Public perceptions of cancer risk factors: a Western Australian study
Anna MacTiernan A , Lin Fritschi B , Terry Slevin C , Geoffrey Jalleh D , Rob Donovan D and Jane Heyworth A EA School of Population Health, Faculty of Medicine, Dentistry and Health Sciences, The University of Western Australia, 35 Stirling Highway, Crawley, WA 6009, Australia.
B Harry Perkins Institute of Medical Research, The University of Western Australia, 35 Stirling Highway, Crawley, WA 6009, Australia.
C Cancer Council Western Australia, 15 Bedbrook Place, Shenton Park, WA 6008, Australia.
D Centre for Behavioural Research in Cancer Control, Curtin University, GPO Box U1987, Curtin University, Perth, WA 6845, Australia.
E Corresponding author. Email: jane.heyworth@uwa.edu.au
Health Promotion Journal of Australia 25(2) 90-96 https://doi.org/10.1071/HE13081
Submitted: 27 September 2013 Accepted: 13 March 2014 Published: 25 July 2014
Abstract
Issue addressed: People’s perceptions of risk may influence health-related behaviours. The aim of this study was to investigate the perception of cancer risk factors among Western Australian adults in order to inform health promotion policies.
Methods: Cross-sectional surveys of 2094 adults were undertaken in 2007/2008 in which respondents were asked whether they thought factors increased or decreased the risk of cancer. Factors included both established and unestablished risk factors for cancer. The distribution of perceptions was compared according to age and sex.
Results: The study found high levels of endorsement for some unestablished risk factors (74–91%) and comparatively lower levels of endorsement for many established risk factors (33–80%). The established risk factors of smoking and asbestos received high levels of endorsement (94–98%).
Conclusion: It appears that the alignment between scientifically established risk factors and the Western Australian public’s perception of cancer risk factors could be improved.
So what?: Health promotion strategies are needed to improve the public’s awareness of cancer risk factors. The high levels of endorsement attributed to unestablished risk factors highlight the need to dispel myths surrounding cancer and to reinforce the key factors in cancer prevention. Ongoing assessment of the alignment between community perceptions of cancer risk and the scientific evidence for cancer risk is important for guiding prioritisation within public health organisations.
Introduction
Cancer is the leading cause of the total burden of disease in Australia,1 yet it has been estimated that more than 30% of cancer cases are preventable.2 A study in the UK found 43% of cancers were attributable to 14 lifestyle-related or environmental risk factors.3 Smoking, inappropriate diet, alcohol and physical inactivity were the top four risk factors, accounting for 39% of cancer cases. Apart from smoking, the prevalence of these factors is high in Australia. For example, the prevalence of obesity in Australian adults is 25%, which is one of the highest levels of obesity in the OECD.1 Australian adults also have low levels of adequate fruit consumption (50% of Australian adults reported adequate consumption) and vegetable consumption (<10% of Australian adults reported adequate consumption), high levels of physical inactivity (60% of Australian adults reported physical inactivity) and high levels of alcohol consumption (20% of Australian adults reported high levels of alcohol consumption).1
Research into the public awareness of cancer risk factors has highlighted the relatively low level of understanding of some well-established cancer risk factors.4–18 While smoking has consistently been shown to have the highest level of recognition as a risk factor for cancer,4,7,8,14,17,19–23 diet, being overweight or obese, alcohol and physical inactivity have been underestimated as risk factors in many populations.7,9,12,14,16–18
In contrast, studies have shown that some factors for which there is inadequate or no evidence of association with cancer have high levels of public endorsement as risk factors for cancer.7,9,18,19,23 A 2013 survey by the American Institute of Cancer Research found that a considerable proportion of the public believe food additives (56%), genetically modified foods (51%), stress (50%) and artificial sweeteners (40%) are risk factors for cancer.19 These factors received higher recognition as cancer risk factors than did evidence-based risks such as overweight/obesity (48%), diet low in vegetables and fruit (43%), alcohol (38%), insufficient physical activity (36%), and diet high in red meat (35%).19 In contrast, other studies have shown relatively low endorsement of unestablished cancer risk factors, with the exception of stress.4,8 Several studies suggest that the public rate risk factors that are out of their control as more serious risks than those factors that are controllable by the individual.9,13,16,18–20,22,23
An association between knowledge of cancer risk factors and preventative behaviour has been found in several studies.7,8,24 A 2004 UK study found participants with low levels of fruit and vegetable intake, and participants with low physical activity levels were less likely to endorse these as cancer risk factors.8 A recent Australian study on the perception of cancer risk factors found overweight and obese participants were less likely than normal-weight participants to acknowledge weight as a risk factor for cancer.21 Knowledge of cancer risk factors has the potential to engage the public in preventative behaviours.25
The aims of this study were to investigate the public perception of cancer risk factors among West Australian adults, to compare ratings of established risk factors and unestablished risk factors, and to investigate whether there were differences in perception of cancer risk according to sex or age.
Methods
Data were obtained from two cross-sectional computer-assisted telephone-interviewing surveys. In Survey 1, data were collected in 2007 as part of a Cancer Council Western Australia survey to assess the perception of the organisation and cancer education in Western Australia. Survey 2 was conducted in 2007 and 2008. Households were randomly selected from the Western Australian White Pages directories for inclusion in both surveys. In Survey 1, interviewers asked to speak with the adult resident who had most recently had a birthday. In Survey 2, interviewers alternated between asking to speak to the youngest male of the household and the youngest female of the household.
In both surveys, five attempts were made to contact households. Interviews were conducted on weekdays between 10.00 a.m. and 8.30 p.m. (from 4.30 p.m. for Survey 1) and on weekends between 10.00 a.m. and 4.30 p.m. to maximise the availability of household members. Eligible respondents were residents of Western Australia who were not employed full-time in a charitable institution. Eligible respondents were invited to participate in a survey on behalf of one of the major charities in WA in Survey 1 or in a survey conducted by a university in Survey 2.
Participants
Of the 6098 telephone numbers randomly selected for the surveys, 1833 were either disconnected, or were business or fax numbers; no contact was made for 204 numbers; the resident was ineligible to participate (i.e. non-resident of WA or full-time employee of a charitable institution) for four numbers; for 1963 numbers the resident refused to participate; and for 2094 the resident completed the interview. Thus, the participation rate was 52%, with 408 of the participants in Survey 1 and 1686 in Survey 2.
Survey instrument
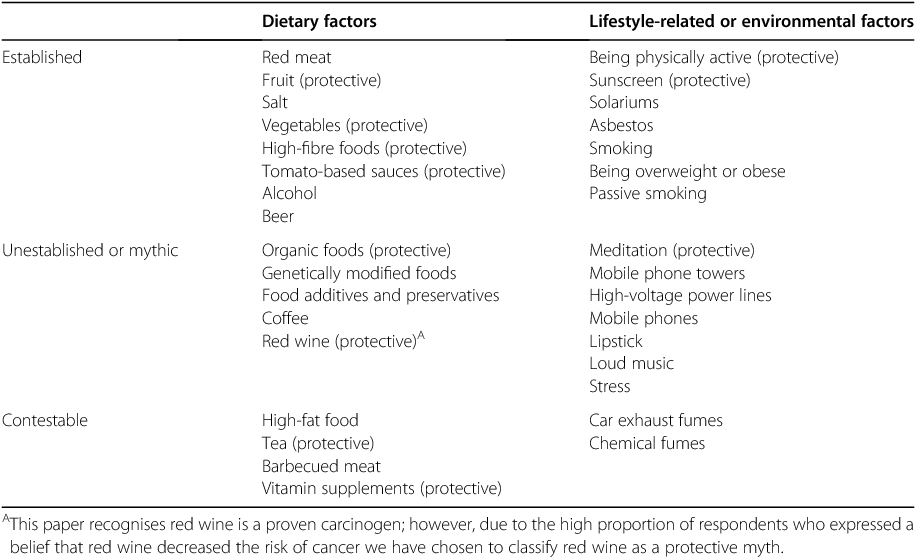
In both surveys, the participants (n = 2094) were randomly assigned one of two sets of survey questions on either diet-related risk factors or lifestyle-related or environmental risk factors. To minimise response fatigue, respondents were asked only one set of questions (Table 1). A total of 1072 participants completed the survey on 17 diet-related risk factors. Of these 17 factors, eight factors were established cancer risk factors (i.e. there was adequate evidence that these factors cause at least one type of cancer), five factors were unestablished or mythical, and four factors were in a ‘contestable’ category, meaning they were currently debated in the scientific literature (e.g. tea, barbequed meat) or the term used was not sufficiently specific to make a clear judgment (e.g. chemical fumes, car exhaust) (Table 1).
The remaining 1022 participants completed a survey on 16 environmental or lifestyle-related risk factors, of which seven were established risk factors, seven were unestablished or mythic risk factors, and two were contestable.
The category for each factor was based on the Cancer Council Western Australia website (http://www.cancerwa.asn.au, accessed 4 February 2013). This website is a primary source of information on cancer risk factors for Western Australian adults.
For the diet-related risk factors, respondents were asked: ‘Do you think eating any of the following types of food on a regular basis increases, decreases or has no effect on cancer risk?’ For the environmental and lifestyle risk factors, respondents were asked: ‘Which of the following do you think increase, decrease or have no effect on cancer risk?’ The risk factors were read out in a random order. There were no questions asked directly about cancer risk factors before the risk perception questions in either survey. The response categories were ‘increase a little’, ‘increase a lot’, ‘decrease a little’ or ‘decrease a lot’. The categories of ‘increase a little’ and ‘increase a lot’ were combined to determine percentage endorsement of established cancer risk factors, and the categories ‘decrease a little’ or ‘decrease a lot’ were combined to determine percentage endorsement of established protective cancer factors.
During the data analysis, two scores (either diet or lifestyle/environment) were determined for participants based on the sum of their endorsement of (1) established risk factors, and (2) unestablished risk factors (Table 1). The contestable factors were omitted from both scores. The maximum score for established dietary factors was 8, for unestablished dietary factors was 5, for established lifestyle-related or environmental factors was 7, and for unestablished lifestyle-related or environmental factors was 7.
Analysis
Analyses were carried out using Statistical Package for the Social Sciences (SPSS) for Windows version 7. Cross-tabulations with Chi-square tests were used to assess differences in perception according to sex or age. The mean number of endorsements of established factors and mean number of endorsements for unestablished factors were determined. Multiple linear regression models were used to determine associations between endorsement of established and unestablished factors according to age or sex.
Results
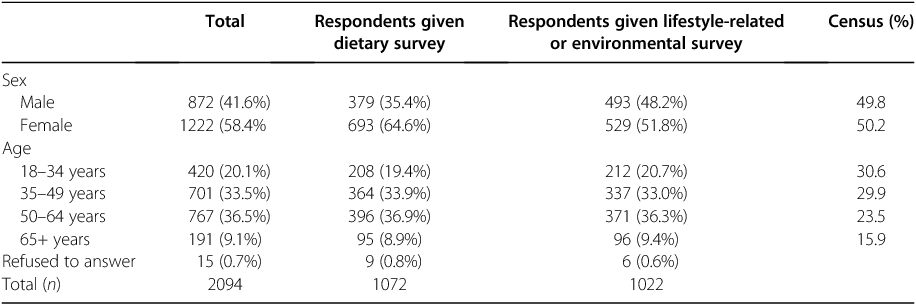
The sample contained smaller proportions of males and respondents in the youngest and oldest age groups than the general population26 (Table 2).
|
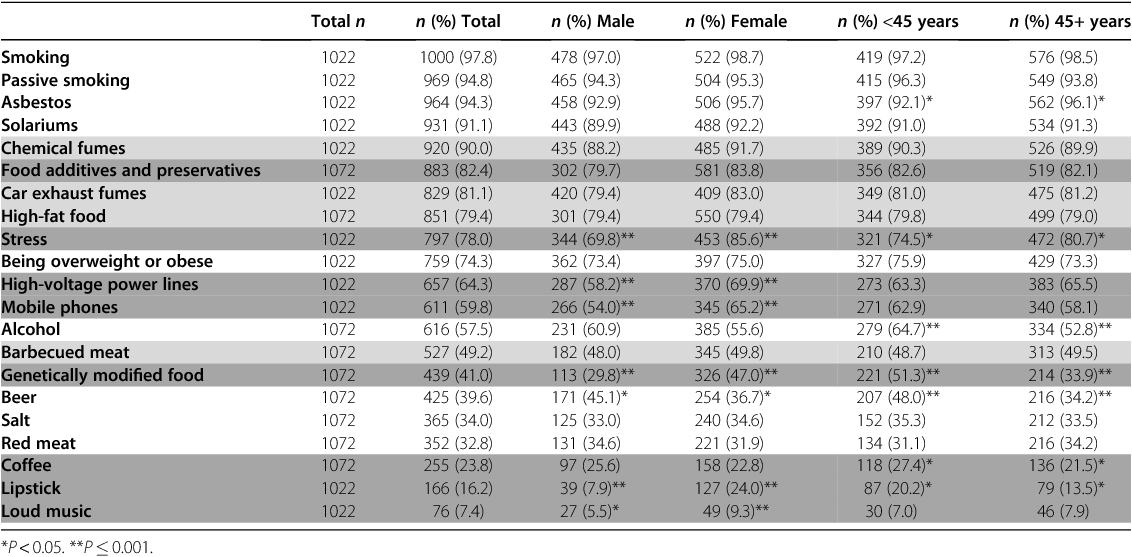
Endorsement of cancer risk factors (Table 3)
The factors with the highest levels of public recognition as cancer risk factors were smoking (98%), passive smoking (95%), asbestos (94%), solariums (91%) and chemical fumes (90%). Established risk factors that had low levels of public recognition were alcohol (58%), beer (40%), salt (34%) and red meat (33%). Unestablished factors that had high endorsement percentages included food additives (82%) and stress (78%).
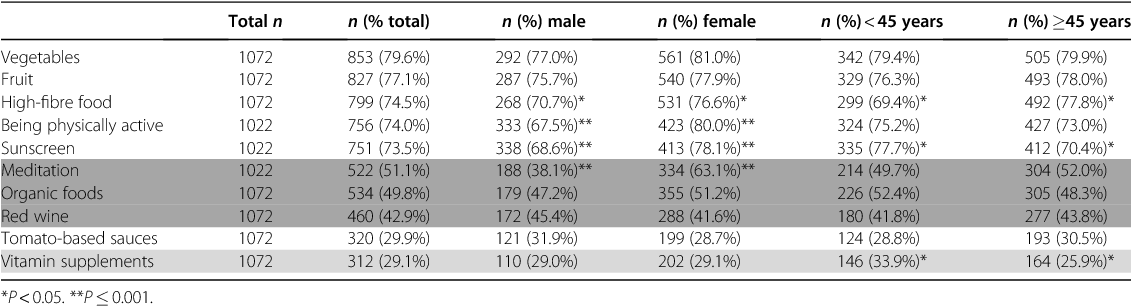
Endorsement of protective factors for cancer (Table 4)
The factors with the highest levels of public recognition as protective factors were vegetables (80%), fruit (77%), high-fibre food (75%) and being physically active (74%). Meditation and organic foods, as unestablished factors, were endorsed by almost half the sample. Red wine was endorsed as a protective factor by 43% of the sample.
Age and sex differences in endorsement of factors
Overall women endorsed more individual established and unestablished risk factors than men (Tables 3 and 4). Women were more likely than men to endorse the established factors of being physically active (80% vs 68%), sunscreen (78% vs 69%) and high-fibre food (77% vs 71%) as protective factors against cancer, whereas men were more likely than women to endorse beer as a risk factor (45% vs 37%). Women were also more likely than men to endorse the unestablished risk factors of stress (86% vs 70%), high-voltage power lines (70% vs 58%), mobile phones (65% vs 54%), genetically modified foods (47% vs 30%), lipstick (24% vs 8%) and loud music (9% vs 6%). Women were more likely than men to endorse meditation (63% vs 38%) as protective against cancer.
Overall, people under 45 years endorsed more established and unestablished factors than people over 45 years. Participants under 45 years were more likely to endorse alcohol as causative of cancer than participants aged 45+ years (65% vs 53%).
Beliefs regarding established and unestablished risk factors
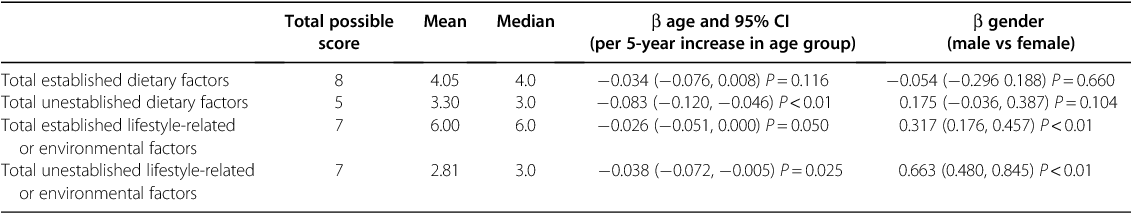
On average, participants endorsed 4.05 out of 8 established dietary factors and 3.30 out of 5 unestablished dietary factors (Table 5). There were no significant differences according to age or sex for established dietary factors, but for every 5-year increase in age the number of endorsements of unestablished diet factors decreased by 0.083 (P < 0.001).
|
Participants endorsed on average 6 out of 7 established lifestyle-related or environmental factors as cancer risk factors (Table 5). Women were more likely than men to endorse established lifestyle-related or environmental factors (6.30 vs 5.99, P < 0.001). Participants endorsed on average 2.81 out of 7 unestablished lifestyle-related or environmental factors, with women more likely to endorse unestablished lifestyle-related or environmental factors (3.36 vs 2.69, P < 0.001). For every 5-year increase in age the total number of endorsements of unestablished lifestyle-related or environmental factors decreased by 0.038 (P = 0.025).
Discussion
This study found a high level of public recognition of the established lifestyle-related or environmental risk factors of smoking, passive smoking, asbestos and solariums. Tobacco use and asbestos are factors that have been shown to be widely recognised as risk factors by the public.8,17,19,20,23,27 The risks associated with solarium use have received media attention in Australia because of the melanoma-related death of a young female who had used solariums regularly, and several public campaigns warning about the risks of solarium use occurred during the years of the surveys presented here.28,29
This study found a high level of endorsement of unestablished cancer risk factors. High proportions of respondents considered that chemical fumes, high-voltage power lines, food additives and preservatives, and car exhaust fumes increased the risk of cancer. However, other studies have found lower levels of endorsement of unestablished risk factors.4,8,22 A 2008 UK study found percentage endorsements of 21% for power lines and 16% for mobile phones as increasing cancer risk, and 12% for organic food and 9% for vitamin supplements as decreasing cancer risk.20 Stress has consistently received a high level of endorsement as a risk factor for cancer in this study and in other4,8,9,18,22 studies.5,10,13,22,25
Although knowledge by itself is not sufficient, it is an important influence on subsequent behavioural change.25 A recent study showed people who perceive cancer prevention as out of their control were less likely to engage in preventative behaviours.30 A heightened focus on environmental risk factors that are out of the individual’s control has the potential to divert attention away from the established lifestyle-related factors and the behavioural changes that could effectively contribute to cancer prevention.31
Despite consistent evidence linking alcohol consumption to cancer causation, recognition of alcohol as a risk factor for cancer was found to be low; in particular the recognition of beer and red wine as risk factors for cancer was low. Further, red wine consumption was seen by 43% of the sample as being protective against cancer. This proportion is considerably higher than in similar studies conducted at the same time in the UK, in which the percentage endorsement was ~15%.20 A 2005 study in Spain found 81% of the participants endorsed alcohol as a cancer risk factor compared with only 58% of the respondents in our study.23
There was a low level of recognition of salt and red meat as foods likely to increase cancer risk. The level of recognition of fruit and vegetable intake as protective against cancer was similar to the findings of a recent Australian study in which 73% of participants recognised dietary measures as being protective against cancer.21 A 2010 Australian study found that less than 50% of participants recognised overweight or obesity and lack of exercise as cancer risk factors,21 whereas the present study found that 74% of participants recognised these factors. A 2004 European study on colorectal cancer found similar levels of recognition of relevant dietary factors as preventive, but lower levels of awareness of the role of overweight or obesity and physical inactivity in increasing the risk of cancer.11 A 2004 UK study found significantly lower numbers (<35%) of respondents recognised low fruit and vegetable intake, being overweight, physical inactivity and alcohol as associated with cancer risk.8
The results from this study are consistent with research that has found women display a greater awareness of established risk factors,4,7–9,12,15,20,23 but also endorse a higher number of unestablished risk factors.8,20,23 Health promotion strategies can assist in dispelling the myths around unestablished cancer risk factors and in raising awareness of the factors established as protective against cancer; certain factors such as physical activity and sunscreen protection may be targeted at males.
This study found younger people were more likely to endorse unestablished diet and lifestyle-related or environmental factors as increasing the risk of cancer. There was no relationship found between age and the endorsement of established diet and lifestyle-related or environmental factors. Whilst knowledge of cancer risk factors is commonly higher among middle-aged participants,12,13,32 some studies have found older participants to have both lower5,6,16,18 and higher levels of knowledge of cancer risk factors.8,10 The relationship between age and cancer knowledge remains inconclusive.
There is ongoing research into factors that might prevent or cause cancer, and there is ongoing scientific debate on these issues. As such, the precise language used in this study in identifying established and unestablished risk factors is subject to such debate with reference to the strength of evidence linking the nominated risk factors to cancer causality or prevention. These scientific debates can create conflicting messages about the factors that influence an individual’s risk of cancer. Hence, it is not surprising that there is variation in the degree of endorsement of factors subject to ongoing debate.
As the popular mass media is a key source of health information in Australia,29 it is perhaps not surprising that there is some misalignment between public perceptions of cancer risk factors and the current evidence on factors linked to cancer risk. By investigating Australian adults’ perception of cancer risk factors, this study reveals some of the cancer ‘myths’ that exist in our society.
By way of historical context, a 1964 survey of Perth residents’ beliefs about cancer causes found the most commonly cited cause of cancer was ‘a knock’ (25%). Smoking was endorsed as a cause of cancer by 22%, sun exposure by 5%, diet by 4%, and stress by 3%.33 In a 1988 Australian survey, 36% of participants acknowledged diet as a cancer prevention strategy, and 13% mentioned protecting skin from sun exposure.32 In contrast, our surveys indicated a higher recognition of the role of smoking (98%), diet (80%), and sun protection (74%). So, while there has been progress in the public’s understanding, more needs to be done to ensure the public’s beliefs are aligned with current scientific knowledge.
The findings of this study are likely to be an overestimation of the public’s awareness of risk factors as prompted questions receive significantly higher recognition than open-ended questions that rely on recall.7,14,15,17,20,21 An analysis that directly compared the two survey methods found significantly lower levels of cancer knowledge using unprompted methods.12 Furthermore, risk factors differ across cancers, and responses may have been influenced by both the prevalence of risk factors and also individual cancer types. Participants may have been able to attribute risk factors more accurately if they were asked to consider them with regards to individual cancer types.
Further limitations of the study include the potential for bias as a consequence of the low response fraction and the limited generalisability of a sample that did not reflect the age demographic of the general population. Other demographic factors such as education and socioeconomic status, which were not collected in the surveys reported here, may also have influenced respondents’ awareness of risk factors. However, the data provides a population-level overview of the perceptions of the general population about cancer risk factors.
The survey data have been used by Cancer Council Western Australia to pursue health promotion activities in lifestyle-related cancer prevention. Cancer Council Western Australia in conjunction with the Western Australian Drug and Alcohol Office established an alcohol and cancer campaign as a response to the large number of respondents who did not endorse alcohol as a cancer risk factor. The data were also used in the development of the Live Lighter campaign in conjunction with the Heart Foundation (http://livelighter.com.au, accessed 4 April 2013).
Conclusions
The results of this study highlight gaps in the knowledge of cancer risk factors in a sample of Western Australian adults. Of note, the high level of endorsement of unestablished risk factors highlights the need to dispel myths surrounding cancer and to reinforce the key factors in cancer prevention. Specific areas of concern include the low level of endorsement of alcohol as a cancer risk factor and the number of participants endorsing red wine as protective against cancer. Men had particularly low levels of endorsement of physical activity as a cancer prevention strategy, which reinforces the need for targeted health promotion in this area. The greatest potential for cancer prevention lies in the known modifiable cancer risk factors, and it appears that Australians are yet to fully recognise these.
Acknowledgements
Cancer Council Western Australia.
References
[1] Australian Institute of Health and Welfare. Australia’s Health, no. 13. Canberra: AIHW; 2012.[2] World Health Organization. Cancer. Fact sheet no. 297. Geneva: World Health Organization; 2013. Available from: http://www.who.int/topics/cancer/en/ [Verified 2 February 2013]
[3] Parkin D, Boyd L, Walker LC (2011) The fraction of cancer attributable to lifestyle and environmental factors in the UK in 2010. Br J Cancer 105, S77–81.
| The fraction of cancer attributable to lifestyle and environmental factors in the UK in 2010.Crossref | GoogleScholarGoogle Scholar | 22158327PubMed |
[4] Wardle J, Waller J, Brunswick N, Jarvis MJ (2001) Awareness of risk factors for cancer among British adults. Public Health 115, 173–4.
| Awareness of risk factors for cancer among British adults.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD3MzntFGjtw%3D%3D&md5=a74b99f5a694326e7a0cbc7c9cbede01CAS | 11429711PubMed |
[5] Breslow R, Sorkin JD, Frey CM, Kessler LG (1997) Americans’ knowledge of cancer risk and survival. Prev Med 26, 170–7.
| Americans’ knowledge of cancer risk and survival.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK2s3jvFOhtg%3D%3D&md5=be7e2091d7270e184857044042f31de3CAS | 9085385PubMed |
[6] Paul C, Barrat A, Redman S, Cockburn J, Lowe J (1999) Knowledge and perceptions about breast cancer incidence, fatality and risk among Australian women. Aust N Z J Public Health 23, 396–400.
| Knowledge and perceptions about breast cancer incidence, fatality and risk among Australian women.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK1Mzpt1WhsA%3D%3D&md5=10843a40b840d8a4a9de4776cdf0260aCAS | 10462863PubMed |
[7] Hawkins N, Berkowitz Z, Lucy AP (2010) What does the public know about preventing cancer? Results from the Health Information National Trends Survey (HINTS). Health Educ Behav 37, 490–503.
| What does the public know about preventing cancer? Results from the Health Information National Trends Survey (HINTS).Crossref | GoogleScholarGoogle Scholar | 17478600PubMed |
[8] Redeker C, Wardle J, Wilder D, Hiom S, Miles A (2009) The launch of Cancer Research UK’s ‘Reduce the Risk’ campaign: baseline measurements of public awareness of cancer risk factors in 2004. Eur J Cancer 45, 827–36.
| The launch of Cancer Research UK’s ‘Reduce the Risk’ campaign: baseline measurements of public awareness of cancer risk factors in 2004.Crossref | GoogleScholarGoogle Scholar | 19054666PubMed |
[9] Inoue M, Iwasaki M, Otani T, Sasazuki S, Tsugane S. Public awareness of risk factors for cancer among the Japanese general population: a population-based survey. BMC Public Health 2006; 6: 2.
[10] Marlow L, Waller J, Wardle J (2007) Public awareness that HPV is a risk factor for cervical cancer. Br J Cancer 97, 691–4.
| Public awareness that HPV is a risk factor for cervical cancer.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD2srgsFGqtg%3D%3D&md5=6de39099652024bc70d2b7672a90d61dCAS | 17687335PubMed |
[11] Keighley M, O’Morain C, Giacosa A, Ashorn M, Burroughs A, Crespi M, et al (2004) Public awareness of risk factors and screening for colorectal cancer in Europe. Eur J Cancer Prev 13, 257–62.
| Public awareness of risk factors and screening for colorectal cancer in Europe.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD2crnvVahug%3D%3D&md5=7f015b2f0633eb7b7b4cc28a7bbadc02CAS | 15554552PubMed |
[12] Waller J, McCaffery K, Wardle J (2004) Measuring cancer knowledge: comparing prompted and unprompted recall. Br J Psychol 95, 219–34.
| Measuring cancer knowledge: comparing prompted and unprompted recall.Crossref | GoogleScholarGoogle Scholar | 15142303PubMed |
[13] Waller J, McCaffery K, Wardle J (2004) Beliefs about the risk factors for cervical cancer in a British population sample. Prev Med 38, 745–53.
| Beliefs about the risk factors for cervical cancer in a British population sample.Crossref | GoogleScholarGoogle Scholar | 15193894PubMed |
[14] Sanderson SC, Waller J, Jarvis MJ, Humphries SE, Wardle J (2009) Awareness of lifestyle risk factors for cancer and heart disease among adults in the UK. Patient Educ Couns 74, 221–7.
| Awareness of lifestyle risk factors for cancer and heart disease among adults in the UK.Crossref | GoogleScholarGoogle Scholar | 19059747PubMed |
[15] McCaffery K, Wardle J, Waller J (2003) Knowledge, attitudes, and behavioral intentions in relation to the early detection of colorectal cancer in the United Kingdom. Prev Med 36, 525–35.
| Knowledge, attitudes, and behavioral intentions in relation to the early detection of colorectal cancer in the United Kingdom.Crossref | GoogleScholarGoogle Scholar | 12689797PubMed |
[16] Grunfeld E, Ramirez AJ, Hunter MS, Richards MA (2002) Women’s knowledge and beliefs regarding breast cancer. Br J Cancer 86, 1373–8.
| Women’s knowledge and beliefs regarding breast cancer.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD383kslWmsA%3D%3D&md5=cbbbe172cf692c3ddda595e7bdd576baCAS | 11986766PubMed |
[17] Reeder A, Trevena J. Adults’ perceptions of the causes and primary prevention of common fatal cancers in New Zealand. N Z Med J 2003; 116(1182): 1–10.
[18] Peacey V, Steptoe A, Davidsdottir S, Baban A, Wardle J (2006) Low levels of breast cancer risk awareness in young women: an international survey. Eur J Cancer 42, 2585–9.
| Low levels of breast cancer risk awareness in young women: an international survey.Crossref | GoogleScholarGoogle Scholar | 16829071PubMed |
[19] American Institute for Cancer Research. The AICR 2013 cancer risk awareness survey report. 2013. Available from: http://www.aicr.org/assets/docs/pdf/education/aicr-cancer-awareness-report-2012.pdf [Verified 7 January 2013]
[20] Cancer Research UK. Perceptions of risk survey 2008: key findings. 2010. Available from: http://www.cancerresearchuk.org/prod_consump/groups/cr_common//@nre/@hea/documents/generalcontent/014219.pdf [Verified 7 January 2013]
[21] Cameron M, Scully M, Herd N, Jamsen K, Hill D (2010) The role of overweight and obesity in perceived risk factors for cancer: implications for education. J Cancer Educ 25, 506–11.
| The role of overweight and obesity in perceived risk factors for cancer: implications for education.Crossref | GoogleScholarGoogle Scholar | 20217292PubMed |
[22] Baghurst K, Baghurt PA, Record SJ (1992) Public perceptions of the role of dietary and other environmental factors in cancer causation or prevention. J Epidemiol Community Health 46, 120–6.
| Public perceptions of the role of dietary and other environmental factors in cancer causation or prevention.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK383mtVWgtg%3D%3D&md5=682ff7b0676ac898c48237f6e28a2f41CAS | 1583425PubMed |
[23] Garcia M, Fernandez E, Borras JM, Nieto FJ, Schiaffino A, Peris M, et al (2005) Cancer risk perceptions in an urban Mediterranean population. Int J Cancer 117, 132–6.
| Cancer risk perceptions in an urban Mediterranean population.Crossref | GoogleScholarGoogle Scholar | 1:CAS:528:DC%2BD2MXhtVaht7vK&md5=7090fe1e9472b87e0470a5aa76c47635CAS | 15880362PubMed |
[24] Jones S, Carter O, Donovan RJ, Jalleh G (2005) Western Australians’ perceptions of the survivability of different cancers: implications for public education campaigns. Health Promot J Austr 16, 124–8.
[25] Viswanath K, Breen N, Meissner H, Moser RP, Hesse B, Steele WR, et al (2006) Cancer knowledge and disparities in the information age. J Health Commun 11, 1–17.
| Cancer knowledge and disparities in the information age.Crossref | GoogleScholarGoogle Scholar | 16641071PubMed |
[26] Australian Bureau of Statistics. 2006 Census 2006. Available from: http://www.censusdata.abs.gov.au/census_services/getproduct/census/2006 [Verified 15 January 2013]
[27] Halpern A, Kopp LJ (2005) Awareness, knowledge and attitudes to non-melanoma skin cancer and actinic keratosis among the general public. Int J Dermatol 44, 107–11.
| Awareness, knowledge and attitudes to non-melanoma skin cancer and actinic keratosis among the general public.Crossref | GoogleScholarGoogle Scholar | 15689206PubMed |
[28] Jalleh G, Donovan RJ, Lin C, Slevin T (2008) Changing perceptions of solaria and cancer risk: the role of the media. Med J Aust 188, 735
[29] MacKenzie R, Imison M, Chapman S, Holding S (2008) Mixed messages and a missed opportunity: Australian news media coverage of Clare Oliver’s campaign against solaria. Med J Aust 189, 371–4.
[30] Stewart B (2008) Banding carcinogenic risks in developed countries: a procedural basis for qualitative assessment. Mutat Res 658, 124–51.
[31] Stewart B (2012) Priorities for cancer prevention: lifestyle choices versus unavoidable exposures. Lancet 13, 126–33.
| Priorities for cancer prevention: lifestyle choices versus unavoidable exposures.Crossref | GoogleScholarGoogle Scholar |
[32] Hill D, White V, Borland R, Cockburn J (1991) Cancer-related beliefs and behaviours in Australia. Aust J Public Health 15, 14–23.
| Cancer-related beliefs and behaviours in Australia.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK3M3itlahtA%3D%3D&md5=e2aae736d7789dd4d337f1414c443a64CAS | 2025669PubMed |
[33] Donovan R, Carter OBJ, Jalleh G, Jones SC (2004) Changes in beliefs about cancer in Western Australia, 1964–2001. Med J Aust 181, 23–5.