Trends and predicted trends in presentations of older people to Australian emergency departments: effects of demand growth, population aging and climate change
Ellen Burkett A B G , Melinda G. Martin-Khan C D , Justin Scott E , Mayukh Samanta F and Leonard C. Gray C DA Princess Alexandra Hospital, Ipswich Road, Woolloongabba, Qld 4102, Australia.
B South-side Clinical School, School of Medicine, University of Queensland, Princess Alexandra Hospital, Ipswich Road, Woolloongabba, Qld 4102, Australia.
C Centre for Research in Geriatric Medicine, University of Queensland, Princess Alexandra Hospital, Ipswich Road, Woolloongabba, Qld 4102, Australia.
D Centre for Online Health, School of Medicine, University of Queensland, Princess Alexandra Hospital, Ipswich Road, Woolloongabba, Qld 4102, Australia. Email: m.martinkhan@uq.edu.au; len.gray@uq.edu.au
E Queensland Facility for Advanced Bioinformatics, University of Queensland, 306 Carmody Road, St Lucia, Qld 4072, Australia. Email: j.scott@qfab.org
F Clinical Trials and Biostatistics Unit, QIMR Berghofer Medical Research Institute, 300 Herston Road, Herston, Qld 4006, Australia. Email: Mayukh.Samanta@qimrberghofer.edu.au
G Corresponding author. Email: ellen.burkett@health.qld.gov.au
Australian Health Review 41(3) 246-253 https://doi.org/10.1071/AH15165
Submitted: 8 September 2015 Accepted: 23 May 2016 Published: 29 July 2016
Journal Compilation © AHHA 2017 Open Access CC BY-NC-ND
Abstract
Objectives The aim of the present study was to describe trends in and age and gender distributions of presentations of older people to Australian emergency departments (EDs) from July 2006 to June 2011, and to develop ED utilisation projections to 2050.
Methods A retrospective analysis of data collected in the National Non-admitted Patient Emergency Department Care Database was undertaken to assess trends in ED presentations. Three standard Australian Bureau of Statistics population growth models, with and without adjustment for current trends in ED presentation growth and effects of climate change, were examined with projections of ED presentations across three age groups (0–64, 65–84 and ≥85 years) to 2050.
Results From 2006–07 to 2010–11, ED presentations increased by 12.63%, whereas the Australian population over this time increased by only 7.26%. Rates of presentation per head of population were greatest among those aged ≥85 years. Projections of ED presentations to 2050 revealed that overall ED presentations are forecast to increase markedly, with the rate of increase being most marked for older people.
Conclusion Growth in Australian ED presentations from 2006–07 to 2010–11 was greater than that expected from population growth alone. The predicted changes in demand for ED care will only be able to be optimally managed if Australian health policy, ED funding instruments and ED models of care are adjusted to take into account the specific care and resource needs of older people.
What is known about the topic? Rapid population aging is anticipated over coming decades. International studies and specific local-level Australian studies have demonstrated significant growth in ED presentations. There have been no prior national-level Australian studies of ED presentation trends by age group.
What does this paper add? The present study examined national ED presentation trends from July 2006 to June 2011, with specific emphasis on trends in presentation by age group. ED presentation growth was found to exceed population growth in all age groups. The rate of ED presentations per head of population was highest among those aged ≥85 years. ED utilisation projections to 2050, using standard Australian Bureau of Statistics population modelling, with and without adjustment for current ED growth, were developed. The projections demonstrated linear growth in ED presentation for those aged 0–84 years, with growth in ED presentations of the ≥85 year age group demonstrating marked acceleration after 2030.
What are the implications for practitioners? Growth in ED presentations exceeding population growth suggests that current models of acute health care delivery require review to ensure that optimal care is delivered in the most fiscally efficient manner. Trends in presentation of older people emphasise the imperative for ED workforce planning and education in care of this complex patient cohort, and the requirement to review funding models to incentivise investment in ED avoidance and substitutive care models targeting older people.
Introduction
Background and rationale
Older people have complex care needs that are highly time and resource intensive.1–3 They have further been identified as a vulnerable population in the emergency department (ED) environment, having substantially inferior clinical outcomes after discharge from the ED,4–6 with higher rates of missed diagnoses and medication errors compared with younger, severity-matched controls.7–9 Internationally, presentations of older people to EDs are projected to increase markedly as a result of rapid population aging.10
The Madrid International Plan of Action on Ageing stressed the need to integrate issues of aging into all relevant policy arenas, through collection and analysis of age-disaggregated data, this being central to ensuring that policies respond to needs of the elderly and that efficiency of resource utilisation is optimised.11 ED funding models in Australia do not adjust funding based on the age of the patient and, currently, with a focus on activity-based funding, do not incentivise investment in ED substitutive care or avoidance models of care.12,13
In order to better inform Australian health policy and facilitate development of funding models and models of healthcare that deliver optimal acute health care to Australians, a detailed understanding of trends in and effects of population ageing on ED presentations across Australia is essential.
Objectives
The present study involved secondary analysis of age-disaggregated data from July 2006 to June 2011, using the National Non-admitted Patient Emergency Department Care Database (NNAPEDCD). Specific objectives of the study were to: (1) describe the age and gender distribution of people presenting to EDs; (2) describe the trends in number of ED presentations to public EDs across Australia of older people compared with younger people; and (3) develop ED utilisation projections to assess trends in ED presentations to 2050, based on predicted population trends, demonstrated growth in ED presentations and potential effects of climate change.
Methods
Study design
A retrospective analysis of data collected in the NNAPEDCD was undertaken. The NNAPEDCD is a national database administered by the Australian Institute of Health and Welfare (AIHW) that describes episode-level presentations to public EDs across Australia. The research team purchased de-identified data across 15 data elements from the AIHW. The data elements provided were determined by availability, data integrity and consent of state data custodians. State data custodians provided stipulations on data elements to be provided, their format, use and reporting. The data custodians further required that no comparative state-level data be published. The study was granted ethics approval by the University of Queensland Medical Research Ethics Committee.
Variables
NNAPEDCD variables
Data representativeness was assessed by distribution of presentations by state or territory of hospitalisation, by year and by hospital peer group (hospital groupings that allow for comparison of hospital performance across hospitals with similar characteristics).
As a requirement of state data custodians, all visits to EDs from July 2006 to June 2011 were stratified by age group. The age groups used were based on the groupings that fulfilled study requirements and were broadly consistent with the age ranges defined by both the National Health Data Dictionary14 and demographic projections of the Australian Bureau of Statistics (ABS),15 specifically 0–64 years (young people), 65–84 years (older people) and ≥85 years (oldest old). Trends over time of ED presentations by age group were assessed. Gender and hospital peer group of ED presentations by age group were also examined.
ABS variables
Projected population estimates over three population growth scenarios from the ABS, with their conservative assumptions of fertility, life expectancy and immigration, were used to assess the rate of ED presentations by population.15 These rates, in conjunction with the documented actual population for 2007–11,16 identified trends in ED growth and predicted effects of climate change and were used to forecast demand for ED care to 2050. Three ABS population growth scenarios were used in predictive modelling: high (A), medium (B) and low (C). Scenario A assumes a fertility rate of 2.0 births per woman, net annual overseas migration of 280 000 and life expectancy at birth to be 92.1 years for men and 93.6 years for women by 2060–61, with projections of 5.4% of the population to be ≥85 years by 2054–55. Scenario B assumes a fertility rate at 1.8 births per woman, net annual overseas migration of 240 000 and life expectancy of 85.2 years for men and 88.3 years for women by 2060–61, with 4.3% of the population to be ≥85 years by 2054–55. Scenario C assumes a fertility rate at 1.6 births per woman, net annual overseas migration of 200 000 and a life expectancy of 85.2 years for men and 88.3 years for women by 2060–61, with 4.3% of the population to be ≥85 years by 2054–55.15 Two scenarios were examined for each of these population growth examples: with and without adjustment for current trends in ED presentation growth.
Climate change variables
Three climate change scenarios of the Intergovernmental Panel of Climate Change (IPCC) were examined for effects on ED presentations: no climate change (IPCC scenario U0), unmitigated climate change (IPCC scenario U1) and mitigated climate change (IPCC scenario M4).17 Change in hospitalisation rate was used as relative indicator of change in ED presentation rate in the setting of climate change.
Statistical methods and analysis
All analyses were performed using Microsoft® Excel for Mac Version 14; IBM® SPSS® Statistics, Version 22.0; GraphPad Prism Version 5.0d; and R Foundation for Statistical Computing, R Version 3.1.1.
Stability of the data was investigated by assessing the consistency of states and hospitals contributing data across time.
Demographic profiles of patients presenting to the ED were assessed using descriptive statistics, with results reported for individual age groups and for the population overall. Mean values, 95% confidence intervals (CIs) of the mean, median and interquartile ranges (IQR) were used to report continuous variables, whereas categorical variables are reported as frequency and percentages. Group differences for normally distributed continuous variables were compared with two-tailed t-tests (or analysis of variance (ANOVA) for multiple comparisons, with a post hoc Tukey test), whereas non-parametric variables were compared using the Mann–Whitney test (or Kruskal–Wallis for multiple comparisons). Pearson’s Chi-squared test was used to assess the significance of group differences for categorical variables. For all comparisons, P < 0.05 (two-tailed) was considered significant.
Trends in presentations to ED over time were assessed with linear regression, using only that portion of the dataset where the same hospitals contributed data over time to negate confounding of instability in contributing hospital numbers. To ensure that this population remained representative of the total population, the data from these hospitals were compared with those of the hospitals contributing data for only a portion of the study period.
Linear regression slopes were compared using a method equivalent to analysis of covariance (ANCOVA), with a two-tailed P-value testing the null hypothesis that slopes were all identical and P < 0.05 indicating that the lines were significantly different.18
ED presentation projections were developed using ED trends (assessed via Excel using a complete linear least-squares curve fitting, with uncertainty estimates for the fit values), actual population for 2007–1116 and ABS population growth projections from 2012 to 2050. Presentations were projected using two scenarios: the first involved extrapolations based on the ratio of average ED presentations per head of population between 2007 and 2011, with no adjustment for growth in ED presentations; the second involved extrapolations of the ratio of average ED presentations per head of population adjusted for the trend in ED growth per year between 2007 and 2011.
Results
There were 28 708 035 ED episodes of care in 187 hospitals (plus the hospital/s of the single territory contributing data without hospital identifier/s) reported during the study period. All Australian states and territories contributed data, with 77.1% of data contributed being from eastern mainland states; this distribution of data matched state distribution of population. There were 154 hospitals from all six states and one territory that contributed data for all 5 years, representing 25 816 425 ED episodes of care. Trends did not differ significantly between these hospitals and the further 33 hospitals that contributed data over only a portion of the study time period.
Data contributed by one territory was provided as an entirety rather than by hospital. Therefore, the data used for trending represented presentations to 82.35% of all public hospital EDs contributing data; however, these presentations represented 89.93% of all documented ED episodes of care over this time.
Demographic profiles
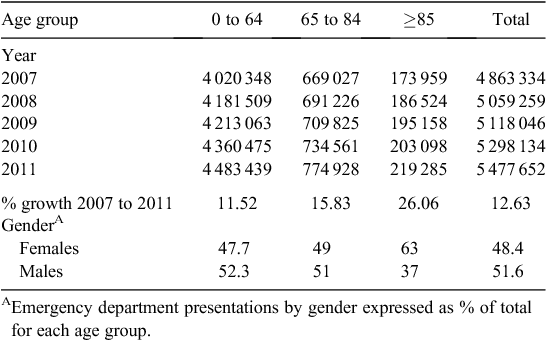
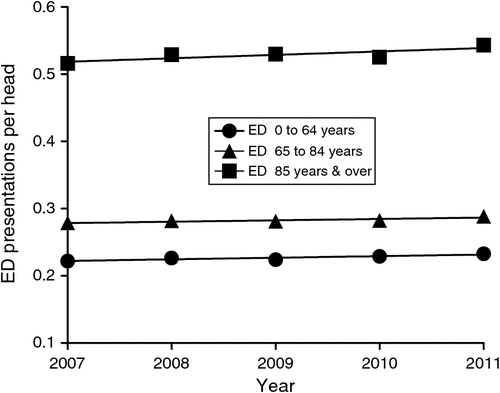
Demographic profiles of patients presenting to EDs in Australia are given in Table 1. Most ED presentations (82%) were by people in the 0–64 years age group, with those aged ≥65 and ≥85 years representing 18% and 3.8% respectively of total ED presentations from 2007 to 2011. Rates of ED presentation per head of population were also assessed (Fig. 1), although these rates likely represent an underestimate of true presentation rates because of data limitations (see below). The crude annual average rate of ED presentations from 2007 to 2011 across all age groups was 0.24 presentations per person. The crude annual average rate of ED presentations per person from 2007 to 2011 was highest among those aged ≥85 years, at 0.53 annual presentations per person, with differences reaching statistical significance among the three age groups (P < 0.001).
|
|
Overall, the proportion of presentations by females and males was similar, with a slight male predominance in those aged 0–84 years. However, among the oldest old (≥85 years), the proportion of female presentations was significantly higher than that of males (62.9% females; 37.1% males; P < 0.001).
Assessment of ED presentations by peer group hospitals revealed significantly fewer older people presenting to A2 hospitals (specialised women and children’s hospitals) and fewer older people presenting to D2 (small non-acute) and D3 (small remote) hospitals compared with A1 or major city hospitals (13.9%, 5.4% and 20.6% respectively; P < 0.001). However, it must be noted that D2 and D3 hospitals accounted for only 0.3% and 0.6% of total ED presentations documented by NNAPEDCD for the study time frame.
ED presentation trends
There was a 12.63% increase in overall ED presentations from 2006–07 to 2010–11 (Table 1). Population growth over this same time period was 7.26%;16 therefore, growth in overall ED presentations occurred at a rate greater than that of population growth.
From 2006–07 to 2010–11, the group accounting for the greatest absolute increase in ED presentations was the 0–64 years age group (ED presentation annual growth trend of 110 515 presentations). However, over the 5-year study period, the percentage growth was greatest in the older age groups (26.06%, 15.83% and 11.52% increases in ED presentations in those aged ≥85, 65–84 and 0–64 years respectively), with these differences being significant (P < 0.001). For each of these age groups, this percentage growth in ED presentations was greater than the percentage population growth over the same period, with population growth for this time period being 19.72%, 11.79% and 6.42% for those aged ≥85, 65–84 and 0–64 years respectively.
Demand projections for ED services to 2050
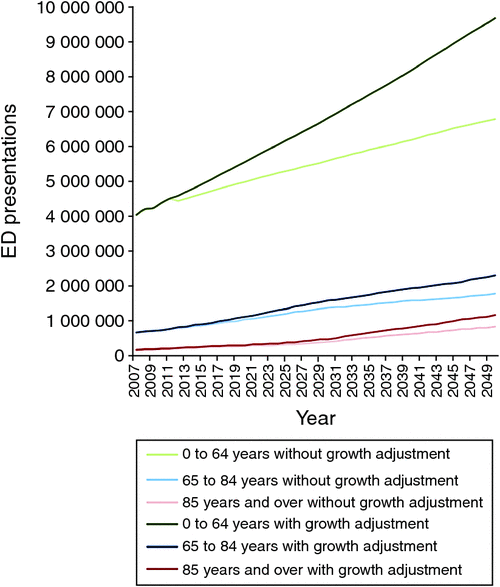
ED presentation projections, taking into account three scenarios of ABS projections of population growth (A, high; B, medium; C, low), revealed that presentations will increase significantly over coming decades regardless of potential population growth scenarios (Fig. 2). In the model that assumed medium population growth (ABS Scenario B), total annual ED presentations increased from 4 863 334 presentations in 2006–7 to 9 350 197 presentations in 2050–51 when no adjustment for growth in ED presentations was undertaken and to 13 164 844 when adjustment for ED growth patterns was performed.
|
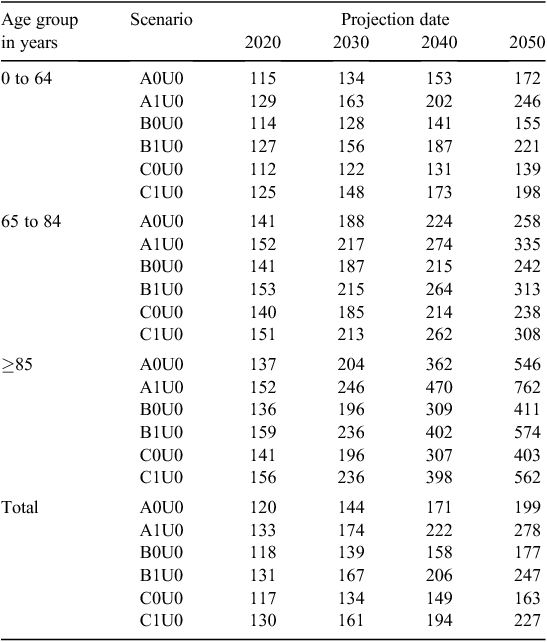
Again assuming medium population growth and with no adjustment for ED growth, compared with 2010 (considered as the baseline of 100%), ED presentation projections in 2050 revealed an increase to 177% of total ED presentations, with an increase to 242% and 411% in ED presentations by those aged 65–84 and ≥85 years respectively (Table 2). With ED growth adjusted for, presentations of those aged ≥85 years in a medium growth population scenario increased to 150% by 2020, 236% by 2030, 402% by 2040 and 574% by 2050.
|
Three climate change scenarios were examined for their effect on ED presentations (no climate change, unmitigated climate change and mitigated climate change). Change in hospitalisations was used as a relative indicator of change in ED presentations. The difference between no climate change and the two climate change scenarios was minimal, around 1%, even out to 2070.
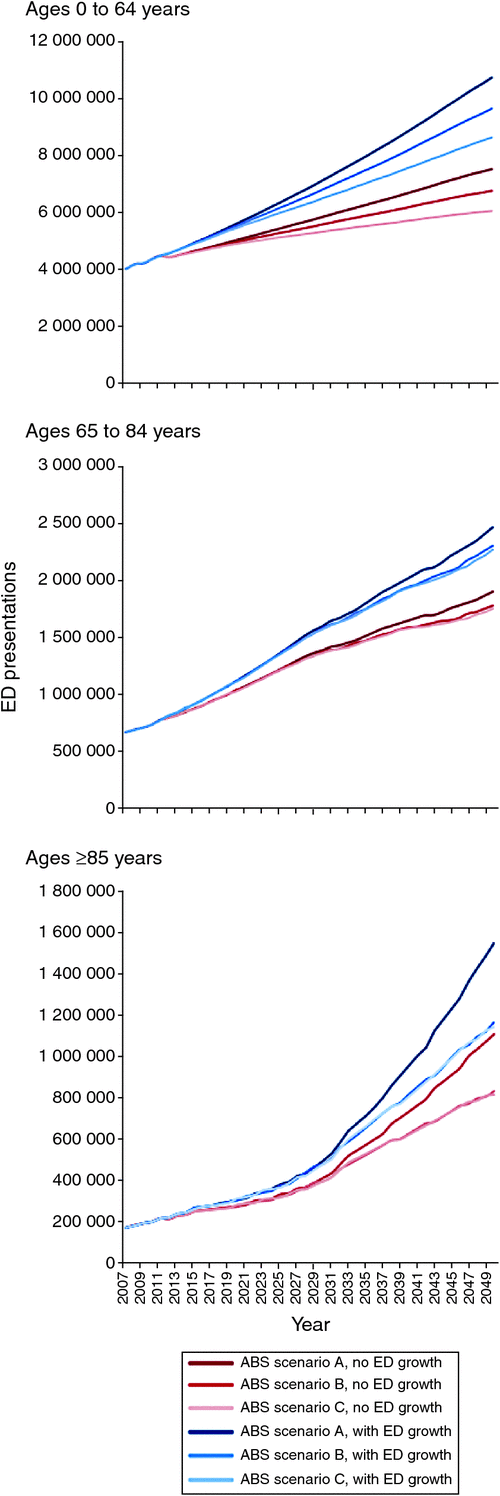
The results of projections for each age group, incorporating the three ABS scenarios with no climate change and with and without ED growth adjustment, are shown in Fig. 3. Although growth is linear for the 0–84 years age groups, the growth in ED presentations of the ≥85 years age group accelerates markedly after 2030.
|
Discussion
Between now and 2050, the Australian population is anticipated to experience significant aging.15 Given the documented sharp increase in health expenditure with age, total health expenditure is projected to increase significantly, in concert with population aging.19,20 The present study has attempted to promote a baseline understanding of age-disaggregated data on ED presentations to facilitate exploration of the potential effect of this aging on ED service delivery in Australia.
The present study has shown that older people represent a significant and increasing sector of ED presentations in Australia. This is in keeping with previous international studies that found similar trends.21,22
Although the rate of population growth within the young-old group is expected to equal that of the old-old group in Australia,23 the rate of presentation to the ED of the 65–84 years cohort increased more from 2006–07 to 2010–11 in absolute terms compared with the ≥85 years age group. However, when assessed per head of population, the growth trend was greater in the ≥85 years age group.
As expected, there was a female predominance in the oldest-old group, with male predominance in the 65–74 year group; this likely reflects changes in gender proportions at the population level with aging.24
The finding that fewer older people presented to D2 (small non-acute) and D3 (small remote) hospitals compared with A1 or major city hospitals may reflect the documented lower proportion of older adults living in remote communities, or earlier mortality of people living in remote areas.25
ED presentation projections were assessed in relation to three ABS population growth scenarios, namely high (A), medium (B) and low (C).15 Of note, the 2015 intergenerational report used assumptions of a fertility rate of 1.9 births per woman, net annual overseas migration of 215 000, life expectancy of 95.1 years for men and 96.6 years for women by 2054–55, with 4.9% of the population aged ≥85 years.26 Therefore, current government policy appears most closely aligned with population projections following a model with population growth between those of ABS Scenarios A and B. If these assumptions are correct, future ED presentations may similarly follow a pattern that falls between modelled Scenarios A and B.
The ED presentation projections were developed for each population scenario both with and without adjustment for observed trends in ED growth. The observed trends in ED growth and the finding that this growth exceeds population growth mirror those previously demonstrated in trend analysis of ED presentations in Australia, although prior studies have assessed these trends at the local level.27 A systematic review of trends in ED presentations concluded that population aging, lack of social supports for older people and reduced rates of home and nursing home visits of primary care providers are all contributors to observed high growth rates of ED presentations.28
Service demand exceeding population growth suggests that alternative models of care may require consideration in order to meet further predicted increases in demand. Although it may be argued that innovations in disease treatments may reduce future demand on hospital services, there is significant potential that emergence of antimicrobial resistance may increase demand for these services.29 The most marked relative increases in ED presentations in each of the population scenarios, both in terms of percentage change relative to 2010 presentations and per head of population, can be expected amongst older Australians. Older people continue to represent only a small proportion of ED presentations in absolute terms. However, given their documented increased time and resource utilisation in the ED,1–3 their multidisciplinary care needs, high case complexity and higher rates of in-patient admission, this projected growth in older person presentations poses a significant challenge for our health systems.30
ED workforce planning is required now to ensure these increasing demands can be adequately met. Aging of the population and the projected proportional increase in older person presentations to the ED requires an urgent review of the ED training curriculum to ensure that the specific care needs of older people are adequately addressed in ED physician training. Unlike the American College of Emergency Physicians,31 the Australasian College for Emergency Medicine (ACEM) does not have a specific, explicitly defined geriatric emergency medicine curriculum. The revised ACEM policy on the care of elderly patients in the ED emphasises the need for access to multidisciplinary assessment and care planning in the ED,32 and although it appears that many EDs have embraced a multidisciplinary approach to geriatric patient assessment, the extent of access to multidisciplinary assessment in EDs across Australia has not been documented. In addition, the projected aging of the population mandates consideration of ED design features that may affect older people’s safety, delirium and falls risk, ability to confidently navigate in the ED and comfort.33
Ensuring sustainability of acute healthcare systems despite this growth in ED presentations and in-patient admissions will require forward planning, with optimisation of healthcare funding models to incentivise ED substitutive care and hospital avoidance programs, with emphasis on avoiding presentations of older people and increasingly managing this demand in the community setting.28 Such programs of ED avoidance34 may include improved chronic disease care,35 management of specific acute illnesses in ED-alternative settings,36 enhancing primary care services or improved used of advance care plans.37,38 ED substitutive care models have been best described in the residential aged care population and encompass either nurse-led or integrated care models, and have been demonstrated to reduce both ED presentations and in-patient length of stay of residents of aged care facilities.37,39 Current emphasis on activity-based funding (ABF) models serves as a disincentive for health services to adopt these innovative programs, because they largely do not attract ABF funding for ED substitutive care elements of the programs. Governments will need to address these funding disincentives to facilitate meeting of future projected growth in ED demand.
Climate change was found to have only a minimal effect on ED presentations (~1%) compared with the very significant effect of demographic change. However, this 1% effect (equating to ~93 501 and ~131 648 patients in medium population growth scenarios with and without adjustment for ED growth respectively) is likely to present as surges concurrent with severe weather events and these events, particularly in the face of concurrent demographic change effects, may further overwhelm EDs.
Limitations
The data available to the research team spanned only July 2006–June 2011. Assessment of data integrity revealed that there was considerable variation in the proportion of hospitals consistently contributing data over time, with trending therefore performed using only those hospitals contributing data for the entire study period. For the 2006–7 and 2010–11 years, the proportion of all emergency occasions of service captured by NNAPEDCD was estimated by the organisation to be 100% for public hospitals in Peer Groups A and B and 78% and 81% respectively in 2006–7 and 2010–11 for all other public hospitals.40,41
Bias may also have been introduced secondary to potential changes in definitions used by the data providers from year to year and between jurisdictions. However, the use of the National Health Data Dictionary by all contributing hospitals ensures potential for a high standard of data comparability between states. In addition, it is likely that such measurement bias is non-differential with regard to the parameter of most interest, namely patient age.
It should be noted that the effects of climate change will vary across Australia; however, the modelling was only assessed at a national level. In addition, because of constraints of the climate change models used, assessment was only performed for years 2020 and 2050.
The predictive modelling in the present study did not incorporate effects on ED presentation of factors such as changes to models of care and the development of new medical therapies, which may influence the need for ED presentation. Furthermore, internal constraints on ED presentations, such as effects on presentations of prolonged waiting times, as reflected in queuing theory, were not accounted for.
Finally, it should not be overlooked that differences in local population demographics may result in variable effects of Australian population aging on individual EDs.42 Therefore, if using the finding of the present study to inform local policy and planning, it would be necessary to explore specific local trends.
Conclusion
The present study has identified that, across all age groups, growth in ED presentations was greater than expected from population growth alone. Older people represent a minority of ED presentations in absolute terms. However, older Australians account for the most marked observed and projected relative increases in ED presentations (in terms of both percentage change and per head of population). Older people’s increased ED resource utilisation, multidisciplinary care needs and documented increased risk of diagnostic and medication error on ED presentation mean there is an imperative for both health policy planners and emergency physicians to consider the following in their planning for future changes in ED utilisation: (1) ED workforce planning to allow for the anticipated increase in ED presentations; (2) emphasis on the management of the complex care needs of the geriatric patient in the emergency fellowship curriculum, as well as in ongoing professional education; (3) implementation of geriatric-friendly ED design principles; and (4) adoption of healthcare funding models that incentivise ED avoidance and substitutive care programs and improve access to primary care, such that demand may be increasingly be managed in the community setting.
Competing interests
Dr Ellen Burkett is clinical lead for a recurrently funded Queensland Health ED substitutive care and hospital avoidance program for residents of aged care facilities; she is also a member of the executive of the Geriatric Emergency Medicine Special Interest Group of the Australasian College for Emergency Medicine.
References
[1] Aminzadeh F, Dalziel WB. Older adults in the emergency department: a systematic review of patterns of use, adverse outcomes, and effectiveness of interventions. Ann Emerg Med 2002; 39 238–47.| Older adults in the emergency department: a systematic review of patterns of use, adverse outcomes, and effectiveness of interventions.Crossref | GoogleScholarGoogle Scholar | 11867975PubMed |
[2] George G, Jell C, Todd BS. Effect of population ageing on emergency department speed and efficiency: a historical perspective from a district general hospital in the UK. Emerg Med J 2006; 23 379–83.
| Effect of population ageing on emergency department speed and efficiency: a historical perspective from a district general hospital in the UK.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD283itVSisQ%3D%3D&md5=f364491c295ba929e7fdd104793a2734CAS | 16627841PubMed |
[3] Salvi F, Morichi V, Grilli A, Giorgi R, De Tommaso G, Dessi-Fulgheri P. The elderly in the emergency department: a critical review of problems and solutions. Intern Emerg Med 2007; 2 292–301.
| The elderly in the emergency department: a critical review of problems and solutions.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1c%2FgsFeksA%3D%3D&md5=9b23c5d86e709d5a440b8dc025a598e1CAS | 18043874PubMed |
[4] Caplan GA, Brown A, Croker WD, Doolan J. Risk of admission within 4 weeks of discharge of elderly patients from the emergency department: the DEED study. Age Ageing 1998; 27 697–702.
| Risk of admission within 4 weeks of discharge of elderly patients from the emergency department: the DEED study.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1MzjsFWnug%3D%3D&md5=b3ee643a490f22e9e5cd51acbb5f989aCAS | 10408663PubMed |
[5] Friedmann PD, Jin L, Karrison TG, Hayley DC, Mulliken R, Walter J, Chin M. Early revisit, hospitalization, or death among older persons discharged from the ED. Am J Emerg Med 2001; 19 125–9.
| Early revisit, hospitalization, or death among older persons discharged from the ED.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3M7psl2ltg%3D%3D&md5=839ab60693bede9d1f6c8a74d579dbb5CAS | 11239256PubMed |
[6] Hastings SN, Purser JL, Johnson KS, Sloane RJ, Whitson HE. Frailty predicts some but not all adverse outcomes in older adults discharged from the emergency department. J Am Geriatr Soc 2008; 56 1651–7.
| Frailty predicts some but not all adverse outcomes in older adults discharged from the emergency department.Crossref | GoogleScholarGoogle Scholar | 18691282PubMed |
[7] Meldon SW, Mion LC, Palmer RM, Drew BL, Connor JT, Lewicki LJ, et al A brief risk-stratification tool to predict repeat emergency department visits and hospitalizations in older patients discharged from the emergency department. Acad Emerg Med 2003; 10 224–32.
| A brief risk-stratification tool to predict repeat emergency department visits and hospitalizations in older patients discharged from the emergency department.Crossref | GoogleScholarGoogle Scholar | 12615588PubMed |
[8] Chin MH, Wang LC, Jin L, Mulliken R, Walter J, Hayley DC, Karrison TG, Nerney MP, Miller A, Friedmann PD. Appropriateness of medication selection for older persons in an urban academic emergency department. Acad Emerg Med 1999; 6 1232–41.
| Appropriateness of medication selection for older persons in an urban academic emergency department.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c%2Fns1Sgug%3D%3D&md5=bcb49641cac270cc5e761a415510ad88CAS | 10609925PubMed |
[9] Lewis LM, Miller DK, Morley JE, Nork MJ, Lasater LC. Unrecognized delirium in ED geriatric patients. Am J Emerg Med 1995; 13 142–5.
| Unrecognized delirium in ED geriatric patients.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DyaK2MXltFejur4%3D&md5=58b7c51837db20f57fbb03ced30a989aCAS | 7893295PubMed |
[10] Roberts DC, McKay MP, Shaffer A. Increasing rates of emergency department visits for elderly patients in the United States, 1993 to 2003. Ann Emerg Med 2008; 51 769–74.
| Increasing rates of emergency department visits for elderly patients in the United States, 1993 to 2003.Crossref | GoogleScholarGoogle Scholar | 18069088PubMed |
[11] Lane R, Serour F. The Madrid international plan of action on ageing: guiding framework and toolkit for practitioners and policy makers. United Nations. 2008. Available at: http://www.un.org/esa/socdev/ageing/documents/building_natl_capacity/guiding.pdf [verified 20 June 2016].
[12] Independent Hospital Pricing Authority. National efficient price determination 2014–15. Canberra: Commonwealth of Australia; 2014.
[13] Queensland Health Department of Health. Health funding principles and guidelines 2013–14. Brisbane: Queensland Health; 2013.
[14] Australian Institute of Health and Welfare (AIHW). National health data dictionary. Version 16. Catalogue no. HWI 119. Canberra: AIHW; 2012.
[15] Australian Bureau of Statistics (ABS). 3222.0 – Population projections, Australia, 2012 (base) to 2101. Canberra: ABS; 2013. Available at: http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/3222.0main+features52012 (base) to 2101 [verified 5 July 2015].
[16] Australian Bureau of Statistics (ABS). 3105.0.65.001 – Australian historical population statistics, 2014 population age–sex structure. 2013. Available at: http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/3222.0main+features52012%20(base)%20to%202101 [verified 1 July 2015].
[17] Bambrick HDK, Woodruff R, Hanigan I, McMichael A. The impacts of climate change on three health outcomes: temperature-related mortality and hospitalisations, salmonellosis and other bacterial gastroeneritis, and population at risk from dengue. Canberra: Commonwealth of Australia; 2008. Available at: http://garnautreview.org.au/CA25734E0016A131/WebObj/03-AThreehealthoutcomes/$File/03-AThreehealth outcomes.pdf [verified 1 June 2015].
[18] Zar JH. Biostatistical analysis. 2nd edn. Englewood Cliffs: Prentice-Hall; 1984.
[19] Banks G. Health costs and policy in an ageing Australia. Canberra: Australian National University; 2008. Available at: http://www.pc.gov.au/news-media/speeches/cs20080328/cs20080701-agedhealthpolicy.pdf [verified 20 June 2016].
[20] Productivity Commission. An ageing Australia: preparing for the future. Commission Research Paper. Canberra: Productivity Commission; 2013.
[21] Wolinsky FD, Liu L, Miller TR, An H, Geweke JF, Kaskie B, Wright KB, Chrischilles EA, Pavlik CE, Cook EA, Ohsfeldt RL, Richardson KK, Rosenthal GE, Wallace RB. Emergency department utilization patterns among older adults. J Gerontol A Biol Sci Med Sci 2008; 63 204–9.
| Emergency department utilization patterns among older adults.Crossref | GoogleScholarGoogle Scholar | 18314459PubMed |
[22] Strange GR, Chen EH, Sanders AB. Use of emergency departments by elderly patients: projections from a multicenter data base. Ann Emerg Med 1992; 21 819–24.
| Use of emergency departments by elderly patients: projections from a multicenter data base.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK38zgtlylsQ%3D%3D&md5=791ad6eb36b41ad13622d31d3fc2fbc6CAS | 1610039PubMed |
[23] Anderson GF, Hussey PS. Population aging: a comparison among industrialized countries. Health Aff (Millwood) 2000; 19 191–203.
| Population aging: a comparison among industrialized countries.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c3nt1Kkuw%3D%3D&md5=aa9c9de426eaec8b2c9f8922adfe4ac0CAS | 10812799PubMed |
[24] Australian Bureau of Statistics (ABS). 2071.0 – Reflecting a nation: stories from the 2011 census, 2012–2013. Who are Australia’s older people? 17 April, 2013 Available at: http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/2071.0main+features752012-2013 [verified 18 April 2015].
[25] Australian Institute of Health and Welfare (AIHW). Rural, regional and remote health: indicators of health status and determinants of health. Rural health series no. 9. Catalogue no. PHE 97. Canberra: AIHW; 2008.
[26] 26 The Commonwealth of Australia. 2015 Intergenerational report: Australia in 2055. Canberra: The Commonwealth of Australia; 2015.
[27] Lowthian JA, Curtis AJ, Jolley DJ, Stoelwinder JU, McNeil JJ, Cameron PA. Demand at the emergency department front door: 10-year trends in presentations. Med J Aust 2012; 196 128–32.
| Demand at the emergency department front door: 10-year trends in presentations.Crossref | GoogleScholarGoogle Scholar | 22304608PubMed |
[28] Lowthian JA, Curtis AJ, Cameron PA, Stoelwinder JU, Cooke MW, McNeil JJ. Systematic review of trends in emergency department attendances: an Australian perspective. Emerg Med J 2011; 28 373–7.
| Systematic review of trends in emergency department attendances: an Australian perspective.Crossref | GoogleScholarGoogle Scholar | 20961936PubMed |
[29] World Health Organization (WHO). WHO global strategy for containment of antimicrobial resistance. World Health Organization; 2001.
[30] Chu K, Brown A, Pillay R. Older patients’ utilisation of emergency department resources: a cross-sectional study. Aust Health Rev 2001; 24 44–52.
| Older patients’ utilisation of emergency department resources: a cross-sectional study.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3Mrms1alsA%3D%3D&md5=7cfb671bade3e7d807413672fe8b808fCAS | 11668924PubMed |
[31] Hogan TM, Losman ED, Carpenter CR, Sauvigne K, Irmiter C, Emanuel L, Leipzig RM. Development of geriatric competencies for emergency medicine residents using an expert consensus process. Acad Emerg Med 2010; 17 316–24.
| Development of geriatric competencies for emergency medicine residents using an expert consensus process.Crossref | GoogleScholarGoogle Scholar | 20370765PubMed |
[32] Australian College for Emergency Medicine (ACEM). Policy on the care of elderly patients in the emergency department. Melbourne: ACEM; 2015.
[33] Rosenberg MCC, Bromley M, Caterino J, Chun A, Gerson L, Greenspan J, Hwang U, John D, Lichtman J, Lyons W, Mortensen B, Platts-Mills T, Ragsdale L, Rispoli J, Seaberg D, Wilber S. The geriatric emergency department guidelines. American College of Emergency Physicians, American Geriatrics Society, Emergency Nurses Association and Society for Academic Emergency Medicine; 2013. Available at: https://www.acep.org/geriedguidelines/ [verified 18 April 2015]
[34] Arendts G, Howard K. The interface between residential aged care and the emergency department: a systematic review. Age Ageing 2010; 39 306–12.
| The interface between residential aged care and the emergency department: a systematic review.Crossref | GoogleScholarGoogle Scholar | 20176712PubMed |
[35] Rice KL, Dewan N, Bloomfield HE, Grill J, Schult TM, Nelson DB, Kumari S, Thomas M, Geist L, Beaner C, Caldwell M, Niewoehner DE. Disease management program for chronic obstructive pulmonary disease: a randomized controlled trial. Am J Respir Crit Care Med 2010; 182 890–6.
| Disease management program for chronic obstructive pulmonary disease: a randomized controlled trial.Crossref | GoogleScholarGoogle Scholar | 20075385PubMed |
[36] Dosa D. Should I hospitalize my resident with nursing home-acquired pneumonia? J Am Med Dir Assoc 2005; 6 327–33.
| Should I hospitalize my resident with nursing home-acquired pneumonia?Crossref | GoogleScholarGoogle Scholar | 16165074PubMed |
[37] Conway J, Dilworth S, Hullick C, Hewitt J, Turner C, Higgins I. A multi-organisation aged care emergency service for acute care management of older residents in aged care facilities. Aust Health Rev 2015; 39 514–6.
| A multi-organisation aged care emergency service for acute care management of older residents in aged care facilities.Crossref | GoogleScholarGoogle Scholar | 25981903PubMed |
[38] Molloy DW, Guyatt GH, Russo R, Goeree R, O’Brien BJ, Bedard M, Willan A, Watson J, Patterson C, Harrison C, Standish T, Strang D, Darzins PJ, Smith S, Dubois S. Systematic implementation of an advance directive program in nursing homes: a randomized controlled trial. JAMA 2000; 283 1437–44.
| Systematic implementation of an advance directive program in nursing homes: a randomized controlled trial.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c7psFSksw%3D%3D&md5=3eaa6ff8d44a32609fc1260774eab143CAS | 10732933PubMed |
[39] Crilly J, Chaboyer W, Wallis M, Thalib L, Polit D. An outcomes evaluation of an Australian hospital in the nursing home admission avoidance programme. J Clin Nurs 2011; 20 1178–87.
| An outcomes evaluation of an Australian hospital in the nursing home admission avoidance programme.Crossref | GoogleScholarGoogle Scholar | 20846245PubMed |
[40] Australian Institute of Health and Welfare (AIHW). Australian hospital statistics 2010–11. Health services series no. 43. Catalogue No. HSE 117. Canberra: AIHW; 2012.
[41] Australian Institute of Health and Welfare (AIHW). Australian hospital statistics 2006–07. Health services series no. 31. Catalogue No. HSE 55. Canberra: AIHW; 2008.
[42] Chu K, Brown A, Lukin W. Local trends in emergency department attendances by older patients in an ageing national population. Aust Health Rev 2009; 33 117–23.
| Local trends in emergency department attendances by older patients in an ageing national population.Crossref | GoogleScholarGoogle Scholar | 19203341PubMed |


