Condom use errors and problems: a global view
Stephanie A. Sanders A B C H , William L. Yarber A C D , Erin L. Kaufman E , Richard A. Crosby A C E , Cynthia A. Graham A C F and Robin R. Milhausen A C GA The Kinsey Institute for Research in Sex, Gender, and Reproduction, Indiana University, Bloomington, IN 47405, USA.
B Department of Gender Studies, Indiana University, Bloomington, IN 47405, USA.
C Rural Center for AIDS/STD Prevention, Indiana University, Bloomington, IN 47405, USA.
D Department of Applied Health Science, Indiana University, Bloomington, IN 47405, USA.
E College of Public Health at the University of Kentucky University, Lexington, KY 40506, USA.
F Department of Psychology, University of Southampton, Southampton SO17 1BJ, UK.
G Department of Family Relations and Applied Nutrition at the University of Guelph, Ontario N1G2W1, Canada.
H Corresponding author. Email: sanders@indiana.edu
Sexual Health 9(1) 81-95 https://doi.org/10.1071/SH11095
Submitted: 3 July 2011 Accepted: 24 November 2011 Published: 17 February 2012
Journal Compilation © CSIRO Publishing 2012 Open Access CC BY-NC-ND
Abstract
Background: Significantly more research attention has been devoted to the consistency of condom use, with far fewer studies investigating condom use errors and problems. The purpose of this review was to present the frequency of various condom use errors and problems reported worldwide. Methods: A systematic literature search was conducted for peer-reviewed articles, published in English-language journals between 1995 and 2011. Results: Fifty articles representing 14 countries met criteria for inclusion. The most common errors included not using condoms throughout sex, not leaving space at the tip, not squeezing air from the tip, putting the condom on upside down, not using water-based lubricants and incorrect withdrawal. Frequent problems included breakage, slippage, leakage, condom-associated erection problems, and difficulties with fit and feel. Prevalence estimates showed great variation across studies. Prevalence varied as a function of the population studied and the period assessed. Conclusion: Condom use errors and problems are common worldwide, occurring across a wide spectrum of populations. Although breakage and slippage were most commonly investigated, the prevalence of other condom use errors and problems found in this review were substantially higher. As a framework for understanding the role of condom errors and problems in inadequate protection, we put forward a new model: the Condom Use Experience model. This model can be used to generate testable hypotheses for future research. Addressing condom use errors and problems in research and interventions is crucial to closing the gap between the perfect use and typical use of condoms.
Additional keywords: condom breakage, condom slippage, sexual behaviour, sexually transmissible infections.
Introduction
The global pandemic of HIV, sexually transmissible infections (STIs) and unintended pregnancy necessitates an accelerated emphasis on correct and consistent male condom use. According to global health organisations, ‘The male latex condom is the single, most efficient, available technology to reduce the sexual transmission of HIV and other sexually transmitted infections.’1 However, condom effectiveness is compromised by user errors and lack of use.2 For example, the World Health Organisation reported that condoms have a 2% perfect use failure rate for pregnancy, but the typical failure rate is 15%.3,4 Magnified over the world population, this 4-fold difference has substantial implications for population growth and, in turn, public health. The gap between perfect and typical use has similar relevance for HIV and STI prevention, suggesting that millions of infections could be avoided by improved user effectiveness. The discrepancy between perfect and typical failure rates is attributable to the combination of both inconsistent and incorrect use, but the respective contribution of user errors to typical use failure rates has never been quantified.5
Significantly more attention has been given to consistency of condom use, with far fewer investigations on the details of user errors and problems. From a methodology perspective, measuring condom use frequency is a relatively straightforward process.6 Unfortunately, the same cannot be said about measuring the numerous errors and problems that individuals may experience when using condoms. Nonetheless, a growing body of literature is documenting the many different condom errors and problems, and their relative prevalence and correlates. We use the term errors to refer to those behaviours that represent incorrect use of condoms (e.g. letting condoms contact sharp objects or other application errors, not using condoms through the entire act of intercourse). Problems refer to those experiences that may be under less direct behavioural control of the condom user, but may compromise condom use or condom protection (e.g. breakage, slippage, erection problems, problems with fit and feel). Failing to account for condom use errors and problems can lead to faulty conclusions regarding condom effectiveness or evaluation of interventions. Additionally, errors and problems may not only compromise condom efficacy, but may also discourage condom use if people become frustrated or have less pleasurable experiences as result of them. Accordingly, the purpose of this review was to present the frequency of various condom use errors and problems reported worldwide. Although the literature is sparse, it is nonetheless important because it can inform efforts to promote effective condom use worldwide.
Methods
We considered all English-language publications from 1995 to the present that were published in peer-reviewed journals available through the university library systems. In March–May 2011, we queried the PubMed Database using the following search terms: condom rate, condom error rate, condom problem rate, condom errors, condom problems, condom failure, condom failure rates, condom failure prevalence, condom failure international, incomplete use, oil-based lubricant condom failure, oil lubrication condom failure, lubrication condom, lubrication male condom, lubrication condom, oil lubrication, oil male condom, and condom with fit or feel. Article information was then extracted and entered into tables, with the principal summary measure being the prevalence of the condom use problem/error in the study population. Although different wording was used across studies, we classified errors as follows:
-
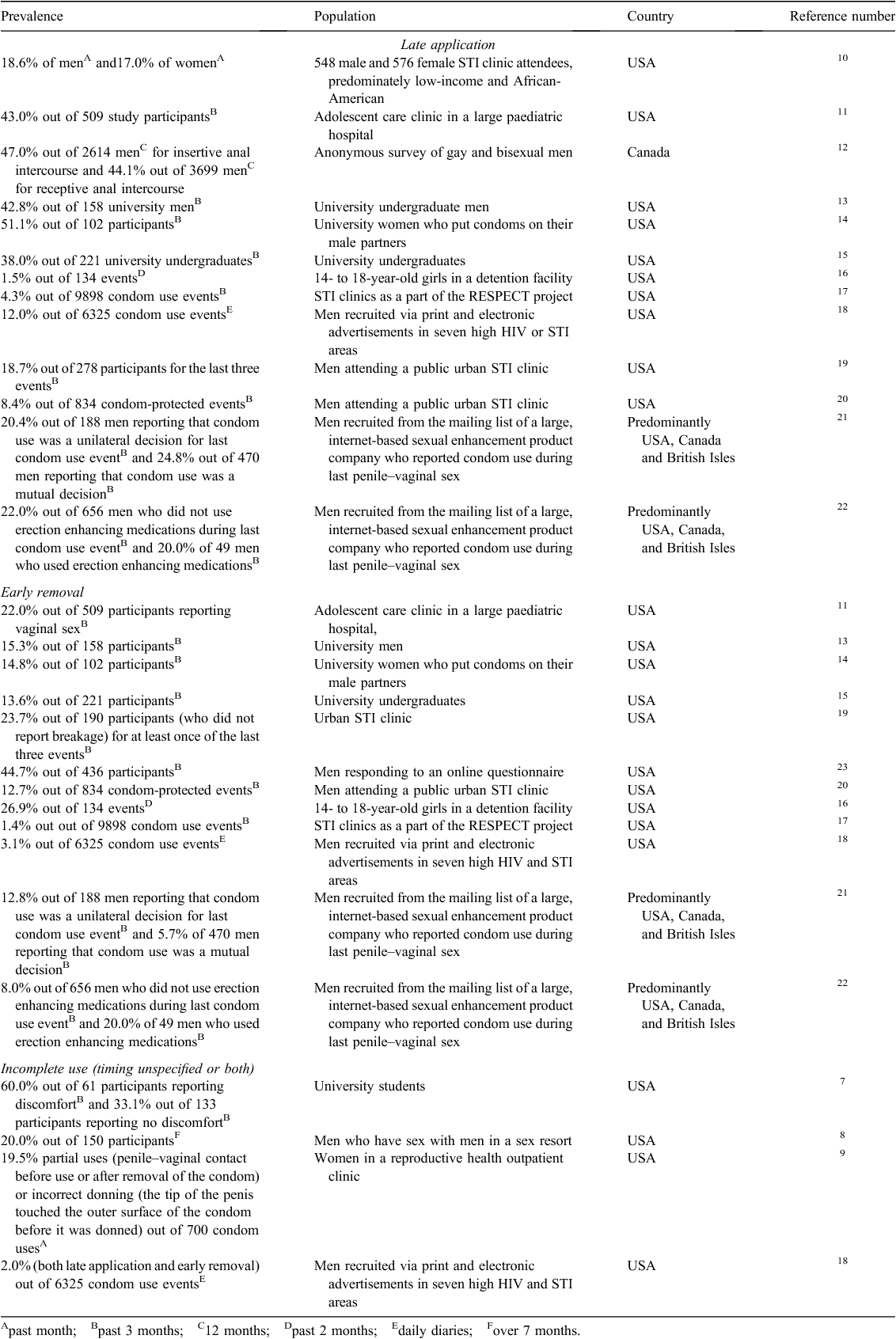
Incomplete use – not using a condom during the entire act of intercourse, including late application and early removal. Late application is when intercourse begins before condom application. Early removal refers to taking the condom off followed by unprotected intercourse (Table 1).
-
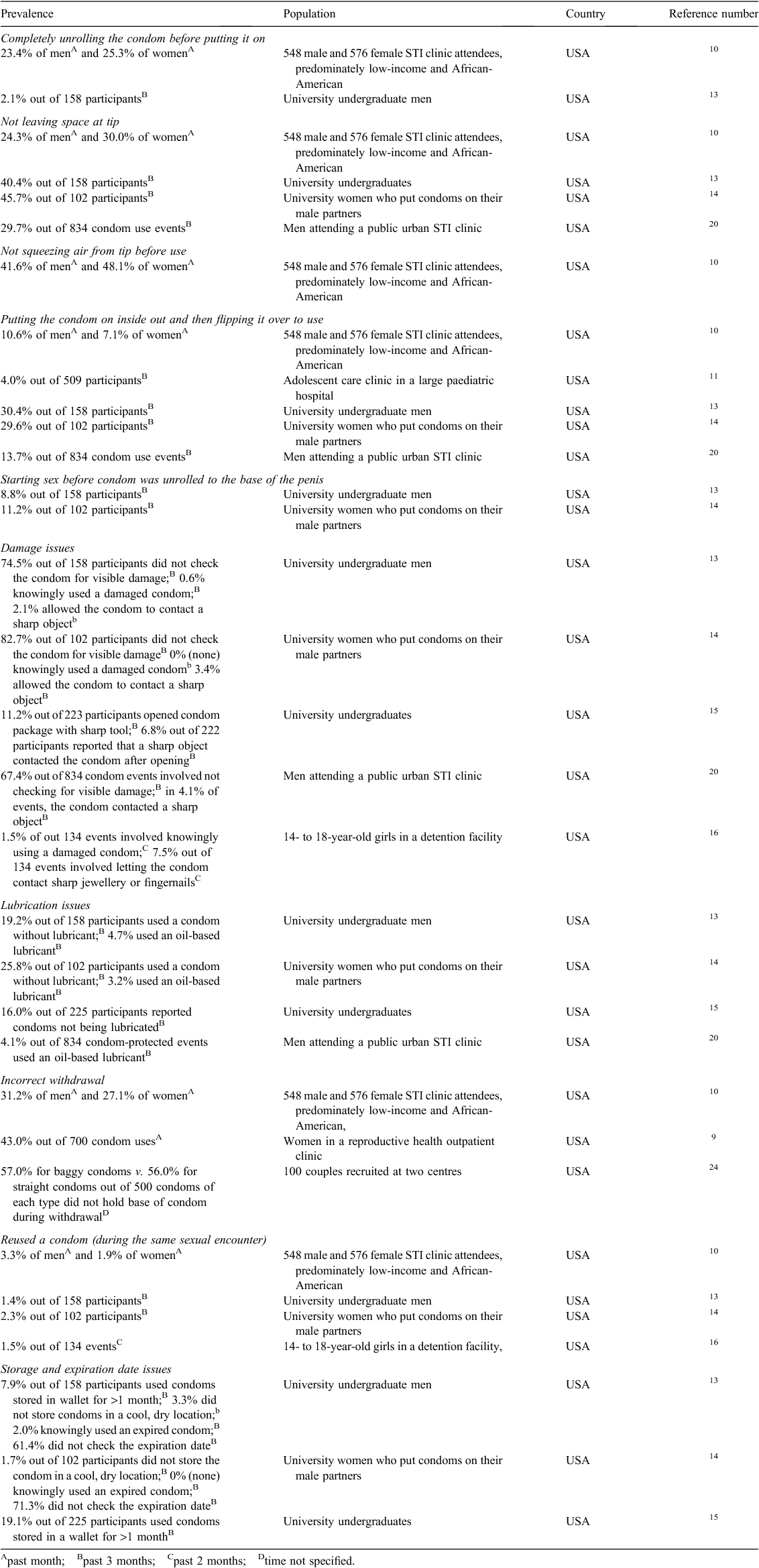
Other condom use errors – including (1) completely unrolling the condom before putting it on, (2) not leaving space at the tip of the condom, (3) not squeezing air from the tip before use, (4) putting the condom on inside out and then flipping it over to use, (5) starting sex before the condom was unrolled to the base of the penis, (6) damage issues (using a sharp object to open the package, letting the condom contact a sharp object, knowingly using a damaged condom, not checking for physical damage), (7) lubrication issues (condom not lubricated, using oil-based lubricant), (8) incorrect withdrawal or not holding base of condom during withdrawal, (9) reuse of a condom (during same sexual encounter) and (10) storage and expiration date issues (Table 2).
-
Problems related to breakage, slippage, leakage or ‘condom failure’ (Table 3).
-
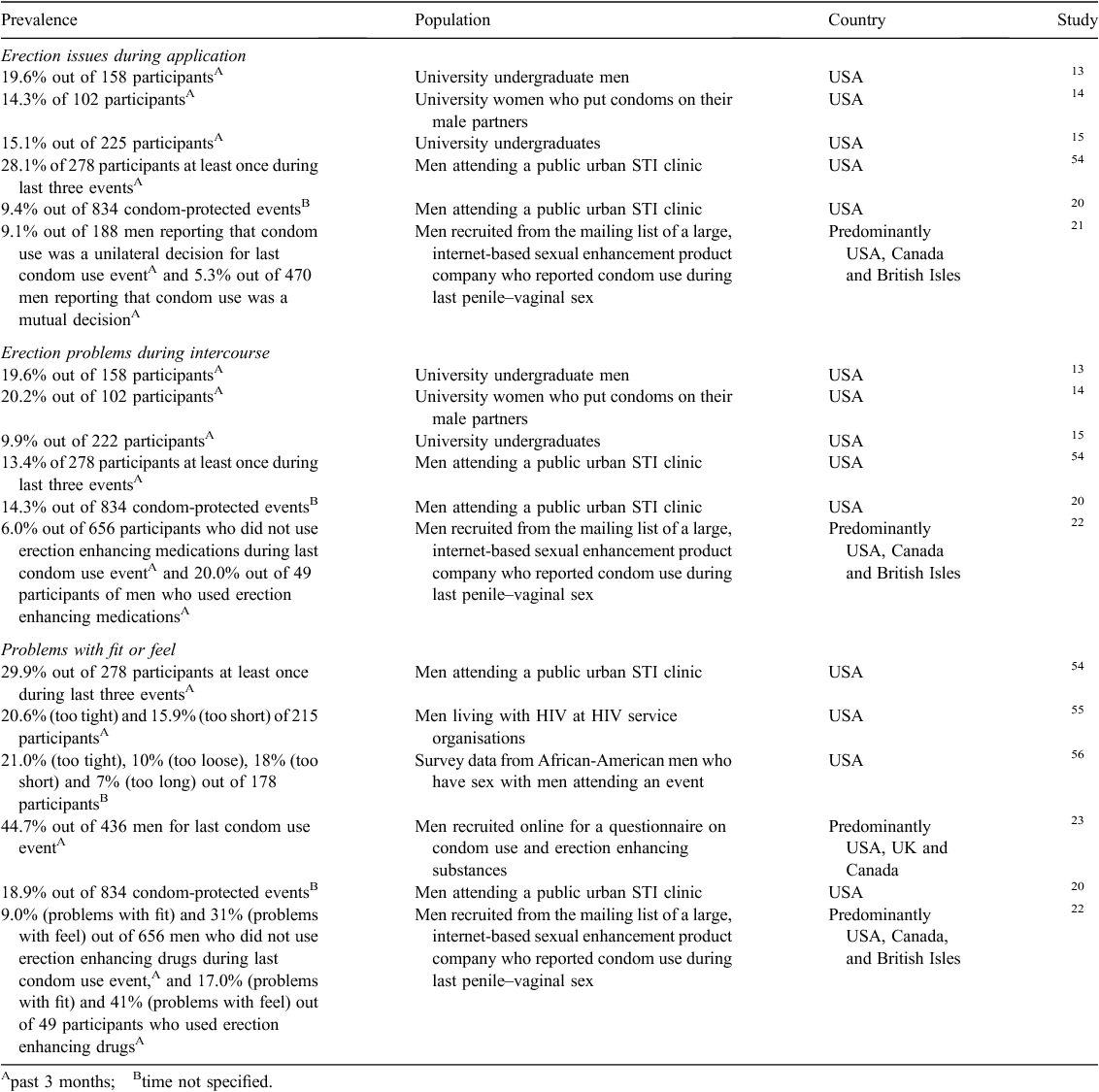
Problems with condom-associated erection problems (either during application or during intercourse while using a condom) and problems with the ‘fit’ or ‘feel’ of condoms, including problems related to the size or shape of the condom, or discomfort or interference with sensation (Table 4).
Results
Fifty articles representing 14 countries met the criteria for inclusion. All studies reviewed below reported findings for condom use for either vaginal or anal intercourse or both. Broadly, two types of prevalence estimates are reported: (1) proportion of individuals reporting an error or problem within a specified recall period; or (2) proportion of events for which an error or problem occurred. The populations studied are noted in the tables, as are the recall periods (in the footnotes) which varied across studies. Given the numbers of studies found in each category, we present the findings in four tables, two for errors and two for problems.
Incomplete use
Table 1 displays findings from 14 studies assessing incomplete use. In some studies, the type of incomplete use was not specified or the errors were combined in reporting;7–9 in some, the terms sex or sexual activity were used without specifying intercourse. Six studies reported the prevalence of late application among participants, with 17.0% to 51.1% of participants reporting this error.10–16 Seven studies reported the prevalence of late application as a proportion of condom use events, with estimates ranging from 1.5% to 24.8%.16–22 Six studies reported early removal at the participant level, with prevalence ranging from 13.6% to 44.7%.11,13–15,19,23 Six studies reported early removal at the event level, with prevalence ranging from 1.4% to 26.9%.16–18,20–22 Finally, two studies reported a combined prevalence (either late application or early removal or both), ranging from 20.0% to 60.0% of participants.7,8 One study found 2% of respondents reported both late application and early removal for the same event.18
|
Other condom use problems
Table 2 displays the 10 categories of other condom use errors. Two studies estimated the prevalence of completely unrolling the condom before putting it on, reported by 2.1% to 25.3% of participants.10,13 Three studies reported prevalence rates for not leaving space at the tip, ranging from 24.3% to 45.7% of participants.10,13,14 One of these studies further reported that 41.6% of men and 48.1% of women reported that air was not squeezed from the tip before use.10 Four studies reported that between 4.0% and 30.4% of participants had put the condom on inside out and then flipped it over.10,11,13,14 Two studies reported 8.8% of men and 11.2% of women started sex before the condom was unrolled to the base of the penis.13,14 Several damage-related issues were reported across five studies. Exposing the condoms to sharp objects was reported by 2.1–11.2% of participants from three studies,13–15 and for 4.1% and 7.5% of events in two other investigations.16,20 Not inspecting the condom for damage was reported by 74.5% of men and 82.7% of women in two studies.13,14 In two studies, knowing use of a damaged condom was reported by 0–0.6% of participants13,14 and, in another study, during 1.5% of events.16 Across three studies, using a condom that was not lubricated was reported by 16.0–25.8% of participants.13–15 Two studies reported 3.2% of women and 4.7% of men used an oil-based lubricant,13,14 with another reporting that oil-based lubricants were used on 4.1% of events.20 Incorrect withdrawal was reported by 31.2% of men and 27.1% of women in one study,10 and in 43.0% and 57.0% of condom use events in two other studies.9,24 Reusing the condom during the same intercourse session was reported for 1.4–3.3% of participants in three studies10,13,14 and for 1.5% of events in another study.16 Incorrect storage was reported by 3.3–19.1% of participants in three studies.13–15
|
Breakage, slippage, leakage or ‘condom failure’
Table 3 shows the studies examining breakage, slippage, leakage and ‘condom failure’ rates. Breakage rates ranged from 0.8% to 40.7% of participants across 15 studies7,8,10,11,13–15,25–32 and 0.0% to 32.8% of condom use events across 23 studies.9,16,17,20,21,24,26,32–47 Studies have reported on slippage in a variety of ways, sometimes specifying timing (during intercourse or upon withdrawal) and sometimes specifying degree of slippage (complete or partial); most of the reports, however, did not specify either of these. It is worth noting that slippage during withdrawal may reflect the user error of not holding the rim of the condom during withdrawal. Estimates for slippage during intercourse ranged from 13.1% to 19.3% of participants in three studies13–15 and from 0.0% to 6.6% for condom use events across five additional studies.20,22,36,40,42 Estimates for slippage during withdrawal ranged from 11.6% to 14.9% of participants in three studies13–15 and from 0.0% to 12.8% of events in four other studies.20,21,36,42 For studies which did not specify timing of slippage, the range of estimates was 0.8%31 to 36.2%27 of participants across eight studies.8,11,26–31 The event level estimates for slippage ranged from a low of 0.0% for a sample of licensed prostitutes in Nevada USA36 to a high of 78.0% reporting partial slippage of less than 1 inch for baggy condoms used by monogamous couples.24 Leakage was reported by 7.6% of men13 and 12.5% of women14, and for 0.4%17 to 6.5% of events.15 Breakage and slippage combined or complete failure was reported by 25.2% to 44.7% of participants in seven studies14,23,27,48–51 and from 0.7% to 7.6% of events in four studies.9,45,52,53

|
Condom-associated erection problems and problems with ‘fit’ and ‘feel’
Table 4 presents data for condom-associated erection problems, and problems with fit and feel. Erection problems can occur during condom application or during intercourse while using a condom. Condom-associated erection problems during application ranged from 14.3% to 28.1% of participants in four studies,13–15,54 and 5.3% and 9.4% of events in two others.20,21 Condom-associated erection problems during intercourse were reported by 9.9% to 20.2% of participants across four studies13–15,54 and in 6.0% and 20.0% of events in two studies.20,22 Problems with fit and feel ranged from 7.0% to 29.9% of participants across three studies54–56 and from 9.0% to 44.7% of events across three studies,20,22,23 depending on the specific aspect assessed.
|
Discussion
This review from studies representing 14 countries suggests that condom use errors and problems are common events worldwide. Moreover, the diversity of samples studied (e.g. sex workers, STI clinic attendees, monogamous married couples, college students) suggest that these errors and problems may be affecting millions of people. Common errors include: incomplete use (i.e. late application of condoms after intercourse began, early removal of condom followed by unprotected intercourse), not leaving space at the tip, not squeezing air from the tip before use, putting the condom on inside out and having to flip it over, not using water-based lubricant and incorrect withdrawal. Common problems include: breakage, slippage, leakage, erection problems during condom application, erection problems during intercourse while using a condom, and problems with the fit or feel of condoms.
The largest number of studies were those documenting the prevalence of breakage and slippage (see Table 3). Clearly, these studies are important, given that breakage and slippage are two of the primary forms of condom use failure. However, other errors and problems may be similarly important. First, these errors may expose a partner to infection via skin-to-skin contact with a penis or ejaculate. For example, frequency estimates of early removal of condoms followed by unprotected intercourse are often greater than those for breakage and slippage. Thus, this error may represent a more likely threat of exposure than that resulting from breakage or slippage.
Second, based on the findings reported in Table 2, it is probable that breakage and slippage often occur as a result of other errors made by users. Indeed, incorrect methods of applying condoms such as letting the condom contact sharp objects have been correlated with condom breakage,25,31,57 as have problems with lubrication (e.g. dryness or use of oil-based lubricants).34 In one study,13 the more errors a person reported, the greater the odds of breakage, slippage or both. Inadequate condom protection results not only from breakage, slippage and leakage, but also from any condom use error that may lead to these outcomes or to potential exposure to pathogens (risk for STIs) or sperm (risk for unintended pregnancy) in and of itself (e.g. incomplete use). Inadequate condom protection also accrues from inconsistent or non-use of condoms across events. Therefore, much may be gained by a broader examination of errors and problems beyond breakage and slippage in terms of both their prevalence and their relationship to inadequate condom protection.
One error that is obviously problematic in terms of risk of exposure is incomplete use. This error has frequently been investigated, and estimates suggest it is very commonly reported. Despite this, the actual duration of condom use during intercourse is unknown; for example, during late application how much time elapses between penetration and condom application? Regarding early removal of condoms, we know that issues related to arousal and pleasure and erectile difficulties can be the impetus for taking off condoms before sex is over.19,22,54
Condom-associated erection difficulties have been surprisingly under-researched. Yet what evidence we have suggests that they may be of crucial importance in terms of their relationship to slippage,54,57 and possibly to attitudes towards condoms and future use. We also have evidence that despite assumptions to the contrary, phosphodiesterase type 5 inhibitors do not fully overcome condom-associated erection problems.22
This initial review provides a guide to the literature. It is important to note that the prevalence estimates in the tables vary tremendously across studies. For example, breakage estimates ranged from less than 1% to more than one-third of events (see Table 3). Logically, estimates depend on the particular sample studied and the period assessed. Some are presented in terms of the number of participants experiencing the condom use error or problem and others in terms of the number of condom use events during which the condom use error and problem occurred. Some event level studies examined a single or specified number of events per person. Others included a range of number of events per person. This latter method can introduce some error in prevalence estimates. For example, one well established finding is that condom breakage is not a random event. A relatively small proportion of condom users experience a disproportionate number of breakages.25,31,36,58,59 Therefore, analytic methods for event-level data should control for the number of reports per person. Both participant- and event-level prevalence estimates can be useful. One strength of event-level analysis is the ability to infer causation. Participant-level analyses may help identify people experiencing multiple episodes of breakage or any other problem or error who may benefit from intensified intervention efforts.
A major limitation of the review is that the overwhelming majority of studies have been conducted in developed countries and mostly in North America. In fact, except for the studies focussed on breakage, slippage, leakage or condom failure (reported in Table 3), all of the studies on errors and other problems reported on participants predominantly from the USA, Canada or the British Isles. Therefore, more research is needed on condom use errors and problems in a wider range of countries, particularly in developing countries, and among varying populations. For example, reuse of condoms was rarely reported in the studies in this review, but may be more common in less economically developed countries or among the poor. Collecting data on condom use errors and problems among a larger diversity of populations may help better inform condom intervention strategies tailored to those populations.
Condom use promotion programs should emphasise that condoms must be used both consistently (on every occasion of intercourse) and correctly. The following guidelines for correct condom use, based largely on the recommendations of Hatcher et al.4 are useful for clients and patients:
-
Before intercourse. Plan ahead to use condoms and discuss condom use with your sexual partner(s). Have an adequate supply of latex (the most common type) or polyurethane condoms and water-based lubricant. Sufficient lubrication is important and more than one condom may be needed if one is damaged or put on incorrectly, for repeated intercourse or when switching behaviours such as from anal to vaginal intercourse. Do not reuse condoms.
-
At time of intercourse.
-
-
o Opening the condom. Check the date on the package and do not use expired condoms. Push the condom away from the corner of the package you are going to tear. When opening the package, carefully avoid contact with sharp objects including teeth and fingernails. Without unrolling it, inspect the condom for damage. Do not use a damaged or deteriorated condom (e.g. holes, brittle, discoloured, sticky) regardless of expiration date. Store condoms in a cool, dry place.
-
o Putting the condom on: Put the condom on the penis before any contact with the partner’s mouth, anus or vagina. If uncircumcised (uncut), pull back the foreskin before putting on the condom. Roll the condom slightly in your fingers to ascertain the direction to put it on so that the rolled ring will be on the outside and can unroll easily. Do not unroll the condom before putting it on. Place the condom on the tip of the erect penis and unroll a short distance to make sure it is being unrolled in the right direction. If the condom does not unroll easily, it is on upside down. If it is on upside down, dispose of that condom and start with a new one. (Pre-ejaculate (‘pre-cum’) may infect or impregnate a partner.) If the condom is unrolling properly, squeeze the tip to leave some space and unroll the condom to the base of the penis, smoothing out air as you unroll. Squeeze out excess air. If you see that the condom is damaged, change to a new one.
-
o Lubrication is important. Even when lubricated condoms are used, additional lubricant can help avoid excessive friction that can be uncomfortable and may damage the condom. For latex condoms, only water-based lubricants (e.g. lubricating jellies; spermicidal creams, jellies, foam or suppositories; water; saliva) should be used. Oil-based lubricants can damage latex condoms. For polyurethane condoms, any type of lubricant can be used. In addition to placing additional lubricant on the outside of the condom or on the partner, some men find it helpful to place a small amount of lubricant in the tip of the condom before placing it on the penis.
-
o Protect the entire act of intercourse. The condom should be put on the penis before intercourse and remain on the penis throughout intercourse (the entire time the penis is in contact with the vagina, anus or mouth). Avoid condom contact with sharp objects (including genital or mouth piercings) throughout use. Put on additional lubricant or change to a new condom for prolonged intercourse if desired. Change condoms between different types of intercourse (vaginal, oral, anal) within a session.
-
-
After intercourse: Soon after ejaculation or when intercourse is over, hold the base of the condom during withdrawal to make sure it does not slip off or leak semen. Do not linger too long letting the penis get soft before withdrawal or semen may leak out. Check the condom for visible damage such as holes. Wrap it in tissue and discard. Do not flush condoms down the toilet.
-
If the condom breaks, falls off, leaks or is not used during intercourse: If the condom breaks or slips off during intercourse and before ejaculation, stop and put on a new one before continuing intercourse. Even if ejaculation has not occurred, your partner may have been exposed to semen and infectious organisms. When a condom has broken or slipped off during intercourse or if a condom was not used for the complete act of intercourse, gently wash the penis, vulva, anus and surrounding areas with soap and water immediately after intercourse to reduce the risk of acquiring an STI. Insert an applicator full of spermicide in the vagina as soon as possible. Do not douche. Discuss the possibility of pregnancy or infection, and consult a health care provider as soon as you can to determine what action should be taken.
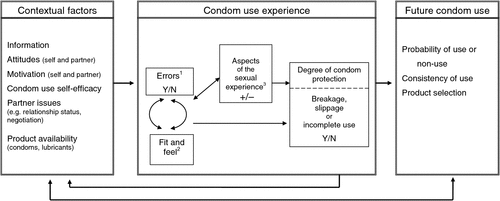
A review of the correlations among condom use errors and problems, consistency of condom use and contextual factors related to condom use is beyond the scope of this paper. However, given the prevalence of the errors and problems reviewed here, a framework for understanding their role in inadequate condom protection and possible avenues for further research and for intervention is warranted. As a way of conceptualising the inter-relationship of the errors and problems presented in this review within the larger context of condom use, we propose the Condom Use Experience (CUE) model, which focuses on the details of condom use experience within the context of other known predictors of condom use (Fig. 1).
|
Contextual factors (the left panel) include personal and situational variables such as information, attitudes (self and partner), motivation (self and partner), condom use self-efficacy, partner issues (e.g. relationship status, negotiation) and product availability (e.g. condoms, lubricants). These influence the probability that a condom will be used for a sexual event as well as the general pattern of future condom use.
Condom use experience during sexual events (the centre panel) mediates the relationship between contextual factors and future condom use. The condom use experience panel is the locus of the condom use errors and problems that are the topic of this review. Specifically, the model suggests that condom use errors (presence or absence; type) interact with issues of condom fit and feel (positive or negative) and that together these are predictive of the degree of condom protection during the event, either directly or mediated through the aspects of the sexual experience (e.g. duration and intensity of intercourse; sensations such as lack of stimulation, or discomfort and sexual arousal issues). For example, problems with fit and feel, or letting a condom touch a sharp object may lead to breakage. An uncomfortable condom may make erection problems more likely, which could lead to slippage or early removal (incomplete use). It is important to note that aspects of the sexual experience may also affect the fit and feel of the condom and whether it is used correctly. For example, lengthy intercourse may lead to condoms drying out, affecting the fit and feel of the condom. This could be dealt with by addition of lubricant or changing to a new condom. Failing to do this may lead to early removal of the condom, or condom breakage or slippage due to high friction compromising condom protection. The degree of condom protection component includes two types of highly correctable errors: incomplete use (delayed application and early removal) and slippage that occurs due to failure to hold the base of the condom during withdrawal. However, because these experiences can directly compromise the efficacy of condom use, we highlight them in the model as inadequate condom protection.
Future condom use (the right panel), including the probability of use or non-use, consistency of use and product selection, is affected by the quality of the condom use experience. For example, difficulties during the sexual experience including breakage, slippage and incomplete use affect the probability of condom use in the future as well as product selection, feeding back to contextual factors influencing future condom use events.
The CUE model provides a framework for understanding the role of user errors and problems in condom use, and generates testable hypotheses to guide future research. We acknowledge that our search strategy may not have identified all of the current relevant literature; selecting appropriate search terms for such a specific area of condom use was challenging. In the interest of serving researchers in this area, we have created an online resource that contains a ‘living’ compendium of citations on condom use errors and problems that currently includes the studies reviewed herein as well as reports published before 1995. We encourage researchers to inform us of their published findings so their citations can be added to the compendium (link on www.kinseyinstitute.org/research/condom_errors.html).
Closing the gap between perfect use and the errors characterising typical use is one of the most crucial challenges of future condom promotion programs. Researchers and intervention specialists alike should address common condom use errors and problems, including those related to fit and feel and aspects of the sexual experience. Doing so is critical to closing this gap and greatly reducing the epidemics of STIs and unintended pregnancies.
Conflicts of interest
None declared.
References
[1] Condoms and HIV Prevention. Position statement by UNAIDS, UNFPA and WHO. UNAIDS, UNFPA, WHO; 2009. Available online at: http://www.unaids.org/en/Resources/PressCentre/Featurestories/2009/March/20090319preventionposition [verified June 2011].[2] Warner L, Stone KM, Macaluso M, Buehler JW, Austin HD. Condom use and risk of gonorrhea and chlamydia: a systematic review of design and measurement factors assessed in epidemiologic studies. Sex Transm Dis 2006; 33 36–51.
| Condom use and risk of gonorrhea and chlamydia: a systematic review of design and measurement factors assessed in epidemiologic studies.Crossref | GoogleScholarGoogle Scholar |
[3] World Health Organization (WHO). Family Planning. Fact sheet No. 351. Geneva: World Health Organization; April 2011. Available online at: http://www.who.int/mediacentre/factsheets/fs351/en/index.html [verified January 2012].
[4] Trussell J. Contraceptive efficacy. In: Hatcher RA, Trussell J, Nelson AL, Cates A, Stewart FH, Kowal D (editors). Contraceptive technology. 19th edn. New York: Ardent Media, Inc., 2007.
[5] Sheeran P, Abraham C, Orbell S. Psychosocial correlates of heterosexual condom use: a meta-analysis. Psychol Bull 1999; 125 90–132.
| Psychosocial correlates of heterosexual condom use: a meta-analysis.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1M7ksVKmtQ%3D%3D&md5=5927c6899f8c5fea0e419a54734dca97CAS |
[6] Crosby R, DiClemente RJ, Holtgrave DR, Wingood GM. Design, measurement, and analytical considerations for testing hypotheses relative to condom effectiveness against non-viral STIs. Sex Transm Infect 2002; 78 228–31.
| Design, measurement, and analytical considerations for testing hypotheses relative to condom effectiveness against non-viral STIs.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD38vjvFehtQ%3D%3D&md5=309ffc63b433761a654aee6878d11949CAS |
[7] Crosby R, Yarber WL, Sanders SA, Graham CA. Condom discomfort and associated problems with their use among university students. J Am Coll Health 2005; 54 143–7.
| Condom discomfort and associated problems with their use among university students.Crossref | GoogleScholarGoogle Scholar |
[8] Crosby R, Mettey A. A descriptive analysis of HIV risk behavior among men having sex with men attending a large sex resort. J Acquir Immune Defic Syndr 2004; 37 1496–9.
| A descriptive analysis of HIV risk behavior among men having sex with men attending a large sex resort.Crossref | GoogleScholarGoogle Scholar |
[9] Macaluso M, Blackwell R, Jamieson DJ, Kulczycki A, Chen MP, Akers R, et al Efficacy of the male latex condom and of the female polyurethane condom as barriers to semen during intercourse: a randomized clinical trial. Am J Epidemiol 2007; 166 88–96.
| Efficacy of the male latex condom and of the female polyurethane condom as barriers to semen during intercourse: a randomized clinical trial.Crossref | GoogleScholarGoogle Scholar |
[10] Grimley DM, Annang L, Houser S, Chen H. Prevalence of condom use errors among STD clinic patients. Am J Health Behav 2005; 29 324–30.
[11] Paz-Bailey G, Koumans EH, Sternberg M, Pierce A, Papp J, Unger ER, et al The effect of correct and consistent condom use on chlamydial and gonococcal infection among urban adolescents. Arch Pediatr Adolesc Med 2005; 159 536–42.
| The effect of correct and consistent condom use on chlamydial and gonococcal infection among urban adolescents.Crossref | GoogleScholarGoogle Scholar |
[12] Allman D, Xu K, Myers T, Aguinaldo J, Calzavara L, Maxwell J, et al Delayed application of condoms with safer and unsafe sex: factors associated with HIV risk in a community sample of gay and bisexual men. AIDS Care 2009; 21 775–84.
| Delayed application of condoms with safer and unsafe sex: factors associated with HIV risk in a community sample of gay and bisexual men.Crossref | GoogleScholarGoogle Scholar |
[13] Crosby RA, Sanders SA, Yarber WL, Graham CA, Dodge B. Condom use errors and problems among college men. Sex Transm Dis 2002; 29 552–7.
| Condom use errors and problems among college men.Crossref | GoogleScholarGoogle Scholar |
[14] Sanders SA, Graham CA, Yarber WL, Crosby RA. Condom use errors and problems among young women who put condoms on their male partners. J Am Med Womens Assoc 2003; 58 95–8.
[15] Crosby R, Sanders S, Yarber WL, Graham CA. Condom-use errors and problems: a neglected aspect of studies assessing condom effectiveness. Am J Prev Med 2003; 24 367–70.
| Condom-use errors and problems: a neglected aspect of studies assessing condom effectiveness.Crossref | GoogleScholarGoogle Scholar |
[16] Crosby R, Salazar LF, DiClemente RJ, Yarber WL, Caliendo AM, Staples-Horne M. Condom misuse among adjudicated girls: associations with laboratory-confirmed chlamydia and gonorrhea. J Pediatr Adolesc Gynecol 2007; 20 339–43.
| Condom misuse among adjudicated girls: associations with laboratory-confirmed chlamydia and gonorrhea.Crossref | GoogleScholarGoogle Scholar |
[17] Warner L, Newman DR, Kamb ML, Fishbein M, Douglas JM, Zenilman J, et al Problems with condom use among patients attending sexually transmitted disease clinics: prevalence, predictors, and relation to incident gonorrhea and chlamydia. Am J Epidemiol 2008; 167 341–9.
| Problems with condom use among patients attending sexually transmitted disease clinics: prevalence, predictors, and relation to incident gonorrhea and chlamydia.Crossref | GoogleScholarGoogle Scholar |
[18] Hensel DJ, Stupiansky NW, Herbenick D, Dodge B, Reece M. When condom use is not condom use: an event-level analysis of condom use behaviors during vaginal intercourse. J Sex Med 2011; 8 28–34.
| When condom use is not condom use: an event-level analysis of condom use behaviors during vaginal intercourse.Crossref | GoogleScholarGoogle Scholar |
[19] Yarber WL, Crosby RA, Graham CA, Sanders SA, Arno J, Hartzell RM, et al Correlates of putting condoms on after sex has begun and of removing them before sex ends: a study of men attending an urban public STD clinic. Am J Men Health 2007; 1 190–6.
| Correlates of putting condoms on after sex has begun and of removing them before sex ends: a study of men attending an urban public STD clinic.Crossref | GoogleScholarGoogle Scholar |
[20] Crosby R, Yarber WL, Sanders SA, Graham CA, Arno JN. Slips, breaks and ‘falls’: condom errors and problems reported by men attending an STD clinic. Int J STD AIDS 2008; 19 90–3.
| Slips, breaks and ‘falls’: condom errors and problems reported by men attending an STD clinic.Crossref | GoogleScholarGoogle Scholar |
[21] Crosby R, Milhausen R, Sanders S, Graham C, Yarber W. Two heads are better than one: the association between condom decision-making and condom use errors and problems. Sex Transm Infect 2008; 84 198–201.
| Two heads are better than one: the association between condom decision-making and condom use errors and problems.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1czksFWksQ%3D%3D&md5=fbfc6536b345eba509498111c82e18e5CAS |
[22] Sanders SA, Milhausen RR, Crosby RA, Graham CA, Yarber WL. Do phosphodiesterase type 5 inhibitors protect against condom-associated erection loss and condom slippage? J Sex Med 2009; 6 1451–6.
| Do phosphodiesterase type 5 inhibitors protect against condom-associated erection loss and condom slippage?Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BD1MXmtFaitLg%3D&md5=deb99f3086e3789e69e9916d195d6c83CAS |
[23] Crosby RA, Yarber WL, Graham CA, Sanders SA. Does it fit okay? Problems with condom use as a function of self-reported poor fit. Sex Transm Infect 2010; 86 36–8.
| Does it fit okay? Problems with condom use as a function of self-reported poor fit.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3c7gvVymtg%3D%3D&md5=cf3096a45e3f87c84e4f1e36d7b02156CAS |
[24] Macaluso M, Blackwell R, Carr B, Meinzen-Derr J, Montgomery M, Roark M, et al Safety and acceptability of a baggy latex condom. Contraception 2000; 61 217–23.
| Safety and acceptability of a baggy latex condom.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c3oslCnsQ%3D%3D&md5=5249b9d669690606071e8f1d1ea98eb1CAS |
[25] Crosby RA, Yarber WL, Sanders SA, Graham CA, McBride K, Milhausen RR, et al Men with broken condoms: who and why? Sex Transm Infect 2007; 83 71–5.
| Men with broken condoms: who and why?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD2s%2FnvVersQ%3D%3D&md5=5c2136628d1b09fc9e05defce270886dCAS |
[26] Messiah A, Dart T, Spencer BE, Warszawski J. Condom breakage and slippage during heterosexual intercourse: a French national survey. French National Survey on Sexual Behavior Group (ACSF). Am J Public Health 1997; 87 421–4.
| Condom breakage and slippage during heterosexual intercourse: a French national survey. French National Survey on Sexual Behavior Group (ACSF).Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2s3ltVylsA%3D%3D&md5=11d2116f097b07b8c1de1db8ca054a3bCAS |
[27] Choi SY, Chen KL, Jiang ZQ. Client-perpetuated violence and condom failure among female sex workers in southwestern China. Sex Transm Dis 2008; 35 141–6.
| Client-perpetuated violence and condom failure among female sex workers in southwestern China.Crossref | GoogleScholarGoogle Scholar |
[28] Steiner MJ, Taylor D, Hylton-Kong T, Mehta N, Figueroa JP, Bourne D, et al Decreased condom breakage and slippage rates after counseling men at a sexually transmitted infection clinic in Jamaica. Contraception 2007; 75 289–93.
| Decreased condom breakage and slippage rates after counseling men at a sexually transmitted infection clinic in Jamaica.Crossref | GoogleScholarGoogle Scholar |
[29] de Visser RO, Smith AM, Rissel CE, Richters J, Grulich AE. Sex in Australia: experience of condom failure among a representative sample of men. Aust N Z J Public Health 2003; 27 217–22.
| Sex in Australia: experience of condom failure among a representative sample of men.Crossref | GoogleScholarGoogle Scholar |
[30] Kirkkola AL, Mattila K, Virjo I. Problems with condoms – a population-based study among Finnish men and women. Eur J Contracept Reprod Health Care 2005; 10 87–92.
| Problems with condoms – a population-based study among Finnish men and women.Crossref | GoogleScholarGoogle Scholar |
[31] Spruyt A, Steiner MJ, Joanis C, Glover LH, Piedrahita C, Alvarado G, et al Identifying condom users at risk for breakage and slippage: findings from three international sites. Am J Public Health 1998; 88 239–44.
| Identifying condom users at risk for breakage and slippage: findings from three international sites.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1c7ltFOitg%3D%3D&md5=cacf2c979696cb07fc94673475d47d36CAS |
[32] Stone E, Heagerty P, Vittinghoff E, Douglas JM, Koblin BA, Mayer KH, et al Correlates of condom failure in a sexually active cohort of men who have sex with men. J Acquir Immune Defic Syndr Hum Retrovirol 1999; 20 495–501.
| Correlates of condom failure in a sexually active cohort of men who have sex with men.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1M3jvFOguw%3D%3D&md5=8d0b8b195548727127ce2356dd8e9913CAS |
[33] Wong ML, Chan RK, Koh D, Wee S. A prospective study on condom slippage and breakage among female brothel-based sex workers in Singapore. Sex Transm Dis 2000; 27 208–14.
| A prospective study on condom slippage and breakage among female brothel-based sex workers in Singapore.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c3kt1ygtA%3D%3D&md5=25a48e4cfeafc14b61b6deccc998e502CAS |
[34] Crosby R, Diclemente RJ, Yarber WL, Snow G, Troutman A. An event-specific analysis of condom breakage among African American men at risk of HIV acquisition. Sex Transm Dis 2008; 35 174–7.
| An event-specific analysis of condom breakage among African American men at risk of HIV acquisition.Crossref | GoogleScholarGoogle Scholar |
[35] Crosby R, Yarber WL, Sanders SA, Graham CA. Is phosphodiesterase type 5 inhibitor use associated with condom breakage? Sex Transm Infect 2009; 85 404–5.
| Is phosphodiesterase type 5 inhibitor use associated with condom breakage?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1MnktF2qtw%3D%3D&md5=78e84083394559f5a2a35d91aa277455CAS |
[36] Albert AE, Warner DL, Hatcher RA, Trussell J, Bennett C. Condom use among female commercial sex workers in Nevada’s legal brothels. Am J Public Health 1995; 85 1514–20.
| Condom use among female commercial sex workers in Nevada’s legal brothels.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK28%2Fjs1Grsg%3D%3D&md5=bff775537cb41f1ccc03bfbc65a55134CAS |
[37] Smith AM, Jolley D, Hocking J, Benton K, Gerofi J. Does additional lubrication affect condom slippage and breakage? Int J STD AIDS 1998; 9 330–5.
| Does additional lubrication affect condom slippage and breakage?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1czjsVehsw%3D%3D&md5=6c67fc563738ff7f5b7aee00bbeac68fCAS |
[38] Rugpao S, Beyrer C, Tovanabutra S, Natpratan C, Nelson KE, Celentano DD, et al Multiple condom use and decreased condom breakage and slippage in Thailand. J Acquir Immune Defic Syndr Hum Retrovirol 1997; 14 169–73.
| Multiple condom use and decreased condom breakage and slippage in Thailand.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2s3gsFahsQ%3D%3D&md5=112b0e4a6fadaf9adeccccf18ab8b6a1CAS |
[39] Rosenberg MJ, Waugh MS. Latex condom breakage and slippage in a controlled clinical trial. Contraception 1997; 56 17–21.
| Latex condom breakage and slippage in a controlled clinical trial.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2svltFSmsw%3D%3D&md5=5d92ecdd90267c4e582199191784ef90CAS |
[40] Reece M, Herbenick D, Sanders SA, Monahan P, Temkit M, Yarber WL. Breakage, slippage and acceptability outcomes of a condom fitted to penile dimensions. Sex Transm Infect 2008; 84 143–9.
| Breakage, slippage and acceptability outcomes of a condom fitted to penile dimensions.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1c3htVSrug%3D%3D&md5=21425284bff4bc9111a2c50f64e7759eCAS |
[41] Macaluso M, Kelaghan J, Artz L, Austin H, Fleenor M, Hook EW, et al Mechanical failure of the latex condom in a cohort of women at high STD risk. Sex Transm Dis 1999; 26 450–8.
| Mechanical failure of the latex condom in a cohort of women at high STD risk.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1MvitlWhtQ%3D%3D&md5=a4c74bc1a117ed2318dfb24b98093ad2CAS |
[42] Walsh TL, Frezieres RG, Peacock K, Nelson AL, Clark VA, Bernstein L, et al Effectiveness of the male latex condom: combined results for three popular condom brands used as controls in randomized clinical trials. Contraception 2004; 70 407–13.
| Effectiveness of the male latex condom: combined results for three popular condom brands used as controls in randomized clinical trials.Crossref | GoogleScholarGoogle Scholar |
[43] Valappil T, Kelaghan J, Macaluso M, Artz L, Austin H, Fleenor ME, et al Female condom and male condom failure among women at high risk of sexually transmitted diseases. Sex Transm Dis 2005; 32 35–43.
| Female condom and male condom failure among women at high risk of sexually transmitted diseases.Crossref | GoogleScholarGoogle Scholar |
[44] Smith AM, Jolley D, Hocking J, Benton K, Gerofi J. Does penis size influence condom slippage and breakage? Int J STD AIDS 1998; 9 444–7.
| Does penis size influence condom slippage and breakage?Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1czmsl2ksQ%3D%3D&md5=777ed520c4f159ab88bb5c78ec588328CAS |
[45] Potter WD, de Villemeur M. Clinical breakage, slippage and acceptability of a new commercial polyurethane condom: a randomized, controlled study. Contraception 2003; 68 39–45.
| Clinical breakage, slippage and acceptability of a new commercial polyurethane condom: a randomized, controlled study.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3szks1ansA%3D%3D&md5=33b2570fba39c062e771006f879ceb76CAS |
[46] Callahan M, Mauck C, Taylor D, Frezieres R, Walsh T, Martens M. Comparative evaluation of three Tactylon(TM) condoms and a latex condom during vaginal intercourse: breakage and slippage. Contraception 2000; 61 205–15.
| Comparative evaluation of three Tactylon(TM) condoms and a latex condom during vaginal intercourse: breakage and slippage.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3c3oslCnsA%3D%3D&md5=a98e4ea3dff5c0cecb105f39fe31d988CAS |
[47] Duerr A, Gallo MF, Warner L, Jamieson DJ, Kulczycki A, Macaluso M. Assessing male condom failure and incorrect use. Sex Transm Dis 2011; 580–6.
[48] Nguyen NT, Nguyen HT, Trinh HQ, Mills SJ, Detels R. Clients of female sex workers as a bridging population in Vietnam. AIDS Behav 2009; 13 881–91.
| Clients of female sex workers as a bridging population in Vietnam.Crossref | GoogleScholarGoogle Scholar |
[49] Crosby RA, DiClemente RJ, Wingood GM, Salazar LF, Rose E, Levine D, et al Condom failure among adolescents: implications for STD prevention. J Adolesc Health 2005; 36 534–6.
| Condom failure among adolescents: implications for STD prevention.Crossref | GoogleScholarGoogle Scholar |
[50] Crosby RA, Diclemente RJ, Wingood GM, Salazar LF, Rose E, Levine D, et al Correlates of condom failure among adolescent males: an exploratory study. Prev Med 2005; 41 873–6.
| Correlates of condom failure among adolescent males: an exploratory study.Crossref | GoogleScholarGoogle Scholar |
[51] Wang D. Contraceptive failure in China. Contraception 2002; 66 173–8.
| Contraceptive failure in China.Crossref | GoogleScholarGoogle Scholar |
[52] Gabbay MB, Thomas J, Gibbs A, Hold P. A randomized crossover trial of the impact of additional spermicide on condom failure rates. Sex Transm Dis 2008; 35 862–8.
| A randomized crossover trial of the impact of additional spermicide on condom failure rates.Crossref | GoogleScholarGoogle Scholar |
[53] Moreau C, Trussell J, Rodriguez G, Bajos N, Bouyer J. Contraceptive failure rates in France: results from a population-based survey. Hum Reprod 2007; 22 2422–7.
| Contraceptive failure rates in France: results from a population-based survey.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD2svosFylsg%3D%3D&md5=e2768a2b60f04185219850684e500570CAS |
[54] Graham CA, Crosby R, Yarber WL, Sanders SA, McBride K, Milhausen RR, et al Erection loss in association with condom use among young men attending a public STI clinic: potential correlates and implications for risk behaviour. Sex Health 2006; 3 255–60.
| Erection loss in association with condom use among young men attending a public STI clinic: potential correlates and implications for risk behaviour.Crossref | GoogleScholarGoogle Scholar |
[55] Reece M, Briggs L, Dodge B, Herbenick D, Glover R. Perceptions of condom fit and feel among men living with HIV. AIDS Patient Care STDS 2010; 24 435–40.
| Perceptions of condom fit and feel among men living with HIV.Crossref | GoogleScholarGoogle Scholar |
[56] Reece M, Dodge B, Herbenick D, Fisher C, Alexander A, Satinsky S. Experiences of condom fit and feel among African-American men who have sex with men. Sex Transm Infect 2007; 83 454–7.
| Experiences of condom fit and feel among African-American men who have sex with men.Crossref | GoogleScholarGoogle Scholar |
[57] Yarber WL, Graham CA, Sanders SA, Crosby RA. Correlates of condom breakage and slippage among university undergraduates. Int J STD AIDS 2004; 15 467–72.
| Correlates of condom breakage and slippage among university undergraduates.Crossref | GoogleScholarGoogle Scholar |
[58] Richters J, Donovan B, Gerofi J. How often do condoms break or slip off in use? Int J STD AIDS 1993; 4 90–4.
| 1:STN:280:DyaK3s3jsleluw%3D%3D&md5=65affbd10aeaa7b4e9995ecc700e328eCAS |
[59] Steiner M, Piedrahita C, Glover L, Joanis C. Can condom users likely to experience condom failure be identified? Fam Plann Perspect 1993; 25 220–3.
| 1:STN:280:DyaK2c%2FosFGgtA%3D%3D&md5=55ba74202ac334f554116987df4e2373CAS |


