Electronic health records and online medical records: an asset or a liability under current conditions?
Judith Allen-Graham A B G , Lauren Mitchell B , Natalie Heriot A , Roksana Armani A , David Langton A C , Michele Levinson A D , Alan Young A E , Julian A. Smith A F , Tom Kotsimbos A B and John W. Wilson A BA Monash University, Wellington Road and Blackburn Road, Clayton, Vic. 3800, Australia. Email: natalie.rose.heriot@gmail.com; armani.roksana@gmail.com; john.wilson@monash.edu.au; david.langton@monash.edu.au
B The Alfred Hospital, 55 Commercial Road, Melbourne, Vic. 3004, Australia. Email: lauren.mitchell@monash.edu.au; t.kotsimbos@alfred.org.au
C Peninsula Health, 2 Hastings Road, Frankston, Vic. 3199, Australia.
D Cabrini Private Hospital, 181–183 Wattletree Road, Malvern, Vic. 3144, Australia. Email: mlevinson@cabrini.com.au
E Eastern Health, Level 2, 5 Arnold Street, Box Hill, Vic. 3128, Australia. Email: alan.young@easternhealth.org.au
F Monash Medical Centre, 246 Clayton Road, Clayton, Vic. 3168, Australia. Email: julian.smith@monash.edu.au
G Corresponding author. Email: j.allen-graham@alfred.org.au
Australian Health Review 42(1) 59-65 https://doi.org/10.1071/AH16095
Submitted: 28 April 2016 Accepted: 13 November 2016 Published: 20 January 2017
Journal compilation © AHHA 2018 Open Access CC BY-NC-ND
Abstract
Objective The aim of the present study was to audit the current use of medical records to determine completeness and concordance with other sources of medical information.
Methods Medical records for 40 patients from each of five Melbourne major metropolitan hospitals were randomly selected (n = 200). A quantitative audit was performed for detailed patient information and medical record keeping, as well as data collection, storage and utilisation. Using each hospital’s current online clinical database, scanned files and paperwork available for each patient audited, the reviewers sourced as much relevant information as possible within a 30-min time allocation from both the record and the discharge summary.
Results Of all medical records audited, 82% contained medical and surgical history, allergy information and patient demographics. All audited discharge summaries lacked at least one of the following: demographics, medication allergies, medical and surgical history, medications and adverse drug event information. Only 49% of records audited showed evidence the discharge summary was sent outside the institution.
Conclusions The quality of medical data captured and information management is variable across hospitals. It is recommended that medical history documentation guidelines and standardised discharge summaries be implemented in Australian healthcare services.
What is known about this topic? Australia has a complex health system, the government has approved funding to develop a universal online electronic medical record system and is currently trialling this in an opt-out style in the Napean Blue Mountains (NSW) and in Northern Queensland. The system was originally named the personally controlled electronic health record but has since been changed to MyHealth Record (2016). In Victoria, there exists a wide range of electronic health records used to varying degrees, with some hospitals still relying on paper-based records and many using scanned medical records. This causes inefficiencies in the recall of patient information and can potentially lead to incidences of adverse drug events.
What does this paper add? This paper supports the concept of a shared medical record system using 200 audited patient records across five Victorian metropolitan hospitals, comparing the current information systems in place for healthcare practitioners to retrieve data. This research identifies the degree of concordance between these sources of information and in doing so, areas for improvement.
What are the implications for practitioners? Implications of this research are the improvements in the quality, storage and accessibility of medical data in Australian healthcare systems. This is a relevant issue in the current Australian environment where no guidelines exist across the board in medical history documentation or in the distribution of discharge summaries to other healthcare providers (general practitioners, etc).
Additional keywords: adverse drug event (ADE), eHealth, electronic medical record (EMR), medical history.
Introduction
Australia has a complex health system1,2 that has evolved to deal with many competing demands, including increasing life expectancy and an aging population in the setting of limited resources, a common issue for health systems in many developed countries. New technologies and information systems offer an opportunity for significant improvements in quality and efficiencies in health care delivery and integrated data management.
It is recognised that the effective use of electronic health records (EHR) can improve aspects of care and reduce the risk of adverse drug events (ADEs).2 In 2010, the Australian Government approved and committed to fund the development of the personally controlled electronic health record (PCEHR).3 In 2015, the government announced an A$485 million rescue package to improve electronic medical records, renaming the PCEHR ‘myHealth Record’.4 For the purposes of this paper, PCEHR will be used because it was the name in place during the present study. By assigning patients an individual healthcare identifier (IHI), this system of health information repository stores a range of health information, including health summaries, medications, hospital discharge summaries, specialist letters, consultant referrals, event summaries and the location of advance care directives. In Australia, an economic review by Deloitte on the expected benefits of the PCEHR estimated a net benefit to the public of A$11.5 billion over the years 2010–25.5 It was concluded that these benefits would result from reduced hospital admissions and visits to general practitioners (GPs) and improved continuity of care.
In the present study we examined the completeness and concordance of various information sources currently used by healthcare providers in Victoria during the transition phase towards a complete EHR. To that end, the effectiveness of current medical data collection, storage, retrieval and communication is described and compared with regard to a clearly identifiable and important outcome variable, namely the incidence of ADEs.
We hypothesise that there is currently discordance in the medical information collected and stored in different hospital systems relating specifically to ADEs, which may lead to inefficient practices and potentially repeated drug-related events.
Methods
Five major university teaching hospitals, including one private hospital, in metropolitan Melbourne were chosen to provide as broad a range of healthcare activity as possible within a well-defined urban region. The healthcare activity, electronic information databases and specific ADE information for all these healthcare providers was evaluated objectively and systematically. In particular, sampling of medical records, discharge summaries, Riskman International Pty Ltd reports and pharmacy records was undertaken to estimate the incidence of chosen indices for both completeness within and concordance between repositories.
Previously, we surveyed a cohort of patients from these hospitals regarding awareness and acceptability of an EHR.6 Medical records for a randomly selected cohort of 40 patients per site from that study were chosen for audit in the present study (n = 200), which occurred approximately 1 month after discharge, allowing the discharge summary from the admission during surveying to be included in the audit. The study sample was stratified into first-time and return patients to the hospital. Patients were excluded if they were still admitted.
Review of medical record and discharge summaries
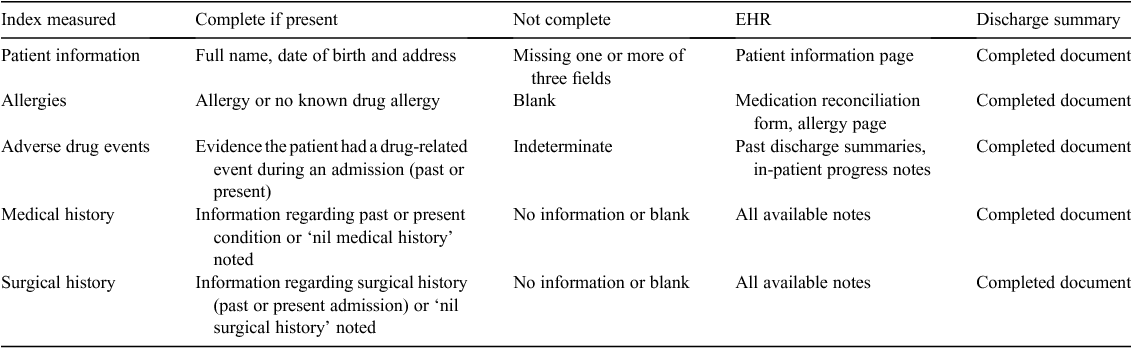
Documentation reviewed included all available material concerning the patient’s medical history at the chosen site; reviewers were allocated 30 min per medical record and discharge summary because this was deemed an appropriate time frame for accessing patient information during a clinical consultation. Fields assessed were taken from, but not limited to, published criteria for Australian electronic records.7–9 The methodology for auditing of the current health records (electronic, online databases, paper) and discharge summaries for chosen indices is explained in Table 1.
|
Medications
Current medications were listed in the patient discharge summary. If a record states ‘nil medications’, this is considered a complete entry. No documentation of medications is considered incomplete.
Correspondence
It was ascertained whether the discharge summary was identified as being sent from the hospital to the relevant medical professional. This was found at the end of the discharge summary and at some sites also within the medical record, with method of correspondence and the details of the recipient recorded.
Review of pharmacy databases
Pharmacy systems that record medications, allergies and ADEs were compared with the medical records. This allowed an index of concordance of the medical records to be determined at institutions using pharmacy dispensing systems.
Review of Riskman mandatory reporting information
The Riskman Enterprise Risk Management System is the incident reporting, risk and complaints management system used by the Victorian Department of Health for incident reporting in public health services.10 This system is in use at all five healthcare services.
Results
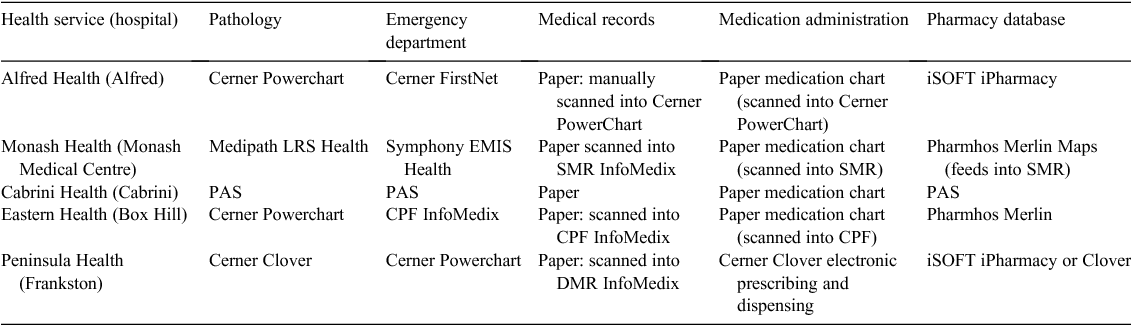
In all, 200 medical records were audited (40 per site). The mean patient age was 59 years (range 17–97 years), with a male to female ratio of 103 : 97 and a first-time to return patient ratio of 91 : 109. Table 2 describes the type of information system in use at the sites audited.
Medical records concordance
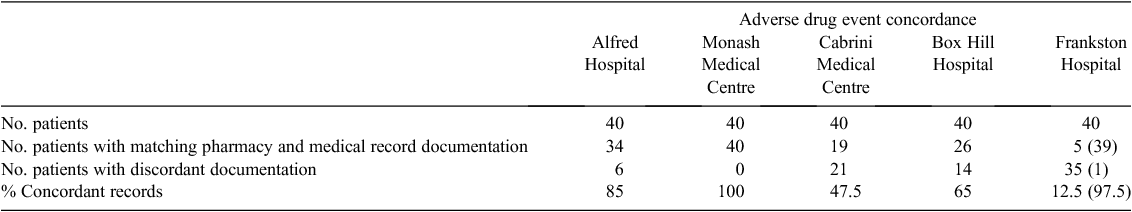
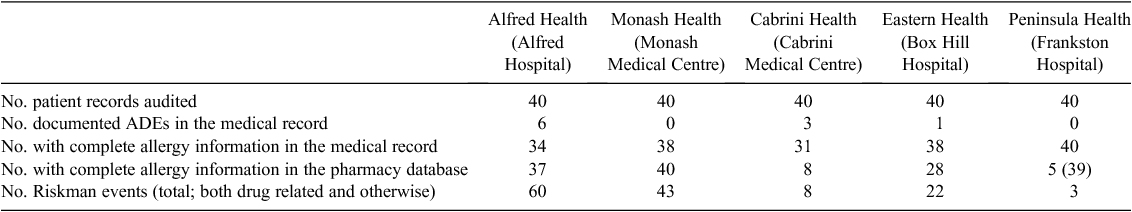
Because health data were captured differently at each site, the results between information sources are not fully comparable beyond their baseline discordance. Some information sources recorded numerous events for an individual patient; hence, the number of events for some of the items in Table 3 exceeds the number of patients. The distinction between missing information and negative information was often unclear, a limitation particularly in relation to auditing ADEs.
|
Medical record and discharge summary audit results
Patient information
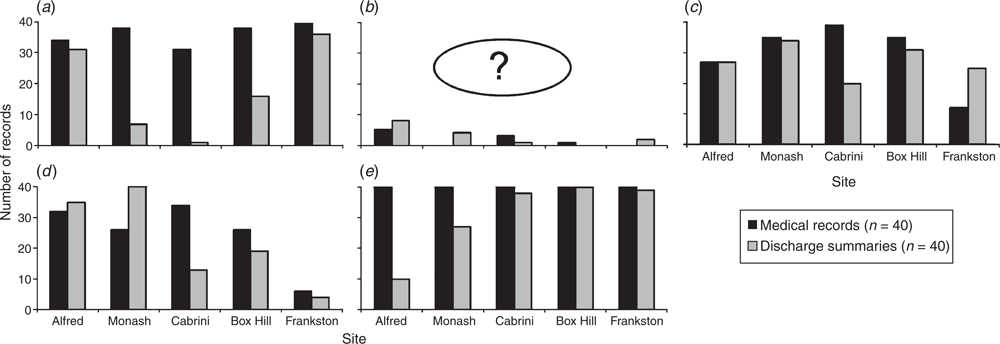
Fig. 1e shows that the recording of patient demographic information in medical records was 100% at all sites. Box Hill Hospital was the only site to have patient demographic details in all discharge summaries audited. The Alfred Hospital had the lowest rate of inclusion of complete patient demographics in the audited discharge summaries.
|
Allergies
No organisation had complete documentation of allergy status in their medical records and discharge summaries (Fig. 1a). Frankston Hospital had complete allergy documentation in the medical record. At Monash, Cabrini and Box Hill hospitals, less than half the discharge summaries audited had allergies or ‘no known drug allergy’ noted (n = 7, 1 and 16 (of 40) respectively). The Alfred and Frankston hospitals showed higher degrees of concordance of allergy status information between the medical record and discharge summary than any other sites.
Adverse drug events
The recording of ADE incidence was low in medical records and discharge summaries at all sites. It could not be ascertained whether patients without an ADE recorded indeed have no history of an ADE (Fig. 1b).
Medical history
No organisation was found to have complete medical history documentation in their medical records. The presence of a medical history is limited by the level of documentation by healthcare providers. The Alfred, Monash and Box Hill hospitals had the highest concordance of medical history contained in the medical records and discharge summaries. Although Cabrini Hospital had the most complete medical records, this sample had the least complete discharge summaries and therefore the highest discordance between these two information sources. Frankston Hospital had the least information within the medical record, whereas more information was found within discharge summaries, hence leading to greater degree of discordance (Fig. 1c).
Surgical history
Surgical history was not documented consistently in the medical records audited. Surgical history was most prevalent at Cabrini Hospital, but only 13 of 40 discharge summaries at Cabrini Hospital contained surgical history. Frankston Hospital the lowest number of recordings of surgical history in the records audited. Monash and Cabrini hospitals report less than half the surgical procedures in their discharge summaries (including past or present admission). The Alfred Hospital had a high number of audited patients with surgical history in both the medical record and the discharge summary (Fig. 1d).
Medications in the discharge summary
No site showed complete medication information within the discharge summaries audited.
Further investigation into the records of discharged patients without medication at the Alfred Hospital confirmed that this group was, in fact, discharged on medication (as determined by the medication reconciliation form, a pharmacy document scanned and entered into Cerner PowerChart, the electronic database in use). This indicates that the discharge summaries for these patients are not a true reflection of their current medication regimens. Discharge summaries at Cabrini Hospital did not contain any medication information.
Correspondence
There was a substantial difference between sites in the documentation of correspondence being sent to other healthcare providers upon discharge. Overall, at none of the sites was there evidence that discharge summaries are sent in a timely manner after discharge.
Review of pharmacy systems
In reviewing the pharmacy databases in use, the medication allergies recorded in the allergy section of the medical record were noted and compared with allergies recorded in the pharmacy repository (or equivalent). The concordance of allergy information in the medical record compared with the pharmacy repository is given in Table 4. Frankston Hospital uses electronic prescribing from Cerner Clover and not iSOFT iPharmacy. This results in 97.5% concordance of allergy information between Clover and the electronic clinical database, but a low concordance when the EHR is compared with iPharmacy. For consistency of analysis across sites, the iPharmacy database at Frankston Hospital was included in the present analysis. At Cabrini Hospital, 10 of the concordant records at had blank entries in the allergy fields in both information sources and are therefore negatively concordant (i.e. lacking patient information in both sources).
Review of Riskman mandatory reporting information
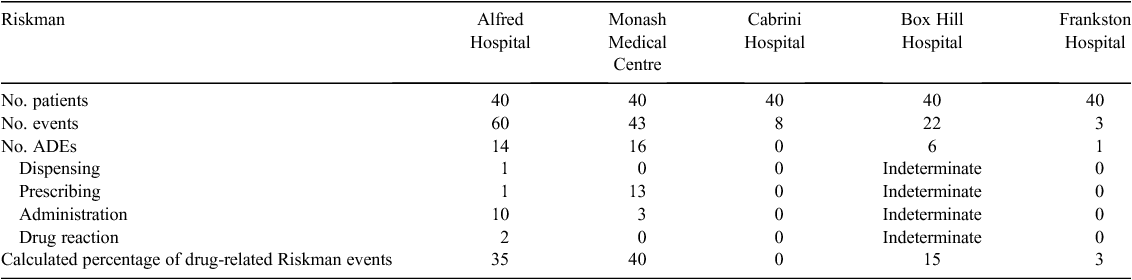
Table 5 highlights the fact that Riskman reporting varied significantly. The Alfred Hospital and Monash Health Riskman events were more detailed, with the surrounding circumstances, whereas Cabrini and Frankston hospitals gave very little background information or detail around the event.
|
Data analysis at Box Hill Hospital was not possible because the description for each event was non-specific, preventing identification of the type of event that occurred and where in the chain of care the event happened.
Discussion
The major finding of the present study is the degree of discordant information present in various components of a patient’s hospital medical record. First, there is little uniformity in the current electronic clinical information systems being used by healthcare providers that have been widely adopted in an attempt to improve efficiencies relating to medical information. Second, the details of the health care information captured, stored and used is variable and site dependent. Third, the overall variability in medical information quality across many categories has created information silos. Patient safety is dependent on complete and efficiently captured health information. Multiple sources of discordant and potentially incomplete information expose the patient to harm. Therefore, the results of the present study have far-reaching implications for both current and future healthcare management strategies.
The use of ADEs as an important index highlighted the level of variability in how a critical piece of patient information may be captured. In particular, the absence of information relating to ADEs was not only a difficulty for the audit process, but also raised a major potential concern regarding patient management protocols. The unclear distinction between missing information and a negative data entry for ADEs transforms an efficient technological system into a dysfunctional one. There are several possible reasons for incomplete entries, including the belief or expectation that specific information may be recorded elsewhere. If the patient’s healthcare records are linked and the information is readily accessible by all who need to know, such as in the case of an EHR, then this would reduce risk of error and harms. The current electronic databases are only as good as the information that is entered and are dependent on patient recall limitations and staff biases in deciding what is relevant to record. The data in the present study relating particularly to ADEs and medical records and discharge summaries demonstrate that there are significant improvements to be made in data capture and management. The findings support transition from paper and scanned medical records to a more complete, accurate and unified patient-centred EHR.
Absent data in the medical records and discharge summary information was especially concerning. The absence of data was a significant problem further compounded by the discordance in patient information between medical records and discharge summaries. Incomplete discharge summaries may reflect the unique nature of services and site-specific protocols, which does not excuse any lack of record keeping. Cabrini is a private hospital and the most common method of communication with GPs is a letter from the private practitioner to the GP issued from private rooms. The Alfred Hospital had significantly more medical and surgical information in both their medical records and discharge summaries. This information was not 100% concordant, particularly regarding discharge medication. The Alfred Hospital is a major tertiary/quaternary centre with many complex patients that routinely require timely out-patient treatment and many repeat hospital visits. There is an incentive for the medical staff to ensure that the information available in out-patients and on readmission is relevant. The documentation regarding communication of discharge summaries to external healthcare providers was clearly lacking in the present study cohort. The results show that the likelihood of a discharge summary being sent ranged between 9 and 31 of 40 patients across the sites; less than half the total records surveyed had evidence of a discharge summary being sent 1 month after discharge. A recent study revealed that only 55% of hospital discharge summaries reached the GP before a patient’s first post-discharge consultation,11 whereas another study identified a trend towards decreased risk of readmission for patients who were reviewed by a clinician who had received the hospital discharge summary.12 Added to this is the problem of incomplete information being received by the GP or other healthcare provider. These deficiencies are even more important in the context of any new diagnostic and/or therapeutic information that may require specific follow-up.13
The pharmacy database audits also showed the highest discordance at Cabrini Hospital, where 10 of 40 records were blank in the medical record and the pharmacy database (perhaps due to a reliance on other practices of managing a patient’s medication list). Frankston Hospital uses electronic prescribing from Clover (not iPharmacy), explaining their discordant results. In Clover, medication allergies are visible to the pharmacist and medical staff; in addition, the system prompts the user when a medication allergy is present, thereby preventing ADEs from known allergies. At Monash Health the medical record and pharmacy database are linked and therefore 100% concordant. These represent an ‘ideal’ model, where numerous systems are replaced by one that incorporates information from a range of sources and, in doing so, minimises the possibility of error.
Drug-related events and allergic reactions contribute to significant morbidity in the acute care setting. These events can recur and can be prevented with adequate information. ADEs were found in patient alert tabs, past discharge summaries and in in-patient and out-patient progress notes. This demonstrates the number of areas that a clinician may need to access (unreasonably) to provide an overview of previous ADEs. Most of the sites’ current medical records are paper documents scanned and uploaded to the electronic system (Table 2). Problems arising from this include the timeliness from scanning to upload (not measured in the present study) and the location in the record to which they are uploaded.
The implementation of a solely electronic system that integrates hospital and GP records in a shared database for all healthcare workers will improve patient safety and has the potential not only to reduce healthcare costs, but also to improve health care quality.14
By using an IHI and the PCEHR (myHealth Record), both currently available under Australian legislation, the management of emergency medical problems and complex cases may be improved in new patients, when substantial medical information is held at another institution. However, the information uploaded to the PCEHR can only be as good as the information contained in clinical systems across the healthcare service.
Lack of concordance between the different information sources means there is no easily identifiable source of truth for healthcare providers. Without comparing individual events, the present study highlights that each database (with the exception of pharmacy at Monash) is separate and is used differently at each of the sites audited. Evaluation of the same index, for example an ADE, between the sources is incredibly difficult and not reliable. For ADEs, this may be in the medical history (paper or scanned), discharge summary, pharmacy database, as a coded event, as a Riskman report or any combination of these. This highlights the exhaustive investigation required by clinicians to locate vital patient information. When analysing data from Riskman, it was apparent that multiple entries were recorded as incidents, many of which were not related to the use of medications. No distinct pattern could be discerned in relation to medication incidents, and descriptors were incomplete in many instances. Reviewers found in some institutions that an incident had been logged in Riskman, but no description of the incident (ADE or other) had been entered in the medical record. It was therefore unclear whether healthcare workers had elected to use an alternative system of reporting or not to report the incident. Riskman has the potential for ADE reporting to be optimised; however, due to the lack of consistency in use across sites, it cannot be used as a baseline measure for any events logged.
Although the health information discordances identified relating to ADEs create the potential for errors, the likelihood of such errors eventuating will largely depend on how specific healthcare providers use each information system, and how they incorporate it into their decision making regarding patient management. A summary healthcare record needs to prioritise major events in a way that helps with patient care decisions in real time. In this setting, an improved focus on the quality of health data capture and the alignment of these data for each patient across the various information systems being used represent an opportunity to both specifically minimise the possibility of ADE errors and, more generally, to improve healthcare efficiencies, effectiveness and, hopefully, patient experiences. How well this is achieved will depend on the quality of local healthcare information capture; at present the paper record interface limits the PCEHR, as does the degree of the current database convergences (e.g. pharmacy and the EHR) and the overall maturity in the EHR. Finally, it is clear that current electronic health systems are simply another tool that used properly can be an excellent asset, but if incorrectly used may be a significant liability.
Competing interests
None declared.
Acknowledgements
This study was supported by a grant from the National E-Health Transition Authority (NeHTA).
References
[1] Australian Institute of Health and Welfare (AIHW). Australia’s health 2012. Canberra: AIHW; 2012.[2] Bishop TF, Press MJ, Mendelsohn JL, Casalino LP. Electronic communication improves access, but barriers to its widespread adoption remain. Health Aff 2013; 32 1361–7.
| Electronic communication improves access, but barriers to its widespread adoption remain.Crossref | GoogleScholarGoogle Scholar |
[3] Australian Digital Health Agency (formerly National E-Health Transition Authority). Sydney: Australian Government; 2014. Available at: http://www.digitalhealth.gov.au/about-the-agency [verified 24 April 2016].
[4] Murphy J, Ley S. Patients to get new myHealth Record: $485m ‘rescue’ package to reboot Labor’s e-health failures. 2015. Available at: https://www.health.gov.au/internet/ministers/publishing.nsf/Content/health-mediarel-yr2015-ley050.htm [verified 24 April 2016].
[5] Deloitte. Expected benefits of the national PCEHR system. Based on economic modelling work undertaken in 2010–2011. 2012. Available at: http://www.aph.gov.au/~/media/Estimates/Live/clac_ctte/estimates/bud_1213/DoHA/tabled_docs/DeloitteExpectedBenefitsPCEHR.ashx [verifed 19 April 2016].
[6] Armani R, Mitchell LE, Allen-Graham J, Heriot NR, Kotsimbos T, Wilson JW. Current patient and healthcare worker attitudes to eHealth and the personally controlled electronic health record in major hospitals. Internal Med J 2016; 46 717–22.
| Current patient and healthcare worker attitudes to eHealth and the personally controlled electronic health record in major hospitals.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC28fmt1ensw%3D%3D&md5=e139628e77aac095691ad787f80596faCAS |
[7] Health Information Management of Australia (HIMAA). General clinical information and documentation requirements. 2006. Available at: http://www.himaa.org.au/Pubs/HIMAA_Practice_Brief_2006.pdf [verified 24 April 2016].
[8] Australian Commission on Safety and Quality in HealthCare (ACSQHC). Electronic discharge summary systems literature scan. 2010. Available at: http://www.safetyandquality.gov.au/wp-content/uploads/2012/02/e-DischargeLiteratureScan.pdf [verified 20 April 2016].
[9] NSW Health. Health care records – documentation and management. 2012. Available at: http://www0.health.nsw.gov.au/policies/pd/2012/pdf/PD2012_069.pdf [verified 24 April 2016].
[10] Riskman Industry experts. 2014. Available at: http://www.riskman.net.au/Methodology/Industry-Experts [verified 16 April 2016].
[11] Belleli E, Naccarella L, Pirotta M. Communication at the interface between hospitals and primary care. A general practice audit of hospital discharge summaries. Aust Fam Physician 2013; 42 886–90.
[12] van Walraven CSR, Austin PC, Laupacis A. Effect of discharge summary availability during post-discharge visits on hospital readmission. J Gen Intern Med 2002; 17 186–92.
| Effect of discharge summary availability during post-discharge visits on hospital readmission.Crossref | GoogleScholarGoogle Scholar |
[13] Australian Government. Australia to 2050: future challenges. Australia to 2050: Future challenges. The 2010 intergenerational report. Overview. 2010. Available at: https://archive.treasury.gov.au/igr/igr2010/Overview/pdf/IGR_2010_Overview.pdf [verified 23 November 2016].
[14] Blumenthal D, Tavenner M. The ‘meaningful use’ regulation for electronic health records. N Engl J Med 2010; 363 501–4.
| The ‘meaningful use’ regulation for electronic health records.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BC3cXpsl2lsL4%3D&md5=ea2596e0c1feaf4ae1e51d9555303677CAS |