Optimising the delivery of sexual health services in Australia: a qualitative study
Varsicka Kularadhan A B , Christopher K. Fairley
A B , Christopher K. Fairley  C D , Marcus Chen C D , Jade Bilardi C D E , Ria Fortune C , Eric P. F. Chow
C D , Marcus Chen C D , Jade Bilardi C D E , Ria Fortune C , Eric P. F. Chow  C D F , Tiffany Philips
C D F , Tiffany Philips  C D § and Jason J. Ong
C D § and Jason J. Ong  C D G § *
C D G § *
A Monash University, School of Rural Health, Bendigo, Vic., Australia.
B Bendigo Health, Bendigo, Vic., Australia.
C Melbourne Sexual Health Centre, Alfred Health, Melbourne, Vic., Australia.
D Central Clinical School, Monash University, Melbourne, Vic., Australia.
E Department of General Practice, University of Melbourne, Melbourne, Vic., Australia.
F Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne, Melbourne, Vic., Australia.
G Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, UK.
Handling Editor: Jane Hocking
Sexual Health 19(4) 376-385 https://doi.org/10.1071/SH22024
Submitted: 29 January 2022 Accepted: 27 July 2022 Published: 23 August 2022
© 2022 The Author(s) (or their employer(s)). Published by CSIRO Publishing. This is an open access article distributed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License (CC BY-NC-ND)
Abstract
Background: With a rise in sexually transmitted infections in Australia, it is important to evaluate and optimise current sexual health services to reduce barriers to access and increase testing. We aimed to describe the range of sexual health services in Australia, focusing on strategies to improve testing among priority populations, and any future strategies participants believed would improve service delivery.
Methods: We conducted 20 semi-structured interviews with key informants working in Australian sexual health services from July to December 2020, and collected data on service characteristics and strategies to improve access. We used content analysis, then coded and categorised the data into recurring themes and sub-themes.
Results: We identified two major themes: ‘Expanding Traditional Service Delivery’ and ‘Thinking Outside the Box’. The first theme outlines strategies that build upon pre-existing service delivery models, such as express clinics and an increased focus on confidentiality. The second theme outlines new strategies introduced to fill gaps in service delivery, such as self-testing and outreach.
Conclusions: To improve access to HIV/STI testing, there is a need for multiple access points to cater for a range of populations and their preferences. Establishing strategies to accomplish this involves utilising a combination of expanding traditional service models and implementing new approaches to service delivery.
Keywords: Australian sexual health services, health service delivery, HIV, priority populations, service providers, sexually transmitted infection, strategies, strategies to optimise.
Introduction
With sexually transmitted infections (STIs) increasing in Australia, demand for sexual health services is growing. Maintaining access to HIV/STI testing for priority populations is important for optimal STI control, which includes addressing potential barriers. These include personal barriers (misperception of risk, fear of negative attitude from health providers, lack of knowledge of HIV/STI), structural barriers (costs, access to services, perceived lack of privacy/confidentiality), and social barriers (fear of stigma and discrimination).1,2
Delayed healthcare seeking prolongs the duration of infectiousness, which leads to greater morbidity and mortality and onward transmission of STIs. Evaluation and optimisation of service delivery may assist services to address the institutional factors and make a meaningful difference to HIV/STI testing access.3 However, there are limited data on how to optimise current HIV/STI service configurations to improve access to, and meet the needs of, priority populations.
This study aimed to describe strategies used by sexual health services in Australia to improve HIV/STI testing and any future strategies to improve service delivery. This study provides an overview of the views and experiences of key informants working in a range of Australian sexual health services, particularly the service characteristics they perceived to be of importance to their patients.
Methods
This study was reported according to the COREQ (COnsolidated criteria for REporting Qualitative research) guidelines (see Supplementary Material).4
Theoretical framework
We used a Qualitative Descriptive approach, common in healthcare research, as it allows researchers to explore and gain insight into specific areas of interest.5 As a pragmatic rather than a theory-driven approach, it describes events or experiences rather than a theoretical or interpretive analysis.6
Method, research team and reflexivity
We conducted semi-structured interviews with key informants working in Australian sexual health services. The interview guide was jointly designed by members of the research team, including JO (FAChSHM, PhD), a male sexual health physician and researcher with a special interest in increasing access to sexual health services to priority populations, TP (PhD), a female research fellow with experience working in sexual health, and VK (MD), a female junior doctor with an interest in sexual health, particularly improving access in regional and rural areas. The questions were developed to explore key areas of clinical interest.
VK conducted interviews from 23 July 2020 to 22 December 2020. Participants had no prior relationship with VK and were informed the study was being undertaken to describe the range of HIV/STI testing services available throughout Australia, focusing on exploring strategies to improve testing among priority populations.
Recruitment
Key informants were recruited from clinics in the Australian Collaboration for Coordinated Enhanced Sentinel Surveillance of Sexually Transmissible Infections and Blood Borne Viruses (ACCESS) network, which is a national sexual health surveillance network involving over 120 Australian clinical services. We approached the medical directors of sexual services within the ACCESS network or their suggested colleagues working in sexual health services in Australia. Clinics were purposively sampled to ensure diversity of services (public sexual health service, general practice), location (at least one from each state, a mix of metropolitan and rural locations) and gender.
Data collection
Invitations to participate in this study were sent via email by JO to key informants. Those interested were emailed a plain language statement and scheduled interview time. Interviews were conducted by telephone, in English by VK, and participants provided verbal consent before the interview commenced. Only the participant and researcher were present at the interview.
The interview comprised of two main sections: the first included 14 structured questions focused on the current HIV/STI testing options offered to patients attending the service, and the second was a series of open-ended questions around the strategies used to improve access to sexual health services, and any future strategies participants believed would be worth investigating. All interviews were audio-recorded and transcribed verbatim. VK made field notes summarising key and interesting strategies discussed after each interview.
Data analysis
The research team met monthly to discuss the preliminary data and developing themes. After two interviews were completed, two additional questions about other services offered in addition to HIV/STI testing were added. The interview guide was not further altered after this stage. After 20 interviews were completed, the research team met to discuss the results and reviewed the interview transcripts and service sample. At this time, it was decided that no further strategies and themes were emerging, and data saturation was met.
Data were analysed using content analysis, a commonly used analysis method in qualitative descriptive studies.5 Transcripts were uploaded to Taguette (an open-source qualitative data analysis tool)7 for data management. Transcripts were re-read, and noteworthy phrases or concepts were coded and categorised into themes and sub-themes derived both deductively from the interview schedule and the data itself. JO and TP read a sub-set of the transcripts to confirm coding and thematic analysis, with no major differences in interpretation evident. Summaries of service models, including data from the first part of the interview, and key strategies in the second part, were summarised in tables.
Ethics statement
Ethics approval for the study was obtained from the Alfred Hospital Ethics Committee (Project number 312/20). The views on improvements and challenges of sexual health services are the interviewees’ personal opinions and are not necessarily representative of their organisation.
Results
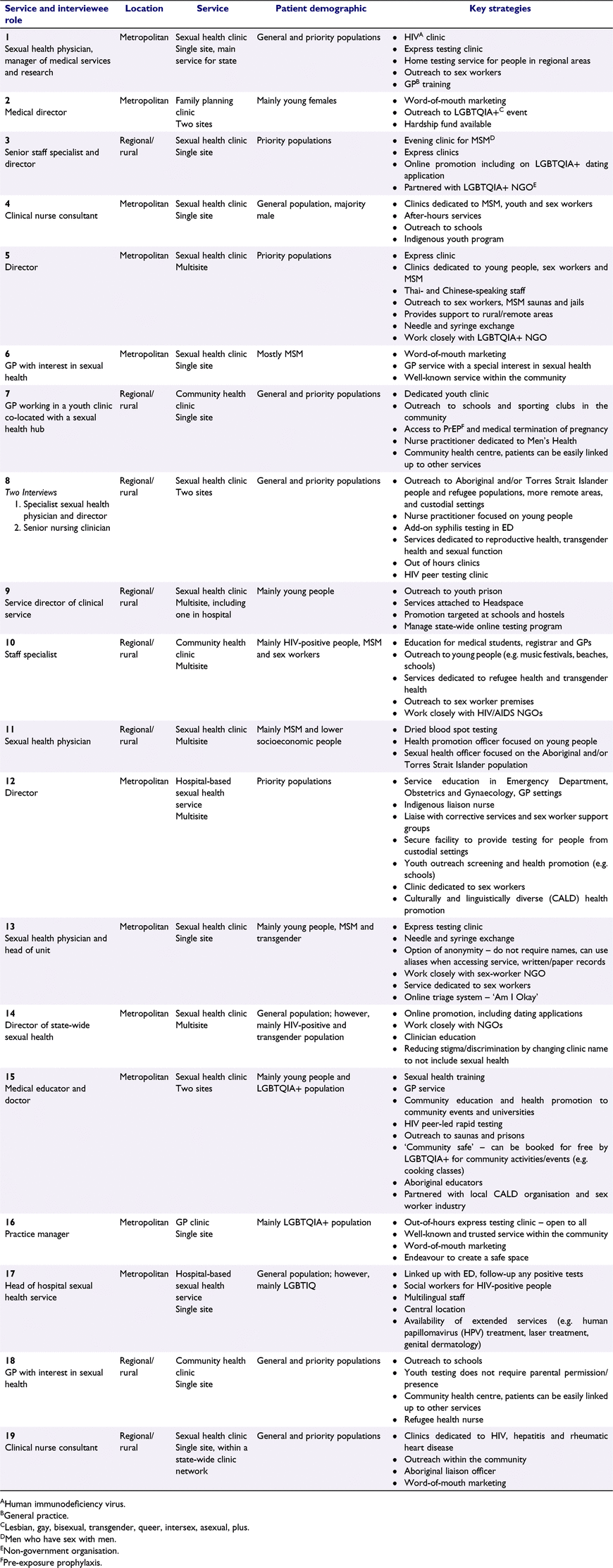
Interviews averaged 40 min in length (range 25–70). Of 30 services approached, 19 participated, three declined (and recommended alternate participants within their service as they were too busy) and eight did not respond. Twenty interviews were undertaken across 19 services, with two key informants from one service participating. Table 1 outlines the key strategies identified. Of 19 services, 11 were metropolitan based, and eight were rural or regional. Twelve were sexual health clinics, three community health clinics, two hospital-based sexual health services, one general practitioner (GP) clinic and one family planning clinic.
|
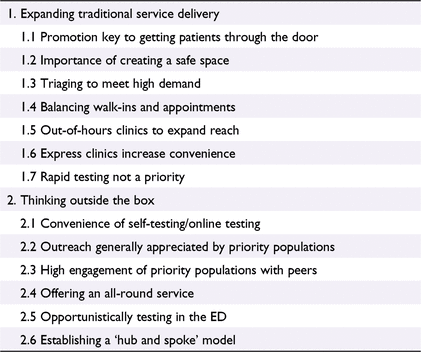
Two major themes arose from the data and 13 sub-themes, as shown in Table 2.
|
Expanding traditional service delivery
This theme describes strategies clinics were using or felt could be useful for optimising HIV/STI testing, which builds upon pre-existing service models. A large aspect involved refining their approach to target priority populations’ needs. Services reported strategies that focused on almost every aspect of service delivery, including advertising to patients, streamlining the testing process and the variety of clinic structures offered, confidentiality measures and express clinics.
Promotion and accessibility
Smaller services and GP clinics, particularly those well-known within their community, depend on word-of-mouth and stated there was no need for promotion. However, larger centres reported trialling various promotional strategies to increase accessibility. These included advertising on social media and online dating platforms to reach gay and bisexual men who have sex with men (gbMSM); and using interactive online campaigns to promote their services and provide sexual health education in the form of an online forum on their service website, which allowed individuals to submit questions regarding sexual health and receive answers from staff. Several services employed dedicated health promotion officers whereas others partnered with local non-government organisations (NGOs) to focus on priority populations. A few discussed employing multilingual staff and making their website translatable to other languages to increase accessibility and provide care for the culturally and linguistically diverse (CALD) community.
Confidentiality
Confidentiality was an important factor in service delivery, particularly for priority populations. Services reported adopting strategies to maintain confidentiality, and foster an environment where patients feel safe and encouraged to attend for testing.
Strategies included allowing patients to use aliases, electronic self-registration to avoid private information being overheard, not requiring identification when attending, and keeping medical records for the sexual health service on a separate system to other services. Using generic or acronym names for clinics and being physically located among other health services were also reported by many services as key strategies to provide a safe and non-judgemental environment.
So we have an acronym that describes the sex worker clinic … and that is an indicator so people can have less things to say publicly at the reception desk, so we try to make the reception desk as confidential a place as possible, and we’re moving to self-collected registration information. (Service 13, metropolitan sexual health clinic)
Regarding priority populations, one service worked with a sex worker NGO to tailor their services to be as acceptable and accessible as possible; this involved establishing a separate waiting room for sex workers. Another service dedicated a day every fortnight to people living with HIV.
On Wednesdays every fortnight is when we run our HIV service. So [we] don’t have any other clinics that run on that day to minimise the traffic on the day to ensure our client group who are accessing the HIV care and or PrEP have the best experience that they can. (Service 19, regional sexual health service)
Triage
Of 19 services, eight used a triage system via a questionnaire before booking or an assessment by a nurse when patients first arrive. These services were specifically public sexual health services that found triage was an effective mechanism to meet the high demand and prioritise patients at high risk, and those with STI symptoms.
We’ve got a triage system which brings about improvements in improving access for the high priority populations and facilitates finding appointments for them. So, we triage in the most important cases and triage out those who can be seen by general practitioners. (Service 3, regional sexual health clinic)
Several participants identified a helpful online tool they used to assist in triaging. The ‘Am I Okay’ website or similar versions assess patients’ risk and advised them to see their general practitioner or present to a sexual health service urgently if required. Participants found the website assisted their service to streamline the triage process and successfully facilitated priority populations to get tested.
So that’s a tool that we use and encourage and people in the priority groups would be channelled into the service and people outside the priority groups would be channelled to primary care unless they had a symptomatic or other urgent reason to see us. (Service 13, metropolitan sexual health clinic)
Walk-in testing
Nine services offered both appointments and walk-ins, with the remaining 10 being appointment only. Services that allowed walk-ins only did so for high-risk or symptomatic patients. Of 10 that only offered appointments, six recently stopped allowing walk-ins, four attributing the change to the coronavirus disease 2019 (COVID-19) pandemic.
Generally, most identified their service preferred an appointment-based system due to the structure and organisation this offers clinicians. However, there were benefits to allowing a few walk-in slots to cater for patients who may not necessarily return for an appointment or required urgent care.
The best model is where you have appointments and you have a couple of spare spots for people to walk in. So it doesn’t overburden the clinician. (Service 15, metropolitan sexual health clinic)
One metropolitan service did not advertise walk-ins; however, it would attempt to see those who walk-in as soon as possible. Another regional service prioritised walk-ins considered at high-risk; for example, people who are Aboriginal and/or Torres Strait Islander and patients requesting post exposure prophylaxis (PEP). Participants felt priority populations could be more easily targeted when offering some walk-ins.
Out-of-hours clinics
Eight services offered out-of-hours clinics; all found them to be generally popular. These clinics captured patients who would normally be deterred from accessing sexual health services due to work or familial commitments during business hours. Most ran evening clinics, but noted weekend clinics would be beneficial, with a few specifically stating they had patient requests for weekend hours. A further eight clinics felt out-of-hours services would reach their priority populations; however, most expressed that funding and staffing were the biggest barriers. A few services noted their location (e.g. in a shopping centre or community hub with their own hours of operation) restricted them from providing out-of-hours services.
Express clinics
Six services offered express clinics; most targeted asymptomatic patients. Rather than 20- to 40-min appointment slots, express clinics aimed to see patients for a shorter period, and focused on maximising the number of patients tested. The clinics appeared to run differently; some for asymptomatic patients only, others specifically targeted priority populations. All were reported to be highly successful for several reasons, including ease and convenience for patients, reduced consultation time and providing a comfortable atmosphere. One service envisioned their express clinic would appeal primarily to priority populations; however, it increased attendance by heterosexual males.
And that’s open to anybody who wants testing because we wanted it to be easy, we wanted it to be quick and we didn’t want people to feel that you know, that they were going to be looked down on or judged… And you know we’re really lucky to be able to provide that service. And we didn’t envisage that we would have the boys from the Army rock up, but we’re glad that they do. Because if they’re getting testing, that’s testing that they may not have undertaken. (Service 16, metropolitan GP clinic)
HIV/STI point-of-care testing
There were mixed opinions and experiences when participants were asked about point-of-care testing (POCT), which involves testing a specimen on-site and providing near-immediate results. Most found that although, in theory, it appeared to be an appealing option, patients preferred not to stay and wait for their results. Most services had standard testing results available within a few days, and reported that most patients did not consider getting immediate results a priority. Concerns regarding the accuracy of POCTs were also raised, with a few noting that test costs seemed to outweigh their benefit.
They preferred just to do the test and then go and know that we would call them with the results. (Service 11, regional sexual health clinic)
Services did see the benefit of POCTs in settings such as peer-led clinics and outreach to attract patients who would not normally get tested. Two clinics offered POCT in their peer-led clinic. Another four clinics that did not provide POCT felt it would benefit their patients, but was not feasible for their service, mostly due to the test costs.
Thinking outside the box
This theme describes relatively new strategies introduced to fill gaps in service delivery or increase HIV/STI testing. Of particular focus was how the services were moulded to meet patient preferences, particularly those of priority populations.
I think having a smorgasbord of different options is important… I think what we’ve learnt … is people have different wants and needs and so you want to offer different types of service deliveries. (Service 1, metropolitan sexual health clinic)
Self-testing and online testing
Self- and online-testing allows patients to organise HIV/STI testing remotely, complete it themselves, and potentially be managed without attending a clinic. This eliminates barriers to access (e.g. long-distance from clinics) and provides both convenience and confidentiality.
Participants highlighted the merits of this method, and many believed that having it readily available would increase testing rates. One service already provided self-testing at home on a small scale, whereas others have it on patient request; however, they do not offer it unless needed.
… People in regional areas can go to the website and ask for home testing, a kit to be sent to them for screening. (Service 1, metropolitan sexual health service)
Participants identified obstacles to implementing self-testing, including managing kit delivery, coordinating with pathology laboratories, funding additional costs, establishing an effective system to provide results, and arranging follow up. Additionally, concerns over data security of testing online were raised. Various participants discussed that although patients may perceive it to be convenient, accessing appropriate counselling, education, and management becomes more complicated following a positive result.
That’s what people are looking for now, aren’t they? I think they’re looking for less of the traditional, mundane ‘come to the clinic and get sorted’ model, particularly for people who are asymptomatic. They’re thinking, ‘Well, why do I have to go somewhere and ask a whole lot of personal questions when I can just get this test done?’ and that’s fine when it’s negative. But our experience has been when it’s positive, it’s not quite so fine. So I think a lot of testing, people think, ‘I’ll just do the test and it’s all going to be negative,’ and then when it isn’t, that’s when it becomes more problematic. (Service 9, regional sexual health clinic)
Several participants discussed established state-wide services, which offer mail-out HIV/STI testing, and found this to be an adequate system for accessing self-testing.
Overall, various factors need to be considered when implementing and streamlining self- and online testing. If an effective system could be designed, participants felt it would benefit service delivery. A few mentioned the Dean Street Express Clinic in London as highly successful and that it should be replicated in Australia. The Dean Street Express Clinic operates as a self-service HIV/STI testing clinic, and provides clients with results via text message on the same day. One service offered a home testing program for chlamydia tests of re-infection, but found it unsuccessful, as most patients did not return the test.
We implemented a chlamydia test of re-infection program, a home testing program. Based on daily findings that demonstrated that it was an effective strategy in a research context. But in our kind of real-world context it hasn’t been that successful and not many people either request the home testing option or if they do request it don’t return the specimen. (Service 5, metropolitan sexual health clinic)
Outreach
The opposite approach of the ‘self-care’ model is bringing the service to the patient. Outreach was used by 12 services, commonly targeting sex workers, young people and Aboriginal and/or Torres Strait Islander peoples. Outreach into Indigenous communities appeared most successful when conducted by dedicated liaison officers or Indigenous people. In some cases, they even go to patients’ homes to provide services.
And we’ve been known to put Implanons in people’s living rooms and things like that. So it’s about taking service to these people rather than them coming to us some of the time. Which is a really important aspect of the work that we do. (Service 8, regional sexual health clinic)
Outreach to youth mostly involved sexual health education rather than testing itself, with most clinics encouraging youth to visit their service. However, only a few services provided testing at the outreach site itself. At one regionally based service, a doctor attended schools once a week to provide STI testing. Another service provided STI testing at boarding schools, which yielded a significant number of positive results.
Numerous participants reported using outreach to increase access for sex workers, with most finding it to be highly successful. One service, however, found themselves pulling away from this strategy as a result of feedback suggesting it was not a service appreciated by everyone.
We’ve been told by [a community base peer organisation] that outreach into sex worker premises is not actually appreciated by everyone. And that in many ways, workers would rather do that in their own time. So, we’ve pulled back quite a bit from that. (Service 10, regional community health clinic)
Several participants spoke of offering STI testing at events directed at, and places frequented by, priority populations, including music festivals, sporting clubs, hostels and universities. Some viewed this strategy as ineffective, as although popular, it yielded very few positive tests. In contrast, others saw merit in the promotion it offered and felt it was one of the most successful strategies they employed.
They didn’t get a particularly high rate of positive tests but it was all about demystifying sexual health screening and encouraging people to talk about sexual health. (Service 10, regional community health clinic)
Peer testing
Two services had peer-led testing clinics aimed at gbMSM and sex workers, and both found it to be successful. One had their peers run a clinic and go into the community to provide sexual health education and vaccinations. The other believed a peer service dedicated to the Aboriginal and/or Torres Strait Islander population would be greatly beneficial, and if funding permitted, they would like to implement it.
Service is run by people living with HIV … workers went out to the local sauna and offered free Hepatitis A and B vaccination and discussed HIV testing as well. So we do use our community education as an opportunity to invite people in. (Service 15, metropolitan sexual health clinic)
Other health services
Participants found that offering more than HIV/STI testing was appealing to patients. Various additional services were discussed, including needle and syringe exchange, an in-house psychologist and clinics focusing on transgender health. A few services already offered these options; however, many highlighted they were hoping to implement them in the future.
So being able to offer a one-stop-shop for a lot of those things. For some patients, that breaks down a lot of barriers… the doctor that they’re seeing and the practice that they’re going to is familiar. (Service 16, metropolitan GP clinic)
Routine testing in the emergency department
One participant discussed their success in opportunistically screening patients in emergency departments (ED) after noting there was a high rate of syphilis within the Aboriginal and/or Torres Strait Islander population compared to the general population. The service added syphilis serology to blood specimens taken from Aboriginal and/or Torres Strait Islander patients, aged 15–34 years, who had not tested in the last month and for people who injected drugs. If patients tested positive for syphilis, HIV testing was then subsequently added. Results and treatment were followed up by dedicated nursing staff. This process was considered as routine testing and did not require individual consent. Before its introduction, this was discussed with the ethics committee, relevant community organisations and Aboriginal health liaison officers. However, a barrier to this strategy was only approximately 25% of Aboriginal and/or Torres Strait Islander patients who presented to the ED required venepuncture, limiting the benefits of add-on testing.
The future is primary care
Most highlighted that although the strategies discussed were important, training GPs to provide similar services would make the biggest difference. A few services described training programs and learning modules they ran for GPs about testing and treating STIs, and prescribing pre-exposure prophylaxis (PrEP).
…that’s the sort of big picture strategy you need to be sustained in primary care to make a dent in the STI rate. (Service 1, metropolitan sexual health clinic)
One participant referred to the ‘Review of Sexual Health Clinical Services in Victoria’ conducted in 2019,8 which recommended a ‘hub and spoke model’ with sexual health centres working as the specialist hub and supporting GPs to provide basic services. Another participant discussed the need to engage clinicians about approaching sexual health in general.
… that’s the biggest barrier, I think. Healthcare workers not feeling comfortable talking about sex. (Service 10, regional community health clinic)
Discussion
This study provided an overview of strategies used by Australian sexual health services to increase accessibility to HIV/STI testing and management, with a focus on priority populations. It explored the views and experiences of a diverse range of sexual health providers across Australia, including sexual health clinics, hospital-based clinics and primary care clinics, covering a variety of locations. We add to the limited literature focused on optimising service delivery to specific priority populations, particularly gbMSM and young people, whereby studies have sampled the population rather than service providers.9–11
When focusing on expanding current models, overall, clinics felt the most successful strategies were programs tailored specifically to priority populations; for example, express clinics. A study conducted in Toronto, Ontario, which surveyed healthcare providers’ opinions about strategies to improve STI testing among gbMSM found express or fast-track testing services were viewed as most likely to improve testing, with 89% of providers (n = 95) identifying it as a useful strategy to implement in their service.9 Interestingly, most study participants did not believe POCT was beneficial for the patients within their clinics, despite previous literature suggesting it to be an effective strategy to increase testing.12 However, they did note it may be effective for outreach and peer-testing. This has been previously reviewed in proof-of-concept studies, which surveyed the experiences of MSM who used the service, and in one study that also interviewed peer testers.10,11 These studies found that POCT appealed to MSM who would not otherwise be tested, supporting our research findings. Overall, the strategies described by clinicians are thought to have been successful at increasing testing for numerous priority populations. However, existing literature primarily focuses on youth and MSM. Further research focused on the use of express clinics and POCT for other priority populations would be beneficial in evaluating the most effective implementation of these strategies.
Service providers described new approaches to fill the gaps of traditional service delivery. Most clinics utilised some form of outreach and found it successful. This is supported by a systemic review of chlamydia and gonorrhoea screening programs in outreach settings, which found that although they tested relatively low numbers, there were high yields of infections.13 However, one service did pull back on outreach in response to patient feedback. This highlights the importance of flexibility in service provision and the need to mould services to suit the communities they cater to. Furthermore, in our study, the clinics had varied opinions about self- and online testing. Although not utilised by most services, the consensus was that self- and online testing offers great potential and is a service model that most clinics are keen to explore. This finding is consistent with studies evaluating self-testing for MSM and youth that found it effective in increasing testing; however, there are limited data for other priority populations.14,15 The importance of education among health practitioners and increasing services within general practice were also key points raised. There was consensus in our study that service delivery is most efficient when based in primary care, with sexual health services focusing their energy on priority populations. Given the number of GPs vastly outnumber staffing in public sexual health services, the potential capacity for expanding sexual health service delivery through primary care is immense.
The strength of this study is that, to our knowledge, it is the first to explore the views and experiences of key informants working in a range of Australian sexual health services to discuss the strategies they used to improve testing among priority populations. However, there were some limitations. First, although a diverse range of services was included, in using a qualitative methodology, the study aimed to understand the range of strategies used rather than generalisable data. Further studies are required to determine if the views and experiences of clinics in this study represent the broader population of service providers in Australia. Second, there was limited discussion to reach other priority populations such as CALD, those in custodial settings, travellers and mobile workers. Third, we conducted these interviews when COVID-19 restrictions affected different parts of the country in varying ways; therefore, COVID-19-related restrictions may have impacted participants’ views and experiences.
Conclusion
Different populations require different service configurations and multiple access points to account for their varying needs and preferences. Australian sexual health services have expanded traditional service models and implemented new approaches to optimise service delivery; however, there are constraints related to the service location, funding, resources and skillset of care providers. It is important to remain adaptable to new strategies, such as self-testing or online sexual health services, and provide patient-centred care.
Supplementary material
Supplementary material is available online.
Data availability
All relevant data have been published in the manuscript or in the supplementary material. Further details can be obtained by writing to the corresponding author.
Conflicts of interest
JJO is the Special Issue Editor of Sexual Health and CKF is the Editor of Sexual Health, but both were blinded from the peer-review process for this paper. All other authors declare no conflicts of interest.
Declaration of funding
JJO and EPFC are supported by the Australian National Health and Medical Research Council (NHMRC) Emerging Leadership Investigator Grant (GNT1193955 and GNT1172873, respectively). CKF is supported by an Australian NHMRC Leadership Investigator Grant (GNT1172900).
Author contributions
JO, TP and VK designed the project. VK interviewed the participants. CF, MC, JB, RF and EC contributed by providing advice throughout the project. VK wrote the manuscript and all authors critically revised the manuscript and approved the final version for publication.
References
[1] Hengel B, Guy R, Garton L, Ward J, Rumbold A, Taylor-Thomson D, et al. Barriers and facilitators of sexually transmissible infection testing in remote Australian Aboriginal communities: results from the Sexually Transmitted Infections in Remote Communities, Improved and Enhanced Primary Health Care (STRIVE) Study. Sex Health 2015; 12 4–12.| Barriers and facilitators of sexually transmissible infection testing in remote Australian Aboriginal communities: results from the Sexually Transmitted Infections in Remote Communities, Improved and Enhanced Primary Health Care (STRIVE) Study.Crossref | GoogleScholarGoogle Scholar |
[2] Denison HJ, Bromhead C, Grainger R, Dennison EM, Jutel A. Barriers to sexually transmitted infection testing in New Zealand: a qualitative study. Aust N Z J Public Health 2017; 41 432–7.
| Barriers to sexually transmitted infection testing in New Zealand: a qualitative study.Crossref | GoogleScholarGoogle Scholar |
[3] Footman A, Dagama D, Smith CH, Van Der Pol B. A systematic review of new approaches to sexually transmitted infection screening framed in the capability, opportunity, motivation, and behavior model of implementation science. Sex Transm Dis 2021; 48 S58–65.
| A systematic review of new approaches to sexually transmitted infection screening framed in the capability, opportunity, motivation, and behavior model of implementation science.Crossref | GoogleScholarGoogle Scholar |
[4] Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care 2007; 19 349–57.
| Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups.Crossref | GoogleScholarGoogle Scholar |
[5] Sandelowski M. Whatever happened to qualitative description? Res Nurs Health 2000; 23 334–40.
| Whatever happened to qualitative description?Crossref | GoogleScholarGoogle Scholar |
[6] Neergaard MA, Olesen F, Andersen RS, Sondergaard J. Qualitative description – the poor cousin of health research? BMC Med Res Methodol 2009; 9 52
| Qualitative description – the poor cousin of health research?Crossref | GoogleScholarGoogle Scholar |
[7] Rampin R, Rampin V. Taguette: open-source qualitative data analysis. J Open Source Software 2021; 6 3522
| Taguette: open-source qualitative data analysis.Crossref | GoogleScholarGoogle Scholar |
[8] Poljski C, Atkin L, Williams H. Review of sexual health clinical services in Victoria. Family Planning Victoria; 2019.
[9] Rana J, Guiang CB, Lisk R, Shahin R, Brunetta J, Mitterni L, et al. Survey of health care providers’ practices and opinions regarding bacterial sexually transmitted infection testing among gay, bisexual, and other men who have sex with men. Sex Transm Dis 2021; 48 94–102.
| Survey of health care providers’ practices and opinions regarding bacterial sexually transmitted infection testing among gay, bisexual, and other men who have sex with men.Crossref | GoogleScholarGoogle Scholar |
[10] Mullens AB, Duyker J, Brownlow C, Lemoire J, Daken K, Gow J. Point-of-care testing (POCT) for HIV/STI targeting MSM in regional Australia at community ‘beat’ locations. BMC Health Serv Res 2019; 19 93
| Point-of-care testing (POCT) for HIV/STI targeting MSM in regional Australia at community ‘beat’ locations.Crossref | GoogleScholarGoogle Scholar |
[11] Mullens AB, Daken K, Lemoire J, Brownlow C, Driver G, Gow J. HIV point of care testing (PoCT) at late-night sex on premises venues (SOPV) for gay and bisexual men and other men who have sex with men (GBMSM): a mixed methods analysis. AIDS Behav 2020; 24 450–66.
| HIV point of care testing (PoCT) at late-night sex on premises venues (SOPV) for gay and bisexual men and other men who have sex with men (GBMSM): a mixed methods analysis.Crossref | GoogleScholarGoogle Scholar |
[12] Turner SD, Anderson K, Slater M, Quigley L, Dyck M, Guiang CB. Rapid point-of-care HIV testing in youth: a systematic review. J Adolesc Health 2013; 53 683–91.
| Rapid point-of-care HIV testing in youth: a systematic review.Crossref | GoogleScholarGoogle Scholar |
[13] Hengel B, Jamil MS, Mein JK, Maher L, Kaldor JM, Guy RJ. Outreach for chlamydia and gonorrhoea screening: a systematic review of strategies and outcomes. BMC Public Health 2013; 13 1040
| Outreach for chlamydia and gonorrhoea screening: a systematic review of strategies and outcomes.Crossref | GoogleScholarGoogle Scholar |
[14] Katz DA, Golden MR, Hughes JP, Farquhar C, Stekler JD. HIV self-testing increases HIV testing frequency in high-risk men who have sex with men: a randomized controlled trial. J Acquir Immune Defic Syndr 2018; 78 505–12.
| HIV self-testing increases HIV testing frequency in high-risk men who have sex with men: a randomized controlled trial.Crossref | GoogleScholarGoogle Scholar |
[15] Habel MA, Brookmeyer KA, Oliver-Veronesi R, Haffner MM. Creating innovative sexually transmitted infection testing options for university students: the impact of an STI self-testing program. Sex Transm Dis 2018; 45 272–7.
| Creating innovative sexually transmitted infection testing options for university students: the impact of an STI self-testing program.Crossref | GoogleScholarGoogle Scholar |
§ Joint senior authors.


