New digital media interventions for sexual health promotion among young people: a systematic review
Erin Wadham A , Clare Green A , Joseph Debattista B , Shawn Somerset A C and Adem Sav A D E
A D E
A School of Allied Health, Australian Catholic University, Banyo, Qld 4014, Australia.
B Metro North Public Health Unit, Metro North Hospital and Health Service, Bryden Street, Windsor, Qld 4030, Australia.
C Present address: Faculty of Health, University of Canberra, 11 Kirinari Street, Bruce, ACT 2617, Australia.
D School of Public Health and Social Work, Queensland University of Technology, Kelvin Grove, Qld 4059, Australia.
E Corresponding author. Email: adem.sav@qut.edu.au
Sexual Health 16(2) 101-123 https://doi.org/10.1071/SH18127
Submitted: 4 July 2018 Accepted: 22 November 2018 Published: 1 March 2019
Journal Compilation © CSIRO 2019 Open Access CC BY-NC-ND
Abstract
New digital media platforms (e.g. social networking sites, web pages and text messaging) have dramatically changed interpersonal communication and present novel opportunities for health interventions. Due to the high uptake and use of digital media among young people, advances in digital media provide potential new opportunities in delivering health interventions to this audience to reduce sexually transmissible infection (STI) risk. The aim of this study was to assess the effectiveness of sexual health interventions delivered via new digital media to young people (aged 13–24 years). A systematic search was conducted of seven databases for peer-reviewed literature published between January 2010 and April 2017 that evaluated a sexual health intervention delivered to young people (aged 13–24 years). Of 2017 papers reviewed, 25 met the inclusion criteria and were assessed. Sixteen studies used web-based platforms to deliver their intervention. A large proportion of studies (11/25) specifically focused on HIV prevention. Seven studies found a statistically significant effect of the intervention on knowledge levels regarding the prevention HIV and other STI, as well as general sexual health knowledge, but only one-fifth of interventions evaluating intentions to use condoms reported significant effects due to the intervention. Nine studies focused on individuals from an African American background. Although new media has the capacity to expand efficiencies and coverage, the technology itself does not guarantee success. It is essential that interventions using new digital media have high-quality, evidence-based content that engages with individual participants.
Additional keywords: adolescent, teenager, social media.
Introduction
New digital media, such as text messaging, web pages, social networking sites (SNS) and location-based social mobile applications, have changed information sharing and communication substantially.1 ‘New digital media’ refers to any user-controlled and shareable and interactive forms of communication.1 The rise in the use of new digital media is particularly common among adolescents and young adults worldwide. For example, adolescents (aged 10–19 years) account for 35% of China’s 298 million Internet users,1 whereas in the US, 97% of Americans aged 18–29 years use the Internet on a regular basis.2 In particular, the use of mobile phones is ostensibly ubiquitous across many populations within developed countries. The anonymity, convenience and accessibility afforded by text messaging, web access and video streaming provides significant potential for innovative interventions to reach communities and individuals otherwise disconnected from mainstream services.3–5
One particular health issue that is of great importance to young people, and one that has been targeted using digital media, is sexual health and sexually transmissible infections (STIs). Today, numerous education interventions, using websites, short message services (SMS) and social networking sites, have been developed to modify the sexual health knowledge and behaviours of adolescents and young adults.1 The high level of use among youth and adolescents has made new digital media a promising delivery mode for sexual health interventions.
Young people are at high risk of contracting STIs due to increased propensity for risk taking behaviour, impulsivity and experimentation, and greater vulnerability through reduced access to information, services, power and social engagement.6,7 The popularity of digital technologies, particularly smartphones, as the often preferred mode for accessing the Internet among this demographic raises the potential for new media to shape the development of targeted sexual health promotion and public health initiatives.5
Such technologies enable rapid, inexpensive, highly reproducible and widespread coverage of interventions, allowing for evidence-based programs to be adapted to digital platforms, precisely directed at individuals through interactive, custom-designed interfaces without increasing demands on staffing or training. Digitised programs provide for greater anonymity, repetition, temporal flexibility and client sensitivity, and appeal to a variety of learning needs. They can be easily updated and adapted to particular social and demographic needs, which have been demonstrated across the age range 12–30 years.7,8 Further, social media and Internet-facilitated communication have enabled the establishment of virtual communities whereby young adults, particularly those often marginalised by society, have the freedom and anonymity to share experiences, learn about sex, initiate meaningful and casual sexual and social relationships and connect with wider networks.9 The ease, speed and geographical coverage of such networks poses both great challenges for infection control and great promise for health promotion.
Although digital media is recognised as a new and important health communication tool, there is little published evidence about the overall effectiveness of sexual health interventions delivered via new digital media. As with many other prevention interventions, digital platforms have sought to enhance knowledge, increase intentions to use condoms and communicate condom use with partners, improve attitudes to condom use and safer sex, increase self-efficacy and the ability to use condoms, practice safer sex and affect perceived vulnerability to infection. These variables are strongly predictive of consistent condom use and safer sex practice.7 However, despite evidence of the effectiveness of new digital media interventions to modify sexual health knowledge, attitudes and behavioural intentions of adolescents, demonstrated longer-term behaviour change is more limited.1
Nonetheless, new digital media continues to attract great interest for its significant population reach, attractiveness for young people, interactive features, efficiency at disseminating messages and connectivity between and within communities of peers.6,10 A systematic review by Guse et al.1 found that digital media interventions had significant potential to enhance the sexual health knowledge of adolescents or young adults (aged 13–24 years), particularly in relation to HIV and other STIs. Like many authors, Guse et al.1 advocated for the great potential of digital media to engage and support youth sexual health.
The review by Guse et al.1 was conducted at a time when the use of digital media was only emerging. Since 2011 there has been a further increase in the use of digital media and an emerging body of literature using digital media interventions for sexual health promotion among adolescents and young adults. The primary aim of this systematic review was to assess the current effectiveness of new digital media interventions to enhance sexual health in those aged 13–24 years. The findings will be beneficial to both researchers and clinicians in designing effective digital media interventions that focus on sexual and other health issues among adolescent and young adult populations.
Methods
Literature search
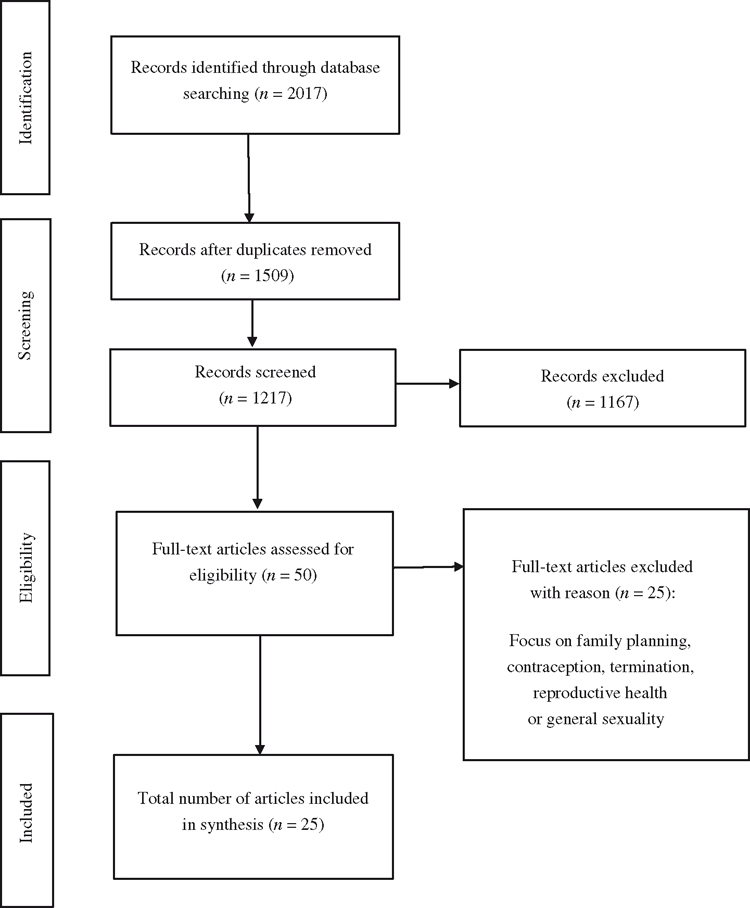
This systematic review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. All researchers built up a search strategy, which incorporated different keywords, their synonyms and various spellings. A search was conducted of peer-reviewed literature published between January 2010 and April 2017 to identify articles that provided an evaluation of a sexual health intervention delivered to young people (aged 13–24 years) through a new digital media platform. In order to gather a range of literature, databases and search terms were identified based on their relevance to the search topic. Seven databases were interrogated: Cumulative Index to Nursing and Allied Health Literature (CINAHL), Medline, PsycINFO, SocINDEX, Informit, PubMed and Scopus. Due to inconsistent definitions, broad search terms were used. Each database search was conducted by combining terms into three separate categories: population (adolescen*, teen*,youth*, ‘young adult*’), intervention (‘social media’, ‘social network*’, SNS, internet*, ‘digital media*’, ‘mobile phone*’, ‘cell* phone*’, ‘text messag*’, technolog*, new media*’, Online*, Web*) and outcome (‘sex* health’, ‘sex* behaviour*’, ‘sex* behavior*’, ‘sex* knowledge’, ‘sex* attitude*’, ‘attitude* to* sex*’, ‘knowledge of sex*’, ‘sex* understand*’, ‘sex* education*’). Where possible, database-specific terms, such as MeSH (PubMed) and CINAHL headings, were supplemented with similar terms and phrases. The literature search and studies included in this systematic review are shown in Fig. 1.
Inclusion and exclusion criteria
In all, 2017 papers were identified through seven electronic databases and processed using Endnote X7 software (Clarivate Analytics, Philadelphia, PA, USA). After duplicates were removed, eligible papers were independently identified by two authors (EW, CG) based on titles and abstracts being read against inclusion criteria. Papers were included in the review if a substantial number of participants were aged 13–24 years and the paper described an evaluation of the effect of an intervention on sexual health knowledge, attitudes and/or behaviours. Studies were included only if 50% or more of the sample size comprised participants in the defined age group. In addition, papers that evaluated the feasibility, useability and acceptability of new digital media interventions on sexual health were included. In addition, to be eligible for inclusion, papers had to be full text, peer reviewed and published in the English language. Editorials, conference papers and other non-peer-reviewed publications were excluded. Because the purpose of the present review relates primarily to communicable disease, papers that focused on gender and sexual identity, family planning and sexual dysfunction were also excluded.
If eligibility was unclear, the study was retained for a second evaluation by another reviewer (AS). During the second stage, the full text of each included study was reviewed to confirm eligibility. Disagreements on eligibility were assessed by a third reviewer (AS) to determine the final decision regarding eligibility. Data from the included papers were extracted using a standardised pro forma, which collected data on year of publication, authors, country, study design, participant number, population, aim and type of intervention, outcome measures, evaluation methodology, overall results, reported facilitators and barriers and study limitations. Furthermore, these study outcomes were classified into different themes with a range of subcategories within each theme: (1) behaviour (number of sexual partners, number of unprotected sexual acts, frequency of condom use, negotiation skills for condom use, sex under the influence of alcohol and other drugs, testing seeking behaviour); (2) Self-efficacy (condom use); (3) Skills and Abilities (sexual communication and risk assessment); (4) Intentions (to use condoms); (5) Attitudes; (6) Knowledge (HIV, STI, general sexual health); (7) Efficacy of the Intervention (feasibility, acceptability, usability, satisfaction); and (8) Well-being (mental health, sexuality, self-acceptance). Appendix 1 provides a summary of the studies (n = 25) included in the systematic review.
Results
Population of interest
There was substantial variability among the studies in relation to setting, sexual preferences, recruitment methods and outcomes measured. Although 16 of 25 studies recruited subjects either from an education setting (n = 7;7,11–16 e.g. high schools, middle schools and universities) or a health setting (n = 9;3–5,8,17–21 including sexual health clinics and hospitals), the remaining nine studies were defined by the recruitment method rather than a particular physical setting. These nine studies recruited participants directly online through new digital media, such as Facebook or location-based social mobile applications.4,8–10,13,22–26 Many of the studies used multiple methods of recruitment, with some (6/25)4,5,9,12,14,15 extending the reach of recruitment through the use of shopping mall and community notice boards, and through collaboration with community-based organisations.5,6,15 One study recruited participants purposively from a larger related study.27
Most (22/25) of the included studies were conducted in industrialised country settings. Within the US, African American communities were the primary focus.3,4,7,8,12,17,20,21,27 One intervention was delivered to a Latino/Hispanic population.13 The three studies conducted in low- to middle-income countries were based in Chile, Uganda and Thailand.11,15,20
Sexual identity and preference were also used as a basis for study, with seven interventions focusing on members of the men who have sex with men (MSM) and wider lesbian, gay, bisexual and transgender (LGBT) community.4,8–10,19,23,24 In 13 studies, participants were predominantly male, with eight of the interventions focusing solely on men.4,8–10,12,19,20,24 Women were the sole focus of five studies,3,5,12,17,21 and women were the predominant participants in 11 of the 25 studies.3,5,12,13,15,17,18,21,25–27 In two studies, the prioritisation of youth focused on the related issue of substance abuse disorders.7,9
Intervention design
Although participants’ age ranged from 12 to >50 years, most participants were in the range 15–24 years (n = 17 studies).
Of the 25 studies, 11 were randomised control trials,4,5,7,11,16,17,19,21,22,24,26 six used a pre-post test evaluation design,6,9,12–14,23 three were uncontrolled longitudinal studies6,10,13 and the remaining studies comprised a mixture of qualitative cohort, observational and mixed methods.3,15,18,27 Thirteen of the studies included a process evaluation of the intervention, six of which comprised process evaluation only with no other outcomes reported.5,6,8,11,20,27 Sample sizes ranged from <20 to >7500 participants, with three studies reporting >1000 participants.16,18,22
Although HIV was the major preventive theme for a large proportion (11/25) of studies,4,5,7–9,11,12,17,19,21,27 many (12/25) based their intervention on sexual health in general.3,6,10,13,15,16,20,22–26 One study each focused on chlamydia or gonorrhoea.14,18 Follow-up frameworks were relatively short, with six studies providing for follow-up beyond 3 months5,8,11,13,14,17 and only two continuing follow-up for 12 months after the intervention.6,14 Both these studies involved web-based campaigns that did not require a recruited cohort of participants.
A large majority of studies used a web-based platform for their intervention (n = 16). These web-based interventions ranged from complex, individually tailored, multimedia modules to more simplified educational modules. Five of the studies used SMS platforms,3,18,22,25,27 including mobile phone messages and web-based instant message services. Transmedia ‘edutainment’, such as webisodes of a serialised drama, were used in three interventions.5,10,13 A small number of interventions used social networking sites, often as an accompaniment to a web-based platform or for live chat purposes.6,7,10 Media variety across multiple platforms (e.g. videos, social media, interactive elements, live chat and quizzes) was also associated with stronger positive responses from participants and improved outcomes.4,17,24 Yet, for some studies, the frequency of intervention or online promotion required to generate a response raised issues about transition from research to practice.14,19 The reinforcement of online interventions through community promotion and engagement was identified as an important consideration.6
Outcomes
Specific details related to main outcome measures and sample size are summarised in Appendix 1. In general, outcome evaluation focused on upstream behavioural determinants of infection risk, with an emphasis on knowledge and practice of condom usage. These behavioural attributes ranged from reported actual usage through to self-efficacy of condom use.
Three interventions reported non-significant behavioural outcomes, specifically condom use.7,22,26 In other studies, Billings et al.17 found that women who enrolled in a web-based multimedia HIV intervention reported an increase in condom use compared with the control group. Another study of a computer-based HIV intervention adapted from an existing evidence-based program21 reported a higher percentage of condom-protected sex acts compared with the control group, with participants more likely to use condoms consistently for vaginal and oral sex. Similarly, a web-based delivery of a pre-existing evidence-based program12 led to a significant increase in self-efficacy related to condom usage. Self-reported condom use increased significantly and the number of sexual partners decreased for all participants of a theory-based, tailored intervention4 from baseline to the 1-month follow-up. However, findings from an SMS-based mobile phone intervention22 demonstrated that although the intervention group reported higher levels of sexual health knowledge, there was no significant change in STI testing behaviour, improvement in condom use or reduction in partner numbers.
Finally, of the five studies evaluating intervention effects on intention to use condoms, one study reported significant effects due to the intervention.13 One study delivering an interactive, customisable web-based intervention with and without an educator7 reported increased intention to use condoms in both study arms. Three of the six studies evaluating the effect of an intervention on attitudes reported significant increases in positive attitudes towards condom use and engaging in safe sex discussions.10,13,15 Again, Marsch et al.,7 who used an interactive, customisable, web-based program with and without an educator, found that both arms of study reported significantly more positive attitudes towards engaging in safe sex practices.
Of the studies reviewed, outcomes related to knowledge centred on HIV and STI prevention, correct condom use and general sexual preventive health. Of the 12 studies evaluating knowledge-based outcomes, seven9,12,13,15,21–23 found a significant effect on knowledge relating to HIV, STIs or general sexual health. However, in studies where both the intervention and control arms received relevant education in some form,7,19 an increase in HIV or STI knowledge was reported equally across both arms. Similarly, in another study in which the control group was offered standard web-based HIV information compared with a theory-based tailored intervention,4 there was no significant increase in knowledge despite increases in protective behaviours among the intervention group. Billings et al.17 also found no significant evidence of increased knowledge despite improvements in condom usage.
Six of the 25 studies only considered process outcomes relating to the overall acceptability, feasibility and satisfaction with the intervention.5,6,8,11,20,27 In all but one study,8 acceptability and satisfaction with the intervention was rated high. Development of programs via ongoing consultation with and active participation by particular communities also led to greater engagement, acceptability and satisfaction.6,8,20
Of the five studies that evaluated the effects of the intervention on well-being, one yielded a statistically significant decrease in levels of worry among those using an SMS or instant messaging service about asking questions concerning reproductive health.25 Hightow-Weidman et al.4 found a reduction (non-significant) in mean scores on the Center for Epidemiologic Studies Depression Scale (CES-D) among participants in the intervention compared with control group. Likewise, although a study of a live chat intervention delivered via Facebook9 reported a reduction in depressive symptoms and gay-related concealment behaviours, the effect was not statistically significant, although significant increases in protective behaviours were reported. Another study of a theory-based multimedia intervention23 reported significant improvements in behaviour and knowledge, but only a small effect size for self-acceptance (e.g. internalised homophobia).
Of the four studies that evaluated sexual communication skills,15,17,20,26 only one17 reported a statistically significant increase in sexual communication by participants to assess the HIV risk of partners compared with the control group.
Many (15/25) studies also reported on outcomes related to sexual behaviour, including the number of sexual partners,12,17,22 the number of unprotected sex acts,9,12,15,19,21,23,24 sex while under the influence of alcohol or drugs,9 seeking STI testing6,14,16,18,22,26 and condom use, including frequency12,15,17,21,22,26 and self-efficacy.4,12,15,19,21,26 Twelve studies reported on knowledge-based outcomes, such as improved knowledge and prevention regarding HIV, STIs and general sexual health.4,7,9,10,12,13,15,17,19,21–23 Attitudes and intentions towards condom use were measured in six studies.4,7,10,13,15,19 Sixteen studies also considered process outcomes relating to the quality of the interventions, including feasibility, acceptability, usability and participant satisfaction.3–6,8–11,13,14,18,20,23,25,27 Five studies also considered outcomes relating to well-being, such as sexuality, self-acceptance and levels of worry.4,9,12,23,25
Several studies did not report the number of human participants, rather reporting the number of SMS or instant messaging transcripts analysed or the number of website views within a specific time frame.10,14,25
Discussion
The rapid development and uptake of new digital media presents significant potential for influencing health behaviours via health education, social marketing and health promotion interventions. New digital media have already been used in a range of health contexts, including chronic disease,28 winter preparedness,29 general school health,30 physical activity,31 substance abuse,32 mental illness,32,33 dietary behaviour change34,35 and breastfeeding.36 Digital media have also been evaluated for efficacy in enabling health promoting capacity through processes such as information seeking37 and holistic self-participatory care.38 Further, these media also have been used in specific disease contexts, such as obesity39 and breast cancer.40
This systematic review focused on the role of new digital media on sexual health knowledge, attitudes and behaviours of 13–24 year olds. The findings reveal a large diversity in intervention designs, settings, populations and evaluation strategies of new digital media in this age group. We believe that this diversity reflects, in part, the expanding range of new digital media available for sexual health promotion in young people. Indeed, as a result of the rapid rise in technology and mobile phone usage over the past decade, new digital media have become popular platforms for reaching young adults, particularly around health-related behaviours. Several key observations emerge from the diversity of research identified in this systematic review.
An interesting observation from our review was that programs that were web-based adaptations of an existing prevention program,12,19,21 were theory based or had been developed from models of behaviour change4 appeared effective regardless of the digital media mode used. Although our sample size was small, this was particularly highlighted for interventions tailored for specific groups. Customised messages towards particular audiences enhanced engagement, knowledge uptake and self-reported protective behaviours.19 The advantages of using a digital platform centred on interactivity with subjects and providing real-time personalised responses to specific needs, risks and concerns. Customisable delivery to many people was an added dimension. The iterative process of the development of programs via ongoing consultation with and active participation by particular communities also led to greater engagement, acceptability and satisfaction,6,8,20 and was considered integral to successful outcomes. Although intervention delivery across a variety of media platforms was associated with improved outcomes,4,17,24 some studies noted that the intervention frequency may be integral to successful transition from research to practice.14,19 In a similar context, community engagement with interventions emerged as an important consideration.6
Many interventions evaluated self-reported satisfaction with regard to acceptability or feasibility of programs,5,6,8,11,20,27 levels of knowledge,4,7,13,15,17,19,22,23 self-reported numbers of sexual partners12,17,22 or acts of unprotected sex,9,12,15,19,21,23,24 self-reported intentions to use condoms or practice safe sex4,7,13,26 or self-reported use of condoms.12,15,17,22,26 However, few measured actual group behaviour change, such as testing or service access.16,18,22,26 Where a control group was used, an intervention effect was often not detected.7,19 The paucity of intervention effects detected by this review may reflect the inherent difficulty in measuring sexual behaviours objectively. It may also indicate that the short-term follow-up of most reviewed studies may not allow sufficient time for measurable changes in complex behaviours to have occurred. However, Wakefield et al.41 argue that behaviour change may also occur indirectly, because health messages can set an agenda and increase discussion about a particular health issue within an individual’s social environment, which, in combination with individual exposure to the message, may reinforce (or undermine) a specific change in behaviour. This reinforces the need for trials with longer-term follow-up and more erudite methodologies to measure actual sexual risk behaviours.
Significant weaknesses were highlighted for many of these studies, either individually or in combination. These included small sample size, the absence of a control group comparison, a short study follow-up, reliance on self-reported behaviours and consequent recall bias, lack of randomisation, poor baseline measurements, low response rates to follow-up, incidental control group exposure to interventions, a lack of specific outcomes and difficulty in identifying the effective elements of complex interventions. Although these are all limitations common to many health promotion contexts, they nonetheless compound the difficulty of interpreting study outcomes. Further, the complexity of the technology and potential for malfunction, damage or poor access was a significant consideration for some studies.5,11–13,17,22
Evaluation was also limited where large broadcast interventions using social networking sites or SMS messaging could only offer aggregated data, restricting more specific analysis of demographic trends.6,10,13,25 Certainly, some studies addressed this through mixed-methods approaches to assess levels of reach, engagement and interaction.10
This systematic review itself has several limitations and potential biases. Studies were limited only to those published in English and, given the focus on young people (aged 13–24 years), many online or digital interventions focusing on predominantly older people were excluded, but may nonetheless be relevant to this age group. Given that this field has emerged only recently, many studies have likely not yet been evaluated or published. Further, the search term ‘new media’ may not yet be sufficiently ubiquitous to have covered all relevant published studies. The term ‘new media’ may also lack sufficient precision, given the nature of this rapidly changing communication environment. In the present review, the search term allowed for the inclusion of a wide range of digital platforms embracing the web, social media, mobile communications, video and personal computer. With regard to other search terms, such as ‘safe sex’ or terms related to contraception, their omission may have excluded relevant papers. Our search was focused on interventions directed at infection prevention and consequently sought to exclude papers related to pregnancy prevention, sexual assault and mental health strategies promoting strengthened sexual identity. We also excluded study protocols in our search criteria. This may have further reduced the range of suitable papers.
The broad range of studies included in this review, with their diversity of methods, populations and objectives, precludes any easily drawn comparisons or conclusions. The small number and large diversity of study designs compromise the stratification of studies to account for samples that were sexually active or inactive, engaged in formal or informal education, or living in high- or middle- to low-income countries, further weakening contextual analysis.
Conclusion
This review highlights the broad potential for digital media to enhance health promotion and service delivery towards better sexual health. There is significant scope for these technologies to interact in real time with participants and create customised programs,16,26 to facilitate networking among participants and health specialists4,6,9,10,20,25 and to reach large numbers at times and places convenient to the individual.5,12,13,19,24 Although new media has the capacity to expand efficiencies and coverage, the technology itself does not guarantee success. As with any delivery platform, high-quality, evidence-based content that engages with individual participants is essential. The rapid pace of change with the various digital platforms will create extra challenges for determining best practice. An important challenge for public health is that the rapidity of change may outpace the currency of evaluation and publication, creating a space for many interventions to flourish without solid evidence and for effective interventions to lose relevance. Such challenges compound the need for ongoing and timely research to monitor and evaluate these new trends while not losing sight of the general evidence-based principles that underlie all effective health promotion.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Acknowledgement
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
[1] Guse K, Levine D, Martins S, Lira A, Gaarde J, Westmorland W, Gilliam M. Interventions using new digital media to improve adolescent sexual health: a systematic review. J Adolesc Health 2012; 51 535–43.| Interventions using new digital media to improve adolescent sexual health: a systematic review.Crossref | GoogleScholarGoogle Scholar | 23174462PubMed |
[2] Lenhart A, Purcell K, Smith A, Zickuhr K. Social media & mobile internet use among teens and young adults. Pew Internet & American Life Project; 2010. Available online at http://www.pewinternet.org/2010/02/03/social-media-and-young-adults/ [verified 7 January 2019].
[3] Broaddus MR, Marsch LA, Fisher CB. Risks and benefits of text-message-delivered and small-group-delivered sexual health interventions among African American women in the Midwestern United States. Ethics Behav 2015; 25 146–68.
| Risks and benefits of text-message-delivered and small-group-delivered sexual health interventions among African American women in the Midwestern United States.Crossref | GoogleScholarGoogle Scholar | 25750497PubMed |
[4] Hightow-Weidman LB, Pike E, Fowler B, Matthews DM, Kibe J, McCoy R, Adimora AA. Healthmpowerment.Org: feasibility and acceptability of delivering an internet intervention to young Black men who have sex with men. AIDS Care 2012; 24 910–20.
| Healthmpowerment.Org: feasibility and acceptability of delivering an internet intervention to young Black men who have sex with men.Crossref | GoogleScholarGoogle Scholar | 22272759PubMed |
[5] Jones R, Lacroix LJ. Streaming weekly soap opera video episodes to smartphones in a randomized controlled trial to reduce HIV risk in young urban African American/Black women. AIDS Behav 2012; 16 1341–58.
| Streaming weekly soap opera video episodes to smartphones in a randomized controlled trial to reduce HIV risk in young urban African American/Black women.Crossref | GoogleScholarGoogle Scholar | 22430640PubMed |
[6] Dowshen N, Lee S, Lehman BM, Castillo M, Mollen C. IknowUshould2: feasibility of a youth-driven social media campaign to promote STI and HIV testing among adolescents in Philadelphia. AIDS Behav 2015; 19 106–11.
| IknowUshould2: feasibility of a youth-driven social media campaign to promote STI and HIV testing among adolescents in Philadelphia.Crossref | GoogleScholarGoogle Scholar | 25563502PubMed |
[7] Marsch LA, Grabinski MJ, Bickel WK, Desrosiers A, Guarino H, Muehlbach B, Solhkhah R, Taufique S, Acosta M. Computer-assisted HIV prevention for youth with substance use disorders. Subst Use Misuse 2011; 46 46–56.
| Computer-assisted HIV prevention for youth with substance use disorders.Crossref | GoogleScholarGoogle Scholar | 21190405PubMed |
[8] Hightow-Weidman LB, Fowler B, Kibe J, McCoy R, Pike E, Calabria M, Adimora A. Healthmpowerment.org: development of a theory-based HIV/STI website for young Black MSM. AIDS Educ Prev 2011; 23 1–12.
| Healthmpowerment.org: development of a theory-based HIV/STI website for young Black MSM.Crossref | GoogleScholarGoogle Scholar | 21341956PubMed |
[9] Lelutiu-Weinberger C, Pachankis JE, Gamarel KE, Surace A, Golub SA, Parsons JT. Feasibility, acceptability, and preliminary efficacy of a live-chat social media intervention to reduce HIV risk among young men who have sex with men. AIDS Behav 2015; 19 1214–27.
| Feasibility, acceptability, and preliminary efficacy of a live-chat social media intervention to reduce HIV risk among young men who have sex with men.Crossref | GoogleScholarGoogle Scholar | 25256808PubMed |
[10] Pedrana A, Hellard M, Gold J, Ata N, Chang S, Howard S, Asselin J, Ilic O, Batrouney C, Stoove M. Queer as f**k: reaching and engaging gay men in sexual health promotion through social networking sites. J Med Internet Res 2013; 15 e25
| Queer as f**k: reaching and engaging gay men in sexual health promotion through social networking sites.Crossref | GoogleScholarGoogle Scholar | 23391459PubMed |
[11] Ybarra ML, Bull SS, Prescott TL, Birungi R. Acceptability and feasibility of CyberSenga: an Internet-based HIV-prevention program for adolescents in Mbarara, Uganda. AIDS Care 2014; 26 441–7.
| Acceptability and feasibility of CyberSenga: an Internet-based HIV-prevention program for adolescents in Mbarara, Uganda.Crossref | GoogleScholarGoogle Scholar | 24093828PubMed |
[12] Danielson CK, McCauley JL, Jones AM, Borkman AL, Miller S, Ruggiero KJ. Feasibility of delivering evidence-based HIV/STI prevention programming to a community sample of African American teen girls via the Internet. AIDS Educ Prev 2013; 25 394–404.
| Feasibility of delivering evidence-based HIV/STI prevention programming to a community sample of African American teen girls via the Internet.Crossref | GoogleScholarGoogle Scholar | 24059877PubMed |
[13] Wang H, Singhal A. East los High: transmedia edutainment to promote the sexual and reproductive health of young Latina/o Americans. Am J Public Health 2016; 106 1002–10.
| East los High: transmedia edutainment to promote the sexual and reproductive health of young Latina/o Americans.Crossref | GoogleScholarGoogle Scholar | 27077336PubMed |
[14] Mann TA, Uddin Z, Hendriks AM, Bouchard CJ, Etches VG. Get tested why not? A novel approach to Internet-based chlamydia and gonorrhea testing in Canada. Can J Public Health 2013; 104 e205–9.
| Get tested why not? A novel approach to Internet-based chlamydia and gonorrhea testing in Canada.Crossref | GoogleScholarGoogle Scholar | 23823883PubMed |
[15] Villegas N, Santisteban D, Cianelli R, Ferrer L, Ambrosia T, Peragallo N, Loreto L. Pilot testing an internet-based STI and HIV prevention intervention with Chilean women. J Nurs Scholarshp 2015; 47 106–16.
| Pilot testing an internet-based STI and HIV prevention intervention with Chilean women.Crossref | GoogleScholarGoogle Scholar |
[16] Lustria MLA, Cortese J, Gerend MA, Schmitt K, Kung YM, McLaughlin C. A model of tailoring effects: a randomized controlled trial examining the mechanisms of tailoring in a web-based STD screening intervention. Health Psychol 2016; 35 1214–24.
| A model of tailoring effects: a randomized controlled trial examining the mechanisms of tailoring in a web-based STD screening intervention.Crossref | GoogleScholarGoogle Scholar |
[17] Billings DW, Leaf SL, Spencer J, Crenshaw T, Brockington S, Dalal RS. A randomized trial to evaluate the efficacy of a web-based HIV behavioral intervention for high-risk African American women. AIDS Behav 2015; 19 1263–74.
| A randomized trial to evaluate the efficacy of a web-based HIV behavioral intervention for high-risk African American women.Crossref | GoogleScholarGoogle Scholar | 25616838PubMed |
[18] Dukers-Muijrers NHTM, Theunissen KATM, Wolffs PT, Kok G, Hoebe CJPA. Acceptance of home-based chlamydia genital and anorectal testing using short message service (SMS) in previously tested young people and their social and sexual networks. Plos One 2015; 10 e0133575
| Acceptance of home-based chlamydia genital and anorectal testing using short message service (SMS) in previously tested young people and their social and sexual networks.Crossref | GoogleScholarGoogle Scholar |
[19] Mustanski B, Garofalo R, Monahan C, Gratzer B, Andrews R. Feasibility, acceptability, and preliminary efficacy of an online HIV prevention program for diverse young men who have sex with men: the Keep It Up! intervention. AIDS Behav 2013; 17 2999–3012.
| Feasibility, acceptability, and preliminary efficacy of an online HIV prevention program for diverse young men who have sex with men: the Keep It Up! intervention.Crossref | GoogleScholarGoogle Scholar | 23673793PubMed |
[20] Kasatpibal N, Viseskul N, Srikantha W, Fongkaew W, Surapagdee N, Grimes RM. Developing a web site for human immunodeficiency virus prevention in a middle income country: a pilot study from Thailand. Cyberpsychol Behav Soc Netw 2012; 15 560–3.
| Developing a web site for human immunodeficiency virus prevention in a middle income country: a pilot study from Thailand.Crossref | GoogleScholarGoogle Scholar | 23002987PubMed |
[21] Wingood GM, Card JJ, Er D, Solomon J, Braxton N, Lang D, Seth P, Cartreine J, Diclemente RJ. Preliminary efficacy of a computer-based HIV intervention for African-American women. Psychol Health 2011; 26 223–34.
| Preliminary efficacy of a computer-based HIV intervention for African-American women.Crossref | GoogleScholarGoogle Scholar | 21318931PubMed |
[22] Gold J, Aitken CK, Dixon HG, Lim MSC, Gouillou M, Spelman T, Wakefield M, Hellard ME. A randomised controlled trial using mobile advertising to promote safer sex and sun safety to young people. Health Educ Res 2011; 26 782–94.
| A randomised controlled trial using mobile advertising to promote safer sex and sun safety to young people.Crossref | GoogleScholarGoogle Scholar | 21447750PubMed |
[23] Mustanski B, Greene GJ, Ryan D, Whitton SW. Feasibility, acceptability, and initial efficacy of an online sexual health promotion program for LGBT youth: the Queer Sex Ed intervention. J Sex Res 2015; 52 220–30.
| Feasibility, acceptability, and initial efficacy of an online sexual health promotion program for LGBT youth: the Queer Sex Ed intervention.Crossref | GoogleScholarGoogle Scholar | 24588408PubMed |
[24] Carpenter KM, Stoner SA, Mikko AN, Dhanak LP, Parsons JT. Efficacy of a web-based intervention to reduce sexual risk in men who have sex with men. AIDS Behav 2010; 14 549–57.
| Efficacy of a web-based intervention to reduce sexual risk in men who have sex with men.Crossref | GoogleScholarGoogle Scholar | 19499321PubMed |
[25] Giorgio MM, Kantor LM, Levine DS, Arons W. Using chat and text technologies to answer sexual and reproductive health questions: planned parenthood pilot study. J Med Internet Res 2013; 15 e203
| Using chat and text technologies to answer sexual and reproductive health questions: planned parenthood pilot study.Crossref | GoogleScholarGoogle Scholar | 24055754PubMed |
[26] Mevissen FEF, Ruiter RAC, Meertens RM, Zimbile F, Schaalma HP. Justify your love: testing an online STI-risk communication intervention designed to promote condom use and STI-testing. Psychol Health 2011; 26 205–21.
| Justify your love: testing an online STI-risk communication intervention designed to promote condom use and STI-testing.Crossref | GoogleScholarGoogle Scholar |
[27] Cornelius JB, St. Lawrence JS, Howard JC, Shah D, Poka A, McDonald D, White AC. Adolescents’ perceptions of a mobile cell phone text messaging‐enhanced intervention and development of a mobile cell phone‐based HIV prevention intervention. J Spec Pediatr Nurs 2012; 17 61–9.
| Adolescents’ perceptions of a mobile cell phone text messaging‐enhanced intervention and development of a mobile cell phone‐based HIV prevention intervention.Crossref | GoogleScholarGoogle Scholar | 22188273PubMed |
[28] Greene JA, Choudhry NK, Kilabuk E, Shrank WH. Online social networking by patients with diabetes: a qualitative evaluation of communication with Facebook. J Gen Intern Med 2011; 26 287–92.
| Online social networking by patients with diabetes: a qualitative evaluation of communication with Facebook.Crossref | GoogleScholarGoogle Scholar | 20945113PubMed |
[29] Bandera C. Design and management of public health outreach using interoperable mobile multimedia: an analysis of a national winter weather preparedness campaign. BMC Public Health 2016; 16 436
| Design and management of public health outreach using interoperable mobile multimedia: an analysis of a national winter weather preparedness campaign.Crossref | GoogleScholarGoogle Scholar | 27225500PubMed |
[30] Wysocki R.. Social media for school nurses: promoting school health in the 21st century. NASN Sch Nurse 2015; 30 180–8.
| Social media for school nurses: promoting school health in the 21st century.Crossref | GoogleScholarGoogle Scholar | 25816429PubMed |
[31] Ridgers ND, Timperio A, Brown H, Ball K, Macfarlane S, Lai SK, Richard K, Ngan W, Salmon J. A cluster-randomised controlled trial to promote physical activity in adolescents: the Raising Awareness of Physical Activity (RAW-PA) study. BMC Public Health 2017; 17 6
| A cluster-randomised controlled trial to promote physical activity in adolescents: the Raising Awareness of Physical Activity (RAW-PA) study.Crossref | GoogleScholarGoogle Scholar | 28052773PubMed |
[32] Elgán TH, Kartengren N, Strandberg AK, Ingemarson M, Hansson H, Zetterlind U, Gripenberg J. A web-based group course intervention for 15–25-year-olds whose parents have substance use problems or mental illness: study protocol for a randomized controlled trial. BMC Public Health 2016; 16 1011
| A web-based group course intervention for 15–25-year-olds whose parents have substance use problems or mental illness: study protocol for a randomized controlled trial.Crossref | GoogleScholarGoogle Scholar | 27663995PubMed |
[33] Naslund JA, Aschbrenner KA, Bartels SJ. How people with serious mental illness use smartphones, mobile apps, and social media. Psychiatr Rehabil J 2016; 39 364–7.
| How people with serious mental illness use smartphones, mobile apps, and social media.Crossref | GoogleScholarGoogle Scholar | 27845533PubMed |
[34] Farley TA, Halper HS, Carlin AM, Emmerson KM, Foster KN, Fertig AR. Mass media campaign to reduce consumption of sugar-sweetened beverages in a rural area of the United States. Am J Public Health 2017; 107 989–95.
| Mass media campaign to reduce consumption of sugar-sweetened beverages in a rural area of the United States.Crossref | GoogleScholarGoogle Scholar | 28426298PubMed |
[35] McGloin AF, Eslami S. Digital and social media opportunities for dietary behaviour change. Proc Nutr Soc 2015; 74 139–48.
| Digital and social media opportunities for dietary behaviour change.Crossref | GoogleScholarGoogle Scholar | 25319345PubMed |
[36] Gross TT, Davis M, Anderson AK, Hall J, Hilyard K. Long-term breastfeeding in African American mothers. J Hum Lact 2017; 33 128–39.
| Long-term breastfeeding in African American mothers.Crossref | GoogleScholarGoogle Scholar | 28061039PubMed |
[37] Kim A, Hansen H, Duke J, Davis K, Alexander R, Rowland A, Mitchko J. Does digital ad exposure influence information-seeking behavior online? Evidence from the 2012 Tips From Former Smokers National Tobacco Prevention Campaign. J Med Internet Res 2016; 18 e64
| Does digital ad exposure influence information-seeking behavior online? Evidence from the 2012 Tips From Former Smokers National Tobacco Prevention Campaign.Crossref | GoogleScholarGoogle Scholar | 27847353PubMed |
[38] Miron-Shatz T, Hansen MM, Grajales FJ, 3rd, Martin-Sanchez F, Bamidis PD. Social media for the promotion of holistic self-participatory care: an evidence based approach. Contribution of the IMIA Social Media Working Group. Yearb Med Inform 2013; 8 162–8.
| 23974565PubMed |
[39] Livingood WC, Monticalvo D, Bernhardt JM, Wells KT, Harris T, Kee K. Engaging adolescents through participatory and qualitative research methods to develop a digital communication intervention to reduce adolescent obesity. Health Educ Behav 2017; 44 570–80.
| Engaging adolescents through participatory and qualitative research methods to develop a digital communication intervention to reduce adolescent obesity.Crossref | GoogleScholarGoogle Scholar | 27811164PubMed |
[40] Theiss SK, Burke RM, Cory JL, Fairley TL. Getting beyond impressions: an evaluation of engagement with breast cancer-related Facebook content. mHealth 2016; 2 41
| 27840816PubMed |
[41] Wakefield MA, Loken B, Hornik RC. Use of mass media campaigns to change health behaviour. Lancet 2010; 376 1261–71.
| Use of mass media campaigns to change health behaviour.Crossref | GoogleScholarGoogle Scholar | 20933263PubMed |
Appendix 1. Summary of studies included in the systematic review
BART, Becoming a Responsible Teen; CHOP, Children’s Hospital of Philadelphia; CT, Chlamydia trachomatis; ELH, East Los High; HMP, HealthMpowerment.org; IM, instant messaging; IMB, information–motivation–behavioural; LGBT, lesbian, gay, bisexual and transgender; MCP, mobile cell phone; MSM, men who have sex with men; NGO, non-governmental organisations; QAF, Queer as F**k; QSE, Queer Sex Ed; RCT, randomised control trial; SNS, social networking sites; STI, sexually transmissible infection

|