Integrated mental health atlas of the Western Sydney Local Health District: gaps and recommendations
Ana Fernandez A B F , James A. Gillespie C , Jennifer Smith-Merry B , Xiaoqi Feng C D E , Thomas Astell-Burt D , Cailin Maas A B and Luis Salvador-Carulla A BA The Mental Health Policy Unit, Brain and Mind Centre, The University of Sydney, 100 Mallett Street, Camperdown, NSW 2050, Australia.
B Centre for Disability Research and Policy, Faculty of Health Sciences, The University of Sydney, 75 East Street, Lidcombe, NSW 2141, Australia. Email: cailin.maas@sydney.edu.au; luis.salvador-carulla@sydney.edu.au
C Menzies Centre for Health Policy and Sydney School of Public Health, The University of Sydney, City Road, Edward Ford Building A27, NSW 2006, Australia. Email: james.gillespie@sydney.edu.au
D School of Health and Society, University of Wollongong, Northfields Avenue, Wollongong, NSW 2522, Australia. Email: xfeng@uow.edu.au; thomasab@uow.edu.au
E Early Start Research Institute, University of Wollongong, Northfields Avenue, Wollongong, NSW 2522, Australia. Email: xfeng@uow.edu.au
F Corresponding author. Email: ana.fernandez@sydney.edu.au
Australian Health Review 41(1) 38-44 https://doi.org/10.1071/AH15154
Submitted: 17 August 2015 Accepted: 1 February 2016 Published: 24 March 2016
Journal Compilation © AHHA 2017 Open Access CC BY-NC-ND
Abstract
Objective Australian mental health care remains hospital centric and fragmented; it is riddled with gaps and does little to promote recovery. Reform must be built on better knowledge of the shape of existing services. Mental health atlases are an essential part of this knowledge base, enabling comparison with other regions and jurisdictions, but must be based on a rigorous classification of services. The main aim of this study is to create an integrated mental health atlas of the Western Sydney LHD in order to help decision makers to better plan informed by local evidence.
Methods The standard classification system, namely the Description and Evaluation of Services and Directories in Europe for Long-term Care model, was used to describe and classify adult mental health services in the Western Sydney Local Health District (LHD). This information provided the foundation for accessibility maps and the analysis of the provision of care for people with a lived experience of mental illness in Western Sydney LHD. All this data was used to create the Integrated Mental Health Atlas of Western Sydney LHD.
Results The atlas identified four major gaps in mental health care in Western Sydney LHD: (1) a lack of acute and sub-acute community residential care; (2) an absence of services providing acute day care and non-acute day care; (3) low availability of specific employment services for people with a lived experience of mental ill-health; and (4) a lack of comprehensive data on the availability of supported housing.
Conclusions The integrated mental health atlas of the Western Sydney LHD provides a tool for evidence-informed planning and critical analysis of the pattern of adult mental health care.
What is known about the topic? Several reports have highlighted that the Australian mental health system is hospital based and fragmented. However, this knowledge has had little effect on actually changing the system.
What does this paper add? This paper provides a critical analysis of the pattern of adult mental health care provided within the boundaries of the Western Sydney LHD using a standard, internationally validated tool to describe and classify the services. This provides a good picture of the availability of adult mental health care at the local level that was hitherto lacking.
What are the implications for practitioners? The data presented herein provide a better understanding of the context in which mental health practitioners work. Managers and planners of services providing care for people with a lived experience of mental illness can use the information herein for better planning informed by local evidence.
Introduction
The failures and scarcities of the Australian mental health system have been well documented.1–6 We have had more than 20 years of warnings that the mental health system is built on a hospital-based and fragmented model, which promotes neither recovery nor inclusion.1,7,8 Despite the evidence reiterated in recent reports,1–5 there are few signs of change.
The model of evidence-informed policy suggests that in order to make changes decision makers (i.e. policy makers and planners) should be provided with tools to help them make better, more intelligent choices about future investments in mental health care. This must be built on knowledge of which services are needed and where and how they can be most effectively delivered. That is, decision makers would benefit from a map of where current resources are invested to guide them through their reform journey.
Integrated atlases of mental health have been developed to fulfil this need. They start from accurate local data on service availability and care capacity. These provide the foundation for maps and graphics to analyse local information on social and demographic characteristics and health-related needs.9 Integrated atlases allow comparison between territories, highlighting variations of care and detecting gaps in the system.10 The holistic service maps produced through integrated atlases allow decision makers to build bridges between the different sectors (i.e. health, family and community services, social housing, non-governmental organisations (NGOs)) and to better allocate services. This is particularly important because mental health services are becoming more ‘person centred’ and public investment is focusing on care coordination programs such as Partners in Recovery (PIR) and the National Disability Insurance Scheme (NDIS).
As a visual form of communicating health information, integrated atlases have proved to be an invaluable tool for bridging the gap between research and policy makers, translating complex statistics into forms easily communicated to audiences with varied educational backgrounds.11 Decision makers may use the information presented in the atlas as a visual reference to quickly present and structure their ideas. Consequently, they would be more able to make and communicate steps needed to implement any change in the system.12
The main aim of this study is to create an integrated mental health atlas of the Western Sydney LHD in order to help decision makers to better plan informed by local evidence. Starting from an analysis of the pattern of adult mental health care, with a focus on the gaps detected, we identify some of the main reforms that may close these gaps.
Methods
Study population
The Western Sydney LHD is a large area with a population of over 800 000 inhabitants. It is one of Australia’s fastest growing urban populations, with a diverse ethnic and linguistic mix. It has areas of extreme social and economic disadvantage, characterised by high unemployment, low education attainment rates and poor physical health.13 A recent study mapping the distribution of risk of psychological distress across New South Wales (NSW) showed above average levels in the area of the Western Sydney LHD.14
Measures
We used the Description and Evaluation of Services and Directories in Europe for Long-term Care (DESDE-LTC)15 to assess all the services providing care for people with a lived experience of mental illness within the boundaries of Western Sydney Local Health District. The DESDE-LTC is an internationally validated instrument for the standardised description and classification of services for long-term care. The DESDE-LTC instrument has been used in Chile and Canada, and in various countries in Europe with very little in common (i.e. Finland, UK, Spain and Romania).12,16–19 The DESDE-LTC system is based on local area comparisons, which allow local planning and resource allocation at the local level.
The DESDE-LTC system allows identification of the primary object for coding, namely the basic stable inputs of care (BSICs). The BSICs are the smallest identifiable distinct units of production of care within a service organisation; a BSIC is defined as a team of professionals working together to provide care for a group of people. BSICs have time stability (e.g. they may have been funded for more than 3 years), as well as structural stability, meaning they have their administrative support, their own space, their own finances (e.g. a specific cost centre) and their own forms of documentation to enable tracking of their activity (e.g. annual report or other published sources). By using a common unit of analysis, different areas can be compared.
Once BSICs are identified, the type of care provided by the BSIC is broken down into a smaller unit of analysis that identifies the main type(s) of care (MTC) offered by the BSIC. Each service is described using one or more MTC codes based on the main care structure and activity offered by the service. This classification of services based on the actual activity of the service reflects the real provision of care in the territory. Box 1 summarises the six main types of care.15
| Box 1. Main types of care identified in the Description and Evaluation of Services and Directories in Europe for Long-term Care15 |
| Residential care: The codes related to residential care are used to classify facilities that provide beds overnight for clients for a purpose related to the clinical and social management of their health condition. Residential care can be divided into acute (services dealing with crisis) and non-acute branches, with each of these subsequent branches taking into account whether the setting was the community or the hospital, and the intensity of the support. |
| Day care: The day care branch is used to classify facilities that: (1) are normally available to several clients at a time (rather than delivering services to individuals one at a time); (2) provide some combinations of treatment for problems related to long-term care needs (e.g. providing structured activities or social contact and/or support); (3) have regular opening hours during which they are normally available; and (4) expect clients to stay at the facility beyond the periods during which they have face-to-face contact with staff. This type of care can also be divided into acute and non-acute branches. In addition, it also takes into account whether the facility is targeting the health or social needs of the clients-related needs of the clients. |
| Out-patient care: The out-patient care branch is used to code facilities that: (1) involve contact between staff and clients for some purpose related to the management of the client’s condition and associated clinical and social needs; and (2) are not provided as a part of delivery of residential or day care services, as defined above. Similar to the other branches, out-patient care can be divided in acute and non-acute care, and takes into account whether the service is mobile (50% or more of the contacts are made outside the office) or non-mobile and whether the main aim is related to the health or social needs of the clients. |
| Accessibility to care: This type of care classifies facilities whose main aim is to facilitate accessibility to care for clients with long-term care needs. These services do not provide any therapeutic care. |
| Information for care: Facilities that provide clients with information and/or an assessment of their needs are classified as providing information for care. Services providing information are not involved in subsequent monitoring, follow-up or the direct provision of care. |
| Self-help and voluntary care: Facilities that aim to provide clients with support, self-help or social contact, with un-paid staff that offer any type of care described above (i.e. residential, day, out-patient, accessibility or information) are classified as providing self-help and voluntary care. |
Inclusion criteria
In order to be included in the atlas, a service had to meet the following inclusion criteria.
-
The service targets people with a lived experience of mental ill health: at least 20% of its clients have a lived experience of mental health problems.
-
The service is universally accessible. The present study focused on services that are publicly funded and/or universally accessible.
-
The service has received funding for more than 3 years. The inclusion of stable services provides an indicator of the robustness of the system. The funding could have come from different sources, but overall had to sum more than 3 years. If the service was a pilot program or already knew it was not going to be funded for any length of time beyond the point of the present study or thought it was highly unlikely, the service was not included in the atlas.
-
The service is within the boundaries of the Western Sydney LHD.
-
The service provides direct care or support to clients. Services that were only concerned with the coordination of other services or system improvement, without any type of contact with people with a lived experience of mental ill health, were excluded from the present study.
Procedures
This study was funded by Western Sydney Partners in Recovery (PIR). The PIR program attempts to bring together different organisations to deliver person-centred recovery-oriented services that meet the needs of individuals experiencing long-term, complex mental ill health.20 Western Sydney PIR assisted the researchers to identify and make contact with the service providers in the area. Service providers could choose between filling in an online survey or having a telephone or face-to-face interview with a member of the research team.
Data were collected from 13 October 2014 to 28 February 2015. Preliminary results were presented to the Western Sydney PIR Steering committee in two different meetings (December 2014 and February 2105). On May 2015, the data were presented to an audience of more than 200 service providers, consumers and advocates in the Western Sydney LHD, in public meetings organised by Western Sydney PIR. The first version of the atlas was open for public comment for 2 months. As a result of this, an additional four services were included in the atlas that were missed in the first version, and three codes were corrected (2.5% of all codes were changed after the revision).
Ethics approval was granted by the Human Research Ethics Committee (HREC) at The University of Sydney (2013/678).
Analysis
The availability and capacity of services were analysed by MTC. Rates were calculated per 100 000 inhabitants.
Availability
A service was defined as being available in a defined catchment area when it is operable or usable on demand to perform its designated or required function.
Placement capacity
The placement capacity is the maximum number of beds in residential care and of places in day care in a care delivery organisation or a catchment area at a given time.
Results
Seventy online responses were received that were supplemented with 15 face-to-face interviews with large mental health provider organisations. In all, there were 114 BSICs identified that provided care for people with a lived experience of mental illness. Approximately 93% of these BSICs received only one MTC code. The total number of MTC codes was 122. More than 74% of the MTCs were devoted to the adult population.
Pattern of adult mental health care in the Western Sydney LHD
Figure 1 shows the availability of the main components of adult mental health care per 100 000 inhabitants.
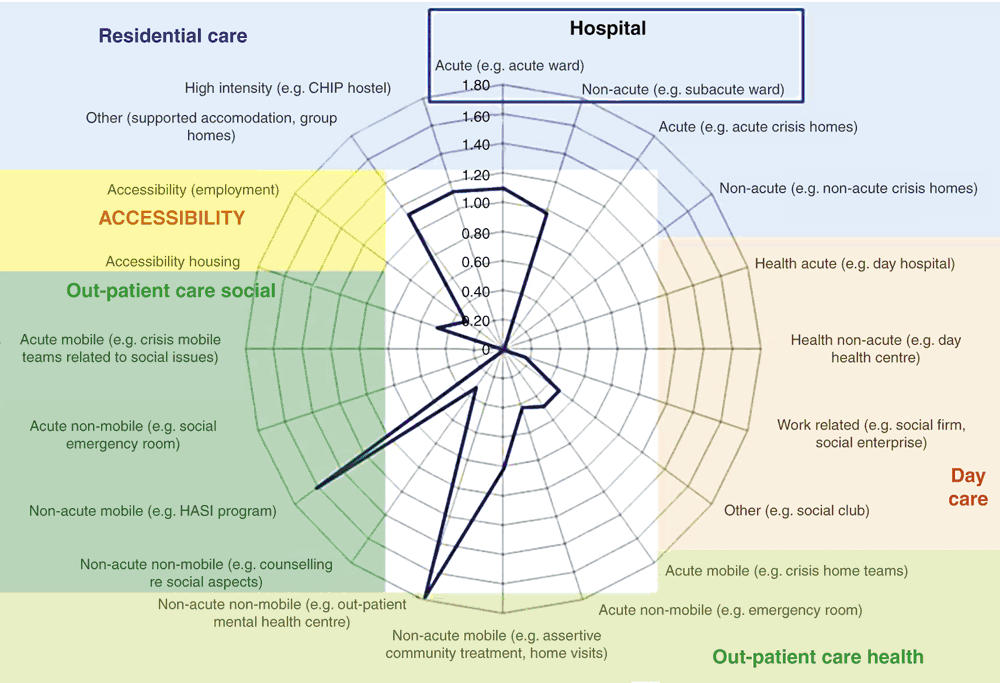
|
Residential care
The availability of acute and subacute wards in the hospital was approximately 1.10 and 0.97 per 100 000 inhabitants, respectively. The number of available beds per 100 000 inhabitants in acute and subacute wards was 20.59 and 16.83, respectively. No service was found that provided acute or subacute residential care in the community (e.g. crisis homes or transitional step-up or step-down programs). The availability of other types of residential services, such as group homes and boarding houses, was approximately 1.13 per 100 000 inhabitants. The capacity of other types of residential services was 6.31 beds per 100 000 inhabitants. The availability of high-intensity residential facilities (24-h support provided by non-clinical staff only) was also 1.13 per 100 000 inhabitants, with 5.66 places per 100 000 inhabitants.
Day care
There was no facility found in the Western Sydney LHD providing acute or non-acute day care related to the health needs of people with a lived experience of mental illness. There were only 0.16 services per 100 000 inhabitants related to employment and 0.49 providing day care related to culture or leisure (e.g. social clubs).
Out-patient care
There were 0.49 services per 100 000 inhabitants providing acute mobile care in the Western Sydney LHD (e.g. crisis homes teams) and 0.42 per 100 000 inhabitants providing acute non-mobile care related to health needs (e.g. emergency room), but none providing acute care related to social needs (e.g. social care emergency team). With regard to non-acute mobile care, there were 0.81 services per 100 000 inhabitants providing care related to health (e.g. assertive community treatment and non-acute home visits) and 1.62 services per 100 000 inhabitants related to social needs (e.g. Housing and Accommodation Support Initiative or Personal Helpers and Mentors Service). Finally, 1.78 MTCs per 100 000 inhabitants were providing non-acute, non-mobile out-patient care related to health (e.g. a visit with an allied health worker at a mental health-focused community centre), and 0.32 services per 100 000 inhabitants providing services related to social needs (e.g. debt counselling).
Accessibility to different type of care
The number of services in the Western Sydney LHD providing access to housing was 0.49 per 100 000 inhabitants, whereas there were 0.32 services per 100 000 inhabitants providing access to employment.
Discussion
The integrated mental health atlas of Western Sydney LHD has revealed some important systemic gaps in the provision of adult mental health care that can be used to focus discussion on the planning of an equitable, sustainable and effective mental health system. These gaps are related primarily to the lack of an alternative to hospitalisation and an absence of services providing day care. As such, the findings of the present study align with the recommendations made recently by the National Mental Health Commission in its Report of the National Review of Mental Health Programs and Services.1
According to several international models,21–23 specialised adult mental health services should include the following components: specialised out-patient/ambulatory clinics; assertive community treatment (ACT) teams; alternatives to acute in-patient care; alternative types of long-stay community residential care; and specialised forms of work and occupation. Community-based care and living arrangements are only sustainable if located within a broader system of care that provides short-term expert acute care to manage crisis.
Specialised out-patient/ambulatory clinic services are coded as out-patient non-mobile care because <50% of the care is provided outside the centre; these services are well developed in the Western Sydney LHD. ACT is coded as mobile non-acute out-patient care. Only one team was found providing this type of care in the Western Sydney LHD. There is good-quality evidence of the effectiveness of ACT;24 consequently, there is a need to promote the development of these services in Western Sydney.
Alternatives to acute in-patient care
Two major gaps identified in the Western Sydney LHD were in residential acute and non-acute care outside the hospital (i.e. in the community) and acute day care.
Acute beds within hospitals remain a key component of an integrated care system. However, it is also important to implement residential alternatives located in the community because these may be less stigmatising and more cost-effective than hospital admission.22 A recent quasi-experimental study performed in Brisbane (Qld, Australia) demonstrated that ‘crisis houses’ provide a cost-effective option.25 These services can also function as ‘step-down’ transitions from a period of acute psychiatric hospitalisation. The development of these types of services in the Western Sydney LHD would fill a gap in the provision of mental health care services.
Conversely, acute day care (ADC) is completely missing in the services offered by the Western Sydney LHD. ADC is a less restrictive alternative to in-patient admission for people who are acutely mentally ill. ACD delivers personalised, intensive and structured acute health care interventions outside the hospital setting. A recent systematic review26 concluded that ADC is at least as effective as traditional methods and provides a suitable option in situations where demand for in-patient care is high and facilities exist that can be converted to these uses. However, it is less attractive where the demand for in-patient care is low and can be covered by other options.26 Another study27 indicated that ADC was more useful for female, educated patients with moderate to severe symptoms than those with the most severe symptoms (regardless of gender and education), who may benefit from acute hospital care. Because of the high demand for beds in the Western Sydney LHD, ADC services could be a beneficial addition to services in the area, diverting demand from overstretched (and more expensive) acute in-patient services.
Alternative types of long-stay community residential care
Supported housing is another key component of a community mental health system. However, it has not been possible to obtain comprehensive information on the public and community housing properties assigned to people with a lived experience of mental ill health, primarily because the health status of the clients of public housing is not recorded. This lack of information on supportive accommodation jeopardises evidence-informed policy and planning, especially as more attention is given to integrating care across clinical, residential and social care services.
Specialised forms of work and occupation
Employment plays a critical role in promoting recovery.28 Unfortunately, we have found a lack of variety of services related to work and occupation. Some organisations support people with a lived experience of mental ill health to work in jobs that pay competitive wages in integrated settings in the community. However, it could be the case that many people with a lived experience of mental illness may find it difficult to enter the mainstream workforce. It is important to guarantee that there are other options available for people who may have other abilities and may require more support, such as ‘social firms’, market-oriented businesses that employ people with disabilities or ‘social enterprises’ that are primarily focused on training and rehabilitation.29 The availability of these other options may also allow a smoother transition to ordinary employment.
Further findings
The present study also located problems in the general robustness of the system. Many mental health services are provided by short-term programs lacking a recurrent funding base. The common 3-year time frame is an insufficient period to demonstrate any benefits (or lasting problems) from interventions. In Australia, as in other high-income countries, decision makers and/or policy planners take a ‘component view’ rather than a ‘system view’ of the whole pattern of care at the local level and how the different components are related.22 The problem of the component approach is that it results in a highly inefficient use of scarce resources, because investments are made in new services, whereas the core services are absent or not appropriately resourced. This leads to a ‘reactive’ system rather than a ‘proactive’ system. In addition, most of these programs are community based. Consequently, the community mental health system in the Western Sydney LHD is very ‘fragile’. More long-term funding for the NGO sector is needed. This would stabilise operations and promote long-term planning. The incorporation of systems thinking into policy and planning would ease the development of an integrated mental health model of care.
The atlas also becomes a base on which other information can be layered in order to understand and prioritise the gaps that need to be filled. For example, an evaluation of the PIR program has collected data from 791 people with severe and complex mental ill health in the Western Sydney region. An analysis of the unmet needs of this population derived from the Camberwell Assessment of Need Short Assessment (CANSAS) scale demonstrates that the highest levels of need (in order) are psychological distress, company, daytime activities, physical health, employment and volunteering, and accommodation.30 When this is layered on the atlas, we can see that there are very limited services in the region that are directly meeting these most highly rated needs.
Study limitations
Although preliminary results were presented to the Steering Committee of Western Sydney PIR and they agreed that the majority of services had been included and coded, some services that are not specific to mental health but are used by people experiencing mental ill health may be absent from the atlas. In addition, information related to the capacity of some services (i.e. number of places) is lacking because this may vary according to demand. Furthermore, private providers were not included in the present study. The inclusion of private providers in the mapping of publicly available services may increase noise, hamper the interpretation of the results and misrepresent the universality of access to services. In fact, a recent paper focused on the evaluation of the ‘Better Access’ initiative concluded that it ‘…is not providing universality or consistent equity of delivery in mental health care’ because the access is conditioned by economic barriers.31 Private services should be included as an additional map in future analyses. The present study also only mapped services that did not have time-limited funding (<3 years). In this process, nine services were excluded that had <3 years funding or were pilot programs for a time-limited period. The inclusion of care programs that are time-limited would have distorted the analysis, decreasing the usefulness of the atlas for evidence-informed planning. Finally, we only included services within the boundaries of the Western Sydney LHD. We acknowledge that some of the inhabitants in this area may use services from other adjacent LHDs, such as Nepean/Blue Mountains and South West Sydney. A complete atlas of NSW would eventually solve this problem.
Future research
The information presented in this atlas can be complemented with a pathway and network analysis. In addition, it may be useful for the development of benchmark analyses of small areas.
The Australian Government response to the review made by the National Mental Health Commission highlights the need for ‘locally planned and commissioned mental health services through Primary Health Networks (PHNs) and the establishment of a flexible primary mental health care funding pool’32. The atlas developed in the present study was funded by WentWest as the lead agency in Western Sydney PIR. WentWest is now the PHN for Western Sydney and is involved in the local use of the atlas. We are currently completing more detailed studies of its use by planners and policy makers, similar to what has been done with other atlases.12 The impact analysis of the mental health atlas of Western Sydney will be reported when completed.
Conclusion
The information presented in this atlas highlights key specific areas for system improvement in the provision of mental health services in the Western Sydney LHD. Policy makers can use the information presented in the atlas to develop service plans that are better informed by local evidence and to reform the pattern of adult mental health care in the Western Sydney LHD.
Competing interests
The authors declare they have no competing interests.
Acknowledgement
This project was funded by WentWest/Western Sydney Partners in Recovery (PIR), as part of their flexible funding. The project was overseen by the PIR Steering Committee. This committee is composed of representatives from the following organisations: Mental Health Service from Western Sydney Local Health District, AfterCare, Uniting Care Mental Health, Wise Employment, Mission Australia, RichmondPRA, CareConnect, University of Sydney, and WentWest. The authors are grateful to all for their valuable comments during the project. The authors particularly thank Western Sydney PIR, who assisted with provider contact and helped give meaning to the data: Ian Corless, Bill Campos, Angela Van Dyke, Bronwyn Howlett and Natalie Healy. The authors are also thankful to Alan Rosen and Paul O’Halloran for their critical review of the final report. Finally, the authors are grateful to the managers of the organisations and services providing care for people with a lived experience of mental illness who shared their information with us.
References
[1] National Mental Health Commission. Report of the national review of mental health programmes and services. Canberra: Australian Government; 2014.[2] Mental Health Commission of NSW. Living well report: Putting people at the centre of mental health reform in NSW. Sydney: NSW Mental Health Commission; 2014.
[3] Mendoza J, Bresnan A, Rosenberg S, Elson A, Gilbert Y, Long P, Wilson K, Hopkins J. Obsessive hope disorder: reflections on 30 years of mental health reform in Australia and visions for the future. Technical report. Caloundra: ConNetica; 2013.
[4] Medibank Private. The case for mental health reform in Australia: a review of expenditure and system design. 2013 [cited 2014 27 November]. Available at: https://www.medibankhealth.com.au/files/editor_upload/File/Mental%20Health%20Full%20Report.pdf [verified 14 January 2015].
[5] Department of Health. Fourth National Mental Health Plan: an agenda for collaborative government action in mental health 2009–2014. Canberra: Commonwealth of Australia; 2009.
[6] Australian Health Ministers. National Mental Health Plan. Canberra: Department of Health and Ageing; 1992.
[7] Rosen A, Gurr R, Fanning P. The future of community-centred health services in Australia: lessons from the mental health sector. Aust Health Rev 2010; 34 106–15.
| The future of community-centred health services in Australia: lessons from the mental health sector.Crossref | GoogleScholarGoogle Scholar | 20334766PubMed |
[8] Rosen A, Gurr R, Fanning P, Owen A. The future of community-centred health services in Australia: ‘When too many beds are not enough’. Aust Health Rev 2012; 36 239–43.
| The future of community-centred health services in Australia: ‘When too many beds are not enough’.Crossref | GoogleScholarGoogle Scholar | 22935108PubMed |
[9] Saxena S, Sharan P, Cumbrera MG, Saraceno B. World Health Organization’s mental health atlas 2005: implications for policy development. World Psychiatry 2006; 5 179–84.
| 17139355PubMed |
[10] Saxena S, Thornicroft G, Knapp M, Whiteford H. Global mental health 2 – resources for mental health: scarcity, inequity, and inefficiency. Lancet 2007; 370 878–89.
| Global mental health 2 – resources for mental health: scarcity, inequity, and inefficiency.Crossref | GoogleScholarGoogle Scholar | 17804062PubMed |
[11] Parrott R, Hopfer S, Ghetian C, Lengerich E. Mapping as a visual health communication tool: promises and dilemmas. Health Commun 2007; 22 13–24.
| Mapping as a visual health communication tool: promises and dilemmas.Crossref | GoogleScholarGoogle Scholar | 17617010PubMed |
[12] Fernandez A, Salinas-Perez JA, Gutierrez-Colosia MR, Prat-Pubill B, Serrano-Blanco A, Molina C, Jorda E, Garcia-Alonso CR, Salvador-Carulla L. Use of an integrated atlas of mental health care for evidence informed policy in Catalonia (Spain). Epidemiol Psychiatr Sci 2014; 16 1–13.
| 1:CAS:528:DC%2BC2cXhs1yisbY%3D&md5=8be37b4b1eae0257b81bfdf3bf15072eCAS |
[13] Montoya D. Western Sydney: An economic Profile. Briefing Paper No 6/2012. NSW Parlimentary Research Service. Available at: https://www.parliament.nsw.gov.au/prod/parlment/publications.nsf/0/1003F4B4BE8C5699CA257A5B00205266/$File/Western%20Sydney%20An%20Economic%20Profile%20Briefing%20Paper%2006%202012.pdf [verified 18 Feb 2016].
[14] Astell-Burt T, Feng X. Investigating ‘place effects’ on mental health: implications for population-based studies in psychiatry. Epidemiol Psychiatr Sci 2015; 24 27–37.
| Investigating ‘place effects’ on mental health: implications for population-based studies in psychiatry.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC2MzgslCltg%3D%3D&md5=793c893b4aafb150cb0fb3a07a559f27CAS | 25424460PubMed |
[15] Salvador-Carulla L, Alvarez-Galvez J, Romero C, Gutierrez-Colosia MR, Weber G, McDaid D, Dimitrov H, Sprah L, Kalseth B, Tibaldi G, Salinas-Perez JA, Lagares-Franco C, Roma-Ferri MT, Johnson S. Evaluation of an integrated system for classification, assessment and comparison of services for long-term care in Europe: the eDESDE-LTC study. BMC Health Serv Res 2013; 13 218
| Evaluation of an integrated system for classification, assessment and comparison of services for long-term care in Europe: the eDESDE-LTC study.Crossref | GoogleScholarGoogle Scholar | 23768163PubMed |
[16] The Refinement Research Consortium. The refinement project. 2011. Available at: http://www.refinementproject.eu/results.php [verified 14 January 2015].
[17] Salvador-Carulla L, Saldivia S, Martinez-Leal R, Vicente B, Garcia-Alonso C, Grandon P, Haro JM. Meso-level comparison of mental health service availability and use in Chile and Spain. Psychiatr Serv 2008; 59 421–8.
| Meso-level comparison of mental health service availability and use in Chile and Spain.Crossref | GoogleScholarGoogle Scholar | 18378842PubMed |
[18] Lesage A, Rhéaume J, Laberge F. L’application Québécoise du modèle Européen de cartographie des services de santé mentale pour les personnes souffrant de troubles mentaux graves. JASP 2002. 2002. Available at: http://jasp.inspq.qc.ca/Data/Sites/1/SharedFiles/presentations/2002/20021120-Rheaume-ModeleEuropeenCartographie.pdf [verified 14 January 2015].
[19] Salvador-Carulla L, Amaddeo F, Gutierrez-Colosia MR, Salazzari D, Gonzalez-Caballero JL, Montagni I, Tedeschi F, Cetrano G, Chevreul K, Kalseth J, Hagmair G, Strabmyr C, Park A, Sfetcu R, Wahlbeck K, Garcia , Alonso C. Developing a tool for mapping adult mental health care provision in Europe: the REMAST research protocol and its contribution to better integrated care Int J Integr Care 2015; 15
| Developing a tool for mapping adult mental health care provision in Europe: the REMAST research protocol and its contribution to better integrated careCrossref | GoogleScholarGoogle Scholar |
[20] Department of Health. Partners in recovery. 2014. Available at: http://www.health.gov.au/internet/main/publishing.nsf/Content/mental-pir [verified 14 January 2015].
[21] Department of Health. National service framework for mental health. London: Department of Health; 1999.
[22] Thornicroft G, Tansella M. The balanced care model for global mental health. Psychol Med 2013; 43 849–63.
| The balanced care model for global mental health.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC38jpt1ajug%3D%3D&md5=b2f0a79e150a694f5cb8bb9e403a8967CAS | 22785067PubMed |
[23] Thornicroft G, Tansella M. Components of a modern mental health service: a pragmatic balance of community and hospital care: overview of systematic evidence. Br J Psychiatry 2004; 185 283–90.
| Components of a modern mental health service: a pragmatic balance of community and hospital care: overview of systematic evidence.Crossref | GoogleScholarGoogle Scholar | 15458987PubMed |
[24] Marshall M, Lockwood A. Assertive community treatment for people with severe mental disorders. Cochrane Database Syst Rev 2000; 2 CD001089
| 10796415PubMed |
[25] Siskind D, Harris M, Kisely S, Brogan J, Pirkis J, Crompton D, Whiteford H. A retrospective quasi-experimental study of a community crisis house for patients with severe and persistent mental illness. Aust N Z J Psychiatry 2013; 47 667–75.
| A retrospective quasi-experimental study of a community crisis house for patients with severe and persistent mental illness.Crossref | GoogleScholarGoogle Scholar | 23567635PubMed |
[26] Marshall M, Crowther R, Sledge WH, Rathbone J, Soares-Weiser K. Day hospital versus admission for acute psychiatric disorders. Cochrane Database Syst Rev 2011; 12 CD004026
| 22161384PubMed |
[27] Priebe S, McCabe R, Schutzwohl M, Kiejna A, Nawka P, Raboch J, Reininghaus U, Wang D, Kallert TW. Patient characteristics predicting better treatment outcomes in day hospitals compared with inpatient wards. Psychiatr Serv 2011; 62 278–84.
| Patient characteristics predicting better treatment outcomes in day hospitals compared with inpatient wards.Crossref | GoogleScholarGoogle Scholar | 21363899PubMed |
[28] Walsh FP, Tickle AC. Working towards recovery: the role of employment in recovery from serious mental health problems: a qualitative meta-synthesis. Int J Psychosoc Rehabil 2013; 17 35–49.
[29] Grove B. Mental health and employment: shaping a new agenda. J Ment Health 1999; 8 131–40.
| Mental health and employment: shaping a new agenda.Crossref | GoogleScholarGoogle Scholar |
[30] Smith-Merry J, Gillespie J, Hancock N, Yen I. Integrating care for chronic mental ill-health: the Partners in Recovery Western Sydney study. Int J Integr Care 2014; 14
| Integrating care for chronic mental ill-health: the Partners in Recovery Western Sydney study.Crossref | GoogleScholarGoogle Scholar |
[31] Meadows GN, Enticott JC, Inder B, Russell GM, Gurr R. Better access to mental health care and the failure of the Medicare principle of universality. Med J Aust 2015; 202 190–4.
| Better access to mental health care and the failure of the Medicare principle of universality.Crossref | GoogleScholarGoogle Scholar | 25716601PubMed |
[32] Department of Health. Australian Government response to Contributing Lives, Thriving Communities: review of mental health programmes and services. Commonwealth of Australia; 2015. Available at: http://www.health.gov.au/internet/main/publishing.nsf/Content/0DBEF2D78F7CB9E7CA257F07001ACC6D/$File/response.pdf [verified 10 December 2015].


