health- Temeke specialized laboratory, Dar Es Salaam, Tanzania.
Background: In Tanzania, the efforts against the existing challenges of climate change and HIV interventions have a complex landscape, efforts marked by unpredictable rainfall patterns and varying sunny days. These climatic dynamics pose significant barriers to the successful interventions of community-based HIV programs hence affecting the reaching and sustainability of health care services to key and vulnerable populations, the program made the demand creations to explore the climate challenges to provide effectiveness of community-based HIV interventions for KVP’s at Ubungo municipality in Tanzania.
Description: The demand creations for local government authorities to observe the challenges of climate changes which affect the community HIV interventions for KVPs was conducted in September–December 2022. We had 10 facilities doing community HIV testing services for KVp’s, we demand for having gumboots, umbrellas, jackets, phone, transports, local government leaders. These demands helped us in implementations of the program regarding how worse climate changes were troubled.
Lessons learned: Increased number of client from 2000 in June 2020 to 9500 in December 2022 for HIV care and treatment services was observed. the sustainability and utilizations of the health services during climate changes depend on sensitization and demand creation from local government authorities, donors, funders, partners and stakeholders. Community sensitizations with LGAS are essential to the success of dealing with climate changes which are the barriers of community HIV interventions.
Conclusions/Next steps: We recommend that, for sustainability and success community HIV interventions which are challenged by climate changes, is better to have demand creations from LGAs, donors, funders and partners in order to smooth interventions for Key and vulnerable populations.
PP05.31 – AIDS2024: 1328 Enhancing Emotional Support for MSM Living with HIV: Insights and Strategies from PLWHIV in Nairobi County
Mr. Harrison Wanjohi1
1Hoymas, Kenya.
2FAHARI YA JAMII, Kenya.
Background: Living with HIV presents not only physical challenges but also emotional hurdles that greatly impact an individual’s well-being. This study aimed to delve into the emotional landscape of MSM with HIV, understanding the emotional challenges is a key component in providing support for MSM living with HIV. To understand the emotional hurdles faced by MSM living with HIV and their effect on the care they receive. To identify effective strategies to support the emotional well-being of MSM living with HIV.
Description: Study ran from Jan 2022 to Aug 2023 with MSM in Kibera, Kenya. Used Focus Group Discussions for emotions and mental health talks, and One-on-One Interviews with 5 HIV+ MSM for detailed mental health insights.
Lessons learned: The FGDs and one on one interviews provided key insights on the importance of MSM living with HIV in having access to mental health services. Having toll- free numbers for free online counsellors and free health medication assistance is an integral part in ensuring the well being of MSM living with HIV. The interactions highlighted several programs and approaches that positively impacted the emotional well-being of individuals living with HIV namely professional counselling services, peer support groups in providing comfort and empowerment, art and expression therapy to express feelings and relieve stress, mindfulness and relaxation techniques to manage stress and community engagement programs to provide a sense of purpose and to uplifted spirits.
Conclusions: It is important to have readily available mental health services for the MSM living with HIV. Having toll-free numbers for free counselors and free mental health medication, as well as providing safe houses for those dealing with mental issues will work to enhance their mental status. It’s important to integrate these services with HIV care. Regularly checking and improving these support systems.
PP06.01 – Lessons Learned: Implementing Point of Care Tests at an Adolescent and Young Adult Clinic System
Dr. Allyssa Abacan1, Michelle Nong1, Dr. Meghna Raphael1
1Baylor College of Medicine, Houston, United States.
Background: Adolescents and young adults (AYA) account for over half of the new sexually transmitted infections (STI) in the United States. AYAs face many barriers to healthcare access. The purpose of this study was to implement a free chlamydia (CT) and gonorrhea (GC) point of care (POC) testing service line for AYA. The CT/GC POC test was implemented at a pilot clinic site of an AYA clinic system that provides free sexual health services to 13–24 years in Southeast Texas.
Description: A matched-pair study comparing patients who received a POC test versus patients who received the standard urine test was used to assess POC process and patient outcomes. The POC patients were then matched to a control patient by sex and birth and date of visit (+/– 2 days). In addition to whether the patient received a POC or urine screening, data collected for both case and matched patients also included patient demographics (eg. age, sex at birth), whether the patient was symptomatic or asymptomatic at the time of visit, GC/CT diagnosis, and sexual behaviors (eg. condom use, previous testing behaviors, past STI diagnoses). Chi-square and t-tests were used to analyze the differences between POC and matched patients’ demographic, sexual behaviors and STI outcomes.
Findings: The study included 228 samples (114 cases and 114 matches). There were no statistically significant differences in demographics, STI outcomes and sexual behaviors. Patients who received a POC test were statistically more likely to have been symptomatic (P = 0.006) and less likely to have had a previous HIV test (P = 0.015).
Conclusions: POC tests allows patients, especially those experiencing symptoms, the ability to get STI testing, diagnosis and treatment same day. Providing free POC tests for AYA is convenient for patients with no reliable transportation and experience cost barriers to care.
PP06.02 – Barriers and Facilitators to Discontinuation of Routine Chlamydia Testing in Asymptomatic Clients at Public Sexual Health Services in the Netherlands
Ms. Zoïe Alexiou1,2,4, Dr. Bernice M. Hoenderboom2, Dr Nicole H. T. M. Dukers-Muijrers1,3, Dr Birgit van Benthem2
1Department of Health Promotion, Care and Public Health Research Institute (CAPHRI), Maastricht University, Maastricht, The Netherlands.
2Centre for Infectious Disease Control, National Institute for Public Health and the Environment, Bilthoven, The Netherlands.
3Department of Sexual Health, Infectious Diseases and Environmental Health, Living Lab Public Health Mosa, Public Health Service South Limburg, Heerlen, The Netherlands.
4GROW Research Institute for Oncology and Reproduction, Maastricht University, Maastricht, The Netherlands.
Background: The Dutch chlamydia guideline has been updated, citing growing evidence that routine testing in asymptomatic individuals offers limited benefit and may cause harm. After years of emphasizing the importance of (asymptomatic) chlamydia testing, starting January 2025, routine testing at Dutch sexual health centers (SHCs) is no longer advised. This marks a major behavioral and organizational shift for SHCs and involved professionals. Understanding barriers and facilitators for this policy change is important for effective implementation.
Description: We developed an online questionnaire based on the Measurement Instrument for Determinants of Innovations (MIDI), assessing determinants related to the innovation, user, organization, and socio-political context on a 5-point Likert scale. We supplemented MIDI with themes identified during national coordination meetings, where SHC representatives discussed implementation experiences. The questionnaire was distributed via snowball sampling among SHC professionals. Determinants were categorized as barriers or facilitators using predefined thresholds; open-text responses were analyzed thematically.
Findings: Between 18 February and 12 March 2025, 158 professionals responded: 57.0% nurses, 22.2% doctors, 12.7% physician assistants, and 8.1% other staff. Most identified as female (86.1%), and 50.0% had ≥5 years of work experience. Key facilitators included clarity and perceived correctness of the policy (innovation), sufficient knowledge and skills (user), expected benefits like reduced antibiotic use (user), and colleague support (organization). Main barriers were limited perceived relevance for some clients (innovation), dealing with client resistance (user), and lab logistics (organization). Some (5.1%) indicated that clients generally are not satisfied. 73% agreed that tailored care can outweigh strict policy adherence, citing unclear symptoms, clients’ emotional well-being, and continued engagement with sex workers.
Conclusion: Though many professionals support the policy change and perceive potential benefits, de-implementation remains complex and gradual. Addressing identified barriers such as the relevance for all clients, understanding client resistance and optimizing lab logistics is important for continuation of implementation.
PP06.03 – Discontinuation of PrEP Users in PrEP Implementation Program Under Thailand’s Universal Health Coverage (UHC) Scheme: Missing Opportunities to Prevent Newly HIV Acquisition Among High-Risk Population in Thailand
Prof. Suwat Chariyalertsak1, Asso. Prof. Kannikar Intawong1, Ms Jutatip Thungthnog2, Mr Poonchana Wareechai2
1Faculty of Public Health, Chiang Mai University, Chiang Mai, Thailand.
2National Health Security Office, Bangkok, Thailand.
Background: UHC scheme in Thailand have been successfully implemented as the benefit packages for HIV prevention services since 2022. PrEP services were provided mainly by Key Population-Led Health Services (KPLHS) run by Community Based Organizations (CBOs) and hospital-based facilities (Hosp) distributed throughout the country.
Methods: All PrEP and HIV VCT services under UHC were recorded under National AIDS Program (NAP) through online system. We used linked de-identified PrEP users and HIV testing results who newly registered under NAP and initiated PrEP under UHC in 2022 and then follow up them till October 2024 to explore PrEP persistency and newly HIV seroconvert among PrEP users under PrEP services. HIV testing results were used to explore HIV status among continued PrEP users and discontinued PrEP users who stopped PrEP but returned for VCT services during study period.
Results: There were 10,084 people who registered and initiated PrEP under UHC in 2022 which 7,817(77.5%) received PrEP by KPLHS and 2,267 (22.5%) by hospitals. Most common key population were MSM (77.40%) and TGW (9.84%) by KPLHS and MSM (72.96%) and partner of PLHIV (14.78%) by hospital-based services. At the end of study period, 3,395 (33.67%) people still persisted in PrEP (mostly 99% ever stopped for sometimes and restarted PrEP) and 6,698 (66.33%) people discontinued from PrEP services. There were 3 newly HIV seroconverts in person who were still on PrEP (all related to inconsistency adherence). Among people who discontinued PrEP, 3,490 (52.11%) had come back for VCT services at least one time or more and found 177 (5.1%) newly HIV seroconverts. Among them, 158(89.27%) were MSM, 10(5.65%) were TGW, 75.86% aged 20–29 yrs. Estimated time to seroconvert after stopped using PrEP, 9.20% within 3 months, 13.22% 3–6 months, 33.33% 6–12 months and 46% after 1 year.
Conclusions: Factors associated with reasons for PrEP discontinuation need to be explored and better comprehensive HIV prevention strategies.
PP06.04 – Impact of an EMR-Based Syphilis Screening Prompt Among Hospitalized Adults with Substance Use Disorder
Dr. Megan Rose Curtis1, Dr. L. Madeline McCrary, Dr. Benjamin Hoemann, Tracey Habrock-Bach, Dr. Michael J. Durkin, Dr. Laura Marks
1Washington University School of Medicine, St. Louis, United States.
Background: Syphilis prevalence is rising in the United States. People with substance use disorder (SUD) are a priority population for syphilis screening. Inpatient hospitalizations present an opportunity for syphilis care. This study evaluated the impact of an electronic medical record (EMR)–based syphilis screening prompt on testing rates, diagnostic yield, and responsiveness by provider type.
Description: We implemented an EMR advisory for rapid plasma regain (RPR) testing among hospitalized adults with documented SUD. Using data from 4-months pre-implementation and 12-months post-implementation, we assessed syphilis screening rates and results. A subanalysis examined outcomes among women of reproductive age (15–49 years). Multivariable logistic regression estimated the adjusted odds ratio of responsiveness to the prompt by provider type, adjusted for patient age, patient sex, and day of alert activation (weekday versus weekend).
Findings: Syphilis screening increased from 16.2% to 57.0% post-implementation. Among those tested, 5.8% were RPR-positive pre-intervention compared to 3.6% post-intervention. Of the 479 women in the post-implementation group, 275 (57.4%) had a syphilis screen, of which 10 (3.6%) were positive. Fellows were more likely than residents to order an RPR in response to the alert (aOR 3.13; 95% CI, 1.05–9.36), while nurse practitioners and physician assistants were less likely to do so (aOR 0.55, 95% CI, 0.44–0.68; and aOR 0.66, 95% CI, 0.44–1.00), respectively). Attendings did not differ significantly from residents.
Conclusions: An EMR-based prompt increased syphilis screening 3.5-fold among hospitalized patients with SUD. The diagnostic yield declined post-intervention, likely due to broader screening of asymptomatic individuals. Following implementation, 10 syphilis cases were identified in women of reproductive age, highlighting the intervention’s potential for preventing congenital syphilis. Variation in provider response suggests opportunities to optimize implementation through targeted engagement with advanced practice providers. EMR-based inpatient alerts can improve identification of syphilis among priority populations with limited access to outpatient care.
PP06.05 – Offering the New At-Home Syphilis Test Through TakeMeHome, an Online Self-Testing Program
Ms. Jen Hecht1, Shalika Gupta1, Melissa Papp-Green2
1BHOC, Richmond, USA.
2Los Angeles County Department of Health, Los Angeles, USA.
Background: Self-testing has found strong acceptance among many populations globally and is substantially increasing access to HIV/STI testing for many people who have never tested. However, questions remain about the best options for offering self-testing, including self-testing versus self-collection. For syphilis, additional questions remain about confirmatory testing and accurate identification of acute infections.
Description: TakeMeHome, an online ordering platform for self-testing in the US, recently added the newly-approved NowDx syphilis test. The website was modified to offer a free syphilis test to users ordering an OraQuick in participating locations, with Los Angeles County becoming the first pilot location in January 2025. Users indicating interest in the syphilis test completed an additional question about prior syphilis diagnoses; affirmative responses were not mailed the test.
To support user education, supplemental information was added to the order process, email confirmation, FAQs, and social media.
We used a Poisson regression model to assess the associations between user demographics and interest in and eligibility for at-home syphilis testing using order data.
Findings: Between Jan 3 and Mar 26, 2025, 858 orders were placed through TakeMeHome by users in Los Angeles. 697 (81%) expressed interest in the syphilis test and 608 (71%) were both interested and eligible. 26% indicated it was their first HIV/STI test.
We found that cis women were significantly more likely than men (RR = 1.26, 95% CI = 1.14, 1.40) to be interested and eligible for an at-home syphilis test, after adjustment for age, race/ethnicity, time since last HIV/STI test, and prior testing with TakeMeHome.
Conclusions: Preliminary findings suggest strong acceptance and uptake of an offer of free syphilis home test in the context of an online self-testing program. Given the high rates of syphilis and congenital syphilis, home syphilis screening may help address barriers to testing.
PP06.06 – Perceptions of Acceptability and Preferences Surrounding a Hypothetical Syphilis Vaccine in Lima, Peru
Mx. Vale Fulqui2, Ms. Wendy Hamasaki2, Dr. Jessica Perez1, Mr. Gilbert Orta Portillo1, Dr. Jeffrey D. Klausner1, Assoc. Prof. Kelika Konda1
1University of Southern California, United States.
2Universidad Peruana Cayetano Heredia, Lima, Peru.
Background: Syphilis causes substantial morbidity and mortality worldwide; however, there is no vaccine against syphilis infection. There are research efforts to advance understanding of syphilis pathogenesis to inform vaccine development. Parallel to vaccine development efforts, there is a critical need to identify the drivers of willingness to receive new vaccines. Therefore, we conducted focus groups discussions (FDGs) with different population groups to understand their views of a hypothetical syphilis vaccine.
Description: In early 2025, we conducted 10 FDGs to understand syphilis knowledge, hypothetical syphilis vaccine acceptability important attributes, and implementation characteristics. Two FDGs were conducted with each of these five groups: 1) health professionals (n = 16); 2) sexual/gender minorities (n = 20); 3) general population (n = 18); 4) cis-gender female sex workers (n = 15); and 5) parents with children under 18 years old (n = 16).
Findings: Participants expressed high acceptability of a hypothetical syphilis vaccine. All groups were interested in a vaccine with high efficacy demonstrated in clinical trials, non-significant adverse effects, government health authority approval, production by recognized pharmaceutical companies, inclusion as part of free government health care; and availability via a single dose. Participants wanted assurance that vaccines would be available nationwide and with a guaranteed supply, avoiding stock-outs; some of these specifications were based on their COVID vaccination experiences. Notably, the possibility of persistent positivity and post-vaccination scarring would diminish vaccine acceptability. Members of key population groups, sexual and gender minorities and female sex workers, thought that to avoid stigma the vaccine should be available to the general population.
Conclusion: There was interest in and acceptability of a hypothetical syphilis vaccine. While the vaccine characteristics mentioned (high efficacy, low side-effects, and free availability) are expected, the relative importance of these characteristics should be explored further. Importantly, issues such as persistent positivity should be considered by vaccine developers given the potential to diminish acceptability.
PP06.07 – Mapping Global Syphilis Research: A Scoping Review to Support Implementation of the World Health Organisation’s Global Research Agenda for Sexually Transmitted Infections
Dr. Rosie Matthews1
1LSHTM, Keppel Street, United Kingdom.
Background: The World Health Organization’s (WHO) Global Research Agenda for Sexually Transmitted Diseases (STIs), launched in 2024, identified 22 priority areas for syphilis research to accelerate innovation and close evidence gaps in support of the 2030 STI strategy. These priorities were developed through a global research prioritisation process to guide future coordination and accountability. However, the extent to which existing syphilis research aligns with them remains unclear. This is the first study to assess the global syphilis research landscape against WHO’s research priority framework.
Description: As part of a larger mixed-methods study, we conducted a global scoping review to support implementation of the WHO STI Research Agenda. An ongoing Delphi process with global stakeholders will complement the review by validating findings and generating expert consensus on how to address identified gaps.
We systematically searched academic databases and grey literature for completed or ongoing syphilis-related research from February 2020 onward. Studies were included if they addressed at least one of WHO’s 22 syphilis research priorities and were mapped to four domains: diagnostics, prevention, management, and epidemiology.
Findings: Nearly half (47.5%) addressed the epidemiology domain, with Priority Area 16 (estimating prevalence and incidence) alone comprising 29.5% of all included studies (Fig. 1). Diagnostics and management accounted for just 13.0% and 16.1%, respectively.
The least studied areas: antimicrobial resistance, multipurpose prevention technologies, and vaginal microbiome research, each represented <1% of studies. The current research landscape remains focused on describing the problem, with limited attention to solution-oriented innovation.
Conclusion: This review provides a baseline to monitor alignment with global research priorities. Together with the ongoing Delphi process, it will help guide future STI research investments, support repeat mapping for other STI pathogens, especially gonorrhoea and chlamydia, and hold the field accountable to the priorities it has collectively defined.
PP06.08 – Evaluation of AnkaSmart!, a Multimodal Innovation for Enhanced Sexual and Reproductive Health in Peri-urban India
Miss Olivia Vaikla1,2, Dr. Suma Nair3, Miss Elizabeth Woolhouse2, Miss Needa Shaikh3, Dr. Shaveta Menon3, Dr. Daksha Parmar3, Dr. Roni Deli-Houssein2, Dr. Qihuang Zhang1,2, Dr. Sudha Rani4, Dr. Nitika Pant Pai1,2
1McGill University, Montreal, Canada.
2Research Institute of the McGill University Health Centre, Montreal, Canada.
3D.Y. Patil University, Navi Mumbai, India.
4D.Y. Patil Hospital, Navi Mumbai, India.
Background: Access to evidence-based, comprehensive sexual and reproductive health (SRH) education and services remains challenging for young populations residing in peri-urban areas of India. Key challenges include a lack of evidence-based information for SRH care; inadequate knowledge about appropriate use of contraception; shame and stigma associated with seeking care and services; and delays in pursuing timely testing and vaccinations for sexually transmitted infections.
Funded by Grand Challenges Canada and the Canadian Institutes of Health Research, we developed AnkaSmart!, a multimodal solution to improve comprehensive SRH care service delivery. We evaluated the solution for usability and feasibility in menstruating young adults of peri-urban India.
Description: We recruited participants from a higher education institution in India (18–30 years old, all gender identities, sex assigned female at birth, menstruating) in a cross-sectional study. We conducted pre- and post-intervention knowledge assessments and gathered user experience data with an adapted validated Usability Metric for User Experience (UMUX) scale. Feasibility was assessed with established metric completion rate and participants’ feedback documented.
Findings: Of 103 eligible participants, 78 have completed all study tasks, while 19 are actively enrolled. Overall, the majority of participants (88.89%, 72/81) found the innovation addressed their SRH needs. AnkaSmart! received an UMUX score of 70.79 [95% CI: 67.17, 74.41], n = 88. Knowledge assessments revealed a slight increase in understanding of SRH topics (Mean (SD) 8.48 (2.07) to 8.87 (2.29), P = 0.180, n = 83).
Conclusion: AnkaSmart! demonstrated high usability and feasibility among educated young populations. Participants found the platform user-friendly and relevant, though sustained wearable device engagement posed challenges. Findings highlight the need for targeted content, personalized features, culturally relevant innovations, language additions, and improved engagement solutions to impact outcomes and service delivery. Findings generate evidence to guide the design of clinical trials for global applicability.
PP06.09 – Protecting Providers: Programmatic Gaps and Implementation Challenges in HIV/STI Care in Nairobi’s Informal Settlements
Ms. Joyce Wangariria1
1Suruvi Care For Caregivers, Nairobi, Kenya.
Background: Healthcare providers serving in HIV/AIDS and STI clinics in Nairobi’s informal settlements (Mukuru, Kibera, and Korogocho) face significant risks, including exposure to infectious diseases, emotional burnout, stigma, and lack of institutional support. Despite being frontline workers in high-prevalence areas, the programs designed to protect them are often under-resourced or poorly implemented.
Description: This qualitative study explores the design and implementation of interventions aimed at safeguarding care providers in three informal settlements. Using purposive sampling, 25 in-depth interviews and 5 focus group discussions were conducted with clinical staff, peer educators, and program managers. Data were analyzed thematically using NVivo software to identify key gaps in program delivery, provider perceptions of risk, and systemic bottlenecks in protection protocols.
Findings: Preliminary analysis revealed inconsistent availability of personal protective equipment (PPE), minimal psychosocial support, and weak enforcement of workplace safety policies. 72% of providers reported emotional fatigue, while 60% cited fear of occupational exposure as a persistent concern. Providers also highlighted gaps in training on post-exposure prophylaxis (PEP) and inadequate follow-up mechanisms for incidents of occupational exposure. Community-level stigma further compounded provider vulnerability, especially among peer educators.
Conclusion: Findings highlight urgent gaps in program design and implementation related to provider protection in high-risk HIV/STI settings. Interventions must integrate consistent supply chains for PPE, institutionalize mental health support, and reinforce provider-centered safety protocols. Community stigma must also be addressed as part of a broader risk mitigation strategy. Strengthening these components is vital not only for provider well-being but also for sustaining quality HIV/STI service delivery in resource-constrained, high-burden settings.
PP06.10 – Gamifying Prevention: Engaging Youth with AI-Powered STI/HIV Prevention Games
Mrs Tolulope Adebisi1, Mrs Ronke Adeoye, Mr Emmanuel Clement
1National Agency for the Control of AIDS, Abuja, Nigeria.
Background: HIV/STI prevention interventions need to be targeted and packaged to meet the needs of high-risk groups. Significant progress in the discovery and adoption of HIV/STI prevention and treatment measures has resulted in a global decline in the incidence rate by 23% in the last 10 years. Engaging youth in STI/HIV prevention is crucial as they remain one of the most vulnerable groups to new infections. Traditional awareness campaigns often fail to captivate this tech-savvy generation. Gamification, combined with artificial intelligence (AI), presents an innovative avenue to enhance learning and behavioral change. This study explores the development, deployment, and impact of AI-powered games designed to educate youth on STI/HIV prevention.
Descriptions: We designed an interactive suite of games, “HealthQuest,” powered by AI to deliver personalized, engaging prevention messages. These games include role-playing scenarios, quizzes, and decision-making tasks, allowing players to navigate realistic challenges related to STI/HIV risks and prevention. AI algorithms adapt content based on users’ responses, age, and risk factors to ensure relevance and cultural sensitivity. The games were piloted among 2,000 youths aged 15–24 across urban and rural settings in Nigeria.
Findings: After 6 months of gameplay, knowledge of STI/HIV prevention improved by 65%, as measured by pre-and post-intervention surveys. Condom usage rates among participants increased from 38% to 62%, and stigma toward HIV-positive individuals decreased by 42%. Youth engagement with the platform was high, with 85% completing all game levels and 74% recommending it to peers. The AI adaptation feature was cited as a favorite, making the experience relatable and empowering.
Conclusion: Gamification, supported by AI, offers a transformative approach to STI/HIV prevention among youth, combining education with entertainment to achieve measurable outcomes. This innovative tool can be scaled to reach broader populations, particularly in low-resource settings where traditional methods are limited.
PP06.100 – A Pilot of a Real Time Syphilis Dashboard to Prevent Congenital Syphilis
Dr. Hilary Reno1, Dr. Germysha Little1, Nick Cardoza1, Dustin Hampton2, Benjamin Cooper1
1Washington University in St. Louis, Saint Louis, USA.
2DHSS State of Missouri, Jefferson City, USA.
Background: Preventing congenital syphilis requires diagnosing and treating pregnant people with syphilis but also people that could become pregnant. Treatment of syphilis before pregnancy would reduce treatment of babies born to people with syphilis. EMR data dashboards can identify people with reactive syphilis testing to provide a priority list for disease intervention specialists to contact, follow for treatment assurance, and offer partner services.
Methods: Using STI testing results (Q1 2024) from a large health care system, included cases had positive syphilis testing, assigned female at birth, age 15–44, living in Missouri. Test results were compared to Websurv, the state database for STI surveillance. The primary outcome was the % of people with positive syphilis testing included in Websurv while the secondary outcome included % of tests shared in both systems.
Results: In Q1 2024, a total of 112 people met inclusion criteria and had positive syphilis testing; 110 of the 112 people had records in Websurv (98.2%). One patient without a record in Websurv had a false positive (FP) test; the other patient had secondary syphilis but was not reported to the health department. Of the 166 tests from included people, 17 had not been included in Websurv. These 10.4% of tests were from people with a history of treated syphilis or people who had a known FP test.
Conclusions: Additional validation is ongoing, but this trial demonstrated the ability to identify at least one patient with syphilis whose tests were not communicated to DIS. Health care data platforms containing real time syphilis testing, treatment and contact information helps DIS focus efforts upstream for congenital syphilis prevention.
PP06.101 – Empowering Care: Recognizing Nurses to Boost Engagement in HIV Opt-Out Testing in Emergency Departments
Ms. Annae Saldivar1
1Dignity Health- St. Joseph’s Hospital and Medical Center, Phoenix, United States.
Background: Routine HIV opt-out testing in emergency departments (EDs) is a vital strategy in early detection. At St. Joseph’s Hospital and Medical Center in Phoenix, AZ, initial numbers were lower than expected. Nurses, as key implementers of the program, required additional engagement and support to enhance testing rates and program success.
Description: Several strategies were introduced to address low testing rates and bolster nurse involvement. A series of “lunch and learns” provided education on the importance of HIV testing and allowed for open discussions (Fig. 1). Opt-out testing form tracking was implemented, and the results were shared with ED managers, who recognized high-performing nurses with gift cards. Additionally, a monthly newsletter highlighted program updates, including testing numbers, reactive results, success stories, HIV facts and events. Nurses conducting the most tests were prominently acknowledged in this newsletter. This initiative drew inspiration from a successful program at a sister hospital. Daily huddles with multidisciplinary teams, including charge nurses, social workers, registration staff, and laboratory personnel, further reinforced the importance of the program and addressed challenges in real time.
Findings: Following the interventions, HIV testing numbers improved significantly. Nurses reported feeling more well informed, and connected with the program when receiving regular updates. Despite initial growth, testing rates have plateaued, suggesting the need for further innovation to sustain engagement and expand the program’s reach.
Conclusion: Recognizing and engaging nurses through targeted interventions significantly improved HIV opt-out testing rates in the ED. However, maintaining momentum requires continuous evaluation and adaptation of strategies. Future efforts should focus on addressing the plateau by exploring new recognition methods and fostering a culture of sustained collaboration. This model of nurse engagement may serve as a blueprint for other institutions looking to help end the HIV epidemic.
PP06.102 – HIV and Syphilis Universal Screening in the Emergency Department: Implementation and Comprehensive One Year Review
Dr. Julieta Sanchez-Ruiz1, Mrs. Julieta Sanchez-Ruiz1, Mrs. Chermane Stringfield1, Dr. KayLynn Bowman1
1St. Rose Dominican Dignity Health, Henderson, United States.
Background: Nevada has one of the highest rates of new HIV diagnosis in the nation and the highest rate in the entire western United States. Clark County is the most populous county in Nevada and has a new HIV infection rate of 19.8, higher than the state rate. To address this growing public health issue, Frontlines of Communities in the United States (FOCUS) program was integrated into Dignity Health St. Rose Hospitals Emergency Department (ED) policies that encourage universal opt-out HIV and syphilis screenings.
Methods: The implementation process began with leadership approval and support from ED providers. Key changes included developing workflows for lab testing, creating informational handouts, and conducting frequent rounds to review processes with providers. Screening criteria targeted patients over 18 requiring blood work, with an opt-out option. Provider engagement was emphasized through relationship building, sharing success stories, and presenting data results. Through the use of Cerner software, the team manually collected daily data from three EDs, enabling analysis of test results, demographics, and linkage to care (LTC) efforts. Eligible patients were referred to the Dignity Health Medical Group and Ryan White Program for comprehensive medical and support services.
Results: Between November 1, 2023, and November 30, 2024, 9,976 patients were screened, with 8 providers completing 70% of screenings. Of 67 participating providers, the screenings identified 71 HIV cases and 115 reactive syphilis cases. All eligible patients received LTC or HIV comprehensive prevention services (CPS).
Conclusion: Implementing universal HIV and syphilis screenings in the ED is a successful method for identifying persons living with HIV and connecting at-risk patients to HIV CPS. Bridging internal structural programs along with developing community partnerships has proven as an effective universal screening program, allowing care teams to link persons to care thus lowering the incidence of HIV in the community.
PP06.103 – Reconceptualizing Gender-Based Violence in HIV Prevention Research and Programming for Adolescent Girls and Young Women: An Integrative Review
Ms. Emma Sandstrom1, Dr. Robert Lorway1, Dr. Souradet Shaw1, Ms. Mê-Linh Lê2, Dr. Marissa Becker1
1Institute for Global Public Health, University of Manitoba, Winnipeg, Canada.
2Neil John Maclean Health Sciences Library, University of Manitoba, Winnipeg, Canada.
Background: Adolescent girls and young women, particularly those engaged in transactional sex and sex work, experience disproportionate rates of gender-based violence. While public health scholarship and practice acknowledge that gender-based violence may render an individual more susceptible to adverse health outcomes, this understanding often conceives of gender-based violence at the individual as opposed to the structural levels where risk and vulnerability are shaped.
Description: Using Relational Gender Theory and the Ecological Framework of Violence to locate gender as a multidimensional structure, an integrative review of 31 peer-reviewed articles on gender-based violence interventions in HIV prevention research and programming targeting adolescent girls and young women in low- and middle-income countries was conducted.
Findings: The results revealed a predominant focus on sexual and physical violence perpetrated by partners, with limited attention given to emotional and economic forms of violence in approaches to defining and measuring gender-based violence. Moreover, interventions have focused primarily on individual level factors, neglecting broader community and structural drivers.
Conclusion: By applying a robust gendered lens, this review revealed an opportunity to broaden both the conceptualization and operationalization of gender-based violence within HIV prevention programming and research for adolescent girls and young women.
PP06.104 – Acceptability of Gonorrhoea Vaccination by Potential Efficacy in an Online Sample of Men Who Have Sex with Men in New Zealand
Dr Adrian Ludlam1, Professor Felicity Goodyear-Smith1, Dr Janine Paynter1, Associate Professor Helen Petousis-Harris1, Assoc. Prof. Peter Saxton1
1University of Auckland, Auckland, New Zealand.
Background: Many countries report increasing cases of gonorrhoea and the development of antimicrobial resistance is a major global concern, limiting future treatment options. Studies have shown that vaccines developed for Neisseria meningiditis may be effective against gonorrhoea infection, however, acceptability of such vaccines among key populations outside clinics is understudied. We aimed to estimate vaccine acceptability among a community sample of gay, bisexual and other men who have sex with men (GBM).
Methods: We examined data from the 2022 round of SPOTS, a cross-sectional HIV behavioural surveillance programme among GBM in New Zealand. Participants were asked “If there was a vaccine against gonorrhoea, how likely would you be to have it?” alongside four vaccine efficacy (VE) scenarios: “If it were 90%/50%/30%/15% effective against gonorrhoea”. Response options for each scenario were “very likely”, “likely” “neutral”, unlikely”, “very unlikely”. We report overall acceptability (“very likely”/”likely”) and univariate associations with acceptability at a VE up to 30%, based on a prior New Zealand case-control study.
Results: Among n = 2991 participants, vaccine acceptability was 88%, 67%, 37%, 27% based on hypothetical VE scenarios of 90%, 50%, 30%, 15% respectively. Vaccine acceptability at VE up to 30% was associated with age (P < 0.001), gay social connections (P < 0.001), number of partners (P < 0.001), HIV post-exposure prophylaxis (P < 0.001), chemsex (P < 0.001), HIV status (P = 0.011), history of any STI <12 months (P < 0.001) and gonorrhoea <12 months (P < 0.001). Vaccine acceptability was not associated with ethnicity (P = 0.068), disposable income (P = 0.948), outness (P = 0.792) or comfort discussing sexuality with healthcare professionals (P = 0.322).
Conclusion: In this large, diverse GBM community sample, a moderately effective vaccine against gonorrhoea was acceptable to over a third. Acceptability was higher among GBM reporting behavioural risk factors for gonorrhoea acquisition, and younger age. Encouragingly for implementation planning, equity-related factors such as ethnicity, income and outness were not associated with acceptability.
PP06.105 – Implementation of Community-Based HIV-Self-Testing (CB-HIVST) to Improve Awareness of HIV Exposure: Centre for Population Health Initiatives Experience
Mrs. Elizabeth Shoyemi, Kanayochukwu Okeke, Dooshima Uganden, Ikenna Michael
1Centre For Population Health Initiatives, Lagos, Nigeria.
Background: HIV testing involving blood poses significant barriers, including fear of stigma, dislike of needles, and difficulties accessing testing, especially for marginalized communities. HIV self-testing (HIVST) using oral swabs was introduced as a more accessible, confidential, and non-invasive testing option. Community-based HIV self-testing (CB-HIVST) was established to bridge gaps in conventional HIV testing services.
Description: In October 2020, the Centre for Population Health Initiatives (CPHI) implemented HIVST in Lagos, Nigeria, for key populations, including men who have sex with men (MSM), female sex workers (FSW), people who inject drugs (PWID), and transgender women (TGW). Using the national HIVST guidelines, CPHI trained community health workers (CHWs) to assist clients with self-testing, result interpretation, and follow-up support. Individuals with reactive results were referred for confirmatory blood tests at preferred facilities. The program also conducted community sensitization and targeted sessions in mobile hotspots like brothels, bars, and dating sites, along with media campaigns to increase awareness of HIVST.
Findings: The CB-HIVST program enhanced HIV testing access in a stigma-free and confidential setting. Between October 2020 and July 2024, 6,192 HIVSTs were conducted, with the following breakdown: 35% MSM, 43% FSW, 19% PWID, and 4% TGW. Ten percent (630) of tests were reactive, with a 59% reactivity rate among MSM. All reactive cases confirmed their HIV status via blood tests, and 99% commenced antiretroviral therapy. The CB-HIVST initiative addressed barriers such as transportation costs, stigma, and discomfort with blood tests, providing a pathway to comprehensive care.
Conclusion: CB-HIVST has proven effective in reaching individuals unaware of their HIV exposure, contributing significantly to increased access to testing and supporting UNAIDS’ 95-95-95 goals. Scaling up this approach, particularly amongst marginalized populations, could further improve testing coverage and reduce undiagnosed HIV cases. CPHI plans to expand CB-HIVST to more communities, enhancing HIV prevention and care efforts.
PP06.106 – Art4PrEP: Enhancing HIV Prevention and Sexual Health Care for High-Risk Adolescents and Young Persons in Nigeria
Mrs. Elizabeth Shoyemi1, Mr Kanayochukwu Okeke, Dooshima Uganden
1Centre For Population Health Initiatives, Lagos, Nigeria.
Background: In Nigeria, high-risk adolescents and young persons (AYPs), such as children of key populations and adolescent key populations, face significant barriers to accessing HIV prevention and sexual health services. Poor risk perception, limited awareness of HIV prevention options, and inadequate knowledge of sexual and reproductive health (SRH) services heighten their vulnerability to HIV.
Description: Art4PrEP, a campaign led by the Centre for Population Health Initiatives (CPHI) with support from HJFMRI, to promote awareness and uptake of pre-exposure prophylaxis (PrEP) and SRH services by combining edutainment, youth-focused outreach, and multisectoral collaboration. Interactive events, including talk shows with experts, SRH-focused games, and activities integrated into existing sex education programs, bring essential health services closer to students in schools and community centers. Events like “Paint and Sip” provide engaging opportunities for HIV testing, PrEP counseling, and referrals to other services. Social media platforms such as Instagram, TikTok, and Facebook feature youth-driven content amplified by ambassadors who use humor and storytelling to connect with diverse audiences, including LGBTQ+ youth and young women. Collaboration with the Ministry of Health, educators, and community-based clinics ensures sustainability and scalability.
Findings: Between March and September 2024, Art4PrEP organized 28 events, reaching over 10,000 high-risk adolescents and young persons, distributing 1,500 HIV self-test kits, and enrolling 420 individuals on PrEP. The campaign’s online presence garnered over 1.3 million views, with inclusive messaging tailored for diverse youth groups, including gay, transgender, and nonbinary individuals.
Conclusion: Art4PrEP effectively addresses gaps in high-risk AYPs’ access to HIV prevention and SRH services by embedding these services within familiar environments and using relatable, youth-driven content. Building on its success, CPHI plans to scale Art4PrEP to underserved rural areas, expand digital engagement, and foster stakeholder collaboration, ensuring sustained impact and improved HIV prevention outcomes among the AYPs.
PP06.107 – Comprehensive At-Home Sexually Transmitted and Blood Borne Infection (STBBI) Testing Program: A Pilot Study
Dr. Caley Shukalek1, Dr Brandon Christensen, Dr Kevin Fonseca, Dr Ranjani Somayaji
1University of Calgary, Calgary, Canada.
Background: Rates of sexually transmitted and blood borne infections (STBBI) are rapidly increasing. Despite the high diagnostic accuracy of self-testing, no fully remote STBBI testing programs are available in Canada. We aimed to evaluate feasibility and acceptability of fully-remote, web-based, at-home STBBI testing in Calgary, Canada.
Methods: Participants who were Alberta residents aged 16 years self-enrolled into a web-based platform between February 2023-March 2024 including consent and intake questionnaire consisting of demographic and sexual health data. Kits were mailed, and samples were self-collected including swabs, urine and dried blood spot testing. Results of processed kits were communicated securely to participants. Surveys to assess feasibility and acceptability of the process were completed.
Results: Of the total 156 participants (39.7% men, 37.3 ± 10.5 years) from diverse sex and gender backgrounds who completed the intake, 67 participants returned their testing kits (43%). In the cohort, there was low reported condom use in more than 50%, and 40% had not had STBBI testing in the past 12 months. There were six participants with new positive tests for an STBBI (7.5%) and all were connected with treatment as appropriate. Participants largely reported satisfaction with the web-based platform and testing process as well as ease with testing modalities with the exception of dried blood spot testing which led to some challenges.
Conclusions: Our web-based comprehensive testing pilot was feasible and acceptable and may serve as an important tool as we work to dimmish the threat of rising STBBI rates.
PP06.108 – Opportunities and Limitations to HIV and STBBI Program Delivery for On-Reserve Populations in Saskatchewan
Dr. Cara Spence1, Ms. Trisha Campbell1,2, Ms. Mary Zettl1, Ms. Michelle Dornan1,2, Ms. Visna Rampersad3, Ms. Noreen Reed2, Dr. Stuart Skinner1,2
1University of Saskatchewan, Saskatoon, Canada.
2Wellness Wheel Clinic, Regina, Canada.
3Indigenous Services Canada, Regina, Canada.
Background: The ‘Know Your Status’ (KYS) (2016–2025) project is a CIHR team grant funded to implement and expand HIV and STBBI clinical care to on-reserve Indigenous communities across Saskatchewan (SK). The community-engaged project aimed to increase prevention, diagnosis, linkage to and engagement in care through mobile and remote infectious disease care and on-reserve community partnerships.
Description: Adapted from the ‘Community Readiness Assessment Tool’, semi-structured, mixed-method interviews were administered to 19 providers across 5 partnering on-reserve communities. Two reviewers conducted a thematic analysis of the interview transcripts using NVivo software and co-developed a codebook using a sample of 3 transcripts. Once inter-reviewer reliability was established, the analysts divided and rigorously coded the remaining transcripts.
Findings: A total of 18 themes were identified. Among these, gaps and barriers to service provision (n = 136), challenges to providing care (n = 41), confounding factors facing clientele (n = 108), and recommendations (n = 189) highlighted the needs and limitations to improving care uptake and engagement. Barriers and gaps were identified at all levels, from lacking basic needs to insufficient organizational resources, community stigma, and systemic barriers.
The interviews yielded 11 recommendations, including programming suggestions (mental health care and peer support), additional staff roles, improved training and staffing policies, more resources for provider organizations and clientele, and improved communication and partnering between health systems, researchers, and communities.
Conclusion: The KYS project supported on-reserve Indigenous communities that were facing high rates of mental health, addictions, HIV and STBBI transmission. However, realities within partnering communities and challenges for individuals without stable housing, food, income, transportation and phone access, with limited organizational resources to provide sufficient tailored programming, highlighted key lessons of why researchers and program developers must work with communities to ensure the intended project outcomes align with the needs, priorities and readiness of the communities in addressing HIV and STBBIs.
PP06.109 – Recommendations from a Participatory Action Program Evaluation to Improve HIV Care Outcomes in Saskatoon, Saskatchewan
Dr. Cara Spence1,3, Ms. Mary Zettl1, Ms. Emmanuelle Morin2, Dr. Larissa Keisman1,3, Dr. Beverly Wudel1,4, Ms. Lisa Clatney3, Ms. Katelyn Roberts5, Ms. Cristina Ugolini4, Ms. Ashley Hrabowy6, Ms. Dessie Jo Sutherland1,3, Ms. Stacy Naytowhow1,3
1University of Saskatchewan, Saskatoon, Canada.
2Cambiar Consulting, Saskatoon, Canada.
3Westside Community Clinic, Saskatoon, Canada.
4Saskatchewan Health Authority, Saskatoon, Canada.
5Sanctum Care Group, Saskatoon, Canada.
6Saskatoon Tribal Council, Saskatoon, Canada.
Background: Saskatoon has been without an HIV strategy since 2018 and is facing a syndemic crisis of HIV, syphilis, homelessness, mental health and opioid addiction. Saskatoon has the highest number of infections at 6x the national average, and UNAIDS 95-95-95, with outcomes reported at 61-61-42 (2023). Most of HIV care in Saskatoon is delivered through the Positive Living Program (acute care), the Westside Saskatoon Community Clinic (community-based care), and Sanctum Care Group (intensive short-term and palliative care), whose 2023 UNAIDS outcomes are 53-52-43, 82-74-46, and 90-94-43 respectively.
Description: Guided by the WHO program review guide (2013), the community-based evaluation design conducted a 2-year, 4-phase evaluation design with semi-structured interviews, focus group, peer-led sharing circles, clinical data, organizational audits, care process mapping, research literature and environmental scan of HIV policies and programs. Final recommendations and community consultation sessions co-developed a vision for the future of HIV care and clinical pathways to create an integrated HIV care ecosystem in Saskatoon.
Findings:
Final recommendations:
-
Establish a provincial HIV strategy
-
Strengthen provider relationships
-
Establish & implement shared data and reporting definitions
-
Establish cross-agency data-sharing policies, protocols & procedures
-
Develop & implement an enhanced consent process
-
Develop & implement shared approaches to address care linkages and engagement gaps
-
Enhance culturally competent & trauma-informed care
-
Hire a provincial HIV Coordinator
-
Hire a Saskatoon Care Coordinator
-
Establish a Peer Support Network
Conclusions: Recommendations were well received, and stakeholders committed to developing an HIV strategy, a more equitable resource allocation, and implementing coordinated HIV care pathways. However, ongoing relationship challenges/conflicts between provider groups, competition for resources, and failure to appropriately acknowledge the support received by partner organizations were evident throughout the two-year evaluation and remain barriers to effectively improving HIV care in Saskatoon.
PP06.11 – A Five-Year Review of the HIV Prevention Efforts Among Key Populations in Nigeria: Using the Prevention Self-Assessment Tool Lite
Dr. Rose Aguolu1, Joy Egwuonwu1, Chukwuebuka Ejeckam
1National Agency for the Control of AIDS, Abuja, Nigeria.
2WACPHD, Abuja, Nigeria.
Background: Key populations in Nigeria, including men who have sex with men (MSM), transgender persons (TG), female sex workers (FSW), and people who inject drugs (PWID), face heightened HIV risks. Understanding the effectiveness of prevention interventions and gaps in service delivery is crucial for targeted public health interventions. This study evaluated the effectiveness of HIV prevention interventions for these key populations from 2016 to 2021 using the Prevention Self-Assessment Tool Lite (PSAT Lite).
Description: The assessment was conducted across eighteen states with significant key population presence. PSAT Lite sessions were administered to program implementers and key population representatives in each state. The tool evaluated programs using a 5-point scale across two domains: program management and implementation. A score of 1.0 indicated minimal or absent performance, while 5.0 represented optimal performance.
Findings: In program management, FSW and MSM programs achieved the highest scores (3.0), with leadership and coordination scoring 3.5 and financing scoring 2.5. TG programs scored lowest (2.6), with particularly low financing scores (2.0). In program implementation, FSW and MSM programs again led with scores of 3.9. Implementation arrangements, service delivery, and program monitoring achieved the highest scores (4.4 each) within these programs. Structural interventions and targeting/planning received lower scores but remained above 3.0. PWID programs scored 3.8 in implementation, while TG programs scored 3.2, with notably low scores in structural interventions (2.9) and targeting/planning (2.8).
Conclusion: While Nigeria’s HIV prevention programs for key populations show promise, several areas require strengthening. Priority areas for improvement include structural interventions, planning processes, program financing, and services specifically tailored for transgender individuals. These enhancements are crucial for developing more effective and comprehensive HIV prevention strategies for key populations in Nigeria.
PP06.110 – National Survey of U.S. Emergency Department Sexually Transmitted Infection Notification and Treatment Practices
Assoc. Prof. Kimberly Stanford1, Joseph Mason1, Eleanor Friedman1, Christopher Buresh2, Douglas White3, Rachel Solnick4, Lauren Walter5, Elissa Schechter-Perkins6, Jason Wilson7, Yu-Hsiang Hsieh8, Emily Parker1, Kiran Faryar9
1University of Chicago, Chicago, United States.
2University of Washington, Seattle, United States.
3Highland Hospital, Oakland, United States.
4Mount Sinai Hospital, New York, United States.
5University of Alabama, Birmingham, United States.
6Boston Medical Center, Boston, United States.
7University of South Florida, Tampa, United States.
8Johns Hopkins University, Baltimore, United States.
9University Hospitals Cleveland Medical Center, Case Western Reserve University, Cleveland, United States.
Background: As syphilis and other sexually transmitted infections (STIs) increase across the U.S., the emergency department (ED) has emerged as a critical venue for screening. However, as results are often unavailable during the ED visit, testing creates an additional burden for result notification and treatment that may deter clinicians from testing. This study aims to evaluate the current national landscape of result notification and treatment for STIs diagnosed in the ED.
Methods: Electronic surveys were distributed via email to departmental leadership at 281 institutions with emergency medicine residency programs. Survey responses were also solicited utilizing relevant professional society listservs and in-person recruitment from October 2023 through May 2024. To avoid duplication, if more than one survey from the same institution was received, the responses of the most academically senior respondent were retained. Non-academic EDs were excluded due to a low response rate.
Results: A total of 98 academic EDs caring for adult patients (34.9% response rate) were represented. Responses were distributed similarly across census regions. In addition to diagnostic testing, 64 (60.6%) of EDs had an HIV screening program and 15 (15.3%) a syphilis screening program. Result notification was most often the responsibility of the ordering clinician (OC) and/or designated ED staff (DS) (syphilis 29.5% OC, 69.4% DS; gonorrhea/chlamydia (GC/CT) 30.6% OC, 67.3% DS; HIV 41.8% OC, 48.0% DS). Individuals with syphilis or GC/CT returned to the ED for treatment in 40.8% and 42.8% of EDs, respectively. Only 6.1% of EDs reported providing HIV treatment, whereas 72.4% was provided by Infectious Diseases.
Conclusion: A large proportion of EDs rely on ED staff to notify patients about their STI testing results and arrange treatment. Developing partnerships with outpatient clinics or health departments to shift this burden off of the ED could be an effective strategy to increase STI screening in EDs.
PP06.111 – Expanding Clinical Education Through On-Demand Interactive E-Learning
Ms. Jessica Steinke1,2, Ms. Gowri Nagendra1,2, Ms. Cindy Truong1,2, Dr. Jason Zucker1,3
1New York City STI/HIV Prevention Training Center, New York, United States.
2Mailman School of Public Health at Columbia University, New York, United States.
3Columbia University Irving Medical Center, New York, United States.
The New York City STI/HIV Prevention Training Center (PTC) is CDC-funded to provide training to clinical providers on sexual health topics. PTC traditionally provides in-person or live virtual training, though these may not meet the diverse requirements of learners. On-demand, interactive e-learning modules offer a potential solution, allowing learners to engage with content at their convenience.
To address the diverse needs of learners, PTC developed and launched seven on-demand modules in 2024 using Articulate Rise (AR), an e-learning platform, chosen for its ease of use, interactivity, and features. These modules cover sexual health topics identified by PTC as areas of need, including sexual history taking, syphilis, and congenital syphilis. Five courses are accredited for continuing education (CE) credits via CDC. Courses are designed for clinical providers, utilizing AR’s capabilities for case studies and quizzes to enhance learner experience. Learners access the content via an online account to complete at their own pace, with capacity to retake; each module takes roughly one-hour to complete.
Across the seven courses there were a total of 1,294 registrants (per course (PC) range: 100-329), with 457 completions (PC range: 40–114). PTC’s five CE-accredited courses were rated five stars by an average of 71.4% of users (4 stars = 27.6%). The usability of the AR platform provided PTC the ability and flexibility to quickly create courses on emerging topics, namely doxyPEP and the Bicillin-LA shortage.
On-demand interactive training modules are a flexible method for providing clinical education. PTC recently translated five courses into Spanish to broaden its reach. Future courses will include short modules that can be used as staff onboarding training, given the need of many clinics with high turnover. E-learning modules can serve as valuable tools for ongoing professional development for clinical providers, offering an additional option for clinical education in diverse healthcare settings.
| Course | Registration | Completion* | CE Claimed | CE Rating | Qualitative Feedback | |
|---|---|---|---|---|---|---|
| Taking a sexual history | 303 | 98 | 131 | 5 stars: 74% | “Very thorough” | |
| 4 stars: 21% | ||||||
| Congenital syphilis | 329 | 114 | 118 | 5 stars: 75% | “Very informative with case scenarios” | |
| 4 stars: 25% | “Very helpful supplementary tables that I have incorporated into my practice for interpreting syphilis serology.” | |||||
| PrEP guidelines | 136 | 52 | 43 | 5 stars: 57% | “Helpful, updated w/ case scenarios” | |
| 4 stars: 43% | ||||||
| HIV prevention benefits navigation | 104 | 45 | 28 | 5 stars: 69% | “This is extremely helpful information for helping clients navigate paying for PrEP and PEP. Considering how quickly PEP needs to be prescribed, it’s great to have a solid base of information so we don’t have a lag in patient care.” | |
| 4 stars: 31% | ||||||
| Syphilis | 100 | 40 | 28 | 5 stars: 82% | “This was a great course that provided easy to understand and navigate.” | |
| 4 stars: 18% | “Great information” | |||||
| “This was the best syphilis education for clinicians I’ve ever studied.” | ||||||
| DoxyPEP (no CE) | 172 | 60 | n/a | n/a | n/a | |
| Bicillin L-A shortage (no CE) | 150 | 48 | n/a | n/a | n/a |
*‘CE Claimed’ may be higher than ‘Completion’ due to those who retake the course without completing it, thus resetting their progress and status.
PP06.112 – Implementation and Acceptability of Point-Of-Care Sexually Transmitted Infection Testing at a Mobile Clinic for Women Who Inject Drugs in Seattle, WA
Dr. Abigail G. Fessler1, Dr. Lauren R. Violette1,2,3, Dr. Maria A. Corcorran1, Dr. Tom Fitzpatrick1, Dr. Elizabeth Austin1, Dr. Sara Glick1,4, Dr. Shireesha Dhanireddy1, Dr. Jenell Stewart5,6
1University of Washington, Seattle, United States.
2Harvard Medical School, Boston, United States.
3Harvard Pilgrim Health Care Institute, Boston, United States.
4Public Health Seattle & King County, Seattle, United States.
5Hennepin Healthcare, Minneapolis, United States.
6University of Minnesota, Minneapolis, United States.
Background: Women who inject drugs (WWID) face complex barriers to testing and treatment for sexually transmitted infections (STI). This study assessed demographics, STI prevalence and risk factors, and acceptability of point-of-care (POC) STI testing at a mobile clinic for WWID in Seattle, Washington.
Methods: We implemented a weekly mobile clinic offering substance use and sexual health services to women ≥18 years who had ever used injection drugs and were not known to have HIV. Visits occurred at enrollment, 3, and 6 months. To measure STI prevalence, we offered POC testing for Treponema pallidum and HIV (fingerstick), Neisseria gonorrhoeae and Chlamydia trachomatis, and Trichomonas vaginalis (vaginal swab) using ChemBio DPP, Binx io, and OSOM platforms, respectively. Surveys assessed substance use, sexual practices, and POC testing acceptability. We identified factors associated with STI positivity using chi-square/Fisher’s exact and Wilcoxon rank-sum tests for categorical and continuous variables, respectively. We present results from enrollment visits (March–August 2024).
Results: Among 50 WWID, median age was 35 (interquartile range [IQR] = 29–42), 73% were unstably housed, and 56% reported a previous STI. In the prior 3 months, 34% reported transactional sex, 82% used opioids, 43% injected drugs, and the median number of sexual partners was 1 (IQR = 1–4). At enrollment, STI prevalence was 30%, including trichomonas (11/42), gonorrhea (1/24), chlamydia (1/24), syphilis (2/50), and HIV (0/50). Women with an STI were more likely to report transactional sex (P = 0.02) and more sexual partners (5 vs 1; P = 0.02). Nearly all participants (96%) reported feeling comfortable receiving POC testing, and 88% preferred it over traditional methods.
Conclusion: STI prevalence was high among this cohort of WWID. Mobile POC STI testing is an acceptable healthcare delivery strategy for this population. Long-term feasibility and impact of POC testing remains unknown for WWID facing complex care barriers.
| Total N = 50 n (%) | STI detected N = 13 n (%) | No STI detected N = 37 n (%) | P-valuea | ||
|---|---|---|---|---|---|
| Median age [IQR] | 35 [29–42] | 33 [27-42] | 38 [31-42] | 0.4379 | |
| Race/Ethnicity | |||||
| American Indian or Alaska Native | 3/50 (6%) | 1/13 (8%) | 2/37 (5%) | 0.2574 | |
| Asian | 2/50 (4%) | 0/13 (0%) | 2/37 (5%) | ||
| Black or African American | 3/50 (6%) | 0/13 (0%) | 3/37 (8%) | ||
| Hispanic or Latinxb | 3/50 (6%) | 2/13 (15%) | 1/37 (3%) | ||
| Native Hawaiian or Pacific Islander | 0/50 (0%) | 0/13 (0%) | 0/37 (0%) | ||
| White | 28/50 (56%) | 9/13 (69%) | 19/37 (51%) | ||
| Multiple races | 11/50 (22%) | 1/13 (8%) | 10/37 (27%) | ||
| Gender | |||||
| Cisgender woman | 48/50 (96%) | 13/13 (100%) | 35/37 (95%) | – | |
| Transgender woman | 2/50 (4%) | 0/0 (0%) | 2/37 (5%) | ||
| Current Living Situation | |||||
| Homeless/Unstably housedc | 36/49 (73%) | 8/13 (62%) | 28/36 (78%) | 0.2884 | |
| Stably housed | 13/49 (27%) | 5/13 (38%) | 8/36 (22%) | ||
| Any opioid use in the past 3 monthsd | 41/50 (82%) | 11/13 (85%) | 30/37 (81%) | – | |
| Any meth use in the past 3 months | 42/50 (84%) | 11/13 (85%) | 31/37 (84%) | – | |
| Injection drug use in past 3 months | 21/49 (43%) | 4/13 (31%) | 17/36 (47%) | 0.3477 | |
| Shared injection equipment in past 3 months | 3/21 (14%) | 1/4 (25%) | 2/17 (12%) | 0.4887 | |
| Median sex partners in past 3 months [IQR] | 1 [1-4] | 5 [1-15] | 1 [1-2] | 0.0171 | |
| Condomless sex in past 3 months | 39/50 (78%) | 11/13 (85%) | 28/37 (76%) | 0.7044 | |
| Transactional sex in past 3 months | 17/50 (34%) | 8/13 (62%) | 9/37 (24%) | 0.0210 | |
| Self-reported history of any prior STI | 28/50 (56%) | 8/13 (62%) | 20/37 (54%) | 0.6400 |
PP06.113 – Enhancing HIV and Hepatitis C Care for People Experiencing Criminalization by Addressing Digital Exclusion
Ms. Amrit Tiwana1,2, Nicola Gale1,3, Mike Mahay1, Tiffany Barker1, Rebecca Hasdell1, Pam Young4, Mo Korchinski4, Deb Schmitz5, Daryl Luster5, Alnoor Ramji6,7, Julia MacIsaac6,7, Brian Conway8,9, Chris Fraser10, Sofia Bartlett1,7
1BC Centre For Disease Control, Vancouver, Canada.
2Faculty of Applied Science, University of British Columbia, Vancouver, Canada.
3CUPS Liver Clinic, Calgary, Canada.
4Unlocking the Gates Services Society, Maple Ridge, Canada.
5BC Hepatitis Network, Richmond, Canada.
6St. Paul’s Hospital, Vancouver, Canada.
7Faculty of Medicine, University of British Columbia, Vancouver, Canada.
8Vancouver Infectious Diseases Centre, Vancouver, Canada.
9Faculty of Health Sciences, Simon Fraser University, Burnaby, Canada.
10Cool Aid Community Health Centre, Victoria, Canada.
People with lived experiences of criminalization, including incarceration, homelessness, and substance use, face high rates of HIV and/or hepatitis C virus (HCV) infections and low treatment uptake in Canada. A significant barrier to care is the lack of having a cell phone, which hinders healthcare providers’ ability to contact individuals and coordinate follow-up care. This barrier particularly affects access to services which use virtual platforms.
Test, Link, Call (TLC) Project aims to improve access to HIV and/or HCV care for people experiencing criminalization in British Columbia. Clients receive a cell phone with 6-months unlimited talk and text and pre-installed health apps. They are also paired with peer health mentors (PHMs) to assist with navigating health services. A mixed-methods evaluation was conducted from October 2021–March 2024 to determine the outcomes and acceptability of TLC and its impact on care engagement. Qualitative data were collected using semi-structured interviews with healthcare providers (n = 8), PHMs (n = 6), and clients (n = 20). Demographic and clinical data were collected using program records and cross-sectional clinical chart reviews. Factors associated with HCV treatment uptake were assessed among HCV RNA positive clients (n = 245) using multivariate logistic regression.
TLC enrolled 273 clients in HCV care and 26 in HIV care. Clients reported that TLC was highly acceptable, with increased access to health services, improved connections with loved ones, and enhanced independence and safety. Challenges included phone theft and digital literacy issues. Among HCV clients, 57% initiated treatment within 12 months of enrollment. Multivariate analysis identified cis-gendered men, stable housing, safer supply prescriptions, and longer program involvement as significant predictors of HCV treatment uptake.
This evaluation demonstrates that the TLC Project significantly improves engagement in HIV and/or HCV care for people experiencing criminalization. The program can be adapted to other regions and health conditions, such as syphilis and substance use disorder.
PP06.114 – Amplifying Voices: Using Storytelling and Music to Address Gaps in HIV Prevention Research for Cisgender Bisexual Black Women
Miss Mystkue Woods1
1Mystkue Publications, LLC, Philadelphia, United States.
Background: Cisgender bisexual Black women are underrepresented in HIV prevention research, despite being disproportionately affected by systemic healthcare inequities. Existing prevention programs often fail to address their unique intersections of identity, leaving critical gaps in outreach and intervention.
Description:
This workshop utilizes storytelling and music to address these gaps:
-
Storytelling Activity: Participants reflect on personal or community experiences with HIV prevention, sharing narratives that highlight systemic barriers and resilience.
-
Music Creation Workshop: Groups collaborate to produce songs or spoken word pieces that convey empowerment and culturally relevant prevention themes.
-
Educational Segment: The Facilitator will provide context on the gaps in research and the importance of culturally tailored approaches.
Findings:
Evaluation of past workshop data showed:
Qualitative Data: Stories reveal recurring themes, including distrust in healthcare systems, stigma, and lack of tailored resources.
Quantitative Data: 85% of participants reported an increased understanding of the role of cultural identity in HIV prevention after the workshop.
Output: Advocacy tools (songs, spoken word pieces) were created, with 90% of participants expressing intent to use them in community education efforts.
Conclusion: The workshop demonstrates the potential of art modalities to bridge research gaps and engage marginalized populations in HIV prevention. Lessons learned include the importance of centering lived experiences and using culturally relevant tools to foster engagement. Attendees can replicate these methods to enhance outreach and advocacy within their own communities.
PP06.115 – Accelerating Progress Towards AIDS-Free Generation in Nigeria: A Sustainable Multi-Sectoral Approach
Mrs Hidayat Bukola Yahaya1, Dr Babayemi Olakunde2, Dr Mojisola Bello3, Mr Seun Oshagbami1, Mrs Ibironke Adeoye1, Mrs Tolulope Adebisi1, Dr Chizurum Okey1, Dr James Anenih1
1National Agency for the Control of AIDS, Abuja, Nigeria.
2College of Public Health, University of North Texas Science Centre, United State of America.
3National AIDS and STI Control Programme, Abuja, Nigeria.
Background: Nigeria faces a significant gap in PMTCT coverage, contributing to 14% of new HIV infections in infants and 12% of child deaths from AIDS-related causes. In response, the National AIDS, STI, and Viral Hepatitis Division (NASCP) and the National Agency for the Control of AIDS (NACA), in partnership with stakeholders, developed a comprehensive plan to eliminate mother-to-child transmission of HIV (eMTCT). This study highlights the progress of the implementation plan.
Description: With funding from the Global Fund, NASCP coordinated a strategic approach emphasizing service delivery, data quality, community engagement, and program coordination across all states and the Federal Capital Territory. NACA led the non-health sector innovation by initiating the AIDS-Free Generation campaign to empower communities, ensuring no child is born HIV-positive, and developing a medium-term resource mobilization strategy. Stakeholders’ collaboration was strengthened to link communities and health facilities, aligning efforts with sustainability agenda.
Findings: A total of 296 state and 3,870 local government area management team were trained in PMTCT program management, including representatives from the Ministry of Health, Primary Healthcare Development Agency, and people living with HIV networks. 39,000 Service Delivery Points (SDPs) including birth homes and health facilities, were mapped and assessed. SDP Focal persons received training on PMTCT service delivery and data management.
Additionally, 12,340 community mobilizers were trained, complemented by media campaigns featuring posters and radio jingles to create demand for PMTCT services. The AIDS-Free Generation campaign was launched in four states with key champions, including governors’ wives and religious leaders. The First Lady of Nigeria pledged her support as a campaign ambassador to drive political will and resource mobilization.
Next steps: Effective coordination of strategic approaches, ongoing quality improvement, strengthened multi-sectoral collaboration, and unwavering political commitment are essential to successfully eliminate mother-to-child transmission of HIV in Nigeria and ensure the sustainable HIV programs.
PP06.116 – Sexual Health Promotion for Sexual and Gender Minorities in Primary Care: Results of a Scoping Review
Dr. Anna Yeung1, Paige Homme1,2,5, Jenny Gong3,4, Robinson Truong1,5, Carolyn Ziegler6, Cassandra Freitas1,3, Morgan Martin1,5, Moyosola Ogunsuyi7, Dr. Darrell HS Tan1,8, Dr. Ann N Burchell1,2,3,9
1Unity Health Toronto, Toronto, Canada.
2Department of Family and Community Medicine, University of Toronto, Toronto, Canada.
3Dalla Lana School of Public Health, University of Toronto, Toronto, Canada.
4Nuffield Department of Population Health, University of Oxford, Oxford, United Kingdom.
5Temerty Faculty of Medicine, University of Toronto, Toronto, Canada.
6Library Services, Unity Health Toronto, Toronto, Canada.
7Toronto Metropolitan University, Toronto, Canada.
8Division of Infectious Diseases, Unity Health Toronto, Toronto, Canada.
9Department of Family and Community Medicine, Unity Health Toronto, Toronto, Canada.
Background: Sexual and gender minorities (SGM) face health inequities such as reduced or delayed access to care/health insurance, discrimination by healthcare providers, and a higher burden of sexual health issues including sexually transmitted infections (STIs) and human immunodeficiency virus (HIV). We conducted a scoping review to synthesize the current evidence regarding sexual health promotion interventions for SGM in primary care, and identify areas of priority, improvement and future research.
Description: Guided by the Sexual and Gender Minority Health Disparities Framework (SGM HDF) and the Gender-based Analysis Plus (GBA+) framework, we searched eleven databases between 01/2000-05/2022. We included articles if they addressed 1) SGM aged 12+ years 2) sexual health promotion in primary care and 3) were set in high-income countries. Two reviewers independently screened publications using Covidence and extracted data on study design, aims, populations, and results. The protocol is registered on the Open Science Framework Registries (https://doi.org/10.17605/OSF.IO/X5R47). We tabulated results and broadly categorized by the content area of the study’s primary aim.
Findings: 110/4606 publications screened met the inclusion criteria. Of these 110, 45 addressed STI/HIV testing, 34 addressed HIV pre-exposure prophylaxis (PrEP), 20 addressed HIV prevention and care (excluding HIV PrEP), 5 addressed viral STIs, 4 addressed gender-affirming care and 2 addressed other aspects of sexual health. 106/110 (96%) papers included gay, bisexual, or other men who have sex with men (GBM), and only 13 (12%) addressed racialized populations. Table 1 summarizes the frequency of primary factors from the SGM HDF at the individual, interpersonal, community and societal levels.
Conclusion: Interventions largely focused on biomedical aspects such as uptake and adherence of HIV PrEP. Few interventions addressed non-GBM and racialized communities. Our review found an emphasis on medical intervention but many of these studies highlighted other factors such as affirming patient-provider relationships to reduce the burden of STIs and HIV.
| Aspect of SGM Health Disparities Framework | Factor | # of Publications included | |
|---|---|---|---|
| Individual Factors | Coping mechanisms | 11 | |
| Interpersonal Factors | Affirming patient-provider relationships | 7 | |
| Community Factors | Access to PrEP | 32 | |
| Access to SGM-specific clinical and researcher training | 8 | ||
| Availability of safe spaces and SGM-specific resources | 49 | ||
| Societal Factors | Gender-affirming therapies | 2 | |
| SGM-specific screening and care guidelines | 1 |
PP06.117 – Rapid Diagnostic Tests for Sexually Transmitted Infections: A Review for Clinic- and Community-Based Testing
Ms. Shengruo Zhang1, Amber Lauff2, Jennifer Morton2, Noel Kalanga2, Dr. Paul Drain1,2,3
1Department of Epidemiology, University of Washington, Seattle, United States.
2Department of Global Health, University of Washington, Seattle, United States.
3Department of Medicine, University of Washington, Seattle, United States.
Background: One million sexually active people between ages 15–49 years acquire a new sexually transmitted infection (STI) each day. The likelihood of spreading an STI to others and/or developing more serious infection will rise when testing and care seeking are delayed. Rapid diagnostic tests (RDTs) may improve global access to STI testing and diagnostic services, which may accelerate diagnosis, reduce transmission, and improve patient outcomes.
Methods: We conducted a landscape analysis for five STI pathogens of interest: Chlamydia trachomatis (CT), Neisseria gonorrhea (NG), Trichomonas vaginalis (TV), Mycoplasma genitalium (MG), and Treponema pallidum (TP). We sought to obtain relevant information to inform the implementation of RDTs, information on RDTs that are still in development or undergoing clinical evaluation, and the characteristics of available and marketed RDTs suitable for clinic- and community-based testing.
Results: We identified 34 RDTs that are either being developed or have been approved for the screening or diagnosis of STIs, including 16 tests for CT or NG, 6 for TV, 3 for MG, and 16 for TP. Many RDTs have been approved by the World Health Organization, the US Food and Drug Administration, and/or China’s National Medical Products Administration. Tests have various characteristics, such as single or multiplex tests, sample types, and collection processes. Diagnostic accuracy, including sensitivity and specificity, were generally above 90% for most RDTs. The time-to-result ranged from 3–90 min, and most provided a result within 30 min. Many people can access STI testing in various clinical and community locations, including homes, churches, and schools.
Conclusion: Many RDTs for STIs have been developed and approved for use in clinical and community-based settings. Optimal RDTs have reduced test time, enable use of a self-collected specimen, lowered the costs of testing, and improved diagnostic accuracy, which may play a pivotal role in reducing STI incidence worldwide.
| Chlamydia | Gonorrhea | Trichomonas | Syphilis | ||
|---|---|---|---|---|---|
| Specimen type | Minimal: Vaginal swab or urine | Minimal: Vaginal swab or urine | Minimal: Vaginal swab | Minimal: Finger prick capillary blood (maximum 50 µL) | |
| Optimal: Urine, vaginal, rectal and pharyngeal swabs | Optimal: Urine, vaginal, rectal and pharyngeal swabs | Optimal: Urine | Optimal: Finger prick capillary blood (maximum 20 µL) and oral fluids | ||
| Specimen collection | Minimal: By a health-care worker | Minimal: By a health care provider | Minimal: By a health worker | Minimal: By a healthcare worker | |
| Optimal: Self-collection by the health service user | Optimal: Self-collection by the health service user | Optimal: Self-collection by health service user | Optimal: Self-collection by the health service user | ||
| Clinical sensitivity | Minimal: >90% (LL > 90%) (genital) | Minimal: 90% (genital) | Minimal: 85% | TPPA: Minimal: >80%; | |
| Optimal: 100% (genital) | Optimal: 98% (genital) | Optimal: 98% | Optimal: >90% | ||
| RPR: Minimal: >95% of high titer (>1 in 8) specimens | |||||
| Optimal: >99% of high titer (>1 in 8) specimens | |||||
| Clinical specificity | Minimal: 98% (LL > 95%) (genital) | Minimal: 90% (genital) | Minimal: 99% | TPPA: Minimal: >90%; | |
| Optimal: 100% (genital) | Optimal: >98% (genital) | Optimal: 100% | Optimal: >95% | ||
| RPR: Minimal: >90% of high titer (>1 in 8) specimens | |||||
| Optimal: >95% of high titer (>1 in 8) specimens | |||||
| Time to result | Minimal: <=60 min | Minimal: <=60 min | Minimal: <=60 min | Minimal: <=30 min | |
| Optimal: <=15 min | Optimal: <=15 min | Optimal: <=30 min | Optimal: <=15 min | ||
| Target price per test | Minimal: <US $5 | Minimal: <US $5 | Minimal: <US $5 | Minimal: <US $3 | |
| Optimal: <US $1 | Optimal: <US $1 | Optimal: <US $1 | Optimal: <US $1 |
*We were unable to identify a TPP document for a rapid diagnostic test for M. genitalium.
PP06.118 – Impact and Cost-Effectiveness of Regular Self-Digital Anal Rectal Examination on the Epidemic of Syphilis in Men Who Have Sex with Men: A Mathematical Modelling Study
Mr Hao Lai2, Prof Christopher Fairley1, Prof Mingwang Shen2, Prof. Lei Zhang1
1Monash University, Carlton, Australia.
2Xi’an Jiaotong University, Xi’an, China.
Introduction: Regular self-digital anal rectal examination (self-DARE) may reduce the incidence of syphilis among men who have sex with men (MSM) by detecting asymptomatic anorectal syphilis. This study aimed to evaluate the epidemic impact and cost-effectiveness of self-DARE among Australian MSM.
Methods: We developed an integrated transmission-dynamic health-economic model of syphilis to simulate the intervention for 10 years based on different scenarios including combinations of coverage (10%–100%), frequency (every 7, 30, and 90 days), sensitivity (10%–100%), and specificity (10%–100%) of self-DARE. We conducted a cost-effective analysis from a healthcare system’s perspective with a 3% annual discount rate. We calculated the outcomes including the cumulative diagnoses, incident cases, and incremental cost-effectiveness ratio (ICER).
Results: The moderate use of self-DARE (conducted by 50% of MSM every 30 days with a sensitivity and specificity of 50%) could reduce cumulative syphilis diagnoses over 10 years from 45,697 (95% confidence interval (CI): 41,352–50,042) in the base case to 20,346 (95% CI: 18,120–22,572). The corresponding ICER is AUD $868 (95% CI: 714–1,022) per quality-adjusted life year gained, and the cost to avert one incident infection is AUD $328 (95% CI: 279–377). Various scenarios could reduce cumulative diagnoses by 2,909–45,184 cases. In all self-DARE scenarios, the ICER is below the willing-to-pay threshold of AUD $50,000, and in 51.7% of scenarios, the cost to avert one incident infection is less than the cost to treat one early syphilis case. Self-DARE’s impact could be enhanced by higher coverage, frequency, and sensitivity, while its cost-effectiveness benefits from higher sensitivity in high-frequency and coverage scenarios, and from higher specificity in low-frequency and coverage scenarios.
Conclusions: Self-DARE would be effective and cost-effective for reducing syphilis cases among Australian MSM. Further empirical research should validate the real-world effectiveness and feasibility of this intervention.
PP06.119 – Accelerating HIV Care Through Lean Management: A Systems Strengthening Approach at Ibulanku Community Health Centre IV
Mr. Paul Kasu1, Dr. Peter Mikago
1Uganda Protestant Medical Bureau, Iganga Town, Uganda.
2Accelerating HIV Care through Lean Management: A Systems Strengthening Approach at Ibulanku Community Health Centre IV
Background: Despite advancements in HIV care, many ART clinics in Uganda still face challenges such as long waiting times, poor resource utilization, and high patient dropout rates. Ibulanku Community Health Centre IV was experiencing these issues, which hindered its ability to provide effective care. In January 2024, the facility implemented Lean management principles, particularly a Kanban system, to streamline workflows, reduce inefficiencies, and support the goal of ending AIDS by 2030.
Objective: The goal of this project was to evaluate the use of a Kanban board as an innovative approach to improve HIV care, reduce waiting times, optimize resource use, and enhance patient retention.
Project Description: Over 6 months, the Kanban board was used to manage patient appointments and services. Patients’ statuses were updated from “Pending” to “In Progress” as they received care, and finally to “Completed” once all services were finished. This process improved patient flow, minimized delays, and enhanced overall satisfaction.
Results:
The implementation of the Kanban system yielded significant improvements:
-
Wait times decreased from 2 h to 45 min
-
Dropout rates dropped from 20% to 0%
-
Patients on treatment increased from 178 to 212
-
Viral load suppression improved from 68% to 97%
-
Viral load testing within 12 months improved from 78% to 98%
-
Additionally, the system helped reduce drug expiries and stock-outs by improving procurement planning.
Recommendations: The Kanban system proved to be a cost-effective and innovative tool for strengthening health systems. It improved both immediate care delivery and long-term operational efficiency. Further research is needed to assess the scalability of this approach in other healthcare settings.
| Week 44 | From 28 Oct 2024 | To 3 Nov 2024 | Date of review 4 Nov 2024 | |
| Service required | Pending (Patient IDs) | In progress (patient IDs) | Completed (patient IDs) | |
| MMD | 423, 508, 208, 650 | 433 | 206, 315, 277 | |
| Viral load bleeding | 433, 508, 208 | 104 | 206, 315, 277 | |
| IAC initiation | 433, 508, 208 | 107, 287 | 167 | |
| CD4 testing | 433, 508, 208 | 107, 287 | 167 | |
| OVE screening | 433, 508, 208 | 880, 233 | ||
| Cervical cancer screening | 433, 508, 208 and 660 | 421, 377, 289, 14, 415 and 208 |
PP06.12 – Facilitators and Barriers to the Rollout of Doxycycline Post-Exposure Prophylaxis for Sexually Transmitted Infections in a Boston Community Health Center
Dr. Lao-Tzu Allan-Blitz1,2, Dr. Michael Traeger2, Dr. Sy Gitin2, Kevin Smith2, Prof Kenneth Mayer1,2, Dr. Taimur Khan2
1Harvard Medical School, Boston, United States.
2The Fenway Institute, Boston, USA.
Background: Doxycycline post-exposure prophylaxis (doxyPEP) has emerged as a promising strategy to prevent bacterial sexually transmitted infections. Real-world implementation is ongoing, yet limited data exist evaluating patient and provider experiences since doxyPEP has become widely available. We aimed to explore such factors among providers and patients during real-world implementation within one community health center.
Methods: DoxyPEP was rolled out on February 2, 2023. To support rollout, we developed electronic health record tools, implemented three provider training sessions, and held a community town hall. We surveyed all providers who participated in doxyPEP trainings. We retrospectively identified patients with evidence of a doxyPEP discussion during a clinic encounter (both those prescribed and not prescribed doxyPEP) and invited them to participate in the survey. Survey items were based on recurring questions, concerns, and comments raised during provider training sessions, as well as insights gathered from the earlier town hall.
Results: Between rollout and September 3, 2024, there were 3,770 doxyPEP prescriptions. We surveyed 45 providers and 150 patients. After the third training session, the median score of comfort having conversations about doxyPEP was 100 (IQR 88–100) out of 100 – increased from a median score was 78 (IQR 52–100) after the second training. Of 150 patient responses, 90 (60.0%) were from individuals prescribed doxyPEP; reasons for use included sex with a random partner (65.6%) and condomless anal intercourse (63.3%). Among 60 not prescribed doxyPEP, 25 (41.7%) reported they did not feel it was warranted due to low perceived risk, while 11 (18.3%) reported they felt their concerns outweighed the benefits.
Conclusion: Without national guidelines, the uptake of doxyPEP was robust, supported by electronic support tools for clinicians, a series of provider training sessions, and community engagement efforts. Differences in risk perception were important factors in the choice to use doxyPEP.
PP06.13 – Knowing Your HIV Status: Integrated HIV and Sexually Transmitted Infections, Mozambique 2023–2024
Mrs Guita Amane1, Mrs Isabel Sathane1, Mr Irenio Gaspar1, Mr Emilton Cumbana1, Mrs Aleny Couto2
1National STI, HIV and AIDS Control Program, Ministry of Health of Mozambique, Maputo, Mozambique.
2Public Health Directorate, Ministry of Health of Mozambique, Maputo, Mozambique.
Background: Achieve 95 95 95 global goals in Mozambique still a challenge. 71.6% of people living with HIV know their status. To identify cases with HIV, aligning with WHO guidelines, Mozambique adopts the strategy of testing all clients with Sexually Transmitted Infections STI, who are in high risk of HIV infection to control HIV epidemic.
Description: Mozambique implement STI screening in all HTS services, to facilitate the access for HIV diagnosis and the identification of PLHIV. In August 2022 the MoH updated STI data tools to enable collection of HIV status at all public facilities in Mozambique (n = 1,634). Providers were trained to screen, test and report the HIV status among all STI clients. Routine data was extracted from the information database system which has the aggregated data from clinical level.
Finding: We analyzed routine data from 24 months (January 2023 to December 2024). A total of 920,561 new STI cases were diagnosed compared to 1,042,518 in 2024, an increased aware of their HIV status was observed, 84% in 2023 compared with 92% in 2024 of all were aware of their HIV status at the time of leaving the consultation. Among those with aware HIV status 200,652 were HIV positive (83,638 in 2023 and 117,014 in 2024). Data demonstrated 11% of HIV positive rate in 2023 compared to 13% in 2024 among new STI cases reported during this period.
Conclusions: Mozambique is one of the highest HIV prevalence countries (12,5%). Data shows that clients with STI are at high risk of having or acquiring HIV and confirms the feasibility of capturing HIV data into STI service. Additionally, integration of services can improve access to rapid identification of PLHIV and ensure linkage to care and treatment and prevention services. However, data showing feasibility HIV testing rates among STIs remain suboptimal.
PP06.14 – Giving Consent for Test, Ensure the Acceptance of HIV Testing Results, Mozambique 2024
Mrs Guita Amane1, Mrs Isabel Sathane1, Mrs Edna Paunde1, Mrs Aleny Couto2
1National STI, HIV and AIDS Control Program, Ministry of Health of Mozambique.
2Public Health Directorate, Ministry of Health of Mozambique.
Background: To understand the current situation and evaluate the different types of stigma and discrimination against PLHIV, in partnership with MOH, a survey was carried out. Also to observed the consent for HIV testing. According to a Mozambican law, the clients should not be tested for HIV without giving consent. This procedure is crucial to ensure the acceptance of an HIV result and reduce stigma and discrimination based in integration of human rights issues.
Description: Mozambique conducted an evaluation of Stigma and Discrimination in STI and ART services. Was identified an indicator to verify the compliance of HIV testing protocols, related to obtaining consent before testing. Respondents (N = 1896) were asked about the existence of a law which does not allow testing for HIV without consent of clients. Questionnaires were adapted for use in the study, considering ethical standards. Participants were informed about the confidentiality of the data collected.
Findings: Asked about obtain consent for HIV testing, the majority of health providers (77%), responding that they know and proceed according to the law during HIV testing. However, 16% of health providers disagree and respond that it is not necessary to ask clients for consent before HIV test.
Conclusions: Data shows that although the majority of health providers observe the client’s right’s to consent before HIV test, there are a few number of providers who do not observe the importance of test consent. Health providers must be trained to proceed according of the legislation and country guidelines. In Mozambique only 71.6% of people living with HIV know their status. Giving consent for testing is crucial for acceptance of the result and to facilitate the access to HIV care and treatment, preventions services and to reduce stigma and discrimination against PLHIV.
PP06.15 – One Size Doesn’T Fit All: A Canadian Approach to Increase HIV Testing by Meeting People Where They Are
Ms. Reena Anthonyraj1, Ms. Kristin MacLennan1, Mr. Anderson Webber1, Dr. Jason Lo Hog Tian1, Dr. Wale Ajiboye1, Ms. Wangari Tharao2, Ms. Maureen Owino3, Dr. David Este4, Ms. Margaret Kisikaw Pieysis5, Mr. Albert McLeod5,6, Mr. Jody Jolimore7, Dr. Nathan Lachowsky8,9, Dr. Sean B. Rourke1,10
1Reach Nexus, Map Centre For Urban Health Solutions, St. Michael’s Hospital, Unity Health Toronto, Toronto, Canada.
2Women’s Health in Women’s Hands Community Health Centre, Toronto, Canada.
3York University, Toronto, Canada.
4University of Calgary, Calgary, Canada.
5Communities, Alliances & Networks (CAAN), Fort Qu’Appelle, Canada.
62Spirit Consultants of Manitoba, Winnipeg, Canada.
7Canadian AIDS Treatment Information Exchange (CATIE), Toronto, Canada.
8University of Victoria, Victoria, Canada.
9Community-based Research Centre (CBRC), Vancouver, Canada.
10University of Toronto, Toronto, Canada.
Background: HIV self-testing (HIVST) improves testing and reduces stigma, particularly in underserved populations. While various countries have implemented self-testing, the first HIVST was approved in Canada in November 2020. Recognizing that “one size doesn’t fit all”, we implemented a multi-pronged low-barrier approach to promote HIVST uptake through two discrete access options for Canada’s diverse populations.
Description: The I’m Ready program launched in June 2021 uses a mobile app for participants to order HIVST kits for home delivery or local pick-up from participating locations. The Community Link program involves community-based distribution of HIVST kits through 400 frontline and community agencies (AIDS Service Organizations, health centers, pharmacies and public health clinics) during 1:1 client interaction or community events. Both strategies allowed participants to access 3–5 kits for multiple use or distribution to secondary testers.
Findings: From program launch, until December 2024, both programs distributed 130,000+ kits to 50,000+ Canadians. 33% of I’m Ready users and 44% of Community Link participants were first-time testers. Both programs reached rural populations (14%–16%) with limited facility-based testing, and people who identified as heterosexual (41%–60%), non-binary or transgender (4%–5%), and sexual minorities (12%–16%). While racialized and underserved groups accessed kits through both programs, I’m Ready engaged more gay, bisexual and men who have sex with men (44%) compared to Community Link, and community-based distribution was more effective in reaching Black (26%) and Indigenous (15%) populations, and people who use and inject drugs (12%) compared to mobile app-based distribution.
Conclusion: A multi-pronged low-barrier approach using technology and community partnerships are effective evidence-based strategies for increasing HIV self-testing uptake among those who are undiagnosed, in underserved areas, and from key populations. By giving people options to know their status and get tested, this adaptable model offers pathways for scaling testing access for other STBBIs, supporting “Sexual Health for All”.
PP06.16 – Inclusive Conversations, Confident Care: Transforming Sexual Health Training with Clinical Simulations
Ms. Chidimma Anunobi1, Mr. Nicholas Kummer1, Mrs. Erica Mann1, Dr. Olivia Van Gerwen2, Dr. Nicholas Van Wagoner2
1UAB Heersink School of Medicine, Birmingham, United States.
2Division of Infectious Diseases, University of Alabama at Birmingham, Birmingham, United States.
Background: Sexual health is a vital yet often overlooked aspect of patient care. Despite rising sexually transmitted infection (STI) rates, less than 25% of physician encounters include a documented sexual history, and topics like sexual behavior, gender identity, and sexuality are rarely addressed in medical training. Addressing these gaps is critical to equipping clinicians with the skills and confidence needed to provide inclusive, effective sexual health care. This project aimed to enhance clinician competency and understanding of sexual health through immersive, simulation-based training.
Description: We developed immersive training sessions to build clinicians’ confidence and skills in discussing sex and gender health with patients. The sessions began with a pre-test questionnaire assessing baseline knowledge and comfort in areas such as using inclusive language, taking a gender and sexual history, and addressing sexual health goals. Participants engaged in six simulations covering diverse clinical scenarios involving sex, sexuality, and gender identity. The session concluded with a debrief and post-training survey to assess progress.
Findings: Participants rated the importance of sexual health at an average of 8.7/10, with most feeling confident discussing related topics. However, only half regularly conducted sexual histories, and they reported challenges including using inclusive language, addressing sexual satisfaction, navigating transgender-specific topics, and compassionately delivering STI diagnoses. Knowledge gaps emerged in key areas like DoxyPEP, PrEP, sexual subcultures, and nuanced aspects of sexuality.
Conclusion: While clinicians feel generally comfortable discussing sexual health, significant knowledge and skill gaps persist. The training sessions provided valuable opportunities to practice navigating sensitive conversations and to build confidence in areas often perceived as “challenging” or “uncomfortable.” Continued education should emphasize HIV prophylaxis, inclusive transgender care, and complex aspects of sexual health. Going forward, simulation-based training is a powerful tool that can be used to integrate sexual health education into medical training at all levels.
PP06.17 – Nurse-Led Implementation of Doxycycline Post Exposure Prophylaxis (Doxy-PEP) at a Community Health Centre in Victoria, British Columbia (BC), Canada
Prof. Marion Selfridge1,2, Ms. Tamara Barnett1,3, Ms Katie Besko1, Ms Anne Drost1, Ms Denise Geib1, Ms Kellie Guarasci1, Ms Karen Lundgren1, Ms Hannah Roy1,4, Dr. Chris Fraser1,5
1Cool Aid Community Health Centre, Victoria, Canada.
2University of Victoria, Victoria, Canada.
3York University, Toronto, Canada.
4University of Alberta, Edmonton, Canada.
5University of British Columbia, Vancouver, Canada.
Background: Infection rates for bacterial sexually transmitted infections (STBBIs) like syphilis, chlamydia and gonorrhea are increasing, and gay, bisexual, and other men who have sex with men (gbMSM) and transgender women are disproportionately affected in British Columbia (BC). Recent studies have demonstrated efficacy of doxycycline post exposure prophylaxis (doxy-PEP) for STBBI prevention in this population.
The Cool Aid Community Health Centre (CACHC), an inner-city, interdisciplinary primary health centre in Victoria, BC, serves over 7,000 clients. Its weekly drop-in nurse-led STBBI clinic, Prism Wellness, offers education, screening, treatment, and pre-exposure prophylaxis (PrEP) services, staffed by STI certified nurses in partnership with AVI Health and Community Services.
Description: In December 2022, CACHC introduced doxy-PEP for eligible individuals: people living with HIV, PrEP users, gbMSM, transgender women, and those at high risk of bacterial STIs. Eligibility criteria include a history of syphilis, chlamydia, or gonorrhea in the past year, or clinical assessment of increased risk. Since December 2023, the BC Centre for Excellence in HIV has publicly funded doxy-PEP.
A retrospective chart review was conducted to identify clients accessing doxy-PEP through CACHC. All gbMSM and transgender clients who initiated doxy-PEP from December 27, 2022, to December 1, 2024, were included.
Findings: A total of 153 clients accessed doxy-PEP: 147 gbMSM, 1 woman, 3 transwomen, 2 non-binary, 14 living with HIV, 136 on PrEP, 38 previous syphilis, 22 rectal chlamydia/gonorrhea (within the last year). Clients were provided with 200mg of doxy-PEP to take within 72 h (10–200 doses) and 77 clients refilled prescriptions. To date, 21 clients have documented STBBI’s (1 syphilis, 3 rectal chlamydia, 1 throat chlamydia, 1 urine chlamydia, 9 rectal gonorrhea, 18 throat gonorrhea) since receiving doxy-PEP.
Conclusions: This innovative nurse-led program at a community health centre facilitated access to doxy-PEP for people at high risk of contracting STBBIs.
PP06.18 – Neisseria Gonorrhoeae Bacterial Load: A Standardization for Lyophilized Panels Production for the External Quality Assessment Program in Brazil
Miss Larissa Victória Backes da Cunha1, PhD Jéssica Motta Martins2, PhD Renata Cristina Messores Rudolf1, MSc Fernando Hartmann Barazzetti1, Miss Adriane Wendling Leismann1, Miss Julia Kinetz Wachter1, Mr. Rafael Emmanuel Godoy Martinez1, Mrs. Ana Duarte Cardoso2, Mrs. Cristina Duarte Cardoso da Silva2, PhD Marcos André Schörner1, Prof. Maria Luiza Bazzo1
1Laboratório de Biologia Molecular, Microbiologia e Sorologia (LBMMS) -Federal University of Santa Catarina, Florianópolis, Brazil.
2Central Public Health Laboratory of Santa Catarina, Florianópolis, Brazil.
Background: External quality assessment (EQA) programs prepare panels for testing in several methods with different sensitivities and detection ranges. High bacterial load could be misinterpreted as negative in equipment that does not have “high load” information.
Methods: Neisseria gonorrhoeae (NG) ATCC 49226 strain was cultured in Thayer Martin medium. With the isolates, 12 aliquots were produced for each dilution (10−3 to 10−10) from a 0.5 McF bacterial suspension, totaling 96 cryotubes. Of these, 48 were used for direct analysis by qPCR (Seenege®/Bio-Rad CFX96™, Cepheid® GeneXpert®, and Roche® Cobas® 5800), and 48 were lyophilized. To evaluate potential bacterial load loss during the lyophilization process. These 48 lyophilized aliquots were tested by qPCR on the same three platforms. The risk of cross-contamination was assessed in the two stages of the EQA panel production: the preparation of bacterial dilutions and the lyophilization process, using bench and lyophilization negative controls.
Results: NG was detected in dilutions ranging from 10−3 to 10−7 in both lyophilized and non-lyophilized samples using the Seegene®/CFX96™ and GeneXpert®, while the range for the Cobas® 5800 was 10−3 to 10−8 due to its lower detection limit. Dilutions of 10−9 and 10−10 consistently showed “not detected” results. The three qPCR methodologies also indicated an increase in Cycle Threshold (Ct) with increasing dilution level. There was no detection of NG in the negative control samples (bench and lyophilization).
Conclusion: Comparing the detection range of non-lyophilized and lyophilized samples (10−3 to 10−7), it was confirmed that the lyophilization process does not cause bacterial load loss. The ideal range of bacterial dilutions for producing EQA panels with lyophilized samples and low, intermediate, and high Ct values is from 10−3 to 10−7.
PP06.19 – Identifying Critical Opportunities for Care Engagement by Analyzing Patients’ Healthcare Engagement and Pre-Exposure Prophylaxis (PrEP) Utilization Prior to HIV Diagnosis
Ms. Alexa Beacham1, Ms. Lila Starbuck1, Dr. Sarit Golub1, Mr. Bryant Gomez1, Mr. Elí Andrade2, Dr. Debjyoti Datta2, Dr. Robert Beil2, Dr. Viraj Patel2
1Hunter College at The City University of New York, New York, United States.
2Albert Einstein College of Medicine, New York, USA.
Background: Despite the availability and effectiveness of PrEP some patients are diagnosed with HIV. Understanding patients’ care prior to HIV diagnosis is important for creating implementation strategies that keep people from slipping between the cracks of care engagement. We aim to understand individuals’ care engagement surrounding diagnosis at a granular level, focusing on patients who were prescribed PrEP but who were later diagnosed with HIV. Prior literature has focused on large cohort studies, but this in-depth perspective offers us a novel lens through which we can understand patients’ engagement prior to diagnosis and potentially identify critical missed opportunities.
Methods: Data were extracted from electronic medical records (EMR) at a large urban healthcare system in New York City for patients prescribed PrEP between January 2015 and April 2022. We analyzed patients’ individual healthcare visits including HIV testing and PrEP prescription prior to diagnosis to identify critical period(s) and potential opportunities for intervention.
Results: Of the 2033 patients, 32 (1.6%) were diagnosed with HIV during the study period. Of patients who seroconverted, 22% had their last negative HIV test within 3 months of their HIV diagnosis, and 31% had their last negative test 3–6 months before their diagnosis. Many patients had an active PrEP prescription at the time of their diagnosis (28%) and 19% had a PrEP prescription that ended within 3 months of diagnosis. We identified important missed opportunities for PrEP continuation: 30% of diagnosed patients had a sexual healthcare visit after their PrEP prescription ended, and 39% of patients had another healthcare visit after their PrEP prescription ended.
Conclusion: These data allow us to identify opportunities for care engagement. Orienting care engagement around missed opportunities where patients may be reached before diagnosis may be an effective method of reducing HIV diagnoses and ending the HIV epidemic.
HIV tests and PrEP prescriptions prior to HIV diagnosis (N = 32). Each circle represents an HIV test. Each X indicates the beginning of a PrEP prescription, and each square represents the end of a PrEP prescription, lines connecting the two indicate active PrEP prescription.
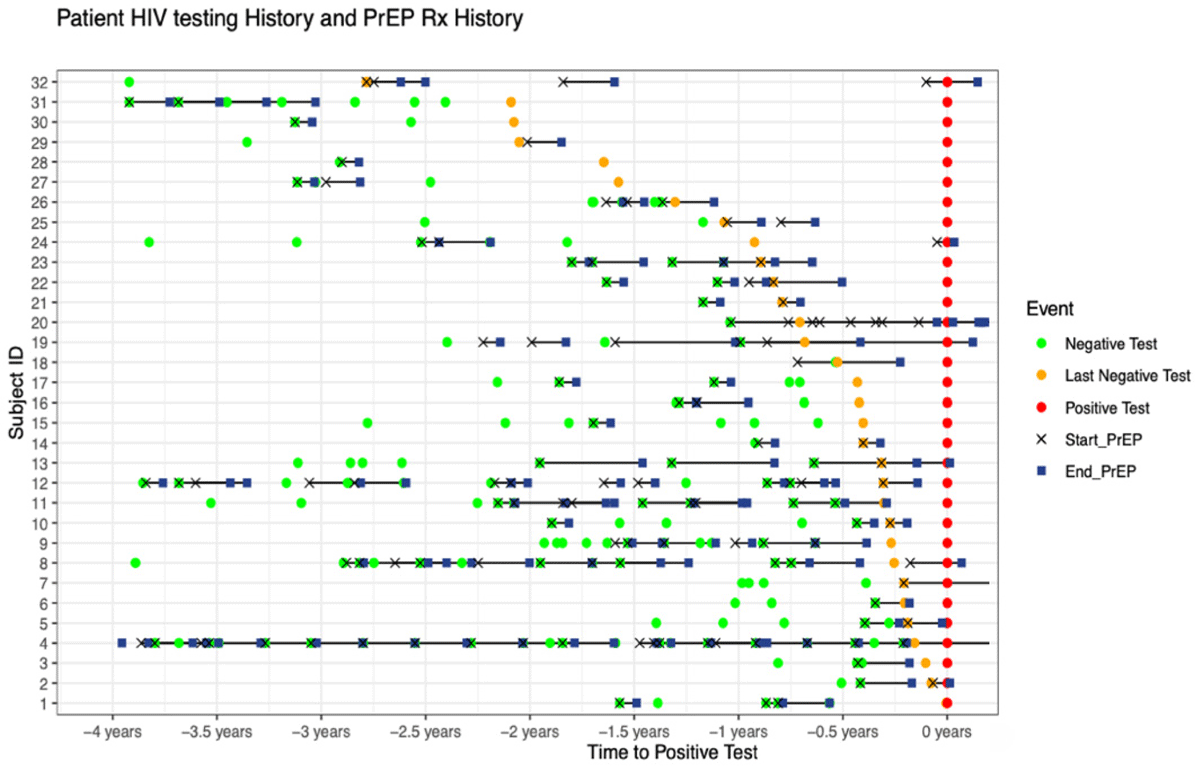
PP06.20 – The Impact of Arv Treatment Duration (≥12 Months) on Viral Effectiveness Among Women Living with HIV in 2023 in Guinea
Mr. Balla Beavogui1, Madame Aissata Camara1, Sir Mamadou Aliou Diallo1
1Programme National de lutte contre le Sida et les Hépatites, Conakry, Guinée.
Context: ARV treatments are crucial for controlling viral load (VL) in people living with HIV, reducing transmission and facilitating disease management. In Guinea, this study aims to evaluate the impact of ARV treatment of 12 months or longer on viral suppression. It seeks to determine the proportion of PLHIV achieving an undetectable viral load and to analyse possible differences between men and women, making it possible to optimise the effectiveness of treatments and to better adapt therapeutic strategies.
Method: The study is based on a quantitative analysis of viral loads measured in PLHIV who have undergone ARV treatment (≥ 12 months). The data are divided into detectable and undetectable viral loads, differentiated by sex.
Results: Among the 33,779 people living with HIV who achieved viral load by December 31, 2023 after 12 months or more of their follow-up, 30,323 suppressed their viral load (89.77%) and (2880) did not suppress it, (8.53%). Of the total viral load performed, 576 were invalid 1.71%.
The majority of people living with HIV who suppressed their viral load were women (21,798) or 71.89% compared to (8525) men (28.11%).
Conclusion: This study shows that a majority of PLHIV on ARV treatment for at least 12 months achieve an undetectable viral load, with an overall undetectability rate of 89.77%. This is a testament to the effectiveness of ARV treatments in Guinea. Undetectability rates are slightly higher among women (71.89%) compared to men (28.11%). This difference could be related to social, behavioral or biological factors, and would merit further research for a better understanding and adaptation of treatment strategies.
Keywords: PLHIV; ARV; Viral Load (VL).
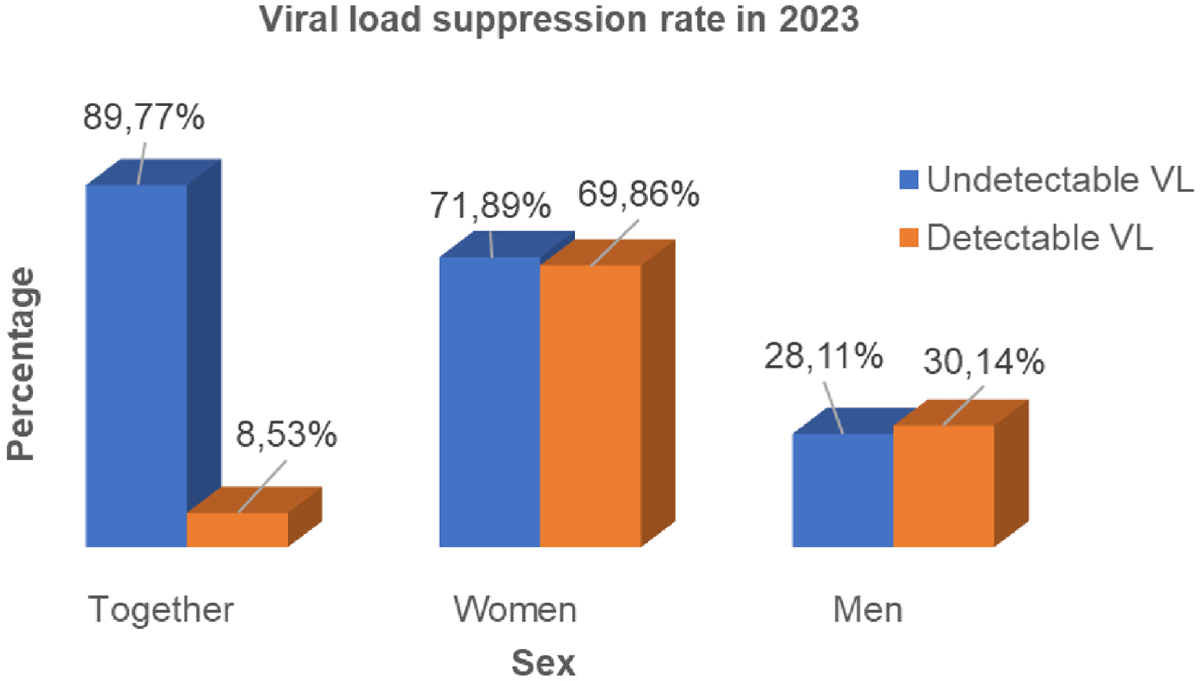
PP06.21 – Increasing Prevention Access: Oral HIV Pre-Exposure Prophylaxis (PrEP) and Doxycycline for Bacterial STI Prevention (doxy-PEP) Delivered Remotely in U.S. TelePrEP Program Sees Exponential Growth in First 16 Months
Dr. Jennifer Belfry1, Dr. Christopher Hall2, Dr. Daniel Stec1, Mr. Anthony Interrante1
1Q Care Plus, Atlanta, United States.
2Avita Care Solutions, Plano, United States.
Background: In the U.S., patient access to HIV pre-exposure prophylaxis (PrEP) and sexual health care demonstrates disparities across geography and demographic indices. Since 2020, telehealth delivery of sexual health care has increased and offers a new tool to overcome access barriers. Q Care Plus, a nationally scaled digital health practice, offers comprehensive sexual health care in 36 states and Washington D.C. Through its HIV PrEP program, Q Care Plus maximizes patient convenience and privacy, offering remote visits, at-home STI testing, and home delivery of medication. Telehealth sexual health care models facilitate rapid deployment of new STI prevention methods to populations at risk for STIs, such as doxy-PEP (STI-PEP) for bacterial STI prevention. In August of 2023, Q Care Plus successfully introduced doxy-PEP services in conjunction with HIV PrEP for patients identifying as gay and bisexual cisgender men and transgender women.
Description/Methods: Data were collected via electronic medical records of PrEP encounters from August 1, 2023, to December 31, 2024, in 36 states and Washington D.C. Data were de-identified and aggregated. Data analysis was completed using standard statistical methods.
Findings: The Q Care Plus PrEP + Doxy-PEP program experienced exponential uptake, reaching 13,596 new doxy-PEP users by December 31, 2024. More patients started doxy-PEP at initial PrEP visits than at quarterly PrEP renewal visits, suggesting that patients new to Q Care Plus PrEP services were seeking access to doxy-PEP. Several barriers to doxy-PEP were reported by patients, including no prior knowledge of doxy-PEP, challenges finding a provider who would prescribe it, and barriers to getting enough medication refilled for use.
Conclusions: Patients experiencing barriers to STI prevention, specifically doxy-PEP, gained access to sexual health care via telehealth. Doxy-PEP, which decreased STI incidence in Q Care Plus PrEP users, was shown to correlate with improved HIV PrEP uptake and retention rates.
PP06.22 – Comprehensive STI Clinics Improve Access to Etiologic STI Diagnosis and Identification of Undiagnosed HIV Infection
Dr. Adele Benzaken1, Jan van den Hombergh1, Fernanda Fonseca1, Wilfred Odoke1, Dr. Vivian Avelino-Silva1
1AIDS Healthcare Foundation, Los Angeles, United States.
Background: Widely adopted syndromic treatment of sexually transmitted infections (STIs) fails to identify asymptomatic and antibiotic-resistant cases. Expanding specialized care services with etiologic diagnostic capacity is key to control STI dissemination, providing additional opportunities to identify undiagnosed HIV infections.
Description: Three decades ago, pivotal studies showed that syndromic STI management could improve care indicators and reduce HIV transmission. However, the relevance of providing etiologic diagnosis for STIs cannot be disregarded. Laboratory tests allow the identification of asymptomatic STI cases, antibiotic-resistant infections, and a more assertive case/partner management.
Together with the increasing accuracy/accessibility of STI diagnostic assays, epidemiologic trends with increase in syphilis and antibiotic-resistant microorganisms suggest that it is time to globally implement/expand specialized STI clinics with etiologic diagnostic capacity.
Currently, AIDS Healthcare Foundation (AHF) Global Program supports 36 STI specialized STI clinics (Wellness Centers) providing free-off-charge care in 22 countries. Here, we describe the expansion of AHF Wellness Centers in 2024, including indicators of improved access to etiologic STI diagnosis and detection of undiagnosed HIV cases.
Findings: The implementation of new STI Wellness Centers was based on a feasibility and local needs assessment, considering regional epidemiology; existing services/infrastructure; prior partnerships with local governments and community organizations; and operational aspects. In 2024, AHF opened 20 new Wellness Centers in 16 countries in Africa, Asia, and Latin America and The Caribbean.
Between Jan–October/2024, AHF Wellness Centers performed 71,181 visits, 31,038 syphilis tests, and 42,126 HIV tests, with positivity rates of 17.8% and 4.4% respectively. The availability of etiologic diagnostic resources is expected to increase in 2025–2026 (Fig. 1).
Conclusion: Expanding the availability of specialized clinics with etiologic diagnostic capacity is a key public health strategy to respond to the growing STI epidemic, including identification of HIV infections that would otherwise remain undiagnosed.
PP06.23 – Mitigating the Concerning Trends of Sexually Transmitted Infections in the U.S. – the Role of Sexual Health Wellness Centers
Dr. Vivian Avelino-Silva1, Alexander Goncalvez1, Whitney Engeran1, Laura Boudreau1, Michael Weinstein1, Dr. Adele Benzaken1
1AIDS Healthcare Foundation, Los Angeles, United States.
Background: Sexually transmitted infections (STIs) are a long-standing public health issue with increasing incidence even though most STIs can be effectively treated or even cured with simple, inexpensive medications. Barriers for STI diagnosis and care include low availability of free-of-charge and walk-in services; shifts in STI models of care from specialized clinics to primary care units; cutbacks in STI services during the COVID-19 pandemic; administrative hurdles in insurance-covered services; inability to extend investigation and treatment for uninsured sexual partners; limited working hours in health facilities; and stigma in healthcare.
Description: Here, we discuss the approach adopted by AIDS Healthcare Foundation (AHF) to mitigate STI trends, focusing on the innovative strategies implemented by AHF’s Wellness Centers.
Findings:
AHF’s has implemented 35 Wellness Centers across 13 U.S. States, with free and confidential services designed to reduce the barriers for STI care using the following approaches:
-
Convenience and efficiency: No appointment needed; accessible venues; operations in post-commercial hours and weekends; digital health resources; waiting time minimized by the specific menu of care; quick turnaround time for diagnostic resources.
-
Sex-positive culture: Healthcare teams include peer professionals, facilitating kinship with service users. AHF’s sex-positive culture acknowledges behaviors and practices as part of one’s values and identity.
-
Volume capacity: Between January–May/2024, AHF’s Wellness Centers in the U.S. provided services to 68,449 persons. Considering HIV, syphilis, Chlamydia and gonorrhea combined, 10% of all STIs notified across 11 U.S. health jurisdictions were diagnosed at an AHF facility.
-
Advertising: AHF has continuously invested in advertising, promoting STI awareness, informing of the availability of testing and care services, and combating stigma (Fig. 1).
Conclusion: AHF’s Wellness Centers have employed innovative strategies aiming to remove barriers for STI diagnosis and care. This experience could be adapted and expanded to other settings, helping mitigate the spread and detrimental outcomes of STIs.
PP06.24 – HIV Test Positivity by Sex Strata in Facility-, Outreach-, and Community-Based Testing
Betty Biwot1, Wilfred Odoke1, Jan van den Hombergh1, Fernanda Fonseca1, Dr. Adele Benzaken1, Dr. Vivian Avelino-Silva1
1AIDS Healthcare Foundation Global Program, Los Angeles, United States.
Background: HIV-testing programs frequently monitor the rates of positive results as an indicator of undiagnosed infections in targeted populations. Sex-related patterns of healthcare utilization may influence one’s access to HIV testing and the underlying prevalence of undiagnosed HIV. HIV testing using community-based and outreach strategies could expand testing opportunities beyond health facilities and reduce sex-related access inequity.
Description: We extracted data from the AIDS Healthcare Foundation Global HIV-testing Program to investigate sex-stratified percentages of HIV-reactive results, categorizing the testing setting into healthcare facility (permanent health units); community; and facility outreach (mobile clinics or outreach services).
Findings: We included data from 14,666,028 HIV tests performed in 44 countries between 2020 and 2023. Tests performed in health facility settings yielded between 5.4 and 6.2% positive results among men and between 3.1 and 3.4% positive results among women. In facility outreach settings, positive results varied from 4.0 and 6.2% among men and from 2.1 to 2.9% among women. The percentage of positive results in community-based testing varied from 2.9% to 3.9% among men and from 2.6 to 3.9% among women (Fig. 1).
Conclusion: HIV diagnosis is a crucial component of the HIV care cascade. Expanding testing opportunities could help reduce the contingent of PLWH who remain unaware of their HIV status. Sex-related differences in access to HIV diagnosis suggest that testing in non-traditional settings, including community and facility outreach programs, could help reduce undiagnosed infections with greater impact for males. This hypothesis is supported by the higher percentage of positive HIV test results among males in health facility and its outreach settings as compared with community test settings in this study. The overall impact of expanding diagnostic opportunities into non-traditional testing settings should be examined using additional measures and outcomes, taking local epidemiological data and programmatic characteristics into consideration.
Sex-stratified percentages of positive HIV test results by testing setting between 2020 and 2023 in AIDS Healthcare Foundation-supported facilities.
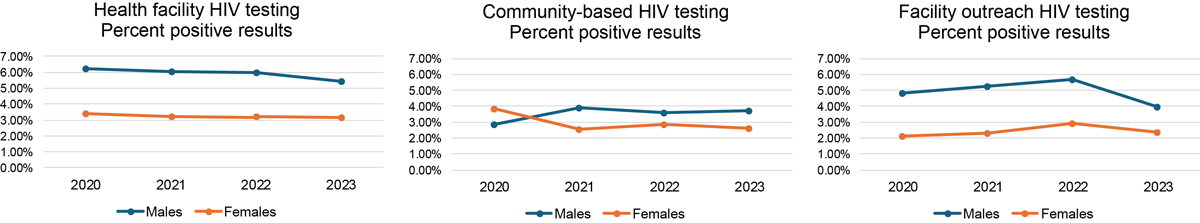
PP06.25 – Brazil’s National Molecular Biology Network: A Leading Example of Automated and Integrated STI Diagnostics
Dr. Amanda Morais1, Dr. Fernanda Conte1, Dr. Ana Claudia Philippus1, Dr. Alisson Bigolin1, Nivea Guedes1, Rogger Diquique1, Dr Draurio Barreira1
1Ministry of Health of Brazil, Brasilia, Brazil.
Background: Access to timely diagnosis and monitoring is crucial for the prevention, control, and treatment of HIV, viral hepatitis B (HBV) and C (HCV), and Chlamydia/Gonococcus (CT/NG). The Brazilian Ministry of Health (MoH) established the National Molecular Biology Network (NMBN) with an integrated platform for these four exams across all federal units, optimizing logistics, reducing costs, and ensuring efficient high-quality care.
Description: Data from the laboratory management platform, encompassing results produced by the 83 laboratories within the NMBN – which conduct integrated exams for HIV, HBV, and HCV viral loads (VL) as well as CT/NG detection – were analyzed for the period from January to November 2024.
Findings: A total of 1,075,679 HIV-VL, 80,582 HBV-VL, 56,624 HCV-VL, and 58,481 CT/NG tests were reported in the information systems. The average result release times were approximately 5.0 days for HIV-VL, 6.5 days for HBV-VL, 6.8 days for HCV-VL, and 7.9 days for CT/NG. Of the total exams performed, only 2% were invalidated due to issues such as result confirmation, equipment problems, electrical failures, or sample quality. In 2024, the MoH conducted one round of theoretical External Quality Assessment (EQA) and two practical rounds, achieving a 100% success rate in the theoretical assessment and an average of 97% approval in the practical evaluations.
Conclusion: The NMBN has proven highly effective in integrating and automating STI diagnostics across Brazil. With a high volume of exams, rapid turnaround times of results, and minimal loss rates of tests. It ensures reliable, equitable access to timely, accurate diagnostics while maintaining high quality, setting a benchmark for public health interventions worldwide.
PP06.26 – Enhancing STI Diagnosis in Brazil: Leveraging a Hybrid Lab/POCT Network for Chlamydia and Gonorrhea Detection
Dr. Alisson Bigolin1, Dr Amanda Alencar Cabral Morais1, Dr. Ana Claudia Philippus1, MSc Mayra Gonçalves Aragón1, Dr. Luiz Fernando Aires Júnior1, Dr. Pamela Cristina Gaspar1, Dr Draurio Barreira1
1Brazilian Ministry of Health, Brasília, Brazil.
Background: In 2023, the Brazilian National Network for HIV, HBV, and HCV testing integrated molecular detection for Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) into its laboratory-based strategy, focusing on high-demand centers. In 2024, a pilot initiative expanded CT/NG detection to the Point-of-Care Testing (POCT) network, improving access in underserved areas and enabling etiological diagnosis of these infections, previously limited to laboratory-based methods.
Description: This study compared the laboratory-based and POCT approaches using data from the National Laboratory Management Platform (January–December 2024), focusing on population profiles, sample types, and positivity rates.
Findings: The laboratory network processed 64,061 tests across 50 laboratories, while the POCT network performed 2,690 tests at six health facilities. The average age of tested individuals was 31 years in the laboratory and 30 years in the POCT. Men represented 67% of those tested in laboratories but only 52% in POCT. Regarding race/ethnicity, 52% of laboratory users were White and 38% Black/Mixed-race, while in POCT, 52% were Black/Mixed-race and 34% White. The POCT network primarily used swabs (vaginal/endocervical: 29%, Oropharyngeal: 29%, and urine: 27%), while the laboratory network predominantly used urine samples (56%). CT positivity was 8% in laboratories and 9% in the POCT, while NG positivity was higher in the POCT (14%) compared to laboratories (7%). In laboratories, NG positivity was highest in urine (4%) and anal swabs (2%), like CT. In POCT, NG positivity was highest in urine and oropharyngeal swabs (5% and 4%, respectively), while CT positivity peaked in urine (3%) and vaginal/endocervical and anal swabs (both 2%).
Conclusion: The laboratory network efficiently supports high-demand screening of asymptomatic individuals, while the POCT network improves access in underserved areas and detects higher NG positivity rates, supporting the etiological approach. This hybrid network strategy expands diagnostic coverage and addresses multiple public health needs.
PP06.27 – Implementing Rapid Molecular Testing of Chlamydia and Gonorrhea in Brazil: Impact on Diagnosis, Treatment, and Sexually Transmitted Infections Management
Dr. Amanda Morais1, Dr. Ana Philippus1, Dr. Mayra Aragón1, Dr. Alisson Bigolin1, Dr. Pâmela Gaspar1, Dr. Draurio Barreira1
1Department of HIV/AIDS, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasilia, Brazil.
Background: Sexually transmitted infections (STIs), especially Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG), are prevalent globally. The syndromic approach is limited, especially in asymptomatic cases, and can contribute to antibiotic resistance. Etiological diagnostics are considered the gold standard for effective treatment.
Description: The Brazilian Ministry of Health launched a pilot strategy to introduce molecular tests for rapid CT/NG detection in seven Testing and Counseling Centers. Urine, oropharyngeal and/or anal samples tested with Xpert® CT/NG. Epidemiological and implementation data were collected via Research Electronic Data Capture (REDCap) system, and test results via National Laboratory Management Platform (NLMP), from January to November/2024.
Findings: A total of 2,415 results were released in NLMP, and 1,948 forms were registered in RedCap. Most individuals (45%/n = 485) were aged 20–29 years. The majority identified as Brown/Pardo (44%/n = 1,059) or White (37%/n = 889). Of the tests, 40% (n = 771) were for asymptomatic individuals with recent STI risk exposure or those using PrEP/PEP. The average time from sample collection to result release was one day, with 79% (n = 1,336) of individuals receiving results during the same appointment. Oropharyngeal (31%/n = 744) and urine (26%/n = 629) samples were most common. Among test results, 8% (n = 195) were detected for CT, 13% (n = 319) for NG, of which 2% (n = 62) were co-infections. Of those indicated for treatment, 8% (n = 37) were treated syndromically, 78% (n = 340) received treatment based on the results (etiological approach), and 14% (n = 61) did not receive treatment due to a lack of licensed professionals to prescribe antibiotics.
Conclusion: The high proportion of individuals treated following detected results highlights the potential of rapid molecular testing in improving treatment outcomes. However, challenges such as limited access to licensed professionals to prescribe antibiotics must be addressed to ensure comprehensive care. The pilot strategy demonstrated the value of rapid molecular diagnostics for improving STI management, reducing transmission, and combating antibiotic resistance.
PP06.28 – Awareness and Intention to Uptake the Human Papillomavirus Vaccine Among Men Who Have Sex with Men Using HIV Pre-Exposure Prophylaxis in Hanoi, Vietnam
Dr. Hao Bui1, Dr. Paul C. Adamson2, Dr. Giang M. Le3
1Center for Training and Research on Substance Abuse - HIV, Hanoi Medical University, Hanoi, Vietnam.
2Division of Infectious Diseases, David Geffen School of Medicine, University of California, Los Angeles, Los Angeles, USA.
3Center for Training and Research on Substance Abuse - HIV; and School for Preventive Medicine and Public Health, Hanoi Medical University, Hanoi, Vietnam.
Background: Men who have sex with men (MSM) in Vietnam face high rates of human papillomavirus (HPV) infections and HPV-related cancers. In 2023, the Gardasil-9 HPV vaccine was approved in Vietnam. This study aimed to describe awareness of and intention to uptake the HPV vaccine among MSM attending an HIV Pre-Exposure Prophylaxis (PrEP) clinic in Hanoi, Vietnam.
Methods: From November 2022 to January 2023, MSM aged 16–26 years participating in the HIV-PrEP program at the Sexual Health Promotion (SHP) clinic, which provides comprehensive HIV prevention services in Hanoi, were recruited. Participants completed an online questionnaire assessing demographics, sexual behavior, and knowledge of HPV and the Gardasil-9 vaccine. Brief information about HPV and Gardasil-9, including its full cost (~$400 USD), was provided, then participants were asked about their intention to uptake the vaccine.
Results: A total of 198 MSM completed the survey (median age: 22 years [IQR: 21–24]; median monthly income: 14 million VND [~$630 USD] [IQR: 9–21]). Most (86.9%) were aware of HPV and its health consequences, while 30.3% had heard of Gardasil-9. Only 1% (n = 2) had been vaccinated. Following the information, 70.9% (139/196) of unvaccinated participants expressed vaccination intent. Of those, 38.1% could afford the full price, and 66.9% could afford half-price. Among those unwilling to vaccinate, key barriers included cost (47.4%), concerns about vaccine safety and efficacy (22.8%), and confidence in avoiding HPV through safe sexual behavior (23.8%).
Conclusions: Awareness and uptake of the HPV vaccine were low among young MSM on HIV-PrEP in Hanoi, though vaccination intent was high. Cost emerged as a significant barrier, with only one-third able to afford the full price. Efforts to reduce costs and improve HPV vaccination outreach are essential to increase uptake among this priority population.
PP06.29 – Self-Reported Anal Cancer Screening Among People Living with HIV in Ontario, Canada, Prior to Release of New Clinical Guidelines
Prof. Ann Burchell1,2, Lucia Light3, Dr. Troy Grennan4, Dr. Gordon Arbess1,2, Dr. Christine Fahim1,2, Prof. Daniel Grace2, Dr. Irving Salit2,6, Dr. Michael Silverman7, Dr. Paul MacPherson5, ACCESS Study Team1
1Unity Health Toronto, Toronto, Canada.
2University of Toronto, Toronto, Canada.
3Ontario HIV Treatment Network, Toronto, Canada.
4BC Centre for Disease Control, Vancouver, Canada.
5Ottawa Hospital, Ottawa, Canada.
6University Health Network, Toronto, Canada.
7St. Joseph’s Hospital London, London, Canada.
Background: In 01/2024, the International Anal Neoplasia Society (IANS) released new guidelines recommending anal precancer screening in high-risk populations, including men who have sex with men (MSM) and transgender women living with HIV starting at age 35, and all others living with HIV starting at age 45 (Stier et al. Int J Cancer 2024). Our aim was to estimate the proportions undergoing anal screening in 2023 as a baseline for future monitoring of guideline implementation in Ontario, Canada.
Methods: We analysed data from the Ontario HIV Treatment Network Cohort Study, a multi-site clinical HIV cohort. During interviews in 2023, respondents were asked whether they had undergone either of two anal screening modalities in the past 12 months: (1) an anal Pap test (for precancer); and (2) a digital anal rectal exam (DARE, for early-stage cancer). We estimated the proportions reporting anal screening and examined their correlates using multiple logistic regression.
Results: Among the 2,238 respondents, 18% were aged 35–44 and 72% were aged 45 and older. Among the 1720 respondents who were assigned male sex at birth, 24 identified as transgender women or genderqueer, and 1692 identified as cisgender men. We observed statistically-significant (P < 0.05) differences in screening by guideline-defined cancer risk category and age (Table 1). Screening also varied by region but was not associated with race, viral load suppression, CD4 cell count, tobacco smoking, or history of AIDS.
Conclusion: Limitations include volunteer participation and self-report. As expected, only a minority reported screening in the period immediately preceding the release of the IANS guidelines. It was more often reported by MSM/transgender women and among older respondents, and least reported by cisgender women and heterosexual men. Ideally, post-guideline implementation will incorporate strategies to facilitate equitable scale-up among all recommended for anal screening.
| MSM and transgender women (n = 1390) | Cisgender women (n = 508) | Heterosexual men (n = 283) | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Pap | DARE | Either | Pap | DARE | Either | Pap | DARE | Either | ||
| Age (years) | ||||||||||
| <35 | 20.1 | 9.8 | 21.0 | 3.4 | 0.0 | 3.4 | 0.0 | 0.0 | 0.0 | |
| 35–44 | 24.3 | 13.6 | 28.5 | 2.3 | 1.5 | 2.3 | 5.1 | 2.6 | 5.3 | |
| 45–54 | 25.5 | 19.2 | 29.9 | 7.1 | 3.2 | 7.1 | 2.8 | 1.4 | 4.2 | |
| 55–64 | 26.0 | 16.8 | 31.1 | 2.5 | 3.3 | 5.0 | 5.1 | 7.1 | 9.2 | |
| 65 and older | 31.8 | 24.7 | 39.2 | 6.7 | 4.4 | 8.9 | 4.1 | 12.8 | 12.8 | |
PP06.30 – Implementation of Pre-Exposure Prophylaxis (PrEP) Within a Housing First Model: A Case Study of Uptake in People Who Use Drugs
Mrs. Morgan Cole1, Ms. Laura Guy1, Mrs. Lisa Cambron1
1Solutions Health, Louisville, United States.
Background: Pre-exposure prophylaxis (PrEP) uptake among people who use drugs (PWUD) remains suboptimal despite its proven efficacy in preventing HIV transmission in this hard-to-reach population. Barriers to PrEP access include housing instability, transportation, disengagement from healthcare, and low awareness of the potential benefits of PrEP for PWUD. This case study describes early findings from a linkage to PrEP intervention at a collocated community health clinic and supportive housing facility in Louisville that serves chronically unhoused PWUD and other populations at high risk for HIV acquisition.
Description: In October 2024, Solutions Health established a new standard of care in which trusted staff support all residents of their collocated supportive housing facility to complete sexual (CDC - The Five P’s + Pleasure) and drug use histories, comprehensive STI testing, including HCV and HBV, and referral to treatment as needed. During this first visit, staff provide patient-tailored education on HIV and share CDC recommendations for PrEP use. The clinic aims to further build patient trust by employing a trauma-informed care approach and shared patient/ provider decision making.
Findings: Over the course of 10 weeks, a total of 7 PWUD and housing insecure patient, 4 male and 3 female – started PrEP.
Conclusion: By collocating our health clinic within a housing first facility, we removed barriers and leveraged the trust they built to effectively engage PWUD. Furthermore, by uniformly implementing CDC STI screening and PrEP guidelines and talking with patients about their risk factors for HIV acquisition, we successfully increased PrEP access and uptake in nontraditional, PWUD and housing insecure populations.
We plan to expand this model by integrating a street nursing component, to provide these services to marginalized populations. Organizations seeking to implement a more inclusive PrEP program may want to consider our approach.
| Patient Demographic Profiles | ||||||
|---|---|---|---|---|---|---|
| Race | Age | Gender | Relevant Medical History | Sexual History | Housing Status | |
| White | 48 | Male (cis gender) | Multiple female partners, condomless sex | Chronic Unhoused | ||
| Hispanic | 27 | Male (cis gender) | Multiple female partners, condomless sex | Chronic Unhoused | ||
| White | 36 | Female (cis gender) | Male Partners, not currently sexually active | housing first facility | ||
| White | 27 | Female (cis gender) | Condomless sex with 1 male partner | Chronic Unhoused | ||
| White | 38 | Female (cis gender) | Multiple male partners | Housing first facility | ||
| Black/African American | 51 | Male (cis gender) | Not currently sexually active | Chronic Unhoused | ||
| Black/African American | 32 | Male (cis gender | Multiple female partners, condomless sex | Chronic Unhoused | ||
PP06.31 – Cascade of Syphilis and Treatment at Ante-Natal Care: Case of Mozambique
Dr. Aleny Couto1, Mr Morais Da Cunha2, Ms Isabel Sathane2, Ms Guita Amane2, Mr Valdo Mega2, Dr Maira Marra2, Dr Namita Eliseu2, Dr Irenio Gaspar2
1Ministry of Health Mozambique, Maputo, Mozambique.
2National STI, HIV and AIDS Control Program, Maputo, Mozambique.
Background: Syphilis is a curable and exclusive Sexually Transmitted Infection (STI) of humans, caused by the bacterium Treponema pallidum. It can present several clinical manifestations and different stages. Syphilis infection can endanger not only the health of the adult but can also be transmitted to the baby during pregnancy. The monitoring of pregnant women and sexual partners during prenatal care prevents congenital syphilis and is essential and protect maternal and child health.
Description: Routine data from 2024 (January to September), were collected by MCH tools, aggregated into the Information System (SIS-MA) at national level. It was possible to report in the number of the women in the cohort that attended ante natal care service (ANC) and out of that how many were tested for syphilis and not tested, positive cases, how many completed the treatment, partners treated
Findings: ANC routine data from January to September 2024 demonstrated 1,585,590 pregnant women attended ante natal care service, and 99.2% were tested for Syphilis. 36,053 tested positive (positivity rate of 2.3 %) and 34.751 completed the treatment (96.4%). In other hand 12,974 pregnant women who attend the health facility were not tested for syphilis, corresponding to 0.8% of eligible women that should have tested. For better antenatal syphilis surveillance partners should be treated, 34,481(95.6%) of them were treated after the diagnose of the pregnant women.
Conclusions: Finding shown feasibility to monitor syphilis cascade, results are aligned with country and WHO policies that contribute to the elimination of vertical transmission of HIV, Hepatitis B and Syphilis. Despite, gaps identified, particularly in ensuring treatment for all eligible pregnant women and their partners. Addressing these gaps should remain a priority to break the transmission chain and improve maternal and child health outcomes, also guide improvement of delivery and monitoring of syphilis screening and treatment in ANC.
PP06.32 – Responding to STI in Adolescents and Young Adults: Trend of STI Cases in the Last 5 Years (2019–2023) in Mozambique
Dr. Aleny Couto1, Ms Isabel Sathane2, Ms Guita Amane2, Mr Valdo Mega2, Dr Mercia Matsinhe2, Dr Irenio Gaspar2, Ms Isabel Menetiane3
1Ministry Of Health Mozambique, Maputo, Mozambique.
2National STI, HIV and AIDS Control Program, Maputo, Mozambique.
3Adolescents and Youth Program, Maputo, Mozambique.
Background: Sexually transmitted infections (STI) at the global level continue to be a public health problem, especially among adolescents and young adults. According to the World Health Organization (WHO), in 2024 more than 1 million curable STIs are acquired every day globally in people 15–49 years, increasing the risk of acquiring HIV. In Mozambique, the STIs scenario is also worrisome, aggregated routine data reports about 4 million STI cases in the last 5 years, of which 41% were in adolescents and young people.
Description: Routine data were analyzed, between 2019 to 2023 using MOH STI data tools that enable collection of adolescent and young people at all public facilities in Mozambique (n = 1,634) disaggregated by age, sex and syndrome. All providers who screen, diagnose, and treat syndromic management of STIs were trained to correctly use STI paper-based forms. Every month those data were aggregated at the clinic level and digitized into a national database.
Finding: STI aggregated routine program data from 2019 to 2023 demonstrated 4,419,054 cases diagnosed and treated, of those 1,812,604 were adolescents and young people (AYP) aged 15 to 24 years (41%). Among AYP more female (58%) was diagnosed with STI compared to men (42%). STI cases have been increasing over the year from 797,431 in 2019 to 895,755 in 2023. Analyzing data by syndrome, most correspond to vaginal discharge (41%) followed by urethral discharge (31%) and genital ulcer (25%).
Conclusions: Cases of STIs among adolescents and young people suggest that they continue to be of concern and non-use of condoms remains a challenge, which could contribute to the increase in new HIV infections. In settings with low STI prevalence among AYP, granular analyses are recommended as routine-based analysis for better prioritization of combined prevention interventions, with emphasis of the correctly and consistently condom use.
PP06.33 – Missed Opportunities for Syphilis Testing Among Pregnant Women in Mozambique 2019–2023
Dr. Aleny Couto1, Mr Morais Da Cunha2, Ms Isabel Sathane2, Ms Guita Amane2, Mr Valdo Mega2, Dr Maira Marra2, Dr Namita Eliseu2, Dr Irenio Gaspar2
1Ministry Of Health Mozambique, Maputo, Mozambique.
2National STI, HIV and AIDS Control Program, Maputo, Mozambique.
Background: Syphilis is a curable and exclusive Sexually Transmitted Infection (STI) of humans and can endanger not only the health of the adult but can also be transmitted to the baby during pregnancy. Untreated syphilis in pregnancy is associated with adverse clinical outcomes for the infant, therefore the monitoring of pregnant women and sexual partners during prenatal care is essential to promote health to mothers and partners and preventing congenital syphilis.
Description: Routine data in the past 5 years (2019–2023), were collected at Ante-Natal Care (ANC) within the Health Facilities and aggregated into the Information System (SIS-MA) at national level. Analyzing the data it was possible to report in the number of the women in the cohort that attended ANC and out of that how many were tested for syphilis, positive and the number of women not tested for syphilis even knowing that were presented at ANC.
Findings: As we can observe a total of 9,213,411 pregnant women were attended in ANC, 7,834,963 of them were tested for syphilis and 1,378,448 were not tested along the 5 years. Of those women who have not been tested for syphilis data disaggregated by year shows different variations, in 2019: 290.340 of 1.680.94 (17.3%); 2020: 354.812 of 1.637.627 (21.7%); 2021: 224.442 of 1.815.219 (12.4%); 2022: 433.089 of 2.059.155 (21%); 2023: 75.765 of 2.020.469 (3.7%).
Conclusion: Syphilis testing in the country has made great progress despite all challenges, however we can observe there are still many women who attend their antenatal appointments but did not have access to a syphilis test, except the year 2023, in this sense policies that improve service quality, availability of supplies, and strengthen the training of health professionals, must be reinforced and putted in place like we did in 2023.
PP06.34 – Technological Innovation in the Subnational Certification Process of Elimination of Vertical Transmission of HIV, Syphilis, and Hepatitis B in Brazil, 2024
Sra. Nádia M S Machado1, Sra. Ana Paula Betaressi da Silva1, Sra. Pâmela Cristina Gaspar1, Sr. Rodrigo Calado da Silva2, Sra. Mayra G Aragón1, Sr. Cristiano Francisco da Silva1, Sra. Márcia Colombo1, Sra. Leila S A Barreto1, Sra. Ariane T B de Matos1, Sr. Vinícius J da Silva Lôbo1, Sr. Draurio Barreira1
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
2ISANTACASA – Instituto Santa Casa de Educação, Pesquisa e Inovação, São Paulo, Brasil.
Background: Brazil is committed to eliminating vertical transmission (VT) of HIV, syphilis, and hepatitis B as a public health problem. Due to this, the country implemented the subnational certification process of VT of HIV, syphilis and hepatitis B elimination, since 2017. However, robust and systematic data collection was still a challenge, especially considering the country’s dimension and the 95 specialists in the process validation team. Thus, this work aims to report a successful experience in implementing a technological tool for data collection, analysis, and management in certification process to maximize its response, and increase the data quality.
Description: In 2024, the Research Electronic Data Capture (REDCap) was employed as a data collection tool during on-site visits to municipalities seeking certification. The developed forms contained semi-structured and unstructured fields under four thematic axes: healthcare; epidemiological surveillance; diagnostic capacity; and human rights. Then, online training was conducted with the specialists, each with individual access and according to their respective axes; only to team coordinators access to all axes was granted. The project was inserted in mobile devices.
Results: Eighty-five municipalities were visited. In all of them it was possible to collect, insert and validate data, offline or online, using REDCap, and to issue a final report with strategic information, main results and recommendations to the territory; and if necessary, it was possible to provide subsequent complementation. Additionally, its use resulted in operational efficiency, mainly due to simultaneous collaboration; and at the national level, real time evaluation of difficulties and information quality while the team was still in the field.
Conclusion: The use of new technological tools and permanent updating in technological approaches, such as REDCap in our scenario, reflected better response strategies and processes in public health as well as data reliability and accuracy, and improvement in health surveillance.
PP06.35 – National Strategic Planning as a Tool for the Elimination of Vertical Transmission of HIV, Syphilis, Hepatitis B, and HTLV in Brazil, 2024
Sra. Nádia M S Machado1, Sra. Ana Paula Betaressi da Silva1, Sra. Pâmela Cristina Gaspar1, Sra. Mayra G Aragón1, Sr. Cristiano Francisco1, Sr. Vinícius J da S Lôbo1, Sra. Márcia Regina Colombo1, Sra. Leila S A Barreto1, Sra. Ariane T B de Matos1, Sra. Isabella M C D de Souza1, Sr. Fabio Moherdaui1, Sr. Draurio Barreira1
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
Background: The elimination of vertical transmission (VT) of sexually transmitted infections (STIs) is a Brazilian government commitment under the 2030 Sustainable Development Goals (SDGs). Thus, in 2024, goals were developed to enhance health actions on this topic. The objective is to present the results of the national strategic planning goals to achieve ETV of HIV, syphilis, hepatitis B and HTLV in Brazil.
Methods: Within the strategic objectives of the Department of HIV/AIDS, Tuberculosis, Viral Hepatitis and STIs, Brazilian Ministry of Health (MoH), the following goals were listed: (a) support the implementation of state committees for investigation of VT in five states; (b) make the notification of pregnant/parturient/puerperal women and children exposed to HTLV mandatory; (c) Incorporation of universal HTLV screening in pregnant women into the national health system; (d) training 500 health professionals in the management of syphilis; (e) implementation of rapid DUO tests (HIV/syphilis) in the prenatal care of pregnant women in the states.
Results: Three of the five proposed goals were fully achieved: (b) publication of the national ordinance Number 3,148/2024 about HTLV; (d) national webinars about syphilis, regional Question & Answer sessions, quick-reference guides, and on-site training for priority state; and (e) technical notes were published, and 4,000,000 DUO tests were procured and distributed. Regarding goal (a) it was partially achieved with the implementation of VT committees in two of five targeted federal units, while goal (c) progressed with approval for universal HTLV screening, currently in the implementation phase.
Conclusion: The expansion of knowledge on syphilis management and innovation in testing HIV/syphilis by DUO rapid tests in prenatal care, the establishment of VT committees, and the institution of mandatory notification of HTLV to understand the national epidemiological scenario demonstrate an integrated and synergistic approach to early intervention and progress towards the national elimination of STIs and TV.
PP06.36 – After Certification, What to Do? Sustainability of Health Actions in Municipalities Certified with Elimination or a Seal of Good Practices Towards the Elimination of Vertical Transmission of HIV, Syphilis, And/Or Hepatitis B in Brazil
Sra. Nádia M S Machado1, Sra. Ana Paula Betaressi da Silva1, Sra. Pâmela Cristina Gaspar1, Sra. Mayra G Aragón1, Sr. Cristiano Francisco da Silva1, Sra. Márcia Regina Colombo1, Sra. Leila SA Barreto1, Sra. Ariane TB de Matos1, Sra. Aparecida P Lima1, Sra. Maria G Oliveira1, Sra. Leonor H Lannoy1, Sr. Luiz F A Júnior1, Sr. Ítalo V A Diniz1, Sr. Esdras D S Pereira1, Sra. Romina S M Oliveira1, Sr. Vinicius J S Lôbo1, Sra. Juliana S Moreno1, Sr. Draurio Barreira1
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
Background: The subnational certification of the elimination of vertical transmission (EVT) of HIV, syphilis, and hepatitis B in Brazil for municipalities with a population >= 100,000 is an adaptation of the World Health Organization and Pan American Health Organization initiatives for country certification. The strategy was adopted by Brazil in 2017 for HIV certification, expanding to syphilis in 2021, and hepatitis B in 2024. Until 2024, the recertification rule was every 2 years for municipalities with populations between 100,000–1,000,000, and every 3 years for those with populations >1,000,000. This study describes the actions undertaken by the Ministry of Health to monitor certified municipalities with elimination and/or good practice seals in Brazil from 2017 to 2024.
Description: The EVT certification process involves on-site visits by specialists, with reports issued and sent to the National Validation Commission, which approves or disapproves the certification. Subsequently, the certification result and the visit report containing suggestions for qualification and sustainability of health and human rights actions are forwarded to municipal managers. The progress of actions and indicators in these municipalities are monitored in partnership with the respective states.
Results: The main recommendations to municipalities are related to improving prenatal care, especially for pregnant women in vulnerable situations; strengthening epidemiological surveillance and diagnosis; integrating health services, access to actions and services, improving community and civil society engagement, and qualification and communication. Between 2017 and 2024, Brazil certified 151 municipalities in 19 States, totaling 258 certifications or recertifications for HIV, syphilis, and/or hepatitis B, with 23 municipalities being recertified during this period.
Conclusion: Continuous monitoring of the qualification of actions and EVT indicators in certified municipalities contributes to promoting good practices and the continuous improvement of health surveillance and care, providing sustainability to the process and driving the achievement of recertification.
 |
Note: A detailed attached table with recommendations is available for consultation.
PP06.37 – HIV Testing Increases Among Minority Young Adults Through an Urban Emergency Department Intervention
Ms. Isioma Nwonye, Ms. Katie Huynh, Dr. Rachel Alinsky, Mr. Erik Peevy, Dr. Mustapha Saheed, Dr. Christopher Hammond, Mrs Gaby Dashler, Dr. Renata Arrington-Sanders, Dr. Marc Fishman, Dr. Mitchell Goldstein, Dr. Richard Rothman, Ms. Marla Oros, Dr. Yu-Hsiang Hsieh
1Johns Hopkins University, Baltimore, United States.
Background: Despite recommendations for annual HIV testing, only 18.9% of adolescents and young adults (AYA) aged 18–24 tested in the past year, and 31.5% ever tested, according to the 2017 CDC national survey. This study evaluates the impact of an ED-integrated HIV/substance use (SU) intervention to increase HIV testing among racial and ethnic minority AYAs.
Methods: This study was conducted in an urban adult ED utilizing an established triage nurse-delivered HIV testing program and a peer-navigated SU screening, brief intervention, and referral-to-treatment (SBIRT) program. In April 2021, a peer-facilitated HIV/SU brief intervention (BI) was introduced to increase awareness and testing among minority AYAs aged 18–24 using motivational interviewing. Participants who declined HIV testing at the triage were offered testing after a peer-facilitated one-on-one BI. Data of HIV testing 1-year post-enrollment were obtained for 270 participants enrolled April 2021 to April 2023. HIV testing rates among demographic-matched AYAs in the same ED from January to February 2021, served as reference. Logistic regression identified factors associated with HIV testing.
Results: 81 of 270 (30.0%) enrollees were tested for HIV at the index ED visit. This was significantly higher than the 63 of 301 (20.9%) of the reference period (proportion difference: 9.1%, 95% CI: 1.9%, 16.2%). Of the 189 participants not tested during enrollment, 51 (27.0%) received testing within one year. Combining index ED and follow-up testing, 132 (48.9%) were tested. Non-male enrollees and those positive for both alcohol and drug use were more likely to have HIV testing (OR = 1.8; OR = 2.3). Of these, 1.2% tested positive, compared to 0% during the reference period.
Conclusion: HIV testing rates at baseline and the following year among our HIV/SU BI participants were significantly higher than their counterparts in the study ED and general population, showing the potential of ED-based peer interventions to improve HIV testing.
PP06.38 – Applying FRAME-IS to Document Modifications to Implementation Strategies for Improving PrEP Use Among Black Women in the United States
Ms. Samantha A. Devlin1, Dr. Jessica P. Ridgway1, Dr. Lisa R. Hirschhorn2, Dr. Maria Pyra2, Dr. Jodi Simon3, Dr. Sadia Haider4, Dr. Kelly Ducheny5, Dr. Eleanor E. Friedman1, Dr. Katherine Chung-Bridges6, Ms. Angela Reese7, Ms. Elizabeth Tumiel8, Dr. Amy K. Johnson2,9
1University of Chicago, Chicago, United States.
2Northwestern University, Chicago, United States.
3AllianceChicago, Chicago, United States.
4Rush University, Chicago, United States.
5Howard Brown Health, Chicago, United States.
6Health Choice Network, Miami, United States.
7FQHC, United States.
8FQHC, United States.
9Ann & Robert H. Lurie Children’s Hospital of Chicago, Chicago, United States.
Background: Implementation strategies are frequently modified to fit the local setting and context; understanding modifications is critical to determine the mechanisms by which implementation strategies affect implementation outcomes. The FRAME-IS (Framework for Reporting Adaptations and Modifications for Implementation Strategies) can be used to collect structured adaptation data. We used FRAME-IS to systematically document adaptations to implementation strategies for improving pre-exposure prophylaxis (PrEP) uptake among Black cisgender women in two federally qualified health centers (FQHCs) in the United States.
Methods: Five interrelated implementation strategies were modified: provider training, electronic medical record (EMR) optimization, clinical champions, patient education, and PrEP navigation. Multiple data sources were used to identify adaptations: notes from implementation meetings, focus groups with providers and patients, and summary reports completed by implementation leads at FQHCs. FQHCs were involved in the decision-making progress regarding adaptations. Text was extracted from the data sources according to the FRAME-IS modules and inputted into a master spreadsheet for content analysis by one author; a second author conducted validation. Discussion of findings ensured agreement and consistency.
Results: Modifications entailed changing the content and context of strategies, as well as personnel who delivered the strategies. Provider training and patient education were modified according to the local context (i.e., FQHC) and the population of focus (i.e., Black women). The majority of adaptations were proactively planned based on findings from the pre-implementation focus groups. However, clinical champions and EMR optimization were reactively modified, such as drifting and returning to the strategy, according to organizational needs. PrEP navigation was the least-modified strategy.
Conclusion: We demonstrate the ability to document our adaptations across FRAME-IS modules, attesting to its applicability for multi-faceted implementation strategies. Tracking iterative and ongoing adaptations will help inform the dissemination of our strategies to implement PrEP across diverse settings for use among Black women in the U.S.
PP06.39 – HIV Prevention and Harm Reduction Service Coverage Gaps Among People Who Inject Drugs in Nigeria: Insights from the 2020 Integrated Biological and Behavioural Surveillance Survey
Mr. Chukwuebuka Ejeckam2, Dr Temitope Ilori1, Mr Francis Agbo1, Dr Rose Aguolu1, Dr Kalada Green3, Dr Chukwuemeka Agi2, Mr Kufre Ndueso2, Mr Adediran Adesina2, Prof Souradet Shaw3, Prof Leigh McClarty3, Prof James Blanchard3
1National Agency for the Control of AIDs, Abuja, Nigeria.
2West Africa Centre for Public Health and Development, Abuja, Nigeria.
3Institute for Global Public Health, University of Manitoba, Winnipeg, Canada.
Background: People Who Inject Drugs (PWID) in Nigeria face criminalization and substantial marginalization, placing them at disproportionate risk for acquiring HIV and other sexually transmitted and blood-borne infections (STBBI). Comprehensive HIV services for PWID, including harm reduction services, are essential to reduce these risks. This study highlights HIV/STBBI prevention program coverage and service gaps for PWID in 12 Nigerian states using data from the 2020 Integrated Biological and Behavioral Surveillance Survey (IBBSS).
Methods: Biobehavioral data were collected from a random sample of 4,414 PWID aged ≥15 years following informed consent. Behavioral data examined self-reported injecting practices, prevention program coverage, and service access, and biological data (whole blood draw and dried blood spot) were collected to estimate HIV prevalence. Reported harm reduction program coverage is examined relative to national needs. Univariate analyses of service access, injecting practices, and HIV prevalence were performed using SPSS and STATA.
Results: Of 4,414 PWID participants, only 12% accessed sterile needles through needle exchange programs, while 58% sourced needles from chemists. About 32% reported sharing needles. HIV prevalence was 10.9%, with state-level variation from 23.4% in Benue to 0.8% in Nasarawa. Only 63% received free condoms in the last 12 months prior to study, and 11% had ever used pre-exposure prophylaxis (PrEP). Stigma, discrimination, and law enforcement threats discouraged service use, with 31% avoiding HIV services due to stigma and 45% reporting harassment by law enforcement.
Conclusion: The findings reveal insufficient harm reduction services for PWID in Nigeria. Expanding needle exchange programs, improving access to PrEP, and addressing stigma through advocacy and community-led initiatives are critical. Additionally, reallocating resources and engaging policymakers can help scale up harm reduction services nationwide to reduce HIV transmission and support PWID health.
PP06.40 – Suboptimal HIV Prevention Outcomes Among Key Populations in Nigeria: Results from 2024 Key Population Programme Review
Mr. Chukwuebuka Ejeckam2, Dr Temitope Ilori1, Mr Francis Agbo1, Dr Fatimah Jajere1, Dr Kalada Green3, Dr Chukwuemeka Agi2, Mr Soladoye Oladayo2, Mr Osayende Ayewah2, Ms Oletta Ogio2, Prof Leigh McClarty3, Prof Souradet Shaw3, Prof James Blanchard3
1National Agency for the Control of AIDS, Abuja, Nigeria.
2West Africa Centre for Public Health and Development, Abuja, Nigeria.
3Institute for Global Public Health, University of Manitoba, Winnipeg, Canada.
Background: Key populations (KP),including female sex workers (FSW),men who have sex with men (MSM),people who inject drugs (PWID), and transgender individuals (TG), represent 2% of Nigeria’s population but account for 91% of new adult HIV infections. Recent national bio-behavioral survey revealed high HIV prevalence among KP, low condom use, and gaps in achieving 95-95-95 targets. In 2024, the National Agency for the Control of AIDS (NACA) conducted a Key Population Programme Review (KPPR) in 18 states to assess HIV prevention and treatment outcomes and identify challenges towards HIV epidemic control in Nigeria.
Methods: A polling booth survey (PBS) component of the KPPR collected HIV prevention outcome data from anonymous, unlinked ballot responses among KP in 13 KPPR states, across six geopolitical zones. Data on HIV testing, condom use, antiretroviral therapy (ART), pre- and post-exposure prophylaxis (PrEP and PEP) were collected from 936 FSW, 936 MSM, 936 PWID, and 780 TG, through 299 PBS sessions. Data analysis was done using SPSS vs 23.
Results: Condom use at last sex was highest among FSW (84%), followed by PWID (69%), MSM (57%), and TG (52%), with variation by geopolitical zone. Among FSW, it ranged from 75% in Northeast to 92% in the Northwest. HIV testing in the past 12 months ranged from 61% among MSM in the Northwest to 86% among FSW in the Southeast. ART uptake among people living with HIV was suboptimal across KP groups and geopolitical zone, with lowest ART coverage among MSM in the Northwest (16%). PrEP use in the last 12 months ranged from 22% among FSW in Northcentral to 75% among MSM in the Northwest. PEP uptake in the last 12 months was lowest among FSW in the Southwest (7%).
Conclusion: Findings from the KPPR PBS highlight critical gaps in HIV prevention outcome targets among KP in Nigeria. Low condom use, especially amongst MSM and TG, low ART and PEP uptake emphasize the need for targeted interventions and strengthened peer-led, community-based approaches to improve HIV service access.
PP06.41 – Assessing Service Availability Coverage in One-Stop Shops for Key Populations in Nigeria: Results from the 2024 Key Population Programme Review
Mr. Chukwuebuka Ejeckam2, Dr Temitope Ilori1, Mr Francis Agbo1, Dr James Anenih1, Dr Kalada Green3, Dr Chukwuemeka Agi2, Mr Kuifre Ndueso2, Dr Achama Eluwa3, Prof Souradet Shaw3, Prof Leigh McClarty3, Prof James Blanchard3
1National Agency for the Control of AIDS, Abuja, Nigeria.
2West Africa Centre for Public Health and Development, Abuja, Nigeria.
3Institute for Global Public Health, University of Manitoba, Winnipeg, Canada.
Background: One-stop shops (OSS) provide comprehensive, integrated services for prevention and treatment of sexually transmitted and blood-borne infections (STBBI), including HIV, to key populations (KP) in Nigeria. In 2024, a KP Programme Review (KPPR) used mixed methods to assess 41 OSS facilities across 18 of 37 Nigerian states. Prior to the KPPR, the country had used the Progammatic Mapping method to estimate a total of 932,664 Key population across the 18 states including 373,329 female sex workers (FSW), 334,763 men who have sex with men (MSM), 213,997 people who inject drugs (PWID), and 10,175 transgender persons (TG). However, only 44 OSS facilities are operational across the 18 states, mostly in urban areas, leaving rural and underserved regions with limited-service access.
Methods: The KPPR collected quantitative data using structured questionnaires to describe STBBI prevention services offered and the number of KP clients served. Our descriptive analyses compare OSS client loads to global recommendations for HIV prevention programs and examine gaps in service availability coverage. Data analysis was done using SPSS v23 and STATA.
Results: The OSS served 62% of FSW,52% of MSM and PWID, and 42% of TG populations across the 18 states.On average, one OSS facility served 5,806 FSW,4,437 MSM,2,940 PWID, and 171 TG. Staffing levels were inadequate, with one doctor serving thousands of clients, far above recommended ratios for effective HIV prevention. Service availability coverage was limited: only 44% of OSS offered Needle and Syringe programs, 51% provided family planning, and 56% conducted substance abuse screening. Legal support services were available at 71% of OSS. These services are critical for reducing health disparities among KPs and ensuring comprehensive care.
Conclusion: The current OSS coverage does not meet the needs of Nigeria’s KP. Expanding OSS to both underserved areas and increasing their numbers in areas with high KP client loads, improving staff capacity, and aligning services with global standards are vital to addressing gaps in STBBI/HIV prevention and care.
PP06.42 – Understanding HIV Prevalence and Vulnerability Indices Among Men Who Have Sex with Men in Nigeria: Insights from the 2020 Integrated Biological and Behavioral Surveillance Survey
Mr. Chukwuebuka Ejeckam2, Dr Temitope Ilori1, Mr Francis Agbo1, Dr Rose Aguolu1, Dr Kalada Green3, Dr Chukwuemeka Agi2, Mr Osayende Ayewah2, Dr Faran Emmanuel3, Prof Leigh McClarty3, Prof Souradet Shaw3, Prof James Blanchard3
1National Agency for the Control of AIDS, Abuja, Nigeria.
2West Africa Centre for Public Health, Abuja, Nigeria.
3Institute for Global Public Health, University of Manitoba, Winnipeg, Nigeria.
Background: Nigeria, Africa’s most populous nation, remains a significant global HIV hotspot. With a general population prevalence of 1.3% among adults aged 15–49, approximately 1.9-million people were living with HIV in Nigeria as of 2022.The HIV epidemic in Nigeria disproportionately affects Key Populations, including men who have sex with men (MSM). The 2020 IBBSS study examined behavioral indices that influences HIV vulnerabilities amongst Key Populations, including MSM in Nigeria.
Methods: The 2020 Integrated Biological and Behavioral Surveillance Survey (IBBSS) employed a multistage cluster sampling design to recruit a total of 4397 MSM aged ≥15 years. Mapped and validated hotspots such as hostels, campuses, massage parlors and brothels served as recruitment sites across 12 states. Behavioral data, focusing on sexual practices, condom use, and prevention service access, were collected using structured questionnaires. Blood sample collection with consenting study participants was done in line with national guidelines standards. Analysis was done using SPSS vs 23 and STATA.
Results: Result show that 97% of respondents had tested in the last year. However, risk behaviors such as inconsistent condom use (despite 82% usage in the last encounter) and high rates of unprotected receptive anal intercourse persisted. Awareness of PrEP was 50%, but uptake was only 27%, while PEP use was even lower at 11%, reflecting significant service access delivery gaps. HIV prevalence amongst MSM was 25%, which revealed a 9 % increase from the 2014 rate (22.9%). Violence and harassment also increased amongst MSM as about 36% of MSM were forced to have sex without using condom while 17% were harassed or arrested by law enforcement in the 6 months preceding the study.
Conclusions: The findings underscore the persistent vulnerabilities of MSM in Nigeria due to violence, legal constraints, and inadequate prevention and care services. Targeted, inclusive strategies are crucial to achieving UNAIDS’ 95-95-95 goals and reducing HIV transmission amongst this KP sub-typology, a step critical in the drive towards comprehensive HIV epidemic control in Nigeria.
PP06.43 – Enhancing PrEP Accessibility in STI Clinics: A Decision Tree Approach
Miss Darya Fridman1
1The LGBTQ Center, Las Vegas, United States.
Background: The rise in HIV infections highlights the need for effective prevention strategies, particularly among high-risk populations. Pre-exposure prophylaxis (PrEP) is effective but underutilized due to stigma, misinformation, and access barriers. This project aims to enhance PrEP accessibility in an STI clinic using a decision tree model that tailors discussions to individual patient risk profiles.
Description: Our clinic implemented a structured Social Assessment to identify HIV risk factors. Patients answered questions about their sexual history and lifestyle, allowing advocates to categorize them into low, medium, or high-risk groups. This personalized approach enabled tailored discussions about PrEP and empowered patients to make informed choices aligned with their lifestyles. Advocates created a safe space for open conversations, addressing stigma and misinformation while providing resources. Once patients expressed interest in PrEP, providers facilitated the setup process, ensuring seamless access to care, including options for PrEP administration based on individual preferences and financial situations, such as programs covering medication costs through our in-house pharmacy.
Findings: In 2023, our STI clinic assessed 5,137 individuals who tested HIV-negative, enrolling 477 new patients in PrEP. Patients were classified based on their risk factors, allowing for targeted education. Low-risk patients received safe sex kits with PrEP information, moderate-risk patients learned safer practices and PrEP options, while high-risk patients engaged in comprehensive discussions about PrEP benefits. This approach increased patient understanding and engagement.
Conclusion: The decision tree model significantly improved PrEP accessibility and patient engagement. By personalizing education and facilitating open discussions, we increased interest in PrEP and promoted informed decision-making in sexual health, serving as a valuable framework for addressing health disparities in underserved communities.
PP06.44 – Enhancing Hepatitis C Testing and Treatment Access Through Expanded Services and Community Partnerships
Miss Darya Fridman1
1The LGBTQ Center, Las Vegas, United States.
Background: Hepatitis C (HCV) disproportionately affects underserved populations, particularly racial and ethnic minorities. Our clinic serves a majority-minority population (70.8%), making it an ideal site to evaluate the effectiveness of existing HCV testing protocols. This study explores expanding service access through partnerships with Medication-Assisted Treatment (MAT) centers, methadone clinics, and the development of a mobile clinic to improve outreach and care delivery.
Description: From January 2023 to December 2024, the clinic conducted 1,000 rapid INSTI Hepatitis C tests on 8,100 patients at the clinic and outreach events. Patients who tested positive were promptly scheduled for follow-up appointments for lab work, risk factor assessments, and treatment planning. Testing was expanded to MAT facilities, where patients who tested positive received same-day follow-up care. Transportation support, including ride-share services and bus passes, was provided to improve accessibility. A mobile clinic, launching in January 2025, will offer on-site lab work at MAT centers to further enhance access.
Findings: Of the 1,000 tests conducted, 55 patients tested positive for Hepatitis C and received timely follow-up care. Expanding testing services to MAT centers led to a significant increase in the identification of HCV cases. Integrating testing, consultation, and treatment in one setting improved care continuity. Same-day follow-up and the involvement of the Linkage to Care (LTC) team boosted patient engagement and adherence. The mobile clinic is expected to further improve access by providing lab work directly at MAT facilities.
Conclusion: The clinic’s HCV testing and treatment model has been effective in identifying and treating Hepatitis C, particularly in underserved populations. Expanding services through MAT partnerships and the mobile clinic will increase access to care, especially for uninsured and underinsured individuals. Lessons learned include the importance of integrated testing and treatment services, timely follow-up, and consistent patient support.
PP06.45 – Implementation of Anal Precancer Screening Among People Living with HIV: Needs Assessment Among Health System Stakeholders in Ontario, Canada
Dr. Dina Gaid1, Dr. Troy Grennan2, Dr. Meghan Walker3, Dr. Gordon Arbess1, Dr. Tyler Chesney1, Dr. Christine Fahim1, Dr. Daniel Grace4, Dr. Aisha Lofters5, Dr. Paul MacPherson6, Mr. Devan Nambiar7, Mary Ndung’u8, Dr. Apondi J. Odhiambo1, Dr. Irving Salit9, Dr. Michael Silverman10, Dr. Kevin Woodward11, Dr. Anna Yeung1, Dr. Ann Burchell1
1Unity Health Toronto, Toronto, Canada.
2BC Centre for Disease Control, Vancouver, Canada.
3Ontario Health, Toronto, Canada.
4University of Toronto, Toronto, Canada.
5Women’s College Hospital, Toronto, Canada.
6Ottawa Hospital, Ottawa, Canada.
7Gay Men’s Sexual Health Alliance, Toronto, Canada.
8Women’s Health in Women’s Hands, Toronto, Canada.
9University Health Network, Toronto, Canada.
10St. Joseph’s Hospital London, London, Canada.
11HQ Toronto, Toronto, Canada.
Background: In 2024, the International Anal Neoplasia Society released clinical recommendations for anal precancer screening in high-risk populations, including people living with HIV. The recommended screening test is Pap cytology or human papillomavirus testing, accompanied by a digital anal rectal exam (DARE). We are conducting a needs assessment for guideline implementation according to the healthcare provider, organization, and health system levels in Ontario, Canada.
Methods: We used a phenomenology qualitative design with semi-structured, virtual interviews with key informants, guided by the Theoretical Domains Framework (TDF) and the Consolidated Framework for Implementation Research (CFIR). Eligible participants were professionals with experience with the healthcare system in Ontario involving the provision, administration, or management of services. Recruitment was purposive via email networks and announcements at presentations. One coder (DG) has deductively and inductively analyzed recorded transcripts to identify themes within TDF and CFIR theoretical domains.
Results: To date, we conducted 12 interviews out of an anticipated 30. Identified themes covered all CFIR domains (innovation, individual, and implementation domains, and inner and outer setting) and five TDF domains (environmental context, professional role and identity, skills, emotions, and knowledge). Barriers include a lack of knowledge about the guidelines, who is recommended for screening, and how to screen; lack of resources, namely high resolution anoscopy (HRA) services; and, among patients, limited awareness of the need for screening and trauma and stigma associated with screening. Facilitators include increased access to HRA specialists, simplification of the guidelines for providers, opinion leaders who can offer guidance, and, among patients, education, fostering positive beliefs about the process, and patient-peers to support implementation.
Conclusion: Our findings suggest ways to guide the equitable implementation of anal pre-cancer screening guidelines tailored to local settings. These will be used to inform the development of an implementation toolkit to support scale-up.
PP06.46 – Addressing Neisseria Gonorrhoeae Antimicrobial Resistance in Brazil: Advancing Through Coordinated Public Health Initiatives
Dr. Pâmela Cristina Gaspar1, Dr Alisson Bigolin1, Msc, MD Mayra Aragon, BSc Amanda Krummenauer1, Dr Amanda Morais1, BSc Adson Paixão1, Dr Ana Pascom1, Dr, MD Carmen Domingues1, Dr José Morais1, BSc Renatto Carrijo1, BSc Ronaldo Coelho1, Dr Maria Luiza Bazzo2, Dr Angélica Miranda3, MD Dráurio Barreira1
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
2Molecular Biology, Microbiology, and Serology Laboratory (LBMMS), Federal University of Santa Catarina, Florianópolis, Brazil.
3Federal University of Espírito Santo, Vitória, Brazil.
Background: Monitoring antimicrobial susceptibility of Neisseria gonorrhoeae (NG) is crucial but addressing treatment resistance and promoting rational use of medications requires a comprehensive approach.
Description: The Brazilian Gonococcal Antimicrobial Surveillance Programme (Brazilian-GASP) initiated in 2015, involving a partnership between the Ministry of Health, sentinel sites and a National Reference Laboratory (NRL). It integrates sentinel urethral discharge notifications, NG isolation for antimicrobial susceptibility testing, molecular etiological diagnosis, and epidemiological data collection. A national laboratory network for molecular diagnosis of Chlamydia trachomatis (CT) and NG was established, focusing on key populations. Additionally, a pilot for a rapid molecular test in STI clinics is ongoing, aiming to establish the etiological management of symptomatic STI cases. All types of molecular testing (laboratory or rapid) analyzes samples from urine, oropharyngeal, anal, urethral, and vaginal discharge.
Results: Brazilian-GASP data showed over 50% resistance to ciprofloxacin and 100% susceptibility to ceftriaxone, justifying update to national guidelines. Ciprofloxacin was replaced with ceftriaxone in dual therapy with azithromycin for uncomplicated gonorrhea. Additionally, increasing azithromycin resistance has been observed. Between September 2022 and November 2024, 79,229 samples were analyzed through the national laboratory network. A total of 7.1% (5,652) were positive for CT, 6.8% (5,413) for NG, and among these 1.6% (1,301) had CT/NG co-infection. In the pilot for rapid molecular testing, 2,415 samples were analyzed, detecting 8% for CT and 13% for NG, with 3% co-infection. Seventy-nine percent of the people tested received results during the same clinical appointment. Furthermore,1,061 urethral discharge notifications were registered from 7 sentinel sites (January/2023–December/2024). Worryingly, 30% of cases were treated with non-standard for syndromic management in Brazil.
Conclusion: To address NG resistance, it is important to integrate epidemiological surveillance, strengthen diagnostic capacity, adopt and continuously update technologies, and regularly revise national prevention, diagnosis, and treatment guidelines based on surveillance data.
PP06.47 – The Brazilian Gonococcal Antimicrobial Surveillance Programme (Brazilian-GASP): 10 Years of Implementation
Dr. Pâmela Cristina Gaspar1, Dr Alisson Bigolin1, Dr Marcos André Schörner2, Dr Jéssica Martins2, MSc Felipe de Rocco2, Msc, MD Mayra Aragon1, Dr, MD Adele Schwartz Benzaken3, MD Draurio Barreira1, Dr, MD Angélica Miranda4, Dr Maria Luiza Bazzo2
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
2Molecular Biology, Microbiology, and Serology Laboratory (LBMMS), Federal University of Santa Catarina, Florianópolis, Brazil.
3AIDS Healthcare Foundation, Los Angeles, United States of America.
4Federal University of Espírito Santo, Vitória, Brazil.
Background: Monitoring the antimicrobial susceptibility of Neisseria gonorrhoeae (NG) is crucial due to its ability to develop resistance. The Brazilian Gonococcal Antimicrobial Surveillance Programme (Brazilian-GASP) has been implemented for 10 years and is well-established.
Description: In 2014, the Brazilian Ministry of Health (MoH) initially selected STI clinics with expertise in gonococcal culture. A national reference laboratory (NRL) was designated to oversee procurement, supply distribution, training all the sites and centralized inhibitory concentration testing using the agar dilution method. The Pan-American Health Organization, Malbrán Institute/Argentina and the World Health Organization (WHO) STI reference laboratory technically supported Brazilian-GASP, including quality control and genome analysis. Two editions have been completed, and the third is ongoing. After successful editions, Brazilian-GASP became part of the National Surveillance System, which includes sentinel urethral discharge notification, NG analysis, molecular diagnosis, and epidemiological data collection. The MoH funds this initiative, complementing the infrastructure at the NRL and sentinel sites.
Results: In the first round (2015–2016), 550 NG isolates from men with urethral discharge were collected at seven sentinel sites, revealing over 50% resistance to ciprofloxacin and 100% susceptibility to ceftriaxone/cefixime. This led to an update of the national treatment protocol from ciprofloxacin 500mg plus azithromycin 1g to ceftriaxone 500mg plus azithromycin 1g. In the second round (633 isolates), azithromycin resistance increased from 1.3% to 10.9%, while ceftriaxone susceptibility remained at 100%. Preliminary third-round results corroborate these findings. The national STI protocol is being updated to consider shifting to monotherapy for gonorrhea, replacing azithromycin with doxycycline in dual therapy for urethral and vaginal discharge.
Conclusion: The collaboration between the MoH, NRL, sentinel sites, and international institutions has been essential to Brazilian-GASP’s success. The results are supporting updates to national STI guidelines and public policy. It also, strengthened Brazil’s role in the WHO-GASP initiative, now advancing to implement Enhanced GASP.
PP06.48 – Sustaining a Digital Sexually Transmitted and Blood-Borne Infection Testing Program in British Columbia: from Planning to Scale-Up, What Have We Learned?
Janice Duddy, Hsiu-Ju Chang1,2, Devon Haag1, Heather Pedersen1, Mark Bondyra1, Dr. Ihoghosa Iyamu1,2, Dr. Cathy Worthington4, Dr. Daniel Grace3, Dr. Mark Gilbert1,2
1British Columbia Centre for Disease Control, Vancouver, Canada.
2University of British Columbia, Vancouver, Canada.
3University of Toronto, Toronto, Canada.
4University of Victoria, Victoria, Canada.
Background: Digital sexually transmitted and blood-borne infection (STBBI) testing programs are complex health system interventions, with many parts interacting across multiple health organizations, systems and contexts, and requiring substantial financial investment. We aimed to understand how best to implement these services to maximize their sustainability over time.
Description: As a case study we used GetCheckedOnline, a digital STBBI testing service in British Columbia, Canada that has demonstrated effectiveness and has been scaled up and sustained. We conducted interviews and focus groups with 38 staff from multiple regional and provincial organizations involved in implementing GetCheckedOnline from initial planning (2009) to current scale-up (2024). Organizations spanned clinical, public health, laboratory, government and community sectors. Factors perceived as contributing to sustainability of the service were identified from observer notes using framework analysis based on the Consolidated Framework for Sustainability Constructs in Health Care.
Findings: Factors perceived to have contributed to sustainability are shown in Table 1. The most commonly identified factors were related to the framework’s constructs of People Involved, Resources, and Negotiating Initiative Processes. Building innovative digital testing solutions requires interdisciplinary teams, collaborations, and new partnerships across health system program silos and organizations, as well as identifying g the required teams and functions needed for implementation. Building and maintaining relationships by program staff – which takes time and resources – was recognized as critical and cut across multiple framework constructs.
Conclusion: Based on our study of GetCheckedOnline, multiple factors contribute to sustaining digital STBBI testing services, speaking to their complexity and inherent requirement for interdisciplinary teams, new partnerships within and across organizations and systems, integrated operations, and a foundation of strong relationships. Incorporating and appropriately resourcing processes that reflect these factors during the planning, implementation and scale-up of digital testing or other digital sexual health services may maximize their sustainability.
PP06.49 – Strengthening Chlamydia Management in Australian General Practice Using Interventions That Align with Clinic Workflow
Dr. Jane Goller1, Ms Zoie Alexiou1,2, Dr Helen Bittleston1, Dr Stephanie Munari1,3, Prof Meridith Temple-Smith4, Prof Lena Sanci4, Prof Jane Hocking1, Dr Jacqueline Coombe1
1Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
2National Institute for Public Health and the Environment, The Netherlands.
3Burnet Institute, Melbourne, Australia.
4Department of General Practice and Primary Care, The University of Melbourne, Melbourne, Australia.
Background: In Australia and many countries, chlamydia control focuses on optimising management to reduce risk of reproductive sequelae. The Management of Chlamydia Cases in Australia (MoCCA) study co-designed an intervention to support best practice chlamydia care, including partner management, timely retesting for reinfection and pelvic inflammatory disease (PID) detection. In an implementation and feasibility trial, we evaluated MoCCA in Australian general practice.
Description: MoCCA included a website (www.mocca.org.au), shortcut text, prescription templates, patient factsheets, patient-delivered partner therapy resources, and postal retesting and was implemented in 14 general practices across three Australian states. Qualitative and quantitative data were analysed to understand adoption and impact on chlamydia management. Our approach was guided by the Consolidated Framework for Implementation Research and Normalisation Process Theory. Chlamydia retesting (2–4 months) and PID diagnoses were compared between a 12-month pre-intervention and intervention for patients 16–44 years.
Findings: Chlamydia tests were conducted in 17.2% patients’ pre-intervention (n = 7695/44,847, 4.6%=positive) and intervention = 17.8% (n = 9823/55,333, 5.0%=positive). Proportions retested were 13.5% (95% CI 10.9–16.4) pre-intervention and 18.8% (95% CI 14.7%–23.5%) intervention (difference = 5.4%, 95% CI 0.4–10.4). PID proportions pre-intervention (0.97%, 95% CI 0.86–1.08) and intervention (1.03% 95% CI 0.93%–1.13%) were similar (difference = 0.06%, 95% CI –0.09–0.20). Clinician perspectives (doctors = 40, nurses = 17) mostly indicated MoCCA integrated with clinic workflows, was simple to set-up and use, but not used by all. Reported improvements in care included better quality, continuity and time-efficiency (e.g. website simplified chlamydia management) and patient communication (e.g. shortcuts/factsheets remind to discuss retesting/partners) “MoCCA for chlamydia and PID, we spend better time, we structure the appointment, it’s made it a more targeted or quality consult.” Many clinicians wanted access to MoCCA resources post-study, particularly the website, shortcuts, factsheets and suggested this be via organisations with STI-care responsibilities or practice software.
Conclusion: MoCCA supported improved chlamydia management. MoCCA resources could be made routinely available via existing mechanisms and adapted to other STIs.
PP06.50 – Operationalizing Opt-Out HIV Screening Guidelines in Pediatric Emergency Departments
Dr. Mark Griffiths1,2, Ms Sandy Francois1, Ms Melissa N. Cameron1, Ms Jordan E. Bryant1, Ms. Bridget A. Wynn1, Sara P. Brown2, Sarah Thompson2, Rebekah Carter2, Kelly DeNaples2, Dr. Swaminathan Kandaswamy1, Dr. Evan Orenstein1,2, Dr. Andres Camacho-Gonzalez1,2, Dr. Claudia R. Morris1,2, Dr. Lauren Middlebrooks1,2
1Emory University, Atlanta, United States.
2Children’s Healthcare of Atlanta, Atlanta, United States.
The Centers for Disease Control and Prevention recommends HIV screening for all patients ≥13 years. Parts of Atlanta have HIV positive rates at 8-times the national average. Adolescents are least likely to know their HIV status, have the lowest rate of linkage to care, and viral suppression. Children’s Healthcare of Atlanta (Children’s) implemented opt-out HIV testing in its emergency departments for patients ≥13 years undergoing venipuncture at all their sites. The objective is to increase testing in adolescents leading to earlier HIV diagnosis and linkage-to-care.
Children’s electronic medical record EPIC and its population discovery tool were used to compare HIV testing volumes of 13–24-year-olds, 17 months pre and post the July 6, 2023, clinical implementation. Results were cross-referenced to determine newly diagnosed adolescents living with HIV (ALHIV) from known positives. The data was compared using descriptive statistics.
There were 1956 patients tested pre-implementation, 1417 (72%) girls and 539 (28%) boys. Nine new ALHIV were identified; mean age 17.4 ± 1.7, assignment at birth was (6) male, 1 coinfected with syphilis and (3) female. Post-implementation, 4183 patients were tested: 2763 (66%) girls and 1420 (34%) boys. Ten new ALHIV were identified; mean age 15.8 ± 1.8, assignment at birth was (8) male, 2 coinfected with syphilis, and (2) female. This demonstrates a positivity rate of 0.2%; 1 in 177 boys tested positive (0.6%). All newly diagnosed cases were linked to care with a median of 3.5 days.
Atlanta remains a hotspot for HIV cases. Ten cases in 17 months highlights the importance of HIV testing and reflects a public health crisis. The initiative drastically increased HIV screening and will likely identify ALHIV at an earlier stage of infection, facilitating timely access to medical care. This can lead to improved clinical and immunological outcomes, and a reduced risk of secondary transmission.
PP06.51 – Exploring the 6 C’S Framework for Cultural Sensitivity in HIV Care: Insights from Community-Based Programs in the Philippines
Dr. Ryan Guinaran1
1AIDS Healthcare Foundation (AHF) Philippines, Cubao, Philippines.
Background: In HIV/AIDS prevention and care, adopting a cultural approach leverages a population’s cultural references and resources to create strategies that drive impact. Addressing diversity requires health services to adapt to target populations, especially in Low and Middle-income countries with limited resources and sociocultural complexity. Despite its importance, disparities persist in HIV care, highlighting the need for culturally sensitive, patient-centered approaches to improve prevention, testing, and treatment outcomes. However, gaps remain in analyzing how culture is integrated into HIV interventions. This study applies the 6 C’s framework developed from the author’s dissertation as a novel model for analyzing cultural sensitivity in HIV programs.
Description: The study employed qualitative content analysis to assess the utility of the 6 C’s framework for cultural sensitivity. It analyzed 120 monthly reports from 10 community-based organizations partnered with the AIDS Healthcare Foundation (AHF) Philippines, covering programs from January to December 2024. The activities were coded according to their alignment with the framework.
Findings: All the 6 C’s were observed in the CBO strategies. The Character strategy was seen in client-appropriate visual aids, information materials, and facilities. The Count strategy included utilizing the demographic data of clients to inform tailored approaches. Closeness strategy bridged distance problems through outreach, home visits, courier services, and digital means. The Communication strategy engaged adaptive messaging through local languages and culturally relatable lingo. The Community involvement approach empowered clients as co-producers of care as volunteers and advocates and engaged multiple stakeholders from the academe, workplace, and community. Context and Care strategy featured integrated HIV care and consideration of social determinants of health of client groups.
Conclusion: The 6 C’s framework is helpful in analyzing and guiding culturally sensitive HIV program implementation. This framework’s intersection with the WHO’s health system six building blocks may be explored to enhance HIV program effectiveness.
PP06.52 – Enhancing HIV Re-Linkage to Care: Findings from an Emergency Department-Based Intervention
Ms. Haley Haines1, Gabriella Dashler1, Nyah Johnson1, Dante Brown1, Mun Heol Cho1, Genevieve Barrow2, Dr. Adena Greenbaum2, Kaye Park3, Dr. Joyce Jones3, Dr. Mustapha Saheed1, Dr. Richard Rothman1, Dr. Yu-Hsiang Hsieh1
1Johns Hopkins University School of Medicine Department of Emergency Medicine, Baltimore, United States.
2Baltimore City Health Department, Baltimore, United States.
3Johns Hopkins University School of Medicine Departent of Medicine/Division of Infectious Diseases, Baltimore, United States.
Background: Emergency departments (EDs) across the U.S. have successfully linked 93% of newly diagnosed HIV patients to care within one month. Some EDs have extended these programs to re-link people living with HIV (PLWH) who have poor care engagement, potentially reducing complications and transmission. However, factors affecting success with ED-based re-LTC interventions remain unclear. This quality improvement project identified socio-demographics (SDs) and clinical factors associated with sustained poor HIV care engagement following a re-LTC intervention in an urban ED.
Methods: At an urban academic ED in Baltimore, Maryland, with routine HIV/HCV testing, program staff identified PLWH with poor HIV care engagement (missing ≥1 HIV care appointment and not refilling ART prescriptions within 3 months) using Epic reports. Staff provided bedside intake appointment scheduling to local HIV clinics. Data on SDs, HCV coinfection, substance use disorder (SUD), insurance type, and intervention outcomes (scheduled HIV care appointments, attendance, and ART reinitiation within 3 months) were collected from January 2023 to June 2024 during program shifts (16 h, 5 days/week). Binomial logistic regressions in R identified predictors of unsuccessful re-engagement.
Results: Among 893 ED PLWH, 116 had poor HIV care engagement. Most were Black or African American (69%, n = 80), < 50 years old (60%, n = 70), and assigned Male at birth (65%, n = 75). Among those receiving re-LTC interventions, younger PLWH (<50 years old) were 71% less likely (OR: 0.29, 95% CI: 0.11–0.67, reference: >50 years old) and PLWH with SUD were 85% less likely (OR: 0.15, 95% CI: 0.05–0.41, reference: no SUD) to attend scheduled appointments or reinitiate ART. No significant differences were observed based on race.
Conclusion: In Baltimore, factors negatively affecting HIV care engagement include age (<50) and living with an SUD. EDs, often a primary healthcare contact for younger PLWH, should tailor strategies to these populations.
| Attending Scheduled Appointment | Reinitiate ART | |||||
|---|---|---|---|---|---|---|
| Patient Factors | n (%), N = 116 | OR (95% CI) | P-value | OR (95% CI) | P-value | |
| Age | ||||||
| 50 years old and older | 46 (40) | – | – | – | – | |
| Under 50 years old | 70 (60) | 0.29 (0.12 - 0.67) | 0.02* | 0.29 (0.12 - 0.67) | 0.02* | |
| Ethnicity** | ||||||
| Non-Hispanic or Latino | 112 (97) | |||||
| Hispanic or Latino | 4 (3) | |||||
| Assigned Sex at Birth | ||||||
| Female | 41 (35) | – | – | – | – | |
| Male | 75 (65) | 1.01 (0.45 - 2.31) | 0.98 | 1.01 (0.45 - 2.31) | 0.98 | |
| Race | ||||||
| BIPOC | 88 (76) | – | – | – | – | |
| White | 28 (24) | 1.56 (0.55 - 4.41) | 0.48 | 1.56 (0.55 - 4.41) | 0.48 | |
| Coinfection Status | ||||||
| Monoinfection | 71 (61) | – | – | – | – | |
| Coinfection with HCV | 45 (39) | 1.13 (0.42 - 3.00) | 0.84 | 1.13 (0.42 - 3.00) | 0.84 | |
| History of Housing Instability | ||||||
| No History of Housing Instability | 54 (47) | – | – | – | – | |
| History of Housing Instability | 62 (53) | 1.51 (0.67 - 3.50) | 0.41 | 1.51 (0.67 - 3.50) | 0.41 | |
| Active IDU | ||||||
| No Active IDU | 90 (78) | – | – | – | – | |
| Active IDU | 26 (22) | 1.16 (0.38 - 3.53) | 0.82 | 1.16 (0.38 - 3.53) | 0.82 | |
| History of SUD | ||||||
| No History of SUD | 29 (25) | – | – | – | – | |
| History of SUD | 87 (75) | 0.15 (0.05 - 0.41) | < 0.01* | 0.15 (0.05 - 0.41) | < 0.01* | |
| Insurance Type | ||||||
| Public | 100 (86) | – | – | – | – | |
| Other (Private, Uninsured) | 16 (14) | 0.58 (0.17 - 1.77) | 0.44 | 0.58 (0.17 - 1.77) | 0.44 | |
*Statistically significant: P-value<0.05.
**Excluded ethnicity from analysis due to unequal distribution.
-- Patient factor served as reference group.
BIPOC = Black, Indigenous, and People of Color.
PP06.53 – Awareness and Knowledge of and Barriers to Accessing PrEP for HIV Prevention in Allegheny County, Pennsylvania, 2024
Emma Roth2, Elizabeth Klusman2, Kell Wilkinson2, Richard Smith2, Therese Cushing3, Zack Bickel3, Emily Galeza3, Assoc. Prof. Ken Ho1, Professor Harold Wiesenfeld1
1University of Pittsburgh, Pittsburgh, United States.
2Jewish Healthcare Foundation, Pittsburgh, United States.
3CAMPOS, Pittsburgh, United States.
Background: PrEP (pre-exposure prophylaxis) is a key prevention tool critical to ending the HIV epidemic. Multiple clinical trials have demonstrated that PrEP is safe and highly effective with good adherence. Assessing regional PrEP awareness and knowledge may help guide local prevention efforts and inform interventions.
Description: We conducted a survey to assess awareness and knowledge of PrEP among Allegheny County, Pennsylvania residents (June – July 2024). Responses were collected via an online research panel representative of the county, in-person with tablets at predetermined locations (e.g., bars, bus stops), social media, dating app advertisements, flyers, and community groups distribution lists. Efforts were made to oversample populations disproportionately impacted by HIV.
Findings: Of the 1,334 respondents, 100 (7.5%) respondents identified as non-cisgender, and 132 (9.9%) respondents were men who have sex with men (MSM). Overall, 46.0% had heard of and were familiar with PrEP (14.6% heard of but not familiar; 39.4% never heard of). Among 18–29-year-olds, 33.9% had never heard of PrEP (23.7% 30–39-year-olds, 50.0% 40+ year olds) and 48.9% of Black individuals had never heard of it (38.5% white individuals, 30.3% other races). Most MSM (78.8%), non-cisgender individuals (87.0%), individuals who participate in in-person sex work (75.6%), and those recently diagnosed with a sexually transmitted infection (81.6%) had heard of and knew what PrEP was for. In contrast, 53.5% of people who inject drugs had heard of and knew what PrEP was for. One third (37.1%) reported knowing where to access PrEP if needed.
Conclusion: Awareness and knowledge of PrEP varied by subgroup. Awareness was low among both people who inject drugs and participate in in-person sex work, populations disproportionally impacted by HIV. Results indicate opportunities for improved and subgroup-specific education and messaging. As the HIV epidemic continues to evolve, it is important to continue monitoring PrEP awareness and knowledge.
PP06.54 – Integrating STI and Harm Reduction Services to Reach New Populations with Comprehensive Services
Ms. Rebekah Horowitz, Ms. Kat Kelley1
1National Association of County and City Health Officials (NACCHO), Washington, United States.
Background: STIs and substance use (SU) are closely intertwined: SU is a leading risk factor for STIs, particularly congenital syphilis, and people who use drugs face significant barriers to accessing STI services and prenatal care. Integrating STI and harm reduction (HR) services is a promising strategy to reach new populations and address STIs and SU-related health outcomes.
Description: In 2023, the National Association of County and City Health Officials (NACCHO) funded 10 organizations to participate in a mixed-methods evaluation of STI/HR integration models. This included three rounds of interviews and collection of service delivery data (e.g., STI/HR services provided and STI test results).
Findings: The project identified pros and cons of common service delivery models, motivations for integration, activities to start up and maintain integrated services, and challenges. Common motivations for service integration included desires to reach new populations and offer comprehensive services to medically underserved clients. Sites reported challenges related to funding (quantity, flexibility, siloes), interoperability of STI/HR data systems, physical space, and balancing the desire to offer comprehensive vs low-threshold, accessible services. Hiring and cross-training staff and changing workflows and protocols were critical for startup. Passionate staff with strong interpersonal skills were essential to success. STI positivity rates varied but suggest integrated service providers are effectively identifying and treating STIs.
Conclusion: This project provides insight into the pros and cons of various STI/HR integration models, what it takes to initiate and maintain integrated services, and what challenges and benefits an organization might experience. This session will highlight project findings, including implications for implementation, scale up, and further evaluation of STI/HR integration.
PP06.55 – Trends and Outcomes of STI/HIV Testing at CPACS Cosmo Health Center: An Evaluation of Demographics and Diagnostic Results from 2022–2024
Miss Lamiya Hussain1
1Cosmos Health, Norcross, United States.
Background: Access to timely STI/HIV screenings is crucial for early diagnosis and treatment, especially in underserved populations. The Center for Pan Asian Community Services (CPACS) Cosmo Health Center has been providing STI/HIV screenings in a diverse community. This formative evaluation seeks to assess ongoing screening processes, identify barriers, and guide improvements for greater impact.
Descriptions: A retrospective review of STI/HIV screening data from 2022 to 2024 was conducted to analyze patient demographics, screening coverage, and diagnostic outcomes. Variables included patient age, gender, race, ethnicity, and test results for HIV and Hepatitis. Trends were examined to identify gaps and opportunities for improvement.
Findings: Preliminary data from over 2,345 screenings revealed diverse patient demographics, with 60% of patients identifying as Asian and 25% as African American. HIV positivity rates remained stable at 4%, with significant gender differences (6% in males and 2% in females). Hepatitis screenings indicated a higher positivity rate among African American populations. These challenges contributed to delays in accessing services, highlighting the need for targeted interventions to address these obstacles.
Conclusion: The evaluation indicates that while the screening process is strong, challenges like access and engagement require attention. Recommendations include enhancing patient outreach, addressing cultural barriers, and improving follow-up services to ensure better linkage to care. These findings will inform adjustments to screening protocols and support broader public health goals.
PP06.56 – Does Digital Recruitment Influence Evaluation of Awareness and Use of Digital STBBI Testing Services? Insights from GetCheckedOnline’s 2022 Community Survey in British Columbia, Canada
Dr. Ihoghosa Iyamu1,2, Aidan Ablona2, Dr. Rodrigo Sierra-Rosales1,2, Heather Pedersen2, Dr. Paul Flowers3, Dr. Nathan Lachowsky4, Dr. Troy Grennan2,5, Dr. Sofia Bartlett1,2, Devon Haag2, Dr. Catherine Worthington4, Dr. Daniel Grace6, Dr. Mark Gilbert1,2
1School of Population and Public Health, University of British Columbia, Langley, Canada.
2British Columbia Centre for Disease Control, Vancouver, Canada.
3School of Psychology & Health, University of Strathclyde, Glasgow, United Kingdom.
4School of Public Health and Social Policy, University of Victoria, Victoria, Canada.
5Division of Infectious Diseases, University of British Columbia, Vancouver, Canada.
6Dalla Lana School of Public Health, University of Toronto, Toronto, Canada.
Background: Online surveys are often used to evaluate digital sexually transmitted and bloodborne infections (STBBI) care services but risk selection bias towards respondents with better digital access and literacy. We compared awareness and use of GetCheckedOnline, BC’s online testing service, between participants recruited digitally vs in-person.
Methods: Between June and September 2022, we recruited English-speaking, sexually active BC residents (≥16 years, ≥1 partner in the past year), using two modalities: (1) digitally mediated recruitment using social media ads and digital survey links at sexual health clinics and community sites, and (2) in-person paper surveys at community events/sites (e.g. Pride festivals, colleges), targeting populations facing STBBI testing barriers (e.g., low-income earners, gay men). We assessed awareness and use of GetCheckedOnline (Yes/No), recruitment modality (digital/in-person), socio-demographics, e-health literacy, digital access, and sexual health characteristics. Differences in awareness and use were analyzed using bivariable and multivariable logistic regression models, accounting for plausible confounders. Intersectionality theory informed the testing and inclusion of significant interaction terms.
Results: Among 1,657 participants (mean age: 33.0 years, SD: 11.77), 52.5% (784) were women, 36.2% (600) were recruited digitally, and 35.8% (584) were aware of GetCheckedOnline, of whom 57.4% (324) had used it (Table 1). Digitally-recruited participants had higher odds of awareness (OR: 5.27, 95% CI: 4.23–6.57) and use (OR: 3.13, 95% CI: 2.20–4.45) compared with participants recruited in-person. Differences persisted after adjusting for socio-demographics, digital literacy and access, region, STBBI testing history and previous experience of testing barriers: awareness (aOR: 3.17, 95% CI: 2.18–4.60) and use (aOR: 2.47, 95% CI: 1.43–4.26). Covariate interactions were not significant.
Conclusion: Digitally recruited participants had greater awareness and use of GetCheckedOnline. Recruitment modalities strongly influence survey evaluations of awareness and use of digital STBBI services like GetCheckedOnline. Combined recruitment strategies are essential for more inclusive and accurate evaluations of awareness and use of these services.
| Variable* | In-person survey N (%) | Online survey N (%) | P-Value | |
|---|---|---|---|---|
| 1057 | 600 | |||
| Aware of GetCheckedOnline | ||||
| No | 812 (77.9) | 237 (40.1) | <0.001 | |
| Yes | 230 (22.1) | 354 (59.9) | ||
| Used GetCheckedOnline | ||||
| No | 132 (59.2) | 108 (31.7) | <0.001 | |
| Yes | 91 (40.8) | 233 (68.3) | ||
| Age in years (mean (SD)) | 34.74 (13.08) | 29.49 (7.42) | <0.001 | |
| Gender | ||||
| Gender minority | 134 (13.3) | 106 (21.6) | <0.001 | |
| Men | 319 (31.8) | 151 (30.8) | ||
| Women | 551 (54.9) | 233 (47.6) | ||
| Sexuality | ||||
| Sexual minority | 514 (52.1) | 306 (63.0) | <0.001 | |
| Straight | 473 (47.9) | 180 (37.0) | ||
| Ethnicity | ||||
| Racialized minority | 331 (29.8) | 769 (60.2) | <0.001 | |
| White | 780 (70.2) | 508 (39.8) | ||
| Annual income | ||||
| <$20,000 | 303 (34.1) | 86 (18.9) | <0.001 | |
| $20,000-$39,999 | 206 (23.2) | 112 (24.6) | ||
| $40,000-$59,999 | 152 (17.1) | 132 (28.9) | ||
| $60,000-$79,999 | 92 (10.4) | 86 (18.9) | ||
| $80,000 or more | 135 (15.2) | 40 (8.8) | ||
| Education | ||||
| High school or less | 292 (30.4) | 123 (25.4) | 0.138 | |
| Post-Secondary School | 320 (33.3) | 175 (36.2) | ||
| Bachelor or higher | 348 (36.2) | 186 (38.4) | ||
| eHeals Score (mean (SD)) | 30.34 (5.79) | 31.07 (5.04) | 0.023 | |
| Ease of going online (Digital access) | ||||
| Easy | 904 (90.2) | 430 (92.9) | 0.154 | |
| Neither easy nor difficult | 58 (5.8) | 23 (5.0) | ||
| Difficult | 40 (4.0) | 10 (2.2) | ||
| Health Authority | ||||
| Fraser Health | 183 (22.6) | 46 (14.8) | <0.001 | |
| Interior Health | 348 (43.1) | 97 (31.3) | ||
| Island Health | 245 (30.3) | 133 (42.9) | ||
| Vancouver Coastal Health/Northern Health | 32 (4.0) | 34 (11.0) | ||
| Previous STBBI diagnosis | ||||
| No | 691 (71.2) | 268 (52.7) | <0.001 | |
| Yes | 279 (28.8) | 241 (47.3) | ||
| Previous experience of STBBI testing barriers | ||||
| No | 380 (40.0) | 113 (21.2) | <0.001 | |
| Yes | 569 (60.0) | 421 (78.8) |
*Percentages exclude missing values.
STBBI: Sexually transmitted and blood-borne infection; SD: Standard Deviation.
PP06.57 – Early Data from Real World Use of Lenacapavir in Heavily Treatment Experienced People with HIV
Dr. Christopher Kaperak1, Paul Djuricich1, Andrew Merker1, Dr. Aniruddha Hazra1
1University of Chicago Medicine, Chicago, United States.
Background: Lenacapavir (LEN) is a long-acting injectable antiretroviral therapy (ART) option for heavily treatment experienced (HTE) people with HIV (PWH). We present real-world experience with LEN in HTE individuals at a large academic Ryan White clinic serving the Chicago South Side.
Description: We conducted a single-center retrospective cohort study of PWH who initiated LEN through December 31, 2024. Demographic and clinical characteristics were collected, including previous ART, HIV drug resistance mutations, HIV viral loads (VL), and self-reported adherence to optimized background regimen (OBR) after LEN initiation.
Findings: Ten patients received at least one dose of LEN. Six were cisgender males and 4 were cisgender females. Median age was 49 (range 27–72). Nine patients were non-Hispanic Black or multiracial. Six of 10 had stable housing. Median time living with HIV was 22.5 years (IQR 9.75–31.5). Seven had NRTI, NNRTI, PI, and INSTI class treatment history. Regarding resistance mutations, 8 patients had NRTI mutations, 7 patients had NNRTI mutations, 6 had INSTI mutations, and 6 had PI mutations. Seven of nine patients with subsequent VL testing available were suppressed with most recent VL <200 copies/mL (Fig. 1). One patient demonstrated non-adherence to their OBR after LEN initiation, resulting LEN discontinuation due to persistently elevated VLs. Median time on LEN for the other 9 patients was 350 days (IQR 238.5–447). One patient experienced a significant injection site reaction 4 days after their 2nd injection but chose to continue LEN.
Conclusions: Most HTE PWH in our cohort achieved virologic suppression with LEN, with one patient experiencing uncontrolled viremia concerning for LEN resistance. Our experience shows promise for LEN as salvage therapy for patients adherent to an OBR. Our results underscore the need for commercially available LEN resistance assays and implementation studies investigating how to support HTE individuals receiving LEN salvage therapy as use increases.
PP06.58 – Understanding Preferences for Long-Acting Injectable HIV Treatment Among Two-Spirit, Gay, Bisexual, Trans, and Queer Men and Non-Binary People and Advocating for Improved Access in Canada
Mr. Ben Klassen1, Malhar Shah1, Chris Draenos1, Stephanie Arthur2, Kimia Rohani2, Dr. Tyrone Curtis2, Dr. Jose Benito Tovillo2, Dr. Francisco Ibáñez-Carrasco3, Sarah Chown4, Dr. Nathan J. Lachowsky1,2
1Community-Based Research Centre, Vancouver, Canada.
2University of Victoria, Victoria, Canada.
3University of Toronto, Toronto, Canada.
4Ribbon Community, Vancouver, Canada.
Background: Long-acting HIV treatment (LA-treatment) can improve quality of life and address key adherence challenges with daily oral treatments among people living with HIV (PLHIV). Currently, one LA-treatment regimen is approved in Canada, but access remains limited across different provinces and territories.
Methods: We assessed Two-Spirit, gay, bisexual, trans, and queer men and non-binary (2S/GBTQ) people’s preferences for LA-treatment in Canada through CBRC’s 2024 online Sex Now survey. Participants were 2S/GBTQ PLHIV who were aged 15+, living in Canada, and self-completed a questionnaire in English, French, or Spanish. Recruitment occurred through social media, community-based organizations, and sociosexual websites/apps. Pearson’s chi-square and Fisher exact tests were used to assess statistically significant differences (P < 0.1) in preference for LA-treatment across explanatory variables.
Results: Overall, 42% of participants (n = 232) reported preferring LA-treatment over daily pills. Preference for LA-treatment was higher among participants reporting financial strain (53%, P = 0.033), sexualized substance use in the past 6 months (57%, P = 0.007), and lower satisfaction with their connection to 2SLGBTQQIA+ communities (46%, P = 0.091). The most frequently reported benefits of LA-treatment included not needing to take a daily pill (75%) and not worrying about forgetting to take daily meds (63%), while drawbacks included more frequent visits to healthcare providers (54%) and concern that LA-treatment was less effective than daily pills (50%). Participants preferred receiving LA-treatment at a clinic (76%), home (53%), or a pharmacy (46%) and from a primary care provider (79%), themselves (50%), or infectious disease specialist (48%).
Conclusion: Our findings can inform improvements in the rollout of LA-treatment among 2S/GBTQ people in Canada, including across diverse healthcare settings and within key sub-populations who would most benefit. Given the potential quality of life benefits of LA-treatment, access must be expanded and awareness about treatment efficacy must be enhanced among healthcare providers and PLHIV.
PP06.59 – Partner Variables as Risk Factors for Sexually Transmitted Infections in Adolescent Girls and Young Women in South Africa
Dr. Ranmini Kularatne1,2,3, Dr Etienne Muller4, Dr Aurelie Nelson5, Dr Massimo Mirandola6, Mr Firdavs Kurbonov7, Mr Karel Blondeel8, Dr Igor Toskin9, Prof Paul Milligan10
1Clinical Microbiology Department, Awanui Labs Northern, Auckland, New Zealand.
2Faculty of Epidemiology and Population Health, London School of Hygiene & Tropical Medicine, UK.
3Department of Clinical Microbiology & Infectious Diseases, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa.
4Sexually Transmitted Infections Section, Centre for HIV & STI, National Institute for Communicable Diseases, Johannesburg, South Africa.
5Medecins Sans Frontieres, Cape Town, South Africa.
6WHO Collaborating Centre for Sexual Health and Vulnerable Populations, Department of Diagnostics and Public Health, University of Verona, Verona, Italy.
7World Health Organization, Department of Sexual and Reproductive Health and Research, Geneva, Switzerland.
8Faculty of Medicine & Health Sciences, Ghent University, Ghent, Belgium.
9World Health Organization, Department of Sexual and Reproductive Health and Research, Geneva, Switzerland.
10Faculty of Epidemiology and Population Health, London School of Hygiene & Tropical Medicine, London, UK.
Background: There is a high prevalence of sexually transmitted infections (STI) among adolescent girls and young women (AGYW) in South Africa, which independently increase the incidence risk of HIV. We determined whether partner age disparity (age gap of >=5 years in the regular male partner) and multiple (>=2) sexual partnerships in the preceding 3 months were independently associated with laboratory-confirmed STI in sexually-experienced AGYW.
Description: We enrolled consecutive, consenting AGYW (18–25 years) at a Youth Clinic in Cape Town in 2018-2019. Sociodemographic and clinical information were collected by questionnaire interview. Participants self-collected vaginal swab specimens for STI pathogen molecular testing. Logistic regression was used to determine independent association with STI for the two main exposure variables.
Findings: Of 791 AGYW enrolled, 125/786 (15.9%) had an age-disparate partner. 158/789 (20%) reported >=2 partners. Overall, STI pathogens were detected in 434/791 (54.9%; 95% CI 51.3–58.4), including in 52% of those who reported no recent sexual activity. Most participants (85%) with detectable STI were asymptomatic. There were lower odds of STI in those with age-disparate partner, compared to no partner (aOR 0.49; 95% CI 0.27–0.86); but no difference in odds when compared to those with age-concordant partner. Multiple partners increased odds of STI compared to no partner (aOR 1.84; 95% CI 1.23–2.76) or 1 partner only (aOR 2.44; 95% CI 1.50–3.97). However, prediction using the logistic model (probability cutoff 0.5) had only 65% sensitivity for STI, and 60% probability of correct STI classification.
Conclusion: Partner-age disparity was not a risk factor for STI among AGYW; however, recent multiple sex partners was associated with a two-fold increase in STI odds. Considering the high underlying burden of STI among AGYW, the exposure variables investigated were not sufficiently reliable for STI screening. Regular, universal STI screening, preferably using rapid, accurate point-of-care tests would be an important intervention in this population.
PP06.60 – Synthesis and Dissemination of HIV-Related Research Evidence Using the Rapid Response Service
Mr. Ryan LaPenna1, Danielle Giliauskas1, David Gogolishvili1,2
1The Ontario HIV Treatment Network, Toronto, Canada.
2McMaster University, Hamilton, Canada.
Background: Decision makers increasingly seek high quality research evidence but are constrained with limited time and resources. Since 2009, the Ontario HIV Treatment Network (OHTN) operates the Rapid Response Service (RRS), which provides research evidence summaries to inform policy decisions, intervention planning, and adoption of best practices in the HIV sector in Ontario, Canada.
Description: The Rapid Response process starts by collaborating with the requestor to develop research question(s). A systematic search is conducted in relevant electronic database(s). Grey literature, relevant websites, and experts may be also consulted. Key findings from identified literature are synthesized into a concise and clear summary. After incorporating feedback from the requestor, the finalized Rapid Responses are published online at: www.ohtn.on.ca/rapid-responses/ and disseminated among internal and external stakeholders using the OHTN’s communication and dissemination tools (Fig. 1). RRS evaluation has been implemented to inform quality improvement measures. Using Google Analytics, the RRS website also allows ongoing collection of metrics regarding its utilization.
Findings: By December 2024, the total number of published Rapid Responses reached 183. The analysis of the most recent 12-month period (January–December 2024) shows that the total number of pageviews was 95,824. Pageviews vary significantly between the Rapid Responses, and the Rapid Response with the highest pageviews in 2024 was on sexualized drug use (chemsex) among men who have sex with men (n = 11,681). About 40% of all site visits are from within Canada, and the remaining 60% are from about 187 countries worldwide. Since its initiation, the RRS has both informed organizational programming and contributed to service delivery and policy changes at the provincial level.
Conclusion: By synthesizing and disseminating research evidence, the RRS provides a platform to ensure that research is accessible to people living with HIV, policymakers, clinicians, and other stakeholders in the HIV sector in Ontario and beyond.
PP06.61 – Lateralizing Community-Led Health Service Delivery: Integrating Comprehensive Anogenital Health Care Into HIV Programs for Gay, Bisexual, and Other Men Who Have Sex with Men (GBMSM) in Kenya
Dr. Lisa Lazarus1, Samuel Anyula Gorigo2, Pascal Macharia2, Zipporah Mwangangi2, Marissa Becker1, Souradet Shaw1, Stephen Moses1, Parinita Bhattacharjee1,3, Joshua Kimani1,3, John Mathenge2, Lyle R. McKinnon1, Matthew Thomann4, James Blanchard1, Sushena Reza-Paul1, Robert Lorway1
1University of Manitoba, Winnipeg, Canada.
2Health Options for Young Men Against STIs, Nairobi, Kenya.
3Partners for Health and Development in Africa, Nairobi, Kenya.
4University of Maryland, College Park, USA.
Background: Amidst shifting political and funding landscapes for HIV prevention, how do we capitalize on decades of investment in community-led health service delivery for key populations? Lateralization provides a model for a new generation of HIV programs that not only meet the goal of integrative health but expand upon the gains we have made in HIV prevention science. Innovations in community-led HIV care can be lateralized towards addressing other health needs of populations who are often left behind due to criminalization, marginalization, and poverty.
Description: Gay, bisexual, and other men who have sex with men (GBMSM) have only recently begun to be included in HPV screening and vaccination programs. However, in settings where GBMSM are criminalized, they continue to be left out of HPV interventions. In Nairobi, Kenya, GBMSM are presenting for care at extremely late stages of anal disease. In response, Health Options for Young Men Against STIs (HOYMAS), a community-based organization serving GBMSM, lateralized lessons learned from their HIV program towards integrating comprehensive HPV care into their healthcare services.
Findings: Beginning in 2022, HOYMAS, in collaboration with the University of Manitoba, worked to: 1) strengthen anogenital health services in their community clinic through clinician assessment, treatment, and referral; 2) raise awareness on anogenital health through community discussion groups; 3) share knowledge and experiences with clinicians/clinician students working in community-led organizations in 14 counties across the country; and 4) develop standard operating procedures and clinical reporting tools, with government feedback and approval.
Conclusion: Decades of investments in community infrastructure and expertise to respond to the HIV epidemic hold valuable lessons and insights towards addressing other health needs of marginalized populations more widely. Lateralizing community-led health services offers important roadmaps towards ensuring that “no one is left behind”, while capitalizing on the expertise of communities in addressing emerging health needs.
PP06.62 – Barriers and Facilitators to HIV Pre-Exposure Prophylaxis Implementation for Key Populations in India
Ms. Katherine Lewis1, Suchith Kumar2, Jayee Chowdhury3, Sukanta Paul3, Asim Sen3, Akram Pasha4, Bhagyma Lakshmi4, Pranathi Prakash4, Syed Hafeez Ur Rahman4, KT Venukumar4, Sara Piao5, Katarina Scala5, Natasha Glendening6, Dr. Dallas Swendeman5, Dr. Protim Ray3, Dr. Sushena Reza-Paul4, Dr. Anne Fehrenbacher1
1University of Southern California, Los Angeles, United States.
2SK Professional Translation and Transcription Services, Mysore, India.
3Durbar Mahila Samanwaya Committee, Kolkata, India.
4Ashodaya Samithi, Mysore, India.
5University of California Los Angeles, Los Angeles, United States.
6University of California Irvine, Irvine, United States.
Background: India has the second largest HIV epidemic in the world, but HIV Pre-Exposure Prophylaxis (PrEP) has not been implemented into national HIV Targeted Intervention programs. This study aims to identify barriers and facilitators to PrEP implementation and PrEP use in India to inform advocacy and risk reduction programs.
Description: This research was guided by the EPIS Framework for Implementation Science (Exploration, Preparation, Implementation, Sustainment). Individual in-depth interviews were conducted through Durbar Mahila Samanwaya Committee in Kolkata and Ashodaya Samithi in Mysore to explore factors influencing PrEP implementation, including how strategies should be tailored for key populations. Interviews were conducted with 23 external stakeholders and 20 stakeholders internal to Targeted Intervention programs. External stakeholders represented individuals from Indian national, state, and regional agencies; medical practitioners; and individuals from Indian and global non-governmental organizations, universities, and pharmaceutical companies. Interview transcripts were analyzed using deductive thematic coding in Dedoose.
Findings: Institutional Barriers: Participants described a need for operational guidelines on PrEP for Targeted Intervention programs, funding for PrEP efforts, and the need to overcome supply chain challenges. Institutional Facilitators: Stakeholders described community groups for peer educators, raising community awareness, PrEP-related advocacy efforts, and the existing Targeted Intervention programs through which PrEP could be distributed.
Community Barriers: Barriers to PrEP use included stigma towards sex workers and other key populations, some key populations being highly mobile, and concerns about PrEP adherence and potential condom use impacts. Community Facilitators: Participants described the role of existing community-based organizations, peer educators, and community education efforts as facilitators for PrEP use among key populations.
Conclusion: We identified community and institutional level barriers to PrEP implementation in India. We also identified facilitators of PrEP implementation and use which can be leveraged to address existing barriers. Our findings highlight future targets to improve PrEP implementation and advocacy efforts.
PP06.63 – Improving Pre- Exposure Prophylaxis Uptake Among Sexually Transmitted Infections Clients Through Integrated Service Delivery: Lessons from Pre-Exposure Prophylaxis Up! Quality Improvement Collaborative in Blantyre, Malawi
Mrs Suzike Likumbo1
1Ministry of Health, Blantyre district health Office, Blantyre, Malawi.
Background: In 2019, the Malawi Ministry of Health approved oral PrEP for HIV prevention, with widespread rollout in public facilities by 2021. Despite its availability, only one public facility in Blantyre – Malawi’s district with the highest HIV prevalence – had integrated PrEP with Sexually Transmitted Infections (STI) services. A significant number of STI clients were being missed despite being a population at high risk of HIV acquisition. To address this gap, the Blantyre Prevention Strategy (BPS), a collaboration between the Government of Malawi and Georgetown University, launched an STI-focused Quality Improvement Collaborative (QIC) affinity group in 2023. This initiative aimed to increase PrEP uptake among STI clients across 18 facilities, including 4 hospitals and 14 health centers.
Description: A one-day orientation on the affinity group approach was conducted, followed by the establishment of a district-based STI-PrEP affinity group comprissed of STI and PrEP providers. Standardized indicators for STI and PrEP services were introduced. Facilities developed tailored client flow processes and implemented Quality Improvement (QI) changes. Key changes contributing to these outcomes included demand creation for PrEP services, redesigning client flows, peer-to-peer service navigation, and a “same-room, same-provider” service model. The group held monthly virtual meetings, and progress was reviewed quarterly during QIC learning sessions and data was analyzed.
Findings: The integration of PrEP into STI services via the QIC affinity group led to significant improvements. Public facilities offering integrated PrEP-STI services increased from 1 (6%) to 12 (67%) out of 18. PrEP uptake rose by 75% and PrEP initiation among STI clients increasing substantially to 82% from 16%.
Conclusion: Integrating PrEP into existing HIV prevention services, such as STI clinics and QIC affinity group approach is an effective strategy for improving PrEP uptake.
| INDICATORS | PUBLIC FACILITIES | 2023 PERFOMANCE | 2024 PERFOMANCE | |
|---|---|---|---|---|
| Percentage of STI-PrEP services integration | 18 | 1 (6%) | 12 (67%) | |
| Total STI diagnosed | 18 | 19,922 | 18,540 | |
| Total STI clients HIV Negative | 18 | 82.6% | 86.5% | |
| Total PrEP initiations | 18 | 16% | 75% |
PP06.64 – Evaluating the Impact of a Marketing Plan on Sexually Transmitted Infections (STIs) and Sexual Reproductive Health (SRH) Consultations at Ahf Manzini Wellness Centre
Dr. Yves Mafulu1, Sr Khetsiwe Maseko1, Mrs Nonkululeko Dlamini1, Dr. Adele Benzaken, Dr Nkululeko Dube1
1AIDS Healthcare Foundation, Manzini, Eswatini.
Background: STIs in Eswatini represent a significant public health challenge. A study showed a 25% STI rate among HIV-positive females, with asymptomatic cases accounting for nearly 29%. STIs increase the risks of HIV acquisition and cause negative outcomes on the SRH systems. In response, the AHF Manzini Wellness Centre implemented a focused marketing plan aimed at increasing awareness about service provision in the facility. We evaluate the impact of a marketing plan on the rates of STI and SRH consultations.
Description: We used a quantitative approach to assess client attendance from June to December 2024. The marketing strategy included community outreach, educational campaigns, partnerships with local organizations, deployment of outreach vehicles at night to offer services to sex workers, dissemination of educational materials via social networks and social media, and erection of billboards at busy places.
Findings: Client attendance rose from 20 in June to 445 in December. The number of new patients attending STI consultations escalated from 14 to 119, representing an increase exceeding 750%. Sex workers accounted for 11.28% of total clinic attendees in October 2024. Male client numbers surged from 10 in June to 166 in December, and females from 10 to 279. Consultation for syndromic STIs declined from 100% in June to approximately 30% in December, while the demand for SRH and HIV prevention services increased. The Pre-exposure Prophylaxis (PrEP) increased from 14 in June to 101 in December, even reaching 154 in October. Syphilis testing rose from 15 tests in June to 126 by December. Statistical analysis confirmed significant differences in attendance patterns across months (p < 0.05).
Conclusion: These findings underscore the effectiveness of a comprehensive marketing plan in fostering awareness about STIs and SRH services. The findings emphasize the significance of community participation and tailored and diversified communication strategies.
PP06.65 – Organizational Factors Affecting Implementation Effectiveness of Pay-It-Forward Strategy in Improving STI Test-Uptake: A Sequential Mixed Methods Analysis in China
Miss Zixuan Zhu1, PhD Dan Wu2, MD Katherine T. Li3, MD Thomas Fitzpatrick1,4, Miss Liyuan Zhang5, Miss Ye Liu1, PhD Rayner K.J Tan6, Dr. Gifty Marley1, MD Weiming Tang1,7, MD, PhD Rohit Ramaswamy8, MD, PhD Joseph D. Tucker1,7
1University of North Carolina - Project China, Guangzhou, China.
2Nanjing Medical University, Nanjing, China.
3University of California, Los Angeles, Los Angeles, USA.
4University of Washington, Washington D.C, USA.
5Johns Hopkins University, Baltimore, USA.
6National University of Singapore, Singapore, Singapore.
7University of North Carolina at Chapel Hill, Chapel Hill, USA.
8Cincinnati Children’s Hospital Medical Center, Cincinnati, USA.
Background: Pay-it-forward is an evidence-based implementation strategy that offers individuals free STI testing and optional donation opportunities towards providing this service for future participants. We organized a 12-site cluster randomized controlled trial evaluating a chlamydia/gonorrhoea testing pay-it-forward program for Chinese men at public STI clinics and community-based organization (CBO) clinics (NCT05723263). This study is a secondary data analysis of the RCT examining the organizational factors affecting implementation effectiveness.
Description: We organized a sequential mixed methods analysis to identify organizational-level factors associated with implementation effectiveness (test-uptake). Quantitative data were collected from site visits, participant surveys, and clinical records, and analysed using multivariable logistic regression. Qualitative data were collected from 13 semi-structured interviews conducted with 9 health professional implementers from 5 public clinics and 5 staff from 4 CBO clinics. Rapid thematic analysis was applied.
Findings: A total of 800 adult men were recruited into the pay-it-forward intervention arm, with 484 (60.5%) aged over 30, 424 (53%) were MSM, and equal numbers (400,50%) recruited from public and community-based organization (CBO) clinics. Among these, 751/800 (93.9%) of men tested.
Quantitative analysis in Table 1 revealed that the involvement of multiple implementers (e.g., physicians, CBO staff, volunteers) in the implementation significantly increased testing uptake, whereas competing STI testing projects in clinics were negatively associated with uptake. Fast-paced implementation hindered testing in public clinics but facilitated it in CBO settings.
Qualitative data showed that involving multiple implementers fostered team-based work infrastructure that improved adoption and enhanced effectiveness of test uptake. Competing STI projects and fast-paced delivery reduced the intervention fidelity by limiting time and attention for the intervention process. Despite this, CBO settings, with their strong community connections and flexible service integration, may transform fast-paced implementation into a facilitator for intervention effectiveness.
Conclusion: Organizational factors had impacted the implementation effectiveness and diverged across settings.
| Organizational-level factors* | Categories | Test uptake of public clinics | Test uptake of CBO clinics | |||||
|---|---|---|---|---|---|---|---|---|
| aOR | 95% CI | P value | aOR | 95% Cl | P value | |||
| Number of implementers delivering PIF strategy | 1 | Ref. | Ref. | |||||
| 2 and above | 10.2 | 2.53-41.10 | 0.001 | 43.7 | 5.92-322.04 | 0.001 | ||
| Has competing STI testing projects | No | Ref. | Ref. | |||||
| Yes | 0.07 | 0.01-0.57 | 0.013 | 0.02 | 0.01-0.17 | 0.001 | ||
| Implemented fast-paced intervention | No | Ref. | Ref. | |||||
| Yes | 0.07 | 0.01-0.57 | 0.013 | 176.89 | 22.84-1369.93 | 0.001 | ||
*Logistic models were adjusted for age group, income, education, marriage status, MSM. Multiple implementers were defined as more than one full-time physicians joined in the implementation in public clinics, and more than one staff joined in the implementation (volunteers included) in CBO clinics. Competing projects were defined as similar STI testing projects, i.e. Gonococcal AMR or Surveillance project; Fast paced implementation was defined as averagely less than 10/min per visit in public clinics and averagely less than 30/min per visit in CBO clinics.
PP06.66 – Adaption and Implementation of a Collective Intelligence-Based Participatory COVID-19 Surveillance in Accra, Ghana: Implications for STI Programs
Dr. Gifty Marley1, Dr Phyllis Dako-Gyeke2, Dr Sean Sylvia3
1UNC at Chapel Hill - Project China, Guangzhou, China.
2University of Ghana, Legon/Accra, Ghana.
3University of North Carolina at Chapel Hill, Chapel Hill, USA.
Background: Infectious disease surveillance is difficult in many low- and middle-income countries. Information market (IM)–based participatory surveillance (IM surveillance) is a crowdsourcing method that encourages individuals to actively report health symptoms and observed trends by trading web-based virtual “stocks” with payoffs tied to a future event. We assessed the feasibility and acceptability of a tailored IM surveillance system to monitor population-level COVID-19 outcomes in Accra, Ghana.
Methods: Using a mixed methods study approach, we designed and evaluated a prediction markets IM system from October to December 2021 among healthcare workers and community volunteers aged ≥18 in Accra. Participants received 10,000 virtual credits to trade on 12 questions on COVID-19–related outcomes. Payoffs were tied to the cost estimation of new and cumulative cases in Greater Accra and nationwide at specified future time points. Phone credits were awarded based on the tally of virtual credits left and percentile ranking. In-depth interviews explored the factors associated with user journey experience, feasibility, and acceptability.
Findings: Of 105 invited participants, 36 signed up, and 21 (58.3%) traded at least once on the platform. The average age of traders was 28 years (SD = 5.2). Estimating the national-level number of COVID-19 cases received the highest trades (13 to 19) and obtaining COVID–19–related information mainly from television and radio was negatively associated with trading (marginal effect: −0.184). Active trading by friends with a communal discussion about the trades facilitated reach. 6/10(60%) interviewed participants signed up because their friends participated, and 5/10 (50%) believed friends/family would be more trusting and willing to try trading. Interviewed participants found the onboarding process effective and agreed that seeing others engaged on the platform motivated their continued trading.
Conclusion: Implementing IM surveillance for infectious diseases was feasible and successful and has significant potential for STI incidence and prevention program surveillance in LMICs with limited monitoring resources.
PP06.67 – Integrating Screening for Curable Sexually Transmitted Infections in Antenatal Care in Zimbabwe: A Mixed Methods Process Evaluation
Dr. Kevin Martin1,2, Dr. Constance RS Mackworth-Young1,2, Dr. Chido Dziva Chikwari1,2, Ethel Dauya2, Rangarirayi Nyamwanza2, Professor Joseph D Tucker1, Dr Victoria Simms1,2, Tsitsi Bandason2, Dr. Francis Ndowa3, Dr. Leolin Katsidzira4, Dr. Owen Mugurungi5, Anna Machiha5, Professor Remco Peters6,7,8, Professor Michael Marks1,9,10, Professor Katharina Kranzer1,2,11, Professor Rashida A Ferrand1,2
1London School of Hygiene & Tropical Medicine, London, United Kingdom.
2The Health Research Unit Zimbabwe, Biomedical Research and Training Institute, Harare, Zimbabwe.
3Skin and Genito-Urinary Medicine Clinic, Zimbabwe.
4University of Zimbabwe, Zimbabwe.
5AIDS and TB Unit, Ministry of Health and Child Care, Zimbabwe.
6Foundation for Professional Development, South Africa.
7University of Pretoria, South Africa.
8University of Cape Town, South Africa.
9Hospital for Tropical Diseases, University College London Hospital, United Kingdom.
10University College London, United Kingdom.
11LMU University Hospital, LMU Munich, Germany.
Background: Sexually transmitted infections (STIs) in pregnancy are associated with adverse birth outcomes. In resource-limited settings syndromic management of STIs is used. As such, most STIs, being asymptomatic, are not identified. We conducted a mixed methods process evaluation to investigate an integrated strategy of point-of-care screening for Chlamydia trachomatis, Neisseria gonorrhoeae, Trichomonas vaginalis, syphilis, hepatitis B virus (HBV) and HIV screening in antenatal care (ANC) in Zimbabwe.
Methods: A prospective interventional study was conducted in two public-sector ANC clinics in Harare. Clients attending for ANC were screened for C. trachomatis, N. gonorrhoeae, T. vaginalis, syphilis, HBV, and HIV, using point-of-care tests. Uptake of screening and treatment was calculated. Interviews (n = 57) and group discussions (n = 2) with pregnant women, healthcare professionals, and the intervention team were conducted and analysed thematically. Implementation, mechanisms of impact, and context were explored using the MRC Process Evaluation Framework (Fig. 1).
Results: There were 13,500 ANC attendances over 207 implementation days. Of 1105 (8.2%) women assessed for eligibility, 1103 (99.8%) were eligible, of whom uptake of the full screening package was 91.0% (1004/1103). Although the intervention was highly acceptable, recruitment was limited by workload and diagnostic capacity of the GeneXpert device for C. trachomatis/N. gonorrhoeae. Furthermore, the testing of multiple sample types with different tests, with a range of reading times, was challenging. Finally, implementation occurred within an overburdened healthcare system, and integration with routine care was inhibited by a reliance on regularly changing locum staff.
Conclusion: Despite high levels of acceptability, current technological limitations likely preclude this screening strategy from being scaled beyond low-throughput settings. Future priorities include the development of STI point-of-care tests with shorter analytic times alongside consideration of alternative strategies involving laboratory-based high-throughput testing. Furthermore, given the significant structural and financial barriers, our data underline the need for more resources to address STI screening for pregnant women.
Diagram showing the interaction of the themes and sub-themes with the process evaluation domains and the pathway to impact.
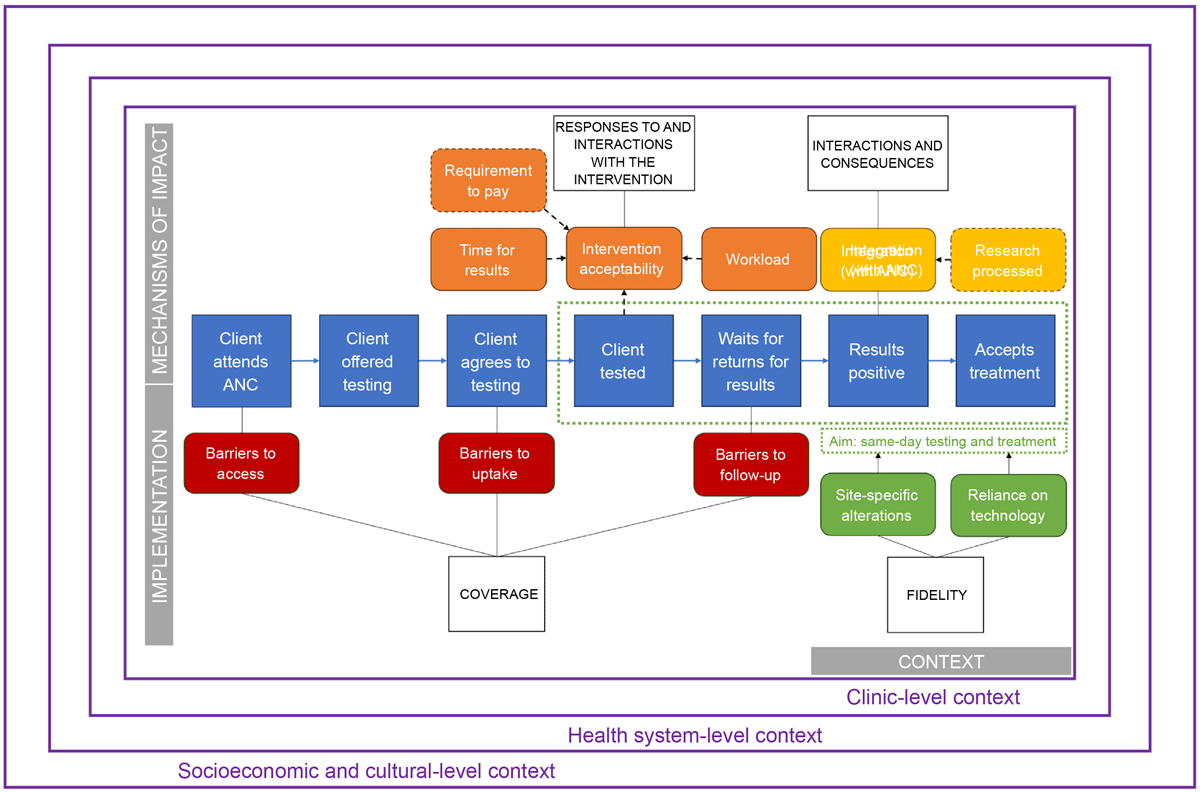
PP06.68 – The Malawi WHO Enhanced Gonococcal Antimicrobial Surveillance Program – Implementation and Results 2023–2024
Dr. Mitch Matoga1, Dr. Jane Chen2, Mr. Edward Jere1, Dr. Gomezgani Lukhanda1, Mr. Claightone Chirombo1, Mrs. Beatrice Ndalama1, Mrs. Naomi Bonongwe1, Mrs. Esther Mathiya1, Mrs. Naomi Nyirenda1, Mr. Gabriel Banda1, Mr. Robert Krysiak2, Mr. James Kaphatika1, Dr. Daniel Golparian3, Prof. Magnus Unemo3, Dr. Ismail Maatouk4, Prof. Irving Hoffman2
1University of North Carolina Project Malawi, Lilongwe, Malawi.
2UNC Department of Medicine, Division of Infectious Diseases, Chapel Hill, United States.
3The WHO Collaborating Centre for Gonorrhea and other Sexually Transmitted Infections, Orebro, Sweden.
4The Department of Global HIV, Hepatitis and STI Programmes, World Health Organization, Geneva, Switzerland.
Malawi has a rich history of antimicrobial resistance (AMR) surveillance for Neisseria gonorrhoeae (NG) including tests of cure (TOC). Since 2023, Malawi has participated in the global WHO enhanced gonococcal antimicrobial surveillance program (EGASP).
Each year, men ≥18 years presenting with purulent urethral discharge (UD) at Bwaila Hospital’s STI clinic in Lilongwe are recruited. Gram staining is performed from a urethral swab and men with Gram-negative intracellular diplococci are enrolled. After enrollment, culture from a second urethral swab, antimicrobial susceptibility testing using Etest, and whole genome sequencing are performed. Per Malawian guidelines, participants are treated syndromically with gentamicin 240 mg IM stat, doxycycline 100 mg orally twice daily for 7 days and metronidazole 2 g orally as a single dose. Participants are invited for a TOC visit 14 days post-enrollment for evaluation of clinical and microbiological cure. Data is collected using Open Data Kit and uploaded to the WHO NET data platform.
During year 1 (2023/24), 126 men were enrolled. The mean age was 31 years (±SD 8), 4% (5/126) were HIV co-infected. 122/126 (97%) had culture confirmed NG isolates saved. 112/122 (92%) returned for a TOC-1 and 9 (8%) were symptomatic and were re-treated with gentamicin and doxycycline (n = 7) or ceftriaxone 1g IM stat and azithromycin 1g orally as a single dose (n = 2). 8/122 (7%) remained culture positive (6 symptomatic, 2 asymptomatic). Of these, 5 returned for TOC-2 and all were culture negative and asymptomatic. Using the EGASP standardized alert values, all isolated were fully susceptible to ceftriaxone, cefixime, azithromycin and gentamicin (Table 1).
Full susceptibility of NG isolates to cephalosporins and azithromycin is encouraging as it provides treatment options for Malawi. Despite full in vitro susceptibility to gentamicin, we observed suspected clinical treatment failures, highlighting the lack of reliable standards for the classification of resistance for gentamicin.
| Antimicrobial susceptibility testing | Total NG isolates (%) | |
|---|---|---|
| MIC Ceftriaxone | ||
| ≤0.125 mg/L | 122 (100%) | |
| >0.125 mg/L | 0 (0%) | |
| MIC Cefixime | ||
| ≤0.125 mg/L | 122 (100%) | |
| >0.125 mg/L | 0 (0%) | |
| MIC Azithromycin | ||
| ≤1 mg/L | 122 (100%) | |
| >1 mg/L | 0 (0%) | |
| MIC Gentamicin | ||
| ≤16 mg/L | 122 (100%) | |
| >16 mg/L | 0 (0%) | |
| MIC Ciprofloxacin* | ||
| ≤0.06 mg/L | 26 (21%) | |
| >0.06 mg/L | 94 (77%) |
*2 specimens were not tested for Ciprofloxacin antimicrobial susceptibility due to
NG – Neisseria gonorrhoeae.
MIC – minimally inhibitory concentration.
PP06.69 – Targeted Syphilis Screening Initiative in an Urban Academic Emergency Department Provides Access to Diagnosis and Treatment Among Key Populations
Mrs Cammeo Mauntel-Medici1, Mrs Anjana Maheswaran1, Miss Riley Hunt1, Mr Andrew Trotter, Ms Janet Lin, Ms Samantha Hay
1UI Health/University of Illinois at Chicago, Chicago, United States.
Background: The U.S. is facing a Syphilis epidemic, with a 2,140% increase in incidence between 2000 and 2020 and a tenfold increase in congenital syphilis between 2012 and 2022. The UI Health Emergency Department (ED) began offering targeted Syphilis screening in order to provide timely diagnosis and access to treatment to key populations with limited healthcare access.
Description: From May 16 to October 16, 2024, ED patients meeting CDC syphilis screening criteria and women ages 13–40 had a provider alert for a treponemal test using the reverse Syphilis testing algorithm. All patients with positive or equivocal treponemal test results were chart reviewed to determine treatment history and status of presumed active infection (PAI). Patients with no documentation of treatment were contacted by a patient navigator, ED PharmD, or provider for result notification and linkage to treatment.
Findings: During the study period, ED Syphilis screening increased by 384% compared to the 5 months prior. 11% of ED patients aged 13 and over met the screening criteria, triggering 1686 automated provider alerts for 1590 unique patients, and resulting in 1089 (68%) unique treponemal tests (57% women and 43% men) and 55 abnormal results (5% positivity rate). Among those with abnormal results, 14 were determined to have PAI, including 7 (50%) women of childbearing age. Of the 14 patients with PAI, 3 received empiric treatment in the ED, 5 received treatment during hospital stay, 1 was linked to outpatient treatment, 1 returned to the ED for treatment, 3 were unreachable, and 1 was pending follow-up titer testing.
Conclusions: ED Syphilis screening and linkage to treatment is feasible and offers opportunities to identify key populations in need of diagnosis and treatment. Notification of results and gathering treatment history to interpret results after discharge can be challenging due to poor contact information.
PP06.70 – An Innovative Virtual Testing Approach for HIV and Other Sexually Transmitted Infections
Ms. Michaela A Maynard1,4, Alexi Almonte2, Thomas Betrand3, Dr. Philip A Chan1,2,3,4
1Open Door Health, Providence, United States.
2Brown University Health, Providence, United States.
3Rhode Island Department of Health, Providence, United States.
4Department of Medicine, Brown University, Providence, United States.
Background: Sexually transmitted infections (STIs) including HIV continue to be a significant burden across the United States and elsewhere. Novel approaches to increasing access to HIV/STI testing are needed.
Methods: The Testing 1-2-3 Program in Rhode Island is a collaboration between the Rhode Island Department of Health (RIDOH) and local clinical partners. The program allows asymptomatic people to request HIV/STI testing online via a secure form. The platform is bilingual and generates a physician-signed laboratory order for testing (HIV, HCV, syphilis, gonorrhea, and chlamydia) under standing orders at any walk-in lab location across the state associated with any clinic (>70 sites). Symptomatic patients or those with clinical concerns are referred to a network of community-based clinics which offer sexual healthcare services. The Testing 1-2-3 Program was promoted through social media and internet dating sites. We evaluate program use from January 1, 2022 to December 31, 2024.
Results: A total of N = 1,002 people requested HIV/STI testing during the time period. Of these, 446 (44.5%) completed testing, and 9 (2.0%) were positive (77.8% (N = 7) Chlamydia, 11.1% (N = 1) Gonorrhea, 11.1% (N = 1) Syphilis, 0% HIV, 0% HCV). Participants ranged in age from 18–74 years (median 30 years). 56.8% of people identified as male, while 39.7% identified as female and 2.3% identified as another gender identity. Of people who requested HIV/STI testing, 22.9% reported a prior STI diagnosis, 9.3% reported 5+ sexual partners, 4.6% reported using inhalants (poppers), 12.1% reported condomless receptive anal sex, 21.2% reported sex while intoxicated, and 15.2% reported sex with an anonymous partner. All individuals who tested positive were successfully linked to clinical care.
Conclusions: Individuals engaging in a virtual HIV/STI testing program reported significant behaviors associated with HIV/STI infection. Virtual testing offers improved access for HIV/STI care and prevention.
PP06.71 – Development and Evaluation of an Algorithm to Identify Doxycycline Prescribed for STI Prevention (DoxyPEP) from Clinical Databases
Dr. Abigail G. Fessler1, Dr. Tim Menza1, Dr. Patrick S. Sullivan2, Dr. Susan P. Buchbinder3, Dr. Anne F. Luetkemeyer4, Dr. Connie Celum1
1University of Washington, Seattle, United States.
2Emory University, Atlanta, United States.
3San Francisco Department of Public Health, San Francisco, United States.
4University of California, San Francisco, United States.
Background: Doxycycline post-exposure prophylaxis (doxyPEP) reduces the risk of gonorrhea, chlamydia, and syphilis in men who have sex with men and transwomen. Research on doxyPEP’s population impact is hindered by non-standardized prescribing practices, complicating extraction and measurement of doxyPEP data. We developed an algorithm to identify doxyPEP prescriptions in clinical databases, supporting research on this STI prevention strategy.
Methods: We performed a retrospective chart review of a random sample of doxycycline prescriptions at the Madison HIV clinic in Seattle, WA from October 2023–October 2024. We reviewed prescriptions for dosing schedule, dose, refills, dispense quantity, and ICD codes, classifying each prescription as “doxyPEP” or “non-doxyPEP” based on prescriber documentation. DoxyPEP predictors were identified two ways: 1) characteristics appearing in >10% of prescriptions with a significant difference in usage between doxyPEP and non-doxyPEP prescriptions (chi-square p < 0.01) were iteratively combined and tested for predictive accuracy; 2) machine learning was used to identify influential variables and train a random forest classifier, a model that leverages decision trees to predict outcomes based on key data features.
Results: In review of 200 doxycycline prescriptions, the highest accuracy algorithm (98.0% accuracy, 98.1% sensitivity, 97.8% specificity) utilized inclusion criteria of as-needed dosing schedule (i.e. “As directed”, “Daily as-needed”, and “Once as-needed”), 1 or 2 refills, and 200 mg dose, with an exclusion criterion of dispense quantity of 14. Eighteen ICD codes were associated with doxyPEP prescriptions, but their inclusion did not improve model accuracy. The random forest classifier, using dose and frequency, demonstrated a similar accuracy (97.5%), sensitivity (96.2%), and specificity (98.9%).
Conclusion: Identification of doxycycline prescribed for STI prevention from clinical databases is essential for evaluating doxyPEP implementation, including through a doxyPEP-to-need ratio. As-needed dosing schedule, 200 mg dose and the presence of refills can accurately identify doxyPEP prescriptions, enabling better monitoring of this public health intervention.
| DoxyPEP N = 107 n (%) | Non-DoxyPEP N = 93 n (%) | P-value | ||
|---|---|---|---|---|
| Dosing Schedule | ||||
| As directed | 27 (100%) | 0 (0%) | <0.01 | |
| Daily as needed | 29 (100%) | 0 (0%) | <0.01 | |
| Once as needed | 36 (100%) | 0 (0%) | <0.01 | |
| Twice daily | 4 (4.3%) | 88 (95.7%) | <0.01 | |
| Other | 11 | 5 | ||
| Dose | ||||
| 100mg | 7 (7.1%) | 92 (92.9%) | <0.01 | |
| 200mg | 77 (98.7%) | 1 (1.3%) | <0.01 | |
| Other | 23 | 0 | ||
| Refills | ||||
| 0 | 22 (20.0%) | 88 (80.0%) | <0.01 | |
| 1 | 36 (97.3%) | 1 (2.7%) | <0.01 | |
| 2 | 31 (100%) | 0 (0%) | <0.01 | |
| 3+ | 18 | 4 | ||
| Dispense Quantity | ||||
| 14 | 0 (0%) | 64 (100%) | <0.01 | |
| 30 | 52 (96.3%) | 2 (3.7%) | <0.01 | |
| 60 | 38 (88.4%) | 5 (11.6%) | <0.01 | |
| Other | 17 | 22 |
PP06.72 – Dual Rapid HIV/Syphilis Tests Have the Potential to Increase Syphilis Screening Coverage Among Pregnant Women in Botswana
Ms. Aamirah Mussa1,2, Ms Anjana Baradwaj3, Ms Neo Ndlovu1, Ms Lefhela Tamuthiba1, Ms Maipelo Tsuaneng1, Mr Bame Bame1, Dr Natasha Martin3, Dr Jeffrey Klausner4, Dr Chelsea Morroni1,5, Dr Adriane Wynn
1Botswana Harvard Health Partnership, Gaborone, Botswana.
2Usher Institute, The University of Edinburgh, Edinburgh, United Kingdom.
3University of California, San Diego, California, USA.
4University of Southern California, California, USA.
5Centre for Reproductive Health, The University of Edinburgh, Edinburgh, United Kingdom.
Background: Dual rapid HIV/syphilis diagnostic tests present an opportunity to close the gap between antenatal syphilis and HIV screening coverage. We assessed uptake and preferences related to dual rapid HIV/syphilis screening among pregnant women in Botswana and compared time to results and treatment between rapid syphilis screening and the standard-of-care.
Methods: The study was conducted in Gaborone, Botswana (October 2022–August 2023) in two antenatal clinics, one intervention clinic and one standard-of-care clinic. Pregnant women aged ≥15, ≤27 weeks’ gestation and attending first antenatal care were eligible. In the intervention clinic, dual rapid HIV/syphilis or single rapid syphilis screening (SD BIOSENSOR Korea) was offered. Participants in both clinics received routine syphilis (lab-based VDRL/RPR tests) and HIV screening. Screening results and treatment were assessed through record abstraction.
Results: Among 404 eligible women, 400 enrolled. The four who declined were in the intervention clinic representing an uptake rate of 98% (200/204). Most participants (97%, 361/372) preferred rapid testing over delayed methods, and 89% (278/312) favoured dual HIV/syphilis over single tests. Among those who received rapid syphilis screening (n = 200), all received same-day results, and 100% (n = 5) with a reactive result were treated within 2 days; 60% same-day. Routine VDRL/RPR syphilis screening coverage within one month of the first antenatal care visit was 48% (95/198) and 53% (106/200) in the standard-of-care and intervention clinics, respectively. Routine HIV screening coverage was 99%. Stockouts of laboratory reagents were the main barrier to VDRL/RPR screening. In a historical cohort of 500 pregnant women receiving care in the study clinics between September 2021–April 2022, three had a reactive VDRL/RPR test. Average time to treatment was 47 days (range 2-112).
Conclusion: Integrating syphilis screening with routine rapid HIV screening during antenatal care may leverage the existing infrastructure and prioritization of HIV services to decrease the syphilis screening gap during pregnancy.
PP06.73 – Assessing Knowledge and Practice Change Associated with Two Experiential Sexual Healthcare Training Models in the Southeastern United States
Ms. Jennifer Nall1,2,3, Dr. Stefania Carmona3,4, Ms. Katherine White3,4, Dr. Kristal Aaron3,4, Ms. Aiesha Gentry3,4, Mr. Joshua O’Neal3,4, Dr. Candice McNeil1,2,3, Dr. Nicholas Van Wagoner3,4
1Wake Forest University School of Medicine, Winston Salem, United States.
2Guilford County Department of Public Health, Greensboro, United States.
3Southeast STI/HIV Prevention Training Center, Birmingham, United States.
4University of Alabama at Birmingham Heersink School of Medicine, Birmingham, United States.
Background: Effective provider training in sexual healthcare is critical to improving screening and management of sexually transmitted infections (STIs) in the Southeastern United States, a region with high STI/human immunodeficiency virus (HIV) morbidity. The Southeast STI/HIV Prevention Training Center (SE PTC) has utilized two experiential training models, Foundations of STI/HIV Management Intensive through the University of Alabama at Birmingham (UAB) and North Carolina (NC) New Public Health STI Provider Training, to enhance knowledge and skills in the screening, management, and prevention of STIs/HIV.
Description: Training programs are in-person and cover obtaining respectful, age-appropriate sexual history with cultural humility and trauma-informed care, diagnostic test selection and interpretation, the comprehensive STI physical examination, evidence-based treatment, and patient education and counseling. Pre/post assessments of STI/HIV knowledge and practice are conducted with each training. The Foundations Intensive program, delivered over multiple days, takes place at UAB and local health departments. The NC Public Health program, conducted over 1–2 days at a local health department, covers both clinical and laboratory competencies designated by the state STI program (Fig. 1).
Findings: June 2022–December 2024 pre/post training knowledge assessments were analyzed. Both training models showed increases in participants’ knowledge of STIs/HIV including hands-on components such as history taking and completing an appropriate physical examination. Pre/post answers reflected an increase in knowledge of epidemiology, symptomology, diagnosis, and treatment of STIs/HIV.
Conclusion: Experiential training models offer a unique opportunity to enhance sexual health provider knowledge and skills. Overall, training sessions conducted by the SE PTC have enhanced the participants’ ability to conduct comprehensive sexual health assessments and manage STIs. The presented models create an opportunity to identify best practices for effective experiential training and monitoring practice change. Improving these programs may sustain and bolster the confidence and competence of sexual health providers and contribute to better public health outcomes.
PP06.74 – Optimizing Pre-Exposure Prophylaxis (PrEP) Continuity Through Locator Information Among Cis-Gender Women of Childbearing Age at Four Facilities in Eastern Province, Zambia
Dr. Liswani Khutwelo Nyau1, Justine Nkaama1, Melinda Luhana1, Dr. Mathew Ng’ambi1
1Eastern Provincial Health Office - Ministry of Health, Chipata, Zambia.
Background: Primary prevention of HIV among women of childbearing potential through Pre-exposure prophylaxis (PrEP) is a key intervention in eliminating vertical transmission. PrEP interruption, however, remains a concerning gap among this population in the HIV program in Zambia. One strategy to improving PrEP continuity is the utilization of PrEP recipients’ locator information. Locator information enhances follow-up and optimizes communication between providers and recipients of PrEP. Recipients may be followed-up for many reasons, including pre-appointment reminders and missed appointment. Here, we describe the effect of locator information utilization in augmenting PrEP continuity in four facilities of the Eastern Province of Zambia.
Methods: March 2024 SmartCare and facility program data from four facilities was reviewed. Counts of age-specific female PrEP recipients scheduled for a PrEP refill appointment between January and March 2024 were categorized into two subgroups: with locator information and without locator information. Demographic characteristics of PrEP recipients and their appointment outcomes were summarized by descriptive statistics. Differences in appointment outcomes between the two subgroups were assessed using Chi-square test. Correlation analysis was used to demonstrate relationship between appointment outcome and locator information status.
Results: Eight hundred and eighty-seven (887) PrEP recipients, with median age within the 19–34 years age band were scheduled for a PrEP refill appointment. 58% (513) had locator information on record, while 42%, representing 374 did not. PrEP continuity (97%; 498/513) was significantly higher among this subgroup compared to 16% (61/374) among PrEP recipients without locator information (P < 0.001). There was strong association between locator information and kept appointments (r = 0.83).
Conclusions: This analysis demonstrates the positive association between locator information utilization and favorable appointment outcomes among PrEP recipients, underscoring the utility of locator information in supporting PrEP continuity. Increased investment in and scale-up of locator information utilization is recommended in averting PrEP interruptions in resource limited settings.
PP06.75 – Locator Information Utilization: A Retention Strategy to Improving Antiretroviral Treatment Continuity at Four Health Facilities in Eastern Province, Zambia
Dr. Liswani Khutwelo Nyau1, Justine Nkaama1, Dr. Mathew Ng’ambi1
1Eastern Provincial Health Office - Ministry of Health, Chipata, Zambia.
Background: By March 2024, the Zambia HIV response reached more than 94% of people living with HIV (PLHIV) with antiretroviral therapy (ART). However, among those not on treatment were people who had started ART but had treatment interruption. Efforts supporting treatment continuity and optimal viral suppression for PLHIV remain critical to improving health outcomes and attaining epidemic control. We will assess the usage of locator information and its effect on treatment continuity in four facilities of the Eastern Province of Zambia.
Methods: Retrospective review of March 2024 SmartCare data was conducted. RoCs scheduled for pharmacy appointment between January and March were categorized into two subgroups: with and without locator information. Appointment outcomes were evaluated 28 days post-appointment date. Treatment interruption was defined as missing an appointment for more than 28 days. Demographic characteristics and appointment outcomes were summarized by descriptive statistics. Chi-square test, P < 0.05 statistical significance, was utilized to assess inter-group differences in appointment outcomes. Correlation analysis was done between locator information and kept appointments.
Results: A total of 8170 RoCs, median age within the 25–34 years age band, 57% were females, were scheduled for an appointment. Among these, 6536 (80%) had locator information, while 1634 (20%) did not. Of 6502 (99%) with locator information pre-reminded of their appointment, 6128 (94%) kept their appointment. Among 408 (6%) who missed appointment and were followed up, a total of 403 (99%) were retained in care. Pre and post-appointment follow-ups were more successful among those with locator information (P < 0.001). Treatment continuity (99%; 6531/6536) was significantly higher among this subgroup compared to those (9%;143/1634) without locator information (P < 0.001). There was strong correlation between locator information and kept appointments (r = 0.91).
Conclusions: These results show positive association between locator information use and favorable appointment outcomes among RoCs, highlighting the usefulness of locator information in supporting treatment continuity.
PP06.76 – Utility of Pre-Exposure Prophylaxis in Averting Postnatal Seroconversion Among Infants Born from Breastfeeding Mothers Testing HIV Negative at Delivery in Four Facilities of Eastern Province of Zambia
Dr. Liswani Khutwelo Nyau1, Justine Nkaama1, Melinda Luhana1, Joseph Tembo1, Dr. Mathew Ng’ambi1
1Eastern Provincial Health Office - Ministry of Health, Chipata, Zambia.
Background: In Zambia, HIV negative pregnant and breastfeeding women require routine HIV retesting as part of elimination of mother-to-child transmission (EMTCT). Pregnant women attending antenatal are retested during these visits. After delivery, however, postnatal mothers often elude HIV retesting. In such settings, maternal postpartum HIV acquisition contributes to a significant proportion of infants with HIV. Pre-exposure prophylaxis (PrEP) is a safe and effective prevention strategy to reduce women‘s risk of HIV in pregnancy and postpartum. We will describe and assess the utility of PrEP in averting seroconversion among infants born from breastfeeding mothers testing HIV negative at delivery.
Methods: This retrospective review utilized 2021 program data from SmartCare. The data included counts of HIV negative breastfeeding women (BFW) which we categorized into those receiving PrEP and those not receiving PrEP. Descriptive statistics were used to summarize demographic characteristics of the BFW and the mother-infant HIV status outcomes at 24 months postnatal. Chi-square test was employed to assess differences in the mother–infant HIV status outcomes between the two subgroups. Statistical significance was set at P < 0.05.
Results: In December 2021, 261 (27%) BFW were receiving PrEP, while 704 (73%) were not. Maternal seroconversion was significantly lower among the PrEP cohort at 0.8%, compared to those not on PrEP (4%) (P < 0.001). Similarly, infant seroconversion was not observed in the infants of seroconverted mothers from the PrEP cohort, but was significant (21%) among infants from mothers who seroconverted and not receiving PrEP (P < 0.001).
Conclusions: Though only 27% of PBW during the review period were receiving PrEP, this analysis shows low postnatal maternal incident HIV and vertical transmission outcomes. In contrast, unfavourable HIV serostatus outcomes persisted among BFW not receiving PrEP and their infants. These findings underscore the critical role of PrEP services in complementing other interventions to optimize EMTCT efforts.
PP06.77 – Leaving no Child Behind: Sungani Bana, a Local Initiative to Optimize Paediatric and Adolescent HIV Treatment Outcomes in Eastern Province of Zambia
Dr. Liswani Khutwelo Nyau1, Kevile Fred1, Dr. Wezi Mutambo1, Dr. Mathew Ng’ambi1
1Eastern Provincial Health Office - Ministry of Health, Chipata, Zambia.
Background: In Zambia, attaining optimal viral load coverage (VLC) > 95% and suppression (VLS) >95% among children and adolescents living with HIV (CALHIV) has been a concerning gap. One strategy to improve VLC and VLS among CALHIV is the Sungani Bana (SB) initiative. SB is a child-centered community case management strategy to improve HIV treatment outcomes. Case management is done by trained caseworkers from the local health facilities, who support the CALHIV through monthly home visits, appointment reminders, TB-screening, and nutrition assessments. We will describe and assess the effect of Sungani Bana on VLC and VLS among C/ALHIV in the Eastern Province.
Method: Program data from four consecutive years was utilized for this retrospective review. This included baseline data for the year prior to SB implementation and 3 years following implementation. Treatment outcomes, measured by VLC and VLS, before and after implementation were determined, compared and evaluated using Chi-square test, with P < 0.05 statistical significance.
Results: Pre-implementation, 2,996 CALHIV were reported in care in September 2021, with 81% VLC and 89% VLS. In the first year of SB initiative, with 2,590 CALHIV enrolled, VLC and VLS increased to 90% and 96% respectively. A further increase in the treatment outcome indictors was registered by September 2023, with 92% VLC, 97% VLS and a total of 2,550 CALHIV enrolled in the initiative. By the end of the third implementation year in September 2024, with a total enrollment of 3,103 CALHIV, VLC and VLS were documented at 95% and 98% respectively, representing a significant increase (P < 0.007) in both VLC (14%) and VLS (9%) from baseline data.
Conclusion: These results demonstrate the effectiveness of a child-centered community case management strategy in optimizing paediatric and adolescent HIV treatment outcomes. Increased investment in Sungani Bana is recommended as part of the efforts to ending AIDS in children.
PP06.78 – Resilience in the Face of Violence: FSWs Combating GBV in Benue State
Mrs Chukwudera B Okeke1, Ms Becky Gbihi1, Ms Onyinyechi Chidozie1, Mr Okechukwu Maduabum1
1CWIDI, Makurdi, Nigeria.
Background: Female Sex Workers (FSWs) in Benue State have an HIV prevalence rate 10 to 15 times higher than the general population, compounded by their frequent exposure to gender-based violence (GBV). GBV increases their vulnerability to HIV. To address these challenges, Concerned Women International Development Initiative (CWIDI) has implemented GBV activities within its HIV prevention, treatment, and care program.
Description: CWIDI’s GBV reporting, prevention, and care program aims to empower FSWs through psychosocial education, capacity building, and legal support. The initiative improves FSWs’ understanding of their legal rights, de-normalizes GBV, and strengthens reporting pathways. Survivors of GBV receive legal and psychosocial services, and advocacy sessions are held with justice sector actors, including the National Human Rights Commission, to create a more survivor-centered system.
Findings:
From 2022 to 2023, 63 GBV cases were reported by FSWs, categorized as follows:
| Type of Violence | Number of Cases | Percentage | |
|---|---|---|---|
| Physical Assault | 35 | 55.6% | |
| Sexual Violence | 12 | 19.0% | |
| Social Violence: | 10 | 15.9% | |
| Emotional Violence | 6 | 9.5% |
Of the 12 cases of sexual violence, 100% of survivors underwent HIV and STI testing, with no HIV cases recorded but 3% treated for other STIs. Two survivors (16.7%) reported within 24 h and received post-exposure prophylaxis (PEP). Advocacy sessions engaged eight authorities, and 300 FSWs participated in capacity-building programs on GBV, enhancing awareness and resilience.
Conclusions/Next Steps: Despite progress, GBV remains a barrier to HIV prevention among FSWs in Benue. In 2025, CWIDI will expand its GBV reporting network to six local government areas, incorporate community leaders, and strengthen referral systems and national advocacy efforts.
PP06.79 – Optimal Testing Frequency for Sexually Transmitted Infections Among Men Who Have Sex with Men and Transgender Women Who Use HIV Pre-Exposure Prophylaxis in Australia, Thailand and Brazil: A Cost-Effectiveness Analysis
Dr. Rui Zhao1, Dr. Maeve Mello2, Dr. Pâmela Gaspar3, Dr. Angelica Miranda4, Dr. Nittaya Phanuphak5,6, Dr. Philippe Mayaud7, Dr. Angela Freitas8, Dr. Katia Bassichetto9, Dr. Maria Veras10, Dr. Daniel McCartney7, Mr. Jiajun Sun1, Dr. Hao Lai1, Dr. Jason Ong1,11,12,13, Prof. Dr. Jason Ong1,11,12,13, Dr. Lei Zhang1,11,12
1China-Australia Joint Research Center for Infectious Diseases, School of Public Health, Xi’an Jiaotong University Health Science Center, Xian, China.
2Global HIV, Hepatitis and STI Programmes, World Health Organization, Geneva, Switzerland.
3Departamento de HIV/AIDS, Tuberculose, Hepatites Virais e Infecçoes Sexualmente Transmissíveis, Secretaria de Vigilância em Saúde e Ambiente, Ministério da Saúde, Brasilia, Brazil.
4Departamento de Medicina Social, Universidade Federal do Espírito Santo, Espírito Santo, Brazil.
5Institute of HIV Research and Innovation, Bangkok, Thailand.
6Center of Excellence in Transgender Health, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand.
7Clinical Research Department, London School of Hygiene & Tropical Medicine, London, United Kingdom.
8Departamento de Infectologia e Medicina Tropical, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, Brazil.
9Faculty of Medical Sciences of Santa Casa de São Paulo, São Paulo, Brazil.
10Faculdade de Ciências Médicas da Santa Casa de São Paulo, São Paulo, Brazil.
11School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
12Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
13Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: PrEP is highly effective in preventing HIV, but not other STIs in MSM and TGW. PrEP users are offered periodic STI testing for early detection of STIs including CT, NG and syphilis. However, the optimal and most cost-effective frequency for STI testing in PrEP users has yet to be established.
Methods: We constructed dynamic transmission models and simulated the epidemic trajectories of three STIs (CT, NG and syphilis) among MSM/TGW using PrEP in Australia, Brazil and Thailand. Two testing scenarios were considered: single pathogen testing for CT, NG or syphilis, and combined pathogens testing for all three STIs simultaneously. From a healthcare system perspective, cost-effectiveness analysis was used to explore the optimal testing strategy for STIs across three countries over a 5-year time horizon. The incremental cost-effectiveness ratio (ICER) and benefit-cost ratio (BCR) were calculated for each country.
Results: For Australian MSM, the optimal combined pathogens testing strategy was 6-monthly dual testing for CT/NG, along with 3-monthly syphilis testing (BCR = 4.14, cost-saving). In contrast, for Brazilian MSM, the optimal strategy was annual dual testing for CT/NG, along with 3-monthly syphilis testing (BCR = 35.50, cost-saving). Further, for Thai MSM, the optimal strategy was annual dual testing for CT/NG, along with 6-monthly syphilis testing (ICER = $2,667/QALY gained). For Brazilian TGW, the optimal strategy was 3-monthly dual testing for CT/NG, along with 3-monthly syphilis testing (BCR = 1.92, cost-saving). In comparison, for Thai TGW, the optimal strategy was annual dual testing for CT/NG, along with 3-monthly syphilis testing (ICER = $2,402/QALY gained).
Conclusion: Our study suggests that more frequent syphilis testing for PrEP users (every 3 months) provides good value for money among both MSM and TGW in all three countries. However, less frequent CT and NG testing may be considered, depending on the country’s background epidemic and the local costs associated with testing and management.
CT = Chlamydia trachomatis. NG = Neisseria gonorrhoeae. ICER = incremental cost-effectiveness ratio. MSM = men who have sex with men. TGW = transgender women. PrEP = pre-exposure prophylaxis. QALY = quality-adjusted life-year. WTP = willingness-to-pay.
| Cost, $, thousand | Effectiveness | Cost-effectiveness | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Strategy | PrEP related | STI testing | STI treatment | Total | No. STI cases | No. identified STI cases | QALYs | Cost per case averted, $a | Cost per case identified, $ | ICER ($/QALY gained)b | Benefit to cost ratio | |
| Single testing for CT | ||||||||||||
| 12m_CT | 46,861 | 86,206 | 237,742 | 370,809 | 66,151 | 31,075 | 620,423 | … | 11933 | … | … | |
| 6m_CT* | 42,450 | 98,385 | 229,942 | 370,778 | 26,041 | 15,994 | 620,581 | -1 | 23183 | -195 | 0.64 | |
| 3m_CT* | 40,929 | 120,809 | 226,682 | 388,420 | 12,289 | 9,045 | 620,641 | 327 | 42941 | 80784 | 0.32 | |
| Single testing for NG | ||||||||||||
| 12m_NG* | 41,181 | 109,203 | 229,895 | 380,279 | 14,071 | 5,987 | 620,362 | … | 63516 | … | … | |
| 6m_NG* | 40,835 | 123,355 | 228,449 | 392,639 | 10,932 | 5,899 | 620,429 | 3938 | 66564 | 184487 | 0.10 | |
| 3m_NG* | 40,568 | 151,176 | 227,337 | 419,082 | 8,590 | 5,759 | 620,480 | 7079 | 72764 | 328839 | 0.06 | |
| Single testing for Syphilis | ||||||||||||
| 12m_Syphilis | 66,951 | 3,925 | 298,099 | 368,975 | 206,828 | 157,044 | 614,936 | … | 2349 | … | … | |
| 6m_Syphilis | 48,647 | 4,726 | 264,666 | 318,038 | 144,172 | 115,140 | 617,886 | -813 | 2762 | -17266 | 41.75 | |
| 3m_Syphilis* | 39,143 | 5,993 | 240,260 | 285,396 | 78,985 | 59,951 | 619,118 | -654 | 4760 | -19985 | 27.97 | |
| Multiple testing for (CT+NG) + Syphilis | ||||||||||||
| 12m_(CT+NG)+12m_Syphilis | 66,951 | 113,128 | 765,735 | 945,815 | 287,050 | 194,106 | 1,855,722 | … | 4872 | … | … | |
| 6m_(CT+NG)+12m_Syphilis | 66,951 | 127,280 | 756,491 | 950,722 | 243,801 | 178,936 | 1,855,946 | 113 | 5313 | 21909 | 0.65 | |
| 3m_(CT+NG)+12m_Syphilis | 66,951 | 155,101 | 752,118 | 974,170 | 227,707 | 171,849 | 1,856,058 | 478 | 5669 | 84392 | 0.32 | |
| 12m_(CT+NG)+6m_Syphilis | 48,647 | 113,929 | 732,302 | 894,878 | 224,394 | 152,202 | 1,858,672 | -813 | 5879 | -17266 | 41.75 | |
| 6m_(CT+NG)+6m_Syphilis | 48,647 | 128,081 | 723,057 | 899,785 | 181,145 | 137,032 | 1,858,896 | -435 | 6566 | -14502 | 2.85 | |
| 3m_(CT+NG)+6m_Syphilis | 48,647 | 155,902 | 718,684 | 923,234 | 165,051 | 129,944 | 1,859,008 | -185 | 7105 | -6872 | 1.10 | |
| 12m_(CT+NG)+3m_Syphilis* | 46,861 | 115,196 | 707,897 | 869,953 | 159,207 | 97,013 | 1,859,904 | -593 | 8967 | -18140 | 27.97 | |
| 6m_(CT+NG)+3m_Syphilis* | 42,450 | 129,348 | 698,652 | 870,450 | 115,958 | 81,843 | 1,860,128 | -440 | 10636 | -17105 | 4.14 | |
| 3m_(CT+NG)+)+3m_Syphilis* | 40,929 | 157,169 | 694,279 | 892,376 | 99,864 | 74,756 | 1,860,240 | -285 | 11937 | -11828 | 1.62 | |
*: undominated strategy; a: compared with the strategy producing the highest number of STI cases; b: compared with 12-monthly STI testing strategy.
CT = Chlamydia trachomatis. NG = Neisseria gonorrhoeae. ICER = incremental cost-effectiveness ratio. MSM = men who have sex with men. PrEP = pre-exposure prophylaxis. STI = sexually transmitted infections. TGW = transgender women. QALY = quality-adjusted life-year. WTP = willingness-to-pay.
| Cost, $, thousand | Effectiveness | Cost-effectiveness | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Strategy | PrEP related | STI testing | STI treatment | Total | No. STI cases | No. identified STI cases | QALYs | Cost per case averted, $a | Cost per case identified, $ | ICER ($/QALY gained)b | Benefit to cost ratio | |
| Single testing for CT | ||||||||||||
| 12m_CT* | 51,456 | 45,543 | 1,752,851 | 1,849,850 | 579,899 | 127,667 | 7,720,200 | … | 14,490 | … | … | |
| 6m_CT* | 49,713 | 78,282 | 1,738,485 | 1,866,480 | 455,513 | 97,070 | 7,720,981 | 134 | 19,228 | 21,293 | 0.44 | |
| 3m_CT* | 48,995 | 143,182 | 1,732,329 | 1,924,506 | 411,963 | 83,731 | 7,721,391 | 445 | 22,984 | 62,683 | 0.21 | |
| Single testing for NG | ||||||||||||
| 12m_NG* | 49,532 | 45,893 | 1,712,672 | 1,808,097 | 92,998 | 20,148 | 7,721,227 | … | 89,739 | … | … | |
| 6m_NG* | 49,390 | 79,454 | 1,710,388 | 1,839,232 | 84,774 | 26,397 | 7,721,387 | 3,786 | 69,675 | 194,594 | 0.07 | |
| 3m_NG* | 49,246 | 145,795 | 1,708,183 | 1,903,224 | 76,970 | 32,542 | 7,721,549 | 5935 | 58,485 | 295,425 | 0.04 | |
| Single testing for Syphilis | ||||||||||||
| 12m_Syphilis | 66,722 | 2,509 | 1,996,050 | 2,065,281 | 1,809,374 | 1,026,515 | 7,642,286 | … | 2,012 | … | … | |
| 6m_Syphilis | 50,853 | 3,663 | 1,904,967 | 1,959,483 | 1,294,162 | 714,189 | 7,668,450 | -205 | 2,744 | -4,044 | 78.93 | |
| 3m_Syphilis* | 46,634 | 5,950 | 1,873,928 | 1,926,512 | 1,081,967 | 542,242 | 7,674,789 | -191 | 3,553 | -4,269 | 35.49 | |
| Multiple testing for (CT+NG)+Syphilis | ||||||||||||
| 12m_(CT+NG)+12m_Syphilis | 66,722 | 48,402 | 5,461,572 | 5,576,696 | 2,482,271 | 1,174,330 | 23,083,713 | … | 4,749 | … | … | |
| 6m_(CT+NG)+12m_Syphilis | 66,722 | 81,963 | 5,444,923 | 5,593,608 | 2,349,661 | 1,149,982 | 23,084,653 | 128 | 4,864 | 17,991 | 0.50 | |
| 3m_(CT+NG)+12m_Syphilis | 66,722 | 148,305 | 5,436,562 | 5,651,589 | 2,298,307 | 1,142,788 | 23,085,226 | 407 | 4,945 | 49,500 | 0.25 | |
| 12m_(CT+NG)+6m_Syphilis | 51,456 | 49,556 | 5,370,490 | 5,471,502 | 1,967,060 | 862,005 | 23,109,878 | -204 | 6,347 | -4,020 | 78.93 | |
| 6m_(CT+NG)+6m_Syphilis | 50,853 | 83,117 | 5,353,841 | 5,487,811 | 1,834,449 | 837,657 | 23,110,818 | -137 | 6,551 | -3,279 | 3.10 | |
| 3m_(CT+NG)+6m_Syphilis | 50,853 | 149,459 | 5,345,480 | 5,545,792 | 1,783,095 | 830,463 | 23,111,391 | -44 | 6,678 | -1,117 | 1.15 | |
| 12m_(CT+NG)+3m_Syphilis* | 51,456 | 51,843 | 5,339,450 | 5,442,749 | 1,754,864 | 690,057 | 23,116,217 | -184 | 7,887 | -4,121 | 35.49 | |
| 6m_(CT+NG)+3m_Syphilis* | 49,713 | 85,404 | 5,322,802 | 5,457,919 | 1,622,254 | 665,709 | 23,117,157 | -138 | 8,199 | -3,552 | 3.75 | |
| 3m_(CT+NG)+3m_Syphilis* | 49,246 | 151,746 | 5,314,440 | 5,515,432 | 1,570,899 | 658,515 | 23,117,730 | -67 | 8,376 | -1,801 | 1.42 | |
*: undominated strategy; a: compared with the strategy producing the highest number of STI cases; b: compared with 12-monthly STI testing strategy.
CT = Chlamydia trachomatis. NG = Neisseria gonorrhoeae. ICER = incremental cost-effectiveness ratio. MSM = men who have sex with men. PrEP = pre-exposure prophylaxis. QALY = quality-adjusted life-year. STI = sexually transmitted infection. TGW = transgender women. WTP = willingness-to-pay.
| Cost, $, thousand | Effectiveness | Cost-effectiveness | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Strategy | PrEP related | STI testing | STI treatment | Total | No. STI cases | No. identified STI cases | QALYs | Cost per case averted, $a | Cost per case identified, $ | ICER ($/QALY gained)b | Benefit to cost ratio | |
| Single testing for CT | ||||||||||||
| 12m_CT | 6,925 | 4,683 | 194,753 | 206,361 | 233,239 | 75,889 | 770,889 | -49 | 2,719 | … | … | |
| 6m_CT* | 6,527 | 7,966 | 190,774 | 205,267 | 237,716 | 107,297 | 771,085 | -324 | 1,913 | -5,582 | 1.21 | |
| 3m_CT* | 6,113 | 14,295 | 186,409 | 206,817 | 242,503 | 141,315 | 771,306 | … | 1,464 | 1,094 | 0.87 | |
| Single testing for NG | ||||||||||||
| 12m_NG* | 2,368 | 1,516 | 15,057 | 18,935 | 62,214 | 10,839 | 224,539 | -7,544 | 1,747 | … | … | |
| 6m_NG* | 2,346 | 2,573 | 14,984 | 19,903 | 62,369 | 16,914 | 224,531 | -8,424 | 1,177 | -121,000 | 0.07 | |
| 3m_NG* | 2,321 | 4,640 | 14,871 | 21,832 | 62,598 | 25,604 | 224,519 | … | 853 | -144,850 | 0.06 | |
| Single testing for Syphilis | ||||||||||||
| 12m_Syphilis | 10,055 | 254 | 224,247 | 234,556 | 217,940 | 143,331 | 758,196 | 526 | 1,636 | … | … | |
| 6m_Syphilis | 8,696 | 388 | 218,433 | 227,517 | 231,501 | 173,273 | 760,999 | 535 | 1,313 | -2,511 | 43.39 | |
| 3m_Syphilis* | 7,666 | 636 | 213,555 | 221,857 | 242,073 | 195,901 | 762,729 | … | 1,132 | -2,801 | 27.99 | |
| Multiple testing for CT+NG+Syphilis | ||||||||||||
| 12m_(CT+NG)+12m_Syphilis | 10,055 | 4,937 | 434,057 | 449,049 | 513,393 | 230,058 | 1,753,625 | 344 | 1,952 | … | … | |
| 6m_(CT+NG)+12m_Syphilis | 10,055 | 8,220 | 430,005 | 448,280 | 518,025 | 267,542 | 1,753,812 | 372 | 1,676 | -4,112 | 1.23 | |
| 3m_(CT+NG)+12m_Syphilis | 10,055 | 14,549 | 425,526 | 450,130 | 523,042 | 310,249 | 1,754,021 | 526 | 1,451 | 2,730 | 0.89 | |
| 12m_(CT+NG)+6m_Syphilis | 8,696 | 5,071 | 428,243 | 442,010 | 526,954 | 260,000 | 1,756,428 | 226 | 1,700 | -2,511 | 43.39 | |
| 6m_(CT+NG)+6m_Syphilis | 8,696 | 8,354 | 424,191 | 441,241 | 531,586 | 297,484 | 1,756,615 | 244 | 1,483 | -2,611 | 2.89 | |
| 3m_(CT+NG)+6m_Syphilis | 8,696 | 14,683 | 419,713 | 443,092 | 536,603 | 340,191 | 1,756,824 | 535 | 1,302 | -1,862 | 1.47 | |
| 12m_(CT+NG)+3m_Syphilis | 7,666 | 5,319 | 423,365 | 436,350 | 537,526 | 282,629 | 1,758,158 | -112 | 1,544 | -2,801 | 27.99 | |
| 6m_(CT+NG)+3m_Syphilis | 7,666 | 8,602 | 419,313 | 435,581 | 542,158 | 320,112 | 1,758,345 | -369 | 1,361 | -2,853 | 4.02 | |
| 3m_(CT+NG)+3m_Syphilis* | 7,666 | 14,931 | 414,835 | 437,432 | 547,175 | 362,819 | 1,758,554 | … | 1,206 | -2,357 | 1.92 | |
*: undominated strategy; a: compared with the strategy producing the highest number of STI cases; b: compared with 12-monthly STI testing strategy.
CT = Chlamydia trachomatis. NG = Neisseria gonorrhoeae. ICER = incremental cost-effectiveness ratio. MSM = men who have sex with men. PrEP = pre-exposure prophylaxis. STI = sexually transmitted infection. TGW = transgender women. QALY = quality-adjusted life-year. WTP = willingness-to-pay.
| Cost, $, thousand | Effectiveness | Cost-effectiveness | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Strategy | PrEP related | STI testing | STI treatment | Total | No. STI cases | No. identified STI cases | QALYs | Cost per case averted, $a | Cost per case identified, $ | ICER ($/QALY gained)b | Benefit to cost ratio | |
| Single testing for CT | ||||||||||||
| 12m_CT* | 27,444 | 138,499 | 70,042 | 235,985 | 68,291 | 22,122 | 3,139,742 | … | 10668 | … | … | |
| 6m_CT* | 27,040 | 201,405 | 69,630 | 298,076 | 58,286 | 21,305 | 3,139,828 | 6206 | 13991 | 721984 | 0.01 | |
| 3m_CT* | 26,791 | 325,695 | 69,374 | 421,861 | 52,600 | 20,740 | 3,139,889 | 11846 | 20340 | 1264459 | 0.003 | |
| Single testing for NG | ||||||||||||
| 12m_NG* | 26,635 | 138,331 | 69,412 | 234,378 | 22,398 | 5,403 | 3,139,812 | … | 43376 | … | … | |
| 6m_NG* | 26,581 | 201,544 | 69,329 | 297,453 | 21,160 | 6,871 | 3,139,835 | 50949 | 43289 | 2742404 | 0.001 | |
| 3m_NG* | 26,522 | 326,502 | 69,241 | 422,266 | 19,873 | 8,374 | 3,139,860 | 74411 | 50423 | 3914331 | 0.001 | |
| Single testing for Syphilis | ||||||||||||
| 12m_Syphilis* | 27,574 | 15,092 | 75,536 | 118,202 | 246,672 | 93,852 | 3,128,450 | … | 1259 | … | … | |
| 6m_Syphilis* | 25,733 | 21,350 | 73,601 | 120,684 | 208,079 | 69,750 | 3,130,022 | 64 | 1730 | 1578 | 0.31 | |
| 3m_Syphilis* | 25,319 | 33,983 | 73,051 | 132,353 | 199,969 | 63,257 | 3,130,351 | 303 | 2092 | 7444 | 0.13 | |
| Multiple testing for CT+NG+Syphilis | ||||||||||||
| 12m_(CT+NG)+12m_Syphilis* | 27,574 | 153,591 | 214,990 | 396,155 | 337,362 | 121,377 | 9,408,004 | … | 3264 | … | … | |
| 6m_(CT+NG)+12m_Syphilis | 27,574 | 216,635 | 214,495 | 458,705 | 326,119 | 122,028 | 9,408,114 | 5563 | 3759 | 568634 | 0.01 | |
| 3m_(CT+NG)+12m_Syphilis | 27,574 | 341,594 | 214,151 | 583,319 | 319,145 | 122,967 | 9,408,199 | 10274 | 4744 | 959816 | 0.004 | |
| 12m_(CT+NG)+6m_Syphilis* | 27,444 | 159,849 | 213,055 | 400,348 | 298,769 | 97,275 | 9,409,576 | 109 | 4116 | 2667 | 0.31 | |
| 6m_(CT+NG)+6m_Syphilis | 27,040 | 222,894 | 212,560 | 462,493 | 287,526 | 97,926 | 9,409,685 | 1331 | 4723 | 39464 | 0.04 | |
| 3m_(CT+NG)+6m_Syphilis | 26,791 | 347,852 | 212,216 | 586,859 | 280,551 | 98,864 | 9,409,771 | 3357 | 5936 | 107925 | 0.01 | |
| 12m_(CT+NG)+3m_Syphilis* | 27,444 | 172,482 | 212,504 | 412,431 | 290,659 | 90,782 | 9,409,905 | 349 | 4543 | 8562 | 0.13 | |
| 6m_(CT+NG)+3m_Syphilis* | 27,040 | 235,527 | 212,010 | 474,576 | 279,416 | 91,433 | 9,410,014 | 1353 | 5190 | 39016 | 0.04 | |
| 3m_(CT+NG)+3m_Syphilis* | 26,791 | 360,485 | 211,666 | 598,942 | 272,442 | 92,372 | 9,410,100 | 3124 | 6484 | 96749 | 0.02 | |
*: undominated strategy; a: compared with the strategy producing the highest number of STI cases; b: compared with 12-monthly STI testing strategy.
CT = Chlamydia trachomatis. NG = Neisseria gonorrhoeae. ICER = incremental cost-effectiveness ratio. MSM = men who have sex with men. PrEP = pre-exposure prophylaxis. STI = sexually transmitted infection. TGW = transgender women. QALY = quality-adjusted life-year. WTP = willingness-to-pay.
| Cost, $, thousand | Effectiveness | Cost-effectiveness | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Strategy | PrEP related | STI testing | STI treatment | Total | No. STI cases | No. identified STI cases | QALYs | Cost per case averted, $a | Cost per case identified, $ | ICER ($/QALY gained)b | Benefit to cost ratio | |
| Single testing for CT | ||||||||||||
| 12m_CT* | 5,173 | 12,337 | 7,534 | 25,044 | 96,129 | 36,598 | 232,003 | -4131 | 684 | … | … | |
| 6m_CT* | 4,850 | 19,220 | 7,292 | 31,362 | 98,314 | 49,046 | 232,054 | -5270 | 639 | 123885 | 0.04 | |
| 3m_CT* | 4,508 | 32,369 | 7,016 | 43,893 | 100,692 | 62,723 | 232,114 | … | 700 | 169813 | 0.03 | |
| Single testing for NG | ||||||||||||
| 12m_NG* | 4,281 | 12,228 | 7,120 | 23,629 | 69,269 | 18,430 | 232,027 | -19163 | 1282 | … | … | |
| 6m_NG* | 4,193 | 19,174 | 7,011 | 30,377 | 69,722 | 26,234 | 232,055 | -22427 | 1158 | 241009 | 0.02 | |
| 3m_NG* | 4,081 | 32,710 | 6,863 | 43,654 | 70,314 | 36,410 | 232,094 | … | 1199 | 298881 | 0.01 | |
| Single testing for Syphilis | ||||||||||||
| 12m_Syphilis* | 4,827 | 1,433 | 8,174 | 14,434 | 40,306 | 26,255 | 229,991 | -460 | 550 | … | … | |
| 6m_Syphilis* | 4,358 | 2,187 | 8,025 | 14,570 | 41,606 | 30,360 | 230,471 | -923 | 480 | 283 | 0.20 | |
| 3m_Syphilis* | 4,012 | 3,596 | 7,884 | 15,492 | 42,605 | 33,415 | 230,772 | … | 464 | 1355 | 0.13 | |
| Multiple testing for CT+NG+Syphilis | ||||||||||||
| 12m_(CT+NG)+12m_Syphilis* | 5,173 | 13,770 | 22,828 | 41,771 | 205,704 | 81,284 | 694,021 | -2631 | 514 | … | … | |
| 6m_(CT+NG)+12m_Syphilis | 4,850 | 20,653 | 22,477 | 47,979 | 208,342 | 101,536 | 694,101 | -2771 | 473 | 77603 | 0.05 | |
| 3m_(CT+NG)+12m_Syphilis | 4,827 | 34,143 | 22,053 | 61,024 | 211,312 | 125,389 | 694,199 | -676 | 487 | 108160 | 0.04 | |
| 12m_(CT+NG)+6m_Syphilis* | 5,173 | 14,524 | 22,679 | 42,376 | 207,004 | 85,388 | 694,501 | -3058 | 496 | 1260 | 0.20 | |
| 6m_(CT+NG)+6m_Syphilis | 4,850 | 21,406 | 22,328 | 48,584 | 209,642 | 105,640 | 694,581 | -3526 | 460 | 12166 | 0.07 | |
| 3m_(CT+NG)+6m_Syphilis | 4,508 | 34,897 | 21,904 | 61,309 | 212,612 | 129,493 | 694,680 | -1270 | 473 | 29648 | 0.04 | |
| 12m_(CT+NG)+3m_Syphilis* | 5,173 | 15,933 | 22,538 | 43,644 | 208,003 | 88,443 | 694,801 | -3376 | 493 | 2402 | 0.13 | |
| 6m_(CT+NG)+3m_Syphilis* | 4,850 | 22,815 | 22,187 | 49,853 | 210,641 | 108,696 | 694,881 | -4284 | 459 | 9397 | 0.07 | |
| 3m_(CT+NG)+3m_Syphilis* | 4,508 | 36,306 | 21,764 | 62,577 | 213,611 | 132,549 | 694,980 | … | 472 | 21696 | 0.05 | |
*: undominated strategy; a: compared with the strategy producing the highest number of STI cases; b: compared with 12-monthly STI testing strategy.
CT = Chlamydia trachomatis. NG = Neisseria gonorrhoeae. ICER = incremental cost-effectiveness ratio. MSM = men who have sex with men. PrEP = pre-exposure prophylaxis. STI = sexually transmitted infection. TGW = transgender women. QALY = quality-adjusted life-year. WTP = willingness-to-pay.
PP06.80 – Pathways for Transitioning to a Diagnostic-Led Approach for STI Management in Kenya
Dr. Dismas Ouma1, Dr. Daniel Were2, Dr. Patricia Ongwen2, Ms Kristina Grabbe3, Dr. Hannah Tappis3, Dr. Lisa Noguchi3, Ms Naoko Doi3, Mr. Paul Gathi2, Professor Yuka Manabe4, Dr. Susan Ontiri1
1International Centre for Reproductive Health, Nairobi, Kenya.
2Jheigo-Kenya, Nairobi, Kenya.
3Jpheigo, Baltimore, USA.
4John Hopkins School of Medicine, Baltimore, USA.
Background: The WHO advocates for a diagnostic-led approach to STI management, prioritizing rapid point-of-care (POC) testing. Transitioning from syndromic to diagnostic-based STI management in low- and middle-income countries requires understanding local health systems. This study explored pathways for such a transition in Kenya.
Methods: We conducted qualitative research in Nairobi and Kilifi counties in Kenya in August 2024, including 39 key informant interviews with national-level researchers, policymakers, service providers, and regulators; county-level managers and policymakers; and facility-level managers and service providers. We held four focus group discussions with healthcare providers and two human-centered design workshops with providers and clients. Data were analyzed using QSR NVivo 14, applying both deductive and inductive coding with multiple coders to ensure reliability and capture rich, emergent insights.
Results: Stakeholders highlighted effective leadership and stakeholder collaboration, led by national government, as required for successful implementation of STI POC diagnostics. Community STI awareness and integration with routine services can reduce stigma, enhance health-seeking behavior, and increase demand for diagnostics. High-performance devices with strong quality control systems will build trust among healthcare providers, promoting effective use and care. However, participants were concerned about challenges within the healthcare system, such as limited physical infrastructure to support sample collection and testing, high workload and poor staffing, especially in public hospitals, inadequate data collection and reporting, suboptimal training of service providers, and perennial stock-outs of diagnostics and medication in public facilities. Participants want these concerns to be addressed to advance adoption of etiological STI management.
Conclusion: Effective leadership and collaboration, along with reliable diagnostic devices and strong quality control, are essential for successful implementation of STI POC diagnostics. Addressing healthcare system challenges such as infrastructure, inadequate staffing, data collection, and stock shortages is crucial to improving services and supporting adoption of etiological STI management.
PP06.81 – Stakeholder Perspectives on Adopting Point-Of-Care Diagnostics for Sexually Transmitted Infections Management in Kenya
Dr. Dismas Ouma1, Dr. Daniel Were2, Dr. Patricia Ongweni Ongwen2, Ms Kristina Grabbe3, Dr. Hannah Tappis3, Dr. Lisa Noguchi3, Ms Naoko Doi3, Mr. Paul Gathi2, Professor Yuka Manabe4, Dr. Susan Ontiri1
1International Centre for Reproductive Health, Nairobi, Kenya.
2Jpheigo-Kenya, Nairobi, Kenya.
3Jpheigo, Baltimore, USA.
4John Hopkins University School of Medicine, Baltimore, USA.
Background: The WHO recommends transitioning from syndromic STI management to diagnostic-led approaches, including rapid point-of-care (POC) testing. This study examined stakeholder perspectives on Kenya’s readiness to shift from syndromic to diagnostic-led STI management.
Method: A qualitative formative assessment was conducted in Kilifi and Nairobi Counties through 39 key informant interviews with national policymakers, county decision-makers, facility managers, and healthcare providers. Four focus group discussions were held with healthcare providers from service delivery points with potential for STI POC diagnostic integration. Two human-centered design workshops were conducted with STI clients and service providers to explore user perspectives and preferences for POC diagnostic tools. Data were analyzed using QSR NVivo 14, applying both deductive and inductive coding with multiple coders to ensure reliability and capture rich, emergent insights.
Results: Stakeholders supported transitioning to diagnostic-led STI management, citing the potential for improved treatment accuracy, better decision-making, and reduced costs from misdiagnoses and repeat visits. However, concerns were raised about increased provider workload, device costs, resistance from healthcare workers, task-shifting conflicts, and community stigma surrounding STIs. Participants highlighted the need for accurate, user-friendly diagnostics that require minimal training and can be used by non-laboratory staff. Affordability emerged as a critical factor due to limited health insurance coverage.
Stakeholders emphasized the importance of strong national leadership, collaboration, and community awareness to drive demand for POC STI testing. Quality assurance, including reliable devices, robust quality control, and updated reporting tools, was seen as vital for maintaining trust among providers and patients.
Conclusion: Stakeholders recognize the value of POC diagnostics for STI management in Kenya, contingent on affordability, ease-of-use, quality assurance processes, and evidence-based implementation. Effective leadership and early stakeholder engagement will be critical to scaling up rapid, cost-effective, diagnostic-led approaches to improve STI care in resource-limited settings.
PP06.82 – Pathways for Transitioning to a Diagnostic-Led Approach for STI Management in Kenya
Dr. Dismas Ouma1, Dr. Daniel Were2, Dr. Patricia Ongwen2, Ms Kristina Grabbe3, Dr. Hannah Tappis3, Dr. Lisa Noguchi3, Ms Naoko Doi3, Mr. Paul Gathi2, Professor Yuka Manabe4, Dr. Susan Ontiri1
1International Centre for Reproductive Health, Nairobi, Kenya.
2Jheigo-Kenya, Nairobi, Kenya.
3Jpheigo, Baltimore, USA.
4John Hopkins School of Medicine, Baltimore, USA.
Background: The WHO advocates for a diagnostic-led approach to STI management, prioritizing rapid point-of-care (POC) testing. Transitioning from syndromic to diagnostic-based STI management in low- and middle-income countries requires understanding local health systems. This study explored pathways for such a transition in Kenya.
Methods: We conducted qualitative research in Nairobi and Kilifi counties in Kenya in August 2024, including 39 key informant interviews with national-level researchers, policymakers, service providers, and regulators; county-level managers and policymakers; and facility-level managers and service providers. We held four focus group discussions with healthcare providers and two human-centered design workshops with providers and clients. Data were analyzed using QSR NVivo 14, applying both deductive and inductive coding with multiple coders to ensure reliability and capture rich, emergent insights.
Results: Stakeholders highlighted effective leadership and stakeholder collaboration, led by national government, as required for successful implementation of STI POC diagnostics. Community STI awareness and integration with routine services can reduce stigma, enhance health-seeking behavior, and increase demand for diagnostics. High-performance devices with strong quality control systems will build trust among healthcare providers, promoting effective use and care. However, participants were concerned about challenges within the healthcare system, such as limited physical infrastructure to support sample collection and testing, high workload and poor staffing, especially in public hospitals, inadequate data collection and reporting, suboptimal training of service providers, and perennial stock-outs of diagnostics and medication in public facilities. Participants want these concerns to be addressed to advance adoption of etiological STI management.
Conclusion: Effective leadership and collaboration, along with reliable diagnostic devices and strong quality control, are essential for successful implementation of STI POC diagnostics. Addressing healthcare system challenges such as infrastructure, inadequate staffing, data collection, and stock shortages is crucial to improving services and supporting adoption of etiological STI management.
PP06.83 – Minding the Gaps in Treatment Practices for Bacterial STIs: Insights from Online Survey Among Physicians
Mr. Victor Passarelli1, Ms Flora Goldemberg1, Dr Ricardo Vasconcelos1, Dr Gwenda Hughes2, Dr Silvia Figueiredo Costa1
1Faculdade De Medicina Da Universidade De São Paulo, São Paulo, Brazil.
2The London School of Hygiene & Tropical Medicine, London, England.
Background: Inadequate treatments for sexually transmitted infections (STIs) may contribute to antimicrobial resistance (AMR), particularly with Neisseria gonorrhoeae (Ng) and Mycoplasma genitalium (Mg). Therefore understanding prescription practices for bacterial STIs is important to help improve public policies and AMR surveillance strategies.
Methods: This was a prospective transversal observational study. We used the platform SurveyMonkey™ to develop an online self-applied questionnaire (table) targeting Brazilian physicians. It was disseminated through social media and contact lists.
Findings: Between August and December of 2024, 250 physicians completed the survey. The majority were women (139, 55,6%) aged 25-35 (131, 52,4%), working in both public and private sectors (130, 52%), primarily with Infectious Diseases (ID): (82; 32,8%), Gynecology and Obstetrics (56; 22,4%), Family Medicine (47; 18.8%), and Internal Medicine (30; 12%). Responses were predominantly from Brazillian Southeast (181; 72,4%), South (30; 12%) and Northeast (26; 10,4%) regions.
Ceftriaxone plus azithromycin was the most common empirical treatment for both urethritis (153; 61,2%) and cervicitis (76; 30,4%), while ceftriaxone plus doxycycline was the most common choice for proctitis (74; 29,6%). Ceftriaxone doses for gonorrhea varied widely (from 250 mg to 1g) among all specialties. For Mg, while azithromycin 1g was the most popular choice overall (45; 18%), 104 respondents (41.6%) had never prescribed a specific treatment for it.
When stratified by medical specialty and compared to non-ID responses, ID respondents’ prescriptions were seemingly more precise regarding drug choice for empirical treatments, but posology also varied greatly among them. Two-step treatments including moxifloxacin for Mg were more common among ID physicians. Treatments for syphilis and chlamydia were more uniform (table).
Conclusion: Discrepant and outdated treatments highlight the need for continuous medical education among all specialties to enhance evidence-based and uptodate care, therefore reducing STI burden and AMR risks, especially regarding pathogens of concern such as Ng and Mg.
| Question | Answer | Overall (n = 250) | ID* Respondents (n = 82) | Non-ID* Respondents (n = 168) | P-Value | |
|---|---|---|---|---|---|---|
| Empirical choice for urethritis treatment | ||||||
| Ceftriaxone + Azithromycin | 61.20% (153) | 70,73% (58) | 56,55% (95) | 0,043 | ||
| Ceftriaxone + Doxycycline | 16% (40) | 23,17% (19) | 12,5% (21) | 0,048 | ||
| Azithromycin | 7.6% (19) | 1,22% (1) | 10,71% (18) | 0,016 | ||
| Ciprofloxacin | 1.2% (3) | 0 | 1,79% (3) | 0,54 | ||
| Ciprofloxacin + Azithromycin | 4.8% (12) | 1,2% (1) | 6,55% (11) | 0,12 | ||
| Ciprofloxacin + Doxycycline | 4.4% (11) | 2,44% (2) | 5,36% (9) | 0,46 | ||
| Levofloxacin | 0.8% (2) | 0 | 1,19% (2) | 0,81 | ||
| I don’t know | 2.02% (5) | 0 | 2,98% (5) | – | ||
| Other | 2,02% (5) | 1,22% (1) | 2,38% (4) | – | ||
| Empirical choice for cervicitis treatment | ||||||
| Ceftriaxone + Azithromycin | 30.4% (76) | 30.49% (25) | 30.36% (51) | 1 | ||
| Ceftriaxone + Azithromycin + Metronidazole | 25.20% (63) | 31,71% (26) | 22,02% (37) | 0,13 | ||
| Ceftriaxone + Doxycycline | 19.6% (49) | 26,8% (22) | 16,07% (27) | 0,06 | ||
| Azithromycin | 6.80% (17) | 0 | 10,12% (17) | 0,006 | ||
| Ciprofloxacin + Doxycycline | 2.8% (7) | 2.44% (2) | 2.98% (5) | 1 | ||
| Ciprofloxacin + Azithromycin | 2.8% (7) | 0 | 4,17% (7) | 0,14 | ||
| Ciprofloxacin + Metronidazole | 4.0% (10) | 1,22% (1) | 4.17% (9) | 0,22 | ||
| Ceftriaxone + Azithromycin + Metronidazole + Fluconazole | 1.6% (4) | 2,44% (2) | 1,19% (2) | 0,84 | ||
| I don’t know | 2.8% (7) | 0 | 4,17% (7) | – | ||
| Other | 4.0% (10) | 4,88% (4) | 3,57% (6) | – | ||
| Empirical choice for proctitis treatment | ||||||
| Ceftriaxone + Doxycycline | 29.6% (74) | 48,78% (40) | 20,24% (34) | <0,001 | ||
| Ceftriaxone + Azithromycin | 24.8% (62) | 37,8% (31) | 18,45% (31) | <0,001 | ||
| Ciprofloxacin | 8.4% (21) | 1,22% (1) | 11,9% (20) | <0,001 | ||
| Ciprofloxacin + Azithromycin | 4.4% (11) | 2,44% (2) | 5,36% (9) | 0,46 | ||
| Ciprofloxacin + Metronidazole | 4.0% (10) | 3,66% (3) | 4,17% (7) | 1 | ||
| Ciprofloxacin + Doxycycline | 3.6% (9) | 2,44% (2) | 4,17% (7) | 0,74 | ||
| Azithromycin | 2.4% (6) | 0 | 3,57% (6) | 0,19 | ||
| I don’t know | 19.35% (47) | 2,44% (2) | 26,79% (45) | – | ||
| Other | 4% (10) | 1,22% (1) | 5,3% (9) | – | ||
| Prescription choice for a confirmed case of uncomplicated Gonorrhea | ||||||
| Ceftriaxone 500mg IM single dose | 38.8% (97) | 54,88% (45) | 30,95% (52) | <0,001 | ||
| Ceftriaxone 500mg IM single dose + Azithromycin 1g PO single dose | 24.4% (61) | 25,61% (21) | 23,81% (40) | 0,87 | ||
| Ceftriaxone 1g IM single dose | 9.6% (24) | 12,2% (10) | 8,33% (14) | 0,45 | ||
| Ceftriaxone 250mg IM in a single dose | 8.8% (22) | 2,44% (2) | 11,9% (20) | 0,02 | ||
| Ceftriaxone 250mg IM single dose + Azithromycin 1g PO single dose | 5.2% (13) | 2,44% (2) | 6,55% (11) | 0,28 | ||
| Azithromycin 2g PO in a single dose | 4.4% (11) | 0 | 6,55% (11) | 0,04 | ||
| Ciprofloxacin 1g PO in a single dose | 0.40% (1) | 0 | 0,60% (1) | 1 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 3.2% (8) | 1,22% (1) | 4,17% (7) | 0,38 | ||
| Penicillin G Benzathine 2.4 million IU IM single dose | 1.2% (3) | 0 | 1,79% (3) | 0,54 | ||
| I don’t know | 1.21% (3) | 0 | 1,79% (3) | 0,54 | ||
| Other | 2.42% (6) | 1,22% (1) | 3,57% (6) | 0,51 | ||
| Prescription choice for a confirmed case of Chlamydia | ||||||
| Azithromycin 1g PO in a single dose | 61.6% (154) | 65,85% (54) | 59,52% (100) | 0,4 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 29.6% (74) | 31,71% (26) | 28,57% (48) | 0,71 | ||
| Azithromycin 500mg PO, once a day for 5 days | 4.8% (12) | 1,22% (1) | 6,55% (11) | 0,12 | ||
| Ciprofloxacin 500mg PO every 12 h for 7 days | 0.40% (1) | 0 | 0,60% (1) | 1 | ||
| Levofloxacin 500mg PO, once a day for 7 days | 0.40% (1) | 0 | 0,60% (1) | 1 | ||
| I don’t know | 1.61% (4) | 0 | 2,38% (4) | – | ||
| Other | 1.61% (4) | 1,22% (1) | 1,79% (3) | – | ||
| Prescription choice for a confirmed case of Mycoplasma genitalium | ||||||
| I have never prescribed a specific treatment for this infection | 41.6% (104) | 26,83%% (22) | 48,81% (82) | 0,001 | ||
| Azithromycin 1g PO in a single dose | 18% (45) | 15,85% (13) | 19,05% (32) | 0,65 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 14.4% (36) | 17,07% (14) | 13,1% (22) | 0,51 | ||
| Doxycycline 100mg PO every 12 h for 7 days followed by Moxifloxacin 400mg/day PO for another 7 days | 9.6% (24) | 23,17% (19) | 2,98% (5) | <0,001 | ||
| Doxycycline 100mg PO every 12h for 7 days followed by Azithromycin 500mg/day PO for another 5 days | 5.6% (14) | 9,76% (8) | 3,57% (6) | 0,08 | ||
| Azithromycin 500mg PO once a day for 5 days | 1.6% (4) | 1,22% (1) | 1,79% (3) | 1 | ||
| Moxifloxacin 400mg PO once a day for 7 days | 4.4% (11) | 4,88% (4) | 4,17% (7) | 1 | ||
| Levofloxacin 500mg PO once a day for 7 days | 0.8% (2) | 0 | 1,19% (2) | 0,81 | ||
| I don’t know | 3.23% (8) | 0 | 4,76% (8) | – | ||
| Other | 1.21% (3) | 1,22% (1) | 0,6% (1) | – | ||
| Prescription choice for Primary Syphilis | ||||||
| Penicillin G Benzathine 2.4 million IU IM, single dose | 90.8% (227) | 95,12% (78) | 88,69% (149) | 0,15 | ||
| Penicillin G Benzathine 7.2 million IU IM, once a week for 3 weeks | 4.40% (11) | 2,44% (2) | 5,36% (9) | 0,46 | ||
| Penicillin G Benzathine 4.8 million IU IM, once a week for 2 weeks | 1.6% (4) | 0 | 2,38% (4) | 0,38 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 0.40% (1) | 1,22% (1) | 0 | 0,71 | ||
| Ceftriaxone 1g IM, once a day for 7 days | 0.40% (1) | 0.40% (0) | 0,6% (1) | 1 | ||
| Azithromycin 2g PO in a single dose | 0.40% (1) | 0.40% (0) | 0,6% (1) | 1 | ||
| I don’t know | 1.6% (4) | 0 | 1,6% (4) | |||
*ID respondents = Infectious Diseases Specialists who responded the survey; Non-ID respondents: respondents from medical specialties other than ID.
P-values were calculated using the Chi-Squared test with Free Statistics Software, and a threshold of p < 0.05 was considered statistically significant.
PP06.84 – Acceptance and Prescription Practices of Doxycycline Post-Exposure Prophylaxis (DoxyPEP) Among Brazilian Physicians: A Nationwide Study
Mr. Victor Passarelli1, Ms Flora Goldemberg1, Dr Ricardo Vasconcelos1, Dr Gwenda Hughes2, Dr Silvia Figueiredo Costa1
1Faculdade De Medicina Da Universidade De São Paulo, São Paulo, Brazil.
2The London School of Hygiene & Tropical Medicine, London, England.
Background: Post Exposure Prophylaxis with Doxycycline (DoxyPEP) is a groundbreaking method to prevent some of the most common bacterial STIs. Controversies regarding antimicrobial resistance (AMR) surveillance and acceptance for its implementation provoke discussions among different medical specialties, therefore understanding the current scenario is of utmost importance.
Methods: This was a prospective transversal observational study. We used the platform SurveyMonkey™ to develop an online self-applied questionnaire targeting Brazilian physicians. It was disseminated through social media and contact lists. Questions are shown in Table.
Findings: Between August and December of 2024, 250 physicians completed the survey. The majority were women (139, 55.6%), aged between 25–35 (131, 52.4%), working in both public and private sectors (130, 52%), mainly with Infectious Diseases (ID): (82; 32.8%), Gynecology and Obstetrics (56; 22.4%), Family Medicine (47; 18.8%), and Internal Medicine (30; 12%). Responses were received from all five Brazilian regions, predominantly from the Southeast (181; 72.4%), South (30; 12%) and Northeast (26; 10.4%)
DoxyPEP acceptance was high overall, with 55.6% of respondents either 'agreeing’ or 'strongly agreeing’ with its implementation.
However, non-Infectious Diseases (Non-ID) practitioners more commonly stated they did not know enough about it to give an opinion (35.12% vs 3.66%, P < 0.001).
Among ID physicians, 41 (50%) had already prescribed DoxyPEP to their patients, while 29 (17.2%) had done it among the non-ID (P < 0.001). Results are summarized in the table.
Conclusion: The high acceptance of DoxyPEP across various medical specialties is promising. However, limited awareness of this intervention outside the field of Infectious Diseases warrants attention. Additionally, the current practice of DoxyPEP prescription in the absence of specific public policies raises concerns, particularly regarding its proper integration into healthcare services and its implications for AMR surveillance strategies.
| Question | Response | Overall (n = 250) | ID Respondents1 (n = 82) | Non-ID Respondents2 (n = 168) | P-Value | |
|---|---|---|---|---|---|---|
| How much do you agree with the implementation of Post-Exposure Prophylaxis with Doxycycline (DoxyPEP)3 to prevent STIs such as syphilis in vulnerable populations? | ||||||
| Strongly agree | 24% (60) | 26,83% (22) | 22,62% (38) | 0,56 | ||
| Agree | 31.6% (79) | 47,56% (39) | 23,81% (40) | <0,001 | ||
| Neither agree nor disagree | 10% (25) | 12,2% (10) | 8,93% (15) | 0,55 | ||
| Disagree | 5.2% (13) | 6,1% (5) | 4,76% (8) | 0,88 | ||
| Strongly disagree | 2.8% (7) | 2,44% (2) | 2.98% (5) | 1 | ||
| I don’t know enough to give an opinion. | 24.80% (62) | 3,66% (3) | 35,12% (59) | <0,001 | ||
| I prefer not to answer. | 1.6% (4) | 1.22% (1) | 1,79% (3) | 1 | ||
| Do you prescribe DoxyPEP to your patients? | ||||||
| Yes, I already prescribe it. | 28% (70) | 50% (41) | 17,26% (29) | <0,0001 | ||
| No, I don’t prescribe it. | 67,6% (169) | 48,78% (40) | 76,79% (129) | <0,0001 | ||
| I prefer not to answer. | 4.4% (11) | 1,22% (1) | 5,95% (10) | 0,16 | ||
P-values were calculated using the Chi-Squared test with Free Statistics Software, and a threshold of P < 0.05 was considered statistically significant.
PP06.85 – Performance Analysis of Clinical Service Providers in HIV Care and Treatment: Results from the 2024 Digital Certification Exams for Clinical Mentorship Training in Mozambique
Dr. Yara Paulo1, Dr Leuchim Gemo2, Dr Orlando Munguambe1, Dr António Paúnde2, Dr Irénio Gaspar1, Dra Aleny Couto1
1MoH Mozambique, Maputo, Moçambique.
2I-TECH Mozambique, Maputo, Moçambique.
Background: Mozambique ranks 8th globally for HIV prevalence, with 2.4 million people living with HIV (PLHIV). Currently, the country is at 71-96-89 for the 95-95-95 targets, highlighting the need for improvements in HIV care delivery. One major factor contributing to this challenge is the quality of clinical mentors, which affects the effectiveness of ART services.In response, a new exam was introduced in 2023 as a prerequisite for accessing the clinical mentorship training package.
Description For these evaluations, provinces request the assessment from the Ministry of Health’s (MoH) Quality Improvement team, which is conducted remotely using the providers’ own electronic devices. Providers must belong to clinicprofessional categories: and have at least 12 months of experience in the ART service. Providers who score above 66% are considered to have passed the exam.
Findings: The 2024 evaluations involved 747 healthcare providers from 10 provinces, including Maputo City, Maputo Province, Gaza, Inhambane, Sofala, Manica, Tete, Zambézia, Nampula, and Cabo Delgado. The approval rates across these provinces varied significantly, with some provinces like Maputo City and Maputo Province achieving higher approval rates (80% and 71%), while others like Zambézia and Nampula had much lower rates (39% and 29%). The overall average approval rate was 59%, reflecting the need for targeted interventions to improve clinical mentoring and ART service delivery.
Conclusion: Data shows considerable regional disparities, with 90% of the provinces reporting approval rates below 75%. The introduction of the new exam in 2023 was a step in the right direction, MoH must define strategies to improve the perfomance of the provinces with low perfomance, addressing regional disparities.
PP06.86 – A Comparative Retention Among Women Living with HIV in Mozambique
Mrs Edna Paunde Xavier1, Dr Aleny Couto1, Dr Irenio Gaspar1, Dr Yara Paulo1, Mr Orlando Munguambe, Mr Fernando Boene1
1Moh Mozambique, Maputo, Mozambique.
Background: The impact of HIV in Mozambique is visible in women, with the epidemic in the country being more feminised. According to spectrum data (version 6.36) by December 2023 in Mozambique 60 per cent of people living with HIV are women. In Mozambique 1,470,000 women are living with HIV and of these 125,000, 8.5% are pregnant women. Early retention refers to the process of ensuring that pregnant women are followed up from the beginning of pregnancy for proper monitoring and prevention of complications.
Description: a follow-up flow has been drawn up and standardised which recommends that all pregnant and breastfeeding women living with HIV who are diagnosed in the antenatal clinic or at-risk child clinic, or who arrive at these clinics with the diagnosis, receive psychosocial support according to their needs. At every monthly consultation, pregnant and breastfeeding women should be assessed for risk factors for adherence.
Findings: In the 3 regions of the country, retention is higher in the first 33 days after starting ART than at 99 days after starting treatment. In the southern region of the country, retention at 33 days is 89 % and at 99 days 84 %. In the Centre region, retention at 33 days is 81% and at 99 days 74%. In the Northern region, retention at 33 days is 78 % and at 99 days 66 %, with the Southern region of the country having the best early retention of pregnant women on antiretroviral treatment.
Conclusion: The implementation of early retention strategies for WLHIV is fundamental to guaranteeing maternal and neonatal health, improving the quality of life and preventing mother-to-child transmission of HIV. WLHIV face additional challenges during pregnancy, such as the need for constant adherence to antiretroviral treatment (ART), monitoring viral load and preventing complications associated with the infection.
PP06.87 – Pilot Study in Brazil: Fourth-Generation Immunochromatographic HIV Tests Show no Added Benefit Over Third-Generation Tests
Ms. Ana Philippus1, Ms. Amanda Alencar Cabral Morais1, Alisson Bigolin1, Adson Belém Ferreira da Paixão1, José Boullosa1, Gilvane Casimiro1, Draurio Barreira1
1Brazilian Ministry of Health, Brasília, Brazil.
Background: HIV infection remains a significant public health challenge, particularly among vulnerable populations. Early diagnosis is crucial to prevent transmission and complications. From 2023–2024, the Brazilian Ministry of Health led a pilot project in four Testing and Counseling Centers to evaluate the benefits of implementing fourth-generation rapid combined antigen and antibody tests (RT-Ag/Ab) in healthcare services that cater to populations at higher risk of HIV infection and to assess whether the current strategy in Brazil, using antibody-only tests, might be missing diagnoses.
Description: Guidelines and an algorithm supported the project implementation, allowing diagnostic completion in health services (Fig. 1), performing both fourth- and third-generation HIV tests simultaneously. Data were collected using the Research Electronic Data Capture (REDCap) system.
Findings: A total of 1,631 forms were recorded in RedCap. Most participants were Black/Brown (70.3%) or White (28.2%), and the majority completed high school (32.5%) or held college degrees (30.9%). Among participants, 74.7% identified as cisgender men, 23.3% as cisgender women. Regarding sexual orientation, 43.9% identified as heterosexual, 42.8% as homosexual. A significant portion (70.8%) sought testing voluntarily. Notably, 95.7% reported unprotected sex, with 52.1% within less than 15 days, 18.6% between 15–30 days, and 29.3% over 30 days ago. Furthermore, 44.2% were starting PrEP, and 13.6% were under PrEP follow-up. Of the RT-Ag/Ab tests, 67 individuals tested positive: one for antigen only, 29 for both antigen and antibody, and 37 for antibody only. Comparable RT-Ab test results identified 73 positive cases. Based on guidelines, 61 individuals were diagnosed with HIV using RT-Ag/Ab, and 69 with RT-Ab.
Conclusion: The study found no significant advantage in case detection with RT-Ag/Ab compared to RT-Ab. Additionally, more cases were diagnosed using RT-Ab. Public health-wise in Brazil, the cost of the RT-Ab test (US$0.16) is much lower than the RT-Ag/Ab test (US$1.49).
PP06.88 – Ensuring Quality and Performance in Brazil’s Rapid HIV, Syphilis, and Hepatitis Testing: An Overview of the 2024 Monitoring and Evaluation Results
Ms. Ana Philippus1, Mr. Alisson Bigolin1, Ms. Pamela Gaspar1
1Brazilian Ministry of Health, Brasília, Brazil.
Background: The Brazilian Ministry of Health (MoH) distributes around 25 million anti-HIV, treponemal, anti-HCV, and HBsAg rapid tests (RT) annually, recommending them as the primary diagnostic tool. Despite their reliability and ease of use, maintaining their quality is essential for accurate diagnoses.
Methods: MoH manages RT quality through technical criteria definition for acquisition (e.g., registration with the Brazilian Health Regulatory Agency, performance criteria), offering distance learning [webinars and online training platform (OTP) with practical guides covering test precautions, report models, testing traceability, stock controls], monitoring work process organization across Brazil using forms, and post-market surveillance [verifying the performance of all test lots distributed and monitoring customer service (CS) reports]. External Quality Assessment for Rapid Tests (EQA-RT) is also conducted for all RT, (HBsAg to be included next year). Data from 2024 were analyzed.
Results: All RT acquired by MoH met technical criteria. A total of 3,357 professionals attended webinars and 33,251 accessed the OTP. All 116 RT lots were approved based on performance criteria. In the EQA-RT practical assessment, 6,203 professionals participated, with approval rates of 91.7%, 96.2%, and 92.2% for HIV, Syphilis, and HCV tests, respectively. In the theoretical assessment, 92.4% of 5,534 professionals passed. The main errors were related to diagnostic flowcharts and results interpretation. CS reported 220 non-conformities (0.0006% of RTs distributed), most of which were not confirmed in the manufacturer’s assessment. Additionally, 6,256 professionals responded to word process forms. Key findings indicated thar 51% open the test device at the time of testing, 78% use the correct pipette for adequate blood volume and 98% start tests with the device requiring the most blood, following MoH recommendations.
Conclusion: The 2024 data demonstrates that MoH’s quality tools are effective in ensuring compliance and high performance. However, errors in diagnostic flowcharts and result interpretation indicate areas for further improvement.
PP06.89 – Rising Syphilis and HIV Trends Among Rural Populations in India: A Clarion Call Towards Sexual Health for All
Mr. Mohnish Kumar1, Dr. V Sam Prasad2, Dr. V Sam Prasad2, Miss Elizabeth Michael3, Mr. Shivam Dwivedi4, Mr. Lyle Honig Mojica5
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
2AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
3AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
4AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
5AIDS Healthcare Foundation (AHF), Los Angeles, United States of America.
Background: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across ten states in India to screen and track trends of syphilis and HIV co-infections. Syphilis and HIV co-infections pose significant public health concern, particularly among rural populations.
Description: This retrospective study analyzed data randomly selected from the pre and post-test counselling notes and the test results of men (n = 500) and women (n = 500) community-based STI/ HIV screening program for 2 years, that included men (n = 317,597) and women (n = 230,693) from rural areas across 9 states in India. Syphilis and HIV screening were conducted using rapid diagnostic tests, and data was analyzed to identify age- and gender-wise trends of syphilis and HIV co-infections.
Findings:
The study revealed a rising trend of syphilis cases among rural populations, with significant increases among:
-
Men over 50 years (35%)
-
Young women aged 30 years (28%)
-
Migrant workers (40%)
-
Individuals with low knowledge on STI/HIV (30%)
HIV co-infection rates were also high among these groups:
Multivariate analysis revealed that:
-
Lack of knowledge on STI/HIV (OR: 2.5)
-
Poverty (OR: 3.1)
-
Limited access to healthcare services (OR: 2.2)
-
Migrating for work (OR: 1.8)
were significant predictors of syphilis and HIV co-infections.
Conclusion: This study highlights the need for targeted interventions to address the rising trend of syphilis and HIV co-infections among rural populations in India. Policymakers, healthcare providers, and community organisations must work together to promote comprehensive sexual health education, condom promotion, and regular testing for syphilis and HIV, while addressing the social determinants of health.
PP06.90 – Promoting Access to HIV Services Among Men Who Have Sex With Men Under a Harsh Environment in the Wake of the Anti-LGBTQ+Debate in Ghana
Mrs. Hellen Mawuli Quarshie1, Mr Samuel Elliot Owusu1, Mr Solomon Atsuvia
1Maritime Life Precious Foundation, Kumasi, Ghana.
Background: In Ghana, men who have sex with men (MSM) often face challenges accessing HIV services due to stigma and discrimination. Approval of an anti-LGBTQ+ bill by parliament has further facilitated an environment where MSM constantly experience societal homophobia and human-rights abuses which affect uptake of HIV services. Maintaining uninterrupted access to HIV services for MSM under this harsh climate requires using integrated, community-based strategies.
Description: Various community-based approaches to HIV service delivery for MSM were introduced during the period.
Peer-Educators halted group outreach and engaged peers with one-on-one meetings to reduce public visibility. M-Friends/M-Watchers were deployed to facilitate access to needed legal services and address HIV-related abuses directed at MSM.
Flexible community-based strategies were implemented to preserve access to HIV services and promote safety of KP implementers and MSM during the period: (1) Social media platforms were used to engage peers for HTS and support PLHIVs through virtual case management; (2) HTS and treatment took place at homes and safe locations agreed to by peers; (3) Condoms, lubricants and HIV self-test kits were made available at outlets, community-led DICs and outlets for easy access; (4) Multi-month dispensing of ART and PrEP were promoted to eliminate clinic visits.
Findings: Introduction of community-based strategies reached out to more MSM and increased HIV+ yield. During the period of anti-LGBTQ+ debate from September 2023–February 2024, 608 MSM were reached and tested for HIV; 48 were diagnosed positive. After the introduction of community-based strategies, from March–August 2024, 844 MSM were reached and tested; 162 were diagnosed positive.
Conclusions: Tailored community-based approaches to HIV service delivery proved to be effective during the anti-LGBTQ+ climate. Nevertheless, the influence of the anti LGBTQ+ bill on HIV&AIDS programming is enormous affecting MSM and KP organizations. We call for high-level stakeholder advocacy on the effect of the anti-LGBT bill against sexual minorities in the fight against HIV&AIDS.
The table and graph below show results before and after the introduction of integrated, community-based approaches during the anti-LGBTQ+ period in Ghana. Table 1 and Fig. 1 show that New MSM Reached increased after these innovative strategies were introduced from March to August 2024.
Introduction of community-based strategies during the anti-LGBTQ+ bill period reached out to more MSM.
Testing and HIV positivity rate were higher after the introduction of community-based strategies.
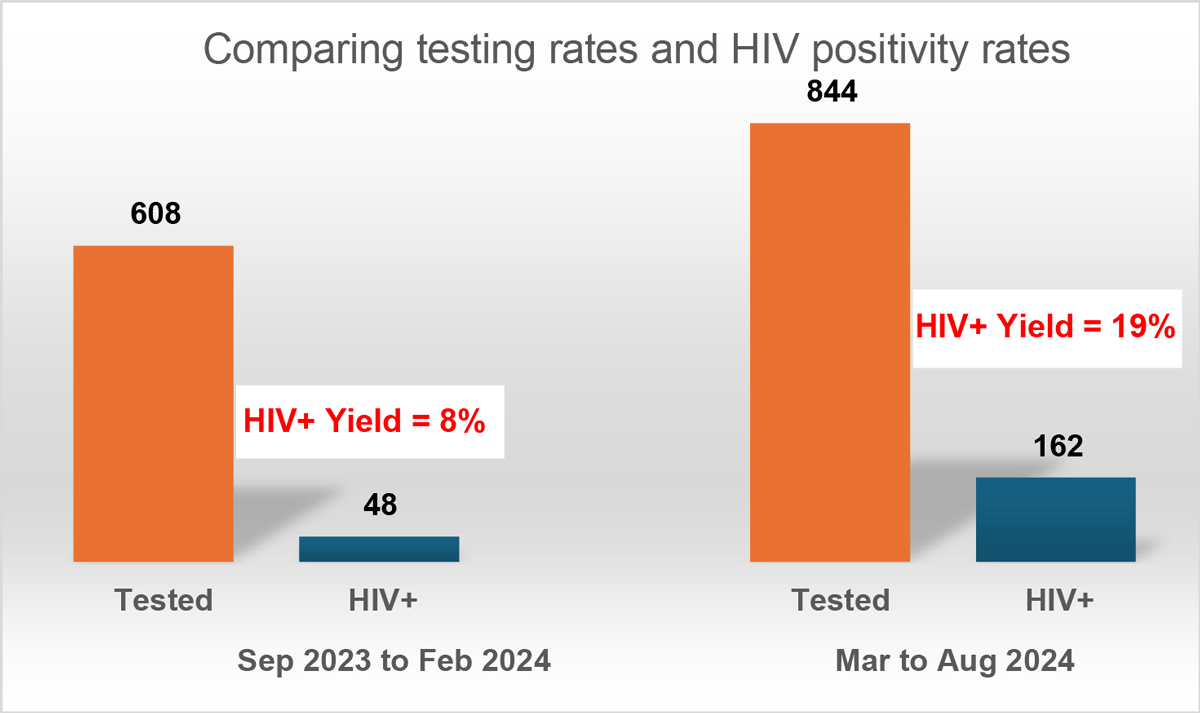
Table 2 and Fig. 2 also indicate that both testing rates and HIV+ yield increased after the introduction of community-based strategies from March to August 2024.
PP06.91 – Peer-Driven Approaches to Increase Uptake of HIV Testing Services Among Fetish Priests Who Are Men Who Have Sex with Men (MSM) in the Western Region of Ghana
Mrs. Hellen Mawuli Quarshie1, Mr Agbesi Wosornu1
1Maritime Life Precious Foundation, Kumasi, Ghana.
Background: Key populations are recognized as significant drivers of the HIV epidemic in Ghana. According to the National Strategic Plan, 18.5% of men who have sex with men (MSM) are living with HIV. Certain high-risk MSM subgroups, such as fetish priests, often avoid HIV testing services (HTS). Reaching fetish priests is particularly challenging due to prevailing superstitions and the belief that HIV is a spiritual disease that does not affect them. Peer-driven approaches are essential to effectively reach this population.
Description: A snowball approach was implemented where an HIV-positive MSM was encouraged to refer his sexual partners from the past year to a trained counselor for HIV testing. This referral chain led the outreach team to a fetish priest at his shrine. Through ongoing visits and HIV education, the priest was counseled on the importance of HIV testing. After ensuring confidentiality, the priest agreed to undergo HIV testing and was motivated to refer other MSM fetish priests for testing.
Findings: The peer-driven strategy, utilizing a referral chain initiated by an HIV-positive fetish priest, successfully reached more MSM fetish priests in the Tarkwa district. A total of 25 shrines led by MSM fetish priests were identified, with 19 priests agreeing to HIV testing after continuous education and engagement. Of the 19 priests tested, 4 refused to accept their HIV-positive status and declined ART initiation. However, 15 accepted their results and were linked to ART via differentiated service delivery at their shrines.
Conclusions: The snowball and referral chain strategy for HTS is effective in reaching hidden MSM populations and should be expanded to other districts. Providing confidential and accessible differentiated service delivery encourages MSM, including fetish priests, to seek HIV services. Ongoing education and monitoring are essential to promote ART acceptance among those who initially refused treatment and ensure viral suppression in those who have started ART.
PP06.92 – Enhancing HIV Testing Rates Among Men Who Have Sex with Men in Ghana Through Free STI Treatment
Mrs. Hellen Mawuli Quarshie1, Mr James Martin2, Mr Samuel Elliot Owusu1
1Maritime Life Precious Foundation (MLPF), Kumasi, Ghana.
2HeHeF, Kumasi, Ghana.
Background: In Ghana, the screening of sexually transmitted infections (STIs) among men-who-have-sex-with-men (MSM) often results in prescriptions without actual treatment due to financial constraints faced by key population (KP) implementers and the high cost of STI medications. This leads to delayed or neglected treatment, increasing the risk of HIV transmission. This abstract examines the impact of providing free STI treatment on both STI service uptake and HIV testing services (HTS) among MSM.
Methods: In response to low STI treatment completion rates, MLPF realigned its project budget to offer free STI treatment for MSM. The medications were made available at Community Drop-In-Centers and selected health facilities for easier access. Peer educators raised awareness about the availability of free STI drugs and referred MSM for screening and treatment services.
Results: Programmatic data showed a significant increase in both STI screening and HIV testing following the introduction of free STI treatment. Between December 2023 and January 2024, 235 MSM were referred for STI services, with 148 receiving treatment, representing a 62% completion rate. After the provision of free treatment, between February and March 2024, 231 MSM were referred, and all received STI treatment, achieving a 100% completion rate. Consequently, the number of MSM receiving HTS increased from 405 in December–January to 583 in February-March, reflecting a 43.9% rise in HIV testing uptake.
Conclusions: The provision of free STI treatment is a feasible strategy to enhance HIV testing rates among MSM in Ghana. By removing financial barriers to STI treatment, health systems can foster a more proactive approach to HIV prevention, which may ultimately reduce HIV incidence among MSM. We strongly advocate for policy changes and public health initiatives that integrate free STI medications into comprehensive HIV prevention programs, recognizing the critical interconnection between STI treatment and HIV prevention for this key population.
PP06.93 – Availability and Readiness of STI and HIV Services in Bangladesh: Insights from a Nationally Representative Mixed-Method Study
Dr. Farah Naz Rahman1,3, Dr Mohammad Jahangir Hossain2, Professor AKM Fazlur Rahman2
1International Centre for Diarrhoeal Disease Research Bangladesh, Dhaka, Bangladesh.
2Centre for Injury Prevention and Research Bangladesh (CIPRB), Dhaka, Bangladesh.
3School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia.
Background: Sexually transmitted infections (STIs) and HIV continue to pose public health challenges in Bangladesh. This study assessed the readiness of healthcare facilities to deliver STI and HIV services and to identify key bottlenecks that require policy attention.
Methods: Bangladesh Medical Research Council (BMRC) conducted a facility-assessment survey across 490 public, private, and NGO healthcare-facilities in Bangladesh, selected through weighted cluster-staged sampling to ensure national representation. The adapted WHO’s Service Availability and Readiness Assessment tool was utilized to evaluate service readiness. Readiness was measured across three domains for both STI and HIV services – staff and guidelines, essential medicines, diagnostics – with an additional equipment domain for HIV services. A composite readiness index (RI) was calculated using a weighted additive procedure. Additionally, 12 key informant interviews with national-level policymakers provided qualitative insights.
Results: Among the surveyed facilities, 332 (67%) reported offering STI and HIV services. The overall readiness index for STI services was 46%, indicating that facilities are underprepared compared to the WHO-benchmark of 70–80% for adequate readiness. Public tertiary-facilities exhibited higher readiness (78%), while public primary-facilities were notably deficient at 54%. Availability of diagnostic services was limited, especially in public primary and private facilities. HIV services demonstrated a national readiness index of only 28%, with critical shortages in essential medicines (5%) and basic equipment (19%). KII findings underscored systemic issues, including inadequate resource allocation, weak coordination mechanisms, lack of involvement of key population, and persistent stigma, further impeding service delivery.
Conclusion: Healthcare facilities in Bangladesh are critically underprepared to provide STI and HIV services, with only 28% readiness to deliver comprehensive HIV care. Gaps in essential medicines, diagnostics, and frontline service delivery must be urgently addressed to meet global health targets. Targeted, equity-focused interventions are essential to bridge the readiness gap and ensure vulnerable populations have access to life-saving STI and HIV care.
PP06.94 – Prevalence and Treatment of Syphilis Co-Infection Among Newly Enrolled People Living with HIV: A Study from AHF Nepal’s Collaborative Art Centers
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1, Dr. Unnat Shrestha1, Mr. Ajij Prasad Poudyal1, Ms. Sangita Bhatta1, Mr. Madhab Raj Pant1, Mr. Sanjaya Paudel1, Ms. Bidhya Koirala1, Mr. Radheshyam Shrestha1, Mr. Krishna Hari Sapkota1, Mr. Dharma Raj Bhattarai1, Mr. Bimal Sah1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
AIDS Healthcare Foundation (AHF) Nepal, in collaboration with 19 government ART centers, is dedicated to providing quality HIV treatment services to people living with HIV (PLHIV). In fiscal year 2024, AHF Nepal tested all newly enrolled PLHIV for syphilis to determine the prevalence of syphilis among those receiving HIV services at these centers. Out of 1,384 newly enrolled PLHIV, 72 children and 7 deaths excluded and 1,305 PLHIVs were tested for syphilis. Of these, 193 tested positive, resulting in a syphilis prevalence of 14.8%.
Statistical analysis using a chi-square test revealed a significant association between syphilis positivity and key population groups, including migrants, sexual minorities, and MSM/TG individuals (χ2 = 27.34, P-value < 0.05). The highest syphilis prevalence was observed in migrants (53.33%), sexual minorities (26.67%), and MSM/TG individuals (20%). Age and gender analysis showed that the 25–39 age group had the highest prevalence of syphilis (40%), with a significant age-related difference (P-value = 0.02). Additionally, syphilis positivity was higher in males (68%) compared to females (32%) (P-value = 0.03).
Treatment for syphilis was administered to 60% of the 193 individuals who tested positive. The treatment rates varied across key population groups, with migrants receiving the highest treatment rate (75%), followed by MSM/TG individuals (66.67%) and sexual minorities (25%). Logistic regression analysis indicated that sexual minorities were significantly less likely to receive treatment (OR = 0.22, P-value = 0.01) compared to other groups.
The study also found a significant correlation between syphilis positivity and untreated HIV (P-value = 0.04), highlighting the need for improved co-management of syphilis and HIV.
These findings underscore the high syphilis prevalence among PLHIV, especially within vulnerable populations. The results highlight the necessity for targeted interventions and enhanced services to address both syphilis and HIV, ultimately improving health outcomes and treatment adherence for PLHIV in Nepal.
PP06.95 – Sustainable Health Financing for Marginalized Groups: Nepal’s Free Health Insurance Model for PLHIV
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1, Mr. Ajij Poudyal1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
Nepal introduced its Health Insurance scheme in 2016 to reduce financial barriers to healthcare and improve access to quality services for all citizens. In 2019, a free Health Insurance scheme for People Living with HIV (PLHIV) and their families was launched. However, the uptake was limited, with only 21% of PLHIV enrolled by 2021 at the 16 ART centers collaborating with the AIDS Healthcare Foundation (AHF) Nepal. The primary barrier identified was the stigma and discrimination associated with HIV status disclosure during registration at local ward offices. By 2024, AHF Nepal was supporting 60.4% of the 25,728 PLHIV receiving antiretroviral treatment (ART) in Nepal.
To address these challenges, AHF Nepal initiated a collaborative effort with the Health Insurance Board to modify the registration process, incorporating ART centers as the primary site for insurance registration. Peer Educators were enlisted to support PLHIV during the process, reducing the stigma associated with enrollment. ART centers, where PLHIV have already disclosed their HIV status, were identified as a more suitable environment for integration.
This strategic shift led to a significant increase in enrollment: by 2022, the registration rate increased to 53%, 82% by 2023 and by 2024, it reached 88%. The results suggest that embedding the health insurance registration process within ART services, where individuals are already receiving care and have disclosed their HIV status, improved enrollment rates significantly.
The study demonstrates that merely offering free health insurance is not enough for high enrollment rates. Stigma and the need for a supportive environment are key factors. ART centers, with their established patient trust and privacy, offer an effective setting for registration. The integration of health insurance registration within ART centers, with continuous support from peer educators and other community-based interventions, has proven to be an effective strategy for increasing enrollment among PLHIV.
PP06.96 – Assessing the Shift in HIV Detection Rates Pre- and Post-Community-Led HIV Testing (CLT) Intervention in Nepal
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1, Dr. Unnat Shrestha1, Mr. Bobby Singh1, Mr. Ajij Prasad Poudyal1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
Nepal introduced Community-led HIV Testing (CLT) as “Test-for-Triage” in 2017 to enhance testing uptake, improve case yield, and prevent HIV transmission. The epidemic predominantly affects key populations (KPs), yet over 50% of new HIV infections in 2022 were observed in non-KP individuals. This shift presents challenges in reaching these populations. AIDS Healthcare Foundation (AHF) Nepal has implemented CLT among sexual partners of HIV-negative individuals within KPs to address unsafe sexual behaviors.
This study aimed to assess the difference in the percentage of new HIV cases before and after the CLT intervention among sexual partners of HIV-negative individuals from KPs in Nepal.
A retrospective cross-sectional comparative study was conducted using secondary data from AHF Nepal’s program database between January 2020 and December 2024. Data from January 2020 to July 2021 (pre-CLT intervention) were compared with data from August 2021 to December 2024 (post-CLT intervention). Only data on sexual partners of HIV-negative individuals within KPs were included.
The study revealed a significant increase in HIV positivity following the implementation of CLT. The positivity rate rose from 0.38% in 2020 to 4.36% in 2022, to 4.48% in 2023 and further to 4.74% in 2024. The male population saw a notable increase, from 0% in 2020 to 2.48% in early 2021, 6.71% from August to December 2021, 5.15% in 2022, 5.19% in 2023 and 5.42% in 2024. These findings suggest that CLT has been highly effective in detecting new HIV cases in Nepal.
CLT among sexual partners of HIV-negative individuals from KPs has proven effective in identifying a higher number of new HIV cases, indicating the intervention’s potential to enhance HIV detection and prevention efforts in Nepal.
PP06.97 – Enhancing STI Management Among People Living with HIV in Nepal: Insights from Sudurpaschim Province
Mr. Amrit Bikram Rai1, Dr. Rita Dhungel2
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
2University of the Fraser Valley, Abbotsford, Canada.
Sudurpaschim Province in Nepal faces challenges in the prevention, diagnosis, and treatment of sexually transmitted infections (STIs), particularly among key populations such as sex workers (SWs), people living with HIV (PLHIVs), and migrants. This study analyzes STI testing, confirmation, and treatment trends across multiple districts based on program data from July 2023 to June 2024, aiming to identify gaps and performance disparities in STI management for high-risk groups.
Data on STI testing, confirmed cases, and treatment status were collected from 6,521 individuals across 9 districts in Sudurpaschim Province during the fiscal year from July 2023 to June 2024. The analysis focused on key populations, including PLHIVs, sex workers, people who inject drugs (PWIDs), men who have sex with men (MSM), transgender individuals (TG), and pregnant women. Key performance indicators like confirmation rate and treatment success rates were evaluated to assess the effectiveness of STI care in the region, with particular emphasis on PLHIVs.
A total of 6,521 individuals were tested, with Kailali and Kanchanpur reporting the highest numbers. Darchula had the highest confirmation rate at 100%, while Bajura and Dadeldhura reported no confirmed cases. Overall treatment success was 89.6%. Testing among PLHIVs included 980 individuals, with Kailali testing 645 and reporting 32 confirmed cases, 31 of which received treatment. Achham and Kanchanpur showed 100% confirmation and treatment rates for PLHIVs, while Bajura reported no confirmed cases despite testing 164 PLHIVs, indicating potential diagnostic issues. Disparities in testing and confirmation rates were observed across districts, suggesting the need for improved diagnostic practices and resource allocation.
The study reveals significant disparities in STI testing, diagnosis, and treatment across Sudurpaschim Province. Although treatment rates are high, targeted interventions are needed to improve diagnostics, expand outreach, and address resource gaps, particularly for PLHIVs, to ensure comprehensive care and reduce vulnerability to STIs.
PP06.98 – Using the RE-AIM Framework to Evaluate the Reach of Pre-Exposure Prophylaxis Services in a Sexual Health Clinic in Ontario, Canada
Miss Carmela Rapino1,2, Dr. Emma Nagy2, Dr. Sahar Saeed1, Dr. Beatriz Alvarado1, Ms. Nicole Szumlanski2, Ms. Miriam Kamotho2, Dr. Hugh Guan2, Dr. Jorge Martinez-Cajas1
1Queen’s University, Kingston, Canada.
2South East Public Health Unit, Kingston, Canada.
Background: HIV diagnoses in Canada have increased by 35.2% from 2022-2023, challenging the attainment of the UNAIDS 95-95-95 targets. Scaling access to pre-exposure prophylaxis (PrEP) is critical, yet uptake remains low, particularly in suburban and rural areas. Since 2018, the Kingston, Frontenac, Lennox, and Addington Public Health Unit (KFL&A PHU) has offered PrEP services through its sexual health clinic (SHC) to address these gaps. This study aims to evaluate the clinic’s reach.
Methods: The SHC operates with an interdisciplinary team, initially targeting gay, bisexual, and other men who have sex with men (gbMSM), but later expanding to all populations at risk of HIV. Clients are referred by healthcare providers or self-initiate care. The clinic offers in-person and remote services, including SMS reminders and phone appointments, for eligibility assessments, prescriptions, and follow-ups. Using the RE-AIM framework, client characteristics were developed in consultation with SHC staff and analyzed from electronic medical records to define reach. Risk was stratified using the high-incidence risk index (HIRI), a screening tool that assesses demographics, sexual behaviours, and substance use.
Results: Between October 1, 2018, to December 15, 2024, 171 clients consulted the PrEP clinic, and 71.8% initiated PrEP. Most clients were male (97.8%), aged 29–40 (35.5.%), who lived locally (74.5%), and had primary care attachment (57.4%). Due to low sample size, clients reporting heterosexuality and shared injection drug use are not reported. As seen in Fig. 1, high-risk behaviours were predominately observed in two HIRI categories: age (60.3%) and condomless receptive anal sex with a man (51.1%). Additionally, 46.1% of clients reported a history of an STBBI, with chlamydia being the most common (24.1%).
Conclusion: While the SHC effectively reaches gbMSM, other populations remain underserved. Addressing these gaps requires tailored outreach strategies and inclusive screening practices to optimize HIV prevention.
Client Distribution of High Incident Risk Index (HIRI) Responses Stratified by Level of Risk.
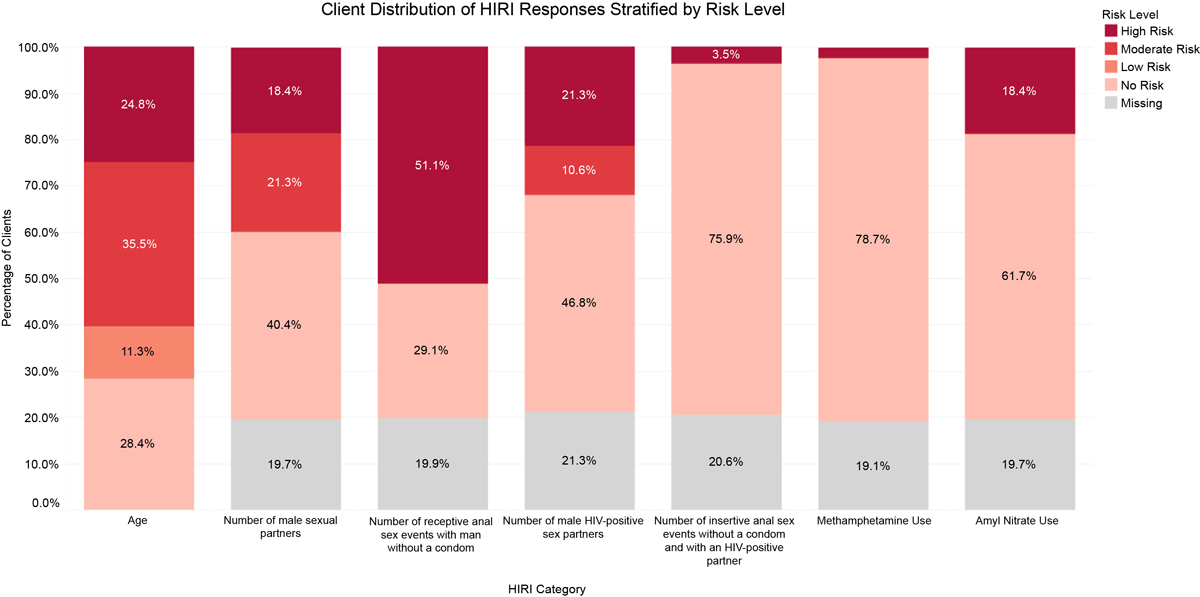
Note. Stratification based on level of risk within each HIRI category are as follows: ages < 18 and 49 represent no risk, 18–28 represent high risk, 29–40 represent moderate risk, and 41–48 represent low risk. For number of male sexual partners in the last 6 months, >10 represents high risk, 6–10 represents moderate risk, and 0–5 represents no risk. For number of receptive anal sex events with a man without a condom, >1 positive partner represents high risk and <1 time represents no risk. For number of make HIV-positive sex partners, >1 positive represents high risk, 1 positive partner represents moderate risk, and <1 positive partner represents no risk. For the number of insertive anal sex events without a condom and with an HIV-positive partner, 5 or more times represents high risk, and 0–4 represents no risk. For methamphetamine and amyl nitrate use, “Yes” represents high risk and “No” represents no risk.
PP06.99 – A Human-Centered Design Approach to Re-Designing Sexual Health Care in St Louis
Ms. Anne Trolard1, Dr. Hilary Reno
1Washington University in St Louis, St Louis, United States.
Background: Public health strategies for sexually transmitted infections have limited reach into communities that bear the greatest burden from infections. Limited evidence exists on the fit between these communities and STI services intended to reach them. In contrast to traditional public health inquiries, human-centered design methods place the system under the microscope instead of people, and assess how services should meet people’s needs. HCD methods assert it can be difficult to accurately characterize problems involving complex interactions between people and processes. This is especially true for (1) those who seek healthcare without access to the required resources (e.g. transportation, flexible schedule, adequate finances), and (2) stigmatized health conditions like an STI.
Methods: This study explores from the vantage point of patients the pain points and opportunities in accessing the sexual health care system in St. Louis through (1) secret shopper reports; and (2) a think-aloud exercise simulating a sexual health clinic experience. We recruited participants through advisory groups and clinics. Rapid qualitative analysis methods were used to analyze audio-transcriptions and shopper reports to summarize data and produce insights.
Results: Two of 3 secret shopper reports and 5 of 7 interviews have been completed. Preliminary results from secret shopper reports showed that requests for sensitive personal information made without an explanation for how that information is used or why it is collected raised concerns; and the presence of security guards sent unintended messages to patients with a history with law enforcement. Preliminary results from the think-aloud exercises mirrored secret shopper findings in that requests for personal and health information were met with both trusting and distrusting reactions, but could be easily re-designed to build trust.
Conclusion: When collecting information on stigmatized conditions it would help patients to know why sensitive information is collected and with whom it could potentially be shared.
PT01.01 – ABI-5366, a Potent HSV Helicase-Primase Inhibitor, with Potential for Weekly or Monthly Oral Dosing for Recurrent Genital Herpes
Dr Michael Shen1, Dr Carl Li1, Dr Zhixin Zong1, Dr Heidi Contreras1, Dr Ran Yan1, Dr Michel Perron1, Dr William Delaney1, Dr Katie Kitrinos1
1Assembly Biosciences, South San Francisco, United States.
Background: Recurrent genital herpes (RGH), primarily caused by herpes simplex virus type 2 (HSV-2) infection, results in painful genital lesions. RGH suppression standard of care is nucleoside analogues (NA, e.g. valacyclovir); however, NAs are limited by suboptimal efficacy. Helicase primase inhibitors (HPIs), a novel class of antivirals, have shown improved efficacy compared to NAs. ABI-5366 is a long-acting oral investigational HPI in development for RGH treatment.
Methods: HSV antiviral assays were conducted in Vero cells. Metabolic stability was measured in rat, dog, monkey, and human liver microsomes. Pharmacokinetic (PK) studies evaluated 0.1–1 mg/kg ABI-5366 IV in rats, dogs, and monkeys, and an oral (PO) dose of 100 mg ABI-5366 in dogs. A bile-duct cannulated (BDC) study was conducted in rats with 0.5 mg/kg ABI-5366 IV. Reabsorption of 5366 following intestinal secretion was evaluated in dogs dosed with 0.1 mg/kg ABI-5366 IV ± 25 g/kg activated charcoal PO dosed every 2–8 h from 2 h pre-ABI-5366 dosing to 120 h post-ABI-5366 dosing. Tissue distribution was evaluated in rats after a single 15 mg/kg PO dose.
Results: In vitro, ABI-5366 inhibited HSV-1 and HSV-2 clinical isolates with low nanomolar potency (4–39 nM). ABI-5366 was metabolically stable in liver microsomes (CLint <9 mL/min/kg). Preclinical PK studies demonstrated that ABI-5366 has a very low clearance (CL = 0.002–0.02 L/h/kg) and an extended half-life (20–71 h). A rat BDC study showed ABI-5366 is mainly eliminated unchanged through feces. Co-dosing ABI-5366 with activated charcoal resulted in higher clearance and shorter half-life, suggesting intestinal reabsorption contributes to the extended half-life. ABI-5366 was well distributed in all tissues evaluated, including the ganglia (the HSV reservoir).
Conclusion: ABI-5366 is a potent HPI with broad activity against HSV-1 and HSV-2 and a PK profile supporting potential weekly or monthly dosing. A phase 1b study of ABI-5366 in RGH patients is ongoing.
PT01.02 – Investigating the Bacterial Side of the Host-Pathogen Interaction: Treponema Pallidum Proteome Response to Brain Endothelial Cell Exposure
Ms. Angela Mitchell1, Dr. Simon Houston1, Mr. Alloysius Gomez1, Dr. Mara Goodyear1, Mr. Derek Smith2, Dr. David Goodlett1,2, Dr. Caroline Cameron1,3
1University of Victoria, Victoria, Canada.
2University of Victoria-Genome BC Proteomics Centre, Victoria, Canada.
3University of Washington, Seattle, United States.
Background: Syphilis vaccine development requires a comprehensive understanding of the pathogenic mechanisms used by Treponema pallidum to infect the host, including how the bacterium crosses the blood-brain barrier (BBB) to cause neurosyphilis. Current understanding of the molecular mechanisms used by T. pallidum to cross the BBB is limited. Here, we use mass spectrometry (MS)-based label-free quantitative proteomic analyses to investigate T. pallidum protein expression following exposure to brain microvascular endothelial cells (BECs), a model for the BBB.
Methods: Treponema pallidum was co-incubated for 4 and 24 h with BECs or rabbit epithelial cells (Sf1Eps; serves as a control for in vitro T. pallidum growth). Bacteria were isolated using an in-house developed gentle sample preparation method optimized for T. pallidum proteomics studies. Protein identification was accomplished using liquid chromatography-tandem MS (LC-MS/MS) and T. pallidum protein expression levels were determined using label-free quantification (LFQ) based on peptide ion peak intensities from three biological replicates.
Results: Quantitative proteomic analysis of T. pallidum following co-incubation with BECs allowed identification of expression level changes in T. pallidum proteins in response to endothelial cells. Global protein expression levels were also determined for proteins that mapped to the categories of predicted pathogenesis-related proteins, proteins involved in transport or regulatory networks, and predicted/known outer membrane proteins (OMPs). Analysis of expression levels of T. pallidum OMPs was prioritized since these proteins reside at the host-pathogen interface and are therefore promising targets for syphilis vaccine development.
Conclusion: These analyses identified T. pallidum proteins and protein categories that are altered in expression levels in response to brain endothelial cell exposure. This study informs our understanding of T. pallidum pathogenesis, and in particular syphilis vaccine development, by providing a nuanced approach to identifying T. pallidum proteins that are important for blood-brain barrier traversal and neurosyphilis.
PT01.03 – The Role of Estradiol in Sequestration of HIV-1 R5 in Endometrial Epithelial Cells
Dr. Aisha Nazli1, Dr Charu Kaushic1
1McMaster University, Hamilton, Canada.
Background: Women, who make up majority of HIV-1 infections globally, contract HIV-1 primarily through heterosexual intercourse via the female reproductive tract (FRT). Although both R5 and X4 HIV-1 strains are present in semen, initial infection in the FRT mainly occurs through the R5 strain. Previously we found that X4 HIV exposure induced a strong anti-viral response by genital epithelial cells (GECs), that was not seen in response to R5 HIV. This resulted in X4 HIV getting sequestered in GECs while R5 HIV crossed the epithelium unhindered. Since sex hormones influence the immune response of FRT GECs to viruses, we examined the effect of sex hormones on the interactions between HIV-1 strains and genital epithelial cells.
Methods: Human endometrial tissues were obtained with informed consent from women undergoing elective hysterectomy. GECs were grown in monolayer cultures with no hormone or in the presence of estradiol (10–9 M) or progesterone (10–7 M). HIV-1 leakage through GEC monolayers was observed in basolateral supernatants by TZMbl assay. Intracellular trafficking of HIV-1 was studied by immunofluorescence microscopy.
Results: When GECs were exposed to HIV-1 in the absence of hormones, significant upregulation of the TLR2-signaling pathway was observed only in response to X4 but not R5 HIV-1. In contrast in the presence of estradiol, GEC induced comparable anti-viral immunity to both X4 and R5 HIV. TLR2 pathway activation by estradiol resulted in the upregulation of anti-viral factors BST-2 and ISG-15, and sequestration of both X4 and R5 HIV-1 in the endosomal compartment. In contrast, GECs grown in the presence of progesterone downregulated IFN signaling in response to both strains of HIV.
Conclusion: Results showed that in the absence of hormones, only HIV-1 X4 triggers a strong antiviral response. Estradiol treatment targets anti-viral immunity against X4 and R5, trapping both viruses in GECs.
PT01.04 – In Vitro Selection and Characterization of Resistance to Josamycin and Pristinamycin in Mycoplasma Genitalium
Dr. Chloé Le Roy1, Dr. Otgonjargal Byambaa1, Dr. Jennifer Guiraud2, Mrs. Carla Balcon2, Mr. Léo Gilet2, Dr. Jorgen Skov Jensen3, Pr. Cécile Bébéar1,2, Prof. Sabine Pereyre1,2
1University of Bordeaux – CNRS, Bordeaux, France.
2CHU Bordeaux – French National Reference Center for Bacterial STIs, Bordeaux, France.
3Department of Bacteria, Parasites and Fungi, Statens Serum Institut, Copenhagen, Denmark.
Background: Pristinamycin is a recommended third-line treatment of Mycoplasma genitalium infections according to the European guidelines. No data regarding mechanisms of pristinamycin resistance have been available to date. In M. pneumoniae, crossed resistance to pristinamycin and josamycin was associated with mutations at position 2062 (Escherichia coli numbering) of 23S rRNA.
We investigated the in vitro development of resistance in M. genitalium in the presence of subinhibitory concentrations of josamycin and pristinamycin.
Methods: Selection of resistant mutants was performed by serial passages of M. genitalium G37 reference strain in subinhibitory concentrations of josamycin or pristinamycin. Resistant mutants were characterized by Sanger sequencing of 23S rRNA, L4 and L22 ribosomal protein genes and MICs of seven antibiotics were determined. Whole genome sequencing (WGS) was performed on selected mutants using the Illumina technology.
Results: A mutant selected in the presence of josamycin harbored the A2059G mutation in 23S rRNA. This mutant showed a strong increase in the MICs of erythromycin, azithromycin, josamycin, and clindamycin (16–32 µg/mL), but no changes in MICs of pristinamycin, doxycycline, and moxifloxacin (all three at 0.125 µg/mL). Two mutants selected in the presence of pristinamycin harbored mutation A2062C or A2062G. Both mutants showed a strong increase of the MICs of pristinamycin (8 and 2 µg/mL, respectively) and josamycin (32 and 16 µg/mL, respectively) and a slight 4 to 8-fold increase of erythromycin MIC. Azithromycin, clindamycin, doxycycline and moxifloxacin MICs remained unchanged. No mutations in L4 and L22 gene were detected in any mutants. WGS of the three mutants confirmed the 23S rRNA mutations associated with antibiotic resistance and revealed 6 to 10 additional SNPs not likely to be involved in resistance.
Conclusion: Resistant mutants can be selected in vitro in M. genitalium using josamycin and pristinamycin. These laboratory-derived mutants may predictive for mutations observed in clinical strains.
PT01.05 – Genomic Surveillance of Neisseria Gonorrhoeae Isolates from Cameroon and Madagascar: Resistance Patterns and Phylogenetic Insights
Dr. Lala Rafetrarivony1, Dr. Rosanne Ngome2, Mr. Arsène Djoko2, Dr. Elisoa Ratsima Hariniaina3, Dr. Frédérique Randrianirina3, Dr. Lovasoa Ramparany3, Dr. Solène Cottis4, Dr. Chiara Crestani4, Pr. Sylvain Brisse4, Dr. Tania Crucitti1
1Bacteriology Experimental Unit, Institut Pasteur Madagascar, Antananarivo, Madagascar.
2Centre Pasteur Cameroon, Yaoundé, Cameroon.
3Clinical Biology Centre, Institut Pasteur Madagascar, Antananarivo, Madagascar.
4Institut Pasteur, Université Paris Cité, Biodiversity and Epidemiology of Bacterial Pathogens, Paris, France.
Background: Antibiotic resistance poses a global health threat, significantly impacting sexual health. In Africa, weak regulation of antibiotic use exacerbates the problem, with resistance rates and genomic data underreported. To address this gap, the ‘Surveillance of Antimicrobial Resistance in Africa’ (SARA) project was initiated. This project included surveillance of Neisseria gonorrhoeae, a major threat to sexual health globally, in Cameroon and Madagascar.
Methods: Within this framework, gonococcal isolates with antimicrobial susceptibility test (AST) data were obtained from medical laboratories. Forty isolates from Cameroon (2018–2023) and 73 isolates from Madagascar (2021–2023) were sequenced using Illumina technology. These sequences were analyzed together with public PubMLST genomic sequences, comprising 50 for Cameroon and 119 for Madagascar.
Results: High phenotype-genotype concordance was observed for isolates from Madagascar, whereas discrepancies were detected in Cameroon, particularly for azithromycin. In 2023, an azithromycin-resistant ST9363 isolate from clonal complex (CC)168 carrying a mosaic mtrD gene and a genotypically cefixime-resistant ST7363 (CC348) isolate carrying a penA (10.001) mosaic allele were detected in Cameroon and Madagascar, respectively. ST1588 is prevalent and persistent in both countries, while ST17783, undocumented elsewhere, exhibits similar prevalence and persistence over time in Madagascar. Core genome and SNP analysis revealed clusters in each country (8 in Madagascar and 7 in Cameroon). Using the threshold of 300 allele differences, only two of 40 clusters were shared between the two countries (Ng_cgc_300: 133 and 239). In Madagascar, the majority of core genome clusters comprising at least two isolates (13 out of 19) had not been previously identified in other countries.
Conclusion: This work highlights that Madagascar has its own circulating clones of N. gonorrhoeae which evolve over time, whereas those in Cameroon follow the trend observed in Africa. However, continued and extended surveillance is needed to better understand the molecular epidemiology of N. gonorrhoeae in these countries and more broadly in Africa.
PT01.06 – Genomic Variations in the Chlamydia Trachomatis Polymorphic Membrane Protein Gene Pmpe Exhibit Anatomic Site-Specific Tissue Tropism in a Non-Human Primate Model
Mr. Robert Suchland1, Mrs. Yvonne Cosgrove-Sweeney2, Dr. Dorothy Patton2, Dr. Lucia Vojtech2, Dr. Olusegun Soge3, Dr. Christine Khosropour4, Dr. Kevin Hybiske1
1Department of Medicine, University of Washington, Seattle, WA, United States.
2Department of Obstetrics and Gynecology, University of Washington, Seattle, United States.
3Department of Global Health, University of Washington, Seattle, United States.
4Department of Epidemiology, University of Washington, Seattle, United States.
Background: Chlamydia trachomatis (CT) infects the mucous membranes of the genital tract, anorectum, and conjunctiva. Genomic studies have revealed clear lineages and distinct genomic profiles of the CT strains that exhibit tropism for these different anatomic sites. We previously showed that specific pmpE genotypes are strongly associated with genital infections in females vs rectal tropism in males. PmpE is a surface-exposed membrane protein which we hypothesize promotes differential infection across distinct anatomic sites. To investigate how these varying genotypes might lead to tissue site-specific infection phenotypes, we performed in vivo studies utilizing a non-human primate (NHP) CT infection model.
Methods: Seven pig-tailed macaques were inoculated either in the cervix (N = 3) or rectum (N = 4) with inocula containing equal titers of three CT clinical strains. These strains were selected based on their isolation from different anatomic sites and pmpE genotypes: D (female rectal isolate with cervical pmpE), G (cervical isolate with cervical pmpE), and Ga (MSM rectal isolate with rectal pmpE). Infected pig-tailed macaques were monitored by cell culture for 8 weeks with weekly swab collections.
Results: Strain D was isolated from both the cervix and rectum by cell culture each week in two of both the cervically and the rectally inoculated macaques, while the Ga strain was only isolated from the cervix periodically through the first 4 weeks of the cervically inoculated macaques. In contrast, strain Ga was isolated from the rectum weekly in three of the rectally inoculated macaques throughout the 8-week study. The G strain was only isolated intermittently from either site, regardless of the site of inoculation.
Conclusions: These results strengthen the hypothesis that pmpE genotypes correlate with tissue-specific tropism. Continued exploration of PmpE function both in vitro and in the NHP model could further facilitate the understanding of CT infections and promote future vaccine development.
PT01.07 – Unveiling the Vaginal Microbiome: A Metagenomic Study of Bacterial Vaginosis in Women from Northern India
Ms Gurmeet1, Dr Rakesh Yadav1, Dr Rashmi Bagga1, Dr Amit Arora1, Dr Sunil Sethi1
1Postgraduate Institute of Medical Education and Research (PGIMER), Chandigarh, India.
Background: Bacterial vaginosis (BV) is a clinical state of microbial dysbiosis among women of reproductive age. The diagnosis of BV remains problematic due to its polymicrobial etiology. The current diagnostic methods Amsel’s criteria and Nugent scoring system are subjective and can’t identify new morphotypes. In this study, we compared the vaginal microbiome of BV-positive with BV-intermediate and BV-negative population to assess the distinct shifts in bacterial communities and identify key changes in microbial composition.
Methods: A total of 701 women with complaints of abnormal discharge, or for routine gynecological check-ups were enrolled between November 2021 to May 2024 from the Department of Obstetrics and Gynaecology, PGIMER, Chandigarh. Two high vaginal swabs were collected from each participant along with medical history and demographic details. Amsel’s criteria was determined clinically and smear microscopy was performed for Nugent scoring. DNA was extracted followed by V3-V4 16SrRNA gene sequencing on Illumina MiSeq platform.
Results: Based on Nugent scoring, 95/680 (13.9%) samples were found to be BV-positive, 174/680 (25.5%) BV-intermediate and 411/680 (60.4%) BV-negative. BV was most prevalent among women aged between 28–37 and strongly associated with symptoms, including abnormal discharge (87.3%), odor (50.5%) and vaginal itching (40%). The 16S metagenomic sequencing was performed for 265 (77 BV-positive, 88 BV-intermediate and 100 BV-negative) samples. Metagenomic analysis revealed the predominance of Gardnerella, Sneathia, Atopobium and Prevotella in BV-positive samples while BV-intermediate group had abundant lactobacilli, Gardnerella and Sneathia. The alpha diversity was found to be higher in BV-positive group. In contrast, BV-negative group was marked by high prevalence of lactobacilli and comparatively low evenness (Fig. 1).
Conclusion: Metagenomic sequencing could comprehensively elucidate the distinct microbial profiles associated with BV-positive and BV-negative women, unravelling intricate microbial signatures, which would be helpful in the early detection of BV, and development of targeted management strategies, thus advancing and enhancing women health outcomes.
(a) Taxa bar plots representing relative abundance of Top 10 genus in different groups; (b, c) Alpha diversity analysed using Kruska–Wallis test and D-PCoA (Principal Coordinate Analysis) generated using Bray–Curtis distance indicating distinct clustering of samples from each group.
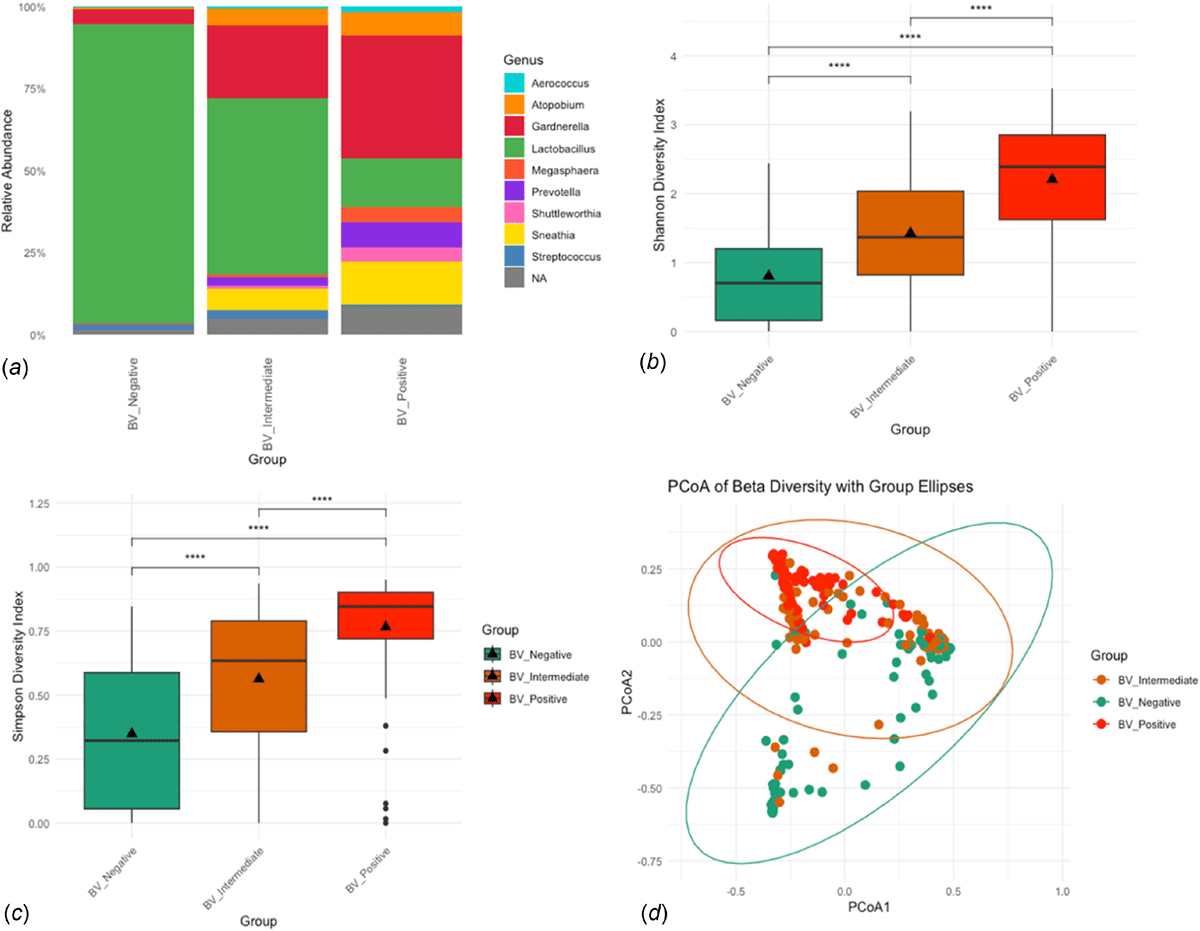
PT02 .01 – The Impact of ‘Undetectable=Untransmittable’ on Health Outcomes: A Systematic Review and Qualitative Synthesis
Mr Daniel Zhao Yang Chong1, Mr Andrew Amadeus Susilo1, Mr Judd Denzel Garcia Mondina1, Ms Jia Wen Tay1, Mr Clifton Liu Ziheng1, Mr Micheal Ighodaro2, Dr Christina Misa Wong1, Dr Joseph D Tucker3,4, Dr Rayner Kay Jin Tan1
1Saw Swee Hock School of Public Health, National University of Singapore and National University Health System, Singapore, Singapore.
2Global Black Gay Men Connect Corporation, New York City, USA.
3Institute for Global Health and Infectious Diseases, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA.
4Clinical Research Department, Faculty of Infectious and Tropical Diseases, London School of Hygiene & Tropical Medicine, London, UK.
Background: The ‘Undetectable=Untransmittable’ (U=U) campaign revolutionized HIV care through affirming that people living with HIV who are virally suppressed cannot sexually transmit HIV. Given its public health impact, this systematic review and qualitative analysis was undertaken to examine the impact of U=U on health outcomes of individuals globally.
Methods: We used the Cochrane Handbook and registered the review (PROSPERO: CRD42024525175). PubMed, CINAHL, PsycINFO, ProQuest, and Scopus were searched for relevant studies. The purpose of the review is to examine how knowledge of U=U impacted a wide range of outcomes. Thematic analysis was employed to derive our themes. We assessed study quality using the Critical Appraisal Skills Programme checklist.
Results: The search identified 4065 studies, of which 82 were included in the synthesis. Study populations included people living with HIV (k = 41), gender and sexual minority men (k = 24), and individuals in serodiscordant relationships (k = 14). Study settings included high- (k = 50), middle- (k = 34), and low-income countries (k = 6). Knowledge of U=U impacted health outcomes in five health areas: behavioral, psycho-emotional, relational, socio-cultural, and health communications. A summary can be found in Fig. 1. In the behavioral domain, U=U contributed to greater treatment adherence (k = 15). In the psycho-emotional domain, U=U provided a return to normalcy for individuals (k = 11). In the relational domain, U=U encouraged open communication (k = 9) and provided certainty within serodiscordant relationships (k = 8). In the socio-cultural domain, U=U has decreased societal stigma within varying populations (k = 11). In the domain of health communications, individuals and healthcare workers were motivated (k = 11), and confident (k = 15), in communicating U=U. Nevertheless, these were met with confusion on how HIV is transmitted when an individual is undetectable (k = 11).
Conclusion: We found that the concept of U=U has demonstrated a positive impact on various health outcomes at multiple levels. U=U should be incorporated as part of key messaging in HIV care communications.
PT02 .02 – Does the Crowd Want to Crowdsource? Crowdsourcing Acceptability for PrEP Promotional Messaging in the Southern United States
Kevin M. Joseph1, Dr. Latesha Elopre1, Dr. Lynn T. Matthews1, Dr. Barbara Van Der Pol1, Dr. Joseph D. Tucker2,3, Dr. Ronnie Gravett1
1University of Alabama at Birmingham, Birmingham, United States.
2University of North Carolina – Chapel Hill, Chapel Hill, United States.
3London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: HIV pre-exposure prophylaxis (PrEP) uptake in the Southern United States (US) remains poor due to stigma, medical mistrust, and structural barriers, thus perpetuating HIV disparities, especially among sexual minority men (SMM) of color. Crowdsourcing engages the community to create and share solutions. Little formative research has been done on organizing crowdsourcing for HIV prevention services, especially in the Southern US context. We explored the acceptability of crowdsourcing and identified practical tips for crowdsourcing to develop PrEP promotions among SMM and sexual health providers.
Methods: Grounded in the Theoretical Framework of Acceptability (TFA), we conducted focus group discussions (FGD) with HIV-negative SMM ages 18–39 years and interviews with sexual health providers using topic guides grounded in the TFA. FGDs and interviews were recorded and transcribed. We deductively and inductively coded transcripts to develop and iteratively revise the codebook. We utilized thematic analysis to develop themes with sub-themes for richer context and mapped themes to TFA constructs.
Results: We conducted 2 FGDs (n = 10, 60% Black, 50% younger than 30 years) and 6 provider interviews. We identified 4 themes: (1) Participant identity/background informs the participation and the products of crowdsourcing, (2) Motivation to participate in crowdsourcing is strong, (3) Crowdsourcing participants require resources (e.g. compensation, skilled support) to effectively engage, and (4) Logistic and social barriers (e.g. scheduling/timing, stigma) may prevent inclusive crowdsourcing participation. Table 1 shows themes and sub-themes mapping to TFA constructs with exemplar quotes.
Conclusion: SMM and sexual health providers found that crowdsourcing to create PrEP promotions in the Southern US is acceptable and would be effective. These novel findings demonstrate new understanding of how SMM would consider participating in crowdsourcing events and provide insight into the future design of crowdsourcing events. Sexual health stakeholders should use this participatory tool to create authentic, inclusive messaging to increase PrEP uptake.
| Theme | Sub-theme | Construct | Exemplar Quotes | |
|---|---|---|---|---|
| Participant identity/background informs the participation and products of crowdsourcing | SMM and non-SMM should participate and be the audience in crowdsourcing. | Affective Attitude, Perceived Effectiveness | So, it’ll be great if it was created by the community that is directly affecting. But I also think that in some cases, I just think that it needs to be a little bit more of a broader spectrum. (FG1, Interviewee 3) | |
| Non-LGBTQ+ providers express caution about participating in crowdsourcing past sharing medical expertise. | Affective Attitude, Ethicality | I do feel like my experience would be more limited just because I would only feel like I could really comment on the accuracy of the content from a scientific point of view. I couldn’t comment on the acceptability of the content. […] I’m not the target demographic. (Provider 1) | ||
| Crowdsourcing processes and products should intentionally have diverse representation. | Perceived Effectiveness | A gay, Black man is more inclined to listen to another gay, Black man…I think if there are more commercials where there are more gay, Black men or even straight, Black men there are just more black people expressing that it is okay to protect yourself from HIV (FG2, Interviewee 4) | ||
| Motivation to participate in crowdsourcing is strong | SMM want to participate in crowdsourcing and give back to their community. | Affective Attitude | I think I would be able to participate. And feel…proud to have done such…And you kind of begin to give back to the community that way, silently almost, (FG2, Interviewee 5) | |
| Providers want to participate in crowdsourcing to serve the community while addressing the HIV epidemic | Affective Attitude | I would think that anything that pushes us out of the provider space, and into a more community space, and maybe what we can learn globally, and bring to our prevention portfolio, would be beneficial. I think for that crowd sourcing would be really good for this. (Provider 2) | ||
| Crowdsourcing participants require resources to effectively engage | Community heroes could increase crowdsourcing’s promotional messaging products’ appeal | Perceived Effectiveness | It needs to be highly specific and also huge emphasis on community heroes because…they don’t stop scrolling unless it’s someone they recognize (FG1, Interviewee 2) | |
| Effective crowdsourcing needs funding to produce and media to share the product | Perceived Effectiveness | When you were speaking about challenges or problems or creating that, like I think another issue would be having proper funding to make sure that the message could be told correctly. (FG1, Interviewee 3) | ||
| Participants may have or may not have sufficient HIV knowledge or skill sets to effectively participate | Self-Efficacy | You know, we can come up with a bunch of solutions. But if no one understands the problem, then what are we solving? (FG1, Interviewee 2) | ||
| The expectations of the plan and process of crowdsourcing must be clear to recruit participants | Intervention Coherence | I think you would have to just be a little more specific than just saying, “We’re doing crowdsourcing”…If they know what’s being asked of them, they’re probably going to be more apt to participate. (Provider 3]) | ||
| Logistic and social barriers may prevent inclusive crowdsourcing participation | The time to crowdsource must be convenient, organized, and reasonable for participation | Burden, Opportunity Costs | And how strongly you feel about it. So that would kinda dictate and determine what time you allow it to take away from other prospects. (FG2, Interviewee 5) | |
| Compensation for the time spent on crowdsourcing could be necessary for participation | Burden | If it’s for free, because I can’t do nothing for free. (FG1, Interviewee 1) If you can comp people [for] their time, they will be more inclined to doing it. (FG1, Interviewee 2) | ||
| Both medical providers and community members may have differing beliefs and comfort discussing HIV as part of crowdsourcing | Ethicality, Affective Attitude | [Providers] who are not in it and doing it all the time may think this is a moral dilemma, because it’s promoting promiscuity or all these things that we know are not true (Provider 3) Some of the crowd, even in that community, will not appreciate it. Everyone is not always going to agree with that, but this is something that has to be done. (FG1, Interviewee 5) | ||
| Privacy and stigma concerns for both SMM and providers surrounding sexual health/HIV | Affective Attitude, Opportunity Costs | For me personally, I probably would not want to be a face [whose] involved. But I’m offering ideas or my own personal experiences maybe. (FG2, Interviewee 2) |
PT02 .03 – Women’s Preferences for Hypothetical PoCT for STIs in Madagascar, South Africa and Zimbabwe – a Discrete Choice Experiment
Prof. Ayako Honda1, Dr Timothy Barry Bolt2, Dr Chido Dziva Chikwari3,6, Dr Katherine Gill4, Dr Aina Harimanana5, Ms Lucia Jola4, Ms Tinashe Mwaturura3, Dr Thandeka Nkosi4, Ms Vaomalala Raharimanga5, Dr Emma Harding-Esch6, Dr Kimie Kitai7
1Hitotsubashi University, Kunitachi, Japan.
2Saitama University, Saitama, Japan.
3Organization for Public Health Interventions and Development, Harare, Zimbabwe.
4Desmond Tutu Health Foundation, Cape Town, South Africa.
5Institut Pasteur de Madagascar, Antananarivo, Madagascar.
6London School of Hygiene and Tropical Medicine, London, United Kingdom.
7Japanese Red Cross College of Nursing, Shibuya, Japan.
Background: Most women with laboratory-confirmed sexually transmitted infections (STIs) or bacterial vaginosis (BV) are asymptomatic. In low- and middle-income countries, due to both supply and demand-side issues, STIs and BV are only treated if women present with clinical symptoms, despite asymptomatic women being at increased risk of HIV infection and pregnancy complications. Point of Care Testing (PoCT) to detect genital inflammation and asymptomatic infection can significantly improve health outcomes by enabling timely treatment of asymptomatic STIs.
Methods: A discrete choice experiment (DCE) was undertaken in Madagascar, South Africa and Zimbabwe to examine patient preferences for various aspects of STI management that includes PoCT. Results from qualitative interviews were supplemented by a literature review to inform attributes and levels selected for the DCE. At each study site, locally-trained interviewers administered face-to-face choice experiment interviews with 200 women aged 18–35. Mixed logit models were estimated for analysis.
Results: Most participants indicated they were likely to use PoCT for STI. Attributes consistently increasing acceptance of the implementation of PoCT for STIs include provision of HIV preventive medication upon a positive result, medicine availability at the facility undertaking PoCT, and detailed explanation of STI PoCT before testing. Socio-economic status influenced preferences for some attributes. Variations in relative importance of attributes exist in the three study sites, possibly reflecting different health system contexts.
Conclusion: Women in the study settings are interested in PoCT for STI. Broader health system factors need to be improved to effectively deliver STI PoCT services. Availability of sustainable medicine supplies at PoCT health facilities was highly valued by women in all study settings. Successful integration of STI PoCT in day-to-day healthcare service delivery requires contextualizing implementation strategies and considering target population.
PT02 .04 – Prospective Acceptability of a Novel Point-Of-Care Genital Inflammation Test to Identify Women with Sexually Transmitted Infections and Bacterial Vaginosis in Zimbabwe and South Africa
Mr Jayjay Karumazondo1,2, Mr Jason Naidoo3, Dr Sarah Bernays4, Ms Thulisa Mayekiso3, Ms Maureen Tshuma1, Ms Tinashe Mwaturura1, Dr Chido Dziva-Chikwari1,5, Dr Eneyi Kpokiri6, Dr Katherine Gill3, Dr L Becker3, Dr Lindi Masson7,8, Dr Jo-Ann Passmore8,9, Dr Emma Harding-Esch6, Dr Constance Mackworth-Young1,10
1The Health Research Unit, Biomedical Research and Training Institute, Harare, Zimbabwe.
2Department of Demography Settlement and Development, University of Zimbabwe, Harare, Zimbabwe.
3Desmond Tutu Health Foundation, Cape Town, South Africa.
4Faculty of Medicine and Health, University of Sydney, Sydney, Australia.
5Infectious Disease Epidemiology and International Health Department, London School of Hygiene & Tropical Medicine, London, United Kingdom.
6Clinical Research Department, Faculty of Infectious and Tropical Diseases, London School of Hygiene & Tropical Medicine, London, United Kingdom.
7Burnet Institute, Melbourne, Australia.
8Institute of Infectious Disease and Molecular Medicine, University of Cape Town, Cape Town, South Africa.
9National Health Laboratory Service, Cape Town, South Africa.
10Department of Global Health and Development, London School of Hygiene & Tropical Medicine, London, United Kingdom.
Background: The Genital InFlammation Test (GIFT) is a novel point-of-care test under development to detect genital inflammation associated with STIs or BV, which can increase the risk of HIV, adverse birth outcomes, and infertility. This study assessed the prospective acceptability of GIFT as a screening tool, which would be followed by STI diagnostic tests among women, healthcare professionals, and decision-makers. This study was set within national healthcare sector in LMICs where STI diagnostics are limited.
Methods: Sixty-five in-depth interviews were conducted with women (n = 33), healthcare professionals (n = 20), and decision-makers (n = 12) across Zimbabwe and South Africa, along with seven focus group discussions (women n = 2, healthcare professionals n = 5). Interviews and FGDs were audio-recorded, transcribed, and analysed thematically using Sekhon’s framework of acceptability, which covers seven domains: affective attitude, burden, ethicality, intervention coherence, opportunity costs, perceived effectiveness, and self-efficacy.
Results: Women showed a strong desire for novel tools to manage their sexual health. Acceptability of GIFT was often due to a misunderstanding that it was as a diagnostic test rather than a screening tool. Women who understood GIFT as a screening tool expressed concern about the cost implications of follow-up STI tests. Healthcare professionals had a better understanding of GIFT. They welcomed the attention needed for more STI screening, diagnostics, and treatment investment. However, they expressed concerns about GIFT’s clinical utility and the lack of accessible follow-up STI diagnostics. Decision-makers echoed these concerns: GIFT’s utility as a screening tool was limited by follow-up diagnostic availability and affordability. Some decision-makers saw potential for GIFT to support advocacy for improved STI diagnostic development and infrastructure.
Conclusion: This study reinforces the idea that a technological device’s acceptability cannot be separated from the context of its use. As such, intervention design must consider the feasibility of implementation within existing health systems and leverage opportunities for system strengthening.
PT02 .05 – Anxiety Responses and Testing Intentions Among Gay and Bisexual, and Other Men Who Have Sex with Men Using an AI-Powered Risk Assessment Tool for Sexually Transmitted Infections: A Quasi-Experimental Study
Dr. Phyu Mon Latt1,2, Dr. Nyi Nyi Soe1,2, Dr. Xianglong Xu2,3, Ms. Yining Bao2,4, Dr. David Lee2, Prof. Jason Ong1,2,5, Prof. Eric Chow1,2,6, Prof. Lei Zhang1,2,7, Prof. Christopher Fairley1,2
1Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
3School of Public Health, Shanghai University of Traditional Chinese Medicine, Shanghai, China.
4China–Australia Joint Research Centre for Infectious Diseases, School of Public Health, Xi’an Jiaotong University Health Science Centre, Xi’an, China.
5Department of Clinical Research, London School of Hygiene and Tropical Medicine, London, United Kingdom.
6Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
7Clinical Medical Research Centre, Children’s Hospital of Nanjing Medical University, Nanjing, China.
Background: Web-based tools for the assessment of the risk of sexually transmitted infections (STI) may increase testing but also may induce anxiety. We evaluated anxiety responses and testing intentions among gay, bisexual and other men who have sex with men (GBMSM) using MySTIRisk, an artificial intelligence-powered STI risk assessment tool, compared to a standard sexual health information webpage for GBMSM.
Methods: We conducted a quasi-experimental pre-post study at the Melbourne Sexual Health Centre between April and October 2024. Participants were allocated to either MySTIRisk, which provides personalised STI risk assessment, or a standard webpage providing general sexual health information for GBMSM on alternating days. We measured anxiety using the State-Trait Anxiety Inventory (STAI-6) before and after participants viewed their assigned websites. We defined clinically significant anxiety changes as ≥3 points on STAI-6. We used multivariable ordinal logistic regression analysis to evaluate clinically significant anxiety changes while controlling for baseline scores and demographic variables.
Results: Our study population had a median age of 34 years (IQR: 28–42); 48% were born in Australia, and 69.7% had tertiary education. The baseline characteristics were similar between MySTIRisk (n = 150) and control groups (n = 150). In the MySTIRisk group, STAI-6 scores increased significantly from baseline (median [IQR]: 10 [8, 12]) to post-intervention (11 [8, 13], P = 0.001). The control group showed a decrease from baseline (11 [9, 12]) to post-intervention (10 [8, 13], P = 0.01). Despite increased anxiety, MySTIRisk users maintained high user acceptability (92.0%) with similar testing intentions between groups (87.3% vs 82.7%, P = 0.6). The multivariable regression analysis showed that the intervention’s effect on anxiety was independent of demographic characteristics, except for employment status.
Conclusion: While MySTIRisk increased anxiety in some users, it maintained high acceptability and did not deter testing intentions. These findings support implementing such tools with anxiety management strategies.
PT02 .06 – The Unseen Burden: Sexually Transmitted Infections and Mental Health Among Transgender Individuals in India – A Clarion Call Towards Sexual Health for All!
Dr. V Sam Prasad1, Ms. Elizabeth Michael1, Mr. Mohnish Kumar1, Mr. Shivam Dwivedi1, Mr. Lyle Honig Mojica2
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
5AIDS Healthcare Foundation (AHF), Los Angeles, United States.
Background: Transgender individuals in India face significant social, economic, and healthcare challenges, increasing their vulnerability to sexually transmitted infections (STIs). The intersection of STIs and mental health issues can exacerbate the overall well-being of this marginalized community.
Methods: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across 10 states. The retrospective study of program data (n = 390) and qualitative in-depth interviews (n = 25) with transgender individuals in India. Participants were recruited randomly through a community-based STI/HIV testing program. The study used the WHO 5 mental well-being scale for all (390) to assess the mental well-being of transgender participants in the STI HIV screening program. Around 73% of the transgender community were practicing sex work for their livelihood.
Results: The mental well-being of transgender people without any physical symptoms (11%) were good while 89% said that they were curious to know the results of the STI/HIV tests. 17% of the participants were detected with HIV while 36% reported one or more symptoms of STI during the pre and post-test counselling. The in-depth interviews showed that 27% experiencing symptoms of depression and 22% experiencing symptoms of anxiety. Qualitative findings also highlighted the stigma, shame, and social isolation associated with STIs/ HIV they face daily, exacerbating mental health issues. Participants reported difficulty accessing STI testing, treatment, and mental health services due to fear of discrimination and losing their clients.
Conclusion: This study shows the critical need for comprehensive healthcare services addressing the intersection of STIs and mental health among transgender individuals in India. Findings emphasize the importance of culturally sensitive healthcare providers, accessible STI testing and treatment, and mental health support services. Policymakers, healthcare providers, and community organizations must work together to address the social determinants of health and promote inclusive, equitable care for transgender individuals in India.
PT02 .07 – Association Between Availability of Non-English Language Services and HIV-Related Services in Substance Use Disorder Treatment Facilities in the United States
Dr. Khairul Siddiqi1, Fahima Nasrin Eva2, Gazi Sakir Mohammad Pritom3, A. M. Khairul Islam4, Mary A. Hatch5, Michael G. McDonell1
1Washington State University Elson S. Floyd College of Medicine, Spokane, United States.
2North South University, Dhaka, Bangladesh.
3University of South Carolina, Columbia, SC.
4University of Rochester School of Nursing, Rochester, NY.
5University of Washington, Seattle, WA.
Background: This study investigated the association between non-English language services and the availability of HIV-related services in substance use disorder (SUD) treatment facilities across the United States (US), addressing the need for culturally competent care.
Methods: This study analyzed data from the 2023 National Substance Use and Mental Health Services Survey (N-SUMHSS), representing two types of US SUD treatment facilities: SUD treatment only (n = 6,746) and mixed mental health and SUD treatment services (n = 7,662). Descriptive statistics and bivariate comparisons using chi-square tests assessed the association between the availability of non-English language services and HIV/STI-related services, with statistical significance set at P < 0.01.
Results: Among 14,408 SUD treatment facilities, 39.8% have sign language services, and 54.6% have non-English language services (51.0% in SUD only and 57.8% mixed facilities). Among those non-English programs, Spanish was the most widely available language service (89.2% vs 85.7%), followed by Russian (14.7% vs 15.2%), French (10.8% vs 16.6%), Portuguese (8.8% vs 12.1%), and Creole (7.1% vs 15.7%). HIV prevention services were significantly higher in facilities with non-English services compared to other facilities (P < 0.001), both in SUD-only settings [HIV testing (41.1 vs 30.4%), HIV/AIDS education/counseling/support (73.9% vs 61.5%), early intervention for HIV (28.8% vs 18.7%)] and mixed setting [HIV testing (38.3% vs 32.7%), HIV/AIDS education, counseling, or support (64.1% vs 52.2%), early intervention for HIV (25.2% vs 19.6%)]. Similarly, testing for Hepatitis B and C and STDs was more prevalent in facilities that have non-English services and provide mixed services.
Conclusion: SUD treatment facilities with non-English language services had higher HIV preventive care, suggesting they are better equipped to prevent new HIV infections among people with SUD. However, non-English services other than Spanish are less available in SUD-only treatment, revealing opportunities for improving the availability of culturally competent HIV prevention via access to interpretive services.
PT03.01 – In Vitro Activity of Gepotidacin Against a Challenging Panel of Ceftriaxone Resistant Neisseria Gonorrhoeae Isolates
Dr Michelle Cole1, Dr Michel Doumith1, Dr Anna Vickers1, Dr Sarah Alexander1, Dr Helen Fifer1, Dr Nicole Scangarella-Oman2, Dr Charles Jakielaszek2, Dr Rachel Pitt-Kendall1
1UK Health Security Agency, London, United Kingdom.
2GSK, Collegeville, USA.
Background: New gonorrhoea treatments are required urgently. GSK’s novel triazaacenaphthylene topoisomerase inhibitor, gepotidacin, was shown to be non-inferior to the combination of 500 mg IM ceftriaxone and 1 g oral azithromycin in the treatment of uncomplicated urogenital gonorrhoea (EAGLE-1 [NCT04010539]). Gepotidacin selectively inhibits bacterial replication by a distinct binding site, unique mechanism of action and for most pathogens, well-balanced inhibition of two topoisomerase enzymes. An evaluation of gepotidacin’s in vitro activity against a panel of ceftriaxone-resistant Neisseria gonorrhoeae isolates was performed.
Methods: Gepotidacin and comparator antimicrobials were tested by agar dilution against 23 different ceftriaxone-resistant (MICs 0.25–1 mg/L) N. gonorrhoeae isolates and seven control strains. Genomic sequences of all isolates were examined for known resistance determinants and MLST.
Results: Gepotidacin inhibited the majority (96%) of isolates at ≤2 mg/L, with a MIC range of 0.25–4 mg/L and MIC50 and MIC90 values of 0.5 mg/L and 2 mg/L, respectively. Four isolates with the highest gepotidacin MICs (2–4 mg/L) all belonged to ST8123 and carried both GyrA S91F and D95Y and ParC S87N, amino-acid modifications associated with ciprofloxacin resistance. The rare A92P alteration in GyrA was also identified within these isolates. All had mutations causing the overexpression of the MtrCDE and NorM efflux pumps.
Conclusion: For the GyrA alterations identified in the isolates with the highest gepotidacin MICs, there is evidence to suggest that these substitutions do not affect gepotidacin binding. The contribution of efflux in isolates with the highest gepotidacin MICs needs further assessment. Overall, gepotidacin showed good in vitro activity against the panel of ceftriaxone-resistant gonococcal clinical isolates. The MIC distribution was similar to other studies, suggesting that gepotidacin should work equally effectively in patients with gonorrhoea caused by ceftriaxone-susceptible or ceftriaxone-resistant N. gonorrhoeae.
PT03.02 – Biofilm Formation in STIs: A Hidden Challenge in Infection Management
Prof. Svetlana Dubrovina1, MD Elena Trizna2, MD Diana Baidamshina2, Prof. Airat Kaumov2
1Rostov State Medical University, Rostov, Russian Federation.
2Federal State Autonomous Educational Institution of Higher Education, Kazan, Russian Federation.
Background: Quite often STIs are combined with diseases of the lower genital tract in women, particularly bacterial vaginosis. It is evidence that bacterial vaginosis increases the risk of HIV infection by 2–3.7 times, gonorrhea – 4 times, chlamydia infection by 3.5 times, and susceptibility to HSV-2 increases twofold. It is known that hyaluronic acid, a component of the biofilm matrix and envelope, can lose its properties under the action of hyaluronidase.
Methods: The drug bovgialuronidase azoximer (Longidaza®) was studied to reveal its effect on formed bacterial and mixed biofilms of various microorganisms. The study was carried out in vitro. Escherichia coli, Enterococcus faecalis, Staphylococcus aureus strains were used in the study. Biofilm formation was analyzed by spectrophotometry. The minimum bactericidal concentration was determined according to EUCAST recommendations as the lowest concentration of the substance at which bacterial growth was completely absent. Cell viability was assessed by confocal laser microscopy. Then, bovgialuronidase azoximer in combination with antibiotics was added to the newly cultured biofilms. The experiment was performed in 3 biological repeats.
Results: The results showed that 2 h incubation of bovgialuronidase azoximers at a concentration of 750–1500 IU/mL causes a twofold decrease in the biomass of the matrix of mature biofilms of E. faecalis and E. coli and a 60% decrease in S. aureus. Moreover, it can increase antibiotic activity against bacteria in biofilms: the concentration of ciprofloxacin and amoxicillin required to reduce the biofilm biomass by 3 orders of magnitude in the E. faecalis biofilm is reduced 16-fold in the presence of bovgialuronidase azoximer.
Conclusion: The use of enzyme preparations, in particular bovgialuronidase azoximer, is a promising method of bacterial vaginosis treatment and as a consequence may have an effect on reducing the burden of sexually transmitted infections.
PT03.03 – A Study on Cases of Congenital Syphilis Reported in Mongolia from 2020 to 2024
Хатагтай Otgonjargal Ganbold1, Dr. Bayandorj Oyunbeleg1, Dr. Oyun Mandal1, Dr. Bazarragchaa Purevdagva1, Dr. Saule Egshiglen1, Dr. Magsar Tungalag1, Dr. Vangan Nyamtsengel2, Dr. Badrakh Jugderjav1
1National Center for Communicable Diseases, Ulaanbaatar, Mongolia.
2Mongolian National University of Medical Sciences, Mongolia, Ulaanbaatar, Mongolia.
Background: Congenital syphilis arises when syphilis is transmitted from an infected mother to the fetus during pregnancy or delivery. Such transmission can lead to severe outcomes, including miscarriage, preterm birth, or neonatal death. In Mongolia, the syphilis incidence rate was 13.6 per 10,000 population in 2024. Syphilis accounted for 41.1% of sexually transmitted infections (STIs), with 1.3% of pregnant women testing positive.
Objective: To identify the epidemiological and clinical characteristics, causes of congenital syphilis cases reported in Mongolia.
Methods: Data from the HIV/STI Surveillance and Research Department at the NCCD and the ‘Health Statistics Information’ of the Health Development Center (HDC) were analyzed for the period 2020–2024. Records included syphilis and congenital syphilis surveillance reports, pregnancy monitoring data, and detailed clinical information on infants diagnosed with congenital syphilis.
Results: From 2020 to 2024, 120 cases of congenital syphilis were reported nationwide. Of these, 73 cases (60.8%) were in Ulaanbaatar, and 47 cases (39.2%) were from rural areas. Among the mothers of these infants, 67 (55.8%) received antenatal care, but 4 (3.3%) were not tested for syphilis despite attending care, and 53 (44.2%) did not attend antenatal care at all. The average birth weight of affected infants was 2,040 g, with 71.6% classified as low birth weight and 28.4% as normal (≥2,500 g). Based on the Apgar score, 78.3% of infants were in severe or moderately severe conditions. Clinical signs associated with congenital syphilis included hepatosplenomegaly in 95%, syphilitic skin lesions in 84.1%, and pneumonia in 87.5% of cases.
Conclusion: Of the mothers of infants born with congenital syphilis, 53 (44.2%) had no antenatal care. Additionally, 63.3% of the affected infants were preterm, and 71.6% had low birth weights. Each infant exhibited at least 2–3 specific symptoms of congenital syphilis. Therefore, improving the coverage and quality of antenatal care is essential.
PT03.04 – Bacterial Load and Clearance of Treponema Pallidum from Oral and Anal Sites in Men and Transgender-Women Who Have Sex with Men, with Secondary Syphilis
Dr Janet Towns1,2, Mr Janath A Fernando3, Ms Rebecca Wigan1,2, Dr Marcelina Krysiak3, Professor David A Lewis4, Dr Rick Varma5,13, Professor Anna McNulty5, Professor Deborah A Williamson6, Dr Carole Khaw7, Ms Jayne Howard1, Ms Kate Potappel1, Professor Louise Owen8, Dr Caroline Thng9, Dr Nathan Ryder10, Professor Eric PF Chow1,2,14, Professor Christopher K Fairley1,2, Professor Stephen Graves11, Dr Sarah Huffam12, Dr Shivani Pasricha2, Professor Marcus Y Chen1,2
1Melbourne Sexual Health Centre, Alfred Health, Carlton, Australia.
2School of Translational Medicine, Faculty of Medicine and Health Sciences, Monash University, Melbourne, Australia.
3University of Melbourne, Department of Infectious Diseases at The Peter Doherty Institute for Infection and Immunity, Melbourne, Australia.
4Western Sydney Sexual Health Centre, Western Sydney Local Health District, Parramatta, Australia.
5Sydney Sexual Health Centre, Sydney, Australia.
6UK Health Security Agency, London, England.
7Adelaide Sexual Health Centre, Infectious Diseases Unit, Royal Adelaide Hospital, Adelaide, Australia.
8Statewide Sexual Health Service, Hobart, Australia.
9Gold Coast Sexual Health, Southport, Australia.
10Pacific Clinic, Newcastle Sexual Health, Hunter New England Local Health District, Newcastle, Australia.
11Australian Rickettsial Reference Laboratory, Barwon Health, Geelong, Australia.
12BRaSH Clinic, University Hospital, Barwon Health, Geelong, Australia.
13The Kirby Institute, University of New South Wales, Kensington, Australia.
14Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Secondary syphilis is emerging as the most infectious stage. We aimed to determine the frequency of Treponema pallidum shedding, load, and time to clearance from mucosal sites after treatment to further understand transmission.
Methods: MSM and TGW with secondary syphilis were recruited from Australian clinics. At baseline (Day 0), syphilis treatment was given, mucocutaneous lesions were tested for diagnostic T. pallidum PCR, and non-lesion samples (blood, oral cavity and anal canal) with T. pallidum polA quantitative PCR for bacterial load. Non-lesion samples were repeated on Days 3, 7, 14, and 30 after treatment.
Results: Between January 2023 and August 2024, 80 MSM and 1 TGW were recruited. Most, 93%, received benzathine penicillin 2.4 mU. Baseline oral T. pallidum detection was in 81.3% (65/80) of participants: 58 had a positive oral cavity swab alone, and 7 had an additional positive oral lesion swab. Oral cavity cycle threshold (CT) increased from baseline to Day 3 (median 35.7 [Ξ53.9 copies/uL] to 37.7 [Ξ15.2 copies/uL] P = 0.012). Baseline, anal T. pallidum detection was in 67.5% (54/80) of participants; 14 were positive on both anal canal and anal lesion swabs. Anal CT increased from baseline to Day 3 (median 30.1 [Ξ1878.3 copies/uL] to 38.2 [Ξ11.0 copies/uL] P < 0.001). 50.6% (40/79) had T. pallidum detected at baseline at both oral and anal sites (Fig. 1). T. pallidum was detected in baseline blood in 23.5% (19/81), with median CT of 38.4 (Ξ9.7 copies/uL). By Day 7, T. pallidum was not detected in 99.4% (161/162) of infected sites.
Conclusion: This is the largest study to examine T. pallidum clearance after treatment of secondary syphilis, when T. pallidum shedding from oral and/or anal sites occurs in the majority of MSM, fuelling transmission risk. Loads fell significantly by Day 3 with clearance in almost all by Day 7.
PT03.05 – Increase of Ocular and Disseminated Gonorrhea in the Netherlands in Recent Years
Dr Alje Van Dam1,2, Feline Velthuis3, Dr Thijs Van de Laar4, Dr Rogier Jansen4, Arjen Stam1,2, Dr Annelot Schoffelen3
1Public Health Laboratory, Infectious Diseases, Amsterdam Health Service, Amsterdam, Netherlands.
2Department of Medical Microbiology, Amsterdam UMC, Amsterdam, Netherlands.
3On behalf of the ISIS-AR Study Group, Centre for Infectious Disease Control (CIb), National Institute for Public Health and the Environment (RIVM), Bilthoven, Netherlands.
4Laboratory of Medical Microbiology, OLVG laboratory, Amsterdam, Netherlands.
Background: Albeit rare, infections with Neisseria gonorrhoeae (Ng) can cause infections outside the genital, anal and pharyngeal area, such as bacteremia, arthritis and ocular and other infections. In recent years, the number of patients with gonorrhea diagnosed in STD clinics rose markedly. We investigated whether a similar increase of cases of gonorrhea outside the classical STI domain was found.
Methods: Ng culture data from non-genital samples (1 isolate per patient) for 2018–2023 were collected from ISIS-AR, a nationwide system in which clinical microbiology laboratories report resistance data of cultures of bacterial species to the National Institute for Public Health. Nationwide coverage was >90% (n = 48) of the laboratories in 2023. Additional molecular data for the period 2020–2024 were obtained from the laboratory systems of the three major laboratories in Amsterdam.
Results: In 2023, 95 positive Ng non-genital cultures were reported, from the eye (n = 59), sterile body fluids (n = 9), blood (n = 5) and other pus/wound/ulcers (n = 22). Of these, 58% were diagnosed in men and 42% in women. From 39 labs continuously reporting data during the entire study period the number of isolates varied between 24 and 38 in 20182021 but increased to 52 in 2022 and 84 in 2023. In Amsterdam 62 cases of gonorrhea outside the classical domain were diagnosed during 2020–2024, of which 40 (62%) by molecular tests only, suggesting that real nationwide number of cases could be threefold higher compared to culture-based numbers only (>285 in 2023). These might have been detected if a surveillance system including molecular diagnosis of gonorrhea had been in place.
Conclusion: The incidence of ocular and disseminated gonorrhea rose markedly during recent years in the Netherlands.
PT03.06 – Real-World Effect of Decreasing the Frequency of Screening for Neisseria Gonorrhoeae and Chlamydia Trachomatis on the Incidence of These Infections and Antimicrobial Use in Men Who Have Sex with Men Taking HIV Pre-Exposure Prophylaxis in Belgium: A Retrospective Cohort Study
Dr. Thibaut Vanbaelen1, Dr. Irith De Baetselier1, Achilleas Tsoumanis1, Dr. Bernadette Hensen1, Dr. Chris Kenyon1
1Institute of Tropical Medicine, Antwerp, Belgium.
Background: There is growing evidence that the benefits of systematic screening for Neisseria gonorrhoeae and Chlamydia trachomatis in men who have sex with men (MSM) taking HIV pre-exposure prophylaxis (PrEP) are limited, and that screening leads to high antimicrobial consumption. Since 2019, we have been reducing the frequency of screening for N. gonorrhoeae and C. trachomatis. In this study, we estimated the real-world effect of reducing screening frequency on the incidence of these infections and antimicrobial use among MSM taking PrEP in Belgium.
Methods: Retrospective analysis of medical records, laboratory results, and antimicrobial prescriptions for MSM taking PrEP at the Institute of Tropical Medicine clinic in Antwerp, Belgium between January 2019, and June 2024. We estimated yearly testing rates for N. gonorrhoeae and C. trachomatis, incidence rates of overall and symptomatic infections, and antimicrobial prescription rates (azithromycin, doxycycline, ceftriaxone). Trends were analyzed using a Poisson regression model.
Results: Overall, 3644 MSM attended the PrEP clinic in the study period. Testing rates decreased over fourfold between 2019 and 2024 (yearly rate ratio (RR) 0.77 [95% CI 0.76–0.78], P-value <0.001, Fig. 1). The incidence of all N. gonorrhoeae and C. trachomatis infections decreased in the same period (yearly incidence RR (IRR) 0.92 [95% CI 0.89–0.96], P-value < 0.001, and IRR 0.86 [95% CI 0.82–0.89], P-value < 0.001, respectively). There was no increase in the incidence of symptomatic infections. Doxycycline and azithromycin prescriptions decreased (RR 0.5 [95% CI 0.45–0.55], P-value < 0.001, and RR 0.92 [95% CI 0.88–0.97], P-value < 0.001, respectively).
Conclusion: Our findings provide evidence that the incidence of symptomatic N. gonorrhoeae and C. trachomatis infections did not increase over time despite less frequent screening in MSM taking PrEP, and antimicrobial prescriptions decreased. Our findings underline the potential of decreasing frequency of screening as a safe and effective antimicrobial stewardship intervention in MSM taking PrEP.
Incidence rates of all and symptomatic Neisseria gonorrhoeae, Chlamydia trachomatis, and LGV infections over time (panel A), and prescription rates of Azithromycin, Ceftriaxone, and Doxycycline over time (panel B).
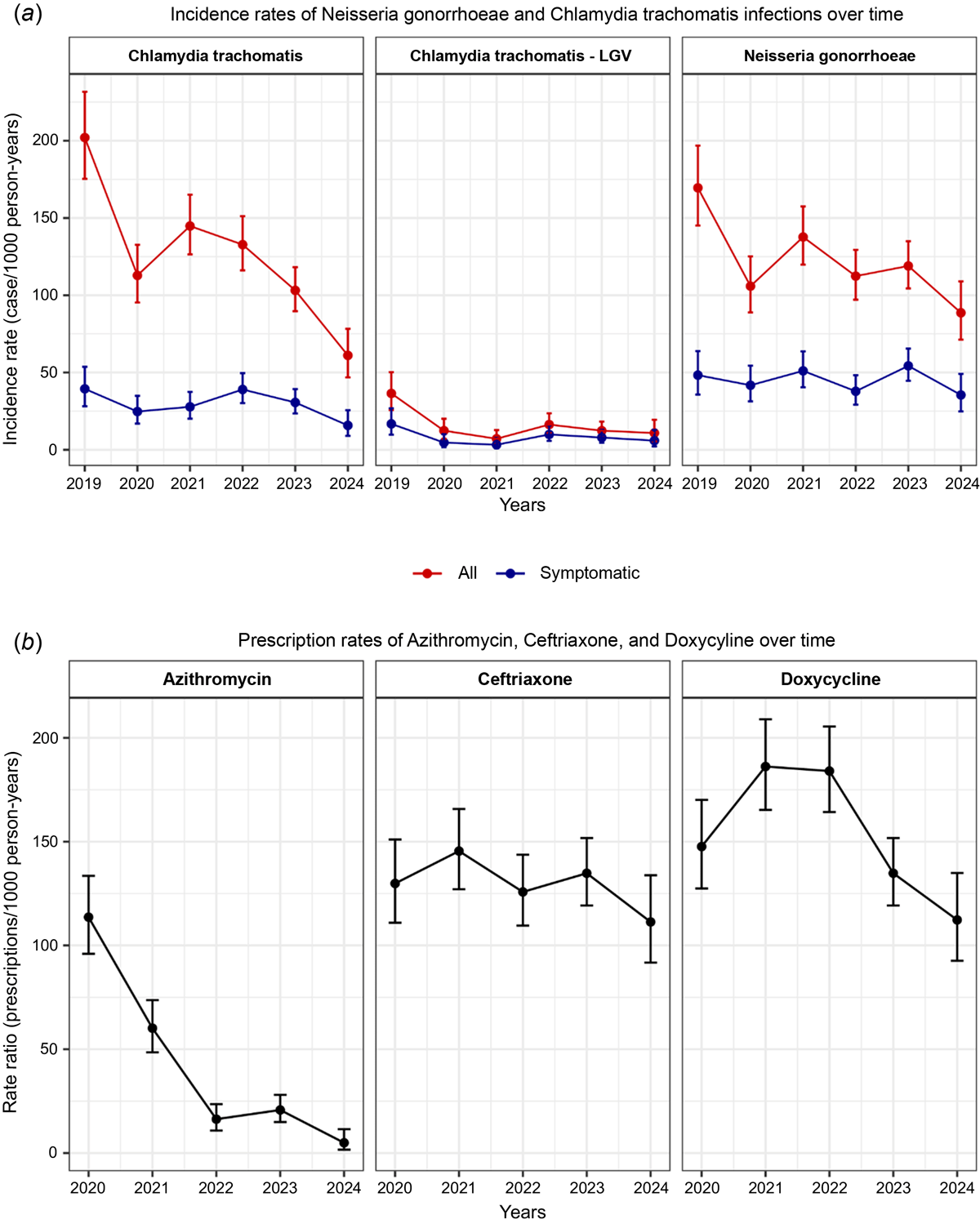
PT03.07 – ABI-5366, a Novel, Oral, Long-Acting Herpes Simplex Virus Helicase-Primase Inhibitor: Interim Safety and Pharmacokinetic Results from a Phase 1A Study in Healthy Participants
Prof. Edward Gane1, Dr Christian Schwabe2, Dr Grace Wang3, Mr Jieming Liu3, Mr Steven Knox3, Ms Kathryn Kitrinos3, Dr Anuj Gaggar3, Dr Katie Zomorodi3
1University of Auckland, Auckland, New Zealand.
2New Zealand Clinical Research, Auckland, New Zealand.
3Assembly Biosciences, South San Francisco, United States.
Background: Approximately 491.5 million people aged 15–49 years worldwide have herpes simplex virus type 2 (HSV-2) infection, the primary cause of genital herpes. Nucleoside analogue suppression is suboptimal, and recurrence is associated with pain and psychological stress. HSV-2 infection increases risk of acquiring HIV-1 infection. ABI-5366, an investigational, orally administered, long-acting HSV helicase-primase inhibitor is under development for suppression of recurrent genital herpes (RGH). In vitro, ABI-5366 potently inhibits HSV-1, HSV-2 laboratory strains and clinical isolates. Single-dose safety and PK data in healthy participants are reported.
Methods: ABI-5366-101 (NCT06385327) is a randomized, blinded, placebo-controlled Phase 1a/b study. Phase 1a, evaluating the safety and PK of single, oral ABI-5366 doses in healthy participants is ongoing. Each group includes participants randomized 6:2 to ABI-5366 or placebo with up to 98-day follow-up. Safety was assessed by physical examination, adverse events (AEs), laboratory parameters. ABI-5366 plasma concentrations were measured by LCMS.
Results: 32 participants received treatment in four ABI-5366 groups (10, 30, 100, 350 mg). Most were male (24/32), white (16/32), aged 19–59 years with BMI 19.3–31.6 kg/m2. Treatment was well tolerated. After median 70-day follow-up, 26/32 participants reported an AE; 90.4% Grade 1. No Grade 3/4 AEs or treatment-related lab abnormalities, serious AEs or deaths were reported. ABI-5366 plasma concentrations increased from 10 to 350 mg. The PK profile suggests intestinal reabsorption with a t1/2 >20 days and projected Ctrough values in multifold excess of protein-adjusted EC50 for HSV replication achievable with weekly and monthly dosing.
Conclusion: ABI-5366 was well tolerated when administered orally as single doses up to 350 mg. Plasma concentrations exceeded in vitro EC50’s for inhibition of HSV replication and the observed t1/2 >20 days supports weekly and monthly dosing. Antiviral activity following multiple doses in participants with RGH will be explored in Phase 1b.
PT04.01 – High Prevalence and Incidence of Curable Sexually Transmitted Infections Among Young Girls and Women Using HIV Pre-Exposure Prophylaxis in Sub-Saharan Africa
Dr. Irene Mukui1, Sue Peacock1, Deborah Donnell1,2, Brenda Gati3, Katherine Gill4, Shannon Bosman5, Remco Peters6, Sinead Delany-Moretlwe7, Renee Heffron8, Prof. Connie Celum1,9
1Department of Global Health, University of Washington, Seattle, United States.
2Fred Hutchinson Cancer Center, Seattle, United States.
3Makerere University-Johns Hopkins University, Makerere, Uganda.
4Desmond Tutu HIV Centre, University of Cape Town, South Africa.
5Human Sciences Research Council, Center for Community Based Research (CCBR), South Africa.
6Foundation for Professional Development, South Africa.
7Wits Reproductive Health and HIV Unit, University of the Witwatersrand, South Africa.
8Department of Medicine, University of Alabama at Birmingham, Birmingham, United States.
9Departments of Medicine, and Epidemiology, University of Washington, Seattle, United States.
Background: Women in sub-Saharan Africa have a high burden of curable sexually transmitted infections (STIs) and related reproductive health sequelae; women eligible for HIV pre-exposure prophylaxis (PrEP) are at risk of both HIV and curable STIs. We assessed the prevalence, incidence, and factors associated with curable STIs among women using PrEP.
Methods: Between August 2022 and December 2022, sexually active women ages 16–30 were enrolled into a 6-month cohort and offered PrEP from 15 South African sites, and one site each in Eswatini, Kenya, Malawi, Uganda, and Zambia. At enrolment and month 6, nucleic acid amplification tests (NAATs) were conducted for Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), and Trichomonas vaginalis (TV), and at enrolment, rapid plasma reagin with confirmatory Treponema pallidum particle agglutination for syphilis. Baseline prevalence and month 6 incidence rates were calculated, and multivariable regression used to assess predictors.
Results: Of 3,087 participants, 96.7% initiated Tenofovir/emtricitabine oral PrEP; 97.4% had baseline STI results. Median age was 23 years (IQR: 21–27). At baseline, 30.3% had at least one STI, with 76.3% asymptomatic. Cross-site STI prevalence was 20.8% chlamydia, 6.8% gonorrhea, 6.1% trichomoniasis, and 3.5% syphilis with highest prevalence in eSwatini (40.8%) and South Africa (33.0%), and lowest in Kenya and Zambia (14.0%). Month 6 incidence of any STI was 49.3/100 person-years (95% CI: 45.3–53.3); 30.3/100 p-y (95% CI 27.3–33.4) for CT; 11.5/100 p-y (95% CI 10.0–13.4) for TV, and 10.8/100 p-y (95% CI 9.0–12.6) for NG. Alcohol use (aIRR 1.3, 95% CI: 1.0–1.6) and baseline STI (aIRR 1.9, 95% CI: 1.6–2.2) were associated with incident STIs.
Conclusion: Among African women with high PrEP uptake, STI burden was high, highlighting gaps in sexual health services. Most STIs were asymptomatic, underscoring the need for etiologic testing. In resource limited settings, women with prior STIs should be prioritized for repeat testing.
PT04.02 – Exploratory Examination of Time Between Chlamydia And/Or Gonorrhea Diagnosis and Future Syphilis Diagnosis in British Columbia, 2014 –2023
Dr. Theodora B. Consolacion1, Amanda Yu1, Hannah M. Baer1, Heather Burgess1,2, Robert Higgins1, Justin Sorge1,2, Venessa Ryan1, Ina Chen1, Sven Dong1, Jennifer Vines1, Sofia R. Bartlett1,3
1British Columbia Centre for Disease Control, Vancouver, Canada.
2Public Health Agency of Canada, Vancouver, Canada.
3University of British Columbia, Vancouver, Canada.
Background: Infectious syphilis (IS) diagnoses (Dx) rates in British Columbia (BC) rose from 11.7 per 100,000 population in 2014 to 37.4 in 2023. Efficient strategies targeting syphilis screening to at-risk groups are needed. Rates are much higher in Chlamydia (CT) and gonorrhea (GC). The study’s purpose is to examine the time between incident CT and/or GC (CT/GC) Dx to subsequent IS Dx.
Methods: All genital CT, GC and IS Dx from provincial Electronic Medical Record system (2014 to 2023) were included (N = 139,486) with sex (males = 62,496; females = 76,990), age (median = 26, IQR: 21, 32), time between first CT/GC Dx to IS Dx, and a flag denoting an IS Dx after first CT/GC Dx, excluding those under 15 years, missing sex, or with CT/GC Dx after December 15, 2023. Kaplan-Meier curves by sex and age-group and Cox proportional hazard ratios with sex, age and time between CT/GC to IS Dx were calculated. Incidence rates of IS after a CT/GC Dx were calculated by sex and age-group using the median.
Results: Kaplan-Meier curves show sex and age group time differences in acquiring syphilis. Cox proportional models show that sex, age and the interaction (sex*age) were significant. Males were 3.3 times more likely to have an IS Dx after CT/GC Dx compared to females. Comparing sex across increasing ages show an increased likelihood for IS among older males (see Table 1). Incidence for females <26 years was 91.91; males <26 years was 266.4; females ≥26 years was 208.06; and males ≥26 years was 770.46 per 100,000 person-years.
Conclusion: Older males with a CT/GC Dx have an IS Dx sooner compared to females of the same age-group, suggesting the length of time for follow-up syphilis testing may vary by age and sex. With the current syphilis outbreak, universal syphilis testing after CT/GC Dx could be recommended in BC.
| Point Estimate | 95% Wald Confidence Limits | ||||
|---|---|---|---|---|---|
| Model 1: Effect of sex across ages | Male (Ref = Female) | 3.33 | 3.02 | 3.66 | |
| Model 2 Interaction: Effect of 1 unit change in age by sex | Age Unit = 1 At Sex = Male | 1.04 | 1.04 | 1.04 | |
| Age Unit = 1 At Sex = Female | 1.03 | 1.02 | 1.04 | ||
| Model 2 Interaction: Effect of sex across ages | Male (Ref = Female) At Age = 21 | 2.99 | 2.64 | 3.38 | |
| Male (Ref = Female) At Age = 26 | 3.17 | 2.86 | 3.51 | ||
| Male (Ref = Female) At Age = 26 | 3.40 | 3.08 | 3.76 | ||
PT04.03 – High Burden of Sexually Transmitted Infections Among Pregnant Women in Governmental Hospitals of Southern Ethiopia: Findings from a Baseline Study
Mrs Meskerem Ebido1,2, Professor Zeleke Mekonnen3, Professor Carl Lachat2, Professor Bruno Levecke2, Doctor Taye Gari1, Professor Elizaveta Padalko2,4
1Hawassa University, Hawassa, Ethiopia.
2Ghent University, Ghent, Belgium.
3Jimma University, Jimma, Ethiopia.
4Ghent University Hospital, Ghent, Belgium.
Background: Sexually transmitted infections (STIs) significantly threaten maternal and neonatal health in resource-limited settings like Ethiopia. The World Health Organization’s syndromic management (SM) often leads to over-treatment and missed diagnoses of asymptomatic STIs, emphasizing the need for accurate lab-based data on STIs prevalence during pregnancy. This study aims to determine STIs prevalence and associated factors among women attending antenatal care (ANC) clinics in southern Ethiopia, addressing these diagnostic gaps.
Methods: This study is part of a prospective cohort, assessing the impact of STIs on birth outcomes. A baseline survey was conducted with 743 pregnant women from July to December 2024. Vaginal swabs were collected using eNAT Copan swabs and screened for Neisseria gonorrhoeae and Trichomonas vaginalis (via wet mount and Gram stain) and syphilis and HIV (using the SD BIOLINE HIV/Syphilis Duo test). PCR tests for additional STIs will be performed later. Predictors of STIs were analyzed through multivariable logistic regression.
Results: From 743 recruited women, 91 (12.2%, 95% confidence interval (CI): 10.1–14.8) were infected with at least one STIs; 64.8% of these cases were asymptomatic (Table 1). Predictors for overall STIs include those women who have sex without desire (adjusted odds ratio (AOR) = 2.09 (95% CI: 1.15–3.81)), have economic autonomy (AOR = 12.72 (95% CI: 2.86–6.52)), have vaginal odour (AOR = 2.14 (95% CI: 1.12–4.08)), and are positive for clue cell (AOR = 3.76 (95% CI: 2.26–6.24)).
Conclusion: STIs prevalence is high, with a high proportion of asymptomatic cases. STIs diagnoses through SM exceeded lab results. Desire to have sex, vaginal odour, and also economic decision-making power are main predictors of STIs. These findings emphasise the need for routine lab-based STIs screening, and economic factors and sexual health education should be addressed to mitigate the risks associated with STIs.
| STIs Type | ANC 1st visit (≤16 weeks) | Percent (%) | |
|---|---|---|---|
| Gram-negative diplococci (suggestive of gonorrhea) | 55 | 7.4 | |
| Trichomonas vaginalis | 23 | 3.1 | |
| Syphilis | 11 | 1.5 | |
| HIV/AIDS | 8 | 1.1 | |
| Total lab-confirmed STIs | 91 | 12.2 | |
| Cases positive for syndromic management | 202 | 27.3 | |
| Asymptomatic STI | 59 | 8.3 |
PT04.04 – Impact of Declines in HIV Testing Volumes on HIV Status Awareness and Time to Diagnosis in Africa
Mr. Andrey Kutsyh1, Dr. Ahmadou Alioum4, Dr. Jeffery W Imai-Eaton2,3, Dr. Mathieu Maheu-Giroux1
1Mcgill University, Montréal, Canada.
2Imperial College London, London, United Kingdom.
3Harvard University, Cambridge, United States.
4University of Bordeaux, Bordeaux, France.
Background: HIV testing services are the entry point to HIV diagnosis and treatment. In Africa, where 2/3 people living with HIV reside, annual numbers tested for HIV have declined since peaking in 2017. This study aims to assess the impact of these reductions on diagnosis coverage and time-to-diagnosis by gender in African countries.
Methods: We collated information on total and antenatal care (ANC) HIV testing volumes in all African countries with available data, as reported in their UNAIDS Spectrum files. To capture gender differences, we modified a previously validated mathematical model of HIV testing rates (Shiny90) and calibrated it to ANC testing. For each country, we constructed a counterfactual scenario in which peak pre-decline rates of HIV testing are maintained and compared across knowledge of HIV status and time-to-diagnosis by gender.
Results: Program data from 37 countries showed that HIV testing declined in 65% of countries over 2016–2023, mostly attributed to reduced HIV testing outside of ANC. Among countries with a decline, HIV testing volumes decreased by a median of 28% (interquartile range [IQR]: 24%–52%) (Fig. 1). Although awareness of status increased in most countries between 2017 and 2023, it would have further increased by 1.2%-points (Credible Interval [CrI]: 1.0%–1.6%) to 87% (CrI: 86%–87%) in men and 1.0%-points (CrI: 0.8%–1.1%) to 91% (CrI: 91%–91%) in women had there been no decline in HIV testing. In countries with an HIV testing decline, time-to-diagnosis increased by an additional 0.5 years (CrI: 0.4–0.6) to 2.7 years (CrI: 2.6–2.9) among women and 0.7 years (CrI: 0.6–0.8) to 3.3 years (CrI: 3.1–3.5) among men in 2023, if there had been no decline in HIV testing.
Conclusion: Recent declines in HIV testing did not affect testing at ANC. These reductions in testing volumes have worsened HIV testing outcomes, especially for men. Longer time-to-diagnosis may lead to increased time spent infectious and a slower decline of incidence.
Median [line] and 95% credible interval [shaded] of median time-to-diagnosis in men [dark blue] and women [dark red] in 24 countries in which HIV testing rates declined from 2015 to 2023, pooled by new infections. Counterfactual scenario in men [bright blue] and women [bright red] indicate time-to-diagnosis without an HIV testing decline. Counterfactual scenarios begin in the year of peak HIV testing in each country; as early as 2016, but 83% of the counterfactual scenarios begin on or after 2018.
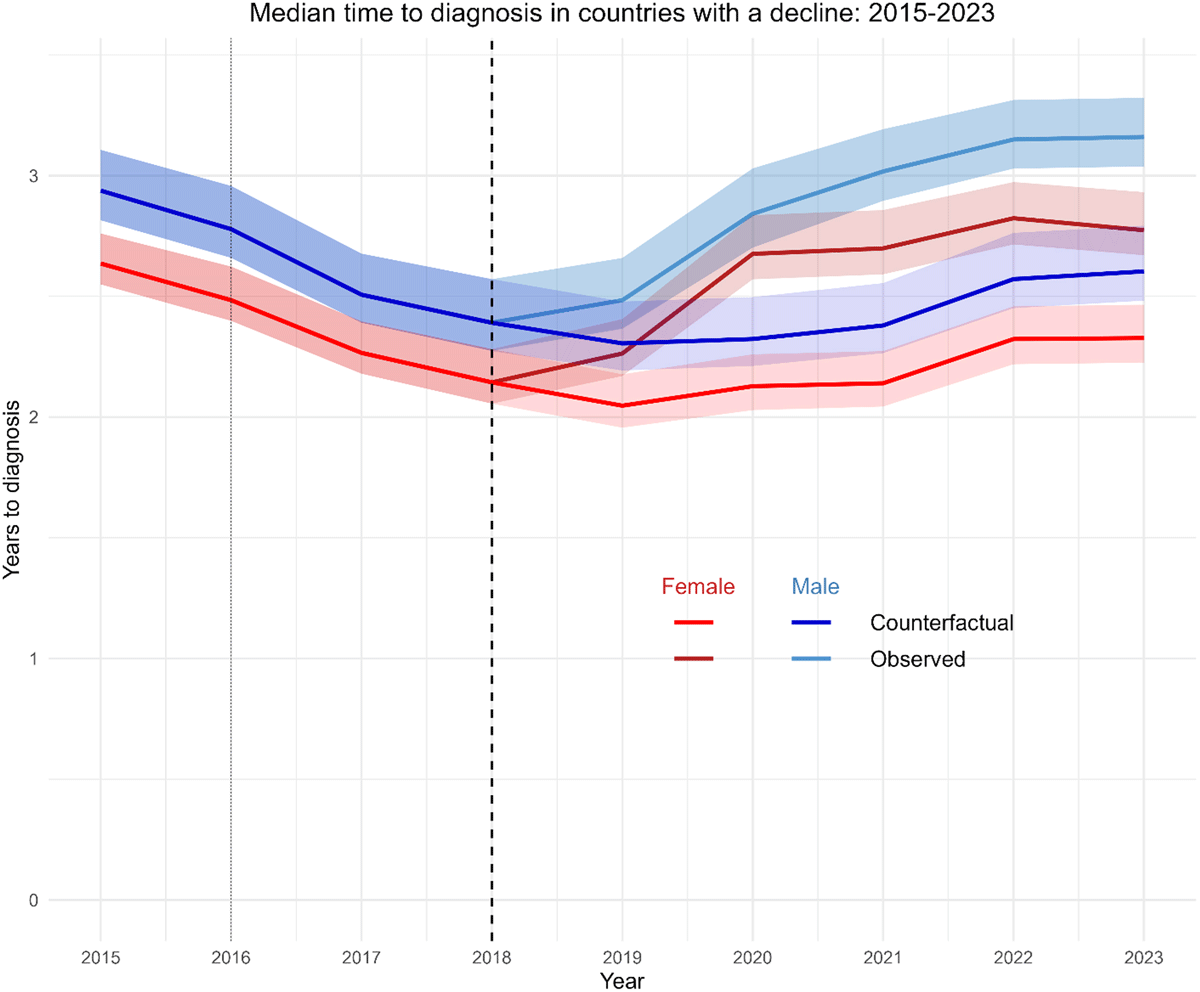
PT04.05 – Syphilis and Mortality in Denmark – A Nationwide, Population-Based, Matched Cohort Study
Ms. Emilie With Hall Petersen1, Ms. Laura Nina Glismann2,3, Ms. Maria Wessman2, Ms. Lene Holm Harritshøj1,4, Mr. Jan Gorm Lisby5, Ms. Terese Katzenstein1, Mr. Steen Hoffmann2, Mr. Jørgen Skov Jensen2, Ms. Kirsten Salado-Rasmussen2,3,4, Mr. Lars Haukali Omland1,2,4
1Copenhagen University Hospital, Rigshospitalet, Copenhagen, Denmark.
2Statens Serum Institute, Copenhagen, Denmark.
3Bispebjerg University Hospital, Copenhagen, Denmark.
4Faculty of Health and Medical Sciences, University of Copenhagen, Copenhagen, Denmark.
5Copenhagen University Hospital – Amager and Hvidovre, Copenhagen, Denmark.
Background: Syphilis incidence has risen substantially in recent decades. Updated and valid information on mortality among individuals infected with syphilis is missing, and there is a need for more appropriate comparators than healthy controls that account for confounding by test activity.
Methods: We performed a nationwide, population-based, matched cohort study of all Danish patients with syphilis between 2000 and 2023. To form the syphilis patient cohort, we identified all patients with positive syphilis serology in Denmark (i.e. a positive test for non-treponemal and treponemal antibodies). Patients notified through the mandatory notification system were also included in the syphilis patient cohort. We identified a test negative comparison cohort matched in a ratio of 1:1 of individuals with a negative syphilis test, to account for confounding by test activity. We used Kaplan Meier analysis to illustrate survival curves. Time-updated Cox regression was used to compute hazard ratios as an estimate of mortality rate ratios (MRR) (<10 years and >=10 years after study inclusion).
Results: We identified 5,085 patients in the syphilis cohort and test negative cohort, 3,991 (78%) were male and the median age was 36 years at study inclusion (Fig. 1). We did not observe an increased mortality among patients with syphilis compared to the test negative comparison cohort (MRR<10 years 1.01 (95% CI: 0.81–1.26) and MRR >=10 years 1.29 (95% CI: 0.84–1.97)). The absolute difference in mortality between the two cohorts was 3% (95% CI: –1%–7%) after 20 years of follow-up.
Conclusion: Despite a very big study population and 20 years of follow-up time, we did not observe an increased mortality among patients with syphilis compared to the test negative comparison cohort, which should serve as a reassurance for people with syphilis.
PT04.06 – The Dynamics of HIV Genetic Diversity in Cameroon from 1990 to 2023: Lessons and Implications for Achieving Elimination by 2030
Mr Derrick Tambe Ayuk Ngwese1,2,3,4, Dr Joseph Fokam1,2,5,6, Dr Alex Nka1, Dr Aude Ka’e1, Mr Desire Takou1, Dr Ezechiel Ngoufack1, Dr Collins Chenwi1,7, Dr Georges Teto1, Mrs Grace Angong Beloumou1,7, Mrs Sandrine Djupsa Djeyep1, Dr Bouba Yagai1, Dr Luna Colagrossi7, Prof Maria Mercedes Santoro7, Prof Francesca Ceccherini-Silberstein7, Dr Linda Esso8, Dr Alain Georges Etoundi Mballa9, Prof Edie-G. Halle-Ekane5, Prof Nicaise Ndembi10, Prof Vittorio Collizzi1,7, Dr Marta Giovanetti11, Dr Eduan Wilkinson12, Dr Cheryl Baxter12, Prof Tulio de Oliviera12, Prof Marcel Yotebieng13, Prof Charles Fokunang2, Prof Wilfred Fon Mbacham2,3,4, Prof Akinde Nji Mbuh3,4, Prof Carlo-F Perno1,14, Prof Alexis Ndjolo1
1Chantal Biya International Reference Centre, Yaounde, Cameroun.
2Faculty of Medicine and Biomedical Sciences; University of Yaounde 1, Yaounde, Cameroun.
3Fobang Institutes for Innovations In Science And Technology, Yaounde, Cameroun.
4The Biotechnology Centre, University of Yaounde 1, Yaounde, Cameroun.
5Faculty of Health Sciences, University of Yaounde 1, Yaounde, Cameroun.
6Central Technical Group, National AIDS Control Committee, Yaounde, Cameroun.
7University of Rome, Tor Vergata, Rome, Italy.
8Operational Research and Health Department, Ministry of Public Health, Yaoundé, Yaounde, Cameroun.
9Disease Control department, Ministry of Public Health, Cameroon, Yaounde, Cameroun.
10Africa, Centre of Disease and Control (CDC), Addis-Abeba, Addis Abeba, Ethiopia.
11Laboratório de Flavivírus, Instituto Oswaldo Cruz, Fundação Oswaldo Cruz, Rio de Janeiro, Brazil.
12Centre for Epidemic Response and Innovation (CERI), School of Data Science and Computational Thinking, Stellenbosch University, Cape Town, South Africa.
13Department of Medicine, Albert Einstein College of Medicine, Bronx, NY, United States of America.
14Ospedale Pediatrico Bambino Gesu, Rome, Italy.
Background: Interestingly, some HIV-clades have impact on public health strategies through diagnostic escape, suboptimal therapeutic response and natural resistance to some treatment regimens. Following changing treatment-paradigm, we sought to study the dynamics of HIV-clades in Cameroon.
Methods: A study was conducted on 12,230 Cameroonian-HIV-sequences between 1990and 2023 retrieved from HIV-Genbank. Sequences were grouped by 10 years’ interval and dynamics of each viral clade over the 3-time points was evaluated with P-values < 0.05 considered statistically significant using the proportion trend test. Furthermore, prediction analysis was done using generalised additive models to model the temporal trends of clade proportions for future investigations.
Results: Our results revealed that HIV-1 group-M prevailed (93.59%), followed by group-O (4.99%), group-N (0.99%), group-P (0.18%) and HIV-2 (0.12%). Circulating recombinant forms (CRFs) were most prevalent (72.83%), followed by pure subtype (19.57%) and unclassified recombinants (1.12%). Between 1990–2000 (period-1: limited-treatment-coverage; (1,304-sequences), CRFs represented 49.1% and pure-subtypes; 14.6%; where CRF02_AG was the predominant clade; 30.5%. This time-point was experienced by a high-group-O prevalence; 32.2%. Between 2001–2011 (period-2: NNRTI-based ART; 5995-sequences), CRFs and pure-subtypes slightly increased (77.2% and 18.9% respectively), with high prevalence of non-CRF02_AG recombinants (40.6%) as compared to CRF02_AG clades (36.6%), P = <0.01 a significant decrease of HIV-1-Group-O (2.3%, P = <0.01); a 1.2%-group-N prevalence and 0.04% group-P prevalence. Between 2012–2023 (period-3: test-and-treat and early-TLD-era, 4452-sequences), we noticed constant rates of pure subtypes and recombinant forms with prevalences of 21.8% and 77.3% respectively. Overall, CRFs significant increased over the three-time points (P < 0.01), with increasing CRF02_AG-(59.1 % at period-3). HIV-1-Group-O (0.4% at period-3) and Group-N (0.4% at period-3) decreased significantly (P < 0.01 respectively) while group-P completely disappeared. From 2024–2030 (extended TLD era, long acting and pandemic control), prediction analyses show declining trends in which group-P and -N would not reappear this period, group-O may completely disappear, and group-M would continue to maintain its dominance driven by recombinant forms with-CRF02_AG-emerging as a competitive clade by 2030.
Conclusion: HIV-dynamics in Cameroon over the past 30-years reveals an evolutionary pathway, characterised by an increasing CRFs-(driven by CRF02_AG)-and a significant declining trend of the HIV-1-group-O.Thus,in the current-dolutegravir-era in Cameroon, achieving elimination requires targeting in priority HIV-1-CRFs for diagnosis and monitoring in a context of disappearance of HIV-1-group-O, group-P and HIV-2.
PT04.07 – Neisseria Gonorrhoeae Antimicrobial Susceptibility Patterns: Comparing Anatomical Locations Between and within Persons in the Netherlands
Mrs Maartje Visser1,2, Dr Petra F G Wolffs3, Prof Christian J P A Hoebe2,3,4, Dr Birgit H B van Benthem1, Dr Alje P van Dam5, Dr Denise E Twisk6, Dr Nicole H T M Dukers-Muijrers2,4, Dr Janneke C M Heijne5,7
1National Institute for Public Health and the Environment (RIVM), Bilthoven, Netherlands.
2Maastricht University, Maastricht, Netherlands.
3Maastricht University Medical Center+ (MUMC+), Maastricht, Netherlands.
4Public Health Service South Limburg, Heerlen, Netherlands.
5Public Health Service Amsterdam, Amsterdam, Netherlands.
6Municipal Public Health Service Rotterdam-Rijnmond, Rotterdam, Netherlands.
7Amsterdam UMC, Amsterdam, Netherlands.
Background: Pharyngeal gonorrhoea infections may contribute to developing antimicrobial resistance, but observational evidence is conflicting. Some studies find higher resistance in pharyngeal isolates compared to genital isolates; others do not, possibly due to single isolate sampling per person. We aim to study antimicrobial susceptibility patterns across anatomical sites, using both population-level and within-person analyses.
Methods: We used Dutch gonococcal antimicrobial resistance surveillance (GRAS) data of men who have sex with men (MSM) and women (2016–2023). Ceftriaxone and azithromycin susceptibility was measured by Minimum Inhibitory Concentration (MIC)-values. We calculated anatomical-site specific proportions decreased susceptible (CRO-DS; MIC >0.032 mg/L) for ceftriaxone and resistant (AZI-RES; MIC >1 mg/L) for azithromycin. Anatomical-site differences were tested using chi2-test for total population and persons with multiple MICs at one visit. In the latter, we also analysed within-person discordant MIC pairs (>1 doubling dilution difference), and determinants of discordant MICs by logistic regression.
Results: This study included 16,916 MSM and 2,521 women with at least 1 MIC reported. Proportions CRO-DS were higher in pharyngeal isolates for both MSM and women. AZI-RES was higher in pharyngeal isolates for MSM but not women. 1,217 MSM and 457 women had multiple MICs reported. Among them, proportions of DS/RES did not differ across anatomical sites, except among MSM for azithromycin. Discordant MIC-pairs were seen in 9.6% (95% CI: 8.1–11.2%) of MSM and 4.8% (95% CI: 3.1–6.7%) of women for ceftriaxone, and 12.1% (95% CI: 10.4–14.0%) of MSM and 9.2% (95% CI: 6.8–11.8%) of women for azithromycin. In discordant pairs, pharyngeal MICs were on average not higher than urogenital or anal MICs. No sexual behavioural determinants were associated with discordant MICs.
Conclusions: Pharyngeal isolates showed higher levels of DS/RES on a population level, but not within persons. However, discordance of MICs within persons occurred, potentially leading to missed resistant cases. Culturing multiple anatomical sites per individual is recommended to optimise detection of resistant cases.
PT05.01 – A Digital Citizen Science Intervention to Reduce HIV Stigma and Promote HIV Testing: A Randomized Clinical Trial Among Adolescents and Young Adults in Kazakhstan
Dr. Alissa Davis1, Dr. Laura Nyblade, Yi Yihang Sun, Olga Balabekova, Sara Landers, Denis Gryazev, Joseph Tucker, Valera Gulyaev, Susan Rosenthal, Karsten Lunze, Weiming Tang, Azamat Kuskulov, Assel Terlikbayeva, Sholpan Primbetova, Mingway Chang, Alfiya Denebayeva, Aikerim Akhmetova, Ainur Absemetova, Sholpan Karzhaubayeva, Sairankul Kassymbekova, Marina Maximova, Zhannat Mussina, Gulnar Bekenova, Zhamilya Nugmanova, Zhanna Kalmatayeva, Ludmila Polyakova, Zhanneta Zhazykbaeva, Vitaliy Vinogradov, Amir Shaikezhanov, Meruyert Darisheva, Bella Orynbetova, Elena Norakidze, Mashirov Kozhakhmet, Akbota Tolgenova, Aknur Imadillda, Dariga Satkhozhina, Alikhan Kartamyssov, Zhamilya Kanieva, Albina Aleshina, Olzhas Makhan, Aida Muravyova, Adema Rahimzanova, Arman Duisenbayev, Zhanerke Tursynbek, Nurgazy Dias, Malika Beken, Miras Murzakhan, Zhandos Brown, Daniyal Maitekov, Artur Li, Sandizaira Mergen, Dautali Mergenov, Amirali Kuanysh, Anuar Rakhimbekov, Yenlik Baisbay, Alibek Aruzhan, Zhasmina Kozhambet, Denis Grebenchsishikov, Dmitriy Bekker, Sultan Kozhamberdiev, Dauren Salykov, Madina Sagimbayeva, Kamila Yussupova, Guakhar Mergenova
1Columbia University, New York, United States.
Background: Kazakhstan has a HIV high incidence among adolescents and young adults (AYA), and high HIV stigma contributing to low HIV testing uptake. We examined whether an AYA-developed digital crowdsourced intervention reduced HIV stigma compared to conventional public health materials among AYA in Almaty, Kazakhstan.
Methods: 216 AYA (Females: 116/Males: 110) ages 16–24 were recruited to the online study cohort and randomized 1:1 to the intervention or control arm. AYA were exposed to the crowdsourced intervention or control materials once a week for 5 weeks, with equivalent exposures between arms. Outcomes included a total HIV stigma score assessed at baseline, immediately post-intervention and 2 months post-intervention from January to August 2023. We conducted multilevel mixed models to compare changes over time by arm and sex.
Results: AYA in the intervention arm had significantly lower HIV testing stigma 2 months post-intervention (adjusted mean change (AMC): –0.73 [–1.07, –0.39]) than AYA in the control arm (AMC: –0.06 [–0.42, 0.30]) (P = 0.032). Female AYA in the intervention arm had significantly lower total HIV stigma immediately post intervention (AMC: –4.91 [–7.25, –2.58]) and 2 months post-intervention (AMC: –5.16 [–7.48, –2.84]) than females in the control arm (immediately post-intervention AMC: –0.03 [–2.63, 2.57] and 2-months post-intervention AMC: –0.07 [–2.70, 2.56]) (P = 0.012, P = 0.012).
Conclusions: The AYA-developed crowdsourced intervention decreased HIV testing stigma, though this effect was moderated by sex, and decreased total HIV stigma among female AYA. Crowdsourced interventions may be a promising way to engage communities to develop interventions to decrease HIV stigma.
PT05.02 – Brazilian Experience Towards Eliminating of Vertical Transmission of HIV, Syphilis and Viral Hepatitis B: A Human Rights Perspective Addressing Gender and Racial/Ethnic Inequalities and Community Participation
Sra. Márcia Rejane Colombo1, Dr. Pâmela Cristina Gaspar1, Sra Leila Sueli Barreto1, Sra Ariane T B Matos1, Phd Leonor Lannoy1, Sra Nádia Machado1, Phd Sérgio Ferreira Junior1, Phd Dráurio Barreira1
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
Introduction: The Brazilian experience with the Subnational Certification for the Elimination of Vertical Transmission (TVE) of HIV, syphilis, and hepatitis B highlights the importance of measures to protect human rights, address inequalities, and encourage community participation. Brazil adopts public policies aimed at combating socially determined diseases and mitigating stigma and discrimination.
Description: In the certification process, states and municipalities report, through documents, questionnaires, and interviews, the actions undertaken to promote human rights and address social, gender, and ethnic-racial inequalities. Community participation is also evaluated, with a focus on the involvement of women-led social organizations.
Results: Between 2022 and 2024, 151 municipalities with populations over 100,000 were certified. Significant progress was observed in the areas of human rights, gender equality, and racial/ethnic equality, driven by the implementation of laws and public policies. Key achievements include guarantees of professional confidentiality, combating discrimination, addressing violence against women, and strengthening social participation through Health Councils. Additionally, inclusive policies have benefited vulnerable groups, such as pregnant women living in poverty, Black and Indigenous women, people experiencing homelessness, and drug users. Health professional training proved to be a critical factor, varying significantly across municipalities. Subjective and moral aspects continue to pose barriers to including pregnant women who face challenges in accessing prenatal care and preventive services. In some locations, discrepancies between self-reported data and in loco observations revealed ongoing challenges linked to conservatism and social stigma.
Conclusion: The Subnational Certification Strategy contributes on promoting the elimination of vertical transmission diseases, which are socially determined. Its contribution hinges on ensuring human rights, addressing social, gender, and racial/ethnic inequalities, and expanding social and community participation in the certification process.
PT05.03 – Rural Australian Grassroots Movements for the Collective Future
Ms Anne-Marie Kelly1, Ms Ashleigh Colquhoun1, Professor Jane Tomnay1
1Centre for Excellence in Rural Sexual Health, Department of Rural Health, University of Melbourne, Shepparton, Australia.
Background: In rural and regional Victorian communities, sexual health is often shaped by longstanding cultural, social, and religious norms, leading to stigma, limited investment, and reluctance to address these issues. To address these challenges, the Centre for Excellence in Rural Sexual Health (CERSH) partnered with rural communities to develop five Sexual Wellness Action Plans (SWAPs). Using an appreciative inquiry approach, SWAPs established unified community visions and strategic plans to embed sexual health into local agendas, aiming to shift entrenched attitudes, reduce stigma, and promote evidence-based sexual health practices.
Methods: SWAPs were implemented across five rural Victorian Local Government Areas (LGAs), focusing on Indigenous communities, migrant workers, and socioeconomically disadvantaged populations. CERSH collaborated with local health services, Aboriginal-controlled community health organisations, schools, local governments, and diversity and settlement services. The approach prioritised grassroots engagement, cultural sensitivity, and community-driven strategies to normalise sexual health.
Findings: Preliminary results indicate significant improvements in the coordination of sexual health initiatives. Feedback suggests a positive shift in community attitudes and reduced stigma, as evidenced by local funding reallocations to support sexual health initiatives. Early observations highlight growing acceptance of sexual health as a community priority. A formal evaluation is ongoing to assess the long-term impact on service uptake and behavioural changes, with findings to be presented at the conference.
Conclusion: SWAPs demonstrate the potential for grassroots strategies to transform sexual health in rural communities. Sustained success requires evolving the plans to meet changing community needs, strengthening partnerships, and maintaining cultural sensitivity. Insights from the formal evaluation will guide future improvements, ensuring CERSH’s approach continues to create lasting change in rural and regional Victorian communities.
PT05.04 – Locating ‘Risk’ in the Australian Government’s National Sexually Transmissible Infections Strategy: An Analysis of Problem Representation
Dr. Heather Mccormack1,2, A/Prof Niamh Stephenson3
1Kirby Institute, Unsw Sydney, Sydney, Australia.
2Australian Human Rights Institute, UNSW Sydney, Sydney, Australia.
3School of Population Health, UNSW Sydney, Sydney, Australia.
Background: Since its inception in 2005, the Australian Government’s National Sexually Transmissible Infections (STI) Strategy has played a central role in shaping public health responses, influencing the resourcing and reach of STI prevention interventions We critically analysed its representations of ‘STI risk’ to identify alignment or misalignment with best practices in health promotion.
Method: We used Carol Bacchi’s “What’s the Problem Represented to Be?” (WPR) framework to analyse all editions of the National STI Strategy published since 2005. WPR offers a rigorous method to identify underpinning assumptions, interrogate gaps, and examine the effects of the problem representation. Specifically, we focussed on the framing of ‘risk’ within the strategy over the past two decades.
Results: The initial strategy framed the problem it purported to address as a lack of a nationally coordinated response to address risk associated with individual behaviour and lack of education. More recent strategies invoked a ‘healthy settings’ health promotion strategy. Healthy Settings approaches aim to forge multisectoral collaborations to change policies and programs that shape inequities where people live, work and play. Yet, recent strategies have increasingly framed STI risk as a problem of inadequate knowledge, education and awareness, widening the framing of educational need to now include health professionals. Moreover, responsibility for policy change is, in the most recent document, envisioned as lying with proactive communities in the first instance.
Conclusion: There has been some shift in the National STI Strategy’s representation of “STI risk”. Acknowledgment of how ‘settings’ shape STI transmission and of the importance of identifying and addressing inequities has increased. However, the strategy still emphasises interventions that aim to change individuals’ knowledge and awareness. Our findings suggest the need for a balanced approach that maintains focused support for populations subject to health and healthcare inequities while also addressing broader determinants of health.
PT05.05 – Healing and Harm Reduction: Indigenous-Led Approaches to Overdose Prevention and Care Within, By, and for Indigenous Peoples Living with and Without HIV
Ms. Melanie Grace Medina1,2, Claudette Cardinal2, Dr. Surita Parashar1,2, Sandy Lambert3, Dr. Kathleen Inglis1,2,4, Delilah Gregg5, Dr. Navneet Kaur Gill2, Hazel Cardinal6, Silke Hansen2, Miriam Muirhead2, Michael Budu2, Glyn Townson6, Dr. Katherine Kooij1,2, Wayne Campbell6, Valerie Nicholson3, Dr. Robert Hogg1,2
1Faculty of Health Sciences, Simon Fraser University, Burnaby, Canada.
2British Columbia Centre for Excellence in HIV/AIDS, Vancouver, Canada.
3Independent, Vancouver, Canada.
4School of Public Health and Social Policy, University of Victoria, Victoria, Canada.
5The Vancouver Area Network of Drug Users, Vancouver, Canada.
6The Ribbon Community, Vancouver, Canada.
Background: Indigenous harm reduction (IHR) moves beyond conventional ideas and forms of harm reduction. This approach emphasizes Indigenous (First Nations, Inuit, Métis) Peoples as experts and leaders in their lived/living experiences, connection to culture and community, integration of Indigenous values, and collective accountability for community well-being. Importantly, this approach is rooted in culturally safe, and trauma-informed practices. Emerging literature and harm reduction resources have highlighted significant calls to further Indigenize harm reduction, toward improving equitable access to substance use treatment for Indigenous Peoples, aligned with community members’ unique values and needs.
Methods: This study is a subset of a broader mixed-methods study, aimed at alleviating overdose risk and adverse long-term health effects among people living with and without HIV, who were at risk of, or experienced an overdose, in Vancouver, British Columbia, within the COVID-19 context. Indigenous Elders and academic researchers co-conducted two focus group discussions (FGD) with a total of ten Indigenous community members from Vancouver’s Downtown Eastside. The FGD interviews were professionally transcribed, and coded and analyzed using NVivo 14.0.
Results: IHR principles were consistently reflected across the interview transcripts, demonstrating how community actively practiced and sought out IHR. Indigenous community members shared their experiences looking after their fellow Indigenous brothers and sisters during an overdose event, highlighting their imperative role as first responders. Community members stressed the significance and utilization of Indigenous community-based harm reduction programs, Indigenous-led peer supports, and the value of community connection in their harm reduction journey. Community echoed the need for hiring Indigenous healthcare providers with lived/living experience, and more wholistic and compassionate care.
Conclusions: Findings illustrate the critical role of IHR, reinforcing the need to Indigenize harm reduction. This is vital for reducing substance use-related harms and addressing the ongoing impacts of colonization on Indigenous Peoples, both living with and without HIV.
PT05.06 – Barriers to HIV Prevention and Care Among Indigenous Populations in Canada: A Systematic Review
Ms. Sabina Rajkumar1, Ms Aditi Agarwal1, Mr. Sahith Rajkumar2, Dr. Patricia Farrugia3
1Faculty of Health Science, McMaster University, Hamilton, Canada.
2Faculty of Science, McMaster University, Hamilton, Canada.
3Department of Orthopedic Surgery, McMaster University, Hamilton, Canada.
Background: Indigenous populations face disproportionate rates of HIV compared to non-Indigenous groups, driven by systemic, socio-economic, and cultural barriers exacerbated by colonial legacies. This review examines the intersection of these factors and their influence on the prevalence, prevention, and treatment of HIV within Canadian Indigenous communities.
Methods: Electronic searches were conducted on MEDLINE, EMBASE, iPortal from inception to October 2024, supplemented with manual citation search. The search strategy included forward and backward citation tracking. Two reviewers independently and in duplicate assessed titles, abstracts, and full-text articles, with discrepancies resolved by a third member. Eligible studies consisted of randomized controlled trials (RCTs), cohort studies, cross-sectional research, and qualitative analyses. Data were extracted on key themes, including HIV prevalence, barriers to healthcare access, and cultural influences. Qualitative data were synthesized using thematic analysis.
Results: Indigenous populations in Canada have HIV prevalence rates 3.6 times higher than non-Indigenous populations, with disproportionate impacts on women (45% of cases) and youth (12–36% HIV-positive). Systemic barriers, including healthcare inaccessibility and stigma, delay HIV diagnosis and treatment. Racism, stereotyping, and distrust in healthcare create significant obstacles. Socioeconomic factors such as poverty, housing instability, and unemployment restrict access to consistent care and drive high-risk behaviours, including substance use and unsafe sex practices. Cultural disconnection from traditional practices and intergenerational trauma stemming from colonial systems, such as residential schools, exacerbate vulnerabilities. Lack of culturally competent care further alienates Indigenous patients, perpetuating disparities and undermining health outcomes.
Conclusion: Findings highlight the urgent need for culturally competent, community-driven healthcare strategies to address the compounded impact of systemic inequities and socio-economic barriers. Congress attendees will gain insights into integrating Indigenous voices in healthcare planning and implementing tailored interventions to bridge these disparities. These strategies can inform global approaches to reducing HIV disparities among marginalized populations.
PT05.07 – A Designathon to Co-Create Accessible Sexual Health Services for Adults Aged 45+ Including Those with Disabilities in the UK: Findings from a Community-Led Participatory Event
Dr. Eneyi Kpokiri1, Hayley Conyers1, Arushi Subba1, Ms Yoshiko Sakuma1, Tracey Jannaway2, Prof Joseph D Tucker3, Prof Dan Wu4
1London School of Hygiene and Tropical Medicine, London, United Kingdom.
2Independent Living Alternatives, London, United Kingdom.
3University of North Carolina, Chapel Hill, United States of America.
4Nanjing Medical University, Nanjing, China.
Background: There is limited tailored sexual health services for middle aged, older (45+) and disabled adults in the United Kingdom (UK). Existing services mostly cater to younger people. We organized a Designathon to identify community-led, innovative approaches to improve access to sexual health services for this population in the UK. A designathon is a three-phase participatory process informed by design thinking that includes the preparation phase by soliciting innovative ideas from end-users, an intensive collaborative event to co-create intervention components, and follow-up activities.
Methods: We organized co-creation sessions and a crowdsourcing open call to solicit suggestions to improve sexual health services for older adults. Findings from the crowdsourcing call and co-creation sessions generated five themes: adapting existing sexual health services, improving patient-provider relationships, improving sexual health communication, breaking down sexual health taboos, and community-led sexual health support. These themes informed a 2-day designathon in London (7–8 March 2024), consisting of five teams (3–4 individuals per team) supported by mentors and facilitators (Fig. 1). As for follow-up activities, final designathon ideas were reviewed by judges and top-scored ideas were publicly disseminated.
Results: Eighteen participants, 7 facilitators, 5 mentors, and 3 judges supported participated in the designathon. Attendees included older adults, community-based organizations representatives, policy makers, clinicians, disabled adults, activists, and researchers. The event facilitated rich discussions of implementation strategies to improve sexual healthcare for adults aged 45+. Themes from the designathon included community-led strategies, leveraging existing resources, peer education, and inclusive and accessible messaging. These were disseminated via stakeholder panels, online webinars, conferences and on the study website.
Conclusion: Our designathon engaged key stakeholders to co-develop practical strategies to improve uptake of sexual health services for adults aged 45+, including those with disabilities in the UK. Implementation research is needed to assess the effectiveness and sustainability of the strategies identified.
PT06.01 – Trichomonas Vaginalis Infection Among Adolescent Girls and Young Women Accessing Sexual and Reproductive Health Services at Retail Pharmacies in Kenya
Dr. Felix Mogaka1, Mr Benard Rono1, Mr Bernard Nyerere1, Dr Greshon Rota1, Mr Harrison Lagat2, Mrs Josephine Odoyo1, Dr Katrina Ortblad3, Ms Meena Lenn2, Dr Monisha Sharma2, Miss Omolara Akingba2, Dr Victor Omollo1, Dr Zachary Kwena1, Prof. Elizabeth Bukusi1,2, Dr Jillian Pintye2
1Kenya Medical Research Institute, Kisumu, Kenya.
2University of Washington, Seattle, United States.
3Fred Hutchinson Cancer Research Center, Seattle, United States.
Background: Trichomonas vaginalis (TV) infection increases susceptibility to HIV, yet limited data are available on TV infection among adolescent girls and young women (AGYW) who are at high risk of HIV infectin in Kenya. We evaluated the prevalence of TV among AGYW seeking sexual and reproductive health (SRH) services at retail pharmacies in Kisumu, Kenya.
Methods: We analyzed baseline data from AGYW enrolled in an ongoing cluster randomized controlled trial (NCT05467306) assessing pharmacy-based HIV PrEP delivery models at 20 retail pharmacies in Kisumu. AGYW (15–24 years) purchasing contraception, who tested HIV negative were offered an option of either oral PrEP or the dapivirine vaginal ring (DPV-VR) per national guidelines. A subset was offered TV testing using Xpert® TV assays. Poisson regression was used to identify correlates of TV infection.
Results: As of December 2024, 481 AGYW were tested for TV. Median age was 20 years (IQR 18-22), 81% were unmarried, and 39% were currently in school. One-third (32%) reported having casual sexual partners and 40% had a prior pregnancy. Condomless sex was common (84%) and 11% recently engaged in transactional sex. TV prevalence was 6.4% (31/481), and only 23% (7/31) were symptomatic. AGYW who reported STI symptoms were twice as likely to have TV as asymptomatic AGYW (PR = 2.88, 95% CI:1.32–6. 28, P = 0.008). A prior diagnosis of an STI was associated with current TV infection (PR = 3.21,95% CI:1.47–6.99, P = 0.003). HIV PrEP uptake was higher among AGYW with TV detected (93% vs 79 %, P = 0.047). Among AGYW who accepted HIV PrEP (n = 392), the frequency of selecting DPV-VR over oral PrEP was similar among AGYW with symptomatic TV (17%), asymptomatic TV (17%), and no TV (18%, P = 0.998).
Conclusion: TV was relatively common and frequently asymptomatic. Offering TV screening within pharmacies in Kenya could be beneficial for AGYW with a history of STIs or among those considering HIV PrEP.
PT06.02 – “We Have the Tools”: Health System Stakeholders’ Perspectives on Implementation of Injectable Cabotegravir as HIV-PrEP Among Two-Spirit, Gay, Bisexual, Queer, and Other Men Who Have Sex with Men (2SGBQM) in Canada
Dr. Tyrone J Curtis1, Mr Lucas Gergyek2, Mr Ben Klassen2, Mr Chris Draenos2, Dr Clemon George3, Dr Daniel Grace4, Mr Kenneth Monteith5, Dr Aniela dela Cruz6, Mr Harlan Pruden7, Mr Michael Kwag2, Dr Darrell H S Tan4,8
1University of Victoria, Victoria, Canada.
2Community-Based Research Centre, Vancouver, Canada.
3Buffalo State University, Buffalo, USA.
4University of Toronto, Toronto, Canada.
5COCQ-SIDA, Montreal, Canada.
6University of Calgary, Calgary, Canada.
7BC Centre for Disease Control, Vancouver, Canada.
8St Michael’s Hospital, Toronto, Canada.
Background: Long-acting injectable cabotegravir (CAB-LA) was recently approved as HIV pre-exposure prophylaxis (PrEP) in Canada. To maximize the benefit of CAB-LA PrEP within key populations, including Two-Spirit, gay, bisexual, queer, and other men who have sex with men (2SGBQM), we must understand existing challenges with oral PrEP, adapt PrEP delivery to reduce structural inequities, and proactively address anticipated challenges of CAB-LA PrEP implementation.
Methods: Nine focus groups and ten semi-structured interviews with health system stakeholders (N = 37) involved in PrEP provision across Canada were conducted to explore readiness to implement CAB-LA PrEP, resources required for delivery, and potential approaches to maximize access for 2SGBQM. Data were analyzed using reflexive thematic analysis.
Results: Participants emphasized that CAB-LA PrEP could address PrEP inequities for some 2SGBQM who face challenges with oral PrEP access and adherence, including people who travel frequently, experience homelessness, or have limited privacy. Implementation of CAB-LA PrEP in rural communities via pharmacies and among people experiencing homelessness via mobile delivery were highlighted as novel approaches to challenge inequities. Some participants had experience administering long-acting HIV treatment and reported readiness to implement CAB-LA PrEP, while others raised logistical barriers to implementation, including staffing and space requirements for administration and follow-up, discrepancies between STBBI testing and CAB-LA PrEP dosing frequencies, and providers’ inexperience administering gluteal injections. Participants highlighted structural barriers to implementation, including drug cost and provider reimbursement challenges, scope of practice limitations which restrict who can administer injections, and resistance from government stakeholders to adapt and expand PrEP delivery.
Conclusion: CAB-LA PrEP implementation requires learning from existing oral PrEP inequities while adapting PrEP delivery models to meet community needs and address feasibility constraints. Clear guidelines and decision-making tools, innovative approaches to delivery, and additional space and staffing resources are essential for ensuring CAB-LA PrEP works for providers and patients.
PT06.03 – A Review of Public Health Surveillance Data to Inform Doxy-PEP Use: Results from Ottawa, Canada for Bacterial STI Diagnoses Among Gay, Bi, and Other Men Who Have Sex with Men
Dr. Dara Spatz Friedman1, Dr. Patrick O’Byrne1,2, Ms. Lauren Orser1
1Ottawa Public Health, Ottawa, Canada.
2University of Ottawa, School of Nursing, Ottawa, Canada.
Background: Gay, bi, and other men who have sex with men (gbMSM) account for a disproportionate number of bacterial sexually transmitted infections (bac-STIs). A new preventative tool, “doxy-PEP,” is taken as a one-time 200 mg oral dose of doxycycline after condomless oral or anal sex as post-exposure prophylaxis (PEP). We reviewed surveillance data to understand the potential public health impact of offering doxy-PEP to gbMSM who have been diagnosed with 0, 1 or ≥ 2 bac-STI diagnoses.
Description: We analyzed episodes during 2022 –2024 in which a bac-STI was confirmed in 18+-year-old gbMSM to determine the number of individuals with one or more positive bac-STIs testing episodes (PTEs) within 12 months of a previous diagnosis. We calculated the number of PTEs and bac-STIs that might be prevented, and the number needed to treat (NNT), using either 0, ≥1 or ≥ 2 PTEs in a 12-month period as a threshold for prescribing doxy-PEP.
Findings: We found that approximately 3% of gbMSM had one or more PTEs within 12 months, 26% with one PTE had a second PTE within 12 months; and 32% with two PTEs, a third. Based on this analysis, the NNT for doxy-PEP taken by all gbMSM to prevent a first PTE is 50; by gbMSM following a first PTE to prevent a second, 7; and following a second PTE to prevent a third, 6. Taking doxy-PEP following a single PTE would avert approximately one-third of subsequent PTEs and one-fifth of bac-STIs.
Conclusion: This analysis enables informed decisions about prescribing doxy-PEP to achieve the best prevention outcomes while minimizing antibiotic overuse. Doxy-PEP use in gbMSM with at least one bac-STI diagnosis in the preceding 12 months would result in a high population-level prevention outcome with a low NNT, consistent with recent US CDC guidelines.
| Number of gbMSM* | Number of gbMSM with 1+ PTE | Percent of gbMSM with 1+ PTE | Total number of PTEs | Number of chlamydia infections | Number of gonorrhea infections | Number of syphilis infections | Total number of infections | ||
|---|---|---|---|---|---|---|---|---|---|
| 2021 | 20,497 | 413 | 2.0% | 471 | 231 | 169 | 125 | 231 | |
| 2022 | 20,884 | 644 | 3.1% | 770 | 388 | 368 | 120 | 388 | |
| 2023 | 21,290 | 749 | 3.5% | 889 | 399 | 449 | 150 | 399 | |
| 2024 | 21,650 | 692 | 3.2% | 792 | 330 | 456 | 102 | 888 | |
| Sum | N/A | 1,912** | N/A | 2,922 | 1,348 | 1,442 | 497 | 3,287 | |
| 2022–24 average | 21,274 | 695 | 3.3% | 817 | 372 | 424 | 124 | 921 |
Notes: *Based on population growth following 2019 estimate from SexNow.
** Individuals are counted in each calendar year in which they experience a PTE.
| Year | Number of PTEs/individual | Number of individuals with given number of PTEs | Percent of individuals with given number of PTEs who have another PTE | Percent of individuals with given number of PTEs who would have another PTE were doxy-PEP used | NNT to have prevented another PTE | |
|---|---|---|---|---|---|---|
| 2022 | 0+ | 20,884 | 3.2% | 1.2% | 52 | |
| 1 | 485 | 26.3% | 10.2% | 6 | ||
| 2 | 117 | 32.4% | 12.6% | 5 | ||
| 3+ | 42 | |||||
| 2023 | 0+ | 21,290 | 3.6% | 1.4% | 46 | |
| 1 | 577 | 24.0% | 9.3% | 7 | ||
| 2 | 116 | 36.3% | 14.1% | 5 | ||
| 3+ | 56 | |||||
| 2024 | 0+ | 21,650 | 3.2% | 1.3% | 51 | |
| 1 | 511 | 26.8% | 10.4% | 6 | ||
| 2 | 140 | 25.1% | 9.7% | 6 | ||
| 3+ | 41 | |||||
| 2022-24 average | 0+ | 21,274 | 3.3% | 1.3% | 50 | |
| 1 | 524 | 24.6% | 9.5% | 7 | ||
| 2 | 124 | 27.1% | 10.5% | 6 | ||
| 3+ | 46 |
Note: The calculation of PTEs averted takes average efficacy of doxy-PEP into account.
| Number of previous PTEs/individual in a 12-month period ending with the individual’s most recent PTE | Average number of PTEs averted in the following 12 months if given doxy-PEP following a given PTE | % of PTEs in the following 12 months averted if given doxy-PEP | Average number of bac-STIs averted in the following 12 months if given doxy-PEP following a given PTE | % of bac-STIs in the following 12 months averted if given doxy-PEP | |
|---|---|---|---|---|---|
| 0 | 426 | 61.2% | 564 | 61.2% | |
| 1 | 209 | 30.1% | 160 | 17.4% | |
| 2 | 85 | 12.2% | 46 | 5.0% |
Note: The calculation of PTEs and bac-STIs averted takes average efficacy of doxy-PEP into account.
PP06.80 – Pathways for Transitioning to a Diagnostic-Led Approach for STI Management in Kenya
Dr. Dismas Ouma1, Dr. Daniel Were2, Dr. Patricia Ongwen2, Ms Kristina Grabbe3, Dr. Hannah Tappis3, Dr. Lisa Noguchi3, Ms Naoko Doi3, Mr. Paul Gathi2, Professor Yuka Manabe4, Dr. Susan Ontiri1
1International Centre for Reproductive Health, Nairobi, Kenya.
2Jheigo-Kenya, Nairobi, Kenya.
3Jpheigo, Baltimore, USA.
4John Hopkins School of Medicine, Baltimore, USA.
Background: The WHO advocates for a diagnostic-led approach to STI management, prioritizing rapid point-of-care (POC) testing. Transitioning from syndromic to diagnostic-based STI management in low- and middle-income countries requires understanding local health systems. This study explored pathways for such a transition in Kenya.
Methods: We conducted qualitative research in Nairobi and Kilifi counties in Kenya in August 2024, including 39 key informant interviews with national-level researchers, policymakers, service providers, and regulators; county-level managers and policymakers; and facility-level managers and service providers. We held four focus group discussions with healthcare providers and two human-centered design workshops with providers and clients. Data were analyzed using QSR NVivo 14, applying both deductive and inductive coding with multiple coders to ensure reliability and capture rich, emergent insights.
Results: Stakeholders highlighted effective leadership and stakeholder collaboration, led by national government, as required for successful implementation of STI POC diagnostics. Community STI awareness and integration with routine services can reduce stigma, enhance health-seeking behavior, and increase demand for diagnostics. High-performance devices with strong quality control systems will build trust among healthcare providers, promoting effective use and care. However, participants were concerned about challenges within the healthcare system, such as limited physical infrastructure to support sample collection and testing, high workload and poor staffing, especially in public hospitals, inadequate data collection and reporting, suboptimal training of service providers, and perennial stock-outs of diagnostics and medication in public facilities. Participants want these concerns to be addressed to advance adoption of etiological STI management.
Conclusion: Effective leadership and collaboration, along with reliable diagnostic devices and strong quality control, are essential for successful implementation of STI POC diagnostics. Addressing healthcare system challenges such as infrastructure, inadequate staffing, data collection, and stock shortages is crucial to improving services and supporting adoption of etiological STI management.
PP06.81 – Stakeholder Perspectives on Adopting Point-Of-Care Diagnostics for Sexually Transmitted Infections Management in Kenya
Dr. Dismas Ouma1, Dr. Daniel Were2, Dr. Patricia Ongweni Ongwen2, Ms Kristina Grabbe3, Dr. Hannah Tappis3, Dr. Lisa Noguchi3, Ms Naoko Doi3, Mr. Paul Gathi2, Professor Yuka Manabe4, Dr. Susan Ontiri1
1International Centre for Reproductive Health, Nairobi, Kenya.
2Jpheigo-Kenya, Nairobi, Kenya.
3Jpheigo, Baltimore, USA.
4John Hopkins University School of Medicine, Baltimore, USA.
Background: The WHO recommends transitioning from syndromic STI management to diagnostic-led approaches, including rapid point-of-care (POC) testing. This study examined stakeholder perspectives on Kenya’s readiness to shift from syndromic to diagnostic-led STI management.
Method: A qualitative formative assessment was conducted in Kilifi and Nairobi Counties through 39 key informant interviews with national policymakers, county decision-makers, facility managers, and healthcare providers. Four focus group discussions were held with healthcare providers from service delivery points with potential for STI POC diagnostic integration. Two human-centered design workshops were conducted with STI clients and service providers to explore user perspectives and preferences for POC diagnostic tools. Data were analyzed using QSR NVivo 14, applying both deductive and inductive coding with multiple coders to ensure reliability and capture rich, emergent insights.
Results: Stakeholders supported transitioning to diagnostic-led STI management, citing the potential for improved treatment accuracy, better decision-making, and reduced costs from misdiagnoses and repeat visits. However, concerns were raised about increased provider workload, device costs, resistance from healthcare workers, task-shifting conflicts, and community stigma surrounding STIs. Participants highlighted the need for accurate, user-friendly diagnostics that require minimal training and can be used by non-laboratory staff. Affordability emerged as a critical factor due to limited health insurance coverage.
Stakeholders emphasized the importance of strong national leadership, collaboration, and community awareness to drive demand for POC STI testing. Quality assurance, including reliable devices, robust quality control, and updated reporting tools, was seen as vital for maintaining trust among providers and patients.
Conclusion: Stakeholders recognize the value of POC diagnostics for STI management in Kenya, contingent on affordability, ease-of-use, quality assurance processes, and evidence-based implementation. Effective leadership and early stakeholder engagement will be critical to scaling up rapid, cost-effective, diagnostic-led approaches to improve STI care in resource-limited settings.
PP06.82 – Pathways for Transitioning to a Diagnostic-Led Approach for STI Management in Kenya
Dr. Dismas Ouma1, Dr. Daniel Were2, Dr. Patricia Ongwen2, Ms Kristina Grabbe3, Dr. Hannah Tappis3, Dr. Lisa Noguchi3, Ms Naoko Doi3, Mr. Paul Gathi2, Professor Yuka Manabe4, Dr. Susan Ontiri1
1International Centre for Reproductive Health, Nairobi, Kenya.
2Jheigo-Kenya, Nairobi, Kenya.
3Jpheigo, Baltimore, USA.
4John Hopkins School of Medicine, Baltimore, USA.
Background: The WHO advocates for a diagnostic-led approach to STI management, prioritizing rapid point-of-care (POC) testing. Transitioning from syndromic to diagnostic-based STI management in low- and middle-income countries requires understanding local health systems. This study explored pathways for such a transition in Kenya.
Methods: We conducted qualitative research in Nairobi and Kilifi counties in Kenya in August 2024, including 39 key informant interviews with national-level researchers, policymakers, service providers, and regulators; county-level managers and policymakers; and facility-level managers and service providers. We held four focus group discussions with healthcare providers and two human-centered design workshops with providers and clients. Data were analyzed using QSR NVivo 14, applying both deductive and inductive coding with multiple coders to ensure reliability and capture rich, emergent insights.
Results: Stakeholders highlighted effective leadership and stakeholder collaboration, led by national government, as required for successful implementation of STI POC diagnostics. Community STI awareness and integration with routine services can reduce stigma, enhance health-seeking behavior, and increase demand for diagnostics. High-performance devices with strong quality control systems will build trust among healthcare providers, promoting effective use and care. However, participants were concerned about challenges within the healthcare system, such as limited physical infrastructure to support sample collection and testing, high workload and poor staffing, especially in public hospitals, inadequate data collection and reporting, suboptimal training of service providers, and perennial stock-outs of diagnostics and medication in public facilities. Participants want these concerns to be addressed to advance adoption of etiological STI management.
Conclusion: Effective leadership and collaboration, along with reliable diagnostic devices and strong quality control, are essential for successful implementation of STI POC diagnostics. Addressing healthcare system challenges such as infrastructure, inadequate staffing, data collection, and stock shortages is crucial to improving services and supporting adoption of etiological STI management.
PP06.83 – Minding the Gaps in Treatment Practices for Bacterial STIs: Insights from Online Survey Among Physicians
Mr. Victor Passarelli1, Ms Flora Goldemberg1, Dr Ricardo Vasconcelos1, Dr Gwenda Hughes2, Dr Silvia Figueiredo Costa1
1Faculdade De Medicina Da Universidade De São Paulo, São Paulo, Brazil.
2The London School of Hygiene & Tropical Medicine, London, England.
Background: Inadequate treatments for sexually transmitted infections (STIs) may contribute to antimicrobial resistance (AMR), particularly with Neisseria gonorrhoeae (Ng) and Mycoplasma genitalium (Mg). Therefore understanding prescription practices for bacterial STIs is important to help improve public policies and AMR surveillance strategies.
Methods: This was a prospective transversal observational study. We used the platform SurveyMonkey™ to develop an online self-applied questionnaire (table) targeting Brazilian physicians. It was disseminated through social media and contact lists.
Findings: Between August and December of 2024, 250 physicians completed the survey. The majority were women (139, 55,6%) aged 25-35 (131, 52,4%), working in both public and private sectors (130, 52%), primarily with Infectious Diseases (ID): (82; 32,8%), Gynecology and Obstetrics (56; 22,4%), Family Medicine (47; 18.8%), and Internal Medicine (30; 12%). Responses were predominantly from Brazillian Southeast (181; 72,4%), South (30; 12%) and Northeast (26; 10,4%) regions.
Ceftriaxone plus azithromycin was the most common empirical treatment for both urethritis (153; 61,2%) and cervicitis (76; 30,4%), while ceftriaxone plus doxycycline was the most common choice for proctitis (74; 29,6%). Ceftriaxone doses for gonorrhea varied widely (from 250 mg to 1g) among all specialties. For Mg, while azithromycin 1g was the most popular choice overall (45; 18%), 104 respondents (41.6%) had never prescribed a specific treatment for it.
When stratified by medical specialty and compared to non-ID responses, ID respondents’ prescriptions were seemingly more precise regarding drug choice for empirical treatments, but posology also varied greatly among them. Two-step treatments including moxifloxacin for Mg were more common among ID physicians. Treatments for syphilis and chlamydia were more uniform (table).
Conclusion: Discrepant and outdated treatments highlight the need for continuous medical education among all specialties to enhance evidence-based and uptodate care, therefore reducing STI burden and AMR risks, especially regarding pathogens of concern such as Ng and Mg.
| Question | Answer | Overall (n = 250) | ID* Respondents (n = 82) | Non-ID* Respondents (n = 168) | P-Value | |
|---|---|---|---|---|---|---|
| Empirical choice for urethritis treatment | ||||||
| Ceftriaxone + Azithromycin | 61.20% (153) | 70,73% (58) | 56,55% (95) | 0,043 | ||
| Ceftriaxone + Doxycycline | 16% (40) | 23,17% (19) | 12,5% (21) | 0,048 | ||
| Azithromycin | 7.6% (19) | 1,22% (1) | 10,71% (18) | 0,016 | ||
| Ciprofloxacin | 1.2% (3) | 0 | 1,79% (3) | 0,54 | ||
| Ciprofloxacin + Azithromycin | 4.8% (12) | 1,2% (1) | 6,55% (11) | 0,12 | ||
| Ciprofloxacin + Doxycycline | 4.4% (11) | 2,44% (2) | 5,36% (9) | 0,46 | ||
| Levofloxacin | 0.8% (2) | 0 | 1,19% (2) | 0,81 | ||
| I don’t know | 2.02% (5) | 0 | 2,98% (5) | – | ||
| Other | 2,02% (5) | 1,22% (1) | 2,38% (4) | – | ||
| Empirical choice for cervicitis treatment | ||||||
| Ceftriaxone + Azithromycin | 30.4% (76) | 30.49% (25) | 30.36% (51) | 1 | ||
| Ceftriaxone + Azithromycin + Metronidazole | 25.20% (63) | 31,71% (26) | 22,02% (37) | 0,13 | ||
| Ceftriaxone + Doxycycline | 19.6% (49) | 26,8% (22) | 16,07% (27) | 0,06 | ||
| Azithromycin | 6.80% (17) | 0 | 10,12% (17) | 0,006 | ||
| Ciprofloxacin + Doxycycline | 2.8% (7) | 2.44% (2) | 2.98% (5) | 1 | ||
| Ciprofloxacin + Azithromycin | 2.8% (7) | 0 | 4,17% (7) | 0,14 | ||
| Ciprofloxacin + Metronidazole | 4.0% (10) | 1,22% (1) | 4.17% (9) | 0,22 | ||
| Ceftriaxone + Azithromycin + Metronidazole + Fluconazole | 1.6% (4) | 2,44% (2) | 1,19% (2) | 0,84 | ||
| I don’t know | 2.8% (7) | 0 | 4,17% (7) | – | ||
| Other | 4.0% (10) | 4,88% (4) | 3,57% (6) | – | ||
| Empirical choice for proctitis treatment | ||||||
| Ceftriaxone + Doxycycline | 29.6% (74) | 48,78% (40) | 20,24% (34) | <0,001 | ||
| Ceftriaxone + Azithromycin | 24.8% (62) | 37,8% (31) | 18,45% (31) | <0,001 | ||
| Ciprofloxacin | 8.4% (21) | 1,22% (1) | 11,9% (20) | <0,001 | ||
| Ciprofloxacin + Azithromycin | 4.4% (11) | 2,44% (2) | 5,36% (9) | 0,46 | ||
| Ciprofloxacin + Metronidazole | 4.0% (10) | 3,66% (3) | 4,17% (7) | 1 | ||
| Ciprofloxacin + Doxycycline | 3.6% (9) | 2,44% (2) | 4,17% (7) | 0,74 | ||
| Azithromycin | 2.4% (6) | 0 | 3,57% (6) | 0,19 | ||
| I don’t know | 19.35% (47) | 2,44% (2) | 26,79% (45) | – | ||
| Other | 4% (10) | 1,22% (1) | 5,3% (9) | – | ||
| Prescription choice for a confirmed case of uncomplicated Gonorrhea | ||||||
| Ceftriaxone 500mg IM single dose | 38.8% (97) | 54,88% (45) | 30,95% (52) | <0,001 | ||
| Ceftriaxone 500mg IM single dose + Azithromycin 1g PO single dose | 24.4% (61) | 25,61% (21) | 23,81% (40) | 0,87 | ||
| Ceftriaxone 1g IM single dose | 9.6% (24) | 12,2% (10) | 8,33% (14) | 0,45 | ||
| Ceftriaxone 250mg IM in a single dose | 8.8% (22) | 2,44% (2) | 11,9% (20) | 0,02 | ||
| Ceftriaxone 250mg IM single dose + Azithromycin 1g PO single dose | 5.2% (13) | 2,44% (2) | 6,55% (11) | 0,28 | ||
| Azithromycin 2g PO in a single dose | 4.4% (11) | 0 | 6,55% (11) | 0,04 | ||
| Ciprofloxacin 1g PO in a single dose | 0.40% (1) | 0 | 0,60% (1) | 1 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 3.2% (8) | 1,22% (1) | 4,17% (7) | 0,38 | ||
| Penicillin G Benzathine 2.4 million IU IM single dose | 1.2% (3) | 0 | 1,79% (3) | 0,54 | ||
| I don’t know | 1.21% (3) | 0 | 1,79% (3) | 0,54 | ||
| Other | 2.42% (6) | 1,22% (1) | 3,57% (6) | 0,51 | ||
| Prescription choice for a confirmed case of Chlamydia | ||||||
| Azithromycin 1g PO in a single dose | 61.6% (154) | 65,85% (54) | 59,52% (100) | 0,4 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 29.6% (74) | 31,71% (26) | 28,57% (48) | 0,71 | ||
| Azithromycin 500mg PO, once a day for 5 days | 4.8% (12) | 1,22% (1) | 6,55% (11) | 0,12 | ||
| Ciprofloxacin 500mg PO every 12 h for 7 days | 0.40% (1) | 0 | 0,60% (1) | 1 | ||
| Levofloxacin 500mg PO, once a day for 7 days | 0.40% (1) | 0 | 0,60% (1) | 1 | ||
| I don’t know | 1.61% (4) | 0 | 2,38% (4) | – | ||
| Other | 1.61% (4) | 1,22% (1) | 1,79% (3) | – | ||
| Prescription choice for a confirmed case of Mycoplasma genitalium | ||||||
| I have never prescribed a specific treatment for this infection | 41.6% (104) | 26,83%% (22) | 48,81% (82) | 0,001 | ||
| Azithromycin 1g PO in a single dose | 18% (45) | 15,85% (13) | 19,05% (32) | 0,65 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 14.4% (36) | 17,07% (14) | 13,1% (22) | 0,51 | ||
| Doxycycline 100mg PO every 12 h for 7 days followed by Moxifloxacin 400mg/day PO for another 7 days | 9.6% (24) | 23,17% (19) | 2,98% (5) | <0,001 | ||
| Doxycycline 100mg PO every 12h for 7 days followed by Azithromycin 500mg/day PO for another 5 days | 5.6% (14) | 9,76% (8) | 3,57% (6) | 0,08 | ||
| Azithromycin 500mg PO once a day for 5 days | 1.6% (4) | 1,22% (1) | 1,79% (3) | 1 | ||
| Moxifloxacin 400mg PO once a day for 7 days | 4.4% (11) | 4,88% (4) | 4,17% (7) | 1 | ||
| Levofloxacin 500mg PO once a day for 7 days | 0.8% (2) | 0 | 1,19% (2) | 0,81 | ||
| I don’t know | 3.23% (8) | 0 | 4,76% (8) | – | ||
| Other | 1.21% (3) | 1,22% (1) | 0,6% (1) | – | ||
| Prescription choice for Primary Syphilis | ||||||
| Penicillin G Benzathine 2.4 million IU IM, single dose | 90.8% (227) | 95,12% (78) | 88,69% (149) | 0,15 | ||
| Penicillin G Benzathine 7.2 million IU IM, once a week for 3 weeks | 4.40% (11) | 2,44% (2) | 5,36% (9) | 0,46 | ||
| Penicillin G Benzathine 4.8 million IU IM, once a week for 2 weeks | 1.6% (4) | 0 | 2,38% (4) | 0,38 | ||
| Doxycycline 100mg PO every 12 h for 7 days | 0.40% (1) | 1,22% (1) | 0 | 0,71 | ||
| Ceftriaxone 1g IM, once a day for 7 days | 0.40% (1) | 0.40% (0) | 0,6% (1) | 1 | ||
| Azithromycin 2g PO in a single dose | 0.40% (1) | 0.40% (0) | 0,6% (1) | 1 | ||
| I don’t know | 1.6% (4) | 0 | 1,6% (4) | |||
*ID respondents = Infectious Diseases Specialists who responded the survey; Non-ID respondents: respondents from medical specialties other than ID.
P-values were calculated using the Chi-Squared test with Free Statistics Software, and a threshold of p < 0.05 was considered statistically significant.
PP06.84 – Acceptance and Prescription Practices of Doxycycline Post-Exposure Prophylaxis (DoxyPEP) Among Brazilian Physicians: A Nationwide Study
Mr. Victor Passarelli1, Ms Flora Goldemberg1, Dr Ricardo Vasconcelos1, Dr Gwenda Hughes2, Dr Silvia Figueiredo Costa1
1Faculdade De Medicina Da Universidade De São Paulo, São Paulo, Brazil.
2The London School of Hygiene & Tropical Medicine, London, England.
Background: Post Exposure Prophylaxis with Doxycycline (DoxyPEP) is a groundbreaking method to prevent some of the most common bacterial STIs. Controversies regarding antimicrobial resistance (AMR) surveillance and acceptance for its implementation provoke discussions among different medical specialties, therefore understanding the current scenario is of utmost importance.
Methods: This was a prospective transversal observational study. We used the platform SurveyMonkey™ to develop an online self-applied questionnaire targeting Brazilian physicians. It was disseminated through social media and contact lists. Questions are shown in Table.
Findings: Between August and December of 2024, 250 physicians completed the survey. The majority were women (139, 55.6%), aged between 25–35 (131, 52.4%), working in both public and private sectors (130, 52%), mainly with Infectious Diseases (ID): (82; 32.8%), Gynecology and Obstetrics (56; 22.4%), Family Medicine (47; 18.8%), and Internal Medicine (30; 12%). Responses were received from all five Brazilian regions, predominantly from the Southeast (181; 72.4%), South (30; 12%) and Northeast (26; 10.4%)
DoxyPEP acceptance was high overall, with 55.6% of respondents either 'agreeing’ or 'strongly agreeing’ with its implementation.
However, non-Infectious Diseases (Non-ID) practitioners more commonly stated they did not know enough about it to give an opinion (35.12% vs 3.66%, P < 0.001).
Among ID physicians, 41 (50%) had already prescribed DoxyPEP to their patients, while 29 (17.2%) had done it among the non-ID (P < 0.001). Results are summarized in the table.
Conclusion: The high acceptance of DoxyPEP across various medical specialties is promising. However, limited awareness of this intervention outside the field of Infectious Diseases warrants attention. Additionally, the current practice of DoxyPEP prescription in the absence of specific public policies raises concerns, particularly regarding its proper integration into healthcare services and its implications for AMR surveillance strategies.
| Question | Response | Overall (n = 250) | ID Respondents1 (n = 82) | Non-ID Respondents2 (n = 168) | P-Value | |
|---|---|---|---|---|---|---|
| How much do you agree with the implementation of Post-Exposure Prophylaxis with Doxycycline (DoxyPEP)3 to prevent STIs such as syphilis in vulnerable populations? | ||||||
| Strongly agree | 24% (60) | 26,83% (22) | 22,62% (38) | 0,56 | ||
| Agree | 31.6% (79) | 47,56% (39) | 23,81% (40) | <0,001 | ||
| Neither agree nor disagree | 10% (25) | 12,2% (10) | 8,93% (15) | 0,55 | ||
| Disagree | 5.2% (13) | 6,1% (5) | 4,76% (8) | 0,88 | ||
| Strongly disagree | 2.8% (7) | 2,44% (2) | 2.98% (5) | 1 | ||
| I don’t know enough to give an opinion. | 24.80% (62) | 3,66% (3) | 35,12% (59) | <0,001 | ||
| I prefer not to answer. | 1.6% (4) | 1.22% (1) | 1,79% (3) | 1 | ||
| Do you prescribe DoxyPEP to your patients? | ||||||
| Yes, I already prescribe it. | 28% (70) | 50% (41) | 17,26% (29) | <0,0001 | ||
| No, I don’t prescribe it. | 67,6% (169) | 48,78% (40) | 76,79% (129) | <0,0001 | ||
| I prefer not to answer. | 4.4% (11) | 1,22% (1) | 5,95% (10) | 0,16 | ||
P-values were calculated using the Chi-Squared test with Free Statistics Software, and a threshold of P < 0.05 was considered statistically significant.
PP06.85 – Performance Analysis of Clinical Service Providers in HIV Care and Treatment: Results from the 2024 Digital Certification Exams for Clinical Mentorship Training in Mozambique
Dr. Yara Paulo1, Dr Leuchim Gemo2, Dr Orlando Munguambe1, Dr António Paúnde2, Dr Irénio Gaspar1, Dra Aleny Couto1
1MoH Mozambique, Maputo, Moçambique.
2I-TECH Mozambique, Maputo, Moçambique.
Background: Mozambique ranks 8th globally for HIV prevalence, with 2.4 million people living with HIV (PLHIV). Currently, the country is at 71-96-89 for the 95-95-95 targets, highlighting the need for improvements in HIV care delivery. One major factor contributing to this challenge is the quality of clinical mentors, which affects the effectiveness of ART services.In response, a new exam was introduced in 2023 as a prerequisite for accessing the clinical mentorship training package.
Description For these evaluations, provinces request the assessment from the Ministry of Health’s (MoH) Quality Improvement team, which is conducted remotely using the providers’ own electronic devices. Providers must belong to clinicprofessional categories: and have at least 12 months of experience in the ART service. Providers who score above 66% are considered to have passed the exam.
Findings: The 2024 evaluations involved 747 healthcare providers from 10 provinces, including Maputo City, Maputo Province, Gaza, Inhambane, Sofala, Manica, Tete, Zambézia, Nampula, and Cabo Delgado. The approval rates across these provinces varied significantly, with some provinces like Maputo City and Maputo Province achieving higher approval rates (80% and 71%), while others like Zambézia and Nampula had much lower rates (39% and 29%). The overall average approval rate was 59%, reflecting the need for targeted interventions to improve clinical mentoring and ART service delivery.
Conclusion: Data shows considerable regional disparities, with 90% of the provinces reporting approval rates below 75%. The introduction of the new exam in 2023 was a step in the right direction, MoH must define strategies to improve the perfomance of the provinces with low perfomance, addressing regional disparities.
PP06.86 – A Comparative Retention Among Women Living with HIV in Mozambique
Mrs Edna Paunde Xavier1, Dr Aleny Couto1, Dr Irenio Gaspar1, Dr Yara Paulo1, Mr Orlando Munguambe, Mr Fernando Boene1
1Moh Mozambique, Maputo, Mozambique.
Background: The impact of HIV in Mozambique is visible in women, with the epidemic in the country being more feminised. According to spectrum data (version 6.36) by December 2023 in Mozambique 60 per cent of people living with HIV are women. In Mozambique 1,470,000 women are living with HIV and of these 125,000, 8.5% are pregnant women. Early retention refers to the process of ensuring that pregnant women are followed up from the beginning of pregnancy for proper monitoring and prevention of complications.
Description: a follow-up flow has been drawn up and standardised which recommends that all pregnant and breastfeeding women living with HIV who are diagnosed in the antenatal clinic or at-risk child clinic, or who arrive at these clinics with the diagnosis, receive psychosocial support according to their needs. At every monthly consultation, pregnant and breastfeeding women should be assessed for risk factors for adherence.
Findings: In the 3 regions of the country, retention is higher in the first 33 days after starting ART than at 99 days after starting treatment. In the southern region of the country, retention at 33 days is 89 % and at 99 days 84 %. In the Centre region, retention at 33 days is 81% and at 99 days 74%. In the Northern region, retention at 33 days is 78 % and at 99 days 66 %, with the Southern region of the country having the best early retention of pregnant women on antiretroviral treatment.
Conclusion: The implementation of early retention strategies for WLHIV is fundamental to guaranteeing maternal and neonatal health, improving the quality of life and preventing mother-to-child transmission of HIV. WLHIV face additional challenges during pregnancy, such as the need for constant adherence to antiretroviral treatment (ART), monitoring viral load and preventing complications associated with the infection.
PP06.87 – Pilot Study in Brazil: Fourth-Generation Immunochromatographic HIV Tests Show no Added Benefit Over Third-Generation Tests
Ms. Ana Philippus1, Ms. Amanda Alencar Cabral Morais1, Alisson Bigolin1, Adson Belém Ferreira da Paixão1, José Boullosa1, Gilvane Casimiro1, Draurio Barreira1
1Brazilian Ministry of Health, Brasília, Brazil.
Background: HIV infection remains a significant public health challenge, particularly among vulnerable populations. Early diagnosis is crucial to prevent transmission and complications. From 2023–2024, the Brazilian Ministry of Health led a pilot project in four Testing and Counseling Centers to evaluate the benefits of implementing fourth-generation rapid combined antigen and antibody tests (RT-Ag/Ab) in healthcare services that cater to populations at higher risk of HIV infection and to assess whether the current strategy in Brazil, using antibody-only tests, might be missing diagnoses.
Description: Guidelines and an algorithm supported the project implementation, allowing diagnostic completion in health services (Fig. 1), performing both fourth- and third-generation HIV tests simultaneously. Data were collected using the Research Electronic Data Capture (REDCap) system.
Findings: A total of 1,631 forms were recorded in RedCap. Most participants were Black/Brown (70.3%) or White (28.2%), and the majority completed high school (32.5%) or held college degrees (30.9%). Among participants, 74.7% identified as cisgender men, 23.3% as cisgender women. Regarding sexual orientation, 43.9% identified as heterosexual, 42.8% as homosexual. A significant portion (70.8%) sought testing voluntarily. Notably, 95.7% reported unprotected sex, with 52.1% within less than 15 days, 18.6% between 15–30 days, and 29.3% over 30 days ago. Furthermore, 44.2% were starting PrEP, and 13.6% were under PrEP follow-up. Of the RT-Ag/Ab tests, 67 individuals tested positive: one for antigen only, 29 for both antigen and antibody, and 37 for antibody only. Comparable RT-Ab test results identified 73 positive cases. Based on guidelines, 61 individuals were diagnosed with HIV using RT-Ag/Ab, and 69 with RT-Ab.
Conclusion: The study found no significant advantage in case detection with RT-Ag/Ab compared to RT-Ab. Additionally, more cases were diagnosed using RT-Ab. Public health-wise in Brazil, the cost of the RT-Ab test (US$0.16) is much lower than the RT-Ag/Ab test (US$1.49).
PP06.88 – Ensuring Quality and Performance in Brazil’s Rapid HIV, Syphilis, and Hepatitis Testing: An Overview of the 2024 Monitoring and Evaluation Results
Ms. Ana Philippus1, Mr. Alisson Bigolin1, Ms. Pamela Gaspar1
1Brazilian Ministry of Health, Brasília, Brazil.
Background: The Brazilian Ministry of Health (MoH) distributes around 25 million anti-HIV, treponemal, anti-HCV, and HBsAg rapid tests (RT) annually, recommending them as the primary diagnostic tool. Despite their reliability and ease of use, maintaining their quality is essential for accurate diagnoses.
Methods: MoH manages RT quality through technical criteria definition for acquisition (e.g., registration with the Brazilian Health Regulatory Agency, performance criteria), offering distance learning [webinars and online training platform (OTP) with practical guides covering test precautions, report models, testing traceability, stock controls], monitoring work process organization across Brazil using forms, and post-market surveillance [verifying the performance of all test lots distributed and monitoring customer service (CS) reports]. External Quality Assessment for Rapid Tests (EQA-RT) is also conducted for all RT, (HBsAg to be included next year). Data from 2024 were analyzed.
Results: All RT acquired by MoH met technical criteria. A total of 3,357 professionals attended webinars and 33,251 accessed the OTP. All 116 RT lots were approved based on performance criteria. In the EQA-RT practical assessment, 6,203 professionals participated, with approval rates of 91.7%, 96.2%, and 92.2% for HIV, Syphilis, and HCV tests, respectively. In the theoretical assessment, 92.4% of 5,534 professionals passed. The main errors were related to diagnostic flowcharts and results interpretation. CS reported 220 non-conformities (0.0006% of RTs distributed), most of which were not confirmed in the manufacturer’s assessment. Additionally, 6,256 professionals responded to word process forms. Key findings indicated thar 51% open the test device at the time of testing, 78% use the correct pipette for adequate blood volume and 98% start tests with the device requiring the most blood, following MoH recommendations.
Conclusion: The 2024 data demonstrates that MoH’s quality tools are effective in ensuring compliance and high performance. However, errors in diagnostic flowcharts and result interpretation indicate areas for further improvement.
PP06.89 – Rising Syphilis and HIV Trends Among Rural Populations in India: A Clarion Call Towards Sexual Health for All
Mr. Mohnish Kumar1, Dr. V Sam Prasad2, Dr. V Sam Prasad2, Miss Elizabeth Michael3, Mr. Shivam Dwivedi4, Mr. Lyle Honig Mojica5
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
2AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
3AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
4AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
5AIDS Healthcare Foundation (AHF), Los Angeles, United States of America.
Background: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across ten states in India to screen and track trends of syphilis and HIV co-infections. Syphilis and HIV co-infections pose significant public health concern, particularly among rural populations.
Description: This retrospective study analyzed data randomly selected from the pre and post-test counselling notes and the test results of men (n = 500) and women (n = 500) community-based STI/ HIV screening program for 2 years, that included men (n = 317,597) and women (n = 230,693) from rural areas across 9 states in India. Syphilis and HIV screening were conducted using rapid diagnostic tests, and data was analyzed to identify age- and gender-wise trends of syphilis and HIV co-infections.
Findings:
The study revealed a rising trend of syphilis cases among rural populations, with significant increases among:
-
Men over 50 years (35%)
-
Young women aged 30 years (28%)
-
Migrant workers (40%)
-
Individuals with low knowledge on STI/HIV (30%)
HIV co-infection rates were also high among these groups:
Multivariate analysis revealed that:
-
Lack of knowledge on STI/HIV (OR: 2.5)
-
Poverty (OR: 3.1)
-
Limited access to healthcare services (OR: 2.2)
-
Migrating for work (OR: 1.8)
were significant predictors of syphilis and HIV co-infections.
Conclusion: This study highlights the need for targeted interventions to address the rising trend of syphilis and HIV co-infections among rural populations in India. Policymakers, healthcare providers, and community organisations must work together to promote comprehensive sexual health education, condom promotion, and regular testing for syphilis and HIV, while addressing the social determinants of health.
PP06.90 – Promoting Access to HIV Services Among Men Who Have Sex With Men Under a Harsh Environment in the Wake of the Anti-LGBTQ+Debate in Ghana
Mrs. Hellen Mawuli Quarshie1, Mr Samuel Elliot Owusu1, Mr Solomon Atsuvia
1Maritime Life Precious Foundation, Kumasi, Ghana.
Background: In Ghana, men who have sex with men (MSM) often face challenges accessing HIV services due to stigma and discrimination. Approval of an anti-LGBTQ+ bill by parliament has further facilitated an environment where MSM constantly experience societal homophobia and human-rights abuses which affect uptake of HIV services. Maintaining uninterrupted access to HIV services for MSM under this harsh climate requires using integrated, community-based strategies.
Description: Various community-based approaches to HIV service delivery for MSM were introduced during the period.
Peer-Educators halted group outreach and engaged peers with one-on-one meetings to reduce public visibility. M-Friends/M-Watchers were deployed to facilitate access to needed legal services and address HIV-related abuses directed at MSM.
Flexible community-based strategies were implemented to preserve access to HIV services and promote safety of KP implementers and MSM during the period: (1) Social media platforms were used to engage peers for HTS and support PLHIVs through virtual case management; (2) HTS and treatment took place at homes and safe locations agreed to by peers; (3) Condoms, lubricants and HIV self-test kits were made available at outlets, community-led DICs and outlets for easy access; (4) Multi-month dispensing of ART and PrEP were promoted to eliminate clinic visits.
Findings: Introduction of community-based strategies reached out to more MSM and increased HIV+ yield. During the period of anti-LGBTQ+ debate from September 2023–February 2024, 608 MSM were reached and tested for HIV; 48 were diagnosed positive. After the introduction of community-based strategies, from March–August 2024, 844 MSM were reached and tested; 162 were diagnosed positive.
Conclusions: Tailored community-based approaches to HIV service delivery proved to be effective during the anti-LGBTQ+ climate. Nevertheless, the influence of the anti LGBTQ+ bill on HIV&AIDS programming is enormous affecting MSM and KP organizations. We call for high-level stakeholder advocacy on the effect of the anti-LGBT bill against sexual minorities in the fight against HIV&AIDS.
The table and graph below show results before and after the introduction of integrated, community-based approaches during the anti-LGBTQ+ period in Ghana. Table 1 and Fig. 1 show that New MSM Reached increased after these innovative strategies were introduced from March to August 2024.
Introduction of community-based strategies during the anti-LGBTQ+ bill period reached out to more MSM.

Testing and HIV positivity rate were higher after the introduction of community-based strategies.

Table 2 and Fig. 2 also indicate that both testing rates and HIV+ yield increased after the introduction of community-based strategies from March to August 2024.
PP06.91 – Peer-Driven Approaches to Increase Uptake of HIV Testing Services Among Fetish Priests Who Are Men Who Have Sex with Men (MSM) in the Western Region of Ghana
Mrs. Hellen Mawuli Quarshie1, Mr Agbesi Wosornu1
1Maritime Life Precious Foundation, Kumasi, Ghana.
Background: Key populations are recognized as significant drivers of the HIV epidemic in Ghana. According to the National Strategic Plan, 18.5% of men who have sex with men (MSM) are living with HIV. Certain high-risk MSM subgroups, such as fetish priests, often avoid HIV testing services (HTS). Reaching fetish priests is particularly challenging due to prevailing superstitions and the belief that HIV is a spiritual disease that does not affect them. Peer-driven approaches are essential to effectively reach this population.
Description: A snowball approach was implemented where an HIV-positive MSM was encouraged to refer his sexual partners from the past year to a trained counselor for HIV testing. This referral chain led the outreach team to a fetish priest at his shrine. Through ongoing visits and HIV education, the priest was counseled on the importance of HIV testing. After ensuring confidentiality, the priest agreed to undergo HIV testing and was motivated to refer other MSM fetish priests for testing.
Findings: The peer-driven strategy, utilizing a referral chain initiated by an HIV-positive fetish priest, successfully reached more MSM fetish priests in the Tarkwa district. A total of 25 shrines led by MSM fetish priests were identified, with 19 priests agreeing to HIV testing after continuous education and engagement. Of the 19 priests tested, 4 refused to accept their HIV-positive status and declined ART initiation. However, 15 accepted their results and were linked to ART via differentiated service delivery at their shrines.
Conclusions: The snowball and referral chain strategy for HTS is effective in reaching hidden MSM populations and should be expanded to other districts. Providing confidential and accessible differentiated service delivery encourages MSM, including fetish priests, to seek HIV services. Ongoing education and monitoring are essential to promote ART acceptance among those who initially refused treatment and ensure viral suppression in those who have started ART.
PP06.92 – Enhancing HIV Testing Rates Among Men Who Have Sex with Men in Ghana Through Free STI Treatment
Mrs. Hellen Mawuli Quarshie1, Mr James Martin2, Mr Samuel Elliot Owusu1
1Maritime Life Precious Foundation (MLPF), Kumasi, Ghana.
2HeHeF, Kumasi, Ghana.
Background: In Ghana, the screening of sexually transmitted infections (STIs) among men-who-have-sex-with-men (MSM) often results in prescriptions without actual treatment due to financial constraints faced by key population (KP) implementers and the high cost of STI medications. This leads to delayed or neglected treatment, increasing the risk of HIV transmission. This abstract examines the impact of providing free STI treatment on both STI service uptake and HIV testing services (HTS) among MSM.
Methods: In response to low STI treatment completion rates, MLPF realigned its project budget to offer free STI treatment for MSM. The medications were made available at Community Drop-In-Centers and selected health facilities for easier access. Peer educators raised awareness about the availability of free STI drugs and referred MSM for screening and treatment services.
Results: Programmatic data showed a significant increase in both STI screening and HIV testing following the introduction of free STI treatment. Between December 2023 and January 2024, 235 MSM were referred for STI services, with 148 receiving treatment, representing a 62% completion rate. After the provision of free treatment, between February and March 2024, 231 MSM were referred, and all received STI treatment, achieving a 100% completion rate. Consequently, the number of MSM receiving HTS increased from 405 in December–January to 583 in February-March, reflecting a 43.9% rise in HIV testing uptake.
Conclusions: The provision of free STI treatment is a feasible strategy to enhance HIV testing rates among MSM in Ghana. By removing financial barriers to STI treatment, health systems can foster a more proactive approach to HIV prevention, which may ultimately reduce HIV incidence among MSM. We strongly advocate for policy changes and public health initiatives that integrate free STI medications into comprehensive HIV prevention programs, recognizing the critical interconnection between STI treatment and HIV prevention for this key population.
PP06.93 – Availability and Readiness of STI and HIV Services in Bangladesh: Insights from a Nationally Representative Mixed-Method Study
Dr. Farah Naz Rahman1,3, Dr Mohammad Jahangir Hossain2, Professor AKM Fazlur Rahman2
1International Centre for Diarrhoeal Disease Research Bangladesh, Dhaka, Bangladesh.
2Centre for Injury Prevention and Research Bangladesh (CIPRB), Dhaka, Bangladesh.
3School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia.
Background: Sexually transmitted infections (STIs) and HIV continue to pose public health challenges in Bangladesh. This study assessed the readiness of healthcare facilities to deliver STI and HIV services and to identify key bottlenecks that require policy attention.
Methods: Bangladesh Medical Research Council (BMRC) conducted a facility-assessment survey across 490 public, private, and NGO healthcare-facilities in Bangladesh, selected through weighted cluster-staged sampling to ensure national representation. The adapted WHO’s Service Availability and Readiness Assessment tool was utilized to evaluate service readiness. Readiness was measured across three domains for both STI and HIV services – staff and guidelines, essential medicines, diagnostics – with an additional equipment domain for HIV services. A composite readiness index (RI) was calculated using a weighted additive procedure. Additionally, 12 key informant interviews with national-level policymakers provided qualitative insights.
Results: Among the surveyed facilities, 332 (67%) reported offering STI and HIV services. The overall readiness index for STI services was 46%, indicating that facilities are underprepared compared to the WHO-benchmark of 70–80% for adequate readiness. Public tertiary-facilities exhibited higher readiness (78%), while public primary-facilities were notably deficient at 54%. Availability of diagnostic services was limited, especially in public primary and private facilities. HIV services demonstrated a national readiness index of only 28%, with critical shortages in essential medicines (5%) and basic equipment (19%). KII findings underscored systemic issues, including inadequate resource allocation, weak coordination mechanisms, lack of involvement of key population, and persistent stigma, further impeding service delivery.
Conclusion: Healthcare facilities in Bangladesh are critically underprepared to provide STI and HIV services, with only 28% readiness to deliver comprehensive HIV care. Gaps in essential medicines, diagnostics, and frontline service delivery must be urgently addressed to meet global health targets. Targeted, equity-focused interventions are essential to bridge the readiness gap and ensure vulnerable populations have access to life-saving STI and HIV care.
PP06.94 – Prevalence and Treatment of Syphilis Co-Infection Among Newly Enrolled People Living with HIV: A Study from AHF Nepal’s Collaborative Art Centers
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1, Dr. Unnat Shrestha1, Mr. Ajij Prasad Poudyal1, Ms. Sangita Bhatta1, Mr. Madhab Raj Pant1, Mr. Sanjaya Paudel1, Ms. Bidhya Koirala1, Mr. Radheshyam Shrestha1, Mr. Krishna Hari Sapkota1, Mr. Dharma Raj Bhattarai1, Mr. Bimal Sah1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
AIDS Healthcare Foundation (AHF) Nepal, in collaboration with 19 government ART centers, is dedicated to providing quality HIV treatment services to people living with HIV (PLHIV). In fiscal year 2024, AHF Nepal tested all newly enrolled PLHIV for syphilis to determine the prevalence of syphilis among those receiving HIV services at these centers. Out of 1,384 newly enrolled PLHIV, 72 children and 7 deaths excluded and 1,305 PLHIVs were tested for syphilis. Of these, 193 tested positive, resulting in a syphilis prevalence of 14.8%.
Statistical analysis using a chi-square test revealed a significant association between syphilis positivity and key population groups, including migrants, sexual minorities, and MSM/TG individuals (χ2 = 27.34, P-value < 0.05). The highest syphilis prevalence was observed in migrants (53.33%), sexual minorities (26.67%), and MSM/TG individuals (20%). Age and gender analysis showed that the 25–39 age group had the highest prevalence of syphilis (40%), with a significant age-related difference (P-value = 0.02). Additionally, syphilis positivity was higher in males (68%) compared to females (32%) (P-value = 0.03).
Treatment for syphilis was administered to 60% of the 193 individuals who tested positive. The treatment rates varied across key population groups, with migrants receiving the highest treatment rate (75%), followed by MSM/TG individuals (66.67%) and sexual minorities (25%). Logistic regression analysis indicated that sexual minorities were significantly less likely to receive treatment (OR = 0.22, P-value = 0.01) compared to other groups.
The study also found a significant correlation between syphilis positivity and untreated HIV (P-value = 0.04), highlighting the need for improved co-management of syphilis and HIV.
These findings underscore the high syphilis prevalence among PLHIV, especially within vulnerable populations. The results highlight the necessity for targeted interventions and enhanced services to address both syphilis and HIV, ultimately improving health outcomes and treatment adherence for PLHIV in Nepal.
PP06.95 – Sustainable Health Financing for Marginalized Groups: Nepal’s Free Health Insurance Model for PLHIV
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1, Mr. Ajij Poudyal1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
Nepal introduced its Health Insurance scheme in 2016 to reduce financial barriers to healthcare and improve access to quality services for all citizens. In 2019, a free Health Insurance scheme for People Living with HIV (PLHIV) and their families was launched. However, the uptake was limited, with only 21% of PLHIV enrolled by 2021 at the 16 ART centers collaborating with the AIDS Healthcare Foundation (AHF) Nepal. The primary barrier identified was the stigma and discrimination associated with HIV status disclosure during registration at local ward offices. By 2024, AHF Nepal was supporting 60.4% of the 25,728 PLHIV receiving antiretroviral treatment (ART) in Nepal.
To address these challenges, AHF Nepal initiated a collaborative effort with the Health Insurance Board to modify the registration process, incorporating ART centers as the primary site for insurance registration. Peer Educators were enlisted to support PLHIV during the process, reducing the stigma associated with enrollment. ART centers, where PLHIV have already disclosed their HIV status, were identified as a more suitable environment for integration.
This strategic shift led to a significant increase in enrollment: by 2022, the registration rate increased to 53%, 82% by 2023 and by 2024, it reached 88%. The results suggest that embedding the health insurance registration process within ART services, where individuals are already receiving care and have disclosed their HIV status, improved enrollment rates significantly.
The study demonstrates that merely offering free health insurance is not enough for high enrollment rates. Stigma and the need for a supportive environment are key factors. ART centers, with their established patient trust and privacy, offer an effective setting for registration. The integration of health insurance registration within ART centers, with continuous support from peer educators and other community-based interventions, has proven to be an effective strategy for increasing enrollment among PLHIV.
PP06.96 – Assessing the Shift in HIV Detection Rates Pre- and Post-Community-Led HIV Testing (CLT) Intervention in Nepal
Mr. Amrit Bikram Rai1, Mr. Divya Raj Joshi1, Dr. Unnat Shrestha1, Mr. Bobby Singh1, Mr. Ajij Prasad Poudyal1
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
Nepal introduced Community-led HIV Testing (CLT) as “Test-for-Triage” in 2017 to enhance testing uptake, improve case yield, and prevent HIV transmission. The epidemic predominantly affects key populations (KPs), yet over 50% of new HIV infections in 2022 were observed in non-KP individuals. This shift presents challenges in reaching these populations. AIDS Healthcare Foundation (AHF) Nepal has implemented CLT among sexual partners of HIV-negative individuals within KPs to address unsafe sexual behaviors.
This study aimed to assess the difference in the percentage of new HIV cases before and after the CLT intervention among sexual partners of HIV-negative individuals from KPs in Nepal.
A retrospective cross-sectional comparative study was conducted using secondary data from AHF Nepal’s program database between January 2020 and December 2024. Data from January 2020 to July 2021 (pre-CLT intervention) were compared with data from August 2021 to December 2024 (post-CLT intervention). Only data on sexual partners of HIV-negative individuals within KPs were included.
The study revealed a significant increase in HIV positivity following the implementation of CLT. The positivity rate rose from 0.38% in 2020 to 4.36% in 2022, to 4.48% in 2023 and further to 4.74% in 2024. The male population saw a notable increase, from 0% in 2020 to 2.48% in early 2021, 6.71% from August to December 2021, 5.15% in 2022, 5.19% in 2023 and 5.42% in 2024. These findings suggest that CLT has been highly effective in detecting new HIV cases in Nepal.
CLT among sexual partners of HIV-negative individuals from KPs has proven effective in identifying a higher number of new HIV cases, indicating the intervention’s potential to enhance HIV detection and prevention efforts in Nepal.
PP06.97 – Enhancing STI Management Among People Living with HIV in Nepal: Insights from Sudurpaschim Province
Mr. Amrit Bikram Rai1, Dr. Rita Dhungel2
1AIDS Healthcare Foundation (AHF), Nepal Country Office, Lalitpur, Nepal.
2University of the Fraser Valley, Abbotsford, Canada.
Sudurpaschim Province in Nepal faces challenges in the prevention, diagnosis, and treatment of sexually transmitted infections (STIs), particularly among key populations such as sex workers (SWs), people living with HIV (PLHIVs), and migrants. This study analyzes STI testing, confirmation, and treatment trends across multiple districts based on program data from July 2023 to June 2024, aiming to identify gaps and performance disparities in STI management for high-risk groups.
Data on STI testing, confirmed cases, and treatment status were collected from 6,521 individuals across 9 districts in Sudurpaschim Province during the fiscal year from July 2023 to June 2024. The analysis focused on key populations, including PLHIVs, sex workers, people who inject drugs (PWIDs), men who have sex with men (MSM), transgender individuals (TG), and pregnant women. Key performance indicators like confirmation rate and treatment success rates were evaluated to assess the effectiveness of STI care in the region, with particular emphasis on PLHIVs.
A total of 6,521 individuals were tested, with Kailali and Kanchanpur reporting the highest numbers. Darchula had the highest confirmation rate at 100%, while Bajura and Dadeldhura reported no confirmed cases. Overall treatment success was 89.6%. Testing among PLHIVs included 980 individuals, with Kailali testing 645 and reporting 32 confirmed cases, 31 of which received treatment. Achham and Kanchanpur showed 100% confirmation and treatment rates for PLHIVs, while Bajura reported no confirmed cases despite testing 164 PLHIVs, indicating potential diagnostic issues. Disparities in testing and confirmation rates were observed across districts, suggesting the need for improved diagnostic practices and resource allocation.
The study reveals significant disparities in STI testing, diagnosis, and treatment across Sudurpaschim Province. Although treatment rates are high, targeted interventions are needed to improve diagnostics, expand outreach, and address resource gaps, particularly for PLHIVs, to ensure comprehensive care and reduce vulnerability to STIs.
PP06.98 – Using the RE-AIM Framework to Evaluate the Reach of Pre-Exposure Prophylaxis Services in a Sexual Health Clinic in Ontario, Canada
Miss Carmela Rapino1,2, Dr. Emma Nagy2, Dr. Sahar Saeed1, Dr. Beatriz Alvarado1, Ms. Nicole Szumlanski2, Ms. Miriam Kamotho2, Dr. Hugh Guan2, Dr. Jorge Martinez-Cajas1
1Queen’s University, Kingston, Canada.
2South East Public Health Unit, Kingston, Canada.
Background: HIV diagnoses in Canada have increased by 35.2% from 2022-2023, challenging the attainment of the UNAIDS 95-95-95 targets. Scaling access to pre-exposure prophylaxis (PrEP) is critical, yet uptake remains low, particularly in suburban and rural areas. Since 2018, the Kingston, Frontenac, Lennox, and Addington Public Health Unit (KFL&A PHU) has offered PrEP services through its sexual health clinic (SHC) to address these gaps. This study aims to evaluate the clinic’s reach.
Methods: The SHC operates with an interdisciplinary team, initially targeting gay, bisexual, and other men who have sex with men (gbMSM), but later expanding to all populations at risk of HIV. Clients are referred by healthcare providers or self-initiate care. The clinic offers in-person and remote services, including SMS reminders and phone appointments, for eligibility assessments, prescriptions, and follow-ups. Using the RE-AIM framework, client characteristics were developed in consultation with SHC staff and analyzed from electronic medical records to define reach. Risk was stratified using the high-incidence risk index (HIRI), a screening tool that assesses demographics, sexual behaviours, and substance use.
Results: Between October 1, 2018, to December 15, 2024, 171 clients consulted the PrEP clinic, and 71.8% initiated PrEP. Most clients were male (97.8%), aged 29–40 (35.5.%), who lived locally (74.5%), and had primary care attachment (57.4%). Due to low sample size, clients reporting heterosexuality and shared injection drug use are not reported. As seen in Fig. 1, high-risk behaviours were predominately observed in two HIRI categories: age (60.3%) and condomless receptive anal sex with a man (51.1%). Additionally, 46.1% of clients reported a history of an STBBI, with chlamydia being the most common (24.1%).
Conclusion: While the SHC effectively reaches gbMSM, other populations remain underserved. Addressing these gaps requires tailored outreach strategies and inclusive screening practices to optimize HIV prevention.
Client Distribution of High Incident Risk Index (HIRI) Responses Stratified by Level of Risk.

Note. Stratification based on level of risk within each HIRI category are as follows: ages < 18 and 49 represent no risk, 18–28 represent high risk, 29–40 represent moderate risk, and 41–48 represent low risk. For number of male sexual partners in the last 6 months, >10 represents high risk, 6–10 represents moderate risk, and 0–5 represents no risk. For number of receptive anal sex events with a man without a condom, >1 positive partner represents high risk and <1 time represents no risk. For number of make HIV-positive sex partners, >1 positive represents high risk, 1 positive partner represents moderate risk, and <1 positive partner represents no risk. For the number of insertive anal sex events without a condom and with an HIV-positive partner, 5 or more times represents high risk, and 0–4 represents no risk. For methamphetamine and amyl nitrate use, “Yes” represents high risk and “No” represents no risk.
PP06.99 – A Human-Centered Design Approach to Re-Designing Sexual Health Care in St Louis
Ms. Anne Trolard1, Dr. Hilary Reno
1Washington University in St Louis, St Louis, United States.
Background: Public health strategies for sexually transmitted infections have limited reach into communities that bear the greatest burden from infections. Limited evidence exists on the fit between these communities and STI services intended to reach them. In contrast to traditional public health inquiries, human-centered design methods place the system under the microscope instead of people, and assess how services should meet people’s needs. HCD methods assert it can be difficult to accurately characterize problems involving complex interactions between people and processes. This is especially true for (1) those who seek healthcare without access to the required resources (e.g. transportation, flexible schedule, adequate finances), and (2) stigmatized health conditions like an STI.
Methods: This study explores from the vantage point of patients the pain points and opportunities in accessing the sexual health care system in St. Louis through (1) secret shopper reports; and (2) a think-aloud exercise simulating a sexual health clinic experience. We recruited participants through advisory groups and clinics. Rapid qualitative analysis methods were used to analyze audio-transcriptions and shopper reports to summarize data and produce insights.
Results: Two of 3 secret shopper reports and 5 of 7 interviews have been completed. Preliminary results from secret shopper reports showed that requests for sensitive personal information made without an explanation for how that information is used or why it is collected raised concerns; and the presence of security guards sent unintended messages to patients with a history with law enforcement. Preliminary results from the think-aloud exercises mirrored secret shopper findings in that requests for personal and health information were met with both trusting and distrusting reactions, but could be easily re-designed to build trust.
Conclusion: When collecting information on stigmatized conditions it would help patients to know why sensitive information is collected and with whom it could potentially be shared.
PT01.01 – ABI-5366, a Potent HSV Helicase-Primase Inhibitor, with Potential for Weekly or Monthly Oral Dosing for Recurrent Genital Herpes
Dr Michael Shen1, Dr Carl Li1, Dr Zhixin Zong1, Dr Heidi Contreras1, Dr Ran Yan1, Dr Michel Perron1, Dr William Delaney1, Dr Katie Kitrinos1
1Assembly Biosciences, South San Francisco, United States.
Background: Recurrent genital herpes (RGH), primarily caused by herpes simplex virus type 2 (HSV-2) infection, results in painful genital lesions. RGH suppression standard of care is nucleoside analogues (NA, e.g. valacyclovir); however, NAs are limited by suboptimal efficacy. Helicase primase inhibitors (HPIs), a novel class of antivirals, have shown improved efficacy compared to NAs. ABI-5366 is a long-acting oral investigational HPI in development for RGH treatment.
Methods: HSV antiviral assays were conducted in Vero cells. Metabolic stability was measured in rat, dog, monkey, and human liver microsomes. Pharmacokinetic (PK) studies evaluated 0.1–1 mg/kg ABI-5366 IV in rats, dogs, and monkeys, and an oral (PO) dose of 100 mg ABI-5366 in dogs. A bile-duct cannulated (BDC) study was conducted in rats with 0.5 mg/kg ABI-5366 IV. Reabsorption of 5366 following intestinal secretion was evaluated in dogs dosed with 0.1 mg/kg ABI-5366 IV ± 25 g/kg activated charcoal PO dosed every 2–8 h from 2 h pre-ABI-5366 dosing to 120 h post-ABI-5366 dosing. Tissue distribution was evaluated in rats after a single 15 mg/kg PO dose.
Results: In vitro, ABI-5366 inhibited HSV-1 and HSV-2 clinical isolates with low nanomolar potency (4–39 nM). ABI-5366 was metabolically stable in liver microsomes (CLint <9 mL/min/kg). Preclinical PK studies demonstrated that ABI-5366 has a very low clearance (CL = 0.002–0.02 L/h/kg) and an extended half-life (20–71 h). A rat BDC study showed ABI-5366 is mainly eliminated unchanged through feces. Co-dosing ABI-5366 with activated charcoal resulted in higher clearance and shorter half-life, suggesting intestinal reabsorption contributes to the extended half-life. ABI-5366 was well distributed in all tissues evaluated, including the ganglia (the HSV reservoir).
Conclusion: ABI-5366 is a potent HPI with broad activity against HSV-1 and HSV-2 and a PK profile supporting potential weekly or monthly dosing. A phase 1b study of ABI-5366 in RGH patients is ongoing.
PT01.02 – Investigating the Bacterial Side of the Host-Pathogen Interaction: Treponema Pallidum Proteome Response to Brain Endothelial Cell Exposure
Ms. Angela Mitchell1, Dr. Simon Houston1, Mr. Alloysius Gomez1, Dr. Mara Goodyear1, Mr. Derek Smith2, Dr. David Goodlett1,2, Dr. Caroline Cameron1,3
1University of Victoria, Victoria, Canada.
2University of Victoria-Genome BC Proteomics Centre, Victoria, Canada.
3University of Washington, Seattle, United States.
Background: Syphilis vaccine development requires a comprehensive understanding of the pathogenic mechanisms used by Treponema pallidum to infect the host, including how the bacterium crosses the blood-brain barrier (BBB) to cause neurosyphilis. Current understanding of the molecular mechanisms used by T. pallidum to cross the BBB is limited. Here, we use mass spectrometry (MS)-based label-free quantitative proteomic analyses to investigate T. pallidum protein expression following exposure to brain microvascular endothelial cells (BECs), a model for the BBB.
Methods: Treponema pallidum was co-incubated for 4 and 24 h with BECs or rabbit epithelial cells (Sf1Eps; serves as a control for in vitro T. pallidum growth). Bacteria were isolated using an in-house developed gentle sample preparation method optimized for T. pallidum proteomics studies. Protein identification was accomplished using liquid chromatography-tandem MS (LC-MS/MS) and T. pallidum protein expression levels were determined using label-free quantification (LFQ) based on peptide ion peak intensities from three biological replicates.
Results: Quantitative proteomic analysis of T. pallidum following co-incubation with BECs allowed identification of expression level changes in T. pallidum proteins in response to endothelial cells. Global protein expression levels were also determined for proteins that mapped to the categories of predicted pathogenesis-related proteins, proteins involved in transport or regulatory networks, and predicted/known outer membrane proteins (OMPs). Analysis of expression levels of T. pallidum OMPs was prioritized since these proteins reside at the host-pathogen interface and are therefore promising targets for syphilis vaccine development.
Conclusion: These analyses identified T. pallidum proteins and protein categories that are altered in expression levels in response to brain endothelial cell exposure. This study informs our understanding of T. pallidum pathogenesis, and in particular syphilis vaccine development, by providing a nuanced approach to identifying T. pallidum proteins that are important for blood-brain barrier traversal and neurosyphilis.
PT01.03 – The Role of Estradiol in Sequestration of HIV-1 R5 in Endometrial Epithelial Cells
Dr. Aisha Nazli1, Dr Charu Kaushic1
1McMaster University, Hamilton, Canada.
Background: Women, who make up majority of HIV-1 infections globally, contract HIV-1 primarily through heterosexual intercourse via the female reproductive tract (FRT). Although both R5 and X4 HIV-1 strains are present in semen, initial infection in the FRT mainly occurs through the R5 strain. Previously we found that X4 HIV exposure induced a strong anti-viral response by genital epithelial cells (GECs), that was not seen in response to R5 HIV. This resulted in X4 HIV getting sequestered in GECs while R5 HIV crossed the epithelium unhindered. Since sex hormones influence the immune response of FRT GECs to viruses, we examined the effect of sex hormones on the interactions between HIV-1 strains and genital epithelial cells.
Methods: Human endometrial tissues were obtained with informed consent from women undergoing elective hysterectomy. GECs were grown in monolayer cultures with no hormone or in the presence of estradiol (10–9 M) or progesterone (10–7 M). HIV-1 leakage through GEC monolayers was observed in basolateral supernatants by TZMbl assay. Intracellular trafficking of HIV-1 was studied by immunofluorescence microscopy.
Results: When GECs were exposed to HIV-1 in the absence of hormones, significant upregulation of the TLR2-signaling pathway was observed only in response to X4 but not R5 HIV-1. In contrast in the presence of estradiol, GEC induced comparable anti-viral immunity to both X4 and R5 HIV. TLR2 pathway activation by estradiol resulted in the upregulation of anti-viral factors BST-2 and ISG-15, and sequestration of both X4 and R5 HIV-1 in the endosomal compartment. In contrast, GECs grown in the presence of progesterone downregulated IFN signaling in response to both strains of HIV.
Conclusion: Results showed that in the absence of hormones, only HIV-1 X4 triggers a strong antiviral response. Estradiol treatment targets anti-viral immunity against X4 and R5, trapping both viruses in GECs.
PT01.04 – In Vitro Selection and Characterization of Resistance to Josamycin and Pristinamycin in Mycoplasma Genitalium
Dr. Chloé Le Roy1, Dr. Otgonjargal Byambaa1, Dr. Jennifer Guiraud2, Mrs. Carla Balcon2, Mr. Léo Gilet2, Dr. Jorgen Skov Jensen3, Pr. Cécile Bébéar1,2, Prof. Sabine Pereyre1,2
1University of Bordeaux – CNRS, Bordeaux, France.
2CHU Bordeaux – French National Reference Center for Bacterial STIs, Bordeaux, France.
3Department of Bacteria, Parasites and Fungi, Statens Serum Institut, Copenhagen, Denmark.
Background: Pristinamycin is a recommended third-line treatment of Mycoplasma genitalium infections according to the European guidelines. No data regarding mechanisms of pristinamycin resistance have been available to date. In M. pneumoniae, crossed resistance to pristinamycin and josamycin was associated with mutations at position 2062 (Escherichia coli numbering) of 23S rRNA.
We investigated the in vitro development of resistance in M. genitalium in the presence of subinhibitory concentrations of josamycin and pristinamycin.
Methods: Selection of resistant mutants was performed by serial passages of M. genitalium G37 reference strain in subinhibitory concentrations of josamycin or pristinamycin. Resistant mutants were characterized by Sanger sequencing of 23S rRNA, L4 and L22 ribosomal protein genes and MICs of seven antibiotics were determined. Whole genome sequencing (WGS) was performed on selected mutants using the Illumina technology.
Results: A mutant selected in the presence of josamycin harbored the A2059G mutation in 23S rRNA. This mutant showed a strong increase in the MICs of erythromycin, azithromycin, josamycin, and clindamycin (16–32 µg/mL), but no changes in MICs of pristinamycin, doxycycline, and moxifloxacin (all three at 0.125 µg/mL). Two mutants selected in the presence of pristinamycin harbored mutation A2062C or A2062G. Both mutants showed a strong increase of the MICs of pristinamycin (8 and 2 µg/mL, respectively) and josamycin (32 and 16 µg/mL, respectively) and a slight 4 to 8-fold increase of erythromycin MIC. Azithromycin, clindamycin, doxycycline and moxifloxacin MICs remained unchanged. No mutations in L4 and L22 gene were detected in any mutants. WGS of the three mutants confirmed the 23S rRNA mutations associated with antibiotic resistance and revealed 6 to 10 additional SNPs not likely to be involved in resistance.
Conclusion: Resistant mutants can be selected in vitro in M. genitalium using josamycin and pristinamycin. These laboratory-derived mutants may predictive for mutations observed in clinical strains.
PT01.05 – Genomic Surveillance of Neisseria Gonorrhoeae Isolates from Cameroon and Madagascar: Resistance Patterns and Phylogenetic Insights
Dr. Lala Rafetrarivony1, Dr. Rosanne Ngome2, Mr. Arsène Djoko2, Dr. Elisoa Ratsima Hariniaina3, Dr. Frédérique Randrianirina3, Dr. Lovasoa Ramparany3, Dr. Solène Cottis4, Dr. Chiara Crestani4, Pr. Sylvain Brisse4, Dr. Tania Crucitti1
1Bacteriology Experimental Unit, Institut Pasteur Madagascar, Antananarivo, Madagascar.
2Centre Pasteur Cameroon, Yaoundé, Cameroon.
3Clinical Biology Centre, Institut Pasteur Madagascar, Antananarivo, Madagascar.
4Institut Pasteur, Université Paris Cité, Biodiversity and Epidemiology of Bacterial Pathogens, Paris, France.
Background: Antibiotic resistance poses a global health threat, significantly impacting sexual health. In Africa, weak regulation of antibiotic use exacerbates the problem, with resistance rates and genomic data underreported. To address this gap, the ‘Surveillance of Antimicrobial Resistance in Africa’ (SARA) project was initiated. This project included surveillance of Neisseria gonorrhoeae, a major threat to sexual health globally, in Cameroon and Madagascar.
Methods: Within this framework, gonococcal isolates with antimicrobial susceptibility test (AST) data were obtained from medical laboratories. Forty isolates from Cameroon (2018–2023) and 73 isolates from Madagascar (2021–2023) were sequenced using Illumina technology. These sequences were analyzed together with public PubMLST genomic sequences, comprising 50 for Cameroon and 119 for Madagascar.
Results: High phenotype-genotype concordance was observed for isolates from Madagascar, whereas discrepancies were detected in Cameroon, particularly for azithromycin. In 2023, an azithromycin-resistant ST9363 isolate from clonal complex (CC)168 carrying a mosaic mtrD gene and a genotypically cefixime-resistant ST7363 (CC348) isolate carrying a penA (10.001) mosaic allele were detected in Cameroon and Madagascar, respectively. ST1588 is prevalent and persistent in both countries, while ST17783, undocumented elsewhere, exhibits similar prevalence and persistence over time in Madagascar. Core genome and SNP analysis revealed clusters in each country (8 in Madagascar and 7 in Cameroon). Using the threshold of 300 allele differences, only two of 40 clusters were shared between the two countries (Ng_cgc_300: 133 and 239). In Madagascar, the majority of core genome clusters comprising at least two isolates (13 out of 19) had not been previously identified in other countries.
Conclusion: This work highlights that Madagascar has its own circulating clones of N. gonorrhoeae which evolve over time, whereas those in Cameroon follow the trend observed in Africa. However, continued and extended surveillance is needed to better understand the molecular epidemiology of N. gonorrhoeae in these countries and more broadly in Africa.
PT01.06 – Genomic Variations in the Chlamydia Trachomatis Polymorphic Membrane Protein Gene Pmpe Exhibit Anatomic Site-Specific Tissue Tropism in a Non-Human Primate Model
Mr. Robert Suchland1, Mrs. Yvonne Cosgrove-Sweeney2, Dr. Dorothy Patton2, Dr. Lucia Vojtech2, Dr. Olusegun Soge3, Dr. Christine Khosropour4, Dr. Kevin Hybiske1
1Department of Medicine, University of Washington, Seattle, WA, United States.
2Department of Obstetrics and Gynecology, University of Washington, Seattle, United States.
3Department of Global Health, University of Washington, Seattle, United States.
4Department of Epidemiology, University of Washington, Seattle, United States.
Background: Chlamydia trachomatis (CT) infects the mucous membranes of the genital tract, anorectum, and conjunctiva. Genomic studies have revealed clear lineages and distinct genomic profiles of the CT strains that exhibit tropism for these different anatomic sites. We previously showed that specific pmpE genotypes are strongly associated with genital infections in females vs rectal tropism in males. PmpE is a surface-exposed membrane protein which we hypothesize promotes differential infection across distinct anatomic sites. To investigate how these varying genotypes might lead to tissue site-specific infection phenotypes, we performed in vivo studies utilizing a non-human primate (NHP) CT infection model.
Methods: Seven pig-tailed macaques were inoculated either in the cervix (N = 3) or rectum (N = 4) with inocula containing equal titers of three CT clinical strains. These strains were selected based on their isolation from different anatomic sites and pmpE genotypes: D (female rectal isolate with cervical pmpE), G (cervical isolate with cervical pmpE), and Ga (MSM rectal isolate with rectal pmpE). Infected pig-tailed macaques were monitored by cell culture for 8 weeks with weekly swab collections.
Results: Strain D was isolated from both the cervix and rectum by cell culture each week in two of both the cervically and the rectally inoculated macaques, while the Ga strain was only isolated from the cervix periodically through the first 4 weeks of the cervically inoculated macaques. In contrast, strain Ga was isolated from the rectum weekly in three of the rectally inoculated macaques throughout the 8-week study. The G strain was only isolated intermittently from either site, regardless of the site of inoculation.
Conclusions: These results strengthen the hypothesis that pmpE genotypes correlate with tissue-specific tropism. Continued exploration of PmpE function both in vitro and in the NHP model could further facilitate the understanding of CT infections and promote future vaccine development.
PT01.07 – Unveiling the Vaginal Microbiome: A Metagenomic Study of Bacterial Vaginosis in Women from Northern India
Ms Gurmeet1, Dr Rakesh Yadav1, Dr Rashmi Bagga1, Dr Amit Arora1, Dr Sunil Sethi1
1Postgraduate Institute of Medical Education and Research (PGIMER), Chandigarh, India.
Background: Bacterial vaginosis (BV) is a clinical state of microbial dysbiosis among women of reproductive age. The diagnosis of BV remains problematic due to its polymicrobial etiology. The current diagnostic methods Amsel’s criteria and Nugent scoring system are subjective and can’t identify new morphotypes. In this study, we compared the vaginal microbiome of BV-positive with BV-intermediate and BV-negative population to assess the distinct shifts in bacterial communities and identify key changes in microbial composition.
Methods: A total of 701 women with complaints of abnormal discharge, or for routine gynecological check-ups were enrolled between November 2021 to May 2024 from the Department of Obstetrics and Gynaecology, PGIMER, Chandigarh. Two high vaginal swabs were collected from each participant along with medical history and demographic details. Amsel’s criteria was determined clinically and smear microscopy was performed for Nugent scoring. DNA was extracted followed by V3-V4 16SrRNA gene sequencing on Illumina MiSeq platform.
Results: Based on Nugent scoring, 95/680 (13.9%) samples were found to be BV-positive, 174/680 (25.5%) BV-intermediate and 411/680 (60.4%) BV-negative. BV was most prevalent among women aged between 28–37 and strongly associated with symptoms, including abnormal discharge (87.3%), odor (50.5%) and vaginal itching (40%). The 16S metagenomic sequencing was performed for 265 (77 BV-positive, 88 BV-intermediate and 100 BV-negative) samples. Metagenomic analysis revealed the predominance of Gardnerella, Sneathia, Atopobium and Prevotella in BV-positive samples while BV-intermediate group had abundant lactobacilli, Gardnerella and Sneathia. The alpha diversity was found to be higher in BV-positive group. In contrast, BV-negative group was marked by high prevalence of lactobacilli and comparatively low evenness (Fig. 1).
Conclusion: Metagenomic sequencing could comprehensively elucidate the distinct microbial profiles associated with BV-positive and BV-negative women, unravelling intricate microbial signatures, which would be helpful in the early detection of BV, and development of targeted management strategies, thus advancing and enhancing women health outcomes.
(a) Taxa bar plots representing relative abundance of Top 10 genus in different groups; (b, c) Alpha diversity analysed using Kruska–Wallis test and D-PCoA (Principal Coordinate Analysis) generated using Bray–Curtis distance indicating distinct clustering of samples from each group.

PT02 .01 – The Impact of ‘Undetectable=Untransmittable’ on Health Outcomes: A Systematic Review and Qualitative Synthesis
Mr Daniel Zhao Yang Chong1, Mr Andrew Amadeus Susilo1, Mr Judd Denzel Garcia Mondina1, Ms Jia Wen Tay1, Mr Clifton Liu Ziheng1, Mr Micheal Ighodaro2, Dr Christina Misa Wong1, Dr Joseph D Tucker3,4, Dr Rayner Kay Jin Tan1
1Saw Swee Hock School of Public Health, National University of Singapore and National University Health System, Singapore, Singapore.
2Global Black Gay Men Connect Corporation, New York City, USA.
3Institute for Global Health and Infectious Diseases, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA.
4Clinical Research Department, Faculty of Infectious and Tropical Diseases, London School of Hygiene & Tropical Medicine, London, UK.
Background: The ‘Undetectable=Untransmittable’ (U=U) campaign revolutionized HIV care through affirming that people living with HIV who are virally suppressed cannot sexually transmit HIV. Given its public health impact, this systematic review and qualitative analysis was undertaken to examine the impact of U=U on health outcomes of individuals globally.
Methods: We used the Cochrane Handbook and registered the review (PROSPERO: CRD42024525175). PubMed, CINAHL, PsycINFO, ProQuest, and Scopus were searched for relevant studies. The purpose of the review is to examine how knowledge of U=U impacted a wide range of outcomes. Thematic analysis was employed to derive our themes. We assessed study quality using the Critical Appraisal Skills Programme checklist.
Results: The search identified 4065 studies, of which 82 were included in the synthesis. Study populations included people living with HIV (k = 41), gender and sexual minority men (k = 24), and individuals in serodiscordant relationships (k = 14). Study settings included high- (k = 50), middle- (k = 34), and low-income countries (k = 6). Knowledge of U=U impacted health outcomes in five health areas: behavioral, psycho-emotional, relational, socio-cultural, and health communications. A summary can be found in Fig. 1. In the behavioral domain, U=U contributed to greater treatment adherence (k = 15). In the psycho-emotional domain, U=U provided a return to normalcy for individuals (k = 11). In the relational domain, U=U encouraged open communication (k = 9) and provided certainty within serodiscordant relationships (k = 8). In the socio-cultural domain, U=U has decreased societal stigma within varying populations (k = 11). In the domain of health communications, individuals and healthcare workers were motivated (k = 11), and confident (k = 15), in communicating U=U. Nevertheless, these were met with confusion on how HIV is transmitted when an individual is undetectable (k = 11).
Conclusion: We found that the concept of U=U has demonstrated a positive impact on various health outcomes at multiple levels. U=U should be incorporated as part of key messaging in HIV care communications.
PT02 .02 – Does the Crowd Want to Crowdsource? Crowdsourcing Acceptability for PrEP Promotional Messaging in the Southern United States
Kevin M. Joseph1, Dr. Latesha Elopre1, Dr. Lynn T. Matthews1, Dr. Barbara Van Der Pol1, Dr. Joseph D. Tucker2,3, Dr. Ronnie Gravett1
1University of Alabama at Birmingham, Birmingham, United States.
2University of North Carolina – Chapel Hill, Chapel Hill, United States.
3London School of Hygiene and Tropical Medicine, London, United Kingdom.
Background: HIV pre-exposure prophylaxis (PrEP) uptake in the Southern United States (US) remains poor due to stigma, medical mistrust, and structural barriers, thus perpetuating HIV disparities, especially among sexual minority men (SMM) of color. Crowdsourcing engages the community to create and share solutions. Little formative research has been done on organizing crowdsourcing for HIV prevention services, especially in the Southern US context. We explored the acceptability of crowdsourcing and identified practical tips for crowdsourcing to develop PrEP promotions among SMM and sexual health providers.
Methods: Grounded in the Theoretical Framework of Acceptability (TFA), we conducted focus group discussions (FGD) with HIV-negative SMM ages 18–39 years and interviews with sexual health providers using topic guides grounded in the TFA. FGDs and interviews were recorded and transcribed. We deductively and inductively coded transcripts to develop and iteratively revise the codebook. We utilized thematic analysis to develop themes with sub-themes for richer context and mapped themes to TFA constructs.
Results: We conducted 2 FGDs (n = 10, 60% Black, 50% younger than 30 years) and 6 provider interviews. We identified 4 themes: (1) Participant identity/background informs the participation and the products of crowdsourcing, (2) Motivation to participate in crowdsourcing is strong, (3) Crowdsourcing participants require resources (e.g. compensation, skilled support) to effectively engage, and (4) Logistic and social barriers (e.g. scheduling/timing, stigma) may prevent inclusive crowdsourcing participation. Table 1 shows themes and sub-themes mapping to TFA constructs with exemplar quotes.
Conclusion: SMM and sexual health providers found that crowdsourcing to create PrEP promotions in the Southern US is acceptable and would be effective. These novel findings demonstrate new understanding of how SMM would consider participating in crowdsourcing events and provide insight into the future design of crowdsourcing events. Sexual health stakeholders should use this participatory tool to create authentic, inclusive messaging to increase PrEP uptake.
| Theme | Sub-theme | Construct | Exemplar Quotes | |
|---|---|---|---|---|
| Participant identity/background informs the participation and products of crowdsourcing | SMM and non-SMM should participate and be the audience in crowdsourcing. | Affective Attitude, Perceived Effectiveness | So, it’ll be great if it was created by the community that is directly affecting. But I also think that in some cases, I just think that it needs to be a little bit more of a broader spectrum. (FG1, Interviewee 3) | |
| Non-LGBTQ+ providers express caution about participating in crowdsourcing past sharing medical expertise. | Affective Attitude, Ethicality | I do feel like my experience would be more limited just because I would only feel like I could really comment on the accuracy of the content from a scientific point of view. I couldn’t comment on the acceptability of the content. […] I’m not the target demographic. (Provider 1) | ||
| Crowdsourcing processes and products should intentionally have diverse representation. | Perceived Effectiveness | A gay, Black man is more inclined to listen to another gay, Black man…I think if there are more commercials where there are more gay, Black men or even straight, Black men there are just more black people expressing that it is okay to protect yourself from HIV (FG2, Interviewee 4) | ||
| Motivation to participate in crowdsourcing is strong | SMM want to participate in crowdsourcing and give back to their community. | Affective Attitude | I think I would be able to participate. And feel…proud to have done such…And you kind of begin to give back to the community that way, silently almost, (FG2, Interviewee 5) | |
| Providers want to participate in crowdsourcing to serve the community while addressing the HIV epidemic | Affective Attitude | I would think that anything that pushes us out of the provider space, and into a more community space, and maybe what we can learn globally, and bring to our prevention portfolio, would be beneficial. I think for that crowd sourcing would be really good for this. (Provider 2) | ||
| Crowdsourcing participants require resources to effectively engage | Community heroes could increase crowdsourcing’s promotional messaging products’ appeal | Perceived Effectiveness | It needs to be highly specific and also huge emphasis on community heroes because…they don’t stop scrolling unless it’s someone they recognize (FG1, Interviewee 2) | |
| Effective crowdsourcing needs funding to produce and media to share the product | Perceived Effectiveness | When you were speaking about challenges or problems or creating that, like I think another issue would be having proper funding to make sure that the message could be told correctly. (FG1, Interviewee 3) | ||
| Participants may have or may not have sufficient HIV knowledge or skill sets to effectively participate | Self-Efficacy | You know, we can come up with a bunch of solutions. But if no one understands the problem, then what are we solving? (FG1, Interviewee 2) | ||
| The expectations of the plan and process of crowdsourcing must be clear to recruit participants | Intervention Coherence | I think you would have to just be a little more specific than just saying, “We’re doing crowdsourcing”…If they know what’s being asked of them, they’re probably going to be more apt to participate. (Provider 3]) | ||
| Logistic and social barriers may prevent inclusive crowdsourcing participation | The time to crowdsource must be convenient, organized, and reasonable for participation | Burden, Opportunity Costs | And how strongly you feel about it. So that would kinda dictate and determine what time you allow it to take away from other prospects. (FG2, Interviewee 5) | |
| Compensation for the time spent on crowdsourcing could be necessary for participation | Burden | If it’s for free, because I can’t do nothing for free. (FG1, Interviewee 1) If you can comp people [for] their time, they will be more inclined to doing it. (FG1, Interviewee 2) | ||
| Both medical providers and community members may have differing beliefs and comfort discussing HIV as part of crowdsourcing | Ethicality, Affective Attitude | [Providers] who are not in it and doing it all the time may think this is a moral dilemma, because it’s promoting promiscuity or all these things that we know are not true (Provider 3) Some of the crowd, even in that community, will not appreciate it. Everyone is not always going to agree with that, but this is something that has to be done. (FG1, Interviewee 5) | ||
| Privacy and stigma concerns for both SMM and providers surrounding sexual health/HIV | Affective Attitude, Opportunity Costs | For me personally, I probably would not want to be a face [whose] involved. But I’m offering ideas or my own personal experiences maybe. (FG2, Interviewee 2) |
PT02 .03 – Women’s Preferences for Hypothetical PoCT for STIs in Madagascar, South Africa and Zimbabwe – a Discrete Choice Experiment
Prof. Ayako Honda1, Dr Timothy Barry Bolt2, Dr Chido Dziva Chikwari3,6, Dr Katherine Gill4, Dr Aina Harimanana5, Ms Lucia Jola4, Ms Tinashe Mwaturura3, Dr Thandeka Nkosi4, Ms Vaomalala Raharimanga5, Dr Emma Harding-Esch6, Dr Kimie Kitai7
1Hitotsubashi University, Kunitachi, Japan.
2Saitama University, Saitama, Japan.
3Organization for Public Health Interventions and Development, Harare, Zimbabwe.
4Desmond Tutu Health Foundation, Cape Town, South Africa.
5Institut Pasteur de Madagascar, Antananarivo, Madagascar.
6London School of Hygiene and Tropical Medicine, London, United Kingdom.
7Japanese Red Cross College of Nursing, Shibuya, Japan.
Background: Most women with laboratory-confirmed sexually transmitted infections (STIs) or bacterial vaginosis (BV) are asymptomatic. In low- and middle-income countries, due to both supply and demand-side issues, STIs and BV are only treated if women present with clinical symptoms, despite asymptomatic women being at increased risk of HIV infection and pregnancy complications. Point of Care Testing (PoCT) to detect genital inflammation and asymptomatic infection can significantly improve health outcomes by enabling timely treatment of asymptomatic STIs.
Methods: A discrete choice experiment (DCE) was undertaken in Madagascar, South Africa and Zimbabwe to examine patient preferences for various aspects of STI management that includes PoCT. Results from qualitative interviews were supplemented by a literature review to inform attributes and levels selected for the DCE. At each study site, locally-trained interviewers administered face-to-face choice experiment interviews with 200 women aged 18–35. Mixed logit models were estimated for analysis.
Results: Most participants indicated they were likely to use PoCT for STI. Attributes consistently increasing acceptance of the implementation of PoCT for STIs include provision of HIV preventive medication upon a positive result, medicine availability at the facility undertaking PoCT, and detailed explanation of STI PoCT before testing. Socio-economic status influenced preferences for some attributes. Variations in relative importance of attributes exist in the three study sites, possibly reflecting different health system contexts.
Conclusion: Women in the study settings are interested in PoCT for STI. Broader health system factors need to be improved to effectively deliver STI PoCT services. Availability of sustainable medicine supplies at PoCT health facilities was highly valued by women in all study settings. Successful integration of STI PoCT in day-to-day healthcare service delivery requires contextualizing implementation strategies and considering target population.
PT02 .04 – Prospective Acceptability of a Novel Point-Of-Care Genital Inflammation Test to Identify Women with Sexually Transmitted Infections and Bacterial Vaginosis in Zimbabwe and South Africa
Mr Jayjay Karumazondo1,2, Mr Jason Naidoo3, Dr Sarah Bernays4, Ms Thulisa Mayekiso3, Ms Maureen Tshuma1, Ms Tinashe Mwaturura1, Dr Chido Dziva-Chikwari1,5, Dr Eneyi Kpokiri6, Dr Katherine Gill3, Dr L Becker3, Dr Lindi Masson7,8, Dr Jo-Ann Passmore8,9, Dr Emma Harding-Esch6, Dr Constance Mackworth-Young1,10
1The Health Research Unit, Biomedical Research and Training Institute, Harare, Zimbabwe.
2Department of Demography Settlement and Development, University of Zimbabwe, Harare, Zimbabwe.
3Desmond Tutu Health Foundation, Cape Town, South Africa.
4Faculty of Medicine and Health, University of Sydney, Sydney, Australia.
5Infectious Disease Epidemiology and International Health Department, London School of Hygiene & Tropical Medicine, London, United Kingdom.
6Clinical Research Department, Faculty of Infectious and Tropical Diseases, London School of Hygiene & Tropical Medicine, London, United Kingdom.
7Burnet Institute, Melbourne, Australia.
8Institute of Infectious Disease and Molecular Medicine, University of Cape Town, Cape Town, South Africa.
9National Health Laboratory Service, Cape Town, South Africa.
10Department of Global Health and Development, London School of Hygiene & Tropical Medicine, London, United Kingdom.
Background: The Genital InFlammation Test (GIFT) is a novel point-of-care test under development to detect genital inflammation associated with STIs or BV, which can increase the risk of HIV, adverse birth outcomes, and infertility. This study assessed the prospective acceptability of GIFT as a screening tool, which would be followed by STI diagnostic tests among women, healthcare professionals, and decision-makers. This study was set within national healthcare sector in LMICs where STI diagnostics are limited.
Methods: Sixty-five in-depth interviews were conducted with women (n = 33), healthcare professionals (n = 20), and decision-makers (n = 12) across Zimbabwe and South Africa, along with seven focus group discussions (women n = 2, healthcare professionals n = 5). Interviews and FGDs were audio-recorded, transcribed, and analysed thematically using Sekhon’s framework of acceptability, which covers seven domains: affective attitude, burden, ethicality, intervention coherence, opportunity costs, perceived effectiveness, and self-efficacy.
Results: Women showed a strong desire for novel tools to manage their sexual health. Acceptability of GIFT was often due to a misunderstanding that it was as a diagnostic test rather than a screening tool. Women who understood GIFT as a screening tool expressed concern about the cost implications of follow-up STI tests. Healthcare professionals had a better understanding of GIFT. They welcomed the attention needed for more STI screening, diagnostics, and treatment investment. However, they expressed concerns about GIFT’s clinical utility and the lack of accessible follow-up STI diagnostics. Decision-makers echoed these concerns: GIFT’s utility as a screening tool was limited by follow-up diagnostic availability and affordability. Some decision-makers saw potential for GIFT to support advocacy for improved STI diagnostic development and infrastructure.
Conclusion: This study reinforces the idea that a technological device’s acceptability cannot be separated from the context of its use. As such, intervention design must consider the feasibility of implementation within existing health systems and leverage opportunities for system strengthening.
PT02 .05 – Anxiety Responses and Testing Intentions Among Gay and Bisexual, and Other Men Who Have Sex with Men Using an AI-Powered Risk Assessment Tool for Sexually Transmitted Infections: A Quasi-Experimental Study
Dr. Phyu Mon Latt1,2, Dr. Nyi Nyi Soe1,2, Dr. Xianglong Xu2,3, Ms. Yining Bao2,4, Dr. David Lee2, Prof. Jason Ong1,2,5, Prof. Eric Chow1,2,6, Prof. Lei Zhang1,2,7, Prof. Christopher Fairley1,2
1Monash University, Melbourne, Australia.
2Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
3School of Public Health, Shanghai University of Traditional Chinese Medicine, Shanghai, China.
4China–Australia Joint Research Centre for Infectious Diseases, School of Public Health, Xi’an Jiaotong University Health Science Centre, Xi’an, China.
5Department of Clinical Research, London School of Hygiene and Tropical Medicine, London, United Kingdom.
6Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
7Clinical Medical Research Centre, Children’s Hospital of Nanjing Medical University, Nanjing, China.
Background: Web-based tools for the assessment of the risk of sexually transmitted infections (STI) may increase testing but also may induce anxiety. We evaluated anxiety responses and testing intentions among gay, bisexual and other men who have sex with men (GBMSM) using MySTIRisk, an artificial intelligence-powered STI risk assessment tool, compared to a standard sexual health information webpage for GBMSM.
Methods: We conducted a quasi-experimental pre-post study at the Melbourne Sexual Health Centre between April and October 2024. Participants were allocated to either MySTIRisk, which provides personalised STI risk assessment, or a standard webpage providing general sexual health information for GBMSM on alternating days. We measured anxiety using the State-Trait Anxiety Inventory (STAI-6) before and after participants viewed their assigned websites. We defined clinically significant anxiety changes as ≥3 points on STAI-6. We used multivariable ordinal logistic regression analysis to evaluate clinically significant anxiety changes while controlling for baseline scores and demographic variables.
Results: Our study population had a median age of 34 years (IQR: 28–42); 48% were born in Australia, and 69.7% had tertiary education. The baseline characteristics were similar between MySTIRisk (n = 150) and control groups (n = 150). In the MySTIRisk group, STAI-6 scores increased significantly from baseline (median [IQR]: 10 [8, 12]) to post-intervention (11 [8, 13], P = 0.001). The control group showed a decrease from baseline (11 [9, 12]) to post-intervention (10 [8, 13], P = 0.01). Despite increased anxiety, MySTIRisk users maintained high user acceptability (92.0%) with similar testing intentions between groups (87.3% vs 82.7%, P = 0.6). The multivariable regression analysis showed that the intervention’s effect on anxiety was independent of demographic characteristics, except for employment status.
Conclusion: While MySTIRisk increased anxiety in some users, it maintained high acceptability and did not deter testing intentions. These findings support implementing such tools with anxiety management strategies.
PT02 .06 – The Unseen Burden: Sexually Transmitted Infections and Mental Health Among Transgender Individuals in India – A Clarion Call Towards Sexual Health for All!
Dr. V Sam Prasad1, Ms. Elizabeth Michael1, Mr. Mohnish Kumar1, Mr. Shivam Dwivedi1, Mr. Lyle Honig Mojica2
1AIDS Healthcare Foundation (AHF) India Cares, South Delhi, India.
5AIDS Healthcare Foundation (AHF), Los Angeles, United States.
Background: Transgender individuals in India face significant social, economic, and healthcare challenges, increasing their vulnerability to sexually transmitted infections (STIs). The intersection of STIs and mental health issues can exacerbate the overall well-being of this marginalized community.
Methods: AIDS HEALTHCARE FOUNDATION – India implements STI/ HIV rapid community-based testing across 10 states. The retrospective study of program data (n = 390) and qualitative in-depth interviews (n = 25) with transgender individuals in India. Participants were recruited randomly through a community-based STI/HIV testing program. The study used the WHO 5 mental well-being scale for all (390) to assess the mental well-being of transgender participants in the STI HIV screening program. Around 73% of the transgender community were practicing sex work for their livelihood.
Results: The mental well-being of transgender people without any physical symptoms (11%) were good while 89% said that they were curious to know the results of the STI/HIV tests. 17% of the participants were detected with HIV while 36% reported one or more symptoms of STI during the pre and post-test counselling. The in-depth interviews showed that 27% experiencing symptoms of depression and 22% experiencing symptoms of anxiety. Qualitative findings also highlighted the stigma, shame, and social isolation associated with STIs/ HIV they face daily, exacerbating mental health issues. Participants reported difficulty accessing STI testing, treatment, and mental health services due to fear of discrimination and losing their clients.
Conclusion: This study shows the critical need for comprehensive healthcare services addressing the intersection of STIs and mental health among transgender individuals in India. Findings emphasize the importance of culturally sensitive healthcare providers, accessible STI testing and treatment, and mental health support services. Policymakers, healthcare providers, and community organizations must work together to address the social determinants of health and promote inclusive, equitable care for transgender individuals in India.
PT02 .07 – Association Between Availability of Non-English Language Services and HIV-Related Services in Substance Use Disorder Treatment Facilities in the United States
Dr. Khairul Siddiqi1, Fahima Nasrin Eva2, Gazi Sakir Mohammad Pritom3, A. M. Khairul Islam4, Mary A. Hatch5, Michael G. McDonell1
1Washington State University Elson S. Floyd College of Medicine, Spokane, United States.
2North South University, Dhaka, Bangladesh.
3University of South Carolina, Columbia, SC.
4University of Rochester School of Nursing, Rochester, NY.
5University of Washington, Seattle, WA.
Background: This study investigated the association between non-English language services and the availability of HIV-related services in substance use disorder (SUD) treatment facilities across the United States (US), addressing the need for culturally competent care.
Methods: This study analyzed data from the 2023 National Substance Use and Mental Health Services Survey (N-SUMHSS), representing two types of US SUD treatment facilities: SUD treatment only (n = 6,746) and mixed mental health and SUD treatment services (n = 7,662). Descriptive statistics and bivariate comparisons using chi-square tests assessed the association between the availability of non-English language services and HIV/STI-related services, with statistical significance set at P < 0.01.
Results: Among 14,408 SUD treatment facilities, 39.8% have sign language services, and 54.6% have non-English language services (51.0% in SUD only and 57.8% mixed facilities). Among those non-English programs, Spanish was the most widely available language service (89.2% vs 85.7%), followed by Russian (14.7% vs 15.2%), French (10.8% vs 16.6%), Portuguese (8.8% vs 12.1%), and Creole (7.1% vs 15.7%). HIV prevention services were significantly higher in facilities with non-English services compared to other facilities (P < 0.001), both in SUD-only settings [HIV testing (41.1 vs 30.4%), HIV/AIDS education/counseling/support (73.9% vs 61.5%), early intervention for HIV (28.8% vs 18.7%)] and mixed setting [HIV testing (38.3% vs 32.7%), HIV/AIDS education, counseling, or support (64.1% vs 52.2%), early intervention for HIV (25.2% vs 19.6%)]. Similarly, testing for Hepatitis B and C and STDs was more prevalent in facilities that have non-English services and provide mixed services.
Conclusion: SUD treatment facilities with non-English language services had higher HIV preventive care, suggesting they are better equipped to prevent new HIV infections among people with SUD. However, non-English services other than Spanish are less available in SUD-only treatment, revealing opportunities for improving the availability of culturally competent HIV prevention via access to interpretive services.
PT03.01 – In Vitro Activity of Gepotidacin Against a Challenging Panel of Ceftriaxone Resistant Neisseria Gonorrhoeae Isolates
Dr Michelle Cole1, Dr Michel Doumith1, Dr Anna Vickers1, Dr Sarah Alexander1, Dr Helen Fifer1, Dr Nicole Scangarella-Oman2, Dr Charles Jakielaszek2, Dr Rachel Pitt-Kendall1
1UK Health Security Agency, London, United Kingdom.
2GSK, Collegeville, USA.
Background: New gonorrhoea treatments are required urgently. GSK’s novel triazaacenaphthylene topoisomerase inhibitor, gepotidacin, was shown to be non-inferior to the combination of 500 mg IM ceftriaxone and 1 g oral azithromycin in the treatment of uncomplicated urogenital gonorrhoea (EAGLE-1 [NCT04010539]). Gepotidacin selectively inhibits bacterial replication by a distinct binding site, unique mechanism of action and for most pathogens, well-balanced inhibition of two topoisomerase enzymes. An evaluation of gepotidacin’s in vitro activity against a panel of ceftriaxone-resistant Neisseria gonorrhoeae isolates was performed.
Methods: Gepotidacin and comparator antimicrobials were tested by agar dilution against 23 different ceftriaxone-resistant (MICs 0.25–1 mg/L) N. gonorrhoeae isolates and seven control strains. Genomic sequences of all isolates were examined for known resistance determinants and MLST.
Results: Gepotidacin inhibited the majority (96%) of isolates at ≤2 mg/L, with a MIC range of 0.25–4 mg/L and MIC50 and MIC90 values of 0.5 mg/L and 2 mg/L, respectively. Four isolates with the highest gepotidacin MICs (2–4 mg/L) all belonged to ST8123 and carried both GyrA S91F and D95Y and ParC S87N, amino-acid modifications associated with ciprofloxacin resistance. The rare A92P alteration in GyrA was also identified within these isolates. All had mutations causing the overexpression of the MtrCDE and NorM efflux pumps.
Conclusion: For the GyrA alterations identified in the isolates with the highest gepotidacin MICs, there is evidence to suggest that these substitutions do not affect gepotidacin binding. The contribution of efflux in isolates with the highest gepotidacin MICs needs further assessment. Overall, gepotidacin showed good in vitro activity against the panel of ceftriaxone-resistant gonococcal clinical isolates. The MIC distribution was similar to other studies, suggesting that gepotidacin should work equally effectively in patients with gonorrhoea caused by ceftriaxone-susceptible or ceftriaxone-resistant N. gonorrhoeae.
PT03.02 – Biofilm Formation in STIs: A Hidden Challenge in Infection Management
Prof. Svetlana Dubrovina1, MD Elena Trizna2, MD Diana Baidamshina2, Prof. Airat Kaumov2
1Rostov State Medical University, Rostov, Russian Federation.
2Federal State Autonomous Educational Institution of Higher Education, Kazan, Russian Federation.
Background: Quite often STIs are combined with diseases of the lower genital tract in women, particularly bacterial vaginosis. It is evidence that bacterial vaginosis increases the risk of HIV infection by 2–3.7 times, gonorrhea – 4 times, chlamydia infection by 3.5 times, and susceptibility to HSV-2 increases twofold. It is known that hyaluronic acid, a component of the biofilm matrix and envelope, can lose its properties under the action of hyaluronidase.
Methods: The drug bovgialuronidase azoximer (Longidaza®) was studied to reveal its effect on formed bacterial and mixed biofilms of various microorganisms. The study was carried out in vitro. Escherichia coli, Enterococcus faecalis, Staphylococcus aureus strains were used in the study. Biofilm formation was analyzed by spectrophotometry. The minimum bactericidal concentration was determined according to EUCAST recommendations as the lowest concentration of the substance at which bacterial growth was completely absent. Cell viability was assessed by confocal laser microscopy. Then, bovgialuronidase azoximer in combination with antibiotics was added to the newly cultured biofilms. The experiment was performed in 3 biological repeats.
Results: The results showed that 2 h incubation of bovgialuronidase azoximers at a concentration of 750–1500 IU/mL causes a twofold decrease in the biomass of the matrix of mature biofilms of E. faecalis and E. coli and a 60% decrease in S. aureus. Moreover, it can increase antibiotic activity against bacteria in biofilms: the concentration of ciprofloxacin and amoxicillin required to reduce the biofilm biomass by 3 orders of magnitude in the E. faecalis biofilm is reduced 16-fold in the presence of bovgialuronidase azoximer.
Conclusion: The use of enzyme preparations, in particular bovgialuronidase azoximer, is a promising method of bacterial vaginosis treatment and as a consequence may have an effect on reducing the burden of sexually transmitted infections.
PT03.03 – A Study on Cases of Congenital Syphilis Reported in Mongolia from 2020 to 2024
Хатагтай Otgonjargal Ganbold1, Dr. Bayandorj Oyunbeleg1, Dr. Oyun Mandal1, Dr. Bazarragchaa Purevdagva1, Dr. Saule Egshiglen1, Dr. Magsar Tungalag1, Dr. Vangan Nyamtsengel2, Dr. Badrakh Jugderjav1
1National Center for Communicable Diseases, Ulaanbaatar, Mongolia.
2Mongolian National University of Medical Sciences, Mongolia, Ulaanbaatar, Mongolia.
Background: Congenital syphilis arises when syphilis is transmitted from an infected mother to the fetus during pregnancy or delivery. Such transmission can lead to severe outcomes, including miscarriage, preterm birth, or neonatal death. In Mongolia, the syphilis incidence rate was 13.6 per 10,000 population in 2024. Syphilis accounted for 41.1% of sexually transmitted infections (STIs), with 1.3% of pregnant women testing positive.
Objective: To identify the epidemiological and clinical characteristics, causes of congenital syphilis cases reported in Mongolia.
Methods: Data from the HIV/STI Surveillance and Research Department at the NCCD and the ‘Health Statistics Information’ of the Health Development Center (HDC) were analyzed for the period 2020–2024. Records included syphilis and congenital syphilis surveillance reports, pregnancy monitoring data, and detailed clinical information on infants diagnosed with congenital syphilis.
Results: From 2020 to 2024, 120 cases of congenital syphilis were reported nationwide. Of these, 73 cases (60.8%) were in Ulaanbaatar, and 47 cases (39.2%) were from rural areas. Among the mothers of these infants, 67 (55.8%) received antenatal care, but 4 (3.3%) were not tested for syphilis despite attending care, and 53 (44.2%) did not attend antenatal care at all. The average birth weight of affected infants was 2,040 g, with 71.6% classified as low birth weight and 28.4% as normal (≥2,500 g). Based on the Apgar score, 78.3% of infants were in severe or moderately severe conditions. Clinical signs associated with congenital syphilis included hepatosplenomegaly in 95%, syphilitic skin lesions in 84.1%, and pneumonia in 87.5% of cases.
Conclusion: Of the mothers of infants born with congenital syphilis, 53 (44.2%) had no antenatal care. Additionally, 63.3% of the affected infants were preterm, and 71.6% had low birth weights. Each infant exhibited at least 2–3 specific symptoms of congenital syphilis. Therefore, improving the coverage and quality of antenatal care is essential.
PT03.04 – Bacterial Load and Clearance of Treponema Pallidum from Oral and Anal Sites in Men and Transgender-Women Who Have Sex with Men, with Secondary Syphilis
Dr Janet Towns1,2, Mr Janath A Fernando3, Ms Rebecca Wigan1,2, Dr Marcelina Krysiak3, Professor David A Lewis4, Dr Rick Varma5,13, Professor Anna McNulty5, Professor Deborah A Williamson6, Dr Carole Khaw7, Ms Jayne Howard1, Ms Kate Potappel1, Professor Louise Owen8, Dr Caroline Thng9, Dr Nathan Ryder10, Professor Eric PF Chow1,2,14, Professor Christopher K Fairley1,2, Professor Stephen Graves11, Dr Sarah Huffam12, Dr Shivani Pasricha2, Professor Marcus Y Chen1,2
1Melbourne Sexual Health Centre, Alfred Health, Carlton, Australia.
2School of Translational Medicine, Faculty of Medicine and Health Sciences, Monash University, Melbourne, Australia.
3University of Melbourne, Department of Infectious Diseases at The Peter Doherty Institute for Infection and Immunity, Melbourne, Australia.
4Western Sydney Sexual Health Centre, Western Sydney Local Health District, Parramatta, Australia.
5Sydney Sexual Health Centre, Sydney, Australia.
6UK Health Security Agency, London, England.
7Adelaide Sexual Health Centre, Infectious Diseases Unit, Royal Adelaide Hospital, Adelaide, Australia.
8Statewide Sexual Health Service, Hobart, Australia.
9Gold Coast Sexual Health, Southport, Australia.
10Pacific Clinic, Newcastle Sexual Health, Hunter New England Local Health District, Newcastle, Australia.
11Australian Rickettsial Reference Laboratory, Barwon Health, Geelong, Australia.
12BRaSH Clinic, University Hospital, Barwon Health, Geelong, Australia.
13The Kirby Institute, University of New South Wales, Kensington, Australia.
14Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Secondary syphilis is emerging as the most infectious stage. We aimed to determine the frequency of Treponema pallidum shedding, load, and time to clearance from mucosal sites after treatment to further understand transmission.
Methods: MSM and TGW with secondary syphilis were recruited from Australian clinics. At baseline (Day 0), syphilis treatment was given, mucocutaneous lesions were tested for diagnostic T. pallidum PCR, and non-lesion samples (blood, oral cavity and anal canal) with T. pallidum polA quantitative PCR for bacterial load. Non-lesion samples were repeated on Days 3, 7, 14, and 30 after treatment.
Results: Between January 2023 and August 2024, 80 MSM and 1 TGW were recruited. Most, 93%, received benzathine penicillin 2.4 mU. Baseline oral T. pallidum detection was in 81.3% (65/80) of participants: 58 had a positive oral cavity swab alone, and 7 had an additional positive oral lesion swab. Oral cavity cycle threshold (CT) increased from baseline to Day 3 (median 35.7 [Ξ53.9 copies/uL] to 37.7 [Ξ15.2 copies/uL] P = 0.012). Baseline, anal T. pallidum detection was in 67.5% (54/80) of participants; 14 were positive on both anal canal and anal lesion swabs. Anal CT increased from baseline to Day 3 (median 30.1 [Ξ1878.3 copies/uL] to 38.2 [Ξ11.0 copies/uL] P < 0.001). 50.6% (40/79) had T. pallidum detected at baseline at both oral and anal sites (Fig. 1). T. pallidum was detected in baseline blood in 23.5% (19/81), with median CT of 38.4 (Ξ9.7 copies/uL). By Day 7, T. pallidum was not detected in 99.4% (161/162) of infected sites.
Conclusion: This is the largest study to examine T. pallidum clearance after treatment of secondary syphilis, when T. pallidum shedding from oral and/or anal sites occurs in the majority of MSM, fuelling transmission risk. Loads fell significantly by Day 3 with clearance in almost all by Day 7.
PT03.05 – Increase of Ocular and Disseminated Gonorrhea in the Netherlands in Recent Years
Dr Alje Van Dam1,2, Feline Velthuis3, Dr Thijs Van de Laar4, Dr Rogier Jansen4, Arjen Stam1,2, Dr Annelot Schoffelen3
1Public Health Laboratory, Infectious Diseases, Amsterdam Health Service, Amsterdam, Netherlands.
2Department of Medical Microbiology, Amsterdam UMC, Amsterdam, Netherlands.
3On behalf of the ISIS-AR Study Group, Centre for Infectious Disease Control (CIb), National Institute for Public Health and the Environment (RIVM), Bilthoven, Netherlands.
4Laboratory of Medical Microbiology, OLVG laboratory, Amsterdam, Netherlands.
Background: Albeit rare, infections with Neisseria gonorrhoeae (Ng) can cause infections outside the genital, anal and pharyngeal area, such as bacteremia, arthritis and ocular and other infections. In recent years, the number of patients with gonorrhea diagnosed in STD clinics rose markedly. We investigated whether a similar increase of cases of gonorrhea outside the classical STI domain was found.
Methods: Ng culture data from non-genital samples (1 isolate per patient) for 2018–2023 were collected from ISIS-AR, a nationwide system in which clinical microbiology laboratories report resistance data of cultures of bacterial species to the National Institute for Public Health. Nationwide coverage was >90% (n = 48) of the laboratories in 2023. Additional molecular data for the period 2020–2024 were obtained from the laboratory systems of the three major laboratories in Amsterdam.
Results: In 2023, 95 positive Ng non-genital cultures were reported, from the eye (n = 59), sterile body fluids (n = 9), blood (n = 5) and other pus/wound/ulcers (n = 22). Of these, 58% were diagnosed in men and 42% in women. From 39 labs continuously reporting data during the entire study period the number of isolates varied between 24 and 38 in 20182021 but increased to 52 in 2022 and 84 in 2023. In Amsterdam 62 cases of gonorrhea outside the classical domain were diagnosed during 2020–2024, of which 40 (62%) by molecular tests only, suggesting that real nationwide number of cases could be threefold higher compared to culture-based numbers only (>285 in 2023). These might have been detected if a surveillance system including molecular diagnosis of gonorrhea had been in place.
Conclusion: The incidence of ocular and disseminated gonorrhea rose markedly during recent years in the Netherlands.
PT03.06 – Real-World Effect of Decreasing the Frequency of Screening for Neisseria Gonorrhoeae and Chlamydia Trachomatis on the Incidence of These Infections and Antimicrobial Use in Men Who Have Sex with Men Taking HIV Pre-Exposure Prophylaxis in Belgium: A Retrospective Cohort Study
Dr. Thibaut Vanbaelen1, Dr. Irith De Baetselier1, Achilleas Tsoumanis1, Dr. Bernadette Hensen1, Dr. Chris Kenyon1
1Institute of Tropical Medicine, Antwerp, Belgium.
Background: There is growing evidence that the benefits of systematic screening for Neisseria gonorrhoeae and Chlamydia trachomatis in men who have sex with men (MSM) taking HIV pre-exposure prophylaxis (PrEP) are limited, and that screening leads to high antimicrobial consumption. Since 2019, we have been reducing the frequency of screening for N. gonorrhoeae and C. trachomatis. In this study, we estimated the real-world effect of reducing screening frequency on the incidence of these infections and antimicrobial use among MSM taking PrEP in Belgium.
Methods: Retrospective analysis of medical records, laboratory results, and antimicrobial prescriptions for MSM taking PrEP at the Institute of Tropical Medicine clinic in Antwerp, Belgium between January 2019, and June 2024. We estimated yearly testing rates for N. gonorrhoeae and C. trachomatis, incidence rates of overall and symptomatic infections, and antimicrobial prescription rates (azithromycin, doxycycline, ceftriaxone). Trends were analyzed using a Poisson regression model.
Results: Overall, 3644 MSM attended the PrEP clinic in the study period. Testing rates decreased over fourfold between 2019 and 2024 (yearly rate ratio (RR) 0.77 [95% CI 0.76–0.78], P-value <0.001, Fig. 1). The incidence of all N. gonorrhoeae and C. trachomatis infections decreased in the same period (yearly incidence RR (IRR) 0.92 [95% CI 0.89–0.96], P-value < 0.001, and IRR 0.86 [95% CI 0.82–0.89], P-value < 0.001, respectively). There was no increase in the incidence of symptomatic infections. Doxycycline and azithromycin prescriptions decreased (RR 0.5 [95% CI 0.45–0.55], P-value < 0.001, and RR 0.92 [95% CI 0.88–0.97], P-value < 0.001, respectively).
Conclusion: Our findings provide evidence that the incidence of symptomatic N. gonorrhoeae and C. trachomatis infections did not increase over time despite less frequent screening in MSM taking PrEP, and antimicrobial prescriptions decreased. Our findings underline the potential of decreasing frequency of screening as a safe and effective antimicrobial stewardship intervention in MSM taking PrEP.
Incidence rates of all and symptomatic Neisseria gonorrhoeae, Chlamydia trachomatis, and LGV infections over time (panel A), and prescription rates of Azithromycin, Ceftriaxone, and Doxycycline over time (panel B).

PT03.07 – ABI-5366, a Novel, Oral, Long-Acting Herpes Simplex Virus Helicase-Primase Inhibitor: Interim Safety and Pharmacokinetic Results from a Phase 1A Study in Healthy Participants
Prof. Edward Gane1, Dr Christian Schwabe2, Dr Grace Wang3, Mr Jieming Liu3, Mr Steven Knox3, Ms Kathryn Kitrinos3, Dr Anuj Gaggar3, Dr Katie Zomorodi3
1University of Auckland, Auckland, New Zealand.
2New Zealand Clinical Research, Auckland, New Zealand.
3Assembly Biosciences, South San Francisco, United States.
Background: Approximately 491.5 million people aged 15–49 years worldwide have herpes simplex virus type 2 (HSV-2) infection, the primary cause of genital herpes. Nucleoside analogue suppression is suboptimal, and recurrence is associated with pain and psychological stress. HSV-2 infection increases risk of acquiring HIV-1 infection. ABI-5366, an investigational, orally administered, long-acting HSV helicase-primase inhibitor is under development for suppression of recurrent genital herpes (RGH). In vitro, ABI-5366 potently inhibits HSV-1, HSV-2 laboratory strains and clinical isolates. Single-dose safety and PK data in healthy participants are reported.
Methods: ABI-5366-101 (NCT06385327) is a randomized, blinded, placebo-controlled Phase 1a/b study. Phase 1a, evaluating the safety and PK of single, oral ABI-5366 doses in healthy participants is ongoing. Each group includes participants randomized 6:2 to ABI-5366 or placebo with up to 98-day follow-up. Safety was assessed by physical examination, adverse events (AEs), laboratory parameters. ABI-5366 plasma concentrations were measured by LCMS.
Results: 32 participants received treatment in four ABI-5366 groups (10, 30, 100, 350 mg). Most were male (24/32), white (16/32), aged 19–59 years with BMI 19.3–31.6 kg/m2. Treatment was well tolerated. After median 70-day follow-up, 26/32 participants reported an AE; 90.4% Grade 1. No Grade 3/4 AEs or treatment-related lab abnormalities, serious AEs or deaths were reported. ABI-5366 plasma concentrations increased from 10 to 350 mg. The PK profile suggests intestinal reabsorption with a t1/2 >20 days and projected Ctrough values in multifold excess of protein-adjusted EC50 for HSV replication achievable with weekly and monthly dosing.
Conclusion: ABI-5366 was well tolerated when administered orally as single doses up to 350 mg. Plasma concentrations exceeded in vitro EC50’s for inhibition of HSV replication and the observed t1/2 >20 days supports weekly and monthly dosing. Antiviral activity following multiple doses in participants with RGH will be explored in Phase 1b.
PT04.01 – High Prevalence and Incidence of Curable Sexually Transmitted Infections Among Young Girls and Women Using HIV Pre-Exposure Prophylaxis in Sub-Saharan Africa
Dr. Irene Mukui1, Sue Peacock1, Deborah Donnell1,2, Brenda Gati3, Katherine Gill4, Shannon Bosman5, Remco Peters6, Sinead Delany-Moretlwe7, Renee Heffron8, Prof. Connie Celum1,9
1Department of Global Health, University of Washington, Seattle, United States.
2Fred Hutchinson Cancer Center, Seattle, United States.
3Makerere University-Johns Hopkins University, Makerere, Uganda.
4Desmond Tutu HIV Centre, University of Cape Town, South Africa.
5Human Sciences Research Council, Center for Community Based Research (CCBR), South Africa.
6Foundation for Professional Development, South Africa.
7Wits Reproductive Health and HIV Unit, University of the Witwatersrand, South Africa.
8Department of Medicine, University of Alabama at Birmingham, Birmingham, United States.
9Departments of Medicine, and Epidemiology, University of Washington, Seattle, United States.
Background: Women in sub-Saharan Africa have a high burden of curable sexually transmitted infections (STIs) and related reproductive health sequelae; women eligible for HIV pre-exposure prophylaxis (PrEP) are at risk of both HIV and curable STIs. We assessed the prevalence, incidence, and factors associated with curable STIs among women using PrEP.
Methods: Between August 2022 and December 2022, sexually active women ages 16–30 were enrolled into a 6-month cohort and offered PrEP from 15 South African sites, and one site each in Eswatini, Kenya, Malawi, Uganda, and Zambia. At enrolment and month 6, nucleic acid amplification tests (NAATs) were conducted for Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), and Trichomonas vaginalis (TV), and at enrolment, rapid plasma reagin with confirmatory Treponema pallidum particle agglutination for syphilis. Baseline prevalence and month 6 incidence rates were calculated, and multivariable regression used to assess predictors.
Results: Of 3,087 participants, 96.7% initiated Tenofovir/emtricitabine oral PrEP; 97.4% had baseline STI results. Median age was 23 years (IQR: 21–27). At baseline, 30.3% had at least one STI, with 76.3% asymptomatic. Cross-site STI prevalence was 20.8% chlamydia, 6.8% gonorrhea, 6.1% trichomoniasis, and 3.5% syphilis with highest prevalence in eSwatini (40.8%) and South Africa (33.0%), and lowest in Kenya and Zambia (14.0%). Month 6 incidence of any STI was 49.3/100 person-years (95% CI: 45.3–53.3); 30.3/100 p-y (95% CI 27.3–33.4) for CT; 11.5/100 p-y (95% CI 10.0–13.4) for TV, and 10.8/100 p-y (95% CI 9.0–12.6) for NG. Alcohol use (aIRR 1.3, 95% CI: 1.0–1.6) and baseline STI (aIRR 1.9, 95% CI: 1.6–2.2) were associated with incident STIs.
Conclusion: Among African women with high PrEP uptake, STI burden was high, highlighting gaps in sexual health services. Most STIs were asymptomatic, underscoring the need for etiologic testing. In resource limited settings, women with prior STIs should be prioritized for repeat testing.
PT04.02 – Exploratory Examination of Time Between Chlamydia And/Or Gonorrhea Diagnosis and Future Syphilis Diagnosis in British Columbia, 2014 –2023
Dr. Theodora B. Consolacion1, Amanda Yu1, Hannah M. Baer1, Heather Burgess1,2, Robert Higgins1, Justin Sorge1,2, Venessa Ryan1, Ina Chen1, Sven Dong1, Jennifer Vines1, Sofia R. Bartlett1,3
1British Columbia Centre for Disease Control, Vancouver, Canada.
2Public Health Agency of Canada, Vancouver, Canada.
3University of British Columbia, Vancouver, Canada.
Background: Infectious syphilis (IS) diagnoses (Dx) rates in British Columbia (BC) rose from 11.7 per 100,000 population in 2014 to 37.4 in 2023. Efficient strategies targeting syphilis screening to at-risk groups are needed. Rates are much higher in Chlamydia (CT) and gonorrhea (GC). The study’s purpose is to examine the time between incident CT and/or GC (CT/GC) Dx to subsequent IS Dx.
Methods: All genital CT, GC and IS Dx from provincial Electronic Medical Record system (2014 to 2023) were included (N = 139,486) with sex (males = 62,496; females = 76,990), age (median = 26, IQR: 21, 32), time between first CT/GC Dx to IS Dx, and a flag denoting an IS Dx after first CT/GC Dx, excluding those under 15 years, missing sex, or with CT/GC Dx after December 15, 2023. Kaplan-Meier curves by sex and age-group and Cox proportional hazard ratios with sex, age and time between CT/GC to IS Dx were calculated. Incidence rates of IS after a CT/GC Dx were calculated by sex and age-group using the median.
Results: Kaplan-Meier curves show sex and age group time differences in acquiring syphilis. Cox proportional models show that sex, age and the interaction (sex*age) were significant. Males were 3.3 times more likely to have an IS Dx after CT/GC Dx compared to females. Comparing sex across increasing ages show an increased likelihood for IS among older males (see Table 1). Incidence for females <26 years was 91.91; males <26 years was 266.4; females ≥26 years was 208.06; and males ≥26 years was 770.46 per 100,000 person-years.
Conclusion: Older males with a CT/GC Dx have an IS Dx sooner compared to females of the same age-group, suggesting the length of time for follow-up syphilis testing may vary by age and sex. With the current syphilis outbreak, universal syphilis testing after CT/GC Dx could be recommended in BC.
| Point Estimate | 95% Wald Confidence Limits | ||||
|---|---|---|---|---|---|
| Model 1: Effect of sex across ages | Male (Ref = Female) | 3.33 | 3.02 | 3.66 | |
| Model 2 Interaction: Effect of 1 unit change in age by sex | Age Unit = 1 At Sex = Male | 1.04 | 1.04 | 1.04 | |
| Age Unit = 1 At Sex = Female | 1.03 | 1.02 | 1.04 | ||
| Model 2 Interaction: Effect of sex across ages | Male (Ref = Female) At Age = 21 | 2.99 | 2.64 | 3.38 | |
| Male (Ref = Female) At Age = 26 | 3.17 | 2.86 | 3.51 | ||
| Male (Ref = Female) At Age = 26 | 3.40 | 3.08 | 3.76 | ||
PT04.03 – High Burden of Sexually Transmitted Infections Among Pregnant Women in Governmental Hospitals of Southern Ethiopia: Findings from a Baseline Study
Mrs Meskerem Ebido1,2, Professor Zeleke Mekonnen3, Professor Carl Lachat2, Professor Bruno Levecke2, Doctor Taye Gari1, Professor Elizaveta Padalko2,4
1Hawassa University, Hawassa, Ethiopia.
2Ghent University, Ghent, Belgium.
3Jimma University, Jimma, Ethiopia.
4Ghent University Hospital, Ghent, Belgium.
Background: Sexually transmitted infections (STIs) significantly threaten maternal and neonatal health in resource-limited settings like Ethiopia. The World Health Organization’s syndromic management (SM) often leads to over-treatment and missed diagnoses of asymptomatic STIs, emphasizing the need for accurate lab-based data on STIs prevalence during pregnancy. This study aims to determine STIs prevalence and associated factors among women attending antenatal care (ANC) clinics in southern Ethiopia, addressing these diagnostic gaps.
Methods: This study is part of a prospective cohort, assessing the impact of STIs on birth outcomes. A baseline survey was conducted with 743 pregnant women from July to December 2024. Vaginal swabs were collected using eNAT Copan swabs and screened for Neisseria gonorrhoeae and Trichomonas vaginalis (via wet mount and Gram stain) and syphilis and HIV (using the SD BIOLINE HIV/Syphilis Duo test). PCR tests for additional STIs will be performed later. Predictors of STIs were analyzed through multivariable logistic regression.
Results: From 743 recruited women, 91 (12.2%, 95% confidence interval (CI): 10.1–14.8) were infected with at least one STIs; 64.8% of these cases were asymptomatic (Table 1). Predictors for overall STIs include those women who have sex without desire (adjusted odds ratio (AOR) = 2.09 (95% CI: 1.15–3.81)), have economic autonomy (AOR = 12.72 (95% CI: 2.86–6.52)), have vaginal odour (AOR = 2.14 (95% CI: 1.12–4.08)), and are positive for clue cell (AOR = 3.76 (95% CI: 2.26–6.24)).
Conclusion: STIs prevalence is high, with a high proportion of asymptomatic cases. STIs diagnoses through SM exceeded lab results. Desire to have sex, vaginal odour, and also economic decision-making power are main predictors of STIs. These findings emphasise the need for routine lab-based STIs screening, and economic factors and sexual health education should be addressed to mitigate the risks associated with STIs.
| STIs Type | ANC 1st visit (≤16 weeks) | Percent (%) | |
|---|---|---|---|
| Gram-negative diplococci (suggestive of gonorrhea) | 55 | 7.4 | |
| Trichomonas vaginalis | 23 | 3.1 | |
| Syphilis | 11 | 1.5 | |
| HIV/AIDS | 8 | 1.1 | |
| Total lab-confirmed STIs | 91 | 12.2 | |
| Cases positive for syndromic management | 202 | 27.3 | |
| Asymptomatic STI | 59 | 8.3 |
PT04.04 – Impact of Declines in HIV Testing Volumes on HIV Status Awareness and Time to Diagnosis in Africa
Mr. Andrey Kutsyh1, Dr. Ahmadou Alioum4, Dr. Jeffery W Imai-Eaton2,3, Dr. Mathieu Maheu-Giroux1
1Mcgill University, Montréal, Canada.
2Imperial College London, London, United Kingdom.
3Harvard University, Cambridge, United States.
4University of Bordeaux, Bordeaux, France.
Background: HIV testing services are the entry point to HIV diagnosis and treatment. In Africa, where 2/3 people living with HIV reside, annual numbers tested for HIV have declined since peaking in 2017. This study aims to assess the impact of these reductions on diagnosis coverage and time-to-diagnosis by gender in African countries.
Methods: We collated information on total and antenatal care (ANC) HIV testing volumes in all African countries with available data, as reported in their UNAIDS Spectrum files. To capture gender differences, we modified a previously validated mathematical model of HIV testing rates (Shiny90) and calibrated it to ANC testing. For each country, we constructed a counterfactual scenario in which peak pre-decline rates of HIV testing are maintained and compared across knowledge of HIV status and time-to-diagnosis by gender.
Results: Program data from 37 countries showed that HIV testing declined in 65% of countries over 2016–2023, mostly attributed to reduced HIV testing outside of ANC. Among countries with a decline, HIV testing volumes decreased by a median of 28% (interquartile range [IQR]: 24%–52%) (Fig. 1). Although awareness of status increased in most countries between 2017 and 2023, it would have further increased by 1.2%-points (Credible Interval [CrI]: 1.0%–1.6%) to 87% (CrI: 86%–87%) in men and 1.0%-points (CrI: 0.8%–1.1%) to 91% (CrI: 91%–91%) in women had there been no decline in HIV testing. In countries with an HIV testing decline, time-to-diagnosis increased by an additional 0.5 years (CrI: 0.4–0.6) to 2.7 years (CrI: 2.6–2.9) among women and 0.7 years (CrI: 0.6–0.8) to 3.3 years (CrI: 3.1–3.5) among men in 2023, if there had been no decline in HIV testing.
Conclusion: Recent declines in HIV testing did not affect testing at ANC. These reductions in testing volumes have worsened HIV testing outcomes, especially for men. Longer time-to-diagnosis may lead to increased time spent infectious and a slower decline of incidence.
Median [line] and 95% credible interval [shaded] of median time-to-diagnosis in men [dark blue] and women [dark red] in 24 countries in which HIV testing rates declined from 2015 to 2023, pooled by new infections. Counterfactual scenario in men [bright blue] and women [bright red] indicate time-to-diagnosis without an HIV testing decline. Counterfactual scenarios begin in the year of peak HIV testing in each country; as early as 2016, but 83% of the counterfactual scenarios begin on or after 2018.

PT04.05 – Syphilis and Mortality in Denmark – A Nationwide, Population-Based, Matched Cohort Study
Ms. Emilie With Hall Petersen1, Ms. Laura Nina Glismann2,3, Ms. Maria Wessman2, Ms. Lene Holm Harritshøj1,4, Mr. Jan Gorm Lisby5, Ms. Terese Katzenstein1, Mr. Steen Hoffmann2, Mr. Jørgen Skov Jensen2, Ms. Kirsten Salado-Rasmussen2,3,4, Mr. Lars Haukali Omland1,2,4
1Copenhagen University Hospital, Rigshospitalet, Copenhagen, Denmark.
2Statens Serum Institute, Copenhagen, Denmark.
3Bispebjerg University Hospital, Copenhagen, Denmark.
4Faculty of Health and Medical Sciences, University of Copenhagen, Copenhagen, Denmark.
5Copenhagen University Hospital – Amager and Hvidovre, Copenhagen, Denmark.
Background: Syphilis incidence has risen substantially in recent decades. Updated and valid information on mortality among individuals infected with syphilis is missing, and there is a need for more appropriate comparators than healthy controls that account for confounding by test activity.
Methods: We performed a nationwide, population-based, matched cohort study of all Danish patients with syphilis between 2000 and 2023. To form the syphilis patient cohort, we identified all patients with positive syphilis serology in Denmark (i.e. a positive test for non-treponemal and treponemal antibodies). Patients notified through the mandatory notification system were also included in the syphilis patient cohort. We identified a test negative comparison cohort matched in a ratio of 1:1 of individuals with a negative syphilis test, to account for confounding by test activity. We used Kaplan Meier analysis to illustrate survival curves. Time-updated Cox regression was used to compute hazard ratios as an estimate of mortality rate ratios (MRR) (<10 years and >=10 years after study inclusion).
Results: We identified 5,085 patients in the syphilis cohort and test negative cohort, 3,991 (78%) were male and the median age was 36 years at study inclusion (Fig. 1). We did not observe an increased mortality among patients with syphilis compared to the test negative comparison cohort (MRR<10 years 1.01 (95% CI: 0.81–1.26) and MRR >=10 years 1.29 (95% CI: 0.84–1.97)). The absolute difference in mortality between the two cohorts was 3% (95% CI: –1%–7%) after 20 years of follow-up.
Conclusion: Despite a very big study population and 20 years of follow-up time, we did not observe an increased mortality among patients with syphilis compared to the test negative comparison cohort, which should serve as a reassurance for people with syphilis.
PT04.06 – The Dynamics of HIV Genetic Diversity in Cameroon from 1990 to 2023: Lessons and Implications for Achieving Elimination by 2030
Mr Derrick Tambe Ayuk Ngwese1,2,3,4, Dr Joseph Fokam1,2,5,6, Dr Alex Nka1, Dr Aude Ka’e1, Mr Desire Takou1, Dr Ezechiel Ngoufack1, Dr Collins Chenwi1,7, Dr Georges Teto1, Mrs Grace Angong Beloumou1,7, Mrs Sandrine Djupsa Djeyep1, Dr Bouba Yagai1, Dr Luna Colagrossi7, Prof Maria Mercedes Santoro7, Prof Francesca Ceccherini-Silberstein7, Dr Linda Esso8, Dr Alain Georges Etoundi Mballa9, Prof Edie-G. Halle-Ekane5, Prof Nicaise Ndembi10, Prof Vittorio Collizzi1,7, Dr Marta Giovanetti11, Dr Eduan Wilkinson12, Dr Cheryl Baxter12, Prof Tulio de Oliviera12, Prof Marcel Yotebieng13, Prof Charles Fokunang2, Prof Wilfred Fon Mbacham2,3,4, Prof Akinde Nji Mbuh3,4, Prof Carlo-F Perno1,14, Prof Alexis Ndjolo1
1Chantal Biya International Reference Centre, Yaounde, Cameroun.
2Faculty of Medicine and Biomedical Sciences; University of Yaounde 1, Yaounde, Cameroun.
3Fobang Institutes for Innovations In Science And Technology, Yaounde, Cameroun.
4The Biotechnology Centre, University of Yaounde 1, Yaounde, Cameroun.
5Faculty of Health Sciences, University of Yaounde 1, Yaounde, Cameroun.
6Central Technical Group, National AIDS Control Committee, Yaounde, Cameroun.
7University of Rome, Tor Vergata, Rome, Italy.
8Operational Research and Health Department, Ministry of Public Health, Yaoundé, Yaounde, Cameroun.
9Disease Control department, Ministry of Public Health, Cameroon, Yaounde, Cameroun.
10Africa, Centre of Disease and Control (CDC), Addis-Abeba, Addis Abeba, Ethiopia.
11Laboratório de Flavivírus, Instituto Oswaldo Cruz, Fundação Oswaldo Cruz, Rio de Janeiro, Brazil.
12Centre for Epidemic Response and Innovation (CERI), School of Data Science and Computational Thinking, Stellenbosch University, Cape Town, South Africa.
13Department of Medicine, Albert Einstein College of Medicine, Bronx, NY, United States of America.
14Ospedale Pediatrico Bambino Gesu, Rome, Italy.
Background: Interestingly, some HIV-clades have impact on public health strategies through diagnostic escape, suboptimal therapeutic response and natural resistance to some treatment regimens. Following changing treatment-paradigm, we sought to study the dynamics of HIV-clades in Cameroon.
Methods: A study was conducted on 12,230 Cameroonian-HIV-sequences between 1990and 2023 retrieved from HIV-Genbank. Sequences were grouped by 10 years’ interval and dynamics of each viral clade over the 3-time points was evaluated with P-values < 0.05 considered statistically significant using the proportion trend test. Furthermore, prediction analysis was done using generalised additive models to model the temporal trends of clade proportions for future investigations.
Results: Our results revealed that HIV-1 group-M prevailed (93.59%), followed by group-O (4.99%), group-N (0.99%), group-P (0.18%) and HIV-2 (0.12%). Circulating recombinant forms (CRFs) were most prevalent (72.83%), followed by pure subtype (19.57%) and unclassified recombinants (1.12%). Between 1990–2000 (period-1: limited-treatment-coverage; (1,304-sequences), CRFs represented 49.1% and pure-subtypes; 14.6%; where CRF02_AG was the predominant clade; 30.5%. This time-point was experienced by a high-group-O prevalence; 32.2%. Between 2001–2011 (period-2: NNRTI-based ART; 5995-sequences), CRFs and pure-subtypes slightly increased (77.2% and 18.9% respectively), with high prevalence of non-CRF02_AG recombinants (40.6%) as compared to CRF02_AG clades (36.6%), P = <0.01 a significant decrease of HIV-1-Group-O (2.3%, P = <0.01); a 1.2%-group-N prevalence and 0.04% group-P prevalence. Between 2012–2023 (period-3: test-and-treat and early-TLD-era, 4452-sequences), we noticed constant rates of pure subtypes and recombinant forms with prevalences of 21.8% and 77.3% respectively. Overall, CRFs significant increased over the three-time points (P < 0.01), with increasing CRF02_AG-(59.1 % at period-3). HIV-1-Group-O (0.4% at period-3) and Group-N (0.4% at period-3) decreased significantly (P < 0.01 respectively) while group-P completely disappeared. From 2024–2030 (extended TLD era, long acting and pandemic control), prediction analyses show declining trends in which group-P and -N would not reappear this period, group-O may completely disappear, and group-M would continue to maintain its dominance driven by recombinant forms with-CRF02_AG-emerging as a competitive clade by 2030.
Conclusion: HIV-dynamics in Cameroon over the past 30-years reveals an evolutionary pathway, characterised by an increasing CRFs-(driven by CRF02_AG)-and a significant declining trend of the HIV-1-group-O.Thus,in the current-dolutegravir-era in Cameroon, achieving elimination requires targeting in priority HIV-1-CRFs for diagnosis and monitoring in a context of disappearance of HIV-1-group-O, group-P and HIV-2.
PT04.07 – Neisseria Gonorrhoeae Antimicrobial Susceptibility Patterns: Comparing Anatomical Locations Between and within Persons in the Netherlands
Mrs Maartje Visser1,2, Dr Petra F G Wolffs3, Prof Christian J P A Hoebe2,3,4, Dr Birgit H B van Benthem1, Dr Alje P van Dam5, Dr Denise E Twisk6, Dr Nicole H T M Dukers-Muijrers2,4, Dr Janneke C M Heijne5,7
1National Institute for Public Health and the Environment (RIVM), Bilthoven, Netherlands.
2Maastricht University, Maastricht, Netherlands.
3Maastricht University Medical Center+ (MUMC+), Maastricht, Netherlands.
4Public Health Service South Limburg, Heerlen, Netherlands.
5Public Health Service Amsterdam, Amsterdam, Netherlands.
6Municipal Public Health Service Rotterdam-Rijnmond, Rotterdam, Netherlands.
7Amsterdam UMC, Amsterdam, Netherlands.
Background: Pharyngeal gonorrhoea infections may contribute to developing antimicrobial resistance, but observational evidence is conflicting. Some studies find higher resistance in pharyngeal isolates compared to genital isolates; others do not, possibly due to single isolate sampling per person. We aim to study antimicrobial susceptibility patterns across anatomical sites, using both population-level and within-person analyses.
Methods: We used Dutch gonococcal antimicrobial resistance surveillance (GRAS) data of men who have sex with men (MSM) and women (2016–2023). Ceftriaxone and azithromycin susceptibility was measured by Minimum Inhibitory Concentration (MIC)-values. We calculated anatomical-site specific proportions decreased susceptible (CRO-DS; MIC >0.032 mg/L) for ceftriaxone and resistant (AZI-RES; MIC >1 mg/L) for azithromycin. Anatomical-site differences were tested using chi2-test for total population and persons with multiple MICs at one visit. In the latter, we also analysed within-person discordant MIC pairs (>1 doubling dilution difference), and determinants of discordant MICs by logistic regression.
Results: This study included 16,916 MSM and 2,521 women with at least 1 MIC reported. Proportions CRO-DS were higher in pharyngeal isolates for both MSM and women. AZI-RES was higher in pharyngeal isolates for MSM but not women. 1,217 MSM and 457 women had multiple MICs reported. Among them, proportions of DS/RES did not differ across anatomical sites, except among MSM for azithromycin. Discordant MIC-pairs were seen in 9.6% (95% CI: 8.1–11.2%) of MSM and 4.8% (95% CI: 3.1–6.7%) of women for ceftriaxone, and 12.1% (95% CI: 10.4–14.0%) of MSM and 9.2% (95% CI: 6.8–11.8%) of women for azithromycin. In discordant pairs, pharyngeal MICs were on average not higher than urogenital or anal MICs. No sexual behavioural determinants were associated with discordant MICs.
Conclusions: Pharyngeal isolates showed higher levels of DS/RES on a population level, but not within persons. However, discordance of MICs within persons occurred, potentially leading to missed resistant cases. Culturing multiple anatomical sites per individual is recommended to optimise detection of resistant cases.
PT05.01 – A Digital Citizen Science Intervention to Reduce HIV Stigma and Promote HIV Testing: A Randomized Clinical Trial Among Adolescents and Young Adults in Kazakhstan
Dr. Alissa Davis1, Dr. Laura Nyblade, Yi Yihang Sun, Olga Balabekova, Sara Landers, Denis Gryazev, Joseph Tucker, Valera Gulyaev, Susan Rosenthal, Karsten Lunze, Weiming Tang, Azamat Kuskulov, Assel Terlikbayeva, Sholpan Primbetova, Mingway Chang, Alfiya Denebayeva, Aikerim Akhmetova, Ainur Absemetova, Sholpan Karzhaubayeva, Sairankul Kassymbekova, Marina Maximova, Zhannat Mussina, Gulnar Bekenova, Zhamilya Nugmanova, Zhanna Kalmatayeva, Ludmila Polyakova, Zhanneta Zhazykbaeva, Vitaliy Vinogradov, Amir Shaikezhanov, Meruyert Darisheva, Bella Orynbetova, Elena Norakidze, Mashirov Kozhakhmet, Akbota Tolgenova, Aknur Imadillda, Dariga Satkhozhina, Alikhan Kartamyssov, Zhamilya Kanieva, Albina Aleshina, Olzhas Makhan, Aida Muravyova, Adema Rahimzanova, Arman Duisenbayev, Zhanerke Tursynbek, Nurgazy Dias, Malika Beken, Miras Murzakhan, Zhandos Brown, Daniyal Maitekov, Artur Li, Sandizaira Mergen, Dautali Mergenov, Amirali Kuanysh, Anuar Rakhimbekov, Yenlik Baisbay, Alibek Aruzhan, Zhasmina Kozhambet, Denis Grebenchsishikov, Dmitriy Bekker, Sultan Kozhamberdiev, Dauren Salykov, Madina Sagimbayeva, Kamila Yussupova, Guakhar Mergenova
1Columbia University, New York, United States.
Background: Kazakhstan has a HIV high incidence among adolescents and young adults (AYA), and high HIV stigma contributing to low HIV testing uptake. We examined whether an AYA-developed digital crowdsourced intervention reduced HIV stigma compared to conventional public health materials among AYA in Almaty, Kazakhstan.
Methods: 216 AYA (Females: 116/Males: 110) ages 16–24 were recruited to the online study cohort and randomized 1:1 to the intervention or control arm. AYA were exposed to the crowdsourced intervention or control materials once a week for 5 weeks, with equivalent exposures between arms. Outcomes included a total HIV stigma score assessed at baseline, immediately post-intervention and 2 months post-intervention from January to August 2023. We conducted multilevel mixed models to compare changes over time by arm and sex.
Results: AYA in the intervention arm had significantly lower HIV testing stigma 2 months post-intervention (adjusted mean change (AMC): –0.73 [–1.07, –0.39]) than AYA in the control arm (AMC: –0.06 [–0.42, 0.30]) (P = 0.032). Female AYA in the intervention arm had significantly lower total HIV stigma immediately post intervention (AMC: –4.91 [–7.25, –2.58]) and 2 months post-intervention (AMC: –5.16 [–7.48, –2.84]) than females in the control arm (immediately post-intervention AMC: –0.03 [–2.63, 2.57] and 2-months post-intervention AMC: –0.07 [–2.70, 2.56]) (P = 0.012, P = 0.012).
Conclusions: The AYA-developed crowdsourced intervention decreased HIV testing stigma, though this effect was moderated by sex, and decreased total HIV stigma among female AYA. Crowdsourced interventions may be a promising way to engage communities to develop interventions to decrease HIV stigma.
PT05.02 – Brazilian Experience Towards Eliminating of Vertical Transmission of HIV, Syphilis and Viral Hepatitis B: A Human Rights Perspective Addressing Gender and Racial/Ethnic Inequalities and Community Participation
Sra. Márcia Rejane Colombo1, Dr. Pâmela Cristina Gaspar1, Sra Leila Sueli Barreto1, Sra Ariane T B Matos1, Phd Leonor Lannoy1, Sra Nádia Machado1, Phd Sérgio Ferreira Junior1, Phd Dráurio Barreira1
1Department of HIV/aids, Tuberculosis, Viral Hepatitis and Sexually Transmitted Infections, Ministry of Health of Brazil, Brasília, Brazil.
Introduction: The Brazilian experience with the Subnational Certification for the Elimination of Vertical Transmission (TVE) of HIV, syphilis, and hepatitis B highlights the importance of measures to protect human rights, address inequalities, and encourage community participation. Brazil adopts public policies aimed at combating socially determined diseases and mitigating stigma and discrimination.
Description: In the certification process, states and municipalities report, through documents, questionnaires, and interviews, the actions undertaken to promote human rights and address social, gender, and ethnic-racial inequalities. Community participation is also evaluated, with a focus on the involvement of women-led social organizations.
Results: Between 2022 and 2024, 151 municipalities with populations over 100,000 were certified. Significant progress was observed in the areas of human rights, gender equality, and racial/ethnic equality, driven by the implementation of laws and public policies. Key achievements include guarantees of professional confidentiality, combating discrimination, addressing violence against women, and strengthening social participation through Health Councils. Additionally, inclusive policies have benefited vulnerable groups, such as pregnant women living in poverty, Black and Indigenous women, people experiencing homelessness, and drug users. Health professional training proved to be a critical factor, varying significantly across municipalities. Subjective and moral aspects continue to pose barriers to including pregnant women who face challenges in accessing prenatal care and preventive services. In some locations, discrepancies between self-reported data and in loco observations revealed ongoing challenges linked to conservatism and social stigma.
Conclusion: The Subnational Certification Strategy contributes on promoting the elimination of vertical transmission diseases, which are socially determined. Its contribution hinges on ensuring human rights, addressing social, gender, and racial/ethnic inequalities, and expanding social and community participation in the certification process.
PT05.03 – Rural Australian Grassroots Movements for the Collective Future
Ms Anne-Marie Kelly1, Ms Ashleigh Colquhoun1, Professor Jane Tomnay1
1Centre for Excellence in Rural Sexual Health, Department of Rural Health, University of Melbourne, Shepparton, Australia.
Background: In rural and regional Victorian communities, sexual health is often shaped by longstanding cultural, social, and religious norms, leading to stigma, limited investment, and reluctance to address these issues. To address these challenges, the Centre for Excellence in Rural Sexual Health (CERSH) partnered with rural communities to develop five Sexual Wellness Action Plans (SWAPs). Using an appreciative inquiry approach, SWAPs established unified community visions and strategic plans to embed sexual health into local agendas, aiming to shift entrenched attitudes, reduce stigma, and promote evidence-based sexual health practices.
Methods: SWAPs were implemented across five rural Victorian Local Government Areas (LGAs), focusing on Indigenous communities, migrant workers, and socioeconomically disadvantaged populations. CERSH collaborated with local health services, Aboriginal-controlled community health organisations, schools, local governments, and diversity and settlement services. The approach prioritised grassroots engagement, cultural sensitivity, and community-driven strategies to normalise sexual health.
Findings: Preliminary results indicate significant improvements in the coordination of sexual health initiatives. Feedback suggests a positive shift in community attitudes and reduced stigma, as evidenced by local funding reallocations to support sexual health initiatives. Early observations highlight growing acceptance of sexual health as a community priority. A formal evaluation is ongoing to assess the long-term impact on service uptake and behavioural changes, with findings to be presented at the conference.
Conclusion: SWAPs demonstrate the potential for grassroots strategies to transform sexual health in rural communities. Sustained success requires evolving the plans to meet changing community needs, strengthening partnerships, and maintaining cultural sensitivity. Insights from the formal evaluation will guide future improvements, ensuring CERSH’s approach continues to create lasting change in rural and regional Victorian communities.
PT05.04 – Locating ‘Risk’ in the Australian Government’s National Sexually Transmissible Infections Strategy: An Analysis of Problem Representation
Dr. Heather Mccormack1,2, A/Prof Niamh Stephenson3
1Kirby Institute, Unsw Sydney, Sydney, Australia.
2Australian Human Rights Institute, UNSW Sydney, Sydney, Australia.
3School of Population Health, UNSW Sydney, Sydney, Australia.
Background: Since its inception in 2005, the Australian Government’s National Sexually Transmissible Infections (STI) Strategy has played a central role in shaping public health responses, influencing the resourcing and reach of STI prevention interventions We critically analysed its representations of ‘STI risk’ to identify alignment or misalignment with best practices in health promotion.
Method: We used Carol Bacchi’s “What’s the Problem Represented to Be?” (WPR) framework to analyse all editions of the National STI Strategy published since 2005. WPR offers a rigorous method to identify underpinning assumptions, interrogate gaps, and examine the effects of the problem representation. Specifically, we focussed on the framing of ‘risk’ within the strategy over the past two decades.
Results: The initial strategy framed the problem it purported to address as a lack of a nationally coordinated response to address risk associated with individual behaviour and lack of education. More recent strategies invoked a ‘healthy settings’ health promotion strategy. Healthy Settings approaches aim to forge multisectoral collaborations to change policies and programs that shape inequities where people live, work and play. Yet, recent strategies have increasingly framed STI risk as a problem of inadequate knowledge, education and awareness, widening the framing of educational need to now include health professionals. Moreover, responsibility for policy change is, in the most recent document, envisioned as lying with proactive communities in the first instance.
Conclusion: There has been some shift in the National STI Strategy’s representation of “STI risk”. Acknowledgment of how ‘settings’ shape STI transmission and of the importance of identifying and addressing inequities has increased. However, the strategy still emphasises interventions that aim to change individuals’ knowledge and awareness. Our findings suggest the need for a balanced approach that maintains focused support for populations subject to health and healthcare inequities while also addressing broader determinants of health.
PT05.05 – Healing and Harm Reduction: Indigenous-Led Approaches to Overdose Prevention and Care Within, By, and for Indigenous Peoples Living with and Without HIV
Ms. Melanie Grace Medina1,2, Claudette Cardinal2, Dr. Surita Parashar1,2, Sandy Lambert3, Dr. Kathleen Inglis1,2,4, Delilah Gregg5, Dr. Navneet Kaur Gill2, Hazel Cardinal6, Silke Hansen2, Miriam Muirhead2, Michael Budu2, Glyn Townson6, Dr. Katherine Kooij1,2, Wayne Campbell6, Valerie Nicholson3, Dr. Robert Hogg1,2
1Faculty of Health Sciences, Simon Fraser University, Burnaby, Canada.
2British Columbia Centre for Excellence in HIV/AIDS, Vancouver, Canada.
3Independent, Vancouver, Canada.
4School of Public Health and Social Policy, University of Victoria, Victoria, Canada.
5The Vancouver Area Network of Drug Users, Vancouver, Canada.
6The Ribbon Community, Vancouver, Canada.
Background: Indigenous harm reduction (IHR) moves beyond conventional ideas and forms of harm reduction. This approach emphasizes Indigenous (First Nations, Inuit, Métis) Peoples as experts and leaders in their lived/living experiences, connection to culture and community, integration of Indigenous values, and collective accountability for community well-being. Importantly, this approach is rooted in culturally safe, and trauma-informed practices. Emerging literature and harm reduction resources have highlighted significant calls to further Indigenize harm reduction, toward improving equitable access to substance use treatment for Indigenous Peoples, aligned with community members’ unique values and needs.
Methods: This study is a subset of a broader mixed-methods study, aimed at alleviating overdose risk and adverse long-term health effects among people living with and without HIV, who were at risk of, or experienced an overdose, in Vancouver, British Columbia, within the COVID-19 context. Indigenous Elders and academic researchers co-conducted two focus group discussions (FGD) with a total of ten Indigenous community members from Vancouver’s Downtown Eastside. The FGD interviews were professionally transcribed, and coded and analyzed using NVivo 14.0.
Results: IHR principles were consistently reflected across the interview transcripts, demonstrating how community actively practiced and sought out IHR. Indigenous community members shared their experiences looking after their fellow Indigenous brothers and sisters during an overdose event, highlighting their imperative role as first responders. Community members stressed the significance and utilization of Indigenous community-based harm reduction programs, Indigenous-led peer supports, and the value of community connection in their harm reduction journey. Community echoed the need for hiring Indigenous healthcare providers with lived/living experience, and more wholistic and compassionate care.
Conclusions: Findings illustrate the critical role of IHR, reinforcing the need to Indigenize harm reduction. This is vital for reducing substance use-related harms and addressing the ongoing impacts of colonization on Indigenous Peoples, both living with and without HIV.
PT05.06 – Barriers to HIV Prevention and Care Among Indigenous Populations in Canada: A Systematic Review
Ms. Sabina Rajkumar1, Ms Aditi Agarwal1, Mr. Sahith Rajkumar2, Dr. Patricia Farrugia3
1Faculty of Health Science, McMaster University, Hamilton, Canada.
2Faculty of Science, McMaster University, Hamilton, Canada.
3Department of Orthopedic Surgery, McMaster University, Hamilton, Canada.
Background: Indigenous populations face disproportionate rates of HIV compared to non-Indigenous groups, driven by systemic, socio-economic, and cultural barriers exacerbated by colonial legacies. This review examines the intersection of these factors and their influence on the prevalence, prevention, and treatment of HIV within Canadian Indigenous communities.
Methods: Electronic searches were conducted on MEDLINE, EMBASE, iPortal from inception to October 2024, supplemented with manual citation search. The search strategy included forward and backward citation tracking. Two reviewers independently and in duplicate assessed titles, abstracts, and full-text articles, with discrepancies resolved by a third member. Eligible studies consisted of randomized controlled trials (RCTs), cohort studies, cross-sectional research, and qualitative analyses. Data were extracted on key themes, including HIV prevalence, barriers to healthcare access, and cultural influences. Qualitative data were synthesized using thematic analysis.
Results: Indigenous populations in Canada have HIV prevalence rates 3.6 times higher than non-Indigenous populations, with disproportionate impacts on women (45% of cases) and youth (12–36% HIV-positive). Systemic barriers, including healthcare inaccessibility and stigma, delay HIV diagnosis and treatment. Racism, stereotyping, and distrust in healthcare create significant obstacles. Socioeconomic factors such as poverty, housing instability, and unemployment restrict access to consistent care and drive high-risk behaviours, including substance use and unsafe sex practices. Cultural disconnection from traditional practices and intergenerational trauma stemming from colonial systems, such as residential schools, exacerbate vulnerabilities. Lack of culturally competent care further alienates Indigenous patients, perpetuating disparities and undermining health outcomes.
Conclusion: Findings highlight the urgent need for culturally competent, community-driven healthcare strategies to address the compounded impact of systemic inequities and socio-economic barriers. Congress attendees will gain insights into integrating Indigenous voices in healthcare planning and implementing tailored interventions to bridge these disparities. These strategies can inform global approaches to reducing HIV disparities among marginalized populations.
PT05.07 – A Designathon to Co-Create Accessible Sexual Health Services for Adults Aged 45+ Including Those with Disabilities in the UK: Findings from a Community-Led Participatory Event
Dr. Eneyi Kpokiri1, Hayley Conyers1, Arushi Subba1, Ms Yoshiko Sakuma1, Tracey Jannaway2, Prof Joseph D Tucker3, Prof Dan Wu4
1London School of Hygiene and Tropical Medicine, London, United Kingdom.
2Independent Living Alternatives, London, United Kingdom.
3University of North Carolina, Chapel Hill, United States of America.
4Nanjing Medical University, Nanjing, China.
Background: There is limited tailored sexual health services for middle aged, older (45+) and disabled adults in the United Kingdom (UK). Existing services mostly cater to younger people. We organized a Designathon to identify community-led, innovative approaches to improve access to sexual health services for this population in the UK. A designathon is a three-phase participatory process informed by design thinking that includes the preparation phase by soliciting innovative ideas from end-users, an intensive collaborative event to co-create intervention components, and follow-up activities.
Methods: We organized co-creation sessions and a crowdsourcing open call to solicit suggestions to improve sexual health services for older adults. Findings from the crowdsourcing call and co-creation sessions generated five themes: adapting existing sexual health services, improving patient-provider relationships, improving sexual health communication, breaking down sexual health taboos, and community-led sexual health support. These themes informed a 2-day designathon in London (7–8 March 2024), consisting of five teams (3–4 individuals per team) supported by mentors and facilitators (Fig. 1). As for follow-up activities, final designathon ideas were reviewed by judges and top-scored ideas were publicly disseminated.
Results: Eighteen participants, 7 facilitators, 5 mentors, and 3 judges supported participated in the designathon. Attendees included older adults, community-based organizations representatives, policy makers, clinicians, disabled adults, activists, and researchers. The event facilitated rich discussions of implementation strategies to improve sexual healthcare for adults aged 45+. Themes from the designathon included community-led strategies, leveraging existing resources, peer education, and inclusive and accessible messaging. These were disseminated via stakeholder panels, online webinars, conferences and on the study website.
Conclusion: Our designathon engaged key stakeholders to co-develop practical strategies to improve uptake of sexual health services for adults aged 45+, including those with disabilities in the UK. Implementation research is needed to assess the effectiveness and sustainability of the strategies identified.
PT06.01 – Trichomonas Vaginalis Infection Among Adolescent Girls and Young Women Accessing Sexual and Reproductive Health Services at Retail Pharmacies in Kenya
Dr. Felix Mogaka1, Mr Benard Rono1, Mr Bernard Nyerere1, Dr Greshon Rota1, Mr Harrison Lagat2, Mrs Josephine Odoyo1, Dr Katrina Ortblad3, Ms Meena Lenn2, Dr Monisha Sharma2, Miss Omolara Akingba2, Dr Victor Omollo1, Dr Zachary Kwena1, Prof. Elizabeth Bukusi1,2, Dr Jillian Pintye2
1Kenya Medical Research Institute, Kisumu, Kenya.
2University of Washington, Seattle, United States.
3Fred Hutchinson Cancer Research Center, Seattle, United States.
Background: Trichomonas vaginalis (TV) infection increases susceptibility to HIV, yet limited data are available on TV infection among adolescent girls and young women (AGYW) who are at high risk of HIV infectin in Kenya. We evaluated the prevalence of TV among AGYW seeking sexual and reproductive health (SRH) services at retail pharmacies in Kisumu, Kenya.
Methods: We analyzed baseline data from AGYW enrolled in an ongoing cluster randomized controlled trial (NCT05467306) assessing pharmacy-based HIV PrEP delivery models at 20 retail pharmacies in Kisumu. AGYW (15–24 years) purchasing contraception, who tested HIV negative were offered an option of either oral PrEP or the dapivirine vaginal ring (DPV-VR) per national guidelines. A subset was offered TV testing using Xpert® TV assays. Poisson regression was used to identify correlates of TV infection.
Results: As of December 2024, 481 AGYW were tested for TV. Median age was 20 years (IQR 18-22), 81% were unmarried, and 39% were currently in school. One-third (32%) reported having casual sexual partners and 40% had a prior pregnancy. Condomless sex was common (84%) and 11% recently engaged in transactional sex. TV prevalence was 6.4% (31/481), and only 23% (7/31) were symptomatic. AGYW who reported STI symptoms were twice as likely to have TV as asymptomatic AGYW (PR = 2.88, 95% CI:1.32–6. 28, P = 0.008). A prior diagnosis of an STI was associated with current TV infection (PR = 3.21,95% CI:1.47–6.99, P = 0.003). HIV PrEP uptake was higher among AGYW with TV detected (93% vs 79 %, P = 0.047). Among AGYW who accepted HIV PrEP (n = 392), the frequency of selecting DPV-VR over oral PrEP was similar among AGYW with symptomatic TV (17%), asymptomatic TV (17%), and no TV (18%, P = 0.998).
Conclusion: TV was relatively common and frequently asymptomatic. Offering TV screening within pharmacies in Kenya could be beneficial for AGYW with a history of STIs or among those considering HIV PrEP.
PT06.02 – “We Have the Tools”: Health System Stakeholders’ Perspectives on Implementation of Injectable Cabotegravir as HIV-PrEP Among Two-Spirit, Gay, Bisexual, Queer, and Other Men Who Have Sex with Men (2SGBQM) in Canada
Dr. Tyrone J Curtis1, Mr Lucas Gergyek2, Mr Ben Klassen2, Mr Chris Draenos2, Dr Clemon George3, Dr Daniel Grace4, Mr Kenneth Monteith5, Dr Aniela dela Cruz6, Mr Harlan Pruden7, Mr Michael Kwag2, Dr Darrell H S Tan4,8
1University of Victoria, Victoria, Canada.
2Community-Based Research Centre, Vancouver, Canada.
3Buffalo State University, Buffalo, USA.
4University of Toronto, Toronto, Canada.
5COCQ-SIDA, Montreal, Canada.
6University of Calgary, Calgary, Canada.
7BC Centre for Disease Control, Vancouver, Canada.
8St Michael’s Hospital, Toronto, Canada.
Background: Long-acting injectable cabotegravir (CAB-LA) was recently approved as HIV pre-exposure prophylaxis (PrEP) in Canada. To maximize the benefit of CAB-LA PrEP within key populations, including Two-Spirit, gay, bisexual, queer, and other men who have sex with men (2SGBQM), we must understand existing challenges with oral PrEP, adapt PrEP delivery to reduce structural inequities, and proactively address anticipated challenges of CAB-LA PrEP implementation.
Methods: Nine focus groups and ten semi-structured interviews with health system stakeholders (N = 37) involved in PrEP provision across Canada were conducted to explore readiness to implement CAB-LA PrEP, resources required for delivery, and potential approaches to maximize access for 2SGBQM. Data were analyzed using reflexive thematic analysis.
Results: Participants emphasized that CAB-LA PrEP could address PrEP inequities for some 2SGBQM who face challenges with oral PrEP access and adherence, including people who travel frequently, experience homelessness, or have limited privacy. Implementation of CAB-LA PrEP in rural communities via pharmacies and among people experiencing homelessness via mobile delivery were highlighted as novel approaches to challenge inequities. Some participants had experience administering long-acting HIV treatment and reported readiness to implement CAB-LA PrEP, while others raised logistical barriers to implementation, including staffing and space requirements for administration and follow-up, discrepancies between STBBI testing and CAB-LA PrEP dosing frequencies, and providers’ inexperience administering gluteal injections. Participants highlighted structural barriers to implementation, including drug cost and provider reimbursement challenges, scope of practice limitations which restrict who can administer injections, and resistance from government stakeholders to adapt and expand PrEP delivery.
Conclusion: CAB-LA PrEP implementation requires learning from existing oral PrEP inequities while adapting PrEP delivery models to meet community needs and address feasibility constraints. Clear guidelines and decision-making tools, innovative approaches to delivery, and additional space and staffing resources are essential for ensuring CAB-LA PrEP works for providers and patients.
PT06.03 – A Review of Public Health Surveillance Data to Inform Doxy-PEP Use: Results from Ottawa, Canada for Bacterial STI Diagnoses Among Gay, Bi, and Other Men Who Have Sex with Men
Dr. Dara Spatz Friedman1, Dr. Patrick O’Byrne1,2, Ms. Lauren Orser1
1Ottawa Public Health, Ottawa, Canada.
2University of Ottawa, School of Nursing, Ottawa, Canada.
Background: Gay, bi, and other men who have sex with men (gbMSM) account for a disproportionate number of bacterial sexually transmitted infections (bac-STIs). A new preventative tool, “doxy-PEP,” is taken as a one-time 200 mg oral dose of doxycycline after condomless oral or anal sex as post-exposure prophylaxis (PEP). We reviewed surveillance data to understand the potential public health impact of offering doxy-PEP to gbMSM who have been diagnosed with 0, 1 or ≥ 2 bac-STI diagnoses.
Description: We analyzed episodes during 2022 –2024 in which a bac-STI was confirmed in 18+-year-old gbMSM to determine the number of individuals with one or more positive bac-STIs testing episodes (PTEs) within 12 months of a previous diagnosis. We calculated the number of PTEs and bac-STIs that might be prevented, and the number needed to treat (NNT), using either 0, ≥1 or ≥ 2 PTEs in a 12-month period as a threshold for prescribing doxy-PEP.
Findings: We found that approximately 3% of gbMSM had one or more PTEs within 12 months, 26% with one PTE had a second PTE within 12 months; and 32% with two PTEs, a third. Based on this analysis, the NNT for doxy-PEP taken by all gbMSM to prevent a first PTE is 50; by gbMSM following a first PTE to prevent a second, 7; and following a second PTE to prevent a third, 6. Taking doxy-PEP following a single PTE would avert approximately one-third of subsequent PTEs and one-fifth of bac-STIs.
Conclusion: This analysis enables informed decisions about prescribing doxy-PEP to achieve the best prevention outcomes while minimizing antibiotic overuse. Doxy-PEP use in gbMSM with at least one bac-STI diagnosis in the preceding 12 months would result in a high population-level prevention outcome with a low NNT, consistent with recent US CDC guidelines.
| Number of gbMSM* | Number of gbMSM with 1+ PTE | Percent of gbMSM with 1+ PTE | Total number of PTEs | Number of chlamydia infections | Number of gonorrhea infections | Number of syphilis infections | Total number of infections | ||
|---|---|---|---|---|---|---|---|---|---|
| 2021 | 20,497 | 413 | 2.0% | 471 | 231 | 169 | 125 | 231 | |
| 2022 | 20,884 | 644 | 3.1% | 770 | 388 | 368 | 120 | 388 | |
| 2023 | 21,290 | 749 | 3.5% | 889 | 399 | 449 | 150 | 399 | |
| 2024 | 21,650 | 692 | 3.2% | 792 | 330 | 456 | 102 | 888 | |
| Sum | N/A | 1,912** | N/A | 2,922 | 1,348 | 1,442 | 497 | 3,287 | |
| 2022–24 average | 21,274 | 695 | 3.3% | 817 | 372 | 424 | 124 | 921 |
Notes: *Based on population growth following 2019 estimate from SexNow.
** Individuals are counted in each calendar year in which they experience a PTE.
| Year | Number of PTEs/individual | Number of individuals with given number of PTEs | Percent of individuals with given number of PTEs who have another PTE | Percent of individuals with given number of PTEs who would have another PTE were doxy-PEP used | NNT to have prevented another PTE | |
|---|---|---|---|---|---|---|
| 2022 | 0+ | 20,884 | 3.2% | 1.2% | 52 | |
| 1 | 485 | 26.3% | 10.2% | 6 | ||
| 2 | 117 | 32.4% | 12.6% | 5 | ||
| 3+ | 42 | |||||
| 2023 | 0+ | 21,290 | 3.6% | 1.4% | 46 | |
| 1 | 577 | 24.0% | 9.3% | 7 | ||
| 2 | 116 | 36.3% | 14.1% | 5 | ||
| 3+ | 56 | |||||
| 2024 | 0+ | 21,650 | 3.2% | 1.3% | 51 | |
| 1 | 511 | 26.8% | 10.4% | 6 | ||
| 2 | 140 | 25.1% | 9.7% | 6 | ||
| 3+ | 41 | |||||
| 2022-24 average | 0+ | 21,274 | 3.3% | 1.3% | 50 | |
| 1 | 524 | 24.6% | 9.5% | 7 | ||
| 2 | 124 | 27.1% | 10.5% | 6 | ||
| 3+ | 46 |
Note: The calculation of PTEs averted takes average efficacy of doxy-PEP into account.
| Number of previous PTEs/individual in a 12-month period ending with the individual’s most recent PTE | Average number of PTEs averted in the following 12 months if given doxy-PEP following a given PTE | % of PTEs in the following 12 months averted if given doxy-PEP | Average number of bac-STIs averted in the following 12 months if given doxy-PEP following a given PTE | % of bac-STIs in the following 12 months averted if given doxy-PEP | |
|---|---|---|---|---|---|
| 0 | 426 | 61.2% | 564 | 61.2% | |
| 1 | 209 | 30.1% | 160 | 17.4% | |
| 2 | 85 | 12.2% | 46 | 5.0% |
Note: The calculation of PTEs and bac-STIs averted takes average efficacy of doxy-PEP into account.
PT06.04 – Enhancing HIV PrEP Uptake Among Black Women: Perspectives from PrEP and OB-GYN Providers in New Orleans, Louisiana (NOLA)
Ms. Clare Kelsey, Dr. Whitney Irie, Mr. Brian Perry, Ms. Jacquelyn Bickham, Ms. Tamachia Davenport, Dr. Meredith Clement, Dr. Amy Corneli
1Louisiana State University Health Sciences Center, New Orleans, United States.
Prior formative research identified barriers that Black cisgender women in New Orleans face with HIV pre-exposure prophylaxis (PrEP) uptake, including infrequent mention of PrEP from their providers. To address this barrier, an educational initiative was proposed to train OB-GYN residents to discuss and prescribe PrEP.
We conducted in-depth interviews (IDIs) with PrEP providers, OB-GYN residents, and OB-GYN residency program leadership to inform the implementation strategy. Guided by the Consolidated Framework for Implementation Research (CFIR), we explored the perceptions of HIV prevention context for Black cisgender women in NOLA (outer setting), integrating the initiative into an OB-GYN residency program (inner setting), provider perceptions on the appropriateness of residents offering PrEP (innovation), and the perceived self-efficacy and needs of residents to provide PrEP.
Interviews were conducted with 4 PrEP providers, 4 OB-GYN residents, and 4 leadership. Participants identified systemic obstacles that they believe disproportionately impact Black cisgender women’s HIV risk. Providers perceived that Black cisgender women have “dueling interests” (e.g., work, child care) that, in their view, make accessing PrEP challenging, particularly if PrEP is not regarded as essential or relevant to their lives. Both PrEP and OB-GYN providers strongly endorsed PrEP provision in OB-GYN resident clinics. Residents and program leadership reported that PrEP conversations appropriately fit their current care model, as residents already discuss STIs and sexual health with patients. OB-GYN leadership noted the feasibility of incorporating PrEP labs and prescriptions into their existing workflows; however, residents were not currently knowledgeable about PrEP and would need training. Additional concerns included insufficient time with patients, and that residents’ rotating schedules would limit continuity, negatively impacting follow-up.
PrEP and OB-GYN providers strongly supported an OB-GYN resident training program to improve PrEP uptake and access for Black cisgender women in NOLA. While challenges were noted, providers believed the existing infrastructure would facilitate program implementation.
PT06.05 – Two-Spirit, Gay, Bisexual, Trans, and Queer Men and Non-Binary People’s Preferences for Doxycycline as Sexually Transmitted Infection PrEP/PEP: A Qualitative Study Across British Columbia, Canada
Lucas Gergyek1, Mr. Ben Klassen1, Kartik Arora1, Anuar Chain-Haddad1, Jose Gamboa1, Evan Hall1, Samuel Salvati1, Dr. Jose Benito Tovillo2, Chris Draenos1, Dr. Troy Grennan3, Dr. Nathan J. Lachowsky1,2, Dr. Mark Hull4
1Community-Based Research Centre, Vancouver, Canada.
2University of Victoria, Victoria, Canada.
3BC Centre for Disease Control, Vancouver, Canada.
4University of British Columbia, Vancouver, Canada.
Background: Doxycycline as prophylaxis (doxy PrEP/PEP) may help ameliorate the impact of some bacterial sexually transmitted infections (STIs), including syphilis and chlamydia, that Two-Spirit, gay, bisexual, trans and queer men and non-binary (2S/GBTQ) people disproportionately face. In December 2023, British Columbia (BC) became the first province in Canada to introduce a public doxy PEP (i.e., post-exposure) program. We sought to understand 2S/GBTQ people’s experiences with and preferences for the implementation of doxy PrEP/PEP across BC.
Methods: We conducted semi-structured individual interviews with 2S/GBTQ community members (N = 20) across BC from late 2024 to early 2025 to identify key preferences for delivery of doxy PrEP/PEP. We recruited participants through clinics, community-based organizations, and social media. We purposively selected participants to maximize diversity based on race, HIV status, and geography. We recorded, transcribed, and analyzed interviews using reflexive thematic analysis.
Results: Participants had primarily accessed doxy PEP through 2S/GBTQ-friendly sexual health clinics and community-based organizations where they had previously accessed other STI prevention, including HIV PrEP. Experiences were largely positive. Participants described few barriers to access and minimal side effects that were outweighed by the confidence provided by doxyPEP. Participants also reported confusion between doxy PrEP/PEP and HIV PrEP/PEP, concerns around antimicrobial resistance, and existing preference for other STI prevention methods (e.g., condoms, routine testing). Preferences for implementation included building doxy PrEP/PEP into existing online or telehealth HIV PrEP delivery services and ensuring doxy PrEP/PEP accessibility through pharmacies, particularly those in rural regions.
Conclusion: Overall, successful implementation of doxy PrEP/PEP requires tailored and culturally competent health promotion for 2S/GBTQ community members that situate doxy PrEP/PEP within the broader landscape of existing HIV/STI prevention. Key lessons from BC’s initial public program implementation, including the importance of leveraging existing 2S/GBTQ-friendly STI prevention and care infrastructure, can enhance rollout across Canada and beyond.
PT06.06 – Integration of the Dual HIV/Syphilis Test Within HIV Prevention Services in South Africa
Dr. Catherine Martin1, Mr Sydney Ncube1, Ms Nthabiseng Koloane1, Ms Maserame Mojapele1, Mr Sean Arries1, Ms Siphokazi Dada1, Ms Vusile Butler1, Prof Saiqa Mullick1
1Wits RHI, University of the Witwatersrand, Johannesburg, South Africa.
Background: There has been an unprecedented increase in syphilis cases globally in recent years. Dual HIV/syphilis rapid diagnostic tests hold the potential to improve access to diagnosis and treatment, yet are not routinely implemented outside of antenatal care settings in South Africa. We evaluated the introduction of the dual HIV/syphilis test within HIV prevention services.
Description: This evaluation was undertaken within an existing implementation study focused on the introduction of HIV pre-exposure prophylaxis (PrEP) within routine primary care services. The study is implemented in eight primary care facilities and three linked mobile clinics in four areas of South Africa. Project lay counsellors were trained on the use of the dual HIV/syphilis test, including pre-and post-test counselling and quality control; implementation was overseen and supported on-site by trained nurses.
Findings: Between April and October 2024, 3020 clients (2160/3020 [71.5%] females 15–24 years) presented for services for the first time at project sites and were seen by a trained counsellor. Of these, 2788 (92.3%) were offered a dual test and 2446/2788 (87.7%) accepted; 2343/2446 (95.8%) tested and had results documented, of whom 157/2343 (6.7%) tested positive for syphilis, 67/2343 (2.9%) positive for HIV and 17/2343 (0.7%) positive for both. Of those who tested positive for syphilis, 118/157 had a specimen sent to the laboratory and 60/71 (84.5%) with results available were confirmed rapid plasma reagin (RPR) positive. There were 136/157 (86.6%) clients treated for syphilis at project sites, 132/136 (97.0%) on the day of testing.
Conclusion: There was high acceptability of the dual HIV/syphilis test among clients accessing HIV prevention services and a high prevalence of syphilis detected. The majority were active cases of syphilis and received treatment the same day. Point of care testing can improve syphilis diagnosis and treatment when integrated with HIV prevention services.
PT06.07 – Should Etiological Diagnosis Be Encouraged to Treat Urethral Discharge in Brazil? Preliminary Data from a National STI Monitoring Platform
Mr. Adson Belém Ferreira da Paixão1, Ms. Ana Philippus1, Mayra Aragon1, Isabella Nepomuceno de Souza1, Carmen Silvia Bruniera Domingues1, Ronaldo de Almeida Coelho1, Renatto Carrijo1, Jessica Motta Martins2, Marcos André Schörner2, Maria Luiza Bazzo2, Pâmela Cristina Gaspar1, Álisson Bigolin1
1Ministry of Health, Brasília, Brazil.
2Molecular Biology, Microbiology, and Serology Laboratory (LBMMS), Federal University of Santa Catarina, Florianópolis, Brazil.
Etiological diagnosis of urethral discharge (UD) is not mandatory in Brazil. The control of these infections is related to effective treatment. However, knowledge of the national epidemiological scenario remains limited and syndromic management is the mostly used for treatment.
Since 2015, Brazil has led a project to evaluate gonococcal antimicrobial resistance, showing an increase in azithromycin resistance. In 2020, this project was incorporated into the Urethral Discharge Sentinel Surveillance, making it mandatory to report treated UD cases, collect biological samples for Molecular Biology Tests for Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG), and NG strains for antimicrobial susceptibility testing. In 2023, there were 11 sentinels and a National STI Monitoring Platform (NSMP) was developed. Sentinel surveillance includes people with penis, ≥18 years of age, with UD and no recent NG treatment.
From January 2023 to December 2024, 1,061 notifications (528 under investigation) were registered from 7 sentinel sites on the NSMP. Cis men represented 93.78%, and trans women/non-binary 1.32%. Regarding sexual partnerships, 54.38% had sex with cis men, 46.56% with cis women, 2.26% with trans women and 1.79% with trans men. Most individuals had 1 (27.14%) or 2 (23.94%) partners in the past 30 days. Transmission routes included oral (65.60%), anal (58.81%), and vaginal sex (45.62%). Among collected samples, 50.33% were tested for CT/NG (41.31% NG positive, 5.99% CT positive, and 10.86% co-infected), and 16.68% were tested for mycoplasma and trichomoniasis (10.17% mycoplasma positive – 2 co-infected with CT and 1 with NG). Most common treatment (70.59%) was the standard for the syndromic management in Brazil (azithromycin-1g + ceftriaxone-500mg).
Sentinel surveillance may support updates to guidelines for screening and treatment based on epidemiology, main pathogens and antimicrobial resistance. Brazilian data highlights the importance of the etiological management, since most cases were treated with azithromycin, despite NG being the main pathogen.
PT07.01 – Impacts of Methamphetamine Use and Bacterial STIs on Systemic Inflammatory Cytokine Levels Among a Longitudinal Cohort of Sexual Minority Men
Asst. Prof. Cherie Blair1, Jennifer Fulcher1, Pamina Gorbach1, Steven Shoptaw1, Jesse Clark1
1University of California Los Angeles, Los Angeles, United States.
Background: Methamphetamine (MA) use and STIs are independently associated with sexual risk behavior and inflammation, particularly among sexual minority men (SMM). These factors may drive HIV/STI co-transmission and exacerbate inflammation-related comorbidities. However, the independent and combined effects of MA use and STIs on systemic inflammation remain unclear. Understanding these dynamics is critical to addressing mechanisms of HIV/STI transmission and associated inflammation.
Methods: This is a secondary analysis of data from a longitudinal cohort of SMM in Los Angeles, CA (mSTUDY). Every 6 months, participants reported sexual behaviors and substance use, underwent STI testing for gonorrhea/chlamydia (GC/CT), syphilis, and HIV, and provided serum samples. Inflammatory cytokines, including interferon (INF)-gamma, tumor necrosis factor (TNF)-alpha, and interleukins (IL-6, -10, -12, -23), were measured using a custom Milliplex High-Sensitivity multiplex panel. Associations between systemic cytokine levels, bacterial STIs, and MA use were analyzed using mixed-effects generalized linear models, adjusting for HIV status and body mass index. Interaction terms assessed joint effects of MA use with syphilis, GC, and CT on cytokines.
Results: Among 140 participants (median age 35 years; 100 living with HIV) across 560 visits, bacterial STIs were detected at 17% of visits, including CT (8.2%), GC (6.6%), and syphilis (5%). MA use was absent at 61.6% of visits, while 19.3% reported weekly/daily use. Syphilis was positively associated with INF-gamma, TNF-alpha, IL-6, -10, -12, and -23. MA use was associated with elevated IL-6 and -10, while CT was associated with IL-23, and GC with TNF-alpha. However, no significant interactions were found between MA use and STIs on systemic cytokine levels.
Conclusion: Both MA use and bacterial STIs independently contribute to systemic inflammation without synergistic effects. Syphilis significantly drives pro-inflammatory cytokines, underscoring the importance of STI prevention and treatment strategies to mitigate inflammation-related comorbidities and the potential for HIV transmission.
PT07.02 – Neutrophil Extracellular Traps Impair Vaginal Barrier Function and Increase HIV Acquisition in Responde to Non-Optimal Bacteria Species
Miss Marina Costa Fujishima1, Miss Deesha Nayar1, Mr Morgan Taverner1, Ms Oluwaseun Ajibola1, Miss Riley Greenslade1, Mr Thomas Murooka1
1University of Manitoba, Winnipeg, Canada.
Background: Analysis from >700 women from the CAPRISA004 cohort show that women with a non-Lactobacillus dominant vaginal microbiome (non-optimal microbiome) were at significantly higher risk of sexual HIV acquisition, and that this strongly correlated with loss of barrier integrity, inflammation and neutrophil accumulation. Despite these strong associations, the cellular and molecular mechanisms that mediate this risk remain largely unknown. Here, we will test that hypothesis that neutrophil recruitment and neutrophil extracellular traps (NETs) in response to non-optimal bacterial species initiate an inflammatory cascade that results in vaginal barrier dysfunction and enhances HIV acquisition.
Methods: Balb/c mice were intravaginally inoculated with either PBS, Lactobacillus crispatus, Mobiluncus mulieris or Gardnerella vaginalis. Vaginal barrier integrity was assessed in the presence or absence of NETs (DNAse I treatment) by inoculating mice with lucifer yellow (0.45Da) and measuring dye penetration into the submucosa by immunohistochemistry. Finally, to evaluate the impact of different bacteria species on HIV transmission, humanized BLT (bone marrow/liver/thymus) mice were weekly challenged with a low dose of HIV transmitted/founder (T/F) REJO.c virus and plasma viremia was monitored by RT-qPCR.
Results: We found that the presence of non-optimal bacteria species in the vaginal mucosa causes substantial damage to the vaginal epithelium and results in high neutrophil recruitment along with an increase in the release of NETs. Excitingly, we also show that NET formation directly impacts the FGT biology and drives barrier breakdown in the vaginal mucosa. Finally, we demonstrate that these changes in barrier dysfunction directly impact HIV acquisition rates by ~10–14 days compared to PBS controls, suggesting that increased HIV translocation across the FGT barrier contribute to systemic viremia.
Conclusions: Together, our work provides a mechanistic understanding of how non-optimal bacteria species can alter innate immune responses and increase barrier breakdown in the vaginal mucosa to modulate HIV acquisition risk in vivo.
PT07.03 – Association of Prenatal Ultrasound Findings and Congenital Syphilis
Assoc. Prof. Irene Stafford1, Dr Edgar Edgar Hernandez-Andrade, Dr Donatella Gerulewicz, Dr Kaitlyn Stark, Dr Kathryn Miele, Dr Melanie Taylor, Dr Sean Blackwell, Dr. Ana Luisa Davie
1The University of Texas Health Science Center, Houston, United States.
Background: Sonographic evaluation of fetuses exposed to syphilis can contribute to a congenital syphilis (CS) diagnosis. This analysis describes sonographic stigmata of CS among fetuses exposed to syphilis and the association of these findings with CDC-defined neonatal CS categories.
Methods: We performed a prospective study of pregnant patients with syphilis between 05/2023–06/2024. Serial sonographic evaluation of all exposed fetuses ≥18 weeks gestational age (GA) was performed within 7 days of treatment and monthly thereafter. We tested the association of known sonographic finding of CS, including placentomegaly (>2 SD above mean for GA), hepatomegaly (>90% for GA), and/or elevated middle cerebral artery peak systolic velocity (MCA PSV ≥1.5 MoM) with CS categories at birth (less-likely, possible, and highly probable/proven CS). Femur length (FL) <10% for GA, estimated fetal weight (EFW) <10%, and fetal growth with moderate (≥20%) and severe (≥40%) decreases in growth velocity percentiles were added to known CS-associated findings as predictors. Multivariate ordinal logistic regression models evaluated sonographic measurements as predictors of neonatal CS category.
Results: Among 40 enrolled patients, 38 (95%) had serial sonographic evaluation, and 37 (93%) had serial growth scans. Thirteen (33%) neonates were identified as possible or highly probable/proven CS cases. Known CS-associated sonographic findings were reported in 89% (n = 24) of neonates in the less-likely CS category and 100% (n = 13) in the possible or highly probable/proven CS category. FL <10% and a decrease in growth velocity ≥20% increased detection of CS to 100% in all CS categories (Table 1). The odds ratio for progression of CS risk category at birth was 2.0 for FL <10% (95% CI: 0.91,4.42) and 1.3 for a severe decrease in growth velocity (95% CI: 0.68,2.58) (Table 2).
Conclusion: When growth-related abnormalities are added to known CS-associated sonographic findings, all cases in this cohort were identified as CS cases by sonographic data alone.
| CS less likely | CS possible | CS case/highly probable | ||||||
|---|---|---|---|---|---|---|---|---|
| n = 28 | % | n = 3 | % | n = 10 | % | P-value | ||
| Any known CS-associated findings* | 24/27 | 88.9 | 3/3 | 100.0 | 8/8 | 100.0 | 1.00 | |
| Above plus growth-related findings** | 27/27 | 100.0 | 3/3 | 100.0 | 8/8 | 100.0 | -- | |
*Known CS-associated findings: placentomegaly (> 2 SD above mean for GA), hepatomegaly with > 90% for GA, and/or elevated MCP PSV ≥ 1.5 MoM.
**Growth-related findings: femur length < 10% for GA, estimated fetal weight <10% for GA, and fetal growth with moderate (≥ 20%) decrease in growth velocity.
| Sonographic Finding | OR* | 95% CI** | P-value | |
|---|---|---|---|---|
| Decrease in growth velocity ≥40% | 1.3 | 0.68, 2.58 | 0.41 | |
| Femur length <10% for GA | 2.0 | 0.91, 4.42 | 0.09 | |
| Estimated fetal weight <10% for GA | 2.3 | 0.78, 6.93 | 0.13 |
*OR = odds ratio.
**CI = confidence interval.
PT07.04 – Chlamydia and Gonorrhea Prevalence and Molecular Characteristics Among Female Sex Workers in Nairobi, Kenya
Ms. Clarissa Klenke1,2, Ms. Vanessa Schulz2, Ms. Paige Adams2, Dr. Irene Martin2, Mrs. Suzanne Gibbons2, Ms. Kibii Belindah1,4, Mr. Fred Owino1,4, Mr. Erastus Irungu4, Ms. Monica Okumu4, Ms. Mary Kungu4, Ms. Rhoda Kabuti4, Dr. Joshua Kimani1,3,4, Dr. Lyle McKinnon1,3, Dr. Aida Sivro1,2,5
1University of Manitoba, Winnipeg, Canada.
2National Microbiology Lab Branch, Public Health Agency of Canada, Winnipeg, Canada.
3University of Nairobi, Nairobi, Kenya.
4Partners for Health and Development in Africa, Nairobi, Kenya.
5University of KwaZulu-Natal, Durban, South Africa.
Background: In Kenya, sexually transmitted infection (STI) management is syndromic. As a result, the current prevalence and incidence of chlamydia and gonorrhea infections are underreported. Additionally, the distribution of circulating strains and antibiotic resistance remain poorly characterized.
Methods: This project aims to characterize the burden and molecular characteristics of STIs in a cohort of Kenyan sex workers. Recruited through the Sex Worker Outreach Program(SWOP), HPV-positive enrolled participants had urine samples collected bi-monthly over 12 months. STIs were diagnosed by GeneXpert and confirmatory tests were performed using rRNA amplification by the Hologic Aptima Combo 2 assay. Chlamydia-positive samples were genotyped by Sanger sequencing of the ompA gene, which can differentiate between all 19 chlamydia serovars. Gonorrhea-positive samples were typed by Neisseria gonorrhoeae Multi-Antigen Sequence Typing (NG-MAST), targeting the porB and tbpB genes, and then tested by qPCR to predict resistance to cephalosporins, ciprofloxacin, and azithromycin.
Results: 1868 sex workers were screened for the study, where 40.3% (95% CI 38.1–42.6) tested positive for high-risk HPV. Female sex workers with HPV (n = 701) were enrolled in the longitudinal study, having a median age of 31 (IQR: 25–37). Participants were 94% cis-women, 13% HIV-positive, and 71% reported condom use during most recent intercourse. At screening, there was a chlamydia prevalence of 8.8% (95% CI 7.6–10.1) and a gonorrhea prevalence of 3.2% (95% CI 2.5–4.1). Chlamydia typing revealed serovars D (13.0%), E (16.5%), F (26.1%), G (22.6%), I (11.3%), J (0.9%) and K (9.6%). Gonorrhea testing identified all new NG-MAST sequence types with high ciprofloxacin resistance (89%). Testing and characterization of the follow-up samples are ongoing.
Conclusion: The prevalence of chlamydia and gonorrhea in this population was slightly higher than the overall estimates for the African region. A diverse assortment of chlamydia and gonorrhea types is evident. Further identification of bacterial types and antimicrobial resistance in this cohort will impact Kenyan STI prevention and treatment policies, contributing to global STI control.
PT07.05 – Prevalence and Correlates of Chemsex, Injection Drug Use and Injection Risk Behaviors Among Men Who Have Sex with Men and Transgender Women in 16 Asia-Pacific Countries: Insights from the PrEP Appeal Study
Mr. Wen Zhi Ng1, Kuhanesan Naidu1, Eleanor Joan Ong1, Danyang Luo2, Benjamin R Bavinton3, Curtis Chan3, Heather-Marie Schmidt4,5, Warittha Tieosapjaroen6,7, Lei Zhang7, Nittaya Phanuphak8, Kimberly E Green9, Weiming Tang10, Nicky Suwandi11, Rayner Kay Jin Tan1
1Saw Swee Hock School of Public Health, National University of Singapore, Singapore, Singapore.
2Rollins School of Public Health, Emory University, Atlanta, United States.
3Kirby Institute, University of New South Wales Sydney, Sydney, Australia.
4World Health Organization, Geneva, Switzerland.
5UNAIDS, Geneva, Switzerland.
6Central Clinical School, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
7Melbourne Sexual Health Centre, Alfred Health, Melbourne, Australia.
8Institute of HIV Research and Innovation, Bangkok, Thailand.
9PATH, Hanoi, Vietnam.
10University of North Carolina, Chapel Hill, United States.
11APCOM Foundation, Bangkok, Thailand.
Background: Chemsex and injection drug use are pressing public health issues among men who have sex with men (MSM) and transgender women (TGW). This analysis examines the correlates of chemsex, injection drug use, and associated risk behaviors in the Asia-Pacific region.
Methods: The PrEP APPEAL cross-sectional survey of MSM and TGW populations collected data between May 2022 and November 2022 across 16 countries and territories in Asia-Pacific. Behavioral outcomes included chemsex engagement, injection drug use, and shared equipment. Country level variables included GDP per capita and availability of harm reduction policies. Mixed-effects logistic regression models were used to identify predictors of behavioral risks, accounting for country-level clustering.
Results: Among 18,290 participants (MSM: 93.1%, TGW: 6.9%), the past 6-month prevalence of chemsex was 19.1% (MSM:18.2%,TGW:31.0%), with significant variability across countries (range = 3.39%–41.48%). Past 6-month prevalence of injection drug use was 7.40%, with 15.21% of these sharing equipment. PrEP awareness was high (84.31%), and 31.1% reported PrEP use. Key correlates of chemsex included being a transgender man (adjusted Odds Ratio[aOR]=1.58,95% confidence interval[CI]=1.21,2.07), being retired (aOR = 1.57, 95% CI = 1.01, 2.44) or unemployed (aOR = 1.23, 95% CI = 1.02, 1.48), and being paid for sex in the last 6 months (aOR = 1.56, 95% CI = 1.2, 2.03). Injection drug use was correlated with being TGW (aOR = 1.37, 95% CI = 1.02, 1.83), unemployment (aOR = 1.68, 95% CI = 1.30, 2.17), and sex work ever being a primary income source (aOR = 1.43, 95% CI = 1.03, 1.99). Likelihood of sharing injecting equipment was associated with being paid for sex in the last 6 months (aOR = 5.64, 95% CI = 2.25, 14.15), sex work ever being a primary income source (aOR = 3.38, 95% CI = 1.28, 8.94), and a sexually transmitted infection diagnosis in the last 6 months (aOR = 3.01, 95% CI = 1.63, 5.55).
Conclusion: The findings underscore the need for policy makers to prioritize funding of tailored interventions for MSM and TGW to address chemsex and injection risk behaviours in the Asia-Pacific. Interventions considering the compounding vulnerabilities of sex work could mitigate health-related risks, particularly for individuals with socioeconomic vulnerabilities, reducing disparities and improving health outcomes in key populations.
PT07.06 – A Habitus of Insecurity and Sexual Healthcare Among Sexually Diverse Muslim Men: An Ethnographic Study in Winnipeg, Canada
Dr. Muhammad Naveed Noor1, Dr Souradet Shaw1, Dr Robert Lorway1
1University of Manitoba, Winnipeg, Canada.
Background: In Winnipeg, sexually diverse Muslim men (SDMM) are often reluctant to utilize sexual healthcare, which can place them at an increased risk of HIV and other sexually transmitted infections (STI).
Description: This study adopted a qualitative ethnographic approach, conducting fieldwork with SDMM in Winnipeg, Manitoba, from March 2024 to December 2025. Pierre Bourdieu’s concept of habitus was used to analyze fieldnotes, informal communications, and semi-structured interviews with 10 participants. Habitus refers to a system of individuals’ dispositions structured by the their past and ongoing social experiences, that also shape their worldviews and social practices.
Findings: Participants’ narratives revealed lives shaped by insecurity stemming from intersecting layers of exclusion and discrimination. Despite Canada’s progressive stance on lesbian, gay, bisexual, and queer (LGBTQ) rights, SDMM face dual marginalization: homophobia within Muslim communities and exclusion from mainstream LGBTQ spaces. Homophobia results in rejection by families and faith communities, while xenophobia and societal heteropatriarchy amplify their marginalization. Perceptions of Islam as incompatible with queer identities, combined with cultural differences, further obstruct their integration into LGBTQ spaces. These intersecting oppressions cultivate a habitus of instability that shapes SDMM’s understanding of their social position. To avoid stigma and discrimination, many SDMM hesitate to seek sexual healthcare, increasing their risk of HIV/STI and perpetuating their social disadvantage.
Conclusion: Stigma surrounding sex between men is further compounded for individuals with multiple intersecting identities, such as SDMM. To enhance accessibility and equity in sexual healthcare, it is essential to design policies that foster non-judgmental care and build trust between SDMM, healthcare providers, and the broader healthcare system.
PT07.07 – Accuracy of Symptom Checker for the Diagnosis of Sexually Transmitted Infections Using Machine Learning and Bayesian Network Algorithms
Dr. Nyi Nyi Soe1,2, Dr. Janet M Towns1,2, Dr. Phyu Mon Latt1,2, Owen Woodberry3, Mark Chung1, Dr. David Lee1, Dr. Jason J Ong1,2, Dr. Eric P.F. Chow1,2,5, Dr. Lei Zhang1,2,4, Dr. Christopher K. Fairley1,2
1Melbourne Sexual Health Centre, Melbourne, Australia.
2School of Translational Medicine, Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, Australia.
3Faculty of Information Technology, Monash Data Futures Institute, Monash University, Melbourne, Australia.
4China-Australia Joint Research Centre for Infectious Diseases, School of Public Health, Xi’an Jiaotong University Health Science Centre, Xi’an, China.
5Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Australia.
Background: Many individuals with STI symptoms delay healthcare, but digital diagnostic tools might encourage earlier visits. Unfortunately, no current tools fully replicate clinical assessments or cover a wide range of STIs.
Methods: Between 2015 and 2018, we invited attendees with STI-related symptoms at Melbourne Sexual Health Centre to complete gender-specific questionnaires about 12 common STIs via a computer-assisted self-interview system. We then developed an online symptom checker (iSpySTI.org) using Bayesian networks. This study evaluated several machine learning (ML) algorithms for predicting STIs and anogenital conditions. We compared the ML algorithms with Bayesian networks for diagnostic accuracy.
Results: The study population included 6,162 men (median age 30, IQR: 26–38) and 4,358 women (median age 27, IQR: 24–31). The most common conditions in men were non-gonococcal urethritis (23.6%), genital warts (11.7%), and balanitis (8.9%). The most common conditions in women were candidiasis (16.6%) and bacterial vaginosis (16.2%). ML models excelled on unseen datasets for most male conditions, with AUCs averaging 0.81 to 0.95, except for UTIs at 0.72. AUCs ranged from 0.75 to 0.95 for female conditions, except for cervicitis at 0.58. Urethral discharge and other urinary symptoms were important features for predicting urethral gonorrhoea, NGU and UTIs. Similarly, participants selected skin images that were similar to their lesions, and the location of the anogenital skin lesions were also strong predictors. The vaginal discharge (odour, colour) and itchiness were important predictors for bacterial vaginosis and candidiasis. The performance of the machine learning models was significantly better than Bayesian models for male balanitis, molluscum contagiosum and genital warts (P < 0.05) but was similar for the other conditions.
Conclusion: Both machine learning and Bayesian models could reasonably predict correct diagnoses. Further work should explore a wider coverage of disease conditions and improvements in diagnostic accuracy.
The AUC for the best performing machine learning models throughout validation, testing and external testing across different diseases.
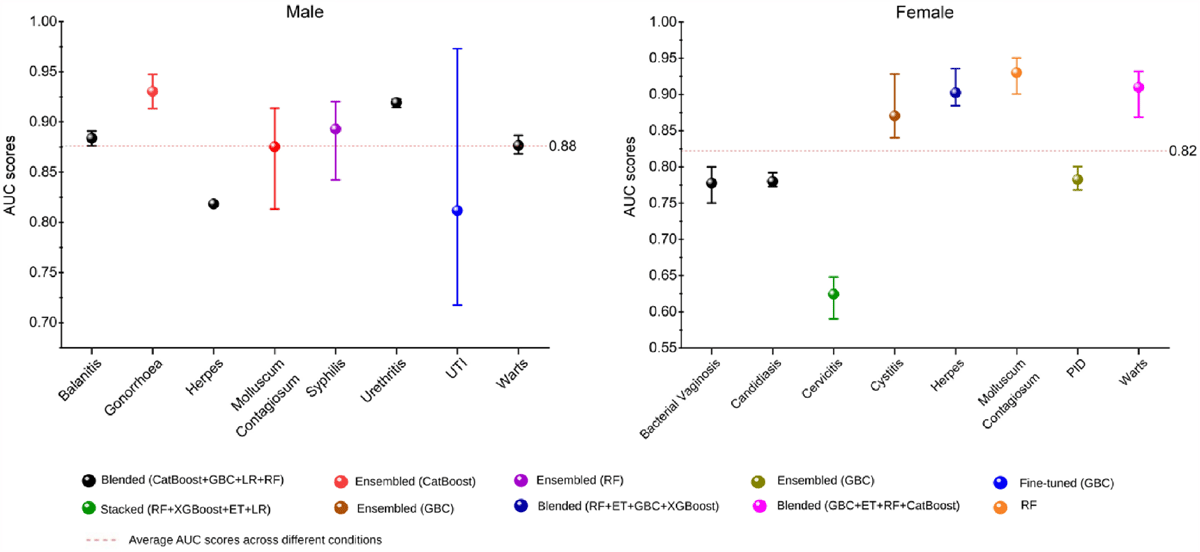
Substantial Increase in the Proportion of Females Who Ever Had Anal Sex over Generations in Canada
Prof. Marc Brisson
Background: Although anal sex has mostly been associated with homosexuality, this practice seems to be increasing among heterosexuals, which would have important public health implications. However, little quantitative data exist to document age-cohort changes in the proportion of heterosexuals that have anal sex. We aimed to examine the evolution of anal sex across generations, among Canadian heterosexual females.
Methods: CONNECT is a pan Canadian population-based study of social/sexual contacts conducted in 2018–2019. Participants were recruited by random digit dialing and data was collected using self-administered online questionnaires. Questionnaires documented sociodemographic, behavioral and sexual characteristics (including insertive/receptive anal sex). Our main analysis focussed on receptive anal sex among heterosexual females. Anal sex among heterosexual/non-heterosexuel males was examined in additional anayses. The main outcome was the proportion of females who ever had receptive anal sex by age (e.g., age 20, 30,., 60 years) by generation (silent generation, baby boomers, and generations X, Y and Z). Sociodemographic and behavioral characteristics associated with ever having anal sex were examined by generation.
Results: The study included 1,288 heterosexual females. The lifetime proportion of females who ever had anal sex increased substantially over generations (Fig. 1). For example, the propropotion of heterosexual females who ever had anal sex by age 20 years was 1% for the silent generation, 3% for baby boomers, 8% for generation X, and >20% for generations Y and Z. Factors associated with ever having anal sex were smoking, alcohol/drug use, and having had an STI. Patterns were similar for heterosexual males, but there were little differences for non-heterosexual males (incertive/receptive) over generations.
Conclusion: Ever having anal sex increased dramatically over generations among Canadian females, with earlier age of initiation. Better understanding the evolution of anal sex behaviours is essential to predict the evolution of STIs linked to this practice, and optimise prevention strategies.
Substantial Rise in Anal Cancer Projected Among Heterosexual Females Due to Increasing Anal Sex Practice Over Generations in Canada: A Modeling Study
Prof. Marc Brisson
Background: The CONNECT study estimated that the percentage of heterosexual females who ever had anal sex (ASex) is increasing in Canada; from 8%/17% by age 30 years among the silent/baby boomer generations, to 34% among generation X to >50% for generation Y. Currently, anal cancer (AC) is rising among females in high income countries. Given the long lag time between HPV infection and AC, current trends are driven by females from the silent/baby boomer generations. The substantial increase in receptive ASex over generations could lead to an accelerated rise in female AC in the next decades. Our aim was to project AC incidence among Canadian females.
Methods: A mathematical model of trends in AC incidence among females was developed, based on 1) trends among heterosexual females who ever had ASex by birth-cohort (CONNECT), and 2) Canadian age-specific trends in AC (Statistics Canada). To reproduce past and project future trends in age-specific AC incidence, key model parameters include: 1) distribution of ASex debut by birth-cohort, 2) time between ASex debut and HPV infection, 3) proportion of infections that progress to AC, and 4) distribution of time from infection to AC. Least squares were used to fit the model to yearly age-specific AC incidence (1992–2017). For projections, sexual behavior of future birth-cohorts was assumed stable. HPV vaccination impact was examined using a best-case scenario, where individuals born after 1995, eligible for vaccination, would be 100% protected against HPV/AC.
Results: The model projects a 3-fold increase in AC incidence among females between 2020 and 2050, which would not be mitigated by HPV vaccination (Fig. 1). In 2050, AC incidence would be comparable to 2017 cervical cancer incidence.
Conclusion: Increased practice of ASex over generations is projected to raise AC incidence substantially amongst females over the next decades. Screening and additional preventive measures should be explored.
SY05.04 – Provincial Surveillance of Mycoplasma Genitalium Antimicrobial Resistance in Québec, Canada: 2018–2022
Brigitte Lefebvre1, Emilie Vallières2,3, Fafard Judith1,2, Shelley Peterson5, Irene Martin5, Anissa Brahami6, Kyle Vaughn Roerick4, Annie-Claude Labbé2,4
1Laboratoire de santé publique du Québec, Institut national de santé publique du Québec, Sainte-Anne-de-Bellevue, Canada.
2Université de Montréal, Montréal, Canada.
3Centre Hospitalier Universitaire (CHU) Sainte-Justine, Montréal, Canada.
4Hôpital Maisonneuve-Rosemont, Montréal, Canada.
5National Microbiology Laboratory (NML), Public Health Agency of Canada (PHAC), Winnipeg, Canada.
6University of Manitoba, Winnipeg, Canada.
Background: This study aims to estimate the prevalence of macrolide resistance mutations (MRM) and quinolone resistance-associated mutations (QRAM) in cases of Mycoplasma genitalium (MG) infections detected in individuals who sought care in various clinical settings in the province of Québec, Canada.
Methods: Between 2018 and 2022, urine or genital swabs were collected from individuals who displayed symptoms compatible with MG infection. These samples were sent to the CHU Sainte-Justine laboratory for testing (in-house real-time PCR assay targeting the pdhD gene). DNA extracts of positive samples were forwarded to the National microbiology laboratory (NML), where sequencing of MRM and QRAM genes (23S rRNA, parC, and gyrA) gene.
Results: Over this period, 5361 samples were tested for MG, of which 711 (13.3%) were positive. MG was three times more prevalent in samples from men (629/3714; 16.9%) than from women (81/1647; 5.0%; p < 0.001). After eliminating duplicates (n = 70) and non-typable results, 631 and 604 samples remained for MRM and QRAM testing, respectively (Table). The most common MRM were 23S rRNA A2058G (n = 233), A2059G (n = 222) and A2058T (n = 44). QRAM found in parC were S83I (n = 102), D87N (n = 9) and S83R (n = 6). QRAM found in gyrA were M95I (n = 9) and D99Y (n = 2). Seven specimens were found to have both parC and gyrA mutations, all of which had the parC S83I mutation.
Conclusion: MRM were found in 80% of samples and QRAM in 21%, higher than reported elsewhere. This can be partly explained by a selection bias since most individuals likely received azithromycin for STI symptom management before being tested for MG. Still, more than 100 individuals (18%) had dual resistance infections, for which no highly effective treatment is readily available. Continued surveillance will be critical to determine if guidelines restricting the use of azithromycin for gonorrhea and chlamydia management will reduce the spread of macrolide-resistant MG.
| Predicted antibiotic resistance | TOTAL n/N (%; 95% CI) | Women n/N (%; 95% CI) | Men n/N (%; 95% CI) | p | |
|---|---|---|---|---|---|
| Azithromycin (MRM) | 506/631 (80.2%; 76.9–83.2) | 56/74 (75.7%; 66.3–85.7) | 450/557 (80.8%; 77.7–84.3) | 0.31 | |
| Moxifloxacin (QRAM) | 128/604 (21.2%; 18.0–24.7) | 7/69 (10.1%; 4.2–19.8) | 121/535 (22.6%; 19.1–26.4) | 0.02 | |
| Both | 109/598 (18.2%; 15.2–21.6) | 7/69 (10.1%; 4.2–19.8) | 102/529 (19.3%; 16.0–22.9) | 0.06 |
SY11.04 – Comparing the Effect of On-site vs Off-site Models of Care on Pre-exposure Prophylaxis (PrEP) Initiation Among People Who Inject Drugs: The M2HepPrEP Trials
Dr. Valérie Martel-Laferrière1, Daniel J Feaster2, Dr. Julie Bruneau1, Yue Pan2, Dr. Hansel Tookes2, Tyler Scott Bartholomew2, Kyle Grealis2, Rania Khemiri1, Iveth Gabriela Yanez2, Lauren K Gooden3, Aïssata Sako1, Lisa Rosen-Metsch3
1Centre de recherche du Centre hospitalier de l’Université de Montréal, Montréal, Canada.
2University of Miami, Miami, United States.
3Columbia University, New York, United States.
Background: As the co-occurring epidemics of HIV and Hepatitis C (HCV) among people who use drugs (PWID) are still ongoing, evaluation of innovative multi-modal approaches, integrating harm reduction, pre-exposure prophylaxis (PrEP), and HCV treatment is required. The aim of this study is to assess the effectiveness of an integrated care model in syringe services programs or opioids agonist therapy (OAT) programs for PrEP initiation among people who inject drugs.
Methods: The Miami-Montreal HCV and PrEP trial (M2HepPrEP) is an open-label, multi-site, multi-center, randomized, controlled, superiority trial. Persons who injected drugs in the prior 6 months and were eligible for PrEP were randomized to either on-site care, with adherence counseling, or referral to off-site clinics assisted by a patient navigator. All participants were offered PrEP and, if interested, were provided with daily, oral tenofovir disoproxil fumarate/emtricitabine (TDF/FTC). PrEP initiation was assessed 6 months post-randomization.
Results: Of 446 enrolled participants (224 off-site; 222 on-site), majority were men (78%), White (82%) and unemployed (85%). In the past month, most commonly injected substances were fentanyl (47% of participants), heroin (39%) and cocaine (30%). PrEP initiation was higher in the on-site arm compared to off-site (23% vs 7%). In logistic regression models, on-site randomization was associated with significantly higher odds of PrEP initiation (OR = 4.2, 95% CI: 2.3–7.8, P < 0.0001). Stratified by site, initiation was higher on-site in Miami (29%) and Montreal (13%) compared to off-site Miami (4%) and Montreal (10%). Significant interaction (P = 0.003) indicated variation in on-site effects by city.
Conclusion: Overall, PrEP initiation was relatively low. On-site delivery significantly increased initiation rates, this effect being driven by Miami. These findings highlight the effectiveness of integrated care models in improving PrEP uptake among PWID and support their implementation in settings where traditional referral approaches may fall short.