Skin health in northern Australia
Hannah M. M. Thomas A * , Stephanie Enkel A B , Tracy McRae A B , Victoria Cox C D , Heather-Lynn Kessaris C , Abbey J. Ford A , Rebecca Famlonga A E , Rebekah Newton A F , Ingrid Amgarth-Duff A , Alexandra Whelan A and Asha C. Bowen A B GA Wesfarmers Centre of Vaccines and Infectious Diseases, Telethon Kids Institute, 15 Hospital Avenue, Nedlands, WA 6009, Australia.
B University of Western Australia, 35 Stirling Highway, Crawley, WA 6009, Australia.
C Royal Darwin Hospital, 105 Rocklands Drive, Tiwi, NT 0810, Australia.
D Menzies School of Health Research, John Matthew Building, Royal Darwin Hospital Campus, Rocklands Drive, Casuarina, NT 0810, Australia.
E Murdoch University, 90 South Street, Murdoch, WA 6150, Australia.
F Royal Perth Hospital, Victoria Square, Perth, WA 6000, Australia.
G Perth Children’s Hospital, 15 Hospital Avenue, Nedlands, WA 6009, Australia.

Dr Hannah M. M. Thomas is an early career postdoctoral researcher at the Wesfarmers Centre of Vaccines and Infectious Diseases, Telethon Kids Institute. Hannah’s research aims to reduce the burden of skin infections for children living in the remote Kimberley region of Western Australia through the implementation of a holistic package of clinical, preventative, and capacity-building skin health interventions. |

Stephanie Enkel is a PhD Candidate at the School of Medicine, University of Western Australia and the Wesfarmers Centre of Vaccines and Infectious Diseases, Telethon Kids Institute. Her research focuses on environmental health initiatives to halt the transmission of Streptococcus pyogenes infection in remote Australian Aboriginal and Torres Strait Islander communities. |

Tracy McRae is a PhD Candidate and Research Assistant at the Telethon Kids Institute. Her research focuses on prevention initiatives to help reduce the burden of skin infections in remote Aboriginal communities. Through this work, Tracy has been working with communities to embed local language into healthy skin resources. |

Dr Victoria Cox is a medical doctor at Royal Darwin Hospital and a PhD student at the Menzies School of Health Research with an interest in Neglected Tropical Diseases with skin manifestations. She undertook the MPhil in Evidence Based Social Intervention and Policy Evaluation at the University of Oxford as a General Sir John Monash Scholar between 2016 and 2018. Victoria is currently working on a collaborative project to estimate the burden of scabies in Indigenous communities and consider the impact of undertaking an ivermectin-based MDA treatment program in northern Australia. |

Dr Heather-Lynn Kessaris is an Alawa and Marra woman from the Northern Territory. She initially completed a Bachelor of Science at the University of Western Australia in 2014, majoring in Population Health and Aboriginal Health and Wellbeing, before going on to complete her Doctor of Medicine in 2018 in Perth, Western Australia. She is currently a resident medical officer based at the Royal Darwin Hospital and has a keen interest in dermatology. |

Abbey J. Ford is a Project Officer on the See, Treat, Prevent Skin Sores and Scabies (SToP) Trial. She works with East Kimberley Aboriginal communities to coordinate data collection visits and run health promotion projects, with the ultimate aim to decrease skin infections in remote communities. |

Rebecca Famlonga is an Aboriginal woman descending from the Wadawurrung people in Southwestern Victoria. She has more than 20 years of experience in Education and has held teaching and leadership positions in secondary schools across Western Australia. Rebecca is currently a Senior Research Officer at the Telethon Kids Institute and is completing her Masters by Research at Murdoch University. |

Dr Rebekah Newton is a Doctor of Medicine graduate from the University of Western Australia, and recipient of the Australian Medical Association WA Prize for 2021. She is an aspiring paediatrician, with a special interest in rural medicine and infectious diseases, and has worked on the SToP Trial to examine the relationship between head lice and impetigo. |

Dr Ingrid Amgarth-Duff is an early-career, postdoctoral researcher at the Telethon Kids Institute in Perth, Western Australia. She is leading the development of the 2nd Edition of the National Healthy Skin Guidelines, which has been developed for treating clinicians. The guidelines focus on the prevention and treatment of skin infections for Aboriginal populations living in remote areas of Australia. |

Alexandra Whelan is Program Manager for the ENDRHD Program at the Telethon Kids Institute, a team of researchers committed to ending Rheumatic Heart Disease (RHD) in Australia. Alexandra manages their portfolio of research, which aims to accelerate research, clinical trials, treatment methods, policy and advocacy; ultimately working to prevent diseases caused by Strep A, including skin infections, which contribute to the development of RHD. |

Associate Professor Asha C. Bowen is a clinician scientist working across the Perth Children’s Hospital as a paediatric infectious disease specialist and the Telethon Kids Institute as Head of the Healthy Skin and ARF Prevention Team and the ENDRHD Program. Asha and her team launched the inaugural National Healthy Skin Guidelines to guide clinicians in the recognition and evidence-based treatment of skin infections, and are updating this resource in 2022. Asha has more than 10 years’ experience leading infectious diseases research and investigator-initiated clinical trials focused on issues significant to Aboriginal child health. |
Microbiology Australia 43(3) 98-103 https://doi.org/10.1071/MA22033
Submitted: 15 June 2022 Accepted: 20 September 2022 Published: 10 October 2022
© 2022 The Author(s) (or their employer(s)). Published by CSIRO Publishing on behalf of the ASM. This is an open access article distributed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND)
Abstract
Achieving healthy skin requires the prevention of infectious diseases that affect the skin. Prevention activities range from environmental health improvements to address inequities in living situations, through to community-wide treatment programs to reduce transmission and improve skin health. In this paper we discuss the pathogens that cause and conditions that arise when skin is infected, the burden of disease in northern Australia, and some of the current research underway to address this high burden, which predominantly affects remote-living Aboriginal and Torres Strait Islander children and families.
Keywords: Aboriginal and Torres Strait Islander populations, environmental health, health promotion, impetigo, infectious diseases, northern Australia, scabies, skin health.
Introduction
The skin is the largest and only externally visible organ of the body, and healthy skin is crucial for holistic physical and social-emotional wellbeing. In remote northern Australia, a variety of skin infections are endemic, which can impact on wellbeing. These include pruritic infections such as scabies, tinea,1 and headlice that can lead to skin disruption and subsequent impetigo.2,3
In remote northern Australia, up to 75% of all community members attend a clinic at least once each year for the treatment of a skin or soft tissue infection,4 and there has been a long history of skin infection programs in individual communities to address this burden. In the Northern Territory (NT) these efforts include scabies mass drug administration (MDA) in Wadeye,5 the East Arnhem Healthy Skin Program6 and, more recently, a focus to prevent skin infections upstream of rheumatic heart disease (RHD) in Maningrida.7 In the Kimberley region of Western Australia (WA), an outbreak of acute post-streptococcal glomerulonephritis (APSGN) from 2013 to 20178,9 has led to a strong focus on healthy skin, and the inclusion of prevention activities alongside diagnosis and treatment in the SToP (See, Treat, Prevent) Trial currently underway.10 In northern Queensland (QLD), several older studies have documented the burden of skin infections,3 with newer work emerging from the Torres Strait.11
Here we summarise the work to date in understanding the burden and control of skin infections in northern Australia and describe a potential road map for future action.
Burden
Impetigo
Impetigo, also known as skin sores, is a frequent diagnosis for children and adults living in remote northern Australia. Impetigo is a bacterial skin infection, and in northern Australia is driven by Streptococcus pyogenes12,13 with Staphylococcus aureus also present independently or as a co-infection at high rates.12 Impetigo begins as a blister that fills with pus, crusts and then eventually heals following re-epithelialisation of the skin surface.14 At any one time, 45% of remote-living Aboriginal children in northern Australia are suffering from impetigo – this is by far the highest documented burden in the world.2,3
Skin infections, predominantly scabies with secondary infection with S. pyogenes and S. aureus, affect many infants in the first month of life, with the median timing of first clinic presentation in the NT at 2 months of age15 and 82% of children presenting to the clinic with an episode of impetigo before 12 months of age.16 In WA skin infections, predominantly impetigo, are the chief reason for presentation to the clinic, with 72% of all children aged 0–5 years presenting at least once each year for skin infections.17 This heavy, early burden of skin infections results in 15% of infants admitted to hospital in the first year of life18 and this early S. pyogenes exposure increases the risk of subsequent acute rheumatic fever (ARF).19 Despite their frequency, skin sores may be ‘normalised’ by clinicians in endemic regions, leading to under-recognition and under-treatment of impetigo in remote Australia.20 Left untreated, bacterial skin infections can become complicated by S. pyogenes and S. aureus sepsis,21 bone and joint infections,22 and pneumonia,23 as well as post-infectious sequelae including acute rheumatic fever (ARF) (and therefore RHD) and acute post streptococcal glomerulonephritis (APSGN)24 (Fig. 1).
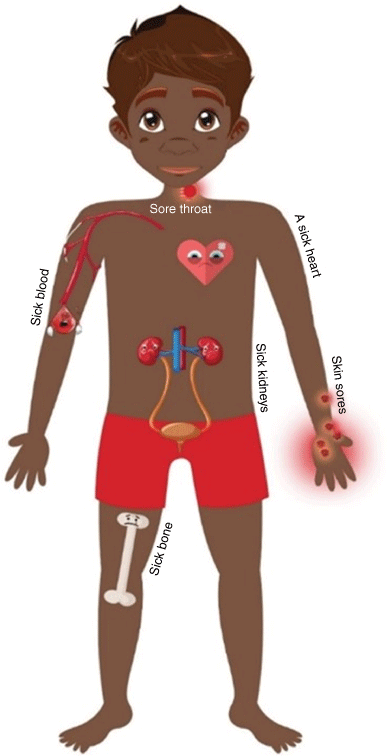
|
Scabies
The scabies mite, Sarcoptes scabiei, is transmitted from human to human, and is endemic in remote northern Australia. Remote Australian children have some of the highest reported rates of scabies in the world,25 with up to 35% of children affected at any time.2 Scabies infestations can also be complicated by bacterial skin infectious, with common pathogens including S. pyogenes and S. aureus.
Attempts to control scabies through MDA of permethrin5,26 and ivermectin27 have been somewhat successful, but not sustained. Recently, community engagement in consideration of scabies treatment with an ivermectin mass drug administration approach has been important, and this has informed the recent change to make ivermectin available across Australia for first line treatment of scabies in Aboriginal or Torres Strait Islander people.28 More recently, mathematical modelling has shown that up to seven rounds of MDA in a community might be required for sustained impact29 – an approach that has not been trialled to date in Australia or globally.
In a hospital study in WA, no children with scabies were identified in a retrospective chart review, compared to 8% of children who were prospectively assessed for skin conditions when admitted to hospital.20 This demonstrates that normalisation of scabies by health care providers may be a contributory factor to the ongoing burden, with education and training packages that can be accessed through the National Healthy Skin Guidelines30 a key strategy to address this normalisation among healthcare workers. Similarly, the SToP Trial10 has been designed to deliver the continuity of training required for healthcare workers in a heavy burden context. Empowering families as well as Aboriginal health workers to work alongside families and support access to culturally informed diagnosis, treatment and prevention activities will be key to successful change. With this in mind, further resources are available in the National Healthy Skin Guideline community care workers manual.
Crusted scabies in all age groups may be a critical contributor to the heavy burden of classical scabies in young children due to stigma, ‘shame’, under-diagnosis, and frequent recurrences.31 Crusted scabies is notifiable in the Northern Territory,32 and considerable progress has been made in improving recognition, treatment, and facilitating a ‘scabies-free environment’ approach for those affected with crusted scabies to reduce recurrences.33 Crusted scabies may be less common in other states of Australia, but there is limited data available to confirm this, as it is not a notifiable disease in WA or QLD.
Tinea
Tinea is a pruritic, scaly skin condition transmitted from human to human. Alternatively, it can also be acquired from the environment1 or household pets,34 and in northern Australia is caused by Microsporum spp. and Trichophyton spp. Estimates of the tinea burden in northern Australia are not well established;1 however, tinea was recorded in 7% of children prospectively assessed for skin infections on admission to hospital in WA,20 and 4.3% of participants had skin sores associated with tinea in the Skin Sore Trial conducted across the NT.13
Kerion, onychomycosis, and other complications of tinea are well documented,35 but may be misclassified as they are frequently under-recognised. Similar to bacterial skin infections, ‘normalisation’ of fungal infections by clinicians has also been noted in remote Australia.20 As with other pruritic skin conditions, tinea predisposes to bacterial skin infections and the other sequelae previously mentioned, can be stigmatised, and is challenging to treat.
Head lice
The head louse is a hematophagous ectoparasite, Pediculus humanus capitis, readily transmitted by direct head-to-head contact. In Australia, head lice is the third most commonly reported outbreak in day-care centres and schools, with rates of up to 35% reported in school-aged children.36 There are no published studies on the prevalence of head lice in remote Australia; however, the SToP Trial is measuring this burden in remote Kimberley communities of WA.10 Breaks in the epidermis due to intense itching from head lice can be complicated by secondary bacterial infection37 and have been known to cause severe impetigo of the scalp in remote-living Australian Aboriginal children.38 In this way, ectoparasitic diseases like headlice and scabies can predispose to S. pyogenes infection and post-infectious complications, such as glomerulonephritis and rheumatic fever.39
Less common skin infections
Other skin infections occur with less frequency but remain present in northern Australia. Leprosy, a chronic granulomatous infection characterised by anaesthetic skin lesions and caused by Mycobacterium leprae, is diagnosed infrequently in Australia but remains at the highest burden in remote-living Aboriginal and Torres Strait Islander Australians.40 Buruli ulcer is a neglected tropical skin disease which leads to skin and soft tissue destruction, predominantly on the lower limbs, after infection with slow-growing Mycobacterium ulcerans. This is endemic in coastal regions in south-east Victoria and in Far North Queensland but is uncommon in Western Australia and in the Northern Territory.41
The road to healthy skin
We offer guidance on treatment for skin infections in remote settings in the Australian National Healthy Skin Guidelines;30 however, strengths-based, integrated, Aboriginal community-led and co-designed programs across the region will be required to comprehensively address the heavy burden of skin infections in northern Australia. In order to be successful, these programs must be informed by timely and consistent estimations of disease burden, give attention to the social and environmental determinants of health which underpin this burden, and employ holistic approaches to public health intervention which empower and support individuals and communities to improve health outcomes.
A contemporary understanding of prevalence to inform public health action
Studies of skin infection burden across northern Australia over the last few decades have been intermittent and community-based.3 While this has informed community-based interventions,5,27,42 broader regional skin disease control is needed. The prototype for this has been the East Arnhem Healthy Skin program6 in the NT and, more recently, the SToP Trial in WA;10 however, both are limited to small regions within their respective jurisdictions. Ongoing Aboriginal- and community-led skin burden studies across the entire northern region of Australia are crucial to inform skin disease control, improve quality of life and reduce the downstream consequences.
However, the barriers of remote distance and competing heavy burdens of chronic disease (further exacerbated by events such as the recent pandemic) make ongoing assessment of skin infection prevalence in remote regions of northern Australia challenging. The development and validation of accurate, sustainable, and community-led mechanisms to determine skin infection prevalence will be key to a contemporary understanding of the burden of these diseases, which is in turn crucial to advocate for and monitor the success of public health interventions. Empowering community-based health workers to facilitate skin assessments may be a way forward, such as described by Tsoi et al. in Fiji and the Solomon Islands,43 and work is under way to explore the cultural security and accuracy of this approach in northern Australia. While prevalence studies can be informative to disease control, primordial prevention by addressing housing, environmental, and other determinants of health remains critical.
Environmental health
Environmental health occurs at the interface between humans and the broader environment in which we live.44 It is a strong determinant of health, including skin health, existing within a socio-ecological model whereby external factors constrain and limit an individual’s health behaviours. Colonisation and historical polices and determinants of health have impeded Aboriginal peoples’ rights to access safe, effective, and culturally responsive healthcare and housing.45 For populations in remote Australia, this has led to overcrowding, inadequate housing, and limited access to functional and regularly repaired health hardware (e.g. showers, washing machines) and software (e.g. soap, towels) in the home. To make real change, researchers and policy-makers must look beyond reducing overcrowding only through the provision of new housing stock, and instead invest in co-designed environmental health initiatives with significant community input to achieve the Healthy Living Practices.46 Recent and ongoing work in WA and the NT suggests that the focus should be placed on functional hand and body washing facilities, functional washing machines, and regular maintenance cycles for housing as essential strategies to improve skin health, with additional benefits for other infectious diseases.47
Health promotion
As part of a holistic approach to addressing skin infections, health promotion and prevention programs must be developed using a ground-up approach, to ensure they are meaningful to the environment in which they are implemented.48 Approaching biomedical science from an Aboriginal cultural standpoint has the potential to transcend traditional Western prevention programs and create inclusive, empowering, and contemporary methods of promoting health and wellbeing.49 Embedding of culture, language, and Aboriginal peoples’ voices specific to the target communities within health messaging is likely to increase engagement and improve sustainability,50 and this has been shown in previous work to improve the diagnosis, treatment, and prevention of a range of diseases in northern Australia including wet cough,51 RHD52 and skin infections.53 In the Kimberley region of WA, work is underway in partnership with remote Aboriginal communities to co-design and implement culturally appropriate healthy skin resources.10 At the request of community Elders, local language and culture are embedded within these resources with an aim to reduce the burden of skin infections. Moving forwards, initiatives to promote healthy skin across northern Australia will require this multifocal lens, with Aboriginal people’s worldviews and ways of knowing, being, and doing central to the narratives and messaging of programs.
Conclusions
Skin infections remain a longstanding challenge across northern Australia, predominantly affecting Aboriginal children and families. While prevalence assessments followed by community-wide treatment is one approach to address this, more comprehensive co-designed and community-led programs with attention to the environments in which people live, achieving the healthy living practices, and culturally informed health promotion will be critical to achieve real change.
Data availability
Data sharing is not applicable as no new data were generated or analysed during this study.
Conflicts of interest
The authors declare no conflicts of interest.
Declaration of funding
This research did not receive any specific funding.
Acknowledgements
The authors acknowledge the Nyoongar Wadjuk, Yawuru, Kariyarra and Kaurna Elders, their people, and their land upon which the Telethon Kids Institute is located, as well as the traditional owners of the lands across northern Australia.
References
[1] Currie, BJ and Carapetis, JR (2000) Skin infections and infestations in Aboriginal communities in northern Australia. Australas J Dermatol 41, 139–143.| Skin infections and infestations in Aboriginal communities in northern Australia.Crossref | GoogleScholarGoogle Scholar |
[2] Bowen, AC et al.. (2015) The global epidemiology of impetigo: a systematic review of the population prevalence of impetigo and pyoderma. PLoS One 10, e0136789.
| The global epidemiology of impetigo: a systematic review of the population prevalence of impetigo and pyoderma.Crossref | GoogleScholarGoogle Scholar |
[3] Davidson, L et al.. (2020) Skin infections in Australian Aboriginal children: a narrative review. Med J Aust 212, 231–237.
| Skin infections in Australian Aboriginal children: a narrative review.Crossref | GoogleScholarGoogle Scholar |
[4] Thomas, L et al.. (2019) Burden of skin disease in two remote primary healthcare centres in northern and central Australia. Intern Med J 49, 396–399.
| Burden of skin disease in two remote primary healthcare centres in northern and central Australia.Crossref | GoogleScholarGoogle Scholar |
[5] Wong, L-CF et al.. (2001) Outcome of an interventional program for scabies in an Indigenous community. Med J Aust 175, 367–370.
| Outcome of an interventional program for scabies in an Indigenous community.Crossref | GoogleScholarGoogle Scholar |
[6] Andrews, RM et al.. (2009) A regional initiative to reduce skin infections amongst Aboriginal children living in remote communities of the Northern Territory, Australia. PLoS Negl Trop Dis 3, e554.
| A regional initiative to reduce skin infections amongst Aboriginal children living in remote communities of the Northern Territory, Australia.Crossref | GoogleScholarGoogle Scholar |
[7] Francis, JR et al.. (2020) Hyperendemic rheumatic heart disease in a remote Australian town identified by echocardiographic screening. Med J Aust 213, 118–123.
| Hyperendemic rheumatic heart disease in a remote Australian town identified by echocardiographic screening.Crossref | GoogleScholarGoogle Scholar |
[8] Speers, DJ et al.. (2017) M protein gene (emm type) analysis of group A Streptococcus isolates recovered during an acute glomerulonephritis outbreak in northern Western Australia. Pathology 49, 765–769.
| M protein gene (emm type) analysis of group A Streptococcus isolates recovered during an acute glomerulonephritis outbreak in northern Western Australia.Crossref | GoogleScholarGoogle Scholar |
[9] Custodio, J et al.. (2016) Working in partnership with communities at risk: the potential of integrated public health action during an outbreak of APSGN in remote Australia. Aust Indig Health Bull 16, .
[10] Mullane, MJ et al.. (2019) SToP (See, Treat, Prevent) skin sores and scabies trial: study protocol for a cluster randomised, stepped-wedge trial for skin disease control in remote Western Australia. BMJ Open 9, e030635.
| SToP (See, Treat, Prevent) skin sores and scabies trial: study protocol for a cluster randomised, stepped-wedge trial for skin disease control in remote Western Australia.Crossref | GoogleScholarGoogle Scholar |
[11] Kris, E et al.. (2021) Breathing life into community-driven research in the Torres Strait. Med J Aust 215, 304–304.e1.
| Breathing life into community-driven research in the Torres Strait.Crossref | GoogleScholarGoogle Scholar |
[12] Bowen, AC et al.. (2014) The microbiology of impetigo in Indigenous children: associations between Streptococcus pyogenes, Staphylococcus aureus, scabies, and nasal carriage. BMC Infect Dis 14, 727.
| The microbiology of impetigo in Indigenous children: associations between Streptococcus pyogenes, Staphylococcus aureus, scabies, and nasal carriage.Crossref | GoogleScholarGoogle Scholar |
[13] Bowen, AC et al.. (2014) Short-course oral co-trimoxazole versus intramuscular benzathine benzylpenicillin for impetigo in a highly endemic region: an open-label, randomised, controlled, non-inferiority trial. Lancet 384, 2132–2140.
| Short-course oral co-trimoxazole versus intramuscular benzathine benzylpenicillin for impetigo in a highly endemic region: an open-label, randomised, controlled, non-inferiority trial.Crossref | GoogleScholarGoogle Scholar |
[14] Bowen, AC et al.. (2014) Standardising and assessing digital images for use in clinical trials: a practical, reproducible method that blinds the assessor to treatment allocation. PLoS One 9, e110395.
| Standardising and assessing digital images for use in clinical trials: a practical, reproducible method that blinds the assessor to treatment allocation.Crossref | GoogleScholarGoogle Scholar |
[15] Clucas, DB et al.. (2008) Disease burden and health-care clinic attendances for young children in remote Aboriginal communities of northern Australia. Bull World Health Organ 86, 275–281.
| Disease burden and health-care clinic attendances for young children in remote Aboriginal communities of northern Australia.Crossref | GoogleScholarGoogle Scholar |
[16] McMeniman, E et al.. (2011) Skin disease in the first two years of life in Aboriginal children in East Arnhem Land. Australas J Dermatol 52, 270–273.
| Skin disease in the first two years of life in Aboriginal children in East Arnhem Land.Crossref | GoogleScholarGoogle Scholar |
[17] Hendrickx, D et al.. (2018) Ascertaining infectious disease burden through primary care clinic attendance among young Aboriginal children living in four remote communities in Western Australia. PLoS One 13, e0203684.
| Ascertaining infectious disease burden through primary care clinic attendance among young Aboriginal children living in four remote communities in Western Australia.Crossref | GoogleScholarGoogle Scholar |
[18] Abdalla, T et al.. (2017) Hospital admissions for skin infections among Western Australian children and adolescents from 1996 to 2012. PLoS One 12, e0188803.
| Hospital admissions for skin infections among Western Australian children and adolescents from 1996 to 2012.Crossref | GoogleScholarGoogle Scholar |
[19] McDonald, M et al.. (2004) Acute rheumatic fever: a chink in the chain that links the heart to the throat? Lancet Infect Dis 4, 240–245.
| Acute rheumatic fever: a chink in the chain that links the heart to the throat?Crossref | GoogleScholarGoogle Scholar |
[20] Yeoh, DK et al.. (2017) Are scabies and impetigo “normalised”? A cross-sectional comparative study of hospitalised children in northern Australia assessing clinical recognition and treatment of skin infections. PLoS Negl Trop Dis 11, e0005726.
| Are scabies and impetigo “normalised”? A cross-sectional comparative study of hospitalised children in northern Australia assessing clinical recognition and treatment of skin infections.Crossref | GoogleScholarGoogle Scholar |
[21] Skull, SA et al.. (1999) Investigation of a cluster of Staphylococcus aureus invasive infection in the Top End of the Northern Territory. Aust NZ J Med 29, 66–72.
| Investigation of a cluster of Staphylococcus aureus invasive infection in the Top End of the Northern Territory.Crossref | GoogleScholarGoogle Scholar |
[22] Brischetto, A et al.. (2016) A retrospective case-series of children with bone and joint infection from Northern Australia. Medicine (Baltimore) 95, e2885.
| A retrospective case-series of children with bone and joint infection from Northern Australia.Crossref | GoogleScholarGoogle Scholar |
[23] Engelman, D et al.. (2014) Invasive Staphylococcus aureus infections in children in tropical northern Australia. J Pediatric Infect Dis Soc 3, 304–311.
| Invasive Staphylococcus aureus infections in children in tropical northern Australia.Crossref | GoogleScholarGoogle Scholar |
[24] Oliver, J et al.. (2021) Preceding group A streptococcus skin and throat infections are individually associated with acute rheumatic fever: evidence from New Zealand. BMJ Glob Health 6, e007038.
| Preceding group A streptococcus skin and throat infections are individually associated with acute rheumatic fever: evidence from New Zealand.Crossref | GoogleScholarGoogle Scholar |
[25] Romani, L et al.. (2015) Prevalence of scabies and impetigo worldwide: a systematic review. Lancet Infect Dis 15, 960–967.
| Prevalence of scabies and impetigo worldwide: a systematic review.Crossref | GoogleScholarGoogle Scholar |
[26] Wong, L-C et al.. (2002) Factors supporting sustainability of a community-based scabies control program. Australas J Dermatol 43, 274–277.
| Factors supporting sustainability of a community-based scabies control program.Crossref | GoogleScholarGoogle Scholar |
[27] Kearns, TM et al.. (2015) Impact of an ivermectin mass drug administration on scabies prevalence in a remote Australian Aboriginal community. PLoS Negl Trop Dis 9, e0004151.
| Impact of an ivermectin mass drug administration on scabies prevalence in a remote Australian Aboriginal community.Crossref | GoogleScholarGoogle Scholar |
[28] Australian Government Department of Health (2022) The Pharmaceutical Benefits Scheme. https://www.pbs.gov.au/pbs/home
[29] Lydeamore, MJ et al.. (2019) A biological model of scabies infection dynamics and treatment informs mass drug administration strategies to increase the likelihood of elimination. Math Biosci 309, 163–173.
| A biological model of scabies infection dynamics and treatment informs mass drug administration strategies to increase the likelihood of elimination.Crossref | GoogleScholarGoogle Scholar |
[30] The Australian Healthy Skin Consortium (2018) National Healthy Skin Guideline: for the Prevention, Treatment and Public Health Control of Impetigo, Scabies, Crusted Scabies and Tinea for Indigenous Populations and Communities in Australia. 1st edn, Telethon Kids Institute, Perth, Western Australia.
[31] Lokuge, B et al.. (2014) Crusted scabies in remote Australia, a new way forward: lessons and outcomes from the East Arnhem Scabies Control Program. Med J Aust 200, 644–648.
| Crusted scabies in remote Australia, a new way forward: lessons and outcomes from the East Arnhem Scabies Control Program.Crossref | GoogleScholarGoogle Scholar |
[32] Hasan, T et al.. (2020) Crusted scabies; a 2-year prospective study from the Northern Territory of Australia. PLoS Negl Trop Dis 14, e0008994.
| Crusted scabies; a 2-year prospective study from the Northern Territory of Australia.Crossref | GoogleScholarGoogle Scholar |
[33] OneDisease (2021) Annual report 2020–2021.
[34] Cafarchia, C et al.. (2006) Isolation of Microsporum canis from the hair coat of pet dogs and cats belonging to owners diagnosed with M. canis tinea corporis. Vet Dermatol 17, 327–331.
| Isolation of Microsporum canis from the hair coat of pet dogs and cats belonging to owners diagnosed with M. canis tinea corporis.Crossref | GoogleScholarGoogle Scholar |
[35] Nguyen, T et al.. (2020) Case report: scald burn to the scalp complicated by fungal kerion. Burns Open 4, 191–193.
| Case report: scald burn to the scalp complicated by fungal kerion.Crossref | GoogleScholarGoogle Scholar |
[36] Grieve, K et al.. (2007) A randomised, double-blind, comparative efficacy trial of three head lice treatment options: malathion, pyrethrins with piperonyl butoxide and MOOV Head Lice Solution. Aust Pharmacist 26, 738–743.
[37] Amanzougaghene, N et al.. (2020) Where are we with human lice? A review of the current state of knowledge. Front Cell Infect Microbiol 9, 474.
| Where are we with human lice? A review of the current state of knowledge.Crossref | GoogleScholarGoogle Scholar |
[38] Cook, S et al.. (2007) Headlice: a precursor to Group A Streptococcal infection in remote Indigenous children. Prim Intention Aust J Wound Manage 15, 181–184.
| Headlice: a precursor to Group A Streptococcal infection in remote Indigenous children.Crossref | GoogleScholarGoogle Scholar |
[39] Currie, MJ et al.. (2010) A pilot study of the use of oral ivermectin to treat head lice in primary school students in Australia. Pediatr Dermatol 27, 595–599.
| A pilot study of the use of oral ivermectin to treat head lice in primary school students in Australia.Crossref | GoogleScholarGoogle Scholar |
[40] Hempenstall, A et al.. (2019) Leprosy in Far North Queensland: almost gone, but not to be forgotten. Med J Aust 211, 182–183.
| Leprosy in Far North Queensland: almost gone, but not to be forgotten.Crossref | GoogleScholarGoogle Scholar |
[41] O’Brien, DP et al.. (2000) Nontuberculous mycobacterial disease in northern Australia: a case series and review of the literature. Clin Infect Dis 31, 958–967.
| Nontuberculous mycobacterial disease in northern Australia: a case series and review of the literature.Crossref | GoogleScholarGoogle Scholar |
[42] Carapetis, JR et al.. (1995) Skin sores in Aboriginal children. J Paediatr Child Health 31, 563.
| Skin sores in Aboriginal children.Crossref | GoogleScholarGoogle Scholar |
[43] Tsoi, SK et al.. (2021) Estimation of scabies prevalence using simplified criteria and mapping procedures in three Pacific and southeast Asian countries. BMC Public Health 21, 2060.
| Estimation of scabies prevalence using simplified criteria and mapping procedures in three Pacific and southeast Asian countries.Crossref | GoogleScholarGoogle Scholar |
[44] World Health Organization (2021) Environment, Climate Change and Health.
[45] United Nations General Assembly (2011) United Nations Declaration on the Rights of Indigenous Peoples.
[46] Healthabitat (2019) The Healthy Living Practices.
[47] McLoughlin, F et al.. (2022) Skin health situational analysis to inform skin disease control programs for the Kimberley. Med J Aust 217, 58.
| Skin health situational analysis to inform skin disease control programs for the Kimberley.Crossref | GoogleScholarGoogle Scholar |
[48] Thomas, S et al.. (2017) Reducing recurrence of bacterial skin infections in Aboriginal children in rural communities: new ways of thinking, new ways of working. Aust J Prim Health 23, 229–235.
| Reducing recurrence of bacterial skin infections in Aboriginal children in rural communities: new ways of thinking, new ways of working.Crossref | GoogleScholarGoogle Scholar |
[49] Brown, AD et al.. (2006) Uncovering the determinants of cardiovascular disease among Indigenous people. Ethn Health 11, 191–210.
| Uncovering the determinants of cardiovascular disease among Indigenous people.Crossref | GoogleScholarGoogle Scholar |
[50] Bond, C et al.. (2012) ‘It had to be my choice’ Indigenous smoking cessation and negotiations of risk, resistance and resilience. Health Risk Soc 14, 565–581.
| ‘It had to be my choice’ Indigenous smoking cessation and negotiations of risk, resistance and resilience.Crossref | GoogleScholarGoogle Scholar |
[51] Laird, P et al.. (2020) We won’t find what we don’t look for: identifying barriers and enablers of chronic wet cough in Aboriginal children. Respirology 25, 383–392.
| We won’t find what we don’t look for: identifying barriers and enablers of chronic wet cough in Aboriginal children.Crossref | GoogleScholarGoogle Scholar |
[52] Haynes, E et al.. (2019) Community-based participatory action research on rheumatic heart disease in an Australian Aboriginal homeland: evaluation of the ‘On track watch’ project. Eval Program Plann 74, 38–53.
| Community-based participatory action research on rheumatic heart disease in an Australian Aboriginal homeland: evaluation of the ‘On track watch’ project.Crossref | GoogleScholarGoogle Scholar |
[53] Shield, JM et al.. (2018) Cross-cultural, Aboriginal language, discovery education for health literacy and informed consent in a remote Aboriginal community in the Northern Territory, Australia. Trop Med Infect Dis 3, 15.
| Cross-cultural, Aboriginal language, discovery education for health literacy and informed consent in a remote Aboriginal community in the Northern Territory, Australia.Crossref | GoogleScholarGoogle Scholar |