Recurrent episodes of injury in children: an Australian cohort study
Cate M. Cameron A G , Anneliese B. Spinks B C , Jodie M. Osborne A , Tamzyn M. Davey D , Neil Sipe E and Roderick J. McClure FA Menzies Health Institute Queensland, Griffith University, Logan campus, University Drive, Meadowbrook, Qld 4131, Australia. Email: j.osborne@griffith.edu.au
B Commonwealth Scientific and Industrial Research Organisation (CSIRO), 41 Boggo Road, Dutton Park, Qld 4102, Australia. Email: Anneliese.Spinks@csiro.au
C School of Medicine, Griffith University, 170 Kessels Road, Nathan, Qld 4111, Australia.
D Faculty of Medicine and Biomedical Science, School of Public Health Room 429A, Level 4 Public Health Building, Herston Campus, The University of Queensland, Qld 4006, Australia. Email: t.davey@uq.edu.au
E School of Geography, Planning and Environmental Management, Chamberlain Building (35), The University of Queensland, St Lucia, Brisbane, Qld 4072, Australia. Email: n.sipe@uq.edu.au
F Visiting Scientist, Department of Health Policy and Management, Harvard School of Public Health, 677 Huntington Avenue, Kresge Building, Boston, MA 02115, USA. Email: rmcclure@hsph.harvard.edu
G Corresponding author. Email: cate.cameron@griffith.edu.au
Australian Health Review 41(5) 485-491 https://doi.org/10.1071/AH15193
Submitted: 15 October 2015 Accepted: 12 July 2016 Published: 19 August 2016
Journal Compilation © AHHA 2017 Open Access CC BY-NC-ND
Abstract
Objective The aim of the present study was to compare sociodemographic characteristics of children with single versus recurrent episodes of injury and provide contemporary evidence for Australian injury prevention policy development.
Methods Participants were identified from the Environments for Healthy Living: Griffith Birth Cohort Study 2006–11 (n = 2692). Demographic data were linked to the child’s hospital emergency and admissions data from birth to December 2013. Data were dichotomised in two ways: (1) injured or non-injured; and (2) single or recurrent episodes of injury. Multivariate logistic regression was used for analysis.
Results The adjusted model identified two factors significantly associated with recurrent episodes of injury in children aged <3 years. Children born to mothers <25 years were almost fourfold more likely to have recurrent episodes of injury compared with children of mothers aged ≥35 years (adjusted odds ratio (aOR) = 3.68; 95% confidence interval (CI) 1.44–9.39) and, as a child’s age at first injury increased, odds of experiencing recurrent episodes of injury decreased (aOR = 0.97; 95% CI 0.94–0.99). No differences were found in sociodemographic characteristics of children aged 3–7 years with single versus recurrent episodes of injury (P > 0.1).
Conclusion National priorities should include targeted programs addressing the higher odds of recurrent episodes of injury experienced by children aged <3 years with younger mothers or those injured in the first 18 months of life.
What is known about the topic? Children who experience recurrent episodes of injury are at greater risk of serious or irrecoverable harm, particularly when repeat trauma occurs in the early years of life.
What does the paper add? The present study identifies key factors associated with recurrent episodes of injury in young Australian children. This is imperative to inform evidence-based national injury prevention policy development in line with the recent expiry of the National Injury Prevention and Safety Promotion Plan: 2004–2014.
What are the implications for practitioners? Injury prevention efforts need to target the increased injury risk experienced by families from lower socioeconomic backgrounds and, as a priority, children under 3 years of age with younger mothers and children who are injured in the first 18 months of life. These families require access to education programs, resources, equipment and support, particularly in the child’s early years. These programs could be provided as part of the routine paediatric and child health visits available to families after their child’s birth or incorporated into hospital and general practitioner injury treatment plans.
Introduction
Injury prevention is a key public health priority within Australia.1 With the recent expiry of the National Injury Prevention and Safety Promotion Plan: 2004–2014 (http://www.health.gov.au/internet/main/publishing.nsf/Content/health-pubhlth-strateg-injury-index.htm, accessed 9 July 2015), broad discussion is required across the sector to identify new national injury prevention plans and priorities. This requires input from a range of stakeholders, as well as a strong and contemporary evidence base of injury-related data and research.
A particularly vulnerable group within the Australian population are children who experience recurrent episodes of injury, because they are at greater risk of sustaining serious or irrecoverable harm.2 Injury prevention efforts need to identify the individual and social factors associated with recurrent episodes of injury in these children and ensure they receive targeted early intervention and support. A few recent international studies have highlighted the effect of child characteristics, maternal behaviour and lifestyle as antecedents of recurrent episodes of injury.3–5 An association between different measures of social disadvantage and recurrent injury events has also been reported.4,6,7 The heterogeneity of these studies with regard to methodology, target populations and factors analysed means that the findings of this research are broad and complex.
Studies examining risk factors for recurrent episodes of injury largely compare children with recurrent injury events to a combined group of children with one and no episodes of injury.3–6 This provides insight into the factors associated with recurrent episodes of injury in the broader population. However, it is also important that we examine the injured population exclusively so we can isolate which factors, over and above the sociodemographic factors associated with overall injury risk, increase the likelihood of recurrent episodes of injury in this vulnerable population.
Commonly used cross-sectional surveillance data, although invaluable for monitoring injury rates in the community, are unable to provide insight into recurrent episodes of injury or associated sociodemographic factors in the way that longitudinal research can. The Environments for Healthy Living (EFHL): Griffith Birth Cohort Study followed health and social outcomes of children born within a selected geographical region in Australia.8 It provides a timely opportunity to follow children’s injury patterns and, in particular, patterns of recurrent injury events in an Australian context. The aim of the present study was to compare sociodemographic characteristics of children with single versus recurrent episodes of injury and provide contemporary evidence for Australian injury prevention policy development.
Methods
Study design
The present study was a prospective cohort study.
Participants
Participants were children enrolled in EFHL, whose family resided in Queensland at the time of enrolment. EFHL investigates the impact of social, environmental, family and individual factors on child health and development.8 Pregnant women were recruited in their third trimester from the antenatal clinics of the Logan and Gold Coast public hospitals from 2006 to 2011. Detailed project methodology and baseline participant characteristics have been provided elsewhere.8,9 EFHL is listed on the Australian and New Zealand Clinical Trials Registry (ACTRN12610000931077).
Ethics approval
Ethics approval for the study was provided by the human research ethics committees of Griffith University, The University of Queensland and the participating hospitals. Maternal participants provided written informed consent regarding their involvement in baseline and subsequent surveys, the release of hospital perinatal information and linkage of their child’s health department hospital records.
Data sources and collection
Baseline social, maternal and household variables
Participating women completed a self-administered baseline survey during pregnancy covering a range of maternal, household and neighbourhood factors. Baseline information was also drawn from hospital perinatal records. The baseline child characteristic included in the present analysis was gender, whereas the maternal characteristics included education level, age at enrolment in the study and cigarette smoking during pregnancy. Baseline household characteristics included marital status, whether other children were residing in the home, employment status of the partner and families’ housing status. Gross annual household income was reported in $10 000 increments and standardised in 2010 Australian dollars using published Consumer Price Index10,11 then divided into income quintiles, median $62 946.9
Administrative health data
Emergency department (ED) data were drawn from the Queensland Emergency Department Information Systems (EDIS). Hospital admissions data were drawn from Queensland Hospital Admitted Patients Data Collection (QHAPDC). Demographic, child and maternal information were linked by the Queensland Department of Health, through linkage software using deterministic and probabilistic methods. Where required, the Queensland Health Data Linkage Unit conducted manual clerical reviews of the data.
Outcome measure
The outcome of interest was injury related hospital or ED ‘episodes of care’. Dates of hospital admissions and ED presentations, transfer codes and diagnostic fields were used to identify multiple and nested admissions and any corresponding hospital and ED presentations that were likely to relate to one injury incident. These records were collapsed into a single episode of care for that event.
Children with recurrent episodes of injury were defined as those who had received hospital treatment for more than one episode of injury at different times across the study period. Recurrent injuries did not include multiple injuries related to the one injury event and may or may not have been the same type or cause as the child’s first injury event.
Injury classification
The International Classifications of Diseases, 10th Revision, Australian Modification (ICD-10-AM)12 was used to classify injury presentations. Injury records were identified from Chapter 19, Injury and Poisonings (codes S00–T98)12 and Chapter 20, External Causes (codes U50–Y98).12 Any late effects from injury were excluded. EDIS data contain only a single diagnostic field in which to describe the reason for presentation, whereas the QHAPDC contains a primary diagnosis field and multiple other diagnostic fields in which external causes and activity codes may be recorded. Researchers checked text descriptions in the EDIS data to identify any injuries that were not captured in the single diagnosis field. Almost all ED records used the one available diagnostic field to classify the nature of the injury (S00–T98). External cause codes (V01–Y98) were used in less than 4% of ED records. As a result, injury cause codes were only available comprehensively for the in-patient episodes of care. Injury subgroups were defined and matched to the ICD-10-AM chapter subcategories.
Calculation of person-years
The length of follow-up for injury-related hospital treatment varied considerably across participants. Individual person-years (PYs) were calculated for each child, based on the time between birth and 31 December 2013 in which he or she was residing in the state of Queensland, alive and eligible for health care.
Analysis
Data cleaning and analyses were undertaken using SAS version 9.4 software (SAS Institute).13 Because of a priori hypothesised developmental differences,14–16 data were analysed separately for the first 3 years of life and for children aged 3–7 years. Data was dichotomised in two ways: (1) injured or non-injured; and then, for children who had sustained an injury, (2) single or recurrent episodes of injury. The statistical significance of differences between groups was assessed by Pearson’s Chi-squared test for categorical data and two-sample t-test for continuous data.
Direct multivariate logistic regression was performed to estimate adjusted odds ratios (aORs) between multiple exposure factors (child, maternal and household characteristics) and the likelihood of the outcome (single vs recurrent episodes of injury) for child participants in the first 3 years of life and separately for children aged 3–7 years. All factors significant in the univariate analyses associated with injury were included in the model. The log of individual PYs of exposure time was included as an offset. The final model included age of the child at first injury, child gender, maternal age, maternal education, maternal smoking, household marital status, partner employment and housing status. Complete case analysis was used with significance set at a level of 5% (two-tailed).
Results
In total, 2663 families who enrolled in the EFHL study at the two participating Queensland hospitals were included in the present analysis. The number of children totalled 2692 (including 29 sets of twins). Maternal age ranged from 16 to 52 years, with a mean age of 28.9 years. At the time of enrolment, 14.6% of households were sole parent families, 35.7% had no other children living in the household and 22.2% of the maternal participants had not completed secondary school education.
Follow-up
Follow-up consisted of a total of 13 113.3 PYs from birth to 7 years of age, with a mean 4.9 PYs per child (range 0–7). Automated linkage and manual searching found records in QHAPDC for 97.1% of the child participants, including their birth record, and records in EDIS for 44.7% of the child participants.
Child injury
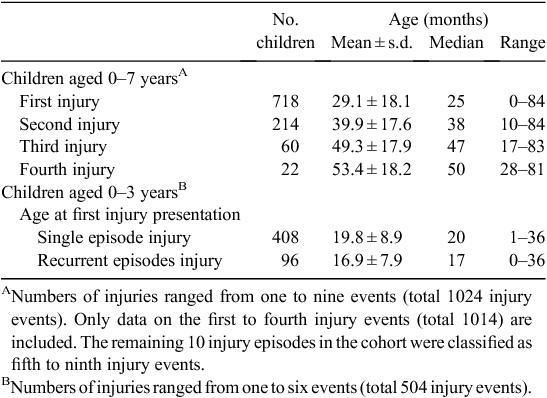
In the total cohort (all children aged 0–7 years), 718 children (26.7%) presented to hospital for treatment of an injury during the study period. After removal of hospital transfers and matching of ED presentations to admission records, there was a total of 1024 injury-related ‘episodes of care’. Of those, 158 (15.4%) required hospital admission. The number of injury episodes per child in the total cohort ranged from zero to nine events, with 214 children presenting more than once for an injury, 29.8% of the injured population. The mean age at first injury presentation for the total cohort was 29 months and almost 40 months for second injury presentation (Table 1).
|
In the first 3 years of life, the number of injury episodes per child ranged from zero to six events, with 96 children presenting more than once for an injury, 19.1% of the injured population. Children who experienced recurrent episodes of injury before the age of 3 years were significantly younger at their first injury presentation (mean age 16.9 months; 95% confidence interval (CI) 15.3–18.5) than children with only one injury event (mean age 19.8 months; 95% CI 19.0–20.7; P = 0.001; Table 1).
Cause and type of injury
ICD-10-AM nature and type of injury codes were present for 96.7% of in-patient and ED records, whereas cause of injury codes were available for in-patient records only. There were no differences in the most common cause of in-patient injury admissions for children injured once compared with children who had recurrent episodes of injury, regardless of age (P > 0.1). Falls were the most common cause of all injuries (38.6% for those aged <3 years and 48.3% for those aged 3–7 years). Accidental poisonings was the second highest injury for children <3 years of age (21.6%), whereas being struck or crushed by inanimate mechanical forces was the second highest injury for children aged 3–7 years (20.0%). Where place of injury was specified, most injuries occurred in the home, but this proportion decreased with child age (60.2% for those aged <3 years and 41.7% for those aged 3–7 years).
The leading types of injury (both single and recurrent injuries) experienced by children differed between in-patient and ED records. Open wounds and fractures accounted for 30.0% of in-patient injury admissions in children <3 years of age, compared with 66.7% of admissions for children aged 3–7 years. In contrast, superficial injuries dominated ED presentations, followed by open wounds and dislocations, sprains and strains for all ages. No particular nature, types or places of injury occurrence were more prevalent for the children with recurrent episodes of injury compared with children who experienced a single episode of injury (P > 0.1).
Comparison of the nature and type of the first injury event and subsequent injury events for children with recurrent injuries demonstrated no significant or consistent pattern, regardless of age. Subsequent injury events were varied and, in most cases, differed from the type of the first injury event.
Maternal and household characteristics
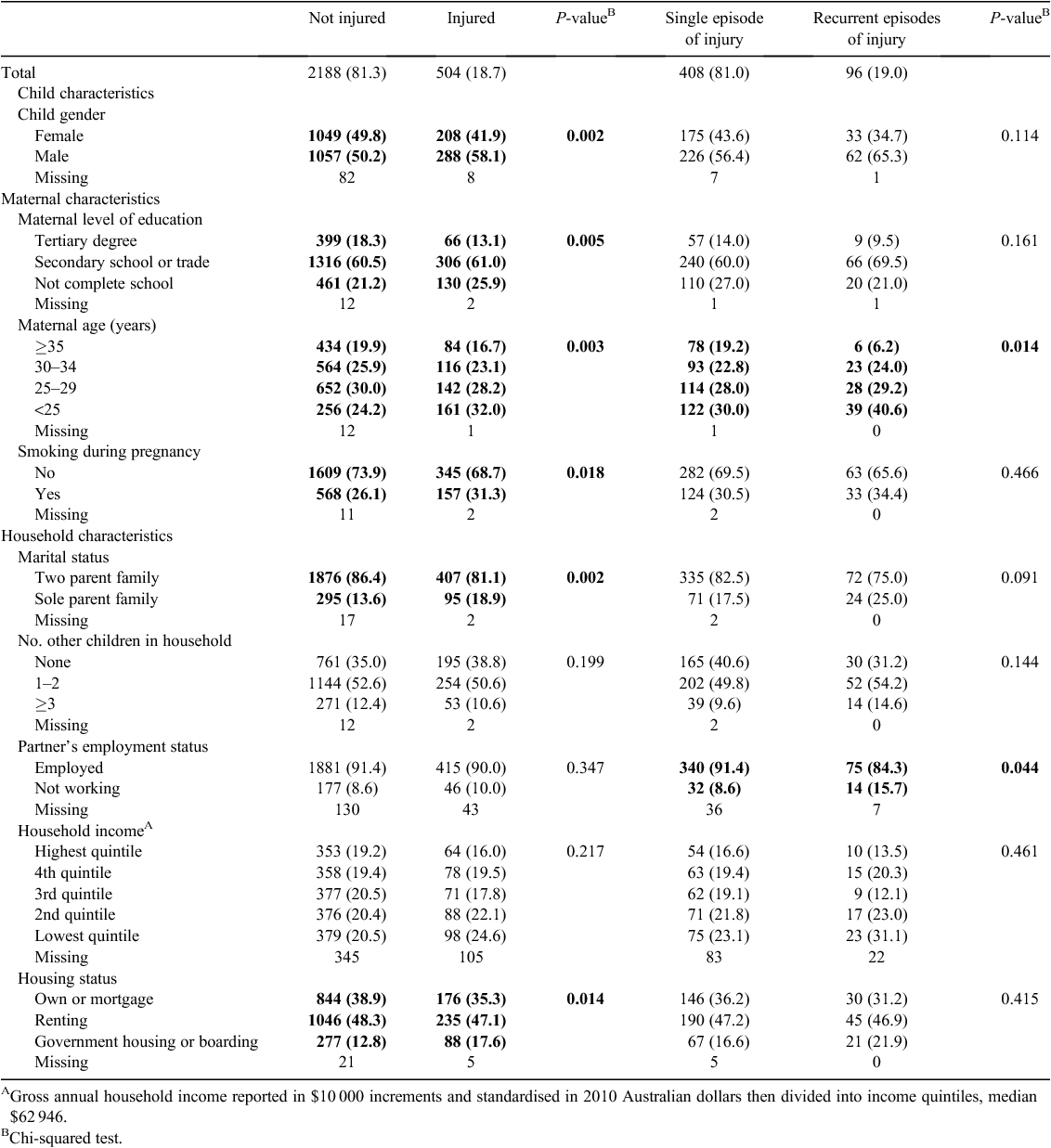
There was a significant difference in sociodemographic factors between children who were injured compared with those not injured in the first 3 years of life (Table 2). Significant variables included child gender, maternal education, maternal age, maternal smoking in pregnancy and household marital and housing status (P < 0.05).
Children who experienced recurrent episodes of injury before 3 years of age were more likely than children injured once to come from families with younger mothers (P = 0.014) and from a household in which the father or partner was not working (P = 0.044; Table 2). Only younger maternal age was associated with recurrent injury episodes for children in the cohort aged 3–7 years compared with children injured once (P = 0.05; data not shown). Although factors such as child gender, maternal education, maternal smoking and household marital and housing status were associated with overall injury occurrence, none of these factors was significantly different for children with recurrent versus single episodes of injury at any age (P > 0.05).
Adjusted regression analyses
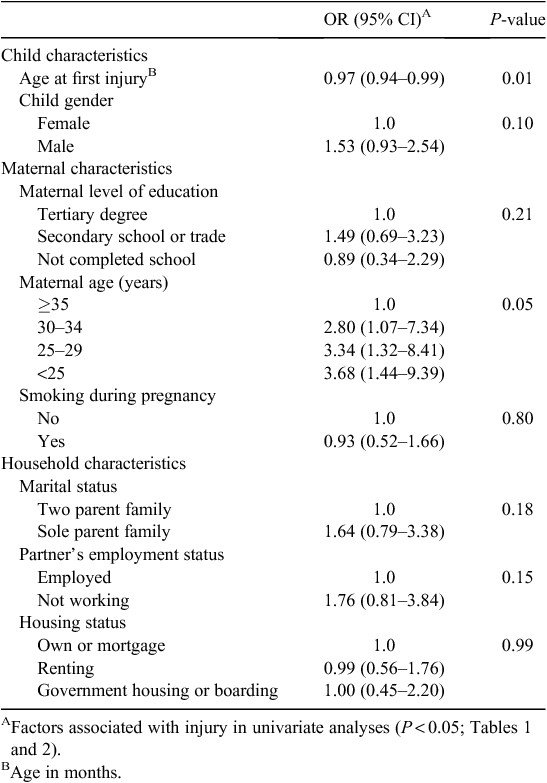
Multivariate logistic regression was used to model the eight factors found to be associated with single or recurrent episodes of injury in the univariate analyses, accounting for individual PYs of exposure time. The full model for the first 3 years of life, containing all predictors, was statistically significant (χ212 = 28.2; n = 441; P = 0.005). Only two factors made a statistically significant contribution to the model: maternal age and child’s age at first injury (Table 3). Children who had a mother aged less than 25 years when the child was born were almost fourfold more likely to have recurrent episodes of injury in the early years of life compared with children of mothers aged 35 years or older, after controlling for other factors in the model (aOR = 3.68; 95% CI 1.44–9.39). As maternal age increased, the likelihood of recurrent child injury events decreased; however, all maternal age groups less than 35 years had increased adjusted odds. In addition, as the age of the child at first injury presentation increased, the odds of the child experiencing recurrent episodes of injury decreased (aOR = 0.97; 95% CI 0.94–0.99).
|
The full model for the children with data from 3 to 7 years of age was not statistically significant (χ212 = 14.3; n = 266; P = 0.284). No differences were found for any of the child, maternal or household factors for children aged 3–7 years of age with single versus recurrent episodes of injury (P > 0.1; data not shown).
Discussion
The present study provides contemporary data on recurrent episodes of injury in a peri-urban cohort of Australian children to support an evidence-based approach to Australian injury prevention policy development. Injuries continue to be a major concern, with just over one-quarter of children in the present study aged 0–7 years recording at least one episode of hospital treated injury and 30% of those receiving treatment for recurrent episodes of injury. Consistent with previous research,17–20 there was clear evidence of a link between sociodemographic factors and overall injury risk (injured vs non-injured), making families from socially disadvantaged backgrounds an ongoing priority for injury prevention.
Of particular concern, approximately 20% of children who experienced an injury in the early years of life experienced up to six recurrent episodes of hospital-treated injury before 3 years of age. The present study identified two factors that were significantly associated with increased odds of recurrent episodes of injury in children under three: children with younger mothers and children who presented for an injury in the first 18 months of life. The relationship between younger maternal age and recurrent episodes of injury has been demonstrated in recent research,4,6 as has the relationship between earlier age at first injury and recurrent injury episodes.7
Interestingly, this relationship was only evident in the first 3 years of life. No significant differences were found in any child, maternal or household factors for children aged 3–7 years with single versus recurrent injuries. These differences may reflect developmental changes in the child requiring less intense parental supervision or environmental changes, with many moving on towards more structured child care, school and recreational activities. This was also suggested by the decrease in the proportion of injuries occurring in the home in the older ages. The finding that sociodemographic differences in child injury may vary with age has been demonstrated in previous research, although no clear model has been established.21–23 Because there were limited data on older children in the present study (not all children reached 7 years of age in the study period), further examination of this relationship would be beneficial.
Interventions that target the broader association between social disadvantage and child injury would clearly have benefits for children who experience recurrent episodes of injury by reducing overall injury risk. However, given the heightened vulnerability of recurrently injured children, there is a need for targeted, evidence-based early intervention programs that are responsive to this increased risk. The present research identifies two priorities for these programs: (1) infant children with younger mothers; and (2) children who experience an episode of injury in the first 18 months of life. These programs should account for the developmental level of the child and include access to an array of education, services, resources and supports. They could be included as part of the routine paediatric and child health visits available to families after their child’s birth or be incorporated directly into hospital and general practitioner treatment plans for children under 18 months of age who experience an injury.
The present study did not find child gender, marital or partner status, household income or maternal smoking to be associated with recurrent episodes of injury, unlike previous studies.3–7 This may be due to differences in the study design, sample characteristics and injury measures assessed. In particular, the present study focused only on the injured population when analysing the odds of recurrent episodes of injury, whereas previous studies included the broader non-injured population for comparison.
A key strength of the present study is its linkage of survey data with state-wide hospital injury data. By using data linkage, we minimised recall bias from proxy-reported injury events,24 as well as loss to follow-up and attrition that may be experienced by other longitudinal studies.8
Although state-wide in-patient data were available from all public and private hospitals, ED data were only available for public hospitals. ED records also contained only a single diagnostic field in which to describe the reason for presentation. External cause codes were used in only 3.3% of ED records. As a result, cause of injury could only be examined for in-patient episodes of care; these cases only represented a small proportion of the outcomes data and differed in level of severity to the remaining cases.
The EFHL population from which our participants were drawn is largely representative of births in the region but included a higher representation than the national average of families with lower incomes, younger age, more overseas born and high proportions of maternal smoking in pregnancy.9 The present findings pertain to injuries severe enough to require hospital attendance and do not include injuries treated at a clinic, general practitioner or by family and friends. Because of the smaller sample size of the group of participants with recurrent episodes of injury, the study may also have been underpowered to detect differences between groups for some characteristics.
Conclusions
The findings of the present study have clear injury prevention policy implications. At the broader level, priorities for injury prevention should include families from lower sociodemographic backgrounds to address the broader socioeconomic differentials in child health. Given the heightened vulnerability of children who experience recurrent episodes of injury, there is also a need for developmentally appropriate, funded early intervention programs, particularly targeting children under 3 years of age with younger mothers and children who are injured in the first 18 months of life. It is recommended that these programs include a range of services and supports and be incorporated into existing routine paediatric health visits and hospital injury treatment plans.
Competing interests
None declared.
Acknowledgements
This study was funded by an Australian Research Council Discovery Grant (DP110105423). The research reported is part of the Griffith Study of Population Health: Environments for Healthy Living (EFHL), which is registered with the Australian and New Zealand Clinical Trials Registry (ACTRN12610000931077). Core funding to support EFHL is provided by Griffith University. The EFHL project was conceived by Rod McClure, Cate Cameron, Judy Searle and Ronan Lyons. The authors are thankful for the contributions of the project manager, Rani Scott, and the current and past database managers. The authors gratefully acknowledge the administrative staff, research staff and the hospital antenatal and birth suite midwives of the participating hospitals for their valuable contributions to the study, in addition to the expert advice provided by research investigators throughout the project. C. Cameron was supported by a Public Health Fellowship (428254) from the National Health and Medical Research Council of Australia.
References
[1] Australian Institute of Health and Welfare. National health priority areas. 2015. Available at: http://www.aihw.gov.au/national-health-priority-areas/ [verified 9 September 2015].[2] Deans KJ, Thackeray J, Groner JI, Cooper JN, Minneci PC. Risk factors for recurrent injuries in victims of suspected non-accidental trauma: a retrospective cohort study. BMC Pediatr 2014; 14 217
| Risk factors for recurrent injuries in victims of suspected non-accidental trauma: a retrospective cohort study.Crossref | GoogleScholarGoogle Scholar | 25174531PubMed |
[3] Junger M, Japel C, Cote S, Xu Q, Boivin M, Tremblay RE. Smoking and medication during pregnancy predict repeated unintentional injuries in early childhood but not single unintentional injuries. Prev Sci 2013; 14 13–24.
| Smoking and medication during pregnancy predict repeated unintentional injuries in early childhood but not single unintentional injuries.Crossref | GoogleScholarGoogle Scholar | 23212766PubMed |
[4] Braun PA, Beaty BL, DiGuiseppi C, Steiner JF. Recurrent early childhood injuries among disadvantaged children in primary care settings. Inj Prev 2005; 11 251–5.
| Recurrent early childhood injuries among disadvantaged children in primary care settings.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD2Mvhslaruw%3D%3D&md5=6f68afcf488483c7281cb820d460627bCAS | 16081757PubMed |
[5] Russell KM. Preschool children at risk for repeat injuries. J Community Health Nurs 1998; 15 179–90.
| Preschool children at risk for repeat injuries.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1cvhvFWlsw%3D%3D&md5=9aefadcf636576d08c8356d924b62763CAS | 9747024PubMed |
[6] Ordonana JR, Caspi A, Moffitt TE. Unintentional injuries in a twin study of preschool children: environmental, not genetic, risk factors. J Pediatr Psychol 2008; 33 185–94..
| Unintentional injuries in a twin study of preschool children: environmental, not genetic, risk factors.Crossref | GoogleScholarGoogle Scholar | 17569713PubMed |
[7] Spady DW, Saunders DL, Schopflocher DP, Svenson LW. Patterns of injury in children: a population-based approach. Pediatrics 2004; 113 522–9.
| Patterns of injury in children: a population-based approach.Crossref | GoogleScholarGoogle Scholar | 14993544PubMed |
[8] Cameron CM, Scuffham PA, Spinks A, Scott R, Sipe N, Ng S, Wilson A, Searle J, Lyons RA, Kendall E, Halford K, Griffiths LR, Homel R, McClure RJ. Environments for Healthy Living (EFHL) Griffith birth cohort study: background and methods. Maternal Child Health J 2012; 16 1896–905.
| Environments for Healthy Living (EFHL) Griffith birth cohort study: background and methods.Crossref | GoogleScholarGoogle Scholar |
[9] Cameron CM, Scuffham PA, Shibl R, Ng S, Scott R, Spinks A, Mihala G, Wilson A, Kendall E, Sipe N, McClure RJ. Environments for Healthy Living (EFHL) Griffith birth cohort study: characteristics of sample and profile of antenatal exposures. BMC Public Health 2012; 12 1080
| Environments for Healthy Living (EFHL) Griffith birth cohort study: characteristics of sample and profile of antenatal exposures.Crossref | GoogleScholarGoogle Scholar | 23241307PubMed |
[10] Australian Bureau of Statistics. Consumer Price Index, Australia 2006–10. Canberra: ABS; 2010.
[11] Australian Bureau of Statistics. Household Income and Income Distribution, Australia, 2009–10. Canberra: ABS; 2011.
[12] National Centre for Classification in Health, ICD-10-AM. Fifth ed. Sydney: National Centre for Classification in Health; 2006.
[13] SAS Institute. Sample 42514: tests for comparing nested and nonnested models (program). Cary, NC: SAS Institute; 2011.
[14] Flavin MP, Dostaler SM, Simpson K, Brison RJ, Pickett W. Stages of development and injury patterns in the early years: a population-based analysis. BMC Public Health 2006; 6 187
| Stages of development and injury patterns in the early years: a population-based analysis.Crossref | GoogleScholarGoogle Scholar | 16848890PubMed |
[15] MacInnes K, Stone DH. Stages of development and injury: an epidemiological survey of young children presenting to an emergency department. BMC Public Health 2008; 8 120
| Stages of development and injury: an epidemiological survey of young children presenting to an emergency department.Crossref | GoogleScholarGoogle Scholar | 18410685PubMed |
[16] Agran PF, Anderson C, Winn D, Trent R, Walton-Haynes L, Thayer S. Rates of pediatric injuries by 3-month intervals for children 0 to 3 years of age. Pediatrics 2003; 111 e683–92.
| Rates of pediatric injuries by 3-month intervals for children 0 to 3 years of age.Crossref | GoogleScholarGoogle Scholar | 12777586PubMed |
[17] Laursen B, Nielsen JW. Influence of sociodemographic factors on the risk of unintentional childhood home injuries. Eur J Public Health 2008; 18 366–70.
| Influence of sociodemographic factors on the risk of unintentional childhood home injuries.Crossref | GoogleScholarGoogle Scholar | 18515863PubMed |
[18] Myhre MC, Thoresen S, Grogaard JB, Dyb G. Familial factors and child characteristics as predictors of injuries in toddlers: a prospective cohort study. BMJ Open 2012; 2 e000740
| Familial factors and child characteristics as predictors of injuries in toddlers: a prospective cohort study.Crossref | GoogleScholarGoogle Scholar | 22403343PubMed |
[19] Orton E, Kendrick D, West J, Tata LJ. Persistence of health inequalities in childhood injury in the UK: a population-based cohort study of children under 5. PLoS One 2014; 9 e111631
| Persistence of health inequalities in childhood injury in the UK: a population-based cohort study of children under 5.Crossref | GoogleScholarGoogle Scholar | 25347771PubMed |
[20] Kendrick D, Mulvaney C, Burton P, Watson M. Relationships between child, family and neighbourhood characteristics and childhood injury: a cohort study. Soc Sci Med 2005a; 61 1905–15.
| Relationships between child, family and neighbourhood characteristics and childhood injury: a cohort study.Crossref | GoogleScholarGoogle Scholar | 15927334PubMed |
[21] Chen E, Matthews KA, Boyce WT. Socioeconomic differences in children’s health: how and why do these relationships change with age? Psychol Bull 2002; 128 295–329.
| Socioeconomic differences in children’s health: how and why do these relationships change with age?Crossref | GoogleScholarGoogle Scholar | 11931521PubMed |
[22] Chen E, Martin AD, Matthews KA. Socioeconomic status and health: do gradients differ within childhood and adolescence? Soc Sci Med 2006; 62 2161–70.
| Socioeconomic status and health: do gradients differ within childhood and adolescence?Crossref | GoogleScholarGoogle Scholar | 16213644PubMed |
[23] Hippisley-Cox J, Groom L, Kendrick D, Coupland C, Webber E, Savelyich B. Cross sectional survey of socioeconomic variations in severity and mechanism of childhood injuries in Trent 1992–7. BMJ 2002; 324 1132
| Cross sectional survey of socioeconomic variations in severity and mechanism of childhood injuries in Trent 1992–7.Crossref | GoogleScholarGoogle Scholar | 12003886PubMed |
[24] Cummings P, Rivara FP, Thompson RS, Reid RJ. Ability of parents to recall the injuries of their young children. Inj Prev 2005; 11 43–7.
| Ability of parents to recall the injuries of their young children.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD2M%2FmtlClsg%3D%3D&md5=cb05b2920f4488c048b228943823ab76CAS | 15691989PubMed |