Understanding health talk in an urban Aboriginal and Torres Strait Islander primary healthcare service: a cross-sectional study
Prabha Lakhan A F , Deborah Askew A B , Mark F. Harris C , Corey Kirk A D and Noel Hayman A EA Southern Queensland Centre of Excellence in Aboriginal and Torres Strait Islander Primary Health Care (Inala Indigenous Health Service), Metro South Health, PO Box 52, Inala, Qld 4077, Australia.
B Discipline of General Practice, Primary Care Clinical Unit, Faculty of Medicine, The University of Queensland, Level 8 Health Sciences Building, Building 16/910, Royal Brisbane & Women’s Hospital, Brisbane Qld 4029, Australia.
C Centre for Primary Health Care and Equity, University of New South Wales, Sydney, NSW 2052, Australia.
D Present address: Aboriginal Employment Strategy Ltd, Shop 5/12 Queen Street, Goodna, Qld 4300, Australia.
E Primary Care Clinical Unit, School of Clinical Medicine, The University of Queensland, Level 8 Health Sciences Building, Building 16/910, Royal Brisbane & Women’s Hospital, Brisbane, Qld 4029, Australia.
F Corresponding author. Email: prabha.lakhan@health.qld.gov.au
Australian Journal of Primary Health 23(4) 335-341 https://doi.org/10.1071/PY16162
Submitted: 30 November 2016 Accepted: 15 March 2017 Published: 9 June 2017
Journal Compilation © La Trobe University 2017 Open Access CC BY-NC-ND
Abstract
Health literacy is an important determinant of health status. This cross-sectional study aimed to describe the prevalence of adequate health literacy among Aboriginal and Torres Strait Islander patients or their carers including parents of sick children attending an urban primary healthcare clinic in Australia, and their experiences of communication with General Practitioners (GPs). A questionnaire, including questions from the Brief Health Literacy Screen (BHLS) and questions from the Consumer Assessment of Healthcare Providers and Systems (CAHPS): Communication with Provider, was administered to 427 participants. Descriptive statistics, Pearson’s Chi-Square test and logistic regression analysis were used to describe the prevalence and risk factors associated with health literacy and any associations between the CAHPS questions and health literacy. In total, 72% of participants had adequate health literacy. An age of ≥50 years was independently associated with inadequate health literacy, and completion of secondary or post-secondary schooling was protective. Communication questions that identified areas for improvement included less use of incomprehensible medical words and more frequent use of visual aids. The study provides useful information on health literacy among Aboriginal and Torres Strait Islander patients, or their carers, and their experiences of communication with GPs. Further population-based research is required to investigate the effect of health literacy on health outcomes of Aboriginal and Torres Strait Islander patients.
Additional keywords: communication, General Practitioner, health literacy.
| What is known about the topic? |
• The adequacy of health literacy and healthcare providers’ communication skills will influence patients’ abilities to critically appraise and use health information to manage their illness and subsequently their health outcomes. |
| What does this paper add? |
• General Practitioners can communicate effectively when providing health information to patients with inadequate health literacy by using interpersonal skills, visual aids and avoiding the use of medical terminology. |
Introduction
Health literacy is being recognised globally as an important determinant of health. There is a greater understanding of the complexity and multidimensional nature of the concept of health literacy, reflected in the extension of its definition from an individual’s ability to understand health information to include one’s ability to access, understand, critically appraise and apply the information when making health-related decisions, managing illness, communicating with healthcare providers and navigating an increasingly complex and modern healthcare system. Multidimensional models are beginning to highlight the complexity of the concept, incorporating its core components, the multitude of patient, healthcare provider and health system level factors affecting one’s health literacy, and the association between health literacy and health outcomes at the individual, population and broader healthcare system level (Paasche-Orlow and Wolf 2007; Sørensen et al. 2012). A systematic review conducted to investigate the association between health literacy and health outcomes, with most of the included studies investigating associations between functional literacy (numeracy and literacy) and health outcomes, reported that low health literacy was associated with poorer health outcomes, but the association between numeracy and health outcomes was inconclusive (Berkman et al. 2011).
Inequality in the health status of Aboriginal and Torres Strait Islander people compared to non-Indigenous Australians is widely acknowledged (Commonwealth of Australia 2016). Inadequate health literacy may contribute to the poorer health status of Aboriginal and Torres Strait Islander people. Information on health literacy among Aboriginal and Torres Strait Islander people is limited to a few studies identifying an association between inadequate dental health literacy and poorer dental health outcomes among Aboriginal Australians residing in rural South Australia (Jamieson et al. 2008; Parker and Jamieson 2010; Jamieson et al. 2013). Assessment of health literacy will provide some indication of the prevalence of adequate health literacy, increase health professionals’ awareness of the need to provide health information that is easily understood by patients and assist Indigenous Australians to better manage their illness.
General Practitioners (GPs) deliver primary health services in Australia (Harris 2016). Health literacy adequacy influences the quality of patient–healthcare provider interaction (Paasche-Orlow and Wolf 2007; Davies et al. 2014; Faruqi et al. 2015). Difficulties communicating with health practitioners are a major barrier to Aboriginal and Torres Strait Islander patients seeking health care (Lin et al. 2016). A simple screening tool to identify patients’ health literacy adequacy may help GPs adapt communication styles when providing health information (Chew et al. 2004; Paasche-Orlow and Wolf 2007; Davies et al. 2014).
The purpose of this study was to identify the prevalence of adequate health literacy among patients or their carers or parents of sick children (henceforth participants) attending an urban Aboriginal and Torres Strait Islander primary healthcare clinic, and their experiences of communication of health information by GPs.
Methods
This cross-sectional study was conducted at the Southern Queensland Centre of Excellence (CoE) in Aboriginal and Torres Strait Islander Primary Health Care Clinic from 4 May to 11 June 2015. The CoE is located at Inala, a suburb in Brisbane, Queensland, Australia. It aims to improve health outcomes for Aboriginal and Torres Strait Islander people through access to a range of primary and secondary healthcare services provided in a culturally appropriate environment (Hayman et al. 2014). The study included Aboriginal and Torres Strait Islander participants aged ≥18 years, including those visiting the Clinic for the first time. Patients who were acutely ill (such as those experiencing severe chest pain) or experiencing any cognitive impairment were not included.
Metro South Human Research Ethics Committee provided ethical approval for the study. An ‘op-out’ approach for obtaining consent was used (The National Health and Medical Research Council 2015). Verbal consent and completion of the survey questionnaire was deemed as providing consent. Participants were provided a written Participant Information Form, detailing the reasons for the study and maintenance of anonymity of participants and confidentiality of survey responses. Participants were informed of the voluntary nature of the study and their right to not participate or withdraw at any time without affecting the care provided at the Clinic in any way. The Inala Community Jury for Aboriginal and Torres Strait Islander Health Research (Bond et al. 2016) provided community support for the study. As a gesture of reciprocity, each participant was offered a pen inscribed with the CoE’s name and telephone number, and included in a healthy food hamper draw, drawn at the recruitment of every 25th participant.
Data collection and recruitment
A questionnaire comprising three sections was used to survey participants in the waiting room. The demographic section included the following variables: age, gender, highest level of education achieved, duration of attendance at the Clinic and attendance at the Clinic in the previous 12 months. The Brief Health Literacy Screen (BHLS) section included three questions that obtained information on the frequency of requiring assistance with reading health materials; experiencing problems learning about their medical condition because of difficulty reading health materials; and confidence in completing health forms. The BHLS is easily administered in clinical settings (Chew et al. 2008; Cawthon et al. 2014; Faruqi et al. 2015), with studies supporting its internal consistency, predictive ability and concurrent validity (Chew et al. 2008; Wallston et al. 2014). The third section comprised nine questions from the ‘Communication with Provider’ CAHPS (Health literacy program) survey tool, a component of the Consumer Assessment of Healthcare Providers and Systems (CAHPS) program. Participants rate the frequency of experiencing each of the following: difficulty understanding the doctor because of an accent or way English was spoken; not understanding medical words; doctor speaking too fast; doctor using different aids when explaining things; doctor ignoring information provided; being interrupted by the doctor when talking; doctor showing interest in questions and concerns; satisfaction with answers provided to questions; and being encouraged to ask questions or discuss concerns. The CAHPS health literacy questions are a validated measure for consumers to provide feedback on their experiences of communication with providers (Lake et al. 2005; Horowitz et al. 2012; Agency for Healthcare Research and Quality 2016; Shirk et al. 2016; Thiels et al. 2016). The BHLS questions and the CAHPS questions have not been validated for their use with Aboriginal and Torres Strait Islander people. Additional space following the nine CAHPS questions was provided for participants to provide written comments describing their communication experiences with GPs.
Two Research Officers (ROs) conducted the survey (P. Lakhan, C. Kirk) in the Clinic’s waiting room. Before approaching any potential participant, Administration Officers confirmed inclusion criteria or informed the ROs of reasons not to approach a participant such as family bereavement. All participants completed the demographic and BHLS questions. To minimise recall bias, participants who attended the Clinic at least once in the previous 12 months completed the CAHPS questions. Participants frequently requested the RO to read aloud each question and tick their chosen response on the questionnaire. The ROs checked each questionnaire for completion before participant’s departure from the Clinic. Age, gender and reason for refusal were recorded on a separate sheet if eligible participants declined participation.
Data analysis
Data were analysed using STATA (ver. 11; StataCorp, TX, USA). The five response options for BHLS questions were: never, occasionally, sometimes, often, always (first two questions); OR extremely, quite a bit, somewhat, a little bit, not at all (third question) and were allocated scores one to five respectively. Adequate health literacy was defined as a combined score of ≤10 for the three BHLS questions and ≤2 for the third question (confidence in completing medical forms). Inadequate health literacy was defined as either a combined score of >10 for all three questions or a score of ≥3 for the third item, if the combined score was ≤10. The inclusion of those with scores <3 was based on the higher sensitivity and comparable specificity of this question, as described in previous research (Chew et al. 2004; Collins et al. 2012). Each CAHPS question had four response options: ‘Never’, ‘Sometimes’, ‘Usually’, ‘Always’, scored from one to four respectively. Lower scores for the first six, and higher scores for the last three questions indicated a positive communication experience.
Descriptive statistics were used to describe the demographic characteristics, BHLS, health literacy and CAHPS scores. Pearson’s Chi-Square test, univariate and multivariate logistic regression analyses were used to investigate any associations between demographic factors, CAHPS questions and health literacy adequacy. Participants’ written comments describing communication experiences with GPs were analysed thematically.
Results
Sample
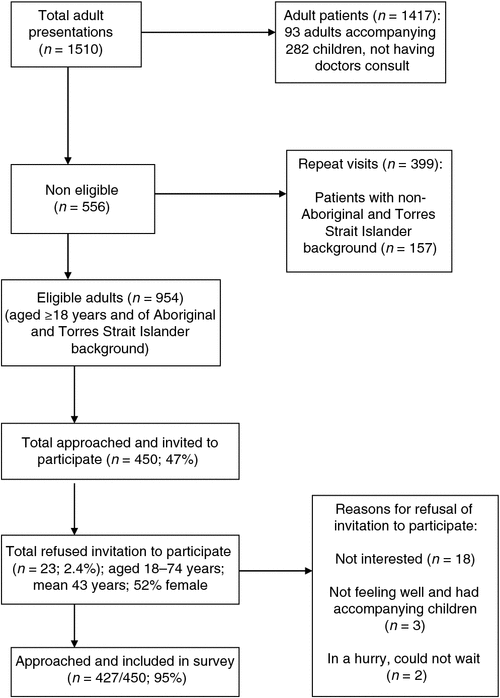
Of 954 potentially eligible participants, 450 were approached and 427 participated (95% response rate; Fig. 1).
|
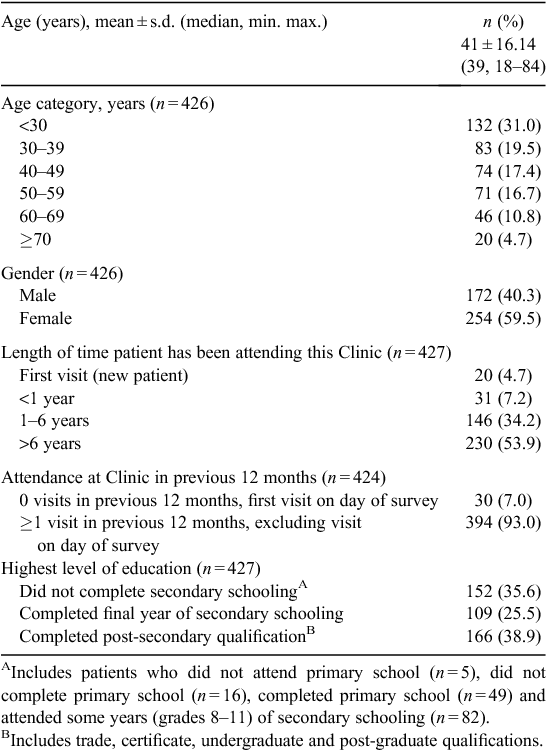
Table 1 describes the demographic characteristics of the sample. Participants were aged between 18 and 84 years (mean 41 years) and the majority (60%) were female. There was a significant association between age and highest level of education completed (P < 0.001), with 48% of participants aged ≥50 years completing secondary schooling or post-secondary qualifications compared with 72% of participants aged <50 years.
|
Brief Health Literacy Screen responses and scores
A majority of participants never or occasionally required assistance with reading health information materials or experienced difficulty learning about their medical illness because of difficulty understanding health information materials (80 and 75% respectively), and 72% were extremely, or quite a bit, confident in completing medical forms (Table 2).

|
The combined BHLS scores for the three questions ranged between 3 and 15 (mean 5.6). A majority of participants (305/424; 72%) had adequate health literacy.
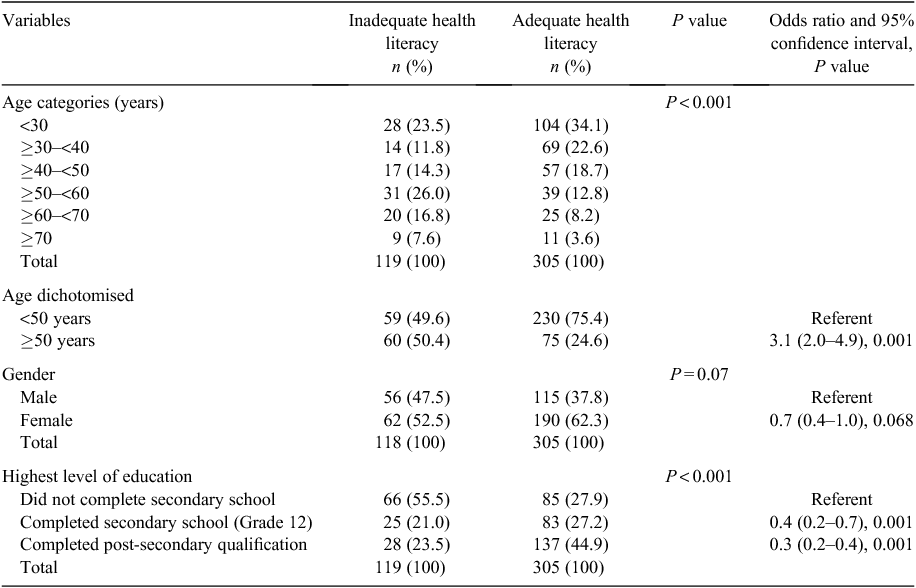
The univariate logistic regression analysis found age ≥50 years to be significantly associated with inadequate health literacy and completing secondary or post-secondary qualification was protective (Table 3). Both factors were included in the multivariate logistic regression model. Age ≥50 years was independently associated with inadequate health literacy (OR 2.7; 95% CI 1.7–4.3; P = 0.0001), and completion of secondary and post-secondary qualification was protective (OR 0.5, 95% CI 0.4–0.7; P = 0.001). The model had moderate discriminatory ability; Area under ROC 0.70 (95% CI 0.64–0.75).
Consumer assessment of healthcare providers and systems: communication with health provider
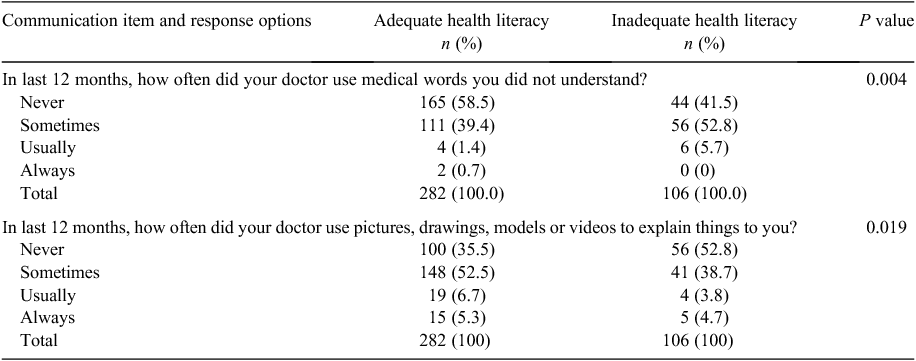
Of the 394 participants attending the Clinic in the previous 12 months (Table 1), 392 completed this section. A majority of participants identified positive experiences with all except two of the nine CAHPS questions: 46% stated GPs sometimes, usually or always used medical words they did not understand; and 40% stated GPs never used visual aids when providing information (Table 4).

|
There was a significant association between difficulty understanding medical words and health literacy adequacy (P = 0.004; Table 5). Similar results were found among participants aged ≥50 years (P = 0.023).
|
There was a significant association between GPs using visual aids to provide information and health literacy adequacy (P = 0.02; Table 5). Although similar experiences were reported among participants aged ≥50 years (54% with inadequate and 42% with adequate health literacy stating the GP never used visual aids), this difference did not reach significance (P = 0.58).
Participant experiences of information provided by GPs
Participants providing comments on their communications with GPs were satisfied with information provided, as described by a participant:
I find the medical staff very helpful, they are aware of cultural concerns as well as personal health matters. I have been to other Aboriginal and Torres Strait Islander health services, and … come back to Inala because of the level of care and professionalism [40–45-year-old female participant].
Effective communication techniques used by GPs were identified and included interpersonal communication skills (such as being friendly, courteous, understanding, helpful, knowledgeable); simplifying information by ‘breaking down’ medical terminology; explaining reasons for prescribing medications; providing information in small segments; and using visual aids, as one participant stated:
If they did use medical terms I did not understand, they always explained it to me and showed me where to access info on the web [50–55-year-old female participant].
Suggested strategies to communicate effectively included: using simple clear language, tailoring the words to the participant’s level of understanding, encouraging participants to ask questions, seeking feedback and being aware that participants may not ask questions because they do not know what to ask.
[Doctors] … talk at my level not theirs. Saying ‘you got to ask the questions’ means I have to know what I should ask … simple, plain facts, for example if you don’t do this, this is what will happen [60-65-year-old male participant].
Discussion
This is the first study describing the prevalence of, and factors associated with, health literacy among Aboriginal and Torres Strait Islander people attending an urban Indigenous primary healthcare clinic in Australia, and experiences of communication with GPs. The combined use of the BHLS and CAHPS questions in the survey has strengthened the study by providing information on the multiple dimensions of health literacy, consistent with its current definition. A high proportion of participants surveyed in this study reported having adequate health literacy. Methodological differences made it difficult to compare prevalence rates from other international and Australian studies.
A majority of participants in our study experienced positive communication with GPs, except for difficulty understanding medical words and infrequent use of visual aids. Some qualitative studies have highlighted the negative outcomes of ineffective communication of health information by health professionals to Aboriginal and Torres Strait Islander people living with chronic diseases in remote areas of Australia, and suggested some useful communication strategies when providing information (Cass et al. 2002; Anderson et al. 2008; Davies et al. 2014). Lin et al. (2016) describe a culturally meaningful communication framework described as ‘clinical yarning’. It is a relaxed, open-style conversation with story-telling as the medium to discuss health issues with health practitioners.
Our convenience sample of English-speaking Aboriginal and Torres Strait Islander participants attending one Indigenous-specific primary healthcare clinic limits generalisability of the study findings. Accessing primary health care in this environment may reduce the demand on patients to possess adequate health literacy to understand health information. The use of simple oral language and easy access to the same GP provides opportunities to seek answers to questions over multiple visits and minimises reliance on written health information materials. Information provision in this environment also confirms that health literacy arises from the interaction between patient knowledge, skill and confidence, and the information demands of health and health services (Parker 2009). Therefore, risk for our participants arises when they access other healthcare services that do not have the same empathetic relationships observed in our study.
Given the association between health literacy and health outcomes, further research is required to identify strategies to ensure effectiveness of communication between Aboriginal and Torres Strait Islander peoples and health professionals in all circumstances.
Practice implications
The study findings identify patients or their carers at a greater risk of inadequate health literacy and highlight the need to screen patient’s health literacy adequacy. Interpersonal skills of GPs are important in effectively communicating with patients. Patients vary in their requirements for, and preferred method of, communication of health information. A variety of visual aids, such as simple colourful drawings, pictures, photos and anatomical models, should be used when providing information. Use of medical terms should be avoided.
Conclusion
The study findings contribute to evidence on the adequacy of health literacy among Aboriginal and Torres Strait Islander people attending a suburban Indigenous-specific primary healthcare clinic, and their experiences of communication of health information from GPs. Future population-based studies into health literacy and its effect on health status are required to address the inequity in health status of Aboriginal and Torres Strait Islander people.
Conflicts of interest
N. Hayman, D. Askew and P. Lakhan are all employed at the primary health care Clinic where the study was undertaken. C. Kirk was employed at the Clinic when the study was being conducted.
Acknowledgements
We sincerely thank all participants who took part in the survey; administration staff, all doctors and nurses employed at the Clinic for their support; Ms Michelle Bowles (Registered Nurse) for assistance with obtaining data on total eligible patients and response rate for the survey; and all members of the Inala Community Jury for Aboriginal and Torres Strait Islander Health Research for their advice and support of this study. The research reported in this paper is a project of COMPaRE-PHC (Centre for Obesity Management and Prevention Research Excellence in Primary Health Care), which is funded by the Australian Primary Health Care Research Institute and the Australian Government Department of Health.
References
Agency for Healthcare Research and Quality (2016) Supplemental Health Literacy Items for the CAHPS Hospital Survey: Adult. (Agency for Healthcare Research and Quality: Rockville, MD, USA) Available at https://www.ahrq.gov/cahps/surveys-guidance/cg/instructions/12monthsurvey.html [Verified 17 February 2017]Anderson K, Devitt J, Cunningham J, Preece C, Cass A (2008) ‘All they said was my kidneys were dead’: Indigenous Australian patients’ understanding of their chronic kidney disease. The Medical Journal of Australia 189, 499–503.
Berkman ND, Sheridan SL, Donahue KE, Halpern DJ, Crotty K (2011) Low health literacy and health outcomes: an updated systematic review. Annals of Internal Medicine 155, 97–107.
| Low health literacy and health outcomes: an updated systematic review.Crossref | GoogleScholarGoogle Scholar |
Bond C, Foley W, Askew D (2016) ‘It puts a human face on the researched’ – a qualitative evaluation of an Indigenous health research governance model. Australian and New Zealand Journal of Public Health 40, S89–S95.
| ‘It puts a human face on the researched’ – a qualitative evaluation of an Indigenous health research governance model.Crossref | GoogleScholarGoogle Scholar |
Cass A, Lowell A, Christie M, Snelling P, Flack M, Marrnganyin B, Brown I (2002) Sharing the true stories: improving communication between Aboriginal patients and healthcare workers. The Medical Journal of Australia 176, 466–470.
Cawthon C, Mion L, Willens D, Roumie C, Kripalani S (2014) Implementing routine health literacy assessment in hospital and primary care patients. Joint Commission Journal on Quality and Patient Safety 40, 68–76.
| Implementing routine health literacy assessment in hospital and primary care patients.Crossref | GoogleScholarGoogle Scholar |
Chew LD, Bradley KA, Boyko EJ (2004) Brief questions to identify patients with inadequate health literacy. Family Medicine 36, 588–594.
Chew LD, Griffin JM, Partin MR, Noorbaloochi S, Grill JP, Snyder A, Bradley KA, Nugent SM, Baines AD, Vanryn M (2008) Validation of screening questions for limited health literacy in a large VA outpatient population. Journal of General Internal Medicine 23, 561–566.
| Validation of screening questions for limited health literacy in a large VA outpatient population.Crossref | GoogleScholarGoogle Scholar |
Collins SA, Currie LM, Bakken S, Vawdrey DK, Stone PW (2012) Health literacy screening instruments for eHealth applications: a systematic review. Journal of Biomedical Informatics 45, 598–607.
| Health literacy screening instruments for eHealth applications: a systematic review.Crossref | GoogleScholarGoogle Scholar |
Commonwealth of Australia (2016) Closing the Gap. Prime Minister’s Report 2016. (Department of the Prime Minster and Cabinet: Canberra, ACT, Australia) Available at http://closingthegap.dpmc.gov.au/assets/pdfs/closing_the_gap_report_2016.pdf [Verified 27 July 2016]
Davies J, Bukulatjpi S, Sharma S, Davis J, Johnston V (2014) ‘Only your blood can tell the story’ – a qualitative research study using semi-structured interviews to explore the hepatitis B related knowledge, perceptions and experiences of remote dwelling Indigenous Australians and their health care providers in northern Australia. BMC Public Health 14, 1233
| ‘Only your blood can tell the story’ – a qualitative research study using semi-structured interviews to explore the hepatitis B related knowledge, perceptions and experiences of remote dwelling Indigenous Australians and their health care providers in northern Australia.Crossref | GoogleScholarGoogle Scholar |
Faruqi N, Lloyd J, Ahmad R, Yeong L-L, Harris M (2015) Feasibility of an intervention to enhance preventive care for people with low health literacy in primary health care. Australian Journal of Primary Health 21, 321–326.
| Feasibility of an intervention to enhance preventive care for people with low health literacy in primary health care.Crossref | GoogleScholarGoogle Scholar |
Harris M (2016) The interface between primary health care and population health: challenges and opportunities for prevention. Public Health Research & Practice 26, e2611601
| The interface between primary health care and population health: challenges and opportunities for prevention.Crossref | GoogleScholarGoogle Scholar |
Hayman NE, Askew DA, Spurling GK (2014) From vision to reality: a centre of excellence for Aboriginal and Torres Strait Islander primary health care. The Medical Journal of Australia 200, 623–624.
| From vision to reality: a centre of excellence for Aboriginal and Torres Strait Islander primary health care.Crossref | GoogleScholarGoogle Scholar |
Horowitz AM, Wang MQ, Kleinman DV (2012) Opinions of Maryland adults regarding communication practices of dentists and staff. Journal of Health Communication 17, 1204–1214.
| Opinions of Maryland adults regarding communication practices of dentists and staff.Crossref | GoogleScholarGoogle Scholar |
Jamieson LM, Parker EJ, Richards L (2008) Using qualitative methodology to inform an Indigenous-owned oral health promotion initiative in Australia. Health Promotion International 23, 52–59.
| Using qualitative methodology to inform an Indigenous-owned oral health promotion initiative in Australia.Crossref | GoogleScholarGoogle Scholar | 1:STN:280:DC%2BD1c7htFWlsQ%3D%3D&md5=3d195a876bc3298a897faf2e2c1abe32CAS |
Jamieson LM, Divaris K, Parker EJ, Lee JY (2013) Oral health literacy comparisons between Indigenous Australians and American Indians. Community Dental Health 30, 52–57.
Lake T, Kvam C, Gold M (2005) Literature review: using quality information for health care decisions and quality improvement. 2005. Contract number 233–02–0086; MPR Reference number 6110–230. (Mathematica Policy Research, Inc.: Cambridge, MA, USA) Available at https://cahps.ahrq.gov/about-cahps/cahps-program/qualityinfo.pdf [Verified 3 February 2015]
Lin I, Green C, Bessarab D (2016) ‘Yarn with me’: applying clinical yarning to improve clinician-patients communication in Aboriginal health care. Australian Journal of Primary Health 22, 377–382.
| ‘Yarn with me’: applying clinical yarning to improve clinician-patients communication in Aboriginal health care.Crossref | GoogleScholarGoogle Scholar |
Paasche-Orlow MK, Wolf MS (2007) The causal pathways linking health literacy to health outcomes. American Journal of Health Behavior 31, S19–S26.
| The causal pathways linking health literacy to health outcomes.Crossref | GoogleScholarGoogle Scholar |
Parker R (2009) Measuring health literacy: why? So what? Now what? In ‘Measures of Health Literacy: Workshop Summary’, 26 February 2009, Washington, DC, USA. (Ed. L Hernandez) pp. 91–94. (National Academies Press: Washington, DC, USA)
Parker EJ, Jamieson LM (2010) Associations between Indigenous Australian oral health literacy and self-reported oral health outcomes. BMC Oral Health 10, 3
| Associations between Indigenous Australian oral health literacy and self-reported oral health outcomes.Crossref | GoogleScholarGoogle Scholar |
Shirk JD, Tan HJ, Hu JC, Saigal CS, Litwin MS (2016) Patient experience and quality of urologic cancer surgery in US hospitals. Cancer 122, 2571–2578.
| Patient experience and quality of urologic cancer surgery in US hospitals.Crossref | GoogleScholarGoogle Scholar |
Sørensen K, Van den Broucke S, Fullam J, Doyle G, Pelikan J, Slonska Z, Brand H (2012) Health literacy and public health: a systematic review and integration of definitions and models. BMC Public Health 12, 80
| Health literacy and public health: a systematic review and integration of definitions and models.Crossref | GoogleScholarGoogle Scholar |
The National Health and Medical Research Council (2015) National statement on ethical conduct in human research. 2015 update. (The National Health and Medical Research Council; the Australian Research Council; Australian Vice-Chancellors’ Committee; Commonwealth of Australia: Canberra, ACT, Australia) Available at https://www.nhmrc.gov.au/_files_nhmrc/publications/attachments/e72_national_statement_may_2015_150514_a.pdf [Verified 18 July 2016]
Thiels CA, Hanson KT, Yost KJ, Mathis KL, Cima RR, Zielinski MD, Habermann EB (2016) Achieving a 5-star rating: analysis of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) scores among patients undergoing elective colorectal operations. Surgery 160, 902–914.
| Achieving a 5-star rating: analysis of Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) scores among patients undergoing elective colorectal operations.Crossref | GoogleScholarGoogle Scholar |
Wallston KA, Cawthon C, McNaughton CD, Rothman RL, Osborn CY, Kripalani S (2014) Psychometric properties of the brief health literacy screen in clinical practice. Journal of General Internal Medicine 29, 119–126.
| Psychometric properties of the brief health literacy screen in clinical practice.Crossref | GoogleScholarGoogle Scholar |