Skill sharing and delegation practice in two Queensland regional allied health cancer care services: a comparison of tasks
Juanine Passfield A E , Ilsa Nielsen B , Neil Brebner C and Cara Johnstone DA Central Integrated Regional Cancer Services, Queensland Health Corporate Office, GPO Box 48, Brisbane, Qld 4001, Australia.
B Allied Health Professions’ Office of Queensland, Level 6, Building 2, William McCormack Place II, 5B Sheridan Street, Cairns, Qld 4870, Australia. Email: Ilsa.Nielsen@health.qld.gov.au
C Cancer Care Support Team, Wide Bay Hospital and Health Service, PO Box 592, Hervey Bay, Qld 4655, Australia. Email: Neil.Brebner@health.qld.gov.au
D Cancer Care Team, Cairns and Hinterland Hospital and Health Service, Liz Plummer Cancer Centre, PO Box 902, Cairns, Qld 4870, Australia. Email: Cara.Johnstone@health.qld.gov.au
E Corresponding author. Email: Juanine.Passfield@health.qld.gov.au
Australian Health Review 42(6) 656-660 https://doi.org/10.1071/AH16160
Submitted: 19 July 2016 Accepted: 22 May 2017 Published: 24 July 2017
Journal Compilation © AHHA 2018 Open Access CC BY-NC-ND
Abstract
Objective Delegation and skill sharing are emerging service strategies for allied health (AH) professionals working in Queensland regional cancer care services. The aim of the present study was to describe the consistency between two services for the types and frequency of tasks provided and the agreement between teams in the decision to delegate or skill share clinical tasks, thereby determining the potential applicability to other services.
Methods Datasets provided by two similar services were collated. Descriptive statistical analyses were used to assess the extent of agreement.
Results In all, 214 tasks were identified as being undertaken by the services (92% agreement). Across the services, 70 tasks were identified as high frequency (equal to or more frequently than weekly) and 29 as not high frequency (46% agreement). Of the 68 tasks that were risk assessed, agreement was 66% for delegation and 60% for skill sharing, with high-frequency and intervention tasks more likely to be delegated.
Conclusions Strong consistency was apparent for the clinical tasks undertaken by the two cancer care AH teams, with moderate agreement for the frequency of tasks performed. The proportion of tasks considered appropriate for skill sharing and/or delegation was similar, although variation at the task level was apparent. Further research is warranted to examine the range of factors that affect the decision to skill share or delegate.
What is known about the topic? There is limited research evidence regarding the use of skill sharing and delegation service models for AH in cancer care services. In particular, the extent to which decisions about task safety and appropriateness for delegation or skill sharing can be generalised across services has not been investigated.
What does this paper add? This study investigated the level of clinical task consistency between two similar AH cancer care teams in regional centres. It also examined the level of agreement with regard to delegation and skill sharing to provide an indication of the level of local service influence on workforce and service model decisions.
What are the implications for practitioners? Local factors have a modest influence on delegation and skill sharing decisions of AH teams. Practitioners need to be actively engaged in decision making at the local level to ensure the clinical service model meets local needs. However, teams should also capitalise on commonalities between settings to limit duplication of training and resource development through collaborative networks.
Introduction
Sustainable public health services require health professionals and support workers to be used effectively and that clinically unnecessary task duplication is minimised.1–4 Increases in cancer diagnosis and improving survival are predicted to increase demand for services and place pressure on the cancer care workforce.5 The recent expansion of regional cancer centres, including radiation therapy,6 has improved accessibility to care for regional and rural patients. It has also generated challenges for health services needing to recruit and retain staff with cancer care expertise, including allied health (AH) professions. The effective and efficient use of this workforce is a challenge for new regional services. Suitable indicators to support AH workforce planning in cancer care are not readily available.7 Delegation to support workers has been demonstrated to improve access and efficiency in the cancer care setting.8 Delegation is defined as the process by which an AH professional delegates activities to a support worker who has appropriate education, knowledge and skills to undertake the activity safely.9
Consumers use the analogy of a ‘train trip across Australia’ to describe their cancer experience, emphasising that patients are the only ones to complete the whole cancer journey.5 Clinicians, including AH, often work within professional silos, resulting in duplication of history taking, assessment and intervention, and necessitating the consumer to have contact with multiple professionals, leading to role confusion and decreased consumer satisfaction.10,11 Skill sharing occurs when two or more health professionals share knowledge, skills and responsibilities across professional boundaries in assessment, diagnosis, planning and/or implementation.12 Consumer satisfaction has been shown to be high in skill share service models.13
There is interest in the increased use of delegation and skill sharing in cancer care AH teams in regional areas to improve workforce flexibility, service efficiency and responsiveness, as well as to increase access for patients. Development of a common model of delegation and skill sharing, with associated training and competency assessment resources, would support replication of this work by multiple teams. However, the degree to which a generic delegation and/or skills sharing model may be developed and implemented is unclear. Variation in the clinical tasks undertaken by different teams, the task frequency (which reduces the feasibility of training and maintaining competence of another worker undertaking the task) and local context (factors potentially limiting the safety and appropriateness of skill sharing or delegation of specific clinical tasks) may also affect the ability to develop a multisite workforce model. The present study examined the degree of consistency between two Queensland public regional cancer care AH teams for clinical task frequency and decisions regarding the appropriateness of the task for delegation or skill sharing.
Methods
Two cancer care AH services in regional Queensland were involved in separate workforce redesign projects using the same methodology. This allowed opportunistic pooling and comparison of data. Both services provided in-patient and out-patient care for medical, surgical, radiation oncology, haematology and palliative care units. The staffing establishment of each service was similar, with 12 full-time equivalent staff at the time of data collection from the professions of dietetics, occupational therapy, physiotherapy, psychology, social work and speech pathology. AH assistants (AHA) were to be trialled in Site 1, whereas Site 2 was scoping the role of an AHA to contribute to workforce redesign strategies. Site 2 services were delivered through two facilities 120 km apart (referred to as Site 2a and Site 2b herein when reported as separate centres). The service at Site 1 was provided at a single hospital.
Both services undertook a task mapping and analysis process using the Calderdale Framework (CF), a workforce redesign tool.14 Each of the two services were supported by a trained external CF facilitator. (The two CF facilitators were both AH professionals with workforce development expertise who were external to the cancer care team and had received training in the CF method.)
The task mapping data collection process involved AH professionals at each centre self-identifying and recording clinical tasks undertaken during a 4-week period, and providing a self-reported estimate of task frequency. Clinical tasks were defined as those involved in direct patient care and related to clinical activities. ‘Non-clinical’ task data were excluded from the project data collation and reporting.
Site 1 developed the task list by recording all clinical tasks undertaken in the course of daily practice. For efficiency, Site 2 used the Site 1 task list as a checklist, noting tasks on the list that were delivered (tasks not undertaken were recorded as zero frequency) and adding tasks relevant to their practice that were not evident on the Site 1 list. Frequency could be recorded as daily, two to three times weekly, weekly, fortnightly, monthly or less than monthly. Tasks were then collated and validated by the team, including the addition of a task descriptor and discussion of the scope of activities in the task, and the frequency reports by all team members confirmed. Task frequency was considered as an aggregate of all team members delivering the task, such that the data recorded represented the frequency with which the task was done by the team, as opposed to by individual staff.
Services used the CF task risk assessment tool to determine whether a task could be delegated and/or skill shared, or whether it should remain with the existing AH professional. The tool prompts the team to consider risk factors, including task complexity, the extent of technical skill and clinical reasoning requirements, as well as the degree to which the task may be protocolised for the client group relevant to the team’s casemix. The task analysis decisions were collated as part of the project outcomes.
Task mapping and analysis were undertaken at Site 1 between September 2012 and March 2013 and at Site 2 between January and May 2015. The resulting datasets (Sites 2a and 2b) were combined into one service (Site 2) for task analysis.
Data analysis
Datasets developed by both services were collated in January 2016 for frequency and decision to delegate (i.e. to an AHA), skill share with another AH professional or neither (i.e. remain with the profession/s currently providing the task). Descriptive statistical analysis was used to examine the agreement between the available datasets. ‘Agreement’ was considered to have occurred if sites had the same outcome; that is, both sites reported the same frequency (either high or not-high) or suitability/or not to delegate and/or skill share the task.
Frequency
Frequency was analysed as a dichotomous discrete variable: ‘high-frequency’ and ‘not high-frequency’ tasks. High-frequency tasks were defined as tasks reported being undertaken equal to or more frequently than weekly. Experience in other projects indicated that tasks conducted weekly or more often and assessed at an appropriate risk level for skill sharing or delegation are more likely to be implemented. Analysis entailed counts and proportions of the number of tasks identified as high frequency by all three teams, two teams, one team or no teams. Tasks were compared in subsets of clinical functions that had already been defined in the dataset (e.g. social, musculoskeletal, swallowing). Tasks were also identified as assessment or intervention.
Task analysis decision making (delegate, skill share, neither)
The project spreadsheets, available for task analysis by the two services (Site 1 and Site 2), were compared for decision making outcomes. Site 2 chose a subset of 68 tasks for analysis based on the frequency of performance, the task being performed by more than one AH professional and the likelihood of implementation. Tasks were coded for each site as either determined by the team to be suitable for delegation, suitable for skill sharing or remain with the profession that has historically delivered the task.
Results
In all, 214 tasks were identified as being undertaken in the three regional AH cancer care services (Site 1, 204 tasks; Sites 2a and 2b, 208 tasks). Most tasks (n = 195/214; 91% agreement) were identified as being undertaken by all three sites. Seven tasks (3%) were identified as unique to one of the three sites. These tasks related to differences in lymphoedema care including use of perometry, laser, screening tools and treatment contracts, as well as use of a clinical outcome measure specific to just one service and the use of fibre optic endoscopic evaluation of swallow (FEES), which was available at one site.
Frequency
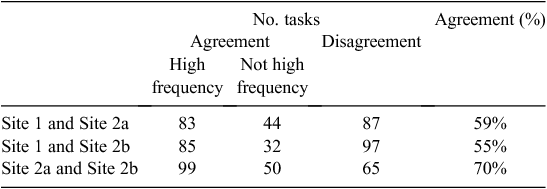
Of the 214 tasks, agreement was apparent at all three sites for 70 high-frequency and 29 not high-frequency tasks (99/214; 46% agreement). Comparisons of the agreement between individual sites are given in Table 1.
|
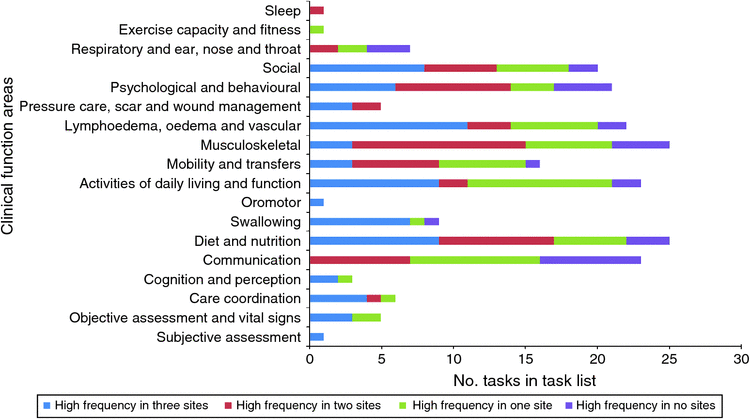
Tasks identified as high-frequency tasks by all services were most numerous in the clinical areas of musculoskeletal, lymphoedema, oedema and vascular, diet and nutrition, activities of daily living and function, social and swallowing (Fig. 1).
|
Task analysis decision making (delegate, skill share, neither)
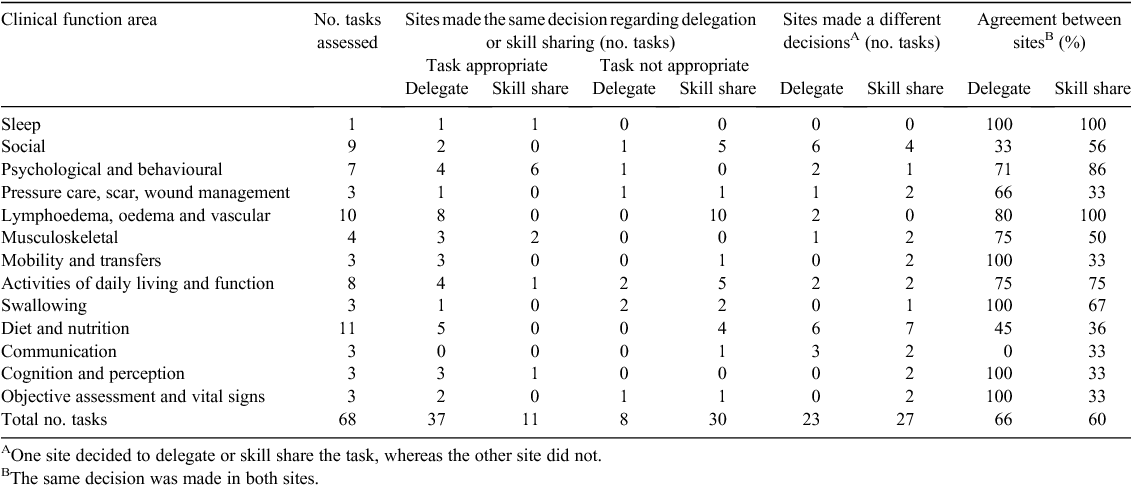
Of the collated list of tasks, 68 tasks were analysed for appropriateness to delegate or skill share by both Site 1 and Site 2. Twenty-four tasks were assessment tasks and 44 were intervention tasks. Different risks and mitigation strategies affect the decision to delegate or to skill share a task; these were considered separate decisions for the purpose of analysis. Consequently, 136 decisions were examined for agreement between sites. Sites were considered to agree if both decided to delegate or to skill share a task or neither did so. Sites were not in agreement if one determined a task could be delegated or skill shared but the other did not. The decisions for each task are detailed in Table 2.
Delegate
Of the 68 tasks analysed, 37 were deemed suitable and eight tasks unsuitable for delegation by both services (66% agreement). The remaining 23 tasks (34%) were analysed as suitable for delegation by one service but not the other. The overall proportion of tasks delegated by each service was similar (69% Site 1, 74% Site 2). Of those tasks suitable for delegation, high-frequency tasks appear more likely to be delegated than not high-frequency tasks. (38/47 (81%) at Site 1; 43/50 (86%) at Site 2). Intervention tasks (32/47 (68%) at Site 1; 36/50 (72%) at Site 2) appear to be more frequently delegated than assessment tasks (32% Site 1, 28% Site 2).
Agreement in the decision to delegate, or not, appears lowest for clinical function areas of communication (0/3 tasks; 0%), social (3/9 tasks; 33%) and diet and nutrition (5/11 tasks; 45%). A 100% agreement for the decision to delegate, or not, was apparent for five of the 13 clinical function areas (Table 2).
Skill share
Of the 68 tasks analysed, 11 were deemed suitable and 30 tasks unsuitable for skill sharing by both services (60% agreement). The remaining 27 tasks (40%) were analysed as suitable for skill sharing by one service but not the other. The decision to skill share tasks was lower at Site 1 (20/68; 29%) than Site 2 (29/68; 43%). Task frequency does not appear to influence the decision to skill share, with Site 1 finding 11 of 20 (55%) high-frequency tasks suitable and Site 2 finding 13 of 29 (45%) high-frequency tasks suitable for skill sharing. Similarly, the type of task (assessment or intervention) appears to not affect the decision to skill share, with proportions being almost even (11 and nine respectively at Site 1; 13 and 16 respectively Site 2).
Neither delegate nor skill share (remain with the profession/s)
Of the 68 tasks analysed, 22 were deemed as unsuitable for either delegation or skill sharing in one or both sites. Site 1 identified 17 tasks (25%) and Site 2 identified 11 tasks (16%) that were to remain with the existing profession/s. Six of the 22 profession-specific tasks were identified by both sites.
Discussion
This paper describes the consistency of clinical task delivery in two Queensland regional AH cancer care services that are similar in size, purpose, context and workforce structure. The teams’ independent decisions regarding task appropriateness for delegation or skill sharing were also compared. The overall number and types of tasks undertaken by each service were similar, with moderate agreement for task frequency. Variation in task frequency may be affected by how the task descriptors were interpreted, local service delivery models (including availability of equipment and/or access to other services) and clinician preference and/or expertise for particular tasks. Despite the number of referrals and patient diagnoses not being examined, the tasks performed by AH professionals in regional cancer care services appear relatively consistent. Comparison with other regional cancer care services is indicated to further investigate the consistency of the clinical task requirements of these services to inform decisions on the application of common workforce models across centres.
Of the 68 tasks analysed for delegation, the proportion of tasks deemed suitable for delegation by each service was similar (69% Site 1 vs 74% Site 2); however, a higher proportion of tasks was deemed suitable for skill sharing at Site 2 than Site 1 (43% vs 29% respectively). The Site 1 workforce included the development of an AHA role in the workforce redesign project, whereas Site 2 did not. The lack of an AHA within the Site 2 team may have resulted in the prioritisation of opportunities for skill sharing as an efficiency measure in the interim.
The types of tasks delegated by both services were more likely to be intervention (68% Site 1, 72% Site 2) than assessment tasks. This is related, in part, to the higher number of intervention tasks that were identified and analysed. It may also be related to the strong inter-relationship between administration of an assessment process and the interpretation of the outcome that a clinician would generally complete in parallel. Particularly for standardised or repeated testing, separating the time-consuming administration from the clinical reasoning element of an assessment can be feasible and efficient. However, delegation was found to favour the more repetitious intervention tasks. Of the clinical function areas analysed, the tasks areas that most strongly identified as suitable for delegation were in the physical rehabilitation areas (lymphoedema, musculoskeletal, mobility and transfer, cognition and perception). This may be due, in part, to the long history of support workers in physiotherapy and occupational therapy.
The agreement for the decision to skill share tasks was 60%. When deciding to skill share, teams discussed the current care arrangements. Tasks undertaken by more than one AH profession (e.g. physiotherapy and occupational therapy) at all sites were objective assessment of skin, wounds and scars, scar massage and management, relaxation and stress management. Site 2 viewed skill sharing these tasks as an opportunity to improve consistency in management between AH clinicians. Site 1 regarded it as an area of shared practice and that the health professionals skill set covered the task with adequate consistency to be considered functionally equivalent from a professional perspective and that there was probably greater variance between individual practitioners than variation between two professions. This local discussion potentially contributed to Site 2’s increased number of skill sharing tasks and highlights the requirement for local context application.
Conclusion
The self-reported clinical tasks delivered by two Queensland regional AH cancer care teams were found in the present study to have strong consistency, with moderate agreement between teams with regard to the frequency with which the tasks are performed. The teams also had moderate agreement in relation to the proportion of the total number of tasks that were considered appropriate for delegation and/or skill sharing. However, there was more substantial variation at the specific task level in the delegation or skill sharing decisions. Factors affecting the delegation and skill sharing decisions were not formally investigated in the present study. Context, including access to assistant staff in the facility, familiarity and previous experiences of staff with these workforce models, may have positively or negatively disposed the team to delegation or skill sharing. These factors warrant further research because they will be important considerations for teams seeking to replicate delegation and skill sharing models implemented in other regional cancer care services.
Competing interests
None declared.
Acknowledgements
The authors thank the cancer care teams who participated in these workforce redesign projects with a view to improving the delivery of care and meeting the needs of these patients.
References
[1] Queensland Health. Innovations in models of care for the health practitioner workforce in Queensland Health. Brisbane, Australia. Allied Health Workforce Advice and Coordination Unit, Queensland Government; 2011.[2] Duckett SJ. Health workforce design for the 21st century. Aust Health Rev 2005; 29 201–10.
| Health workforce design for the 21st century.Crossref | GoogleScholarGoogle Scholar |
[3] Nancarrow SA, Borthwick AM. Dynamic professional boundaries in the healthcare workforce. Sociol Health Illn 2005; 27 897–919.
| Dynamic professional boundaries in the healthcare workforce.Crossref | GoogleScholarGoogle Scholar |
[4] Leggat S. Changing health professionals’ scope of practice: how do we continue to make progress? 2014. Available at: http://ahha.asn.au/publication/issue-briefs/changing-health-professionals%E2%80%99-scope-practice-how-do-we-continue-make [verified 17 May 2016].
[5] Health Workforce Australia. National cancer workforce strategic framework. Australian Government Department of Health, Canberra, Australia 2013.
[6] Radiation Oncology Tripartite Committee. Planning for the best. Tripartite national strategic plan for radiation oncology 2012–2022. 2012. Available at: http://www.radiationoncology.com.au/ [verified 17 May 2015].
[7] Passfield J, McQueen L, Hulcombe J. Workforce profile for allied health professions in Queensland public health cancer care services with linear accelerators. J Oncol Pract 2014; 10 244–7.
| Workforce profile for allied health professions in Queensland public health cancer care services with linear accelerators.Crossref | GoogleScholarGoogle Scholar |
[8] Johnstone C, Johnson L, Cibau L, Harvey D, Nielsen I. Improving patient access: outcomes from an allied health cancer redesign project. In: Proceedings of the 11th National Allied Health Conference; 9–11 November 2015; Melbourne, Australia. 2015.
[9] Queensland Health. Governance guidelines for allied health assistants. Brisbane: Queensland Government; 2016.
[10] Thylefors I, Persson O, Hellström D. Team types, perceived efficiency and team climate in Swedish cross-professional teamwork. J Interprof Care 2005; 19 102–14.
| Team types, perceived efficiency and team climate in Swedish cross-professional teamwork.Crossref | GoogleScholarGoogle Scholar |
[11] Nancarrow S, Enderby P, Moran AM, Dixon S, Parker S, Bradburn M, Mitchell C, John A, McClimens A The relationship between workforce flexibility and the costs and outcomes of older peoples’ services. Report for the National Institute of Health Research Service Delivery and Organisation Programme. University of Sheffield, Sheffield, UK; 2010. Available at: http://www.sdo.nihr.ac.uk/projdetails.php?ref=08-1519-95# [verified 17 May 2015].
[12] State of Queensland (Queensland Health). Guidelines for skill sharing between allied health professionals. Workplace Instruction (WPI3) for allied health professionals. Brisbane: Queensland Government; 2013. Available at: https://www.health.qld.gov.au/__data/assets/pdf_file/0020/155513/wpi-three.pdf [verified 22 June 2017].
[13] Bradford M. Patients’ experiences of healthcare systems: a qualitative study. Internal project report Mackay Hospital and Health Service. 2013.
[14] Smith R, Duffy J. The Calderdale Framework information sheet. 2015. Available at: https://www.health.qld.gov.au/ahwac/docs/calderdale-framework.pdf [verified 17 May 2015].