Is the Counterweight Program a feasible and acceptable option for structured weight management delivered by practice nurses in Australia? A mixed-methods study
Jodi Gray A B D , Elizabeth A. Hoon A , Hossein Haji Ali Afzali A , Catherine Spooner B C , Mark F. Harris B C and Jonathan Karnon A BA School of Public Health, University of Adelaide, Level 7, 178 North Terrace, Adelaide, SA 5005, Australia.
B Centre for Obesity Management and Prevention Research Excellence in Primary Health Care (COMPaRE-PHC), c/o CPHCE, University of NSW, Level 3, AGSM Building, Sydney, NSW 2052, Australia.
C Centre for Primary Health Care and Equity (CPHCE), University of NSW, Level 3, AGSM Building, Sydney, NSW 2052, Australia.
D Corresponding author. Email: jodi.gray@adelaide.edu.au
Australian Journal of Primary Health 23(4) 348-363 https://doi.org/10.1071/PY16105
Submitted: 26 August 2016 Accepted: 5 February 2017 Published: 11 May 2017
Journal Compilation © La Trobe University 2017 Open Access CC BY-NC-ND
Abstract
Nurse-led weight management programs, like the Counterweight Program in the United Kingdom, may offer a way for Australian general practices to provide weight management support to adults who are overweight or obese. During Counterweight, nurses provide patients with six fortnightly education sessions and three follow-up sessions to support weight maintenance. This study examined the feasibility, acceptability and perceived value of the Counterweight Program in the Australian primary care setting using a mixed-methods approach. Six practice nurses, from three general practices, were trained and subsidised to deliver the program. Of the 65 patients enrolled, 75% (n = 49) completed the six education sessions. General practitioners and practice nurses reported that the training and resource materials were useful, the program fitted into general practices with minimal disruption and the additional workload was manageable. Patients reported that the program created a sense of accountability and provided a safe space to learn about weight management. Overall, Counterweight was perceived as feasible, acceptable and valuable by Australian practice staff and patients. The key challenge for future implementation will be identifying adequate and sustainable funding. An application to publically fund Counterweight under the Medicare Benefits Schedule would require stronger evidence of effectiveness and cost-effectiveness in Australia.
Additional keywords: general practice, obesity, overweight, primary care.
| What is known about the topic? |
• The Counterweight Program is an evidence-based, structured, practice nurse-led weight management program that has been successfully implemented in the United Kingdom. |
| What does this paper add? |
• The Counterweight Program was demonstrated to be a feasible, acceptable and valued option for weight management care in Australian general practice from the perspective of practice staff and patients. |
Introduction
Australia has one of the highest rates of overweight and obesity (63%) among developed nations (Australian Institute of Health and Welfare 2014). Overweight and obesity are associated with an increased risk of a range of chronic conditions (National Health and Medical Research Council 2013) and place a substantial burden on the Australian healthcare system (Colagiuri et al. 2010). There is a need to identify effective obesity management interventions. Allied health professionals, specialist physicians and bariatric surgeons all have a role to play in obesity management. However, given its prevalence, less intensive, intermediate-level services are also needed to reduce the potentially overwhelming demand on specialist providers. In the United Kingdom (UK), where the commissioning of health services is well established, guidelines for the commissioning of lifestyle-based weight management services recommend programs that achieve a 60% completion rate, where at least 30% of participants achieve a weight loss of 5% or more (National Institute for Health and Care Excellence 2014).
The regularity of general practice attendance by Australian adults means that the primary care team is well placed to identify and manage obesity (Department of Health 2014). For the patient, general practice provides a reputable, convenient, familiar and accessible setting with the opportunity for long-term follow up and support. There is evidence that nurse-led programs are effective in providing risk assessment, patient education, counselling and obesity management in primary care (Counterweight Project Team 2008, 2012; Wood et al. 2008; Sargent et al. 2012; Karnon et al. 2013) and that patients report high levels of satisfaction with nurses providing chronic disease management (Halcomb et al. 2015). However, international evidence suggests that the perceived self-efficacy and legitimacy of GPs and practice nurses in providing weight management care is impeded by a lack of obesity-specific training (Nolan et al. 2012; Henderson 2015).
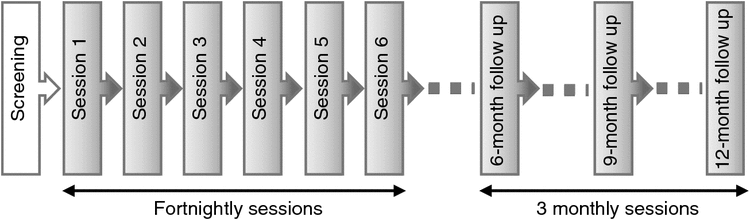
The Counterweight Program was launched in the UK in 2000. It provides a structured, evidence-based model for managing obesity in adults that can be delivered by practice nurses as part of routine clinical care (Counterweight Project Team 2008, 2012). In the program, practice nurses are trained and supported to deliver weight management care to their patients. Prior to patient enrolment, practice nurses and patients discuss the program’s aims and requirements, and consider the patients’ readiness to make weight-related lifestyle changes using Prochaska and DiClemente’s Stage of Change model (Prochaska et al. 1992). During the program, patients receive six fortnightly education sessions on healthy lifestyle and behaviour modification techniques. Topics include: healthy eating, food labelling, alcohol, eating habits, emotional drivers, physical activity, recovering from short-term lapses and long-term weight maintenance. Follow-up sessions are provided at 6, 9 and 12 months to support weight-loss maintenance (Fig. 1).
Australian primary care is predominantly funded by fee-for-service payments provided under the Medicare Benefits Schedule (MBS), which is part of the national public health insurance scheme. Prior to receiving funding under the MBS, new services require careful evaluation of their costs and benefits. However, before the significant investment of time and resources required to establish the cost-effectiveness of Counterweight in Australia, the program’s transferability needed to be explored. This paper reports on a mixed-methods study to explore the feasibility, acceptability and perceived value of the Counterweight Program to Australian practice nurses, GPs, practice managers and patients.
Methods
Setting
The study was conducted from September 2014 to September 2015 in Adelaide, South Australia. Qualitative and quantitative methods were used to evaluate the Counterweight Program and its processes (Fig. 2). In particular, the study examined: whether the program could be implemented in Australian general practice given existing activities and constraints, and the financial reimbursements required to support program delivery (feasibility); whether the aims, content and delivery methods of the intervention were perceived to be appropriate (acceptability); and whether the program was perceived as useful, important and offered a means to address an unmet need (perceived value).
The Northern Health Network (NHN) and their predecessor, the Northern Adelaide Medicare Local (NAML), collaborated on the project. Ethical approval was obtained from the Human Research Ethics Committee at the University of Adelaide.
The feasibility study had a limited time frame and budget. It was calculated that three practices and 15–25 patients per practice were the maximum number that could be recruited and funded in the time available, and would be sufficient to provide insight into the feasibility, acceptability and perceived value of the program. General practices were recruited by a short presentation at a NHN education event for GPs and practice nurses. Six practices expressed an interest, and three were selected to participate based on the eligibility criteria (use of electronic medical records and employment of at least two practice nurses) and the order in which they responded.
Practices received reimbursement for delivering the Counterweight Program and for nurses’ time during training sessions. Sessions one and two (expected duration 30 min) were reimbursed at a fee of A$25, whereas sessions three to six (expected duration 20 min) were reimbursed at a fee of A$20. Options for funding the delivery of the Counterweight Program were discussed with the NHN (to clarify the amount) and with participating providers (to ensure an appropriate payment method).
The NHN provided local support to the practices, assisting with patient recruitment and data collection, and supporting ongoing delivery of the program following the completion of the study.
Practice nurse training and resource materials
Practice nurses received 12 h of interactive, online training from an experienced, UK-based, Counterweight dietitian. The training sessions were scheduled early or late in the day (at 0730 or 1930 hours) to accommodate time zone differences between the UK-based trainer and Australian nurses. Practices received reimbursement for the time nurses participated in training. Ongoing support was provided, as needed, by email or telephone. After 6 months, the nurses received four additional hours of training to consolidate their knowledge.
Nurses were provided with a training manual that included information on the assessment, causes, health consequences and treatment of obesity. Patients received a folder with educational inserts added at each Counterweight session. To promote consistency and enhance the quality of intervention delivery, nurses used a quick reference guide alongside the patient resource folder to guide each Counterweight session.
Patient screening, recruitment and program delivery
Once trained, the nurses discussed the Counterweight Program with potentially eligible patients who attended the practice for routine care. GPs also referred potentially eligible patients to the nurse. To be eligible to enrol in the Counterweight Program, patients needed to have a body mass index (BMI) greater than 25 kg m–2 and be ready to make weight-related behaviour changes. Additionally, patients needed to be aged 18 years and over, have regularly attended the general practice (three visits in the previous 12 months), not have reduced their weight by 10 kg or more in the previous 12 months and be able to communicate in English (as resource materials were only available in English). Practices were asked to recruit 15–25 patients into the study, which was determined to be sufficient to assess the feasibility of the recruitment processes, indicate program completion rates and inform the planned qualitative analyses.
Nurses then delivered the six fortnightly education sessions and the follow-up appointments to the enrolled patients.
Quantitative data collection and analysis
During enrolment, patients provided consent for routinely collected data recorded in their general practice medical records to be extracted by the research team. Demographic characteristics, comorbidities, Counterweight session attendance and measurements of height and weight were extracted. Baseline characteristics and program completion rates were calculated using Stata, ver. 14.1 (StataCorp, College Station, TX, USA).
Qualitative data collection and analysis
To explore the program’s feasibility, acceptability and perceived value, in-depth, semi-structured interviews were conducted with practice staff and patients between May and September 2015.
All practice nurses delivering the program, all practice managers and a sample of GPs from participating practices were invited to be interviewed. Practice nurses and managers were asked to suggest GPs with a range of engagement and attitudes towards the program (both positive and negative) for interview. Interviews were conducted either by telephone or face-to-face in a private room at the practice. Reimbursement was offered to offset the time away from professional obligations (A$40 for practice nurses and managers; A$75 for GPs).
Patients in the feasibility study indicated on their consent form if they were willing to be contacted about further research on the program. Willing patients were invited to be interviewed by a letter with a follow-up telephone call. The invitation was issued a minimum of 3 months after program enrolment. Purposive sampling was used to recruit 12–20 patients across all three general practices, with a range of ages, genders and number of Counterweight sessions attended (e.g. complete attendance at the initial six sessions or early program disengagement). Depending on the patients’ preference, interviews were conducted by telephone or face-to-face in a private room at the offices of the NHN. During the interviews, patients were asked about their past experiences of weight loss and weight gain, and their experience of the Counterweight Program. Patient interviewees were offered A$15 to offset travel and time costs.
All interviews were conducted by J. Gray (see Appendix 1 for interview guides). They were audio recorded and transcribed by a professional service. J. Gray reviewed transcripts and recordings to ensure accuracy of the transcript. Under a pragmatic epistemology, the analysis focussed on the explicit, stated meaning of the data. Thematic analysis (Braun and Clarke 2006) was used to develop themes from the data. NVivo 10 for Windows (QSR International Pty Ltd, Melbourne, Vic., Australia) was used for data management. J. Gray undertook the initial coding of all transcripts. E. A. Hoon reviewed and coded selected transcripts. Regular discussions between J. Gray and E. A. Hoon explored, challenged and redefined the emerging themes. Feedback from the broader research team clarified the salience and contextualised the themes.
Results
Participant characteristics
Three general practices participated in the study. Two practices had more than five GPs and were located in metropolitan regions of low socioeconomic status, and one practice had a single GP and was located in a non-metropolitan region of medium socioeconomic status. Two nurses from each practice were trained to deliver Counterweight. The nurses’ background in weight management varied. Some had very little experience or training, others had attended multiple lifestyle modification training programs or had been responsible for diabetic education within their practice.
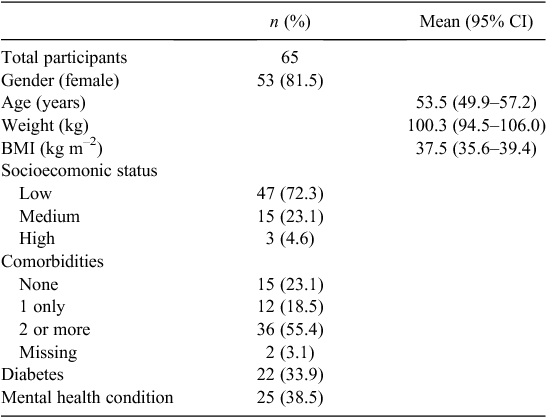
Across the three practices, 65 patients were enrolled within 3 months (Table 1). Patients were predominantly female (82%), lived in an area of low socioeconomic status (72%) and 55% had two or more comorbidities. The mean BMI of enrolled patients was 38 kg m–2 (s.d.: 7.6, range: 25–58). The initial six Counterweight sessions were completed by 75% of patients (n = 49), with patients taking between 68 and 197 days to reach session six (median: 83 days).
|
All six practice nurses, all three practice managers, four GPs and 18 patients agreed to be interviewed about their experience of the program. Thematic saturation was reached in interviews with practice nurses, practice managers and patients, but was unable to be reached in interviews with GPs. The spread of patient interviewees across practices and nurses reflected the spread for all enrolled patients. On average, patient interviews were conducted 2.7 months (s.d.: 1.8) from the last Counterweight session attended (range 12 days to 7 months). Similar to the characteristics of all enrolled patients, interviewees were predominately female (83%), had a mean age of 55 years (s.d. 17.2) and most lived in an area of low socioeconomic status (78%). Compared to all those enrolled, a higher proportion of interviewees had completed the six sessions (89% compared to 75%) and lost 5% or more of their baseline weight (44% compared to 28%).
Feasibility
The online training, with its interactive classroom environment, was well received by the nurses. Some nurses experienced technical issues but were able to resolve these with the support of the trainers. The convenience of the online training was emphasised, particularly by nurses who would normally need to travel long distances to attend training events. The timing of the training sessions (early or late in the day) was perceived as manageable but ‘not ideal’ (Table 2, Quotation 1); however, scheduling training during work hours would also have been problematic for the nurses.

|
Practice staff reported that Counterweight fitted into the practice with minimal disruption (Table 2, Quotation 2). Both nurses and practice managers felt that the additional workload for the nurses was manageable, provided the appointments were distributed across the week and not clustered on a single day. GPs reported the program did not affect their workload (Table 2, Quotation 3).
Although some patients found it easy to regularly attend the fortnightly appointments, others required additional flexibility due to work and other commitments. This flexibility was facilitated by the one-to-one delivery of the program and the relatively small number of appointments required; that is, nine appointments over 12 months, compared to weekly sessions required by other weight management programs (Table 2, Quotation 4).
Practice staff indicated that the biggest challenge to continuing to deliver the Counterweight Program was finding adequate and sustained funding. It was suggested that asking patients to pay could create a barrier to engaging them (Table 2, Quotation 5), or alternatively, it might help identify those who are strongly motivated. Practices indicated they would require some reimbursement for session delivery to make Counterweight sustainable and to be able to allocate significant nurse time to the program (Table 2, Quotations 6, 7).
Acceptability
The content of the program and the resource materials provided for nurses and patients were considered useful and appropriate (Table 2, Quotation 8), requiring only minor changes to adapt the content to the Australian context (e.g. reference to Australian rather than UK guidelines for dietary intake, physical activity and alcohol consumption).
Patients described how the Counterweight Program created a safe space for them to explore their weight, learn about weight management and to make changes towards a healthier lifestyle. The broad definitions of success, the non-judgemental and non-prescriptive approach, and the delivery of the program in their general practice helped to create this safe space.
The program was seen as being non-prescriptive and ‘not a diet’ (Table 2, Quotation 9). Patients appreciated being offered information, guidelines and suggestions on how to shift towards a healthier lifestyle. In particular, they valued being able to work with the nurse to problem-solve challenges they were experiencing rather than being told what they should or should not do (Table 2, Quotation 10). The non-judgemental approach of the nurses meant that patients felt they could openly discuss difficulties and seek support during challenging times, including when they plateaued, put on weight or ‘fell off the wagon’ (Table 2, Quotation 11). Some patients described the sense of having a champion: someone who was on their side, cheering them on and recognising when they achieved something. This was supported by the broad definitions of success used by the program – emphasising the value of small weight losses or keeping weight stable (not gaining), setting realistic goals and focussing on creating a healthier lifestyle rather than weight loss alone.
Patients considered the practice to be their regular general practice before enrolment in Counterweight, thus they had an established relationship with the practice, even if they had not met the practice nurse. Regardless of whether they knew the nurse before starting the program, patients described how having the program delivered in general practice made it more comfortable, trustworthy, accessible and convenient for them (Table 2, Quotations 12–14). They trusted the education provided because it was recommended and delivered by the general practice staff. For most patients, having the program in general practice positioned it as part of their broader medical care, which had already been entrusted to the general practice. Combined with the non-judgemental support from the nurses, the delivery through general practice reinforced the sense that if a patient needed additional help they could always ask for it.
Perceived value
Practice staff recognised that many of their patients had a high BMI and could benefit from a program like Counterweight (Table 2, Quotation 15). Both GPs and nurses recognised that GPs often had limited time within routine appointments to provide weight management advice to patients (Table 2, Quotations 16, 17). Training nurses to deliver Counterweight allowed the practice to offer a structured weight-management program, without placing additional workload on the GPs (Table 2, Quotation 18). One GP pointed to the ‘fine line between criticism and advice’, suggesting that offering a coordinated program helped patients remain receptive, rather than feeling lectured by the GP.
GPs were pleased with the feedback they received from patients and the results they saw. All GPs were keen to see the program become part of standard care; however, they were clear that further evidence of effectiveness was needed, particularly over the longer term (Table 2, Quotations 19–21). All nurses expressed an interest in continuing to deliver the program.
Many nurses reported that the extended, one-to-one time with patients during Counterweight sessions allowed them to become aware of deeper issues that were affecting the patients’ lives, health and capacity to manage their weight. These issues could be raised with the GP and the patients referred for further support (Table 2, Quotation 22).
Patients described how the regular, fortnightly visits created a sense of accountability and helped to build and sustain their motivation for behaviour change (Table 2, Quotations 23, 24). They emphasised that the program was not a ‘quick fix’ but provided information and strategies that empowered them to shift towards a healthier lifestyle and manage their weight (Table 2, Quotation 25). Some patients spoke of encouraging friends and family members to enrol in the program, whereas others spoke of informally sharing the knowledge they had gained.
Challenges
For some patients, moving from the fortnightly visits to the 3-monthly follow ups created a challenge (Table 2, Quotations 26, 27). They keenly felt the reduced support and found it harder to sustain their motivation and recover from lapses. Having a very brief, monthly check-in assisted with this transition. In contrast, other patients felt this gap less acutely, and some described becoming accountable to themselves for achieving the goals they had set.
Some of the nurses questioned the usefulness of the screening questions. They recognised that some patients could give positive answers and have the best of intentions, but once enrolled were not able to engage with or complete the program (Table 2, Quotation 28). For some of these patients, the nurses recognised that ‘real life gets in the way’ leading to program drop-out, but there was also a concern that others might be seeking a ‘quick fix’ or lacking sufficient motivation.
Nurses identified that it was important to allocate time to maintaining a recall register and following up with patients who missed Counterweight appointments (Table 2, Quotation 29). Follow-up telephone calls allowed nurses to talk with patients who may have ‘drifted’ and to help ‘get them back on track’ if the patient was interested in doing so.
Although many of the patients who left the program early were not willing to talk with us, those who did pointed to conflicting commitments; for example, increased hours at work, a changed work schedule or the need to care for family members (Table 2, Quotation 30). These patients expressed a desire to return to the program but were unsure if it was still available to them (which may be why they were willing to be interviewed). One patient described how telephone calls from the nurse to check if she was coming back helped her return after a lengthy gap.
Discussion
The reported study demonstrated the feasibility, acceptability and perceived value of the Counterweight Program for nurse-led management of obesity in an Australian primary healthcare setting. Participating practices were able to enrol patients, and program completion was high with 75% of patients completing the initial 3 months. This is compared to a 55% completion rate in the UK evaluation of Counterweight (Counterweight Project Team 2008) and the 60% completion rate recommended in the National Institute for Health and Care Excellence (NICE) commissioning guidelines (National Institute for Health and Care Excellence 2014). The study was designed to evaluate the feasibility, acceptability and perceived value of the program. The study did not include a sample size calculation or a control group, both of which would be required to generate evidence on weight change outcomes and determine effectiveness. However, it is reassuring to note that 28% of all enrolled patients (39% of completers) reduced their weight by 5% or more at 3 months, which is comparable with those participating in Counterweight in the UK where 14% (95% CI: 12.5–16.2) of enrolees lost 5% or more at 3 months (26% of completers, 95% CI: 23.1–29.3) (Counterweight Project Team 2008).
The qualitative evaluation found that the Counterweight Program provided nurses with relevant training, support and materials, and fitted into general practices with minimal disruption. By providing obesity-specific training, the program enhanced the perceived self-efficacy and legitimacy of nurses and removed a barrier to their involvement in providing weight management care (Nolan et al. 2012; Henderson 2015).
Patients saw the program as a non-judgemental, non-prescriptive way to learn about weight management in an environment that was convenient, accessible and trusted. Given the stigma and discrimination often experienced by patients who are overweight or obese (Puhl and Heuer 2009; Malterud and Ulriksen 2011; Spahlholz et al. 2016), the finding that the program created a safe space for patients to explore weight-related issues with their healthcare provider is an important one.
The perceived value of the program went beyond weight management outcomes. The additional time spent with patients during program delivery enabled nurses to identify and seek to address deeper, previously unrecognised issues that were affecting patients’ health and wellbeing.
Several challenges were identified by the study. These challenges did not, however, negate the feasibility of the program. Rather, the issues raised tended to be typical issues for any weight management program; for example, patient motivation and sustained attendance (Moroshko et al. 2011).
Limitations of the study included the enrolment of only three general practices, and that the practices were self-selecting. However, self-selection would also be expected if the program was rolled out more broadly. We were unable to reach thematic saturation in interviews with GPs; however, common themes still arose and have been discussed. The patients interviewed may have been more likely to report a positive experience of Counterweight compared to all enrolled patients, given their high completion rates and the higher proportion achieving a weight loss of 5% or more from baseline. However, the interviewees had experienced a range of weight change outcomes (from no loss to significant loss) and a range of perspectives were obtained.
Current options for weight management support in Australian primary care include the provision of care by general practice staff, or referral to allied health providers, community programs or telephone counselling. Under existing MBS funding, patients with chronic conditions (including patients with obesity who have co-morbidities or multiple risk factors) are eligible for a GP Management Plan (GPMP), which includes five subsidised allied health visits. However, these five visits are often insufficient to meet all the care needs of patients and to provide care consistent with best-practice guidelines; for example, weight management guidelines produced by the Dietitians Association of Australia (Cant 2010). This is particularly the case for patients with obesity and complex comorbidities who require care across multiple allied health specialties.
The Healthy Eating Activity & Lifestyle (HEAL) Program was a community-based healthy lifestyle program funded until June 2013 under the Commonwealth’s Healthy Communities Initiative (HCI) (Hetherington et al. 2015). The program continued beyond the end of HCI funding; however, even with a low fee per participant, program enrolments fell from 1755 in 2012 to 320 in the first 6 months of 2014 (J. Borodzicz, pers. comm., 24 November 2014). The experience of the HEAL Program illustrates the need to plan for the long-term sustainability of new programs.
The Australian practice nurse workforce remains an underutilised resource (Hoare et al. 2012). Funding mechanisms have the power to direct and expand the nurse’s role; for example, under a GPMP, MBS service payments enable five visits to a practice nurse for chronic disease management (Halcomb et al. 2008; Pearce et al. 2011; McInnes et al. 2017). Additional service payments to promote practice nurse involvement in obesity management have been suggested (Afzali et al. 2014), as without adequate funding, practice nurse time is likely to be directed to other, more financially rewarded priorities (Nolan et al. 2012).
This study replicated potential MBS service payments to fund program delivery by practice nurses, which were acceptable to practices. Following completion of the study, some participating practices continued to deliver Counterweight using the five nurse visits funded under a GPMP. However, this has restricted patient eligibility and offers only limited session funding. It is likely to limit the wider uptake and sustainability of the program. An application to the Medical Services Advisory Committee (MSAC) to fund the Counterweight Program through new, more appropriate MBS item numbers would require stronger evidence on the effectiveness and cost-effectiveness of the program.
Conclusions and implications
General practice has a role to play in supporting patients who are overweight or obese, but there are currently no widely implemented weight management programs in general practice in Australia. The Counterweight Program had been implemented in the UK and may provide an effective and cost-effective option in Australia. This study has demonstrated that the Counterweight Program is feasible, acceptable and perceived as valuable by Australian general practice staff and patients. Funding limitations were identified as the biggest challenge to continued program delivery. The existing evidence may support limited investment in the program, but stronger evidence of effectiveness in Australia is required to enable MBS funding for widespread and sustainable program delivery.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Acknowledgements
We thank the participating practice staff and patients for their willingness to be involved and share their experiences. We also acknowledge the support of Veronica Hunter-Riviere (NHN), Hazel Ross and Anna Bell-Higgs (Counterweight Ltd UK). This research was a project of the Australian Primary Health Care Research Institute, which was supported by a grant from the Australian Government Department of Health. The information and opinions contained in it do not necessarily reflect the views or policy of the Australian Primary Health Care Research Institute or the Australian Government Department of Health.
References
Afzali HHA, Karnon J, Beilby J, Gray J, Holton C, Banham D (2014) Practice nurse involvement in general practice clinical care: policy and funding issues need resolution. Australian Health Review 38, 301–305.| Practice nurse involvement in general practice clinical care: policy and funding issues need resolution.Crossref | GoogleScholarGoogle Scholar |
Australian Bureau of Statistics (2013) Census of population and housing: Socio-Economic Indexes for Areas (SEIFA), Australia, 2011. (ABS: Canberra, ACT, Australia) Available at http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2033.0.55.0012011?OpenDocument [Verified 1 February 2017].
Australian Institute of Health and Welfare (2014) ‘Australia’s Health 2014.’ (AIHW: Canberra, ACT, Australia)
Braun V, Clarke V (2006) Using thematic analysis in psychology. Qualitative Research in Psychology 3, 77–101.
| Using thematic analysis in psychology.Crossref | GoogleScholarGoogle Scholar |
Cant R (2010) Today’s profession: views and practices of private practice dietitians re Medicare Chronic Disease Management program. Nutrition & Dietetics: the Journal of the Dietitians Association of Australia 67, 77–83.
| Today’s profession: views and practices of private practice dietitians re Medicare Chronic Disease Management program.Crossref | GoogleScholarGoogle Scholar |
Colagiuri S, Lee CM, Colagiuri R, Magliano D, Shaw JE, Zimmet PZ, Caterson ID (2010) The cost of overweight and obesity in Australia. The Medical Journal of Australia 192, 260–264.
Counterweight Project Team (2008) Evaluation of the Counterweight Programme for obesity management in primary care: a starting point for continuous improvement. The British Journal of General Practice 58, 548–554.
| Evaluation of the Counterweight Programme for obesity management in primary care: a starting point for continuous improvement.Crossref | GoogleScholarGoogle Scholar |
Counterweight Project Team (2012) The implementation of the Counterweight Programme in Scotland, UK. Family Practice 29, i139–i144.
| The implementation of the Counterweight Programme in Scotland, UK.Crossref | GoogleScholarGoogle Scholar |
Department of Health (2014) ‘Annual Medicare Statistics – Financial Year 2007–2008 to 2013–14.’ (Commonwealth of Australia: Canberra, ACT, Australia)
Halcomb EJ, Davidson PM, Salamonson Y, Ollerton R, Griffiths R (2008) Nurses in Australian general practice: implications for chronic disease management. Journal of Clinical Nursing 17, 6–15.
| Nurses in Australian general practice: implications for chronic disease management.Crossref | GoogleScholarGoogle Scholar |
Halcomb EJ, Salamonson Y, Cook A (2015) Satisfaction and comfort with nursing in Australian general practice. Collegian 22, 199–205.
| Satisfaction and comfort with nursing in Australian general practice.Crossref | GoogleScholarGoogle Scholar |
Henderson E (2015) Obesity in primary care: a qualitative synthesis of patient and practitioner perspectives on roles and responsibilities. The British Journal of General Practice 65, e240–e247.
| Obesity in primary care: a qualitative synthesis of patient and practitioner perspectives on roles and responsibilities.Crossref | GoogleScholarGoogle Scholar |
Hetherington SA, Borodzicz JA, Shing CM (2015) Assessing the real world effectiveness of the Healthy Eating Activity and Lifestyle (HEALTM) program. Health Promotion Journal of Australia 26, 93–98.
| Assessing the real world effectiveness of the Healthy Eating Activity and Lifestyle (HEALTM) program.Crossref | GoogleScholarGoogle Scholar |
Hoare KJ, Mills J, Francis K (2012) The role of Government policy in supporting nurse‐led care in general practice in the United Kingdom, New Zealand and Australia: an adapted realist review. Journal of Advanced Nursing 68, 963–980.
| The role of Government policy in supporting nurse‐led care in general practice in the United Kingdom, New Zealand and Australia: an adapted realist review.Crossref | GoogleScholarGoogle Scholar |
Karnon J, Afzali HHA, Gray J, Holton C, Banham D, Beilby J (2013) A risk adjusted cost‐effectiveness analysis of alternative models of nurse involvement in obesity management in primary care. Obesity 21, 472–479.
| A risk adjusted cost‐effectiveness analysis of alternative models of nurse involvement in obesity management in primary care.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3srlvFSmuw%3D%3D&md5=641543fb866e648ca4431c87f4c8f37cCAS |
Malterud K, Ulriksen K (2011) Obesity, stigma, and responsibility in health care: a synthesis of qualitative studies. International Journal of Qualitative Studies on Health and Well-being 6, 8404
| Obesity, stigma, and responsibility in health care: a synthesis of qualitative studies.Crossref | GoogleScholarGoogle Scholar |
McInnes S, Peters K, Bonney A, Halcomb E (2017) The influence of funding models on collaboration in Australian general practice. Australian Journal of Primary Health 23, 31–36.
| The influence of funding models on collaboration in Australian general practice.Crossref | GoogleScholarGoogle Scholar |
Moroshko I, Brennan L, O’Brien P (2011) Predictors of dropout in weight loss interventions: a systematic review of the literature. Obesity Reviews 12, 912–934.
| Predictors of dropout in weight loss interventions: a systematic review of the literature.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC3MbhslGrsw%3D%3D&md5=e0e683a2323e15f4be767f241ad4d341CAS |
National Health and Medical Research Council (2013) ‘Clinical practice guidelines for the management of overweight and obesity in adults, adolescents and children in Australia.’ (NHMRC: Melbourne, Vic., Australia)
National Institute for Health and Care Excellence (2014) Managing overweight and obesity in adults – lifestyle weight management services: NICE public health guidance 53. (NICE: London, UK) Available at www.nice.org.uk/guidance/ph53 [Verified 1 February 2017]
Nolan C, Deehan A, Wylie A, Jones R (2012) Practice nurses and obesity: professional and practice-based factors affecting role adequacy and role legitimacy. Primary Health Care Research and Development 13, 353–363.
| Practice nurses and obesity: professional and practice-based factors affecting role adequacy and role legitimacy.Crossref | GoogleScholarGoogle Scholar |
Pearce C, Phillips C, Hall S, Sibbald B, Porritt J, Yates R, Dwan K, Kljakovic M (2011) Following the funding trail: financing, nurses and teamwork in Australian general practice. BMC Health Services Research 11, 38
| Following the funding trail: financing, nurses and teamwork in Australian general practice.Crossref | GoogleScholarGoogle Scholar |
Prochaska JO, Diclemente CC, Norcross JC (1992) In search of how people change. The American Psychologist 47, 1102–1114.
| In search of how people change.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DyaK3s%2Fjs1OnsA%3D%3D&md5=4255e31aae6be521ece1cb7e9b9d926eCAS |
Puhl RM, Heuer CA (2009) The stigma of obesity: a review and update. Obesity (Silver Spring) 17, 941–964.
| The stigma of obesity: a review and update.Crossref | GoogleScholarGoogle Scholar |
Sargent GM, Forrest LE, Parker RM (2012) Nurse delivered lifestyle interventions in primary health care to treat chronic disease risk factors associated with obesity: a systematic review. Obesity Reviews 13, 1148–1171.
| Nurse delivered lifestyle interventions in primary health care to treat chronic disease risk factors associated with obesity: a systematic review.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC38bmsFOnsg%3D%3D&md5=031050c073d532fede054420e5b66829CAS |
Spahlholz J, Baer N, König H-H, Riedel-Heller S, Luck-Sikorski C (2016) Obesity and discrimination – a systematic review and meta-analysis of observational studies. Obesity Reviews 17, 43–55.
| Obesity and discrimination – a systematic review and meta-analysis of observational studies.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BC28vksVejug%3D%3D&md5=2d63de2edad93ea501001afc2c5c46ffCAS |
Wood DA, Kotseva K, Connolly S, Jennings C, Mead A, Jones J, Holden A, De Bacquer D, Collier T, De Backer G, Faergeman O (2008) Nurse-coordinated multidisciplinary family based cardiovascular disease prevention programme (EUROACTION) for patients with coronary heart disease and asymptomatic individuals at high risk of cardiovascular disease: a paired cluster-randomised controlled trial. Lancet 371, 1999–2012.
| Nurse-coordinated multidisciplinary family based cardiovascular disease prevention programme (EUROACTION) for patients with coronary heart disease and asymptomatic individuals at high risk of cardiovascular disease: a paired cluster-randomised controlled trial.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1czoslWktA%3D%3D&md5=1c79861100db815ccc7f4d093e2da606CAS |

|