Comparing clinical and demographic characteristics of people with mental illness in hospital- and community-based residential rehabilitation units in Queensland
Tom Meehan A B E , Terry Stedman A B , Stephen Parker C D , Bretine Curtis A and Donna Jones AA Queensland Mental Health Benchmarking Unit, The Park, Centre for Mental Health, Locked Bag 500, Archerfield, Qld 4108, Australia. Email: Bretine.Curtis@health.qld.gov.au; Donna.Jones3@health.qld.gov.au; Terry.Stedman@health.qld.gov.au
B Department of Psychiatry, University of Queensland, Herston, Qld 4066, Australia.
C Rehabilitation Clinical Academic Unit, Metro South Addiction and Mental Health Service, 519 Kessels Road, MacGregor, Qld 4109, Australia. Email: Stephen.Parker@health.qld.gov.au
D School of Public Health, University of Queensland, Herston, Qld 4066, Australia.
E Corresponding author. Email: Tom.Meehan@health.qld.gov.au
Australian Health Review 41(2) 139-143 https://doi.org/10.1071/AH15207
Submitted: 3 November 2015 Accepted: 14 March 2016 Published: 28 April 2016
Journal Compilation © AHHA 2017 Open Access CC BY-NC-ND
Abstract
Objective The aim of the present study was to examine care pathways and characteristics of mental health consumers participating in both hospital- and community-based residential rehabilitation programs.
Methods An audit of consumers (n = 240) in all publicly funded residential rehabilitation units in Queensland was performed on the same day in 2013. Data collection focused on demographic characteristics, clinical information and measures of consumer functioning.
Results Significant differences emerged for consumers in community- and hospital-based services with regard to age, length of stay, functioning, Mental Health Act status, guardianship status, family contact and risk of violence. Consumers in hospital-based programs have more severe and complex problems.
Conclusions Consumers in residential rehabilitation units have high levels of disability, poor physical health and high levels of vulnerability. Nonetheless, it is likely that a sizeable proportion of consumers occupying rehabilitation beds in Queensland could be discharged if more ‘step-down’ options to move patients on were available.
What is known about the topic? A small subgroup of people with severe and complex mental health problems is likely to require time in a residential rehabilitation program. This group is characterised by failure to respond to treatment, severe negative symptoms and some degree of cognitive impairment.
What does this paper add? Patients currently occupying residential rehabilitation beds in Queensland have high levels of disability, poor physical health and high levels of vulnerability. Patients in hospital-based programs are more severely disabled than those in community-based programs.
What are the implications for practitioners? It is likely that a sizeable proportion of patients occupying rehabilitation beds in Queensland could be discharged if more ‘step-down’ options were available. Future planning initiatives need to focus on developing a greater array of community support options to facilitate the discharge of people from residential services.
Additional keywords: benchmarking, patient characteristics, service profile.
Introduction
In keeping with trends in other developed countries, recent mental health policy in Australia has focused on the closure of long-stay hospitals and the development of community alternatives. There is now a growing realisation that a broad range of service models is required to support the recovery of individuals with more complex problems.1 However, recent commentary has raised questions about this service mix, especially in relation to subacute beds2 and community-based services.3 A clearer understanding of the available service models and the characteristics of the consumers who use them offers a pathway to understanding the adequacy of current service models.
Most people with mental illness admitted to acute in-patient care will respond to treatment and be discharged to some form of community support. However, a small subgroup of patients is likely to require more intensive treatment in a residential rehabilitation setting. In the UK, this group is characterised by failure to respond to treatment, severe negative symptoms and some degree of cognitive impairment.4 Similar patients undergoing residential rehabilitation in Australia were found to have medication non-compliance, treatment resistance, frequent and lengthy periods of hospitalisation, lack of insight and self-care deficits.5 It has been estimated that up to 10% of people diagnosed with psychosis will develop these complex problems and require access to rehabilitation services.6 Although these patients represent only a small proportion of the overall population with mental illness, they experience a disproportionately large illness burden, leading to greater need for mental health services.4
In Australia, a range of service models has emerged to meet the needs of people with complex mental health problems. The need for 24-h staffed residential rehabilitation is now widely accepted as a key component of contemporary mental health service provision.1 In Queensland, these residential service models take two forms: (1) hospital-based rehabilitation services, which emerged in the early 1990s and are more likely to be located on the grounds of former long-stay psychiatric hospitals; and (2) community care units (CCUs), which have been established more recently and are located in community settings.
Although both service types were intended to operate according to the same model of service delivery and recovery principles, some significant differences have evolved. Although hospital-based services remain ‘authorised’ mental health services, most community-based services do not serve this function. However, consumers can be treated involuntarily in CCUs by way of an Involuntary Treatment Order (ITO). It is also clear that community-based services are less governed by ‘institutional’ policies, tending to be less restrictive, and offer greater opportunity for community integration than hospital-based services.7 Notwithstanding these differences, the philosophy of both service models is to provide a similar service to similar patients.8
Twelve residential rehabilitation units have been established in Queensland over the past 15 years with an additional six community-based units (CCUs) due to be commissioned by mid-2016. These units are designed for purpose and provide cluster style housing of up to 20 beds arranged in mostly self-contained, single-occupancy units. Consumers are supported to manage their own affairs and undertake activities of daily living to the maximum extent possible. Nonetheless, 24-h mental health care with living skill enhancement is provided through a multidisciplinary team. Although most consumers accessing these services are expected to be reintegrated back into their community within 6–24 months, a small subgroup of consumers with severe deficits in functioning may require extended periods in residential rehabilitation.8
Despite the ongoing development of rehabilitation services in Queensland and elsewhere in Australia, there is a paucity of information on the clients accessing such services. The aim of the present study was to define and compare the characteristics of consumers in Queensland’s residential rehabilitation services. It is anticipated that this information will facilitate improved understanding of how these services are being used and provide valuable information to guide future planning initiatives.
Methods
The study data were derived from a benchmarking exercise in 2013 of all 240 consumers resident in the 12 publicly funded community- and hospital-based residential rehabilitation services in Queensland. Secure rehabilitation, older people and acquired brain injury programs were excluded. The Queensland Mental Health Benchmarking Unit (QMHBU) was established in 2006 to assist with performance measurement and service reform of extended care in-patient programs in Queensland. The QMHBU works with services to coordinate the development of clinical and performance indicators, the collection of indicator data and the analysis and reporting of such data.9,10 Data for each benchmarking round are collected from all in-scope services on an agreed date (‘survey’ day). Treatment staff familiar with the patients at each site collect the required data and provide it to the QMHBU for processing. Benchmarking staff visit each service before data collection to ensure that staff responsible for data collection understand each indicator and the data collection process. In the present benchmarking round, data were entered onto a pro forma to ensure consistency in data collection. Outliers were discussed and clarified with service staff before being accepted.
The data reported herein were deemed by the West Moreton Hospital and Health Service Ethics Committee to constitute an audit of data already in the public domain and, as such, the publication of these data does not require additional ethics clearance. Descriptive and analytical statistics using Chi-squared tests and t-tests were used to assess between-group differences. Given the large number of comparisons performed, the level of significance was lowered to 0.01 to reduce the risk of Type I error.11
Results
Data were collected on all patients in the 12 facilities on the same day in August 2013. On this survey day there were 115 consumers in the six community-based CCUs (93% occupancy of the total 124 beds) and 125 consumers in the six hospital-based units (87% occupancy of the total 144 beds). In the 12 months before the survey day, 122 consumers had been admitted to the six community-based services and 265 had been admitted to the hospital-based services. Forty-three of the consumers (35.2%) admitted to the community-based services were referred from acute in-patient units and 79 (64.8%) from community mental health services or other extended in-patient units. Of the 265 consumers admitted to the hospital-based services, 167 (63%) were referred from acute in-patient units and 98 (37.0%) were referred from community mental health or other extended inpatient services (χ2 = 25.9, P < 0.001).
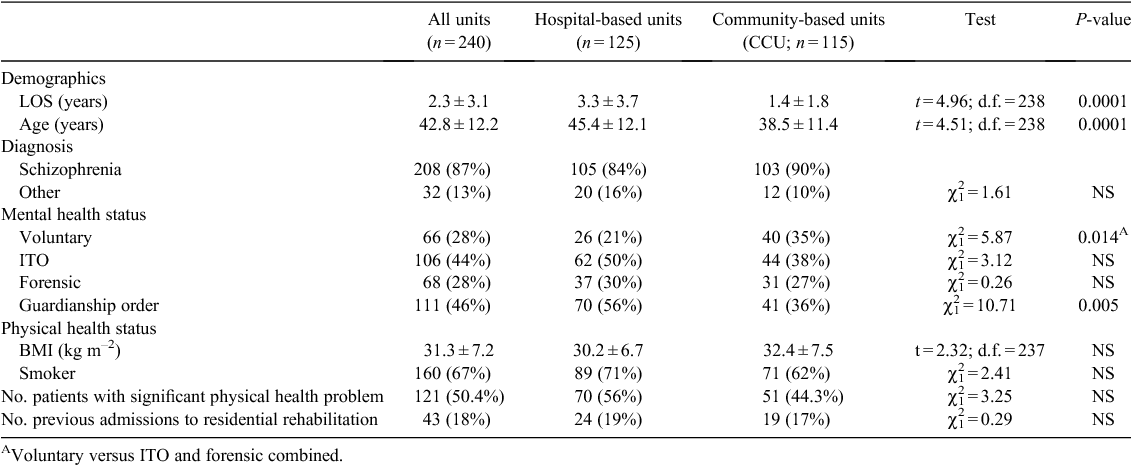
Most consumers were male (70%) and the overall mean age was 43.8 years, with the community-based cohort being significantly younger than the hospital-based sample (Table 1). Length of stay for those present in the services on the survey day ranged from 1 month to 13.9 years, with an overall mean of 2.7 years. The mean length of stay for the CCU sample (1.3 years) was significantly less than that of the hospital-based cohort (3.2 years; t = 4.96, P < 0.0001). Although 48% of the overall sample had been in a rehabilitation service for less than 1 year, 36% had been in a service for 1–5 years and 16% for more than 5 years.
|
Most consumers (86.6%) had a diagnosis of schizophrenia and more than one-quarter (27.5%) were receiving treatment as a voluntary patient. More than half the patients (50.4%) were classified as having a significant health problem (defined as requiring specialist medical treatment). Two-thirds (66%) smoked and the mean weight was 98 kg (range 37–159 kg), with 60% in the obese category (body mass index >30 kg m–2).
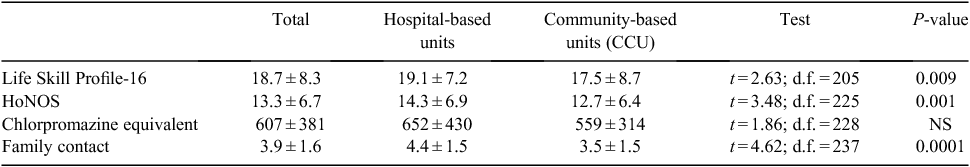
Family contact was assessed using a scale ranging from 1 (= daily) to 6 (= never). Family members were significantly more likely to have contact with patients in the community-based CCUs than those in hospital-based units (Table 2). All antipsychotic medications were converted to chlorpromazine equivalents12 and although hospital-based patients were receiving almost 100 mg day–1 more than their community-based counterparts, this difference did not reach statistical significance.
|
Patients differed significantly in their level of functioning. The Life Skill Profile-1613 and Health of the Nation Outcome Scales (HoNOS)14 are administered routinely in residential rehabilitation facilities to monitor consumer functioning. The measures completed closest to the survey day were considered; 86% of these had been completed within the previous 3 months. Hospital-based consumers had significantly higher scores (more severe problems) on both the HoNOS (P < 0.001) and the Life Skills Profile-16 (P < 0.009). Using the modified version of Lelliott’s classification15 to convert HoNOS scores to a measure of severity, 29.2% of CCU clients and 58.3% of hospital clients were classified as having ‘very severe’ disability.
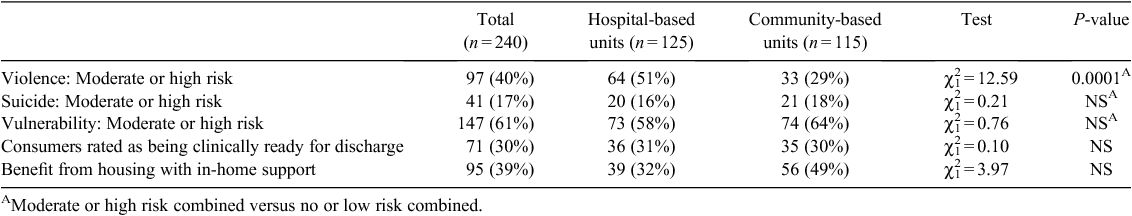
Over 40% of consumers were rated by staff as having a moderate to high risk for violence (Table 3). There was a difference in violence risk across service settings, with significantly more hospital-based consumers rated as having a moderate to high risk of violence (P < 0.0001). Nonetheless, almost one-third of the overall cohort (30%) was rated by staff as being clinically ready for discharge, but this was not feasible because of a lack of appropriate ‘step-down’ accommodation. Staff felt that over 40% of those present in the units on the survey day would benefit from independent housing with in-home supports (i.e. accommodation such as the Housing and Support Program (HASP) in Queensland, and the Housing and Support Initiative (HASI) in New South Wales).
|
Discussion
The consumers in this review had high levels of disability, with 42% remaining in their current rehabilitation unit for between 1 and 5 years and 16% remaining there for more than 5 years. Nonetheless, on the day of the survey, one-third of consumers were rated by staff as being clinically ready for discharge. However, this was not possible because of a lack of appropriate step-down accommodation. This finding supports greater investment in community-based options to improve the throughput of consumers through in-patient rehabilitation services. In Australian research, Meehan et al.16 demonstrated that community housing with adequate supports was preferred by consumers, was less expensive and offered no disadvantage to consumers in terms of outcomes.
There was variation in the way in which rehabilitation beds were used across the state. Some community-based services had accumulated a high proportion of patients on forensic orders and had little throughput. Conversely, one of the hospital-based units seemed to be operating as a subacute unit, admitting large numbers of patients from the local acute unit for brief periods. This variation in the operation of individual units resulted in the hospital-based services having both longer lengths of stay and higher patient turnover. This variation in the use of rehabilitation beds is frequently driven by the lack of other service options (e.g. medium secure units and subacute units) within a district.
The commissioning of six new CCUs in Queensland by mid-2016 will increase the number of rehabilitation beds to 320. This provides just over 10 beds per 100 000 population (18–65 years). The number of rehabilitation beds available may appear low when one considers the level of psychiatric disability in the community.17 However, bed provision is in keeping with national planning estimates, which recommend 10 rehabilitation beds per 100 000 adult population.1 It is clear that both service types have accumulated a significant number of consumers from the former psychiatric hospitals. These are severely disabled and would have difficulty managing their lives in the absence of 24-h care. However, these patients are now elderly and, as they move to aged care accommodation, the services will have greater capacity to treat ‘new’ patients emerging from the system.
Residential rehabilitation beds must be reserved for consumers with the most complex mental health needs and who require intensive support to successfully transition to more independent living options.8 Moving people from high-cost in-patient beds to less-expensive community options is in keeping with the recommendations outlined in the recent National Mental Health Commission Report.17 The Report recommends that integrated packages of care should be provided for those with severe problems to keep them out of avoidable high-cost care.
Findings from the present study indicate that hospital-based rehabilitation programs treat consumers with more severe and complex problems. Because the ‘new’ community services were largely funded through reductions in long-stay hospital beds, establishing these services involved a process of relocating some patients from existing long-stay beds. This process was subject to intense negotiation and resulted in the more disabled people remaining in hospital-based services. Despite rehabilitation efforts over several years, hospital-based services have had greater difficulty discharging these patients to less intensive levels of care (as indicated by the significantly longer length of stay in hospital-based services). Notwithstanding this, the length of stay in either service type is much less than the stay of 3 years in community-based services and 5 years in hospital-based rehabilitation services reported in the UK.4
The cross-sectional nature of the present study is a limitation and, in the absence of longitudinal data, it is impossible to draw conclusions about the advantages of community-based rehabilitation programs. Indeed, the cross-sectional approach is likely to have resulted in an over-representation of long-stay and difficult-to-discharge consumers. There is a need for further research to establish the outcome of residential rehabilitation programs because the data from the present study describe the consumers currently in the services, not those who have improved functional outcomes (and who are likely to have been discharged).
Conclusions
The findings from the present study provide a comprehensive description of consumers undergoing psychiatric rehabilitation services in Queensland. Patients in residential rehabilitation have high levels of disability, poor physical health and high levels of vulnerability. Hospital-based rehabilitation programs tend to treat consumers with more severe and complex problems. Notwithstanding these differences, it is likely that a considerable number of patients occupying rehabilitation beds in Queensland could be discharged if more ‘step-down’ options to move patients on were available. The findings of the study have implications for the future planning of mental health services for those requiring rehabilitation services.
Competing interests
The authors report no conflicts of interest.
References
[1] Harris M, Buckingham B, Pirkis J, Groves A, Whiteford H. Planning estimates for the provision of core mental health services in Queensland 2007–2017. Aust N Z J Psychiatry 2012; 46 982–94.| Planning estimates for the provision of core mental health services in Queensland 2007–2017.Crossref | GoogleScholarGoogle Scholar | 22802553PubMed |
[2] Allison S, Bastiampillai T, Goldney R. Acute versus sub-acute care beds: should Australia invest in community beds at the expense of hospital beds? Aust N Z J Psychiatry 2014; 48 952–4.
| Acute versus sub-acute care beds: should Australia invest in community beds at the expense of hospital beds?Crossref | GoogleScholarGoogle Scholar | 25136059PubMed |
[3] Parker S, Siskind D, Harris M. Community based residential mental health services: what do we need to know. Aust N Z J Psychiatry 2015; 49 86–7.
| Community based residential mental health services: what do we need to know.Crossref | GoogleScholarGoogle Scholar | 25360002PubMed |
[4] Killaspy H. The ongoing need for local services for people with complex mental health problems. Psychiatr Bull 2014; 38 257–9.
| The ongoing need for local services for people with complex mental health problems.Crossref | GoogleScholarGoogle Scholar |
[5] Gonda T, Deane F. Predicting clinically significant change in an inpatient program for people with severe mental illness. Aust N Z J Psychiatry 2012; 46 651–8.
| Predicting clinically significant change in an inpatient program for people with severe mental illness.Crossref | GoogleScholarGoogle Scholar | 22528976PubMed |
[6] Craig T, Garety P, Power P, Rahaman N, Colbert S, Fornella-Ambrojo M, Dunn G. The Lambeth Early Onset (LEO) team: randomised controlled trial of the effectiveness of specialised care for early psychosis. BMJ 2004; 329 1067–71.
| The Lambeth Early Onset (LEO) team: randomised controlled trial of the effectiveness of specialised care for early psychosis.Crossref | GoogleScholarGoogle Scholar | 15485934PubMed |
[7] Trauer T, Farhall J, Newton R, Cheung P. From long-stay psychiatric hospital to community care unit: evaluation at 1 year. Soc Psychiatry Psychiatr Epidemiol 2001; 36 416–9.
| From long-stay psychiatric hospital to community care unit: evaluation at 1 year.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD38%2FjvFCntg%3D%3D&md5=7e0f8e6863bdf37d55358accd0ae8a73CAS | 11766972PubMed |
[8] Queensland Health. Community care unit: model of service delivery. Brisbane: Queensland Health; 2012.
[9] Meehan TJ, Stedman TJ, Neuendorf KE, Francisco ID, Neilson MG. Benchmarking Australia’s mental health services: is it possible and useful? Aust Health Rev 2007; 34 623–7.
| Benchmarking Australia’s mental health services: is it possible and useful?Crossref | GoogleScholarGoogle Scholar |
[10] Shepherd N, Meehan T, Davidson F, Stedman T. An evaluation of benchmarking initiative in extended treatment mental health services. Aust Health Rev 2010; 34 328–33.
| An evaluation of benchmarking initiative in extended treatment mental health services.Crossref | GoogleScholarGoogle Scholar | 20797366PubMed |
[11] Tabachnick B, Fidell L. Using multivariate statistics. 4th edn. Needham Heights, MA: Allyn & Bacon; 2001.
[12] Woods S. Chlorpromazine equivalent doses for newer atypical antipsychotics. J Clin Psychiatry 2003; 64 663–7.
| Chlorpromazine equivalent doses for newer atypical antipsychotics.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BD3sXls12ktb0%3D&md5=00f61905606b278767e74cd0b048464fCAS | 12823080PubMed |
[13] Buckingham W, Burgess P, Solomon S, Pirkis J, Eagar K. Developing a casemix classification for mental health services: summary. Canberra: Commonwealth Department of Health and Family Services; 1998.
[14] Wing JK, Beevor AS, Curtis RH, Park SB, Hadden S, Burns A. Health of the Nation Outcome Scales (HoNOS). Research and development. Br J Psychiatry 1998; 172 11–18.
| Health of the Nation Outcome Scales (HoNOS). Research and development.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1c7ps1ehtg%3D%3D&md5=f925fa53a6683e4df86fd98f4589e39dCAS | 9534825PubMed |
[15] Parabiaghi A, Barbato A, D’Avanzo B, Erlicher A, Lora A. Assessing reliable and clinically significant change on the Health of the Nation Outcome Scales: method for displaying longitudinal data. Aust N Z J Psychiatry 2005; 39 719–45.
| Assessing reliable and clinically significant change on the Health of the Nation Outcome Scales: method for displaying longitudinal data.Crossref | GoogleScholarGoogle Scholar | 16050926PubMed |
[16] Meehan T, Stedman T, Robertson S, Drake S, King R. Do supported housing models improve clinical and social outcomes for people with severe mental illness? Aust N Z J Psychiatry 2011; 45 586–92.
| Do supported housing models improve clinical and social outcomes for people with severe mental illness?Crossref | GoogleScholarGoogle Scholar | 21534823PubMed |
[17] National Mental Health Commission (NHMC). Contributing lives, thriving communities: the national review of mental health programs and services. Sydney: NMHC; 2014.


