Major trauma: the unseen financial burden to trauma centres, a descriptive multicentre analysis
Kate Curtis A B C G , Mary Lam D , Rebecca Mitchell E , Cara Dickson B and Karon McDonnell FA Sydney Nursing School, University of Sydney, 88 Mallet Street, Camperdown, NSW 2050, Australia.
B St George Hospital, Gray Street, Kogarah, NSW 2217, Australia. Email: cara.dickson@sesiahs.health.nsw.gov.au
C The George Institute for Global Health, George Street, Sydney, NSW 2000, Australia.
D Faculty of Health Sciences, University of Sydney, Sydney, NSW 2141, Australia. Email: mary.lam@sydney.edu.au
E Transport and Road Safety Research, University of New South Wales, NSW 2033, Australia. Email: r.mitchell@unsw.edu.au
F St Vincent’s Hospital, Darlinghurst, Sydney, NSW 2010, Australia. Email: kmcdonell@stvincents.com.au
G Corresponding author. Email: kate.curtis@sydney.edu.au
Australian Health Review 38(1) 30-37 https://doi.org/10.1071/AH13061
Submitted: 22 March 2013 Accepted: 18 September 2013 Published: 18 November 2013
Journal Compilation © AHHA 2014
Abstract
Objective This research examines the existing funding model for in-hospital trauma patient episodes in New South Wales (NSW), Australia and identifies factors that cause above-average treatment costs. Accurate information on the treatment costs of injury is needed to guide health-funding strategy and prevent inadvertent underfunding of specialist trauma centres, which treat a high trauma casemix.
Methods Admitted trauma patient data provided by 12 trauma centres were linked with financial data for 2008–09. Actual costs incurred by each hospital were compared with state-wide Australian Refined Diagnostic Related Groups (AR-DRG) average costs. Patient episodes where actual cost was higher than AR-DRG cost allocation were examined.
Results There were 16 693 patients at a total cost of AU$178.7 million. The total costs incurred by trauma centres were $14.7 million above the NSW peer-group average cost estimates. There were 10 AR-DRG where the total cost variance was greater than $500 000. The AR-DRG with the largest proportion of patients were the upper limb injury categories, many of whom had multiple body regions injured and/or a traumatic brain injury (P < 0.001).
Conclusions AR-DRG classifications do not adequately describe the trauma patient episode and are not commensurate with the expense of trauma treatment. A revision of AR-DRG used for trauma is needed.
What is known about this topic? Severely injured trauma patients often have multiple injuries, in more than one body region and the determination of appropriate AR-DRG can be difficult. Pilot research suggests that the AR-DRG do not accurately represent the care that is required for these patients.
What does this paper add? This is the first multicentre analysis of treatment costs and coding variance for major trauma in Australia. This research identifies the limitations of the current AR-DRGS and those that are particularly problematic. The value of linking trauma registry and financial data within each trauma centre is demonstrated.
What are the implications for practitioners? Further work should be conducted between trauma services, clinical coding and finance departments to improve the accuracy of clinical coding, review funding models and ensure that AR-DRG allocation is commensurate with the expense of trauma treatment.
Additional keywords: cost, injury, health economics, health services.
Background
Worldwide, traumatic injury accounts for 11% of mortality1 and is increasing as a leading cause of death and disability.2 Injury impacts society significantly on a physical, psychological and economic level.3 In Australia, injuries are one of the most costly disease groups,4 responsible for over half a million hospitalisations, making it the second highest in-hospital cost after cardiovascular disease.5 In 2008–09, New South Wales (NSW), the most populous state in Australia, received over one-third (34.3%, n = 137 088) of all hospital admissions relating to injury.6
Trauma treatment represents a significant cost to the community and different funding models are used to resource the healthcare sector with varying degrees of accuracy.7,8 In NSW, an episode-based funding model (also known as casemix-based funding) has been adopted for acute healthcare services9 where a healthcare facility is allocated a predetermined financial payment for each type of patient episode, defined by an Australian Refined Diagnosis-Related Group (AR-DRG).10
For some health conditions, such as rehabilitation or palliative care, episode funding models and AR-DRG have not been found to be good indicators of the ‘true’ types of patient episodes.11 Internationally, episode funding models are not commensurate with the cost of treating trauma and may leave trauma centres at a financial disadvantage.12–14 The same has been suggested for the Australian episode funding model.15 Severely injured trauma patients often have complex care needs as they can have multiple injuries, in more than one body region,16 thus the determination of appropriate AR-DRG can be difficult.10
In an environment of increasing healthcare costs and competition for finite resources, economic data relating to the cost of injury and illness is integral to guiding health services policy. Therefore, it is important to have appropriately costed hospital treatment and service-utilisation funding models and subsequent resource allocation to avoid under-resourcing of the hospital sector. The present study aims to: determine whether AR-DRG adequately describe the in-hospital trauma patient episode; identify AR-DRG groupings where average AR-DRG costs are not commensurate with total actual cost; and identify factors, including demographics, specific treatment and circumstances of the injury event, that are associated with above-average treatment costs.
Methods
Data capture, costing methods and linkage
All 12 hospitals designated Level I trauma centres by the NSW Ministry of Health17 at the time of the study provided both trauma and health service cost data. Each trauma centre has a trauma registry. As a minimum, data are collected on every major trauma admission (that is, an injury severity score greater than 12), although most centres collect data on all patients with a significant injury mechanism, regardless of injury severity, such as high-speed motor vehicle collision, stabbing, fall from greater than 3 m or assault. Each trauma centre provided demographic, injury and treatment-related data on all trauma patients admitted between 1 July 2008 and 30 June 2009. Due to the variance in data classifications for some site trauma centre registries, the codes for each data variable required manual review and recoding. Further, medical record numbers and admission dates from the trauma data were provided to the casemix or performance units at each health service or hospital to obtain health service cost data. The trauma and financial cost data were linked using medical record number, date of birth and admission date. Any discrepancies were individually resolved using a manual review.
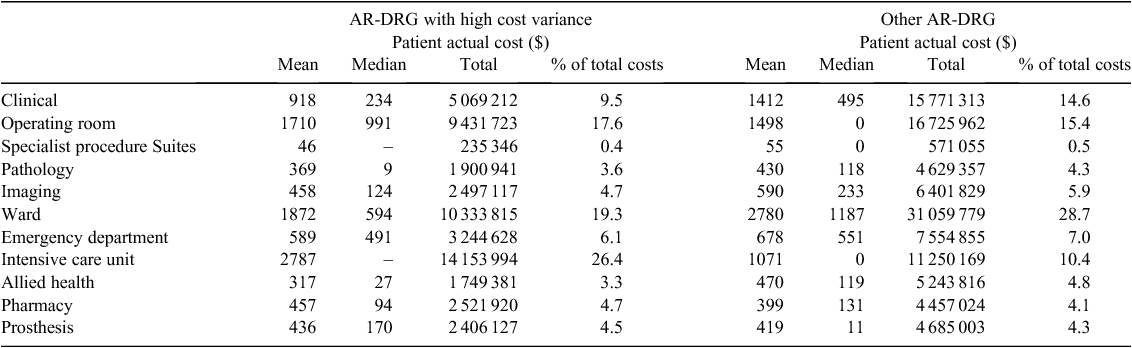
The costing tool used by the NSW Ministry of Health at the time of the study was the Power Performance Management Reporting System,18 which employs both clinical costing and cost-modelling methods in the cost-allocation process. The system has two main components: financial and clinical. Financial information is extracted from the hospital’s general ledger at cost centre and account code level. Indirect costs are allocated to patient care cost centres, during the costing process, using appropriate allocation statistics (e.g. human resources using staffing head count, cleaning expense using floor space). The clinical information is based on patient data from the hospital patient administration system, which is accessed via an interface with the Health Information Exchange. The Health Information Exchange is the NSW Ministry of Health’s corporate data warehouse and acts as a repository for several data collections. Patient-level resource use from both state and local information systems, such as diagnostic, theatre, pharmacy allied health and imaging, is linked to the patient administration system data facilitating patient-level costing. Episode costs are reported broken down into 10 cost buckets, including clinical (e.g. medical wages), operating room, pathology, imaging, ward, emergency department, Intensive Care Unit (ICU), allied health, pharmacy and prostheses. All patient costing was conducted in accordance with 2008–09 NSW Program and Product Data Collection.19
Each inpatient episode was grouped to an AR-DRG according to diagnoses and interventions coded after hospital discharge. The 2008–09 state-wide average costs for the AR-DRG were obtained from the NSW Ministry of Health Inter-Government and Funding Strategies Branch.20 All costs are presented in Australian dollars for 2008–09. The 2008–09 average exchange rates for the US dollar and British pound were 76 cents and 47 cents (Australian), respectively.21 Ethics approval was received from each site.
Injury severity
Injury severity was categorised using the Injury Severity Score (ISS), an anatomic diagnosis system derived from the Abbreviated Injury Scale (AIS).22 ISS range from 0 to 75, with a score of less than 9 considered minor, 9–15 major and greater than 15 severe.23,24 Further development of the AIS system has led to an ISS greater than 12 being considered reflective of severe injury in NSW.25 Traumatic brain injury was calculated using an AIS greater than 2 (definition of serious traumatic brain injury26) and polytrauma the presence of more than two body regions injured.
Data management and analysis
Data were analysed using SPSS 20.0.27 The direct cost and AR-DRG estimated cost of treating trauma patients are described for the 2008–09 financial year. There were 837 trauma patients where no AR-DRG code was allocated and these cases were excluded from cost analyses.
Descriptive analyses were conducted. The actual cost of treating the trauma patient was compared with peer-group hospitals (i.e. the reported AR-DRG average costs of NSW hospitals of similar size and resources) to determine any variance between the actual costs incurred by the trauma patient and the average costs of all patients with the same AR-DRG.
For the 10 AR-DRG with the most variance between actual and peer-group average total costs, non-parametric univariate analyses (Mann–Whitney Test) were performed to investigate variables that were associated with large cost variance. These variables included demographics, specific treatment and mechanism of injury.
Results
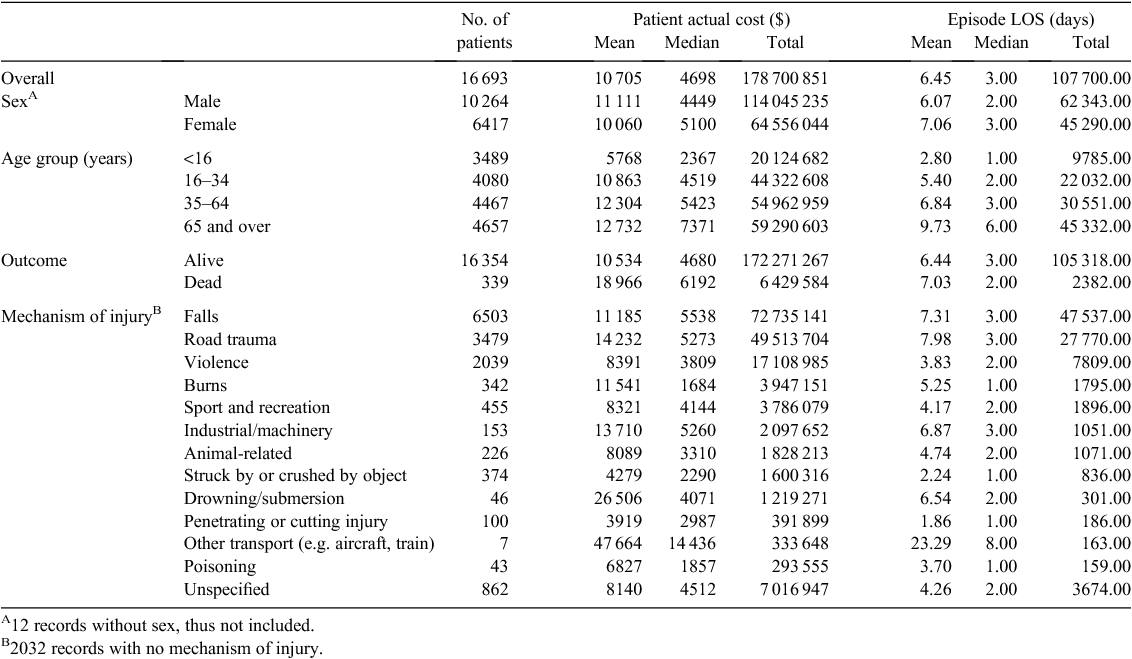
There were 16 693 trauma patients who had AR-DRG assigned and costing information available. The average trauma patient cost was $10 705 (median $4698, quartile range (QR): $2222–$10 231) and the average length of stay (LOS) was 6.5 days. The average cost for males was higher than for females ($11 111 and $10 060, respectively). Patients aged 65 years and older had the highest average cost at $12 732. Patients who did not survive their injuries cost $8 432 more than those who survived. Patients with an injury mechanism of other transport ($47 664), drowning/submersion ($26 506) and road trauma ($14 232) had the highest average costs of trauma care, although both other transport and drowning/submersion accounted for only a relatively small number of patients (Table 1).
|
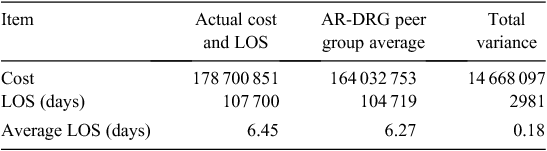
There were 386 AR-DRG groupings identified for the trauma patients. Comparison of the actual trauma costs for trauma patients with the peer-group hospital average found that there were 267 (69.2%) instances where the trauma patient cost was above average, totalling $19 993 525. There were 119 (30.8%) instances where the trauma patient costs were below average, equivalent to $3 724 009. Overall, trauma patient costs were $14 668 097 above average (Table 2).
|
For the AR-DRG allocated to trauma patients the actual treatment costs versus NSW peer-group average costs of all patients with the same AR-DRG were examined. There were 10 AR-DRG that had total variance greater than $500 000. The largest cost variances by AR-DRG classification were for treatments that required ‘tracheostomy or ventilation >95 h’ (A06Z), ‘injury to the forearm, wrist, hand or foot for patients aged <75 years without complications of care’ (I74C), ‘hand procedures’ (I30Z) and ‘humerus, tibia, fibula and ankle procedures for patients age <60 years without catastrophic or severe complications of care’ (I13C). The AR-DRG with the most patients was ‘injuries, age <65 years’ (X60C). Mean LOS did not differ significantly between the trauma centres in the study and the NSW peer-group hospital, except for ‘other knee procedures’ (I18Z) (Table 3).
On closer examination of these 10 high-variance AR-DRG, 84% (n = 3963) of patients had minor injuries (ISS <9). The average treatment cost of patients increased exponentially with the number of body regions injured (from $7598 for patients with an isolated injury to $64 652 for patients with four or more regions injured), although patients with four or more body regions injured represented only 2% of patients. The median cost for patients with a traumatic brain injury was significantly higher than for patients without a traumatic brain injury (P < 0.001). Falls, road trauma and violence were the most predominant injury mechanisms, although patients who fell from a height greater than 5 m had a higher median cost than those that fell less than 5 m (P < 0.001). Similarly, motorcycle crashes and pedestrians had higher median costs than those injured in a motor vehicle collision (P = 0.035 and P = 0.01, respectively) (Table 4).
As the hospital LOS was not significantly different in the high-variance AR-DRG group, the cost components where hospital LOS was not the main cost driver were compared. Patients in the high-variance group had higher ICU, operating room, prosthesis and pharmacy costs compared with those who were not in the high-variance AR-DRG group (Table 5).
The AR-DRG that had both a high cost variance compared with the NSW peer-group average and the largest proportion of patients were those from the upper limb injury or ‘I’ category (i.e. I74C, I13C, I30Z and I19Z). When examining the injury characteristics of patients allocated the ‘I’ AR-DRG, patients were predominantly aged less than 60 years, and a large proportion of patients in each ‘I’ category had multiple body regions injured and/or a traumatic brain injury (Table 6). For example, in AR-DRG I74C, a 57-year-old who fell from 1–5 m had a fractured (#) radius, panfacial fractures, cheek degloving and a concussion. A 64-year-old pedestrian had a # radius, # ulna, arm degloving and a concussion, a 42-year-old who fell from a horse had bilateral ulna fractures, a radius fracture and multiple rib fractures. In other instances there were likely incorrect AR-DRG allocations, for example in I19Z a 30-year-old motorcycle rider had a severe head injury (diffuse axonal injury), cerebral contusions, facial laceration and a fractured radius.
The mechanisms with the highest proportions of patients in the high-variance AR-DRG were sport (50%), fall from unspecified height (44%), violence, and motorcycle and pedal cycle crashes (36%). Large proportions of each of these injury-mechanism groups were allocated the AR-DRG I74C and I13C.
Discussion
This multicentre study describes the trauma casemix treated at major trauma centres and demonstrates that traumatic injury cost NSW trauma centres AU$178.7 million in 2008–09. Average per patient costs for severely injured patients in this study were less than those reported internationally7 and locally.28 In comparing costs, it is necessary to collect data across multiple sites so that discrepancies caused by variations in efficiency across centres are offset. The high financial cost of treating trauma highlights the need to ensure that injury-prevention interventions remain a priority in Australia.
When severely injured individuals are treated at specialist trauma centres, their chances of surviving their injury are greatly improved.26,29–31 Trauma centres are major teaching hospitals that provide services for the full spectrum of illness, as well as major trauma. The present study highlighted that AR-DRG classifications used as the basis for funding are not commensurate with the trauma patient episode of care. Within the AR-DRG examined in this study, trauma patients are only one patient group. It is expected that there is a range of patient illnesses and associated individual comorbidities. The mean cost for reimbursement assumes that within a hospital, some patients fall below the average cost and others fall above. However, the findings of this study demonstrate that hospitals with a high trauma casemix are likely to have a higher proportion of AR-DRG where patient costs are above average.
The allocation of AR-DRG for trauma patients can be complicated, as trauma patients often have multiple injuries32 that are not easily defined by a single AR-DRG classification. This was demonstrated by the examination of a series of cases that were allocated to the problematic upper-limb injury AR-DRG. This could be a result of inaccurate coding or the inadequacy of AR-DRG in describing the trauma patient episode. Further work should be undertaken between trauma services, clinical coders and health-strategy services to review funding models and ensure that AR-DRG allocation is commensurate with the expense of trauma treatment, as has been suggested previously.15,33,34
The most recent AR-DRG classification and International Classification of Diseases (ICD)-10-AM were implemented in Australia on 1 July 2013. Previous research and our findings should be taken into account when these systems are refined by the National Centre for Classification in Health in 2014. For example, as LOS is not predicative of trauma treatment cost variance, perhaps a new AR-DRG should be developed, or a higher clinical complexity National Weighted Activity Unit allocated to trauma patients with polytrauma and traumatic brain injury, which are known predictors of higher treatment costs and cost variance.8
Institutions around the world have attempted to enhance their coding accuracy by directly engaging clinicians to document clearly and comprehensively, but this strategy has proven to be both unsuccessful and difficult to sustain. Healthcare organisations need to continue to assess clinical documentation and identify problems,35 as well as adopt site-specific strategies known to improve coding quality, such as: improved coder career opportunities; higher staffing levels; reduced throughput; and increased coder interactions with clinical staff.36 A study in 2002 demonstrated that when trauma nurse case managers who routinely collected trauma data and coordinated patient care collaborated with clinical coding staff, coding accuracy and financial return for the hospital were improved.10 More recently in NSW, the Health Education and Training Institute has implemented a Clinical Coding Workforce Enhancement project and will be more closely involved in the recruitment, education and training of clinical coders.37
Patients in the high-variance group had polytrauma and high ICU and operating room costs. Polytrauma occurs when the severity of injury in each body regions rises above an AIS of 2. It is intuitive that polytrauma is associated with higher treatment costs as it requires the involvement of multiple health teams, is highly resource intensive, and often involves massive resuscitation efforts, extensive imaging, multiple operations, extended ICU stays and complex rehabilitation programs.38 Admission to ICU as a predictor of cost has been demonstrated previously. The challenge for critical care practitioners is to meticulously assess new innovations in therapy and to adopt the most efficient technologies that improve unit function and staff efficiency, and enhance patient outcome at a reasonable cost.39
As trauma increases as a significant aspect of the global burden of disease, it is imperative that the most common mechanisms are adequately represented in funding models, particularly as trauma patients are likely to sustain injury to multiple body regions.38,39 In the current study, trauma patients who had the highest cost variance commonly sustained their injury as a result of a fall, a road traffic crash or violence, which is reflective of wider injury patterns. Injurious falls in the older person population are the leading cause of injury-related mortality and hospitalised morbidity in most developed countries.40 By 2030, road traffic injuries are expected to become the fifth leading cause of death and the third leading cause of disability worldwide, prompting the United Nations General Assembly to proclaim 2011–20 as the Decade of Action for Road Safety.41 The road trauma patients in the present study with the highest cost variance were vulnerable road users, such as pedestrians, pedal cyclists and motorcyclists, who have less protection from high-energy impact. There is an increasing rate of interpersonal violence in Australia.42,43 Early intervention and education while young males are at school has become a focus of prevention strategies to address this,44 as well as other programs, such as the prevention of alcohol-related trauma in youth, which was found to effectively reduce the incidence of traumatic injuries among its participants, although more so in women than men.45
There are several limitations of the current research. It only included those injured individuals admitted to one of the 12 major trauma centres, some of which were only able to provide information on severely injured patients. The acute treatment costs of trauma represent a fraction of the overall financial costs of trauma3 and the present study did not include any post-acute rehabilitative treatment costs or individual costs incurred by the patients’ families. Longitudinal costing studies are required in order to determine the complete financial burden of traumatic injury to the healthcare system. There was some variability in trauma data classifications between trauma centres. The authors undertook stringent quality processes to address these problems. The implementation of a mandatory NSW state-wide trauma registry and an increase in the data items recorded in the NSW trauma minimum dataset will go some way toward reducing these problems.
Conclusion
With the globally increasing burden of injury, accurate costing information is essential for health service resource strategies. AR-DRG classifications do not adequately describe the trauma patient episode of care. Future research should examine the process of allocation of AR-DRG for trauma and a revision of trauma-related AR-DRG should be conducted to prevent the underfunding of trauma patient episodes.
Competing interests
The authors declare there are no competing interests.
Acknowledgements
The authors thank the trauma coordinators and data managers of participating centres for assistance with ethics and provision of data. Funding support for statistical analysis was provided by the St George Honda Trauma and Critical Care Research program. Associate Professor Curtis was supported by a Sydney Nursing School, University of Sydney post-doctoral fellowship.
References
[1] Peden M, McGee K, Krug E. Injury: a leading cause of the global burden of disease, 2000. Geneva: World Health Organisation; 2002.[2] Horton R. GBD 2010: understanding disease, injury, and risk. Lancet 2012; 380 2053–4.
| GBD 2010: understanding disease, injury, and risk.Crossref | GoogleScholarGoogle Scholar | 23245595PubMed |
[3] Lyons RA, Finch CF, McClure R, van Beeck E, Macey S. The injury list of all deficits (LOAD) framework – conceptualising the full range of deficits and adverse outcomes following injury and violence. Int J Inj Contr Saf Promot 2010; 17 145–59.
| The injury list of all deficits (LOAD) framework – conceptualising the full range of deficits and adverse outcomes following injury and violence.Crossref | GoogleScholarGoogle Scholar | 19946813PubMed |
[4] Australian Institute of Health and Welfare (AIHW). Australia’s health 2010. Canberra: AIHW; 2010.
[5] Australian Institute of Health and Welfare. Health expenditure Australia 2008–09. Health and welfare expenditure series no. 42. Cat. no. HWE 51. Canberra: AIHW; 2010.
[6] Australian Institute of Health and Welfare. Australian hospital statistics 2008–09. Health services series no. 17. Cat. no. HSE 84. Canberra: AIHW; 2010.
[7] Willenberg L, Curtis K, Taylor C, Jan S, Glass P, Myburgh J. The variation of acute treatment costs of trauma in high-income countries. BMC 2012; 12 267
| The variation of acute treatment costs of trauma in high-income countries.Crossref | GoogleScholarGoogle Scholar |
[8] Curtis K, Lam M, Mitchell R, Black DA, Taylor C, Dickson C, et al Acute costs and predictors of higher treatment costs of trauma in New South Wales, Australia. Injury 2010;
| Acute costs and predictors of higher treatment costs of trauma in New South Wales, Australia.Crossref | GoogleScholarGoogle Scholar |
[9] NSW Health Department. NSW health episode funding policy 2008/2009. 2010. Available at http://www.health.nsw.gov.au/policies/pd/2008/PD2008_063.html v[verified 16 April 2010]
[10] Curtis K, Bollard L, Dickson C. Coding errors and the trauma patient – is nursing case management the solution? Aust Health Rev 2002; 25 73–80.
| Coding errors and the trauma patient – is nursing case management the solution?Crossref | GoogleScholarGoogle Scholar | 12404969PubMed |
[11] Eager K, Harvey R. Australia not ready to implement ‘best practice’ health financing model. Healthcover 2001; 10 52–6.
[12] Rotondo MF, Bard MR, Sagraves SG, Toschlog EA, Schenarts PJ, Goettler CE, et al What price commitment: What benefit? The cost of a saved life in a developing level 1 Trauma Center. J Trauma Inj Infect Crit Care 2009; 67 915–23.
| What price commitment: What benefit? The cost of a saved life in a developing level 1 Trauma Center.Crossref | GoogleScholarGoogle Scholar |
[13] Campbell A, Vittinghoff E, Morabito D, Paine P, Shagoury C, Praetz P, et al Trauma centres in a managed care environment. J Trauma Inj Infect Crit Care 1995; 39 246–53.
| Trauma centres in a managed care environment.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2MvgsVOjug%3D%3D&md5=673ff2a1e79456659feb433a17eb3996CAS |
[14] Grotz M, Schwermann T, Lefering R, Ruchholtz S, Schulenburg JMGVD, Krettek C, et al [G-DRG reimbursement for polytrauma patients – a comparison with the comprehensive hospital costs using the German trauma registry Unfallchirurgische 2004; 107 68–75.
| 1:STN:280:DC%2BD2c%2FkvFejtQ%3D%3D&md5=9b0ade9ce0792e04a1203e26f9a521f0CAS |
[15] Curtis K, Mitchell R, Dickson C, Black D, Lam M. Do AR-DRGs adequately describe the trauma patient episode in New South Wales, Australia? Health Information Management Journal 2011; 40 7–13.
| 21430303PubMed |
[16] Jacobs B, Jacobs L. The effect of the new trauma DRGs on reimbursement. J Trauma Inj Infect Crit Care 1992; 33 495–503.
| The effect of the new trauma DRGs on reimbursement.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK3s%2FlvFGjtQ%3D%3D&md5=6db96f26725c290f57559a0eb3601309CAS |
[17] NSW Health. Selected specialty and statewide services plans number six. NSW Trauma Services Plan. North Sydney: NSW Health; 2009.
[18] PowerHealth Solutions. Powerperformance management Adelaide 2006. Available at http://www.powerhealthsolutions.com/products/PPM/ [verified 14 February 2012]
[19] NSW Health Department. 2006–2007 NSW program and product data collection standards incorporating subacute and non-acute and national minimum dataset for mental health establishments’ data collection requirements. North Sydney: NSW Health Department; 2007.
[20] NSW Health Department. Episode funding policy 2008/2009 NSW. Sydney: NSW Health; 2008. Available at: http://www.health.nsw.gov.au/policies/pd/2008/PD2008_063.html. 1–30 [verified October 2013]
[21] Australian Tax Office. Foreign currency exchange rates for financial year 2009 foreign currency equivalent to $1 Aust. Canberra: Australian Government; 2010. Available at http://www.ato.gov.au/taxprofessionals/content.aspx?doc=/content/00228489.htm [verified October 2013]
[22] Association for the Advancement of Automotive Medicine. The abbreviated injury scale 2005 – update 2008. Barrington, IL: Association for the Advancement of Automotive Medicine; 2008.
[23] Palmer C. Major trauma and the injury severity score – where should we set the bar? Annu Proc Assoc Adv Automot Med 2007; 51 13
| 18184482PubMed |
[24] Holbrook T, Hoyt D, Anderson J. The impact of major in-hospital complications on functional outcome and quality of life after trauma. J Trauma Inj Infect Crit Care 2001; 50 91–5.
| The impact of major in-hospital complications on functional outcome and quality of life after trauma.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3MzmslWhtA%3D%3D&md5=1f72b5f00a9cee42fad8904cc6189fb6CAS |
[25] NSW Institute of Trauma and Injury Management. The NSW trauma registry profile of serious to critical injuries 2007. Sydney: NSW Institute of Trauma and Injury Management; 2012. Available at http://www.itim.nsw.gov.au [verified 29 August 2012]
[26] Cameron PA, Gabbe BJ, Cooper DJ, Walker T, Judson R, McNeil J. A statewide system of trauma care in Victoria: effect on patient survival. Med J Aust 2008; 189 546–50.
| 19012550PubMed |
[27] SPSS. SPSS: Statistical Program for the Social Sciences version 20. Armonk: IBM; 2012.
[28] Rowell D, Connelly L, Webber J, Tippett V, Thiele D, Schuetz M. What are the true costs of major trauma? J Trauma Inj Infect Crit Care 2011; 70 1086–95.
| What are the true costs of major trauma?Crossref | GoogleScholarGoogle Scholar |
[29] Gabbe BJ, Biostat GD, Lecky FE, Bouamra O, Woodford M, Jenks T, et al The effect of an organized trauma system on mortality in major trauma involving serious head injury: a comparison of the United Kingdom and Victoria, Australia. Ann Surg 2011; 253 138–43.
| The effect of an organized trauma system on mortality in major trauma involving serious head injury: a comparison of the United Kingdom and Victoria, Australia.Crossref | GoogleScholarGoogle Scholar | 21233612PubMed |
[30] Celso B, Tepas J, Langland-Orban B, Pracht E, Papa L, Lottenberg L, et al A systematic review and meta-analysis comparing outcome of severely injured patients treated in trauma centers following the establishment of trauma systems. J Trauma Inj Infect Crit Care 2006; 60 371–8.
| A systematic review and meta-analysis comparing outcome of severely injured patients treated in trauma centers following the establishment of trauma systems.Crossref | GoogleScholarGoogle Scholar |
[31] Curtis KA, Mitchell RJ, Chong SS, Balogh ZJ, Reed DJ, Clark PT, et al Injury trends and mortality in adult patients with major trauma in New South Wales. Med J Aust 2012; 197 233–7.
| Injury trends and mortality in adult patients with major trauma in New South Wales.Crossref | GoogleScholarGoogle Scholar | 22900875PubMed |
[32] Taheri P, Butz D, Watts C, Giffes L, Greenfield L. Trauma services: a profit center? J Am Coll Surg 1999; 188 349–54.
| Trauma services: a profit center?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1M3htVSqsA%3D%3D&md5=d74b7bef1da79c34a8b47394f2af1f9aCAS | 10195717PubMed |
[33] Curtis K, Bollard L, Dickson C.. Coding errors and the trauma patient – is nursing case management the solution? Aust Health Rev 2002; 25 73–80.
| Coding errors and the trauma patient – is nursing case management the solution?Crossref | GoogleScholarGoogle Scholar | 12404969PubMed |
[34] Watson WL, Ozanne-Smith J, Monash University Accident Research Centre. The cost of injury to Victoria. Melbourne: Monash University Accident Research Centre; 1997.
[35] Moczygemba J, Fenton SH. Lessons learned from an ICD-10-CM clinical documentation pilot study. Perspec Health Info Manag 2012; (Winter): 9.
[36] Santos S, Murphy G, Baxter K, Robinson KM. Organisational factors affecting the quality of hospital clinical coding. Health Inf Manag 2008; 37 25–37.
[37] Health Education and Training Institute. Clinical Coding Workforce Enhancement Project. Sydney: NSW Ministry of Health 2012. Available at http://www.heti.nsw.gov.au/programs/clinical-coding-workforce-enhancement-project/ [verified 15 October 2013]
[38] Butcher N, Balogh ZJ. The definition of polytrauma: the need for international consensus. Injury 2009; 40 S12–22.
| The definition of polytrauma: the need for international consensus.Crossref | GoogleScholarGoogle Scholar | 19895948PubMed |
[39] Pape HC, Neugebauer E, Ridley SA, Chiara O, Nielsen TG, Christensen MC. Cost-drivers in acute treatment of severe trauma in Europe: a systematic review of literature. Eur J Trauma Emerg Surg. 2009; 35 61–6.
| Cost-drivers in acute treatment of severe trauma in Europe: a systematic review of literature.Crossref | GoogleScholarGoogle Scholar |
[40] Callaway DW, Wolfe R. Geriatric trauma. Emerg Med Clin North Am 2007; 25 837–60.
| Geriatric trauma.Crossref | GoogleScholarGoogle Scholar | 17826220PubMed |
[41] World Health Organization. Global status report on road safety: time for action. Geneva: WHO; 2009.
[42] Hayen A, Mitchell R. A description of interpersonal violence-related hospitalisations in NSW. NSW Public Health Bull 2006; 17 8–12.
[43] Forum on Global Violence Prevention Institute of Medicine. Medicine Io. Social and economic costs of violence: workshop summary. Washington DC: National Academies Press; 2012.
[44] Ivers R. School based programs for prevention of violence: do they work? Inj Prev 2006; 12 351
| School based programs for prevention of violence: do they work?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD28rovVOrsA%3D%3D&md5=540d09e7d58a2f9fbb4829d9717ffa77CAS | 17018681PubMed |
[45] Banfield JM, Gomez M, Kiss A, Redelmeier DA, Brenneman F. Effectiveness of the PARTY (prevent alcohol and risk-related trauma in youth) program in preventing traumatic injuries: a 10-year analysis. J Trauma 2011; 70 732–5.
| Effectiveness of the PARTY (prevent alcohol and risk-related trauma in youth) program in preventing traumatic injuries: a 10-year analysis.Crossref | GoogleScholarGoogle Scholar | 21610366PubMed |